Review Article Focus Issue on Male Infertility
|
|
|
- Willa McDonald
- 5 years ago
- Views:
Transcription
1 Advances in Urology Volume 2012, Article ID , 6 pages doi: /2012/ Review Article Focus Issue on Male Infertility Hideyuki Kobayashi, Koichi Nagao, and Koichi Nakajima Department of Urology, Toho University School of Medicine, Tokyo , Japan Correspondence should be addressed to Hideyuki Kobayashi, hideyukk@med.toho-u.ac.jp Received 14 July 2011; Revised 20 October 2011; Accepted 22 October 2011 Academic Editor: Edward Kim Copyright 2012 Hideyuki Kobayashi et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Male infertility problems can occur when sperms are limited in number or function. In this paper, we describe the clinical evaluation of male infertility. A detailed history, physical examination, and basic semen analysis are required. In addition, ultrasound, karyotyping, and hormonal studies are needed to determine specific causes of infertility. In addition, the World Health Organization (WHO, 2009) has developed a manual to provide guidance in performing a comprehensive semen analysis. Among the possible reasons for male infertility, nonobstructive azoospermia is the least treatable, because few or no mature sperm may be produced. In many cases, men with nonobstructive azoospermia typically have small-volume testes and elevated FSH. Although treatment may not completely restore the quality of semen from men with subnormal fertility, in some cases a successful pregnancy can still be achieved through assisted reproductive technology. 1. Introduction About 1 in 7 couples have problems conceiving, with a similar incidence worldwide. Over 80% of couples who have regular sexual intercourse and do not use contraception will achieve a pregnancy within one year, and approximately 92% can achieve a pregnancy within 2 years [1]. Infertility affects males and females equally, although many people believe that infertility is a female problem. In Japan, especially, couples oppose insemination or adoption as an alternative to having a child carrying both parents genes, which means that males are likely to seek infertility evaluations when a couple has difficulty conceiving. The clinical evaluation of male infertility includes a detailed history, physical examination, laboratory tests, ultrasound study, and karyotyping. The two main purposes of the evaluation are (1) to identify any modifiable factors that can improve the man s fertility status and (2) to identify any serious underlying conditions, such as testis cancer, osteoporosis, and endocrine or genetic problems that present first as infertility [2]. 2. History-Taking for the Male Infertility Workup The infertility history should include a detailed account of the patient s reproductive and sexual history, developmental, family, medical, and surgical history. The information to be included in each portion of the history is detailed below Reproductive and Sexual History. For the reproductive history, any prior conceptions for the male with present or past partners, details of any prior difficulty achieving conception, past evaluations and treatments for infertility, and previous use of contraception should all be recorded, along with the frequency and timing of intercourse with the man s current partner. Information about erectile and ejaculatory function and frequency of masturbation should be requested, as well as the timing of first masturbation and intercourse Developmental History. A history of specific childhood illness or conditions may be informative. For example,
2 2 Advances in Urology bilateral cryptorchidism causes a significant decrease in spermatogenesis, but unilateral cryptorchidism usually has much less impact. Studies of patients who underwent orchiopexy to treat cryptorchidism report decreased sperm densities in about 30% of men, on average, with unilateral cryptorchidism (range 28 82%), although two studies have reported abnormal sperm densities in only 17% of patients [3, 4]. In contrast, an average of about 50% of patients with bilateral cryptorchidism (range 9 88%) show decreased sperm densities. Despite the trend of performing orchidopexies at an earlier age, improved fertility rates have yet to be demonstrated with this approach. On the other hand, testes that remain undescended after puberty do not function, and fertility rates are not improved by postpubertal repair [5, 6]. Testicular trauma or a history of torsion should be noted, since both may result in atrophic testes. Approximately 30 40% of men with a history of testicular torsion have abnormal results upon semen analysis [7 14]. In up to 11% of patients with testicular torsion, antisperm antibodies are present at the time of or after the event [15, 16]. The timing of pubertal development should be noted. Significantly delayed or incomplete development may suggest an endocrinopathy. In addition, although early childhood mumps does not appear to affect the testis, after the age of 11 or 12, 30% of male patients who contract mumps develop unilateral orchitis. Bilateral orchitis occurs in approximately 10% of peripubertal and adult males who contract mumps [17]. Unilateral and bilateral orchitis from mumps can cause severe testicular damage Medical History. Diabetes may affect erectile and/or ejaculatory function [18], and any systemic illness accompanied by fever or viremia can lead to impaired testicular function, although the effects may not be measurable in the ejaculate for 1 4 months. A history of pyospermia or prostatitis should be noted, although both are uncommon and neither is proved to cause infertility [19]. Primary ciliary dyskinesia (also known as immotile cilia syndrome), which should be suspected when there is a history of chronic upper respiratory infections, causes severe defects in sperm motility. When this condition is associated with situs inversus, it is known as Kartagener syndrome, which is a rare cause of male infertility [20]. Frequent respiratory infections associated with azoospermia raise the possibility of Young syndrome [21], in which epididymal obstruction is caused by the inspissation of secretions. Neurologic issues can lead to male infertility as a variety of hormonal abnormalities including thyroid disorders, hyperprolactinemia, and elevated estrogen levels. Finally, any history of urinary tract infections or sexually transmitted disease should be recorded, particularly if associated with epididymitis, as these conditions can lead to epididymal obstruction Past Surgical History and Cancer Treatments. Details of past surgeries should be obtained. Pelvic and retroperitoneal surgery may impair ejaculatory function. Patients with testicular cancer may present with infertility either before or after treatment. Approximately, 50% of testicular cancer patients have subnormal sperm densities prior to chemotherapy [11, 13, 22, 23]. Following cisplatinum-based chemotherapy for testicular cancer, most patients will develop azoospermia. However, most will recoverspermproductionwithinfouryears[24, 25]. Most patients with lymphoma, leukemia, or sarcoma become permanent sterility after chemotherapy Medication and Drug Use. A detailed history of medications should be obtained. Unfortunately, for many substances, data detailing potential effects on male fertility are lacking. Online sources include databases such as Reprotox and Reprotext. Both are often available through online hospital and university databases. Exogenous androgens are well known to induce hypogonadotropic hypogonadism, which may be induced directly by testosterone or by synthetic anabolic steroids. The subsequent suppression of endogenous testosterone production usually results in azoospermia, which is frequently reversible over a 3 6-month period. Importantly, some patients do not recover normal pituitary function Lifestyle Exposure. Exposure to potential environmental toxins including pesticides, mercury, cadmium, arsenic, and hydrocarbons can impair spermatogenesis. In particular, the soil fumigants amebicide and nematocide, and 2- bromopropane (a substitute for chlorofluorocarbons) can cause decreased spermatogenesis [26 32]. Alcohol dependency is frequently associated with testicular atrophy, but moderate alcohol consumption does not appear to impair fertility [33 36]. The effect of cigarette smoking on male infertility remains controversial, with some studies showing decreased semen health and others showing no effect [37 43]. However, the sum of the accumulating evidence suggests that cigarettes smoking can impact male fertility. 3. Physical Examination The physical examination for male infertility should focus on identifying abnormalities that could affect fertility. Endocrine disorders should be suspected in cases of abnormal androgenization. Gynecomastia can result from excessive estrogens, an improper estrogen-to-androgen ratio, or elevated prolactin levels. Penile curvature, angulation, and the location of the urethral meatus should be assessed. The scrotum should be carefully palpated with the patient standing, noting the size and consistency of the testicles; the room should be kept warm for this exam. The testicle size can be measured with an orchidometer. This measurement is important because impaired spermatogenesisoftenaccompaniessmall-volumetestes[44]. The normal volume is at least 20 ml [45, 46]. Note, however, that Asian men typically have smaller testes than men of other races. The epididymis should be examined carefully, noting the presence of the caput, corpus, and cauda as well as whether the epididymis feels full or indurated. Fullness can suggest obstruction of the genital ducts.
