Intradialytic Parenteral Nutrition
|
|
|
- Marcia Gordon
- 5 years ago
- Views:
Transcription
1 Intradialytic Parenteral Nutrition Policy Number: Last Review: 8/2014 Origination: 8/2014 Next Review: 8/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Intradialytic Parenteral Nutrition when it is determined to be medically necessary because the criteria shown below are met. When Policy Topic is covered Intradialytic parenteral nutrition may be considered medically necessary when it is offered as an alternative to a regularly scheduled regimen of total parenteral nutrition only in patients who would be considered candidates for total parenteral nutrition (TPN), i.e., a severe pathology of the alimentary tract that does not allow absorption of sufficient nutrients to maintain weight and strength commensurate with the patient s general condition. When Policy Topic is not covered Intradialytic parenteral nutrition is considered not medically necessary in patients who would be considered a candidate for TPN, but for whom the intradialytic parenteral nutrition is not offered as an alternative to TPN, but in addition to regularly scheduled infusions to TPN. Intradialytic parenteral nutrition is considered investigational in patients who would not otherwise be considered candidates for TPN. Description of Procedure or Service Intradialytic parenteral nutrition (IDPN) is the infusion of an intravenous nutritional formula of hyperalimentation, such as amino acids, glucose, and lipids, during dialysis, to treat protein calorie malnutrition in an effort to decrease the associated morbidity and mortality experienced in patients with renal failure. Background Protein calorie malnutrition occurs in an estimated 25 40% of those undergoing dialysis. The clinical evaluation of malnutrition is multifactorial but typically includes measurement of serum albumin. Serum albumin levels correlate with nutritional status but are imperfect measures of nutrition because they can be affected by multiple other disease states. Protein calorie malnutrition is an important clinical consideration, since it is associated with increased morbidity and mortality. For example, the risk of death is increased more than 10-fold in those whose serum albumin levels are less than 2.5 g/dl, and those with a serum albumin near the normal range (i.e., from 3.5 to 3.9 g/dl) have a mortality rate twice as high as those with albumin greater than 4.0 g/dl. In patients receiving chronic dialysis, the National Kidney Foundation currently recommends a daily protein intake of equal to or greater than 1.2 g/kg in patients undergoing hemodialysis and equal to or greater than 1.3 g/kg in patients undergoing peritoneal dialysis. Intradialytic parenteral nutrition, i.e., infusing hyperalimentation fluids at the time of either hemodialysis or peritoneal dialysis, has been investigated as a technique to treat protein calorie malnutrition in an effort to decrease the associated morbidity and mortality. In hemodialysis, the intradialytic parenteral nutrition (IDPN) infusion is administered through the venous port of the dialysis tubing, typically, 30 minutes after dialysis has
2 begun, and continued throughout the remainder of a dialysis session. In peritoneal dialysis, sometimes referred to as intraperitoneal parenteral nutrition (IPPN) or intraperitoneal nutrition (IP), parenteral nutrition is infused into the peritoneal cavity during peritoneal dialysis. Rationale This policy was originally created with searches of the MEDLINE database. The most recent literature search was performed for the period of April 2012 through May 14, The following is a summary of the key findings to date. Systematic Reviews While intradialytic parenteral nutrition (IDPN) has been available for many years, there has never been a consensus regarding either its efficacy or patient selection criteria. In 1993, the Office of Health Technology Assessment, the technology assessment arm of Medicare, published a review concluding that studies of IDPN reported equivocal results and the data did not validate its efficacy. (1) Subsequently, in 1999, Foulks reported on an evidenced-based evaluation of IDPN. (2) The analysis concluded that the overall quality of the literature was poor; only 3 randomized controlled trials (RCTs) were identified, and 1 was a feasibility study only; the other 2 had methodologic flaws or used types of IDPN that were not routinely used or were not available in the United States. The remaining literature consists of case series, which obviously cannot control for the many variables in the renal dialysis population that may contribute to increased morbidity and mortality. According to Foulks analysis, the majority of case series had methodologic flaws including heterogeneity in study design, patient selection criteria, types of IDPN used, and adequacy of dialysis. Dukkipati and colleagues conducted a systematic review of IDPN for the treatment of malnutrition in hemodialysis patients in (3) The authors identified only 3 RCTs and found the data were insufficient to conduct a meta-analysis and to demonstrate net benefits in health outcomes with the use of IDPN. The authors concluded further clinical trials on IDPN are needed, and those trials should measure survival, quality of life, and nutritional status. Randomized Controlled Trials An RCT of 186 malnourished hemodialysis patients from 38 treatment centers in France studied the effects of adding IDPN to oral supplementation compared to oral supplementation alone (1 year of treatment with 2-year follow up). (4) Based on intention-to-treat analysis, no differences were found in 2-year survival, hospitalizations, Karnofsky score, body mass index (BMI), or serum albumin and prealbumin levels between treatment groups. The study was powered to detect a 10% reduction in mortality with 78% power (5% α error). Meeting the stated nutritional goals (orally or parenterally) may have improved outcomes; an editorialist suggests that both groups had approximately 15% improved survival compared to historical controls. (5) Nonrandomized Comparative Studies The largest study is a retrospective case series comparing the morbidity of 1,679 IDPN-treated patients with that of 22,517 nontreated patients. (6) This study found that dialysis patients with a serum albumin level of less than 3.4 g/dl who were treated with IDPN had significant increases in albumin and creatinine over time. In addition, these patients experienced a significant decrease in the odds ratio for death at 1 year compared to those who were not treated with IDPN. Interestingly, the odds ratio for death increased for IDPN-treated patients who had an albumin level of greater than 3.4 mg/dl. Pupim and colleagues performed a detailed analysis of protein metabolism in 7 patients receiving IDPN during hemodialysis. (7) These patients would not have been considered candidates for IDPN on the basis of their nutritional status. While the administration of IDPN was associated with a sharp increase in protein anabolism, the effect was only transient. An accompanying editorial points out that in patients with renal disease, malnutrition is a multifaceted problem that is not related to insufficient or improper food or diet and probably cannot be corrected by simply supplying more or a different balance of nutrition. (8)
3 A case series was published of 22 hemodialysis patients with acute illnesses (major surgery, infection) treated with IDPN for 1.5 to 48 months as nutritional supplementation (not support). (9) IDPN was discontinued when the following were met: weight ceased to decline, stabilized, or increased; protein catabolic rate was greater than 1.0 g/kg/d; and serum albumin levels were greater than 3.8 g/dl. IDPN was well-tolerated and associated with improvements from baseline of several nutritional parameters. Without a comparison group, it is impossible to conclude that the effects were due to IDPN, and therefore this study does not affect the policy statement regarding patients who would otherwise not be candidates for TPN. Predictors of IDPN response on hypoalbuminemia were examined in a study of 196 hypoalbumineic patients receiving maintenance hemodialysis who underwent IDPN. (10) The study suggested that IDPN treatment can improve hypoalbuminemia in patients receiving maintenance hemodialysis and that the likelihood and magnitude of response to IDPN in these patients is associated with the baseline severity of hypoalbuminemia. The authors suggest that this association may be useful in risk stratification of malnourished dialysis patients and recommend that their findings be confirmed through further controlled trials. Also of potential future interest, Pupim et al. reported that in a small series (n=8) of chronic hemodialysis patients, intradialytic oral nutrition or IDPN both led to highly positive whole-body net balance during hemodialysis. (11) Two other uncontrolled studies also suggest an improved outcome associated with IDPN. (12, 13) Due to the numerous biases inherent in any uncontrolled trial, these studies cannot validate whether IDPN is associated with an improved mortality. The observed treatment effect could be related to a selection bias in which very ill patients, i.e., those expected to die, were not offered IDPN. In addition, IDPN administration may be associated with an increased attentiveness to dialysis parameters, counseling, and nutritional advice, etc. These studies suggest that being selected for IDPN may be associated with an improved mortality rate, but analysis of the direct contribution of IDPN will require controlled trials. No studies were identified addressing IDPN in peritoneal dialysis patients. Ongoing Clinical Trials A May 24, 2013 search of online site ClinicalTrials.gov identified only one multicenter