Comparison of Hallux Rigidus Surgical Treatment Outcomes Between Active Duty and Non Active Duty Populations
|
|
|
- Leslie Dawson
- 5 years ago
- Views:
Transcription
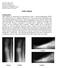
1 ORIGINAL ARTICLES Comparison of Hallux Rigidus Surgical Treatment Outcomes Between Active Duty and Non Active Duty Populations A Retrospective Review Marc D. Jones, DPM* Kerry J. Sweet, DPM Background: Our aim in this study was to compare the long-term outcomes of three different surgical procedures for the treatment of hallux rigidus (ie, cheilectomy, decompressive osteotomy, and arthrodesis) between active duty military and non active duty patients. Methods: A retrospective review of 80 patients (95 feet) undergoing surgical treatment for hallux rigidus was performed. Telephone survey was used to obtain postoperative outcome measures and subjective satisfaction. Additional data recorded and analyzed included age, sex, status of patient (active duty or non active duty), grade of hallux rigidus, surgical procedure performed, date of surgery, time to return to full activity, ability to return to full duty, and follow-up time postoperatively. Results: The decompressive osteotomy group had the highest return-to-duty rate, satisfaction rate, and Maryland Foot Scores of all three surgical groups, although these differences were not statistically significant. Active duty and non active duty patients did not have statistically significant differences in outcomes measures (ie, time to return to full activity, ability to return to full duty, satisfaction, or postoperative Maryland Foot Score) in any of the three surgical groups. Conclusions: Decompressive osteotomy, cheilectomy, and first metatarsophalangeal joint arthrodesis are all reliable and effective procedures for treatment of hallux rigidus in both active duty military and non active duty patients. Active duty military personal have a high rate of returning to their prior military activities after surgical treatment of hallux rigidus. (J Am Podiatr Med Assoc 108(4): , 2018) Hallux rigidus is a common disorder affecting the first metatarsophalangeal joint (MTPJ), accounting for up to 9.3% of patients visiting a podiatrist. 1 Hallux rigidus is characterized by degenerative changes to the first MTPJ leading to a painful restriction of motion of the joint. The restriction of the joint motion and pain with motion is most pronounced on dorsiflexion rather than plantarflexion. 2,3 There are many proposed causes of hallux rigidus, including anatomical and structural factors such as congenital squaring of the metatarsal head, an elevated first ray, hallux valgus, hypermobility, and pronation. 4-7 Trauma and repetitive loading of *Mann-Grandstaff VA Medical Center, Spokane, WA. Surgery/Podiatry Service, VA Puget Sound Healthcare System, Lakewood, WA. Corresponding author: Marc D. Jones, DPM, Mann-Grandstaff VA Medical Center, 4815 N Assembly, Spokane, WA ( marc.jones@va.gov) the joint through high-impact activities such as running and jumping, over a long period, have also been identified as contributing to hallux rigidus. 8,9 Conservative treatment can be effective early on in the disease process, including trials of rigid shoe gear, rocker-bottom shoes, orthotics with modification such as Morton s or reverse Morton s extensions, activity modification, steroid injection, and nonsteroidal anti-inflammatory drugs Once conservative treatment has failed to relieve a patient s symptoms, surgical treatment is most often the option of choice. Many different surgical techniques have been described for treatment hallux rigidus, 13 and are commonly placed into two categories: joint-preserving and joint-destructive procedures. Joint-preserving operations include cheilectomy and first metatarsal and phalangeal osteotomies. Joint-destructive 272 July/August 2018 Vol 108 No 4 Journal of the American Podiatric Medical Association
2 procedures include excisional with interpositional arthroplasties, arthrodesis, and implant arthroplasty. Generally, joint-preserving surgical treatments are used for early-stage disease and joint-destructive procedure are used for late-stage disease. 14 Although there is significant published literature on surgical treatment options for hallux rigidus, there is little reporting of the outcomes of surgical procedures in athletes or active duty military populations. After our extensive review of the literature, we were unable to find published results on outcomes of surgical management of hallux rigidus in the active duty military population. In light of this, it was the aim of this study to compare the long-term outcomes of three different surgical procedures (ie, cheilectomy, decompressive osteotomy, and arthrodesis) between active duty military and non active duty patients. Methods A retrospective review of patients treated surgically for hallux rigidus by means of electronic medical records between January 2005 and December 2012 was performed. One hundred four patients were identified who had a diagnosis of hallux rigidus and were treated surgically with a first MTPJ arthrodesis, a cheilectomy, or a first metatarsal decompressive osteotomy. These