Reproductive organ transplantation: advances and controversies
|
|
|
- Bryan Charles
- 5 years ago
- Views:
Transcription
1 MODERN TRENDS Reproductive organ transplantation: advances and controversies Mohamed A. Bedaiwy, M.D., Ph.D., a Ahmed Y. Shahin, M.D., b and Tommaso Falcone, M.D. a a Department of Obstetrics Gynecology, The Cleveland Clinic Foundation, Cleveland, Ohio; and b Department of Obstetrics and Gynecology, Women s Health Centre, Assiut University, Assiut City, Egypt Objective: To review the advances and controversies in the field of reproductive organ transplantation. Result(s): Although many cancer treatments can damage female reproductive organs, leading to temporary or permanent infertility, recent advances in cancer management have translated into improved patient survival, making preservation of reproductive function a more important priority than ever before. Reproductive organ transplantation represents a new potential treatment for patients facing infertility as a result of cancer treatment. Pregnancies have now been reported from several centers after transplanting fresh and frozen ovarian tissue pieces. The longevity of the graft and its potential long-term complications are unknown. However, it seems clear that the ovarian tissue graft has a shortened life span. Allogeneic reproductive organ transplants are under investigation. Patients must take immunosuppressive medications following heterologus transplantation, and these medications can cause adverse side effects. The effects on the fetus are largely unknown. Conclusion(s): Despite the recent biologic and clinical advances, reproductive organ transplantation remains experimental and controversial. (Fertil Steril Ò 2008;90: Ó2008 by American Society for Reproductive Medicine.) Key Words: Ovarian transplantation, immunosuppression, cryopreservation, uterine transplantation Recent trends in the management of cancer have not only given new hope for survival but also improved quality of life. Women undergoing cancer treatment were advised against pregnancy or urged to undergo medical termination if they were pregnant. Even today there is a lack of awareness of potential fertility preserving options. Recent publications reporting births from ovarian tissue transplantation (1 4) have attached a clinical relevance to a previously academic discussion. Reproductive organ loss or damage includes ovarian insufficiency because of premature failure, exposure to radiotherapy and/or chemotherapy, and systemic and genital tract malignancies that result in organ removal. The ovary is susceptible to permanent damage from a variety of medical treatments. There is a limited endowment of follicles in the ovary at birth, which declines naturally over time (5). The number of patients facing the risk of premature ovarian failure (POF) or loss of their uteri who are seeking out help in preserving their fertility has increased dramatically. There are multiple reasons for this increase, including cancer treatment regimens that have proven successful because of Received August 5, 2008; revised and accepted August 5, M.A.B. has nothing to disclose. A.Y.S. has nothing to disclose. T.F. has nothing to disclose. Reprint requests: Tommaso Falcone, M.D., Department of Obstetrics and Gynecology, A81, The Cleveland Clinic Foundation, 9500 Euclid Avenue, Cleveland, OH (FAX: ; falcont@ccf. org). their aggressive nature. Furthermore, because many women are delaying childbearing, there is a higher probability of encountering patients with a malignancy who have no children and require treatment that is potentially sterilizing. Primary POF is defined as the spontaneous and irreversible cessation of menses before 40 years of age. Abnormal karyotype, translocations, point mutations, ovarian autoimmunity, pelvic infection, cytotoxic drugs, radiotherapy, and ovarian surgery can lead to the failure of follicles to reach maturity, either by exhausting the store of primordial follicles or making them refractory to growth stimuli (6). The disappearance of ovarian follicular endowment is accelerated by exposure to alkylating agents and ionizing radiation. The expanding use of alkylating agents in combination with ionizing radiotherapy is particularly gonadotoxic. When given to premenopausal breast cancer patients, cyclophosphamide, methotrexate, and 5-fluorouracil resulted in ovarian failure with no effect on pituitary and adrenal functions (7). Another catastrophic event in the reproductive life of a woman is the loss of her uterus, secondary to congenital disorders, malignancies, surgery, or accidents. The Mayer-Rokitansky-K uster-hauser syndrome involves vaginal agenesis and variable remnants of uterine tissue; the incidence is 1 per 5,000 female births (8). The syndrome represents the most common cause of vaginal absence and the second most frequent cause of primary amenorrhea (9). Uterine loss is a problem that cannot be overcome in some countries where surrogacy is facing legal and/or social /08/$34.00 Fertility and Sterility â Vol. 90, No. 6, December doi: /j.fertnstert Copyright ª2008 American Society for Reproductive Medicine, Published by Elsevier Inc.
2 prohibitions. However, recent work has investigated the potential for uterine transplantation (10). CANCER AND REPRODUCTION The National Cancer Institute indicated that as of January 2000, almost 10 million Americans were living with a history of cancer (11). Childhood cancer survivors will, by 2010, comprise 1 in 250 young adults in the industrialized world (12).In addition, the overall relative 5-year survival rate improved from 56% to 64% in women and from 56% to 75% children. Moreover, there is a trend toward early detection of malignancies and more aggressive treatment to optimize survival. Chemotherapy The probability of POF after chemotherapy is influenced by the type of chemotherapeutic agents, the cumulative dose of the cytotoxic drugs, and the patient s age at the time of exposure. The type and dose of chemotherapeutic agent influence the progression to ovarian failure, with alkylating agents increasing the risk of POF by a factor of 9 (13). The outcome of the deleterious sterilizing effect of these agents is age sensitive. Growing follicles are more susceptible to cytotoxic agents than are primordial follicles. Once all primordial follicles in the ovary are destroyed, permanent ovarian failure sets in. Using a mathematical model, Faddy and Gosden (14) predicted that POF would set in by the age of 27 years if the germ cell population was reduced by 90% before the age of 14 years. Cyclophosphamide is the agent most commonly implicated in damaging oocytes and granulosa cells in a dose-dependent manner (15 18). Doses of 5, 9, and 20 g can cause complete amenorrhoea in women over 40, years, and years of age, respectively (19). There was a fourfold increased risk of POF in teenagers treated for cancer with an alkylating agent, and this risk increased by a factor of 27 in women between the ages of 21 and 25 years (20). Sanders et al. (16) reported that no pregnancies occurred after hematopoietic cell transplantation in a group pretreated with busulfan in combination with cytoxan. Combined chemotherapeutic regimens like MOPP/ABV (chlorethamine, vincristine, procarbazine, prednisone, doxorubicin, bleomycin, vinblastine) induced an age-related, gradual ovarian failure (21). Chemotherapy induces acute follicular damage, reducing the number of follicles and leading to chronic follicular damage as they easily undergo atresia. Features of early atresia include intracytoplasmic vacuoles, multivesicular bodies, altered mitochondria, and myelinic-like structures, which have been demonstrated in primordial follicles by electron microscopy studies after chemotherapy (22). Granulosa cells are highly involved in the process of apoptosis, which is triggered by chemotherapy. The end result is the eventual destruction of primordial follicles (23 25). High-dose chemotherapy and/or total body irradiation before bone marrow transplantation (BMT) present the greatest risk of POF in almost all cases, regardless of patient age (16, 25, 26). Radiotherapy Radiotherapy regimens affect both ovarian and uterine function. The risk of ovarian damage after radiotherapy is related to the patient s age, the total dose, and the number of doses. The radiation doses used with standard pelvic radiation therapy will uniformly induce ovarian failure, and the risk of POF is increased with combined radio- and chemotherapy (27, 28). The combination of abdominal ionizing radiation with alkylating agents often induces POF, rendering patients infertile in almost 100% of cases. A dose of 5 Gy to 20 Gy administered to the ovary is sufficient to completely impair gonadal function depending on the age (29). Less than 2 Gy destroys 50% of the oocyte reserve (30). Single-dose radiation is more toxic than fractionated regimens (25). The break point for radiation-induced ovarian failure is approximately 300 cgy to the ovaries, only 11% to 13% experience ovarian failure below 300 cgy, while 60% to 63% will do so above this threshold value (31). Uterine dysfunction has been also reported to follow radiation doses between 14 and 30 Gy (32 34). Uterine irradiation at a young age reduces adult uterine volume (35). FERTILITY PRESERVATION Current cancer treatments include conservative surgeries, radiotherapy, advanced patient-friendly chemotherapeutic regimens, and allogeneic bone marrow transplantation. These strategies have raised patients expectations of a better quality of life, among which fertility preservation represents an imminent wish. A recent survey evaluated the fertility issues for young women with a history of early-stage breast cancer revealed that fertility after treatment is a major concern, but one that was not adequately addressed in 51% of the patients (36). Most currently available strategies to preserve fertility in women are still experimental and do not guarantee the recovery of fertility. The only established methods are sperm cryopreservation in men and in vitro fertilization (IVF) with embryo cryopreservation in women (37). Most promising options are oocyte and ovarian tissue cryobanking before cancer therapy (38). Proposed strategies to preserve fertility in women with cancer include: [1] storage of frozen embryos, [2] storage of frozen oocytes for future fertilization and embryo transfer, [3] storage of frozen ovarian tissue or the whole ovary for future transplantation, [4] frozen storage of ovarian tissue or isolated follicles for in vitro growth and maturation, [5] ovarian transposition before radiotherapy, [6] hormonal protection with GnRH analogs, and [7] pharmacologic protection with antiapoptotic agents (e.g., sphingosine-1-phospate) and [8] in patients with an absent or nonfunctional uterus a uterine transplant. Only option 1 is considered nonexperimental and could be offered to willing patients as an established fertility preservation strategy. In this review, we will focus on the recent advances in reproductive organ transplantation. REPRODUCTIVE ORGAN TRANSPLANTATION Nonreproductive solid organ transplantation has been practiced with variable success rates all over the world for 2032 Bedaiwy et al. Reproductive organ transplantation Vol. 90, No. 6, December 2008
3 many decades. These transplantations typically occur with a human lypmphocyte antigen (HLA)-matched genetically different donor, which means that the patient must take immunosuppressive medications for the rest of her life. Patients taking these medication regimens require close follow-up to monitor and deal effectively with any side effects. In contrast, transplantation of reproductive organs could be either an autotransplantation or heterologous transplantation. Autotransplantation is the process of transplanting tissue back into the body such as with ovarian tissue transplantation or from one part of the body to another in the same individual. Heterologous transplantation means the transplantation of tissues into another person. The process of heterologous transplantataion is already well established for many solid organs such as the kidney, pancreas, liver, heart, lung and bone marrow. However, the dynamics and the logistics of solid organ transplantation are not same for reproductive organs. Ovarian Tissue Transplantation Ovarian tissue can be transplanted to different sites (Fig. 1). Thus far, the most commonly practiced approach to ovarian transplantation is the reimplantation of small pieces of cryopreserved ovarian tissue that were removed from the patient before treatment. The thawed cryopreserved tissue is autotransplanted back into the patient after she has completed her treatment and is in remission. Autotransplantation of ovarian cortical pieces in humans can be performed at orthotopic and/or heterotopic locations (Fig. 1). Orthotopic ovarian tissue transplants involve grafting these strips in a pocket beneath or on the ovary where the tissues originated or onto the contralateral side. With the orthotopic approach, patients must undergo abdominal surgery and general anesthesia. A laparoscopic approach makes this surgery less invasive but technically more challenging. Autotransplanting tissue to a heterotopic site is a well-established technique that has been utilized for implanting fresh or frozen thawed parathyroid tissue following total parathyroidectomy (39, 40). Ovarian tissue transplants can be grafted subcutaneously at various locations including the forearm and abdominal wall. The main concern of human ovarian tissue transplantation of avsacular grafts are the quality of oocytes in the graft and the longevity of the transplant given that ischemia occurs until neovascularization occurs. For this reason, transplantation of the ovary along with its vascular pedicle was proposed (41). Initial clinical experience with ovarian transplantation Oktay et al. (42 44) reported three cases of autotransplantation with ovarian cortical tissues into the subcutaneous space above the FIGURE 1 This diagram illustrates the various proposed sites of ovarian tissue transplantation with and without vascular anastomosis. (A) Those with vascular anastomosis could be at orthotopic or heterotopic locations. The microvascular anastomosis could be performed using end-to-end, endo-to-side, or fish-mouth modification approaches. The heterotopic sites are the upper limb to the humeral vessels and the abdominal wall to the inferior epigastric vessels. (B) Those without vascular anatomosis entail transplantation of parts or most of the cortical tissue orthotopically or heterotopically. Bedaiwy. Reproductive organ transplantation. Fertil Steril Fertility and Sterility â 2033
