IN 1996, BLACKWELL et al1 reported. The Bridging Lateral Mandibular Reconstruction Plate Revisited ORIGINAL ARTICLE
|
|
|
- Dwain Owens
- 5 years ago
- Views:
Transcription
1 The Bridging Lateral Mandibular Reconstruction Plate Revisited Keith E. Blackwell, MD; Victor Lacombe, MD ORIGINAL ARTICLE Background: Lateral oromandibular reconstruction using a soft tissue free flap with a first-generation locking mandibular reconstruction plate (MRP) was rejected in a previous series by the senior author (K.E.B.) owing to a high incidence of delayed plate extrusion through the cheek skin. Objective: To reexamine this method of reconstruction using a second-generation, low-profile MRP. Patients and Design: A prospective case series of 27 patients with segmental defects of the lateral mandible after treatment of head and neck cancer. Setting: An academic tertiary care referral center. Intervention: All patients had mandibular continuity restored using the Leibinger Locking System (Stryker Leibinger Inc, Kalamazoo, Mich) MRP. Associated soft tissue defects were repaired using radial forearm (n = 22) or rectus abdominis (n = 5) free flaps. Main Outcome Measure: Incidence of hardwarerelated complications. Results: All microvascular flap transfers were successful. One patient experienced a plate fracture 9 months after reconstruction. Only 1 patient experienced external plate exposure, 6 months after undergoing reconstruction of a through-and-through defect. Reconstruction was successful in 25 (93%) of the cases after a median follow-up period of 19.5 months. Conclusions: The high incidence of external plate exposure in patients undergoing lateral oromandibular reconstruction using soft tissue free flaps and firstgeneration locking MRPs may have resulted from a plate geometry that was prone to result in extrusion. After a similar length of follow-up, the incidence of reconstructive failure was reduced by using a low-profile, roundedcontour MRP. Final assessment of the durability of this technique will require long-term follow-up. Arch Otolaryngol Head Neck Surg. 1999;125: From the Division of Head and Neck Surgery, the Department of Surgery, University of California Los Angeles School of Medicine, Los Angeles. IN 1996, BLACKWELL et al1 reported a series of 14 patients who underwent lateral oromandibular reconstruction using soft tissue free flaps in conjunction with bridging titanium hollow screw reconstruction plate (THORP) mandibular reconstruction plates (MRPs). This method of reconstruction was rejected owing to a high incidence of delayed hardwarerelated complications. The incidence of hardware-related reconstructive failure was 29% in 14 patients after a median follow-up period of 16.5 months. One patient experienced fracture of a THORP MRP, while 3 patients suffered from hardware extrusion through the cheek skin. Analysis of this experience led to the conclusion that segmental defects of the lateral mandible were optimally reconstructed using a vascularized bone containing free flap. Because of the critical role of the tongue for speech and swallowing and the complex 3-dimensional anatomy of the oropharynx, it was recognized that the soft tissue component of vascularized bone containing free flaps would be inadequate to reconstruct the soft tissue component of some lateral oromandibular defects. In this situation, it would be necessary to carry out a vascularized bone containing free flap to restore mandibular continuity and a simultaneous soft tissue free flap to reconstruct the soft tissues. The THORP MRP was the first system of mandibular fixation that achieved an added degree of hardware stability by allowing for screw osteointegration and a mechanism to lock the screw heads to the screw holes of the plate. As a result of these properties, this first-generation locking MRP has achieved a very low incidence of hardware complications related to screw loosening. 2 However, the THORP system has a high plate profile height, projecting 3.5 mm away from the underlying mandible or bone graft. In addition, the plate contour contains obtuse angles and straight edges. A second generation of locking MRPs has been introduced that has a low plate profile and smooth, rounded contour at the screw holes compared with the THORP MRP. The current study was undertaken to determine if the high inci- 988
2 PATIENTS AND METHODS This series includes 15 men and 12 women who underwent segmental resection of the lateral mandible for squamous cell carcinoma of the oral cavity or oropharynx. Data were recorded prospectively using a personal computer spreadsheet database. The patients ages at the time of treatment ranged from 32 to 88 years. Primary tumors were classified as stage II in 6 cases, stage III in 4 cases, and stage IV in 17 cases. Oromandibular defects were classified using a previously published classification. 3 All surgical procedures were carried out after obtaining appropriate informed consent. The Leibinger Locking System (Stryker Leibinger Inc, Kalamazoo, Mich) MRP was used to bridge the segmental mandibular defects in all cases. The MRPs were applied to the buccal cortex of the remaining native mandible using standard techniques. An effort was made to use a minimum of 3 fixation screws in each mandibular segment, although short condylar segments would sometimes accommodate only 2 screws. Whenever oncologically feasible, the MRP was contoured and applied to the buccal cortex of the mandible before performing the segmental resection. The indication for soft tissue free flap and bridging plate reconstruction was largely determined by the nature of the soft tissue defect in patients undergoing lateral segmental mandibulectomy. Patients in this series had complex or extensive soft tissue defects that in our judgment were poorly suited for reconstruction using the skin or muscle component of a fibula or iliac crest free flap. Soft tissue defects were reconstituted using radial forearm (n = 22) or rectus abdominis (n = 5) free flaps. Radial forearm flaps were selected for patients with lateral mandibulectomy defects associated with complex 3-dimensional soft tissue resections of the oropharynx, where the thin and pliable radial forearm flap was folded for reconstruction of the base of the tongue, lateral and posterior oropharynx, and the soft palate. Rectus abdominis flaps were often selected for soft tissue reconstruction in patients who underwent subtotal or total glossectomy. Twenty-three patients (85%) in this series received high-dose, external-beam radiation therapy. Five patients received preoperative, and 17 patients, postoperative radiation therapy. One patient received both preoperative and postoperative radiation therapy. dence of THORP extrusion reported by Blackwell et al 1 might be secondary to a plate geometry that was prone to extrusion. A follow-up series of patients underwent lateral oromandibular reconstruction using soft tissue free flaps in conjunction with a bridging, secondgeneration, low-profile locking MRP. The incidence of hardware-related complications was analyzed and compared with the previous series of patients. RESULTS Patient and tumor characteristics, defect classification, reconstructive method, and outcome are summarized in Figure 1. Plate extrusion occurred through the skin of the lateral chin 6 months after reconstruction of a through-and-through oromandibular defect using a radial forearm free flap and a bridging mandibular reconstruction plate. the Table. Tumor was confined to the lingual aspect of the mandible in 22 of the 27 patients. One patient had tumor involving the masseter muscle that necessitated thinning of the cheek flap to achieve negative surgical margins. Four patients underwent through-andthrough resection of mucosa, mandible, and skin to treat advanced cancers. All free tissue transfers were successful, and there were no perioperative deaths. There were no serious early perioperative reconstructive complications (eg, total or partial flap necrosis, fistula, hematoma, or infection). Major perioperative medical complications occurred in 10 patients (37%). Three patients (11%) experienced delayed hardware-related reconstructive complications. One of the reconstructive complications did not require plate removal. This patient experienced malocclusion of her remaining teeth as a result of poor contouring of the MRP. This was corrected at a second surgery to recontour the plate 7 months after the initial reconstruction. Two patients experienced hardware-related complications that required plate removal. One patient with intact contralateral maxillary and mandibular dentition and a long-standing history of tooth grinding experienced plate fracture 9 months after reconstruction. A second patient experienced delayed external plate exposure, with external extrusion of the MRP through the skin. She underwent reconstruction of a through-andthrough oromandibular defect using a radial forearm free flap that was partially deepithelialized and folded to reconstruct the floor of the mouth and the external facial skin. After receiving postoperative radiation therapy, the plate extruded 6 months postoperatively through the portion of the free flap that was used to reconstruct the lateral chin skin (Figure 1). In both of these patients, plate removal resulted in swing of the mandibular remnant toward the side of the segmental mandibulectomy and some loss of cheek contour. Four patients died of recurrent cancer during the study period, while 3 were alive with recurrent cancer. The remaining 20 patients were alive and free of evidence of recurrent disease at the end of follow-up. The follow-up period ranged from 6 to 32 months, with a median follow-up of 19.5 months. The MRP remained in 989
