Semiconstrained Primary and Revision Total Elbow Arthroplasty with Use of the Coonrad-Morrey Prosthesis
|
|
|
- Tyrone Robertson
- 5 years ago
- Views:
Transcription
1 1467 COPYRIGHT 2007 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Semiconstrained Primary and Revision Total Elbow Arthroplasty with Use of the Coonrad-Morrey Prosthesis By Lewis L. Shi, MD, David Zurakowski, PhD, Deryk G. Jones, MD, Mark J. Koris, MD, and Thomas S. Thornhill, MD Investigation performed at the Department of Orthopaedic Surgery, Brigham and Women s Hospital, Boston; Children s Hospital Boston, Boston, Massachusetts, and at the Department of Orthopaedic Surgery, Tulane University Health Sciences Center, New Orleans, Louisiana Background: Semiconstrained total elbow prostheses are used routinely by many surgeons to treat a variety of severe elbow disorders. Our objective was to review the results of primary and revision total elbow arthroplasty with use of the Coonrad-Morrey prosthesis. The selected use of this semiconstrained implant in patients with instability and poor bone stock was hypothesized to provide inferior results compared with those in the published reports. Methods: The results of sixty-seven semiconstrained total elbow arthroplasties that were performed in fifty-six patients between 1990 and 2003 were evaluated. Thirty-seven elbows had a primary arthroplasty and were followed for a mean of eighty-six months, and thirty elbows had a revision arthroplasty and were followed for a mean of sixty-eight months. Mayo elbow performance scores and radiographic analyses were used to assess the clinical results. Results: In the primary arthroplasty group, the average flexion improved from 116 to 135 ; average extension, from 40 to 33 ; average pronation, from 60 to 81 ; and average supination, from 60 to 69. The improvements in flexion and pronation were significant (p < for both). Preoperatively, twenty-five (74%) of thirty-four elbows with data available had moderate or severe pain, whereas only four (11%) had pain postoperatively. The average postoperative Mayo score (and standard deviation) was 84 ± 16. Eleven of the thirty-seven primary replacements failed, and the five-year survival rate was 72%. In the revision arthroplasty group, average flexion improved from 124 to 131 ; average extension, from 32 to 22 ; average pronation, from 66 to 75 ; and average supination, from 64 to 76 ; the improvement in supination was significant (p < 0.05). Preoperatively, eighteen (64%) of the twenty-eight elbows with data available had moderate or severe pain, while only five (17%) had pain postoperatively. The average postoperative Mayo score was 85 ± 16. Eleven of the thirty revision replacements failed, and the fiveyear survival rate was 64%. Conclusions: A Coonrad-Morrey semiconstrained total elbow arthroplasty provides excellent pain relief and good functional return in patients with severe destructive arthropathy. The higher prevalence of failure in this cohort compared with series reported elsewhere is likely due to adverse patient selection as this implant was reserved for more complex arthroplasties with severe bone loss and ligamentous laxity. Level of Evidence: Therapeutic Level IV. See Instructions to Authors for a complete description of levels of evidence. Total elbow arthroplasty has been reported to be successful with use of both linked, or semiconstrained, and unlinked, or resurfacing, prostheses 1. In the last thirty years, advancements in the design of total elbow prostheses have reduced the rate of complications, but patients with complex elbow disorders continue to pose surgical challenges. The initial use of single-axis, metal-hinged total elbow prostheses was associated with high failure rates because of aseptic loosening 2-5. As a Disclosure: The authors did not receive any outside funding or grants in support of their research for or preparation of this work. Neither they nor a member of their immediate families received payments or other benefits or a commitment or agreement to provide such benefits from a commercial entity. No commercial entity paid or directed, or agreed to pay or direct, any benefits to any research fund, foundation, division, center, clinical practice, or other charitable or nonprofit organization with which the authors, or a member of their immediate families, are affiliated or associated. J Bone Joint Surg Am. 2007;89: doi: /jbjs.f.00715
2 1468 result, the use of unlinked, or resurfacing, prostheses has become popular. Several groups of investigators have reported lower rates of aseptic loosening with unlinked implants, but they also noted early postoperative complications such as dislocation, subluxation, and transient nerve palsy 6-9. As a result, semiconstrained prostheses are used in many centers and are used routinely by some surgeons. The Coonrad-Morrey total elbow prosthesis (Zimmer, Warsaw, Indiana) is a semiconstrained implant that was used first at our institution in Investigators at the Mayo Clinic and elsewhere have described long-term outcomes of the Coonrad-Morrey prosthesis when they were used routinely All reported that >80% of the patients had excellent or good results at the time of the latest follow-up. Most patients had good elbow function and good pain relief. The studies had failure rates, defined as the need for revision surgery, ranging from 5% to 22%. At our institution, the Coonrad-Morrey prosthesis has not been used routinely but rather has been the elbow implant of choice for patients with extensive capsuloligamentous injury, atrophic musculature, and loss of considerable bone stock. Moreover, it was the most common revision total elbow arthroplasty used during the period of this study. Typical patients include those with end-stage rheumatoid arthritis with extensive bone loss, severe posttraumatic arthritis, or failed resurfacing and semiconstrained replacements. The objective of the present study was to review the results of the primary and revision Coonrad-Morrey total elbow arthroplasties in these selected patients. Primary and revision total elbow replacements were analyzed separately with regard to functional outcome, survival rate, and complications. Materials and Methods ne hundred and two Coonrad-Morrey total elbow ar- were performed for eighty-six patients at our Othroplasties institution between July 1990 and November 2003, as identified by hospital records. Sixty patients were alive at the time of this review, according to the Social Security Death Index ( Every patient was contacted by telephone to urge them to return for a follow-up evaluation. A previously described protocol was used to ascertain the contact information of the patients who were lost to follow-up 15. All but one of the sixty patients were reached on the telephone. Thirty-nine patients (forty-six elbows) returned to the clinic, eleven (fifteen elbows) were evaluated in their homes or offices, and, for one patient (one elbow), the outside hospital records were reviewed. At the time of writing, nine patients had not yet returned for follow-up. Twenty-six patients died prior to the review, and only five of those patients (five elbows) are included in this report as they had greater than twenty-four months of follow-up, defined as the elapsed time from the index procedure to the most recent clinic visit that included a history, a physical examination, and radiographs. All subjects gave informed consent to participate in the study, and the study was approved by our institutional review board. Sixty-seven Coonrad-Morrey total elbow arthroplasties are included in the data analyses (Table I). The average age of the thirty patients (thirty-seven elbows) who had primary total elbow arthroplasty was sixty-one years (range, thirty-five to eighty-seven years) at the time of surgery, and they had a mean length of follow-up of eighty-six months (range, twenty-seven to 168 months). The diagnoses were rheumatoid arthritis (six- TABLE I Characteristics of the Study Cohorts Primary Total Elbow Arthroplasty (N = 37) Revision Total Elbow Arthroplasty (N = 30) Age at time of surgery* (yr) 61 ± 14 (35-87) 65 ± 9 (43-77) Gender No. (%) of elbows in female patients 28 (76) 26 (87) No. (%) of elbows in male patients 9 (24) 4 (13) Side Left 11 (30) 10 (33) Right 26 (70) 20 (67) Diagnosis Rheumatoid arthritis 16 (43) 24 (80) Posttraumatic osteoarthritis 10 (27) 0 (0) Trauma 9 (24) 4 (13) Osteoarthritis 1 (3) 2 (7) Hemophiliac arthropathy 1 (3) 0 (0) Dominant arm 19 (51) 19 (63) Failures 11 (30) 11 (37) *The values are given as the mean and the standard deviation, with the range in parentheses. The values are given as the number of elbows, with the percentage in parentheses.
