Recent advances have improved the
|
|
|
- Sybil Perry
- 5 years ago
- Views:
Transcription
1 SURGICAL TECHNIQUES BY NEERAJ KOHLI, MD, MBA, and JOHN R. MIKLOS, MD Meeting the challenge of vesicovaginal fistula repair: Conservative and surgical measures A number of simple adjustments to technique and timing of repair can improve the outlook for this troublesome complication. Here, 2 experts offer tips and caveats. Recent advances have improved the success of vesicovaginal fistula (VVF) repair a challenge that can test even the most experienced gynecologic surgeon. For example, it now is apparent that some small uncomplicated fistulae respond to conservative treatment. Further, in selected cases, laparoscopic repair can eliminate the need for complicated laparotomy. In addition, timing of fistula repair no longer requires long periods of observation, and good surgical technique for identifying and repairing bladder injuries at the time of KEY POINTS Surgical risk factors include prior pelvic surgery, history of pelvic inflammatory disease, pelvic malignancy, endometriosis, infection, diabetes, and anatomic distortion. Conservative therapy should be reserved for simple fistulae that are less than 1 cm in size, diagnosed within 7 days of the index surgery, lacking associated carcinoma or radiation, and subject to at least 4 weeks of constant bladder drainage. In surgical repair, the Latzko partial colpocleisis or fistulectomy with flapsplitting closure is preferred. the index surgery can often prevent the development or reduce the severity of VVF. Vesicovaginal fistula is the most common type of urogenital fistula. Presentation and prognosis vary, depending on location and size of the defect, as well as coexisting factors such as tissue devascularization and previous radiation. However, surgical repair is associated with a high cure rate if it is performed by an experienced surgeon. Most US cases follow gynecologic surgery Vesicovaginal fistula was first documented in the mummified remains of Egyptian Queen Henhenit (11th Dynasty, 2050 BC), which were examined in 1923 by Derry. 1 Although the exact incidence of VVF in the United States is unknown, the primary cause is gynecologic surgery, especially hysterectomy. The defect is estimated to occur in 0.01% Dr. Kohli is chief, division of urogynecology and reconstructive pelvic surgery, Brigham and Women s Hospital, and assistant professor, department of obstetrics and gynecology, Harvard Medical School, in Boston, Mass. Dr. Miklos is director, Atlanta Urogynecology Associates, and clinical instructor, department of obstetrics and gynecology, Medical College of Georgia, Atlanta, Ga. 16 OBG MANAGEMENT August 2003
2 Meeting the challenge of vesicovaginal fistula repair TABLE CLASSIFICATION Simple Classification of vesicovaginal fistulae 17 Complicated DESCRIPTION Fistula is less than 2 to 3 cm in size and near the cuff (supratrigonal) Patient has no history of radiation or malignancy Vaginal length is normal Patient has had previous radiation therapy Pelvic malignancy is present Vaginal length is shortened Fistula is greater than 3 cm in size Fistula is distant from cuff or has trigonal involvement to 0.04% of gynecologic procedures. A study of 303 women with genitourinary fistula found that the defect was related to gynecologic surgery in 82% of cases, obstetric events in 8%, radiation therapy in 6%, and trauma or fulguration in 4%. 2 Rare causes of VVF include lymphogranuloma venereum, tuberculosis, syphilis, bladder stones, and a retained foreign body in the vagina. In rare instances, spontaneous vesicouterine fistulae were reported following uncomplicated vaginal birth after cesarean section. 3 Gynecologic surgery may lead to VVF due to extensive dissection between the bladder and the uterus, unrecognized bladder laceration, inappropriate stitch placement, and/or devascularization injury to the tissue planes. Concurrent ureteric involvement has been reported in as many as 10% to 15% of vesicovaginal fistula cases. In developing countries, vesicovaginal fistulae are far more common and generally related to obstetric factors such as obstructed labor (due to unattended deliveries), small pelvic dimensions, malpresentation, poor uterine contractions, and introital stenosis. Risk factors. Conditions that may predispose patients to VVF include prior pelvic surgery, a history of pelvic inflammatory disease, pelvic malignancy, endometriosis, infection, diabetes, and anatomic distortion. If these risk factors are present, the patient should be counseled accordingly prior to gynecologic surgery. Correct classification crucial to surgical success classification of VVF Proper can help the gynecologic surgeon plan operative intervention. Obstetric vesicovaginal fistulae usually are categorized according to their cause, complexity, and site of obstruction. In contrast, gynecologic fistulae are generally classified as simple or complicated (TABLE). These levels may have important implications for the surgical approach and prognosis. 4 For example, simple vesicovaginal fistulae are usually uncomplicated surgical cases with good prognosis. Complicated vesicovaginal fistulae, on the other hand, can challenge even highly practiced and skilled gynecologic surgeons and are associated with a high rate of recurrence. Women typically present within specific intervals after the various antecedent events (pelvic surgery, childbirth, radiation therapy) with a primary complaint of constant, painless urinary incontinence. If the fistula is related to traumatic childbirth, most patients experience urine leakage within the first 24 to 48 hours. Following pelvic surgery, symptoms usually occur within the first 30 days. In contrast, radiation-induced fistulae develop over a much longer interval secondary to progressive devascularization necrosis, and may present 30 days to 30 years after the antecedent event. Some patients report exacerbation during physical activities, which can sometimes 18 OBG MANAGEMENT August 2003
3 Meeting the challenge of vesicovaginal fistula repair FIGURE 1 Vesicovaginal fistula Bladder Mucosa Pubocervical fascia Vesicovaginal fistula Vaginal epithelium Rectum Vagina Urethra Anus Pelvic cross section depicting high vesicovaginal fistula. IMAGE: Maura Flynn lead to erroneous diagnosis of uncomplicated stress incontinence. If the fistula is small, intermittent leakage with increased bladder distention or physical activity may be noted. Other patients may complain of vaginal discharge or hematuria. If there is concurrent ureteric involvement, the patient may experience constitutional symptoms (such as fever, chills, and flank pain) or even gastrointestinal symptoms. Physical findings. Any pooling of fluid in the vagina that is noted should be sent for analysis if the diagnosis is unclear. Next, perform a careful speculum exam that allows visualization of the entire anterior vaginal wall to identify the fistula tract (FIGURE 1). In many cases, the fistula is grossly visible. Determine the location of the fistula in relation to the vaginal apex and bladder trigone and assess the quality of surrounding tissue (eg, presence of inflammation, edema, or infection). Fistulas near the vaginal apex may require a more complicated abdominal approach, and those close to the trigone may be associated with increased risk of ureteral injury during repair. If the fistula is particularly small, no tract may be apparent. In such cases, bimanual exam with careful palpation of the anterior wall may help isolate the fistula (eg, when there is a surrounding zone of induration). Office tests. If no fistula is noted despite highly suspicious signs and symptoms and careful examination, a simple office test can August 2003 OBG MANAGEMENT 21
