Diseases of the Renal System
|
|
|
- Isabel Morton
- 5 years ago
- Views:
Transcription
1 Diseases of the Renal System Chapter 20 1
2 2
3 Kidneys - Anatomy Regulatory and metabolic functions Nephron - functional unit; approx. 1.2 million in each kidney Glomerulus within Bowman s capsule Afferent arteriole carries blood to glomerulus Efferent arteriole - carries blood from glomerulus 3
4 Kidneys - Anatomy Nephron Tubules see Fig Proximal convoluted tubule Loop of Henle Distal convoluted tubule Colleting duct 4
5 5
6 Kidneys - Anatomy Nephron Ultrafiltrate formed by glomerulus Similar to composition of blood Filters large proteins and blood cells Modified by tubules Reabsorption of amino acids, glucose, select minerals, water Secretion of solutes, water 65% of filtered sodium and water reabsorbed (active transport in proximal tubule) 6
7 Kidneys - Anatomy Nephron - functions Maintain extracellular environment for cell function Excretion of waste products of metabolism Maintain fluid, electrolyte and acidbase balance Vasopressin in response to blood volume, maintains fluid balance 7
8 Kidneys - Anatomy Nephron - functions Secretion of hormones that modulate hemodynamics Erythropoietin - red blood cell production Vitamin D bone metabolism 8
9 The Kidneys Diagnostic Procedures GFR - glomerular filtration rate; rate at which substances are cleared from plasma normal L/day Clearance calculations see p. 613 Tubular function tests Microscopic evaluation of the urine Radiologic evaluation (IVP, MRI, ultrasound) Biopsy 9
10 Nephrotic Syndrome Deficiency of albumin in blood and its excretion in the urine d/t altered glomerular function large-molecule proteins and RBCs leak into urine Proteinuria >3.5 Hyperlipidemia Hypoalbuminemia Result of underlying disease More prevalent in children 10
11 Nephrotic Syndrome Clinical Manifestations Frothy urine Anorexia, malaise, puffy eyelids, abdominal pain, muscle wasting Anascarca with ascites, plural effusion Altered blood pressure Oliguria d/t hypovolemia Edema Loss of zinc, copper, vitamin D; iron bound to proteins lost 11
12 Nephrotic Syndrome Treatment Treat underlying cause Reduce cholesterol Control blood pressure Reduce protein in urine ACE inhibitors and ARBs Check potassium levels 12
13 Nephrotic Syndrome Nutrition Therapy See Table 20.1 Control intake of protein g/kg/day Soy- or flaxseed-based proteins Protein supplementation no benefit 13
14 Chronic Kidney Disease (CKD) Syndrome in which progressive loss of kidney function occurs Not reversible Progression to end-stage renal disease (ESRD or CKD stage 5) Renal replacement therapy or transplant Requires medication and specialized diet 14
15 Chronic Kidney Disease (CKD) Risk factors Proteinuria Ethnicity African American with diabetes highest Gender males Smoking Heavy consumption of non-narcotic analgesics Obesity??? 15
16 Chronic Kidney Disease (CKD) Most frequent causes Diabetes Hypertension Glomerulonephritis Hereditary and cystic congenital renal disease Interstitial nephritis Neoplasm/tumor 16
17 Chronic Kidney Disease (CKD) Common complications Malnutrition CVD aggressive management recommended Bone and mineral disorders Anemia 17
18 Chronic Kidney Disease (CKD) Stages see Table 20.2 Stages 1 & 2 kidney damage with: Normal or increased GFR, mild decrease in GFR Stage 3 Moderate decrease: GFR ml/min Stage 4 Severe decrease: GFR ml/min Stage 5 Inadequate to sustain life 18
19 Chronic Kidney Disease (CKD) Pathophysiology Advanced impairment in control of fluid and electrolyte balance Uremia, hyperphosphatemia, azotemia, oliguria Kidney function < 15 ml/min Sodium retention, edema, hypertension Metabolic acidosis Hyperkalemia 19
20 Chronic Kidney Disease (CKD) Pathophysiology Microcytic anemia and iron deficiency Inadequate erythropoietin Renal osteodystrophy d/t impaired intestinal calcium absorption and secondary hyperparathyroidism 20
21 21
22 Chronic Kidney Disease (CKD) Treatment Treat underlying disease, delay progression Stages 1 & 2 EPO replacement, vitamin D supplementation Stage 5 renal replacement therapy, nutrition therapy crucial, transplant Post transplant immunosuppresants 22
23 Chronic Kidney Disease (CKD) Renal Replacement Therapy - Dialysis removal of excessive and toxic by-products of metabolism from the blood, replacing the filtering function of the kidney Fluid and electrolyte balance must be maintained Passing blood across selective membrane exposed to rinsing fluid (dialysate) 23
24 CKD - Renal Replacement Therapy Serum creatinine 6 mg/dl for nondiabetics or Creatine clearance < 15 ml per minute for diabetics Definite indicators: Pericarditis, uncontrolled fluid overload, pulmonary edema, uncontrolled and repeated hyperkalemia, coma, lethargy 24
25 CKD - Renal Replacement Therapy Hemodialysis (HD) or Peritoneal Dialysis (PD) Type based on underlying kidney disease and co-morbid factors See Box role of health team Both require selective, permeable membrane Allows passage of water and small molecules Excludes larger molecules such as protein 25
26 CKD - Renal Replacement Therapy Hemodialysis(HD) Membrane is manmade dialyzer artificial kidney See Fig. 20.5, 20.7 Preferred access site AVF, AVG Typical regimen 3 days/week for 4 hrs/treatment 26
27 27
28 28
29 CKD - Renal Replacement Therapy Peritoneal dialysis (PD) Lining of patient s peritoneal wall is the selective membrane see Fig Types CAPD - continuous ambulatory CCPD - continuous cycling Access via catheter into peritoneal cavity Range of dextrose concentrations Dwell time and number of exchanges 29
30 30
31 CKD - Stages 1 & 2 Nutrition Therapy Focus on co-morbid conditions: diabetes, hypertension, hyperlipidemia, progression of CVD K/DOQI guidelines for GFR 20 SGA every 1 3 mo. Dietary interviews and food intake, or npna every 3-4 mo. More frequent if GFR 15 Protein: g/kg Energy: kcal/kg 31
32 CKD - Stages 3 & 4 Nutrition Therapy See ADA guidelines Nutrition assessment recommendations see p. 624 Nutrient recommendations see Table 20.4 Protein (inc), energy, sodium (dec), potassium, phosphorus, calcium, vitamins, minerals, fluid may need adjustment Emphasize usual foods 32