3 1469 Fig. 1 Kaplan-Meier survivorship curve for primary total elbow replacements. Each stepwise decline between the beginning point and the end point on the curve represents a failure that happened at a specific time after the index procedure. With each of the eleven failures, there is a lowering of the survivorship percentage. The bars bracketing each point indicate the 95% confidence interval for the survivorship at that time. The numbers in parentheses on the x-axis represent the number of total elbow replacements that survived at a given time after surgery; the decreasing trend in these numbers is due to a combination of failures and those that were no longer being followed. The five-year survival rate is 72% (95% confidence interval, 62% to 82%). teen elbows), posttraumatic arthritis (ten), trauma (nine), osteoarthritis (one), and hemophiliac arthritis (one). There were thirty revision total elbow arthroplasties. The average age of the twenty-six patients (thirty elbows) who had revision arthroplasty was sixty-five years (range, forty-three to seventyseven years) at the time of surgery, and they had a mean length of follow-up of sixty-eight months (range, twenty-four to 167 months); the diagnoses were rheumatoid arthritis (twentyfour elbows), trauma (four), and osteoarthritis (two). Only one patient who had a total elbow arthroplasty with less than twenty-four months of follow-up is included in the data analyses because the elbow was found to be infected at ten months after the surgery. Fifty-eight of the sixty-seven total elbow arthroplasties were performed by the two senior authors (M.J.K. and T.S.T.); the remaining nine were performed by five surgeons who also had hand and/or upper extremity or arthroplasty fellowship training. The Coonrad-Morrey Total Prosthesis The semiconstrained Coonrad-Morrey prosthesis with fixation of both stems with cement was used in all patients. The implant allows for 7 to 10 of varus-valgus movement and 7 to 10 of axial rotation 16. There were minor changes in the component design during the study period: the central locking pin was redesigned in 1996, and the ulnar component changed from a beaded surface to a precoat of polymethylmethacrylate in 1992 and then back to a beaded surface in The modified Kocher or triceps-splitting surgical approach was used in all patients. The ulnar nerve was isolated but was not routinely transposed. On occasion, the medial epicondyle was excised. When possible, the medial head of the triceps was preserved. If it was removed, it was reattached through holes in the ulna and, if possible, was fortified with the anconeus. The radial head was excised in all patients. Of note, humeral allografts were required in seven revision arthroplasties, one of which also needed an ulnar allograft. Data Collection For each patient, hand dominance, range of motion (flexion, extension, supination, and pronation), stability, pain level, and functionality of the affected elbow(s) were recorded. Preoperative data were gathered from the written and electronic
4 1470 TABLE II Range of Motion and Evaluation Scores for Thirty-seven Elbows That Had Primary Total Elbow Arthroplasty Variable Preop. Postop. P Value Range of motion* (deg) Flexion 116 ± ± 13 <0.001 Extension 40 ± ± Pronation 60 ± ± 17 <0.001 Supination 60 ± ± Pain score* 12 ± ± 12 <0.001 Mayo score* 44 ± ± 16 <0.001 Level of pain <0.001 None 3 (9) 23 (62) Mild 6 (18) 10 (27) Moderate 10 (29) 4 (11) Severe 15 (44) 0 (0) *The values are given as the mean and standard deviation. The difference was significant. The values are given as the number of elbows with the percentage in parentheses. Preoperative pain scores were not obtained for three patients. medical record. Postoperative data were gathered from the medical record, clinic evaluations, or home visit evaluations. Mayo elbow performance scores were used in the analyses 17 ; the 100-point system contains four components: pain, motion (flexion arc), stability, and function and/or activity. Some patients with elbow injuries had incomplete preoperative data, as a thorough evaluation (i.e., range of motion) was not appropriate in some of those situations. Also of note, the function and/or activity component of the preoperative Mayo scores for approximately one-quarter of the patients was estimated from the history if specific activities were not noted. Postoperative anteroposterior and lateral radiographs of the elbows were analyzed to evaluate component position, cementing technique, and radiolucent lines. Radiolucencies were examined for progression over time. Failures were defined as arthroplasties that required revision or resection, or those that had radiographic signs of failure (i.e., progressive radiolucencies over time or a radiolucency of >2 mm between the implant and cement on any one radiograph). Dates of the onset of failure were noted. Statistical Analysis All continuous variables were tested for normality with use of the Kolmogorov-Smirnov test, and no significant skewness was detected. Therefore, age, range of motion, pain scores, and Mayo scores are presented as means and standard deviations. Primary and revision groups were compared with respect to age, gender, side, dominant arm, and diagnosis by univariate analysis with the two-sample Student t test for continuous variables and the Fisher exact test for categorical variables. Preoperative and postoperative range of motion as well as pain scores and Mayo scores were tested for each of the two cohorts (primary and revision groups) with use of paired t tests. Changes in the level of pain (none, mild, moderate, or severe) were evaluated with use of the nonparametric Wilcoxon signed-rank test 18. For each group, time to failure was analyzed with use of the Kaplan-Meier product-limit method with 95% confidence intervals around the curves as calculated by the Greenwood formula 19. This survivorship method accounts for so-called censoring (i.e., elbows that had not had failure but continued to be at risk for failure). For multivariate analysis, both multiple logistic regression (stepwise backward selection) and the Cox proportional-hazards model were applied to control for confounding and to evaluate possible predictors of failure, including age, gender, side, dominant arm, diagnosis, and preoperative Mayo score 20. Statistical analysis was performed with the SPSS software package (version 14.0; SPSS, Chicago, Illinois). All two-tailed p values of <0.05 were considered significant. Power analysis indicated that the patient sample sizes of the primary (thirty-seven elbows) and revision groups (thirty elbows) provided 90% power to detect significant changes of at least one standard deviation in each of the range-of-motion variables, pain scores, and Mayo scores on the basis of paired t tests (two-tailed α = 0.05, β = 0.10). In addition, precision of the Kaplan-Meier survivorship curves as determined by error bars representing 95% confidence intervals would be to within 10% to 15% of the estimated steps along the curves (version 6.0, nquery Advisor; Statistical Solutions, Saugus, Massachusetts). Results Primary Arthroplasties n the thirty-seven elbows that had primary total arthroplasty, all range-of-motion measurements improved after I the elbow replacement (Table II). Average flexion improved from 116 ± 21 to 135 ± 13 (p < 0.001). Average extension improved from 40 ± 29 to 33 ± 23 (p = 0.30). Average pronation improved from 60 ± 24 to 81 ± 17 (p < 0.001).
5 1471 TABLE III List of Failed Primary Total Elbow Replacements Case Gender Diagnosis Length of Survival of Total Elbow Replacement (mo) Reasons for Failure Treatment 1 F Rheumatoid arthritis 48.8 Loose humeral component and broken bushing Revision 2 F Posttraumatic arthritis Loose ulnar and humeral components, broken bushing, bone loss, and triceps avulsion Revision 3 F Rheumatoid arthritis 61.1 Loose humeral component and osteolysis Revision 4 F Osteoarthritis 26.3 Periprosthetic fracture of distal end of humerus Revision 5 F Trauma 51.5 Loose humeral component Revision 6 M Rheumatoid arthritis 14.4 Loose ulnar component and periprosthetic fracture Revision 7 F Posttraumatic arthritis 25.9 Loose ulnar and humeral components and severe osteolysis Revision 8 M Posttraumatic arthritis 1.6 Infection Resection 9 F Traumatic 0.5 Infection Resection 10 M Traumatic 22.1 Infection Resection 11 M Posttraumatic arthritis 52.2 Loose ulnar component None Supination improved from 60 ± 24 to 69 ± 24 (p = 0.16). Twenty-five (74%) of the thirty-four elbows with data available had moderate or severe pain preoperatively, and only four (11%) had moderate or severe pain postoperatively. This difference was significant (p < 0.001). When converted to a numerical measure as a component of the Mayo score (with 0 Fig. 2 Kaplan-Meier survivorship curve for revision total elbow replacements. With each of the eleven failures, there is a lowering of the survivorship percentage. The five-year survival rate is 64% (95% confidence interval, 50% to 78%).
6 1472 TABLE IV Comparison of Primary Total Elbow Replacements That Failed and Those That Survived Variable Replacements That Survived (n = 26) Replacements That Failed (n = 11) P Value Age* (yr) 59 ± ± Preop. Mayo score* 50 ± ± 16 <0.01 Gender 0.40 No. (%) of elbows in female patients 21 (81) 7 No. (%) of elbows in male patients 5 (19) 4 Diagnosis 0.47 Rheumatoid arthritis 12 (46) 3 Other 14 (54) 8 Dominant arm 11 (42) *The values are given as the mean and the standard deviation. According to multivariate analysis, the preoperative Mayo score was the only significant predictor of radiographic failure. The values are given as the number of elbows, with the percentage in parentheses. indicating severe pain; 15, moderate pain; 30, mild pain; and 45, no pain), the average pain score improved significantly from 12 ± 12 preoperatively to 36 ± 12 postoperatively (p < 0.001). In the primary total elbow arthroplasty group, the Mayo score increased from an average of 44 ± 21 preoperatively to an average of 84 ± 16 postoperatively (p < 0.001). Eleven of the thirty-seven primary total elbow replacements failed. Seven of the failed elbows were revised, three were resected, and one was treated nonoperatively (Table III). The primary reason for the seven revisions was periprosthetic fracture in two, humeral component loosening in three, and loosening of both components in two. All three total elbow replacements that were resected had an infection around the prosthesis. In one patient who had failure, progressive radiolucencies of the ulnar component were seen on radiographs; the prosthesis was not revised because the patient preferred to tolerate the symptoms. Multiple logistic regression analysis and the Cox proportional-hazards model were used to evaluate possible predictors of failure, including age, gender, side, dominant arm, diagnosis of rheumatoid arthritis, and preoperative Mayo