Reflection. Constrained Liner
|
|
|
- Clement Cain
- 5 years ago
- Views:
Transcription
1 Reflection Constrained Liner S u r g i c a l T e c h n i q u e S M I T H & N E P H E W
2
3 R EFLECTION C ONSTRAINED L INER S URGICAL T ECHNIQUE Produced in conjunction with: Robert Barrack, M.D., Ph.D., Tulane University School of Medicine, New Orleans, Louisiana Robert Bourne, M.D., F.R.C.S.(C), Chief of Orthopedics, London Health Sciences Centre, London, Ontario, Canada Cecil Rorabeck, M.D., F.R.C.S.(C), University of Western Ontario, London, Ontario, Canada Michael Ries, M.D., Ph.D., Professor, Chief of Arthoplasty, Department of Orthopaedics University of California at San Francisco Todd Swanson, M.D., Desert Orthopedic Center, Las Vegas, Nevada Introduction The Reflection Microstable liner locking mechanism is a robust design that allows easy liner insertion and removal, and outstanding liner/shell stability. With the addition of an adapter ring, the Reflection shell provides the pull-out strength necessary for constrained liner applications. The adapter ring is a three-piece construct packaged assembled on a Y- shaped holder that helps align the rings when being impacted into the shell. The constrained liner is made of conventional, non-irradiated UHMWPE to retain the polyethylene material properties. The liner provides 4mm of lateralization. The design of constrained liners involves a trade-off between head lever-out resistance and ROM. Typically, the higher the lever-out resistance, the smaller the ROM the device can achieve. The Reflection constrained liner was optimized to balance range of motion requirements with increased resistance to head lever-out. The head lever-out of at least 270 inch-pounds for a 28mm head, is approximately 80% greater than a constrained device with multiple cases of re-dislocation reported in the literature and comparable to the smaller size tripolar constrained liners which have few reported re-dislocations. The adapter/liner assembly resists liner lever-out to levels of over 1300 inch-pounds. This is higher than all measurable lever-out loads of standard liners reported by Greenwald, et al, in the AAOS 1996 scientific exhibit. Combined with Smith & Nephew circulo-trapezoidal neck, 87 o of motion is achieved with a 28mm head. This exceeds reported measrurements with a commonly used tripolar design. Using the constrained liner in combination with a skirted head is not recommended. Skirted heads may reduce prosthetic ROM to clinically unacceptable levels. Nota Bene: The technique description herein is made available to the healthcare professional to illustrate the authors suggested treatment for the uncomplicated procedure. In the final analysis, the preferred treatment is that which addresses the needs of the patient.
4 R EFLECTION C ONSTRAINED L INER S URGICAL T ECHNIQUE Surgical Technique Constrained liners should be used only as a last resort, and only when all other available options to avoid dislocations have been exhausted. Such options include, but are not limited to, reorienting or using a different liner option (e.g. lateralized, anteverted etc), using a prosthesis with a larger head diameter, a stem with increased offset, or a head with increased length. Shell preparation When inserting a new Reflection shell: Prepare the acetabulum and insert the shell per respective surgical technique. The use of pegs or screws is recommended. For a Reflection liner revision: Remove the existing liner using the liner removal tool. Remove the apex hole cover using a screwdriver 1. Insert the appropriately sized Constrained Liner Adapter into the shell. The adapter should be placed into the liner lock mechanism. For ease of insertion and visual check, place the open end of the adapter rings over the removal slot on the shell or where best visibility of opening is possible. 2. Insert the Alignment rod through the center of the adapter and screw into the apex hole in the shell. This may be performed by hand or using any of the standard Reflection 3.5mm hex screwdrivers. 4
5 R EFLECTION C ONSTRAINED L INER S URGICAL T ECHNIQUE 3. Select the respectively sized impactor and slide it over the end of the alignment rod. Place the legs of the impactor between the arms of the plastic holder of the adapter (see picture). Use a mallet to strike the platform on the impactor. When impacted sufficiently, the adapter device will be locked into the shell. When the ring is locked in place, the plastic holder is loose, and can be easily pulled from the adapter rings. If the plastic adapter is not loose, strike the impactor again and repeat check. 4. Remove the plastic holder. This piece is disposable. At this point, the apex hole cover may be inserted into the shell. 5. Insert the liner into the shell. Rotating the liner may be necessary to match up the anti-ratation splines of the liner with the inner adapter ring. When liner has been pushed as far as possible into the shell by hand, use the liner impactor tool to seat completely. After liner is assembled, visually check the liner lock ring to see if it has closed back together. 5
6 R EFLECTION C ONSTRAINED L INER S URGICAL T ECHNIQUE 6. Place the retainer ring over the head of the femoral implant with the "tabs" facing away from the femur. Reduce the femoral implant head into the opening of the acetabular liner. Rotate the femur to check mobility of the head in the liner. After the head is in the liner, position the retainer ring tabs into the mating slots on the liner face. To find the slots, place the tabs onto the groove in the face and rotate the ring until they drop in the slots. 7. Once all tabs are started into the slots, push the retainer ring down until the tabs are seated fully. To seat all the way, the use of the horseshoe shaped retainer impactor may be desired. Place the retainer impactor around the neck of the femoral component and push on the retainer ring, using a mallet if needed. Use of other tools to push the impactor ring could cause damage, which could lead to ring fracture. 6
7 R EFLECTION C ONSTRAINED L INER S URGICAL T ECHNIQUE Finished Assembly A B C Adapter Ring Assembly A. Split Ring B. Inner Adapter Ring C. Liner Lock Ring Liner Assembly D. Liner E. Constraining Ring F. Retaining Ring D E F 7
8 Catalog Information Implants Part No.Description Reflection Constrained Liner 0 Degree Reflection Constrained Liner 0 Degree Reflection Constrained Liner 0 Degree Reflection Constrained Liner 0 Degree Reflection Constrained Liner 0 Degree Reflection Constrained Liner Adapter Reflection Constrained Liner Adapter Reflection Constrained Liner Adapter Reflection Constrained Liner Adapter Reflection Constrained Liner Adapter Instruments Part No.Description Constrained Liner Alignment Rod Constrained Liner Retaining Ring Pusher Constrained Liner Lock Ring Retractor Constrained Liner Impactor Constrained Liner Impactor Constrained Liner Impactor Constrained Liner Impactor Constrained Liner Impactor Constrained Liner Impactor Constrained Liner Impactor Constrained Liner Instrument Tray
9 IMPORTANT MEDICAL INFORMATION Warnings and Precautions Reflection Constrained Liner Acetabular System IMPORTANT NOTE The Reflection Constrained Liner Acetabular System is designed for those total hip replacement patients who suffer from or are at risk for recurrent dislocations. The Reflection Constrained Liner Acetabular System will not restore function to the level expected with a normal healthy joint, and the patient should be instructed as to the limitations of the device. The range of motion achievable with a constrained liner is less than the range of motion of a normal joint, and less than with a semi-constrained prosthesis. The patient should be told that, although the constrained hip liner provides resistance to dislocation, it can dislocate if subjected to excessive loading. Once dislocated, additional surgery will be required to reduce the joint. Patients should also be instructed that significant reduction in the range of motion is inherent to the design characteristic of a constrained acetabular liner, and activities that may force the joint to exceed those range of motion limits should be avoided. MATERIALS Acetabular shells and locking rings are manufactured from titanium alloy (Ti-6Al-4V). The acetabular liner and poly ring are manufactured from ultra high molecular weight polyethylene (UHMWPE). The adapter holder is manufactured from copolymer acetal resin. Some of the alloys needed to produce orthopedic implants contain some metallic components that may be carcinogenic in tissue cultures or intact organism under very unique circumstances. Questions have been raised in the scientific literature as to whether or not these alloys may be carcinogenic in implant recipients. Studies conducted to evaluate this issue have not identified conclusive evidence of such phenomenon, in spite of the millions of implants in use. DESCRIPTION OF SYSTEM The Reflection Constrained Liner and Shell Construct is a multi-piece component made up of any Reflection Shell, the Constrained Liner Adapter and the Constrained Liner Construct. The Constrained Liner Adapter includes a plastic holder (disposed after adapter insertion) and locking rings that are inserted into the shell so that the shell can be used with the Constrained Liner. The Constrained Liner Construct includes the liner, poly ring and retaining ring. Therefore, the entire implanted Reflection Constrained Shell and Liner Construct includes the following: metal shell with locking rings in place and the liner, poly ring and retaining ring. The Constrained Liner may be used with previously implanted femoral stems, femoral heads and acetabular shells as in a revision case, or it may be used in primary cases and implanted along with the shell, head and stem. Any Reflection shell may be utilized, provided it will accept a 28 mm metal femoral head. The Constrained Liner should not be used with ceramic femoral heads or skirted femoral heads of any material. All implantable devices are designed for single use only. Please see the package insert for the femoral stems and femoral heads for Warnings and Precautions for these devices. INDICATIONS, CONTRAINDICATIONS, AND ADVERSE EFFECTS The Reflection Constrained Liner Acetabular System is a cemented or uncemented prosthesis intended to replace a hip joint. The Constrained Liner is intended for primary or revision patients at high risk for hip dislocation due to a history of prior dislocation, bone loss, soft tissue laxity, neuromuscular disease, or intra-operative instability and for whom all other options to constrained acetabular components have been considered. Contraindications 1. Conditions that would eliminate or tend to eliminate adequate implant support or prevent the use of an appropriately- sized implant, e.g.: a. blood supply limitations; b. insufficient quantity or quality of bone support, e.g., osteoporosis, or metabolic disorders which may impair bone formation, and osteomalacia; and c. infections or other conditions which lead to increased bone resorption. 2. Mental or neurological conditions which tend to impair the patient s ability or willingness to restrict activities. 3. Physical conditions or activities which tend to place extreme loads on implants, e.g., Charcot joints, muscle deficiencies, multiple joint disabilities, etc. 4. Skeletal immaturity. Contraindications may be relative or absolute and must be carefully weighted against the patient s entire evaluation and the prognosis for possible alternative procedures such as non-operative treatment, arthrodesis, femoral osteotomy, pelvic osteotomy, resection arthroplasty, hemiarthroplasty and others. Conditions presenting increased risk of failure include: osteoporosis, metabolic disorders which may impair bone formation, and osteomalacia. Possible Adverse Effects 1. Wear of the polyethylene articulating surfaces of acetabular components may occur. Higher rates of wear may be initiated by the presence of particles of cement, metal, or other debris which can develop during or as a result of the surgical procedure and cause abrasion of the articulating surfaces. Higher rates of wear may shorten the useful life of the prosthesis, and lead to early revision surgery to replace the worn prosthetic components. 2. With all joint replacements, asymptomatic, localized, progressive bone resorption (osteolysis) may occur around the prosthetic components as a consequence of foreign-body reaction to particu late wear debris. Particles are generated by interaction between components, as well as between the components and bone, primarily through wear mechanisms of adhesion, abrasion, and fatigue. Secondarily, particles may also be generated by third-body particles lodged in the polyethylene articular surfaces. Osteolysis can lead to future complications necessitating the removal or replacement of prosthetic components. 3. Loosening, bending, cracking, or fracture of implant components may result from failure to observe the Warnings and Precautions that follow. Fracture of the implant can occur as a result of trauma, strenuous activity, improper alignment, or duration of service. 4. Dislocation or fracture of the locking ring may occur and may increase the risk for device dislocation. Periodic x-rays are recommended for close comparison with immediate postoperative conditions to detect evidence of ring disassociation or fracture. With evidence of ring disassociation or fracture, patients should be closely observed, the possibilities of further deterioration evaluated, and the benefits of early revision considered. In addition, the patient should be advised that ring disassociation or fracture may require additional surgery.