German study on IDPN, NCT , which has been completed. In this study, 140 malnourished hemodialysis patients were randomized to receive hemodialysis without IDPN or hemodialysis with 16 weeks of IDPN during each dialysis session followed by 12 weeks without IDPN. The study completion date was December 2010; the results have not been published. In addition, results from one comparative study that addressed changes of serum prealbumin levels of IDPN in malnourished hemodialysis patients have been published in abstract form in (14) No fulllength publication is available for this study. Statistical calculation was undertaken for 32 patients per study group. IDPN was reported to lead to a significant increase of prealbumin during the 16-week course of treatment (26.31 mg/l), compared to the non-interventional control group (1.84 mg/l, p=.02). Due to the small sample size, there was a lack of statistical power to evaluate responsiveness of the secondary endpoints in this study (e.g., albumin, transferrin, quality of life). (14) Summary Intradialytic parenteral nutrition (IDPN) is the infusion of an intravenous nutritional formula of hyperalimentation, such as amino acids, glucose, and lipids, during dialysis, to treat protein calorie malnutrition in an effort to decrease the associated morbidity and mortality experienced in patients with renal failure. Evidence of efficacy of IDPN treatment is limited. Available evidence demonstrates improvements in intermediate outcomes such as increases in serum albumin and catabolic rate. However, long-term data on survival, quality of life, and other nutritional status outcomes are unavailable. Therefore, IDPN may only be considered medically necessary when it is offered as an alternative to a regularly
4 scheduled regimen of total parenteral nutrition (TPN) in patients who would be considered candidates for TPN. IDPN is considered not medically necessary when added to regularly scheduled infusions of TPN and may be harmful due to the excess administration of lipids. Finally, due to the limited availability of data on IDPN in patients who would not otherwise be considered TPN candidates, the impact on net health outcome is not known and therefore, is considered investigational in these patients. Practice Guidelines and Position Statements As noted in the Description section, clinical guidelines published by the National Kidney Foundation have established target daily protein requirements in patients undergoing chronic dialysis. (15) The National Kidney Foundation updated their pediatric nutrition guideline to recommend a trial of IDPN to augment inadequate nutritional intake for malnourished children (BMI for height and age below the fifth percentile) receiving maintenance hemodialysis who are unable to meet their nutritional requirements through oral and tube feeding. (16) It has been suggested that intradialytic nutrition may be reasonable in patients who cannot meet these requirements. However, this patient population is already addressed by the published medical literature, and thus scientific evidence is inadequate to determine whether intradialytic nutrition in these patients leads to improved outcomes. The German Association for Nutritional Medicine guidelines indicate IDPN should only be carried out when modifiable causes of malnutrition are excluded and enhanced oral or enteral supply is unsuccessful or cannot be carried out. (17) These guidelines note the following international criteria for malnutrition have been suggested, even though they are not based on firm evidence: Middle predialysis serum albumin <3.4 g/l for >3 months Middle predialysis serum creatinine <8.0 mg/l for >3 months Weight loss >10% of ideal body weight or >20% of normal body weight (no time limit) Clinical examination indicates moderate to severe malnutrition Dietary history indicating protein intake <0.8 g/kg, reduced calorie intake <25 kcal/kg Subjective Global Assessment (SGA) C = severe malnutrition IDPN should be considered when three of the above-mentioned criteria are associated with the following conditions: Aborted attempts to increase oral/enteral food intake Refusal of enteral gavage The American Society for Parenteral and Enteral Nutrition issued 2010 Clinical Guidelines: Nutrition Support in Adults in Acute and Chronic Renal Failure. They issued a level C (supported by at least 1 level II investigation) that stated that IDPN should not be used as a nutritional supplement in malnourished chronic kidney disease-v hemodialysis patients. The rationale was that a large RCT found that mortality rates did not differ between malnourished patients receiving IDPN versus malnourished patients who received oral supplements with no IDPN. An additional concern was that IDPN is limited by the need to complete the entire nutrient infusion during the hemodialysis treatment, which may cause adverse effects because of the rapid infusion of glucose and lipids. They further recommended larger RCTs in malnourished patients to ensure that a clinical benefit does not exist.(19) Medicare National Coverage Medicare Policy/Benefit The coverage eligibility of intradialytic parenteral nutrition for Medicare beneficiaries is summarized in a Health Care Financing Administration (HCFA) ruling from December 1996, which established that intradialytic nutrition would be considered eligible for coverage only if the patient would otherwise be a candidate for total parenteral nutrition. (18, 19) This ruling reads in part:
5 Medicare coverage policies which apply to parenteral and enteral nutrition therapy items and services apply identically to intradialytic parenteral nutrition therapy items and services, because intradialytic parenteral nutrition therapy is a subset of parenteral and enteral nutrition therapy. Coverage of parenteral and enteral nutrition therapy is amplified in Medicare Coverage Issues manual section Daily parenteral therapy is considered reasonable and necessary for a patient with severe pathology of the alimentary tract which does not allow absorption of sufficient nutrients to maintain weight and strength commensurate with the patient s general condition. Intradialytic parenteral nutrition therapy is administered to end stage renal disease (ESRD) patients while they are receiving dialysis. ESRD patients sometimes undergo parenteral therapy to replace fluids and nutrients lost during dialysis. ESRD patients must meet all of the parenteral nutrition therapy coverage requirements to receive intradialytic parenteral nutrition therapy. Those patients who do not meet all of the parenteral nutrition therapy coverage requirements are ineligible to receive Medicare coverage of intradialytic parenteral nutrition therapy under the prosthetic device benefit. The HCFA ruling goes on to clarify the benefits for patients who would be considered candidates for total parenteral nutrition and when the intradialytic parenteral nutrition is designed to be offered in lieu of a regularly scheduled infusion of total parenteral nutrition. However, parenteral and enteral nutrition, including intradialytic parenteral nutrition therapy, services and items which are otherwise covered under section 1861(s)(8) can be denied under section 1862(a)(1) for lack of medical necessity: Example, if a Medicare beneficiary with ESRD, a dialysis patient who meets all of the requirements for coverage of parenteral nutrition therapy, receives intradialytic parenteral nutrition therapy during dialysis and also receives parenteral nutrition therapy on the other days of the week when the patient is not on dialysis, it may be determined that the patient is receiving an excessive number of lipids. A claim for Medicare payment that is denied because the patient, who qualifies for parenteral nutrition therapy coverage, is receiving an excessive number of lipids would be denied as not reasonable and necessary under section 1862(a)(1)(A) of the Act Therefore the precise statutory basis for the coverage or denial of parenteral and enteral nutrition therapy, including intradialytic parenteral nutrition therapy, services and items is crucial and determinative as to whether or not limitation on liability protections can be applied. References 1. Office of Health Technology Assessment (OHTA). Intradialytic parenteral nutrition for hemodialysis patients. Health Technology Review, No. 6, August, AHCPR Pub. No Available online at: 2. Foulks CJ. An evidence-based evaluation of intradialytic parenteral nutrition. Am J Kidney Dis 1999; 33(1): Dukkipati R, Kalantar-Zadeh K, Kopple JD. Is there a role for intradialytic parenteral nutrition? A review of the evidence. Am J Kidney Dis 2010; 55(2): Sigrist MK, Levin A, Tejani AM. Systematic review of evidence for the use of intradialytic parenteral nutrition in malnourished hemodialysis patients. J Ren Nutr 2010; 20(1): Cano NJ, Fouque D, Roth H et al. Intradialytic parenteral nutrition does not improve survival in malnourished hemodialysis patients: a 2-year multicenter, prospective, randomized study. J Am Soc Nephrol 2007; 18(9): Ikizler TA. Parenteral nutrition offers no benefit over oral supplementation in malnourished hemodialysis patients. Nat Clin Pract Nephrol 2008; 4(2): Chertow GM, Ling J, Lew NL et al. The association of intradialytic parenteral nutrition administration with survival in hemodialysis patients. Am J Kidney Dis 1994; 24(6): Pupim LB, Flakoll PJ, Brouillette JR et al. Intradialytic parenteral nutrition improves protein and energy homeostasis in chronic hemodialysis patients. J Clin Invest 2002; 110(4): Mitch WE. Malnutrition: a frequent misdiagnosis for hemodialysis patients. J Clin Invest 2002; 110(4): Korzets A, Azoulay O, Ori Y et al. The use of intradialytic parenteral nutrition in acutely ill haemodialysed patients. J Ren Care 2008; 34(1):14-8.