33 CKD - Stages 3 & 4 Outcome measures Clinical Biochemical see Table 20.3 Anthropometrics Clinical signs and symptoms Behavioral Meal planning, meeting nutrient needs, awareness of food/drug interactions, exercise See Table
34 CKD - Stage 5 Nutrition Assessment On dialysis measures not different Dietary intake Biochemical: serum albumin See Table 20.7 for other indicators Goals: meet nutritional requirements, prevent malnutrition, minimize uremia, minimize complications Maintain blood pressure, fluid status 34
35 CKD - Stage 5 Nutrition Intervention HD high in protein, control intake of potassium, phosphorus, fluids and sodium Modifications in fat, cholesterol, TG if warranted PD more liberalized; higher in pro., sodium, potassium and fluid, limit phosphorus See Table 20.8 nutrients to monitor 35
36 CKD - Stage 5 Nutrition Intervention Protein g/kg (HD), at least 50% HBV PD same except during peritonitis increase protein Losses increase % and may remain elevated 36
37 CKD - Stage 5 Nutrition Intervention Energy to prevent catabolism; needs slightly higher; individualized PD - account for kcal in dialysate Caloric load PET Box kcal/kg/day average intake 37
38 CKD - Stage 5 Nutrition Intervention Adjusted Edema-Free Body Weight should be used to calculate body weight for calculating protein and kcal For those < 95% or > 115% median standard weight NHANESII For maintenance in HD and PD pts. Obtained postdialysis for HD pts., and after drainage for PD patients 38
39 CKD - Stage 5 Nutrition Intervention Fat - increased risk for CAD and stroke HD typically have normal LDL, HDL, TG PD higher TC, LDL, TG Recommend TLC diet guidelines for both 39
40 CKD - Stage 5 Nutrition Intervention Fluid and Sodium highly individualized based on residual urine output and dialysis modality Interdialytic weight gain (HD) should not exceed 5% of body weight 2 gram sodium diet Not more than 1 L fluid daily If urine output > 1 L/day sodium and fluid can be liberalized to 2-4 g and 2 L 40
41 CKD - Stage 5 Nutrition Intervention Fluid and Sodium PD based on ultrafiltration; kg fluid/day Fluid 2 L Sodium 2-4 g Fluid overload: shortness of breath, htn., CHF, edema 41
42 CKD - Stage 5 Nutrition Intervention Phosphorus Hyperphospatemia - GFR ml/min Dietary phosphorus restriction: mg/day, < 17 mg/kg body IBW See Table Phosphate binders; calcium salts Limit calcium intake 42
43 CKD - Stage 5 Nutrition Intervention Calcium requirements higher in CKD Restrict foods high in calcium Take supplements on empty stomach Limit to 2000 mg/day from all sources 43
44 CKD - Stage 5 Nutrition Intervention Vitamin Supplementation Water-soluble vitamins Daily requirements Table Renal vitamins include B 12, folic acid, vitamin C Avoid high doses of vitamins A & C May need vitamin K if on antibiotics 44
45 CKD - Stage 5 Nutrition Intervention Mineral supplementation Avoid Mg-containing phosphate binders, antacids, and supplements Iron Zinc 45
46 Comorbid Conditions - Nutrition Therapy Cardiovascular Disease - more likely to die from CVD than progress to Stage 4 CKD Heart failure, LVH, atherosclerosis Accelerated atherogenesis Other non-traditional risk factors Elevated CRP 46
47 Comorbid Conditions - Nutrition Therapy Secondary Hyperparathyroidism (SHPT) Can progress to severe, intractable forms of bone disease Prolonged PTH exposure osteitis fibrosa More prone to fracture Restrict dietary phosphorus Supplementation of vitamin D 47
48 Comorbid Conditions - Nutrition Therapy Anemia d/t low Hgb from inadequate endogenous erythropoietin Treatment with rhuepo and iron 48
49 Medicare Coverage for MNT Part B Medicare, renal disease dg of GFR ml/min or kidney transplant qualify Dialysis patients excluded 49
50 Post Transplant Nutrition therapy differs between: Acute phase up to 8 weeks Chronic phase after 9 weeks See Table for summary 50
51 Post Transplant Protein and Energy Increased for up to 6 8 weeks After 8 weeks: RDA for protein and low in saturated fat Carbohydrate Glucose intolerance common; insulin or OHA may be warranted Emphasize dietary fiber 51
52 Post Transplant Fat Low-fat diet Sodium Hypertension common; restrict sodium Potassium Potassium restriction in acute period 52
53 Post Transplant Immunosuppressants Used to prevent acute rejection Avoid grapefruit and grapefruit juice Cardiovascular Disease TLC Lipid-lowering agents Hypomagnesemia Supplementation of Mg to lower LDL and apolipoprotein B 53
54 Post Transplant Obesity Weight gain common; may complicate hyperlipidemia and glucose intolerance Emphasize diet, behavior modification, exercise 54
55 Post Transplant Calcium, Phosphorus, Altered Bone Metabolism Osteoporosis and altered vitamin D Hypercalcuria from corticosteroids Supplement with calcium, vitamin D, anti-resorptive agents Increase phosphorus Monitor serum potassium 55
56 Acute Renal Failure ARF - when kidneys suddenly stop functioning and abrupt cessation or reduction in GFR and accumulation of nitrogenous wastes occurs Stress or injury induced hypercatabolic state Status declines rapidly, loss in lean body mass, toxicity-related symptoms 56
57 Acute Renal Failure Clinical manifestations Fluid and electrolyte disorders, azotemia, wasting Electrolytes increases or decreases in potassium, Mg, phosphorus; monitor frequently BUN and creatinine elevated even if ratio is normal; maintain BUN mg/dl 57
58 Acute Renal Failure Treatment Treat underlying cause Nutrition therapy depends on type of dialysis or CRRT 58
59 Acute Renal Failure Nutrition Implications Trace Minerals and Vitamins May develop trace mineral toxicity Daily infusion not recommended Vitamins A, D, K and C may need to be adjusted Triglycerides May need lipid-free formula 59
60 Acute Renal Failure Nutrition Interventions Energy and protein May need enteral nutrition Protein.6 to 1.4 g/kg/d; essential and nonessential amino acids Kcal kcal/kg/d 60% CHO, 20-35% fat TPN > 5 days; g lipids as emulsion 60
61 Acute Renal Failure Nutrition Interventions Fluid status should be monitored Supplementation of minerals, electrolytes, and trace elements Monitor serum and urine levels Vitamin A not recommended Vitamin K recommended B 12 ; 10 mg pyridoxine Limit ascorbic acid to mg/d 61
