Disaster Medical Operations Part 1. Unit 3
|
|
|
- Megan Johnson
- 5 years ago
- Views:
Transcription
1 CERT Disaster Medical Operations Part 1 Unit 3
2 Airways Bleeding/Wound Care Shock Burns Fractures, dislocations, splinting Head-To-Toe Assessment First Aid
3 Why Disaster Medical Ops? Need for CERT members to learn disaster medical operations is based on two assumptions: Number of victims could exceed local capacity for treatment Survivors will assist others They will do whatever they know how to do They need to know lifesaving first aid or postdisaster survival techniques
4 3 Phases of Death from Trauma Phase 1 Death within minutes due to overwhelming injuries to major organs Phase 2 Death within hours due to excessive bleeding Phase 3 Death in days/weeks due to infection or multiple organ failure complications from an injury Peter Safer s research after earthquakes in Chile, Peru, and Italy indicated that more than 40 percent of disaster victims in the second and third phases of death from trauma could be saved by providing simple medical care.
5 Treatment of Life-Threatening Conditions The Killers : Airway obstruction Excessive bleeding Shock First priority of medical operations: Open airway Control excessive bleeding Treat for shock
6 START STart = Simple Triage Victims sorted based on priority of treatment start = And Rapid Treatment Rapid treatment of injuries assessed and prioritized in first phase Greatest good for the greatest number.
7 Public Health Considerations Maintain proper hygiene Maintain proper sanitation Main Goal: Prevent the spread of disease!
8 Steps to Maintain Hygiene Wash hands frequently using soap and water OR use alcohol based hand sanitizer Wear latex gloves; change or disinfect after each patient Wear a mask and goggles Keep dressings sterile Avoid contact with body fluids If it is warm, wet, and not yours, DON T TOUCH IT!!!
9 Water Sanitation Methods Boil water for 1 minute Water purification tablets Non-perfumed liquid bleach 8 drops/gal of water 16 drops/gal if water is cloudy Let stand for 30 minutes before use
10 DEMONSTRATION Glove Use
11 How to Approach a Victim Be sure victim can see you Identify yourself Your name and name of your organization Request permission to treat, if possible Respect cultural differences
12 Components of a respiratory system: Lung Bronchus Larynx Pharynx Nasal Air Passage Trachea Airway Obstruction
13 Open Versus Obstructed Airway
14 Head-Tilt/Chin-Lift Opening the Airway
15 Jaw Thrust Opening the Airway
16 Look for the chest to rise Listen for air exchange Feel for air exchange Look, Listen and Feel
17 Triage - Are they breathing? YES NO Maintain Open Airway Walking wounded, or Elevate shoulders Reposition: 1. Return to neutral 2. Re-tilt (further back) Tag Immediate and move on Are they breathing? YES NO Tag Deceased and move on
18 Any questions?
19 Main Function Transport oxygen to cells Circulatory System
20 Result of ineffective circulation of the blood Primary cause in a disaster: blood loss Remaining in shock will result in Cell, Tissue and Organ death Important to continually re-evaluate and monitor victims for symptoms of shock Shock
21 Recognizing Shock Rapid Breathing >30 breaths per minute (very shallow) Inadequate circulation Capillary blanch >2 seconds Mental Status Unconscious, or Unable to follow simple command, squeeze my hand Symptoms of shock are easily missed pay careful attention to your patient!
22 Treating for Shock Lay victim on back Maintain open airway Elevate feet Control bleeding Maintain body temperature
23 Treating for Shock ALL shock victims, except for. Head injury Difficulty Breathing Unconscious: must be left alone or vomiting Spinal Cord injury/ Unsure/leg fracture
24 Three Types of Bleeding: Arterial spurting Venous flowing Capillary oozing Excessive Bleeding
25 Types of Bleeding - 2
26 Wound Classification
27 Controlling Bleeding 3 Main Methods to Control Bleeding: Direct Pressure Pressure bandage Elevation Above heart Pressure Points Arm, leg Direct Pressure Elevation Pressure Point
28 Pressure Points
29 Tourniquet Use direct pressure, elevation and pressure points to control bleeding first If bleeding can t be stopped and getting professional treatment will be delayed a tourniquet may be a viable option to save a person from bleeding to death Using a tourniquet is a LAST RESORT
30 Tourniquet A tourniquet is a tight bandage which, when placed around a limb and tightened, cuts off the blood supply to the part of the limb beyond it. Use any long, flat, soft material (bandage, neck tie, belt, or stocking). Do not use materials like rope, wire, or string that can cut into the patient s flesh.
31 Apply a Tourniquet To tie a tourniquet: 1. Place the tourniquet between the wound and the heart (for example, if the wound is on the wrist, you would tie the tourniquet around the forearm). 2. Tie the piece of material around the limb. 3. Place a stick, pen, ruler, or other sturdy item against the material and tie a knot around the item, so that the item is knotted against the limb. 4. Use the stick or other item as a lever to twist the knot more tightly against the limb, tightening the bandage until the bleeding stops.
32 Tourniquet 5. Tie one or both ends of the lever against the limb to secure it and maintain pressure. 6. Mark the patient in an obvious way that indicates that a tourniquet was used and include the time it was applied. 7. Do not loosen a tourniquet once it has been applied. 8. Only proper medical authorities should remove a tourniquet. 9. Monitor patient for symptoms of shock.
33 Tourniquet Video U tube video:
34 Control bleeding add dressings over existing dressings maintain pressure - use pressure dressing Elevate/pressure points Tourniquet Prevent infection: Clean wound Apply dressing & bandage Wound Care
35 Cleaning and Bandaging Wounds Clean by irrigating with clean, room temperature water NEVER use hydrogen peroxide Irrigate but do not scrub Apply dressing and bandage Dressing applied directly to wound Bandage holds dressing in place
36 Rules of Dressing If active bleeding: Redress OVER existing dressing If no active bleeding: Remove bandage and dressing to flush wound Check for infection every 4-6 hours
37 Rules of Dressing In the absence of active bleeding, remove dressing and flush, check wound at least every 4-6 hours. If there is active bleeding, redress over existing dressing and maintain pressure and elevation. Check for signs of infection swelling discoloration - redness discharge (pus) from wound
38 Signs of Infection Signs of possible infection Swelling around wound site Discoloration Discharge from wound Red striations from wound site
39 Treating Amputations Control bleeding Clean wound Treat for shock Save tissue parts, wrapped in clean cloth and place in a plastic bag Keep tissue cool, but NOT directly on ice Keep severed part with the victim Tag Immediate during Triage!
40 Treating Amputations
41 Treating Impaled Objects Immobilize affected body part Don t move or remove Control bleeding at entrance wound Clean and dress wound making sure impaled object is stabilized
42 Impaled Objects USC Drill Oklahoma Tornado - Teacher
43 Nasal Bleeding Causes: Blunt force Skull fracture Nontrauma-related conditions sinus infection, high blood pressure, and bleeding disorders Blood loss can lead to shock may not know how much blood has been lost because victim will swallow some Victims may become nauseated and vomit if they swallow blood.