6 11. Dezfuli A, Scholl D, Lindenfeld SM et al. Severity of hypoalbuminemia predicts response to intradialytic parenteral nutrition in hemodialysis patients. J Ren Nutr 2009; 19(4): Pupim LB, Majchrzak KM, Flakoll PJ et al. Intradialytic oral nutrition improves protein homeostasis in chronic hemodialysis patients with deranged nutritional status. J Am Soc Nephrol 2006; 17(11): Foulks CJ. The effect of intradialytic parenteral nutrition on hospitalization rate and mortality in malnourished hemodialysis patients. J Renal Nutr 1994; 4(1): Capelli JP, Kushner H, Camiscioli TC et al. Effect of intradialytic parenteral nutrition on mortality rates in end-stage renal disease care. Am J Kidney Dis 1994; 23(6): Marsen TA, Degenhardt S, Hoffmann C et al. Intradialytic parenteral nutrition (IDPN) leads to sustained increase of serum prealbumin (PA) levels in malnourished hemodialysis (HD) patients a prospective, multicenter, open, phase-iv-study. Clin Nutr Suppl 2012; 7(1): Kopple JD. The National Kidney Foundation K/DOQI clinical practice guidelines for dietary protein intake for chronic dialysis patients. Am J Kidney Dis 2001; 38(4 Suppl 1):S KDOQI Clinical Practice Guideline for Nutrition in Children with CKD: 2008 update. Executive summary. Am J Kidney Dis 2009; 53(3 Suppl 2):S Druml W, Kierdorf HP. Parenteral nutrition in patients with renal failure - Guidelines on Parenteral Nutrition, Chapter 17. Ger Med Sci 2009; 7:Doc American Society for Parenteral and Enteral Nutrition (ASPEN). Clinical Guidelines: Nutrition support in adults in acute and chronic renal failure Last accessed March, Kopple JD, Foulks CJ, Piraino B et al. Proposed Health Care Financing Administration guidelines for reimbursement of enteral and parenteral nutrition. Am J Kidney Dis 1995; 26(6): HCFA Rulings. December Available online at: Guidance/Guidance/Rulings/downloads//hcfar963.pdf Billing Coding/Physician Documentation Information Hemodialysis procedure with single evaluation by a physician or other qualified health care professional Hemodialysis procedure requiring repeated evaluation(s) with or without substantial revision of dialysis prescription Hemodialysis access flow study to determine blood flow in grafts and arteriovenous fistulae by an indicator method Dialysis procedure other than hemodialysis (eg, peritoneal dialysis, hemofiltration, or other continuous renal replacement therapies), with single evaluation by a physician or other qualified health care professional Dialysis procedure other than hemodialysis (eg, peritoneal dialysis, hemofiltration, or other continuous renal replacement therapies) requiring repeated evaluations by a physician or other qualified health care professional, with or without substantial revision of dialysis prescription End-stage renal disease (ESRD) related services monthly, for patients younger than 2 years of age to include monitoring for the adequacy of nutrition, assessment of growth and development, and counseling of parents; with 4 or more face-to-face visits by a physician or other qualified health care professional per month End-stage renal disease (ESRD) related services monthly, for patients younger than 2 years of age to include monitoring for the adequacy of nutrition, assessment of growth and development, and counseling of parents; with 2-3 face-to-face visits by a physician or other qualified health care professional per month End-stage renal disease (ESRD) related services monthly, for patients younger than 2 years of age to include monitoring for the adequacy of nutrition, assessment of growth and development, and counseling of parents; with 1 face-to-face visit by a physician or other qualified health care professional per month End-stage renal disease (ESRD) related services monthly, for patients 2-11 years of age to include monitoring for the adequacy of nutrition, assessment of growth and development, and counseling of parents; with 4 or more face-to-face visits by a physician or other qualified health care professional per month
7 90955 End-stage renal disease (ESRD) related services monthly, for patients 2-11 years of age to include monitoring for the adequacy of nutrition, assessment of growth and development, and counseling of parents; with 2-3 face-to-face visits by a physician or other qualified health care professional per month End-stage renal disease (ESRD) related services monthly, for patients 2-11 years of age to include monitoring for the adequacy of nutrition, assessment of growth and development, and counseling of parents; with 1 face-to-face visit by a physician or other qualified health care professional per month End-stage renal disease (ESRD) related services monthly, for patients years of age to include monitoring for the adequacy of nutrition, assessment of growth and development, and counseling of parents; with 4 or more face-to-face visits by a physician or other qualified health care professional per month End-stage renal disease (ESRD) related services monthly, for patients years of age to include monitoring for the adequacy of nutrition, assessment of growth and development, and counseling of parents; with 2-3 face-to-face visits by a physician or other qualified health care professional per month End-stage renal disease (ESRD) related services monthly, for patients years of age to include monitoring for the adequacy of nutrition, assessment of growth and development, and counseling of parents; with 1 face-to-face visit by a physician or other qualified health care professional per month End-stage renal disease (ESRD) related services monthly, for patients 20 years of age and older; with 4 or more face-to-face visits by a physician or other qualified health care professional per month End-stage renal disease (ESRD) related services monthly, for patients 20 years of age and older; with 2-3 face-to-face visits by a physician or other qualified health care professional per month End-stage renal disease (ESRD) related services monthly, for patients 20 years of age and older; with 1 face-to-face visit by a physician or other qualified health care professional per month End-stage renal disease (ESRD) related services for home dialysis per full month, for patients younger than 2 years of age to include monitoring for the adequacy of nutrition, assessment of growth and development, and counseling of parents End-stage renal disease (ESRD) related services for home dialysis per full month, for patients 2-11 years of age to include monitoring for the adequacy of nutrition, assessment of growth and development, and counseling of parents End-stage renal disease (ESRD) related services for home dialysis per full month, for patients years of age to include monitoring for the adequacy of nutrition, assessment of growth and development, and counseling of parents End-stage renal disease (ESRD) related services for home dialysis per full month, for patients 20 years of age and older End-stage renal disease (ESRD) related services for dialysis less than a full month of service, per day; for patients younger than 2 years of age End-stage renal disease (ESRD) related services for dialysis less than a full month of service, per day; for patients 2-11 years of age End-stage renal disease (ESRD) related services for dialysis less than a full month of service, per day; for patients years of age End-stage renal disease (ESRD) related services for dialysis less than a full month of service, per day; for patients 20 years of age and older B4164 Parenteral nutrition solution: carbohydrates (dextrose), 50% or less (500 ml = 1 unit), home mix B4168 Parenteral nutrition solution; amino acid, 3.5%, (500 ml = 1 unit) - home mix B4172 Parenteral nutrition solution; amino acid, 5.5% through 7%, (500 ml = 1 unit) - home mix B4176 Parenteral nutrition solution; amino acid, 7% through 8.5%, (500 ml = 1 unit) - home mix B4178 Parenteral nutrition solution: amino acid, greater than 8.5% (500 ml = 1 unit), home mix B4180 Parenteral nutrition solution: carbohydrates (dextrose), greater than 50% (500 ml = 1 unit),
8 B4185 B4189 B4193 B4197 B4199 B4216 B4220 B4222 B4224 B5000 B5100 B5200 home mix Parenteral nutrition solution, per 10 grams lipids trace elements, and vitamins, including preparation, any strength, 10 to 51 g of protein, premix trace elements, and vitamins, including preparation, any strength, 52 to 73 g of protein, premix Parenteral nutrition solution; compounded amino acid and carbohydrates with electrolytes, trace elements and vitamins, including preparation, any strength, 74 to 100 grams of protein - premix Parenteral nutrition solution; compounded amino acid and carbohydrates with electrolytes, trace elements and vitamins, including preparation, any strength, over 100 grams of protein - premix Parenteral nutrition; additives (vitamins, trace elements, Heparin, electrolytes), home mix, per day Parenteral nutrition supply kit; premix, per day Parenteral nutrition supply kit; home mix, per day Parenteral nutrition administration kit, per day trace elements, and vitamins, including preparation, any strength, renal - Amirosyn RF, NephrAmine, RenAmine - premix trace elements, and vitamins, including preparation, any strength, hepatic - FreAmine HBC, HepatAmine - premix trace elements, and vitamins, including preparation, any strength, stress - branch chain amino acids - premix Additional Policy Key Words N/A Policy Implementation/Update Information 8/1/14 New policy. Check for medical necessity. State and Federal mandates and health plan contract language, including specific provisions/exclusions, take precedence over Medical Policy and must be considered first in determining eligibility for coverage. The medical policies contained herein are for informational purposes. The medical policies do not constitute medical advice or medical care. Treating health care providers are independent contractors and are neither employees nor agents Blue KC and are solely responsible for diagnosis, treatment and medical advice. No part of this publication may be reproduced, stored in a retrieval system or transmitted, in any form or by any means, electronic, photocopying, or otherwise, without permission from Blue KC.
