Results of Treatment of 111 Patients With Nonunion of Femoral Shaft Fractures
|
|
|
- Alexis Powell
- 6 years ago
- Views:
Transcription
1 The University of Pennsylvania Orthopaedic Journal 12: 52 56, The University of Pennsylvania Orthopaedic Journal Results of of 111 Patients With onunion of Femoral Shaft Fractures P. K. BEREDJIKLIA, M.D., R. J. ARAJA, M.D., R. B. HEPPESTALL, M.D., C. T. BRIGHTO, M.D., PH.D., AD J. L. ESTERHAI, M.D. Abstract: The purpose of this study is to report our experience with the treatment of femoral shaft fracture nonunion and to define poor prognostic indicators in the treatment of this complication. The records and available radiographs of 111 patients treated for nonunion of the femoral shaft in our institution were retrospectively reviewed. The mean duration of follow-up after establishment of nonunion was 62 months. The following factors were found to have an adverse effect on nonunion healing (p < 0.05): (1) advanced patient age; (2) presence of osteomyelitis; (3) presence of synovial pseudarthrosis; (4) duration of nonunion; (5) treatment with flexible intramedullary devices; (6) treatment with compression plating; (7) poor bone stock; (8) malalignment in the anteroposterior plane of more than 10 degrees; and (9) malalignment in the lateral plane of more than 20 degrees. Introduction In spite of increased understanding of biomechanics and implant design, nonunion of femoral shaft fractures continues to hinder the treatment of these injuries. This complication presents a difficult treatment challenge for the surgeon and a formidable personal and economic hardship for the patient [8,15]. In most series of femoral fractures treated with modern intramedullary nailing techniques, the incidence of this complication is estimated to be 0.9% [28]. This frequency appears to be on the rise due to advances in trauma care leading to increased survivorship among severely injured patients [28,29]. The treatment of long bone fracture nonunion has been extensively discussed in the orthopaedic literature. The evolution of treatment began with traction and prolonged immobilization as described by Watson-Jones. This was later surpassed by the concept of bony apposition to stimulate primary healing by removing fibrous tissue interposed between the fracture fragments [10,21]. In contrast, Harkins and Phemister [12] contended that this fibrous tissue was necessary for nonunion healing and advocated the use of onlay bone grafts. Other adjuvant methods to stimulate healing have included conventional bone grafting as well as electrical stimulation of osteogenesis in various forms [2,5,6]. In the 1950s, the application of internal fixation in From the Department of Orthopaedic Surgery, University of Pennsylvania School of Medicine, Philadelphia, PA. Address correspondence to: P.K. Beredjiklian, M.D., Department of Orthopaedic Surgery, University of Pennsylavania, Philadelphia, PA the form of compression plating as described by Danis and others gained popularity [16,21,22,24]. A few years later, the use of external fixation was introduced as a therapeutic alternative for the treatment of nonunions [1 3,10,25]. Whereas the treatment of femoral shaft fractures has been extensively described in the orthopaedic literature, the data regarding treatment of femoral shaft fracture nonunion are sparse and conflicting. Most of the discussion on long bone nonunions is centered around tibial injuries. Most series available in the current orthopaedic literature comprise a small number of femoral shaft nonunions. The accepted standard of therapy for femoral shaft fracture nonunion invariably includes surgical intervention in the form of closed intramedullary nailing with reaming. More specifically, several authors [4,7,13,14,18,23] recommend removing the present intramedullary nail, reaming the intramedullary canal, and inserting a larger diameter nail. Open autogenous bone grafting in addition to intramedullary reaming has been recommended only in cases of synovial pseudarthrosis or in nonunions with bony defects at the site of injury. The purpose of this study is to report our experience with the treatment of femoral shaft fracture nonunion and to define poor prognostic indicators in the treatment of this complication. Materials and Methods Between 1970 and 1992, 111 patients with nonunion of the shaft of the femur were evaluated and cared for at our institution. For the purposes of this study, nonunion is defined as absence of clinical or radiographic healing 9 months postinjury. The shaft of the femur is defined as the area 5 cm distal to the lesser trochanter proximally and 5 cm proximal to the epicondylar axis distally. All hospital inpatient and outpatient records were reviewed to determine the following factors: patient age, type of initial injury, description of initial care, number of previous surgeries, treatment for nonunion, complications associated with care, time to union, duration of follow-up, and final status. Available roentgenograms were evaluated to determine bone stock as assessed by the ratio of cortical thickness to shaft width (poor if the ratio was less than one half, adequate if greater than one half), type of nonunion (hypertrophic, oligotrophic, or atrophic), and fracture align- 52
2 OUIO OF FEMORAL STRESS FRACTURES 53 Table 1. Initial treatment of femoral fractures Table 3. Ineffective treatment modalities for nonunion Intramedullary nailing 53 Compression plating 27 Skeletal traction 23 Traction followed by casting 4 External fixation 4 Table 2. modalities for delayed union Capacitive coupling (CC) 15 Intramedullary nailing (IM) 6 Compression plating (P) 5 Direct Current (DC) 5 Autogenous bone grafting (BG) 3 External fixation (EX) 1 IM + BG 15 P+BG 5 IM + CC 3 EX + CC 3 P+BG+DC 2 IM + BG + CC 1 EX + DC 1 ment in the anteroposterior (AP) and lateral planes (as measured with a standard goniometer). Mean patient age at the time of injury was 39.5 years, ranging from 17 to 82 years of age. There were 60 men and 51 women. Fifty-eight nonunions involved the left femur and 53 involved the right. The mechanism of initial injury included motor vehicle accidents (65%, n 72); falls (19%, n 21); osteotomy (6%, n 7); gunshot wounds (3%, n 3); and miscellaneous injuries (7%, n 8). Eighty-nine of the fractures were closed injuries, 15 were open, and seven patients had elective open femoral osteotomies. In the course of treatment, 34 (31%) nonunions developed culture-proven osteomyelitis and 18 (16%) developed synovial pseudarthroses as determined by either biopsy or bone scan. Patient treatment was temporally classified into three separate categories: initial treatment at the time of femoral fracture; treatment of the delayed union (i.e., surgical intervention performed after the initial fracture treatment but before the establishment of nonunion defined at 9 months postinjury); and treatment of the established nonunion. Initial treatment of the femoral fracture included intramedullary nailing (48%, n 53); compression plating (24%, n 27); traction (20%, n 23); traction followed by casting or cast bracing (3%, n 4); and external fixation (3%, n 4) (Table 1). of delayed union in our patient population was varied. Fifty-nine (53%) of the patients in the study were treated either surgically (a total of 50 surgical procedures) or with capacitive coupling alone (12 patients) as described in Table 2. Six of these patients went on to heal the femoral nonunion without any further intervention. Capacitive coupling (CC) 20 Intramedullary nailing (IM) 7 Compression plating (P) 4 Direct Current (DC) 20 Autogenous bone grafting (BG) 15 External fixation (EX) 3 IM + BG 14 P+BG 8 IM + CC 1 P+CC 2 P+DC 1 EX + BG 1 P+BG+CC 2 IM + BG + CC 2 BG + CC 2 Table 4. Effective treatment modalities for nonunion Capacitive coupling (CC) 12 Intramedullary nailing (IM) 4 Compression plating (P) 1 Direct Current (DC) 11 Autogenous bone grafting (BG) 6 IM + BG 13 P+BG 1 P+DC 1 IM + BG + CC 4 BG + CC 1 of the established nonunion was also varied and included several forms of internal and external fixation, as well as adjunctive treatment with bone grafting and/or electrical stimulation of osteogenesis in the form of capacitive coupling or direct current. modalities were considered failures if (1) the femur remained ununited during the available documented follow-up after the intervention in question or if (2) another treatment modality was instituted during the time of recorded follow-up, in all cases due to an absence of bony healing. A total of 82 failed surgical interventions were recorded, with an additional 20 patients undergoing capacitive coupling (Table 3). modalities were considered successful if bony healing was achieved following the intervention in question. Healing was achieved in these patients with a total of 42 surgical interventions with an additional 12 patients undergoing capacitive coupling (Table 4). Statistical analysis was performed using the Student s t test for numeric data and chi square analysis for nonparametric data. Results The mean time from fracture to care at our institution was 24.5 months (range 0 144) and the patients had undergone
3 54 BEREDJIKLIA ET AL. Fig. 1. onunion treatment with intramedullary nails. Fig. 2. ail type versus healing. an average of two surgical procedures (range 0 8) prior to presentation. The mean duration of follow-up after establishment of nonunion was 62 months. Fifty-five (49%) of the nonunions healed and 56 (51%) did not heal as determined by the available follow-up. Data analysis revealed a significant difference in the average age of those patients who healed (35.9 years, range 17 82) versus those who did not (42.9 years, range 18 81) (p 0.026). The presence of osteomyelitis adversely influenced healing, as only 10 of 34 (29.4%) infected nonunions healed (p 0.007). As expected, open fractures resulted in a significantly higher incidence of infected nonunions (11 of 23, 48%; p 0.021). In addition, only 4 of 18 (22.2%) patients with synovial pseudarthroses went on to heal their femoral nonunion (p 0.013). The mode of initial treatment of the femoral shaft fracture did not significantly impact the result of nonunion treatment. However, statistically significant differences in healing rates were found between different treatment modalities for established nonunions. Intramedullary rodding with reaming (with and without open adjuvant bone grafting and/ or electrical stimulation of osteogenesis) was the most successful mode of therapy for the established nonunion. Of the patients treated in this fashion, 21 of 45 (47%) went on to heal their nonunion (p 0.031) (Fig. 1). Furthermore, in 34 of 45 patients treated with intramedullary nails, we were able to assess the type of device used (rigid [e.g., Kuntschner or Russell-Taylor type nails] versus flexible [e.g., Enders or Rush rods]). otably, patients treated with rigid devices had a significantly higher rate of nonunion healing (18 of 23) than those treated with flexible nails (3 of 11; p 0.004) (Fig. 2). It is unclear from our data whether the addition of bone grafting and/or electrical stimulation of osteogenesis as adjuvants to intramedullary rodding improved the outcome of treatment. In contrast, compression plating of the established nonunion (with and without adjuvant bone grafting and/or electrical stimulation of osteogenesis) generally resulted in a poor outcome. In comparison to all other treatment modalities, only 3 of 20 (15%) patients treated in this fashion went on to heal their nonunion (p 0.044; Fig. 3). It is unclear from our data whether the addition of bone grafting and/or electrical stimulation of osteogenesis as adjuvants to plating improved the outcome of treatment. We found no statistically significant differences regarding other types of treatment and nonunion healing. either capacitive coupling alone (12 of 33 healed versus 43 of 130 healed for all other treatment types, p 0.72) nor direct current alone (11 of 31 healed versus 44 of 132 healed for all other treatment types, p 0.82) revealed differences in healing rates. Bone grafting alone also proved no more effective than other types of treatment (6 of 21 healed versus 49 of 142 healed for all other treatment types, p 0.59). Radiographic analysis revealed that significant predictors of poor outcome included bone stock and malalignment in the AP and lateral planes. Bone stock Only 4 of 26 patients determined to have poor bone stock by the earliest available radiographs obtained after the establishment of the nonunion went on to heal. In contrast, 23 of 50 patients with adequate bone stock healed their nonunions (p 0.008). Malalignment of the fracture in the AP plane greater than 10 degrees Twenty-five of 51 (49%) patients with adequate alignment in the AP plane went on to heal, whereas 19 of 25 (76%) patients with deformity of more than 10 degrees in this plane did not heal their nonunions (p 0.03). Malalignment of the fracture ends in the lateral plane greater than 20 degrees Thirty-one of 57 (54%) patients with adequate alignment in the lateral plane went on to heal, whereas 15 of 19 (79%) patients with deformity of more than 20 degrees in this plane did not heal their nonunions (p 0.011). otably, nonunion type (e.g., hypertrophic versus atrophic) did not yield significant differences in healing rates. Fig. 3. onunion treatment with compression plating.
