Outcomes after free tissue transfer for composite oral cavity resections involving skin
|
|
|
- Whitney Joseph
- 5 years ago
- Views:
Transcription
1 Received: 21 March 2017 Revised: 13 September 2017 Accepted: 22 November 2017 DOI: /hed ORIGINAL ARTICLE Outcomes after free tissue transfer for composite oral cavity resections involving skin Sameer A. Alvi MD Chelsea S. Hamill MD Jason P. Lepse MD Marco Ayala MD Douglas A. Girod MD Terance T. Tsue MD Yelizaveta Shnayder MD Kiran Kakarala MD Department of Otolaryngology - Head and Neck Surgery, University of Kansas Medical Center, Kansas City, Kansas Correspondence Kiran Kakarala, Department of Otolaryngology - Head and Neck Surgery, University of Kansas Medical Center, 3901 Rainbow Boulevard, Kansas City, KS kkakarala@kumc.edu Abstract Background: Resections involving oral cavity mucosa, bone, and skin present a unique challenge. Optimizing outcomes often requires technically demanding reconstruction. The purpose of this study is to evaluate outcomes of several reconstructive approaches for patients with composite through-and-through defects, with a focus on the osteocutaneous radial forearm free flap (RFFF). Methods: We conducted a retrospective evaluation of the cohort of patients treated for composite through-and-through defects with cutaneous involvement who underwent free flap reconstruction from August 2012 through October Results: Seventeen patients received a single flap (12 cases of osteocutaneous RFFF), whereas 10 patients underwent a combination of flaps. Complication rates and functional outcomes were favorable in patients who underwent osteocutaneous RFFFs. The supraclavicular artery island flap (SCAIF) was used as a second flap in 3 cases. Conclusion: The osteocutaneous RFFF provides a valuable reconstructive option for complex composite resection defects involving skin. When 2 flaps are required, the SCAIF is a viable alternative to a second free flap or pectoralis flap. KEYWORDS composite resection, free flap reconstruction, head and neck cancer, microvascular reconstruction, oral cavity cancer, osteocutaneous radial forearm free flap 1 INTRODUCTION Free tissue transfer provides a safe and reliable method to reconstruct complex surgical defects that arise from head and neck cancer resection. 1,2 Despite progress in microsurgery, extensive composite mandibular resections with cutaneous involvement can create challenging defects for reconstruction. 3 Patients requiring these types of procedures often have This article was presented as a poster at the American Head and Neck Society ninth International Conference on Head and Neck Cancer, Seattle, Washington, July 16-20, very advanced disease and poor survival outcomes despite aggressive treatment. Therefore, the ideal reconstruction maximizes function and quality of life and does not delay the initiation of adjuvant treatments. Free flap reconstruction techniques are the first choice for major composite through-and-through defects. 4 Various reconstructive techniques have been described using single free flaps, double free flaps, or free flaps combined with local or regional flaps. 5 8 Osteocutaneous free flap donor sites best suited for single flap reconstruction of these defects include the scapula, 5 fibula, 6 and the radius. 7 Various permutations of 2 flaps have been described, ranging from the use Head & Neck. 2018;40: wileyonlinelibrary.com/journal/hed VC 2018 Wiley Periodicals, Inc. 973
2 974 ALVI ET AL. of 2 separate free flaps, such as the combination of the anterolateral thigh flap with the fibula, as proposed by Koshima et al 8 in 1998, or using a free flap with a local or regional flap, as suggested by Deleyiannis et al 9 in Although these articles have carefully described each reconstructive technique, there is limited information in the literature regarding the comparisons between approaches for these complicated defects. 7 The use of the RFFF as a single flap for this application has also not been previously well described. Additionally, the supraclavicular artery island flap (SCAIF) has recently emerged as a versatile option for head and neck reconstruction; its use as a second flap in complex reconstruction has not been previously described, to the best of our knowledge. The purpose of this study was to review our experience in the reconstruction of extensive composite oral cavity resections creating through-and-through defects. We examined the different surgical options used, with particular focus on the osteocutaneous RFFF, and evaluated the functional and survival outcomes. 2 MATERIALS AND METHODS Approval was sought and obtained by the Institutional Review Board at the University of Kansas before commencement of this research study. A retrospective cohort was assembled of all patients with free flap operations by the corresponding author between August 2012 and October Patients were identified utilizing the Healthcare Enterprise Repository for Ontological Narration database. These charts were reviewed and all patients with composite through-andthrough defects with cutaneous involvement who underwent free flap reconstruction were included. Patients without a full thickness defect were excluded from the study. These charts were then further reviewed to collect demographics, cancer staging, surgical procedures, and patient outcomes. Statistical analysis was performed using the SPSS software version 22 (IBM, Armonk, NY). Descriptive statistics were utilized to describe demographic variables. 3 RESULTS Twenty-seven patients with through-and-through defects of the oral cavity were identified in our review. There were 18 men and 9 women with a mean age of 62.5 years (SD 11.22). Twenty-four patients underwent surgery for squamous cell cancer of the oral cavity, whereas 3 surgeries were performed for osteoradionecrosis of the mandible. These patients were examined based on reconstructive technique. Seventeen patients underwent reconstruction with a single free flap, and 10 patients underwent reconstruction with more than just a single free flap. The various reconstructive techniques used within each cohort are described in Table 1. The majority of patients (12; 71%) who received a single free flap underwent an osteocutaneous RFFF for reconstruction. Two of these single flap cases involved the latissimus dorsi scapular mega free flap for repair. This flap included both the parascapular and latissimus skin paddles with the scapular bone for mandibular repair. In patients requiring 2 flaps, the majority (8; 80%) underwent an osteocutaneous fibula free flap for intraoral bony reconstruction, with the addition of either a regional pectoralis myocutaneous flap or SCAIF for internal or external coverage. Patients 1 and 19 were reconstructed without an osteocutaneous free flap because they were edentulous with lateral mandibular defects and the soft tissue reconstruction was optimized without bone. Patients were followed up for a mean of days (SD 293.9). A description of the defects, including sizes, is included in Table Complications In our series of 27 patients, there were 3 cases of partial flap loss, but no cases of total flap loss. In the 12 patients who received the osteocutaneous RFFFs, there were no cases of partial or total flap loss. Flap complications were classified as either immediate (ie, occurring intraoperatively or during the postoperative hospitalization) or delayed (ie, any flap complication that happened after discharge from the hospital). These can be seen in detail in Table 3. Overall, 12 patients (45%) experienced immediate complications, including 2 flap takebacks for evaluation or revision of the microvascular anastomosis. In the patients who underwent osteocutaneous RFFF for reconstruction, 2 (17%) underwent immediate complications, including 1 flap takeback, which was salvaged. Overall, 5 patients (19%) experienced delayed complications with hardware exposure. In patients reconstructed with the osteocutaneous RFFF, 3 patients (25%) experienced delayed wound breakdown. Depending on the complication, patients were managed either conservatively or taken back to the operating room (Table 3). 3.2 Functional outcomes To assess functional outcomes, we first examined tracheostomy decannulation according to data available at the last follow-up visit. Overall, the average time to decannulation was 62 days (SD 127). Four patients remained tracheostomy dependent at last follow-up. These data are outlined in Table 4. When looking at patients with osteocutaneous RFFF specifically, all 12 were able to be decannulated, with a mean tracheostomy duration time of 13 days (SD 12). We also evaluated clearance for oral diet based on their postoperative swallow study results. Our swallow studies are performed by a dedicated team of head and neck speech
3 ALVI ET AL. 975 TABLE 1 Patient characteristics ID Sex Age, years Indication TNM Reconstruction 1 F 66 Cutaneous SCC T3N0M0 RFFF 2 M 87 Oral cavity SCC T2N2bM0 Osteocutaneous RFFF 3 M 54 Oral cavity SCC T4aN2cM0 Osteocutaneous RFFF 4 F 80 ORN mandible j N/A Osteocutaneous RFFF 5 F 78 Oral cavity SCC T2N0M0 Osteocutaneous RFFF 6 M 65 Oral cavity SCC T4aN0M0 Osteocutaneous RFFF 7 F 65 Oral cavity SCC T4aN0M0 Osteocutaneous RFFF 8 M 67 Oral cavity SCC T4aN1M0 Osteocutaneous RFFF 9 M 54 Oral cavity SCC T4aN2bM0 Osteocutaneous RFFF 10 M 60 Oral cavity SCC 1 BCC T4N0M0 Osteocutaneous RFFF 11 F 68 ORN mandible N/A Osteocutaneous RFFF 12 M 47 Oral cavity SCC T3N0M0 Osteocutaneous RFFF 13 M 70 ORN mandible N/A Osteocutaneous RFFF 14 M 68 ORN mandible N/A Fibula 15 F 55 Oral cavity SCC T4aN1M0 Fibula 16 M 63 Oral cavity SCC T4aN2bM0 Fibula 1 pectoralis 17 F 79 Oral cavity SCC T4aN0M0 Fibula 1 pectoralis 18 M 52 Oral cavity SCC T4aN2cM0 Fibula 1 pectoralis 19 M 63 Oral cavity SCC T4aN0M0 ALT 1 pectoralis 20 M 60 Oral cavity SCC T4aN2bM0 Fibula 1 pectoralis 21 F 70 Oral cavity SCC T4aN1M0 Fibula 1 supraclavicular 22 M 48 Oral cavity SCC T4aN0M0 Fibula 1 supraclavicular 23 F 67 Oral cavity SCC T4aN0M0 Fibula 1 supraclavicular 24 M 53 Oral cavity SCC T4aN2cM0 Osteocutaneous RFFF 1 pectoralis 25 M 47 Oral cavity SCC T4aN2bM0 Scapula 1 latissimus 26 M 61 Oral cavity SCC T4aN1M0 Fibula 1 RFFF 27 M 40 Oral cavity SCC T3N0M0 Scapula 1 latissimus Abbreviations: ALT, anterolateral thigh flap; BCC, basal cell carcinoma; N/A, not applicable; ORN, j osteoradionecrosis; RFFF, radial forearm free flap; SCC, squamous cell carcinoma. language pathologists, and studies are based on the National Outcomes Measurement System grading scale. For the purposes of this study, any patient who was cleared to begin a trial of oral nutrition was deemed as passing their swallow study. In total, 17 of our 27 patients (63%) with through-andthrough defects were able to pass their swallow study at last follow-up. The average strict NPO time was 43 days (SD 48). In the patients who underwent osteocutaneous RFFFs, all but 2 patients were cleared to start an oral diet. The average NPO duration in these patients was 35 days (SD 39). 3.3 Additional outcomes In addition to the functional outcomes discussed above, we also looked at operative times and duration of hospital stay.
