Rectal Incontinence After Childbirth and Surgery Webcast November 24, 2009 Anne-Marie Boller, M.D. Introduction
|
|
|
- Paulina McKenzie
- 5 years ago
- Views:
Transcription
1 Rectal Incontinence After Childbirth and Surgery Webcast November 24, 2009 Anne-Marie Boller, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of Northwestern Memorial Hospital, its medical staff or Patient Power. Our discussions are not a substitute for seeking medical advice or care from your own doctor. That s how you ll get care that s most appropriate for you. Introduction Childbirth can take its toll on a woman's body, and there also can be complications of chronic conditions and obesity, and that can often you cause issues that are difficult to discuss such as urinary and fecal incontinence and constipation. Coming up you'll hear an expert discuss emerging treatments and ways to improve pelvic floor health next on Patient Power. Hello and welcome to Patient Power sponsored by Northwestern Memorial Hospital. I'm Andrew Schorr. So as a man I have not certainly felt the pain of childbirth, but my wife has delivered vaginally three times, and it took her a while to recover. And sometimes there are complications that can happen related to pelvic floor problems. Now, on other programs we've discussed pelvic organ prolapse, and part of that, one of the problems that can happen is even rectal problems. And we're going to discuss that with a colorectal surgeon, Dr. Anne-Marie Boller, and also understand how even this problem can happen with men as well, not of course from childbirth, but we're going to understand the problem and what can be done about it. Dr. Boller, thank you so much for being with us. Thank you. It's a pleasure to be here. Dr. Boller, so let's talk about the trauma of childbirth. It's a big medical event, and when you deliver vaginally I know it can move things around, and it can stretch muscles and organs and things. How common it is that some people have ongoing issues and what percentage maybe needs to be addressed surgically. Well, it's hard to put an actual percentage on it or number because this is actually fairly underreported in terms of long-term follow up, and many of these women get seen later in life and it's not directly linked to a birthing injury. But the obstetric trauma that can happen has to do with many different things, not only factors like the baby, how large is the baby, how is the baby oriented, but difficulty, how difficult the actual birth is. Was a vacuum used? Were forceps used? And then of course also do you have to voluntarily make a cut, like an episiotomy, sometimes all the way back through the rectal and anal sphincter complex. Or is there a tear,
2 and they have degrees of these tears of which third- and fourth- degree are tears that go all the way and sometimes through the anal sphincter complex disrupting the anterior portion of your anal sphincter. So these factors all play a role. And then also how were you repaired? Was there infection afterward? Were you seen by someone after these repairs in terms of how well these things do after the fact. So all these things play into your long-term outcomes after what I would term obstetric trauma. Symptoms of Problems Okay. And it's something that women may be embarrassed to talk about. What would be the symptoms? There are urinary symptoms, and there are fecal incontinence symptoms too, right? There's a number of different symptoms and some of them can occur immediately after, you know, in your acute recovery period, and some of them can gradually occur in the years that follow the childbirth, and some of them can occur later in your life as the rest of your body is relaxing and muscles are giving way. So there's different stages of when you would see symptoms. But acutely you could have a tear and have some incontinence problems, meaning you can't make it to the bathroom the way you used to, or you don't have the sense of when you have to go to the bathroom like you used to, or you just can't actually hold it. There are some injuries that disrupt and then connect the vagina and the rectum, and these are called rectovaginal fistulas. In this case you would then have maybe stool coming through your vagina or having mucus from your vagina coming back through your rectum. You can also have similar problems with your bladder although that's a little bit more common in men after some of their disease problems. So those would be the acute problems. The middle- and long-term problems are the ones that kind of gradually come about. Say maybe you did have a fairly good recovery after an obstetric trauma but gradually you've noticed that you really can't afford to go to Target for two hours with your three children because you don't know where the bathrooms are or that you don't have the urge and so you're afraid to go on that nine-hole golf course because you can't be out on the ninth hole because you know you won't make it to a bathroom. And these people tend to adapt around and often don't come to the doctor because of their adaptation kind of behaviors. But those medium- to long-term outcomes are the ones that are a little bit more insidious. And embarrassing for people. Now, in previous programs we've discussed pelvic organ prolapse, and we've talked about different surgeries there, but if it's okay I 2
3 wanted to focus a little more on the rectal issues because I think people just don't discuss them. I imagine there are people who just don't even bring it up with their doctor. Absolutely. And more often than not people also don't ask, so it's a problem on both sides of the physician-patient relationship. Non-Surgical Treatment All right. You're a colorectal surgeon, so what are the approaches that can be done to help someone? First, are there nonsurgical approaches, and then help us understand if surgery is indicated how can it be done in the most minimally invasive way. Well, the most important intervention is, as we just discussed, is to intervene, meaning talk to your doctor about your problems at any of those stages that I talked about, the acute, the mid or the long-term outcomes. And make sure that they're aware and that you're talking to them about what is going on. Because of the psychological stigma around fecal incontinence people tend not only not to talk about it but they tend to hide it as much as possible, and that's the wrong thing to do because we know that the earlier we intervene the better our results usually are in the long run. The initial evaluation is a number of tests that I would do to kind of assess what the damage is and what the exact disorder is. But many people, even if they have gross sphincter disruption, will benefit from a physical therapy that we call biofeedback. This is a therapy that strengthens the pelvic muscles as well as the anal-sphincter complex but more importantly can recoordinate all of these muscles so that they work together to restore a patient's continence. And biofeedback has been proven to work in the literature very, very effectively. Now, having said that, if it doesn't work in terms of biofeedback there are a number of surgical interventions that we can initiate if the patient is an adequate candidate and is going to benefit from the surgery. If they have a sphincter disruption we can do what is called a sphincteroplasty, meaning we can dissect out to where those sphincter muscles are and rewrap them, recreating the anal sphincter complex. If it's an acute problem that's more along the lines of a rectovaginal fistula there are also a number of repairs for these including things like a Martius flap, which would be putting a flap of muscle or fat, a Martius flap is a labial fat pad, in between the rectum and the vagina to recreate the soft tissue that normally separates the rectum and the vagina. Again, if it's an attenuated sphincter that means it's just thinner than normal because of the trauma from the childbirth. We not only start with biofeedback but 3
4 we would maybe consider some other interventions. On the research side of things there are some people who are injecting bulking agents into the anal sphincter. And soon to be hopefully approved here in America is sacral nerve stimulation which has also been proven in the literature from Europe to help a large percentage of women restore their continence following these types of injuries. Let me just understand what that term means. So this is like electrical stimulation, or how does that work? It is, actually. It's a pacemaker that we would go into your buttock and the electrode would go into the holes in your bony sacrum, your pelvis, and right to where your spinal cord, the nerves come around to enervate your pelvis and the perineum. Sacral nerve stimulation has been used for a number of years by urologists for urinary incontinence. That's actually how we discovered that it works for fecal incontinence because there's a crossover of about 30 percent of people, 30 to 50 percent of people who have urinary incontinence also have some degree of fecal incontinence undiagnosed. And when these patients were having the sacral nerve stimulators placed to help them with their urine incontinence we found out through surveys that they were also having vast benefits from a fecal incontinence standpoint. So what you would do is you would place a temporary electrode into the foramen, the sacral foramen, that's the hole in the bone, and have them keep a journal to see if they benefit from this, meaning less accidents a week, more warning in terms of being able to make it to a bathroom and in some people even more warning and a more urge capacitance response from the rectum itself. If they then respond to the sacral nerve stimulator that is temporary, European studies have known that they then would be the ones who would benefit from a permanent implantation, and that is when they would go to the operating room and have a pacemaker placed in their buttock, and the node, the electrode, permanently placed. Is that done investigationally at Northwestern yet? It is not yet. We are going to be doing it here as soon as the FDA approves it. It is in the FDA's approval process as we speak. Surgical Treatment Doctor, let's talk about the degree of surgery. So we talked about the possibility of sort of a pacemaker to help with nerve stimulation related to rectal incontinence. I know there can be minimally invasive approaches and sometimes there needs to be abdominal surgery. How do you decide which? 4
