Viable versus frozen meniscus allografts. A clinical and imaging short term evaluation
|
|
|
- Allyson McLaughlin
- 5 years ago
- Views:
Transcription
1 Professional paper/stručni članak Viable versus frozen meniscus allografts. A clinical and imaging short term evaluation Viabilni i smrznuti transplantat meniska. Rana klinička i radiološka evaluacija Jaap van der Maas 1, Pieter Vansintjan 1, Rene Verdonk 2*, Peter Verdonk 3 Abstract. Aim: To perform a clinical and imaging short term evaluation of viable and frozen meniscus allografts. Methods and materials: Between 2005 and 2006, 12 meniscal allograft transplantations were performed in our institution. The study population consisted of 5 men and 7 women with a mean age of 36.4 years (range ). Six patients received a viable allograft and six a deep-frozen one. All allografts were harvested from donors who died after a short disease. All patients were operated with an open surgical technique (medial or lateral arthrotomy) and soft tissue fixation with secure anterior and posterior horn fixation, performed by one senior surgeon. All patients were scored pre-operatively, at 6 weeks, 3 months, 6 months, 1 and 2 years postoperatively. Three questionnaires were used to score the patients clinically (KOOS, modified HSS and SF-36 questionnaire). Every patient received radiographs pre-operatively and at 6 months and 1 year. Results: Clinically, there was no difference in patient self-reported results through questionnaires or in a questionnaire based on clinical examination. There was no significant progress in joint space narrowing on weight bearing and Rosenberg view radiographs. Conclusion: Our results suggest that there are no clinical significant differences between the viable and the deep frozen subgroup after two years. 1 Department of Orthopaedic Surgery & Traumatology, University Hospital Ghent, Ghent, Belgium 2 Department of Orthopaedic Surgery & Traumatology, Jan Palfijn Hospital, Ghent, Belgium 3 Department of Orthopaedic Surgery & Traumatology Monica Ziekenhuizen, Antwerpen, Belgium Received: Accepted: Key words: cartilage; frozen; menisci; transplantation; viable Sažetak. Cilj: Učiniti ranu kliničku i radiološku evaluaciju vijabilnog i smrznutog transplantata meniska. Metoda i materijali: Tijekom i godine, u našoj ustanovi izvedeno je 12 alotransplantacija meniska. U studiju je bilo uključeno 5 muškaraca i 7 žena, s prosječnom dobi od 36,4 godina (raspon od 17,1 do 42,5). U šest pacijenata presađen je vijabilni transplantat, a u šest duboko smrznuti transplantat. Svi transplantati su dobiveni od davatelja koji su umrli nakon kratke bolesti. Svi pacijenti operirani su otvorenim kirurškim zahvatom (medijalna ili lateralna artrotomija), uz fiksaciju mekih tkiva i fiksaciju prednjeg i stražnjeg roga. Svi pacijenti su evaluirani preoperativno, te 6 tjedana, 3 mjeseca, 6 mjeseci, jednu i dvije godine nakon operacije. Za kliničku evaluaciju bolesnika korištena su tri upitnika (KOOS, adaptirani HSS i SF-36 upitnik). Svakom pacijentu je učinjena rendgenska slika preoperativno, nakon 6 mjeseci i nakon jedne godine. Rezultati: Klinički, nije bilo razlika između rezultata koje su bolesnici samostalno naveli u upitnicima i onih dobivenih temeljem kliničkog pregleda. Rendgenska slika po Rosenbergu nije pokazala značajni pomak u suženju zglobne pukotine pod opterećenjem. Zaključak: Naši rezultati ukazuju na to da nakon dvije godine ne postoje klinički značajne razlike između transplantacije vijabilnog i duboko smrznutog transplantata. Ključne riječi: hrskavica; menisci; transplantat; vijabilni; zamrznuti *Corresponding author: Rene Verdonk, MD Department of Orthopaedic Surgery & Traumatology, Jan Palfijn Hospital, Ghent, Belgium rene.verdonk@ugent.be 175
2 INTRODUCTION Ever since Fairbank described the radiographic degenerative evolution of the post-meniscectomized knee in , the functional importance of the meniscus has been more appreciated. Locht et al. performed the first work in meniscal allograft transplantation in the beginning of the eighties with the transplantation of proximal tibial osteochondral grafts in combination with meniscal allograft 2. In 1948 it was Milachowski who performed Study population The study population consisted of 5 men and 7 women with a mean age of 36.4 years (range 17.1 to 42.5). Six patients received a viable and six a deep-frozen allograft. There were eight lateral allografts (5 deep-frozen and 3 viable) and four medial allografts (1 deep-frozen and 3 viable). Seven patients received a concomitant procedure with the meniscal transplantation (microfracture in 5, and a corrective valgus high tibial osteotomy in 3 patients). Meniscal allograft transplantation is a good option in a young, symptomatic, post-meniscectomized knee for pain relief and improvement of function. the first meniscal allograft transplantation in a human being 3. Now there is more and more growing evidence in literature that a meniscal allograft transplantation, given the right indications, results in significant improvements in knee function and pain relief, in the short- as well as in the long term 4-9. Many variables contribute to the result, such as surgical technique and sizing of the allograft, but also the preservation technique of the allografts. The hypothesis was that by keeping the cells viable, they could maintain the extracellular matrix and so the mechanical integrity of the meniscus. METHODS AND MATERIALS Between 2005 and 2006, 12 meniscal allograft transplantations were performed in our institution. The indications for the surgery were: a young, active patient (< 50 years) who sustained a previous total meniscectomy, presenting with (medial or lateral) pain and swelling and unable to perform daily professional activities. The knee should be normally aligned and stable. The contra-indications included progressed articular cartilage damage (> grade III ICRS), degenerative changes on radiographs, malalignment, instability, a history of septic arthritis in the knee and other inflammatory diseases. In case of malalignment or focal cartilage damage, a concomitant procedure was performed (corrective valgus high tibial osteotomy or focal cartilage repair). Meniscal allograft preservation All allografts were harvested from donors who died after a short disease. The maximum age for the donors was set at 45 years. None had received corticosteroids or cytostatic drugs. All grafts were obtained within 24 hours postmortem. The deep-frozen allografts were obtained from the tissue bank of the University Hospital of Ghent after comparative sizing with the acceptor. Sizing was done through radiographs. After graft prelevation in the sterile operating room, it was immediately transported to the tissue bank and conserved at -80 C. After screening for transmittable diseases, the grafts were released from the tissue bank for transplantation. Viable allografts were harvested likewise and immediately conserved in a solution of Dulbecco s Modified Eagle Medium (D-MEM; Gibco Invitrogen, Merelbeke, Belgium) enriched with 20 % of autologous serum from the acceptor which had been obtained before and stored at min 80 C. The graft stayed in this medium for a period of 14 days at 37 C and the medium was replaced every three days in a sterile fashion. During this conservation time, the donor was screened for transmittable diseases 10. Surgical technique All patients were operated with an open surgical technique (medial or lateral arthrotomy) and soft tissue fixation with secure anterior and posterior horn fixation by one senior surgeon (RV) 11. The lateral allograft transplantation was performed through a classic lateral parapatellar arthrotomy (Figure 1). Proximal insertion of the lateral collateral ligament and popliteus tendon were re
3 leased by creating an osteotomy with a curved osteotome (Figure 2). The bone block was fixated with a screw after the transplantation was performed. For the fixation of the graft, first the remaining rim and posterior and anterior horns were trimmed to fit the donor meniscus. This was fixed with non-resorbable Prolene 2/0 sutures every 3 mm from posterior to anterior, and extra horizontal sutures to fixate the posterior and anterior horns (Figure 3). Subsequently, the bone block from the osteotomy was fixated and the arthrotomy closed. The medial allograft transplantation was performed through a classic medial parapatellar arthrotomy of approximately 8 cm (Figure 4). This incision can easily be extended if a concomitant Figure 1. Lateral incision of approximately 8 cm is performed with the knee in 90 of flexion. Figure 2. Curvilinear osteotomy of the proximal insertion of the lateral collateral ligament and popliteus tendon to get better access to the lateral compartment. Figure 3. The allograft is tightly fixed with horizontal, non-resorbable sutures every 3 mm
