SCREENING THE NEWBORN FOR DEVELOPMENTAL DYSPLASIA OF THE HIP: REVIEW
|
|
|
- Caroline Wells
- 5 years ago
- Views:
Transcription
1 SCREENING THE NEWBORN FOR DEVELOPMENTAL DYSPLASIA OF THE HIP: REVIEW Dr. Upendra Yadav *1, 3, Dr. Zhu Xiao Fang 3, Dr. Ajit Kumar Yadav 1, 2, Dr. Sudhir Kumar Yadav 4 and Dr. Jeetendra Yadav 4 1 Yangtze University, 1 Nanhuan Road Jingzhou Hubei , P.R. China 2 Department of Orthopedic, First Hospital of Yangtze University, Jingzhou Hubei , P.R. China 3 Department of Peadiatrics, Clinical Medical College of Yangtze University, Jingzhou Central Hospital, Jingzhou, Hubei Province, PR China 4 Department of Radiology, The first affiliated hospital of Dali University,Dali Yunnan ,P.R China ABSTRACT Developmental dysplasia of the hip is the preferred term to describe the condition in which the femoral head has an abnormal relationship to the acetabulum. Developmental dysplasia of the hip includes frank dislocation (luxation), partial dislocation (subluxation), instability wherein the femoral head comes in and out of the socket, and an array of radiographic abnormalities that reflect inadequate formation of the acetabulum, The precise cause of DDH is unknown, with a combination of genetic and environmental influences associated with DDH and hip dislocation including family history, fetal crowding, vaginal delivery, breech presentation and female gender [1]. Early screening for DDH has the potential to prevent long term hip dysplasia and arthritis requiring hip replacement. Delayed diagnosis requires more complex treatment and has a less successful outcome than dysplasia diagnosed early. For all infants, a competent newborn physical examination using the Ortolani maneuver is the most useful procedure to detect hip instability. Early treatment of an unstable hip with a Pavlik harness or similarly effective orthosis is effective, safe, and strongly advised. Despite having had normal newborn and infant hip examinations, there remains the possibility of a late-onset hip dislocation needing treatment in approximately 1 in 5000 infants. Keywords: developmental dysplasia of the hip (DDH), newborn, dislocation 474
2 INTRODUCTION Early diagnosis and treatment of developmental dysplasia of the hip (DDH) is important to provide the best possible clinical outcome. DDH encompasses a spectrum of physical and imaging findings, from mild instability and developmental variations to frank dislocation. DDH is asymptomatic during infancy and early childhood, and, therefore, screening of otherwise healthy infants is performed to detect this uncommon condition. The incidence of developmental dislocation of the hip is approximately 1 in 1000 live births. The incidence of the entire spectrum of DDH is undoubtedly higher but not truly known because of the lack of a universal definition. [2].Important risk factors for DDH include breech position, female sex, incorrect lowerextremity swaddling, and positive family history. These risk factors are thought to be additive. Other suggested findings, such as being the first born or having torticollis, foot abnormalities, or oligohydramnios, have not been proven to increase the risk of nonsyndromic DDH. [3]Breech presentation may be the most important single risk factor, with DDH reported in 2% to 27% of boys and girls presenting in the breech position. [4, 5].Traditional methods of screening have included the newborn and periodic physical examination and selected use of radiographic imaging. The term Congenital Dislocation of the Hip (CDH) was superseded by the new name of Developmental Dislocation of the Hip (DDH) in 1989.[6]This was in recognition of the fact that not all cases of pathological hip conditions associated with DDH were present at birth. This opinion has important legal ramifications. If some hip joint conditions that are stable at birth deteriorate and are diagnosed at a later date as an irreducible hip dislocation, they cannot be considered to be missed cases following negative neonatal clinical hip screening by a competent screener. DDH is a dynamic condition in which the hip abnormality may improve or deteriorate with growth.[7]the spectrum of presentation varies from hip dysplasia, to reducible subluxation/dislocation and eventually irreducible hip joint dislocation.[7]neurological, neuromuscular, syndromes and skeletal dysplasia s are excluded, as the hip abnormality is secondary to a primary pathology and is not idiopathic.[6]the traditional outcome measure is that of irreducible hip dislocation.[8]the diagnosis of hip pathology in DDH screening may be clinical and or sonographic. DISCUSSION Neonatal screening in dedicated centres has led to a marked reduction in missed cases of DDH. Risk factors such as family history, breech presentation, oligohydramnios and the presence of other congenital abnormalities are taken into account in selecting newborn infants for special examination and ultrasonography. Ideally all neonates should be examined, but if the programme is to be effective those doing the examining should receive special training [9] SCREENING METHODS Serial clinical examination: Serial clinical examination includes the Ortolani and Barlow tests during the first several months of life and testing for limited hip abduction or leg length discrepancy in older infants and children. The Ortolani 475
3 test involves flexion and abduction of the hips. This movement relocates the dislocated hip into the normal acetabular position and is accompanied with a palpable clunk. [10-12] The Barlow test is a provocative test of dislocation of the hip joint. The hips are tested individually, both in the flexed position. The tested hip is adducted, with gentle pressure exerted on the upper femur in a posteriolateral direction. Key components of the serial clinical examination include leg length discrepancy (Galeazzi sign), limitation of normal abduction of the hip and asymmetry of posterior thigh or gluteal folds.[11, 12] identified too late for nonsurgical therapy to be effective. In clinically screened populations, the detection rate of hip joint instability at birth has ranged from 5 to 20 cases per 1000 infants, depending mainly on age at testing and examiner experience. An observant mother may spot asymmetry, a clicking hip, or difficulty in applying the napkin (diaper) because of limited abduction. With unilateral dislocation the skin creases look asymmetrical and the leg is slightly short (Galeazzi s sign) and externally rotated; a thumb in the groin may feel that the femoral head is missing. With bilateral dislocation there is an abnormally wide perineal gap. Abduction is decreased. Contrary to popular belief, late walking is not a marked feature; nevertheless, in children who do not walk by 18 months dislocation must be excluded. Likewise, a limp or Trendelenburg gait, or a waddling gait could be a sign of missed dislocation Radiography: X-rays of infants are difficult to interpret and in the newborn they can be frankly misleading. This is because the acetabulum and femoral head are largely (or entirely) cartilaginous and therefore not visible on x-ray. X-ray examination is more useful after the first 6 months, and assessment is helped by drawing lines on the x-ray plate to define three geometric indice.limited evidence supports obtaining a properly positioned anteroposterior radiograph of the pelvis. If the pelvis is rotated or if a gonadal shield obscures the hip joint, then the radiograph should be repeated. Hip asymmetry, subluxation, and dislocation can be detected on radiographs when dysplasia is present. There is debate about whether early minor radiographic variability (such as increased acetabular index) constitutes actual disease. [13]Radiography is traditionally indicated for diagnosis of the infant with risk factors or an abnormal examination after 4 months of age. [4, 14] Ultrasonography: Ultrasound scanning has replaced radiography for imaging hips in the newborn. The radiographically invisible acetabulum and femoral head can, with practice, be displayed with static and dynamic ultrasound. Sequential assessment is straightforward and allows monitoring of the hip during a period of splintage. Ultrasonography can provide detailed static and dynamic imaging of the hip before femoral head ossification. The American Institute of Ultrasound in Medicine and the American College of Radiology published a joint guideline for the standardized performance of the infantile hip ultrasonographic examination. [15].Static ultrasonography shows coverage of the femoral head by the cartilaginous acetabulum (α angle) at rest, and dynamic ultrasonography demonstrates a real-time image of the Barlow and Ortolani tests. 476
4 COMPLICATIONS Failed reduction multiple attempts at treatment, with failure to achieve concentric reduction, may be worse than no treatment. The acetabulum remains undeveloped, the femoral head may be deformed, the neck is usually anteverted and the capsule is thickened and adherent. It is important to enquire also why reduction failed: is the dislocation part of a generalized condition, or a neuromuscular disorder associated with muscle imbalance? The principles of treatment for children over 8 years are the same as those discussed above. Avascular necrosis a much-feared complication of treatment is ischaemia of the immature femoral head. It may occur at any age and any stage of treatment and is probably due to vascular injury or obstruction resulting from forceful reduction and hip splintage in abduction. The effects vary considerably: in the mildest cases the changes are confined to the ossific nucleus, which appears to be slightly distorted and irregular on x-ray. The cartilaginous epiphysis retains the shape and physical growth is normal. After months the appearances return to normal. In more severe cases the epiphyseal and physeal growth plates also suffer; the ossific nucleus looks fragmented, the epiphysis is distorted to greater or lesser extent and metaphyseal changes lead to shortening and deformity of the femoral neck. Prevention is the best cure: forced manipulative reduction should not be allowed; traction should be gentle and in the neutral position; positions of extreme abduction must be avoided; soft-tissue release (adductor tenotomy) should precede closed reduction; and if difficulty is anticipated open reduction is preferable. Once the condition is established, there is no effective treatment except to avoid manipulation and weight bearing until the epiphysis has healed. In the mildest cases there will be no residual deformity, or at worst a femoral neck deformity which can be corrected by osteotomy. In severe cases the outcome may be flattening and mushrooming of the femoral head, shortening of the neck (with or without coxa vara), acetabular dysplasia and in congruency of the hip. Surgical correction of the proximal femur and pelvic osteotomy to reposition or deepen the acetabulum may be needed MANAGEMENT THE FIRST 3 6 MONTHS: Where facilities for ultrasound scanning are available, all newborn infants with a high-risk background or a suggestion of hip instability are examined by ultrasonography. If this shows that the hip is reduced and has a normal cartilaginous outline, no treatment is required but the child is kept under observation for 3 6 months. In the presence of acetabular dysplasia or hip instability, the hip is splinted in a position of flexion and abduction and ultrasound scanning is repeated at intervals until stability and normal anatomy are restored or a decision is made to abandon splintage in favor of more aggressive treatment. If ultrasound is not available, the simplest policy is to regard all infants with a high-risk background or a positive Ortolani or Barlow test, as suspect and to nurse them in double napkins or an abduction pillow for the first 6 weeks. At that stage they are re-examined: those with stable hips are left free but kept under observation for at least 6 months; those with persistent instability are treated by more formal abduction splintage until the hip is stable and x-ray shows that the acetabular roof is developing satisfactorily (usually 477
