Oxford Phase 3 unicompartmental knee arthroplasty: medium-term results of a minimally invasive surgical procedure
|
|
|
- Rhoda Gibbs
- 5 years ago
- Views:
Transcription
1 Knee Surg Sports Traumatol Arthrosc (2011) 19: DOI /s KNEE Oxford Phase 3 unicompartmental knee arthroplasty: medium-term results of a minimally invasive surgical procedure Lukas A. Lisowski Michel P. J. van den Bekerom Peter Pilot C. Niek van Dijk Andrzej E. Lisowski Received: 7 December 2009 / Accepted: 29 June 2010 / Published online: 17 July 2010 Ó The Author(s) This article is published with open access at Springerlink.com Abstract Purpose In the last decade, a major increase in the use of and interest in unicompartmental knee arthroplasty (UKA) has developed. The Oxford Phase 3 UKA is implanted with a minimally invasive technique using newly developed instruments. The objective of this prospective study was to evaluate the outcome of UKA in patients with medial osteoarthritis of the knee in a high-volume unit. Methods Two-hundred and forty-four UKAs were performed with a minimally invasive approach. The median age was 72 (43 91) years. The median follow-up was 4.2 years (range years). Fourteen patients died, and nine were considered to be lost to follow-up, but all had a well-functioning prosthesis in situ until their last follow-up. Pain, function and health-related quality of life were evaluated pre- and postoperatively using patient- and assessor-based outcome scores, as well as radiographic evidence. Results The mean Knee Society knee and function scores, WOMAC-scores, Oxford-score and VAS pain and satisfaction all improved. Nine knees required revision. Eleven L. A. Lisowski M. P. J. van den Bekerom C. N. van Dijk Department of Orthopedic Surgery, Academic Medical Center Amsterdam, Amsterdam, The Netherlands P. Pilot Department of Orthopedic Surgery, Reinier de Graaf Gasthuis, Delft, The Netherlands A. E. Lisowski Department of Orthopedic Surgery, Atrium Medical Centre, Kerkrade/Heerlen/Brunssum, The Netherlands L. A. Lisowski (&) Het Bergske 4, 6417 GN Heerlen, The Netherlands lalisowski@gmail.com patients required an additional arthroscopic procedure due to persisting pain secondary to intra-articular pathology, and four patients required manipulation under anaesthesia because of limited range of motion. The 7-year cumulative survival rate of the arthroplasty was 94.4%. A low incidence (21%) of a radiolucent line beneath the tibial component was observed at 5 years of follow-up. Conclusion This study showed a high survival rate of the Oxford Phase 3 UKA. Patient satisfaction and functional performance were also very high. Major complication rate was low; in addition, the incidence of radiolucency under the tibial component, when compared to present literature, was low. When strict indication criteria are followed, excellent, durable, and in our opinion reliable, results can be expected for this procedure. Keywords Unicompartmental knee arthroplasty Results Survival Radiolucency Introduction Interest in unicompartmental knee arthroplasty (UKA) for medial osteoarthritis has increased rapidly over the last two decades [42]. The main reasons for its rising popularity are the introduction of minimally invasive surgical (MIS) techniques [31, 41] with modified surgical equipment, the publication of the excellent medium- and long-term results of the Oxford Phase 2 arthroplasty [14, 39, 44, 45] and the well-documented improved polyethylene wear characteristics of the mobile bearing device [18, 38]. Medial osteoarthritis of the knee is considered to be a unicompartmental disease and, when left untreated, it may later progress to involve the other knee compartments [1]. This has given rise to the rationale for the treatment of only one
2 278 Knee Surg Sports Traumatol Arthrosc (2011) 19: compartment, either with a high tibial osteotomy (HTO) or a unicompartmental knee arthroplasty. In the 1970s, the pioneers of UKA developed and introduced their first designs [11, 16, 28], but the results of these early UKAs were controversial due to high early failure rates. This changed in 1998 when Goodfellow and colleagues reported encouraging results for the unicondylar Oxford knee arthroplasty [13]. Today s opinion is that early failures are mainly attributable to a surgeon s inadequate technique and/or lack of experience with the technically demanding procedure [25, 43]. The designer group of the Oxford Phase 3 prosthesis has reported excellent results with their implant [33]. These results were reinforced by Svard and co-workers who reported favourably on a 15- and 20-year follow-up (FU) of the Oxford prosthesis [35, 44]. Although some reports show satisfactory results in shorter or long-term FU periods [21, 39, 49], others show less favourable results compared to the series of Pandit et al. and Svard et al. [10, 23, 29]. The survival and outcomes as reported in various arthroplasty registers are, however, even less satisfying [22]. This may be attributed to their lesser experience with this technique, patient selection or to the lower number of patients treated. The purpose of the present study is to report the functional and radiological outcome of 244 consecutive Oxford Phase 3 unicompartmental knee arthroplasties performed using a MIS technique by a single orthopaedic surgeon. Our hypothesis is that results generated by an experienced high-volume surgeon treating a large number of patients will be comparable to those of the designer group, and better than those reported in the arthroplasty registers. We will report the medium-term results as previous research has shown that most complications and failures occur in the early follow-up phase, and as a result medium-term data can indicate comparable longer-term results [13]. This study describes our experiences of using the Oxford Phase 3 prosthesis implanted by a single surgeon and focuses on postoperative knee function, early complications, number and reason of revision operations, number of additional procedures, pain and radiological results. Materials and methods Between 1999 and 2008, 244 medial Oxford Phase 3 arthroplasties (216 patients) (Biomet Ltd., Swindon, UK) were performed in a district general hospital and form the cohort for this study. The study was uncontrolled, nonblinded and prospective. Patients demographic details are shown in Table 1. All knees were diagnosed with medial compartment osteoarthritis. The mean preoperative tibiofemoral angle was 0.2 (SD 4.1) degrees varus. After 2001, Table 1 Demographic baseline characteristics of 216 patients treated by means of UKA for medial compartment osteoarthritis Number of prostheses N = 244 (N = 216 patients) Follow-up [5 years N = 96 Bilateral N = 28 Side 122 right; 122 left Age (years), median (range) 72 (43 91) Body mass index (kg/m 2 ), 28 ± 5 ( ) mean ± SD (range) Operation time (min), 66 ± 14 (45 120) mean ± SD (range) due to controversial reports appearing in the literature, we considered previous HTO a contraindication for Oxford arthroplasty [45]. Prior to 2001, five patients had a HTO prior to their UKA. The strict indication criteria for unicompartmental knee arthroplasty defined by White et al. [55] and Keyes et al. [19] were followed. Osteoarthritis of the patellofemoral joint and obesity were not considered contraindications for this procedure. Fourteen patients deceased during the study period (average 34 months postoperative), none of them as a result of the surgery. These patients were included until latest follow-up. Among these patients, one UKA was revised to a total knee arthroplasty (TKA). Nine patients did not attend the outpatient clinic for their latest FU due to general health reasons and were considered as lost to FU (LTFU). These patients or their relatives were subsequently interviewed by phone, and none of them had had a revision operation (median FU 57 months, range months). For this surveillance, patients informed consent was obtained. This study was performed as routine FU, and examination was performed in accordance with generally accepted practice. Approval was obtained from our institutional review board. Surgical technique The cemented Oxford Phase 3 unicompartmental knee arthroplasty consists of cobalt chromium molybdenum spherical femoral and flat tibial components and a fully congruent polyethylene mobile bearing device. The MIS operation technique has been described in detail by Murray et al. [32] and was performed with newly developed instruments. These instruments not only allow better component positioning, but also create a perfect balance of the flexion and extension gap to achieve improved stability. The minimally invasive approach is the recommended standard approach for this procedure. The operation is performed under tourniquet and via a short paramedial incision running from the medial pole of the patella to the medial border of the tuberosity. This approach does not
3 Knee Surg Sports Traumatol Arthrosc (2011) 19: compromise the extensor mechanism or the suprapatellar pouch. Before cementing, pulsed lavage is used to rinse the subchondral bone. Full weight bearing was allowed postoperatively, and thromboprophylaxis was prescribed. Outcome measures The clinical FU consisted of physical examination, registration of pain and complications and a standard series of radiographs. Patients attended the routine FU assessments in the outpatient clinic scheduled at 6 weeks, 6 months and 1, 2, 5 and 10 years. Revision was defined as any surgical procedure that resulted in the removal or exchange of any of the arthroplasty components. Additional procedures were defined as additional operations that did not result in the removal of parts of the original arthroplasty. Pain, function and health-related quality of life were evaluated pre- and postoperatively by patient- and assessor-based outcome scores. The WOMAC Questionnaire [3], the Knee Society Score (KSS) [17], Oxford Knee Score (OKS) [9] and postoperative visual analogue scale (VAS) for pain and satisfaction were used [54]. The accuracy of implant positioning was determined by standing anteroposterior and lateral radiographs on first outpatient review and then at routine outpatient clinic visits (including skyline views). The alignment was determined by means of the tibiofemoral angle. Osteoarthritic changes in the non-replaced compartments were graded according to the Ahlbäck classification modified by Mont et al. [30]. A fluoroscopic-centred technique was used to assess any radiolucency at the bone cement interface above the femoral component and under the tibial component. All measurements were based on manufacturer s guidelines [32]. A radiolucent line of less than 2 mm width with a sclerotic line beneath the tibial component was considered to be physiological [47, 53]. Postoperative radiographs examining the progression of osteoarthritis in the lateral and patellofemoral (PF) compartments, the tibiofemoral angle and the presence and extent of radiolucency were investigated in 96 cases with a minimum follow-up of 5 years. Radiological examination including the fluoroscopic-centred technique was evaluated by consensus of two independent radiologists. Statistical analysis Data were analysed using SPSS software (SPSS Ó 15.0, SPSS Inc., Chicago, IL, USA). The non-parametric Wilcoxon test was used for all non-parametric data. The general linear model (GLM) was used to compare the repeated measurements, a post hoc Bonferroni test was used to analyse the location of the difference, and p-values of P \ 0.05 were considered significant. Using revision of the arthroplasty for any cause as an end-point, a life-table was constructed, and rates of survival determined using the Kaplan Meier survival analysis. Results The median FU was 4.2 years (range years). Baseline characteristics are shown in Table 1, and outcome scores are shown in Table 2. A total of 84.3% of knees had good (70 84 points) or excellent ( points) results for Table 2 Outcome results of 216 patients treated by means of UKA for medial compartment osteoarthritis Pre 6 months 12 months 24 months [30 months Latest FU total (Mean FU 4.4 years)* VAS Satisfied 1.1 ± ± ± ± ± 1.1 VAS Pain 1.5 ± ± ± ± ± 1.6 Oxford total 13.0 ± ± 10.2* 36.2 ± ± ± ± 8.5 Oxford pain 6.1 ± ± 4.4* 14.9 ± ± ± ± 3.9 Oxford function 6.9 ± ± 6.2* 21.3 ± ± ± ± 4.9 WOMAC pain 42.4 ± ± 17.4* 85.7 ± ± ± ± 17.0 WOMAC stiffness 45.9 ± ± 19.6* 76.4 ± ± ± ± 19.3 WOMAC function 44.1 ± ± 17.6* 82.0 ± ± ± ± 18.0 ROM ± ± 10.5* ± ± ± ± 9.8 Tibiofemoral angle ± ± 3.4* 5.0 ± ± ± ± 3.0 KSS knee 44.2 ± ± 13.4* 90.8 ± ± ± ± 8.7 KSS function 45.0 ± ± 15.9* 88.2 ± ± ± ± 17.8 The GLM showed that all scores increased postoperatively, P \ for all scores. The Bonferroni post hoc test showed that the difference was only between preoperative and 6 month; afterwards the scores remained constant * P \ 0.001: compared preoperative with 6-month postoperative with paired t-test
