CIC Edizioni Internazionali. original article. Transanal repair of rectocele with high frequency radio scalpel. Patients and methods.
|
|
|
- Nicholas Carroll
- 5 years ago
- Views:
Transcription
1 G Chir Vol n. 5 - pp September-October 2018 Transanal repair of rectocele with high frequency radio scalpel D. SFORZA, C. BELARDI, M. PELLICCIARO, V. FILINGERI SUMMARY: Transanal repair of rectocele with high frequency radio scalpel. D. SFORZA, C. BELARDI, M. PELLICCIARO, V. FILINGERI Aim. This is a prospective randomized study to analyze results obtained in two groups of patients, affected by stage 2 rectocele and treated with rectum anterior wall repair and strength, performed with standard or modified Khubchandani technique, using High Frequency (HF) Radio Scalpel. Materials and methods. A cohort of 24 patients with stage 2 rectocele (Mellgren s classification) have been included. Twelve (group A) underwent surgery with standard technique and twelve (group B) underwent surgery using the HF Radio Scalpel, which cuts and coagulates tissues without damage thanks to its low working temperature (45-70 C). Each patient underwent proctolo- Introduction KEY WORDS: Rectocele - Rectocele repair - Transanal surgery - Radiofrequency scalpel. Surgical treatment of rectocele represents a controversial issue among colorectal surgeons. Many techniques have been considered and this means that the ideal one has not been chosen yet. In fact, each procedure has its own advantages and disadvantages from a technical, clinical and economical point of view. Transanal surgical treatment seems to have the best clinical results so it is the favourite treatment of the majority of authors at the moment. The aim of this study is to estimate the results obtained with modified Khubchandani technique performed with High Frequency (HF) Radio Scalpel (1, 2), compared to the standard technique (3). Patients and methods original article gical examination and anoscopy in 7th, 15th, 45th POD and after 6 and 12 months. Results. During post-operative follow-up 5 patients from group A and 1 from group B didn t show up so that they drop out the study. As a result, group A is composed by 7 patients and group B by 11 patients. Mean operating time was significantly favourable in group B (51 vs 33 minutes, p< 0.01). The differences between other parameters weren t statistically significant, even if post-operative course was less difficult in HF Radio Scalpel group. Conclusions. The surgical technique to repair and reinforce anterior rectal wall is easier and faster if performed with HF Radio Scalpel respect to the standard procedure described by Khubchandani. Post-operative course was less painful and, even more importantly considering the patient age, surgical time was shorter. Therefore, the results obtained cast positive light on using this technique to treat uncomplicated grade 2 rectocele. For this study we used the CONSORT criteria (4). Once we received the approval of the ethical committee, we informed patients and obtained their consent. Twenty-four patients with stage 2 rectocele (according to Mellegren s classification) (5) were selected and divided into 2 groups: 12 underwent surgery with standard Khubchandani s technique (group A) and 12 underwent surgery using the HF Radio Scalpel (group B). The surgeon was always the same one. Diagnoses were obtained using defecography o defeco-mr. Exclusion criteria were: recto-anal prolapse and other proctological disorders (each patient underwent proctological examination and proctosigmoidoscopy), previous proctological surgery, pregnancy and high anaesthesia risk (ASA III or IV). Anticoagulant drugs were stopped 7 days before surgery. No particular diet was advised. Department of Experimental Medicine and Surgery, Transplant Unit, University of Rome Tor Vergata, Rome, Italy Corresponding author: Vincenzino Filingeri, v.filingeri@tiscali.it Copyright 2018, CIC Edizioni Internazionali, Roma 303
2 An enema was administered 4 hours before surgery as preoperative preparation. At the induction of anaesthesia prophylactic antibiotics were used: metronidazole 500 mg and ceftriaxone 2 g by intravenous infusion (iv). General and epidural anaesthesia were alternatively used according to anaesthesiologist evaluation. Post-operative treatment consisted of Metronidazole 500 mg iv every 8 hours in the first postoperative day and Ketorolac 30 mg if needed for pain control. After hours, we administered a mild laxative (lactulose mg) to facilitate the first evacuation or paraffin oil (3 spoons/day) in order to make stool softer and reduce traumatisms in the anal canal. After procedure a highfiber diet was prescribed with administration of Flavonoid pills Deflanil Plus (quercetin 200 mg and hesperidin 50 mg, with Resveratrol, Bromelain, Folic acids, vitamin C and D). We preferred this product because it is more complete and it is sold in single use packages (6). Every patient underwent proctological examination and anoscopy on the 7 th, 15 th, 45 th POD and after 6 and 12 months. D. Sforza et al. Surgical technique Surgical technique adopted derives from Khubchandani s one modified using HF Radio Scalpel. The aim was to correct the deformation of the anterior anorectal wall using a trans-anal approach trying to reconstitute the solidity of the pathological wall through the use of internal sutures to allow the formation of scarring fibrosis. The patient is positioned in gynaecological and slightly Trendelenburg position, and for optimum exposure of the rectocele, the Parks retractor is used. The mucosal tissue is infiltrated with adrenaline, diluted with saline solution (concentration 1: ), to facilitate the detachment and hemostasis maneuvers. Using the HF Radio Scalpel a lozenge surface incision is performed with a transversal axis relative to the intestinal lumen, only on the margin of the rectocele. The mucosa covering the rectocele is delicately detached and removed to promote the development of scarring fibrosis. After an accurate hemostasis the rectal wall is repaired. Two stitch are positioned on the end of lozenge, held in tension to facilitate the suture. Interrupted suture is performed, usually with 7-8 stitches, using absorbable sutures (Vycril 2/0). In order to obtain a plication of the rectocele wall and therefore its reduction and correction (Figure 1), the suture of the upper margin is first performed, then the muscular layer with at least two passes and finally the lower margin (Figures 1, 2). During the plication it is advisable to insert a finger into the vagina both to facilitate the suture and to verify that the vagina is not involved in the suture. HF Radio Scalpel, used for the detachment and removal of the mucosa, allowed to cut and coagulate without damaging the tissues. This is made possible by the lower operating temperature of the HF Radio Figure 1 - After the transverse incision at the dentate line and removing a mucosa rectal flap, a vertical plication sutures starting. Figure 2 - Final suture vision. 304