3 Patient and Tumor Characteristics, Defect Classifications, and Reconstructive Methods* Patient No./ Sex/Age, y Tumor Location and Stage Soft Tissue Defect Bone Defect 1/F/ 80 SCCA floor of mouth T4 N2c M0 FOM A,L BR N IA,L Nerve Defect 2/F/61 SCCA tonsil T2 N0 M0 T B1/2,SP 1/2,PH L BR N IA,L 3/M/55 SCCA tongue T4 N0 M0 SP 1/2, FOM L, TG, PH L BR N IA,L B, H B 4/M/50 SCCA tonsil T2 N1 M0 SP 1/2, FOM L,T B1/4,PH L BR N IA,L 5/F/52 SCCA tonsil T1 N1 M0 SP 1/2, FOM L,PH L,T B1/4 BR N IA,L 6/F/84 SCCA tonsil T3 N0 M0 SP 1/2, FOM L,PH L,T B1/2 BR N IA,L 7/M/54 SCCA floor of mouth T2 N0 M0 B, FOM L,PH L,T B1/4 BRS H N IA,L,H 8/M/67 SCCA tonsil T2 N0 M0 SP 1/2, FOM L,PH L,T B3/4,T M1/4 BR N IA,L,H 9/M32 SCCA tonsil T4 N2b M0 T B3/4,SP 3/4,PH L BR N IA,L,H 10/M/56 SCCA tonsil T3 N2b M0 SP 1/2, FOM L,PH L,T B1/4 BR N IA,L,H 11/F/69 SCCA posterior pharynx T4 N2b M0 SPT, FOM L,PH L,T B1/2,T M1/4 BR N IA,L,H 12/M/61 SCCA floor of mouth T2 N0 M0 FOM L,T M1/4 BS H N IA,L 13/F/50 SCCA tonsil T3 N2b M0 SP 1/2,PH L,T B1/4 BR N IA,L 14/F/73 SCCA lip TX N3 M0 FOM L,A,C CH,N,M BRS H N IA,L,F 15/M/67 SCCA tonguet4 N3 M0 FOM L,T B,T M1/4, laryngectomy B N IA,L,N H B 16/M/65 SCCA tonsil T3 N0 M0 SP 3/4,PH L,T B1/2 BR N IA,L 17/F/75 SCCA buccal T4 N2a M0 FOM L, B,C CH B N IA,L,F 18/F/75 SCCA floor of mouth T3 N0 M0 FOM L,PH L,T B1/2 BR N IA,L,H 19/M/55 SCCA tonsil T2 N2c M0 SP 1/4,PH L,T B1/4 BR N IA,L,H 20/M/80 SCCA tongue T3 N2b M0 SP 1/4, FOM L PH L,T B3/4,T M1/2 BR N IA,L,H 21/M/61 SCCA tongue T4 N2c M0 TG, SP 1/4 FOM L,A,PH L, BR N IA,L B N H B supraglottic laryngectomy 22/M/65 SCCA tonsil T3 N2b M0 SP 3/4, FOM L,PH L,T B1/2 BR N IA,L 23/M/71 SCCA tongue T4 N0 M0 SP 3/4, FOM L,PH L,T B3/4 T M1/2 BR N IA,L,H 24/F/88 SCCA lip T4 N0 M0 B, L L1/4,C CH,M BS H N IA,F 25/M/69 SCCA tonsil T2 N2a M0 SP 1/4, FOM L,PH L,T B1/4 BR N IA 26/F/80 SCCA palate T2 N2b M0 FOM L,C CH,N BP N IA,F 27/F/61 SCCA tongue T3 N2b M0 SP 1/4, FOM L,PH L,T B3/4, TM1/2 BR N IA,L,N H B *SCCA indicates squamous cell carcinoma; preop, preoperative; postop, postoperative; GI, gastrointestinal; and NED, no evidence of disease. For an explanation of the soft tissue, bone, and nerve defect classification system, see the tables and text of reference 3. place and functioning well in 25 (93%) of the 27 patients at the end of the follow-up period. COMMENT Vascularized bone containing free flaps are a reliable and effective method of oromandibular reconstruction. 4 Of the available donor sites, fibula free flaps, iliac crest free flaps, and scapula free flaps are selected frequently for mandibular reconstruction. However, the soft tissue components available in the fibula and iliac crest free flaps may be ill suited for reconstruction of certain composite oromandibular defects. In the case of the fibula flap, the skin paddle is attached to the fibula bone at the site of one or more cutaneous perforating branches of the peroneal vascular pedicle. This sometimes limits the mobility and arc of rotation of the skin paddle relative to the bone graft, making it difficult to use the skin component of the flap for reconstruction of complex 3-dimensional defects of the oropharynx that include portions of the tongue, lateral and posterior pharyngeal wall, and soft palate. In addition, the thickness of the subcutaneous fat in the leg often provides inadequate bulk for tongue reconstruction after total or subtotal glossectomy. The considerable bulk of the skin paddle of the iliac crest flap is better suited for reconstruction of substantial glossectomy defects. However, it may be too bulky to fold for reconstruction of soft tissues within the oropharynx. In addition, when an iliac crest flap is harvested from the ipsilateral hip for reconstruction of lateral mandibulectomy defects without osteotomy, the skin paddle is located on the lateral aspect of the reconstructed mandible after bone graft insetting. This anatomic relationship may limit the arc of rotation of the skin paddle for reconstruction of lateral oromandibular defects. Both the iliac crest and fibula flaps offer a second soft tissue component in the form of the internal oblique muscle and the soleus muscle. 5-6 However, it is more difficult to achieve a watertight wound closure when using these muscle components for soft tissue repair, and the transferred muscle will undergo a considerable degree of denervation atrophy after insetting. The soft tissue components of the scapula system of flaps offers the most versatility of the vascularized bone containing free flaps that are commonly used for oromandibular reconstruction. However, flap harvest requires intraoperative patient repositioning to the decubitus position for most cases of head and neck reconstruction, which eliminates the ability to decrease the length of the surgery by performing simultaneous tumor resection and free flap harvest. 990
4 Free Flap Irradiation Complications Outcome/Length of Follow-up, mo Radial forarm flap Preop Atrial fibrillation; upper GI bleed; NED/32 forearm tendon exposure Radial forearm flap None None NED/31 Rectus flap Postop None NED /30 Radial forearm flap Preop & postop None Dead of cancer/21 Radial forearm flap Preop Plate fracture after 10 mo; NED/29 plate removed. Radial forearm flap None Stroke NED/29 Radial forearm flap Preop None NED/27 Rectus flap Postop None NED/27 Radial forearm flap Postop None Dead of cancer/23 Rectus flap Postop None NED/23 Radial forearm flap Postop None Dead of cancer/19 Radial forearm flap Postop None NED/22 Radial forearm flap Postop Malocclusion, plate recontoured NED/22 Radial forearm flap Postop External plate exposure 6 months; NED/21 plate removed Radial forearm flap Postop None NED/20 Radial forearm flap Postop Delerium tremens; upper GI bleed; NED/19 fluid overload; pseudomembranous colitis Radial forearm flap Postop Atrial fibrillation Alive with cancer/13 Radial forearm flap None Colon perforation NED/13 Radial forearm flap Preop Readmission for transfusion Alive with cancer/13 Rectus flap Postop Atrial fibrillation; fluid overload NED/13 Rectus flap Postop Readmission for pneumonia NED/11 Radial forearm flap Postop None NED/10 Rectus flap Preop Atrial fibrillation; pulmonary embolism; NED/10 pneumonia Radial forearm flap None None NED/7 Radial forearm flap Postop None NED/7 Radial forearm flap Postop Stroke Alive with cancer/7 Radial forearm flap Postop None Dead of cancer/6 To overcome the limitations of the soft tissue components of vascularized bone containing free flaps for complex cases of oromandibular reconstruction, Wenig and Keller 7 introduced the concept of using a soft tissue free flap that has attributes that are well suited for the defect in conjunction with a bridging mandibular reconstruction plate. Subsequent series of bridging mandibular reconstruction plates documented a high incidence of intraoral plate extrusion after reconstruction of anterior segmental mandibulectomy defects. 8,9 However, these series reported a favorable outcome when free flaps and bridging plates were used to reconstruct lateral oromandibular defects. Schusterman and associates 8 reported a 93% success rate in 14 patients with lateral mandibular resections who underwent reconstruction using soft tissue flaps and bridging MRPs. Boyd et al 9 reported a 95% success rate in 20 patients who underwent lateral oromandibular reconstruction using fasciocutaneous free flaps in conjunction with bridging MRPs. 9 In 1996, Blackwell et al 1 reported a series of 14 patients who underwent lateral oromandibular reconstruction usingsofttissuefreeflapsinconjunctionwithbridgingthorp MRPs. While the incidence and nature of early postoperative reconstructive complications were acceptable, there was a 29% incidence of delayed reconstructive failure after a median follow-up period of 16.5 months. The most common cause of delayed reconstructive failure was external extrusion of the plate through the cheek skin, which occurred in 3 patients after postoperative intervals of 7, 15, and 15 months, respectively. It was postulated that delayed external plate extrusion occurred as a result of soft tissue contraction within the dead space medial to the MRP. The authors concluded that most simple lateral oromandibular defects were optimally reconstructed using a composite soft tissue vascularized bone free flap, while some complex lateral defects would require transfer of 2 simultaneous free flaps for separate osseous and soft tissue reconstruction. In the current series, the incidence of hardwarerelated reconstructive failure was reduced to 7% in 27 patients who underwent reconstruction using a secondgeneration, low-profile locking MRP after a similar median follow-up period of 19.5 months. Detailed analysis of the patient and defect characteristics failed to reveal discernible differences between the subjects of the 2 series that might account for the different outcomes. Tumor type and stage, defect classification, and flap selection were similar in the 2 series, and the incidence of radiation therapy in the previous series (100%) was only incrementally higher than in the current series (85%). The prevalence of throughand-through oromandibular defects, which is probably a 991
