Preface. Hvidovre, d. 12. September, Anders Troelsen, Michael Brix, Kirill Gromov
|
|
|
- Gervais Wilson
- 5 years ago
- Views:
Transcription
1 Preface The annual report from the Danish Fracture Database (DFDB) 215 is the third of its kind. It contains data based on over 4. fracture related surgeries, of which over 3. are primary surgeries registered at The purpose of DFDB is web based quality monitoring of fracture related surgery and today these efforts are joined by 2 orthopaedic departments in Denmark, covering close to 9% of the Danish population. The effort to monitor quality of fracture related surgery in Denmark is unique and important: Unique because DFDB is the fracture register with the highest national coverage in the world and important given the high number of surgeries performed each year probably making fracture surgery/traumatology one of the busiest specialties within orthopaedic surgery. Previously it has not been possible to assess nationwide quality of all fracture related surgeries. We wish to thank all the participating surgeons and departments taking part in this unique and important task. It is truly inspirational to realize the unity DFDB has brought into orthopaedic traumatology in Denmark. Also the continued support from The Danish Orthopaedic Society (DOS) and Danish Orthopaedic Trauma Society (DOT), and the possibility to present the annual report at the DOS Congress is much appreciated. The annual report is structured as previously with general data overview of registered parameters followed by department specific data, and finally the major body of the report with specific data for each anatomic region, e.g. proximal humerus, distal radius, and proximal femur. This years focus area is surgically treated clavicular fractures, a hot topic in recent years, and currently under scrutiny with new national treatment guidelines being recently published by DOT. A basic principle surrounding DFDB is that surgeons reporting to the database should get feedback concerning the quality of treatment. This is delivered via and entails surgeon specific (only to be seen by the individual surgeon), department specific (the surgeon can only see data from his/her own department), and nationwide feedback on the rate of reoperations performed. The level of detail send by can be configured by the surgeon when logged in to DFDB. It is our hope that with time this feedback from DFDB can support surgeons in making decisions about best practice in fracture related surgery. In Sweden a Fracture Register has been established too ( DFDB has engaged in cooperation with colleagues in Sweden and Norway to establish a core dataset of common parameters that will make it possible to join data and efforts across Scandinavia. Further, the efforts to become a national clinical quality monitoring database are ongoing. Finally, a platform to scan, trace and monitor orthopaedic implants has been introduced and taken in use at one department. The scanned implants are linked together with registrations in DFDB. It is a hope that the needed and important task of monitoring quality of specific implants and groups of implants can soon be undertaken in DFDB. We hope to see more departments join DFDB in the future. Hvidovre, d. 12. September, 215 Anders Troelsen, Michael Brix, Kirill Gromov
2 Table on contents About the Danish Fracture Database.1 Summary and comments 2 Data limitations 3 General overview of data.5 Department specific data 19 Focus area - Clavicle..39 Adult Proximal Humerus.44 Humeral shaft 49 Distal humerus..54 Proximal antebrachium 59 Antebrachium.64 Distal radius..69 Hand.74 Proximal femur..79 Acetabulum..84 Femur..89 Distal femur..94 Patella.99 Proximal tibia..14 Tibia shaft 19 Distal tibia 114 Malleoli 119 Foot 124 Shoulder 129 Pediatric Humerus..134 Radius/Ulna.139 Femur..144 Tibia/Fibula..149 Hand.154 Foot 158 Appendix 1 - Registered parameters...162
3 About the Danish Fracture Database Background and recent development The aim of the Danish Fracture Database is to monitor the quality of surgical fracture treatment by assessing the rate of revision surgery both in general and for each fracture type specifically. This assessment results in a potential quality improvement through focus on specific fracture types where the quality of treatment is not considered high enough. Lastly, epidemiologic research in fracture surgery will contribute to identify surgical and fracture related prognostic factors for a good or poor outcome of surgery. The use of DFDB provides each participating department the possibility to monitor own data and thus the quality of their fracture treatment. The educational level of both the surgeon and the supervisor is registered and can therefore also be monitored. During the past year, there has been a marked escalation of data entry. The number of registered surgeries has increased from approximately 28. in 214 to more than 4. in 215. Secretariat and daily operations Each participating department has a controller in daily charge of complete reporting. The daily operation is also supported by a secretariat, which was established last year at the Department of Orthopaedic Surgery, Hvidovre Hospital. The secretariat consists of an administrator, Alina Hansen, and a statistician, Thomas Kallemose. Together the developers of DFDB and the secretariat has the responsibility and right to development and changes of the registry in cooperation with the provider Procordo Aps. Steering Committee The idea behind DFDB and the registry s recent progress are attributed to Michael Brix and Anders Troelsen. Kirill Gromov contributed substantially to the registry s developmental phase. Michael, Anders and Kirill are today a part of the DFDB steering committee and are responsible for the registry s overall administration, quality monitoring, and research. In addition, each participating department is represented in the steering committee. Both DOT (Danish Orthopaedic Trauma Society) and DOS (Danish Orthopaedic Society) are represented in the steering committee. A minimum of one annual meeting is held in order to correct inexpediencies, increase the usability, and optimize the database through the members feedback. 1
4 Summary and comments In this annual report from DFDB we present a general overview of registered data as well as data for specific anatomical regions. The general overview covers basic demographics (age, gender and ASA score) for all primary surgeries as well as reoperations. Anatomical distribution of registered primary surgeries and reoperations as well as indications for reoperations are described. We describe the educational level of the primary surgeon and level of supervision for primary surgeries. Anatomical distribution for primary surgeries for all separate departments participating in the DFDB collaboration is described in the first part of the report. For definitions and specifications of the different parameters please see Appendix 1. Demographics 84% of primary procedures were due to adult fractures and 16% due to pediatric fractures. Age distribution was biphasic, with first peak at age -2 and second peak at age 6-9. More males were surgically treated for fractures when age <5, while more female were surgically treated for fractures when age >5. 76% of patients with primary surgeries had ASA score 1-2 while 78% of patients with reoperations had ASA score % of all registered patients were female. Reoperations Proximal femur (27%), malleoli (2%), and distal radius (7%) were the 3 most frequently reoperated anatomical regions in adults. Radius/ulna (47%), humerus (21%) and tibia (18%) were the 3 most frequently reoperated anatomical regions in children. Pain and discomfort due to osteosynthesis material (38%), secondary fracture dislocation (15%), and infection 13%) were the 3 most frequent indications for adult reoperations. Secondary fracture dislocation (39%), suboptimal osteosynthesis (21%), and pain and discomfort due to osteosynthesis material (22%) were the 3 most frequent indications for paediatric reoperations. Level of education 6% of all primary surgeries were performed by surgeons in training (intern- 5th year resident). Interns, 1 st year resident, 2 nd year resident, and 3 rd year residents performed more procedures under supervision than without supervision, while 4-5 th year residents, attending surgeons, and traumatologist performed more procedures without supervision than with supervision Anatomical distribution Proximal femur (35%), distal radius (15%), and malleoli (12%) were the 3 most frequent operated regions for primary adult surgical procedures. Radius/ulna (58%), humerus (22%), and tibia (9%) were the 3 most frequently operated regions for primary paediatric surgical procedures. 2
5 Data limitations There are some limitations to the data in this report. Essential limitations are: 1) Data completeness for treatment of primary fractures 2) Data completeness for reoperations Initially, after full implementation of DFDB at the orthopaedic departments in Hvidovre and Odense, an evaluation of data validity and data completeness for treatment of primary fractures and reoperations was performed (Gromov 213). Two plausible factors to limit data completeness were identified: 1) that the registry had only been implemented for few months, and 2) that both departments are large, with regularly 5-9 possible surgeons. The results of the study showed that the validity of data (the percentage of data that was correct when compared to the best external data source outside of DFDB) was 9-1% for all parameters, and most above 97%. The total degree of completeness for data entry of primary fracture treatment was 88% and for reoperations it was 77%. Thus, there was, at an early point in time after initiation of DFDB, a satisfactory degree of data validity and data completeness under the prevailing circumstances. Similar evaluations of data completeness should be performed continuously. Another limitation is lacking reoperation data performed at non-participating departments where the primary operation was performed and registered at a participating department. The extent of this phenomenon can be investigated by using data from the National Patient Registry (Landspatientregistret, LPR). For this year s report, data was not extracted from LPR with regards to knowing the true number of reoperations, why the rates of reoperations and survival curves are underestimated. However, as the number of departements participating in DFDB collaboration has risen to 2, covering close to 9% of the Danish population, such underestimation is significantly reduced. Reoperation rates and curves are presented to illustrate the potential of data analysis with the DFDB. Currently, work is ongoing to validate the primary fracture codes that are registered in the LPR, to know the validity of these codes if they are to be used as a data source for the DFDB. Furthermore, definition and validation of the reoperation codes in LPR to investigate the applicability of the LPR as a data source for the DFDB is ongoing. Fracture diagnosis in Danish National Patient Registry (NPR) have been investigated by Andersen et al. The overall validity of data was 86%. The NPR diagnosis code was correct in 94% of all cases and the NPR anatomic region was correct in 99% of all cases. In 91% of all cases the operation code was correct and the anatomic region for the operation was correct in 99% of all cases. NPR coding will be used in the future for continuous completeness monitoring of DFDB data. Data was extracted from DFDB on August 8 th 215. References Gromov K, Fristed JV, Brix M, Troelsen A. Completeness and data validity for the Danish Fracture Database. Danish medical journal. 213 Oct;6 (1):A4712. PubMed PMID:
6 Participating departments Aabenraa Aalborg Aarhus Bispebjerg Esbjerg Farsø Gentofte Herlev Hillerød Holbæk Horsens Hvidovre Kolding Køge Nykøbing Falster Odense Randers Rigshospitalet Slagelse Vejle Viborg 4
7 General overview of data The graphs in this section covers general areas such as surgery type distribution, primary indication for reoperation, and primary surgeon, which uses data from all participating departments. 4 Fracture types (41856) 84% % Adult Pediatric 4 Procedure types (38262) 9% % Primary Reoperation 5
