Risk factors for the need of hip arthroscopy following periacetabular osteotomy
|
|
|
- Brook Eaton
- 5 years ago
- Views:
Transcription
1 Journal of Hip Preservation Surgery Vol. 2, No. 4, pp doi: /jhps/hnv053 Advance Access Publication 27 August 2015 Research Article Risk factors for the need of hip arthroscopy following periacetabular osteotomy Charlotte Hartig-Andreasen 1 *, Anders Troelsen 2, Theis M. Thillemann 3, John Gelineck 4 and Kjeld Søballe 3 1. Orthopaedic Research Unit, Aarhus University Hospital, Tage-Hansens Gade 2, Building 10A, DK-8000 Aarhus C, Denmark, 2. Department of Orthopaedics, Clinical and Orthopeadic Research Hvidovre, Copenhagen University Hospital, Kettegård Allé 30, DK-2650 Hvidovre, Denmark, 3. Department of Orthopaedics, Aarhus University Hospital, Tage-Hansens Gade 2, DK-8000 Aarhus C, Denmark and 4. Department of Radiology, Aarhus University Hospital, Nørrebrogade 44, DK-8000 Aarhus C, Denmark *Correspondence to: C. Hartig-Andreasen. hartig@dadlnet.dk Submitted 2 September 2014; Revised 18 December 2014; revised version accepted 29 June 2015 ABSTRACT Despite the frequency of labral tears in symptomatic developmental dysplasia of the hip, no consensus exists regarding the treatment of coexisting dysplasia of the hip and tearing of the acetabular labrum. The purpose of this prospective, MR arthrography (MRA) based 2-year follow-up study was to identify risk factors predicting the need for a hip arthroscopy (HA) after periacetabular osteotomy (PAO). Ninety-nine patients (104 hips) scheduled for PAO were evaluated preoperatively and at 2-year follow-up. MRA was performed in all patients prior to PAO. At follow-up, patients were divided into a non-arthroscopy and arthroscopy group. The two groups were compared clinical and radiological, and risk factors for HA after PAO were calculated. Patient reported outcome measures (WOMAC, Oxford Hip and SF36) were filled out before PAO and at follow-up. Ninety-five hips (91.3%) were evaluated. Twenty-six hips (27%) required an arthroscopy within 2 years of the PAO. Risk factors were preoperative borderline dysplasia, acetabular retroversion and complete labral detachment. Labral tearing, or hypertrophy did not negatively affect the outcome of PAO. Patients not requiring an arthroscopy had a statistically significant better outcome measured by patients reported outcome measures. After PAO, 27% of the hips needed intra-articular assessment. Conventional radiographs and MRA analysis can be used to identify predictors for patients requiring HA after PAO. At 2-year follow-up, the clinical outcome improved in all patients. However, those patients who had no need of a HA after their PAO had superior results. INTRODUCTION The Bernese periacetabular osteotomy (PAO) has become the preferred joint preserving treatment for symptomatic developmental dysplasia of the hip (DDH) [1]. Dorrell and Caterall [2] were among the first to report on the relationship between dysplastic osseous abnormalities and labrum pathology. Since then literature describing how the osseous abnormalities and the resulting pathological joint biomechanics in developmental DDH may frequently lead to damage of the acetabular labrum has been evolving [3 6]. Recently, Ross et al. found only 5 normal labrums in 73 dysplastic hips [7]. Despite the frequency of labral tears in symptomatic DDH and the increasing literature concerning labral pathology, no consensus exists regarding the treatment strategy for DDH with coexisting acetabular labral tear. Tearing of the labrum is recognized being involved in joint and this may untreated lead to osteoarthritis. This has lead to new concepts and treatment strategies regarding the treatment of labral tearing in DHH. Open arthrotomy during PAO was the first means of addressing intraarticular pathology during PAO surgery [8]. Later hip arthroscopy assisted PAO was introduced to assess and address any present intraarticular pathology [9]. There is no evidence that intraarticular assessment, open or arthroscopic, is superior to not assessing the joint during PAO. However, hip arthroscopy alone without addressing the bony VC The Author Published by Oxford University Press. This is an Open Access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted reuse, distribution, and reproduction in any medium, provided the original work is properly cited. 374
2 Risk factors for the need of hip arthroscopy 375 abnormalities in DDH is in general not recommended, and studies have showed failure in DDH hips undergoing hip arthroscopy with debridement of the labrum [10], and resulted in high reoperation rates comparing mild DDH hips with normal hips [11]. Studies reporting the outcome of PAO performed without simultaneous assessment of the joint have shown high hip joint survival rates [12, 13]. However, femoroacetabular impingement after PAO has been observed with poor outcome, and some patients will require a subsequent hip arthroscopy, and it would be valuable to identify predictors for hip arthroscopy as well as assessment of the results after hip arthroscopy in PAO patients. The purpose of this prospective, MR arthrography (MRA) based 2-year follow-up study was to identify risk factors predicting the frequency of the need for a hip arthroscopy after PAO, and finally to compare clinical and radiographic outcomes between patients require a subsequent arthroscopy and patients not requiring arthroscopy after PAO. MATERIAL AND METHODS Ninety-nine patients (104 hips) consecutively scheduled for PAO due to DDH were enrolled in the study. Patients were included from January 2010 to August 2011 and all surgeries were performed or assisted by the senior author in Aarhus, Denmark. Five patients were excluded from the study, because of multiple complaints from several joints and thus, were not considered being representative for this PAO cohort. Four patients failed to show up at 2-year follow-up. Hence, the study group consisted of 90 patients (95 hips, 79 females, 52 right hips). Mean age of the patients at the time of PAO surgery was 34.1 years (range years). Before PAO eight hips had a hip arthroscopy (Table I) and one patient had had a combined femoral and pelvic osteotomy. Twenty-three patients underwent PAO surgery on the opposite hip within the 2-year study period, and three patients had screws removed following PAO. One complication among the 95 was observed: an obturator nerve affection resulting in pain and paralysis of the adductor muscles. Another hip developed osteoarthritis. Beside that no intra- or postoperative complications was observed. Bilateral dysplasia was seen in 78% of the patients. Indication for PAO were persisting hip pain, a center edge angle of Wiberg [14] <25 o, pelvic bone maturity, internal rotation >15 o, hip flexion <110 o and Tönnis grade of osteoarthritis 0 or 1. The minimally invasive transsartorial approach was used in all cases [15]. Preoperatively and at 2-year follow-up, the clinical and radiographic outcome were evaluated. Follow-up was done primarily by one investigator (CHA), except for four patients seen by the senior author (KSO). For data analysis, the patients were divided into an arthroscopy group if a hip arthroscopy was required within the 2-year follow-up period and a non-arthroscopy group. Clinical evaluation At 2-year follow-up, patients were interviewed regarding continued mechanical symptoms (clicking, locking and instability) from the hip joint, dysesthesia of the dermatome Table I. Description of the eight hips undergoing hip arthroscopy (HA) prior to the PAO Hip Time from HA to PAO HA findings HA procedures HA after PAO 12 a NA NA NA, but no effect of surgery No 13 1 year Torn labrum Labrum resection, short term effect No 15 a NA NA NA, but no effect of surgery No 38 a NA Labrum tear Reinsertion of labrum No 45 3 years Intact labrum, cartilage pieces Removal of several cartilage pieces No 46 6 years Thin cartilage, loose pieces of cartilage, labrum tear Resection of the damaged parts years Labrum a little frayed Resection of the frayed part of the labrum Yes 59 4 years Labrum-cartilage separation, hypertrophic labrum, pincer, CAM a Information from patient, journal records not available. HA findings, Findings during hip arthroscopy; HA procedures, Procedures performed during hip arthroscopy. Yes Yes
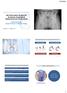
3 376 C. Hartig-Andreasen et al. innervated by the lateral femoral cutaneous nerve, any kind of surgical and non-surgical treatment since the PAO. Signs of trochanteric bursitis, internal and external snapping hip were noted. Any leg length discrepancy and range of motion was measured. Impingement test and FABER test [16] were performed; however, in three hips, the tests were left out due to recent hip arthroscopy, and in two hips due to severe hip pain. Preoperatively and at 2-year follow-up, patients were requested to fill out the Western Ontario and McMaster Universities Osteoarthritis index (WOMAC) [17], the Oxford hip score (OHS)[18] and the general health questionnaire short form 36, version 1 [19]. Each subscale of the WOMAC score was calculated. To enhance the comparability with other studies, the summarized WOMAC total score were normalized with 100 indicating the best possible score. The OHS score was given as a total score with 48 indicating the best possible score. From the SF36 data, the physical and mental component scores were subsequently calculated. Five patients failed to fill out the questionnaires preoperatively, hence only 90 hips were evaluated by questionnaires. Radiographic evaluation Conventional standing pelvic radiographs recorded preoperatively and at 2-year follow-up were analyzed. One investigator (CHA) assessed the following radiographic parameters: the center edge (CE) angle of Wiberg [14], the acetabular index (AI) angle [20], the presence of an os acetabuli [21], the Tönnis grade of osteoarthritis [20] and signs of retroversion (cross over sign) [21]. Hips were characterized dysplastic if the CE angle was between <25 o. AI angles were considered normal if within 0 o 10 o. For the hip arthroscopy group, CE angles and AI angles after PAO were analyzed at the postoperative supine radiographs, since the arthroscopy may have changed the angles. Using supine exposures were justified by an earlier study showing no significant changes in these two angles when repositioning from the supine to the weight-bearing position [22]. The acetabulum was considered retroverted if the crossover sign [21, 23, 24] was present prior to PAO. All patients had a magnetic resonance arthrography (MRA) performed. The MRA were performed with a 1.5 Tesla Scanner (Siemens Magnetom Symphony) preceded by guided injection of 10 ml of diluted gadolinium contrast medium (Gd-DTPA, 2 mmol l 1 ) into the hip joint. The MRA was assessed for labral pathology in terms of, hypertrophic changes, tears and paralabral cysts. Labral lesions were graded according to the Czerny grading [25]. Czerny stages the labrum into groups according to shape, homogeneity and attachment to the acetabular rim. Cystic changes in the femoral head or in the Fig. 1. MRA measurement of the a-angle of Notzli on the oblique plane. After identification of the center of the femoral head, a line along the middle of the femoral neck and a line from the center to the point where the femoral head-neck junction left the best fitted circle of the femoral head make up the a-angle. acetabulum were noted. The a-angle was measured on oblique axial MRA images (Fig. 1) [26]. An a-angle 55 o was considered pathological. One senior radiologist (J.G.) performed all intraarticular injections and analysis of MRA scans. Measurement of the a-angles was also performed by the C.H.A. In five hips, the a-angle could not be assessed due to imprecise oblique MRA images. Intra- and interobserver variability of the a-angle measurement was assessed by the C.H.A and the senior radiologist by doing rereadings of the MRA scan separated by 4 weeks. The mean of difference for intraobserver variability was 0.48 o (SD o ). The 95% limits of agreement (LOA) were 3.31 o to 4.27 o, and for the interobserver variability the mean difference was 1.52 o (SD o ), 95% LOA was 4.76 o to 7.80 o. Indication for hip arthroscopy All patients with continuous symptoms in this study were primarily referred to the Sports Traumatology unit at Aarhus University Hospital, Denmark and evaluated by two experts in hip arthroscopy. Relevant patient history, continuous groin pain after PAO, a positive impingement or Faber test were indications for hip arthroscopy. Labral pathology diagnosed on MRA supported the diagnosis and indication. All patients referred in this study underwent hip arthroscopy.