44 Control nasal bleeding: Pinch nostrils or put pressure on upper lip under nose Have victim sit with head forward, NOT back Ensure that airway remains open Keep victim calm Treatment of Nasal Injuries
45 Any questions?
46 Burns Skin protection from infection retains body water maintains body temperature Causes Heat Radiation Chemical Electrical current
47 Burn Severity Factors that affect burn severity: Temperature of burning agent Period of time victim exposed Area of body affected Size of area burned Depth of burn
48 Classifications of Burns Classification Skin Layers Affected Signs 1 st Degree Epidermis (superficial) Reddened, dry skin Pain Swelling (possible) 2 nd Degree Epidermis Partial destruction of dermis Reddened, blistered skin Wet appearance Pain Swelling (possible) 3 rd Degree (Full Thickness Burns) Complete destruction of epidermis and dermis Possible subcutaneous damage (destroys all layers of skin and some or all underlying structures) Whitened, leathery, or charred (brown or black) Painful or relatively painless 1 st Degree 2 nd Degree 3 rd Degree
49 Burn Treatment: DOs When treating a burn victim, DO: Cool skin or clothing if they are still hot Cover burn loosely with dry, sterile dressings to keep air out, reduce pain, and prevent infection Elevate burned extremities
50 Burn Treatment: DON Ts When treating a burn victim, DO NOT: Use ice Apply antiseptics, ointments, or other remedies Remove shreds of tissue, break blisters, or remove adhered particles of clothing
51 Treatment for Chemical Burns Remove cause of burn + affected clothing/jewelry If irritant is dry, gently brush away as much as possible Always brush away from eyes, victim, and you Flush with lots of cool running water Apply cool, wet compress to relieve pain Cover wound loosely with dry, sterile or clean dressing Treat for shock if appropriate
52 Inhalation Burns Signs and Symptoms Sudden loss of consciousness Evidence of respiratory distress or upper airway obstruction Soot around mouth or nose Singed facial hair Burns around face or neck
53 Any questions?
54 Indicators of Injury Labored or shallow breathing Bleeding Bruising Swelling Severe pain Disfigurement/Deformity How the person may have been hurt Signs of a head, neck, or spinal injury
55 Treating Muscle/Bone/Joint Injuries Objective: Immobilize the joints above and below the injury. If questionable, treat as a fracture.
56 Fractures 2 types of fractures: Closed Open Broken bone with no wound May or may not be deformed Swelling and pain over site Broken bone with some kind of wound that allows contaminates to enter into fracture site Higher priority due to infection bleeding
57 Types of Fractures
58 DO NOT: Draw exposed bones back into tissue. Irrigate wound. DO: Cover wound. Splint fracture without disturbing wound. Place a moist 4" x 4" dressing over bone end to prevent drying. Treating an Open Fracture
59 Dislocations Dislocation is injury to ligaments around joint So severe that it permits separation of bone from its normal position in joint Treatment Immobilize; do NOT relocate Check PMS before and after splinting/ immobilization
60 Sprains and Strains Sprains: Tearing of a ligament or a tendon Ligament connects one bone to the other Tendon connects a muscle to a bone. Strains: Overstretching a muscle.
61 Strains and Sprains Signs and Symptoms Tenderness at injury site Swelling and/or bruising Restricted use or loss of use Treatment Immobilize and elevate
62 Support the injured area. Guidelines for Splinting Assess Pulse, Motor, Sensation (PMS) Splint injury in the position that you find it. Soft splint Rigid splint Anatomical splint Immobilize above and below the injury. Don t try to realign bones. Fill the voids to stabilize & immobilize After splinting reassess PMS
63 Splinting
64 Any questions?
65 Heat-Related Injuries Heat cramps: Muscle spasms brought on by over-exertion in extreme heat Heat exhaustion: Occurs when exercising or working in extreme heat results in loss of body fluids Heat stroke: Victim s temperature control system shuts down Body temperature rises so high that brain damage and death may result
66 Cool, moist, pale or flushed skin Heavy sweating Headache Nausea or vomiting Dizziness Exhaustion Symptoms of Heat Exhaustion
67 Symptoms of Heat Stroke Hot, red skin Lack of perspiration Changes in consciousness Rapid, weak pulse and rapid, shallow breathing This is very serious!
68 Treatment of Heat-Related Injuries Remove from heat to cool environment Cool body slowly Have the victim drink water, SLOWLY No food or drink if victim is experiencing vomiting, cramping, or is losing consciousness
69 Treatment for Bites/Stings If bite or sting is suspected, and situation is nonemergency: Remove stinger if still present by scraping edge of credit card or other stiff, straight-edged object across stinger Wash site thoroughly with soap and water Place ice on site for 10 minutes on and 10 minutes off
70 Any questions?
71 A head-to-toe assessment: Determines the extent of injuries and treatment. Determines the type of treatment needed. Documents injuries. Conducting Victim Assessment
72 Conducted on ALL victims Verbal, hands-on Head-to-Toe Assessment Wear protective gear Look, listen, and feel for anything unusual. Assess from top to bottom Assess completely before beginning treatment Document: injuries and treatment Treat all victims as if they have a spinal injury until certain they do not Check color, warmth, and sensation on all extremities Look for medical identification
73 1. Head 2. Neck 3. Shoulders 4. Chest 5. Arms 6. Abdomen 7. Pelvis 8. Legs Order of Assessment
74 Indicators of Head, Neck or Spine Injury Unconsciousness Unable to move one or more body parts Severe pain in head, neck, or back Tingling or numbness in extremities Bleeding, bruising, or deformity of the head or spine Seizures Blood or fluid in the nose or ears Bruising behind the ear or Raccoon eyes
75 Deformities Contusions Abrasions Punctures Burns Tenderness Lacerations Swelling DCAP-BTLS
76 Head, Neck, and Spinal Cord Injuries
77 Closed-Head, Neck, Spinal Injuries Do no harm Minimize movement of head and neck Keep spine in straight line Stabilize head
78 Any questions?
79 Mass Casualty Triage
Disaster Medical Operations Part 2. CERT Basic Training Unit 4
 Disaster Medical Operations Part 2 Unit 4 Unit 3 Review 3 Killers Airway obstruction Excessive bleeding Shock 4-1 CERT Sizeup 1. Gather Facts 2. Assess Damage 3. Consider Probabilities 4. Assess Your Situation
Disaster Medical Operations Part 2 Unit 4 Unit 3 Review 3 Killers Airway obstruction Excessive bleeding Shock 4-1 CERT Sizeup 1. Gather Facts 2. Assess Damage 3. Consider Probabilities 4. Assess Your Situation
Disaster Medical Operations-Part 2
 Disaster Medical Operations-Part 2 Community Emergency Response Team Disaster Medical Operations Part 1 Review The killers Airway obstruction Excessive bleeding Shock All immediate receive airway control,
Disaster Medical Operations-Part 2 Community Emergency Response Team Disaster Medical Operations Part 1 Review The killers Airway obstruction Excessive bleeding Shock All immediate receive airway control,
UNIT 4: DISASTER MEDICAL OPERATIONS
 UNIT 4: DISASTER MEDICAL OPERATIONS PART 2 Patient Evaluation: How to perform a head-to-toe assessment to identify and treat injuries. Basic Treatment How to: Treat burns Dress and bandage wounds Treat
UNIT 4: DISASTER MEDICAL OPERATIONS PART 2 Patient Evaluation: How to perform a head-to-toe assessment to identify and treat injuries. Basic Treatment How to: Treat burns Dress and bandage wounds Treat
OV United Soccer Club
 Preventing disease transmission Place an effective barrier between you and the victim s blood when you give first aid. Examples of such barriers are: the victim s hand, a piece of plastic, clean folded
Preventing disease transmission Place an effective barrier between you and the victim s blood when you give first aid. Examples of such barriers are: the victim s hand, a piece of plastic, clean folded
Disaster Medical Operations Part 2
 Disaster Medical Operations Part 2 Unit 4 Spring 2017 Unit 3 Review RPM, 30-2-Can Do 3 Killers! Airway obstruction! Excessive Bleeding! Shock (Circulatory) 4-1 1 Review - CERT Sizeup 1. Gather Facts 2.
