TRM06.02 PELVIC BINDER GUIDELINE
|
|
|
- Adam Sharp
- 6 years ago
- Views:
Transcription
1 Trauma Service Guidelines Title: Pelvic Binder Guideline Developed by: K. Gumm, D. McDonald, M. Richardson & ACT Created: December 2007 Version 1.0 Revised: Version 3.0 August 2016, Version 2.1 June 2016 Reviewed by: K. Gumm, K. Liersch, R. Judson, A. Bucknill, A. Oppy & ACT TRM06.02 PELVIC BINDER GUIDELINE Background Pelvic Trauma Pelvic fractures result from high velocity mechanisms. They cause life threatening blood loss, are amongst the most devastating musculoskeletal injuries and are associated with a high incidence of mortality 19% 1. Survival rates have increased over recent years and patients usually die as a result of concomitant injuries rather than isolated pelvic fractures 2, 3. Pelvis Anatomy Pelvic fractures, especially with ring disruption allow an increased volume of blood to accumulate in the pelvic cavity before tamponading 2. Bleeding in pelvic ring fractures is usually venous from the pelvic veins and from the pre sacral venous plexus in 80% of cases or the marrow of the broken pelvic bones. Arterial bleeding is a direct result of damage to the vessel close to a bony injury. Injured vessels are typically branches of the internal iliac artery 1, 2, 4. Other organs that can be affected in pelvic ring injuries include the genitourinary and gastrointestinal systems, vagina and prostate and also the lumbar and sacral plexuses which run posteriorly 1, 2, 4. Mechanism of Injury and Classification of Pelvic Ring Injuries The most common causes of pelvic fractures, listed in order of frequency are MVA, pedestrian hit by motor vehicle, motor bike accidents, falls, crush injuries and sport or recreational accidents 4, 5. The pelvis is relatively immobile due to the SI joints, hence displacement of the pelvic ring requires a break in two places to become unstable. Young and Burgess describe three forces involved in pelvic ring 6 LC (Lateral Compression) This is the most common force and usually occurs in association with abdominal thoracic and cervical spine injuries. LC results from side impact and causes inward rotation of the hemi pelvis and rotational instability i.e. pedestrian struck by motor vehicle, motor vehicle accidents with side impact. If the force is not strong enough to open the pelvis, there can be organ damage from the bony fragment. Caution with binder use in LC fractures, use should be confirmed with orthopaedic team. APC (Anterior Posterior Compression) This compression force is directed either anterior posterior or posterior anterior such as motor vehicle or motorbike accidents. Injuries are mostly ligamentous with possible pubic rami fractures i.e. open book pelvis. AP injuries associated with severe arterial damage, involving the internal iliac artery and adjacent veins. Lumbosacral plexus injuries also occur. These injuries have the potential to lead to haemodynamic instability VS (Vertical Shear) VS injuries transmit energy through the femurs and produce varying injury patterns i.e. someone jumping from a great height and landing on an extended lower limb causing ipsilateral disruption of all ligaments restraining the hemi pelvis. This mechanism does not usually involve major arterial injuries. Melbourne Health [2012/2013] The information made available on [these web pages/in these guidelines] is produced for guidance purposes only and is designed as a general reference. The information made available does not, and does not purport to, contain all the information that the user may desire or require. Users should always exercise independent judgement and, when necessary, refer to other reference sources including obtaining professional assistance. [Melbourne Health/Trauma Service], its officers, employees, agents and advisers: are not, and will not be, responsible or liable for the accuracy or completeness of the information [on these web pages/in these guidelines]; expressly disclaim any and all liability arising from, or use of, such information; except so far as liability under any statute cannot be excluded, accepts no responsibility arising from errors or omissions in such information; accepts no liability for any loss or damage suffered by any person as a result of that person, or any other person, placing any reliance on the content of such information, including any stated or inferred interpretation or opinion.
2 Treatment Key points in treating pelvic fractures are 2-5, 7, 8 reduction in intraperitoneal volume reduction in bleeding splinting of fractures pain reduction definitive pelvic stabilisation and resuscitation. PELVIC BINDER GUIDELINE Early reduction and stabilisation of pelvic fractures can be lifesaving; application of external compression devices such as the pelvic binder is quick, safe, and easy. It can assist in stabilising the disrupted pelvic ring, reducing the volume and assisting with tamponade and clot formation, decrease mobility and can have an effect on bleeding and pain 2, 3. Circumferential compression via wrapping or a commercially available external compression device such as Sam Sling, RMH Pelvic Binder External Fixation or C/clamp Open reduction internal fixation (ORIF) invasive, requires theatre, and delays angiography. Mast Suit Circumferential Wrapping C/Clamp Pelvic Binder Open reduction internal fixation & External Fixation Stabilisation of the Pelvis (please refer to the guideline for the management of haemodynamically unstable patient with a pelvic fracture) 1-5, Rotationally unstable fractures benefit most from pelvic stabilisation. Vertical instability requires accompanying ipsilateral skeletal traction 2. The optimal external pelvic stabilisation device is non-invasive. Placement should allow both laparotomy access and bilateral femoral artery access. 3. Invasive anterior external fixation devices should be applied when venous bleeding is ongoing or if more time is needed until definitive internal fixation. Caution should be taken as any motion between the torso and lower limbs can cause a shifting of the pelvic ring fracture and jeopardise the coagulation and blood clot formation 10. V3 Endorsed by the Advisory Committee on Trauma August 2016 Page 2 of 8
3 Pelvic Circumferential Compressive Devices PELVIC BINDER GUIDELINE Pelvic Circumferential Compression Devices (PCCD s) are most commonly used in pelvic fractures where there has been separation of the pelvic ring, particularly the symphysis pubis. PCCD s can be used for cases where operative intervention is unsuitable or patient s haemodynamic status is labile. The PCCD s are easy to apply, provide controlled pressure delivery and do not hinder ongoing resuscitation efforts 2, 3, The most effective application site is the greater trochanters and symphysis pubis regions (see figure). The sling should be tightened to 180 Newton which is equivalent to lifting an eighteen kilo weight 3, 13, 14. PCCD s are not without complications which include pressure sores and skin abrasions 2, 3. Complication risk factors include 2, 3 immobilisation on a spine board moistness between the sling and skin hypotension BMI/ waist size age and gender. Figure Greater trochanters and symphysis pubic region It s recommended that patients are removed early from spine boards, intermitted skin checks when stable, and early removal of sling when definition management decisions made. The Royal Melbourne Hospital Pelvic Binder Guideline Best practice guidelines and The Royal Melbourne Hospital Haemodynamically Unstable Pelvic Fracture Guideline dictates that the following patients are fitted with a Pelvic Binder 5, 15 suspected pelvic fracture fall from a height haemodynamic instability. The Royal Melbourne Hospital Pelvic Binder Application Figure 11 Three-Strap Pelvic Binder Closed Figure 12 Three Strap Pelvic Binder Opened Figure 15: Straps rolled up ready for application Correct application of the pelvic binder should Figure ensure 12 Three Strap that PFix open the flat square portion is under the patient s buttocks (see figure 14), and that the middle strap is overlapping the patients greater trochanteric and symphysis pubis region (see figure 15). V3 Endorsed by the Advisory Committee on Trauma August 2016 Page 3 of 8
