A Ware Injury in Collegiate Athletics- The Lisfranc Fracture-Dislocation
|
|
|
- Wilfred Harmon
- 6 years ago
- Views:
Transcription
1 Journal of Sport Rehabilitation, 1993, 2, O 1993 Human Kinetics Publishers, Inc. A Ware Injury in Collegiate Athletics- The Lisfranc Fracture-Dislocation Keith M. Gorse, Graham Johnstone, and Jennifer Cruse A rare injury in collegiate athletics is the Lisfranc fracture-dislocation of the foot. This case study will give team physicians and athletic trainers an idea of what to look for in this type of injury. It will be shown how an 18- year-old college football player received the injury, how it was evaluated by the sports medicine staff, and how it was surgically treated by the team physician. Finally, the athlete's rehabilitation will be summarized and the time frame during which full activities were started again will be outlined. This case study will give sports medicine specialists a better understanding of the Lisfranc topic and how to deal with it. The Lisfranc fracture-dislocation is an injury rarely seen in athletics. But when it occurs, it is extremely important that the athletic trainer and physician recognize it immediately. The injury itself occurs in the midfoot. A direct or indirect force that causes midfoot eversion produces this type of injury. The metatarsals are the bones most involved with the Lisfranc injury. The cuneiforms and the cuboid are the secondary bones involved (5). Pain and swelling to the area involved should be carefully evaluated by the athletic trainer and physician. Immobilization should occur with transport to a hospital if necessary. Usual treatment includes surgery to the injured area with an extended rehabilitation period (I). This report was written in hopes that other sports medicine personnel will gain some understanding of how to diagnose and treat this injury. Since the Lisfranc injury is very rare in athletics, it is important that it be diagnosed and treated early, so chronic disabilities do not occur. History On August 31, 1992, an 18-year-old Carnegie Mellon University football player was practicing with the team on the grass intramural field. It was in the late Keith M. Gorse and Graham Johnstone are with the Athletic Department, Carnegie Mellon University, 5000 Forbes Ave., Pittsburgh, PA Jennifer Cmse is with Allentown Sports Medicine, 2724 Elm Court, Allentown, PA
2 Gorse, Johnstone, and Cruse Figure - 1 -Athlete with his left \ A foot field the opposing player in front of him. The force, which is a pushing and downward force, causes the left foot to be twisted and pushed in the hole, thus causing the injury. afternoon and practice was about halfway over. During a certain play of the drill the player, a tight end, got his left foot caught in a hole in the field. As the opposing defensive player came up to block him, he put all his weight on the left side of his body. His left foot was planted in the hole and his forefoot was hyperextended. As more weight was forced on top of him, his left foot rotated and snapped (Figure 1). The play ended immediately with the player lying on the ground in a lot of pain. Evaluation The injured athlete was calmed down and stabilized on his back. He said he felt a sharp pain in his midfoot-up to his toes. The athlete said he felt a "pop" in the middle of his foot when the injury occurred. On initial evaluation, half of his left shoe had to be cut off in order to carefully slide his foot out. Moderate swelling was present in the midfoot to forefoot area. When the injured area was palpated, most of the pain and discomfort were found to be between the first and third metatarsals. There was no definite evidence of a fracture or dislocation
3 Lisfranc Fracture-Dislocation 283 at that time. There was no severe deformity to the area. The pain was moderate and the injured area was swelling very quickly. The foot and lower leg were immobilized and the athlete was carried to the training room from the practice field. His foot, still immobilized, was elevated on a treatment table and ice was placed around it. The team physician came into the training room almost immediately after ice was placed on the athlete. He did an initial evaluation and felt there could be a fracture of one of the bones in the midfoot. The physician then placed a temporary posterior splint on the athlete's foot and lower leg. An X ray and further evaluation were to be done early the next morning in his office. The athlete was placed on crutches and transported to his dormitory room. Treatment The athlete was taken to the team physician's office the next morning. He was X-rayed and reevaluated. His pain and discomfort were about the same as the previous night. The physician's examination revealed that he had suffered a Lisfranc fracture-dislocation of the first and second metatarsals. At that time it was decided to do a surgical repair on the injury that afternoon (Figure 2). With surgery, it was discovered that the first metatarsal base was subluxated 40-50%. There was also a small fracture in the fit metatarsal. The second metatarsal was fractured, but nondisplaced. The medial joint ligaments of the second metatarsal were disrupted superiorly. With the first and second metatarsals reduced and holding nicely, a K-wire was inserted percutaneously through the base of the first metatarsal of the lateral comer of the cuneiform into the second metatarsal into the cuneiform. A second K-wire was inserted transversely through the first and second metatarsal bases into one cortex of the third metatarsal. X rays (fluoroscopy) showed this to be in excellent position. The athlete was placed into a short leg cast with the foot placed in a neutral position. The pins were left protruding and were bent over, and Vaseline gauze was placed around them (3). The athlete was seen 2 weeks postsurgery for cast change and evaluation. X rays showed pin and bone placement still to be excellent (Figure 3). Six weeks postsurgery, the cast and pins were removed from the foot. X rays taken at this time showed almost complete healing of the area. Rehabilitation Rehabilitation for the injury started 1 week after the surgery; the athlete was given isometric calf exercises to do while he was in the cast. He performed these exercises 1-2 times a day on his own. It was opted not to use electrical stimulation on the calf muscles until the cast was taken off. The athlete was allowed to do light resistance work on his hamstrings, quadriceps, and hips. This phase of rehabilitation lasted 6 weeks. Six weeks postoperation, the cast was removed. Active and passive range of motion exercises, without any resistance, were started on the athlete's foot and ankle. Muscle stimulation was started on the calf muscles, which would help strengthen those muscles. The athlete was partial weight bearing at this time, for a period of 1 week.