3 Advances in Urology 3 Table 1: Semen parameters. Volume >1.5 ml Sperm concentration >15million/mL Total sperm count per ejaculate 39 million Sperm progressive motility >32% Total sperm motility >40% Sperm vitality >58% alive Normal morphology >3% WBC (white blood cells) <1 million/ml During palpation of the spermatic cords, the clinician should confirm the presence or absence of the vas deferens and note any vasal atrophy or nodularity, or the presence of a varicocele within the spermatic cord and surrounding the testicle. An enlarged venous diameter can be detected with the patient performing the Valsalva maneuver. Alternatively, the patient can often increase intra-abdominal pressure without contracting the cremaster muscles, by distending the abdomen. Varicoceles are graded as small (grade I) if palpable only when the patient performs the Valsalva maneuver, moderate (grade II) if palpable when the patient is standing but does not perform the Valsalva maneuver, and large (grade III) when veins can be seen through the scrotal skin. Varicoceles should decrease in size when the patient is in the supine position. 4. Laboratory Tests After the above exams have been completed, appropriate laboratory tests should be performed. The first step in laboratory testing is to identify patients who are likely to be infertile, subfertile, and fertile, for which only semen analysis is required. Since most infertile men have some motile sperm in the semen, threshold values are used to indicate whether fertility is more or less likely. Azoospermic patients, however, are sterile. Importantly, although the number of motile sperm is suggestive of fertility, there can be considerable variation in the fertility of men with equal motile sperm counts Semen Analysis. The World Health Organization (WHO, 2009) has published a guide to semen analysis in humans. Because semen parameters fluctuate from day to day, at least two semen samples are usually required to diagnose belownormal semen quality. A recent study of over 4500 samples from men living in four continents was used to determine the reference range for adults. The lower reference limits (5th percentile) for semen parameters in fertile adult men are given in Table 1 [47] Collection. Patients should be given specific instructions on collecting semen specimens for analysis. Semen is collected by masturbation. Patients should be encouraged to abstain from ejaculation for 72 hours prior to collecting a semen sample in the laboratory. We provide adult videos and books for patients in a room dedicated to semen collection. The specimen container should be clean, although sterility is not required, and wide-mouthed, to minimize collection error. The specimen should be transported to the laboratory at room temperature. Note that fresh semen is a coagulum that liquefies 5 25 min after ejaculation Concentration. The term, sperm count, typically refers to sperm density, reported as millions of sperm per milliliter of semen. Total sperm count refers to the total number of sperm in the ejaculate Interpretation of the Initial Evaluation. Once the data from the physical examination, history, and semen analysis have been acquired, a differential diagnosis should be developed. Additional laboratory studies may then be ordered to refine the diagnosis and determine management options. The results from the semen analysis are categorized as all parameters normal, oligozoospermia, asthenospermia (defects in motility), teratozoospermia (defects in morphology), and azoospermia (complete lack of sperm) Interpretation of Normal Semen Parameters. A finding of normal semen parameters in the context of infertility raises the possibility of a female factor, erectile dysfunction, and/or antisperm antibodies. 5. Diagnosis 5.1. Differential Diagnosis of Azoospermia. Azoospermia is categorized as either obstructive or nonobstructive. Nonobstructive azoospermia refers to a lack of sperm production, whereas obstructive azoospermia implies adequate sperm production but failure to deliver the sperm into the ejaculate because of a ductal obstruction. The data on the testicular size and presence of the vas deferens relate to this diagnosis, and congenital bilateral absence of the vas deferens (CBAVD), an obstructive azoospermia, is diagnosed by physical examination. Atrophic testes may be primary, due to an inherent testicular dysfunction, or secondary, due to a hormonal deficiency. Azoospermic patients with normal semen volumes and a palpable vas deferens should have their FSH and testosterone levels measured. The finding of small testes in association with low FSH and testosterone suggests hypogonadotropic hypogonadism, and the patient s LH and prolactin levels should be evaluated as well. Low gonadotropin levels associated with elevated prolactin raise the possibility of a pituitary prolactinoma, and a pituitary MRI should be performed. The finding of atrophic testes and elevated FSH levels indicates germ cell failure. Patients with normal sperm production typically have FSH values in the lower end of the normal range, and levels above this should raise suspicion of a defect in spermatogenesis. In addition, patients with unilateral testicular disease may have elevated FSH levels. A diagnostic testicular biopsy is not indicated in patients with elevated FSH levels. Instead, patients with nonobstructive azoospermia due to a primary testicular defect and not to a hormonal deficiency should be offered genetic testing,
4 4 Advances in Urology consisting of a karyotype and a Y-chromosome microdeletion analysis. If abnormalities are found, a couple should be offered genetic counseling prior to proceeding with assisted reproductive techniques. Normal-sized testes accompanied by normal FSH and azoospermia suggest the possibility of obstruction, and a testicular biopsy is required to differentiate between obstruction and maturation arrest. If mature sperms are found in the biopsy, sperm may be cryopreserved for later use in an IVF/ICSI cycle. Low-volume azoospermic semen specimens may be caused by hypogonadism (low testosterone levels), ejaculatory duct obstruction, or seminal vesicle absence or hypofunction. Patients with bilateral ejaculatory duct obstruction and those with congenital bilateral absence of the vas deferens (CBAVD) produce low-volume, acidic, and azoospermic semen specimens Multiple Semen Abnormalities. The finding of defects in sperm density, motility, and morphology is commonly referred to as oligoasthenoteratozoospermia (OAT). By far the most common cause of this pattern is varicocele, which is a clinical diagnosis determined by a physical examination and ultrasound study. Additional causes of OAT include environmental toxins, drugs or medications, and cryptorchidism Defects in Isolated Semen Parameters. Complete ejaculatory failure, also called aspermia, exists when no fluid is produced during the male orgasm, and it is due to retrograde ejaculation. Common causes of ejaculatory failure include neurogenic abnormalities, such as spinal cord injury, diabetes mellitus, multiple sclerosis, and the use of α-blockers. Retroperitoneal surgeries, including pelvic surgery and retroperitoneal lymph node dissections, can also result in impaired ejaculation. True absence of ejaculation should be differentiated from the complete inability to obtain orgasm, which can be caused by medications such as serotonin reuptake inhibitors and/or by psychological disturbances. However, much more common than complete lack of ejaculation are low-volume ejaculate specimens. The most common cause of this finding is an incomplete collection. Complete bilateral ejaculatory duct obstruction will result in azoospermic, low-volume, and acidic semen specimens Defects in Sperm Concentration. In patients with less than sperm/ml, serum FSH and testosterone levels should be determined. In patients with less than sperm/ml, a karyotype and Y-chromosome microdeletion analysis should be considered as well. Elevated serum FSH may indicate a primary testicular defect. Although varicoceles are a common cause of low sperm density, other abnormal sperm parameters are also usually present with varicocele Defects in Motility. The term asthenospermia refers to defects in sperm movement. Such cases show only a low percentage of sperm that have any motility. Antisperm antibodies and varicoceles may account for this defect Defects in Morphology. The term teratozoospermia refers to defects in sperm morphology. This has been reported with the application of strict criteria. The majority of the cases are idiopathic, while varicoceles and temperature insults to spermatogenesis are also potential causes. 6. Additional Laboratory Tests 6.1. Hormonal Studies. Hormonal evaluation for male subfertility is done to (1) identify causative endocrine abnormalities or (2) obtain prognostic information. Endocrine studies should include serum levels of PRL, LH, FSH, testosterone, and E2 (estradiol). As mentioned above, the most common endocrine abnormality associated with male infertility or subfertility is elevated FSH, which generally indicates the impairment of spermatogenesis. However, FSH levels may be normal in cases of impaired spermatogenesis. True endocrine causes of male infertility account for less than 3% of cases [48] Antisperm Antibodies. Immunologic infertility is an autoimmune disorder that can involve both the humoral and cellular immune system. However, the mechanism is still poorly understood. Note that other causes may account for cases of male infertility, even when antisperm antibodies are detected. Treatment of antisperm antibodies is the use of ICSI to bypass potential fertilization problems induced by the antibodies. 7. Conclusions While many assays can be used in the diagnosis of male infertility, the foundation of any workup should be obtaining a detailed history, thorough physical examination, and a basic semen analysis. Additional tests, including an antisperm antibody assay and hormonal, karyotype, and ultrasound studies are needed only to investigate specific causes of infertility. In addition, there are some significant health issues which are diagnosed only with presentation of male infertility, testis tumor and significant endocrinopathies amongst them. A careful evaluation that considers all of the possible explanations for a man s infertility is not only critical for a good diagnosis, it is an ethical imperative for the reproductive specialist. Acknowledgments This study was supported in part by the 5th Young Research Grant of the Japanese Urological Association and Grant of Strategic Research Foundation Grant-aided Project for Private schools at Heisei 23th from Ministry of Education, Culture, Sports, Science and Technology of Japan,