5 Figure 2. Size and shape comparison of a THORP (titanium hollow screw reconstruction plate) system (upper plate) vs the Leibinger Locking System (lower plate) shown from a lateral view (left) and profile height (right). risk factor for external plate extrusion, was higher in the current series than in the previous series. In 1994, a second-generation locking MRP was introduced by Stryker Leibinger Inc. This system has a plate profile height of 2.8 mm, compared with a THORP system profile height of 3.5 mm. Perhaps more important than this difference in profile height, the Leibinger Locking System plate has a smooth, rounded contour compared with the geometry of the THORP system (Figure 2). More recently, additional second-generation locking MRPs have been introduced by Synthes U.S.A. (Paoli, Pa), Walter Lorenz Surgical Inc (Jacksonville, Fla), and KLS Martin, LP (Jacksonville, Fla). Most of these systems also offer a lower profile and rounded plate contour when compared with the THORP system. To our knowledge, the current series is the first to investigate the potential role of lowprofile locking MRPs as a bridging plate system. In the current series of low-profile bridging MRPs, there was only 1 case of external plate extrusion, and this occurred after reconstruction of a through-and-through defect. It is possible that the low-profile height and smooth contour of the second-generation locking MRP contributedtoalowincidenceofplateextrusionthroughthecheek skin when compared with the first-generation locking MRP. If this is the case, then it is likely that external plate extrusions previously reported in patients with bridging THORP MRPs resulted from a plate geometry that was prone to extrude rather than from soft tissue contraction within the dead space medial to a bridging plate. Indeed, experience with the THORP system for fixation of vascularized bone grafts indicates that there is a notable incidence of plate extrusion even when the plate is used in conjunction with a vascularized bone graft. 4 Defects were described in the current series and in the previous series by Blackwell et al 1 using the most detailed method of oromandibular defect classification reported in the literature, 4 and this analysis failed to reveal significant differences between the 2 groups of patients. However, we recognize the possibility that the decreased incidence of plate extrusion seen in the current series when compared with the previous series of patients who underwent THORP reconstruction may be the result of unidentified variables between the 2 series of patients. For instance, evidence suggests that the length of the segmental mandibular defect and the volume of the resection specimen have an impact on the likelihood of failure after bridging plate reconstruction. 10 These factors were not considered in the current analysis. The incidence of plate fracture was not increased when using a low-profile locking MRP in the current series compared with previous series of bridging plates using the larger THORP system. Possible explanations for why a smaller plate is not more prone to fracture may relate to differences in the titanium alloys used in the 2 plating systems or to differences in plate geometry. When a bending force is applied to a THORP MRP, there is a tendency for plate deformation to occur at the screw holes. Plate deformation occurs primarily between the screw holes when contouring a Leibinger Locking System MRP. In general, plate fractures tend to occur at these sites of plate deformation due to metal fatigue. A THORP plate fracture usually occurs through a screw hole where the plate has a minimum crosssectional area, while the Leibinger Locking System plate fracture that occurred in the current series occurred between 2 screw holes, where the plate has a maximum crosssectional area (Figure 3). Regardless of intrinsic plate strength, all patients who are able to chew using remaining maxillary and mandibular dentition are at risk to eventually experience fracture of a bridging MRP. Therefore, longer follow-up will be necessary before the durability of bridging Leibinger Locking System MRPs can be assessed. A series by Cordeiro and Hildalgo 11 reported that the average operative time for patients who underwent oromandibular reconstruction using soft tissue free flaps and bridging MRPs was 721 minutes, which falls within the range of most osteocutaneous flap oromandibular reconstructions. Therefore, the soft tissue free flap with bridging plate option should not be selected for cases of lateral oromandibular reconstruction in an attempt to decrease surgical time or perioperative medical morbidity in patients who are acceptable candidates to undergo a vascularized bone containing free flap on the basis of defect analysis. Indeed, the incidence of major medical complications in the current series was 39%, compared with a 17% incidence of major medical complications seen during the senior author s (K.E.B.) career experience with 119 microvascular head and neck reconstructions. 12 However, the increased incidence of medical complications in the current series probably reflects our bias to limit the 992
6 Figure 3. Left, Panoramic radiograph of a fractured titanium hollow-screw reconstruction plate reconstruction occurring through a screw hole, where the plate has minimal cross-sectional area. Right, Panoramic radiograph of a fractured Leibinger Locking System reconstruction occurring between 2 screw holes (arrow), where the plate has maximum cross-sectional area. complexity of reconstruction in a patient population with substantial preoperative comorbidity who are at high risk to experience complications. Most of the patients in this series would have required 2 simultaneous free flaps to achieve an osseous reconstruction with a good-quality soft tissue reconstruction. Performance of 2 simultaneous free flaps adds approximately 2 hours to the length of surgery when compared with performance of a single free flap. 13 It is doubtful that this incremental increased length of surgery would result in a significantly increased incidence of medical complications. However, use of 2 simultaneous free flaps results in increased donor site morbidity; there is no doubt that performance of 2 simultaneous free flaps adds to the complexity of reconstruction when compared with using a single soft tissue free flap with a bridging plate. The increased morbidity resulting from the complexity of simultaneous free flap transfer is reflected in the 7% incidence of total flap failure reported in 43 cases of dual free flap oromandibular reconstruction described in the literature, compared with the 100% flap survival achieved in the current series. In addition, Nakatsuka et al 15 reported a 41% incidence of early perioperative reconstructive complications in a series of dual free flap oromandibular reconstruction, while there were no cases of significant perioperative reconstructive complications in the current series. CONCLUSIONS Reconstruction was successful in 93% of 27 cases of lateral oromandibular reconstruction using soft tissue free flaps in conjunction with second-generation bridging locking MRPs. The high incidence of delayed external plate extrusion seen previously with THORP plates used in this manner was reduced by using a low-profile, roundedcontour plate in the current series, and use of a smaller plating system did not result in an increased incidence of plate fracture after a similar length of follow-up. Vascularized bone containing free flaps remain the preferred method for reconstruction of most lateral oromandibular defects. However, preliminary analysis of the current series indicates that a soft tissue free flap used with a low-profile bridging plate might suffice in cases where a significant soft tissue resection would otherwise require transfer of 2 simultaneous free flaps. Final assessment of the durability of this technique will require long-term follow-up. Accepted for publication May 14, Reprints: Keith E. Blackwell, MD, Box , UCLA Medical Center, Los Angeles, CA REFERENCES 1. Blackwell KE, Buchbinder D, Urken ML. Lateral oromandibular reconstruction using soft tissue free flaps and plates. Arch Otolaryngol Head Neck Surg. 1996; 122: Vuillemin T, Raveh J, Sutter F. Mandibular reconstruction with the titanium hollow screw reconstruction plate (THORP) system: evaluation of 62 cases. Plast Reconstr Surg. 1988;82: Urken ML, Weinberg H, Vickery C, Buchbinder D, Lawson W, Biller HF. Oromandibular reconstruction using microvascular composite free flaps: report of 71 cases and a new classification scheme for bony, soft tissue, and neurologic defects. Arch Otolaryngol Head Neck Surg. 1991;117: Urken ML, Buchbinder D, Costantino PD, et al. Oromandibular reconstruction using microvascular composite flaps: report of 210 cases. Arch Otolaryngol Head Neck Surg. 1998;124: Urken ML, Weinberg H, Vickery C, Buchbinder D, Lawson W, Biller HF. The internal oblique-iliac crest free flap in composite defects of the oral cavity involving bone, skin, and mucosa. Laryngoscope. 1991;101: Haughey BH, Fredrickson JM, Lerrick AJ, Sclaroff A, Gay WD. Fibular and iliac crest osteomuscular free flap reconstruction of the oral cavity. Laryngoscope. 1994;104: Wenig BL, Keller AJ. Microvascular free-tissue transfer with rigid internal fixation for reconstruction of the mandible following tumor resection. Otolaryngol Clin North Am. 1987;20: Schusterman MA, Reece GP, Kroll SS, Weldon ME. Use of the AO plate for immediate mandibular reconstruction in cancer patients. Plast Reconstr Surg. 1991; 88: Boyd JB, Mulholland RS, Davidson J, et al. The free flap and plate in oromandibular reconstruction: long-term review and indications. Plast Reconstr Surg. 1995;95: Arden RL, Rachel JD, Marks SC, Dang K. Volume-length impact of lateral jaw resections on complication rates. Arch Otolaryngol Head Neck Surg. 1999;125: Cordeiro PG, Hildago DA. Soft tissue coverage of mandibular reconstruction plates. Head Neck Surg. 1994;16: Blackwell KE. Unsurpassed reliability of free flaps for head and neck reconstruction. Arch Otolaryngol Head Neck Surg. 1999;125: Urken ML, Weinberg H, Vickery C, et al. The combined sensate radial forearm and iliac crest free flaps for reconstruction of significant glossectomymandibulectomy defects. Laryngoscope. 1992;102: Sanger JR, Matloub HS, Yousif NJ. Sequential connection of flaps: a logical approach to customized mandibular reconstruction. Am J Surg. 1990;160: Nakatsuka T, Harii K, Yamada A, Ueda K, Ebihara S. Dual free flap transfer using forearm flap for mandibular reconstruction. Head Neck. 1992;14: Wells MD, Luce EA, Edwards AL, Vasconez H, Sadove R, Bouzaglou S. Sequentially linked free flaps in head and neck reconstruction. Clin Plast Surg. 1994; 21:
Plate Exposure after Reconstruction by Plate and Anterolateral Thigh Flap in Head and Neck Cancer Patients with composite mandibular Defects
 Plate Exposure after Reconstruction by Plate and Anterolateral Thigh Flap in Head and Neck Cancer Patients with composite mandibular Defects Chia-Hsuan Tsai/ Huang-Kai Kao M. D. Introduction Malignant
Plate Exposure after Reconstruction by Plate and Anterolateral Thigh Flap in Head and Neck Cancer Patients with composite mandibular Defects Chia-Hsuan Tsai/ Huang-Kai Kao M. D. Introduction Malignant
Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap.
