Identify the risk management issues involved in caring for patient with orthopedic complaints.
|
|
|
- Jessie Collins
- 6 years ago
- Views:
Transcription
1 MACEP Risk Management Course Module 4: Emergency Orthopedics Matthew B. Mostofi, D.O., FACEP Course Objectives Identify the risk management issues involved in caring for patient with orthopedic complaints. Recognize that Failure to Diagnose significant orthopedic injuries is currently the highest cause of both claims made against emergency physicians and in percentage of claims with indemnity (pay-outs). Recognize that cervical spine injuries, pelvic fractures, compartment syndrome and occult extremity fractures are high risk orthopedic situations. Identify the risk that patients with unreliable history and physical exams pose to identification of significant orthopedic injuries. List the pertinent history, physical findings, testing, management, documentation and follow-up essential in the evaluation of patients with high risk orthopedic injuries. Fracture Management Fractures and other orthopedic injuries account for more than 11% of malpractice claims against emergency physicians. From , 42% of these claims ended with indemnity or payout. The average indemnity for these cases was $314,285. Two missed cervical spine fractures were settled during this time frame for amounts in excess of 1 million dollars. Orthopedic claims have the highest likelihood to have indemnity when compared to any other system cases. 2 There are several themes that emerge when reviewing closed claims data which can be useful in managing risk. The vast majority of claims made against emergency physicians for orthopedic injuries are based on failure to diagnose an existing injury. Factors involved include: Failure to suspect a fracture: There are often patient factors which render history and physical unreliable, resulting in failure to order an x-ray of an affected body part because history and physical do not suggest injury. This is most dramatically associated with the intoxicated trauma patient who has an unsuspected vertebral fracture, but young children, elderly, patients with mental disorders and distracting injuries are also high risk patients. Care should be given to avoid over reliance on Module 4: Emergency Orthopedics Page 1 of 9
2 exam in these patients and when in doubt appropriate imaging should be obtained. Failure to diagnose additional fractures when the first fracture is identified is also a pitfall. Misread of radiograph or ordering wrong views/study: Often an x-ray is interpreted as normal when in fact a fracture/injury exists. Good clinical judgment coupled with a robust and reliable radiographic follow-up system is essential to minimize this risk. Look at all films ordered, as pathology is often seen on only one view. Do not accept partial or incomplete x-ray studies. When in doubt, other imaging modalities like CT or MRI may be necessary and consultation with radiologist or orthopedist encouraged. Failure to recognize or prevent complications associated with fractures: Missed associated injuries, hemorrhage/vascular injury, nerve injury and compartment syndrome are known complications of orthopedic injuries that frequently lead to disability and may result in legal action. Documentation of neurovascular function, tendon injuries, and compartment pressure in suspected compartment syndrome is essential. Missed or delayed pelvic fractures which are associated with significant occult hemorrhage and often catastrophic disabilities have resulted in large settlements. However, the most catastrophic disabilities and largest settlements result from problems in the management of vertebral fractures and a subsequent neurologic dysfunction. Poor discharge instructions: The most common missed fractures are of extremities. Although most of these fractures are not serious injuries, significant disability can result. Giving clear after-care instructions, describing warning signs for potential complications, and providing mechanism for follow up care, are essential to mitigate risk. Vertebral Fractures Fractures and subluxations of the cervical spine account for some of the highest dollar loss claims in emergency medicine. Again, failure to diagnose is the most frequent claim associated with malpractice. After reviewing closed claims it is clear emergency physicians can incorporate practice concepts to minimize risk. Strategies include: Suspect cervical fractures in all trauma patients. These include alert trauma patients with neck pain, all intoxicated patients, unresponsive or head injured patients, and any trauma patient with new neurologic deficit. Immobilize all suspected spine fractures and document that immobilization was performed and maintained. Significant vertebral injury may be present without cord injury. Evaluation of suspected fractures must be performed without injuring the cord or exacerbating a cord injury. Cervical immobilization requires rigid collars, tape, sand bags, back boards, or other immobilization devices in various combinations. Soft collars do not immobilize the neck. When emergent airway management is needed, Module 4: Emergency Orthopedics Page 2 of 9
3 care should be used to maintain cervical immobilization and should be documented. Options include in-line immobilization, nasal intubation, and flexible fiber optic intubation. Newer difficult airway devices like Glidescope or optical stylets may also be helpful. While controversy exists as to the optimal technique for airway management in a patient with suspect cervical spine fracture, it is clear that documenting that care was taken to consider and immobilize the cervical spine is an effective risk management approach. Image all patients that require imaging. Not all trauma patients need cervical spine imaging. There are currently two validated clinical decision rules which may be used as a guide when considering who needs radiographs. The National Emergency X-ray Utilization Study (NEXUS) looked at 34,069 patients and identified 810/818 clinically significant fractures. This gives the NEXUS rules sensitivity (positive in disease) of 99.0%. The negative predictive value of rules was 99.8%. NEXUS criteria 1. No midline tenderness 2. No focal neurological deficits 3. Normal alertness 4. No intoxication 5. No painful or distracting injury The Canadian C-Spine Rules (CCR) has also been validated and is a useful guide as to which patients will need cervical spine imaging. This study looked at 8924 patients and identified 151/151 important fractures, giving it a sensitivity of 100%. CCR 1. Are there any high risk factors (Age >65, dangerous mechanism*, paraesthesia in extremities)? 2. Are there any low risk factors (Simple rear-end MVC**, sitting positioning ED, ambulatory at any time, delayed onset of neck pain, absence of midline tenderness)? 3. Can patient rotate neck 45 degrees to the right and left? * Dangerous mechanisms: Fall from height >3 ft/5 stairs, axial load to head, ejection, MVC >100km/hr, rollover, motorized recreational vehicle, bicycle struck or collision **Simple rear-end MVC excludes: pushed into oncoming traffic, hit by bus/large truck, rollover, hit by high speed vehicle While both rules are reasonable tools to decide who does and does not require imaging, no rule should take place of good clinical judgment and neither rule is perfect. The Canadian C-spine rules have some very specific definitions and exclusion criteria, so caution is advised when employing them. Module 4: Emergency Orthopedics Page 3 of 9
4 Computerized tomography of the c-spine is the gold standard for blunt trauma patients that require imaging. With the increased availability of CT scan, there is decreased use of cervical plain film to evaluate for fracture. A meta-analysis of seven studies involving 3,834 blunt trauma patients with cervical spine injuries showed pooled sensitivity of 98% for CT scan vs. 52% for plain films. If plain radiographs of the cervical spine are to be used, at least 3 views should be obtained: AP, lateral and odontoid view. For adequate evaluation, all seven cervical vertebrae (including the upper part of T1) must be seen. This may require special views, such as a pull-down or swimmer s view. When unable to get a complete study, CT scan should be obtained. If you can t read the study, consult someone who can. Consult radiologist freely when reading vertebral radiographs/ct. This is a high risk injury and a mistake in an x-ray/ct read can have a bad outcome for you and your patient. In some cases, when the radiologist is unsure, further evaluation with MRI or orthopedist/neurosurgeon may be warranted. Remember to maintain c-spine immobilization throughout this often timely process. Good discharge instructions. Most spine injuries involve soft tissue rather than bone. Since certain soft tissue injuries can potentially cause disability, even with normal radiographs, always instruct patient to obtain follow-up if symptoms persist or worsen. Warning signs like numbness, weakness, and