5 Advances in Urology 5 References [1] B. Robaire and P. Chan, Handbook of Andrology, The American Society of Andrology, 2nd edition, [2] L. I. Lipshultz, L. I. Howards, and C. S. Niederberger, Infertility in the Male, Cambridge University Press, Cambridge, UK, 4th edition, [3] P. A. Lee, Fertility after cryptorchidism: epidemiology and other outcome studies, Urology, vol. 66, no. 2, pp , [4] P. A. Lee, Fertility in cryptorchidism: does treatment make adifference? Endocrinology and Metabolism Clinics of North America, vol. 22, no. 3, pp , [5] M. Grasso, A. Buonaguidi, C. Lania, F. Bergamaschi, M. Castelli, and P. Rigatti, Postpubertal cryptorchidism: review and evaluation of the fertility, European Urology, vol. 20, no. 2, pp , [6] A. Okuyama, N. Nonomura, M. Nakamura et al., Surgical management of undescenced testis: retrospective study of potential fertility in 274 cases, JournalofUrology, vol. 142, no. 3, pp , [7] J. B. Anderson and R. C. N. Williamson, The fate of the human testes following unilateral torsion of the spermatic cord, British Urology, vol. 58, no. 6, pp , [8] J. B. Anderson and R. C. N. Williamson, Fertility after torsion of the spermatic cord, British Urology, vol. 65, no. 3, pp , [9] G.Bartsch,S.Frank,H.Marberger,andG.Mikuz, Testicular torsion: late results with special regard to fertility and endocrine function, Urology, vol. 124, no. 3, pp , [10] F. Dondero, A. Lenzi, M. Picardo, R. Pastore, and G. Valesini, Cell-mediated antisperm immunity in selected forms of male infertility, Andrologia, vol. 12, no. 1, pp , [11] I. Fraser, N. Slater, C. Tate, and J. G. Smart, Testicular torsion does not cause autoimmunization in man, British Surgery, vol. 72, no. 3, pp , [12] I. Mastrogiacomo, R. Zanchetta, P. Graziotti, C. Betterle, P. Scrufari, and A. Lembo, Immunological and clinical study in patients after spermatic cord torsion, Andrologia, vol. 14, no. 1, pp , [13] P.Puri,D.Barton,andB.O Donnell, Prepubertaltesticular torsion: subsequent fertility, Pediatric Surgery, vol. 20, no. 6, pp , [14] W. E. G. Thomas, M. J. Cooper, and G. A. Crane, Testicular exocrine malfunction after torsion, The Lancet, vol. 2, no. 8416, pp , [15] P. Hagen, M. M. Buchholz, J. Eigenmann, and K. Bandhauer, Testicular dysplasia causing disturbance of spermiogenesis in patients with unilateral torsion of the testis, Urologia Internationalis, vol. 49, no. 3, pp , [16] M. J. Anderson, J. K. Dunn, L. I. Lipshultz, and M. Coburn, Semen quality and endocrine parameters after acute testicular torsion, Urology, vol. 147, no. 6, pp , [17] C. A. Werner, Mumps orchitis and testicular atrophy; a factor in male sterility, Annals of Internal Medicine, vol. 32, no. 6, pp , [18] L. F. Greene and P. P. Kelalis, Retrograde ejaculation of semen dueto diabetic neuropathy, Urology, vol. 98, no. 6, p. 696, [19] W. Weidner, W. Krause, and M. Ludwig, Relevance of male accessory gland infection for subsequent fertility with special focus on prostatitis, Human Reproduction Update, vol. 5, no. 5, pp , [20] L. J. Wilton, H. Teichtahl, P. D. Temple-Smith, and D. M. de Kretser, Kartagener s syndrome with motile cilia and immotile spermatozoa: axonemal ultrastructure and function, American Review of Respiratory Disease, vol. 134, no. 6, pp , [21] L. J. Wilton, H. Teichtahl, P. D. Temple-Smith et al., Young s syndrome (obstructive azoospermia and chronic sinobronchial infection): a quantitative study of axonemal ultrastructure and function, Fertility and Sterility, vol. 55, no. 1, pp , [22] P. R. Carroll, W. F. Whitmore Jr., H. W. Herr et al., Endocrine and exocrine profiles of men with testicular tumors before orchiectomy, JournalofUrology, vol. 137, no. 3, pp , [23] L. Dubin and R. D. Amelar, Sexual causes of male infertility, Fertility and Sterility, vol. 23, no. 8, pp , [24] S. P. Boyers, M. D. Corrales, G. Huszar, and A. H. DeCherney, The effects of Lubrin on sperm motility in vitro, Fertility and Sterility, vol. 47, no. 5, pp , [25] D. A. Ohl and J. Sonksen, What are the chances of infertility and should sperm be banked? Seminars in Urologic Oncology, vol. 14, no. 1, pp , [26] L. I. Lipshultz, C. E. Ross, D. Whorton, T. Milby, R. Smith, and R. E. Joyner, Dibromochloropropane and its effect on testicular function in man, Urology, vol. 124, no. 4, pp , [27] R. de Celis, A. Feria-Velasco, M. González-Unzaga, J. Torres- Calleja, and N. Pedrón-Nuevo, Semen quality of workers occupationally exposed to hydrocarbons, Fertility and Sterility, vol. 73, no. 2, pp , [28] Y. Kim, J. Park, and Y. Moon, Hematopoietic and reproductive toxicity of 2-bromopropane, a recently introduced substitute for chlorofluorocarbons, Toxicology Letters, vol. 108, no. 2-3, pp , [29] I. Lancranjan, H. I. Popescu, O. GAvǎnescu, I. Klepsch, and M. Serbǎnescu, Reproductive ability of workmen occupationally exposed to lead, Archives of Environmental Health, vol. 30, no. 8, pp , [30] S. Tališman, P. Cvitković, J. Jurasović, A. Pizent, M. Gavella, and B. Ročić, Semen quality and reproductive endocrine function in relation to biomarkers of lead, cadmium, zinc, and copper in men, Environmental Health Perspectives, vol. 108, no. 1, pp , [31] A. Toth, Reversible toxic effect of salicylazosulfapyridine on semen quality, Fertility and Sterility, vol. 31, no. 5, pp , [32] D. H. van Thiel, J. S. Gavaler, W. I. Smith Jr., and G. Paul, Hypothalamic-pituitary-gonadal dysfunction in men using cimetidine, The New England Medicine, vol. 300, no. 18, pp , [33]K.M.Curtis,D.A.Savitz,and T.E.Arbuckle, Effects of cigarette smoking, caffeine consumption, and alcohol intake on fecundability, American Epidemiology, vol. 146, no. 1, pp , [34] B.C.Dunphy,C.L.R.Barratt,andI.D.Cooke, Malealcohol consumption and fecundity in couples attending an infertility clinic, Andrologia, vol. 23, no. 3, pp , [35] H. J. M. Goverde, H. S. Dekker, H. J. G. Janssen, B. A. Bastiaans, R. Rolland, and G. A. Zielhuis, Semen quality and frequency of smoking and alcohol consumption an explorative study, International Fertility and Menopausal Studies, vol. 40, no. 3, pp , 1995.
6 6 Advances in Urology [36] J. Olsen, F. Bolumar, J. Boldsen, and L. Bisanti, Does moderate alcohol intake reduce fecundability? A European multicenter study on infertility and subfecundity. European Study Group on Infertility and Subfecundity, Alcoholism: Clinical and Experimental Research, vol. 21, no. 2, pp , [37] M.F.Vine,C.K.J.Tse,P.C.Hu,andK.Y.Truong, Cigarette smoking and semen quality, Fertility and Sterility, vol. 65, no. 4, pp , [38] C. E. Close, P. L. Roberts, and R. E. Berger, Cigarettes, alcohol and marijuana are related to pyospermia in infertile men, Urology, vol. 144, no. 4, pp , [39] S. E. Chia, S. T. A. Lim, S. K. Tay, and S. T. Lim, Factors associated with male infertility: a case-control study of 218 infertile and 240 fertile men, British Obstetrics and Gynaecology, vol. 107, no. 1, pp , [40] R.K.Dikshit,J.G.Buch,andS.M.Mansuri, Effect of tobacco consumption on semen quality of a population of hypofertile males, Fertility and Sterility, vol. 48, no. 2, pp , [41] H. J. Evans, J. Fletcher, M. Torrance, and T. B. Hargreave, Sperm abnormalities and cigarette smoking, The Lancet, vol. 1, no. 8221, pp , [42] P. B. Marshburn, C. S. Sloan, and M. G. Hammond, Semen quality and association with coffee drinking, cigarette smoking, and ethanol consumption, Fertility and Sterility, vol. 52, no. 1, pp , [43] S. Osser, A. Beckman-Ramirez, and P. Liedholm, Semen quality of smoking and non-smoking men in infertile couples in a Swedish population, Acta Obstetricia et Gynecologica Scandinavica, vol. 71, no. 3, pp , [44] L. I. Lipshultz and J. N. Corriere Jr., Progressive testicular atrophy in the varicocele patient, Urology, vol. 117, no. 2, pp , [45] C. W. Charny, The spermatogenic potential of the undescended testis before and after treatment, Urology, vol. 83, pp , [46] S. Gunalp, C. Onculoglu, T. Gurgan, T. F. Kruger, and C. J. Lombard, A study of semen parameters with emphasis on sperm morphology in a fertile population: an attempt to develop clinical thresholds, Human Reproduction, vol. 16, no. 1, pp , [47] World Health Organization, Laboratory Manual for the Examination of Human Semen, World Health Organization, Geneva, Switzerland, 5th edition, [48] M.SigmanandJ.P.Jarow, Endocrineevaluationofinfertile men, Urology, vol. 50, no. 5, pp , 1997.
7 MEDIATORS of INFLAMMATION The Scientific World Journal Gastroenterology Research and Practice Diabetes Research International Endocrinology Immunology Research Disease Markers Submit your manuscripts at BioMed Research International PPAR Research Obesity Ophthalmology Evidence-Based Complementary and Alternative Medicine Stem Cells International Oncology Parkinson s Disease Computational and Mathematical Methods in Medicine AIDS Behavioural Neurology Research and Treatment Oxidative Medicine and Cellular Longevity
DEFINITION HX & PH/EX
 DEFINITION HX & PH/EX Because of the success of the assisted reproductive techniques (ART), the evaluation of the man is often ignored. The physician should not forget the fact that many causes of male
DEFINITION HX & PH/EX Because of the success of the assisted reproductive techniques (ART), the evaluation of the man is often ignored. The physician should not forget the fact that many causes of male
What You Need to Know
 UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
Male History, Clinical Examination and Testing
 Male History, Clinical Examination and Testing Dirk Vanderschueren, MD, PhD Case Jan is 29 years old and consults for 1 year primary subfertility partner 28 years old and normal gynaecological investigation
Male History, Clinical Examination and Testing Dirk Vanderschueren, MD, PhD Case Jan is 29 years old and consults for 1 year primary subfertility partner 28 years old and normal gynaecological investigation
What to do about infertility?