10 5. Dislocations, subluxation, decreased range of motion, or lengthening or shortening of the femur caused by improper neck selection, positioning, looseness of acetabular or femoral components, extraneous bone, penetration of the femoral prosthesis through the shaft of the femur, fracture of the acetabulum, intrapelvic protrusion of acetabular component, femoral impingement, periarticular calcification, and/or excessive reaming. 6. Fracture of the pelvis or femur: post-operative pelvic fractures are usually stress fractures. Femoral fractures are often caused by defects in the femoral cortex due to misdirected reaming, etc. Intraoperative fractures are usually associated with old congenital deformity, improper stem selection, improper broaching, and/or severe osteoporosis. 7. Infection, both acute post-operative wound infection and late deep wound sepsis. 8. Neuropathies; femoral, sciatic, peroneal nerve, and lateral femoral cutaneous neuropathies have been reported. Temporary or permanent nerve damage resulting in pain or numbness of the affected limb. 9. Wound hematoma, thromboembolic disease including venous thrombosis, pulmonary embolus, or myocardial infarction. 10. Myositis ossificans, especially in males with hypertrophic arthritis, limited pre-operative range of motion and/or previous myositis. Also, periarticular calcification with or without impediment to joint mobility can cause decreased range of motion. 11. Trochanteric nonunion usually associated with early weight bearing and/or improper fixation of the trochanter, when a transtrochanteric surgical approach is used. 12. Although rare, metal sensitivity reactions and/or allergic reactions to foreign materials have been reported in patients following joint replacement. 13. Damage to blood vessels. 14. Traumatic arthrosis of the knee from intraoperative positioning of the extremity. 15. Delayed wound healing. 16. Aggravated problems of the affected limb or contralateral extremity caused by leg length discrepancy, excess femoral medialization, or muscle deficiency. 17. Failure of the porous coating/ substrate interface or hydroxylapatite coating/ porous coating bonding may result in bead separation delamination. 18. Stem migration or subsidence has occurred in conjunction with compaction grafting procedures usually resulting from insufficient graft material or improper cement techniques. Varus stem alignment may also be responsible. WARNINGS AND PRECAUTIONS The patient should be warned of surgical risks, and made aware of possible adverse effects including the risk of ring failure and device dislocations. The patient should be warned that the device does not replace normal healthy bone, that the implant can break or become damaged as a result of strenuous activity or trauma, and that it has a finite expected service life and may need to be replaced in the future. Do not mix components from different manufacturers. Additional Warnings and Precautions may be included in component literature. Preoperative 1. Use extreme care in handling and storage of implant components. Cutting, bending, or scratching the surface of components can significantly reduce the strength, fatigue resistance, and/or wear characteristics of the implant system. These, in turn, may induce internal stresses that are not obvious to the eye and may lead to fracture of the component. Implants and instruments should be protected from corrosive environments such as salt air during storage. Do not allow the porous surfaces to come in contact with cloth or other fiber-releasing materials. 2. Allergies and other reactions to device materials, although infrequent, should be considered, tested for (if appropriate), and ruled out preoperatively. 3. Fixation and expected longevity of components expected to be left in place at revision surgery should be thoroughly assessed. 4. Surgical technique information is available upon request. The surgeon should be familiar with the technique. Refer to medical or manufacturer literature for specific product information. 5. Intraoperative fracture or breaking of instruments can occur. Instruments which have experienced extensive use or excessive force are susceptible to fracture. Instruments should be examined for wear, or damage, prior to surgery. Intraoperative 1. The general principles of patient selection and sound surgical judgment apply. The correct selection of the implant is extremely important. The appropriate type and size should be selected for patients with consideration of anatomical and biomechanical factors such as patient age and activity levels, weight, bone and muscle conditions, any prior surgery and anticipated future surgeries, etc. Generally, the largest cross-section component which will allow adequate bone support to be maintained is preferred. Failure to use the optimum-sized component may result in loosening, bending, cracking, or fracture of the component and/or bone. 2. Correct selection of the neck length and cup, and stem positioning, are important. Muscle looseness and/or malpositioning of components may result in loosening, subluxation, dislocation, and/or fracture of components. Increased neck length and varus positioning will increase stresses which must be borne by the stem. The component should be firmly seated with the component insertion instruments. 3. Care should be taken not to scratch, bend or cut implant components during surgery for the reasons stated in Number One of the Pre-Operative section of Warnings and Precautions. 4. When using modular heads with sleeves and extended liners with the Reflection Constrained System, use caution and consider component malposition, component placement, and the effect on range of motion. Malposition of the Constrained Acetabular Component may cause impingement, premature dislocation, and revision. 5. Use only Reflection Liners with Reflection Shells. 6. Take care, when positioning and drilling screw and peg holes, to avoid penetration of the inner cortex of the pelvis, penetration of the sciatic notch, or damage to vital neurovascular structures. Perforation of the pelvis with screws that are too long can rupture blood vessels causing the patient to hemorrhage. Do not place a screw in the center hole of the acetabular prosthesis. Placement of drills and screws in the anterior or medial portions of the prosthesis is associated with a high risk of potentially fatal vascular injury. Bone screws must be completely seated in the holes of the shell to allow proper locking for the acetabular component liner. If the tapered pegs need to be removed from the shell after impaction of the pegs, do not reuse the pegs or the peg shell holes. Use new pegs and different shell holes, or a new shell if necessary. 7. USE ONLY REFLECTION TITANIUM BONE SCREWS, UNI- VERSAL CANCELLOUS BONE SCREWS, TAPERED PEGS, AND HOLE COVERS with the Reflection Acetabular Component. The Reflection InterFit and the Reflection For Screws Only (FSO) shells accept Universal Cancellous, Reflection screws, and tapered screw-hole covers, not pegs. Tapered pegs can only be used with Reflection V Shells. The threaded center hole in Reflection Shells only accepts the threaded hole cover, not screws or pegs. The InterFit threaded hole cover is only for use with Reflection InterFit. The Reflection threaded hole cover can be used with both Reflection and InterFit shells. Refer to product literature for proper adjunctive fixation and hole cover usage.
