Osteochondral Lesions of the Talus: From Birth to Near Death
|
|
|
- Rachel Aileen Paul
- 6 years ago
- Views:
Transcription
1 AOFAS Symposium 6 Arthroscopy: Incisions are Too Complicated Tuesday, September 23, :50 12:05 pm Moderator: Annunziato Amendola, MD Iowa City, Iowa Osteochondral Lesions of the Talus: From Birth to Near Death Richard D. Ferkel, MD Van Nuys, California I. Terminology A. Multiple terms used to describe similar problem, including: 1. transchondral fracture 2. osteochondral fracture 3. osteochondritis dissecans 4. talar dome fracture 5. flake fracture B. Best term probably is Osteochondral Lesion of Talus (OLT) II. III. Incidence A. OLT comprise 4% of all O.D. B. Average age of patients between 20 and 30 years, with males slightly predominant C. Medial dome lesions more common than lateral D. Bilateral lesions about 10%. Recent study by Hermanson & Ferkel found the incidence to be 10% in a group of 526 patients with OLT Location and Characteristics of Lesion A. Medial lesions are deeper, larger, cup-shaped and are usually non-displaced B. Medial dome of talus in mid or posterior third. Medial talar dome/middle row (Raikin zone 4) most common (53% of 428 lesions) C. Lateral dome of talus in mid or anterior portion. These are located in lateral/middle second most common (26%) D. Lateral lesions are usually shallow and wafer-shaped and often displaced and elevated by levering effect of distal tibia E. Lateral lesions occur more in shear, while medial lesions occur more with compression F. There are exceptions to the above rules
2 IV. Staging A. Berndt & Harty classified OLT as to their appearance on x-ray into four stages: 1. small compression fracture without displacement (intact) 2. partially detached osteochondral fragment 3. completely detached fragment remaining in its bed 4. completely displaced fragment of loose body B. Ferkel, Cheng & Sgaglione developed a CT scan staging 1-4. This correlates better with treatment & outcome (Table 1) C. MRI staging has been done by Anderson and others D. Arthroscopic staging 1. Pritsch et al. classified lesions by arthroscopic appearance of overlying cartilage into 3 grades: a. intact, firm shiny articular cartilage b. intact but soft cartilage c. frayed cartilage 2. Lesion can progress from Grade I to III during course of treatment 3. Correlation poor between x-ray appearance and arthroscopic findings a. Scope appearance is more important determinant of treatment 4. Arthroscopic classification of Ferkel & Chen is probably best way to stage lesion (Table 2) a. Ferkel, Cheng & Applegate found correlation between CT, MRI and new arthroscopic classification V. Radiologic Features A. Three views of ankle done on all patients. Weight bearing views and special views are occasionally helpful. Stress x-rays done when appropriate B. Tomography in two planes can be helpful but is presently rarely used C. CT in coronal and axial planes with sagittal reconstructions is one of the best ways to study lesion and most helpful for preop planning. Adding contrast and air can help determine if the lesion is loose. I prefer a bilateral study to check the asymptomatic side. D. Bone scans helpful in Stage I lesions E. MRI helpful in diagnosing OLT, and in future may provide information on vascularity of lesion, treatment and subsequent healing. Gadolinium injection can help determine if lesion is loose VI. VII. Surgical Indications A. Staging determined by CT and/or MRI scan and arthroscopic evaluation B. Stage 1 & 2, and Stage 3 in children fail 8-12 weeks of casting and conservative treatment C. All Stage 3 and 4 lesions in adults Arthroscopic Technique (Ferkel) A. Use thigh and ankle holder in supine position with ankle distractor B. 2.7-mm 30- and 70-degree arthroscopes with interchangeable cannulae C. Use anteromedial, anterolateral and posterolateral portals to visualize and treat the lesion. Use 2.9 and 3.5 shavers and burrs for debridement of the lesion. Small curettes (3.5-, 4.5- mm with different angulations) critical for removal of lesion. Small joint graspers are needed for loose body removal
3 D. Treatment of chronic OLT 1. unroof or remove separated or loose fragment 2. curettage and/or drill OLT bed using standard, transmalleolar or transtalar approaches with mm or mm K-wires and drill guide 3. alternatively, microfracture can be done with or without drilling; abrasion arthroplasty does not appear to be as useful E. Anteromedial lesion (rare) drilled or microfractured through anteromedial portal, visualize through anterolateral portal F. Posteromedial lesion best approached by visualization through posterolateral portal and drilling transmalleolarly or transtalarly with the drill guide. Microfracture also is used through either anteromedial or posterolateral portal. In larger lesion, use a combination of drilling and microfracture. Shaver and curettes through anteromedial portal G. Anterolateral lesions drilled and/or microfractured through anterolateral portal and visualized through anteromedial portal. Occasionally drill through tibia using drill guide. Microfracture also used as noted above. H. When articular cartilage is intact and lesion cystic, transtalar bone grafting can be done using the drill guide, but in our experience, these lesions are rare. VIII. Large Cystic OLT A. Introduction 1. in the past, large unstable cystic OLT have been treated with excision, drilling and/or microfracture through an arthroscopic approach 2. results are variable in these large lesions when treated as described above 3. better results with debridement, drilling or microfracture and bone grafting B. Technique for bone grafting 1. ankle arthroscopy done as described 2. arthroscopic bone grafting equipment 3. patient should be paralyzed for maximum distraction 4. lesion is excised and all loose articular cartilage and cystic membrane is removed down to healthy bleeding bone 5. edges of the cystic lesion should be cut at 90 o to promote blood pooling 6. incision over distal tibia with exposure of the distal tibia and elliptical bone graft taken from the medial side of the distal tibia metaphyseal region 7. morselizing of bone graft so it can be inserted through a 3- or 5-mm cannula arthroscopically 8. insertion of the bone graft into the cannula and placement of the cannula into the cystic lesion 9. using an obturator, the bone graft is advanced in the cystic lesion and continuously impacted with a Freer Elevator through the anterolateral portal while the bone graft is inserted through the anteromedial portal (on a medial lesion); visualization is done through the posterolateral portal and the bone graft is slowly compacted 10. insertion of fibrin glue (optional) 11. tourniquet and distraction are released while pressure is held on the bone graft with two Freer Elevators. After 2 minutes, the bone graft site has had enough bleeding to form an adhesive clot to hold the graft in place 12. posterior splint for 2 weeks, then removable splint for gentle dorsi and plantar flexion exercising 4 times a day 13. patient is non-weight bearing 6-8 weeks, depending on the size of the lesion
4 IX. Postoperative Arthroscopic Surgical Treatment A. Posterior splint and compression dressing applied at surgery B. Remove splint in 1 week for arthroscopic procedures that involve excision and/or drilling and microfracture; then start ROM and strengthening with removable splint non-weight bearing C. Drilling with or without curettage 1. non-weight bearing 2-4 weeks if lesion <1.0cm 2 in diameter 2. non-weight bearing 6-8 weeks if lesion >1.0cm 2 D. Curettage and debridement alone weight bearing in 1 week E. Follow-up CT scan or MRI in 6 months to assess healing X. Arthroscopic Results A. Kumai, Takakura (1999) patients/18 ankles, f/u 2 to 9.5 years 2. all patients drilled, with immediate weight bearing, no cast 3. results good in 13, fair in 5 4. best results for patients under 30 years of age and non-cystic lesion B. Kelberine, Frank (1999) patients with different treatments 2. acute did best, with 16 G/E out of chronic 20 G/E out of 30 C. Erggelet (2000) patients over 5 years percutaneous drilling and 13 bone grafting 3. hindfoot score improved in most patients D. Tol et al. (2000) 1. meta analysis of electronic databases of all cases excision alone, 38% G/E 3. excision and curettage, 78% G/E 4. excision and drilling, 85% G/E 5. nonoperative, 45% G/E E. Hinterman (2001) cases 2. results better in most grades I and II, especially laterally 3. results unsatisfactory in grade II and III medial lesions 4. recommend stage 1 conservative and stage IV surgery 5. grade II to III conservative with medial and surgery with lateral F. van Dijk (2002) patients 2. curettage and drilling 3. follow-up 56 months 4. primary 86% G/E; revision 75% G/E G. Ferkel (2008) cases treated arthroscopically % G/E 3. f/u 71 months
