The Valenti technique in the treatment of hallux rigidus
|
|
|
- Milo Bruno Webster
- 6 years ago
- Views:
Transcription
1 Orthopaedics & Traumatology: Surgery & Research (2009) 95, ORIGINAL ARTICLE The Valenti technique in the treatment of hallux rigidus A. Harisboure, P. Joveniaux, K. Madi, E. Dehoux Department of orthopaedics and traumatology, Maison Blanche Hospital, 45, avenue Cognacq Jay, Reims, France Accepted: 2 February 2009 KEYWORDS Metatarsophalangeal joint osteoarthritis; Hallux rigidus; Cheilectomy; Arthrodesis Summary Introduction. Metatarsophalangeal joint osteoarthritis of the great toe (hallux rigidus) is a frequent condition for which numerous surgical techniques have been proposed. The most used ones are cheilectomy and arthrodesis. The objectives of this retrospective study are to present the midterm results of the Valenti procedure and to compare these results with those from other recognized surgical techniques. Materials and methods. We conducted a retrospective analysis of a continuous group of 32 patients (41 cases) presenting hallux rigidus and treated using the Valenti technique from November 1999 to July The mean age of these patients at the time of surgery was 57 years. Forty-one percent of these patients also presented a static disorder of the foot. One or several additional procedures were undertaken, at the time of surgery, in 24% of these cases. Patients were assessed using the AOFAS score completed by the walking distance test, the gait test, the tiptoe test and self-evaluation of patient satisfaction. The radiographic work-up before surgery and at follow-up showed the progression of the joint space changes and allowed us to evaluate plantar subluxation at the base of the first phalanx under the metatarsal head. Results. Twenty-four patients (32 cases) were reviewed and evaluated with a mean follow-up of 5.5 years. Two cases of reflex sympathetic dystrophy were observed as complications. The mean final score was 81 out of 100 from a preoperative score of 47 out of 100. Pain was absent or only occasional in 94% of the cases. Discomfort wearing shoes was absent or moderate in 91% of the cases. Joint range of movement was greater than 30 in 72% of the cases and the toes were stable. Walking distance was unlimited in 79% of the cases. A mean 30% plantar subluxation at the base of the first phalanx was noted at follow-up, with no clinical consequence. The results were comparable irrelevantly of the hallux rigidus grade being treated. Discussion. The numerous techniques proposed achieve comparable results both in terms of pain relief and functional result but each one has its own limitations. Only arthroplasties with silastic implants and the Keller technique give less satisfactory results. Arthrodesis remains Corresponding author. address: aharisboure@chu-reims.fr (A. Harisboure) /$ see front matter 2009 Published by Elsevier Masson SAS. doi: /j.otsr
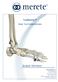
2 The Valenti technique in the treatment of hallux rigidus 203 the first-choice treatment for advanced hallux rigidus but failure is possible in case of technical error or malunion. Cheilectomy, a conservative intervention, is ideal for lesions that are not too advanced or remain limited to the dorsal part of the joint; this conservative option presents generally no specific complications. Prosthetic replacement with, to date, little long-term experience for total arthroplasty remains controversial because the results deteriorate over time. The Valenti procedure exposes the patient to a possible risk of metatarsophalangeal joint destabilization if the resection is too great, but this does not impair the final functional outcome. Conclusion. The arthrectomy described by Valenti is a highly reproducible intervention. We find it to be a good compromise between mobility and stability, providing good results for all hallux rigidus grades and entailing a low complication rate. Level of clinical evidence: Level IV. Therapeutic Study Published by Elsevier Masson SAS. Introduction Hallux rigidus is the clinical manifestation of osteoarthritis of the metatarsophalangeal joint of the great toe. It was described for the first time in 1887 by Davies-Colley (hallux flexus) [1] and then by Cotteril in 1888 [2] as hallux rigidus. Its clinical progression begins with intermittent joint pain during gait (grade I), it continues with painful limitation of joint range of movement (grade II) and ends in ankylosis (grade III). For more than a century, many surgical techniques have been developed to relieve pain and restore function in the great toe in patients suffering from this condition. The Valenti procedure [3] is a partial arthrectomy, a technique designed by the Italian surgeon Valente Valenti, who began using it in 1976 and presented it at the Hershey Seminar in Pennsylvania in This procedure involves an 80 angular V resection of the metatarsal head and the proximal phalanx of two-thirds of the joint height, while preserving the plantar joint space. Thus, the length of the first ray and the intrinsic plantar musculature from the metatarsalsesamoid joint is not altered by the resection. The objectives of this retrospective study were to present the midterm results of the Valenti procedure in the treatment of hallux rigidus and to demonstrate the clinical or radiographic factors that can influence these results. Starting with a review of the literature, the authors compared their results with other recognized surgical techniques in the treatment of hallux rigidus to establish a better understanding of the role and indications for the Valenti procedure. Material and methods Patients This retrospective, descriptive and continuous study collected 32 patients (41 feet) presenting osteoarthritis of the first-ray metatarsophalangeal joint operated on with the Valenti procedure from November 1999 to July During this period, all patients suffering from hallux rigidus operated in our unit underwent this technique. One patient who had had an additional bone procedure on the first ray was excluded from the study. The study included 25 women and seven men, with hallux rigidus on the right side in 19 cases and on the left side in 22 cases (nine patients presented bilateral hallux rigidus treated during the same operative time). The mean age at surgery was 57 years (range: years). In 47% of the cases, the patient had an Egyptian-type forefoot, 37% had a Greek-type forefoot and 16% had a square-type forefoot. In all, 41% of the patients presented gait disturbances involving the foot: 17% presented pies cavus and 24% flatfoot. Frequent wear of high heels was reported by 61% of the women. A history of injury to the great toe was found in two cases. Clinically, we treated five cases of grade I hallux rigidus, 29 grade II and four grade III. Based on the radiographs, there were six cases of grade I hallux rigidus, 19 grade II and ten grade III. The metatarsal-sesamoidal joint was modified in 22 cases (0 grade I, 12 grade II and ten grade III). The preoperative AOFAS score was 47 out of 100; the mean range of movement was 34. There was a correlation with the grade as determined from the radiographs (Table 1). One or several complementary acts were performed in 24% of the cases (eight tendon transpositions, two tenotomies and two osteotomies of the lateral metatarsals). The joint space was a mean 1.4 mm (range: 0 4 mm). One or several osteophytes were present on the first metatarsal in 89% of the cases, all located dorsally. The osteophytosis was circumferential in 34% of the cases. Operative technique The surgery required only a short hospital stay (48 h). The patients presenting bilateral involvement preferred that both sides be treated in the same surgical time. The procedure was performed with rachianesthesia, with the patient in the dorsal decubitus position, with a pneumatic tourniquet inflated at mid-calf. A medial incision was made at the point where the plantar and dorsal skin meet (Fig. 1 A). Capsulotomy and arthrolysis exposed the dorsal and medial parts of the joint. After ablation of the osteophytes, the arthroplastic resection began with the osteotomy of the metatarsal head. The osteotomy line, cut with the oscillating saw, extended from the dorsal cortex at the neck to the joint at the junction of the upper two-thirds and the
3 204 A. Harisboure et al. Table 1 Preoperative and final scores for each radiological grade. Preoperative radiological stages I 5 cases II 17 cases III 10 cases Overall AOFAS score (/100) Preoperative 71 (57 77) 44.8 (30 65) 34 (20 42) Final 83.4 (75 100) 81.5 (53-100) 86.4 (67 100) AOFAS pain score (/40) Preoperative 24 (20 30) 7.1 (0 20) 4.4 (0 20) Final 32 (30 40) 32.1 (20 40) 33.5 (30 40) AOFAS function score (/45) Preoperative 33.4 (25 42) 24.6 (15 37) 16.1 (14 19) Final 37.8 (32 40) 36.4 (24 45) 36.3 (22 45) MTP 1 joint range of movement Preoperative 63.2 (40 80) 38.8 (15 50) 7.4 (0 20) Final 57 (45 90) 51.8 (50 80) 25.6 (0 55) (p = 0.004) lower third, forming a 30 angle with the diaphyseal axis. At the first phalanx, the osteotomy cut extended in the same manner from the dorsal cortex up to the joint, forming a 45 angle with the diaphyseal axis (Fig. 1 B). Intraoperative mobilization allowed us to obtain dorsal flexion close to 90. The capsular suture at the end of the procedure retightened the dorsal capsule above the resected zone. Joint stability was ensured by maintaining the plantar joint and by capsuloplasty. The wound was closed using simple skin stitches with no drainage. The postoperative x-ray provided evaluation of the angle and height of the resected part. Weightbearing was allowed immediately postoperative with no immobilization. Oral pain relief was necessary for approximately 2 weeks. The bandage was changed regularly until the stitches were removed toward the 15th day. During the first 2 weeks, patients wore a postoperative shoe with rigid soles. Normal shoe wear was possible beginning after 6 months. Methodology Data were collected on a data collection sheet, with the statistical analysis carried out