paraesthesia, with an action plan should also be discussed with patient and documented in the discharge instructions. Pelvic Fractures While pelvic fractures represent a tiny percentage of all fractures, the mortality rate from severe pelvis injury is high. High risk pelvic fractures occur in multiple trauma patients and evaluation of such patients must include thorough evaluation of the pelvis. The following factors have been reported in the literature to increase the risk of mortality: Pelvic ring injury-particularly with posterior injury/instability High injury severity score (other associated injuries) Hemorrhagic shock on admission (blood pressure < 90) Large transfusion requirement Any perineal laceration Advanced age Think of pelvic fracture in trauma patient with a history of shock. The typical pelvic fracture malpractice suit is the result of a patient s death from unsuspected hemorrhage. Injuries to the lower GI tract (blood in rectum) or urinary system (blood at meatus or high riding prostate) are often signs of pelvic injury. Pedestrian versus auto collisions are a common cause. The critical risk management strategy is to suspect pelvic fractures in the multi-injured patient and always consider pelvic fracture as a cause of shock. Early recognition can expedite definitive care which may include transfer to trauma center or involvement of Module 4: Emergency Orthopedics Page 4 of 9
5 orthopedist/interventional radiologist. Often pelvic stabilization, a commercially available pelvic stabilization/compression device, and massive fluid resuscitation may be the only treatment while arranging definitive care. Historically, bed sheets or other straps were used to provide pelvic compression and stabilization but there are now commercially available pelvic stabilization/compression devices. Good documentation of your actions will be imperative as frequently there is a poor outcome. Extremity Fractures Emergency physicians see a great deal of extremity trauma and the majority of malpractice suits related to fractures arise from extremity injuries. These cases are generally decided in the physicians favor or result in small payouts. Certain injuries, such as hip fractures, slipped capital femoral epiphysis, and compartment syndromes are associated with significant disability and can result in significant judgments against the physician. Like the rest of orthopedic claims, areas of risk when evaluating an extremity injury include: 1. Failure to suspect a fracture and therefore not ordering an x-ray of the affected part. 2. Failure to get appropriate views. 3. Misreading of radiographs. 4. Failure to identify and splint potential occult fractures. 5. Poor discharge instructions. 6. Breakdown in the follow-up system for radiographs. Some methods to mitigate risk are as follows: 1. Get the radiograph, and make sure it is the right one. Take a careful history, especially to determine the mechanism of injury. Perform thorough examination with documentation or pertinent positive and negative findings. Beware of the multiple trauma patients, as other more acute injuries may take your attention away from the extremities. Any missed fracture in the ED, which results in a bad outcome for the patient, will likely be your responsibility. Listen to the patient. If your patient says it hurts, believe it. If your patient says they can not use the extremity (i.e. cannot walk), believe it. Many malpractice suits result from a patient s perception that the physician did not take the complaint seriously, and did not adequately examine (physically and with radiographs) the injured area. 2. Never accept poor quality radiographs or inadequate views. Repeat the study, or if needed get a study (CT or MRI) that will answer the question asked. 3. Improved interpretation of radiographs. ED physician leadership should have in place a system for quality control and improvement. Reviews of missed x-ray findings and a mechanism to identify an individual physician for addressing substandard quality should be in place and followed. Internet portal applications can now allow consult viewing of radiographs remotely and in real time. Advocate for these systems Module 4: Emergency Orthopedics Page 5 of 9
6 to be available for all orthopedic consultants. For concerning cases, ask consultants to review the images and work together on planning next evaluation/treatment steps. 4. Know the signs, symptoms, mechanism of injury, and radiographic findings of occult fractures. Such occult fractures include, the carpal navicular bone, tibial plateau fractures, the radial head, calcaneal fractures, stress fractures, and Salter I growth plate fractures. Use CT or MRI on patients where there is a strong clinical suspicion of an extremity fracture with normal x-ray finding. Also, good communication with patient and family is important. Informing the patient to the possibility of an occult fracture, and treating the area with immobilization and referral for orthopedic follow up is an effective strategy. This open communication often satisfies the expectation of the patient and minimizes the surprise if there is a change in diagnosis and treatment plan. 5. Develop an efficient follow-up system. Timely radiology follow-up is critical to risk management in emergency orthopedics. Prompt notification of a missed fracture and initiation of appropriate therapy and referral is essential. Discharge instructions should reflect the fact that the ED x-ray read is preliminary and that a formal interpretation by radiologist will follow. Patients should be notified for any significant discrepancy. Any significant delay in this notification will be scrutinized by a patient s attorney if there is a bad outcome or significant disability. A few complications of orthopedic injuries should also be in the forefront of the mind of any practicing emergency physician. These complications include open fractures, neurovascular compromise and compartment syndrome. The common factor for all of these entities is that a delayed or missed diagnosis of any complications is frequently associated with significant disability, so care in the evaluation and treatment are critical elements in mitigating legal risk. Ensure all patients (with extra care to multi-injured and those with unreliable history and physical exam) are undressed and examined, so as not to miss a small open fracture. Documentation of this exam and its findings are the protection needed if an infectious complication occurs. Injured extremities should be reassessed before and after splinting/casting for signs of neurovascular compromise. When splints are applied in the emergency department, careful instructions should be given to patients and caregivers regarding reevaluation of neurovascular function and warning signs warranting a return to ED. In lower extremity injury, failure to instruct the patient to remain nonweight bearing can worsen a recognized or unrecognized condition such as stress fracture, slipped capital femoral epiphysis in a child, Salter-Harris (growth-plate) fractures or others. Compartment syndrome is increased pressure in a confined space (with and without fracture), which interferes with proper circulation. Pain is the earliest and most reliable sign and often it is out of proportion to physical exam. Other findings include pain with passive motion, tenderness of a tense compartment, anesthesia, Module 4: Emergency Orthopedics Page 6 of 9
7 weakness and paresis. Risk factors include long bone fractures, crush and significant soft tissue injuries and patients with coagulopathy or on anticoagulants. All patients with risk and findings suggestive of compartment syndrome should be evaluated emergently by an orthopedist for measurements of compartment pressures. The average award for delay in diagnosis of compartment syndrome in 1993 was $280,000. Discharge Instructions Discharge instructions are critical. This is your last chance; take advantage of it by giving thorough instructions, particularly concerning follow-up. Every patient with orthopedic injury should be referred to an orthopedist or their primary care physician. Good discharge instructions should tell the patient how to care for the injury. This should include use, care and cautions regarding immobilization devices, when and how to arrange follow-up and potential complications (neuro-vascular problems, etc.) that may result from the injury. If there is a significant injury and concern that the patient may not be able to arrange a follow-up appointment with orthopedist in a timely manner, it is advisable to call the orthopedist and make the arrangement prior to patient s departure from the ED. Summary Points History: Discover and document mechanism and circumstances of injury. Read all accompanying documents, including nurse notes and EMS reports. Document pertinent past medical history, family history, and social history. Carefully assess and document patient s mental status and level of consciousness, with the understanding that impaired patients have unreliable history and physical findings. Evaluation: Suspect fractures. Failure to image or choosing the wrong imaging modality is a significant factor in failure to diagnose claim. 1 Young children, elderly, patients with language barriers, mental disorders, distracting injuries and intoxication frequently have unreliable history and physical findings. Beware of these patients; often a more liberal use of imaging is indicated. Assume cervical spine fracture and pelvic fracture in any multiple trauma patients. Evaluate and document neurologic, vascular and tendon integrity in all areas of injury. Be sure to repeat if any manipulation was performed. Use your Radiology and orthopedic consultant when there is doubt about the presence of an injury or treatment plan. Consider asking orthopedic consultants not present in the ED to review images remotely if possible in order to assist in determining extent of the injury and treatment plan. Consider compartment syndrome in patients with risk and pain out of proportion to physical findings. Module 4: Emergency Orthopedics Page 7 of 9