8 4 Procedure types by fracture types (37815) Primary (33992) Reoperation (2418) Pain from osteosynthesis (145) 3 89% 2 1 Adult 95% 7% 4% Pediatric 4% 1% 12 Anatomical distribution Primary procedure Adult fractures (2918) 1 35% % 12% 2 4% 3% 1% 2% 1% Humeral shaft Proximal humerus 8% Patella Distal femur Femur Acetabulum Proximal femur Hand Distal radius Antebrachium Proximal antebrachium Distal humerus Foot Malleoli Distal tibia Tibia shaft Proximal tibia 1% 2% 1% 1% 3% 3% 1% 2% 3% % Scapula Clavicle 6
9 2 Anatomical distribution Reoperations Adult fractures (3555) % 2% 5 7% 5% 3% 1% 2% 1% 2% Proximal antebrachium Distal humerus Humeral shaft Proximal humerus Proximal femur Hand Distal radius Antebrachium 7% 2% 4% 3% 3% 4% 2% Patella Distal femur Femur Acetabulum Malleoli Distal tibia Tibia shaft Proximal tibia 5% 2% Shoulder Foot 4 Anatomical distribution Primary procedure Pediatric fracture (4985) 3 58% 2 22% 1 Humerus Radius/Ulna 4% Femur 9% Tibia/Fibula 6% Hand 1% Foot 7
10 2 Anatomical distribution Reoperation Pediatric fractures (267) % 5 21% Humerus Radius/Ulna 9% Femur 18% Tibia/Fibula 5% Hand % Foot 2 Primary indication for reoperation Adult fractures (3532) 15 38% % 9% 15% 9% 9% Infection Hematoma Bone necrosis Arthroplasty dislocation Pain or discomfort from osteosynthesis Pseudarthrosis / delayed union Secondary fracture dislocation or osteosynthesis failure Suboptimal osteosynthesis Not identified preoperative fracture New fracture Neurovascular complication 1% 1% 2% % Muscle and soft-tissue revision 2% % 8
11 14 Primary indication for reoperation Pediatric fractures (263) % % 22% 4 2 5% Infection 1% 1% 5% New fracture Neurovascular complication Muscle and soft-tissue revision 1% Bone necrosis Pain or discomfort from osteosynthesis Pseudarthrosis / delayed union Secondary fracture dislocation or osteosynthesis failure Suboptimal osteosynthesis 5% Not identified preoperative fracture 1% ASA-score for procedure types Adult fractures (32563) 4% Primary (297) Reoperation (3556) 36% % 4 2 4% 38% 21% 2% 1% % %
12 6 ASA-score for procedure types Pediatric fractures (525) Primary (4983) Reoperation (267) 5 98% % 2% 3% % % % % Gender (42316) 25 56% % 5 Female Male 1
13 3 Time of primary procedure Adult fractures (297) Time of day 6 Time of primary procedure Pediatric fracture (4983) Time of day 11
14 14 Surgeon level Primary procedure (3439) 12 33% % 13% 13% 14% 4 6% 2 % Intern Attending 4-5 year resident 3 year resident 2 year resident 1 year resident Traumatologist Surgeon level by procedure types Adult fractures (3252) Primary (28965) Reoperation (3555) 1 33% 8 6 2% 4 14% 13% 14% 2 % 1% Intern 17% 1 year resident 7% 4-5 year resident 3 year resident 2 year resident 44% 11% 1% Attending 7% 9% Traumatologist 12
15 25 Surgeon level by procedure types Pediatric (5246) Primary (4979) Reoperation (267) 2 35% % 16% 13% 13% 5 % % Intern 11% 1 year resident 9% 2 year resident 7% 3 year resident 14% Attending 4-5 year resident 5% 49% 1% Traumatologist 5 4 Time of primary procedure by surgeons level Adult fractures (28963) Intern (88) 1 year resident (5813) 2 year resident (3962) 3 year resident (3695) 4-5 year resident (49) Attending (9425) Traumatologist (189) Time of day 13
16 Time of primary surgery by surgeons level Pediatric fractures (4979) 8 6 Intern (15) 1 year resident (95) 2 year resident (635) 3 year resident (63) 4-5 year resident (778) Attending (1763) Traumatologist (253) Time of day 25 Level of supervision for all fracture types Primary procedure (33457) 2 58% % 5 % % 1% 2% Intern 1 year resident 2 year resident 8% Attending 4-5 year resident 3 year resident 4% Unsupervised Traumatologist 14
17 5 Level of supervision for interns and residents Adult fractures (17559) Below attending (3566) Attending or above (7596) Unsupervised (6397) % 5% 41% 35% 53% 39% 71% 1 13% 24% 26% 48%44% 8% Intern 1 year resident 2 year resident 8% 3 year resident 3% 4-5 year resident 1 Level of supervision for interns and residents Pediatric fractures (2943) Below attending (564) Attending or above (1183) Unsupervised (1196) % 5% 49% 77% 38%38% 4% 2 36%64% % Intern 13% 1 year resident 24% 2 year resident 11% 3 year resident 22% 1% 4-5 year resident 15
18 Survival for primary procedure with reoperation due to any reason as endpoint All procedures (3436) probability days 1. Survival for primary procedure with reoperation due to any reason except pain and discomfort from surgical hardware All procedures (3436).98 probability days 16
19 1. Survival for primary procedure with reoperation due to any reason Adult and pediatric fractures (33989).98 probability Adult Pediatric days 5 Age distribution for gender Primary procedure (34285) Female (1954) Male (14745) 4 19% 21% 18% % 16% 1% 1% 11% 12% 11% 1% 8% 6% 8% 9% 1 5% 5% 3% 3% 2% 2% 2% Age Group 17
20 12 1 Trauma patients by anatomical distribution Adult fractures (2912) 2% No (27329) Yes (1683) % 4% 3% 2 4% 12% 6% 6% 2% Proximal antebrachium Distal humerus Humeral shaft Proximal humerus Patella Distal femur Femur Acetabulum Proximal femur Hand Distal radius Antebrachium 59% 2% 14% 7% 1% 18% 15% Malleoli Distal tibia Tibia shaft Proximal tibia 12% 12% 24% Scapula Clavicle Foot 35 3 Trauma patients by anatomical distribution Pediatric fractures (4984) 1% No (4859) Yes (125) % 5 Humerus 19% Femur Radius/Ulna 5% Tibia/Fibula 2% Hand 7% Foot 18
21 Department specific data This section provides department specific data for all 2 participating departments. The data covers anatomical distribution for primary procedure for adults and pediatric. Aabenraa 14 Anatomical distribution for Aabenraa Primary procedure Adult fractures (227) % 4 12% 15% 2 6% 4% 2% 1% 1% Proximal antebrachium Distal humerus Humeral shaft Proximal humerus 6% Distal femur Femur Proximal femur Hand Distal radius Antebrachium Foot Malleoli Distal tibia Tibia shaft Proximal tibia Patella 2% 1% 1% 2% 3% 1% 1% 5% % Scapula Clavicle 3 Anatomical distribution for Aabenraa Primary procedure Pediatric fractures (363) 25 59% % 5 Humerus Femur Radius/Ulna 5% 7% Tibia/Fibula 6% Hand 1% Foot 19
22 Aalborg 2 Anatomical distribution for Aalborg Primary procedure Adult fractures (38) % 26% 18% 5 11% 8% 3% 3% Femur Proximal femur Distal femur Tibia shaft Proximal tibia Distal tibia Malleoli 2
23 Aarhus 25 Anatomical distribution for Aarhus Primary procedure Adult fractures (33) 2 52% % 5 9% Distal radius 3% Hand Proximal femur 3% Femur Malleoli 1 Anatomical distribution for Aarhus Primary procedure Pediatric fractures (6) % 2 17% Humerus Radius/Ulna 21
24 Bispebjerg 5 Anatomical distribution for Bispebjerg Primary procedure Adult fractures (934) % 33% 16% 1 2% 1% 2% 7% Proximal antebrachium Distal humerus Humeral shaft Proximal humerus Femur Proximal femur Hand Distal radius Antebrachium 1% 6% Distal tibia Tibia shaft Proximal tibia Patella Distal femur 2% 1% 2% 4% 2% 2% 1% Foot Malleoli 5% Clavicle 2. Anatomical distribution for Bispebjerg Primary procedure Pediatric fractures (2) % 5%.5. Radius/Ulna Tibia/Fibula 22
25 Esbjerg 8 Anatomical distribution for Esbjerg Primary procedure Adult fractures (1574) 6 33% 4 2 6% Proximal antebrachium Distal humerus Humeral shaft Proximal humerus 1% 2% 3% 1% 15% 1% Patella Distal femur Femur Acetabulum Proximal femur Hand Distal radius Antebrachium Foot Malleoli Distal tibia Tibia shaft Proximal tibia % 2% 1% 1% 2% 3% 1% 14% 1% 3% % Scapula Clavicle 2 Anatomical distribution for Esbjerg Primary procedure Pediatric fractures (268) 15 52% 1 23% 5 13% Humerus Radius/Ulna 3% Femur Tibia/Fibula 6% Hand 2% Foot 23
26 Gentofte 5 Anatomical distribution for Gentofte Primary procedure Adult fractures (57) 4 72% % 1 Distal radius Hand 5 Anatomical distribution for Gentofte Primary procedure Pediatric fractures (2) % 1 Hand 24
27 Herlev 1 Anatomical distribution for Herlev Primary procedure Adult fractures (147) % 21% 2 Humeral shaft Proximal humerus Acetabulum Proximal femur Hand Distal radius Antebrachium Proximal antebrachium Distal humerus 4% 1% 2% 4% 6% 1% 1% Foot Malleoli Distal tibia Tibia shaft Proximal tibia Patella Distal femur Femur % 3% 1% 2% 3% 3% 1% 1% 1% % Scapula Clavicle 25 Anatomical distribution for Herlev Primary procedure Pediatric fractures (311) 2 65% % 5 Humerus Radius/Ulna 2% Femur 8% Tibia/Fibula % 1% Hand Foot 25
28 Hillerød 6 Anatomical distribution for Hillerød Primary procedure Adult fractures (883) % 38% 19% 1 3% 1% % 1% % Proximal antebrachium Distal humerus Humeral shaft Proximal humerus Distal femur Femur Proximal femur Hand Distal radius Antebrachium 6% Foot Malleoli Distal tibia Tibia shaft Proximal tibia Patella 2% 1% 1% 3% 3% 2% 2% 3% Clavicle 2 Anatomical distribution for Hillerød Primary procedure Pediatric fractures (234) 15 61% % 13% Humerus Radius/Ulna 2% Femur Tibia/Fibula 2% Hand 26
29 Holbæk 6 Anatomical distribution for Holbæk Primary procedure Adult fractures (891) % 1 Scapula Clavicle Foot Malleoli Distal tibia Tibia shaft Proximal tibia Patella Distal femur Femur Acetabulum Proximal femur Hand Distal radius Antebrachium Proximal antebrachium Distal humerus Humeral shaft Proximal humerus 1% 2% 1% 3% 1% 7% 2% % 2% 2% 1% 4% 2% 1% 13% 1% 2% % 2 Anatomical distribution for Holbæk Primary procedure Pediatric fractures (236) 15 59% % Humerus Femur Radius/Ulna 6% 1% Tibia/Fibula % 2% Hand Foot 27
30 Horsens 35 Anatomical distribution for Horsens Primary procedure Adult fractures (542) % 1 15% 15% 5 Clavicle Foot Malleoli Distal tibia Tibia shaft Proximal tibia Patella Distal femur Femur Acetabulum Proximal femur Hand Distal radius Antebrachium Proximal antebrachium Distal humerus Humeral shaft Proximal humerus 5% 2% 1% 1% 2% 6% % 2% 1% 1% 2% 3% 1% 3% 2% 8 Anatomical distribution for Horsens Primary procedure Pediatric fractures (15) 63% % 15% Humerus Radius/Ulna 2% Femur Tibia/Fibula 5% Hand 28
31 Hvidovre 3 Anatomical distribution for Hvidovre Primary procedure Adult fractures (4624) Clavicle Foot Malleoli Distal tibia Tibia shaft Proximal tibia Patella Distal femur Femur Acetabulum Proximal femur Hand Distal radius Antebrachium Proximal antebrachium Distal humerus Humeral shaft Proximal humerus 3% 1% 2% 4% 1% 14% 5% 37% % 2% 2% 1% 3% 4% 1% 17% 1% 2% 1 Anatomical distribution for Hvidovre Primary procedure Pediatric fractures (1384) 62% % 2 Humerus Femur Radius/Ulna 4% 5% Tibia/Fibula 4% Hand 1% Foot 29
32 Kolding 14 Anatomical distribution for Kolding Primary procedure Adult fractures (2678) % 27% 4 2 Acetabulum Proximal femur Hand Distal radius Antebrachium Proximal antebrachium Distal humerus Humeral shaft Proximal humerus 6% 2% 2% 3% 2% 9% 3% 2% 1% % Distal femur Femur Foot Malleoli Distal tibia Tibia shaft Proximal tibia Patella 4% 2% 2% 12% 1% 4% % Scapula Clavicle 4 Anatomical distribution for Kolding Primary procedure Pediatric fractures (63) 3 45% 2 31% 1 13% Humerus Femur Radius/Ulna 7% Tibia/Fibula 4% Hand 1% Foot 3
33 Køge 12 Anatomical distribution for Køge Primary procedure Adult fractures (223) % 32% 13% 2 5% 1% 2% 4% 1% Proximal antebrachium Distal humerus Humeral shaft Proximal humerus 6% Femur Acetabulum Proximal femur Hand Distal radius Antebrachium % 2% 4% 3% 1% 1% 1% Tibia shaft Proximal tibia Patella Distal femur Scapula Clavicle Foot Malleoli Distal tibia 1% 3% % 35 Anatomical distribution for Køge Primary procedure Pediatric fractures (399) % % 5 Humerus Femur Radius/Ulna 3% 1% Tibia/Fibula 5% Hand 1% Foot 31
34 Nykøbing Falster 3 Anatomical distribution for Nykøbing F Primary procedure Adult fractures (557) 25 41% % 12% 5 Acetabulum Proximal femur Hand Distal radius Antebrachium Proximal antebrachium Distal humerus Humeral shaft Proximal humerus 6% 2% 1% 3% 1% 4% Distal femur Femur Foot Malleoli Distal tibia Tibia shaft Proximal tibia Patella 3% 2% 3% 3% 3% % 1% 1% % Clavicle 6 Anatomical distribution for Nykøbing F Primary procedure Pediatric fractures (88) 5 49% % 1 Humerus Radius/Ulna 2% Femur 7% Tibia/Fibula 11% Hand 32
35 Odense 2 Anatomical distribution for Odense Primary procedure Adult fractures (3836) % 1% 1% 3% 2% 1% Proximal antebrachium Distal humerus Humeral shaft Proximal humerus 7% 29% Femur Acetabulum Proximal femur Hand Distal radius Antebrachium 5% 5% 6% 4% 2% 2% 1% Patella Distal femur Distal tibia Tibia shaft Proximal tibia 15% 4% 1% % Scapula Clavicle Foot Malleoli 4 Anatomical distribution for Odense Primary procedure Pediatric fractures (52) 3 56% 2 1 2% Humerus Femur Radius/Ulna 8% 9% Tibia/Fibula 5% Hand 1% Foot 33