4 Gorse, Johnstone, and Cruse Figure 2 - X ray of the injury before surgery. Eight weeks postoperation, and 2 weeks after the cast was taken off, the athlete started more aggressive rehabilitation. Range of motion exercises with resistance were instituted. When it was seen that the foot and ankle could handle light resistance through normal range, the athlete was placed on a heavier resistance program. A slant board was used for stretching of the lower leg muscles. A BAPS board was used with varying weights and movements. Different resistances of theraband were used to increase range of motion and strength. Other exercises such as toe raises, heel cord, and towel curls were incorporated with the rehab program to add endurance. At the end of each exercise program the athlete either rode the stationary bike or swam in the gymnasium pool for 15 to 20 min. The final phase of the organized rehabilitation program was started at 12 weeks postoperation. This phase started with the athlete jogging straight lines
5 Lisfranc Fracture-Dislocation Figure 3 - X ray of the injury, postsurgery, with the pins in place. (50 yd). He then progressed to running circles and figure eights, and then sprinting. By the end of the program he was able to sprint and turn, and then backpedal without pain. During this phase he was still working out in the swimming pool and the weight room, trying to gain more strength and endurance (4). At about 4 months postoperation the athlete was given clearance by the team physician to do any activity on his own, as long as he had no pain. He was instructed to stay away from contact sports and to do everything on smooth surfaces. He was also fitted with a special arch support, to be used in all of his shoes. This would give the foot more comfort and support with activity. He was expected to be given medical clearance to play football in Conclusion The Lisfranc fracture-dislocation can be caused by either a direct or an indirect force on the foot. The area injured is in the midfoot region and includes the 5
6 286 Gorse, Johnstone, and Cruse metatarsals, 3 cuneiforms, and cuboid. The ligaments in this area also can be involved and often become unstable. The injury suffered by our athlete was caused by an indirect force. His foot was stuck in a hole in the field, and an opposing player was placing a force from the front and top. The forefoot was twisted and hyperextended from the force, causing injury to the midfoot region. The injury was detected mainly by X rays taken the next day, but in most cases there is more of a gross deformity evident. Athletic trainers should always observe for deformity of bony areas, swelling, and discoloration. The dorsalis pedis pulse should also be checked during the evaluation. In severe cases, the dorsalis pedis artery could be severed from the displacement of bones caused by the injury (2). Finally, it is important for athletic trainers and physicians to check the shoes their athletes are wearing and the type of surface they are playing on. This type of foot injury can be controlled by playing on a smooth, regular surface and wearing supportive shoes. References 1. American Academy of Orthopaedic Surgeons. Athletic Training and Sports Medicine (2nd ed.). Chicago: AAOS, 1991, pp Brown, D., and R. Gumbs. Lisfranc fracture4islocation: Report of two cases. J. Natl. Med. Assoc. 83: , Johnstone, G. Head Team Physician, Carnegie Mellon University. Orthopaedic Surgeon-4.S.A. Group. Evaluation and surgical notes, September Prentice, W. Rehabilitation Techniques in Sports Medicine (1st ed.). St. Louis: Mosby, 1990, pp Saurs, R., E. Deloreo, and C. Weiss. A Lisfranc's fracture-dislocation in a collegiate football player. Athletic Training, JNATA, 27: 24-26, 1992.
ANKLE SPRAINS. Explanation. Causes. Symptoms
 ANKLE SPRAINS Explanation Ankle sprains occur when ligaments in the ankle are partially or completely torn due to sudden stretching, either laterally or medially, or when the ankle is suddenly twisted
ANKLE SPRAINS Explanation Ankle sprains occur when ligaments in the ankle are partially or completely torn due to sudden stretching, either laterally or medially, or when the ankle is suddenly twisted
Hip Arthroscopy with CAM resection/labral Repair Protocol
 Hip Arthroscopy with CAM resection/labral Repair Protocol As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp, swelling, or other undesirable factors are
Hip Arthroscopy with CAM resection/labral Repair Protocol As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp, swelling, or other undesirable factors are
Lateral Collateral Ligament Sprain
 What is lateral collateral ligament sprain? Lateral Collateral Ligament Sprain A sprain is a joint injury that causes a stretch or tear in a ligament, a strong band of tissue connecting one bone to another.
What is lateral collateral ligament sprain? Lateral Collateral Ligament Sprain A sprain is a joint injury that causes a stretch or tear in a ligament, a strong band of tissue connecting one bone to another.
Common Athletic Injuries of the Ankle
 Common Athletic Injuries of the Ankle Common Injuries of the Ankle in Athletes Ankle Sprains Chronic Lateral Ankle Instability Peroneal Tendon Injuries Achilles Tendon Tears Ankle Sprains What s an Ankle
Common Athletic Injuries of the Ankle Common Injuries of the Ankle in Athletes Ankle Sprains Chronic Lateral Ankle Instability Peroneal Tendon Injuries Achilles Tendon Tears Ankle Sprains What s an Ankle
TIBIAL PLATEAU FRACTURE
 TIBIAL PLATEAU FRACTURE Description Preventive Measures A tibial plateau fracture is a complete or incomplete break Appropriately warm up and stretch before practice or in the larger of the two leg bones
TIBIAL PLATEAU FRACTURE Description Preventive Measures A tibial plateau fracture is a complete or incomplete break Appropriately warm up and stretch before practice or in the larger of the two leg bones
ANKLE SPRAIN, ACUTE. Description
 Description ANKLE SPRAIN, ACUTE An acute ankle sprain involves the stretching and tearing of one or more ligaments in the ankle. A two-ligament sprain causes more disability than a single-ligament sprain.