4 Risk factors for the need of hip arthroscopy 377 Statistical analysis Depending on distribution data was presented as means with 95% confidence intervals, or as medians with interquartile ranges. Odds ratios for hip arthroscopy were calculated using logistic regression. Non-parametric variables were evaluated with Wilcoxson sign rank test or Fisher s exact test. Intra- and interobserver variability was assessed using the Bland Altman approach [27 29], and data was presented as means of the difference with SD and 95% LOA. RESULTS Twenty-six of 95 hips (27%) had a hip arthroscopy within 2 years after PAO. One of these hips was converted to total hip arthroplasty two months after hip arthroscopy (7 months after PAO) (Table II). No significant differences in sex were found between the non-arthroscopy and arthroscopy group Significant adjusted predictors of need for hip arthroscopy after PAO were (i) mild dysplasia (OR 2.92); (ii) presence of the cross-over sign on preoperative radiographs (OR 3.30) and (iii) labrum detachment (Table III). The MRA analysis of the acetabular labrum revealed only six labrum (five in the non-arthroscopy group) without any signs of, hypertrophy or pathology according to the Czerny grading. No significant differences in labral pathology were found between the non-arthroscopy and arthroscopy group (Table IV). For the arthroscopy group, the median preoperative CE angle for was 20 o (range 11 o 24 o ) and the AI angle was 14 o (range 8 o 21 o ). The postoperative CE angle and the AI angle was 34 o (range 17 o 46 o ) and 3 o (range 8 o to 16 o ), respectively (Table V). At follow-up, the median CE angle and AI angle was 34 o (range 25 o 40 o ) and 1 o (range 8 o to 16 o ), respectively. For the hip arthroscopy group, both the CE angle and AI angle changed significantly after arthroscopy (Table VI). The median a-angle for the arthroscopy group was 50 o (range 37 o 72. o ), with no significant difference between the nonarthroscopy and arthroscopy groups. About 18 of 95 hips were retroverted preoperatively, and four hips at 2-year follow-up, all in the non-arthroscopy group. Clinical testing after PAO for signs of impingement, trochanteric bursitis or persisting dysplasia revealed no significant difference between groups (Table VII). For both groups, the median normalized WOMAC total score increased from 66 (range 3 100) preoperatively to 89 (range ) postoperatively and the median OHS increased from 28 (range 8 47) to 43 (range 12 48). The overall SF36 physical and mental component scores increased from 38 (range 16 55) to 48 (range 18 60) and from 54 (range 29 69) to 58 (range 27 78), respectively, (Table VIII). Improvements between the preoperative and 2-year follow-up assessment were observed in 7 of 8 subscales of the SF36 (Fig. 2). The total WOMAC score, the OHS and the physical component score of the SF36 differed statistically significant with superior results in the non-arthroscopy group compared to the arthroscopy group (P ) (Table VIII). The preoperative scores for all patient reported outcome measures did not show any statistically significant differences between the arthroscopy and non-arthroscopy groups (P ). DISCUSSION This study identifies radiographic predictors for the need of a hip arthroscopy 2 years after PAO. At 2-year followup, a statistical difference in patient reported outcome measures between the non-arthroscopy and arthroscopy group were found. In mild dysplasia, only little reorientation is possible before overcorrection may occur, which could be the reason for the finding of a CE angle of 20 o 25 o being a significant predictor for subsequent arthroscopy. However, in this study a negative AI angle is not a significant factor similar to earlier findings reported by Steppacher [30]. Though, femoroacetabular impingement after PAO for hip dysplasia is well known [8].This could advocate for a thorough intraoperative assessment of femoroacetabular impingement. By restricting simultaneously intraarticular surgery only to patients with mild dysplasia the majority of the patients will avoid over-treatment and thereby the risk of unnecessary complications. However, a recent study of 26 patients with mild dysplasia undergoing arthroscopic treatment alone, demonstrates at 2-year follow-up significant improvement in patient reported outcome measures and VAS score [31]. In the present study, the non-arthroscopy group and the arthroscopy group showed improved WOMAC, OXFORD and the SF36 scores at 2-year follow-up. For all scores, the results for the non-arthroscopy group are superior to that in the arthroscopy group. However, when dichotomizing the WOMAC pain score into a no or low pain score group (WOMAC pain score <10) or a high pain score group (WOMAC pain score of 10 or more), 90% of patients (21 in the arthroscopy group and 60 patients in the non-arthroscopy group) had no or low pain. No statistical difference was found between groups. Finally, the intention to treat analysis of this study evaluated outcome at 2 years after PAO. The statistical difference found in patient reported outcome measures may be a result of the arthroscopy group only having mean 11.5 months (range months) of follow-up between hip
5 378 C. Hartig-Andreasen et al. Table II. Description of the 26 hips undergoing hip arthroscopy (HA) after PAO Hip Time from PAO to HA MRA labrum diagnosis MRA a-angle HA findings 9 9 months Czerny 3A 46 o Labrum damage anteriorly, mildly hypertrophic, pincer, CAM a 10 b 21 months Czerny 3A, months Czerny 1A, 55 o Frayed labrum, pincer, minor CAM 51 o Labrum-cartilage separation, pincer, CAM, loose cartilage 26 6 months Czerny 2B 53 o Labrum-cartilage separation, pincer, minor CAM months Czerny 3A, 33 b 15 months Czerny 3A, 40 7 months Czerny 3B, 46 4 months No tears, mild hypertrophy 44 o Labrum-cartilage separation, pincer, minor CAM, area with osteoarthritis 58 o Labrum lesion with minor impact on the cartilage, pincer, bump on collum 44 o Labrum-cartilage separation, frayed labrum, pincer, CAM 43 o Labrum-cartilage separation, synovitis, pincer, CAM months Czerny 3A 44 o Minor labrum-cartilage resection, minor pincer, CAM months Czerny 3A, 52 8 months Czerny 3A, 54 b 7 months Czerny 3A, 48 o Labrum-cartilage separation, pincer, CAM 69 o Labrum-cartilage separation, pincer, CAM 58 o Voluminous labrum, labrumcartilage separation, minor CAM months Czerny 3A 49 o Lesion of the cartilage at acetabulum and femur. Labrum attached months No tears, crushed and 49 o Osteoarthritis acetabulum and caput femoris, labrum attached to the rim months Czerny 2A 48 o Labrum-cartilage separation, minor pincer, minor CAM months Czerny 3A, 42 o Labrum-cartilage separation, pincer, minor CAM HA procedures minor, mircrofracture treatment minor Rimtrim, minor minor Minor rimtrim, Labrum reinsertion, minor Minor rimtrim,, synovectomy Synovectomy minor (continued)
6 Risk factors for the need of hip arthroscopy 379 Table II. (continued) Hip Time from PAO to HA MRA labrum diagnosis MRA a-angle HA findings HA procedures months Czerny 3A 37 o Labrum not described, pincer minor CAM 67 7 months Czerny 3B,, hypertrophy 61 o Labrum-cartilage separation, mild osteoarthritis, pincer, CAM 71 b 18 months Czerny 3B 66 o Degeneration of labrum, no tears, CAM osteoarthritis at acetabulum and femur 72 5 months Czerny 3A 72 o Labrum-cartilage separation and influence of the cartilage, pincer, CAM Cheilectomy 75 b 7 months Czerny 3A 57 o Not available According to the patient some bone work. No effect months Czerny 3B 54 o 82 9 months Czerny 3A, NA 85 b 4 months Normal 50 o Labrum tear months Czerny 3A 45 o Labrum tear Labrum reinsertion months Czerny 3A 56 o Labrum tear, minimal pincer Minimal rimtrim, labrum reinsertion a CAM term for the exostose on the femoral head neck junction. b (10) Repeat arthroscopy 11 months after first HA: refixation of labrum, minor rimtrim of the acetabulum and extended on femur. (33) Repeat arthroscopy 14 months after first HA: labrum healed, acetabular cartilage with wave-sign, minor rimtrim, minor, screw removal. (54) Repeat arthroscopy 8 months after first HA: labrum healed, minor pincer removed, minor, psoastenotomy. (71) Hip arthroplasty 6 months after HA. (75) Repeat arthroscopy 3 months after first HA. Labrum attached but anterior lesion. Pincer and minor CAM. Detachment of the labrum, rimtrim, reinsertion of labrum and minor. Psoastenotomy. (85) Repeat arthroscopy 11 months after first HA. (95) Repeat HA 9 months after HA:. arthroscopy and the 2-year follow-up after PAO. Thus longer follow-up is needed to evaluate the final clinical result after delayed hip arthroscopy. However, excluding seven patients (seven hips) who had a hip arthroscopy within 6 months from 2-year follow-up did not change association. By including patients who previously underwent hip arthroscopy, the result of this study could possibly be biased. However, since this is a prospective cohort study illustrating daily clinical practice, these patients were not excluded. Hip arthroscopy is offered to the patient by two experts at the Sports Traumatology unit, if the clinical findings suggest intraarticular pathology. However, the decision to offer a hip arthroscopy is multifactorial and it is difficult to apply narrow clinical indications regarding this end-point. MRA is considered the gold standard in imaging labral tears, but hip arthroscopy gives a direct view of the intraarticular status including any chondral damage. This means relying only on MRA findings and clinical tests, chondral damage may be overlooked. A study by Mechlenburg et al. showed unchanged status of cartilage thickness 2 1 = 2 years after PAO assessed on MRI preoperatively and at followup indicating that osteoarthritis do not progress during follow-up even in the presence of a labral tear [32]. Fujii et al. [33] however, did find that advanced intra-articular lesions at the time of hip joint preserving surgery were a significant risk factor for high rate postoperative progression of osteoarthritis of the hip joint. Czerny s classification of labral tears was in an earlier study found not to be
7 380 C. Hartig-Andreasen et al. Table III. Odds ratios for predictors of clinical failure in terms of hip arthroscopy (n ¼ 95 a ) Parameter OR (95% CI) P value Adjusted OR (95% CI) b P value Borderline dysplasia (CE-angle 20 to <25 ) 2.82 ( ) ( ) AI angle <0 or > ( ) ( ) Preoperatively cross over sign present 3.52 ( ) ( ) a-angle 55 o 1.47 ( ) ( ) Labrum detachment 2.28 ( ) ( ) Labrum 0.73 ( ) ( ) Labrum hypertrophy 3.62 ( ) ( ) Presence of paralabral cyst 2.31 ( ) ( ) a Five hips excluded from the analyses involving the a-angle. b Adjusted for age (35 years)and borderline dysplasia. Table IV. Magnetic resonance arthrography characteristics (results for all hips and in groups, number of hips) Parameter All hips Arthroscopy group (n ¼ 26) Degeneration of the labrum Yes No Hypertrophied labrum Yes No Paralabral cyst Yes No Classification of labrum pathology A B A B A B Non-arthroscopy group (n ¼ 69) a No significant differences in labral pathology were found between the nonarthroscopy and arthroscopy group. prognostic for outcome [34] and Matheney et al. [35] found that a labral tear did not predict failure in terms of conversion to a THA after PAO. However, in this study a complete detachment of the acetabular labrum from the rim seen at MRA (Czerny 3A or 3B lesions), is a predictor for the need of a hip arthroscopy after PAO. An interesting finding in this present study was that almost all patients with dysplasia had MRA verified pathology of the labrum and it is interesting to note that a great deal of the patients had a positive effect of PAO alone without addressing the labrum. We believe that redirection of the acetabulum results in significantly reduced load on the labrum which probably explains the good clinical result even when lesions of the labrum are present. In conclusion, 27% (26 hips out of 95) of the hips underwent hip arthroscopy within the first 2 years after PAO. Predictors for hip arthroscopy were mild hip dysplasia, cross-over sign and a detached labrum evaluated on MRA. At follow-up 2 years after PAO, the clinical outcome in the non-arthroscopic group is superior to that in the arthroscopy group with statistically significant differences in patient reported outcome measures. In the majority of patients, a PAO without subsequent intraarticular assessment resulted in joint preservation with excellent clinical outcome, and currently we recommend PAO as first choice in patients with hip dysplasia. However, patient with mild dysplasia, cross over sign and detached labrum is at particular risk for the need of a hip arthroscopy and future studies must clarify treatment strategies for this patient group. We agree with Parvizi et al. [10] that hip arthroscopy alone without addressing the bony abnormalities in DDH is in general not recommended since a high reoperation rate has been observed.
