Audit of two-week rule referrals for suspected testicular cancer in Cornwall,
|
|
|
- Louisa McBride
- 6 years ago
- Views:
Transcription
1 The Royal College of Surgeons of England UROLOGY doi / X Audit of two-week rule referrals for suspected testicular cancer in Cornwall, PRAKASH KUMARASWAMY, ROBERT COX, JOHN S O ROURKE, ROBERT G. WILLIS Department of Urology, Royal Cornwall Hospital, Truro, Cornwall, UK ABSTRACT INTRODUCTION The objective was to evaluate the two-week wait referral system for suspected testicular cancer and to compare waiting times from referral to treatment before and after the introduction of the two-week wait process. PATIENTS AND METHODS We reviewed 241 case notes for patients referred under the two-week wait system with suspected testicular tumour during a complete 3-year period ( ) and recorded information from the referral letter, findings in the urology clinic, results of ultrasound and final outcomes. We also identified 42 cases of testicular tumour treated during a complete 3-year period ( ) just before the two-week wait system was introduced. The journey from referral to treatment for tumour cases was compared during these two periods. RESULTS Testicular cancer was only found in 8% of patients referred by the two-week wait system. We judged the referral to be inappropriate in 48% of cases. Of referred cases, 78% required no surgical treatment. There was a significant improvement of 9 days in the average time from general practitioner (GP) referral to urology clinic attendance but all other journey intervals remained the same. CONCLUSIONS The performance of GPs in examining scrotal swellings and applying the two-week wait guidelines was very poor, resulting in many unnecessary urgent clinic visits. The referral system speeds up the visit to a urology clinic but the overall effect is probably not of clinical significance. We suggest that it would be much more cost-effective for all these patients to have an ultrasound scan within 2 weeks instead of a urology clinic appointment. KEYWORDS Testes Tumour Cancer Two-week referral CORRESPONDENCE TO Prakash Kumaraswamy, Department of Urology, Royal Cornwall Hospital, Truro, Cornwall TR1 3LJ, UK T: +44 (0) ; F: +44 (0) ; E: dr_prakashk@yahoo.com In February 2000, the UK Department of Health introduced a range of cancer rules and targets which directly impacted upon general practitioners (GPs) and hospital departments responsible for managing cancer patients. This was prompted by evidence that, in some areas of cancer treatment, cancer survival in the UK was inferior to figures from Europe and North America. A number of changes were introduced to tackle this problem and this included a series of speciality and tumour-specific two-week wait rules. For urology this included suspected prostate cancer, bladder/urothelial cancer, kidney cancer, testis and penile cancer. Central guidance criteria were issued by the Department of Health covering each speciality and GPs were encouraged to fax referrals for cases which fitted the criteria direct to their local hospital centre. It should be noted that there were no preliminary studies to pilot this system and demonstrate benefit or cost-effectiveness. For suspected testicular cancer, the 2000 referral guidelines stipulated swellings in the body of the testis. In addition, some general guidance was included (Table 1). In June 2005, the original guidance was replaced by guidance from the National Institute for Health and Clinical Excellence (NICE). The referral criterion was refer urgently patients with a swelling or mass in the body of the testis. Within the full guidance document, the original general advice was replaced with the information given in Table 2. This audit was stimulated by the impression of one consultant author (RGW) that a large proportion of two-week wait referrals for suspected testicular cancer seen in his clinic were inappropriate and often consisted of elderly men with clinically obvious hydroceles and epididymal cysts. We decided to audit these referrals, first to assess the quality of referrals, and second to see if the introduction of 239
2 Table 1 Original February 2000 two-week wait referral guidance for testis cancer Table 2 Revised guidance from NICE, 2005, for testicular cancer Scrotal swellings are relatively common in general practice Solid swellings affecting the body of the testis have a high probability (> 50%) of being due to cancer Indeterminate swellings of the testicle have a low probability of being due to cancer especially in men over 55 years and should be considered for ultrasound before urological referral Swellings outside the body of the testis are hardly ever due to cancer and need not be referred urgently the two-week wait system made any significant difference to time taken from referral to treatment. Patients and Methods Cornwall is a long, narrow peninsula and the county has a single major hospital. With the exception of areas in North Cornwall close to Plymouth and Barnstaple, we knew that the vast majority of testicular tumours from Cornwall would be seen and treated in the Royal Cornwall Hospital and that their histology would be accessible in our pathology laboratory. We also discovered that all two-week wait referrals to our hospital are processed by a single dedicated office with an electronic database and they were able to list all referrals for suspected testicular cancer. We performed a retrospective audit for the period January 2003 to December 2005 inclusive and we asked for a list of referrals for suspected testicular cancer seen under the two-week wait system for all three urology consultants (RC, JSOR and RGW). The hospital notes were retrieved and Table 3 Data collected from hospital notes Name and hospital number Age at referral A history of a vasectomy Did the swelling relate to vasectomy? GP description of examination Did the referral fit the criterion for two-week wait referral? Urologist s findings Ultrasound findings Was a tumour found? Histology of tumours Final outcome Any patient with a swelling or mass in the body of the testis should be referred urgently An urgent ultrasound should be considered in men with a scrotal mass that does not transilluminate and/or when the body of the testis cannot be distinguished studied jointly by two of the authors (PK and RGW). A proforma was designed for data collection (PK) and a Microsoft Access database was created for data storage and analysis (RGW). The data fields used for this part of the study are listed in Table 3. For every referral, the description of physical signs from the GP letter was recorded verbatim and then compared with the two-week wait guidelines. A joint decision was agreed as to whether the referral was correct or not under this scheme. If there was any disagreement or doubt about the appropriateness of a referral, it was marked as valid. It was, of course, possible that some two-week wait referrals might be missed and we approached the pathology department to see if we could double-check the list of tumour cases found from the review of notes. A print-out of all histology reports which included testis was obtained for the study period and was carefully vetted by one author (PK) to identify testicular tumours. This method was repeated for the 3-year period January 1997 to December 1999 to identify all testicular tumours treated in the 3-year period immediately before the introduction of the two-week wait rule. For all cases so identified, additional data were recorded (Table 4). The intervals along the patient journey from GP referral to orchidectomy were calculated for each patient and a comparison was made between those patients referred before the twoweek wait rule was introduced ( , inclusive) and with those referred after the introduction of the two-week wait system ( , inclusive). Differences between these groups Table 4 Additional data collected for proven cases of testicular cancer Date of referral Date seen in clinic Date of operation Histology 240
3 Table 5 Examples of inappropriate referrals Table 6 Testicular tumours found in two-week wait referrals Can feel the left testicle as normal swelling attached to it Mass at lower pole of scrotum distinct from either testicle No testicular swelling or abnormality on examination A soft lump adjacent to [R] testis I do not expect this to be a malignant lump Left hydrocele transilluminates completely to exclude underlying neoplasm He has a very large hydrocele transilluminates may be due to malignancy This may well be a cyst of the [R] epididymis Appears to have a hydrocele on the [L] side Swelling not attached to the [L] testis feels like a varicocele Painless lump on his [R] testicle appearance of epididymal cyst which transilluminates Cystic swelling separate from testis Lump in [L] scrotum I felt it was a hydrocele were analysed using the Kaplan Meier survival analysis using orchidectomy for suspected tumour as the survival end-point. This method was chosen on the advice of Dr Colin Pritchard, statistician to our hospital and he performed the analysis using SPSS software. Results Two-week wait referrals, inclusive A total of 241 patients were referred to the urology department under the two-week wait rule with suspicion of testicular cancer. The age range was years of age (average, 42 years). We have compared this with the age distribution for all of the 65 testicular cancer patients found in our study ( and ). For these tumour cases, the age range was years (average, 41.1 years). Therefore, the age characteristics of patients referred under the twoweek wait rule were similar to the patients with testicular cancer. For 37 patients, there was a history of a previous vasectomy; usually