Description ANKLE SPRAIN, ACUTE An acute ankle sprain involves the stretching and tearing of one or more ligaments in the ankle. A two-ligament sprain causes more disability than a single-ligament sprain.
METATARSAL FRACTURE (Including Jones and Dancer s Fractures)
 METATARSAL FRACTURE (Including Jones and Dancer s Fractures) Description Possible Complications Metatarsal fracture is a broken bone (fracture) in the middle Nonunion (fracture does not heal, particularly
METATARSAL FRACTURE (Including Jones and Dancer s Fractures) Description Possible Complications Metatarsal fracture is a broken bone (fracture) in the middle Nonunion (fracture does not heal, particularly
Knee OCD Repair/Fixation/Grafting Protocol
 Knee OCD Repair/Fixation/Grafting Protocol As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp, swelling, or other undesirable factors are indicators that
Knee OCD Repair/Fixation/Grafting Protocol As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp, swelling, or other undesirable factors are indicators that
Review relevant anatomy of the foot and ankle. Learn the approach to examining the foot and ankle
 Objectives Review relevant anatomy of the foot and ankle Learn the approach to examining the foot and ankle Learn the basics of diagnosis and treatment of ankle sprains Overview of other common causes
Objectives Review relevant anatomy of the foot and ankle Learn the approach to examining the foot and ankle Learn the basics of diagnosis and treatment of ankle sprains Overview of other common causes
ACHILLES TENDON RUPTURE
 ACHILLES TENDON RUPTURE Description Expected Outcome Achilles tendon rupture is a complete tear of the Achilles tendon. This tendon, sometimes called the heel cord, is the tendon attachment of the calf
ACHILLES TENDON RUPTURE Description Expected Outcome Achilles tendon rupture is a complete tear of the Achilles tendon. This tendon, sometimes called the heel cord, is the tendon attachment of the calf
Anterior Cruciate Ligament (ACL) Reconstruction Protocol. Hamstring Autograft, Allograft, or Revision
 Anterior Cruciate Ligament (ACL) Reconstruction Protocol Hamstring Autograft, Allograft, or Revision As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp,
Anterior Cruciate Ligament (ACL) Reconstruction Protocol Hamstring Autograft, Allograft, or Revision As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp,
Postoperative Days 1-7
 ACL RECONSTRUCTION REHABILITATION PROTOCOL Postoperative Days 1-7 *IT IS EXTREMELY IMPORTANT THAT YOU WORK ON EXTENSION IMMEDIATELY Goals: * Control pain and swelling * Care for the knee and dressing *
ACL RECONSTRUCTION REHABILITATION PROTOCOL Postoperative Days 1-7 *IT IS EXTREMELY IMPORTANT THAT YOU WORK ON EXTENSION IMMEDIATELY Goals: * Control pain and swelling * Care for the knee and dressing *
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction
 Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY
 Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
Hany El-Rashidy and Anand Vora
 Chapter 194 Lisfranc Injuries Chapter 194 Lisfranc Injuries Hany El-Rashidy and Anand Vora 8 ICD-9 CODE 838.03 Lisfranc (Tarsometatarsal) Fracture-Dislocation Key Concepts The Lisfranc joint represents
Chapter 194 Lisfranc Injuries Chapter 194 Lisfranc Injuries Hany El-Rashidy and Anand Vora 8 ICD-9 CODE 838.03 Lisfranc (Tarsometatarsal) Fracture-Dislocation Key Concepts The Lisfranc joint represents
.org. Tibia (Shinbone) Shaft Fractures. Anatomy. Types of Tibial Shaft Fractures
 Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
What is arthroscopy? Normal knee anatomy
 What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
Brennen Lucas, M.D. Advanced Orthopaedic Associates
 Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GUIDELINES FOR REHABILITATION FOLLOWING SURGICAL RECONSTRUCTION
Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GUIDELINES FOR REHABILITATION FOLLOWING SURGICAL RECONSTRUCTION
AMERICAN RED CROSS FIRST AID RESPONDING TO EMERGENCIES FOURTH EDITION Copyright 2006 by The American National Red Cross All rights reserved.
 Musculoskeletal injuries are most commonly caused by Mechanical forms of energy. Chemicals. Electrical energy. Heat Mechanical energy produces direct, indirect, twisting and contracting forces. Can be
Musculoskeletal injuries are most commonly caused by Mechanical forms of energy. Chemicals. Electrical energy. Heat Mechanical energy produces direct, indirect, twisting and contracting forces. Can be
Calcaneus (Heel Bone) Fractures
 Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
Rehabilitation After Patellar Tendon Debridement Surgery
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Rehabilitation Guidelines for Meniscal Repair
 Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Prevention and Treatment of Injuries. Anatomy. Anatomy. Tibia: the second longest bone in the body
 Prevention and Treatment of Injuries The Ankle and Lower Leg Westfield High School Houston, Texas Anatomy Tibia: the second longest bone in the body Serves as the principle weight-bearing bone of the leg.
Prevention and Treatment of Injuries The Ankle and Lower Leg Westfield High School Houston, Texas Anatomy Tibia: the second longest bone in the body Serves as the principle weight-bearing bone of the leg.