4 questionnaire is validated in Dutch for the followup of meniscal allograft transplantation. KOOS and SF-36 were filled out by the patient and the modified HSS questionnaire was filled out by an independent orthopedic surgeon after conducting clinical examination in a standardized fashion. Radiological evaluation Figure 4. Medial parapatellar incision of approximately 8 cm, made with the knee in 90 flexion. procedure has to be performed, such as a corrective valgus high tibial osteotomy or an ACL reconstruction. To further open the arthrotomy, a flake osteotomy of the femoral attachment of the medial collateral ligament was performed at the level of the medial femoral epicondyle. Fixation of the allograft was performed in the same fashion as described above for the lateral allograft. The postoperative rehabilitation program consisted of a non-weight-bearing and restricted flexion until 60 for the first three weeks. After that, progressive weight bearing and flexion until 90 was allowed. After six weeks the crutches were progressively removed and full flexion was allowed. Clinical evaluation and follow up All patients were scored pre-operatively, at 6 weeks, 3 months, 6 months, 1 and 2 years postoperatively. Three questionnaires were used to score the patients clinically: the KOOS, the modified HSS and SF-36 questionnaire. The KOOS Every patient received radiographs (AP, PA and full leg) pre-operatively and at 6 months and 1 year. Joint-space narrowing was scored according to the IKDC-classification (Table 1). Each patient also had consecutive MRI s on a 1.5T scanner (Magnetom Symphony or Avanto; Siemens Medical Solutions, Erlangen, Germany) at 6 weeks and 1 year. All examinations were done in 3 mm sagittal slices with proton density and T2 weighted fast spin echo images, followed by 2 mm coronal slices and 3 mm axial slices according to a 3D dual echo steady state sequence for optimal visualization of the menisci and the articular cartilage. Each allograft was scored according to following parameters: signal intensity, ruptures and extrusion 12. The articular cartilage of the femur condyle as well as on the tibial plateau was graded according to Yulish with minor adjustments (Table 2) 13. Statistical analysis Statistical analysis was performed with SPSS v13.0 for Windows XP. First the population was checked with the Shapiro-Wilk test, but this showed no normal distribution. Therefore, further statistical analysis was performed using nonparametric tests. The Mann-Whitney U test was used to show significant differences between the deep frozen and viable group. Comparison of the pre-operative data and the post-operative data was performed using the Wilcoxon Signed Ranks test. Statistical significance was set at P < Table 1. IKDC classification of joint-space narrowing Grade 0 Grade 1 Grade 2 Grade 3 IKDC classification No narrowing of the joint-space < 50 % narrowing > 50 % narrowing Joint space obliteration 178
5 Table 2. Yulish MRI classification of articular cartilage damage MRI Classification of articular cartilage Grade 0 Normal Grade 1 Normal contour ± abnormal signal Grade 2 Superficial fraying: erosion or ulceration of less than 50 % Grade 3 Partial thickness defect of more than 50 % but less than 100 % Grade 4 Full-thickness cartilage loss Clinical outcome RESULTS At first, the deep-frozen and viable subgroup were compared for all the clinical parameters at 6 weeks, 3 months, 6 months, 1 and 2 year postoperatively. Out of a total of 82 parameters, there were 9 statistically significant differences between the two groups at different follow-up times. Because there was no obvious relation between the significantly different parameters, the two groups were considered clinically equal, none of them being superior to the other. Therefore, the entire population was studied as one group for further analysis. The modified HSS score improved for pain, function and range of motion applied after 6 months gave results that were statistically significantly better compared to those at 6 weeks postoperatively. This continued to improve up to year 2, but there was no statistically significant improvement compared to 6 months postop (Table 3, Figure 5). Table 3. Overview of modified HSS scores 6 weeks postoperative compared to 6 months postoperative Modified HSS score (Mean ± SD) 6 weeks 1 year p-value Pain 27.3 ± ± ROM 17.3 ± ± function 33.5 ± ± Figure 5. Evolution of modified HSS scores, comparing 6 weeks post-op to 2 years post-op
6 In the KOOS questionnaire, there was also a statistically significant improvement in the pain and function subscores obtained at 6 months when compared to those measured preoperatively. After one year, the ADL, sport & recreation and quality of life -scores, also improved statistically significantly. After another one year, there was no statistically significant improvement anymore in any of the subscores (Table 4, Figure 6). The SF-36 parameters all improved over time but did not all reach statistically significant improved results after 2 years. There was a trend of declin- Figure 6. Evolution of modhss scores, comparing pre-operative post-op to 1 and 2 years post-op. ADL = activities of daily live, S&R = sports and recreation, QoL = quality of life Table 4. KOOS scores compared preoperative to 1 year post-op. KOOS score (Mean ± SD) pre-operative 1 year p-value pain 52.8 ± ± symptoms 47.3 ± ± ADL 63.4 ± ± S&R 17.3 ± ± QoL 31.3 ± ± ADL = activities of daily live, S&R = sports and recreation, QoL = quality of life Table 5. SF-36 scores compared preoperative to 1 year post-op. SF-36 scores (Mean±SD) pre-operative 1 year p-value PF (physical functioning) 45.1 ± ± RP (role physical) 18.2 ± ± BP (bodily pain) 39.3 ± ± SF (social functioning) 67.2 ± ± MH (mental health) 67.6 ± ± RE (role emotional) 54.5 ± ± VT (vitality) 55.5 ± ± GH (general health) 68.6 ± ± HCLY (health compared to last year) 45.5 ± ±
7 ing scores after 6 weeks, after which they improved (Table 5). Radiological outcome There was no significant decline in the grading of the joint space in all study subjects. In the short term, there was no progressive joint-space narrowing either in the viable or in the deep-frozen group. The images from the MRI were also compared for the viable and deep-frozen subgroups. There was hardly any difference in the signal intensity of all menisci at six weeks post-op and one year postop. There were more tears in the posterior root of the viable menisci (50 %), in contrast to no tears in the deep-frozen subgroup. Meniscal body extrusion was seen in all allografts after one year. After one year, five viable and four deep-frozen allografts presented complete extrusion, and one viable and two deep-frozen were partially extruded. The status of the articular cartilage remained constant over 1 year in both subgroups. DISCUSSION Since the first meniscal allograft transplantation in 1984 by Milachowski 3, there have been numerous studies in search of the perfect conservation technique. At the end of the eighties, the philosophy to start using viable allografts emerged in the University Hospital of Ghent. The hypothesis was that by keeping the cells viable, they could maintain the extracellular matrix and so the mechanical integrity of the meniscus. Earlier studies showed that long-term survival of the viable meniscal allograft transplants was excellent with good results in 70 % of cases after 10 years 5. This is comparable to other published data using deep-frozen and cryopreserved allografts 4,7,8. This study was conducted to see if these results would be noticed also in the short term because this had not been investigated before. After two years, no group proved to be superior to the other clinically or radiologically. This was expected, given the small population and the short-term follow-up. Because there is not enough weight in this study, the results need to be interpreted with caution. A second remark refers to the interpretation of the incorporation and survival of the graft with MRI. Evaluation with arthroscopy and biopsies with histological analysis of the cellularity