4 Meeting the challenge of vesicovaginal fistula repair FIGURE 2 Abdominal repair Placement of omental flap Bladder and vaginal closure Abdominal repair of vesicovaginal fistula, with closure of bladder defect and posterior cystotomy and separate closure of vaginal defect. Note the omental flap pictured in the insert. be performed. Using a catheter, fill the bladder with a dyed solution such as normal saline with indigo carmine and repeat the pelvic exam with a half-speculum to visualize the anterior wall. Ask the patient to cough and bear down, and identify the fistula by visualizing urine leakage. If this test fails to locate the fistula, insert a tampon and ask the patient to perform 10 to 15 minutes of exertional maneuvers, including stair climbing and jumping in place. Then remove the tampon. Visualization of dye beyond the most distal edge of the tampon confirms the presence of a fistula. A variation of this technique is the doubledye test: Give the patient oral phenazopyridine (Pyridium), fill the bladder with the blue-tinted solution, and insert a tampon. The presence of blue staining suggests vesicovaginal or urethrovaginal fistula, while red staining (Pyridium) suggests ureterovaginal fistula. Other testing. Further assessment is recommended to rule out concurrent pathology and formulate an appropriate treatment plan. Routine testing should include a urinalysis and culture to exclude coexisting urinary tract infection, an electrolyte panel to evaluate renal function, and a complete blood cell count to rule out systemic infection. Cystoscopy should be performed to visualize the fistulous tract, assess its location in relation to the ureters and trigone, assure bilateral ureteral patency, and exclude the presence of a foreign body or suture in the bladder. In patients with a history of urogenital IMAGE: Maura Flynn 22 OBG MANAGEMENT August 2003
5 Meeting the challenge of vesicovaginal fistula repair malignancy, biopsy of the fistula tract and urine cytology is warranted. Radiologic studies are recommended prior to surgical repair of a vesicovaginal fistula to fully assess the defect and exclude the presence of multiple fistulae. An intravenous Comparable success rates have been reported for early and late repair of surgery-induced fistulae. pyelogram is helpful to exclude concurrent ureterovaginal fistulae or ureteral obstruction. A targeted fistulogram may be indicated if conservative therapy is planned, including expectant management, continuous bladder drainage, fulguration, or fibrin occlusion. Indications for conservative management Because spontaneous closure is uncommon, symptomatic VVF merits treatment. Appropriate therapy depends on various factors, including fistula size and location, timing from the antecedent event, severity of symptoms, quality of surrounding tissue, and clinician experience and surgical skills. Occasionally, a fistula heals following prolonged bladder drainage through a transurethral or suprapubic catheter provided it is diagnosed within a few days of surgery. Zimmern 5 recommends a conservative approach to small fistulae if the patient s complaints of urinary incontinence are resolved with insertion of a Foley catheter. In this case, bladder drainage should be continued for 3 weeks, followed by reevaluation of the fistula. If the fistula has diminished in size, an additional 3 weeks of catheter drainage is associated with a high rate of spontaneous closure; if there is no change, the fistula is unlikely to resolve spontaneously. 5 Varying success rates have been reported August 2003 OBG MANAGEMENT 25
6 FIGURE 3 Laparoscopic repair Laparoscopic repair of vesicovaginal fistula. for conservative management, ranging from 2% to 80%. 4,6 The chances of success are apparently greater if the fistula is: diagnosed within 7 days of the index surgery, less than 1 cm in size, simple, without associated carcinoma or radiation, and subject to at least 4 weeks of constant bladder drainage. Persistent, large, or complex fistulae are best treated surgically. Indications for surgical management The basic principles of fistula closure apply. They are: adequate exposure, good hemostasis, wide mobilization of the bladder and vagina, resection of devascularized tissue, removal of any foreign bodies, tension-free closure, nonopposition of suture lines, confirmation of a water-tight seal on bladder closure, and bladder drainage for 10 to 14 days following the repair. Timing of the repair has been the subject of controversy and can pose a dilemma to physician and patient alike. Traditionally, an interval of 3 months was recommended between the index surgery and fistula repair, with a delay of up to 1 year when the fistula was radiation-induced. However, little data support these recommendations. Today most experts recommend an individualized approach, delaying the surgery until inflammation and infection of the surrounding tissue have resolved. The use of estrogen, antibiotics, or steroids to facilitate healing during this period also has been recommended. 7 Comparable success rates have been reported for early and late repair of surgery-induced fistulae based on these principles Vaginal approach. Most vesicovaginal fistulae can be surgically corrected using a vaginal approach. Traditionally, a Latzko partial colpocleisis or fistulectomy with flap-splitting closure has been advocated. Debate continues about whether resection of the fistulous tract is necessary. Some experts believe that wide resection increases the size of the fistula and, therefore, the risk of recurrence. They also maintain that the fibrous tissue surrounding the fistula helps to reinforce the surgical repair. Proponents of fistulectomy counter that resection of the fistula and exposure of healthy tissue optimizes wound healing and improves surgical success rates. Comparable success has been reported for both techniques. 11,12 We prefer an individualized approach, with minimal resection of the fistulous tract to simplify the procedure and minimize associated complications, including recurrence. Latzko partial colpocleisis. This technique, first reported in 1942, remains a common procedure, with success rates of 90% to 100%. 13 Advantages include a short operative IMAGE: Copyright John Miklos, MD 26 OBG MANAGEMENT August 2003
7 Meeting the challenge of vesicovaginal fistula repair time, low intraoperative and postoperative morbidity, and low risk of ureteral injury. Make a circumferential incision in the vagina approximately 2 cm from the fistulous tract. Mobilize the vagina and close it over the fistulous tract, with delayed absorbable suture in a double layer, without disturbing the bladder mucosa. The vaginal mucosa is then closed, completing the repair. Fistulectomy technique. Alternatively, to perform fistulectomy with a flap-splitting closure, begin by resecting the fistulous tract to expose healthy tissue at the wound margins. Then close the defect in a multilayer fashion, beginning with the bladder mucosa, bladder serosa, pubocervical fascia, and vaginal mucosa. Be careful to avoid tension on suture lines. In addition, create a fascial flap to prevent opposition of the incision planes and reduce the risk of recurrence. Grafts. In cases with a high risk of recurrence, such as complex or large fistulae, a Martius fat-pad graft should be interposed between the closure layers to promote vascularization and reduce the risk of recurrence. 14 Placement of a cadaveric biomaterial graft also has been reported, reducing the need for complicated flap procedures. 15 Perform cystoscopy prior to and following the procedure to exclude ureteral compromise. Abdominal approach. Although most vesicovaginal fistulae can be surgically corrected via the vaginal approach, the abdominal route may be preferred when the fistula is high and inaccessible, large and complex, multiple in number, or when there is concurrent uterine or bowel involvement or a need for ureteral reimplantation. The abdominal approach may be facilitated by cystoscopically guided placement of a catheter through the fistulous tract to assist in subsequent identification and dissection. To begin, make a vertical skin incision to optimize visualization and allow mobilization of an omental flap, if necessary. Expose the bladder and perform a high extraperitoneal cystotomy to visualize the fistulous tract. Place ureteral stents if the fistula is in close proximity to the ureteral orifice. Extend the bladder incision to the fistulous tract and completely excise it following mobilization of the vagina. Then close the vagina and bladder with interrupted, delayed absorbable suture in a double layer. Transpose an omental flap between the vaginal and bladder incisions to promote vascularization, minimize opposition of suture lines, and reduce the risk of recurrence (FIGURE 2). Laparoscopic approach. A similar laparoscopic repair has been reported with comparable results, but requires advanced skills with endoscopic suturing and knot tying (FIGURE 3). 