this was noted in the urology clinic and not in the GP referral letter. In 17 of these cases (46%), the referred swelling was thought to relate to the previous vasectomy. However, a previous vasectomy did not avoid a risk of tumour and three were subsequently diagnosed in this group (1 seminoma, 1 lymphoma and 1 benign Leydig cell tumour). The two authors who reviewed the referral letters judged that, in 115 patients (48%), the referral did not fit the Testicular tumours found (n = 23) from 241 referrals (10%) Testicular carcinomas (20) * Seminomas (14) * Teratomas (2) * Embryonal/yolk-sac tumours (2) * Lymphomas (2) Benign tumours (3) * Leydig cell tumours (2) * Epidermoid cyst (1) Overall cancer detection rate 8% Only tumour cases from correct two-week wait referrals guidelines. In 43 instances (18%), we judged that there was a flagrant breach of protocol. Some examples of these are given in Table 5. In two cases, the referral letter suggested that the GP had not actually examined the patient. Overall, 158 (66%) of the two-week wait referrals underwent an ultrasound scan of the testes and every tumour found in our series had ultrasound confirmation before surgery. Although GPs had referred 241 patients as suspected of having a testicular tumour, a diagnosis of testicular tumour was only made on initial examination in 29 cases by a urologist and a total of 23 tumours were subsequently confirmed. Therefore, the final yield of tumours was only 10% and for malignant tumours was just 8% of two-week wait referrals. The tumour characteristics are given in Table 6. It is important to note that not a single tumour was found from an inappropriate referral. Two testicular tumours were identified in patients thought to have a benign epididymal swelling on initial examination by a urologist; one was a benign adenomatoid tumour of the epididymis and the second was a spermatocytic seminoma in a 74-year-old patient. The final outcomes for the 241 two-week wait referred patients is given in Table 7. The majority of patients (56%) Table 7 Outcomes in two-week wait referred cases (n = 241) Orchidectomy for suspected tumour 26 Re-assured and discharged 134 (56%) Follow-up with scans 8 Surgery for hydrocele, cyst, etc. 28 Treated for epididymitis 19 DNA follow-up 25 Other unrelated treatment 1 241
4 Table 8 Average journey intervals in days (± SD) Interval Pre-two-week wait Post-two-week wait P-value (n = 42) (n = 23) Referral to clinic 16 (± 13.2) 6.8 (± 5.1) Clinic to operation 25.7 (± 31.3) 25 (± 25.5) Referral to operation 41.8 (± 35.3) 31.8 (± 27.3) Statistical comparison by Kaplan Meier survival analysis. were re-assured and discharged with no treatment after initial assessment. In total, 187 patients (78%) did not require any surgical intervention at all and only 28 (12%) went on to have elective surgery for hydroceles and epididymal cysts, etc. Overall, 74 cases (31%) received treatment of some kind following referral, including antibiotics. When the pathology laboratory database was compared with this list of two-week wait referrals only two other tumour case were found one of which had been referred to the private sector and the other via a traditional letter. Referral to treatment times before and after the two-week wait rule In total, we found 23 patients with a testicular tumour from two-week wait referrals ( , inclusive) and identified a further 42 patients with tumours in the period inclusive immediately before the two-week wait rules were introduced. Using the data collected as outlined in Table 4, we compared the patient s journey from referral to orchidectomy for tumour in these two groups and time periods. These data are summarised in Table 8. Tumours in the over 55-year-old age group It was apparent that the age characteristics of referred patients and tumour cases was higher than we expected. Of the 65 testicular tumours found from the two periods of this study, 14 (22%) were aged 55 years or over; Table 9 shows the tumour types found. Discussion The impression that GPs in Cornwall were referring too many older men for suspected testicular cancer is correct in comparison to UK data. From the 241 cases referred under the two-week wait rule in this study, 30% of men were > 55 years of age. Cancer Research UK has published data on the internet suggesting that this type of malignancy affects only 8% of men > 55 years of age. 1 However, when we looked at the total series of 65 testicular tumour patients from the two phases of this study, we were surprised to find that 22% were > 55 years of age. We have no data to explain this observation but it may reflect the popularity of Cornwall for retirement and a more elderly population in the county. We carefully examined the notes and referral letter for evidence of a previous vasectomy. It is clear that the referring GP rarely mentioned such a history when this was identified by the urologist and it was obvious that hardly any GPs appreciated that vasectomy can cause swelling of the epididymis 2 or other masses such as a palpable vasectomy site or sperm granuloma. We have shown that vasectomy patients can develop a testicular tumour but, nonetheless, the frequent referral of worried men with no abnormality other than the postoperative features from a vasectomy might merit some discussion in guidelines. The principal findings of this study are that GPs are very poor at examination of the scrotum and weak at interpreting their own findings. The nature of many of the referred swellings was easily determined using a pen torch and there was scant reference to trans-illumination in the referral letters. From the 241 referrals from GPs of suspected testicular tumour, only 29 tumours were suspected on clinical examination by a urologist, only 23 (10%) tumours confirmed by ultrasound and 20 (8%) of these were malignant. These cancer detection rates are lower than in another report where figures of 17% from two-week wait referrals and 15% for all suspected testicular tumour referrals were found. 3 When comparing the GP s description of the examination with the guidelines, 48% of the referrals were judged not to fit the criteria and 18% flagrantly broke protocol. Table 9 Tumours found in men aged 55 years or older Lymphoma 5 Spermatocystic seminoma 2 Seminoma 6 Leydig cell 1 242
5 From a smaller study in Liverpool, the authors found that up to 83% of their referrals were inappropriate. 4 In another report from Gloucestershire, it was observed that 81% of two-week wait referrals did not fit the guidance. 3 Clearly, many GPs feel that they have a right to over-ride the guidelines. However, our data clearly show that not a single tumour was found other than in correctly referred patients, a finding confirmed in the study from Liverpool. 4 This and our own study clearly show that GPs should strictly abide by the referral criteria and that to do so would dramatically reduce the burden from these patients in urology clinics. The cases cited in Table 5 demonstrate a belief by some GPs that testicular tumour can hide behind an associated hydrocele. Whilst the original guidance from February 2000 (Table 1) was re-assuring in this regard, the revised guidance from NICE (Table 2) if anything tends to encourage this concern about hydroceles. From our study, there was no case where a testicular tumour was associated with, or concealed by, a hydrocele. A computerised population study from Denmark of 183 boys diagnosed with testicular cancer reported a higher risk associated with cryptorchidism, hypospadias, inguinal hernia, and hydrocele. 5 However, this relates to congenital patent processus variants and not adult (acquired) hydrocele. A literature search of PubMed failed to find any clear account of association between the common varieties of testicular tumour and adult hydrocele other than occasional case reports usually involving rare pathologies. In Table 7, we list the outcomes for the 241 two-week wait referral cases. It is clear that the majority of these patients do not require anything other than re-assurance that they do not have cancer. Excluding those patients (29) who had an orchidectomy for suspected cancer, only 28 (12%) went on to have elective surgery for their scrotal swelling and a further 19 (8%) required antibiotic therapy for epididymitis. This latter group could, of course, have been treated by the GP. The final part of our project was to assess the impact of the two-week wait system on the journey from referral to orchidectomy for testicular cancer (Table 8). The data clearly show that the only significant change has been the shortened time from referral to being seen in the urology clinic (reduced by an average of 9 days). This reduction is almost certainly explained by the more streamlined process faxing of the referral letters and direct booking of cases into clinic without preliminary vetting by the urologists. Once seen in the urology clinic, the interval from then until orchidectomy has not altered at all since the two-week wait rule was introduced, showing that urologists have always treated these cases expeditiously. Although we have no data on survival rates, we would doubt that the overall 10-day improvement from referral to orchidectomy would have any significant effect on cancer survival, especially as this tumour group has such a good survival prospect overall. It is important to appreciate the invaluable role of ultrasound in assessing this group of patients. Ultrasound scanning has become the gold standard in determining the presence of a testicular tumours 6 9 and is the final arbiter where there is doubt or dispute. Although the urologists dispensed with a scan in 34% of the referred cases, without doubt many patients were scanned to re-assure the patient in the face of opposing clinical diagnoses from GP and urologist. From the outcome data in Table 7, clearly this is what many patients and GPs require. Given the very small tumour and cancer detection rate and high probability that a scan will be required, we would argue that this group of patients would be better served by having an ultrasound scan within 2 weeks rather than being seen by a urologist. This conclusion has also been suggested by others. 