VARIABLES THAT AFFECT TREATMENT DECISIONS STABILIZING THE MANDIBLE INTERMAXILLARY FIXATION WITH ARCH BARS IMMEDIATE REPAIR VERSUS DELAYED REPAIR
|
|
|
- Jeffery Lang
- 5 years ago
- Views:
Transcription
1 Mandible Fractures Chapter 26 MANDIBLE FRACTURES JEFFREY A. FAULKNER, MD, DDS* INTRODUCTION VARIABLES THAT AFFECT TREATMENT DECISIONS TREATMENT STABILIZING THE MANDIBLE INTERMAXILLARY FIXATION WITH ARCH BARS ANTIBIOTIC COVERAGE IMMEDIATE REPAIR VERSUS DELAYED REPAIR SUMMARY CASE PRESENTATIONS Case Study 26-1: Immediate Treatment Case Study 26-2: Delayed Treatment Case Study 26-3: Immediate Treatment *Colonel (Retired), Medical Corps, US Army; Physician, Otolaryngology, th Street, Floresville, Texas
2 Otolaryngology/Head and Neck Combat Casualty Care INTRODUCTION World War I saw the introduction of the first military medical unit devoted solely to maxillofacial surgery and plastic surgery. Dr Harold Gillies, an English otolaryngologist who volunteered for the Red Cross in France, established the unit and reported seeing more than 2,000 facial casualties on the first day of the Battle of the Somme. 1 5 In comparison, the total number of patients with facial injuries from Operation Iraqi Freedom (OIF) and Operation Enduring Freedom over an 8-year period was 7, In the face of such large numbers of casualties, it is inspiring that Dr Gillies and his team developed and documented innovations in the reconstruction of massive facial injuries. Those innovations were primarily in the area of bone grafting and skin flap reconstructions. In the same conflict, the American dentist Varistad Kazanjian advanced the management of facial fractures from conservative splinting techniques to simple wiring techniques. 7,8 Although wiring fractures is a more invasive technique than splinting, the value was recognized and eventually adopted as the standard of care for facial fractures until the advent of modern open reduction and internal fixation (ORIF) using titanium plates and screws or resorbable materials. Although the total volume of casualties has been lower in more recent conflicts, the percentage of casualties with head and neck injuries is increasing. This trend has been noted in urban conflicts, such as the Battle of the Black Sea, fought in the streets of Mogadishu, Somalia, in Contemporary articles document the increase in facial injuries as well. Owens et al 10 reported a 30% rate of head and neck wounds, whereas Belmont et al 11 showed a 36% rate of head and neck injuries. Perhaps the most definitive study of 10 years of war in Operation Enduring Freedom and OIF showed a 42% rate of craniomaxillofacial injury for those evacuated to a Role 4 center. 12 First reports concerning the best management of facial wounds and fractures at the beginning of OIF counseled against immediate treatment of most facial fractures in theater because of the risk of infection and complications (based on information from the Annual 2004 San Antonio Military Trauma Conference). A study conducted by Zapour and Moran, 13 published in 2005, supported that delayed treatment. Those recommendations for facial fractures were mostly anecdotal, and later studies showed that patients injured in combat have a lower rate of complications if their facial fractures can be repaired within a few days of injury A study of 3,000 facial fractures from World War II treated by the Number 4 Maxillofacial Surgery Unit in North Africa and Italy concluded that immediate treatment resulted in fewer complications. 17 A noncombat injury study conducted at the San Francisco General Hospital in 2002 concluded that a delay in treatment was associated with an increase in the technical difficulty of repair. 18 A study published in 2008 that evaluated gunshot wounds to the face in the American civilian community also recommended facial fracture repair within 48 hours unless the wound is complex with comminuted and avulsive bony injuries accompanied by avulsive soft-tissue injury. 19 Perhaps the study that is most reflective of the challenges of managing facial injuries incurred in combat comes from the Maxillofacial Unit of the Specialized Surgeries Hospital, Medical City, Baghdad, Unlike a current US Army Combat Support Hospital with a robust staff and logistical support, the more constrained resources in the hospitals of Central Baghdad during the early years of the war would dictate what treatments were possible, given local availability of supplies and personnel. In this study, the authors also recommend primary repair and closure within 24 hours. If primary closure is not feasible, then their recommendation is to pack the wounds open. Active treatment was undertaken in 74% of patients. Fifty-two percent of patients were treated with closed reduction and stabilization. This historical review is presented to provide a basic philosophical framework based on clinical research related to facial fractures caused by combat and noncombat ballistic injuries. Clinical research provides a guide to the surgeon faced with the daunting task of providing the earliest and best treatment to a patient with the complex injuries that occur in combat. Whether caused by combat or noncombat trauma, randomized controlled trials comparing repair within 12 to 24 hours with delayed repair do not exist. However, there are studies that demonstrate fewer complications with facial fracture repaired in the combat zone compared with reconstruction following the delays that accompany evacuation. With those studies in mind, and in consideration of patient comfort, greater safety in transport, and ease of patient management, early repair of mandible fractures should be the goal of the surgeon in combat. However, there are many factors that will impact the ability of the surgeon to provide a definitive repair within 48 hours (Figure 26-1).The following section describes nonclinical factors that may impact clinical decision-making when repairing a mandible under combat conditions. 330
3 Mandible Fractures Figure Concurrent operations in one operating room during Operation Iraqi Freedom (2006). VARIBLES THAT AFFECT TREATMENT DECISIONS Equipment, Personnel Availability, and Logistical Support In the initial stages of any armed conflict, there is a period of time where medical facilities are in transition. The rapid advancement of a Combat Support Hospital and the need for mobility will preclude any treatment beyond stabilization and evacuation. Even the larger evacuation hospitals will have a period of growth during which time the option for immediate definitive treatment is not advisable or possible. Brennan21 describes the evolution of the first deployed otolaryngology team in OIF and documents the decision-making that occurs during the mass casualty that resulted from the Second Battle of Fallujah in November Local personnel resources and supplies were also mentioned as a critical determinant of treatment options at the Specialized Surgeries Hospital, Medical City, Baghdad, These limitations can occur at any time during combat and require the surgeon to be adept at several techniques for managing fractures. Hospital Census and Air Evacuation Schedule During periods of high patient volume, there are often limitations to the availability of operating room suites or hospital beds. Delaying treatment in favor of stabilization and evacuation is preferable, as well as reserving operating room resources for those in the most critical condition. Surgeon Experience and Training Although the experience in a combat zone pushes the limits of one s capability, it is good to know your boundaries. When a case is beyond your surgical 331
4 Otolaryngology/Head and Neck Combat Casualty Care experience or capability, it is in the best interest of the patient to perform stabilization and evacuation. Patient Condition In recent armed conflicts, it is not uncommon for a patient to suffer multiple extremity injuries, which may include vascular compromise, traumatic amputations, and severe blood loss. Those injuries can lead to hypothermia, acidosis, and coagulopathy (commonly called the lethal triad). These patients are often too critically ill to sustain lengthy surgical procedures for reconstruction and are best treated by stabilization and evacuation. Patients with cerebral edema secondary to craniofacial trauma also require a period of convalescence prior to undertaking reconstructive surgery. TREATMENT Immediate combat life support management prioritizes the control of bleeding prior to addressing the airway. Injuries of the face complicate that recommendation because of the intimate association of the airway with the bleeding source and the difficulties associated with applying pressure to wounds that involve flail mandibular segments and lacerated oral and pharyngeal mucosae. Mandible fractures caused by ballistic injury are commonly associated with airway compromise. In a review of trauma at the Specialized Surgeries Hospital, Medical City, Baghdad, Kummoona et al 20 found that 86% of the cases requiring airway management had mandible fractures, and 59% of those needing airway management were injured with high-velocity missiles. As a result, intubation or cricothyrotomy may be required immediately, followed by control of hemorrhage and stabilization of the patient. Once stabilized, a decision must be made concerning the long-term airway management following treatment. Figure Actual Operation Enduring Freedom critical care airport transport team patient transition at Landstuhl Regional Medical Center occurring during a mock mass casualty exercise in Patient is transferred from a converted school bus to the ground outside the Landstuhl Regional Medical Center emergency department. 332
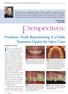
5 Mandible Fractures If the patient will be transported to higher levels of care with intermaxillary fixation (IMF) in place, in most cases that patient should have a tracheostomy. The primary reason for that recommendation is for safety and airway security during transport. The patient will make several transitions from vehicles to helicopters, airplanes, and buses during the evacuation process (Figure 26-2). There are many opportunities during those transfers for a nasotracheal tube to be dislodged. If that happens, the conditions for reintubation are at their worst with a compromised airway in a patient with wire fixation, a confined area, and low lighting. If a surgical airway was indicated to repair the facial fractures or if a cricothyrotomy was placed in the field, it is best to keep that airway until the patient has been evacuated out of the combat theater. Definitive control of bleeding is also best performed at the time of repair of the mandible fracture with meticulous dissection to find the bleeding source. This is often in combination with a neck exploration when the fracture results from a ballistic injury. STABILIZING THE MANDIBLE Even if immediate repair is not possible because of the clinical or nonclinical indicators, stabilization of the fractured mandible will immediately reduce the pain experienced by the patient and reduce the need for heavy sedation. A tracheotomy placed at the time of IMF will allow for removal of the endotracheal tube. This has many advantages for the patient. Once extubated, the patient will not require as much sedation. Without sedation, the cervical spine can be clinically cleared, and mental status can be better assessed. It also makes transportation easier on the patient and safer with regard to airway management. Techniques for stabilization of the mandible are discussed in the next section. INTERMAXILLARY FIXATION WITH ARCH BARS Erich arch bars are commonly used to achieve good IMF when adequate dentition is present. The arch bar is cut to span each arch from the most posterior tooth on each side. It is then wired into position typically capturing all teeth from the canine posteriorly. The fragments are aligned so that the teeth achieve their premorbid dentition, and then the upper and lower arch bars are wired together (Figure 26-3). This typically provides a stable reduction that simplifies the task of open reduction and internal fixation. It is not uncommon for IMF to be used as the definitive treatment for some fractures. 