4 Figure 13: Velcro straps removed Application by log rolling: Step 1: Ensure the patient is lying supine Figure 14: Square flat portion placed under patients buttocks Step 2: Prepare the Pelvic Binder for application: undo the clips and remove the velcro straps to enable the long straps to be rolled small enough to pass under the patient (see figure 13 & 15). Figure 13 Flat square portion placed under patients backside. Figure 15: Patient on their backs and Pelvic Binder Figure 15: Pelvic Binder position for application straps rolled ready for application Figure 16: Straps rolled up ready for application Step 3: Line the Pelvic Binder up so that the middle strap will pass under the patient s great trochanteric and pubic region (see figures 10 & 15) Step 4: Log roll the patient as part of secondary survey. Insert the Pelvic Binder by pushing the rolled straps through as far as possible (see figure 16) Step 5: Log roll the patient back and ensure that the flat square portion is under the patients buttocks (see figure 14) pull the straps through (see figure 17 & 18) In the emergency department if a patient is expected who will require a Pelvic Binder, it can be put on the trolley ready for application rather than applying it via a log roll. Figure 17& 18: Straps being pulled through V3 Endorsed by the Advisory Committee on Trauma August 2016 Page 4 of 8
5 Step 6: Reattach the velcro tabs and apply the straps: the most important strap is the middle strap or the one positioned between the symphysis pubis and the greater trochanteric region, the other straps are fastened above and below this area for example: Strap 1: positioned between the anterior superior iliac spine and iliac crests (placed above strap 2) Strap 2: positioned over the symphysis pubis and the greater trochanteric region Strap 3: positioned strap at the level of the symphysis pubis and ischial tuberosity (placed below strap 2) In a time critical situation if the middle strap does not align with the greater trochanteric pubic region fasten the straps closest to this region; the Pelvic Binder can be readjusted at a later stage. Figure 19: Fasten the straps beginning with the middle strap if Pelvic Binder is placed as directed Figure 20: 3 straps fastened Figure 21: Strap 1 left unfastened as it is above the iliac crests At no time should any strap above the iliac crests be applied. If the Pelvic Binder is fitted with a strap in this position it should be left undone (see figure 21,) to prevent increasing abdominal pressure. Fastening this strap will have no effect on pelvic stabilisation. Ensure that the velcro section is attached and the Pelvic Binder is tightened to approximately 180 newtons which is equivalent to lifting an 18 kilogram weight with manual tension 10. If a procedure needs to be attended i.e. femoral vascular access, FAST scan or a catheterisation, the appropriate strap can be loosened and refastened on completion of the procedure. Application By Sliding the Pelvic Binder Under the Patient s Buttocks The Pelvic Binder can be applied in emergency situations (i.e. prehospital, patient who cannot log roll), by sliding it under the patient s legs and then buttocks. In this case there will be no need to remove the buckles; the Pelvic Binder can be opened by pulling apart the Velcro. Nursing Care of a Patient in a Pelvic Binder The Pelvic Binder is used in the haemodynamically unstable trauma patient with a pelvic fracture. These injuries are treated with PCCD s (Pelvic Binder), angiography +/- external or internal fixation. In the acute phase of care the Pelvic Binder should not be released or re-tensioned until the patient is stabilised evidenced by: normothermia correction of acidosis normal coagulation no evidence of ongoing haemorrhage adequate resuscitation V3 Endorsed by the Advisory Committee on Trauma August 2016 Page 5 of 8
6 Pressure Area Care Nursing care of the patient with a Pelvic binder requires close monitoring of the patients, haemodynamic status as well as skin integrity. Rotation of Straps Rotating the straps may assist in prevention of potential skin break down. Straps can be released 1-2 hourly in ICU and up to 4 hourly on the wards, on a rotational basis (as long as the sling is placed correctly). Only two straps are required to be tensioned at a time to maintain pelvic stability. For example one strap of the three can be released at any one time. When undoing the straps ensure that the skin is checked for any early signs of skin breakdown (See figure 22 & 23). If the patient demonstrates any signs of haemodynamic compromise when undoing straps they should be refastened ASAP and the patient reassessed. Replacement of the Pelvic Binder Replacement of the Pelvic Binder should only be considered in the haemodynamically stable patient as outlined above, or when markedly soiled, wet or offensive (i.e. blood soaked). If it is anticipated that the Pelvic Binder is going to become soiled (ie ongoing bleeding or incontinence), insert a bluesheet inside the Pelvic Binder to provide some protection. Before removal ensure that there is clear documentation regarding pelvic stability and position restrictions. Pelvic Binder replacement is similar to Pelvic binder application (See figure 24). Using the Bedpan Figure 22: PAC Strap Rotation Figure 23: PAC Strap Rotation Figure 24: Replacing the binder If a patient needs to use the bedpan, they can be log rolled and a slipper pan used (See figure 25). For this procedure the bottom strap should be loosened. Ensure that a blue sheet is placed under the bedpan to prevent soling of the linen and the Pelvic Binder. Monitoring Patients should be monitored throughout all of the above Figure 25: Using bedpan procedures. If at any time there are signs of haemodynamic compromise the patient should be immediately returned to the supine position and the Pelvic Binder re-tensioned. Neurovascular Observations Neurovascular observations should be attended after Pelvic Binder application, re-tensioning or replacement. Cleaning and Maintenance of Pelvic Binders Once Pelvic Binder use is complete they should be placed in the red linen skips for processing by Princess Linen. Once washed and returned, prior to returning to stock it should be checked for quality. Slings that do not pass inspection or are damaged in any way are disposed of. V3 Endorsed by the Advisory Committee on Trauma August 2016 Page 6 of 8
7 Pelvic Binder (PB) Flow Diagram Yes Patient expected with: Suspected pelvic fracture? Fall from a height? Heamodynamic instability? No Patient arrived meeting above criteria? Have a PB prepared on patient trolley with velcro open and straps unrolled, ensure that the flat square portion will be under the patients buttocks Yes Prepare the PB for application: undo clips remove velcro and roll up the 3 straps Ensure that the patient is rolled onto the sling so the the middle strap will be inline with the greater trochanteric and pubic region Log roll the patient and insert the PB so the middle strap will be inline with the greater trochanteric and pubic region pushing the straps through as far as possible Log roll the patient back onto their back and ensure that the flat square portion is under the patients buttocks. Pull the 3 straps through Reattach the velcro straps and buckle up the sling Step 1: Line up strap two with the symphysis pubis and the greater trochanteric region (this is the most important strap to have correctly positioned) Step 2: Strap one should be positioned between the anterior superior iliac spine and iliac crests Step 3: Strap three should be positioned midway between the ischeal tuberosity and the iliac crests If the middle strap does not align with the greater trochanteric pubic region fasten the strap closest to this region. The PB can be readjusted at a later stage. The PB should be tensioned to approximatly 180 newtons which is equivalent to 18 kilograms of manual tension at no time should a strap be applied above the iliac crests. If there is a strap in this region leave it unfastened. If a procedure is required (eg FAST, Femoral Access, IDC) an appropriate strap can be unfastened for the procedure Pressure Area Care (one haemodynamically stable) One strap can be loosened at a time for up to 1/24 Skin should be monitored for signs of early breakdown V3 Endorsed by the Advisory Committee on Trauma August 2016 Page 7 of 8