5 If the incontinence is because of a sphincter issue, meaning muscle, sphincter is just a fancy word for the muscle around your anus. It helps you hold your feces in so that you can make it to a bathroom. And those repairs that I talked about previously, sphincteroplasties, are a major repair. They do require general anesthesia, but certainly they are not abdominal. We do that from underneath, a direct repair of the anal sphincter complex. The same can be said for a rectovaginal fistula. But then we get into the area where if you have a rectal prolapse or a sagging of your entire rectal complex or a fistula that is too high to repair from below, meaning between the legs, then we have to do an abdominal surgery, whether laparoscopic or open surgery. We can make that decision based on other patient factors. But a rectal prolapse or an internal sagging that's causing some thinning of the sphincter muscle leading to fecal incontinence or a fistula from traumatic events, there are a few of those that can only be addressed through the abdomen. Dr. Boller, so if someone has one of these surgeries does it last, or might they need surgery sometime in the future? There's a good study that was out from the University of Minnesota that showed that even sphincteroplasties in the best of hands tend to start to not perform as well after ten years. We don't have long-term results for sacral nerve stimulation yet. And in terms of fistula repairs and prolapse, those are a bit sturdier in terms of long-term results. Having said that, because of this fact that sphincteroplasties can break down and that recurrent surgery is difficult, it's important to make sure you institute physical therapy before and after the surgery and make sure that you're doing everything possible to give the patient a fighting chance, meaning modulate the consistency of their stool so that they get the most sense of urgency that they can. Make sure that you work with them on their diet and make sure that they have colonoscopies to make sure there aren't other problems affecting them. So it's very, very important that these medical and conservative management tools are used prior to any surgery and also after the surgery. The Risk for Problems Dr. Boller, I was looking at a study from Kaiser Permanente from California, and this study from 2008 said 80 percent of the 4,000 women studied had given birth, and of those 4,000 women 25 percent suffered from anal incontinence and then 15 percent from stress urinary incontinence, 13 percent from overactive bladder and then 6 percent pelvic organ prolapse where they felt that organs were dropping out 5
6 at the bottom. But what I was surprised about was how common it was, these anal issues. So then a woman says, okay, I don't want to go there. Is there anything I can do in preparing for childbirth to make that less likely? You know, we have studies that broadcast or publish the risk factors for tearing or needing episiotomies, but not everyone who tears or needs an episiotomy then has fecal incontinence, so there's clearly some other issues that contribute to this. We're just getting a study up here at Northwestern to look at what is the relationship between obstetric trauma and fecal incontinence, and what are these risk factors that we need to look at. Having said that, the important intervention that we know now can help is that once you have had obstetric trauma, meaning even episiotomy or a third- or a fourth-degree tear or even just an infection in that area, we call it the perineum, after childbirth it's important to have the doctors, a multidisciplinary team of doctors see you at that time. Because we know that if we can get healing to occur that that is better to do in the acute setting. So I think the most appropriate intervention is to have this multidisciplinary team of obstetrics and gynecologist doctors, your primary doctor and a colorectal doctor and perhaps a urogynecologist on board if you have any problems after giving birth to your baby. Now, my wife did have bladder problems that persisted for a long time after the birth of our third child, fortunately not the other issues. So how do we get women to start talking about it? First of all, things like IBS are real common in women, and we have TV commercials. A woman might say, well, I've got IBS or some other issue, you know, just food doesn't agree with me. How do we identify that this is the problem and they need to speak about it? Well, I think that that's another thing that we're trying to work on here at Northwestern is in developing and starting our pelvic floor center here getting almost a public service announcement out that these problems are out there and if you have them there are people who can help you. Unfortunately I don't see those kind of public service announcements or even ads out there right now. And I think that that's probably the biggest issue because until you identify a problem and make a patient feel at home with their symptoms, make them understand that this is a legitimate medical surgical problem and that there are many other people out there that have these problems and there are also many of us out here who want to help them, and that's the message that has to start getting across to the general public and certainly to the obstetric population postpartum. Well, we're working on that today and hopefully people will hear this message far and wide. So what should a woman say? If it's not brought up by the doctor, what should a woman say? Should she say, you know, I can't seem to hold my stools as 6
7 well, I just have to run to the bathroom, I don't even know when I need to go? What would be things that they would bring up to sort of put it on the radar of the medical team? I think the first thing to do if you've had a baby is to, because the labor suite is not, you don't always know what's going on there, and of course I think most people's priority is to see a healthy baby, but I think it should be of great importance to every woman to ask their doctor after the fact, what happened? Did I tear? Did you have to sew me up? How much did you have to sew me up? And I think that those are important questions, and I'm constantly struck by how many women don't know if they had a third-degree tear or a fourth-degree tear or an episiotomy. And when I see them, even though I can see the sutures down there in the perineum, that area between the vagina and the anus, they are unaware of why they were sewn up. So I think the first thing that any woman has had a baby should do whether or not there are problems or not is ask, how did the birth go and did you have to sew me up? Did I rip? Certainly if forceps or vacuums were used or there was a breech birth you should know these things so that we can all get together, as I said, in a multidisciplinary fashion and evaluate you and see if you are someone who is going to have problems. Having said that, even if you do know and were told that nothing happened, nothing went awry and everything was just fine, you can still have a sphincter tear just from the actual birth itself, and if you start to have leakage when you didn't have leakage before, if you start to not have the normal urge that you used to have giving you enough time to get to the bathroom, heaven forbid, if you start to have frank accidents, which does happen, then you need to get to your doctor, your gynecologist, and get referred to someone who deals with these sorts of problems and get the right workup. That could be a gastroenterologist at your institution. That could be a colorectal surgeon. It could be a general surgeon that specializes in this. It could be a urogynecologist. But there are people around the country that specialize in this, and it's important once you have those symptoms, lack of urge, lack of warning, increased leakage, unable to hold solid stools, unable to hold liquid stool, unable to take walks, difficulty exercising without having leakage, these kinds of problems you need to bring to your doctor's attention. We've talked about this in the setting of childbirth and trauma from childbirth. Let's talk about a couple of other situations. Does obesity or obesity with childbirth come into play in putting more pressure that then can cause damage? Obesity is certainly evaluated in terms of obstetric outcomes in the literature, but even just from a pelvic floor dysfunction standpoint people who are obese are at marked increased risk for pelvic floor dysfunction and fecal incontinence. Actually 7
