Non-QPP Measures 3 AQUA12. 6 AQUA15 Stones: Urinalysis documented 30 days before
|
|
|
- Buck Fowler
- 5 years ago
- Views:
Transcription
1 Non-QPP Measures 1 Measure ID Measure Title Definition Type Domain AQUA3 (inverse) Cryptorchidism: Inappropriate use of scrotal/groin ultrasound on boys Percentage of patients (boys) =< 18 years of age newly diagnosed with undescended testis or retractile testis with an order for ultrasound (scrotal or groin) placed Efficiency and Cost Reduction 2 AQUA8 (inverse) Hospital re admissions / complications within 30 days of TRUS Biopsy Percentage of patients who had TRUS biopsy performed who had 24h after the biopsy): infection, hematuria, new antibiotic Rx after biopsy, or inpatient consultation within 30 days Patient Safety 3 AQUA12 Benign Prostate Hyperplasia: IPSS improvement after diagnosis Percentage of patients with NEW diagnosis of clinically significant BPH who had IPSS (international prostate symptoms score) or AUASS (American urological association symptom score) improvement by 20% Person & giver Centered Experience s 4 AQUA13 (inverse) Stress Urinary Incontinence (SUI): Revision surgery within 12 months of incontinence procedure Percentage of women who undergo surgery for stress incontinence who require revision surgery within 12 months 5 AQUA14 (inverse) Stones: Repeat Shock Wave Lithotripsy (SWL) within 6 months of treatment Percentage of patients who underwent endoscopic procedures following SWL Efficiency and Cost Reduction 6 AQUA15 Stones: Urinalysis documented 30 days before surgical stone procedures Percentage of patients with a documented urinalysis30 days before surgical stone procedures Patient Safety 2018 QCDR Measures 2018 American Urological Association All Rights Reserved 1 Page
2 Non-QPP Measures Measure ID Measure Title Definition Type Domain 7 AQUA16 Non Muscle Invasive Bladder Cancer: Repeat Transurethral Resection of Bladder Tumor (TURBT) for T1 disease Percentage of patients with T1 disease, that had a second TURBT within 6 weeks of the initial TURBT Efficiency and Cost Reduction 8 AQUA17 Non Muscle Invasive Bladder Cancer: Initiation of BCG within 3 months of diagnosis of high grade T1 bladder cancer and/or CIS Percentage of patients who initiate BCG treatment within 3 months of diagnosis of high grade T1 bladder cancer and/or CIS 9 AQUA18 Non Muscle Invasive Bladder Cancer: Early surveillance cystoscopy within 4 months of initial diagnosis Percentage of patients who receive surveillance cystoscopy within 4 months of TURBT for bladder cancer 10 AQUA19 Diagnosis of Type of Azoospermia and Diagnostic Testing for Obstructive Azoospermia Percentage of patients who had minimum necessary concepts discussed as part of diagnosis of azoospermia alone, to determine possibility of obstructive versus non obstructive azoospermia and underwent diagnostic testing for obstructive azoospermia 11 AQUA20 Genetic Testing of the Azoospermic Male Percentage of patients with non obstructive azoospermia due to primary testis failure who were offered genetic testing 12 AQUA21 Appropriate Management of Obstructive Azoospermia Percentage of obstructive azoospermia patients managed appropriately 2018 QCDR Measures 2018 American Urological Association All Rights Reserved 2 Page
3 Non QPP Measures Measure ID Measure Title Definition Type Domain 13 AQUA22 Bone imaging and soft tissue imaging at the time of diagnosis of metastatic CPRC Percentage of patients who receive bone imaging and soft tissue imaging at the time of diagnosis of metastatic CPRC 14 AQUA23 Blood work for patients receiving abiraterone Percentage of patients receiving abiraterone who receive monthly blood work and serum transaminases (ALT and AST) and bilirubin levels prior to starting treatment and every two weeks for the first three months of treatment and monthly thereafter 15 AQUA24 Testosterone and PSA levels checked for CRPC patients Percentage of patients on hormonal therapy who have their testosterone and PSA levels checked before starting treatment for CRPC 16 AQUA25 Use of Prednisone for CRPC patients on abiraterone Percentage of patients who are receiving abiraterone who are also receiving prednisone 17 AQUA26 (inverse) Benign Prostate Hyperplasia : Benign Prostate Hyperplasia (Formerly AQUA5 & AQUA6 in 2017) Percentage of patients with new diagnosis of BPH who had a creatinine lab order placed or had a CT abdomen, MRI abdomen, ultrasound abdomen ordered or performed. Efficiency and Cost Reduction 18 AQUA27 Appropriate Testing for Vasectomy Patients Percentage of patients where a Post Vasectomy Semen Analysis (PVSA) was ordered and confirmed sterility within 6 months of undergoing a vasectomy 2018 QCDR Measures 2018 American Urological Association All Rights Reserved 3 Page
4 Non QPP Measures Measure ID Measure Title Definition Type Domain 19 AQUA28 20 AQUA29 21 AQUA30 Hypogonadism: Testosterone and hematocrit within 6 months of starting testosterone replacement (Formerly AQUA4 in 2017; added hematocrit in 2018 ) Prostate Cancer: Patient report of Urinary function after treatment (Formerly AQUA10 in 2017) Prostate Cancer: Patient report of Sexual function after treatment (Formerly AQUA11 in 2017) Percentage of patients with hypogonadism, starting testosterone medication (any formulation of testosterone) or rec d testosterone injection in clinic have testosterone level ordered and hematocrit ordered/reported within 6 months of first testosterone Rx or injection Percentage of patients who had a reported urinary function score at 12 months after treatment that is within 80% of the reported urinary function score at baseline (before treatment) Percentage of patients who had a reported sexual function score at 24 months after treatment that is within 60% of the reported sexual function score at baseline (before treatment) Person & giver Centered Experience s Person & giver Centered Experience s 22 MUSIC4 Prostate Cancer: Active surveillance / watchful waiting for low risk prostate cancer Percentage of patients with low risk prostate cancer receiving active surveillance or watchful waiting 23 MUSIC10 Prostate Cancer: Confirmation Testing in low risk AS eligible patients Percentage of low risk patients that are eligible for active surveillance who receive confirmation testing within 6 months of diagnosis Efficiency and Cost Reduction 24 MUSIC11 Prostate Cancer: Follow Up Testing for patients on active surveillance for at least 30 months Percentage of patients on active surveillance that have 2 tumor burden reassessments and 3 PSA tests in first 30 months since diagnosis 2018 QCDR Measures 2018 American Urological Association All Rights Reserved 4 Page
5 QPP Measures QPP Measure Title Definition Type Domain 25 1* Diabetes: Hemoglobin A1c (HbA1c) Poor Control (>9%) Percentage of patient years of age with diabetes who had hemoglobin A1c>9.0% during the measurement period Intermediate Perioperative : Venous Thromboembolism (VTE) Prophylaxis (When indicated in ALL patients) Percentage of surgical patients aged 18 years and older undergoing procedures for which VTE prophylaxis is indicated in all patients, who had an order for Low Molecular Weight Heparin (LMWH), Low Dose Unfractionated Heparin(LDUH), adjusted dose warfarin, fondaparinux or mechanical prophylaxis to be given within 24 hours prior to incision time or within 24 hours after Patient Safety Medication Reconciliation Percentage of patients aged 65 years and older discharged from any inpatient facility (e.g. hospital, skilled nursing facility, or rehabilitation facility) and seen within 30 days following discharge in the office by the physician, prescribing practitioner, registered nurse, or clinical pharmacist providing on going care who had a reconciliation of the discharge medications with the current medication list in the outpatient medical record documented. Communication & Coordination Advance Plan Percentage of patients aged 65 years and older who have an advance care plan or surrogate decision maker documented in the medical record or documentation in the medical record that an advance care plan was discussed but the patient did not wish or was not able to name a surrogate decision maker or provide an advance care plan Communication & Coordination 2018 QCDR Measures 2018 American Urological Association All Rights Reserved 5 Page
