LIMITED INFLUENCE OF PROSTHETIC POSITION ON ASEPTIC LOOSENING OF THE SOUTER-STRATHCLYDE TOTAL ELBOW PROSTHESIS
|
|
|
- Victoria Simpson
- 6 years ago
- Views:
Transcription
1 6 LIMITED INFLUENCE OF PROSTHETIC POSITION ON ASEPTIC LOOSENING OF THE SOUTER-STRATHCLYDE TOTAL ELBOW PROSTHESIS J.C.T. van der Lugt R.B. Geskus P.M. Rozing Acta Orthop. 2005;76(5):654-61
2 Chapter 6 Abstract Introduction: Aseptic loosening of elbow replacements with long-term followup remains a problem. In this study, we attempted to ascertain the influence of cementing technique, prosthetic position, different component sizes, usage of a bone plug and intraoperative fractures on the development and progression of radiolucent lines and aseptic loosening. Methods: Standard radiographs of 125 primary Souter-Strathclyde total elbow prostheses were studied using the Wrightington method. Additionally, 104 preoperative radiographs were available for analysis. A Markow statistical model was used to detect relationships among all factors described above. Results: The mean followup of the radiographs was 67.4 months. Twenty-one prostheses loosened radiographically (16,8%) after an average period of 62.5 months (10-years survival 64,6 %). When the humeral component was tilted more medially or more anteriorly we found, respectively, the development of radiolucent lines at the medial condyle and at the posterior side of the humeral component. However, the progression of these lines was not influenced by these positions. No other prognostic factors on radiolucent lines or aseptic loosening were found. Interpretation: Despite the small number of elbows studied in this study, the poor influence of prosthetic position on aseptic loosening gives more ground for a multifactorial cause of aseptic loosening of the Souter-Strathclyde total elbow prosthesis. 86
3 Limited influence of prosthetic position on aseptic loosening of the Souter-Strathclyde Total Elbow Prosthesis Introduction Total elbow replacement is a well-established treatment for the destructed elbow 1-6. The clinical results of most types of total elbow replacements are promising, but the survival rates are still not comparable to, for example, the survival rates for total hip replacements (THRs) 7. In recent literature 74 to 90 % of the implanted total elbow prostheses was still in situ after more than 10 years of followup 2,5,8. The most important factor that diminished the survival rate of elbow replacements was aseptic loosening of the humeral component Since the beginning of the 1980s we have used the Souter-Strathclyde total elbow prosthesis at our center, and we have also found high aseptic loosening rates of the humeral component 8,11. In this series of 125 elbow prosthesis we tried to determine different factors that affect aseptic loosening. First the survival of the 125 elbows is given for the endpoint radiological loosening. In most studies only the time to revision is taken to calculate the survival rate. Consequently, this would cause an underestimation of the actual survival rate, because not all loosened prostheses were revised immediately. Secondly the cementing technique of the prosthesis in the bone is analyzed. Little is known about the correct cementing technique, but the current opinion is that the prosthesis should be covered totally with a cement mantle of 1 mm thickness. The prosthetic position is of importance. Trail et al. used the Wrightington method for determination the prosthetic position and they found that more anterior tilting of the humeral component was related to aseptic loosening 12. We applied the same method in our series to obtain detailed information about the position of the prosthesis and the relationship to radiolucent lines and aseptic loosening during the followup. The recent tendency to use larger components of the Souter-Strathclyde prosthesis for primary surgery have improved the survival rates, but no scientific reason for this phenomenon has been stated 13. In this study the different humeral component sizes of the Souter-Strathclyde were related to the size of the patients humeral bone. The hypothesis is that a relative small prosthesis is fixed in cancellous bone, has therefore less cortical support and will, for that reason, loose more easily. Bone plugs have been proven in knees and hips arthroplasties, but the influence on elbow replacements is unclear One-third of the patients have received a humeral bone plug in this study and therefore this factor is taken separately into analysis. Intra-operative fractures may jeopardize the survival of prostheses 4,6. All fractures and their consequences at followup are described in this series. Finally, we have tried to determine the influence of preoperative radiographs on aseptic loosening. Unfortunately no standard scoring methods exists for the preoperative amount of bone resorption or dislocation of elbows. A new method was developed to accomplish this additional analysis. All data were analyzed using a Markov 87
4 Chapter 6 model, which was the first time this statistical model was employed for radiological evaluation of joint replacements Patients and Methods We retrospectively studied the standard radiographs of 125 primary Souter-Strathclyde total elbow prostheses (Stryker Howmedica Osteonics, Limerick, Ireland) inserted at our center. Standard radiographs were made as follows: the patient sits on a chair while resting the upper extremity on a table; the radiographs were made for the anteroposterior and lateral direction. For the anteriorposterior direction the shoulder is anteflexed and the elbow should be extended as much as possible and for the lateral view the elbow should be flexed 90 degrees whereas the shoulder is rotated internally. In this way the flexed elbow rests on the table (which consists the plate) in a horizontal position. All patients were observed for at least 2 years. The preoperative diagnosis was seropositive rheumatoid arthritis in 94 patients (108 elbows), seronegative rheumatoid arthritis in nine patients (nine elbows), juvenile chronic arthritis in two patients (three elbows), psoriatic arthritis in one patient (one elbow), synovial chondromatosis in one patient (one elbow), and posttraumatic osteoarthrosis in three patients (three elbows). The Larsen classification for the 120 elbows affected by rheumatoid arthritis was Larsen Class III in 10 elbows, Larsen Class IV in 62 elbows, and Larsen Class V in 48 elbows 20. The size of the components was determined before the operation by templating on radiographs. The size of the humeral components were small (48 elbows), medium (64 elbows), or large (13 elbows), and the ulnar components differed among small (66 elbows), medium (54 elbows), and metal- backed (five elbows, with the snap-fit option in four elbows) component. The latter component was used because of insufficient ulnar bone stock. When there was an additional tendency for dislocation after the trial reduction during the operation the snap-fit insert was used. We used the Wrightington method for assessing all radiographs (Fig. 1) 12. This method consists of 12 position measurements and 21 radiolucent line measurements. All measurements were done by the first author, who was not the operating surgeon, by using a universal goniometer. For assessing the position of the prosthesis we used only the first postoperative radiograph. All elbow prostheses were successively taken into analysis, but only if the first postoperative radiograph has been made more than 6 months after the operation (18 elbows) or when aseptic loosening was not the reason of failure (22 elbows) the elbow was excluded from this study. Radiolucent lines were defined as demarcation lines between the cement-bone interfaces seen on a standard 88
5 Limited influence of prosthetic position on aseptic loosening of the Souter-Strathclyde Total Elbow Prosthesis Fig. 1. The Wrightington method for measuring radiolucent lines (RLLs) and position of the Souter-Strathclyde total elbow prosthesis. The RLLs are divided into zones and are scored in two directions (anterioposterior and lateral direction). radiograph and were classified as none, less than 1 mm, 1 to 2 mm, 2 mm, and greater than 2 mm. Loosening was defined as complete radiolucency (> 1 mm) around one or two components that was progressive in time. Cementing technique was classified as adequate as the thickness of the cement mantle was more than 1 mm and covered the prosthesis completely. When there was a defect in the cement mantle in one zone (see Wrightington method, Fig. 1) the mantle was classified as sufficient. In case of defects in more than one zone the cement mantle was classified as poor. For determination of the component size related to the size of the humeral bone two measurements were performed. First the distance between the medial and lateral condyle of the humeral bone, and secondly the distance between the prosthetic condyles of the humeral component were determined and, finally, the ratio of these two distances was calculated. In 46 elbows (37%) a humeral bone plug was applied and the influence of this factor on aseptic loosening was taken into analysis. Four intra-operative fractures were seen in this series and the consequences at postoperative outcome is discussed. Of the 125 elbows, 104 preoperative radiographs (made within 6 months before the operation) were available for additional analysis. First we classified bone resorption at four locations (medial and lateral condyles of the humerus, the olecranon, and the coronoid process), rated as none, minimal, moderate, or severe (Fig 2). Secondly, we measured narrowing of the humeroulnar joint space (in mm). Finally, horizontal and vertical dislocation of the elbow were measured (also in mm; Fig 3). All these observations were done by the first author and made on standard radiographs as described above. A Markov model was used to analyze the relationship between the position of the prosthesis and the development (from none to < 1 mm) or progression of radiolucent 89
6 Chapter 6 Fig. 2. Preoperative measurements of the horizontal (A.) and vertical dislocation (B.) on lateral view. Horizontal dislocation is the distance between the posterior cortex of the humerus and the most proximal cortex of the olecranon when the elbow is flexed 90 degrees. Vertical dislocation is the distance between the humero-ulnar joint surface and the lowest tip of the humeral medial condyle when the elbow is flexed 90 degrees. In elbows with severe destruction the dislocation increased in both directions. Fig. 3. The amount of bone resorption in the epicondyles, the olecranon and the coronoid process. coronoideus. The resorption is classified as non, minimal, moderate and severe. 90