8 across the literature we know that these are the people who have the problems earlier, have more difficult problems, and more importantly are more difficult to solve their problems. So certainly obesity, even aside from the obstetric factors, obesity is a risk factor for pelvic floor dysfunction. On the other side of the coin, you can also talk about men have these problems, and they're even less talked about than the females. And certain risk factors seem to be for them long-standing bowel problems, prostate cancer that was treated with radiation. These all can be in their medical history and their surgical history. Certainly if they have had surgery on their prostate or rectum or they have a history of radiation then these factors can also predispose males to fecal incontinence. Males at Risk Can you help in that setting? Absolutely. They can also get sphincteroplasties, but having said that all of these patients get a comprehensive workup which includes an ultrasound of the sphincter complex. Remember, that's the muscles. They also get manometry testing, which is a dynamic test which tells us how strong the muscles are and how well they relax and how coordinated they are. It can also tell us how their urge is in terms of how much volume and the rectal capacitance, whether it's working for them or working against them. We can also do nerve testing, which we do for all of these patients to tell whether their nerves are actually functioning, and if they are functioning are they functioning at the right time and place. Because a nerve that's been stretched or broken from a trauma, obstetric or otherwise, often will not convey the signals in a normal timely manner. Lastly we can also get what's called a defecating proctogram, which is where we take a radiologic picture of someone as they are defecating so that we can see if anything else is causing these problems, meaning causing them not to have the control they used to have. Is there bowel coming down in on itself? We call that intussusception. Is their rectum prolapsing so that their sphincter is stretched and they don't have control anymore? Or is their anatomic and pelvic dysfunction where they're just not able to coordinate all of these muscles and all of these nerves and all of the rectal capacitance and get that coordinated together? So all of these tests go into the workup for fecal incontinence and give us a complete picture. And you should always have that picture before you operate because you don't want to operate on the muscles if what the problem is is the 8
9 nerves. You don't want to operate on the muscles if what the problem is is the rectum. So it's very important to get the entire workup and look at the entire picture before intervening. Dr. Boller, as I hear about this, you talk about things that are difficult for people to discuss, and then these exams you talk about, I know it's useful information for you, but you think, we were that way with colonoscopy, and I think more people are having it. Thank god for Katie Couric and other people who have spoken out about it. Yes. So can we get there with these issues of fecal incontinence, because, sure, it can be a complication for men related to prostate surgery or radiation. We talked about childbirth, and the studies show it's not at all uncommon. I'm sure you want to help people, and we do need to talk about it more. Prevention Absolutely. I think that the number one thing that has to happen is that these issues have to be acceptable in some way. We have to get our society to stop marginalizing these symptoms so that people can talk about them. Because if you don't tell your doctor, that's the first step, so there's a very real way in which the first step is the patient's. If as a society we don't empower the patient instead of as we do now ostracizing anybody with these symptoms, we're not going to get the patients and all the people out there with these problems to make that first step. I want to go back to one thing. We all think, though, is there something we can do. So I know my wife and some of her friends, they worked out really hard at the gym. They would keep in shape anyway, were not obese, for muscle tone going into childbirth. Can that be preventative? Or women are instructed about Kegel exercises before or even after childbirth. Those sorts of things, can that help? I think that anybody who is in shape going into a surgery or a surgical trauma, which can be a descriptive term for childbirth, unfortunately, but anybody who is more physically fit rather than less is going to have an advantage. I have not seen any data on doing the physical therapy that I called biofeedback earlier in this conversation. I certainly know that it helps my patients to have it done before and after my surgeries because, as I always tell my patients, biofeedback is like doing pushups and getting cardiovascularly fit just down here in your perineum. And so I 9
10 think that certainly in a perisurgical atmosphere biofeedback and physical therapy and exercises that those therapies entail are very important to pursue and take seriously. It sounds like we'll be learning more. As more people talk about it, then more studies knowing risk factors. Exactly. We talked about obesity, but diet, all sorts of things, even can these conditions run in families and I read that maybe some, but we'll understand that a lot better. I want to thank you for talking about it today, Dr. Anne-Marie Boller, colorectal surgeon, and helping women and men to better understand that we need to talk about it more and that there is help available. Thank you very much. Thank you very much, Dr. Boller. This is what we do on Patient Power. Special thanks to Northwestern Memorial for connecting with us leading experts who can help you understand both common issues that are discussed a lot and even in this case a fairly common condition that needs to be discussed a lot more. So please, please if you're having these issue that certainly affect your quality of life, bring it up with your doctor and connect with a team that can help. I'm Andrew Schorr. Remember, knowledge can be the best medicine of all. Please remember the opinions expressed on Patient Power are not necessarily the views of Northwestern Memorial Hospital, its medical staff or Patient Power. Our discussions are not a substitute for seeking medical advice or care from your own doctor. That s how you ll get care that s most appropriate for you. 10
Pelvic Organ Prolapse: What Can I Do About This Problem? Webcast July 27, 2010 Christina Lewicky-Gaupp, M.D. Joanne s Story
 Pelvic Organ Prolapse: What Can I Do About This Problem? Webcast July 27, 2010 Christina Lewicky-Gaupp, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of Northwestern
Pelvic Organ Prolapse: What Can I Do About This Problem? Webcast July 27, 2010 Christina Lewicky-Gaupp, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of Northwestern
URINARY INCONTINENCE
 Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Bladder Cancer Knowing the Risks and Warning Signs. Part II: Warning Signs
 Bladder Cancer Knowing the Risks and Warning Signs Part II: Warning Signs May 8, 2018 Presented by: is the Director of Urologic Oncology at MedStar Washington Hospital Center and an Assistant Professor
Bladder Cancer Knowing the Risks and Warning Signs Part II: Warning Signs May 8, 2018 Presented by: is the Director of Urologic Oncology at MedStar Washington Hospital Center and an Assistant Professor
Tracking Genetic-Based Treatment Options for Inflammatory Bowel Disease
 Tracking Genetic-Based Treatment Options for Inflammatory Bowel Disease Recorded on: June 25, 2013 Melvin Heyman, M.D. Chief of Pediatric Gastroenterology UCSF Medical Center Please remember the opinions
Tracking Genetic-Based Treatment Options for Inflammatory Bowel Disease Recorded on: June 25, 2013 Melvin Heyman, M.D. Chief of Pediatric Gastroenterology UCSF Medical Center Please remember the opinions
Minimally Invasive Surgery Offers Promise for Pancreatic Cancer Patients
 Minimally Invasive Surgery Offers Promise for Pancreatic Cancer Patients Recorded on: August 1, 2012 Venu Pillarisetty, M.D. Surgical Oncologist Seattle Cancer Care Alliance Please remember the opinions
Minimally Invasive Surgery Offers Promise for Pancreatic Cancer Patients Recorded on: August 1, 2012 Venu Pillarisetty, M.D. Surgical Oncologist Seattle Cancer Care Alliance Please remember the opinions
Treatments for Fecal Incontinence A Review of the Research for Adults
 Treatments for Fecal Incontinence A Review of the Research for Adults e Is This Information Right for Me? This information is right for you if: Your health care professional* said you or your loved one
Treatments for Fecal Incontinence A Review of the Research for Adults e Is This Information Right for Me? This information is right for you if: Your health care professional* said you or your loved one
Postpartum Complications
 ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
One of the areas where it's certainly made it difference is with the transplantation of the liver. Dr. Roberts thinks so much for joining us.