8 References 1. Gabbe B, De Steiger R, Bucknill A, Russ M, Cameron P. Predictors Of Mortality Following Severe Pelvic Ring Fracture: Results Of A Population-Based Study. Injury. October 2011;42(10): Bakhshayesh P, Boutrfnouchet T, Totterman A. Effectiveness Of Non Invasice External Pelvice Compression: A Systematic Review Of The Litreature. Scandinavian Journal Of Trauma, Resusitation And Emergency Medicine 2016;24(73). 3. Knops S, Goossens R, Hofwegen M, Patka P. Development Of Circumferential Compression Device: The Guardian. Treatment of pelvic ring fractures with pelvic circumferential compression devices. 2014: Vaidya R, Scott A, Tonnos F, Hudson I, Martin A, Sethi A. Patients With Pelvic Fractures From Blunt Trauma. What Is The Cause Of Mortality And When?. The American Journal Of Surgery 2016;211: Heeveld M. The Management Of Haemodynamically Unstable Patients With Pelvic Fractures: NSW Insitute Of Trauma And Injury Management; Alton T, Gee A. Classifications In Brief: Young And Burgess Classification of Pelvic Ring Injuries Clinical Orthopeadics Relat Res August 2014;472(8): Surgeons Aco. Advanced Trauma Life Support : Program For Doctors. 9E Ed. Chicago: American College Of Surgeons; Curtis K, Ramsden C. Emergency and Trauma Care For Nurses and Paramedics. 2nd Ed: Elsevier; Garlapati A, Ashwood N. An Overview of Pelvic Ring Disruption. Trauma. Apr 2012;14(2): Bottlang M, Krieg JC. Introducing The Pelvic Sling: Pelvic Fracture Stabilization Made Simple. JEMS: Journal of Emergency Medical Services. 2003;28(9): Qureshi A, Mcgee A, Cooper JP, Porter K. Reduction Of The Posterior Pelvic Ring By Non- Invasive Stabilisation: A Report of Two Cases. Emergency Medicine Journal. 2005;22(12): Toth L, King K, Mcgrath B, Zsolt J. Efficacy And Saftey Of Emergency Non-Invasive Pelvic Ring Stabilisation. Injury. 2012;43(2012): Jain S BS, Marciniak J, Pace A. A National Survey Of United Kingdom Trauma Units On The Use Of Pelvic Binders. International Orthopaedics. 2013;31: Bottlang M, Simpson T, Sigg J, Krieg J, Madey S, Long W. Noninvasive Reduction Of Open- Book Pelvic Fractures By Circumferential Compression. Journal of Orthopaedic Trauma. ; 2002;16(6): Gumm K, Judson R, Bucknill A, et al. Haemodynamically Unstable Pelvic Fracture Guideline Melbourne: The Royal Melbourne Hospital; July V3 Endorsed by the Advisory Committee on Trauma August 2016 Page 8 of 8
Pelvic fractures. Dr Raymond Yean, MBBS Surgical SRMO
 Pelvic fractures Dr Raymond Yean, MBBS Surgical SRMO PELVIC FRACTURES Pelvic fracture account for 2-8% all skeletal injuries Associated with High energy trauma Soft tissue injuries and blood loss. Shock,
Pelvic fractures Dr Raymond Yean, MBBS Surgical SRMO PELVIC FRACTURES Pelvic fracture account for 2-8% all skeletal injuries Associated with High energy trauma Soft tissue injuries and blood loss. Shock,
RMH TRAUMA CALL GUIDELINES
 Trauma Service Guidelines Title: Trauma Team Activation ( Call and Alert) TRM 08.05 TRAUMA TEAM ACTIVATION (CALL AND ALERT) Developed by: K. Gumm, J. Papson, P. Morley, R. Judson, M. Van Den Driesen &
Trauma Service Guidelines Title: Trauma Team Activation ( Call and Alert) TRM 08.05 TRAUMA TEAM ACTIVATION (CALL AND ALERT) Developed by: K. Gumm, J. Papson, P. Morley, R. Judson, M. Van Den Driesen &
Haemodynamic deterioration in lateral compression pelvic fracture after prehospital pelvic circumferential compression device application
 Haemodynamic deterioration in lateral compression pelvic fracture after prehospital pelvic circumferential compression device application Authors Alan A Garner Retrieval consultant CareFlight Northmead,
Haemodynamic deterioration in lateral compression pelvic fracture after prehospital pelvic circumferential compression device application Authors Alan A Garner Retrieval consultant CareFlight Northmead,
Musculoskeletal System
 CHAPTER 28 Musculoskeletal Injuries Musculoskeletal System Anatomy & Physiology Bones provide framework. Joints allow for bending. Muscles allow for movement. Cartilage provides flexibility. Tendons connect
CHAPTER 28 Musculoskeletal Injuries Musculoskeletal System Anatomy & Physiology Bones provide framework. Joints allow for bending. Muscles allow for movement. Cartilage provides flexibility. Tendons connect
CHAPTER 28 Musculoskeletal Injuries
 CHAPTER 28 Musculoskeletal Injuries Musculoskeletal System Anatomy & Physiology Bones provide framework. Joints allow for bending. Muscles allow for movement. Cartilage provides flexibility. Tendons connect
CHAPTER 28 Musculoskeletal Injuries Musculoskeletal System Anatomy & Physiology Bones provide framework. Joints allow for bending. Muscles allow for movement. Cartilage provides flexibility. Tendons connect
Emergent Management of Pelvic Ring Fractures with Use of Circumferential Compression
 This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. Emergent Management of Pelvic Ring Fractures with Use of Circumferential
This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. Emergent Management of Pelvic Ring Fractures with Use of Circumferential
T-PODResponder Pelvic Stabilization Device
 T-PODResponder Pelvic Stabilization Device Training Session Pyng Medical Corp. 1-604-303-7964 2014 Pyng Medical Corp. August 2014 PM-176a Why T-PODResponder? Pelvic fractures have a mortality rate of 5%
T-PODResponder Pelvic Stabilization Device Training Session Pyng Medical Corp. 1-604-303-7964 2014 Pyng Medical Corp. August 2014 PM-176a Why T-PODResponder? Pelvic fractures have a mortality rate of 5%
Classification, management and outcomes of severe pelvic ring fractures
 Classification, management and outcomes of severe pelvic ring fractures School of Public Health and Preventive Medicine, Monash University The Alfred Hospital, Royal Melbourne Hospital, Epworth Health
Classification, management and outcomes of severe pelvic ring fractures School of Public Health and Preventive Medicine, Monash University The Alfred Hospital, Royal Melbourne Hospital, Epworth Health
Pelvic Fractures. AOCP National Course Belfast City Hospital. 11 th June D Swain BSc; FRCSI; FRCS (Orth.)
 Pelvic Fractures AOCP National Course Belfast City Hospital 11 th June 2010 Who s this bloke? Consultant orthopaedic surgeon RVH Trained in Belfast, England and Toronto Interests - pelvic and acetabular
Pelvic Fractures AOCP National Course Belfast City Hospital 11 th June 2010 Who s this bloke? Consultant orthopaedic surgeon RVH Trained in Belfast, England and Toronto Interests - pelvic and acetabular
Clinical Module. Pelvic Injury Trauma. Princess Alexandra Hospital Emergency Department. 1 Introduction
 Princess Alexandra Hospital Emergency Department Clinical Module Trauma Review Officers: Katherine Isoardi / Glenn Ryan Version no: 2 Review date: Aug 2015 Key Words: Pelvic Trauma, Pelvic Injury, Pelvic
Princess Alexandra Hospital Emergency Department Clinical Module Trauma Review Officers: Katherine Isoardi / Glenn Ryan Version no: 2 Review date: Aug 2015 Key Words: Pelvic Trauma, Pelvic Injury, Pelvic
10/2/2018. Acute Management of Pelvic Injuries. Learning Objectives. 17 yo male ped struck by truck
 17 yo male ped struck by truck Acute Management of Pelvic Injuries David Volgas, MD CoxHealth University of Missouri HD unstable Open pelvic wound superior gluteal fold through rectum to scrotum Open rami
17 yo male ped struck by truck Acute Management of Pelvic Injuries David Volgas, MD CoxHealth University of Missouri HD unstable Open pelvic wound superior gluteal fold through rectum to scrotum Open rami
2018 SAM MEDICAL PRODUCTS. ALL RIGHTS RESERVED. SLI-PED-G-01 FEB 2018
 https://www.youtube.com/watch?time_continue=2&v=-my1ctcxad4 WHY WE NEED PELVIC BINDERS WHY WE NEED PELVIC BINDERS Pelvic fractures are a common result of high energy impacts such as falls, crushing injuries,
https://www.youtube.com/watch?time_continue=2&v=-my1ctcxad4 WHY WE NEED PELVIC BINDERS WHY WE NEED PELVIC BINDERS Pelvic fractures are a common result of high energy impacts such as falls, crushing injuries,
Activity Three: Where s the Bleeding?