 Case Report Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF, Patient Specific Plate Contouring (PSPC) and the MatrixMANDIBLE Plating
Case Report Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF, Patient Specific Plate Contouring (PSPC) and the MatrixMANDIBLE Plating
CASE REPORT Reconstruction and Characterization of Composite Mandibular Defects Requiring Double Skin Paddle Fibular Free Flaps
 CASE REPORT Reconstruction and Characterization of Composite Mandibular Defects Requiring Double Skin Paddle Fibular Free Flaps Austin M. Badeau, BA, a and Frederic W.-B. Deleyiannis, MD, MPhil, MPH b
CASE REPORT Reconstruction and Characterization of Composite Mandibular Defects Requiring Double Skin Paddle Fibular Free Flaps Austin M. Badeau, BA, a and Frederic W.-B. Deleyiannis, MD, MPhil, MPH b
Screw hole-positioning guide and plate-positioning guide: A novel method to assist mandibular reconstruction
 Journal of Dental Sciences (2012) 7, 301e305 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Screw hole-positioning guide and plate-positioning guide: A novel method
Journal of Dental Sciences (2012) 7, 301e305 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Screw hole-positioning guide and plate-positioning guide: A novel method
REINNERVATED ANTEROLATERAL THIGH FLAP FOR TONGUE RECONSTRUCTION
 REINNERVATED ANTEROLATERAL THIGH FLAP FOR TONGUE RECONSTRUCTION Peirong Yu, MD Department of Plastic Surgery, FC-8.2000, 1400 Holcombe Boulevard, Houston, TX 77030. E-mail: peirongyu@mdanderson.org Accepted
REINNERVATED ANTEROLATERAL THIGH FLAP FOR TONGUE RECONSTRUCTION Peirong Yu, MD Department of Plastic Surgery, FC-8.2000, 1400 Holcombe Boulevard, Houston, TX 77030. E-mail: peirongyu@mdanderson.org Accepted
Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases
 J Oral Maxillofac Surg 58:1104-1108, 2000 Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases Yadranko Ducic, MD, FRCS (C),* and Mark Burye, DDS Purpose: This article describes
J Oral Maxillofac Surg 58:1104-1108, 2000 Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases Yadranko Ducic, MD, FRCS (C),* and Mark Burye, DDS Purpose: This article describes
Surgery in Head and neck cancers.principles. Dr Diptendra K Sarkar MS,DNB,FRCS Consultant surgeon,ipgmer
 Surgery in Head and neck cancers.principles Dr Diptendra K Sarkar MS,DNB,FRCS Consultant surgeon,ipgmer Email:diptendrasarkar@yahoo.co.in HNC : common inclusives Challenges Anatomical preservation R0 Surgical
Surgery in Head and neck cancers.principles Dr Diptendra K Sarkar MS,DNB,FRCS Consultant surgeon,ipgmer Email:diptendrasarkar@yahoo.co.in HNC : common inclusives Challenges Anatomical preservation R0 Surgical
A review of the advantages of the anterolateral thigh flap in head and neck reconstruction
 The British Association of Plastic Surgeons (2004) 57, 603 609 A review of the advantages of the anterolateral thigh flap in head and neck reconstruction Jagdeep S. Chana, Fu-chan Wei* Department of Plastic
The British Association of Plastic Surgeons (2004) 57, 603 609 A review of the advantages of the anterolateral thigh flap in head and neck reconstruction Jagdeep S. Chana, Fu-chan Wei* Department of Plastic
Disclosures. The Expanding Role of Microvascular Reconstruction. Overview. Things they are a Changing. Surgical Advisory Board, Genentech Corp
 Disclosures Surgical Advisory Board, Genentech Corp The Expanding Role of Microvascular Reconstruction P. Daniel Knott, MD FACS Associate Professor Director, Facial Plastic and Reconstructive Surgery UCSF
Disclosures Surgical Advisory Board, Genentech Corp The Expanding Role of Microvascular Reconstruction P. Daniel Knott, MD FACS Associate Professor Director, Facial Plastic and Reconstructive Surgery UCSF
Survey of Laryngeal Cancer at SBUH comparing 108 cases seen here from to the NCDB of 9,256 cases diagnosed nationwide in 2000
 Survey of Laryngeal Cancer at comparing 108 cases seen here from 1998 2002 to the of 9,256 cases diagnosed nationwide in 2000 Stony Brook University Hospital Cancer Program Annual Report 2002-2003 Gender
Survey of Laryngeal Cancer at comparing 108 cases seen here from 1998 2002 to the of 9,256 cases diagnosed nationwide in 2000 Stony Brook University Hospital Cancer Program Annual Report 2002-2003 Gender
Reconstruction of large mandibular defects
 Immediate Reconstruction of a Large Mandibular Defect of Locally Invasive Benign Lesions (A New Method) Gholamreza Shirani, OMFS, DDS, MS,* Mahnaz Arshad, DDS, 1 Farnoush Mohammadi, OMFS, DDS, MS* Tehran,
Immediate Reconstruction of a Large Mandibular Defect of Locally Invasive Benign Lesions (A New Method) Gholamreza Shirani, OMFS, DDS, MS,* Mahnaz Arshad, DDS, 1 Farnoush Mohammadi, OMFS, DDS, MS* Tehran,
Reconstruction for Oral Neoplasms in Indian Setup: Redebating the Utility of Radial Artery Free Flaps
 World Articles of Ear, Nose and Throat ---------------------Page 1 Reconstruction for Oral Neoplasms in Indian Setup: Redebating the Utility of Radial Artery Free Flaps Authors: Ranjan G Aiyer*, Rahul
World Articles of Ear, Nose and Throat ---------------------Page 1 Reconstruction for Oral Neoplasms in Indian Setup: Redebating the Utility of Radial Artery Free Flaps Authors: Ranjan G Aiyer*, Rahul
A novel classification system for the evaluation and reconstruction of oral defects following oncological surgery
 ONCOLOGY LETTERS 14: 7049-7054, 2017 A novel classification system for the evaluation and reconstruction of oral defects following oncological surgery WEI WEI LIU, CHU YI ZHANG, JIAN YIN LI, MING FANG
ONCOLOGY LETTERS 14: 7049-7054, 2017 A novel classification system for the evaluation and reconstruction of oral defects following oncological surgery WEI WEI LIU, CHU YI ZHANG, JIAN YIN LI, MING FANG
Multi-dimensional analysis of oral cavity and oropharyngeal defects following cancer extirpation surgery, a cadaveric study
 Idris et al. Journal of Otolaryngology - Head and Neck Surgery (2018) 47:27 https://doi.org/10.1186/s40463-018-0276-9 ORIGINAL RESEARCH ARTICLE Open Access Multi-dimensional analysis of oral cavity and
Idris et al. Journal of Otolaryngology - Head and Neck Surgery (2018) 47:27 https://doi.org/10.1186/s40463-018-0276-9 ORIGINAL RESEARCH ARTICLE Open Access Multi-dimensional analysis of oral cavity and
BUILDING A. Achieving total reconstruction in a single operation. 70 OCTOBER 2016 // dentaltown.com
 BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
ORIGINAL ARTICLE. Condylar Prostheses in Head and Neck Cancer Reconstruction
 Condylar Prostheses in Head and Neck Cancer Reconstruction Alpen Patel, MD; Robert Maisel, MD ORIGINAL ARTICLE Objective: To discuss the use of condylar prostheses after mandibular resection for tumor.
Condylar Prostheses in Head and Neck Cancer Reconstruction Alpen Patel, MD; Robert Maisel, MD ORIGINAL ARTICLE Objective: To discuss the use of condylar prostheses after mandibular resection for tumor.
RECONSTRUCTION OF SEGmental
 ORIGINAL ARTICLE Combining Use of Resin Models With External Fixation in Mandibular Reconstruction Emre Vural, MD; James C. Yuen, MD Objective: To obtain accurate occlusion in mandibular reconstruction
ORIGINAL ARTICLE Combining Use of Resin Models With External Fixation in Mandibular Reconstruction Emre Vural, MD; James C. Yuen, MD Objective: To obtain accurate occlusion in mandibular reconstruction
Adipofascial anterolateral thigh free flap for tongue repair
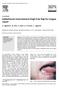 The British Association of Plastic Surgeons (2003) 56, 614 618 CASE REPORT Adipofascial anterolateral thigh free flap for tongue repair V. Agostini*, M. Dini, A. Mori, A. Franchi, T. Agostini Department
The British Association of Plastic Surgeons (2003) 56, 614 618 CASE REPORT Adipofascial anterolateral thigh free flap for tongue repair V. Agostini*, M. Dini, A. Mori, A. Franchi, T. Agostini Department
Reconstruction of a Maxillary Oncologic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF and the MatrixMIDFACE Plating System.
 Case Report Reconstruction of a Maxillary Oncologic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF and the MatrixMIDFACE Plating System. Reconstruction of a Maxillary Oncologic Defect
Case Report Reconstruction of a Maxillary Oncologic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF and the MatrixMIDFACE Plating System. Reconstruction of a Maxillary Oncologic Defect
Case Report. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System.
 Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
THE USE OF FREE AUTOGENOUS RIB GRAFTS IN MAXILLOFACIAL RECONSTRUCTION
 THE USE OF FREE AUTOGENOUS RIB GRAFTS IN MAXILLOFACIAL RECONSTRUCTION * P. DONKOR, D.O. BANKAS, G. BOAKYE 1, S. ANSAH and A.O. ACHEAMPONG Oral and Maxillofacial Unit, Departments of Surgery and 1 Anaesthesia,
THE USE OF FREE AUTOGENOUS RIB GRAFTS IN MAXILLOFACIAL RECONSTRUCTION * P. DONKOR, D.O. BANKAS, G. BOAKYE 1, S. ANSAH and A.O. ACHEAMPONG Oral and Maxillofacial Unit, Departments of Surgery and 1 Anaesthesia,
Craniomaxillofacial. Customized Mandible Reconstruction Plate. Patient Specific Design Powered by BluePrint Technology
 Craniomaxillofacial Customized Mandible Reconstruction Plate Patient Specific Design Powered by BluePrint Technology We re putting the control in your hands Customized Mandible gives you the flexibility
Craniomaxillofacial Customized Mandible Reconstruction Plate Patient Specific Design Powered by BluePrint Technology We re putting the control in your hands Customized Mandible gives you the flexibility
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
Use of the Teres Major Muscle in Chimeric Subscapular System Free Flaps for Head and Neck Reconstruction
 Research Original Investigation Use of the Teres Major Muscle in Chimeric Sub System Free Flaps for Head and Neck Reconstruction Andrew R. Tomlinson, MD; Mark J. Jameson, MD, PhD; Nitin A. Pagedar, MD,
Research Original Investigation Use of the Teres Major Muscle in Chimeric Sub System Free Flaps for Head and Neck Reconstruction Andrew R. Tomlinson, MD; Mark J. Jameson, MD, PhD; Nitin A. Pagedar, MD,
Outcomes after free tissue transfer for composite oral cavity resections involving skin
 Received: 21 March 2017 Revised: 13 September 2017 Accepted: 22 November 2017 DOI: 10.1002/hed.25062 ORIGINAL ARTICLE Outcomes after free tissue transfer for composite oral cavity resections involving
Received: 21 March 2017 Revised: 13 September 2017 Accepted: 22 November 2017 DOI: 10.1002/hed.25062 ORIGINAL ARTICLE Outcomes after free tissue transfer for composite oral cavity resections involving
Maxillary Reconstruction with the Free Fibula Flap
 Maxillary Reconstruction with the Free Fibula Flap Xin Peng, D.D.S., Ph.D., Chi Mao, D.D.S., Ph.D., Guang-yan Yu, D.D.S., Ph.D., Chuan-bin Guo, D.D.S., Ph.D., Min-xian Huang, D.D.S., and Yi Zhang, D.D.S.,
Maxillary Reconstruction with the Free Fibula Flap Xin Peng, D.D.S., Ph.D., Chi Mao, D.D.S., Ph.D., Guang-yan Yu, D.D.S., Ph.D., Chuan-bin Guo, D.D.S., Ph.D., Min-xian Huang, D.D.S., and Yi Zhang, D.D.S.,
Customized Mandible Reconstruction Plate
 Craniomaxillofacial Customized Mandible Reconstruction Plate Patient Specific Design Powered by BluePrint Technology We re putting the control in your hands Customized Mandible gives you the flexibility
Craniomaxillofacial Customized Mandible Reconstruction Plate Patient Specific Design Powered by BluePrint Technology We re putting the control in your hands Customized Mandible gives you the flexibility
(loco-regional disease)
 (loco-regional disease) (oral cavity) (circumvillae papillae) (subsite) A (upper & lower lips) B (buccal membrane) C (mouth floor) D (upper & lower gingiva) E (hard palate) F (tongue -- anterior 2/3 rds
(loco-regional disease) (oral cavity) (circumvillae papillae) (subsite) A (upper & lower lips) B (buccal membrane) C (mouth floor) D (upper & lower gingiva) E (hard palate) F (tongue -- anterior 2/3 rds
Primary closure of the deltopectoral flap-donor site without skin grafting
 Primary closure of the deltopectoral flap-donor site without skin grafting Received: 4/3/2013 Accepted: 14/5/2013 Introduction Reliable and simultaneous reconstruction of head-and-neck defects has been
Primary closure of the deltopectoral flap-donor site without skin grafting Received: 4/3/2013 Accepted: 14/5/2013 Introduction Reliable and simultaneous reconstruction of head-and-neck defects has been
Osteoradionecrosis of Jaw in Head and Neck Cancer Patient Treated with Free Iliac Bone and Umbilical Fat Pad Graft
 Maxillofac Plast Reconstr Surg 2014;36(2):62-66 http://dx.doi.org/10.14402/jkamprs.2014.36.2.62 ISSN 2288-8101(Print) ISSN 2288-8586(Online) Case Report Osteoradionecrosis of Jaw in Head and Neck Cancer
Maxillofac Plast Reconstr Surg 2014;36(2):62-66 http://dx.doi.org/10.14402/jkamprs.2014.36.2.62 ISSN 2288-8101(Print) ISSN 2288-8586(Online) Case Report Osteoradionecrosis of Jaw in Head and Neck Cancer
Interesting Case Series. Scalp Reconstruction With Free Latissimus Dorsi Muscle
 Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
The learning curve in head and neck reconstruction with microvascular free flaps: a retrospective review
 Asian Biomedicine Vol. 4 No. 6 December 2010; 907-912 Brief communication (Original) The learning curve in head and neck reconstruction with microvascular free flaps: a retrospective review Patnarin Mahattanasakul
Asian Biomedicine Vol. 4 No. 6 December 2010; 907-912 Brief communication (Original) The learning curve in head and neck reconstruction with microvascular free flaps: a retrospective review Patnarin Mahattanasakul
ORIGINAL ARTICLE. The Palatal Island Flap for Reconstruction of Palatal and Retromolar Trigone Defects Revisited. decades, the range of reconstructive
 ORIGINAL ARTICLE The Palatal Island Flap for Reconstruction of Palatal and Retromolar Trigone Defects Revisited Eric M. Genden, MD; Bryant B. Lee, MD; Mark L. Urken, MD Background: Although a host of local
ORIGINAL ARTICLE The Palatal Island Flap for Reconstruction of Palatal and Retromolar Trigone Defects Revisited Eric M. Genden, MD; Bryant B. Lee, MD; Mark L. Urken, MD Background: Although a host of local
COMPARISON OF MINIPLATES AND RECONSTRUCTION PLATES IN MANDIBULAR RECONSTRUCTION
 COMPARISON OF MINIPLATES AND RECONSTRUCTION PLATES IN MANDIBULAR RECONSTRUCTION Richard J. Shaw, FRCS, 1 A. N. Kanatas, MFDS, 2 Derek Lowe, C Stat, MSc, 1 James S. Brown, FRCS, MD, 1 Simon N. Rogers, FRCS,
COMPARISON OF MINIPLATES AND RECONSTRUCTION PLATES IN MANDIBULAR RECONSTRUCTION Richard J. Shaw, FRCS, 1 A. N. Kanatas, MFDS, 2 Derek Lowe, C Stat, MSc, 1 James S. Brown, FRCS, MD, 1 Simon N. Rogers, FRCS,
Value of preoperative mandibular plating in reconstruction of the mandible
 ORIGINAL ARTICLE Value of preoperative mandibular plating in reconstruction of the mandible Eitan Prisman, MD, FRCSC, * Stephan K. Haerle, MD, MSc, FRCSC, Jonathan C. Irish, MD, Michael Daly, MSc, Brett
ORIGINAL ARTICLE Value of preoperative mandibular plating in reconstruction of the mandible Eitan Prisman, MD, FRCSC, * Stephan K. Haerle, MD, MSc, FRCSC, Jonathan C. Irish, MD, Michael Daly, MSc, Brett
SIMPLIFYING HEAD AND NECK MICROVASCULAR RECONSTRUCTION
 SIMPLIFYING HEAD AND NECK MICROVASCULAR RECONSTRUCTION Eben Rosenthal, MD, 1 William Carroll, MD, 1 Mathew Dobbs, BA, 1 J. Scott Magnuson, MD, 1 Mark Wax, MD, 2 Glenn Peters, MD 1 1 Department of Surgery,
SIMPLIFYING HEAD AND NECK MICROVASCULAR RECONSTRUCTION Eben Rosenthal, MD, 1 William Carroll, MD, 1 Mathew Dobbs, BA, 1 J. Scott Magnuson, MD, 1 Mark Wax, MD, 2 Glenn Peters, MD 1 1 Department of Surgery,
The gastrocnemius with soleus bi-muscle flap
 The British Association of Plastic Surgeons (2004) 57, 77 82 The gastrocnemius with soleus bi-muscle flap Ikuo Hyodo a, *, Bin Nakayama b, Mitsuru Takahashi c, Kazuhiro Toriyama d, Yuzuru Kamei d, Shuhei
The British Association of Plastic Surgeons (2004) 57, 77 82 The gastrocnemius with soleus bi-muscle flap Ikuo Hyodo a, *, Bin Nakayama b, Mitsuru Takahashi c, Kazuhiro Toriyama d, Yuzuru Kamei d, Shuhei
THE SUBMENTAL ISLAND FLAP IN HEAD AND NECK RECONSTRUCTION
 THE SUBMENTAL ISLAND FLAP IN HEAD AND NECK RECONSTRUCTION Emre Vural, MD, James Y. Suen, MD Department of Otolaryngology-Head and Neck Surgery, University of Arkansas for Medical Sciences, 4301 West Markham,
THE SUBMENTAL ISLAND FLAP IN HEAD AND NECK RECONSTRUCTION Emre Vural, MD, James Y. Suen, MD Department of Otolaryngology-Head and Neck Surgery, University of Arkansas for Medical Sciences, 4301 West Markham,
Combined tongue flap and V Y advancement flap for lower lip defects
 British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
For the Attention of the Operating Surgeon: IMPORTANT INFORMATION ON THE MATRIXRIB FIXATION SYSTEM
 For the Attention of the Operating Surgeon: IMPORTANT INFORMATION ON THE MATRIXRIB FIXATION SYSTEM 10/16 GP2685-E-CAN DESCRIPTION The MatrixRIB Fixation System consists of locking plates, locking screws,
For the Attention of the Operating Surgeon: IMPORTANT INFORMATION ON THE MATRIXRIB FIXATION SYSTEM 10/16 GP2685-E-CAN DESCRIPTION The MatrixRIB Fixation System consists of locking plates, locking screws,
Accepted 13 March 2008 Published online 18 July 2008 in Wiley InterScience ( DOI: /hed.20874
 ORIGINAL ARTICLE ZYGOMATICOMAXILLARY BUTTRESS RECONSTRUCTION OF MIDFACE DEFECTS WITH THE OSTEOCUTANEOUS RADIAL FOREARM FREE FLAP Patricio Andrades, MD, Eben L. Rosenthal, MD, William R. Carroll, MD, Christopher
ORIGINAL ARTICLE ZYGOMATICOMAXILLARY BUTTRESS RECONSTRUCTION OF MIDFACE DEFECTS WITH THE OSTEOCUTANEOUS RADIAL FOREARM FREE FLAP Patricio Andrades, MD, Eben L. Rosenthal, MD, William R. Carroll, MD, Christopher
Fibular Bone Graft for Nasal Septal Reconstruction: A Case Report
 220 Nasal septal reconstruction Case Report Fibular Bone Graft for Nasal Septal Reconstruction: A Case Report Yakup Cil1* Diyarbakır Military Hospital, Department of Plastic Surgery 21000 Diyarbakır, Turkey
220 Nasal septal reconstruction Case Report Fibular Bone Graft for Nasal Septal Reconstruction: A Case Report Yakup Cil1* Diyarbakır Military Hospital, Department of Plastic Surgery 21000 Diyarbakır, Turkey
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/31632 holds various files of this Leiden University dissertation. Author: Mensink, Gertjan Title: Bilateral sagittal split osteotomy by the splitter-separator
Cover Page The handle http://hdl.handle.net/1887/31632 holds various files of this Leiden University dissertation. Author: Mensink, Gertjan Title: Bilateral sagittal split osteotomy by the splitter-separator
Technique Guide. Compact 2.0 LOCK Mandible. The locking system for the mandible.