 Benefits and Risks of Living Donor Liver Transplant Webcast May 28, 2008 John Roberts, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center,
Benefits and Risks of Living Donor Liver Transplant Webcast May 28, 2008 John Roberts, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center,
Surgical Treatment For Prostate Cancer Webcast May 6, 2010 John W. Davis, M.D., F.A.C.S. Mike Whyte. Mike s Story
 Surgical Treatment For Prostate Cancer Webcast May 6, 2010 John W. Davis, M.D., F.A.C.S. Mike Whyte Please remember the opinions expressed on Patient Power are not necessarily the views of M. D. Anderson
Surgical Treatment For Prostate Cancer Webcast May 6, 2010 John W. Davis, M.D., F.A.C.S. Mike Whyte Please remember the opinions expressed on Patient Power are not necessarily the views of M. D. Anderson
Fine-Tuning Immunotherapy to Treat Prostate Cancer Recorded on: April 24, 2013
 Fine-Tuning Immunotherapy to Treat Prostate Cancer Recorded on: April 24, 2013 John Corman, M.D. Medical Director, Floyd & Delores Jones Cancer Institute at Virginia Mason Virginia Mason Medical Center
Fine-Tuning Immunotherapy to Treat Prostate Cancer Recorded on: April 24, 2013 John Corman, M.D. Medical Director, Floyd & Delores Jones Cancer Institute at Virginia Mason Virginia Mason Medical Center
PROSTATE CANCER SCREENING SHARED DECISION MAKING VIDEO
 PROSTATE CANCER SCREENING SHARED DECISION MAKING VIDEO 1 00:00:00,067 --> 00:00:10,968 2 00:00:10,968 --> 00:00:12,701 So, you were given a decision aid sheet 3 00:00:12,701 --> 00:00:14,567 about prostate
PROSTATE CANCER SCREENING SHARED DECISION MAKING VIDEO 1 00:00:00,067 --> 00:00:10,968 2 00:00:10,968 --> 00:00:12,701 So, you were given a decision aid sheet 3 00:00:12,701 --> 00:00:14,567 about prostate
Female Urinary Incontinence: What It Is and What You Can Do About It
 Female Urinary Incontinence: What It Is and What You Can Do About It Urogynecology Patient Information Sheet What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for example,
Female Urinary Incontinence: What It Is and What You Can Do About It Urogynecology Patient Information Sheet What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for example,
Communication Methods for Proper Engagement in a Discussion about Overactive Bladder and Recommended Treatment Options
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Incontinence. Anatomy The human body has two kidneys. The kidneys continuously filter the blood and make urine.
 Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
Breast Cancer Imaging Webcast October 21, 2009 Peter Eby, M.D. Introduction
 Breast Cancer Imaging Webcast October 21, 2009 Peter Eby, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle Cancer Care Alliance, its medical staff or
Breast Cancer Imaging Webcast October 21, 2009 Peter Eby, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle Cancer Care Alliance, its medical staff or
Hello and welcome to Patient Power sponsored by Northwestern Memorial Hospital. I'm Andrew Schorr.
 Brain Tumor Clinical Trials Webcast November 22, 2011 Sean Grimm, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of Northwestern Memorial Hospital, its medical
Brain Tumor Clinical Trials Webcast November 22, 2011 Sean Grimm, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of Northwestern Memorial Hospital, its medical
Surgical Options for Breast Cancer October 28, 2009 Kristine Calhoun, M.D. Suzie Hagerland. Introduction
 Surgical Options for Breast Cancer October 28, 2009 Kristine Calhoun, M.D. Suzie Hagerland Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle Cancer Care Alliance,
Surgical Options for Breast Cancer October 28, 2009 Kristine Calhoun, M.D. Suzie Hagerland Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle Cancer Care Alliance,
Surgery for stress incontinence:
 Surgery for stress incontinence: information for you aashara Published February 2005 by the RCOG Contents Key points About this information What is stress incontinence? Do I need an operation? What operation
Surgery for stress incontinence: information for you aashara Published February 2005 by the RCOG Contents Key points About this information What is stress incontinence? Do I need an operation? What operation
Dr. Coakley, so virtual colonoscopy, what is it? Is it a CT exam exactly?
 Virtual Colonoscopy Webcast January 26, 2009 Fergus Coakley, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center, its medical staff or Patient
Virtual Colonoscopy Webcast January 26, 2009 Fergus Coakley, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center, its medical staff or Patient
Robotic Surgery: A Better Option for Many Head & Neck Cancers
 Robotic Surgery: A Better Option for Many Head & Neck Cancers Neal Futran, MD, DMD Director of Head and Neck Surgery, Department of Otolaryngology UW Medicine Eduardo Mendez, MD Assistant Professor, Otolaryngology:
Robotic Surgery: A Better Option for Many Head & Neck Cancers Neal Futran, MD, DMD Director of Head and Neck Surgery, Department of Otolaryngology UW Medicine Eduardo Mendez, MD Assistant Professor, Otolaryngology:
Advances in Pediatric Bone Marrow Transplant Webcast March 4, 2011 Scott Baker, M.D., M.S. Anna Robinson. Introduction
 Advances in Pediatric Bone Marrow Transplant Webcast March 4, 2011 Scott Baker, M.D., M.S. Anna Robinson Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle
Advances in Pediatric Bone Marrow Transplant Webcast March 4, 2011 Scott Baker, M.D., M.S. Anna Robinson Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle
Kegel Exercises for Men
 Kegel Exercises for Men The following information is based on the general experiences of many prostate cancer patients. Your experience may be different. If you have any questions about what prostate cancer
Kegel Exercises for Men The following information is based on the general experiences of many prostate cancer patients. Your experience may be different. If you have any questions about what prostate cancer
Laparoscopic Surgical Approaches for Ulcerative Colitis
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/laparoscopic-surgicalapproaches-for-ulcerative-colitis/7261/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/laparoscopic-surgicalapproaches-for-ulcerative-colitis/7261/
Robotic Ventral Rectopexy
 Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
Loss of Bladder Control
 BLADDER HEALTH Loss of Bladder Control SURGERY TO TREAT URINARY INCONTINENCE AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is Urinary Incontinence? Urinary incontinence
BLADDER HEALTH Loss of Bladder Control SURGERY TO TREAT URINARY INCONTINENCE AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is Urinary Incontinence? Urinary incontinence
Urinary Incontinence
 Urinary Incontinence Q: What is urinary incontinence and what causes it? A: When you are not able to hold your urine until you can get to a bathroom, you have what s called urinary incontinence (also called
Urinary Incontinence Q: What is urinary incontinence and what causes it? A: When you are not able to hold your urine until you can get to a bathroom, you have what s called urinary incontinence (also called
Cognitive Challenges After Hormone Therapy August 26, 2009 Webcast Monique Cherrier, Ph.D. Celestia Higano, M.D. Introduction
 Cognitive Challenges After Hormone Therapy August 26, 2009 Webcast Monique Cherrier, Ph.D. Celestia Higano, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of
Cognitive Challenges After Hormone Therapy August 26, 2009 Webcast Monique Cherrier, Ph.D. Celestia Higano, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of
Surgery for vaginal vault prolapse. Patient decision aid
 Surgery for vaginal vault prolapse Patient decision aid? i What is vaginal vault prolapse? Vaginal vault prolapse happens when the top of the vagina (the vault) slips from its normal position and sags
Surgery for vaginal vault prolapse Patient decision aid? i What is vaginal vault prolapse? Vaginal vault prolapse happens when the top of the vagina (the vault) slips from its normal position and sags
Brachytherapy for Prostate Cancer Webcast November 4, 2008 David Swanson, M.D. Steven Frank, M.D. Introduction
 Brachytherapy for Prostate Cancer Webcast November 4, 2008 David Swanson, M.D. Steven Frank, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of M. D. Anderson
Brachytherapy for Prostate Cancer Webcast November 4, 2008 David Swanson, M.D. Steven Frank, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of M. D. Anderson
Coping with urges and leaks?