Intradialytic Parenteral Nutrition. Description
 Subject: Intradialytic Parenteral Nutrition Page: 1 of 9 Last Review Status/Date: September 2015 Intradialytic Parenteral Nutrition Description Intradialytic parenteral nutrition (IDPN) is the infusion
Subject: Intradialytic Parenteral Nutrition Page: 1 of 9 Last Review Status/Date: September 2015 Intradialytic Parenteral Nutrition Description Intradialytic parenteral nutrition (IDPN) is the infusion
Intradialytic Parenteral Nutrition
 Intradialytic Parenteral Nutrition Policy Number: 8.01.44 Last Review: 8/2017 Origination: 8/2014 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for
Intradialytic Parenteral Nutrition Policy Number: 8.01.44 Last Review: 8/2017 Origination: 8/2014 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for
Intradialytic Parenteral Nutrition
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Intradialytic Parenteral Nutrition in Hemodialysis Patients. Hamdy Amin, Pharm.D., MBA, BCNSP Riyadh, Saudi Arabia
 Intradialytic Parenteral Nutrition in Hemodialysis Patients Hamdy Amin, Pharm.D., MBA, BCNSP Riyadh, Saudi Arabia Disclosure Information Intradialytic Parenteral Nutrition in Hemodialysis Patients Hamdy
Intradialytic Parenteral Nutrition in Hemodialysis Patients Hamdy Amin, Pharm.D., MBA, BCNSP Riyadh, Saudi Arabia Disclosure Information Intradialytic Parenteral Nutrition in Hemodialysis Patients Hamdy
Prevalence of malnutrition in dialysis
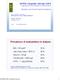 ESPEN Congress Cannes 2003 Organised by the Israel Society for Clinical Nutrition Education and Clinical Practice Programme Session: Nutrition and the Kidney Malnutrition and Haemodialysis Doctor Noël
ESPEN Congress Cannes 2003 Organised by the Israel Society for Clinical Nutrition Education and Clinical Practice Programme Session: Nutrition and the Kidney Malnutrition and Haemodialysis Doctor Noël
Intracellular Micronutrient Analysis
 Intracellular Micronutrient Analysis Policy Number: 2.04.73 Last Review: 1/2019 Origination: 1/2013 Next Review: 1/2020 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
Intracellular Micronutrient Analysis Policy Number: 2.04.73 Last Review: 1/2019 Origination: 1/2013 Next Review: 1/2020 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
MEDICAL POLICY: Enteral and Parenteral Nutrition
 POLICY: PG0114 ORIGINAL EFFECTIVE: 02/15/07 LAST REVIEW: 08/14/18 MEDICAL POLICY: Enteral and Parenteral Nutrition GUIDELINES This policy does not certify benefits or authorization of benefits, which is
POLICY: PG0114 ORIGINAL EFFECTIVE: 02/15/07 LAST REVIEW: 08/14/18 MEDICAL POLICY: Enteral and Parenteral Nutrition GUIDELINES This policy does not certify benefits or authorization of benefits, which is
Clinical Policy: Total Parenteral Nutrition and Intradialytic Parenteral Nutrition Reference Number: CP.PHAR.205
 Clinical Policy: Reference Number: CP.PHAR.205 Effective Date: 05.16 Last Review Date: 02.18 See Important Reminder at the end of this policy for important regulatory and legal information. Coding Implications
Clinical Policy: Reference Number: CP.PHAR.205 Effective Date: 05.16 Last Review Date: 02.18 See Important Reminder at the end of this policy for important regulatory and legal information. Coding Implications
End stage renal disease and Protein Energy wasting
 End stage renal disease and Protein Energy wasting Dr Goh Heong Keong MBBS,MRCP(UK) www.passpaces.com/kidney.htm Introduction Chronic kidney disease- increasing health burden in many countries. The estimated
End stage renal disease and Protein Energy wasting Dr Goh Heong Keong MBBS,MRCP(UK) www.passpaces.com/kidney.htm Introduction Chronic kidney disease- increasing health burden in many countries. The estimated
Epidemiology, Diagnostic and treatment for Protein Energy Wasting in Dialysis
 Epidemiology, Diagnostic and treatment for Protein Energy Wasting in Dialysis Pr Denis FOUQUE Department of Nephrology Centre de Recherche en Nutrition Humaine University Claude Bernard Lyon - France ESRD
Epidemiology, Diagnostic and treatment for Protein Energy Wasting in Dialysis Pr Denis FOUQUE Department of Nephrology Centre de Recherche en Nutrition Humaine University Claude Bernard Lyon - France ESRD
Nutrition Therapy. Medical Coverage Policy Enteral/Parenteral EFFECTIVE DATE: POLICY LAST UPDATED: 11/20/2018 OVERVIEW
 Medical Coverage Policy Enteral/Parenteral Nutrition Therapy EFFECTIVE DATE: 01 20 2007 POLICY LAST UPDATED: 11/20/2018 OVERVIEW This policy describes the reimbursement for enteral and parenteral nutrition
Medical Coverage Policy Enteral/Parenteral Nutrition Therapy EFFECTIVE DATE: 01 20 2007 POLICY LAST UPDATED: 11/20/2018 OVERVIEW This policy describes the reimbursement for enteral and parenteral nutrition
Facet Arthroplasty. Policy Number: Last Review: 9/2018 Origination: 9/2009 Next Review: 3/2019
 Facet Arthroplasty Policy Number: 7.01.120 Last Review: 9/2018 Origination: 9/2009 Next Review: 3/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for total facet
Facet Arthroplasty Policy Number: 7.01.120 Last Review: 9/2018 Origination: 9/2009 Next Review: 3/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for total facet
Home Total Parenteral Nutrition for Adults
 Home Total Parenteral Nutrition for Adults Policy Number: Original Effective Date: MM.08.007 05/21/1999 Line(s) of Business: Current Effective Date: PPO, HMO, QUEST Integration 05/27/2016 Section: Home
Home Total Parenteral Nutrition for Adults Policy Number: Original Effective Date: MM.08.007 05/21/1999 Line(s) of Business: Current Effective Date: PPO, HMO, QUEST Integration 05/27/2016 Section: Home
ISN Mission: Advancing the diagnosis, treatment and prevention of kidney diseases in the developing and developed world
 ISN Mission: Advancing the diagnosis, treatment and prevention of kidney diseases in the developing and developed world Nutrition in Kidney Disease: How to Apply Guidelines to Clinical Practice? T. Alp
ISN Mission: Advancing the diagnosis, treatment and prevention of kidney diseases in the developing and developed world Nutrition in Kidney Disease: How to Apply Guidelines to Clinical Practice? T. Alp
Bioimpedance Devices for Detection and Management of Lymphedema
 Bioimpedance Devices for Detection and Management of Lymphedema Policy Number: 2.01.82 Last Review: 5/2017 Origination: 1/2011 Next Review: 5/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue
Bioimpedance Devices for Detection and Management of Lymphedema Policy Number: 2.01.82 Last Review: 5/2017 Origination: 1/2011 Next Review: 5/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue
Aspetti nutrizionali nel paziente in emodialisi cronica
 Aspetti nutrizionali nel paziente in emodialisi cronica Enrico Fiaccadori enrico.fiaccadori@unipr.it Università degli Studi di Parma Agenda Diagnosis of protein-energy wasting (PEW) in ESRD on HD Epidemiology
Aspetti nutrizionali nel paziente in emodialisi cronica Enrico Fiaccadori enrico.fiaccadori@unipr.it Università degli Studi di Parma Agenda Diagnosis of protein-energy wasting (PEW) in ESRD on HD Epidemiology
Pr Denis FOUQUE. Department of Nephrology Centre de Recherche en Nutrition Humaine University Claude Bernard Lyon - France
 Pr Denis FOUQUE Department of Nephrology Centre de Recherche en Nutrition Humaine University Claude Bernard Lyon - France Observatoire Phosphocalcique, January 2011 1200 36.1 ± 5.0 g/l 1050 900 PEW
Pr Denis FOUQUE Department of Nephrology Centre de Recherche en Nutrition Humaine University Claude Bernard Lyon - France Observatoire Phosphocalcique, January 2011 1200 36.1 ± 5.0 g/l 1050 900 PEW
The revision date appears in the footer of the document. Links within the document are updated as changes occur throughout the year.
 An Independent Licensee of the Blue Cross Blue Shield Association. APPENDIX C HOME INFUSION THERAPY MANUAL This appendix to the Business Procedure Manual briefly describes home infusion therapy benefits
An Independent Licensee of the Blue Cross Blue Shield Association. APPENDIX C HOME INFUSION THERAPY MANUAL This appendix to the Business Procedure Manual briefly describes home infusion therapy benefits
Nutrition and Renal Disease Update
 Nutrition and Renal Disease Update Denis FOUQUE Department of Nephrology Centre de Recherche en Nutrition Humaine University Claude Bernard Lyon - France What have we learned? 1. Chronic kidney disease:
Nutrition and Renal Disease Update Denis FOUQUE Department of Nephrology Centre de Recherche en Nutrition Humaine University Claude Bernard Lyon - France What have we learned? 1. Chronic kidney disease:
Surgical Treatment of Bilateral Gynecomastia
 Surgical Treatment of Bilateral Gynecomastia Policy Number: 7.01.13 Last Review: 4/2018 Origination: 4/2006 Next Review: 4/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage
Surgical Treatment of Bilateral Gynecomastia Policy Number: 7.01.13 Last Review: 4/2018 Origination: 4/2006 Next Review: 4/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage
Potential Impact of Nutritional Intervention on End-Stage Renal Disease Hospitalization, Death, and Treatment Costs
 ORIGINAL RESEARCH Potential Impact of Nutritional Intervention on End-Stage Renal Disease Hospitalization, Death, and Treatment Costs Eduardo Lacson, Jr., MD,* T. Alp Ikizler, MD, J. Michael Lazarus, MD,*
ORIGINAL RESEARCH Potential Impact of Nutritional Intervention on End-Stage Renal Disease Hospitalization, Death, and Treatment Costs Eduardo Lacson, Jr., MD,* T. Alp Ikizler, MD, J. Michael Lazarus, MD,*
TO EAT OR NOT TO EAT DURING HEMODIALYSIS TREATMENT?