Disaster Medical Operations Part 2 Unit 4 Spring 2017 Unit 3 Review RPM, 30-2-Can Do 3 Killers! Airway obstruction! Excessive Bleeding! Shock (Circulatory) 4-1 1 Review - CERT Sizeup 1. Gather Facts 2.
Note: This CareKit does not replace expert medical care. Be Prepared
 Note: This CareKit does not replace expert medical care. Be Prepared EMS #: 9-1-1 Poison Control #: 800.222.1222 Take a first aid course. Learn CPR and first aid for choking. Before you give first aid,
Note: This CareKit does not replace expert medical care. Be Prepared EMS #: 9-1-1 Poison Control #: 800.222.1222 Take a first aid course. Learn CPR and first aid for choking. Before you give first aid,
First Aid Policy. One member of every coaching staff (competitive) is "required" to be first aid certified.
 First Aid Policy When you accept the role of coach with LSSC, regardless of what level, you accept a major responsibility for the care and safety of your players. Although the athletes share in the responsibility
First Aid Policy When you accept the role of coach with LSSC, regardless of what level, you accept a major responsibility for the care and safety of your players. Although the athletes share in the responsibility
First Aid Fact Sheet 2005 Standards
 First Aid Fact Sheet 2005 Standards Five Leading Causes of Unintentional death: 1. Motor vehicle accidents 2. Falls 3. Poisonings 4. Drownings 5. Choking Good Samaritan Laws laws that give legal protection
First Aid Fact Sheet 2005 Standards Five Leading Causes of Unintentional death: 1. Motor vehicle accidents 2. Falls 3. Poisonings 4. Drownings 5. Choking Good Samaritan Laws laws that give legal protection
QI. Read the following questions and choose the most correct answer (20 Marks):
 Question One: QI. Read the following questions and choose the most correct answer (20 Marks): 1- Some people are very allergic to some drugs like penicillin. This condition is called: a) Septic shock.
Question One: QI. Read the following questions and choose the most correct answer (20 Marks): 1- Some people are very allergic to some drugs like penicillin. This condition is called: a) Septic shock.
Key Words. clammy closed fracture dislocation fainting ligament open fracture splint sprain strain trauma. Linked Core Abilities
 Lesson 4 Treating for Shock and Immobilizing Fractures Key Words clammy closed fracture dislocation fainting ligament open fracture splint sprain strain trauma What You Will Learn to Do Determine first
Lesson 4 Treating for Shock and Immobilizing Fractures Key Words clammy closed fracture dislocation fainting ligament open fracture splint sprain strain trauma What You Will Learn to Do Determine first
Aviation Rescue Swimmer Course
 Aviation Rescue Swimmer Course Primary Survey LT 5.4 December 2003 1 Objectives List the procedures used in a primary survey. Demonstrate primary survey procedures used in a mock trauma (moulage) scenario
Aviation Rescue Swimmer Course Primary Survey LT 5.4 December 2003 1 Objectives List the procedures used in a primary survey. Demonstrate primary survey procedures used in a mock trauma (moulage) scenario
NOTE If it is necessary to perform abdominal thrusts, expose the abdominal area prior to pressing on the abdomen.
 ENABLING OBJECTIVES: 4.7 List the procedures used in a primary survey. 4.8 Demonstrate primary survey procedures used in a mock trauma (moulage) scenario without injury to personnel or damage to equipment.
ENABLING OBJECTIVES: 4.7 List the procedures used in a primary survey. 4.8 Demonstrate primary survey procedures used in a mock trauma (moulage) scenario without injury to personnel or damage to equipment.
Skin Anatomy and Physiology
 Skin Anatomy and Physiology Body s largest organ Three layers: Epidermis Dermis Subcutaneous tissue 1 2 Skin Anatomy and Physiology Complex system, variety of functions Sensation Control of water loss
Skin Anatomy and Physiology Body s largest organ Three layers: Epidermis Dermis Subcutaneous tissue 1 2 Skin Anatomy and Physiology Complex system, variety of functions Sensation Control of water loss
OUTLINE SHEET 5.4 PRIMARY SURVEY
 ENABLING OBJECTIVES: 4.7 List the procedures used in a primary survey. 4.8 Demonstrate primary survey procedures used in a mock trauma (moulage) scenario without injury to personnel or damage to equipment.
ENABLING OBJECTIVES: 4.7 List the procedures used in a primary survey. 4.8 Demonstrate primary survey procedures used in a mock trauma (moulage) scenario without injury to personnel or damage to equipment.
Unit 7 INJURY MANAGEMENT Review Game
 Unit 7 INJURY MANAGEMENT Review Game Print and cut out the playing cards. Divide the class into groups of 3 or 4. Each group will need a set of playing cards. Directions for the Review game 1. Stack all
Unit 7 INJURY MANAGEMENT Review Game Print and cut out the playing cards. Divide the class into groups of 3 or 4. Each group will need a set of playing cards. Directions for the Review game 1. Stack all
Have an Emergency Plan. Injury Prevention. Stretches for All Players
 Have an Emergency Plan It is important to have a well thought out plan for dealing with injuries. It is best to have a written response plan for emergencies. Keep this in your coaching bag where you can
Have an Emergency Plan It is important to have a well thought out plan for dealing with injuries. It is best to have a written response plan for emergencies. Keep this in your coaching bag where you can
Providing for Players Safety 31. Emergency Plan
 Providing for Players Safety 31 Emergency Plan An emergency plan is the final step in preparing to take appropriate action for severe or serious injuries. The plan calls for three steps: 1. Survey the
Providing for Players Safety 31 Emergency Plan An emergency plan is the final step in preparing to take appropriate action for severe or serious injuries. The plan calls for three steps: 1. Survey the
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Hatfield & McCoy Mine Safety Competition First-Aid Contest JULY 15, Page 1
 Hatfield & McCoy Mine Safety Competition First-Aid Contest JULY 15, 2014 Page 1 PROBLEM Billy is a maintenance person that has been conducting clean-up and service duties on the number one conveyor belt
Hatfield & McCoy Mine Safety Competition First-Aid Contest JULY 15, 2014 Page 1 PROBLEM Billy is a maintenance person that has been conducting clean-up and service duties on the number one conveyor belt
Basic First Aid. Sue Fisher Emergency Management Coordinator CSUF University Police
 Basic First Aid Sue Fisher Emergency Management Coordinator CSUF University Police Information given for this lecture is not meant to replace any official training by the American Red Cross, or any other
Basic First Aid Sue Fisher Emergency Management Coordinator CSUF University Police Information given for this lecture is not meant to replace any official training by the American Red Cross, or any other
Lesson 9: Bone & Joint Injuries. Emergency Reference Guide p
 Lesson 9: Bone & Joint Injuries Emergency Reference Guide p. 33-43 Objectives Define strain, sprain, fracture and dislocation List Signs & Symptoms of strain, sprain, fracture & dislocation Demonstrate
Lesson 9: Bone & Joint Injuries Emergency Reference Guide p. 33-43 Objectives Define strain, sprain, fracture and dislocation List Signs & Symptoms of strain, sprain, fracture & dislocation Demonstrate
Chapter 24 Soft Tissue Injuries Presentation Notes
 Names: Chapter 24 Soft Tissue Injuries Presentation Notes Anatomy of the Skin - Function of the Skin control Soft-Tissue Injuries injuries Soft-tissue damage the skin injuries Break in the of the skin
Names: Chapter 24 Soft Tissue Injuries Presentation Notes Anatomy of the Skin - Function of the Skin control Soft-Tissue Injuries injuries Soft-tissue damage the skin injuries Break in the of the skin
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions
 Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What is caused by overexerting or tearing of a muscle? p. 375 A.) Dislocation B.) Sprain C.) Fracture *D.)