8 Treatment: Until cervical spine is cleared, maintain cervical immobilization. For those patients who walk in with traumatic neck pain, protocols should be in place for immobilization in triage. Immobilize injured extremities liberally. Know when to call a consultant or transfer to trauma center, when in doubt consult. Discharge instructions: Give complete instructions on the care of the injury. Always include warning signs for when to return to the emergency department. Always provide a mechanism for appropriate follow up. Administrative: Advocate/Assist in enabling remote image viewing by orthopedic related consultants for better real time consultant input/follow up care arrangement. Develop a system to monitor missed x-rays and to inform patients of corrected findings. Develop a system to notify patient of any positive culture result, crucial in case of septic arthritis. Module 4: Emergency Orthopedics Page 8 of 9
9 Module 4: Orthopedics References 1. Medical Professional Mutual Insurance Company ( ProMutual ); Closed Case Analysis, Emergency Medicine Closed Claim Studies, ProMutual Germann C; Perron, A. Risk Management and Avoiding Legal Pitfalls in the Emergency Treatment of High-Risk Orthopedic Injuries. Emerg Med Clin N AM 28 (2010) Yu, K; Green, R. Critical Aspects of Emergency Department Documentation and Communication. Emerg Med Clin N AM 27 (2009) Gulli B, Templeman D: Compartment syndrome of the lower extremity. Orthop Clin North Am 25: , 1994 Module 4: Emergency Orthopedics Page 9 of 9
Indications for cervical spine immobilisation: -
 Paediatric Trauma Cervical Spine Guidelines UHW Traumatic injuries of the cervical spine (C-spine) are uncommon in children. However, it is safer assume there is a cervical spine injury until examination
Paediatric Trauma Cervical Spine Guidelines UHW Traumatic injuries of the cervical spine (C-spine) are uncommon in children. However, it is safer assume there is a cervical spine injury until examination
Introduction. Objectives C-Spine: Where Are We Now? NAEMSP Medical Director Course 1/9/2013
 NAEMSP Medical Director Course 1/9/2013 Objectives C-Spine: Where Are We Now? Robert M. Domeier, MD EMS Medical Director Washtenaw/Livingston Medical Control Authority Department of Emergency Medicine
NAEMSP Medical Director Course 1/9/2013 Objectives C-Spine: Where Are We Now? Robert M. Domeier, MD EMS Medical Director Washtenaw/Livingston Medical Control Authority Department of Emergency Medicine
Selective Spine Assessment & Spinal Motion Restriction
 Selective Spine Assessment & Spinal Motion Restriction Supersedes: 02-09-15 Effective: 10-20-15 Spinal cord injury may be the result of direct blunt and/or penetrating trauma, compression forces (axial
Selective Spine Assessment & Spinal Motion Restriction Supersedes: 02-09-15 Effective: 10-20-15 Spinal cord injury may be the result of direct blunt and/or penetrating trauma, compression forces (axial
3/10/17 Spinal a Injury 1
 Spinal Injury 1 'Paralysed' Watmough vows he'll have the backbone for Game Two after treatment for neck injury Watmough will have cortisone injected into his spine this morning to speed up the recovery
Spinal Injury 1 'Paralysed' Watmough vows he'll have the backbone for Game Two after treatment for neck injury Watmough will have cortisone injected into his spine this morning to speed up the recovery
The Prehospital Validation of the Canadian C-Spine Rule by Paramedics
 The Prehospital Validation of the Canadian C-Spine Rule by Paramedics CAEP, Victoria 2007 Study Coordinating Center: C Vaillancourt MD IG Stiell MD GA Wells PhD Ottawa Health Research Institute University
The Prehospital Validation of the Canadian C-Spine Rule by Paramedics CAEP, Victoria 2007 Study Coordinating Center: C Vaillancourt MD IG Stiell MD GA Wells PhD Ottawa Health Research Institute University
Spinal, or Suspected Spinal Injury
 Approved by: Spinal, or Suspected Spinal Injury Vice President and Chief Medical Officer; and Vice President and Chief Operating Officer Corporate Policy & Procedures Manual Number: VII-B-150 Date Approved
Approved by: Spinal, or Suspected Spinal Injury Vice President and Chief Medical Officer; and Vice President and Chief Operating Officer Corporate Policy & Procedures Manual Number: VII-B-150 Date Approved
To Backboard or Not To Backboard, That is the Question? Selective Spinal Immobilization
 To Backboard or Not To Backboard, That is the Question? Selective Spinal Immobilization Will Smith, MD, NREMT-P Medical Director, Jackson Hole Fire/EMS, Grand Teton National Park Emergency Medicine, St.
To Backboard or Not To Backboard, That is the Question? Selective Spinal Immobilization Will Smith, MD, NREMT-P Medical Director, Jackson Hole Fire/EMS, Grand Teton National Park Emergency Medicine, St.
3/14/2014 USED TO BE SIMPLE.. TO IMMOBILIZE OR NOT TO IMMOBILIZE.THAT IS THE QUESTION THE PROBLEM OLD THINKING
 USED TO BE SIMPLE.. TO IMMOBILIZE OR NOT TO IMMOBILIZE.THAT IS THE QUESTION Immobilization following injury used to be a simple decision--but no one was thinking. Up to 5 million people per year receive
USED TO BE SIMPLE.. TO IMMOBILIZE OR NOT TO IMMOBILIZE.THAT IS THE QUESTION Immobilization following injury used to be a simple decision--but no one was thinking. Up to 5 million people per year receive
Objective 1 Review Research on spine injuries and evaluation standards.
 To Backboard or Not To Backboard? Spinal Clearance Protocols Will Smith, MD, NREMT-P Medical Director, Jackson Hole Fire/EMS, Grand Teton National Park Wilderness and Emergency Medicine Consulting (WEMC),
To Backboard or Not To Backboard? Spinal Clearance Protocols Will Smith, MD, NREMT-P Medical Director, Jackson Hole Fire/EMS, Grand Teton National Park Wilderness and Emergency Medicine Consulting (WEMC),
Evaluation and Stabilization of the Athlete with Possible Spine Injury
 Evaluation and Stabilization of the Athlete with Possible Spine Injury Jeffrey H. Bohmer, MD, FACEP Emergency Physician Northwestern Medicine Central DuPage Hospital June 12, 2015 Introduction Goals: 1.
Evaluation and Stabilization of the Athlete with Possible Spine Injury Jeffrey H. Bohmer, MD, FACEP Emergency Physician Northwestern Medicine Central DuPage Hospital June 12, 2015 Introduction Goals: 1.
Controversies in Spinal Immobilization
 Controversies in Spinal Immobilization Ken Berumen, BSN, MD, FACEP Medical Director El Paso Fire Department Medical Director Emergency Services District #1 Network Director EM Sierra Providence Health
Controversies in Spinal Immobilization Ken Berumen, BSN, MD, FACEP Medical Director El Paso Fire Department Medical Director Emergency Services District #1 Network Director EM Sierra Providence Health
Time Equals Neurons - Spinal Cord Injury Management in the first 4 Hours
 Time Equals Neurons - Spinal Cord Injury Management in the first 4 Hours William D. Whetstone M.D. Clinical Professor UCSF Department of Emergency Medicine SFGH ED Center for Neuro-Critical Emergencies
Time Equals Neurons - Spinal Cord Injury Management in the first 4 Hours William D. Whetstone M.D. Clinical Professor UCSF Department of Emergency Medicine SFGH ED Center for Neuro-Critical Emergencies
Clinical Radiology: A Pragmatic Perspective. Agenda. Clinical Practice The Art of Hypothesis S APTA CSM /17/12. APTA CSM 2013, San Diego 1
 Clinical Radiology: A Pragmatic Perspective Dan Rhon, PT, DPT, DSc Madigan Army Medical Center APTA CSM 2013 Agenda Background Clinical Approach (Tool in your Toolbox) Inherent Limitations of Imaging Hierarchy
Clinical Radiology: A Pragmatic Perspective Dan Rhon, PT, DPT, DSc Madigan Army Medical Center APTA CSM 2013 Agenda Background Clinical Approach (Tool in your Toolbox) Inherent Limitations of Imaging Hierarchy
SPINE EVALUATION AND CLEARANCE Basic Principles
 SPINE EVALUATION AND CLEARANCE Basic Principles General 1. Entire spine is immobilized during primary survey. 2. Radiographic clearance of the spine is not required before emergent surgical procedures.