62 Nephrolithiasis Kidney stones form when calcium, oxalate or uric acid in urine in higher than normal amounts Can become lodged in urinary tract and obstruct urine flow Typically consist of calcium salts, cystine, uric acid or struvite 62
63 Nephrolithiasis Risk factors: family hx, hypercalciuria, hyperuricosuria, hyperoxaluria and low urine volume Other causes: gout, excess intake of vitamin D, UTIs, and urinary tract blockages Asymptomatic until blockage occurs Acute pain, hematuria, nausea, vomiting, pain with urination, urgency to urinate 63
64 Nephrolithiasis Treatment/Nutrition Therapy Most can pass with plenty of fluid and pain medications Medical procedures if unable to pass ESWL most common Increase fluid intake by 3 L/day in divided doses Avoid calcium supplementation, dairy OK 64
65 Nephrolithiasis Treatment/Nutrition Therapy Limit oxalate intake to mg/d Avoid foods that increase urinary oxalate beets, chocolate, cola, coffee/tea, nuts, berries, wheat bran, spinach, rhubarb 65
RENAL FAILURE IN CHILDREN Dr. Mai Mohamed Elhassan Assistant Professor Jazan University
 RENAL FAILURE IN CHILDREN Dr. Mai Mohamed Elhassan Assistant Professor Jazan University OBJECTIVES By the end of this lecture each student should be able to: Define acute & chronic kidney disease(ckd)
RENAL FAILURE IN CHILDREN Dr. Mai Mohamed Elhassan Assistant Professor Jazan University OBJECTIVES By the end of this lecture each student should be able to: Define acute & chronic kidney disease(ckd)
HIHIM 409 7/26/2009. Kidney and Nephron. Fermamdo Vega, M.D. 1
 Function of the Kidneys Nephrology Fernando Vega, M.D. Seattle Healing Arts Center Remove Wastes Regulate Blood Pressure Regulate Blood Volume Regulates Electrolytes Converts Vitamin D to active form Produces
Function of the Kidneys Nephrology Fernando Vega, M.D. Seattle Healing Arts Center Remove Wastes Regulate Blood Pressure Regulate Blood Volume Regulates Electrolytes Converts Vitamin D to active form Produces
Kidneys and Homeostasis
 16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
Case Study: Chronic Kidney Disease
 Taylor Zwimpfer Joan Rupp Nutrition 409 23 September 2014 Case Study: Chronic Kidney Disease 1. Kidneys act to maintain the balance of fluids, electrolytes and organic solutes in the body through filtration
Taylor Zwimpfer Joan Rupp Nutrition 409 23 September 2014 Case Study: Chronic Kidney Disease 1. Kidneys act to maintain the balance of fluids, electrolytes and organic solutes in the body through filtration
Nephrology - the study of the kidney. Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system
 Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
End-Stage Renal Disease. Anna Vinnikova, M.D. Associate Professor of Medicine Division of Nephrology
 End-Stage Renal Disease Anna Vinnikova, M.D. Associate Professor of Medicine Division of Nephrology ESRD : Life with renal replacement therapy CASE: 18 month old male with HUS develops ESRD PD complicated
End-Stage Renal Disease Anna Vinnikova, M.D. Associate Professor of Medicine Division of Nephrology ESRD : Life with renal replacement therapy CASE: 18 month old male with HUS develops ESRD PD complicated
The Urinary System. BIOLOGY OF HUMANS Concepts, Applications, and Issues. Judith Goodenough Betty McGuire
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 16 The Urinary System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 16 The Urinary System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009
 The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009 Teresa Northcutt, RN BSN Primaris Program Manager, Prevention - CKD MO-09-01-CKD This material was prepared by Primaris,
The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009 Teresa Northcutt, RN BSN Primaris Program Manager, Prevention - CKD MO-09-01-CKD This material was prepared by Primaris,
The Urinary S. (Chp. 10) & Excretion. What are the functions of the urinary system? Maintenance of water-salt and acidbase
 10.1 Urinary system The Urinary S. (Chp. 10) & Excretion 10.1 Urinary system What are the functions of the urinary system? 1. Excretion of metabolic wastes (urea, uric acid & creatinine) 1. Maintenance
10.1 Urinary system The Urinary S. (Chp. 10) & Excretion 10.1 Urinary system What are the functions of the urinary system? 1. Excretion of metabolic wastes (urea, uric acid & creatinine) 1. Maintenance
Alterations of Renal and Urinary Tract Function
 Alterations of Renal and Urinary Tract Function Chapter 29 Urinary Tract Obstruction Urinary tract obstruction is an interference with the flow of urine at any site along the urinary tract The obstruction
Alterations of Renal and Urinary Tract Function Chapter 29 Urinary Tract Obstruction Urinary tract obstruction is an interference with the flow of urine at any site along the urinary tract The obstruction
network of thin-walled capillaries closely surrounded by a pear-shaped epithelial membrane called the Bowman s capsule
 Renal Terminology Renal-Root Words & Combining Forms calyx cortex glomerul/o medulla nephr/o pyel/o py/o ur/o ren/o cuplike division of the kidney outer layer of kidney glomerula inner or central portion
Renal Terminology Renal-Root Words & Combining Forms calyx cortex glomerul/o medulla nephr/o pyel/o py/o ur/o ren/o cuplike division of the kidney outer layer of kidney glomerula inner or central portion
Dr.Nahid Osman Ahmed 1
 1 ILOS By the end of the lecture you should be able to Identify : Functions of the kidney and nephrons Signs and symptoms of AKI Risk factors to AKI Treatment alternatives 2 Acute kidney injury (AKI),
1 ILOS By the end of the lecture you should be able to Identify : Functions of the kidney and nephrons Signs and symptoms of AKI Risk factors to AKI Treatment alternatives 2 Acute kidney injury (AKI),
NATIONAL KIDNEY MONTH
 NATIONAL KIDNEY MONTH According to the WebMD website, kidneys have several specific roles: Maintain your body s balance of water and concentration of minerals, such as sodium, potassium, magnesium and
NATIONAL KIDNEY MONTH According to the WebMD website, kidneys have several specific roles: Maintain your body s balance of water and concentration of minerals, such as sodium, potassium, magnesium and
Case Study: Renal Disease