4 976 ALVI ET AL. TABLE 2 Defect sizes ID Reconstruction Mucosal defect surface area, cm 2 Bone length, cm Skin defect surface area, cm 2 1 RFFF 35 N/A 42 2 Osteocutaneous RFFF Osteocutaneous RFFF Osteocutaneous RFFF Osteocutaneous RFFF Osteocutaneous RFFF Osteocutaneous RFFF Osteocutaneous RFFF Osteocutaneous RFFF Osteocutaneous RFFF Osteocutaneous RFFF Osteocutaneous RFFF Osteocutaneous RFFF Fibula Fibula Fibula 1 pectoralis Fibula 1 pectoralis Fibula 1 pectoralis ALT 1 pectoralis 96 N/A Fibula 1 pectoralis Fibula 1 supraclavicular Fibula 1 supraclavicular Fibula 1 supraclavicular Osteocutaneous RFFF 1 pectoralis Scapula 1 latissimus Fibula 1 RFFF Scapula 1 latissimus Abbreviations: ALT, anterolateral thigh flap; N/A, not applicable; RFFF, radial forearm free flap. Using our available data, the mean operative time, including resection, was 10 hours and 27 minutes (SD 2 hours 18 minutes). In patients who underwent osteocutaneous RFFFs, the mean operative time was 9 hours and 6 minutes (SD 1 hour and 1 minute). The mean hospital stay in all patients after reconstruction of through-and-through defects was 12 days (SD 10 days). Patients who underwent a single osteocutaneous RFFF had an average stay of 9 days in the hospital (SD 3 days). These additional outcomes are listed in Table 5. Survival outcomes are detailed in Table Selected cases Figures 1 and 2 show composite through-and-through defects, which illustrate the use of a single osteocutaneous RFFF with 2 skin paddles. The radius bone is first used to
5 ALVI ET AL. 977 TABLE 3 Complications ID Reconstruction Immediate flap complication Delayed complications Complication management Flap survival 1 RFFF No failure 2 Osteocutaneous RFFF No failure 3 Osteocutaneous RFFF Hardware exposure Conservative No failure 4 Osteocutaneous RFFF Superior flap dehiscence Hardware exposure Hardware removal No failure 5 Osteocutaneous RFFF No failure 6 Osteocutaneous RFFF No failure 7 Osteocutaneous RFFF Venous congestion Flap takeback No failure 8 Osteocutaneous RFFF No failure 9 Osteocutaneous RFFF No failure 10 Osteocutaneous RFFF No failure 11 Osteocutaneous RFFF No failure 12 Osteocutaneous RFFF Hardware exposure, wound breakdown Unknown No failure 13 Osteocutaneous RFFF No failure 14 Fibula Fluid collection/ hematoma Wound breakdown Conservative No failure 15 Fibula No failure 16 Fibula 1 pectoralis No failure 17 Fibula 1 pectoralis Wound infection, wound dehiscence Conservative No failure 18 Fibula 1 pectoralis Intraoral necrosis Conservative Partial failure 19 ALT 1 pectoralis Seroma at ALT Conservative No failure 20 Fibula 1 pectoralis Venous clot, hematoma Flap takeback No failure 21 Fibula 1 supraclavicular Wound dehiscence Hardware exposure Pectoralis salvage, Hardware repair with supraclavicular No failure 22 Fibula 1 supraclavicular Supraclavicular flap breakdown, partial necrosis 23 Fibula 1 supraclavicular Fibula seroma, wound dehiscence 24 Osteocutaneous RFFF 1 pectoralis 25 Scapula 1 latissimus Scapula oral skin paddle loss Pectoralis salvage Hardware removal Pectoralis salvage Partial Failure No failure No failure Partial failure 26 Fibula 1 RFFF Venous congestion Flap takeback No failure 27 Scapula 1 latissimus No failure Abbreviations: ALT, anterolateral thigh flap; RFFF, radial forearm free flap.
6 978 ALVI ET AL. TABLE 4 Functional outcomes ID Reconstruction Decannulation Days to decannulation Passed swallow study NPO duration, days 1 RFFF Y 7 Y 7 2 Osteocutaneous RFFF Y 11 Y 7 3 Osteocutaneous RFFF Y 8 Y 7 4 Osteocutaneous RFFF Y 6 N N/A 5 Osteocutaneous RFFF Y 7 N N/A 6 Osteocutaneous RFFF Y 7 Y 20 7 Osteocutaneous RFFF Y 7 Y 76 8 Osteocutaneous RFFF Y 6 Y Osteocutaneous RFFF Y 47 Y Osteocutaneous RFFF Y 26 Y Osteocutaneous RFFF Y 7 Y Osteocutaneous RFFF Y 6 Y Osteocutaneous RFFF Y 19 Y Fibula Y 4 Y 6 15 Fibula N N/A Y Fibula 1 pectoralis Y 16 N N/A 17 Fibula 1 pectoralis Y 297 N N/A 18 Fibula 1 pectoralis Y 246 N N/A 19 ALT 1 pectoralis N N/A N N/A 20 Fibula 1 pectoralis Y 523 N N/A 21 Fibula 1 supraclavicular Y 132 Y Fibula 1 supraclavicular Y 21 Y Fibula 1 supraclavicular Y 8 N N/A 24 Osteocutaneous RFFF 1 pectoralis N N/A N N/A 25 Scapula 1 latissimus N N/A N N/A 26 Fibula 1 RFFF Y 9 Y Scapula 1 latissimus Y 10 Y 48 Abbreviations: ALT, anterolateral thigh flap; N/A, not applicable; RFFF, radial forearm free flap. reconstruct the mandible with or without 1 or 2 osteotomies as needed. The microvascular anastomosis is then performed, followed by the reconstruction of the oral cavity and external skin defects. The oral cavity defect is first addressed and then a strip of skin is deepithelialized to create an external skin paddle, which is then inset to complete the reconstruction. Figure 3 demonstrates the use of a scapula latissimus mega flap in a patient with a lateral mandible defect with large soft tissue volume loss. This flap allows for harvest of 2 independent skin paddles (scapular or parascapular fasciocutaneous and latissimus myocutaneous) along with 10 to 12 cm of bone from the scapula. In this case, the parascapular skin paddle was inset intraorally, and the latissimus myocutaneous paddle was used to replace the large soft tissue volume deficit and provide external coverage. Composite defects with a bony defect of >10 cm are usually reconstructed with the fibula osteocutaneous free
7 ALVI ET AL. 979 TABLE 5 Additional outcomes ID Reconstruction Operative time Hospital stay, days 1 RFFF 8 h 53 min 8 2 Osteocutaneous RFFF 9 h 27 min 11 3 Osteocutaneous RFFF 9 h 11 min 8 4 Osteocutaneous RFFF 7 h 54 min 7 5 Osteocutaneous RFFF 7 h 54 min 8 6 Osteocutaneous RFFF 9 h 24 min 7 7 Osteocutaneous RFFF 11 h 30 min 7 8 Osteocutaneous RFFF 8 h 15 min 7 9 Osteocutaneous RFFF 10 h 12 min Osteocutaneous RFFF 9 h 1 min Osteocutaneous RFFF 8 h 42 min 7 12 Osteocutaneous RFFF 8 h 24 min 7 13 Osteocutaneous RFFF 9 h 20 min 7 14 Fibula 8 h 53 min 8 15 Fibula 9 h 45 min 7 16 Fibula 1 pectoralis 14 h 43 min Fibula 1 pectoralis 13 h 9 min Fibula 1 pectoralis 13 h 10 min 7 19 ALT 1 pectoralis 10 h 38 min 7 20 Fibula 1 pectoralis N/A Fibula 1 supraclavicular 11 h Fibula 1 supraclavicular 10 h 11 min Fibula 1 supraclavicular 12 h 2 min 8 24 Osteocutaneous RFFF 1 pectoralis 17 h 33 min 8 25 Scapula 1 latissimus 8 h 57 min Fibula 1 RFFF 12 h 48 min 9 27 Scapula 1 latissimus 10 h 58 min 12 Abbreviations: ALT, anterolateral thigh flap; N/A, not applicable; RFFF, radial forearm free flap. flap. Figure 4 shows a large composite defect of the lower lip, oral cavity mucosa, anterior mandible, and mental skin and soft tissue. An osteocutaneous fibula free flap was used to repair the mandibular defect, and an additional fasciocutaneous RFFF was used to repair the lower lip orbicularis sling, mental soft tissue, and skin. The palmaris tendon was harvested with the forearm and was suspended to the modiolus bilaterally to give some tone to the lower lip and restore oral competence. Figure 5 shows a large composite resection of the right hemimandible, intraoral mucosa, and facial soft tissue with skin. The mandible bone defect was 12-cm long, which required the use of the fibula free flap for mandibular reconstruction. However, a large defect of the external skin remained, and, thus, a right SCAIF was harvested from the right shoulder for repair of this skin defect.
8 980 ALVI ET AL. TABLE 6 Survival outcomes ID Reconstruction Disease-free interval, months Recurrence Overall survival, months Death 1 RFFF 9 Y 32 N 2 Osteocutaneous RFFF 40 N 40 Y 3 Osteocutaneous RFFF 10 Y 21 N 4 Osteocutaneous RFFF (ORN j ) N/A N/A N/A N/A 5 Osteocutaneous RFFF 1 N 1 Y 6 Osteocutaneous RFFF 8 Y 11 Y 7 Osteocutaneous RFFF 17 Y 23 N 8 Osteocutaneous RFFF 13 N 13 Y 9 Osteocutaneous RFFF 18 N 18 N 10 Osteocutaneous RFFF 17 N 17 Y 11 Osteocutaneous RFFF (ORN) N/A N/A N/A N/A 12 Osteocutaneous RFFF 14 Y 17 N 13 Osteocutaneous RFFF (ORN) N/A N/A N/A N/A 14 Fibula (ORN) N/A N/A N/A N/A 15 Fibula 6 N 6 Y 16 Fibula 1 pectoralis 2 N 2 Y 17 Fibula 1 pectoralis 19 N 19 Y 18 Fibula 1 pectoralis 8 N 8 Y 19 ALT 1 pectoralis N/A N/A 9 Y 20 Fibula 1 pectoralis 31 N 31 N 21 Fibula 1 supraclavicular 41 N 41 N 22 Fibula 1 supraclavicular 5 N 19 Y 23 Fibula 1 supraclavicular 16 Y 16 Y 24 Osteocutaneous RFFF 1 pectoralis 10 N 10 N 25 Scapula 1 latissimus 5 N 5 Y 26 Fibula 1 RFFF 21 Y 23 N 27 Scapula 1 latissimus 19 N 19 N Abbreviations: ALT, anterolateral thigh flap; N/A, not applicable; ORN, j osteoradionecrosis; RFFF, radial forearm free flap. 4 DISCUSSION This study explored reconstructive techniques utilizing free tissue transfer in patients with complex defects involving the oral cavity mucosa, bone, and soft tissue with skin. We observed that patients who underwent reconstruction with a single osteocutaneous RFFF had favorable outcomes with respect to the complication rate, operative time, hospital stay, decannulation, and resumption of oral intake. We also demonstrated a novel used for the SCAIF as a second flap for complex head and neck reconstruction in lieu of a free flap or other regional flap. There are many advantages to the osteocutaneous RFFF that have made it a popular choice among some
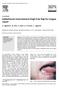
9 ALVI ET AL. 981 FIGURE 1 Use of 2 skin paddles in a radial forearm free flap for reconstruction. A, Defect after composite resection of cm oral cavity mucosa, 8cmmandible,and735cm skin. B, The mid portion of the skin paddle of the osteocutaneous radial forearm is de-epithelialized after bone inset. C, Partial inset with proximal skin paddle intraoral and distal skin paddle external, commissure recreated with Estlander flap [Color figure can be viewed at wileyonlinelibrary.com] reconstructive surgeons. The osteocutaneous RFFF allows for simultaneous resection and harvest with no repositioning of the patient needed. The flap can be raised with a long vascular pedicle that is usually less affected by peripheral vascular disease than the fibula free flap vessels. 10 A large and pliable skin paddle can be harvested that is relatively free from the bone and, therefore, has the ability to be customized and contorted to provide more functional soft tissue reconstruction compared with other bulkier flaps. Deepithelializing a small portion allows one portion of the flap to be closed to the intraoral mucosa and the remaining skin paddle to be used externally for repair of the skin defect. Depending on the size and bulk of the forearm donor site, even large volume and surface area defects can be reconstructed with this single flap. However, the osteocutaneous RFFF is not without its limitations. The forearm does not easily allow for dental implants due to limited bone stock, although implants can be achieved with additional bone grafting or by double-barreling the bony reconstruction. In our center s experience, very few patients pursue dental implants secondary to cost and reluctance to undergo further procedures. Another suggested concern with the osteocutaneous RFFF is high donor site morbidity secondary to radial fractures. 7,11 The rate of this potential morbidity after harvest of the osteocutaneous RFFF has significantly decreased with the introduction of donor site prophylactic plating. In a previous study from our institution, the risk of pathologic fracture of the radius after routine prophylactic plating in a large cohort was roughly 1% with mean follow-up of 25.9 months. 12 No fractures are reported in our present series. Our series of osteocutaneous RFFF reconstructions did well from a functional standpoint. The rate of resumption of oral intake in the subgroup of patients who underwent osteocutaneous RFFF in our study is similar to a study conducted by Bianchi et al, 7 in which the majority of osteocutaneous flaps were fibula free flaps. Patients with increased bulk from the use of multiple flaps for reconstruction may do worse with aerodigestive function in the immediate postoperative period. This is particularly true with the pectoralis major flap, where the muscle bulk can compromise the airway and impede swallowing function. 13 In certain composite through-and-through defects, other reconstructive choices may be preferred over the osteocutaneous RFFF. Baker and Sullivan 14 and Sullivan et al 15 popularized the subscapular system of flaps for head and neck reconstruction. A single vascular pedicle can be used to supply a variety of reconstructive flaps, including bone with multiple, independent skin paddles. Deschler and Hayden 3 described using the composite scapular free flap with scapular and parascapular skin paddles, allowing one paddle to be used for intraoral coverage and the second for external coverage with good success for through-and-through defects. A FIGURE 2 Use of 2 skin paddles in a radial forearm free flap for reconstruction. A, Defect after composite resection of cm oral cavity mucosa, 8cmmandible,and635cm skin. B, The mid portion of the skin paddle of the osteocutaneous radial forearm is de-epithelialized after bone inset. C, Final inset with distal skin paddle placed intraorally and proximal skin paddle externally [Color figure can be viewed at wileyonlinelibrary.com]