20 Ivy loops are also used for temporary fixation (Figure 26-4). Other methods of rapidly achieving IMF involve screws drilled into the maxilla and mandible with wire or rubber band fixation between them. This technique is also discussed in Case Study External fixators are also very useful for stabilization of comminuted fractures that do not lend themselves to immediate repair. The external fixator is less invasive than open reduction and internal fixation, and provides stabilization without further compromise to the vascular supply. 22 ANTIBIOTIC COVERAGE Studies of noncombat mandibular fractures indicate that 24 hours of postoperative antibiotic coverage is sufficient In a comprehensive review of combat injuries and head and neck infections, Petersen et al 26 recommend perioperative prophylaxis and postoperative coverage for 24 hours. The primary antibiotic recommendation is Cefazolin 2 grams every 8 hours preoperatively and for 24 hours following surgery. If the patient is beta-lactam allergic, then Clindamycin 600 mg IV can be given every 8 hours preoperatively and for 24 hours postoperatively. An alternative antibiotic is Ceftriaxone 1 gram every 12 hours preoperatively and for 24 hours postoperatively. IMMEDIATE REPAIR VERSUS DELAYED REPAIR There is no consensus regarding the optimal timing of repair for mandibular fractures. A literature review by Hermund et al 27 concluded that there was no strong evidence for either acute or delayed treatment of mandibular fractures to minimize healing complications. The review study was hampered by the fact that none of the reviewed studies were randomized, and only six studies included sufficient documentation to allow for statistical analysis. In addition, none of the studies included cases treated within 12 to 24 hours. A 5-year 333
6 Otolaryngology/Head and Neck Combat Casualty Care Figure Example of mandibulomaxillary fixation in a patient with a mandible fracture, missing teeth, and a significant premorbid malocclusion. Figure Ivy loops demonstrated on a manikin. 334 retrospective study by Furr et al,28 published in 2006, concluded that the lag time to repair did not influence the development of postoperative complications. There are many studies reviewing civilian trauma that recommend immediate repair with primary closure, if possible.23,29,30 A few recent studies demonstrate an increase in complications following repair of combatrelated facial fractures as the time-to-repair increases.15 Patients with large avulsive injuries of the mandible, especially with concurrent loss of soft-tissue coverage, should undergo immediate debridement and stabilization with delayed reconstruction.19 Combat injuries seen in the war zone are typically more complex than those seen at a Level I trauma center in the United States. The mandible fractures are typically comminuted or have a significant loss of the bony framework. The soft-tissue envelope is commonly lacerated by projectiles, thus compromising the vascular supply; frequently, the skin
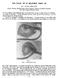
7 Mandible Fractures is burned. These factors complicate the decisionmaking concerning both the timing and the use of local flaps for reconstruction. In the acute setting, if primary repair cannot be accomplished, the bony fragments should at least be stabilized and softtissue coverage provided following debridement of the wound. If the wound is significantly contaminated or the skin is burned, performing a rotational flap to provide coverage may not be prudent. This is a judgment made by the surgeon based on the conditions of the wound. With high-velocity ballistic injury, the wound tends to worsen over the first few days. This evolution of the wound is because of the delayed effects of the transference of the kinetic energy (KE) of the projectile KE = 1/2Mass Velocity 2 to the surrounding tissues. It is perfectly acceptable to stage the reconstruction of these complex injuries. 22,31 SUMMARY The decision to repair mandibular fractures in the combat environment involves more environmental and logistical consideration than is typically required in a noncombat environment. 32 Immediate repair can be provided in theater if the patient s physiology permits and the operational tempo or transportation demands do not preclude taking the patient to the operating room. If bone grafting or a vascularized free flap will be required for reconstruction, those patients are best served by stabilization of the fractured segments, adequate soft-tissue coverage, and delayed reconstruction. CASE PRESENTATIONS Case Study 26-1: Immediate Treatment Presentation A 47-year-old male fell while running in Afghanistan, sustaining blunt trauma to the mandible. Preoperative Workup/Radiology On evaluation at Landstuhl Regional Medical Center, the patient was sedated and intubated with a nasotracheal tube. He was in IMF using four screws, had a diathesis between his lower incisors, and had a posterior crossbite. The patient was taken to the operating room. The lower IMF screws were removed and an arch bar placed. He was then put into a good class I occlusion, A CT (computerized tomography) scan was performed noting bilateral condylar fractures through the capsule and a symphysis fracture with lingual splaying of the mandible anteriorly and widening of the ramus segment (Figures 26-5 to 26-7). Operative Planning/Timing of Surgery On the day of injury, his C-spine was cleared clinically, and he was taken to the operating room at a Forward Surgical Hospital. Operation The patient was intubated with a nasotracheal tube and placed in IMF using screws placed in the right and left maxilla and mandible (Figure 26-8). The patient was placed on the protocol for ventilator-associated pneumonia, deep venous thrombosis prophylaxis (sequential compression devices, LOVENOX [Bridgewater, NJ], and a duplex scan), prophylactically treated with a proton pump inhibitor, and then transported sedated and intubated to Landstuhl Regional Medical Center. Figure CT (computed tomography) scan shows bilateral condylar fractures through the capsule. 335
8 Otolaryngology/Head and Neck Combat Casualty Care Figure Open lingual cortex by 1 to 2 mm translates to posterior cross-bite. Complications The patient required a second operation with general anesthesia. Lessons Learned Figure Symphysis fracture. taking care to close the anterior gap and correct the posterior cross-bite. Through an incision in the labial vestibule, the periosteum of the mandible was elevated to the inferior border and laterally to each first bicuspid. A mandible matrix, 6-hole locking titanium plate was secured across the reduced symphysis fracture with three screws on either side of the fracture. The incision was irrigated with bacitracin. The mentalis was resuspended with 3-0 chromic suture and the mucosal incision closed with a running 3-0 chromic suture. The IMF was released to check the occlusion. The occlusion was Class I. Without IMF, he had an anterior open bite consistent with the bilateral condylar fractures. He was left out of IMF for extubation and overnight due to concerns for his airway. The patient did well overnight and was placed in IMF with elastics the following day. At postoperative day 10, the patient had no open bite, a Class I occlusion, and an oral opening of 1.5 cm. He was placed on an aggressive oral physiotherapy regimen and achieved an oral opening of 40 mm in 2 weeks. At 6 weeks, the elastics were removed. At 12 weeks, there was no relapse. The arch bar and screws were removed in the clinic. A panorex showed good bony healing of the symphysis and a slight shortening of the right condyle. At 16 weeks, the patient reported normal occlusion without pain and was discharged from treatment. In this case, it would have been best to provide definitive treatment for the patient in-theater. The case took 30 minutes in the operating room and would have eliminated the risks of transporting a sedated Figure Rapid intermaxillary fixation using screws. Note the lever arm created by the extension of the screw laterally, potentially contributing to increased posterior crossbite, and opening of the lingual cortex in a mandible with bilateral condylar instability and a symphysis fracture. 336
9 Mandible Fractures patient with a nasotracheal intubation, an unstable mandible, and IMF. Immediate treatment would have obviated the need for ventilator-associated pneumonia prophylaxis and deep venous thrombosis prophylaxis, as well. In addition, the choice of IMF screws increased the displacement of the fractures causing the patient more pain and increasing the level of sedation required for transport. Case Study 26-2: Delayed Treatment Presentation A 22-year-old male was injured in an improvised explosive device blast in Iraq. He suffered third-degree burns over 64% of his body, including the head and neck (Figure 26-9). Preoperative Workup/Radiology A CT scan showed a comminuted fracture of the mandible with a bilateral condylar fracture, a fractured ulna, a fractured femur, and a penetrating wound to the abdomen (Figure 26-10). Operative Planning/Timing of Surgery The patient presented to the hospital at Balad sedated with a cricothyrotomy in place. He was immediately taken to the operating room for stabilization and debridement of his wounds. Once the life-threatening wounds were addressed, an otolaryngologist was consulted to evaluate his facial injuries. The patient was reasonably stable, but his facial burns had caused significant edema. With multiple injuries and 64% burns, this patient was scheduled for immediate transport to the burn unit at Brooke Army Medical Center (San Antonio, TX). It was concluded that it would be in his best interest to stabilize his injuries and prepare him for transport immediately rather than attempt a definitive repair immediately. Figure Patient on presentation with severe facial burns, lacerations, open fracture of the mandible, and a cricothyrotomy in position. was treated with open reduction and internal fixation of the mandibular symphysis, with a bone graft and bilateral costochondral grafts to the condyle and ramus. Six months later through a transcervical approach, an anterior sliding osteotomy was performed along with bilateral neck advancement flaps. Approximately 2 months later, he required excision of fistula tracts in Operation In the operating room, the patient s cricothyrotomy was converted to a formal tracheostomy, arch bars were placed, and IMF was obtained. His facial wounds were then debrided and closed. Following air evacuation to the continental United States, he was in IMF for 6 weeks because he was being treated for severe burn injuries, and receiving multiple escharotomies and split-thickness skin grafts. On evaluation for reconstruction of his mandible, he had bilateral temporomandibular joint ankylosis. He Figure CT (computed tomography) scan shows a severely comminuted anterior mandible. 337
10 Otolaryngology/Head and Neck Combat Casualty Care Figure Iraqi soldier on presentation with a severely comminuted open fracture of the mandible, fractures of the midface, and a left globe injury. the left submandibular region and removal of a broken wire. A month later, he required an additional excision of fistulas, removal of multiple teeth, and removal of the dental splint. One year later, he underwent contracture releases of the lower lip and eyelid with fullthickness skin grafts and debulking of a nasolabial flap. Complications Late complications included bilateral temporomandibular joint ankylosis, multiple fistulas, and infected hardware. Lessons Learned This case demonstrates the factors that influence immediate versus delayed treatment. Prolonged immobilization of a mandible that has sustained condylar and subcondylar trauma has a high risk for ankylosis because 338 Figure CT (computed tomography) scan shows one area of comminution of the mandible.