by an independent operator. The osteoarthritis grade was evaluated radiologically before surgery. Different radiological classifications are in use today. The three-stage classification is widely used and Figure 1 Operating procedure. A. Medial-surgical approach of the metatarsophalangeal joint. B. Articular resection. has the advantage of being simple [4]. Grade 1 corresponds to beginning involvement with minimal or absent joint space reduction associated with beginning dorsal and lateral osteophytosis (Fig. 2). Grade 2 is characterized by progressive joint space reduction, substantial osteophytosis, as well as the appearance of geodes in condensed subchondral bone. Grade 3 corresponds to nearly complete joint space loss associated with deformation of the metatarsal head, circumferential osteophytosis and involvement of the metatarsal-sesamoidal joint (Fig. 3). The radiological workup included: preoperative: anteroposterior and lateral views of the forefoot with load, a Meary view and a Guntz view; final: anteroposterior and lateral views of the forefoot with load. The radiological criteria studied were: joint space, in millimeters, on the anteroposterior view at the central part of the joint preoperatively and on the final lateral view at the remaining plantar joint; the number and location of the osteophytes; subluxation of the remaining plantar joint corresponding to the displacement of the base of the first phalanx under the head of the first metatarsal. This was checked on the final lateral radiograph with load. The AOFAS score [5] was the preoperative and final evaluation criterion. This is a 100-point clinical score comprising three parts: a function scored out of 45 points, a pain out of 40 and alignment of the first ray out of 15. The result was judged excellent for a score higher than or equal to 95 out of 100, good between 80 and 94, fair between 50 and 79 and poor for a score less than 50. The evaluation was completed by measuring walking distance, gait quality and patient satisfaction. The evaluation of walking was based on the clinical analysis of the gait and sought to see whether the patient could achieve painless digitigrade walking. The degree of patient satisfaction was collected without any particular questionnaire. The statistical analysis was carried out with the following tests: the Chi square and Fisher tests (to compare qualitative data), the Anova test (a parametric test comparing means),
4 The Valenti technique in the treatment of hallux rigidus 205 Figure 2 Grade I hallux rigidus: pre- and postoperative radiographs. A. Anteroposterior preoperative radiograph. B. Lateral preoperative radiograph. C. Anteroposterior postoperative radiograph. D. Lateral postoperative radiograph. the Kruskal-Wallis and Wilcoxon tests (nonparametric tests of identity comparing means), and the Bartlett test (testing homogeneity of variances). Significance was set at a 5% margin of error (p = 0.05). Results The mean follow-up was 65 months (range: 33 90). Eight patients were lost to follow-up and complete analysis was therefore done on 32 cases (24 patients). Only two algodystrophy complications occurred. There was no septic nor thromboembolic complication. Postoperative weightbearing was immediate in 26 cases. For the six remaining patients, postoperative antalgics were not used beyond 2 weeks. The mean duration of time off work was 3.5 months (3 weeks to 8.5 months). Pain was totally absent in 12 cases (38%), it was occasionally present primarily when the weather changed in 18 cases (56%) and was daily in two cases (6%). Discomfort when wearing shoes was totally absent in 16 cases (50%), moderate (with comfortable, wider, soft-soled shoes) in 13 cases (41%) and severe in three cases (9%). None of the patients wore orthopaedic shoes. Walking was normal for 20 patients (87%). Three patients (13%) presented slight painful supination in the forefoot when walking. One patient presented transfer metatarsalgia on the second metatarsal. Walking distance was unlimited in 79% of the cases. Tiptoeing was possible in 79% of the cases. Metatarsophalangeal joint mobility was normal in eight patients (25%), in 15 it was reduced, between 30 and 75 (47%), and in nine patients it was sharply reduced to less than 30 (28%). The mean joint range of movement was 40 (range: 0 90 ) with 39 dorsal flexion and 1 plantar flexion; 20% of the patients had plantar flexion at 10 with loss of the toe s pulp bearing. The interphalangeal range of movement was reduced or painful for three toes (9%). The alignment of the first ray was perfect in 24 cases (75%). The eight remaining toes presented a moderate valgus deviation. All the toes were clinically stable. None had a callous in the pulp. The pressure force of the hallux on the ground was not recorded. The mean Kitaoka score of the series was 81.6 out of 100 (range: ), the pain score was 33 out of 40, the function score was 35.3 out of 45 and the alignment score was 13.3 out of 15. The objective results (determined from the AOFAS score) were distributed into four excellent, 20 good, seven fair and one poor. The subjective results (based on patient satisfaction) were distributed into 15 excellent, nine good, five fair and three poor. The results obtained were comparable for the patients who had bilateral treatment. Final radiographic analysis The mean residual joint space (measured on the lateral view with load measuring the joint space at the plantar joint) was Figure 3 Grade III hallux rigidus: preoperative, postoperative and final radiographs. A. Anteroposterior preoperative radiograph. B. Lateral preoperative radiograph. C. Anteroposterior postoperative radiograph. D. Lateral postoperative radiograph. E. Final anteroposterior radiograph. F. Final lateral radiograph.
5 206 A. Harisboure et al. 1.2 mm, a mean, nonsignificant reduction of 0.2 mm. This reduction had no clinical repercussions. A plantar subluxation of the base of the first phalanx under the head of the first metatarsal was found in 30% of the cases. This was identical for all degrees of osteophytosis. It has no clinical consequences, notably on joint mobility. The joint range of movement was 49. The AOFAS score was 86 out of 100. The objective, subjective, functional and toe alignment results were not altered. Results of radiographic grades (Table 1) The functional result after the Valenti procedure (measured by the AOFAS score) was relatively constant for all hallux rigidus radiological grades. Only metatarsophalangeal joint range of movement was significantly less in stage III cases (p < 0.004). When metatarsal-sesamoidal involvement was associated, the AOFAS score was not modified (81 out of 100) and only the range of movement was significantly reduced to 28 (p = 0.04). The results were unchanged in cases of circumferential osteophytosis. Results of associated surgical acts Associating a complementary act to the arthroplasty did not significantly modify the result obtained for any of these acts. Only the complementary transposition of the abductor onto the extensor muscles significantly improved the metatarsophalangeal mobility at follow-up (p = 0.02). The mobility of the metatarsophalangeal joint did not improve the quality of shoe wear. Discussion The Valenti procedure presents several advantages. It restores joint range of movement in the most useful sector of the gait. It preserves the length of the first ray because it maintains the plantar joint. It also respects the sesamoid ligament complex and the intrinsic plantar musculature that provide stable weightbearing of the metatarsal head. The results of this series are comparable to those of other series investigating the Valenti procedure (Table 2). There were few complications beyond transfer metatarsalgia on the external rays. Curvale et al. [6] found 6% in their series. We report 9% of patients experiencing pain or stiffness of the great toe s interphalangeal joint. Saxena [7] and Grady and Axe [8] found 25% and 86% sesamoiditis at follow-up, respectively. This is transitory (resolving in less than 6 months). This sesamoid and interphalangeal pain is responsible for a delay in resuming normal walking and shoe wear. The sector of joint mobility is nearly totally dorsal, with a loss of the toe s pulp bearing in 20% of the cases. The functional repercussions are limited since the mobility sector essentially corresponds to the zone necessary to swing. Saxena [7] and Kurtz et al. [9] obtained comparable results with 6.8 and 13 mean plantar flexion, respectively, and 40.4 and 44.8 mean dorsal flexion. A number of biases make it difficult to interpret the results of the different surgical treatments of hallux rigidus. Although cheilectomy and Valenti resection are reserved for hallux rigidus treatment, this is not necessarily true for arthrodesis. The series studying arthrodesis for the most part are not highly homogeneous, grouping different indications (hallux rigidus, hallux valgus, rheumatoid arthritis and surgical revision) [10 13]. The classification of hallux rigidus lesions differs from one series to another. Some authors use a three-grade classification [14 17]; others use a four-grade classification [7,9,13,18]. This makes it difficult to compare the different indications proposed for the different surgical techniques. The criteria retained to assess the final result vary from one study to another. In the series studied by Kurtz et al. [9], the result was judged based on the AOFAS score. In other series, it is established using different objective criteria pain, gait and shoe wear quality, and joint range of movement [10,11] or subjectively based on patient satisfaction [12,18,19]. Some studies do not specify these criteria [7]. The results of the Valenti procedure are also similar to the results of arthrodesis and cheilectomy (Table 2). The Keller technique gives less satisfactory results. Méary and Ficat [20] found 61% good and excellent results, Curvalle et al. [6] only 48%. They noted that walking distance was limited in 81% of the cases. Associating interposition of the dorsal capsule