 Case Study: Renal Disease Laboratory Values: Lab Units Patient Normal Source Interpretation GFR ml/min 46 above 90 Renal Lecture 2 BUN mg/dl 40 10-20 NTP A-90 Serum creatinine mg/dl 2.5 0.6-1.2 NTP A-90
Case Study: Renal Disease Laboratory Values: Lab Units Patient Normal Source Interpretation GFR ml/min 46 above 90 Renal Lecture 2 BUN mg/dl 40 10-20 NTP A-90 Serum creatinine mg/dl 2.5 0.6-1.2 NTP A-90
Understanding. Your Kidneys. Laurie Biel, RN,BSN, CNN The MGH Center For Renal Education March 28, 2016
 Understanding Your Kidneys Laurie Biel, RN,BSN, CNN The MGH Center For Renal Education March 28, 2016 Today s Discussion - The Role of your kidneys Common causes of kidney disease Treatment for kidney
Understanding Your Kidneys Laurie Biel, RN,BSN, CNN The MGH Center For Renal Education March 28, 2016 Today s Discussion - The Role of your kidneys Common causes of kidney disease Treatment for kidney
Urinary System. Analyze the Anatomy and Physiology of the urinary system
 Urinary System Analyze the Anatomy and Physiology of the urinary system Kidney Bean-shaped Located between peritoneum and the back muscles (retroperitoneal) Renal pelvis funnelshaped structure at the beginning
Urinary System Analyze the Anatomy and Physiology of the urinary system Kidney Bean-shaped Located between peritoneum and the back muscles (retroperitoneal) Renal pelvis funnelshaped structure at the beginning
TABLE OF CONTENTS T-1. A-1 Acronyms and Abbreviations. S-1 Stages of Chronic Kidney Disease (CKD)
 A-1 Acronyms and Abbreviations TABLE OF CONTENTS S-1 Stages of Chronic Kidney Disease (CKD) Chapter 1: Nutrition Assessment Charts, Tables and Formulas 1-2 Practical Steps to Nutrition Assessment Adult
A-1 Acronyms and Abbreviations TABLE OF CONTENTS S-1 Stages of Chronic Kidney Disease (CKD) Chapter 1: Nutrition Assessment Charts, Tables and Formulas 1-2 Practical Steps to Nutrition Assessment Adult
Final Case Study: Renal Disease Due 3/19/14 60 points
 NUT 116BL Name: CHRISTINE WOO Winter 2014 Section: 1 Final Case Study: Renal Disease Due 3/19/14 60 points Part I: Initial Presentation Present Illness: Jenny is a 19 yo F student referred to the renal
NUT 116BL Name: CHRISTINE WOO Winter 2014 Section: 1 Final Case Study: Renal Disease Due 3/19/14 60 points Part I: Initial Presentation Present Illness: Jenny is a 19 yo F student referred to the renal
EXCRETION QUESTIONS. Use the following information to answer the next two questions.
 EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
Chapter 12. Excretion and the Interaction of Systems
 Chapter 12 Excretion and the Interaction of Systems 1 2 Goals for This Chapter 1. Identify the main structures and functions of the human excretory system 2. Explain the function of the nephron 3. Describe
Chapter 12 Excretion and the Interaction of Systems 1 2 Goals for This Chapter 1. Identify the main structures and functions of the human excretory system 2. Explain the function of the nephron 3. Describe
Chronic Kidney Disease. Basics of CKD Terms Diagnosis Management
 Chronic Kidney Disease Basics of CKD Terms Diagnosis Management Review the prevalence of chronic kidney disease (CKD) Review how CKD develops Review populations at risk for CKD Review CKD diagnosis Objectives
Chronic Kidney Disease Basics of CKD Terms Diagnosis Management Review the prevalence of chronic kidney disease (CKD) Review how CKD develops Review populations at risk for CKD Review CKD diagnosis Objectives
Acute Kidney Injury (AKI)
 (Last Updated: 08/22/2018) Created by: Socco, Samantha Acute Kidney Injury (AKI) Thambi, M. (2017). Acute Kidney Injury. Lecture presented at PHAR 503 Lecture in UIC College of Pharmacy, Chicago. AKI This
(Last Updated: 08/22/2018) Created by: Socco, Samantha Acute Kidney Injury (AKI) Thambi, M. (2017). Acute Kidney Injury. Lecture presented at PHAR 503 Lecture in UIC College of Pharmacy, Chicago. AKI This
Exer Ex cise Pa P tien tien with End End stag sta e g renal Disease
 Exercise in Patients with End stage Exercise in Patients with End stage renal Disease Chronic renal failure : gradual and progressive loss of the ability of the kidneys to function Structural kidney damage
Exercise in Patients with End stage Exercise in Patients with End stage renal Disease Chronic renal failure : gradual and progressive loss of the ability of the kidneys to function Structural kidney damage
A. Correct! Flushing acids from the system will assist in re-establishing the acid-base equilibrium in the blood.
 OAT Biology - Problem Drill 16: The Urinary System Question No. 1 of 10 1. Which of the following would solve a drop in blood ph? Question #01 (A) Decreased retention of acids. (B) Increased excretion
OAT Biology - Problem Drill 16: The Urinary System Question No. 1 of 10 1. Which of the following would solve a drop in blood ph? Question #01 (A) Decreased retention of acids. (B) Increased excretion
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
CKD FOR INTERNISTS. Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College
 CKD FOR INTERNISTS Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College INTRODUCTION In 2002, the National Kidney Foundation s Kidney Disease Outcomes Quality Initiative(KDOQI)
CKD FOR INTERNISTS Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College INTRODUCTION In 2002, the National Kidney Foundation s Kidney Disease Outcomes Quality Initiative(KDOQI)
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Chapter 10: Urinary System & Excretion
 Chapter 10: Urinary System & Excretion Organs of Urinary System Kidneys (2) form urine Ureters (2) Carry urine from kidneys to bladder Bladder Stores urine Urethra Carries urine from bladder to outside
Chapter 10: Urinary System & Excretion Organs of Urinary System Kidneys (2) form urine Ureters (2) Carry urine from kidneys to bladder Bladder Stores urine Urethra Carries urine from bladder to outside
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
Nephron Function and Urine Formation. Ms. Kula December 1, 2014 Biology 30S
 Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
7. Dryness of the mouth from lack of normal secretions is called A. xerostomia. B. cheilosis. C. gingivitis. D. dysphagia.
