Chromosome Studies in 150 Sexually Abnormal Patients (A Summarized Report)1,2
|
|
|
- Alvin Freeman
- 5 years ago
- Views:
Transcription
1 Studies in 150 Sexually Abnormal Patients (A Summarized Report)1,2 Part II Received October 12, 1965 Sajiro Makino Zoological Institute, Hokkaido University, Sapporo, Japan Part II describes cytogenetical and clinical features of 150 sexually abnormal patients data of which were collected during a period from September 1959 to July 1965 in the writer's laboratory in collaboration with his co-workers and clinicians of various medical fields. General remarks and conclusion were given in Part I, together with some repre sentative karyotypes and related references (Makino, S. 1957: studies in 150 sexually abnormal patients (a summarized report), Part I. Cytologia 31: ). DESCRIPTION OF 150 CASES Phenotypic males Klinefelter's syndrome with an XXXXY sex chromosome complement (1 case) Case #1 Male, 12 years Clinical features: Height 142cm. Weight 23.5kg. Both parents normal and healthy. Maternal age 21 years. Paternal age 25 years. Widely spaced eyes characterized by a divergent strabismus and mongoloid slant. Broad and flat nasal bridge. Hypoplastic maxilla. Prognathic mandible. Short peg-shaped and widely spaced teeth. Normal palate, neck and chest. The elbow-joints had a limited supination due to the bilateral radio-ulnar synostosis. The fifth finger was short and curved in both hands. Small penis, 4cm long showing pseudophimosis. Scrotum normal size. Extremely small testes. Severe mental deficiency (IQ 30). High gonadotropin. Normal 17-KS. Atrophic and hyalinized semi niferous tubules. No germ cells. Sex chromatin: One-positive 20.0%, two-positive 33.6%, three-positive 37.4%, four-positive 2.1%, and negative 8.0%. < >50 total Blood Karyotype: 49-XXXXY. Reference: Makino et al. 1964b. Klinefelter's syndrome with an XXXY sex chromosome complement (1 case) Case #2 Male, 16 years Clinical features: Height 163cm. Weight 43.5kg. Last born of six siblings. Maternal age 45 years. Paternal age 45 years. Slight epicanthus. Atrophic optic fundi. Normal palate. Slightly funnel shaped chest. Marked gynecomastia. Small penis, 4.6cm long. 1 Contribution No. 770 from the Zoological Institute, Faculty of Science, Hokkaido University, Sapporo, Japan. 2 With the cooperation of Dr. Motomichi Sasaki in organizing data.
2 350 S. Makino Cytologia 31 Normal scrotum. Small testes. Atrophic seminiferous tubules with hyalinized basement membrane. No germ cells. Leydig cells present in edematous stroma with lipoid granules. High gonadotropin. Estrogen beyond normal limits. Sex chromatin: One-positive 34.6%, two-positive 42.6%, three-positive 1.6%, and negative 21.6%. < >49 total Blood Karyotype: 48-XXXY. Reference: Makino et al. 1964b Klinefelter's syndrome with an XXYY sex chromosome complement (1 case) Case #3 Male, 14 years Clinical features: Height 162cm. Weight 44kg. Upper measurement 75cm. Symphy sis to sole 87cm. IQ 63. Maternal age 38 years. Paternal age 39 years. Both parents and two siblings normal and healthy. Epicanthic folds noted in both eyes. Clinodactyly on the fifth fingers. No gynecomastia. Normal-sized penis and scrotum. Extremely small testes; right 1.7 ~1.1 ~1.0cm, left 1.9 ~1.1 ~1.1cm. Prostate not palpable. No pubic hair. Normal bone age. Testicular biopsy revealed a few hyalinized tubules showing thickening of the lamina propria, and a few tubules containing many Sertoli cells and a few sper matogonia. Leydig cells formed large clumps. 17.KS mg/day. Gonadotropin 48 muu/day. 17-OHCS mg/day. Sex chromatin: One-positive 65.0%, two-positive 0.5%, and negative 34.5%. < >48 total Blood Karyotype: 48-XXYY. Reference: Takagi et at Klinefelter's syndrome with an XX/XXY sex chromosome complement (1 case) Case #4 Male, 17 years Clinical features: Underdeveloped genitalia. Eunuchoid body proportions. Testicular biopsy revealed hyalinized tubules, absence of spermatogonia. Sex chromatin positive. Blood Skin Karyotype: 46-XX/47-XXY. Rererence: Dave Klinefelter's syndrome with an XXY sex chromosome complement (29 cases) Case #5 Male, 44 years Clinical features: Testicular biopsy revealed small atrophic hyalinized tubules with atrophic spermatogenesis. 17-KS 11.23mg/day. Gonadotropin 48muu/day. Sex chromatin positive. Bone marrow
3 1966 Studies in 150 Sexually Abnormal Patients, II 351 Karyotype: 47-XXY. Reference: Makino et al Case #6 Male, 30 years. 1962b. Clinical features: Underdeveloped external genitalia. Testes; right 1.8 ~0.9 ~1.2cm, left 1.6 ~1.2 ~1.1cm. Impotent. No child during four years married life. IQ KS 3.86mg/day. Gonadotropin 80muu/day. < >48 total Blood Karyotype: 47-XXY. Reference: Makino et al. 1963b. Case #7 Male, 25 years Clinical features: Gynecomastia present. Penis of a normal size. Atrophic testes, 2.2 ~ 2.0 ~2.0cm. Hypoplastic prostate. Pubic hair of a normal male type. < >48 total Blood Karyotype: 47-XXY. Reference: Makino et al. 1963b. Case #8 Male, 31 years Clinical features: Eunuchoid proportions. Atrophic testes with hyalinized seminiferous tubules. Arrest of spermatogenesis. Aspermia. No obesity. 17-KS 7.1mg/day. < >48 total Blood Karyotype: 47-XXY. Reference: Makino and Sofuni Case #9 Male, 20 years Clinical features: No gynecomastia. Very small penis, about 3cm long. Hypoplastic scrotum and testes. Atrophic hyalinized seminiferous tubules. Arrest of spermatogenesis. Aspermia. No pubic hair. Increase of Leydig cells. 17-KS 2.6mg/day. Gonadotropin 48 muu/day. Sex chromatin positive. < >48 total Blood Karyotype: 47-XXY. Reference: Makino and Sofuni Case #10 Male, 29 years Clinical features: Eunuchoid proportions. Hypoplastic scrotum and penis. Atrophic testes. No pubic hair. No beard. Arrest of spermatogenesis. 17-KS 5.6mg/day. Gona dotropin 64muu/day. 17-OHCS 10.4mg/day. < >48 total Blood Karyotype: 47-XXY. Reference: Makino and Sofuni Case #11 Male, 20 years Clinical features: Eunuchoid proportions. No gynecomastia. Atrophic testes. Left testis 2cm long. Right testis 3cm long. Penis normal, 9cm long. Atrophic hyalinized seminiferous tubules. Arrest of spermatogenesis. Aspermia. Increase of Leydig cells. Normal pubic hair.
4 352 S. Makino Cytologia 31 Blood Karyotype: 47-XXY. Reference: Makino and Sofuni Case #12 Male, 13 years Clinical features: Height 153cm. Weight 37kg. Pubis to crown 68cm. Pubis to sole 85cm. IQ 68. Maternal age 32 years. Paternal age 40 years. Penis and scrotum normal size. No gynecomastia. Testes; right 2.9 ~1.8 ~2.0cm, left 2.8 ~1.9 ~1.5cm. Well formed prepuberal seminiferous tubules with thickening of lamina propria and hyaliniza tion. A few Leydig cells. 17-KS mg/day. Gonadotropin 24-48muu/day. 17-OHCS mg/day. Sex chromatin: One-positive 57.5%, two-positive 4.5%, and negative 38.0%. < >48 total Blood Karyotype: 47-XXY. Reference: Takagi et al Case #13 Male, 13 years Clinical features: Height 154.5cm. Weight 37kg. Upper measurement 73.5cm. Symphysis to sole 81cm. IQ 76. Maternal age 19 years. Paternal age 28 years. Penis and scrotum normal in size. No gynecomastia. Right testis 2.4 ~1.7 ~1.6cm. Left testis, 2.5 ~1.8 ~1.5cm. Well-formed prepuberal seminiferous tubules with thickening of lamina propria and hyalinization. A few Leydig cells. 17-KS mg/day. Gonadotropin 24-48muu/day. 17-OHCS mg/day. Sex chromatin: One-positive 66.0%, two-positive 1.5%, and negative 32.5%. < >48 total Blood Karyotype: 47-XXY. Reference: Takagi et al Case #14 Male, 18 years Clinical features: Small penis and testes. No gynecomastia. Scanty pubic hair. Hy poplastic prostate. High excretion of gonadotropin, estrogen and 17-KS. Atrophic testes containing scanty seminiferous tubules and clumps of Leydig cells. < >48 total Blood Karyotype: 47-XXY. Reference: Makino et al. 1964c. Case #15 Male, 22 years Clinical features: Small penis, 4.0cm long. Small testes; right 1.8 ~1.3 ~1.0cm, left 1.7 ~1.2 ~1.0cm. Atrophy of seminiferous tubules. Clumps of Leydig cells. Hypoplastic prostate. High exeretion of gonadotropin. Cleft palate with hare-lip. Sex chromatin positive (63%). IQ 59. Blood Karyotype: 47-XXY. Reference: Makino et al. 1964c.