4 OUIO OF FEMORAL STRESS FRACTURES 55 Finally, the presence of implant failure or frank loosening also did not reliably predict poor outcome. Three patients in this study group underwent above the knee amputations for treatment of a recalcitrant nonunion. All of the significant clinical and radiographic predictors of outcome are outlined in Table 5. Discussion Historically, nonunion of long bone fractures has been the subject of intensive study in the orthopaedic literature. This fact undoubtedly stems not only from the inherent difficulty in treating this complication, but also from the enormous physical and psychological demands placed on the patient. Of 602 long bone nonunions, Connolly [8] estimated that 62% were located in the tibia, with only 23% occurring in the femur. The higher incidence of tibial nonunion may explain why most of the discussion concerning treatment has focused on tibial injuries. evertheless, femoral nonunion remains a relatively common occurrence with catastrophic consequences. The existing orthopaedic literature is lacking in an analysis of a large series of femoral shaft nonunions. However, careful review of the existing literature regarding femoral nonunion does provide some answers regarding management. Taylor [26] advocated the use of two slotted plates at 90 degrees to each other with cortical bone graft for the definitive treatment of femoral nonunion. A few year later, Brav [4] advocated the use of open intramedullary nailing with bone grafting as the procedure of choice in the treatment of femoral shaft nonunion. Rigid fixation and early rehabilitation were noted as the key factors in the success of this procedure. Klemm [19], Kostuik and Harrington [20], and Varma and Rao [27] expanded the indications of intramedullary nailing to include infected nonunions of the femoral shaft. They found this method of treatment superior to compression plating for nonunion healing. In the early 1980s, Brighton et al. [5] and Bassett et al. [3] added electrical stimulation of osteogenesis to the treatment armamentarium. The advent of improved implant design has helped achieve excellent results treating femoral shaft delayed and nonunions with a success rate approaching 100%. Webb et al. [28] reported a total of 44 nonunions of the femur, all treated with reamed intramedullary nails. onunion was Table 5. Clinical and radiographic predictors of poor outcome (p < 0.05) Advanced patient age Presence of osteomyelitis Presence of Synovial Pseudarthrosis Duration of nonunion with flexible intramedullary devices with compression plating Poor bone stock Malalignment in the anteroposterior plane > 10 degrees Malalignment in the lateral plane > 20 degrees defined as an ununited fracture lasting longer than 1 year. It is unclear, however, how many of these injuries involved the femoral shaft. The authors do not state the average length of nonunion duration nor the number of surgical procedures that patients had undergone prior to the assumption of care by the authors. Our data highlight significant risk factors in the treatment of femoral shaft nonunions. Advanced patient age, the number of surgical procedures, and the duration of nonunion all were demographic factors inversely proportional in treatment success rates. The first two factors likely relate to the physiologic capacity of patients to heal their nonunion. The orthopaedic surgeon should be aware of the patient s general medical condition and nutritional status, as these factors may be requisite in successful nonunion treatment. Other factors related to poor prognosis include the presence of osteomyelitis and synovial pseudarthrosis at the nonunion site. The nonunions complicated by osteomyelitis probably represent a subgroup of more severe injuries than the rest of the group. Open fractures, injuries resulting from high energy trauma, and fractures occurring in debilitated hosts are more likely to develop infection and predispose patients to a poor outcome. Synovial pseudarthroses are thought to result from gross motion at the fracture site due to inadequate immobilization [15]. It is believed that poor fixation results in metaplasia of the lining tissue at the fracture site consisting of fibroblasts and histiocytes, tissue comparable to that present in synovial joints. Given the poor healing rates in these cases, it is clear that this environment is not conducive to fracture healing. Our data support this assertion. In a similar study, Brighton et al. [6] identified risk factors adversely associated with the treatment of tibial nonunion. Using logistic regression analysis, the authors reviewed the treatment results of 271 tibial fracture nonunions with an average follow-up of 23.5 months. In this group of patients, the authors identified duration of nonunion, prior bone graft surgery, prior electrical treatment, open fracture, osteomyelitis, comminuted or oblique fracture, and atrophic nonunion as poor prognostic indicators in the treatment of tibial nonunion. With regard to the radiographic analysis in our study, the presence of poor bone stock and malalignment in the AP and lateral planes presaged a precarious outcome. The evaluation of bone stock from plain radiographs is technique dependent and inexact. There exist no reproducible objective parameters for this determination. In fact, it is believed that between 30 50% of bone mass must be lost before any degree of osteopenia becomes apparent in plain films. Recently, the advent of dual energy x-ray absorptiometry (DEXA) scanning has provided an accurate and reproducible method of quantitating bone [11]. This modality was not available during the treatment of patients in this study. Comparing the cortical width to the width of the shaft does provide a rough guideline for the determination of bone stock. These measurements significantly correlated with nonunion healing potential. The best results were achieved with rigid intramedullary
5 56 BEREDJIKLIA ET AL. nail fixation of the established nonunion. Court-Brown et al. [9] hypothesized that intramedullary nailing with reaming may stimulate bony union in tibial injuries for the following reasons: (1) increased stability, (2) autografting of osteoinductive reaming products, and (3) increased periosteal new bone formation and blood flow. It is interesting to note that the nonunions in our study treated with flexible intramedullary devices had significantly lower healing rates when compared to stiff nails. These data highlight the importance of stability as it relates to rigid fixation and the potential osteoinductive properties of the reaming process in the management of femoral shaft nonunion. In contrast, compression plating of the injuries under study yielded poor results. Several factors may account for this finding. First, application of the plate necessitates the devascularization of a segment of bone at the nonunion site. Damage to the soft tissues as well as disruption of the periosteal blood supply at the site of injury may inhibit the healing potential of the nonunion. Second, a single plate is biomechanically inferior to an intramedullary rod in regard to the torsion and bending characteristics [14]. It is possible that compression plating may have a role in the treatment of proximal or distal femoral nonunion. However, it appears as if its use in femoral shaft nonunions is not tenable. At the time of treatment of the patients in this study, our institution was a large referral center for the treatment of long bone nonunion. Thus, the data presented in this study may describe a group of nonunions recalcitrant in nature, those that were not responsive to initial treatment by the primary orthopaedist. This fact may explain the marginal success rate in treating the nonunions reported here. In addition, most of the implants used in this study reflect technology used as long as 10 to 20 years ago, and thus our results do not reflect the benefits gained from advances in implant design. The development of newer implants, as well as the use of osteoinductive substances such as bone morphogenetic protein (BMP), may substantially improve the results of treatment of femoral shaft fracture nonunion [17]. References 1. Alonso JG and Hughes JL: External fixation of femoral fractures. Clin Orthop 241:83 88, Barquet A, Silva R, Massaferro J, et al.: The AO tubular external fixator in the treatment of open fractures and infected non-unions of the shaft of the femur. Injury 19: , Bassett CA, Mitchell S, Schink MM: of therapeutically resistant non-unions with bone grafts and pulsing electromagnetic fields. J Bone Joint Surg 64A: , Brav EA: The use of intramedullary nailing for nonunion of the femur. Clin Orthop 60:69 75, Brighton CT, Friedenberg ZB, Esterhai JL, et al.: of nonunion with constant direct current. J Bone Joint Surg 63A:2 13, Brighton CT, Shaman P, Heppenstall RB, et al.: Tibial nonunion treated with direct current, capacitive coupling, or bone graft. Clin Orthop 321: , Christensen O: Kuntscher intramedullary reaming and nail fixation for non-union of fracture of the femur and the tibia. J Bone Joint Surg 55B: , Connolly JF: Common avoidable problems in nonunions. Clin Orthop 194: , Court-Brown CM, Keating JF, Christie J, et al.: Exchange intramedullary nailing. J Bone Joint Surg 77B:407???,????. 