5 H. Guo et al. (2010) patients with OLT 2. all had debridement and 36 had microfracture 3. 5 lost to follow-up. 4. average follow-up 24 months 5. 82% G/E; AOFAS strong correlation found between the size of the lesion and successful outcome I. Kennedy et al. (2011) used bone marrow aspirate concentrate (BMAC) as a biological adjunct for the treatment of OLT XI. XII. Future A. Long term solution to treating full thickness cartilage defects involve cartilage growth enhancement instead of drilling or abrasion B. Techniques of cartilage growth enhancement 1. osteochondral autograft 2. osteochondral allograft 3. autologous chondrocyte implantation 4. scaffolds with autologous chondrocytes 5. particulated juvenile articular cartilage allograft 6. others Osteochondral Autograft Transplantation (OATS) A. Robs Peter to pay Paul B. Uses osteochondral graft plugs from the sulcus terminalis of knee, anterior talar head, or medial or lateral non-articulating portions of the talus for graft sources C. Advantage of single setting procedure D. Size limitations for autograft transplantations usually between 8 and 20 mm E. Question of long-term problems with femoral plug holes and subsequent pain F. Anteromedial talar lesions 1. Arthroscopy and debridement 2. Arthrotomy establish lesion size 3. Core out or drill out lesion to at least 10 mm deep 4. Compact the base and measure depth 5. Harvest donor graft from the knee or ankle 6. Insert donor graft into the defect G. Posterolateral lesions 1. Arthroscopy and debridement 2. Arthrotomy and release the anterior talofibular and calcaneofibular ligaments 3. Sublux talus anteriorly 4. Insert graft as above H. Posteromedial talar lesions 1. Arthroscopy and debridement 2. Medial malleolar osteotomy, including pre-drilling the medial malleolus for later screw insertion 3. Same as above I. Allograft OATS core grafting or en bloc 1. Steps as above
6 2. Try to match the exact location and morphology on the allograft to the insertion site J. Retrograde OATS tibial plateau or tibial plafond 1. Arthroscopically define the size of the lesion 2. Use angle drill guide to retrograde drill at 70-degrees into the plateau or plafond lesion 3. Harvest graft and insert with special instrumentation, as described by Scranton K. Results OATS 1. Sammarco (2002) did 12 patients and harvested graft from medial or lateral facet of talus for OATS a. AOFAS scores 64 to Scranton et al. (2005) did 50 OATS cases with 2 to 6 year follow-up a. 64% had failed one or more surgeries prior to grafting b. 90% good/excellent c. 15 required either screw removal or second-look for scar debridement d. 2 failed required ankle arthrodesis L. Results Allograft OATS 1. Gross (2001) did 9 patients; 6 patients remain in situ with mean survival 11 years. 3 cases required fusion; 2. Gortz et al. (2010) reported on 12 ankles in 11 patients with fresh osteochondral allografts for OLT; all involved partial unipolar grafts of the talar dome implanted through an anterior approach without osteotomy a. Mean follow-up 38 months b. Mean OMAS improved from 28 to 71 c. 30% excellent; 20% good; 30% fair; 20% poor 3. El-Rashidy et al. (2011) reported on 42 patients using fresh osteochondral allograft for OLT a. Mean follow-up 38 months b. Mean AOFAS 52 to 79 c. Graft failure in 4 patients XIII. Autologous Chondrocyte Implantation A. Definition implantation of in vitro cultured autologous chondrocytes using a periosteal tissue cover or membrane after expansion of isolated chondrocytes B. Cartilage Repair Registry (Genzyme Tissue Repair, vol. 6:3-00) 1. Prospective multicenter data from 636 surgeons, 47 patients at 4 year follow-up 2. Mean total defect size = 4.6cm 2 3. Average age 38 years (15-55) 4. 81% of condyle group improved on Modified Cincinnati Score 5. 78% had at least one associated procedure 6. Overall debridement 4.3%, AF 1.9%, hypertrophy 1.3%, 3.2% failure XIV. Indications for ACI in the Ankle A. Indications 1. Patients aged 15 to Focal defect 3. Unipolar (only talus affected) 4. Contained
7 5. Edge loading 6. Failed previous surgery 7. Large lesions with extensive subchondral cystic changes B. Relative Indications 1. Multifocal unipolar lesions 2. Uncontained lesions XV. ACI Generations A. Generation 1 Carticel suspended under a periosteal flap B. Generation 2 Carticel inserted under a tissue patch or onto a carrier scaffold C. Generation 3 Carrier-free, immature cartilage tissue XVI. Surgical Technique ACI Generation 1 A. Medial or lateral malleolar osteotomy performed under fluoroscopic control B. Defect preparation includes removing all damaged cartilage from subchondral bone and debriding defect on the calcified cartilage layer without penetrating bone C. Harvest periosteum from distal tibia along the medial malleolus or from just distal to the pes anserinus and the proximal anterior tibia D. Mark non-cambium layer of periosteum E. Periosteum fixation 1. Place periosteum in the defect with the cambium layer down, suture with 5.0 or 6.0 Vicryl suture and seal with fibrin glue F. BioGide membrane 1. Absorbable porcine bilayer collagen I/III membrane used by dentists in the United States for a number of years 2. Recently has been used in knee and ankle ACI in place of periosteum, but this indication is not FDA approved 3. Has a rough and smooth layer 4. Made by the same company as Chondro-gide and very similar G. Aspirate cell vial contents and resuspend cells H. Implant via catheter through opening in the periosteum I. Close hole in the periosteum and use fibrin glue; then reattach osteotomy J. Wound closure 1. Re-insert pre-drilled guide pins and insert appropriate length screws in the medial malleolus 2. Insert lag screws in fibula, then appropriate size plate and screws 3. The patient goes into short leg cast in neutral position XVII. Postoperative Care for OATS and ACI A. Four phases B. Immobilization 2-3 weeks, until wounds are healed C. Then start partial weight bearing with removable CAM walker and TED stocking D. At 6 weeks, go to full weight bearing and start physical therapy 1. Progress through Phase 1, 2, 3 and 4 with specific protocol XVIII. Results of ACI First Generation (ACI-P) A. Baums et al. (2006)
8 1. 12 patients 2. Mean follow-up 63 months 3. Hannover score increased from 40 to 86 points 4. AOFAS increased 45 points 5. Patients involved in competitive sports were able to return to their full activity level B. Ferkel (2010) patients done; the first 11 patients have been reviewed and published in AJSM 2. Current study: Follow-up on 29 of 32 (91%) 3. Average age: 34 (18-54) 4. Average follow-up: 70 months (24-129) 5. 9 sandwich procedures done, with bone grafting of large cystic underlying defect and use of two periosteal grafts back to back 6. 2nd look arthroscopy on 90% of patients (26/29) 7. Results: Excellent: 8; Good: 15; Fair: 5; Poor: 1 8. Entire paper presented at AAOS 2011 XIX. ACI Periosteal Problems A. First Generation ACI complications include: 1. Periosteal hypertrophy 2. Delamination 3. Graft failure B. USFDA estimated 3.8 complication rate in knees 1. 18% graft hypertrophy C. Type I/III bilayer porcine collagen membranes available in United States to be used in place of periosteum 1. Gomoll et al. compared subsequent surgeries with periosteum versus collagen membrane 2. Results similar except hypertrophy related surgery: 52% with periosteum and 3.4% with collagen membrane XX. Second Generation ACI A. A variety of scaffolds being used in Europe, implanted either through a small arthrotomy or arthroscopically. 1. Used as a patch and cells inserted underneath 2. Cells seeded onto the scaffold membrane B. Collagen-covered autologous chondrocyte implantation (CACI or ACI-C) 1. Absorbable porcine bilayer collagen I/III membrane 2. Chondro-Gide membrane with one compact and one porous surface 3. Gooding found no difference in results between periosteum and membrane cover in knees with CACI C. Hyalograft C 1. Benzyl ester of Hyaluronic acid 2. Bioabsorbs in 3 months 3. Marcacci et al. presented 175 patients with grafts in the knee with 46 month mean follow-up. Results were 93% improvement at ICRS Giannini et al. (2008) 46 patients in ankle a. Mean age 32; follow-up 3 years
9 b. Preop 57; postop 90 mean AOFAS score c. Biopsies collagen type II D. Membrane/matrix autologous chondrocyte implantation (MACI) 1. Highly purified type I/III collagen membrane 2. Guillen and Abelow presented first 50 cases (42 knees; 8 ankles) 3. 8 ankles (ages 22-46) 4. Large full thickness cartilage lesions of the talus (2-6 cm) 5. 5/6 good & excellent results with follow-up 4 months-2 1/2 years 6. Giza et al. did MACI on 10 patients; AOFAS 61 to 73 XXI. Third generation ACI A. Use carrier-free, immature cartilage tissue B. Lack of carrier scaffold C. Avoids carrier integration, degradation and biocompatibility complications D. Jubel et al. used an alginate matrix to produce cell-rich chondrocyte disc in MFC of 48 sheep E. Chondral defects treated with De Novo cartilage transplantation showed qualitatively better micro and macroscopic regeneration than those with periosteal flaps alone 1. Farr and Yao reported earlier results in the knee 2. Adams et al. reported particulated juvenile articular cartilage allograft transplant for OLT with early good results F. DeNovo particulated juvenile cartilage results 1. Coetzee, Giza, Schon et al. reported on 24 ankles, average age failed at least one prior bone marrow stimulation procedure with average lesion size 125 mm 2 and average depth 7 mm 3. AOFAS score 85 with 18 (78%) ankles showing G-E scores 4. 92% G-E in lesions mm XXII. Recommended reading on current and future innovations on ACI and treatment of osteochondral lesions of the talus A. Safran, Kim and Zaffagnini in JAAOS, 2008 B. Mitchell, Giza, Sullivan in JAAOS, 2009 C. Getgood, Brooks, Fortier, Rushton in JBJS (Br) 2009 D. Gikas, Bayliss, Bentley, Briggs in JBJS (Br) 2009 E. O Loughlin, Heyworth, Kennedy in AJSM 2009 F. Ferkel, Scranton, Stone in Instructional Course Lectures 2010 G. McGahan, Pinney in FAI 2010 H. Easley, Latt, Santangelo et al in JAAOS 2010 I. Harris, Siston, Pan, Flanigan in JBJS 2010 J. Zengerink, Struijs, Tol, van Dijk in Knee Surg Sports Traumatol Arthrosc K. Dhollander, Guevara Sanchez, Almqvist et al. in J Knee Surg L. Coetzee, Giza, Schon, et al. in Foot Ankle Int M. Murawski, Kennedy in JBJS N. Moran, Pascual-Garrido, Chubinskaya et al. in JBJS (Am) XXIII. Summary A. Zengerink et al. has nicely summarized when to use which treatment for OLT (see Table 3) B. Is there a critical defect size for poor outcome?