6 QPP Measures QPP Measure Title Definition Type Domain Urinary Incontinence: Assessment of Presence or Absence of Urinary Incontinence in Women Aged 65 Years and Older Percentage of female patients aged 65 years and older who were assessed for the presence or absence of urinary incontinence within 12 months Urinary Incontinence: Plan of for Urinary Incontinence in Women Aged 65 Years and Older Percentage of female patients aged 65 years and older with a diagnosis of urinary incontinence with a documented plan of care for urinary incontinence at least once within 12 months Person & giver Centered Experience & s * Prostate Cancer: Avoidance of Overuse of Bone Scan for Staging Low Risk Prostate Cancer Patients Percentage of patients, regardless of age, with a diagnosis of prostate cancer at low risk of recurrence receiving interstitial prostate brachytherapy, OR external beam radiotherapy to the prostate, OR radical prostatectomy, OR cryotherapy who did not have a bone scan performed at any time since diagnosis of prostate cancer Efficiency and Cost Reduction Prostate Cancer: Adjuvant Hormonal Therapy for High Risk Prostate Cancer Patients Percentage of patients, regardless of age, with a diagnosis of prostate cancer at high risk of recurrence receiving external beam radiotherapy to the prostate who were prescribed adjuvant hormonal therapy (GnRH agonist or antagonist) * Influenza Immunization Percentage of patients aged 6 months and older seen for a visit between October 1 and March 31 who received an influenza immunization OR who reported previous receipt of an influenza immunization Population Health * Pneumococcal Vaccination Status for Older Adults Percentage of patients 65 years of age and older who have ever received a pneumococcal vaccine 2018 QCDR Measures 2018 American Urological Association All Rights Reserved 6 Page
7 QPP Measures QPP Measure Title Definition Type Domain * Breast Cancer Screening Percentage of women years of age who had a mammogram to screen for breast cancer * Colorectal Cancer Screening Percentage of patients 50 through 75 years of age who had appropriate screening for colorectal cancer * Diabetes: Eye Exam Percentage of patients years of age with diabetes who had a retinal or dilated eye exam by an eyecare professional during the measurement period or a negative retinal or dilated eye exam (no evidence of retinopathy) in the 12 months prior to the measurement period * Diabetes: Medical Attention for Nephropathy The percentage of patients years of age with diabetes who had a nephropathy screening test or evidence of nephropathy during the measurement period * Preventive and Screening: Body Mass Index (BMI) Screening and Follow Up Percentage of patients aged 18 years and older with a documented BMI during the current encounter or during the previous six months AND when the BMI is outside of normal parameters, a follow up plan is documented during the encounter or during the previous six months of the encounter 2018 QCDR Measures 2018 American Urological Association All Rights Reserved 7 Page
8 QPP Measures QPP Measure Title Definition Type Domain * Documentation of Current Medications in the Medical Record Percentage of specified visits for patients aged 18 years and older for which the eligible professional attests to documenting a list of current medications to the best of his/her knowledge and ability. This list must include ALL prescriptions, over the counters, herbals, and vitamin/mineral/dietary (nutritional) supplements AND must contain the medications name, dosage, frequency and route of administration Patient Safety Pain Assessment and Follow Up Percentage of visits for patients aged 18 years and older with documentation of a pain assessment using a standardized tool(s) on each visit AND documentation of a follow up plan when pain is present * Preventive and Screening: Screening for Depression and Follow Up Plan Percentage of patients aged 12 years and older screened for depression on the date of the encounter using an age appropriate standardized depression screening tool AND if positive, a follow up plan is documented on the date of the positive screen * Ischemic Vascular Disease (IVD): Use of Aspirin or another Antiplatelet Percentage of patients 18 years of age and older who were diagnosed with acute myocardial infarction (AMI), coronary artery bypass graft (CABG) or percutaneous coronary interventions (PCI) in the 12 months prior to the measurement period, or who had an active diagnosis of ischemic vascular disease (IVD) during the measurement period, and who had documentation of aspirin or another antiplatelet during the measurement period 2018 QCDR Measures 2018 American Urological Association All Rights Reserved 8 Page
9 QPP Measures * QPP Measure Title Definition Type Domain Preventive and Screening Tobacco Use: Screening and Cessation Intervention Percentage of patients aged 18 years and older who were screened for tobacco use one or more times within 24 months AND who received cessation counseling intervention if identified as a tobacco user * Controlling High Blood Pressure Percentage of patients 18 through 85 years of age who had a diagnosis of hypertension and whose blood pressure was adequately controlled (< 140/90 mmhg) during the measurement period Intermediate Biopsy Follow Up Percentage of new patients whose biopsy results have been reviewed and communicated to the primary care/referring physician and patient by the performing physician Communication & Coordination * Preventive and Screening: Screening for High Blood Pressure and Follow Percentage of patients aged 18 years and older seen during the reporting period who were screened for high blood pressure AND a recommended follow up plan is documented based on the current blood pressure (BP) reading as indicated * Preventive and Falls: Screening for Future Fall Risk Percentage of patients 65 years of age and older who were screened for future fall risk during the measurement period Surgical Site Infection Percentage of patients aged 18 years and older who had a surgical site infection (SSI) 2018 QCDR Measures 2018 American Urological Association All Rights Reserved 9 Page
10 QPP Measure QPP Measure Title Definition Type Domain Patient Centered Surgical Risk Assessment and Communication Percentage of patients who underwent a non emergency surgery who had their personalized risks of postoperative complications assessed by their surgical team prior to surgery using a clinical data based, patient specific risk calculator and who received personal discussion of those risks with the surgeon Person & giver Centered Experience & s * Depression Remission at Twelve Months The percentage of patients 18 years of age or older with major depression or dysthymia who reached remission 12 months (+/ 30 days) after an index visit Preventive and Screening Unhealthy Alcohol Use Screening & Brief Counseling Percentage of patients aged 18 years and older who were screened at least once within the last 24 months for unhealthy alcohol use using a systematic screening method AND who received brief counseling if identified as an unhealthy alcohol user * Statin Therapy for the Prevention and Treatment of Cardiovascular Disease Percentage of the following patients all considered at high risk of cardiovascular events who were on statin therapy during the performance period: Adults aged > 21 years who were previously diagnosed with or currently have an active diagnosis of clinical atherosclerotic cardiovascular disease (ASCVD); OR Adults > 21 years who ever had a fasting or direct low density lipoprotein cholesterol (LDL C) level > 190 mg/dl or were previously diagnosed with or currently have an active diagnosis of familial or pure hypercholesterolemia; OR Adults aged years with a diagnosis of diabetes with a fasting or direct LDL C level of mg/dl 2018 QCDR Measures 2018 American Urological Association All Rights Reserved 10 Page
Percentage of patients who underwent endoscopic procedures following SWL