3 Scalpel (45-70 ) compared to the traditional electro-centric scalpel ( ) (1, 2). Statistical analysis The statistical analysis was performed with the Statistical Package for the Social Science Windows version 1.7 (SPSS Inc., Chicago, IL, USA). Descriptive statistics for quantitative variables were the mean and Standard Deviation (mean ± SD). The comparison was performed with the Fisher s exact test for categorical variables and the Student s t-test. Results In the period between January 2006 and December 2014, 24 patients with stage 2 rectocele, using Mellgren s classification, were randomized into two groups before surgery. During post-operative followup 5 patients from group A and 1 from group B didn t show up so they drop out the study. As a result, group A was composed by 7 patients (mean age 60,3 ± 7,8) and group B by 11 patients (mean age 63,8 ± 7,2). In Table 1 there is a list of the preoperative symptoms described by patients, lasting for at least 4 years. Six patients from group A and (85,7%) and 9 from group B (81,8%) reported constipation with feces type 1-2 on the Bristol stool scale (7); 6 patients from group A (85,7%) and 9 from group B (81,8%) reported pain during and after defecation and necessity of fingers inserted into the vagina to assist evacuation (group A 42,8% and group B 72,7%). No cases of incontinence have been reported. Defecation in two or more times concerned 6 patients from group A Transanal repair of rectocele with high frequency radio scalpel TABLE 1 - PREOPERATIVE REPORTED SYMPTOMS FOR AT LEAST 4 YEARS. (85,7%) and 10 patients from group B (90,1%). Four patients from group A (57,1%) and 7 patients from group B (63,6%) needed laxatives at least once a week (Table 2). The quality of life regarding defecation was estimated according to Agachan-Wexner s criteria (8), with a mean value of 19,5 for patients from group A and 19,1 for patients from group B. This score, also known as Cleveland Clinic Constipation Score, includes 8 variables (number of evacuations, time needed to defecate, abdominal pain, attempts of defecation, difficult defecation, incomplete defecation, manual support and constipation duration) with an increasing score from 0 to 4 and a total score from 0 to 30. No meaningful complications or problems have been reported during surgery and hospitalization. No cases of post-operative hypotonic sphincter were observed. Mean operative time was 51 minutes for group A and 33 minutes for group B (p<0.01). Only 4 patients from group A (57,1%) and 4 patients from group B (36,7%) referred severe pain, successfully treated with Ketorolac 30 mg i.m. All the patients were discharged in the first postoperative day. Table 2 shows symptoms reported during the follow-up. In both groups pain is particularly evident during the first week. Moreover, the permanence of constipation, which required laxatives, was observed in almost all patients. All the problems reported before the surgery seems to be significantly improved. No relapse was reported after 12 months and no one required enema. All the patients were satisfied with the results of surgery. All the data recorded were not statistically Group A Group B Standard technique HF Radio Scalpel Constipation 6 (85,7%) 9 (81,8%) Pain during and after defecation 6 (85,7%) 9 (81,8%) Defecation in two or more times 6 (85,7%) 10 (90,1%) Need to insert fingers inside the vagina 3 (42,8%) 8 (72,7%) Incontinence - - Need of laxatives at least once a week 4 (57,1%) 7 (63,6%) Need of enema at least once a week 1 (14,3%) 1 (9,1%) 305
4 D. Sforza et al. TABLE 2 - POST-OPERATIVE RESULTS. significant, exception made for the mean operative time. Discussion Group A Standard technique 7 th POD 15 th POD 45 th POD 6 th Month 12 th Month Post-Operative Pain 4 (57,1%) 2 (28,6%) Constipation 3 (42,1%) 3 (42,1%) 3 (42,1%) 2 (28,6%) 2 (28,6%) Pain during and after defecation 1 (14,2%) 1 (14,2%) Defecation in two or more times (14,2%) 1 (14,2%) Need to insert fingers inside the vagina 1 (14,2%) 1 (14,2%) 1 (14,2%) 1 (14,2%) 1 (14,2%) Incontinence Need of laxatives at least once a week 7 (100%) 7 (100%) 6 (86,7%) 2 (28,6%) 2 (28,6%) Need of enema at least once a week Group B HF Radio Scalpel 7 th POD 15 th POD 45 th POD 6 th Month 12 th Month Post-Operative Pain 4 (36,7%) 2 (18,2%) Constipation 4 (36,7%) 4 (36,7%) 4 (36,7%) 4 (36,7%) 4 (36,7%) Pain during and after defecation 1 (9,1%) 1 (9,1%) Defecation in two or more times (28,6%) 2 (28,6%) Need to insert fingers inside the vagina (28,6%) 2 (28,6%) 2 (28,6%) Incontinence Need of laxatives at least once a week 10 (90,1%) 10 (90,1%) 6 (54,2%) 4 (36,7%) 4 (36,7%) Need of enema at least once a week Rectocele is a frequent pathological condition characterized by the herniation of the anterior wall of rectum through the rectovaginal septum. So both proctologist and gynecologist are involved. Defecography or Defeco-MR and Anorectal Manometry allow an accurate diagnosis, dimensions of rectocele and the presence of potential dynamic alteration of the pelvic floor. The Obstructed Defecation Syndrome (ODS) represents the more frequent problem in this disorder. It consists of an anatomical and functional obstacle to evacuation, despite the stimulus and with a feeling of incomplete emptying. Defecation is particularly laborious. Often to be completed need to push for a long time and use of hands to complete the evacuation. This causes in patients prostration and shame. Abuse of enemas and laxatives is often frequent. In the most severe cases perianal pain may be present, sometimes with difficulty treatment. The symptomatology influences negatively the quality of life of these patients. The large dimension of rectocele is not an absolute indication for surgical treatment. In fact, the symptoms are not always related to size: the large rectocele can be asymptomatic and often are occasional finds while the small one can be very annoy- 306
5 Transanal repair of rectocele with high frequency radio scalpel ing. Only symptomatic rectocele justifies surgical treatment. Over the last years many surgical techniques have been proposed and there is not a gold standard treatment at the moment. The surgical procedures can be divided into trans-vaginal, trans-anal or by abdominal access. Trans-vaginal techniques, preferred by gynaecologists, involve reconstruction of muscle fascial defects using prosthesis. The aim of trans-anal techniques is to eliminate the pathological lesion in the rectum. The most popular techniques are Delorme (the pathological mucosa is removed circumferentially to expose the muscle of the intestinal wall and is sutured with single stitch readsorbable), Sullivan and Khubchandani procedures (correction of the anterior rectal deformation by plication with single stitches). Recently two techniques have been described: STARR with PPH01 and STARR with Contour Transtar (rectal trans-anal resection and reconstruction using mechanical stapler) (9-12). Trans-anal techniques have the advantage of being less invasive, easier and faster. They maintain normal morphology and physiology of the rectum especially during the evacuation. When rectocele is associated to a complete prolapse the correct surgical treatment is rectopexy (fixation of the rectal trough the abdomen). The abdominal laparoscopic techniques reconstruct the anatomical planes to sustain pelvic organs in the correct position. There are several techniques for example suture rectopexy in which the rectum is directly anchored to the sacrum using sutures or mesh. D Hoore s anterior rectopexy is the most common, it can be laparoscopic and consists of the anterior mobilization of the rectum accessing the recto-vaginal space. Using mesh, which is fixed between rectum and vagina, the reinforcing of the anterior wall of the rectum is obtained. In the superior part, the mesh is fixed to the sacrum hanging up the rectum and therefore reducing prolapse. With this technique, lateral and posterior mobilization is not necessary with an important reduction of the risk of denervation and postoperative constipation (very common in rectopexy surgeries) (13). In our opinion, the choice of surgical technique should be based on the clinical and radiological evaluation of the rectocele. Voluminous rectoceles with dimensions over than 4 cm surely have less chances of success, higher probability of relapse and higher incidence of functional complications. To obtain homogeneity in our results with the technique that we adopted, in this study we limited the indication only to second stage rectocele (Mellgren s classification). We believe that the surgical treatment of the rectocele should be quick and easy, improving the quality of life of the patients. It is important that the technique is minimally invasive and preserves the morphology, the physiology of the