10. Fellander M: of fractures and pseudarthroses of the long bones by Hoffmann s transfixation method (osteotaxis). Acta Orthop Scand 33: , Genant HK, et al.: Appropriate use of bone densitometry. Radiology 170: , Harkins H and Phemister DB: Simplified technique of onlay grafts for all ununited fractures in acceptable position. JAMA 109: , Harper MC: Ununited fractures of the femur stabilized with a fluted rod. Clin Orthop 190: , Heiple KG, Figgie HE, Lacey SH, et al.: Femoral shaft nonunion treated by a fluted intramedullary rod. Clin Orthop 194: , Heppenstall RB, Brighton CT, Esterhai JL, et al.: Synovial pseudarthrosis: A clinical, roentgenographic, scintigraphic, and pathologic study. J Trauma 27: , Johnson EE: Custom titanium plating for failed nonunion or delayed internal fixation of femoral fractures. Clin Orthop 234: , Johnson EE, Urist MR, Finerman GA: Bone morphogenetic protein augmentation grafting of resistant femoral nonunions. A preliminary report. Clin Orthop 230: , Kempf I, Grosse A, Rigaut P: The treatment of noninfected pseudarthrosis of the femur and tibia with locked intramedullary nailing. Clin Orthop 212: , Klemm KW: of infected pseudarthrosis of the femur and tibia with an interlocking nail. Clin Orthop 212: , Kostuik JP and Harrington IJ: of infected un-united femoral shaft fractures. Clin Orthop 108:90 94, Muller ME: of nonunion by compression. Clin Orthop 43: 83 91, Muller ME and Thomas RJ: of non-union in fractures of long bones. Clin Orthop 138: , Oh I, ahigian SH, Rascher JJ, et al.: Closed intramedullary nailing for ununited femoral shaft fractures. Clin Orthop 106: , Rosen H: Compression treatment of long bone pseudarthroses. Clin Orthop 138: , Slatis P and Paavolainen P: External fixation of infected non-unions of the femur. Injury 16: , Taylor LW: Principles of treatment of fractures and non-union of the shaft of the femur. J Bone Joint Surg 45A: , Varma BP and Rao YP: An evaluation of the results of medullary nailing in the treatment of infected diaphyseal fractures. Clin Orthop 100: , Webb LX, Winquist RA, Hansen ST: Intramedullary nailing and reaming for delayed union or nonunion of the femoral shaft: A report of 105 consecutive cases. Clin Orthop 212: , Winquist RA, Hansen ST, Clawson DK: Closed intramedullary nailing of femoral fractures: A report of five hundred and twenty cases. J Bone Joint Surg 66A: , 1984.
Fractures of the tibia shaft treated with locked intramedullary nail Retrospective clinical and radiographic assesment
 ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
Intramedullary Nailing: History & Rationale
 Intramedullary Nailing: History & Rationale Overview 1. What is IM Nailing? 2. History 3. Design Rationale & Evolution 4. Modern IM Nails 5. The Future What is IM Nailing? Method of internal fixation in
Intramedullary Nailing: History & Rationale Overview 1. What is IM Nailing? 2. History 3. Design Rationale & Evolution 4. Modern IM Nails 5. The Future What is IM Nailing? Method of internal fixation in
Use of Unlocked Intramedullary Nailing in Winquist Type I and II Femoral Isthmus Fracture
 Use of Unlocked Intramedullary Nailing in Winquist Type I and II Femoral Isthmus Fracture HT Ling, MBBS (UM), WM Ng, MS Ortho (UM), MK Kwan, MS Ortho (UM), LK Fathi Aizuddeen, MBBS (UM), PCM Tay, MBBS
Use of Unlocked Intramedullary Nailing in Winquist Type I and II Femoral Isthmus Fracture HT Ling, MBBS (UM), WM Ng, MS Ortho (UM), MK Kwan, MS Ortho (UM), LK Fathi Aizuddeen, MBBS (UM), PCM Tay, MBBS
Ethan M. Braunstein, M.D. 1, Steven A. Goldstein, Ph.D. 2, Janet Ku, M.S. 2, Patrick Smith, M.D. 2, and Larry S. Matthews, M.D. 2
 Skeletal Radiol (1986) 15:27-31 Skeletal Radiology Computed tomography and plain radiography in experimental fracture healing Ethan M. Braunstein, M.D. 1, Steven A. Goldstein, Ph.D. 2, Janet Ku, M.S. 2,
Skeletal Radiol (1986) 15:27-31 Skeletal Radiology Computed tomography and plain radiography in experimental fracture healing Ethan M. Braunstein, M.D. 1, Steven A. Goldstein, Ph.D. 2, Janet Ku, M.S. 2,
.org. Tibia (Shinbone) Shaft Fractures. Anatomy. Types of Tibial Shaft Fractures
 Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Surgical treatment of aseptic nonunion in long bones: review of 193 cases
 J Orthopaed Traumatol (2007) 8:11 15 DOI 10.1007/s10195-007-0155-z ORIGINAL A. Megaro S. Marchesi U.E. Pazzaglia Surgical treatment of aseptic nonunion in long bones: review of 193 cases Received: 5 September
J Orthopaed Traumatol (2007) 8:11 15 DOI 10.1007/s10195-007-0155-z ORIGINAL A. Megaro S. Marchesi U.E. Pazzaglia Surgical treatment of aseptic nonunion in long bones: review of 193 cases Received: 5 September
Tibial Nonunions: Should I Tackle and How
 Tibial Nonunions: Should I Tackle and How Frank R. Avilucea, MD Assistant Professor Department of Orthopaedic Surgery University of Cincinnati Medical Center Disclosures Journal Reviewer Journal of Bone
Tibial Nonunions: Should I Tackle and How Frank R. Avilucea, MD Assistant Professor Department of Orthopaedic Surgery University of Cincinnati Medical Center Disclosures Journal Reviewer Journal of Bone
Neurologic Damage. The most common neurologic injury following intramedullary tibial nailing is injury to the peroneal nerve.
 COMPLICATIONS Knee Pain Anterior knee pain was present in 55% Affects younger more than older patients A significant number of the patients with anterior knee pain had pain with kneeling [90%] They also
COMPLICATIONS Knee Pain Anterior knee pain was present in 55% Affects younger more than older patients A significant number of the patients with anterior knee pain had pain with kneeling [90%] They also
MANAGEMENT OF BILATERAL FRACTURE FEMUR WITH IMPLANT FAILURE: A CASE REPORT
 CASE REPORT East African Orthopaedic Journal MANAGEMENT OF BILATERAL FRACTURE FEMUR WITH IMPLANT FAILURE: A CASE REPORT J.C. Mwangi, MBChB, MMed(Surg), Lecturer, and A.A. Admani, MBChB, Resident, Department
CASE REPORT East African Orthopaedic Journal MANAGEMENT OF BILATERAL FRACTURE FEMUR WITH IMPLANT FAILURE: A CASE REPORT J.C. Mwangi, MBChB, MMed(Surg), Lecturer, and A.A. Admani, MBChB, Resident, Department
A Clinical Study For Evaluation Of Results Of Closed Interlocking Nailing Of Fractures Of The Shaft Of The Tibia
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 17 Number 2 A Clinical Study For Evaluation Of Results Of Closed Interlocking Nailing Of Fractures Of The Shaft Of R Gupta, T Motten, N Kalsotra,
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 17 Number 2 A Clinical Study For Evaluation Of Results Of Closed Interlocking Nailing Of Fractures Of The Shaft Of R Gupta, T Motten, N Kalsotra,
Unlocked Nailing vs. Interlocking Nailing for Winquist Type I and II Femoral Isthmus Fractures. Is there a Difference?
 Unlocked Nailing vs. Interlocking Nailing for Winquist Type I and II Femoral Isthmus Fractures. Is there a Difference? CK Yu, MBBS (UM), HY Wong*, MD (UKM), AS Vivek, FRCS (Edin), BC Se To*, FRCS (Edin)
Unlocked Nailing vs. Interlocking Nailing for Winquist Type I and II Femoral Isthmus Fractures. Is there a Difference? CK Yu, MBBS (UM), HY Wong*, MD (UKM), AS Vivek, FRCS (Edin), BC Se To*, FRCS (Edin)
7/23/2018 DESCRIBING THE FRACTURE. Pattern Open vs closed Location BASIC PRINCIPLES OF FRACTURE MANAGEMENT. Anjan R. Shah MD July 21, 2018.
 BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
CASE REPORT. Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur
 PRODUCTS CASE REPORT Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur Robert D. Fitch, M.D. Duke University Health System 1 1 CONDITION Infected nonunion
PRODUCTS CASE REPORT Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur Robert D. Fitch, M.D. Duke University Health System 1 1 CONDITION Infected nonunion
BRIDGE PLATING OF COMMINUTED SHAFT OF FEMUR FRACTURES
 BRIDGE PLATING OF COMMINUTED SHAFT OF FEMUR FRACTURES Mohammad Abul kalam, Pradeep Kumar, Mohammad Afzal Hussain and Iqbal Ahmad Abstract A prospective study of forty comminuted femoral shaft fractures,
BRIDGE PLATING OF COMMINUTED SHAFT OF FEMUR FRACTURES Mohammad Abul kalam, Pradeep Kumar, Mohammad Afzal Hussain and Iqbal Ahmad Abstract A prospective study of forty comminuted femoral shaft fractures,
Locked plating constructs are creating a challenge for surgeons.