5 3 6 months) There are two drawbacks to this approach: (1) the sensitivity of the clinical tests is not high enough to ensure that all cases will be spotted [16]; and (2) of those hips that are unstable at birth, per cent will stabilize spontaneously in 2 3 weeks. It therefore seems more sensible not to start splintage immediately unless the hip is already dislocated. This reduces the small (but significant) risk of epiphyseal necrosis that attends any form of restrictive splintage in the neonate. Thus: if a hip is dislocatable but not habitually dislocated, the baby is left untreated but reexamined weekly; if at 3 weeks the hip is still unstable, abduction splintage is applied. If the hip is already dislocated at the first examination, it is gently placed in the reduced position and abduction splintage is applied from the outset. Reduction is maintained until the hip is stable. This situation must be avoided; if the hip fails to locate, splintage should be abandoned in favor of closed or operative reduction at a later date. Follow-up whatever policy is adopted, follow-up is continued until the child is walking. Sometimes, even with the most careful treatment, the hip may later show some degree of acetabular dysplasia. PERSISTENT DISLOCATION: 6 18 MONTHS: If, after early treatment, the hip is still incompletely reduced, or if the child presents late with a missed dislocation, the hip must be reduced preferably by closed methods but if necessary by operation and held reduced until acetabular development is satisfactory. Closed reduction Closed reduction is suitable after the age of 3 months and is performed under general anesthesia with an arthrogram to confirm a concentric reduction. To minimize the risk of avascular necrosis, reduction must be gentle and may be preceded by gradual traction to both legs. Failure to achieve concentric reduction should lead to abandoning this method in favor of an operative approach at approximately 1 year of age. The hips should be stable in a safe zone of abduction, which may be increased with a closed adductor tenotomy. Splintage The concentrically reduced hip is held in a plaster spica at 60 degrees of flexion, 40 degrees of abduction and 20 degrees of internal rotation. After 6 weeks the spica is changed and the stability of the hips assessed under anaesthesia. Provided the position and stability are satisfactory the spica is retained for a further 6 weeks. Following plaster removal the hip is either left unsplinted or managed in a removable abduction splint which is retained for up to 6 months depending on radiological evidence of satisfactory acetabular development. Operation if, at any stage, concentric reduction has not been achieved, open operation is needed. The psoas tendon is divided; obstructing tissues (redundant capsule and thickened ligamentum teres) are removed and the hip is reduced. It is usually stable in 60 degrees of flexion, 40 degrees of abduction and 20 degrees of internal rotation. A spica is applied and the hip is splinted as described above. If stability can be achieved only by markedly internally rotating the hip, a corrective subtrochanteric osteotomy of the femur is carried out, either at the time of open reduction or 6 weeks later. In young children this usually gives a good result PERSISTENT DISLOCATION: 18 MONTHS 4 YEARS: In the older child, closed reduction is less likely to succeed; many surgeons would proceed straight to arthrography and open reduction. Traction Even if closed reduction is unsuccessful, a period of traction (if 478
6 necessary combined with psoas and adductor tenotomy) may help to loosen the tissues and bring the femoral head down opposite the acetabulum. Arthrography An arthrogram at this stage will clarify the anatomy of the hip and show whether there is an inturned limbus or any marked degree of acetabular dysplasia Operation The joint capsule is opened anteriorly, any redundant capsule is removed along with any other blocks to reduction including the hypertrophied ligamentum teres and transverse acetabular ligament and the femoral head is seated in the acetabulum. Usually a derotation femoral osteotomy held by a plate and screws will be required. At the same time a 1 cm segment can be removed from the proximal femur to reduce pressure on the hip (Klisic and Jankovic, 1976). If there is marked acetabular dysplasia, some form of acetabuloplasty will also be needed either a pericapsular reconstruction of the acetabular roof (Pemberton s operation) or an innominate (Salter) osteotomy which repositions the entire innominate bone and acetabulum Splintage After operation, the hip is held in a plaster spica for 3 months and then left unsupported to allow recovery of movement. The child is kept under intermittent clinical and radiological surveillance until skeletal maturity. DISLOCATION IN CHILDREN OVER 4 YEARS: Reduction and stabilization become increasingly difficult with advancing age. Nevertheless, in children between 4 and 8 years especially if the dislocation is unilateral it is still worth attempting, bearing in mind that the risk of avascular necrosis and hip stiffness is reported as being in excess of 25 per cent. The principles of treatment are as described immediately above. Unilateral dislocation in the child over 8 years often leaves the child with a mobile hip and little pain. This is the justification for non-intervention, though in that case the child must accept the fact that gait is distinctly abnormal. If reduction is attempted it will require an open operation and acetabular reconstruction. These procedures are best undertaken in centres specializing in this area. With bilateral dislocation the deformity and the waddling gait is symmetrical and therefore not so noticeable; the risk of operative intervention is also greater because failure on one or other side turns this into an asymmetrical deformity. Therefore, in these cases, most surgeons avoid operation above the age of 6 years unless the hip is painful or deformity unusually severe. The untreated patient walks with a waddle but may be surprisingly uncomplaining CONCLUSION Late diagnosis of DDH might cause serious public health problems. Screening for and treatment of hip dislocation (positive Ortolani test result) and initially observing milder early forms of dysplasia and instability (positive Barlow test result) infants should be examined for hip instability at birth, with periodic follow-up exams until the child is walking, which helps to prevent further complication of hip joint. Early diagnosis and treatment of developmental dysplasia of the hip (DDH) is important to provide the best possible clinical outcome. 479
7 REFERENCES 1. Sewell, M.D., K. Rosendahl, and D.M. Eastwood, Developmental dysplasia of the hip. Bmj, : p. b Rosendahl, K., et al., Immediate treatment versus sonographic surveillance for mild hip dysplasia in newborns. Pediatrics, (1): p. e Barr, L.V. and A. Rehm, Should all twins and multiple births undergo ultrasound examination for developmental dysplasia of the hip?: A retrospective study of 990 multiple births. Bone Joint J, b(1): p Imrie, M., et al., Is ultrasound screening for DDH in babies born breech sufficient? J Child Orthop, (1): p Suzuki, S. and T. Yamamuro, Avascular necrosis in patients treated with the Pavlik harness for congenital dislocation of the hip. J Bone Joint Surg Am, (7): p Bialik, V., et al., Developmental dysplasia of the hip: a new approach to incidence. Pediatrics, (1): p Klisic, P.J., Congenital dislocation of the hip--a misleading term: brief report. J Bone Joint Surg Br, (1): p Macnicol, M.F., Results of a 25-year screening programme for neonatal hip instability. J Bone Joint Surg Br, (6): p Harcke, H.T. and S.J. Kumar, The role of ultrasound in the diagnosis and management of congenital dislocation and dysplasia of the hip. J Bone Joint Surg Am, (4): p Weinstein, S.L., S.J. Mubarak, and D.R. Wenger, Fundamental concepts of developmental dysplasia of the hip. Instr Course Lect, : p Staheli, L.T., et al., Congenital hip dysplasia. Instr Course Lect, : p Mooney, J.F., 3rd and J.B. Emans, Developmental dislocation of the hip: a clinical overview. Pediatr Rev, (8): p ; quiz Mladenov, K., et al., Natural history of hips with borderline acetabular index and acetabular dysplasia in infants. J Pediatr Orthop, (5): p Karmazyn, B.K., et al., ACR Appropriateness Criteria on developmental dysplasia of the hip--child. J Am Coll Radiol, (8): p AIUM practice guideline for the performance of an ultrasound examination for detection and assessment of developmental dysplasia of the hip. J Ultrasound Med, (1): p Jones, D.A., Principles of screening and congenital dislocation of the hip. Ann R Coll Surg Engl, (4): p
Clinical Practice & Referral Guideline - Developmental Dysplasia of the Hip
 Clinical Practice & Referral Guideline - Developmental Dysplasia of the Hip *This guideline was developed from the American Academy of Pediatrics Clinical Practice Guideline: Early Detection of Developmental
Clinical Practice & Referral Guideline - Developmental Dysplasia of the Hip *This guideline was developed from the American Academy of Pediatrics Clinical Practice Guideline: Early Detection of Developmental
Hip Dysplasia for the Primary Care Physician George Gantsoudes, MD. November 4, 2017
 Hip Dysplasia for the Primary Care Physician George Gantsoudes, MD November 4, 2017 Introduction Developmental Dysplasia of the Hip DDH - preferred term Teratologic hips Subluxation Dislocation-usually
Hip Dysplasia for the Primary Care Physician George Gantsoudes, MD November 4, 2017 Introduction Developmental Dysplasia of the Hip DDH - preferred term Teratologic hips Subluxation Dislocation-usually
Developmental Dysplasia of the Hip
 Developmental Dysplasia of the Hip Abnormal relationship of femoral head to the acetabulum Formerly known as congenital hip dislocation Believed to be developmental Most dislocations are evident at births
Developmental Dysplasia of the Hip Abnormal relationship of femoral head to the acetabulum Formerly known as congenital hip dislocation Believed to be developmental Most dislocations are evident at births
Childhood hip conditions. Belen Carsi Paediatric Orthopaedic Consultant
 Childhood hip conditions Belen Carsi Paediatric Orthopaedic Consultant Developmental Dysplasia of the Hip Legg-Calve-Perthes disease Slipped Capital femoral epiphysis Limp Arthritis Developmental Dysplasia
Childhood hip conditions Belen Carsi Paediatric Orthopaedic Consultant Developmental Dysplasia of the Hip Legg-Calve-Perthes disease Slipped Capital femoral epiphysis Limp Arthritis Developmental Dysplasia
Hip Dysplasia David S. Feldman, MD
 Hip Dysplasia David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone Medical Center & NYU Hospital for Joint Diseases Overview Hip dysplasia
Hip Dysplasia David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone Medical Center & NYU Hospital for Joint Diseases Overview Hip dysplasia
DDH. Abnormal hip development Traditionally CDH (congenital dysplasia of the hip) Today DDH(developmental dysplasia of the hip)
 DDH Update on Screening Kathryn A Keeler, MD Assistant Professor University of Missouri-Kansas City School of Medicine, Department of Orthopaedic Surgery and Department of Pediatrics Children s Mercy Kansas
DDH Update on Screening Kathryn A Keeler, MD Assistant Professor University of Missouri-Kansas City School of Medicine, Department of Orthopaedic Surgery and Department of Pediatrics Children s Mercy Kansas
What is a Hip Dysplasia?