10 982 ALVI ET AL. FIGURE 3 Use of a scapular and latissimus mega free flap for reconstruction. A, Composite resection defect including cmoralcavitymucosa, 10 cm mandible, cm skin. B, Subscapular system mega flap with the fasciocutaneous parascapular and myocutaneous latissimus dorsi skin paddles and 11 cm of scapula bone. C, Parascapular skin paddle inset intraorally, bone inset to the mandible. D, Latissimus used for volume replacement and external coverage [Color figure can be viewed at wileyonlinelibrary.com] major downside of this flap is the need to reposition the patient for flap harvest after the completion of the resection; this adds time and complexity to an already lengthy procedure. Another drawback of this flap is the donor site morbidity, in particular, pain and decreased shoulder function; physical therapy services may be required to optimize arm function. Despite these limitations, the subscapular system of flaps is an excellent choice for selected patients with bony defects <12 cm who require large volume soft tissue reconstruction. The soft tissue skin paddles have almost complete freedom from the bone, allowing for functional reconstruction of complex structures, such as the mobile tongue, which are often included in these resections. For these cases, we have used a combination of the latissimus myocutaneous and parascapular fasciocutaneous skin paddles with the scapula bone. The fibula osteocutaneous free flap is certainly an excellent option for reconstruction of composite resection defects, and is indeed the flap of choice for bony reconstruction at many institutions. It can be harvested with multiple skin paddles to facilitate a single flap reconstruction of through-andthrough composite defects. 6 Alternatively, it can be used either with a second free flap or with a local or regional pedicled flap. Although there has been reported success of the use of double free flaps in these advanced cases, 8,16 19 one study by Gabr et al 20 showed that single flap use had a lower complication rate when compared with cases utilizing 2 free flaps. Furthermore, these patients have a return to only modest functional outcomes. 21 Our data also show that there is an increased operative time as well as an increased hospital stay in these patients. Longer hospital stay in cases of double flap reconstruction may be accounted for by the increased morbidity, drain management, and pain control associated with 2 donor sites. This idea of days of life lost becomes increasingly important as it has been shown that patient quality of life improves if they can spend more time at home. 22 Despite these drawbacks, in selected patients, a second free flap may be used to optimize functional and aesthetic outcomes, as demonstrated in Figure 4, where the radial forearm flap harvested with palmaris longus tendon was combined with the fibula flap to optimize oral competence in a patient with near total lower lip loss. In this series, we demonstrated the use of the SCAIF as a second flap for complex head and neck reconstruction. The SCAIF is a fasciocutaneous regional flap based off of the supraclavicular artery that is pliable and has a wide arc of rotation, allowing it to be used for many sites in the head and neck The SCAIF can be used in this setting for either intraoral mucosal reconstruction or external skin reconstruction. The flap is suitable for large surface area defects that may not require a large amount of soft tissue volume. Care must be taken when insetting the flap not to place too much FIGURE 4 Use of fibula free flap with radial forearm free flap for reconstruction. A, Defect after composite resection of cmoralcavity mucosa, 12 cm mandible, and cm skin. B, Fibula osteocutaneous free flap with 2 osteotomies. C, Radial forearm fasciocutaneous free flap including palmaris longus for lower lip resuspension. D, Fibula used for intraoral and mandible defects, radial forearm used for lower lip and chin reconstruction, palmaris tendon suspended to modiolus [Color figure can be viewed at wileyonlinelibrary.com]
11 ALVI ET AL. 983 FIGURE 5 Use of fibula free flap plus supraclavicular artery island flap (SCAIF) for reconstruction. A, Composite resection, including cm oral cavity mucosa, 12 cm mandible, cm external skin. B, The SCAIF harvested from the right shoulder for external coverage. C, Fibula flap used for the oral cavity and mandible and the SCAIF used externally (the proximal SCAIF can also be de-epithelialized and tunneled) [Color figure can be viewed at wileyonlinelibrary.com] tension on the pedicle as this is the most common cause of partial flap loss, as occurred in 1 of our patients. There is relatively low morbidity with this reconstructive technique with complications reported to be as low as 4%, with more recent reports suggesting between 13% and 28%. 26,27 Comparatively, pectoralis major flap complication rates have been reported to be between 16% and 63%. 13,28 Pectoralis flaps have also been associated with arm morbidity with increased stiffness and decreased range of motion, which is not the case with the SCAIF. 29 The majority of patients in our study had stage IV cancer of the oral cavity, and survival outcomes were poor, in keeping with other series on this subject. The 5-year survival in patients requiring this type of reconstruction has been reported to be between 30% and 50%. 19,20,30 It may be suggested that T4a tumors extending to the skin have a worse prognosis, but we cannot make this conclusion definitively with this small sample size without a comparison group. Despite the poor survival outcomes, other series have also demonstrated that these procedures are safe and effective leading to improved quality of life and increasing the number of days spent outside the hospital. 19,31 An efficient and reliable reconstruction could benefit patients in terms of quality of life, days of life lost, as well as giving a last chance for a curative resection. In addition to optimizing the functional and aesthetic outcomes, the reconstructive surgeon must optimize healing to allow timely initiation of adjuvant therapy. Simplifying the reconstruction may sometimes be the best the way to achieve this last goal. Limitations of this study include its retrospective nature and small patient cohort. Naturally, it is not feasible to blind patients and surgeons as to what reconstructive operation the patient will undergo. A retrospective analysis of outcomes is our best attempt to evaluate these operations. Additionally, a true comparison between the osteocutaneous RFFF and other reconstructive options in terms of complications and functional outcomes is not possible because patients were not matched in terms of the defect. There is also a natural bias toward reconstructive technique based on the experience at our institution; however, we do believe success with the osteocutaneous RFFF can be reproduced elsewhere by reconstructive surgeons. 5 CONCLUSION Composite oral cavity defects involving the intraoral mucosa, mandible, and cutaneous tissue are challenging reconstructions from both a functional and cosmetic standpoint. Various reconstructive techniques have been utilized, including single free flaps with multiple skin paddles, double free flaps, and combinations of free flaps with local or regional flaps. The subscapular system of using free flaps and fibula free flaps has been previously well described for these defects. We show that the use of a single osteocutaneous RFFF provides an alternative reconstructive option for these challenging defects. The flap provides up to 10 cm of bone and can accommodate 2 osteotomies. The osteocutaneous RFFF has a pliable and versatile skin paddle that can be used for intraoral mucosa and extraoral skin reconstruction simultaneously. Prophylactic plating of the radius bone has minimized donor site morbidity. In this study, patients reconstructed with a single osteocutaneous RFFF had favorable outcomes in terms of operative time, hospital stay, complications, and functional status. The SCAIF provides an alternative to the pectoralis flap if a regional flap without significant volume is required to augment a free flap reconstruction. It can be used for facial or neck coverage, and is pliable in nature with relatively low complication rate and donor site morbidity. These flaps provide valuable additional options for reconstructive surgeons to use in addressing these challenging defects. ORCID Sameer A. Alvi MD Chelsea S. Hamill MD
12 984 ALVI ET AL. REFERENCES [1] Haughey BH, Wilson E, Kluwe L, et al. Free flap reconstruction of the head and neck: analysis of 241 cases. Otolaryngol Head Neck Surg. 2001;125(1): [2] Suh JD, Sercarz JA, Abemayor E, et al. Analysis of outcome and complications in 400 cases of microvascular head and neck reconstruction. Arch Otolaryngol Head Neck Surg. 2004;130(8): [3] Deschler DG, Hayden RE. The optimum method for reconstruction of complex lateral oromandibular-cutaneous defects. Head Neck. 2000;22(7): [4] Boyd JB, Morris S, Rosen IB, Gullane P, Rotstein L, Freeman JL. The through-and-through oromandibular defect: rationale for aggressive reconstruction. Plast Reconstr Surg. 1994;93(1): [5] Takushima A, Harii K, Asato H, Nakatsuka T, Kimata Y. Mandibular reconstruction using microvascular free flaps: a statistical analysis of 178 cases. Plast Reconstr Surg. 2001;108(6): [6] Gal TJ, Jones KA, Valentino J. Reconstruction of the throughand-through oral cavity defect with the fibula free flap. Otolaryngol Head Neck Surg. 2009;140(4): [7] Bianchi B, Ferri A, Ferrari S, et al. Reconstruction of lateral through and through oro-mandibular defects following oncological resections. Microsurgery. 2010;30(7): [8] Koshima I, Hosoda S, Inagawa K, Urushibara K, Moriguchi T. Free combined anterolateral thigh flap and vascularized fibula for wide, through-and-through oromandibular defects. J Reconstr Microsurg. 1998;14(8): [9] Deleyiannis FW, Rogers C, Lee E, et al. Reconstruction of the lateral mandibulectomy defect: management based on prognosis and location and volume of soft tissue resection. Laryngoscope. 2006;116(11): [10] M uller-richter UD, Driemel O, M ortl M, et al. The value of Allen s test in harvesting a radial forearm flap: correlation of exvivo angiography and histopathological findings. Int J Oral Maxillofac Surg. 2008;37(7): [11] Clark S, Greenwood M, Banks RJ, Parker R. Fracture of the radial donor site after composite free flap harvest: a ten-year review. Surgeon. 