36 Randers 2 Anatomical distribution for Randers Primary procedure Adult fractures (349) 15 4% 1 17% 5 13% 5% Proximal antebrachium Distal humerus Humeral shaft Proximal humerus 1% 1% 2% 1% 7% Femur Proximal femur Hand Distal radius Antebrachium 4% 1% 2% 2% 3% % Proximal tibia Patella Distal femur Distal tibia Tibia shaft Foot Malleoli % 1% Clavicle 5 Anatomical distribution for Randers Primary procedure Pediatric fractures (56) 4 61% % 4% 9% 9% Humerus Radius/Ulna Femur Tibia/Fibula Hand 34
37 Rigshospitalet 5 Anatomical distribution for Rigshospitalet Primary procedure Adult fractures (1354) % 1% 14% 1 5% 6% 4% 5% 4% 3% 3% 3% Proximal antebrachium Distal humerus Humeral shaft Proximal humerus Femur Acetabulum Proximal femur Hand Distal radius Antebrachium 7% 5% 5% 3% 4% 1% Proximal tibia Patella Distal femur Foot Malleoli Distal tibia Tibia shaft 5% 1% Scapula Clavicle 1 Anatomical distribution for Rigshospitalet Primary procedure Pediatric fractures (163) 8 44% % 17% 2 1% Humerus Radius/Ulna Femur Tibia/Fibula 4% Hand 3% Foot 35
38 Slagelse 14 Anatomical distribution for Slagelse Primary procedure Adult fractures (2851) % 19% 3% 4 12% 2 Acetabulum Proximal femur Hand Distal radius Antebrachium Proximal antebrachium Distal humerus Humeral shaft Proximal humerus % % 2% 3% 1% Distal femur Femur Foot Malleoli Distal tibia Tibia shaft Proximal tibia Patella 2% 2% 2% 3% 3% 1% % 1% 1% Clavicle 4 Anatomical distribution for Slagelse Primary procedure Pediatric fractures (519) % 5% 15% 12% Humerus Radius/Ulna 2% Femur Tibia/Fibula Hand % Foot 36
39 Vejle 14 Anatomical distribution for Vejle Primary procedure Adult fractures (235) % 31% 4 14% 16% 2 1% 1% 2% 2% Proximal antebrachium Distal humerus Proximal humerus Proximal tibia Patella Distal femur Proximal femur Hand Distal radius Antebrachium Foot Malleoli Distal tibia Tibia shaft 1% 3% 2% 1% 1% 3% 2% Clavicle 4 Anatomical distribution for Vejle Primary procedure Pediatric fractures (35) 3 86% 2 1 Radius/Ulna 9% Tibia/Fibula 6% Hand 37
40 Viborg 4 Anatomical distribution for Viborg Primary procedure Adult fractures (763) % Proximal antebrachium Distal humerus Humeral shaft Proximal humerus 1% 2% 2% 2% 2% 9% 31% Femur Proximal femur Hand Distal radius Antebrachium Foot Malleoli Distal tibia Tibia shaft Proximal tibia Patella Distal femur 2% 1% 2% 2% 2% 1% 14% 1% 2% % Scapula Clavicle 14 Anatomical distribution for Viborg Primary procedure Pediatric fractures (186) % % 15% 2 Humerus Femur Radius/Ulna 1% Tibia/Fibula 5% Hand 1% Foot 38
41 Focus area - Clavicle 12 Fracture classification for Shoulder fractures (958) 1 96% Clavicle 4% Scapula 1 Method of osteosynthesis Clavicle fractures Primary procedure (913) 92% % Plate Other 39
42 4 Indication for reoperations of Clavicle fractures (56) 3 54% 2 23% 1 9% Infection 2% New fracture 4% Suboptimal osteosynthesis 9% Secondary fracture dislocation or osteosynthesis failure Pain or discomfort from osteosynthesis Pseudarthrosis / delayed union 6 Surgeon level for Clavicle fractures (917) 5 55% % 14% 1 6% 5% 5% 2 year resident 1 year resident Attending 4-5 year resident 3 year resident Traumatologist 4
43 8 Level of supervision for Clavicle fractures (886) 75% % % % 2 year resident 3% 4-5 year resident 3 year resident Attending 3% Traumatologist Unsupervised 2 Level of supervision for interns and residents Clavicle fractures (282) Below attending (3) Attending or above (166) Unsupervised (86) % 38% 5 76% 73% 89% 24% 1 year resident % 18% 2 year resident 9% 4% 3 year resident 6% 6% 4-5 year resident 41
44 Surgical delay for Clavicle fractures (577) % 22 % 2 % 16 % 12 % 8 % 5 % Hours (Proportion of patients operated in 24 hour intervals) 2 Time of primary Clavicle procedure Adult fractures (917) Time of day 42
45 1. Survival for primary procedure with reoperation due to any reason Clavicle fractures (917).95 probability days 1. Survival for primary procedure with reoperation due to any reason except pain and discomfort from surgical hardware Clavicle fractures (917).95 probability days 43
46 Adult Proximal Humerus 1 Method of osteosynthesis proximal humerus fractures (1136) 8 6% % 2 9% Arthroplasty Plate Other 6 Indication for reoperations of proximal humerus fractures (114) % 3% 27% 1 7% 1% 7% Infection 1% New fracture Pain or discomfort from osteosynthesis Pseudarthrosis / delayed union Secondary fracture dislocation or osteosynthesis failure Suboptimal osteosynthesis 1% Arthroplasty dislocation 2% Bone necrosis Hematoma 44
47 1 Surgeon level for proximal humerus fractures (1147) 8 68% % 3% 4% 1 year resident 2 year resident 1% 4-5 year resident 3 year resident Attending 14% Traumatologist 1 Level of supervision for proximal humerus fractures (181) 8 76% % % % Intern 4-5 year resident Attending 4% Traumatologist Unsupervised 45
48 14 12 Level of supervision for interns and residents proximal humerus fractures (21) Below attending (3) Attending or above (176) Unsupervised (31) 1 76% % 4 91% 24% 2 94% % 1 year resident 6% 9% 2 year resident % % 3 year resident 5% % 4-5 year resident Surgical delay for proximal humerus fractures (794) 2 14 % 23 % 18 % 16 % 12 % 9 % 7 % Hours (Proportion of patients operated in 24 hour intervals) 46
49 1. Survival for primary procedure with reoperation due to any reason proximal humerus fractures (1147).95 probability days 1. Survival for primary procedure with reoperation due to any reason except pain and discomfort from surgical hardware proximal humerus fractures (1147).95 probability days 47
50 5 Fracture classification for proximal humerus fractures (1147) A 11B 11C 48
51 Humeral shaft 35 Method of osteosynthesis humeral shaft fractures (347) 3 75% % 5 6% Intramedullary nail(s) Plate Other 35 Indication for reoperations of humeral shaft fractures (47) % 1 19% 17% 5 4% Infection 2% 2% New fracture Neurovascular complication Muscle and soft-tissue revision 4% 4% Secondary fracture dislocation or osteosynthesis failure Suboptimal osteosynthesis Pain or discomfort from osteosynthesis Pseudarthrosis / delayed union 49
52 3 Surgeon level for humeral shaft fractures (351) 25 66% % 5 % 1% Intern 2 year resident 1 year resident 3% 3% 8% 4-5 year resident 3 year resident Attending Traumatologist 35 Level of supervision for humeral shaft fractures (34) 3 78% % % 3 year resident Attending 4-5 year resident 17% 5% Traumatologist Unsupervised 5
53 3 25 Level of supervision for interns and residents humeral shaft fractures (55) Below attending (1) Attending or above (43) Unsupervised (11) % 91% 64% 32% 5 1% 1% % % Intern 9% 4% % % % % % 1 year resident 2 year resident 3 year resident 4-5 year resident Surgical delay for humeral shaft fractures (21) 8 24 % 23 % 15 % 13 % 12 % 6 % 5 % Hours (Proportion of patients operated in 24 hour intervals) 51
54 1. Survival for primary procedure with reoperation due to any reason humeral shaft fractures (351).95 probability days 1. Survival for primary procedure with reoperation due to any reason except pain and discomfort from surgical hardware humeral shaft fractures (351).95 probability days 52
55 2 Fracture classification for humeral shaft fractures (351) A 12B 12C 53
56 Distal Humerus 4 Method of osteosynthesis distal humerus fractures (462) 72% % 11% 6% External fixation Plate Screw(s) Other 6 Indication for reoperations of distal humerus fractures (85) 5 52% % Infection 2% 2% 4% New fracture Neurovascular complication Muscle and soft-tissue revision 6% 16% Secondary fracture dislocation or osteosynthesis failure Suboptimal osteosynthesis 6% Pain or discomfort from osteosynthesis Pseudarthrosis / delayed union 54
57 4 Surgeon level for distal humerus fractures (466) 3 58% 2 1 5% 2% 1 year resident 3 year resident 2 year resident 18% 6% Attending 4-5 year resident 11% Traumatologist 4 Level of supervision for distal humerus fractures (454) 3 68% % % % 2 year resident 3% 4-5 year resident 3 year resident Attending 8% Traumatologist Unsupervised 55
58 1 Level of supervision for interns and residents distal humerus fractures (145) Below attending (13) Attending or above (97) Unsupervised (35) % 32% 76% 2 9% 91% 1 year resident % 38% 48% 14% 7% 2 year resident 3 year resident 17% 2% 4-5 year resident Surgical delay for distal humerus fractures (392) 12 3 % 29 % 16 % 12 % 5 % 5 % 4 % Hours (Proportion of patients operated in 24 hour intervals) 56
59 1. Survival for primary procedure with reoperation due to any reason distal humerus fractures (468).95 probability days 1. Survival for primary procedure with reoperation due to any reason except pain and discomfort from surgical hardware distal humerus fractures (468).95 probability days 57
60 25 Fracture classification for distal humerus fractures (468) A 13B 13C 58
61 Proximal antebrachium 6 Method of osteosynthesis proximal antebrachium fractures (937) 5 54% % 1 6% 1% Plate Screw(s) Wire(s) Other 14 Indication for reoperations of proximal antebrachium fractures (172) 12 63% % Infection New fracture Muscle and soft-tissue revision 1% 3% 5% 12% Secondary fracture dislocation or osteosynthesis failure Suboptimal osteosynthesis 7% Pain or discomfort from osteosynthesis Pseudarthrosis / delayed union 59
62 6 Surgeon level for proximal antebrachium fractures (948) % 2 15% 13% 13% 16% 1 6% 3 year resident 2 year resident 1 year resident Attending 4-5 year resident Traumatologist 8 Level of supervision for proximal antebrachium fractures (927) 6 6% 4 24% 2 % 1% 1 year resident 3 year resident 2 year resident 8% 3% Attending 4-5 year resident 5% Traumatologist Unsupervised 6
63 2 Level of supervision for interns and residents proximal antebrachium fractures (54) Below attending (19) Attending or above (24) Unsupervised (191) % 52% 67% 5 38% 28% 41% 31% 37% 29% 5% 11% 4% 1 year resident 2 year resident 3 year resident 4-5 year resident 35 Surgical delay for proximal antebrachium fractures (832) 31 % 27 % 16 % 11 % 6 % 6 % 3 % Hours (Proportion of patients operated in 24 hour intervals) 61
64 1. Survival for primary procedure with reoperation due to any reason proximal antebrachium fractures (95).95 probability days 1. Survival for primary procedure with reoperation due to any reason except pain and discomfort from surgical hardware proximal antebrachium fractures (95).95 probability days 62
65 1 Fracture classification for proximal antebrachium fractures (95) A 21B 21C 63
66 Antebrachium 4 Method of osteosynthesis antebrachium fractures (386) 88% % 6% External fixation Plate Other 35 Indication for reoperations of antebrachium fractures (43) % 1 5 9% Infection 2% 7% 7% New fracture Neurovascular complication 5% Secondary fracture dislocation or osteosynthesis failure Suboptimal osteosynthesis 16% Pain or discomfort from osteosynthesis Pseudarthrosis / delayed union 64
67 25 Surgeon level for antebrachium fractures (41) % 36% 5 11% 12% 15% 6% % Intern Attending 4-5 year resident 3 year resident 2 year resident 1 year resident Traumatologist 3 Level of supervision for antebrachium fractures (393) 25 56% % 5 % 1% 1 year resident 3 year resident 2 year resident 7% 3% Attending 4-5 year resident 5% Traumatologist Unsupervised 65
68 1 Level of supervision for interns and residents antebrachium fractures (233) Below attending (42) Attending or above (116) Unsupervised (75) % 66% 56% 52% 31% 2 44% 33% 25% % 1% % Intern % 1 year resident 15% 2 year resident 7% 3 year resident 2% 4-5 year resident Surgical delay for antebrachium fractures (35) % 23 % 11 % 5 % 1 % 2 % 3 % Hours (Proportion of patients operated in 24 hour intervals) 66
69 1. Survival for primary procedure with reoperation due to any reason antebrachium fractures (41).95 probability days 1. Survival for primary procedure with reoperation due to any reason except pain and discomfort from surgical hardware antebrachium fractures (41).95 probability days 67
70 25 Fracture classification for antebrachium fractures (41) A 22B 22C 68
71 Distal radius 5 Method of osteosynthesis distal radius fractures (4284) 4 93% % Plate Other 14 Indication for reoperations of distal radius fractures (233) 12 48% % 16% 2 3% 3% Infection 8% 1% New fracture Neurovascular complication Muscle and soft-tissue revision 4% Secondary fracture dislocation or osteosynthesis failure Suboptimal osteosynthesis Hematoma Pain or discomfort from osteosynthesis Pseudarthrosis / delayed union 1% 69
