CASE STUDIES STUDII DE CAZ. Palestrica of the third millennium Civilization and Sport Vol. 16, no. 1, January-March 2015, 41 45
|
|
|
- Norah Copeland
- 5 years ago
- Views:
Transcription
1 CASE STUDIES STUDII DE CAZ Palestrica of the third millennium Civilization and Sport Vol. 16, no. 1, January-March 2015, Rehabilitation after total shoulder arthroplasty for a giantcell tumor of bone - a case report Reabilitarea după artroplastia totală de umăr pentru tumoră cu celule gigante a osului - prezentare de caz Alina Popa 1, Alexandrina Nicu 1, Monica Borda 1,2, László Irsay 1,2, Rodica Ungur 1,2, Ioan Onac 1,2, Viorela Ciortea 1,2 1 Clinical Rehabilitation Hospital, Cluj-Napoca, Romania 2 Rehabilitation Department, Iuliu Haţieganu University of Medicine and Pharmacy, Cluj-Napoca, Romania Abstract Background. Total shoulder arthroplasty is a standard operative treatment for a variety of disorders of the glenohumeral joint. Successful outcome of total shoulder arthroplasty depends on a well-designed and a well-executed physical therapy program. The rehabilitation program needs to respect a logical sequence: tissue healing, joint mobility and muscle strength. Aims. The purpose of this study was to emphasize the best therapeutic options to functionally rehabilitate a shoulder that was surgically replaced after a giant-cell tumor excision. Methods. The case report describes a 24-year-old female patient who presented in September 2013 to the Clinical Rehabilitation Hospital in Cluj-Napoca for rehabilitation after undergoing total shoulder arthroplasty for a giant-cell bone tumor located in the proximal region of the right humerus. Although they are considered benign in 90% of the cases, giant-cell tumors show a tendency for significant bone destruction, local recurrence, and occasional metastasis in the lung or lymph nodes. The objective examination of the patient at her first hospital admission: normal weight (BMI=19 kg/m 2 ), two postoperative scars in the anterior region of the right arm with minimal sensitivity when palpated, hypotonia and hypotrophy of the right upper limb, spontaneous pain at the mobilization of the right shoulder and limited active and passive range of motion (especially for flexion, abduction and external rotation), pain on the VAS = 30 mm, Constant Shoulder Score = 42, DASH score = 35, SPADI score = 53%. In our hospital, she underwent the current Neer protocol for postoperative total shoulder arthroplasty rehabilitation, which is widely used and is based on the basic science of soft tissue and bone healing. Results. The functional outcome was good, as the range of motion and strength of the upper right limb improved after attending our physical therapy program. Conclusions. When a well-performed surgical procedure is supplemented with a well-designed and frequently monitored therapy program, an excellent outcome of shoulder replacement should be expected. Key words: rehabilitation, shoulder arthroplasty, giant-cell tumor. Rezumat Premize. Artroplastia totală de umăr reprezintă o intervenţie chirurgicală standard pentru diverse afecţiuni ale articulaţiei gleno-humerale. Succesul endoprotezării de umăr depinde de calitatea programului de reabilitare instituit cât mai precoce. Programul de reabilitare trebuie să respecte o secvenţă logică: vindecarea ţesuturilor, mobilitatea articulaţiei şi forţa musculară. Obiective. Obiectivul acestui studiu este de a pune în evidenţă cea mai bună conduită terapeutică pentru reabilitarea funcţională a unui umăr endoprotezat, după excizia unei tumori cu celule gigante. Metode. Prezentarea de caz aduce în discuţie cazul unei paciente în vârstă de 24 ani, care s-a prezentat în septembrie 2013 în Spitalul Clinic de Recuperare Cluj Napoca pentru recuperarea mobilităţii umărului drept după implantarea unei endoproteze totale la acest nivel pentru o tumoră cu celule gigante a osului, localizată în regiunea proximală a humerusului drept. Chiar dacă sunt considerate benigne în 90% din cazuri, tumorile cu celule gigante tind să evolueze spre distrucţie osoasă, recidivă locală şi, ocazional, metastaze în plămân şi ganglionii limfatici. La examenul obiectiv la prima internare se evidenţiază: pacientă normoponderală (IMC=19 kg/m 2 ), două cicatrici postoperatorii în curs de vindecare la nivelul feţei anterioare a braţului drept, cu minimă sensibilitate dureroasă la palpare, hipotonie şi Received: 2015, February 17; Accepted for publication: 2015, February 20; Address for correspondence: Iuliu Haţieganu University of Medicine and Pharmacy Cluj-Napoca, Clinical Rehabilitation Hospital, Rehabilitation Department, No , Viilor St Cluj-Napoca viorela.ciortea@yahoo.com; alina_med87@yahoo.com; monicampop@yahoo.fr Corresponding author: Ileana Monica Borda, monicampop@yahoo.fr Copyright 2010 by Iuliu Haţieganu University of Medicine and Pharmacy Publishing 41
2 Alina Popa et al. hipotrofie a membrului superior drept, limitarea mobilităţii umărului operat (mai ales pentru flexie, abducţie şi rotaţie externă), durerea pe scala VAS = 30mm, Scorul Constant = 42, scorul DASH = 35, scorul SPADI = 53%. În spitalul nostru, pacienta a urmat protocolul curent Neer pentru reabilitarea umărului după artroplastie, care se bazează pe vindecarea ţesuturilor moi şi a osului. Rezultate. Evoluţia după programul de reabilitare a fost favorabilă, cu creşterea amplitudinii de mişcare şi a forţei musculare la nivelul membrului superior drept. Concluzie. Când o intervenţie chirurgicală de implantare a unei endoproteze este continuată de un program de reabilitare instituit precoce, bine controlat şi individualizat, prognosticul funcţional este favorabil. Cuvinte cheie: reabilitare, artroplastie de umăr, tumoră cu celule gigante. Introduction Total shoulder arthroplasty (TSA) is a standard operative treatment for a variety of disorders of the glenohumeral joint (Boudreau et al., 2007). Complications after TSA may include infection, instability, neurovascular injury, stiffness, cuff tear, periprosthetic fractures, glenoid erosion and component loosening (Sanchez-Sotelo et al., 2011). The success of TSA depends on surgery, i.e. on the correct placement of the prosthesis, as well as on the quality of the rehabilitation program initiated as early as possible, which needs to respect a logical sequence: tissue healing, joint mobility and periarticular muscle strength (Brems, 2007). It is also critical for the surgical team to communicate to the rehabilitation team important and relevant information about the surgical procedure, to ensure proper progression, so that the specific exercises are not advanced too rapidly in efforts to quickly provide functional rehabilitation (Cahill et al., 2014). Rehabilitation after TSA is more challenging when the integrity of the rotator cuff is poor and the functional outcome is generally not as good as it is for patients with an intact rotator cuff (Frankle et al., 2005). Hawkins et al. (1989) concluded based on a series of 65 patients, followed up over an average of 40 months, that the underlying etiology of the disease process and the status of the rotator cuff are the best predictors of outcome for individuals treated with TSA. Giant-cell tumors (GCT) are osteolytic primitive tumors with a rich vascularization, consisting of two predominant cell types: many multinuclear osteoclastic giant cells and mononuclear stromal cells, whose cytological appearance reflects the degree of aggressiveness, establishing in this way histological prognosis (Formasier et al., 1996). GCT represent 20% of all benign tumors and about 5% of primary bone tumors (Niu et al., 2012). The tumor commonly occurs during the second to fourth decades of life, with a female-to-male ratio of :1 (Schajowicz et al., 2001), and it usually originates from the epiphysis of long bones (Szendröi, 2004). The radiographic appearance of the GCT is that of a lytic lesion with a well-defined non-sclerotic margin, eccentric in location, which extends near the articular surface. However, GCT may present aggressive features, such as cortical expansion or destruction of the softtissue components (Chakarun et al., 2013) and has a potential risk of local recurrence (0-65%) depending on the type of treatment (Klenke et al., 2011). Magnetic resonance imaging (MRI) is often performed to evaluate the extent of the tumor. In typical GCT, the signal intensity is homogeneous, and the lesion is well circumscribed, with low signal intensity on T1-weighted images and intermediate signal