 TO EAT OR NOT TO EAT DURING HEMODIALYSIS TREATMENT? Rana G. Rizk, PhD, MPH, LD Maastricht University, The Netherlands November, 2017 Learning objectives Review the evidence behind benefits and concerns
TO EAT OR NOT TO EAT DURING HEMODIALYSIS TREATMENT? Rana G. Rizk, PhD, MPH, LD Maastricht University, The Netherlands November, 2017 Learning objectives Review the evidence behind benefits and concerns
LOUISIANA MEDICAID PROGRAM ISSUED:
 37.12 TOTAL PARENTERAL NUTRITION Overview Introduction In This Section This Section explains the LMPBM program s Total Parenteral Nutrition (TPN) therapy coverage, limitations, prior authorization, reimbursement
37.12 TOTAL PARENTERAL NUTRITION Overview Introduction In This Section This Section explains the LMPBM program s Total Parenteral Nutrition (TPN) therapy coverage, limitations, prior authorization, reimbursement
LLL Session - Nutritional support in renal disease
 ESPEN Congress Leipzig 2013 LLL Session - Nutritional support in renal disease Peritoneal dialysis D. Teta (CH) Nutrition Support in Patients undergoing Peritoneal Dialysis (PD) Congress ESPEN, Leipzig
ESPEN Congress Leipzig 2013 LLL Session - Nutritional support in renal disease Peritoneal dialysis D. Teta (CH) Nutrition Support in Patients undergoing Peritoneal Dialysis (PD) Congress ESPEN, Leipzig
Nutrition in hemodialysis patients with focus on Intradialytic Parenteral Nutrition (IDPN)
 Nutrition in hemodialysis patients with focus on Intradialytic Parenteral Nutrition (IDPN) Enrico Fiaccadori enrico.fiaccadori@unipr.it Acute and Chronic Renal Failure Unit Medicine & Surgery Dept. Parma
Nutrition in hemodialysis patients with focus on Intradialytic Parenteral Nutrition (IDPN) Enrico Fiaccadori enrico.fiaccadori@unipr.it Acute and Chronic Renal Failure Unit Medicine & Surgery Dept. Parma
Nutrient/Nutritional Panel Testing
 Nutrient/Nutritional Panel Testing Policy Number: 2.04.136 Last Review: 10/2017 Origination: 10/2015 Next Review: 10/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
Nutrient/Nutritional Panel Testing Policy Number: 2.04.136 Last Review: 10/2017 Origination: 10/2015 Next Review: 10/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
Bioimpedance Devices for Detection and Management of Lymphedema
 Bioimpedance Devices for Detection and Management of Lymphedema Policy Number: 2.01.82 Last Review: 5/2018 Origination: 1/2011 Next Review: 5/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
Bioimpedance Devices for Detection and Management of Lymphedema Policy Number: 2.01.82 Last Review: 5/2018 Origination: 1/2011 Next Review: 5/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
Clinical Policy: Total Parenteral Nutrition and Intradialytic Parenteral Nutrition
 Clinical Policy: Reference Number: CP.MP.163 Last Review Date: 04/18 See Important Reminder at the end of this policy for important regulatory and legal information. Coding Implications Revision Log Parenteral
Clinical Policy: Reference Number: CP.MP.163 Last Review Date: 04/18 See Important Reminder at the end of this policy for important regulatory and legal information. Coding Implications Revision Log Parenteral
SAMPLE. Chronic Kidney Disease, Evidence-Based Practice, and the Nutrition Care Process. Chapter 1
 Chapter 1 Chronic Kidney Disease, Evidence-Based Practice, and the Nutrition Care Process This guide follows the steps of the Nutrition Care Process (NCP) nutrition assessment, nutrition diagnosis, nutrition
Chapter 1 Chronic Kidney Disease, Evidence-Based Practice, and the Nutrition Care Process This guide follows the steps of the Nutrition Care Process (NCP) nutrition assessment, nutrition diagnosis, nutrition
Parenteral Nutrition. The Health Plan PARENTERAL NUTRITION
 Parenteral Nutrition Adopted from National Government Services website For any item to be covered by The Health Plan, it must: 1. Be eligible for a defined Medicare or The Health Plan benefit category
Parenteral Nutrition Adopted from National Government Services website For any item to be covered by The Health Plan, it must: 1. Be eligible for a defined Medicare or The Health Plan benefit category
1. Reggie J. Divina, M.D. (1) 2. Fe S. Felicilda, M.D., DPBCN (1,2) 3. Rufino E. Chan, M.D. (1) 4. Luisito O. Llido, M.D.
 82 TITLE: Nutritional status of hemodialysis patients in the Philippines: a cross sectional survey in four out- patient dialysis centers Submitted: January 10, 2010 Posted: August 30, 2010 AUTHOR(S) 1.
82 TITLE: Nutritional status of hemodialysis patients in the Philippines: a cross sectional survey in four out- patient dialysis centers Submitted: January 10, 2010 Posted: August 30, 2010 AUTHOR(S) 1.
PARENTERAL NUTRITION THERAPY
 UnitedHealthcare Benefits of Texas, Inc. 1. UnitedHealthcare of Oklahoma, Inc. 2. UnitedHealthcare of Oregon, Inc. UnitedHealthcare of Washington, Inc. UnitedHealthcare West BENEFIT INTERPRETATION POLICY
UnitedHealthcare Benefits of Texas, Inc. 1. UnitedHealthcare of Oklahoma, Inc. 2. UnitedHealthcare of Oregon, Inc. UnitedHealthcare of Washington, Inc. UnitedHealthcare West BENEFIT INTERPRETATION POLICY
Full Title of Guideline: Author (include and role): Division & Speciality:
 Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date (when this version goes out of date): Explicit definition of patient
Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date (when this version goes out of date): Explicit definition of patient
Biofeedback as a Treatment of Headache
 Biofeedback as a Treatment of Headache Policy Number: 2.01.29 Last Review: 7/2018 Origination: 7/2008 Next Review: 7/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) may provide coverage
Biofeedback as a Treatment of Headache Policy Number: 2.01.29 Last Review: 7/2018 Origination: 7/2008 Next Review: 7/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) may provide coverage
Macro- and Micronutrient Homeostasis in the Setting of Chronic Kidney Disease. T. Alp Ikizler, MD Vanderbilt University Medical Center
 Macro- and Micronutrient Homeostasis in the Setting of Chronic Kidney Disease T. Alp Ikizler, MD Vanderbilt University Medical Center Nutrition and Chronic Kidney Disease What is the disease itself and
Macro- and Micronutrient Homeostasis in the Setting of Chronic Kidney Disease T. Alp Ikizler, MD Vanderbilt University Medical Center Nutrition and Chronic Kidney Disease What is the disease itself and
Claim Filing Information INSIDE THIS ISSUE: FEP Point-of-Service identification numbers
 May 30, 2000 INSIDE THIS ISSUE: CLAIMS FILING INFORMATION Pages 1-4 FEP Point-Of-Service Identification Numbers Guidelines For Newborn Care Claims Mailing Address for Claims and Customer Service Inquiries
May 30, 2000 INSIDE THIS ISSUE: CLAIMS FILING INFORMATION Pages 1-4 FEP Point-Of-Service Identification Numbers Guidelines For Newborn Care Claims Mailing Address for Claims and Customer Service Inquiries
Vertebral Axial Decompression
 Vertebral Axial Decompression Policy Number: 8.03.09 Last Review: 11/2017 Origination: 11/2005 Next Review: 11/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
Vertebral Axial Decompression Policy Number: 8.03.09 Last Review: 11/2017 Origination: 11/2005 Next Review: 11/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
Dynamic Spinal Visualization and Vertebral Motion Analysis
 Dynamic Spinal Visualization and Vertebral Motion Analysis Policy Number: 6.01.46 Last Review: 2/2019 Origination: 2/2006 Next Review: 2/2020 Policy Blue Cross and Blue Shield of Kansas City (Blue KC)
Dynamic Spinal Visualization and Vertebral Motion Analysis Policy Number: 6.01.46 Last Review: 2/2019 Origination: 2/2006 Next Review: 2/2020 Policy Blue Cross and Blue Shield of Kansas City (Blue KC)
Nutritional Management of Criticallly Ill Patients with Acute Kidney Injury
 Nutritional Management of Criticallly Ill Patients with Acute Kidney Injury 3 rd International Conference of European Renal Nutrition Working Group of ERA-EDTA T. Alp Ikizler, MD Catherine McLaughlin-Hakim
Nutritional Management of Criticallly Ill Patients with Acute Kidney Injury 3 rd International Conference of European Renal Nutrition Working Group of ERA-EDTA T. Alp Ikizler, MD Catherine McLaughlin-Hakim
Evaluation and management of nutrition in children
 Evaluation and management of nutrition in children Date written: May 2004 Final submission: January 2005 Author: Elisabeth Hodson GUIDELINES No recommendations possible based on Level I or II evidence
Evaluation and management of nutrition in children Date written: May 2004 Final submission: January 2005 Author: Elisabeth Hodson GUIDELINES No recommendations possible based on Level I or II evidence
Vertebral Axial Decompression
 Vertebral Axial Decompression Policy Number: 8.03.09 Last Review: 11/2018 Origination: 11/2005 Next Review: 11/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
Vertebral Axial Decompression Policy Number: 8.03.09 Last Review: 11/2018 Origination: 11/2005 Next Review: 11/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
Peripheral Subcutaneous Field Stimulation
 Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 9/2014 Origination: 7/2013 Next Review: 1/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 9/2014 Origination: 7/2013 Next Review: 1/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Nutritional support in advanced kidney disease: Role of oral and parenteral nutrition. T. Alp Ikizler, MD Vanderbilt University Medical Center
 Nutritional support in advanced kidney disease: Role of oral and parenteral nutrition T. Alp Ikizler, MD Vanderbilt University Medical Center Goals To delineate the mechanisms through which wasting syndrome
Nutritional support in advanced kidney disease: Role of oral and parenteral nutrition T. Alp Ikizler, MD Vanderbilt University Medical Center Goals To delineate the mechanisms through which wasting syndrome
Ingrezza (valbenazine)
 Ingrezza (valbenazine) Policy Number: 5.01.635 Last Review: 7/2018 Origination: 07/2017 Next Review: 7/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Ingrezza
Ingrezza (valbenazine) Policy Number: 5.01.635 Last Review: 7/2018 Origination: 07/2017 Next Review: 7/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Ingrezza
Influenza Therapies. Considerations Prescription influenza therapies require prior authorization through pharmacy services.