pelvic floor and the functionality of the anal sphincter. The technique we have adopted is simple and allows you to repair the anterior wall of the rectum resolving the clinical symptomatology. Unlike the Khubchandani technique, we remove excess mucosa to work directly on the sphincter, without changing the normal proportions of the anorectal angle and reducing the possibility of potential damage. The HF Radio Scalpel, thanks to its peculiar characteristics, facilitates the surgical maneuvers of preparation and dissection of the mucosa. The use of 4 MHz Radio Waves produces heat and this allows cutting and coagulating the tissues without any trauma. In the section line, each vessel with a diameter less than mm is coagulated, reducing bleeding at the capillaries. Thus, operating time has been significantly reduced. This improvement should not be underestimated considering the age of the patients. This also entails a significant reduction in costs and other immediate problems such as postoperative pain and bleeding. It is very important explain to the patients that surgery can solve symptoms related to rectocele but not other disorders associated like constipation, irritable bowel syndrome or perineal descent. The permanence of constipations might be related to the pain during the first two weeks, as showed in our results, and to psychological reasons. Constipation may be treated with high-fiber diet to reduce the incidence of relapses. Conclusions The surgical treatment, modified respect to the Khubchandani s using the HF Radio Scalpel, is easier and with a good results. The reduction of operative time is particularly significant, especially considering the patient s age, as well as the postoperative problems like pain and bleeding. In conclusion, this technique seems to be a good choice for the treatment of uncomplicated grade 2 rectocele, according to Mellgren s classification. 307
6 References 1. Filingeri V, Gravante G, Cassisa D. Physics of radiofrequency in proctology. Eur Rev Med Pharmacol Sci. 2005;9: Filingeri V, Gravante G, Cassisa D. Clinical applications of radiofrequency in proctology: a review. Eur Rev Med Pharmacol Sci. 2006;10: Khubchandani It, Clancy JP, Rosen L, Riether RD, Stasik JJ Jr. Endorectal repair of rectocele revisited. Br J Surg. 1997;84: Moher D, Schulz KF, Altman DG. The CONSORT statement: revised commentations for improving the quality of reports of parallel-group randomized trials. Lancet. 2001;357: Mellgren A, Anzén B, Nilsson BY, Johansson C, Dolk A, Gillgren P, Bremmer S, Holmström B. Results of rectocele repair. A prospective study. Dis Colon Rectum. 1995;38: Filingeri V, Buonomo O, Sforza D. Use of Flavonoids for the treatment of symptoms after hemorrhoidectomy with radiofrequency scalpel. Eur Rev Med Pharmacol Sci. 2014;18: Lewis SJ, Heaton KW. Stool form scale as a useful guide to intestinal transit time. Scandinavian Jorunal of Gastroenterology. 1997;32: Agachan F, Chen T, Pfeifer J, Reissman P, Wexner SD. A D. Sforza et al. constipation scoring system to simplify evaluation and management of constipated patients. Dis Colon Rectum. 1996; 39: A.Gaj F, Trecca A, Andreucetti j, Crispino P. Trattamento del rettocele e del prolasso mucoso del retto con escissione a lembi della mucosa con sutura manuale. Clin Ter. 2011;162:e Gagliardi G, Pescatori M, Altomare DF, Binda GA, Bottini C, Dodi G, Filingeri V, Milito G, Rinaldi M, Romano G, Spazzafumo L, Trompetto M. Results, outcome predictors, and complications after stapled transanal rectal resection for obstructed defecation. Dis Colon Rectum. 2008;51: Gentile M, De Rosa M, Cestaro G, Vitiello C, Sivero L. Internal Delorme vs. STARR procedure for correction of obstructed defecation from rectocele and rectal intussusception. Ann Ital Chir;85: L Lenisa, O Schwandner, A Stuto, D Jayne, F Pigot, JJ Tuech, R Scherer, K Nugent, F Corbisier, E Espin-Basany, FH Hetzer. STARR with Contour Transtar : prospective multicentre European study. Colorectal Dis. 2009;11: D Hoore A, Cadoni R, Penninckx F. Long-term outcome of laparoscopic ventral rectopexy for total rectal prolapse. Br J Surg. 2004;91:
Original Article. Keywords Obstructive Resection Iran. Introduction
 IJMS Vol 39, No 5, September 2014 Original Article Comparing the Outcomes of Stapled Transanal Rectal Resection, Delorme Operation and Electrotherapy Methods Used for the Treatment of Obstructive Defecation
IJMS Vol 39, No 5, September 2014 Original Article Comparing the Outcomes of Stapled Transanal Rectal Resection, Delorme Operation and Electrotherapy Methods Used for the Treatment of Obstructive Defecation
Perineale Rektumprolapsoperation: Gute Resultate bei geringem Aufwand! F.H. Hetzer
 Perineale Rektumprolapsoperation: Gute Resultate bei geringem Aufwand! F.H. Hetzer STARR: Wunderwaffe beim Obstructed Defecation Syndrom (ODS) F.H. Hetzer Stapled TransAnal Rectal Resection STARR PPH 01
Perineale Rektumprolapsoperation: Gute Resultate bei geringem Aufwand! F.H. Hetzer STARR: Wunderwaffe beim Obstructed Defecation Syndrom (ODS) F.H. Hetzer Stapled TransAnal Rectal Resection STARR PPH 01
Stapled transanal rectal resection for obstructed defaecation syndrome
 Stapled transanal rectal resection for obstructed Issued: June 2010 www.nice.org.uk/ipg351 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Stapled transanal rectal resection for obstructed Issued: June 2010 www.nice.org.uk/ipg351 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 6, Issue 1 Article 3 Starr Surgery In ODS: A Case Series Of 500 ODS Patients Operated At India s Largest Proctology Clinic Ashwin Dhanarajji Porwal Paresh Manilal
World Journal of Colorectal Surgery Volume 6, Issue 1 Article 3 Starr Surgery In ODS: A Case Series Of 500 ODS Patients Operated At India s Largest Proctology Clinic Ashwin Dhanarajji Porwal Paresh Manilal
B I O L I F E R E S E A R C H A R T I C L E. Trans rectal rectocele repair vs standard posterior colporaphy in the treatment of obstructed defecation
 AN INTERNATIONAL QUARTERLY JOURNAL OF BIOLOGY & LIFE SCIENCES 3(2):361-366 B I O L I F E R E S E A R C H A R T I C L E Trans rectal rectocele repair vs standard posterior colporaphy in the treatment of
AN INTERNATIONAL QUARTERLY JOURNAL OF BIOLOGY & LIFE SCIENCES 3(2):361-366 B I O L I F E R E S E A R C H A R T I C L E Trans rectal rectocele repair vs standard posterior colporaphy in the treatment of
Robotic Ventral Rectopexy
 Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
3D Dynamic Ultrasound In Obstructed Defecation
 3D Dynamic Ultrasound In Obstructed Defecation By Ramy Salahudin Abdelkader Assist. Lecturer of General Surgery Cairo University Introduction Pelvic floor is complex system, with passive and active components
3D Dynamic Ultrasound In Obstructed Defecation By Ramy Salahudin Abdelkader Assist. Lecturer of General Surgery Cairo University Introduction Pelvic floor is complex system, with passive and active components
Summary and conclusion. Summary And Conclusion
 Summary And Conclusion Summary and conclusion Rectal prolapse remain a disorder for which no single ideal treatment was approved for all cases. Complete rectal prolapse (procidentia) is the circumferential
Summary And Conclusion Summary and conclusion Rectal prolapse remain a disorder for which no single ideal treatment was approved for all cases. Complete rectal prolapse (procidentia) is the circumferential
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Pelvic Floor Disorders. Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon
 Pelvic Floor Disorders Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon What is Pelvic Floor Disorder Surgical perspective symptoms of RED, FI or prolapse on the background
Pelvic Floor Disorders Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon What is Pelvic Floor Disorder Surgical perspective symptoms of RED, FI or prolapse on the background