72 25 Surgeon level for distal radius fractures (4366) % 17% 12% 15% 31% % Intern 4-5 year resident 3 year resident 2 year resident 1 year resident Attending 4% Traumatologist 35 Level of supervision for distal radius fractures (4265) 3 61% % 5 % 1% Intern 2 year resident 1 year resident 2% 3% Attending 4-5 year resident 3 year resident 9% 3% Unsupervised Traumatologist 7
73 1 Level of supervision for interns and residents distal radius fractures (284) Below attending (632) Attending or above (963) Unsupervised (129) % 41% 43% 82% 37% 44% 47% 2 67% 33% % Intern 13% 1 year resident 2% 2 year resident 1% 3 year resident 3% 14% 4-5 year resident Surgical delay for distal radius fractures (38) % 27 % 15 % 1 % 8 % 5 % 3 % Hours (Proportion of patients operated in 24 hour intervals) 71
74 1. Survival for primary procedure with reoperation due to any reason distal radius fractures (4376).95 probability days 1. Survival for primary procedure with reoperation due to any reason except pain and discomfort from surgical hardware distal radius fractures (4376).95 probability days 72
75 25 Fracture classification for distal radius fractures (4375) A 23B 23C 73
76 Hand 25 Method of osteosynthesis hand fractures (2352) 2 8% % 1% K-wire(s) Screw(s) Other 4 Indication for reoperations of hand fractures (8) % 31% 21% 1 8% 8% 1% Infection 1% 1% New fracture Neurovascular complication Muscle and soft-tissue revision Secondary fracture dislocation or osteosynthesis failure Suboptimal osteosynthesis Bone necrosis Pain or discomfort from osteosynthesis Pseudarthrosis / delayed union 2% 74
77 14 Surgeon level for hand fractures (2381) 12 44% % 13% 11% 12% 2 % Intern Attending 4-5 year resident 3 year resident 2 year resident 1 year resident 5% Traumatologist Level of supervision for hand fractures (2328) 2 69% % % 1% 1% 1 year resident 2 year resident 5% 4-5 year resident 3 year resident Attending 2% Traumatologist Unsupervised 75
78 4 Level of supervision for interns and residents hand fractures (1199) Below attending (171) Attending or above (488) Unsupervised (54) % 53% 46% 41% 45% 52% 83% 1 14% 14% 17% 83% 17% % Intern 1 year resident 2 year resident 3% 3 year resident 1% 4-5 year resident Surgical delay for hand fractures (1964) 6 36 % 25 % 13 % 1 % 7 % 5 % 3 % Hours (Proportion of patients operated in 24 hour intervals) 76
79 1. Survival for primary procedure with reoperation due to any reason hand fractures (238).95 probability days 1. Survival for primary procedure with reoperation due to any reason except pain and discomfort from surgical hardware hand fractures (238).95 probability days 77
80 14 Fracture classification for hand fractures (2381) 12 45% % 4% 4% 1. metacarpal Wrist bones 1% 1. distal phalanx 1. proximal phalanx 18% 1% 2-5 middle phalanx 2-5 proximal phalanx 2-5 metacarpal 6% 2-5 distal phalanx 78
81 Proximal femur 6 Method of osteosynthesis proximal femur fractures (1127) % 34% 14% 16% 1 4% Arthroplasty Screw(s) Intramedullary nail(s) Other Sliding hip screw(s) 6 Indication for reoperations of proximal femur fractures (953) % 18% 16% 34% 1 Infection % Bone necrosis Arthroplasty dislocation Pain or discomfort from osteosynthesis Pseudarthrosis / delayed union Secondary fracture dislocation or osteosynthesis failure Suboptimal osteosynthesis Not identified preoperative fracture New fracture 4% % 3% Muscle and soft-tissue revision 5% 6% % Hematoma 79
82 6 Surgeon level for proximal femur fractures (111) % 17% 16% 13% 2% 1 1% Intern Attending 4-5 year resident 3 year resident 2 year resident 1 year resident 2% Traumatologist 6 Level of supervision for proximal femur fractures (986) 5 49% % 12% 1 % Intern 1% 2 year resident 1 year resident 4% 2% 4-5 year resident 3 year resident 4% Traumatologist Attending Unsupervised 8
83 25 Level of supervision for interns and residents proximal femur fractures (7827) Below attending (1837) Attending or above (376) Unsupervised (2914) % 47% 82% 37% 38% 47% 44% 5 44%51% 5% Intern 15% 1 year resident 25% 2 year resident 9% 3 year resident 3% 15% 4-5 year resident Surgical delay for proximal femur fractures (9631) 6 68 % 26 % 4 % 1 % % % % Hours (Proportion of patients operated in 24 hour intervals) 81
84 1. Survival for primary procedure with reoperation due to any reason proximal femur fractures (1132).95 probability days 1. Survival for primary procedure with reoperation due to any reason except pain and discomfort from surgical hardware proximal femur fractures (1132).95 probability days 82
85 6 Fracture classification for proximal femur fractures (1133) A 31B 31C 83
86 Acetabulum 3 Method of osteosynthesis acetabulum fractures (347) % 33% 5 7% External fixation Plate Screw(s) 3% Other 5 Indication for reoperations of acetabulum fractures (72) % 1 Infection 1% 1% Secondary fracture dislocation or osteosynthesis failure Suboptimal osteosynthesis 7% 14% 1% Pain or discomfort from osteosynthesis Pseudarthrosis / delayed union 1% Arthroplasty dislocation Bone necrosis 4% Hematoma 84
87 25 Surgeon level for acetabulum fractures (348) 2 5% % 5 1% 1 year resident 5% 3 year resident 1% 4-5 year resident Attending Traumatologist 3 Level of supervision for acetabulum fractures (348) 25 7% % 15% % % 1 year resident 4-5 year resident Attending Traumatologist Unsupervised 85
88 4 Level of supervision for interns and residents acetabulum fractures (24) Below attending (2) Attending or above (22) Unsupervised () % 1 67% 33% % 1 year resident 1% 5% % % % 3 year resident 4-5 year resident Surgical delay for acetabulum fractures (286) 8 17 % 13 % 13 % 18 % 16 % 13 % 9 % Hours (Proportion of patients operated in 24 hour intervals) 86
89 1. Survival for primary procedure with reoperation due to any reason acetabulum fractures (348).95 probability days 1. Survival for primary procedure with reoperation due to any reason except pain and discomfort from surgical hardware acetabulum fractures (348).95 probability days 87
90 5 Fracture classification for acetabulum fractures (145) % 16% 14% 14% 12% 1% 1 4% 3% 6% 3% Posterior wall Anterior wall Posterior column Anterior column Transverse Posterior column/wall Both column Ant. Column/ post hemitransverse T-type Transverse/posterior wall 88
91 Femur 6 Method of osteosynthesis femur fractures (674) 5 71% % 1 7% External fixation Intramedullary nail(s) Plate 3% Other 8 Indication for reoperations of femur fractures (141) % 27% 2 11% 11% 9% 14% Infection 1% New fracture Muscle and soft-tissue revision Secondary fracture dislocation or osteosynthesis failure Suboptimal osteosynthesis 3% Pain or discomfort from osteosynthesis Pseudarthrosis / delayed union Hematoma 89
92 4 Surgeon level for femur fractures (678) 3 2 2% 32% 1 15% 9% 15% 8% % Intern 3 year resident 2 year resident 1 year resident Attending 4-5 year resident Traumatologist Level of supervision for femur fractures (672) % % 1 1% 1% 2 year resident 6% 4-5 year resident 3 year resident Attending 8% Traumatologist Unsupervised 9
93 14 12 Level of supervision for interns and residents femur fractures (46) Below attending (55) Attending or above (248) Unsupervised (13) % 77% 45% 51% 4 2 % 33% 67% Intern 24% 1 year resident 56% 7% 31% 12% 2 year resident 6% 17% 3 year resident 4% 4-5 year resident Surgical delay for femur fractures (648) 4 61 % 26 % 7 % 3 % 2 % 1 % 1 % Hours (Proportion of patients operated in 24 hour intervals) 91
94 1. Survival for primary procedure with reoperation due to any reason femur fractures (678).95 probability days 1. Survival for primary procedure with reoperation due to any reason except pain and discomfort from surgical hardware femur fractures (678).95 probability days 92
95 5 Fracture classification for femur fractures (678) A 32B 32C 93
96 Distal femur 4 Method of osteosynthesis distal femur fractures (379) 82% % 6% 5% External fixation Plate Screw(s) Other 7 Indication for reoperations of distal femur fractures (13) % 2% 44% 1 9% Infection New fracture Neurovascular complication 1% 3% 5% Secondary fracture dislocation or osteosynthesis failure Suboptimal osteosynthesis Pain or discomfort from osteosynthesis Pseudarthrosis / delayed union 94
97 25 Surgeon level for distal femur fractures (387) 2 41% % 5 6% 4% 13% 14% 2 year resident 1 year resident Attending 4-5 year resident 3 year resident Traumatologist 3 Level of supervision for distal femur fractures (38) 25 57% % 5 1% 1% 1 year resident 3% 4-5 year resident 3 year resident Attending 13% Traumatologist Unsupervised 95
98 1 Level of supervision for interns and residents distal femur fractures (171) Below attending (13) Attending or above (128) Unsupervised (3) % 63% 33% 92% 2 76% 8% 1 year resident % 24% 2 year resident % 8% 3 year resident 8% 4% 4-5 year resident Surgical delay for distal femur fractures (35) % 31 % 17 % 7 % 6 % 3 % 1 % Hours (Proportion of patients operated in 24 hour intervals) 96
99 1. Survival for primary procedure with reoperation due to any reason distal femur fractures (387).95 probability days 1. Survival for primary procedure with reoperation due to any reason except pain and discomfort from surgical hardware distal femur fractures (387).95 probability days 97
100 Fracture classification for distal femur fractures (387) A 33B 33C 98
101 Patella 4 Method of osteosynthesis patella fractures (343) 3 88% 2 1 6% Screw(s) Wire(s) 6% Other 8 Indication for reoperations of patella fractures (94) 6 6% % 18% Infection 1% New fracture 3% Suboptimal osteosynthesis 2% Secondary fracture dislocation or osteosynthesis failure Pain or discomfort from osteosynthesis Pseudarthrosis / delayed union 99
102 2 Surgeon level for patella fractures (342) % 17% 32% 5 14% 13% 6% 4-5 year resident 3 year resident 2 year resident 1 year resident Attending Traumatologist 25 Level of supervision for patella fractures (33) 2 54% % 5 11% 1% 2% 2% 1 year resident 2 year resident Attending 4-5 year resident 3 year resident 3% Traumatologist Unsupervised 1
103 1 Level of supervision for interns and residents patella fractures (212) Below attending (51) Attending or above (97) Unsupervised (64) % 72% 2 1 year resident 2 year resident 57% 35% 3% 39% 32% 15% % 3 year resident 28% 11% 17% 4-5 year resident Surgical delay for patella fractures (311) 2 42 % 32 % 13 % 5 % 4 % 2 % 3 % Hours (Proportion of patients operated in 24 hour intervals) 11
104 1. Survival for primary procedure with reoperation due to any reason patella fractures (343).95 probability days 1. Survival for primary procedure with reoperation due to any reason except pain and discomfort from surgical hardware patella fractures (343).95 probability days 12
The Danish Fracture Database can monitor quality of fracture-related surgery, surgeons experience level and extent of supervision
 Dan Med J 61/6 June 2014 danish medical JOURNAL 1 The Danish Fracture Database can monitor quality of fracture-related surgery, surgeons experience level and extent of supervision Morten Jon Andersen 1,
Dan Med J 61/6 June 2014 danish medical JOURNAL 1 The Danish Fracture Database can monitor quality of fracture-related surgery, surgeons experience level and extent of supervision Morten Jon Andersen 1,
Orthopedic Injury Coding. Bryant Oliphant 10:20
 Orthopedic Injury Coding Bryant Oliphant 10:20 Orthopaedic Trauma in MTQIP Bryant Oliphant, MD, MBA, MSc Research Investigator bryantol@med.umich.edu @BonezNQuality DEPARTMENT OF ORTHOPAEDIC SURGERY None
Orthopedic Injury Coding Bryant Oliphant 10:20 Orthopaedic Trauma in MTQIP Bryant Oliphant, MD, MBA, MSc Research Investigator bryantol@med.umich.edu @BonezNQuality DEPARTMENT OF ORTHOPAEDIC SURGERY None
EFORT Expert Meet Expert Forum. ExMex Forum. Periarticular Fractures. Case Discussions/Workshops
 ExMex Forum Copenhagen, Denmark 25-26 April 2014 Case Discussions/Workshops EFORT Expert Meet Expert Forum Copenhagen, Denmark: 25-26 April 2014 Periarticular Fractures Subtrochanteric fractures Complex
ExMex Forum Copenhagen, Denmark 25-26 April 2014 Case Discussions/Workshops EFORT Expert Meet Expert Forum Copenhagen, Denmark: 25-26 April 2014 Periarticular Fractures Subtrochanteric fractures Complex
Forearm Fracture Solutions. Product Overview
 Forearm Fracture Solutions Product Overview Acumed Forearm Fracture Solutions Acumed Forearm Fracture Solutions includes plating and rodding systems with a range of diaphyseal radius and ulna fracture
Forearm Fracture Solutions Product Overview Acumed Forearm Fracture Solutions Acumed Forearm Fracture Solutions includes plating and rodding systems with a range of diaphyseal radius and ulna fracture
What is Tuberous Sclerosis Complex?