 What is a Hip Dysplasia? Hip dysplasia, developmental dysplasia of the hip (DDH)[1] or congenital dysplasia of the hip (CDH)[2] is a congenital or acquired deformation or misalignment of the hip joint.
What is a Hip Dysplasia? Hip dysplasia, developmental dysplasia of the hip (DDH)[1] or congenital dysplasia of the hip (CDH)[2] is a congenital or acquired deformation or misalignment of the hip joint.
Subluxation of the hip presenting for the first time
 The treatment of subluxation of the hip in children over the age of four years John A. Fixsen, Patrick L. S. Li From the Hospitals for Sick Children, Great Ormond Street, London, England Subluxation of
The treatment of subluxation of the hip in children over the age of four years John A. Fixsen, Patrick L. S. Li From the Hospitals for Sick Children, Great Ormond Street, London, England Subluxation of
Society for Pediatric Radiology 2015 Hands on Session. DDH: Pitfalls and Practical Tips
 Society for Pediatric Radiology 2015 Hands on Session DDH: Pitfalls and Practical Tips Michael A. DiPietro, M.D. John F. Holt Collegiate Professor of Radiology Professor of Pediatrics and Communicable
Society for Pediatric Radiology 2015 Hands on Session DDH: Pitfalls and Practical Tips Michael A. DiPietro, M.D. John F. Holt Collegiate Professor of Radiology Professor of Pediatrics and Communicable
DDH: Pathology Diagnosis, and Treatment before Walking Age
 DDH: Pathology Diagnosis, and Treatment before Walking Age 영남의대 김세동 Ⅰ. Terminology of hip dysplasia a. Congenital dysplasia or dislocation of the hip(cdh): Hippocrates Congenital -Existing at Birth but
DDH: Pathology Diagnosis, and Treatment before Walking Age 영남의대 김세동 Ⅰ. Terminology of hip dysplasia a. Congenital dysplasia or dislocation of the hip(cdh): Hippocrates Congenital -Existing at Birth but
Successful Pavlik treatment in late-diagnosed developmental dysplasia of the hip
 International Orthopaedics (SICOT) (2012) 36:1661 1668 DOI 10.1007/s00264-012-1587-5 ORIGINAL PAPER Successful Pavlik treatment in late-diagnosed developmental dysplasia of the hip Michiel A. J. van de
International Orthopaedics (SICOT) (2012) 36:1661 1668 DOI 10.1007/s00264-012-1587-5 ORIGINAL PAPER Successful Pavlik treatment in late-diagnosed developmental dysplasia of the hip Michiel A. J. van de
Combined Pelvic Osteotomy in the Treatment of Both Deformed and Dysplastic Acetabulum Three Years Prospective Study
 Prague Medical Report / Vol. 106 (2005) No. 2, p. 159 166 159) Combined Pelvic Osteotomy in the Treatment of Both Deformed and Dysplastic Acetabulum Three Years Prospective Study Al Razi Orthopedic Hospital,
Prague Medical Report / Vol. 106 (2005) No. 2, p. 159 166 159) Combined Pelvic Osteotomy in the Treatment of Both Deformed and Dysplastic Acetabulum Three Years Prospective Study Al Razi Orthopedic Hospital,
Developmental Dysplasia of the Hip From Birth to Six Months
 From Birth to Six Months James T. Guille, MD, Peter D. Pizzutillo, MD, and G. Dean MacEwen, MD Abstract The term developmental dysplasia or dislocation of the hip (DDH) refers to the complete spectrum
From Birth to Six Months James T. Guille, MD, Peter D. Pizzutillo, MD, and G. Dean MacEwen, MD Abstract The term developmental dysplasia or dislocation of the hip (DDH) refers to the complete spectrum
ORDER OF VERBAL EXAMS
 ORDER OF VERBAL EXAMS The students are able to register for the exam on the NEPTUN system. The students pick two titles, from the title list available at the beginning of the Semester. This list can be
ORDER OF VERBAL EXAMS The students are able to register for the exam on the NEPTUN system. The students pick two titles, from the title list available at the beginning of the Semester. This list can be
The Hip Baby?? Baby Hippie??
 In Need of a Title? The Hip Baby?? Baby Hippie?? Review of Developmental Dysplasia of the Hip in the Newborn OCR Symposium 2018 Ryan L. Hartman, MD Specialty: Pediatric and Sports Orthopaedics 23 month
In Need of a Title? The Hip Baby?? Baby Hippie?? Review of Developmental Dysplasia of the Hip in the Newborn OCR Symposium 2018 Ryan L. Hartman, MD Specialty: Pediatric and Sports Orthopaedics 23 month
Developmental Dysplasia of the Hip, (DDH) including Femoral and Pelvic Osteotomy
 Developmental Dysplasia of the Hip, (DDH) including Femoral and Pelvic Osteotomy Leicester Children s Hospital Information for Patients, Parents and Carers DRAFT What is developmental dysplasia of the
Developmental Dysplasia of the Hip, (DDH) including Femoral and Pelvic Osteotomy Leicester Children s Hospital Information for Patients, Parents and Carers DRAFT What is developmental dysplasia of the
Ultrasound Scanning of Neonatal Hips
 Ultrasound Scanning of Neonatal Hips Dr. Dickson S F Tsang Associate Consultant Queen Mary Hospital Why? How? What? Outline IAAHS 2nd April, 2011 Outline Why? Why performing hip ultrasound (USG)? Why USG?
Ultrasound Scanning of Neonatal Hips Dr. Dickson S F Tsang Associate Consultant Queen Mary Hospital Why? How? What? Outline IAAHS 2nd April, 2011 Outline Why? Why performing hip ultrasound (USG)? Why USG?