4 280 Knee Surg Sports Traumatol Arthrosc (2011) 19: the knee score, and 74.7% had a good or excellent functional score. The general linear model revealed no significant change in scores after the 12-month FU period. The cumulative survival at 7 years was 94.4% (95% CI ) (Fig. 1). Preoperatively, 90.1% of the patients with medial osteoarthritis of the knee had moderate (KSS 5 10 points) or severe pain (KSS 0 points). At 1-year postoperatively, 17 patients (7.3%) had moderate or severe pain. At final FU, of the patients with a UKA in place, only 2 (1%) had moderate pain. Early complications One fracture of the proximal tibia occurred intra-operatively. The patient was treated by continuous passive motion for 7 days followed by casting for another 4 weeks and has achieved a good outcome in regard to pain and function (125 degrees flexion, KS knee score 95 points, KS function score 100 points). In our series, no wound dehiscence, deep or superficial infection, deep venous thrombosis, pulmonary embolus or death related to the orthopaedic procedure were observed. Revisions Nine patients underwent a revision procedure at a mean of 33 ± 27 months after primary surgery. Details of the revised UKAs are summarised in Table 3. Additional procedures Fifteen additional procedures were performed. Four patients, with limited flexion postoperatively, required manipulation of the knee under anaesthesia (MUA) (mean 3.5 weeks after primary surgery) to improve ROM. Flexion of less than 90 degrees 3 6 weeks postoperatively was considered an indication for MUA. At latest FU, the ROM of these patients was degrees. Eleven patients underwent an arthroscopic procedure for pain related to intraarticular causes (e.g. synovitis, haemorrhage, lateral meniscal lesion, loose bodies). Three patients in this group with additional procedures were revised. The other eight arthroscopic procedures were all successful in relieving the complaints. High tibial osteotomy One of the five patients with a previous high tibial osteotomy was revised to a TKA. This patient still experienced pain after revision surgery to TKA. The other four patients had fair scores (range points) and moderate function at 1-year FU (mean KS knee and function score both 61.7 points, ROM 122 degrees). These four patients eventually progressed to good and excellent scores 6.8 years after surgery (mean KSS knee: 70 points; KSS function: 83.3 points; ROM 133 degrees). Radiology Complete physiological radiolucency (\2 mm) as measured by means of the fluoroscopic-centred technique was observed in 5 tibial components. There were 15 tibial components with partial radiolucent lines. All these radiolucencies were visible at year one postsurgery and thereafter remained unchanged in extent and thickness. In two patients, pathological signs of radiolucency (i.e. a line [2 mm without a thin sclerotic bordering line) beneath the tibial component were observed. These arthroplasties were still in place and functioning well at final follow-up. No radiolucency was seen between the surface of the femoral component and the bone. Progression of medial facet PF osteoarthritis was observed in two non-symptomatic patients. The occurrence of lateral facet PF osteoarthritis was observed in four patients of whom two were symptomatic. Five patients had a postoperative valgus angle of more than 10 degrees and were considered overcorrected. This angle was not altered at 5-year FU except in one knee, which was revised. Discussion Fig. 1 Kaplan Meier survival analysis using revision for any reason as an end-point The most important finding of this study was the good medium-term results of the Oxford Phase 3 UKA with a cumulative survival rate of 94.4% at 7-year FU obtained in a high-volume district general hospital. These results are comparable with the series of Pandit et al. [34] and to the series of Robertsson et al. [43] who reported an 8-year
5 Knee Surg Sports Traumatol Arthrosc (2011) 19: Table 3 Details of the revised UKAs Revision History Indication for revision Operative findings Time to revision (years) Procedure Outcome 1 HTO Pain PF arthritis 3.3 Revision to TKA Poor ( ) Components fixed 2 ACL reinsertion 10 years prior Pain Unknown 2.2 Revision to TKA elsewhere Unknown 3 Fibromyalgia Pain PF and lateral osteoarthritis 5.3 Revision to TKA Poor Polyarthritis Components fixed elsewhere 4 None 1st Dislocation Malposition components Open bearing reposition Poor 2nd dislocation Revision to TKA Excellent 5 None Dislocation Flexion/extension gap disbalance 6 None Lateral compartment arthritis MCL insufficiency ACL absent 7 Trauma Lateral compartment arthritis 0.3 Revision to Tibial Vanguard UKA Components fixed 2.5 Revision to Hinged TKA elsewhere Good Good Components fixed 6.8 Revision to TKA Good 8 Trauma Dislocation Undersized bearing 0.5 Open bearing reposition; Good Thicker bearing 9 None Synovitis; Cobalt allergy Synovitis; secondary PE wear 3.7 Revision to Titanium AGC TKA Good survival rate of 93%. The importance of high-volume units was stressed by Koskinen et al. [22] who reported high failure rates of the technically demanding Oxford arthroplasty in their Finnish Arthroplasty Register study. The results in this study compare favourably to those reported by the Finnish Arthroplasty Register which mainly reported procedures performed in low-volume clinics [22]. The average number of procedures annually in this series was 23, the same as in the series of Robertsson et al. [43]. This study reflects the experience of one single highvolume surgeon using one single implant and might not reflect the results obtained in a general community practice, with different surgeons, varying indications and numerous designs. The present study reports the outcome of patients with a medium-term FU, since functional recovery is almost complete after 1 year and does not improve significantly thereafter [34]. Almost none of the reported outcome measures improved during further FU compared to the 1-year results. Revisions for all causes occurred at a mean follow-up of 2.8 years after primary surgery. Other authors state that revisions occur mostly within 2 years after surgery [12, 20, 26, 27]. Because of these two reasons, a medium-term FU could be justified. However, as with any design one has to keep in mind that other factors (e.g. aseptic loosening, instability and progressive lateral OA) that reduce the longevity of the prosthesis will influence the survival negatively with longer FU. The series by Svard et al. showed very few revisions in the second decade after the index procedure and suggests that the implant is durable in this period after implantation. So, on the other hand, the medium-term FU and a lack of control group might be considered a limitation of the study; however, complications arise usually in early follow-up [44]. In this series, two UKAs were revised due to progression of osteoarthritis of the lateral compartment. One had overcorrection at primary surgery and its alignment changed from 11 to 18 degrees valgus postoperatively. Both of these patients had a history of trauma; one sustained medial collateral ligament insufficiency and had to be revised to a hinged TKA, the other received a Vanguard TKA. In recent literature on UKAs, it has been stated that progression of arthritis in the lateral compartment is the most important reason for revision surgery [8, 10]. Kumar et al. [24] described this phenomenon as a natural progression of the disease, and Price et al. [36] reported seven revisions due to lateral OA in their series of Oxford knees. Although in our series the knee with overcorrection was revised 6.8 years after primary surgery, Weale et al. [52] showed that failures due to lateral OA often occur within 2 years, especially in overcorrected knees. Previous studies conclude that patellofemoral osteoarthritis (PFOA) does not influence revision rate. However, they did not differentiate between medial and lateral facet degeneration [4, 24]. We agree with Weale et al. [51] that progression of medial and lateral PFOA is rare after medial
6 282 Knee Surg Sports Traumatol Arthrosc (2011) 19: UKA. Two of the patients with progression of medial patellofemoral facet degeneration are still doing well after 6.3 and 7.3 years FU. One patient with progression of the lateral PF facet required revision surgery. Beard et al. [2] stated that the presence of lateral PF degeneration might negatively influence the outcome of the UKA and that caution in these cases should be observed, this is contrary to the apparent lack of negative impact of worsening medial PF facet osteoarthritis. One might argue, however, that the patient with progression of lateral PF facet osteoarthritis might not have been a suitable candidate for the UKA in the first place. The most frequent cause for revision surgery in the present series was early dislocation of the meniscal bearing (1.2%). Lewold et al. [25] observed a dislocation of the bearing in 2.3% of their cases and three out of 688 cases (0.4%) in the series of Pandit et al. [34] also had a bearing dislocation. Dislocation of the mobile bearing in the Oxford knee primarily occurs shortly after implantation; it can probably be attributed to a technical error during surgery. A mismatch between the tibial and femoral component, and/or size of the bearing itself, might lead to failure. In this series, two dislocations are considered to have resulted from technical errors in the surgical procedure. One of these had a malposition of the components and was revised to a TKA. The other demonstrated a flexion extension gap imbalance, and in this patient the tibial component was revised to a unilateral non-mobile tibial component. One further patient suffered a traumatic dislocation of the bearing and received a thicker insert by a conventional open procedure. One knee was revised to a titanium AGC TKA due to a cobalt allergy (confirmed by dermatology), and secondary macroscopic polyethylene wear 3.5 years after surgery. Polyethylene wear has not been reported as a cause of failure of the Oxford knee [5, 25, 41]. No revisions were performed due to deep infection, primary polyethylene wear or loosening of the components. In contrast to the present study, the most common reason for revision in the series of Koskinen et al. [22] was aseptic loosening. As reported by others, we conclude that the indication for surgery and operative technique are predictors for failure of the arthroplasty [48]. As confirmed by others [7], arthroscopy has shown to be a successful and safe procedure post-uka implantation for the treatment of subsequent intra-articular pathology. Psychoyios et al. [38] state that revision surgery is not always a solution, as in one of every four revisions the problem is not solved. This series suggests that patients with complaints of pain should be investigated, carefully followed up, and revision for unexplained pain must be avoided as it may not be warranted in these cases [23]. The five patients with a previous HTO required a longer time to reach their highest functional score. Vorlat et al. [50] did not show successful outcome of UKAs after HTO. Likewise, the revision rate after HTO was 28% in Rees series [40] after a FU period of 2.9 years. One patient with a previous HTO in this series was revised from UKA to TKA. This evidence of unacceptably high failure rates emerged after the study began and was deemed reason to abandon the implantation of a UKA following HTO. Compared to previous authors, a low incidence of radiolucency at 5-year FU was found (21%, 20/96), for instance Pandit et al. [33] who reported radiolucent lines in 70% of their arthroplasties (40% complete and 60% partial). Like others, we conclude that these radiolucent lines have no clinical relevance [6, 15]. We hypothesise that the use of thorough pulsed lavage and a dry surgical field before cementing in all the implant procedures might have played a positive role. This is further supported by the recent study of Clarius et al. [6] who also showed a lower incidence of radiolucent lines after the use of pulsed lavage in the cemented Oxford Phase 3 prosthesis after a FU of 1 year. In patients with anteromedial osteoarthritis with persisting or progressive complaints after appropriate application of non-surgical treatment, the performance of an unicompartmental knee replacement can be recommended as long as the strict indication criteria for unicompartmental knee arthroplasty previously defined are considered [19, 55]. Recent studies suggest that the results of unicompartmental knee arthroplasty compare well with the results of total knee arthroplasty in similar age groups [35, 46]. Long-term FU results of UKA demonstrate predictably good results comparable with those of total knee replacement [20, 33]. With appropriate patient selection, prosthetic design and surgical technique, a surgeon can achieve good outcomes once he is well trained on its indications and technique. Although a specific number of implantations a year cannot be given, high volume for this technique is important in our opinion. With the MIS technique, patients experience a rapid recovery after the unicompartmental knee arthroplasty [37]. Conclusion This independent prospective study showed a high survival rate of the Oxford Phase 3 UKA performed by a single surgeon. Major complication rate was low. The newly developed instruments that were introduced with the Oxford Phase 3 UKA allow the surgeon to create a good balance of the flexion and extension gap, resulting in a reduction in the risk of dislocation of the mobile bearing and overcorrection. We would not recommend the use of this procedure after HTO or in the presence of lateral facet