4,10 We have attempted to compare the costs between a scan first or a urology clinic first approach in Table 10. Although there are many pitfalls in constructing such estimates, there is little doubt that the scan first method would save money for the NHS. It should also be borne in mind that, in order to meet waiting-time targets, all three urology consultants in our department are currently carrying out extra out-patient clinics and any process which reduces demand for clinic appointments would be beneficial. Despite introducing such a costly fast-track referral system with no evidence-basis, it must be profoundly disappointing to all involved health professionals that there was also no attempt to put in place any on-going audit measures Table 10 Cost estimates Based on: Urology new appointment = 168 (includes subsequent investigations) Scrotal ultrasonography (trust tariff for GP) = Current two-week wait system 241 appointments = 40,488 Total = 40,488 A scan first system Cases needing clinic after scan: 26 Underwent orchidectomy 8 Followed up with scans 28 Had benign surgery Total = appointments = 10, ultrasound scans = 15,000 Total = 25,
6 (other than target compliance) to assess cost, benefit or improved outcomes. Several publications on the two-week wait system report high rates of inappropriate referral, low detection rates of cancer, large numbers of cancers coming via other referral methods and increased delays for nontwo-week wait appointments One study has looked at differences in survival for colon cancer before and after the introduction of the two-week wait; no difference was found, although the 2-year survival figure used is rather short. 15 A survey of GPs suggested that they appreciated that they are over-referring cases under the two-week wait rule, in part because of concerns that cases referred by more traditional methods would inevitably wait longer. 16 Conclusions The application of the two-week wait criteria for suspected testicular cancer by GPs is very poor and their ability to compare scrotal examination with referral guidelines is weak, resulting in a large number of unnecessary urology clinic appointments. The faster journey from referral to orchidectomy was not statistically significant and is almost certainly not clinically significant. We would suggest that the current two-week wait system should be modified to provide an ultrasound scan within 2 weeks so that urologists can concentrate their clinic service on those with a tumour confirmed or suspected on ultrasound. Acknowledgements The authors thank Dr Colin Pritchard (Statistician to the Royal Cornwall Hospital) for his advice on statistical matters, Dr Alison StJohn for providing information from the pathology database, and Mrs Melanie Walsh (secretary) who retrieved the hospital notes for this study. These results were first presented in poster form at the annual scientific meeting of BAUS Oncology, Birmingham, November References 1. Cancer Research UK. Testicular Cancer: UK Testicular Cancer Incidence Statistics. 2006; < 2. Jarvis LJ, Dubbins PA. Changes in the epididymis after vasectomy: sonographic findings. AJR Am J Roentgenol 1989; 152: Foster PW, Ritchie AW, Jones DJ. Prospective analysis of scrotal pathology referrals are referrals appropriate and accurate? Ann R Coll Surg Engl 2006; 88: Ravichandran S, Reddy G, O Sullivan D, Williamson E, Machin D. Is The Two- Week Cancer Rule Working? In: Manchester: British Association of Urological Surgeons, Prener A, Engholm G, Jensen OM. Genital anomalies and risk for testicular cancer in Danish men. Epidemiology 1996; 7: Lesnik G, Nickl S, Kuschnig P, Sinzig M, Hausegger K, Jeschke K. [Sonography of the scrotum]. Rofo 2006; 178: Micallef M, Torreggiani WC, Hurley M, Dinsmore WW, Hogan B. The ultrasound investigation of scrotal swelling. Int J STD AIDS 2000; 11: Polak V, Hornak M. The value of scrotal ultrasound in patients with suspected testicular tumour. Int Urol Nephrol 1990; 22: London NJ, Smart JG, Kinder RB, Watkin EM, Rees Y, Haley P. Prospective study of routine scrotal ultrasonography in urological practice. Br J Urol 1989; 63: Allen D, Popert R, O Brien T. The two-week-wait cancer initiative in urology: useful modernization? J R Soc Med 2004; 97: Rai S, Kelly MJ. Prioritization of colorectal referrals: a review of the 2-week wait referral system. Colorectal Dis 2007; 9: Morrison J, Gillespie S, MacKenzie IZ. Two week wait standards for suspected gynaecological malignancy. On target, but missing the point? J Br Menopause Soc 2003; 9: Debnath D, Dielehner N, Gunning KA. Guidelines, compliance, and effectiveness: a 12 months audit in an acute district general healthcare trust on the two week rule for suspected colorectal cancer. Postgrad Med J 2002; 78: Cox NH. Evaluation of the UK 2-week referral rule for skin cancer. Br J Dermatol 2004; 150: Walsh SR, Gilson NL, Brown K, Novell JR. Trends in colorectal cancer survival following the 2-week rule. Colorectal Dis 2007; 9: Dodds W, Morgan M, Wolfe C, Raju KS. Implementing the 2-week wait rule for cancer referral in the UK: general practitioners views and practices. Eur J Cancer Care (Engl) 2004; 13:
A 15-year longitudinal analysis of trends in elective urological surgery an evidence base for Modernising Medical Careers
 The Royal College of Surgeons of England UROLOGY doi 10.1308/003588407X168226 A 15-year longitudinal analysis of trends in elective urological surgery an evidence base for Modernising Medical Careers C
The Royal College of Surgeons of England UROLOGY doi 10.1308/003588407X168226 A 15-year longitudinal analysis of trends in elective urological surgery an evidence base for Modernising Medical Careers C
COLOR DOPPLER ULTRASOUND IN EVALUATION OF SCROTAL LESIONS
 COLOR DOPPLER ULTRASOUND IN EVALUATION OF SCROTAL LESIONS Desai Sanjay D Associate Professor, Department of Radiology, RCSM Govt. Medical College, Kolhapur. ABSTRACT: Color Doppler ultrasound is a non-invasive,
COLOR DOPPLER ULTRASOUND IN EVALUATION OF SCROTAL LESIONS Desai Sanjay D Associate Professor, Department of Radiology, RCSM Govt. Medical College, Kolhapur. ABSTRACT: Color Doppler ultrasound is a non-invasive,
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 2/19/2011 Radiology Quiz of the Week # 8 Page 1 CLINICAL PRESENTATION AND RADIOLOGY QUIZ
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 2/19/2011 Radiology Quiz of the Week # 8 Page 1 CLINICAL PRESENTATION AND RADIOLOGY QUIZ
REVERSAL OF VASECTOMY INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk INFORMATION
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk INFORMATION
Cardiff MRCS OSCE Courses Testicular Cancer
 Testicular Cancer Scenario: A 40-year-old male presents to the surgical out-patient clinic with a 6-8 week history of a painless lump in his left scrotum. He however complains of a dull ache in the scrotum
Testicular Cancer Scenario: A 40-year-old male presents to the surgical out-patient clinic with a 6-8 week history of a painless lump in his left scrotum. He however complains of a dull ache in the scrotum
Miss Rashmi Singh Consultant urological Surgeon. Men s Health Seminar Parkside Hospital November 2016
 Miss Rashmi Singh Consultant urological Surgeon Men s Health Seminar Parkside Hospital November 2016 Hernia Hydrocele Varicocele Infections Epididymal cyst Testicular Ca Miscellaneous Phimosis Paraphimosis
Miss Rashmi Singh Consultant urological Surgeon Men s Health Seminar Parkside Hospital November 2016 Hernia Hydrocele Varicocele Infections Epididymal cyst Testicular Ca Miscellaneous Phimosis Paraphimosis
West Midlands Sarcoma Advisory Group
 West Midlands Sarcoma Advisory Group Guideline for the Initial Investigation and Referral to Sarcoma Specialist Multi Disciplinary Team for Suspected Sarcoma of Soft Tissue Extremities (limbs and trunk
West Midlands Sarcoma Advisory Group Guideline for the Initial Investigation and Referral to Sarcoma Specialist Multi Disciplinary Team for Suspected Sarcoma of Soft Tissue Extremities (limbs and trunk
Commissioning Policy Individual Funding Request
 Commissioning Policy Individual Funding Request Surgical Intervention for Treatment of Hydrocele (also known as Hydroecoele) in Males Policy Prior Approval Policy Date Adopted: 16 th September 2016 Version:
Commissioning Policy Individual Funding Request Surgical Intervention for Treatment of Hydrocele (also known as Hydroecoele) in Males Policy Prior Approval Policy Date Adopted: 16 th September 2016 Version:
6 UROLOGICAL CANCERS. 6.1 Key Points
 6 UROLOGICAL CANCERS 6.1 Key Points Prostate Cancer Commonest cancer in males in Scotland Approximately 99% of cases occur in men aged > 50 years About 40% of cases present in men aged < 70 years when
6 UROLOGICAL CANCERS 6.1 Key Points Prostate Cancer Commonest cancer in males in Scotland Approximately 99% of cases occur in men aged > 50 years About 40% of cases present in men aged < 70 years when
HYPOSPADIAS NEONATAL CLINICAL GUIDELINE. 1. Aim/Purpose of this Guideline. 2. The Guidance
 HYPOSPADIAS NEONATAL CLINICAL GUIDELINE 1. Aim/Purpose of this Guideline 1.1. This guideline applies to all staff managing the initial care of infants born with hypospadias. It includes assessment and