16 REFERENCES 1. Kremling H. Labor-induced bladder injuries: historical observations. Gynakol Geburtshilfliche Rundsch. 1996;36: Lee RA, Symmonds RE, Williams TJ. Current state of genitourinary fistula. Obstet Gynecol. 1998;72: Miklos JR, Sze EHM, Parobeck D, et al. Vesicouterine fistula: a rare complication of vaginal birth after cesarean. Obstet Gynecol. 1995;86: Elkins TE, Thompson JR. Lower urinary tract fistulas. In: Walters M, Karram MM, eds. Urogynecology and Reconstructive Pelvic Surgery. 2nd ed. St. Louis, Mo: Mosby; 1999: Zimmern PE, Hadley HR, Staskin D. Genitourinary fistulas: vaginal approach for repair of vesicovaginal fistulas. Clin Obstet Gynaecol. 1985;12: Davits RJ, Miranda SI. Conservative treatment of vesicovaginal fistulas by bladder drainage alone. Br J Urol. 1991;68: Margolis T, Mercer LJ. Vesicovaginal fistula. Obstet Gynecol Surv. 1995;49: Blaivas JG, Heritz DM, Romanzi LJ. Early versus late repair of vesicovaginal fistulas: vaginal and abdominal approaches. J Urol. 1995;153: Blandy JP, Badenoch DF, Fowler CG. Early repair of iatrogenic injury to the ureter or bladder after gynecological surgery. J Urol. 1991;146: Cruikshank SH. Early closure of posthysterectomy vesicovaginal fistulas. South Med J. 1988;81: Raz S, Bregg KJ, Nitti VW. Transvaginal repair of vesicovaginal fistula using a peritoneal flap. J Urol. 1993;150: Iselin CE, Aslan P, Webster GD. Transvaginal repair of vesicovaginal fistulas after hysterectomy by vaginal cuff excision. J Urol. 1998;160(3 Pt 1): Latzko W. Postoperative vesicovaginal fistulas: genesis and therapy. Am J Surg. 1942;58: Punekar SV, Buch DN, Soni AB. Martius labial fat pad interposition and its modification in complex lower urinary fistulae. J Postgrad Med. 1999;10: Miklos JR, Kohli N. Rectovaginal fistula repair utilizing a cadaveric dermal allograft. Int Urogynecol J Pelvic Floor Dysfunct. 1999;10: Nezhat CH, Nezhat F, Nezhat C. Laparoscopic repair of a vesicovaginal fistula: a case report. Obstet Gynecol. 1994;83(5 Pt 2): Walters MD, Karram MM, eds. Urogynecology and Reconstructive Pelvic Surgery. 2nd ed. St. Louis, Mo: Mosby; The authors report no financial relationship with any companies whose products are mentioned in this article. August 2003 OBG MANAGEMENT 27
Sara Schaenzer Grand Rounds January 24 th, 2018
 Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
11 th Dynasty- Egyptian mummies : Queen Henhenit circa 2050 BC wife of King Mentuhotep II VVF 550 BC- Ancient Egyptian documents (papyri)
 February 2019 11 th Dynasty- Egyptian mummies : Queen Henhenit circa 2050 BC wife of King Mentuhotep II VVF 550 BC- Ancient Egyptian documents (papyri) Prescription for a woman whose urine is in an irksome
February 2019 11 th Dynasty- Egyptian mummies : Queen Henhenit circa 2050 BC wife of King Mentuhotep II VVF 550 BC- Ancient Egyptian documents (papyri) Prescription for a woman whose urine is in an irksome
Case Based Urology Learning Program
 Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 19 CBULP 2011 044 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 19 CBULP 2011 044 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
SciFed Journal of Public Health. Endoscopic Management of Obstetrical Uretero-Uterine Fistula. Case Report and Review of Literature
 SciFed Journal of Public Health Case Report Open Access Endoscopic Management of Obstetrical Uretero-Uterine Fistula. Case Report and Review of Literature * Yasin Idweini * Chairperson of Urology Department
SciFed Journal of Public Health Case Report Open Access Endoscopic Management of Obstetrical Uretero-Uterine Fistula. Case Report and Review of Literature * Yasin Idweini * Chairperson of Urology Department
A New Dimension in Vesicovaginal Fistula Management: An 8-year Experience at Ramathibodi Hospital
 Original Article A New Dimension in Vesicovaginal Fistula Management: An 8-year Experience at Ramathibodi Hospital Wachira Kochakarn and Wipaporn Pummangura, 1 Division of Urology, Department of Surgery,
Original Article A New Dimension in Vesicovaginal Fistula Management: An 8-year Experience at Ramathibodi Hospital Wachira Kochakarn and Wipaporn Pummangura, 1 Division of Urology, Department of Surgery,
Postoperative Care for Pelvic Fistulae. Peter Jeppson, MD October 3, 2017
 Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Paravaginal Repair: A Laparoscopic Approach
 44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
Laparoscopic extravesical vesicovaginal fistula repair: our technique and 15-year experience
 DOI 10.1007/s00192-014-2458-y ORIGINAL ARTICLE Laparoscopic extravesical vesicovaginal fistula repair: our technique and 15-year experience John R. Miklos & Robert D. Moore Received: 26 March 2014 /Accepted:
DOI 10.1007/s00192-014-2458-y ORIGINAL ARTICLE Laparoscopic extravesical vesicovaginal fistula repair: our technique and 15-year experience John R. Miklos & Robert D. Moore Received: 26 March 2014 /Accepted:
Research Article Transvesicoscopic Repair of Vesicovaginal Fistula
 Diagnostic and Therapeutic Endoscopy Volume 2010, Article ID 760348, 4 pages doi:10.1155/2010/760348 Research Article Transvesicoscopic Repair of Vesicovaginal Fistula R. B. Nerli and Mallikarjun Reddy
Diagnostic and Therapeutic Endoscopy Volume 2010, Article ID 760348, 4 pages doi:10.1155/2010/760348 Research Article Transvesicoscopic Repair of Vesicovaginal Fistula R. B. Nerli and Mallikarjun Reddy
For personal use only. Injury-free vaginal surgery: Case-based protective tactics
 For mass reproduction, content licensing and permissions contact Dowden Health Media. OBG MANAGEMENT Lennox Hoyte, MD Director of Female Pelvic Medicine and Reconstructive Surgery, Department of Obstetrics
For mass reproduction, content licensing and permissions contact Dowden Health Media. OBG MANAGEMENT Lennox Hoyte, MD Director of Female Pelvic Medicine and Reconstructive Surgery, Department of Obstetrics
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF)
 Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF) Blair B. Washington MD, MHA Urogynecology & Reconstructive Pelvic Surgery Virginia Mason Medical Center Disclosures
Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF) Blair B. Washington MD, MHA Urogynecology & Reconstructive Pelvic Surgery Virginia Mason Medical Center Disclosures
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
5 DIAGNOSIS. History taking
 5 DIAGNOSIS All of the photographs in Chapter 4 were taken in theatre before operation. This chapter deals with how one can recognize the type of fistula by history taking and examination. (Note that the
5 DIAGNOSIS All of the photographs in Chapter 4 were taken in theatre before operation. This chapter deals with how one can recognize the type of fistula by history taking and examination. (Note that the
THE operation of reimplantation of the ureter into the bladder has undergone
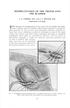 REIMPLANTATION OF THE URETER INTO THE BLADDER J. G. WARDEN, M.D., and C. C. HIGGINS, M.D. Department of Urology THE operation of reimplantation of the ureter into the bladder has undergone a stormy course
REIMPLANTATION OF THE URETER INTO THE BLADDER J. G. WARDEN, M.D., and C. C. HIGGINS, M.D. Department of Urology THE operation of reimplantation of the ureter into the bladder has undergone a stormy course
8 A SIMPLE FISTULA REPAIR, STEP BY STEP
 8 A SIMPLE FISTULA REPAIR, STEP BY STEP The first step is to suture the labia to the thighs and cover the anus with a swab (Figure 31). Figure 31 The labia are sutured to the thighs and the anus is covered
8 A SIMPLE FISTULA REPAIR, STEP BY STEP The first step is to suture the labia to the thighs and cover the anus with a swab (Figure 31). Figure 31 The labia are sutured to the thighs and the anus is covered
Management of Urethrovaginal Fistulas
 european urology 50 (2006) 1000 1005 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Management of Urethrovaginal Fistulas Dmitri Y. Pushkar *, Vladimir V.