Resected specimen evaluation, anorectal manometry, endoanal ultrasonography and clinical follow-up after STARR procedures
 Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v17.i19.2411 World J Gastroenterol 2011 May 21; 17(19): 2411-2416 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v17.i19.2411 World J Gastroenterol 2011 May 21; 17(19): 2411-2416 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Motility Disorders. Pelvic Floor. Colorectal Center for Functional Bowel Disorders (N = 701) January 2010 November 2011
 Motility Disorders Pelvic Floor Colorectal Center for Functional Bowel Disorders (N = 71) January 21 November 211 New Patients 35 3 25 2 15 1 5 Constipation Fecal Incontinence Rectal Prolapse Digestive-Genital
Motility Disorders Pelvic Floor Colorectal Center for Functional Bowel Disorders (N = 71) January 21 November 211 New Patients 35 3 25 2 15 1 5 Constipation Fecal Incontinence Rectal Prolapse Digestive-Genital
A Constipation Scoring System to Simplify Evaluation and Management of Constipated Patients
 A Constipation Scoring System to Simplify Evaluation and Management of Constipated Patients Feran Agachan, M.D., Teng Chen, M.D., Johann Pfeifer, M.D., Petachia Reissman, M.D., Steven D. Wexner, M.D.,
A Constipation Scoring System to Simplify Evaluation and Management of Constipated Patients Feran Agachan, M.D., Teng Chen, M.D., Johann Pfeifer, M.D., Petachia Reissman, M.D., Steven D. Wexner, M.D.,
Rectal Prolapse: A 10-Year Experience
 24 The Ochsner Journal Volume 7, Number 1, Spring 2007 25 Rectal Prolapse: A 10-Year Experience Figure 2. Physical examination. A. Concentric folds of prolapsed rectum. B. Radial folds of hemorrhoids (mucosal
24 The Ochsner Journal Volume 7, Number 1, Spring 2007 25 Rectal Prolapse: A 10-Year Experience Figure 2. Physical examination. A. Concentric folds of prolapsed rectum. B. Radial folds of hemorrhoids (mucosal
TYPES OF RECTAL PROLAPSE
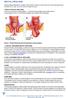 RECTAL PROLPASE Rectal prolapse describes a condition where either the lining or entire wall of the rectum becomes loose and falls into, or even out of, the rectum through the anus. TYPES OF RECTAL PROLAPSE
RECTAL PROLPASE Rectal prolapse describes a condition where either the lining or entire wall of the rectum becomes loose and falls into, or even out of, the rectum through the anus. TYPES OF RECTAL PROLAPSE
Hemorrhoids. Carlos R. Alvarez-Allende PGY-III Colorectal Surgery
 Hemorrhoids Carlos R. Alvarez-Allende PGY-III Colorectal Surgery Overview Anatomy Classification Etiology Incidence Symptoms Differential Diagnosis Medical Management Surgical Management Anatomy Anal canal
Hemorrhoids Carlos R. Alvarez-Allende PGY-III Colorectal Surgery Overview Anatomy Classification Etiology Incidence Symptoms Differential Diagnosis Medical Management Surgical Management Anatomy Anal canal
Surgical repair of vaginal wall prolapse using mesh
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
Maurizio Gentile, Michele De Rosa, Gabriele Carbone, Vincenzo Pilone, Francesca Mosella, and Pietro Forestieri. 1. Introduction
 International Scholarly Research Network ISRN Gastroenterology Volume 2011, Article ID 467258, 6 pages doi:10.5402/2011/467258 Clinical Study Haemorrhoidectomy versus Conventional for IV-Degree Haemorrhoids:
International Scholarly Research Network ISRN Gastroenterology Volume 2011, Article ID 467258, 6 pages doi:10.5402/2011/467258 Clinical Study Haemorrhoidectomy versus Conventional for IV-Degree Haemorrhoids:
Hesham M. Hasan 1 and Hani M. Hasan Introduction
 International Scholarly Research Network ISRN Surgery Volume 2012, Article ID 652345, 6 pages doi:10.5402/2012/652345 Clinical Study Stapled Transanal Rectal Resection for the Surgical Treatment of Obstructed
International Scholarly Research Network ISRN Surgery Volume 2012, Article ID 652345, 6 pages doi:10.5402/2012/652345 Clinical Study Stapled Transanal Rectal Resection for the Surgical Treatment of Obstructed
Anorectal malformations include a wide spectrum of
 JOURNAL OF LAPAROENDOSCOPIC & ADVANCED SURGICAL TECHNIQUES Volume 20, Number 1, 2010 ª Mary Ann Liebert, Inc. DOI: 10.1089=lap.2008.0343 Laparoscopic-Assisted Pull-Through for Congenital Rectal Stenosis
JOURNAL OF LAPAROENDOSCOPIC & ADVANCED SURGICAL TECHNIQUES Volume 20, Number 1, 2010 ª Mary Ann Liebert, Inc. DOI: 10.1089=lap.2008.0343 Laparoscopic-Assisted Pull-Through for Congenital Rectal Stenosis
What the radiologist needs to know!
 What the radiologist needs to know! Clare Molyneux Sam Treadway Sathi Sukumar Wal Baraza Abhiram Sharma Karen Telford University Hospital of South Manchester Manchester UK Introduction Indications Investigations
What the radiologist needs to know! Clare Molyneux Sam Treadway Sathi Sukumar Wal Baraza Abhiram Sharma Karen Telford University Hospital of South Manchester Manchester UK Introduction Indications Investigations
Magnetic resonance follow-up protocol for patients after stapled transanal rectal resection for intussusception and rectocele
 Magnetic resonance follow-up protocol for patients after stapled transanal rectal resection for intussusception and rectocele Poster No.: C-2659 Congress: ECR 2013 Type: Scientific Exhibit Authors: S.
Magnetic resonance follow-up protocol for patients after stapled transanal rectal resection for intussusception and rectocele Poster No.: C-2659 Congress: ECR 2013 Type: Scientific Exhibit Authors: S.
Prospective randomised comparison of rubber band ligation (RBL) and combined. hemorrhoidal radiocoagulation (CHR).
 European Review for Medical and Pharmacological Sciences Prospective randomised comparison of rubber band ligation (RBL) and combined hemorrhoidal radiocoagulation (CHR) V. FILINGERI, R. ANGELICO, M.I.
European Review for Medical and Pharmacological Sciences Prospective randomised comparison of rubber band ligation (RBL) and combined hemorrhoidal radiocoagulation (CHR) V. FILINGERI, R. ANGELICO, M.I.
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015
 Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Prolaps: Anteriore Rektopexie nach D Hoore. Prof. Dr. med. F. Hetzer
 Prolaps: Anteriore Rektopexie nach D Hoore Prof. Dr. med. F. Hetzer franc.hetzer@spital-linth.ch Rectal prolapse pathophysiology 24 22 20 18 congenital female pathology (90%) 16 14 straining weakened pelvic
Prolaps: Anteriore Rektopexie nach D Hoore Prof. Dr. med. F. Hetzer franc.hetzer@spital-linth.ch Rectal prolapse pathophysiology 24 22 20 18 congenital female pathology (90%) 16 14 straining weakened pelvic
ARTIFICIAL MESH REPAIR FOR TREATMENT OF PELVIC ORGAN PROLAPSE
 Pelvic Floor Unit / Department of Gynaecology Ward 17, Singleton Hospital, Sketty, Swansea, SA2 8QA 01792 205666 Secretary Direct Line: 01792 285688. Fax: 01792 285874 ARTIFICIAL MESH REPAIR FOR TREATMENT
Pelvic Floor Unit / Department of Gynaecology Ward 17, Singleton Hospital, Sketty, Swansea, SA2 8QA 01792 205666 Secretary Direct Line: 01792 285688. Fax: 01792 285874 ARTIFICIAL MESH REPAIR FOR TREATMENT
Anus,Rectum and Colon
 JOURNAL OF THE Anus,Rectum and Colon http://journal-arc.jp CLINICAL RESEARCH Laparoscopic ventral rectopexy with sacrocolpopexy for coexisting pelvic organ prolapse and external rectal prolapse Yoshiyuki
JOURNAL OF THE Anus,Rectum and Colon http://journal-arc.jp CLINICAL RESEARCH Laparoscopic ventral rectopexy with sacrocolpopexy for coexisting pelvic organ prolapse and external rectal prolapse Yoshiyuki
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Accidental Bowel Leakage (Fecal Incontinence)
 Accidental Bowel Leakage (Fecal Incontinence) What is Accidental Bowel Leakage (ABL)? Accidental bowel leakage is the inability to control solid or liquid stool. This is the inability to control gas and
Accidental Bowel Leakage (Fecal Incontinence) What is Accidental Bowel Leakage (ABL)? Accidental bowel leakage is the inability to control solid or liquid stool. This is the inability to control gas and
Fecal Incontinence. What is fecal incontinence?
 Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 3, Issue 2 2013 Article 7 Delayed Bleeding Following LigaSure Hemorrhoidectomy Alexander Becker, MD Yakov Khromov, MD Joel Sayfan,MD, FACS Department of Surgery
World Journal of Colorectal Surgery Volume 3, Issue 2 2013 Article 7 Delayed Bleeding Following LigaSure Hemorrhoidectomy Alexander Becker, MD Yakov Khromov, MD Joel Sayfan,MD, FACS Department of Surgery
The American Society of Colon and Rectal Surgeons
 CLINICAL PRACTICE GUIDELINES Downloaded from https://journals.lww.com/dcrjournal by BhDMf5ePHKav1zEoum1tQfN4a+kJLhEZgbsIHo4XMi0hCywCX1AWnYQp/IlQrHD3IJrtBKuSsQVRz8fA4yAY0a8W1YLRn6mHykFpaZ5LFvI= on 03/16/2018
CLINICAL PRACTICE GUIDELINES Downloaded from https://journals.lww.com/dcrjournal by BhDMf5ePHKav1zEoum1tQfN4a+kJLhEZgbsIHo4XMi0hCywCX1AWnYQp/IlQrHD3IJrtBKuSsQVRz8fA4yAY0a8W1YLRn6mHykFpaZ5LFvI= on 03/16/2018
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 6, Issue 5 2016 Article 8 Sigmoidocele: A Rare Cause Of Constipation In Males Noor Shah MD Milind Kachare MD Craig Rezac MD Rutgers Robert Wood Johnson Medical
World Journal of Colorectal Surgery Volume 6, Issue 5 2016 Article 8 Sigmoidocele: A Rare Cause Of Constipation In Males Noor Shah MD Milind Kachare MD Craig Rezac MD Rutgers Robert Wood Johnson Medical
Single Stage Transanal Pull-Through for Hirschsprung s Disease in Neonates: Our Early Experience
 Journal of Neonatal Surgery 2013;2(4):39 ORIGINAL ARTICLE Single Stage Transanal Pull-Through for Hirschsprung s Disease in Neonates: Our Early Experience Pradeep Bhatia,* Rakesh S Joshi, Jaishri Ramji,
Journal of Neonatal Surgery 2013;2(4):39 ORIGINAL ARTICLE Single Stage Transanal Pull-Through for Hirschsprung s Disease in Neonates: Our Early Experience Pradeep Bhatia,* Rakesh S Joshi, Jaishri Ramji,
Index. Note: Page numbers of article title are in boldface type.
 Index Note: Page numbers of article title are in boldface type. A Abscess(es) in Crohn s disease, 168 169 IPAA and, 110 114 as unexpected finding in colorectal surgery, 46 Adhesion(s) trocars-related laparoscopy
Index Note: Page numbers of article title are in boldface type. A Abscess(es) in Crohn s disease, 168 169 IPAA and, 110 114 as unexpected finding in colorectal surgery, 46 Adhesion(s) trocars-related laparoscopy
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
Guide to Pelvic Floor Multicompartment Scanning
 Guide to Pelvic Floor Multicompartment Scanning These guidelines have been prepared by Giulio A. Santoro, MD, PhD, Head Pelvic Floor Unit, Section of Anal Physiology and Ultrasound, Coloproctology Service,
Guide to Pelvic Floor Multicompartment Scanning These guidelines have been prepared by Giulio A. Santoro, MD, PhD, Head Pelvic Floor Unit, Section of Anal Physiology and Ultrasound, Coloproctology Service,
ORIGINAL CONTRIBUTION 686 DISEASES OF THE COLON &RECTUM VOLUME54: 6 (2011)
 ORIGINAL CONTRIBUTION Prospective Multicenter Trial Comparing With in the Assessment of Anorectal Dysfunction in Patients With Obstructed Defecation F. Sergio P. Regadas, Ph.D. 1 Eric M. Haas, M.D. 2 Maher
ORIGINAL CONTRIBUTION Prospective Multicenter Trial Comparing With in the Assessment of Anorectal Dysfunction in Patients With Obstructed Defecation F. Sergio P. Regadas, Ph.D. 1 Eric M. Haas, M.D. 2 Maher
Laparoscopic Ventral. Mesh Rectopexy (LVMR)
 Laparoscopic Ventral Mesh Rectopexy (LVMR) Questions & Answers GLASGOW COLORECTAL CENTRE Ross Hall Hospital 221 Crookston Road Glasgow G52 3NQ e-mail: info@colorectalcentre.co.uk Ph: Main hospital switchboard
Laparoscopic Ventral Mesh Rectopexy (LVMR) Questions & Answers GLASGOW COLORECTAL CENTRE Ross Hall Hospital 221 Crookston Road Glasgow G52 3NQ e-mail: info@colorectalcentre.co.uk Ph: Main hospital switchboard
To inject, to band or to excise? These were the alternatives for a colorectal surgeon
 CHAPTER 2 Hemorrhoids To inject, to band or to excise? These were the alternatives for a colorectal surgeon some 50 years ago, when sclerosant injection, rubber band ligation and hemorrhoidectomy were
CHAPTER 2 Hemorrhoids To inject, to band or to excise? These were the alternatives for a colorectal surgeon some 50 years ago, when sclerosant injection, rubber band ligation and hemorrhoidectomy were
Pelvic Floor Ultrasound Imaging. Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague)
 Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
Laparoscopic ventral rectopexy for obstructed defecation syndrome
 Surg Endosc (2008) 22:2728 2732 DOI 10.1007/s00464-008-9771-9 Laparoscopic ventral rectopexy for obstructed defecation syndrome J. W. van den Esschert Æ A. A. W. van Geloven Æ N. Vermulst Æ A. Groenedijk
Surg Endosc (2008) 22:2728 2732 DOI 10.1007/s00464-008-9771-9 Laparoscopic ventral rectopexy for obstructed defecation syndrome J. W. van den Esschert Æ A. A. W. van Geloven Æ N. Vermulst Æ A. Groenedijk
CHAU KHAC TU M.D., Ph.D.
 CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
Robot Assisted Rectopexy
 1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
UvA-DARE (Digital Academic Repository) Rectal prolapse: enlightenment of the obscure Wijffels, N.A.T. Link to publication
 UvA-DARE (Digital Academic Repository) Rectal prolapse: enlightenment of the obscure Wijffels, N.A.T. Link to publication Citation for published version (APA): Wijffels, N. A. T. (2012). Rectal prolapse:
UvA-DARE (Digital Academic Repository) Rectal prolapse: enlightenment of the obscure Wijffels, N.A.T. Link to publication Citation for published version (APA): Wijffels, N. A. T. (2012). Rectal prolapse:
Saint-Petersburg State Pediatric Medical University, Saint-Petersburg, Russia
 Saint-Petersburg State Pediatric Medical University, Saint-Petersburg, Russia Modern technologies in treatment of fecal incontinence in children Komissarov Igor Alexeevich- Ph.D, M.D, Prof. Kolesnikova
Saint-Petersburg State Pediatric Medical University, Saint-Petersburg, Russia Modern technologies in treatment of fecal incontinence in children Komissarov Igor Alexeevich- Ph.D, M.D, Prof. Kolesnikova
Delorme's operation plus sphincteroplasty for complete rectal prolapse associated with traumatic fecal incontinence
 Available online at www.jbr-pub.org Open Access at PubMed Central The Journal of Biomedical Research, 2015, 29(4):326-331 Original Article Delorme's operation plus sphincteroplasty for complete rectal
Available online at www.jbr-pub.org Open Access at PubMed Central The Journal of Biomedical Research, 2015, 29(4):326-331 Original Article Delorme's operation plus sphincteroplasty for complete rectal
LONG TERM OUTCOME OF ELECTIVE SURGERY
 LONG TERM OUTCOME OF ELECTIVE SURGERY Roberto Persiani Associate Professor Mini-invasive Oncological Surgery Unit Institute of Surgical Pathology (Dir. prof. D. D Ugo) Dis Colon Rectum, March 2000 Dis
LONG TERM OUTCOME OF ELECTIVE SURGERY Roberto Persiani Associate Professor Mini-invasive Oncological Surgery Unit Institute of Surgical Pathology (Dir. prof. D. D Ugo) Dis Colon Rectum, March 2000 Dis
Clinical Study Delorme s Procedure for Complete Rectal Prolapse: A Study of Recurrence Patterns in the Long Term
 Surgery Research and Practice Volume 215, Article ID 92154, 6 pages http://dx.doi.org/1.1155/215/92154 Clinical Study Delorme s Procedure for Complete Rectal Prolapse: A Study of Recurrence Patterns in
Surgery Research and Practice Volume 215, Article ID 92154, 6 pages http://dx.doi.org/1.1155/215/92154 Clinical Study Delorme s Procedure for Complete Rectal Prolapse: A Study of Recurrence Patterns in
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy
 Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
Articles. Funding None.
 Bowel function after laparoscopic posterior sutured versus ventral mesh for rectal prolapse: a double-blind, randomised single-centre study Lilli Lundby, Lene H Iversen, Steen Buntzen, Pål Wara, Katrine
Bowel function after laparoscopic posterior sutured versus ventral mesh for rectal prolapse: a double-blind, randomised single-centre study Lilli Lundby, Lene H Iversen, Steen Buntzen, Pål Wara, Katrine
A Comparitive Study of Laying Open of Wound Vs Primary Closure In Fistula in Ano
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-853, p-issn: 2279-861.Volume 13, Issue 9 Ver. III (Sep. 214), PP 39-45 A Comparitive Study of Laying Open of Wound Vs Primary Closure
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-853, p-issn: 2279-861.Volume 13, Issue 9 Ver. III (Sep. 214), PP 39-45 A Comparitive Study of Laying Open of Wound Vs Primary Closure
Benign anorectal diseases
 Benign anorectal diseases Symptoms Bleeding Pruritus Discharge Fecal incontinence Diarrhea Constipation False need to defecate Examinations Clinical exam Anuscopy Rectosigmoidoscopy Endosonography MRI
Benign anorectal diseases Symptoms Bleeding Pruritus Discharge Fecal incontinence Diarrhea Constipation False need to defecate Examinations Clinical exam Anuscopy Rectosigmoidoscopy Endosonography MRI
Transanal Stapling Techniques for Anorectal Prolapse
 Transanal Stapling Techniques for Anorectal Prolapse Transanal Stapling Techniques for Anorectal Prolapse Edited by David Jayne Department of Colorectal Surgery, Leeds General Hospital, Great George Street,
Transanal Stapling Techniques for Anorectal Prolapse Transanal Stapling Techniques for Anorectal Prolapse Edited by David Jayne Department of Colorectal Surgery, Leeds General Hospital, Great George Street,
Haemorrhoidal disorders -What is the optimal treatment?
 Haemorrhoidal disorders -What is the optimal treatment? Per-Olof Nyström, M.D., Ph.D. Professor of Surgery Karolinska Institutet and Karolinska University Hospital Huddinge Stockholm, Sweden The methods
Haemorrhoidal disorders -What is the optimal treatment? Per-Olof Nyström, M.D., Ph.D. Professor of Surgery Karolinska Institutet and Karolinska University Hospital Huddinge Stockholm, Sweden The methods
Rectal Cancer. About the Colon and Rectum. Symptoms. Colorectal Cancer Screening
 Patient information regarding care and surgery associated with RECTAL CANCER by Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou., M.D. location: Michigan Heart and Vascular Institute,
Patient information regarding care and surgery associated with RECTAL CANCER by Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou., M.D. location: Michigan Heart and Vascular Institute,
JNM Journal of Neurogastroenterology and Motility
 JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 19 No. 1 January, 2013 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm.2013.19.1.78 Original Article Successful
JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 19 No. 1 January, 2013 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm.2013.19.1.78 Original Article Successful
Citation Acta medica Nagasakiensia. 2003, 48
 NAOSITE: Nagasaki University's Ac Title Author(s) Surgical Strategy for Low Imperfora Anal Transplantation or Limited Pos Obatake, Masayuki; Yamashita, Hidek Norihisa; Nakagoe, Tohru Citation Acta medica
NAOSITE: Nagasaki University's Ac Title Author(s) Surgical Strategy for Low Imperfora Anal Transplantation or Limited Pos Obatake, Masayuki; Yamashita, Hidek Norihisa; Nakagoe, Tohru Citation Acta medica
The use of conventional defecography in clinical practice
 The use of conventional defecography in clinical practice Poster No.: C-1564 Congress: ECR 2014 Type: Educational Exhibit Authors: A. Šmite, R. Laguns ; Lielvarde/LV, Riga/LV Keywords: Pelvic floor dysfunction,
The use of conventional defecography in clinical practice Poster No.: C-1564 Congress: ECR 2014 Type: Educational Exhibit Authors: A. Šmite, R. Laguns ; Lielvarde/LV, Riga/LV Keywords: Pelvic floor dysfunction,
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
GI Physiology - Investigating and treating patients with pelvic floor dysfunction. Lynne Smith Department of GI Physiology NGH Sheffield
 GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
Surgical Management for Defecation Dysfunction
 Defecatory Dysfunction Surgical Management for Defecation Dysfunction JMAJ 46(9): 378 383, 2003 Tatsuo TERAMOTO Professor, 1st Department of Surgery, School of Medicine, Toho University Abstract: Typical
Defecatory Dysfunction Surgical Management for Defecation Dysfunction JMAJ 46(9): 378 383, 2003 Tatsuo TERAMOTO Professor, 1st Department of Surgery, School of Medicine, Toho University Abstract: Typical
The use of conventional defecography in clinical practice
 The use of conventional defecography in clinical practice Poster No.: C-1564 Congress: ECR 2014 Type: Educational Exhibit Authors: A. Šmite, R. Laguns ; Lielvarde/LV, Riga/LV Keywords: Pelvic floor dysfunction,
The use of conventional defecography in clinical practice Poster No.: C-1564 Congress: ECR 2014 Type: Educational Exhibit Authors: A. Šmite, R. Laguns ; Lielvarde/LV, Riga/LV Keywords: Pelvic floor dysfunction,
19th Annual International Colorectal Disease Symposium An International Exchange of Medical and Surgical Concepts
 Wednesday, February 13, 2008 7-9:00p Early Check-In / Registration (Grand Ballroom Foyer) Thursday, February 14, 2008 6:45 AM Breakfast (Caribbean Ballroom and Foyer) 7:00 AM Registration (Grand Ballroom
Wednesday, February 13, 2008 7-9:00p Early Check-In / Registration (Grand Ballroom Foyer) Thursday, February 14, 2008 6:45 AM Breakfast (Caribbean Ballroom and Foyer) 7:00 AM Registration (Grand Ballroom
Management of Neurogenic Bowel Dysfunction. Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders
 Management of Neurogenic Bowel Dysfunction Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders DEFECATION Delivery of colon contents to the rectum Rectal compliance
Management of Neurogenic Bowel Dysfunction Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders DEFECATION Delivery of colon contents to the rectum Rectal compliance
Viscous Fluid Retention: A New Method for Evaluating Anorectal Function