and ingrowth would be more ideal, but are not easy to obtain. In a recent study 14 comparing both viable and fresh frozen meniscal allografts, evidence of both fibroblasts and fibrochondrocytes was found in all specimen types. Specifically, the main cell type seen was a fibrochondroblast in both allograft types. However, it has been noted that there is no unique cell-specific marker for meniscal cells. In the short term, there are no statistical differences in clinical or radiological outcomes between viable or deep-frozen allografts. Identifying the exact phenotype of the re-populating cells requires analysis of the RNA produced by these cells in comparison with the RNA produced by normal meniscal fibrochondrocytes 15. In the same study, when cell density is considered, the density seen in the central area of biopsies from deep-frozen allografts was significantly lower than that seen in viable allografts. This result is reflected in the data from previous reports on deep-frozen allografts, where repopulation was limited to the superficial zone, while the core of the transplant remained acellular 16. This may relate to the processing of the deep frozen allografts, with the resulting loss of cells. CONCLUSION In conclusion, these results suggest that there are no clinical significant differences between the viable and the deep-frozen subgroups after two years. Clinically, there was no difference between the results self-reported by patients in questionnaires and those based on clinical examination. The results for both groups after two years showed a statistically significant improvement in pain scores and function, as well as in the range of motion. This finding is in positive contrast with microscopic evidence suggesting obvious depletion of viable cells in the core of the meniscal body in case of deep-freezing preservation
8 However this does not seem to be illustrated in clinical findings in the short term (min 2 y FU). There was no significant progress in the joint space narrowing on weight bearing or on Rosenberg view radiographs. MRI also showed some extrusion of all allografts after 2 years, but no difference between the two subgroups. Articular cartilage in the affected compartment minimally declined on MRI in both groups after two years. The higher tearing rate in the viable subgroup should be interpreted with caution because of the small size of the subgroups, and the fact that it was not reflected in the clinical outcome. In the future, further studies with biopsies are needed to elucidate the biological histological fate of both viable and deep-frozen allografts. Standardized, longer-term follow-up is mandatory if clinical or radiological differences appear in the long term. Conflicts of interest statement: The authors report no conflicts of interest. references 1. Fairbank TJ. Knee joint changes after meniscectomy. J Bone Joint Surg Br 1948;30B: Locht RC, Gross AE, Langer F. Late osteochondral resurfacing for tibial plateau fractures. J Bone Joint Surg Am 1984;66: Wirth CJ, Milachowski KA, Weismeier K. Meniscus transplantation in animal experiments and initial clinical results. Z Orthop Ihre Grenzgeb 1986;124: Saltzman BM, Bajaj S, Salata M, Daley EL, Strauss E, Verma N et al. Prospective long-term evaluation of meniscal allograft transplantation procedure: a minimum of 7-year follow-up. J Knee Surg 2012;25: Verdonk PC, Demurie A, Almqvist KF, Veys EM, Verbruggen G, Verdonk R. Transplantation of viable meniscal allograft. Survivorship analysis and clinical outcome of one hundred cases. J Bone Joint Surg Am 2005;87: Verdonk PC, Verstraete KL, Almqvist KF, De Cuyper K, Veys EM, Verbruggen G et al. Meniscal allograft transplantation: long-term clinical results with radiological and magnetic resonance imaging correlations. Knee Surg Sports Traumatol Arthrosc 2006;14: von Lewinski G, Milachowski KA, Weismeier K, Kohn D, Wirth CJ. Twenty-year results of combined meniscal allograft transplantation, anterior cruciate ligament reconstruction and advancement of the medial collateral ligament. Knee Surg Sports Traumatol Arthrosc 2007;15: Vundelinckx B, Vanlauwe J, Bellemans J. Long-term Subjective, Clinical, and Radiographic Outcome Evaluation of Meniscal Allograft Transplantation in the Knee. Am J Sports Med. 2014;42: Wirth CJ, Peters G, Milachowski KA, Weismeier KG, Kohn D. Long-term results of meniscal allograft transplantation. Am J Sports Med 2002;30: Verdonk R, Kohn D. Harvest and conservation of meniscal allografts. Scand J Med Sci Sports 1999;9: Verdonk PC, Demurie A, Almqvist KF, Veys EM, Verbruggen G, Verdonk R. Transplantation of viable meniscal allograft. Surgical technique. J Bone Joint Surg Am 2006;88 Suppl 1 Pt 1: Verdonk P, Depaepe Y, Desmyter S, De Muynck M, Almqvist KF, Verstraete K et al. Normal and transplanted lateral knee menisci: evaluation of extrusion using magnetic resonance imaging and ultrasound. Knee Surg Sports Traumatol Arthrosc 2004;12: Yulish BS, Montanez J, Goodfellow DB, Bryan PJ, Mulopulos GP, Modic MT. Chondromalacia patellae: assessment with MR imaging. Radiology 1987;164: Moran CJ, Atmaca S, Declercq HA, Cornelissen MJ, Verdonk PC. Cell distribution and regenerative activity following meniscus replacement. Int Orthop 2014;38: Rodeo SA, Seneviratne A, Suzuki K, Felker K, Wickiewicz TL, Warren RF. Histological analysis of human meniscal allografts. A preliminary report. J Bone Joint Surg Am 2000;82-A: Hutchinson ID, Moran CJ, Potter HG, Warren RF, Rodeo SA. Restoration of the meniscus: form and function. Am J Sports Med 2014;42:
Outcome after meniscectomy? Val D Isere 2014 update
 Outcome after meniscectomy? Val D Isere 2014 update Meniscus Allograft Transplantation and New Options by Peter Verdonk, MD, PhD Department of Orthopaedic Surgery, Monica Hospitals, Antwerp, Belgium Peter
Outcome after meniscectomy? Val D Isere 2014 update Meniscus Allograft Transplantation and New Options by Peter Verdonk, MD, PhD Department of Orthopaedic Surgery, Monica Hospitals, Antwerp, Belgium Peter
Meniscal Allografts and Collagen Meniscus Implants. Original Policy Date
 MP 7.01.11 Meniscal Allografts and Collagen Meniscus Implants Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return
MP 7.01.11 Meniscal Allografts and Collagen Meniscus Implants Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return
Meniscal Tears/Deficiency in Athletes
 Meniscal Tears/Deficiency in Athletes A. Amendola MD Professor of Orthopaedic Surgery Director of Sports Medicine Duke University 1 2 Meniscal tears Introduction Meniscal tears are one of the most frequent
Meniscal Tears/Deficiency in Athletes A. Amendola MD Professor of Orthopaedic Surgery Director of Sports Medicine Duke University 1 2 Meniscal tears Introduction Meniscal tears are one of the most frequent
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries
 What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT
 OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
Survivorship After Meniscal Allograft Transplantation According To Articular Cartilage Status
 # 154134 Survivorship After Meniscal Allograft Transplantation According To Articular Cartilage Status Jun-Gu Park, Seong-Il Bin, Jong-Min Kim, Bum Sik Lee Department of Orthopaedic Surgery, Asan Medical
# 154134 Survivorship After Meniscal Allograft Transplantation According To Articular Cartilage Status Jun-Gu Park, Seong-Il Bin, Jong-Min Kim, Bum Sik Lee Department of Orthopaedic Surgery, Asan Medical
Cartilage Repair Center Brigham and Women s Hospital Harvard Medical School
 Brigham and Women s Hospital Harvard Medical School Safety, feasibility, and radiographic outcomes of the anterior meniscal takedown technique to approach chondral defects on the tibia and posterior femoral
Brigham and Women s Hospital Harvard Medical School Safety, feasibility, and radiographic outcomes of the anterior meniscal takedown technique to approach chondral defects on the tibia and posterior femoral
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
TREATMENT OF CARTILAGE LESIONS
 TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
Meniscus cartilage replacement with cadaveric
 Technical Note Meniscal Allografting: The Three-Tunnel Technique Kevin R. Stone, M.D., and Ann W. Walgenbach, R.N.N.P., M.S.N. Abstract: This technical note describes an improved arthroscopic technique
Technical Note Meniscal Allografting: The Three-Tunnel Technique Kevin R. Stone, M.D., and Ann W. Walgenbach, R.N.N.P., M.S.N. Abstract: This technical note describes an improved arthroscopic technique