intensity on T2-weighted images. Being aggressive and potentially malignant lesions, GCT pose a challenging problem in accurately predicting their tendency to recur or metastasize. It is considered that 80% of GCT have a benign course, with a local recurrence rate of 10-50%, and about 10% undergo malignant transformation through their recurrences. The principal aim of the management of GCT is to eliminate the tumor and still save the joint function (Rahim et al., 2015). It is advised that each patient with GCT should be treated individually. Regardless of non-malignant features, the local behavior of tumors determines the treatment approach according to treatment principles for malignant tumors of bone (Maric et al., 2012). Surgical and oncological treatment takes into account tumor location, previous treatments (in case of recurrence), histological aggressiveness and the presence or not of lung metastases, which are a cause of death in 16-25% of the cases (Kay et al., 1994). Surgical treatment consists of curettage and filling with cancellous bone or acrylic cement or mixed filling, in inactive forms (Kivioja et al., 2008). In case of recurrence, if histological examination evidences an inactive appearance, curettage is repeated, and if an active or aggressive appearance is evidenced, tumor resection will be performed (Becker et al., 2008). In case of an aggressive tumor, oncologic resection with or without reconstruction, depending on the tumor site (bone reconstruction or modular prosthesis), is carried out. Amputations or disarticulations are indicated in untreatable cases (Klenke et al., 2011). The postoperative rehabilitation program for patients with TSA has a long duration (12-18 months), is intense, sustained and regular in nature, and includes the following main objectives: increase of the quality-of-life index, maximization of mobility in the replaced shoulder, as well as restoration of motor control in the entire upper limb. It is based on the protocol initiated by Neer, structured in three phases. Phase I of the Neer protocol has the following main objectives: wound healing, maintenance of the integrity of the replaced joint, gradual increase in the passive range of motion of the shoulder, initiation of active elbow and wrist movements, reduction of pain and inflammation, reduction of muscle inhibition. The methods used are continuous orthosis use for up to 4 weeks, avoidance of shoulder overextension in clinostatism, avoidance of active shoulder 42
3 Rehabilitation after total shoulder arthroplasty movements, weight lifting and rotations, cryotherapy, passive and self-passive shoulder mobilization, passive, self-passive, isometric and balancing exercises (Coodman type). The objectives of phase II of the Neer protocol are to obtain a maximum passive range of motion, to gradually initiate active mobilizations, using active resistance-free, stretching exercises, and to restore the rotator cuff muscle strength. Phase III of the Neer protocol is aimed at the gradual restoration of the strength and resistance of the shoulder, using stretching and active resistance exercises. The full achievement of the objectives of a specific phase is mandatory before passing to the next phase, which particularizes the functional rehabilitation treatment. Although individuals undergoing TSA have less difficulty regaining range of motion initially than those undergoing arthroscopic or open rotator cuff repair, it is still imperative to restore and maintain as much shoulder joint range of motion as possible. It is important to note that although the literature consistently shows significant improvements in strength, range of motion, and functional outcomes after TSA, full range of motion and restoration of full strength are generally not obtained and in some cases not expected (Kasten et al., 2010; Sperling et al., 2008). mass effect (Fig. 1). The suspicion of a malignant giant-cell tumor was raised. For the confirmation of diagnosis, bone puncture biopsy was indicated, which was performed in June Anatomo-pathological examination evidenced tissue fragments containing bone tissue, periosteum and reactive bone, as well as images of cell proliferation including a component of mononuclear cells with abundant cytoplasm and a histiocytic appearance with numerous mitoses without atypias, and a component of multinuclear cells, osteogenesis foci apparently located towards the periphery of the tumor proliferations, aneurysmal spaces present inside the proliferation; tumor cells were CD68 positive, CD56 staining was focally positive on cells with osteoblastic appearance, the proliferation index assessed with Ki67 was expressed almost exclusively in the mononuclear component and had a mean value of 30%. The morphological picture, correlated with radiological data, corresponded to a giant-cell tumor of bone. Hypothesis We assessed a young female patient with total shoulder arthroplasty after the excision of a giant-cell tumor of the right proximal humerus as an example for clinical management. Fig. 1a T1 sequence Material and methods The study was performed in accordance with all current deontological rules. The patient s informed consent was obtained. Research protocol Period and place of the research We report the case of a 24-year-old female patient from a rural area, who presented to the Rehabilitation Hospital in Cluj-Napoca in September 2013, for the restoration of right shoulder mobility after the placement of a total shoulder endoprosthesis. Subjects and groups The current disease started insidiously in January 2012, by mixed pain in the right shoulder, of low/moderate intensity, persistent and deep, which was not improved by the administration of analgesics or rest. About 3 months later, in March 2012, the patient observed a progressive limitation of mobility at this level, which is why she presented to the service of Orthopedics of the Baia Mare County Hospital. On radiological examination, a tumor of the right proximal humerus was described. Contrast MRI of the right shoulder was indicated, which evidenced a 4.6/3.6/3.7 cm tumor formation occupying the entire neck of the humerus, with an inhomogeneous structure, with intense contrast uptake, located 7 mm from the scapulohumeral joint in the lower half, which invaded the bone cortex, the subdeltoid bursa, the bicipital sulcus, the insertions of the infraspinatus and supraspinatus muscles, as well as the inner side of the deltoid muscle, with fascial invasion and Fig. 1b T1 sequence, TIRM Fig. 1c T2 sequence Fig. 1 Right shoulder MRI, March 2012 In August 2012, surgery was carried out in the Orthopedic Clinic in Munich. The tumor was removed, and metal osteosynthesis with a plate and screws was performed. Postoperative evolution was favorable (Fig. 2). Approximately 6 months after surgery, in January 2013, pain in the right shoulder recurred, and imaging 43
4 Alina Popa et al. investigations supported local recurrence. In August 2013, another surgery was performed for the excision of the recurrent tumor, and a titanium total right shoulder endoprosthesis was placed in the same clinic in Munich (Fig. 3). Fig. 2 Right shoulder X-Ray (AP), August 2012 Fig. 3 Right shoulder X-Ray (AP), August 2013 At the first presentation of the patient (September 2013) to the medical rehabilitation service of the Clinical Rehabilitation Hospital Cluj-Napoca, general objective and locomotor system examination was performed, which evidenced: a patient with normal weight (BMI=19 kg/m 2 ), general good status, postoperative scar in the process of healing on the anterior side of the right arm, with minimum painful sensitivity on palpation, hypotonia and hypotrophy of the right upper limb, and limitation of the mobility of the operated shoulder in all movement planes. Tests applied The right shoulder joint was evaluated using goniometry, which showed low range of motion values in all planes, particularly for flexion (5 ), abduction (15 ) and external rotation (0 ). The range of motion values on the first evaluation in September 2013 can be seen in Table I. The patient was also assessed using specific scales: Constant Shoulder Score, Disabilities of the Arm, Shoulder and Hand Score (DASH), Shoulder Pain and Disability Index (SPADI). The values obtained on the first evaluation in September 2013 are presented in Table II. Results and discussion By correlating clinical and paraclinical data, the objectives of the rehabilitation treatment were formulated: functional rehabilitation of the right shoulder and upper limb, oncologic follow-up, family and socio-professional reintegration, and improvement of the quality of life. Rehabilitation was important because a young adult woman, in full process of developing her personal evolution potential, had lost the optimal function of her dominant upper limb. To the specific rehabilitation objectives, oncologic objectives were added, i.e. monitoring locoregional recurrence and the development of metastases by imaging methods (MRI, CT). Hence, the importance of multidisciplinary collaboration, between the medical rehabilitation specialist, the oncologist, the imaging radiologist, and the family doctor. The rehabilitation methods used were: kinetotherapy according to phase I of the Neer protocol, associated with water gymnastics in the pool, psychotherapy, occupational therapy, massage and administration of systemic or topical analgesics when needed. It was decided not to use any other form of physiokinetotherapy (e.g. high-frequency short waves), because of the increased recurrence potential of the malignant tumor. The parameters of the rehabilitation program were as follows: 14 days continuous hospitalization, 10 days kinetotherapy (30 minutes twice a day), 10 days water gymnastics in the pool (60 minutes), 10 days sedative massage (20 minutes). At the end of the first rehabilitation program, the range of motion in the right shoulder was significantly improved (Table I), and the Table I Range of motion (ROM) of the right shoulder. Range of motion September 2013 September 2013 January 2014 January 2014 August 2014 August 2014 Admission Discharge Admission Discharge Admission Discharge Flexion Extension Abduction Internal rotation External rotation Table II Shoulder scores. Score September 2013 September 2013 January 2014 January 2014 August 2014 August 2014 Admission Discharge Admission Discharge Admission Discharge Constant Shoulder Score DASH score SPADI score 54% 50% 43% 35% 30% 28% 44
5 Rehabilitation after total shoulder arthroplasty assessed scores had decreasing values (Table II). The patient was discharged with the following recommendations: continuation of the kinetic program at home, low protein diet, homeopathic treatment, psychotherapy, cognitivebehavioral therapy, and maintenance of contact with the rehabilitation team (consultant doctor, resident doctor, kinetotherapist) by phone or Internet. The patient returned for follow-up after 6 months, in January 2014, with improved range of motion values in the shoulder (the patient reported the daily program of exercises performed at home), and thus, phase II of the Neer protocol could be initiated, following which results were satisfactory (Tables I, II). In August 2014, the patient returned to continue inpatient rehabilitation treatment, and phase III of the Neer protocol was started, with favorable results (Tables I, II). The patient was discharged with the recommendation to continue the kinetotherapeutic program at home, in order to maintain the obtained values. Prognosis Prognosis ad functionem is favorable, as there was an increase in the passive and active range of motion, an improvement of muscle strength in the right upper limb, with the amelioration of activities of daily living, as well as family and socio-professional reintegration. Prognosis ad vitam is reserved because of the high risk of local and/or distant recurrence. Also, there are some difficulties in interpreting CT or MRI images due to artefacts generated by the metal endoprosthesis. Long-term monitoring can be done using musculoskeletal ultrasound, which can provide important information on local status. Particularities of the case The particularities of the case are the location of the tumor with a starting point in bone that invaded periarticular soft tissues, tumor recurrence requiring surgical reintervention with the placement of a total shoulder endoprosthesis, and the need to adapt kinetotherapy to the residual anatomic function. The limitations of functional recovery are due to the surgical protocol, which required the resection of the insertions of the rotator cuff muscles in order to remove the head of the humerus, and their subsequent block reinsertion. Conclusions 1. Physical therapy is an essential determinant of clinical outcome after total shoulder arthroplasty. 2. A graduated rehabilitation program allows patients to obtain a satisfactory overall function of the upper limb. 3. When surgery for the placement of an endoprosthesis is complemented by an early, well-controlled and individualized rehabilitation program, functional prognosis is favorable, and an optimal autonomy of the upper limb, depending on the new anatomical situation, can be obtained. Conflicts of interests There are no conflicts of interest. References Becker WT, Dohle J, Bernd L, Braun A, Cserhati M, Enderle A, Hovy L, Matejovsky Z, Szendroi M, Trieb K, Tunn PU. Local recurrence of giant cell tumor of bone after intralesional treatment with and without adjuvant therapy. The J Bone Joint Surg Am, 2008;90(5): Boudreau S, Boudreau E, Higgins L, Wilcox R. Rehabilitation following reverse total shoulder arthoplasty. J Orthop and Sports Phys Ther, 2007;37: Brems JJ. Rehabilitation after total shoulder arthroplasty: current concepts. Seminars in Arthroplasty, 2007;18(1): Cahill JB, Cavanaugh JT, Craig EV. Total Shoulder Arthroplasty Rehabilitation. Techniques in Shoulder & Elbow Surgery, 2014;15(1): Chakarun CJ, Forrester DM, Gottsegen CJ, Patel DB, White EA, Matcuk GR. Giant cell tumor of bone: review, mimics, and new developments in treatment. Radiographics, 2013;33(1): Fornasier VL, Protzner K, Zhang I et al. The prognostic significance of histomorphometry and immunohistochemistry in giant cell tumors of bone. Hum pathol, 1996;27(8): Frankle M, Siegal S, Pupello D, Saleem A, Mighell M, Vasey M. The Reverse Shoulder Prosthesis for glenohumeral arthritis associated with severe rotator cuff deficiency. A minimum two-year follow-up study of sixty patients. J Bone Joint Surg Am, 2005;87(8): Hawkins RJ, Bell RH, Jallay B. Total shoulder arthroplasty. Clin Orthop Relar Res, 1989;242: Kasten P, Maier M, Wendy P, Rettig O, Raiss P, Wolf S, Loew M. Can shoulder arthroplasty restore the range of motion in activities of daily living? A prospective 3D video motion analysis study. J Shoulder Elbow Surg, 2010;19(2Suppl.): Kay RM, Eckardt JJ, Seeger LL, Mirra JM, Hak DJ. Pulmonary Metastasis of Benign Giant Cell Tumor of Bone: Six Histologically Confirmed Cases, Including One of Spontaneous Regression. Clin Orthop Relat Res, 1994;(302): Kivioja AH, Blomqvist C, Hietaniemi K, Trovik C, Walloe A, Bauer HC, Jorgensen PH, Bergh P, Follerås G. Cement is recommended in intralesional surgery of giant cell tumors: a Scandinavian Sarcoma Group study of 294 patients followed for a median time of 5 years. Acta Orthop, 2008;79(1): Klenke FM, Wenger DE, Inwards CY, Rose PS, Sim FH. Giant cell tumor of bone: risk factors for recurrence. Clin Orthop Relat Res, 2011;469(2): Maric M, Bergovec M, Viskovic A, Kolundzic R, Smerdelj M, Orlic D. Treatment and complications in patients with giant cell tumor of bone. J Bone Joint Surg Br, 2012;94-B(SUPP XXXVII): Niu X, Zhang Q, Hao L et al. Giant Cell Tumor of the Extremity. J Bone Joint Surg Am, 2012;94(5): Rahim A, Tiwari M, Khan G, Gupta G, Sharma S. Total knee arthroplasty with Mesh technique in management of juxta-articular giant cell tumor around the knee. Int Surg J, 2015;2(1): Sanchez-Sotelo J. Total shoulder arthroplasty. Open Orthop J, 2011;5: doi: / Schajowicz F, Granato DB, McDonald DJ, Sundaram M. Clinical and radiological features of atypical giant cell tumours of bone. Brit J Radiol, 1991;64(766): Sperling JW, Kaufman KR, Schleck CD, Cofield RH. A biomechanical analysis of strength and motion following total shoulder arthroplasty. Int J Shoulder Surg, 2008;2(1):1-3. Szendröi M. Giant-cell tumour of bone. J Bone Joint Surg Br 2004;86(1):
Not relevant to this presentation.
 Nolan R. May, MD Kearney, NE Heartland Surgery Center, Kearney NE Not relevant to this presentation. 1 What are the indications for total shoulder arthroplasty? What are the differences between total shoulder
Nolan R. May, MD Kearney, NE Heartland Surgery Center, Kearney NE Not relevant to this presentation. 1 What are the indications for total shoulder arthroplasty? What are the differences between total shoulder
Why are these shoulder replacements called a reverse prosthesis?