 Non-QPP Measures Measure ID Measure Title Definition Type Domain 1 AQUA12 Benign Prostate Hyperplasia: IPSS improvement after diagnosis Percentage of patients with NEW diagnosis of clinically significant
Non-QPP Measures Measure ID Measure Title Definition Type Domain 1 AQUA12 Benign Prostate Hyperplasia: IPSS improvement after diagnosis Percentage of patients with NEW diagnosis of clinically significant
creatinine lab order placed abdomen, MRI abdomen, ultrasound abdomen ordered or performed
 Non-QPP Measures # Measure Title Definition Type Domain 1 Cryptorchidism: Inappropriate use of scrotal/groin ultrasound on boys Percentage of patients (boys) =< 18 years of age newly diagnosed with undescended
Non-QPP Measures # Measure Title Definition Type Domain 1 Cryptorchidism: Inappropriate use of scrotal/groin ultrasound on boys Percentage of patients (boys) =< 18 years of age newly diagnosed with undescended
Non-QPP Measures. # Measure Title Definition Type Domain. Cryptorchidism: Inappropriate use of scrotal/groin ultrasound on boys
 Non-QPP Measures # Measure Title Definition Type Domain 1 Cryptorchidism: Inappropriate use of scrotal/groin ultrasound on boys Percentage of patients (boys) =< 18 years of age newly diagnosed with undescended
Non-QPP Measures # Measure Title Definition Type Domain 1 Cryptorchidism: Inappropriate use of scrotal/groin ultrasound on boys Percentage of patients (boys) =< 18 years of age newly diagnosed with undescended
Measure ID Domain Measure Title Measure Description/Definition Numerator Denominator Denominator Exclusions Denominator Exceptions
 n-qpp s ID Domain Title Description/Definition Numerator Denominator Denominator Exclusions Denominator Exceptions Riskadjustment AQUA3 (inverse) Cryptorchidism: Inappropriate use of scrotal/groin ultrasound
n-qpp s ID Domain Title Description/Definition Numerator Denominator Denominator Exclusions Denominator Exceptions Riskadjustment AQUA3 (inverse) Cryptorchidism: Inappropriate use of scrotal/groin ultrasound
AQUA Registry 2019 Non-QPP Measure Specifications. Denominator Exceptions. IPSS<8 None None Yes Patient Reported Outcome (PRO)
 AQUA12 Benign Prostate Hyperplasia: IPSS improvement after diagnosis with NEW diagnosis of clinically significant BPH who had IPSS (international prostate symptoms score) or AUASS (American urological
AQUA12 Benign Prostate Hyperplasia: IPSS improvement after diagnosis with NEW diagnosis of clinically significant BPH who had IPSS (international prostate symptoms score) or AUASS (American urological
The table below includes the quality measures an ACO is required to submit to CMS as a participant in an MSSP Track 3 ACO
 The table below includes the quality measures an ACO is required to submit to CMS as a participant in an MSSP Track 3 ACO ACO-1 ACO-2 Getting Timely Care, Appointments, and Information How Well Your Providers
The table below includes the quality measures an ACO is required to submit to CMS as a participant in an MSSP Track 3 ACO ACO-1 ACO-2 Getting Timely Care, Appointments, and Information How Well Your Providers
IQSS 2019 QCDR and MIPS Measure Specifications
 IQSS1 Hypogonadism: Serum T, CBC, PSA, IPSS within 6 months of Rx Percentage of patients with a Effective Clinical Patients with documented new diagnosis of hypogonadism receiving androgen replacement
IQSS1 Hypogonadism: Serum T, CBC, PSA, IPSS within 6 months of Rx Percentage of patients with a Effective Clinical Patients with documented new diagnosis of hypogonadism receiving androgen replacement
2015 PQRS Registry. Source Measure Title Measure Description CITIUS1
 1 CQ-IQ covers 65 CMS defined measures that Eligible Providers (EPs) have to report on to assess quality of care provided to the patients. Version Supported: PQRS Registry 2015 65 measures Reporting Period:
1 CQ-IQ covers 65 CMS defined measures that Eligible Providers (EPs) have to report on to assess quality of care provided to the patients. Version Supported: PQRS Registry 2015 65 measures Reporting Period:
Date Modified: March 31, Clinical Quality Measures for PQRS
 Date Modified: March 31, 2015 2015 Clinical Quality s for PQRS # Domain Title Description Type Denominator Numerator Denominator Exclusions/Exceptions 1 Patient Safety Prostate Biopsy Antibiotic Process
Date Modified: March 31, 2015 2015 Clinical Quality s for PQRS # Domain Title Description Type Denominator Numerator Denominator Exclusions/Exceptions 1 Patient Safety Prostate Biopsy Antibiotic Process
Quality Payment Program: Cardiology Specialty Measure Set
 Quality Payment Program: Cardiology Specialty Set Title Number CMS Reporting Method(s) Heart Failure (HF): Angiotensin- Converting Enzyme (ACE) Inhibitor or Angiotensin Receptor Blocker (ARB) Therapy for
Quality Payment Program: Cardiology Specialty Set Title Number CMS Reporting Method(s) Heart Failure (HF): Angiotensin- Converting Enzyme (ACE) Inhibitor or Angiotensin Receptor Blocker (ARB) Therapy for
Meaningful Use Clinical Quality Measures for Eligible Professionals
 Meaningful Use Clinical Quality Measures for Eligible Professionals Measure Type NQF ID CMS ID Description Title: Adult Weight Screening and Follow-Up 1 NQF 0421 PQRI 128 calculated BMI in the past six
Meaningful Use Clinical Quality Measures for Eligible Professionals Measure Type NQF ID CMS ID Description Title: Adult Weight Screening and Follow-Up 1 NQF 0421 PQRI 128 calculated BMI in the past six
2016 Internal Medicine Preferred Specialty Measure Set
 1 0059 Diabetes: Hemoglobin A1c (HbA1c) Poor Control (>9%): Percentage of patients 18-75 years of age with diabetes who had hemoglobin A1c > 9.0% during the measurement period 5 0081 Registry, EHR, 9 0105
1 0059 Diabetes: Hemoglobin A1c (HbA1c) Poor Control (>9%): Percentage of patients 18-75 years of age with diabetes who had hemoglobin A1c > 9.0% during the measurement period 5 0081 Registry, EHR, 9 0105
Quality Payment Program: Cardiology Specialty Measure Set
 Measure Title * Reportable via PINNACLE α Reportable via Diabetes Collaborative CQMC v1.0 Measure High Priority Measure Cross Cutting Measure Heart Failure (HF): Angiotensin- Converting Enzyme (ACE) Inhibitor
Measure Title * Reportable via PINNACLE α Reportable via Diabetes Collaborative CQMC v1.0 Measure High Priority Measure Cross Cutting Measure Heart Failure (HF): Angiotensin- Converting Enzyme (ACE) Inhibitor
Clinical Quality Measures for Submission by Medicare or Medicaid EP/s for the 2011 and 2012 Payment Year
 1 NQF 0059 1 NQF 0064 2 NQF 0061 3 Title: Diabetes: Hemoglobin A1c Poor Control Description: Percentage of patients 18-75 years of age with diabetes (type 1 or type 2) who had hemoglobin A1c > 9.0%. Title:
1 NQF 0059 1 NQF 0064 2 NQF 0061 3 Title: Diabetes: Hemoglobin A1c Poor Control Description: Percentage of patients 18-75 years of age with diabetes (type 1 or type 2) who had hemoglobin A1c > 9.0%. Title:
The NOF & NBHA Quality Improvement Registry
 In collaboration with CECity The NOF & NBHA Quality Improvement Registry This registry is approved by CMS as a Qualified Clinical Data Registry (QCDR) for Eligible Professionals and GPRO Practices for
In collaboration with CECity The NOF & NBHA Quality Improvement Registry This registry is approved by CMS as a Qualified Clinical Data Registry (QCDR) for Eligible Professionals and GPRO Practices for
2017 MSSP Clinical Quality Measures
 *The information contained in this document relies heavily on information supplied by CMS. GPRO CARE-1 (NQF 0097): Medication Reconciliation Post-Discharge DESCRIPTION: Percentage of discharges from any
*The information contained in this document relies heavily on information supplied by CMS. GPRO CARE-1 (NQF 0097): Medication Reconciliation Post-Discharge DESCRIPTION: Percentage of discharges from any
Clinical Quality Measures
 Core Measures Preventive Care and Screening Measure Pair: a. Tobacco Use Assessment, b. Tobacco Cessation Intervention. Percentage of patients aged 18 years and older who have been seen for at least 2
Core Measures Preventive Care and Screening Measure Pair: a. Tobacco Use Assessment, b. Tobacco Cessation Intervention. Percentage of patients aged 18 years and older who have been seen for at least 2
DataDerm Quality Measures