7 Limited influence of prosthetic position on aseptic loosening of the Souter-Strathclyde Total Elbow Prosthesis Fig. 4. Markov model to analyse the radiographs of the Souter-Strathclyde total elbow prosthesis. The RLL were analysed for different zones around the prosthesis according to the Wrightington method. Fig. 4. RLL = Radio Lucent Line(s) Fig. 4. a. Influence of position of the prosthesis on the development and progression of RLL Fig. 4. b. Development and progression of RLL Fig. 4. c. Influence of RLL on aseptic loosening Fig. 4. d. Influence of position of the prosthesis on aseptic loosening, independent on RLL lines (significance at p < 0.05 level; Fig 4). 1,2,24 The program we used allows the time of transition to the next category of radiolucent line width to be interval censored. This means that the exact transition time is only known to lie between two observation times. For the survival of the prosthesis (time to aseptic loosening), related to the preoperative radiographs and to the position of the prosthesis, we used a Cox model (significance at p < 0.05 level). The Kaplan-Meier survival curve was obtained for the overall survival of the prosthesis (end-point aseptic loosening). Results The mean followup of the radiographs was 67.4 months (range months, S.E. 3.6 months). Of the 125 elbow prostheses analyzed, 21 (16,8%) loosened radio- 91
8 Chapter 6 Fig. 5. Kaplan-Meier survival curve for endpoint aseptic loosening. The 95% confidence interval is given. graphically after an average period of 62.5 months (S.E. 7.3 months). In 17 elbows there was aseptic loosening of the humeral component, in one elbow there was aseptic loosening of the ulnar component, and in three elbows both components loosened simultaneously (Fig 5). The probability to remain free of aseptic loosening was 88.8 % (S.E. 3.3%) after 5 years and 64.6 % (S.E. 8.0%) after 10 years. No clear differences were seen in the cementing techniques. In all 125 elbows the cement mantle was 1 mm or more around both components directly after the operation and no cement defects were noticed; therefore, the quality of the cement mantles were classified as adequate. The position of components was not obvious related to radiolucent lines in this study. On anterioposterior view the humeral component was placed in lateral (102 elbows), neutral (21 elbows) or medial (2 elbows) position, whereas the ulnar component was placed in lateral (79 elbows), neutral (40 elbows) or medial position (6 elbows). On lateral view the humeral component was tilted anteriorly (61 elbows), posteriorly (30 elbows) or placed in neutral position (34 elbows) while the ulnar component was inserted in extension (99 elbows), flexion (7 elbows) or in neutral position. First we looked at the influence of position (as a continuous variable, in degrees) of the prosthesis on the development or progression of radiolucent lines in all Wrightington zones on AP and lateral views (see figure 1). Within one year after the replacement 92
9 Limited influence of prosthetic position on aseptic loosening of the Souter-Strathclyde Total Elbow Prosthesis Fig. 6. Lateral and anteroposterior (AP) radiographs of two elbows with small humeral components taken 5 years after insertion. A. Lateral view of a well-fixed humeral component. B. Lateral view of a migrating humeral component with anterior tilting. C. AP view of a well-fixed humeral component D. AP view of a migrating humeral component (with a fracture of the medial epicondyle). The ulnar components in all figures show radiolucent lines, but no aseptic loosening was seen. 93
10 Chapter 6 Table I. Position Development radiolucent line Progression radiolucent line Humaral angle anterioposterior view Hap (S.E. 0.02), P= (S.E. 0.03), P=0.09 Hap (S.E. 0.02), P= (S.E. 0.03), P=0.49 Hap (S.E. 0.02), P= (S.E. 0.03), P=0.97 Hap (S.E. 0.02), P= (S.E. 0.03), P=0.95 Hap (S.E. 0.02), P= (S.E. 0.04), P=0.13 Humeral angle lateral view Hap (S.E. 0.04), P= (S.E. 0.06), P=0.42 Hap (S.E. 0.03), P= (S.E. 0.06), P=0.04 Hap (S.E. 0.03), P= (S.E. 0.04), P=0.73 Hap (S.E. 0.03), P< (S.E. 0.04), P=0.37 Hap (S.E. 0.04), P= (S.E. 0.06), P=0.71 Humeral angle anterioposterior view Hlat (S.E. 0.02), P= (S.E. 0.04), P=0.01 Hlat (S.E. 0.03), P= (S.E. 0.03), P=0.40 Hlat (S.E. 0.02), P= (S.E. 0.03), P=0.70 Hlat (S.E. 0.02), P= (S.E. 0.02), P=0.81 Hlat (S.E. 0.03), P= (S.E. 0.03), P=0.07 Humeral angle lateral view Hlat (S.E. 0.04), P= (S.E. 0.06), P=0.28 Hlat (S.E. 0.04), P= (S.E. 0.06), P=0.54 Hlat (S.E. 0.04), P= (S.E. 0.04), P=0.62 Hlat (S.E. 0.03), P= (S.E. 0.04), P<0.01 Hlat (S.E. 0.03), P= (S.E. 0.05), P=0.18 The relationship between the angle of the humeral component in the bone (as a continuous variable) and the development en progressional of radiolucent lines. On anteriorposterior view the humeral angle is given from valgus (positive value) to varus postion (negative value). On lateral view the humeral angle is given from posterior tilting (postive value) to anterior tilting (negative value). For all relationships the standard errors (S.E.) as well as the level of significance are given. Significance at p<
11 Limited influence of prosthetic position on aseptic loosening of the Souter-Strathclyde Total Elbow Prosthesis Table II. Angle of components Humeral component Anterioposterior angle Lateral angle Ulnar component Anterioposterior angle Lateral angle Relation to aseptic loosening (S.E. 0.04), P= (S.E. 0.07), P= (S.E. 0.07), P= (S.E. 0.07), P=0.15 The relationship between the angle of the components (according to the Wrightington method, see figure 1) and aseptic loosening. The angles have been taken sa continuous variables. For all relationships the standard errors (S.E.) as well as the level of significance are given. Significance at p<0.05. surgery RLLs were found in 17,6 percent of the humeral and in 29,6 percent of the ulnar components. At latest followup these percentages increased respectively to 80,0 and 76,0 percent. When the humeral component was tilted more medially ( valgus position on the AP view) we found the development of radiolucent lines at the medial condyle and at the posterior distal zone (Hap 4, p = 0.02 and Hlat3, p=0.0, see table I). On the other hand, the progression of these lines was not influenced by this position. The same trend was seen for the development of radiolucent lines on the anterior and posterior side of the humeral component on the lateral view. If the humeral component was positioned in a more anterior tilting, radiolucent lines occurred more often in Hap4 (p=0.02) and Hlat2 (p=0.03), but the progression of these radiolucent lines did not depend on the prosthetic position. In contrast in three zones only progression of radiolucent lines was noticed whereas no influence on development of lines was seen in the same zones. For all other humeral and ulnar zones we could not demonstrate any other clear effect of the position of the humeral component on radiolucent lines. Even no effect of the position was found on the AP view after combining the radiolucent lines of zones Hap2 en Hap3 (lateral side of the prosthesis) and the humeral zones Hap4 and Hap5 (medial side of the component). In 69 elbows (55,2 %) radiolucent lines were seen around the ulnar component in Ulat4 en Ulat5 immediately after the operation, but also this finding had no effect on the progression of radiolucent lines or aseptic loosening in this study. We analyzed the relationship between the position of the humeral and ulnar components as categorical variables and radiolucent lines, but the outcomes were not divergent. The relationship between the position (also as a continuous variable, in degrees) of the prosthesis and aseptic loosening was analyzed, independent of the occurrence of radiolucent lines (Table II). The position of the components differed, but no prediction 95
12 Chapter 6 could be made on aseptic loosening. If we took the humeral angle on the lateral view as a categorical variable (anterior, neutral, or posterior position) instead of a continuous variable (in degrees), the outcome also did not change. A valgus or a varus position of the humeral component also did not have predictive value for aseptic loosening for continuous (in degrees) and categorical analysis, but only two humeral components were placed in medial position on AP view. None of the ulnar positions enhanced the risk of aseptic loosening. We measured the distances between the medial and lateral cortices of the epicondyles and the humeral component (humeral distances 1 and 2 on the AP view, Fig 1) and the ratio was calculated. However, although this ratio did differ in the 125 elbows (ratio range, ), we could not demonstrate a relationship to aseptic loosening. Intraoperative fractures occurred in four elbows. In three elbows the medial component fractured and in one elbow the lateral condyle of the humeral bone fractured. The peroparative alignment of these four prostheses had not been changed. Two of these elbows with intraoperative fractures had aseptic loosening (after 99 and 36 months), but both fractures had healed within 3 months after the surgery. For that reason an evident relationship between the fractures and aseptic loosening was not supposed. Three medial supracondylar ridges fractured after a average period of 31 months postoperatively (range months) after migration of the humeral component. In all these patients anterior migration (tilting) of the humeral tip had already occurred. The humeral bone plug did not prevent the occurrence of radiolucent lines in our series. No differences could be found in radiolucent lines or aseptic loosening between elbows with and without a humeral bone plug. Assessment of preoperative radiographs of the elbow had restricted weight in the prediction of aseptic loosening (Table III). First, the Larsen score did not predict the elbows which were at risk for aseptic loosening and, secondly, on our own scoring method could only prove that bone resorption around the lateral condyle was related (p = 0.02) to aseptic loosening of the prosthesis. None of the other items measured on the preoperative radiographs had an influence on aseptic loosening. Discussion The survival rate was approximately 10% lower after 5 and 10 years of followup when radiographic loosening, as previously defined, was used as the end point, compared with when the removal of the prosthesis was used as the end point 4,8. This can be explained by the absence of pain while the prosthesis loosened and, for that reason, the delay of the revision operation. 96