11 Mandible Fractures of the scarring within the temporomandibular joint or as a result of trauma to the coronoid process and zygoma, thus creating zygomaticocoronal ankylosis.33 It is very likely that if his mandibular fractures had been addressed immediately and he then underwent oral physiotherapy early, then he may not have suffered the complication of ankylosis. However, he was at a high risk for succumbing to the lethal triad, and it would have been inadvisable to undertake a long reconstructive surgery, including bone grafting from other donor sites under those conditions. Case Study 26-3: Immediate Treatment Presentation Figure Displaced segments of the mandible. An Iraqi soldier presented with injuries sustained by a blast from an improvised explosive device to the face, with multiple facial fractures and injuries throughout his body. Figure Intraoperative placement of the reconstruction bar through a transcervical incision. 339
12 Otolaryngology/Head and Neck Combat Casualty Care Preoperative Workup/Radiology A CT scan on arrival showed that the fragment caused a nasal fracture, left globe laceration, a comminuted mandible fracture, and multiple facial lacerations (Figures to 26-13). Operative Planning/Timing of Surgery The patient was taken immediately to the operating room. Operation Anesthesia was delivered through the cricothyrotomy. The first procedure was conversion of the cricothyrotomy to a tracheostomy. The ophthalmologist performed repair of the left globe laceration. Closed reduction of his nasal fracture was performed, and Doyle splints were sutured into position. The oral cavity was inspected. Multiple maxillary and mandibular teeth were extracted, and the oral cavity debrided of devitalized tissue. Erich arch bars were placed on the remaining teeth, and the patient was placed into IMF. The neck was prepped and draped, and a cervical incision was made 4 cm inferior to the border of the mandible. Dissection was carried through the platysma and the Hayes-Martin procedure performed to gain access to the inferior border of the mandible. The mandible was reconstructed with a 2.4 mm reconstruction bar, and the wound was irrigated and closed (Figures and 26-15). Arch bars were removed at the end of the case to allow normal function. The patient was put on a soft diet, recovered without incident, and was decanulated 1 week later. Figure Postoperative view of reconstruction. (For more details, see article by Güven O. Zygomaticocoronoid ankylosis: a rare clinical condition leading to limitation of mouth opening. J Craniofac Surg. 2012;23: ) 340
13 Mandible Fractures Complications None. Lessons Learned This case illustrates some of the indications for immediate treatment. The patient s physiology was stable, allowing immediate reconstructive surgery. The operating room tempo, although busy, did not preclude scheduling the 3-hour operation, and there was no advantage to delaying the procedures. Because the patient was Iraqi, evacuation out of theater was not an option, so delaying treatment would not benefit the hospital census and could potentially complicate the patient s recovery and healing. If this patient had been an American or other coalition soldier with the option of evacuation, the treatment plan would have been the same, while opting for immediate treatment unless there was a pressing logistical reason not to operate. Transporting a patient with this type of open wound would increase the risk of transport, subject the patient to more blood loss, and potentially increase the complication rate. REFERENCES 1. Chambers JA, Davis MR, Rasmussen TE. A band of surgeons, a long healing line: development of craniofacial surgery in response to armed conflict. J Craniofac Surg. 2010;21: Crumley R. Some pioneers in plastic surgery of facial region. Arch Facial Plast Surg. 2003;5: Rosdeutscher J. The history of otolaryngology in plastic surgery. Plast Reconstr Surg. 1969;111: Gillies H. The Principles and Art of Plastic Surgery. Boston, MA: Little Brown; Simpson D, David J. World War I: the genesis of craniomaxillofacial surgery? ANZ J Surg. 2004;74: Feldt B, Salinas N, Rasmussen T, Brennan J. The Joint Facial and Invasive Neck Trauma (J-FAINT) Project, Iraq and Afghanistan Otolaryngol Head Neck Surg. 2013;148: Hallock G. The plastic surgeon of the 20th century. Plast Reconstr Surg. 2001;107: Anonymous. Massachusetts General Hospital, Department of Plastic Surgery, Departments_and_Services/surgery/medical_professionals/surged/PlasticSurgery/AboutKazanjian.aspx. Accessed September 3, Mabry R, Holcomb J, Baker A, et al. United States Army rangers in Somalia: an analysis of combat casualties on an urban battlefield. J Trauma. 2000;49: Owens B, Kragh J, Wenke J, Macaitis J, Wade C, Holcomb J. Combat wounds in Operation Iraqi Freedom and Operation Enduring Freedom. J Trauma. 2008;64: Belmont P, Goodman G, Zacchilli M, Posner M, Evans C, Owens B. Incidence and epidemiology of combat injuries sustained during the surge portion of Operation Iraqi Freedom by a U.S. Army Brigade Combat Team. J Trauma. 2010;68: Chan R, Siller-Jackson A, Verrett A, Wu J, Hale R. Ten years of war: a characterization of craniomaxillofacial injuries incurred during Operations Enduring Freedom and Iraqi Freedom. J Trauma Acute Care Surg. 2012;73:S453 S Zapour MJ, Moran KA. Infectious diseases during wartime. Curr Opin Infect Dis. 2005;18: Lopez M, Arnholt J. Safety of definitive in-theater repair of facial fractures. Arch Facial Plast Surg. 2007;9: Salinas N, Faulkner J. Facial trauma in Operation Iraqi Freedom casualties: an outcomes study of patients treated from April 2006 through October J Craniofac Surg. 2010;21: Petersen K, Colyer M, Hayes D, Hale R, Bell R. Prevention of infections associated with combat-related eye, maxillofacial, and neck injuries. J Trauma. 2011;71:S264 S
14 Otolaryngology/Head and Neck Combat Casualty Care 17. Clarkson J, Kirkpatrick J, Lawrie R. Prevention by organization: the story of no. 4 maxillofacial surgical unit in North Africa and Italy during the Second World War. Plastic Reconstr Surg. 2008;121: Biller J, Pletcher S, Goldberg A, Murr A. Complications and the time to repair of mandible fractures. Laryngoscope. 2005;115: Kaufman Y, Cole P, Hollier L. Contemporary issues in facial gunshot wound management. J Craniofac Surg. 2008;19: Kummoona R, Muna A. Evaluation of immediate phase of management of missile injuries affecting maxillofacial region in Iraq. J Craniofac Surg. 2006;17: Brennan J. Experience of first deployed otolaryngology team in Operation Iraqi Freedom: the changing face of combat injuries. Otolaryngol Head Neck Surg. 2006;134: Maki M. Management outline of oral and maxillofacial missile injuries in Iraq: the value of the intermediate phase. J Craniofac Surg. 2009;20: Abubaker AO, Rollert MK. Postoperative antibiotic prophylaxis in mandibular fractures: a preliminary randomized, double-blind, and placebo-controlled clinical study. J Oral Maxillofac Surg. 2001;59: Chole RA, Yee J. Antibiotic prophylaxis for facial fractures. A prospective, randomized clinical trial. Arch Otolaryngol- Head Neck Surg. 1987;113: Andreasen JO, Jensen SS, Schwartz O, Hillerup Y. A systematic review of prophylactic antibiotics in the surgical treatment of maxillofacial fractures. J Oral Maxillofac Surg. 1987;64: Petersen K, Hayes D, Blice J, Hale R. Prevention and management of infections associated with combat-related head and neck injuries. J Trauma. 2008;64:S265 S Hermund N, Hillerup S, Kofod T, Schwartz O, Andreasen J. Effect of early or delayed treatment upon healing of mandibular fractures: a systematic literature review. Dent Traumatol. 2008;24: Furr A, Schweinfurth J, May W. Factors associated with long-term complications after repair of mandibular fractures. Laryngoscope. 2006;116: Ellis E III, Muniz O, Anand K. Treatment considerations for comminuted mandibular fractures. J Oral Maxillofac Surg. 2003;61: Peleg M, Sawatari Y. Management of gunshot wounds to the mandible. J Craniofac Surg. 2010;21: Doctor VS, Farwell DG. Gunshot wounds to the head and neck. Curr Opin Otolaryngol Head Neck Surg. 2007;15: Salinas N, Eller R, Davis M, Rasmussen T. Mass casualty response of a modern deployed head and neck surgical team. J Craniofac Surg. 2010;21: Güven O. Zygomaticocoronoid ankylosis: a rare clinical condition leading to limitation of mouth opening. J Craniofac Surg. 2012;23:
Head and Neck Trauma in Iraq and Afghanistan: Different War, Different Surgery, Lessons Learned
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. TRIOLOGICAL SOCIETY CANDIDATE THESIS Head and Neck Trauma in Iraq and Afghanistan: Different War, Different
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. TRIOLOGICAL SOCIETY CANDIDATE THESIS Head and Neck Trauma in Iraq and Afghanistan: Different War, Different
More than 43,000 US military personnel have been
 Original Research Facial Plastic and Reconstructive Surgery The Joint Facial and Invasive Neck Trauma (J-FAINT) Project, Iraq and Afghanistan 2003-2011 Otolaryngology Head and Neck Surgery 148(3) 403 408
Original Research Facial Plastic and Reconstructive Surgery The Joint Facial and Invasive Neck Trauma (J-FAINT) Project, Iraq and Afghanistan 2003-2011 Otolaryngology Head and Neck Surgery 148(3) 403 408
DEMOGRAPHICS OF HEAD AND NECK INJURIES IN IRAQ AND AFGHANISTAN
 Demographics of Head and Neck Injuries in Iraq and Afghanistan Chapter 6 DEMOGRAPHICS OF HEAD AND NECK INJURIES IN IRAQ AND AFGHANISTAN JOSEPH A BRENNAN, MD, FACS* INTRODUCTION GENERAL DEMOGRAPHICS PRETREATMENT
Demographics of Head and Neck Injuries in Iraq and Afghanistan Chapter 6 DEMOGRAPHICS OF HEAD AND NECK INJURIES IN IRAQ AND AFGHANISTAN JOSEPH A BRENNAN, MD, FACS* INTRODUCTION GENERAL DEMOGRAPHICS PRETREATMENT
Case Report. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System.
 Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
Bundeswehrkrankenhaus Ulm Abteilung HNO Kopf-Halschirurgie
 Kai Johannes Lorenz and Klaus Effinger Department of Otorhinolaryngology, Head and Neck Surgery Department of Radiology and interventional Radiology German Armed Forces Hospital Incidence of hemorrhage
Kai Johannes Lorenz and Klaus Effinger Department of Otorhinolaryngology, Head and Neck Surgery Department of Radiology and interventional Radiology German Armed Forces Hospital Incidence of hemorrhage
MEDICAL CODING FOR FACIAL INJURIES & RECONSTRUCTION
 MEDICAL CODING FOR FACIAL INJURIES & RECONSTRUCTION Tirbod Fattahi, MD, DDS, FACS Chief & Associate Professor Division of Oral & Maxillofacial Surgery University of Florida Health Science Center, Jacksonville
MEDICAL CODING FOR FACIAL INJURIES & RECONSTRUCTION Tirbod Fattahi, MD, DDS, FACS Chief & Associate Professor Division of Oral & Maxillofacial Surgery University of Florida Health Science Center, Jacksonville
Oral and Maxillofacial Surgeons and the seriously injured patient. Barts and The London NHS Trust
 Oral and Maxillofacial Surgeons and the seriously injured patient Barts and The London NHS Trust How do you assess this? Primary Survey A B C D E Airway & Cervical Spine Breathing & Ventilation Circulation
Oral and Maxillofacial Surgeons and the seriously injured patient Barts and The London NHS Trust How do you assess this? Primary Survey A B C D E Airway & Cervical Spine Breathing & Ventilation Circulation
PARANASAL SINUS FRACTURES
 Paranasal Sinus Fractures Chapter 23 PARANASAL SINUS FRACTURES MARK GIBBONS, MD, FACS,* and NATHAN SALINAS, MD INTRODUCTION ANATOMY DIAGNOSIS: CLINICAL AND IMAGING STUDIES MANAGEMENT ISSUES AND ALGORITHM
Paranasal Sinus Fractures Chapter 23 PARANASAL SINUS FRACTURES MARK GIBBONS, MD, FACS,* and NATHAN SALINAS, MD INTRODUCTION ANATOMY DIAGNOSIS: CLINICAL AND IMAGING STUDIES MANAGEMENT ISSUES AND ALGORITHM
Outcomes of Internal Fixation in a Combat Environment. Consistent with previous conflicts, the vast majority
 Outcomes of Internal Fixation in a Combat Environment CPT Daniel J. Stinner, MD, 1 Lt Col James A. Keeney, MD, 2 MAJ(P) Joseph R. Hsu, MD, 1 CPT Jeremy K. Rush, MD, 3 MAJ Mickey S. Cho, MD, 3 Joseph C.
Outcomes of Internal Fixation in a Combat Environment CPT Daniel J. Stinner, MD, 1 Lt Col James A. Keeney, MD, 2 MAJ(P) Joseph R. Hsu, MD, 1 CPT Jeremy K. Rush, MD, 3 MAJ Mickey S. Cho, MD, 3 Joseph C.
Craniomaxillofacial Battle Injuries: Injury Patterns, Conventional Treatment Limitations and Direction of Future Research
 Review Article Craniomaxillofacial Battle Injuries: Injury Patterns, Conventional Treatment Limitations and Direction of Future Research Robert G Hale, 1 Timothy Lew 2 and Joseph C Wenke 3 1 Craniomaxillofacial
Review Article Craniomaxillofacial Battle Injuries: Injury Patterns, Conventional Treatment Limitations and Direction of Future Research Robert G Hale, 1 Timothy Lew 2 and Joseph C Wenke 3 1 Craniomaxillofacial
ISPUB.COM. GSW To The Face: "Hunting Camp" C Perry, B Phillips CASE REPORT
 ISPUB.COM The Internet Journal of Rescue and Disaster Medicine Volume 2 Number 2 C Perry, B Phillips Citation C Perry, B Phillips.. The Internet Journal of Rescue and Disaster Medicine. 2000 Volume 2 Number
ISPUB.COM The Internet Journal of Rescue and Disaster Medicine Volume 2 Number 2 C Perry, B Phillips Citation C Perry, B Phillips.. The Internet Journal of Rescue and Disaster Medicine. 2000 Volume 2 Number
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery FACIAL FRACTURES
 Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Mandible Fractures May 2004
 TITLE: Mandible Fractures SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: May 26, 2004 RESIDENT PHYSICIAN: Jacques Peltier, MD FACULTY ADVISOR: Matthew W. Ryan, MD SERIES EDITORS:
TITLE: Mandible Fractures SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: May 26, 2004 RESIDENT PHYSICIAN: Jacques Peltier, MD FACULTY ADVISOR: Matthew W. Ryan, MD SERIES EDITORS:
Surgical technique. IMF Screw Set. For temporary, peri opera tive stabilisation of the occlusion in adults.
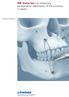 Surgical technique IMF Screw Set. For temporary, peri opera tive stabilisation of the occlusion in adults. Table of contents Features and benefits 2 Indications and contraindications 3 Surgical technique
Surgical technique IMF Screw Set. For temporary, peri opera tive stabilisation of the occlusion in adults. Table of contents Features and benefits 2 Indications and contraindications 3 Surgical technique
Technique Guide. IMF Screw Set. For intermaxillary fixation.
 Technique Guide IMF Screw Set. For intermaxillary fixation. Table of Contents Introduction IMF Screw Set 2 Indications and Contraindications 3 Surgical Technique Preparation 4 Insert IMF Screw 6 Insert
Technique Guide IMF Screw Set. For intermaxillary fixation. Table of Contents Introduction IMF Screw Set 2 Indications and Contraindications 3 Surgical Technique Preparation 4 Insert IMF Screw 6 Insert
TRAUMA TO THE FACE AND MOUTH
 Dr.Yahya A. Ali 3/10/2012 F.I.C.M.S TRAUMA TO THE FACE AND MOUTH Bailey & Love s 25 th edition Injuries to the orofacial region are common, but the majority are relatively minor in nature. A few are major
Dr.Yahya A. Ali 3/10/2012 F.I.C.M.S TRAUMA TO THE FACE AND MOUTH Bailey & Love s 25 th edition Injuries to the orofacial region are common, but the majority are relatively minor in nature. A few are major
A Novel Technology for Maxillomandibular Fixation: Universal SMARTLock Hybrid MMF
 A Novel Technology for Maxillomandibular Fixation: Universal SMARTLock Hybrid MMF INTRODUCTION Maxillomandibular Fixation (MMF) is a critical step in the management of facial trauma and reconstruction.
A Novel Technology for Maxillomandibular Fixation: Universal SMARTLock Hybrid MMF INTRODUCTION Maxillomandibular Fixation (MMF) is a critical step in the management of facial trauma and reconstruction.