 01 MIPS 224 NQF 0562 DataDerm Quality s Melanoma: Overutilization of Imaging Studies 02 a & b MIPS 138 Melanoma: Coordination of Care 03 MIPS 137 NQF 0650 Melanoma: Continuity of Care Recall System Percentage
01 MIPS 224 NQF 0562 DataDerm Quality s Melanoma: Overutilization of Imaging Studies 02 a & b MIPS 138 Melanoma: Coordination of Care 03 MIPS 137 NQF 0650 Melanoma: Continuity of Care Recall System Percentage
Date Modified: May 29, Clinical Quality Measures for PQRS
 Date Modified: May 29, 2014 Clinical Quality s for PQRS # Domain Type Denominator Numerator Denominator Exclusions/Exceptions Rationale QCDR-1 QCDR-2 Patient Safety 102 Efficiency and Cost Reduction QCDR-3
Date Modified: May 29, 2014 Clinical Quality s for PQRS # Domain Type Denominator Numerator Denominator Exclusions/Exceptions Rationale QCDR-1 QCDR-2 Patient Safety 102 Efficiency and Cost Reduction QCDR-3
2016 General Practice/Family Practice Preferred Specialty Measure Set
 1 0059 5 0081 41 N/A 50 N/A 65 0069, EHR 66 0002, EHR Effective Clinical Care Effective Clinical Care Effective Clinical Care Diabetes: Hemoglobin A1c (HbA1c) Poor Control (>9%): Percentage of patients
1 0059 5 0081 41 N/A 50 N/A 65 0069, EHR 66 0002, EHR Effective Clinical Care Effective Clinical Care Effective Clinical Care Diabetes: Hemoglobin A1c (HbA1c) Poor Control (>9%): Percentage of patients
Possible Denominator Codes Applicable to OMS * Le Fort Fractures 21346, 21347, 21348, 21422, 21423, 21432, 21433, 21435, 21436
 2015 Individual PQRS s Eligible OMS #22: Perioperative Care: Discontinuation of Prophylactic Antibiotics (Non- Cardiac Procedures) Percentage of noncardiac surgical patients aged 18 years and older undergoing
2015 Individual PQRS s Eligible OMS #22: Perioperative Care: Discontinuation of Prophylactic Antibiotics (Non- Cardiac Procedures) Percentage of noncardiac surgical patients aged 18 years and older undergoing
CLINICAL QUALITY MEASURES Stage 1 Meaningful Use
 CLINICAL QUALITY MEASURES Stage 1 Meaningful Use * Eligible professionals (EPs) must report on 3 required core clinical quality measures (CQMs). If the denominator of 1 or more of the required core measures
CLINICAL QUALITY MEASURES Stage 1 Meaningful Use * Eligible professionals (EPs) must report on 3 required core clinical quality measures (CQMs). If the denominator of 1 or more of the required core measures
NQF Measure Number & PQRI Implementation Number
 Title NQF Steward s Adult Weight Screening and Follow-Up Hypertension: Blood Pressure ment Preventive Care and Screening Pair: a. Tobacco Use Assessment, b. Tobacco Cessation Intervention with a calculated
Title NQF Steward s Adult Weight Screening and Follow-Up Hypertension: Blood Pressure ment Preventive Care and Screening Pair: a. Tobacco Use Assessment, b. Tobacco Cessation Intervention with a calculated
For Electronic Measure Specification Information go to:
 Diabetes Recognition NQF 0421 PQRI 128 Title: Adult Weight Screening and Follow-Up Description: Percentage of patients aged 18 years and older with a calculated BMI in the past six months or during the
Diabetes Recognition NQF 0421 PQRI 128 Title: Adult Weight Screening and Follow-Up Description: Percentage of patients aged 18 years and older with a calculated BMI in the past six months or during the
2016 Cross-Cutting Measure Set
 1 0059 Diabetes: Hemoglobin A1c Poor Control: Percentage of patients 18-75 years of age with diabetes who had hemoglobin A1c > 9.0% during the 46 0097 Claims, Registry Medication Reconciliation Post Discharge:
1 0059 Diabetes: Hemoglobin A1c Poor Control: Percentage of patients 18-75 years of age with diabetes who had hemoglobin A1c > 9.0% during the 46 0097 Claims, Registry Medication Reconciliation Post Discharge:
American College of Physicians Genesis Registry
 Powered by Premier American College of Physicians Genesis Registry This registry has been approved by CMS as a Qualified Clinical Data Registry (QCDR) for Eligible Clinicians and group practices for the
Powered by Premier American College of Physicians Genesis Registry This registry has been approved by CMS as a Qualified Clinical Data Registry (QCDR) for Eligible Clinicians and group practices for the
The Renal Physicians Association Quality Improvement Registry
 In collaboration with CECity The Renal Physicians Association Quality Improvement Registry This registry is approved by CMS as a Qualified Clinical Data Registry (QCDR) for Eligible Professionals and GPRO
In collaboration with CECity The Renal Physicians Association Quality Improvement Registry This registry is approved by CMS as a Qualified Clinical Data Registry (QCDR) for Eligible Professionals and GPRO
American College of Physicians Genesis Registry
 Powered by Premier American College of Physicians Genesis Registry This registry has been approved by CMS as a Qualified Clinical Data Registry (QCDR) for Eligible Clinicians and group practices for the
Powered by Premier American College of Physicians Genesis Registry This registry has been approved by CMS as a Qualified Clinical Data Registry (QCDR) for Eligible Clinicians and group practices for the
Consensus Core Set: ACO and PCMH / Primary Care Measures Version 1.0
 Consensus Core Set: ACO and PCMH / Primary Care s 0018 Controlling High Blood Pressure patients 18 to 85 years of age who had a diagnosis of hypertension (HTN) and whose blood pressure (BP) was adequately
Consensus Core Set: ACO and PCMH / Primary Care s 0018 Controlling High Blood Pressure patients 18 to 85 years of age who had a diagnosis of hypertension (HTN) and whose blood pressure (BP) was adequately
Table 1. Proposed Measures for Use in Establishing Quality Performance Standards that ACOs Must Meet for Shared Savings
 CMS-1345-P 174 Table 1. Proposed Measures for Use in Establishing Quality Performance Standards that ACOs Must Meet for Shared Savings AIM: Better Care for Individuals 1. Patient/Care Giver Experience
CMS-1345-P 174 Table 1. Proposed Measures for Use in Establishing Quality Performance Standards that ACOs Must Meet for Shared Savings AIM: Better Care for Individuals 1. Patient/Care Giver Experience
ADDITIONAL INFORMATION REGARDING EP CLINICAL QUALITY MEASURES FOR 2014 EHR INCENTIVE PROGRAMS
 ADDITIONAL INFORMATION REGARDING EP CLINICAL QUALITY MEASURES FOR 2014 EHR INCENTIVE PROGRAMS The table below entitled Clinical s for 2014 CMS EHR Incentive Programs for Eligible Professionals contains
ADDITIONAL INFORMATION REGARDING EP CLINICAL QUALITY MEASURES FOR 2014 EHR INCENTIVE PROGRAMS The table below entitled Clinical s for 2014 CMS EHR Incentive Programs for Eligible Professionals contains
2017 CMS Web Interface Reporting
 2017 CMS Web Interface Reporting Measure Specification Review May 18, 2017 Sherry Grund, Telligen Mary Schrader, Telligen Medicare Shared Savings Program and Next Generation ACO Model DISCLAIMER This presentation
2017 CMS Web Interface Reporting Measure Specification Review May 18, 2017 Sherry Grund, Telligen Mary Schrader, Telligen Medicare Shared Savings Program and Next Generation ACO Model DISCLAIMER This presentation
Comprehensive ESRD Care (CEC) Model Proposed Quality Measures for Public Comment. Table of Contents
 Comprehensive ESRD Care (CEC) Model Proposed Quality s for Public Comment Table of Contents Page # Introduction 3 Summaries by Domain Technical Expert Panel Recommended CEC Quality s 4 s that were recommended
Comprehensive ESRD Care (CEC) Model Proposed Quality s for Public Comment Table of Contents Page # Introduction 3 Summaries by Domain Technical Expert Panel Recommended CEC Quality s 4 s that were recommended
2017 Eligible Measure Applicability (EMA) for Claims Data Submission of Individual Quality Measures
 2017 Eligible Measure Applicability (EMA) for Claims Data Submission of Individual Quality Measures QPP Clinically Related Measures Analysis Used in EMA Step 1: Clinical Relation including an Outcome/High
2017 Eligible Measure Applicability (EMA) for Claims Data Submission of Individual Quality Measures QPP Clinically Related Measures Analysis Used in EMA Step 1: Clinical Relation including an Outcome/High
PQRS in TRAKnet 2015 GUIDE TO SUBMIT TING AND REPORTING PQRS IN 2015 THROUGH TRAKNET