 PATIENT GUIDE TO REVERSE PROSTHESIS Edward G. McFarland MD The Division of Sports Medicine and Shoulder Surgery The Department of Orthopaedic Surgery The Johns Hopkins University Baltimore MD Why are these
PATIENT GUIDE TO REVERSE PROSTHESIS Edward G. McFarland MD The Division of Sports Medicine and Shoulder Surgery The Department of Orthopaedic Surgery The Johns Hopkins University Baltimore MD Why are these
Total Shoulder Arthroplasty
 1 Total Shoulder Arthroplasty Surgical indications and contraindications Anatomical Considerations: Total shoulder arthroplasty surgery involves the replacement of the humeral head and the glenoid articulating
1 Total Shoulder Arthroplasty Surgical indications and contraindications Anatomical Considerations: Total shoulder arthroplasty surgery involves the replacement of the humeral head and the glenoid articulating
Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty
 Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
D Degenerative joint disease, rotator cuff deficiency with, 149 Deltopectoral approach component removal with, 128
 Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
Shawn Hennigan, MD Total Shoulder Arthroplasty Protocol. Phase 1 Maximum Protection (0-4 weeks)
 Shawn Hennigan, MD Total Shoulder Arthroplasty Protocol Goals for phase 1 Minimize Pain and inflammation Protect integrity of repair Initiate shoulder PROM Reduce muscular inhibition Maintain AROM of elbow,
Shawn Hennigan, MD Total Shoulder Arthroplasty Protocol Goals for phase 1 Minimize Pain and inflammation Protect integrity of repair Initiate shoulder PROM Reduce muscular inhibition Maintain AROM of elbow,
Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD
 General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
ROTATOR CUFF DISORDERS/IMPINGEMENT
 ROTATOR CUFF DISORDERS/IMPINGEMENT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH
ROTATOR CUFF DISORDERS/IMPINGEMENT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH
Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol
 Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol The intent of this protocol is to provide the therapist with a guideline of the postoperative rehabilitation course of a patient that has
Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol The intent of this protocol is to provide the therapist with a guideline of the postoperative rehabilitation course of a patient that has
Biomechanical concepts of total shoulder replacement. «Shoulder Course» Day 1. Richard W. Nyffeler Orthopädie Sonnenhof Bern. 11. Sept.
 Biomechanical concepts of total shoulder replacement Richard W. Nyffeler Orthopädie Sonnenhof Bern First total shoulder prosthesis Jules Emile Péan, 1830-1898 Monobloc prostheses Charles Neer, 1917-2011
Biomechanical concepts of total shoulder replacement Richard W. Nyffeler Orthopädie Sonnenhof Bern First total shoulder prosthesis Jules Emile Péan, 1830-1898 Monobloc prostheses Charles Neer, 1917-2011
Reverse Total Shoulder Arthroplasty Protocol
 General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
DISTINGUISHING BETWEEN ACUTE AND CHRONIC ROTATOR CUFF INJURIES IN WORKERS COMPENSATION PATIENTS
 DISTINGUISHING BETWEEN ACUTE AND CHRONIC ROTATOR CUFF INJURIES IN WORKERS COMPENSATION PATIENTS Lyndon B. Gross M.D. Ph.D. The Orthopedic Center of St. Louis SHOULDER PAIN Third most common musculoskeletal
DISTINGUISHING BETWEEN ACUTE AND CHRONIC ROTATOR CUFF INJURIES IN WORKERS COMPENSATION PATIENTS Lyndon B. Gross M.D. Ph.D. The Orthopedic Center of St. Louis SHOULDER PAIN Third most common musculoskeletal
 www.fisiokinesiterapia.biz Shoulder Problems Fractures Instability Impingement Miscellaneous Anatomy Bones Joints / Ligaments Muscles Neurovascular Anatomy Anatomy Supraspinatus Anterior Posterior Anatomy
www.fisiokinesiterapia.biz Shoulder Problems Fractures Instability Impingement Miscellaneous Anatomy Bones Joints / Ligaments Muscles Neurovascular Anatomy Anatomy Supraspinatus Anterior Posterior Anatomy
Total Shoulder Arthroplasty / Hemiarthroplasty Protocol
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Shoulder Arthroplasty / Hemiarthroplasty Protocol The intent of this protocol is to provide the
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Shoulder Arthroplasty / Hemiarthroplasty Protocol The intent of this protocol is to provide the
Reverse Total Shoulder Protocol
 Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
Shoulder Arthroplasty
 Shoulder Arthroplasty Nathan G. Everding, MD Specializing in Hand, Wrist, Elbow & Shoulder Surgery Syracuse Orthopedic Specialists SJH Family Practice Refresher course 3/8/19 Shoulder Arthroplasty Rate
Shoulder Arthroplasty Nathan G. Everding, MD Specializing in Hand, Wrist, Elbow & Shoulder Surgery Syracuse Orthopedic Specialists SJH Family Practice Refresher course 3/8/19 Shoulder Arthroplasty Rate
Massive Rotator Cuff Tears. Rafael M. Williams, MD
 Massive Rotator Cuff Tears Rafael M. Williams, MD Rotator Cuff MRI MRI Small / Partial Thickness Medium Tear Arthroscopic View Massive Tear Fatty Atrophy Arthroscopic View MassiveTears Tear is > 5cm
Massive Rotator Cuff Tears Rafael M. Williams, MD Rotator Cuff MRI MRI Small / Partial Thickness Medium Tear Arthroscopic View Massive Tear Fatty Atrophy Arthroscopic View MassiveTears Tear is > 5cm
Acute Orthopaedic Injuries Developing a Diagnostic Approach to the Shoulder
 Acute Orthopaedic Injuries Developing a Diagnostic Approach to the Shoulder WWW.FISIOKINESITERAPIA.BIZ Overview To be able to quickly categorize shoulder injuries To take appropriate history and conduct
Acute Orthopaedic Injuries Developing a Diagnostic Approach to the Shoulder WWW.FISIOKINESITERAPIA.BIZ Overview To be able to quickly categorize shoulder injuries To take appropriate history and conduct
Rehabilitation Guidelines for Labral/Bankert Repair
 Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
SICOT Online Report E057 Accepted April 23th, in Fibula and Rib
 Metachronous, multicentric giant cell tumors in Fibula and Rib Toshihiro Akisue, Tetsuji Yamamoto ( ), Teruya Kawamoto, Toshiaki Hitora, Takashi Marui, Tetsuya Nakatani, Takafumi Onga, and Masahiro Kurosaka
Metachronous, multicentric giant cell tumors in Fibula and Rib Toshihiro Akisue, Tetsuji Yamamoto ( ), Teruya Kawamoto, Toshiaki Hitora, Takashi Marui, Tetsuya Nakatani, Takafumi Onga, and Masahiro Kurosaka
Shoulder Ultrasonography as a Diagnostic Tool for Rotator Cuff Disease
 Shoulder Ultrasonography as a Diagnostic Tool for Rotator Cuff Disease Jay D Keener, MD Associate Professor Shoulder and Elbow Service Washington University Disclosure No relevant financial disclosures
Shoulder Ultrasonography as a Diagnostic Tool for Rotator Cuff Disease Jay D Keener, MD Associate Professor Shoulder and Elbow Service Washington University Disclosure No relevant financial disclosures
REVERSE SHOULDER REPLACEMENT
 REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is designed specifically for the use in shoulders with a deficient rotator cuff and arthritis, as well as other difficult shoulder reconstructive
REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is designed specifically for the use in shoulders with a deficient rotator cuff and arthritis, as well as other difficult shoulder reconstructive
PROM is not stretching!
 Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
ADHESIVE CAPSULITIS (FROZEN SHOULDER)
 ADHESIVE CAPSULITIS (FROZEN SHOULDER) Frozen shoulder, or adhesive capsulitis is a condition that generally begins with the gradual onset of pain followed by a limitation of shoulder motion. The discomfort
ADHESIVE CAPSULITIS (FROZEN SHOULDER) Frozen shoulder, or adhesive capsulitis is a condition that generally begins with the gradual onset of pain followed by a limitation of shoulder motion. The discomfort
Orthopedic Surgery and Sports Medicine FL License:
 Reverse Shoulder Arthroplasty Protocol: The intent of this protocol is to provide the therapist with a guideline for the post-operative rehabilitation course of a patient that has undergone a Reverse Shoulder
Reverse Shoulder Arthroplasty Protocol: The intent of this protocol is to provide the therapist with a guideline for the post-operative rehabilitation course of a patient that has undergone a Reverse Shoulder
CASE PRESENTATION. Dr. Faseeh Shahab PGY3 Orthopaedic Resident, Khyber Teaching Hospital, Peshawar, PAKISTAN
 CASE PRESENTATION Dr. Faseeh Shahab PGY3 Orthopaedic Resident, Khyber Teaching Hospital, Peshawar, PAKISTAN CASE PRESENTATION - History Ms. SB, 30yo Afghan National Presented with 3 months history of Swelling
CASE PRESENTATION Dr. Faseeh Shahab PGY3 Orthopaedic Resident, Khyber Teaching Hospital, Peshawar, PAKISTAN CASE PRESENTATION - History Ms. SB, 30yo Afghan National Presented with 3 months history of Swelling
Type Three Rotator Cuff Repair Arthroscopic Assisted with SAD Large to Massive Tears (Greater than 4 cm)
 Type Three Rotator Cuff Repair Arthroscopic Assisted with SAD Large to Massive Tears (Greater than 4 cm) Therapist Phone I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity
Type Three Rotator Cuff Repair Arthroscopic Assisted with SAD Large to Massive Tears (Greater than 4 cm) Therapist Phone I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity
Type II SLAP lesions are created when the biceps anchor has pulled away from the glenoid attachment.
 Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
Pseudotumor Deltoideus in the Left Humerus of a Young Adult Female Patient with Acute Lateral Shoulder Pain: A Case Report
 of a Young Adult Female Patient with Acute Lateral Shoulder Pain: A Gulsen Aykol 1, Senol Fatih Elbir 2 1 Physical Medicine and Rehabilitation, Private Sevgi Medical Centre, Malatya, Turkey 2 Radiology
of a Young Adult Female Patient with Acute Lateral Shoulder Pain: A Gulsen Aykol 1, Senol Fatih Elbir 2 1 Physical Medicine and Rehabilitation, Private Sevgi Medical Centre, Malatya, Turkey 2 Radiology
Disclosures. Giant Cell Rich Tumors of Bone. Outline. The osteoclast. Giant cell rich tumors 5/21/11
 Disclosures Giant Cell Rich Tumors of Bone Andrew Horvai, MD, PhD Associate Clinical Professor, Pathology This lecture discusses "off label" uses of a number of pharmaceutical agents. The speaker is describing
Disclosures Giant Cell Rich Tumors of Bone Andrew Horvai, MD, PhD Associate Clinical Professor, Pathology This lecture discusses "off label" uses of a number of pharmaceutical agents. The speaker is describing
TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY
 Teodoro P. Nissen, M.D., Q.M.E. Fellowship Trained Board Certified Joseph M. Centeno, M.D. Fellowship Trained Board Certified TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY Protocol: The intent of this
Teodoro P. Nissen, M.D., Q.M.E. Fellowship Trained Board Certified Joseph M. Centeno, M.D. Fellowship Trained Board Certified TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY Protocol: The intent of this
REHABILITATION FOR SHOULDER FRACTURES & SURGERIES. Clavicle fractures Proximal head of humerus fractures
 REHABILITATION FOR SHOULDER FRACTURES & SURGERIES Clavicle fractures Proximal head of humerus fractures By Dr. Mohamed Behiry Lecturer Department of physical therapy for Orthopaedic and its surgery. Delta
REHABILITATION FOR SHOULDER FRACTURES & SURGERIES Clavicle fractures Proximal head of humerus fractures By Dr. Mohamed Behiry Lecturer Department of physical therapy for Orthopaedic and its surgery. Delta
WILLIAM M. ISBELL, MD Jeremy R. Stinson PA-C
 WILLIAM M. ISBELL, MD Jeremy R. Stinson PA-C Post-Operative Rehabilitation Guidelines for Total Shoulder Arthroplasty (TSA) The intent of this protocol is to provide the physical therapist with a guideline/treatment
WILLIAM M. ISBELL, MD Jeremy R. Stinson PA-C Post-Operative Rehabilitation Guidelines for Total Shoulder Arthroplasty (TSA) The intent of this protocol is to provide the physical therapist with a guideline/treatment
Rehab protocol. Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits. Goals:
 Reverse Total shoulder arthroplasty Rehab protocol Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase
Reverse Total shoulder arthroplasty Rehab protocol Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase
Shoulder Arthroplasty. Valentin Lance 3/24/16
 Shoulder Arthroplasty Valentin Lance 3/24/16 Outline Background Pre-operative imaging assessment Total Shoulder Arthroplasty: Standard and Reverse Complications Other shoulder hardware Hemiarthroplasty
Shoulder Arthroplasty Valentin Lance 3/24/16 Outline Background Pre-operative imaging assessment Total Shoulder Arthroplasty: Standard and Reverse Complications Other shoulder hardware Hemiarthroplasty
Dr. Denard s Rehabilitation Protocols Arthroscopic Shoulder Surgery
 2780 E. Barnett Rd Medford, OR 97530 541-779-6250 Dr. Denard s Rehabilitation Protocols Arthroscopic Shoulder Surgery These rehabilitation protocols are based on current studies detailing healing time
2780 E. Barnett Rd Medford, OR 97530 541-779-6250 Dr. Denard s Rehabilitation Protocols Arthroscopic Shoulder Surgery These rehabilitation protocols are based on current studies detailing healing time
Harold Schock III, MD Rotator Cuff Repair Rehabilitation Protocol
 Harold Schock III, MD Rotator Cuff Repair Rehabilitation Protocol The following document is an evidence-based protocol for arthroscopic rotator cuff repair rehabilitation. The protocol is both chronologically
Harold Schock III, MD Rotator Cuff Repair Rehabilitation Protocol The following document is an evidence-based protocol for arthroscopic rotator cuff repair rehabilitation. The protocol is both chronologically
 Use of a partial humeral head resurfacing system for management of an osseous mechanic... Page 1 of 12 Int J Shoulder Surg. 2011 Jan-Mar; 5(1): 17 20. doi: 10.4103/0973-6042.80465. PMCID: PMC3109768 Copyright
Use of a partial humeral head resurfacing system for management of an osseous mechanic... Page 1 of 12 Int J Shoulder Surg. 2011 Jan-Mar; 5(1): 17 20. doi: 10.4103/0973-6042.80465. PMCID: PMC3109768 Copyright
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Shoulder Hemi-arthroplasty (Trauma)
 Shoulder Hemi-arthroplasty (Trauma) Sling What can I do from day 1? Restrictions? Commence strengthening? Trauma: Up to 6 Active assisted/active supported within safe zone* Mobilise unaffected joints e.g
Shoulder Hemi-arthroplasty (Trauma) Sling What can I do from day 1? Restrictions? Commence strengthening? Trauma: Up to 6 Active assisted/active supported within safe zone* Mobilise unaffected joints e.g
Shoulder Arthroscopy. Dr. J.J.A.M. van Raaij. NOV Jaarvergadering Den Bosch 25 jan 2018
 Shoulder Arthroscopy Dr. J.J.A.M. van Raaij NOV Jaarvergadering Den Bosch 25 jan 2018 No disclosures Disclosure Shoulder Instability Traumatic anterior Traumatic posterior Acquired atraumatic Multidirectional
Shoulder Arthroscopy Dr. J.J.A.M. van Raaij NOV Jaarvergadering Den Bosch 25 jan 2018 No disclosures Disclosure Shoulder Instability Traumatic anterior Traumatic posterior Acquired atraumatic Multidirectional
Bradley C. Carofino, M.D. Shoulder Specialist 230 Clearfield Avenue, Suite 124 Virginia Beach, Virginia Phone