8 Risk factors for the need of hip arthroscopy 381 Table V. Radiographic characteristics before and after PAO Parameter Nonarthroscopy group (n ¼ 69) Arthroscopy group (n ¼ 26) P value Before PAO Center-edge angle Median (interquartile range) 17 (13 to 20 ) 20 (17 to 21 ) Range 10 to to 24 Acetabular index angle Median (interquartile range) 15 (12 to 20 ) 14 (12 to 18 ) Range 0 to 33 8 to 21 After PAO Center-edge angle Median (interquartile range) 34 (29 to 36 ) 34 (32 to 37 ) Range 17 to to 46 Acetabular index angle Median (interquartile range) 3 (1 to 6 ) 1 o ( 1 to 3 ) Range 3 to 16 8 to 16 Crossover sign before PAO a Before PAO At 2-year followup a Crossover sign before arthroscopy were not possible to evaluate, since postoperative radiographs after PAO were supine taken. Table VI. Description of the changes in CE-angle in the arthroscopy group (n ¼ 25 a ) Parameter Before PAO Before arthroscopy After arthroscopy P value b Center-edge angle Median (interquartile range) 20 (17 to 21 ) 34 (32 to 37 ) 32 (29 to 36 ) Range 11 to to to 40 Acetabular index angle Median (interquartile range) 14 (12 to 18 ) 1 ( 1 to 3 ) 4 (0 to 5 ) <0.001 Range 8 to 21 8 v to 16 4 to 16 a One hip had only pre-arthroscopy radiographs and was left out for this analysis. b Statistically significant difference between CE angles and AI angles before and after arthroscopy. The poor results in the arthroscopy group might be explained by the fact that the problem does not come from the hip joint itself, and that the need for hip arthroscopy after PAO might be lower. As a consequence of the present study, we do not refer our patients directly to arthroscopy if the present with pain at follow-up. Instead we focus on extra-articular reasons for pain. Our regimen at follow-up has changed in direction to ultrasound examination in
9 382 C. Hartig-Andreasen et al. Table VII. Clinical findings at 2-year follow-up Parameter Arthroscopy group Nonarthroscopy group P value Positive impingement Positive FABER Positive impingement and FABER Trochanteric bursitis Persisting dysesthesia Table VIII. Patient reported outcome measures for arthroscopy and nonarthroscopy group (n ¼ 90 hips) Parameter WOMAC b Stiff Pain Preoperative a All (n ¼ 90) All (n ¼ 90) Arthroscopy (n ¼ 26) nonarthroscopy (n ¼ 64) P value Median (interquartile range) 7 (5 10) 2 (0 6) 5 (1 9) 1 (0 4) <0.001 Range Median (interquartile range) 3 (2 4) 2 (0 2) 2 (1 3) 1 (0 2) Range <0.001 Physical function Median (interquartile range) 19 (11 29) 4 (0 11) 10 (3 24) 2 (0 7) Range <0.001 Total scores Median (interquartile range) 30 (17 41) 8 (1 22) 18 (8 36) 5 (1 14) Range Normalized Median (interquartile range) 66 (56 78) 89 (73 98) 78 (62 89) 91 (82 100) Range Oxford hip score c SF36 Total score (0 48) Median (interquartile range) 28 (23 33) 43 (35 47) 36 (28 42) 43 (37 47) <0.001 Range Physical component score (0 100) Median (interquartile range) 38 (33 44) 48 (38 55) 39 (32 48) 51 (44 56) <0.001 (continued)
10 Table VIII. (continued) Parameter Preoperative a All (n ¼ 90) All (n ¼ 90) Arthroscopy (n ¼ 26) Range Mental component score (0 100) nonarthroscopy (n ¼ 64) Median (interquartile range) 54 (43 61) 58 (52 61) 56 (50 61) 58 (52 61) Range a The preoperative scores did not show any statistically significant differences between the arthroscopy and nonarthroscopy groups (P values ). b Raw scores with 0 indicating best results. Normalized score with 100 indicating best result. c Score with 48 indicating best results. Risk factors for the need of hip arthroscopy 383 P value Fig. 2. Changes in SF36 subscale parameters for 90 patients before PAO and at 2-year follow-up after PAO. The postoperative subscale parameters are also illustrated separately for the nonarthroscopy group (dash) and the arthroscopy group (dot). SF36 consist of eight subscales with health-related parameters: physical functioning (PF), role-physical (RP), bodily pain (BP), general health (GH), vitality (VT), social functioning (SF), role emotional (RE) and mental health (MH). order to address soft tissues around the hip, and we also refer the patients to iliopsoas exercises [36], since we often observe weakness and inflammation of iliopsoas. Currently, we are performing an ongoing prospective study focusing on soft tissue around the dysplastic hip. Which eventually might result in more knowledge about persisting pain in these patients since arthroscopy does not seem to be the answer. Funding Danish Rheumatism Association (R99-A1830) to C.H.A. CONFLICT OF INTEREST STATEMENT None declared. REFERENCES 1. Ganz R, Klaue K, Vinh TS et al. A new periacetabular osteotomy for the treatment of hip dysplasias. technique and preliminary results. Clin Orthop Relat Res 1988; 232: Dorrell JH, Catterall A. The torn acetabular labrum. J Bone Joint Surg Br 1986; 68: Domb BG, Lareau JM, Baydoun H et al. Is intraarticular pathology common in patients with hip dysplasia undergoing periacetabular osteotomy? Clin Orthop Relat Res 2014; 472: Klaue K, Durnin CW,Ganz R. The acetabular rim syndrome. A clinical presentation of dysplasia of the hip. J Bone Joint Surg Br 1991; 73: McCarthy JC, Lee JA. Acetabular dysplasia: A paradigm of arthroscopic examination of chondral injuries. Clin Orthop Relat Res 2002; 405: Pitto RP, Klaue K, Ganz R et al. Acetabular rim pathology secondary to congenital hip dysplasia in the adult. A radiographic study. Chir Organi Mov 1995; 80: Ross JR, Zaltz I, Nepple JJ et al. Arthroscopic disease classification and interventions as an adjunct in the treatment of acetabular dysplasia. Am J Sports Med 2011; 39 (Suppl): 72S 8S. 8. Myers SR, Eijer H,Ganz R. Anterior femoroacetabular impingement after periacetabular osteotomy. Clin Orthop Relat Res 1999; 363: Kim KI, Cho YJ, Ramteke AA et al. Peri-acetabular rotational osteotomy with concomitant hip arthroscopy for treatment of hip dysplasia. J Bone Joint Surg Br 2011; 93: Parvizi J, Bican O, Bender B et al. Arthroscopy for labral tears in patients with developmental dysplasia of the hip: A cautionary note. J Arthroplasty 2009; 24: Kalore NV, Jiranek WA. Save the torn labrum in hips with borderline acetabular coverage. Clin Orthop Relat Res 2012; 470: Hartig-Andreasen C, Troelsen A, Thillemann TM et al. What factors predict failure 4 to 12 years after periacetabular osteotomy?. Clin Orthop Relat Res 2012; 470: Troelsen A, Elmengaard B, Soballe K. Medium-term outcome of periacetabular osteotomy and predictors of conversion to total hip replacement. J Bone Joint Surg Am 2009; 91:
11 384 C. Hartig-Andreasen et al. 14. Wiberg G. Studies on dysplastic acetabula and congenital subluxation of the hip joint with special reference to the complication of osteoarthritis. Acta Chir Scand 1939; 83 (Suppl): Troelsen A, Elmengaard B, Soballe K. A new minimally invasive transsartorial approach for periacetabular osteotomy. J Bone Joint Surg Am 2008; 90: Troelsen A, Mechlenburg I, Gelineck J et al. What is the role of clinical tests and ultrasound in acetabular labral tear diagnostics?. Acta Orthop 2009; 80: Bellamy N, Buchanan WW, Goldsmith CH et al. Validation study of WOMAC: A health status instrument for measuring clinically important patient relevant outcomes to antirheumatic drug therapy in patients with osteoarthritis of the hip or knee. J Rheumatol.1988; 15: Dawson J, Fitzpatrick R, Carr A et al. Questionnaire on the perceptions of patients about total hip replacement. J Bone Joint Surg.Br 1996; 78: Bjorner JB, Thunedborg K, Kristensen TS et al. The Danish SF-36 health survey: Translation and preliminary validity studies. J Clin Epidemiol 1998; 51: Tönnis D. Congenital Dysplasia and Dislocation of the Hip in Children and Adults. New York: Springer, Reynolds D, Lucas J, Klaue K. Retroversion of the acetabulum. A cause of hip pain. J Bone Joint Surg Br 1999; 81: Troelsen A, Jacobsen S, Romer L et al. Weightbearing anteroposterior pelvic radiographs are recommended in DDH assessment. Clin Orthop Relat Res 2008; 466: Jamali AA, Mladenov K, Meyer DC et al. Anteroposterior pelvic radiographs to assess acetabular retroversion: High validity of the cross-over-sign. J Orthop Res 2007; 25: Troelsen A, Romer L, Jacobsen S et al. Cranial acetabular retroversion is common in developmental dysplasia of the hip as assessed by the weight bearing position. Acta Orthop 2010; 81: Czerny C, Hofmann S, Neuhold A et al. Lesions of the acetabular labrum: Accuracy of MR imaging and MR arthrography in detection and staging. Radiology 1996; 200: Notzli HP, Wyss TF, Stoecklin CH et al. The contour of the femoral head-neck junction as a predictor for the risk of anterior impingement. J Bone Joint Surg Br 2002; 84: Altman RD, Bloch DA, Dougados M et al. Measurement of structural progression in osteoarthritis of the hip: The Barcelona consensus group. Osteoarthr Cartilage 2004; 12: Bland JM, Altman DG. Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1986; 1: Bland JM, Altman DG. Applying the right statistics: Analyses of measurement studies. Ultrasound Obstet Gynecol 2003; 22: Steppacher SD, Tannast M, Ganz R et al. Mean 20-year followup of Bernese periacetabular osteotomy. Clin Orthop Relat Res 2008; 466: Domb BG, Stake CE, Lindner D et al. Arthroscopic capsular plication and labral preservation in borderline hip dysplasia: Two-year clinical outcomes of a surgical approach to a challenging problem. Am J Sports Med 2013; 41: Mechlenburg I, Nyengaard JR, Gelineck J et al. Cartilage thickness in the hip measured by MRI and stereology before and after periacetabular osteotomy. Clin Orthop Relat Res 2010; 468: Fujii M, Nakashima Y, Noguchi Y et al. Effect of intra-articular lesions on the outcome of periacetabular osteotomy in patients with symptomatic hip dysplasia. J Bone Joint Surg Br 2011; 93: Freedman BA, Potter BK, Dinauer PA et al. Prognostic value of magnetic resonance arthrography for Czerny stage II and III acetabular labral tears. Arthroscopy 2006; 22: Matheney T, Kim YJ, Zurakowski D et al. Intermediate to longterm results following the bernese periacetabular osteotomy and predictors of clinical outcome. J Bone Joint Surg Am 2009; 91: Holmich P. Long-standing groin pain in sportspeople falls into three primary patterns, a clinical entity approach: A prospective study of 207 patients. Br J Sports Med 2007; 41:
What level of pain reduction can be expected up to two years after periacetabular osteotomy? A prospective cohort study of 146 patients
 Journal of Hip Preservation Surgery Vol. 5, No. 3, pp. 274 281 doi: 10.1093/jhps/hny031 Advance Access Publication 10 August 2018 Research article What level of pain reduction can be expected up to two
Journal of Hip Preservation Surgery Vol. 5, No. 3, pp. 274 281 doi: 10.1093/jhps/hny031 Advance Access Publication 10 August 2018 Research article What level of pain reduction can be expected up to two
FAI syndrome with or without labral tear.
 Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Rapidly Progressive Osteoarthritis after Arthroscopic Labral Repair for Dysplasia. Dean K. Matsuda, MD Monti Khatod, MD Los Angeles, California, USA
 Rapidly Progressive Osteoarthritis after Arthroscopic Labral Repair for Dysplasia Dean K. Matsuda, MD Monti Khatod, MD Los Angeles, California, USA Recent reports of poor clinical outcomes after arthroscopic
Rapidly Progressive Osteoarthritis after Arthroscopic Labral Repair for Dysplasia Dean K. Matsuda, MD Monti Khatod, MD Los Angeles, California, USA Recent reports of poor clinical outcomes after arthroscopic
Periacetabular osteotomy for developmental hip dysplasia with labral tears: is arthrotomy or arthroscopy required?
 Journal of Hip Preservation Surgery Vol. 5, No. 1, pp. 23 33 doi: 10.1093/jhps/hnx048 Advance Access Publication 11 January 2018 Research article Periacetabular osteotomy for developmental hip dysplasia
Journal of Hip Preservation Surgery Vol. 5, No. 1, pp. 23 33 doi: 10.1093/jhps/hnx048 Advance Access Publication 11 January 2018 Research article Periacetabular osteotomy for developmental hip dysplasia
Combined Hip Arthroscopy and Periacetabular Osteotomy: Intra-Articular Pathology
 Combined Hip Arthroscopy and Periacetabular Osteotomy: Intra-Articular Pathology University of Rochester Department of Orthopaedics and Rehabilitation Raymond J. Kenney, MD P. Christopher Cook, MD Kelly
Combined Hip Arthroscopy and Periacetabular Osteotomy: Intra-Articular Pathology University of Rochester Department of Orthopaedics and Rehabilitation Raymond J. Kenney, MD P. Christopher Cook, MD Kelly
Combined Hip Arthroscopy and Periacetabular Osteotomy: Intra-Articular Pathology
 Combined Hip Arthroscopy and Periacetabular Osteotomy: Intra-Articular Pathology URMC Sports Medicine and Hip Preservation Raymond J. Kenney, MD Kelly L. Adler, MEd, ATC P. Christopher Cook, MD Brian D.
Combined Hip Arthroscopy and Periacetabular Osteotomy: Intra-Articular Pathology URMC Sports Medicine and Hip Preservation Raymond J. Kenney, MD Kelly L. Adler, MEd, ATC P. Christopher Cook, MD Brian D.
The condition occurs when the proximal femur repeatedly comes into contact with the native acetabular rim during normal hip range of motion.
 RIM SYNDROME [femoroacetabular impingement] It has been suggested to be a preosteoarthritic mechanism. The condition occurs when the proximal femur repeatedly comes into contact with the native acetabular
RIM SYNDROME [femoroacetabular impingement] It has been suggested to be a preosteoarthritic mechanism. The condition occurs when the proximal femur repeatedly comes into contact with the native acetabular
Who Doesn t Need a Hip Scope?
 AOSSM 2013 Annual Meeting Chicago, Illinois July 14, 2013 I. Hip arthroscopy only helps if it is a hip joint problem A. Not always evident - Among athletes, 60% of intraarticular disorders treated for
AOSSM 2013 Annual Meeting Chicago, Illinois July 14, 2013 I. Hip arthroscopy only helps if it is a hip joint problem A. Not always evident - Among athletes, 60% of intraarticular disorders treated for
Case Report Unusual Bilateral Rim Fracture in Femoroacetabular Impingement
 Case Reports in Orthopedics Volume 2015, Article ID 210827, 4 pages http://dx.doi.org/10.1155/2015/210827 Case Report Unusual Bilateral Rim Fracture in Femoroacetabular Impingement Claudio Rafols, Juan
Case Reports in Orthopedics Volume 2015, Article ID 210827, 4 pages http://dx.doi.org/10.1155/2015/210827 Case Report Unusual Bilateral Rim Fracture in Femoroacetabular Impingement Claudio Rafols, Juan
Periacetabular osteotomy: sporting, social and sexual activity 9-12 years post surgery
 Hip Int 2014; 24 ( 1) : 27-31 DOI: 10.5301/hipint.5000077 Original Article Periacetabular osteotomy: sporting, social and sexual activity 9-12 years post surgery Jakob Klit 1, Charlotte Hartig-Andreasen
Hip Int 2014; 24 ( 1) : 27-31 DOI: 10.5301/hipint.5000077 Original Article Periacetabular osteotomy: sporting, social and sexual activity 9-12 years post surgery Jakob Klit 1, Charlotte Hartig-Andreasen
Outcomes of Hip Arthroscopy for Patients with Symptomatic Borderline Dysplasia: A Comparison to a Matched Cohort of Patients with FAI
 Outcomes of Hip Arthroscopy for Patients with Symptomatic Borderline Dysplasia: A Comparison to a Matched Cohort of Patients with FAI Danyal Nawabi MD Kara Fields MS Catherine Wentzel BS Alexander McLawhorn,
Outcomes of Hip Arthroscopy for Patients with Symptomatic Borderline Dysplasia: A Comparison to a Matched Cohort of Patients with FAI Danyal Nawabi MD Kara Fields MS Catherine Wentzel BS Alexander McLawhorn,
CLINICS IN SPORTS MEDICINE
 Clin Sports Med 25 (2006) 365 369 CLINICS IN SPORTS MEDICINE A Acetabular labrum, tears of, hip arthroscopy in, 264 Acetabular rim, trimming of, and labral repair, new method for, 293 297 Acetabulum, femoral
Clin Sports Med 25 (2006) 365 369 CLINICS IN SPORTS MEDICINE A Acetabular labrum, tears of, hip arthroscopy in, 264 Acetabular rim, trimming of, and labral repair, new method for, 293 297 Acetabulum, femoral
The Relationship Between Hip Physical Examination Findings and Intra-articular Pathology Seen at the Time of Hip Arthroscopy
 The Relationship Between Hip Physical Examination Findings and Intra-articular Pathology Seen at the Time of Hip Arthroscopy Craig M. Capeci, MD Mohaned Al-Humadi, MD Malachy P. McHugh, PhD Alexis Chiang-Colvin,
The Relationship Between Hip Physical Examination Findings and Intra-articular Pathology Seen at the Time of Hip Arthroscopy Craig M. Capeci, MD Mohaned Al-Humadi, MD Malachy P. McHugh, PhD Alexis Chiang-Colvin,
October 1999, Supplement 1 Volume 15 Number 7
 October 1999, Supplement 1 Volume 15 Number 7
October 1999, Supplement 1 Volume 15 Number 7
Accelerated Degenerative Joint Disease After Staged Hip Arthroscopy and Periacetabular Osteotomy in a Patient with Hip Dysplasia
 220 Accelerated Degenerative Joint Disease After Staged Hip Arthroscopy and Periacetabular Osteotomy in a Patient with Hip Dysplasia Michael S. Guss, M.D., and Thomas Youm, M.D. Abstract Hip dysplasia,
220 Accelerated Degenerative Joint Disease After Staged Hip Arthroscopy and Periacetabular Osteotomy in a Patient with Hip Dysplasia Michael S. Guss, M.D., and Thomas Youm, M.D. Abstract Hip dysplasia,
1/15/ year old male. Hip Preservation Surgery for Acetabular Dysplasia in Adolescents and Young Adults PATHOMECHANICS OF ACETABULAR DYSPLASIA
 29 year old male Hip Preservation Surgery for Acetabular Dysplasia in Adolescents and Young Adults Eduardo Novais, MD Assistant Professor of Orthopedic Surgery PATHOMECHANICS OF ACETABULAR DYSPLASIA Static
29 year old male Hip Preservation Surgery for Acetabular Dysplasia in Adolescents and Young Adults Eduardo Novais, MD Assistant Professor of Orthopedic Surgery PATHOMECHANICS OF ACETABULAR DYSPLASIA Static
Arthroscopy of the hip for patients with mild to moderate developmental dysplasia of the hip and femoroacetabular impingement
 HIP Arthroscopy of the hip for patients with mild to moderate developmental dysplasia of the hip and femoroacetabular impingement K. Fukui, C. A. C. Trindade, K. K. Briggs, M. J. Philippon From Steadman
HIP Arthroscopy of the hip for patients with mild to moderate developmental dysplasia of the hip and femoroacetabular impingement K. Fukui, C. A. C. Trindade, K. K. Briggs, M. J. Philippon From Steadman
Arthroscopic Treatment of Femoroacetabular Impingement in Patients over 60 Years Old: Preliminary Report of a Pilot Study
 Original Article Arthroscopic Treatment of Femoroacetabular Impingement in Patients over 60 Years Old: Preliminary Report of a Pilot Study Cartilage 1(3) 188 193 The Author(s) 2010 Reprints and permission:
Original Article Arthroscopic Treatment of Femoroacetabular Impingement in Patients over 60 Years Old: Preliminary Report of a Pilot Study Cartilage 1(3) 188 193 The Author(s) 2010 Reprints and permission:
The Birmingham Interlocking Pelvic Osteotomy (BIPO) for Acetabular Dysplasia: 13 to 21 Year Survival Outcomes
 The Birmingham Interlocking Pelvic Osteotomy (BIPO) for Acetabular Dysplasia: 13 to 21 Year Survival Outcomes Omer Mei-Dan, MD Dylan Jewell, BSc, MSc, FRCS Tigran Garabekyan, MD Jason Brockwell, FRCSEdOrth