score (Table IV). Among these factors, the preoperative Mayo score was the only significant predictor of failure (p < 0.01). A Kaplan-Meier survivorship curve was generated to depict the eleven failures among the thirty-seven primary total elbow replacements (Fig. 1). The five-year survival rate was 72% (95% confidence interval, 62% to 82%). Of the twenty-six primary total elbow replacements that did not fail, six elbows had a flexion contracture of >45, one elbow had transient ulnar neuropathy (less than six months), one had persistent ulnar neuropathy (greater than one year), and one had triceps avulsion. Revision Arthroplasties In the thirty elbows that had revision arthroplasty, all rangeof-motion measurements improved after the surgery (Table V), although not by as great a magnitude as they had in the primary arthroplasty group. Average flexion improved from 124 ± 22 to 131 ± 18 (p = 0.19). Average extension improved from 32 ± 27 to 22 ± 18 (p = 0.17). Average pronation improved from 66 ± 23 to 75 ± 25 (p = 0.07). Average supination improved from 64 ± 25 to 76 ± 21 (p < 0.05). Eighteen (64%) of the twenty-eight elbows with data available had moderate or severe pain preoperatively, and five (17%) had moderate or severe pain postoperatively (p < 0.001). When converted to a numerical measure, the average pain scores demonstrated a significant improvement from 18 ± 11 preoperatively to 36 ± 13 postoperatively (p < 0.001). The Mayo score increased from an average of 56 ± 17 preoperatively to an average of 85 ± 16 postoperatively (p < 0.001). Among the thirty revision total elbow replacements, eleven failed (Table VI). Of the five that were revised, two had humeral component loosening, one had ulnar component loosening, one dislocated with a worn bushing, and one was precipitated by a fall that led to a nonunion of a mid-shaft humeral periprosthetic fracture. Moreover, five additional failures were detected radiographically and were treated nonoperatively because of patient preference and/or lack of symptoms. These included one with humeral loosening and a humeral allograft nonunion, one with a periprosthetic fracture of an ulnar graft and graft nonunion, one with loosening of the ulnar component, and two with loosening of both the ulnar and humeral components. Another patient with a loose humeral component and nonunion of a humeral allograft was scheduled for revision with a custom prosthesis. Multiple logistic regression analysis and the Cox proportional-hazards model were used to evaluate possible predictors of failure (Table VII), yet none proved to be significant. A Kaplan- Meier survivorship curve for the thirty revision total elbow replacements was generated to depict the eleven failures (Fig. 2). The five-year survival rate was 64% (95% confidence interval, 50% to 78%). Of the nineteen revision total elbow replacements that did not fail, three elbows had a flexion contracture of >45. Four elbows had a persistent ulnar neuropathy lasting more
7 1473 TABLE V Range of Motion and Evaluation Scores for the Thirty Elbows That Had Revision Total Elbow Arthroplasty Variable Preop. Postop. P Value Range of motion* (deg) Flexion 124 ± ± Extension 32 ± ± Pronation 66 ± ± Supination 64 ± ± 21 <0.05 Pain score* 18 ± ± 13 <0.001 Mayo score* 56 ± ± 16 <0.001 Level of pain <0.001 None 0 (0) 18 (60) Mild 10 (36) 7 (23) Moderate 14 (50) 4 (13) Severe 4 (14) 1 (3) *The values are given as the mean and the standard deviation. The difference was significant. The values are given as the number of elbows, with the percentage in parentheses. Preoperative pain scores were not obtained for two elbows. than one year. Two elbows had an intraoperative humeral fracture, resulting in transient radial neuropathy in one of them and transient ulnar neuropathy in the other; these symptoms resolved within six months in both patients. One elbow had triceps avulsion. Ulnar component loosening was examined because of reports by other investigators that precoated ulnar components had a higher rate of loosening 21. At our institution, precoated ulnar components were used between February 1993 and June 2001, and six (12%) of fifty-one total elbow replacements had ulnar component loosening. Of the sixteen total elbow replacements with a beaded ulnar component surface, two had ulnar component loosening. With the numbers studied, there was no significant difference in the prevalence of loosening between the precoated and the beaded component surface components (p = 0.94). TABLE VI Failed Revision Total Elbow Replacements Case Gender Diagnosis Allograft Length of Survival of Total Elbow Replacement (mo) Reason for Failure Treatment 1 F Rheumatoid arthritis 56.4 Fall led to mid-humeral fracture that led to nonunion of periprosthetic fracture Revision 2 F Rheumatoid arthritis 48.1 Loose humeral component Revision 3 F Rheumatoid arthritis 7.2 Worn bushing and dislocation Revision 4 F Rheumatoid arthritis 18.9 Loose humeral component Revision 5 F Rheumatoid arthritis 10.3 Loose ulnar component Revision 6 F Rheumatoid arthritis Humerus 29.6 Allograft nonunion and loose humeral component None 7 M Trauma Humerus and ulna 2.5 Allograft nonunion and periprosthetic fracture of ulnar graft None 8 F Rheumatoid arthritis 28.9 Loose ulnar and humeral components None 9 F Rheumatoid arthritis 36.7 Loose ulnar and humeral components, osteolysis 10 M Rheumatoid arthritis 91.3 Loose ulnar component, plate fracture, and nonunion of periprosthetic fracture 11 F Rheumatoid arthritis Humerus 26.1 Allograft nonunion and loose humeral component None None Scheduled for revision with custom prosthesis
8 1474 TABLE VII Comparison of Revision Total Elbow Replacements That Failed and Those That Survived Variable Total Elbow Replacements That Survived (n = 19) Total Elbow Replacements That Failed (n = 11) P Value Age* (yr) 66 ± ± Preop. Mayo score* 59 ± ± Gender 0.61 No. of elbows in female patients 17 9 No. of elbows in male patients 2 2 Diagnosis 0.37 Rheumatoid arthritis Other 5 1 Dominant arm Use of allograft *The values are given as the mean and the standard deviation. Discussion he Mayo elbow performance scores in this study were T compared with those reported in other studies. The mean postoperative scores for the patients who had primary total elbow arthroplasty (84 ± 16) and those who had revision total elbow arthroplasty (85 ± 16) were lower than the mean scores in the other published series. The investigators who studied patients with rheumatoid arthritis have reported Mayo scores in the range of 87 to 94 11,13,14,22. Those who studied patients with traumatic or posttraumatic conditions have reported Mayo scores ranging from 84 to 95, with one outlier of 79 10,12,13,23,24. A common complication in the present series was dysfunction of the ulnar nerve. In both complex primary and revision total elbow arthroplasty, we routinely identified the ulnar nerve and protected it during the procedure. Despite these efforts, six (13%) of the forty-five elbows in which the replacement did not fail had ulnar neuropathy develop postoperatively, and the neuropathy persisted beyond one year for five of the six elbows. This is consistent with the findings in other studies in which ulnar neuropathy occurred within a few days after surgery in as many as 21% of the patients, with the rate of permanent ulnar nerve dysfunction ranging from 0 to 10% 4,10,11,25. Two elbows had intraoperative fracture of the humeral shaft; both were in the revision total elbow arthroplasty group and, in both elbows, the surgeon had noted particular difficulty with removal of the cement. Both patients were postmenopausal women, and underlying osteoporosis may have been a factor that contributed to the intraoperative fracture. This fracture rate is comparable with the reported frequency of this complication, which has ranged from 0% to 4% 4,11,12,22. In addition, one of them had an ulnar neuropathy and the other had a radial neuropathy develop postoperatively; both neuropathies resolved within six months of surgery. Cement removal in revision total elbow arthroplasty can be extremely difficult, and we frequently identify the radial and ulnar nerves and protect them during the cement removal. Triceps avulsion following total elbow arthroplasty is another common problem. In a recently published study of 887 arthroplasties, sixteen elbows (1.8%) had a triceps avulsion 26. In the current series, two elbows experienced this complication. Both arthroplasties were performed with a modified Kocher approach, and the triceps tendon was reflected, leaving the medial head intact. One patient had a reconstruction of the triceps mechanism; however, the triceps was still not able to overcome gravity thirty months after the reconstruction. It is our opinion that release and repair of the medial head of the triceps is associated with substantial morbidity and meticulous repair is essential to preserve function. Postoperative infection requiring implant resection occurred in three elbows (4%). This rate is comparable with other studies, in which the rate of deep infection has ranged from 0% to 9% 27. All three patients were in the primary arthroplasty group, and all three were treated by resection arthroplasty. Two of the three patients remained on chronic antibiotic suppression. The five-year survival rates for primary and revision total elbow replacements (72% and 64%, respectively) in the present study are notably lower than those reported in the Mayo Clinic series, in which elbow replacements in patients with rheumatoid arthritis had a five-year survival rate of 94.4% (95% confidence interval, 89% to 99.9%), with seventyeight prostheses at risk, and those in patients with posttraumatic arthritis had a survival rate of 80% (thirty-three of forty-one elbows) at a mean follow-up of 5.6 years 11,12. This is likely due to the broader definition of failure used in the present study and the characteristics of our patient population. Unlike many other reports that have defined failure as the need for additional surgery, our study also included radiographic and clinical failures that were treated nonoperatively because of the lack of patient symptoms, the preference of the patient, or anesthesia considerations. Moreover, at our institution, the Coonrad-Morrey prosthesis is reserved for patients