2004;2(5): [12] Arganbright JM, Tsue TT, Girod DA, et al. Outcomes of the osteocutaneous radial forearm free flap for mandibular reconstruction. JAMA Otolaryngol Head Neck Surg. 2013;139(2): [13] You YS, Chung CH, Chang YJ, Kim KH, Jung SW, Rho YS. Analysis of 120 pectoralis major flaps for head and neck reconstruction. Arch Plast Surg. 2012;39(5): [14] Baker SR, Sullivan MJ. Osteocutaneous free scapular flap for one-stage mandibular reconstruction. Arch Otolaryngol Head Neck Surg. 1988;114(3): [15] Sullivan MJ, Baker SR, Crompton R, Smith-Wheelock M. Free scapular osteocutaneous flap for mandibular reconstruction. Arch Otolaryngol Head Neck Surg. 1989;115(11): [16] Koshima I, Fukuda H, Soeda S. Free combined anterolateral thigh flap and vascularized iliac bone graft with double vascular pedicle. J Reconstr Microsurg. 1989;5(1): [17] Wei FC, Celik N, Chen HC, Cheng MH, Huang WC. Combined anterolateral thigh flap and vascularized fibula osteoseptocutaneous flap in reconstruction of extensive composite mandibular defects. Plast Reconstr Surg. 2002;109(1): [18] Wei FC, Celik N, Yang WG, Chen IH, Chang YM, Chen HC. Complications after reconstruction by plate and soft-tissue free flap in composite mandibular defects and secondary salvage reconstruction with osteocutaneous flap. Plast Reconstr Surg. 2003;112(1): [19] Wei FC, Demirkan F, Chen HC, Chen IH. Double free flaps in reconstruction of extensive composite mandibular defects in head and neck cancer. Plast Reconstr Surg. 1999;103(1): [20] Gabr E, Kobayashi MR, Salibian AH, et al. Mandibular reconstruction: are two flaps better than one? Ann Plast Surg. 2004;52(1): [21] Posch NA, Mureau MA, Dumans AG, Hofer SO. Functional and aesthetic outcome and survival after double free flap reconstruction in advanced head and neck cancer patients. Plast Reconstr Surg. 2007;120(1): [22] Boyd JB, Mulholland RS, Davidson J, et al. The free flap and plate in oromandibular reconstruction: long-term review and indications. Plast Reconstr Surg. 1995;95(6): [23] Emerick KS, Herr MA, Deschler DG. Supraclavicular flap reconstruction following total laryngectomy. Laryngoscope. 2014;124(8): [24] Emerick KS, Herr MW, Lin DT, Santos F, Deschler DG. Supraclavicular artery island flap for reconstruction of complex parotidectomy, lateral skull base, and total auriculectomy defects. JAMA Otolaryngol Head Neck Surg. 2014;140(9): [25] Giordano L, Bondi S, Toma S, Biafora M. Versatility of the supraclavicular pedicle flap in head and neck reconstruction. Acta Otorhinolaryngol Ital. 2014;34(6): [26] Kokot N, Mazhar K, Reder LS, Peng GL, Sinha UK. Use of the supraclavicular artery island flap for reconstruction of cervicofacial defects. Otolaryngol Head Neck Surg. 2014;150(2): [27] Kozin ED, Sethi RK, Herr M, et al. Comparison of perioperative outcomes between the supraclavicular artery island flap and fasciocutaneous free flap. Otolaryngol Head Neck Surg. 2016;154(1): [28] Avery CM, Gandhi N, Peel D, Neal CP. Indications and outcomes for 100 patients managed with a pectoralis major flap within a UK maxillofacial unit. Int J Oral Maxillofac Surg. 2014;43(5): [29] Refos JW, Witte BI, de Goede CJ, de Bree R. Shoulder morbidity after pectoralis major flap reconstruction. Head Neck. 2016; 38(8): [30] Jeng SF, Kuo YR, Wei FC, Su CY, Chien CY. Reconstruction of extensive composite mandibular defects with large lip involvement by using double free flaps and fascia lata grafts for oral sphincters. Plast Reconstr Surg. 2005;115(7): [31] Jang DW, Teng MS, Ojo B, Genden EM. Palliative surgery for head and neck cancer with extensive skin involvement. Laryngoscope. 2013;123(5): How to cite this article: Alvi SA, Hamill CS, Lepse JP, et al. Outcomes after free tissue transfer for composite oral cavity resections involving skin. Head & Neck. 2018;40:
CASE REPORT Reconstruction and Characterization of Composite Mandibular Defects Requiring Double Skin Paddle Fibular Free Flaps
 CASE REPORT Reconstruction and Characterization of Composite Mandibular Defects Requiring Double Skin Paddle Fibular Free Flaps Austin M. Badeau, BA, a and Frederic W.-B. Deleyiannis, MD, MPhil, MPH b
CASE REPORT Reconstruction and Characterization of Composite Mandibular Defects Requiring Double Skin Paddle Fibular Free Flaps Austin M. Badeau, BA, a and Frederic W.-B. Deleyiannis, MD, MPhil, MPH b
Plate Exposure after Reconstruction by Plate and Anterolateral Thigh Flap in Head and Neck Cancer Patients with composite mandibular Defects
 Plate Exposure after Reconstruction by Plate and Anterolateral Thigh Flap in Head and Neck Cancer Patients with composite mandibular Defects Chia-Hsuan Tsai/ Huang-Kai Kao M. D. Introduction Malignant
Plate Exposure after Reconstruction by Plate and Anterolateral Thigh Flap in Head and Neck Cancer Patients with composite mandibular Defects Chia-Hsuan Tsai/ Huang-Kai Kao M. D. Introduction Malignant
Disclosures. The Expanding Role of Microvascular Reconstruction. Overview. Things they are a Changing. Surgical Advisory Board, Genentech Corp
 Disclosures Surgical Advisory Board, Genentech Corp The Expanding Role of Microvascular Reconstruction P. Daniel Knott, MD FACS Associate Professor Director, Facial Plastic and Reconstructive Surgery UCSF
Disclosures Surgical Advisory Board, Genentech Corp The Expanding Role of Microvascular Reconstruction P. Daniel Knott, MD FACS Associate Professor Director, Facial Plastic and Reconstructive Surgery UCSF
Use of the Teres Major Muscle in Chimeric Subscapular System Free Flaps for Head and Neck Reconstruction
 Research Original Investigation Use of the Teres Major Muscle in Chimeric Sub System Free Flaps for Head and Neck Reconstruction Andrew R. Tomlinson, MD; Mark J. Jameson, MD, PhD; Nitin A. Pagedar, MD,
Research Original Investigation Use of the Teres Major Muscle in Chimeric Sub System Free Flaps for Head and Neck Reconstruction Andrew R. Tomlinson, MD; Mark J. Jameson, MD, PhD; Nitin A. Pagedar, MD,
A review of the advantages of the anterolateral thigh flap in head and neck reconstruction
 The British Association of Plastic Surgeons (2004) 57, 603 609 A review of the advantages of the anterolateral thigh flap in head and neck reconstruction Jagdeep S. Chana, Fu-chan Wei* Department of Plastic
The British Association of Plastic Surgeons (2004) 57, 603 609 A review of the advantages of the anterolateral thigh flap in head and neck reconstruction Jagdeep S. Chana, Fu-chan Wei* Department of Plastic
Fascia Lata Free Flap Reconstruction of Limited Hard Palate Defects
 Open Access Original Article DOI: 10.7759/cureus.2356 Fascia Lata Free Flap Reconstruction of Limited Hard Palate Defects Rhorie P. Kerr 1, Andrea Hanick 1, Michael A. Fritz 1 1. Head and Neck Institute,
Open Access Original Article DOI: 10.7759/cureus.2356 Fascia Lata Free Flap Reconstruction of Limited Hard Palate Defects Rhorie P. Kerr 1, Andrea Hanick 1, Michael A. Fritz 1 1. Head and Neck Institute,
Stomal recurrence after total laryngectomy is 1
 CASE REPORT Eben L. Rosenthal, MD, Section Editor ANTEROLATERAL THIGH FREE FLAP FOR TRACHEAL RECONSTRUCTION AFTER PARASTOMAL RECURRENCE Umberto Caliceti, MD, 1 Ottavio Piccin, MD, 1 Ottavio Cavicchi, MD,
CASE REPORT Eben L. Rosenthal, MD, Section Editor ANTEROLATERAL THIGH FREE FLAP FOR TRACHEAL RECONSTRUCTION AFTER PARASTOMAL RECURRENCE Umberto Caliceti, MD, 1 Ottavio Piccin, MD, 1 Ottavio Cavicchi, MD,
Reconstruction for Oral Neoplasms in Indian Setup: Redebating the Utility of Radial Artery Free Flaps
 World Articles of Ear, Nose and Throat ---------------------Page 1 Reconstruction for Oral Neoplasms in Indian Setup: Redebating the Utility of Radial Artery Free Flaps Authors: Ranjan G Aiyer*, Rahul
World Articles of Ear, Nose and Throat ---------------------Page 1 Reconstruction for Oral Neoplasms in Indian Setup: Redebating the Utility of Radial Artery Free Flaps Authors: Ranjan G Aiyer*, Rahul
Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases
 J Oral Maxillofac Surg 58:1104-1108, 2000 Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases Yadranko Ducic, MD, FRCS (C),* and Mark Burye, DDS Purpose: This article describes
J Oral Maxillofac Surg 58:1104-1108, 2000 Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases Yadranko Ducic, MD, FRCS (C),* and Mark Burye, DDS Purpose: This article describes
Interesting Case Series. Scalp Reconstruction With Free Latissimus Dorsi Muscle
 Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
Case Report Dorsalis Pedis Free Flap: The Salvage Option following Failure of the Radial Forearm Flap in Total Lower Lip Reconstruction
 Case Reports in Medicine, Article ID 458286, 4 pages http://dx.doi.org/10.1155/2014/458286 Case Report Dorsalis Pedis Free Flap: The Salvage Option following Failure of the Radial Forearm Flap in Total
Case Reports in Medicine, Article ID 458286, 4 pages http://dx.doi.org/10.1155/2014/458286 Case Report Dorsalis Pedis Free Flap: The Salvage Option following Failure of the Radial Forearm Flap in Total
Modern Oral Cavity Reconstruction with Free Flaps and Pedicled Flaps
 Editorial imedpub Journals http://www.imedpub.com Journal of Aesthetic & Reconstructive Surgery DOI: 10.4172/2472-1905.10004 Modern Oral Cavity Reconstruction with Free Flaps and Pedicled Flaps Received:
Editorial imedpub Journals http://www.imedpub.com Journal of Aesthetic & Reconstructive Surgery DOI: 10.4172/2472-1905.10004 Modern Oral Cavity Reconstruction with Free Flaps and Pedicled Flaps Received:
The earlier clinic experience of the reverse-flow anterolateral thigh island flap
 British Journal of Plastic Surgery (2005) 58, 160 164 The earlier clinic experience of the reverse-flow anterolateral thigh island flap Gang Zhou, Qi-Xu Zhang*, Guang-Yu Chen Scar Multiple Treatment Centre,
British Journal of Plastic Surgery (2005) 58, 160 164 The earlier clinic experience of the reverse-flow anterolateral thigh island flap Gang Zhou, Qi-Xu Zhang*, Guang-Yu Chen Scar Multiple Treatment Centre,
Flap Selection and Functional Outcomes in Total Glossectomy with Laryngeal Preservation
 Original Research Facial Plastic and Reconstructive Surgery Flap Selection and Functional Outcomes in Total Glossectomy with Laryngeal Preservation Otolaryngology Head and Neck Surgery 149(4) 547 553 Ó
Original Research Facial Plastic and Reconstructive Surgery Flap Selection and Functional Outcomes in Total Glossectomy with Laryngeal Preservation Otolaryngology Head and Neck Surgery 149(4) 547 553 Ó
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty
 CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
Survey of Laryngeal Cancer at SBUH comparing 108 cases seen here from to the NCDB of 9,256 cases diagnosed nationwide in 2000
 Survey of Laryngeal Cancer at comparing 108 cases seen here from 1998 2002 to the of 9,256 cases diagnosed nationwide in 2000 Stony Brook University Hospital Cancer Program Annual Report 2002-2003 Gender
Survey of Laryngeal Cancer at comparing 108 cases seen here from 1998 2002 to the of 9,256 cases diagnosed nationwide in 2000 Stony Brook University Hospital Cancer Program Annual Report 2002-2003 Gender
STAIR-STEP FLAP FOR SECONDARY LOWER LIP REVISION AFTER LIP AND CHEEK COMPOSITE DEFECTS RECONSTRUCTION
 ORIGINAL ARTICLE STAIR-STEP FLAP FOR SECONDARY LOWER LIP REVISION AFTER LIP AND CHEEK COMPOSITE DEFECTS RECONSTRUCTION Takashi Fujiwara, MD, Chien-Chang Chen, MD, Hsiang-Shun Shih, MD, Rico P. Nebres,
ORIGINAL ARTICLE STAIR-STEP FLAP FOR SECONDARY LOWER LIP REVISION AFTER LIP AND CHEEK COMPOSITE DEFECTS RECONSTRUCTION Takashi Fujiwara, MD, Chien-Chang Chen, MD, Hsiang-Shun Shih, MD, Rico P. Nebres,
Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap.