Acute Achilles Tendon Repair Protocol
 Acute Achilles Tendon Repair Protocol As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp, swelling, or other undesirable factors are indicators that you
Acute Achilles Tendon Repair Protocol As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp, swelling, or other undesirable factors are indicators that you
ACL REHABILITATION PROTOCOL
 Name: ID: Date Of Surgery :DD / MM / YYYY Procedure: ACL REHABILITATION PROTOCOL Note :If another procedure like meniscus repair or OATS (Osteochondralautograft transfer) has been done along with ACL reconstruction
Name: ID: Date Of Surgery :DD / MM / YYYY Procedure: ACL REHABILITATION PROTOCOL Note :If another procedure like meniscus repair or OATS (Osteochondralautograft transfer) has been done along with ACL reconstruction
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: PCL RECONSTRUCTION +/- ACL / MCL / LCL / POSTEROLATERAL CORNER 1. General Guidelines: Time lines in this rehabilitation
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: PCL RECONSTRUCTION +/- ACL / MCL / LCL / POSTEROLATERAL CORNER 1. General Guidelines: Time lines in this rehabilitation
Foot Injuries. Dr R B Kalia
 Foot Injuries Dr R B Kalia Overview Dramatic impact on the overall health, activity, and emotional status More attention and aggressive management Difficult appendage to study and diagnose. Aim- a stable
Foot Injuries Dr R B Kalia Overview Dramatic impact on the overall health, activity, and emotional status More attention and aggressive management Difficult appendage to study and diagnose. Aim- a stable
Patella Instability in Children and Adolescents
 Patella Instability in Children and Adolescents Description Patella Instability is an injury to the kneecap (patella) affecting the joint it forms with the thigh bone (femur) Patella Instability can occur
Patella Instability in Children and Adolescents Description Patella Instability is an injury to the kneecap (patella) affecting the joint it forms with the thigh bone (femur) Patella Instability can occur
Week 1 Orthotics- 1. Knee brace locked in full extension at all times except for rehab exercises 2. Elastic bandage as needed to control swelling
 General Principles: This protocol was designed to provide the rehabilitation professional with a guideline of postoperative care. It should be stressed that this is only a protocol and should not be a
General Principles: This protocol was designed to provide the rehabilitation professional with a guideline of postoperative care. It should be stressed that this is only a protocol and should not be a
A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY
 A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY Georgia Bouffard Student Physiotherapist Colin Walker Orthopaedic Knee Specialist Frank Gilroy BSc MSCP 1 CONTENTS Anatomy of the knee
A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY Georgia Bouffard Student Physiotherapist Colin Walker Orthopaedic Knee Specialist Frank Gilroy BSc MSCP 1 CONTENTS Anatomy of the knee
REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL. WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches.
 REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL IMMEDIATE POST OPERATIVE PHASE Week 1: WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches. Ankle Pumps Passive knee extension
REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL IMMEDIATE POST OPERATIVE PHASE Week 1: WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches. Ankle Pumps Passive knee extension
Post Operative ACL Reconstruction Protocol Brian J. White, MD
 Post Operative ACL Reconstruction Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve as
Post Operative ACL Reconstruction Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve as
Anterior Cruciate Ligament Hamstring Rehabilitation Protocol
 Anterior Cruciate Ligament Hamstring Rehabilitation Protocol Focus on exercise quality avoid overstressing the donor area while it heals. Typically, isolated hamstring strengthening begins after the 6
Anterior Cruciate Ligament Hamstring Rehabilitation Protocol Focus on exercise quality avoid overstressing the donor area while it heals. Typically, isolated hamstring strengthening begins after the 6
KNEE AND LEG EXERCISE PROGRAM
 KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
Ankle Rehabilitation with Wakefield Sports Clinic
 Ankle Rehabilitation with Wakefield Sports Clinic With Michael Woodcock Adelaide 36ERS & Wakefield Sports Clinic Physiotherapist The ankle joint is one of the major weight bearing structures in the body.
Ankle Rehabilitation with Wakefield Sports Clinic With Michael Woodcock Adelaide 36ERS & Wakefield Sports Clinic Physiotherapist The ankle joint is one of the major weight bearing structures in the body.
Mr. Siva Chandrasekaran Orthopaedic Surgeon MBBS MSpMed MPhil (surg) FRACS
 Sprained Ankle An ankle sprain occurs when the strong ligaments that support the ankle stretch beyond their limits and tear. Ankle sprains are common injuries that occur among people of all ages. They
Sprained Ankle An ankle sprain occurs when the strong ligaments that support the ankle stretch beyond their limits and tear. Ankle sprains are common injuries that occur among people of all ages. They
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
Ankle Sprain Recovery and Rehabilitation Protocol:
 Ankle Sprain Recovery and Rehabilitation Protocol: ***NOTE: Depending on the severity of your injury, you may be placed into a boot, brace, or similar type of supportive device for a brief period of time
Ankle Sprain Recovery and Rehabilitation Protocol: ***NOTE: Depending on the severity of your injury, you may be placed into a boot, brace, or similar type of supportive device for a brief period of time
Lesser toe sequential repair
 Lesser toe sequential repair For the correction of lesser toe deformity Information for patients Department of Podiatric Surgery What is lesser toe deformity? The lesser toes are those other than your
Lesser toe sequential repair For the correction of lesser toe deformity Information for patients Department of Podiatric Surgery What is lesser toe deformity? The lesser toes are those other than your
Post-Operative Meniscus Repair Protocol Brian J.White, MD
 Post-Operative Meniscus Repair Protocol Brian J.White, MD www.western-ortho.com (This protocol should be used with combined a ACL Reconstruction and meniscus repair) The intent of this protocol is to provide
Post-Operative Meniscus Repair Protocol Brian J.White, MD www.western-ortho.com (This protocol should be used with combined a ACL Reconstruction and meniscus repair) The intent of this protocol is to provide
James R. Romanowski, M.D.