9 1475 with gross elbow instability and/or poor bone stock, whereas at the Mayo Clinic it has been routinely used for most elbow arthroplasties. In summary, the thirty-seven primary and thirty revision Coonrad-Morrey elbow replacements reviewed showed significant improvement in range of motion, function, and pain. The rates of common complications were comparable with those in other reports. The higher rates of failure may have been due to the broader definition of a surgical failure in this study and our practice of reserving the Coonrad-Morrey prosthesis for the more complex cases of elbows with severe bone loss and ligamentous laxity. Lewis L. Shi, MD Mark J. Koris, MD Thomas S. Thornhill, MD Department of Orthopaedic Surgery, Brigham and Women s Hospital, 75 Francis Street, Boston, MA address for T.S. Thornhill: tthornhill@partners.org David Zurakowski, PhD Children s Hospital Boston, 300 Longwood Avenue, Boston, MA Deryk G. Jones, MD Department of Orthopaedic Surgery, Tulane University Health Sciences Center, 1430 Tulane Avenue, S132, New Orleans, LA References 1. Cooney WP 3rd. Elbow arthroplasty: indications and implant selection. In: Morrey BF, editor. The elbow and its disorders. 2nd ed. Philadelphia: WB Saunders; p Dee R. Total replacement of the elbow joint. Orthop Clin North Am. 1973; 4: Garrett JC, Ewald FC, Thomas WH, Sledge CB. Loosening associated with G.S.B. hinge total elbow replacement in patients with rheumatoid arthritis. Clin Orthop Relat Res. 1977;127: Morrey BF, Bryan RS. Complications of total elbow arthroplasty. Clin Orthop Relat Res. 1982;170: Souter WA. Arthroplasty of the elbow with particular reference to metallic hinge arthroplasty in rheumatoid patients. Orthop Clin North Am. 1973;4: Ewald FC, Simmons ED Jr, Sullivan JA, Thomas WH, Scott RD, Poss R, Thornhill TS, Sledge CB. Capitellocondylar total elbow replacement in rheumatoid arthritis. Long-term results. J Bone Joint Surg Am. 1993;75: Erratum in: J Bone Joint Surg Am. 1993;75: Ruth JT, Wilde AH. Capitellocondylar total elbow replacement. A long-term follow-up study. J Bone Joint Surg Am. 1992;74: Ljung P, Jonsson K, Rydholm U. Short-term complications of the lateral approach for non-constrained elbow replacement. Follow-up of 50 rheumatoid elbows. J Bone Joint Surg Br. 1995;77: Weissman BN, Simmons BP, Thomas WH. Replacement of other joints. Radiol Clin North Am. 1995;33: Cobb TK, Morrey BF. Total elbow arthroplasty as primary treatment for distal humeral fractures in elderly patients. J Bone Joint Surg Am. 1997;79: Gill DR, Morrey BF. The Coonrad-Morrey total elbow arthroplasty in patients who have rheumatoid arthritis. A ten to fifteen-year follow-up study. J Bone Joint Surg Am. 1998;80: Schneeberger AG, Adams R, Morrey BF. Semiconstrained total elbow replacement for the treatment of post-traumatic osteoarthrosis. J Bone Joint Surg Am. 1997;79: Hildebrand KA, Patterson SD, Regan WD, MacDermid JC, King GJ. Functional outcome of semiconstrained total elbow arthroplasty. J Bone Joint Surg Am. 2000;82: Morrey BF, Adams RA. Semiconstrained arthroplasty for the treatment of rheumatoid arthritis of the elbow. J Bone Joint Surg Am. 1992;74: King PJ, Malin AS, Scott RD, Thornhill TS. The fate of patients not returning for follow-up five years after total knee arthroplasty. J Bone Joint Surg Am. 2004; 86: O Driscoll SW, An KN, Korinek S, Morrey BF. Kinematics of semi-constrained total elbow arthroplasty. J Bone Joint Surg Br. 1992;74: Morrey BF, An K. Functional evaluation of the elbow. In: Morrey BF, editor. The elbow and its disorders. 3rd ed. Philadelphia: WB Saunders; p Kocher MS, Zurakowski D. Clinical epidemiology and biostatistics: a primer for orthopaedic surgeons. J Bone Joint Surg Am. 2004;86: Harris EK, Albert A. Survivorship analysis for clinical studies. New York: Marcel Dekker; p Vittinghoff E, Glidden DV, Shiboski SC, McCulloch CE. Regression methods in biostatistics: linear, logistic, survival, and repeated measures models. New York: Springer; p Morrey BF. Personal communication; Connor PM, Morrey BF. Total elbow arthroplasty in patients who have juvenile rheumatoid arthritis. J Bone Joint Surg Am. 1998;80: Morrey BF, Adams RA. Semiconstrained elbow replacement for distal humeral nonunion. J Bone Joint Surg Br. 1995;77: Ramsey ML, Adams RA, Morrey BF. Instability of the elbow treated with semiconstrained total elbow arthroplasty. J Bone Joint Surg Am. 1999;81: King GJ, Adams RA, Morrey BF. Total elbow arthroplasty: revision with use of a non-custom semiconstrained prosthesis. J Bone Joint Surg Am. 1997; 79: Celli A, Arash A, Adams RA, Morrey BF. Triceps insufficiency following total elbow arthroplasty. J Bone Joint Surg Am. 2005;87: Morrey BF. Complications of elbow replacement surgery. In: Morrey BF, editor. The elbow and its disorders. 3rd ed. Philadelphia: WB Saunders; p
Kudo type-5 total elbow arthroplasty in mutilating rheumatoid arthritis
 Upper limb Kudo type-5 total elbow arthroplasty in mutilating rheumatoid arthritis A 5- TO 11-YEAR FOLLOW-UP T. Mori, H. Kudo, K. Iwano, T. Juji From the National Hospital Organization Sagamihara Hospital,
Upper limb Kudo type-5 total elbow arthroplasty in mutilating rheumatoid arthritis A 5- TO 11-YEAR FOLLOW-UP T. Mori, H. Kudo, K. Iwano, T. Juji From the National Hospital Organization Sagamihara Hospital,
Recurrent subluxation or dislocation after surgical
 )263( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY CASE REPORT Persistent Medial Subluxation of the Ulna with Radiotrochlear Articulation Amir R. Kachooei, MD; David Ring, MD, PhD Research
)263( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY CASE REPORT Persistent Medial Subluxation of the Ulna with Radiotrochlear Articulation Amir R. Kachooei, MD; David Ring, MD, PhD Research
Total Elbow Arthroplasty in Patients Who Have Juvenile Rheumatoid Arthritis
 This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. Total Elbow Arthroplasty in Patients Who Have Juvenile Rheumatoid Arthritis
This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. Total Elbow Arthroplasty in Patients Who Have Juvenile Rheumatoid Arthritis
Total Elbow Arthroplasty: an Update
 Total Elbow Arthroplasty: an Update Emilie Cheung, M.D. Associate Professor Chief, Shoulder and Elbow Service Stanford University Department of Orthopedic Surgery Procedure volumes and rates increased
Total Elbow Arthroplasty: an Update Emilie Cheung, M.D. Associate Professor Chief, Shoulder and Elbow Service Stanford University Department of Orthopedic Surgery Procedure volumes and rates increased
Elbow Fractures ORIF VS Arthroplasty
 Elbow Fractures ORIF VS Arthroplasty Oke Anakwenze, M.D. Olympus Orthopedics No disclosures Disclosures Distal humerus fractures 0.5-0.7% of all fractures 30% of all elbow fractures Bimodal etiology Young
Elbow Fractures ORIF VS Arthroplasty Oke Anakwenze, M.D. Olympus Orthopedics No disclosures Disclosures Distal humerus fractures 0.5-0.7% of all fractures 30% of all elbow fractures Bimodal etiology Young
From 1984 to 1995, 68 ankylosed elbows and 11
 Sloppy hinge prosthetic elbow replacement for post-traumatic ankylosis or instability D. P. Baksi From the Medical College and Hospitals, Calcutta, India From 1984 to 1995, 68 ankylosed elbows and 11 which
Sloppy hinge prosthetic elbow replacement for post-traumatic ankylosis or instability D. P. Baksi From the Medical College and Hospitals, Calcutta, India From 1984 to 1995, 68 ankylosed elbows and 11 which
11/9/15. Total Elbow Arthroplasty. Who would not want this Patient? I have 3 hours of Free Time!!! KRISTOPHER R. AVANT, DO
 Total Elbow Arthroplasty KRISTOPHER R. AVANT, DO SOUTH W E ST ORTH OP A E DIC SP EC IALISTS BONE & JOINT HOSPITAL OKLAHOMA CITY, OK Who would not want this Patient? I have 3 hours of Free Time!!! 1 A comparison
Total Elbow Arthroplasty KRISTOPHER R. AVANT, DO SOUTH W E ST ORTH OP A E DIC SP EC IALISTS BONE & JOINT HOSPITAL OKLAHOMA CITY, OK Who would not want this Patient? I have 3 hours of Free Time!!! 1 A comparison
Normal elbow function requires
 Review Article Total Elbow Arthroplasty: Current Options Andrew Choo, MD Matthew L. Ramsey, MD From the Department of Orthopaedic Surgery, The Rothman Institute, Thomas Jefferson University, Philadelphia,
Review Article Total Elbow Arthroplasty: Current Options Andrew Choo, MD Matthew L. Ramsey, MD From the Department of Orthopaedic Surgery, The Rothman Institute, Thomas Jefferson University, Philadelphia,
E ORIGINAL ARTICLE Low extra-articular (transcondylar) fractures of the distal humerus
 Shoulder & Elbow. ISSN 1758-5732 E ORIGINAL ARTICLE Low extra-articular (transcondylar) fractures of the distal humerus Alexander A. Weening, Kim M. Brouwer, Margaritha Adams & David Ring Orthopaedic Hand
Shoulder & Elbow. ISSN 1758-5732 E ORIGINAL ARTICLE Low extra-articular (transcondylar) fractures of the distal humerus Alexander A. Weening, Kim M. Brouwer, Margaritha Adams & David Ring Orthopaedic Hand
Int J Clin Exp Med 2015;8(8): /ISSN: /IJCEM Guoqing Zha, Xiaofeng Niu, Weiguang Yu, Liangbao Xiao
 Int J Clin Exp Med 2015;8(8):14214-14220 www.ijcem.com /ISSN:1940-5901/IJCEM0011204 Case Report Severe injury of bilateral elbow joints with unilateral terrible triad of the elbow and unilateral suspected
Int J Clin Exp Med 2015;8(8):14214-14220 www.ijcem.com /ISSN:1940-5901/IJCEM0011204 Case Report Severe injury of bilateral elbow joints with unilateral terrible triad of the elbow and unilateral suspected
Anterior Elbow Capsulodesis
 7(1):72 76, 2006 m R E V I E W m Anterior Elbow Capsulodesis Donald H. Lee, MD, Douglas R. Weikert, and Jeffry T. Watson Department of Orthopaedic Surgery Vanderbilt Orthopaedic Institute Nashville, TN
7(1):72 76, 2006 m R E V I E W m Anterior Elbow Capsulodesis Donald H. Lee, MD, Douglas R. Weikert, and Jeffry T. Watson Department of Orthopaedic Surgery Vanderbilt Orthopaedic Institute Nashville, TN
ELBOW ARTHROSCOPY WHERE ARE WE NOW?
 ELBOW ARTHROSCOPY WHERE ARE WE NOW? Christian Veillette M.D., M.Sc., FRCSC Assistant Professor, University of Toronto Shoulder & Elbow Reconstructive Surgery Toronto Western Hospital @ University Health
ELBOW ARTHROSCOPY WHERE ARE WE NOW? Christian Veillette M.D., M.Sc., FRCSC Assistant Professor, University of Toronto Shoulder & Elbow Reconstructive Surgery Toronto Western Hospital @ University Health
The Journal of the Korean Society of Fractures Vol.11, No.3, July, 1998
 The Journal of the Korean Society of Fractures Vol11, No3, July, 1998 Department of Orthopaedic Surgery, College of Medicine, Gyeong-Sang National Univeristy, Chinju, Korea Post-traumatic elbow stiffness
The Journal of the Korean Society of Fractures Vol11, No3, July, 1998 Department of Orthopaedic Surgery, College of Medicine, Gyeong-Sang National Univeristy, Chinju, Korea Post-traumatic elbow stiffness
This is an author-deposited version published in : Eprints ID : 18546
 Open Archive TOULOUSE Archive Ouverte (OATAO) OATAO is an open access repository that collects the work of Toulouse researchers and makes it freely available over the web where possible. This is an author-deposited
Open Archive TOULOUSE Archive Ouverte (OATAO) OATAO is an open access repository that collects the work of Toulouse researchers and makes it freely available over the web where possible. This is an author-deposited
Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty
 Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Citation for published version (APA): Bruinsma, W. E. (2014). Classification and management of shoulder and elbow trauma.