 Rehabilitation following Arthroscopic Rotator Cuff Repair: Medium Tears Phase I: Immediate Postsurgical Phase (Days 10-14) Precautions: No lifting of objects; No excessive arm motions; No excessive external
Rehabilitation following Arthroscopic Rotator Cuff Repair: Medium Tears Phase I: Immediate Postsurgical Phase (Days 10-14) Precautions: No lifting of objects; No excessive arm motions; No excessive external
Chondrosarcoma with a late local relapse
 Chondrosarcoma with a late local relapse J. Shinoda, T. Ozaki, T. Oka, T. Kunisada, H. Inoue Department of Orthopaedic Surgery, Okayama University Medical School, Okayama, 700-8558, Japan Correspondence:
Chondrosarcoma with a late local relapse J. Shinoda, T. Ozaki, T. Oka, T. Kunisada, H. Inoue Department of Orthopaedic Surgery, Okayama University Medical School, Okayama, 700-8558, Japan Correspondence:
Jennifer L. Cook, MD Stephen A. Hanff, MD. Rotator Cuff Type I Repair (Small Large Tear)
 Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 Rotator Cuff Type I Repair (Small Large Tear) This
Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 Rotator Cuff Type I Repair (Small Large Tear) This
Common Shoulder Problems and Treatment Options. Benjamin W. Szerlip D.O. Austin Shoulder Institute
 Common Shoulder Problems and Treatment Options Benjamin W. Szerlip D.O. Austin Shoulder Institute Speaker Disclosure Dr. Szerlip has disclosed that he has no actual or potential conflict of interest in
Common Shoulder Problems and Treatment Options Benjamin W. Szerlip D.O. Austin Shoulder Institute Speaker Disclosure Dr. Szerlip has disclosed that he has no actual or potential conflict of interest in
ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME
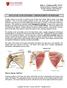 ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME Shoulder injuries are common in patients across all ages, from young, athletic people to the aging population. Two of the most common problems occur in the
ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME Shoulder injuries are common in patients across all ages, from young, athletic people to the aging population. Two of the most common problems occur in the
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears:
 Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty
 Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty Josef K. Eichinger, MD General Information Total Recovery time is between 4-6 months depending on factors such as injury
Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty Josef K. Eichinger, MD General Information Total Recovery time is between 4-6 months depending on factors such as injury
2015 OPSC Annual Convention. syllabus. February 4-8, 2015 Hyatt Regency Mission Bay San Diego, California
 2015 OPSC Annual Convention syllabus February 4-8, 2015 Hyatt Regency Mission Bay San Diego, California THURSDAY, FEBRUARY 5, 2015: 3:30pm - 4:30pm The Shoulder: 2 View or Not 2 View * Presented by Alexandra
2015 OPSC Annual Convention syllabus February 4-8, 2015 Hyatt Regency Mission Bay San Diego, California THURSDAY, FEBRUARY 5, 2015: 3:30pm - 4:30pm The Shoulder: 2 View or Not 2 View * Presented by Alexandra
A Patient s Guide to Adult Forearm Fractures
 A Patient s Guide to Adult Forearm Fractures Orthopedic and Sports Medicine 825 South 8th Street, #550 Minneapolis, MN 55404 Phone: 612-333-5000 Fax: 612-333-6922 1 DISCLAIMER: The information in this
A Patient s Guide to Adult Forearm Fractures Orthopedic and Sports Medicine 825 South 8th Street, #550 Minneapolis, MN 55404 Phone: 612-333-5000 Fax: 612-333-6922 1 DISCLAIMER: The information in this
Latissimus dorsi tendon transfer protocol
 Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the physical therapist with a guideline/treatment protocol for the postoperative rehabilitation management
Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the physical therapist with a guideline/treatment protocol for the postoperative rehabilitation management
(PROTOCOL #18) REVERSE TOTAL SHOULDER ARTHROPLASTY PROTOCOL
 The following is a set of general guidelines. It is important to remember that each patient is different. The progression of the patient depends on many factors including age and medical health of the
The following is a set of general guidelines. It is important to remember that each patient is different. The progression of the patient depends on many factors including age and medical health of the
Total Shoulder Arthroplasty / Hemi-arthroplasty (Elective)
 Total Shoulder Arthroplasty / Hemi-arthroplasty (Elective) Sling What can I do from day 1? Restrictions? Commence strengthening? Up to 3 weeks Active assisted/active supported within safe zone* Mobilise
Total Shoulder Arthroplasty / Hemi-arthroplasty (Elective) Sling What can I do from day 1? Restrictions? Commence strengthening? Up to 3 weeks Active assisted/active supported within safe zone* Mobilise
Elbow Fractures ORIF VS Arthroplasty
 Elbow Fractures ORIF VS Arthroplasty Oke Anakwenze, M.D. Olympus Orthopedics No disclosures Disclosures Distal humerus fractures 0.5-0.7% of all fractures 30% of all elbow fractures Bimodal etiology Young
Elbow Fractures ORIF VS Arthroplasty Oke Anakwenze, M.D. Olympus Orthopedics No disclosures Disclosures Distal humerus fractures 0.5-0.7% of all fractures 30% of all elbow fractures Bimodal etiology Young
THE REVERSE SHOULDER REPLACEMENT
 THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
Anatomy Your shoulder is made up of three bones: your upper arm bone (humerus), your shoulder blade (scapula), and your collarbone (clavicle).
 Shoulder Impingement/Rotator Cuff Tendinitis One of the most common physical complaints is shoulder pain. Your shoulder is made up of several joints combined with tendons and muscles that allow a great
Shoulder Impingement/Rotator Cuff Tendinitis One of the most common physical complaints is shoulder pain. Your shoulder is made up of several joints combined with tendons and muscles that allow a great
Biceps Tenodesis Protocol
 Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
Christopher K. Jones, MD Colorado Springs Orthopaedic Group
 Christopher K. Jones, MD Colorado Springs Orthopaedic Group 719-632-7669 Total Shoulder Replacement You have undergone a shoulder replacement procedure. The performance of the procedure is complete, but
Christopher K. Jones, MD Colorado Springs Orthopaedic Group 719-632-7669 Total Shoulder Replacement You have undergone a shoulder replacement procedure. The performance of the procedure is complete, but
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery. By: Aun Lauriz E. Macuja SAC_SN4
 Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Limb Salvage Surgery for Musculoskeletal Oncology
 Editorial Limb Salvage Surgery for Musculoskeletal Oncology Wan Faisham Nu man Bin Wan Ismail Submitted: 2 May 2015 Accepted: 18 June 2015 Orthopaedic Oncology Unit, Orthopaedic Department, School of Medical
Editorial Limb Salvage Surgery for Musculoskeletal Oncology Wan Faisham Nu man Bin Wan Ismail Submitted: 2 May 2015 Accepted: 18 June 2015 Orthopaedic Oncology Unit, Orthopaedic Department, School of Medical
A GUIDE TO TOTAL SHOULDER REPLACEMENT
 A GUIDE TO TOTAL SHOULDER REPLACEMENT Making the decision to have a total shoulder replacement should be a topic discussed between the individual considering the surgery as well as the individual s family,
A GUIDE TO TOTAL SHOULDER REPLACEMENT Making the decision to have a total shoulder replacement should be a topic discussed between the individual considering the surgery as well as the individual s family,
Arthroscopic Rotator Cuff Repair Protocol:
 Arthroscopic Rotator Cuff Repair Protocol: The intent of this protocol is to provide the therapist and patient with guidelines for the post-operative rehabilitation course after arthroscopic SLAP repair.
Arthroscopic Rotator Cuff Repair Protocol: The intent of this protocol is to provide the therapist and patient with guidelines for the post-operative rehabilitation course after arthroscopic SLAP repair.