10 1. Choi et al (2009) found initial defect size is important prognostic factor for OLT and can serve as a basis for preop surgical decisions 2. OLT defect of 150 mm 2 or greater as calculated from MRI has a high correlation of having a poor clinical outcome XXIV. Is there a critical defect size for poor outcome? A. Chuckpaiwong et al. (2008) did debridement and microfracture on 105 patients with mean follow-up of 32 months. 1. Lesions smaller than 15 mm, no failures 2. Lesions great than 15 mm, one patient successful 3. Factors affecting negative outcome: increasing age, higher BMI, trauma history and presence of osteophytes B. Guo et al. (2010) treated 43 patients arthroscopically with mean age of 32 years 1. AOFAS 70 to 90; 81% good/excellent 2. Strong correlation with size of lesion (<10 mm) and successful outcome C. Choi et al (2009) found initial defect size is important prognostic factor for OLT and can serve as a basis for preop surgical decisions 1. OLT defect of 150 mm 2 or greater as calculated from MRI has a high correlation of having a poor clinical outcome 2. OLT defect of <150 mm 2 has a high correlation of a good clinical outcome XXV. Summary A. Zengerink et al. has nicely summarized when to use which treatment for OLT (see Table 3) Stage 1 Stage IIA Stage IIB Stage III Stage IV Grade A Grade B Grade C Grade D Grade E Grade F Table 1. CT Classification 17 Cystic lesion within dome of talus, intact room on all views Cystic lesion with communication to talar dome surface Open articular surface lesion with overlying displaced fragment Undisplaced lesion with lucency Displaced fragment Table 2. Surgical Grade Based on Articular Cartilage 17 Smooth, intact but soft or ballottable Rough surface Fibrillations/fissures Flap present or bone exposed Loose, undisplaced fragment Displaced fragment Table 3. Guideline for Treatment of Osteochondral Talar Lesions 51 Lesion Type 1: asymptomatic lesions, low-symptomatic lesions Type 2: symptomatic lesions < 10 mm Type 3: symptomatic lesions mm Treatment Conservative Debridement and drilling/microfracturing Consider debridement & drilling, fixation, an osteochondral graft or ACI
11 Type 4: symptomatic lesions > 15 mm Type 5: large talar cystic lesions Type 6: secondary lesions Consider fixation, graft or ACI Consider retrograde drilling + bone transplant, or ACI with sandwich procedure Consider osteochondral transplant For types 4 through 6, debridement and bone marrow stimulation can always be considered a treatment option. * Zengerink M, Szerb I, Hangody L, et al.: Current Concepts: Treatment of Osteochondral Ankle Defects References 1. Adams SB, Yao JQ, Schon LC: Particulated juvenile articular cartilage allograft transplantation for osteochondral lesions of the talus. Tech Foot Ankle Surg 2011;10: Barnes CJ, Ferkel RD: Arthroscopic debridement and drilling of osteochondral lesions of the talus. Foot Ankle Clin North Am 8: , Bassett FH, Gates HS, Billys JB, et al. Talar impingement by the anteroinferior tibiofibular ligament. A cause of chronic pain in the ankle after inversion sprain. J Bone Joint Surg 72A:55, Baums MH, Heidrich G, Schultz W, et al.: Autologous chondrocyte transplantation for treating cartilage defects of the talus. J Bone Joint Surg 88A: , Bazaz R, Ferkel RD: Treatment of osteochondral lesions of the talus with autologous chondrocyte implantation. Tech Foot Ankle Surg 3:45-52, Brown JE, Branch TP: Surgical alternatives for treatment of articular cartilage lesions. J Am Acad Orthop Surg 8: , Choi et al. Osteochondral lesion of the talus: Is there a critical defect size for poor outcome? Am J Sports Med 37: , Coetzee JC, Giza E, Schon LC, et al.: Treatment of osteochondral lesions of the talus with particulated juvenile cartilage. Foot Ankle Int 2013;34: Easley ME, Latt LD, Santangelo JR, Merian-Genast M, Nunley JA II: Osteochondral lesions of the talus. J Amer Acad Orthop Surg 18: , Easley ME, Scranton PE: Osteochondral autologous transfer system. Foot Ankle Clin North Am 8: , El-Rashidy H, Villacis D, Omar I, Kelikian AS: Fresh osteochondral allograft for the treatment of cartilage defects of the talus: a retrospective review. J Bone Joint Surg Am 2011;93: Farr J, Yao JQ: Chondral defect repair with particulated juvenile cartilage allograft. Cartilage 2011;2: Ferkel RD: Arthroscopic Surgery: The Foot and Ankle. Philadelphia, PA: J.B. Lippincott, Ferkel RD, Karzel RJ, Del Pizzo W, Friedman MJ, Fischer SP: Arthroscopic treatment of anterolateral impingement of the ankle. Am J Sports Med 19: , Ferkel RD, Scranton PE: Current concepts review: Arthroscopy of the ankle and foot. J Bone Joint Surg 75A:1233, Ferkel RD, Scranton PE Jr., Stone JW, Kern B: Chronic osteochondral lesions of the talus: therapeutic dilemmas. Part II: Surgical treatment of osteochondral lesions of the talus. Inst Course Lect 59: , Ferkel RD, Zanotti RM, Komenda GA, et al.: Arthroscopic treatment of chronic osteochondral lesions of the talus. Am J Sports Med 36: , Getgood A, Brooks R, Fortier L, Rushton N: Articular cartilage tissue engineering. J Bone Joint Surg 91B: , Giannini S, Buda R, Faldini C, et al.: Surgical treatment of osteochondral lesions of the talus in young active patients. J Bone Joint Surg 87A(suppl 2):28-41, 2005.
12 20. Giannini S, Buda R, Vannini F, DiCaprio F, Grigolo B: Arthroscopic autologous chondrocyte implantation in osteochondral lesions of the talus: surgical technique and results. Am J Sports Med 36: , Gikas PD, Bayliss L, Bentley G, Briggs TWR: An overview of autologous chondrocyte implantation. J Bone Joint Surg 91B: , Giza E, Sullivan M, Ocel D, et al.: Matrix-induced autologous chondrocyte implantation of talus articular defects. Foot Ankle Int 2010;31: Gortz S, DeYoung A, Bugbee W: Fresh osteochondral allografting for osteochondral lesions of the talus. Foot Ankle Int 31: , Gras F, Marintschev I, Muller M, et al: Arthroscopic-controlled navigation for retrograde drilling of osteochondral lesions of the talus. Foot Ankle Int 31: , Gross AE, Agnidis Z, Hutchison CR: Osteochondral defects of the talus treated with fresh osteochondral allograft transplantation. Foot Ankle Int 22: , Guo Q-W, Hu Y-L, Jiao C, et al.: Arthroscopic treatment for osteochondral lesions of the talus: analysis of outcome predictors. Clin Med J 2010;123: Hahn DB, Aanstoos ME, Wilkins RM: Osteochondral lesions of the talus treated with fresh talar allografts. Foot Ankle Int 31: , Harris JD, Siston RA, Pan X, Flanigan DC: Autologous chondrocyte implantation: A systematic review. J Bone Joint Surg 92A: , Hermanson E, Ferkel RD: Bilateral osteochondral lesions of the talus. Foot Ankle Int 30: , Jones DG, Peterson L: Autologous chondrocyte implantation. J bone Joint Surg 88A: , Lee C-H, Chao K-H, Huang G-S, Wu S-S: Osteochondral autografts for osteochondritis dissecans of the talus. Foot ankle Int 24: , Liu SH, Raskin BS, Osti L, et al. Arthroscopic treatment of anterolateral ankle impingement. Arthroscopy 10:215, Martin DF, Baker CL, Curl WW, et al. Operative ankle arthroscopy: long-term follow-up. Am J Sports Med 17:16, McGahan PJ, Pinney SJ: Current concept review: Osteochondral lesions of the talus. Foot Ankle Int 31:90-101, Meislin RJ, Rose DJ, Parisien S, Springer S. Arthroscopic treatment of synovial impingement of the ankle. Am J Sports Med 21:186, Mitchell ME, Giza E, Sullivan MR: Cartilage transplantation techniques for talar cartilage lesions. J am Acad Orthop Surg 17: , Moran CJ, Pascual-Garrido C, Chubinskaya S, et al.: Restoration of articular cartilage. J Bone Joint Surg Am 2014;96: Murawski CD, Duke GL, Deyer TW, Kennedy JG: Bone marrow aspirate concentrate (BMAC) as a biological adjunct to the surgical treatment of osteochondral lesions of the atlus. Tech Foot Ankle Surg 2011;10: Nam EK, Ferkel RD, Applegate GR: Autologous chondrocyte implantation of the ankle: a 2 to 5 year followup. Am J Sports Med 37: , Niemeyer P, Lenz P, Kreuz PC, et al.: Chondrocyte-seeded type I/III collegen membrane for autologous chondrocyte transplantation: prospective 2-year results in patients with cartilage defects of the knee joint. Arthroscopy 26: , Ogilvie-Harris DJ, Reed SC: Disruption of the ankle syndesmosis: Diagnosis and treatment by arthroscopic surgery. Arthroscopy 10:561, Peterson L, Vasiliadis HS, Brittberg M, Lindahl A: Autologous chondrocyte implantation: a long-term followup. Am J sports Med 38: , Raikin SM: Fresh osteochondral allografts for large-volume cystic osteochondral defects of the talus. J Bone Joint Surg 91A: , Rubin DA, Tishkoff NW, Britton CA, Conti SF, Towers JD: Anterolateral soft-tissue impingement of the ankle: diagnosis using MR imaging. AJR 169: , Safran MR, Kim H, Zaffagnini S: The use of scaffolds in the management of articular cartilage injury. J Am Acad Orthop Surg 16: , 2008.