 Treatment of patients with Tuberous Sclerosis Complex in Denmark- results from a survey amongst the patient population- a case study Sarah Lysdal Krøtel, Department of Management, Aarhus University Liselotte
Treatment of patients with Tuberous Sclerosis Complex in Denmark- results from a survey amongst the patient population- a case study Sarah Lysdal Krøtel, Department of Management, Aarhus University Liselotte
Country Health SA Medical Imaging
 Country Health SA Medical Imaging REMOTE OPERATORS POSITIONING GUIDE Contents Image Evaluation Page 4 Positioning Guides Section 1 - THORAX 1.1 Chest Page 5 1.2 Bedside Chest Page 7 1.3 Ribs Page 8 Section
Country Health SA Medical Imaging REMOTE OPERATORS POSITIONING GUIDE Contents Image Evaluation Page 4 Positioning Guides Section 1 - THORAX 1.1 Chest Page 5 1.2 Bedside Chest Page 7 1.3 Ribs Page 8 Section
EPOS-EFORT Instructional Course. Paediatrics: Trauma Course. Workshops / Case discussions. Instructional Course
 xxxxxxxxx EPOS-EFORT Instructional Course 12-14 October 2011 Workshops / Case discussions EPOS-EFORT Instructional Course Vienna, Austria: 12-14 October 2011 Paediatrics: Trauma Course Fractures in the
xxxxxxxxx EPOS-EFORT Instructional Course 12-14 October 2011 Workshops / Case discussions EPOS-EFORT Instructional Course Vienna, Austria: 12-14 October 2011 Paediatrics: Trauma Course Fractures in the
AAOS/OTA Daily Dilemmas in Trauma: Your Topics, Expert Solutions
 AAOS/OTA Daily Dilemmas in Trauma: Your Topics, Expert Solutions You pick the topics. We bring the expertise. May 2 4, 2019 Orlando, FL Paul Tornetta III, MD & J. Tracy Watson, MD Course Directors AAOS/OTA
AAOS/OTA Daily Dilemmas in Trauma: Your Topics, Expert Solutions You pick the topics. We bring the expertise. May 2 4, 2019 Orlando, FL Paul Tornetta III, MD & J. Tracy Watson, MD Course Directors AAOS/OTA
Results of tibia nailing with Angular Stable Locking Screws (ASLS); A retrospective study of 107 patients with distal tibia fracture.
 Results of tibia nailing with Angular Stable Locking Screws (ASLS); A retrospective study of 107 patients with distal tibia fracture. stud. med. David Andreas Lunde Hatfield stud. med. Mohammed Sherif
Results of tibia nailing with Angular Stable Locking Screws (ASLS); A retrospective study of 107 patients with distal tibia fracture. stud. med. David Andreas Lunde Hatfield stud. med. Mohammed Sherif
Log Book. Diploma In Orthopaedic Surgery (D-Ortho) For. Bangabandhu Sheikh Mujib Medical University Shahbagh, Dhaka-1000
 Log Book For Diploma In Orthopaedic Surgery (D-Ortho) Bangabandhu Sheikh Mujib Medical University Shahbagh, Dhaka-1000 1 Table of Contents Page No Personal details of the candidate 3 Section-A 4 Purpose
Log Book For Diploma In Orthopaedic Surgery (D-Ortho) Bangabandhu Sheikh Mujib Medical University Shahbagh, Dhaka-1000 1 Table of Contents Page No Personal details of the candidate 3 Section-A 4 Purpose
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Unified Classification System (UCS) for peri-prosthetic fractures (PPFx)
 Unified Classification System (UCS) for peri-prosthetic fractures (PPFx) Waleed A Abdulwahid Consultant surgeon Medical City, Iraq 6th Emirates International Orthopedic Congress Dubai, UAE May 3-5, 2018
Unified Classification System (UCS) for peri-prosthetic fractures (PPFx) Waleed A Abdulwahid Consultant surgeon Medical City, Iraq 6th Emirates International Orthopedic Congress Dubai, UAE May 3-5, 2018
7/23/2018 DESCRIBING THE FRACTURE. Pattern Open vs closed Location BASIC PRINCIPLES OF FRACTURE MANAGEMENT. Anjan R. Shah MD July 21, 2018.
 BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
Hand Fracture System with Small Bone External Fixation System. Product Overview
 Hand Fracture System with Small Bone External Fixation System Product Overview Acumed Hand Fracture System The Acumed Hand Fracture System is designed to provide both standard and fracture-specific fixation
Hand Fracture System with Small Bone External Fixation System Product Overview Acumed Hand Fracture System The Acumed Hand Fracture System is designed to provide both standard and fracture-specific fixation
Shoulder Position: Supine arm in the neutral position. Collateral arm above head Indication: fracture humerus, fracture scapula
 Shoulder Position: Supine arm in the neutral position. Collateral arm above head Indication: fracture humerus, fracture scapula No instrumentation With metal or cast KV/ Effective mas/rotation time 140/300/1.0
Shoulder Position: Supine arm in the neutral position. Collateral arm above head Indication: fracture humerus, fracture scapula No instrumentation With metal or cast KV/ Effective mas/rotation time 140/300/1.0
AO Trauma Course Advances in Operative Fracture Management for Surgeons
 AO Course Zagreb, Croatia _ AO Trauma Course Advances in Operative Fracture Management for Surgeons 8 10 November 2013 Overall Chairperson: Course Chairpersons: Bore Bakota, MD PhD Candidate(HR) Ivan Dobric,
AO Course Zagreb, Croatia _ AO Trauma Course Advances in Operative Fracture Management for Surgeons 8 10 November 2013 Overall Chairperson: Course Chairpersons: Bore Bakota, MD PhD Candidate(HR) Ivan Dobric,
1:00 pm Welcome and Introduction Paul Tornetta III, MD and J. Tracy Watson, MD
 AAOS/OTA Daily Dilemmas in Trauma: Your Topics, Expert Solutions #3248 May 2-4, 2019 Orlando, FL Paul Tornetta III, MD and J. Tracy Watson, MD; Course Directors SCHEDULE THURSDAY, MAY 2 12:00 1:00 pm Registration/Exhibits
AAOS/OTA Daily Dilemmas in Trauma: Your Topics, Expert Solutions #3248 May 2-4, 2019 Orlando, FL Paul Tornetta III, MD and J. Tracy Watson, MD; Course Directors SCHEDULE THURSDAY, MAY 2 12:00 1:00 pm Registration/Exhibits
FLT105 12/02.
 FLT105 12/02 www.biometmerck.co.uk Disclaimer Biomet Merck Ltd, as the manufacturer of this device, does not practice medicine and does not recommend this or any other surgical technique for use on a
FLT105 12/02 www.biometmerck.co.uk Disclaimer Biomet Merck Ltd, as the manufacturer of this device, does not practice medicine and does not recommend this or any other surgical technique for use on a
Dr.Israa H. Mohsen. Lecture 5. The vertebral column
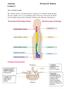 Anatomy Lecture 5 Dr.Israa H. Mohsen The vertebral column The vertebral column a flexible structure consisting of 33 vertebrae holds the head and torso upright, serves as an attachment point for the legs,
Anatomy Lecture 5 Dr.Israa H. Mohsen The vertebral column The vertebral column a flexible structure consisting of 33 vertebrae holds the head and torso upright, serves as an attachment point for the legs,
Complex fractures of the humeral shaft. Janos Solyom Sahlgrenska University Hospital Gothenburg, Sweden
 Complex fractures of the humeral shaft Janos Solyom Sahlgrenska University Hospital Gothenburg, Sweden Kopenhagen 2018 Complex fracture Changes in the AO/OTA classification system Complex Multifragmentary
Complex fractures of the humeral shaft Janos Solyom Sahlgrenska University Hospital Gothenburg, Sweden Kopenhagen 2018 Complex fracture Changes in the AO/OTA classification system Complex Multifragmentary
THE NANCY NAIL. The End Caps ADVANTAGES OF NANCY NAIL
 NANCY NAIL THE NANCY NAIL Nancy nails are manufactured from a specific titanyum alloy with proprietary surface treatment, which provides increased fatigue resistance. Six nail diameters (1.5 mm 2.0 mm
NANCY NAIL THE NANCY NAIL Nancy nails are manufactured from a specific titanyum alloy with proprietary surface treatment, which provides increased fatigue resistance. Six nail diameters (1.5 mm 2.0 mm
The study of distal ¼ diaphyseal extra articular fractures of humerus treated with antegrade intramedullary interlocking nailing
 2018; 4(4): 46-50 ISSN: 2395-1958 IJOS 2018; 4(4): 46-50 2018 IJOS www.orthopaper.com Received: 01-08-2018 Accepted: 03-09-2018 Dr. Ankur Parikh Orthopaedics, Jehangir Hospital, Sassoon road, Pune, Dr.
2018; 4(4): 46-50 ISSN: 2395-1958 IJOS 2018; 4(4): 46-50 2018 IJOS www.orthopaper.com Received: 01-08-2018 Accepted: 03-09-2018 Dr. Ankur Parikh Orthopaedics, Jehangir Hospital, Sassoon road, Pune, Dr.