Departement of Stomatology, The Second Hospital of Lanzhou University, 82 Cuiyingmwen, Chengguan District, Lanzhou City, Gansu Province, China
 European Review for Medical and Pharmacological Sciences Comparative evaluation of 2.0 mm locking plate system vs 2.0 mm non-locking plate system for mandibular angle fracture fixation: a prospective randomized
European Review for Medical and Pharmacological Sciences Comparative evaluation of 2.0 mm locking plate system vs 2.0 mm non-locking plate system for mandibular angle fracture fixation: a prospective randomized
MASS CASUALTIES AND TRIAGE
 Mass Casualties and Triage Chapter 15 MASS CASUALTIES AND TRIAGE JOSEPH A. BRENNAN, MD, FACS* INTRODUCTION PATTERN OF HEAD AND NECK INJURIES DURING MASS CASUALTIES MASS CASUALTY EVACUATIONS INCIDENCE OF
Mass Casualties and Triage Chapter 15 MASS CASUALTIES AND TRIAGE JOSEPH A. BRENNAN, MD, FACS* INTRODUCTION PATTERN OF HEAD AND NECK INJURIES DURING MASS CASUALTIES MASS CASUALTY EVACUATIONS INCIDENCE OF
King's College Hospital Dental School, London, S.E. 5.
 OSTECTOMY AT THE MANDIBULAR SYMPHYSIS J. H. SOWRAY, B.D.S., F.D.S.R.C.S. (Eng.), L.R.C.P., M.R.C.S. and R. HASKELL, M.B., B.S., F.D.S.R.C.S. (Eng.). King's College Hospital Dental School, London, S.E.
OSTECTOMY AT THE MANDIBULAR SYMPHYSIS J. H. SOWRAY, B.D.S., F.D.S.R.C.S. (Eng.), L.R.C.P., M.R.C.S. and R. HASKELL, M.B., B.S., F.D.S.R.C.S. (Eng.). King's College Hospital Dental School, London, S.E.
Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap.
 Case Report Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF, Patient Specific Plate Contouring (PSPC) and the MatrixMANDIBLE Plating
Case Report Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF, Patient Specific Plate Contouring (PSPC) and the MatrixMANDIBLE Plating
ROTATIONAL PILON FRACTURES
 CHAPTER 31 ROTATIONAL PILON FRACTURES George S. Gumann, DPM The opinions and commentary of the author should not be construed as refl ecting offi cial U.S. Army Medical Department policy. Pilon injuries
CHAPTER 31 ROTATIONAL PILON FRACTURES George S. Gumann, DPM The opinions and commentary of the author should not be construed as refl ecting offi cial U.S. Army Medical Department policy. Pilon injuries
Mandible fracture - Management. Dr Dinesh Kumar Verma OMFS SDCRI, SGNR
 Mandible fracture - Management Dr Dinesh Kumar Verma OMFS SDCRI, SGNR MANAGEMENT OPEN! CLOSE! DIRECT! INDIRECT! IMMEDIATE (PRIMARY) 1. ABC 2. Temporary stabilization 3. Tetanus prophylaxis 4. Antibiotics
Mandible fracture - Management Dr Dinesh Kumar Verma OMFS SDCRI, SGNR MANAGEMENT OPEN! CLOSE! DIRECT! INDIRECT! IMMEDIATE (PRIMARY) 1. ABC 2. Temporary stabilization 3. Tetanus prophylaxis 4. Antibiotics
Damage Control in Abdominal and Pelvic Injuries
 Damage Control in Abdominal and Pelvic Injuries Raul Coimbra, MD, PhD, FACS The Monroe E. Trout Professor of Surgery Surgeon-in Chief UCSD Medical Center Hillcrest Campus Executive Vice-Chairman Department
Damage Control in Abdominal and Pelvic Injuries Raul Coimbra, MD, PhD, FACS The Monroe E. Trout Professor of Surgery Surgeon-in Chief UCSD Medical Center Hillcrest Campus Executive Vice-Chairman Department
Use of Modified Retro-mandibular subparotid approach for treatment of Condylar fracture: a Technical note
 Original article: Use of Modified Retro-mandibular subparotid approach for treatment of Condylar fracture: a Technical note 1 DR.Sonal Anchlia, 2 DR.BIPIN.S.SADHWANI, 3 DR.ROHIT KUMAR, 4 Dr.Vipul 1Assistant
Original article: Use of Modified Retro-mandibular subparotid approach for treatment of Condylar fracture: a Technical note 1 DR.Sonal Anchlia, 2 DR.BIPIN.S.SADHWANI, 3 DR.ROHIT KUMAR, 4 Dr.Vipul 1Assistant
IMF Screw Set. For temporary, peri opera tive stabilisation of the occlusion in adults.
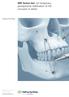 IMF Screw Set. For temporary, peri opera tive stabilisation of the occlusion in adults. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved
IMF Screw Set. For temporary, peri opera tive stabilisation of the occlusion in adults. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved
Property Latmedical, LLC.
 Dr. Goed provides a complete and innovate product portfolio solution to the growing healthcare need within the field of non-invasive orthopedics, sports medicine, bandaging, wound care and compression
Dr. Goed provides a complete and innovate product portfolio solution to the growing healthcare need within the field of non-invasive orthopedics, sports medicine, bandaging, wound care and compression
The resident will be assigned to be on call with the Oral and Maxillofacial service. Call will be set according to PARO guidelines.
 Goals and Objectives for the Otolaryngology-Head & Neck Resident on the Oral and Maxillofacial Surgery (OMFS) Rotation St. Catharines General Hospital (1 four-week rotational block) During the second year
Goals and Objectives for the Otolaryngology-Head & Neck Resident on the Oral and Maxillofacial Surgery (OMFS) Rotation St. Catharines General Hospital (1 four-week rotational block) During the second year
North Oaks Trauma Symposium Friday, November 3, 2017
 + Evaluation and Management of Facial Trauma D Antoni Dennis, MD North Oaks ENT an Allergy November 3, 2017 + Financial Disclosure I do not have any conflicts of interest or financial interest to disclose
+ Evaluation and Management of Facial Trauma D Antoni Dennis, MD North Oaks ENT an Allergy November 3, 2017 + Financial Disclosure I do not have any conflicts of interest or financial interest to disclose
Mandibular Fractures June 2000
 TITLE: Mandibular Fractures DATE: June 14, 2000 RESIDENT PHYSICIAN: Karen L. Stierman, M.D. FACULTY ADVISOR: Byron J. Bailey, M.D., FACS SERIES EDITOR: Francis B. Quinn, Jr., M.D. FACS ARCHIVIST: Melinda
TITLE: Mandibular Fractures DATE: June 14, 2000 RESIDENT PHYSICIAN: Karen L. Stierman, M.D. FACULTY ADVISOR: Byron J. Bailey, M.D., FACS SERIES EDITOR: Francis B. Quinn, Jr., M.D. FACS ARCHIVIST: Melinda
Three Dimensional Titanium Mini Plates in Management of Mandibular Fractures
 Biomedical & Pharmacology Journal Vol. 7(1), 241-246 (2014) Three Dimensional Titanium Mini Plates in Management of Mandibular Fractures R. BALAKRISHNAN, VIJAY EBENEZER and ABU DAKIR Department of Oral
Biomedical & Pharmacology Journal Vol. 7(1), 241-246 (2014) Three Dimensional Titanium Mini Plates in Management of Mandibular Fractures R. BALAKRISHNAN, VIJAY EBENEZER and ABU DAKIR Department of Oral
PRE-OP and POST-OP SURGICAL CONSIDERATIONS
 PRE-OP and POST-OP SURGICAL CONSIDERATIONS Darlene Sorrell, DMD, is not an oral surgeon. AIDC is an out-patient facility. 29 years of experience in IHS. Advanced General Practice Residency. No access
PRE-OP and POST-OP SURGICAL CONSIDERATIONS Darlene Sorrell, DMD, is not an oral surgeon. AIDC is an out-patient facility. 29 years of experience in IHS. Advanced General Practice Residency. No access
THE pedicled flap, commonly used by the plastic surgeon in the reconstruction
 THE PEDICLE!) SKIN FLAP ROBIN ANDERSON, M.D. Department of Plastic Surgery THE pedicled flap, commonly used by the plastic surgeon in the reconstruction of skin and soft tissue defects, differs from the
THE PEDICLE!) SKIN FLAP ROBIN ANDERSON, M.D. Department of Plastic Surgery THE pedicled flap, commonly used by the plastic surgeon in the reconstruction of skin and soft tissue defects, differs from the
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #1 Facial Trauma
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #1 Facial Trauma The face is vital to human appearance and function. Facial injuries can impair a patient
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #1 Facial Trauma The face is vital to human appearance and function. Facial injuries can impair a patient
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/31632 holds various files of this Leiden University dissertation. Author: Mensink, Gertjan Title: Bilateral sagittal split osteotomy by the splitter-separator
Cover Page The handle http://hdl.handle.net/1887/31632 holds various files of this Leiden University dissertation. Author: Mensink, Gertjan Title: Bilateral sagittal split osteotomy by the splitter-separator
Oral & Maxillofacial Surgery
 Chapter 2 Oral & Maxillofacial Surgery Ruchi Singhal 1 ; Virendra Singh 2 ; Amrish Bhagol* 1 Jaipur Dental College, Jaipur, India 2 Senior Professor, PGIDS, Rohtak, India Amrish Bhagol Condylar Fractures
Chapter 2 Oral & Maxillofacial Surgery Ruchi Singhal 1 ; Virendra Singh 2 ; Amrish Bhagol* 1 Jaipur Dental College, Jaipur, India 2 Senior Professor, PGIDS, Rohtak, India Amrish Bhagol Condylar Fractures
Clinical Study Open Reduction of Subcondylar Fractures Using a New Retractor
 Plastic Surgery International Volume 2011, Article ID 421245, 5 pages doi:10.1155/2011/421245 Clinical Study Open Reduction of Subcondylar Fractures Using a New Retractor Akira Sugamata, 1 Naoki Yoshizawa,
Plastic Surgery International Volume 2011, Article ID 421245, 5 pages doi:10.1155/2011/421245 Clinical Study Open Reduction of Subcondylar Fractures Using a New Retractor Akira Sugamata, 1 Naoki Yoshizawa,
Maxillofacial and Ocular Injuries