HYPOSPADIAS NEONATAL CLINICAL GUIDELINE 1. Aim/Purpose of this Guideline 1.1. This guideline applies to all staff managing the initial care of infants born with hypospadias. It includes assessment and
ACE Programme SOMERSET INTEGRATED LUNG CANCER PATHWAY. Phases One and Two Final Report
 ACE Programme SOMERSET INTEGRATED LUNG CANCER PATHWAY Phases One and Two Final Report July 2017 Introduction This paper presents the learning and actions that have been generated from phase One and Two
ACE Programme SOMERSET INTEGRATED LUNG CANCER PATHWAY Phases One and Two Final Report July 2017 Introduction This paper presents the learning and actions that have been generated from phase One and Two
9/13/2017. Highgate Private Hospital & Whittington Health NHS Trust. London Cancer Urology Guidelines for Target Referrals. Urological Cancer Groups
 London Cancer Urology Guidelines for Target Referrals Mr Paul Erotocritou MBBS BSc MSc, MRCS, FRCS (Urol)Eng Highgate Private Hospital & Whittington Health NHS Trust Urological Cancer Groups 5 groups:
London Cancer Urology Guidelines for Target Referrals Mr Paul Erotocritou MBBS BSc MSc, MRCS, FRCS (Urol)Eng Highgate Private Hospital & Whittington Health NHS Trust Urological Cancer Groups 5 groups:
Urgent referral for suspected cancer in Scotland
 270 Oncology Urgent referral for suspected cancer in Scotland Cancer is a common problem, but an individual GP may only see about seven to eight new cases of cancer per annum (although they will see many
270 Oncology Urgent referral for suspected cancer in Scotland Cancer is a common problem, but an individual GP may only see about seven to eight new cases of cancer per annum (although they will see many
Faster Cancer Treatment Indicators: Use cases
 Faster Cancer Treatment Indicators: Use cases 2014 Date: October 2014 Version: Owner: Status: v01 Ministry of Health Cancer Services Final Citation: Ministry of Health. 2014. Faster Cancer Treatment Indicators:
Faster Cancer Treatment Indicators: Use cases 2014 Date: October 2014 Version: Owner: Status: v01 Ministry of Health Cancer Services Final Citation: Ministry of Health. 2014. Faster Cancer Treatment Indicators:
West Midlands Sarcoma Advisory Group
 West Midlands Sarcoma Advisory Group Guideline for the Initial Investigation and Referral to Specialist Sarcoma Multi Disciplinary Team for Suspected Bone Sarcoma Version History Version Date Brief Summary
West Midlands Sarcoma Advisory Group Guideline for the Initial Investigation and Referral to Specialist Sarcoma Multi Disciplinary Team for Suspected Bone Sarcoma Version History Version Date Brief Summary
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons
 General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: ABDOMINAL WALL, RETROPERITONEUM, UROGENITAL 5-May-2013
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: ABDOMINAL WALL, RETROPERITONEUM, UROGENITAL 5-May-2013
Briefing Paper. Single Cancer Pathway
 Briefing Paper Single Cancer Pathway Author: Tom Crosby, Clinical Director, Wales Cancer Network Owner: Wales Cancer Network Date: 27 th November 2017 Version: 1.0 Publication/ Distribution: Wales Cancer
Briefing Paper Single Cancer Pathway Author: Tom Crosby, Clinical Director, Wales Cancer Network Owner: Wales Cancer Network Date: 27 th November 2017 Version: 1.0 Publication/ Distribution: Wales Cancer
One Stop Prostate Biopsy Protocol Author Consultation Date Approved
 One Stop Prostate Biopsy Protocol Author Consultation Date Approved Urology Nurse Practioner PROTOCOL FOR MEN ATTENDING A ONE STOP PROSTATE BIOPSY CLINIC RATIONALE Prostate cancer is the most common cancer
One Stop Prostate Biopsy Protocol Author Consultation Date Approved Urology Nurse Practioner PROTOCOL FOR MEN ATTENDING A ONE STOP PROSTATE BIOPSY CLINIC RATIONALE Prostate cancer is the most common cancer
T his article is based on a recent report from
 62 EFFECTIVENESS BULLETIN A systematic review of cancer waiting time audits R Lewis, R Collins, A Flynn, M Emmans Dean, L Myers, P Wilson, A Eastwood... A summary of a systematic review of clinical audits
62 EFFECTIVENESS BULLETIN A systematic review of cancer waiting time audits R Lewis, R Collins, A Flynn, M Emmans Dean, L Myers, P Wilson, A Eastwood... A summary of a systematic review of clinical audits
controversial topics in surgery
 doi 10.1308/003588408X261717 The Royal College of Surgeons of England Tom Dehn, Series Editor E: thomas.dehn@royalberkshire.nhs.uk controversial topics in surgery Who should run breast clinics, surgeons
doi 10.1308/003588408X261717 The Royal College of Surgeons of England Tom Dehn, Series Editor E: thomas.dehn@royalberkshire.nhs.uk controversial topics in surgery Who should run breast clinics, surgeons
Improving diagnostic pathways for patients with vague symptoms
 Improving diagnostic pathways for patients with vague symptoms Executive summary Accelerate, Coordinate, Evaluate (ACE) Programme An early diagnosis of cancer initiative supported by: NHS England, Cancer
Improving diagnostic pathways for patients with vague symptoms Executive summary Accelerate, Coordinate, Evaluate (ACE) Programme An early diagnosis of cancer initiative supported by: NHS England, Cancer
What you need to know about having a vasectomy
 University Teaching Trust What you need to know about having a vasectomy Urology Hope Building 0161 206 5380 All Rights Reserved 2017. Document for issue as handout. What is a vasectomy? A vasectomy is
University Teaching Trust What you need to know about having a vasectomy Urology Hope Building 0161 206 5380 All Rights Reserved 2017. Document for issue as handout. What is a vasectomy? A vasectomy is
North Trent Cancer Network. Referral Guidelines, Head & Neck Cancer (including Thyroid), for Primary Care Practitioners
 North Trent Cancer Network Fulwood House Sheffield S10 3TH http://nww.barnsleyhealth.nhs.uk/pct/norcom/cancer/ Tel: 0114 2263436 Fax: 0114 2263407 Email: Kim.Fell@ntcn.nhs.uk Referral Guidelines, Head
North Trent Cancer Network Fulwood House Sheffield S10 3TH http://nww.barnsleyhealth.nhs.uk/pct/norcom/cancer/ Tel: 0114 2263436 Fax: 0114 2263407 Email: Kim.Fell@ntcn.nhs.uk Referral Guidelines, Head
Information leaflet for women with an increased lifetime risk of breast and ovarian cancer. Hereditary Breast and Ovarian Cancer (HBOC)
 Information leaflet for women with an increased lifetime risk of breast and ovarian cancer Hereditary Breast and Ovarian Cancer (HBOC) What is Hereditary Breast and Ovarian Cancer (HBOC)? Hereditary Breast
Information leaflet for women with an increased lifetime risk of breast and ovarian cancer Hereditary Breast and Ovarian Cancer (HBOC) What is Hereditary Breast and Ovarian Cancer (HBOC)? Hereditary Breast
REMOVAL OF PART OR ALL OF THE EPIDIDYMIS
 Procedure Specific Information What is the evidence base for this information? This publication includes advice from consensus panels, the British Association of Urological Surgeons, the Department of
Procedure Specific Information What is the evidence base for this information? This publication includes advice from consensus panels, the British Association of Urological Surgeons, the Department of
INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk INFORMATION
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk INFORMATION
Guidelines for the Management of Acute Scrotal Pain in Children (V 1.0)
 Guidelines for the Management of Acute Scrotal Pain in Children (V 1.0) Clinical Director Signed Name... Mr C. Hendrickse.. Date 14/10/2011.. Meta Data Guideline Title: Guidelines for the Management of
Guidelines for the Management of Acute Scrotal Pain in Children (V 1.0) Clinical Director Signed Name... Mr C. Hendrickse.. Date 14/10/2011.. Meta Data Guideline Title: Guidelines for the Management of
Ultrasound of malignant testicular lesions. Arne Hørlyck Department of Radiology Aarhus University Hospital, Skejby
 Ultrasound of malignant testicular lesions Arne Hørlyck Department of Radiology Aarhus University Hospital, Skejby Testis Ultrasound is fantastic!! Scrotum Extratesticular mass: Benign Intratesticular
Ultrasound of malignant testicular lesions Arne Hørlyck Department of Radiology Aarhus University Hospital, Skejby Testis Ultrasound is fantastic!! Scrotum Extratesticular mass: Benign Intratesticular
The International Ovarian Tumour Analysis (IOTA) criteria
 The International Ovarian Tumour Analysis (IOTA) criteria Elizabeth Bullivant Specialist Sonographer Sheffield Teaching Hospitals NHS Foundation Trust Contents Ultrasound reports. What is IOTA? What the
The International Ovarian Tumour Analysis (IOTA) criteria Elizabeth Bullivant Specialist Sonographer Sheffield Teaching Hospitals NHS Foundation Trust Contents Ultrasound reports. What is IOTA? What the
The Urology One-Stop Clinic
 The Urology One-Stop Clinic Exceptional healthcare, personally delivered The aim of this leaflet is to answer any questions you may have about the Urology One-Stop Clinic. What is the Urology One-Stop
The Urology One-Stop Clinic Exceptional healthcare, personally delivered The aim of this leaflet is to answer any questions you may have about the Urology One-Stop Clinic. What is the Urology One-Stop
Appendix 4 Urology Care Pathways
 Appendix 4 Urology Care Pathways Cancer Care Pathways outline the steps and stages in the patient journey from referral through to diagnostics, staging, treatment, follow up, rehabilitation and if applicable
Appendix 4 Urology Care Pathways Cancer Care Pathways outline the steps and stages in the patient journey from referral through to diagnostics, staging, treatment, follow up, rehabilitation and if applicable
What does the procedure involve? What are the alternatives to this procedure? What should I expect before the procedure?...