Four weeks of Intrauterine life
 Objective Congenital & Developmental Malformation Overview of Musculoskeletal dev. Abnormal pattern of dev. Common upper & lower ext. abnormalities READ : SPINE and more information in text book Definition
Objective Congenital & Developmental Malformation Overview of Musculoskeletal dev. Abnormal pattern of dev. Common upper & lower ext. abnormalities READ : SPINE and more information in text book Definition
Peggers Super Summaries: Paediatric Hip
 EMBRYOLOGY Development o Mesenchymal stem cells cartilage blood supply bone Dates o 6/40 Limb development o 8-11/40 hip development (acetabulum and hip formed from one bone splitting by apoptosis) o 16/40
EMBRYOLOGY Development o Mesenchymal stem cells cartilage blood supply bone Dates o 6/40 Limb development o 8-11/40 hip development (acetabulum and hip formed from one bone splitting by apoptosis) o 16/40
Radiological Sequelae of developmental dysplasia of the hip: a Review
 Radiological Sequelae of developmental dysplasia of the hip: a Review Poster No.: P-0037 Congress: ESSR 2012 Type: Scientific Exhibit Authors: S. G. Flanagan, J. Sarkodieh, K. Mcdonald, M. Ramachandran,
Radiological Sequelae of developmental dysplasia of the hip: a Review Poster No.: P-0037 Congress: ESSR 2012 Type: Scientific Exhibit Authors: S. G. Flanagan, J. Sarkodieh, K. Mcdonald, M. Ramachandran,
Treatment of DDH before Walking Age 고려대학안암병원
 Treatment of DDH before Walking Age 이 순혁 고려대학안암병원 Subluxated Hip Always to deg. hip The more, the earlier Even in 2nd Decade Dysplastic Hip Eventually to osteoarthritis but later Etiology of end-stage
Treatment of DDH before Walking Age 이 순혁 고려대학안암병원 Subluxated Hip Always to deg. hip The more, the earlier Even in 2nd Decade Dysplastic Hip Eventually to osteoarthritis but later Etiology of end-stage
PROBLEMS IN THE EARLY RECOGNITION OF DYSPLASIA
 PROBLEMS IN THE EARLY RECOGNITION OF HIP DYSPLASIA STUART J. M. DAVIES, GEOFFREY WALKER From Queen Mary s Hospitalfor Children, Carshalton Ten children who had clinically stable hips at birth were radiographed
PROBLEMS IN THE EARLY RECOGNITION OF HIP DYSPLASIA STUART J. M. DAVIES, GEOFFREY WALKER From Queen Mary s Hospitalfor Children, Carshalton Ten children who had clinically stable hips at birth were radiographed
Case Developmental dysplasia of hip
 Case 13303 Developmental dysplasia of hip Hidayatullah Hamidi, Sahar Maroof French medical institute for children, Kabul, Afghanistan Email: Hedayatullah.hamidi@gmail.com Maroofsahar1@gmail.com French
Case 13303 Developmental dysplasia of hip Hidayatullah Hamidi, Sahar Maroof French medical institute for children, Kabul, Afghanistan Email: Hedayatullah.hamidi@gmail.com Maroofsahar1@gmail.com French
Adult Hip Dysplasia David S. Feldman, MD
 Adult Hip Dysplasia David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone Medical Center & NYU Hospital for Joint Diseases Overview Adult hip
Adult Hip Dysplasia David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone Medical Center & NYU Hospital for Joint Diseases Overview Adult hip
Developmental dysplasia of the hip: What has changed in the last 20 years?
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5312/wjo.v6.i11.886 World J Orthop 2015 December 18; 6(11): 886-901 ISSN 2218-5836 (online)
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5312/wjo.v6.i11.886 World J Orthop 2015 December 18; 6(11): 886-901 ISSN 2218-5836 (online)
L side 65% Torticollis, Plagiocephaly, Metatarsus varus Flat foot.
 DEVELOPMENTAL DISLOCATION OF THE HIP [DDH] Older terminology was Congenital dislocation of the hip. DDH means developmental dysplasia of the hip. DDH is better than CDH as dislocation is not always congenital.
DEVELOPMENTAL DISLOCATION OF THE HIP [DDH] Older terminology was Congenital dislocation of the hip. DDH means developmental dysplasia of the hip. DDH is better than CDH as dislocation is not always congenital.
CLINICAL GUIDELINES ID TAG Developmental Dysplasia of hips Regional Guideline Mr Aidan Cosgrove. Title:
 Title: Author: Designation: Speciality / Division: Directorate: CLINICAL GUIDELINES ID TAG Developmental Dysplasia of hips Regional Guideline Mr Aidan Cosgrove Paediatric Orthopaedics Orthopaedic Orthopaedics
Title: Author: Designation: Speciality / Division: Directorate: CLINICAL GUIDELINES ID TAG Developmental Dysplasia of hips Regional Guideline Mr Aidan Cosgrove Paediatric Orthopaedics Orthopaedic Orthopaedics
The Efficacy of Pavlik Harness as a Treatment of Developmental Dislocation of the Hip
 The Efficacy of Pavlik Harness as a Treatment of Developmental Dislocation of the Hip Firas A. Suleiman, MD*, Fadi Al Rousan, MD*, Ahmad Almarzoq, MD *, Razi Altarawneh, MD*, Hidar Soudi, MD* ABSTRACT
The Efficacy of Pavlik Harness as a Treatment of Developmental Dislocation of the Hip Firas A. Suleiman, MD*, Fadi Al Rousan, MD*, Ahmad Almarzoq, MD *, Razi Altarawneh, MD*, Hidar Soudi, MD* ABSTRACT
DEVELOPMENTAL DYSPLASIA OF THE HIP CURRENT TRENDS APLLIED IN ARAD
 DEVELOPMENTAL DYSPLASIA OF THE HIP CURRENT TRENDS APLLIED IN ARAD PAVEL Adrian Ionel 1, BOIA Eugen Sorin 2, 1 PhD, Victor Babes University of Medicine and Pharmacy, Timisoara, Romania 2 Prof., PhD, MD,
DEVELOPMENTAL DYSPLASIA OF THE HIP CURRENT TRENDS APLLIED IN ARAD PAVEL Adrian Ionel 1, BOIA Eugen Sorin 2, 1 PhD, Victor Babes University of Medicine and Pharmacy, Timisoara, Romania 2 Prof., PhD, MD,
Ultrasound in the selective screening of developmental dysplasia of the hip
 European Review for Medical and Pharmacological Sciences 2011; 15: 394-398 Ultrasound in the selective screening of developmental dysplasia of the hip A.A. AFAQ, S. STOKES, H. FAREED*, H.G. ZADEH*, M.
European Review for Medical and Pharmacological Sciences 2011; 15: 394-398 Ultrasound in the selective screening of developmental dysplasia of the hip A.A. AFAQ, S. STOKES, H. FAREED*, H.G. ZADEH*, M.
RESULTS OF THE EARLY TREATMENT OF DEVELOPMENTAL DYSPLASIA OF THE HIP
 RESULTS OF THE EARLY TREATMENT OF DEVELOPMENTAL DYSPLASIA OF THE HIP Dana Vasilescu, Dan Cosma University of Medicine and Pharmacy Iuliu Haţieganu Cluj-Napoca 13, E. Isac st., 400023 Cluj-Napoca, România
RESULTS OF THE EARLY TREATMENT OF DEVELOPMENTAL DYSPLASIA OF THE HIP Dana Vasilescu, Dan Cosma University of Medicine and Pharmacy Iuliu Haţieganu Cluj-Napoca 13, E. Isac st., 400023 Cluj-Napoca, România
Guidelines, Policies and Statements. Statement on the Use of Ultrasound in the Diagnosis of Developmental Hip Dysplasia and Dislocation
 Guidelines, Policies and Statements Statement on the Use of Ultrasound in the Diagnosis of Developmental Hip Dysplasia and Dislocation Approved by Council June 2018 Disclaimer and Copyright The ASUM Standards
Guidelines, Policies and Statements Statement on the Use of Ultrasound in the Diagnosis of Developmental Hip Dysplasia and Dislocation Approved by Council June 2018 Disclaimer and Copyright The ASUM Standards
Friday Teaching. Bones
 Friday Teaching Bones Regarding slipped femoral capital epiphysis It represents Salter Harris type V injury 20% are bilateral There is slight widening of the joint space Slip is typically posteromedial
Friday Teaching Bones Regarding slipped femoral capital epiphysis It represents Salter Harris type V injury 20% are bilateral There is slight widening of the joint space Slip is typically posteromedial
Outcome of surgical management of late presenting developmental dysplasia of hip with pelvic and femoral osteotomies
 Original Research Article DOI: 10.18231/2395-1362.2018.0012 Outcome of surgical management of late presenting developmental dysplasia of hip with pelvic and femoral osteotomies G. Jagadesh 1, Venugopal
Original Research Article DOI: 10.18231/2395-1362.2018.0012 Outcome of surgical management of late presenting developmental dysplasia of hip with pelvic and femoral osteotomies G. Jagadesh 1, Venugopal
Hip Biomechanics and Osteotomies
 Hip Biomechanics and Osteotomies Organization Introduction Hip Biomechanics Principles of Osteotomy Femoral Osteotomies Pelvic Osteotomies Summary Inroduction Osteoarthritis is very prevalent Primary OA
Hip Biomechanics and Osteotomies Organization Introduction Hip Biomechanics Principles of Osteotomy Femoral Osteotomies Pelvic Osteotomies Summary Inroduction Osteoarthritis is very prevalent Primary OA
Treatment of congenital subluxation and dislocation of the hip by knee splint harness
 Prosthetics and Orthotics International, 1994,18, 34-39 Treatment of congenital subluxation and dislocation of the hip by knee splint harness M. FUKUSHIMA Fukushima Orthopaedic Clinic, Hiroshima City,
Prosthetics and Orthotics International, 1994,18, 34-39 Treatment of congenital subluxation and dislocation of the hip by knee splint harness M. FUKUSHIMA Fukushima Orthopaedic Clinic, Hiroshima City,
COMMON MUSCULOSKELETAL PROBLEMS GROWTH AND DEVELOPMENT PATHOLOGIC VS. NORMAL
 COMMON MUSCULOSKELETAL PROBLEMS GROWTH AND DEVELOPMENT PATHOLOGIC VS. NORMAL Clifford L. Craig, M.D. M2 Musculoskeletal Fall 2008 I. ANGULAR AND TORSIONAL DEFORMITIES OF THE LOWER LIMBS Examination Relaxed,
COMMON MUSCULOSKELETAL PROBLEMS GROWTH AND DEVELOPMENT PATHOLOGIC VS. NORMAL Clifford L. Craig, M.D. M2 Musculoskeletal Fall 2008 I. ANGULAR AND TORSIONAL DEFORMITIES OF THE LOWER LIMBS Examination Relaxed,
ONE STAGE COMBINED SURGICAL TREATMENT FOR DEVELOPMENTAL DISLOCATION OF THE HIP IN OLDER CHILDREN INCLUDING FEMORAL SHORTENING
 Basrah Journal Original Article Of Surgery Bas J Surg, March, 17, 2011 ONE STAGE COMBINED SURGICAL TREATMENT FOR DEVELOPMENTAL DISLOCATION OF THE HIP IN OLDER CHILDREN INCLUDING FEMORAL SHORTENING MBChB,
Basrah Journal Original Article Of Surgery Bas J Surg, March, 17, 2011 ONE STAGE COMBINED SURGICAL TREATMENT FOR DEVELOPMENTAL DISLOCATION OF THE HIP IN OLDER CHILDREN INCLUDING FEMORAL SHORTENING MBChB,
EARLY OPEN REDUCFION FOR CONGENITAL DISLOCATION OF THE HIP
 EARLY OPEN REDUCFION FOR CONGENITAL DISLOCATION OF THE HIP SUNIL DHAR, J. F. TAYLOR, W. A. JONES, R. OWEN From Alder Hey Children s Hospital, Liverpool We have reviewed 82 children with congenital dislocation
EARLY OPEN REDUCFION FOR CONGENITAL DISLOCATION OF THE HIP SUNIL DHAR, J. F. TAYLOR, W. A. JONES, R. OWEN From Alder Hey Children s Hospital, Liverpool We have reviewed 82 children with congenital dislocation
Is ultrasound screening for DDH in babies born breech sufficient?