13 Limited influence of prosthetic position on aseptic loosening of the Souter-Strathclyde Total Elbow Prosthesis Table III. Preoperative data Ulno-humeral joint space Resorption medial condyle Resorption lateral condyle Resorption olecranon Resorption coronoid process Horizontal dislocation Vertical dislocation Aseptic loosening (S.E. 0.39), P= (S.E. 0.34), P= (S.E. 0.32), P= (S.E. 0.38), P= (S.E. 0.41), P= (S.E. 0.08), P= (S.E. 0.06), P=0.52 The relationship between preopartive radiographs and septic loosening. Narrowing of the preoperative joint space, increased preoperative resorption of medial condyle, olecranon, coronoid process or increased preoperative dislocation was not significantly related. Only preoperative resorption of the lateral condyle showed a significant relationship to aseptic loosening. For all relationships the standard errors (S.E.) as well as the level of significance are given. Significance at p<0.05. Making measurements on standard radiographs, as is done frequently in the outpatient clinic, has some pitfalls. The doctor who does the assessment should realize that such measurements depend on the rotation angle of the upper extremity and on the quality of the radiograph. The Wrightington method was developed to standardize measurements on standard radiographs of the Souter-Strathclyde total elbow prosthesis, but this method requires standarized radiographs of good quality. In contrast to Trail et al our series showed only minor influence of prosthetic position on aseptic loosening, maybe because the placement of most prostheses was around the average level and abnormal situations were hardly seen 12. We could postulate that the extremely divergent positions of the prosthesis could be related to aseptic loosening. Hermann and Egund found that the position of hip prostheses can be accurately and reproducibly ascertained from routine radiographs 21. Furthermore Pollock et al showed that liner thickness of acetabular components can be adequately determined on radiographs 22. Therefore we argue that measuring component-position on standard radiographs is also adequate for clinical assessment of elbow prostheses but, in our opinion, more detailed position measurements (migration up to 0.4 mm) should be performed with the RSA method in of a universal goniometer (with a 1-mm scale). Valstar et al showed that, with the application of radiostereometry (RSA) in cases of humeral loosening, the tip of the humeral component migrated anteriorly (anterior tilting). Unfortunately they did not look at the development and progression of RLLs in relation to this anterior tilting
14 Chapter 6 Radiolucent lines are difficult to interpret. The definition varies and, furthermore, the meaning of radiolucent lines is not clear 23,24. As in hip replacements, a radiolucent line around an elbow prosthesis will not always be the same as loosening 24. The value of radiolucent lines is restricted for this reason. The Markov model allows use to intergrate all different factors in one model. Because of that the Markov model provides a useful way to analyze the complex process of aseptic loosening. Weakness of our study is the relative small amount of elbows related to the large number of different factors. On the other hand, even no obvious statistical trend was seen after analysing 125 elbows. Probably the patterns of development and progression of RLLs and aseptic loosening are not as clear as one may have thought. The use of a bone plug in elbow prostheses is not well studied. Whereas in hip and knee replacements the efficacy of a bone plug has been proven (better cement mantle and less blood loss), the effect of bone plugs in elbow replacements is not well established In this series the cement mantle was of similar quality in all elbows and could therefore not predict aseptic loosening. In the preoperative radiographs, the elbows we analyzed were all destroyed by rheumatoid arthritis. The frequently applied Larsen score cannot classify the amount of dislocation or bone loss (resorption) before the operation 20. Because of this we developed an additional scoring list. More validated bone resorption-scores are necessary for research purposes and to understand the value of bone resorption prior to joint replacement surgery. Fracturing the medial epicondylar ridge during migration of the humeral component should be prevented. When the migration becomes obvious (progression of complete radiolucent lines) revision must be considered if fracture of the epicondyle is imminent. The preoperative radiologic scoring might be of importance, but could not be answered by this study. The factors that cause aseptic loosening of the primary Souter-Strathclyde total elbow prosthesis remain uncertain after preforming this study, but despite the relative small number of elbows, a multifactorial cause of aseptic loosening seemed to be most plausible. 98
15 Limited influence of prosthetic position on aseptic loosening of the Souter-Strathclyde Total Elbow Prosthesis References 1. Ferlec D C Total elbow arthroplasty for treatment of elbow arthritis. J Shoulder Elbow Surg 1999; 8(4): Gschwend N, Scheier N H, and Baehler A R. Longterm results of the GSB III elbow arthroplasty. J Bone Joint Surg (Br) 1999; 81(6): Mackay D C, Hudson B, Williams J R. Which primary shoulder and elbow replacement? A review of the results of prostheses available in the UK. Ann R Coll Surg Engl 2001; 83(4): Rozing P. Souter-Strathclyde total elbow arthroplasty. J Bone Joint Surg (Br) 2000; 82(8): Tanaka N, Kudo H, Iwano K, Sakahashi H, Sato E, Ishii S. Kudo total elbow arthroplasty in patients with rheumatoid arthritis. J Bone Joint Surg (Am) 2001; 83(10): Trancik T, Wilde A H, Borden L S. Captillocondylar total elbow arthroplasty. Two to eight year experience. Clin Orthop 1987; 233 : Herberts P, Malchau H. Long-term registration has improved the quality of hip replacement: a review of the Swedish THR Register comparing 160,000 cases. Acta Orthop Scand 2000; 71(2): Van der Lugt J C, Geskus R B, Rozing P M. Primary Souter-Strathclyde total elbow prosthesis for rheumatoid arthritis. J Bone Joint Surg (Am) 2004; 86 (3): Hargreaves D, Emery R. Total elbow replacement in the treatment of rheumatoid disease. Clin Orthop 1999; 366: Kudo H, Iwano K. Total elbow arthroplasty with a non-constrained surface-replacement prosthesis in patients who have rheumatoid arthritis: a long- term follow-up study. J Bone Joint Surg (Am) 1990; 72(3): Valstar E R, Garling E H, Rozing P M. Micromotion of the Souter-Strathclyde total elbow prosthesis in patients with rheumatoid arthritis: 21 elbows followed for 2 years. Acta Orthop Scand 2002; 73(3): Trail I A, Nuttall D, Stanley J K. Survivorship and radiological analysis of the standard Souter- Strathclyde total elbow arthroplasty. J Bone Joint Surg (Br) 1999; 81(1): Ikävalko M, Belt E A, Kautiainen H, Lehto M U. Revisions for aseptic loosening in Souter-Strathclyde elbow arthroplasty. Incidence of revision of different components used in 522 consecutive cases. Acta Orthop Scand 2002; 73(3): Klapach A S, Callaghan J J, Goetz D D, Olejniczak J P, Johnston R C. Charnley total hip arthroplasty with use of improved cementing techniques: a minimum twenty-year follow-up study. J Bone Joint Surg (Am) 2001; 83(12): Kligman M, Roffman M. The effect of intramedullary bone plug on femoral stem migration of hydroxyapatite-coated hip arthroplasty. Orthopedics 2000; 23(7): Kumar N, Saleh J, Gardiner E, Devadoss V G, Howell F R. Plugging the intramedullary canal of the femur in total knee arthroplasty: reduction in postoperative blood loss. J Arthroplasty 2000; 15(7): Andersen P K. Repeated assessment of risk factors in survival analysis. Stat Methods Med Res 1992; 1(3): Commenges D. Inference for multi-state models from interval-censored data. Stat Methods Med Res 2002; 11(2): Van Houwelingen H C. The future of biostatistics: expecting the unexpected. Stat Med 1997; 16(24): Larsen A, Dale K, Eek M. Radiographic evaluation of rheumatoid arthritis and related conditions by standard reference films. Acta Radiol Diagn (Stockh) 1997; 18(4): Hermann K L, Egund N. Measuring anteversion in the femoral neck from routine radiographs. Acta Radiol 1998; 39(4): Pollock D, Sychterz C J, Engh C A. A clinically practical method of manually assessing polyethylene liner thickness. J.Bone Joint Surg (Am) 2001; 83(12): Freeman M A. Radiolucent lines: a question of nomenclature. J Arthroplasty 1999; 14(1): Kwong L M, Jasty M, Mulroy R D, Maloney W J, Bragdon C, Harris W H. The histology of the radiolucent line. J Bone Joint Surg (Br) 1992; 74(1):
16 100
PRIMARY SOUTER-STRATHCLYDE TOTAL ELBOW
 4 PRIMARY SOUTER-STRATHCLYDE TOTAL ELBOW PROSTHESIS IN RHEUMATOID ARTHRITIS, SURGICAL TECHNIQUE J.C.T. van der Lugt R.B. Geskus P.M. Rozing J Bone Joint Surg Am. 2005 (supp 1);87:67-77 Chapter 4 Abstract
4 PRIMARY SOUTER-STRATHCLYDE TOTAL ELBOW PROSTHESIS IN RHEUMATOID ARTHRITIS, SURGICAL TECHNIQUE J.C.T. van der Lugt R.B. Geskus P.M. Rozing J Bone Joint Surg Am. 2005 (supp 1);87:67-77 Chapter 4 Abstract
Kudo type-5 total elbow arthroplasty in mutilating rheumatoid arthritis
 Upper limb Kudo type-5 total elbow arthroplasty in mutilating rheumatoid arthritis A 5- TO 11-YEAR FOLLOW-UP T. Mori, H. Kudo, K. Iwano, T. Juji From the National Hospital Organization Sagamihara Hospital,
Upper limb Kudo type-5 total elbow arthroplasty in mutilating rheumatoid arthritis A 5- TO 11-YEAR FOLLOW-UP T. Mori, H. Kudo, K. Iwano, T. Juji From the National Hospital Organization Sagamihara Hospital,
General Introduction. Development of elbow prostheses
 1INTRODUCTION Chapter 1 10 Introduction General Introduction Development of elbow prostheses The elbow joint is a semi-constrained joint with three articulations: ulnotrochlear, radiocapitellar and proximal
1INTRODUCTION Chapter 1 10 Introduction General Introduction Development of elbow prostheses The elbow joint is a semi-constrained joint with three articulations: ulnotrochlear, radiocapitellar and proximal
Continuing the Tradition. VerSys Heritage Hip System
 Continuing the Tradition VerSys Heritage Hip System Heritage Following the Tradition The low-friction hip prosthesis developed by Sir John Charnley has more than a 20-year history of outstanding results.