 Maxillofacial and Ocular Injuries Objectives At the conclusion of this presentation the participant will be able to: Identify the key anatomical structures of the face and eye and the impact of force on
Maxillofacial and Ocular Injuries Objectives At the conclusion of this presentation the participant will be able to: Identify the key anatomical structures of the face and eye and the impact of force on
Amputations. Chapter 23
 Amputations Chapter 23 Amputations Introduction Battle casualties who sustain amputations have the most severe extremity injuries. Historically, 1 in 3 patients with a major amputation (proximal to the
Amputations Chapter 23 Amputations Introduction Battle casualties who sustain amputations have the most severe extremity injuries. Historically, 1 in 3 patients with a major amputation (proximal to the
EVOS MINI with IM Nailing
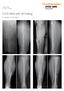 Case Series Dr. John A. Scolaro EVOS MINI with IM Nailing A series of studies Introduction Intramedullary nailing has become the standard for many long bone fractures. Fracture reduction prior to nail
Case Series Dr. John A. Scolaro EVOS MINI with IM Nailing A series of studies Introduction Intramedullary nailing has become the standard for many long bone fractures. Fracture reduction prior to nail
ALTERNATE OCCLUSAL SCHEMES
 ALTERNATE OCCLUSAL SCHEMES The same basic concepts need to be applied to all occlusal schemes. Some challenges include missing teeth, transposed teeth, crossbites, and anterior open bites. POSTERIOR CROSSBITES
ALTERNATE OCCLUSAL SCHEMES The same basic concepts need to be applied to all occlusal schemes. Some challenges include missing teeth, transposed teeth, crossbites, and anterior open bites. POSTERIOR CROSSBITES
BUILDING A. Achieving total reconstruction in a single operation. 70 OCTOBER 2016 // dentaltown.com
 BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
COMPLEX HEAD AND NECK RECONSTRUCTION IN THEATER
 Complex Head and Neck Reconstruction in Theater Chapter 27 COMPLEX HEAD AND NECK RECONSTRUCTION IN THEATER CHRISTOPHER KLEM, MD, FACS* INTRODUCTION TYPES OF WOUNDS MANAGEMENT OF SMALL WOUNDS RECONSTRUCTIVE
Complex Head and Neck Reconstruction in Theater Chapter 27 COMPLEX HEAD AND NECK RECONSTRUCTION IN THEATER CHRISTOPHER KLEM, MD, FACS* INTRODUCTION TYPES OF WOUNDS MANAGEMENT OF SMALL WOUNDS RECONSTRUCTIVE
MAXILLOFACIAL TRAUMATOLOGY Department of Maxillofacial Surgery Semmelweis University, Budapest. Dr. Huszár Tamás
 MAXILLOFACIAL TRAUMATOLOGY Department of Maxillofacial Surgery Semmelweis University, Budapest Dr. Huszár Tamás Maxillofacial injuries isolated maxillofacial injury multiple injuries polytrauma (injury
MAXILLOFACIAL TRAUMATOLOGY Department of Maxillofacial Surgery Semmelweis University, Budapest Dr. Huszár Tamás Maxillofacial injuries isolated maxillofacial injury multiple injuries polytrauma (injury
No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture
 CALCANEUS FRACTURES No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture lecture series INCIDENCE 2% of all fractures
CALCANEUS FRACTURES No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture lecture series INCIDENCE 2% of all fractures
I. Introduction CASE REPORT
 CASE REPORT http://dx.doi.org/10.5125/jkaoms.2014.40.3.135 pissn 2234-7550 eissn 2234-5930 Treatment of extensive comminuted mandibular fracture between both mandibular angles with bilateral condylar fractures
CASE REPORT http://dx.doi.org/10.5125/jkaoms.2014.40.3.135 pissn 2234-7550 eissn 2234-5930 Treatment of extensive comminuted mandibular fracture between both mandibular angles with bilateral condylar fractures
SURGICAL TREATMENT OF MANDIBULAR ASYMMETRY By MARIAN GORSKI, M.D., 1 and IRENA HALINA TARCZYNSKA, M.D. Maxillo-Facial Clinic, Warsaw Medical Academy
 SURGICL TRETMENT OF MNDIULR SYMMETRY y MRIN GORSKI, M.D., 1 and IREN HLIN TRCZYNSK, M.D. Maxillo-Facial Clinic, Warsaw Medical cademy UNILTERL mandibular deformities may be due to either overgrowth or
SURGICL TRETMENT OF MNDIULR SYMMETRY y MRIN GORSKI, M.D., 1 and IREN HLIN TRCZYNSK, M.D. Maxillo-Facial Clinic, Warsaw Medical cademy UNILTERL mandibular deformities may be due to either overgrowth or
The treatment of malocclusion after open reduction of maxillofacial fracture: a report of three cases
 CASE REPORT http://dx.doi.org/10.5125/jkaoms..40.2.91 pissn 2234-7550 eissn 2234-5930 The treatment of malocclusion after open reduction of maxillofacial fracture: a report of three cases Sung-Suk Lee,
CASE REPORT http://dx.doi.org/10.5125/jkaoms..40.2.91 pissn 2234-7550 eissn 2234-5930 The treatment of malocclusion after open reduction of maxillofacial fracture: a report of three cases Sung-Suk Lee,
Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience
 80 Original Article THIEME Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience V. Velho 1 Hrushikesh U. Kharosekar 1 Jasmeet S. Thukral 1 Shonali Valsangkar
80 Original Article THIEME Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience V. Velho 1 Hrushikesh U. Kharosekar 1 Jasmeet S. Thukral 1 Shonali Valsangkar
Investigation of Severe Craniomaxillofacial Battle Injuries Sustained by U.S. Service Members: A Case Series
 Case Report 243 Investigation of Severe Craniomaxillofacial Battle Injuries Sustained by U.S. Service Members: A Case Series Pamela R. Brown Baer, DDS, MEd 1 Joseph C. Wenke, PhD 2 Steven J. Thomas, MD
Case Report 243 Investigation of Severe Craniomaxillofacial Battle Injuries Sustained by U.S. Service Members: A Case Series Pamela R. Brown Baer, DDS, MEd 1 Joseph C. Wenke, PhD 2 Steven J. Thomas, MD
Recurrent subluxation or dislocation after surgical
 )263( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY CASE REPORT Persistent Medial Subluxation of the Ulna with Radiotrochlear Articulation Amir R. Kachooei, MD; David Ring, MD, PhD Research
)263( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY CASE REPORT Persistent Medial Subluxation of the Ulna with Radiotrochlear Articulation Amir R. Kachooei, MD; David Ring, MD, PhD Research
Pelvic Injuries. Chapter 21
 Chapter 21 Introduction Injuries of the pelvis are an uncommon, but potentially lethal, battlefield injury. Blunt injuries may be associated with major hemorrhage and early mortality. Death within the
Chapter 21 Introduction Injuries of the pelvis are an uncommon, but potentially lethal, battlefield injury. Blunt injuries may be associated with major hemorrhage and early mortality. Death within the
Case Study. Micrognathia Secondary to Pierre Robin Sequence. Treated with distraction osteogenesis using an internal mandible distractor.
 Case Study Micrognathia Secondary to Pierre Robin Sequence. Treated with distraction osteogenesis using an internal mandible distractor. Micrognathia Secondary to Pierre Robin Sequence Patient profile
Case Study Micrognathia Secondary to Pierre Robin Sequence. Treated with distraction osteogenesis using an internal mandible distractor. Micrognathia Secondary to Pierre Robin Sequence Patient profile
DR. SAAD AL-MUHAYAWI, M.D., FRCSC. ORL Head & Neck Surgery
 TRAUMA IN ORL DR. SAAD AL-MUHAYAWI, M.D., FRCSC Associate Professor & Consultant ORL Head & Neck Surgery TYPES OF TRAUMA EAR & TEMPORAL BONE TRAUMA NOSE & FACIAL BONES TRAUMA LARYNGEAL TRAUMA NECK TRAUMA
TRAUMA IN ORL DR. SAAD AL-MUHAYAWI, M.D., FRCSC Associate Professor & Consultant ORL Head & Neck Surgery TYPES OF TRAUMA EAR & TEMPORAL BONE TRAUMA NOSE & FACIAL BONES TRAUMA LARYNGEAL TRAUMA NECK TRAUMA
Dentistry and OMFS. Dalhousie Mini-Medical School 2018 Dr. Trish Brady BSc, DDS Dr. James Brady BSc, DDS, MD, MSc, FRCDC
 Dentistry and OMFS Dalhousie Mini-Medical School 2018 Dr. Trish Brady BSc, DDS Dr. James Brady BSc, DDS, MD, MSc, FRCDC Introduction Dr. Trish Brady, BSc, DDS Grew up in Halifax Bachelor of Science degree
Dentistry and OMFS Dalhousie Mini-Medical School 2018 Dr. Trish Brady BSc, DDS Dr. James Brady BSc, DDS, MD, MSc, FRCDC Introduction Dr. Trish Brady, BSc, DDS Grew up in Halifax Bachelor of Science degree
Maxillo-facial and Oral Surgery Department, Withington Hospital, Manchester
 FRACTURE OF THE MIDLINE OF THE MANDIBLE ASSOCIATED WITH COMPLETE UNILATERAL DISLOCATION OF THE JAW By IAN H. HESLOV, M.B., B.S., B.D.S., F.D.S.R.C.S.(Eng.) Maxillo-facial and Oral Surgery Department, Withington
FRACTURE OF THE MIDLINE OF THE MANDIBLE ASSOCIATED WITH COMPLETE UNILATERAL DISLOCATION OF THE JAW By IAN H. HESLOV, M.B., B.S., B.D.S., F.D.S.R.C.S.(Eng.) Maxillo-facial and Oral Surgery Department, Withington
Postoperative malocclusion after maxillofacial fracture management: a retrospective case study
 Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2018) 40:27 https://doi.org/10.1186/s40902-018-0167-z Maxillofacial Plastic and Reconstructive Surgery REVIEW Open Access Postoperative malocclusion
Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2018) 40:27 https://doi.org/10.1186/s40902-018-0167-z Maxillofacial Plastic and Reconstructive Surgery REVIEW Open Access Postoperative malocclusion
Class II. Bilateral Cleft Lip and Palate. Clinician: Dr. Mike Mayhew, Boone, NC Patient: R.S. Cleft Lip and Palate.