european urology 50 (2006) 1000 1005 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Management of Urethrovaginal Fistulas Dmitri Y. Pushkar *, Vladimir V.
REPAIR OF LARGE CYSTOCELE
 REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
Pan African Urological Surgeons Association. African Journal of Urology.
 African Journal of Urology (2012) 18, 175 179 Pan African Urological Surgeons Association African Journal of Urology www.ees.elsevier.com/afju www.sciencedirect.com Martius flap and anterior vaginal wall
African Journal of Urology (2012) 18, 175 179 Pan African Urological Surgeons Association African Journal of Urology www.ees.elsevier.com/afju www.sciencedirect.com Martius flap and anterior vaginal wall
The circumferential obstetric fistula: characteristics, management and outcomes
 DOI: 10.1111/j.1471-0528.2007.01329.x www.blackwellpublishing.com/bjog Short communication The circumferential obstetric fistula: characteristics, management and outcomes A Browning Barhirdar Hamlin Fistula
DOI: 10.1111/j.1471-0528.2007.01329.x www.blackwellpublishing.com/bjog Short communication The circumferential obstetric fistula: characteristics, management and outcomes A Browning Barhirdar Hamlin Fistula
WOMEN subject to urinary incontinence often are reluctant and ashamed
 THE CLASSIFICATION AND DIAGNOSIS OF URINARY INCONTINENCE IN WOMEN JAMES S. KRIEGER, M.D., Department of Obstetrics and Gynecology and RALPH A. STRAFFON, M.D. Department of Urology WOMEN subject to urinary
THE CLASSIFICATION AND DIAGNOSIS OF URINARY INCONTINENCE IN WOMEN JAMES S. KRIEGER, M.D., Department of Obstetrics and Gynecology and RALPH A. STRAFFON, M.D. Department of Urology WOMEN subject to urinary
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Unlocking the Challenges of Diagnosing Fistulas in the Pelvis
 Unlocking the Challenges of Diagnosing Fistulas in the Pelvis Lucy Chow, MD & Simin Bahrami, MD Department of Radiological Sciences David Geffen School of Medicine at UCLA Goals and Objectives Understand
Unlocking the Challenges of Diagnosing Fistulas in the Pelvis Lucy Chow, MD & Simin Bahrami, MD Department of Radiological Sciences David Geffen School of Medicine at UCLA Goals and Objectives Understand
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
SURGICAL. How to manage the cuff at vaginal hysterectomy. For personal use only. Copyright Dowden Health Media TECHNIQUES
 For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Marietta Mahendeka, M.D. Obstetrician and Gynaecologist Bugando Medical Centre Tanzania. Tutor: Dr Luc de Bernis, WHO
 A COMPARATIVE STUDY OF THE MANAGEMENT OF VESICO AND/OR RECTO-VAGINAL FISTULAE AT BUGANDO MEDICAL CENTRE, MWANZA, TANZANIA, EAST AFRICA: A RETROSPECTIVE STUDY Marietta Mahendeka, M.D. Obstetrician and Gynaecologist
A COMPARATIVE STUDY OF THE MANAGEMENT OF VESICO AND/OR RECTO-VAGINAL FISTULAE AT BUGANDO MEDICAL CENTRE, MWANZA, TANZANIA, EAST AFRICA: A RETROSPECTIVE STUDY Marietta Mahendeka, M.D. Obstetrician and Gynaecologist
Surgical repair of vaginal wall prolapse using mesh
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
Prevention of Surgical Injuries in Gynecology
 in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
Chatzipapas I., Kathopoulis N., Protopapas A., Kyritsis N., Vlachos D. E., Loutradis D.