7 Knee Surg Sports Traumatol Arthrosc (2011) 19: PFOA. The technically demanding Oxford procedure should be performed in a high-volume unit and pulsed lavage should be used in a dry operating field with the cementing technique. Another important recommendation is that complaints of pain should be thoroughly investigated as revision for unexplained pain has been shown to produce poor results. Compared to present literature, a very low percentage of radiolucency was detected. Outcome scores after 1 year do not change significantly so a minimum FU of 1 year in this series is justified. When strict indication criteria are followed, excellent, durable, and in our opinion reliable, results can be expected for this procedure in the medium-term. Acknowledgments The authors wish to thank Joanne Bloemsaat- Minekus and Matthew Easdale for their assistance. The authors did not receive any outside funding or grants in support of their research for or preparation of this work. Neither they nor a member of their immediate families received payments or other benefits or a commitment or agreement to provide such benefits from a commercial entity. No commercial entity paid or directed, or agreed to pay or direct, any benefits to any research fund, foundation, division, centre, clinical practice, or other charitable or non-profit organisation with which the authors, or a member of their immediate families, are affiliated or associated. Open Access This article is distributed under the terms of the Creative Commons Attribution Noncommercial License which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited. References 1. Ahlback S (1968) Osteoarthrosis of the knee. A radiographic investigation. Acta Radiol Diagn (Stockh) Suppl 277: Beard DJ, Pandit H, Ostlere S, Jenkins C, Dodd CA, Murray DW (2007) Pre-operative clinical and radiological assessment of the patellofemoral joint in unicompartmental knee replacement and its influence on outcome. J Bone Joint Surg Br 89: Bellamy N, Buchanan WW, Goldsmith CH, Campbell J, Stitt LW (1988) Validation study of WOMAC: a health status instrument for measuring clinically important patient relevant outcomes to antirheumatic drug therapy in patients with osteoarthritis of the hip or knee. J Rheumatol 15: Callaghan JJ, Squire MW, Goetz DD, Sullivan PM, Johnston RC (2000) Cemented rotating-platform total knee replacement. A nine to twelve-year follow-up study. J Bone Joint Surg Am 82: Carr A, Keyes G, Miller R, O Connor J, Goodfellow J (1993) Medial unicompartmental arthroplasty. A survival study of the Oxford meniscal knee. Clin Orthop Relat Res 295: Clarius M, Hauck C, Seeger JB, James A, Murray DW, Aldinger PR (2009) Pulsed lavage reduces the incidence of radiolucent lines under the tibial tray of Oxford unicompartmental knee arthroplasty: pulsed lavage versus syringe lavage. Int Orthop 33(6): Clark M, Campbell DG, Kiss G, Dobson PJ, Lewis PL (2010) Reintervention after mobile-bearing Oxford unicompartmental knee arthroplasty. Clin Orthop Relat Res 468(2): Collier MB, Engh CA Jr, Engh GA (2004) Shelf age of the polyethylene tibial component and outcome of unicondylar knee arthroplasty. J Bone Joint Surg Am 86: Dawson J, Fitzpatrick R, Murray D, Carr A (1998) Questionnaire on the perceptions of patients about total knee replacement. J Bone Joint Surg Br 80: Emerson RH Jr, Higgins LL (2008) Unicompartmental knee arthroplasty with the oxford prosthesis in patients with medial compartment arthritis. J Bone Joint Surg Am 90: Engelbrecht E (1971) Sliding prosthesis, a partial prosthesis in destructive processes of the knee joint. Chirurg 42: Gesell MW, Tria AJ Jr (2004) MIS unicondylar knee arthroplasty: surgical approach and early results. Clin Orthop Relat Res 428: Goodfellow JW, Kershaw CJ, Benson MK, O Connor JJ (1988) The Oxford Knee for unicompartmental osteoarthritis. The first 103 cases. J Bone Joint Surg Br 70: Goodfellow JW, O Connor J, Murray DW (2002) The Oxford meniscal unicompartmental knee. J Knee Surg 15: Gulati A, Chau R, Pandit HG, Gray H, Price AJ, Dodd CA, Murray DW (2009) The incidence of physiological radiolucency following Oxford unicompartmental knee replacement and its relationship to outcome. J Bone Joint Surg Br 91: Gunston FH (1971) Polycentric knee arthroplasty. Prosthetic simulation of normal knee movement. J Bone Joint Surg Br 53: Insall JN, Dorr LD, Scott RD, Scott WN (1989) Rationale of the Knee Society clinical rating system. Clin Orthop Relat Res 248: Kendrick BJ, Longino D, Pandit H, Svard U, Gill HS, Dodd CA, Murray DW, Price AJ (2010) Polyethylene wear in Oxford unicompartmental knee replacement: a retrieval study of 47 bearings. J Bone Joint Surg Br 92: Keyes GW, Carr AJ, Miller RK, Goodfellow JW (1992) The radiographic classification of medial gonarthrosis. Correlation with operation methods in 200 knees. Acta Orthop Scand 63: Keys GW, Ul-Abiddin Z, Toh EM (2004) Analysis of first forty Oxford medial unicompartmental knee replacement from a small district hospital in UK. Knee 11: Kort NP, van Raay JJ, Cheung J, Jolink C, Deutman R (2007) Analysis of Oxford medial unicompartmental knee replacement using the minimally invasive technique in patients aged 60 and above: an independent prospective series. Knee Surg Sports Traumatol Arthrosc 15: Koskinen E, Paavolainen P, Eskelinen A, Pulkkinen P, Remes V (2007) Unicondylar knee replacement for primary osteoarthritis: a prospective follow-up study of 1, 819 patients from the Finnish Arthroplasty Register. Acta Orthop 78: Kuipers BM, Kollen BJ, Bots PC, Burger BJ, van Raay JJ, Tulp NJ, Verheyen CC (2010) Factors associated with reduced early survival in the Oxford phase III medial unicompartment knee replacement. Knee 17: Kumar A, Chambers I, Wong P (2008) Periprosthetic fracture of the proximal tibia after lateral unicompartmental knee arthroplasty. J Arthroplasty 23: Lewold S, Goodman S, Knutson K, Robertsson O, Lidgren L (1995) Oxford meniscal bearing knee versus the Marmor knee in unicompartmental arthroplasty for arthrosis. A Swedish multicenter survival study. J Arthroplasty 10: Lewold S, Robertsson O, Knutson K, Lidgren L (1998) Revision of unicompartmental knee arthroplasty: outcome in 1, 135 cases from the Swedish Knee Arthroplasty study. Acta Orthop Scand 69: Luscombe KL, Lim J, Jones PW, White SH (2007) Minimally invasive Oxford medial unicompartmental knee arthroplasty. A note of caution! Int Orthop 31:
8 284 Knee Surg Sports Traumatol Arthrosc (2011) 19: Marmor L (1973) The modular knee. Clin Orthop Relat Res 94: Mercier N, Wimsey S, Saragaglia D (2009) Long-term clinical results of the Oxford medial unicompartmental knee arthroplasty. Int Orthop. doi: /s z 30. Mont MA, Haas S, Mullick T, Hungerford DS (2002) Total knee arthroplasty for patellofemoral arthritis. J Bone Joint Surg Am 84: Murray DW, Goodfellow JW, O Connor JJ (1998) The Oxford medial unicompartmental arthroplasty: a ten-year survival study. J Bone Joint Surg Br 80: Murray DW, Goodfellow JW, O Connor JJ, Dodd CA (1999) Oxford Unicompartmental knee: manual of the surgical technique. Biomet UK Ltd, Bridgend, pp Pandit H, Jenkins C, Barker K, Dodd CA, Murray DW (2006) The Oxford medial unicompartmental knee replacement using a minimally-invasive approach. J Bone Joint Surg Br 88: Pandit H, Jenkins C, Beard DJ et al (2009) Cementless Oxford unicompartmental knee replacement shows reduced radiolucency at one year. J Bone Joint Surg Br 91: Price AJ, Dodd CA, Svard UG, Murray DW (2005) Oxford medial unicompartmental knee arthroplasty in patients younger and older than 60 years of age. J Bone Joint Surg Br 87: Price AJ, Waite JC, Svard U (2005) Long-term clinical results of the medial Oxford unicompartmental knee arthroplasty. Clin Orthop Relat Res 435: Price AJ, Webb J, Topf H, Dodd CA, Goodfellow JW, Murray DW (2001) Oxford Hip and Knee Group. Rapid recovery after oxford unicompartmental arthroplasty through a short incision. J Arthroplasty 16(8): Psychoyios V, Crawford RW, O Connor JJ, Murray DW (1998) Wear of congruent meniscal bearings in unicompartmental knee arthroplasty: a retrieval study of 16 specimens. J Bone Joint Surg Br 80: Rajasekhar C, Das S, Smith A (2004) Unicompartmental knee arthroplasty. 2- to 12-year results in a community hospital. J Bone Joint Surg Br 86: Rees JL, Price AJ, Lynskey TG, Svard UC, Dodd CA, Murray DW (2001) Medial unicompartmental arthroplasty after failed high tibial osteotomy. J Bone Joint Surg Br 83: Repicci JA, Eberle RW (1999) Minimally invasive surgical technique for unicondylar knee arthroplasty. J South Orthop Assoc 8: Ritter MA, Faris PM, Thong AE, Davis KE, Meding JB, Berend ME (2004) Intra-operative findings in varus osteoarthritis of the knee. An analysis of pre-operative alignment in potential candidates for unicompartmental arthroplasty. J Bone Joint Surg Br 86: Robertsson O, Knutson K, Lewold S, Lidgren L (2001) The routine of surgical management reduces failure after unicompartmental knee arthroplasty. J Bone Joint Surg Br 83: Svard U (2009) Long term results after partial knee arthroplasty with the oxford Knee. Dissertation, University of Gothenburg 45. Svard UC, Price AJ (2001) Oxford medial unicompartmental knee arthroplasty. A survival analysis of an independent series. J Bone Joint Surg Br 83: Tabor OB Jr, Tabor OB, Bernard M, Wan JY (2005) Unicompartmental knee arthroplasty: long-term success in middle-age and obese patients. J Surg Orthop Adv 14: Tibrewal SB, Grant KA, Goodfellow JW (1984) The radiolucent line beneath the tibial components of the Oxford meniscal knee. J Bone Joint Surg Br 66: Vardi G, Strover AE (2004) Early complications of unicompartmental knee replacement: the Droitwich experience. Knee 11: Verdonk R, Cottenie D, Almqvist KF, Vorlat P (2005) The Oxford unicompartmental knee prosthesis: a 2 14 year followup. Knee Surg Sports Traumatol Arthros 13: Vorlat P, Verdonk R, Schauvlieghe H (2000) The Oxford unicompartmental knee prosthesis: a 5-year follow-up. Knee Surg Sports Traumatol Arthrosc 8: Weale AE, Murray DW, Baines J, Newman JH (2000) Radiological changes five years after unicompartmental knee replacement. J Bone Joint Surg Br 82: Weale AE, Murray DW, Crawford R et al (1999) Does arthritis progress in the retained compartments after Oxford medial unicompartmental arthroplasty? A clinical and radiological study with a minimum ten-year follow-up. J Bone Joint Surg Br 81: Weale AE, Murray DW, Newman JH, Ackroyd CE (1999) The length of the patellar tendon after unicompartmental and total knee replacement. J Bone Joint Surg Br 81: Wewers ME, Lowe NK (1990) A critical review of visual analogue scales in the measurement of clinical phenomena. Res Nurs Health 13: White SH, Ludkowski PF, Goodfellow JW (1991) Anteromedial osteoarthritis of the knee. J Bone Joint Surg Br 73:
Pre-operative clinical and radiological
 Pre-operative clinical and radiological assessment of the patellofemoral joint in unicompartmental knee replacement and its influence on outcome D. J. Beard, H. Pandit, S. Ostlere, C. Jenkins, C. A. F.