 Influenza Therapies Policy Number: 5.01.515 Last Review: 10/2017 Origination: 10/2002 Next Review: 10/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for influenza
Influenza Therapies Policy Number: 5.01.515 Last Review: 10/2017 Origination: 10/2002 Next Review: 10/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for influenza
IDPN. A Piece of the Puzzle for Dialysis Patients Nutrition. Toll Free: Toll Free:
 IDPN A Piece of the Puzzle for Dialysis Patients Nutrition Toll Free: 844-633-3448 Toll Free: 844-633-3448 Executive Infusion is pleased to announce our nutritional services which include Intradialytic
IDPN A Piece of the Puzzle for Dialysis Patients Nutrition Toll Free: 844-633-3448 Toll Free: 844-633-3448 Executive Infusion is pleased to announce our nutritional services which include Intradialytic
Artificial Nutritional Support in Chronic Hemodialysis Patients: A Narrative Review
 REVIEW Artificial Nutritional Support in Chronic Hemodialysis Patients: A Narrative Review Maurizio Bossola, MD,* Luigi Tazza, MD,* Stefania Giungi, MD,* Fausto Rosa, MD, and Giovanna Luciani, MD* Objective:
REVIEW Artificial Nutritional Support in Chronic Hemodialysis Patients: A Narrative Review Maurizio Bossola, MD,* Luigi Tazza, MD,* Stefania Giungi, MD,* Fausto Rosa, MD, and Giovanna Luciani, MD* Objective:
Saturation Biopsy for Diagnosis and Staging and Management of Prostate Cancer
 Saturation Biopsy for Diagnosis and Staging and Management of Prostate Cancer Policy Number: 7.01.121 Last Review: 2/2018 Origination: 8/2006 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas
Saturation Biopsy for Diagnosis and Staging and Management of Prostate Cancer Policy Number: 7.01.121 Last Review: 2/2018 Origination: 8/2006 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas
By; Ashraf El Houfi MD MS (pulmonology) MRCP (UK) FRCP (London) EDIC Consultant ICU Dubai Hospital
 By; Ashraf El Houfi MD MS (pulmonology) MRCP (UK) FRCP (London) EDIC Consultant ICU Dubai Hospital Introduction The significance of nutrition in hospital setting (especially the ICU) cannot be overstated.
By; Ashraf El Houfi MD MS (pulmonology) MRCP (UK) FRCP (London) EDIC Consultant ICU Dubai Hospital Introduction The significance of nutrition in hospital setting (especially the ICU) cannot be overstated.
Takhzyro (lanadelumab-flyo)
 Takhzyro (lanadelumab-flyo) Policy Number: 5.01.675 Last Review: 1/2019 Origination: 1/2019 Next Review: 1/2020 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Takhzyro
Takhzyro (lanadelumab-flyo) Policy Number: 5.01.675 Last Review: 1/2019 Origination: 1/2019 Next Review: 1/2020 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Takhzyro
TABLE OF CONTENTS T-1. A-1 Acronyms and Abbreviations. S-1 Stages of Chronic Kidney Disease (CKD)
 A-1 Acronyms and Abbreviations TABLE OF CONTENTS S-1 Stages of Chronic Kidney Disease (CKD) Chapter 1: Nutrition Assessment Charts, Tables and Formulas 1-2 Practical Steps to Nutrition Assessment Adult
A-1 Acronyms and Abbreviations TABLE OF CONTENTS S-1 Stages of Chronic Kidney Disease (CKD) Chapter 1: Nutrition Assessment Charts, Tables and Formulas 1-2 Practical Steps to Nutrition Assessment Adult
Hematopoietic Cell Transplantation for Epithelial Ovarian Cancer
 Hematopoietic Cell Transplantation for Epithelial Ovarian Cancer Policy Number: 8.01.23 Last Review: 1/2018 Origination: 9/2002 Next Review: 1/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
Hematopoietic Cell Transplantation for Epithelial Ovarian Cancer Policy Number: 8.01.23 Last Review: 1/2018 Origination: 9/2002 Next Review: 1/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
Addyi (flibanserin) When Policy Topic is covered Coverage of Addyi is recommended in those who meet the following criteria:
 Addyi (flibanserin) Policy Number: 5.01.605 Last Review: 10/2018 Origination: 10/2015 Next Review: 10/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Addyi when
Addyi (flibanserin) Policy Number: 5.01.605 Last Review: 10/2018 Origination: 10/2015 Next Review: 10/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Addyi when
Vosevi (sofosbuvir/velpatasvir/voxilaprevir)
 Vosevi (sofosbuvir/velpatasvir/voxilaprevir) Policy Number: 5.01.646 Last Review: 10/2017 Origination: 10/2017 Next Review: 11/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide
Vosevi (sofosbuvir/velpatasvir/voxilaprevir) Policy Number: 5.01.646 Last Review: 10/2017 Origination: 10/2017 Next Review: 11/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide
Antigen Leukocyte Antibody Test
 Antigen Leukocyte Antibody Test Policy Number: 2.01.93 Last Review: 4/2018 Origination: 4/2014 Next Review: 4/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for
Antigen Leukocyte Antibody Test Policy Number: 2.01.93 Last Review: 4/2018 Origination: 4/2014 Next Review: 4/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for
Transtympanic Micropressure Applications as a Treatment of Meniere s Disease
 Transtympanic Micropressure Applications as a Treatment of Meniere s Disease Policy Number: 1.01.23 Last Review: 8/2014 Origination: 2/2006 Next Review: 8/2015 Policy Blue Cross and Blue Shield of Kansas
Transtympanic Micropressure Applications as a Treatment of Meniere s Disease Policy Number: 1.01.23 Last Review: 8/2014 Origination: 2/2006 Next Review: 8/2015 Policy Blue Cross and Blue Shield of Kansas
Antigen Leukocyte Antibody Test
 Antigen Leukocyte Antibody Test Policy Number: 2.01.93 Last Review: 4/2014 Origination: 4/2014 Next Review: 4/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for
Antigen Leukocyte Antibody Test Policy Number: 2.01.93 Last Review: 4/2014 Origination: 4/2014 Next Review: 4/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for
Saturation Biopsy for Diagnosis and Staging and Management of Prostate Cancer
 Saturation Biopsy for Diagnosis and Staging and Management of Prostate Cancer Policy Number: 7.01.121 Last Review: 2/2019 Origination: 8/2006 Next Review: 8/2019 Policy Blue Cross and Blue Shield of Kansas
Saturation Biopsy for Diagnosis and Staging and Management of Prostate Cancer Policy Number: 7.01.121 Last Review: 2/2019 Origination: 8/2006 Next Review: 8/2019 Policy Blue Cross and Blue Shield of Kansas
Medical Policy Enteral Nutrition Formulas and Supplements
 Document Number: 017 Medical Policy Enteral Nutrition Formulas and Supplements Commercial and Qualified Health Plans MassHealth Authorization required X X No notification or authorization Not covered Overview
Document Number: 017 Medical Policy Enteral Nutrition Formulas and Supplements Commercial and Qualified Health Plans MassHealth Authorization required X X No notification or authorization Not covered Overview
MEASURE INFORMATION FORM
 MEASURE INFORMATION FORM Project Title: Comprehensive Reevaluation Dialysis Adequacy Project Overview: The Centers for Medicare & Medicaid Services (CMS) has contracted with the University of Michigan
MEASURE INFORMATION FORM Project Title: Comprehensive Reevaluation Dialysis Adequacy Project Overview: The Centers for Medicare & Medicaid Services (CMS) has contracted with the University of Michigan
Nutrition Dilemmas, Controversies & Issues CHRONIC KIDNEY DISEASE (CKD)
 Nutrition Dilemmas, Controversies & Issues CHRONIC KIDNEY DISEASE (CKD) Objectives To discuss the role of nutrition in clinical outcomes of chronic kidney disease (CKD) To discuss and update on the nutrition
Nutrition Dilemmas, Controversies & Issues CHRONIC KIDNEY DISEASE (CKD) Objectives To discuss the role of nutrition in clinical outcomes of chronic kidney disease (CKD) To discuss and update on the nutrition
Electrical Stimulation for Scoliosis
 Electrical Stimulation for Scoliosis Policy Number: 1.01.509 Last Review: 8/2017 Origination: 8/2008 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
Electrical Stimulation for Scoliosis Policy Number: 1.01.509 Last Review: 8/2017 Origination: 8/2008 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
Clinical Policy: Ferumoxytol (Feraheme) Reference Number: CP.PHAR.165