 PQRS in TRAKnet 2015 GUIDE TO SUBMITTING AND REPORTING PQRS IN 2015 THROUGH TRAKNET What is PQRS? PQRS is a quality reporting program that uses negative payment adjustments to promote reporting of quality
PQRS in TRAKnet 2015 GUIDE TO SUBMITTING AND REPORTING PQRS IN 2015 THROUGH TRAKNET What is PQRS? PQRS is a quality reporting program that uses negative payment adjustments to promote reporting of quality
Meaningful Use Criteria for Pediatric Providers
 SET OF CRITERIA - 15 REQUIRED These 15 core criteria are called the core set and are required elements for demonstrating meaningful use. This document was prepared for pediatric providers so language pertaining
SET OF CRITERIA - 15 REQUIRED These 15 core criteria are called the core set and are required elements for demonstrating meaningful use. This document was prepared for pediatric providers so language pertaining
Meaningful Use for Eligible Providers
 Meaningful Use for Eligible Providers Summary of Core and Menu objectives and Clinical Quality s Healthcare Technical Assistance Program, March 11, 2011 V.1.0Copyright 2011, Purdue Research Foundation
Meaningful Use for Eligible Providers Summary of Core and Menu objectives and Clinical Quality s Healthcare Technical Assistance Program, March 11, 2011 V.1.0Copyright 2011, Purdue Research Foundation
proposed set to a required subset of 3 to 5 measures based on the availability of electronic
 CMS-0033-P 143 proposed set to a required subset of 3 to 5 measures based on the availability of electronic measure specifications and comments received. We propose to require for 2011 and 2012 that EP's
CMS-0033-P 143 proposed set to a required subset of 3 to 5 measures based on the availability of electronic measure specifications and comments received. We propose to require for 2011 and 2012 that EP's
Validating and Reporting the 2017 ACO Clinical Measures (Version 1)
 Validating and Reporting the 2017 ACO Clinical Measures Author: Ben Fouts, Informatics Redwood Community Health Coalition 1310 Redwood Way Petaluma, California 94954 support@rchc.net Document Last Updated:
Validating and Reporting the 2017 ACO Clinical Measures Author: Ben Fouts, Informatics Redwood Community Health Coalition 1310 Redwood Way Petaluma, California 94954 support@rchc.net Document Last Updated:
QUALIFIED CLINICAL DATA REGISTRY (QCDR) 2017 MEASURE SPECIFICATIONS
 QOPI5 Chemotherapy administered to patients with metastatic solid tumor with performance status of 3, 4, or undocumented (Lower Score - Better) Percentage of adult patients with metastatic solid tumors
QOPI5 Chemotherapy administered to patients with metastatic solid tumor with performance status of 3, 4, or undocumented (Lower Score - Better) Percentage of adult patients with metastatic solid tumors
MEASURING CARE QUALITY
 MEASURING CARE QUALITY Region December 2013 For Clinical Effectiveness of Care Measures of Performance From: Healthcare Effectiveness Data and Information Set (HEDIS ) HEDIS is a set of standardized performance
MEASURING CARE QUALITY Region December 2013 For Clinical Effectiveness of Care Measures of Performance From: Healthcare Effectiveness Data and Information Set (HEDIS ) HEDIS is a set of standardized performance
2017 CMS Quality Reporting - ABSTRACTION PROCESS OVERVIEW
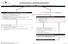 2017 CMS Quality Reporting - ABSTRACTION PROCESS OVERVIEW REMEMBER! Abstract only those cases belonging to your ACO and use only MiShare (https://mishare.med.umich.edu/) when communicating PHI! STEP 1:
2017 CMS Quality Reporting - ABSTRACTION PROCESS OVERVIEW REMEMBER! Abstract only those cases belonging to your ACO and use only MiShare (https://mishare.med.umich.edu/) when communicating PHI! STEP 1:
MEASURE SPECIFICATIONS
 QOPI REPTING REGISTRY (QCDR) 2018 QOPI 5 QOPI 11 Chemotherapy administered to patients with metastatic solid tumor with performance status of 3, 4, or undocumented (Lower Score - Better) Combination chemotherapy
QOPI REPTING REGISTRY (QCDR) 2018 QOPI 5 QOPI 11 Chemotherapy administered to patients with metastatic solid tumor with performance status of 3, 4, or undocumented (Lower Score - Better) Combination chemotherapy
MEASURE SPECIFICATIONS
 QOPI REPTING REGISTRY (QCDR) 2018 QOPI5 Title Chemotherapy administered to patients with metastatic solid tumor with performance status of 3, 4, or undocumented (Lower Score - Better) Description Percentage
QOPI REPTING REGISTRY (QCDR) 2018 QOPI5 Title Chemotherapy administered to patients with metastatic solid tumor with performance status of 3, 4, or undocumented (Lower Score - Better) Description Percentage
Preferred Care Partners. HEDIS Technical Standards
 Preferred Care Partners HEDIS Technical Standards 1 HEDIS What is HEDIS HEDIS Overview Adults HEDIS Overview Pediatrics HEDIS is a registered trademark of the National Committee for Quality Assurance 2
Preferred Care Partners HEDIS Technical Standards 1 HEDIS What is HEDIS HEDIS Overview Adults HEDIS Overview Pediatrics HEDIS is a registered trademark of the National Committee for Quality Assurance 2
Compass PTN Core Measures
 Compass PTN Core Measures emeasure ID: CMS122v5 NQF: 0059 QualityID: 001 Diabetes: Hemoglobin A1c (HbA1c) Poor Control (>9%) Patients 18-75 years of age with diabetes with a visit during the measurement
Compass PTN Core Measures emeasure ID: CMS122v5 NQF: 0059 QualityID: 001 Diabetes: Hemoglobin A1c (HbA1c) Poor Control (>9%) Patients 18-75 years of age with diabetes with a visit during the measurement
CMS-5522-FC TABLE C.1: MIPS Measures Finalized for Removal Only from Specialty Sets for the 2018 Performance Period and Future Years
 CMS-5522-FC 1569 MIPS s Finalized for Removal Only from Sets for the 2018 Performance Period and Future Years Note: In the CY 2018 Payment Program proposed rule (82 FR 30455 through 30462), CMS proposed
CMS-5522-FC 1569 MIPS s Finalized for Removal Only from Sets for the 2018 Performance Period and Future Years Note: In the CY 2018 Payment Program proposed rule (82 FR 30455 through 30462), CMS proposed
HEDIS 2014 MQIC MEASURES SUMMARY LISTING FOR ANNUAL PERFORMANCE REPORTING
 HEDIS 2014 MQIC MEASURES SUMMARY LISTING FOR ANNUAL PERFORMANCE REPORTING DIABETES 1. Comprehensive Diabetes Care (CDC): Percentage of members 18-75 years of age with diabetes (type 1 and type 2) who had
HEDIS 2014 MQIC MEASURES SUMMARY LISTING FOR ANNUAL PERFORMANCE REPORTING DIABETES 1. Comprehensive Diabetes Care (CDC): Percentage of members 18-75 years of age with diabetes (type 1 and type 2) who had
2014 Oncology Measures Group Overview
 2014 Oncology Measures Group Overview The Oncology Measures Group is a reporting option that significantly reduces the burden of participation in the Physician Quality Reporting System (PQRS). Source:
2014 Oncology Measures Group Overview The Oncology Measures Group is a reporting option that significantly reduces the burden of participation in the Physician Quality Reporting System (PQRS). Source:
2017 HEDIS Measures. PREVENTIVE SCREENING 2017 Measure Quality Indicator
 PREVENTIVE SCREENING Childhood Immunization Children who turn 2 during the Adolescent Immunization Adolescents who turn 13 during the Lead Screening Children who turn 2 during the Breast Cancer Screening
PREVENTIVE SCREENING Childhood Immunization Children who turn 2 during the Adolescent Immunization Adolescents who turn 13 during the Lead Screening Children who turn 2 during the Breast Cancer Screening
2012 Core Measures. Acute Myocardial Infarction (AMI)
 2012 Core Measures Acute Myocardial Infarction (AMI) Aspirin at Arrival Aspirin Prescribed at Discharge Angiotensin converting enzyme inhibitor (ACEI) or angiotensin receptor blocker (ARB) for left ventricular
2012 Core Measures Acute Myocardial Infarction (AMI) Aspirin at Arrival Aspirin Prescribed at Discharge Angiotensin converting enzyme inhibitor (ACEI) or angiotensin receptor blocker (ARB) for left ventricular
Program Metrics. New Unique ID. Old Unique ID. Metric Set Metric Name Description. Old Metric Name
 Program Metrics The list below includes the metrics that will be calculated by the PINNACLE Registry for the outpatient office setting. These include metrics for, Atrial Fibrillation, Hypertension and.