Pre-operative clinical and radiological assessment of the patellofemoral joint in unicompartmental knee replacement and its influence on outcome D. J. Beard, H. Pandit, S. Ostlere, C. Jenkins, C. A. F.
Ten- to 15-year results of the Oxford Phase III mobile unicompartmental knee arthroplasty
 L. A. Lisowski, L. I. Meijer, M. P. J. van den Bekerom, P. Pilot, A. E. Lisowski From BovenIJ Hospital, Statenjachtstraat 1, 1034 CS Amsterdam, The Netherlands L. A. Lisowski, MD, PhD, Orthopaedic Surgeon,
L. A. Lisowski, L. I. Meijer, M. P. J. van den Bekerom, P. Pilot, A. E. Lisowski From BovenIJ Hospital, Statenjachtstraat 1, 1034 CS Amsterdam, The Netherlands L. A. Lisowski, MD, PhD, Orthopaedic Surgeon,
The young patient and the medial unicompartmental knee replacement
 Acta Orthop. Belg., 2015, 81, 283-288 ORIGINAL STUDY The young patient and the medial unicompartmental knee replacement Omar Faour Martín, Jose Antonio Valverde García, Miguel Ángel Martín Ferrero, Aurelio
Acta Orthop. Belg., 2015, 81, 283-288 ORIGINAL STUDY The young patient and the medial unicompartmental knee replacement Omar Faour Martín, Jose Antonio Valverde García, Miguel Ángel Martín Ferrero, Aurelio
The Oxford phase III unicompartmental knee replacement in patients less than 60 years of age Kort, Nanne P.; van Raay, Jos J. A. M.; van Horn, Jim J.
 University of Groningen The Oxford phase III unicompartmental knee replacement in patients less than 60 years of age Kort, Nanne P.; van Raay, Jos J. A. M.; van Horn, Jim J. Published in: Knee surgery
University of Groningen The Oxford phase III unicompartmental knee replacement in patients less than 60 years of age Kort, Nanne P.; van Raay, Jos J. A. M.; van Horn, Jim J. Published in: Knee surgery
Assessment of radiolucent lines around the Oxford unicompartmental knee replacement
 KNEE Assessment of radiolucent lines around the Oxford unicompartmental knee replacement SENSITIVITY AND SPECIFICITY FOR LOOSENING S. Kalra, T. O. Smith, B. Berko, N. P. Walton From Norfolk and Norwich
KNEE Assessment of radiolucent lines around the Oxford unicompartmental knee replacement SENSITIVITY AND SPECIFICITY FOR LOOSENING S. Kalra, T. O. Smith, B. Berko, N. P. Walton From Norfolk and Norwich
With over 40 years clinical experience, the Oxford Partial Knee is the most widely used, 1 clinically proven 2 partial knee system in the world.
 Oxford Partial Knee A Definitive Implant With over 40 years clinical experience, the Oxford Partial Knee is the most widely used, 1 clinically proven 2 partial knee system in the world. Compared with total
Oxford Partial Knee A Definitive Implant With over 40 years clinical experience, the Oxford Partial Knee is the most widely used, 1 clinically proven 2 partial knee system in the world. Compared with total
Bilateral total knee arthroplasty: One mobile-bearing and one fixed-bearing
 Journal of Orthopaedic Surgery 2001, 9(1): 45 50 Bilateral total knee arthroplasty: One mobile-bearing and one fixed-bearing KY Chiu, TP Ng, WM Tang and P Lam Department of Orthopaedic Surgery, The University
Journal of Orthopaedic Surgery 2001, 9(1): 45 50 Bilateral total knee arthroplasty: One mobile-bearing and one fixed-bearing KY Chiu, TP Ng, WM Tang and P Lam Department of Orthopaedic Surgery, The University
Cementless Oxford unicompartmental knee replacement shows reduced radiolucency at one year
 Cementless Oxford unicompartmental knee replacement shows reduced radiolucency at one year H. Pandit, C. Jenkins, D. J. Beard, J. Gallagher, A. J. Price, C. A. F. Dodd, J. W. Goodfellow, D. W. Murray From
Cementless Oxford unicompartmental knee replacement shows reduced radiolucency at one year H. Pandit, C. Jenkins, D. J. Beard, J. Gallagher, A. J. Price, C. A. F. Dodd, J. W. Goodfellow, D. W. Murray From
Oxford. Partial Knee
 Oxford Partial Knee Oxford Partial Knee A Definitive Implant The Oxford Partial Knee is the most widely used 38 and clinically proven 22 partial knee replacement (PKR) system in the world, offering industry
Oxford Partial Knee Oxford Partial Knee A Definitive Implant The Oxford Partial Knee is the most widely used 38 and clinically proven 22 partial knee replacement (PKR) system in the world, offering industry
Functional Outcome of Uni-Knee Arthroplasty in Asians with six-year Follow-up
 Functional Outcome of Uni-Knee Arthroplasty in Asians with six-year Follow-up Ching-Jen Wang, M.D. Department of Orthopedic Surgery Kaohsiung Chang Gung Memorial Hospital Chang Gung University College
Functional Outcome of Uni-Knee Arthroplasty in Asians with six-year Follow-up Ching-Jen Wang, M.D. Department of Orthopedic Surgery Kaohsiung Chang Gung Memorial Hospital Chang Gung University College
The Survivorship and Clinical Results of Minimally Invasive Unicompartmental Knee Arthroplasty at 10-Year Follow-up
 Original Article Clinics in Orthopedic Surgery 2015;7:199-206 http://dx.doi.org/10.4055/cios.2015.7.2.199 The Survivorship and Clinical Results of Minimally Invasive Unicompartmental Knee Arthroplasty
Original Article Clinics in Orthopedic Surgery 2015;7:199-206 http://dx.doi.org/10.4055/cios.2015.7.2.199 The Survivorship and Clinical Results of Minimally Invasive Unicompartmental Knee Arthroplasty
Minimally invasive unicompartmental knee arthroplasty in treatment of osteonecrosis versus osteoarthritis : a matched-pair comparison
 Acta Orthop. Belg., 2015, 81, 333-339 ORIGINAL STUDY Minimally invasive unicompartmental knee arthroplasty in treatment of osteonecrosis versus osteoarthritis : a matched-pair comparison Qidong Zhang,
Acta Orthop. Belg., 2015, 81, 333-339 ORIGINAL STUDY Minimally invasive unicompartmental knee arthroplasty in treatment of osteonecrosis versus osteoarthritis : a matched-pair comparison Qidong Zhang,
Mid-Term Results of Oxford Medial Unicompartmental Knee Arthroplasty
 Original Article Clinics in Orthopedic Surgery 2011;3:178-183 http://dx.doi.org/10.4055/cios.2011.3.3.178 Mid-Term Results of Oxford Medial Unicompartmental Knee Arthroplasty Won-Sik Choy, MD, Kap Jung
Original Article Clinics in Orthopedic Surgery 2011;3:178-183 http://dx.doi.org/10.4055/cios.2011.3.3.178 Mid-Term Results of Oxford Medial Unicompartmental Knee Arthroplasty Won-Sik Choy, MD, Kap Jung
The Knee. The Twin Peg Oxford partial knee replacement: The first 100 cases. Stephen H. White a,, Sharon Roberts a, Peter W.
 The Knee 19 (2012) 36 40 Contents lists available at ScienceDirect The Knee The Twin Peg Oxford partial knee replacement: The first 100 cases Stephen H. White a,, Sharon Roberts a, Peter W. Jones b a Department
The Knee 19 (2012) 36 40 Contents lists available at ScienceDirect The Knee The Twin Peg Oxford partial knee replacement: The first 100 cases Stephen H. White a,, Sharon Roberts a, Peter W. Jones b a Department
Alignment of the femoral component in a mobile-bearing unicompartmental knee arthroplasty Kort, N. P.; van Raay, J. J. A. M.; Thomassen, B. J. W.