Continuing the Tradition VerSys Heritage Hip System Heritage Following the Tradition The low-friction hip prosthesis developed by Sir John Charnley has more than a 20-year history of outstanding results.
N Plain films are usually sufficient to assess the state of. N Criteria for loosening depends on site and make of
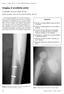 Imaging, 15 (2003), 270 285 E 2003 The British Institute of Radiology Imaging of prosthetic joints S OSTLERE, FRCR and S SOIN, MB BChir Nuffield Orthopaedic Centre and Oxford Radcliffe Hospital, Oxford,
Imaging, 15 (2003), 270 285 E 2003 The British Institute of Radiology Imaging of prosthetic joints S OSTLERE, FRCR and S SOIN, MB BChir Nuffield Orthopaedic Centre and Oxford Radcliffe Hospital, Oxford,
A clinical and radiographic 13-year follow-up study of 138 Charnley hip arthroplasties in patients years old
 Acta Orthopaedica 2008; 79 (5): x x 1 9 A clinical and radiographic 13-year follow-up study of 138 Charnley hip arthroplasties in patients 50 70 years old Comparison of university hospital data and registry
Acta Orthopaedica 2008; 79 (5): x x 1 9 A clinical and radiographic 13-year follow-up study of 138 Charnley hip arthroplasties in patients 50 70 years old Comparison of university hospital data and registry
Preoperative Planning. The primary objectives of preoperative planning are to:
 Preoperative Planning The primary objectives of preoperative planning are to: - Determine preoperative leg length discrepancy. - Assess acetabular component size and placement. - Determine femoral component
Preoperative Planning The primary objectives of preoperative planning are to: - Determine preoperative leg length discrepancy. - Assess acetabular component size and placement. - Determine femoral component
CLINICAL PAPER / ORTHOPEDIC
 HIP LEG LENGTH AND OFFSET Kelley T.C. and Swank M.L. (2009) Using CAS leads to more accurate positioning within the safe zone (inclination between 30 and 50, anteversion between 5 and 25 ) CAS improves
HIP LEG LENGTH AND OFFSET Kelley T.C. and Swank M.L. (2009) Using CAS leads to more accurate positioning within the safe zone (inclination between 30 and 50, anteversion between 5 and 25 ) CAS improves
Optimum implant geometry
 Design Rationale Optimum implant geometry Extending the proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Design Rationale Optimum implant geometry Extending the proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
4/28/2010. Fractures. Normal Bone and Normal Ossification Bone Terms. Epiphysis Epiphyseal Plate (physis) Metaphysis
 Fractures Normal Bone and Normal Ossification Bone Terms Epiphysis Epiphyseal Plate (physis) Metaphysis Diaphysis 1 Fracture Classifications A. Longitudinal B. Transverse C. Oblique D. Spiral E. Incomplete
Fractures Normal Bone and Normal Ossification Bone Terms Epiphysis Epiphyseal Plate (physis) Metaphysis Diaphysis 1 Fracture Classifications A. Longitudinal B. Transverse C. Oblique D. Spiral E. Incomplete
Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 366, pp. 39-45 0 1999 Lippincott Williams & Wilkins, Inc. Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis Jens 0. S@jbjerg,
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 366, pp. 39-45 0 1999 Lippincott Williams & Wilkins, Inc. Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis Jens 0. S@jbjerg,
Bipolar Radial Head System
 Bipolar Radial Head System Katalyst Surgical Technique DESCRIPTION The Katalyst Telescoping Bipolar Radial Head implant restores the support and bearing surface of the radial head in the face of fracture,
Bipolar Radial Head System Katalyst Surgical Technique DESCRIPTION The Katalyst Telescoping Bipolar Radial Head implant restores the support and bearing surface of the radial head in the face of fracture,
Integra. Katalyst Bipolar Radial Head System SURGICAL TECHNIQUE
 Integra Katalyst Bipolar Radial Head System SURGICAL TECHNIQUE Surgical Technique As the manufacturer of this device, Integra does not practice medicine and does not recommend this or any other surgical
Integra Katalyst Bipolar Radial Head System SURGICAL TECHNIQUE Surgical Technique As the manufacturer of this device, Integra does not practice medicine and does not recommend this or any other surgical
Bone Bangalore
 Dr Suresh Annamalai MBBS, MRCS(Edn), FRCS( Tr & Orth)(Edn), FEBOT(European Board), Young Hip and Knee Fellowship(Harrogate, UK) Consultant Arthroplasty and Arthroscopic Surgeon Manipal Hospital, Whitefield,
Dr Suresh Annamalai MBBS, MRCS(Edn), FRCS( Tr & Orth)(Edn), FEBOT(European Board), Young Hip and Knee Fellowship(Harrogate, UK) Consultant Arthroplasty and Arthroscopic Surgeon Manipal Hospital, Whitefield,
PLR. Proximal Loading Revision Hip System
 PLR Proximal Loading Revision Hip System The PLR splined revision stem is designed to recreate the natural stresses in the revised femur, where proximal bone may be compromised. PLR Hip System Design Considerations
PLR Proximal Loading Revision Hip System The PLR splined revision stem is designed to recreate the natural stresses in the revised femur, where proximal bone may be compromised. PLR Hip System Design Considerations
Distal Cut First Femoral Preparation
 Surgical Technique Distal Cut First Femoral Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Femoral preparation Contents Introduction...3 DCF femoral highlights...4 Preoperative planning...6
Surgical Technique Distal Cut First Femoral Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Femoral preparation Contents Introduction...3 DCF femoral highlights...4 Preoperative planning...6
FLH /11
 FLH 225 04/11 This publication has been issued by: European Central Marketing Waterton Industrial Estate Bridgend, South Wales CF31 3XA, United Kingdom Tel: +44 (0)1656 655221 Fax: +44 (0)1656 645454 www.biomet.com
FLH 225 04/11 This publication has been issued by: European Central Marketing Waterton Industrial Estate Bridgend, South Wales CF31 3XA, United Kingdom Tel: +44 (0)1656 655221 Fax: +44 (0)1656 645454 www.biomet.com
ORIGINAL PAPER. Department of Orthopedic Surgery, Hamamatsu Medical Center ABSTRACT
 Nagoya J. Med. Sci. 71. 145 ~ 150, 2009 ORIGINAL PAPER AUTOGENOUS BULK STRUCTURAL BONE GRAFTING FOR RECONSTRUCTION OF THE ACETABLUM IN PRIMARY TOTAL HIP ARTHROPLASTY: AVERAGE 12-YEAR FOLLOW-UP TETSUO MASUI,
Nagoya J. Med. Sci. 71. 145 ~ 150, 2009 ORIGINAL PAPER AUTOGENOUS BULK STRUCTURAL BONE GRAFTING FOR RECONSTRUCTION OF THE ACETABLUM IN PRIMARY TOTAL HIP ARTHROPLASTY: AVERAGE 12-YEAR FOLLOW-UP TETSUO MASUI,
Taperloc Complete Hip System. Surgical Technique
 Taperloc Complete Hip System Surgical Technique One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide personalized care to one patient. The science and art of medical
Taperloc Complete Hip System Surgical Technique One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide personalized care to one patient. The science and art of medical
Bone Preservation Stem
 TRI-LOCK Bone Preservation Stem Featuring GRIPTION Coating Surgical Technique Implant Geometry Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
TRI-LOCK Bone Preservation Stem Featuring GRIPTION Coating Surgical Technique Implant Geometry Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty
 Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Optimum implant geometry
 Design Rationale Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Design Rationale Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Charnley Total Hip Arthroplasty with Use of Improved Cementing Techniques A MINIMUM TWENTY-YEAR FOLLOW-UP STUDY
 1840 COPYRIGHT 2001 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Charnley Total Hip Arthroplasty with Use of Improved Cementing Techniques A MINIMUM TWENTY-YEAR FOLLOW-UP STUDY BY AIMEE S. KLAPACH,
1840 COPYRIGHT 2001 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Charnley Total Hip Arthroplasty with Use of Improved Cementing Techniques A MINIMUM TWENTY-YEAR FOLLOW-UP STUDY BY AIMEE S. KLAPACH,
TOTAL HIP REPLACEMENT:
 THR Prosthesis Design TOTAL HIP REPLACEMENT: PROSTHESIS DESIGN FEATURES JESS JOHNSTON & MELINDA ZIETH History of Hip Prosthesis Joint Replacement Registry Implant Design Technology & Future History and