 What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
Clinical evaluation of infertility
 Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
Chris Davies & Greg Handley
 Chris Davies & Greg Handley Contents Definition Epidemiology Aetiology Conditions for pregnancy Female Infertility Male Infertility Shared infertility Treatment Definition Failure of a couple to conceive
Chris Davies & Greg Handley Contents Definition Epidemiology Aetiology Conditions for pregnancy Female Infertility Male Infertility Shared infertility Treatment Definition Failure of a couple to conceive
Testosterone Therapy-Male Infertility
 Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
GUIDELINES ON THE INVESTIGATION AND TREATMENT OF MALE INFERTILITY
 GUIDELINES ON THE INVESTIGATION AND TREATMENT OF MALE INFERTILITY G. Dohle (chairman), A. Jungwirth and W. Weidner. Eur Urol 2002;42(4):313-322 Eur Urol 2004;46(5):555-558 1. Introduction Infertility is
GUIDELINES ON THE INVESTIGATION AND TREATMENT OF MALE INFERTILITY G. Dohle (chairman), A. Jungwirth and W. Weidner. Eur Urol 2002;42(4):313-322 Eur Urol 2004;46(5):555-558 1. Introduction Infertility is
Information for Patients. Male infertility. English
 Information for Patients Male infertility English Table of contents What is male infertility?... 3 Diagnosis... 3 Medical history... 3 Physical examination... 3 Hormone blood tests... 3 Semen analysis...
Information for Patients Male infertility English Table of contents What is male infertility?... 3 Diagnosis... 3 Medical history... 3 Physical examination... 3 Hormone blood tests... 3 Semen analysis...
Male factors can be identified as the cause of infertility in 30~40% of couples and a
 Focused Issue of This Month Causes and Diagnosis of Male Infertility Nam Cheol Park, MD Department of Urology, Pusan National University College of Medicine Email : pnc@pusan.ac.kr J Korean Med Assoc 2007;
Focused Issue of This Month Causes and Diagnosis of Male Infertility Nam Cheol Park, MD Department of Urology, Pusan National University College of Medicine Email : pnc@pusan.ac.kr J Korean Med Assoc 2007;
GUIDELINES FOR THE INVESTIGATION AND TREATMENT OF MALE INFERTILITY
 GUIDELINES FOR THE INVESTIGATION AND TREATMENT OF MALE INFERTILITY G.R. Dohle, Z. Kopa, A. Jungwirth, T.B. Hargreave. Eur Urol 2002;42(4):313-322 Eur Urol 2004;46(5):555-558 Definition Infertility is the
GUIDELINES FOR THE INVESTIGATION AND TREATMENT OF MALE INFERTILITY G.R. Dohle, Z. Kopa, A. Jungwirth, T.B. Hargreave. Eur Urol 2002;42(4):313-322 Eur Urol 2004;46(5):555-558 Definition Infertility is the
Evaluation and Treatment of the Subfertile Male. Karen Baker, MD Associate Professor Duke University, Division of Urology
 Evaluation and Treatment of the Subfertile Male Karen Baker, MD Associate Professor Duke University, Division of Urology Disclosures: None Off label uses: There are no oral medications approved by the
Evaluation and Treatment of the Subfertile Male Karen Baker, MD Associate Professor Duke University, Division of Urology Disclosures: None Off label uses: There are no oral medications approved by the
Postgraduate Training in Reproductive Health
 SURGICAL TREATMENT OF MALE INFERTILITY Georges A. de Boccard, M.D. Consultant Urologist F.M.H., F.E.B.U. Postgraduate Training in Reproductive Health Geneva Foundation for Medical Education and Research
SURGICAL TREATMENT OF MALE INFERTILITY Georges A. de Boccard, M.D. Consultant Urologist F.M.H., F.E.B.U. Postgraduate Training in Reproductive Health Geneva Foundation for Medical Education and Research
EVALUATION OF MALE AND FEMALE INFERTILITY ANDREA BARRUECO AMERICAN CENTER FOR REPRODUCTIVE MEDICINE CLEVELAND CLINIC ART TRAINING 2018
 EVALUATION OF MALE AND FEMALE INFERTILITY ANDREA BARRUECO AMERICAN CENTER FOR REPRODUCTIVE MEDICINE CLEVELAND CLINIC ART TRAINING 2018 The evaluation of an infertile couple requires an understanding of
EVALUATION OF MALE AND FEMALE INFERTILITY ANDREA BARRUECO AMERICAN CENTER FOR REPRODUCTIVE MEDICINE CLEVELAND CLINIC ART TRAINING 2018 The evaluation of an infertile couple requires an understanding of
FERTILITY & TCM. On line course provided by. Taught by Clara Cohen
 FERTILITY & TCM On line course provided by Taught by Clara Cohen FERTILITY & TCM FERTILITY AND TCM THE PRACTITIONER S ROLE CAUSES OF INFERTILITY RISK FACTORS OBJECTIVES UNDERSTANDING TESTS Conception in
FERTILITY & TCM On line course provided by Taught by Clara Cohen FERTILITY & TCM FERTILITY AND TCM THE PRACTITIONER S ROLE CAUSES OF INFERTILITY RISK FACTORS OBJECTIVES UNDERSTANDING TESTS Conception in
Reproductive System Purpose General Structures Male Structures Functions Female Anatomy Structures Functions Clinical Applications
 The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
Information Sheet. Male Infertility
 Infertility National Public Awareness Campaign Information Sheet Male Infertility In approximately half of couples complaining of infertility part of the problem lies with the male. Male infertility has
Infertility National Public Awareness Campaign Information Sheet Male Infertility In approximately half of couples complaining of infertility part of the problem lies with the male. Male infertility has
Male Factor Infertility
 Male Factor Infertility Simplified Evaluaon and Treatment* ^ * In 20 minutes or less In 20 slides ^ 5 minute office visit ALWAYS EVALUATE THE MALE & THE FEMALE Why 1. To help the coupleachieve a pregnancy
Male Factor Infertility Simplified Evaluaon and Treatment* ^ * In 20 minutes or less In 20 slides ^ 5 minute office visit ALWAYS EVALUATE THE MALE & THE FEMALE Why 1. To help the coupleachieve a pregnancy
Infertility. Rhian Allen & David Rogers.
 Infertility Rhian Allen & David Rogers http://www.worldofsurrogacy.com Objectives Definition & Epidemiology Female Gonadal Axis Normal Menstrual Cycle Causes Patient History Patient Examination Investigations
Infertility Rhian Allen & David Rogers http://www.worldofsurrogacy.com Objectives Definition & Epidemiology Female Gonadal Axis Normal Menstrual Cycle Causes Patient History Patient Examination Investigations
Getting Help for Obstructive Azoospermia A BASIC GUIDE TO MALE. A doctor s guide for patients developed by the American Urological Association, Inc.
 A BASIC GUIDE TO MALE Getting Help for Obstructive Azoospermia A doctor s guide for patients developed by the American Urological Association, Inc. Based on the AUA Best Practice Policy and ASRM Practice
A BASIC GUIDE TO MALE Getting Help for Obstructive Azoospermia A doctor s guide for patients developed by the American Urological Association, Inc. Based on the AUA Best Practice Policy and ASRM Practice
MALE INFERTILITY & SEMEN ANALYSIS
 MALE INFERTILITY & SEMEN ANALYSIS DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and mitigate potential
MALE INFERTILITY & SEMEN ANALYSIS DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and mitigate potential
BIOCHEMICAL TESTS FOR THE INVESTIGATION OF COMMON ENDOCRINE PROBLEMS IN THE MALE
 Authoriser: Moya O Doherty Page 1 of 7 BIOCHEMICAL TESTS FOR THE INVESTIGATION OF COMMON ENDOCRINE PROBLEMS IN THE MALE The purpose of this protocol is to describe common tests used for the investigation
Authoriser: Moya O Doherty Page 1 of 7 BIOCHEMICAL TESTS FOR THE INVESTIGATION OF COMMON ENDOCRINE PROBLEMS IN THE MALE The purpose of this protocol is to describe common tests used for the investigation
Abnormalities of Spermatogenesis
 Abnormalities of Spermatogenesis Male Factor 40% of the cause for infertility Sperm is constantly produced by the germinal epithelium of the testicle Sperm generation time 73 days Sperm production is thermoregulated
Abnormalities of Spermatogenesis Male Factor 40% of the cause for infertility Sperm is constantly produced by the germinal epithelium of the testicle Sperm generation time 73 days Sperm production is thermoregulated
TESTOSTERONE DEFINITION
 DEFINITION A hormone that is a hydroxyl steroid ketone (C19H28O2) produced especially by the testes or made synthetically and that is responsible for inducing and maintaining male secondary sex characteristics.