 UvA-DARE (Digital Academic Repository) Classification and management of shoulder and elbow trauma Bruinsma, W.E. Link to publication Citation for published version (APA): Bruinsma, W. E. (2014). Classification
UvA-DARE (Digital Academic Repository) Classification and management of shoulder and elbow trauma Bruinsma, W.E. Link to publication Citation for published version (APA): Bruinsma, W. E. (2014). Classification
the radial collateral ligament, the lateral ulnar collateral ligament, and the annular ligament 13
 1823 COPYRIGHT 2001 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Ligamentous Stabilizers Against Posterolateral Rotatory Instability of the Elbow BY CYNTHIA E. DUNNING, PHD, ZANE D.S. ZARZOUR,
1823 COPYRIGHT 2001 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Ligamentous Stabilizers Against Posterolateral Rotatory Instability of the Elbow BY CYNTHIA E. DUNNING, PHD, ZANE D.S. ZARZOUR,
Twenty-five-Year Results After Charnley Total Hip Arthroplasty in Patients Less than Fifty Years Old A CONCISE FOLLOW-UP OF A PREVIOUS REPORT*
 1066 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Twenty-five-Year Results After Charnley Total Hip Arthroplasty in Patients Less than Fifty Years Old A CONCISE FOLLOW-UP OF A
1066 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Twenty-five-Year Results After Charnley Total Hip Arthroplasty in Patients Less than Fifty Years Old A CONCISE FOLLOW-UP OF A
SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY
 SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY Th. KARACHALIOS, P. P. SARANGI, J. H. NEWMAN From Winford Orthopaedic Hospital, Bristol, England We report a prospective case-controlled
SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY Th. KARACHALIOS, P. P. SARANGI, J. H. NEWMAN From Winford Orthopaedic Hospital, Bristol, England We report a prospective case-controlled
Unstable elbow dislocations: a case report of a new surgical technique
 SICOT J 2016, 2, 15 Ó The Authors, published by EDP Sciences, 2016 DOI: 10.1051/sicotj/2016010 Available online at: www.sicot-j.org CASE REPORT OPEN ACCESS Unstable elbow dislocations: a case report of
SICOT J 2016, 2, 15 Ó The Authors, published by EDP Sciences, 2016 DOI: 10.1051/sicotj/2016010 Available online at: www.sicot-j.org CASE REPORT OPEN ACCESS Unstable elbow dislocations: a case report of
Rehabilitation after Total Elbow Arthroplasty
 Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
MANAGEMENT OF INTRAARTICULAR FRACTURES OF ELBOW JOINT. By Dr B. Anudeep M. S. orthopaedics Final yr pg
 MANAGEMENT OF INTRAARTICULAR FRACTURES OF ELBOW JOINT By Dr B. Anudeep M. S. orthopaedics Final yr pg INTRAARTICULAR FRACTURES Intercondyar fracture Elbow dislocation Capitellum # Trochlea # Radial head
MANAGEMENT OF INTRAARTICULAR FRACTURES OF ELBOW JOINT By Dr B. Anudeep M. S. orthopaedics Final yr pg INTRAARTICULAR FRACTURES Intercondyar fracture Elbow dislocation Capitellum # Trochlea # Radial head
Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 366, pp. 39-45 0 1999 Lippincott Williams & Wilkins, Inc. Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis Jens 0. S@jbjerg,
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 366, pp. 39-45 0 1999 Lippincott Williams & Wilkins, Inc. Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis Jens 0. S@jbjerg,
What Are the Risk Factors and Complications Associated With Intraoperative and Postoperative Fractures in Total Wrist Arthroplasty?
 Clin Orthop Relat Res (2017) 475:2694 2700 DOI 10.1007/s11999-017-5442-2 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH What Are
Clin Orthop Relat Res (2017) 475:2694 2700 DOI 10.1007/s11999-017-5442-2 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH What Are
Total elbow arthroplasty: A pictorial review of its associated complications
 Total elbow arthroplasty: A pictorial review of its associated complications Poster No.: C-624 Congress: ECR 2009 Type: Topic: Authors: Keywords: DOI: Educational Exhibit Musculoskeletal D. Y. F. Chung,
Total elbow arthroplasty: A pictorial review of its associated complications Poster No.: C-624 Congress: ECR 2009 Type: Topic: Authors: Keywords: DOI: Educational Exhibit Musculoskeletal D. Y. F. Chung,
Surgical techniques for reconstruction of chronic insufficiency of the triceps
 Surgical techniques for reconstruction of chronic insufficiency of the triceps ROTATION FLAP USING ANCONEUS AND TENDO ACHILLIS ALLOGRAFT Joaquin Sanchez-Sotelo, Bernard F. Morrey From the Mayo Clinic,
Surgical techniques for reconstruction of chronic insufficiency of the triceps ROTATION FLAP USING ANCONEUS AND TENDO ACHILLIS ALLOGRAFT Joaquin Sanchez-Sotelo, Bernard F. Morrey From the Mayo Clinic,
PRIMARY SOUTER-STRATHCLYDE TOTAL ELBOW
 4 PRIMARY SOUTER-STRATHCLYDE TOTAL ELBOW PROSTHESIS IN RHEUMATOID ARTHRITIS, SURGICAL TECHNIQUE J.C.T. van der Lugt R.B. Geskus P.M. Rozing J Bone Joint Surg Am. 2005 (supp 1);87:67-77 Chapter 4 Abstract
4 PRIMARY SOUTER-STRATHCLYDE TOTAL ELBOW PROSTHESIS IN RHEUMATOID ARTHRITIS, SURGICAL TECHNIQUE J.C.T. van der Lugt R.B. Geskus P.M. Rozing J Bone Joint Surg Am. 2005 (supp 1);87:67-77 Chapter 4 Abstract
Elbow dislocations represent 10% to 25% of all injuries. Elbow Fracture-Dislocations. The Role of Hinged External Fixation
 33 Elbow Fracture-Dislocations The Role of Hinged External Fixation Nader Paksima, D.O., M.P.H., and Anand Panchal, B.S. Abstract Fracture-dislocations of the elbow remain a complex problem in orthopaedics.
33 Elbow Fracture-Dislocations The Role of Hinged External Fixation Nader Paksima, D.O., M.P.H., and Anand Panchal, B.S. Abstract Fracture-dislocations of the elbow remain a complex problem in orthopaedics.
EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY
 EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY Benkovich V. Perry T., Bunin A., Bilenko V., Unit for Joint Arthroplasty, Soroka Medical Center Ben Gurion University of Negev Beer
EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY Benkovich V. Perry T., Bunin A., Bilenko V., Unit for Joint Arthroplasty, Soroka Medical Center Ben Gurion University of Negev Beer
Bipolar Radial Head System
 Bipolar Radial Head System Katalyst Surgical Technique DESCRIPTION The Katalyst Telescoping Bipolar Radial Head implant restores the support and bearing surface of the radial head in the face of fracture,
Bipolar Radial Head System Katalyst Surgical Technique DESCRIPTION The Katalyst Telescoping Bipolar Radial Head implant restores the support and bearing surface of the radial head in the face of fracture,
Slide 1. Slide 2. Slide 3. The Thrower s Elbow: When to Operate. Medial Elbow Pain in the Athlete. Goal of This Talk
 Slide 1 The Thrower s Elbow: When to Operate Luke S. Oh, MD Massachusetts General Hospital Team Physician, Boston Red Sox Team Physician, New England Revolution Consultant, Harvard University Athletics
Slide 1 The Thrower s Elbow: When to Operate Luke S. Oh, MD Massachusetts General Hospital Team Physician, Boston Red Sox Team Physician, New England Revolution Consultant, Harvard University Athletics
Case Presentation: Comminuted Fractures of the Proximal Ulna 11/28/2017. Disclosures. Surgical Strategy. Implant Choice. Melvin P.
 Current Solutions in Orthopaedic Trauma Case Presentation: Comminuted Fracture of the Proximal Ulna Melvin P. Rosenwasser, MD Robert E. Carroll Professor of Surgery of the Hand Chief, Orthopaedic Hand
Current Solutions in Orthopaedic Trauma Case Presentation: Comminuted Fracture of the Proximal Ulna Melvin P. Rosenwasser, MD Robert E. Carroll Professor of Surgery of the Hand Chief, Orthopaedic Hand
Investigation performed at the Department of Orthopedics, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
 1090 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Total Knee Arthroplasty in Young Patients with Juvenile Rheumatoid Arthritis BY JAVAD PARVIZI, MD, FRCS, CLAUDETTE M. LAJAM, MD,
1090 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Total Knee Arthroplasty in Young Patients with Juvenile Rheumatoid Arthritis BY JAVAD PARVIZI, MD, FRCS, CLAUDETTE M. LAJAM, MD,
Radial Head Fractures Save or Replace?
 Radial Head Fractures Save or Replace? Current Solutions in Orthopedic Trauma Sepember 19, 2015 Jorge L. Orbay MD. Disclosure Skeletal Dynamics Elbow Joint Ulno-Humeral and Radio-Capitellar The key joint
Radial Head Fractures Save or Replace? Current Solutions in Orthopedic Trauma Sepember 19, 2015 Jorge L. Orbay MD. Disclosure Skeletal Dynamics Elbow Joint Ulno-Humeral and Radio-Capitellar The key joint
Revision of the humeral component for aseptic loosening in arthroplasty of the shoulder
 Revision of the humeral component for aseptic loosening in arthroplasty of the shoulder A. Cil, C. J. H. Veillette, J. Sanchez-Sotelo, J. W. Sperling, C. Schleck, R. H. Cofield From the Mayo Clinic, Rochester,
Revision of the humeral component for aseptic loosening in arthroplasty of the shoulder A. Cil, C. J. H. Veillette, J. Sanchez-Sotelo, J. W. Sperling, C. Schleck, R. H. Cofield From the Mayo Clinic, Rochester,
TORNIER LATITUDE EV. Total Elbow Arthroplasty
 TORNIER LATITUDE EV Total Elbow Arthroplasty LATITUDE EV TOTAL ELBOW ARTHROPLASTY Welcome to the EVOLUTION of elbow replacement The LATITUDE EV total elbow arthroplasty system is designed to replicate
TORNIER LATITUDE EV Total Elbow Arthroplasty LATITUDE EV TOTAL ELBOW ARTHROPLASTY Welcome to the EVOLUTION of elbow replacement The LATITUDE EV total elbow arthroplasty system is designed to replicate
Long-term sequel of posterolateral rotatory instability of the elbow: a case report
 CASE REPORT Open Access Long-term sequel of posterolateral rotatory instability of the elbow: a case report Chun-Ying Cheng * Abstract The natural course of untreated posterior lateral rotatory instability
CASE REPORT Open Access Long-term sequel of posterolateral rotatory instability of the elbow: a case report Chun-Ying Cheng * Abstract The natural course of untreated posterior lateral rotatory instability
Unicondylar Knee Vs Total Knee Replacement: Is Less Better In the Middle Aged Athlete
 Unicondylar Knee Vs Total Knee Replacement: Is Less Better In the Middle Aged Athlete Chair: Maurilio Marcacci, MD Alois Franz "Basic principles and considerations of the Unis" Joao M. Barretto "Sport
Unicondylar Knee Vs Total Knee Replacement: Is Less Better In the Middle Aged Athlete Chair: Maurilio Marcacci, MD Alois Franz "Basic principles and considerations of the Unis" Joao M. Barretto "Sport
Terrible triad of the elbow
 Terrible triad of the elbow Vasu Pai ? Terrible triad of the elbow" Posterior dislocation of the elbow + Fractures of the radial head + Fracture of coronoid process Uncommon injury 5% of dislocation Problems
Terrible triad of the elbow Vasu Pai ? Terrible triad of the elbow" Posterior dislocation of the elbow + Fractures of the radial head + Fracture of coronoid process Uncommon injury 5% of dislocation Problems
MEDIAL EPICONDYLE FRACTURES
 MEDIAL EPICONDYLE FRACTURES Demographic 20% of elbow fractures 60% of which are associated with elbow dislocation. 75% in boys between 6-12 years 20% of elbow dislocation with ME fracture, the ME is incarcerated
MEDIAL EPICONDYLE FRACTURES Demographic 20% of elbow fractures 60% of which are associated with elbow dislocation. 75% in boys between 6-12 years 20% of elbow dislocation with ME fracture, the ME is incarcerated
Traumatic Elbow Instability
 Traumatic Elbow Instability David Ring MD PhD Updated April 2016 Simple Elbow Dislocation No associated fractures Complete or near complete capuloligamentous injury Extensive muscle injury Nearly always
Traumatic Elbow Instability David Ring MD PhD Updated April 2016 Simple Elbow Dislocation No associated fractures Complete or near complete capuloligamentous injury Extensive muscle injury Nearly always
Biomechanical concepts of total shoulder replacement. «Shoulder Course» Day 1. Richard W. Nyffeler Orthopädie Sonnenhof Bern. 11. Sept.