 James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
Achilles Tendonitis and Tears
 Achilles Tendonitis and Tears The Achilles tendon is an important structure for normal ankle motion and normal function, even for daily activities such as walking. Achilles tendonitis can occur in patients
Achilles Tendonitis and Tears The Achilles tendon is an important structure for normal ankle motion and normal function, even for daily activities such as walking. Achilles tendonitis can occur in patients
ACHILLES TENDON REPAIR REHAB GUIDELINES
 ACHILLES TENDON REPAIR REHAB GUIDELINES Typically patients are discharged on the day of the operation or the next day. The leg is usually immobilized in a cast or hinged brace, ranging from 4-8 weeks.
ACHILLES TENDON REPAIR REHAB GUIDELINES Typically patients are discharged on the day of the operation or the next day. The leg is usually immobilized in a cast or hinged brace, ranging from 4-8 weeks.
REHABILITATION FOLLOWING ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION (using Hamstring Graft)
 REHABILITATION FOLLOWING ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION (using Hamstring Graft) PHASE 1: (0-3 WEEKS) Goal: Protect graft, manage pain, decrease swelling and improve range of movement. To optimise
REHABILITATION FOLLOWING ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION (using Hamstring Graft) PHASE 1: (0-3 WEEKS) Goal: Protect graft, manage pain, decrease swelling and improve range of movement. To optimise
Bones = phalanges 5 metatarsals 7 tarsals
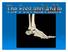 The Foot (Bones) Bones = 26 14 phalanges 5 metatarsals 7 tarsals Toes (Phalanges) Designed to give wider base for balance and propelling the body forward. 1st toe (Hallux) Two sesamoid bones located under
The Foot (Bones) Bones = 26 14 phalanges 5 metatarsals 7 tarsals Toes (Phalanges) Designed to give wider base for balance and propelling the body forward. 1st toe (Hallux) Two sesamoid bones located under
1. Split the evaluation form into four sections 2. Different sections on form
 1. Split the evaluation form into four sections a. 1 st year student does history/observation/palpation b. 2 nd year student does muscle testing/rom c. 3 rd year student does stress testing d. 4 th year
1. Split the evaluation form into four sections a. 1 st year student does history/observation/palpation b. 2 nd year student does muscle testing/rom c. 3 rd year student does stress testing d. 4 th year
ACL Reconstruction Protocol. Weeks 0 2
 ACL Reconstruction Protocol This is an outline of the major exercises that are commonly incorporated. Individual patient response should be considered and therefore modifications may need to be made. Communication
ACL Reconstruction Protocol This is an outline of the major exercises that are commonly incorporated. Individual patient response should be considered and therefore modifications may need to be made. Communication
LOWER LEG FRACTURES. Contents Anatomy of the lower leg...3
 Contents Anatomy of the lower leg.............................................................3 What is a fracture?....................................................................3 YOUR GUIDE TO LOWER
Contents Anatomy of the lower leg.............................................................3 What is a fracture?....................................................................3 YOUR GUIDE TO LOWER
Rehab and Return to Swimming for Breaststroker's Knee
 Page 1 of 9 Back Rehab and Return to Swimming for Breaststroker's Knee by June Quick, PT, ATC, CPI DIAGNOSIS Breaststrokers knee or sore knees from swimming usually involves inflammation around the kneecap.
Page 1 of 9 Back Rehab and Return to Swimming for Breaststroker's Knee by June Quick, PT, ATC, CPI DIAGNOSIS Breaststrokers knee or sore knees from swimming usually involves inflammation around the kneecap.
Page 1 of 5 SPECTRUM MEDICAL
 Page 1 of 5 SPECTRUM MEDICAL HOME INSTRUCTIONS Total Knee Replacement I. Walking A. Use walker/crutches until your doctor says you no longer need them. Your foot should be flat on the floor with on it.
Page 1 of 5 SPECTRUM MEDICAL HOME INSTRUCTIONS Total Knee Replacement I. Walking A. Use walker/crutches until your doctor says you no longer need them. Your foot should be flat on the floor with on it.