13 46. Scranton PE, Frey CC, Feder KS: Outcome of osteochondral autograft transplantation for type V cystic osteochondral lesions of the talus. J Bone Joint Surg 88B: m, Scranton PE, McDermott JE: Anterior tibiotalar spurs: A comparison of open versus arthroscopic debridement. Foot Ankle 13:125, Stetson WB, Ferkel RD: Ankle arthroscopy. Part I: Technique and complications. Part II: Indications and results. J Amer Acad Orthop Surg 4:17, Tol JL, Struijs PA, Bossuyt PM, Verhagen RA, van Dijk CN: Treatment strategies in osteochondral defects of the talar dome: A systematic review. Foot Ankle Int 21: , Verhagen RAW, Struijs PAA, Bossuyt PMM, van Dijk CN: Systematic review of treatments strategies for osteochondral defects of the talar dome. Foot Ankle Clin North Am 8: , Zengerink M, Szerb I, Hangody L, et al.: Current concepts: treatment of osteochondral ankle defects. Foot Ankle Clin 11: , Zengerink M, Struijs PAA, Tol JL, van Dijk CN: Treatment of osteochondral lesions of the talus: a systematic review. Knee Surg Sports Traumatol Arthrosc 2010;18: Recommended Reading 1. Ferkel RD, Dierckman B, Phisitkul P: Arthroscopy of the ankle and foot. In: Coughlin MJ, Saltzman CL (eds): Mann s Surgery of the foot and ankle, 9 th edition. Philadelphia; Elsevier, Ferkel RD, Jackson J: Arthroscopy of the ankle and subtalar joints. In Thordarson (ed.): Orthopedic Surgery Essentials: Foot and Ankle. Philadelphia; Elsevier, 2013.
11:40 11:45 am Clinical Outcome of Autologous Chondrocyte Implantation - ACI of the Talus Richard D. Ferkel, MD Van Nuys, California
 11:40 11:45 am Clinical Outcome of Autologous Chondrocyte Implantation - ACI of the Talus Richard D. Ferkel, MD Van Nuys, California I. INTRODUCTION A. In 1743, Hunter stated that From Hippocrates down
11:40 11:45 am Clinical Outcome of Autologous Chondrocyte Implantation - ACI of the Talus Richard D. Ferkel, MD Van Nuys, California I. INTRODUCTION A. In 1743, Hunter stated that From Hippocrates down
Greetings From SCOI. Richard D. Ferkel, M.D
 Greetings From SCOI Richard D. Ferkel, M.D OLT In the Athlete Operative Treatment and Return to Play The Following relationships exist: Royalties and stock options Smith and Nephew Consulting income
Greetings From SCOI Richard D. Ferkel, M.D OLT In the Athlete Operative Treatment and Return to Play The Following relationships exist: Royalties and stock options Smith and Nephew Consulting income
OCD: Beyond Microfracture. Disclosures. OCD Talus: My Approach 2/23/2018
 OCD: Beyond Microfracture Gregory C Berlet MD, FRCS(C), FAOA Orthopedic Foot and Ankle Center Columbus Ohio Disclosures Consultant/Speaker Bureau/Royalties/ Stock: Wright Medical, Stryker, ZimmerBiomet,
OCD: Beyond Microfracture Gregory C Berlet MD, FRCS(C), FAOA Orthopedic Foot and Ankle Center Columbus Ohio Disclosures Consultant/Speaker Bureau/Royalties/ Stock: Wright Medical, Stryker, ZimmerBiomet,
POSITION STATEMENT The Use of Osteochondral Transplantation for the Treatment of Osteochondral Lesions of the Talus
 Position Statement POSITION STATEMENT The Use of Osteochondral Transplantation for the Treatment of Osteochondral Lesions of the Talus The American Orthopaedic Foot & Ankle Society (AOFAS) endorses the
Position Statement POSITION STATEMENT The Use of Osteochondral Transplantation for the Treatment of Osteochondral Lesions of the Talus The American Orthopaedic Foot & Ankle Society (AOFAS) endorses the
Comparison of Outcomes of Osteochondral Transplantation with Autografts and Allografts for Osteochondral Lesions of the Talus
 Comparison of Outcomes of Osteochondral Transplantation with Autografts and Allografts for Osteochondral Lesions of the Talus Yoshiharu Shimozono, MD, Eoghan T Hurley, MB, BCh, Timothy W Deyer, MD, John
Comparison of Outcomes of Osteochondral Transplantation with Autografts and Allografts for Osteochondral Lesions of the Talus Yoshiharu Shimozono, MD, Eoghan T Hurley, MB, BCh, Timothy W Deyer, MD, John
Osteochondral Lesions: Medial Versus Lateral, Persistent Pain, Cartilage Restoration Options and Indications
 Osteochondral Lesions: Medial Versus Lateral, Persistent Pain, Cartilage Restoration Options and Indications AnnunziatoAmendola, MD a,b, *, Ludovico Panarella, MD, PhD c,d KEYWORDS Talus Osteochondral
Osteochondral Lesions: Medial Versus Lateral, Persistent Pain, Cartilage Restoration Options and Indications AnnunziatoAmendola, MD a,b, *, Ludovico Panarella, MD, PhD c,d KEYWORDS Talus Osteochondral
Ankle Arthroscopy PAULO ROCKETT, M.D. Porto Alegre Brazil
 Ankle Arthroscopy PAULO ROCKETT, M.D. Porto Alegre Brazil Ankle sprains are among the most common injuries in sports and at work. Between 20 and 40% of patients treated with conservative therapy may have
Ankle Arthroscopy PAULO ROCKETT, M.D. Porto Alegre Brazil Ankle sprains are among the most common injuries in sports and at work. Between 20 and 40% of patients treated with conservative therapy may have
Arthroscopy Of the Ankle.
 Arthroscopy Of the Ankle www.fisiokinesiterapia.biz Ankle Arthroscopy Anatomy Patient setup Portal placement Procedures Complications Anatomy Portals Anterior Anteromedial Anterolateral Anterocentral Posterior
Arthroscopy Of the Ankle www.fisiokinesiterapia.biz Ankle Arthroscopy Anatomy Patient setup Portal placement Procedures Complications Anatomy Portals Anterior Anteromedial Anterolateral Anterocentral Posterior
Arthroscopic Management of Osteochondral Lesions of the Talus
 Med. J. Cairo Univ., Vol. 77, No. 3, June: 147-153, 2009 www.medicaljournalofcairouniversity.com Arthroscopic Management of Osteochondral Lesions of the Talus AHMAD KHOLEIF, M.D.*; KAMAL SAMY ABDEL MEGUID,
Med. J. Cairo Univ., Vol. 77, No. 3, June: 147-153, 2009 www.medicaljournalofcairouniversity.com Arthroscopic Management of Osteochondral Lesions of the Talus AHMAD KHOLEIF, M.D.*; KAMAL SAMY ABDEL MEGUID,
Cartilage Repair Options
 Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
Osteochondral Lesions of the Talus A Unique Surgical Approach. Mark J. Mendeszoon, DPM, FACFAS, FACFAOM
 Osteochondral Lesions of the Talus A Unique Surgical Approach Mark J. Mendeszoon, DPM, FACFAS, FACFAOM Introduction Osteochondral lesions of the talar dome can cause significant functional impairment and
Osteochondral Lesions of the Talus A Unique Surgical Approach Mark J. Mendeszoon, DPM, FACFAS, FACFAOM Introduction Osteochondral lesions of the talar dome can cause significant functional impairment and
Craig S. Radnay, M.D. 1/27/2016. Access to the Talus for Treatment of Osteochondral Lesions. Epidemiology of OLT. Treatment of OLT
 Access to the Talus for Treatment of Osteochondral Lesions Craig S. Radnay, MD, MPH ISK Institute for Orthopaedics and Sports Medicine NYU/Hospital for Joint Diseases Tampa, FL January 23, 2016 Epidemiology
Access to the Talus for Treatment of Osteochondral Lesions Craig S. Radnay, MD, MPH ISK Institute for Orthopaedics and Sports Medicine NYU/Hospital for Joint Diseases Tampa, FL January 23, 2016 Epidemiology
NORTHERN OHIO FOUNDATION
 NORTHERN OHIO FOOT & ANKLE FOUNDATION! The!Northern!Ohio!Foot!and!Ankle!Journal!!!!!!!!!!!!!!!Official!Publication!of!the!NOFA!Foundation!! Osteochondral Lesions of the Talus: Literature Review by Neil
NORTHERN OHIO FOOT & ANKLE FOUNDATION! The!Northern!Ohio!Foot!and!Ankle!Journal!!!!!!!!!!!!!!!Official!Publication!of!the!NOFA!Foundation!! Osteochondral Lesions of the Talus: Literature Review by Neil
Reinsertion of an inverted osteochondral lesion of the talus; a case report
 Reinsertion of an inverted osteochondral lesion of the talus; a case report T. Schepers MD PhD, P.P. De Rooij MD, E.M.M. Van Lieshout PhD, P. Patka MD PhD Erasmus MC, University Medical Center Rotterdam,
Reinsertion of an inverted osteochondral lesion of the talus; a case report T. Schepers MD PhD, P.P. De Rooij MD, E.M.M. Van Lieshout PhD, P. Patka MD PhD Erasmus MC, University Medical Center Rotterdam,
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT
 OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
Osteochondritis Dissecans of the Knee. M Lucas Murnaghan MD, MEd, FRCSC
 Osteochondritis Dissecans of the Knee M Lucas Murnaghan MD, MEd, FRCSC Outline 1. Clinical Presentation 2. Investigations 3. Classification 4. Non-operative Treatment 5. Operative Treatment 6. Treatment
Osteochondritis Dissecans of the Knee M Lucas Murnaghan MD, MEd, FRCSC Outline 1. Clinical Presentation 2. Investigations 3. Classification 4. Non-operative Treatment 5. Operative Treatment 6. Treatment
Osteochondral transplantation of autologous graft for the treatment of osteochondral lesions of talus: 5- to 7-year follow-up
 DOI 10.1007/s00167-014-3389-3 ANKLE Osteochondral transplantation of autologous graft for the treatment of osteochondral lesions of talus: 5- to 7-year follow-up Dimitrios Georgiannos Ilias Bisbinas Athanasios
DOI 10.1007/s00167-014-3389-3 ANKLE Osteochondral transplantation of autologous graft for the treatment of osteochondral lesions of talus: 5- to 7-year follow-up Dimitrios Georgiannos Ilias Bisbinas Athanasios
TREATMENT OF CARTILAGE LESIONS
 TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
June 2013 Case Study. Author: T. Walker Robinson, MD, MPH, Nationwide Children s Hospital