 1. The term used to describe difficulty in swallowing is A. gag reflex. B. dysfunction. C. dysphagia. D. dysphoria. 2. An example of a meal that may cause an increase in symptoms for a patient with peptic
1. The term used to describe difficulty in swallowing is A. gag reflex. B. dysfunction. C. dysphagia. D. dysphoria. 2. An example of a meal that may cause an increase in symptoms for a patient with peptic
Filters 1600 L of blood/day Makes 180 L of ultrafiltrate Kidney contains 600,000 to 1.4 million nephrons
 Filters 1600 L of blood/day Makes 180 L of ultrafiltrate Kidney contains 600,000 to 1.4 million nephrons Filtered: Ammonia Protein Amino acids Creatinine Uric acid Electrolytes Some are then reabsorbed
Filters 1600 L of blood/day Makes 180 L of ultrafiltrate Kidney contains 600,000 to 1.4 million nephrons Filtered: Ammonia Protein Amino acids Creatinine Uric acid Electrolytes Some are then reabsorbed
Renal System and Excretion
 Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
HEALTHYSTART TRAINING MANUAL. Living well with Kidney Disease
 HEALTHYSTART TRAINING MANUAL Living well with Kidney Disease KIDNEY DISEASE CAN AFFECT ANYONE! 1 HEALTHYSTART PROGRAMME HEALTHYSTART is a lifestyle management programme to assist you to remain healthy
HEALTHYSTART TRAINING MANUAL Living well with Kidney Disease KIDNEY DISEASE CAN AFFECT ANYONE! 1 HEALTHYSTART PROGRAMME HEALTHYSTART is a lifestyle management programme to assist you to remain healthy
The UK Renal Registry collects national data about the causes and treatment of kidney failure.
 1 Kidney failure is a serious condition. Many kidney patients receive some form of renal replacement therapy (RRT) such as dialysis. The UK Renal Registry collects national data about the causes and treatment
1 Kidney failure is a serious condition. Many kidney patients receive some form of renal replacement therapy (RRT) such as dialysis. The UK Renal Registry collects national data about the causes and treatment
A&P of the Urinary System
 A&P of the Urinary System Week 44 1 Objectives Identify the organs of the urinary system, from a Identify the parts of the nephron (the functional unit List the characteristics of a normal urine specimen.
A&P of the Urinary System Week 44 1 Objectives Identify the organs of the urinary system, from a Identify the parts of the nephron (the functional unit List the characteristics of a normal urine specimen.
Excretory System. Biology 2201
 Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations ORGANS
Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations ORGANS
Excretory System. Excretory System
 Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations 1
Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations 1
EXCRETION IN HUMANS 31 JULY 2013
 EXCRETION IN HUMANS 31 JULY 2013 Lesson Description In this lesson we: Discuss organs of excretion Look at the structure of the urinary system Look at the structure and functioning of the kidney Discuss
EXCRETION IN HUMANS 31 JULY 2013 Lesson Description In this lesson we: Discuss organs of excretion Look at the structure of the urinary system Look at the structure and functioning of the kidney Discuss
Physio 12 -Summer 02 - Renal Physiology - Page 1
 Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
1. remove: waste products: urea, creatinine, and uric acid foreign chemicals: drugs, water soluble vitamins, and food additives, etc.
 Making Water! OR is it really Just Water Just Ask the Nephron!! Author: Patricia L. Ostlund ostlundp@faytechcc.edu (910) 678-9892 Fayetteville Technical Community College Fayetteville, NC 28303 Its just
Making Water! OR is it really Just Water Just Ask the Nephron!! Author: Patricia L. Ostlund ostlundp@faytechcc.edu (910) 678-9892 Fayetteville Technical Community College Fayetteville, NC 28303 Its just
Chronic Kidney Disease. Heidi Anderson Erica Bailey Anai Villalobos Katie Pearce
 Chronic Kidney Disease Heidi Anderson Erica Bailey Anai Villalobos Katie Pearce Anatomy of the Kidney 2 major parts: Cortex Medulla Functional Unit Nephrons Renal Pyramid Renal Pelvis Ureter Nephrons
Chronic Kidney Disease Heidi Anderson Erica Bailey Anai Villalobos Katie Pearce Anatomy of the Kidney 2 major parts: Cortex Medulla Functional Unit Nephrons Renal Pyramid Renal Pelvis Ureter Nephrons
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology
 Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
The Excretory System
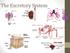 The Excretory System The excretory system The excretory system includes the skin, lungs and kidneys which all release metabolic wastes from the body. The kidneys, skin and the lungs are the principle organs
The Excretory System The excretory system The excretory system includes the skin, lungs and kidneys which all release metabolic wastes from the body. The kidneys, skin and the lungs are the principle organs
Chronic Kidney Disease (CKD) Stages. CHRONIC KIDNEY DISEASE Treatment Options. Incident counts & adjusted rates, by primary diagnosis Figure 2.