5 1966 Studies in 150 Sexually Abnormal Patients, II 353 Case #16 Male, 20 years Clinical features: Small penis, 5.8cm long. Small testes; right 1.5 ~1.0 ~0.8cm, left 1.6 ~1.0 ~0.8cm. Gynecomastia present. Hypoplastic prostate. Slight epicanthus. IQ 90. Sex chromatin positive (78%). < >48 total Blood Karyotype: 47-XXY. Reference: Makino et al. 1964c. Case #17 Male, 29 years Clinical features: Small penis. Small testes; right 2.0 ~1.5 ~1.4cm, left 1.7 ~0.8 ~0.8 cm. Left testes undescended. Atrophic seminiferous tubules. Hypoplastic prostate. Scanty pubic hair. Sex chromatin positive (47.5%). IQ 59. Blood Karyotype; 47-XXY. Reference: Makino et al. 1964c. Case #18 Male, 23 years Clinical features: Gynecomastir Normal penis. Atrophic testes. Hypoplastic prostate. Normal pubic hair. Deep voice. Blood Karyotype: 47-XXY. Reference: Makino et al. 1964c. Case #19 Male, 14 years Clinical features: Gynecomastia. Small testes. Atrophy of seminiferous tubules. No spermatogenesis. Drumstick positive. 17-KS 1.26mg/day. Gonadotropin 48muu/day. Bone marrow Karyotype: 47-XXY. Reference: Makino et al Case #20 Male, 53 years Clinical features: Small testes. Atrophic seminiferous tubules. Gynecomastia. No spermatogenesis. Drumstick positive. 17-KS 2.7mg/day. Gonadotropin 12muu/day. Bone marrow Karyotype: 47-XXY. Reference: Makino et al Case #21 Male, 11 years Clinical features: Normal external genitalia. Normal testes; right 2.4 ~1.7 ~1.5cm, left 2.5 ~1.6 ~1.3cm. Histologically normal for his age. High excretion of estrogen and gonadotropin. Hypoplastic prostate. Sex chromatin positive (65%). IQ 77. Blood Karyotype 47-XXY. Reference: Takagi et al
6 354 S. Makino Cytologia 31 Case #22 Male, 12 years Clinical features: Normal external genitalia. Normal testes, 2.3 ~1.6 ~1.3cm, with normal bistology for his age. High urinary excretion of 17-KS, estrogen and gonadotropin. Sex chromatin positive (62%). IQ 69. Blood Karyotype: 47-XXY. Reference: Takagi et al Case #23 Male, 14 years Clinical features: Normal external genitalia with scanty pubic hair. Right testis 2.5 ~ 1.8 ~1.3cm. Left testis 2.5 ~1.8 ~1.3cm. Hyaline-degeneration of seminiferous tubules with increase of Leydig cells. Small prostate. High excretion of estrogen and gonado tropin. Sex chromatin positive (44%). IQ 78. Blood Karyotype: 47-XXY. Reference: Takagi et al Case #24 Male, 15 years Clinical features: Normal external genitalia without pubic hair. Right testis 2.0 ~1.5 ~ 1.3cm. Left testis 2.0 ~1.6 ~1.0cm. Hyalinized seminiferous tubules with numerous Leydig cells. Hypoplastic prostate. High excretion of estrogen and gonadotropin. Sex chromatin positive (61%). IQ 74. Clinodactyly of the fifth fingers. <47 47 >47 total Blood Karyotype: 47-XXY. Reference: Takagi et al Case #25 Male, 15 years Clinical features: Normal external genitalia. Right testis 2.2 ~1.4 ~1.1cm. Left testis 2.0 ~1.5 ~1.2cm. Atrophic seminiferous tubules with many Leydig cells. High excretion of 17-KS, 17-OHCS, estrogen and gonadotropin. Sex chromatin positive (55%). IQ 76. Blood Karyotype: 47-XXY. Reference: Takagi et. al Case #26 Male, 28 years Clinical features: Normal external genitalia. Pubic hair normal. Small prostate. Small testes; right 2.0 ~1.5 ~1.2cm, containing scanty degenerated seminiferous tubules and clumps of Leydig cells. Sex chromatin positive (64.5%). Normal intelligence. Blood Karyotype: 47-XXY. Reference: Takagi et al Case #27 Male, 29 years Clinical features: Diagnosed as Klinefelter's syndrome. Clinical details not available.
7 1966 Studies in 150 Sexually Ab normal Patients, II 355 Blood Karyotype: 47-XXY. Reference: Muramoto, unpublished. Case #28 Male, 37 years Clinical features: Diagnosed as Klinefelter's syndrome. Clinical details not available. < >47 total Blood Karyotype: 47-XXY. Reference: Muramoto, unpublished. Case #29 Male; 25 years Clinical features: No clinical data available < >48 total Blood (?) - 14 Karyotype: 47-XXY. Reference: Ikeuchi Case #30 Male, 21 years., unpublished. chromatin Clinical features: Small testes positive., 1.8 ~1.5 ~1.2cm in both. Scanty pubic hair. Sex <47 47 >47 total Blood Karyotype: 47-XXY. Reference: Sasaki, unpublished. Case #31 Male, 25 years Clinical features: Diagnosed as Klinefelter's syndrome. Details not available. Mode at 47 in 20 cells counted. Karyotype: 47-XXY. Reference: Makino Case #32 Male, 34 years Clinical features: Diagnosed as Klinefelter's syndrome. Details not available. Mode at 47 in 60 cells counted. Karyotype: 47-XXY. Reference: Makino Case #33 Male, 37 years Clinical features: Diagnosed as Klinefelter's syndrome. Clinical details not available. Mode at 47 in 53 cells counted. Karyotype: 47-XXY. Reference: Makino Suspected Klinefelter's syndrome with an XY sex mechanism (3 cases) Case #34 Male, 32 years Clinical features: Atrophic hyalinized seminiferous tubules. Arrest of spermatogenesis. Aspermia. Normal history of development and puberty. Normal penis and scrotum. 17 KS 3.6mg/day. Gonadotropin 16muu/day. Blood Karyotype: 46-XY. Reference: Makino et al. 1963b. Case #35 Male, 10 years Clinical features: Underdeveloped external genitalia. Small testes. 17-KS 3.6mg/day. Cytotogia 31,
8 356 S. Makino Cytologia 31 Gonadotropin 4muu/day. Blood Karyotype: 46-XY. Reference: Makino et al. 1963b. Case #36 Male, 26 years Clinical features: Data not available. Mode at 46 in 10 cells counted. Karyotype: 46-XY. Reference: Makino Patients with hypospadias (9 cases) Case #37 Male, 22 years Clinical features: Hypospadia penoscrotalis. Urethral groove failed to close completely and opened in the peno-scrotal angle with chordee. Blood Karyotype: 46-XY. Reference: Makino et al. 1963b. Case #38 Male, 14 years Clinical features: Hypospadia. Palpable testes in hypoplastic scrotum. Small crooked penis, about 2.5cm long. Prostate not palpated digitally. < >46 total Blood Karyotype: 46-XY. Reference: Makino et al. 1963b. Case #39 Male, 5 years Clinical features: Hypospadia penis. Abnormal urethral opening at the base of the crooked penis. Blood Karyotype: 46/X+a long Y. Y corresponds in length to group chromosomes. Reference: Makino et al. 1964c. Case #40 Male, 15 years Clinical features: Hypospadia penis. Urethral groove failed to close completely and opened on the ventral surface of the penis with chordee. < >46 total Blood Karyotype: 46-XY Reference: Makino et al. 1964c. Case #41 Male, 6 years Clinical features: Hypospadia penis. Urethral opening on the ventral surface of the penis. Hypoplastic scrotum. Small testes. Blood
9 1966 Studies in 150 Sexually Abnormal Patients, II 357 Karyotype: 46-XY. Reference: Makino et al. 1964c. Case #42 Male, 15 years Clinical features: Hypospadia penoscrotalis. Bifid scrotum. Urethral opening at the base of the crooked penis. Blood Karyotype: 46-XY. Reference: Takagi et al Case #43 Male, 5 years Clinical features: Hypospadia penis. Urethral opening at the base of the penis. Blood Karyotype: 46-XY. Reference: Takagi et al Case #44 Male, 30 years Clinical features: Hypospadia. < >47 total Blood Case #45 Male, 18 years Clinical features: Hypospadia penis. Testes and scrotum normal in size. No other abnormality. Sex Chromatin negative. Blood Karyotype: 46-XY. Reference: Sasaki, unpublished. Patients with cryptorchism (25 cases) Case #46 Male, 18 months Clinical features: Bilateral undescended testes. Congenital dislocation of the hip joints. Mental and some other physical developmental features apparently normal. No sign of Down's syndrome. Maternal age 25 years. Paternal age 27 years. Both parents, physically and mentally normal. counts; Blood Karyotype: 46-XY. One of no. 15 chromosomes had an unusually enlarged short arm. The same abnormality was found in the patient's father, paternal grandfather and two paternal aunts. Reference: Kato et al. 1965, Makino et al Case #47 Male, 6 years Clinical features: Bilateral inguinal testes. Other external genitalia, normal as a male. Blood *
10 358 S. Makino Cytologia 31 Karyotype: 46-XY. Reference: Makino and Sofuni Case #48 Male, 5 years Clinical features: Bilateral inguinal testes. Normal male genitalia. Body under developed for his age. Rickety. Sex chromatin negative. Blood Karyotype: 46-XY. Reference: Dave Case #49 Male, 14 years Clinical features: Bilateral undescended testes. Blood Karyotype: 46-XY. Reference: Dave Case #50 Male, 2 years Clinical features: Bilateral inguinal testes. Blood Case #51 Male, 5 years Clinical features: Bilateral inguinal testes. Blood Case #52 Male, 7 years Clinical features: Bilateral undescended testes. Further data not available. Blood Case #53 Male, 3 years Clinical features: Bilateral undescended testes. Further data not available. Blood Case #54 Male, 5 years Clinical features: Bilateral inguinal testes. Further details not available. Blood
11 1966 Studies in 150 Sexually Abnormal Patients, II 359 Case #55 Male, 33 years Clinical features: Right inguinal and left abdominal testes. Azoospermia. Normal penis. Blood Karyotype: 46-XY. Reference: Takagi et al Case #56 Male, 18 years Clinical features: Left undescended testes, atrophic histologically. 17-KS 7mg/day. Bone marrow Karyotype: 46-XY. Reference: Makino and Kikuchi Case #57 Male, 6 years Clinical features: Left undescended testis. Other external genitalia normal as a male. Blood Karyotype: 46-XY. Reference: Makino and Sofuni Case #58 Male, 5 years Clinical features: Left undescended testis. General body weakness, slightly under developed for his age. External genitalia normal. < >47 total Blood Karyotype: 46-XY. Reference: Dave Case #59 Male, 22 years Clinical features: Left undescended testis. Body hair growth normal as a male. His tologically the left testis infantile. Sex chromatin negative. < >47 total Blood Karyotype: 46-XY. Reference: Dave Case #60 Male, 5 years Clinical features: Left undescended testis. Blood Case #61 Male, 11 years Clinical features: Right abdominal testis. Blood
12 360 S. Makino Cytologia 31 Case #62 Male, 15 years Clinical features: Right inguinal testis. Details not available. < >46 total Blood Karyotype: 46-XY. Reference: Makino et al. 1964d. Case #63 Male, 15 years Clinical features: Right inguinal testes. Further data not available. Blood Case #64 Male, 12 years Clinical features: Right inguinal testis. Further details not available. Blood Case #65 Male, age unknown Clinical features: Undescended testes. Further details not available. Mode at 46 in 25 cells counted. Karyotype: 46-XY. Reference: Makino Case #66 Male, 10 years Clinical features: Undescended testes. Further data not available. Mode at 46 in 8 cells counted. Karyotype: 46-XY. Reference: Makino Case #67 Male, 11 years Clinical features: Undescended testes. Further data not available. counts : Mode at 46 in 25 cells counted. Karyotype: 46-XY. Reference: Makino Case #68 Male, 7 years Clinical features: Undescended testes. Further data not available. Mode at 46 in 62 cells counted. Karyotype: 46-XY. Reference: Makino Case #69 Male, 52 years Clinical features: Left undescended testis. Absence of right testis. Other external genitalia, normal as a male. 17-KS 3.85mg/day. Blood Karyotype: 46-XY. Reference: Makino et al. 1963b. Case #70 Male, 5 years Clinical features: Left testis undescended. Absence of right testis.