The Birmingham Interlocking Pelvic Osteotomy (BIPO) for Acetabular Dysplasia: 13 to 21 Year Survival Outcomes Omer Mei-Dan, MD Dylan Jewell, BSc, MSc, FRCS Tigran Garabekyan, MD Jason Brockwell, FRCSEdOrth
Radiographic and Clinical Risk Factors for the Extent of Labral Injury at the Time of Hip Arthroscopy
 Radiographic and Clinical Risk Factors for the Extent of Labral Injury at the Time of Hip Arthroscopy John M. Redmond, MD Jon E. Hammarstedt, BS Asheesh Gupta, MD MPH Christine E. Stake, DHA Kevin F. Dunne,
Radiographic and Clinical Risk Factors for the Extent of Labral Injury at the Time of Hip Arthroscopy John M. Redmond, MD Jon E. Hammarstedt, BS Asheesh Gupta, MD MPH Christine E. Stake, DHA Kevin F. Dunne,
Femoroacetabular impingement in adolescents and young adults an update
 U N I V E R S I T E T E T I B E R G E N Femoroacetabular impingement in adolescents and young adults an update Lene Bjerke Laborie, MD, PhD Paediatric Radiology Department, Haukeland University Hospital
U N I V E R S I T E T E T I B E R G E N Femoroacetabular impingement in adolescents and young adults an update Lene Bjerke Laborie, MD, PhD Paediatric Radiology Department, Haukeland University Hospital
The Young Adult Hip: FAI. Jason Snibbe, M.D. Snibbe Orthopedics Team Physician, University of Southern California
 The Young Adult Hip: FAI Jason Snibbe, M.D. Snibbe Orthopedics Team Physician, University of Southern California Introduction Femoroacetabular Impingment(FAI) Presentation and Exam Imaging Surgical Management
The Young Adult Hip: FAI Jason Snibbe, M.D. Snibbe Orthopedics Team Physician, University of Southern California Introduction Femoroacetabular Impingment(FAI) Presentation and Exam Imaging Surgical Management
Cartilage Thickness and Cyst Volume Are Unchanged 10 Years After Periacetabular Osteotomy in Patients Without Hip Symptoms
 Clin Orthop Relat Res (2015) 473:2644 2649 DOI 10.1007/s11999-015-4273-2 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons BASIC RESEARCH Cartilage
Clin Orthop Relat Res (2015) 473:2644 2649 DOI 10.1007/s11999-015-4273-2 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons BASIC RESEARCH Cartilage
Mitchell McDowell, DO**, Daljeet Sagoo, DO*, Michael P. Muldoon, MD*, Richard Santore, MD*
 Mitchell McDowell, DO**, Daljeet Sagoo, DO*, Michael P. Muldoon, MD*, Richard Santore, MD* *Orthopedic Medical Group,7910 Frost St. #200 San Diego, California 92123, USA **Riverside County Regional Medical
Mitchell McDowell, DO**, Daljeet Sagoo, DO*, Michael P. Muldoon, MD*, Richard Santore, MD* *Orthopedic Medical Group,7910 Frost St. #200 San Diego, California 92123, USA **Riverside County Regional Medical
Hip Arthroscopy in Patients with Mild to Moderate Dysplasia: When do they Fail?
 Hip Arthroscopy in Patients with Mild to Moderate Dysplasia: When do they Fail? Andrew J. Bryan 1, MD K. Poehling-Monaghan 1, MD Rohith Mohan 1, BA Nick R Johnson 1, BS Aaron J. Krych 1, MD Bruce A. Levy
Hip Arthroscopy in Patients with Mild to Moderate Dysplasia: When do they Fail? Andrew J. Bryan 1, MD K. Poehling-Monaghan 1, MD Rohith Mohan 1, BA Nick R Johnson 1, BS Aaron J. Krych 1, MD Bruce A. Levy
Hip Preservation Timothy J Sauber MD Orthopaedic Update March 22, 2015 Nemacolin Woodlands Resort
 Hip Preservation Timothy J Sauber MD Orthopaedic Update March 22, 2015 Nemacolin Woodlands Resort Disclosures No disclosures relevant to this topic Objectives Evaluate and recognize common hip pathology
Hip Preservation Timothy J Sauber MD Orthopaedic Update March 22, 2015 Nemacolin Woodlands Resort Disclosures No disclosures relevant to this topic Objectives Evaluate and recognize common hip pathology
Bone Bangalore
 Dr Suresh Annamalai MBBS, MRCS(Edn), FRCS( Tr & Orth)(Edn), FEBOT(European Board), Young Hip and Knee Fellowship(Harrogate, UK) HOD & Consultant Arthroplasty and Arthroscopic Surgeon Manipal Hospital,
Dr Suresh Annamalai MBBS, MRCS(Edn), FRCS( Tr & Orth)(Edn), FEBOT(European Board), Young Hip and Knee Fellowship(Harrogate, UK) HOD & Consultant Arthroplasty and Arthroscopic Surgeon Manipal Hospital,
F.A.I. indications. E. Sabetta. Arcispedale S. Maria Nuova Struttura Complessa Ortopedia e Traumatologia Direttore: Ettore Sabetta
 F.A.I. indications E. Sabetta Arcispedale S. Maria Nuova Struttura Complessa Ortopedia e Traumatologia Direttore: Ettore Sabetta !.FAI treatment might become a mainstay in joint-preserving treatment of
F.A.I. indications E. Sabetta Arcispedale S. Maria Nuova Struttura Complessa Ortopedia e Traumatologia Direttore: Ettore Sabetta !.FAI treatment might become a mainstay in joint-preserving treatment of
InTRoDucTIon. METHoDS. M. Jäger 1 *, b. bittersohl 1 *, c. Zilkens 1, H. S. Hosalkar 2, K. Stefanovska 1, S. Kurth 1, R. Krauspe 1
 May 12, 2011 Eu Ro PE an JouR nal of MED I cal RE SEaRcH 217 Eur J Med Res (2011) 16: 217-222 I. Holzapfel Publishers 2011 SuRgIcal HIP DISlocaTIon In SyMPToMaTIc cam FEMoRoacETabulaR IMPIngEMEnT: WHaT
May 12, 2011 Eu Ro PE an JouR nal of MED I cal RE SEaRcH 217 Eur J Med Res (2011) 16: 217-222 I. Holzapfel Publishers 2011 SuRgIcal HIP DISlocaTIon In SyMPToMaTIc cam FEMoRoacETabulaR IMPIngEMEnT: WHaT
Disclosures. Objectives 11/18/2015. Hip Preservation in the Adolescent and Young Adult. Financial - None I do not perform total joint arthroplasty
 Hip Preservation in the Adolescent and Young Adult Alfred A. Mansour, III, MD Pediatric Sports Medicine and Hip Preservation UT-Ortho 59th Annual Edward T. Smith Orthopaedic Lectureship November 5-6, 2015
Hip Preservation in the Adolescent and Young Adult Alfred A. Mansour, III, MD Pediatric Sports Medicine and Hip Preservation UT-Ortho 59th Annual Edward T. Smith Orthopaedic Lectureship November 5-6, 2015
Adolescent Hip Dysplasia
 Adolescent Hip Dysplasia The hip is a "ball-and-socket" joint. In a normal hip, the ball at the upper end of the femur (thighbone) fits firmly into the socket, which is a curved portion of the pelvis called
Adolescent Hip Dysplasia The hip is a "ball-and-socket" joint. In a normal hip, the ball at the upper end of the femur (thighbone) fits firmly into the socket, which is a curved portion of the pelvis called
Efficacy of Osseous Abnormalities Correction with Arthroscopic Surgery in Femoroacetabular Impingement
 Original Article Efficacy of Osseous Abnormalities Correction with Arthroscopic Surgery in Femoroacetabular Impingement Cartilage 1(3) 233 237 The Author(s) 2010 Reprints and permission: sagepub.com/journalspermissions.nav
Original Article Efficacy of Osseous Abnormalities Correction with Arthroscopic Surgery in Femoroacetabular Impingement Cartilage 1(3) 233 237 The Author(s) 2010 Reprints and permission: sagepub.com/journalspermissions.nav
21 year-old collegiate rower: R/O labral tear
 Hip MRI Primer AOSSM 2014 Hollis G. Potter, MD Chair, Department of Radiology & Imaging The Coleman Chair, MRI Research Hospital for Special Surgery Professor of Radiology Weill Medical College of Cornell
Hip MRI Primer AOSSM 2014 Hollis G. Potter, MD Chair, Department of Radiology & Imaging The Coleman Chair, MRI Research Hospital for Special Surgery Professor of Radiology Weill Medical College of Cornell
Hip arthroscopy. Anatomy The hip is functionally a ball and socket joint.
 Hip arthroscopy The term arthroscopy (or keyhole surgery) refers to the viewing of the inside of a joint through a small operating telescope. First described in the 1970s, arthroscopic techniques have
Hip arthroscopy The term arthroscopy (or keyhole surgery) refers to the viewing of the inside of a joint through a small operating telescope. First described in the 1970s, arthroscopic techniques have
A Patient s Guide to Femoroacetabular Impingement (FAI) of the Hip
 A Patient s Guide to Femoroacetabular Impingement (FAI) of the Hip 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com DISCLAIMER: The information in this booklet
A Patient s Guide to Femoroacetabular Impingement (FAI) of the Hip 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com DISCLAIMER: The information in this booklet
Circles are Pointless - Angles in the assessment of adult hip dysplasia are not!