 This leaflet explains: What does the procedure involve?... 2 What are the alternatives to this procedure?... 2 What should I expect before the procedure?... 2 What happens during the procedure?... 2 What
This leaflet explains: What does the procedure involve?... 2 What are the alternatives to this procedure?... 2 What should I expect before the procedure?... 2 What happens during the procedure?... 2 What
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM)
 SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician CSCCN PORTSMOUTH HOSPITALS Portsmouth Colorectal MDT (11-2D-1) - 2011/12 Daniel OLeary Compliance Self Assessment COLORECTAL
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician CSCCN PORTSMOUTH HOSPITALS Portsmouth Colorectal MDT (11-2D-1) - 2011/12 Daniel OLeary Compliance Self Assessment COLORECTAL
Testicular Germ Cell Cancer Explained
 The Beatson West of Scotland Cancer Centre Pan Glasgow Urology / Oncology Patient Information Testicular Germ Cell Cancer Explained The Beatson West of Scotland Cancer Centre 1053 Great Western Road, Glasgow
The Beatson West of Scotland Cancer Centre Pan Glasgow Urology / Oncology Patient Information Testicular Germ Cell Cancer Explained The Beatson West of Scotland Cancer Centre 1053 Great Western Road, Glasgow
Surgical Presentations in Children
 From Gums to Bums: Surgical Presentations in Children Sebastian King Paediatric Colorectal Surgeon From Gums to Bums (and the rest): Surgical Presentations in Children Sebastian King Paediatric Colorectal
From Gums to Bums: Surgical Presentations in Children Sebastian King Paediatric Colorectal Surgeon From Gums to Bums (and the rest): Surgical Presentations in Children Sebastian King Paediatric Colorectal
Suspected testicular cancer
 Suspected testicular cancer Urology Department Patient Information Leaflet Introduction Your consultant has informed you that you may have testicular cancer. This leaflet gives the facts about your condition
Suspected testicular cancer Urology Department Patient Information Leaflet Introduction Your consultant has informed you that you may have testicular cancer. This leaflet gives the facts about your condition
BENIGN & MALIGNANT TESTIS DISEASES. Gary J. Faerber, M.D. Associate Professor, Dept of Urology March 2009 OBJECTIVES
 BENIGN & MALIGNANT TESTIS DISEASES Gary J. Faerber, M.D. Associate Professor, Dept of Urology March 2009 OBJECTIVES 1. Become familiar with the scrotal contents and their anatomical relationship with each
BENIGN & MALIGNANT TESTIS DISEASES Gary J. Faerber, M.D. Associate Professor, Dept of Urology March 2009 OBJECTIVES 1. Become familiar with the scrotal contents and their anatomical relationship with each
Single Suspected Cancer Pathway Definitions pathway start date
 Single Suspected Cancer Pathway Definitions pathway start date Date: March 2018 Version: 1.2.1 Wales Cancer Owner: Network and Welsh Government Status Published 1 P a g e Purpose of Document This document
Single Suspected Cancer Pathway Definitions pathway start date Date: March 2018 Version: 1.2.1 Wales Cancer Owner: Network and Welsh Government Status Published 1 P a g e Purpose of Document This document
Transforming Cancer Services for London
 Programme Director Paul Roche Status Draft Owner Laura Boyd Version 0.4 Author Jennifer Layburn Date 15/05/13 Transforming Cancer Services for London Best Practice Commissioning Pathway for the early detection
Programme Director Paul Roche Status Draft Owner Laura Boyd Version 0.4 Author Jennifer Layburn Date 15/05/13 Transforming Cancer Services for London Best Practice Commissioning Pathway for the early detection
There are a number of national guidelines and performance standards which support the implementation of a straight to CT pathway.
 December 2015 CONTENTS Contents... 2 1 Introduction... 3 2 Case for Change... 3 3 Evidence... 3 3.1 National and regional policy... 3 3.2 Local audit... 4 4 Supporting Work Initiatives... 5 4.1 Identification
December 2015 CONTENTS Contents... 2 1 Introduction... 3 2 Case for Change... 3 3 Evidence... 3 3.1 National and regional policy... 3 3.2 Local audit... 4 4 Supporting Work Initiatives... 5 4.1 Identification
Richard Watson, Chief Transformation Officer. Dr P Holloway, GP Clinical Lead for Cancer Lisa Parrish, Senior Transformation Lead
 GOVERNING BODY Agenda Item No. 08 Reference No. IESCCG 18-02 Date. 23 January 2018 Title Lead Chief Officer Author(s) Purpose Cancer Services Update Richard Watson, Chief Transformation Officer Dr P Holloway,
GOVERNING BODY Agenda Item No. 08 Reference No. IESCCG 18-02 Date. 23 January 2018 Title Lead Chief Officer Author(s) Purpose Cancer Services Update Richard Watson, Chief Transformation Officer Dr P Holloway,
REVERSAL OF VASECTOMY
 Procedure Specific Information What is the evidence base for this information? This publication includes advice from consensus panels, the British Association of Urological Surgeons, the Department of
Procedure Specific Information What is the evidence base for this information? This publication includes advice from consensus panels, the British Association of Urological Surgeons, the Department of
Streamlining the lung diagnostic pathway (A87)
 Streamlining the lung diagnostic pathway (A87) Crawley CCG with Surrey and Sussex Healthcare NHS Trust Evaluation January 2017 Summary A new Straight-to-CT pathway for patients with an abnormal CXR result
Streamlining the lung diagnostic pathway (A87) Crawley CCG with Surrey and Sussex Healthcare NHS Trust Evaluation January 2017 Summary A new Straight-to-CT pathway for patients with an abnormal CXR result
What is a hydrocele? It is a swelling caused by a build-up of fluid in the fluid sac surrounding the testicle. It is very common.