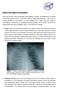 Activity Three: Where s the Bleeding? There are five main sites of potentially fatal bleeding in trauma, remembered by the phrase on the floor and four more. On the floor refers to losing blood externally
Activity Three: Where s the Bleeding? There are five main sites of potentially fatal bleeding in trauma, remembered by the phrase on the floor and four more. On the floor refers to losing blood externally
Pelvic Injuries. Chapter 21
 Chapter 21 Introduction Injuries of the pelvis are an uncommon, but potentially lethal, battlefield injury. Blunt injuries may be associated with major hemorrhage and early mortality. Death within the
Chapter 21 Introduction Injuries of the pelvis are an uncommon, but potentially lethal, battlefield injury. Blunt injuries may be associated with major hemorrhage and early mortality. Death within the
Initial Management of Pelvic Injuries
 Initial Management of Pelvic Injuries Olav Røise, MD, PhD Chairman Division of Neuroscience and Skeletal Medicine Ullevål University Hospital Trauma treatment Represent a chain of health services in which
Initial Management of Pelvic Injuries Olav Røise, MD, PhD Chairman Division of Neuroscience and Skeletal Medicine Ullevål University Hospital Trauma treatment Represent a chain of health services in which
LESSON ASSIGNMENT. After completing this lesson, you should be able to:
 LESSON ASSIGNMENT LESSON 3 Traction Splints. LESSON ASSIGNMENT Paragraphs 3-1 through 3-5. LESSON OBJECTIVES After completing this lesson, you should be able to: 3-1. Identify the purpose of a traction
LESSON ASSIGNMENT LESSON 3 Traction Splints. LESSON ASSIGNMENT Paragraphs 3-1 through 3-5. LESSON OBJECTIVES After completing this lesson, you should be able to: 3-1. Identify the purpose of a traction
Chapter 30 - Musculoskeletal_Trauma
 Introduction to Emergency Medical Care 1 OBJECTIVES 30.1 Define key terms introduced in this chapter. Slides 11 12, 19 20, 22 23, 37 30.2 Describe the anatomy of elements of the musculoskeletal system.
Introduction to Emergency Medical Care 1 OBJECTIVES 30.1 Define key terms introduced in this chapter. Slides 11 12, 19 20, 22 23, 37 30.2 Describe the anatomy of elements of the musculoskeletal system.
Northern Trauma Network. Management of Haemodynamically Unstable Patients with Pelvic Injury
 Management of Haemodynamically Unstable Patients with Pelvic Injury Northern Trauma Network This guideline focuses on the assessment of haemodynamic instability related to haemorrhage associated with a
Management of Haemodynamically Unstable Patients with Pelvic Injury Northern Trauma Network This guideline focuses on the assessment of haemodynamic instability related to haemorrhage associated with a
THE INITIAL MANAGEMENT OF PELVIC AND ACETABULAR TRAUMA LOUIS LEBLOND MD FRCSC DEPT OF ORTHOPAEDICS THE MONCTON HOSPITAL - L HÔPITAL DE MONCTON
 THE INITIAL MANAGEMENT OF PELVIC AND ACETABULAR TRAUMA LOUIS LEBLOND MD FRCSC DEPT OF ORTHOPAEDICS THE MONCTON HOSPITAL - L HÔPITAL DE MONCTON DISCLOSURES + BACKGROUND No. Centre de formation médicale
THE INITIAL MANAGEMENT OF PELVIC AND ACETABULAR TRAUMA LOUIS LEBLOND MD FRCSC DEPT OF ORTHOPAEDICS THE MONCTON HOSPITAL - L HÔPITAL DE MONCTON DISCLOSURES + BACKGROUND No. Centre de formation médicale
Overview. Overview. Chapter 30. Injuries to the Head and Spine 9/11/2012. Review of the Nervous and Skeletal Systems. Devices for Immobilization
 Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
Pelvis injuries Fractures of the femur (proximal,shaft) Dr Tamás Bodzay
 Pelvis injuries Fractures of the femur (proximal,shaft) Dr Tamás Bodzay Pelvis anatomy Pelvis function - axial load bearing - protection: abdominal, pelvic structures Pelvic injury mechanism Falling from
Pelvis injuries Fractures of the femur (proximal,shaft) Dr Tamás Bodzay Pelvis anatomy Pelvis function - axial load bearing - protection: abdominal, pelvic structures Pelvic injury mechanism Falling from
Initial Pelvic Fracture Management. Patrick M Reilly MD FACS February 27, 2010
 Initial Pelvic Fracture Management Patrick M Reilly MD FACS February 27, 2010 John Pryor MD Field Triage* * Step One : Physiology * Step Two : Anatomy * Step Three : Mechanism * Step Four : Co-Morbid Conditions
Initial Pelvic Fracture Management Patrick M Reilly MD FACS February 27, 2010 John Pryor MD Field Triage* * Step One : Physiology * Step Two : Anatomy * Step Three : Mechanism * Step Four : Co-Morbid Conditions
Fractures of the Thoracic and Lumbar Spine
 A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
.org. Tibia (Shinbone) Shaft Fractures. Anatomy. Types of Tibial Shaft Fractures
 Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Unstable fractures of the pelvis treated with a trapezoid compression frame
 Acta Orthop Scand 55, 325-329, 1984 Unstable fractures of the pelvis treated with a trapezoid compression frame Sixteen patients with unstable pelvic fractures were treated by early reduction and fixation
Acta Orthop Scand 55, 325-329, 1984 Unstable fractures of the pelvis treated with a trapezoid compression frame Sixteen patients with unstable pelvic fractures were treated by early reduction and fixation
Abdominal Trauma. Nat Krairojananan M.D., FRCST Department of Trauma and Emergency Medicine Phramongkutklao Hospital
 Abdominal Trauma Nat Krairojananan M.D., FRCST Department of Trauma and Emergency Medicine Phramongkutklao Hospital overview Quick review abdominal anatomy Review of mechanism of injury Review of investigation
Abdominal Trauma Nat Krairojananan M.D., FRCST Department of Trauma and Emergency Medicine Phramongkutklao Hospital overview Quick review abdominal anatomy Review of mechanism of injury Review of investigation
LESSON ASSIGNMENT. After completing this lesson, you should be able to: be able to:
 LESSON ASSIGNMENT LESSON 4 Fractures of the Lower Extremities. LESSON ASSIGNMENT Paragraphs 4-1 through 4-8. LESSON OBJECTIVES After completing this lesson, you should be able to: be able to: 4-1. Identify
LESSON ASSIGNMENT LESSON 4 Fractures of the Lower Extremities. LESSON ASSIGNMENT Paragraphs 4-1 through 4-8. LESSON OBJECTIVES After completing this lesson, you should be able to: be able to: 4-1. Identify
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 17 Orthopedic Techniques Key Points 2 17.1 Traction Use an appropriate method of traction to treat fractures of the extremities and cervical spine Apply extremity
Surgical Care at the District Hospital 1 17 Orthopedic Techniques Key Points 2 17.1 Traction Use an appropriate method of traction to treat fractures of the extremities and cervical spine Apply extremity
Management of Pelvic Fracture
 Management of Pelvis Fracture with Hemodynamic Instability James W. Davis MD Professor of Clinical Surgery, UCSF/Fresno Chief of Trauma Management of Pelvic Fracture How NOT to do it The basics Evaluation
Management of Pelvis Fracture with Hemodynamic Instability James W. Davis MD Professor of Clinical Surgery, UCSF/Fresno Chief of Trauma Management of Pelvic Fracture How NOT to do it The basics Evaluation
SPINAL IMMOBILIZATION
 Spinal Immobilization Decision Assessment Recent studies have shown an increase in mortality for patients with isolated penetrating trauma who are spinally immobilized. Therefore spinal immobilization
Spinal Immobilization Decision Assessment Recent studies have shown an increase in mortality for patients with isolated penetrating trauma who are spinally immobilized. Therefore spinal immobilization
The Acute Management of Pelvic Ring Injuries
 The Acute Management of Pelvic Ring Injuries Brian J Ladner, MD North Oaks Medical Center Original Author: Kyle F. Dickson, MD; Created March 2004 Sean E. Nork, MD; Revised December 2010 New Author: October