Original Report. The Reverse Segond Fracture: Association with a Tear of the Posterior Cruciate Ligament and Medial Meniscus
 Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Meniscal Allograft Transplantation Without Bone Blocks: A 5- to 8-Year Follow-Up of 33 Patients
 Meniscal Allograft Transplantation Without Bone Blocks: A 5- to 8-Year Follow-Up of 33 Patients Gemma González-Lucena, M.D., Pablo Eduardo Gelber, M.D., Ph.D., Xavier Pelfort, M.D., Marc Tey, M.D., and
Meniscal Allograft Transplantation Without Bone Blocks: A 5- to 8-Year Follow-Up of 33 Patients Gemma González-Lucena, M.D., Pablo Eduardo Gelber, M.D., Ph.D., Xavier Pelfort, M.D., Marc Tey, M.D., and
Anterior Cruciate Ligament (ACL) Injuries
 Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Clinical Application of Scaffolds for Partial Meniscus Replacement
 1 Clinical Application of Scaffolds for Partial Meniscus Replacement 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 Cathal&J.&Moran,&MD,&FRCS(Orth)& 1,&Daniel&P&Withers&MB,&FRCS&(Orth)&
1 Clinical Application of Scaffolds for Partial Meniscus Replacement 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 Cathal&J.&Moran,&MD,&FRCS(Orth)& 1,&Daniel&P&Withers&MB,&FRCS&(Orth)&
Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes
 Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes William M Weiss, MD MSc FRCSC Orthopedic Surgery & Rehabilitation Sports Medicine, Arthroscopy & Extremity Reconstruction
Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes William M Weiss, MD MSc FRCSC Orthopedic Surgery & Rehabilitation Sports Medicine, Arthroscopy & Extremity Reconstruction
Joint Preservation Clinical Case
 Joint Preservation Clinical Case Jason M. Scopp, M.D. Director of Joint Preservation Peninsula Orthopaedic Associates, 1/19/19 Rational Rationale There are no absolutes. There is no dogma. Organize thoughts,
Joint Preservation Clinical Case Jason M. Scopp, M.D. Director of Joint Preservation Peninsula Orthopaedic Associates, 1/19/19 Rational Rationale There are no absolutes. There is no dogma. Organize thoughts,
Meniscal Root Tears: Evaluation, Imaging, and Repair Techniques
 Meniscal Root Tears: Evaluation, Imaging, and Repair Techniques R O B E R T N A S C I M E N TO, M D, M S C H I E F OF S P O RT S M E D I C I N E & SH O U L D E R S U R G E RY N E W TO N- W E L L E S L
Meniscal Root Tears: Evaluation, Imaging, and Repair Techniques R O B E R T N A S C I M E N TO, M D, M S C H I E F OF S P O RT S M E D I C I N E & SH O U L D E R S U R G E RY N E W TO N- W E L L E S L
MENISCUS IMPLANT AND ALLOGRAFT
 MENISCUS IMPLANT AND ALLOGRAFT UnitedHealthcare Commercial Medical Policy Policy Number: SUR063 Effective Date: January 1, 2019 Table of Contents Page COVERAGE RATIONALE... 1 APPLICABLE CODES... 1 DESCRIPTION
MENISCUS IMPLANT AND ALLOGRAFT UnitedHealthcare Commercial Medical Policy Policy Number: SUR063 Effective Date: January 1, 2019 Table of Contents Page COVERAGE RATIONALE... 1 APPLICABLE CODES... 1 DESCRIPTION
TABLE E-1 Search Terms and Number of Resulting PubMed Search Results* Sear Search Terms
 Moksnes eappendix Page 1 of 15 TABLE E-1 Search Terms and Number of Resulting PubMed Search Results* Sear ch Search Terms No. of Studies #1 Anterior cruciate ligament [MeSH] 7768 #2 Child [MeSH] 1,371,559
Moksnes eappendix Page 1 of 15 TABLE E-1 Search Terms and Number of Resulting PubMed Search Results* Sear ch Search Terms No. of Studies #1 Anterior cruciate ligament [MeSH] 7768 #2 Child [MeSH] 1,371,559
Lateral Location of the Tibial Tunnel Increases Lateral Meniscal Extrusion After Anatomical Single Bundle Anterior Cruciate Ligament Reconstruction
 Lateral Location of the Tibial Tunnel Increases Lateral Meniscal Extrusion After Anatomical Single Bundle Anterior Cruciate Ligament Reconstruction Takeshi Oshima Samuel Grasso David A. Parker Sydney Orthopaedic
Lateral Location of the Tibial Tunnel Increases Lateral Meniscal Extrusion After Anatomical Single Bundle Anterior Cruciate Ligament Reconstruction Takeshi Oshima Samuel Grasso David A. Parker Sydney Orthopaedic
Life. Uncompromised. The KineSpring Knee Implant System Surgeon Handout
 Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: meniscal_allografts_and_other_meniscal_implants 9/1993 6/2018 6/2019 6/2018 Description of Procedure or Service
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: meniscal_allografts_and_other_meniscal_implants 9/1993 6/2018 6/2019 6/2018 Description of Procedure or Service
Lateral ligament injuries of the knee
 Knee Surg, Sports Traumatol, Arthrosc (1998) 6:21 25 KNEE Springer-Verlag 1998 Y. Krukhaug A. Mølster A. Rodt T. Strand Lateral ligament injuries of the knee Received: 22 January 1997 Accepted: 20 June
Knee Surg, Sports Traumatol, Arthrosc (1998) 6:21 25 KNEE Springer-Verlag 1998 Y. Krukhaug A. Mølster A. Rodt T. Strand Lateral ligament injuries of the knee Received: 22 January 1997 Accepted: 20 June
Meniscal Allografts and Other Meniscal Implants. Populations Interventions Comparators Outcomes Individuals: Who are undergoing partial meniscectomy
 Protocol Meniscal Allografts and Other Meniscal Implants (70115) Medical Benefit Effective Date: 01/01/14 Next Review Date: 09/18 Preauthorization No Review Dates: 02/07, 02/08, 03/09, 01/10, 01/11, 01/12,
Protocol Meniscal Allografts and Other Meniscal Implants (70115) Medical Benefit Effective Date: 01/01/14 Next Review Date: 09/18 Preauthorization No Review Dates: 02/07, 02/08, 03/09, 01/10, 01/11, 01/12,
Knee MRI Update Case Review 2009 Russell C. Fritz, M.D. National Orthopedic Imaging Associates San Francisco, CA
 Knee MRI Update Case Review 2009 Russell C. Fritz, M.D. National Orthopedic Imaging Associates San Francisco, CA Meniscal Tears -linear increased signal extending to an articular surface is the hallmark
Knee MRI Update Case Review 2009 Russell C. Fritz, M.D. National Orthopedic Imaging Associates San Francisco, CA Meniscal Tears -linear increased signal extending to an articular surface is the hallmark
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Meniscus Reconstruction: Trough Surgical Technique
 Meniscus Reconstruction: Trough Surgical Technique Technique Consultant Jeffrey L. Halbrecht, M.D. San Francisco, CA ABOUT THE TROUGH TECHNIQUE The trough technique for meniscal allograft reconstruction
Meniscus Reconstruction: Trough Surgical Technique Technique Consultant Jeffrey L. Halbrecht, M.D. San Francisco, CA ABOUT THE TROUGH TECHNIQUE The trough technique for meniscal allograft reconstruction
IKDC DEMOGRAPHIC FORM
 IKDC DEMOGRAPHIC FORM Your Full Name Your Date of Birth / / Your Social Security Number - - Your Gender: Male Female Occupation Today s Date / / The following is a list of common health problems. Please
IKDC DEMOGRAPHIC FORM Your Full Name Your Date of Birth / / Your Social Security Number - - Your Gender: Male Female Occupation Today s Date / / The following is a list of common health problems. Please
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of partial replacement of the meniscus of the knee using a biodegradable scaffold
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of partial replacement of the meniscus of the knee using a biodegradable scaffold
All-Soft Tissue Quadriceps Tendon Autograft for Anterior Cruciate Ligament Reconstruction: Short to Intermediate-Term Clinical Outcomes
 All-Soft Tissue Quadriceps Tendon Autograft for Anterior Cruciate Ligament Reconstruction: Short to Intermediate-Term Clinical Outcomes William Godfrey, BS Aaron Gebrelul, BA; John Xerogeanes, MD; Ajay
All-Soft Tissue Quadriceps Tendon Autograft for Anterior Cruciate Ligament Reconstruction: Short to Intermediate-Term Clinical Outcomes William Godfrey, BS Aaron Gebrelul, BA; John Xerogeanes, MD; Ajay
BASELINE QUESTIONNAIRE (SURGEON)
 SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
PATIENT GUIDE TO CARTILAGE INJURIES
 Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
The American Journal of Sports Medicine
 The American Journal of Sports Medicine http://ajs.sagepub.com/ Long-term Survivorship and Function of Meniscus Transplantation Frank R. Noyes and Sue D. Barber-Westin Am J Sports Med 2016 44: 2330 originally
The American Journal of Sports Medicine http://ajs.sagepub.com/ Long-term Survivorship and Function of Meniscus Transplantation Frank R. Noyes and Sue D. Barber-Westin Am J Sports Med 2016 44: 2330 originally
ASSESSMENT AND MANAGEMENT OF THE KNEE AND LOWER LIMB.