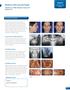 Bilateral Cleft Lip and Palate Clinician: Dr. Mike Mayhew, Boone, NC Patient: R.S. Class II Cleft Lip and Palate Pretreatment Diagnosis Class II dolichofacial female, age 22 years 11 months, presented
Bilateral Cleft Lip and Palate Clinician: Dr. Mike Mayhew, Boone, NC Patient: R.S. Class II Cleft Lip and Palate Pretreatment Diagnosis Class II dolichofacial female, age 22 years 11 months, presented
Lesson Plans and Objectives: Review material for article Prep work for article Picture recovery Review for placement on-line.
 Lesson Plans and Objectives: Review material for article Prep work for article Picture recovery Review for placement on-line. After reading the article, the staff will be able to: Define facial trauma
Lesson Plans and Objectives: Review material for article Prep work for article Picture recovery Review for placement on-line. After reading the article, the staff will be able to: Define facial trauma
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Patient information booklet Orthognathic Surgery
 Patient information booklet Orthognathic Surgery 2 Table of contents This patient information booklet contains all the answers to your questions regarding orthognathic surgery. + + + + + + What is Orthognathic
Patient information booklet Orthognathic Surgery 2 Table of contents This patient information booklet contains all the answers to your questions regarding orthognathic surgery. + + + + + + What is Orthognathic
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
The application of the Risdon approach for mandibular condyle fractures
 Nam et al. BMC Surgery 2013, 13:25 RESEARCH ARTICLE Open Access The application of the Risdon approach for mandibular condyle fractures Seung Min Nam 1, Jang Hyun Lee 2* and Jun Hyuk Kim 3 Abstract Background:
Nam et al. BMC Surgery 2013, 13:25 RESEARCH ARTICLE Open Access The application of the Risdon approach for mandibular condyle fractures Seung Min Nam 1, Jang Hyun Lee 2* and Jun Hyuk Kim 3 Abstract Background:
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Interesting Case Series. Virtual Surgical Planning in Orthognathic Surgery
 Interesting Case Series Virtual Surgical Planning in Orthognathic Surgery Suraj Jaisinghani, MS, a Nicholas S. Adams, MD, b,c Robert J. Mann, MD, b,c,d John W. Polley, MD, b,c,d, and John A. Girotto, MD,
Interesting Case Series Virtual Surgical Planning in Orthognathic Surgery Suraj Jaisinghani, MS, a Nicholas S. Adams, MD, b,c Robert J. Mann, MD, b,c,d John W. Polley, MD, b,c,d, and John A. Girotto, MD,
The Melbourne Temporomandibular Total Joint Replacement System
 The Melbourne Temporomandibular Total Joint Replacement System Device Description: The Melbourne TMJ Total Joint Replacement System is used to reconstruct a damaged or diseased temporomandibular joint
The Melbourne Temporomandibular Total Joint Replacement System Device Description: The Melbourne TMJ Total Joint Replacement System is used to reconstruct a damaged or diseased temporomandibular joint
Independent italian ngo founded in EMERGENCY. Promotes a culture of peace, solidarity and respect for human rights.
 Independent italian ngo founded in 1994. EMERGENCY Promotes a culture of peace, solidarity and respect for human rights. 2 34% 26% 17% 16% 7% The victims War Victims WWI WWII after Combatants Civilians
Independent italian ngo founded in 1994. EMERGENCY Promotes a culture of peace, solidarity and respect for human rights. 2 34% 26% 17% 16% 7% The victims War Victims WWI WWII after Combatants Civilians
For many years, patients with
 Dr. Robert Lowe is one of the great teachers in dentistry. Recently, he received the Gordon J. Christensen Award from the Chicago Dental Society in recognition of his excellence in teaching. Some of my
Dr. Robert Lowe is one of the great teachers in dentistry. Recently, he received the Gordon J. Christensen Award from the Chicago Dental Society in recognition of his excellence in teaching. Some of my
Management of Pediatric Mandibular Fracture Using Orthodontic Vacuum formed Thermoplastic Splint: A Case Report and Review of Literature
 Case Report Management of Pediatric Mandibular Fracture Using Orthodontic Vacuum formed Thermoplastic Splint: A Case Report and Review of Literature OO Sanu, AOS Ayodele 1, MO Akeredolu 1 Department of
Case Report Management of Pediatric Mandibular Fracture Using Orthodontic Vacuum formed Thermoplastic Splint: A Case Report and Review of Literature OO Sanu, AOS Ayodele 1, MO Akeredolu 1 Department of
Treatment Considerations in Management of Soft Tissues Injuries A Case Report. Key Words: Facial Injuries, Delayed Treatment, Antibiotics, Scar, etc.
 ISSN-0975-8437 INTERNATIONAL JOURNAL OF DENTAL CLINICS: 2 (1):22-27 CASE REPORT Treatment Considerations in Management of Soft Tissues Injuries A Case Report Siddqua Aaisha MDS 1 and Thakur Nitin MDS 2
ISSN-0975-8437 INTERNATIONAL JOURNAL OF DENTAL CLINICS: 2 (1):22-27 CASE REPORT Treatment Considerations in Management of Soft Tissues Injuries A Case Report Siddqua Aaisha MDS 1 and Thakur Nitin MDS 2
Post-operative stability of the maxilla treated with Le Fort I and horseshoe osteotomies in bimaxillary surgery
 European Journal of Orthodontics 24 (2002) 471 476 2002 European Orthodontic Society Post-operative stability of the maxilla treated with Le Fort I and horseshoe osteotomies in bimaxillary surgery Kiyoshi
European Journal of Orthodontics 24 (2002) 471 476 2002 European Orthodontic Society Post-operative stability of the maxilla treated with Le Fort I and horseshoe osteotomies in bimaxillary surgery Kiyoshi
Reconstruction of large mandibular defects
 Immediate Reconstruction of a Large Mandibular Defect of Locally Invasive Benign Lesions (A New Method) Gholamreza Shirani, OMFS, DDS, MS,* Mahnaz Arshad, DDS, 1 Farnoush Mohammadi, OMFS, DDS, MS* Tehran,
Immediate Reconstruction of a Large Mandibular Defect of Locally Invasive Benign Lesions (A New Method) Gholamreza Shirani, OMFS, DDS, MS,* Mahnaz Arshad, DDS, 1 Farnoush Mohammadi, OMFS, DDS, MS* Tehran,
15. Facial and dental injuries
 15. Facial and dental injuries Priorities in management Best practice is based on current APLS / ATLS guidelines. Maxillofacial injuries will often take a lower priority than other potentially life or
15. Facial and dental injuries Priorities in management Best practice is based on current APLS / ATLS guidelines. Maxillofacial injuries will often take a lower priority than other potentially life or
Injuries to the Hands and Feet
 Injuries to the Hands and Feet Chapter 26 Injuries to the Hands and Feet Introduction Combat injuries to the hands and feet differ from those of the arms and legs in terms of mortality and morbidity. Death
Injuries to the Hands and Feet Chapter 26 Injuries to the Hands and Feet Introduction Combat injuries to the hands and feet differ from those of the arms and legs in terms of mortality and morbidity. Death
CASE REPORT. Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur
 PRODUCTS CASE REPORT Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur Robert D. Fitch, M.D. Duke University Health System 1 1 CONDITION Infected nonunion
PRODUCTS CASE REPORT Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur Robert D. Fitch, M.D. Duke University Health System 1 1 CONDITION Infected nonunion
SCOPE OF PRACTICE PGY-6 PGY-7 PGY-8
 PGY-6 Round on all plastic surgery inpatients every day. Assess progress of patients and identify real or potential problems. Review patients progress with attending physicians daily and participate in
PGY-6 Round on all plastic surgery inpatients every day. Assess progress of patients and identify real or potential problems. Review patients progress with attending physicians daily and participate in
CHAPTER 8 SECTION 1.4 ORAL SURGERY TRICARE/CHAMPUS POLICY MANUAL M DEC 1998 SPECIAL BENEFIT INFORMATION
 TRICARE/CHAMPUS POLICY MANUAL 6010.47-M DEC 1998 SPECIAL BENEFIT INFORMATION CHAPTER 8 SECTION 1.4 Issue Date: October 8, 1986 Authority: 32 CFR 199.4(e)(10) I. DESCRIPTION There are certain oral surgical
TRICARE/CHAMPUS POLICY MANUAL 6010.47-M DEC 1998 SPECIAL BENEFIT INFORMATION CHAPTER 8 SECTION 1.4 Issue Date: October 8, 1986 Authority: 32 CFR 199.4(e)(10) I. DESCRIPTION There are certain oral surgical
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007 Hosted by: Australian Small Animal Veterinary Association (ASAVA) Australian Small Animal Veterinary Association (ASAVA)
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007 Hosted by: Australian Small Animal Veterinary Association (ASAVA) Australian Small Animal Veterinary Association (ASAVA)
Fixed Twin Blocks. Guidelines for case selection are similar to those for removable Twin Block appliances.