The Acute Management of Pelvic Ring Injuries Brian J Ladner, MD North Oaks Medical Center Original Author: Kyle F. Dickson, MD; Created March 2004 Sean E. Nork, MD; Revised December 2010 New Author: October
Overview. Background. Table of Contents
 Trauma Service Guidelines Title: Cervical Spine Guidelines Developed by: P. Page, R. Judson, K. Gumm, M. Kennedy, D. McDonald & Advisory Committee on Trauma Created: Version 1.0 October 2005, Revised:
Trauma Service Guidelines Title: Cervical Spine Guidelines Developed by: P. Page, R. Judson, K. Gumm, M. Kennedy, D. McDonald & Advisory Committee on Trauma Created: Version 1.0 October 2005, Revised:
Combat Ready Clamp. Medic/Corpsman carried device Aidbag-based. Partially broken down 1.5 lbs
 Combat Ready Clamp Combat Ready Clamp Medic/Corpsman carried device Aidbag-based Partially broken down 1.5 lbs Assembly of the CRoC FDA-Approved CRoC Application Points The Combat Ready Clamp is indicated
Combat Ready Clamp Combat Ready Clamp Medic/Corpsman carried device Aidbag-based Partially broken down 1.5 lbs Assembly of the CRoC FDA-Approved CRoC Application Points The Combat Ready Clamp is indicated
Selective Spine Assessment & Spinal Motion Restriction
 Selective Spine Assessment & Spinal Motion Restriction Supersedes: 02-09-15 Effective: 10-20-15 Spinal cord injury may be the result of direct blunt and/or penetrating trauma, compression forces (axial
Selective Spine Assessment & Spinal Motion Restriction Supersedes: 02-09-15 Effective: 10-20-15 Spinal cord injury may be the result of direct blunt and/or penetrating trauma, compression forces (axial
PediLoc Extension Osteotomy Plate (PLEO)
 PediLoc Extension Osteotomy Plate (PLEO) Left PLEO Plates Sizes: 6, 8 and 10 hole plates Right PLEO Plates Sizes: 6, 8 and 10 hole plates PediLoc Extension Osteotomy Plate The technique description herein
PediLoc Extension Osteotomy Plate (PLEO) Left PLEO Plates Sizes: 6, 8 and 10 hole plates Right PLEO Plates Sizes: 6, 8 and 10 hole plates PediLoc Extension Osteotomy Plate The technique description herein
1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles. Striated Skeletal. Smooth
 1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles Striated Skeletal Smooth 3 Anatomy and Physiology of the Musculoskeletal System 4 Skeletal System 5 Skeletal System Functions
1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles Striated Skeletal Smooth 3 Anatomy and Physiology of the Musculoskeletal System 4 Skeletal System 5 Skeletal System Functions
Shenandoah Co. Fire & Rescue. Injuries to. and Spine. December EMS Training Bill Streett Training Section Chief
 Shenandoah Co. Fire & Rescue Injuries to the Head and Spine December EMS Training Bill Streett Training Section Chief C.E. Card Information BLS Providers 2 Cards / Provider Category 1 Course # Blank Topic#
Shenandoah Co. Fire & Rescue Injuries to the Head and Spine December EMS Training Bill Streett Training Section Chief C.E. Card Information BLS Providers 2 Cards / Provider Category 1 Course # Blank Topic#
DISTRACTION EXTERNAL FIXATIONS OF PELVIC FRACTURES CAUSED BY A LATERAL COMPRESSION
 DOI: 10.5272/jimab.2011171.161 Journal of IMAB - Annual Proceeding (Scientific Papers) 2011, vol. 17, book 1 DISTRACTION EXTERNAL FIXATIONS OF PELVIC FRACTURES CAUSED BY A LATERAL COMPRESSION Pavlin Apostolov,
DOI: 10.5272/jimab.2011171.161 Journal of IMAB - Annual Proceeding (Scientific Papers) 2011, vol. 17, book 1 DISTRACTION EXTERNAL FIXATIONS OF PELVIC FRACTURES CAUSED BY A LATERAL COMPRESSION Pavlin Apostolov,
Junctional Emergency Treatment Tool Item#: NSN#:
 Junctional Emergency Treatment Tool Item#: 30-0088 NSN#: 6515-01-616-5841 35 Tedwall Ct. Greer, SC 29650 Anatomy of the JETT (Junctional Emergency Treatment Tool) Instructions Overview The Junctional Emergency
Junctional Emergency Treatment Tool Item#: 30-0088 NSN#: 6515-01-616-5841 35 Tedwall Ct. Greer, SC 29650 Anatomy of the JETT (Junctional Emergency Treatment Tool) Instructions Overview The Junctional Emergency
Hemorrhage Control. Chapter 6
 Chapter 6 The hemorrhage that take[s] place when a main artery is divided is usually so rapid and so copious that the wounded man dies before help can reach him. Colonel H. M. Gray, 1919 Stop the Bleeding!
Chapter 6 The hemorrhage that take[s] place when a main artery is divided is usually so rapid and so copious that the wounded man dies before help can reach him. Colonel H. M. Gray, 1919 Stop the Bleeding!
ABC of Emergency Radiology
 ABC of Emergency Radiology It is possible for the non-specialist to interpret pelvic radiographs accurately Important anatomical considerations THE PELVIS P A Driscoll, R Ross, D A Nicholson FIG i-line
ABC of Emergency Radiology It is possible for the non-specialist to interpret pelvic radiographs accurately Important anatomical considerations THE PELVIS P A Driscoll, R Ross, D A Nicholson FIG i-line
North West London Trauma Network Spinal Pathway and Protocols
 North West London Trauma Network Spinal Pathway and Protocols 1. Spinal Clearance in the Trauma Patient Inclusions: All trauma patients who are not alert and orientated, unable to cooperate (including
North West London Trauma Network Spinal Pathway and Protocols 1. Spinal Clearance in the Trauma Patient Inclusions: All trauma patients who are not alert and orientated, unable to cooperate (including
Information within the handout. Brief Introduction Anatomy & Biomechanics Assessment & Diagnosis Treatment through Muscle Energy
 Manual Medicine Diagnosis and Treatment for Somatic Dysfunction of the Pelvis Through Muscle Energy Greenman s Priciples of Manual Medicine (5 th Ed.)- Lisa DeStefano,DO Speaker disclosure I declare I
Manual Medicine Diagnosis and Treatment for Somatic Dysfunction of the Pelvis Through Muscle Energy Greenman s Priciples of Manual Medicine (5 th Ed.)- Lisa DeStefano,DO Speaker disclosure I declare I
MASSACHUSETTS DEPARTMENT OF PUBLIC HEALTH OFFICE OF EMERGENCY MEDICAL SERVICES Basic EMT Practical Examination Cardiac Arrest Management
 Basic EMT Practical Examination 6.0 - Cardiac Arrest Management Station 1 RESUSCITATION & DEFIBRILLATION No Point WHILE FUNCTIONING AS FIRST RESCUER: Point 1. Verbalizes or takes body substance isolation
Basic EMT Practical Examination 6.0 - Cardiac Arrest Management Station 1 RESUSCITATION & DEFIBRILLATION No Point WHILE FUNCTIONING AS FIRST RESCUER: Point 1. Verbalizes or takes body substance isolation
Trauma Alert Step 2 Additions
 Trauma Alert Step 2 Additions MANGLED, DEGLOVED OR PULSELESS EXTREMITY PELVIC INJURY WITH HIGH-RISK MECHANISM OF INJURY Many thanks to Paramedic FTO Justin Bramlette for assembling this training presentation
Trauma Alert Step 2 Additions MANGLED, DEGLOVED OR PULSELESS EXTREMITY PELVIC INJURY WITH HIGH-RISK MECHANISM OF INJURY Many thanks to Paramedic FTO Justin Bramlette for assembling this training presentation
Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles
 1 2 3 4 5 6 7 Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles Striated Skeletal Smooth Anatomy and Physiology of the Musculoskeletal System Skeletal System Skeletal System Functions
1 2 3 4 5 6 7 Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles Striated Skeletal Smooth Anatomy and Physiology of the Musculoskeletal System Skeletal System Skeletal System Functions
Large Distractor Femur
 Fracture Reduction and Provisional Stabilization Large Distractor Femur Surgical Technique Table of Contents Introduction Standard Femoral Distraction 2 Large Distractor System 4 Surgical Technique Prepare