Ankle Program Range of Motion Exercises Stretches:
 Ankle Program Range of Motion Exercises Due to injury, immobilization or a combination of both your ankle has become stiff. These exercises are designed to help regain the motion and strength lost. You
Ankle Program Range of Motion Exercises Due to injury, immobilization or a combination of both your ankle has become stiff. These exercises are designed to help regain the motion and strength lost. You
REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT. Brace E-Z Wrap locked at zero degree extension, sleep in Brace
 Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
Treating the Ankle Sprain
 Treating the Ankle Sprain Ankle 'sprains' are very common injuries. Typically the ankle is rolled either inward (inversion sprain) or outward (eversion sprain). Inversion sprains cause pain along the outside
Treating the Ankle Sprain Ankle 'sprains' are very common injuries. Typically the ankle is rolled either inward (inversion sprain) or outward (eversion sprain). Inversion sprains cause pain along the outside
Ankle Sprains. Treatment and Restoration of Motion
 Ankle Sprains Treatment and Restoration of Motion Ankle sprains Ankle anatomy The ankle is a complex joint made up of three bones: the tibia, the fibula and the talus. These three bones are connected by
Ankle Sprains Treatment and Restoration of Motion Ankle sprains Ankle anatomy The ankle is a complex joint made up of three bones: the tibia, the fibula and the talus. These three bones are connected by
A Patient s Guide to Collateral Ligament Injuries
 A Patient s Guide to Collateral Ligament Injuries 264 Pleasant Street Concord, NH 03301 Phone: 6032243368 Fax: 6032287268 marketing.copa@concordortho.com DISCLAIMER: The information in this booklet is
A Patient s Guide to Collateral Ligament Injuries 264 Pleasant Street Concord, NH 03301 Phone: 6032243368 Fax: 6032287268 marketing.copa@concordortho.com DISCLAIMER: The information in this booklet is
Mosaicplasty and OATS Rehabilitation Protocol
 Mosaicplasty and OATS Rehabilitation Protocol PHASE 1: 0 2 weeks after surgery You will go home with crutches, cryocuff cold therapy unit and a CPM machine. GOALS: 1. Protect the cartilage transfer avoid
Mosaicplasty and OATS Rehabilitation Protocol PHASE 1: 0 2 weeks after surgery You will go home with crutches, cryocuff cold therapy unit and a CPM machine. GOALS: 1. Protect the cartilage transfer avoid
9180 KATY FREEWAY, STE. 200 (713)
 OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
.org. Ankle Fractures (Broken Ankle) Anatomy
 Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
9180 KATY FREEWAY, STE. 200 (713)
 AUTOLOGOUS CHONDROCYTE IMPLANTATION Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protect healing tissue from load and shear forces - Decrease pain and effusion
AUTOLOGOUS CHONDROCYTE IMPLANTATION Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protect healing tissue from load and shear forces - Decrease pain and effusion
Diagnosis: s/p ( LEFT / RIGHT ) Injury to MCL of the Knee -- Surgery Date:
 UCLA OUTPATIENT REHABILITATION SERVICES! SANTA MONICA! WESTWOOD 1000 Veteran Ave., A level Phone: (310) 794-1323 Fax: (310) 794-1457 1260 15 th St, Ste. 900 Phone: (310) 319-4646 Fax: (310) 319-2269 FOR
UCLA OUTPATIENT REHABILITATION SERVICES! SANTA MONICA! WESTWOOD 1000 Veteran Ave., A level Phone: (310) 794-1323 Fax: (310) 794-1457 1260 15 th St, Ste. 900 Phone: (310) 319-4646 Fax: (310) 319-2269 FOR
Femoral Condyle Rehabilitation Guidelines
 Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Brace: Protect healing tissue from load and shear forces Decrease pain and effusion Restore full passive knee extension
Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Brace: Protect healing tissue from load and shear forces Decrease pain and effusion Restore full passive knee extension
NICHOLAS J. AVALLONE, M.D.
 NICHOLAS J. AVALLONE, M.D. www.dravallone.com ACHILLES TENDON REPAIR REHAB GUIDELINES DISCLAIMER: The intent of this protocol is to provide therapists with guidelines for rehabilitation based on a review
NICHOLAS J. AVALLONE, M.D. www.dravallone.com ACHILLES TENDON REPAIR REHAB GUIDELINES DISCLAIMER: The intent of this protocol is to provide therapists with guidelines for rehabilitation based on a review
REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING Allograft
 Sports Medicine and Rehabilitation Center Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING Allograft I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation
Sports Medicine and Rehabilitation Center Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING Allograft I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: MENISCAL REPAIR: 1. General Guidelines: Time lines in this rehabilitation protocol are approximate. If the
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: MENISCAL REPAIR: 1. General Guidelines: Time lines in this rehabilitation protocol are approximate. If the
Bone-Patellar tendon-bone Autograft ACL Recon. Date of Surgery: Patient Name:
 Dx: o Right o Left Bone-Patellar tendon-bone Autograft ACL Recon Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: GENERAL
Dx: o Right o Left Bone-Patellar tendon-bone Autograft ACL Recon Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: GENERAL
Knee Conditioning Program
 Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon
 Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon Ph: (03) 9598 0691 Post op Instructions: Achilles Tendon Repair Recommended appliances for after your surgery: Crutches, walking frame
Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon Ph: (03) 9598 0691 Post op Instructions: Achilles Tendon Repair Recommended appliances for after your surgery: Crutches, walking frame