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What is caused by overexerting or tearing of a muscle? p. 375 A.) Dislocation B.) Sprain C.) Fracture *D.)
Face and Throat Injuries. Chapter 26
 Face and Throat Injuries Chapter 26 Anatomy of the Head Landmarks of the Neck Injuries to the Face Injuries around the face can lead to upper airway obstructions. Bleeding from the face can be profuse.
Face and Throat Injuries Chapter 26 Anatomy of the Head Landmarks of the Neck Injuries to the Face Injuries around the face can lead to upper airway obstructions. Bleeding from the face can be profuse.
Module Summaries: The emergency plan is a crucial part of the total sports program.
 Module Summaries: Summary - The Emergency Plan The emergency plan is a crucial part of the total sports program. Prior to each season and game, those individuals responsible for the program and athletes
Module Summaries: Summary - The Emergency Plan The emergency plan is a crucial part of the total sports program. Prior to each season and game, those individuals responsible for the program and athletes
Chapter IV Disaster Medical Operations Part 2
 Chapter IV Disaster Medical Operations Part 2 In this chapter you will learn about: Patient evaluation: How to perform a head-to-toe patient evaluation in order to identify and treat injuries. Disaster
Chapter IV Disaster Medical Operations Part 2 In this chapter you will learn about: Patient evaluation: How to perform a head-to-toe patient evaluation in order to identify and treat injuries. Disaster
WOUNDS. Emergency Procedures in PT
 WOUNDS Emergency Procedures in PT Types of Wounds Abrasions uppermost layer scraped away, minor capillary bleeding occurs, nerve endings exposed Lacerations skin tear with edges jagged and uneven Incisions
WOUNDS Emergency Procedures in PT Types of Wounds Abrasions uppermost layer scraped away, minor capillary bleeding occurs, nerve endings exposed Lacerations skin tear with edges jagged and uneven Incisions
Frontline First Aid 2012 Emergency Care Manual Treatments
 Heart Attack/Angina (p. 132) 1. Recognize signals of a heart attack 2. Assist with Nitroglycerin 3. Assist with ASA 4. Rest and Comfort 6. More advanced medical care Breathing Emergencies (p. 105) Anaphylaxis
Heart Attack/Angina (p. 132) 1. Recognize signals of a heart attack 2. Assist with Nitroglycerin 3. Assist with ASA 4. Rest and Comfort 6. More advanced medical care Breathing Emergencies (p. 105) Anaphylaxis
AMERICAN RED CROSS FIRST AID RESPONDING TO EMERGENCIES FOURTH EDITION Copyright 2006 by The American National Red Cross All rights reserved.
 Musculoskeletal injuries are most commonly caused by Mechanical forms of energy. Chemicals. Electrical energy. Heat Mechanical energy produces direct, indirect, twisting and contracting forces. Can be
Musculoskeletal injuries are most commonly caused by Mechanical forms of energy. Chemicals. Electrical energy. Heat Mechanical energy produces direct, indirect, twisting and contracting forces. Can be
68W COMBAT MEDIC POCKET GUIDE
 GTA 08-05-058 68W COMBAT MEDIC POCKET GUIDE PART I: TRAUMA TREATMENT This publication contains technical information that is for official Government use only. Distribution is limited to U.S. Government
GTA 08-05-058 68W COMBAT MEDIC POCKET GUIDE PART I: TRAUMA TREATMENT This publication contains technical information that is for official Government use only. Distribution is limited to U.S. Government
Football First Aid: An Overview. Steven Richmond 95# Commissioner --BRYC Firefighter II, EMT-B, HTR & HZMT Tech City of Alexandria Fire and EMS
 Football First Aid: An Overview Steven Richmond 95# Commissioner --BRYC Firefighter II, EMT-B, HTR & HZMT Tech City of Alexandria Fire and EMS Overview Hyperthermia (Heat Related Injuries) Concussions
Football First Aid: An Overview Steven Richmond 95# Commissioner --BRYC Firefighter II, EMT-B, HTR & HZMT Tech City of Alexandria Fire and EMS Overview Hyperthermia (Heat Related Injuries) Concussions
Musculoskeletal Injuries
 Musculoskeletal Injuries KNOWLEDGE OBJECTIVES 1. Identify the four main structures of the musculoskeletal system. 2. List five common signs or symptoms of musculoskeletal injuries. 3. List seven signs
Musculoskeletal Injuries KNOWLEDGE OBJECTIVES 1. Identify the four main structures of the musculoskeletal system. 2. List five common signs or symptoms of musculoskeletal injuries. 3. List seven signs
Medical & Safety. Stay safe at Kamp Dovetail 2011
 Medical & Safety Stay safe at Kamp Dovetail 2011 Seizures Seizures are very misunderstood and may be caused by many different types of conditions, such as: Insulin shock High fevers Viral infections of
Medical & Safety Stay safe at Kamp Dovetail 2011 Seizures Seizures are very misunderstood and may be caused by many different types of conditions, such as: Insulin shock High fevers Viral infections of
Overview. Overview. Chapter 30. Injuries to the Head and Spine 9/11/2012. Review of the Nervous and Skeletal Systems. Devices for Immobilization
 Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
You Are the Emergency Medical Responder
 Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
SSA Player Injury Prevention and Care Guide
 SSA Player Injury Prevention and Care Guide Prevention of Injuries The first line of defense in the treatment of athletic injuries is to prevent them. There are a variety of ways to accomplish this: 1.
SSA Player Injury Prevention and Care Guide Prevention of Injuries The first line of defense in the treatment of athletic injuries is to prevent them. There are a variety of ways to accomplish this: 1.