 ASSESSMENT AND MANAGEMENT OF THE KNEE AND LOWER LIMB www.fisiokinesiterapia.biz Overview History Examination X-rays Fractures and Dislocations. Soft Tissue Injuries Other Knee/Lower limb Problems Anatomy
ASSESSMENT AND MANAGEMENT OF THE KNEE AND LOWER LIMB www.fisiokinesiterapia.biz Overview History Examination X-rays Fractures and Dislocations. Soft Tissue Injuries Other Knee/Lower limb Problems Anatomy
Assessment of the Knee Articular Cartilage through MRI-T2 Mapping at Five Year Follow-Up of Meniscal Allograft Transplantation
 Assessment of the Knee Articular Cartilage through MRI-T2 Mapping at Five Year Follow-Up of Meniscal Allograft Transplantation Luis T. Llano-Rodriguez, MD, Mexico City, MEXICO Francisco Cruz-Lopez, Mexico
Assessment of the Knee Articular Cartilage through MRI-T2 Mapping at Five Year Follow-Up of Meniscal Allograft Transplantation Luis T. Llano-Rodriguez, MD, Mexico City, MEXICO Francisco Cruz-Lopez, Mexico
The influence of preserving Infrapatellar fatpad in ACL reconstruction
 The influence of preserving Infrapatellar fatpad in ACL reconstruction Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1) Department of Orthopaedic Surgery,
The influence of preserving Infrapatellar fatpad in ACL reconstruction Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1) Department of Orthopaedic Surgery,
evicore MSK joint surgery procedures requiring prior authorization
 evicore MSK joint surgery procedures requiring prior authorization Moda Health Commercial Group and Individual Members* Updated 1/30/2018 *Check EBT to verify member enrollment in evicore program Radiology
evicore MSK joint surgery procedures requiring prior authorization Moda Health Commercial Group and Individual Members* Updated 1/30/2018 *Check EBT to verify member enrollment in evicore program Radiology
ACL AND PCL INJURIES OF THE KNEE JOINT
 ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
American Journal of Sports Medicine
 American Journal of Sports Medicine http://ajs.sagepub.com Prospective Evaluation of Concurrent Meniscus Transplantation and Articular Cartilage Repair: Minimum 2-Year Follow-Up LCDR John-Paul H. Rue,
American Journal of Sports Medicine http://ajs.sagepub.com Prospective Evaluation of Concurrent Meniscus Transplantation and Articular Cartilage Repair: Minimum 2-Year Follow-Up LCDR John-Paul H. Rue,
Articular Cartilage Surgical Restoration Options
 Articular Cartilage Surgical Restoration Options Randy Schwartzberg, M.D. Assistant Professor - UCF College of Medicine Rationale Our bodies do not make articular/hyaline cartilage. gics injections to
Articular Cartilage Surgical Restoration Options Randy Schwartzberg, M.D. Assistant Professor - UCF College of Medicine Rationale Our bodies do not make articular/hyaline cartilage. gics injections to
What s your diagnosis?
 Case Study 58 A 61-year-old truck driver man presented with a valgus injury to the left knee joint when involved in a truck accident. What s your diagnosis? Diagnosis : Avulsion of Deep MCL The medial
Case Study 58 A 61-year-old truck driver man presented with a valgus injury to the left knee joint when involved in a truck accident. What s your diagnosis? Diagnosis : Avulsion of Deep MCL The medial
Medical Diagnosis for Michael s Knee
 Medical Diagnosis for Michael s Knee Introduction The following report mainly concerns the diagnosis and treatment of the patient, Michael. Given that Michael s clinical problem surrounds an injury about
Medical Diagnosis for Michael s Knee Introduction The following report mainly concerns the diagnosis and treatment of the patient, Michael. Given that Michael s clinical problem surrounds an injury about
ACL RECONSTRUCTION HAMSTRING METHOD. Presents ACL RECONSTRUCTION HAMSTRING METHOD. Multimedia Health Education
 HAMSTRING METHOD Presents HAMSTRING METHOD Multimedia Health Education Disclaimer Stephen J. Incavo MD This movie is an educational resource only and should not be used to make a decision on Anterior Cruciate
HAMSTRING METHOD Presents HAMSTRING METHOD Multimedia Health Education Disclaimer Stephen J. Incavo MD This movie is an educational resource only and should not be used to make a decision on Anterior Cruciate
Meniscal Allograft Transplantation in the Adolescent Population
 Meniscal Allograft Transplantation in the Adolescent Population Jonathan C. Riboh, M.D., Annemarie K. Tilton, B.S., Gregory L. Cvetanovich, M.D., Kirk A. Campbell, M.D., and Brian J. Cole, M.D., M.B.A.
Meniscal Allograft Transplantation in the Adolescent Population Jonathan C. Riboh, M.D., Annemarie K. Tilton, B.S., Gregory L. Cvetanovich, M.D., Kirk A. Campbell, M.D., and Brian J. Cole, M.D., M.B.A.