11 8. Prior to seating modular components, surgical debris including tissue must be cleaned from the surfaces. Debris, including bone cement, may inhibit the component locking mechanism. If the shell is to be cemented in place, remove extraneous cement with a plastic sculps tool to ensure proper locking of the liner. During liner insertion, make sure soft tissue does not interfere with the shell/liner interface. Modular components must be assembled securely to prevent disassociation. Debris inhibits the proper fit and locking of modular components which may lead to early failure of the procedure. Failure to properly seat the acetabular liner into the shell can lead to disassociation of the liner from the shell. 9. Avoid repeated assembly and disassembly of the modular components which could compromise the critical locking action of the locking mechanism. 10. Care is to be taken to assure complete support of all parts of the device embedded in bone cement to prevent stress concentration which may lead to failure of the procedure. During curing of the cement, care should be taken to prevent movement of the implant components. 11. If the head is removed from a femoral component that will be left in place at revision surgery, a metal head must be used. 12. If components are to be left in place at revision surgery, they should first be thoroughly checked for signs of looseness, etc. and replaced if necessary. The head/neck component should be changed only when clinically necessary. 13. Once removed from the patient, implants previously implanted should never be reused, since internal stresses which are not visible may lead to early bending or fracture of these components. 14. With the congenitally dislocated hip, special care should be taken to prevent sciatic nerve palsy. Also, note that the femoral canal is often very small and straight and may require an extra-small straight femoral prosthesis; however, a regular-sized prosthesis should be used when possible. Note that the true acetabulum is rudimentary and shallow. A false acetabulum should not ordinarily be utilized as a cup placement site for anatomical and biomechanical reasons. 15. With rheumatoid arthritis, especially for those patients on steroids, bone may be extremely osteoporotic. Care should be taken to prevent excessive penetration of the acetabular floor or fracture of the medial acetabular wall, femur, or greater trochanter. 16. Revision procedures for previous arthroplasty, Girdlestone, etc., are technically demanding and difficult to exercise. Common errors include misplacement of the incision, inadequate exposure or mobilization of the femur, inadequate removal of ectopic bone, or improper positioning of components. Postoperative instability as well as excessive blood loss can result. In summary, increased operative time, blood loss, increased incidence of pulmonary embolus and wound hematoma can be expected with revision procedures. 17. Prior to closure, the surgical site should be thoroughly cleaned of cement, bone chips, ectopic bone, etc. Ectopic bone and/or bone spurs may lead to dislocation or painful or restricted motion. Range of motion should be thoroughly checked for early contact or instability. 18. Proper positioning of the components is important to minimize impingement which could lead to early failure, premature wear, and/or dislocation. 19. In order to minimize the risks of dislocation and loosening of the shell-acetabular bone or shell-bone cement interface that may occur when using a metallic shell intended for biological fixation or cemented use only, surgeons should consider providing immediate resistance to tensile forces between the metallic shell and the acetabular bone or bone cement interface through the use of orthopedic bone fixation devices such as bone screws, spikes, screw threads, fins, or other bone fixation devices. 20. To correctly position the metallic locking ring that is a part of the Constrained Liner assembly, surgeons should consult the Reflection Constrained Liner System surgical technique for appropriate device assembly. Postoperative 1. Postoperative directions and warnings to patients by physicians, and patient care, are extremely important. Gradual weight bearing is begun after surgery in ordinary total hip arthroplasty. However, with trochanter osteotomy or certain complex cases, weight-bearing status should be individualized with the non or partial weight-bearing period extended. 2. Patients should be warned against unassisted activity, particularly use of toilet facilities and other activities requiring excessive motion of the hip. 3. Use extreme care in patient handling. Support should be provided to the operative leg when moving the patient. While placing the patient on bedpans, changing dressings, and clothing, and similar activities, precautions should be taken to avoid placing excessive load on the operative part of the body. 4. Postoperative therapy should be structured to regain muscle strength around the hip and a gradual increase of activities. 5. Periodic x-rays are recommended for close comparison with immediate postoperative conditions to detect long-term evidence of changes in position, loosening, bending and/or cracking of components or bone loss. With evidence of these conditions, patients should be closely observed, the possibilities of further deterioration evaluated, and the benefits of early revision considered. 6. Prophylactic antibiotics should be recommended to the patient similar to those suggested by the American Heart Association for conditions or situations that may result in bacteremia. 7. If the Constrained Liner dislocates, closed reduction is not possible. Patients should be advised that if the Constrained Liner dislocates, additional surgery will be required. PACKAGING AND LABELING Components should only be accepted if received by the hospital or surgeon with the factory packaging and labeling intact. STERILIZATION/RESTERILIZATION Implants and the plastic adapter holder are supplied sterile and have been packaged in protective trays. Other instruments are supplied non-sterile and must be sterilized prior to use. Inspect packages for punctures or other damage prior to surgery. If the sterile barrier has been broken and the components have not contacted blood, the components may be resterilized using ethylene oxide gas. If the components have contacted blood, they may not be reused. The following parameters are recommended as starting points for cycle validation by the health care facility: Sterilant 100% EtO Temp. 131 F (55 o C) Humidity 40-80% (70% Target) Maximum Pressure 10 PSIA (689 millibar) Concentration 725 mg/l Exposure Time minutes Suggested initial starting point for aeration validation is 12 hours at 120 F (49 C) with power aeration. Consult aerator manufacturer for more specific instructions. INFORMATION For further information, please contact Customer Service at (800) for calls within the continental USA and (901) for all international calls. Smith & Nephew, Inc., Orthopaedic Division, 1450 Brooks Road, Memphis, Tennessee, U.S.A. Caution: Federal Law (USA) restricts this device to sale by or on the order of a physician. Trademark of Smith & Nephew, Reg. U.S. Pat. & Tm. Off Rev. A 12/02
12 Smith & Nephew, Inc Brooks Road Memphis, TN U.S.A. (901) For information: For orders and order inquiries: Reflection and Microstable are trademarks of Smith & Nephew, Inc Smith & Nephew, Inc. 01/03
REFLECTION Constrained Liner Introduction
 Surgical Technique REFLECTION Constrained Liner Introduction Surgical treatment of recurrent dislocation should be directed toward correction of any mechanical abnormalities. If dislocation is caused
Surgical Technique REFLECTION Constrained Liner Introduction Surgical treatment of recurrent dislocation should be directed toward correction of any mechanical abnormalities. If dislocation is caused
ESC. Enhanced Stability Liners. Design Rationale & Surgical Technique
 ESC Enhanced Stability Liners Design Rationale & Surgical Technique Choice Without Compromise DePuy Synthes PINNACLE Hip Solutions are designed with a wide range of acetabular cup options, biological and
ESC Enhanced Stability Liners Design Rationale & Surgical Technique Choice Without Compromise DePuy Synthes PINNACLE Hip Solutions are designed with a wide range of acetabular cup options, biological and
CAUTION Federal law (USA) restricts this device to sale, by or on the order of a physician.
 CAUTION Federal law (USA) restricts this device to sale, by or on the order of a physician. ENGLISH Mpact 3D Metal Implants and Augments 3D Metal INSTRUCTION FOR USE Important notice: the device(s) can
CAUTION Federal law (USA) restricts this device to sale, by or on the order of a physician. ENGLISH Mpact 3D Metal Implants and Augments 3D Metal INSTRUCTION FOR USE Important notice: the device(s) can
Duraloc CONSTRAINED LINER
 SURGICAL TECHNIQUE Duraloc CONSTRAINED LINER A COMPREHENSIVE ACETABULAR REVISION SYSTEM DURALOC CONSTRAINED LINER Introduction Dislocation is the most common postoperative complication in total hip reconstruction.
SURGICAL TECHNIQUE Duraloc CONSTRAINED LINER A COMPREHENSIVE ACETABULAR REVISION SYSTEM DURALOC CONSTRAINED LINER Introduction Dislocation is the most common postoperative complication in total hip reconstruction.
Reflection. Ceramic. Acetabular System
 S M I T H & N E P H E W Reflection Ceramic Acetabular System S U R G I C A L T E C H N I Q U E Ceramic Acetabular System Technique As described by James P. Waddell, M.D., F.R.C.S.(C) Toronto, Ontario,
S M I T H & N E P H E W Reflection Ceramic Acetabular System S U R G I C A L T E C H N I Q U E Ceramic Acetabular System Technique As described by James P. Waddell, M.D., F.R.C.S.(C) Toronto, Ontario,
Important notice: the device(s) can be prescribed and implanted only by a doctor legally authorized to perform this type of surgery.