with the extensor hallucis brevis tendon at the joint resection improves the result [17,21]. The complications of arthrodesis are more numerous and more frequent. Metatarsalgia is present in 21% of cases [14]. Depending on the case, this can be first-ray metatarsalgia or transfer metatarsalgia if there has been a technical error during the arthrodesis procedure (first metatarsal overshortened, excessive dorsal flexion, greater than 30 ) or with malunion [11]. The interphalangeal joint is the most often painful or arthritic. It is involved in 20% of Curvale et al. s series [6]. According to Groulier et al. [22], it results from insufficient valgus when adjusting the arthrodesis. Méary and Ficat [20] and Ettl et al. [23] found only 4% and 0%, respectively. There are many poor adjustments and this can have repercussions on function. The extension defect is better tolerated than the valgus defect [10]. Malunion is not rare but its frequency varies greatly from one series to another. Méary and Ficat [20] found 17%. On the other hand, Ettl et al. [23] report none in their series. The series investigating cheilectomy do not report specific complications. Lau and Daniels [17] found 4% metatarsalgia. The results obtained with prosthetic replacements are heterogenous and controversial. The main types of prostheses used are implants in silastic that were initially developed by Swanson [24 26], unipolar interposition implants whose concept is close to capsular interposition arthroplasty [27,28] and the total nonconstrained endoprostheses [29 31]. The diversity of the results is related to the type of prosthesis but also to the varying length of follow-up periods. The silastic implants have encouraging short-term results, but they deteriorate with time. Wenger and Whalley [24] obtained 88% good results at 2 years. Shankar and Orth [25] had only 64% at 9 years. Mahieu et al. [26] found 88% good results at 8 years but recommend limiting the use of these implants because of the frequent associated complications (44% metatarsalgia, 33% delay in healing and
6 Table 2 Results of the different surgical treatments of hallux rigidus. Number Mean follow-up (years) Good and excellent result (%) AOFAS score Pain-free (%) Joint range of movement Limitation of walking distance (%) Arthrodesis Curvale et al. [6] Fitzgerald [13] Beertema et al. [14] Ettl et al. [23] Cheilectomy Beertema et al. [14] Hattrup [16] Lau and Daniels [17] Coughlin and Shurnas [18] Mann and Clanton [32] Keller Curvale et al. [6] Méary et Ficat [20] Capsular interpostion arthroplasty Lau and Daniels [17] Kennedy et al. [21] Prosthesis replacement Wenger and Whalley [24] Shankar and Orth [25] Mahieu et al. [26] Jarde et al. [27] Konkel and Menger [28] Ess et al. [29] Fuhrmann et al. [30] Olms and Dietze [31] Valenti Saxena [7] Grady and Axe [8] Kurtz et al. [9] Our series Shoe wear problem (%) The Valenti technique in the treatment of hallux rigidus 207
7 208 A. Harisboure et al. Table 3 Indications for the different operating procedures in the literature. Grade I Grade II Grade III Hattrup and Johnson [16] Cheilectomy Arthrodesis Arthrodesis Ettl et al. [23] Not specified Not specified Arthrodesis Coughlin and Shurnas [18] Cheilectomy Cheilectomy Arthrodesis Beertema et al. [14] Cheilectomy Cheilectomy Arthrodesis Curvale et al. [6] Cheilectomy Cheilectomy Arthrodesis Olms and Dietze [31] Not specified Arthroplasty Arthroplasty Fuhrmann et al. [30] Not specified Not specified Arthroplasty Kurtz et al. [9] Valenti Valenti Not specified Saxena [7] Valenti Valenti Not specified Our series Valenti Valenti Valenti 14% infection). As a rule, these implants are poorly tolerated (foreign-body reaction) and they are not highly resistant. Curvale et al. [6] recommend abandoning these implants, whose biomechanical characteristics are not well adapted to this joint. The unipolar interposition prostheses give results that are comparable to the conservative techniques at the midterm. They improve the Keller technique in that they preserve the first phalanx [27]. The results of total endoprostheses are less conclusive. Ess et al. [29] only obtained 60% good and excellent results at 2 years and do not recommend these implants for young or active patients. Fuhrmann et al. [30] reported medial instability in 16% of their cases causing poor toe alignment. Olms and Dietze [31] obtained better results but the follow-up period remains short (2 years). The Valenti procedure gives reproducible results in terms of function and pain-free activity for all grades of hallux rigidus. Complications are rare. Inversely, arthrodesis, arthroplasty and the Keller technique have a high rate of complications, in particular transfer metatarsalgia. The indications proposed in the literature for each technique are concordant (Table 3). None of the techniques seems ideal, whatever the grade of pathology presented by the patient. Cheilectomy is proposed for beginning and moderate pathology. Arthrodesis and arthroplasty are proposed in cases of advanced disease or for surgical revision. The Valenti procedure is classically proposed up to advanced grade II, as described in the Hattrup and Johnson [16] classification. Conclusion The partial arthrectomy described by Valenti for the treatment of hallux rigidus is a procedure that can be easily reproduced with little risk of technical error. The results of this series are stable over time and comparable to the results reported in the literature for all grades of hallux rigidus, with a low complication rate. Conflicts of interests None. References [1] Davies colley N. Contraction of the metatarso-phalangeal joint of the great toe (hallux flessus). Br Med J 1887;1:728. [2] Cotterill SM. Stiffness of the great toe in adolescent. Br Med J 1888;1:1158. [3] Bonnel F, Claustre J. Traitement chirurgical de l hallux rigidus. Technique de Valenti. In: Actualités en médecine et chirurgie du pied. Paris: Masson; p [4] Karasick D, Wapner KL. Hallux rigidus deformity: radiologic assessment. AJR Am J Roentgenol 1991;157: [5] Kitaoka HB, Alexander IJ, Adelaar RS, Nunley JA, Myerson MS, Sanders M. Clinical rating systems for the ankle-hindfoot, midfoot, hallux and lesser toes. Foot Ankle Int 1994;15: [6] Curvale G, Diebold P, Jarde O, Mainard D, Tourne Y, Valtin B. Traitement chirurgical de l hallux rigidus. Table ronde SOFCOT, Rev Chir Orthop 1997;83(suppl III): [7] Saxena A. The Valenti procedure for hallux limitus/rigidus. J Foot Ankle Surg 1995;34: [8] Grady JF, Axe TM. The modified Valenti procedure for the treatment of hallux limitus. J Foot Ankle Surg 1994;33: [9] Kurtz DH, Harrill JC, Kaczander BI, Solomon MG. The Valenti procedure for hallux limitus: a long-term follow-up and analysis. J Foot Ankle Surg 1999;38: [10] Girard F, Mazas F, Balc h LE, Margeot TM. L arthrodèse métatarso-phalangienne du gros orteil par vissage axial en compression. Rev Chir Orthop 1988;74(suppl II): [11] Rosset P, Champion P, Burdin P. Étude rétrospective d une série continue de 49 arthrodèses de l articulation métatarsophalangienne du gros orteil. Rev Chir Orthop 1988;74(suppl II): [12] O Doherty DP, Lowrie IG, Magnussen PA, Gregg PJ. The management of the painful first metatarsophalangeal joint in the older patient. J Bone Joint Surg Br 1990;72: [13] Fitzgerald JAW. A review of long-term results of arthrodesis of the first metatarso-phalangeal joint. J Bone Joint Surg Br 1969;51: [14] Beertema W, Draijer WF, Van Os JJ, Pilot P. A retrospective analysis of surgical treatment in patients with symptomatic hallux rigidus: long-term follow-up. J Foot Ankle Surg 2006;45: [15] Curvale G, Croisille H, Tracol P, Groulier P. L arthrodèse métatarsophalangienne du gros orteil. Rev Chir Orthop 1987;73(suppl II): [16] Hattrup SJ, Johnson KA. Subjective results of hallux rigidus following treatment with cheilectomy. Clin Orthop 1988;226: [17] Lau JTC, Daniels TR. Outcomes following cheilectomie and interpositional arthroplasty in hallux rigidus. Foot Ankle Int 2001;22:
8 The Valenti technique in the treatment of hallux rigidus 209 [18] Coughlin MJ, Shurnas PS. Grading and long-term results of operative treatment. J Bone Joint Surg Am 2003;85: [19] Taylor DT, Sage RA, Pinzur MS. Arthrodesis of the first metatarsophalangeal joint. Am J Orthop 2004;33: [20] Meary R, Ficat C. L arthrose de la première métatarsophalangienne. Rev Chir Orthop 1975;61: [21] Kennedy JG, Chow FY, Dines J, Gardner M, Bohne WH. Outcomes after interposition arthroplasty for treatment of hallux rigidus. Clin Orthop 2006;445: [22] Groulier P, Curvale G, Piclet-Legre B, Kelberine F. L arthrodèse de la première articulation métatarso-phalangienne. Rev Chir Orthop 1994;80: [23] Ettl V, Radke S, Gaertner M, Walther M. Arthrodesis in the treatment of hallux rigidus. Int Orthop 2003;27: [24] Wenger RJ, Whalley RC. Total replacement of the first metatarsophalangeal joint. J Bone Joint Surg Br 1978;60: [25] Shankar NS, Orth MC. Silastic single-stem implants in the treatment of hallux rigidus. Foot Ankle Int 1995;16: [26] Mahieu C, Chaput A, Bouillet R. Traitement de l hallux rigidus par les implants en silastic de Swanson (single et double stem). Revue clinique, radiologique et podobarographique avec 16 ans de recul maximum. Acta Orthop Belg 1992;58: [27] Jarde O, Wable E, Havet E, De Lestang M, Vives P. Prothèse métallique d interposition dans l hallux rigidus. Rev Chir Orthop 2001;87: [28] Konkel KF, Menger AG. Mid-term results of titanium hemi-great toe implants. Foot Ankle Int 2006;27: [29] Ess P, Hamalainen M, Leppilahti J. Non-constrained titaniumpolyethylene total endoprosthesis in the treatment of hallux rigidus. A prospective clinical 2-year follow-up study. Scand J Surg 2002;91: [30] Fuhrmann RA, Wagner A, Anders JO. First metatarsophalangeal joint replacement: the method of choice for end-stage hallux rigidus? Foot Ankle Clin 2003;8: [31] Olms K, Dietze A. Replacement arthroplasty for hallux rigidus. 21 patients with a 2-year follow-up. Int Orthop 1999;23: [32] Mann RA, Clanton TO. Hallux rigidus: treatment by cheilectomy. J Bone Joint Surg Am 1988;70:400 5.