 OAB AND YOU Coping with urges and leaks? Let me help you learn more about overactive bladder (OAB) symptoms and ways to help manage them 1 HOW DOES THE BLADDER WORK? Within the urinary tract, the kidneys
OAB AND YOU Coping with urges and leaks? Let me help you learn more about overactive bladder (OAB) symptoms and ways to help manage them 1 HOW DOES THE BLADDER WORK? Within the urinary tract, the kidneys
Loss of Bladder Control
 BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
Fecal Incontinence. What is fecal incontinence?
 Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Hello and welcome to Patient Power sponsored by UCSF Medical Center. I'm Andrew Schorr.
 Managing Pain from Shingles Webcast August 22, 2011 George Pasvankas, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center, its medical staff
Managing Pain from Shingles Webcast August 22, 2011 George Pasvankas, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center, its medical staff
Dr. Gopal, are you encouraged in the direction of where research is headed and its benefit for patients?
 Targeting the Tumor in Lymphoma July 8, 2009 Ajay Gopal Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle Cancer Care Alliance, its medical staff or Patient
Targeting the Tumor in Lymphoma July 8, 2009 Ajay Gopal Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle Cancer Care Alliance, its medical staff or Patient
Accidental Bowel Leakage (Fecal Incontinence)
 Accidental Bowel Leakage (Fecal Incontinence) What is Accidental Bowel Leakage (ABL)? Accidental bowel leakage is the inability to control solid or liquid stool. This is the inability to control gas and
Accidental Bowel Leakage (Fecal Incontinence) What is Accidental Bowel Leakage (ABL)? Accidental bowel leakage is the inability to control solid or liquid stool. This is the inability to control gas and
Lets talk about Faecal incontinence (FI) in Scleroderma
 Lets talk about Faecal incontinence (FI) in Scleroderma Dr. Shamaila Butt Gastroenterology Research Registrar GI Physiology unit University College Hospital London GI manifestations in Scleroderma Oesophagus
Lets talk about Faecal incontinence (FI) in Scleroderma Dr. Shamaila Butt Gastroenterology Research Registrar GI Physiology unit University College Hospital London GI manifestations in Scleroderma Oesophagus
Section 4 Decision-making
 Decision-making : Decision-making Summary Conversations about treatments Participants were asked to describe the conversation that they had with the clinician about treatment at diagnosis. The most common
Decision-making : Decision-making Summary Conversations about treatments Participants were asked to describe the conversation that they had with the clinician about treatment at diagnosis. The most common
Northwest Rehabilitation Associates, Inc.
 Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Pelvic Organ Prolapse. Natural Solutions
 Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
Carrier Screening in your Practice Is it Time to Expand your View?
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-industry-feature/carrier-screening-your-practice-it-time-expandyour-view/9648/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-industry-feature/carrier-screening-your-practice-it-time-expandyour-view/9648/
Stress. incontinence FACTS, ADVICE, AND EXERCISES.
 Stress incontinence FACTS, ADVICE, AND EXERCISES Facts about incontinence Urinary incontinence is a common problem; one in every four women has problems with some form of leakage. Incontinence can be anything
Stress incontinence FACTS, ADVICE, AND EXERCISES Facts about incontinence Urinary incontinence is a common problem; one in every four women has problems with some form of leakage. Incontinence can be anything
Benefits of Survivorship Treatment Care Plans Webcast May 13, 2009 Scott Baker, M.D., M.S. Donald Wilhelm. Introduction
 Benefits of Survivorship Treatment Care Plans Webcast May 13, 2009 Scott Baker, M.D., M.S. Donald Wilhelm Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle
Benefits of Survivorship Treatment Care Plans Webcast May 13, 2009 Scott Baker, M.D., M.S. Donald Wilhelm Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle
Beyond The Data: Promoting Well-being in Older Adults
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/grand-rounds-nation/beyond-data-promoting-well-being-olderadults/9844/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/grand-rounds-nation/beyond-data-promoting-well-being-olderadults/9844/
Sacral Nerve Stimulation for Faecal Incontinence
 Sacral Nerve Stimulation for Faecal Incontinence Questions & Answers GLASGOW COLORECTAL CENTRE Ross Hall Hospital 221 Crookston Road Glasgow G52 3NQ e-mail: info@colorectalcentre.co.uk Ph: Main hospital
Sacral Nerve Stimulation for Faecal Incontinence Questions & Answers GLASGOW COLORECTAL CENTRE Ross Hall Hospital 221 Crookston Road Glasgow G52 3NQ e-mail: info@colorectalcentre.co.uk Ph: Main hospital
Breakthrough Understanding in Pancreatic Cancer Therapy
 Breakthrough Understanding in Pancreatic Cancer Therapy Recorded on: May 28, 2013 Sunil R. Hingorani, M.D., Ph.D. Associate Member Fred Hutchinson Cancer Research Center Please remember the opinions expressed
Breakthrough Understanding in Pancreatic Cancer Therapy Recorded on: May 28, 2013 Sunil R. Hingorani, M.D., Ph.D. Associate Member Fred Hutchinson Cancer Research Center Please remember the opinions expressed
Hello and welcome to Patient Power sponsored by UCSF Medical Center. I m Andrew Schorr.
 The Integrated Approach to Treating Cancer Symptoms Webcast March 1, 2012 Michael Rabow, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center,
The Integrated Approach to Treating Cancer Symptoms Webcast March 1, 2012 Michael Rabow, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center,
Pelvic Floor Exercises
 Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
Defeating Colon Cancer with Surgery
 Defeating Colon Cancer with Surgery Recorded on: September 19, 2012 Alessandro Fichera, M.D. Director, Colorectal Surgical Oncology Program, Seattle Cancer Care Alliance Please remember the opinions expressed
Defeating Colon Cancer with Surgery Recorded on: September 19, 2012 Alessandro Fichera, M.D. Director, Colorectal Surgical Oncology Program, Seattle Cancer Care Alliance Please remember the opinions expressed
IF YOU VE GOT TO GO, WE VE GOT SOLUTIONS.
 IF YOU VE GOT TO GO, WE VE GOT SOLUTIONS. Get the facts about urinary incontinence and get real solutions. HENRY FORD PELVIC HEALTH & CONTINENCE CENTER HENRY FORD WOMEN S HEALTH SERVICES INCONVENIENCE?
IF YOU VE GOT TO GO, WE VE GOT SOLUTIONS. Get the facts about urinary incontinence and get real solutions. HENRY FORD PELVIC HEALTH & CONTINENCE CENTER HENRY FORD WOMEN S HEALTH SERVICES INCONVENIENCE?
Parkinson s Disease Webcast January 31, 2008 Jill Ostrem, M.D. What is Parkinson s Disease?