 Clinical Policy: (Feraheme) Reference Number: CP.PHAR.165 Effective Date: 03/16 Last Review Date: 03/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory
Clinical Policy: (Feraheme) Reference Number: CP.PHAR.165 Effective Date: 03/16 Last Review Date: 03/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory
SUBJECT INDEX. Tvedegaard, E., 20. Ulerich, L., E1 (July) Wapensky, T., 45 Warner, J., 116 Warsaba, D., 52
 268 Supasyndh, O., 134 Suraci, C., 208 Tatangelo, P., 208 Tavares, I., 157 Tozzo, C., 208 Tvedegaard, E., 20 Ulerich, L., E1 (July) Wapensky, T., 45 Warner, J., 116 Warsaba, D., 52 Wells, L.M., 26 Winkler,
268 Supasyndh, O., 134 Suraci, C., 208 Tatangelo, P., 208 Tavares, I., 157 Tozzo, C., 208 Tvedegaard, E., 20 Ulerich, L., E1 (July) Wapensky, T., 45 Warner, J., 116 Warsaba, D., 52 Wells, L.M., 26 Winkler,
Measure #403: Adult Kidney Disease: Referral to Hospice National Quality Strategy Domain: Patient and Caregiver-Centered Experience and Outcomes
 Measure #403: Adult Kidney Disease: Referral to Hospice National Quality Strategy Domain: Patient and Caregiver-Centered Experience and Outcomes 2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE
Measure #403: Adult Kidney Disease: Referral to Hospice National Quality Strategy Domain: Patient and Caregiver-Centered Experience and Outcomes 2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE
Peripheral Subcutaneous Field Stimulation
 Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 3/2018 Origination: 7/2013 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 3/2018 Origination: 7/2013 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Clinical Policy: Ferric Carboxymaltose (Injectafer) Reference Number: CP.PHAR.234
 Clinical Policy: (Injectafer) Reference Number: CP.PHAR.234 Effective Date: 06/16 Last Review Date: 03/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important
Clinical Policy: (Injectafer) Reference Number: CP.PHAR.234 Effective Date: 06/16 Last Review Date: 03/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important
Avastin (bevacizumab)
 Avastin (bevacizumab) Policy Number: 5.02.502 Last Review: 04/2018 Origination: 03/2017 Next Review: 04/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Avastin
Avastin (bevacizumab) Policy Number: 5.02.502 Last Review: 04/2018 Origination: 03/2017 Next Review: 04/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Avastin
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: Methoxy polyethylene glycol-epoetin beta (Mircera) Reference Number: CP.CPA.322 Effective Date: 06.01.18 Last Review Date: 05.18 Line of Business: Commercial Coding Implications Revision
Clinical Policy: Methoxy polyethylene glycol-epoetin beta (Mircera) Reference Number: CP.CPA.322 Effective Date: 06.01.18 Last Review Date: 05.18 Line of Business: Commercial Coding Implications Revision
Corporate Medical Policy
 Corporate Medical Policy Insulin Therapy, Chronic Intermittent Intravenous (CIIIT) File Name: Origination: Last CAP Review: Next CAP Review: Last Review: insulin_therapy_chronic_intermittent_intravenous
Corporate Medical Policy Insulin Therapy, Chronic Intermittent Intravenous (CIIIT) File Name: Origination: Last CAP Review: Next CAP Review: Last Review: insulin_therapy_chronic_intermittent_intravenous
Corporate Medical Policy Investigational (Experimental) Services
 Corporate Medical Policy Investigational (Experimental) Services File Name: Origination: investigational_(experimental)_services 1/1996 Description of Procedure or Service BCBSNC defines the terms "investigational"
Corporate Medical Policy Investigational (Experimental) Services File Name: Origination: investigational_(experimental)_services 1/1996 Description of Procedure or Service BCBSNC defines the terms "investigational"
Chapter Five Clinical indicators & preventive health
 Chapter Five Clinical indicators & preventive health The painter who draws merely by practice and by eye, without any reason, is like a mirror which copies every thing placed in front of it without being
Chapter Five Clinical indicators & preventive health The painter who draws merely by practice and by eye, without any reason, is like a mirror which copies every thing placed in front of it without being
ESPEN Congress Vienna Nutritional implications of renal replacement therapy in ICU Nutritional support - how much nitrogen? W.
 ESPEN Congress Vienna 2009 Nutritional implications of renal replacement therapy in ICU Nutritional support - how much nitrogen? W. Druml (Austria) Nutritional Implications of Renal Replacement Therapy
ESPEN Congress Vienna 2009 Nutritional implications of renal replacement therapy in ICU Nutritional support - how much nitrogen? W. Druml (Austria) Nutritional Implications of Renal Replacement Therapy
PARSABIV (etelcalcetide)
 PARSABIV (etelcalcetide) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and
PARSABIV (etelcalcetide) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and
Nutrition in Acute Kidney Injury Enrico Fiaccadori
 Nutrition in Acute Kidney Injury Enrico Fiaccadori Nephrology Dept. Parma University Medical School Parma, Italy Diagnosis, epidemiology and prognostic impact of proteinenergy wasting (PEW) in AKI Pathogenetic
Nutrition in Acute Kidney Injury Enrico Fiaccadori Nephrology Dept. Parma University Medical School Parma, Italy Diagnosis, epidemiology and prognostic impact of proteinenergy wasting (PEW) in AKI Pathogenetic
Clinical Policy: Iron Sucrose (Venofer) Reference Number: CP.PHAR.167
 Clinical Policy: (Venofer) Reference Number: CP.PHAR.167 Effective Date: 03/16 Last Review Date: 03/17 Revision Log Coding Implications See Important Reminder at the end of this policy for important regulatory
Clinical Policy: (Venofer) Reference Number: CP.PHAR.167 Effective Date: 03/16 Last Review Date: 03/17 Revision Log Coding Implications See Important Reminder at the end of this policy for important regulatory
The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009
 The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009 Teresa Northcutt, RN BSN Primaris Program Manager, Prevention - CKD MO-09-01-CKD This material was prepared by Primaris,
The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009 Teresa Northcutt, RN BSN Primaris Program Manager, Prevention - CKD MO-09-01-CKD This material was prepared by Primaris,
Peripheral Subcutaneous Field Stimulation
 Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 9/2018 Origination: 7/2013 Next Review: 3/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 9/2018 Origination: 7/2013 Next Review: 3/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Medical Policy Enteral Nutrition Formulas and Supplements
 Medical Policy Enteral Nutrition Formulas and Supplements Document Number: 017 Commercial and MassHealth Connector/Qualified Health Plans Authorization required X X Notification within 24 hours of service
Medical Policy Enteral Nutrition Formulas and Supplements Document Number: 017 Commercial and MassHealth Connector/Qualified Health Plans Authorization required X X Notification within 24 hours of service
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: Darbepoetin Alfa (Aranesp) Reference Number: CP.PHAR.236 Effective Date: 06.01.16 Last Review Date: 05.18 Line of Business: HIM, Medicaid Coding Implications Revision Log See Important
Clinical Policy: Darbepoetin Alfa (Aranesp) Reference Number: CP.PHAR.236 Effective Date: 06.01.16 Last Review Date: 05.18 Line of Business: HIM, Medicaid Coding Implications Revision Log See Important
DOWNLOAD OR READ : NUTRITION DURING DIALYSIS TREATMENT PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : NUTRITION DURING DIALYSIS TREATMENT PDF EBOOK EPUB MOBI Page 1 Page 2 nutrition during dialysis treatment nutrition during dialysis treatment pdf nutrition during dialysis treatment
DOWNLOAD OR READ : NUTRITION DURING DIALYSIS TREATMENT PDF EBOOK EPUB MOBI Page 1 Page 2 nutrition during dialysis treatment nutrition during dialysis treatment pdf nutrition during dialysis treatment