 Chronic Kidney Disease (CKD) Stages Stage 1 GFR > 90 (evidence of renal disease) Stage 2 GFR 60-89 Stage 3 GFR 30-59 Stage 4 GFR 15-29 Stage 5 GFR
Chronic Kidney Disease (CKD) Stages Stage 1 GFR > 90 (evidence of renal disease) Stage 2 GFR 60-89 Stage 3 GFR 30-59 Stage 4 GFR 15-29 Stage 5 GFR
A&P 2 CANALE T H E U R I N A R Y S Y S T E M
 A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
THE KIDNEY AND SLE LUPUS NEPHRITIS
 THE KIDNEY AND SLE LUPUS NEPHRITIS JACK WATERMAN DO FACOI 2013 NEPHROLOGY SIR RICHARD BRIGHT TERMINOLOGY RENAL INSUFFICIENCY CKD (CHRONIC KIDNEY DISEASE) ESRD (ENDSTAGE RENAL DISEASE) GLOMERULONEPHRITIS
THE KIDNEY AND SLE LUPUS NEPHRITIS JACK WATERMAN DO FACOI 2013 NEPHROLOGY SIR RICHARD BRIGHT TERMINOLOGY RENAL INSUFFICIENCY CKD (CHRONIC KIDNEY DISEASE) ESRD (ENDSTAGE RENAL DISEASE) GLOMERULONEPHRITIS
Pediatric Nutrition and Kidney Disease
 Pediatric Nutrition and Kidney Disease Loai Eid, MD, MSHS, FAAP Consultant Pediatric Nephrologist Pediatric Nephrology & Hypertension Division Chief Dubai Hospital - DHA 26 th October, 2017 Objectives
Pediatric Nutrition and Kidney Disease Loai Eid, MD, MSHS, FAAP Consultant Pediatric Nephrologist Pediatric Nephrology & Hypertension Division Chief Dubai Hospital - DHA 26 th October, 2017 Objectives
Renal Disease and PK/PD. Anjay Rastogi MD PhD Division of Nephrology
 Renal Disease and PK/PD Anjay Rastogi MD PhD Division of Nephrology Drugs and Kidneys Kidney is one of the major organ of drug elimination from the human body Renal disease and dialysis alters the pharmacokinetics
Renal Disease and PK/PD Anjay Rastogi MD PhD Division of Nephrology Drugs and Kidneys Kidney is one of the major organ of drug elimination from the human body Renal disease and dialysis alters the pharmacokinetics
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
WHY DO WE NEED AN EXCRETORY SYSTEM? Function: To eliminate waste To maintain water and salt balance To maintain blood pressure
 EXCRETORY SYSTEM WHY DO WE NEED AN EXCRETORY SYSTEM? Function: To eliminate waste To maintain water and salt balance To maintain blood pressure These wastes include: Carbon dioxide Mostly through breathing
EXCRETORY SYSTEM WHY DO WE NEED AN EXCRETORY SYSTEM? Function: To eliminate waste To maintain water and salt balance To maintain blood pressure These wastes include: Carbon dioxide Mostly through breathing
Non-protein nitrogenous substances (NPN)
 Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
April 08, biology 2201 ch 11.3 excretion.notebook. Biology The Excretory System. Apr 13 9:14 PM EXCRETORY SYSTEM.
 Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin
![KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin](/thumbs/87/96174332.jpg) Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Outline Urinary System
 Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
Morbidity & Mortality from Chronic Kidney Disease
 Morbidity & Mortality from Chronic Kidney Disease Dr. Lam Man-Fai ( 林萬斐醫生 ) Honorary Clinical Assistant Professor MBBS, MRCP, FHKCP, FHKAM, PDipID (HK), FRCP (Edin, Glasg) Hong Kong Renal Registry Report
Morbidity & Mortality from Chronic Kidney Disease Dr. Lam Man-Fai ( 林萬斐醫生 ) Honorary Clinical Assistant Professor MBBS, MRCP, FHKCP, FHKAM, PDipID (HK), FRCP (Edin, Glasg) Hong Kong Renal Registry Report
CCRN Review - Renal. CCRN Review - Renal 10/16/2014. CCRN Review Renal. Sodium Critical Value < 120 meq/l > 160 meq/l
 CCRN Review Renal Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Sodium 136-145 Critical Value < 120 meq/l > 160 meq/l Sodium Etiology
CCRN Review Renal Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Sodium 136-145 Critical Value < 120 meq/l > 160 meq/l Sodium Etiology
Guidelines for the Management of Nutrition
 S 42 Indian Journal of Nephrology Introduction Protein-energy malnutrition (PEM) is very common among patients with advanced chronic kidney disease (CKD). In the Indian scenario, where malnutrition is
S 42 Indian Journal of Nephrology Introduction Protein-energy malnutrition (PEM) is very common among patients with advanced chronic kidney disease (CKD). In the Indian scenario, where malnutrition is
Chapter 23. Composition and Properties of Urine
 Chapter 23 Composition and Properties of Urine Composition and Properties of Urine (1 of 2) urinalysis the examination of the physical and chemical properties of urine appearance - clear, almost colorless
Chapter 23 Composition and Properties of Urine Composition and Properties of Urine (1 of 2) urinalysis the examination of the physical and chemical properties of urine appearance - clear, almost colorless
Chapter 11 Lecture Outline
 Chapter 11 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. Permission required for reproduction
Chapter 11 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. Permission required for reproduction
Chronic kidney disease : The role of the Pharmacist
 Chronic kidney disease : The role of the Pharmacist Dr. Alladin-Karan (MBBS) Kidney Foundation of Guyana (KFG) Caribbean Association of Pharmacists Annual Convention Guyana Marriott Hotel 13 th August
Chronic kidney disease : The role of the Pharmacist Dr. Alladin-Karan (MBBS) Kidney Foundation of Guyana (KFG) Caribbean Association of Pharmacists Annual Convention Guyana Marriott Hotel 13 th August
1. Disorders of glomerular filtration
 RENAL DISEASES 1. Disorders of glomerular filtration 2. Nephrotic syndrome 3. Disorders of tubular transport 4. Oliguria and polyuria 5. Nephrolithiasis 6. Disturbances of renal blood flow 7. Acute renal
RENAL DISEASES 1. Disorders of glomerular filtration 2. Nephrotic syndrome 3. Disorders of tubular transport 4. Oliguria and polyuria 5. Nephrolithiasis 6. Disturbances of renal blood flow 7. Acute renal
Excretion Chapter 29. The Mammalian Excretory System consists of. The Kidney. The Nephron: the basic unit of the kidney.
 Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
Urinary System and Excretion. Bio105 Lecture 20 Chapter 16
 Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Case Study: Renal Disease
 Name: Melissa Hayes Case Study: Renal Disease Part I: Initial Presentation Chief Complaint: progressive anorexia with N/V, 5 kg weight gain in the past 10 days, edema, fatigue, worsening SOB with 2 pillow
Name: Melissa Hayes Case Study: Renal Disease Part I: Initial Presentation Chief Complaint: progressive anorexia with N/V, 5 kg weight gain in the past 10 days, edema, fatigue, worsening SOB with 2 pillow
Patient Description and Diagnosis: Sarah Jones is a 50-year-old female, 5 4, 131
 Julia Kaesberg Counseling Session KNH 413 February 27 th, 2014 Patient Description and Diagnosis: Sarah Jones is a 50-year-old female, 5 4, 131 pounds and her usual body weight is 125 pounds. Her %UBW
Julia Kaesberg Counseling Session KNH 413 February 27 th, 2014 Patient Description and Diagnosis: Sarah Jones is a 50-year-old female, 5 4, 131 pounds and her usual body weight is 125 pounds. Her %UBW
School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PLB SEMINAR
 1 School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PLB SEMINAR URINARY (RENAL) STONE FORMATION An Overview What are Urinary (Renal)
1 School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PLB SEMINAR URINARY (RENAL) STONE FORMATION An Overview What are Urinary (Renal)
Excretion and Water Balance
 Excretion and Water Balance 1. Osmoregulation (water balance) a. Most marine invertebrates are osmoconformers in which the concentration of solutes in their body fluid is equal to that of their environment.