LESSON 2.1 Minor Wound Management Process
 LESSON 2.1 Minor Wound Management Process How do we make use of the four different kinds of first aid items such as gauze, melolin, padding (triangular bandage), and plaster to cover up the wounds? Cleaning
LESSON 2.1 Minor Wound Management Process How do we make use of the four different kinds of first aid items such as gauze, melolin, padding (triangular bandage), and plaster to cover up the wounds? Cleaning
B) Sprains cause swelling in the injured area, but strains do not have a tendency to swell
 Lesson U4C2L4 FIT Questions 1. (U4C2L4:F1) How many times have you broken a bone? A) none B) one C) two D) more than two 2. (U4C2L4:F2) How many times have you sprained an arm, leg, or other body part?
Lesson U4C2L4 FIT Questions 1. (U4C2L4:F1) How many times have you broken a bone? A) none B) one C) two D) more than two 2. (U4C2L4:F2) How many times have you sprained an arm, leg, or other body part?
Chapter 30 - Musculoskeletal_Trauma
 Introduction to Emergency Medical Care 1 OBJECTIVES 30.1 Define key terms introduced in this chapter. Slides 11 12, 19 20, 22 23, 37 30.2 Describe the anatomy of elements of the musculoskeletal system.
Introduction to Emergency Medical Care 1 OBJECTIVES 30.1 Define key terms introduced in this chapter. Slides 11 12, 19 20, 22 23, 37 30.2 Describe the anatomy of elements of the musculoskeletal system.
Session 3 or 6: Being Active: A Way of Life.
 Session 3 or 6: Being Active: A Way of Life. You can find the time to be active. Set aside one block of time every day to be active. When can you set aside 20 to 30 minutes to do an activity you like?
Session 3 or 6: Being Active: A Way of Life. You can find the time to be active. Set aside one block of time every day to be active. When can you set aside 20 to 30 minutes to do an activity you like?
FIRST AID & EMERGENCIES
 FIRST AID & EMERGENCIES Kelly Pederson, RN Chris DeLapp, CCH Education Manager Safety & Emergencies What is First Aid? Scene Survey Victim Assessment Bleeding Control Shock Burns Choking Basic First Aid
FIRST AID & EMERGENCIES Kelly Pederson, RN Chris DeLapp, CCH Education Manager Safety & Emergencies What is First Aid? Scene Survey Victim Assessment Bleeding Control Shock Burns Choking Basic First Aid
Injuries to the Extremities
 Injuries to the Extremities KNOWLEDGE OBJECTIVES 1. List seven signs and symptoms that suggest a serious extremity injury. 2. Describe how to care for injuries to the shoulder, upper arm, and elbow. 3.
Injuries to the Extremities KNOWLEDGE OBJECTIVES 1. List seven signs and symptoms that suggest a serious extremity injury. 2. Describe how to care for injuries to the shoulder, upper arm, and elbow. 3.
 55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
( PLUM BOROUGH SCHOOL DISTRICT
 No. 209.1 ( PLUM BOROUGH SCHOOL DISTRICT SECTION: PUPILS TITLE: FIRST AID STANDING ORDERS ADOPTED: March 27,1990 REVISED: February 27, 2001 209.1. FIRST AID STANDING ORDERS 1. Guidelines When a student
No. 209.1 ( PLUM BOROUGH SCHOOL DISTRICT SECTION: PUPILS TITLE: FIRST AID STANDING ORDERS ADOPTED: March 27,1990 REVISED: February 27, 2001 209.1. FIRST AID STANDING ORDERS 1. Guidelines When a student
Patient Assessment. Chapter 8
 Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
MUSCULOSKELETAL INJURIES
 WHAT ARE THEY They are injuries to muscles, nerves, tendons ligaments, joints, cartilage and spinal discs. WHAT KIND OF INJURIES ARE MUSCULOSKELETAL INJURIES 1. Fractures- -Open -Closed 2. Dislocations
WHAT ARE THEY They are injuries to muscles, nerves, tendons ligaments, joints, cartilage and spinal discs. WHAT KIND OF INJURIES ARE MUSCULOSKELETAL INJURIES 1. Fractures- -Open -Closed 2. Dislocations
Injuries to Muscles, Bones and Joints. Emergency Medical Response
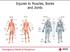 Injuries to Muscles, Bones and Joints Lesson 33: Injuries to Muscles, Bones and Joints You Are the Emergency Medical Responder You are patrolling the state park where you are the emergency medical responder
Injuries to Muscles, Bones and Joints Lesson 33: Injuries to Muscles, Bones and Joints You Are the Emergency Medical Responder You are patrolling the state park where you are the emergency medical responder
Wellness 360 Online Nutrition Counseling* Session 6: Being Active A Way of Life
 Wellness 360 Online Nutrition Counseling* Session 6: Being Active A Way of Life. powered by WELLSTAR 360 Session 6: Overview Be Active It s Your Choice! This session focuses on how to become more physically
Wellness 360 Online Nutrition Counseling* Session 6: Being Active A Way of Life. powered by WELLSTAR 360 Session 6: Overview Be Active It s Your Choice! This session focuses on how to become more physically
Heat Injuries caoches should be aware of...4
 Coaches Handbook 2018 Part D Items that don't relate directly to coaching but are things a coach needs to know - Injuries/first aid - Table of Contents Overview...2 Care and prevention of injuries...2
Coaches Handbook 2018 Part D Items that don't relate directly to coaching but are things a coach needs to know - Injuries/first aid - Table of Contents Overview...2 Care and prevention of injuries...2
Facial Sports Injuries
 Facial Sports Injuries Playing catch, shooting hoops, bicycling on a scenic path or just kicking around a soccer ball have more in common than you may think. On the up side, these activities are good exercise
Facial Sports Injuries Playing catch, shooting hoops, bicycling on a scenic path or just kicking around a soccer ball have more in common than you may think. On the up side, these activities are good exercise
MODULE 5 THE EMERGENCY
 HEALTH EDUCATION II MODULE 5 THE EMERGENCY What this Module is all about You and your friends are biking when suddenly you hear car tires screeching behind you. You turn around and see your friend hit
HEALTH EDUCATION II MODULE 5 THE EMERGENCY What this Module is all about You and your friends are biking when suddenly you hear car tires screeching behind you. You turn around and see your friend hit
MEDICAL JEOPARDY. Q. This is the first thing you check when you find an unconscious victim
 MEDICAL JEOPARDY This is a Medical Jeopardy game with rules similar to Jeopardy on television. Use 3x5 cards with a hole punched in one end on a bulletin board for the game board. Each contestant will
MEDICAL JEOPARDY This is a Medical Jeopardy game with rules similar to Jeopardy on television. Use 3x5 cards with a hole punched in one end on a bulletin board for the game board. Each contestant will
POLICY/PROCEDURE. Issued By: Clinical Services. Policy No.: TX.009. Reference: Code 99 - TX.012. Date Issued: 2/99