 Parkinson s Disease Webcast January 31, 2008 Jill Ostrem, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center, its medical staff or Patient
Parkinson s Disease Webcast January 31, 2008 Jill Ostrem, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center, its medical staff or Patient
Understanding Acute Kidney Injury and Its Impact
 Understanding Acute Kidney Injury and Its Impact Recorded on: March 7, 2013 Chi-Yuan Hsu, M.D., M.S. Chief of the Division of Nephrology, UCSF Department of Medicine UCSF Medical Center Raymond Hsu, M.D.
Understanding Acute Kidney Injury and Its Impact Recorded on: March 7, 2013 Chi-Yuan Hsu, M.D., M.S. Chief of the Division of Nephrology, UCSF Department of Medicine UCSF Medical Center Raymond Hsu, M.D.
Pathology Driving Decisions
 Pathology Driving Decisions Part I: Understanding Your Diagnosis and Your Treatment Options May 7, 2018 Presented by: Dr. Matthew Mossanen completed his college and medical school training at UCLA. He
Pathology Driving Decisions Part I: Understanding Your Diagnosis and Your Treatment Options May 7, 2018 Presented by: Dr. Matthew Mossanen completed his college and medical school training at UCLA. He
Comparing Liquid-Based Cytology Methods in the Detection of Cervical Cancer: Perspectives from Dr. Daniel Ferrante
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/advances-in-womens-health/comparing-liquid-based-cytology-methodsdetection-cervical-cancer-perspectives-dr-daniel-ferrante/7592/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/advances-in-womens-health/comparing-liquid-based-cytology-methodsdetection-cervical-cancer-perspectives-dr-daniel-ferrante/7592/
Detecting Coronary Artery Disease: The Role of Non-Invasive Cardiac Stress Testing Webcast September 28, 2010 Preeti Kansal, M.D.
 Detecting Coronary Artery Disease: The Role of Non-Invasive Cardiac Stress Testing Webcast September 28, 2010 Preeti Kansal, M.D. Please remember the opinions expressed on Patient Power are not necessarily
Detecting Coronary Artery Disease: The Role of Non-Invasive Cardiac Stress Testing Webcast September 28, 2010 Preeti Kansal, M.D. Please remember the opinions expressed on Patient Power are not necessarily
The Latest in Non-Hodgkin Lymphoma News From ASCO
 Patient Power Knowledge. Confidence. Hope. The Latest in Non-Hodgkin Lymphoma News From ASCO John Leonard, MD Associate Dean for Clinical Research Weill Cornell Medical College Please remember the opinions
Patient Power Knowledge. Confidence. Hope. The Latest in Non-Hodgkin Lymphoma News From ASCO John Leonard, MD Associate Dean for Clinical Research Weill Cornell Medical College Please remember the opinions
MS Learn Online Feature Presentation Managing Symptoms: Bladder Dysfunction Nancy Holland, Ed.D, RN, MSCN
 MS Learn Online Feature Presentation Managing Symptoms: Bladder Dysfunction Nancy Holland, Ed.D, RN, MSCN Tom>> Hi, I m Tom Kimball Tracey>> And I m Tracey Kimball. Bladder dysfunction can be a very embarrassing
MS Learn Online Feature Presentation Managing Symptoms: Bladder Dysfunction Nancy Holland, Ed.D, RN, MSCN Tom>> Hi, I m Tom Kimball Tracey>> And I m Tracey Kimball. Bladder dysfunction can be a very embarrassing
Interstitial Cystitis - Painful Bladder Syndrome
 Interstitial Cystitis - Painful Bladder Syndrome Interstitial cystitis (in-tur-stish-ul sis-tie-tis) also called painful bladder syndrome is a chronic condition in which you experience bladder pressure,
Interstitial Cystitis - Painful Bladder Syndrome Interstitial cystitis (in-tur-stish-ul sis-tie-tis) also called painful bladder syndrome is a chronic condition in which you experience bladder pressure,
Andrew Schorr: Hello and welcome once again to Patient Power, sponsored by the Seattle Cancer Care Alliance. I'm Andrew Schorr.
 The Latest in Gynecological Cancers Webcast May 21, 2008 Banjamin Greer, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle Cancer Care Alliance, its
The Latest in Gynecological Cancers Webcast May 21, 2008 Banjamin Greer, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle Cancer Care Alliance, its
Parkinson s Disease: An Update Webcast November 27, 2007 Cindy Zadikoff, M.D.
 Parkinson s Disease: An Update Webcast November 27, 2007 Cindy Zadikoff, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of Northwestern Memorial Hospital, its
Parkinson s Disease: An Update Webcast November 27, 2007 Cindy Zadikoff, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of Northwestern Memorial Hospital, its
Urinary Incontinence
 Urinary Incontinence Q: What is urinary incontinence (UI)? A: UI is also known as loss of bladder control or urinary leakage. UI is when urine leaks out before you can get to a bathroom. If you have UI,
Urinary Incontinence Q: What is urinary incontinence (UI)? A: UI is also known as loss of bladder control or urinary leakage. UI is when urine leaks out before you can get to a bathroom. If you have UI,
Expert Strategies for Working with Anxiety
 Expert Strategies for Working with Anxiety Bonus 1 - Transcript - pg. 1 Expert Strategies for Working with Anxiety An EMDR Approach for Healing Generalized Anxiety Disorder with Laurel Parnell, PhD; Rick
Expert Strategies for Working with Anxiety Bonus 1 - Transcript - pg. 1 Expert Strategies for Working with Anxiety An EMDR Approach for Healing Generalized Anxiety Disorder with Laurel Parnell, PhD; Rick
MS Learn Online Feature Presentation MS and Your Emotions, part two Deborah Miller, PhD. Tracey>> Welcome to MS Learn Online, I m Tracey Kimball.