 Biomechanical concepts of total shoulder replacement Richard W. Nyffeler Orthopädie Sonnenhof Bern First total shoulder prosthesis Jules Emile Péan, 1830-1898 Monobloc prostheses Charles Neer, 1917-2011
Biomechanical concepts of total shoulder replacement Richard W. Nyffeler Orthopädie Sonnenhof Bern First total shoulder prosthesis Jules Emile Péan, 1830-1898 Monobloc prostheses Charles Neer, 1917-2011
Why are these shoulder replacements called a reverse prosthesis?
 PATIENT GUIDE TO REVERSE PROSTHESIS Edward G. McFarland MD The Division of Sports Medicine and Shoulder Surgery The Department of Orthopaedic Surgery The Johns Hopkins University Baltimore MD Why are these
PATIENT GUIDE TO REVERSE PROSTHESIS Edward G. McFarland MD The Division of Sports Medicine and Shoulder Surgery The Department of Orthopaedic Surgery The Johns Hopkins University Baltimore MD Why are these
Competence of the Deltoid Ligament in Bimalleolar Ankle Fractures After Medial Malleolar Fixation *
 Competence of the Deltoid Ligament in Bimalleolar Ankle Fractures After Medial Malleolar Fixation * BY PAUL TORNETTA, III, M.D. Investigation performed at Kings County Hospital, New York, N.Y. Abstract
Competence of the Deltoid Ligament in Bimalleolar Ankle Fractures After Medial Malleolar Fixation * BY PAUL TORNETTA, III, M.D. Investigation performed at Kings County Hospital, New York, N.Y. Abstract
Fractures and dislocations around elbow in adult
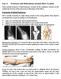 Lec: 3 Fractures and dislocations around elbow in adult These include fractures of distal humerus, fracture of the capitulum, fracture of the radial head, fracture of the olecranon & dislocation of the
Lec: 3 Fractures and dislocations around elbow in adult These include fractures of distal humerus, fracture of the capitulum, fracture of the radial head, fracture of the olecranon & dislocation of the
Terrible Triad: Tricks for Dealing with the Unstable Elbow
 Terrible Triad: Tricks for Dealing with the Unstable Elbow Mark A. Mighell, MD Kaitlyn N. Christmas, BS Disclosure Paid Consultation Research Support Speakers Bureau Paid Consultation Speakers Bureau The
Terrible Triad: Tricks for Dealing with the Unstable Elbow Mark A. Mighell, MD Kaitlyn N. Christmas, BS Disclosure Paid Consultation Research Support Speakers Bureau Paid Consultation Speakers Bureau The
D Degenerative joint disease, rotator cuff deficiency with, 149 Deltopectoral approach component removal with, 128
 Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
ORIGINAL ARTICLE. Department of Orthopedic Surgery, Mashad University of Medical Sciences, Mashad, Iran
 Arch Iranian Med 2003; 6 (3): 196 199 ORIGINAL ARTICLE INJECTION OF METHYLPREDNISOLONE AND LIDOCAINE IN THE TREATMENT OF MEDIAL EPICONDYLITIS: A RANDOMIZED CLINICAL TRIAL Mahmood Bahari MD, Mohammad Gharehdaghi
Arch Iranian Med 2003; 6 (3): 196 199 ORIGINAL ARTICLE INJECTION OF METHYLPREDNISOLONE AND LIDOCAINE IN THE TREATMENT OF MEDIAL EPICONDYLITIS: A RANDOMIZED CLINICAL TRIAL Mahmood Bahari MD, Mohammad Gharehdaghi
TREATMENT OF NONUNION OF OLECRANON FRACTURES
 TREATMENT OF NONUNION OF OLECRANON FRACTURES PANAYIOTIS J. PAPAGELOPOULOS, BERNARD F. MORREY From the Mayo Clinic and Mayo Foundation, Rochester, USA We report the results in 24 consecutive patients treated
TREATMENT OF NONUNION OF OLECRANON FRACTURES PANAYIOTIS J. PAPAGELOPOULOS, BERNARD F. MORREY From the Mayo Clinic and Mayo Foundation, Rochester, USA We report the results in 24 consecutive patients treated
Anatomical Considerations Regarding the Posterior Interosseous Nerve During Posterolateral Approaches to the Proximal Part of the Radius *
 Anatomical Considerations Regarding the Posterior Interosseous Nerve During Posterolateral Approaches to the Proximal Part of the Radius * BY THOMAS DILIBERTI, M.D., MICHAEL J. BOTTE, M.D., AND REID A.
Anatomical Considerations Regarding the Posterior Interosseous Nerve During Posterolateral Approaches to the Proximal Part of the Radius * BY THOMAS DILIBERTI, M.D., MICHAEL J. BOTTE, M.D., AND REID A.
T O T A L E L B O W P R O S T H E S I S
 H A N D, W R I S T A N D E L B O W Solutions by Tornier T O TA L E L B O W P R O S T H E S I S EVOLUTION WELCOME TO THE NEW OF ELBOW REPLACEMENT The Latitude TM EV prosthesis is designed to replicate the
H A N D, W R I S T A N D E L B O W Solutions by Tornier T O TA L E L B O W P R O S T H E S I S EVOLUTION WELCOME TO THE NEW OF ELBOW REPLACEMENT The Latitude TM EV prosthesis is designed to replicate the
Debridement arthroplasty for osteoarthritis of the elbow (Outerbridge-Kashiwagi procedure)
 Acta Orthop. Belg., 2004, 70, 306-310 ORIGINAL STUDIES Debridement arthroplasty for osteoarthritis of the elbow (Outerbridge-Kashiwagi procedure) Bart VINGERHOEDS, Ilse DEGREEF, Luc DE SMET From the University
Acta Orthop. Belg., 2004, 70, 306-310 ORIGINAL STUDIES Debridement arthroplasty for osteoarthritis of the elbow (Outerbridge-Kashiwagi procedure) Bart VINGERHOEDS, Ilse DEGREEF, Luc DE SMET From the University
Outcome of surgically treated displaced medial epicondyle fracture of humerus in children: A prospective study
 2017; 3(3): 287-291 ISSN: 2395-1958 IJOS 2017; 3(3): 287-291 2017 IJOS www.orthopaper.com Received: 08-05-2017 Accepted: 10-06-2017 Sahu RL M.S. Orthopaedics, Professor, Dr. Nadeem Ahmad Outcome of surgically
2017; 3(3): 287-291 ISSN: 2395-1958 IJOS 2017; 3(3): 287-291 2017 IJOS www.orthopaper.com Received: 08-05-2017 Accepted: 10-06-2017 Sahu RL M.S. Orthopaedics, Professor, Dr. Nadeem Ahmad Outcome of surgically
TRICEPS TENDON INJURY AFTER ELBOW ARTHROPLASTY
 TRICEPS TENDON INJURY AFTER ELBOW ARTHROPLASTY Sławomir Dudko Damian Kusz Michał Wójcik Department of Orthopedics and Traumatology Medical University of Silesia in Katowice Distal triceps tendon injury:
TRICEPS TENDON INJURY AFTER ELBOW ARTHROPLASTY Sławomir Dudko Damian Kusz Michał Wójcik Department of Orthopedics and Traumatology Medical University of Silesia in Katowice Distal triceps tendon injury:
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD
 Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Radial - Head Fractures. Christophe Spormann Endoclinic Zürich
 Radial - Head Fractures Christophe Spormann Endoclinic Zürich Elbow Func6on > 90% Ac6vi6es of daily living : 100 Flexion Extension : 130-30 Pro Supina9on : 50-0 - 50 Extension deficit beeer tolerated than
Radial - Head Fractures Christophe Spormann Endoclinic Zürich Elbow Func6on > 90% Ac6vi6es of daily living : 100 Flexion Extension : 130-30 Pro Supina9on : 50-0 - 50 Extension deficit beeer tolerated than
Posterolateral elbow dislocation with entrapment of the medial epicondyle in children: a case report Juan Rodríguez Martín* and Juan Pretell Mazzini
 Open Access Case report Posterolateral elbow dislocation with entrapment of the medial epicondyle in children: a case report Juan Rodríguez Martín* and Juan Pretell Mazzini Address: Department of Orthopaedic
Open Access Case report Posterolateral elbow dislocation with entrapment of the medial epicondyle in children: a case report Juan Rodríguez Martín* and Juan Pretell Mazzini Address: Department of Orthopaedic
Nearly all of these fractures are displaced, given the paucity of soft tissue attachments.