 POLICY/PROCEDURE Title: Emergency Medical Care / First Aid Procedures Hanging Bleeding Poison/Overdose Nose Bleeds Drowning Foreign Bodies in the Eye Burns Fractures Fainting Anaphylactic Reactions Hypoglycemic
POLICY/PROCEDURE Title: Emergency Medical Care / First Aid Procedures Hanging Bleeding Poison/Overdose Nose Bleeds Drowning Foreign Bodies in the Eye Burns Fractures Fainting Anaphylactic Reactions Hypoglycemic
Ears. Mouth. Jowls 6 Major Bones of the Face Nasal bone Two
 1 2 3 4 5 Chapter 25 Injuries to the Face, Neck, and Eyes Injuries to the Face and Neck Face and neck are to injury Relatively unprotected positions on body Some injuries are life-threatening. trauma to
1 2 3 4 5 Chapter 25 Injuries to the Face, Neck, and Eyes Injuries to the Face and Neck Face and neck are to injury Relatively unprotected positions on body Some injuries are life-threatening. trauma to
4 inch laceration traversing down the front of forearm. Fracture of lower leg midway between knee and ankle
 2 inch wound on forehead 3 inch wound on top of shoulder islocated elbow in flexed position 4 inch laceration traversing down the front of forearm 3 inch wound on inner thigh Fracture of lower leg midway
2 inch wound on forehead 3 inch wound on top of shoulder islocated elbow in flexed position 4 inch laceration traversing down the front of forearm 3 inch wound on inner thigh Fracture of lower leg midway
Acting in an emergency. Dr. Samer Sara
 Acting in an emergency Dr. Samer Sara 1 Acting in an emergency basic steps to follow: 1. Recognize the emergency. 2. Check the scene. 3. Call 110. 4. Check the victim. 5. Give first aid. 2 Dr. Samer Sara
Acting in an emergency Dr. Samer Sara 1 Acting in an emergency basic steps to follow: 1. Recognize the emergency. 2. Check the scene. 3. Call 110. 4. Check the victim. 5. Give first aid. 2 Dr. Samer Sara
First Aid in Agriculture
 A Publication of the National Center for Farmworker Health First Aid in Agriculture Mario works at Orange Peel Farm. His job is to bend over, pick up boxes of oranges, and place the boxes on a truck. A
A Publication of the National Center for Farmworker Health First Aid in Agriculture Mario works at Orange Peel Farm. His job is to bend over, pick up boxes of oranges, and place the boxes on a truck. A
5/2/2018. Notice. Putting Humpty Dumpty Back Together Again
 Notice All EMS Live@Nite presentations will be recorded (both audio and video) and available for public viewing online. By participating in EMS Live@Nite, you consent to audio and video recording and its/their
Notice All EMS Live@Nite presentations will be recorded (both audio and video) and available for public viewing online. By participating in EMS Live@Nite, you consent to audio and video recording and its/their
Difficulty breathing Altered level of consciousness Amputated arm
 Difficulty breathing 22-year-old male, severe difficulty breathing, chest sinks in on inspiration, respirations over 30/min, radial pulse present, responds to instructions. Altered level of consciousness
Difficulty breathing 22-year-old male, severe difficulty breathing, chest sinks in on inspiration, respirations over 30/min, radial pulse present, responds to instructions. Altered level of consciousness
FIRST AID TEST Practice Test
 FIRST AID TEST Practice Test www.schoolbusing.com West County Transportation Agency This test was developed to help school bus driver s study and prepare for the California Special Drivers Certificate
FIRST AID TEST Practice Test www.schoolbusing.com West County Transportation Agency This test was developed to help school bus driver s study and prepare for the California Special Drivers Certificate
Skill Evaluation Sheets
 Skill Evaluation Sheets Skill Drill 2-: How to Remove Gloves Skill Drill 4-: Primary Check: RAP-CAB Skill Drill 4-2: Perform a Secondary Check Skill Drill 5-: Adult CPR Skill Drill 5-2: Child CPR Skill
Skill Evaluation Sheets Skill Drill 2-: How to Remove Gloves Skill Drill 4-: Primary Check: RAP-CAB Skill Drill 4-2: Perform a Secondary Check Skill Drill 5-: Adult CPR Skill Drill 5-2: Child CPR Skill
Emergency Care Progress Log
 Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
First Aid Training (Materials provided by the MAYO Clinic and the American Safety & Health institute)
 Copper Hills Little League P. O. Box 194 Sahuarita, AZ 85629 First Aid Training (Materials provided by the MAYO Clinic and the American Safety & Health institute) Page 1 PREVENTION Following safety rules
Copper Hills Little League P. O. Box 194 Sahuarita, AZ 85629 First Aid Training (Materials provided by the MAYO Clinic and the American Safety & Health institute) Page 1 PREVENTION Following safety rules
FIRST AID WRITTEN EXAM. Team Name: 1. Participation in a critical incident stress debriefing (CISD) is mandatory. a. TRUE b. FALSE
 2015 NEW IBERIA MINE RESCUE CONTEST FIRST AID WRITTEN EXAM Name: Date: 1. Participation in a critical incident stress debriefing (CISD) is mandatory. 2. The use of accessory muscles in the chest, abdomen
2015 NEW IBERIA MINE RESCUE CONTEST FIRST AID WRITTEN EXAM Name: Date: 1. Participation in a critical incident stress debriefing (CISD) is mandatory. 2. The use of accessory muscles in the chest, abdomen
Review. 1. Which of the following is NOT a component of the cardiovascular system? A. Heart B. Lungs C. Venules D. Plasma
 Chapter 23 Review 1. Which of the following is NOT a component of the cardiovascular system? A. Heart B. Lungs C. Venules D. Plasma Answer: B Rationale: Components of the cardiovascular system include
Chapter 23 Review 1. Which of the following is NOT a component of the cardiovascular system? A. Heart B. Lungs C. Venules D. Plasma Answer: B Rationale: Components of the cardiovascular system include
Extremity Injuries and Splinting
 CHAPTER 15 Extremity Injuries and Splinting Lesson Objectives 1. Describe the 3 general types of splints and how to improvise splints with common materials. 2. List the general guidelines for splinting
CHAPTER 15 Extremity Injuries and Splinting Lesson Objectives 1. Describe the 3 general types of splints and how to improvise splints with common materials. 2. List the general guidelines for splinting
Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing
 1 2 3 4 5 6 Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing D-Disability Chief complaint and/or Mechanism
1 2 3 4 5 6 Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing D-Disability Chief complaint and/or Mechanism
Chapter 25 - Bleeding
 1 2 3 National EMS Education Standard Competencies (1 of 3) Trauma Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely injured patient.
1 2 3 National EMS Education Standard Competencies (1 of 3) Trauma Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely injured patient.