THR Prosthesis Design TOTAL HIP REPLACEMENT: PROSTHESIS DESIGN FEATURES JESS JOHNSTON & MELINDA ZIETH History of Hip Prosthesis Joint Replacement Registry Implant Design Technology & Future History and
VerSys LD/Fx Cemented and Press-Fit Hip Prostheses. Surgical Technique IMAGE TO COME. Versatile solutions for total and partial hip replacement
 VerSys LD/Fx Cemented and Press-Fit Hip Prostheses Surgical Technique IMAGE TO COME Versatile solutions for total and partial hip replacement VerSys LD/Fx Cemented and Press-Fit Hip Prostheses VerSys
VerSys LD/Fx Cemented and Press-Fit Hip Prostheses Surgical Technique IMAGE TO COME Versatile solutions for total and partial hip replacement VerSys LD/Fx Cemented and Press-Fit Hip Prostheses VerSys
Bilateral total knee arthroplasty: One mobile-bearing and one fixed-bearing
 Journal of Orthopaedic Surgery 2001, 9(1): 45 50 Bilateral total knee arthroplasty: One mobile-bearing and one fixed-bearing KY Chiu, TP Ng, WM Tang and P Lam Department of Orthopaedic Surgery, The University
Journal of Orthopaedic Surgery 2001, 9(1): 45 50 Bilateral total knee arthroplasty: One mobile-bearing and one fixed-bearing KY Chiu, TP Ng, WM Tang and P Lam Department of Orthopaedic Surgery, The University
21st Century Fracture Management ETS. Surgical Protocol
 21st Century Fracture Management ETS Surgical Protocol ETS Operative Technique Step 1 Confirm that a cemented hemiarthroplasty is indicated. An X-ray template of the ETS is provided. This should be used
21st Century Fracture Management ETS Surgical Protocol ETS Operative Technique Step 1 Confirm that a cemented hemiarthroplasty is indicated. An X-ray template of the ETS is provided. This should be used
The shape and size of femoral components in revision total hip arthroplasty among Chinese patients
 Journal of Orthopaedic Surgery 2003: 11(1): 53 58 The shape and size of femoral components in revision total hip arthroplasty among Chinese patients KY Chiu, TP Ng, WM Tang Department of Orthopaedic Surgery,
Journal of Orthopaedic Surgery 2003: 11(1): 53 58 The shape and size of femoral components in revision total hip arthroplasty among Chinese patients KY Chiu, TP Ng, WM Tang Department of Orthopaedic Surgery,
AGGRESSIVE GRANULOMATOUS LESIONS AFTER HIP ARTHROPLASTY
 AGGRESSIVE GRANULOMATOUS LESIONS AFTER HIP ARTHROPLASTY KAJ TALLROTH, ANTTI ESKOLA, SEPPO SANTAVIRTA, YRJ T. KONTTINEN, T. SAM LINDHOLM From the Orthopaedic Hospitalofthe Invalid Foundation, Helsinki We
AGGRESSIVE GRANULOMATOUS LESIONS AFTER HIP ARTHROPLASTY KAJ TALLROTH, ANTTI ESKOLA, SEPPO SANTAVIRTA, YRJ T. KONTTINEN, T. SAM LINDHOLM From the Orthopaedic Hospitalofthe Invalid Foundation, Helsinki We
Optimum implant geometry
 Surgical Technique Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Surgical Technique Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Socket wall addition device in the treatment of recurrent hip prosthesis dislocation
 Acta Orthopaedica 2006; 77 (1): 87 91 87 Socket wall addition device in the treatment of recurrent hip prosthesis dislocation Good outcome in 12 patients followed for 4.5 (1 9) years Anders G Enocson 1,
Acta Orthopaedica 2006; 77 (1): 87 91 87 Socket wall addition device in the treatment of recurrent hip prosthesis dislocation Good outcome in 12 patients followed for 4.5 (1 9) years Anders G Enocson 1,
Ovation Hip System. Surgical Technique
 Ovation Hip System Surgical Technique Ovation Hip System Surgical Technique Ovation Designing Surgeons: Andrew Petrella, M.D. Lecanto, FL Richard Vlasak, M.D. Gainesville, FL Ovation Tribute Designing
Ovation Hip System Surgical Technique Ovation Hip System Surgical Technique Ovation Designing Surgeons: Andrew Petrella, M.D. Lecanto, FL Richard Vlasak, M.D. Gainesville, FL Ovation Tribute Designing
28 Surgical Technique
 Surgical Technique 10 12 14 16 18 20 22 24 28 26 Technique described by James L. Guyton, MD Campbell Clinic Memphis, Tennessee James W. Harkess, MD Campbell Clinic Memphis, Tennessee David G. LaVelle,
Surgical Technique 10 12 14 16 18 20 22 24 28 26 Technique described by James L. Guyton, MD Campbell Clinic Memphis, Tennessee James W. Harkess, MD Campbell Clinic Memphis, Tennessee David G. LaVelle,
Alignment of the femoral component in a mobile-bearing unicompartmental knee arthroplasty Kort, N. P.; van Raay, J. J. A. M.; Thomassen, B. J. W.
 University of Groningen Alignment of the femoral component in a mobile-bearing unicompartmental knee arthroplasty Kort, N. P.; van Raay, J. J. A. M.; Thomassen, B. J. W. Published in: Knee DOI: 10.1016/j.knee.2007.04.007
University of Groningen Alignment of the femoral component in a mobile-bearing unicompartmental knee arthroplasty Kort, N. P.; van Raay, J. J. A. M.; Thomassen, B. J. W. Published in: Knee DOI: 10.1016/j.knee.2007.04.007
Following a tradition of success. VerSys Heritage Primary Hip Prosthesis Surgical Technique
 Following a tradition of success VerSys Heritage Primary Hip Prosthesis Surgical Technique VerSys Heritage Primary Hip Prosthesis 1 Surgical Technique For VerSys Heritage Primary Hip Prosthesis Dennis
Following a tradition of success VerSys Heritage Primary Hip Prosthesis Surgical Technique VerSys Heritage Primary Hip Prosthesis 1 Surgical Technique For VerSys Heritage Primary Hip Prosthesis Dennis
AFTER TOTAL KNEE REPLACEMENT
 CORONAL ALIGNMENT AFTER TOTAL KNEE REPLACEMENT ROBERT S. JEFFERY, RICHARD W. MORRIS, ROBIN A. DENHAM From Queen Alexandra Hospital, Portsmouth Maquet s line passes from the centre of the femoral head to
CORONAL ALIGNMENT AFTER TOTAL KNEE REPLACEMENT ROBERT S. JEFFERY, RICHARD W. MORRIS, ROBIN A. DENHAM From Queen Alexandra Hospital, Portsmouth Maquet s line passes from the centre of the femoral head to
Featuring. Technology. Product Rationale
 Featuring Technology Product Rationale 2 Optimum implant geometry Extending proven TRI-LOCK heritage The original TRI-LOCK Stem was introduced in 1981. This implant was the first proximally coated tapered-wedge
Featuring Technology Product Rationale 2 Optimum implant geometry Extending proven TRI-LOCK heritage The original TRI-LOCK Stem was introduced in 1981. This implant was the first proximally coated tapered-wedge
This publication is not intended for distribution in the USA.
 This publication is not intended for distribution in the USA. Extraction of a CORAIL Stem Surgical Technique Introduction Given the excellent long-term results of the CORAIL stem, 1,2,3 its extraction
This publication is not intended for distribution in the USA. Extraction of a CORAIL Stem Surgical Technique Introduction Given the excellent long-term results of the CORAIL stem, 1,2,3 its extraction
The effect of a lateral flare feature on implant stability
 International Orthopaedics DOI 10.1007/s00264-002-0355-3 Original Paper The effect of a lateral flare feature on implant stability Alex Leali( ) Joseph Fetto Harvey Insler David Elfenbein A. Leali J. Fetto
International Orthopaedics DOI 10.1007/s00264-002-0355-3 Original Paper The effect of a lateral flare feature on implant stability Alex Leali( ) Joseph Fetto Harvey Insler David Elfenbein A. Leali J. Fetto
Long-term Outcome of Polished Stems in Total Hip Arthroplasty
 ORIGINAL ARTICLE Hip Pelvis 27(2): 83-89, 2015 http://dx.doi.org/10.5371/hp.2015.27.2.83 Print ISSN 2287-3260 Online ISSN 2287-3279 Long-term Outcome of Polished Stems in Total Hip Arthroplasty Jin-Young
ORIGINAL ARTICLE Hip Pelvis 27(2): 83-89, 2015 http://dx.doi.org/10.5371/hp.2015.27.2.83 Print ISSN 2287-3260 Online ISSN 2287-3279 Long-term Outcome of Polished Stems in Total Hip Arthroplasty Jin-Young
ADDRESSING CLINICAL ISSUES OF CEMENTLESS HIP ARTHROPLASTY
 E C H E L O N P R I M A R Y H I P S Y S T E M P R O D U C T R A T I O N A L E ADDRESSING CLINICAL ISSUES OF CEMENTLESS HIP ARTHROPLASTY Echelon Primary Total Hip System HIGH OFFSET STANDARD OFFSET Cementless
E C H E L O N P R I M A R Y H I P S Y S T E M P R O D U C T R A T I O N A L E ADDRESSING CLINICAL ISSUES OF CEMENTLESS HIP ARTHROPLASTY Echelon Primary Total Hip System HIGH OFFSET STANDARD OFFSET Cementless
UDHT08.1.qxd:UDHT /03/08 17:14 Page 1. Surgical. Technique. Elbow Prosthesis. RHS Radial Head System.