13 1966 Studies in 150 Sexually Abnormal Patients, II 361 Blood Karyotype: 46-XY. Reference: Makino et at. 1964a. Patients with gynecomastia (4 cases) Case #71 Male, 13 years Clinical features: Gynecomastia. Mental retardation. No symptom of Klinefelter's syndrome. Bone marrow Karyotype: 46-XY. Reference: Makino et al. 1963a. Case #72 Male, 10 years Clinical features: Unilateral gynecomastia, on the right breast, with marked fibrosis and hyaline degeneration. Normal external genitalia. Histologically normal testes. Drumstick positive. 17-KS 3.0mg/day. Bone marrow (?) - 17 Karyotype: 46-XY. Reference: Makino et al Case #73 Male, 21 years Clinical features: Gynecomastia. Scanty axillary hair. Spermatogenesis ( }). Blood Karyotype: 46-XY. Reference: Takagi et at Case #74 Male, 14 years Clinical features: Gynecomastia. Atrophic left testis showing hypoplastic seminiferous tubules without sperm. Blood Karyotype: 46-XY. Reference: Takagi et at., Patients with an XO/XY sex chromosome complement (3 cases) Case #75 Male, 56 years Clinical features: Apparently normal man with recently developed gynecomastia on both sides. Testis slightly larger than the normal and soft. He has fathered seven ap parently normal children by two wives. Testicular biopsy showed an oligospermic picture. Sex chromatin negative. < >47 total Blood Skin Karyotype: 45-XO/46-XY. Reference: Dave 1966.
14 362 S. Makino Cytologia 31 Case #76 Male, 28 years Clinical features: Height 180cm. Weight 75kg. Infantile external genitalia. No facial hair growth. Pelvis, shoulder and chest of a female type. Bone age of 16.5 years. Testicular biopsy revealed infantile tissue. One or two sections from both testes showed no evidence of the ovarian tissue. Sex chromatin negative. < >47 total Blood Karyotype: 45-XO/46-XY. Reference: Dave Case #77 Male, 6 years Clinical features: Urogenital sinus formed by vagina and abnormal opening of urethra. Bifid scrotum. Left testis undescended. A pea-sized right testis containing slightly hy poplastic seminiferous tubules with a few germ cells. Left uterus-like tube. Normal gonadotropin excretion. High estrogen excretion ( ug/day). Sex chromatin nega tive. < >46 total Blood Karyotype: 45-XO/46-XY. Reference: Makino et al. 1964c. Miscellaneous sex abnormalities (19 cases) Case #78 Male, 4 years Clinical features: Obesity. Mental retardation. Convulsion. Ataxia. Small penis and scrotum. Undescended testes. Blood Karyotype: 46-XY. Reference: Makino et al 1962d. Case #79 Male, 6 years Clinical features: Normal penis with underdeveloped scrotum. Right abdominal ectopic testis (1.4 ~0.8 ~0.6cm). Left perineal ectopic testis (1.4 ~0.7 ~0.6cm). Normal excretion of urinary hormones. Blood Case #80 Male, 17 years Clinical features: Eunuchoidism. Slight gynecomastia. Small penis, 1.5cm long. Small testes; right 1.0 ~1.3 ~1.0cm, left 1.5 ~1.0 ~0.5cm, with hyaline-degenerated semini ferous tubules containing spermatogonia, clumps of Leydig cells and no sperm. Normal excretion of gonadotropin and estrogen but high 17-KS excretion. Blood Case #81 Male, 19 years Clinical features: Hypergonadotropic eunuchoidism. Small penis. High excretion of urinary gonadotropin. Normal intelligence. Sex chromatin negative.
15 1966 Studies in 150 Sexually Abnormal Patients, II 363 < >47 total Blood Case #82 Male, 25 years Clinical features: Eunuchoidism. Hypoplastic external genitalia. No gynecomastia. Three sibships show similar clinical features. < >46 total Blood Karyotype: 46-XY. Reference: Takagi et al., Case #83 Male, 6 years Clinical features: Eunuchoidism. Small penis. Normal scrotum. Small testes. Hy poplastic prostate. High excretion of estrogen. Retarded development of secondary sexual characters. High intelligence. Blood Case #84 Male, 28 years Clinical features: Very small-sized penis. Histologically atrophic testes. Blood Karyotype: 46-XY. Reference: Makino et al. 1962d. Case #85 Male, 5 years Clinical features: Hospitalized due to chordee of the penis. Very small penis without hypospadia. Labia-like bifurcated scrotum. Congenital diverticulum of urethra. 17-KS 2mg/day. Bone marrow and blood Karyotype: 46-XY. Reference: Makino and Kikuchi Case #86 Male, 28 years Clinical features: Very small-sized penis. Histologically atrophic testes. 17-KS 6.4 mg/day. Bone marrow Karyotype: 46-XY. Reference: Makino and Kikuchi Case #87 Male, 18 years Clinical features: Hypoplastic scrotum. Small penis, about 4cm long. Intra-abdominal testes with atrophic structure. Prepubertal mentality. Semi-high-pitched voice. No beard. Scanty pubic hair. 17-KS 41mg/day. Gonadotropin 32muu/day. 17-OHCS 6.1mg/day.
16 364 S. Makino Cytologia 31 Blood Karyotype: 46-XY. Reference: Makino et al. 1963b. Case #88 Male, 27 years Clinical features: Hypoplastic scrotum and penis. Eunuchoid proportions. Obesity. No pubic hair. 17-KS 4.1mg/day. Gonadotropin 64muu/day. 17-OHCS 6.1mg/day. Dia gnosed as hypergonadotropic hypogonadism. Blood Karyotype: 46-XY. Reference: Makino et al. 1963b. Case #89 Male, 29 years Clinical features: Eunuchoid proportions. Small penis, 4 ~1.5cm. Gynecomastia. 17- KS mg/day. Gonadotropin 12muu/day. Sex chromatin negative. Diagnosed as hy pogonadotropic hypogonadism. Blood Karyotype: 46-XY. Reference: Makino and Sofuni Case #90 Male, 9 years Clinical features: Hypogonadism. Undescended right testis. Underdeveloped penis and scrotum. Normal mentality. Blood Karyotype: 46-XY. Reference: Makino et al. 1962c. Case #91 Male, 26 years Clinical features: Infantile genitalia and small penis. Bone age of 14 years. Testicular biopsy revealed hyalinization of tubules, stroma filled with fibrous cells. Spermatogoni a present but no spermatogenesis. Sex chromatin negative. Blood Karyotype 46-XY. Reference: Dave Case #92 Male, 16 years Clinical features: Infantile genitalia and small penis. Bone age of 13.5 years. Tes ticular biopsy revealed infa tile tissue, a few Leydig cells, no spermatogenesis. Sex chro matin negative. Blood Karyotype: 46-XY. Reference: Dave Case #93 Male, 26 years Clinical features: External genitalia apparently normal. Pubic hair of a female type
17 1966 Studies in 150 Sexually Abnormal Patie nts, II 365 Body and facial hair growth scanty. Sperm counts normal but sperms mostly non-motile ex chromatin. S negative. Blood Karyotype: 46-XY. Reference: Dave Case #94 Male, 18 years Clinical features: Small testes. Pubic hair and axillary hair scanty. Blood Karyotype: 46-XY. Reference: Dave Case #95 Male, 1 year Clinical features: Hypoplastic scrotum. Limitted extensibility of arms and legs. Polydactyly. High arched palate. Blood Karyotype: 46-XY. Reference: Makino et al. 1962a. Case #96 Male, 6 months Clinical features: Diagnosed as male pseudohermaphroditism. Clinical data not avail able. Mode at 46 in 22 cells counted in leucocytes. Karyotype: 46/X+a long Y. Y corresponds in length to group chromosomes. His father possessed a long Y chromosome of an apparently similar size. Reference: Makino Patients with Azoospermia or oligospermia (17 cases) Case #97 Male, 30 years Clinical features: Azoospermia. Penis and scrotum normally developed. Arrest of spermatogenesis. Normal Leydig cells. Blood Karyotype: 46-XY. Reference: Makino and Sofuni Case #98 Male, 29 years Clinical features: Azoospermia with a normal volume of semen. Penis and scrotum normally developed. Blood Karyotype: 46-XY. Reference: Makino and Sofuni Case #99 Male, 30 years Clinical features: Azoospermia. No child during three years of married life. < >46 total Blood
18 366 S. Makino Cytologia 31 Karyotype: 46-XY. Reference: Makino et al. 1964d. Case #100 Male, 39 years Clinical features: Azoospermia. Atrophic testes. Arrested spermatogenesis. No child during seven years of married life. < >47 total Blood Karyotype: 46-XY. Reference: Makino et al. 1964d. Case #101 Male, 28 years Clinical features: Azoospermia. Normal sized testes. No child during four years of married life. No sperm in semen. < >46 92 total Blood Karyotype: 46/X+ a long Y. Y corresponds in length to group chromosomes. Reference: Makino and Muramoto Case #102 Male, 25 years Clinical features: Azoospermia. Sterility. Small testes with atrophic seminiferous tubules. < >47 total Blood Case #103 Male, 38 years Clinical features: Azoospermia. Sterility. Atrophy of testes. Blood Case #104 Male, 31 years Clinical features: Azoospermia. Sterility. Small testes with atrophic seminiferous tubules. Blood Case #105 Male, 38 years Clinical features: Azoospermia. External genitalia normal. Sterility. Blood Case #106 Male, 31 years Clinical features: Azoospermia. Sterility.
19 1966 Studies in 150 Sexually Abnormal Patients, II 367 Blood Case #107 Male, 28 years Clinical features: Azoospermia. Sterility. Small penis and testes. showing atrophic seminiferous tubules. Blood Case #108 Male, 28 years Clinical features: Azoospermia. Sterility. Normal external genitalia. Normal testes with normal histological features. Blood Case #109 Male, 34 years Clinical features: Azoospermia. Sterility. Blood Case #110 Male, 18 years Clinical features: Azoospermia. Further data not available. Blood Karyotype: 46-XY. Reference: Muramoto, unpublished. Case #111 Male, 32 years Clinical features: Azoospermia. Small testes. Small prostate. No sperm in semen. Blood Karyotype: 46-XY. Reference: Muramoto, unpublished. Case #112 Male, 27 years Clinical features: Azoospermia. Further data not available. Blood Karyotype: 46-XY. Reference: Sasaki, unpublished. Case #113 Male, 58 years Clinical features: Oligospermia. Further data not available.