What is an ACL Tear?...2. Treatment Options...3. Surgical Techniques...4. Preoperative Care...5. Preoperative Requirements...6
 Table of Contents What is an ACL Tear?....2 Treatment Options...3 Surgical Techniques...4 Preoperative Care...5 Preoperative Requirements...6 Postoperative Care...................... 7 Crutch use...8 Initial
Table of Contents What is an ACL Tear?....2 Treatment Options...3 Surgical Techniques...4 Preoperative Care...5 Preoperative Requirements...6 Postoperative Care...................... 7 Crutch use...8 Initial
Post Operative Total Hip Replacement Protocol Brian J. White, MD
 Post Operative Total Hip Replacement Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Post Operative Total Hip Replacement Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
ANTERIOR KNEE PAIN. Explanation. Causes. Symptoms
 ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL
 ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain
ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain
Post-Operative Physical Therapy Protocol for Autograft ACL Reconstruction
 Adam J. Farber, MD Sports Medicine and Orthopaedic Surgery Board Certified; Fellowship-trained in Sports Medicine & Arthroscopic Surgery P: 480-219-3342; F: 480-219-3271 Post-Operative Physical Therapy
Adam J. Farber, MD Sports Medicine and Orthopaedic Surgery Board Certified; Fellowship-trained in Sports Medicine & Arthroscopic Surgery P: 480-219-3342; F: 480-219-3271 Post-Operative Physical Therapy
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction
 Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
ANTERIOR CRUCTIATE LIGAMENT RECONSTRUCTION COLLATERAL LIGAMENT RECONSTRUCION/REPAIR AND MENISCUS REPAIR REHABILITATION PROTOCOL
 ANTERIOR CRUCTIATE LIGAMENT RECONSTRUCTION COLLATERAL LIGAMENT RECONSTRUCION/REPAIR AND MENISCUS REPAIR REHABILITATION PROTOCOL GENERAL GUIDELINES - The local anesthetic (similar to novacaine) in your
ANTERIOR CRUCTIATE LIGAMENT RECONSTRUCTION COLLATERAL LIGAMENT RECONSTRUCION/REPAIR AND MENISCUS REPAIR REHABILITATION PROTOCOL GENERAL GUIDELINES - The local anesthetic (similar to novacaine) in your
STRETCHING. Low Back Rotation. Double Leg Pull. Single Leg Pull. Core Home Exercise Program
 Core Home Exercise Program Seth L. Sherman, M.D. Tamara L. Young, ATC, OTC, M.Ed Department of Sports Medicine STRETCHING Low Back Rotation While lying on your back with both of your knees bent. Rotate
Core Home Exercise Program Seth L. Sherman, M.D. Tamara L. Young, ATC, OTC, M.Ed Department of Sports Medicine STRETCHING Low Back Rotation While lying on your back with both of your knees bent. Rotate
ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL
 ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
PATELLAR DISLOCATION AND SUBLUXATION
 PATELLAR DISLOCATION AND SUBLUXATION Description For jumping (basketball, volleyball) or contact sports, Patellar dislocation and subluxation are injuries to the protect the patella with supportive devices,
PATELLAR DISLOCATION AND SUBLUXATION Description For jumping (basketball, volleyball) or contact sports, Patellar dislocation and subluxation are injuries to the protect the patella with supportive devices,
GUIDELINES FOR REHABILITATION Arthroscopic Meniscectomy/Loose Body Removal/Debridement
 GENERAL GUIDELINES Cryotherapy: Change ice packs or apply cryocuff every 4 hours while awake for first 72 hrs. GENERAL PROGRESSION OF ACTIVITIES OF DAILY LIVING Patients may begin the following activities
GENERAL GUIDELINES Cryotherapy: Change ice packs or apply cryocuff every 4 hours while awake for first 72 hrs. GENERAL PROGRESSION OF ACTIVITIES OF DAILY LIVING Patients may begin the following activities
Introduction. Anatomy
 the patella is called the quadriceps mechanism. Though we think of it as a single device, the quadriceps mechanism has two separate tendons, the quadriceps tendon on top of the patella and the patellar
the patella is called the quadriceps mechanism. Though we think of it as a single device, the quadriceps mechanism has two separate tendons, the quadriceps tendon on top of the patella and the patellar
Lesser metatarsal cuneiform joint fusion for the treatment of midfoot osteoarthritis. Information for patients Department of Podiatric Surgery
 Lesser metatarsal cuneiform joint fusion for the treatment of midfoot osteoarthritis Information for patients Department of Podiatric Surgery What is midfoot osteoarthritis? Midfoot arthritis is 'wear
Lesser metatarsal cuneiform joint fusion for the treatment of midfoot osteoarthritis Information for patients Department of Podiatric Surgery What is midfoot osteoarthritis? Midfoot arthritis is 'wear
WHAT IS PLANTAR FASCIITIS?
 WHAT IS PLANTAR FASCIITIS? If you're finding when you climb out of bed each morning that your first couple steps cause your foot and heel to hurt, this might be a sign of plantar fasciitis. A common condition
WHAT IS PLANTAR FASCIITIS? If you're finding when you climb out of bed each morning that your first couple steps cause your foot and heel to hurt, this might be a sign of plantar fasciitis. A common condition
Musculoskeletal Age Related Changes That Lead to Movement Loss
 Objectives Review the factors that can lead to movement loss (age related changes and previous injuries) Discuss the role that posture plays affecting movement loss Discuss exercises to prevent movement
Objectives Review the factors that can lead to movement loss (age related changes and previous injuries) Discuss the role that posture plays affecting movement loss Discuss exercises to prevent movement
MEDIAL TIBIAL STRESS SYNDROME (Shin Splints)
 MEDIAL TIBIAL STRESS SYNDROME (Shin Splints) Description Expected Outcome Shin splints is a term broadly used to describe pain in the lower extremity brought on by exercise or athletic activity. Most commonly