DEFINITION A hormone that is a hydroxyl steroid ketone (C19H28O2) produced especially by the testes or made synthetically and that is responsible for inducing and maintaining male secondary sex characteristics.
Al-Anbar Medical Journal
 Clinical Patterns and Major Causes of Male Infertility In Fallujah City Ziad H. Abd FIBMS(Urology) College of Medicine, University of Anbar Qais Abdul-Rahman Thamer FIBMS(Urology) College of Medicine,
Clinical Patterns and Major Causes of Male Infertility In Fallujah City Ziad H. Abd FIBMS(Urology) College of Medicine, University of Anbar Qais Abdul-Rahman Thamer FIBMS(Urology) College of Medicine,
What should the clinician ask and look for in the initial consultation?
 What should the clinician ask and look for in the initial consultation? ESHRE Campus Course, Thessaloniki, Greece, 1-3 October 2009 Reproductive andrology: linking laboratory to clinical practice Tim Hargreave
What should the clinician ask and look for in the initial consultation? ESHRE Campus Course, Thessaloniki, Greece, 1-3 October 2009 Reproductive andrology: linking laboratory to clinical practice Tim Hargreave
Male Reproductive Physiology
 Male Reproductive Physiology Overview Anatomy Function Endocrine and spermatogenesis Testis epididymus,vas deferens,seminal vesicles and prostate Hypothalamic pituitary testicular axis Hormones of the
Male Reproductive Physiology Overview Anatomy Function Endocrine and spermatogenesis Testis epididymus,vas deferens,seminal vesicles and prostate Hypothalamic pituitary testicular axis Hormones of the
Importance of the testicular torsion in the male infertility. A. Rusz, Gy. Papp Military Hospital-State Health Centre (ÁEK) EAA Centre
 Importance of the testicular torsion in the male infertility A. Rusz, Gy. Papp Military Hospital-State Health Centre (ÁEK) EAA Centre Budapest, Hungary Acute scrotum Torsion of the testis Torsion of the
Importance of the testicular torsion in the male infertility A. Rusz, Gy. Papp Military Hospital-State Health Centre (ÁEK) EAA Centre Budapest, Hungary Acute scrotum Torsion of the testis Torsion of the
Index. urologic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Acquired hypogonadism, prevalence of, 165 167 primary, 165 secondary, 167 Adipose tissue, as an organ, 240 241 Adrenal hyperplasia, congenital,
Note: Page numbers of article titles are in boldface type. A Acquired hypogonadism, prevalence of, 165 167 primary, 165 secondary, 167 Adipose tissue, as an organ, 240 241 Adrenal hyperplasia, congenital,
Semen Quality in Infertile Men with a History of Unilateral Cryptorchidism
 Journal of Reproduction & Contraception (2004) 15 (3):139-143 Semen Quality in Infertile Men with a History of Unilateral Cryptorchidism P. Tzvetkova 1, Wei-Jie ZHU 2, D. Tzvetkov 3 1. Department of Immunoneuroendocrinology,
Journal of Reproduction & Contraception (2004) 15 (3):139-143 Semen Quality in Infertile Men with a History of Unilateral Cryptorchidism P. Tzvetkova 1, Wei-Jie ZHU 2, D. Tzvetkov 3 1. Department of Immunoneuroendocrinology,
Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia
 Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia Thomas A. Masterson; Aubrey B. Greer; Ranjith Ramasamy University of Miami, Miami, FL, United
Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia Thomas A. Masterson; Aubrey B. Greer; Ranjith Ramasamy University of Miami, Miami, FL, United
Chapter 11 Guidelines and Best Practice Statements for the Evaluation and Management of Infertile Adult and Adolescent Males with Varicocele
 Chapter 11 Guidelines and Best Practice Statements for the Evaluation and Management of Infertile Adult and Adolescent Males with Varicocele With the continuous growth of medical knowledge and the need
Chapter 11 Guidelines and Best Practice Statements for the Evaluation and Management of Infertile Adult and Adolescent Males with Varicocele With the continuous growth of medical knowledge and the need
Reversible Conditions Organising More Information semen analysis Male Infertility at Melbourne IVF Fertility Preservation
 Male Infertility Understanding fertility in men Conceiving a baby depends on a number of factors, including healthy sperm. After a woman s age, this can be the biggest issue. Reproduction, although simple
Male Infertility Understanding fertility in men Conceiving a baby depends on a number of factors, including healthy sperm. After a woman s age, this can be the biggest issue. Reproduction, although simple
Sexual dysfunction of chronic kidney disease. Razieh salehian.md psychiatrist
 Sexual dysfunction of chronic kidney disease Razieh salehian.md psychiatrist Disturbances in sexual function are a common feature of chronic renal failure. Sexual dysfunction is inversely associated with
Sexual dysfunction of chronic kidney disease Razieh salehian.md psychiatrist Disturbances in sexual function are a common feature of chronic renal failure. Sexual dysfunction is inversely associated with
ACUPUNCTURE AND MALE INFERTILITY
 ACUPUNCTURE AND MALE INFERTILITY About male infertility The clinical definition of male infertility is the presence of abnormal semen parameters in the male partner of a couple who have been unable to
ACUPUNCTURE AND MALE INFERTILITY About male infertility The clinical definition of male infertility is the presence of abnormal semen parameters in the male partner of a couple who have been unable to
EVALUATION FORM FOR MALE FACTOR SUBFERTILITY UT ERLANGER MEN S HEALTH
 Date: Patient MR #: _ EVALUATION FORM FOR MALE FACTOR SUBFERTILITY UT ERLANGER MEN S HEALTH Name Medical Record Number Age _ Date of Birth Occupation Religion How did you hear about our Male Infertility
Date: Patient MR #: _ EVALUATION FORM FOR MALE FACTOR SUBFERTILITY UT ERLANGER MEN S HEALTH Name Medical Record Number Age _ Date of Birth Occupation Religion How did you hear about our Male Infertility
Male infertility too often ignored & forgotten
 Male infertility too often ignored & forgotten The journey 1. of the men A review of the guidelines Joo Teoh FRANZCOG MRCP(Ire) MRCOG MBBCh MSc(Lon) MD(Glasgow) SubspecialtyRepromed(UK) Consultant Obstetrician
Male infertility too often ignored & forgotten The journey 1. of the men A review of the guidelines Joo Teoh FRANZCOG MRCP(Ire) MRCOG MBBCh MSc(Lon) MD(Glasgow) SubspecialtyRepromed(UK) Consultant Obstetrician
Imaging of Male Infertility: Pictorial Review
 JR Integrative Imaging LIFELONG LERNING FOR RDIOLOGY Imaging of Male Infertility: Pictorial Review William L. Simpson, Jr. 1 and Dana R. Rausch STRCT Objective This article will review the workup of infertility
JR Integrative Imaging LIFELONG LERNING FOR RDIOLOGY Imaging of Male Infertility: Pictorial Review William L. Simpson, Jr. 1 and Dana R. Rausch STRCT Objective This article will review the workup of infertility
Appendix D Answers to the KAP Survey
 From Trainer s Resource Book to accompany Management of Men s Reproductive Health Problems 2003 EngenderHealth Appendix D Answers to the KAP Survey In the answer key that follows: The answers appear in
From Trainer s Resource Book to accompany Management of Men s Reproductive Health Problems 2003 EngenderHealth Appendix D Answers to the KAP Survey In the answer key that follows: The answers appear in
ACUPUNCTURE AND MALE INFERTILITY
 ACUPUNCTURE AND MALE INFERTILITY About male infertility The clinical definition of male infertility is the presence of abnormal semen parameters in the male partner of a couple who have been unable to
ACUPUNCTURE AND MALE INFERTILITY About male infertility The clinical definition of male infertility is the presence of abnormal semen parameters in the male partner of a couple who have been unable to
Male Reproductive System Dr. Gary Mumaugh
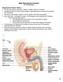 Male Reproductive System Dr. Gary Mumaugh Reproductive System Basics Primary sex organs (gonads) testes in males, ovaries in females Gonads produce sex cells called gametes (gametes means spouses) and
Male Reproductive System Dr. Gary Mumaugh Reproductive System Basics Primary sex organs (gonads) testes in males, ovaries in females Gonads produce sex cells called gametes (gametes means spouses) and