ABOS/CORD Surgical Skills Assessment Program
 American Board of Orthopaedic Surgery Establishing Education & Performance Standards for Orthopaedic Surgeons ABOS/CORD Surgical Skills Assessment Program ABOS Essential Knowledge, Skills, and Behaviors
American Board of Orthopaedic Surgery Establishing Education & Performance Standards for Orthopaedic Surgeons ABOS/CORD Surgical Skills Assessment Program ABOS Essential Knowledge, Skills, and Behaviors
AOTrauma / AORecon Masters Course Periprosthetic Fractures (Course with Anatomical Specimen)
 Sunday, 13 May 2018 (Day 1) 15:00 17:00 Other Registration of participants 17:00 18:00 Opening remarks Opening ceremony 18:00 19:00 Other AOTRAUMA RECEPTION 120 1 / 10 Monday, 14 May 2018 (Day 2) 08:00
Sunday, 13 May 2018 (Day 1) 15:00 17:00 Other Registration of participants 17:00 18:00 Opening remarks Opening ceremony 18:00 19:00 Other AOTRAUMA RECEPTION 120 1 / 10 Monday, 14 May 2018 (Day 2) 08:00
Orthopedics in Motion Tristan Hartzell, MD January 27, 2016
 Orthopedics in Motion 2016 Tristan Hartzell, MD January 27, 2016 Humerus fractures Proximal Shaft Distal Objectives 1) Understand the anatomy 2) Epidemiology and mechanisms of injury 3) Types of fractures
Orthopedics in Motion 2016 Tristan Hartzell, MD January 27, 2016 Humerus fractures Proximal Shaft Distal Objectives 1) Understand the anatomy 2) Epidemiology and mechanisms of injury 3) Types of fractures
ORTHOSCAN MOBILE DI POSITIONING GUIDE
 ORTHOSCAN MOBILE DI POSITIONING GUIDE Table of Contents SHOULDER A/P of Shoulder... 4 Tangential (Y-View) of Shoulder... 5 Lateral of Proximal Humerus... 6 ELBOW A/P of Elbow... 7 Extended Elbow... 8 Lateral
ORTHOSCAN MOBILE DI POSITIONING GUIDE Table of Contents SHOULDER A/P of Shoulder... 4 Tangential (Y-View) of Shoulder... 5 Lateral of Proximal Humerus... 6 ELBOW A/P of Elbow... 7 Extended Elbow... 8 Lateral
Types of Plates 1. New Dynamic Compression Plate: Diaphyseal fracture: Radius, Ulna, Humerus, Rarely tibia
 Types of Plates 1. New Dynamic Compression Plate: DCP Diaphyseal fracture: Radius, Ulna, Humerus, Rarely tibia 1. Undercut adjacent to the holes low contact: less stress shield 2. Undercut at the undersurface
Types of Plates 1. New Dynamic Compression Plate: DCP Diaphyseal fracture: Radius, Ulna, Humerus, Rarely tibia 1. Undercut adjacent to the holes low contact: less stress shield 2. Undercut at the undersurface
Trauma fixation choices chart your fracture
 Trauma fixation choices chart your fracture This brochure is intended for informational and educational purposes only. It is the responsibility of operating physicians to determine and utilize the appropriate
Trauma fixation choices chart your fracture This brochure is intended for informational and educational purposes only. It is the responsibility of operating physicians to determine and utilize the appropriate
Part II; Paediatric trauma
 4th EPOS-EFORT BAT INSTRUCTIONAL COURSE TRILOGY Part II; Paediatric trauma 5-7 October 2016 Orthopaedic Hospital Speising, Vienna, Austria Characteristics of Fractures in Children Initial Assessment of
4th EPOS-EFORT BAT INSTRUCTIONAL COURSE TRILOGY Part II; Paediatric trauma 5-7 October 2016 Orthopaedic Hospital Speising, Vienna, Austria Characteristics of Fractures in Children Initial Assessment of
Basic Radiographic Principles Part II
 Basic Radiographic Principles Part II Kristopher Avant, D.O. October 19 th, 2016 I have no disclosures relevant to the material presented in this discussion. Good Stuff!!! 1 Really? Really! Musculoskeletal
Basic Radiographic Principles Part II Kristopher Avant, D.O. October 19 th, 2016 I have no disclosures relevant to the material presented in this discussion. Good Stuff!!! 1 Really? Really! Musculoskeletal
Pediatric Fractures. Objectives. Epiphyseal Complex. Anatomy and Physiology. Ligaments. Bony matrix
 1 Pediatric Fractures Nicholas White, MD Assistant Professor of Pediatrics Eastern Virginia Medical School Attending, Pediatric Emergency Department Children s Hospital of The King s Daughters Objectives
1 Pediatric Fractures Nicholas White, MD Assistant Professor of Pediatrics Eastern Virginia Medical School Attending, Pediatric Emergency Department Children s Hospital of The King s Daughters Objectives
Injuries of the upper extremity
 Injuries of the upper extremity Dep. of Traumatology M.Szebeny Egon Schiele Sternoclavicular dislocation Direction: towards the outside or inside (what is behind the dislocation!) Reduction? Retention?
Injuries of the upper extremity Dep. of Traumatology M.Szebeny Egon Schiele Sternoclavicular dislocation Direction: towards the outside or inside (what is behind the dislocation!) Reduction? Retention?
NE Nebraska Trauma Conference Tristan Hartzell, MD November 8, 2017
 NE Nebraska Trauma Conference 2017 Tristan Hartzell, MD November 8, 2017 Traumatic arm injuries in the elderly Fractures Hand Wrist Elbow Shoulder Soft tissue injuries Definitions Elderly? old or aging
NE Nebraska Trauma Conference 2017 Tristan Hartzell, MD November 8, 2017 Traumatic arm injuries in the elderly Fractures Hand Wrist Elbow Shoulder Soft tissue injuries Definitions Elderly? old or aging
Practical Reduction Techniques: Diaphyseal Reduction. Philip Wolinsky University of California at Davis Medical Center
 OTA Specialty Day 2016 Practical Reduction Techniques: Diaphyseal Reduction Philip Wolinsky University of California at Davis Medical Center 8:55 am 9:55 am Tips and Tricks: Practical Reduction Techniques
OTA Specialty Day 2016 Practical Reduction Techniques: Diaphyseal Reduction Philip Wolinsky University of California at Davis Medical Center 8:55 am 9:55 am Tips and Tricks: Practical Reduction Techniques
SOLID CLEAR CATALOG A Division of Pacific Research Laboratories, Inc.
 SOLID CLEAR CATALOG 2016 A Division of Pacific Research Laboratories, Inc. WWW.SAWBONES.COM Solid clear plastic bones are ideal for product display and procedure visualization. Great care is taken so that
SOLID CLEAR CATALOG 2016 A Division of Pacific Research Laboratories, Inc. WWW.SAWBONES.COM Solid clear plastic bones are ideal for product display and procedure visualization. Great care is taken so that
Fracture Classification
 Fracture Classification Lisa K. Cannada MD Updated: 05/2016 18 th & 19 th century History of Fracture History based on clinical appearance of limb alone Classification Colles Fracture Dinner Fork Deformity
Fracture Classification Lisa K. Cannada MD Updated: 05/2016 18 th & 19 th century History of Fracture History based on clinical appearance of limb alone Classification Colles Fracture Dinner Fork Deformity
Clinical Practice Guidelines: Can I Learn to Live With Them? What s in the News These Days 2/11/2016. Excessive Costs of Medical Care
 Orthopaedic Trauma Fracture Care: Pushing the Envelope San Diego Clinical Practice Guidelines: Can I Learn to Live With Them? Andrew H. Schmidt, MD What s in the News These Days Excessive Costs of Medical
Orthopaedic Trauma Fracture Care: Pushing the Envelope San Diego Clinical Practice Guidelines: Can I Learn to Live With Them? Andrew H. Schmidt, MD What s in the News These Days Excessive Costs of Medical
Osteosynthesis involving a joint Thomas P Rüedi
 Osteosynthesis involving a joint Thomas P Rüedi How to use this handout? The left column contains the information given during the lecture. The column at the right gives you space to make personal notes.
Osteosynthesis involving a joint Thomas P Rüedi How to use this handout? The left column contains the information given during the lecture. The column at the right gives you space to make personal notes.
Report of reversed fellowship in Eritrea, Marc Lottenbach
 Report of reversed fellowship in Eritrea, 29.6.-27.8.2005 Marc Lottenbach Introduction My wife me and were the second persons which went to Eritrea for the reversed fellow ship. I spent there for 8 weeks
Report of reversed fellowship in Eritrea, 29.6.-27.8.2005 Marc Lottenbach Introduction My wife me and were the second persons which went to Eritrea for the reversed fellow ship. I spent there for 8 weeks
PROFESSIONAL RELIABLE TRAUMA MANUAL. Health is Important
 PROFESSIONAL RELIABLE TRAUMA MANUAL Health is Important 1 Vision In the past, the Treasure Voyages of Zheng He started the epoch-making communication and fusion by sea between the Oriental and the Occidental.
PROFESSIONAL RELIABLE TRAUMA MANUAL Health is Important 1 Vision In the past, the Treasure Voyages of Zheng He started the epoch-making communication and fusion by sea between the Oriental and the Occidental.
What can a redesigned facture pathway look like?
 GRI FRACTURE CLINIC MODERNISATION What can a redesigned facture pathway look like? Lech Rymaszewski Consultant Orthopaedic Surgeon DETROIT BAILOUT TRADITIONAL ORTHOPAEDIC FRACTURE (#) CLINIC All non operated
GRI FRACTURE CLINIC MODERNISATION What can a redesigned facture pathway look like? Lech Rymaszewski Consultant Orthopaedic Surgeon DETROIT BAILOUT TRADITIONAL ORTHOPAEDIC FRACTURE (#) CLINIC All non operated
Increasing surgical freedom Restoring patient function
 Increasing surgical freedom Restoring patient function Fracture specific plating solutions for the most common tibia and fibula fractures Frequency of fracture occurrences* 66% 61% 36% 36% 28% 14% 20%
Increasing surgical freedom Restoring patient function Fracture specific plating solutions for the most common tibia and fibula fractures Frequency of fracture occurrences* 66% 61% 36% 36% 28% 14% 20%
EXAMPLE OF STRONG APPLICATION Includes Entries from COTA Awarded Programs
 EXAMPLE OF STRONG APPLICATION Includes Entries from COTA Awarded Programs (NOTE only blinded submissions will be accepted and distributed for COTA review) Orthopaedic Trauma Fellowship Program Goals and
EXAMPLE OF STRONG APPLICATION Includes Entries from COTA Awarded Programs (NOTE only blinded submissions will be accepted and distributed for COTA review) Orthopaedic Trauma Fellowship Program Goals and
Ref. Number Stainless Steel
 Section of humerus plates for operation on distal humerus Y - Distal Humerus Plate 4. Y - Distale Humerusplatte 4. Plaque pour humerus distal en Y 4. Indication : Used to treat coinuted distal humerus
Section of humerus plates for operation on distal humerus Y - Distal Humerus Plate 4. Y - Distale Humerusplatte 4. Plaque pour humerus distal en Y 4. Indication : Used to treat coinuted distal humerus
Interlocking Nailing Course for Surgeons
 Credit Points Program Interlocking Nailing Course for Surgeons 6-7 February 2017 Berlin Germany Preface Dear Colleagues, Intramedullary nailing has gained widespread acceptance among orthopaedic trauma
Credit Points Program Interlocking Nailing Course for Surgeons 6-7 February 2017 Berlin Germany Preface Dear Colleagues, Intramedullary nailing has gained widespread acceptance among orthopaedic trauma
5/31/2018. Ipsilateral Femoral Neck And Shaft Fractures. Ipsilateral Neck-Shaft Fractures Introduction. Ipsilateral Neck-Shaft Fractures Introduction
 Ipsilateral Femoral Neck And Shaft Fractures Exchange Nailing For Non- Union Donald Wiss MD Cedars-Sinai Medical Center Los Angeles, California Introduction Uncommon Injury Invariably High Energy Trauma
Ipsilateral Femoral Neck And Shaft Fractures Exchange Nailing For Non- Union Donald Wiss MD Cedars-Sinai Medical Center Los Angeles, California Introduction Uncommon Injury Invariably High Energy Trauma
Austin Hill MD MPH. Assistant Professor Dell Medical School Dept of Surgery and Perioperative Care Orthopaedic Trauma
 Austin Hill MD MPH Assistant Professor Dell Medical School Dept of Surgery and Perioperative Care Orthopaedic Trauma Disclosures Orthopedic Implant Company ownership, stock, or options Increasing volume
Austin Hill MD MPH Assistant Professor Dell Medical School Dept of Surgery and Perioperative Care Orthopaedic Trauma Disclosures Orthopedic Implant Company ownership, stock, or options Increasing volume
Research Group Name: Prof. Dr. NYÁRÁDY, József
 Musculoskeletal 1 RECOOP HST Research Activity Inventory Please complete the template for each selected project your organization would like to share with the partners of the RECOOP HST Consortium and
Musculoskeletal 1 RECOOP HST Research Activity Inventory Please complete the template for each selected project your organization would like to share with the partners of the RECOOP HST Consortium and
GENERAL ORTHOPAEDIC PROGRAM SCHEDULE 18. January 25 26, 2019 Rosemont, IL. Albert J. Aboulafia, MD & Isador H. Lieberman, MD, MBA, FRCSC
 AAOS Board Maintenance of Certification Preparation and Review GENERAL ORTHOPAEDIC PROGRAM SCHEDULE 18 CME Credits January 25 26, 2019 Rosemont, IL Albert J. Aboulafia, MD & Isador H. Lieberman, MD, MBA,
AAOS Board Maintenance of Certification Preparation and Review GENERAL ORTHOPAEDIC PROGRAM SCHEDULE 18 CME Credits January 25 26, 2019 Rosemont, IL Albert J. Aboulafia, MD & Isador H. Lieberman, MD, MBA,
Orthopaedic & Rheumatologic Institute Outcomes
 Orthopaedic & Rheumatologic Institute 213 Outcomes Measuring Outcomes Promotes Quality Improvement Measuring and understanding outcomes of medical treatments promotes quality improvement. Cleveland Clinic
Orthopaedic & Rheumatologic Institute 213 Outcomes Measuring Outcomes Promotes Quality Improvement Measuring and understanding outcomes of medical treatments promotes quality improvement. Cleveland Clinic
Danish Pacemaker and ICD Register Annual report 2015
 Danish Pacemaker and ICD Register Annual report 2015 Preface The Danish Pacemaker Register was founded in 1982 by physicians from all Danish hospitals where pacemakers were implanted. When the first implantable
Danish Pacemaker and ICD Register Annual report 2015 Preface The Danish Pacemaker Register was founded in 1982 by physicians from all Danish hospitals where pacemakers were implanted. When the first implantable
Danish Pacemaker and ICD Register Annual Report 2016
 Danish Pacemaker and ICD Register Annual Report 2016 Preface The Danish Pacemaker Register was founded in 1982 by physicians from all Danish hospitals where pacemakers were implanted. When the first implantable
Danish Pacemaker and ICD Register Annual Report 2016 Preface The Danish Pacemaker Register was founded in 1982 by physicians from all Danish hospitals where pacemakers were implanted. When the first implantable
Index. B Backslap technique depth assessment, 82, 83 diaphysis distal trocar, 82 83
 Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
AOTrauma Course Fragility Fractures and Orthogeriatrics
 Thursday, 22 Oct 2015 (Day 1) 09:00 09:30 Other REGISTATION AND WELCOME COFFEE Sokos Hotel Viru, Bolero venue 30 09:30 12:25 Module 1: The Geriatric Patient and Fracture 175 09:30 09:50 Lecture The Morbidity
Thursday, 22 Oct 2015 (Day 1) 09:00 09:30 Other REGISTATION AND WELCOME COFFEE Sokos Hotel Viru, Bolero venue 30 09:30 12:25 Module 1: The Geriatric Patient and Fracture 175 09:30 09:50 Lecture The Morbidity
Surgical Technique. Targeter Systems Overview
 Surgical Technique Targeter Systems Overview PERI-LOC Locked Plating System Targeter Systems Overview Table of contents Product overview... 2 Introduction... 2 Indications... 2 Design features and benefits...