20 368 S. Makino Cytologia 31 Blood Karyotype: 46-XY. Reference: Makino et al. 1964d. Phenotypic Turner's syndrome (3 cases) females Case #114 Female, 20 years Clinical features: Short stature. Primary amenorrhea. No neck webbing. Sex chro matin negative. 17-KS 3.96mg/day. <45 45 >45 total Bone marrow Karyotype: 45-XO. Reference: Makino et al. 1963a. Case #115 Female, 18 years Clinical features: Typical facial configuration of Turner's syndrome with obvious epicanthus. Alveolar process of upper jaw protruded sharply and hard palate is ogival palate-like. Incomplete development of mandible. Neck webbing slightly developed. Broad shield-like chest. Short stature and stocky build. Cubitus valgus at 25 degree in the region of the elbow joint. Atrophic female genitalia. Small uterus, 4 ~0.6cm. Rudi mentary ovaries, 3 ~0.3cm. Normal-sized oviducts, 10cm in length. Histologically the ovary is composed of stroma cells without germ cells. 17-KS 1.09mg/day. Gonadotropin 20muu/day. Sex chromatin negative. Bone marrow Karyotype: 45-XO. Reference: Makino et al. 1962b. Case #116 Female, 1 year Clinical features: Characteristic facial appearance with epicanthus. Low set malformed ears. Anti-mongolian slant of eyes. Hypertelorism. High arched palate. Neck webbing present. Funnel chest. Widely spaced nipples. Dolichocephaly. Short stature. Heart failure of unknown etiology. Bilateral simian lines. Hyperconvex finger nails. Sex chro matin negative. < >45 total Blood Karyotype: 45-XO. Reference: Takagi et al Patients with an enlarged clitoris (13 cases) Case #117 Female, brought up as a male, 5 years Clinical features: Enlarged clitoris with penile configuration. Mis-diagnosed as crooked penis with hypospadia. Uterus and ovary present. < >46 total Blood Skin
21 1966 Studies in 150 Sexually Abnormal Patients, II 369 Karyotype: 46-XX. Reference: Makino and Sofuni Case #118 Female, 1 month Clinical features: Enlarged clitoris, 1.5 ~1.0cm, with penile configuration. Enlarged major labia. Normal ovary, 3 ~1.5cm. Normal oviducts. Drumstick positive. 17-KS 0.08 mg/day. Bone marrow - 1(?) 3 1(?) - 5 Karyotype: 46-XX. Reference: Makino et al Case #119 Female, 4 years Clinical features: Enlarged clitoris. Sex chromatin positive. Blood Karyotype: 46-XX. Reference: Dave Case #120 Female, 29 years Clinical features: Enlarged clitoris. No child during eight years of married life. Menstruation irregular. Sex chromatin positive (20%). Blood Karyotype: 46-XX. Reference: Sasaki, unpublished. Case #121 Female, 4 months Clinical features: Enlarged clitoris. Further data not available. Mode at 46 in 22 cells counted in leucocytes. Karyotype: 46-XX. Reference: Makino Case #122 Female; 12 years Clinical features: Enlarged clitoris. Further details not available. Mode at 46 in 33 cells counted in leucocytes. Karyotype: 46-XX. Reference: Makino Case #123 Female, new born Clinical features: Enlarged clitoris. Further data not available. Mode at 46 in 33 cells counted in leucocytes. Karyotype: 46-XX. Reference: Makino Case #124 Female, 5 years Clinical features: Enlarged clitoris. Further data not available. Mode at 46 in 67 cells counted in leucocytes. Karyotype: 46-XX. Reference: Makino Case #125 Female, 18 years Clinical features: Enlarged clitoris. Further data not available. Mode at 46 in 33 cells counted in leucocytes. Karyotype: 46-XX. Reference: Makino Case #126 Female, 4.5 years years. Clinical features: Enlarged clitoris. Defective vaginal opening. Maternal age 35
22 370 S. Makino Cytologia 31 < >46 total Blood Karyotype: 46-XX. Reference: Dave Case #127 Female, 1 month Clinical features: Enlarged clitoris. Scrotum-like labia majora. No vaginal opening. Her mother was treated with lutenic hormone at the 5th month of gestation. Blood Karyotype: 46-XX. Reference: Takagi et al Case #128 Female, 1 month Clinical features: Enlarged clitoris. Scrotum-like labia majora. No vaginal opening. Unable to suck. Suspicion of some abnormalities in internal organs. Blood Karyotype: 46-XX. Reference: Takagi et al Case #129 Female, 1 year Clinical features: Enlarged clitoris. Further data not available. Bone marrow Karyotype: 46-XX. Reference: Makino et al. 1963a. Patients without vagina (7 cases). Case #130 Female, 2 years Clinical features: Absence of vagina. Abnormal external genitalia. Her mother received progesterone therapy during pregnancy. 17-KS 0.44mg/day. Bone marrow Karyotype: 46-XX. Reference: Makino and Kikuchi Case #131 Female, 24 years Clinical features: Absence of vagina. Bicornuated uterus, very small in size. Oviducts and ovaries, normal in size and histological structure. Gonadotropin, G. A. 225r/day, G. B. 120r/day, by Crooke's method. Sex chromatin positive. Bone marrow Karyotype: 46-XX. Reference: Makino et al. 1962b. Case #132 Female, 23 years Clinical features: Height 153.4cm. Weight 51.0kg. Primary Amenorrhea. Absence of vagina. Underdeveloped uterus. Small-sized ovary. Sex chromatin positive (31%).
23 1966 Studies in 150 Sexually Abnormal Patients, II 371 < >47 total Blood Karyotype: 46-XX. Reference: Makino et al. 1963b. Case #133 Female, 20 years Clinical featuoes: Height 157.2cm. Weight 56.0kg. Absence of vagina. Primary amenorrhea. Normal secondary sexual characters. Laparotomy revealed small uterus, hard string like structures in place of fallopian tubes and small ovaries on both sides. Sex chro matin positive (39%). < >46 total Blood Skin Bone marrow Karyotype: 46-XX. Reference: Dave Case #134 Female, 20 years Clinical features: Absence of vagina and uterus. Primary amenorrhea. Full develop ment of secondary sexual characters. Normal ovaries, right 3.0 ~2.0 ~1.5cm, left 3.5 ~2.0 ~ 1.5cm. Sex chromatin positive (32%). Blood Karyotype: 46-XX. Reference: Takagi et al Case #135 Female, 25 years Clinical features: Height 149cm. Weight 50kg. Absence of vagina. Primary amenor rhea. Small uterus. Ovary not palpable. Sex chromatin positive (38%). < >47 total Blood Karyotype: 46-XX. Reference: Sasaki unpublished. Case #136 Female, 23 years Clinical features: Height 150cm. Weight 54kg. Absence of vagina. Primary amenor rhea. Small uterus. Normal secondary sexual character. Normal ovary. 17-KS 10.6mg/ day. 17-OHCS 6.7mg/day. Sex chromatin positive (32%). Blood Karyotype: 46-XX. Reference: Dave Adrenogenital syndrome (6 cases) Case #137 Female, 6 years Clinical features: Unusually enlarged clitoris. 17-KS 15-20mg/day. Pregnanetriol 2.4mg/day. Diagnosed as adrenogenital syndrome. Bone marrow Cytologia 31,
24 372 S. Makino Cytologia 31 Karyotype: 46-XX. Reference: Makino and Kikuchi Case #138 Female, 4 years Clinical features: Enlarged clitoris. Urogenital sinus. Poorly developed labio-scrotum. 17-KS 20-30mg/day. Pregnanetriol 10.3mg/day. Diagnosed as adrenogenital syndrome. Bone marrow Karyotype: 46-XX. Reference: Makino and Kikuchi Case #139 Female, 22 years Clinical features: Enlarged clitoris, about 4cm long. Uterus normal. Major labia slightly fused. Male-type pubic hair. 17-KS 20.15mg/day. Gonadotropin, G A. 220r/day, G. B. 75r/day by Crooke's method. Estrogen 17.7r/day. Pregnanediol 1.24mg/day. Sex chromatin positive. Diagnosed as adrenogenital syndrome. < >47 total Bone marrow Karyotype: 46-XX. Reference: Makino et al. 1962b. Case #140 Female brought up as a male, 18 years Clinical features: Enlarged clitoris. Uterus and ovary present. Sex chromatin posi tive. Diagnosed as adrenogenital syndrome. Blood Karyotype: 46-XX. Reference: Makino and Sofuni Case #141 Female, 12 years Clinical features: Male type external genitalia. Enlarged clitoris. Pseudopubertas praecox. Her sister shows similar clinical features. Diagnosed as adrenogenital syndrome. Blood Karyotype: 46-XX. Reference: Takagi et al Case #142 Female, 5 years Clinical features: Diagnosed as adrenogenital syndrome. Further data not available. < >46 total Blood Karyotype: 46-XX. Reference: Muramoto unpublished. Miscellaneous sex abnormalities 3 (cases) Case #143 Female, 17 years Clinical features: Hypoplastic uterus and mammary gland. Scanty pubic and axillary hair. Normal menstruation. IQ 59. Two sex chromatin bodies. Diagnosed as sexual hypoplasia. Blood Karyotype: 47-XXX. Reference: Makino et al. 1964c.
25 1966 Studies in 150 Sexually Abnormal Patients, II 373 Case #144 Female, 22 years Clinical features: Hypoplastic uterus. Primary amenorrhea. < >48 total Blood Karyotype: 46-XX. Reference: Makino et al. 1964d. Case #145 Female, 2 years Clinical features: Epispadia. Further data not available. Blood Karyotype: 46-XX. Reference: Takagi et al Testicularr feminization (3 cases) Case #146 Female, 28 years Clinical features: Female type external genitalia including vagina. Scanty pubic and axillary hair. Primary amenorrhea. Absence of uterus. Inguinal tumor (testis?). Bone marrow Karyotype: 46-XY. Reference: Makino et al. 1963a. Case #147 Female, 21 years Clinical features: Primary amenorrhea. Cryptorchism. Female type external genitalia. Well developed breast. Biopsy of a gonadal specimen showed no spermatogenesis. 17-KS 22.0mg/day. Gonadotropin 24muu/day. Sex chromatin negative. < >46 total Bone marrow Karyotype: 46-XY. Reference: Makino et al. 1962b. Case #148 Female, 17 years Clinical features: Female type external genitalia. Well-developed breast. No pubic and axillary hair. Internal organs of a male type except for the remnant of vagina. Ovaries, oviducts and uterus not detected. Undescended testes. 17-KS 3.85mg/day. Blood Karyotype: 46-XY. Reference: Makino et al. 1963b. True hermaphroditism and agonadism True hermaphroditism (1 case) Case #149 Brought up as a female, 25 years Clinical features: Large clitoris with a penile configuration, about 5cm long. Rudi mentary vagina. Female type urethral opening. Unusually thickened major labia. Poorly developed breast. Man-like voice. Bipartite uterus. Ovo-testis on the right side only, which contained atrophic follicles, follicular cysts and ovarian stroma. The ovarian stroma showed structures resembling testicular tissue including atrophic seminiferous tubules and interstitial tissues. Germ cells showed no gametogenetic activity. 25*
26 374 S. Makino Cytologia 31 < >47 total Bone marrow Karyotype: 46-XX. Reference: Sasaki and Makino Agonadism (1 case) Case #150 Ambiguous sex, 3 years Clinical features: Tiny clitoris-like protrusion. No gonad and internal genital organs except for bilateral small tubular structures (Wolffian remnants). Sex chromatin negative. Drumstick negative. Diagnosed as agonadism. Blood Karyotype: 46-XY. Reference: Makino et al. 1963b. For the literature, refer to Part I.