 Locked plating constructs are creating a challenge for surgeons. Three recent studies examining supracondylar femur fractures show concern for the high degree of stiffness of locked plating constructs
Locked plating constructs are creating a challenge for surgeons. Three recent studies examining supracondylar femur fractures show concern for the high degree of stiffness of locked plating constructs
The study of distal ¼ diaphyseal extra articular fractures of humerus treated with antegrade intramedullary interlocking nailing
 2018; 4(4): 46-50 ISSN: 2395-1958 IJOS 2018; 4(4): 46-50 2018 IJOS www.orthopaper.com Received: 01-08-2018 Accepted: 03-09-2018 Dr. Ankur Parikh Orthopaedics, Jehangir Hospital, Sassoon road, Pune, Dr.
2018; 4(4): 46-50 ISSN: 2395-1958 IJOS 2018; 4(4): 46-50 2018 IJOS www.orthopaper.com Received: 01-08-2018 Accepted: 03-09-2018 Dr. Ankur Parikh Orthopaedics, Jehangir Hospital, Sassoon road, Pune, Dr.
Study of Ender s Nailing in Paediatric Tibial Shaft Fractures
 Study of Ender s Nailing in Paediatric Tibial Shaft Fractures Dr. Himanshu G. Ladani 1* 1 Ex. Assistant Professor of Orthopaedics, M.P.Shah Medical College, Jamnagar, Gujarat. ABSTRACT Background: Closed
Study of Ender s Nailing in Paediatric Tibial Shaft Fractures Dr. Himanshu G. Ladani 1* 1 Ex. Assistant Professor of Orthopaedics, M.P.Shah Medical College, Jamnagar, Gujarat. ABSTRACT Background: Closed
Outcome of surgical implant generation network nail initiative in treatment of long bone shaft fractures in Kenya
 Original Article Outcome of surgical implant generation network nail initiative in treatment of long bone shaft fractures in Kenya O.O. Soren, MBChB (Moi), MMed (Orthopaedics) (Makerere), Consultant Orthopaedic
Original Article Outcome of surgical implant generation network nail initiative in treatment of long bone shaft fractures in Kenya O.O. Soren, MBChB (Moi), MMed (Orthopaedics) (Makerere), Consultant Orthopaedic
Surgical Management of aseptic Femoral Shaft Non-union after Intramedullary Fixation
 The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (7), Page 4946-4950 Surgical Management of aseptic Femoral Shaft Non-union after Intramedullary Fixation Eissa Ragheb Refaie 1, Ahmed Abd El
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (7), Page 4946-4950 Surgical Management of aseptic Femoral Shaft Non-union after Intramedullary Fixation Eissa Ragheb Refaie 1, Ahmed Abd El
Techique. Results. Discussion. Materials & Methods. Vol. 2 - Year 1 - December 2005
 to each other. The most distal interlocking hole is 3 mm proximal to distal end of nail, is in anteroposterior direction & proximal distal interlocking hole is in medial to lateral direction i.e. at right
to each other. The most distal interlocking hole is 3 mm proximal to distal end of nail, is in anteroposterior direction & proximal distal interlocking hole is in medial to lateral direction i.e. at right
EVOS MINI with IM Nailing
 Case Series Dr. John A. Scolaro EVOS MINI with IM Nailing A series of studies Introduction Intramedullary nailing has become the standard for many long bone fractures. Fracture reduction prior to nail
Case Series Dr. John A. Scolaro EVOS MINI with IM Nailing A series of studies Introduction Intramedullary nailing has become the standard for many long bone fractures. Fracture reduction prior to nail
Of approximately 2 million long bone fractures
 Proceedings S.Z.P.G.M.I vol: 13(1-2) 1999, pp. 71-75. Treatment of Tibial Non-Union with the Ilizarov Method Pervaiz Iqbal, Muhammad Maq, Hamid Qayum Department of Orthopaedics, Shaikh Zayed Hospital,.
Proceedings S.Z.P.G.M.I vol: 13(1-2) 1999, pp. 71-75. Treatment of Tibial Non-Union with the Ilizarov Method Pervaiz Iqbal, Muhammad Maq, Hamid Qayum Department of Orthopaedics, Shaikh Zayed Hospital,.
Femoral Fractures in Adolescents: A Comparison of Four Methods of Fixation
 Femoral Fractures in Adolescents: A Comparison of Four Methods of Fixation By Leonhard E. Ramseier, MD, Joseph A. Janicki, MD, Shannon Weir, BSc, and Unni G. Narayanan, MBBS, MSc, FRCSC Investigation performed
Femoral Fractures in Adolescents: A Comparison of Four Methods of Fixation By Leonhard E. Ramseier, MD, Joseph A. Janicki, MD, Shannon Weir, BSc, and Unni G. Narayanan, MBBS, MSc, FRCSC Investigation performed
Principles of intramedullary nailing. Management for ORP
 Principles of intramedullary nailing Eakachit Sikarinklul,MD Basic Principles of Fracture Management for ORP Bangkok Medical Center Bangkok, 22-24 July 2016 Learning outcomes At the end of this lecture
Principles of intramedullary nailing Eakachit Sikarinklul,MD Basic Principles of Fracture Management for ORP Bangkok Medical Center Bangkok, 22-24 July 2016 Learning outcomes At the end of this lecture
Tobacco and Bone Health
 Tobacco and Bone Health Prof. Dr. Alok Chandra Agrawal MS Orthopaedics, DNB Orthopaedics, PhD Orthopaedics MAMS All India Institute of Medical Sciences Raipur CG Cigarette smoking is commonly identified
Tobacco and Bone Health Prof. Dr. Alok Chandra Agrawal MS Orthopaedics, DNB Orthopaedics, PhD Orthopaedics MAMS All India Institute of Medical Sciences Raipur CG Cigarette smoking is commonly identified
COMPARATIVE STUDY OF MANAGEMENT OF DIAPHYSEAL FEMUR FRACTURE WITH INTRAMEDULLARY INTERLOCKING NAIL AND K. NAIL
 International Journal of Innovation and Applied Studies ISSN 2028-9324 Vol. 15 No. 3 Apr. 2016, pp. 560-564 2016 Innovative Space of Scientific Research Journals http://www.ijias.issr-journals.org/ COMPARATIVE
International Journal of Innovation and Applied Studies ISSN 2028-9324 Vol. 15 No. 3 Apr. 2016, pp. 560-564 2016 Innovative Space of Scientific Research Journals http://www.ijias.issr-journals.org/ COMPARATIVE
Results of tibia nailing with Angular Stable Locking Screws (ASLS); A retrospective study of 107 patients with distal tibia fracture.
 Results of tibia nailing with Angular Stable Locking Screws (ASLS); A retrospective study of 107 patients with distal tibia fracture. stud. med. David Andreas Lunde Hatfield stud. med. Mohammed Sherif
Results of tibia nailing with Angular Stable Locking Screws (ASLS); A retrospective study of 107 patients with distal tibia fracture. stud. med. David Andreas Lunde Hatfield stud. med. Mohammed Sherif
Treatment Alternatives for Pediatric Femoral Fractures
 Treatment Alternatives for Pediatric Femoral Fractures Gregory A. Schmale, MD Seattle Children's Hospital, USA, gregory.schmale@seattlechildrens.org version 2 I have no conflicts of interest to report
Treatment Alternatives for Pediatric Femoral Fractures Gregory A. Schmale, MD Seattle Children's Hospital, USA, gregory.schmale@seattlechildrens.org version 2 I have no conflicts of interest to report
Angular Malalignment in Subtrochanteric and Proximal Shaft Femur Fractures after Intramedullary Nailing using SIGN Nails
 Angular Malalignment in Subtrochanteric and Proximal Shaft Femur Fractures after Intramedullary Nailing using SIGN Nails Rolando Junior L. Torres, MD Jeremiah R. Morales, MD, FPOA Subtrochanteric Femur
Angular Malalignment in Subtrochanteric and Proximal Shaft Femur Fractures after Intramedullary Nailing using SIGN Nails Rolando Junior L. Torres, MD Jeremiah R. Morales, MD, FPOA Subtrochanteric Femur
A comparative study of locking plate by MIPO versus closed interlocking intramedullary nail in extraarticular distal tibia fractures
 2018; 4(3): 145-149 ISSN: 2395-1958 IJOS 2018; 4(3): 145-149 2018 IJOS www.orthopaper.com Received: 26-05-2018 Accepted: 27-06-2018 Kanachur Institute of Medical Sciences Mangalore University Road, Natekal,
2018; 4(3): 145-149 ISSN: 2395-1958 IJOS 2018; 4(3): 145-149 2018 IJOS www.orthopaper.com Received: 26-05-2018 Accepted: 27-06-2018 Kanachur Institute of Medical Sciences Mangalore University Road, Natekal,
Outcome of Treatment of Nonunion Tibial Shaft Fracture by Intramedullary Interlocking Nail augmentated with Autogenous Cancellous Bone Graft.