Surgical Technique Targeter Systems Overview PERI-LOC Locked Plating System Targeter Systems Overview Table of contents Product overview... 2 Introduction... 2 Indications... 2 Design features and benefits...
Proximal Humerus Fractures
 Proximal Humerus Fractures Trafford General Hospital, June 2010 Nehmat Singh, Jawad Sultan Anatomy of the Proximal Humerus Consists of four parts: humeral head, surgical neck and greater and lesser tubercles
Proximal Humerus Fractures Trafford General Hospital, June 2010 Nehmat Singh, Jawad Sultan Anatomy of the Proximal Humerus Consists of four parts: humeral head, surgical neck and greater and lesser tubercles
10/12/2010. Upper Extremity. Pectoral (Shoulder) Girdle. Clavicle (collarbone) Skeletal System: Appendicular Skeleton
 Skeletal System: Appendicular Skeleton Pectoral girdle Pelvic girdle Upper limbs Lower limbs 8-1 Pectoral (Shoulder) Girdle Consists of scapula and clavicle Clavicle articulates with sternum (Sternoclavicular
Skeletal System: Appendicular Skeleton Pectoral girdle Pelvic girdle Upper limbs Lower limbs 8-1 Pectoral (Shoulder) Girdle Consists of scapula and clavicle Clavicle articulates with sternum (Sternoclavicular
Part II; Paediatric trauma
 3rd EPOS-EFORT BAT INSTRUCTIONAL COURSE TRILOGY Workshops / Case discussions Part II; Paediatric trauma 11-13 March 2015 Orthopaedic Hospital Speising, Vienna, Austria Characteristics of fractures in children
3rd EPOS-EFORT BAT INSTRUCTIONAL COURSE TRILOGY Workshops / Case discussions Part II; Paediatric trauma 11-13 March 2015 Orthopaedic Hospital Speising, Vienna, Austria Characteristics of fractures in children
Fractures and dislocations around elbow in adult
 Lec: 3 Fractures and dislocations around elbow in adult These include fractures of distal humerus, fracture of the capitulum, fracture of the radial head, fracture of the olecranon & dislocation of the
Lec: 3 Fractures and dislocations around elbow in adult These include fractures of distal humerus, fracture of the capitulum, fracture of the radial head, fracture of the olecranon & dislocation of the
Flower Medium Headless & Cannulated Screws
 Flower Medium Headless & Cannulated Screws PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
Flower Medium Headless & Cannulated Screws PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
WHAT YOU IS BACK WITHIN ARM S REACH
 YOUR TOTAL SHOULDER REPLACEMENT SURGERY STEPS TO RETURNING TO A LIFESTYLE YOU DESERVE WHAT YOU IS BACK WITHIN ARM S REACH Nathan Richardson, MD Orthopedics, Shoulder & Elbow Surgeon Board Certified in
YOUR TOTAL SHOULDER REPLACEMENT SURGERY STEPS TO RETURNING TO A LIFESTYLE YOU DESERVE WHAT YOU IS BACK WITHIN ARM S REACH Nathan Richardson, MD Orthopedics, Shoulder & Elbow Surgeon Board Certified in
2018 OAOS Annual Orthopaedic Conference Objectives
 2018 OAOS Annual Orthopaedic Conference Objectives PANEL: The Opioid Crisis in America: Orthopaedic Responsibility & Response 300 Seconds to Save a Life: The Opioid Epidemic at Your Doorstep The pervasive
2018 OAOS Annual Orthopaedic Conference Objectives PANEL: The Opioid Crisis in America: Orthopaedic Responsibility & Response 300 Seconds to Save a Life: The Opioid Epidemic at Your Doorstep The pervasive
Radiographic Positioning Summary (Basic Projections RAD 222)
 Lower Extremity Radiographic Positioning Summary (Basic Projections RAD 222) AP Pelvis AP Hip (Unilateral) (L or R) AP Femur Mid and distal AP Knee Lateral Knee Pt lies supine on table Align MSP to Center
Lower Extremity Radiographic Positioning Summary (Basic Projections RAD 222) AP Pelvis AP Hip (Unilateral) (L or R) AP Femur Mid and distal AP Knee Lateral Knee Pt lies supine on table Align MSP to Center
St Mary Orthopaedic Conference. Steven A. Caruso, MD Trenton Orthopaedic Group Trauma and Complex Fracture Surgeon October 25, 2014
 St Mary Orthopaedic Conference Steven A. Caruso, MD Trenton Orthopaedic Group Trauma and Complex Fracture Surgeon October 25, 2014 Nothing to disclose Goals To discuss common orthopaedic pathologies and
St Mary Orthopaedic Conference Steven A. Caruso, MD Trenton Orthopaedic Group Trauma and Complex Fracture Surgeon October 25, 2014 Nothing to disclose Goals To discuss common orthopaedic pathologies and
Course Template for AOTrauma Course Advanced Principles of Fracture Management
 Course Template for AOTrauma Course Advanced Principles of Fracture Management This template is prepared for a 3-day course. It includes all core (C) content and some optional (O) content for the AOTrauma
Course Template for AOTrauma Course Advanced Principles of Fracture Management This template is prepared for a 3-day course. It includes all core (C) content and some optional (O) content for the AOTrauma
The Flower Proximal Humerus Plate
 The Flower Proximal Humerus Plate PROCEDURE GUIDE www.flowerortho.com The Flower Upper Extremity Application PROXIMAL HUMERUS PLATE SMALL BONE PLATES FOUR CORNER FUSION PLATE ANATOMIC DISTAL RADIUS PLATE
The Flower Proximal Humerus Plate PROCEDURE GUIDE www.flowerortho.com The Flower Upper Extremity Application PROXIMAL HUMERUS PLATE SMALL BONE PLATES FOUR CORNER FUSION PLATE ANATOMIC DISTAL RADIUS PLATE
Part I : Study of Osteoporotic Fractures (SOF) Fractures and Falls History: History of Fractures Questionnaire
 PhenX Measure: Fracture History (#170900) PhenX Protocol: Fracture History (#170901) Date of Interview/Examination (MM/DD/YYYY): Part I : Study of Osteoporotic Fractures (SOF) Fractures and Falls History:
PhenX Measure: Fracture History (#170900) PhenX Protocol: Fracture History (#170901) Date of Interview/Examination (MM/DD/YYYY): Part I : Study of Osteoporotic Fractures (SOF) Fractures and Falls History:
ORTHOPAEDICS & M MEDICAL DEVICES GENERAL CATALOGUE
 ORTHOPAEDICS OR RTH & M MEDICAL DEVICES GENERAL CATALOGUE 2 GENERAL CATALOGUE INDEX TRAUMA PRODUCT CATALOGUE NEW GENERATION TRAUMA PRODUCTS 4-14 PLATES INTRAMEDULLARY NAILS EXTERNAL FIXATORS 15-76 77-95
ORTHOPAEDICS OR RTH & M MEDICAL DEVICES GENERAL CATALOGUE 2 GENERAL CATALOGUE INDEX TRAUMA PRODUCT CATALOGUE NEW GENERATION TRAUMA PRODUCTS 4-14 PLATES INTRAMEDULLARY NAILS EXTERNAL FIXATORS 15-76 77-95
Development and validation of the new AO Pediatric Comprehensive Classification of Long-Bone Fractures (PCCF)
 41 Theddy Slongo and Laurent Audigé Development and validation of the new AO Pediatric Comprehensive Classification of Long-Bone Fractures (PCCF) Introduction Over the last six years, the AO Classification
41 Theddy Slongo and Laurent Audigé Development and validation of the new AO Pediatric Comprehensive Classification of Long-Bone Fractures (PCCF) Introduction Over the last six years, the AO Classification
Flower Opening Wedge Plate
 Flower Opening Wedge Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION T-PLATE, OBLIQUE
Flower Opening Wedge Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION T-PLATE, OBLIQUE
Design Team Vipul Nanavati, MD James M. Paci, MD Frederick W. Werner, MME Levi G. Sutton, MS
 Design Team Vipul Nanavati, MD James M. Paci, MD Frederick W. Werner, MME Levi G. Sutton, MS SUNY Upstate Medical University Scott Macfarlane Office of Technology Transfer 315-464-7613 Anatomically shaped
Design Team Vipul Nanavati, MD James M. Paci, MD Frederick W. Werner, MME Levi G. Sutton, MS SUNY Upstate Medical University Scott Macfarlane Office of Technology Transfer 315-464-7613 Anatomically shaped
Intramedullary Nailing: History & Rationale
 Intramedullary Nailing: History & Rationale Overview 1. What is IM Nailing? 2. History 3. Design Rationale & Evolution 4. Modern IM Nails 5. The Future What is IM Nailing? Method of internal fixation in
Intramedullary Nailing: History & Rationale Overview 1. What is IM Nailing? 2. History 3. Design Rationale & Evolution 4. Modern IM Nails 5. The Future What is IM Nailing? Method of internal fixation in
Orthopaedic Surgery Clinical Privileges
 Name: Effective from / / to / / Initial privileges (initial appointment) Renewal of privileges (reappointment) All new applicants should meet the following requirements as approved by the governing body,
Name: Effective from / / to / / Initial privileges (initial appointment) Renewal of privileges (reappointment) All new applicants should meet the following requirements as approved by the governing body,
PEDIATRIC MODELS A Division of Pacific Research Laboratories, Inc.
 PEDIATRIC MODELS A Division of Pacific Research Laboratories, Inc. www.sawbones.com CMF / SPINE #1337-7 #1337-8 CMF #1337-7 Mandible with hemifacial microsomia. Solid foam. #1337-8 Mandible with nalgers
PEDIATRIC MODELS A Division of Pacific Research Laboratories, Inc. www.sawbones.com CMF / SPINE #1337-7 #1337-8 CMF #1337-7 Mandible with hemifacial microsomia. Solid foam. #1337-8 Mandible with nalgers
A Patient s Guide to Adult Forearm Fractures
 A Patient s Guide to Adult Forearm Fractures Orthopedic and Sports Medicine 825 South 8th Street, #550 Minneapolis, MN 55404 Phone: 612-333-5000 Fax: 612-333-6922 1 DISCLAIMER: The information in this
A Patient s Guide to Adult Forearm Fractures Orthopedic and Sports Medicine 825 South 8th Street, #550 Minneapolis, MN 55404 Phone: 612-333-5000 Fax: 612-333-6922 1 DISCLAIMER: The information in this
Coopera ve and Innova ve MANUAL OF ORTHOPEDICS PROFESSIONAL RELIABLE
 Coopera ve and Innova ve 2019 MANUAL OF ORTHOPEDICS PROFESSIONAL RELIABLE Introduction ZENER MEDTEC (CHANGZHOU) CO., LTD is set up and led by SHANGHAI GUANKE DATA TECHNOLOGY CO., LTD, who is expert in
Coopera ve and Innova ve 2019 MANUAL OF ORTHOPEDICS PROFESSIONAL RELIABLE Introduction ZENER MEDTEC (CHANGZHOU) CO., LTD is set up and led by SHANGHAI GUANKE DATA TECHNOLOGY CO., LTD, who is expert in
Introduction to the Taylor Spatial Frame Hardware. Trademark of Smith & Nephew. Certain marks Reg. US Pat. & TM Off.