SPINE EVALUATION AND CLEARANCE Basic Principles General 1. Entire spine is immobilized during primary survey. 2. Radiographic clearance of the spine is not required before emergent surgical procedures.
Heidi Lako-Adamson, MD, NRP, FAEMS FM Ambulance and Sanford EMS Education Medical Director
 Heidi Lako-Adamson, MD, NRP, FAEMS FM Ambulance and Sanford EMS Education Medical Director Spinal cord injury statistics. Definition of spinal motion restriction. Difference between spinal motion restriction
Heidi Lako-Adamson, MD, NRP, FAEMS FM Ambulance and Sanford EMS Education Medical Director Spinal cord injury statistics. Definition of spinal motion restriction. Difference between spinal motion restriction
Overview. Overview. Chapter 30. Injuries to the Head and Spine 9/11/2012. Review of the Nervous and Skeletal Systems. Devices for Immobilization
 Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
of Trauma Assembly 27 th Page 1
 Eastern Association for the Surgery of Trauma 27 th Annual Scientific Assembly Sunrise Session 08 To Scan or Not To Scan Thatt is the Question January 16, 2014 Waldorf Astoria Naples Naples, Floridaa Page
Eastern Association for the Surgery of Trauma 27 th Annual Scientific Assembly Sunrise Session 08 To Scan or Not To Scan Thatt is the Question January 16, 2014 Waldorf Astoria Naples Naples, Floridaa Page
Shenandoah Co. Fire & Rescue. Injuries to. and Spine. December EMS Training Bill Streett Training Section Chief
 Shenandoah Co. Fire & Rescue Injuries to the Head and Spine December EMS Training Bill Streett Training Section Chief C.E. Card Information BLS Providers 2 Cards / Provider Category 1 Course # Blank Topic#
Shenandoah Co. Fire & Rescue Injuries to the Head and Spine December EMS Training Bill Streett Training Section Chief C.E. Card Information BLS Providers 2 Cards / Provider Category 1 Course # Blank Topic#
Cervical Spine Injury Guidelines
 6/15/2018 Cervical Spine Injury Guidelines Benjamin Oshlag, MD, CAQSM Assistant Professor of Emergency Medicine Assistant Professor of Sports Medicine Columbia University Medical Center Nothing to Disclose
6/15/2018 Cervical Spine Injury Guidelines Benjamin Oshlag, MD, CAQSM Assistant Professor of Emergency Medicine Assistant Professor of Sports Medicine Columbia University Medical Center Nothing to Disclose
EMS Update Spinal Motion Restriction Training
 EMS Update Spinal Motion Restriction Training 700-M11 Spinal Motion Restriction Spinal Motion Restriction, also called SMR Formally known as Spinal Immobilization or C-Spine Effective February 9, 2016
EMS Update Spinal Motion Restriction Training 700-M11 Spinal Motion Restriction Spinal Motion Restriction, also called SMR Formally known as Spinal Immobilization or C-Spine Effective February 9, 2016
Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing
 1 2 3 4 5 6 Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing D-Disability Chief complaint and/or Mechanism
1 2 3 4 5 6 Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing D-Disability Chief complaint and/or Mechanism
Cervical Spine Precautions A quick review. By Joseph Lewis, M.D. Medical Director, Honolulu EMS Board Certified in Emergency Medicine
 Cervical Spine Precautions A quick review By Joseph Lewis, M.D. Medical Director, Honolulu EMS Board Certified in Emergency Medicine 1 Goals of this Cervical Spine Immobilization In-service Learn Objectives:
Cervical Spine Precautions A quick review By Joseph Lewis, M.D. Medical Director, Honolulu EMS Board Certified in Emergency Medicine 1 Goals of this Cervical Spine Immobilization In-service Learn Objectives:
Imaging in the Trauma Patient
 Imaging in the Trauma Patient David A. Spain, MD Department of Surgery Stanford University Pan Scan Instead of Clinical Exam? 1 Granted, some patients don t need CT scan Platinum Package Stanford Special
Imaging in the Trauma Patient David A. Spain, MD Department of Surgery Stanford University Pan Scan Instead of Clinical Exam? 1 Granted, some patients don t need CT scan Platinum Package Stanford Special
PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT
 PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT Board Approved June 2007 Revised December 2009 Revised July 2011 Revised June 2015 435 Hunter Street Fredericksburg, VA 22401
PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT Board Approved June 2007 Revised December 2009 Revised July 2011 Revised June 2015 435 Hunter Street Fredericksburg, VA 22401
XXX Spinal Motion Restriction
 Nor-Cal EMS Policy & Procedure Manual NAME OF MODULE XXX Purpose: The purpose of this protocol is to protect patients with signs and symptoms of spinal injuries and those who have the potential for spinal
Nor-Cal EMS Policy & Procedure Manual NAME OF MODULE XXX Purpose: The purpose of this protocol is to protect patients with signs and symptoms of spinal injuries and those who have the potential for spinal
vel 2 Level 2 3,034 c-spine evaluations with CSR Level 3 detected injury only 53% of the time. Level 3 False (-) rate 47%
 Objectives Blunt and Penetrating Neck Trauma Julie Mayglothling, MD, FACEP Virginia Commonwealth University Richmond, VA Summit to Sound, May 20 th, 2011 Blunt Neck Trauma Evaluation of the low mechanism,
Objectives Blunt and Penetrating Neck Trauma Julie Mayglothling, MD, FACEP Virginia Commonwealth University Richmond, VA Summit to Sound, May 20 th, 2011 Blunt Neck Trauma Evaluation of the low mechanism,
SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services OBJECTIVES DEFINITION 11/8/2017. Identify SCIWORA.
 SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services Identify SCIWORA. OBJECTIVES Identify the population at risk. To identify anatomic and physiologic reasons for SCIWORA. To
SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services Identify SCIWORA. OBJECTIVES Identify the population at risk. To identify anatomic and physiologic reasons for SCIWORA. To
TALK TRAUMA Clearing the C-Spine. David Ouellette
 TALK TRAUMA 2011 Clearing the C-Spine David Ouellette Case #1 - Mother / Daughter MVC 34 y/o female Dangerous mechanism CHI Mumbling incoherently Femur # - distracting injury ETOH - 22 9 y/o female Dangerous
TALK TRAUMA 2011 Clearing the C-Spine David Ouellette Case #1 - Mother / Daughter MVC 34 y/o female Dangerous mechanism CHI Mumbling incoherently Femur # - distracting injury ETOH - 22 9 y/o female Dangerous
CERVICAL SPINE CLEARANCE
 DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
The Assessment & Management of Spine & Spinal Cord Injuries in the Field:
 The Assessment & Management of Spine & Spinal Cord Injuries in the Field: Where We Started, Where We are Now, & Why WMTC Wilderness Medicine Training Center International Paul Nicolazzo Director Wilderness
The Assessment & Management of Spine & Spinal Cord Injuries in the Field: Where We Started, Where We are Now, & Why WMTC Wilderness Medicine Training Center International Paul Nicolazzo Director Wilderness
OBJECTIVES: Define basic assessments skills needed to identify orthopedic injuries. Differentiate when an orthopedic injury is a medical emergency
 1 2 How to Triage Orthopaedic Care David W. Gray, M.D. OBJECTIVES: Define basic assessments skills needed to identify orthopedic injuries Differentiate when an orthopedic injury is a medical emergency
1 2 How to Triage Orthopaedic Care David W. Gray, M.D. OBJECTIVES: Define basic assessments skills needed to identify orthopedic injuries Differentiate when an orthopedic injury is a medical emergency
Upper Cervical Spine - Occult Injury and Trigger for CT Exam
 Upper Cervical Spine - Occult Injury and Trigger for CT Exam Main Menu Introduction Clinical clearance of C-SpineC Radiographic evaluation Norms for C-spineC Triggers for CT exam: Odontoid Lateral view
Upper Cervical Spine - Occult Injury and Trigger for CT Exam Main Menu Introduction Clinical clearance of C-SpineC Radiographic evaluation Norms for C-spineC Triggers for CT exam: Odontoid Lateral view
Pan Scan Instead of Clinical Exam? David A. Spain, MD
 Pan Scan Instead of Clinical Exam? David A. Spain, MD Granted, some patients don t t need CT scan Platinum Package Stanford Special CT Scan Head Neck Chest Abdomen Pelvis Takes about 20 minutes to do
Pan Scan Instead of Clinical Exam? David A. Spain, MD Granted, some patients don t t need CT scan Platinum Package Stanford Special CT Scan Head Neck Chest Abdomen Pelvis Takes about 20 minutes to do
Comparing the Canadian Cervical Spine Rule and Radiology Confirmed Cervical Spine Injury in the Emergency Department
 Rhode Island College Digital Commons @ RIC Master's Theses, Dissertations, Graduate Research and Major Papers Overview Master's Theses, Dissertations, Graduate Research and Major Papers 5-13-2017 Comparing
Rhode Island College Digital Commons @ RIC Master's Theses, Dissertations, Graduate Research and Major Papers Overview Master's Theses, Dissertations, Graduate Research and Major Papers 5-13-2017 Comparing
North West London Trauma Network Spinal Pathway and Protocols
 North West London Trauma Network Spinal Pathway and Protocols 1. Spinal Clearance in the Trauma Patient Inclusions: All trauma patients who are not alert and orientated, unable to cooperate (including
North West London Trauma Network Spinal Pathway and Protocols 1. Spinal Clearance in the Trauma Patient Inclusions: All trauma patients who are not alert and orientated, unable to cooperate (including
Subaxial Cervical Spine Trauma
 Subaxial Cervical Spine Trauma Pooria Salari, MD Assistant Professor Of Orthopaedics Department of Orthopaedic Surgery St. Louis University School of Medicine St. Louis, Missouri, USA Initial Evaluation
Subaxial Cervical Spine Trauma Pooria Salari, MD Assistant Professor Of Orthopaedics Department of Orthopaedic Surgery St. Louis University School of Medicine St. Louis, Missouri, USA Initial Evaluation
Orthopedics. 1. GOAL: Understand the pediatrician's role in preventing and screening for
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Orthopedics 1. GOAL: Understand the pediatrician's role in preventing and screening for orthopedic injury, disease and dysfunction.
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Orthopedics 1. GOAL: Understand the pediatrician's role in preventing and screening for orthopedic injury, disease and dysfunction.
Spinal injury. Structure of the spine
 Spinal injury Structure of the spine Some understanding of the structure of the spine (spinal column) and the spinal cord is important as it helps your Neurosurgeon explain about the part of the spine
Spinal injury Structure of the spine Some understanding of the structure of the spine (spinal column) and the spinal cord is important as it helps your Neurosurgeon explain about the part of the spine
10O SPLINTING OF INJURIES ADULT & PEDIATRIC. 10Oa: Axial/Spine with Selective Spinal Motion Restriction Adult & Pediatric:
 10O SPLINTING OF INJURIES ADULT & PEDIATRIC EMERGENCY MEDICAL RESPONDER EMT EMT-INTERMEDIATE 85 ADVANCED EMT PARAMEDIC 10Oa: Axial/Spine with Selective Spinal Motion Restriction Adult & Pediatric: Many
10O SPLINTING OF INJURIES ADULT & PEDIATRIC EMERGENCY MEDICAL RESPONDER EMT EMT-INTERMEDIATE 85 ADVANCED EMT PARAMEDIC 10Oa: Axial/Spine with Selective Spinal Motion Restriction Adult & Pediatric: Many
Annually in the United States, 1 million patients will require
 ORIGINAL RESEARCH SPINE Screening Cervical Spine CT in the Emergency Department, Phase 2: A Prospective Assessment of Use B. Griffith, M. Kelly, P. Vallee, M. Slezak, J. Nagarwala, S. Krupp, C.P. Loeckner,
ORIGINAL RESEARCH SPINE Screening Cervical Spine CT in the Emergency Department, Phase 2: A Prospective Assessment of Use B. Griffith, M. Kelly, P. Vallee, M. Slezak, J. Nagarwala, S. Krupp, C.P. Loeckner,
ATLS: Initial Assessment and Management. SAUSHEC Medical Student Lecture Series
 ATLS: Initial Assessment and Management SAUSHEC Medical Student Lecture Series Objectives Identify sequence of priorities in assessing the multiply injured patient Apply principles outlined in primary
ATLS: Initial Assessment and Management SAUSHEC Medical Student Lecture Series Objectives Identify sequence of priorities in assessing the multiply injured patient Apply principles outlined in primary
PEM GUIDE CHILDHOOD FRACTURES
 PEM GUIDE CHILDHOOD FRACTURES INTRODUCTION Skeletal injuries account for 10-15% of all injuries in children; 20% of those are fractures, 3 out of 4 fractures affect the physis or growth plate. Always consider
PEM GUIDE CHILDHOOD FRACTURES INTRODUCTION Skeletal injuries account for 10-15% of all injuries in children; 20% of those are fractures, 3 out of 4 fractures affect the physis or growth plate. Always consider
Spinal Cord Injuries: The Basics. Kadre Sneddon POS Rounds October 1, 2003
 Spinal Cord Injuries: The Basics Kadre Sneddon POS Rounds October 1, 2003 Anatomy Dorsal columntouch, vibration Corticospinal tract- UMN Anterior horn-lmn Spinothalamic tractpain, temperature (contralateral)
Spinal Cord Injuries: The Basics Kadre Sneddon POS Rounds October 1, 2003 Anatomy Dorsal columntouch, vibration Corticospinal tract- UMN Anterior horn-lmn Spinothalamic tractpain, temperature (contralateral)
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Chapter 32. Objectives. Objectives 01/09/2013. Spinal Column and Spinal Cord Trauma
 Chapter 32 Spinal Column and Spinal Cord Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1.
Chapter 32 Spinal Column and Spinal Cord Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1.
Pre-hospital Response to Trauma and Brain Injury. Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center
 Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Chapter 32. Injuries to the Spine by Pearson Education, Inc. Upper Saddle River, New Jersey
 Chapter Injuries to the Spine Topics Anatomy and physiology of the spine Spinal injuries Guidelines for immobilization Special considerations Enrichment Introduction Injuries to the spine are among the
Chapter Injuries to the Spine Topics Anatomy and physiology of the spine Spinal injuries Guidelines for immobilization Special considerations Enrichment Introduction Injuries to the spine are among the
Pre-hospital Spinal Motion Restriction Standard update. Presented by: Dr. Tatiana Jevremovic CCFP (EM)(SEM), Dip.