4 brachioradialis facia of the forearm, and recently, the lower abdomen. They performed the first subcutaneous ovarian transplantation in a 35-year-old woman with stage III squamous cervical carcinoma before pelvic radiation (42). Successful ovulation was confirmed. They also reported a case of a 36-year-old woman with stage IIIB nodular sclerosing Hodgkin s lymphoma who received two doses of chemotherapy. Ovarian tissue was obtained from a right oophorectomy and cryopreserved. The tissue was later thawed and transplanted to her left ovary as well as the site of the removed ovary. Menopausal symptoms were relieved several months after transplantation, which denoted the return of ovarian function; this was confirmed by the rise of serum estradiol up to 352 pmol/l and visualization by ultrasound of a 10- mm thick endometrium and a 20 mm follicle on the right side. However, progesterone levels were never higher than 2 nmol/l, and no ovulation was detected. This patient had nearly 3 years of ovarian function but never ovulated spontaneously. Cortex of the frozen thawed ovary, as well as biopsy samples of the retained left ovary, did not show evidence of neoplasia. In another 37-year-old woman, fresh ovarian tissue was transplanted subcutaneously to the forearm after oophorectomy because of recurrent benign ovarian cysts (42). Resumption of menstrual periods and spontaneous ovulation occurred as early as 3 months after the transplant, and ovarian function lasted for 3 years with an irregular cycle length (14 45 days). The world s first pregnancy and live birth with frozen thawed ovarian tissue auto transplantation was reported by Donnez and associates (1). The patient presented with stage IV Hodgkin s lymphoma and received multiagent chemotherapy and radiotherapy. Subsequently, she developed POF. Upon completion of treatment, her frozen thawed ovarian cortical tissue was transplanted into the furrow created by the peritoneal window near the ovarian vessels and fimbria. The patient attempted natural conception for 1 year, and at 9.5 months, FSH levels returned to normal and a follicle of 2.6 cm in size developed. This was followed by spontaneous conception ending with the live birth of a healthy girl (44). Meirow et al. (2) reported the first case of oocyte retrieval, IVF, and pregnancy in a 28-year-old sterilized non-hodgkin s lymphoma patient, following orthotopic transplantation of cryopreserved thawed ovarian tissue. Small frozen fragments were initially thawed for detection of possible malignant cells and follicular assessment for bcr-abl m-rna using real-time polymerase chain reaction, which showed a large number of primordial follicles in the harvested tissue. The ovarian tissue was placed under the surface of the in situ ovary. The patient regained endocrine activity 9 months after transplantation, and a single mature oocyte was retrieved in the fourth IVF trial. Embryo transfer resulted in a normal pregnancy and delivery of a healthy baby. Although spontaneous menstruation resumed after delivery, endocrine profile performed at 22 months after transplantation indicated a low reserve (45). Demeestere et al. (46) reported a spontaneous pregnancy following mixed orthotopic and heterotopic autotransplantation of 18 cryopreserved ovarian tissue pieces in a 29-yearold patient who was previously treated with conditioning chemotherapy and BMT for Hodgkin s disease. Follicular development and activity were observed at all transplantation sites (predominantly at the ovarian site) 5 months after the autotransplantation. Six natural menstrual cycles were fully documented and analyzed. The patient became spontaneously pregnant following the sixth cycle. A 7-week gestation ended in miscarriage because of aneuploidy (46). Two years later, the same group described a full-term spontaneous pregnancy in the same patient who was then 31 years old. After their initial report of spontaneous conception and miscarriage at 12 week gestation, the initial graft seemed nonfunctional with exhaustion of its oocyte pool. Consequently, they performed another combined autologus ovarian transplantation orthotopically and heterotopically. This woman conceived spontaneously after five cycles following the second ovarian tissue transplantation and delivered a healthy baby (47). Silber et al. (48) reported the first successful spontaneous pregnancy in a prematurely menopausal monozygotic twin who received fresh ovarian tissue grafts obtained from her healthy, fertile twin by unilateral oophorectomy. They were tailored to dimensions suitable for the resected surface of the recipient ovarian medulla. The grafts were approximately 1 mm thick, which would promote early revascularization. A series of seven cases of heterologous ovarian tissue transplants between monozygotic twins was recently published by the same investigator (4). The concept in these cases is similar to autotransplantation because the donor and recipient are genetically similar. A hemiovariectomy was performed in the donor by laparotomy and the cortex transplanted in the ovarian bed of the recipient. Orthotopic versus heterotopic transplantation The return of ovarian function following ovarian tissue transplantation depends upon many factors: the freezing protocol, ovarian reserve of the transplanted tissue, whether the graft was vascularized or not at the time of freezing, the microanastomosis method, site of the graft, and the ischemia time after thawing and before transplantation. The process of folliculogenesis from primordial follicles takes 16 to 24 weeks, during which time the oocyte and surrounding somatic cells undergo a series of changes that end with the development of a large antral follicle capable of producing a mature oocyte (49). There is a wide time range reported of return of ovarian function after human ovarian transplantation (Tables 1 and 2). Both tables summarize the ovarian functions after transplantation to orthotopic and heterotopic locations. Patients who underwent combined orthotopic and heterotopic transplantations demonstrated a return of functions are not included in the tables but detailed above. Most of the studies have shown that ovarian tissue grafts transplanted to the ovarian fossa or peritoneal sites recovered their function 8 to Bedaiwy et al. Reproductive organ transplantation Vol. 90, No. 6, December 2008
5 Fertility and Sterility â 2035 TABLE 1 Ovarian function outcome following orthotopic approach of ovarian autotransplantation. Reference Oktay and Karlikaya, 2000 (50) Radford et al., 2001 (51) Donnez et al., 2004 (1) Meirow et al., 2005 (2) Schmidt et al., 2005 (52) Donnez et al., 2006 (53) Aproach of transplantation O: Pelvic peritoneum Number and size of the graft eight pieces each mm O: Ovarian 2 pieces each O: ovarian fossa 67 pieces each O: ovarian 3 þ 8 pieces, sized O: ovarian þ 12 pieces in three peritoneum differrent H: abdominal wall undetermined Orthotopic: ovarian (a) þ ovarian fossa peritoneum (b) Note: ICSI ¼ intracytoplasmic sperm injection. Bedaiwy. Reproductive organ transplantation. Fertil Steril sizes (4 þ 4 þ 4) 69 pc (2 2 1 mm): 45 (a) þ 24 (b) Chemo before freezing Recovery time Follicular development after transplantation Laboratory findings No 16 weeks folliculogenesis, [E 2, Ovulation, menses Yes 8 weeks folliculogenesis YFSHYLH[E 2 Ovulation, menses (onecycle) No 18 weeks folliculogenesis Yes 32 weeks folliculogenesis, No 19/22 weeks folliculogenesis, No 16 weeks A follicle of 20 mm in diameter YFSH[AMH & inhibin B modified natural cycle IVF, oocyte retrieval, one MII oocytes, IVF-ICSI, four-cell embryo, pregnancy, live birth
6 2036 Bedaiwy et al. Reproductive organ transplantation Vol. 90, No. 6, December 2008 TABLE 2 Ovarian function outcome following heterotopic approach of ovarian autotransplantation. Reference Oktay et al., 2001 (41, 42) Callejo et al., 2001 (58) Kim et al., 2004 (57, 59) Oktay et al., 2004 (44) Wolner-Hanssen et al. (2005) Hilders et al., 2004 (61) Oktay et al., 2006 (54) Aproach of transplantation Number and size of the graft Chemo before freezing Recovery time Follicular development after transplantation H: forearm 16 strips of 1 50 No weeks Folliculogenesis, menstruation, documented ovulation and egg retrieval H: rectus pieces No weeks folliculogenesis abdominis each 2 3 mm (20 mm) H: breast H: rectus H: SC abdominal wall Heterotopic: SC forearm Laboratory findings YFSH[E 2 Ovulation retrieval of MII oocyte 40 pieces each No 14 weeks folliculogenesis YFSH[E 2 Ovulation 15 pieces each No 12 weeks Folliculoenesis, retrieval, 20 oocytes, eight IVF-ICSI, four-cell embryos and one aneuploid embryo 10 pc ( mm) No 18 weeks Folliculogenesis of two follicles: 12.6 and 6.7 mm in diameter after local gonadotrophin stimulation [E 2 YFSHYLH[E 2. Ovulation, regular cycles, pregnancy, live birth Heterotopic: arm whole fresh ovary No No comment Doppler indicating normal blood flow in anastomosed artery and vein, local vault reccurence Heterotopic: SC abdominal wall Note: ICSI ¼ intracytoplasmic sperm injection. Bedaiwy. Reproductive organ transplantation. Fertil Steril Left ovary in pieces Yes 8 weeks Folliculogenesis, documented ovulation YFSH[E 2, menses, no stimulation, empty follicle (20 mm)
7 weeks after transplantation (1, 2, 50 54). This time interval between transplantation of cortical tissue and the first E 2 peak is consistent with the expected course in light of data obtained from sheep (55, 56), although some variations were observed. Such variations could be explained by a difference in follicular reserve at the time of cryopreservation. The aforementioned studies used a wide range of thawed cryopreserved ovarian tissue pieces, ranging from whole ovary (54) to sectioned ovarian tissue (53) (Table 1). No correlation could be seen between the time required for recovery of the ovarian function and the size of utilized grafts or their number. All these data are consistent with the proposed concept that after transplantation all developing follicles originate from primordial follicles. Ovarian function returned after 12 to 18 weeks following heterotopic transplantation to tissues of the breast (57), rectus abdominis, and abdominal wall. From Table 2, we noted that transplanting a large number of ovarian tissue pieces to heterotopic sites is associated with the slowest return of ovarian function among patients receiving heterotopic transplantation (58). Return is even slower when larger size individual grafts are used (59). Other studies have demonstrated that the function of transplants is limited by the small mass of ovarian tissue and the percentage of primordial follicles surviving ischemia until revascularization occurs, so that they fail to provide a full span of menstrual life (55, 60). One study by Hilders et al. (61), which transplanted whole fresh ovary into upper arm for a patient with cancer of the cervix, did not comment on the return of ovarian function as local recurrence in the vaginal vault malignant terminated their follow-up. The advantages of heterotopic over orthotopic transplantation include the potentially less invasive surgery on the abdominal wall or arm rather then the peritoneal cavity. This may avoid general anesthesia and have a swifter recovery. However, there are several disadvantages such as no potential for spontaneous pregnancy and difficulties in follicular monitoring. Furthermore, there have been no pregnancies reported from autotransplantation to heterotopic sites compared to orthoptopic sites. Whole ovary transplantation Whole ovary auto transplantation was reported in early studies where ovaries were removed from their pelvic location and immediately transplanted at other sites. The implementation of heterotopic sites for ovarian autotransplantation dates back to 1988, when the first case was reported (62). These investigators documented normal follicular growth and regularity of the cycles after the end of pelvic radiotherapy. The main drawback of avascular ovarian tissue transplantation is that the graft is completely dependent on the establishment of blood supply via neovascularization. Avascular grafts suffer an initial period of ischemia during which neovascularization takes place, and consequently, a