 J Child Orthop (2010) 4:3 8 DOI 10.1007/s11832-009-0217-2 ORIGINAL CLINICAL ARTICLE Is ultrasound screening for DDH in babies born breech sufficient? Meghan Imrie Vanessa Scott Philip Stearns Tracey Bastrom
J Child Orthop (2010) 4:3 8 DOI 10.1007/s11832-009-0217-2 ORIGINAL CLINICAL ARTICLE Is ultrasound screening for DDH in babies born breech sufficient? Meghan Imrie Vanessa Scott Philip Stearns Tracey Bastrom
)371( COPYRIGHT 2016 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE. Research performed at Dr. Sheikh Children Hospital, Mashhad, Iran
 )371( COPYRIGHT 2016 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE Assessment of Diagnostic Value of Single View Static & Dynamic Technique in Diagnosis of Developmental Dysplasia of Hip:
)371( COPYRIGHT 2016 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE Assessment of Diagnostic Value of Single View Static & Dynamic Technique in Diagnosis of Developmental Dysplasia of Hip:
CONGENITAL DISLOCATION O,F THE HIP
 J. roy. Army med. Cps. 1976. 122,73-79 CONGENITAL DISLOCATION O,F THE HIP Lieutenant-Colonel J. T. COULL, M.B., Ch.B., F.R.C.S., R.A,M.C. British Military Hospital, Rinteln SUMMARY: The problems of diagnosis
J. roy. Army med. Cps. 1976. 122,73-79 CONGENITAL DISLOCATION O,F THE HIP Lieutenant-Colonel J. T. COULL, M.B., Ch.B., F.R.C.S., R.A,M.C. British Military Hospital, Rinteln SUMMARY: The problems of diagnosis
DDH: Pathology, Diagnosis & Treatment before Walking Age 고려대학안암병원
 DDH: Pathology, Diagnosis & Treatment before Walking Age 이 순혁 고려대학안암병원 Developmental Hip Dysplasia (DDH) Klisic 1988 AAOS 1991 Congenital Hip Dislocation Not always congenital or dislocated Causes, Risk
DDH: Pathology, Diagnosis & Treatment before Walking Age 이 순혁 고려대학안암병원 Developmental Hip Dysplasia (DDH) Klisic 1988 AAOS 1991 Congenital Hip Dislocation Not always congenital or dislocated Causes, Risk
Developmental Dysplasia of the Hip
 1 Developmental Dysplasia of the Hip Developmental dysplasia of the hip (DDH) or otherwise known as congenital dislocation of the hip (CDH) is a developmental (ongoing) process, which can often go undetected
1 Developmental Dysplasia of the Hip Developmental dysplasia of the hip (DDH) or otherwise known as congenital dislocation of the hip (CDH) is a developmental (ongoing) process, which can often go undetected
Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH)
 Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH) Poster No.: C-2049 Congress: ECR 2012 Type: Scientific Exhibit Authors: E. M. D. B. Pacheco,
Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH) Poster No.: C-2049 Congress: ECR 2012 Type: Scientific Exhibit Authors: E. M. D. B. Pacheco,
Ultrasound Evaluation of Pavlik Harness in Treatment of Infants with Developmental Dysplasia of the Hip: Prone Axial Approach to Harness in Situ
 Ultrasound Evaluation of Pavlik Harness in Treatment of Infants with Developmental Dysplasia of the Hip: Prone Axial Approach to Harness in Situ C Fernández, MD; M Guasp, MD; J Gómez Fernández-Montes,
Ultrasound Evaluation of Pavlik Harness in Treatment of Infants with Developmental Dysplasia of the Hip: Prone Axial Approach to Harness in Situ C Fernández, MD; M Guasp, MD; J Gómez Fernández-Montes,
THE IMPORTANCE OF ULTRASONOGRAPHY IN EARLY DIAGNOSIS AND TREATMENT OF DDH
 THE IMPORTANCE OF ULTRASONOGRAPHY IN EARLY DIAGNOSIS AND TREATMENT OF DDH Pavel Adrian Ionel 1, Boia Eugen Sorin 2 1 PhD student, Victor Babes University of Medicine and Pharmacy, Timisoara, Romania 2
THE IMPORTANCE OF ULTRASONOGRAPHY IN EARLY DIAGNOSIS AND TREATMENT OF DDH Pavel Adrian Ionel 1, Boia Eugen Sorin 2 1 PhD student, Victor Babes University of Medicine and Pharmacy, Timisoara, Romania 2
A One Stage Open Reduction With Salter's Innominate Osteotomy And Corrective Femoral Osteotomy For The Treatment Of Congenital Dysplasia Of The Hip
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 1 Number 2 A One Stage Open Reduction With Salter's Innominate Osteotomy And Corrective Femoral Osteotomy For The Treatment Of Congenital Dysplasia
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 1 Number 2 A One Stage Open Reduction With Salter's Innominate Osteotomy And Corrective Femoral Osteotomy For The Treatment Of Congenital Dysplasia
Case Presentations The Child with a Limp
 Case Presentations The Child with a Limp Douglas G. Armstrong, M.D. Professor, PennState Hershey College of Medicine Division Head, Pediatric Orthopaedics Dept. of Orthopaedics and Rehabilitation PennState
Case Presentations The Child with a Limp Douglas G. Armstrong, M.D. Professor, PennState Hershey College of Medicine Division Head, Pediatric Orthopaedics Dept. of Orthopaedics and Rehabilitation PennState
Original Article Results of simultaneous open reduction and Salter innominate osteotomy for developmental dysplasia of the hip
 Kathmandu University Medical Journal (2005) Vol. 3, No. 1, Issue 9, 6-10 Original Article Results of simultaneous open reduction and Salter innominate osteotomy for developmental dysplasia of the hip Banskota
Kathmandu University Medical Journal (2005) Vol. 3, No. 1, Issue 9, 6-10 Original Article Results of simultaneous open reduction and Salter innominate osteotomy for developmental dysplasia of the hip Banskota
Surgical treatment for developmental dysplasia of the hip- a single surgeon series of 47 hips with a 7 year mean follow up
 754 Acta Orthop. Belg., 2016, 82, j. 754-761 mcfarlane, j. h. kuiper, n. kiely ORIGINAL STUDY Surgical treatment for developmental dysplasia of the hip- a single surgeon series of 47 hips with a 7 year
754 Acta Orthop. Belg., 2016, 82, j. 754-761 mcfarlane, j. h. kuiper, n. kiely ORIGINAL STUDY Surgical treatment for developmental dysplasia of the hip- a single surgeon series of 47 hips with a 7 year
Epidemiology, Clinical Screening and early Management of Developmental Dysplasia of the Hip in Sulaimani City Center
 Epidemiology, Clinical Screening and early Management of Developmental Dysplasia of the Hip in Sulaimani City Center Dr. Rebwar Abdullah Hasan* Dr. Omar Ali Rafiq** ABSTRACT Background and Objectives:
Epidemiology, Clinical Screening and early Management of Developmental Dysplasia of the Hip in Sulaimani City Center Dr. Rebwar Abdullah Hasan* Dr. Omar Ali Rafiq** ABSTRACT Background and Objectives:
Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH)
 Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH) Poster No.: C-2049 Congress: ECR 2012 Type: Scientific Exhibit Authors: E. M. D. B. Pacheco,
Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH) Poster No.: C-2049 Congress: ECR 2012 Type: Scientific Exhibit Authors: E. M. D. B. Pacheco,
Hip ultrasound for developmental dysplasia: the 50% rule
 Pediatr Radiol (2017) 47:817 821 DOI 10.1007/s00247-017-3802-4 COMMENTARY Hip ultrasound for developmental dysplasia: the 50% rule H. Theodore Harcke 1 & B. Pruszczynski 2 Received: 27 October 2016 /Revised:
Pediatr Radiol (2017) 47:817 821 DOI 10.1007/s00247-017-3802-4 COMMENTARY Hip ultrasound for developmental dysplasia: the 50% rule H. Theodore Harcke 1 & B. Pruszczynski 2 Received: 27 October 2016 /Revised:
The Factor Causing Poor Results in Late Developmental Dysplasia of the Hip (DDH)
 The Factor Causing Poor Results in Late Developmental Dysplasia of the Hip (DDH) Perajit Eamsobhana MD*, Kamwong Saisamorn MD*, Tanatip Sisuchinthara MS* Thunchanok Jittivilai PN*, Kamolporn Keawpornsawan
The Factor Causing Poor Results in Late Developmental Dysplasia of the Hip (DDH) Perajit Eamsobhana MD*, Kamwong Saisamorn MD*, Tanatip Sisuchinthara MS* Thunchanok Jittivilai PN*, Kamolporn Keawpornsawan
DDH New Developments and Timeless Classics. DDH Define Treatment Group. (by age) DDH Imaging Choice in 6wk old Infant?