 HJOG An Obstetrics and Gynecology International Journal Research Article HJOG 2017, 16 (2), 23-28 Mobile Cystoscope Chatzipapas I., Kathopoulis N., Protopapas A., Kyritsis N., Vlachos D. E., Loutradis
HJOG An Obstetrics and Gynecology International Journal Research Article HJOG 2017, 16 (2), 23-28 Mobile Cystoscope Chatzipapas I., Kathopoulis N., Protopapas A., Kyritsis N., Vlachos D. E., Loutradis
Alimited degree of vaginal discharge is expected
 ADULT UROLOGY POSTHYSTERECTOMY VAGINAL CUFF FISTULA: DIAGNOSIS AND MANAGEMENT OF AN UNUSUAL CAUSE OF INCONTINENCE DAVID A. GINSBERG, ERIC S. ROVNER, AND SHLOMO RAZ ABSTRACT Objectives. Connection between
ADULT UROLOGY POSTHYSTERECTOMY VAGINAL CUFF FISTULA: DIAGNOSIS AND MANAGEMENT OF AN UNUSUAL CAUSE OF INCONTINENCE DAVID A. GINSBERG, ERIC S. ROVNER, AND SHLOMO RAZ ABSTRACT Objectives. Connection between
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications
 Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Interposition of Omentum, Perivesical Fat, Martious Fat in Management of Lower Urinary Tract Fistula - A Comparative Study
 ORIGINAL ARTICLE Interposition of Omentum, Perivesical Fat, Martious Fat in Management of Lower Urinary Tract Fistula - A Comparative Study KHIZAR HAYAT 1, SHAH JAHAN UR REHMAN 2, MUJAHID ALAM 3, SAJJAD
ORIGINAL ARTICLE Interposition of Omentum, Perivesical Fat, Martious Fat in Management of Lower Urinary Tract Fistula - A Comparative Study KHIZAR HAYAT 1, SHAH JAHAN UR REHMAN 2, MUJAHID ALAM 3, SAJJAD
The World Health Organization estimates that there are
 FELLOWS ARTICLE Urogenital Fistula Micheline J. Wong, MD, Keri Wong, MD, Azadeh Rezvan, MD, Alison Tate, MD, Narender N. Bhatia, MD, and Tajnoos Yazdany, MD Abstract: This review summarizes the available
FELLOWS ARTICLE Urogenital Fistula Micheline J. Wong, MD, Keri Wong, MD, Azadeh Rezvan, MD, Alison Tate, MD, Narender N. Bhatia, MD, and Tajnoos Yazdany, MD Abstract: This review summarizes the available
Iatrogenic Ureteral Injuries in Non Urological Surgeries: An Institutional Experience
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 11 Ver. I (Nov. 2015), PP 29-33 www.iosrjournals.org Iatrogenic Ureteral Injuries in Non Urological
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 11 Ver. I (Nov. 2015), PP 29-33 www.iosrjournals.org Iatrogenic Ureteral Injuries in Non Urological
Management of Radiation-Induced Vesicovaginal Fistula
 european urology 55 (2009) 131 138 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Management of Radiation-Induced Vesicovaginal Fistula Dmitri Y. Pushkar
european urology 55 (2009) 131 138 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Management of Radiation-Induced Vesicovaginal Fistula Dmitri Y. Pushkar
Risk Factors for De Novo Mixed Urinary Incontinence and Stress Urinary Incontinence Following Surgical Removal of a Urethral Diverticulum
 LUTS (2013) 5, 154 158 ORIGINAL ARTICLE Risk Factors for De Novo Mixed Urinary Incontinence and Stress Urinary Incontinence Following Surgical Removal of a Urethral Diverticulum JaeHeonKIM, 1 Kwang Woo
LUTS (2013) 5, 154 158 ORIGINAL ARTICLE Risk Factors for De Novo Mixed Urinary Incontinence and Stress Urinary Incontinence Following Surgical Removal of a Urethral Diverticulum JaeHeonKIM, 1 Kwang Woo
Bladder Trauma Data Collection Sheet
 Bladder Trauma Data Collection Sheet If there was no traumatic injury with PENETRATION of the bladder DO NOT proceed Date of injury: / / Time of injury: Date of hospital arrival: / / Time of hospital arrival:
Bladder Trauma Data Collection Sheet If there was no traumatic injury with PENETRATION of the bladder DO NOT proceed Date of injury: / / Time of injury: Date of hospital arrival: / / Time of hospital arrival:
A trial placement of a prophylactic ureteral catheter during the excision of a huge pelvic mass with incidental cystotomy
 372 CASE REPORT TRAUMA AND RECONSTRUCTIVE UROLOGY A trial placement of a prophylactic ureteral catheter during the excision of a huge pelvic mass with incidental cystotomy Hussein Warda Department of Obstetrics
372 CASE REPORT TRAUMA AND RECONSTRUCTIVE UROLOGY A trial placement of a prophylactic ureteral catheter during the excision of a huge pelvic mass with incidental cystotomy Hussein Warda Department of Obstetrics
Daniel K Roberts MD, PhD 2014 Annual Clinical Update
 Daniel K Roberts MD, PhD 2014 Annual Clinical Update Kevin E Miller, MD Division of Female Pelvic Medicine and Reconstructive Surgery Dept. of OBGYN University of Kansas School of Medicine- Wichita at
Daniel K Roberts MD, PhD 2014 Annual Clinical Update Kevin E Miller, MD Division of Female Pelvic Medicine and Reconstructive Surgery Dept. of OBGYN University of Kansas School of Medicine- Wichita at
The number following the procedure code is the TRICARE payment group. KIDNEY
 TRICARE/CHAMPUS POLICY MANUAL 6010.47-M JUNE 25, 1999 S POLICY CHAPTER 13 SECTION 9.1 ADDENDUM 1, SECTION 8 TRICARE-APPROVED AMBULATORY SURGERY S - URINARY SYSTEM The number following the procedure code
TRICARE/CHAMPUS POLICY MANUAL 6010.47-M JUNE 25, 1999 S POLICY CHAPTER 13 SECTION 9.1 ADDENDUM 1, SECTION 8 TRICARE-APPROVED AMBULATORY SURGERY S - URINARY SYSTEM The number following the procedure code
Cervical Cancer 3/25/2019. Abnormal vaginal bleeding
 Cervical Cancer Abnormal vaginal bleeding Postcoital, intermenstrual or postmenopausal Vaginal discharge Pelvic pain or pressure Asymptomatic In most patients who are not sexually active due to symptoms
Cervical Cancer Abnormal vaginal bleeding Postcoital, intermenstrual or postmenopausal Vaginal discharge Pelvic pain or pressure Asymptomatic In most patients who are not sexually active due to symptoms
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence
 A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
Posterior Deep Endometriosis. What is the best approach? Posterior Deep Endometriosis. Should we perform a routine excision of the vagina??