large proportion of follicles are lost during the initial ischemia, which occurs after transplantation (55, 63 68). Whole ovary transplantation with a vascular anastomosis was proposed as a mechanism to reduce ischemic time, and in theory, prolong the longevity of the graft (41). In this technique, the whole ovary with its vascular pedicle is removed, cryopreserved, thawed, and then transplanted with a microvascular anastomosis to a heterotopic or orthotopic site. Transplantation of intact ovary with vascular anastomosis reduces the ischemic interval between transplantation and revascularization by allowing immediate revascularization of the transplant (69). We (70) reported the restoration of ovarian function after autotransplantation of intact frozen thawed sheep ovaries with microvascular anastomosis. Imhof et al. (71) demonstrated that the autotransplantation of whole cryopreserved sheep ovaries with microanastomosis of the ovarian vascular pedicle could lead to pregnancy and delivery. However, contrary to the initial hypothesis that follicular loss would be reduced, Imhof and colleagues (71) reported that only 7% of what was observed in control animal ovaries was identified in the transplanted ovaries when removed for analysis after 1 year. An intact human ovary with its vascular pedicle could be cryopreserved without affecting the follicular viability, vascular density or molecular integrity of different ovarian components (72). However, it has yet to be shown that this preserves the follicular pool better than grafting ovarian tissue pieces. Harvesting human ovaries with vascular pedicles When obtaining the whole human ovary with its vascular pedicle, surgeons must ensure that the pedicle is long enough to allow the ovarian artery and veins to be skeletonized and sutured to vessels of similar diameter. During this process, ischemic time must be minimized (69). Although open surgery can help diminish ischemia time, a minimally invasive laparoscopic approach is, however, the preferred approach for the purposes of cryopreservation and subsequent transplantation (73). These approaches can facilitate the dissection of the ovarian pedicle up to the pelvic brim, a technique that has been used for ovarian transposition (74). Implementing laparoscopy in cancer patients ensures better wound healing, which is consistent with the patient s needs to start their chemotherapeutic treatment cycles immediately (69). We (73) summarized the technical and microsurgical principles of laparoscopic approach for ovariectomy. These included severing the utero-ovarian ligament before advancing cephalad through the mesosalpnix and ending at the infundibulopelvic ligament, which should be dealt with last to minimize ischemia time. All through the procedure, sharp dissection and suturing are preferred to electrocoagulation, which may induce desiccation of ovarian tissues through thermal injury to the vascular walls. Longer and wider caliber vessels are ensured through ligating the ovarian vessels as proximal to the origin as possible. An endobag is placed through the 10-mm trocar to deliver the ovary with its vascular pedicle outside the peritoneal cavity. Fertility and Sterility â 2037
8 An extended port incision, which helps avoid crushing the ovary and the blood vessels against the narrow port site, should be used. Another approach, although technically challenging, would be the transvaginal route. We (73) reported one case of human ovarian harvesting through this approach, where oophorectomy was combined with vaginal hysterectomy. To minimize the ischemic time, we suggested handling one ovary at a time for cryopreservation and saving the infundibulopelvic ligament and the ovarian vessels until the very end of the procedure. We found that the dissection of a long portion of the ovarian vessels via the vaginal route is not as easy as by laparoscopy. Transplantation of intact cryopreserved thawed ovary Restoration of fertility after whole frozen ovary transplantation was first described in rats by Wang et al. (75). They described successful vascular transplantation of frozen thawed rat ovaries and the reproductive tract in four of seven (57%) transplants; these transplants survived for R60 days, were ovulatory, and resulted in one pregnancy. Courbiere et al. (76) described cryopreservation of whole ovary with vascular pedicles in 5- to 6-month-old sheep by vitrification. No statistically significant differences were observed in follicle viability or normal primordial follicle rates between the ovaries exposed to cryoprotectants and those that were not exposed, nor were there any significant differences before and after vitrification with the two cryoprotectant solutions (VS1 and VS4 containing dimethyl sulfoxide, formamide, and propylene glycol). Although autotransplantation of frozen thawed sheep ovarian cortex has resulted in a pregnancy (77) and prolonged normal hormone production (55), it was not until 2003 when the first report of successful cryopreservation and transplantation of an intact ovary in sheep (defined as return of hormonal functions) occurred (70). A successful pregnancy and delivery in sheep was reported by Imhof et al. (71) following autotransplantation of whole cryopreserved ovaries with microanastomosis of the ovarian vascular pedicle. To date, all human ovarian whole ovary transplantations have been performed using fresh ovaries. A limited number of human studies (61, 78, 79) have attempted this exhausting and technically challenging approach of fresh ovarian transplantation (Table 3). A team of surgeons is needed that include microvascular surgical expertise. These procedures have been performed in cancer patients who need to commence their chemo- or radiotherapy cycles without delay, but other patient groups as those with POF (Silber, unpublished data) or Turner s syndrome (78) have benefited from it. Leporrier et al. (79) were the first to describe fresh ovarian autotransplantation before pelvic irradiation in a patient with Hodgkin s disease. Hilders et al. (61), transplanted whole fresh ovary into the upper arm of a patient with cervical cancer. The procedure was unfortunately followed by local vault malignant recurrence. No long-term follow-up has been reported. Mhatre et al. (78) successfully implemented the technique in two patients with Turner s syndrome (ovarian function was restored and the patients developed secondary sexual characteristics). An abdominal pfannenstiel incision was used in both cases. Whole ovary freezing protocols The challenges facing whole human ovary transplantation include the lack of cryoprotective agents that can adequately perfuse into the relatively large tissue masses, and the subsequent potential complication of vascular injury following intravascular ice formation (69). The freeze thaw protocols used today still require further optimization. Some cytoprotective agents lead to zona hardening and meiotic spindle depolymerization that may lead to aneuploidy (80). Modifications of slow-freezing cryopreservation protocols were implemented in ovarian tissue freezing as an integrated strategy for fertility preservation. These modifications mainly entailed increasing the concentration of sucrose used as nonpenetrating cryoprotectant and replacing sodium with choline that improved survival rates by 80% (81). Cryoprotectant must adequately penetrate throughout the stroma and granulosa cells without causing cryoprotectant toxicity. Newton et al. (63, 82) demonstrated the importance of the diffusion rate and the diffusion temperature. Ice crystal formation must also be minimized by choosing optimal freezing and thawing rates. The choice of cryoprotectant with maximum permeation capacity but minimum toxicity and ice crystal formation is specific to each cell and tissue type (83). An effective technique of cryoperfusion where the cryoprotectant is perfused into the ovary via the ovarian artery was proposed (84 86). This technique lead to acceptable follicle survival rates and relative ovarian function restoration with one case of restored fertility (70, 71, 76, 85, 87), but the loss of tissue viability among studies was a constant component. Thus, in the ovary, it is a matter of balance between the stroma, the follicular cells, and the oocytes (88). On the basis of current knowledge, the standard method for human ovarian cryopreservation is slow-programmed freezing using human serum albumin-containing medium and propanediol, dimethylsulphoxide, or ethylene glycol as a cryoprotectant, with or without sucrose (88). Martinez-Madrid et al. (89) described a cryopreservation protocol for intact human ovary with its vascular pedicle. Ovarian perfusion with cryoprotective solution and slow freezing with a cryofreezing container was performed. Rapid thawing of the ovaries was performed by perfusion and bathing with a decreased sucrose gradient. High survival rates of follicles (75.1%), small vessels, and stroma, as well as a normal histologic structure, were documented in all the ovarian components after thawing (89). No postthawing induction of apoptosis was observed in any cell types, assessed by both the terminal deoxynucleotidyl transferase biotin-dutp nick-end labeling method and immunohistochemistry for active caspase-3 (90, 91). They confirmed that the majority (96.7%) of primordial follicles were intact, and that their endothelial cells had a completely normal ultrastructure after 2038 Bedaiwy et al. Reproductive organ transplantation Vol. 90, No. 6, December 2008
9 Fertility and Sterility â 2039 TABLE 3 Studies reporting fresh whole ovarian transplantation. Reference Number of patients Ovarian volume and site Indication for transplantation of ovarian tissue Outcomes Leporrier et al., 1987 (87) 1 Whole ovary, heterotopic Hodgkin s disease Ovarian cycles remained regular despite radiotherapy, and follicle growth occurred normally Mhatre et al., 2005 (88) 2 Whole ovary, orthotopic, case one vascular pedicle, case two avascular transplantation Turner s syndrome Case one:serum estradiol showed a significant rise from the pretransplant value of <20 pg/ml to >50 pg/ml. Case two showed after 2.5 years: developed uterus with endometrium, normally functioning transplanted ovary, and her native streak gonads. At the conclusion of 2.5 years, the patient is having spontaneous menstruation, ovulation, and excellent growth of secondary sexual character Hilders et al., 2004 (61) 1 Whole ovary Cervical cancer Normal blood flow in the anastomosed artery and vein. Cyclic swellings of the upper arm without major discomfort. Documented follicular activity at different stages. Adequate blood flow and follicular activity of the transplanted ovary Silber and Gosden, 2007 (4) Bedaiwy. Reproductive organ transplantation. Fertil Steril Series of 10 monozygotic twins, reporting on seven cases Hemiovary, orthotopic Premature ovarian failure First successful spontaneous pregnancy
10 cryopreservation (92). The percentage of active caspase- 3-positive endothelial cells was <1%. In conclusion, it appears that in large mammals and humans, cryopreserving a large, intact ovary may prove more problematic than in small animals because of the difficulty of adequate diffusion of cryoprotective agents into large tissue masses and vascular injury caused by intravascular ice formation. Transport time and method Many studies have attempted to develop strategies to diminish ovarian graft s ischemic injuries. At least a fraction of primordial follicles from thawed ovaries of four patients treated by cryopreservation survived a period of approximately 4 hours on ice before cryopreservation (93). One study found a significantly enhanced survival rate of human ovarian follicles following transport in warm (37 C) medium compared to on ice (94). Although a period of about 1 hour of ischemia was not detrimental to ovarian function, in terms of follicular loss of the fresh transplant, a period of 24 hours of ischemia had negative effects (95). Shipping graft pieces on ice between centers without cryopreservation requires rethinking current cryopreservation protocols and a potential resorting to new strategies such as vitrification. Despite carrying the risk prolonged equilibration with high concentrations of cryoprotectants, ultrarapid freezing techniques used in vitrification can prevent ice formation in tissues (96). The current cryopreservation protocols for intact ovaries and for ovarian cortical strips need to be optimized. Techniques for transplantation On harvesting ovarian tissue, the vascular pedicles including the utero-ovarian ligament and the infundibulopelvic ligament are to be severed at the end of the procedure (75, 79) to help shorten the ischemic time before ovarian artery perfusion with heparinized solution and cryoprotectant (75, 79). It is also recommended that a microsurgeon and biologist should participate in the procedure and have a cooled sterile table with a stereomicroscope and microsurgical instruments ready to handle the ovarian tissue upon procurement. Harvesting of the organ should be performed with the anticipation of a technically challenging vascular anastomosis. In ewes, using an aortic patch, the ovarian artery was reanastomosed to the carotid artery to perform autotransplantation of an intact ovary with its vascular pedicle (97). A primate model was tested for an orthotopic transplantation technique using a microsurgical reanastomosis of the ovarian blood vessels (98). These techniques have a rather limited chance for application in clinical practice because an aortic patch is used for the anastomosis (41). The concept is to access the ovarian artery as proximal as possible. An intact fresh human whole ovary autotransplantation with its vascular pedicle has already been performed (Silber et al., video abstract ASRM, 2007). This report further demonstrated the feasibility of a technically challenging microvascular anastomosis of a 1- to 2-mm ovarian artery and more than one ovarian vein. Guided by the results of animal experiments, we postulated alternate sites for human intact ovary autotransplantation with microvascular anastomosis (73). The neck, pectoral reigon, antecubital fossa, lower part of the anterior abdominal wall, and the upper inner aspect of the thigh are possible transplantation recipient sites in humans. The carotid vessels, the cutaneous branches of the internal mammary vessels, the antecubital vessels, the inferior epigastric vessels, and the femoral vessels are anastomosed to the ovarian vessels in their respective regions. Based on safety, amenability to monitoring, caliber, accessibility, liability to trauma, surgical anatomy, and cosmetic factor, the deep inferior epigastric vessels stand as the best available heterotopic option. Discrepancy between the ovarian vessels and the recipient vessels is an important challenge to the subsequent patency of the anastomosis. The sudden change of caliber between the cut end diameters of the vessels, encountered in approximately one-third of anastomoses, may cause turbulence to the blood flow, thus predisposing the vessel to platelet aggregation (99). The choice of the technique of reanastomosis is affected by the degree of discrepancy. There is no ideal technique to deal with every size discrepancy, and choices may have to be individualized according to case and body area (100). Options range from dilatation with the use of a jeweller s forceps (99) in case of simple discrepancies <1:1.5 to using the oblique cut, fish-mouth cut, or end-to-side anastomosis when discrepancies exceed 1:1.5 (99). Sleeve anastomosis is performed when discrepancies are larger and when the upstream donor vessel is smaller than the recipient one (101). Anastomosis to a heterotopic site requires microvascular technical expertise as well. Animal studies reported by Bedaiwy et al. (73) suggested three different microvascular anastomosis techniques based on the caliber of the ovarian and the deep inferior epigastric vessels: end-to-end, end-toside, and fish-mouth anastomosis. End-to-end anastomosis appears to be the ideal approach to perform the anastomosis procedure, with a patency rate >60%. However, if vascular discrepancy between the ovarian vessels and the inferior epigastric vessels is inevitable, end-to-side anastomosis rather than fish-mouth incisions should be adopted. Advances in the field of plastic surgery, such as vascular clips (69), sutureless approaches, glues or adhesives, and laser-assisted anastomosis are potentially useful (100). All in all the microanastomosis part of reproductive organ transplantation could be the least challenging step toward establishment of a successful reproductive organ transplantation program given the recent developments in plastic microsurgery. Microvascular thrombosis after transplantation In the trial of Bedaiwy et al. (70), long-term patency was lost in 8 of 11 transplanted sheep ovaries because of thrombotic events in the reanastomosed vascular pedicle. Recently, Imhof et al. (71) reported that six of eight ovaries showed major ovarian vessels to be thrombosis free, with the structural integrity of the ovarian stroma largely retained 18 to 19 months after transplantation. However, two transplanted ovaries had 2040 Bedaiwy et al. Reproductive organ transplantation Vol. 90, No. 6, December 2008
11 atrophied completely suggesting major vessel thrombosis or long-term vascular jeopardy. In the vascularized ovaries local damage to 30% to 50% of the ovary suggested local thrombosis. Follicle counts per ovary were only a small fraction of the fresh ovary when analyzed at 18 months after transplantion. This suggests a reduced longevity of the graft even with a vascular pedicle. These complications motivated Jadoul et al. (69) to suggest the necessity of cryopreservation of the contralateral ovarian cortical tissue when whole ovary cryopreservation is attempted, until an efficient ovarian tissue cryopreservation protocol is validated with adequate attention to the postthawing survival of the ovarian vascular system. Another alternative was discussed by Yin et al. (95), who suggested that one of a pair of ovaries would be left in situ so that an intact pedicle is available for exchanging the sterilized organ with the frozen and thawed ones, once the patient is ready for autotransplantation. Research should focus on minimizing the cryopreservation-induced damage not only to the ovarian follicular complex but the ovarian vascular system as well. Ischemia reperfusion injury and follicular loss Generally, a complex cascade of events called reperfusion injury attributed to ischemia, hypothermia, and rewarming and reperfusion is associated with damage to the transplanted organ. These injuries can be slowed down by cold ischemic preservation with a protective buffer. This helps prevent delayed graft function and early graft failure (102, 103). The number of viable primordial follicles in ovarian tissue following transplantation and revascularization is the main determinant of success along with the return of ovulation and longevity of the graft. Animal studies showed that primordial follicle-rich cortical ovarian tissue restored ovarian cyclicity and achieved pregnancy, although in most of the recipients, graft activity was shorter than normal. The length of the ischemic period had a major impact on the grafted organ function (104). This ischemic time may affect follicular function restoration and subsequent neovascularization. According to Kim et al. (59), the ovarian cortex can tolerate ischemia for at least 3 hours at 4 C. Compared to the relative small loss because of freezing (55, 66, 105), up to two-thirds of follicles are lost during the initial ischemia after transplantation. This may limit the use of ovarian tissue cryopreservation and transplantation to only those patients younger than 35 years of age because older patients already have a limited ovarian reserve (50). Even with antioxidant treatment, >50% of the follicles were lost during ischemia (60). Heterologous Ovarian Transplantation Silber et al. (48) have reported ovarian transplantation between monozygotic 24-year-old twins who presented with discordant ovarian function. One had developed POF at the age of 14 years, whereas her sister had normal ovaries and three children that had been conceived naturally. The sterile twin received a transplant of ovarian cortical tissue from her sister by means of a minilaparotomy. Within 3 months after transplantation, the recipient s cycles resumed and serum gonadotropin levels fell into the normal range. During the second follow-up cycle, she conceived, and her pregnancy progressed uneventfully. At 38 weeks gestation, she delivered a healthy appearing female infant (48). More recently, the same group reported on ovarian cortex transplantation in a cohort of seven sets of twins discordant for POF. Ovarian cortical tissue was transplanted from the twin with normal ovarian functions to her sister with POF. Folliculogenesis, hormonal functions, and menses were restored in all recipients. In addition, five spontaneous pregnancies were documented in this cohort (4). This work should be seen as preliminary proof that transplantation of large segments of ovarian tissue can be successful. In cases of identical twins, no immunosuppressive drugs are necessary. A recent publication of an allograft between two nonidentical twins was recently reported by Donnez et al. (106). They used ovarian cortical tissue from the donor sister who had already been the donor of bone marrow for a transplant. The recipient had received chemotherapy, totalbody radiation, and bone marrow transplantation. The recipient developed spontaneous cycles after receiving the transplant. Furthermore, two oocytes and two embryos were obtained (106).However,inmostpatientswithanintactimmunesystem the possibility of acute graft rejection and risks of long-term immunosuppressive complications in the mother such as infection and obstetrical complications may limit its use. The idea of introducing heterologous ovarian transplantation as an option to replace an egg donor program faces many problems. Egg donation is a relatively safe procedure with extensive support in the literature. However, many societies have restricted or banned oocyte donations, making this approach a potential option. In contrast, the effects on reproductive performance as well as the short- and long-term outcomes on children brought about by exposure to immunosuppressive medications in utero carry unknown risks. The problem of tissue compatibility and the technical sophistication and cost of techniques needed to bypass it represent another concern. Ovarian tissue transplantation between genetically different individuals is gaining more attention from different groups. Given the few reported cases so far, there is lack of evidence to support its use on a wide scale. Uterine Transplantation With the exception of minor uterine malformations such as septate uterus, uterine infertility because of congenital hypoplasia/agenesis or hysterectomy is untreatable (107). Surrogacy is not approved in many countries because of legal or ethical considerations. Transplantation of a uterus, followed by an IVF procedure, to a woman with absolute uterine infertility and preserved ovaries could be an alternative solution. Uterine transplantation is an experimental approach aiming at replacement of lost or absent uteri (108). Animal Fertility and Sterility â 2041
FERTILITY PRESERVATION. Juergen Eisermann, M.D., F.A.C.O.G South Florida Institute for Reproductive Medicine South Miami Florida
 FERTILITY PRESERVATION Juergen Eisermann, M.D., F.A.C.O.G South Florida Institute for Reproductive Medicine South Miami Florida 1 2 3 4 Oocyte Cryopreservation Experimental option Offer to single cancer
FERTILITY PRESERVATION Juergen Eisermann, M.D., F.A.C.O.G South Florida Institute for Reproductive Medicine South Miami Florida 1 2 3 4 Oocyte Cryopreservation Experimental option Offer to single cancer
Cancer and Fertility Ashley Munchel, MD Assistant Professor of Pediatrics University of Maryland Medical Center
 Cancer and Fertility Ashley Munchel, MD Assistant Professor of Pediatrics University of Maryland Medical Center Trends in Pediatric Cancer Incidence Rates by Site, Ages Birth to 19 Years, 1975 to 2010.
Cancer and Fertility Ashley Munchel, MD Assistant Professor of Pediatrics University of Maryland Medical Center Trends in Pediatric Cancer Incidence Rates by Site, Ages Birth to 19 Years, 1975 to 2010.
Melanoma-What Every Woman Need to Know about Fertility and Pregnancy
 Melanoma-What Every Woman Need to Know about Fertility and Pregnancy Women diagnosed with melanoma may require counseling for fertility preservation, fertility treatment and safety of pregnancy after treatment.
Melanoma-What Every Woman Need to Know about Fertility and Pregnancy Women diagnosed with melanoma may require counseling for fertility preservation, fertility treatment and safety of pregnancy after treatment.
Planning for Parenthood After a Cancer Diagnosis
 Cancer and Fertility Planning for Parenthood After a Cancer Diagnosis If you or someone you love is facing cancer, preserving fertility may be the last thing on your mind. But if you re a woman of childbearing
Cancer and Fertility Planning for Parenthood After a Cancer Diagnosis If you or someone you love is facing cancer, preserving fertility may be the last thing on your mind. But if you re a woman of childbearing
Optimizing Fertility and Wellness After Cancer. Kat Lin, MD, MSCE
 Optimizing Fertility and Wellness After Cancer Kat Lin, MD, MSCE University Reproductive Care University of Washington Nov. 6, 2010 Optimism in Numbers 5-year survival rate 78% for all childhood cancers
Optimizing Fertility and Wellness After Cancer Kat Lin, MD, MSCE University Reproductive Care University of Washington Nov. 6, 2010 Optimism in Numbers 5-year survival rate 78% for all childhood cancers
Cryopreservation: Whole ovary and ovarian tissue
 Belen Martinez Madrid Consensus Meeting: Fertility preservation update Barcelona, June 6 th -7 th, 2011 Cryopreservation: Whole ovary and ovarian tissue Options for fertility preservation Ovarian tissue
Belen Martinez Madrid Consensus Meeting: Fertility preservation update Barcelona, June 6 th -7 th, 2011 Cryopreservation: Whole ovary and ovarian tissue Options for fertility preservation Ovarian tissue
Gynecologic Considerations in Women with FA
 Gynecologic Considerations in Women with FA RAHEL GHEBRE, M.D., MPH University of Minnesota Medical School Objectives Recommendation for Gynecologic Care FA girls starting at age 16 should establish a
Gynecologic Considerations in Women with FA RAHEL GHEBRE, M.D., MPH University of Minnesota Medical School Objectives Recommendation for Gynecologic Care FA girls starting at age 16 should establish a
Should we offer fertility preservation to all patients with severe endometriosis?