 rev.10 CAUTION Federal law (USA) restricts this device to sale, by or on the order of a physician. ENGLISH - EVOLIS/GMK KNEE PROSTHESIS - INSTRUCTIONS FOR USE Important notice: the device(s) can be prescribed
rev.10 CAUTION Federal law (USA) restricts this device to sale, by or on the order of a physician. ENGLISH - EVOLIS/GMK KNEE PROSTHESIS - INSTRUCTIONS FOR USE Important notice: the device(s) can be prescribed
Enhanced Stability Constrained Liners. Design Rationale Surgical Technique
 Enhanced Stability Constrained Liners Design Rationale Surgical Technique The Pinnacle Acetabular Cup System was designed to maximize the number of options available to the surgeon, and provide those options
Enhanced Stability Constrained Liners Design Rationale Surgical Technique The Pinnacle Acetabular Cup System was designed to maximize the number of options available to the surgeon, and provide those options
Basic Steps. Ream to Size. Broach and Trial. Implant Stem
 E C H E L O N P R I M A R Y H I P S Y S T E M S U R G I C A L T E C H N I Q U E Basic Steps Ream to Size Broach and Trial Implant Stem Echelon Primary Hip System Surgical Technique Harry B. Skinner, M.D.,
E C H E L O N P R I M A R Y H I P S Y S T E M S U R G I C A L T E C H N I Q U E Basic Steps Ream to Size Broach and Trial Implant Stem Echelon Primary Hip System Surgical Technique Harry B. Skinner, M.D.,
REFLECTION I & V POROUS-COATED ACETABULAR COMPONENT SURGICAL TECHNIQUE
 S M I T H & N E P H E W REFLECTION I & V POROUS-COATED ACETABULAR COMPONENT SURGICAL TECHNIQUE REFLECTION I & V POROUS-COATED ACETABULAR COMPONENT designed in conjunction with Ramon B. Gustilo, M.D. Richard
S M I T H & N E P H E W REFLECTION I & V POROUS-COATED ACETABULAR COMPONENT SURGICAL TECHNIQUE REFLECTION I & V POROUS-COATED ACETABULAR COMPONENT designed in conjunction with Ramon B. Gustilo, M.D. Richard
Progeny Hip Stem. Surgical Protocol and Product Specifications
 Progeny Hip Stem Surgical Protocol and Product Specifications Progeny Hip Stem Introduction With emphasis on maximum stability and ease of use, the StelKast ProgenyTM Hip System provides the surgeon with
Progeny Hip Stem Surgical Protocol and Product Specifications Progeny Hip Stem Introduction With emphasis on maximum stability and ease of use, the StelKast ProgenyTM Hip System provides the surgeon with
SURGICAL TECHNIQUE COMPLETED IN CONJUNCTION WITH
 The Power Of Simplicity At Work. Conquest Fx SURGICAL TECHNIQUE TAPERED HIP SYSTEM SURGICAL TECHNIQUE COMPLETED IN CONJUNCTION WITH Peter Brooks, M.D. Cleveland, Ohio Wayne M. Goldstein, M.D. Chicago,
The Power Of Simplicity At Work. Conquest Fx SURGICAL TECHNIQUE TAPERED HIP SYSTEM SURGICAL TECHNIQUE COMPLETED IN CONJUNCTION WITH Peter Brooks, M.D. Cleveland, Ohio Wayne M. Goldstein, M.D. Chicago,
Document No Rev. B Pg. 1 of 5 Approvals / Date Title: INSTRUCTIONS FOR USE DJO SURGICAL MODULAR REVISION HIP SYSTEM AND ACETABULAR CAGE
 Document No. 0400-0205 Rev. B Pg. 1 of 5 Approvals / Date Title: INSTRUCTIONS FOR USE DJO SURGICAL MODULAR REVISION HIP SYSTEM AND ACETABULAR CAGE Revision ECO Date ECO Summary of Changes Deann Rector
Document No. 0400-0205 Rev. B Pg. 1 of 5 Approvals / Date Title: INSTRUCTIONS FOR USE DJO SURGICAL MODULAR REVISION HIP SYSTEM AND ACETABULAR CAGE Revision ECO Date ECO Summary of Changes Deann Rector
ContourTM ACETABULAR RINGS SURGICAL TECHNIQUE
 ContourTM ACETABULAR RINGS SURGICAL TECHNIQUE TM Contour ACETABULAR RINGS SURGICAL TECHNIQUE Technique described by Joseph Schatzker M.D., B.Sc. (Med.), FRCS (C) Allan E. Gross, M.D., FRCS (C) Contour
ContourTM ACETABULAR RINGS SURGICAL TECHNIQUE TM Contour ACETABULAR RINGS SURGICAL TECHNIQUE Technique described by Joseph Schatzker M.D., B.Sc. (Med.), FRCS (C) Allan E. Gross, M.D., FRCS (C) Contour
BASIS Femoral Implant System
 Surgical Technique BASIS Femoral Implant System Surgical Technique Contents Design Features...2 Short Technique...3 Catalog Information...6 Important Medical Information...8 Nota Bene: The technique description
Surgical Technique BASIS Femoral Implant System Surgical Technique Contents Design Features...2 Short Technique...3 Catalog Information...6 Important Medical Information...8 Nota Bene: The technique description
Surgical Technique. *smith&nephew REFLECTION Spiked Acetabular Components
 Surgical Technique *smith&nephew REFLECTION Spiked Acetabular Components Reflecting the Commitment to Low Wear Designed with fixation and surgical efficiency in mind, the REFLECTION Acetabular Cup system
Surgical Technique *smith&nephew REFLECTION Spiked Acetabular Components Reflecting the Commitment to Low Wear Designed with fixation and surgical efficiency in mind, the REFLECTION Acetabular Cup system
THE NATURAL FIT. Surgical Technique. Hip Knee Spine Navigation
 THE NATURAL FIT Surgical Technique Hip Knee Spine Navigation MiniMAX Surgical Technique Hip Knee Spine Navigation INTRODUCTION The MiniMAX TM is a cementless anatomic stem available in 9 right sizes and
THE NATURAL FIT Surgical Technique Hip Knee Spine Navigation MiniMAX Surgical Technique Hip Knee Spine Navigation INTRODUCTION The MiniMAX TM is a cementless anatomic stem available in 9 right sizes and
Design Rationale and Surgical Technique. *smith&nephew TANDEM. Bipolar and Unipolar Hip System
 Design Rationale and Surgical Technique *smith&nephew TANDEM Bipolar and Unipolar Hip System Maximizing performance from every angle Saving time in the operating room is one of the most valuable solutions
Design Rationale and Surgical Technique *smith&nephew TANDEM Bipolar and Unipolar Hip System Maximizing performance from every angle Saving time in the operating room is one of the most valuable solutions
Table of contents. Indications Preoperative planning Specifications Short Technique Posterior Approach... 8
 Surgical Technique Table of contents Indications... 3 Preoperative planning... 4 Specifications... 6 Short Technique Posterior Approach... 8 Short Technique Anterior Approach...10 Surgical Technique...12
Surgical Technique Table of contents Indications... 3 Preoperative planning... 4 Specifications... 6 Short Technique Posterior Approach... 8 Short Technique Anterior Approach...10 Surgical Technique...12
Basic Steps. Ream to Size. Broach and Trial. Implant Stem
 Surgical Technique Basic Steps Ream to Size Broach and Trial Implant Stem ECHELON Primary Hip System Surgical Technique Harry B. Skinner, M.D., Ph.D. Professor and Chairman Department of Orthopaedic Surgery
Surgical Technique Basic Steps Ream to Size Broach and Trial Implant Stem ECHELON Primary Hip System Surgical Technique Harry B. Skinner, M.D., Ph.D. Professor and Chairman Department of Orthopaedic Surgery
*smith&nephew CONTOUR
 Surgical Technique *smith&nephew CONTOUR Acetabular Rings CONTOUR Acetabular Rings Surgical technique completed in conjunction with Joseph Schatzker MD, BSc (Med.), FRCS (C) Allan E. Gross, MD, FRCS (C)
Surgical Technique *smith&nephew CONTOUR Acetabular Rings CONTOUR Acetabular Rings Surgical technique completed in conjunction with Joseph Schatzker MD, BSc (Med.), FRCS (C) Allan E. Gross, MD, FRCS (C)
ACETABULAR CUP SURGICAL TECHNIQUE
 ACETABULAR CUP SURGICAL TECHNIQUE ACETABULAR CUP DEVICE INDICATIONS FOR USE The ICONACY I-Hip total hip replacement is indicated for the following conditions: 1. A severely painful and/or disabled hip
ACETABULAR CUP SURGICAL TECHNIQUE ACETABULAR CUP DEVICE INDICATIONS FOR USE The ICONACY I-Hip total hip replacement is indicated for the following conditions: 1. A severely painful and/or disabled hip
Description Materials Indications Patient selection factors to be considered include: Contraindications Absolute contraindications include:
 Description The Patello-Femoral Wave Arthroplasty Systems incorporate a distal femoral trochlear surface articular component that mates to a taper post via a taper interlock, and an all-polyethylene patella
Description The Patello-Femoral Wave Arthroplasty Systems incorporate a distal femoral trochlear surface articular component that mates to a taper post via a taper interlock, and an all-polyethylene patella
28 Surgical Technique
 Surgical Technique 10 12 14 16 18 20 22 24 28 26 Technique described by James L. Guyton, MD Campbell Clinic Memphis, Tennessee James W. Harkess, MD Campbell Clinic Memphis, Tennessee David G. LaVelle,
Surgical Technique 10 12 14 16 18 20 22 24 28 26 Technique described by James L. Guyton, MD Campbell Clinic Memphis, Tennessee James W. Harkess, MD Campbell Clinic Memphis, Tennessee David G. LaVelle,
TC-PLUS Primary Knee IMPORTANT MEDICAL INFORMATION SPECIAL NOTE. This Package Insert is for product distributed in the US only.
 TC-PLUS Primary Knee IMPORTANT MEDICAL INFORMATION SPECIAL NOTE This Package Insert is for product distributed in the US only. The component material is provided on the outside carton label. Components
TC-PLUS Primary Knee IMPORTANT MEDICAL INFORMATION SPECIAL NOTE This Package Insert is for product distributed in the US only. The component material is provided on the outside carton label. Components
Echelon Reamer Chart. Porous Stem Reamer Chart. 260 mm. 190 mm. Bowed. Straight. Cemented Stem Reamer Chart. 175 mm 225 mm. 260 mm.