 Posterior Deep Endometriosis What is the best approach? Dept Gyn Obst Polyclinique Hotel Dieu CHU Clermont Ferrand France Posterior Deep Endometriosis Organs involved - Peritoneum - Uterine cervix -Rectum
Posterior Deep Endometriosis What is the best approach? Dept Gyn Obst Polyclinique Hotel Dieu CHU Clermont Ferrand France Posterior Deep Endometriosis Organs involved - Peritoneum - Uterine cervix -Rectum
Surgery of urogenital trauma in condition of war or precarity
 Surgery of urogenital trauma in condition of war or precarity C. H. Rochat Multi-disciplinary Center for Robotic Surgery, Geneva (www.beaulieu.ch) Geneva Foundation for Medical Education and Research (www.gfmer.ch)
Surgery of urogenital trauma in condition of war or precarity C. H. Rochat Multi-disciplinary Center for Robotic Surgery, Geneva (www.beaulieu.ch) Geneva Foundation for Medical Education and Research (www.gfmer.ch)
6 THE OPERATIONS BASIC PRINCIPLES
 6 THE OPERATIONS BASIC PRINCIPLES Basic principles are described here; strategies for specific situations are discussed in later sections. The basic principles in the repair of a fistula are: adequate
6 THE OPERATIONS BASIC PRINCIPLES Basic principles are described here; strategies for specific situations are discussed in later sections. The basic principles in the repair of a fistula are: adequate
Use of Martius flap in the complex female urethral surgery
 202 Central European Journal of Urology original PAPEr TRAUMA AND RECONSTRUCTIVE UROLOGY Use of Martius flap in the complex female surgery George Kasyan, Nataliya Tupikina, Dmitry Pushkar Urology Department
202 Central European Journal of Urology original PAPEr TRAUMA AND RECONSTRUCTIVE UROLOGY Use of Martius flap in the complex female surgery George Kasyan, Nataliya Tupikina, Dmitry Pushkar Urology Department
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
MIDLAND MEMORIAL HOSPITAL Delineation of Privileges FEMALE PELVIC MEDICINE AND RECONSTRUCTIVE SURGERY (UROGYNECOLOGY)
 MIDLAND MEMORIAL HOSPITAL Delineation of Privileges FEMALE PELVIC MEDICINE AND RECONSTRUCTIVE SURGERY (UROGYNECOLOGY) Physician Name: Your home for healthcare Female Pelvic Medicine and Reconstructive
MIDLAND MEMORIAL HOSPITAL Delineation of Privileges FEMALE PELVIC MEDICINE AND RECONSTRUCTIVE SURGERY (UROGYNECOLOGY) Physician Name: Your home for healthcare Female Pelvic Medicine and Reconstructive
Le fort s operation for prolapse uterus: A forgotten procedure
 2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
A SIMPLE SURGICAL TECHNIQUE TO MINIMIZE POSTOPERATIVE URINARY RETENTION WITH A PUBOVAGINAL SLING
 Urological Neurology Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 27 (3): 275-280, May - June, 2001 A SIMPLE SURGICAL TECHNIQUE TO MINIMIZE POSTOPERATIVE URINARY
Urological Neurology Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 27 (3): 275-280, May - June, 2001 A SIMPLE SURGICAL TECHNIQUE TO MINIMIZE POSTOPERATIVE URINARY
Dr. Aso Urinary Symptoms
 Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
european urology xxx (2006) xxx xxx
 available at www.sciencedirect.com journal homepage: www.europeanurology.com 1 2 3 4 5 Female Urology - Incontinence Supratrigonal VVF Repair by Modified O Connor s Technique- An Experience of 26 Cases
available at www.sciencedirect.com journal homepage: www.europeanurology.com 1 2 3 4 5 Female Urology - Incontinence Supratrigonal VVF Repair by Modified O Connor s Technique- An Experience of 26 Cases
Clinical Curriculum: Urogynecology
 Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Diagnosis and Management of Enterovesical Fistula
 Società Italiana di Chirurgia ColoRettale www.siccr.org 2009; 23: 200-210 Diagnosis and Management of Enterovesical Fistula Gitana Scozzari, Mario Morino Digestive Surgery and Center for Minimal Invasive
Società Italiana di Chirurgia ColoRettale www.siccr.org 2009; 23: 200-210 Diagnosis and Management of Enterovesical Fistula Gitana Scozzari, Mario Morino Digestive Surgery and Center for Minimal Invasive
Urogynecology ICD-9 to ICD-10 Crosswalks
 1100 Wayne Ave, Suite 825 Silver Spring, MD 20910 301.273.0570 Fax 301.273.0778 info@augs.org www.augs.org Urogynecology ICD-9 to ICD-10 Crosswalks ICD 9 ICD 9 Description ICD 10 Code ICD 10 Description
1100 Wayne Ave, Suite 825 Silver Spring, MD 20910 301.273.0570 Fax 301.273.0778 info@augs.org www.augs.org Urogynecology ICD-9 to ICD-10 Crosswalks ICD 9 ICD 9 Description ICD 10 Code ICD 10 Description
A Case Report Hydronephrosis and Hydrodureter due to Ureteral Deep Infiltrating Endometriosis mimic Ureteral Stricture Suryamanggala SI 1, Satria ML 2
 A Case Report Hydronephrosis and Hydrodureter due to Ureteral Deep Infiltrating Endometriosis mimic Ureteral Stricture Suryamanggala SI 1, Satria ML 2 1 Departement of Obstetric and Gynecology Faculty
A Case Report Hydronephrosis and Hydrodureter due to Ureteral Deep Infiltrating Endometriosis mimic Ureteral Stricture Suryamanggala SI 1, Satria ML 2 1 Departement of Obstetric and Gynecology Faculty
Anorectal malformations include a wide spectrum of
 JOURNAL OF LAPAROENDOSCOPIC & ADVANCED SURGICAL TECHNIQUES Volume 20, Number 1, 2010 ª Mary Ann Liebert, Inc. DOI: 10.1089=lap.2008.0343 Laparoscopic-Assisted Pull-Through for Congenital Rectal Stenosis
JOURNAL OF LAPAROENDOSCOPIC & ADVANCED SURGICAL TECHNIQUES Volume 20, Number 1, 2010 ª Mary Ann Liebert, Inc. DOI: 10.1089=lap.2008.0343 Laparoscopic-Assisted Pull-Through for Congenital Rectal Stenosis
Subspecialty Procedural Volume Guidelines
 Subspecialty Review Committee for Obstetrics and Gynecology In response to requests from program directors, and in an effort to be transparent, the Review Committee for Obstetrics and Gynecology has elected
Subspecialty Review Committee for Obstetrics and Gynecology In response to requests from program directors, and in an effort to be transparent, the Review Committee for Obstetrics and Gynecology has elected
PUBOVAGINAL SLING IN THE TREATMENT OF STRESS URINARY INCONTINENCE FOR URETHRAL HYPERMOBILITY AND INTRINSIC SPHINCTERIC DEFICIENCY