EFFECTS OF VARICOCELECTOMY ON TESTIS VOLUME AND SEMEN PARAMETERS IN ADOLESCENTS: A RANDOMIZED PROSPECTIVE STUDY
 Nagoya J. Med. Sci. 58. 127-132, 1995 EFFECTS OF VARICOCELECTOMY ON TESTIS VOLUME AND SEMEN PARAMETERS IN ADOLESCENTS: A RANDOMIZED PROSPECTIVE STUDY MASANORI YAMAMOTO, HATSUKI HIEI, SATOSHI KATSUNO and
Nagoya J. Med. Sci. 58. 127-132, 1995 EFFECTS OF VARICOCELECTOMY ON TESTIS VOLUME AND SEMEN PARAMETERS IN ADOLESCENTS: A RANDOMIZED PROSPECTIVE STUDY MASANORI YAMAMOTO, HATSUKI HIEI, SATOSHI KATSUNO and
The assessment and investigation of the infertile couple
 The assessment and investigation of the infertile couple BIRUTE ZILAITIENE, MD, PHD, PROF., FECSM DEPARTMENT OF ENDOCRINOLOGY AND INSTITUTE OF ENDOCRINOLOGY, LITHUANIAN UNIVERSITY OF HEALTH SCIENCES, KAUNAS,
The assessment and investigation of the infertile couple BIRUTE ZILAITIENE, MD, PHD, PROF., FECSM DEPARTMENT OF ENDOCRINOLOGY AND INSTITUTE OF ENDOCRINOLOGY, LITHUANIAN UNIVERSITY OF HEALTH SCIENCES, KAUNAS,
INFERTILITY GENETIC TESTING. Dr. Ahmad Ebrahimi Molecular Medical Genetics,PhD Yass Medical Genetics Lab. Tehran University of Medical Science
 INFERTILITY GENETIC TESTING Dr. Ahmad Ebrahimi Molecular Medical Genetics,PhD Yass Medical Genetics Lab. Tehran University of Medical Science INFERTILITY GENETIC TESTING It is estimated that genetics are
INFERTILITY GENETIC TESTING Dr. Ahmad Ebrahimi Molecular Medical Genetics,PhD Yass Medical Genetics Lab. Tehran University of Medical Science INFERTILITY GENETIC TESTING It is estimated that genetics are
A USER S GUIDE WHAT EVERY MAN NEEDS TO KNOW
 A USER S GUIDE WHAT EVERY MAN NEEDS TO KNOW 1. Why men need to know more Good health is vital for a happy and full life. But, with work and family responsibilities, men often overlook their own health
A USER S GUIDE WHAT EVERY MAN NEEDS TO KNOW 1. Why men need to know more Good health is vital for a happy and full life. But, with work and family responsibilities, men often overlook their own health
GPVTS TEACHING APRIL 2016 FERTILITY
 GPVTS TEACHING APRIL 2016 FERTILITY Djavid Alleemudder - Consultant Obstetrics & Gynaecology DEFINITIONS What is the definition of infertility? Failure to conceive after 12 months despite regular, unprotected
GPVTS TEACHING APRIL 2016 FERTILITY Djavid Alleemudder - Consultant Obstetrics & Gynaecology DEFINITIONS What is the definition of infertility? Failure to conceive after 12 months despite regular, unprotected
GENETIC TESTING: IN WHOM AND WHEN
 GENETIC TESTING: IN WHOM AND WHEN Robert D Oates, M.D. Boston University School of Medicine My background in this field I was the first to link Cystic Fibrosis Mutations with Congenital Absence of the
GENETIC TESTING: IN WHOM AND WHEN Robert D Oates, M.D. Boston University School of Medicine My background in this field I was the first to link Cystic Fibrosis Mutations with Congenital Absence of the
Failure to Launch. Impairment of Primary Spermatogenesis & Optimization of Reproductive Techniques
 Failure to Launch. Impairment of Primary Spermatogenesis & Optimization of Reproductive Techniques October 16, 2013 Ryan Flannigan PGY3 UBC Urology http://www.chinahearsay.com/china-lethargic-sperm-economic-development/
Failure to Launch. Impairment of Primary Spermatogenesis & Optimization of Reproductive Techniques October 16, 2013 Ryan Flannigan PGY3 UBC Urology http://www.chinahearsay.com/china-lethargic-sperm-economic-development/
Surgical Sperm Retrieval
 Saint Mary s Hospital Department of Reproductive Medicine Information for Patients Surgical Sperm Retrieval About one man in a hundred produces no sperm (10-15% of all sub fertile men) - a condition known
Saint Mary s Hospital Department of Reproductive Medicine Information for Patients Surgical Sperm Retrieval About one man in a hundred produces no sperm (10-15% of all sub fertile men) - a condition known
Aromatase Inhibitors in Male Infertility:
 Aromatase Inhibitors in Male Infertility: The hype of hypogonadism? BEATRIZ UGALDE, PHARM.D. H-E-B/UNIVERSITY OF TEXAS COMMUNITY PHARMACY PGY1 03 NOVEMBER 2017 PHARMACOTHERAPY ROUNDS Disclosures No conflicts
Aromatase Inhibitors in Male Infertility: The hype of hypogonadism? BEATRIZ UGALDE, PHARM.D. H-E-B/UNIVERSITY OF TEXAS COMMUNITY PHARMACY PGY1 03 NOVEMBER 2017 PHARMACOTHERAPY ROUNDS Disclosures No conflicts
Primary sex organs (gonads): testes and ovaries. Accessory reproductive organs: ducts, glands, and external genitalia
 Male Reproductive System Primary sex organs (gonads): testes and ovaries Produce sex cells (gametes) Secrete steroid sex hormones Androgens (males) Estrogens and progesterone (females) Accessory reproductive
Male Reproductive System Primary sex organs (gonads): testes and ovaries Produce sex cells (gametes) Secrete steroid sex hormones Androgens (males) Estrogens and progesterone (females) Accessory reproductive
Chapter 28: REPRODUCTIVE SYSTEM: MALE
 Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
The Reproductive System
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
AQUA Registry 2019 Non-QPP Measure Specifications. Denominator Exceptions. IPSS<8 None None Yes Patient Reported Outcome (PRO)
 AQUA12 Benign Prostate Hyperplasia: IPSS improvement after diagnosis with NEW diagnosis of clinically significant BPH who had IPSS (international prostate symptoms score) or AUASS (American urological
AQUA12 Benign Prostate Hyperplasia: IPSS improvement after diagnosis with NEW diagnosis of clinically significant BPH who had IPSS (international prostate symptoms score) or AUASS (American urological
Outline. Male Reproductive System Testes and Sperm Hormonal Regulation
 Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
John P. Mulhall Peter J. Stahl Doron S. Stember. Clinical Care Pathways in Andrology
 John P. Mulhall Peter J. Stahl Doron S. Stember Clinical Care Pathways in Andrology 123 Clinical Care Pathways in Andrology John P. Mulhall Peter J. Stahl Doron S. Stember Clinical Care Pathways in Andrology
John P. Mulhall Peter J. Stahl Doron S. Stember Clinical Care Pathways in Andrology 123 Clinical Care Pathways in Andrology John P. Mulhall Peter J. Stahl Doron S. Stember Clinical Care Pathways in Andrology
Male Hypogonadism. Types and causes of hypogonadism. What is male hypogonadism? Symptoms. Testosterone production. Patient Information.
 Patient Information English 31 Male Hypogonadism The underlined terms are listed in the glossary. What is male hypogonadism? Male hypogonadism means the testicles do not produce enough of the male sex
Patient Information English 31 Male Hypogonadism The underlined terms are listed in the glossary. What is male hypogonadism? Male hypogonadism means the testicles do not produce enough of the male sex
Laboratory Investigation of Male Gonadal Function. Dr N Oosthuizen Dept of Chemical Pathology UP 2010
 Laboratory Investigation of Male Gonadal Function Dr N Oosthuizen Dept of Chemical Pathology UP 2010 1 Figure 1. Hypothalamic-pituitary pituitary-testicular testicular axis 2 Testosterone (T) measurement
Laboratory Investigation of Male Gonadal Function Dr N Oosthuizen Dept of Chemical Pathology UP 2010 1 Figure 1. Hypothalamic-pituitary pituitary-testicular testicular axis 2 Testosterone (T) measurement
Maldescended testis in Adults. Dr. BG GAUDJI Urologist STEVE BIKO ACADEMIC HOSPITAL
 Maldescended testis in Adults Dr. BG GAUDJI Urologist STEVE BIKO ACADEMIC HOSPITAL Definitions Cryptorchid: testis neither resides nor can be manipulated into the scrotum Ectopic: aberrant course Retractile:
Maldescended testis in Adults Dr. BG GAUDJI Urologist STEVE BIKO ACADEMIC HOSPITAL Definitions Cryptorchid: testis neither resides nor can be manipulated into the scrotum Ectopic: aberrant course Retractile:
Cancer and Fertility Ashley Munchel, MD Assistant Professor of Pediatrics University of Maryland Medical Center
 Cancer and Fertility Ashley Munchel, MD Assistant Professor of Pediatrics University of Maryland Medical Center Trends in Pediatric Cancer Incidence Rates by Site, Ages Birth to 19 Years, 1975 to 2010.
Cancer and Fertility Ashley Munchel, MD Assistant Professor of Pediatrics University of Maryland Medical Center Trends in Pediatric Cancer Incidence Rates by Site, Ages Birth to 19 Years, 1975 to 2010.