 Original Article Nepal Med Coll J 2014; 16(1): 58-62 Outcome of Treatment of Nonunion Tibial Shaft Fracture by Intramedullary Interlocking Nail augmentated with Autogenous Cancellous Bone Graft. Shah SB,
Original Article Nepal Med Coll J 2014; 16(1): 58-62 Outcome of Treatment of Nonunion Tibial Shaft Fracture by Intramedullary Interlocking Nail augmentated with Autogenous Cancellous Bone Graft. Shah SB,
Treatment of delayed union or non-union of the tibial shaft with partial fibulectomy and an Ilizarov frame
 Acta Orthop. Belg., 2007, 73, 630-634 ORIGINAL STUDY Treatment of delayed union or non-union of the tibial shaft with partial fibulectomy and an Ilizarov frame Jo DUJARDYN, Johan LAMMENS From the University
Acta Orthop. Belg., 2007, 73, 630-634 ORIGINAL STUDY Treatment of delayed union or non-union of the tibial shaft with partial fibulectomy and an Ilizarov frame Jo DUJARDYN, Johan LAMMENS From the University
Treatment of traumatic conditions of the femur using the Huckstep nail
 East and Central African Journal of Sulgey Vol. 2, No. I Treatment of traumatic conditions of the femur using the Huckstep nail T F Wisniewski MD PhD(0rth) Department of Orthopaedic Surgery and Bone and
East and Central African Journal of Sulgey Vol. 2, No. I Treatment of traumatic conditions of the femur using the Huckstep nail T F Wisniewski MD PhD(0rth) Department of Orthopaedic Surgery and Bone and
THE RING BUTTERFLY FRAGMENT
 THE RING BUTTERFLY FRAGMENT Pages with reference to book, From 80 To 82 Philip D`Sousa, Masood Umer, Riaz Hussain Lakdawala ( Department of Surgery (Orthopaedics), The Aga Khan University, Karachi. ) In
THE RING BUTTERFLY FRAGMENT Pages with reference to book, From 80 To 82 Philip D`Sousa, Masood Umer, Riaz Hussain Lakdawala ( Department of Surgery (Orthopaedics), The Aga Khan University, Karachi. ) In
The Journal of the Korean Society of Fractures Vol.13, No.3, July, 2000
 The Journal of the Korean Society of Fractures Vol13, No3, July, 2000 2, 3 ) : 40-12, Tel : (02) 966-1616 Fax : (02) 968-2394 E-mail : adkajs@thrunetcom 471 8, 1 2 ) (Table 1) 1 6 14, 2 1 2 1 Ender 29
The Journal of the Korean Society of Fractures Vol13, No3, July, 2000 2, 3 ) : 40-12, Tel : (02) 966-1616 Fax : (02) 968-2394 E-mail : adkajs@thrunetcom 471 8, 1 2 ) (Table 1) 1 6 14, 2 1 2 1 Ender 29
Factors affecting fracture healing after intramedullary nailing of the tibial diaphysis for closed and grade I open fractures
 Trauma Factors affecting fracture healing after intramedullary nailing of the tibial diaphysis for closed and grade I open fractures G. I. Drosos, M. Bishay, I. A. Karnezis, A. K. Alegakis From Royal United
Trauma Factors affecting fracture healing after intramedullary nailing of the tibial diaphysis for closed and grade I open fractures G. I. Drosos, M. Bishay, I. A. Karnezis, A. K. Alegakis From Royal United
Segmental tibial fractures treated with unreamed interlocking nail A prospective study
 2017; 3(2): 714-719 ISSN: 2395-1958 IJOS 2017; 3(2): 714-719 2017 IJOS www.orthopaper.com Received: 13-02-2017 Accepted: 14-03-2017 Ashok Singhvi Hemant Jain Siddharth Jauhar Kishore Raichandani Segmental
2017; 3(2): 714-719 ISSN: 2395-1958 IJOS 2017; 3(2): 714-719 2017 IJOS www.orthopaper.com Received: 13-02-2017 Accepted: 14-03-2017 Ashok Singhvi Hemant Jain Siddharth Jauhar Kishore Raichandani Segmental
Osteosynthesis involving a joint Thomas P Rüedi
 Osteosynthesis involving a joint Thomas P Rüedi How to use this handout? The left column contains the information given during the lecture. The column at the right gives you space to make personal notes.
Osteosynthesis involving a joint Thomas P Rüedi How to use this handout? The left column contains the information given during the lecture. The column at the right gives you space to make personal notes.
Fracture Classification
 Fracture Classification Lisa K. Cannada MD Updated: 05/2016 18 th & 19 th century History of Fracture History based on clinical appearance of limb alone Classification Colles Fracture Dinner Fork Deformity
Fracture Classification Lisa K. Cannada MD Updated: 05/2016 18 th & 19 th century History of Fracture History based on clinical appearance of limb alone Classification Colles Fracture Dinner Fork Deformity
Primary internal fixation of fractures of both bones forearm by intramedullary nailing
 Original article 21 Primary internal fixation of fractures of both bones forearm by intramedullary nailing Nepal Medical College and Teaching Hospital, Kathmandu, Nepal Correspondenc to: Dr R P Singh,
Original article 21 Primary internal fixation of fractures of both bones forearm by intramedullary nailing Nepal Medical College and Teaching Hospital, Kathmandu, Nepal Correspondenc to: Dr R P Singh,
Nonunion of the Femur Treated with Conventional Osteosynthesis Combined with Autogenous and Strut Allogeneic Bone Grafts
 Original Article 268 Nonunion of the Femur Treated with Conventional Osteosynthesis Combined with Autogenous and Strut Allogeneic Bone Grafts Lin-Hsiu Weng, MD; Jun-Wen Wang, MD Background: In this study,
Original Article 268 Nonunion of the Femur Treated with Conventional Osteosynthesis Combined with Autogenous and Strut Allogeneic Bone Grafts Lin-Hsiu Weng, MD; Jun-Wen Wang, MD Background: In this study,
Distal femoral fracture with subsequent ipsilateral proximal femoral fracture
 Distal femoral fracture with subsequent ipsilateral proximal femoral fracture by M Agarwal, MS FRCS, AA Syed, FRCSI, PV Giannoudis (!), BSc,MB,MD,EEC(Orth) Dept. of Orthopaedics and Trauma, St.James University
Distal femoral fracture with subsequent ipsilateral proximal femoral fracture by M Agarwal, MS FRCS, AA Syed, FRCSI, PV Giannoudis (!), BSc,MB,MD,EEC(Orth) Dept. of Orthopaedics and Trauma, St.James University
ORIGINAL ARTICLE. ABSTRACT: Orthopaedic surgeons often encounter diaphyseal femur fractures, because these
 A PROSPECTIVE STUDY OF SURGICAL MANAGEMENT OF FRACTURE SHAFT FEMUR WITH CLOSED INTRAMEDULLARY INTERLOCKING NAIL. Mahendranath Reddy D 1, Muralidhar B.M 2 HOW TO CITE THIS ARTICLE: Mahendranath Reddy D,
A PROSPECTIVE STUDY OF SURGICAL MANAGEMENT OF FRACTURE SHAFT FEMUR WITH CLOSED INTRAMEDULLARY INTERLOCKING NAIL. Mahendranath Reddy D 1, Muralidhar B.M 2 HOW TO CITE THIS ARTICLE: Mahendranath Reddy D,
Current Concepts: Aseptic Nonunion of Femoral Shaft Diaphysis
 European Journal of Trauma and Emergency Surgery Focus on Intramedullary Nailing Current Concepts: Aseptic Nonunion of Femoral Shaft Diaphysis Elias Lambiris 1, Andreas Panagopoulos 1, Panagiotis Zouboulis
European Journal of Trauma and Emergency Surgery Focus on Intramedullary Nailing Current Concepts: Aseptic Nonunion of Femoral Shaft Diaphysis Elias Lambiris 1, Andreas Panagopoulos 1, Panagiotis Zouboulis
Relationship between the Apex of Flexible Nail and the Level of Fracture: A Biomechanical Study Ahmed N* 1, Gakhar H 2, Cheung G 3, Sharma A 4
 Relationship between the Apex of Flexible Nail and the Level of Fracture: A Biomechanical Study Ahmed N* 1, Gakhar H 2, Cheung G 3, Sharma A 4 Abstract Background Centre of Orthopaedic biomechanics, Bath
Relationship between the Apex of Flexible Nail and the Level of Fracture: A Biomechanical Study Ahmed N* 1, Gakhar H 2, Cheung G 3, Sharma A 4 Abstract Background Centre of Orthopaedic biomechanics, Bath
Fractures (Broken Bones)
 Fractures (Broken Bones) A fracture is a broken bone. A bone may be completely fractured or partially fractured in any number of ways (crosswise, lengthwise, in multiple pieces). Types of Fractures Bones
Fractures (Broken Bones) A fracture is a broken bone. A bone may be completely fractured or partially fractured in any number of ways (crosswise, lengthwise, in multiple pieces). Types of Fractures Bones
Failed Subtrochanteric Fracture How I Decide What to Do?