Arthrodesis of the first metatarsophalangeal joint using convex and concave drills A report on 50 cases
 Acta Orthop. Belg., 2005, 71, 76-82 ORIGINAL STUDY Arthrodesis of the first metatarsophalangeal joint using convex and concave drills A report on 50 cases Olivier JARDÉ, Zaccharie LAYA, Bruno OLORY, Gauthier
Acta Orthop. Belg., 2005, 71, 76-82 ORIGINAL STUDY Arthrodesis of the first metatarsophalangeal joint using convex and concave drills A report on 50 cases Olivier JARDÉ, Zaccharie LAYA, Bruno OLORY, Gauthier
NON-CONSTRAINED TITANIUM-POLYETHYLENE TOTAL ENDOPROSTHESIS IN THE TREATMENT OF HALLUX RIGIDUS A prospective clinical 2-year follow-up study
 Scandinavian Journal of Surgery 91: 202 207, 2002 NON-CONSTRAINED TITANIUM-POLYETHYLENE TOTAL ENDOPROSTHESIS IN THE TREATMENT OF HALLUX RIGIDUS A prospective clinical 2-year follow-up study P. Ess, M.
Scandinavian Journal of Surgery 91: 202 207, 2002 NON-CONSTRAINED TITANIUM-POLYETHYLENE TOTAL ENDOPROSTHESIS IN THE TREATMENT OF HALLUX RIGIDUS A prospective clinical 2-year follow-up study P. Ess, M.
Hallux Valgus Deformity: Preoperative Radiologic Assessment
 119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint
 Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint Subject: Partial or Total Replacement of First Metatarsophalangeal (MTP) Joint Background: Underlying causes of disease or
Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint Subject: Partial or Total Replacement of First Metatarsophalangeal (MTP) Joint Background: Underlying causes of disease or
Investigation performed at the Department of Orthopaedic and Trauma Surgery, Glasgow Royal Infirmary, Glasgow, United Kingdom
 748 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Long-Term Results of the Modified Hoffman Procedure in the Rheumatoid Forefoot BY S. THOMAS, MBCHB, BSC, MRCS, A.W.G. KINNINMONTH,
748 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Long-Term Results of the Modified Hoffman Procedure in the Rheumatoid Forefoot BY S. THOMAS, MBCHB, BSC, MRCS, A.W.G. KINNINMONTH,
Modified Proximal Scarf Osteotomy for Hallux Valgus
 Original Article Clinics in Orthopedic Surgery 2018;10:479-483 https://doi.org/10.4055/cios.2018.10.4.479 Modified Proximal Scarf Osteotomy for Hallux Valgus Ki Won Young, MD, Hong Seop Lee, MD, Seong
Original Article Clinics in Orthopedic Surgery 2018;10:479-483 https://doi.org/10.4055/cios.2018.10.4.479 Modified Proximal Scarf Osteotomy for Hallux Valgus Ki Won Young, MD, Hong Seop Lee, MD, Seong
Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant
 Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant DIEBOLD P.-F., ROCHER H.,, DETERME P., CERMOLACCE C., GUILLO S., AVEROUS C., LEIBER WACKENHEIN F. Interphalangeal Arthrodesis
Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant DIEBOLD P.-F., ROCHER H.,, DETERME P., CERMOLACCE C., GUILLO S., AVEROUS C., LEIBER WACKENHEIN F. Interphalangeal Arthrodesis
First metatarsophalangeal hemiarthroplasty for hallux rigidus
 DOI 10.1007/s00264-010-1012-x ORIGINAL PAPER First metatarsophalangeal hemiarthroplasty for hallux rigidus Eric Giza & Martin Sullivan & Dan Ocel & Gregory Lundeen & Matt Mitchell & Lauren Frizzell Received:
DOI 10.1007/s00264-010-1012-x ORIGINAL PAPER First metatarsophalangeal hemiarthroplasty for hallux rigidus Eric Giza & Martin Sullivan & Dan Ocel & Gregory Lundeen & Matt Mitchell & Lauren Frizzell Received:
Investigation performed at Orthopaedic Hospital Gersthof, Vienna, Austria
 1131 COPYRIGHT 2004 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Salvage of a Failed Keller Resection Arthroplasty BY FELIX MACHACEK JR., MD, MARK E. EASLEY, MD, FLORIAN GRUBER, MD, PETER RITSCHL,
1131 COPYRIGHT 2004 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Salvage of a Failed Keller Resection Arthroplasty BY FELIX MACHACEK JR., MD, MARK E. EASLEY, MD, FLORIAN GRUBER, MD, PETER RITSCHL,
Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity
 REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
The Vilex Hemi-Implant: A Retrospective Analysis of 30 Patients in the Treatment of Hallux Rigidus
 Open Access Publication The Vilex Hemi-Implant: A Retrospective Analysis of 30 Patients in the Treatment of Hallux Rigidus by David M. Davidson, DPM 1, Kenneth T. Goldstein, DPM 2, James D. Yakel, DPM
Open Access Publication The Vilex Hemi-Implant: A Retrospective Analysis of 30 Patients in the Treatment of Hallux Rigidus by David M. Davidson, DPM 1, Kenneth T. Goldstein, DPM 2, James D. Yakel, DPM
Joint Preserving Surgery in Severe Forefoot Disorders
 Joint Preserving Surgery in Severe Forefoot Disorders J ORTHOP TRAUMA SURG REL RES 4 (12) 2008 Review article LOUIS S. BAROUK*, PIERRE BAROUK** * 39, Chemin de la Roche, 33370, Yvrac, France ** Clinique
Joint Preserving Surgery in Severe Forefoot Disorders J ORTHOP TRAUMA SURG REL RES 4 (12) 2008 Review article LOUIS S. BAROUK*, PIERRE BAROUK** * 39, Chemin de la Roche, 33370, Yvrac, France ** Clinique
Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot
 168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
Foot and ankle update
 Foot and ankle update Mr Ian Garnham Consultant Foot and Ankle Surgeon Whipps Cross University Hospital Hallux Rigidus Symptoms first ray and 1st MTP pain and swelling worse with push off or forced dorsiflexion
Foot and ankle update Mr Ian Garnham Consultant Foot and Ankle Surgeon Whipps Cross University Hospital Hallux Rigidus Symptoms first ray and 1st MTP pain and swelling worse with push off or forced dorsiflexion
Intermediate outcome of interpositional arthroplasty for the treatment of hallux rigidus. Anand Vora, MD
 Intermediate outcome of interpositional arthroplasty for the treatment of hallux rigidus Anand Vora, MD CONFLICT TO DISCLOSE Intermediate outcome of interpositional arthroplasty for the treatment of hallux
Intermediate outcome of interpositional arthroplasty for the treatment of hallux rigidus Anand Vora, MD CONFLICT TO DISCLOSE Intermediate outcome of interpositional arthroplasty for the treatment of hallux
A perspective on MPJ implant arthroplasty.