 Should we offer fertility preservation to all patients with severe endometriosis? Daniel S. Seidman, MD Department of Ob/Gyn, Sheba Medical Center, Sackler School of Medicine, Tel-Aviv University Endometriosis
Should we offer fertility preservation to all patients with severe endometriosis? Daniel S. Seidman, MD Department of Ob/Gyn, Sheba Medical Center, Sackler School of Medicine, Tel-Aviv University Endometriosis
LOW RESPONDERS. Poor Ovarian Response, Por
 LOW RESPONDERS Poor Ovarian Response, Por Patients with a low number of retrieved oocytes despite adequate ovarian stimulation during fertility treatment. Diagnosis Female About Low responders In patients
LOW RESPONDERS Poor Ovarian Response, Por Patients with a low number of retrieved oocytes despite adequate ovarian stimulation during fertility treatment. Diagnosis Female About Low responders In patients
Disturbances of female reproductive system in survivors of childhood cancer
 Disturbances of female reproductive system in survivors of childhood cancer Assoc. Prof. Zana Bumbuliene VU Faculty of Medicine Clinic of Obstetrics and Gynaecology 13 SEP 2014 Introduction Cancer is the
Disturbances of female reproductive system in survivors of childhood cancer Assoc. Prof. Zana Bumbuliene VU Faculty of Medicine Clinic of Obstetrics and Gynaecology 13 SEP 2014 Introduction Cancer is the
Evidence tables from the systematic literature search for premature ovarian insufficiency surveillance in female CAYA cancer survivors.
 Evidence tables from the systematic literature search for premature ovarian insufficiency surveillance in female CAYA cancer survivors. Who needs surveillance? Chiarelli et al. Early menopause and Infertility
Evidence tables from the systematic literature search for premature ovarian insufficiency surveillance in female CAYA cancer survivors. Who needs surveillance? Chiarelli et al. Early menopause and Infertility
Preservazione della fertilità nella paziente oncologica
 Preservazione della fertilità nella paziente oncologica Dott.ssa Raffaella Fabbri Unità Operativa Ginecologia e Fisiopatologia della Riproduzione Umana Università degli Studi di Bologna Policlinico S.
Preservazione della fertilità nella paziente oncologica Dott.ssa Raffaella Fabbri Unità Operativa Ginecologia e Fisiopatologia della Riproduzione Umana Università degli Studi di Bologna Policlinico S.
Fertility care for women diagnosed with cancer
 Saint Mary s Hospital Department of Reproductive Medicine Information for Patients Fertility care for women diagnosed with cancer Contents Page Overview... 2 Our service... 2 Effects of cancer treatment
Saint Mary s Hospital Department of Reproductive Medicine Information for Patients Fertility care for women diagnosed with cancer Contents Page Overview... 2 Our service... 2 Effects of cancer treatment
FERTILITY AND PREGNANCY AFTER BREAST CANCER LISA KOLP, MD JOHNS HOPKINS SCHOOL OF MEDICINE OCTOBER 2013
 FERTILITY AND PREGNANCY AFTER BREAST CANCER LISA KOLP, MD JOHNS HOPKINS SCHOOL OF MEDICINE OCTOBER 2013 SPECIAL THANKS TO DR. MINDY CHRISTIANSON INTRODUCTION About 6-7% of breast cancers are diagnosed
FERTILITY AND PREGNANCY AFTER BREAST CANCER LISA KOLP, MD JOHNS HOPKINS SCHOOL OF MEDICINE OCTOBER 2013 SPECIAL THANKS TO DR. MINDY CHRISTIANSON INTRODUCTION About 6-7% of breast cancers are diagnosed
UTERINE LEIOMYOSARCOMA. About Uterine leiomyosarcoma
 UTERINE LEIOMYOSARCOMA Uterine Lms, Ulms Or Just Lms Rare uterine malignant tumour that arises from the smooth muscular part of the uterine wall. Diagnosis Female About Uterine leiomyosarcoma Uterine LMS
UTERINE LEIOMYOSARCOMA Uterine Lms, Ulms Or Just Lms Rare uterine malignant tumour that arises from the smooth muscular part of the uterine wall. Diagnosis Female About Uterine leiomyosarcoma Uterine LMS
Obstetrics, Université Libre de Bruxelles, Erasme Hospital, Brussels, Belgium
 The Oncologist Prevention Fertility Preservation: Successful Transplantation of Cryopreserved Ovarian Tissue in a Young Patient Previously Treated for Hodgkin s Disease ISABELLE DEMEESTERE, a,b PHILIPPE
The Oncologist Prevention Fertility Preservation: Successful Transplantation of Cryopreserved Ovarian Tissue in a Young Patient Previously Treated for Hodgkin s Disease ISABELLE DEMEESTERE, a,b PHILIPPE
Testosterone Therapy-Male Infertility
 Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
Neil Goodman, MD, FACE
 Initial Workup of Infertile Couple: Female Neil Goodman, MD, FACE Professor of Medicine Voluntary Faculty University of Miami Miller School of Medicine Scope of Infertility in the United States Affects
Initial Workup of Infertile Couple: Female Neil Goodman, MD, FACE Professor of Medicine Voluntary Faculty University of Miami Miller School of Medicine Scope of Infertility in the United States Affects
Oocyte Freezing and Ovarian Tissue Cryopreservation:
 Oocyte Freezing and Ovarian Tissue Cryopreservation: Comparing Results of These Two Methods in One Program Dr. César Díaz García cesar.diaz@ivi.uk IVI London 83, Wimpole St. London, UK London Conflict
Oocyte Freezing and Ovarian Tissue Cryopreservation: Comparing Results of These Two Methods in One Program Dr. César Díaz García cesar.diaz@ivi.uk IVI London 83, Wimpole St. London, UK London Conflict
Female Health Issues after Treatment for Childhood Cancer
 Female Health Issues after Treatment for Childhood Cancer The effects of childhood cancer therapy on female reproductive function depend on many factors, including the girl s age at the time of cancer
Female Health Issues after Treatment for Childhood Cancer The effects of childhood cancer therapy on female reproductive function depend on many factors, including the girl s age at the time of cancer
Fertility 101. About SCRC. A Primary Care Approach to Diagnosing and Treating Infertility. Definition of Infertility. Dr.
 Dr. Shahin Ghadir A Primary Care Approach to Diagnosing and Treating Infertility St. Charles Bend Grand Rounds November 30, 2018 I have no conflicts of interest to disclose. + About SCRC State-of-the-art
Dr. Shahin Ghadir A Primary Care Approach to Diagnosing and Treating Infertility St. Charles Bend Grand Rounds November 30, 2018 I have no conflicts of interest to disclose. + About SCRC State-of-the-art
10/16/2014. Adolescents (ages 10 19) and young adults (ages 20 24) together compose about 21% of the population of the United States.
 The purview of pediatrics includes the growth, development, and health of the child and therefore begins in the period before birth when conception is apparent. It continues through childhood and adolescence
The purview of pediatrics includes the growth, development, and health of the child and therefore begins in the period before birth when conception is apparent. It continues through childhood and adolescence
Female Reproductive Physiology. Dr Raelia Lew CREI, FRANZCOG, PhD, MMed, MBBS Fertility Specialist, Melbourne IVF
 Female Reproductive Physiology Dr Raelia Lew CREI, FRANZCOG, PhD, MMed, MBBS Fertility Specialist, Melbourne IVF REFERENCE Lew, R, Natural History of ovarian function including assessment of ovarian reserve
Female Reproductive Physiology Dr Raelia Lew CREI, FRANZCOG, PhD, MMed, MBBS Fertility Specialist, Melbourne IVF REFERENCE Lew, R, Natural History of ovarian function including assessment of ovarian reserve
INDICATIONS OF IVF/ICSI
 PROCESS OF IVF/ICSI INDICATIONS OF IVF/ICSI IVF is most clearly indicated when infertility results from one or more causes having no other effective treatment; Tubal disease. In women with blocked fallopian
PROCESS OF IVF/ICSI INDICATIONS OF IVF/ICSI IVF is most clearly indicated when infertility results from one or more causes having no other effective treatment; Tubal disease. In women with blocked fallopian
Cancer Fertility. Fertility Options to Consider Before Treatment Begins & Parenthood Options After Cancer
 & Cancer Fertility Fertility Options to Consider Before Treatment Begins & Parenthood Options After Cancer If you or someone you care about is faced with a cancer diagnosis, preserving fertility may be
& Cancer Fertility Fertility Options to Consider Before Treatment Begins & Parenthood Options After Cancer If you or someone you care about is faced with a cancer diagnosis, preserving fertility may be
CASE 41. What is the pathophysiologic cause of her amenorrhea? Which cells in the ovary secrete estrogen?
 CASE 41 A 19-year-old woman presents to her gynecologist with complaints of not having had a period for 6 months. She reports having normal periods since menarche at age 12. She denies sexual activity,
CASE 41 A 19-year-old woman presents to her gynecologist with complaints of not having had a period for 6 months. She reports having normal periods since menarche at age 12. She denies sexual activity,
Assisted Reproduction. By Dr. Afraa Mahjoob Al-Naddawi
 Assisted Reproduction By Dr. Afraa Mahjoob Al-Naddawi Learning Objectives: By the end of this lecture, you will be able to: 1) Define assisted reproductive techniques (ART). 2) List indications for various
Assisted Reproduction By Dr. Afraa Mahjoob Al-Naddawi Learning Objectives: By the end of this lecture, you will be able to: 1) Define assisted reproductive techniques (ART). 2) List indications for various
Chapter 4. Managing Fertility in Childhood Cancer Patients T.K. Woodruff and K.A. Snyder (eds.) Oncofertility. Springer 2007
 Chapter 4 Managing Fertility in Childhood Cancer Patients T.K. Woodruff and K.A. Snyder (eds.) Oncofertility. Springer 2007 The original publication of this article is available at www.springerlink.com
Chapter 4 Managing Fertility in Childhood Cancer Patients T.K. Woodruff and K.A. Snyder (eds.) Oncofertility. Springer 2007 The original publication of this article is available at www.springerlink.com
Article Harvesting and autotransplantation of vascularized ovarian grafts: approaches and techniques
 RBMOnline - Vol 14. No 3. 2007 360-371 Reproductive BioMedicine Online; www.rbmonline.com/article/2521 on web 31 January 2007 Article Harvesting and autotransplantation of vascularized ovarian grafts:
RBMOnline - Vol 14. No 3. 2007 360-371 Reproductive BioMedicine Online; www.rbmonline.com/article/2521 on web 31 January 2007 Article Harvesting and autotransplantation of vascularized ovarian grafts:
Reproductive Options for Breast Cancer Patients
 08:36 1 Reproductive Options for Breast Cancer Patients Mr Stuart Lavery Director IVF Hammersmith Consultant Gynaecologist Imperial College London 08:36 2 Reproductive Options for Female Cancer Patients
08:36 1 Reproductive Options for Breast Cancer Patients Mr Stuart Lavery Director IVF Hammersmith Consultant Gynaecologist Imperial College London 08:36 2 Reproductive Options for Female Cancer Patients
Chapter 2 Fertility Management for Women with Cancer
 Chapter 2 Fertility Management for Women with Cancer Sanjay K. Agarwal, MD and R. Jeffrey Chang, MD Cancer is now a disease with a variety of treatment options that are leading to longer and more productive
Chapter 2 Fertility Management for Women with Cancer Sanjay K. Agarwal, MD and R. Jeffrey Chang, MD Cancer is now a disease with a variety of treatment options that are leading to longer and more productive
WOMEN & INFANTS HOSPITAL Providence, RI CONSENT FOR IN VITRO FERTILIZATION USING A GESTATIONAL CARRIER (PATIENT/INTENDED PARENTS) 1.