 June 2013 Case Study Author: T. Walker Robinson, MD, MPH, Nationwide Children s Hospital Chief Complaint: Right ankle pain HPI: A 10 year old female dancer presents to the clinic with a five day history
June 2013 Case Study Author: T. Walker Robinson, MD, MPH, Nationwide Children s Hospital Chief Complaint: Right ankle pain HPI: A 10 year old female dancer presents to the clinic with a five day history
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication
 UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
OATS for the Foot and Ankle Surgical Technique
 OATS for the Foot and Ankle Surgical Technique Osteochondral Autograft Transfer System Scientific Support for Small Joint OATS Outcome of Osteochondral Autograft Transplantation for Type-V Cystic Osteochondral
OATS for the Foot and Ankle Surgical Technique Osteochondral Autograft Transfer System Scientific Support for Small Joint OATS Outcome of Osteochondral Autograft Transplantation for Type-V Cystic Osteochondral
Autologous Osteochondral Transplantation for Osteochondral Lesions of the Talus: Functional and T2 MRI Outcomes at Mid to Long-term follow-up
 Autologous Osteochondral Transplantation for Osteochondral Lesions of the Talus: Functional and T2 MRI Outcomes at Mid to Long-term follow-up September 2014 Seán Flynn, Keir Ross, Charles P. Hannon, Hunter
Autologous Osteochondral Transplantation for Osteochondral Lesions of the Talus: Functional and T2 MRI Outcomes at Mid to Long-term follow-up September 2014 Seán Flynn, Keir Ross, Charles P. Hannon, Hunter
Ankle Arthroscopy.
 Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Arthroscopic Treatment of Osteochondral Talar Defects
 Arthroscopic Treatment of Osteochondral Talar Defects Christiaan J.A. van Bergen, MD, Ruben Zwiers, MSc, and C. Niek van Dijk, MD, PhD Based on an original article: J Bone Joint Surg Am. 2013 Mar 20;95(6):519-25.
Arthroscopic Treatment of Osteochondral Talar Defects Christiaan J.A. van Bergen, MD, Ruben Zwiers, MSc, and C. Niek van Dijk, MD, PhD Based on an original article: J Bone Joint Surg Am. 2013 Mar 20;95(6):519-25.
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR FOCAL ARTICULAR CARTILAGE LESIONS
 CARTILAGE LESIONS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
CARTILAGE LESIONS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication
 UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
Autologous Chondrocyte Implantation. Gerard Hardisty FRACS
 Autologous Chondrocyte Implantation Gerard Hardisty FRACS Disclosure Orthopaedic Surgeons Strong as an OX and half as bright Orthopaedic Innovation Arthroscopy Joint replacement Trauma management MIS Early
Autologous Chondrocyte Implantation Gerard Hardisty FRACS Disclosure Orthopaedic Surgeons Strong as an OX and half as bright Orthopaedic Innovation Arthroscopy Joint replacement Trauma management MIS Early
OSTEOCHONDRAL ALLOGRAFTS AND AUTOGRAFTS IN THE TREATMENT OF FOCAL ARTICULAR CARTILAGE LESIONS
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Particulated Juvenile Articular Cartilage Allograft Transplantation With Bone Marrow Aspirate Concentrate for Treatment of Talus Osteochondral Defects
 SPECIAL FOCUS Particulated Juvenile Articular Cartilage Allograft Transplantation With Bone Marrow Aspirate Concentrate for Treatment of Talus Osteochondral Defects Mark C. Drakos, MD and Conor I. Murphy,
SPECIAL FOCUS Particulated Juvenile Articular Cartilage Allograft Transplantation With Bone Marrow Aspirate Concentrate for Treatment of Talus Osteochondral Defects Mark C. Drakos, MD and Conor I. Murphy,
Osteochondral lesions were first described by Konig
 155 Osteochondral Lesions of the Talar Dome Alexander Finger, M.D., and Steven C. Sheskier, M.D. Osteochondral lesions were first described by Konig in 1888. 1 He theorized that spontaneous necrosis was
155 Osteochondral Lesions of the Talar Dome Alexander Finger, M.D., and Steven C. Sheskier, M.D. Osteochondral lesions were first described by Konig in 1888. 1 He theorized that spontaneous necrosis was
ARTICULAR CARTILAGE RESTORATION: A REVIEW OF CURRENTLY AVAILABLE METHODS FOR REPAIR OF ARTICULAR CARTILAGE DEFECTS
 ARTICULAR CARTILAGE RESTORATION: A REVIEW OF CURRENTLY AVAILABLE METHODS FOR REPAIR OF ARTICULAR CARTILAGE DEFECTS AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 76TH ANNUAL MEETING FEBRUARY 25-28, 2009 LAS
ARTICULAR CARTILAGE RESTORATION: A REVIEW OF CURRENTLY AVAILABLE METHODS FOR REPAIR OF ARTICULAR CARTILAGE DEFECTS AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 76TH ANNUAL MEETING FEBRUARY 25-28, 2009 LAS
Knee Preservation and Articular Cartilage Restoration
 Knee Preservation and Articular Cartilage Restoration With Special Thanks to Aaron Krych, MD and Riley Willims, MD Zak Knutson, MD Articular Cartilage Layer of tissue covering the bone which are part of
Knee Preservation and Articular Cartilage Restoration With Special Thanks to Aaron Krych, MD and Riley Willims, MD Zak Knutson, MD Articular Cartilage Layer of tissue covering the bone which are part of
Justin D. Orr, MD, John C. Dunn, MD, Kenneth A. Heida Jr, MD, Nicholas A. Kusnezov, MD, Brian R. Waterman, MD, and Philip J.
 666924FASXXX10.1177/1938640016666924Foot & Ankle SpecialistFoot & Ankle Specialist research-article2016 vol. 10 / no. 2 Foot & Ankle Specialist 125 Clinical Research Results and Functional Outcomes of
666924FASXXX10.1177/1938640016666924Foot & Ankle SpecialistFoot & Ankle Specialist research-article2016 vol. 10 / no. 2 Foot & Ankle Specialist 125 Clinical Research Results and Functional Outcomes of
Articular Cartilage Surgical Restoration Options
 Articular Cartilage Surgical Restoration Options Randy Schwartzberg, M.D. Assistant Professor - UCF College of Medicine Rationale Our bodies do not make articular/hyaline cartilage. gics injections to
Articular Cartilage Surgical Restoration Options Randy Schwartzberg, M.D. Assistant Professor - UCF College of Medicine Rationale Our bodies do not make articular/hyaline cartilage. gics injections to
First Metatarsal Head Osteochondral Defect Treatment with Particulated Juvenile Cartilage Allograft Transplantation
 First Metatarsal Head Osteochondral Defect Treatment with Particulated Juvenile Cartilage Allograft Transplantation Bryan Van Dyke, DO Gregory C. Berlet, MD Justin L. Daigre, MD Christopher F. Hyer, DPM,
First Metatarsal Head Osteochondral Defect Treatment with Particulated Juvenile Cartilage Allograft Transplantation Bryan Van Dyke, DO Gregory C. Berlet, MD Justin L. Daigre, MD Christopher F. Hyer, DPM,
Case Report. Byung Ill Lee, MD and Byoung Min Kim, MD Department of Orthopedic Surgery, Soonchunhyang University Hospital, Seoul, Korea
 Case Report Knee Surg Relat Res 2015;27(4):263-268 http://dx.doi.org/10.5792/ksrr.2015.27.4.263 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Concomitant Osteochondral utograft Transplantation
Case Report Knee Surg Relat Res 2015;27(4):263-268 http://dx.doi.org/10.5792/ksrr.2015.27.4.263 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Concomitant Osteochondral utograft Transplantation
Impingement Syndromes of the Ankle. Noaman W Siddiqi MD 5/4/2006
 Impingement Syndromes of the Ankle Noaman W Siddiqi MD 5/4/2006 Ankle Impingement Overview Clinical DX Increasingly recognized cause of chronic ankle pain Etiology can be soft tissue or osseous Professional
Impingement Syndromes of the Ankle Noaman W Siddiqi MD 5/4/2006 Ankle Impingement Overview Clinical DX Increasingly recognized cause of chronic ankle pain Etiology can be soft tissue or osseous Professional
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication
 UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
Welcome to the: Orthopaedic Opinion Online Website The website for the answer to all your Orthopaedic Questions
 Welcome to the: Orthopaedic Opinion Online Website The website for the answer to all your Orthopaedic Questions Orthopaedic Opinion Online is a website designed to provide information to patients who have
Welcome to the: Orthopaedic Opinion Online Website The website for the answer to all your Orthopaedic Questions Orthopaedic Opinion Online is a website designed to provide information to patients who have
Rakesh Patel, MD 4/9/09
 Rakesh Patel, MD 4/9/09 Chondral Injuries Very common Present in 63-66% patients undergoing arthroscopy 11-19% full-thickness lesions Up to 79% patients with ACL deficient knee have some form of chondral
Rakesh Patel, MD 4/9/09 Chondral Injuries Very common Present in 63-66% patients undergoing arthroscopy 11-19% full-thickness lesions Up to 79% patients with ACL deficient knee have some form of chondral
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication
 UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
Corporate Medical Policy
 Corporate Medical Policy Autologous Chondrocyte Implantation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: autologous_chondrocyte_implantation 4/1996 6/2017 6/2018 6/2017 Description
Corporate Medical Policy Autologous Chondrocyte Implantation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: autologous_chondrocyte_implantation 4/1996 6/2017 6/2018 6/2017 Description
AMIC or ACI for arthroscopic repair of grade IV acetabular cartilage defects in femoroacetabular impingement.