MEDIAL TIBIAL STRESS SYNDROME (Shin Splints) Description Expected Outcome Shin splints is a term broadly used to describe pain in the lower extremity brought on by exercise or athletic activity. Most commonly
Rehabilitation Guidelines for Knee Arthroscopy
 Rehabilitation Guidelines for Knee Arthroscopy The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Knee Arthroscopy The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION
 OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION FEMORAL CONDYLE REHABILITATION PROGRAM PHASE I - PROTECTION PHASE (WEEKS 0-6) Protection of healing tissue from load and shear forces Decrease pain and effusion
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION FEMORAL CONDYLE REHABILITATION PROGRAM PHASE I - PROTECTION PHASE (WEEKS 0-6) Protection of healing tissue from load and shear forces Decrease pain and effusion
ACL RECONSTRUCTION REHABILITATION PROTOCOL DELAYED DAVID R. MACK, M.D. INTRODUCTION
 ACL RECONSTRUCTION REHABILITATION PROTOCOL DELAYED DAVID R. MACK, M.D. INTRODUCTION This DELAYED protocol is used if any of the following are present: meniscal repair, concomitant ligament repair or patellofemoral
ACL RECONSTRUCTION REHABILITATION PROTOCOL DELAYED DAVID R. MACK, M.D. INTRODUCTION This DELAYED protocol is used if any of the following are present: meniscal repair, concomitant ligament repair or patellofemoral
Dr Schock High Tibial Osteotomy
 Dr Schock High Tibial Osteotomy Goals for phase 1 Control pain Control edema Initiate ROM and quad strengthening Maintain WB restrictions Appropriate brace wear Criteria for progression to Phase 2 Edema
Dr Schock High Tibial Osteotomy Goals for phase 1 Control pain Control edema Initiate ROM and quad strengthening Maintain WB restrictions Appropriate brace wear Criteria for progression to Phase 2 Edema
ANTERIOR CRUCIATE LIGAMENT INJURY
 ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
Understanding. Ankle Sprains
 Understanding Ankle Sprains What Causes Ankle Sprains? The ankle is one of the most common places in the body for a sprain. Every day thousands of people sprain their ankles. Landing wrong on your foot
Understanding Ankle Sprains What Causes Ankle Sprains? The ankle is one of the most common places in the body for a sprain. Every day thousands of people sprain their ankles. Landing wrong on your foot
Midfoot - Reduction & Fixation - ORIF - screw fixation - AO Surgery Reference. ORIF - screw fixation
 Midfoot - TMT (Lisfranc) injury 1. Diagnosis ORIF - screw fixation Authors Mechanism of the injury Tarso-metatarsal (Lisfranc) injuries may be caused by direct or indirect forces. Direct forces include
Midfoot - TMT (Lisfranc) injury 1. Diagnosis ORIF - screw fixation Authors Mechanism of the injury Tarso-metatarsal (Lisfranc) injuries may be caused by direct or indirect forces. Direct forces include
Knee Injuries. PSK 4U Mr. S. Kelly North Grenville DHS. Medial Collateral Ligament Sprain
 Knee Injuries PSK 4U Mr. S. Kelly North Grenville DHS Medial Collateral Ligament Sprain Result from either a direct blow from the lateral side in a medial direction or a severe outward twist Greater injury
Knee Injuries PSK 4U Mr. S. Kelly North Grenville DHS Medial Collateral Ligament Sprain Result from either a direct blow from the lateral side in a medial direction or a severe outward twist Greater injury
Anterior Cruciate Ligament (ACL)
 Anterior Cruciate Ligament (ACL) The anterior cruciate ligament (ACL) is one of the 4 major ligament stabilizers of the knee. ACL tears are among the most common major knee injuries in active people of
Anterior Cruciate Ligament (ACL) The anterior cruciate ligament (ACL) is one of the 4 major ligament stabilizers of the knee. ACL tears are among the most common major knee injuries in active people of
ARTHROSCOPIC MENISECTOMY PROTOCOL
 REHABILITATION PROGRESSION ARTHROSCOPIC MENISECTOMY PROTOCOL The following are guidelines for rehabilitation progression following menisectomy, loose body removed, or debridement etc. Progression through
REHABILITATION PROGRESSION ARTHROSCOPIC MENISECTOMY PROTOCOL The following are guidelines for rehabilitation progression following menisectomy, loose body removed, or debridement etc. Progression through
MEDIAL PATELLOFEMORAL LIGAMENT REPAIR & TIBIAL TUBERCLE OSTEOTOMY
 MEDIAL PATELLOFEMORAL LIGAMENT REPAIR & TIBIAL TUBERCLE OSTEOTOMY Revised SEP 2013 SPECIAL PRECAUTIONS/ LIMITATIONS: 1) CRUTCHES/ WEIGHT BEARING: Partial weight bearing at day 1 in brace locked at 0 extension
MEDIAL PATELLOFEMORAL LIGAMENT REPAIR & TIBIAL TUBERCLE OSTEOTOMY Revised SEP 2013 SPECIAL PRECAUTIONS/ LIMITATIONS: 1) CRUTCHES/ WEIGHT BEARING: Partial weight bearing at day 1 in brace locked at 0 extension
MENISCUS TEAR. Description
 MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
Jennifer L. Cook, MD
 Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE
Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE
CHRONIC FOOT PROBLEMS FOOT and ANKLE BASICS
 CHRONIC FOOT PROBLEMS FOOT and ANKLE BASICS ABC s of Comprehensive Musculoskeletal Care December 1 st, 2007 Stephen Pinney MD Chief, UCSF Foot and Ankle Service Chronic problems typically occur gradually
CHRONIC FOOT PROBLEMS FOOT and ANKLE BASICS ABC s of Comprehensive Musculoskeletal Care December 1 st, 2007 Stephen Pinney MD Chief, UCSF Foot and Ankle Service Chronic problems typically occur gradually
Marathon Running & Knee Injuries
 Marathon Running & Knee Injuries Mr Sanjiv Jari Consultant Knee, Lower Limb & Orthopaedic Sports Medicine Surgeon Honorary Clinical Lecturer, University of Manchester. www.thekneedoc.co.uk www.sportmedclinic.com
Marathon Running & Knee Injuries Mr Sanjiv Jari Consultant Knee, Lower Limb & Orthopaedic Sports Medicine Surgeon Honorary Clinical Lecturer, University of Manchester. www.thekneedoc.co.uk www.sportmedclinic.com