 Pre-hospital Spinal Motion Restriction Standard update Presented by: Dr. Tatiana Jevremovic CCFP (EM)(SEM), Dip. Sport Med (CASEM) Dr. Thomas J. Pashby What is happening Pre-hospital Spinal Motion Restriction
Pre-hospital Spinal Motion Restriction Standard update Presented by: Dr. Tatiana Jevremovic CCFP (EM)(SEM), Dip. Sport Med (CASEM) Dr. Thomas J. Pashby What is happening Pre-hospital Spinal Motion Restriction
Chapter 39 Trauma in the Elderly
 Chapter 39 Trauma in the Elderly Episode Overview 1) 5 Risk Factors for falls in the elderly? 2) What anatomic and physiologic changes in the elderly patient are important for the management of trauma
Chapter 39 Trauma in the Elderly Episode Overview 1) 5 Risk Factors for falls in the elderly? 2) What anatomic and physiologic changes in the elderly patient are important for the management of trauma
SPINAL IMMOBILIZATION
 Spinal Immobilization Decision Assessment Recent studies have shown an increase in mortality for patients with isolated penetrating trauma who are spinally immobilized. Therefore spinal immobilization
Spinal Immobilization Decision Assessment Recent studies have shown an increase in mortality for patients with isolated penetrating trauma who are spinally immobilized. Therefore spinal immobilization
Imaging Decision Making: Acute Cervical Spine Injury (in the Alert and Stable Adult Following Blunt Trauma)
 WSCC Clinics Protocol Imaging Decision Making: Acute Cervical Spine Injury (in the Alert and Stable Adult Following Blunt Trauma) Adopted: 6/02 To be reviewed: 6/05 This protocol is intended for acute
WSCC Clinics Protocol Imaging Decision Making: Acute Cervical Spine Injury (in the Alert and Stable Adult Following Blunt Trauma) Adopted: 6/02 To be reviewed: 6/05 This protocol is intended for acute
Patient Assessment. Chapter 8
 Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
Bones 101: Introduction to Emergency Orthopedics
 Bones 101: Introduction to Emergency Orthopedics Claire Plautz, MD (with special thanks to) Andrew D. Perron, MD University of Virginia Health System Intro to ortho: Overview General Terms & Principles
Bones 101: Introduction to Emergency Orthopedics Claire Plautz, MD (with special thanks to) Andrew D. Perron, MD University of Virginia Health System Intro to ortho: Overview General Terms & Principles
Liability Risks for Physiatrists & Physical Therapists
 Liability Risks for Physiatrists & Physical Therapists Physiatrists and physical therapists work to improve and restore functionality to patients who have injuries and impairments affecting the musculoskeletal
Liability Risks for Physiatrists & Physical Therapists Physiatrists and physical therapists work to improve and restore functionality to patients who have injuries and impairments affecting the musculoskeletal
17. Imaging and interventional radiology
 17. Imaging and interventional radiology These guidelines have been adapted from the Leeds Major Trauma Centre Imaging in Paediatric Major Trauma guidelines Written by Dr Annmarie Jeanes (Consultant Paediatric
17. Imaging and interventional radiology These guidelines have been adapted from the Leeds Major Trauma Centre Imaging in Paediatric Major Trauma guidelines Written by Dr Annmarie Jeanes (Consultant Paediatric
Follow your protocols!
 By Will Dunn, BA, NRP, CCEMTP & Myles Sibley, BA, NREMT P Eagle County Paramedic Services, Eagle County, CO. FIELD ASSESSMENT AND TREATMENT OF CLOSED HEAD AND SPINAL INJURY Follow your protocols! Objectives
By Will Dunn, BA, NRP, CCEMTP & Myles Sibley, BA, NREMT P Eagle County Paramedic Services, Eagle County, CO. FIELD ASSESSMENT AND TREATMENT OF CLOSED HEAD AND SPINAL INJURY Follow your protocols! Objectives
Episode 66 Backboard and Collar Nightmares from EMU Conference. The Risks Associated with Backboard & Collar
 However, backboards and collars are not without risk: Episode 66 Backboard and Collar Nightmares from EMU Conference With Dr. Kylie Bosman Prepared by Dr., edited by Dr. Kylie Bosman & Anton Helman, May
However, backboards and collars are not without risk: Episode 66 Backboard and Collar Nightmares from EMU Conference With Dr. Kylie Bosman Prepared by Dr., edited by Dr. Kylie Bosman & Anton Helman, May
MEDICAL CONTROL POLICY STATEMENT/ADVISORY. Re: Spinal Injury Assessment & Spinal Precautions Procedure
 MEDICAL CONTROL POLICY STATEMENT/ADVISORY No. 2015-01 Date: January 20, 2015 Re: Spinal Injury Assessment & Spinal Precautions Procedure Office of the Medical Director Noel Wagner, MD, NREMT-P 1000 Houghton
MEDICAL CONTROL POLICY STATEMENT/ADVISORY No. 2015-01 Date: January 20, 2015 Re: Spinal Injury Assessment & Spinal Precautions Procedure Office of the Medical Director Noel Wagner, MD, NREMT-P 1000 Houghton
Restore adequate respiratory and circulatory conditions. Reduce pain
 Pre-hospital management of the trauma patient is best performed by an integrated team focused on minimizing the time from injury to definitive care at an appropriate trauma center. Dispatchers, first responders,
Pre-hospital management of the trauma patient is best performed by an integrated team focused on minimizing the time from injury to definitive care at an appropriate trauma center. Dispatchers, first responders,
Trauma Overview. Chapter 22
 Trauma Overview Chapter 22 Kinematics of Trauma Injuries are the leading cause of death among children and young adults. Kinematics introduces the basic physical concepts that dictate how injuries occur
Trauma Overview Chapter 22 Kinematics of Trauma Injuries are the leading cause of death among children and young adults. Kinematics introduces the basic physical concepts that dictate how injuries occur
Determination of Cervical Spine Stability in Trauma Patients (Update of the 1997 EAST Cervical Spine Clearance Document)
 1 Determination of Cervical Spine Stability in Trauma Patients (Update of the 1997 EAST Cervical Spine Clearance Document) Cervical Spine Clearance Committee Donald Marion Robert Domeier C. Michael Dunham
1 Determination of Cervical Spine Stability in Trauma Patients (Update of the 1997 EAST Cervical Spine Clearance Document) Cervical Spine Clearance Committee Donald Marion Robert Domeier C. Michael Dunham
Joint Theater Trauma System Clinical Practice Guideline
 CERVICAL SPINE EVALUATION & N-SURGICAL MANAGEMENT Original Release/Approval: 1 March 2010 Note: This CPG requires an annual review Reviewed: Feb 2012 Approved: 19 Mar 2012 Supersedes: Cervical Spine Evaluation,
CERVICAL SPINE EVALUATION & N-SURGICAL MANAGEMENT Original Release/Approval: 1 March 2010 Note: This CPG requires an annual review Reviewed: Feb 2012 Approved: 19 Mar 2012 Supersedes: Cervical Spine Evaluation,
Radiologic Pitfalls. Objectives: High Risk! Occult Fracture? 2/16/2014
 Objectives: Radiologic Pitfalls Gregory W. Hendey, MD, FACEP Professor of Clinical Emergency Medicine UCSF Fresno, Medical Education Program To discuss plain film and physical findings that suggest an
Objectives: Radiologic Pitfalls Gregory W. Hendey, MD, FACEP Professor of Clinical Emergency Medicine UCSF Fresno, Medical Education Program To discuss plain film and physical findings that suggest an
EM Cases Course 2017 Knee Emergencies Module
 EM Cases Course 2017 Knee Emergencies Module Arun Sayal Podcasts to listen to prior to the course Link to: Occult Knee Injuries Pearls & Pitfalls Knee injuries in the ED are much more than fractures and
EM Cases Course 2017 Knee Emergencies Module Arun Sayal Podcasts to listen to prior to the course Link to: Occult Knee Injuries Pearls & Pitfalls Knee injuries in the ED are much more than fractures and