Infertility. Dafydd Ywain & Kayleigh Hansen
 Infertility Dafydd Ywain & Kayleigh Hansen Terminology Epidemiology Aetiology Male infertility Female infertility Conclusion Content Terminology Fecundability The probability of conceiving during a single
Infertility Dafydd Ywain & Kayleigh Hansen Terminology Epidemiology Aetiology Male infertility Female infertility Conclusion Content Terminology Fecundability The probability of conceiving during a single
The Reproductive System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 16 The Reproductive System Slides 16.1 16.20 Lecture Slides in PowerPoint by Jerry L. Cook The Reproductive System Gonads
Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 16 The Reproductive System Slides 16.1 16.20 Lecture Slides in PowerPoint by Jerry L. Cook The Reproductive System Gonads
Alternative management of hypogonadism Tamoxifen. Emmanuele A. Jannini, MD Tor Vergata University of Rome ITALY
 Alternative management of hypogonadism Tamoxifen Emmanuele A. Jannini, MD Tor Vergata University of Rome ITALY eajannini@gmail.com What hypogonadism is? What hypogonadism is? It is an empty glass The two
Alternative management of hypogonadism Tamoxifen Emmanuele A. Jannini, MD Tor Vergata University of Rome ITALY eajannini@gmail.com What hypogonadism is? What hypogonadism is? It is an empty glass The two
DISORDERS OF MALE GENITALS
 Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 9. Testicular disorders/disorders of male genitals. Horm Res 2007;68(suppl 2):63 66 ESPE Code Diagnosis OMIM ICD10
Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 9. Testicular disorders/disorders of male genitals. Horm Res 2007;68(suppl 2):63 66 ESPE Code Diagnosis OMIM ICD10
BENIGN & MALIGNANT TESTIS DISEASES. Gary J. Faerber, M.D. Associate Professor, Dept of Urology March 2009 OBJECTIVES
 BENIGN & MALIGNANT TESTIS DISEASES Gary J. Faerber, M.D. Associate Professor, Dept of Urology March 2009 OBJECTIVES 1. Become familiar with the scrotal contents and their anatomical relationship with each
BENIGN & MALIGNANT TESTIS DISEASES Gary J. Faerber, M.D. Associate Professor, Dept of Urology March 2009 OBJECTIVES 1. Become familiar with the scrotal contents and their anatomical relationship with each
The Reproductive System
 16 PART A The Reproductive System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Reproductive
16 PART A The Reproductive System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Reproductive
Thi-Qar University - College of medicine. Department of obstetrics and gynecology DONE BY SAMI BASSAM HASSAN RAMADAN ANAS TAWFIQ
 Distributional Study of Infertile Male Causes According to semen fluid analysis In a sample attend infertility center in AL- Hussein teaching hospital in Al-Nasiriyah Thi-Qar University - College of medicine
Distributional Study of Infertile Male Causes According to semen fluid analysis In a sample attend infertility center in AL- Hussein teaching hospital in Al-Nasiriyah Thi-Qar University - College of medicine
Student Academic Learning Services Page 1 of 5 Reproductive System Practice
 Student Academic Learning Services Page 1 of 5 Reproductive System Practice Fill in the blanks using the words listed: accessory glands, vas deferens, penis, scrotum, fallopian tube, testes, urethra, vagina,
Student Academic Learning Services Page 1 of 5 Reproductive System Practice Fill in the blanks using the words listed: accessory glands, vas deferens, penis, scrotum, fallopian tube, testes, urethra, vagina,
THE INCIDENCE OF ANTISPERM ANTmODIES IN PATIENTS WITH SEMINAL TRACT OBSTRUCTIONS
 Nagoya J. Med. Sci. 59. 25-29,1996 THE INCIDENCE OF ANTISPERM ANTmODIES IN PATIENTS WITH SEMINAL TRACT OBSTRUCTIONS MASANORI YAMAMOTO, HATSUKI HIBI, and KOJI MIYAKE Department of Urology, Nagoya University
Nagoya J. Med. Sci. 59. 25-29,1996 THE INCIDENCE OF ANTISPERM ANTmODIES IN PATIENTS WITH SEMINAL TRACT OBSTRUCTIONS MASANORI YAMAMOTO, HATSUKI HIBI, and KOJI MIYAKE Department of Urology, Nagoya University
FACTSHEET FERTILITY INVESTIGATIONS
 FACTSHEET FERTILITY INVESTIGATIONS Most people nowadays know enough about contraception to expect a pregnancy to occur reasonably soon after contraceptive precautions are stopped. If your own fertility
FACTSHEET FERTILITY INVESTIGATIONS Most people nowadays know enough about contraception to expect a pregnancy to occur reasonably soon after contraceptive precautions are stopped. If your own fertility
Subfertility B Y A L I S O N, B E N A N D J O H N
 Subfertility B Y A L I S O N, B E N A N D J O H N Contents Definition Causes Male Female Hx & Ex Investigations Treatment Definition Failure to conceive after a year of frequent, unprotected communion.
Subfertility B Y A L I S O N, B E N A N D J O H N Contents Definition Causes Male Female Hx & Ex Investigations Treatment Definition Failure to conceive after a year of frequent, unprotected communion.
15% ART accounts for ~4% of Australian births
 The General Practice Education Day HealthEd / Generation Next 20 th February Sydney Declarations Male Infertility & Assisted Reproduction Prof Robert I McLachlan FRACP, Ph.D. Consultant Andrologist, Monash
The General Practice Education Day HealthEd / Generation Next 20 th February Sydney Declarations Male Infertility & Assisted Reproduction Prof Robert I McLachlan FRACP, Ph.D. Consultant Andrologist, Monash
MALE REPRODUCTIVE SYSTEM
 MALE REPRODUCTIVE SYSTEM 1. The male reproductive system is made up of the following structures, EXCEPT: a. prostate; b. testicle; c. spermatic ducts; d. vestibular bulbs; e. seminal vesicles. 2.The testicle:
MALE REPRODUCTIVE SYSTEM 1. The male reproductive system is made up of the following structures, EXCEPT: a. prostate; b. testicle; c. spermatic ducts; d. vestibular bulbs; e. seminal vesicles. 2.The testicle:
Male Reproductive System
 21-1 21-2 Reproductive System Male Reproductive System Genital Tract In males the testes, held outside the body in the scrotum (optimum temp of about 35 0 C), produce sperm. Sperm mature in coiled tubes
21-1 21-2 Reproductive System Male Reproductive System Genital Tract In males the testes, held outside the body in the scrotum (optimum temp of about 35 0 C), produce sperm. Sperm mature in coiled tubes
When should I ask my doctor about my fertility?
 Preserving Fertility for Men with Cancer Some cancers and their treatments can affect a man s ability to father a child (his fertility). These changes can last for a short time, or may be permanent. This
Preserving Fertility for Men with Cancer Some cancers and their treatments can affect a man s ability to father a child (his fertility). These changes can last for a short time, or may be permanent. This
Cryptorchidism and its impact on male fertility: a state of art review of current literature. Case 1
 CASE REPORT Cryptorchidism and its impact on male fertility: a state of art review of current literature Eric Chung, MBBS, FRACS; Gerald B. Brock, MD, FRCSC Division of Urology, University of Western Ontario,
CASE REPORT Cryptorchidism and its impact on male fertility: a state of art review of current literature Eric Chung, MBBS, FRACS; Gerald B. Brock, MD, FRCSC Division of Urology, University of Western Ontario,
Male Reproductive System. Anatomy
 Male Reproductive System Medical Terminology Chapter Seven HIT # 141 Anatomy Testis or testicle = main male sex organs, paired, oval shaped, enclosed in a sac called the scrotum. Seminiferous tubules =
Male Reproductive System Medical Terminology Chapter Seven HIT # 141 Anatomy Testis or testicle = main male sex organs, paired, oval shaped, enclosed in a sac called the scrotum. Seminiferous tubules =
15% ART accounts for ~4% of Australian births
 The General Practice Education Day HealthEd / Generation Next 23 rd July Brisbane Declarations Male Infertility & Assisted Reproduction Equity interest in Monash IVF Group Prof Robert I McLachlan FRACP,
The General Practice Education Day HealthEd / Generation Next 23 rd July Brisbane Declarations Male Infertility & Assisted Reproduction Equity interest in Monash IVF Group Prof Robert I McLachlan FRACP,
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization
 Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
Chapter 4. Managing Fertility in Childhood Cancer Patients T.K. Woodruff and K.A. Snyder (eds.) Oncofertility. Springer 2007
 Chapter 4 Managing Fertility in Childhood Cancer Patients T.K. Woodruff and K.A. Snyder (eds.) Oncofertility. Springer 2007 The original publication of this article is available at www.springerlink.com
Chapter 4 Managing Fertility in Childhood Cancer Patients T.K. Woodruff and K.A. Snyder (eds.) Oncofertility. Springer 2007 The original publication of this article is available at www.springerlink.com
MEN S HEALTH AFTER CANCER WHAT YOU NEED TO KNOW: INFERTILITY
 UW MEDICINE TITLE OR EVENT MEN S HEALTH AFTER CANCER WHAT YOU NEED TO KNOW: INFERTILITY KEVIN A. OSTROWSKI, MD OSTROWSK@UW.EDU TOM WALSH, MD WALSHT@UW.EDU LEARNING OBJECTIVES At the conclusion of this
UW MEDICINE TITLE OR EVENT MEN S HEALTH AFTER CANCER WHAT YOU NEED TO KNOW: INFERTILITY KEVIN A. OSTROWSKI, MD OSTROWSK@UW.EDU TOM WALSH, MD WALSHT@UW.EDU LEARNING OBJECTIVES At the conclusion of this
- production of two types of gametes -- fused at fertilization to form zygote
 Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
The epidemiology and etiology of azoospermia
 REVIEW The epidemiology and etiology of azoospermia Marcello Cocuzza, Conrado Alvarenga, Rodrigo Pagani Universidade de São Paulo, Faculdade de Medicina, Department of Urology, São Paulo/SP, Brazil. The
REVIEW The epidemiology and etiology of azoospermia Marcello Cocuzza, Conrado Alvarenga, Rodrigo Pagani Universidade de São Paulo, Faculdade de Medicina, Department of Urology, São Paulo/SP, Brazil. The
Biology of Reproduction-Biol 326
 Biology of Reproduction-Biol 326 READ ALL INSTRUCTIONS CAREFULLY. ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER REGARDLESS OF WHAT YOU MARK ON THE
Biology of Reproduction-Biol 326 READ ALL INSTRUCTIONS CAREFULLY. ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER REGARDLESS OF WHAT YOU MARK ON THE
UROLOGY TOPICS FOR SENIOR CLERKSHIP HEMATURIA
 UROLOGY TOPICS FOR SENIOR CLERKSHIP HEMATURIA Blood in urine is an important presenting symptom for many diseases of the urinary tract as well as for systemic disorders. Degree of hematuria has poor correlation
UROLOGY TOPICS FOR SENIOR CLERKSHIP HEMATURIA Blood in urine is an important presenting symptom for many diseases of the urinary tract as well as for systemic disorders. Degree of hematuria has poor correlation
Study Guide Answer Key Reproductive System
 Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
Hypogonadism 4/27/2018. Male Hypogonadism -- Definition. Epidemiology. Objectives HYPOGONADISM. Men with Hypogonadism. 95% untreated.