 Circles are Pointless - Angles in the assessment of adult hip dysplasia are not! Poster No.: C-1964 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit S. E. West, S. G. Cross, J. Adu,
Circles are Pointless - Angles in the assessment of adult hip dysplasia are not! Poster No.: C-1964 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit S. E. West, S. G. Cross, J. Adu,
Non-Arthroplasty Hip Surgery. Javad Parvizi MD FRCS Professor of Orthopaedic Surgery
 Non-Arthroplasty Hip Surgery Javad Parvizi MD FRCS Professor of Orthopaedic Surgery Subcapital reduction osteotomy Relative lengthening of femoral neck (Perthes) AVN surgery Femoral osteotomy Trap door
Non-Arthroplasty Hip Surgery Javad Parvizi MD FRCS Professor of Orthopaedic Surgery Subcapital reduction osteotomy Relative lengthening of femoral neck (Perthes) AVN surgery Femoral osteotomy Trap door
EBM. Comparative Systematic Review of the Open Dislocation, Mini-Open, and Arthroscopic Surgeries for Femoroacetabular Impingement
 EBM Comparative Systematic Review of the Open Dislocation, Mini-Open, and Arthroscopic Surgeries for Femoroacetabular Impingement ~ Arthroscopy: The Journal of Arthroscopic and Related Surgery, Vol 27,
EBM Comparative Systematic Review of the Open Dislocation, Mini-Open, and Arthroscopic Surgeries for Femoroacetabular Impingement ~ Arthroscopy: The Journal of Arthroscopic and Related Surgery, Vol 27,
EVALUATION OF THE ACETABULAR LABRUM BY MR ARTHROGRAPHY
 EVALUATION OF THE ACETABULAR LABRUM BY MR ARTHROGRAPHY M. LEUNIG, S. WERLEN, A. UNGERSBÖCK, K. ITO, R. GANZ From the University of Berne and the Sonnenhof Clinic, Berne, and the AO/ASIF Research Institute,
EVALUATION OF THE ACETABULAR LABRUM BY MR ARTHROGRAPHY M. LEUNIG, S. WERLEN, A. UNGERSBÖCK, K. ITO, R. GANZ From the University of Berne and the Sonnenhof Clinic, Berne, and the AO/ASIF Research Institute,
A Patient s Guide to Labral Tears of the Hip
 A Patient s Guide to Labral Tears of the Hip 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Labral Tears of the Hip 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled from a variety
Title; Periacetabular Osteotomy for the Treatment of Symptomatic Acetabular Dysplasia in. Patients with and without Labral Tears.
 Title; Periacetabular Osteotomy for the Treatment of Symptomatic Acetabular Dysplasia in Patients with and without Labral Tears Authors; Tomonobu Hagio, MD 1 ; Masatoshi Naito, MD, PhD 1 ; Yoshinari Nakamura,
Title; Periacetabular Osteotomy for the Treatment of Symptomatic Acetabular Dysplasia in Patients with and without Labral Tears Authors; Tomonobu Hagio, MD 1 ; Masatoshi Naito, MD, PhD 1 ; Yoshinari Nakamura,
Viviane Khoury, MD. Assistant Professor Department of Radiology University of Pennsylvania
 U Penn Diagnostic Imaging: On the Cape Chatham, MA July 11-15, 2016 Viviane Khoury, MD Assistant Professor Department of Radiology University of Pennsylvania Hip imaging has changed in recent years: new
U Penn Diagnostic Imaging: On the Cape Chatham, MA July 11-15, 2016 Viviane Khoury, MD Assistant Professor Department of Radiology University of Pennsylvania Hip imaging has changed in recent years: new
A Guide for Patients with Hip and Groin Pain. By - Rob Lawton & Ajay Malviya. Overview
 A Guide for Patients with Hip and Groin Pain By - Rob Lawton & Ajay Malviya Overview - Introduction - Hip Anatomy - Is the pain coming from the hip joint? - Intra-articular causes of hip pain o Impingement
A Guide for Patients with Hip and Groin Pain By - Rob Lawton & Ajay Malviya Overview - Introduction - Hip Anatomy - Is the pain coming from the hip joint? - Intra-articular causes of hip pain o Impingement
Hip Arthroscopy. Christopher J. Utz, MD. Assistant Professor of Orthopaedic Surgery University of Cincinnati
 Hip Arthroscopy Christopher J. Utz, MD Assistant Professor of Orthopaedic Surgery University of Cincinnati Disclosures I have no disclosures relevant to this topic. Outline 1. Brief History 2. Review of
Hip Arthroscopy Christopher J. Utz, MD Assistant Professor of Orthopaedic Surgery University of Cincinnati Disclosures I have no disclosures relevant to this topic. Outline 1. Brief History 2. Review of
Labral Tears / Femoro- Acetabular Impingement / Hip Arthroscopy/THA. Dr Allen Turnbull Hip and Knee Surgery
 Labral Tears / Femoro- Acetabular Impingement / Hip Arthroscopy/THA Hip Anatomy Labrum Fovea Femoral Head Articular Cartilage Ligamentum Teres Labral Tears Function of Labrum Deepens acetabulum by 20%
Labral Tears / Femoro- Acetabular Impingement / Hip Arthroscopy/THA Hip Anatomy Labrum Fovea Femoral Head Articular Cartilage Ligamentum Teres Labral Tears Function of Labrum Deepens acetabulum by 20%
10/15/17. Acknowledgements. The Sporting Hip & Groin. TheSporting. SportingHip. The Sporting. The Sporting. The Sporting.
 Michael O Brien Physiotherapist Acknowledgements The TheSporting SportingHip Hip & Groin Impingement or instability? Andrew Wallis Alesha Coonan (Gledhill-Tunks) Melbourne Orthopaedic Group Mr. Jit Balakumar
Michael O Brien Physiotherapist Acknowledgements The TheSporting SportingHip Hip & Groin Impingement or instability? Andrew Wallis Alesha Coonan (Gledhill-Tunks) Melbourne Orthopaedic Group Mr. Jit Balakumar
Mr Simon Jennings BSc, MB BS, FRCS, Dip Sports Med FRCS (Trauma & Orthopaedics)
 Mr Simon Jennings BSc, MB BS, FRCS, Dip Sports Med FRCS (Trauma & Orthopaedics) Consultant Orthopaedic Surgeon Northwick Park Hospital 107 Harley Street RSM 16 th September 2010 Orthopaedic Surgeon Knee
Mr Simon Jennings BSc, MB BS, FRCS, Dip Sports Med FRCS (Trauma & Orthopaedics) Consultant Orthopaedic Surgeon Northwick Park Hospital 107 Harley Street RSM 16 th September 2010 Orthopaedic Surgeon Knee
Adult Hip Dysplasia David S. Feldman, MD
 Adult Hip Dysplasia David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone Medical Center & NYU Hospital for Joint Diseases Overview Adult hip
Adult Hip Dysplasia David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone Medical Center & NYU Hospital for Joint Diseases Overview Adult hip
ORIGINAL STUDY INTRODUCTION
 Acta Orthop. Belg., 2007, 73, 38-43 ORIGINAL STUDY Influence of labral tears on the outcome of acetabular augmentation procedures in adult dysplastic hips Prospective assessment with a minimum follow-up
Acta Orthop. Belg., 2007, 73, 38-43 ORIGINAL STUDY Influence of labral tears on the outcome of acetabular augmentation procedures in adult dysplastic hips Prospective assessment with a minimum follow-up
1/15/2012. Femoroacetabular impingement. Femoroacetabular Impingement FAI. Femoroacetabular impingement. Femoroacetabular impingement
 Femoroacetabular Impingement FAI Previously known as Acetabular rim syndrome Cervicoacetabular impingement Dr. Tudor H Hughes, M.D., FRCR Department of Radiology University of California School of Medicine
Femoroacetabular Impingement FAI Previously known as Acetabular rim syndrome Cervicoacetabular impingement Dr. Tudor H Hughes, M.D., FRCR Department of Radiology University of California School of Medicine
CAN SOFT TISSUES STRUCTURES DIFFERENTIATE BETWEEN DYSPLASIA AND CAM-FAI OF THE HIP?
 CAN SOFT TISSUES STRUCTURES DIFFERENTIATE BETWEEN DYSPLASIA AND CAM-FAI OF THE HIP? A Le Bouthillier, KS Rakhra 1, PE Beaulé 2, RCB Foster 1 1 Department of Medical Imaging 2 Division of Orthopaedic Surgery
CAN SOFT TISSUES STRUCTURES DIFFERENTIATE BETWEEN DYSPLASIA AND CAM-FAI OF THE HIP? A Le Bouthillier, KS Rakhra 1, PE Beaulé 2, RCB Foster 1 1 Department of Medical Imaging 2 Division of Orthopaedic Surgery
Cam- and pincer-type femoroacetabular impingement
 Case Report With Video Illustration Making a Case for Anterior Inferior Iliac Spine/Subspine Hip Impingement: Three Representative Case Reports and Proposed Concept Christopher M. Larson, M.D., Bryan T.
Case Report With Video Illustration Making a Case for Anterior Inferior Iliac Spine/Subspine Hip Impingement: Three Representative Case Reports and Proposed Concept Christopher M. Larson, M.D., Bryan T.
What is FAI? And Why are we getting Hip Problems?