Selective Spinal Immobilization
 Selective Spinal Immobilization Objectives Understand the background of spinal immobilization. Understand the rationale for developing a current selective spinal immobilization protocol. Review the data
Selective Spinal Immobilization Objectives Understand the background of spinal immobilization. Understand the rationale for developing a current selective spinal immobilization protocol. Review the data
Acute spinal cord injury
 Acute spinal cord injury Thakul Oearsakul Songklanagarind hospital Hat Yai Songkhla Introduction New SCI 10000-12000 cases Approximately 4.0-5.3 per 100000 population Common causes of traumatic SCI :Motor
Acute spinal cord injury Thakul Oearsakul Songklanagarind hospital Hat Yai Songkhla Introduction New SCI 10000-12000 cases Approximately 4.0-5.3 per 100000 population Common causes of traumatic SCI :Motor
Outline. Epidemiology Indications for C-spine imaging Modalities Interpretation Types of fractures
 C-Spine Plain Films Outline Epidemiology Indications for C-spine imaging Modalities Interpretation Types of fractures Epidemiology 7000-10000 c-spine injuries treated each year Additional 5000 die at the
C-Spine Plain Films Outline Epidemiology Indications for C-spine imaging Modalities Interpretation Types of fractures Epidemiology 7000-10000 c-spine injuries treated each year Additional 5000 die at the
INJURY IN HEAD TRAUMA
 The Journal ol Emergency Medfane, Vol 6, pp 203-207, 1988 Punted in the USA l Copyright K 1988 Pergamon Press plc CERVICAL INJURY IN HEAD TRAUMA Gary L. Neifeld, MD*, John G. Keene, MD, * George Hevesy,
The Journal ol Emergency Medfane, Vol 6, pp 203-207, 1988 Punted in the USA l Copyright K 1988 Pergamon Press plc CERVICAL INJURY IN HEAD TRAUMA Gary L. Neifeld, MD*, John G. Keene, MD, * George Hevesy,
EMS Spinal Assessment and Precautions
 EMS Spinal Assessment and Precautions Adapted from a presentation prepared by Chelsea C. White IV, MD, NREMT-P Medical Director, Bernalillo County Fire Department Robert M. Domeier, MD, EMS Medical Director,
EMS Spinal Assessment and Precautions Adapted from a presentation prepared by Chelsea C. White IV, MD, NREMT-P Medical Director, Bernalillo County Fire Department Robert M. Domeier, MD, EMS Medical Director,
Imaging of Cervical Spine Trauma
 Imaging of Cervical Spine Trauma C Craig Blackmore, MD, MPH Professor of Radiology and Adjunct Professor of Health Services University of Washington, Harborview Medical Center Salary support: AHRQ grant
Imaging of Cervical Spine Trauma C Craig Blackmore, MD, MPH Professor of Radiology and Adjunct Professor of Health Services University of Washington, Harborview Medical Center Salary support: AHRQ grant
To Backboard or Not To Backboard? Selective Spinal Immobilization
 To Backboard or Not To Backboard? Selective Spinal Immobilization Will Smith, MD, EMT-P Medical Director Grand Teton National Park and Jackson Hole Fire/EMS, Jackson, WY www.wildmedconsulting.com Objectives
To Backboard or Not To Backboard? Selective Spinal Immobilization Will Smith, MD, EMT-P Medical Director Grand Teton National Park and Jackson Hole Fire/EMS, Jackson, WY www.wildmedconsulting.com Objectives
Fractures of the Thoracic and Lumbar Spine
 A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
Orthopedic X-Rays most commonly missed
 Orthopedic X-Rays most commonly missed Vukiet Tran, MD, MHSc, MBA University Health Network Toronto, Canada 1 COI Disclosure I am the current Medical Director for Best Doctors Canada. Presenter: Dr. Vu
Orthopedic X-Rays most commonly missed Vukiet Tran, MD, MHSc, MBA University Health Network Toronto, Canada 1 COI Disclosure I am the current Medical Director for Best Doctors Canada. Presenter: Dr. Vu
Position Statement from the National Ski Patrol Medical Advisory Committee on the Selective Use of Backboards for Possible Spinal Injuries
 Position Statement from the National Ski Patrol Medical Advisory Committee on the Selective Use of Backboards for Possible Spinal Injuries Approved by the NSP Medical Committee 3/8/ 2017 Approved by the
Position Statement from the National Ski Patrol Medical Advisory Committee on the Selective Use of Backboards for Possible Spinal Injuries Approved by the NSP Medical Committee 3/8/ 2017 Approved by the
Pre-hospital Trauma Life Support. Rattiya Banjungam Emergency Physician, Khon Kaen Hospital
 Pre-hospital Trauma Life Support Rattiya Banjungam Emergency Physician, Khon Kaen Hospital Golden principles of Prehospital Trauma Care Golden Hour There is a golden hour if you are critically injured,
Pre-hospital Trauma Life Support Rattiya Banjungam Emergency Physician, Khon Kaen Hospital Golden principles of Prehospital Trauma Care Golden Hour There is a golden hour if you are critically injured,
Every day thousands of people become the accidental victims of trauma.
 Aurora Health Care South Region EMS 2010 2 nd Quarter CE Packet Spinal Cord Trauma Every day thousands of people become the accidental victims of trauma. Approximately 43,000 people die in motor vehicle
Aurora Health Care South Region EMS 2010 2 nd Quarter CE Packet Spinal Cord Trauma Every day thousands of people become the accidental victims of trauma. Approximately 43,000 people die in motor vehicle
X-ray (Radiography) - Bone
 Scan for mobile link. X-ray (Radiography) - Bone Bone x-ray uses a very small dose of ionizing radiation to produce pictures of any bone in the body. It is commonly used to diagnose fractured bones or
Scan for mobile link. X-ray (Radiography) - Bone Bone x-ray uses a very small dose of ionizing radiation to produce pictures of any bone in the body. It is commonly used to diagnose fractured bones or
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abscess, epidural, 822 824 Achilles tendon rupture, 894 895, 981 982 Acromioclavicular separations, shoulder pain in, 751 753 Adhesive capsulitis,
Note: Page numbers of article titles are in boldface type. A Abscess, epidural, 822 824 Achilles tendon rupture, 894 895, 981 982 Acromioclavicular separations, shoulder pain in, 751 753 Adhesive capsulitis,
Spinal injury: assessment and initial management
 National Clinical Guideline Centre Final Spinal injury: assessment and initial management Spinal injury assessment: assessment and imaging for spinal injury NICE guideline NG41 Appendices G -I February
National Clinical Guideline Centre Final Spinal injury: assessment and initial management Spinal injury assessment: assessment and imaging for spinal injury NICE guideline NG41 Appendices G -I February
PEDIATRIC MILD TRAUMATIC HEAD INJURY
 PEDIATRIC MILD TRAUMATIC HEAD INJURY October 2011 Quality Improvement Resources Illinois Emergency Medical Services for Children is a collaborative program between the Illinois Department of Public Health
PEDIATRIC MILD TRAUMATIC HEAD INJURY October 2011 Quality Improvement Resources Illinois Emergency Medical Services for Children is a collaborative program between the Illinois Department of Public Health
Pilon Fractures - OrthoInfo - AAOS. Copyright 2010 American Academy of Orthopaedic Surgeons. Pilon Fractures
 Copyright 2010 American Academy of Orthopaedic Surgeons Pilon Fractures Pilon fractures affect the bottom of the shinbone (tibia) at the ankle joint. In most cases, both bones in the lower leg, the tibia
Copyright 2010 American Academy of Orthopaedic Surgeons Pilon Fractures Pilon fractures affect the bottom of the shinbone (tibia) at the ankle joint. In most cases, both bones in the lower leg, the tibia