Epidemiology. Meniscal Injury & Repair. Meniscus Anatomy. Meniscus Anatomy
 Epidemiology 60-70/100,000 per year Meniscal Injury & Repair Arthroscopic Mensiscectomy One of the most common orthopaedic procedures 20% of all surgeries at some centers Male:Female ratio - 2-4:1 Younger
Epidemiology 60-70/100,000 per year Meniscal Injury & Repair Arthroscopic Mensiscectomy One of the most common orthopaedic procedures 20% of all surgeries at some centers Male:Female ratio - 2-4:1 Younger
2012 Meniscus Transplantation Study Group Tuesday, February 7, :00 3:30 PM
 2012 Meniscus Transplantation Study Group Tuesday, February 7, 2012 1:00 3:30 PM W Hotel, Industry Room 181 Third Street, San Francisco, CA 94103 At the 2012 AAOS Annual Meeting Meeting Agenda: INTRODUCTION:
2012 Meniscus Transplantation Study Group Tuesday, February 7, 2012 1:00 3:30 PM W Hotel, Industry Room 181 Third Street, San Francisco, CA 94103 At the 2012 AAOS Annual Meeting Meeting Agenda: INTRODUCTION:
Rehab Considerations: Meniscus
 Rehab Considerations: Meniscus Steve Cox, PT, DPT Department of Orthopaedics School of Medicine University of Texas Health Science Center at San Antonio 1 -Anatomy/ Function/ Injuries -Treatment Options
Rehab Considerations: Meniscus Steve Cox, PT, DPT Department of Orthopaedics School of Medicine University of Texas Health Science Center at San Antonio 1 -Anatomy/ Function/ Injuries -Treatment Options
Differential Diagnosis
 Case 31yo M who sustained an injury to L knee while playing Basketball approximately 2 weeks ago. He describes pivoting and hyperextending his knee, which swelled over the next few days. He now presents
Case 31yo M who sustained an injury to L knee while playing Basketball approximately 2 weeks ago. He describes pivoting and hyperextending his knee, which swelled over the next few days. He now presents
In-vivo Evaluation Of The Kinematic Behavior Of An Artificial Medial Meniscus Implant: A Pilot Study Using Open-mri
 In-vivo Evaluation Of The Kinematic Behavior Of An Artificial Medial Meniscus Implant: A Pilot Study Using Open-mri Tineke De Coninck, MD 1, Jonathan J. Elsner, PhD 2, Maoz Shemesh, MSc 2, Michiel Cromheecke,
In-vivo Evaluation Of The Kinematic Behavior Of An Artificial Medial Meniscus Implant: A Pilot Study Using Open-mri Tineke De Coninck, MD 1, Jonathan J. Elsner, PhD 2, Maoz Shemesh, MSc 2, Michiel Cromheecke,
NEW DEVELOPMENTS IN MENISCAL SURGERY
 NEW DEVELOPMENTS IN MENISCAL SURGERY Written by Peter Verdonk, Belgium and Francesco Perdisa, Italy Meniscectomy is one of the most common procedures in orthopaedic surgery, capable of returning the knee
NEW DEVELOPMENTS IN MENISCAL SURGERY Written by Peter Verdonk, Belgium and Francesco Perdisa, Italy Meniscectomy is one of the most common procedures in orthopaedic surgery, capable of returning the knee
Japan Journal of Medicine 2018; 1(3): doi: /jjm
 Jpn J Med 2018,1:3 175 Japan Journal of Medicine 2018; 1(3): 175 182. doi: 10.31488/jjm.1000114 Mini Review Meniscal allograft transplantation, still unaccepted treatment option in Japan? review Yuji Uchio*
Jpn J Med 2018,1:3 175 Japan Journal of Medicine 2018; 1(3): 175 182. doi: 10.31488/jjm.1000114 Mini Review Meniscal allograft transplantation, still unaccepted treatment option in Japan? review Yuji Uchio*
Anterior Cruciate Ligament Injuries
 Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
Your Practice Online
 Your Practice Online Disclaimer P R E S E N T S - PATELLAR TENDON This movie is an educational resource only and should not be used to make a decision on Anterior Cruciate Ligament (ACL) Reconstruction.
Your Practice Online Disclaimer P R E S E N T S - PATELLAR TENDON This movie is an educational resource only and should not be used to make a decision on Anterior Cruciate Ligament (ACL) Reconstruction.
MCL Injuries: When and How to Repair Scott D. Mair, MD
 MCL Injuries: When and How to Repair Scott D. Mair, MD Professor and Team Physician: Orthopaedic Surgery University of Kentucky School of Medicine Disclosure Institution: Research/Education Smith-Nephew
MCL Injuries: When and How to Repair Scott D. Mair, MD Professor and Team Physician: Orthopaedic Surgery University of Kentucky School of Medicine Disclosure Institution: Research/Education Smith-Nephew
Torn ACL - Anatomic Footprint ACL Reconstruction
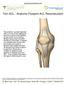 Torn ACL - Anatomic Footprint ACL Reconstruction The anterior cruciate ligament (ACL) is one of four ligaments that are crucial to the stability of your knee. It is a strong fibrous tissue that connects
Torn ACL - Anatomic Footprint ACL Reconstruction The anterior cruciate ligament (ACL) is one of four ligaments that are crucial to the stability of your knee. It is a strong fibrous tissue that connects
Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells,
 What is a Stem Cell? Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells, and so on. These cells can replicate more of their own kind of cell, but they cannot
What is a Stem Cell? Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells, and so on. These cells can replicate more of their own kind of cell, but they cannot
ORIGINAL ARTICLE. ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel
 ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel 1. Associate Professor, Department of Radiodiagnosis & imaging, Bharati Vidyapeeth Medical College and
ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel 1. Associate Professor, Department of Radiodiagnosis & imaging, Bharati Vidyapeeth Medical College and
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping
 Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
Evaluation & Treatment of the Injured Athlete Autograft OATS versus Osteochondral Allograft Technique: Indications, Problems, Outcomes
 Evaluation & Treatment of the Injured Athlete Autograft OATS versus Osteochondral Allograft Technique: Indications, Problems, Outcomes C H R I S T I A N L AT T E R M A N N C H I E F O F S P O R T S M E
Evaluation & Treatment of the Injured Athlete Autograft OATS versus Osteochondral Allograft Technique: Indications, Problems, Outcomes C H R I S T I A N L AT T E R M A N N C H I E F O F S P O R T S M E
Osteochondritis Dissecans
 Osteochondritis Dissecans Introduction Osteochondritis dissecans (OCD) is a problem that affects the knee, mostly at the end of the big bone of the thigh (the femur). A joint surface damaged by OCD doesn't
Osteochondritis Dissecans Introduction Osteochondritis dissecans (OCD) is a problem that affects the knee, mostly at the end of the big bone of the thigh (the femur). A joint surface damaged by OCD doesn't
ANTERIOR CRUCIATE LIGAMENT INJURY
 ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
Imaging the Athlete s Knee. Peter Lowry, MD Musculoskeletal Radiology University of Colorado
 Imaging the Athlete s Knee Peter Lowry, MD Musculoskeletal Radiology University of Colorado None Disclosures Knee Imaging: Radiographs Can be performed weight-bearing or non-weight-bearing View options
Imaging the Athlete s Knee Peter Lowry, MD Musculoskeletal Radiology University of Colorado None Disclosures Knee Imaging: Radiographs Can be performed weight-bearing or non-weight-bearing View options
Systematic Review. Meniscal Allograft Transplantation. David Hergan, M.D., David Thut, M.D., Orrin Sherman, M.D., and Michael S. Day, M.Phil.