 University of Groningen Alignment of the femoral component in a mobile-bearing unicompartmental knee arthroplasty Kort, N. P.; van Raay, J. J. A. M.; Thomassen, B. J. W. Published in: Knee DOI: 10.1016/j.knee.2007.04.007
University of Groningen Alignment of the femoral component in a mobile-bearing unicompartmental knee arthroplasty Kort, N. P.; van Raay, J. J. A. M.; Thomassen, B. J. W. Published in: Knee DOI: 10.1016/j.knee.2007.04.007
The influence of degeneration of the lateral patellofemoral joint on outcome of medial unicompartmental knee replacement
 2015 4 ORTHOPAEDIC BIOMECHANICS MATERIALS AND CLINICAL STUDY.29. doi: 10.3969/j.issn. 1672-5972.2015.02.008 swgk2015-03-0050 * 1 1 2 1 * 1 1 [ ] Oxford 2009 8 2013 12 126 (104 ) Ahlback Weidow 5 1 Hospital
2015 4 ORTHOPAEDIC BIOMECHANICS MATERIALS AND CLINICAL STUDY.29. doi: 10.3969/j.issn. 1672-5972.2015.02.008 swgk2015-03-0050 * 1 1 2 1 * 1 1 [ ] Oxford 2009 8 2013 12 126 (104 ) Ahlback Weidow 5 1 Hospital
Management of Periprosthetic Fracture in Unicompartmental Knee Arthroplasty Patients: A Case Series
 Management of Periprosthetic Fracture in Unicompartmental Knee Arthroplasty Patients: A Case Series Yew Lok Woo, MBBS, Pak Lin Chin, MBBS, FRCS, Ngai Nung Lo, MBBS, FRCS, Shi-Lu Chia, PhD, Darren Keng
Management of Periprosthetic Fracture in Unicompartmental Knee Arthroplasty Patients: A Case Series Yew Lok Woo, MBBS, Pak Lin Chin, MBBS, FRCS, Ngai Nung Lo, MBBS, FRCS, Shi-Lu Chia, PhD, Darren Keng
Implant Overhang after Unicompartmental Knee Arthroplasty: Oxford Prosthesis versus Miller-Galante II Prosthesis
 Original Article Knee Surg Relat Res 2014;26(2):82-87 http://dx.doi.org/10.5792/ksrr.2014.26.2.82 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Implant Overhang after Unicompartmental
Original Article Knee Surg Relat Res 2014;26(2):82-87 http://dx.doi.org/10.5792/ksrr.2014.26.2.82 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Implant Overhang after Unicompartmental
Complications of Medial Unicompartmental Knee Arthroplasty
 Original Article Clinics in Orthopedic Surgery 2014;6:365-372 http://dx.doi.org/10.4055/cios.2014.6.4.365 Complications of Medial Unicompartmental Knee Arthroplasty Jong Hun Ji, MD, Sang Eun Park, MD,
Original Article Clinics in Orthopedic Surgery 2014;6:365-372 http://dx.doi.org/10.4055/cios.2014.6.4.365 Complications of Medial Unicompartmental Knee Arthroplasty Jong Hun Ji, MD, Sang Eun Park, MD,
Does a minimally invasive approach affect positioning of components in unicompartmental knee arthroplasty? Early results with survivorship analysis
 Acta Orthop. Belg., 2006, 72, 709-715 ORIGINAL STUDY Does a minimally invasive approach affect positioning of components in unicompartmental knee arthroplasty? Early results with survivorship analysis
Acta Orthop. Belg., 2006, 72, 709-715 ORIGINAL STUDY Does a minimally invasive approach affect positioning of components in unicompartmental knee arthroplasty? Early results with survivorship analysis
Ten-year in vivo wear measurement of a fully congruent mobile bearing unicompartmental knee arthroplasty
 Ten-year in vivo wear measurement of a fully congruent mobile bearing unicompartmental knee arthroplasty A. J. Price, A. Short, C. Kellett, D. Beard, H. Gill, H. Pandit, C. A. F. Dodd, D. W. Murray From
Ten-year in vivo wear measurement of a fully congruent mobile bearing unicompartmental knee arthroplasty A. J. Price, A. Short, C. Kellett, D. Beard, H. Gill, H. Pandit, C. A. F. Dodd, D. W. Murray From
Conversion of unicompartmental knee arthroplasty to total knee arthroplasty : The challenges and need for augments
 Acta Orthop. Belg., 2013, 79, 699-705 ORIGINAL STUDY Conversion of unicompartmental knee arthroplasty to total knee arthroplasty : The challenges and need for augments Zeeshan Khan, Syed Z. Nawaz, Steven
Acta Orthop. Belg., 2013, 79, 699-705 ORIGINAL STUDY Conversion of unicompartmental knee arthroplasty to total knee arthroplasty : The challenges and need for augments Zeeshan Khan, Syed Z. Nawaz, Steven
Higher revision risk for unicompartmental knee arthroplasty in low-volume hospitals
 Acta Orthopaedica 2014; 85 (4): x x 1 Higher revision risk for unicompartmental knee arthroplasty in low-volume hospitals Data from 5,791 cases in the Norwegian Arthroplasty Register Mona Badawy 1, Birgitte
Acta Orthopaedica 2014; 85 (4): x x 1 Higher revision risk for unicompartmental knee arthroplasty in low-volume hospitals Data from 5,791 cases in the Norwegian Arthroplasty Register Mona Badawy 1, Birgitte
Unicondylar Knee Vs Total Knee Replacement: Is Less Better In the Middle Aged Athlete
 Unicondylar Knee Vs Total Knee Replacement: Is Less Better In the Middle Aged Athlete Chair: Maurilio Marcacci, MD Alois Franz "Basic principles and considerations of the Unis" Joao M. Barretto "Sport
Unicondylar Knee Vs Total Knee Replacement: Is Less Better In the Middle Aged Athlete Chair: Maurilio Marcacci, MD Alois Franz "Basic principles and considerations of the Unis" Joao M. Barretto "Sport
Scandinavian Journal of Surgery 0: 1 8, Department of Surgery, North Karelia Central Hospital, Joensuu, Finland 2
 577022SJS0010.1177/1457496915577022UKA mid-term resultss. S. A. Miettinen et al. research-article2015 ORIGINAL ARTICLE Scandinavian Journal of Surgery 0: 1 8, 2015 Mid-Term Results Of Oxford Phase 3 Unicompartmental
577022SJS0010.1177/1457496915577022UKA mid-term resultss. S. A. Miettinen et al. research-article2015 ORIGINAL ARTICLE Scandinavian Journal of Surgery 0: 1 8, 2015 Mid-Term Results Of Oxford Phase 3 Unicompartmental
Oxford phase 3 unicompartmental knee replacement in Korean patients
 KNEE Oxford phase 3 unicompartmental knee replacement in Korean patients H-C. Lim, J-H. Bae, S-H. Song, S-J. Kim From Guro Hospital, Korea University Medical Center, Seoul, Korea Medium-term survivorship
KNEE Oxford phase 3 unicompartmental knee replacement in Korean patients H-C. Lim, J-H. Bae, S-H. Song, S-J. Kim From Guro Hospital, Korea University Medical Center, Seoul, Korea Medium-term survivorship
H.P. Teng, Y.J. Chou, L.C. Lin, and C.Y. Wong Under general or spinal anesthesia, the knee was flexed gently. In the cases of limited ROM, gentle and
 THE BENEFIT OF ARTHROSCOPY FOR SYMPTOMATIC TOTAL KNEE ARTHROPLASTY Hsiu-Peng Teng, Yi-Jiun Chou, Li-Chun Lin, and Chi-Yin Wong Department of Orthopedic Surgery, Kaohsiung Veterans General Hospital, Kaohsiung,
THE BENEFIT OF ARTHROSCOPY FOR SYMPTOMATIC TOTAL KNEE ARTHROPLASTY Hsiu-Peng Teng, Yi-Jiun Chou, Li-Chun Lin, and Chi-Yin Wong Department of Orthopedic Surgery, Kaohsiung Veterans General Hospital, Kaohsiung,
Unicompartmental Knee Replacement
 Unicompartmental Knee Replacement Results and Techniques Alexander P. Sah, MD California Orthopaedic Association Meeting Laguna Niguel, CA May 20th, 2011 Overview Why partial knee replacement? - versus
Unicompartmental Knee Replacement Results and Techniques Alexander P. Sah, MD California Orthopaedic Association Meeting Laguna Niguel, CA May 20th, 2011 Overview Why partial knee replacement? - versus
Revision surgery for failed unicompartmental knee replacement : Technical aspects and clinical outcome
 Acta Orthop. Belg., 2013, 79, 312-317 ORIGINAL STUDY Revision surgery for failed unicompartmental knee replacement : Technical aspects and clinical outcome Curtis A. Robb, Gulraj S. Matharu, Khalid Baloch,
Acta Orthop. Belg., 2013, 79, 312-317 ORIGINAL STUDY Revision surgery for failed unicompartmental knee replacement : Technical aspects and clinical outcome Curtis A. Robb, Gulraj S. Matharu, Khalid Baloch,
The effect of leg alignment on the outcome of unicompartmental knee replacement
 The effect of leg alignment on the outcome of unicompartmental knee replacement A. Gulati, H. Pandit, C. Jenkins, R. Chau, C. A. F. Dodd, D. W. Murray From Nuffield Orthopaedic Centre, Oxford, England
The effect of leg alignment on the outcome of unicompartmental knee replacement A. Gulati, H. Pandit, C. Jenkins, R. Chau, C. A. F. Dodd, D. W. Murray From Nuffield Orthopaedic Centre, Oxford, England
Clinical Study Cemented versus Uncemented Oxford Unicompartmental Knee Arthroplasty: Is There a Difference?
 Advances in Orthopedics Volume 2013, Article ID 245915, 6 pages http://dx.doi.org/10.1155/2013/245915 Clinical Study Cemented versus Uncemented Oxford Unicompartmental Knee Arthroplasty: Is There a Difference?
Advances in Orthopedics Volume 2013, Article ID 245915, 6 pages http://dx.doi.org/10.1155/2013/245915 Clinical Study Cemented versus Uncemented Oxford Unicompartmental Knee Arthroplasty: Is There a Difference?