 Page 1 MS Learn Online Feature Presentation MS and Your Emotions, part two Deborah Miller, PhD Tracey>> Welcome to MS Learn Online, I m Tracey Kimball. Tom>> and I m Tom Kimball. In the first installment
Page 1 MS Learn Online Feature Presentation MS and Your Emotions, part two Deborah Miller, PhD Tracey>> Welcome to MS Learn Online, I m Tracey Kimball. Tom>> and I m Tom Kimball. In the first installment
Incontinence; Lets talk about it. Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery
 Incontinence; Lets talk about it Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery Select the most appropriate subtitle for this talk A: Bladders gone wild! B: There s no such thing
Incontinence; Lets talk about it Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery Select the most appropriate subtitle for this talk A: Bladders gone wild! B: There s no such thing
Transcript of RELIEF podcast with David Seminowicz:
 Transcript of RELIEF podcast with David Seminowicz: RELIEF: Hello, and thanks for tuning in to RELIEF s podcast series. I'm Neil Andrews, editor of RELIEF. I'm thrilled to have the opportunity to speak
Transcript of RELIEF podcast with David Seminowicz: RELIEF: Hello, and thanks for tuning in to RELIEF s podcast series. I'm Neil Andrews, editor of RELIEF. I'm thrilled to have the opportunity to speak
IMPROVING URINARY INCONTINENCE
 IMPROVING URINARY INCONTINENCE INFORMATION FOR OLDER ADULTS, FAMILIES, AND CAREGIVERS READ THIS PAMPHLET TO LEARN: What Urinary Incontinence is. How to Manage Urinary Incontinence. What Pelvic Floor Exercises
IMPROVING URINARY INCONTINENCE INFORMATION FOR OLDER ADULTS, FAMILIES, AND CAREGIVERS READ THIS PAMPHLET TO LEARN: What Urinary Incontinence is. How to Manage Urinary Incontinence. What Pelvic Floor Exercises
Pelvic Floor Disorders. Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon
 Pelvic Floor Disorders Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon What is Pelvic Floor Disorder Surgical perspective symptoms of RED, FI or prolapse on the background
Pelvic Floor Disorders Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon What is Pelvic Floor Disorder Surgical perspective symptoms of RED, FI or prolapse on the background
Questions & Answers about Sexuality and Intimacy after Bladder Cancer. Part III: Causes and Treatments for Sexual Dysfunction
 Questions & Answers about Sexuality and Intimacy after Bladder Cancer A Valentine's chat with Dr. Trinity Bivalacqua Monday, February 13, 2017 Part III: Causes and Treatments for Sexual Dysfunction Presented
Questions & Answers about Sexuality and Intimacy after Bladder Cancer A Valentine's chat with Dr. Trinity Bivalacqua Monday, February 13, 2017 Part III: Causes and Treatments for Sexual Dysfunction Presented
Conversations: Let s Talk About Bladder Cancer
 Understanding Biomarkers Matt Gaslky, MD, Professor of Medicine Icahn School of Medicine at Mount Sinai Piyush Agarwal, MD, Head, Bladder Cancer Section Urological Oncology Branch, National Cancer Institute
Understanding Biomarkers Matt Gaslky, MD, Professor of Medicine Icahn School of Medicine at Mount Sinai Piyush Agarwal, MD, Head, Bladder Cancer Section Urological Oncology Branch, National Cancer Institute
Perineal Tears. Obstetrics & Gynaecology Women & Children s Group
 Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
Colon Cancer Screening Webcast April 23, 2008 William Grady, M.D. Introduction
 Colon Cancer Screening Webcast April 23, 2008 William Grady, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle Cancer Care Alliance, its medical staff
Colon Cancer Screening Webcast April 23, 2008 William Grady, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle Cancer Care Alliance, its medical staff
Marty: I had my physical in 2006, and my physician said that I had myelofibrosis and said I had three to five years to live.
 Advances in the Treatment of Myeloproliferative Disorders Webcast April 28, 2009 Srdan Verstovsek, M.D., Ph.D. Marty Prager Please remember the opinions expressed on Patient Power are not necessarily the
Advances in the Treatment of Myeloproliferative Disorders Webcast April 28, 2009 Srdan Verstovsek, M.D., Ph.D. Marty Prager Please remember the opinions expressed on Patient Power are not necessarily the
Please Understand Me, Managing ADHD within a Marriage, this is Stay Happily Married episode number 222.
 Announcer: Please Understand Me, Managing ADHD within a Marriage, this is Stay Happily Married episode number 222. Welcome to Stay Happily Married, your source for weekly updates on the latest tips and
Announcer: Please Understand Me, Managing ADHD within a Marriage, this is Stay Happily Married episode number 222. Welcome to Stay Happily Married, your source for weekly updates on the latest tips and
Recording Transcript Wendy Down Shift #9 Practice Time August 2018
 Recording Transcript Wendy Down Shift #9 Practice Time August 2018 Hi there. This is Wendy Down and this recording is Shift #9 in our 6 month coaching program. [Excuse that I referred to this in the recording
Recording Transcript Wendy Down Shift #9 Practice Time August 2018 Hi there. This is Wendy Down and this recording is Shift #9 in our 6 month coaching program. [Excuse that I referred to this in the recording
The Current Research on Stretching and Flexibility is Flawed!
 Transcript from: https://www.youtube.com/watch?v=qz0ot7tbbg0 Original Article: http://stretchcoach.com/articles/proper-stretching/ The Current Research on Stretching and Flexibility is Flawed! Hi. I'm
Transcript from: https://www.youtube.com/watch?v=qz0ot7tbbg0 Original Article: http://stretchcoach.com/articles/proper-stretching/ The Current Research on Stretching and Flexibility is Flawed! Hi. I'm
5 DIAGNOSIS. History taking
 5 DIAGNOSIS All of the photographs in Chapter 4 were taken in theatre before operation. This chapter deals with how one can recognize the type of fistula by history taking and examination. (Note that the
5 DIAGNOSIS All of the photographs in Chapter 4 were taken in theatre before operation. This chapter deals with how one can recognize the type of fistula by history taking and examination. (Note that the
An Oral Fecal Transplant for Lunch?- Frankly Speaking EP 53
 An Oral Fecal Transplant for Lunch?- Frankly Speaking EP 53 Transcript Details This is a transcript of an episode from the podcast series Frankly Speaking accessible at Pri- Med.com. Additional media formats
An Oral Fecal Transplant for Lunch?- Frankly Speaking EP 53 Transcript Details This is a transcript of an episode from the podcast series Frankly Speaking accessible at Pri- Med.com. Additional media formats
EXPECTING A BABY? SOME PREGNANT WOMEN CAN HAVE BLADDER AND BOWEL CONTROL PROBLEMS. YOU CAN GET HELP. HOW DO I KNOW IF I HAVE A PROBLEM?
 11 BLADDER AND BOWEL CONTROL PROBLEMS. When you are pregnant, you get a lot of advice from many people. One topic few people think about is bladder and bowel control problems during pregnancy and after
11 BLADDER AND BOWEL CONTROL PROBLEMS. When you are pregnant, you get a lot of advice from many people. One topic few people think about is bladder and bowel control problems during pregnancy and after
Hereditary Cancer Syndromes and the Obstetrician/Gynecologist
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/clinicians-roundtable/hereditary-cancer-syndromes-and-theobstetriciangynecologist/6990/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/clinicians-roundtable/hereditary-cancer-syndromes-and-theobstetriciangynecologist/6990/
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
Dr. Michael Keating: My Hopes for the Future of CLL Treatment Recorded on December 8, 2014
 Patient Power Knowledge. Confidence. Hope. Dr. Michael Keating: My Hopes for the Future of CLL Treatment Recorded on December 8, 2014 Michael Keating, MB, BS Professor of Medicine, Department of Leukemia
Patient Power Knowledge. Confidence. Hope. Dr. Michael Keating: My Hopes for the Future of CLL Treatment Recorded on December 8, 2014 Michael Keating, MB, BS Professor of Medicine, Department of Leukemia
We know that treatments are now targeting genes, but does genetics play a bigger role in cancer outside of that?
 Welcome to the 3Ps of Cancer podcast, where we'll discuss prevention, preparedness, and progress in cancer treatments and research. Brought to you by the University of Michigan Rogel Cancer Center. I'm
Welcome to the 3Ps of Cancer podcast, where we'll discuss prevention, preparedness, and progress in cancer treatments and research. Brought to you by the University of Michigan Rogel Cancer Center. I'm
Helping Kidney Stones Pass: Use of Alpha Antagonists Frankly Speaking EP7
 Helping Kidney Stones Pass: Use of Alpha Antagonists Frankly Speaking EP7 Transcript Details This is a transcript of an episode from the podcast series Frankly Speaking accessible at Pri- Med.com. Additional
Helping Kidney Stones Pass: Use of Alpha Antagonists Frankly Speaking EP7 Transcript Details This is a transcript of an episode from the podcast series Frankly Speaking accessible at Pri- Med.com. Additional
Uterus (Womb) Rectum. Another problem could be the sensation of something coming down at the birth canal or back passage (prolapse).