 Systematic Review Meniscal Allograft Transplantation David Hergan, M.D., David Thut, M.D., Orrin Sherman, M.D., and Michael S. Day, M.Phil. Purpose: Meniscal allograft transplantation (MAT) has become
Systematic Review Meniscal Allograft Transplantation David Hergan, M.D., David Thut, M.D., Orrin Sherman, M.D., and Michael S. Day, M.Phil. Purpose: Meniscal allograft transplantation (MAT) has become
Meniscal Allografts & Cartilage Surgery in ACL revision surgery
 Meniscal Allografts & Cartilage Surgery in ACL revision surgery Peter Verdonk, MD, PhD Department of Orthopaedic Surgery, Ghent University Hospital, Belgium 1 Introduction Outcome after ACL reconstruction
Meniscal Allografts & Cartilage Surgery in ACL revision surgery Peter Verdonk, MD, PhD Department of Orthopaedic Surgery, Ghent University Hospital, Belgium 1 Introduction Outcome after ACL reconstruction
MRI KNEE WHAT TO SEE. Dr. SHEKHAR SRIVASTAV. Sr.Consultant KNEE & SHOULDER ARTHROSCOPY
 MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
BAD RESULTS OF CONSERVATIVE TREATMENT OF ACL TEARS IN CHILDREN. Guy BELLIER PARIS France
 BAD RESULTS OF CONSERVATIVE TREATMENT OF ACL TEARS IN CHILDREN Guy BELLIER PARIS France TREATMENT OF ACL TEARS IN CHILDREN CONTROVERSIAL DIAGNOSIS clinical exam X-rays (stress) M.R.I. arthroscopy ACL TEARS
BAD RESULTS OF CONSERVATIVE TREATMENT OF ACL TEARS IN CHILDREN Guy BELLIER PARIS France TREATMENT OF ACL TEARS IN CHILDREN CONTROVERSIAL DIAGNOSIS clinical exam X-rays (stress) M.R.I. arthroscopy ACL TEARS
Meniscal Root Tears: A Silent Epidemic
 Meniscal Root Tears: A Silent Epidemic TRIA Orthopedic and Sports Medicine Conference February 9 th, 2018 Robert F. LaPrade, M.D., Ph.D. Chief Medical Officer Steadman Philippon Research Institute Co-Director,
Meniscal Root Tears: A Silent Epidemic TRIA Orthopedic and Sports Medicine Conference February 9 th, 2018 Robert F. LaPrade, M.D., Ph.D. Chief Medical Officer Steadman Philippon Research Institute Co-Director,
Overview Ligament Injuries. Anatomy. Epidemiology Very commonly injured joint. ACL Injury 20/06/2016. Meniscus Tears. Patellofemoral Problems
 Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
Articular cartilage repair using collagen type I hydrogels Clincal results
 Articular cartilage repair using collagen type I hydrogels Clincal results Ulrich Nöth, MD Department of Orthopaedic Surgery, König-Ludwig-Haus University of Würzburg, Germany Orthopädisches Zentrum für
Articular cartilage repair using collagen type I hydrogels Clincal results Ulrich Nöth, MD Department of Orthopaedic Surgery, König-Ludwig-Haus University of Würzburg, Germany Orthopädisches Zentrum für
Medial Meniscal Root Tears: When to rehab? When to repair? When to debride. Christopher Betz, DO Orthopedics Sports Medicine Bristol, CT
 Medial Meniscal Root Tears: When to rehab? When to repair? When to debride Christopher Betz, DO Orthopedics Sports Medicine Bristol, CT Disclosure Consultant Mitek Smith and Nephew-biologic patch Good
Medial Meniscal Root Tears: When to rehab? When to repair? When to debride Christopher Betz, DO Orthopedics Sports Medicine Bristol, CT Disclosure Consultant Mitek Smith and Nephew-biologic patch Good
3/13/2018. Cartilage Cases. Case. Physical exam
 Cartilage Cases Aaron J. Krych, MD Professor, Orthopedic Surgery Sports Medicine Fellowship Director Sports Medicine Research Fellowship Director Mayo Clinic 2014 MFMER slide-1 Case 19 yo F division I
Cartilage Cases Aaron J. Krych, MD Professor, Orthopedic Surgery Sports Medicine Fellowship Director Sports Medicine Research Fellowship Director Mayo Clinic 2014 MFMER slide-1 Case 19 yo F division I
Meniscus Transplantation
 Chapter 18 Meniscus Transplantation Introduction Any significant loss of meniscal function through injury or menisectomy alters the biomechanical and biological environment of the normal knee, eventually
Chapter 18 Meniscus Transplantation Introduction Any significant loss of meniscal function through injury or menisectomy alters the biomechanical and biological environment of the normal knee, eventually
Anterolateral Ligament. Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine
 Anterolateral Ligament Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine What in the world? TIME magazine in November 2013 stated: In an age filled with advanced medical techniques like
Anterolateral Ligament Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine What in the world? TIME magazine in November 2013 stated: In an age filled with advanced medical techniques like
POSTEROLATERAL CORNER RECONSTRUCTION WHEN AND HOW?
 OTHER KNEE SURGERIES POSTEROLATERAL CORNER RECONSTRUCTION WHEN AND HOW? Written by Jacques Ménétrey, Eric Dromzée and Philippe M. Tscholl, Switzerland Injury of the posterolateral corner (PLC) is relatively
OTHER KNEE SURGERIES POSTEROLATERAL CORNER RECONSTRUCTION WHEN AND HOW? Written by Jacques Ménétrey, Eric Dromzée and Philippe M. Tscholl, Switzerland Injury of the posterolateral corner (PLC) is relatively
Ideal Candidate for Cartilage Restoration. Large or Complex Lesions
 Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
The Meniscus. History. Anatomy. Anatomy. Blood Supply. Attachments
 History The Meniscus W. Randall Schultz, MD, MS Austin, TX January 23, 2016 Meniscus originally thought to represent vestigial tissue 1883 first reported meniscal repair (Annandale) Total menisectomy treatment
History The Meniscus W. Randall Schultz, MD, MS Austin, TX January 23, 2016 Meniscus originally thought to represent vestigial tissue 1883 first reported meniscal repair (Annandale) Total menisectomy treatment
SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management
 SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management Gauguin Gamboa Australia has always been a nation where emphasis on health and fitness has resulted in an active population engaged
SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management Gauguin Gamboa Australia has always been a nation where emphasis on health and fitness has resulted in an active population engaged
Does Autologous Chondrocyte Implantation Provide Better Outcomes Than Microfracture in the Repair of Articular Knee Defects?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2012 Does Autologous Chondrocyte Implantation
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2012 Does Autologous Chondrocyte Implantation
Inside-Out Meniscal Repair Still the Gold Standard?
 Inside-Out Meniscal Repair Still the Gold Standard? ERIC BERKSON, MD MGH SPORTS MEDICINE TEAM PHYSICIAN, BOSTON RED SOX ASSISTANT PROFESSOR, HARVARD MEDICAL SCHOOL JULY 26, 2018 Disclosures Neither I nor
Inside-Out Meniscal Repair Still the Gold Standard? ERIC BERKSON, MD MGH SPORTS MEDICINE TEAM PHYSICIAN, BOSTON RED SOX ASSISTANT PROFESSOR, HARVARD MEDICAL SCHOOL JULY 26, 2018 Disclosures Neither I nor
Comparison of high-flex and conventional implants for bilateral total knee arthroplasty
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 14 Number 1 Comparison of high-flex and conventional implants for bilateral total knee arthroplasty C Martin-Hernandez, M Guillen-Soriano, A
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 14 Number 1 Comparison of high-flex and conventional implants for bilateral total knee arthroplasty C Martin-Hernandez, M Guillen-Soriano, A
Introduction Knee Anatomy and Function Making the Diagnosis
 Introduction Knee injuries are a very common problem among active individuals. It is important for us to understand how your knee was injured. Most knee injuries are associated with non-contact mechanisms.
Introduction Knee injuries are a very common problem among active individuals. It is important for us to understand how your knee was injured. Most knee injuries are associated with non-contact mechanisms.