 UDHT08.1.qxd:UDHT08.1 13/03/08 17:14 Page 1 Surgical Technique Elbow Prosthesis RHS Radial Head System www.tornier.com UDHT08.1.qxd:UDHT08.1 13/03/08 17:14 Page 2 TABLE OF CONTENTS DESIGN RATIONALE INDICATIONS
UDHT08.1.qxd:UDHT08.1 13/03/08 17:14 Page 1 Surgical Technique Elbow Prosthesis RHS Radial Head System www.tornier.com UDHT08.1.qxd:UDHT08.1 13/03/08 17:14 Page 2 TABLE OF CONTENTS DESIGN RATIONALE INDICATIONS
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR
 CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
Results of Conversion Total Hip Prosthesis Performed Following Painful Hemiarthroplasty
 M Nomura, S The Journal et al. of International Medical Research Endovascular 2000; 28: Embolization 307 312 of Unruptured Results of Conversion Total Hip Prosthesis Performed Following Painful Hemiarthroplasty
M Nomura, S The Journal et al. of International Medical Research Endovascular 2000; 28: Embolization 307 312 of Unruptured Results of Conversion Total Hip Prosthesis Performed Following Painful Hemiarthroplasty
U2 PSA. Revision Knee. Surgical Protocol
 U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 1 2 Tibial Preparation... 1 2.1 Tibial Canal Preparation... 1 2.2 Proximal Tibial Resection... 2 2.3 Non Offset Tibial
U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 1 2 Tibial Preparation... 1 2.1 Tibial Canal Preparation... 1 2.2 Proximal Tibial Resection... 2 2.3 Non Offset Tibial
Conversion of Anatomic TSA to RSA
 Conversion of Anatomic TSA to RSA Joseph A. Abboud, M.D. Professor of Shoulder and Elbow Surgery Senior Vice-President at the Rothman Institute Philadelphia, PA Disclosures Joseph A. Abboud, MD Depuy Synthes
Conversion of Anatomic TSA to RSA Joseph A. Abboud, M.D. Professor of Shoulder and Elbow Surgery Senior Vice-President at the Rothman Institute Philadelphia, PA Disclosures Joseph A. Abboud, MD Depuy Synthes
Developmental Dysplasia of the Hip Good Results of Later Total Hip Arthroplasty
 The Journal of Arthroplasty Vol. 23 No. 2 2008 Developmental Dysplasia of the Hip Good Results of Later Total Hip Arthroplasty 7135 Primary Total Hip Arthroplasties after Developmental Dysplasia of the
The Journal of Arthroplasty Vol. 23 No. 2 2008 Developmental Dysplasia of the Hip Good Results of Later Total Hip Arthroplasty 7135 Primary Total Hip Arthroplasties after Developmental Dysplasia of the
Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA
 Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA 94065 info@stinsonortho.com www.stinsonortho.com Encina HA Stem Table of Contents Introduction 3 Encina HA Stem Features 4 Surgical
Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA 94065 info@stinsonortho.com www.stinsonortho.com Encina HA Stem Table of Contents Introduction 3 Encina HA Stem Features 4 Surgical
SURGICAL TECHNIQUE. Alpine Cementless Hip Stem
 SURGICAL TECHNIQUE Alpine Cementless Hip Stem The following technique is a general guide for the instrumentation of the Alpine Cementless Hip Stem. It is expected that the surgeon is already familiar with
SURGICAL TECHNIQUE Alpine Cementless Hip Stem The following technique is a general guide for the instrumentation of the Alpine Cementless Hip Stem. It is expected that the surgeon is already familiar with
Early Results of Total Knee Replacements:
 Early Results of Total Knee Replacements: "A Clinical and Radiological Evaluation" K.S. Dhillon, FRCS* Jamal, MS* S. Bhupinderjeet, MBBS** * Dept. of Orthopaedic Surgery University of Malaya, Kuala Lumpur
Early Results of Total Knee Replacements: "A Clinical and Radiological Evaluation" K.S. Dhillon, FRCS* Jamal, MS* S. Bhupinderjeet, MBBS** * Dept. of Orthopaedic Surgery University of Malaya, Kuala Lumpur
EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY
 EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY Benkovich V. Perry T., Bunin A., Bilenko V., Unit for Joint Arthroplasty, Soroka Medical Center Ben Gurion University of Negev Beer
EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY Benkovich V. Perry T., Bunin A., Bilenko V., Unit for Joint Arthroplasty, Soroka Medical Center Ben Gurion University of Negev Beer
Absolut TM Cemented Stem. Surgical Technique
 Absolut TM Cemented Stem Surgical Technique Contents ABSOLUT Cemented Stem 2 Absolut Confidence 2 Absolut Reproducibility 2 Absolut Choice 2 Pre-Operative Planning 3 Suggested Templating Method 3 Surgical
Absolut TM Cemented Stem Surgical Technique Contents ABSOLUT Cemented Stem 2 Absolut Confidence 2 Absolut Reproducibility 2 Absolut Choice 2 Pre-Operative Planning 3 Suggested Templating Method 3 Surgical
Total Hip Arthroplasty Performed Using Conventional and Computer-Assisted, Tissue- Preserving Techniques 6
 Total Hip Arthroplasty Performed Using Conventional and Computer-Assisted, Tissue- Preserving Techniques 6 Stephen B. Murphy, MD, Timo M. Ecker, MD and Moritz Tannast, MD Introduction Less invasive techniques
Total Hip Arthroplasty Performed Using Conventional and Computer-Assisted, Tissue- Preserving Techniques 6 Stephen B. Murphy, MD, Timo M. Ecker, MD and Moritz Tannast, MD Introduction Less invasive techniques
Metal block augmentation for bone defects of the medial tibia during primary total knee arthroplasty
 Tsukada et al. Journal of Orthopaedic Surgery and Research 2013, 8:36 RESEARCH ARTICLE Open Access Metal block augmentation for bone defects of the medial tibia during primary total knee arthroplasty Sachiyuki
Tsukada et al. Journal of Orthopaedic Surgery and Research 2013, 8:36 RESEARCH ARTICLE Open Access Metal block augmentation for bone defects of the medial tibia during primary total knee arthroplasty Sachiyuki
Initial Evaluation on Subsidence of Cemented Collarless Polished Tapered Stem Applied to the Patients with Narrow Femoral Medullar Canal
 The Open Orthopaedics Journal, 2010, 4, 147-151 147 Open Access Initial Evaluation on Subsidence of Cemented Collarless Polished Tapered Stem Applied to the Patients with Narrow Femoral Medullar Canal
The Open Orthopaedics Journal, 2010, 4, 147-151 147 Open Access Initial Evaluation on Subsidence of Cemented Collarless Polished Tapered Stem Applied to the Patients with Narrow Femoral Medullar Canal
Short Term Clinical and Radiographic Results of the Salto Mobile Version Ankle Prosthesis
 Short Term Clinical and Radiographic Results of the Salto Mobile Version Ankle Prosthesis Dong Dong Wan, MD; Dong woo Shim, MD; Yoo Jung Park, MD; Yeokgu Hwang, MD; Jin Woo Lee, MD, PhD Department of Orthopaedic
Short Term Clinical and Radiographic Results of the Salto Mobile Version Ankle Prosthesis Dong Dong Wan, MD; Dong woo Shim, MD; Yoo Jung Park, MD; Yeokgu Hwang, MD; Jin Woo Lee, MD, PhD Department of Orthopaedic
RADIOGRAPHY OF THE ELBOW & HUMERUS
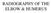 RADIOGRAPHY OF THE ELBOW & HUMERUS Patient Position: ELBOW AP Projection in same plane Part Position: Hand in ; patient Centered to Humeral epicondyles Central Ray: Structures Shown: AP Elbow Criteria
RADIOGRAPHY OF THE ELBOW & HUMERUS Patient Position: ELBOW AP Projection in same plane Part Position: Hand in ; patient Centered to Humeral epicondyles Central Ray: Structures Shown: AP Elbow Criteria
Efficacy Innovation ABG II. Brochure. Surgical Protocol. Cemented Stem
 Efficacy Innovation ABG II Cemented Stem Brochure Surgical Protocol 2 The ABG Hip System The ABG hip implant range has been progressively extended and enhanced over the past years, harnessing extensive
Efficacy Innovation ABG II Cemented Stem Brochure Surgical Protocol 2 The ABG Hip System The ABG hip implant range has been progressively extended and enhanced over the past years, harnessing extensive
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/38039 holds various files of this Leiden University dissertation. Author: Embden, Daphne van Title: Facts and fiction in hip fracture treatment Issue Date:
Cover Page The handle http://hdl.handle.net/1887/38039 holds various files of this Leiden University dissertation. Author: Embden, Daphne van Title: Facts and fiction in hip fracture treatment Issue Date:
Encina Taper Stem. Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA
 Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA 94065 info@stinsonortho.com www.stinsonortho.com Table of Contents Introduction 3 Features 4 Surgical Technique 5 Preoperative
Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA 94065 info@stinsonortho.com www.stinsonortho.com Table of Contents Introduction 3 Features 4 Surgical Technique 5 Preoperative
Inspiring people, Enriching lives
 TM Inspiring people, Enriching lives Encore Medical, L.P. 9800 Metric Blvd. Austin, Texas 78758 512-832-9500 www.encoremed.com Encore Medical, L.P. Cat. # 0177-170 1000 12/04 rev. A Encore and Revelation
TM Inspiring people, Enriching lives Encore Medical, L.P. 9800 Metric Blvd. Austin, Texas 78758 512-832-9500 www.encoremed.com Encore Medical, L.P. Cat. # 0177-170 1000 12/04 rev. A Encore and Revelation
Design Rationale. ECHELON Primary Hip System
 Design Rationale ECHELON Primary Hip System ECHELON Primary Total Hip System Addressing clinical issues of cementless hip arthroplasty Cementless total hip arthroplasty has provided a proven method of
Design Rationale ECHELON Primary Hip System ECHELON Primary Total Hip System Addressing clinical issues of cementless hip arthroplasty Cementless total hip arthroplasty has provided a proven method of
MINIMUM TEN-YEAR FOLLOW-UP OF COMPUTED TOMOGRAPHY BASED, CUSTOM CEMENTLESS STEM AFTER INTERTROCHANTERIC OSTEOTOMY FOR DYSPLASTIC HIPS
 (65) MINIMUM TEN-YEAR FOLLOW-UP OF COMPUTED TOMOGRAPHY BASED, CUSTOM CEMENTLESS STEM AFTER INTERTROCHANTERIC OSTEOTOMY FOR DYSPLASTIC HIPS YOSHIHIDE MASUDA Department of Orthopaedic Surgery, Nara Prefecture
(65) MINIMUM TEN-YEAR FOLLOW-UP OF COMPUTED TOMOGRAPHY BASED, CUSTOM CEMENTLESS STEM AFTER INTERTROCHANTERIC OSTEOTOMY FOR DYSPLASTIC HIPS YOSHIHIDE MASUDA Department of Orthopaedic Surgery, Nara Prefecture
Enhanced Stability Constrained Liners. Design Rationale Surgical Technique
 Enhanced Stability Constrained Liners Design Rationale Surgical Technique The Pinnacle Acetabular Cup System was designed to maximize the number of options available to the surgeon, and provide those options
Enhanced Stability Constrained Liners Design Rationale Surgical Technique The Pinnacle Acetabular Cup System was designed to maximize the number of options available to the surgeon, and provide those options
The Norwegian Arthroplasty Register: 11 years and 73,000 arthroplasties
 Acta Orthopaedica Scandinavica ISSN: 1-647 (Print) (Online) Journal homepage: http://www.tandfonline.com/loi/iort19 The Norwegian Arthroplasty Register: 11 years and 73, arthroplasties Leif I Havelin,
Acta Orthopaedica Scandinavica ISSN: 1-647 (Print) (Online) Journal homepage: http://www.tandfonline.com/loi/iort19 The Norwegian Arthroplasty Register: 11 years and 73, arthroplasties Leif I Havelin,
CAUTION: Ceramic liners are not approved for use in the United States.