Program Metrics The list below includes the metrics that will be calculated by the PINNACLE Registry for the outpatient office setting. These include metrics for, Atrial Fibrillation, Hypertension and.
New PINNACLE Measures The below measures for PINNACLE will be added as new measures to the outcomes reporting starting with Version 2.0.
 New PINNACLE Measures The below measures for PINNACLE will be added as new measures to the outcomes reporting starting with Version 2.0. Measure Steward Measure Name Measure Description Rationale for Adding
New PINNACLE Measures The below measures for PINNACLE will be added as new measures to the outcomes reporting starting with Version 2.0. Measure Steward Measure Name Measure Description Rationale for Adding
2018 MIPS Reporting Family Medicine
 2018 MIPS Reporting Family Medicine Quality Reporting Requirements: Report on 6 quality measures or a specialty measure set Include at least ONE outcome or high-priority measure Report on patients of All-Payers
2018 MIPS Reporting Family Medicine Quality Reporting Requirements: Report on 6 quality measures or a specialty measure set Include at least ONE outcome or high-priority measure Report on patients of All-Payers
2016 Physician Quality Reporting System Data Collection Form: Chronic Obstructive Pulmonary Disease (COPD) (for patients aged 18 and older)
 2016 Physician Quality Reporting System Data Collection Form: Chronic Obstructive Pulmonary Disease (COPD) (for patients aged 18 and older) IMPORTANT: Any measure with a 0% performance rate (100% for inverse
2016 Physician Quality Reporting System Data Collection Form: Chronic Obstructive Pulmonary Disease (COPD) (for patients aged 18 and older) IMPORTANT: Any measure with a 0% performance rate (100% for inverse
HEDIS 2017 MQIC MEASURES SUMMARY LISTING FOR ANNUAL PERFORMANCE REPORTING
 HEDIS 2017 MQIC MEASURES SUMMARY LISTING FOR ANNUAL PERFORMANCE REPORTING ATTENTION-DEFICIT/HYPERACTIVITY DISORDER 1. Follow-up Care for Children Prescribed ADHD Medication (ADD) Percent children newly
HEDIS 2017 MQIC MEASURES SUMMARY LISTING FOR ANNUAL PERFORMANCE REPORTING ATTENTION-DEFICIT/HYPERACTIVITY DISORDER 1. Follow-up Care for Children Prescribed ADHD Medication (ADD) Percent children newly
March 31, Dear colleagues,
 6300 North River Road Rosemont, IL 60018 p: 847-292-0530 f: 847-292-0531 www.ajrr.net March 31, 2014 Dear colleagues, The American Joint Replacement Registry (AJRR) has submitted materials to be considered
6300 North River Road Rosemont, IL 60018 p: 847-292-0530 f: 847-292-0531 www.ajrr.net March 31, 2014 Dear colleagues, The American Joint Replacement Registry (AJRR) has submitted materials to be considered
2017 Eligible Measure Applicability (EMA) for Registry Data Submission of Individual Quality Measures
 2017 Eligible Measure Applicability (EMA) for Registry Data Submission of Individual Quality Measures 07/17/2017 Page 1 of 10 QPP Clinically Related Measure Analysis Used in EMA Clinical Relation including
2017 Eligible Measure Applicability (EMA) for Registry Data Submission of Individual Quality Measures 07/17/2017 Page 1 of 10 QPP Clinically Related Measure Analysis Used in EMA Clinical Relation including
Practice-Level Executive Summary Report
 PINNACLE Registry Metrics 0003, Test Practice_NextGen [Rolling: 1st April 2015 to 31st March 2016 ] Generated on 5/11/2016 11:37:35 AM American College of Cardiology Foundation National Cardiovascular
PINNACLE Registry Metrics 0003, Test Practice_NextGen [Rolling: 1st April 2015 to 31st March 2016 ] Generated on 5/11/2016 11:37:35 AM American College of Cardiology Foundation National Cardiovascular
2017 CMS Web Interface Reporting
 2017 CMS Web Interface Reporting Keys to Successful Reporting Part 2 Measures Refresher November 27, 2017 1:30 3:00 p.m. ET Sherry Grund, Telligen Mary Schrader, Telligen Medicare Shared Savings Program
2017 CMS Web Interface Reporting Keys to Successful Reporting Part 2 Measures Refresher November 27, 2017 1:30 3:00 p.m. ET Sherry Grund, Telligen Mary Schrader, Telligen Medicare Shared Savings Program
WCHQ MEASURES AT A GLANCE
 WCHQ Ambulatory Measures NOTE: s of Tobacco Non-Use and Daily Aspirin or Other Anticoagulant will be added to the Measure in 2014. A1C Blood Sugar A1C Blood Sugar Kidney Function Monitored Blood Pressure
WCHQ Ambulatory Measures NOTE: s of Tobacco Non-Use and Daily Aspirin or Other Anticoagulant will be added to the Measure in 2014. A1C Blood Sugar A1C Blood Sugar Kidney Function Monitored Blood Pressure
UCLA Health System Apr - Jun 2013 (Q2)
 Denom Observed VBP Standard VBP Benchmark Denom Observed VBP Standard VBP Benchmark N Percent x/n N Percent x/n Value Based Purchasing-Clinical Process of Care Measures (%) SCIP-Inf-9 Urinary catheter
Denom Observed VBP Standard VBP Benchmark Denom Observed VBP Standard VBP Benchmark N Percent x/n N Percent x/n Value Based Purchasing-Clinical Process of Care Measures (%) SCIP-Inf-9 Urinary catheter
2014 Clinical Quality Measures: Changes for the Medicaid EHR Incentive Program. Tracy McDonald Medicaid EHR Incentive Program Coordinator
 2014 Clinical Quality Measures: Changes for the Medicaid EHR Incentive Program Tracy McDonald Medicaid EHR Incentive Program Coordinator Agenda Why are Clinical Quality Measures important? Clinical Quality
2014 Clinical Quality Measures: Changes for the Medicaid EHR Incentive Program Tracy McDonald Medicaid EHR Incentive Program Coordinator Agenda Why are Clinical Quality Measures important? Clinical Quality
OCHSNER PHYSICIAN PARTNERS. PQRS Measures by Specialty (FINAL)
 OCHSNER PHYSICIAN PARTNERS PQRS Measures by Specialty (FINAL) Allergy and Immunology 2. Asthma: Pharmacologic Therapy for Persistent Asthma - Ambulatory Care Setting (PQRS 53) 3. Patients aged 18 years
OCHSNER PHYSICIAN PARTNERS PQRS Measures by Specialty (FINAL) Allergy and Immunology 2. Asthma: Pharmacologic Therapy for Persistent Asthma - Ambulatory Care Setting (PQRS 53) 3. Patients aged 18 years
2017 Merit-based Incentive Payment System. Avoiding the Penalty
 2017 Merit-based Incentive Payment System Avoiding the Penalty 1 What is the Quality Reporting Program? Quality Payment Program (also known as MACRA) Advanced Alternative Payment Models (APMs) Merit-based
2017 Merit-based Incentive Payment System Avoiding the Penalty 1 What is the Quality Reporting Program? Quality Payment Program (also known as MACRA) Advanced Alternative Payment Models (APMs) Merit-based
WCHQ MEASURES AT A GLANCE
 WCHQ Ambulatory Measures A1C Blood Sugar Testing A1C Blood Sugar Control Patients with diabetes Patients with diabetes office visit in. Gestational Diabetes (code 648.8) is office visit in. Compliance
WCHQ Ambulatory Measures A1C Blood Sugar Testing A1C Blood Sugar Control Patients with diabetes Patients with diabetes office visit in. Gestational Diabetes (code 648.8) is office visit in. Compliance
IHA P4P Measure Manual Measure Year Reporting Year 2018
 ADULT PREVENTIVE CARE IHA P4P Measure Manual Measure Year 2017 - Reporting Year 2018 *If line of business not labeled, measure is Commercial only Adult BMI (Medicare) 18-74 Medicare members ages 18-74
ADULT PREVENTIVE CARE IHA P4P Measure Manual Measure Year 2017 - Reporting Year 2018 *If line of business not labeled, measure is Commercial only Adult BMI (Medicare) 18-74 Medicare members ages 18-74
SUNY Downstate Medical Center/University Hospital Oct - Dec 2013 (Q4)
 Value Based Purchasing-Clinical Process of Care Measures Denom Observed VBP VBP Benchmark Standard Denom Observed VBP VBP Benchmark Standard N Percent x/n N Percent x/n SCIP-Inf-9 Urinary catheter removed
Value Based Purchasing-Clinical Process of Care Measures Denom Observed VBP VBP Benchmark Standard Denom Observed VBP VBP Benchmark Standard N Percent x/n N Percent x/n SCIP-Inf-9 Urinary catheter removed
Oncology Quality Clinical Data Registry
 Oncology Quality Clinical Data Registry Powered by Premier Inc. This registry has been approved by CMS as a Qualified Clinical Data Registry (QCDR) for eligible clinicians and group practices for the 2019
Oncology Quality Clinical Data Registry Powered by Premier Inc. This registry has been approved by CMS as a Qualified Clinical Data Registry (QCDR) for eligible clinicians and group practices for the 2019
SCORES FOR 4 TH QUARTER, RD QUARTER, 2014
 SCORES FOR 4 TH QUARTER, 2013 3 RD QUARTER, 2014 PATIENT SATISFACTION SCORES (HCAHPS): 4 STARS OUT OF 5 (ONLY 4 AREA ACUTE CARE HOSPITALS RECEIVED A 4-STAR RATING. NONE ACHIEVED 5-STARS). STRUCTURAL MEASURES:
SCORES FOR 4 TH QUARTER, 2013 3 RD QUARTER, 2014 PATIENT SATISFACTION SCORES (HCAHPS): 4 STARS OUT OF 5 (ONLY 4 AREA ACUTE CARE HOSPITALS RECEIVED A 4-STAR RATING. NONE ACHIEVED 5-STARS). STRUCTURAL MEASURES:
2010 Physician Quality Reporting Initiative Measures Groups Specifications Manual
 2010 Physician Quality Reporting Initiative Measures Groups Specifications Manual This manual contains specific guidance for reporting 2010 Physician Quality Reporting Initiative (PQRI) Measures Groups.