Fracture Reduction and Provisional Stabilization Large Distractor Femur Surgical Technique Table of Contents Introduction Standard Femoral Distraction 2 Large Distractor System 4 Surgical Technique Prepare
Balanced Body Movement Principles
 Balanced Body Movement Principles How the Body Works and How to Train it. Module 3: Lower Body Strength and Power Developing Strength, Endurance and Power The lower body is our primary source of strength,
Balanced Body Movement Principles How the Body Works and How to Train it. Module 3: Lower Body Strength and Power Developing Strength, Endurance and Power The lower body is our primary source of strength,
journal ORIGINAL RESEARCH
 texas orthopaedic journal ORIGINAL RESEARCH Mortality with Circumferential Pelvic Compression for Pelvic Ring Disruption in Polytraumatized Patients: A Retrospective Analysis of 1,639 Pelvic Ring Injuries
texas orthopaedic journal ORIGINAL RESEARCH Mortality with Circumferential Pelvic Compression for Pelvic Ring Disruption in Polytraumatized Patients: A Retrospective Analysis of 1,639 Pelvic Ring Injuries
Trauma Overview. Chapter 22
 Trauma Overview Chapter 22 Kinematics of Trauma Injuries are the leading cause of death among children and young adults. Kinematics introduces the basic physical concepts that dictate how injuries occur
Trauma Overview Chapter 22 Kinematics of Trauma Injuries are the leading cause of death among children and young adults. Kinematics introduces the basic physical concepts that dictate how injuries occur
Anatomy & Physiology Pelvic Girdles 10.1 General Information
 Anatomy & Physiology Pelvic Girdles 10.1 General Information ICan2Ed, Inc. In human anatomy, the pelvis (plural pelves or pelvises) is the lower part of. The area of the body that is between the abdomen
Anatomy & Physiology Pelvic Girdles 10.1 General Information ICan2Ed, Inc. In human anatomy, the pelvis (plural pelves or pelvises) is the lower part of. The area of the body that is between the abdomen
Musculoskeletal Trauma. Lesson Goal. Lesson Objectives 9/10/2012. Recognize and manage patients with musculoskeletal trauma
 Musculoskeletal Trauma Lesson Goal Recognize and manage patients with musculoskeletal trauma Lesson Objectives Describe function of muscular system Describe composition of muscular system Describe, compare,
Musculoskeletal Trauma Lesson Goal Recognize and manage patients with musculoskeletal trauma Lesson Objectives Describe function of muscular system Describe composition of muscular system Describe, compare,
Guidelines and Protocols
 TITLE: PELVIC TRAUMA PURPOSE: Develop a protocol of care that will insure rapid identification and treatment of these patients PROCESS: I. CARE OF PATIENTS WITH PELVIC TRAUMA A. Patients in hemorrhagic
TITLE: PELVIC TRAUMA PURPOSE: Develop a protocol of care that will insure rapid identification and treatment of these patients PROCESS: I. CARE OF PATIENTS WITH PELVIC TRAUMA A. Patients in hemorrhagic
Hassan R. Mir, MD, MBA, FACS
 DISCLOSURES Hassan R. Mir, MD, MBA, FACS Paid Consultant for a Company or Supplier Smith & Nephew Zimmer Biomet Trice Medical Stock or Stock Options Core Orthopaedics OrthoGrid Systems Research Support
DISCLOSURES Hassan R. Mir, MD, MBA, FACS Paid Consultant for a Company or Supplier Smith & Nephew Zimmer Biomet Trice Medical Stock or Stock Options Core Orthopaedics OrthoGrid Systems Research Support
Surgical Approaches for Fractures and Injuries of the Pelvic Ring
 Surgical Approaches for Fractures and Injuries of the Pelvic Ring Mara L. Schenker, MD Emory University / Grady Hospital Created by Steven A. Olson, MD in 2004 and Kyle Dickson, MD in 2004 First revised
Surgical Approaches for Fractures and Injuries of the Pelvic Ring Mara L. Schenker, MD Emory University / Grady Hospital Created by Steven A. Olson, MD in 2004 and Kyle Dickson, MD in 2004 First revised
Injuries to the Head and Spine
 Injuries to the Head and Spine Anatomy Review Skull Protects the brain Made up of several bones with seam like sutures Regions of the scalp-frontal, occipital, parietal, temporal Bones of face Orbits Mandible
Injuries to the Head and Spine Anatomy Review Skull Protects the brain Made up of several bones with seam like sutures Regions of the scalp-frontal, occipital, parietal, temporal Bones of face Orbits Mandible
A wheelchair is a body orthosis on wheels. Understanding basic principles of seating. Seating REQUIREMENTS OF SEATING
 Understanding basic principles of seating A wheelchair is a body orthosis on wheels. Bengt Engström Orthosis = splint FUNCTIONS OF AN ORTHOSIS Maintaining alignment Protecting weak muscles Protecting joints
Understanding basic principles of seating A wheelchair is a body orthosis on wheels. Bengt Engström Orthosis = splint FUNCTIONS OF AN ORTHOSIS Maintaining alignment Protecting weak muscles Protecting joints
Dana Alrafaiah. - Amani Nofal. - Ahmad Alsalman. 1 P a g e
 - 2 - Dana Alrafaiah - Amani Nofal - Ahmad Alsalman 1 P a g e This lecture will discuss five topics as follows: 1- Arrangement of pelvic viscera. 2- Muscles of Pelvis. 3- Blood Supply of pelvis. 4- Nerve
- 2 - Dana Alrafaiah - Amani Nofal - Ahmad Alsalman 1 P a g e This lecture will discuss five topics as follows: 1- Arrangement of pelvic viscera. 2- Muscles of Pelvis. 3- Blood Supply of pelvis. 4- Nerve
Fractures Healing & Management. Traumatology RHS 231 Dr. Einas Al-Eisa Lecture 4
 Fractures Healing & Management Traumatology RHS 231 Dr. Einas Al-Eisa Lecture 4 Fractures Despite their strength, bones are susceptible to fractures. In young people, most fractures result from trauma
Fractures Healing & Management Traumatology RHS 231 Dr. Einas Al-Eisa Lecture 4 Fractures Despite their strength, bones are susceptible to fractures. In young people, most fractures result from trauma
Chapter 32. Objectives. Objectives 01/09/2013. Spinal Column and Spinal Cord Trauma
 Chapter 32 Spinal Column and Spinal Cord Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1.
Chapter 32 Spinal Column and Spinal Cord Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1.
ANATYOMY OF The thigh
 ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 5- Intermediate cutaneous nerve of the thigh 1, 2 and 3 are
ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 5- Intermediate cutaneous nerve of the thigh 1, 2 and 3 are
Chapter 2 Triage. Introduction. The Trauma Team
 Chapter 2 Triage Chapter 2 Triage Introduction Existing trauma courses focus on a vertical or horizontal approach to the ABCDE assessment of an injured patient: A - Airway B - Breathing C - Circulation
Chapter 2 Triage Chapter 2 Triage Introduction Existing trauma courses focus on a vertical or horizontal approach to the ABCDE assessment of an injured patient: A - Airway B - Breathing C - Circulation
LAB Notes#1. Ahmad Ar'ar. Eslam
 LAB Notes#1 Ahmad Ar'ar Eslam 1 P a g e Anatomy lab Notes Lower limb bones :- Pelvic girdle: It's the connection between the axial skeleton and the lower limb; it's made up of one bone called the HIP BONE
LAB Notes#1 Ahmad Ar'ar Eslam 1 P a g e Anatomy lab Notes Lower limb bones :- Pelvic girdle: It's the connection between the axial skeleton and the lower limb; it's made up of one bone called the HIP BONE
Monolateral External Fixation System for Trauma and Orthopaedics
 MEFiSTO Monolateral External Fixation System for Trauma and Orthopaedics Surgical Technique Original Instruments and Implants of the Association for the Study of Internal Fixation AO/ASIF MEFiSTO Table
MEFiSTO Monolateral External Fixation System for Trauma and Orthopaedics Surgical Technique Original Instruments and Implants of the Association for the Study of Internal Fixation AO/ASIF MEFiSTO Table
Slide Read the tables it is about the difference between male & female pelvis.