 The 59 th Annual Edward T. Smith Orthopaedic Lectureship Emerging Concepts in the Surgical Management of the Hip: Deformity, Impingement and Fracture DDH New Developments and Timeless Classics Perry L.
The 59 th Annual Edward T. Smith Orthopaedic Lectureship Emerging Concepts in the Surgical Management of the Hip: Deformity, Impingement and Fracture DDH New Developments and Timeless Classics Perry L.
The Pavlik harness is a positioning device commonly
 RESEARCH PAPERS Ultrasound Evaluation of Hip Position in the Pavlik Harness Leslie E. Grissom, MD*, H. Theodore Harcke, MD*, S. Jay Kumar, MOt, George S. Bassett, MOt, G. Dean MacEwen, MOt Fifty infants
RESEARCH PAPERS Ultrasound Evaluation of Hip Position in the Pavlik Harness Leslie E. Grissom, MD*, H. Theodore Harcke, MD*, S. Jay Kumar, MOt, George S. Bassett, MOt, G. Dean MacEwen, MOt Fifty infants
Congenital Dislocation Of The Hip In Newborns Of Mashhad City
 ISPUB.COM The Internet Journal of Pediatrics and Neonatology Volume 4 Number 1 Congenital Dislocation Of The Hip In Newborns Of Mashhad City G Mamouri, F Khatami, A Hamedi Citation G Mamouri, F Khatami,
ISPUB.COM The Internet Journal of Pediatrics and Neonatology Volume 4 Number 1 Congenital Dislocation Of The Hip In Newborns Of Mashhad City G Mamouri, F Khatami, A Hamedi Citation G Mamouri, F Khatami,
Hip Joint DX 612 Orthopedics and Neurology
 Hip Joint DX 612 Orthopedics and Neurology James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Hip Anatomy Palpation Point tenderness Edema Symmetry Hip ROM Hip Contracture
Hip Joint DX 612 Orthopedics and Neurology James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Hip Anatomy Palpation Point tenderness Edema Symmetry Hip ROM Hip Contracture
Hip Anatomy. Hip Joint DX 612 Orthopedics and Neurology. Hip ROM. Palpation
 Hip Joint DX 612 Orthopedics and Neurology Hip Anatomy James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Palpation Hip ROM Point tenderness Edema Symmetry Hip Contracture
Hip Joint DX 612 Orthopedics and Neurology Hip Anatomy James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Palpation Hip ROM Point tenderness Edema Symmetry Hip Contracture
TREATMENT OF DEVELOPMENTAL DISLOCATION OF THE HIP IN CHILDREN AFTER WALKING AGE
 TREATMENT OF DEVELOPMENTAL DISLOCATION OF THE HIP IN CHILDREN AFTER WALKING AGE INDICATIONS FROM TWO-DIRECTIONAL ARTHROGRAPHY SHIGERU MITANI, YOICHI NAKATSUKA, HIROFUMI AKAZAWA, KIYOSHI AOKI, HAJIME INOUE
TREATMENT OF DEVELOPMENTAL DISLOCATION OF THE HIP IN CHILDREN AFTER WALKING AGE INDICATIONS FROM TWO-DIRECTIONAL ARTHROGRAPHY SHIGERU MITANI, YOICHI NAKATSUKA, HIROFUMI AKAZAWA, KIYOSHI AOKI, HAJIME INOUE
Pediatric Orthopedics: ``To Refer or Not to Refer``
 Pediatric Orthopedics: ``To Refer or Not to Refer`` Thierry E. Benaroch, MD, FRCS(C) McGill University Health Centre Intoeing Knock knees Bowlegs Flatfeet Toe walking Knee pain Hip click Intoeing Objectives
Pediatric Orthopedics: ``To Refer or Not to Refer`` Thierry E. Benaroch, MD, FRCS(C) McGill University Health Centre Intoeing Knock knees Bowlegs Flatfeet Toe walking Knee pain Hip click Intoeing Objectives
Reduction of a dislocation of the hip due to developmental dysplasia: Implications for the need for future surgery
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2-1-2003 Reduction of a dislocation of the hip due to developmental dysplasia: Implications for the need for future
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2-1-2003 Reduction of a dislocation of the hip due to developmental dysplasia: Implications for the need for future
The surgical treatment of Perthes disease by
 Lateral shelf acetabuloplasty in Perthes disease A REVIEW AT THE END OF GROWTH K. Daly, C. Bruce, A. Catterall From the Royal National Orthopaedic Hospital, Stanmore, England The surgical treatment of
Lateral shelf acetabuloplasty in Perthes disease A REVIEW AT THE END OF GROWTH K. Daly, C. Bruce, A. Catterall From the Royal National Orthopaedic Hospital, Stanmore, England The surgical treatment of
Popliteal angle as an indicator for successful closed reduction of developmental dysplasia of the hip.