 AMIC or ACI for arthroscopic repair of grade IV acetabular cartilage defects in femoroacetabular impingement. Dr. Andrea Fontana Istituto Auxologico Italiano Milan - Italy Introduction Chondropathies of
AMIC or ACI for arthroscopic repair of grade IV acetabular cartilage defects in femoroacetabular impingement. Dr. Andrea Fontana Istituto Auxologico Italiano Milan - Italy Introduction Chondropathies of
Osteochondritis Dissecans
 P R O C E D U R E 1 4 Ammar Anbari, Adam B. Yanke, and Brian J. Cole ch014-x4397.indd 221 4/11/2008 10:50:21 AM 222 Treatment Options Conservative management Fixation in situ Elevate the OCD lesion, débride
P R O C E D U R E 1 4 Ammar Anbari, Adam B. Yanke, and Brian J. Cole ch014-x4397.indd 221 4/11/2008 10:50:21 AM 222 Treatment Options Conservative management Fixation in situ Elevate the OCD lesion, débride
Immediate Unrestricted Postoperative Weightbearing and Mobilization after Bone Marrow Stimulation of Large Osteochondral Lesions of the Talus
 657639CARXXX10.1177/1947603516657639CartilageLundeen and Dunaway research-article2016 Article Immediate Unrestricted Postoperative Weightbearing and Mobilization after Bone Marrow Stimulation of Large
657639CARXXX10.1177/1947603516657639CartilageLundeen and Dunaway research-article2016 Article Immediate Unrestricted Postoperative Weightbearing and Mobilization after Bone Marrow Stimulation of Large
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3
 AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3 1-EMERGENCY CLINICAL HOSPITAL FLOREASCA BUCHAREST 2-EMERGENCY CLINICAL HOSPITAL SFANTUL
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3 1-EMERGENCY CLINICAL HOSPITAL FLOREASCA BUCHAREST 2-EMERGENCY CLINICAL HOSPITAL SFANTUL
Clinical evaluation where no obvious fracture a. Squeeze test
 7:43 am The Syndesmotic Injury: From Subtle to Severe Robert B. Anderson, MD Chief, Foot and Ankle Carolinas Medical Center OrthoCarolina (Charlotte, North Carolina) 7:30-8:25 am Symposium 1: Management
7:43 am The Syndesmotic Injury: From Subtle to Severe Robert B. Anderson, MD Chief, Foot and Ankle Carolinas Medical Center OrthoCarolina (Charlotte, North Carolina) 7:30-8:25 am Symposium 1: Management
Sequalae of Ankle Sprains: Peri Articular Fractures of the Ankle in Sports Medicine.
 Sequalae of Ankle Sprains: Peri Articular Fractures of the Ankle in Sports Medicine www.fisiokinesiterapia.biz Chronic Ankle Pain The most common cause of chronic pain following an ankle sprain is a missed
Sequalae of Ankle Sprains: Peri Articular Fractures of the Ankle in Sports Medicine www.fisiokinesiterapia.biz Chronic Ankle Pain The most common cause of chronic pain following an ankle sprain is a missed
AOFAS 2016 Annual Convention July 20-23, 2016 Toronto, Canada
 ANKLE ARTHROSCOPY FOR OSTEOCHONDRAL LESIONS OF THE TALUS: THE EFFECT OF LIMITED ANKLE RANGE OF MOTION ON ANTERIOR AND POSTERIOR ARTHROSCOPIC ACCESSIBILITY Phinit Phisitkul, Craig Akoh, Kevin Dibbern, Vinay
ANKLE ARTHROSCOPY FOR OSTEOCHONDRAL LESIONS OF THE TALUS: THE EFFECT OF LIMITED ANKLE RANGE OF MOTION ON ANTERIOR AND POSTERIOR ARTHROSCOPIC ACCESSIBILITY Phinit Phisitkul, Craig Akoh, Kevin Dibbern, Vinay
Page: 1 of 21. Autologous Chondrocyte Implantation for Focal Articular Cartilage Lesions
 Page: 1 of 21 Last Review Status/Date: September 2015 Focal Articular Cartilage Lesions Description A variety of procedures are being developed to resurface articular cartilage defects. Autologous chondrocyte
Page: 1 of 21 Last Review Status/Date: September 2015 Focal Articular Cartilage Lesions Description A variety of procedures are being developed to resurface articular cartilage defects. Autologous chondrocyte
Ankle Fracture in the Athlete: Should I scope? What about the Deltoid? Do I have to repair?
 Ankle Fracture in the Athlete: Should I scope? What about the Deltoid? Do I have to repair? DAVID A PORTER, MDPHD METHODIST SPORTS MEDICINE/THE ORTHOPEDIC SPECIALISTS 201 PENNSYLVANIA PKWY INDIANAPOLIS,
Ankle Fracture in the Athlete: Should I scope? What about the Deltoid? Do I have to repair? DAVID A PORTER, MDPHD METHODIST SPORTS MEDICINE/THE ORTHOPEDIC SPECIALISTS 201 PENNSYLVANIA PKWY INDIANAPOLIS,
Knee Cartilage Transplants
 Knee Cartilage Transplants Date of Origin: 3/2005 Last Review Date: 8/23/2017 Effective Date: 8/23/2017 Dates Reviewed: Developed By: Medical Necessity Criteria Committee I. Description Allograft transplants
Knee Cartilage Transplants Date of Origin: 3/2005 Last Review Date: 8/23/2017 Effective Date: 8/23/2017 Dates Reviewed: Developed By: Medical Necessity Criteria Committee I. Description Allograft transplants
Osteochondral Lesion of the Talus
 AJSM PreView, published on August 4, 2009 as doi:10.1177/0363546509335765 Osteochondral Lesion of the Talus Is There a Critical Defect Size for Poor Outcome? Woo Jin Choi,* MD, Kwan Kyu Park, MD, Bom Soo
AJSM PreView, published on August 4, 2009 as doi:10.1177/0363546509335765 Osteochondral Lesion of the Talus Is There a Critical Defect Size for Poor Outcome? Woo Jin Choi,* MD, Kwan Kyu Park, MD, Bom Soo
The results of arthroscopic treatment for talus osteochondral lesions
 Journal of Clinical & Analytical Medicine Original Research The results of arthroscopic treatment for talus osteochondral lesions Azad Yıldırım Diyarlife Dağ Kapı, Diyarbakır Hospital, Diyarbakır, Turkey
Journal of Clinical & Analytical Medicine Original Research The results of arthroscopic treatment for talus osteochondral lesions Azad Yıldırım Diyarlife Dağ Kapı, Diyarbakır Hospital, Diyarbakır, Turkey
Joint Preservation Clinical Case
 Joint Preservation Clinical Case Jason M. Scopp, M.D. Director of Joint Preservation Peninsula Orthopaedic Associates, 1/19/19 Rational Rationale There are no absolutes. There is no dogma. Organize thoughts,
Joint Preservation Clinical Case Jason M. Scopp, M.D. Director of Joint Preservation Peninsula Orthopaedic Associates, 1/19/19 Rational Rationale There are no absolutes. There is no dogma. Organize thoughts,
Arthroscopic Autologous Chondrocyte Implantation in Osteochondral Lesions of the Talus
 AJSM PreView, published on January 28, 2008 as doi:10.1177/0363546507312644 Arthroscopic Autologous Chondrocyte Implantation in Osteochondral Lesions of the Talus Surgical Technique and Results Sandro
AJSM PreView, published on January 28, 2008 as doi:10.1177/0363546507312644 Arthroscopic Autologous Chondrocyte Implantation in Osteochondral Lesions of the Talus Surgical Technique and Results Sandro
PRONATION-ABDUCTION FRACTURES
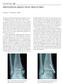 C H A P T E R 1 2 PRONATION-ABDUCTION FRACTURES George S. Gumann, DPM (The opinions of the author should not be considered as reflecting official policy of the US Army Medical Department.) Pronation-abduction
C H A P T E R 1 2 PRONATION-ABDUCTION FRACTURES George S. Gumann, DPM (The opinions of the author should not be considered as reflecting official policy of the US Army Medical Department.) Pronation-abduction
INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement
 016625 REVISION R INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement CASE STUDY Patient History The patient was a 65-year-old
016625 REVISION R INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement CASE STUDY Patient History The patient was a 65-year-old
Osteochondral allografting for all other joints is not covered as the evidence is insufficient to determine the
 Medical Coverage Policy Osteochondral Autologous Chrondrocyte Implantation for Focal Articular Cartilage Lesions EFFECTIVE DATE: 05 20 2008 POLICY LAST UPDATED: 10 16 2018 OVERVIEW A variety of procedures
Medical Coverage Policy Osteochondral Autologous Chrondrocyte Implantation for Focal Articular Cartilage Lesions EFFECTIVE DATE: 05 20 2008 POLICY LAST UPDATED: 10 16 2018 OVERVIEW A variety of procedures
Osteochondral Allograft Transplantation and Autograft Transfer System (OATS/mosaicplasty) in the Treatment of Articular
 Osteochondral Allograft Transplantation and Autograft Transfer System (OATS/mosaicplasty) in the Treatment of Articular Cartilage Lesions Corporate Medical Policy File name: Osteochondral Allograft Transplantation
Osteochondral Allograft Transplantation and Autograft Transfer System (OATS/mosaicplasty) in the Treatment of Articular Cartilage Lesions Corporate Medical Policy File name: Osteochondral Allograft Transplantation