 E C H E L O N R E V I S I O N H I P S Y S T E M S U R G I C A L T E C H N I Q U E Echelon Reamer Chart Porous Stem Reamer Chart 260 mm 245 mm 230 mm 190 mm 175 mm 190 mm Straight 260 mm Bowed Cemented
E C H E L O N R E V I S I O N H I P S Y S T E M S U R G I C A L T E C H N I Q U E Echelon Reamer Chart Porous Stem Reamer Chart 260 mm 245 mm 230 mm 190 mm 175 mm 190 mm Straight 260 mm Bowed Cemented
- October 2013 English
 TOTAL HIP JOINT REPLACEMENT FOR CEMENTED APPLICATIONS FOR THE ATTENTION OF THE OPERATING SURGEON Total hip replacement provides the surgeon with a means of restoring mobility and reducing pain with the
TOTAL HIP JOINT REPLACEMENT FOR CEMENTED APPLICATIONS FOR THE ATTENTION OF THE OPERATING SURGEON Total hip replacement provides the surgeon with a means of restoring mobility and reducing pain with the
BIOLOX delta Option Ceramic Femoral Head System. Product Features and Instructions for Use
 BIOLOX delta Option Ceramic Femoral Head System Product Features and Instructions for Use Product Features BIOLOX delta ceramic heads are composed of 75% aluminum oxide and approximately 25% zirconia.
BIOLOX delta Option Ceramic Femoral Head System Product Features and Instructions for Use Product Features BIOLOX delta ceramic heads are composed of 75% aluminum oxide and approximately 25% zirconia.
CAUTION: Ceramic liners are not approved for use in the United States.
 Total Hip Prostheses, Self-Centering Hip Prostheses and Hemi-Hip Prostheses IMPORTANT: This essential product information sheet does not include all of the information necessary for selection and use of
Total Hip Prostheses, Self-Centering Hip Prostheses and Hemi-Hip Prostheses IMPORTANT: This essential product information sheet does not include all of the information necessary for selection and use of
SURGICAL TECHNIQUE CEMENTED & PRESS-FIT UNIFIED INSTRUMENTATION INTRAOPERATIVE FLEXIBILITY PROVEN BIOMECHANICS
 SURGICAL TECHNIQUE CEMENTED & PRESS-FIT UNIFIED INSTRUMENTATION INTRAOPERATIVE FLEXIBILITY PROVEN BIOMECHANICS INTRODUCTION The Summit Tapered Hip System s comprehensive set of implants and instruments
SURGICAL TECHNIQUE CEMENTED & PRESS-FIT UNIFIED INSTRUMENTATION INTRAOPERATIVE FLEXIBILITY PROVEN BIOMECHANICS INTRODUCTION The Summit Tapered Hip System s comprehensive set of implants and instruments
SURGICAL TECHNIQUE COMPLETED IN CONJUNCTION WITH
 T A P E R E D H I P S Y S T E M SURGICAL TECHNIQUE COMPLETED IN CONJUNCTION WITH Robert B. Bourne, M.D., F.R.C.S.(C) London, Ontario, Canada Professor Ernesto DeSantis Rome, Italy Wayne M. Goldstein, M.D.
T A P E R E D H I P S Y S T E M SURGICAL TECHNIQUE COMPLETED IN CONJUNCTION WITH Robert B. Bourne, M.D., F.R.C.S.(C) London, Ontario, Canada Professor Ernesto DeSantis Rome, Italy Wayne M. Goldstein, M.D.
Pinit Plate Small Bone Fusion System Bone Plate & Screw System
 Pinit Plate Small Bone Fusion System Bone Plate & Screw System Description The Pinit Plate Small Bone Fusion System consists of 2-hole bone plates made available in three length options and two thickness
Pinit Plate Small Bone Fusion System Bone Plate & Screw System Description The Pinit Plate Small Bone Fusion System consists of 2-hole bone plates made available in three length options and two thickness
Optimum implant geometry
 Surgical Technique Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Surgical Technique Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Clinical Evaluation Surgical Technique
 Clinical Evaluation Surgical Technique Table of Contents EMPERION Specifications 3 EMPERION Surgical Technique 9 EMPERION Catalog 18 Nota Bene: This technique description herein is made available to the
Clinical Evaluation Surgical Technique Table of Contents EMPERION Specifications 3 EMPERION Surgical Technique 9 EMPERION Catalog 18 Nota Bene: This technique description herein is made available to the
Surgical Technique. Cup System
 Surgical Technique Cup System INDICATIONS AND USAGE Indications for the use of the CS2 ACETABULAR CUP SYSTEM must be carefully considered with respect to the patient s entire evaluation and alternative
Surgical Technique Cup System INDICATIONS AND USAGE Indications for the use of the CS2 ACETABULAR CUP SYSTEM must be carefully considered with respect to the patient s entire evaluation and alternative
Surgical Technique SYNERGY Cementless Stem
 Surgical Technique SYNERGY Cementless Stem Comprehensive. Simple. Efficient. It s easy to understand why SYNERGY Hip System is one of orthopaedics great success stories. Its rapid adoption by surgeons
Surgical Technique SYNERGY Cementless Stem Comprehensive. Simple. Efficient. It s easy to understand why SYNERGY Hip System is one of orthopaedics great success stories. Its rapid adoption by surgeons
REPIPHYSIS LIMB SALVAGE SYSTEM
 REPIPHYSIS LIMB SALVAGE SYSTEM 150800-0 For additional information please contact the manufacturer or local distributor. M MicroPort Orthopedics Inc. 5677 Airline Rd Arlington, TN 38002 U.S.A. i Y October
REPIPHYSIS LIMB SALVAGE SYSTEM 150800-0 For additional information please contact the manufacturer or local distributor. M MicroPort Orthopedics Inc. 5677 Airline Rd Arlington, TN 38002 U.S.A. i Y October
WristMotion Wrist Hemiarthroplasty System Instructions for Use
 WristMotion Wrist Hemiarthroplasty System Instructions for Use Description The Arthrosurface WristMotion Wrist Hemiarthroplasty System consists of a contoured capitate articular implant designed to articulate
WristMotion Wrist Hemiarthroplasty System Instructions for Use Description The Arthrosurface WristMotion Wrist Hemiarthroplasty System consists of a contoured capitate articular implant designed to articulate
Positioning Sleeve Surgical Technique
 Positioning Sleeve Surgical Technique Surgical Technique The Comprehensive Fracture System offers a unique tool to evaluate and re-establish humeral height, which can be critical to restoring proper biomechanics
Positioning Sleeve Surgical Technique Surgical Technique The Comprehensive Fracture System offers a unique tool to evaluate and re-establish humeral height, which can be critical to restoring proper biomechanics
BIOLOX delta Option Ceramic Femoral Head System
 BIOLOX delta Option Ceramic Femoral Head System Product Features and Instructions for Use Knees Hips Extremities Cement and Accessories PMI Technology Product Features BIOLOX delta ceramic heads are composed
BIOLOX delta Option Ceramic Femoral Head System Product Features and Instructions for Use Knees Hips Extremities Cement and Accessories PMI Technology Product Features BIOLOX delta ceramic heads are composed
Technique Guide Small Bone Fusion System
 Technique Guide Small Bone Fusion System The Pinit Plate Small Bone Fusion System is a super low profile, modular bone plate and screw system designed to stabilize a bunionectomy with a medial to lateral
Technique Guide Small Bone Fusion System The Pinit Plate Small Bone Fusion System is a super low profile, modular bone plate and screw system designed to stabilize a bunionectomy with a medial to lateral
Talar Dome System Surgical Technique
 Talar Dome System Surgical Technique CAP TALAR DOME RESURFACING HEMIARTHROPLASTY IMPLANT Surgical Technique Guide Description The HemiCAP Contoured Articular Prosthetic incorporates an articular resurfacing
Talar Dome System Surgical Technique CAP TALAR DOME RESURFACING HEMIARTHROPLASTY IMPLANT Surgical Technique Guide Description The HemiCAP Contoured Articular Prosthetic incorporates an articular resurfacing
Hip Resurfacing System
 Hip Resurfacing System The Arthrosurface HemiCAP Hip Hemiarthroplasty System restores the articular surface geometry of the femoral head and preserves functional structures using an innovative 3 dimensional
Hip Resurfacing System The Arthrosurface HemiCAP Hip Hemiarthroplasty System restores the articular surface geometry of the femoral head and preserves functional structures using an innovative 3 dimensional
CONSENSUS ORTHOPEDICS INC. UNISYN HIP SYSTEM
 CONSENSUS ORTHOPEDICS INC. UNISYN HIP SYSTEM Instructions for Use (IFU) IMPORTANT INFORMATION FOR SURGEON: PLEASE READ PRIOR TO IMPLANTING THIS DEVICE IN A CLINICAL SETTING. THE SURGEON SHOULD BE FAMILIAR
CONSENSUS ORTHOPEDICS INC. UNISYN HIP SYSTEM Instructions for Use (IFU) IMPORTANT INFORMATION FOR SURGEON: PLEASE READ PRIOR TO IMPLANTING THIS DEVICE IN A CLINICAL SETTING. THE SURGEON SHOULD BE FAMILIAR
SURGICAL TECHNIQUE. Protrusio Cage A COMPREHENSIVE ACETABULAR REVISION SYSTEM
 SURGICAL TECHNIQUE Protrusio Cage A COMPREHENSIVE ACETABULAR REVISION SYSTEM Important: This essential product information does not include all of the information necessary for selection and use of a device.