 CAPITELLAR FRACTURE Vasu Pai Nearly all of these fractures are displaced, given the paucity of soft tissue attachments. Nonsurgical management is fraught with complications including chronic pain, mechanical
CAPITELLAR FRACTURE Vasu Pai Nearly all of these fractures are displaced, given the paucity of soft tissue attachments. Nonsurgical management is fraught with complications including chronic pain, mechanical
Management of arthritis of the shoulder. Omar Haddo Consultant Orthopaedic Surgeon
 Management of arthritis of the shoulder Omar Haddo Consultant Orthopaedic Surgeon Diagnosis Pain - with activity initially. As disease progresses night pain is common and sleep difficult Stiffness trouble
Management of arthritis of the shoulder Omar Haddo Consultant Orthopaedic Surgeon Diagnosis Pain - with activity initially. As disease progresses night pain is common and sleep difficult Stiffness trouble
)532( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY
 )532( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE The Midterm Results of the Delta Xtend Reverse Shoulder System: A Five-Year Outcome Study John G. Horneff, MD; Thema A. Nicholson,
)532( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE The Midterm Results of the Delta Xtend Reverse Shoulder System: A Five-Year Outcome Study John G. Horneff, MD; Thema A. Nicholson,
Charnley Total Hip Arthroplasty with Use of Improved Cementing Techniques A MINIMUM TWENTY-YEAR FOLLOW-UP STUDY
 1840 COPYRIGHT 2001 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Charnley Total Hip Arthroplasty with Use of Improved Cementing Techniques A MINIMUM TWENTY-YEAR FOLLOW-UP STUDY BY AIMEE S. KLAPACH,
1840 COPYRIGHT 2001 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Charnley Total Hip Arthroplasty with Use of Improved Cementing Techniques A MINIMUM TWENTY-YEAR FOLLOW-UP STUDY BY AIMEE S. KLAPACH,
Case Presentation: Comminuted Radial Head Fracture
 11/28/2017 Current Solutions in Orthopaedic Trauma Case Presentation: Comminuted Radial Head Fracture Melvin P. Rosenwasser, MD Robert E. Carroll Professor of Surgery of the Hand Chief, Orthopaedic Hand
11/28/2017 Current Solutions in Orthopaedic Trauma Case Presentation: Comminuted Radial Head Fracture Melvin P. Rosenwasser, MD Robert E. Carroll Professor of Surgery of the Hand Chief, Orthopaedic Hand
Distal Humerus Fractures: How should they be fixed?
 Distal Humerus Fractures: How should they be fixed? Dr. Emil Schemitsch, MD, FRCS(C) Richard Ivey Professor and Chairman, Department of Surgery, Western University Chief of Surgery London Health Sciences
Distal Humerus Fractures: How should they be fixed? Dr. Emil Schemitsch, MD, FRCS(C) Richard Ivey Professor and Chairman, Department of Surgery, Western University Chief of Surgery London Health Sciences
15-Year Follow-up Study of Total Knee Arthroplasty in Patients With Rheumatoid Arthritis
 The Journal of Arthroplasty Vol. 18 No. 8 2003 15-Year Follow-up Study of Total Knee Arthroplasty in Patients With Rheumatoid Arthritis Jun Ito, MD, PhD, Tomihisa Koshino, MD, PhD, Renzo Okamoto, MD, PhD,
The Journal of Arthroplasty Vol. 18 No. 8 2003 15-Year Follow-up Study of Total Knee Arthroplasty in Patients With Rheumatoid Arthritis Jun Ito, MD, PhD, Tomihisa Koshino, MD, PhD, Renzo Okamoto, MD, PhD,
OCCUPATIONAL INJURIES OF THE ELBOW
 PLEASE STAND BY WEBINAR WILL BEGIN AT 12:00 PM PST FOR AUDIO: CALL 866-740-1260 / ACCESS CODE: 764-4915# JAMES VAN DEN BOGAERDE, MD OCCUPATIONAL INJURIES OF THE ELBOW Conflict of Interest Disclosure I,
PLEASE STAND BY WEBINAR WILL BEGIN AT 12:00 PM PST FOR AUDIO: CALL 866-740-1260 / ACCESS CODE: 764-4915# JAMES VAN DEN BOGAERDE, MD OCCUPATIONAL INJURIES OF THE ELBOW Conflict of Interest Disclosure I,
Knee Revision. Portfolio
 Knee Revision Portfolio I use the DePuy Revision Knee System because of its versatility. With this system I can solve nearly any situation I encounter in the OR. Dr. Thomas Fehring, OrthoCarolina Hip and
Knee Revision Portfolio I use the DePuy Revision Knee System because of its versatility. With this system I can solve nearly any situation I encounter in the OR. Dr. Thomas Fehring, OrthoCarolina Hip and
Shoulder Joint Replacement
 Shoulder Joint Replacement Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was first performed
Shoulder Joint Replacement Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was first performed
TERRIBLE TRIAD OF THE ELBOW: EVALUATION OF SURGICAL TREATMENT
 ORIGINAL ARTICLE TERRIBLE TRIAD OF THE ELBOW: EVALUATION OF SURGICAL TREATMENT Leandro Cardoso Gomide 1, Dagoberto de Oliveira Campos 2, José Maria Ribeiro de Sá 1, Marcelo Rangel Pamfílio de Sousa 1,
ORIGINAL ARTICLE TERRIBLE TRIAD OF THE ELBOW: EVALUATION OF SURGICAL TREATMENT Leandro Cardoso Gomide 1, Dagoberto de Oliveira Campos 2, José Maria Ribeiro de Sá 1, Marcelo Rangel Pamfílio de Sousa 1,
Range of Motion of Standard and High-Flexion Posterior Stabilized Total Knee Prostheses A PROSPECTIVE, RANDOMIZED STUDY
 1470 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Range of Motion of Standard and High-Flexion Posterior Stabilized Total Knee Prostheses A PROSPECTIVE, RANDOMIZED STUDY BY YOUNG-HOO
1470 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Range of Motion of Standard and High-Flexion Posterior Stabilized Total Knee Prostheses A PROSPECTIVE, RANDOMIZED STUDY BY YOUNG-HOO
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR
 CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
Functional and radiological outcome of total knee replacement in varus deformity of the knee
 ISSN: 2319-7706 Volume 4 Number 4 (2015) pp. 934-938 http://www.ijcmas.com Original Research Article Functional and radiological outcome of total knee replacement in varus deformity of the knee Sandesh
ISSN: 2319-7706 Volume 4 Number 4 (2015) pp. 934-938 http://www.ijcmas.com Original Research Article Functional and radiological outcome of total knee replacement in varus deformity of the knee Sandesh
A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients
 Original Research Article A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients Ragesh Chandran 1*, Sanath K Shetty 2, Ashwin Shetty 3, Bijith Balan 1, Lawrence J Mathias
Original Research Article A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients Ragesh Chandran 1*, Sanath K Shetty 2, Ashwin Shetty 3, Bijith Balan 1, Lawrence J Mathias
Early failure of total hip replacements implanted at distant hospitals to reduce waiting lists
 : 31 35 doi 10.1308/1478708051450 Audit Early failure of total hip replacements implanted at distant hospitals to reduce waiting lists Jac Ciampolini, Matthew JW Hubble Princess Elizabeth Orthopaedic Centre,
: 31 35 doi 10.1308/1478708051450 Audit Early failure of total hip replacements implanted at distant hospitals to reduce waiting lists Jac Ciampolini, Matthew JW Hubble Princess Elizabeth Orthopaedic Centre,
Condylar constrained system in primary total knee replacement: our experience and literature review
 Original Article Page 1 of 5 Condylar constrained system in primary total knee replacement: our experience and literature review Luigi Sabatini 1, Salvatore Risitano 1, Lorenzo Rissolio 1, Andrea Bonani
Original Article Page 1 of 5 Condylar constrained system in primary total knee replacement: our experience and literature review Luigi Sabatini 1, Salvatore Risitano 1, Lorenzo Rissolio 1, Andrea Bonani
Inspection. Physical Examination of the Elbow. Anterior Elbow 2/14/2017. Inspection. Carrying angle. Lateral dimple. Physical Exam of the Elbow
 of the Elbow Anthony A. Romeo, MD Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Rush University President-Elect, American Shoulder Elbow Surgeons Team Physician, Chicago
of the Elbow Anthony A. Romeo, MD Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Rush University President-Elect, American Shoulder Elbow Surgeons Team Physician, Chicago
Stefan Rahm MD University Hospital Balgrist
 Knee Prosthesis Models & Materials, Surgical Techniques and Approaches Stefan Rahm MD University Hospital Balgrist INTRODUCTION VARUS VALGUS 46 Y OLD MALE Pain in the medial compartment left more than
Knee Prosthesis Models & Materials, Surgical Techniques and Approaches Stefan Rahm MD University Hospital Balgrist INTRODUCTION VARUS VALGUS 46 Y OLD MALE Pain in the medial compartment left more than
Review Article Primary and Posttraumatic Arthritis of the Elbow
 Arthritis Volume 2013, Article ID 473259, 6 pages http://dx.doi.org/10.1155/2013/473259 Review Article Primary and Posttraumatic Arthritis of the Elbow Debdut Biswas, Robert W. Wysocki, and Mark S. Cohen
Arthritis Volume 2013, Article ID 473259, 6 pages http://dx.doi.org/10.1155/2013/473259 Review Article Primary and Posttraumatic Arthritis of the Elbow Debdut Biswas, Robert W. Wysocki, and Mark S. Cohen
Hand Surgery Department Poznan University of Medical Sciences. Piotr Czarnecki
 Hand Surgery Department Poznan University of Medical Sciences Piotr Czarnecki Arthroscopic debridement, bone excision MP, PIP, total wrist replacement PIP, CMC fusion partial wrist fusion proximal row
Hand Surgery Department Poznan University of Medical Sciences Piotr Czarnecki Arthroscopic debridement, bone excision MP, PIP, total wrist replacement PIP, CMC fusion partial wrist fusion proximal row
Integra. Katalyst Bipolar Radial Head System SURGICAL TECHNIQUE
 Integra Katalyst Bipolar Radial Head System SURGICAL TECHNIQUE Surgical Technique As the manufacturer of this device, Integra does not practice medicine and does not recommend this or any other surgical
Integra Katalyst Bipolar Radial Head System SURGICAL TECHNIQUE Surgical Technique As the manufacturer of this device, Integra does not practice medicine and does not recommend this or any other surgical
Bilateral total knee arthroplasty: One mobile-bearing and one fixed-bearing
 Journal of Orthopaedic Surgery 2001, 9(1): 45 50 Bilateral total knee arthroplasty: One mobile-bearing and one fixed-bearing KY Chiu, TP Ng, WM Tang and P Lam Department of Orthopaedic Surgery, The University
Journal of Orthopaedic Surgery 2001, 9(1): 45 50 Bilateral total knee arthroplasty: One mobile-bearing and one fixed-bearing KY Chiu, TP Ng, WM Tang and P Lam Department of Orthopaedic Surgery, The University
Surgical approach to posterior dislocation of the elbow combined with radial head and coronoid fractures (terrible triad): report of 19 cases
 SHAFA ORTHOPEDIC JOURNAL, Original Article Surgical approach to posterior dislocation of the elbow combined with radial head and coronoid fractures (terrible triad): report of 19 cases Kaveh Gharanizadeh
SHAFA ORTHOPEDIC JOURNAL, Original Article Surgical approach to posterior dislocation of the elbow combined with radial head and coronoid fractures (terrible triad): report of 19 cases Kaveh Gharanizadeh
UDHT08.1.qxd:UDHT /03/08 17:14 Page 1. Surgical. Technique. Elbow Prosthesis. RHS Radial Head System.