 Repair of hydrocele Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been recommended to have a procedure to repair a hydrocele. It gives information on what
Repair of hydrocele Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been recommended to have a procedure to repair a hydrocele. It gives information on what
INTERNAL VALIDATION REPORT (MULTI-DISCIPLINARY TEAM)
 INTERNAL VALIDATION REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT NECN N Tees & Hartlepool North Tees And Hartlepool Date Self Assessment Completed 23rd July 2009 Date of IV Review 19th June 2009
INTERNAL VALIDATION REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT NECN N Tees & Hartlepool North Tees And Hartlepool Date Self Assessment Completed 23rd July 2009 Date of IV Review 19th June 2009
The Centre for Men s Health
 96 Harley Street (London) and Manchester All Enquiries - +44 (0)20 7486 2277 www.centreformenshealth.co.uk/ This leaflet provides information about: The Centre for Men s Health The conditions we treat:
96 Harley Street (London) and Manchester All Enquiries - +44 (0)20 7486 2277 www.centreformenshealth.co.uk/ This leaflet provides information about: The Centre for Men s Health The conditions we treat:
The RAPID Programme Rapid Access to Pulmonary Investigation & Diagnosis
 Patient Experience National Network Awards (PENNA) The RAPID Programme 2016-2019 Rapid Access to Pulmonary Investigation & Diagnosis Kath Hewitt Lead Clinical Nurse Specialist Ailsa Rowlands Programme
Patient Experience National Network Awards (PENNA) The RAPID Programme 2016-2019 Rapid Access to Pulmonary Investigation & Diagnosis Kath Hewitt Lead Clinical Nurse Specialist Ailsa Rowlands Programme
Testis Elastography. Paul S. Sidhu. Professor of Imaging Sciences. King s College Hospital London
 Testis Elastography Paul S. Sidhu Professor of Imaging Sciences King s College Hospital London Testicular Elastography Strain elastography Point Shear wave elastography 2D Shear wave elastography Multiparametric
Testis Elastography Paul S. Sidhu Professor of Imaging Sciences King s College Hospital London Testicular Elastography Strain elastography Point Shear wave elastography 2D Shear wave elastography Multiparametric
Identifying distinguishing features of the MDC model within the five ACE projects
 Identifying distinguishing features of the MDC model within the five ACE projects Context: The ACE Programme (Wave 2) has been working with five projects across England to trial and evaluate the concept
Identifying distinguishing features of the MDC model within the five ACE projects Context: The ACE Programme (Wave 2) has been working with five projects across England to trial and evaluate the concept
The London BreasT CenTre
 The London Breast Centre Contents Introduction 4 One-Stop Breast Care Clinic 5 Common breast problems 6 Hereditary breast cancer 8 Breast cancer and cancer screening 9 Breast diagnostic tests 10 Breast
The London Breast Centre Contents Introduction 4 One-Stop Breast Care Clinic 5 Common breast problems 6 Hereditary breast cancer 8 Breast cancer and cancer screening 9 Breast diagnostic tests 10 Breast
An introduction to the multidisciplinary team for Urological Cancers
 An introduction to the multidisciplinary team for Urological Cancers Introduction This leaflet introduces the multidisciplinary team (MDT) for urological cancers. The urological cancer team work at both
An introduction to the multidisciplinary team for Urological Cancers Introduction This leaflet introduces the multidisciplinary team (MDT) for urological cancers. The urological cancer team work at both
REFERRAL GUIDELINES: GALLSTONES
 REFERRAL GUIDELINES: GALLSTONES Document Purpose To ensure patients with gallstones disease are managed appropriately in primary/ secondary care Oxford Radcliffe Hospital Surgical Department Surgical Registrar
REFERRAL GUIDELINES: GALLSTONES Document Purpose To ensure patients with gallstones disease are managed appropriately in primary/ secondary care Oxford Radcliffe Hospital Surgical Department Surgical Registrar
Using patient data to improve. cancer waiting times. May 2018
 Using patient data to improve cancer waiting times May 2018 Summary Background We used patient-level data from Hospital Episode Statistics (HES) for 2016/17 to carry out detailed analysis of what drives
Using patient data to improve cancer waiting times May 2018 Summary Background We used patient-level data from Hospital Episode Statistics (HES) for 2016/17 to carry out detailed analysis of what drives
Radical Orchidectomy. Department of Urology. Patient Information
 Radical Orchidectomy Department of Urology 2 Patient Information This leaflet answers some of the questions people ask about a radical orchidectomy operation. If any further questions are raised after
Radical Orchidectomy Department of Urology 2 Patient Information This leaflet answers some of the questions people ask about a radical orchidectomy operation. If any further questions are raised after
PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM)
 PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM) Network Organisation (Trust) Team DCN POOLE Poole THYROID ONLY MDT (11-2I-2) - 2011/12 Peer Review Visit Date 18th August 2011 Compliance THYROID ONLY
PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM) Network Organisation (Trust) Team DCN POOLE Poole THYROID ONLY MDT (11-2I-2) - 2011/12 Peer Review Visit Date 18th August 2011 Compliance THYROID ONLY
CONSENT FORM UROLOGICAL SURGERY
 CONSENT FORM for UROLOGICAL SURGERY (Designed in compliance with consent form 1) PATIENT AGREEMENT TO INVESTIGATION OR TREATMENT Patient Details or pre-printed label Patient s NHS Number or Hospital number
CONSENT FORM for UROLOGICAL SURGERY (Designed in compliance with consent form 1) PATIENT AGREEMENT TO INVESTIGATION OR TREATMENT Patient Details or pre-printed label Patient s NHS Number or Hospital number
Surgery Illustrated Surgical Atlas Inguinal orchidectomy for testicular cancer
 Surgery Illustrated Focus on Details SURGERY ILLUSTRATED SURGICAL ATLASPIZZOCARO and GUARNERI PIZZOCARO and GUARNERI BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas Inguinal orchidectomy for
Surgery Illustrated Focus on Details SURGERY ILLUSTRATED SURGICAL ATLASPIZZOCARO and GUARNERI PIZZOCARO and GUARNERI BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas Inguinal orchidectomy for
INFORMATION ON MALE STERILISATION. Vasectomy
 INFORMATION ON MALE STERILISATION Vasectomy Please read this leaflet before your operation. Keep it in a safe place, as you may need the information later. Solent Vasectomy Service Sexual Health Service
INFORMATION ON MALE STERILISATION Vasectomy Please read this leaflet before your operation. Keep it in a safe place, as you may need the information later. Solent Vasectomy Service Sexual Health Service
Having a Hydrocele Repair (adult)
 Having a Hydrocele Repair (adult) Information for patients, relatives and carers For more information, please contact: Department of Urology The York Hospital, Wigginton Road, York, YO31 8HE Tel: 01904
Having a Hydrocele Repair (adult) Information for patients, relatives and carers For more information, please contact: Department of Urology The York Hospital, Wigginton Road, York, YO31 8HE Tel: 01904
Integrated Cancer Services Action Plan. Colchester Hospital University NHS Foundation Trust 31 March 2014
 Integrated Cancer Services Action Plan Colchester Hospital University NHS Foundation Trust 31 March KEY Implemented, clearly evidenced and externally approved On Track to deliver Some issues narrative
Integrated Cancer Services Action Plan Colchester Hospital University NHS Foundation Trust 31 March KEY Implemented, clearly evidenced and externally approved On Track to deliver Some issues narrative
4 th Year Urology Core Objectives Keith Rourke (Revised June 1, 2007)
 4 th Year Urology Core Objectives Keith Rourke (Revised June 1, 2007) I. Genitourinary Trauma: 1. Goal: The student will be able to demonstrate a basic clinical approach to the management & diagnosis of
4 th Year Urology Core Objectives Keith Rourke (Revised June 1, 2007) I. Genitourinary Trauma: 1. Goal: The student will be able to demonstrate a basic clinical approach to the management & diagnosis of
Intraparenchymatous adenomatoid tumor dependent on the rete testis: A case report and review of literature
 Intraparenchymatous adenomatoid tumor dependent on the rete testis: A case report and review of literature A. Jiménez Pacheco, J. L. Martínez Torres, F. Valle Díaz de la Guardia, M. A. Arrabal Polo, and
Intraparenchymatous adenomatoid tumor dependent on the rete testis: A case report and review of literature A. Jiménez Pacheco, J. L. Martínez Torres, F. Valle Díaz de la Guardia, M. A. Arrabal Polo, and
Testicular ultrasound in acute scrotal pain - beyond testicular torsion
 Testicular ultrasound in acute scrotal pain - beyond testicular torsion Poster No.: C-1284 Congress: ECR 2015 Type: Educational Exhibit Authors: I. Rolla, M. Nogueira, M. J. Aguiar, D. S. Garrido, J. A.
Testicular ultrasound in acute scrotal pain - beyond testicular torsion Poster No.: C-1284 Congress: ECR 2015 Type: Educational Exhibit Authors: I. Rolla, M. Nogueira, M. J. Aguiar, D. S. Garrido, J. A.