 I didn t include the slides, this is only what the doctor read or said because he skipped a lot of things because we took it previously, very important to go back to the slides (*there is an edited version)
I didn t include the slides, this is only what the doctor read or said because he skipped a lot of things because we took it previously, very important to go back to the slides (*there is an edited version)
The thigh. Prof. Oluwadiya KS
 The thigh Prof. Oluwadiya KS www.oluwadiya.com The Thigh: Boundaries The thigh is the region of the lower limb that is approximately between the hip and knee joints Anteriorly, it is separated from the
The thigh Prof. Oluwadiya KS www.oluwadiya.com The Thigh: Boundaries The thigh is the region of the lower limb that is approximately between the hip and knee joints Anteriorly, it is separated from the
Copyright 2003 Pearson Education, Inc. publishing as Benjamin Cummings. Dr. Nabil Khouri MD, MSc, Ph.D
 Dr. Nabil Khouri MD, MSc, Ph.D Pelvic Girdle (Hip) Organization of the Lower Limb It is divided into: The Gluteal region The thigh The knee The leg The ankle The foot The thigh and the leg have compartments
Dr. Nabil Khouri MD, MSc, Ph.D Pelvic Girdle (Hip) Organization of the Lower Limb It is divided into: The Gluteal region The thigh The knee The leg The ankle The foot The thigh and the leg have compartments
Injuries to the Head and Spine From Bradys Emergency Care 10 th Edition
 Injuries to the Head and Spine From Bradys Emergency Care 10 th Edition 1. When performing the four-rescuer log roll, which responder pulls the board into position? A.) Head B.) Waist C.) Knee D.) Shoulder
Injuries to the Head and Spine From Bradys Emergency Care 10 th Edition 1. When performing the four-rescuer log roll, which responder pulls the board into position? A.) Head B.) Waist C.) Knee D.) Shoulder
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions
 Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What is caused by overexerting or tearing of a muscle? p. 375 A.) Dislocation B.) Sprain C.) Fracture *D.)
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What is caused by overexerting or tearing of a muscle? p. 375 A.) Dislocation B.) Sprain C.) Fracture *D.)
PediLoc 3.5mm and 4.5mm Contour Femur Plate Surgical Technique
 PediLoc 3.5mm and 4.5mm Contour Femur Plate Surgical Technique Surgical Technique Contour Femur Plate The technique description herein is made available to the healthcare professional to illustrate the
PediLoc 3.5mm and 4.5mm Contour Femur Plate Surgical Technique Surgical Technique Contour Femur Plate The technique description herein is made available to the healthcare professional to illustrate the
Access Pelvic Fixator
 Access Pelvic Fixator Attila Poka, MD Director, Orthopedic Trauma Service Grant Medical Center Columbus, OH Patents Pending CONTENTS 1 Introduction...Page 2 Equipment Required...Page 3 Design Rationale...Page
Access Pelvic Fixator Attila Poka, MD Director, Orthopedic Trauma Service Grant Medical Center Columbus, OH Patents Pending CONTENTS 1 Introduction...Page 2 Equipment Required...Page 3 Design Rationale...Page
47b Side-lying and Pregnancy Massage:! Technique Demo and Practice
 47b Side-lying and Pregnancy Massage:! Technique Demo and Practice 47b Side-lying & Pregnancy Massage! Technique Demo and Practice! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders
47b Side-lying and Pregnancy Massage:! Technique Demo and Practice 47b Side-lying & Pregnancy Massage! Technique Demo and Practice! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders
THE HIP. Cooler than cool, the pinnacle of what is "it". Beyond all trends and conventional coolness.
 THE HIP Cooler than cool, the pinnacle of what is "it". Beyond all trends and conventional coolness. Objectives Hip anatomy Causes of hip pain Hip exam Anatomy Bones Ilium Anterior Superior Iliac Spine
THE HIP Cooler than cool, the pinnacle of what is "it". Beyond all trends and conventional coolness. Objectives Hip anatomy Causes of hip pain Hip exam Anatomy Bones Ilium Anterior Superior Iliac Spine
PAL Pelvic Alignment Level
 PAL Pelvic Alignment Level Surgical Protocol For consistency during surgery Pelvic Alignment Level (PAL) Features Pelvic Alignment Level Surgical Protocol To Table To Floor 1. Patient Positioning & Preparation
PAL Pelvic Alignment Level Surgical Protocol For consistency during surgery Pelvic Alignment Level (PAL) Features Pelvic Alignment Level Surgical Protocol To Table To Floor 1. Patient Positioning & Preparation
INGUINAL HERNIA REPAIR PROCEDURE GUIDE
 ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
Major Trauma Scenarios. Ballarat Health Services Emergency Medicine Training Hub
 Major Trauma Scenarios Ballarat Health Services Emergency Medicine Training Hub Trauma Scenario 1 You receive a phone call from the ambulance service. They have a 27 yr old male involved in a MCA, he is
Major Trauma Scenarios Ballarat Health Services Emergency Medicine Training Hub Trauma Scenario 1 You receive a phone call from the ambulance service. They have a 27 yr old male involved in a MCA, he is
To classify the joints relative to structure & shape
 To classify the joints relative to structure & shape To describe the anatomy of the hip joint To describe the ankle joint To memorize their blood & nerve supply JOINTS: Joints are sites where skeletal
To classify the joints relative to structure & shape To describe the anatomy of the hip joint To describe the ankle joint To memorize their blood & nerve supply JOINTS: Joints are sites where skeletal
Fractures and dislocations around elbow in adult
 Lec: 3 Fractures and dislocations around elbow in adult These include fractures of distal humerus, fracture of the capitulum, fracture of the radial head, fracture of the olecranon & dislocation of the
Lec: 3 Fractures and dislocations around elbow in adult These include fractures of distal humerus, fracture of the capitulum, fracture of the radial head, fracture of the olecranon & dislocation of the
EMS SKILL NEUROLOGICAL EMERGENCY / SPINAL MOTION RESTRICTION (SMR) VEST TYPE EXTRICATION DEVICE FOR THE SEATED PATIENT
 EMS SKILL NEUROLOGICAL EMERGENCY / SPINAL MOTION RESTRICTION (SMR) VEST TYPE EXTRICATION DEVICE FOR THE SEATED PATIENT PERFORMANCE OBJECTIVES Demonstrate competency in performing and directing team members
EMS SKILL NEUROLOGICAL EMERGENCY / SPINAL MOTION RESTRICTION (SMR) VEST TYPE EXTRICATION DEVICE FOR THE SEATED PATIENT PERFORMANCE OBJECTIVES Demonstrate competency in performing and directing team members
Spinal or Suspected Spinal, Injury: Logrolling Technique with C- Spine Precautions
 Approved by: Spinal or Suspected Spinal, Injury: Logrolling Technique with C- Spine Precautions Vice President and Chief Medical Officer; and Vice President and Chief Operating Officer Corporate Policy
Approved by: Spinal or Suspected Spinal, Injury: Logrolling Technique with C- Spine Precautions Vice President and Chief Medical Officer; and Vice President and Chief Operating Officer Corporate Policy
DEFINITION OF PRESSURE. Pressure = Force / Area
 PRESSURE & POSTURE IN WHEELCHAIR SEATING DEFINITION OF PRESSURE Pressure = Force / Area ANATOMY OF THE SKIN Epidermis Dermis Subcutaneous Layer EFFECTS OF PRESSURE Occludes capillaries Restricts flow of
PRESSURE & POSTURE IN WHEELCHAIR SEATING DEFINITION OF PRESSURE Pressure = Force / Area ANATOMY OF THE SKIN Epidermis Dermis Subcutaneous Layer EFFECTS OF PRESSURE Occludes capillaries Restricts flow of
Surgical Anatomy of the Hip. Joseph H. Dimon
 Surgical Anatomy of the Hip Joseph H. Dimon The hip joint is a deep joint surrounded by large and powerful muscles necessary for its proper function. Essential neurovascular structures lie in front and