 Case Report Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF, Patient Specific Plate Contouring (PSPC) and the MatrixMANDIBLE Plating
Case Report Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF, Patient Specific Plate Contouring (PSPC) and the MatrixMANDIBLE Plating
JPRAS Open 3 (2015) 1e5. Contents lists available at ScienceDirect. JPRAS Open. journal homepage:
 JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
Primary closure of the deltopectoral flap-donor site without skin grafting
 Primary closure of the deltopectoral flap-donor site without skin grafting Received: 4/3/2013 Accepted: 14/5/2013 Introduction Reliable and simultaneous reconstruction of head-and-neck defects has been
Primary closure of the deltopectoral flap-donor site without skin grafting Received: 4/3/2013 Accepted: 14/5/2013 Introduction Reliable and simultaneous reconstruction of head-and-neck defects has been
REINNERVATED ANTEROLATERAL THIGH FLAP FOR TONGUE RECONSTRUCTION
 REINNERVATED ANTEROLATERAL THIGH FLAP FOR TONGUE RECONSTRUCTION Peirong Yu, MD Department of Plastic Surgery, FC-8.2000, 1400 Holcombe Boulevard, Houston, TX 77030. E-mail: peirongyu@mdanderson.org Accepted
REINNERVATED ANTEROLATERAL THIGH FLAP FOR TONGUE RECONSTRUCTION Peirong Yu, MD Department of Plastic Surgery, FC-8.2000, 1400 Holcombe Boulevard, Houston, TX 77030. E-mail: peirongyu@mdanderson.org Accepted
Reconstructive surgeries in oral cancers
 International Journal of A J Institute of Medical Sciences 1 (2012) 47-54 Original Research Article Reconstructive surgeries in oral cancers Rithin Suvarna, 1 Aravind Pallipady, 2 Ranjith Rao, 3 Ashok
International Journal of A J Institute of Medical Sciences 1 (2012) 47-54 Original Research Article Reconstructive surgeries in oral cancers Rithin Suvarna, 1 Aravind Pallipady, 2 Ranjith Rao, 3 Ashok
MEDIAL SURAL ARTERY PERFORATOR FLAP FOR TONGUE AND FLOOR OF MOUTH RECONSTRUCTION. Adequate speech and swallowing are dependent
 ORIGINAL ARTICLE MEDIAL SURAL ARTERY PERFORATOR FLAP FOR TONGUE AND FLOOR OF MOUTH RECONSTRUCTION Shao-Liang Chen, MD, 1 Tim-Mo Chen, MD, 1 Niann-Tzyy Dai, MD, 1 Yi-Jan Hsia, DDS, MDSC, 2 Yaoh-Shiang Lin,
ORIGINAL ARTICLE MEDIAL SURAL ARTERY PERFORATOR FLAP FOR TONGUE AND FLOOR OF MOUTH RECONSTRUCTION Shao-Liang Chen, MD, 1 Tim-Mo Chen, MD, 1 Niann-Tzyy Dai, MD, 1 Yi-Jan Hsia, DDS, MDSC, 2 Yaoh-Shiang Lin,
Facelift approach for mandibular resection and reconstruction
 ORIGINAL ARTICLE Facelift approach for mandibular resection and reconstruction Bernardo Bianchi, MD, Andrea Ferri, MD, * Silvano Ferrari, MD, Chiara Copelli, MD, Enrico Sesenna, MD Maxillo-Facial Surgery
ORIGINAL ARTICLE Facelift approach for mandibular resection and reconstruction Bernardo Bianchi, MD, Andrea Ferri, MD, * Silvano Ferrari, MD, Chiara Copelli, MD, Enrico Sesenna, MD Maxillo-Facial Surgery
Chest wall reconstruction using a combined musculocutaneous anterolateral anteromedial thigh flap
 Free full text on www.ijps.org Case Report DOI: 10.4103/0970-0358.63966 Chest wall reconstruction using a combined musculocutaneous anterolateral anteromedial thigh flap Pearlie W. W. Tan, Chin-Ho Wong,
Free full text on www.ijps.org Case Report DOI: 10.4103/0970-0358.63966 Chest wall reconstruction using a combined musculocutaneous anterolateral anteromedial thigh flap Pearlie W. W. Tan, Chin-Ho Wong,
ORIGINAL ARTICLE. The Thoracoacromial/Cephalic Vascular System for Microvascular Anastomoses in the Vessel-Depleted Neck
 ORIGINAL ARTICLE The Thoracoacromial/Cephalic Vascular System for Microvascular Anastomoses in the Vessel-Depleted Neck Jeffrey R. Harris, MD; E. Lueg, MD; E. Genden, MD; M. L. Urken, MD Objective: To
ORIGINAL ARTICLE The Thoracoacromial/Cephalic Vascular System for Microvascular Anastomoses in the Vessel-Depleted Neck Jeffrey R. Harris, MD; E. Lueg, MD; E. Genden, MD; M. L. Urken, MD Objective: To
Maxillary Reconstruction with the Free Fibula Flap
 Maxillary Reconstruction with the Free Fibula Flap Xin Peng, D.D.S., Ph.D., Chi Mao, D.D.S., Ph.D., Guang-yan Yu, D.D.S., Ph.D., Chuan-bin Guo, D.D.S., Ph.D., Min-xian Huang, D.D.S., and Yi Zhang, D.D.S.,
Maxillary Reconstruction with the Free Fibula Flap Xin Peng, D.D.S., Ph.D., Chi Mao, D.D.S., Ph.D., Guang-yan Yu, D.D.S., Ph.D., Chuan-bin Guo, D.D.S., Ph.D., Min-xian Huang, D.D.S., and Yi Zhang, D.D.S.,
Original Research. Doi: /jioh
 Received: 15 th June 2016 Accepted: 18 th September 2016 Conflicts of Interest: None Source of Support: Nil Original Research Doi: 10.2047/jioh-08-12-05 Anatomic Variations, Technique, and Clinical Applications
Received: 15 th June 2016 Accepted: 18 th September 2016 Conflicts of Interest: None Source of Support: Nil Original Research Doi: 10.2047/jioh-08-12-05 Anatomic Variations, Technique, and Clinical Applications
Nasolabial flap reconstruction in oral cancer
 Singh et al. World Journal of Surgical Oncology 2012, 10:227 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Open Access Nasolabial flap reconstruction in oral cancer Seema Singh, Rajesh Kumar Singh and Manoj
Singh et al. World Journal of Surgical Oncology 2012, 10:227 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Open Access Nasolabial flap reconstruction in oral cancer Seema Singh, Rajesh Kumar Singh and Manoj
The free thoracodorsal artery perforator flap in head and neck reconstruction
 European Annals of Otorhinolaryngology, Head and Neck diseases (2012) 129, 167 171 Available online at www.sciencedirect.com TECHNICAL NOTE The free thoracodorsal artery perforator flap in head and neck
European Annals of Otorhinolaryngology, Head and Neck diseases (2012) 129, 167 171 Available online at www.sciencedirect.com TECHNICAL NOTE The free thoracodorsal artery perforator flap in head and neck
A new angle to mandibular reconstruction: The scapular tip free flap
 ORIGINAL ARTICLE A new angle to mandibular reconstruction: The scapular tip free flap John Yoo, MD,* Samuel A. Dowthwaite, MBBS, Kevin Fung, MD, Jason Franklin, MD, Anthony Nichols, MD Department of Otolaryngology
ORIGINAL ARTICLE A new angle to mandibular reconstruction: The scapular tip free flap John Yoo, MD,* Samuel A. Dowthwaite, MBBS, Kevin Fung, MD, Jason Franklin, MD, Anthony Nichols, MD Department of Otolaryngology
Role of free tissue transfer in management of chronic venous ulcer
 Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
SIMPLIFYING HEAD AND NECK MICROVASCULAR RECONSTRUCTION
 SIMPLIFYING HEAD AND NECK MICROVASCULAR RECONSTRUCTION Eben Rosenthal, MD, 1 William Carroll, MD, 1 Mathew Dobbs, BA, 1 J. Scott Magnuson, MD, 1 Mark Wax, MD, 2 Glenn Peters, MD 1 1 Department of Surgery,
SIMPLIFYING HEAD AND NECK MICROVASCULAR RECONSTRUCTION Eben Rosenthal, MD, 1 William Carroll, MD, 1 Mathew Dobbs, BA, 1 J. Scott Magnuson, MD, 1 Mark Wax, MD, 2 Glenn Peters, MD 1 1 Department of Surgery,
Regional Myocutaneous Flaps for Head and Neck Reconstruction: Experience of a Head and Neck Cancer Unit
 Original Article Regional Myocutaneous Flaps for Head and Neck Reconstruction: Experience of a Head and Neck Cancer Unit Eyituoyo Okoturo Department of Oral and Maxillofacial Surgery, Regional Head and
Original Article Regional Myocutaneous Flaps for Head and Neck Reconstruction: Experience of a Head and Neck Cancer Unit Eyituoyo Okoturo Department of Oral and Maxillofacial Surgery, Regional Head and
Accepted 16 March 2006 Published online 5 July 2006 in Wiley InterScience (www.interscience.wiley.com). DOI: /hed.20463
 ORIGINAL ARTICLE PROGNOSIS AS A DETERMINANT OF FREE FLAP UTILIZATION FOR RECONSTRUCTION OF THE LATERAL MANDIBULAR DEFECT Frederic W.-B. Deleyiannis, MD, MPhil, MPH, 1,2 Edward Lee, MD, 1 Brian Gastman,
ORIGINAL ARTICLE PROGNOSIS AS A DETERMINANT OF FREE FLAP UTILIZATION FOR RECONSTRUCTION OF THE LATERAL MANDIBULAR DEFECT Frederic W.-B. Deleyiannis, MD, MPhil, MPH, 1,2 Edward Lee, MD, 1 Brian Gastman,
Flaps vs Grafts. Ronen Avram, MD MSc FRCSC
 Flaps vs Grafts Ronen Avram, MD MSc FRCSC POS Keratoacanthoma is not a malignant tumor! Methods of Reconstruction Reconstructive Ladder Primary closure Primary Delayed Secondary Intention Skin Graft Pedicled
Flaps vs Grafts Ronen Avram, MD MSc FRCSC POS Keratoacanthoma is not a malignant tumor! Methods of Reconstruction Reconstructive Ladder Primary closure Primary Delayed Secondary Intention Skin Graft Pedicled
Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect of Upper and Middle Third Leg
 Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
IN 1996, BLACKWELL et al1 reported. The Bridging Lateral Mandibular Reconstruction Plate Revisited ORIGINAL ARTICLE
 The Bridging Lateral Mandibular Reconstruction Plate Revisited Keith E. Blackwell, MD; Victor Lacombe, MD ORIGINAL ARTICLE Background: Lateral oromandibular reconstruction using a soft tissue free flap
The Bridging Lateral Mandibular Reconstruction Plate Revisited Keith E. Blackwell, MD; Victor Lacombe, MD ORIGINAL ARTICLE Background: Lateral oromandibular reconstruction using a soft tissue free flap
Microvascular Free Flaps: Experience in Kwong Wah Hospital
 VOL. VOL.NO. NO. MAYNOVEMBER Microvascular Free Flaps: Experience in Kwong Wah Hospital Dr. Chiu-ming Ho, Dr. Vana SH Chan, Dr. Ming-shiaw Cheng, Dr. Wing-yung Cheung Division of Plastic Surgery, Department
VOL. VOL.NO. NO. MAYNOVEMBER Microvascular Free Flaps: Experience in Kwong Wah Hospital Dr. Chiu-ming Ho, Dr. Vana SH Chan, Dr. Ming-shiaw Cheng, Dr. Wing-yung Cheung Division of Plastic Surgery, Department