Rehabilitation Guidelines for Shoulder Arthroscopy
 Rehabilitation Guidelines for Shoulder Arthroscopy The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Shoulder Arthroscopy The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Endovascular and surgical treatment of giant pelvic tumor
 Endovascular and surgical treatment of giant pelvic tumor Mitrev Z., MD FETCS; Anguseva T., MD; Milev I., MD; Zafiroski G., PhD MD Center for Cardiosurgery, Filip the II, Skopje, Macedonia Background Giant
Endovascular and surgical treatment of giant pelvic tumor Mitrev Z., MD FETCS; Anguseva T., MD; Milev I., MD; Zafiroski G., PhD MD Center for Cardiosurgery, Filip the II, Skopje, Macedonia Background Giant
Balgrist Shoulder Course 2017
 My approach to failed hemiprosthesis Ernst Wiedemann OCM Clinic Munich Consultant to Arthrex Royalties from Arthrex Consultant to Zimmer Disclosures Pathways Hemi-prosthesis Anatomical prosthesis (HSA
My approach to failed hemiprosthesis Ernst Wiedemann OCM Clinic Munich Consultant to Arthrex Royalties from Arthrex Consultant to Zimmer Disclosures Pathways Hemi-prosthesis Anatomical prosthesis (HSA
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
Giant Cell Tumour of the Distal Radius: Wide Resection and Reconstruction by Non-vascularised Proximal Fibular Autograft
 900 Original Article Giant Cell Tumour of the Distal Radius: Wide Resection and Reconstruction by Non-vascularised Proximal Fibular Autograft Ayman Abdelaziz Bassiony, 1 MD Abstract Introduction: Giant
900 Original Article Giant Cell Tumour of the Distal Radius: Wide Resection and Reconstruction by Non-vascularised Proximal Fibular Autograft Ayman Abdelaziz Bassiony, 1 MD Abstract Introduction: Giant
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD
 Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Shoulder Joint Examination. Shoulder Joint Examination. Inspection. Inspection Palpation Movement. Look Feel Move
 Shoulder Joint Examination History Cuff Examination Instability Examination AC Joint Examination Biceps Tendon Examination Superior Labrum Examination Shoulder Joint Examination Inspection Palpation Movement
Shoulder Joint Examination History Cuff Examination Instability Examination AC Joint Examination Biceps Tendon Examination Superior Labrum Examination Shoulder Joint Examination Inspection Palpation Movement
How they begin 8/18/15. Arthroscopic Management of Complex RCT. Disclosures in AAOS Database
 Arthroscopic Management of Complex RCT Brian J. Cole, MD, MBA Professor and Vice-Chairman, Department of Orthopedics Chairman, Department of Surgery, Rush OPH Team Physician, Chicago Whites Sox and Bulls
Arthroscopic Management of Complex RCT Brian J. Cole, MD, MBA Professor and Vice-Chairman, Department of Orthopedics Chairman, Department of Surgery, Rush OPH Team Physician, Chicago Whites Sox and Bulls
SLAP Repair. Pre-operatively. Acute phase (0-4 weeks 1 ) Sling. Restrictions? What can I do from day 1? Commence strengthening?
 SLAP Repair Sling What can I do from day 1? Restrictions? Commence strengthening? Up to 3 weeks Active assisted/active supported within safe zone* No combined AB/ER and end range ER until 6 weeks. Dependent
SLAP Repair Sling What can I do from day 1? Restrictions? Commence strengthening? Up to 3 weeks Active assisted/active supported within safe zone* No combined AB/ER and end range ER until 6 weeks. Dependent
TALLGRASS ORTHOPEDIC & SPORTS MEDICINE. Phase I Immediate Post-Surgical Phase (Weeks 0-2) Date: Maintain/protect integrity of the repair
 TALLGRASS ORTHOPEDIC & SPORTS MEDICINE Name: Date of Surgery: Patient Flow Sheet Arthroscopic Rotator Cuff Repair Small to Medium Tears Benedict Figuerres, MD Phase I Immediate Post-Surgical Phase (Weeks
TALLGRASS ORTHOPEDIC & SPORTS MEDICINE Name: Date of Surgery: Patient Flow Sheet Arthroscopic Rotator Cuff Repair Small to Medium Tears Benedict Figuerres, MD Phase I Immediate Post-Surgical Phase (Weeks
Anterior Labrum Repair Protocol
 Anterior Labrum Repair Protocol Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain scapular
Anterior Labrum Repair Protocol Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain scapular
The role of isokinetic exercises in the rehabilitation of patients with impingement syndrome of the shoulder
 ORIGINAL STUDIES Palestrica of the third millennium Civilization and Sport Vol. 19, no. 1, January-March 2018, 8 12 The role of isokinetic exercises in the rehabilitation of patients with impingement syndrome
ORIGINAL STUDIES Palestrica of the third millennium Civilization and Sport Vol. 19, no. 1, January-March 2018, 8 12 The role of isokinetic exercises in the rehabilitation of patients with impingement syndrome
Laura M. Fayad, MD. Associate Professor of Radiology, Orthopaedic Surgery & Oncology The Johns Hopkins University
 Society of Pediatric Radiology, May 2013 Laura M. Fayad, MD Associate Professor of Radiology, Orthopaedic Surgery & Oncology The Johns Hopkins University Describes surgical techniques that resect and reconstruct
Society of Pediatric Radiology, May 2013 Laura M. Fayad, MD Associate Professor of Radiology, Orthopaedic Surgery & Oncology The Johns Hopkins University Describes surgical techniques that resect and reconstruct
Mini Open Rotator Cuff Repair Large (3 5 cm)
 Mini Open Rotator Cuff Repair Large (3 5 cm) Size: small = < 1 cm, medium = 1 3 cm, large 3 5 cm, massive = > 5 cm **It is the treating therapist s responsibility along with the referring physician s guidance
Mini Open Rotator Cuff Repair Large (3 5 cm) Size: small = < 1 cm, medium = 1 3 cm, large 3 5 cm, massive = > 5 cm **It is the treating therapist s responsibility along with the referring physician s guidance
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines
 Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
The examination of the painful knee. Maja K Artandi, MD, FACP Clinical Associate Professor of Medicine Stanford University
 The examination of the painful knee Maja K Artandi, MD, FACP Clinical Associate Professor of Medicine Stanford University Objectives of the talk By the end of this talk you will know The important anatomy
The examination of the painful knee Maja K Artandi, MD, FACP Clinical Associate Professor of Medicine Stanford University Objectives of the talk By the end of this talk you will know The important anatomy
"Zero-Position" Functional Shoulder Orthosis for Postoperative. management of rotator cuff injuries.
 "Zero-Position" Functional Shoulder Orthosis for Postoperative Management of Rotator Cuff Injuries Jiro Ozaki, M.D. Ichiro Kawamura INTRODUCTION Many shoulder orthoses such as the airplane splint, the
"Zero-Position" Functional Shoulder Orthosis for Postoperative Management of Rotator Cuff Injuries Jiro Ozaki, M.D. Ichiro Kawamura INTRODUCTION Many shoulder orthoses such as the airplane splint, the
CASE STUDY: PRO-DENSE Injectable Regenerative Graft Used to Backfill a Bone Cavity Following Resection of a Giant Cell Tumor
 : PRO-DENSE Used to Backfill a Bone Cavity Following Resection of a Giant Cell Tumor Contributed by: Matthew J. Seidel, MD* Lauren A. Schwartz, NP Scottsdale, AZ *Dr. Seidel is a paid consultant for Wright
: PRO-DENSE Used to Backfill a Bone Cavity Following Resection of a Giant Cell Tumor Contributed by: Matthew J. Seidel, MD* Lauren A. Schwartz, NP Scottsdale, AZ *Dr. Seidel is a paid consultant for Wright
11/13/2017. Disclosures: The Irreparable Rotator Cuff. I am a consultant for Arhtrex, Inc and Endo Pharmaceuticals.