 *40675* 40675 MR-838 (9-2017) WOMEN & INFANTS HOSPITAL Providence, RI 02905 CONSENT FOR IN VITRO FERTILIZATION USING A GESTATIONAL CARRIER (PATIENT/INTENDED PARENTS) 1. I, and (Print Patient s name) (Print
*40675* 40675 MR-838 (9-2017) WOMEN & INFANTS HOSPITAL Providence, RI 02905 CONSENT FOR IN VITRO FERTILIZATION USING A GESTATIONAL CARRIER (PATIENT/INTENDED PARENTS) 1. I, and (Print Patient s name) (Print
Fresh and Frozen Ovary Tissue Transplants: Mechanism of Adult Primordial Follicle Recruitment And Fetal Oocyte Arrest
 Fresh and Frozen Ovary Tissue Transplants: Mechanism of Adult Primordial Follicle Recruitment And Fetal Oocyte Arrest Locking and Unlocking: Oocyte Meiosis and PGC differentiation Yasui et al 2012 Factors
Fresh and Frozen Ovary Tissue Transplants: Mechanism of Adult Primordial Follicle Recruitment And Fetal Oocyte Arrest Locking and Unlocking: Oocyte Meiosis and PGC differentiation Yasui et al 2012 Factors
Ovarian function and pregnancy after Hematopoietic Stem Cell Transplant
 Ovarian function and pregnancy after Hematopoietic Stem Cell Transplant Factors that influence post transplantation fertility and ovarian function in women Total body irradiation (TBI) Drugs prescribed
Ovarian function and pregnancy after Hematopoietic Stem Cell Transplant Factors that influence post transplantation fertility and ovarian function in women Total body irradiation (TBI) Drugs prescribed
How to Select an Egg Donor
 How to Select an Egg Donor How to Select an Egg Donor Egg donation entails the fertilization of eggs of a young woman and transfer of the resulting embryo or embryos into the intended mother uterus. In
How to Select an Egg Donor How to Select an Egg Donor Egg donation entails the fertilization of eggs of a young woman and transfer of the resulting embryo or embryos into the intended mother uterus. In
X-Plain Ovarian Cancer Reference Summary
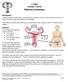 X-Plain Ovarian Cancer Reference Summary Introduction Ovarian cancer is fairly rare. Ovarian cancer usually occurs in women who are over 50 years old and it may sometimes be hereditary. This reference
X-Plain Ovarian Cancer Reference Summary Introduction Ovarian cancer is fairly rare. Ovarian cancer usually occurs in women who are over 50 years old and it may sometimes be hereditary. This reference
Reproduction and Development. Female Reproductive System
 Reproduction and Development Female Reproductive System Outcomes 5. Identify the structures in the human female reproductive system and describe their functions. Ovaries, Fallopian tubes, Uterus, Endometrium,
Reproduction and Development Female Reproductive System Outcomes 5. Identify the structures in the human female reproductive system and describe their functions. Ovaries, Fallopian tubes, Uterus, Endometrium,
Older. Freezing your eggs? Information about the procedure of retrieving and freezing eggs or a section of an ovary.
 Older Freezing your eggs? Information about the procedure of retrieving and freezing eggs or a section of an ovary. Good to know. This information is for younger people who, due to cancer treatment, may
Older Freezing your eggs? Information about the procedure of retrieving and freezing eggs or a section of an ovary. Good to know. This information is for younger people who, due to cancer treatment, may
Ovary Transplantation, VS Oocyte Freezing
 Ovary Transplantation, VS Oocyte Freezing Outline of Talk Ovarian Tissue Cryopreservation Oocyte Cryopreservation Ovary Tissue vs Oocyte Freezing It All Begins Here The Epiblast Primordial Germ Cells Primordial
Ovary Transplantation, VS Oocyte Freezing Outline of Talk Ovarian Tissue Cryopreservation Oocyte Cryopreservation Ovary Tissue vs Oocyte Freezing It All Begins Here The Epiblast Primordial Germ Cells Primordial
Department of Obstetrics and Gynecology, Cleveland Clinic Foundation, Cleveland, Ohio
 FERTILITY AND STERILITY VOL. 81, NO. 2, FEBRUARY 2004 Copyright 2004 American Society for Reproductive Medicine Published by Elsevier Inc. Printed on acid-free paper in U.S.A. MODERN TRENDS Edward E. Wallach,
FERTILITY AND STERILITY VOL. 81, NO. 2, FEBRUARY 2004 Copyright 2004 American Society for Reproductive Medicine Published by Elsevier Inc. Printed on acid-free paper in U.S.A. MODERN TRENDS Edward E. Wallach,
Produce Eggs. Fertility Preservation for Trans People who. LGBTQ Reproductive Options
 for Trans People who Produce Eggs LGBTQ Reproductive Options Many trans people are interested in being parents and want to know their options. While many trans people may conceive on their own, this info
for Trans People who Produce Eggs LGBTQ Reproductive Options Many trans people are interested in being parents and want to know their options. While many trans people may conceive on their own, this info
Minimal Access Surgery in Gynaecology
 Gynaecology & Fertility Information for GPs August 2014 Minimal Access Surgery in Gynaecology Today, laparoscopy is an alternative technique for carrying out many operations that have traditionally required
Gynaecology & Fertility Information for GPs August 2014 Minimal Access Surgery in Gynaecology Today, laparoscopy is an alternative technique for carrying out many operations that have traditionally required
Puerto Rico Fertility Center
 Puerto Rico Fertility Center General Information of the In-Vitro Fertilization Program Dr. Pedro J. Beauchamp First test-tube baby IN PUERTO RICO Dr. Pedro Beauchamp with Adlin Román in his arms. Paseo
Puerto Rico Fertility Center General Information of the In-Vitro Fertilization Program Dr. Pedro J. Beauchamp First test-tube baby IN PUERTO RICO Dr. Pedro Beauchamp with Adlin Román in his arms. Paseo
Age Related fertility Preservation: Should you Consider Multiple Egg Freezing Cycles?
 Age Related Fertility Preservation: Should you Consider Multiple Egg Freezing Cycles? Age Related fertility Preservation: Should you Consider Multiple Egg Freezing Cycles? All what we really know for sure
Age Related Fertility Preservation: Should you Consider Multiple Egg Freezing Cycles? Age Related fertility Preservation: Should you Consider Multiple Egg Freezing Cycles? All what we really know for sure
Causes of Infertility and Treatment Options
 Causes of Infertility and Treatment Options Dr Mrs.Kiran D. Sekhar Former vice President-FOGSI Former Chairperson- Genetics and Foetal medicine-fogsi Founder and Medical Director-Kiran Infertility centre
Causes of Infertility and Treatment Options Dr Mrs.Kiran D. Sekhar Former vice President-FOGSI Former Chairperson- Genetics and Foetal medicine-fogsi Founder and Medical Director-Kiran Infertility centre
NICE fertility guidelines. Hemlata Thackare MPhil MSc MRCOG Deputy Medical Director London Women s Clinic
 NICE fertility guidelines Hemlata Thackare MPhil MSc MRCOG Deputy Medical Director London Women s Clinic About the LWC 4 centres around the UK London Cardiff Swansea Darlington The largest sperm bank in
NICE fertility guidelines Hemlata Thackare MPhil MSc MRCOG Deputy Medical Director London Women s Clinic About the LWC 4 centres around the UK London Cardiff Swansea Darlington The largest sperm bank in
03/14/2019. GnRH Analogs for Fertility Preservation: What are the Data? Educational Objectives. Outline
 GnRH Analogs for Fertility Preservation: What are the Data? AHN-JH SKCCC Current Topics in Breast Cancer Symposium Karen Lisa Smith MD MPH Assistant Professor Johns Hopkins Breast and Cancer Program March
GnRH Analogs for Fertility Preservation: What are the Data? AHN-JH SKCCC Current Topics in Breast Cancer Symposium Karen Lisa Smith MD MPH Assistant Professor Johns Hopkins Breast and Cancer Program March
Age and Fertility. A Guide for Patients Revised 2012 Copyright 2012 by the American Society for Reproductive Medicine
 1 Age and Fertility A Guide for Patients Revised 2012 Copyright 2012 by the American Society for Reproductive Medicine INTRODUCTION Fertility changes with age. Both males and females become fertile in
1 Age and Fertility A Guide for Patients Revised 2012 Copyright 2012 by the American Society for Reproductive Medicine INTRODUCTION Fertility changes with age. Both males and females become fertile in
In Vitro Fertilization What to expect
 Patient Education In Vitro Fertilization What to expect This handout describes how to prepare for and what to expect when you have in vitro fertilization. It provides written information about this process,
Patient Education In Vitro Fertilization What to expect This handout describes how to prepare for and what to expect when you have in vitro fertilization. It provides written information about this process,
CHEMOTHERAPY. Chemo, Ctx, Ctx. A category of cancer treatment that uses one or more anti-cancer drugs. Risk factor Male & Female
 CHEMOTHERAPY Chemo, Ctx, Ctx A category of cancer treatment that uses one or more anti-cancer drugs. Risk factor Male & Female About Chemotherapy Chemotherapy is a category of cancer treatment that uses
CHEMOTHERAPY Chemo, Ctx, Ctx A category of cancer treatment that uses one or more anti-cancer drugs. Risk factor Male & Female About Chemotherapy Chemotherapy is a category of cancer treatment that uses
F REQUENTLY A SKED Q UESTIONS
 Polycystic heart, blood vessels, and appearance. Women with PCOS have these characteristics: Ovarian high levels of male hormones, also called androgens an irregular or no menstrual cycle Syndrome may
Polycystic heart, blood vessels, and appearance. Women with PCOS have these characteristics: Ovarian high levels of male hormones, also called androgens an irregular or no menstrual cycle Syndrome may
Guideline for Fertility Preservation for Patients with Cancer
 Guideline for Fertility Preservation for Patients with Cancer COG Supportive Care Endorsed Guidelines Click here to see all the COG Supportive Care Endorsed Guidelines. DISCLAIMER For Informational Purposes
Guideline for Fertility Preservation for Patients with Cancer COG Supportive Care Endorsed Guidelines Click here to see all the COG Supportive Care Endorsed Guidelines. DISCLAIMER For Informational Purposes
Clinical Policy Committee
 Clinical Policy Committee Commissioning policy: Assisted Conception Fertility assessment and investigations are commissioned where: A woman is of reproductive age and has not conceived after one (1) year
Clinical Policy Committee Commissioning policy: Assisted Conception Fertility assessment and investigations are commissioned where: A woman is of reproductive age and has not conceived after one (1) year
WHAT IS A PATIENT CARE ADVOCATE?
 WHAT IS A PATIENT CARE ADVOCATE? Fertility treatments can be overwhelming. As a member, you have unlimited access to a dedicated Patient Care Advocate (PCA), who acts as your expert resource for discussing
WHAT IS A PATIENT CARE ADVOCATE? Fertility treatments can be overwhelming. As a member, you have unlimited access to a dedicated Patient Care Advocate (PCA), who acts as your expert resource for discussing
INTRODUCTION TABLE OF CONTENTS. If you want to become a parent after cancer, we would like to give you the information you need to make that happen.