 Urological Neurology International Braz J Urol Official Journal of the Brazilian Society of Urology PUBOVAGINAL SLING IN SUI Vol. 29 (6): 540-544, November - December, 2003 PUBOVAGINAL SLING IN THE TREATMENT
Urological Neurology International Braz J Urol Official Journal of the Brazilian Society of Urology PUBOVAGINAL SLING IN SUI Vol. 29 (6): 540-544, November - December, 2003 PUBOVAGINAL SLING IN THE TREATMENT
In the August 2016 issue of OBG Management,
 GYN coding changes to note for your maximized reimbursement Revised ICD-10 gynecologic diagnostic codes go into effect October 1. Here is a look at the added, expanded, and revised codes you will need
GYN coding changes to note for your maximized reimbursement Revised ICD-10 gynecologic diagnostic codes go into effect October 1. Here is a look at the added, expanded, and revised codes you will need
LESIONS OF THE URINARY ORGANS DURING ABDOMINAL AND VAGINAL HYSTERECTOMY
 ESTRATTO DA: UROGYNAECOLOGIA INTERNATIONAL JOURNAL 2000; 15; 2 : 19-2001 Urogynaecologia I. J. LESIONS OF THE URINARY ORGANS DURING ABDOMINAL AND VAGINAL HYSTERECTOMY F. LEANZA, G. BIANCA, G. CINQUERRUI,
ESTRATTO DA: UROGYNAECOLOGIA INTERNATIONAL JOURNAL 2000; 15; 2 : 19-2001 Urogynaecologia I. J. LESIONS OF THE URINARY ORGANS DURING ABDOMINAL AND VAGINAL HYSTERECTOMY F. LEANZA, G. BIANCA, G. CINQUERRUI,
q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE
 493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
Blue Ridge Urogynecology
 Surgery for Stress Urinary Incontinence Surgery has proved to be a very effective treatment for stress incontinence. The best surgical procedures improve or cure the incontinence in 85 to 90 percent of
Surgery for Stress Urinary Incontinence Surgery has proved to be a very effective treatment for stress incontinence. The best surgical procedures improve or cure the incontinence in 85 to 90 percent of
University of Alberta Reconstructive Urology Fellowship
 FACULTY OF MEDICINE AND DENTISTRY DEPARTMENT OF SURGERY DIVISION OF UROLOGY Keith Rourke, MD, FRCSC Reconstructive Urology Professor Chair of Academic Urology Reconstructive Urology Fellowship Director
FACULTY OF MEDICINE AND DENTISTRY DEPARTMENT OF SURGERY DIVISION OF UROLOGY Keith Rourke, MD, FRCSC Reconstructive Urology Professor Chair of Academic Urology Reconstructive Urology Fellowship Director
Laparoscopic Bladder-Preserving Surgery for Enterovesical Fistula Complicated with Benign Gastrointestinal Disease
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
Urologic Surgical Complications In Renal Transplantation
 Urologic Surgical Complications In Renal Transplantation Chris Freise, MD Professor of Surgery UCSF Transplant Division Urologic Complications Review of Bladder Anastomosis Complications and Management
Urologic Surgical Complications In Renal Transplantation Chris Freise, MD Professor of Surgery UCSF Transplant Division Urologic Complications Review of Bladder Anastomosis Complications and Management
Original Article. Abstract. Introduction
 Original Article Surgical Management of Genitourinary Fistula Muhammad Shahbaz Hanif, Khalid Saeed, Masood Ahmed Sheikh Department of Urology, Jinnah Postgraduate Medical Centre, Karachi. Abstract Objective:
Original Article Surgical Management of Genitourinary Fistula Muhammad Shahbaz Hanif, Khalid Saeed, Masood Ahmed Sheikh Department of Urology, Jinnah Postgraduate Medical Centre, Karachi. Abstract Objective:
Avoiding and Managing Urologic Injury
 Avoiding and Managing Urologic Injury Jubilee Brown, MD Professor & Associate Director, Gynecologic Oncology Levine Cancer Institute at the Carolinas HealthCare System Charlotte, North Carolina 1 No relevant
Avoiding and Managing Urologic Injury Jubilee Brown, MD Professor & Associate Director, Gynecologic Oncology Levine Cancer Institute at the Carolinas HealthCare System Charlotte, North Carolina 1 No relevant
Kuwabara, Kaoru; Nonaka, Takashi; H. Citation Journal of Clinical Urology, 7(5),
 NAOSITE: Nagasaki University's Ac Title Author(s) Gluteal-fold adipofascial perforato fistula reconstruction Fujioka, Masaki; Hayashida, Kenji; Kuwabara, Kaoru; Nonaka, Takashi; H Citation Journal of Clinical
NAOSITE: Nagasaki University's Ac Title Author(s) Gluteal-fold adipofascial perforato fistula reconstruction Fujioka, Masaki; Hayashida, Kenji; Kuwabara, Kaoru; Nonaka, Takashi; H Citation Journal of Clinical
THE USE OF DEEPITHELIALIZATION
 THE USE OF DEEPITHELIALIZATION IN URETHROPLASTY - Deepithelialization Stratum corneum - Epidermis Papillary dermis Reticular dermis Skin Healing in any reconstructive surgery depends on not only the intact
THE USE OF DEEPITHELIALIZATION IN URETHROPLASTY - Deepithelialization Stratum corneum - Epidermis Papillary dermis Reticular dermis Skin Healing in any reconstructive surgery depends on not only the intact
Canadian Undergraduate Urology Curriculum (CanUUC): Genitourinary Trauma. Last reviewed June 2014
 Canadian Undergraduate Urology Curriculum (CanUUC): Genitourinary Trauma Last reviewed June 2014 Session Objectives 1. Recognize hematuria as the cardinal symptom of urinary tract trauma. 1. Outline the
Canadian Undergraduate Urology Curriculum (CanUUC): Genitourinary Trauma Last reviewed June 2014 Session Objectives 1. Recognize hematuria as the cardinal symptom of urinary tract trauma. 1. Outline the
We welcome comments and corrections which will be used to improve the system annually.
 ACGME Case Log Instructions: Female Pelvic Medicine and Reconstructive Surgery (FPMRS) Review Committees for Obstetrics and Gynecology, and Urology Updated July 2013 BACKGROUND The ACGME Case Log System
ACGME Case Log Instructions: Female Pelvic Medicine and Reconstructive Surgery (FPMRS) Review Committees for Obstetrics and Gynecology, and Urology Updated July 2013 BACKGROUND The ACGME Case Log System
Management of Female Stress Incontinence
 Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015
 Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Rad Lab 4 Unknowns: Genitourinary!