 Massive Rotator Cuff Tears without Arthritis THE CASE FOR SUPERIOR CAPSULAR RECONSTRUCTION MICHAEL GARCIA, MD NOVEMBER 4, 2017 FLORIDA ORTHOPAEDIC INSTITUTE Disclosures: I am a consultant for Arhtrex,
Massive Rotator Cuff Tears without Arthritis THE CASE FOR SUPERIOR CAPSULAR RECONSTRUCTION MICHAEL GARCIA, MD NOVEMBER 4, 2017 FLORIDA ORTHOPAEDIC INSTITUTE Disclosures: I am a consultant for Arhtrex,
TOTAL SHOULDER ARTHROPLASTY, HEMIARTHROPLASTY OR REVERSE ARTHROPLASTY
 TOTAL SHOULDER ARTHROPLASTY, HEMIARTHROPLASTY OR REVERSE ARTHROPLASTY Philosophy The following is an outline of the standard post-operative rehabilitation program following total shoulder arthroplasty.
TOTAL SHOULDER ARTHROPLASTY, HEMIARTHROPLASTY OR REVERSE ARTHROPLASTY Philosophy The following is an outline of the standard post-operative rehabilitation program following total shoulder arthroplasty.
Biceps Tenotomy Protocol
 Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
Assessment of Approximate Glenoid Size in Thai People
 Assessment of Approximate Glenoid Size in Thai People J Med Assoc Thai 2014; 97 (Suppl. 2): S14-S18 Full text. e-journal: http://www.jmatonline.com Pason Phonphok MD*, Nattha Kulkamthorn MD* * Division
Assessment of Approximate Glenoid Size in Thai People J Med Assoc Thai 2014; 97 (Suppl. 2): S14-S18 Full text. e-journal: http://www.jmatonline.com Pason Phonphok MD*, Nattha Kulkamthorn MD* * Division
Dr. Stefan C. Muzin, MD PM&R Beth Israel Deaconess Medical Center Harvard Medical School Consultant, GE Aviation, OEHN.
 Dr. Stefan C. Muzin, MD PM&R Beth Israel Deaconess Medical Center Harvard Medical School Consultant, GE Aviation, OEHN Work Related Workshop WorkInjuries Related Injuries Workshop Think of the Big Picture
Dr. Stefan C. Muzin, MD PM&R Beth Israel Deaconess Medical Center Harvard Medical School Consultant, GE Aviation, OEHN Work Related Workshop WorkInjuries Related Injuries Workshop Think of the Big Picture
Avon Office 2 Simsbury Rd. Avon, CT Office: (860) Fax: (860) REHABILITATION AFTER REVERSE SHOULDER ARTHROPLASTY
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Iliac aneurysmal bone cyst treated by cystoscopic controlled curettage
 Accepted February 13th, 2004 Iliac aneurysmal bone cyst treated by cystoscopic controlled curettage Ludwig Schwering¹, Markus Uhl² and Georg W. Herget( )¹ ¹ Department of Orthopaedics and Traumatology,
Accepted February 13th, 2004 Iliac aneurysmal bone cyst treated by cystoscopic controlled curettage Ludwig Schwering¹, Markus Uhl² and Georg W. Herget( )¹ ¹ Department of Orthopaedics and Traumatology,
Shoulder Arthroscopy with Posterior Labral Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Revision of the humeral component for aseptic loosening in arthroplasty of the shoulder
 Revision of the humeral component for aseptic loosening in arthroplasty of the shoulder A. Cil, C. J. H. Veillette, J. Sanchez-Sotelo, J. W. Sperling, C. Schleck, R. H. Cofield From the Mayo Clinic, Rochester,
Revision of the humeral component for aseptic loosening in arthroplasty of the shoulder A. Cil, C. J. H. Veillette, J. Sanchez-Sotelo, J. W. Sperling, C. Schleck, R. H. Cofield From the Mayo Clinic, Rochester,
Giant cell tumour of the proximal femur
 ONCOLOGY Giant cell tumour of the proximal femur IS JOINT-SPARING MANAGEMENT EVER SUCCESSFUL? A. E. Wijsbek, B. L. Vazquez- Garcia, R. J. Grimer, S. R. Carter, A. A. Abudu, R. M. Tillman, L. Jeys From
ONCOLOGY Giant cell tumour of the proximal femur IS JOINT-SPARING MANAGEMENT EVER SUCCESSFUL? A. E. Wijsbek, B. L. Vazquez- Garcia, R. J. Grimer, S. R. Carter, A. A. Abudu, R. M. Tillman, L. Jeys From
C. Christopher Smith, M.D. Associate Professor of Medicine Harvard Medical School Beth Israel Deaconess Medical Center
 Evaluation and Treatment of the Painful Shoulder in the Primary Care Setting C. Christopher Smith, M.D. Associate Professor of Medicine Harvard Medical School Beth Israel Deaconess Medical Center A 65-year-old
Evaluation and Treatment of the Painful Shoulder in the Primary Care Setting C. Christopher Smith, M.D. Associate Professor of Medicine Harvard Medical School Beth Israel Deaconess Medical Center A 65-year-old
Radiology Case Reports. Scapular Spine Stress Fracture as a Complication of Reverse Shoulder Arthroplasty
 Radiology Case Reports Volume 2, Issue 2, 2007 Scapular Spine Stress Fracture as a Complication of Reverse Shoulder Arthroplasty Kimberly J. Burkholz, Catherine C. Roberts, and Steven J. Hattrup We report
Radiology Case Reports Volume 2, Issue 2, 2007 Scapular Spine Stress Fracture as a Complication of Reverse Shoulder Arthroplasty Kimberly J. Burkholz, Catherine C. Roberts, and Steven J. Hattrup We report
Monophasic Synovial Carcinoma of knee joint- A Case Report and Review of Literature
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 3 Ver.5 March. (2018), PP 13-17 www.iosrjournals.org Monophasic Synovial Carcinoma of knee
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 3 Ver.5 March. (2018), PP 13-17 www.iosrjournals.org Monophasic Synovial Carcinoma of knee
Chronic Shoulder Disorders
 Chronic Shoulder Disorders Dr. Mustafa Elsingergy Consultant orthopedic surgeon Dallah Hospita Prof. Mamoun Kremli Almaarefa Medical College Contents INTRINSIC Shoulder Pain Due to causes in the shoulder
Chronic Shoulder Disorders Dr. Mustafa Elsingergy Consultant orthopedic surgeon Dallah Hospita Prof. Mamoun Kremli Almaarefa Medical College Contents INTRINSIC Shoulder Pain Due to causes in the shoulder
GIANT CELL-RICH OSTEOSARCOMA: A CASE REPORT
 Nagoya J. Med. Sci. 59. 151-157, 1996 CASE REPORTS GIANT CELL-RICH OSTEOSARCOMA: A CASE REPORT KEIJI SATO!, SHIGEKI YAMAMURA!, HISASHI IWATA!, HIDESHI SUGIURA 2, NOBUO NAKASHIMA 3 and TETSURO NAGASAKA
Nagoya J. Med. Sci. 59. 151-157, 1996 CASE REPORTS GIANT CELL-RICH OSTEOSARCOMA: A CASE REPORT KEIJI SATO!, SHIGEKI YAMAMURA!, HISASHI IWATA!, HIDESHI SUGIURA 2, NOBUO NAKASHIMA 3 and TETSURO NAGASAKA
Conflict of Interest. New Strategies in Rotator Cuff Repair. Objectives. Learner Outcome
 Conflict of Interest New Strategies in Rotator Cuff Repair Sheri Lankford, BSN, CNOR I hereby certify that, to the best of my knowledge, no aspect of my current personal or professional situation might
Conflict of Interest New Strategies in Rotator Cuff Repair Sheri Lankford, BSN, CNOR I hereby certify that, to the best of my knowledge, no aspect of my current personal or professional situation might
Tendinosis & Subacromial Impingement Syndrome. Gene Desepoli, LMT, D.C.
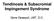 Tendinosis & Subacromial Impingement Syndrome Gene Desepoli, LMT, D.C. What is the shoulder joint? Shoulder joint or shoulder region? There is an interrelatedness of all moving parts of the shoulder and
Tendinosis & Subacromial Impingement Syndrome Gene Desepoli, LMT, D.C. What is the shoulder joint? Shoulder joint or shoulder region? There is an interrelatedness of all moving parts of the shoulder and