For more information about how to cite these materials visit
 Author(s): Gary Faerber, M.D., 2011 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Share Alike 3.0 License: http://creativecommons.org/licenses/by-sa/3.0/
Author(s): Gary Faerber, M.D., 2011 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Share Alike 3.0 License: http://creativecommons.org/licenses/by-sa/3.0/
TitleUltrasonic evaluation of scrotal sw. Author(s) MISAKI, Toshimitsu; HISAZUMI, Haruo. Citation 泌尿器科紀要 (1985), 31(7):
 TitleUltrasonic evaluation of scrotal sw Author(s) MISAKI, Toshimitsu; HISAZUMI, Haruo Citation 泌尿器科紀要 (1985), 31(7): 1151-1158 Issue Date 1985-07 URL http://hdl.handle.net/2433/118548 Right Type Departmental
TitleUltrasonic evaluation of scrotal sw Author(s) MISAKI, Toshimitsu; HISAZUMI, Haruo Citation 泌尿器科紀要 (1985), 31(7): 1151-1158 Issue Date 1985-07 URL http://hdl.handle.net/2433/118548 Right Type Departmental
Treatment Testicular Cancer Guidelines
 Treatment Testicular Cancer Guidelines Thank you very much for reading. As you may know, people have look hundreds times for their chosen readings like this, but end up in infectious downloads. Rather
Treatment Testicular Cancer Guidelines Thank you very much for reading. As you may know, people have look hundreds times for their chosen readings like this, but end up in infectious downloads. Rather
Getting to Diagnosis. Debbie Victor Uro-Oncology CNS Royal Cornwall Hospitals Trust
 Getting to Diagnosis Debbie Victor Uro-Oncology CNS Royal Cornwall Hospitals Trust GP Visit Symptoms Reduced urinary flow Difficulty starting/stopping Urgency Frequency Nocturia Because a friend/relative
Getting to Diagnosis Debbie Victor Uro-Oncology CNS Royal Cornwall Hospitals Trust GP Visit Symptoms Reduced urinary flow Difficulty starting/stopping Urgency Frequency Nocturia Because a friend/relative
An Undergraduate Syllabus for Urology. Produced on behalf of the British Association of Urological Surgeons. March 2012
 An Undergraduate Syllabus for Urology Produced on behalf of the British Association of Urological Surgeons March 2012 Authors H Hashim, P Jones, KJ O Flynn, I Pearce, J Royle, M Shaw, AM Sinclair Correspondence
An Undergraduate Syllabus for Urology Produced on behalf of the British Association of Urological Surgeons March 2012 Authors H Hashim, P Jones, KJ O Flynn, I Pearce, J Royle, M Shaw, AM Sinclair Correspondence
Case 5385 Tubular ectasia of the rete testis: a benign testicular entity diagnosed on imaging
 Case 5385 Tubular ectasia of the rete testis: a benign testicular entity diagnosed on imaging A. C. Tsili 1, C. Tsampoulas 1, D. Giannakis 2, A. Chaidou 1, N. Sofikitis 2, S. C. Efremidis 1 1 Department
Case 5385 Tubular ectasia of the rete testis: a benign testicular entity diagnosed on imaging A. C. Tsili 1, C. Tsampoulas 1, D. Giannakis 2, A. Chaidou 1, N. Sofikitis 2, S. C. Efremidis 1 1 Department
Cancer of Unknown Primary Service
 Cancer of Unknown Primary Service Dr Maurice Fernando Consultant In Specialist Palliative Care and CUP lead Doncaster and Bassetlaw Hospitals NHS FT Wakefield meeting -14-07-2016 CUP service CUP MDT
Cancer of Unknown Primary Service Dr Maurice Fernando Consultant In Specialist Palliative Care and CUP lead Doncaster and Bassetlaw Hospitals NHS FT Wakefield meeting -14-07-2016 CUP service CUP MDT
Clinical Diagnosis. your PR.i.VATES.
 your PR.i.VATES Clinical Diagnosis What is an orchidectomy? What to expect after orchidectomy Results and Confirmed Diagnosis What is the lymphatic system? www.yourprivates.org.uk CONTENTS CLINICAL DIAGNOSIS
your PR.i.VATES Clinical Diagnosis What is an orchidectomy? What to expect after orchidectomy Results and Confirmed Diagnosis What is the lymphatic system? www.yourprivates.org.uk CONTENTS CLINICAL DIAGNOSIS
Role of Colour Doppler Ultrasonography in evaluation of scrotal pain and swelling
 Original Research Article Role of Colour Doppler Ultrasonography in evaluation of scrotal pain and swelling Assistant Professor, Department of Radiodiagnosis, Government Medical College, Rajnandgaon Chattisghar,
Original Research Article Role of Colour Doppler Ultrasonography in evaluation of scrotal pain and swelling Assistant Professor, Department of Radiodiagnosis, Government Medical College, Rajnandgaon Chattisghar,
Appendix 1 - Restorative Dentistry Referral Guidelines for referring practitioners
 Appendix 1 - Restorative Dentistry Referral Guidelines for referring practitioners These guidelines are intended to assist General Dental Practitioners (GDPs), Community Dental Service (CDS) Dentists and
Appendix 1 - Restorative Dentistry Referral Guidelines for referring practitioners These guidelines are intended to assist General Dental Practitioners (GDPs), Community Dental Service (CDS) Dentists and
Urological cancers why we need to change. Stakeholder workshop 14 March 2013
 Urological cancers why we need to change Stakeholder workshop 14 March 2013 Introduction and welcome Today s event aims to cover: 1. Background, clinical evidence and London Cancer s recommendations Q&As
Urological cancers why we need to change Stakeholder workshop 14 March 2013 Introduction and welcome Today s event aims to cover: 1. Background, clinical evidence and London Cancer s recommendations Q&As
Waiting Times for Suspected and Diagnosed Cancer Patients
 Waiting Times for Suspected and Diagnosed Cancer Patients 2015-16 Annual Report Waiting Times for Suspected and Diagnosed Cancer Patients 1 Waiting Times for Suspected and Diagnosed Cancer Patients Prepared
Waiting Times for Suspected and Diagnosed Cancer Patients 2015-16 Annual Report Waiting Times for Suspected and Diagnosed Cancer Patients 1 Waiting Times for Suspected and Diagnosed Cancer Patients Prepared
Adult Patient Information and Consent Form
 The ROAM Trial Radiation versus Observation following surgical resection of Atypical Meningioma: a randomised controlled trial
The ROAM Trial Radiation versus Observation following surgical resection of Atypical Meningioma: a randomised controlled trial
All Men are created. (more or less) Rod Moser, PA, PhD Sutter Roseville Pediatrics Founding President, CAPA
 Rod Moser, PA, PhD Sutter Roseville Pediatrics Founding President, CAPA Balls Stones Family Jewels Meatballs Reece's Pieces Nuts Coconuts Weights Walnuts Gonads / Nads Dumbbells Truffles The sperm factory
Rod Moser, PA, PhD Sutter Roseville Pediatrics Founding President, CAPA Balls Stones Family Jewels Meatballs Reece's Pieces Nuts Coconuts Weights Walnuts Gonads / Nads Dumbbells Truffles The sperm factory
Original Papers ABSTRACT INTRODUCTION
 Original Papers Urgent GP referrals for suspected lung, colorectal, prostate and ovarian cancer Victoria L Allgar, Richard D Neal, Nasreen Ali, Brenda Leese, Phil Heywood, Gill Proctor and Joyce Evans
Original Papers Urgent GP referrals for suspected lung, colorectal, prostate and ovarian cancer Victoria L Allgar, Richard D Neal, Nasreen Ali, Brenda Leese, Phil Heywood, Gill Proctor and Joyce Evans
Bilateral Epididymal Cyst in 65 Years Old Man A Case Report Thorat Nilesh Suresh 1 *, Raut Subhash Y 2 and Kedar Nita M 3
 Int J Ayu Pharm Chem CASE STUDY www.ijapc.com e-issn 2350-0204 Bilateral Epididymal Cyst in 65 Years Old Man A Case Report Thorat Nilesh Suresh 1 *, Raut Subhash Y 2 and Kedar Nita M 3 1-3 Shalyatantra
Int J Ayu Pharm Chem CASE STUDY www.ijapc.com e-issn 2350-0204 Bilateral Epididymal Cyst in 65 Years Old Man A Case Report Thorat Nilesh Suresh 1 *, Raut Subhash Y 2 and Kedar Nita M 3 1-3 Shalyatantra
The Good News. The Comprehensive Approach. Examining the Male Patient: Sexually Transmitted Infections. April 25, 2013 Brittany Grier, M.
 Examining the Male Patient: Sexually Transmitted Infections April 25, 2013 Brittany Grier, M.S, PA-C The Good News Learning how to do a proper male exam can provide high yield information in formulating
Examining the Male Patient: Sexually Transmitted Infections April 25, 2013 Brittany Grier, M.S, PA-C The Good News Learning how to do a proper male exam can provide high yield information in formulating
Acute scrotum. Acute Epididymo-orchitis. Phyllis Yan, APDR (QEH)
 Acute scrotum Acute Epididymo-orchitis Phyllis Yan, APDR (QEH) Conditions leading to acute pain Torsion Acute Epididymitis / Epididymoorchitis Scrotal trauma Inguinal hernias Testicular tumors Epididymitis/epididymo
Acute scrotum Acute Epididymo-orchitis Phyllis Yan, APDR (QEH) Conditions leading to acute pain Torsion Acute Epididymitis / Epididymoorchitis Scrotal trauma Inguinal hernias Testicular tumors Epididymitis/epididymo
CRN SWP Business Intelligence Unit
 CRN SWP Business Intelligence Unit Name of report: Cancer Update Q3 2017/2018 Release date: 26 th February 2018 Data source(s) used: Portfolio ODP Data cut-off: 1 st January 2018 Brief Summary: Summary
CRN SWP Business Intelligence Unit Name of report: Cancer Update Q3 2017/2018 Release date: 26 th February 2018 Data source(s) used: Portfolio ODP Data cut-off: 1 st January 2018 Brief Summary: Summary
What are Varicoceles?