 A perspective on MPJ implant arthroplasty. The BioPro MPJ Hemi Implant System: +65 years of successful clinical use. Pre-op Post-op 20+ year implant survivorship 14 96% Survivorship 1 97% Patient Satisfaction
A perspective on MPJ implant arthroplasty. The BioPro MPJ Hemi Implant System: +65 years of successful clinical use. Pre-op Post-op 20+ year implant survivorship 14 96% Survivorship 1 97% Patient Satisfaction
HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT
 C H A P T E R 1 5 HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT Joe T. Southerland, DPM Mickey D. Stapp, DPM INTRODUCTION Hemi-implant arthroplasty of the first metatarsophalangeal
C H A P T E R 1 5 HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT Joe T. Southerland, DPM Mickey D. Stapp, DPM INTRODUCTION Hemi-implant arthroplasty of the first metatarsophalangeal
Lesser MPJ Hemi Implant
 Lesser MPJ Hemi Implant Surgical Technique Contents Product The BioPro Lesser MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the treatment of arthritis, Freiberg
Lesser MPJ Hemi Implant Surgical Technique Contents Product The BioPro Lesser MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the treatment of arthritis, Freiberg
Course of damage to the hallux over 5 years after forefoot resection arthroplasty in rheumatoid arthritis patients
 International Orthopaedics (SICOT) (2007) 31:477 481 DOI 10.1007/s00264-006-0221-9 ORIGINAL PAPER Course of damage to the hallux over 5 years after forefoot resection arthroplasty in rheumatoid arthritis
International Orthopaedics (SICOT) (2007) 31:477 481 DOI 10.1007/s00264-006-0221-9 ORIGINAL PAPER Course of damage to the hallux over 5 years after forefoot resection arthroplasty in rheumatoid arthritis
Complications associated with Mitchell s Osteotomy for Hallux Valgus Correction: A retrospective hospital review
 The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Complications associated with Mitchell s Osteotomy for Hallux Valgus Correction: A retrospective hospital
The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Complications associated with Mitchell s Osteotomy for Hallux Valgus Correction: A retrospective hospital
6/5/2018. Forefoot Disorders. Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) Hallux Rigidus
 Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Section 6: Preoperative Planning
 Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
ORIGINAL ARTICLE. Keywords Hallux Rigidus; Metatarsophalangeal Joint; Arthroplasty
 ORIGINAL ARTICLE Preliminary Results from the METIS-Newdeal total metatarsophalangeal prosthesis Luís Fernando Nunes Pires Silva 1, Cristina Varino Sousa 1, Ricardo Rodrigues Pinto 2, Claudia Santos 2,
ORIGINAL ARTICLE Preliminary Results from the METIS-Newdeal total metatarsophalangeal prosthesis Luís Fernando Nunes Pires Silva 1, Cristina Varino Sousa 1, Ricardo Rodrigues Pinto 2, Claudia Santos 2,
PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES
 PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES AS PRESENTED BY: JOEL VERNOIS M.D. 016798A Case Study 1 PROstep Minimally
PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES AS PRESENTED BY: JOEL VERNOIS M.D. 016798A Case Study 1 PROstep Minimally
First MPJ Hemi Implant
 First MPJ Hemi Implant Surgical Technique Contents Product The BioPro First MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the hallux metatarsophalangeal joint
First MPJ Hemi Implant Surgical Technique Contents Product The BioPro First MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the hallux metatarsophalangeal joint
A Patient s Guide to Hallux Rigidus
 A Patient s Guide to Hallux Rigidus Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER: The information in this booklet
A Patient s Guide to Hallux Rigidus Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER: The information in this booklet
Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity
 FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2012.0400 Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity Pascal F. Rippstein, MD; Young-Uk
FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2012.0400 Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity Pascal F. Rippstein, MD; Young-Uk
The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY
 60 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY BY J. CHRIS COETZEE,
60 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY BY J. CHRIS COETZEE,
The Ludloff Osteotomy
 Techniques in Foot and Ankle Surgery 4(4):263 268, 2005 Ó 2005 Lippincott Williams & Wilkins, Philadelphia The Ludloff Osteotomy T E C H N I Q U E Hans-Jörg Trnka, MD, PhD and Stefan Hofstätter, MD Foot
Techniques in Foot and Ankle Surgery 4(4):263 268, 2005 Ó 2005 Lippincott Williams & Wilkins, Philadelphia The Ludloff Osteotomy T E C H N I Q U E Hans-Jörg Trnka, MD, PhD and Stefan Hofstätter, MD Foot
THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT. Miss Sue Kendall PhD FRCS (Orth&Trauma)
 THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT Miss Sue Kendall PhD FRCS (Orth&Trauma) Is Minimally Invasive Surgery of the foot a good idea? Minimally invasive surgery, keyhole surgery entering
THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT Miss Sue Kendall PhD FRCS (Orth&Trauma) Is Minimally Invasive Surgery of the foot a good idea? Minimally invasive surgery, keyhole surgery entering
Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair
 Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair Carlos Villas, MD, PhD, 1 Javier Del Río, MD, 3 Andres
Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair Carlos Villas, MD, PhD, 1 Javier Del Río, MD, 3 Andres
A Patient s Guide to Hallux Rigidus
 A Patient s Guide to Hallux Rigidus Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Hallux Rigidus Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled from a variety
How to avoid complications of distraction osteogenesis for first brachymetatarsia
 220 Acta Orthopaedica 2009; 80 (2): 220 225 How to avoid complications of distraction osteogenesis for first brachymetatarsia Keun-Bae Lee, Hyun-Kee Yang, Jae-Yoon Chung, Eun-Sun Moon, and Sung-Taek Jung
220 Acta Orthopaedica 2009; 80 (2): 220 225 How to avoid complications of distraction osteogenesis for first brachymetatarsia Keun-Bae Lee, Hyun-Kee Yang, Jae-Yoon Chung, Eun-Sun Moon, and Sung-Taek Jung
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus
 Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
Results of Metallic Hemi-Great Toe Implant for Grade III and Early Grade IV Hallux Rigidus
 FOOT &ANKLE INTERNATIONAL Copyright 2009 by the American Orthopaedic Foot & Ankle Society DOI: 10.3113/FAI.2009.0653 Results of Metallic Hemi-Great Toe Implant for Grade III and Early Grade IV Hallux Rigidus
FOOT &ANKLE INTERNATIONAL Copyright 2009 by the American Orthopaedic Foot & Ankle Society DOI: 10.3113/FAI.2009.0653 Results of Metallic Hemi-Great Toe Implant for Grade III and Early Grade IV Hallux Rigidus
Scarf osteotomy versus metatarsophalangeal arthrodesis in forefoot first ray disorders: Comparison of functional outcomes
 Orthopaedics & Traumatology: Surgery & Research (2012) 98S, S77 S84 Available online at www.sciencedirect.com ORIGINAL ARTICLE Scarf osteotomy versus metatarsophalangeal arthrodesis in forefoot first ray
Orthopaedics & Traumatology: Surgery & Research (2012) 98S, S77 S84 Available online at www.sciencedirect.com ORIGINAL ARTICLE Scarf osteotomy versus metatarsophalangeal arthrodesis in forefoot first ray
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity
 Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
Or thopaedic Surger y
 Article Lateral hemiepiphysiodesis of the first metatarsal for juvenile hallux valgus Journal of Or thopaedic Surger y Journal of Orthopaedic Surgery 26(3) 1 5 ª The Author(s) 2018 Article reuse guidelines:
Article Lateral hemiepiphysiodesis of the first metatarsal for juvenile hallux valgus Journal of Or thopaedic Surger y Journal of Orthopaedic Surgery 26(3) 1 5 ª The Author(s) 2018 Article reuse guidelines:
Weil osteotomy and flexor to extensor transfer for irreparable plantar plate tear: prospective study
 Weil osteotomy and flexor to extensor transfer for irreparable plantar plate tear: prospective study Daniel Baumfeld, MD Fernando Raduan, MD Fernanda Catena, MD Tania Mann, MD Caio Nery, MD Disclosure
Weil osteotomy and flexor to extensor transfer for irreparable plantar plate tear: prospective study Daniel Baumfeld, MD Fernando Raduan, MD Fernanda Catena, MD Tania Mann, MD Caio Nery, MD Disclosure
Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months.
 Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months. Diagnosis: II MTP instability Demographics of MT instability Lesser MTP joint instability occurs
Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months. Diagnosis: II MTP instability Demographics of MT instability Lesser MTP joint instability occurs
Increased pressures at
 Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
HemiEDGE. Patent No. 8,845,750. Surgical Technique
 HemiEDGE Patent No. 8,845,750 Surgical Technique Contents Product Based on the clinical success of our First MPJ Hemi Implant, the HemiEDGE, incorporates an overlapping edge extending around the medial,
HemiEDGE Patent No. 8,845,750 Surgical Technique Contents Product Based on the clinical success of our First MPJ Hemi Implant, the HemiEDGE, incorporates an overlapping edge extending around the medial,
Index. Clin Podiatr Med Surg 22 (2005) Note: Page numbers of article titles are in boldface type.
 Clin Podiatr Med Surg 22 (2005) 309 314 Index Note: Page numbers of article titles are in boldface type. A Abductor digiti minimi muscle, myectomy of, for tailor s bunionette, 243 Achilles tendon, lengthening
Clin Podiatr Med Surg 22 (2005) 309 314 Index Note: Page numbers of article titles are in boldface type. A Abductor digiti minimi muscle, myectomy of, for tailor s bunionette, 243 Achilles tendon, lengthening
The effectiveness of distal soft tissue procedures in hallux valgus
 J Orthopaed Traumatol (2008) 9:117 121 DOI 10.1007/s10195-008-0017-3 ORIGINAL ARTICLE The effectiveness of distal soft tissue procedures in hallux valgus Cemil Kayali Æ Hasan Ozturk Æ Haluk Agus Æ Taskin
J Orthopaed Traumatol (2008) 9:117 121 DOI 10.1007/s10195-008-0017-3 ORIGINAL ARTICLE The effectiveness of distal soft tissue procedures in hallux valgus Cemil Kayali Æ Hasan Ozturk Æ Haluk Agus Æ Taskin
WHAT IS ARTHRITIS OF THE BIG TOE (HALLUX RIGIDUS)?
 Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT IS ARTHRITIS OF THE BIG TOE (HALLUX RIGIDUS)? A common term for arthritis of the metatarsophalangeal
Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT IS ARTHRITIS OF THE BIG TOE (HALLUX RIGIDUS)? A common term for arthritis of the metatarsophalangeal
NORTHERN OHIO FOUNDATION
 NORTHERN OHIO FOOT & ANKLE FOUNDATION! The!Northern!Ohio!Foot!and!Ankle!Journal!!!!!!!!!!!!!!!Official!Publication!of!the!NOFA!Foundation!! First MPJ Proximal Phalanx Hemi Implant Arthroplasty Literature
NORTHERN OHIO FOOT & ANKLE FOUNDATION! The!Northern!Ohio!Foot!and!Ankle!Journal!!!!!!!!!!!!!!!Official!Publication!of!the!NOFA!Foundation!! First MPJ Proximal Phalanx Hemi Implant Arthroplasty Literature
19 Arthrodesis of the First Metatarsocuneiform Joint
 19 Arthrodesis of the First Metatarsocuneiform Joint CHARLES GUDAS Abduction of the first metatarsal to correct metatarsus primus varus and hallux valgus was first described by Albrecht in 1911. 1 Lapidus
19 Arthrodesis of the First Metatarsocuneiform Joint CHARLES GUDAS Abduction of the first metatarsal to correct metatarsus primus varus and hallux valgus was first described by Albrecht in 1911. 1 Lapidus
University of Groningen. Forefoot disorders Schrier, Joost
 University of Groningen Forefoot disorders Schrier, Joost IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document version
University of Groningen Forefoot disorders Schrier, Joost IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document version
Fixation of first metatarsal basal osteotomy using Acutrak screw
 Available online at www.sciencedirect.com Foot and Ankle Surgery 14 (2008) 21 25 www.elsevier.com/locate/fas Fixation of first metatarsal basal osteotomy using Acutrak screw G.E. Fadel MD FRCS Tr & Orth*,
Available online at www.sciencedirect.com Foot and Ankle Surgery 14 (2008) 21 25 www.elsevier.com/locate/fas Fixation of first metatarsal basal osteotomy using Acutrak screw G.E. Fadel MD FRCS Tr & Orth*,
FREIBERG S INFRACTION TREATMENT WITH METATARSAL NECK DORSAL CLOSING WEDGE OSTEOTOMY: REPORT OF TWO CASES
 FREIBERG S INFRACTION TREATMENT WITH METATARSAL NECK DORSAL CLOSING WEDGE OSTEOTOMY: REPORT OF TWO CASES Sung-Yen Lin, 1 Yuh-Min Cheng, 1,2 and Peng-Ju Huang 1,2 1 Department of Orthopedics, Kaohsiung
FREIBERG S INFRACTION TREATMENT WITH METATARSAL NECK DORSAL CLOSING WEDGE OSTEOTOMY: REPORT OF TWO CASES Sung-Yen Lin, 1 Yuh-Min Cheng, 1,2 and Peng-Ju Huang 1,2 1 Department of Orthopedics, Kaohsiung
Total Ankle Arthroplasty for the Treatment of Symptomatic Nonunion following Tibiotalar Fusion
 Total Ankle Arthroplasty for the Treatment of Symptomatic Nonunion following Tibiotalar Fusion W I L L I A M P. H U N T I N G T O N, M. D. W. H O D G E S D A V I S, M. D. R O B E R T B. A N D E R S O N,
Total Ankle Arthroplasty for the Treatment of Symptomatic Nonunion following Tibiotalar Fusion W I L L I A M P. H U N T I N G T O N, M. D. W. H O D G E S D A V I S, M. D. R O B E R T B. A N D E R S O N,
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow.
 Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities
 Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities NO DISCLOSURES Objectives The main objectives of any procedure in hallux abducto valgus surgery are to correct the deformity,
Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities NO DISCLOSURES Objectives The main objectives of any procedure in hallux abducto valgus surgery are to correct the deformity,
1. Orthoapedic Associates of Michigan, PC, Grand Rapids, MI 2. Michigan State University College of Human Medicine, Grand Rapids, MI
 Second Metatarsal Osteotomy Shortening with Tarsometatarsal Arthrodesis: Comparison of Outcomes Between MSP TM Metatarsal Shortening System and Plates and Screws Donald R. Bohay, MD, FACS 1 ; John G. Anderson,
Second Metatarsal Osteotomy Shortening with Tarsometatarsal Arthrodesis: Comparison of Outcomes Between MSP TM Metatarsal Shortening System and Plates and Screws Donald R. Bohay, MD, FACS 1 ; John G. Anderson,
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION. At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral)
 PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy
 Journal of Orthopaedic Surgery 2005:13(3):245-252 Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy K Yamamoto, A Imakiire, Y Katori,
Journal of Orthopaedic Surgery 2005:13(3):245-252 Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy K Yamamoto, A Imakiire, Y Katori,
Disclosures. 55 year old Male 2/23/2018. Recurrent Hallux Rigidus: Options Other than Arthrodesis
 Recurrent Hallux Rigidus: Options Other than Arthrodesis Gregory C Berlet, MD FRCS(C), FAOA Orthopedic Foot and Ankle Columbus, Ohio Columbus, Ohio orthofootankle.com Disclosures Consultant/Speaker Bureau/Royalties/
Recurrent Hallux Rigidus: Options Other than Arthrodesis Gregory C Berlet, MD FRCS(C), FAOA Orthopedic Foot and Ankle Columbus, Ohio Columbus, Ohio orthofootankle.com Disclosures Consultant/Speaker Bureau/Royalties/
PHALANGEAL BASE AUTOGRAFT FOR THE CORRECTION OF THE SUBLUXED HAMMERTOE
 C H A P T E R 5 PHALANGEAL BASE AUTOGRAFT FOR THE CORRECTION OF THE SUBLUXED HAMMERTOE Raymond G. Cavaliere, DPM INTRODUCTION Hammertoes can be classified as simple, moderate, and severe. The deformities
C H A P T E R 5 PHALANGEAL BASE AUTOGRAFT FOR THE CORRECTION OF THE SUBLUXED HAMMERTOE Raymond G. Cavaliere, DPM INTRODUCTION Hammertoes can be classified as simple, moderate, and severe. The deformities
Columbia/NYOH FOOT and ANKLE ROTATION-SPECIFIC OBJECTIVES
 Updated 2/8/10 Columbia/NYOH FOOT and ANKLE ROTATION-SPECIFIC OBJECTIVES INTERPERSONAL AND COMMUNICATION SKILLS Resident will at all times demonstrate behavior that is beyond reproach. Residents must be
Updated 2/8/10 Columbia/NYOH FOOT and ANKLE ROTATION-SPECIFIC OBJECTIVES INTERPERSONAL AND COMMUNICATION SKILLS Resident will at all times demonstrate behavior that is beyond reproach. Residents must be
SURGICAL TECHNIQUE CHI. Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY
 CHI Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY SURGICAL TECHNIQUE CHI Cannulated Hemi Implants Design Rationale Pain of the great toe joint often leads to altered lifestyles. The goal of MPJ implant
CHI Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY SURGICAL TECHNIQUE CHI Cannulated Hemi Implants Design Rationale Pain of the great toe joint often leads to altered lifestyles. The goal of MPJ implant
Hallux Rigidus & Silastic Total Implants
 Hallux Rigidus & Silastic Total Implants JOSHUA L. MOORE, DPM FACFAS ASSISTANT DEAN OF EDUCATIONAL AFFAIRS TUSPM CLINICAL ASSISTANT PROFESSOR OF SURGERY Definitions Hallux Limitus 1 st MTPJ range of motion
Hallux Rigidus & Silastic Total Implants JOSHUA L. MOORE, DPM FACFAS ASSISTANT DEAN OF EDUCATIONAL AFFAIRS TUSPM CLINICAL ASSISTANT PROFESSOR OF SURGERY Definitions Hallux Limitus 1 st MTPJ range of motion
Mid-Term Results of Triple Osteotomy in Hallux Valgus with Highly Increased Distal Metatarsal Articular Angle
 AOFAS Annual Meeting 2012 The Korean Foot & Ankle Society Mid-Term Results of Triple Osteotomy in Hallux Valgus with Highly Increased Distal Metatarsal Articular Angle Kyung Tai Lee, M.D., Ki Won Young,
AOFAS Annual Meeting 2012 The Korean Foot & Ankle Society Mid-Term Results of Triple Osteotomy in Hallux Valgus with Highly Increased Distal Metatarsal Articular Angle Kyung Tai Lee, M.D., Ki Won Young,
Resection Arthroplasty for Rheumatoid Forefoot Deformity
 Resection Arthroplasty for Rheumatoid Forefoot Deformity Jun-ichi Fukushi, M.D. Yasuharu Nakashima, M.D. Yukihide Iwamoto, M.D. Department of Orthopedic Surgery, Graduate School of Medical Sciences, Kyushu
Resection Arthroplasty for Rheumatoid Forefoot Deformity Jun-ichi Fukushi, M.D. Yasuharu Nakashima, M.D. Yukihide Iwamoto, M.D. Department of Orthopedic Surgery, Graduate School of Medical Sciences, Kyushu
Bunions. A bunion is a painful bony bump that develops on the inside of the foot at the big toe joint. Bunions are often referred to as hallux valgus.