 Introduction to the Taylor Spatial Frame Hardware Trademark of Smith & Nephew. Certain marks Reg. US Pat. & TM Off. What is the Taylor Spatial Frame? Next generation circular fixator capable of 6 axes
Introduction to the Taylor Spatial Frame Hardware Trademark of Smith & Nephew. Certain marks Reg. US Pat. & TM Off. What is the Taylor Spatial Frame? Next generation circular fixator capable of 6 axes
NICE guideline Published: 17 February 2016 nice.org.uk/guidance/ng38
 Fractures (non-complex): assessment and management NICE guideline Published: 17 February 2016 nice.org.uk/guidance/ng38 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Fractures (non-complex): assessment and management NICE guideline Published: 17 February 2016 nice.org.uk/guidance/ng38 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
CHAPTER 8 LECTURE OUTLINE
 CHAPTER 8 LECTURE OUTLINE I. INTRODUCTION A. The appendicular skeleton includes the bones of the upper and lower extremities and the shoulder and hip girdles. B. The appendicular skeleton functions primarily
CHAPTER 8 LECTURE OUTLINE I. INTRODUCTION A. The appendicular skeleton includes the bones of the upper and lower extremities and the shoulder and hip girdles. B. The appendicular skeleton functions primarily
Low revision rate after total hip arthroplasty in patients with pediatric hip diseases
 6 Acta Orthopaedica 2012; 83 (5): x x 1 Low revision rate after total hip arthroplasty in patients with pediatric hip diseases Evaluation of 14,403 THAs due to DDH, SCFE, or Perthes disease and 288,435
6 Acta Orthopaedica 2012; 83 (5): x x 1 Low revision rate after total hip arthroplasty in patients with pediatric hip diseases Evaluation of 14,403 THAs due to DDH, SCFE, or Perthes disease and 288,435
4/28/2010. Fractures. Normal Bone and Normal Ossification Bone Terms. Epiphysis Epiphyseal Plate (physis) Metaphysis
 Fractures Normal Bone and Normal Ossification Bone Terms Epiphysis Epiphyseal Plate (physis) Metaphysis Diaphysis 1 Fracture Classifications A. Longitudinal B. Transverse C. Oblique D. Spiral E. Incomplete
Fractures Normal Bone and Normal Ossification Bone Terms Epiphysis Epiphyseal Plate (physis) Metaphysis Diaphysis 1 Fracture Classifications A. Longitudinal B. Transverse C. Oblique D. Spiral E. Incomplete
AAOS Board Maintenance. Preparation and Review: General Orthopaedic. of Certification. OLC Education & Conference Center. January 25 26, 2019
 AAOS Board Maintenance of Certification Preparation and Review: General Orthopaedic January 25 26, 2019 OLC Education & Conference Center Rosemont, IL Albert J. Aboulafia, MD Isador H. Lieberman, MD, MBA,
AAOS Board Maintenance of Certification Preparation and Review: General Orthopaedic January 25 26, 2019 OLC Education & Conference Center Rosemont, IL Albert J. Aboulafia, MD Isador H. Lieberman, MD, MBA,
Upper Limb Imaging Requirements
 Imaging Requirements Upper Limb Imaging Requirements Instructions for Measurement Radiography and CT Scans Please read before commencing radiography Stanmore Implants 210 Centennial Avenue Centennial Park
Imaging Requirements Upper Limb Imaging Requirements Instructions for Measurement Radiography and CT Scans Please read before commencing radiography Stanmore Implants 210 Centennial Avenue Centennial Park
Pediatric Injuries/Fractures. Rena Heathcote
 Pediatric Injuries/Fractures Rena Heathcote INTRODUCTION Incidence Anatomy of the Growing Bone Injury Patterns What can we X-ray PEDIATRIC FRACTURES INCIDENCE What makes children susceptible to fractures?
Pediatric Injuries/Fractures Rena Heathcote INTRODUCTION Incidence Anatomy of the Growing Bone Injury Patterns What can we X-ray PEDIATRIC FRACTURES INCIDENCE What makes children susceptible to fractures?
EVOS MINI with IM Nailing
 Case Series Dr. John A. Scolaro EVOS MINI with IM Nailing A series of studies Introduction Intramedullary nailing has become the standard for many long bone fractures. Fracture reduction prior to nail
Case Series Dr. John A. Scolaro EVOS MINI with IM Nailing A series of studies Introduction Intramedullary nailing has become the standard for many long bone fractures. Fracture reduction prior to nail
UPDATE ON COMMUNITY TRAUMA. Ericka R. Glass Orthopaedic Traumatologist Spectrum Orthopaedics
 UPDATE ON COMMUNITY TRAUMA Ericka R. Glass Orthopaedic Traumatologist Spectrum Orthopaedics OBJECTIVES Understand common fractures that present to community trauma centers Outline basic treatment principles
UPDATE ON COMMUNITY TRAUMA Ericka R. Glass Orthopaedic Traumatologist Spectrum Orthopaedics OBJECTIVES Understand common fractures that present to community trauma centers Outline basic treatment principles
5.1 BONES: AN OVERVIEW
 Unit 5 Skeletal System 5.1 BONES: AN OVERVIEW Section Objectives Identify the major structures and functions of the skeletal system. Differentiate between the two divisions (axial and appendicular) of
Unit 5 Skeletal System 5.1 BONES: AN OVERVIEW Section Objectives Identify the major structures and functions of the skeletal system. Differentiate between the two divisions (axial and appendicular) of
Hands PA; Obl. Lat.; Norgaard s Thumb AP; Lat. PA. PA; Lat.: Obls.; Elongated PA with ulnar deviation
 Projections Region Basic projections Additional / Modified projections Upper Limbs Hands PA; Obl. Lat.; Norgaard s Thumb ; Lat. PA Fingers PA; Lat. Wrist PA; Lat. Obls. Scaphoid Lunate Trapezium Triquetral
Projections Region Basic projections Additional / Modified projections Upper Limbs Hands PA; Obl. Lat.; Norgaard s Thumb ; Lat. PA Fingers PA; Lat. Wrist PA; Lat. Obls. Scaphoid Lunate Trapezium Triquetral
Young Bones. Characteristics. Klaus Hindsø
 Young Bones Characteristics Klaus Hindsø What s so special Periostium Elasticity Growth The envelope Periostium Elasticity Growth Connects displaced fragments building a bridge during healing Interposed
Young Bones Characteristics Klaus Hindsø What s so special Periostium Elasticity Growth The envelope Periostium Elasticity Growth Connects displaced fragments building a bridge during healing Interposed
Upper limb fractures. Mithun Nambiar Orthopaedic Resident Royal Melbourne Hospital
 Upper limb fractures Mithun Nambiar Orthopaedic Resident Royal Melbourne Hospital http://janeaustensworld.files.wordpress.com/2010/10/17_skeleton.jpg Principles of fracture management Restoration of anatomy
Upper limb fractures Mithun Nambiar Orthopaedic Resident Royal Melbourne Hospital http://janeaustensworld.files.wordpress.com/2010/10/17_skeleton.jpg Principles of fracture management Restoration of anatomy
Fractures of the shoulder girdle, elbow and fractures of the humerus. H. Sithebe 2012
 Fractures of the shoulder girdle, elbow and fractures of the humerus H. Sithebe 2012 Fractures of the Clavicle (mid-shaft). Fractures of the clavicle Fractures of the clavicle Treatment- conservative.
Fractures of the shoulder girdle, elbow and fractures of the humerus H. Sithebe 2012 Fractures of the Clavicle (mid-shaft). Fractures of the clavicle Fractures of the clavicle Treatment- conservative.
Zimmer Patient Specific Instruments (PSI) for Reverse Shoulder Arthroplasty
 Zimmer Patient Specific Instruments (PSI) for Reverse Shoulder Arthroplasty Ryan Krupp, M.D. Norton Orthopaedic Specialists Louisville, KY Anand Murthi, M.D. MedStar Union Memorial Hospital Baltimore,
Zimmer Patient Specific Instruments (PSI) for Reverse Shoulder Arthroplasty Ryan Krupp, M.D. Norton Orthopaedic Specialists Louisville, KY Anand Murthi, M.D. MedStar Union Memorial Hospital Baltimore,
SpeedTip CCS 2.2, 3.0
 PRODUCT INFORMATION SpeedTip CCS 2.2, 3.0 Cannulated Compression Screws APTUS 2 SpeedTip CCS 2.2, 3.0 Cannulated Compression Screws SpeedTip CCS * 2.2, 3.0 Cannulated Compression Screws A new generation
PRODUCT INFORMATION SpeedTip CCS 2.2, 3.0 Cannulated Compression Screws APTUS 2 SpeedTip CCS 2.2, 3.0 Cannulated Compression Screws SpeedTip CCS * 2.2, 3.0 Cannulated Compression Screws A new generation
Important Parts of Bones
 Important Parts of Bones For 2015 Know: Humerus (posterior) Clavical Femur (Anterior) Foot Hand Mandible Os Coxa Scapula Skull (Anterior, Inferior, Lateral) Sternum Humerus (posterior) A. olecranon fossa
Important Parts of Bones For 2015 Know: Humerus (posterior) Clavical Femur (Anterior) Foot Hand Mandible Os Coxa Scapula Skull (Anterior, Inferior, Lateral) Sternum Humerus (posterior) A. olecranon fossa
Orthopedics - Dr. Ahmad - Lecture 2 - Injuries of the Upper Limb
 The shoulder and the upper arm Fractures of the clavicle 1. Fall on the shoulder. 2. Fall on outstretched hand. In mid shaft fractures, the outer fragment is pulled down by the weight of the arm and the
The shoulder and the upper arm Fractures of the clavicle 1. Fall on the shoulder. 2. Fall on outstretched hand. In mid shaft fractures, the outer fragment is pulled down by the weight of the arm and the
TRAUMATOLOGY. Trochanter
 TRAUMATOLOGY Trochanter 1 References Prof. Dr. András Sárváry Head of Department Fővárosi Önkormányzat Péterfy Sándor úti Kórház Rendelőintézet és Baleseti Központ Budapest The following surgical description
TRAUMATOLOGY Trochanter 1 References Prof. Dr. András Sárváry Head of Department Fővárosi Önkormányzat Péterfy Sándor úti Kórház Rendelőintézet és Baleseti Központ Budapest The following surgical description
Immediate post surgical findings of soft tissue swelling, subcutaneous emphysema, and skin staples for reverse total shoulder arthroplasty.
 Immediate post surgical findings of soft tissue swelling, subcutaneous emphysema, and skin staples for reverse total shoulder arthroplasty. REVERSE TOTAL SHOULDER ARTHROPLASTY WITH FRACTURED ACROMION Above:
Immediate post surgical findings of soft tissue swelling, subcutaneous emphysema, and skin staples for reverse total shoulder arthroplasty. REVERSE TOTAL SHOULDER ARTHROPLASTY WITH FRACTURED ACROMION Above:
Traumatic injuries of knee and hip
 Traumatic injuries of knee and hip Martin W. Korn, MD The United States secretary of transportation recently announced that highway deaths had risen from the previously announced 56,000 for 1969 to a new
Traumatic injuries of knee and hip Martin W. Korn, MD The United States secretary of transportation recently announced that highway deaths had risen from the previously announced 56,000 for 1969 to a new
Foot and Ankle Systems Coding Reference Guide
 Foot and Ankle Systems Coding Reference Guide Physician Arthrodesis 27870 Arthrodesis, ankle, open 27871 Arthrodesis, tibiofibular joint, proximal or distal 28705 Arthrodesis; pantalar 28715 Arthrodesis;
Foot and Ankle Systems Coding Reference Guide Physician Arthrodesis 27870 Arthrodesis, ankle, open 27871 Arthrodesis, tibiofibular joint, proximal or distal 28705 Arthrodesis; pantalar 28715 Arthrodesis;
Pectoral (Shoulder) Girdle
 Chapter 8 Skeletal System: Appendicular Skeleton Pectoral girdle Pelvic girdle Upper limbs Lower limbs 8-1 Pectoral (Shoulder) Girdle Consists of scapula and clavicle Clavicle articulates with sternum
Chapter 8 Skeletal System: Appendicular Skeleton Pectoral girdle Pelvic girdle Upper limbs Lower limbs 8-1 Pectoral (Shoulder) Girdle Consists of scapula and clavicle Clavicle articulates with sternum