A CHROMOSOME STUDY IN 20 SEXUALLY ABNORMAL PATIENTS>> WOSAMU MARUYAMA, HACHIRO SHIMBA AND SET-ICHI KOHNO
 JAPAN. J. GENETICS Vol. 43, No. 4: 289-298 (1968) A CHROMOSOME STUDY IN 20 SEXUALLY ABNORMAL PATIENTS>> WOSAMU MARUYAMA, HACHIRO SHIMBA AND SET-ICHI KOHNO Received May 9, 1968 Zoological Institute, Hokkaido
JAPAN. J. GENETICS Vol. 43, No. 4: 289-298 (1968) A CHROMOSOME STUDY IN 20 SEXUALLY ABNORMAL PATIENTS>> WOSAMU MARUYAMA, HACHIRO SHIMBA AND SET-ICHI KOHNO Received May 9, 1968 Zoological Institute, Hokkaido
Intersex Genital Mutilations in ICD-10 Zwischengeschlecht.org / StopIGM.org 2014 (v2.1)
 Intersex Genital Mutilations in ICD-10 Zwischengeschlecht.org / StopIGM.org 2014 (v2.1) ICD-10 Codes and Descriptions: http://apps.who.int/classifications/icd10/browse/2010/en 1. Reference: 17 Most Common
Intersex Genital Mutilations in ICD-10 Zwischengeschlecht.org / StopIGM.org 2014 (v2.1) ICD-10 Codes and Descriptions: http://apps.who.int/classifications/icd10/browse/2010/en 1. Reference: 17 Most Common
CHROMOSOMAL NUMERICAL ABERRATIONS INSTITUTE OF BIOLOGY AND MEDICAL GENETICS OF THE 1 ST FACULTY OF MEDICINE
 CHROMOSOMAL NUMERICAL ABERRATIONS INSTITUTE OF BIOLOGY AND MEDICAL GENETICS OF THE 1 ST FACULTY OF MEDICINE CHROMOSOMAL ABERRATIONS NUMERICAL STRUCTURAL ANEUPLOIDY POLYPLOIDY MONOSOMY TRISOMY TRIPLOIDY
CHROMOSOMAL NUMERICAL ABERRATIONS INSTITUTE OF BIOLOGY AND MEDICAL GENETICS OF THE 1 ST FACULTY OF MEDICINE CHROMOSOMAL ABERRATIONS NUMERICAL STRUCTURAL ANEUPLOIDY POLYPLOIDY MONOSOMY TRISOMY TRIPLOIDY
176 N. TAKAGI, S. MAKINO, S. TAKAI, and M. HIKITA [Vol. 41,
 No. 2] 175 39. A Phenotypical XXYY Human Male with Notes on Two Regular Kline f elter Cases*' By Nobuo TAKAGI, Sajiro MAKINO, Shudo TAKAI, **~ and Masahiro HIKITA**) (Comm. by Yoshimaro TANAKA, M.J.A.,
No. 2] 175 39. A Phenotypical XXYY Human Male with Notes on Two Regular Kline f elter Cases*' By Nobuo TAKAGI, Sajiro MAKINO, Shudo TAKAI, **~ and Masahiro HIKITA**) (Comm. by Yoshimaro TANAKA, M.J.A.,
Chromosome Studies in 150 Sexually Abnormal Patients (A Summarized Report)1,2
 1966 309 Chromosome Studies in 150 Sexually Abnormal Patients (A Summarized Report)1,2 Part I Received October 12, 1965 Sajiro Makino Zoological Institute, Hokkaido University, Sapporo, Japan During the
1966 309 Chromosome Studies in 150 Sexually Abnormal Patients (A Summarized Report)1,2 Part I Received October 12, 1965 Sajiro Makino Zoological Institute, Hokkaido University, Sapporo, Japan During the
Grade 9 Science - Human Reproduction
 Grade 9 Science - Human Reproduction The human reproductive system is a series of organs that work together for one purpose: reproduction (creating new humans). Each part has a specific role in the reproductive
Grade 9 Science - Human Reproduction The human reproductive system is a series of organs that work together for one purpose: reproduction (creating new humans). Each part has a specific role in the reproductive
Sexual Development. 6 Stages of Development
 6 Sexual Development 6 Stages of Development Development passes through distinct stages, the first of which is fertilization, when one sperm enters one ovum. To enter an ovum, a sperm must undergo the
6 Sexual Development 6 Stages of Development Development passes through distinct stages, the first of which is fertilization, when one sperm enters one ovum. To enter an ovum, a sperm must undergo the
SISTEMA REPRODUCTOR (LA IDEA FIJA) Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
Development of the urogenital system
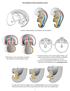 Development of the urogenital system Location of the pronephros, mesonephros and metanephros Differentiation of the intermedierm mesoderm into nephrotome and mesonephric tubules Connection between aorta
Development of the urogenital system Location of the pronephros, mesonephros and metanephros Differentiation of the intermedierm mesoderm into nephrotome and mesonephric tubules Connection between aorta
Let s Talk About Hormones!
 Let s Talk About Hormones! This lesson was created by Serena Reves and Nichelle Penney, with materials from the BCTF and The Pride Education Network. Hormones are responsible for the regulation of many
Let s Talk About Hormones! This lesson was created by Serena Reves and Nichelle Penney, with materials from the BCTF and The Pride Education Network. Hormones are responsible for the regulation of many
Development of the Genital System
 Development of the Genital System Professor Alfred Cuschieri Department of Anatomy University of Malta The mesonephros develops primitive nephrotomes draining into a mesonephric duct nephrotome mesonephric
Development of the Genital System Professor Alfred Cuschieri Department of Anatomy University of Malta The mesonephros develops primitive nephrotomes draining into a mesonephric duct nephrotome mesonephric
Ethiopian patients and a brief review
 Postgraduate Medical Journal (November 1979) 55, 844-848 Testicular feminization syndrome: a report of three Ethiopian patients and a brief review EDEMARIAM TSEGA M.D., D.C.M.T.(L), F.R.C.P.(C) Summary
Postgraduate Medical Journal (November 1979) 55, 844-848 Testicular feminization syndrome: a report of three Ethiopian patients and a brief review EDEMARIAM TSEGA M.D., D.C.M.T.(L), F.R.C.P.(C) Summary
Animal Science 434 Reproductive Physiology"
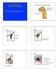 Animal Science 434 Reproductive Physiology" Embryogenesis of the Pituitary and Sexual Development: Part A Development of the Pituitary Gland" Infundibulum" Brain" Rathke s Pouch" Stomodeum" Germ Cell Migration"
Animal Science 434 Reproductive Physiology" Embryogenesis of the Pituitary and Sexual Development: Part A Development of the Pituitary Gland" Infundibulum" Brain" Rathke s Pouch" Stomodeum" Germ Cell Migration"
W.S. O University of Hong Kong
 W.S. O University of Hong Kong Development of the Genital System 1. Sexual differentiation 2. Differentiation of the gonads a. Germ cells extragonadal in origin b. Genital ridge intermediate mesoderm consisting
W.S. O University of Hong Kong Development of the Genital System 1. Sexual differentiation 2. Differentiation of the gonads a. Germ cells extragonadal in origin b. Genital ridge intermediate mesoderm consisting
IN SUMMARY HST 071 NORMAL & ABNORMAL SEXUAL DIFFERENTIATION Fetal Sex Differentiation Postnatal Diagnosis and Management of Intersex Abnormalities
 Harvard-MIT Division of Health Sciences and Technology HST.071: Human Reproductive Biology Course Director: Professor Henry Klapholz IN SUMMARY HST 071 Title: Fetal Sex Differentiation Postnatal Diagnosis
Harvard-MIT Division of Health Sciences and Technology HST.071: Human Reproductive Biology Course Director: Professor Henry Klapholz IN SUMMARY HST 071 Title: Fetal Sex Differentiation Postnatal Diagnosis
- production of two types of gametes -- fused at fertilization to form zygote
 Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
Outline. Male Reproductive System Testes and Sperm Hormonal Regulation
 Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
17. Sex. Being Male and Female
 17. Sex Being Male and Female Reproduction Asexual: more efficient (Only 1 sex) Low genetic variation Sexual: prevalent (2 sexes, separate or not) High genetic variation Need 2 members of the same species
17. Sex Being Male and Female Reproduction Asexual: more efficient (Only 1 sex) Low genetic variation Sexual: prevalent (2 sexes, separate or not) High genetic variation Need 2 members of the same species
REPRODUCCIÓN. La idea fija. Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature
 REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
Recently we had the opportunity of examining a young man with bilateral atrophy of the testes, whose case history may serve to point out the dangers
 From the 2. Medical Clinic, University of Hamburg, Germany (Professor Dr. A. Jores) BILATERAL TESTICULAR ATROPHY AS A RESULT OF SCROTAL HEMATOMA IN THE NEWBORN By Henryk Nowakowski Recently we had the
From the 2. Medical Clinic, University of Hamburg, Germany (Professor Dr. A. Jores) BILATERAL TESTICULAR ATROPHY AS A RESULT OF SCROTAL HEMATOMA IN THE NEWBORN By Henryk Nowakowski Recently we had the
Normal and Abnormal Development of the Genital Tract. Dr.Raghad Abdul-Halim
 Normal and Abnormal Development of the Genital Tract Dr.Raghad Abdul-Halim objectives: Revision of embryology. Clinical presentation, investigations and clinical significance of most common developmental
Normal and Abnormal Development of the Genital Tract Dr.Raghad Abdul-Halim objectives: Revision of embryology. Clinical presentation, investigations and clinical significance of most common developmental
Approach to Disorders of Sex Development (DSD)
 Approach to Disorders of Sex Development (DSD) Old name: The Approach to Intersex Disorders Dr. Abdulmoein Al-Agha, FRCP Ass. Professor & Consultant Pediatric Endocrinologist, KAUH, Erfan Hospital & Ibn
Approach to Disorders of Sex Development (DSD) Old name: The Approach to Intersex Disorders Dr. Abdulmoein Al-Agha, FRCP Ass. Professor & Consultant Pediatric Endocrinologist, KAUH, Erfan Hospital & Ibn
Ch 20: Reproduction. Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition
 Ch 20: Reproduction Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition SLOs Contrast mitosis/meiosis, haploid/diploid, autosomes/sex chromosomes. Outline the hormonal
Ch 20: Reproduction Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition SLOs Contrast mitosis/meiosis, haploid/diploid, autosomes/sex chromosomes. Outline the hormonal
Animal Science 434 Reproductive Physiology
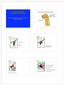 Animal Science 434 Reproductive Physiology Development of the Pituitary Gland Lec 5: Embryogenesis of the Pituitary and Sexual Development Stomodeum Brain Infundibulum Rathke s Pouch Germ Cell Migration
Animal Science 434 Reproductive Physiology Development of the Pituitary Gland Lec 5: Embryogenesis of the Pituitary and Sexual Development Stomodeum Brain Infundibulum Rathke s Pouch Germ Cell Migration
OVOTESTIS Background Pathophysiology
 OVOTESTIS Background Ovotestis refers to the histology of a gonad that contains both ovarian follicles and testicular tubular elements. Such gonads are found exclusively in people with ovotesticular disorder
OVOTESTIS Background Ovotestis refers to the histology of a gonad that contains both ovarian follicles and testicular tubular elements. Such gonads are found exclusively in people with ovotesticular disorder
Action of reproductive hormones through the life span 9/22/99
 Action of reproductive hormones through the life span Do reproductive hormones affect the life span? One hypothesis about the rate of aging asserts that there is selective pressure for either high rate