Excretion and Water Balance 1. Osmoregulation (water balance) a. Most marine invertebrates are osmoconformers in which the concentration of solutes in their body fluid is equal to that of their environment.
Acute renal failure ARF
 Acute renal failure ARF Definition ARF is a clinical syndrome characterized by an abrupt decline in GFR and the accumulation of nitrogenous waste (BUN & creatinine). The decrease in GFR occurs relatively
Acute renal failure ARF Definition ARF is a clinical syndrome characterized by an abrupt decline in GFR and the accumulation of nitrogenous waste (BUN & creatinine). The decrease in GFR occurs relatively
Anatomy/Physiology Study Guide: Unit 9 Excretory System
 Anatomy/Physiology Study Guide: Unit 9 Excretory System 1) In the space below, list the primary structures (organs) and their corresponding functions. Structures: Functions: KIDNEY 1) URETER BLADDER URETHRA
Anatomy/Physiology Study Guide: Unit 9 Excretory System 1) In the space below, list the primary structures (organs) and their corresponding functions. Structures: Functions: KIDNEY 1) URETER BLADDER URETHRA
ONLINE HEMODIALYSIS TRAINING SESSION 1
 ONLINE HEMODIALYSIS TRAINING SESSION 1 This document is a supplement to the Online Training. Do not reproduce. Copyright Dialysis4Career. All Rights Reserved. The Renal System - A highly sophisticated
ONLINE HEMODIALYSIS TRAINING SESSION 1 This document is a supplement to the Online Training. Do not reproduce. Copyright Dialysis4Career. All Rights Reserved. The Renal System - A highly sophisticated
Stages of Chronic Kidney Disease (CKD)
 Early Treatment is the Key Stages of Chronic Kidney Disease (CKD) Stage Description GFR (ml/min/1.73 m 2 ) >90 1 Kidney damage with normal or GFR 2 Mild decrease in GFR 60-89 3 Moderate decrease in GFR
Early Treatment is the Key Stages of Chronic Kidney Disease (CKD) Stage Description GFR (ml/min/1.73 m 2 ) >90 1 Kidney damage with normal or GFR 2 Mild decrease in GFR 60-89 3 Moderate decrease in GFR
Chapter 13 The Urinary System
 Biology 12 Name: Urinary System Per: Date: Chapter 13 The Urinary System Complete using BC Biology 12, page 408-435 13.1 The Urinary System pages 412-413 1. As the kidneys produce urine, they carry out
Biology 12 Name: Urinary System Per: Date: Chapter 13 The Urinary System Complete using BC Biology 12, page 408-435 13.1 The Urinary System pages 412-413 1. As the kidneys produce urine, they carry out
CREATININE: is another nitrogenous waste. Creatinine comes from creatinine phosphate in muscle metabolism (a Phosphate-storage molecule)
 BIOLOGY 12 - EXCRETION: CHAPTER NOTES Your cells are constantly carrying out chemical reactions to maintain homeostasis. Many of these chemical reactions produce wastes that must be removed from cells
BIOLOGY 12 - EXCRETION: CHAPTER NOTES Your cells are constantly carrying out chemical reactions to maintain homeostasis. Many of these chemical reactions produce wastes that must be removed from cells
Chapter 16 Lecture Outline
 Chapter 16 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction
Chapter 16 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction
Lab Values Explained. working at full strength. Other possible causes of an elevated BUN include dehydration and heart failure.
 Patient Education Lab Values Explained Common Tests to Help Diagnose Kidney Disease Lab work, urine samples and other tests may be given as you undergo diagnosis and treatment for renal failure. The test
Patient Education Lab Values Explained Common Tests to Help Diagnose Kidney Disease Lab work, urine samples and other tests may be given as you undergo diagnosis and treatment for renal failure. The test
Macro- and Micronutrient Homeostasis in the Setting of Chronic Kidney Disease. T. Alp Ikizler, MD Vanderbilt University Medical Center
 Macro- and Micronutrient Homeostasis in the Setting of Chronic Kidney Disease T. Alp Ikizler, MD Vanderbilt University Medical Center Nutrition and Chronic Kidney Disease What is the disease itself and
Macro- and Micronutrient Homeostasis in the Setting of Chronic Kidney Disease T. Alp Ikizler, MD Vanderbilt University Medical Center Nutrition and Chronic Kidney Disease What is the disease itself and
* It is proportionate to body size and the reference value is usually expressed after correction for body surface area as 120 ± 25 ml/min/1.