Staff-Assisted Home Hemodialysis
 Medical Coverage Policy Staff-Assisted Home Hemodialysis Table of Contents Coverage Policy... 1 Overview... 1 General Background... 2 Coding/Billing Information... 4 References... 4 Effective Date...11/15/2017
Medical Coverage Policy Staff-Assisted Home Hemodialysis Table of Contents Coverage Policy... 1 Overview... 1 General Background... 2 Coding/Billing Information... 4 References... 4 Effective Date...11/15/2017
The CARI Guidelines Caring for Australians with Renal Impairment. Other criteria for starting dialysis GUIDELINES
 Date written: September 2004 Final submission: February 2005 Other criteria for starting dialysis GUIDELINES No recommendations possible based on Level I or II evidence SUGGESTIONS FOR CLINICAL CARE (Suggestions
Date written: September 2004 Final submission: February 2005 Other criteria for starting dialysis GUIDELINES No recommendations possible based on Level I or II evidence SUGGESTIONS FOR CLINICAL CARE (Suggestions
NATIONAL QUALITY FORUM Renal EM Submitted Measures
 NATIONAL QUALITY FORUM Renal EM Submitted Measures Measure ID/ Title Measure Description Measure Steward Topic Area #1662 Percentage of patients aged 18 years and older with a diagnosis of CKD ACE/ARB
NATIONAL QUALITY FORUM Renal EM Submitted Measures Measure ID/ Title Measure Description Measure Steward Topic Area #1662 Percentage of patients aged 18 years and older with a diagnosis of CKD ACE/ARB
Nutritional management of encapsulating peritoneal sclerosis with intradialytic parenteral nutrition
 Nutritional management of encapsulating peritoneal sclerosis with intradialytic parenteral nutrition Kriel J, BSc(Dietetics); Clinical Dietitian; Esau N, MSc(Dietetics), Clinical Dietitian Tygerberg Academic
Nutritional management of encapsulating peritoneal sclerosis with intradialytic parenteral nutrition Kriel J, BSc(Dietetics); Clinical Dietitian; Esau N, MSc(Dietetics), Clinical Dietitian Tygerberg Academic
Measure #330: Adult Kidney Disease: Catheter Use for Greater Than or Equal to 90 Days National Quality Strategy Domain: Patient Safety
 Measure #330: Adult Kidney Disease: Catheter Use for Greater Than or Equal to 90 Days National Quality Strategy Domain: Patient Safety 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES REGISTRY ONLY This is a
Measure #330: Adult Kidney Disease: Catheter Use for Greater Than or Equal to 90 Days National Quality Strategy Domain: Patient Safety 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES REGISTRY ONLY This is a
Chronic Intermittent Intravenous Insulin Therapy (CIIIT)
 Chronic Intermittent Intravenous Insulin Therapy (CIIIT) Policy Number: 2.01.43 Last Review: 9/2018 Origination: 3/2012 Next Review: 3/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will
Chronic Intermittent Intravenous Insulin Therapy (CIIIT) Policy Number: 2.01.43 Last Review: 9/2018 Origination: 3/2012 Next Review: 3/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will
Handheld Radiofrequency Spectroscopy for Intraoperative Assessment of Surgical Margins During Breast-Conserving Surgery
 7.01.140 Handheld Radiofrequency Spectroscopy for Intraoperative Assessment of Surgical Margins During Breast-Conserving Surgery Section 7.0 Surgery Subsection Description Effective Date November 26, 2014
7.01.140 Handheld Radiofrequency Spectroscopy for Intraoperative Assessment of Surgical Margins During Breast-Conserving Surgery Section 7.0 Surgery Subsection Description Effective Date November 26, 2014
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Neprilysin Inhibitor (Entresto ) Page 1 of 6 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Neprilysin Inhibitor (Entresto ) Prime Therapeutics will review Prior
Neprilysin Inhibitor (Entresto ) Page 1 of 6 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Neprilysin Inhibitor (Entresto ) Prime Therapeutics will review Prior
Corporate Medical Policy
 Corporate Medical Policy Serum Biomarker Human Epididymis Protein 4 (HE4) File Name: Origination: Last CAP Review: Next CAP Review: Last Review: serum_biomarker_human_epididymis_protein_4_(he4) 1/2010
Corporate Medical Policy Serum Biomarker Human Epididymis Protein 4 (HE4) File Name: Origination: Last CAP Review: Next CAP Review: Last Review: serum_biomarker_human_epididymis_protein_4_(he4) 1/2010
Corporate Medical Policy
 Corporate Medical Policy Continuous Monitoring of Glucose in the Interstitial Fluid File Name: Origination: Last CAP Review: Next CAP Review: Last Review: continuous_monitoring_of_glucose_in_the_interstitial_fluid
Corporate Medical Policy Continuous Monitoring of Glucose in the Interstitial Fluid File Name: Origination: Last CAP Review: Next CAP Review: Last Review: continuous_monitoring_of_glucose_in_the_interstitial_fluid
Nutrition Assessment in CKD
 Nutrition Assessment in CKD Shiaw-Wen Chien, MD, EMBA Division of Nephrology, Department of Medicine, Tungs Taichung MetroHarbor Hospital Taichung, Taiwan September 10, 2017 Outline Introduction Composite
Nutrition Assessment in CKD Shiaw-Wen Chien, MD, EMBA Division of Nephrology, Department of Medicine, Tungs Taichung MetroHarbor Hospital Taichung, Taiwan September 10, 2017 Outline Introduction Composite
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Afrezza Page 1 of 7 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Afrezza (human insulin) Prime Therapeutics will review Prior Authorization requests Prior Authorization
Afrezza Page 1 of 7 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Afrezza (human insulin) Prime Therapeutics will review Prior Authorization requests Prior Authorization
Amanda Hernandez FND Parenteral Nutrition Worksheet October 26, 2011
 Amanda Hernandez FND 430-001 Parenteral Nutrition Worksheet October 26, 2011 1. HP needs TPN because he has short bowel syndrome and his GI tract is not functional. His entire jejunum was and proximal
Amanda Hernandez FND 430-001 Parenteral Nutrition Worksheet October 26, 2011 1. HP needs TPN because he has short bowel syndrome and his GI tract is not functional. His entire jejunum was and proximal
Introduction to Clinical Nutrition
 M-III Introduction to Clinical Nutrition Donald F. Kirby, MD Chief, Section of Nutrition Division of Gastroenterology 1 Things We Take for Granted Air to Breathe Death Taxes Another Admission Our Next
M-III Introduction to Clinical Nutrition Donald F. Kirby, MD Chief, Section of Nutrition Division of Gastroenterology 1 Things We Take for Granted Air to Breathe Death Taxes Another Admission Our Next
Clinical Policy: Cinacalcet (Sensipar) Reference Number: CP.PHAR.61 Effective Date: Last Review Date: Line of Business: Medicaid
 Clinical Policy: (Sensipar) Reference Number: CP.PHAR.61 Effective Date: 05.01.11 Last Review Date: 02.18 Line of Business: Medicaid Revision Log See Important Reminder at the end of this policy for important
Clinical Policy: (Sensipar) Reference Number: CP.PHAR.61 Effective Date: 05.01.11 Last Review Date: 02.18 Line of Business: Medicaid Revision Log See Important Reminder at the end of this policy for important
La relation dialyse et nutrition
 Nutrition en dialyse : controverses La relation dialyse et nutrition Charles Chazot, MD NephroCare Tassin-Charcot Sainte Foy Les Lyon, France HEMO study lessons (1) Dose Body weight flux Rocco, Kidney
Nutrition en dialyse : controverses La relation dialyse et nutrition Charles Chazot, MD NephroCare Tassin-Charcot Sainte Foy Les Lyon, France HEMO study lessons (1) Dose Body weight flux Rocco, Kidney
Malnutrition in advanced CKD
 Malnutrition in advanced CKD Malnutrition Lack of proper nutrition, caused by not having enough to eat, not eating enough of the right things or being unable to use the food that one does eat Jessica Stevenson
Malnutrition in advanced CKD Malnutrition Lack of proper nutrition, caused by not having enough to eat, not eating enough of the right things or being unable to use the food that one does eat Jessica Stevenson