 TABLE OF CONTENTS INTRODUCTION INTRODUCTION 1 MEN Fertility Risks 2 Fertility Preservation Options 3 Possible Fertility Outcomes 4 Parenthood After Cancer Options 5 Important Tips for Men 6 WOMEN Fertility
TABLE OF CONTENTS INTRODUCTION INTRODUCTION 1 MEN Fertility Risks 2 Fertility Preservation Options 3 Possible Fertility Outcomes 4 Parenthood After Cancer Options 5 Important Tips for Men 6 WOMEN Fertility
WOMEN & INFANTS HOSPITAL Providence, RI CONSENT FOR THAWING AND TRANSFER OF CRYOPRESERVED EMBRYOS. I and
 *40668* 40668 WOMEN & INFANTS HOSPITAL Providence, RI 02905 CONSENT FOR THAWING AND TRANSFER OF CRYOPRESERVED EMBRYOS FOR inpatients: affix patient label OR I and (Print Patient s name) (Print Partner
*40668* 40668 WOMEN & INFANTS HOSPITAL Providence, RI 02905 CONSENT FOR THAWING AND TRANSFER OF CRYOPRESERVED EMBRYOS FOR inpatients: affix patient label OR I and (Print Patient s name) (Print Partner
Information for Recipient of Donor Oocytes
 Introduction Thank you for expressing an interest as an oocyte recipient in our oocyte donation program at the Family Fertility Center. Our successful program was established since 1994 and is directed
Introduction Thank you for expressing an interest as an oocyte recipient in our oocyte donation program at the Family Fertility Center. Our successful program was established since 1994 and is directed
The Adolescent: A Patient at Risk: Ovarian Failure in Adolescent Cancer Survivors
 The Adolescent: A Patient at Risk: Ovarian Failure in Adolescent Cancer Survivors Avner Hershlag MD Professor and Chief Center for Human Reproduction North Shore LIJ Hofsra university School of Medicine
The Adolescent: A Patient at Risk: Ovarian Failure in Adolescent Cancer Survivors Avner Hershlag MD Professor and Chief Center for Human Reproduction North Shore LIJ Hofsra university School of Medicine
WOMEN & INFANTS HOSPITAL Providence, RI CONSENT FOR IVF WITH EMBRYO TRANSFER
 *40639* 40639 WOMEN & INFANTS HOSPITAL Providence, RI 02905 CONSENT FOR IVF WITH EMBRYO TRANSFER I have requested treatment by the physicians and (Print Patient s name) staff of the Women & Infants Fertility
*40639* 40639 WOMEN & INFANTS HOSPITAL Providence, RI 02905 CONSENT FOR IVF WITH EMBRYO TRANSFER I have requested treatment by the physicians and (Print Patient s name) staff of the Women & Infants Fertility
La preservazione della fertilità in oncologia: il carcinoma mammario come paradigma. Olivia Pagani Centro di Senologia dellasvizzera Italiana
 La preservazione della fertilità in oncologia: il carcinoma mammario come paradigma Olivia Pagani Centro di Senologia dellasvizzera Italiana Centro di Senologia della Svizzera Italiana Pregnancy rate after
La preservazione della fertilità in oncologia: il carcinoma mammario come paradigma Olivia Pagani Centro di Senologia dellasvizzera Italiana Centro di Senologia della Svizzera Italiana Pregnancy rate after
Embryo Selection after IVF
 Embryo Selection after IVF Embryo Selection after IVF Many of human embryos produced after in vitro fertilization carry abnormal chromosomes. Placing a chromosomally normal embryo (s) into a normal uterus
Embryo Selection after IVF Embryo Selection after IVF Many of human embryos produced after in vitro fertilization carry abnormal chromosomes. Placing a chromosomally normal embryo (s) into a normal uterus
Dr Manuela Toledo - Procedures in ART -
 Dr Manuela Toledo - Procedures in ART - Fertility Specialist MBBS FRANZCOG MMed CREI Specialities: IVF & infertility Fertility preservation Consulting Locations East Melbourne Planning a pregnancy - Folic
Dr Manuela Toledo - Procedures in ART - Fertility Specialist MBBS FRANZCOG MMed CREI Specialities: IVF & infertility Fertility preservation Consulting Locations East Melbourne Planning a pregnancy - Folic
Recent Developments in Infertility Treatment
 Recent Developments in Infertility Treatment John T. Queenan Jr., MD Professor, Dept. Of Ob/Gyn University of Rochester Medical Center Rochester, NY Disclosures I don t have financial interest or other
Recent Developments in Infertility Treatment John T. Queenan Jr., MD Professor, Dept. Of Ob/Gyn University of Rochester Medical Center Rochester, NY Disclosures I don t have financial interest or other
Clinical Policy Committee
 Northern, Eastern and Western Devon Clinical Commissioning Group South Devon and Torbay Clinical Commissioning Group Clinical Policy Committee Commissioning policy: Assisted Conception Fertility treatments
Northern, Eastern and Western Devon Clinical Commissioning Group South Devon and Torbay Clinical Commissioning Group Clinical Policy Committee Commissioning policy: Assisted Conception Fertility treatments
Spontaneous recovery of ovarian function and fertility after cancer treatment
 Rigshospitalet The Fertility Clinic Copenhagen, Denmark Spontaneous recovery of ovarian function and fertility after cancer treatment Kirsten Tryde Macklon, Ph.D. 5th society of reproductive medicine and
Rigshospitalet The Fertility Clinic Copenhagen, Denmark Spontaneous recovery of ovarian function and fertility after cancer treatment Kirsten Tryde Macklon, Ph.D. 5th society of reproductive medicine and
Chapter 9. Yasmin Gosiengfiao, MD
 Chapter 9 Progress, History and Promise of Ovarian Cryopreservation and Transplantation for Pediatric Cancer Patients T.K. Woodruff and K.A. Snyder (eds.) Oncofertility. Springer 2007 The original publication
Chapter 9 Progress, History and Promise of Ovarian Cryopreservation and Transplantation for Pediatric Cancer Patients T.K. Woodruff and K.A. Snyder (eds.) Oncofertility. Springer 2007 The original publication
Reproductive function in cancer survivors
 Reproductive function in cancer survivors Professor W Hamish Wallace hamish.wallace@nhs.net Symposium 20: Endocrine consequences of childhood cancer treatment Liffey Hall 2, 0905 19 May 2015 CONFLICT OF
Reproductive function in cancer survivors Professor W Hamish Wallace hamish.wallace@nhs.net Symposium 20: Endocrine consequences of childhood cancer treatment Liffey Hall 2, 0905 19 May 2015 CONFLICT OF
FERTILITY PRESERVATION OPTIONS FOR CANCER PATIENTS
 FERTILITY PRESERVATION OPTIONS FOR CANCER PATIENTS Justo Callejo Olmos, 1 Laura Almeida Toledano 2 1. Professor and Clinical Chief of Gynecology, Department of Obstetrics and Gynaecology, Hospital Sant
FERTILITY PRESERVATION OPTIONS FOR CANCER PATIENTS Justo Callejo Olmos, 1 Laura Almeida Toledano 2 1. Professor and Clinical Chief of Gynecology, Department of Obstetrics and Gynaecology, Hospital Sant
In Vitro Fertilization
 Patient Education In Vitro Fertilization About the treatment This handout describes how to prepare for and what to expect when you have in vitro fertilization. It provides written information about this
Patient Education In Vitro Fertilization About the treatment This handout describes how to prepare for and what to expect when you have in vitro fertilization. It provides written information about this
Infertility treatment
 In the name of God Infertility treatment Treatment options The optimal treatment is one that provide an acceptable success rate, has minimal risk and is costeffective. The treatment options are: 1- Ovulation
In the name of God Infertility treatment Treatment options The optimal treatment is one that provide an acceptable success rate, has minimal risk and is costeffective. The treatment options are: 1- Ovulation
Adoption and Foster Care
 GLOSSARY Family building via Adoption and Foster Care October 2018 www.familyequality.org/resources A Anonymous Donor: A person who donated sperm or eggs with the intention of never meeting resulting children.
GLOSSARY Family building via Adoption and Foster Care October 2018 www.familyequality.org/resources A Anonymous Donor: A person who donated sperm or eggs with the intention of never meeting resulting children.