Mid-Term Results of Oxford Medial Unicompartmental Knee Arthroplasty in Young Asian Patients Less than 60 Years of Age: A Minimum 5-Year Follow-up
 Original Article Knee Surg Relat Res 2017;29(2):122-128 https://doi.org/10.5792/ksrr.16.045 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Mid-Term Results of Oxford Medial Unicompartmental
Original Article Knee Surg Relat Res 2017;29(2):122-128 https://doi.org/10.5792/ksrr.16.045 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Mid-Term Results of Oxford Medial Unicompartmental
Simplifying the Most Clinically Proven 1 Partial Knee in the World. Oxford Partial Knee with Microplasty Instrumentation
 Simplifying the Most Clinically Proven 1 Partial Knee in the World Oxford Partial Knee with Microplasty Instrumentation 1 Microplasty Instrumentation Innovative, Accurate, Reproducible Microplasty Instrumentation
Simplifying the Most Clinically Proven 1 Partial Knee in the World Oxford Partial Knee with Microplasty Instrumentation 1 Microplasty Instrumentation Innovative, Accurate, Reproducible Microplasty Instrumentation
Fixed or Mobile bearing in Unicompartmental Knee Arthroplasty
 Fixed or Mobile bearing in Unicompartmental Knee Arthroplasty Jean-Noel Argenson, Matthieu Ollivier, Xavier Flecher, Sebastien Parratte Institute for Locomotion Sainte Marguerite Hospital, Marseille, France
Fixed or Mobile bearing in Unicompartmental Knee Arthroplasty Jean-Noel Argenson, Matthieu Ollivier, Xavier Flecher, Sebastien Parratte Institute for Locomotion Sainte Marguerite Hospital, Marseille, France
Gender Solutions Patello-Femoral Joint System
 Zimmer Biomet is the leading company in partial knee arthroplasty (PKA) 1 with over 40 years experience, offering a comprehensive range of anatomic and innovative solutions. Research shows that surgeons
Zimmer Biomet is the leading company in partial knee arthroplasty (PKA) 1 with over 40 years experience, offering a comprehensive range of anatomic and innovative solutions. Research shows that surgeons
Simplifying the Most Clinically Proven Partial Knee in the World. Oxford Partial Knee with Microplasty Instrumentation
 Simplifying the Most Clinically Proven Partial Knee in the World Oxford Partial Knee with Microplasty Instrumentation 1 Microplasty Instrumentation Innovative, Accurate, Reproducible Microplasty instrumentation
Simplifying the Most Clinically Proven Partial Knee in the World Oxford Partial Knee with Microplasty Instrumentation 1 Microplasty Instrumentation Innovative, Accurate, Reproducible Microplasty instrumentation
Case Report Meniscal Bearing Dislocation of Unicompartmental Knee Arthroplasty with Faint Symptom
 Case Reports in Orthopedics Volume 2015, Article ID 217842, 5 pages http://dx.doi.org/10.1155/2015/217842 Case Report Meniscal Bearing Dislocation of Unicompartmental Knee Arthroplasty with Faint Symptom
Case Reports in Orthopedics Volume 2015, Article ID 217842, 5 pages http://dx.doi.org/10.1155/2015/217842 Case Report Meniscal Bearing Dislocation of Unicompartmental Knee Arthroplasty with Faint Symptom
Medium term results of the Miller-Galante unicompartmental knee arthroplasty with 10 year survivorship
 Acta Orthop. Belg., 2013, 79, 197-204 ORIGINAL STUDY Medium term results of the Miller-Galante unicompartmental knee arthroplasty with 10 year survivorship Rajesh Rachha, Karunakar Veravalli, Manoj Sood
Acta Orthop. Belg., 2013, 79, 197-204 ORIGINAL STUDY Medium term results of the Miller-Galante unicompartmental knee arthroplasty with 10 year survivorship Rajesh Rachha, Karunakar Veravalli, Manoj Sood
Functional improvement after unicompartmental knee replacement: a follow-up study with a performance based knee test
 Knee Surg Sports Traumatol Arthrosc (2007) 15:1187 1193 DOI 10.1007/s00167-007-0351-7 KNEE Functional improvement after unicompartmental knee replacement: a follow-up study with a performance based knee
Knee Surg Sports Traumatol Arthrosc (2007) 15:1187 1193 DOI 10.1007/s00167-007-0351-7 KNEE Functional improvement after unicompartmental knee replacement: a follow-up study with a performance based knee
Midterm results of cemented Press Fit Condylar Sigma total knee arthroplasty system
 Journal of Orthopaedic Surgery 2005:13(3):280-284 Midterm results of cemented Press Fit Condylar Sigma total knee arthroplasty system S Asif, DSK Choon Department of Orthopaedic Surgery, University of
Journal of Orthopaedic Surgery 2005:13(3):280-284 Midterm results of cemented Press Fit Condylar Sigma total knee arthroplasty system S Asif, DSK Choon Department of Orthopaedic Surgery, University of
Unicompartmental or total knee replacement
 Unicompartmental or total knee replacement THE 15-YEAR RESULTS OF A PROSPECTIVE RANDOMISED CONTROLLED TRIAL J. Newman, R. V. Pydisetty, C. Ackroyd From Avon Orthopaedic Centre, Bristol, England Between
Unicompartmental or total knee replacement THE 15-YEAR RESULTS OF A PROSPECTIVE RANDOMISED CONTROLLED TRIAL J. Newman, R. V. Pydisetty, C. Ackroyd From Avon Orthopaedic Centre, Bristol, England Between
No radiographic difference between patient-specific guiding and conventional Oxford UKA surgery
 DOI 10.1007/s00167-014-2849-0 KNEE No radiographic difference between patient-specific guiding and conventional Oxford UKA surgery Bart Kerens Martijn G. M. Schotanus Bert Boonen Nanne P. Kort Received:
DOI 10.1007/s00167-014-2849-0 KNEE No radiographic difference between patient-specific guiding and conventional Oxford UKA surgery Bart Kerens Martijn G. M. Schotanus Bert Boonen Nanne P. Kort Received:
Comparison of high-flex and conventional implants for bilateral total knee arthroplasty
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 14 Number 1 Comparison of high-flex and conventional implants for bilateral total knee arthroplasty C Martin-Hernandez, M Guillen-Soriano, A
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 14 Number 1 Comparison of high-flex and conventional implants for bilateral total knee arthroplasty C Martin-Hernandez, M Guillen-Soriano, A
EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY
 EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY Benkovich V. Perry T., Bunin A., Bilenko V., Unit for Joint Arthroplasty, Soroka Medical Center Ben Gurion University of Negev Beer
EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY Benkovich V. Perry T., Bunin A., Bilenko V., Unit for Joint Arthroplasty, Soroka Medical Center Ben Gurion University of Negev Beer
A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients
 Original Research Article A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients Ragesh Chandran 1*, Sanath K Shetty 2, Ashwin Shetty 3, Bijith Balan 1, Lawrence J Mathias
Original Research Article A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients Ragesh Chandran 1*, Sanath K Shetty 2, Ashwin Shetty 3, Bijith Balan 1, Lawrence J Mathias
THE KNEE SOCIETY VIRTUAL FELLOWSHIP
 THE KNEE SOCIETY VIRTUAL FELLOWSHIP CHAPTER IX PARTIAL KNEE: MEDIAL, LATERAL AND PFR Revision of Failed Unicompartmental to Total Knee Arthroplasty Presented by: Keith R. Berend, MD COPYRIGHT 2016 THE
THE KNEE SOCIETY VIRTUAL FELLOWSHIP CHAPTER IX PARTIAL KNEE: MEDIAL, LATERAL AND PFR Revision of Failed Unicompartmental to Total Knee Arthroplasty Presented by: Keith R. Berend, MD COPYRIGHT 2016 THE
Clinical Results of Lateral Unicompartmental Knee Arthroplasty: Minimum 2-Year Follow-up
 Original Article Clinics in Orthopedic Surgery 2016;8:386-392 https://doi.org/10.4055/cios.2016.8.4.386 Clinical Results of Lateral Unicompartmental Knee Arthroplasty: Minimum 2-Year Follow-up Kyung Tae
Original Article Clinics in Orthopedic Surgery 2016;8:386-392 https://doi.org/10.4055/cios.2016.8.4.386 Clinical Results of Lateral Unicompartmental Knee Arthroplasty: Minimum 2-Year Follow-up Kyung Tae
Medium-term outcome of cementless, mobile-bearing, unicompartmental knee arthroplasty
 Original Article Page 1 of 12 Medium-term outcome of cementless, mobile-bearing, unicompartmental knee arthroplasty Radosław Stempin 1, Kacper Stempin 2, Wiesław Kaczmarek 3 1 Department of Orthopedic
Original Article Page 1 of 12 Medium-term outcome of cementless, mobile-bearing, unicompartmental knee arthroplasty Radosław Stempin 1, Kacper Stempin 2, Wiesław Kaczmarek 3 1 Department of Orthopedic
The UniSpacer : correcting varus malalignment in medial gonarthrosis
 DOI 10.1007/s00264-009-0908-9 ORIGINAL PAPER The UniSpacer : correcting varus malalignment in medial gonarthrosis Michael Clarius & Justus F. Becker & Holger Schmitt & Joern B. Seeger Received: 20 October
DOI 10.1007/s00264-009-0908-9 ORIGINAL PAPER The UniSpacer : correcting varus malalignment in medial gonarthrosis Michael Clarius & Justus F. Becker & Holger Schmitt & Joern B. Seeger Received: 20 October
SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY
 SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY Th. KARACHALIOS, P. P. SARANGI, J. H. NEWMAN From Winford Orthopaedic Hospital, Bristol, England We report a prospective case-controlled
SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY Th. KARACHALIOS, P. P. SARANGI, J. H. NEWMAN From Winford Orthopaedic Hospital, Bristol, England We report a prospective case-controlled
Functional Outcomes of Revision Total Knee Arthroplasty Following Failed Unicompartmental Knee Arthroplasty
 Reconstructive Review Volume 4, Number 4, December 2014 ORIGINAL ARTICLE Functional Outcomes of Revision Total Knee Arthroplasty Following Failed Unicompartmental Knee Arthroplasty Chris Ironside MBBS,
Reconstructive Review Volume 4, Number 4, December 2014 ORIGINAL ARTICLE Functional Outcomes of Revision Total Knee Arthroplasty Following Failed Unicompartmental Knee Arthroplasty Chris Ironside MBBS,
Medial unicompartmental knee replacement in the under-50s
 Medial unicompartmental knee replacement in the under-50s S. Parratte, J.-N.A.Argenson, O. Pearce, V. Pauly, P. Auquier, J.-M. Aubaniac From Aix-Marseille University, Marseille, France We retrospectively
Medial unicompartmental knee replacement in the under-50s S. Parratte, J.-N.A.Argenson, O. Pearce, V. Pauly, P. Auquier, J.-M. Aubaniac From Aix-Marseille University, Marseille, France We retrospectively
Instrumentation Options
 Instrumentation Options With the introduction of Microplasty and Premier Instrumentation platforms and advancements such as our patented Slidex Technology, the Vanguard Complete Knee System is the surgeon
Instrumentation Options With the introduction of Microplasty and Premier Instrumentation platforms and advancements such as our patented Slidex Technology, the Vanguard Complete Knee System is the surgeon
Functional and radiological outcome of total knee replacement in varus deformity of the knee
 ISSN: 2319-7706 Volume 4 Number 4 (2015) pp. 934-938 http://www.ijcmas.com Original Research Article Functional and radiological outcome of total knee replacement in varus deformity of the knee Sandesh
ISSN: 2319-7706 Volume 4 Number 4 (2015) pp. 934-938 http://www.ijcmas.com Original Research Article Functional and radiological outcome of total knee replacement in varus deformity of the knee Sandesh
Umile Giuseppe Longo, Mattia Loppini, Ugo Trovato, Giacomo Rizzello, Nicola Maffulli,, *, and Vincenzo Denaro. Abstract
 British Medical Bulletin, 2015, 114:65 73 doi: 10.1093/bmb/ldv009 Advance Access Publication Date: 4 March 2015 No difference between unicompartmental versus total knee arthroplasty for the management
British Medical Bulletin, 2015, 114:65 73 doi: 10.1093/bmb/ldv009 Advance Access Publication Date: 4 March 2015 No difference between unicompartmental versus total knee arthroplasty for the management
Stefan Rahm MD University Hospital Balgrist
 Knee Prosthesis Models & Materials, Surgical Techniques and Approaches Stefan Rahm MD University Hospital Balgrist INTRODUCTION VARUS VALGUS 46 Y OLD MALE Pain in the medial compartment left more than
Knee Prosthesis Models & Materials, Surgical Techniques and Approaches Stefan Rahm MD University Hospital Balgrist INTRODUCTION VARUS VALGUS 46 Y OLD MALE Pain in the medial compartment left more than
P a rt i a l Knee Ar t h r o p l a s t y (PKA) Surgical Technique Overview
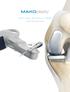 P a rt i a l Knee Ar t h r o p l a s t y (PKA) Surgical Technique Overview Femoral array Medial parapatellar incision Tibial array 1. Perform a medial incision and parapatellar arthrotomy to expose the
P a rt i a l Knee Ar t h r o p l a s t y (PKA) Surgical Technique Overview Femoral array Medial parapatellar incision Tibial array 1. Perform a medial incision and parapatellar arthrotomy to expose the
1. White SH, Nazarian NA, McEwen Smith AM, Balfour TW. Periampullary adenoma causing pancreatitis. Br Med J 1981; 283:527.