 What is FAI? And Why are we getting Hip Problems? Why is Hip pain so common NOW? Greater awareness More accurate imaging MRI Fashionable?? Geography Arthroscopy used to be OP now FAI! Why is Hip pain so
What is FAI? And Why are we getting Hip Problems? Why is Hip pain so common NOW? Greater awareness More accurate imaging MRI Fashionable?? Geography Arthroscopy used to be OP now FAI! Why is Hip pain so
Physical Activity Level Improves After Periacetabular Osteotomy for the Treatment of Symptomatic Hip Dysplasia
 Clin Orthop Relat Res (2013) 471:981 988 DOI 10.1007/s11999-012-2578-y Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH Physical
Clin Orthop Relat Res (2013) 471:981 988 DOI 10.1007/s11999-012-2578-y Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH Physical
Hip Arthroscopy: Intra-articular Saucerization of the Acetabular Cotyloid Fossa
 Hip Arthroscopy: Intra-articular Saucerization of the Acetabular Cotyloid Fossa JAMES K. BRANNON, MD, FAAOS abstract Full article available online at ORTHOSuperSite.com. Search: 20120123-23 Hip arthroscopy
Hip Arthroscopy: Intra-articular Saucerization of the Acetabular Cotyloid Fossa JAMES K. BRANNON, MD, FAAOS abstract Full article available online at ORTHOSuperSite.com. Search: 20120123-23 Hip arthroscopy
Femoroacetabular Impingement in the Throwing Athlete. Michael Banffy, MD Sports Medicine, Hip Preservation Kerlan Jobe Institute
 Femoroacetabular Impingement in the Throwing Athlete Michael Banffy, MD Sports Medicine, Hip Preservation Kerlan Jobe Institute Disclosures None Baseball Hip Injuries - Background Abdominal/groin injuries
Femoroacetabular Impingement in the Throwing Athlete Michael Banffy, MD Sports Medicine, Hip Preservation Kerlan Jobe Institute Disclosures None Baseball Hip Injuries - Background Abdominal/groin injuries
Disclosure. FAI: Imaging Modalities and Dynamic Imaging Software. Acceptance of Hip Arthroscopy & FAI. Public. Payors. Orthopaedic Community
 2015 Chicago Sports Medicine Symposium Chicago, Illinois USA FAI: Imaging Modalities and Dynamic Imaging Software Allston J. Stubbs, M.D., M.B.A. Medical Director Hip Arthroscopy & Associate Professor
2015 Chicago Sports Medicine Symposium Chicago, Illinois USA FAI: Imaging Modalities and Dynamic Imaging Software Allston J. Stubbs, M.D., M.B.A. Medical Director Hip Arthroscopy & Associate Professor
Femoral Acetabular Impingement 10/22/2016
 Femoral Acetabular Impingement 10/22/2016 Disclosures No Disclosures to report Questions Does FAI lead to early development of osteoarthritis? Is surgical correction an effective treatment for FAI? Who
Femoral Acetabular Impingement 10/22/2016 Disclosures No Disclosures to report Questions Does FAI lead to early development of osteoarthritis? Is surgical correction an effective treatment for FAI? Who
Swiss Medical Network Musculoskeletal Conference Surgical Technique and 30-Year Results of the Periacetabular Osteotomy (PAO)
 Swiss Medical Network Musculoskeletal Conference 2017 Surgical Technique and 30-Year Results of the Periacetabular Osteotomy (PAO) Simon D. Steppacher Department of Orthopedic Surgery, Inselspital, University
Swiss Medical Network Musculoskeletal Conference 2017 Surgical Technique and 30-Year Results of the Periacetabular Osteotomy (PAO) Simon D. Steppacher Department of Orthopedic Surgery, Inselspital, University
Labral Tears/FAI. Andrew Parker, MD
 Labral Tears/FAI Andrew Parker, MD Athletic Hip Injuries Incidence of hip injuries has increased dramatically over the last decade In part due to better recognition with improved imaging and arthroscopy,
Labral Tears/FAI Andrew Parker, MD Athletic Hip Injuries Incidence of hip injuries has increased dramatically over the last decade In part due to better recognition with improved imaging and arthroscopy,
Impingement Adversely Affects 10-year Survivorship After Periacetabular Osteotomy for DDH
 Clin Orthop Relat Res (2013) 471:1602 1614 DOI 10.1007/s11999-013-2799-8 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH Impingement
Clin Orthop Relat Res (2013) 471:1602 1614 DOI 10.1007/s11999-013-2799-8 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH Impingement
Classification of Acetabular Cartilage Lesions. Claudio Mella, MD
 Classification of Acetabular Cartilage Lesions Claudio Mella, MD Acetabular cartilage lesions are frequently found during hip arthroscopy. The arthroscopic view offers an exceptional perspective to assess
Classification of Acetabular Cartilage Lesions Claudio Mella, MD Acetabular cartilage lesions are frequently found during hip arthroscopy. The arthroscopic view offers an exceptional perspective to assess
Historically, athletic injuries about the hip and groin
 Sports Medicine and Arthroscopy Review 10:134 140 2002 Lippincott Williams & Wilkins, Inc., Philadelphia : A Clinical Presentation Tania A. Ferguson, M.D.,* and Joel Matta, M.D. SUMMARY Femoroacetabular
Sports Medicine and Arthroscopy Review 10:134 140 2002 Lippincott Williams & Wilkins, Inc., Philadelphia : A Clinical Presentation Tania A. Ferguson, M.D.,* and Joel Matta, M.D. SUMMARY Femoroacetabular
Ganzosteotomy Description and indications. Dr. Jaak Roos - A.Z. Turnhout
 Ganzosteotomy Description and indications Dr. Jaak Roos - A.Z. Turnhout Welcome Turnhout Flanders Cultural Capital 2012 Turnhout: Stad van m n hert Hip Dysplasia Natural history of HD without subluxation:
Ganzosteotomy Description and indications Dr. Jaak Roos - A.Z. Turnhout Welcome Turnhout Flanders Cultural Capital 2012 Turnhout: Stad van m n hert Hip Dysplasia Natural history of HD without subluxation:
Radiographic markers of acetabular retroversion : Correlation of the cross-over sign, ischial spine sign and posterior wall sign
 Acta Orthop. Belg., 2010, 76, 166-173 ORIGINAL STUDY Radiographic markers of acetabular retroversion : Correlation of the cross-over sign, ischial spine sign and posterior wall sign Clément M.L. WERNER,
Acta Orthop. Belg., 2010, 76, 166-173 ORIGINAL STUDY Radiographic markers of acetabular retroversion : Correlation of the cross-over sign, ischial spine sign and posterior wall sign Clément M.L. WERNER,
Evaluation of Hip Pain in Adults. Jerry Ahluwalia, M.D. November 13, 2015
 Evaluation of Hip Pain in Adults Jerry Ahluwalia, M.D. November 13, 2015 Objectives Develop a better understanding of the differential diagnosis of hip pain in active young adults Appreciate key points
Evaluation of Hip Pain in Adults Jerry Ahluwalia, M.D. November 13, 2015 Objectives Develop a better understanding of the differential diagnosis of hip pain in active young adults Appreciate key points
dgemric Effectively Predicts Cartilage Damage Associated with Femoroacetabular Impingement
 Riccardo Lattanzi 1,2 Catherine Petchprapa 2 Daniele Ascani 1 Roy I. Davidovitch 3 Thomas Youm 3 Robert J. Meislin 3 Michael. Recht 2 1 The Bernard and Irene Schwartz Center for Biomedical Imaging, New
Riccardo Lattanzi 1,2 Catherine Petchprapa 2 Daniele Ascani 1 Roy I. Davidovitch 3 Thomas Youm 3 Robert J. Meislin 3 Michael. Recht 2 1 The Bernard and Irene Schwartz Center for Biomedical Imaging, New
Does Salter Innominate Osteotomy Predispose the Patient to Acetabular Retroversion in Adulthood?
 Clin Orthop Relat Res (2015) 473:1755 1762 DOI 10.1007/s11999-014-4053-4 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH Does Salter
Clin Orthop Relat Res (2015) 473:1755 1762 DOI 10.1007/s11999-014-4053-4 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH Does Salter
Young Adult Hip problems. Aresh Hashemi-Nejad FRCS(Orth)
 Young Adult Hip problems Aresh Hashemi-Nejad FRCS(Orth) RNOH founded 1837 by William Little 14 year old presenting with limp Knee pain on and off 4 months Limps Aresh Hashemi-Nejad FRCS(Orth) The Royal
Young Adult Hip problems Aresh Hashemi-Nejad FRCS(Orth) RNOH founded 1837 by William Little 14 year old presenting with limp Knee pain on and off 4 months Limps Aresh Hashemi-Nejad FRCS(Orth) The Royal
University of Bath DOI: / Publication date: Document Version Peer reviewed version. Link to publication
 Citation for published version: Grammatopoulos, G, Davies, O, El-Bakoury, A, Gill, H, Pollard, TC & Andrade, A 2017, 'A traffic light grading system of hip dysplasia to predict the success of arthroscopic
Citation for published version: Grammatopoulos, G, Davies, O, El-Bakoury, A, Gill, H, Pollard, TC & Andrade, A 2017, 'A traffic light grading system of hip dysplasia to predict the success of arthroscopic
A Patient s Guide to Labral Tears of the Hip
 A Patient s Guide to Labral Tears of the Hip Sports-related injuries require specialized care to promote optimum healing. Whether you are a weekend jogger or tennis player, a professional soccer player
A Patient s Guide to Labral Tears of the Hip Sports-related injuries require specialized care to promote optimum healing. Whether you are a weekend jogger or tennis player, a professional soccer player
The interface between periacetabular osteotomy, hip arthroscopy and total hip arthroplasty in the young adult hip
 Syddansk Universitet The interface between periacetabular osteotomy, hip arthroscopy and total hip arthroplasty in the young adult hip Jakobsen, Stig Storgaard; Overgaard, Soren; Søballe, Kjeld; Ovesen,
Syddansk Universitet The interface between periacetabular osteotomy, hip arthroscopy and total hip arthroplasty in the young adult hip Jakobsen, Stig Storgaard; Overgaard, Soren; Søballe, Kjeld; Ovesen,
Non-arthritic anterior hip pain in the younger patient: examination and intervention strategies
 Non-arthritic anterior hip pain in the younger patient: examination and intervention strategies Melodie Kondratek, PT, DScPT, OMPT Bryan Kuhlman, PT, DPT, OMPT Oakland University Orthopedic Spine and Sports
Non-arthritic anterior hip pain in the younger patient: examination and intervention strategies Melodie Kondratek, PT, DScPT, OMPT Bryan Kuhlman, PT, DPT, OMPT Oakland University Orthopedic Spine and Sports
Sports Medicine and Radiology
 Sports Medicine and Radiology The judicious utilization of a thorough history and physical examination and appropriately applied imaging studies will allow for accurate diagnosis and treatment of athletic
Sports Medicine and Radiology The judicious utilization of a thorough history and physical examination and appropriately applied imaging studies will allow for accurate diagnosis and treatment of athletic
Corporate Medical Policy
 Corporate Medical Policy Surgery for Femoroacetabular Impingement File Name: Origination: Last CAP Review: Next CAP Review: Last Review: surgery_for_femoroacetabular_impingement 3/2007 6/2018 6/2019 6/2018
Corporate Medical Policy Surgery for Femoroacetabular Impingement File Name: Origination: Last CAP Review: Next CAP Review: Last Review: surgery_for_femoroacetabular_impingement 3/2007 6/2018 6/2019 6/2018
Hip pain rating after preforming MRI with gadolinium arthrography and intra-articular lidocaine
 Hip pain rating after preforming MRI with gadolinium arthrography and intra-articular lidocaine Poster No.: C-1352 Congress: ECR 2014 Type: Scientific Exhibit Authors: J. García Yavar, J. Cabezudo, S.
Hip pain rating after preforming MRI with gadolinium arthrography and intra-articular lidocaine Poster No.: C-1352 Congress: ECR 2014 Type: Scientific Exhibit Authors: J. García Yavar, J. Cabezudo, S.
Efficacy of Intra-articular Steroid Injection in Patients with Femoroacetabular Impingement
 Case Report Korean J Pain 1 April; Vol. 6, No. : 1-19 pissn 0-919 eissn 9-069 http://dx.doi.org/10./kjp.1.6..1 Efficacy of Intra-articular Steroid Injection in Patients with Femoroacetabular Impingement
Case Report Korean J Pain 1 April; Vol. 6, No. : 1-19 pissn 0-919 eissn 9-069 http://dx.doi.org/10./kjp.1.6..1 Efficacy of Intra-articular Steroid Injection in Patients with Femoroacetabular Impingement
Treatment Of Heterotopic Ossification After Hip Arthroscopy
 Treatment Of Heterotopic Ossification After Hip Arthroscopy ISHA Annual Scientific Meeting 2012 Boston, MA Crispin Ong MD, Michael Hall MD, Thomas Youm MD Disclosures Consultancy: Arthrex, Depuy Lectures/speakers
Treatment Of Heterotopic Ossification After Hip Arthroscopy ISHA Annual Scientific Meeting 2012 Boston, MA Crispin Ong MD, Michael Hall MD, Thomas Youm MD Disclosures Consultancy: Arthrex, Depuy Lectures/speakers
Thousand Oaks High School AP Research STEM
 Investigating open surgical and arthroscopic surgical treatments and non-surgical alternatives for femoral acetabular impingement and torn acetabular labrum Thousand Oaks High School AP Research STEM 2
Investigating open surgical and arthroscopic surgical treatments and non-surgical alternatives for femoral acetabular impingement and torn acetabular labrum Thousand Oaks High School AP Research STEM 2
Hip Injuries & Arthroscopy in Athletes
 Hip Injuries & Arthroscopy in Athletes John P Salvo, MD Sports Medicine Rothman Institute Philadelphia, PA EATA Annual Meeting January, 2011 Hip Injuries & Arthroscopy in Anatomy History Physical Exam
Hip Injuries & Arthroscopy in Athletes John P Salvo, MD Sports Medicine Rothman Institute Philadelphia, PA EATA Annual Meeting January, 2011 Hip Injuries & Arthroscopy in Anatomy History Physical Exam
Degenerative arthritis of Hip Bone Bangalore. Prof Sharath Rao Head, Dept. of Orthopaedics KMC Manipal
 Degenerative arthritis of Hip Prof Sharath Rao Head, Dept. of Orthopaedics KMC Manipal Hip joint Classical Synovial joint Biomechanics of hip Force coincides with trabecular pattern Hip joint Acetabulum
Degenerative arthritis of Hip Prof Sharath Rao Head, Dept. of Orthopaedics KMC Manipal Hip joint Classical Synovial joint Biomechanics of hip Force coincides with trabecular pattern Hip joint Acetabulum
Discrete mineralisation of the acetabular labrum: a novel marker of femoroacetabular impingement?