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL Policy Number: PA.018.MH Last Review Date: 08/04/2016 Effective Date: 01/01/2017
 MedStar Health, Inc. POLICY AND PROCEDURE MANUAL PA.018.MH Infertility- Treatment This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP (Not Covered) MedStar
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL PA.018.MH Infertility- Treatment This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP (Not Covered) MedStar
Symptom Management. Fertility and You
 Symptom Management Fertility and You Table of Contents 3 Will cancer impact my ability to have children? 4 How do I talk to my children about preserving their fertility during cancer treatment? 5 What
Symptom Management Fertility and You Table of Contents 3 Will cancer impact my ability to have children? 4 How do I talk to my children about preserving their fertility during cancer treatment? 5 What
Female Reproductive System. Lesson 10
 Female Reproductive System Lesson 10 Learning Goals 1. What are the five hormones involved in the female reproductive system? 2. Understand the four phases of the menstrual cycle. Human Reproductive System
Female Reproductive System Lesson 10 Learning Goals 1. What are the five hormones involved in the female reproductive system? 2. Understand the four phases of the menstrual cycle. Human Reproductive System
OVARIAN CRYOPRESERVATION: BACKGROUND, FERTILITY PREDICTION AND THE EDINBURGH EXPERIENCE
 OVARIAN CRYOPRESERVATION: BACKGROUND, FERTILITY PREDICTION AND THE EDINBURGH EXPERIENCE Professor W Hamish Wallace Consultant Paediatric Oncologist Royal Hospital for Sick Children Edinburgh hamish.wallace@nhs.net
OVARIAN CRYOPRESERVATION: BACKGROUND, FERTILITY PREDICTION AND THE EDINBURGH EXPERIENCE Professor W Hamish Wallace Consultant Paediatric Oncologist Royal Hospital for Sick Children Edinburgh hamish.wallace@nhs.net
Guideline for Fertility Preservation for Patients with Cancer
 Guideline for Fertility Preservation for Patients with Cancer COG Supportive Care Endorsed Guidelines Click here to see all the COG Supportive Care Endorsed Guidelines. DISCLAIMER For Informational Purposes
Guideline for Fertility Preservation for Patients with Cancer COG Supportive Care Endorsed Guidelines Click here to see all the COG Supportive Care Endorsed Guidelines. DISCLAIMER For Informational Purposes
Review Article Cancer, Fertility Preservation, and Future Pregnancy: AComprehensiveReview
 Obstetrics and Gynecology International Volume 2012, Article ID 953937, 11 pages doi:10.1155/2012/953937 Review Article Cancer, Fertility Preservation, and Future Pregnancy: AComprehensiveReview Michelle
Obstetrics and Gynecology International Volume 2012, Article ID 953937, 11 pages doi:10.1155/2012/953937 Review Article Cancer, Fertility Preservation, and Future Pregnancy: AComprehensiveReview Michelle
Chapter 17 Oncofertility Consortium Consensus Statement: Guidelines for Ovarian Tissue Cryopreservation
 Chapter 17 Oncofertility Consortium Consensus Statement: Guidelines for Ovarian Tissue Cryopreservation Leilah E. Backhus, MD, MS, Laxmi A. Kondapalli, MD, MS, R. Jeffrey Chang, MD, Christos Coutifaris,
Chapter 17 Oncofertility Consortium Consensus Statement: Guidelines for Ovarian Tissue Cryopreservation Leilah E. Backhus, MD, MS, Laxmi A. Kondapalli, MD, MS, R. Jeffrey Chang, MD, Christos Coutifaris,
POST - DOCTORAL FELLOWSHIP PROGRAMME IN REPRODUCTIVE MEDICINE. Anatomy : Male and Female genital tract
 POST - DOCTORAL FELLOWSHIP PROGRAMME IN REPRODUCTIVE MEDICINE DURATION OF THE COURSE : TWO YEARS Detailed syllabus: Part 1 Basic Sciences: Anatomy : Male and Female genital tract Physiology Endocrinology
POST - DOCTORAL FELLOWSHIP PROGRAMME IN REPRODUCTIVE MEDICINE DURATION OF THE COURSE : TWO YEARS Detailed syllabus: Part 1 Basic Sciences: Anatomy : Male and Female genital tract Physiology Endocrinology
OVARIAN FUNCTION AFTER CHILDHOOD CANCER
 OVARIAN FUNCTION AFTER CHILDHOOD CANCER Practicing through Controversy Diane Puccetti MD Leslie Coker Appiah MD NASPAG April 2018 Objectives Review use and limitations of risk stratification. Understand
OVARIAN FUNCTION AFTER CHILDHOOD CANCER Practicing through Controversy Diane Puccetti MD Leslie Coker Appiah MD NASPAG April 2018 Objectives Review use and limitations of risk stratification. Understand
ASSISTED CONCEPTION NHS FUNDED TREATMENT FOR SUBFERTILITY ELIGIBILITY CRITERIA & POLICY GUIDANCE
 ASSISTED CONCEPTION NHS FUNDED TREATMENT FOR SUBFERTILITY ELIGIBILITY CRITERIA & POLICY GUIDANCE Version 1.0 Page 1 of 11 MARCH 2014 POLICY DOCUMENT VERSION CONTROL CERTIFICATE TITLE Title: Assisted Conception
ASSISTED CONCEPTION NHS FUNDED TREATMENT FOR SUBFERTILITY ELIGIBILITY CRITERIA & POLICY GUIDANCE Version 1.0 Page 1 of 11 MARCH 2014 POLICY DOCUMENT VERSION CONTROL CERTIFICATE TITLE Title: Assisted Conception
Restoration of ovarian steroid secretion and histologic assessment after freezing, thawing, and autograft of a hemi-ovary in sheep
 FERTILITY AND STERILITY VOL. 72, NO. 2, AUGUST 1999 Copyright 1999 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Restoration of ovarian
FERTILITY AND STERILITY VOL. 72, NO. 2, AUGUST 1999 Copyright 1999 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Restoration of ovarian
Puberty and Fertility. Normal Female Puberty PUBERTY! What about girls with Galactosemia? E Puberty and Fertility Badik Spencer 1
 Puberty and Fertility Jennifer Badik*, MD Pediatric Endocrinology and Jessica Spencer*, MD, MSc Reproductive Endocrinology and Infertility Part One PUBERTY! *no conflicts of interest to report Every girl
Puberty and Fertility Jennifer Badik*, MD Pediatric Endocrinology and Jessica Spencer*, MD, MSc Reproductive Endocrinology and Infertility Part One PUBERTY! *no conflicts of interest to report Every girl
UW MEDICINE PATIENT EDUCATION. In Vitro Fertilization How to prepare and what to expect DRAFT
 UW MEDICINE PATIENT EDUCATION In Vitro Fertilization How to prepare and what to expect This handout tells how to prepare for and what to expect when you go through a cycle of in vitro fertilization. It
UW MEDICINE PATIENT EDUCATION In Vitro Fertilization How to prepare and what to expect This handout tells how to prepare for and what to expect when you go through a cycle of in vitro fertilization. It
9.4 Regulating the Reproductive System
 9.4 Regulating the Reproductive System The Reproductive System to unite a single reproductive cell from a female with a single reproductive cell from a male Both male and female reproductive systems include
9.4 Regulating the Reproductive System The Reproductive System to unite a single reproductive cell from a female with a single reproductive cell from a male Both male and female reproductive systems include
Fertility, Egg Freezing, and You. If you have questions, we can help you get answers.
 Fertility, Egg Freezing, and You If you have questions, we can help you get answers. Let s talk about fertility If you re thinking about having a baby someday but aren t ready now, you should learn all
Fertility, Egg Freezing, and You If you have questions, we can help you get answers. Let s talk about fertility If you re thinking about having a baby someday but aren t ready now, you should learn all
NHS FUNDED TREATMENT FOR SUBFERTILITY. ELIGIBILITY CRITERIA POLICY GUIDANCE/OPTIONS FOR CCGs
 NHS FUNDED TREATMENT FOR SUBFERTILITY ELIGIBILITY CRITERIA POLICY GUIDANCE/OPTIONS FOR CCGs CONTENTS Page 1. INTRODUCTION 2 2. GENERAL PRINCIPLES 2 3. DEFINITION OF SUBFERTILITY AND TIMING OF ACCESS TO
NHS FUNDED TREATMENT FOR SUBFERTILITY ELIGIBILITY CRITERIA POLICY GUIDANCE/OPTIONS FOR CCGs CONTENTS Page 1. INTRODUCTION 2 2. GENERAL PRINCIPLES 2 3. DEFINITION OF SUBFERTILITY AND TIMING OF ACCESS TO
COMMISSIONING POLICY FOR IN VITRO FERTILISATION (IVF)/ INTRACYTOPLASMIC SPERM INJECTION (ICSI) WITHIN TERTIARY INFERTILITY SERVICES
 COMMISSIONING POLICY FOR IN VITRO FERTILISATION (IVF)/ INTRACYTOPLASMIC SPERM INJECTION (ICSI) WITHIN TERTIARY INFERTILITY SERVICES Version number V2.3 Responsible individual Author(s) Barry Weaver Trish
COMMISSIONING POLICY FOR IN VITRO FERTILISATION (IVF)/ INTRACYTOPLASMIC SPERM INJECTION (ICSI) WITHIN TERTIARY INFERTILITY SERVICES Version number V2.3 Responsible individual Author(s) Barry Weaver Trish
Oncofertility: The Preservation of Fertility Options for Young People with Cancer
 Oncofertility: The Preservation of Fertility Options for Young People with Cancer Teresa K. Woodruff, Ph.D. The Thomas J. Watkins Professor of Obstetrics and Gynecology Northwestern University Feinberg
Oncofertility: The Preservation of Fertility Options for Young People with Cancer Teresa K. Woodruff, Ph.D. The Thomas J. Watkins Professor of Obstetrics and Gynecology Northwestern University Feinberg
Infertility in Women over 35. Alison Jacoby, MD Dept. of Ob/Gyn UCSF
 Infertility in Women over 35 Alison Jacoby, MD Dept. of Ob/Gyn UCSF Learning Objectives Review the effect of age on fertility Fertility counseling for the patient >35 - timing - lifestyle - workup Fertility
Infertility in Women over 35 Alison Jacoby, MD Dept. of Ob/Gyn UCSF Learning Objectives Review the effect of age on fertility Fertility counseling for the patient >35 - timing - lifestyle - workup Fertility
Updated Analysis of Non-Surgical Premature Menopause in the Childhood Cancer Survivor Study
 Analysis Concept Proposal 1. Study Title Updated Analysis of Non-Surgical Premature Menopause in the Childhood Cancer Survivor Study 2. Working Group and Investigators CCSS Working Group: Chronic Disease
Analysis Concept Proposal 1. Study Title Updated Analysis of Non-Surgical Premature Menopause in the Childhood Cancer Survivor Study 2. Working Group and Investigators CCSS Working Group: Chronic Disease
Phases of the Ovarian Cycle
 OVARIAN CYCLE An ovary contains many follicles, and each one contains an immature egg called an oocyte. A female is born with as many as 2 million follicles, but the number is reduced to 300,000 to 400,000
OVARIAN CYCLE An ovary contains many follicles, and each one contains an immature egg called an oocyte. A female is born with as many as 2 million follicles, but the number is reduced to 300,000 to 400,000
Cancer & Fertility: Patient Education Booklet. information suppor t hope
 Cancer & Fertility: Patient Education Booklet information suppor t hope 1 table of contents introduction 1 men Fertility Risks 2 Fertility Preservation Options 3 Possible Fertility Outcomes 4 Parenthood
Cancer & Fertility: Patient Education Booklet information suppor t hope 1 table of contents introduction 1 men Fertility Risks 2 Fertility Preservation Options 3 Possible Fertility Outcomes 4 Parenthood
Blackpool CCG. Policies for the Commissioning of Healthcare. Assisted Conception
 1 Introduction Blackpool CCG Policies for the Commissioning of Healthcare Assisted Conception 1.1 This policy describes circumstances in which NHS Blackpool Clinical Commissioning Group (CCG) will fund
1 Introduction Blackpool CCG Policies for the Commissioning of Healthcare Assisted Conception 1.1 This policy describes circumstances in which NHS Blackpool Clinical Commissioning Group (CCG) will fund
Milder is better? Advantages and disadvantages of "mild" ovarian stimulation for human in vitro fertilization
 Milder is better? Advantages and disadvantages of "mild" ovarian stimulation for human in vitro fertilization Revelli et al. Reproductive Biology and Endocrinology 2011, 9:25 Presenter: R2 孫怡虹 Background
Milder is better? Advantages and disadvantages of "mild" ovarian stimulation for human in vitro fertilization Revelli et al. Reproductive Biology and Endocrinology 2011, 9:25 Presenter: R2 孫怡虹 Background
DCare - Shot Technique
 Ovarian rejuvenation is a procedure that may create new eggs in the ovaries of women who are unable to conceive because of early menopause, advanced maternal age or low oocyte (egg) reserve, yet who wish
Ovarian rejuvenation is a procedure that may create new eggs in the ovaries of women who are unable to conceive because of early menopause, advanced maternal age or low oocyte (egg) reserve, yet who wish
Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature
 REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
Infertility: failure to conceive within one year of unprotected regular sexual intercourse. Primary secondary
 Subfertility Infertility: failure to conceive within one year of unprotected regular sexual intercourse. Primary secondary Infertility affects about 15 % of couples. age of the female. Other factors that
Subfertility Infertility: failure to conceive within one year of unprotected regular sexual intercourse. Primary secondary Infertility affects about 15 % of couples. age of the female. Other factors that
The reproductive lifespan
 The reproductive lifespan Reproductive potential Ovarian cycles Pregnancy Lactation Male Female Puberty Menopause Age Menstruation is an external indicator of ovarian events controlled by the hypothalamicpituitary
The reproductive lifespan Reproductive potential Ovarian cycles Pregnancy Lactation Male Female Puberty Menopause Age Menstruation is an external indicator of ovarian events controlled by the hypothalamicpituitary
COMMISSIONING POLICY FOR IN VITRO FERTILISATION (IVF)/ INTRACYTOPLASMIC SPERM INJECTION (ICSI) WITHIN TERTIARY INFERTILITY SERVICES V2.
 COMMISSIONING POLICY FOR IN VITRO FERTILISATION (IVF)/ INTRACYTOPLASMIC SPERM INJECTION (ICSI) WITHIN TERTIARY INFERTILITY SERVICES V2.3 2017 Agreed at Cannock Chase CCG Signature: Designation: Chair of
COMMISSIONING POLICY FOR IN VITRO FERTILISATION (IVF)/ INTRACYTOPLASMIC SPERM INJECTION (ICSI) WITHIN TERTIARY INFERTILITY SERVICES V2.3 2017 Agreed at Cannock Chase CCG Signature: Designation: Chair of