Surgical Anatomy of the Hip Joseph H. Dimon The hip joint is a deep joint surrounded by large and powerful muscles necessary for its proper function. Essential neurovascular structures lie in front and
The University Of Jordan Faculty Of Medicine THE LOWER LIMB. Dr.Ahmed Salman Assistant Prof. of Anatomy. The University Of Jordan
 The University Of Jordan Faculty Of Medicine THE LOWER LIMB Dr.Ahmed Salman Assistant Prof. of Anatomy. The University Of Jordan Gluteal Region Cutaneous nerve supply of (Gluteal region) 1. Lateral cutaneous
The University Of Jordan Faculty Of Medicine THE LOWER LIMB Dr.Ahmed Salman Assistant Prof. of Anatomy. The University Of Jordan Gluteal Region Cutaneous nerve supply of (Gluteal region) 1. Lateral cutaneous
SURGICAL AND APPLIED ANATOMY
 Página 1 de 6 Copyright 2001 Lippincott Williams & Wilkins Bucholz, Robert W., Heckman, James D. Rockwood & Green's Fractures in Adults, 5th Edition SURGICAL AND APPLIED ANATOMY Part of "37 - HIP DISLOCATIONS
Página 1 de 6 Copyright 2001 Lippincott Williams & Wilkins Bucholz, Robert W., Heckman, James D. Rockwood & Green's Fractures in Adults, 5th Edition SURGICAL AND APPLIED ANATOMY Part of "37 - HIP DISLOCATIONS
PELVIS & SACRUM Dr. Jamila El-Medany Dr. Essam Eldin Salama
 PELVIS & SACRUM Dr. Jamila El-Medany Dr. Essam Eldin Salama Learning Objectives At the end of the lecture, the students should be able to : Describe the bony structures of the pelvis. Describe in detail
PELVIS & SACRUM Dr. Jamila El-Medany Dr. Essam Eldin Salama Learning Objectives At the end of the lecture, the students should be able to : Describe the bony structures of the pelvis. Describe in detail
Introduction to Anatomy. Dr. Maher Hadidi. Tala Ar ar. Mar/10th/2013
 Sheet Introduction to Anatomy Dr. Maher Hadidi Tala Ar ar 15 Mar/10th/2013 Lower limb The skeleton of the lower limb is the lower appendicular skeleton which consists of 2 parts: 1- Pelvic girdle. 2- Bones
Sheet Introduction to Anatomy Dr. Maher Hadidi Tala Ar ar 15 Mar/10th/2013 Lower limb The skeleton of the lower limb is the lower appendicular skeleton which consists of 2 parts: 1- Pelvic girdle. 2- Bones
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #2 Blunt Trauma
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #2 Blunt Trauma Blunt trauma is the most common cause of traumatic death and disability. The definition
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #2 Blunt Trauma Blunt trauma is the most common cause of traumatic death and disability. The definition
A Patient s Guide to Elbow Dislocation
 A Patient s Guide to Elbow Dislocation 2 Introduction When the joint surfaces of an elbow are forced apart, the elbow is dislocated. The elbow is the second most commonly dislocated joint in adults (after
A Patient s Guide to Elbow Dislocation 2 Introduction When the joint surfaces of an elbow are forced apart, the elbow is dislocated. The elbow is the second most commonly dislocated joint in adults (after
ANJON BREMER LIGHT VEST
 PATENTED TECHNOLOGY, TARGETED TO YOUR NEEDS ANJON BREMER APPLICATION, REMOVAL, AND CPR INSTRUCTIONS WWW.GENERIXMEDICAL.COM INTRODUCTORY INFORMATION FOR THE ANJON BREMER MRI Safety Information: Non-clinical
PATENTED TECHNOLOGY, TARGETED TO YOUR NEEDS ANJON BREMER APPLICATION, REMOVAL, AND CPR INSTRUCTIONS WWW.GENERIXMEDICAL.COM INTRODUCTORY INFORMATION FOR THE ANJON BREMER MRI Safety Information: Non-clinical
Spinal injury. Structure of the spine
 Spinal injury Structure of the spine Some understanding of the structure of the spine (spinal column) and the spinal cord is important as it helps your Neurosurgeon explain about the part of the spine
Spinal injury Structure of the spine Some understanding of the structure of the spine (spinal column) and the spinal cord is important as it helps your Neurosurgeon explain about the part of the spine
Lecture 08 THIGH MUSCLES ANTERIOR COMPARTMENT. Dr Farooq Khan Aurakzai. Dated:
 Lecture 08 THIGH MUSCLES ANTERIOR COMPARTMENT BY Dr Farooq Khan Aurakzai Dated: 11.02.2017 INTRODUCTION to the thigh Muscles. The musculature of the thigh can be split into three sections by intermuscular
Lecture 08 THIGH MUSCLES ANTERIOR COMPARTMENT BY Dr Farooq Khan Aurakzai Dated: 11.02.2017 INTRODUCTION to the thigh Muscles. The musculature of the thigh can be split into three sections by intermuscular
MEDICAL CONTROL POLICY STATEMENT/ADVISORY. Re: Spinal Injury Assessment & Spinal Precautions Procedure
 MEDICAL CONTROL POLICY STATEMENT/ADVISORY No. 2015-01 Date: January 20, 2015 Re: Spinal Injury Assessment & Spinal Precautions Procedure Office of the Medical Director Noel Wagner, MD, NREMT-P 1000 Houghton
MEDICAL CONTROL POLICY STATEMENT/ADVISORY No. 2015-01 Date: January 20, 2015 Re: Spinal Injury Assessment & Spinal Precautions Procedure Office of the Medical Director Noel Wagner, MD, NREMT-P 1000 Houghton
FUNCTIONAL ANATOMY AND EXAM OF THE HIP, GROIN AND THIGH
 FUNCTIONAL ANATOMY AND EXAM OF THE HIP, GROIN AND THIGH Peter G Gerbino, MD, FACSM Orthopedic Surgeon Monterey Joint Replacement and Sports Medicine Monterey, CA TPC, San Diego, 2017 The lecturer has no
FUNCTIONAL ANATOMY AND EXAM OF THE HIP, GROIN AND THIGH Peter G Gerbino, MD, FACSM Orthopedic Surgeon Monterey Joint Replacement and Sports Medicine Monterey, CA TPC, San Diego, 2017 The lecturer has no
May Clinical Director, Peninsula Trauma Network (Edited for PTN)
 Network Policy Traumatic vascular injuries Guidelines Purpose Date May 2015 Version Following the national introduction of Regional Trauma Networks, Major Trauma Networks (MTN s) are required to have a
Network Policy Traumatic vascular injuries Guidelines Purpose Date May 2015 Version Following the national introduction of Regional Trauma Networks, Major Trauma Networks (MTN s) are required to have a
ANATYOMY OF The thigh
 ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 5- Intermediate cutaneous nerve of the thigh 1, 2 and 3 are
ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 5- Intermediate cutaneous nerve of the thigh 1, 2 and 3 are
Trauma CT Scanning Protocol
 Northern Trauma Network Trauma CT Scanning Protocol Background Whole body CT (WBCT) has assumed a pivotal position in trauma management. UK trauma is typically described as blunt and blind i.e. blunt trauma
Northern Trauma Network Trauma CT Scanning Protocol Background Whole body CT (WBCT) has assumed a pivotal position in trauma management. UK trauma is typically described as blunt and blind i.e. blunt trauma
DIAGNOSIS ANTERIOR PELVIC ROTATION DIAGNOSIS DIAGNOSIS. Direct techniques to treat sacrum and pelvis somatic dysfunction (HVLA, MET)
 American Academy of Osteopathy Convocation PHYSICIAN STUDENT Thursday, March 18, 2010 Friday, March 19, 2010 2:30 4:00 PM 8:00 9:30 AM 4:30 6:00 PM 10:00 11:30 AM Direct techniques to treat sacrum and
American Academy of Osteopathy Convocation PHYSICIAN STUDENT Thursday, March 18, 2010 Friday, March 19, 2010 2:30 4:00 PM 8:00 9:30 AM 4:30 6:00 PM 10:00 11:30 AM Direct techniques to treat sacrum and
KNEE DISLOCATION. The most common injury will be an anterior dislocation, and this usually results from a hyperextension mechanism.
 KNEE DISLOCATION Introduction Dislocation of the knee is a severe injury associated with major soft tissue injury and a high incidence of damage to the popliteal artery. There is displacement of the tibia
KNEE DISLOCATION Introduction Dislocation of the knee is a severe injury associated with major soft tissue injury and a high incidence of damage to the popliteal artery. There is displacement of the tibia