 Mr Steve White, Consultant Orthopaedic Surgeon Peer-reviewed original papers: 1. White SH, Nazarian NA, McEwen Smith AM, Balfour TW. Periampullary adenoma causing pancreatitis. Br Med J 1981; 283:527.
Mr Steve White, Consultant Orthopaedic Surgeon Peer-reviewed original papers: 1. White SH, Nazarian NA, McEwen Smith AM, Balfour TW. Periampullary adenoma causing pancreatitis. Br Med J 1981; 283:527.
Time-dependent improvement in functional outcome following Oxford medial unicompartmental knee arthroplasty
 46 Acta Orthopaedica 212; 83 (1): 46 52 Time-dependent improvement in functional outcome following Oxford medial unicompartmental knee arthroplasty A prospective longitudinal multicenter study involving
46 Acta Orthopaedica 212; 83 (1): 46 52 Time-dependent improvement in functional outcome following Oxford medial unicompartmental knee arthroplasty A prospective longitudinal multicenter study involving
The Unispacer TM unicompartmental knee implant: Its outcomes in medial compartment knee osteoarthritis
 Orthopaedics & Traumatology: Surgery & Research (2011) 97, 410 417 ORIGINAL ARTICLE The Unispacer TM unicompartmental knee implant: Its outcomes in medial compartment knee osteoarthritis C. Catier, M.
Orthopaedics & Traumatology: Surgery & Research (2011) 97, 410 417 ORIGINAL ARTICLE The Unispacer TM unicompartmental knee implant: Its outcomes in medial compartment knee osteoarthritis C. Catier, M.
Appendix E-1 (Figures and Tables) Fig. E-1
 Page 1 Appendix E-1 (Figures and Tables) Fig. E-1 Survival curves (Kaplan-Meier) for revised knees (failed primary TKAs revised to TKAs [TKA TKA] and failed primary UKAs revised to TKAs [UKA TKA]) according
Page 1 Appendix E-1 (Figures and Tables) Fig. E-1 Survival curves (Kaplan-Meier) for revised knees (failed primary TKAs revised to TKAs [TKA TKA] and failed primary UKAs revised to TKAs [UKA TKA]) according
B i co m pa r t m e n ta l Knee Ar t h r o p l a s t y. Surgical Technique Overview
 B i co m pa r t m e n ta l Knee Ar t h r o p l a s t y Surgical Technique Overview Femoral array Medial parapatellar incision Tibial array 1. Perform a medial incision and parapatellar arthrotomy to expose
B i co m pa r t m e n ta l Knee Ar t h r o p l a s t y Surgical Technique Overview Femoral array Medial parapatellar incision Tibial array 1. Perform a medial incision and parapatellar arthrotomy to expose
Shaoqi Tian 1*, Bin Wang 2, Yuanhe Wang 1, Chengzhi Ha 1, Lun Liu 1 and Kang Sun 1*
 Tian et al. BMC Musculoskeletal Disorders (2016) 17:327 DOI 10.1186/s12891-016-1186-5 RESEARCH ARTICLE Open Access Combined unicompartmental knee arthroplasty and anterior cruciate ligament reconstruction
Tian et al. BMC Musculoskeletal Disorders (2016) 17:327 DOI 10.1186/s12891-016-1186-5 RESEARCH ARTICLE Open Access Combined unicompartmental knee arthroplasty and anterior cruciate ligament reconstruction
)301( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY
 )301( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE Early Results of Oxford Mobile Bearing Medial Unicompartmental Knee Replacement (UKR) with the Microplasty Instrumentation:
)301( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE Early Results of Oxford Mobile Bearing Medial Unicompartmental Knee Replacement (UKR) with the Microplasty Instrumentation:
Functional Outcomes of Uni knee Arthroplasty for Medial Compartment Knee Arthropathy in Asian Patients
 Original Article 406 Functional Outcomes of Uni knee Arthroplasty for Medial Compartment Knee Arthropathy in Asian Patients To Wong 1, Ching Jen Wang 2, Jun Wen Wang 2, Jih Yang Ko 2 Background: Uni knee
Original Article 406 Functional Outcomes of Uni knee Arthroplasty for Medial Compartment Knee Arthropathy in Asian Patients To Wong 1, Ching Jen Wang 2, Jun Wen Wang 2, Jih Yang Ko 2 Background: Uni knee
Gold standard of a TKA. Conflicting goals? POLYETHYLENE WEAR THE SOLUTION: MOBILE BEARING KNEES. MOBILE BEARING A totally new approach (1977)
 Changing designs : the case against mobile bearing? Gold standard of a TKA Goal of a TKA: 1. Pain 2. Motion 3. Longevity Stress Guy BELLIER M.D. PARIS France Conformity = Durability w/o constraints = non
Changing designs : the case against mobile bearing? Gold standard of a TKA Goal of a TKA: 1. Pain 2. Motion 3. Longevity Stress Guy BELLIER M.D. PARIS France Conformity = Durability w/o constraints = non
Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella Treated with a Different Method in Each Knee
 Case Reports in Orthopedics Volume 2015, Article ID 890315, 5 pages http://dx.doi.org/10.1155/2015/890315 Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella
Case Reports in Orthopedics Volume 2015, Article ID 890315, 5 pages http://dx.doi.org/10.1155/2015/890315 Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella
why bicompartmental? A REVOLUTIONARY ALTERNATIVE TO TOTAL KNEE REPLACEMENTS
 why bicompartmental? A REVOLUTIONARY ALTERNATIVE TO TOTAL KNEE REPLACEMENTS TKR is not always the answer Today, many patients with medial or lateral disease and patellofemoral involvement receive a Total
why bicompartmental? A REVOLUTIONARY ALTERNATIVE TO TOTAL KNEE REPLACEMENTS TKR is not always the answer Today, many patients with medial or lateral disease and patellofemoral involvement receive a Total
Why Consider Partial Knee Arthroplasty?
 Why Consider Partial Knee Arthroplasty? Andrew A. Freiberg, MD Chief, Adult Reconstruction Service Massachusetts General Hospital Surgeon, Newton Wellesley Hospital Associate Professor, Harvard Medical
Why Consider Partial Knee Arthroplasty? Andrew A. Freiberg, MD Chief, Adult Reconstruction Service Massachusetts General Hospital Surgeon, Newton Wellesley Hospital Associate Professor, Harvard Medical
Mædica - a Journal of Clinical Medicine
 Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS Total Knee Arthroplasty Following High Tibial Osteotomy a Radiological Evaluation Horia ORBAN, MD, PhD; Emil MARES, MD; Mihaela DRAGUSANU, MD; Gabriel
Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS Total Knee Arthroplasty Following High Tibial Osteotomy a Radiological Evaluation Horia ORBAN, MD, PhD; Emil MARES, MD; Mihaela DRAGUSANU, MD; Gabriel
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR
 CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
15-Year Follow-up Study of Total Knee Arthroplasty in Patients With Rheumatoid Arthritis
 The Journal of Arthroplasty Vol. 18 No. 8 2003 15-Year Follow-up Study of Total Knee Arthroplasty in Patients With Rheumatoid Arthritis Jun Ito, MD, PhD, Tomihisa Koshino, MD, PhD, Renzo Okamoto, MD, PhD,
The Journal of Arthroplasty Vol. 18 No. 8 2003 15-Year Follow-up Study of Total Knee Arthroplasty in Patients With Rheumatoid Arthritis Jun Ito, MD, PhD, Tomihisa Koshino, MD, PhD, Renzo Okamoto, MD, PhD,
There have been conflicting results reported in the
 Bulletin Hospital for Joint Diseases Volume 61, Numbers 1 & 2 2002-2003 5 Total Knee Replacement Following High Tibial Osteotomy Sanjeev Madan, M.Ch.Orth., F.R.C.S. (Orth), M.Sc.(Orth), M.B.A., R. K. Ranjith,
Bulletin Hospital for Joint Diseases Volume 61, Numbers 1 & 2 2002-2003 5 Total Knee Replacement Following High Tibial Osteotomy Sanjeev Madan, M.Ch.Orth., F.R.C.S. (Orth), M.Sc.(Orth), M.B.A., R. K. Ranjith,
The Role of Partial Knee Arthroplasty for Medial OA of the Knee: It s Time has come, Again 34 th Annual Verne T. Inman Lecture.