6/23/2017. What do you see? skull fracture
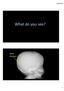 What do you see? skull fracture 1 Head CT On soft tissue windows, posterior soft tissues swelling and hemorrhage, no definite evidence of fracture Head CT On bone windows, fracture now seen subjacent to
What do you see? skull fracture 1 Head CT On soft tissue windows, posterior soft tissues swelling and hemorrhage, no definite evidence of fracture Head CT On bone windows, fracture now seen subjacent to
Massachusetts College of Emergency Physicians RISK MANAGEMENT COURSE REGISTRATION FORM
 Massachusetts College of Emergency Physicians RISK MANAGEMENT COURSE REGISTRATION FORM Tuition fee: $195.00 INSTRUCTIONS: Please print out this document. Then fill in the answers in the appropriate box
Massachusetts College of Emergency Physicians RISK MANAGEMENT COURSE REGISTRATION FORM Tuition fee: $195.00 INSTRUCTIONS: Please print out this document. Then fill in the answers in the appropriate box
Spine and Spinal Cord Injury in Children
 Spine and Spinal Cord Injury in Children S. Danielle Brown, MS, RN, CNRN, SCRN Director, Research Coordination and Education Barrow Neurological Institute at Phoenix Children s Hospital Introduction Trauma
Spine and Spinal Cord Injury in Children S. Danielle Brown, MS, RN, CNRN, SCRN Director, Research Coordination and Education Barrow Neurological Institute at Phoenix Children s Hospital Introduction Trauma
Quiles v Rojas 2015 NY Slip Op 31664(U) January 5, 2015 Supreme Court, Bronx County Docket Number: /11 Judge: Howard H. Sherman Cases posted
 Quiles v Rojas 2015 NY Slip Op 31664(U) January 5, 2015 Supreme Court, Bronx County Docket Number: 306567/11 Judge: Howard H. Sherman Cases posted with a "30000" identifier, i.e., 2013 NY Slip Op 30001(U),
Quiles v Rojas 2015 NY Slip Op 31664(U) January 5, 2015 Supreme Court, Bronx County Docket Number: 306567/11 Judge: Howard H. Sherman Cases posted with a "30000" identifier, i.e., 2013 NY Slip Op 30001(U),
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Date of Admission: [DATE]. Date of Discharge:
![Date of Admission: [DATE]. Date of Discharge: Date of Admission: [DATE]. Date of Discharge:](/thumbs/74/71277118.jpg) Date of Admission: [DATE]. Date of Discharge: History of Present Illness: Mr. [NAME] AKA [NAME] is a 31-year-old male who presents to the [PLACE] Trauma Surgery Service as a moderate trauma on [DATE] following
Date of Admission: [DATE]. Date of Discharge: History of Present Illness: Mr. [NAME] AKA [NAME] is a 31-year-old male who presents to the [PLACE] Trauma Surgery Service as a moderate trauma on [DATE] following
Traumatic Spinal Cord Injury. 39 th CANP Annual Educational Conference March 18 th, :00pm-6:15pm Carl Wherry, ACNP-bc Amanda Severson, ACNP-bc
 Traumatic Spinal Cord Injury 39 th CANP Annual Educational Conference March 18 th, 2016 5:00pm-6:15pm Carl Wherry, ACNP-bc Amanda Severson, ACNP-bc Disclosures No conflicts of interest to disclose. Introduction
Traumatic Spinal Cord Injury 39 th CANP Annual Educational Conference March 18 th, 2016 5:00pm-6:15pm Carl Wherry, ACNP-bc Amanda Severson, ACNP-bc Disclosures No conflicts of interest to disclose. Introduction
Initial Pelvic Fracture Management. Patrick M Reilly MD FACS February 27, 2010
 Initial Pelvic Fracture Management Patrick M Reilly MD FACS February 27, 2010 John Pryor MD Field Triage* * Step One : Physiology * Step Two : Anatomy * Step Three : Mechanism * Step Four : Co-Morbid Conditions
Initial Pelvic Fracture Management Patrick M Reilly MD FACS February 27, 2010 John Pryor MD Field Triage* * Step One : Physiology * Step Two : Anatomy * Step Three : Mechanism * Step Four : Co-Morbid Conditions
7/23/2018 DESCRIBING THE FRACTURE. Pattern Open vs closed Location BASIC PRINCIPLES OF FRACTURE MANAGEMENT. Anjan R. Shah MD July 21, 2018.
 BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
EMS System for Metropolitan Oklahoma City and Tulsa 2018 Medical Control Board Treatment Protocols
 EMERGENCY MEDICAL RESPONDER EMT EMT-INTERMEDIATE 85 ADVANCED EMT PARAMEDIC 14G PATIENT PRIORITIZATION While each patient will receive the best possible EMS care in a humane and ethical manner, proper patient
EMERGENCY MEDICAL RESPONDER EMT EMT-INTERMEDIATE 85 ADVANCED EMT PARAMEDIC 14G PATIENT PRIORITIZATION While each patient will receive the best possible EMS care in a humane and ethical manner, proper patient
102 Results RESULTS. Age Mean=S.D Range 42= years -84 years Number % <30 years years >50 years
 102 Results RESULTS A total of 50 cases were studied 39 males and 11females.Their age ranged between 16 years and 84 years (mean 42years). T1 and T2WI were acquired for all cases in sagittal and axial
102 Results RESULTS A total of 50 cases were studied 39 males and 11females.Their age ranged between 16 years and 84 years (mean 42years). T1 and T2WI were acquired for all cases in sagittal and axial
Focused History and Physical Examination of the
 Henry: EMT Prehospital Care, Revised 3 rd Edition Lecture Notes Chapter 10: Focused History and Physical Examination of Trauma Patients Chapter 10 Focused History and Physical Examination of the Trauma
Henry: EMT Prehospital Care, Revised 3 rd Edition Lecture Notes Chapter 10: Focused History and Physical Examination of Trauma Patients Chapter 10 Focused History and Physical Examination of the Trauma
Overview. Background. Table of Contents
 Trauma Service Guidelines Title: Cervical Spine Guidelines Developed by: P. Page, R. Judson, K. Gumm, M. Kennedy, D. McDonald & Advisory Committee on Trauma Created: Version 1.0 October 2005, Revised:
Trauma Service Guidelines Title: Cervical Spine Guidelines Developed by: P. Page, R. Judson, K. Gumm, M. Kennedy, D. McDonald & Advisory Committee on Trauma Created: Version 1.0 October 2005, Revised:
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery. By: Aun Lauriz E. Macuja SAC_SN4
 Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Trauma Films for Upper Body. LCDR. Naruebade Rungrattanawilai RTN M.D., LL.B. FRCOST, DMOC
 Trauma Films for Upper Body LCDR. Naruebade Rungrattanawilai RTN M.D., LL.B. FRCOST, DMOC Objective A 42 year-old housekeeper with history of motorcycle accident. There was no external wound but she have
Trauma Films for Upper Body LCDR. Naruebade Rungrattanawilai RTN M.D., LL.B. FRCOST, DMOC Objective A 42 year-old housekeeper with history of motorcycle accident. There was no external wound but she have
Lesson Plans and Objectives: Review material for article Prep work for article Picture recovery Review for placement on-line.
 Lesson Plans and Objectives: Review material for article Prep work for article Picture recovery Review for placement on-line. After reading the article, the staff will be able to: Define facial trauma
Lesson Plans and Objectives: Review material for article Prep work for article Picture recovery Review for placement on-line. After reading the article, the staff will be able to: Define facial trauma
Dr. Richard Smith 26/04/16
 BENDIGO HEALTH EMERGENCY DEPARTMENT Spinal Trauma Clinical Practice Guidelines Dr. Richard Smith 26/04/16 1 Contents PURPOSE... 3 PREAMBLE... 3 POLICY... 4 INITIAL CLINICAL MANAGEMENT... 5 Basic exam components...
BENDIGO HEALTH EMERGENCY DEPARTMENT Spinal Trauma Clinical Practice Guidelines Dr. Richard Smith 26/04/16 1 Contents PURPOSE... 3 PREAMBLE... 3 POLICY... 4 INITIAL CLINICAL MANAGEMENT... 5 Basic exam components...