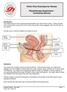 Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
Guide to strengthening the pelvic floor muscles
 Exercise Cones Pelvic Exercise Made Easy Exercise Cones Pelvic Exercise Made Easy This system is clinically proven to strengthen the pelvic floor muscle to help with the control and prevention of stress
Exercise Cones Pelvic Exercise Made Easy Exercise Cones Pelvic Exercise Made Easy This system is clinically proven to strengthen the pelvic floor muscle to help with the control and prevention of stress
Top 10 Tips Bladder Control
 Top 10 Tips Bladder Control for Your Personal Guide to a Sensitive Bladder Dr. Mache Seibel Leading authority on women s wellness and menopause Message from Dr. Mache Seibel Thank you for downloading this
Top 10 Tips Bladder Control for Your Personal Guide to a Sensitive Bladder Dr. Mache Seibel Leading authority on women s wellness and menopause Message from Dr. Mache Seibel Thank you for downloading this
Targeted Therapies in Breast Cancer Webcast October 24, 2007 Julie Gralow, M.D. Hosted By Andrew Schorr
 Targeted Therapies in Breast Cancer Webcast October 24, 2007 Julie Gralow, M.D. Hosted By Andrew Schorr Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle
Targeted Therapies in Breast Cancer Webcast October 24, 2007 Julie Gralow, M.D. Hosted By Andrew Schorr Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle
Urinary incontinence. Urology Department. Patient Information Leaflet
 Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Upper Tract Urothelial Carcinomas (UTUCs)
 Upper Tract Urothelial Carcinomas (UTUCs) Part II: UTUC Treatment Options November 14, 2017 Moderated by: Presented by: Gary D. Steinberg, MD University of Chicago Medical Center Ahmad Shabsigh, MD Ohio
Upper Tract Urothelial Carcinomas (UTUCs) Part II: UTUC Treatment Options November 14, 2017 Moderated by: Presented by: Gary D. Steinberg, MD University of Chicago Medical Center Ahmad Shabsigh, MD Ohio
ONE IN THREE WOMEN WHO EVER HAD A BABY WET THEMSELVES EVERY WOMAN WHO HAS HAD A BABY SHOULD DO PELVIC FLOOR MUSCLE TRAINING.
 08 EVERY WOMAN WHO HAS HAD A BABY SHOULD Women who have even just one baby are nearly three times more likely to leak urine and wet themselves, than women who have not had a baby. The more babies you have,
08 EVERY WOMAN WHO HAS HAD A BABY SHOULD Women who have even just one baby are nearly three times more likely to leak urine and wet themselves, than women who have not had a baby. The more babies you have,
The Pelvic Floor Muscles - a Guide for Women
 The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
Pelvic floor exercises for women. Information for patients Continence Service
 Pelvic floor exercises for women Information for patients Continence Service page 2 of 8 Why do I need to do pelvic floor exercises? Many women experience pelvic floor problems at some time during their
Pelvic floor exercises for women Information for patients Continence Service page 2 of 8 Why do I need to do pelvic floor exercises? Many women experience pelvic floor problems at some time during their
Maternity Information Leaflet. Care of the Perineum (including Pelvic Floor Exercises) Version 2
 Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
Incontinence. Urinary. In Adults. THIS PUBLICATION IS OUT OF DATE. For most current information:
 Urinary Incontinence In Adults A Patient's Guide r I When you eat and drink, your body absorbs the liquid. The kidneys filter out waste products from the body fluids and make urine. Urine travels down
Urinary Incontinence In Adults A Patient's Guide r I When you eat and drink, your body absorbs the liquid. The kidneys filter out waste products from the body fluids and make urine. Urine travels down
How to Foster Post-Traumatic Growth
 How to Foster Post-Traumatic Growth Module 7, Part 2 - Transcript - pg. 1 How to Foster Post-Traumatic Growth Two Ways to Ignite Accelerated Growth Part 2: How Your Choice of Language Can Transform an
How to Foster Post-Traumatic Growth Module 7, Part 2 - Transcript - pg. 1 How to Foster Post-Traumatic Growth Two Ways to Ignite Accelerated Growth Part 2: How Your Choice of Language Can Transform an
Diabetes Remission with Weight Loss - Frankly Speaking EP 49
 Diabetes Remission with Weight Loss - Frankly Speaking EP 49 Transcript Details This is a transcript of an episode from the podcast series Frankly Speaking accessible at Pri- Med.com. Additional media
Diabetes Remission with Weight Loss - Frankly Speaking EP 49 Transcript Details This is a transcript of an episode from the podcast series Frankly Speaking accessible at Pri- Med.com. Additional media
Shoulder Arthritis and Shoulder Replacement Surgery Webcast June 22, 2010 Matthew Saltzman, M.D. Introduction
 Shoulder Arthritis and Shoulder Replacement Surgery Webcast June 22, 2010 Matthew Saltzman, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of Northwestern Memorial
Shoulder Arthritis and Shoulder Replacement Surgery Webcast June 22, 2010 Matthew Saltzman, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of Northwestern Memorial
Surgical Treatment For Pancreatic Cancer Webcast March 22, 2011 Venu Pillarisetty, M.D. Stan Barer. Introduction
 Surgical Treatment For Pancreatic Cancer Webcast March 22, 2011 Venu Pillarisetty, M.D. Stan Barer Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle Cancer
Surgical Treatment For Pancreatic Cancer Webcast March 22, 2011 Venu Pillarisetty, M.D. Stan Barer Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle Cancer
Pelvic Floor Muscle Exercises
 INFORMATION FOR WOMEN OF ALL AGES Pelvic Floor Muscle Exercises How to exercise and strengthen your pelvic floor muscles ASSOCIATION OF CHARTERED PHYSIOTHERAPISTS IN WOMEN S HEALTH This leaflet is supported
INFORMATION FOR WOMEN OF ALL AGES Pelvic Floor Muscle Exercises How to exercise and strengthen your pelvic floor muscles ASSOCIATION OF CHARTERED PHYSIOTHERAPISTS IN WOMEN S HEALTH This leaflet is supported
Life after Bladder Removal Selecting your best urinary diversion. Part IV: Indiana Pouch and Question & Answer Session
 Life after Bladder Removal Selecting your best urinary diversion A candid conversation with Alexander Kutikov MD Tuesday, January 24, 2017 Part IV: Indiana Pouch and Question & Answer Session Presented
Life after Bladder Removal Selecting your best urinary diversion A candid conversation with Alexander Kutikov MD Tuesday, January 24, 2017 Part IV: Indiana Pouch and Question & Answer Session Presented
Hello and welcome to Patient Power sponsored by UW Medicine Health System. I'm Andrew Schorr
 Advanced Techniques for Treating Liver Tumors Webcast James O. Park, M.D. Veena Shankaran, M.D. Raymond S.W. Yeung, M.D., FRCS(C), FACS Derek Epps November 28, 2011 Please remember the opinions expressed
Advanced Techniques for Treating Liver Tumors Webcast James O. Park, M.D. Veena Shankaran, M.D. Raymond S.W. Yeung, M.D., FRCS(C), FACS Derek Epps November 28, 2011 Please remember the opinions expressed