 Technique Guide Compact 2.0 LOCK Mandible. The locking system for the mandible. Table of Contents Introduction Compact 2.0 LOCK Mandible 2 AO Principles 4 Indications and Contraindications 5 Surgical
Technique Guide Compact 2.0 LOCK Mandible. The locking system for the mandible. Table of Contents Introduction Compact 2.0 LOCK Mandible 2 AO Principles 4 Indications and Contraindications 5 Surgical
Versatility of Reverse Sural Artery Flap for Heel Reconstruction
 ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
Fascia Lata Free Flap Reconstruction of Limited Hard Palate Defects
 Open Access Original Article DOI: 10.7759/cureus.2356 Fascia Lata Free Flap Reconstruction of Limited Hard Palate Defects Rhorie P. Kerr 1, Andrea Hanick 1, Michael A. Fritz 1 1. Head and Neck Institute,
Open Access Original Article DOI: 10.7759/cureus.2356 Fascia Lata Free Flap Reconstruction of Limited Hard Palate Defects Rhorie P. Kerr 1, Andrea Hanick 1, Michael A. Fritz 1 1. Head and Neck Institute,
Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect of Upper and Middle Third Leg
 Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
Learning Objectives. Head and Neck Cancer: Post-Treatment Changes. Neck Dissection Classification * Radical neck dissection. Radical Neck Dissection
 Head and Neck Cancer: Post-Treatment Changes Daniel W. Williams III, MD Learning Objectives In patients treated for H/N Cancer: Describe the various types of neck dissections Explain reconstruction techniques
Head and Neck Cancer: Post-Treatment Changes Daniel W. Williams III, MD Learning Objectives In patients treated for H/N Cancer: Describe the various types of neck dissections Explain reconstruction techniques
CASE REPORT. CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration
 Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts
 Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
JPRAS Open 3 (2015) 1e5. Contents lists available at ScienceDirect. JPRAS Open. journal homepage:
 JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
Cancer of the Oral Cavity
 The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology Cancer of the Oral Cavity Ashok Shaha Principals of Management of Oral Cancer A)
The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology Cancer of the Oral Cavity Ashok Shaha Principals of Management of Oral Cancer A)
Accepted 16 March 2006 Published online 5 July 2006 in Wiley InterScience (www.interscience.wiley.com). DOI: /hed.20463
 ORIGINAL ARTICLE PROGNOSIS AS A DETERMINANT OF FREE FLAP UTILIZATION FOR RECONSTRUCTION OF THE LATERAL MANDIBULAR DEFECT Frederic W.-B. Deleyiannis, MD, MPhil, MPH, 1,2 Edward Lee, MD, 1 Brian Gastman,
ORIGINAL ARTICLE PROGNOSIS AS A DETERMINANT OF FREE FLAP UTILIZATION FOR RECONSTRUCTION OF THE LATERAL MANDIBULAR DEFECT Frederic W.-B. Deleyiannis, MD, MPhil, MPH, 1,2 Edward Lee, MD, 1 Brian Gastman,
Facelift approach for mandibular resection and reconstruction
 ORIGINAL ARTICLE Facelift approach for mandibular resection and reconstruction Bernardo Bianchi, MD, Andrea Ferri, MD, * Silvano Ferrari, MD, Chiara Copelli, MD, Enrico Sesenna, MD Maxillo-Facial Surgery
ORIGINAL ARTICLE Facelift approach for mandibular resection and reconstruction Bernardo Bianchi, MD, Andrea Ferri, MD, * Silvano Ferrari, MD, Chiara Copelli, MD, Enrico Sesenna, MD Maxillo-Facial Surgery
Travis G. Boyd, BS, a Katherine M. Huber, BS, a Daniel E. Verbist, BS, a Jeffery M. Bumpous, MD, b and Bradon J. Wilhelmi, MD c INTRODUCTION
 CASE REPORT Removal of Exposed Titanium Reconstruction Plate After Mandibular Reconstruction With a Free Fibula Osteocutaneous Flap With Large Surgical Pin Cutters: A Case Report and Literature Review
CASE REPORT Removal of Exposed Titanium Reconstruction Plate After Mandibular Reconstruction With a Free Fibula Osteocutaneous Flap With Large Surgical Pin Cutters: A Case Report and Literature Review
Case Scenario 1. 7/13/12 Anterior floor of mouth biopsy: Infiltrating squamous cell carcinoma, not completely excised.
 Case Scenario 1 7/5/12 History A 51 year old white female presents with a sore area on the floor of her mouth. She claims the area has been sore for several months. She is a current smoker and user of
Case Scenario 1 7/5/12 History A 51 year old white female presents with a sore area on the floor of her mouth. She claims the area has been sore for several months. She is a current smoker and user of
Vascularized Rib for Facial Reconstruction
 Vascularized Rib for Facial Reconstruction Steven P. Davison, M.D., D.D.S., James H. Boehmler, M.D., Jason C. Ganz, M.D., and Bruce Davidson, M.D. Washington, D.C. The reconstruction of maxillectomy defects
Vascularized Rib for Facial Reconstruction Steven P. Davison, M.D., D.D.S., James H. Boehmler, M.D., Jason C. Ganz, M.D., and Bruce Davidson, M.D. Washington, D.C. The reconstruction of maxillectomy defects
MEDPOR. Oral maxillofacial surgery
 MEDPOR Oral maxillofacial surgery MEDPOR biomaterial MEDPOR has been a trusted name in the industry since 1985, with hundreds of thousands of procedures performed, and hundreds of published clinical reports
MEDPOR Oral maxillofacial surgery MEDPOR biomaterial MEDPOR has been a trusted name in the industry since 1985, with hundreds of thousands of procedures performed, and hundreds of published clinical reports
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty
 CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
LOGIC SURGICAL TECHNIQUE GUIDE. In d i c at i o n s. Co n t r a i n d i c at i o n s. Mandibular Distraction System
 TM SURGICAL TECHNIQUE GUIDE In d i c at i o n s The OSTEOMED Mandibular Distractor system is indicated for use as a mandibular bone lengthener for patients diagnosed with conditions where treatment includes
TM SURGICAL TECHNIQUE GUIDE In d i c at i o n s The OSTEOMED Mandibular Distractor system is indicated for use as a mandibular bone lengthener for patients diagnosed with conditions where treatment includes
SURGICAL TECHNIQUE. Protrusio Cage A COMPREHENSIVE ACETABULAR REVISION SYSTEM
 SURGICAL TECHNIQUE Protrusio Cage A COMPREHENSIVE ACETABULAR REVISION SYSTEM Important: This essential product information does not include all of the information necessary for selection and use of a device.
SURGICAL TECHNIQUE Protrusio Cage A COMPREHENSIVE ACETABULAR REVISION SYSTEM Important: This essential product information does not include all of the information necessary for selection and use of a device.
THE pedicled flap, commonly used by the plastic surgeon in the reconstruction
 THE PEDICLE!) SKIN FLAP ROBIN ANDERSON, M.D. Department of Plastic Surgery THE pedicled flap, commonly used by the plastic surgeon in the reconstruction of skin and soft tissue defects, differs from the
THE PEDICLE!) SKIN FLAP ROBIN ANDERSON, M.D. Department of Plastic Surgery THE pedicled flap, commonly used by the plastic surgeon in the reconstruction of skin and soft tissue defects, differs from the
SENSORY TOPOGRAPHY OF THE ORAL CAVITY AND THE IMPACT OF FREE FLAP RECONSTRUCTION: A PRELIMINARY STUDY
 SENSORY TOPOGRAPHY OF THE ORAL CAVITY AND THE IMPACT OF FREE FLAP RECONSTRUCTION: A PRELIMINARY STUDY Karen B. Zur, MD, Eric M. Genden, MD, Mark L. Urken, MD Department of Otolaryngology Head & Neck Surgery,
SENSORY TOPOGRAPHY OF THE ORAL CAVITY AND THE IMPACT OF FREE FLAP RECONSTRUCTION: A PRELIMINARY STUDY Karen B. Zur, MD, Eric M. Genden, MD, Mark L. Urken, MD Department of Otolaryngology Head & Neck Surgery,
Head and Neck Cancer in FA: Risks, Prevention, Screening, & Treatment Options David I. Kutler, M.D., F.A.C.S.