 Cite this article as: Cooke WR, Gill HS, Murray DW, Ostlere SJ. Discrete mineralisation of the acetabular labrum: a novel marker of femoroacetabular impingement? Br J Radiol 2013;86:20120182. SHORT COMMUNICATION
Cite this article as: Cooke WR, Gill HS, Murray DW, Ostlere SJ. Discrete mineralisation of the acetabular labrum: a novel marker of femoroacetabular impingement? Br J Radiol 2013;86:20120182. SHORT COMMUNICATION
Approach To The Failed Hip Scope. Disclosures. Who/What is to Blame? 8/10/2016
 Approach To The Failed Hip Scope Michael J. Salata, MD Assistant Professor, CWRU UH Sports Medicine Institute Associate Team Physician, Cleveland Browns Director, Joint Preservation and Cartilage Restoration
Approach To The Failed Hip Scope Michael J. Salata, MD Assistant Professor, CWRU UH Sports Medicine Institute Associate Team Physician, Cleveland Browns Director, Joint Preservation and Cartilage Restoration
Supine and Standing AP Pelvis Radiographs in the Evaluation of Pincer Femoroacetabular Impingement
 Clin Orthop Relat Res (2016) 474:1692 1696 DOI 10.1007/s11999-016-4766-7 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH Supine
Clin Orthop Relat Res (2016) 474:1692 1696 DOI 10.1007/s11999-016-4766-7 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH Supine
Technique for Combined Hip Arthroscopy and Periacetabular Osteotomy for the Patient with Hip Dysplasia and Intraarticular Pathology
 DOJ TECHNICAL REPORT Technique for Combined Hip Arthroscopy and Periacetabular 10.5005/jp-journals-10017-1068 Osteotomy for the Patient Technique for Combined Hip Arthroscopy and Periacetabular Osteotomy
DOJ TECHNICAL REPORT Technique for Combined Hip Arthroscopy and Periacetabular 10.5005/jp-journals-10017-1068 Osteotomy for the Patient Technique for Combined Hip Arthroscopy and Periacetabular Osteotomy
Topic: Femoroacetabular Impingement Surgery Date of Origin: July 1, Section: Surgery Last Reviewed Date: January 2014
 Medical Policy Manual Topic: Femoroacetabular Impingement Surgery Date of Origin: July 1, 2008 Section: Surgery Last Reviewed Date: January 2014 Policy No: 160 Effective Date: April 1, 2014 IMPORTANT REMINDER
Medical Policy Manual Topic: Femoroacetabular Impingement Surgery Date of Origin: July 1, 2008 Section: Surgery Last Reviewed Date: January 2014 Policy No: 160 Effective Date: April 1, 2014 IMPORTANT REMINDER
Fovea Alta on MR Images: Is It a Marker of Hip Dysplasia in Young Adults?
 Musculoskeletal Imaging Original Research Beltran et al. MRI of Fovea Alta Musculoskeletal Imaging Original Research Luis S. Beltran 1 Jason D. Mayo 2 Zehava S. Rosenberg 1 Maria Diaz De Tuesta 3 Olga
Musculoskeletal Imaging Original Research Beltran et al. MRI of Fovea Alta Musculoskeletal Imaging Original Research Luis S. Beltran 1 Jason D. Mayo 2 Zehava S. Rosenberg 1 Maria Diaz De Tuesta 3 Olga
Complex Fractures and Hip Dislocations
 IMAGING OF HIP PAIN Patients may present with acute (< 2 weeks) or chronic hip pain. Acute pain may be related or not related to an acute traumatic event such as fall or trauma from a motor vehicle accident.
IMAGING OF HIP PAIN Patients may present with acute (< 2 weeks) or chronic hip pain. Acute pain may be related or not related to an acute traumatic event such as fall or trauma from a motor vehicle accident.
We have observed damage to the labrum as a
 Femoroacetabular impingement and the cam-effect A MRI-BASED QUANTITATIVE ANATOMICAL STUDY OF THE FEMORAL HEAD-NECK OFFSET K. Ito, M.-A. Minka-II, M. Leunig, S. Werlen, R.Ganz From the AO ASIF Research
Femoroacetabular impingement and the cam-effect A MRI-BASED QUANTITATIVE ANATOMICAL STUDY OF THE FEMORAL HEAD-NECK OFFSET K. Ito, M.-A. Minka-II, M. Leunig, S. Werlen, R.Ganz From the AO ASIF Research
Does Surgical Hip Dislocation and Periacetabular Osteotomy Improve Pain in Patients With Perthes-like Deformities and Acetabular Dysplasia?
 Clin Orthop Relat Res (2015) 473:1370 1377 DOI 10.1007/s11999-014-4115-7 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons SYMPOSIUM: 2014 BERNESE HIP
Clin Orthop Relat Res (2015) 473:1370 1377 DOI 10.1007/s11999-014-4115-7 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons SYMPOSIUM: 2014 BERNESE HIP
CONSERVATIVE MANAGEMENT OF FEMOROACETABULAR IMPINGEMENT
 SPORTS REHABILITATION CONSERVATIVE MANAGEMENT OF FEMOROACETABULAR IMPINGEMENT A case study and rationale for treatment Written by Joanne Kemp and Kay Crossley, Australia BACKGROUND The hip joint and FAI
SPORTS REHABILITATION CONSERVATIVE MANAGEMENT OF FEMOROACETABULAR IMPINGEMENT A case study and rationale for treatment Written by Joanne Kemp and Kay Crossley, Australia BACKGROUND The hip joint and FAI
Residual acetabular dysplasia is considered to be. Evolution of Technique and Indications for the Bernese Periacetabular Osteotomy
 S42 Evolution of Technique and Indications for the Bernese Periacetabular Osteotomy Michael Leunig, M.D., and Reinhold Ganz, M.D. Abstract Acetabular dysplasia is among the most frequent causes of secondary
S42 Evolution of Technique and Indications for the Bernese Periacetabular Osteotomy Michael Leunig, M.D., and Reinhold Ganz, M.D. Abstract Acetabular dysplasia is among the most frequent causes of secondary
Total Hip Arthroplasty Performed Using Conventional and Computer-Assisted, Tissue- Preserving Techniques 6
 Total Hip Arthroplasty Performed Using Conventional and Computer-Assisted, Tissue- Preserving Techniques 6 Stephen B. Murphy, MD, Timo M. Ecker, MD and Moritz Tannast, MD Introduction Less invasive techniques
Total Hip Arthroplasty Performed Using Conventional and Computer-Assisted, Tissue- Preserving Techniques 6 Stephen B. Murphy, MD, Timo M. Ecker, MD and Moritz Tannast, MD Introduction Less invasive techniques
RETROSPECTIVE COMPARATIVE STUDY ABSTRACT INTRODUCTION
 RETROSPECTIVE COMPARATIVE STUDY Concomitant Hip Arthroscopy 10.5005/jp-journals-10017-1083 and Periacetabular Osteotomy Concomitant Hip Arthroscopy and Periacetabular Osteotomy: Is there a Difference in
RETROSPECTIVE COMPARATIVE STUDY Concomitant Hip Arthroscopy 10.5005/jp-journals-10017-1083 and Periacetabular Osteotomy Concomitant Hip Arthroscopy and Periacetabular Osteotomy: Is there a Difference in
What Are the Results of Surgical Treatment of Hip Dysplasia With Concomitant Cam Deformity?
 Clin Orthop Relat Res (2017) 475:1128 1137 DOI 10.1007/s11999-016-5054-2 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons SYMPOSIUM: 2016 BERNESE HIP
Clin Orthop Relat Res (2017) 475:1128 1137 DOI 10.1007/s11999-016-5054-2 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons SYMPOSIUM: 2016 BERNESE HIP
Hip Arthroscopy Indications and Latest Techniques
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/clinicians-roundtable/hip-arthroscopy-indications-and-latesttechniques/3801/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/clinicians-roundtable/hip-arthroscopy-indications-and-latesttechniques/3801/
Subject: Hip Arthroscopy and Open, Non-Arthroplasty Hip Repair
 02-20000-55 Original Effective Date: 10/15/16 Reviewed: 06/28/18 Revised: 07/15/18 Subject: Hip Arthroscopy and Open, Non-Arthroplasty Hip Repair THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION,
02-20000-55 Original Effective Date: 10/15/16 Reviewed: 06/28/18 Revised: 07/15/18 Subject: Hip Arthroscopy and Open, Non-Arthroplasty Hip Repair THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION,
Femoroacetabular Impingement: Saving the Joint
 Thomas Jefferson University Jefferson Digital Commons Department of Orthopaedic Surgery Faculty Papers Department of Orthopaedic Surgery 6-2011 Femoroacetabular Impingement: Saving the Joint Ronald Huang
Thomas Jefferson University Jefferson Digital Commons Department of Orthopaedic Surgery Faculty Papers Department of Orthopaedic Surgery 6-2011 Femoroacetabular Impingement: Saving the Joint Ronald Huang
Hip Center Edge Angle and Alpha Angle Morphological Assessment Using Gait Analysis in Femoroacetabular Impingement
 Hip Center Edge Angle and Alpha Angle Morphological Assessment Using Gait Analysis in Femoroacetabular Impingement Gary J. Farkas, BS 1, Marc Haro, MD 1, Simon Lee, MPH 1, Philip Malloy 2, Alejandro A.
Hip Center Edge Angle and Alpha Angle Morphological Assessment Using Gait Analysis in Femoroacetabular Impingement Gary J. Farkas, BS 1, Marc Haro, MD 1, Simon Lee, MPH 1, Philip Malloy 2, Alejandro A.
THE HIP. Cooler than cool, the pinnacle of what is "it". Beyond all trends and conventional coolness.
 THE HIP Cooler than cool, the pinnacle of what is "it". Beyond all trends and conventional coolness. Objectives Hip anatomy Causes of hip pain Hip exam Anatomy Bones Ilium Anterior Superior Iliac Spine
THE HIP Cooler than cool, the pinnacle of what is "it". Beyond all trends and conventional coolness. Objectives Hip anatomy Causes of hip pain Hip exam Anatomy Bones Ilium Anterior Superior Iliac Spine