 Total Hip Prostheses, Self-Centering Hip Prostheses and Hemi-Hip Prostheses IMPORTANT: This essential product information sheet does not include all of the information necessary for selection and use of
Total Hip Prostheses, Self-Centering Hip Prostheses and Hemi-Hip Prostheses IMPORTANT: This essential product information sheet does not include all of the information necessary for selection and use of
SURGICAL TECHNIQUE CEMENTED & PRESS-FIT UNIFIED INSTRUMENTATION INTRAOPERATIVE FLEXIBILITY PROVEN BIOMECHANICS
 SURGICAL TECHNIQUE CEMENTED & PRESS-FIT UNIFIED INSTRUMENTATION INTRAOPERATIVE FLEXIBILITY PROVEN BIOMECHANICS INTRODUCTION The Summit Tapered Hip System s comprehensive set of implants and instruments
SURGICAL TECHNIQUE CEMENTED & PRESS-FIT UNIFIED INSTRUMENTATION INTRAOPERATIVE FLEXIBILITY PROVEN BIOMECHANICS INTRODUCTION The Summit Tapered Hip System s comprehensive set of implants and instruments
Retrospective Study of Patellar Tracking in an Anatomical, Motion Guided Total Knee Design. Adam I. Harris, M.D. & Michelle Ammerman
 Retrospective Study of Patellar Tracking in an Anatomical, Motion Guided Total Knee Design Adam I. Harris, M.D. & Michelle Ammerman History: The Total Condylar knee represented a significant advance in
Retrospective Study of Patellar Tracking in an Anatomical, Motion Guided Total Knee Design Adam I. Harris, M.D. & Michelle Ammerman History: The Total Condylar knee represented a significant advance in
art h ro plasty Heterotopic ossification after total knee 54/61 5 cases after 1-6 years follow-up
 46 Acra Orthop Scand 1997; 68 (1): 46-50 Heterotopic ossification after total knee art h ro plasty 54/61 5 cases after 1-6 years follow-up Christof P Rader, Thomas Barthel, Matthias Haase, Matthias Scheidler
46 Acra Orthop Scand 1997; 68 (1): 46-50 Heterotopic ossification after total knee art h ro plasty 54/61 5 cases after 1-6 years follow-up Christof P Rader, Thomas Barthel, Matthias Haase, Matthias Scheidler
Semiconstrained Primary and Revision Total Elbow Arthroplasty with Use of the Coonrad-Morrey Prosthesis
 1467 COPYRIGHT 2007 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Semiconstrained Primary and Revision Total Elbow Arthroplasty with Use of the Coonrad-Morrey Prosthesis By Lewis L. Shi, MD, David
1467 COPYRIGHT 2007 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Semiconstrained Primary and Revision Total Elbow Arthroplasty with Use of the Coonrad-Morrey Prosthesis By Lewis L. Shi, MD, David
Twenty-five-Year Results After Charnley Total Hip Arthroplasty in Patients Less than Fifty Years Old A CONCISE FOLLOW-UP OF A PREVIOUS REPORT*
 1066 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Twenty-five-Year Results After Charnley Total Hip Arthroplasty in Patients Less than Fifty Years Old A CONCISE FOLLOW-UP OF A
1066 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Twenty-five-Year Results After Charnley Total Hip Arthroplasty in Patients Less than Fifty Years Old A CONCISE FOLLOW-UP OF A
Anterior Approach Surgical Technique. Paragon Stem System. enabling people to enjoy life
 Anterior Approach Surgical Technique Paragon Stem System enabling people to enjoy life Contents Pre-Operative Planning... 2 Suggested Templating Method... 2 Surgical Technique... 3 Surgical Approach...
Anterior Approach Surgical Technique Paragon Stem System enabling people to enjoy life Contents Pre-Operative Planning... 2 Suggested Templating Method... 2 Surgical Technique... 3 Surgical Approach...
Total Knee Original System Primary Surgical Technique
 Surgical Procedure Total Knee Original System Primary Surgical Technique Where as a total hip replacement is primarily a bony operation, a total knee replacement is primarily a soft tissue operation. Excellent
Surgical Procedure Total Knee Original System Primary Surgical Technique Where as a total hip replacement is primarily a bony operation, a total knee replacement is primarily a soft tissue operation. Excellent
Zimmer NexGen MIS Tibial Component. Cemented Surgical Technique IMAGE TO COME
 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique IMAGE TO COME Zimmer NexGen MIS Tibial Component Cemented Surgical Technique 1 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique
Zimmer NexGen MIS Tibial Component Cemented Surgical Technique IMAGE TO COME Zimmer NexGen MIS Tibial Component Cemented Surgical Technique 1 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique
TORNIER AEQUALIS FX. Shoulder System SYSTEM OVERVIEW
 TORNIER AEQUALIS FX Shoulder System SYSTEM OVERVIEW Simple in design, but used for the most complex fractures Each year, approximately 4 million people in the United States seek medical care for shoulder
TORNIER AEQUALIS FX Shoulder System SYSTEM OVERVIEW Simple in design, but used for the most complex fractures Each year, approximately 4 million people in the United States seek medical care for shoulder
Case report: Pain L THR [ post THR 2 years; with history of trivial fall] Your Diagnosis?
![Case report: Pain L THR [ post THR 2 years; with history of trivial fall] Your Diagnosis? Case report: Pain L THR [ post THR 2 years; with history of trivial fall] Your Diagnosis?](/thumbs/78/78456133.jpg) Case report: Pain L THR [ post THR 2 years; with history of trivial fall] Your Diagnosis? Diagnosis: Ceramic head fracture In the 1970 s, Boutin implemented ceramic in modern total hip arthroplasty (THA).
Case report: Pain L THR [ post THR 2 years; with history of trivial fall] Your Diagnosis? Diagnosis: Ceramic head fracture In the 1970 s, Boutin implemented ceramic in modern total hip arthroplasty (THA).
Bone Conserving Hip Replacement Surgical technique
 MiniHip Bone Conserving Hip Replacement Surgical technique MiniHip Contents Operative summary 4 Overview 5 Pre-operative templating 6 Operative technique 7 Neck resection 7 Femoral canal preparation 7
MiniHip Bone Conserving Hip Replacement Surgical technique MiniHip Contents Operative summary 4 Overview 5 Pre-operative templating 6 Operative technique 7 Neck resection 7 Femoral canal preparation 7
Intramedullary Tibial Preparation
 Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
Surgical Care of the Lower Extremity in Rheumatoid Arthritis*
 Surgical Care of the Lower Extremity in Rheumatoid Arthritis* ROBY C. THOMPSON, JR., M. D. Professor of Orthopedic Surgery, University of Virginia School of Medicine, Charlottesville One of the most important
Surgical Care of the Lower Extremity in Rheumatoid Arthritis* ROBY C. THOMPSON, JR., M. D. Professor of Orthopedic Surgery, University of Virginia School of Medicine, Charlottesville One of the most important
Kiernan, Sverrir; Hermann, K L; Wagner, Philippe; Ryd, Leif; Flivik, Gunnar
 The importance of adequate stem anteversion for rotational stability in cemented total hip replacement: A radiostereometric study with ten-year follow-up. Kiernan, Sverrir; Hermann, K L; Wagner, Philippe;
The importance of adequate stem anteversion for rotational stability in cemented total hip replacement: A radiostereometric study with ten-year follow-up. Kiernan, Sverrir; Hermann, K L; Wagner, Philippe;
RECOVERY. P r o t r u s i o
 RECOVERY P r o t r u s i o TM C a g e RECOVERY P r o t r u s i o TM C a g e Design Features Revision acetabular surgery is a major challenge facing today s total joint revision surgeon. Failed endo/bi-polars,
RECOVERY P r o t r u s i o TM C a g e RECOVERY P r o t r u s i o TM C a g e Design Features Revision acetabular surgery is a major challenge facing today s total joint revision surgeon. Failed endo/bi-polars,
Operations included in the National Joint Registry (NJR) Quick links, go to: Hips > Knees > Ankles > Elbows > Shoulders > Trauma >
 Operations included in the National Joint Registry (NJR) Quick links, go to: Hips > Knees > Ankles > Elbows > Shoulders > Trauma > Version 5 December 2013 1 Version control Version number Date Amendments
Operations included in the National Joint Registry (NJR) Quick links, go to: Hips > Knees > Ankles > Elbows > Shoulders > Trauma > Version 5 December 2013 1 Version control Version number Date Amendments
11/9/15. Total Elbow Arthroplasty. Who would not want this Patient? I have 3 hours of Free Time!!! KRISTOPHER R. AVANT, DO
 Total Elbow Arthroplasty KRISTOPHER R. AVANT, DO SOUTH W E ST ORTH OP A E DIC SP EC IALISTS BONE & JOINT HOSPITAL OKLAHOMA CITY, OK Who would not want this Patient? I have 3 hours of Free Time!!! 1 A comparison
Total Elbow Arthroplasty KRISTOPHER R. AVANT, DO SOUTH W E ST ORTH OP A E DIC SP EC IALISTS BONE & JOINT HOSPITAL OKLAHOMA CITY, OK Who would not want this Patient? I have 3 hours of Free Time!!! 1 A comparison
Surgical Technique. Hip System
 Surgical Technique Hip System INDICATIONS FOR USE The TaperSet Hip System is designed for total or partial hip arthroplasty and is intended to be used with compatible components of the Consensus Hip System.