 Bunions A bunion is a painful bony bump that develops on the inside of the foot at the big toe joint. Bunions are often referred to as hallux valgus. Bunions develop slowly. Pressure on the big toe joint
Bunions A bunion is a painful bony bump that develops on the inside of the foot at the big toe joint. Bunions are often referred to as hallux valgus. Bunions develop slowly. Pressure on the big toe joint
Integra. Silicone Toe System SURGICAL TECHNIQUE
 Silicone Toe System SURGICAL TECHNIQUE Silicone Toe System Table of Contents Indications...2 Contraindications...2 Warnings...2 Precautions...2 Adverse Events...2 Flexible Great Toe (FGT)...3 Surgical
Silicone Toe System SURGICAL TECHNIQUE Silicone Toe System Table of Contents Indications...2 Contraindications...2 Warnings...2 Precautions...2 Adverse Events...2 Flexible Great Toe (FGT)...3 Surgical
Finite Element Analysis (FEA) of Swanson Flexible Hinge Toe Implant
 Finite Element Analysis (FEA) of Swanson Flexible Hinge Toe Implant Xiao (Cathy) Zhou (1), Agustín Vidal Lesso (2) 1 Candidate for Bachelors of Science in Mechanical Engineering, Massachusetts Institute
Finite Element Analysis (FEA) of Swanson Flexible Hinge Toe Implant Xiao (Cathy) Zhou (1), Agustín Vidal Lesso (2) 1 Candidate for Bachelors of Science in Mechanical Engineering, Massachusetts Institute
Early Diagnosis. Instability of the lesser MTP joints (Crossover 2 nd toe deformity) -my 25 year journey- Progressive MTP joint subluxation
 Instability of the lesser MTP joints (Crossover 2 nd toe deformity) -my 25 year journey- Conflicts of interest Arthrex- consultant Arthrex- royalties Elsevier-book royalties Michael J Coughlin, M.D. Early
Instability of the lesser MTP joints (Crossover 2 nd toe deformity) -my 25 year journey- Conflicts of interest Arthrex- consultant Arthrex- royalties Elsevier-book royalties Michael J Coughlin, M.D. Early
AUTHOR(S): COUGHLIN, MICHAEL J., M.D., BOISE, IDAHO. An Instructional Course Lecture, The American Academy of Orthopaedic Surgeons
 JBJA Journal of Bone and Joint Surgery - American 1996-1998 June 1996, Volume 78-A, Number 6 932 Instructional Course Lectures, The American Academy of Orthopaedic Surgeons - Hallux Valgus* Instructional
JBJA Journal of Bone and Joint Surgery - American 1996-1998 June 1996, Volume 78-A, Number 6 932 Instructional Course Lectures, The American Academy of Orthopaedic Surgeons - Hallux Valgus* Instructional
Osteotomy vs No Osteotomy Second Ray
 Osteotomy vs No Osteotomy Second Ray Michael D. Dujela DPM, FACFAS Fellowship Trained Foot and Ankle Surgeon Washington Orthopaedic Center, Centralia, WA Chairman, Education and Scientific Affairs Committee
Osteotomy vs No Osteotomy Second Ray Michael D. Dujela DPM, FACFAS Fellowship Trained Foot and Ankle Surgeon Washington Orthopaedic Center, Centralia, WA Chairman, Education and Scientific Affairs Committee
Foot and Ankle Polyvinyl alcohol hemiarthroplasty for first metatarsophalangeal joint arthritis
 SPECIAL FOCUS Foot and Ankle Polyvinyl alcohol hemiarthroplasty for first metatarsophalangeal joint arthritis Alastair S.E. Younger a, Judith F. Baumhauer b and Mark Glazebrook c ABSTRACT End stage arthritis
SPECIAL FOCUS Foot and Ankle Polyvinyl alcohol hemiarthroplasty for first metatarsophalangeal joint arthritis Alastair S.E. Younger a, Judith F. Baumhauer b and Mark Glazebrook c ABSTRACT End stage arthritis
Amputations of the digit, ray and midfoot
 Amputations of the digit, ray and midfoot Dane K. Wukich M.D. Chief, Division of Foot and Ankle Surgery Medical Director, UPMC Foot and Ankle Center University of Pittsburgh School of Medicine Disclosure
Amputations of the digit, ray and midfoot Dane K. Wukich M.D. Chief, Division of Foot and Ankle Surgery Medical Director, UPMC Foot and Ankle Center University of Pittsburgh School of Medicine Disclosure
Scar Engorged veins. Size of the foot [In clubfoot, small foot]
![Scar Engorged veins. Size of the foot [In clubfoot, small foot] Scar Engorged veins. Size of the foot [In clubfoot, small foot]](/thumbs/78/77722241.jpg) 6. FOOT HISTORY Pain: Walking, Running Foot wear problem Swelling; tingly feeling Deformity Stiffness Disability: At work; recreation; night; walk; ADL, Sports Previous Rx Comorbidities Smoke, Sugar, Steroid
6. FOOT HISTORY Pain: Walking, Running Foot wear problem Swelling; tingly feeling Deformity Stiffness Disability: At work; recreation; night; walk; ADL, Sports Previous Rx Comorbidities Smoke, Sugar, Steroid
MiniRail System. Part B: Foot Applications. By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito
 Q U I C K R E F E R E N C E G U I D E 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ORDERING INFORMATION MiniRail System Kit, M190C Contents: M 101 Standard
Q U I C K R E F E R E N C E G U I D E 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ORDERING INFORMATION MiniRail System Kit, M190C Contents: M 101 Standard
First Metatarsophalangeal Arthrodesis: A Clinical, Pedobarographic and Gait Analysis Study
 FOOT & ANKLE INTERNATIONAL Copyright @ 2002 by the American Orthopaedic Foot & Ankle Society, Inc First Metatarsophalangeal Arthrodesis: A Clinical, Pedobarographic and Gait Analysis Study Paul Francis
FOOT & ANKLE INTERNATIONAL Copyright @ 2002 by the American Orthopaedic Foot & Ankle Society, Inc First Metatarsophalangeal Arthrodesis: A Clinical, Pedobarographic and Gait Analysis Study Paul Francis
Forefoot Procedures to Heal and Prevent Recurrence. Watermark. Diabetic Foot Update 2015 San Antonio, Texas
 Forefoot Procedures to Heal and Prevent Recurrence Diabetic Foot Update 2015 San Antonio, Texas J. Randolph Clements, DPM Assistant Professor of Orthopaedics Virginia Tech- Carilion School of Medicine
Forefoot Procedures to Heal and Prevent Recurrence Diabetic Foot Update 2015 San Antonio, Texas J. Randolph Clements, DPM Assistant Professor of Orthopaedics Virginia Tech- Carilion School of Medicine
Mr. Siva Chandrasekaran Orthopaedic Surgeon MBBS MSpMed MPhil (surg) FRACS
 Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
Financial Disclosure. Turf Toe
 Seth O Brien, CP, LP Financial Disclosure Mr. Seth O'Brien has no relevant financial relationships with commercial interests to disclose. Turf Toe Common in athletes playing on firm, artificial turf Forceful
Seth O Brien, CP, LP Financial Disclosure Mr. Seth O'Brien has no relevant financial relationships with commercial interests to disclose. Turf Toe Common in athletes playing on firm, artificial turf Forceful
Long-term results of the Hohmann and Lapidus procedure for the correction of hallux valgus
 FOOT AND ANKLE Long-term results of the Hohmann and Lapidus procedure for the correction of hallux valgus F. W. M. Faber, P. M. van Kampen, M. W. Bloembergen From HAGA Hospital, Den Haag, the Netherlands
FOOT AND ANKLE Long-term results of the Hohmann and Lapidus procedure for the correction of hallux valgus F. W. M. Faber, P. M. van Kampen, M. W. Bloembergen From HAGA Hospital, Den Haag, the Netherlands
Salvage of first metatarsophalangeal joint arthroplasty complications
 Foot Ankle Clin N Am 8 (2003) 37 48 Salvage of first metatarsophalangeal joint arthroplasty complications Judith F. Baumhauer, MD*, Benedict F. DiGiovanni, MD Orthopedic Department, University of Rochester
Foot Ankle Clin N Am 8 (2003) 37 48 Salvage of first metatarsophalangeal joint arthroplasty complications Judith F. Baumhauer, MD*, Benedict F. DiGiovanni, MD Orthopedic Department, University of Rochester
5 COMMON CONDITIONS IN THE FOOT & ANKLE
 5 COMMON CONDITIONS IN THE FOOT & ANKLE MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA IN A NUTSHELL ~ ALL ANATOMY & BIOMECHANICS >90% OF CONDITIONS IN FOOT & ANKLE DIAGNISED FROM GOOD
5 COMMON CONDITIONS IN THE FOOT & ANKLE MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA IN A NUTSHELL ~ ALL ANATOMY & BIOMECHANICS >90% OF CONDITIONS IN FOOT & ANKLE DIAGNISED FROM GOOD
Distal metatarsal osteotomy for hallux varus following surgery for hallux valgus
 FOOT AND ANKLE Distal metatarsal osteotomy for hallux varus following surgery for hallux valgus K. J. Choi, H. S. Lee, Y. S. Yoon, S. S. Park, J. S. Kim, J. J. Jeong, Y. R. Choi From the Asan Medical Center,
FOOT AND ANKLE Distal metatarsal osteotomy for hallux varus following surgery for hallux valgus K. J. Choi, H. S. Lee, Y. S. Yoon, S. S. Park, J. S. Kim, J. J. Jeong, Y. R. Choi From the Asan Medical Center,
)221( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE
 )221( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE First Metatarsophalangeal Joint Arthrodesis: A Retrospective Comparison of Crossed-screws, Locking and Non-Locking Plate
)221( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE First Metatarsophalangeal Joint Arthrodesis: A Retrospective Comparison of Crossed-screws, Locking and Non-Locking Plate
Chevron Osteotomy With Lateral Soft Tissue Release
 5(4):250 256, 2006 T E C H N I Q U E Chevron Osteotomy With Lateral Soft Tissue Release Hans-Jörg Trnka, MD, PhD and Stefan Gerhard Hofstaetter, MD Foot and Ankle Center Vienna Vienna, Austria Ó 2006 Lippincott
5(4):250 256, 2006 T E C H N I Q U E Chevron Osteotomy With Lateral Soft Tissue Release Hans-Jörg Trnka, MD, PhD and Stefan Gerhard Hofstaetter, MD Foot and Ankle Center Vienna Vienna, Austria Ó 2006 Lippincott
ToeMobile. Surgical Technique. Great Toe Endoprosthesis
 Great Toe Endoprosthesis Surgical Technique Merete Medical, Inc. 99 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 Fax: 914-967-1542 E-Mail: service@merete-medical.com www.merete-medical.com - Description
Great Toe Endoprosthesis Surgical Technique Merete Medical, Inc. 99 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 Fax: 914-967-1542 E-Mail: service@merete-medical.com www.merete-medical.com - Description
SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY
 SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY Th. KARACHALIOS, P. P. SARANGI, J. H. NEWMAN From Winford Orthopaedic Hospital, Bristol, England We report a prospective case-controlled
SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY Th. KARACHALIOS, P. P. SARANGI, J. H. NEWMAN From Winford Orthopaedic Hospital, Bristol, England We report a prospective case-controlled
Halux rigidus or arthritis of the big toe
 PATIENT INFORMATION Halux rigidus or arthritis of the big toe Hallux rigidus Metatarso-phalangeal joint What is Hallux rigidus? Hallux rigidus (Latin for a "stiff great toe") is a condition caused by arthritis
PATIENT INFORMATION Halux rigidus or arthritis of the big toe Hallux rigidus Metatarso-phalangeal joint What is Hallux rigidus? Hallux rigidus (Latin for a "stiff great toe") is a condition caused by arthritis
ABSTRACT. Key Words: Hallux Rigidus, toe, arthrodesis, fusion, arthroplasty, MTP, HemiCAP resurfacing. Level of Evidence: Review
 RESURFACING OF THE FIRST METATARSAL HEAD FOR THE TREATMENT OF HALLUX RIGIDUS: EVOLUTION OF IMPLANT DESIGN, REVIEW OF CLINICAL EXPERIENCE AND PRELIMINARY 5 YEAR RESULTS OF METATARSAL HEAD RESURFACING MTP
RESURFACING OF THE FIRST METATARSAL HEAD FOR THE TREATMENT OF HALLUX RIGIDUS: EVOLUTION OF IMPLANT DESIGN, REVIEW OF CLINICAL EXPERIENCE AND PRELIMINARY 5 YEAR RESULTS OF METATARSAL HEAD RESURFACING MTP
innovative and comprehensive product line Metatarsophalangeal Joint Lower Hallux Limitus Hallux Rigidus Extremity
 Surgical Solutions innovative and comprehensive product line Metatarsophalangeal Joint Hallux Limitus Hallux Rigidus Lower Extremity Solutions Hallux Limitus and Hallux Rigidus Hallux limitus is a progressive
Surgical Solutions innovative and comprehensive product line Metatarsophalangeal Joint Hallux Limitus Hallux Rigidus Lower Extremity Solutions Hallux Limitus and Hallux Rigidus Hallux limitus is a progressive
Locked Versus Nonlocked Plate Fixation For Hallux MTP Arthrodesis
 FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2011.0704 Locked Versus Nonlocked Plate Fixation For Hallux MTP Arthrodesis Kenneth J. Hunt, MD; J. Kent Ellington, MD, MS; Robert B. Anderson, MD; Bruce E. Cohen,
FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2011.0704 Locked Versus Nonlocked Plate Fixation For Hallux MTP Arthrodesis Kenneth J. Hunt, MD; J. Kent Ellington, MD, MS; Robert B. Anderson, MD; Bruce E. Cohen,
Health-Related Quality of Life and Functional Outcomes in Ankle Arthritis Patients Based on Treating with and without Total Ankle Replacement Surgery
 Health-Related Quality of Life and Functional Outcomes in Ankle Arthritis Patients Based on Treating with and without Total Ankle Replacement Surgery Chayanin Angthong MD* * Division of Foot and Ankle
Health-Related Quality of Life and Functional Outcomes in Ankle Arthritis Patients Based on Treating with and without Total Ankle Replacement Surgery Chayanin Angthong MD* * Division of Foot and Ankle
Hallux Rigidus. Normal. Normal Arthritis Arthritis
 Richard M. Marks, MD Professor and Director Division of Foot and Ankle Department of Orthopaedic Surgery Medical College of Wisconsin Hallux Rigidus Explanation: Hallux Rigidus is characterized as degeneration
Richard M. Marks, MD Professor and Director Division of Foot and Ankle Department of Orthopaedic Surgery Medical College of Wisconsin Hallux Rigidus Explanation: Hallux Rigidus is characterized as degeneration
A comparison of Chevron and Lindgren-Turan osteotomy techniques in hallux valgus surgery: a prospective randomized controlled study
 ORIGINAL ARTICLE Acta Orthop Traumatol Turc 2016;50(3):255 261 doi: 10.3944/AOTT.2016.14.0272 A comparison of Chevron and Lindgren-Turan osteotomy techniques in hallux valgus surgery: a prospective randomized
ORIGINAL ARTICLE Acta Orthop Traumatol Turc 2016;50(3):255 261 doi: 10.3944/AOTT.2016.14.0272 A comparison of Chevron and Lindgren-Turan osteotomy techniques in hallux valgus surgery: a prospective randomized
NeoFit. Metatarsophal angeal Arthrodesis Pl ate
 NeoFit Metatarsophal angeal Arthrodesis Pl ate 2 NEOFIT - TABLE OF CONTENTS PRODUCT DESCRIPTION 3 INDICATIONS 6 Download «PRINT» version (white background) SURGICAL TECHNIQUE 7 1 - Incision 8 2 - Preparation
NeoFit Metatarsophal angeal Arthrodesis Pl ate 2 NEOFIT - TABLE OF CONTENTS PRODUCT DESCRIPTION 3 INDICATIONS 6 Download «PRINT» version (white background) SURGICAL TECHNIQUE 7 1 - Incision 8 2 - Preparation
A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients
 Original Research Article A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients Ragesh Chandran 1*, Sanath K Shetty 2, Ashwin Shetty 3, Bijith Balan 1, Lawrence J Mathias
Original Research Article A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients Ragesh Chandran 1*, Sanath K Shetty 2, Ashwin Shetty 3, Bijith Balan 1, Lawrence J Mathias
1 st MP Arthrodesis. - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA
 1 st MP Arthrodesis - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA Hallux Limitus Dorsal Bunion Spasm of Short Flexor Immobility of Sesamoids DJD of 1 st MPJ Hallus Limitus Plantar
1 st MP Arthrodesis - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA Hallux Limitus Dorsal Bunion Spasm of Short Flexor Immobility of Sesamoids DJD of 1 st MPJ Hallus Limitus Plantar
ABSTRACT INTRODUCTION
 ORIGINAL ARTICLE Marco Túlio Costa 1, Roberto Zambelli de Almeida Pinto 2, Ricardo Cardenuto Ferreira 1, Minoru Alessandro Sakata 1, Gastão Guilherme Frizzo 1, Roberto Attílio Lima Santin 3 ABSTRACT Objective:
ORIGINAL ARTICLE Marco Túlio Costa 1, Roberto Zambelli de Almeida Pinto 2, Ricardo Cardenuto Ferreira 1, Minoru Alessandro Sakata 1, Gastão Guilherme Frizzo 1, Roberto Attílio Lima Santin 3 ABSTRACT Objective:
Diagnosing and treating hallux valgus: A conservative approach for a common problem
 REVIEW BRIAN G. DONLEY, MD Orthopaedic surgeon, Cleveland Clinic, specializing in foot and ankle disorders. CHRISTOPHER L. TISDEL, MD Orthopaedic surgeon. Cleveland Clinic. JAMES J. SFERRA, MD Orthopaedic
REVIEW BRIAN G. DONLEY, MD Orthopaedic surgeon, Cleveland Clinic, specializing in foot and ankle disorders. CHRISTOPHER L. TISDEL, MD Orthopaedic surgeon. Cleveland Clinic. JAMES J. SFERRA, MD Orthopaedic
Posterior Tibialis Tendon Dysfunction & Repair
 1 Posterior Tibialis Tendon Dysfunction & Repair Surgical Indications and Considerations Anatomical Considerations: The posterior tibialis muscle arises from the interosseous membrane and the adjacent
1 Posterior Tibialis Tendon Dysfunction & Repair Surgical Indications and Considerations Anatomical Considerations: The posterior tibialis muscle arises from the interosseous membrane and the adjacent
PATIENT GUIDE FOR THE TREATMENT OF TOE ARTHRITIS
 arthrosurface.com PATIENT GUIDE FOR THE TREATMENT OF TOE ARTHRITIS A NATIONWIDE SURGEON SURVEY ON OVER 2,000 HEMICAP TOE PROCEDURES INCLUDES: Patient Function and Activity Milestones Patient Rehabilitation
arthrosurface.com PATIENT GUIDE FOR THE TREATMENT OF TOE ARTHRITIS A NATIONWIDE SURGEON SURVEY ON OVER 2,000 HEMICAP TOE PROCEDURES INCLUDES: Patient Function and Activity Milestones Patient Rehabilitation