 Failed Subtrochanteric Fracture How I Decide What to Do? Gerald E. Wozasek Thomas M. Tiefenboeck 5 October 2016, Washington Medical University of Vienna, Department of Trauma Surgery ordination @wozasek.at
Failed Subtrochanteric Fracture How I Decide What to Do? Gerald E. Wozasek Thomas M. Tiefenboeck 5 October 2016, Washington Medical University of Vienna, Department of Trauma Surgery ordination @wozasek.at
REVISING THE DEFICIENT PROXIMAL FEMUR
 REVISING THE DEFICIENT PROXIMAL FEMUR by David Mattingly, Boston, MA Joseph McCarthy, Boston, MA Benjamin E. Bierbaum, Boston, MA Hugh P. Chandler, Boston, MA Roderick H. Turner, Boston, MA Hugh U. Cameron,
REVISING THE DEFICIENT PROXIMAL FEMUR by David Mattingly, Boston, MA Joseph McCarthy, Boston, MA Benjamin E. Bierbaum, Boston, MA Hugh P. Chandler, Boston, MA Roderick H. Turner, Boston, MA Hugh U. Cameron,
ILIZAROV TECHNIQUE IN CORRECTING LIMBS DEFORMITIES: PRELIMINARY RESULTS
 Bahrain Medical Bulletin, Volume 17, Number 2, June 1995 Original ILIZAROV TECHNIQUE IN CORRECTING LIMBS DEFORMITIES: PRELIMINARY RESULTS Saleh W. Al-Harby, FRCS(Glasg)* This is a prospective study of
Bahrain Medical Bulletin, Volume 17, Number 2, June 1995 Original ILIZAROV TECHNIQUE IN CORRECTING LIMBS DEFORMITIES: PRELIMINARY RESULTS Saleh W. Al-Harby, FRCS(Glasg)* This is a prospective study of
ILIZAROV METHOD IN TREATMENT OF TIBIAL AND FEMORAL INFECTED NON-UNIONS IN PATEITNES WITH HIGH-ENERGY TRAUMA AND BATTLE-FIELD WOUNDS
 ILIZAROV METHOD IN TREATMENT OF TIBIAL AND FEMORAL INFECTED NON-UNIONS IN PATEITNES WITH HIGH-ENERGY TRAUMA AND BATTLE-FIELD WOUNDS M. N. Tahmasebi * and Sh. Jalali Mazlouman Department of Orthopedic Surgery,
ILIZAROV METHOD IN TREATMENT OF TIBIAL AND FEMORAL INFECTED NON-UNIONS IN PATEITNES WITH HIGH-ENERGY TRAUMA AND BATTLE-FIELD WOUNDS M. N. Tahmasebi * and Sh. Jalali Mazlouman Department of Orthopedic Surgery,
JMSCR Vol. 03 Issue 08 Page August 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 Index Copernicus Value: 5.88 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v3i8.08 Study of Functional and Radiological Outcome
www.jmscr.igmpublication.org Impact Factor 3.79 Index Copernicus Value: 5.88 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v3i8.08 Study of Functional and Radiological Outcome
PediNail Pediatric Femoral Nail
 PediNail Pediatric Femoral Nail Surgical Technique Table of Contents Indications...3 Patient Positioning...3 Approach...4 Reaming...5 Nail Placement...6 Proximal Interlocking...7 Distal Interlocking...8
PediNail Pediatric Femoral Nail Surgical Technique Table of Contents Indications...3 Patient Positioning...3 Approach...4 Reaming...5 Nail Placement...6 Proximal Interlocking...7 Distal Interlocking...8
2017 Resident Advanced Trauma Techniques Course COMPLICATIONS / CHALLENGES MALUNIONS/DEFORMITY
 2017 Resident Advanced Trauma Techniques Course COMPLICATIONS / CHALLENGES MALUNIONS/DEFORMITY What is a Malunion? Definition: a fracture that has healed in a nonanatomic (i.e. deformed) position Must
2017 Resident Advanced Trauma Techniques Course COMPLICATIONS / CHALLENGES MALUNIONS/DEFORMITY What is a Malunion? Definition: a fracture that has healed in a nonanatomic (i.e. deformed) position Must
5/31/2018. Ipsilateral Femoral Neck And Shaft Fractures. Ipsilateral Neck-Shaft Fractures Introduction. Ipsilateral Neck-Shaft Fractures Introduction
 Ipsilateral Femoral Neck And Shaft Fractures Exchange Nailing For Non- Union Donald Wiss MD Cedars-Sinai Medical Center Los Angeles, California Introduction Uncommon Injury Invariably High Energy Trauma
Ipsilateral Femoral Neck And Shaft Fractures Exchange Nailing For Non- Union Donald Wiss MD Cedars-Sinai Medical Center Los Angeles, California Introduction Uncommon Injury Invariably High Energy Trauma
A prospective study of functional outcome of primary intra-medullary nailing in type 3A and 3B open tibial diaphyseal fractures
 2017; 3(3): 696-700 ISSN: 2395-1958 IJOS 2017; 3(3): 696-700 2017 IJOS www.orthopaper.com Received: 18-05-2017 Accepted: 20-06-2017 Dr. Deepak Shivanna Professor, Dept. of Orthopaedics, BMCRI, Bengaluru,
2017; 3(3): 696-700 ISSN: 2395-1958 IJOS 2017; 3(3): 696-700 2017 IJOS www.orthopaper.com Received: 18-05-2017 Accepted: 20-06-2017 Dr. Deepak Shivanna Professor, Dept. of Orthopaedics, BMCRI, Bengaluru,
Tibia fractures are the third most common long bone
 ORIGINAL ARTICLE Elastic Intramedullary Nailing Versus Open Reduction Internal Fixation of Pediatric Tibial Shaft Fractures Andrew T. Pennock, MD,*w Tracey P. Bastrom, MA,w and Vidyadhar V. Upasani, MD*w
ORIGINAL ARTICLE Elastic Intramedullary Nailing Versus Open Reduction Internal Fixation of Pediatric Tibial Shaft Fractures Andrew T. Pennock, MD,*w Tracey P. Bastrom, MA,w and Vidyadhar V. Upasani, MD*w
Dynamization Versus Static Antegrade Intramedullary Interlocking Nail In Femoral Shaft Fractures
 ORIGINAL ARTICLE Dynamization Versus Static Antegrade Intramedullary Interlocking Nail In Femoral Shaft Fractures Muhammad Khalid, Imtiaz Hashmi, Sohail Rafi, Muhammad Idrees Shah ABSTRACT Objective Study
ORIGINAL ARTICLE Dynamization Versus Static Antegrade Intramedullary Interlocking Nail In Femoral Shaft Fractures Muhammad Khalid, Imtiaz Hashmi, Sohail Rafi, Muhammad Idrees Shah ABSTRACT Objective Study
Management of compound fractures of shaft femur: a study of 55 cases
 International Journal of Research in Orthopaedics Singla G et al. Int J Res Orthop. 2016 Dec;2(4):313-317 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20164160
International Journal of Research in Orthopaedics Singla G et al. Int J Res Orthop. 2016 Dec;2(4):313-317 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20164160
management of sports injuries
 Br J Sp Med 1991; 25(4) Internal fixation of closed tibial fractures for the management of sports injuries A. Abdel-Salam FRCS, K. S. Eyres* FRCS and J. Cleary FRCS Department of Orthopaedics, Huddersfield
Br J Sp Med 1991; 25(4) Internal fixation of closed tibial fractures for the management of sports injuries A. Abdel-Salam FRCS, K. S. Eyres* FRCS and J. Cleary FRCS Department of Orthopaedics, Huddersfield
Treatment of open tibial shaft fractures using intra medullary interlocking
 International Journal of Research in Orthopaedics Reddy GR et al. Int J Res Orthop. 17 May;():66-7 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/1.18/issn.455-451.intjresorthop171574
International Journal of Research in Orthopaedics Reddy GR et al. Int J Res Orthop. 17 May;():66-7 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/1.18/issn.455-451.intjresorthop171574
Closed reduction and internal fixation of fractures of the shaft of the femur by the Titanium Elastic Nailing System in children.
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 17 Number 1 Closed reduction and internal fixation of fractures of the shaft of the femur by the Titanium Elastic Nailing System in children.
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 17 Number 1 Closed reduction and internal fixation of fractures of the shaft of the femur by the Titanium Elastic Nailing System in children.
Designing a Novel Fixation Device for Pediatric Orthopaedic Tibia Fractures
 Designing a Novel Fixation Device for Pediatric Orthopaedic Tibia Fractures Evan Lange, Karl Kabarowski Tyler Max, Sarah Dicker Client: Dr. Matthew Halanski, MD Advisor: Dr. Paul Thompson, PhD Biomedical
Designing a Novel Fixation Device for Pediatric Orthopaedic Tibia Fractures Evan Lange, Karl Kabarowski Tyler Max, Sarah Dicker Client: Dr. Matthew Halanski, MD Advisor: Dr. Paul Thompson, PhD Biomedical
Ankle and subtalar arthrodesis
 OSTEOAMP Allogeneic Morphogenetic Proteins Ankle Nonunions OSTEOAMP Case Report ANKLE NONUNIONS Dr. Jason George DeVries Orthopedic & Sports Medicine, Bay Care Clinic, 501 N. 10th Street, Manitowoc, WI
OSTEOAMP Allogeneic Morphogenetic Proteins Ankle Nonunions OSTEOAMP Case Report ANKLE NONUNIONS Dr. Jason George DeVries Orthopedic & Sports Medicine, Bay Care Clinic, 501 N. 10th Street, Manitowoc, WI
Management of Segmental Tibial Fractures.