2010 Physician Quality Reporting Initiative Measures Groups Specifications Manual This manual contains specific guidance for reporting 2010 Physician Quality Reporting Initiative (PQRI) Measures Groups.
End-Stage Renal Disease Quality Incentive Program (ESRD QIP) Status Type NQF Measure Title
 End-Stage Renal Disease Quality Incentive Program (ESRD QIP) Status Type NQF Measure Title NQF Status ID Implemented Outcome 1454 Proportion of patients with hypercalcemia 0256 Vascular Access Type Catheter
End-Stage Renal Disease Quality Incentive Program (ESRD QIP) Status Type NQF Measure Title NQF Status ID Implemented Outcome 1454 Proportion of patients with hypercalcemia 0256 Vascular Access Type Catheter
Quality Performance Measures. (Starter Set)
 Quality Performance Measures (Starter Set) 1 Contents ADMINISTRATIVE MEASURES.4 HEART AND VASCULAR 5 Cardiology.5 Cardiovascular Surgery 5 Vascular..5 HOSPITAL CLINICAL SERVICES.6 Pathology 6 Radiation
Quality Performance Measures (Starter Set) 1 Contents ADMINISTRATIVE MEASURES.4 HEART AND VASCULAR 5 Cardiology.5 Cardiovascular Surgery 5 Vascular..5 HOSPITAL CLINICAL SERVICES.6 Pathology 6 Radiation
Prostate Cancer Dashboard
 Process Risk Assessment Risk assessment: family history assessment of family history of prostate cancer Best Observed: 97 %1 ; Ideal Benchmark:100% measure P8 2 Process Appropriateness of Care Pre-treatment
Process Risk Assessment Risk assessment: family history assessment of family history of prostate cancer Best Observed: 97 %1 ; Ideal Benchmark:100% measure P8 2 Process Appropriateness of Care Pre-treatment
2017 CMS Quality Reporting - ABSTRACTION PROCESS OVERVIEW
 2017 CMS Quality Reporting - ABSTRACTION PROCESS OVERVIEW STEP 1 - Can you locate the patient's medical record? YES? Proceed to STEP 2 NO? Perform the following actions : Contact the appropriate QROs for
2017 CMS Quality Reporting - ABSTRACTION PROCESS OVERVIEW STEP 1 - Can you locate the patient's medical record? YES? Proceed to STEP 2 NO? Perform the following actions : Contact the appropriate QROs for
ISCHEMIC VASCULAR DISEASE (IVD) MEASURES GROUP OVERVIEW
 ISCHEMIC VASCULAR DISEASE (IVD) MEASURES GROUP OVERVIEW 2014 PQRS OPTIONS F MEASURES GROUPS: 2014 PQRS MEASURES IN ISCHEMIC VASCULAR DISEASE (IVD) MEASURES GROUP: #204. Ischemic Vascular Disease (IVD):
ISCHEMIC VASCULAR DISEASE (IVD) MEASURES GROUP OVERVIEW 2014 PQRS OPTIONS F MEASURES GROUPS: 2014 PQRS MEASURES IN ISCHEMIC VASCULAR DISEASE (IVD) MEASURES GROUP: #204. Ischemic Vascular Disease (IVD):
Cancer Endorsement Maintenance 2011-Maintenance Measures
 Measure Number Title Description Measure Steward 0210 Proportion receiving chemotherapy in the last 14 days of life 0211 Proportion with more than one emergency room visit in the last days of life 0212
Measure Number Title Description Measure Steward 0210 Proportion receiving chemotherapy in the last 14 days of life 0211 Proportion with more than one emergency room visit in the last days of life 0212
TABLE E: 2017 Finalized MIPS Specialty Measure Sets
 TABLE E: 2017 Finalized MIPS Specialty Sets [Discussion of S approach to adding previously identified cross-cutting measures to specialty measure sets.] E- ID Title and Description Steward 1. Allergy/Immunology
TABLE E: 2017 Finalized MIPS Specialty Sets [Discussion of S approach to adding previously identified cross-cutting measures to specialty measure sets.] E- ID Title and Description Steward 1. Allergy/Immunology
2011 Physician Quality Reporting System Measures for Consideration by Oncology Providers: Cancer Care Measures
 2011 Physician Quality Reporting System Measures for Consideration by Oncology Providers: Cancer Care Measures The table below includes measures directly relevant to oncology providers as well as general
2011 Physician Quality Reporting System Measures for Consideration by Oncology Providers: Cancer Care Measures The table below includes measures directly relevant to oncology providers as well as general
Certified Health IT Transparency and Disclosure Information 2014 Edition
 Certified Health IT Transparency and Disclosure Information 2014 Edition 2015 Edition Certified Health IT Transparency and Disclosure Information I. Disclaimer This Complete EHR is 2014 Edition compliant
Certified Health IT Transparency and Disclosure Information 2014 Edition 2015 Edition Certified Health IT Transparency and Disclosure Information I. Disclaimer This Complete EHR is 2014 Edition compliant
2014 ACO GPRO Audit What this means for your practice. Sheree M. Arnold ACO Clinical Transformation Specialist
 2014 ACO GPRO Audit What this means for your practice Sheree M. Arnold ACO Clinical Transformation Specialist Agenda Catholic Medical Partners ACO overview Attribution and sampling of patients ACO quality
2014 ACO GPRO Audit What this means for your practice Sheree M. Arnold ACO Clinical Transformation Specialist Agenda Catholic Medical Partners ACO overview Attribution and sampling of patients ACO quality
MEASURING CARE QUALITY
 MEASURING CARE QUALITY Region November 2016 For Clinical Effectiveness of Care Measures of Performance From: Healthcare Effectiveness Data and Information Set (HEDIS ) HEDIS is a set of standardized performance
MEASURING CARE QUALITY Region November 2016 For Clinical Effectiveness of Care Measures of Performance From: Healthcare Effectiveness Data and Information Set (HEDIS ) HEDIS is a set of standardized performance
Measure Applications Partnership. Hospital Workgroup In-Person Meeting Follow- Up Call
 Measure Applications Partnership Hospital Workgroup In-Person Meeting Follow- Up Call December 21, 2016 Feedback on Current Measure Sets for IQR, HACs, Readmissions, and VBP 2 Previously Identified Crosscutting
Measure Applications Partnership Hospital Workgroup In-Person Meeting Follow- Up Call December 21, 2016 Feedback on Current Measure Sets for IQR, HACs, Readmissions, and VBP 2 Previously Identified Crosscutting
2018 Quality Payment Program (QPP) Merit-Based Incentive Payment System (MIPS) - ABSTRACTION PROCESS OVERVIEW
 2018 Quality Payment Program (QPP) Merit-Based Incentive Payment System (MIPS) - ABSTRACTION PROCESS OVERVIEW STEP 1 Can you locate the patient's medical record? STEP 2 During CY 2018, was the patient
2018 Quality Payment Program (QPP) Merit-Based Incentive Payment System (MIPS) - ABSTRACTION PROCESS OVERVIEW STEP 1 Can you locate the patient's medical record? STEP 2 During CY 2018, was the patient
Overview of Current Quality Measures that can be Impacted by Ambulatory Pharmacists
 Overview of Current Quality Measures that can be Impacted by Ambulatory Pharmacists Measure Name Measure Domain Measure Focus Comment/Explanation CMS Value-based Purchasing Program (CMS VBP) AMI 30-day