Action of reproductive hormones through the life span Do reproductive hormones affect the life span? One hypothesis about the rate of aging asserts that there is selective pressure for either high rate
Chromosome Disease. The general features in autosome abnormalities are a triad of growth retardation, mental
 Medical Genetics Chapter4 Chromosome Disease Chromosome Disease Clinical feature The general features in autosome abnormalities are a triad of growth retardation, mental retardation, and specific somatic
Medical Genetics Chapter4 Chromosome Disease Chromosome Disease Clinical feature The general features in autosome abnormalities are a triad of growth retardation, mental retardation, and specific somatic
DISORDERS OF MALE GENITALS
 Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 9. Testicular disorders/disorders of male genitals. Horm Res 2007;68(suppl 2):63 66 ESPE Code Diagnosis OMIM ICD10
Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 9. Testicular disorders/disorders of male genitals. Horm Res 2007;68(suppl 2):63 66 ESPE Code Diagnosis OMIM ICD10
Unit 15 ~ Learning Guide
 Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
Topic 13 Sex. Being Male and Female
 Topic 13 Sex Being Male and Female Reproduction Asexual (1 individual): more efficient, low genetic variation Sexual: prevalent (2 sexes, separate or not) High genetic variation, need 2 Approaches: External
Topic 13 Sex Being Male and Female Reproduction Asexual (1 individual): more efficient, low genetic variation Sexual: prevalent (2 sexes, separate or not) High genetic variation, need 2 Approaches: External
Clinical evaluation of infertility
 Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
Female Reproduction. Ova- Female reproduction cells stored in the ovaries
 Reproduction Puberty stage of growth and development where males and females become capable of producing offspring. Time of physical and emotional changes. Female *occurs between ages 8 -- 15 *estrogen
Reproduction Puberty stage of growth and development where males and females become capable of producing offspring. Time of physical and emotional changes. Female *occurs between ages 8 -- 15 *estrogen
Study Guide Answer Key Reproductive System
 Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
Chapter 18 Development. Sexual Differentiation
 Chapter 18 Development Sexual Differentiation There Are Many Levels of Sex Determination Chromosomal Sex Gonadal Sex Internal Sex Organs External Sex Organs Brain Sex Gender Identity Gender Preference
Chapter 18 Development Sexual Differentiation There Are Many Levels of Sex Determination Chromosomal Sex Gonadal Sex Internal Sex Organs External Sex Organs Brain Sex Gender Identity Gender Preference
STRUCTURE AND FUNCTION OF THE FEMALE REPRODUCTIVE SYSTEM
 Unit 7B STRUCTURE AND FUNCTION OF THE FEMALE REPRODUCTIVE SYSTEM LEARNING OBJECTIVES 1. Learn the structures of the female reproductive tract. 2. Learn the functions of the female reproductive tract. 3.
Unit 7B STRUCTURE AND FUNCTION OF THE FEMALE REPRODUCTIVE SYSTEM LEARNING OBJECTIVES 1. Learn the structures of the female reproductive tract. 2. Learn the functions of the female reproductive tract. 3.
Embryology /organogenesis/ Week 4 Development and teratology of reproductive system.
 Embryology /organogenesis/ Week 4 Development and teratology of reproductive system. Male or female sex is determined by spermatozoon Y in the moment of fertilization SRY gene, on the short arm of the
Embryology /organogenesis/ Week 4 Development and teratology of reproductive system. Male or female sex is determined by spermatozoon Y in the moment of fertilization SRY gene, on the short arm of the
6.7 IN. Continuity through Reproduction. What are the differences between male and female gametes? Discuss their formation and physical attributes.
 6.7 IN What are the differences between male and female gametes? Discuss their formation and physical attributes. Males - 4 sperm per parent cell; Females - 1 ovum per parent cell Sperm - motile (tail);
6.7 IN What are the differences between male and female gametes? Discuss their formation and physical attributes. Males - 4 sperm per parent cell; Females - 1 ovum per parent cell Sperm - motile (tail);
PHYSIOLOGY AND PATHOLOGY OF SEXUAL DIFFERENTIATION
 PHYSIOLOGY AND PATHOLOGY OF SEXUAL DIFFERENTIATION Prof. Dr med. Jolanta Słowikowska-Hilczer Department of Andrology and Reproductive Endocrinology Medical University of Łódź, Poland Sexual determination
PHYSIOLOGY AND PATHOLOGY OF SEXUAL DIFFERENTIATION Prof. Dr med. Jolanta Słowikowska-Hilczer Department of Andrology and Reproductive Endocrinology Medical University of Łódź, Poland Sexual determination
Intersex is a group of conditions where there is a discrepancy between the external genitals and the internal genitals (the testes and ovaries).
 Intersex to use the sharing features on this page, please enable JavaScript. Share on facebookshare on IwitterBookmark & SharePrintcr-lnendly version Intersex is a group of conditions where
Intersex to use the sharing features on this page, please enable JavaScript. Share on facebookshare on IwitterBookmark & SharePrintcr-lnendly version Intersex is a group of conditions where
Male and Female Reproduction
 Male and Female Reproduction Similarities / Differences Develop very similar structures of sex glands Two genital tubes Manufacture the hormones of the other sex. Hormones of one sex are often used to
Male and Female Reproduction Similarities / Differences Develop very similar structures of sex glands Two genital tubes Manufacture the hormones of the other sex. Hormones of one sex are often used to
CHAPTER-VII : SUMMARY AND CONCLUSIONS
 CHAPTER-VII : SUMMARY AND CONCLUSIONS 199 SUMMARY AND CONCLUSIONS t The rapid development of human genetics during the past couple of decades and the discovery of numerous cytogenetic abnormalities have
CHAPTER-VII : SUMMARY AND CONCLUSIONS 199 SUMMARY AND CONCLUSIONS t The rapid development of human genetics during the past couple of decades and the discovery of numerous cytogenetic abnormalities have
Klinefelter syndrome ( 47, XXY )
 Sex Chromosome Abnormalities, Sex Chromosome Aneuploidy It has been estimated that, overall, approximately one in 400 infants have some form of sex chromosome aneuploidy. A thorough discussion of sex chromosomes
Sex Chromosome Abnormalities, Sex Chromosome Aneuploidy It has been estimated that, overall, approximately one in 400 infants have some form of sex chromosome aneuploidy. A thorough discussion of sex chromosomes
Reproductive physiology. About this Chapter. Case introduction. The brain directs reproduction 2010/6/29. The Male Reproductive System
 Section Ⅻ Reproductive physiology Ming-jie Wang E-Mail: mjwang@shmu.edu.cn About this Chapter The reproductive organs and how they work the major endocrine functions of sexual glands actions of sex hormones
Section Ⅻ Reproductive physiology Ming-jie Wang E-Mail: mjwang@shmu.edu.cn About this Chapter The reproductive organs and how they work the major endocrine functions of sexual glands actions of sex hormones
DEFINITION: Masculinization of external genitalia in patients with normal 46XX karyotype.
 INTERSEX DISORDERS DEFINITION: Masculinization of external genitalia in patients with normal 46XX karyotype. - Degree of masculinization variable: - mild clitoromegaly - complete fusion of labia folds
INTERSEX DISORDERS DEFINITION: Masculinization of external genitalia in patients with normal 46XX karyotype. - Degree of masculinization variable: - mild clitoromegaly - complete fusion of labia folds
Chapter 14 Reproduction Review Assignment
 Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
10. Development of genital system. Gonads. Genital ducts. External genitalia.
 10. Development of genital system. Gonads. Genital ducts. External genitalia. Gonads, genital ducts and the external genital organs initially pass through an indifferent period of development, which is
10. Development of genital system. Gonads. Genital ducts. External genitalia. Gonads, genital ducts and the external genital organs initially pass through an indifferent period of development, which is
IB 140 Midterm #1 PRACTICE EXAM (lecture topics 1-5)
 IB 140 Midterm #1 PRACTICE EXAM (lecture topics 1-5) For all the questions on this exam, the correct answer is the single best answer that is available in the answer key. 1) Which of the following is NOT
IB 140 Midterm #1 PRACTICE EXAM (lecture topics 1-5) For all the questions on this exam, the correct answer is the single best answer that is available in the answer key. 1) Which of the following is NOT
Analysis of the Sex-determining Region of the Y Chromosome (SRY) in a Case of 46, XX True Hermaphrodite
 Clin Pediatr Endocrinol 1994; 3(2): 91-95 Copyright (C) 1994 by The Japanese Society for Pediatric Endocrinology Analysis of the Sex-determining Region of the Y Chromosome (SRY) in a Case of 46, XX True
Clin Pediatr Endocrinol 1994; 3(2): 91-95 Copyright (C) 1994 by The Japanese Society for Pediatric Endocrinology Analysis of the Sex-determining Region of the Y Chromosome (SRY) in a Case of 46, XX True
Goals. Disorders of Sex Development (Intersex): An Overview. Joshua May, MD Pediatric Endocrinology
 Disorders of Sex Development (Intersex): An Overview Joshua May, MD Pediatric Endocrinology Murphy, et al., J Ped Adol Gynecol, 2011 Goals Objectives: Participants will be able to: 1. Apply the medical
Disorders of Sex Development (Intersex): An Overview Joshua May, MD Pediatric Endocrinology Murphy, et al., J Ped Adol Gynecol, 2011 Goals Objectives: Participants will be able to: 1. Apply the medical
ISSN CHROMOSOME STUDY IN SUSPECTED CASES OF TURNER S SYNDROME FROM JAMMU REGION OF JAMMU & KASHMIR
 J. Adv. Zool. 2018: 39(1): 32-36 ISSN-0253-7214 CHROMOSOME STUDY IN SUSPECTED CASES OF TURNER S SYNDROME FROM JAMMU REGION OF JAMMU & KASHMIR Wahied Khawar Balwan and Neelam Saba *Department of Zoology,
J. Adv. Zool. 2018: 39(1): 32-36 ISSN-0253-7214 CHROMOSOME STUDY IN SUSPECTED CASES OF TURNER S SYNDROME FROM JAMMU REGION OF JAMMU & KASHMIR Wahied Khawar Balwan and Neelam Saba *Department of Zoology,
Human Reproductive System
 Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Yutaka; SAKAMOTO, Hiromi. Citation 泌尿器科紀要 (1986), 32(10):
 Title46XX male; report of case OKUYAMA, Akihiko; KONDO, Nobuyuki; Author(s) NAKAMURA, Masahiro; SONODA, Takao; Yutaka; SAKAMOTO, Hiromi Citation 泌尿器科紀要 (1986), 32(10): 1539-1542 Issue Date 1986-10 URL
Title46XX male; report of case OKUYAMA, Akihiko; KONDO, Nobuyuki; Author(s) NAKAMURA, Masahiro; SONODA, Takao; Yutaka; SAKAMOTO, Hiromi Citation 泌尿器科紀要 (1986), 32(10): 1539-1542 Issue Date 1986-10 URL
Testicular feminization. The features of this syndrome in its typical form are these (Fig. 1): (1) Female bodily configuration.