 Head and Neck Cancer in FA: Risks, Prevention, Screening, & Treatment Options David I. Kutler, M.D., F.A.C.S. Associate Professor Division of Head and Neck Surgery Department of Otolaryngology-Head and
Head and Neck Cancer in FA: Risks, Prevention, Screening, & Treatment Options David I. Kutler, M.D., F.A.C.S. Associate Professor Division of Head and Neck Surgery Department of Otolaryngology-Head and
Kuwabara, Kaoru; Nonaka, Takashi; H. Citation Journal of Clinical Urology, 7(5),
 NAOSITE: Nagasaki University's Ac Title Author(s) Gluteal-fold adipofascial perforato fistula reconstruction Fujioka, Masaki; Hayashida, Kenji; Kuwabara, Kaoru; Nonaka, Takashi; H Citation Journal of Clinical
NAOSITE: Nagasaki University's Ac Title Author(s) Gluteal-fold adipofascial perforato fistula reconstruction Fujioka, Masaki; Hayashida, Kenji; Kuwabara, Kaoru; Nonaka, Takashi; H Citation Journal of Clinical
Locking Radial Head Plates
 Locking Radial Head Plates Locking Radial Head Plates Since 1988, Acumed has been designing solutions to the demanding situations facing orthopaedic surgeons, hospitals and their patients. Our strategy
Locking Radial Head Plates Locking Radial Head Plates Since 1988, Acumed has been designing solutions to the demanding situations facing orthopaedic surgeons, hospitals and their patients. Our strategy
A new angle to mandibular reconstruction: The scapular tip free flap
 ORIGINAL ARTICLE A new angle to mandibular reconstruction: The scapular tip free flap John Yoo, MD,* Samuel A. Dowthwaite, MBBS, Kevin Fung, MD, Jason Franklin, MD, Anthony Nichols, MD Department of Otolaryngology
ORIGINAL ARTICLE A new angle to mandibular reconstruction: The scapular tip free flap John Yoo, MD,* Samuel A. Dowthwaite, MBBS, Kevin Fung, MD, Jason Franklin, MD, Anthony Nichols, MD Department of Otolaryngology
ORIGINAL ARTICLE. most commonly result. involving the paranasal sinuses, the overlying facial skin, or both. Such defects may result in substantial
 ORIGINAL ARTICLE Use of Precontoured Positioning Plates and Pericranial Flaps in Midfacial Reconstruction to Optimize Aesthetic and Functional Outcomes Yadranko Ducic, MD, FRCSC; Lance E. Oxford, MD Objectives:
ORIGINAL ARTICLE Use of Precontoured Positioning Plates and Pericranial Flaps in Midfacial Reconstruction to Optimize Aesthetic and Functional Outcomes Yadranko Ducic, MD, FRCSC; Lance E. Oxford, MD Objectives:
A Study of Classification Systems for Maxillectomy Defects
 A Study of Classification Systems for Maxillectomy Defects Zubair Durrani FFDRCS, FRCS, FRCS (OMFS)* Syed Ghazanfar Hassan FFDRCS** Shomaila Ameer Alam BDS*** * Associate Professor & Consultant Oral and
A Study of Classification Systems for Maxillectomy Defects Zubair Durrani FFDRCS, FRCS, FRCS (OMFS)* Syed Ghazanfar Hassan FFDRCS** Shomaila Ameer Alam BDS*** * Associate Professor & Consultant Oral and
An island flap based on the anterior branch of the superficial temporal artery for perioral defects
 Free full text on www.ijps.org Original Article An island flap based on the anterior branch of the superficial temporal artery for perioral defects V. Bhattacharya, Ganji Raveendra Reddy, Sheikh Adil Bashir,
Free full text on www.ijps.org Original Article An island flap based on the anterior branch of the superficial temporal artery for perioral defects V. Bhattacharya, Ganji Raveendra Reddy, Sheikh Adil Bashir,
Increasing surgical freedom Restoring patient function
 Increasing surgical freedom Restoring patient function Fracture specific plating solutions for the most common tibia and fibula fractures Frequency of fracture occurrences* 66% 61% 36% 36% 28% 14% 20%
Increasing surgical freedom Restoring patient function Fracture specific plating solutions for the most common tibia and fibula fractures Frequency of fracture occurrences* 66% 61% 36% 36% 28% 14% 20%
Placement of implants in the mandible reconstructed with free vascularized fibula flap: comparison of 2 cases
 Placement of implants in the mandible reconstructed with free vascularized fibula flap: comparison of 2 cases Mehmet Kürkcü, DDS, MSc, PhD, a Mehmet Emre Benlidayı, DDS, b Cem Kurtoğlu, DDS, PhD, c and
Placement of implants in the mandible reconstructed with free vascularized fibula flap: comparison of 2 cases Mehmet Kürkcü, DDS, MSc, PhD, a Mehmet Emre Benlidayı, DDS, b Cem Kurtoğlu, DDS, PhD, c and
Case Scenario. 7/13/12 Anterior floor of mouth biopsy: Infiltrating squamous cell carcinoma, not completely excised.
 Case Scenario 7/5/12 History A 51 year old white female presents with a sore area on the floor of her mouth. She claims the area has been sore for several months. She is a current smoker and user of alcohol.
Case Scenario 7/5/12 History A 51 year old white female presents with a sore area on the floor of her mouth. She claims the area has been sore for several months. She is a current smoker and user of alcohol.
Nasolabial flap reconstruction in oral cancer
 Singh et al. World Journal of Surgical Oncology 2012, 10:227 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Open Access Nasolabial flap reconstruction in oral cancer Seema Singh, Rajesh Kumar Singh and Manoj
Singh et al. World Journal of Surgical Oncology 2012, 10:227 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Open Access Nasolabial flap reconstruction in oral cancer Seema Singh, Rajesh Kumar Singh and Manoj
Treatment of non-union of forearm bones with a free vascularised cortico - periosteal flap from the medial femoral condyle
 Acta Orthop. Belg., 2009, 75, 611-615 ORIGINAL STUDY Treatment of non-union of forearm bones with a free vascularised cortico - periosteal flap from the medial femoral condyle Luc DE SMET From the University
Acta Orthop. Belg., 2009, 75, 611-615 ORIGINAL STUDY Treatment of non-union of forearm bones with a free vascularised cortico - periosteal flap from the medial femoral condyle Luc DE SMET From the University
Chest wall reconstruction using a combined musculocutaneous anterolateral anteromedial thigh flap
 Free full text on www.ijps.org Case Report DOI: 10.4103/0970-0358.63966 Chest wall reconstruction using a combined musculocutaneous anterolateral anteromedial thigh flap Pearlie W. W. Tan, Chin-Ho Wong,
Free full text on www.ijps.org Case Report DOI: 10.4103/0970-0358.63966 Chest wall reconstruction using a combined musculocutaneous anterolateral anteromedial thigh flap Pearlie W. W. Tan, Chin-Ho Wong,
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Surgical Technique. Calcaneal Locking Plate
 Surgical Technique Calcaneal Locking Plate PERI-LOC Locked Plating System Calcaneal Locking Plate Surgical TechniqueCatalog Infor Table of Contents Introduction...2 Indications...3 Plate Features...3 Patient
Surgical Technique Calcaneal Locking Plate PERI-LOC Locked Plating System Calcaneal Locking Plate Surgical TechniqueCatalog Infor Table of Contents Introduction...2 Indications...3 Plate Features...3 Patient
Interesting Case Series. Reconstruction of Dorsal Wrist Defects
 Interesting Case Series Reconstruction of Dorsal Wrist Defects Maelee Yang, BS, and Joseph Meyerson, MD The Ohio State University Wexner Medical Center, Columbus Correspondence: maelee.yang@osumc.edu Keywords:
Interesting Case Series Reconstruction of Dorsal Wrist Defects Maelee Yang, BS, and Joseph Meyerson, MD The Ohio State University Wexner Medical Center, Columbus Correspondence: maelee.yang@osumc.edu Keywords:
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research report for MSc Dent. University of Witwatersrand. Faculty of health science. Dr J Beukes. Student number: h
 Research report for MSc Dent University of Witwatersrand Faculty of health science Dr J Beukes Student number: 9507510h Supervisor: Prof JP Reyneke October 2011 1 1. Title 2. Aim 3. Introduction 4. Objectives
Research report for MSc Dent University of Witwatersrand Faculty of health science Dr J Beukes Student number: 9507510h Supervisor: Prof JP Reyneke October 2011 1 1. Title 2. Aim 3. Introduction 4. Objectives
Health-related quality of life after mandibular resection for oral cancer: Reconstruction with free fibula flap
 Journal section: Oral Surgery Publication Types: Research doi:10.4317/medoral.19399 http://dx.doi.org/doi:10.4317/medoral.19399 Health-related quality of life after mandibular resection for oral cancer:
Journal section: Oral Surgery Publication Types: Research doi:10.4317/medoral.19399 http://dx.doi.org/doi:10.4317/medoral.19399 Health-related quality of life after mandibular resection for oral cancer:
Technique Guide. Midface Distractor System. For the temporary stabilization and gradual lengthening of the cranial or midfacial bones.