Autologous Chondrocyte Implantation and Other Cell-based Treatments of Focal Articular Cartilage Lesions. Original Policy Date
 MP 7.01.36 Autologous Chondrocyte Implantation and Other Cell-based Treatments of Focal Articular Cartilage Lesions Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review
MP 7.01.36 Autologous Chondrocyte Implantation and Other Cell-based Treatments of Focal Articular Cartilage Lesions Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review
PATIENT GUIDE TO CARTILAGE INJURIES
 Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Autografts and Allografts in the Treatment of Focal Page 1 of 30 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Autografts and Allografts in the Treatment of Focal
Autografts and Allografts in the Treatment of Focal Page 1 of 30 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Autografts and Allografts in the Treatment of Focal
TIBIAXYS ANKLE FUSION
 TIBIAXYS ANKLE FUSION SURGICAL TECHNIQUE TIBIAXYS Ankle Fusion Plate features Anatomically contoured plates The plates are designed to approximate the patient s bony and soft tissue anatomy The plate designs
TIBIAXYS ANKLE FUSION SURGICAL TECHNIQUE TIBIAXYS Ankle Fusion Plate features Anatomically contoured plates The plates are designed to approximate the patient s bony and soft tissue anatomy The plate designs
CARTILAGE LESIONS IN THE PATELLOFEMORAL JOINT
 GENERAL OVERVIEW CARTILAGE LESIONS IN THE PATELLOFEMORAL JOINT Written by Mats Brittberg, Sweden The general low level of understanding of problems in the patellofemoral joint is reflected in the large
GENERAL OVERVIEW CARTILAGE LESIONS IN THE PATELLOFEMORAL JOINT Written by Mats Brittberg, Sweden The general low level of understanding of problems in the patellofemoral joint is reflected in the large
Marrow (MSC) Stimulation Techniques: Microfracture/Microfracture Plus/Cartiform Kai Mithoefer, MD
 Marrow (MSC) Stimulation Techniques: Microfracture/Microfracture Plus/Cartiform Kai Mithoefer, MD Harvard Vanguard Medical Associates New England Baptist Hospital Boston, USA Cartilage Repair Marrow Stimulation
Marrow (MSC) Stimulation Techniques: Microfracture/Microfracture Plus/Cartiform Kai Mithoefer, MD Harvard Vanguard Medical Associates New England Baptist Hospital Boston, USA Cartilage Repair Marrow Stimulation
Disclosures. How to approach cartilage repair. Articular Cartilage Problems: Surface Options
 Disclosures I have the following potential conflicts of interest: Consulting payments/royalties and research support directly related to products discussed: Vericel (ACI) [consultant] SLACK publishing
Disclosures I have the following potential conflicts of interest: Consulting payments/royalties and research support directly related to products discussed: Vericel (ACI) [consultant] SLACK publishing
Why do they fail?? TOM MINAS MD MS. The Management of Failed Cartilage Repair Procedures PALM BEACH FL
 The Management of Failed Cartilage Repair Procedures Why do they fail?? TOM MINAS MD MS DIRECTOR, CARTILAGE REPAIR CENTER, PALEY ORTHOPEDIC INSTITUTE, PALM BEACH FL PROFESSOR EMERITUS, HARVARD MEDICAL
The Management of Failed Cartilage Repair Procedures Why do they fail?? TOM MINAS MD MS DIRECTOR, CARTILAGE REPAIR CENTER, PALEY ORTHOPEDIC INSTITUTE, PALM BEACH FL PROFESSOR EMERITUS, HARVARD MEDICAL
CURRENT TREATMENT OPTIONS
 CURRENT TREATMENT OPTIONS Fix single column or both: Always fix both. A study by Svend-Hansen corroborated the poor results associated with isolated medial malleolar fixation in bimalleolar ankle fractures.
CURRENT TREATMENT OPTIONS Fix single column or both: Always fix both. A study by Svend-Hansen corroborated the poor results associated with isolated medial malleolar fixation in bimalleolar ankle fractures.
MEDICAL POLICY SUBJECT: OSTEOCHONDRAL GRAFTING
 MEDICAL POLICY PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
MEDICAL POLICY PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
Incidence of Occult Chondral Lesions in Weber C Ankle Fractures in Athletes and Their Effect on Time to Return to Play
 Incidence of Occult Chondral Lesions in Weber C Ankle Fractures in Athletes and Their Effect on Time to Return to Play Jefferson B. Sabatini M.D. 1, Kyle T. Aune M.P.H. 2, Norman E. Waldrop III M.D. 3
Incidence of Occult Chondral Lesions in Weber C Ankle Fractures in Athletes and Their Effect on Time to Return to Play Jefferson B. Sabatini M.D. 1, Kyle T. Aune M.P.H. 2, Norman E. Waldrop III M.D. 3
Pilon fractures. Pat Yoon, MD Minneapolis Veterans Affairs Medical Center Associate Professor, University of Minnesota
 Pilon fractures Pat Yoon, MD Minneapolis Veterans Affairs Medical Center Associate Professor, University of Minnesota Disclosures Reviewer Foot and Ankle International Journal of the American Academy of
Pilon fractures Pat Yoon, MD Minneapolis Veterans Affairs Medical Center Associate Professor, University of Minnesota Disclosures Reviewer Foot and Ankle International Journal of the American Academy of
Rehabilitation Protocol:
 Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Autografts and Allografts in the Treatment of Focal Articular Cartilage Lesions
 Autografts and Allografts in the Treatment of Focal Articular Cartilage Lesions Policy Number: 7.01.78 Last Review: 2/2018 Origination: 8/2002 Next Review: 2/2019 Policy Blue Cross and Blue Shield of Kansas
Autografts and Allografts in the Treatment of Focal Articular Cartilage Lesions Policy Number: 7.01.78 Last Review: 2/2018 Origination: 8/2002 Next Review: 2/2019 Policy Blue Cross and Blue Shield of Kansas
Clinical Commissioning Policy: Autologous chrondrocyte implantation for osteochondral lesions of the talus
 Clinical Commissioning Policy: Autologous chrondrocyte implantation for osteochondral lesions of the talus Reference: NHS England: 16012/P NHS England INFORMATION READER BOX Directorate Medical Operations
Clinical Commissioning Policy: Autologous chrondrocyte implantation for osteochondral lesions of the talus Reference: NHS England: 16012/P NHS England INFORMATION READER BOX Directorate Medical Operations
Cartilage Repair Center Brigham and Women s Hospital Harvard Medical School
 Brigham and Women s Hospital Harvard Medical School Safety, feasibility, and radiographic outcomes of the anterior meniscal takedown technique to approach chondral defects on the tibia and posterior femoral
Brigham and Women s Hospital Harvard Medical School Safety, feasibility, and radiographic outcomes of the anterior meniscal takedown technique to approach chondral defects on the tibia and posterior femoral
CARTILAGE REPAIR PROCEDURES IN LARGE CARTILAGE DEFECTS
 CARTILAGE REPAIR TECHNIQUES CARTILAGE REPAIR PROCEDURES IN LARGE CARTILAGE DEFECTS Written by Steffano Zaffagnini, Francesco Perdisa and Giuseppe Filardo, Italy Knee articular cartilage defects greater
CARTILAGE REPAIR TECHNIQUES CARTILAGE REPAIR PROCEDURES IN LARGE CARTILAGE DEFECTS Written by Steffano Zaffagnini, Francesco Perdisa and Giuseppe Filardo, Italy Knee articular cartilage defects greater
Chondral Injuries in the Athlete
 Chondral Injuries in the Athlete Michael J. Stuart MD Professor of Orthopedic Surgery Chair, Division of Sports Medicine Mayo Clinic 2013 MFMER slide-1 Michael J. Stuart MD February 5, 2014 Financial Relationships
Chondral Injuries in the Athlete Michael J. Stuart MD Professor of Orthopedic Surgery Chair, Division of Sports Medicine Mayo Clinic 2013 MFMER slide-1 Michael J. Stuart MD February 5, 2014 Financial Relationships
Osteochondritis Dissecans
 Osteochondritis Dissecans Introduction Osteochondritis dissecans (OCD) is a problem that affects the knee, mostly at the end of the big bone of the thigh (the femur). A joint surface damaged by OCD doesn't
Osteochondritis Dissecans Introduction Osteochondritis dissecans (OCD) is a problem that affects the knee, mostly at the end of the big bone of the thigh (the femur). A joint surface damaged by OCD doesn't
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication
 UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
Histologic change of cartilage layer of osteochondritis dissecans before and after fixation in the knee
 1 Histologic change of cartilage layer of osteochondritis dissecans before and after fixation in the knee Mitsuo Ochi, M.D. PhD Professor and chairman Department of Orthopaedic Surgery Graduate School