 Rad Lab 4 Unknowns: Genitourinary! Peter Clarke MD! Don Di Salvo, MD! Clerkship Directors for Radiology! Harvard Medical School! Brigham and Women s Hospital! Dana Farber Cancer Institute! Case 1: 69 year
Rad Lab 4 Unknowns: Genitourinary! Peter Clarke MD! Don Di Salvo, MD! Clerkship Directors for Radiology! Harvard Medical School! Brigham and Women s Hospital! Dana Farber Cancer Institute! Case 1: 69 year
Robot Assisted Rectopexy
 1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
Urethrolysis; When, Why & How. M Karram Professor of Ob/Gyn & Urology University of Cincinnati
 Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
Post-Traumatic Female Urethral Reconstruction
 Post-Traumatic Female Urethral Reconstruction Jerry G. Blaivas, MD, and Rajveer S. Purohit, MD, MPH Corresponding author Jerry G. Blaivas, MD The New York Presbyterian Hospital, Weill Cornell Medical Center,
Post-Traumatic Female Urethral Reconstruction Jerry G. Blaivas, MD, and Rajveer S. Purohit, MD, MPH Corresponding author Jerry G. Blaivas, MD The New York Presbyterian Hospital, Weill Cornell Medical Center,
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review
 Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Vaginal intraepithelial neoplasia
 Vaginal intraepithelial neoplasia The terminology and pathology of VAIN are analogous to those of CIN (VAIN I-III). The main difference is that vaginal epithelium does not normally have crypts, so the
Vaginal intraepithelial neoplasia The terminology and pathology of VAIN are analogous to those of CIN (VAIN I-III). The main difference is that vaginal epithelium does not normally have crypts, so the
Urethral Injuries: Realignment vs. Delayed Reconstruction
 Urethral Injuries: Realignment vs. Delayed Reconstruction E. Charles Osterberg, MD Assistant Professor of Surgery (Urology) Dell Medical School Chief of Urology and Genitourinary Reconstruction None Disclosures
Urethral Injuries: Realignment vs. Delayed Reconstruction E. Charles Osterberg, MD Assistant Professor of Surgery (Urology) Dell Medical School Chief of Urology and Genitourinary Reconstruction None Disclosures
PRACTICE BULLETIN Female Pelvic Medicine & Reconstructive Surgery Volume 23, Number 4, July/August 2017
 PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
Find Medical Solutions to Your Problems HYDRONEPHROSIS. (Distension of Renal Calyces & Pelvis)
 HYDRONEPHROSIS (Distension of Renal Calyces & Pelvis) Hydronephrosis is the distension of the renal calyces and pelvis due to accumulation of the urine as a result of the obstruction to the outflow of
HYDRONEPHROSIS (Distension of Renal Calyces & Pelvis) Hydronephrosis is the distension of the renal calyces and pelvis due to accumulation of the urine as a result of the obstruction to the outflow of
ENDOMETRIOSIS When and how to implement treatment
 ENDOMETRIOSIS When and how to implement treatment Francisco Carmona Hospital Clínic ENDOMETRIOSIS TREATMENT It depends on the severity of symptoms the patient's desire for pregnancy the extent of disease
ENDOMETRIOSIS When and how to implement treatment Francisco Carmona Hospital Clínic ENDOMETRIOSIS TREATMENT It depends on the severity of symptoms the patient's desire for pregnancy the extent of disease
Appendix 1. Canadian Classification of Health Intervention Codes Used to Identify
 1 2 3 Appendix 1. Canadian Classification of Health Intervention Codes Used to Identify any Vaginal Mesh (Synthetic) Implantation Procedure(s) for Pelvic Organ Prolapse 4 Canadian Classification of health
1 2 3 Appendix 1. Canadian Classification of Health Intervention Codes Used to Identify any Vaginal Mesh (Synthetic) Implantation Procedure(s) for Pelvic Organ Prolapse 4 Canadian Classification of health
Urethral Stricture Management. AUA Guidelines. Michael Coburn, MD Scott Department of Urology Baylor College of Medicine Houston, Texas
 Urethral Stricture Management AUA Guidelines Michael Coburn, MD Scott Department of Urology Baylor College of Medicine Houston, Texas Urethral Stricture Guidelines Systematic peer-reviewed literature review
Urethral Stricture Management AUA Guidelines Michael Coburn, MD Scott Department of Urology Baylor College of Medicine Houston, Texas Urethral Stricture Guidelines Systematic peer-reviewed literature review
ENDOSCOPIC MANAGEMENT OF A URETERAL OBSTRUCTION CAUSED BY ENDOMETRIOSIS: A CASE REPORT
 ENDOSCOPIC MANAGEMENT OF A URETERAL OBSTRUCTION CAUSED BY ENDOMETRIOSIS: A CASE REPORT Hsu-Cheng Juan, 1 Hsin-Chih Yeh, 1 Hsi-Lin Hsiao, 1 Shean-Fang Yang, 2 and Wen-Jeng Wu 1,3 Departments of 1 Urology
ENDOSCOPIC MANAGEMENT OF A URETERAL OBSTRUCTION CAUSED BY ENDOMETRIOSIS: A CASE REPORT Hsu-Cheng Juan, 1 Hsin-Chih Yeh, 1 Hsi-Lin Hsiao, 1 Shean-Fang Yang, 2 and Wen-Jeng Wu 1,3 Departments of 1 Urology
2/25/2013. Speaker Disclosure. Learning Objectives. Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth
 Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth Jaime Sepulveda-Toro MD FACS FACOG Female Pelvic Medicine and Reconstructive Pelvic Surgery South Miami Hospital Speaker
Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth Jaime Sepulveda-Toro MD FACS FACOG Female Pelvic Medicine and Reconstructive Pelvic Surgery South Miami Hospital Speaker
Complication of long indwelling urinary catheter and stent COMPLICATION OF LONG INDWELLING URINARY CATHETER AND STENT
 151 COMPLICATION OF LONG INDWELLING URINARY CATHETER AND STENT Jain A 1 *, Srivastava R 1, Prasad A 1, Marwah K 1 1. Department of surgery, Subharti medical college, Meerut U.P. India Correspondence: Dr.
151 COMPLICATION OF LONG INDWELLING URINARY CATHETER AND STENT Jain A 1 *, Srivastava R 1, Prasad A 1, Marwah K 1 1. Department of surgery, Subharti medical college, Meerut U.P. India Correspondence: Dr.
Program Schedule. 3 rd Annual Collaborative Symposium: Update in Minimally Invasive Gynecologic Surgery
 Program Schedule 3 rd Annual Collaborative Symposium: Update in Minimally Invasive Gynecologic Surgery Thursday, February 5, 2015 6:45 a.m. Registration and Breakfast 7:25 a.m. Welcome / Announcements
Program Schedule 3 rd Annual Collaborative Symposium: Update in Minimally Invasive Gynecologic Surgery Thursday, February 5, 2015 6:45 a.m. Registration and Breakfast 7:25 a.m. Welcome / Announcements
Genitourinary Tract Injuries
 Genitourinary Tract Injuries Chapter 18 Genitourinary Tract Injuries Introduction Genitourinary injuries constitute approximately 5% of the total injuries encountered in combat. Their treatment adheres
Genitourinary Tract Injuries Chapter 18 Genitourinary Tract Injuries Introduction Genitourinary injuries constitute approximately 5% of the total injuries encountered in combat. Their treatment adheres
Retrospective study of 213 cases of female urogenital fistulae at the Department of Urology & Transplantation Civil Hospital Quetta, Pakistan
 Original Article Retrospective study of 213 cases of female urogenital fistulae at the Department of Urology & Transplantation Civil Hospital Quetta, Pakistan Haq Nawaz, Masha Khan, Faiz Muhammed Tareen,
Original Article Retrospective study of 213 cases of female urogenital fistulae at the Department of Urology & Transplantation Civil Hospital Quetta, Pakistan Haq Nawaz, Masha Khan, Faiz Muhammed Tareen,
Quality care in vesico-vaginal obstetric fistula: case series report from the regional hospital of Maroua-Cameroon
 Provisional PDF Published 27 April 2010 Case report, Volume 5, issue 6, 2010 Quality care in vesico-vaginal obstetric fistula: case series report from the regional hospital of Maroua-Cameroon Pierre Marie
Provisional PDF Published 27 April 2010 Case report, Volume 5, issue 6, 2010 Quality care in vesico-vaginal obstetric fistula: case series report from the regional hospital of Maroua-Cameroon Pierre Marie
Case Report Management of Recurrent Rectourethral Fistula by York Mason Posterior Transrectal Transsphincteric Approach
 Case Reports in Urology Volume 2015, Article ID 854365, 6 pages http://dx.doi.org/10.1155/2015/854365 Case Report Management of Recurrent Rectourethral Fistula by York Mason Posterior Transrectal Transsphincteric
Case Reports in Urology Volume 2015, Article ID 854365, 6 pages http://dx.doi.org/10.1155/2015/854365 Case Report Management of Recurrent Rectourethral Fistula by York Mason Posterior Transrectal Transsphincteric