 Popliteal angle as an indicator for successful closed reduction of developmental dysplasia of the hip. Item Type Article Authors Molony, Diarmuid C;Harty, James A;Burke, Thomas E;D'Souza, Lester G Citation
Popliteal angle as an indicator for successful closed reduction of developmental dysplasia of the hip. Item Type Article Authors Molony, Diarmuid C;Harty, James A;Burke, Thomas E;D'Souza, Lester G Citation
Significance of radiological appearance of ossific femoral nucleus in diagnosis of developmental hip dysplasia
 Significance of radiological appearance of ossific femoral nucleus in diagnosis of developmental hip dysplasia, MBChB, D Orth, MSc. Abstract: The aim of the study to determine the benefit of delaying appearance
Significance of radiological appearance of ossific femoral nucleus in diagnosis of developmental hip dysplasia, MBChB, D Orth, MSc. Abstract: The aim of the study to determine the benefit of delaying appearance
Effects of Immobilization. N24 Pedi Musculoskeletal Spring 2012, Week 14. Cabrillo ADN/C. Madsen RN, MSN 1. Physical effects on other systems
 Common Orthopedic Problems of Children Congenital Acquired Bones Neuromuscular Physical effects on other systems Pulmonary Cardiac Skin integrity Elimination GI GU 1 4 General Nursing Considerations any
Common Orthopedic Problems of Children Congenital Acquired Bones Neuromuscular Physical effects on other systems Pulmonary Cardiac Skin integrity Elimination GI GU 1 4 General Nursing Considerations any
HIP DYSPLASIA WITHOUT DISLOCATION IN ONE-YEAR-OLD BOYS
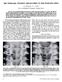 HIP DYSPLASIA WITHOUT DISLOCATION IN ONE-YEAR-OLD BOYS A. B. NEVELOS, p. R. J. BURCH From Leeds/Bradford Orthopaedic Training Schetne Six boys were examined during the second year of life, each with symptoms
HIP DYSPLASIA WITHOUT DISLOCATION IN ONE-YEAR-OLD BOYS A. B. NEVELOS, p. R. J. BURCH From Leeds/Bradford Orthopaedic Training Schetne Six boys were examined during the second year of life, each with symptoms
Improving early detection of developmental dysplasia of the hip through general practitioner assessment and surveillance
 Improving early detection of developmental dysplasia of the hip through general practitioner assessment and surveillance Nicole Williams This article is the third in a series on paediatric health. Articles
Improving early detection of developmental dysplasia of the hip through general practitioner assessment and surveillance Nicole Williams This article is the third in a series on paediatric health. Articles
Subsartorial Approach in Open Reduction of Developmental Dysplasia of Hip
 Med. J. Cairo Univ., Vol. 84, No. 2, March: 287-291, 2016 www.medicaljournalofcairouniversity.net Subsartorial Approach in Open Reduction of Developmental Dysplasia of Hip MOHAMED M. HEGAZY, M.D.; MOHAMED
Med. J. Cairo Univ., Vol. 84, No. 2, March: 287-291, 2016 www.medicaljournalofcairouniversity.net Subsartorial Approach in Open Reduction of Developmental Dysplasia of Hip MOHAMED M. HEGAZY, M.D.; MOHAMED
Surgical treatment of developmental dysplasia of the hip in the periadolescent period
 J Orthop Sci (2005) 10:15 21 DOI 10.1007/s00776-004-0850-z Original article Surgical treatment of developmental dysplasia of the hip in the periadolescent period Vasilios A. Papavasiliou 1 and Athanasios
J Orthop Sci (2005) 10:15 21 DOI 10.1007/s00776-004-0850-z Original article Surgical treatment of developmental dysplasia of the hip in the periadolescent period Vasilios A. Papavasiliou 1 and Athanasios
Ultrasonographic Findings in Developmental Dysplasia of the Hip in Infants
 DEVELOPMENTAL THE IRAQI POSTGRADUATE DYSPLASIA MEDICAL OF JOURNAL THE HIPIN INFANTS Ultrasonographic Findings in Developmental Dysplasia of the Hip in Infants Haider Qasim Hamood ABSTRACT: BACKGROUND:
DEVELOPMENTAL THE IRAQI POSTGRADUATE DYSPLASIA MEDICAL OF JOURNAL THE HIPIN INFANTS Ultrasonographic Findings in Developmental Dysplasia of the Hip in Infants Haider Qasim Hamood ABSTRACT: BACKGROUND:
Adolescent Hip Dysplasia
 Adolescent Hip Dysplasia The hip is a "ball-and-socket" joint. In a normal hip, the ball at the upper end of the femur (thighbone) fits firmly into the socket, which is a curved portion of the pelvis called
Adolescent Hip Dysplasia The hip is a "ball-and-socket" joint. In a normal hip, the ball at the upper end of the femur (thighbone) fits firmly into the socket, which is a curved portion of the pelvis called
Evaluation of the results of operative treatment of hip dysplasia in children after the walking age
 Alexandria Journal of Medicine (2012) 48, 115 122 Alexandria University Faculty of Medicine Alexandria Journal of Medicine www.sciencedirect.com ORIGINAL ARTICLE Evaluation of the results of operative
Alexandria Journal of Medicine (2012) 48, 115 122 Alexandria University Faculty of Medicine Alexandria Journal of Medicine www.sciencedirect.com ORIGINAL ARTICLE Evaluation of the results of operative
Screening for Developmental Dysplasia of the Hip: A Systematic Literature Review for the US Preventive Services Task Force
 REVIEW ARTICLE Screening for Developmental Dysplasia of the Hip: A Systematic Literature Review for the US Preventive Services Task Force Scott A. Shipman, MD, MPH a, Mark Helfand, MD, MPH b, Virginia
REVIEW ARTICLE Screening for Developmental Dysplasia of the Hip: A Systematic Literature Review for the US Preventive Services Task Force Scott A. Shipman, MD, MPH a, Mark Helfand, MD, MPH b, Virginia
Abstract. Introduction
 Outcome of Triple Procedure in Older Children with Developmental Dysplasia of Hip (DDH) Masood Umer, Haq Nawaz 2, Pashtoon Murtaza Kasi 2, Mahmood Ahmed 3, Syed Sohail Ali 2 Department of Surgery, Medical
Outcome of Triple Procedure in Older Children with Developmental Dysplasia of Hip (DDH) Masood Umer, Haq Nawaz 2, Pashtoon Murtaza Kasi 2, Mahmood Ahmed 3, Syed Sohail Ali 2 Department of Surgery, Medical
Ultrasound-guided gradual reduction using flexion and abduction continuous traction for developmental dysplasia of the hip
 K. Fukiage, T. Futami, Y. Ogi, Y. Harada, F. Shimozono, N. Kashiwagi, T. Takase, S. Suzuki From Shiga Medical Center for Children, Japan K. Fukiage, MD, PhD, Paediatric Orthopaedic Surgeon T. Futami, MD,
K. Fukiage, T. Futami, Y. Ogi, Y. Harada, F. Shimozono, N. Kashiwagi, T. Takase, S. Suzuki From Shiga Medical Center for Children, Japan K. Fukiage, MD, PhD, Paediatric Orthopaedic Surgeon T. Futami, MD,
Surgical Therapy for Congenital Dislocation of the Hip in Patients Who Are Twelve to Thirty-six Months Old
 Copyright 984 by The Journal of Bone and Joint Surgers. Incorporated Surgical Therapy for Congenital Dislocation of the Hip in Patients Who Are Twelve to Thirty-six Months Old BY MICHAEL E. BERKELEY, M.D.*,
Copyright 984 by The Journal of Bone and Joint Surgers. Incorporated Surgical Therapy for Congenital Dislocation of the Hip in Patients Who Are Twelve to Thirty-six Months Old BY MICHAEL E. BERKELEY, M.D.*,
After open reduction for developmental dysplasia of
 Test of stability as an aid to decide the need for osteotomy in association with open reduction in developmental dysplasia of the hip A LONG-TERM REVIEW H. G. Zadeh, A. Catterall, A. Hashemi-Nejad, R.
Test of stability as an aid to decide the need for osteotomy in association with open reduction in developmental dysplasia of the hip A LONG-TERM REVIEW H. G. Zadeh, A. Catterall, A. Hashemi-Nejad, R.
Orthopaedics Springer-Verlag 1987
 International Orthopaedics (SICOT) (1987) 11:83-87 International Orthopaedics Springer-Verlag 1987 The correlation of arthrography with the results of treatment in late diagnosed congenital dislocation
International Orthopaedics (SICOT) (1987) 11:83-87 International Orthopaedics Springer-Verlag 1987 The correlation of arthrography with the results of treatment in late diagnosed congenital dislocation
A LONG-TERM FOLLOW-UP OF CONGENITAL DISLOCATION OF THE HIP*
 A LONGTERM FOLLOWUP OF CONGENITAL DISLOCATION OF THE HIP* E. W. SOMERVILLE From The Nuffield Orthopaedic Centre, Oxford Drawing upon a total experience of 450 hips affected by established congenital dislocation
A LONGTERM FOLLOWUP OF CONGENITAL DISLOCATION OF THE HIP* E. W. SOMERVILLE From The Nuffield Orthopaedic Centre, Oxford Drawing upon a total experience of 450 hips affected by established congenital dislocation
Circles are Pointless - Angles in the assessment of adult hip dysplasia are not!