SURGICAL TECHNIQUE Protrusio Cage A COMPREHENSIVE ACETABULAR REVISION SYSTEM Important: This essential product information does not include all of the information necessary for selection and use of a device.
ADDRESSING CLINICAL ISSUES OF CEMENTLESS HIP ARTHROPLASTY
 E C H E L O N P R I M A R Y H I P S Y S T E M P R O D U C T R A T I O N A L E ADDRESSING CLINICAL ISSUES OF CEMENTLESS HIP ARTHROPLASTY Echelon Primary Total Hip System HIGH OFFSET STANDARD OFFSET Cementless
E C H E L O N P R I M A R Y H I P S Y S T E M P R O D U C T R A T I O N A L E ADDRESSING CLINICAL ISSUES OF CEMENTLESS HIP ARTHROPLASTY Echelon Primary Total Hip System HIGH OFFSET STANDARD OFFSET Cementless
StelKast Acetabular. Surgical Protocol and Product Specifications. Including ProForm, Provident, Provident Apical Threaded Hole & Systems
 StelKast Acetabular Surgical Protocol and Product Specifications Including ProForm, Provident, Provident Apical Threaded Hole & Systems StelKast Acetabular Surgical Protocol Introduction StelKast offers
StelKast Acetabular Surgical Protocol and Product Specifications Including ProForm, Provident, Provident Apical Threaded Hole & Systems StelKast Acetabular Surgical Protocol Introduction StelKast offers
Lapidus Arthrodesis System Instructions for Use
 Lapidus Arthrodesis System Instructions for Use Description The AlignMATE Lapidus Arthrodesis System consists of bone plates and bone screws (locking, non-locking and interfragmentary), which are intended
Lapidus Arthrodesis System Instructions for Use Description The AlignMATE Lapidus Arthrodesis System consists of bone plates and bone screws (locking, non-locking and interfragmentary), which are intended
Technique Guide Hip Resurfacing System
 Technique Guide Hip Resurfacing System Approximately 5%-18% of all hip arthroplasties are completed on patients with a primary diagnosis of osteonecrosis. Patients are generally younger adults age 35 years
Technique Guide Hip Resurfacing System Approximately 5%-18% of all hip arthroplasties are completed on patients with a primary diagnosis of osteonecrosis. Patients are generally younger adults age 35 years
Ceramic Femoral Heads and Acetabular Cup Liners
 Important Information: Please read prior to use in a clinical setting. The Surgeon should be familiar with the operative technique. Caution: Federal (U.S.A) law restricts this device to sale by or on the
Important Information: Please read prior to use in a clinical setting. The Surgeon should be familiar with the operative technique. Caution: Federal (U.S.A) law restricts this device to sale by or on the
Cementless Tapered Femoral Stem Surgical technique
 Cementless Tapered Femoral Stem Surgical technique Contents Operative summary 4 Pre-operative planning 5 Femoral neck osteotomy 5 Femoral canal preparation 5 Intra-medullary (IM) reamer 6 Sequential rasping
Cementless Tapered Femoral Stem Surgical technique Contents Operative summary 4 Pre-operative planning 5 Femoral neck osteotomy 5 Femoral canal preparation 5 Intra-medullary (IM) reamer 6 Sequential rasping
Encina Taper Stem. Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA
 Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA 94065 info@stinsonortho.com www.stinsonortho.com Table of Contents Introduction 3 Features 4 Surgical Technique 5 Preoperative
Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA 94065 info@stinsonortho.com www.stinsonortho.com Table of Contents Introduction 3 Features 4 Surgical Technique 5 Preoperative
Optimizing function Maximizing survivorship Accelerating recovery
 Surgical Technique Optimizing Function Maximizing Survivorship Accelerating Recovery The company believes in an approach to patient treatment that places equal importance on: Optimizing function Maximizing
Surgical Technique Optimizing Function Maximizing Survivorship Accelerating Recovery The company believes in an approach to patient treatment that places equal importance on: Optimizing function Maximizing
CC TRIO VERSAFITCUP. Surgical Technique. each to their own. Hip Knee Spine Navigation
 VERSAFITCUP CC TRIO each to their own Surgical Technique Hip Knee Spine Navigation Versafitcup CC TRIO Surgical Technique Hip Knee Spine Navigation EACH TO THEIR OWN The Versafitcup CC Trio is a range
VERSAFITCUP CC TRIO each to their own Surgical Technique Hip Knee Spine Navigation Versafitcup CC TRIO Surgical Technique Hip Knee Spine Navigation EACH TO THEIR OWN The Versafitcup CC Trio is a range
TriboFit Hip System. Issue 3 - August 2013 English
 Important Information: Please read prior to use in a clinical setting. The surgeon should be familiar with the operative technique and all the information in this insert. Description: The TriboFit Hip
Important Information: Please read prior to use in a clinical setting. The surgeon should be familiar with the operative technique and all the information in this insert. Description: The TriboFit Hip
ECHELON Revision Hip System Surgical Technique
 Surgical Technique ECHELON Revision Hip System Surgical Technique Contents ECHELON Reamer Chart...2 Porous Implants...3 Cemented Implants...4 Porous-Coated Implant Specifications...5 Porous-Coated Implant
Surgical Technique ECHELON Revision Hip System Surgical Technique Contents ECHELON Reamer Chart...2 Porous Implants...3 Cemented Implants...4 Porous-Coated Implant Specifications...5 Porous-Coated Implant
Trilogy Acetabular System
 Trilogy Acetabular System Surgical Technique Versatility in a proven design Trilogy Acetabular System 1 Trilogy Acetabular System Surgical Technique Table of Contents Acetabular Reaming 2 Component Sizing
Trilogy Acetabular System Surgical Technique Versatility in a proven design Trilogy Acetabular System 1 Trilogy Acetabular System Surgical Technique Table of Contents Acetabular Reaming 2 Component Sizing
Longevity Offset and Oblique Liners. Surgical Technique
 Longevity Offset and Oblique Liners Surgical Technique Longevity Offset & Oblique Liners Surgical Technique 1 Introduction Complete Acetabular System Joint instability is an important issue in both primary
Longevity Offset and Oblique Liners Surgical Technique Longevity Offset & Oblique Liners Surgical Technique 1 Introduction Complete Acetabular System Joint instability is an important issue in both primary
Precautionary Statement ( )
 Precautionary Statement (21282008) Biomet Sports Medicine, Inc. 21282008 4861 E. Airport Dr. Rev. A Ontario, CA 91761 Date: 06/07 Sleeve and Button Soft Tissue Devices Utilizing ZipLoop Technology ATTENTION
Precautionary Statement (21282008) Biomet Sports Medicine, Inc. 21282008 4861 E. Airport Dr. Rev. A Ontario, CA 91761 Date: 06/07 Sleeve and Button Soft Tissue Devices Utilizing ZipLoop Technology ATTENTION
VerSys LD/Fx Cemented and Press-Fit Hip Prostheses. Surgical Technique IMAGE TO COME. Versatile solutions for total and partial hip replacement
 VerSys LD/Fx Cemented and Press-Fit Hip Prostheses Surgical Technique IMAGE TO COME Versatile solutions for total and partial hip replacement VerSys LD/Fx Cemented and Press-Fit Hip Prostheses VerSys
VerSys LD/Fx Cemented and Press-Fit Hip Prostheses Surgical Technique IMAGE TO COME Versatile solutions for total and partial hip replacement VerSys LD/Fx Cemented and Press-Fit Hip Prostheses VerSys
CMA TM Cemented Modular Augmentable. Baseplate. 2 Knee
 CMA TM Cemented Modular Augmentable Baseplate 2 Knee More can be addressed The U2 Cemented Modular Augmentable Baseplate is an optimal solution for tibial bone defect in primary total knee replacement.
CMA TM Cemented Modular Augmentable Baseplate 2 Knee More can be addressed The U2 Cemented Modular Augmentable Baseplate is an optimal solution for tibial bone defect in primary total knee replacement.
Manza Cup HA SURGICAL TECHNIQUE.