 Technique Guide Midface Distractor System. For the temporary stabilization and gradual lengthening of the cranial or midfacial bones. Table of Contents Introduction Midface Distractor System 2 Indications
Technique Guide Midface Distractor System. For the temporary stabilization and gradual lengthening of the cranial or midfacial bones. Table of Contents Introduction Midface Distractor System 2 Indications
Reconstructive procedures in maxillofacial oncosurgery
 Reconstructive procedures in maxillofacial oncosurgery Richard Pink a, Martin Molitor b, Peter Tvrdy a, Petr Michl a, Jindrich Pazdera a, Vitezslav Zboril a, Bohumil Zalesak b Objective. Oropharyngeal
Reconstructive procedures in maxillofacial oncosurgery Richard Pink a, Martin Molitor b, Peter Tvrdy a, Petr Michl a, Jindrich Pazdera a, Vitezslav Zboril a, Bohumil Zalesak b Objective. Oropharyngeal
MEDIAL SURAL ARTERY PERFORATOR FLAP FOR TONGUE AND FLOOR OF MOUTH RECONSTRUCTION. Adequate speech and swallowing are dependent
 ORIGINAL ARTICLE MEDIAL SURAL ARTERY PERFORATOR FLAP FOR TONGUE AND FLOOR OF MOUTH RECONSTRUCTION Shao-Liang Chen, MD, 1 Tim-Mo Chen, MD, 1 Niann-Tzyy Dai, MD, 1 Yi-Jan Hsia, DDS, MDSC, 2 Yaoh-Shiang Lin,
ORIGINAL ARTICLE MEDIAL SURAL ARTERY PERFORATOR FLAP FOR TONGUE AND FLOOR OF MOUTH RECONSTRUCTION Shao-Liang Chen, MD, 1 Tim-Mo Chen, MD, 1 Niann-Tzyy Dai, MD, 1 Yi-Jan Hsia, DDS, MDSC, 2 Yaoh-Shiang Lin,
King's College Hospital Dental School, London, S.E. 5.
 OSTECTOMY AT THE MANDIBULAR SYMPHYSIS J. H. SOWRAY, B.D.S., F.D.S.R.C.S. (Eng.), L.R.C.P., M.R.C.S. and R. HASKELL, M.B., B.S., F.D.S.R.C.S. (Eng.). King's College Hospital Dental School, London, S.E.
OSTECTOMY AT THE MANDIBULAR SYMPHYSIS J. H. SOWRAY, B.D.S., F.D.S.R.C.S. (Eng.), L.R.C.P., M.R.C.S. and R. HASKELL, M.B., B.S., F.D.S.R.C.S. (Eng.). King's College Hospital Dental School, London, S.E.
Repair of the mandibular nerve by a Title grafting after ablative surgery of. Shibahara, T; Noma, H; Takasaki, Y; Author(s) Fujikawa, M
 Repair of the mandibular nerve by a Title grafting after ablative surgery of Shibahara, T; Noma, H; Takasaki, Y; Author(s) Fujikawa, M Journal Bulletin of Tokyo Dental College, 4 URL http://hdl.handle.net/10130/1019
Repair of the mandibular nerve by a Title grafting after ablative surgery of Shibahara, T; Noma, H; Takasaki, Y; Author(s) Fujikawa, M Journal Bulletin of Tokyo Dental College, 4 URL http://hdl.handle.net/10130/1019
 This article was published in an Elsevier journal. The attached copy is furnished to the author for non-commercial research and education use, including for instruction at the author s institution, sharing
This article was published in an Elsevier journal. The attached copy is furnished to the author for non-commercial research and education use, including for instruction at the author s institution, sharing
Oral cavity landmarks
 By: Dr. Ahmed Rabah Oral cavity landmarks The knowledge of oral anatomy and physiology will help the operator and provides enough landmarks to act as positive guide during denture construction. This subject
By: Dr. Ahmed Rabah Oral cavity landmarks The knowledge of oral anatomy and physiology will help the operator and provides enough landmarks to act as positive guide during denture construction. This subject
CHAPTER 8 SECTION 1.4 ORAL SURGERY TRICARE/CHAMPUS POLICY MANUAL M DEC 1998 SPECIAL BENEFIT INFORMATION
 TRICARE/CHAMPUS POLICY MANUAL 6010.47-M DEC 1998 SPECIAL BENEFIT INFORMATION CHAPTER 8 SECTION 1.4 Issue Date: October 8, 1986 Authority: 32 CFR 199.4(e)(10) I. DESCRIPTION There are certain oral surgical
TRICARE/CHAMPUS POLICY MANUAL 6010.47-M DEC 1998 SPECIAL BENEFIT INFORMATION CHAPTER 8 SECTION 1.4 Issue Date: October 8, 1986 Authority: 32 CFR 199.4(e)(10) I. DESCRIPTION There are certain oral surgical
UCL Repair: Emphasis on Muscle Dissection and Reconstruction
 UCL Repair: Emphasis on Muscle Dissection and Reconstruction Unilateral cleft lip repair is performed using rotation-advancement technique. Markings are made on columella base, redlines, Cupid s bow on
UCL Repair: Emphasis on Muscle Dissection and Reconstruction Unilateral cleft lip repair is performed using rotation-advancement technique. Markings are made on columella base, redlines, Cupid s bow on
ALTHOUGH FIRST described
 The Cervicodeltopectoral Flap for Single-Stage Resurfacing of Anterolateral Defects of the Face and Neck Yadranko Ducic, MD, FRCSC; Jesse E. Smith, MD SURGICAL TECHNIQUE Objective: To evaluate prospectively
The Cervicodeltopectoral Flap for Single-Stage Resurfacing of Anterolateral Defects of the Face and Neck Yadranko Ducic, MD, FRCSC; Jesse E. Smith, MD SURGICAL TECHNIQUE Objective: To evaluate prospectively
SURGICAL TREATMENT OF SEVENTH NERVE PARALYSIS. By B. GRUNDT, M.D. Oslo, Norway
 SURGICAL TREATMENT OF SEVENTH NERVE PARALYSIS By B. GRUNDT, M.D. Oslo, Norway WE are all familiar with the patient who has paralysis of the facial nerve. The oblique mouth and the corresponding oblique
SURGICAL TREATMENT OF SEVENTH NERVE PARALYSIS By B. GRUNDT, M.D. Oslo, Norway WE are all familiar with the patient who has paralysis of the facial nerve. The oblique mouth and the corresponding oblique
ORIGINAL ARTICLE. The Thoracoacromial/Cephalic Vascular System for Microvascular Anastomoses in the Vessel-Depleted Neck
 ORIGINAL ARTICLE The Thoracoacromial/Cephalic Vascular System for Microvascular Anastomoses in the Vessel-Depleted Neck Jeffrey R. Harris, MD; E. Lueg, MD; E. Genden, MD; M. L. Urken, MD Objective: To
ORIGINAL ARTICLE The Thoracoacromial/Cephalic Vascular System for Microvascular Anastomoses in the Vessel-Depleted Neck Jeffrey R. Harris, MD; E. Lueg, MD; E. Genden, MD; M. L. Urken, MD Objective: To
BEAVERTAIL MODIFICATION OF THE RADIAL FOREARM FREE FLAP IN BASE OF TONGUE RECONSTRUCTION: TECHNIQUE AND FUNCTIONAL OUTCOMES
 ORIGINAL ARTICLE BEAVERTAIL MODIFICATION OF THE RADIAL FOREARM FREE FLAP IN BASE OF TONGUE RECONSTRUCTION: TECHNIQUE AND FUNCTIONAL OUTCOMES Hadi Seikaly, MD, FRCSC, 1,2 Jana Rieger, PhD, 2 Daniel O Connell,
ORIGINAL ARTICLE BEAVERTAIL MODIFICATION OF THE RADIAL FOREARM FREE FLAP IN BASE OF TONGUE RECONSTRUCTION: TECHNIQUE AND FUNCTIONAL OUTCOMES Hadi Seikaly, MD, FRCSC, 1,2 Jana Rieger, PhD, 2 Daniel O Connell,
Guide Design in Virtual Planning for Scapular Tip Free Flap Reconstruction
 Laryngoscope Investigative Otolaryngology VC 2018 The Authors Laryngoscope Investigative Otolaryngology published by Wiley Periodicals, Inc. on behalf of The Triological Society Guide Design in Virtual
Laryngoscope Investigative Otolaryngology VC 2018 The Authors Laryngoscope Investigative Otolaryngology published by Wiley Periodicals, Inc. on behalf of The Triological Society Guide Design in Virtual
A Technique for Utilizing Upper Lid Blepharoplasty Full thickness Skin for Peri-Implant Keratinized Tissue Grafting *,y
 A Technique for Utilizing Upper Lid Blepharoplasty Full thickness Skin for Peri-Implant Keratinized Tissue Grafting *,y George R. Deeb D.D.S., M.D. i, Bach T. Le D.D.S., M.D. ii, Brett A. Ueeck D.M.D iii,
A Technique for Utilizing Upper Lid Blepharoplasty Full thickness Skin for Peri-Implant Keratinized Tissue Grafting *,y George R. Deeb D.D.S., M.D. i, Bach T. Le D.D.S., M.D. ii, Brett A. Ueeck D.M.D iii,
Reconstructive surgeries in oral cancers
 International Journal of A J Institute of Medical Sciences 1 (2012) 47-54 Original Research Article Reconstructive surgeries in oral cancers Rithin Suvarna, 1 Aravind Pallipady, 2 Ranjith Rao, 3 Ashok
International Journal of A J Institute of Medical Sciences 1 (2012) 47-54 Original Research Article Reconstructive surgeries in oral cancers Rithin Suvarna, 1 Aravind Pallipady, 2 Ranjith Rao, 3 Ashok
Technique Guide. 3.5 mm LCP Olecranon Plates. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide 3.5 mm LCP Olecranon Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Olecranon Plates 2 AO Principles 3 Indications 3 Clinical
Technique Guide 3.5 mm LCP Olecranon Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Olecranon Plates 2 AO Principles 3 Indications 3 Clinical