 UDHT08.1.qxd:UDHT08.1 13/03/08 17:14 Page 1 Surgical Technique Elbow Prosthesis RHS Radial Head System www.tornier.com UDHT08.1.qxd:UDHT08.1 13/03/08 17:14 Page 2 TABLE OF CONTENTS DESIGN RATIONALE INDICATIONS
UDHT08.1.qxd:UDHT08.1 13/03/08 17:14 Page 1 Surgical Technique Elbow Prosthesis RHS Radial Head System www.tornier.com UDHT08.1.qxd:UDHT08.1 13/03/08 17:14 Page 2 TABLE OF CONTENTS DESIGN RATIONALE INDICATIONS
ORIGINAL PAPER. Department of Orthopedic Surgery, Hamamatsu Medical Center ABSTRACT
 Nagoya J. Med. Sci. 71. 145 ~ 150, 2009 ORIGINAL PAPER AUTOGENOUS BULK STRUCTURAL BONE GRAFTING FOR RECONSTRUCTION OF THE ACETABLUM IN PRIMARY TOTAL HIP ARTHROPLASTY: AVERAGE 12-YEAR FOLLOW-UP TETSUO MASUI,
Nagoya J. Med. Sci. 71. 145 ~ 150, 2009 ORIGINAL PAPER AUTOGENOUS BULK STRUCTURAL BONE GRAFTING FOR RECONSTRUCTION OF THE ACETABLUM IN PRIMARY TOTAL HIP ARTHROPLASTY: AVERAGE 12-YEAR FOLLOW-UP TETSUO MASUI,
Index. orthopedic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acetabular fractures thromboembolic disease after, 341 Achilles tendon rupture ACL. See Anterior cruciate ligament (ACL) Adolescent idiopathic
Index Note: Page numbers of article titles are in boldface type. A Acetabular fractures thromboembolic disease after, 341 Achilles tendon rupture ACL. See Anterior cruciate ligament (ACL) Adolescent idiopathic
The evolution of the elbow can be traced back 20
 24 Bulletin of the Hospital for Joint Diseases 2013;71(1):24-31 The Rise of the Metal Elbow Marc Fajardo, M.D., and Young W. Kwon, M.D., Ph.D. Abstract Painful arthritis of the elbow joint has long been
24 Bulletin of the Hospital for Joint Diseases 2013;71(1):24-31 The Rise of the Metal Elbow Marc Fajardo, M.D., and Young W. Kwon, M.D., Ph.D. Abstract Painful arthritis of the elbow joint has long been
"Stability and Instability of RTSA"
 Orthopedics Update «Reverse Total Shoulder Arthroplasty» Stability and Instability of RTSA A. LÄDERMANN Orthopaedics and Traumatology, La Tour Hospital, Meyrin, Switzerland Orthopaedics and Traumatology,
Orthopedics Update «Reverse Total Shoulder Arthroplasty» Stability and Instability of RTSA A. LÄDERMANN Orthopaedics and Traumatology, La Tour Hospital, Meyrin, Switzerland Orthopaedics and Traumatology,
Ulnar Collateral Ligament Reconstruction in Posttraumatic Elbow Release
 Feature Article Ulnar Collateral Ligament Reconstruction in Posttraumatic Elbow Release KEVIN J. MALONE, MD; PAUL A. MARTINEAU, MD; DOUGLAS P. HANEL, MD abstract Full article available online at ORTHOSuperSite.com.
Feature Article Ulnar Collateral Ligament Reconstruction in Posttraumatic Elbow Release KEVIN J. MALONE, MD; PAUL A. MARTINEAU, MD; DOUGLAS P. HANEL, MD abstract Full article available online at ORTHOSuperSite.com.
McKeever metallic hemiarthroplasty of the knee in unicompartmental degenerative arthritis. Long-term clinical follow-up and current indications
 This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. McKeever metallic hemiarthroplasty of the knee in unicompartmental degenerative
This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. McKeever metallic hemiarthroplasty of the knee in unicompartmental degenerative
Index. B Backslap technique depth assessment, 82, 83 diaphysis distal trocar, 82 83
 Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
Technical Tip for Prosthesis of Antibiotic-Loaded Acrylic Cement (PROSTALAC) Use for Infection after Shoulder Arthroplasty
 SURGICAL TECHNIQUES Technical Tip for Prosthesis of Antibiotic-Loaded Acrylic Cement (PROSTALAC) Use for Infection after Shoulder Arthroplasty ABSTRACT BACKGROUND Shoulder arthroplasty procedures have
SURGICAL TECHNIQUES Technical Tip for Prosthesis of Antibiotic-Loaded Acrylic Cement (PROSTALAC) Use for Infection after Shoulder Arthroplasty ABSTRACT BACKGROUND Shoulder arthroplasty procedures have
Pregnancy After Total Hip Arthroplasty BY CATHY M. MCDOWELL, RN, AND PAUL F. LACHIEWICZ, MD
 1490 COPYRIGHT 2001 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Pregnancy After Total Hip Arthroplasty BY CATHY M. MCDOWELL, RN, AND PAUL F. LACHIEWICZ, MD Investigation performed at the Department
1490 COPYRIGHT 2001 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Pregnancy After Total Hip Arthroplasty BY CATHY M. MCDOWELL, RN, AND PAUL F. LACHIEWICZ, MD Investigation performed at the Department
Coronal Shear Fractures of the Distal End of the Humerus*
 Copyright 1996 by The Journal of Bone and Joint Surgery, Incorporated Coronal Shear Fractures of the Distal End of the Humerus* BY MICHAEL D. McKEE, M.D., F.R.C.S.(C)t, JESSE B. JUPITER, M.D4, BOSTON,
Copyright 1996 by The Journal of Bone and Joint Surgery, Incorporated Coronal Shear Fractures of the Distal End of the Humerus* BY MICHAEL D. McKEE, M.D., F.R.C.S.(C)t, JESSE B. JUPITER, M.D4, BOSTON,
DISTAL HUMERUS FRACTURES WHAT I HAVE LEARNED DISTAL HUMERUS FRACTURES WHAT I HAVE LEARNED 63 YO WOMAN CT FIXABLE OSTEOTOMY NOT NEEDED
 AMERICAN SHOULDER AND ELBOW SURGEONS ORTHOPAEDIC TRAUMA ASSOCIATION SPECIALTY DAY SAN DIEGO, MARCH 2017 Graham JW King MD, MSc, FRCSC 63 YO WOMAN CT FIXABLE OSTEOTOMY NOT NEEDED 64 YO WOMAN FALL OF LADDER
AMERICAN SHOULDER AND ELBOW SURGEONS ORTHOPAEDIC TRAUMA ASSOCIATION SPECIALTY DAY SAN DIEGO, MARCH 2017 Graham JW King MD, MSc, FRCSC 63 YO WOMAN CT FIXABLE OSTEOTOMY NOT NEEDED 64 YO WOMAN FALL OF LADDER
Total Knee Arthroplasty in a Patient with an Ankylosing Knee after Previous Patellectomy
 Case Report Knee Surg Relat Res 2014;26(3):182-186 http://dx.doi.org/10.5792/ksrr.2014.26.3.182 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Total Knee Arthroplasty in a Patient with
Case Report Knee Surg Relat Res 2014;26(3):182-186 http://dx.doi.org/10.5792/ksrr.2014.26.3.182 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Total Knee Arthroplasty in a Patient with
Post-traumatic contracture of the elbow. Operative treatment, including distraction arthroplasty
 This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. Post-traumatic contracture of the elbow. Operative treatment, including
This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. Post-traumatic contracture of the elbow. Operative treatment, including
Biomechanics of Two Reconstruction Techniques for Elbow Ulnar Collateral Ligament Insufficiency
 Biomechanics of Two Reconstruction Techniques for Elbow Ulnar Collateral Ligament Insufficiency Justin E. Chronister, MD 1, Randal P. Morris, BS 2, Clark R. Andersen, MS 2, J. Michael Bennett, MD 3, Thomas
Biomechanics of Two Reconstruction Techniques for Elbow Ulnar Collateral Ligament Insufficiency Justin E. Chronister, MD 1, Randal P. Morris, BS 2, Clark R. Andersen, MS 2, J. Michael Bennett, MD 3, Thomas
LIMITED INFLUENCE OF PROSTHETIC POSITION ON ASEPTIC LOOSENING OF THE SOUTER-STRATHCLYDE TOTAL ELBOW PROSTHESIS
 6 LIMITED INFLUENCE OF PROSTHETIC POSITION ON ASEPTIC LOOSENING OF THE SOUTER-STRATHCLYDE TOTAL ELBOW PROSTHESIS J.C.T. van der Lugt R.B. Geskus P.M. Rozing Acta Orthop. 2005;76(5):654-61 Chapter 6 Abstract
6 LIMITED INFLUENCE OF PROSTHETIC POSITION ON ASEPTIC LOOSENING OF THE SOUTER-STRATHCLYDE TOTAL ELBOW PROSTHESIS J.C.T. van der Lugt R.B. Geskus P.M. Rozing Acta Orthop. 2005;76(5):654-61 Chapter 6 Abstract
Analysis of factors affecting range of motion after Total Knee Arthroplasty
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 9 Ver. II (Sep. 2015), PP 01-10 www.iosrjournals.org Analysis of factors affecting range of
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 9 Ver. II (Sep. 2015), PP 01-10 www.iosrjournals.org Analysis of factors affecting range of
SHOULDER ARTHROPLASTY (TOTAL, HEMI, REVERSE)/ARTHRODESIS
 evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
Shoulder Arthroplasty. Valentin Lance 3/24/16
 Shoulder Arthroplasty Valentin Lance 3/24/16 Outline Background Pre-operative imaging assessment Total Shoulder Arthroplasty: Standard and Reverse Complications Other shoulder hardware Hemiarthroplasty
Shoulder Arthroplasty Valentin Lance 3/24/16 Outline Background Pre-operative imaging assessment Total Shoulder Arthroplasty: Standard and Reverse Complications Other shoulder hardware Hemiarthroplasty