Head and neck free flap surgical site infections in the era of the Surgical Care Improvement Project
 ORIGINAL ARTICLE Head and neck free flap surgical site infections in the era of the Surgical Care Improvement Project Bharat B. Yarlagadda, MD, 1 Daniel G. Deschler, MD, 1 Debbie L. Rich, RN, 2 Derrick
ORIGINAL ARTICLE Head and neck free flap surgical site infections in the era of the Surgical Care Improvement Project Bharat B. Yarlagadda, MD, 1 Daniel G. Deschler, MD, 1 Debbie L. Rich, RN, 2 Derrick
THE SUBMENTAL ISLAND FLAP IN HEAD AND NECK RECONSTRUCTION
 THE SUBMENTAL ISLAND FLAP IN HEAD AND NECK RECONSTRUCTION Emre Vural, MD, James Y. Suen, MD Department of Otolaryngology-Head and Neck Surgery, University of Arkansas for Medical Sciences, 4301 West Markham,
THE SUBMENTAL ISLAND FLAP IN HEAD AND NECK RECONSTRUCTION Emre Vural, MD, James Y. Suen, MD Department of Otolaryngology-Head and Neck Surgery, University of Arkansas for Medical Sciences, 4301 West Markham,
CHARACTERISTICS OF THE ANTEROLATERAL THIGH FLAP IN A WESTERN POPULATION AND ITS APPLICATION IN HEAD AND NECK RECONSTRUCTION
 CHARACTERISTICS OF THE ANTEROLATERAL THIGH FLAP IN A WESTERN POPULATION AND ITS APPLICATION IN HEAD AND NECK RECONSTRUCTION Peirong Yu, MD Department of Plastic Surgery, The University of Texas M. D. Anderson
CHARACTERISTICS OF THE ANTEROLATERAL THIGH FLAP IN A WESTERN POPULATION AND ITS APPLICATION IN HEAD AND NECK RECONSTRUCTION Peirong Yu, MD Department of Plastic Surgery, The University of Texas M. D. Anderson
Robot-Assisted Free Flap in Head and Neck Reconstruction
 Robot-ssisted Free Flap in Head and Neck Reconstruction Han Gyeol Song, In Sik Yun, Won Jai Lee, Dae Hyun Lew, Dong Kyun Rah Department of Plastic and Reconstructive Surgery, Institute for Human Tissue
Robot-ssisted Free Flap in Head and Neck Reconstruction Han Gyeol Song, In Sik Yun, Won Jai Lee, Dae Hyun Lew, Dong Kyun Rah Department of Plastic and Reconstructive Surgery, Institute for Human Tissue
COMPARISON OF MINIPLATES AND RECONSTRUCTION PLATES IN MANDIBULAR RECONSTRUCTION
 COMPARISON OF MINIPLATES AND RECONSTRUCTION PLATES IN MANDIBULAR RECONSTRUCTION Richard J. Shaw, FRCS, 1 A. N. Kanatas, MFDS, 2 Derek Lowe, C Stat, MSc, 1 James S. Brown, FRCS, MD, 1 Simon N. Rogers, FRCS,
COMPARISON OF MINIPLATES AND RECONSTRUCTION PLATES IN MANDIBULAR RECONSTRUCTION Richard J. Shaw, FRCS, 1 A. N. Kanatas, MFDS, 2 Derek Lowe, C Stat, MSc, 1 James S. Brown, FRCS, MD, 1 Simon N. Rogers, FRCS,
A novel classification system for the evaluation and reconstruction of oral defects following oncological surgery
 ONCOLOGY LETTERS 14: 7049-7054, 2017 A novel classification system for the evaluation and reconstruction of oral defects following oncological surgery WEI WEI LIU, CHU YI ZHANG, JIAN YIN LI, MING FANG
ONCOLOGY LETTERS 14: 7049-7054, 2017 A novel classification system for the evaluation and reconstruction of oral defects following oncological surgery WEI WEI LIU, CHU YI ZHANG, JIAN YIN LI, MING FANG
Vascularized Rib for Facial Reconstruction
 Vascularized Rib for Facial Reconstruction Steven P. Davison, M.D., D.D.S., James H. Boehmler, M.D., Jason C. Ganz, M.D., and Bruce Davidson, M.D. Washington, D.C. The reconstruction of maxillectomy defects
Vascularized Rib for Facial Reconstruction Steven P. Davison, M.D., D.D.S., James H. Boehmler, M.D., Jason C. Ganz, M.D., and Bruce Davidson, M.D. Washington, D.C. The reconstruction of maxillectomy defects
Multi-dimensional analysis of oral cavity and oropharyngeal defects following cancer extirpation surgery, a cadaveric study
 Idris et al. Journal of Otolaryngology - Head and Neck Surgery (2018) 47:27 https://doi.org/10.1186/s40463-018-0276-9 ORIGINAL RESEARCH ARTICLE Open Access Multi-dimensional analysis of oral cavity and
Idris et al. Journal of Otolaryngology - Head and Neck Surgery (2018) 47:27 https://doi.org/10.1186/s40463-018-0276-9 ORIGINAL RESEARCH ARTICLE Open Access Multi-dimensional analysis of oral cavity and
Free Flap Surgery at Mengo Hospital, Uganda - A Review of The First 19 Consecutive Microvascular Free Tissue Transfers.
 Free Flap Surgery at Mengo Hospital, Uganda - A Review of The First 19 Consecutive Microvascular Free Tissue Transfers. G.W. Galiwango Mengo Hospital, Kampala - Uganda. Correspondence to: Dr. G.W. Galiwango,
Free Flap Surgery at Mengo Hospital, Uganda - A Review of The First 19 Consecutive Microvascular Free Tissue Transfers. G.W. Galiwango Mengo Hospital, Kampala - Uganda. Correspondence to: Dr. G.W. Galiwango,
Young-Hoon Joo, MD; Kwang-Jae Cho, MD; Jun-Ook Park, MD; Min-Sik Kim, MD
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Usefulness of the Anterolateral Thigh Flap With Vascularized Fascia Lata for Reconstruction of Orbital Floor
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Usefulness of the Anterolateral Thigh Flap With Vascularized Fascia Lata for Reconstruction of Orbital Floor
Anatomical variability of the anterolateral thigh flap perforators between sexes: a cadaveric study
 Eur J Plast Surg (2013) 36:179 184 DOI 10.1007/s00238-012-0778-z ORIGINAL PAPER Anatomical variability of the anterolateral thigh flap perforators between sexes: a cadaveric study Mateusz Zachara & Piotr
Eur J Plast Surg (2013) 36:179 184 DOI 10.1007/s00238-012-0778-z ORIGINAL PAPER Anatomical variability of the anterolateral thigh flap perforators between sexes: a cadaveric study Mateusz Zachara & Piotr
Reconstructive considerations in head and neck surgical oncology: United Kingdom National Multidisciplinary Guidelines
 The Journal of Laryngology & Otology (2016), 130 (Suppl. S2), S191 S197. JLO (1984) Limited, 2016. This is an Open Access article, distributed under the terms of the Creative Commons Attribution licence
The Journal of Laryngology & Otology (2016), 130 (Suppl. S2), S191 S197. JLO (1984) Limited, 2016. This is an Open Access article, distributed under the terms of the Creative Commons Attribution licence
Reconstruction of large mandibular defects
 Immediate Reconstruction of a Large Mandibular Defect of Locally Invasive Benign Lesions (A New Method) Gholamreza Shirani, OMFS, DDS, MS,* Mahnaz Arshad, DDS, 1 Farnoush Mohammadi, OMFS, DDS, MS* Tehran,
Immediate Reconstruction of a Large Mandibular Defect of Locally Invasive Benign Lesions (A New Method) Gholamreza Shirani, OMFS, DDS, MS,* Mahnaz Arshad, DDS, 1 Farnoush Mohammadi, OMFS, DDS, MS* Tehran,
Adipofascial anterolateral thigh free flap for tongue repair
 The British Association of Plastic Surgeons (2003) 56, 614 618 CASE REPORT Adipofascial anterolateral thigh free flap for tongue repair V. Agostini*, M. Dini, A. Mori, A. Franchi, T. Agostini Department
The British Association of Plastic Surgeons (2003) 56, 614 618 CASE REPORT Adipofascial anterolateral thigh free flap for tongue repair V. Agostini*, M. Dini, A. Mori, A. Franchi, T. Agostini Department
Surgery in Head and neck cancers.principles. Dr Diptendra K Sarkar MS,DNB,FRCS Consultant surgeon,ipgmer
 Surgery in Head and neck cancers.principles Dr Diptendra K Sarkar MS,DNB,FRCS Consultant surgeon,ipgmer Email:diptendrasarkar@yahoo.co.in HNC : common inclusives Challenges Anatomical preservation R0 Surgical
Surgery in Head and neck cancers.principles Dr Diptendra K Sarkar MS,DNB,FRCS Consultant surgeon,ipgmer Email:diptendrasarkar@yahoo.co.in HNC : common inclusives Challenges Anatomical preservation R0 Surgical
Reconstruction of a subtotal upper lip defect with a facial artery musculomucosal flap, kite flap, and radial forearm free flap: a case report
 Wang et al. World Journal of Surgical Oncology (2018) 16:194 https://doi.org/10.1186/s12957-018-1492-5 CASE REPORT Open Access Reconstruction of a subtotal upper lip defect with a facial artery musculomucosal
Wang et al. World Journal of Surgical Oncology (2018) 16:194 https://doi.org/10.1186/s12957-018-1492-5 CASE REPORT Open Access Reconstruction of a subtotal upper lip defect with a facial artery musculomucosal
Reconstruction with fibular osteocutaneous free flap in patients with mandibular osteoradionecrosis
 Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2015) 37:7 DOI 10.1186/s40902-015-0007-3 RESEARCH ARTICLE Open Access Reconstruction with fibular osteocutaneous free flap in patients with
Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2015) 37:7 DOI 10.1186/s40902-015-0007-3 RESEARCH ARTICLE Open Access Reconstruction with fibular osteocutaneous free flap in patients with
Endoscopic assisted harvest of the pedicled pectoralis major muscle flap
 British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts
 Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Learning Objectives. Head and Neck Cancer: Post-Treatment Changes. Neck Dissection Classification * Radical neck dissection. Radical Neck Dissection
 Head and Neck Cancer: Post-Treatment Changes Daniel W. Williams III, MD Learning Objectives In patients treated for H/N Cancer: Describe the various types of neck dissections Explain reconstruction techniques
Head and Neck Cancer: Post-Treatment Changes Daniel W. Williams III, MD Learning Objectives In patients treated for H/N Cancer: Describe the various types of neck dissections Explain reconstruction techniques
Scapular & Parascapular flap FLAP TERRITORY ANATOMY. is normally accompanied by two venae comitantes.