Surgical Technique Hip System INDICATIONS FOR USE The TaperSet Hip System is designed for total or partial hip arthroplasty and is intended to be used with compatible components of the Consensus Hip System.
Early failure of total hip replacements implanted at distant hospitals to reduce waiting lists
 : 31 35 doi 10.1308/1478708051450 Audit Early failure of total hip replacements implanted at distant hospitals to reduce waiting lists Jac Ciampolini, Matthew JW Hubble Princess Elizabeth Orthopaedic Centre,
: 31 35 doi 10.1308/1478708051450 Audit Early failure of total hip replacements implanted at distant hospitals to reduce waiting lists Jac Ciampolini, Matthew JW Hubble Princess Elizabeth Orthopaedic Centre,
Predicting the Position of the Femoral Head Center
 The Journal of Arthroplasty Vol. 14 No. 1 1999 Predicting the Position of the Femoral Head Center Nobuhiko Sugano, MD, Philip C. Noble, PhD, and Emir Kamaric, MS Abstract: To find an accurate method to
The Journal of Arthroplasty Vol. 14 No. 1 1999 Predicting the Position of the Femoral Head Center Nobuhiko Sugano, MD, Philip C. Noble, PhD, and Emir Kamaric, MS Abstract: To find an accurate method to
DESIGN RATIONALE AND SURGICAL TECHNIQUE
 DESIGN RATIONALE AND SURGICAL TECHNIQUE ANCHOR PEG GLENOID DESIGN RATIONALE In total shoulder arthroplasty, most cases of clinical and radiographic loosening involve failure of the fixation of the glenoid
DESIGN RATIONALE AND SURGICAL TECHNIQUE ANCHOR PEG GLENOID DESIGN RATIONALE In total shoulder arthroplasty, most cases of clinical and radiographic loosening involve failure of the fixation of the glenoid
INTRAMEDULLARY CANCELLOUS BONE BLOCK TO IMPROVE FEMORAL STEM FIXATION IN CHARNLEY LOW-FRICFION ARTHROPLASTY B. M. WROBLEWSKI, ADRIAN VAN DER RIJT
 INTRAMEDULLARY CANCELLOUS BONE BLOCK TO IMPROVE FEMORAL STEM FIXATION IN CHARNLEY LOW-FRICFION ARTHROPLASTY B. M. WROBLEWSKI, ADRIAN VAN DER RIJT From the Centrefor Hip Surgery, Wrightington, Wigan In
INTRAMEDULLARY CANCELLOUS BONE BLOCK TO IMPROVE FEMORAL STEM FIXATION IN CHARNLEY LOW-FRICFION ARTHROPLASTY B. M. WROBLEWSKI, ADRIAN VAN DER RIJT From the Centrefor Hip Surgery, Wrightington, Wigan In
Revision of the humeral component for aseptic loosening in arthroplasty of the shoulder
 Revision of the humeral component for aseptic loosening in arthroplasty of the shoulder A. Cil, C. J. H. Veillette, J. Sanchez-Sotelo, J. W. Sperling, C. Schleck, R. H. Cofield From the Mayo Clinic, Rochester,
Revision of the humeral component for aseptic loosening in arthroplasty of the shoulder A. Cil, C. J. H. Veillette, J. Sanchez-Sotelo, J. W. Sperling, C. Schleck, R. H. Cofield From the Mayo Clinic, Rochester,
A further enhanced classic. Wagner SL Revision Hip Stem
 A further enhanced classic Wagner SL Revision Hip Stem The original Wagner SL Revision Stem offers a time-proven solution in the treatment of revision hips. While its underlying anchorage philosophy and
A further enhanced classic Wagner SL Revision Hip Stem The original Wagner SL Revision Stem offers a time-proven solution in the treatment of revision hips. While its underlying anchorage philosophy and
SURGICAL TECHNIQUE. Alpine Cemented Hip Stem
 SURGICAL TECHNIQUE Alpine Cemented Hip Stem The following technique is a general guide for the instrumentation of the Alpine Cemented Hip Stem. It is expected that the surgeon is already familiar with
SURGICAL TECHNIQUE Alpine Cemented Hip Stem The following technique is a general guide for the instrumentation of the Alpine Cemented Hip Stem. It is expected that the surgeon is already familiar with
Elbow Fractures ORIF VS Arthroplasty
 Elbow Fractures ORIF VS Arthroplasty Oke Anakwenze, M.D. Olympus Orthopedics No disclosures Disclosures Distal humerus fractures 0.5-0.7% of all fractures 30% of all elbow fractures Bimodal etiology Young
Elbow Fractures ORIF VS Arthroplasty Oke Anakwenze, M.D. Olympus Orthopedics No disclosures Disclosures Distal humerus fractures 0.5-0.7% of all fractures 30% of all elbow fractures Bimodal etiology Young
15-Year Follow-up Study of Total Knee Arthroplasty in Patients With Rheumatoid Arthritis
 The Journal of Arthroplasty Vol. 18 No. 8 2003 15-Year Follow-up Study of Total Knee Arthroplasty in Patients With Rheumatoid Arthritis Jun Ito, MD, PhD, Tomihisa Koshino, MD, PhD, Renzo Okamoto, MD, PhD,
The Journal of Arthroplasty Vol. 18 No. 8 2003 15-Year Follow-up Study of Total Knee Arthroplasty in Patients With Rheumatoid Arthritis Jun Ito, MD, PhD, Tomihisa Koshino, MD, PhD, Renzo Okamoto, MD, PhD,
Integra. Modular Radial Head System SURGICAL TECHNIQUE
 Integra Modular Radial Head System SURGICAL TECHNIQUE Table of Contents System Overview...2 Indications and Contraindications... 3 Modular Radial Head Implant Technique...4 Component Dimensions...8 Implant
Integra Modular Radial Head System SURGICAL TECHNIQUE Table of Contents System Overview...2 Indications and Contraindications... 3 Modular Radial Head Implant Technique...4 Component Dimensions...8 Implant
Aesculap Trilliance Triple Tapered Polished Hip Stem
 Aesculap Trilliance Triple Tapered Polished Hip Stem Aesculap Orthopaedics Trilliance Triple Tapered Polished Hip Stem CONTENTS 2 Contents Page Trilliance Philosophy 4 Trilliance Design 6 Trilliance Implants
Aesculap Trilliance Triple Tapered Polished Hip Stem Aesculap Orthopaedics Trilliance Triple Tapered Polished Hip Stem CONTENTS 2 Contents Page Trilliance Philosophy 4 Trilliance Design 6 Trilliance Implants
10-year results following impaction bone grafting of major bone defects in 29 rotational and hinged knee revision arthroplasties
 Acta Orthopaedica 2013; 84 (4): 387 391 387 10-year results following impaction bone grafting of major bone defects in 29 rotational and hinged knee revision arthroplasties A follow-up of a previous report
Acta Orthopaedica 2013; 84 (4): 387 391 387 10-year results following impaction bone grafting of major bone defects in 29 rotational and hinged knee revision arthroplasties A follow-up of a previous report
Complications of Total Knee Arthroplasty
 Progress in Clinical Medicine Complications of Total Knee Arthroplasty JMAJ 44(5): 235 240, 2001 Shinichi YOSHIYA*, Masahiro KUROSAKA** and Ryosuke KURODA*** *Director, Department of Orthopaedic Surgery,
Progress in Clinical Medicine Complications of Total Knee Arthroplasty JMAJ 44(5): 235 240, 2001 Shinichi YOSHIYA*, Masahiro KUROSAKA** and Ryosuke KURODA*** *Director, Department of Orthopaedic Surgery,
S U R G I C A L T E C H N I Q U E
 SURGICAL TECHNIQUE RECOVERY FUNCTION SURVIVORSHIP DePuy believes in an approach to total hip replacement that places equal importance on recovery, function and survivorship. The DePuy PROXIMA Hip System
SURGICAL TECHNIQUE RECOVERY FUNCTION SURVIVORSHIP DePuy believes in an approach to total hip replacement that places equal importance on recovery, function and survivorship. The DePuy PROXIMA Hip System
TaperFill. Surgical Technique
 TaperFill Surgical Technique Table of Contents Indications and Contraindications 3 TaperFill Hip Size Charts 4-5 DJO Surgical 9800 Metric Boulevard Austin, TX (800) 456-8696 www.djosurgical.com Preoperative
TaperFill Surgical Technique Table of Contents Indications and Contraindications 3 TaperFill Hip Size Charts 4-5 DJO Surgical 9800 Metric Boulevard Austin, TX (800) 456-8696 www.djosurgical.com Preoperative