 Fixed Twin Blocks Development of Fixed Twin Blocks Dr Clark has enjoyed the cooperation of Dynaflex in developing the Fixed Twin Block. Six years of clinical testing has confirmed that this technique produces
Fixed Twin Blocks Development of Fixed Twin Blocks Dr Clark has enjoyed the cooperation of Dynaflex in developing the Fixed Twin Block. Six years of clinical testing has confirmed that this technique produces
CHAPTER. 1. Uncontrolled systemic disease 2. Retrognathic jaw relationship
 CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Hip Fractures. Anatomy. Causes. Symptoms
 Hip Fractures A hip fracture is a break in the upper quarter of the femur (thigh) bone. The extent of the break depends on the forces that are involved. The type of surgery used to treat a hip fracture
Hip Fractures A hip fracture is a break in the upper quarter of the femur (thigh) bone. The extent of the break depends on the forces that are involved. The type of surgery used to treat a hip fracture
Tracheal Trauma: Management and Treatment. Kosmas Iliadis, MD, PhD, FECTS
 Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Plastic Surgeon, Middlesbrough General Hospital, Stockton Children's Hospital, Newcastle Regional Hospital Board
 THE NASAL TIP IN BILATERAL HARE LIP By J. POTTER, F.R.C.S.Ed. Plastic Surgeon, Middlesbrough General Hospital, Stockton Children's Hospital, Newcastle Regional Hospital Board IN the problem of the bilateral
THE NASAL TIP IN BILATERAL HARE LIP By J. POTTER, F.R.C.S.Ed. Plastic Surgeon, Middlesbrough General Hospital, Stockton Children's Hospital, Newcastle Regional Hospital Board IN the problem of the bilateral
INDIANA HEALTH COVERAGE PROGRAMS
 INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization
 Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization Koroush Taheri Talesh, DDS, a Mohammad Hosein Kalantar Motamedi, DDS, b Mahdi Sazavar,
Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization Koroush Taheri Talesh, DDS, a Mohammad Hosein Kalantar Motamedi, DDS, b Mahdi Sazavar,
Screw hole-positioning guide and plate-positioning guide: A novel method to assist mandibular reconstruction
 Journal of Dental Sciences (2012) 7, 301e305 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Screw hole-positioning guide and plate-positioning guide: A novel method
Journal of Dental Sciences (2012) 7, 301e305 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Screw hole-positioning guide and plate-positioning guide: A novel method
PediLoc Extension Osteotomy Plate (PLEO)
 PediLoc Extension Osteotomy Plate (PLEO) Left PLEO Plates Sizes: 6, 8 and 10 hole plates Right PLEO Plates Sizes: 6, 8 and 10 hole plates PediLoc Extension Osteotomy Plate The technique description herein
PediLoc Extension Osteotomy Plate (PLEO) Left PLEO Plates Sizes: 6, 8 and 10 hole plates Right PLEO Plates Sizes: 6, 8 and 10 hole plates PediLoc Extension Osteotomy Plate The technique description herein
Principle Management of Wound and Fracture in Emergency Department
 Principle Management of Wound and Fracture in Emergency Department Presented in Clinical Update Seminar January 15 th 2011 dr. Tedjo Rukmoyo, SpOT (K) Spine Initial Management ATLS Procedure A : airway
Principle Management of Wound and Fracture in Emergency Department Presented in Clinical Update Seminar January 15 th 2011 dr. Tedjo Rukmoyo, SpOT (K) Spine Initial Management ATLS Procedure A : airway
Interview with Vincent KOKICH
 DOI: 10.1051/odfen/2010302 J Dentofacial Anom Orthod 2010;13:218-222 Ó RODF / EDP Sciences Interview with Vincent KOKICH Conducted by and translated by Sophie ROZENCWEIG Dr. Kokich, it has always been
DOI: 10.1051/odfen/2010302 J Dentofacial Anom Orthod 2010;13:218-222 Ó RODF / EDP Sciences Interview with Vincent KOKICH Conducted by and translated by Sophie ROZENCWEIG Dr. Kokich, it has always been
Low-Force Mechanics Nonextraction. Estimated treatment time months (Actual 15 mos 1 week). Low-force mechanics.
 T.S. Age: 43 Years 1 Month Diagnosis: Class I Nonextraction Adult (severe crowding, very flat profile with tissue-grafting indications) Background: This case is very similar to the previous case of a 14-year-old.
T.S. Age: 43 Years 1 Month Diagnosis: Class I Nonextraction Adult (severe crowding, very flat profile with tissue-grafting indications) Background: This case is very similar to the previous case of a 14-year-old.
Case Studies. Flail Chest Acute Pain Chest Wall Deformity Fracture Non-union
 Case Studies Flail Chest Acute Pain Chest Wall Deformity Fracture Non-union Tractor Roll Over Victim Multiple Rib Fractures, Hemothorax Surgeon s Name: John Mayberry, MD Facility Name/ Location: Oregon
Case Studies Flail Chest Acute Pain Chest Wall Deformity Fracture Non-union Tractor Roll Over Victim Multiple Rib Fractures, Hemothorax Surgeon s Name: John Mayberry, MD Facility Name/ Location: Oregon
A lingual orthodontic case with 3M Incognito Appliance System combined with orthognathic surgery.
 SM 3M Health Care Academy A lingual orthodontic case with 3M Incognito Appliance System combined with orthognathic surgery. Dr. B. Iglesias-Sánchez Dr. F. Hernandez-Alfaro Dr. J.C. Pérez-Varela DDS, MS.
SM 3M Health Care Academy A lingual orthodontic case with 3M Incognito Appliance System combined with orthognathic surgery. Dr. B. Iglesias-Sánchez Dr. F. Hernandez-Alfaro Dr. J.C. Pérez-Varela DDS, MS.
Director, Burn Center MetroHealth Medical Center Professor of Surgery Case Western Reserve University
 Director, Burn Center MetroHealth Medical Center Professor of Surgery Case Western Reserve University BLAST INJURY Which of following statements concerning blast lung injury are FALSE? 1)Blast lung injury
Director, Burn Center MetroHealth Medical Center Professor of Surgery Case Western Reserve University BLAST INJURY Which of following statements concerning blast lung injury are FALSE? 1)Blast lung injury
Scholars Journal of Medical Case Reports
 Scholars Journal of Medical Case Reports Sch J Med Case Rep 2017; 5(11):805-809 Scholars Academic and Scientific Publishers (SAS Publishers) (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Medical Case Reports Sch J Med Case Rep 2017; 5(11):805-809 Scholars Academic and Scientific Publishers (SAS Publishers) (An International Publisher for Academic and Scientific Resources)
Virtual Stress Testing of Regenerating Bone in Tibia Fractures
 Virtual Stress Testing of Regenerating Bone in Tibia Fractures Presentation by: Joseph L. Petfield, MD 1 Co-authors: Matthew Kluk, MD 2 ; Emily Shin, MD 2 ; Husain Bharmal, MD 2 ; Paul Hoffman, BS 5 ;
Virtual Stress Testing of Regenerating Bone in Tibia Fractures Presentation by: Joseph L. Petfield, MD 1 Co-authors: Matthew Kluk, MD 2 ; Emily Shin, MD 2 ; Husain Bharmal, MD 2 ; Paul Hoffman, BS 5 ;
Technique Guide. Rapid IMF Device. Temporary mandibular fixation device.
 Technique Guide Rapid IMF Device. Temporary mandibular fixation device. Indications Rapid IMF is an adjustable flexible plastic band that wraps around a tooth to create an anchorage point for temporary
Technique Guide Rapid IMF Device. Temporary mandibular fixation device. Indications Rapid IMF is an adjustable flexible plastic band that wraps around a tooth to create an anchorage point for temporary
Medartis Product Overview MODUS
 Medartis Product Overview MODUS Content 3 Clinical Benefits MODUS 4 5 Technology 6 Clip System 7 0.9 / 1.2, Trauma 0.9 / 1.2 8 1.5, Trauma 1.5 9 Orbital Plating System OPS 1.5 9 Neuro 1.5 10 Trauma 2.0
Medartis Product Overview MODUS Content 3 Clinical Benefits MODUS 4 5 Technology 6 Clip System 7 0.9 / 1.2, Trauma 0.9 / 1.2 8 1.5, Trauma 1.5 9 Orbital Plating System OPS 1.5 9 Neuro 1.5 10 Trauma 2.0
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note
 Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