 Personal Practice Archives of Disease in Childhood, 1970, 45, 595. The XY Female Child C. J. DEWHURST From the Institute of Obstetrics and Gynaecology, Queen Charlotte's Maternity Hospital, and Chelsea
Personal Practice Archives of Disease in Childhood, 1970, 45, 595. The XY Female Child C. J. DEWHURST From the Institute of Obstetrics and Gynaecology, Queen Charlotte's Maternity Hospital, and Chelsea
Hearing on SJR13 -- Proposes to amend the Nevada Constitution by repealing the limitation on the recognition of marriage.
 Written statement of Lauren A. Scott- Executive Director Equality Nevada. 1350 Freeport Blvd, #107 Sparks, Nevada 89431 Testimony and Statement for the Record of Hearing on SJR13 -- Proposes to amend the
Written statement of Lauren A. Scott- Executive Director Equality Nevada. 1350 Freeport Blvd, #107 Sparks, Nevada 89431 Testimony and Statement for the Record of Hearing on SJR13 -- Proposes to amend the
Defining Sex and Gender & The Biology of Sex
 Defining Sex and Gender & The Biology of Sex Today: -Defining Sex and Gender -Conception of a Child -Chromosomes -Defects in Chromosomes Often we hear the terms sex and gender used in our society interchangeably,
Defining Sex and Gender & The Biology of Sex Today: -Defining Sex and Gender -Conception of a Child -Chromosomes -Defects in Chromosomes Often we hear the terms sex and gender used in our society interchangeably,
Disorders of gonadal and sexual development
 Disorders of gonadal and sexual development gonadal embryogenesis, cytogenetics/molecular abnormalities, and clinical aspects Pr I.Maystadt 08/01/2016 IPG Male Genitalia bladder prostate penis Seminal
Disorders of gonadal and sexual development gonadal embryogenesis, cytogenetics/molecular abnormalities, and clinical aspects Pr I.Maystadt 08/01/2016 IPG Male Genitalia bladder prostate penis Seminal
Chromosome pathology
 Chromosome pathology S. Dahoun Department of Gynecology and Obstetrics, University Hospital of Geneva Cytogenetics is the study of chromosomes and the related disease states caused by abnormal chromosome
Chromosome pathology S. Dahoun Department of Gynecology and Obstetrics, University Hospital of Geneva Cytogenetics is the study of chromosomes and the related disease states caused by abnormal chromosome
Human Reproductive System
 Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male=s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male=s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Biology of Reproduction- Zool 346 Exam 2
 Biology of Reproduction- Zool 346 Exam 2 ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER. Some critical words are boldfaced. This exam is 7 pages long.
Biology of Reproduction- Zool 346 Exam 2 ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER. Some critical words are boldfaced. This exam is 7 pages long.
Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems
 CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems 3. Male Reproductive anatomy and physiology. Testes = paired
CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems 3. Male Reproductive anatomy and physiology. Testes = paired
Sex Determination and Development of Reproductive Organs
 Sex Determination and Development of Reproductive Organs Sex determination The SRY + gene is necessary and probably sufficient for testis development The earliest sexual difference appears in the gonad
Sex Determination and Development of Reproductive Organs Sex determination The SRY + gene is necessary and probably sufficient for testis development The earliest sexual difference appears in the gonad
1) Intersexuality - Dr. Huda
 1) Intersexuality - Dr. Huda DSD (Disorders of sex development) occur when there is disruption of either: Gonadal differentiation Fetal sex steroid production or action Mullerian abnormalities and Wolffian
1) Intersexuality - Dr. Huda DSD (Disorders of sex development) occur when there is disruption of either: Gonadal differentiation Fetal sex steroid production or action Mullerian abnormalities and Wolffian
UNIT IX: GENETIC DISORDERS
 UNIT IX: GENETIC DISORDERS Younas Masih Lecturer New Life College Of Nursing Karachi 3/4/2016 1 Objectives By the end of this session the Learners will be able to, 1. Know the basic terms related genetics
UNIT IX: GENETIC DISORDERS Younas Masih Lecturer New Life College Of Nursing Karachi 3/4/2016 1 Objectives By the end of this session the Learners will be able to, 1. Know the basic terms related genetics
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question.
 MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) Which of the following hormones controls the release of anterior pituitary gonadotropins? A) LH
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) Which of the following hormones controls the release of anterior pituitary gonadotropins? A) LH
Hearing on SJR13 -- Proposes to amend the Nevada Constitution by repealing the limitation on the recognition of marriage.
 Written statement of Lauren A. Scott- Executive Director Equality Nevada 1350 Freeport Blvd, #107 Sparks, Nevada 89431 Testimony and Statement for the Record of Hearing on SJR13 -- Proposes to amend the
Written statement of Lauren A. Scott- Executive Director Equality Nevada 1350 Freeport Blvd, #107 Sparks, Nevada 89431 Testimony and Statement for the Record of Hearing on SJR13 -- Proposes to amend the
FLASH CARDS. Kalat s Book Chapter 11 Alphabetical
 FLASH CARDS www.biologicalpsych.com Kalat s Book Chapter 11 Alphabetical alpha-fetoprotein alpha-fetoprotein Alpha-Fetal Protein (AFP) or alpha-1- fetoprotein. During a prenatal sensitive period, estradiol
FLASH CARDS www.biologicalpsych.com Kalat s Book Chapter 11 Alphabetical alpha-fetoprotein alpha-fetoprotein Alpha-Fetal Protein (AFP) or alpha-1- fetoprotein. During a prenatal sensitive period, estradiol
Disordered Sex Differentiation Mixed gonadal dysgenesis Congenital adrenal hyperplasia Mixed gonadal dysgenesis
 Disordered Sex Differentiation DSD has superceded intersex in describing genital anomalies in childhood DSD results from hormonal imbalances due to (i) abnormal genetic status, (ii) enzyme defects, or
Disordered Sex Differentiation DSD has superceded intersex in describing genital anomalies in childhood DSD results from hormonal imbalances due to (i) abnormal genetic status, (ii) enzyme defects, or
Chapter 22 Reproductive Systems. Male Reproductive Organs. Male Reproductive Organs. Specialized to produce, maintain the male sex cells (sperm)
 Chapter 22 Reproductive Systems Male reproductive organs 1 Male Reproductive Organs posterior view 2 Male Reproductive Organs Specialized to produce, maintain the male sex cells (sperm) Transport these
Chapter 22 Reproductive Systems Male reproductive organs 1 Male Reproductive Organs posterior view 2 Male Reproductive Organs Specialized to produce, maintain the male sex cells (sperm) Transport these
Human Anatomy Unit 3 REPRODUCTIVE SYSTEM
 Human Anatomy Unit 3 REPRODUCTIVE SYSTEM In Anatomy Today Male Reproductive System Gonads = testes primary organ responsible for sperm production development/maintenan ce of secondary sex characteristics
Human Anatomy Unit 3 REPRODUCTIVE SYSTEM In Anatomy Today Male Reproductive System Gonads = testes primary organ responsible for sperm production development/maintenan ce of secondary sex characteristics
Chromosomal Abnormalities and Karyotypes Creating a Karyotype
 Chromosomal Abnormalities and Karyotypes Creating a Karyotype The Normal Human Karyotype The normal human karyotype is composed of SEVEN groups of chromosomes A G plus the sex chromosomes X and Y. The
Chromosomal Abnormalities and Karyotypes Creating a Karyotype The Normal Human Karyotype The normal human karyotype is composed of SEVEN groups of chromosomes A G plus the sex chromosomes X and Y. The
 MOCK TEST I (HUMAN REPRODUCTION) 1. In human transfer of sperms into female genital tract is called as 1) Fertilization 2) Implantation 3) Insemination 4) Gestation 2. In male human scrotum maintains the
MOCK TEST I (HUMAN REPRODUCTION) 1. In human transfer of sperms into female genital tract is called as 1) Fertilization 2) Implantation 3) Insemination 4) Gestation 2. In male human scrotum maintains the
Male Reproduction Organs. 1. Testes 2. Epididymis 3. Vas deferens 4. Urethra 5. Penis 6. Prostate 7. Seminal vesicles 8. Bulbourethral glands
 Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
The Reproductive System
 The Reproductive System The Reproductive System Gonads primary sex organs Testes in males Ovaries in females Gonads produce gametes (sex cells) and secrete hormones Sperm male gametes Ova (eggs) female
The Reproductive System The Reproductive System Gonads primary sex organs Testes in males Ovaries in females Gonads produce gametes (sex cells) and secrete hormones Sperm male gametes Ova (eggs) female
Biology of Reproduction-Biol 326
 Biology of Reproduction-Biol 326 READ ALL INSTRUCTIONS CAREFULLY. ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER REGARDLESS OF WHAT YOU MARK ON THE
Biology of Reproduction-Biol 326 READ ALL INSTRUCTIONS CAREFULLY. ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER REGARDLESS OF WHAT YOU MARK ON THE
The Biology of Sex: How We Become Male or Female.