1 Histologic change of cartilage layer of osteochondritis dissecans before and after fixation in the knee Mitsuo Ochi, M.D. PhD Professor and chairman Department of Orthopaedic Surgery Graduate School
Tibial Cartilage Defects
 Tibial Cartilage Defects Kevin C. Wang 1 Rachel M. Frank 2 Brian J. Cole 3 Email brian.cole@rushortho.com 1 2 3 Department of Orthopedics, Icahn School of Medicine at Mount Sinai, New York, NY, USA Department
Tibial Cartilage Defects Kevin C. Wang 1 Rachel M. Frank 2 Brian J. Cole 3 Email brian.cole@rushortho.com 1 2 3 Department of Orthopedics, Icahn School of Medicine at Mount Sinai, New York, NY, USA Department
Talus Fractures: When and Why on Screws and Plates
 Talus Fractures: When and Why on Screws and Plates Frank A. Liporace, MD Associate Professor Director of Orthopaedic Research New York University / Hospital for Joint Diseases, NY, NY Director Orthopaedic
Talus Fractures: When and Why on Screws and Plates Frank A. Liporace, MD Associate Professor Director of Orthopaedic Research New York University / Hospital for Joint Diseases, NY, NY Director Orthopaedic
Osteocartilaginous lesions of the talus in soccer players
 Arch Orthop Trauma Surg (2010) 130:329 333 DOI 10.1007/s00402-008-0783-7 ARTHROSCOPY AND SPORTS MEDICINE Osteocartilaginous lesions of the talus in soccer players Roberto Seijas P. Álvarez O. Ares G. Steinbacher
Arch Orthop Trauma Surg (2010) 130:329 333 DOI 10.1007/s00402-008-0783-7 ARTHROSCOPY AND SPORTS MEDICINE Osteocartilaginous lesions of the talus in soccer players Roberto Seijas P. Álvarez O. Ares G. Steinbacher
Osteochondral Grafting
 Last Review Date: January 19, 2017 Number: MG.MM.SU.68 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: January 19, 2017 Number: MG.MM.SU.68 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER CODING INFORMATION REFERENCES POLICY HISTORY
 Original Issue Date (Created): July 1, 2002 Most Recent Review Date (Revised): January 28, 2014 Effective Date: April 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT
Original Issue Date (Created): July 1, 2002 Most Recent Review Date (Revised): January 28, 2014 Effective Date: April 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT
Autologous Chondrocyte Implantation for Focal Articular Cartilage Lesions
 Autologous Chondrocyte Implantation for Focal Articular Cartilage Lesions Policy Number: Original Effective Date: MM.06.002 8/1/2009 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 12/01/2017
Autologous Chondrocyte Implantation for Focal Articular Cartilage Lesions Policy Number: Original Effective Date: MM.06.002 8/1/2009 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 12/01/2017
8/10/2016. Treatment of Articular Cartilage Injuries: Osteochondral autograft Osteochondral allograft DISCLOSURES CONSIDERATIONS:
 Treatment of Articular Cartilage Injuries: Center for Cartilage Repair and Restoration University of Kentucky Osteochondral autograft Osteochondral allograft Christian Lattermann, MD Professor for Orthopaedics
Treatment of Articular Cartilage Injuries: Center for Cartilage Repair and Restoration University of Kentucky Osteochondral autograft Osteochondral allograft Christian Lattermann, MD Professor for Orthopaedics
Locking Ankle Plating System. Surgical Technique
 Locking Ankle Plating System Surgical Technique Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
Locking Ankle Plating System Surgical Technique Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
Osteochondral lesion of the talus: possible treatment options for Thailand Supachok Rasamimongkol* and Piroon Tangsripong
 Osteochondral lesion of the talus: possible treatment options for Thailand Supachok Rasamimongkol* and Piroon Tangsripong Department of Orthopedic, Faculty of Medicine, Naresuan University Hospital, Tha
Osteochondral lesion of the talus: possible treatment options for Thailand Supachok Rasamimongkol* and Piroon Tangsripong Department of Orthopedic, Faculty of Medicine, Naresuan University Hospital, Tha
Anterior impingement syndrome in dancers
 Curr Rev Musculoskelet Med (2008) 1:12 16 DOI 10.1007/s12178-007-9001-4 Anterior impingement syndrome in dancers John William O Kane Æ Nancy Kadel Published online: 6 November 2007 Ó Humana Press 2007
Curr Rev Musculoskelet Med (2008) 1:12 16 DOI 10.1007/s12178-007-9001-4 Anterior impingement syndrome in dancers John William O Kane Æ Nancy Kadel Published online: 6 November 2007 Ó Humana Press 2007
ACI < > < > +/- MSC MSC MASS
 Articular Cartilage Injury Natural History Management of Small Articular Cartilage Lesions Kai Mithoefer, MD Harvard Vanguard Medical Associates Harvard Medical School New England Baptist Hospital Boston,
Articular Cartilage Injury Natural History Management of Small Articular Cartilage Lesions Kai Mithoefer, MD Harvard Vanguard Medical Associates Harvard Medical School New England Baptist Hospital Boston,
Posterior Ankle Impingement: Don t Get Pinched
 Posterior Ankle Impingement: Don t Get Pinched 11 th Annual Sports Medicine Continuing Education Conference Gregory P Witkowski, MD Orthopaedic Trauma and Foot/Ankle Surgery Disclosures I have nothing
Posterior Ankle Impingement: Don t Get Pinched 11 th Annual Sports Medicine Continuing Education Conference Gregory P Witkowski, MD Orthopaedic Trauma and Foot/Ankle Surgery Disclosures I have nothing
Case Report The Utility and Limitations of the Transfibular Approach in Ankle Trauma Surgery
 Case Reports in Orthopedics, Article ID 234369, 4 pages http://dx.doi.org/10.1155/2014/234369 Case Report The Utility and Limitations of the Transfibular Approach in Ankle Trauma Surgery Mustafa Yassin,
Case Reports in Orthopedics, Article ID 234369, 4 pages http://dx.doi.org/10.1155/2014/234369 Case Report The Utility and Limitations of the Transfibular Approach in Ankle Trauma Surgery Mustafa Yassin,
.org. Ankle Fractures (Broken Ankle) Anatomy
 Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
New Directions in Osteoarthritis Research
 New Directions in Osteoarthritis Research Kananaskis October 22, 2015 Nick Mohtadi MD MSc FRCSC No conflicts of interest related to this presentation 1 Osteoarthritis: Disease? Fact of Life? Strong family
New Directions in Osteoarthritis Research Kananaskis October 22, 2015 Nick Mohtadi MD MSc FRCSC No conflicts of interest related to this presentation 1 Osteoarthritis: Disease? Fact of Life? Strong family
Osteochondral Autologous Transfer and Bulk Allograft for Biological Resurfacing of Large Osteochondral Lesions of the Talus
 SPECIAL FOCUS AND CME ARTICLE for Biological Resurfacing of Large Osteochondral Lesions of the Talus Justin Robbins, MD,* Keir A. Ross, BS,w John G. Kennedy, MD,z and Mark E. Easley, MDy Abstract: Osteochondral
SPECIAL FOCUS AND CME ARTICLE for Biological Resurfacing of Large Osteochondral Lesions of the Talus Justin Robbins, MD,* Keir A. Ross, BS,w John G. Kennedy, MD,z and Mark E. Easley, MDy Abstract: Osteochondral
Autologous Chondrocyte Implantation for Focal Articular Cartilage Lesions
 Autologous Chondrocyte Implantation for Focal Articular Cartilage Lesions Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana,
Autologous Chondrocyte Implantation for Focal Articular Cartilage Lesions Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana,
Ankle Pain After a Sprain.
 Ankle Pain After a Sprain www.fisiokinesiterapia.biz Anterior Drawer Stress Test Talar Tilt Talar Tilt (CFL) Difficult to isolate from subtalar ROM Slight plantar flexion (dorsi = relative subtalar isolation)
Ankle Pain After a Sprain www.fisiokinesiterapia.biz Anterior Drawer Stress Test Talar Tilt Talar Tilt (CFL) Difficult to isolate from subtalar ROM Slight plantar flexion (dorsi = relative subtalar isolation)
AOFAS 2012 ANNUAL SUMMER MEETING. Subtalar Distraction Two Bone-Block Arthrodesis for Calcaneal Malunion
 AOFAS 2012 ANNUAL SUMMER MEETING Subtalar Distraction Two Bone-Block Arthrodesis for Calcaneal Malunion My disclosure is in the Final AOFAS Program Book. I have no potential conflicts with this presentation.
AOFAS 2012 ANNUAL SUMMER MEETING Subtalar Distraction Two Bone-Block Arthrodesis for Calcaneal Malunion My disclosure is in the Final AOFAS Program Book. I have no potential conflicts with this presentation.