Posterolateral Corner Injuries of the Knee: Pearls and Pitfalls
 Posterolateral Corner Injuries of the Knee: Pearls and Pitfalls Robert A. Arciero,MD,Col,ret Professor, Orthopaedics University of Connecticut Incidence of PLC Injuries with ACL Tears Fanelli, 1995 12%
Posterolateral Corner Injuries of the Knee: Pearls and Pitfalls Robert A. Arciero,MD,Col,ret Professor, Orthopaedics University of Connecticut Incidence of PLC Injuries with ACL Tears Fanelli, 1995 12%
Comparative study of sensitivity and specificity of MRI versus GNRB to detect ACL complete and partial tears
 Comparative study of sensitivity and specificity of MRI versus GNRB to detect ACL complete and partial tears Anterior cruciate ligament (ACL) tears are difficult to diagnose and treat (DeFranco). The preoperative
Comparative study of sensitivity and specificity of MRI versus GNRB to detect ACL complete and partial tears Anterior cruciate ligament (ACL) tears are difficult to diagnose and treat (DeFranco). The preoperative
Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury
 Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury I qualified from the Welsh National School of Medicine in Cardiff in 1984. I
Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury I qualified from the Welsh National School of Medicine in Cardiff in 1984. I
Does Every Knee Need a Meniscus?
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/clinicians-roundtable/does-every-knee-need-a-meniscus/3799/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/clinicians-roundtable/does-every-knee-need-a-meniscus/3799/
STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact)
 STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact) David Drez, Jr., M.D. Clinical Professor of Orthopaedics LSU School of Medicine Financial Disclosure Dr. David Drez has no relevant
STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact) David Drez, Jr., M.D. Clinical Professor of Orthopaedics LSU School of Medicine Financial Disclosure Dr. David Drez has no relevant
A comparison of arthroscopic diagnosis of ramp lesion and pre-operative MRI evaluation
 A comparison of arthroscopic diagnosis of ramp lesion and pre-operative MRI evaluation Yasuma S, Nozaki M, Kobayashi M, Kawanishi Y Yoshida M, Mitsui H, Nagaya Y, Iguchi H, Murakami H Department of Orthopaedic
A comparison of arthroscopic diagnosis of ramp lesion and pre-operative MRI evaluation Yasuma S, Nozaki M, Kobayashi M, Kawanishi Y Yoshida M, Mitsui H, Nagaya Y, Iguchi H, Murakami H Department of Orthopaedic
THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE
 THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE Abstract Spontaneous osteonecrosis of the knee (SPONK) and osteonecrosis in the postoperative knee (ONPK) are
THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE Abstract Spontaneous osteonecrosis of the knee (SPONK) and osteonecrosis in the postoperative knee (ONPK) are
The Knee. Two Joints: Tibiofemoral. Patellofemoral
 Evaluating the Knee The Knee Two Joints: Tibiofemoral Patellofemoral HISTORY Remember the questions from lecture #2? Girth OBSERVATION TibioFemoral Alignment What are the consequences of faulty alignment?
Evaluating the Knee The Knee Two Joints: Tibiofemoral Patellofemoral HISTORY Remember the questions from lecture #2? Girth OBSERVATION TibioFemoral Alignment What are the consequences of faulty alignment?
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Outline Coils, Patient Positioning Acquisition Parameters, Planes and Pulse Sequences Knee Arthrography Normal
MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Outline Coils, Patient Positioning Acquisition Parameters, Planes and Pulse Sequences Knee Arthrography Normal
Proximal tibial bony and meniscal slopes are higher in ACL injured subjects than controls: a comparative MRI study
 Proximal tibial bony and meniscal slopes are higher in ACL injured subjects than controls: a comparative MRI study Ashraf Elmansori, Timothy Lording, Raphaël Dumas, Khalifa Elmajri, Philippe Neyret, Sebastien
Proximal tibial bony and meniscal slopes are higher in ACL injured subjects than controls: a comparative MRI study Ashraf Elmansori, Timothy Lording, Raphaël Dumas, Khalifa Elmajri, Philippe Neyret, Sebastien
JMSCR Vol 05 Issue 01 Page January
 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i1.28 Diagnostic Accuracy of Magnetic Resonance
www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i1.28 Diagnostic Accuracy of Magnetic Resonance
High Tibial Osteotomy
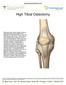 High Tibial Osteotomy With each step, forces equal to three to eight times your body weight travel between the thigh bone (femur) and shin bone (tibia) in your knee. These forces are dampened by a meniscus
High Tibial Osteotomy With each step, forces equal to three to eight times your body weight travel between the thigh bone (femur) and shin bone (tibia) in your knee. These forces are dampened by a meniscus
Meniscal Injuries with Tibial Plateau Fractures: Role of Arthroscopy
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Meniscal Injuries with Tibial Plateau Fractures: Role of Arthroscopy Authors Ansarul Haq Lone 1, Omar Khursheed 2, Shakir Rashid 3, Munir
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Meniscal Injuries with Tibial Plateau Fractures: Role of Arthroscopy Authors Ansarul Haq Lone 1, Omar Khursheed 2, Shakir Rashid 3, Munir
Case Report Reverse Segond Fracture Associated with Anteromedial Tibial Rim and Tibial Attachment of Anterior Cruciate Ligament Avulsion Fractures
 Hindawi Case Reports in Orthopedics Volume 2017, Article ID 9637153, 4 pages https://doi.org/10.1155/2017/9637153 Case Report Reverse Segond Fracture Associated with Anteromedial Tibial Rim and Tibial
Hindawi Case Reports in Orthopedics Volume 2017, Article ID 9637153, 4 pages https://doi.org/10.1155/2017/9637153 Case Report Reverse Segond Fracture Associated with Anteromedial Tibial Rim and Tibial
ACL Updates. Doron Sher. Knee, Shoulder and Elbow Surgeon. MBBS MBiomedE FRACS(Orth) Dr Doron Sher Knee & Shoulder Surgery
 ACL Updates Doron Sher MBBS MBiomedE FRACS(Orth) Knee, Shoulder and Elbow Surgeon What s New in ACL Reconstruction? History Examination Investigations Graft Placement Graft Choice Rehabilitation Routine
ACL Updates Doron Sher MBBS MBiomedE FRACS(Orth) Knee, Shoulder and Elbow Surgeon What s New in ACL Reconstruction? History Examination Investigations Graft Placement Graft Choice Rehabilitation Routine
Hip, Knee and Shoulder Surgery
 Hip, Knee and Shoulder Surgery Policy Number: MM.06.030 Lines of Business: HMO; PPO; QUEST Integration; Medicare Advantage Section: Surgery Place(s) of Service: Outpatient; Inpatient Original Effective
Hip, Knee and Shoulder Surgery Policy Number: MM.06.030 Lines of Business: HMO; PPO; QUEST Integration; Medicare Advantage Section: Surgery Place(s) of Service: Outpatient; Inpatient Original Effective
UNUSUAL ACL CASE: Tibial Eminence Fracture in a Female Collegiate Basketball Player
 UNUSUAL ACL CASE: Tibial Eminence Fracture in a Female Collegiate Basketball Player Cheri Drysdale, MEd,, ATC Margot Putukian,, MD Jeffery Bechler,, MD Princeton University How many of you have done an
UNUSUAL ACL CASE: Tibial Eminence Fracture in a Female Collegiate Basketball Player Cheri Drysdale, MEd,, ATC Margot Putukian,, MD Jeffery Bechler,, MD Princeton University How many of you have done an
Mædica - a Journal of Clinical Medicine
 Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS The Advantage of Arthroscopic Anterior Cruciate Ligament Reconstruction with Autograft from the Tendons of the Semitendinosus Gracilis Muscles for
Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS The Advantage of Arthroscopic Anterior Cruciate Ligament Reconstruction with Autograft from the Tendons of the Semitendinosus Gracilis Muscles for