 Ahmad Al-zoubi Glomerular filtration rate : is the sum of the ultrafiltration rates from plasma into the Bowman s space in each nephron and is a measure of renal excretory function *co : 6L *renal blood
Ahmad Al-zoubi Glomerular filtration rate : is the sum of the ultrafiltration rates from plasma into the Bowman s space in each nephron and is a measure of renal excretory function *co : 6L *renal blood
Urinary System BIO 250. Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat. Routes of Waste Elimination
 Urinary System BIO 250 Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat Routes of Waste Elimination Skin: Variable amounts of heat, salts, and water; small amounts of urea and
Urinary System BIO 250 Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat Routes of Waste Elimination Skin: Variable amounts of heat, salts, and water; small amounts of urea and
Urinary System. consists of the kidneys, ureters, urinary bladder and urethra
 Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Chronic Kidney Disease
 Chronic Kidney Disease Chronic Kidney Disease (CKD) Guideline (2010) Chronic Kidney Disease CKD: Executive Summary of Recommendations (2010) Executive Summary of Recommendations Below are the major recommendations
Chronic Kidney Disease Chronic Kidney Disease (CKD) Guideline (2010) Chronic Kidney Disease CKD: Executive Summary of Recommendations (2010) Executive Summary of Recommendations Below are the major recommendations
Renal Functions: Renal Functions: Renal Function: Produce Urine
 Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015
 RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
NUTRITION CONSIDERATIONS FOR PATIENTS WITH DIABETIC NEPHROPATHY
 NUTRITION CONSIDERATIONS FOR PATIENTS WITH DIABETIC NEPHROPATHY Becca Wallschlaeger, MS RDN CD Transplant Nutritionist University of Wisconsin Transplant Program Fall 2017 OBJECTIVES Recognize kidney disease
NUTRITION CONSIDERATIONS FOR PATIENTS WITH DIABETIC NEPHROPATHY Becca Wallschlaeger, MS RDN CD Transplant Nutritionist University of Wisconsin Transplant Program Fall 2017 OBJECTIVES Recognize kidney disease
Multiphasic Blood Analysis
 Understanding Your Multiphasic Blood Analysis Test Results Mon General thanks you for participating in the multiphasic blood analysis. This test can be an early warning of health problems, including coronary
Understanding Your Multiphasic Blood Analysis Test Results Mon General thanks you for participating in the multiphasic blood analysis. This test can be an early warning of health problems, including coronary
RENAL PHYSIOLOGY. Zekeriyya ALANOGLU, MD, DESA Ahmet Onat Bermede, MD, Ankara University School of Medicine Dept. Anesthesiology and ICM
 RENAL PHYSIOLOGY Zekeriyya ALANOGLU, MD, DESA Ahmet Onat Bermede, MD, Ankara University School of Medicine Dept. Anesthesiology and ICM Kidneys Stabilize the composition of the ECF (electrolyte, H
RENAL PHYSIOLOGY Zekeriyya ALANOGLU, MD, DESA Ahmet Onat Bermede, MD, Ankara University School of Medicine Dept. Anesthesiology and ICM Kidneys Stabilize the composition of the ECF (electrolyte, H
Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012
 Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012 Susan McKenna Renal Clinical Nurse Specialist Cavan General Hospital Renal patient population ACUTE RENAL FAILURE
Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012 Susan McKenna Renal Clinical Nurse Specialist Cavan General Hospital Renal patient population ACUTE RENAL FAILURE
Chronic Kidney Disease. Dr Mohan B. Biyani A. Professor of Medicine University of Ottawa/Ottawa Hospital
 Chronic Kidney Disease Dr Mohan B. Biyani A. Professor of Medicine University of Ottawa/Ottawa Hospital Health Seminar Series Date 12 May 2013 Objectives Normal functioning of Kidneys. Risk factors to
Chronic Kidney Disease Dr Mohan B. Biyani A. Professor of Medicine University of Ottawa/Ottawa Hospital Health Seminar Series Date 12 May 2013 Objectives Normal functioning of Kidneys. Risk factors to
A Review of Renal Diseases
 A Review of Renal Diseases NDFS 356 Amber McArthur April 3, 2014 0 INTRODUCITON Tom Harkin stated, America s health care system is in crisis precisely because we systematically neglect wellness and prevention.
A Review of Renal Diseases NDFS 356 Amber McArthur April 3, 2014 0 INTRODUCITON Tom Harkin stated, America s health care system is in crisis precisely because we systematically neglect wellness and prevention.
SUBJECT INDEX. Tvedegaard, E., 20. Ulerich, L., E1 (July) Wapensky, T., 45 Warner, J., 116 Warsaba, D., 52
 268 Supasyndh, O., 134 Suraci, C., 208 Tatangelo, P., 208 Tavares, I., 157 Tozzo, C., 208 Tvedegaard, E., 20 Ulerich, L., E1 (July) Wapensky, T., 45 Warner, J., 116 Warsaba, D., 52 Wells, L.M., 26 Winkler,
268 Supasyndh, O., 134 Suraci, C., 208 Tatangelo, P., 208 Tavares, I., 157 Tozzo, C., 208 Tvedegaard, E., 20 Ulerich, L., E1 (July) Wapensky, T., 45 Warner, J., 116 Warsaba, D., 52 Wells, L.M., 26 Winkler,
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
LLL Session - Nutritional support in renal disease
 ESPEN Congress Leipzig 2013 LLL Session - Nutritional support in renal disease Peritoneal dialysis D. Teta (CH) Nutrition Support in Patients undergoing Peritoneal Dialysis (PD) Congress ESPEN, Leipzig
ESPEN Congress Leipzig 2013 LLL Session - Nutritional support in renal disease Peritoneal dialysis D. Teta (CH) Nutrition Support in Patients undergoing Peritoneal Dialysis (PD) Congress ESPEN, Leipzig
Osmoregulation and Excretion
 Animal Life and Excretion Harder for multicellular organisms Internal circulation Coordination, information transfer Structural maintenance Movement Maintenance of homeostatic internal environment 15 July
Animal Life and Excretion Harder for multicellular organisms Internal circulation Coordination, information transfer Structural maintenance Movement Maintenance of homeostatic internal environment 15 July
ARE YOU AT INCREASED RISK FOR CHRONIC KIDNEY DISEASE?
 ARE YOU AT INCREASED RISK FOR CHRONIC KIDNEY DISEASE? www.kidney.org National Kidney Foundation s Kidney Disease Outcomes Quality Initiative Did you know that the National Kidney Foundation s Kidney Disease
ARE YOU AT INCREASED RISK FOR CHRONIC KIDNEY DISEASE? www.kidney.org National Kidney Foundation s Kidney Disease Outcomes Quality Initiative Did you know that the National Kidney Foundation s Kidney Disease
Excretory System 1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Nutrition Management in Renal Disease. Dr. Inge Permadhi MS., SpGK
 Nutrition Management in Renal Disease Dr. Inge Permadhi MS., SpGK Kidney functions Excretory of waste products (urea) and drugs Regulation to maintain homeostatic balance from fluids, electrolytes, and
Nutrition Management in Renal Disease Dr. Inge Permadhi MS., SpGK Kidney functions Excretory of waste products (urea) and drugs Regulation to maintain homeostatic balance from fluids, electrolytes, and
Chronic Kidney Disease
 Chronic Kidney Disease Presence of kidney damage or decreased kidney function for three or more months, - necessary to distinguish CKD from acute kidney disease. Ascertained either by kidney biopsy or
Chronic Kidney Disease Presence of kidney damage or decreased kidney function for three or more months, - necessary to distinguish CKD from acute kidney disease. Ascertained either by kidney biopsy or
NUT 116BL Name: Jeana Lim Section: A01 Winter 2013
 NUT 116BL Name: Jeana Lim Section: A01 Winter 2013 Case Study #3: Renal Disease 50 points 1. Please be concise and use only the space provided. 2. Please cite sources as necessary. 3. You may use your
NUT 116BL Name: Jeana Lim Section: A01 Winter 2013 Case Study #3: Renal Disease 50 points 1. Please be concise and use only the space provided. 2. Please cite sources as necessary. 3. You may use your