Skin is the largest, most important organ % of total body weight Functions: - -Sensation - Regulation AKA: System
 1 Chapter 20 Soft-Tissue Injury 2 Introduction to Soft-Tissue Injury Skin is the largest, most important organ % of total body weight Functions: - -Sensation - Regulation AKA: System 3 Epidemiology Most
1 Chapter 20 Soft-Tissue Injury 2 Introduction to Soft-Tissue Injury Skin is the largest, most important organ % of total body weight Functions: - -Sensation - Regulation AKA: System 3 Epidemiology Most
 International Trauma Life Support for Prehospital Care Providers Sixth Edition Patricia M. Hicks, MS, NREMTP Roy Alson, PhD, MD, FACEP Donna Hastings, EMT-P John Emory Campbell, MD, FACEP and Alabama Chapter,
International Trauma Life Support for Prehospital Care Providers Sixth Edition Patricia M. Hicks, MS, NREMTP Roy Alson, PhD, MD, FACEP Donna Hastings, EMT-P John Emory Campbell, MD, FACEP and Alabama Chapter,
At the conclusion of this course the learner will be able to
 Objectives At the conclusion of this course the learner will be able to 1. Discuss basic anatomy and pathophysiology of burns 2. Describe burn injuries in terms of size, depth, coloration and characteristics
Objectives At the conclusion of this course the learner will be able to 1. Discuss basic anatomy and pathophysiology of burns 2. Describe burn injuries in terms of size, depth, coloration and characteristics
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions
 Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What do injuries to the shoulder often produce? p. 393 *A.) Anterior dislocation B.) Superior dislocation
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What do injuries to the shoulder often produce? p. 393 *A.) Anterior dislocation B.) Superior dislocation
Frontline First Aid First Aid - What to Look For and What to Do
 First Aid - What to Look For and Hyperventilation Rapid Shallow Breathing A feeling of suffocating or not getting enough air Relax Reassure Fear Anxiety Breathe slowly Asthma Wheeze when exhaling Unable
First Aid - What to Look For and Hyperventilation Rapid Shallow Breathing A feeling of suffocating or not getting enough air Relax Reassure Fear Anxiety Breathe slowly Asthma Wheeze when exhaling Unable
For the Patient: Fludarabine injection Other names: FLUDARA
 For the Patient: Fludarabine injection Other names: FLUDARA Fludarabine (floo-dare-a-been) is a drug that is used to treat many types of cancer. It is a clear liquid that is injected into a vein. Tell
For the Patient: Fludarabine injection Other names: FLUDARA Fludarabine (floo-dare-a-been) is a drug that is used to treat many types of cancer. It is a clear liquid that is injected into a vein. Tell
DR A.MALIK. Emergency First Aid and CPR
 DR A.MALIK Emergency First Aid and CPR FIRST AID PROCEDURES COVERED Bleeding/Shock/Minor injuries Burn Care Neck and Back Injuries Heat Exhaustion/Heat Stroke Hypothermia/Frost Bite Severe Allergic Reactions
DR A.MALIK Emergency First Aid and CPR FIRST AID PROCEDURES COVERED Bleeding/Shock/Minor injuries Burn Care Neck and Back Injuries Heat Exhaustion/Heat Stroke Hypothermia/Frost Bite Severe Allergic Reactions
HEAT STRESS BLUE COLLAR SILVICULTURE LTD.
 HEAT STRESS BLUE COLLAR SILVICULTURE LTD. TRAINING OVERVIEW What is heat stress Primary contributing factors Sources of heat Removal of heat from the body Personal risk factors Recognizing heat stress
HEAT STRESS BLUE COLLAR SILVICULTURE LTD. TRAINING OVERVIEW What is heat stress Primary contributing factors Sources of heat Removal of heat from the body Personal risk factors Recognizing heat stress
FIRST AID FOR POLICE FIRST RESPONDERS
 FIRST AID FOR POLICE FIRST RESPONDERS ROLES AND RESPONSIBILITIES RESPOND PROMPTLY TO SCENE GAIN ACCESS TO THE PATIENT PERFORM A PATIENT ASSESSMENT ADMINISTER EMERGENCY MEDICAL CARE MOVE PATIENT IF NECESSARY
FIRST AID FOR POLICE FIRST RESPONDERS ROLES AND RESPONSIBILITIES RESPOND PROMPTLY TO SCENE GAIN ACCESS TO THE PATIENT PERFORM A PATIENT ASSESSMENT ADMINISTER EMERGENCY MEDICAL CARE MOVE PATIENT IF NECESSARY
Caring for Bleeding, Shock and Soft-Tissue Injuries From Brady s First Responder (8th Edition) 99 Questions
 Caring for Bleeding, Shock and Soft-Tissue Injuries From Brady s First Responder (8th Edition) 99 Questions 1. Which of the following should NOT be done to treat an internal ear injury? p. 346 A.) Leave
Caring for Bleeding, Shock and Soft-Tissue Injuries From Brady s First Responder (8th Edition) 99 Questions 1. Which of the following should NOT be done to treat an internal ear injury? p. 346 A.) Leave
For the Patient: Trastuzumab emtansine Other names: KADCYLA
 For the Patient: Trastuzumab emtansine Other names: KADCYLA Trastuzumab emtansine (tras tooz' ue mab em tan' seen) is a drug that is used to treat some types of cancer. Trastuzumab emtansine is a clear
For the Patient: Trastuzumab emtansine Other names: KADCYLA Trastuzumab emtansine (tras tooz' ue mab em tan' seen) is a drug that is used to treat some types of cancer. Trastuzumab emtansine is a clear
 TRAUMA LIFE SUPPORT PRE-HOSPITAL EXAMINATION (TLS P) 1. A high-risk bodily fluid for spreading infection is. a. sweat b. saliva c. blood d. urine 2. Items that can be used to reduce the spread of infection
TRAUMA LIFE SUPPORT PRE-HOSPITAL EXAMINATION (TLS P) 1. A high-risk bodily fluid for spreading infection is. a. sweat b. saliva c. blood d. urine 2. Items that can be used to reduce the spread of infection
Theory Assessment Questions Instructions to participant
 Theory Assessment Questions Instructions to participant This section contains 84 questions. Pass Mark is 76/84. You are to mark the correct answers on the table below. This front page and page two must
Theory Assessment Questions Instructions to participant This section contains 84 questions. Pass Mark is 76/84. You are to mark the correct answers on the table below. This front page and page two must
Alix Casler, M.D., F.A.A.P. Orlando, FL
 Alix Casler, M.D., F.A.A.P. Orlando, FL Emergencies in the School Setting Initial triage Basics of History and Exam Specific Scenarios Initial Assessment and Triage First steps in evaluating a potential
Alix Casler, M.D., F.A.A.P. Orlando, FL Emergencies in the School Setting Initial triage Basics of History and Exam Specific Scenarios Initial Assessment and Triage First steps in evaluating a potential
IRECA BLS Challenge 2015 Scenario 1
 Scenario 1 Team Name Team Number Captain Name Judge 1 # Judge 2 # JUDGE S SHEET Overview: This scenario challenges the competitors to use basic triage techniques and then to do the most good for the most
Scenario 1 Team Name Team Number Captain Name Judge 1 # Judge 2 # JUDGE S SHEET Overview: This scenario challenges the competitors to use basic triage techniques and then to do the most good for the most
Competency Log Professional Responder Courses
 Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
Patient Assessment From Brady s First Responder (8th Edition) 83 Questions