 72 Management of Segmental Tibial Fractures. N. S. Motsitsi Chief Specialist / Head of Department.Dept. of Orthopaedic Surgery., Kalafong Hospital Pretoria.Email: silas.motsitsi@up.ac.za. Fax : (012);
72 Management of Segmental Tibial Fractures. N. S. Motsitsi Chief Specialist / Head of Department.Dept. of Orthopaedic Surgery., Kalafong Hospital Pretoria.Email: silas.motsitsi@up.ac.za. Fax : (012);
JOURNALOF ORTHOPAEDIC TRAUMA
 JOT Special Case Report Series CASE REPORTS www.jorthotrauma.com JOURNALOF ORTHOPAEDIC TRAUMA OFFICIAL JOURNAL OF Orthopaedic Trauma Association Belgian Orthopaedic Trauma Association Canadian Orthopaedic
JOT Special Case Report Series CASE REPORTS www.jorthotrauma.com JOURNALOF ORTHOPAEDIC TRAUMA OFFICIAL JOURNAL OF Orthopaedic Trauma Association Belgian Orthopaedic Trauma Association Canadian Orthopaedic
Case Report. Antegrade Femur Lengthening with the PRECICE Limb Lengthening Technology
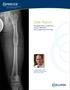 Case Report Antegrade Femur Lengthening with the PRECICE Limb Lengthening Technology S. Robert Rozbruch, MD Hospital for Special Surgery New York, NY, USA ABSTRACT This is a case illustrating a 4.5 cm
Case Report Antegrade Femur Lengthening with the PRECICE Limb Lengthening Technology S. Robert Rozbruch, MD Hospital for Special Surgery New York, NY, USA ABSTRACT This is a case illustrating a 4.5 cm
Percutaneous Reduction Of Femoral Fractures During Intramedullary Fixation: A Technical Tip
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 19 Number 2 Percutaneous Reduction Of Femoral Fractures During Intramedullary Fixation: A Technical Tip P Lorentzos, A Kanawati, G Shyan, F Hoe
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 19 Number 2 Percutaneous Reduction Of Femoral Fractures During Intramedullary Fixation: A Technical Tip P Lorentzos, A Kanawati, G Shyan, F Hoe
Malunion in floating knee injuries An analysis in 30 patients presenting to a tertiary care facility and are surgically treated
 2017; 3(1): 700-705 ISSN: 2395-1958 IJOS 2017; 3(1): 700-705 2017 IJOS www.orthopaper.com Received: 11-11-2016 Accepted: 12-12-2016 Dr. R Ezhilmaran Assistant Professor, Department of Orthopaedics, Chengalpattu
2017; 3(1): 700-705 ISSN: 2395-1958 IJOS 2017; 3(1): 700-705 2017 IJOS www.orthopaper.com Received: 11-11-2016 Accepted: 12-12-2016 Dr. R Ezhilmaran Assistant Professor, Department of Orthopaedics, Chengalpattu
IMPORTANT MEDICAL INFORMATION Advanced Orthopaedic Solutions INTRAMEDULLARY NAILS Warnings and Precautions (SINGLE USE ONLY)
 IMPORTANT MEDICAL INFORMATION Advanced Orthopaedic Solutions INTRAMEDULLARY NAILS Warnings and Precautions (SINGLE USE ONLY) IMPORTANT NOTE Intramedullary nails provide an alternative to open reduction
IMPORTANT MEDICAL INFORMATION Advanced Orthopaedic Solutions INTRAMEDULLARY NAILS Warnings and Precautions (SINGLE USE ONLY) IMPORTANT NOTE Intramedullary nails provide an alternative to open reduction
Orthopedic & Sports Medicine, Bay Care Clinic, 501 N. 10th Street, Manitowoc, WI Procedure. Subtalar arthrodesis
 OSTEOAMP Allogeneic Morphogenetic Proteins Subtalar Nonunions OSTEOAMP Case Report SUBTALAR NONUNIONS Dr. Jason George DeVries and Dr. Brandon M. Scharer Orthopedic & Sports Medicine, Bay Care Clinic,
OSTEOAMP Allogeneic Morphogenetic Proteins Subtalar Nonunions OSTEOAMP Case Report SUBTALAR NONUNIONS Dr. Jason George DeVries and Dr. Brandon M. Scharer Orthopedic & Sports Medicine, Bay Care Clinic,
Minimally Invasive Plating of Fractures:
 Minimally Invasive Plating of Fractures: Advantages, Techniques and Trade-offs Matthew Garner, MD Created January 2016 OUTLINE Principles of fracture management The importance of vascular supply Equipment
Minimally Invasive Plating of Fractures: Advantages, Techniques and Trade-offs Matthew Garner, MD Created January 2016 OUTLINE Principles of fracture management The importance of vascular supply Equipment
Open reduction and internal fixation of humeral non-unions : Radiological and functional results
 Acta Orthop. Belg., 2011, 77, 299-303 ORIGINAL STUDY Open reduction and internal fixation of humeral non-unions : Radiological and functional results Anani ABALO, Ekoué D. DOSSEh, Komlan ADABRA, Atsi WALLA,
Acta Orthop. Belg., 2011, 77, 299-303 ORIGINAL STUDY Open reduction and internal fixation of humeral non-unions : Radiological and functional results Anani ABALO, Ekoué D. DOSSEh, Komlan ADABRA, Atsi WALLA,
The Lateral Trochanteric Wall A Key Element in the Reconstruction of Unstable Pertrochanteric Hip Fractures
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 425, pp. 82 86 2004 Lippincott Williams & Wilkins The Lateral Trochanteric Wall A Key Element in the Reconstruction of Unstable Pertrochanteric Hip Fractures
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 425, pp. 82 86 2004 Lippincott Williams & Wilkins The Lateral Trochanteric Wall A Key Element in the Reconstruction of Unstable Pertrochanteric Hip Fractures
Ilizarov treatment for aseptic delayed union or non-union after reamed intramedullary nailing of the femur
 Acta Orthop. Belg., 2010, 76, 63-68 ORIGINAL STUDY Ilizarov treatment for aseptic delayed union or non-union after reamed intramedullary nailing of the femur Johan LAMMENS, Johan VANLAUWE From Universitair
Acta Orthop. Belg., 2010, 76, 63-68 ORIGINAL STUDY Ilizarov treatment for aseptic delayed union or non-union after reamed intramedullary nailing of the femur Johan LAMMENS, Johan VANLAUWE From Universitair
FUNCTIONAL OUTCOME OF PROXIMAL TIBIA EXTR-ARTICULAR FRACTURES TREATED WITH LOCKING COMPRESSION PLATING
 FUNCTIONAL OUTCOME OF PROXIMAL TIBIA EXTR-ARTICULAR FRACTURES TREATED WITH LOCKING COMPRESSION PLATING Original Article Orthopaedics Pradip B. Patil 1, Dhanish V. Mehendiratta 2, S.A. Lad 3, Rishi K. Doshi
FUNCTIONAL OUTCOME OF PROXIMAL TIBIA EXTR-ARTICULAR FRACTURES TREATED WITH LOCKING COMPRESSION PLATING Original Article Orthopaedics Pradip B. Patil 1, Dhanish V. Mehendiratta 2, S.A. Lad 3, Rishi K. Doshi
Surgical interventions in chronic osteomyelitis
 Kathmandu University Medical Journal (2005) Vol. 3, No. 1, Issue 9, 50-54 Surgical interventions in chronic osteomyelitis Shrestha BK 1, Rajbhandary T 2, Bijukachhe B 2, Banskota AK 3 1 Associate Professor,
Kathmandu University Medical Journal (2005) Vol. 3, No. 1, Issue 9, 50-54 Surgical interventions in chronic osteomyelitis Shrestha BK 1, Rajbhandary T 2, Bijukachhe B 2, Banskota AK 3 1 Associate Professor,
Tibial Shaft Fractures
 Tibial Shaft Fractures Mr Krishna Vemulapalli Consultant Orthopaedics Surgeon Queens & King George Hospitals Queens Hospital 14/03/2018 Google Maps Map data 2018 Google 10 km Orthopaedics Department Covers
Tibial Shaft Fractures Mr Krishna Vemulapalli Consultant Orthopaedics Surgeon Queens & King George Hospitals Queens Hospital 14/03/2018 Google Maps Map data 2018 Google 10 km Orthopaedics Department Covers
Intramedullary nailing without interlocking screws for femoral and tibial shaft fractures
 DOI 10.1007/s00402-013-1775-9 Trauma Surgery Intramedullary nailing without interlocking screws for femoral and tibial shaft fractures Dieuwertje L. Kreb Taco J. Blokhuis Karlijn J. P. van Wessem Mike
DOI 10.1007/s00402-013-1775-9 Trauma Surgery Intramedullary nailing without interlocking screws for femoral and tibial shaft fractures Dieuwertje L. Kreb Taco J. Blokhuis Karlijn J. P. van Wessem Mike
Free vascularized fibular graft for tibial pseudarthrosis in neurofibromatosis
 Acta Orthop Scand 1988;59(4):425-429 Free vascularized fibular graft for tibial pseudarthrosis in neurofibromatosis 03 17878 1 luli lrl Herman H. de Boer', Abraham J. Verbout', Hans K. L. Nielsen2 and
Acta Orthop Scand 1988;59(4):425-429 Free vascularized fibular graft for tibial pseudarthrosis in neurofibromatosis 03 17878 1 luli lrl Herman H. de Boer', Abraham J. Verbout', Hans K. L. Nielsen2 and
Management for Postoperative Infection of Fractures
 The Journal of the Korean Society of Fractures Vol12, No2, April, 1999 = Abstract = Management for Postoperative Infection of Fractures Eui-Hwan Ahn, MD, In-Whan Chung, MD, Jeong-Hwan Oh, MD, Seong-Tae
The Journal of the Korean Society of Fractures Vol12, No2, April, 1999 = Abstract = Management for Postoperative Infection of Fractures Eui-Hwan Ahn, MD, In-Whan Chung, MD, Jeong-Hwan Oh, MD, Seong-Tae
2016 SIGN Conference: Treatment of Difficult Fractures Around The World
 2016 SIGN Conference: Treatment of Difficult Fractures Around The World September 21-24, 2016 Long Bone Osteosynthesis Failure DUONG BUNN Trauma-Orthopedique ward Preah Kossamak Preah Sihaknouk Ville Beach
2016 SIGN Conference: Treatment of Difficult Fractures Around The World September 21-24, 2016 Long Bone Osteosynthesis Failure DUONG BUNN Trauma-Orthopedique ward Preah Kossamak Preah Sihaknouk Ville Beach
Locked Plating: Clinical Indications
 Techniques in Orthopaedics 22(3):181 185 2007 Lippincott Williams & Wilkins, Inc. Locked Plating: Clinical Indications Kyle F. Dickson, M.D., M.B.A., John Munz, M.D. Summary: As shown in the previous article,
Techniques in Orthopaedics 22(3):181 185 2007 Lippincott Williams & Wilkins, Inc. Locked Plating: Clinical Indications Kyle F. Dickson, M.D., M.B.A., John Munz, M.D. Summary: As shown in the previous article,
Crossed Steinmann Pin Fixation In Supracondylar Femur Fractures In Adults A Case Series
 Article ID: WMC005027 ISSN 2046-1690 Crossed Steinmann Pin Fixation In Supracondylar Femur Fractures In Adults A Case Series Peer review status: No Corresponding Author: Dr. Mohit K Jindal, Senior Resident,
Article ID: WMC005027 ISSN 2046-1690 Crossed Steinmann Pin Fixation In Supracondylar Femur Fractures In Adults A Case Series Peer review status: No Corresponding Author: Dr. Mohit K Jindal, Senior Resident,
Cost and Time Considerations: Are Minifragment Plates Worth It? Disclosure. More Disclosures. Are minifragment plates worth it? it depends!