 Scapular & Parascapular flap FLAP TERRITORY This is a composite flap that is situated over the scapula with various incisional arrangements. It can be harvested as a skin and subcutaneous tissue flap,
Scapular & Parascapular flap FLAP TERRITORY This is a composite flap that is situated over the scapula with various incisional arrangements. It can be harvested as a skin and subcutaneous tissue flap,
Hand Microsurgery. A reliable option for lower extremity complex defect reconstructions: Two case reports with free osteocutaneous radial forearm flap
 Hand Microsurgery & Case Report Hand Microsurg 2017;6:51-55 doi:10.5455/handmicrosurg.219016 A reliable option for lower extremity complex defect reconstructions: Two case reports with free osteocutaneous
Hand Microsurgery & Case Report Hand Microsurg 2017;6:51-55 doi:10.5455/handmicrosurg.219016 A reliable option for lower extremity complex defect reconstructions: Two case reports with free osteocutaneous
PECTORALIS MAJOR MYOCUTAJNEUUS FLAP FOR RECONSTRUCTION OF DEFECTS FOLLOWING RESECTIONS IN HEAD AND NECK AREA
 PECTORALIS MAJOR MYOCUTAJNEUUS FLAP FOR RECONSTRUCTION OF DEFECTS FOLLOWING RESECTIONS IN HEAD AND NECK AREA Pages with reference to book, From 72 To 76 Mohammad Arshad Cheema ( Department of Surgery,
PECTORALIS MAJOR MYOCUTAJNEUUS FLAP FOR RECONSTRUCTION OF DEFECTS FOLLOWING RESECTIONS IN HEAD AND NECK AREA Pages with reference to book, From 72 To 76 Mohammad Arshad Cheema ( Department of Surgery,
Role of Latissimus Dorsi Island Flap in Coverage of Mutilating Upper Limb Injuries in Pediatric Age Group
 Original Article Annals of Pediatric Surgery Vol. 6, No 3,4 July, October 2010, PP 154-160 Role of Latissimus Dorsi Island Flap in Coverage of Mutilating Upper Limb Injuries in Pediatric Age Group Ahmed
Original Article Annals of Pediatric Surgery Vol. 6, No 3,4 July, October 2010, PP 154-160 Role of Latissimus Dorsi Island Flap in Coverage of Mutilating Upper Limb Injuries in Pediatric Age Group Ahmed
Chapter 117: Reconstruction of the Hypopharynx and Cervical Esophagus. Richard E. Hayden
 Chapter 117: Reconstruction of the Hypopharynx and Cervical Esophagus Richard E. Hayden In 1877 Czerny performed the first recorded pharyngoesophageal reconstruction, using local cervical skin flaps for
Chapter 117: Reconstruction of the Hypopharynx and Cervical Esophagus Richard E. Hayden In 1877 Czerny performed the first recorded pharyngoesophageal reconstruction, using local cervical skin flaps for
Microvascular reconstruction of traumatic defects requires
 The Journal of TRAUMA Injury, Infection, and Critical Care The Utility of the Anterolateral Thigh Donor Site in Reconstructing the United States Trauma Patient Eduardo D. Rodriguez, DDS, MD, Gedge D. Rosson,
The Journal of TRAUMA Injury, Infection, and Critical Care The Utility of the Anterolateral Thigh Donor Site in Reconstructing the United States Trauma Patient Eduardo D. Rodriguez, DDS, MD, Gedge D. Rosson,
Interesting Case Series. Reconstruction of Dorsal Wrist Defects
 Interesting Case Series Reconstruction of Dorsal Wrist Defects Maelee Yang, BS, and Joseph Meyerson, MD The Ohio State University Wexner Medical Center, Columbus Correspondence: maelee.yang@osumc.edu Keywords:
Interesting Case Series Reconstruction of Dorsal Wrist Defects Maelee Yang, BS, and Joseph Meyerson, MD The Ohio State University Wexner Medical Center, Columbus Correspondence: maelee.yang@osumc.edu Keywords:
Jonathan A. Dunne, MBChB, MRCS, a Daniel J. Wilks, MBChB, MRCS, b and Jeremy M. Rawlins, MBChB, MPhil, FRCS (Plast) c INTRODUCTION
 CASE REPORT A Previously Discounted Flap Now Reconsidered: MatriDerm and Split-Thickness Skin Grafting for Tendon Cover Following Dorsalis Pedis Fasciocutaneous Flap in Lower Limb Trauma Jonathan A. Dunne,
CASE REPORT A Previously Discounted Flap Now Reconsidered: MatriDerm and Split-Thickness Skin Grafting for Tendon Cover Following Dorsalis Pedis Fasciocutaneous Flap in Lower Limb Trauma Jonathan A. Dunne,
The learning curve in head and neck reconstruction with microvascular free flaps: a retrospective review
 Asian Biomedicine Vol. 4 No. 6 December 2010; 907-912 Brief communication (Original) The learning curve in head and neck reconstruction with microvascular free flaps: a retrospective review Patnarin Mahattanasakul
Asian Biomedicine Vol. 4 No. 6 December 2010; 907-912 Brief communication (Original) The learning curve in head and neck reconstruction with microvascular free flaps: a retrospective review Patnarin Mahattanasakul
Osteoradionecrosis of Jaw in Head and Neck Cancer Patient Treated with Free Iliac Bone and Umbilical Fat Pad Graft
 Maxillofac Plast Reconstr Surg 2014;36(2):62-66 http://dx.doi.org/10.14402/jkamprs.2014.36.2.62 ISSN 2288-8101(Print) ISSN 2288-8586(Online) Case Report Osteoradionecrosis of Jaw in Head and Neck Cancer
Maxillofac Plast Reconstr Surg 2014;36(2):62-66 http://dx.doi.org/10.14402/jkamprs.2014.36.2.62 ISSN 2288-8101(Print) ISSN 2288-8586(Online) Case Report Osteoradionecrosis of Jaw in Head and Neck Cancer
OSTEOMYOCUTANEOUS PERONEAL ARTERY PERFORATOR FLAP FOR RECONSTRUCTION OF COMPOSITE MAXILLARY DEFECTS
 OSTEOMYOCUTANEOUS PERONEAL ARTERY PERFORATOR FLAP FOR RECONSTRUCTION OF COMPOSITE MAXILLARY DEFECTS Sukru Yazar, MD, 1 Ming-Huei Cheng, MD, 1 Fu-Chan Wei, MD, FACS, 1 Sheng-Po Hao, MD, FACS, 2 Kai-Ping
OSTEOMYOCUTANEOUS PERONEAL ARTERY PERFORATOR FLAP FOR RECONSTRUCTION OF COMPOSITE MAXILLARY DEFECTS Sukru Yazar, MD, 1 Ming-Huei Cheng, MD, 1 Fu-Chan Wei, MD, FACS, 1 Sheng-Po Hao, MD, FACS, 2 Kai-Ping
Health-related quality of life after mandibular resection for oral cancer: Reconstruction with free fibula flap
 Journal section: Oral Surgery Publication Types: Research doi:10.4317/medoral.19399 http://dx.doi.org/doi:10.4317/medoral.19399 Health-related quality of life after mandibular resection for oral cancer:
Journal section: Oral Surgery Publication Types: Research doi:10.4317/medoral.19399 http://dx.doi.org/doi:10.4317/medoral.19399 Health-related quality of life after mandibular resection for oral cancer:
Accepted 13 March 2008 Published online 18 July 2008 in Wiley InterScience ( DOI: /hed.20874
 ORIGINAL ARTICLE ZYGOMATICOMAXILLARY BUTTRESS RECONSTRUCTION OF MIDFACE DEFECTS WITH THE OSTEOCUTANEOUS RADIAL FOREARM FREE FLAP Patricio Andrades, MD, Eben L. Rosenthal, MD, William R. Carroll, MD, Christopher
ORIGINAL ARTICLE ZYGOMATICOMAXILLARY BUTTRESS RECONSTRUCTION OF MIDFACE DEFECTS WITH THE OSTEOCUTANEOUS RADIAL FOREARM FREE FLAP Patricio Andrades, MD, Eben L. Rosenthal, MD, William R. Carroll, MD, Christopher
Lower Facial Reanimation Techniques Following Cancer Resection and Free Flap Reconstruction
 The Laryngoscope VC 2016 The American Laryngological, Rhinological and Otological Society, Inc. Lower Facial Reanimation Techniques Following Cancer Resection and Free Flap Reconstruction Alexandra E.
The Laryngoscope VC 2016 The American Laryngological, Rhinological and Otological Society, Inc. Lower Facial Reanimation Techniques Following Cancer Resection and Free Flap Reconstruction Alexandra E.
Mentosternal Contracture Treated With an Occipito-Scapular Flap in a 5-year-old Boy: A Case Report
 Mentosternal Contracture Treated With an Occipito-Scapular Flap in a 5-year-old Boy: A Case Report Armin Kraus, MD, Hans-Eberhard Schaller, MD, and Hans-Oliver Rennekampff, MD Department for Hand, Plastic,
Mentosternal Contracture Treated With an Occipito-Scapular Flap in a 5-year-old Boy: A Case Report Armin Kraus, MD, Hans-Eberhard Schaller, MD, and Hans-Oliver Rennekampff, MD Department for Hand, Plastic,
Head and neck cancer - patient information guide
 Head and neck cancer - patient information guide The development of reconstructive surgical techniques in the last 20 years has led to major advances in the treatment of patients with head and neck cancer.
Head and neck cancer - patient information guide The development of reconstructive surgical techniques in the last 20 years has led to major advances in the treatment of patients with head and neck cancer.
The maxilla is the pivotal structure of the midface,
 ORIGINAL ARTICLE MICROVASCULAR FREE FLAP RECONSTRUCTION VERSUS PALATAL OBTURATION FOR MAXILLECTOMY DEFECTS Mauricio A. Moreno, MD, 1,2 Roman J. Skoracki, MD, 1 Ehab Y. Hanna, MD, 2 Matthew M. Hanasono,
ORIGINAL ARTICLE MICROVASCULAR FREE FLAP RECONSTRUCTION VERSUS PALATAL OBTURATION FOR MAXILLECTOMY DEFECTS Mauricio A. Moreno, MD, 1,2 Roman J. Skoracki, MD, 1 Ehab Y. Hanna, MD, 2 Matthew M. Hanasono,
McGregor Flap Reconstruction of Extensive Lower Lip Defects Following Excision of Squamous Cell Carcinoma
 Kasr El Aini Journal of Surgery VOL., 12, NO 2 May 2011 27 McGregor Flap Reconstruction of Extensive Lower Lip Defects Following Excision of Squamous Cell Carcinoma Mohamed A. Albadawy, MD and Bassem M.
Kasr El Aini Journal of Surgery VOL., 12, NO 2 May 2011 27 McGregor Flap Reconstruction of Extensive Lower Lip Defects Following Excision of Squamous Cell Carcinoma Mohamed A. Albadawy, MD and Bassem M.