 Patient Assessment From Brady s First Responder (8th Edition) 83 Questions 1. Which question is important if your patient may be a candidate for surgery? p. 183 *A.) When did you last eat? B.) What is
Patient Assessment From Brady s First Responder (8th Edition) 83 Questions 1. Which question is important if your patient may be a candidate for surgery? p. 183 *A.) When did you last eat? B.) What is
Extreme Heat: A Prevention Guide to Promote Health and Safety
 Extreme Heat: A Prevention Guide to Promote Health and Safety People suffer heat-related illness when their bodies are unable to compensate and properly cool themselves. The body normally cools itself
Extreme Heat: A Prevention Guide to Promote Health and Safety People suffer heat-related illness when their bodies are unable to compensate and properly cool themselves. The body normally cools itself
For the Patient: Paclitaxel Other names: TAXOL
 For the Patient: Paclitaxel Other names: TAXOL Paclitaxel (pak'' li tax' el) is a drug that is used to treat many types of cancer. It is a clear liquid that is injected into a vein. Tell your doctor if
For the Patient: Paclitaxel Other names: TAXOL Paclitaxel (pak'' li tax' el) is a drug that is used to treat many types of cancer. It is a clear liquid that is injected into a vein. Tell your doctor if
Airway and Ventilation. Emergency Medical Response
 Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
MIAMI-DADE COLLEGE. Common Course Number: HSC Course Title: Basic Emergency Care. Course Catalog Description:
 Common Course Number: HSC 2400 MIAMI-DADE COLLEGE Course Title: Basic Emergency Care Course Catalog Description: Designed to provide opportunities to develop, practice, and display skills concerning emergency
Common Course Number: HSC 2400 MIAMI-DADE COLLEGE Course Title: Basic Emergency Care Course Catalog Description: Designed to provide opportunities to develop, practice, and display skills concerning emergency
APPLY FIRST AID ONLINE WORKBOOK
 APPLY FIRST AID ONLINE WORKBOOK STUDENT NAME: ADDRESS: PHONE CONTACT: DATE OF COURSE: Welcome to CYNERGEX GROUP pre-learning package for the APPLY FIRST AID course. This workbook is to be completed in
APPLY FIRST AID ONLINE WORKBOOK STUDENT NAME: ADDRESS: PHONE CONTACT: DATE OF COURSE: Welcome to CYNERGEX GROUP pre-learning package for the APPLY FIRST AID course. This workbook is to be completed in
Basic Assessment and Treatment of Trauma
 Basic Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls 1.2
Basic Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls 1.2
McCann Technical School 70 Hodges Cross Road North Adams, MA Medical Assisting Program
 MA 104 MEDICAL SOCIAL SCIENCE 4 Credits Fall Semester Part IV FIRST RESPONDER Syllabus McCann Technical School 70 Hodges Cross Road North Adams, MA 01247 Medical Assisting Program INSTRUCTORS: Laurie Tuper,
MA 104 MEDICAL SOCIAL SCIENCE 4 Credits Fall Semester Part IV FIRST RESPONDER Syllabus McCann Technical School 70 Hodges Cross Road North Adams, MA 01247 Medical Assisting Program INSTRUCTORS: Laurie Tuper,
BLS ROUTINE MEDICAL CARE
 BLS ROUTINE MEDICAL CARE Scene safety # Assure scene safety prior to patient contact C-spine # Perform manual cervical spine stabilization if indicated (Follow the cervical spine protocol.) ABCs # Assess
BLS ROUTINE MEDICAL CARE Scene safety # Assure scene safety prior to patient contact C-spine # Perform manual cervical spine stabilization if indicated (Follow the cervical spine protocol.) ABCs # Assess
Review. A. abrasion B. contusion C. hematoma D. avulsion
 Chapter 24 Review Review 1. A young male was struck in the forearm with a baseball and complains of pain to the area. Slight swelling and ecchymosis are present, but no external bleeding. What type of
Chapter 24 Review Review 1. A young male was struck in the forearm with a baseball and complains of pain to the area. Slight swelling and ecchymosis are present, but no external bleeding. What type of
Chapter 7 EMERGENCY PLAN AND INITIAL INJURY EVALUATION
 Chapter 7 EMERGENCY PLAN AND INITIAL INJURY EVALUATION Major Concepts. Proper planning of an emergency response is essential for appropriate first aid management of an injury. Anything that can be done
Chapter 7 EMERGENCY PLAN AND INITIAL INJURY EVALUATION Major Concepts. Proper planning of an emergency response is essential for appropriate first aid management of an injury. Anything that can be done
Sorafenib (so-ra-fe-nib) is a drug that is used to treat many types of cancer. It is a tablet that you take by mouth.
 For the Patient: Other names: Sorafenib NEXAVAR Sorafenib (so-ra-fe-nib) is a drug that is used to treat many types of cancer. It is a tablet that you take by mouth. A blood test may be taken before each
For the Patient: Other names: Sorafenib NEXAVAR Sorafenib (so-ra-fe-nib) is a drug that is used to treat many types of cancer. It is a tablet that you take by mouth. A blood test may be taken before each
CENTRAL CARE POLICY SYMPTOMS OF ILLNESS. Policy: Consumers will be observed for symptoms of physical problems, distress, pain, or unusual behaviors.
 Page 1 of 5 CENTRAL CARE POLICY SYMPTOMS OF ILLNESS SUBJECT: SYMPTOMS OF ILLNESS ANNUAL REVIEW MONTH: June RESPONSIBLE FOR REVIEW: Director of Central Care LAST REVISION DATE: June 2009 Policy: Consumers
Page 1 of 5 CENTRAL CARE POLICY SYMPTOMS OF ILLNESS SUBJECT: SYMPTOMS OF ILLNESS ANNUAL REVIEW MONTH: June RESPONSIBLE FOR REVIEW: Director of Central Care LAST REVISION DATE: June 2009 Policy: Consumers
YOUR PATH TO RECOVERY AFTER SHOULDER REPLACEMENT
 YOUR PATH TO RECOVERY AFTER SHOULDER REPLACEMENT Revised 11/2015 Day of Surgery: # 0 After Surgery Day: # 1 Precautions DO NOT actively move your shoulder, lift, carry, reach, bear weight, or reach behind
YOUR PATH TO RECOVERY AFTER SHOULDER REPLACEMENT Revised 11/2015 Day of Surgery: # 0 After Surgery Day: # 1 Precautions DO NOT actively move your shoulder, lift, carry, reach, bear weight, or reach behind
Tips for Teaching ARISE Life Management Skills...3. Introduction...6 Lessons...7. Introduction...12 Lessons Introduction...19 Lessons...
 ARISE Life-Skills for Middle School - Volume 4 Instructor s Manual Table of Contents Tips for Teaching ARISE Life Management Skills...3 SECTION ONE: Health care is self-care Introduction...6 Lessons...7
ARISE Life-Skills for Middle School - Volume 4 Instructor s Manual Table of Contents Tips for Teaching ARISE Life Management Skills...3 SECTION ONE: Health care is self-care Introduction...6 Lessons...7
Table of Contents. Dialysis Port Care Chemotherapy Port Care G-Tube Care Colostomy Bags Wound Dressings
 Table of Contents Dialysis Port Care Chemotherapy Port Care G-Tube Care Colostomy Bags Wound Dressings Dialysis Port Care Know What Type of Vascular Access You Have. Fistula: An artery in your forearm
Table of Contents Dialysis Port Care Chemotherapy Port Care G-Tube Care Colostomy Bags Wound Dressings Dialysis Port Care Know What Type of Vascular Access You Have. Fistula: An artery in your forearm