 Cost and Time Considerations: Are Minifragment Plates Worth It? Andrew Choo, MD Vumedi Webinar November 15, 2016 Disclosure Paid speaker: Depuy Synthes More Disclosures Price quotes are estimates only!
Cost and Time Considerations: Are Minifragment Plates Worth It? Andrew Choo, MD Vumedi Webinar November 15, 2016 Disclosure Paid speaker: Depuy Synthes More Disclosures Price quotes are estimates only!
DifficultTibialNailRemovalusingtheExtendedTrochantericOsteotomyTechniquePriortoTotalKneeArthroplasty
 : H Orthopedic and Musculoskeletal System Volume 14 Issue 3 Version 1.0 Year 2014 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online ISSN: 2249-4618
: H Orthopedic and Musculoskeletal System Volume 14 Issue 3 Version 1.0 Year 2014 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online ISSN: 2249-4618
CASE REPORT. Distal radius nonunion after volar locking plate fixation of a distal radius fracture: a case report
 Nagoya J. Med. Sci. 79. 551 ~ 557, 2017 doi:10.18999/nagjms.79.4.551 CASE REPORT Distal radius nonunion after volar locking plate fixation of a distal radius fracture: a case report Takaaki Shinohara 1
Nagoya J. Med. Sci. 79. 551 ~ 557, 2017 doi:10.18999/nagjms.79.4.551 CASE REPORT Distal radius nonunion after volar locking plate fixation of a distal radius fracture: a case report Takaaki Shinohara 1
Ipsilateral femoral neck and shaft fractures: a retrospective analysis of two treatment methods
 J Orthopaed Traumatol (2008) 9:141 147 DOI 10.1007/s10195-008-0025-3 ORIGINAL ARTICLE Ipsilateral femoral neck and shaft fractures: a retrospective analysis of two treatment methods Roop Singh Æ Rajesh
J Orthopaed Traumatol (2008) 9:141 147 DOI 10.1007/s10195-008-0025-3 ORIGINAL ARTICLE Ipsilateral femoral neck and shaft fractures: a retrospective analysis of two treatment methods Roop Singh Æ Rajesh
InternationalJournalofAgricultural
 www.ijasvm.com IJASVM InternationalJournalofAgricultural SciencesandVeterinaryMedicine ISSN:2320-3730 Vol.5,No.2,May2017 E-Mail:editorijasvm@gmail.com oreditor@ijasvm.comm@gmail.com Int. J. Agric.Sc &
www.ijasvm.com IJASVM InternationalJournalofAgricultural SciencesandVeterinaryMedicine ISSN:2320-3730 Vol.5,No.2,May2017 E-Mail:editorijasvm@gmail.com oreditor@ijasvm.comm@gmail.com Int. J. Agric.Sc &
Fracture Shaft of Femur in Children with Newly Designed Femoral Brace
 18 Fracture Shaft of Femur in Children with Newly Designed Femoral Brace Mahara D P, Lamichhane A, Acharya P, Shrestha G C Department of Orthopaedics, Tribhuvan University Teaching Hospital, Kathmandu,
18 Fracture Shaft of Femur in Children with Newly Designed Femoral Brace Mahara D P, Lamichhane A, Acharya P, Shrestha G C Department of Orthopaedics, Tribhuvan University Teaching Hospital, Kathmandu,
A gift you do not want. Motion Avascularity Gap Infection. Prognostic Issues. BMA & BMP: Alternative to Autologous BG? 11/21/2016.
 BMA & BMP: Alternative to Autologous BG? Frank A. Liporace, MD Associate Professor Dept. of Orthopaedics Director Orthopaedic Trauma Research New York University / Hospital for Joint Diseases, NY, NY Chairman
BMA & BMP: Alternative to Autologous BG? Frank A. Liporace, MD Associate Professor Dept. of Orthopaedics Director Orthopaedic Trauma Research New York University / Hospital for Joint Diseases, NY, NY Chairman
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Study on Surgical Management of Distal Tibial Fractures by Using Minimally Invasive Technique
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Study on Surgical Management of Distal Tibial Fractures by Using Minimally Invasive Technique
Orthopedics in Motion Tristan Hartzell, MD January 27, 2016
 Orthopedics in Motion 2016 Tristan Hartzell, MD January 27, 2016 Humerus fractures Proximal Shaft Distal Objectives 1) Understand the anatomy 2) Epidemiology and mechanisms of injury 3) Types of fractures
Orthopedics in Motion 2016 Tristan Hartzell, MD January 27, 2016 Humerus fractures Proximal Shaft Distal Objectives 1) Understand the anatomy 2) Epidemiology and mechanisms of injury 3) Types of fractures
Treatment of non-union of forearm bones with a free vascularised cortico - periosteal flap from the medial femoral condyle
 Acta Orthop. Belg., 2009, 75, 611-615 ORIGINAL STUDY Treatment of non-union of forearm bones with a free vascularised cortico - periosteal flap from the medial femoral condyle Luc DE SMET From the University
Acta Orthop. Belg., 2009, 75, 611-615 ORIGINAL STUDY Treatment of non-union of forearm bones with a free vascularised cortico - periosteal flap from the medial femoral condyle Luc DE SMET From the University
Abstract. Firas T. Ismaeel, Dept. of Surgery, College of Medicine, Tikrit University
 Bone marrow injection in patients with delayed union and non-union of long Firas T. Ismaeel, Dept. of Surgery, College of Medicine, Tikrit University Abstract In the process of bone formation and healing
Bone marrow injection in patients with delayed union and non-union of long Firas T. Ismaeel, Dept. of Surgery, College of Medicine, Tikrit University Abstract In the process of bone formation and healing
The Use of Ilizarov External Fixation Following Failed Internal Fixation
 Techniques in Orthopaedics 17(4):490 505 2003 Lippincott Williams & Wilkins, Inc., Philadelphia The Use of Ilizarov External Fixation Following Failed Internal Fixation Mark R. Brinker, M.D.*, and Daniel
Techniques in Orthopaedics 17(4):490 505 2003 Lippincott Williams & Wilkins, Inc., Philadelphia The Use of Ilizarov External Fixation Following Failed Internal Fixation Mark R. Brinker, M.D.*, and Daniel
Diaphyseal Humerus Fractures. OTA Course Dallas, TX 1/20/17 Ellen Fitzpatrick MD
 Diaphyseal Humerus Fractures OTA Course Dallas, TX 1/20/17 Ellen Fitzpatrick MD OBJECTIVES TREATMENT OPTIONS SURGICAL INDICATIONS CONTROVERSIES IN MANAGEMENT Humerus Fractures Treatment Goals: Functional
Diaphyseal Humerus Fractures OTA Course Dallas, TX 1/20/17 Ellen Fitzpatrick MD OBJECTIVES TREATMENT OPTIONS SURGICAL INDICATIONS CONTROVERSIES IN MANAGEMENT Humerus Fractures Treatment Goals: Functional
Case Report Bilateral Distal Femoral Nailing in a Rare Symmetrical Periprosthetic Knee Fracture
 Case Reports in Orthopedics, Article ID 745083, 4 pages http://dx.doi.org/10.1155/2014/745083 Case Report Bilateral Distal Femoral Nailing in a Rare Symmetrical Periprosthetic Knee Fracture Marcos Carvalho,
Case Reports in Orthopedics, Article ID 745083, 4 pages http://dx.doi.org/10.1155/2014/745083 Case Report Bilateral Distal Femoral Nailing in a Rare Symmetrical Periprosthetic Knee Fracture Marcos Carvalho,
The Role of Biplanar Distal Locking in Intramedullary Nailing of Tibial Shaft Fractures
 )33( COPYRIGHT 2019 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE The Role of Biplanar Distal Locking in Intramedullary Nailing of Tibial Shaft Fractures Kadir Bahadır Alemdaroğlu, MD; Serkan
)33( COPYRIGHT 2019 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE The Role of Biplanar Distal Locking in Intramedullary Nailing of Tibial Shaft Fractures Kadir Bahadır Alemdaroğlu, MD; Serkan
TECHNIQUE FOR CLOSED REDUCTION OF FEMORAL SHAFT DISPLACED FRACTURE USING INTRAMEDULLARY NAIL WITH STEINMANN PIN SUPPORT: CASE STUDY
 TECHNIQUE FOR CLOSED REDUCTION OF FEMORAL SHAFT DISPLACED FRACTURE USING INTRAMEDULLARY NAIL WITH STEINMANN PIN SUPPORT: CASE STUDY Nitesh Raj Pandey 1, Sumendra raj pandey, Jue-HuaJing 1, XuXin Zhong
TECHNIQUE FOR CLOSED REDUCTION OF FEMORAL SHAFT DISPLACED FRACTURE USING INTRAMEDULLARY NAIL WITH STEINMANN PIN SUPPORT: CASE STUDY Nitesh Raj Pandey 1, Sumendra raj pandey, Jue-HuaJing 1, XuXin Zhong