 1 PRE-OPERATIVE PLANNING. Preoperative assessment of the appropriate size and position of the acetabular component will provide intraoperative guidance for acetabular reaming. To determine the acetabluar
1 PRE-OPERATIVE PLANNING. Preoperative assessment of the appropriate size and position of the acetabular component will provide intraoperative guidance for acetabular reaming. To determine the acetabluar
Intramedullary Tibial Preparation
 Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
Trilogy Acetabular System
 Trilogy Acetabular System Surgical Technique Versatility in a proven design Trilogy Acetabular System 1 Trilogy Acetabular System Surgical Technique Table of Contents Acetabular Reaming 2 Component Sizing
Trilogy Acetabular System Surgical Technique Versatility in a proven design Trilogy Acetabular System 1 Trilogy Acetabular System Surgical Technique Table of Contents Acetabular Reaming 2 Component Sizing
Dual Mobility System Evaluation surgical technique
 Trinity Dual Mobility System Evaluation surgical technique Contents Operative summary 4 Overview 5 Operative technique 6 1. Acetabular reaming 6 Reamer guide 6 2. Acetabular shell trial 6 3. Acetabular
Trinity Dual Mobility System Evaluation surgical technique Contents Operative summary 4 Overview 5 Operative technique 6 1. Acetabular reaming 6 Reamer guide 6 2. Acetabular shell trial 6 3. Acetabular
UTF Stem. reduced. Surgical Protocol
 UTF Stem TM reduced Surgical Protocol Table of Contents Surgical Protocol Device... Preoperative Planning and Templating... Femoral Osteotomy... Femoral Canal Accessing... Canal Reaming... Canal Broaching...
UTF Stem TM reduced Surgical Protocol Table of Contents Surgical Protocol Device... Preoperative Planning and Templating... Femoral Osteotomy... Femoral Canal Accessing... Canal Reaming... Canal Broaching...
Technique Guide KISSloc Suture System
 Technique Guide KISSloc Suture System The KISSloc Suture System consists of a strong self-cinching suture assembly, a unique load-dispersing Arrow Plate and procedure specific instrumentation. Simple,
Technique Guide KISSloc Suture System The KISSloc Suture System consists of a strong self-cinching suture assembly, a unique load-dispersing Arrow Plate and procedure specific instrumentation. Simple,
Dual Mobility System Surgical technique
 Trinity Dual Mobility System Surgical technique 2 Contents Operative summary 4 Overview 5 Operative technique 6 1. Acetabular reaming 6 Reamer guide 6 2. Acetabular shell trial 7 3. Acetabular shell implantation
Trinity Dual Mobility System Surgical technique 2 Contents Operative summary 4 Overview 5 Operative technique 6 1. Acetabular reaming 6 Reamer guide 6 2. Acetabular shell trial 7 3. Acetabular shell implantation
Cementless Tapered Femoral Stem Surgical technique
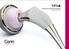 Cementless Tapered Femoral Stem Surgical technique Contents Operative summary 4 Pre-operative planning 5 Femoral neck osteotomy 5 Femoral canal preparation 5 Intra-medullary (IM) reamer 6 Sequential rasping
Cementless Tapered Femoral Stem Surgical technique Contents Operative summary 4 Pre-operative planning 5 Femoral neck osteotomy 5 Femoral canal preparation 5 Intra-medullary (IM) reamer 6 Sequential rasping
Active Articulation. Surgical Technique. Dual Mobility Hip System. Knees Hips Extremities Cement and Accessories PMI Trauma Technology
 Active Articulation Dual Mobility Hip System Surgical Technique Knees Hips Extremities Cement and Accessories PMI Trauma Technology Active Articulation Dual Mobility Hip System Contents Preoperative Planning,
Active Articulation Dual Mobility Hip System Surgical Technique Knees Hips Extremities Cement and Accessories PMI Trauma Technology Active Articulation Dual Mobility Hip System Contents Preoperative Planning,
ECHELON Primary Hip System Surgical Technique
 Surgical Technique ECHELON Primary Hip System Surgical Technique Harry B. Skinner, MD, PhD Professor and Chairman Department of Orthopaedic Surgery University of California, Irvine Orange, California James
Surgical Technique ECHELON Primary Hip System Surgical Technique Harry B. Skinner, MD, PhD Professor and Chairman Department of Orthopaedic Surgery University of California, Irvine Orange, California James
Trilogy Acetabular System
 Trilogy Acetabular System Surgical Technique Versatility in a proven design Trilogy Acetabular System 1 Trilogy Acetabular System Surgical Technique Table of Contents Acetabular Reaming 2 Component Sizing
Trilogy Acetabular System Surgical Technique Versatility in a proven design Trilogy Acetabular System 1 Trilogy Acetabular System Surgical Technique Table of Contents Acetabular Reaming 2 Component Sizing
CONSENSUS ORTHOPEDICS INC. CONSENSUS KNEE SYSTEM
 CONSENSUS ORTHOPEDICS INC. CONSENSUS KNEE SYSTEM IMPORTANT INFORMATION FOR SURGEON: PLEASE READ PRIOR TO IMPLANTING THIS DEVICE IN A CLINICAL SETTING. THE SURGEON SHOULD BE FAMILIAR WITH THE SURGICAL TECHNIQUE.
CONSENSUS ORTHOPEDICS INC. CONSENSUS KNEE SYSTEM IMPORTANT INFORMATION FOR SURGEON: PLEASE READ PRIOR TO IMPLANTING THIS DEVICE IN A CLINICAL SETTING. THE SURGEON SHOULD BE FAMILIAR WITH THE SURGICAL TECHNIQUE.
Constrained Acetabular Insert
 Constrained Acetabular Insert Surgical Protocol Howmedica Osteonics Constrained Acetabular Insert Surgical Protocol Table of Contents Howmedica Osteonics Constrained Acetabular Insert..........................1
Constrained Acetabular Insert Surgical Protocol Howmedica Osteonics Constrained Acetabular Insert Surgical Protocol Table of Contents Howmedica Osteonics Constrained Acetabular Insert..........................1
Technique Guide Wrist Hemiarthroplasty System
 Technique Guide Wrist Hemiarthroplasty System The WristMotion TM Wrist Hemiarthroplasty System restores mobility and maintains native biomechanics using a dual curvature HemiCAPITATE implant that locks
Technique Guide Wrist Hemiarthroplasty System The WristMotion TM Wrist Hemiarthroplasty System restores mobility and maintains native biomechanics using a dual curvature HemiCAPITATE implant that locks
pact SYSTEM Surgical Technique HEMISPHERICAL CEMENTLESS CUP SYSTEM MULTI-HOLE & RIM-HOLE Hip Knee Spine Navigation
 pact SYSTEM HEMISPHERICAL CEMENTLESS CUP SYSTEM MULTI-HOLE & RIM-HOLE Surgical Technique Hip Knee Spine Navigation Mpact Surgical Technique Hip Knee Spine Navigation PREFACE The Mpact Multi-hole and the
pact SYSTEM HEMISPHERICAL CEMENTLESS CUP SYSTEM MULTI-HOLE & RIM-HOLE Surgical Technique Hip Knee Spine Navigation Mpact Surgical Technique Hip Knee Spine Navigation PREFACE The Mpact Multi-hole and the
Surgical Technique. Poly and Ceramic
 Surgical Technique Poly and Ceramic Design surgeon list Smith & Nephew thanks the following surgeons for their participation as part of the R3 system design team: Robert Barrack, MD St. Louis, Missouri
Surgical Technique Poly and Ceramic Design surgeon list Smith & Nephew thanks the following surgeons for their participation as part of the R3 system design team: Robert Barrack, MD St. Louis, Missouri
Surgical Technique. Revision Acetabular System Acetabular Augments
 Surgical Technique Revision Acetabular System Acetabular Augments Design surgeon list Smith & Nephew thanks the following surgeons for their participation as part of the REDAPT Revision Acetabular System
Surgical Technique Revision Acetabular System Acetabular Augments Design surgeon list Smith & Nephew thanks the following surgeons for their participation as part of the REDAPT Revision Acetabular System
Regenerex Primary Tibial Tray
 Cruciate Retaining and Posterior Stabilized Surgical Technique Addendum to the Vanguard Complete Knee System Knees Hips Extremities Cement and Accessories PMI Technology Contents Microplasty Knee Instrumentation
Cruciate Retaining and Posterior Stabilized Surgical Technique Addendum to the Vanguard Complete Knee System Knees Hips Extremities Cement and Accessories PMI Technology Contents Microplasty Knee Instrumentation
Distal Cut First Femoral Preparation
 Surgical Technique Distal Cut First Femoral Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Femoral preparation Contents Introduction...3 DCF femoral highlights...4 Preoperative planning...6
Surgical Technique Distal Cut First Femoral Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Femoral preparation Contents Introduction...3 DCF femoral highlights...4 Preoperative planning...6
TaperFill. Surgical Technique
 TaperFill Surgical Technique Table of Contents Indications and Contraindications 3 TaperFill Hip Size Charts 4-5 DJO Surgical 9800 Metric Boulevard Austin, TX (800) 456-8696 www.djosurgical.com Preoperative
TaperFill Surgical Technique Table of Contents Indications and Contraindications 3 TaperFill Hip Size Charts 4-5 DJO Surgical 9800 Metric Boulevard Austin, TX (800) 456-8696 www.djosurgical.com Preoperative