 The Role of Partial Knee Arthroplasty for Medial OA of the Knee: It s Time has come, Again 34 th Annual Verne T. Inman Lecture David R. Mauerhan, MD Department of Orthopaedic Surgery Carolinas Medical
The Role of Partial Knee Arthroplasty for Medial OA of the Knee: It s Time has come, Again 34 th Annual Verne T. Inman Lecture David R. Mauerhan, MD Department of Orthopaedic Surgery Carolinas Medical
Bicruciate-Retaining or Medial Pivot Total Knee Prosthesis Pritchett 225 Fig. 3. The MP total knee prosthesis. Fig. 1. An anteroposterior radiograph o
 The Journal of Arthroplasty Vol. 26 No. 2 2011 Patients Prefer A Bicruciate-Retaining or the Medial Pivot Total Knee Prosthesis James W. Pritchett, MD, FACS Abstract: Four-hundred forty patients underwent
The Journal of Arthroplasty Vol. 26 No. 2 2011 Patients Prefer A Bicruciate-Retaining or the Medial Pivot Total Knee Prosthesis James W. Pritchett, MD, FACS Abstract: Four-hundred forty patients underwent
Polyethylene wear of mobile-bearing unicompartmental knee replacement at 20 years
 KNEE Polyethylene wear of mobile-bearing unicompartmental knee replacement at 20 years B. J. L. Kendrick, D. J. Simpson, B. L. Kaptein, E. R. Valstar, H. S. Gill, D. W. Murray, A. J. Price From the Nuffield
KNEE Polyethylene wear of mobile-bearing unicompartmental knee replacement at 20 years B. J. L. Kendrick, D. J. Simpson, B. L. Kaptein, E. R. Valstar, H. S. Gill, D. W. Murray, A. J. Price From the Nuffield
For Commercial products, please refer to the following policy: Preauthorization via Web-Based Tool for Procedures
 Medical Coverage Policy Total Joint Arthroplasty Hip and Knee EFFECTIVE DATE: 08/01/2017 POLICY LAST UPDATED: 06/06/2017 OVERVIEW Joint replacement surgery, also known as arthroplasty, has proved to be
Medical Coverage Policy Total Joint Arthroplasty Hip and Knee EFFECTIVE DATE: 08/01/2017 POLICY LAST UPDATED: 06/06/2017 OVERVIEW Joint replacement surgery, also known as arthroplasty, has proved to be
Kinematics Analysis of Different Types of Prosthesis in Total Knee Arthroplasty with a Navigation System
 Showa Univ J Med Sci 29 3, 289 296, September 2017 Original Kinematics Analysis of Different Types of Prosthesis in Total Knee Arthroplasty with a Navigation System Hiroshi TAKAGI 1 2, Soshi ASAI 1, Atsushi
Showa Univ J Med Sci 29 3, 289 296, September 2017 Original Kinematics Analysis of Different Types of Prosthesis in Total Knee Arthroplasty with a Navigation System Hiroshi TAKAGI 1 2, Soshi ASAI 1, Atsushi
Limb alignment in computer-assisted minimally-invasive unicompartmental knee replacement
 Limb alignment in computer-assisted minimally-invasive unicompartmental knee replacement G. Keene, D. Simpson, Y. Kalairajah From Sportsmed-SA Orthopaedic Clinic, Adelaide, South Australia Twenty patients
Limb alignment in computer-assisted minimally-invasive unicompartmental knee replacement G. Keene, D. Simpson, Y. Kalairajah From Sportsmed-SA Orthopaedic Clinic, Adelaide, South Australia Twenty patients
THE KNEE SOCIETY VIRTUAL FELLOWSHIP
 THE KNEE SOCIETY VIRTUAL FELLOWSHIP CHAPTER 16 LONG-TERM FAILURE MECHANISMS AND SURVIVORSHIP Long-Term Failure Mechanisms and Survivorship Presented by: Michael A. Mont, MD, Assem A. Sultan, MD, and Michael
THE KNEE SOCIETY VIRTUAL FELLOWSHIP CHAPTER 16 LONG-TERM FAILURE MECHANISMS AND SURVIVORSHIP Long-Term Failure Mechanisms and Survivorship Presented by: Michael A. Mont, MD, Assem A. Sultan, MD, and Michael
Investigation performed at the Department of Orthopedics, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
 1090 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Total Knee Arthroplasty in Young Patients with Juvenile Rheumatoid Arthritis BY JAVAD PARVIZI, MD, FRCS, CLAUDETTE M. LAJAM, MD,
1090 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Total Knee Arthroplasty in Young Patients with Juvenile Rheumatoid Arthritis BY JAVAD PARVIZI, MD, FRCS, CLAUDETTE M. LAJAM, MD,
Modularity in tibial components for total knee
 CHAPTER 22 Insert Exchange Rahul V. Deshmukh and Richard D. Scott Modularity in tibial components for total knee arthroplasty (TKA) is controversial. Advantages of insert modularity include component inventory
CHAPTER 22 Insert Exchange Rahul V. Deshmukh and Richard D. Scott Modularity in tibial components for total knee arthroplasty (TKA) is controversial. Advantages of insert modularity include component inventory
Clinical Performance of the Optetrak Total Knee Prosthesis: A 11-year Follow-up Study
 Research Article imedpub Journals http://www.imedpub.com/ Journal of Clinical & Experimental Orthopaedics DOI: 10.4172/2471-8416.100045 Clinical Performance of the Optetrak Total Knee Prosthesis: A 11-year
Research Article imedpub Journals http://www.imedpub.com/ Journal of Clinical & Experimental Orthopaedics DOI: 10.4172/2471-8416.100045 Clinical Performance of the Optetrak Total Knee Prosthesis: A 11-year
The Egyptian Journal of Hospital Medicine (January 2019) Vol. 74 (7), Page
 The Egyptian Journal of Hospital Medicine (January 2019) Vol. 74 (7), Page 1599-1603 Elsherbiny Ali Elsherbiny *, Ismail Ahmed Yaseen *, and Hisham Mohamed Safwat * Department of Orthopedic surgery, Faculty
The Egyptian Journal of Hospital Medicine (January 2019) Vol. 74 (7), Page 1599-1603 Elsherbiny Ali Elsherbiny *, Ismail Ahmed Yaseen *, and Hisham Mohamed Safwat * Department of Orthopedic surgery, Faculty
Anterior knee pain following total knee replacement caused by isolated Paget's disease of patella
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 9 Number 2 Anterior knee pain following total knee replacement caused by isolated Paget's disease of patella R Gupta, S Canty, W Ryan Citation
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 9 Number 2 Anterior knee pain following total knee replacement caused by isolated Paget's disease of patella R Gupta, S Canty, W Ryan Citation
Both Knee Re-revision Operations with Different Types of Endoprosthesis after Septic Complications
 DOI: 10.2478/v10163-012-0036-2 ACTA CHIRURGICA LATVIENSIS 2011 (11) CASE REPORT Both Knee Re-revision Operations with Different Types of Endoprosthesis after Septic Complications Silvestris Zebolds*/***,
DOI: 10.2478/v10163-012-0036-2 ACTA CHIRURGICA LATVIENSIS 2011 (11) CASE REPORT Both Knee Re-revision Operations with Different Types of Endoprosthesis after Septic Complications Silvestris Zebolds*/***,
DePuy Attune CR and Attune PS
 Implant Summary Report for: DePuy Comprising PRIMARY knees implanted up to: 06 February 2017 NJR Database extract: 07 April 2017 Produced on: Licensed for use until: 19 April 2017 19 April 2018 Contents
Implant Summary Report for: DePuy Comprising PRIMARY knees implanted up to: 06 February 2017 NJR Database extract: 07 April 2017 Produced on: Licensed for use until: 19 April 2017 19 April 2018 Contents
The KineSpring Knee Implant System Product Information
 The KineSpring Knee Implant System Product Information The Treatment Gap Increasing numbers of young, active OA patients with longer life expectancy and higher activity demands. 1 Large increase in arthroplasty
The KineSpring Knee Implant System Product Information The Treatment Gap Increasing numbers of young, active OA patients with longer life expectancy and higher activity demands. 1 Large increase in arthroplasty
Condylar constrained system in primary total knee replacement: our experience and literature review
 Original Article Page 1 of 5 Condylar constrained system in primary total knee replacement: our experience and literature review Luigi Sabatini 1, Salvatore Risitano 1, Lorenzo Rissolio 1, Andrea Bonani
Original Article Page 1 of 5 Condylar constrained system in primary total knee replacement: our experience and literature review Luigi Sabatini 1, Salvatore Risitano 1, Lorenzo Rissolio 1, Andrea Bonani
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
Stephen R Smith Northeast Nebraska Orthopaedics PC. Ligament Preserving Techniques in Total Knee Arthroplasty
 Stephen R Smith Northeast Nebraska Orthopaedics PC Ligament Preserving Techniques in Total Knee Arthroplasty 10-15% have Fair to poor Results? Why? The complication rate is 2.567% If It happens To You
Stephen R Smith Northeast Nebraska Orthopaedics PC Ligament Preserving Techniques in Total Knee Arthroplasty 10-15% have Fair to poor Results? Why? The complication rate is 2.567% If It happens To You
Tissue-sparing surgery with the bi-unicompartmental knee prosthesis: retrospective study with minimum follow-up of 36 months
 J Orthopaed Traumatol (2006) 7:108 112 DOI 10.1007/s10195-005- - TSS SECTION N. Confalonieri A. Manzotti Tissue-sparing surgery with the bi-unicompartmental knee prosthesis: retrospective study with minimum
J Orthopaed Traumatol (2006) 7:108 112 DOI 10.1007/s10195-005- - TSS SECTION N. Confalonieri A. Manzotti Tissue-sparing surgery with the bi-unicompartmental knee prosthesis: retrospective study with minimum
Day of Surgery Discharge after Unicompartmental Knee Arthroplasty (UKA): An Effective Perioperative Pathway. Jay Patel, MD Hoag Orthopedic Institute
 Day of Surgery Discharge after Unicompartmental Knee Arthroplasty (UKA): An Effective Perioperative Pathway Jay Patel, MD Hoag Orthopedic Institute UKA Rapid Recovery Protocol Purpose of Study Describe
Day of Surgery Discharge after Unicompartmental Knee Arthroplasty (UKA): An Effective Perioperative Pathway Jay Patel, MD Hoag Orthopedic Institute UKA Rapid Recovery Protocol Purpose of Study Describe
Insert dissociation after fixed bearing PS constrained Genesis II total knee arthroplasty. A case series of nine patients
 Acta Orthop. Belg., 2015, 81, 747-751 ORIGINAL STUDY Insert dissociation after fixed bearing PS constrained Genesis II total knee arthroplasty. A case series of nine patients Timothy Voskuijl, Thijs A.
Acta Orthop. Belg., 2015, 81, 747-751 ORIGINAL STUDY Insert dissociation after fixed bearing PS constrained Genesis II total knee arthroplasty. A case series of nine patients Timothy Voskuijl, Thijs A.
Kinematic vs. mechanical alignment: What is the difference?
 Kinematic vs. mechanical alignment: What is the difference? In this 4 Questions interview, Stephen M. Howell, MD, explains the potential benefits of 3D alignment during total knee replacement. Introduction
Kinematic vs. mechanical alignment: What is the difference? In this 4 Questions interview, Stephen M. Howell, MD, explains the potential benefits of 3D alignment during total knee replacement. Introduction
BIOMECHANICAL EVALUATION OF DEGREE OF FREEDOM OF MOVEMENTS OF AN NOVEL HIGH FLEXION KNEE FOR ITS SUITABILITY IN EASTERN LIFESTYLES
 International Journal on Applied Bioengineering, Vol.4, No.2, July 2009 5 BIOMECHANICAL EVALUATION OF DEGREE OF FREEDOM OF MOVEMENTS OF AN NOVEL HIGH FLEXION KNEE FOR ITS SUITABILITY IN EASTERN LIFESTYLES
International Journal on Applied Bioengineering, Vol.4, No.2, July 2009 5 BIOMECHANICAL EVALUATION OF DEGREE OF FREEDOM OF MOVEMENTS OF AN NOVEL HIGH FLEXION KNEE FOR ITS SUITABILITY IN EASTERN LIFESTYLES
1 Introduction. 2 Data and method
 Open Med. 2015; 10: 457 461 Research Article Open Access Si Yulou, Xue Yanqin, Xing Yongjun* Method and effect of total knee arthroplasty osteotomy and soft tissue release for serious knee joint space
Open Med. 2015; 10: 457 461 Research Article Open Access Si Yulou, Xue Yanqin, Xing Yongjun* Method and effect of total knee arthroplasty osteotomy and soft tissue release for serious knee joint space
Validation of a French version of the Oxford knee questionnaire
 Orthopaedics & Traumatology: Surgery & Research (2011) 97, 267 271 ORIGINAL ARTICLE Validation of a French version of the Oxford knee questionnaire J.-Y. Jenny, Y. Diesinger Strasbourg Academic Hospitals
Orthopaedics & Traumatology: Surgery & Research (2011) 97, 267 271 ORIGINAL ARTICLE Validation of a French version of the Oxford knee questionnaire J.-Y. Jenny, Y. Diesinger Strasbourg Academic Hospitals
Knee arthroplasty: What radiologists should know.
 Knee arthroplasty: What radiologists should know. Poster No.: C-2174 Congress: ECR 2014 Type: Educational Exhibit Authors: J. Araújo 1, J. Pires 2, J. Oliveira 3, C. Macedo 1, S. Magalhães 1, I. Ferreira
Knee arthroplasty: What radiologists should know. Poster No.: C-2174 Congress: ECR 2014 Type: Educational Exhibit Authors: J. Araújo 1, J. Pires 2, J. Oliveira 3, C. Macedo 1, S. Magalhães 1, I. Ferreira