 The Biology of Sex: How We Become Male or Female. Dr. Tamatha Barbeau, Dept. of Biology Guest Lecture for Gender 200 March 2017 Objectives: 1. Sex vs. Gender defined. 2. Biological sex based on inheritance
The Biology of Sex: How We Become Male or Female. Dr. Tamatha Barbeau, Dept. of Biology Guest Lecture for Gender 200 March 2017 Objectives: 1. Sex vs. Gender defined. 2. Biological sex based on inheritance
The Male Reproductive System
 The Male Reproductive System Male Reproductive System The male sex cell is a sperm cell The whole purpose is to produce and deliver sperm to the egg Structure of a Human Sperm Cell Streamlined, built to
The Male Reproductive System Male Reproductive System The male sex cell is a sperm cell The whole purpose is to produce and deliver sperm to the egg Structure of a Human Sperm Cell Streamlined, built to
Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes
 Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes Spermatogenesis occurs in the testes after puberty. From the testes they are deposited into the epididymas
Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes Spermatogenesis occurs in the testes after puberty. From the testes they are deposited into the epididymas
Bio 322 Human Anatomy Objectives for the laboratory exercise Female Reproductive System
 Bio 322 Human Anatomy Objectives for the laboratory exercise Female Reproductive System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5 th ed (2017) Chapter 26 For this lab you
Bio 322 Human Anatomy Objectives for the laboratory exercise Female Reproductive System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5 th ed (2017) Chapter 26 For this lab you
Reproduction Lecture Spring 2009
 Reproduction Lecture Spring 2009 Slide #2: The term gonads refer to the sex organs. In the male, these are the testes, and the in the female, the ovary. The produce sex cells, or gametes. The male gamete
Reproduction Lecture Spring 2009 Slide #2: The term gonads refer to the sex organs. In the male, these are the testes, and the in the female, the ovary. The produce sex cells, or gametes. The male gamete
47. Kline f elter's Syndrome with 4d,XY/47,XXY/48,XXXY Mosaicism
 248 Proc. Japan Acad., 5'7, Ser. B (1981) [Vol. 57(B), 47. Kline f elter's Syndrome with 4d,XY/47,XXY/48,XXXY Mosaicism By Kazuyuki IsHITOBI, Noriko NAKADA, Shigeru MIYAGI, Tetsuhiro NINOMIYA, and Yoshimichi
248 Proc. Japan Acad., 5'7, Ser. B (1981) [Vol. 57(B), 47. Kline f elter's Syndrome with 4d,XY/47,XXY/48,XXXY Mosaicism By Kazuyuki IsHITOBI, Noriko NAKADA, Shigeru MIYAGI, Tetsuhiro NINOMIYA, and Yoshimichi
Chapter 46 ~ Animal Reproduction
 Chapter 46 ~ Animal Reproduction Overview Asexual (one parent) fission (parent separation) budding (corals) fragmentation & regeneration (inverts) parthenogenesis Sexual (fusion of haploid gametes) gametes
Chapter 46 ~ Animal Reproduction Overview Asexual (one parent) fission (parent separation) budding (corals) fragmentation & regeneration (inverts) parthenogenesis Sexual (fusion of haploid gametes) gametes
Development of the female Reproductive System. Dr. Susheela Rani
 Development of the female Reproductive System Dr. Susheela Rani Genital System Gonads Internal genitals External genitals Determining sex chronology of events Genetic sex Determined at fertilization Gonadal
Development of the female Reproductive System Dr. Susheela Rani Genital System Gonads Internal genitals External genitals Determining sex chronology of events Genetic sex Determined at fertilization Gonadal
AMBIGUOUS GENITALIA. Dr. HAKIMI, SpAK. Dr. MELDA DELIANA, SpAK
 AMBIGUOUS GENITALIA (DISORDERS OF SEXUAL DEVELOPMENT) Dr. HAKIMI, SpAK Dr. MELDA DELIANA, SpAK Dr. SISKA MAYASARI LUBIS, SpA Pediatric Endocrinology division USU/H. ADAM MALIK HOSPITAL 1 INTRODUCTION Normal
AMBIGUOUS GENITALIA (DISORDERS OF SEXUAL DEVELOPMENT) Dr. HAKIMI, SpAK Dr. MELDA DELIANA, SpAK Dr. SISKA MAYASARI LUBIS, SpA Pediatric Endocrinology division USU/H. ADAM MALIK HOSPITAL 1 INTRODUCTION Normal
To General Embryology Dr: Azza Zaki
 Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
Health Science: the structures & functions of the reproductive system
 Health Science: the structures & functions of the reproductive BELLWORK 1. List (4) careers that are r/t the Reproductive, Urinary, and Endocrine Systems 2. Copy down the following terms: -ologist = one
Health Science: the structures & functions of the reproductive BELLWORK 1. List (4) careers that are r/t the Reproductive, Urinary, and Endocrine Systems 2. Copy down the following terms: -ologist = one
4.05 Remember the structures of the reproductive system
 4.05 Remember the structures of the reproductive system 4.05 Remember the structures of the reproductive system Essential question What are the structures of the reproductive system? 2 Structures of the
4.05 Remember the structures of the reproductive system 4.05 Remember the structures of the reproductive system Essential question What are the structures of the reproductive system? 2 Structures of the
Sexual Reproduction. For most diploid eukaryotes, sexual reproduction is the only mechanism resulting in new members of a species.
 Sex Determination Sexual Reproduction For most diploid eukaryotes, sexual reproduction is the only mechanism resulting in new members of a species. Meiosis in the sexual organs of parents produces haploid
Sex Determination Sexual Reproduction For most diploid eukaryotes, sexual reproduction is the only mechanism resulting in new members of a species. Meiosis in the sexual organs of parents produces haploid
Chapter 2. Reproductive system matures and becomes capable of reproduction
 Chapter 2 Human Reproductive Anatomy and Physiology Key Terms Embryo Menarche Menopause Oxytocin Ovum Prostate gland Puberty Smegma zygote Puberty Involves changes in the whole body and psyche Reproductive
Chapter 2 Human Reproductive Anatomy and Physiology Key Terms Embryo Menarche Menopause Oxytocin Ovum Prostate gland Puberty Smegma zygote Puberty Involves changes in the whole body and psyche Reproductive
Human Sexuality - Ch. 2 Sexual Anatomy (Hock)
 Human Sexuality - Ch. 2 Sexual Anatomy (Hock) penis penile glans corona frenulum penile shaft erection foreskin circumcision corpora cavernosa corpus spongiosum urethra scrotum spermatic cords testicles
Human Sexuality - Ch. 2 Sexual Anatomy (Hock) penis penile glans corona frenulum penile shaft erection foreskin circumcision corpora cavernosa corpus spongiosum urethra scrotum spermatic cords testicles
Obstetrics Content Outline Obstetrics - Fetal Abnormalities
 Obstetrics Content Outline Obstetrics - Fetal Abnormalities Effective February 2007 10 16% renal agenesis complete absence of the kidneys occurs when ureteric buds fail to develop Or degenerate before
Obstetrics Content Outline Obstetrics - Fetal Abnormalities Effective February 2007 10 16% renal agenesis complete absence of the kidneys occurs when ureteric buds fail to develop Or degenerate before
When testes make no testosterone: Identifying a rare cause of 46, XY female phenotype in adulthood
 When testes make no testosterone: Identifying a rare cause of 46, XY female phenotype in adulthood Gardner DG, Shoback D. Greenspan's Basic & Clinical Endocrinology, 10e; 2017 Sira Korpaisarn, MD Endocrinology
When testes make no testosterone: Identifying a rare cause of 46, XY female phenotype in adulthood Gardner DG, Shoback D. Greenspan's Basic & Clinical Endocrinology, 10e; 2017 Sira Korpaisarn, MD Endocrinology
Chapter 26: Reproductive Systems. Male 11/29/2015. Male reproductive system is composed of... BIO 218 Fall Gonads (testes)
 Chapter 26: Reproductive Systems BIO 218 Fall 2015 Male Male reproductive system is composed of... Gonads (testes) Duct system (epididymis, ductus deferens, ejaculatory ducts, urethra) Accessory sex glands
Chapter 26: Reproductive Systems BIO 218 Fall 2015 Male Male reproductive system is composed of... Gonads (testes) Duct system (epididymis, ductus deferens, ejaculatory ducts, urethra) Accessory sex glands
MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure.
 Chapter 27 Exam Due NLT Thursday, July 31, 2015 Name MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure. Figure 27.1 Using Figure 27.1, match the following:
Chapter 27 Exam Due NLT Thursday, July 31, 2015 Name MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure. Figure 27.1 Using Figure 27.1, match the following:
DEVELOPMENT (DSD) 1 4 DISORDERS OF SEX
 Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 4. Disorders of sex development (DSD). Horm Res 2007;68(suppl 2):21 24 ESPE Code Diagnosis OMIM ICD 10 4 DISORDERS
Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 4. Disorders of sex development (DSD). Horm Res 2007;68(suppl 2):21 24 ESPE Code Diagnosis OMIM ICD 10 4 DISORDERS
Chapter 7 DEVELOPMENT AND SEX DETERMINATION
 Chapter 7 DEVELOPMENT AND SEX DETERMINATION Chapter Summary The male and female reproductive systems produce the sperm and eggs, and promote their meeting and fusion, which results in a fertilized egg.
Chapter 7 DEVELOPMENT AND SEX DETERMINATION Chapter Summary The male and female reproductive systems produce the sperm and eggs, and promote their meeting and fusion, which results in a fertilized egg.
The Reproductive System
 C h a p t e r 27 The Reproductive System PowerPoint Lecture Slides prepared by Jason LaPres North Harris College Houston, Texas Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin Cummings
C h a p t e r 27 The Reproductive System PowerPoint Lecture Slides prepared by Jason LaPres North Harris College Houston, Texas Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin Cummings
Urinary System Chapter 16
 Urinary System Chapter 16 1 Urology- the branch of medicine that treats male and female urinary systems as well as the male reproductive system. Nephrology- the scientific study of the anatomy, physiology,
Urinary System Chapter 16 1 Urology- the branch of medicine that treats male and female urinary systems as well as the male reproductive system. Nephrology- the scientific study of the anatomy, physiology,
4.05 Remember the structures of the reproductive system
 4.05 Remember the structures of the reproductive system Scrub In The external area between the vulva and the anus is the : a. Cervix b. Endometrium c. Perineum d. Vagina What structure connects the testes
4.05 Remember the structures of the reproductive system Scrub In The external area between the vulva and the anus is the : a. Cervix b. Endometrium c. Perineum d. Vagina What structure connects the testes
Please Take Seats by Gender as Shown Leave Three Seats Empty in the Middle
 Please Take Seats by Gender as Shown Leave Three Seats Empty in the Middle Women Men Sexual Differentiation & Development Neal G. Simon, Ph.D. Professor Dept. of Biological Sciences Signaling Cascade &
Please Take Seats by Gender as Shown Leave Three Seats Empty in the Middle Women Men Sexual Differentiation & Development Neal G. Simon, Ph.D. Professor Dept. of Biological Sciences Signaling Cascade &