POLARCUP Dual Mobility System. General Safety Instructions. Instructions for Use. Duty to inform the patient. Implant passport
 Important Notice to Users in the United States: This package insert is for product distributed in US only. U.S. Federal law restricts this device to sale by or on the order of a physician. General Safety
Important Notice to Users in the United States: This package insert is for product distributed in US only. U.S. Federal law restricts this device to sale by or on the order of a physician. General Safety
UNDERSTANDING TRADITION, MASTERING INNOVATION. Surgical Technique
 UNDERSTANDING TRADITION, MASTERING INNOVATION Surgical Technique Joint Spine Sports Med MasterLoc Surgical Technique Joint Spine Sports Med INTRODUCTION This document describes the Surgical Technique for
UNDERSTANDING TRADITION, MASTERING INNOVATION Surgical Technique Joint Spine Sports Med MasterLoc Surgical Technique Joint Spine Sports Med INTRODUCTION This document describes the Surgical Technique for
SURGICAL TECHNIQUE GUIDE
 DANGER indicates an imminently hazardous situation which, if not avoided, will result in death or serious injury. WARNING indicates a potentially hazardous situation which, if not avoided, could result
DANGER indicates an imminently hazardous situation which, if not avoided, will result in death or serious injury. WARNING indicates a potentially hazardous situation which, if not avoided, could result
Arcos Modular Femoral Revision System
 Arcos Modular Femoral Revision System Arcos System Simplify the Complex The Arcos Modular Femoral Revision System meets the demands of complex hip revision surgery by offering surgeons and OR staff the
Arcos Modular Femoral Revision System Arcos System Simplify the Complex The Arcos Modular Femoral Revision System meets the demands of complex hip revision surgery by offering surgeons and OR staff the
EVOLVING OUR HERITAGE, MEETING YOUR NEEDS. Surgical Technique
 EVOLVING OUR HERITAGE, MEETING YOUR NEEDS Surgical Technique Joint Spine Sports Med Mpact DM Surgical Technique Joint Spine Sports Med INTRODUCTION The Mpact DM is part of the Mpact Acetabular System and
EVOLVING OUR HERITAGE, MEETING YOUR NEEDS Surgical Technique Joint Spine Sports Med Mpact DM Surgical Technique Joint Spine Sports Med INTRODUCTION The Mpact DM is part of the Mpact Acetabular System and
THE P.F.C. SIGMA FEMORAL ADAPTER. Surgical Technique
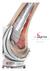 THE P.F.C. SIGMA FEMORAL ADAPTER Surgical Technique Contents P.F.C. Sigma Femoral Adapter and Revision Knee Surgery Introduction 2 Preoperative Planning 2 Overview 3 Surgical Technique Preparation of the
THE P.F.C. SIGMA FEMORAL ADAPTER Surgical Technique Contents P.F.C. Sigma Femoral Adapter and Revision Knee Surgery Introduction 2 Preoperative Planning 2 Overview 3 Surgical Technique Preparation of the
operative technique Kent Hip
 operative technique Kent Hip The Kent Hip Operative Technique The Kent Hip was developed by Mr Cliff Stossel, FRCS in Maidstone, Kent, UK and first implanted in 1986. It was designed to deal with problems
operative technique Kent Hip The Kent Hip Operative Technique The Kent Hip was developed by Mr Cliff Stossel, FRCS in Maidstone, Kent, UK and first implanted in 1986. It was designed to deal with problems
The Leader in Orthopaedic Innovation
 The Leader in Orthopaedic Innovation Wright is a leading international manufacturer and distributor of superior, easy to use, and innovative orthopaedic implants and instrumentation. For over 50 years,
The Leader in Orthopaedic Innovation Wright is a leading international manufacturer and distributor of superior, easy to use, and innovative orthopaedic implants and instrumentation. For over 50 years,
Extramedullary Tibial Preparation
 Surgical Technique Extramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Extramedullary tibial preparation Contents Introduction...2 EM tibial highlights...3 Preoperative
Surgical Technique Extramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Extramedullary tibial preparation Contents Introduction...2 EM tibial highlights...3 Preoperative
asterloc Surgical Technique HIP SYSTEM UNDERSTANDING TRADITION, MASTERING INNOVATION Hip Knee Spine Navigation
 asterloc HIP SYSTEM UNDERSTANDING TRADITION, MASTERING INNOVATION Surgical Technique Hip Knee Spine Navigation Masterloc Surgical Technique Hip Knee Spine Navigation INTRODUCTION This document describes
asterloc HIP SYSTEM UNDERSTANDING TRADITION, MASTERING INNOVATION Surgical Technique Hip Knee Spine Navigation Masterloc Surgical Technique Hip Knee Spine Navigation INTRODUCTION This document describes
Important Notice to Users in the United States: General Safety Instructions
 POLARSTEM Femoral Stems with Ti/HA (Standard, Lateral, Valgus and Collar) Smith & Nephew Orthopaedics AG Oberneuhofstrasse 10d CH-6340 Baar Phone + 41 41 766 22 22 swiss.implants@smith-nephew.com 02/2017
POLARSTEM Femoral Stems with Ti/HA (Standard, Lateral, Valgus and Collar) Smith & Nephew Orthopaedics AG Oberneuhofstrasse 10d CH-6340 Baar Phone + 41 41 766 22 22 swiss.implants@smith-nephew.com 02/2017
Operative Technique Crown Cup Acetabular System
 EXACTECH HIP Operative Technique Crown Cup Acetabular System TABLE OF CONTENTS PRE-OPERATIVE PLANNING... 1 TEMPLATING... 1 INDICATIONS FOR USE... 1 CONTRAINDICATIONS FOR USE... 1 OPERATIVE TECHNIQUE OVERVIEW...
EXACTECH HIP Operative Technique Crown Cup Acetabular System TABLE OF CONTENTS PRE-OPERATIVE PLANNING... 1 TEMPLATING... 1 INDICATIONS FOR USE... 1 CONTRAINDICATIONS FOR USE... 1 OPERATIVE TECHNIQUE OVERVIEW...
Design Rationale. ECHELON Primary Hip System
 Design Rationale ECHELON Primary Hip System ECHELON Primary Total Hip System Addressing clinical issues of cementless hip arthroplasty Cementless total hip arthroplasty has provided a proven method of
Design Rationale ECHELON Primary Hip System ECHELON Primary Total Hip System Addressing clinical issues of cementless hip arthroplasty Cementless total hip arthroplasty has provided a proven method of
OPTIONAL/ADDITIONAL INSTRUMENTS
 20 Elevated 6320-36-22 20 Elevated Rim Liner, 36mm OD x 22mm ID 6320-80-22 20 Elevated Rim Liner, 80mm OD x 22mm ID 6320-42-26 20 Elevated Rim Liner, 42mm OD x 26mm ID 6320-80-26 20 Elevated Rim Liner,
20 Elevated 6320-36-22 20 Elevated Rim Liner, 36mm OD x 22mm ID 6320-80-22 20 Elevated Rim Liner, 80mm OD x 22mm ID 6320-42-26 20 Elevated Rim Liner, 42mm OD x 26mm ID 6320-80-26 20 Elevated Rim Liner,
PMMA Spacer. X-ray Marker
 Full TM Cup 2.5 mm cement thickness PMMA Spacer Uniform 2.5 mm cement thickness; the cement mantle is built within the outer dimension of acetabular cup. Cup O.D. 20 o lipped Prevent joint dislocation
Full TM Cup 2.5 mm cement thickness PMMA Spacer Uniform 2.5 mm cement thickness; the cement mantle is built within the outer dimension of acetabular cup. Cup O.D. 20 o lipped Prevent joint dislocation
Important Notice to Users in the United States: General Safety Instructions
 SLR-PLUS Revision Stem, SLR-PLUS Revision Stem Lateral Smith & Nephew Orthopaedics AG Oberneuhofstrasse 10d CH-6340 Baar Phone + 41 41 766 22 22 swiss.implants@smith-nephew.com non-sterile cemented non-
SLR-PLUS Revision Stem, SLR-PLUS Revision Stem Lateral Smith & Nephew Orthopaedics AG Oberneuhofstrasse 10d CH-6340 Baar Phone + 41 41 766 22 22 swiss.implants@smith-nephew.com non-sterile cemented non-
The short stem hip system Surgical Technique
 The short stem hip system Surgical Technique The short stem hip system cementless The Aida hip system was developed in co-operation with the Aida inventors group, founded by surgeons of 10 surgical department
The short stem hip system Surgical Technique The short stem hip system cementless The Aida hip system was developed in co-operation with the Aida inventors group, founded by surgeons of 10 surgical department
Surgical Technique. CONQUEST FN Femoral Neck Fracture System
 Surgical Technique CONQUEST FN Femoral Neck Fracture System Table of Contents Introduction... 3 Indications... 3 Product Overview... 4 Surgical Technique... 5 Patient Positioning... 5 Reduce the Fracture...
Surgical Technique CONQUEST FN Femoral Neck Fracture System Table of Contents Introduction... 3 Indications... 3 Product Overview... 4 Surgical Technique... 5 Patient Positioning... 5 Reduce the Fracture...
Surgical Technique. Hinge Disassembly and Rebuild Technique
 Surgical Technique Hinge Disassembly and Rebuild Technique Revision Knee Arthroplasty Surgical Technique LEGION HK Hinge Knee System Introduction The LEGION HK Hinge Knee System has been designed as an
Surgical Technique Hinge Disassembly and Rebuild Technique Revision Knee Arthroplasty Surgical Technique LEGION HK Hinge Knee System Introduction The LEGION HK Hinge Knee System has been designed as an