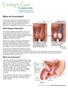 What are Varicoceles? A varicocele is when veins become enlarged inside your scrotum (the pouch of skin that holds your testicles). These veins are called the pampiniform plexus. Ten to 15 of every 100
What are Varicoceles? A varicocele is when veins become enlarged inside your scrotum (the pouch of skin that holds your testicles). These veins are called the pampiniform plexus. Ten to 15 of every 100
International Journal of Case Studies in Clinical Research
 Case Report International Journal of Case Studies in Clinical Research Open Access Acute Vasitis Presenting as an Inguinoscrotal Swelling: A Diagnostic Dilemma 1 Akanji Akinwunmi O, 2 Akinola Oluwaseun
Case Report International Journal of Case Studies in Clinical Research Open Access Acute Vasitis Presenting as an Inguinoscrotal Swelling: A Diagnostic Dilemma 1 Akanji Akinwunmi O, 2 Akinola Oluwaseun
Leicester City, East Leicestershire and Rutland & West Leicestershire Collaborative Commissioning Policy Gamete/Embryo cryopreservation
 Leicester City Clinical Commissioning Group West Leicestershire Clinical Commissioning Group East Leicestershire and Rutland Clinical Commissioning Group Leicester City, East Leicestershire and Rutland
Leicester City Clinical Commissioning Group West Leicestershire Clinical Commissioning Group East Leicestershire and Rutland Clinical Commissioning Group Leicester City, East Leicestershire and Rutland
Genetics and Testicular Cancer
 Genetics and Testicular Cancer Division of Cancer Epidemiology and Genetics Clinical Genetics Branch 7/12/05 Tentative Schedule of Visit 1. Description of the research aspects of the study 3. Genetics
Genetics and Testicular Cancer Division of Cancer Epidemiology and Genetics Clinical Genetics Branch 7/12/05 Tentative Schedule of Visit 1. Description of the research aspects of the study 3. Genetics
Promoting Innovative Practice
 Promoting Innovative Practice Fast-track surgery for pancreatic cancer reduces time to treatment, complications and increases the number of patients undergoing successful surgery 1 Mr Keith Roberts, Consultant
Promoting Innovative Practice Fast-track surgery for pancreatic cancer reduces time to treatment, complications and increases the number of patients undergoing successful surgery 1 Mr Keith Roberts, Consultant
Atlas of Male Reproductive Pathology
 Atlas of Male Reproductive Pathology Current Histopathology Consultant Editor Professor G. Austin Gresham, TO, SeD, MO, FRC Path. Professor of Morbid Anatomy and Histology, University of Cambridge Volume
Atlas of Male Reproductive Pathology Current Histopathology Consultant Editor Professor G. Austin Gresham, TO, SeD, MO, FRC Path. Professor of Morbid Anatomy and Histology, University of Cambridge Volume
Hydrocele repair. Information for parents and carers
 Hydrocele repair Information for parents and carers A hydrocele is a swelling in the scrotum or groin caused by a collection of fluid surrounding the testicle. The testes start developing inside a baby
Hydrocele repair Information for parents and carers A hydrocele is a swelling in the scrotum or groin caused by a collection of fluid surrounding the testicle. The testes start developing inside a baby
LCA Lung Clinical Forum. 21 st October 2014
 LCA Lung Clinical Forum 21 st October 2014 Welcome Dr Liz Sawicka Chair - LCA Lung Pathway Group Succession planning Dr Kate Haire Consultant in Public Health Medicine, LCA Commissioning Intentions for
LCA Lung Clinical Forum 21 st October 2014 Welcome Dr Liz Sawicka Chair - LCA Lung Pathway Group Succession planning Dr Kate Haire Consultant in Public Health Medicine, LCA Commissioning Intentions for
National Institute for Health and Clinical Excellence
 National Institute for Health and Clinical Excellence Ovarian cancer quality standard Quality Standard Consultation Comments Table 25 November 23 December 2011 PLEASE NOTE: Consultation comments have been
National Institute for Health and Clinical Excellence Ovarian cancer quality standard Quality Standard Consultation Comments Table 25 November 23 December 2011 PLEASE NOTE: Consultation comments have been
Cancer of Unknown Primary (CUP)
 Cancer of Unknown Primary (CUP) Pathways and Guidelines V1.0 London Cancer September 2013 The following pathways and guidelines document has been compiled by the London Cancer CUP technical subgroup and
Cancer of Unknown Primary (CUP) Pathways and Guidelines V1.0 London Cancer September 2013 The following pathways and guidelines document has been compiled by the London Cancer CUP technical subgroup and
Cancer in the South West Peninsula - a baseline assessment
 Cancer in the South West Peninsula - a baseline assessment 1 The Cancer Reform Strategy 1.1 The Cancer Reform Strategy, published in December 2007 1, built on the progress already achieved since the publication
Cancer in the South West Peninsula - a baseline assessment 1 The Cancer Reform Strategy 1.1 The Cancer Reform Strategy, published in December 2007 1, built on the progress already achieved since the publication
REPAIR OF HYDROCELE. Procedure Specific Information. What is the evidence base for this information?
 Procedure Specific Information What is the evidence base for this information? This publication includes advice from consensus panels, the British Association of Urological Surgeons, the Department of
Procedure Specific Information What is the evidence base for this information? This publication includes advice from consensus panels, the British Association of Urological Surgeons, the Department of
Vascular Related Torsion Venous compression Hemorrhagic infarct Young men At night Very painful Can be reduced Scrotal Masses Testicular Tumors (solid
 Pathology of the Male Reproductive System Testis and Epididymis Failure of Testis to Descend Testis are not always in scrotum at birth. Testes from in abdomen with kidneys Migrate to scrotum May get stuck
Pathology of the Male Reproductive System Testis and Epididymis Failure of Testis to Descend Testis are not always in scrotum at birth. Testes from in abdomen with kidneys Migrate to scrotum May get stuck
Ultrasonography of intratesticular lesions: its role in
 The Ulster Medical Journal, Volume 68, No. 2, pp. 54-8, November 1999. Ultrasonography of intratesticular lesions: its role in clinical management P T Kennedy, J M Elliott, P F Rice, B E Kelly Accepted
The Ulster Medical Journal, Volume 68, No. 2, pp. 54-8, November 1999. Ultrasonography of intratesticular lesions: its role in clinical management P T Kennedy, J M Elliott, P F Rice, B E Kelly Accepted
DISORDERS OF MALE GENITALS
 Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 9. Testicular disorders/disorders of male genitals. Horm Res 2007;68(suppl 2):63 66 ESPE Code Diagnosis OMIM ICD10
Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 9. Testicular disorders/disorders of male genitals. Horm Res 2007;68(suppl 2):63 66 ESPE Code Diagnosis OMIM ICD10
Prostate Artery Embolisation (PAE)
 Service: Imaging Prostate Artery Embolisation (PAE) Exceptional healthcare, personally delivered Ask 3 Questions The team delivering your healthcare want to encourage you to become as involved as possible
Service: Imaging Prostate Artery Embolisation (PAE) Exceptional healthcare, personally delivered Ask 3 Questions The team delivering your healthcare want to encourage you to become as involved as possible
Direct Access Physiotherapy: Challenges and Benefits of a UK Model
 Dobrodosli Direct Access Physiotherapy: Challenges and Benefits of a UK Model Bradley Scanes MSc BSc (Hons) PGcert Chartered Physiotherapist (CSP, HCPC & ACPSEM Member) Kdo Sem Who Am I? A physio NHS Football
Dobrodosli Direct Access Physiotherapy: Challenges and Benefits of a UK Model Bradley Scanes MSc BSc (Hons) PGcert Chartered Physiotherapist (CSP, HCPC & ACPSEM Member) Kdo Sem Who Am I? A physio NHS Football
MEditorial December Kids Urology
 MEditorial December 2012 Kids Urology Most childhood illnesses are in the realm of infections, usually viral, which although sometimes frightening to parents, go away on their own without any major intervention.
MEditorial December 2012 Kids Urology Most childhood illnesses are in the realm of infections, usually viral, which although sometimes frightening to parents, go away on their own without any major intervention.