 Viscous Fluid Retention: A New Method for Evaluating Anorectal Function Michael Srensen, M.D., Tine Tetzschner, M.D., le 0. Rasmussen, M.D., John Christiansen, M.D. From the Department of Surgery D, Glostrup
Viscous Fluid Retention: A New Method for Evaluating Anorectal Function Michael Srensen, M.D., Tine Tetzschner, M.D., le 0. Rasmussen, M.D., John Christiansen, M.D. From the Department of Surgery D, Glostrup
Laparoscopic Ventral Mesh Rectopexy
 Patient Information Laparoscopic Ventral Mesh Rectopexy Introduction We expect you to make a rapid recovery after your operation and to experience no serious problems. However, it is important that you
Patient Information Laparoscopic Ventral Mesh Rectopexy Introduction We expect you to make a rapid recovery after your operation and to experience no serious problems. However, it is important that you
The Milestones provide a framework for the assessment
 The Colon and Rectal Surgery Milestone Project The Milestones provide a framework for the assessment of the development of the resident physician in key dimensions of the elements of physician competency
The Colon and Rectal Surgery Milestone Project The Milestones provide a framework for the assessment of the development of the resident physician in key dimensions of the elements of physician competency
Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF)
 Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF) Blair B. Washington MD, MHA Urogynecology & Reconstructive Pelvic Surgery Virginia Mason Medical Center Disclosures
Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF) Blair B. Washington MD, MHA Urogynecology & Reconstructive Pelvic Surgery Virginia Mason Medical Center Disclosures
Hernia. emoryhealthcare.org
 Hernia Have you noticed a bulge or pain in your abdominal wall or groin? If so you may have a hernia. You may be in the process of confirming this diagnosis with your Primary Care Physician or already
Hernia Have you noticed a bulge or pain in your abdominal wall or groin? If so you may have a hernia. You may be in the process of confirming this diagnosis with your Primary Care Physician or already
EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May Dr. Annie Leong MBBS, FRANZCOG, CU
 EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May 2011 Dr. Annie Leong MBBS, FRANZCOG, CU Restore normal perineal anatomy Achieve good haemostasis Avoid infection and wound breakdown Avoid coital
EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May 2011 Dr. Annie Leong MBBS, FRANZCOG, CU Restore normal perineal anatomy Achieve good haemostasis Avoid infection and wound breakdown Avoid coital
Bowel dysfunctions following hysterectomy
 Bowel dysfunctions following hysterectomy Marco Scaglia Retrospective studies Retrospective studies 6% of patients developed new symptoms (Carlson 1994) Constipation is more common in women after hysterectomy
Bowel dysfunctions following hysterectomy Marco Scaglia Retrospective studies Retrospective studies 6% of patients developed new symptoms (Carlson 1994) Constipation is more common in women after hysterectomy
The role of biologics in pelvic floor surgery
 Review article doi:10.1111/codi.12045 The role of biologics in pelvic floor surgery M. Ahmad*, P. Sileri, L. Franceschilli and M. Mercer-Jones* *Department of Colorectal Surgery, Queen Elizabeth Hospital,
Review article doi:10.1111/codi.12045 The role of biologics in pelvic floor surgery M. Ahmad*, P. Sileri, L. Franceschilli and M. Mercer-Jones* *Department of Colorectal Surgery, Queen Elizabeth Hospital,
Tertiary, regional and local pelvic floor service providers: the future. model? Andrew Williams
 Tertiary, regional and local pelvic floor service providers: the future Andrew Williams model? Pelvic Floor Unit Guy s and St Thomas NHS Foundation Trust Background 23% women suffer at least one pelvic
Tertiary, regional and local pelvic floor service providers: the future Andrew Williams model? Pelvic Floor Unit Guy s and St Thomas NHS Foundation Trust Background 23% women suffer at least one pelvic
Comparison of Electrotherapy, Rubber Band Ligation and Hemorrhoidectomy in the Treatment of Hemorrhoids: A Clinical and Manometric Study
 Original Article 9 Comparison of Electrotherapy, Rubber Band Ligation and Hemorrhoidectomy in the Treatment of Hemorrhoids: A Clinical and Manometric Study A Izadpanah 1*, SV Hosseini 2, M Mahjoob 1 1.
Original Article 9 Comparison of Electrotherapy, Rubber Band Ligation and Hemorrhoidectomy in the Treatment of Hemorrhoids: A Clinical and Manometric Study A Izadpanah 1*, SV Hosseini 2, M Mahjoob 1 1.
Duc M. Vo, MD, FACS Northwest Surgical Specialists
 Duc M. Vo, MD, FACS Northwest Surgical Specialists Disclosures none Outline Definition Etiologies Exam findings Additional testing Medical management Surgical options What is fecal incontinence? Recurrent
Duc M. Vo, MD, FACS Northwest Surgical Specialists Disclosures none Outline Definition Etiologies Exam findings Additional testing Medical management Surgical options What is fecal incontinence? Recurrent
Delorme s Operation For Rectal Prolapse
 Delorme s Operation For Rectal Prolapse Patient Information Colorectal Surgery Author ID: NM Leaflet Number: Surg 045 Version: 3.1 Name of Leaflet: Delorme s Operation for Rectal Prolapse Date Produced:
Delorme s Operation For Rectal Prolapse Patient Information Colorectal Surgery Author ID: NM Leaflet Number: Surg 045 Version: 3.1 Name of Leaflet: Delorme s Operation for Rectal Prolapse Date Produced:
REPAIR OF LARGE CYSTOCELE
 REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
Appendix B Protocol for management of obstetric anal sphincter injury THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS
 Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
8 A SIMPLE FISTULA REPAIR, STEP BY STEP
 8 A SIMPLE FISTULA REPAIR, STEP BY STEP The first step is to suture the labia to the thighs and cover the anus with a swab (Figure 31). Figure 31 The labia are sutured to the thighs and the anus is covered
8 A SIMPLE FISTULA REPAIR, STEP BY STEP The first step is to suture the labia to the thighs and cover the anus with a swab (Figure 31). Figure 31 The labia are sutured to the thighs and the anus is covered
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS
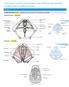 THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
Although disparate topics, these two different pathologic
 34 H E M O R R H O I D S A N D R E C T A L P R O L A P S E CHARLES N. HEADRICK MICHAEL J. STAMOS Although disparate topics, these two different pathologic entities are commonly misdiagnosed by both layperson
34 H E M O R R H O I D S A N D R E C T A L P R O L A P S E CHARLES N. HEADRICK MICHAEL J. STAMOS Although disparate topics, these two different pathologic entities are commonly misdiagnosed by both layperson
Case Report A Case Report of Acute Diverticulitis in (Pseudodiverticulosis) after Hemorpex System Procedure
 Case Reports in Surgery Volume 2016, Article ID 3298048, 4 pages http://dx.doi.org/10.1155/2016/3298048 Case Report A Case Report of Acute Diverticulitis in (Pseudodiverticulosis) after Hemorpex System
Case Reports in Surgery Volume 2016, Article ID 3298048, 4 pages http://dx.doi.org/10.1155/2016/3298048 Case Report A Case Report of Acute Diverticulitis in (Pseudodiverticulosis) after Hemorpex System
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests
 Defecatory Dysfunction Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests JMAJ 46(9): 373 377, 2003 Masatoshi OYA, Masashi UENO, and Tetsuichiro MUTO Department of
Defecatory Dysfunction Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests JMAJ 46(9): 373 377, 2003 Masatoshi OYA, Masashi UENO, and Tetsuichiro MUTO Department of
UvA-DARE (Digital Academic Repository) Rectal prolapse: enlightenment of the obscure Wijffels, N.A.T. Link to publication
 UvA-DARE (Digital Academic Repository) Rectal prolapse: enlightenment of the obscure Wijffels, N.A.T. Link to publication Citation for published version (APA): Wijffels, N. A. T. (2012). Rectal prolapse:
UvA-DARE (Digital Academic Repository) Rectal prolapse: enlightenment of the obscure Wijffels, N.A.T. Link to publication Citation for published version (APA): Wijffels, N. A. T. (2012). Rectal prolapse:
warwick.ac.uk/lib-publications
 Original citation: The Pelvic floor Society, National Institute for Health Research: Chronic Constipation Treatment Pathway (Including: Mercer-Jones, M., Grossi, U., Pares, D., Vollebregt, P. F., Mason,
Original citation: The Pelvic floor Society, National Institute for Health Research: Chronic Constipation Treatment Pathway (Including: Mercer-Jones, M., Grossi, U., Pares, D., Vollebregt, P. F., Mason,
Applied Anatomy and Physiology of the Pelvic Floor. Dr David Tarver Consultant Radiologist, Poole
 Applied Anatomy and Physiology of the Pelvic Floor Dr David Tarver Consultant Radiologist, Poole Pelvic Floor 1. Sacrospinous Ligament 2. Levator Ani A Puborectalis B. Pubococcygeus C. Iliococcygeus 3.