ARTICLE IN PRESS. Postoperative complications in 202 cases of microvascular head and neck reconstruction
 Journal of Cranio-Maxillofacial Surgery (2007) 35, 311 315 r 2007 European Association for Cranio-Maxillofacial Surgery doi:10.1016/j.jcms.2007.05.001, available online at http://www.sciencedirect.com
Journal of Cranio-Maxillofacial Surgery (2007) 35, 311 315 r 2007 European Association for Cranio-Maxillofacial Surgery doi:10.1016/j.jcms.2007.05.001, available online at http://www.sciencedirect.com
Surgical outcomes in cases of postoperative recurrence of primary oral cancer that required reconstruction
 Acta Med. Nagasaki 60: 119 124 MS#AMN 07187 Surgical outcomes in cases of postoperative recurrence of primary oral cancer that required reconstruction Shinya Ji n n o u c h i, MD 1, Kenichi Ka n e ko,
Acta Med. Nagasaki 60: 119 124 MS#AMN 07187 Surgical outcomes in cases of postoperative recurrence of primary oral cancer that required reconstruction Shinya Ji n n o u c h i, MD 1, Kenichi Ka n e ko,
Reconstruction of axillary scar contractures retrospective study of 124 cases over 25 years
 British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
An experience on primary thinning and secondary debulking of anterolateral thigh flap in head and neck reconstruction
 European Review for Medical and Pharmacological Sciences An experience on primary thinning and secondary debulking of anterolateral thigh flap in head and neck reconstruction E. CIGNA, A. MINNI, M. BARBARO,
European Review for Medical and Pharmacological Sciences An experience on primary thinning and secondary debulking of anterolateral thigh flap in head and neck reconstruction E. CIGNA, A. MINNI, M. BARBARO,
Reverse Adipofascial Radial Forearm Flap Surgery for Soft-Tissue Reconstruction of Hand Defects
 Reverse Adipofascial Radial Forearm Flap Surgery for Soft-Tissue Reconstruction of Hand Defects Osman Akdag, MD, a Mehtap Karamese, MD, a Muhammed NebilSelimoglu, MD, a Ahmet Akatekin, MD, a Malik Abacı,
Reverse Adipofascial Radial Forearm Flap Surgery for Soft-Tissue Reconstruction of Hand Defects Osman Akdag, MD, a Mehtap Karamese, MD, a Muhammed NebilSelimoglu, MD, a Ahmet Akatekin, MD, a Malik Abacı,
Comparison of Anterolateral Thigh and Radial Forearm Free Flaps in Head and Neck Reconstruction
 doi:10.21873/invivo.11325 Comparison of Anterolateral Thigh and Radial Forearm Free Flaps in Head and Neck Reconstruction CARLO M. ORANGES, BARBARA LING, MATHIAS TREMP, RETO WETTSTEIN, DANIEL F. KALBERMATTEN
doi:10.21873/invivo.11325 Comparison of Anterolateral Thigh and Radial Forearm Free Flaps in Head and Neck Reconstruction CARLO M. ORANGES, BARBARA LING, MATHIAS TREMP, RETO WETTSTEIN, DANIEL F. KALBERMATTEN
Pedicled medial sural perforator flap for the reconstruction of knee defects
 International Wound Journal ISSN 1742-4801 ORIGINAL ARTICLE Pedicled medial sural perforator flap for the reconstruction of knee defects I-Han Chiang 1, Chia-Chun Wu 2, Shyi-Gen Chen 1 & Chih-Hsin Wang
International Wound Journal ISSN 1742-4801 ORIGINAL ARTICLE Pedicled medial sural perforator flap for the reconstruction of knee defects I-Han Chiang 1, Chia-Chun Wu 2, Shyi-Gen Chen 1 & Chih-Hsin Wang
T. Rapis, S.N. Zanakis, I.F. Letsa, A.P. Karamanos CLINICAL CASE. Summary. Introduction
 Journal of BUON 8: 397-401, 2003 2003 Zerbinis Medical Publications. Printed in Greece CLINICAL CASE Basal cell carcinoma of the posterior neck, reconstructed with lower trapezius island musculocutaneous
Journal of BUON 8: 397-401, 2003 2003 Zerbinis Medical Publications. Printed in Greece CLINICAL CASE Basal cell carcinoma of the posterior neck, reconstructed with lower trapezius island musculocutaneous
Piero Nicolai SURGERY FOR THE TREATMENT OF OROPHARYNGEAL CARCINOMA: STATE OF ART. Department of Otorhinolaryngology University of Brescia
 Biology and technology contribution to clinical advancement: the case of oropharyngeal cancer Brescia May 8 th, 2009 SURGERY FOR THE TREATMENT OF OROPHARYNGEAL CARCINOMA: STATE OF ART Piero Nicolai Department
Biology and technology contribution to clinical advancement: the case of oropharyngeal cancer Brescia May 8 th, 2009 SURGERY FOR THE TREATMENT OF OROPHARYNGEAL CARCINOMA: STATE OF ART Piero Nicolai Department
Int J Clin Exp Med 2015;8(3): /ISSN: /IJCEM Yujie Liang 1, Yaqi Cui 2, Guiqing Liao 1
 Int J Clin Exp Med 2015;8(3):4533-4538 www.ijcem.com /ISSN:1940-5901/IJCEM0004257 Original Article Comparison of quality-of-life in tongue cancer patients undergoing tongue reconstruction with lateral
Int J Clin Exp Med 2015;8(3):4533-4538 www.ijcem.com /ISSN:1940-5901/IJCEM0004257 Original Article Comparison of quality-of-life in tongue cancer patients undergoing tongue reconstruction with lateral
JMSCR Vol 07 Issue 01 Page January 2019
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v7i1.36 Original Article A Study on the
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v7i1.36 Original Article A Study on the
An island flap based on the anterior branch of the superficial temporal artery for perioral defects
 Free full text on www.ijps.org Original Article An island flap based on the anterior branch of the superficial temporal artery for perioral defects V. Bhattacharya, Ganji Raveendra Reddy, Sheikh Adil Bashir,
Free full text on www.ijps.org Original Article An island flap based on the anterior branch of the superficial temporal artery for perioral defects V. Bhattacharya, Ganji Raveendra Reddy, Sheikh Adil Bashir,
Screw hole-positioning guide and plate-positioning guide: A novel method to assist mandibular reconstruction
 Journal of Dental Sciences (2012) 7, 301e305 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Screw hole-positioning guide and plate-positioning guide: A novel method
Journal of Dental Sciences (2012) 7, 301e305 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Screw hole-positioning guide and plate-positioning guide: A novel method
Scapular Flap for Maxillectomy Defect Reconstruction and Preliminary Results Using Three-Dimensional Modeling
 The Laryngoscope VC 2016 The American Laryngological, Rhinological and Otological Society, Inc. Scapular Flap for Maxillectomy Defect Reconstruction and Preliminary Results Using Three-Dimensional Modeling
The Laryngoscope VC 2016 The American Laryngological, Rhinological and Otological Society, Inc. Scapular Flap for Maxillectomy Defect Reconstruction and Preliminary Results Using Three-Dimensional Modeling
Aesthetic surgery techniques after excision of dermatofibrosarcoma protuberans: a case report
 British Journal of Plastic Surgery (2005) 58, 556 560 CASE REPORT Aesthetic surgery techniques after excision of dermatofibrosarcoma protuberans: a case report G. Dagregorio a, *, V. Darsonval b a Department
British Journal of Plastic Surgery (2005) 58, 556 560 CASE REPORT Aesthetic surgery techniques after excision of dermatofibrosarcoma protuberans: a case report G. Dagregorio a, *, V. Darsonval b a Department
Clinical Study Use of the Anterolateral Thigh in Cranio-Orbitofacial Reconstruction
 Hindawi Publishing Corporation Plastic Surgery International Volume 2011, Article ID 941742, 6 pages doi:10.1155/2011/941742 Clinical Study Use of the Anterolateral Thigh in Cranio-Orbitofacial Reconstruction
Hindawi Publishing Corporation Plastic Surgery International Volume 2011, Article ID 941742, 6 pages doi:10.1155/2011/941742 Clinical Study Use of the Anterolateral Thigh in Cranio-Orbitofacial Reconstruction
Accepted 29 May 2009 Published online 11 August 2009 in Wiley InterScience ( DOI: /hed.21204
 CLINICAL REVIEW David W. Eisele, MD, Section Editor ANTEROLATERAL THIGH FLAP Chin-Ho Wong, MBBS, MRCS, MMed (Surgery), FAMS (Plast. Surg.), 1 Fu-Chan Wei, MD 2 1 Department of Plastic Reconstructive and
CLINICAL REVIEW David W. Eisele, MD, Section Editor ANTEROLATERAL THIGH FLAP Chin-Ho Wong, MBBS, MRCS, MMed (Surgery), FAMS (Plast. Surg.), 1 Fu-Chan Wei, MD 2 1 Department of Plastic Reconstructive and
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
ORIGINAL ARTICLE. most commonly result. involving the paranasal sinuses, the overlying facial skin, or both. Such defects may result in substantial
 ORIGINAL ARTICLE Use of Precontoured Positioning Plates and Pericranial Flaps in Midfacial Reconstruction to Optimize Aesthetic and Functional Outcomes Yadranko Ducic, MD, FRCSC; Lance E. Oxford, MD Objectives:
ORIGINAL ARTICLE Use of Precontoured Positioning Plates and Pericranial Flaps in Midfacial Reconstruction to Optimize Aesthetic and Functional Outcomes Yadranko Ducic, MD, FRCSC; Lance E. Oxford, MD Objectives:
Priority of Fibular Reconstruction in Patients with Oral Cavity Cancer Undergoing Segmental Mandibulectomy
 Priority of Fibular Reconstruction in Patients with Oral Cavity Cancer Undergoing Segmental Mandibulectomy Chih-Hung Lin 1,2., Chung-Jan Kang 2,3., Chung-Kan Tsao 1,2, Christopher Glenn Wallace 1,2,3,
Priority of Fibular Reconstruction in Patients with Oral Cavity Cancer Undergoing Segmental Mandibulectomy Chih-Hung Lin 1,2., Chung-Jan Kang 2,3., Chung-Kan Tsao 1,2, Christopher Glenn Wallace 1,2,3,
Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage
 Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage Shareef Jandali, MD, and David W. Low, MD Division of Plastic Surgery, University of Pennsylvania Health System, Philadelphia Correspondence:
Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage Shareef Jandali, MD, and David W. Low, MD Division of Plastic Surgery, University of Pennsylvania Health System, Philadelphia Correspondence:
Complications and Outcome of Free Flap Transfers for Oral and Maxillofacial Reconstruction: Analysis of 213 Cases
 Oral Science International, May 009, p.6 5 Copyright 009, Japanese Stomatology Society. All Rights Reserved. Complications and Outcome of Free Flap Transfers for Oral and Maxillofacial Reconstruction:
Oral Science International, May 009, p.6 5 Copyright 009, Japanese Stomatology Society. All Rights Reserved. Complications and Outcome of Free Flap Transfers for Oral and Maxillofacial Reconstruction:
Anatomical Basis and Clinical Application of the Ulnar Forearm Free Flap for Head and Neck Reconstruction
 The Laryngoscope VC 2012 The American Laryngological, Rhinological and Otological Society, Inc. Anatomical Basis and Clinical Application of the Ulnar Forearm Free Flap for Head and Neck Reconstruction
The Laryngoscope VC 2012 The American Laryngological, Rhinological and Otological Society, Inc. Anatomical Basis and Clinical Application of the Ulnar Forearm Free Flap for Head and Neck Reconstruction