 Circles are Pointless - Angles in the assessment of adult hip dysplasia are not! Poster No.: C-1964 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit S. E. West, S. G. Cross, J. Adu,
Circles are Pointless - Angles in the assessment of adult hip dysplasia are not! Poster No.: C-1964 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit S. E. West, S. G. Cross, J. Adu,
The Hip from Cradle to Grave. Haemish Crawford Ascot Hospital Starship Children s Hospital
 The Hip from Cradle to Grave Haemish Crawford Ascot Hospital Starship Children s Hospital Developmental dysplasia hip DDH Irritable vs. septic hip Perthes disease Slipped Upper Femoral Epiphysis (SUFE)
The Hip from Cradle to Grave Haemish Crawford Ascot Hospital Starship Children s Hospital Developmental dysplasia hip DDH Irritable vs. septic hip Perthes disease Slipped Upper Femoral Epiphysis (SUFE)
The surgical treatment of developmental dislocation of the hip in older children : A comparative study
 Acta Orthop. Belg., 2005, 71, 678-685 ORIGINAL STUDY The surgical treatment of developmental dislocation of the hip in older children : A comparative study Gunduz TEZEREN, Mehmet TUKENMEZ, Okay BULUT,
Acta Orthop. Belg., 2005, 71, 678-685 ORIGINAL STUDY The surgical treatment of developmental dislocation of the hip in older children : A comparative study Gunduz TEZEREN, Mehmet TUKENMEZ, Okay BULUT,
Disparity between Clinical and Ultrasound Examinations in Neonatal Hip Screening
 Original Article Clinics in Orthopedic Surgery 2016;8:203-209 http://dx.doi.org/10.4055/cios.2016.8.2.203 Disparity between Clinical and Ultrasound Examinations in Neonatal Hip Screening Bong Soo Kyung,
Original Article Clinics in Orthopedic Surgery 2016;8:203-209 http://dx.doi.org/10.4055/cios.2016.8.2.203 Disparity between Clinical and Ultrasound Examinations in Neonatal Hip Screening Bong Soo Kyung,
DEVELOPMENTAL HIP DYSPLASIA PREDICTING OUTCOME AND IMPLICATIONS FOR SECONDARY PROCEDURES. Dr G B Firth
 DEVELOPMENTAL HIP DYSPLASIA PREDICTING OUTCOME AND IMPLICATIONS FOR SECONDARY PROCEDURES Dr G B Firth A research report submitted to the Faculty of Health Sciences, University of the Witwatersrand, Johannesburg,
DEVELOPMENTAL HIP DYSPLASIA PREDICTING OUTCOME AND IMPLICATIONS FOR SECONDARY PROCEDURES Dr G B Firth A research report submitted to the Faculty of Health Sciences, University of the Witwatersrand, Johannesburg,
AIUM Practice Guideline for the Performance of an Ultrasound Examination for Detection and Assessment of Developmental Dysplasia of the Hip
 AIUM Practice Guideline for the Performance of an Ultrasound Examination for Detection and Assessment of Developmental Dysplasia of the Hip 2008 by the American Institute of Ultrasound in Medicine The
AIUM Practice Guideline for the Performance of an Ultrasound Examination for Detection and Assessment of Developmental Dysplasia of the Hip 2008 by the American Institute of Ultrasound in Medicine The
Evaluation of the Results of Operative Treatment of Hip Dysplasia in Children after the walking age
 ORIGINAL ARTICLE Evaluation of the Results of Operative Treatment of Hip Dysplasia in Children after the walking age MUHAMMAD KAMRAN SIDDIQUI, MUHAMMAD KAMRAN SHAFI, BASHIR QAISRANI ABSTRACT Background:
ORIGINAL ARTICLE Evaluation of the Results of Operative Treatment of Hip Dysplasia in Children after the walking age MUHAMMAD KAMRAN SIDDIQUI, MUHAMMAD KAMRAN SHAFI, BASHIR QAISRANI ABSTRACT Background:
CliniCal Review what is developmental dysplasia of the hip? Fig 1 How common is it? SummaRy points what do we know about the causes?
 Clinical Review For the full versions of these articles see bmj.com Developmental dysplasia of the hip M D Sewell, 1 K Rosendahl, 2 D M Eastwood 1 2 1 Catterall Unit, Royal National Orthopaedic Hospital,
Clinical Review For the full versions of these articles see bmj.com Developmental dysplasia of the hip M D Sewell, 1 K Rosendahl, 2 D M Eastwood 1 2 1 Catterall Unit, Royal National Orthopaedic Hospital,
Success of Pavlik Harness Treatment Decreases in Patients C 4 Months and in Ultrasonographically Dislocated Hips in Developmental Dysplasia of the Hip
 Clin Orthop Relat Res (2016) 474:1146 1152 DOI 10.1007/s11999-015-4388-5 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons SYMPOSIUM: THE HIP FROM CHILDHOOD
Clin Orthop Relat Res (2016) 474:1146 1152 DOI 10.1007/s11999-015-4388-5 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons SYMPOSIUM: THE HIP FROM CHILDHOOD
A comparison of ultrasonography and radiography in the management of infants with suspected developmental dysplasia of the hip
 Acta Orthop. Belg., 2013, 79, 524-529 ORIGINAL STUDY A comparison of ultrasonography and radiography in the management of infants with suspected developmental dysplasia of the hip Hakan Atalar, Halil Dogruel,
Acta Orthop. Belg., 2013, 79, 524-529 ORIGINAL STUDY A comparison of ultrasonography and radiography in the management of infants with suspected developmental dysplasia of the hip Hakan Atalar, Halil Dogruel,
Results of Surgical Treatment of Coxa Vara in Children: Valgus Osteotomy with Angle Blade Plate Fixation
 Results of Surgical Treatment of Coxa Vara in Children: Valgus Osteotomy with Angle Blade Plate Fixation Chatupon Chotigavanichaya MD*, Duangjai Leeprakobboon MD*, Perajit Eamsobhana MD*, Kamolporn Kaewpornsawan
Results of Surgical Treatment of Coxa Vara in Children: Valgus Osteotomy with Angle Blade Plate Fixation Chatupon Chotigavanichaya MD*, Duangjai Leeprakobboon MD*, Perajit Eamsobhana MD*, Kamolporn Kaewpornsawan
Characterization of Developmental Hip Dysplasia in Saudi infants using Ultrasonography
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 7 Ver. 3 (July. 2018), PP 60-64 www.iosrjournals.org Characterization of Developmental Hip
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 7 Ver. 3 (July. 2018), PP 60-64 www.iosrjournals.org Characterization of Developmental Hip
REDISLOCATION FOLLOWING OPERATIONS TO REDUCE HIP OR TREATING DYSPLASIA IN DEVELOPMENTAL DYSPLASIA OF THE HIP
 Original Article REDISLOCATION FOLLOWING OPERATIONS TO REDUCE HIP OR TREATING DYSPLASIA IN DEVELOPMENTAL DYSPLASIA OF THE HIP Saeid Tabatabaei 1, Ahmad Dashtbozorg 2, Sharareh Shalamzari 3 ABSTRACT Objectives:
Original Article REDISLOCATION FOLLOWING OPERATIONS TO REDUCE HIP OR TREATING DYSPLASIA IN DEVELOPMENTAL DYSPLASIA OF THE HIP Saeid Tabatabaei 1, Ahmad Dashtbozorg 2, Sharareh Shalamzari 3 ABSTRACT Objectives:
Mohamed El-Sayed Tarek Ahmed Sameh Fathy Hosam Zyton. Introduction
 J Child Orthop (2012) 6:471 477 DOI 10.1007/s11832-012-0451-x ORIGINAL CLINICAL ARTICLE The effect of Dega acetabuloplasty and Salter innominate on acetabular remodeling monitored by the acetabular index
J Child Orthop (2012) 6:471 477 DOI 10.1007/s11832-012-0451-x ORIGINAL CLINICAL ARTICLE The effect of Dega acetabuloplasty and Salter innominate on acetabular remodeling monitored by the acetabular index
PAEDIATRIC ORTHOPAEDICS BRENT WEATHERHEAD, MD, FRCSC PAEDIATRIC ORTHOPAEDIC SURGEON MEDICAL DIRECTOR, REBALANCE
 PAEDIATRIC ORTHOPAEDICS BRENT WEATHERHEAD, MD, FRCSC PAEDIATRIC ORTHOPAEDIC SURGEON MEDICAL DIRECTOR, REBALANCE DISCLOSURES I HAVE NO INDUSTRY CONFLICTS TO DECLARE I AM AN ORTHOPAEDIC SURGEON TRAINED IN
PAEDIATRIC ORTHOPAEDICS BRENT WEATHERHEAD, MD, FRCSC PAEDIATRIC ORTHOPAEDIC SURGEON MEDICAL DIRECTOR, REBALANCE DISCLOSURES I HAVE NO INDUSTRY CONFLICTS TO DECLARE I AM AN ORTHOPAEDIC SURGEON TRAINED IN
Developmental dysplasia of the hip
 Developmental dysplasia of the hip Shahryar Noordin, Masood Umer, Kamran Hafeez, Haq Nawaz Section of Orthopedics, Dept. of Surgery, Aga Khan University, Karachi, Pakistan Abstract Developmental dysplasia
Developmental dysplasia of the hip Shahryar Noordin, Masood Umer, Kamran Hafeez, Haq Nawaz Section of Orthopedics, Dept. of Surgery, Aga Khan University, Karachi, Pakistan Abstract Developmental dysplasia
The most relevant diagnostic criteria for developmental dysplasia of the hip: a study of British specialists
 Williams et al. BMC Musculoskeletal Disorders (2016) 17:38 DOI 10.1186/s12891-016-0867-4 RESEARCH ARTICLE Open Access The most relevant diagnostic criteria for developmental dysplasia of the hip: a study
Williams et al. BMC Musculoskeletal Disorders (2016) 17:38 DOI 10.1186/s12891-016-0867-4 RESEARCH ARTICLE Open Access The most relevant diagnostic criteria for developmental dysplasia of the hip: a study
Developmental dysplasia of the hip angle trends after operation in different age groups
 Clinical research Developmental dysplasia of the hip angle trends after operation in different age groups Sonja Milasinovic 1, Radivoj Brdar 2, Ivana Petronic 3, Dejan Nikolic 3, Dragana Cirovic 3 1Institute
Clinical research Developmental dysplasia of the hip angle trends after operation in different age groups Sonja Milasinovic 1, Radivoj Brdar 2, Ivana Petronic 3, Dejan Nikolic 3, Dragana Cirovic 3 1Institute
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and
 This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