 Male Hypogonadism -- Definition - Low T, Low Testosterone Hypogonadism -...a clinical syndrome that results from failure of the testes to produce physiological concentrations of testosterone due to pathology
Male Hypogonadism -- Definition - Low T, Low Testosterone Hypogonadism -...a clinical syndrome that results from failure of the testes to produce physiological concentrations of testosterone due to pathology
Practical Workshop about Fertility in NZ
 Practical Workshop about Fertility in NZ Dr Sarah Wakeman Fertility Associates Christchurch Dr Mary Birdsall Fertility Associates Auckland Professor Wayne Gillett Otago Fertility Service and University
Practical Workshop about Fertility in NZ Dr Sarah Wakeman Fertility Associates Christchurch Dr Mary Birdsall Fertility Associates Auckland Professor Wayne Gillett Otago Fertility Service and University
Hormonal Control of Male Sexual Function
 Hormonal Control of Male Sexual Function A majority of the control of sexual functions in the male (and the female) begins with secretions of gonadotropin-releasing hormone (GnRH) by the hypothalamus.
Hormonal Control of Male Sexual Function A majority of the control of sexual functions in the male (and the female) begins with secretions of gonadotropin-releasing hormone (GnRH) by the hypothalamus.
Male infertility Introduction Definition: Starting a fertility study: Woman s age: Anamnesis Personal history Drugs that cause infertility
 Male infertility Introduction Definition: infertility is defined as the inability to conceive after one year of intercourse without contraception (WHO). 15% of couples cannot have children within the first
Male infertility Introduction Definition: infertility is defined as the inability to conceive after one year of intercourse without contraception (WHO). 15% of couples cannot have children within the first
A. Tes:cular Biopsy B. Adop:on C. IUI D. ICSI E. Scrotal ultrasound to R/O varicocele
 A 36 year old man with azospermia wishes to have children, he underwent Y chromosome microdele:on assay, the results show an AZFa abnormality, what is the next step? A. Tes:cular Biopsy B. Adop:on C. IUI
A 36 year old man with azospermia wishes to have children, he underwent Y chromosome microdele:on assay, the results show an AZFa abnormality, what is the next step? A. Tes:cular Biopsy B. Adop:on C. IUI
What are Varicoceles?
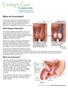 What are Varicoceles? A varicocele is when veins become enlarged inside your scrotum (the pouch of skin that holds your testicles). These veins are called the pampiniform plexus. Ten to 15 of every 100
What are Varicoceles? A varicocele is when veins become enlarged inside your scrotum (the pouch of skin that holds your testicles). These veins are called the pampiniform plexus. Ten to 15 of every 100
Chapter 7. Male Reproductive System
 Chapter 7 Male Reproductive System 1 Sexual Reproduction Sexual reproduction two individuals produce offspring that have genetic characteristics from both parents Sexual reproduction introduces new gene
Chapter 7 Male Reproductive System 1 Sexual Reproduction Sexual reproduction two individuals produce offspring that have genetic characteristics from both parents Sexual reproduction introduces new gene
15% ART accounts for ~4% of Australian births
 The General Practice Education Day HealthEd / Generation Next 5 th March Melbourne Declarations Male Infertility & Assisted Reproduction Prof Robert I McLachlan FRACP, Ph.D. Consultant Andrologist, Monash
The General Practice Education Day HealthEd / Generation Next 5 th March Melbourne Declarations Male Infertility & Assisted Reproduction Prof Robert I McLachlan FRACP, Ph.D. Consultant Andrologist, Monash
EAU GUIDELINES ON MALE HYPOGONADISM
 EAU GUIDELINES ON MALE HYPOGONADISM (Limited text update March 2017) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch Introduction Male hypogonadism is a clinical syndrome caused by androgen
EAU GUIDELINES ON MALE HYPOGONADISM (Limited text update March 2017) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch Introduction Male hypogonadism is a clinical syndrome caused by androgen
Clinical Study Laparoscopic Management of Intra-Abdominal Testis: 5-Year Single-Centre Experience A Retrospective Descriptive Study
 Minimally Invasive Surgery Volume 2012, Article ID 878509, 4 pages doi:10.1155/2012/878509 Clinical Study Laparoscopic Management of Intra-Abdominal Testis: 5-Year Single-Centre Experience A Retrospective
Minimally Invasive Surgery Volume 2012, Article ID 878509, 4 pages doi:10.1155/2012/878509 Clinical Study Laparoscopic Management of Intra-Abdominal Testis: 5-Year Single-Centre Experience A Retrospective
Infertility INA S. IRABON, MD, FPOGS, FPSRM, FPSGE OBSTETRICS AND GYNECOLOGY REPRODUCTIVE ENDOCRINOLOGY AND INFERTILITY
 Infertility INA S. IRABON, MD, FPOGS, FPSRM, FPSGE OBSTETRICS AND GYNECOLOGY REPRODUCTIVE ENDOCRINOLOGY AND INFERTILITY To download lecture deck Reference Comprehensive Gynecology 7 th edition, 2017 (Lobo
Infertility INA S. IRABON, MD, FPOGS, FPSRM, FPSGE OBSTETRICS AND GYNECOLOGY REPRODUCTIVE ENDOCRINOLOGY AND INFERTILITY To download lecture deck Reference Comprehensive Gynecology 7 th edition, 2017 (Lobo
Optimum Time for Orchiopexy in Cryptorchidism
 Optimum Time for Orchiopexy in Cryptorchidism Frank Hinman, Jr., M.D. THE RESULTS of orchiopexy are disappointing. Is it that the surgical procedure is faulty, or can the defect be in the patient or in
Optimum Time for Orchiopexy in Cryptorchidism Frank Hinman, Jr., M.D. THE RESULTS of orchiopexy are disappointing. Is it that the surgical procedure is faulty, or can the defect be in the patient or in
Role Of Serum Hormone Indices Including Inhibin B And Scrotal Ultrasound In Evaluation Of Non Obstructive Male Factor Infertility
 Article ID: WMC001510 ISSN 2046-1690 Role Of Serum Hormone Indices Including Inhibin B And Scrotal Ultrasound In Evaluation Of Non Obstructive Male Factor Infertility Author(s):Dr. Geetika, Dr. Sunita
Article ID: WMC001510 ISSN 2046-1690 Role Of Serum Hormone Indices Including Inhibin B And Scrotal Ultrasound In Evaluation Of Non Obstructive Male Factor Infertility Author(s):Dr. Geetika, Dr. Sunita
Infertility: failure to conceive within one year of unprotected regular sexual intercourse. Primary secondary
 Subfertility Infertility: failure to conceive within one year of unprotected regular sexual intercourse. Primary secondary Infertility affects about 15 % of couples. age of the female. Other factors that
Subfertility Infertility: failure to conceive within one year of unprotected regular sexual intercourse. Primary secondary Infertility affects about 15 % of couples. age of the female. Other factors that