Overview of Current Quality Measures that can be Impacted by Ambulatory Pharmacists Measure Name Measure Domain Measure Focus Comment/Explanation CMS Value-based Purchasing Program (CMS VBP) AMI 30-day
N E R U C Using Certified Electronic Health Record (EHR) Technology to: Improve quality, safety, efficiency, and care coordination
 Due to a last minute ruling on 10/16/2015 O eb K O IS R U C Y L T N E R I 10.14.2014 D I L A V N Meaningful Use IS - Interactive Training Guide TH Using Certified Electronic Health Record (EHR) Technology
Due to a last minute ruling on 10/16/2015 O eb K O IS R U C Y L T N E R I 10.14.2014 D I L A V N Meaningful Use IS - Interactive Training Guide TH Using Certified Electronic Health Record (EHR) Technology
Improving Quality of Care for Medicare Patients: Accountable Care Organizations
 DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services Room 352-G 200 Independence Avenue, SW Washington, DC 20201 Office of Media Affairs MEDICARE FACT SHEET FOR IMMEDIATE RELEASE
DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services Room 352-G 200 Independence Avenue, SW Washington, DC 20201 Office of Media Affairs MEDICARE FACT SHEET FOR IMMEDIATE RELEASE
Individual Quality Measures Applicable to Eligible OMS-MPFS Final Rule 2019
 Individual s Applicable to Eligible OMS-MPFS Final Rule 2019 Indicator* Codes (Patient Safety #21: Perioperative Care: Selection of Prophylactic Antibiotic First Second Generation Cephalospori n National
Individual s Applicable to Eligible OMS-MPFS Final Rule 2019 Indicator* Codes (Patient Safety #21: Perioperative Care: Selection of Prophylactic Antibiotic First Second Generation Cephalospori n National
CMS Hospital IQR Program Measure Comparison Tables FY 2018 (CY 2016) Measures Required to Meet Hospital IQR APU Requirements NHSN Submission
 CMS IQR Program Measure Comparison Tables (CY 2016) NHSN Submission CLABSI Central Line-Associated Bloodstream Infection (CLABSI) Required NHSN CAUTI Catheter-Associated Urinary Tract Infection (CAUTI)
CMS IQR Program Measure Comparison Tables (CY 2016) NHSN Submission CLABSI Central Line-Associated Bloodstream Infection (CLABSI) Required NHSN CAUTI Catheter-Associated Urinary Tract Infection (CAUTI)
Performance and Quality Measures 1. NQF Measure Number. Coronary Artery Disease Measure Set
 Unless indicated, the PINNACLE Registry measures are endorsed by the American College of Cardiology Foundation and the American Heart Association and may be used for purposes of health care insurance payer
Unless indicated, the PINNACLE Registry measures are endorsed by the American College of Cardiology Foundation and the American Heart Association and may be used for purposes of health care insurance payer
Quality Care Plus 2015 Primary Care Physician Incentive Program. Now includes Medicare patients!
 Quality Care Plus 2015 Primary Care Physician Incentive Program Now includes Medicare patients! Health Partners Plans (HPP) would like to express our appreciation for the invaluable role our primary care
Quality Care Plus 2015 Primary Care Physician Incentive Program Now includes Medicare patients! Health Partners Plans (HPP) would like to express our appreciation for the invaluable role our primary care
2013 Physician Quality Reporting System (PQRS) Measures Groups Specifications Manual
 2013 Physician Quality Reporting System (PQRS) Measures Groups Specifications Manual 12/19/2012 CPT only copyright 2012 American Medical Association. All rights reserved. CPT is a registered trademark
2013 Physician Quality Reporting System (PQRS) Measures Groups Specifications Manual 12/19/2012 CPT only copyright 2012 American Medical Association. All rights reserved. CPT is a registered trademark
2014 Physician Quality Reporting System Data Collection Form: Oncology (for patients aged 18 and older)
 2014 Physician Quality Reporting System Data Collection Form: Oncology (for patients aged 18 and older) Physician Name: Patient Name: Last First MI Date of Birth: / / mm dd yyyy Gender: M F Medical Record
2014 Physician Quality Reporting System Data Collection Form: Oncology (for patients aged 18 and older) Physician Name: Patient Name: Last First MI Date of Birth: / / mm dd yyyy Gender: M F Medical Record
What Is Prostate Cancer? Prostate cancer is the development of cancer cells in the prostate gland (a gland that produces fluid for semen).
 What Is Prostate Cancer? Prostate cancer is the development of cancer cells in the prostate gland (a gland that produces fluid for semen). It is a very common cancer in men; some cancers grow very slowly,
What Is Prostate Cancer? Prostate cancer is the development of cancer cells in the prostate gland (a gland that produces fluid for semen). It is a very common cancer in men; some cancers grow very slowly,
NEW JERSEY 2011 HOSPITAL PERFORMANCE REPORT TECHNICAL REPORT: METHODOLOGY RECOMMENDED CARE (PROCESS OF CARE) MEASURES
 NEW JERSEY 2011 HOSPITAL PERFORMANCE REPORT TECHNICAL REPORT: METHODOLOGY RECOMMENDED CARE (PROCESS OF CARE) MEASURES New Jersey Department of Health and Senior Services Health Care Quality Assessment
NEW JERSEY 2011 HOSPITAL PERFORMANCE REPORT TECHNICAL REPORT: METHODOLOGY RECOMMENDED CARE (PROCESS OF CARE) MEASURES New Jersey Department of Health and Senior Services Health Care Quality Assessment
Clinical Quality Measures - Colorado SIM, TCPI
 Clinical Quality s - Colorado SIM, TCPI Aniety AOD Aniety Initiation and Engagement of Alcohol and Other Drug Dependence Treatment Not yet endorsed by 0004 e- - - 137v4 305 General Aniety Disorder GAD-7
Clinical Quality s - Colorado SIM, TCPI Aniety AOD Aniety Initiation and Engagement of Alcohol and Other Drug Dependence Treatment Not yet endorsed by 0004 e- - - 137v4 305 General Aniety Disorder GAD-7
RCCO Quality Indicators Crosswalk
 Aim: Better Care for Individuals (patient s perspective) RCCO Quality Indicators Crosswalk Quality Number 1. Access: timely care, appointments & info Denominator& Numerator ACO patients 18+ Data collection
Aim: Better Care for Individuals (patient s perspective) RCCO Quality Indicators Crosswalk Quality Number 1. Access: timely care, appointments & info Denominator& Numerator ACO patients 18+ Data collection
Appendix 4 Urology Care Pathways
 Appendix 4 Urology Care Pathways Cancer Care Pathways outline the steps and stages in the patient journey from referral through to diagnostics, staging, treatment, follow up, rehabilitation and if applicable
Appendix 4 Urology Care Pathways Cancer Care Pathways outline the steps and stages in the patient journey from referral through to diagnostics, staging, treatment, follow up, rehabilitation and if applicable