Applied Anatomy and Physiology of the Pelvic Floor Dr David Tarver Consultant Radiologist, Poole Pelvic Floor 1. Sacrospinous Ligament 2. Levator Ani A Puborectalis B. Pubococcygeus C. Iliococcygeus 3.
Our Experience in Management of Complete Rectal Prolapse in Children by Delorme Procedure
 Med. J. Cairo Univ., Vol. 84, No. 1, December: 1357-1362, 2016 www.medicaljournalofcairouniversity.net Our Experience in Management of Complete Rectal Prolapse in Children by Delorme Procedure MOHAMED
Med. J. Cairo Univ., Vol. 84, No. 1, December: 1357-1362, 2016 www.medicaljournalofcairouniversity.net Our Experience in Management of Complete Rectal Prolapse in Children by Delorme Procedure MOHAMED
Surgical Management of IBD in the Age of Biologics
 Surgical Management of IBD in the Age of Biologics Lisa S. Poritz, M.D Associate Professor of Surgery Division of Colon and Rectal Surgery Objectives Discuss surgical management of IBD When to operate
Surgical Management of IBD in the Age of Biologics Lisa S. Poritz, M.D Associate Professor of Surgery Division of Colon and Rectal Surgery Objectives Discuss surgical management of IBD When to operate
A Case of Fecal Incontinence: Medical and Interventional Treatment Options
 A Case of Fecal Incontinence: Medical and Interventional Treatment Options HPI JP is a 69 year-old F with a 12-month history of FI. Her symptoms began after a colonoscopy She has been experiencing passive
A Case of Fecal Incontinence: Medical and Interventional Treatment Options HPI JP is a 69 year-old F with a 12-month history of FI. Her symptoms began after a colonoscopy She has been experiencing passive
Clinical Study Long-Term Outcome after Resection Rectopexy for Internal Rectal Intussusception
 International Scholarly Research Network ISRN Gastroenterology Volume 2012, Article ID 824671, 7 pages doi:10.5402/2012/824671 Clinical Study Long-Term Outcome after Resection Rectopexy for Internal Rectal
International Scholarly Research Network ISRN Gastroenterology Volume 2012, Article ID 824671, 7 pages doi:10.5402/2012/824671 Clinical Study Long-Term Outcome after Resection Rectopexy for Internal Rectal
JNM Journal of Neurogastroenterology and Motility
 ㅋ JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 17 No. 4 October, 2011 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm.2011.17.4.416 How to Interpret
ㅋ JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 17 No. 4 October, 2011 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm.2011.17.4.416 How to Interpret
Fig. 1. Clinical condition. before operation.
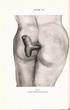 PLATE IX. Fig. 1. Clinical condition before operation. A CASE OF RECTAL PROLAPSE. BY D. Robertson, M.B., Ch.B. (Edin.), AND D. G. C. Tasker, M.S. (Lond.), F.R.C.S. (Eng.). On many occasions in the practice
PLATE IX. Fig. 1. Clinical condition before operation. A CASE OF RECTAL PROLAPSE. BY D. Robertson, M.B., Ch.B. (Edin.), AND D. G. C. Tasker, M.S. (Lond.), F.R.C.S. (Eng.). On many occasions in the practice
STARR with CONTOUR TRANSTAR device for obstructed defecation syndrome: one-year real-world outcomes of the European TRANSTAR registry
 Int J Colorectal Dis (2014) 29:611 622 DOI 10.1007/s00384-014-1836-8 ORIGINAL ARTICLE STARR with CONTOUR TRANSTAR device for obstructed defecation syndrome: one-year real-world outcomes of the European
Int J Colorectal Dis (2014) 29:611 622 DOI 10.1007/s00384-014-1836-8 ORIGINAL ARTICLE STARR with CONTOUR TRANSTAR device for obstructed defecation syndrome: one-year real-world outcomes of the European
The American Journal of Surgery 182 (2001) Manuscript received July 26, 2000; revised manuscript February 14, 2001
 The American Journal of Surgery 182 (2001) 64 68 Randomised controlled trial between stapled circumferential mucosectomy and conventional circular hemorrhoidectomy in advanced hemorrhoids with external
The American Journal of Surgery 182 (2001) 64 68 Randomised controlled trial between stapled circumferential mucosectomy and conventional circular hemorrhoidectomy in advanced hemorrhoids with external
Piotr Walega, *Piotr Krokowicz, Michal Romaniszyn, Jakub Kenig, Jerzy Sałówka, Michał Nowakowski, Roman M Herman, Wojciech Nowak
 Received 8 Feb 2009; Accepted 30 March 2009 Doppler Guided Haemorrhoidal Arterial Ligation with recto-anal-repair (RAR)for the treatment of advanced haemorrhoidal disease. Piotr Walega, *Piotr Krokowicz,
Received 8 Feb 2009; Accepted 30 March 2009 Doppler Guided Haemorrhoidal Arterial Ligation with recto-anal-repair (RAR)for the treatment of advanced haemorrhoidal disease. Piotr Walega, *Piotr Krokowicz,
Prof. Francesco Guarnieri
 Dear Sir / Madam, with today's visit, after evaluation of your clinical status, you may be admitted to the program of surgical treatment in Day Surgery. The organization of our department, in fact, requires
Dear Sir / Madam, with today's visit, after evaluation of your clinical status, you may be admitted to the program of surgical treatment in Day Surgery. The organization of our department, in fact, requires