patients were then contacted by means of telephone and given the option to participate in a follow-up survey regarding the outcome of their survey. The patients were first contacted during regular business hours and then a second time in the evening hours if the first attempt was unsuccessful. A minimum of a 12-month followup was an inclusion criterion. Of the 104 patients, 80 were contacted and agreed to and completed the follow-up telephone interview, including the Maryland Foot Score (MFS) and subjective satisfaction questions (Fig. 1). The Maryland Foot Score measures outcomes of foot surgery in terms of functional activities, pain, and appearance of the foot. A high score is 100 and a low score is 0. Exclusion criteria included 1) patients younger than 18 years, 2) patients who underwent additional concurrent surgical procedures, 3) patients with an additional diagnosis of hallux valgus, and 4) a diagnosis of systemic arthropathies. Data recorded included age, sex, active duty status of patient (active duty or non active duty), grade of hallux rigidus, type of surgical procedure performed, date of surgery (DOS), time to return to full activity (RTA), ability to return to full duty (RTD), MFS, subjective satisfaction, and follow-up time. Return to full activity was defined as the time (in weeks) from the DOS to the date when the patient was able to return to all job, recreational, and/or military duties that were required of them without any physical limitations. Return to full duty was defined as the ability (yes/no) to perform all physical activities required to perform their military or civilian job. Satisfaction was defined as those patients who were either completely satisfied with no reservations or completely satisfied with minor reservations at the time of the telephone survey. Grade of hallux rigidus was determined by means of the Drago, Oloff, and Jacobs scoring system (Fig. 2). 6 Each patient was placed in one of three groups based on the surgical procedure that was performed. Surgery that included first MTPJ arthrodesis was completed using fixation consisting of two crossing screws or a compression screw with dorsal plate. The decompressive osteotomy group included a first metatarsal shortening procedure consisting of either a Youngswick procedure or a distal oblique osteotomy procedure that were fixated with either one or two screws. The cheilectomy surgical procedure was performed by removing approximately the dorsal one-fourth to one-third of the first metatarsal head and joint, as well as removing all loose bodies and osteophytes within the joint. All groups of patients were followed with clinical postoperative appointments until healing was complete and the patients were able to return to full activity. The surgical procedure was determined by radiographic and clinical findings and the surgeon s preference. Informed consent was obtained from all the participants, and the research protocol was approved by the institutional review board at Madigan Army Medical Center (protocol number ). Results Eighty patients, consisting of 58 men and 22 women, 60 active duty and 20 non active duty, were included in our study. Of these 80 patients, there were 95 feet operated on. The mean age of the patients was 42.4 years (range, years). Mean follow-up time was 34.5 months (range, months). The cheilectomy group consisted of 26 total feet, with 23 active duty and three non active duty patients. The decompressive osteotomy group consisted of 27 total feet operated on, with 27 active duty and nine non active duty patients. The Journal of the American Podiatric Medical Association Vol 108 No 4 July/August
3 Figure 1. Survey questions posed to patients, including the Maryland Foot Score and subjective satisfaction. (continued on next page) 274 July/August 2018 Vol 108 No 4 Journal of the American Podiatric Medical Association
4 Figure 1. continued arthrodesis group consisted of 33 total feet, with 20 active duty and 13 non active duty patients. Preoperative grade of hallux rigidus for the cheilectomy group included three (11.5%) grade I, 16 (61.5%) grade II, seven (27.0%) grade III, and zero (0%) grade IV. In the decompressive osteotomy group, 14 (38.9%) were grade I, 20 (55.6%) were grade II, two (5.6%) were grade III, and zero (0%) were grade IV. Within the arthrodesis group, zero (0%) were grade 1, 10 (30.3%) were grade II, 16 (48.5%) were grade III, and seven (21.2%) were grade IV (Table 1). Grade of hallux rigidus was determined by means of the Drago, Oloff, and Jacobs scoring system. 6 A comparison of the outcomes of the patients undergoing a surgical procedure in this study showed a RTD rate of 80.8% (cheilectomy), versus 94.4% (decompressive osteotomy), versus 78.8% (arthrodesis) (P ¼.140). The RTA time was noted to be 12.9 weeks (cheilectomy), versus 19.4 weeks (decompressive osteotomy), versus 20.8 weeks (arthrodesis) (P ¼.002). The mean MFS was 83.1 (cheilectomy), versus 85.2 (decompressive osteotomy), versus 81.3 (arthrodesis) (P ¼.792). The subjective patient satisfaction was noted to be 80.0% (cheilectomy), versus 85.2% (decompressive osteotomy), versus 79.3% (arthrodesis) (P ¼.833) (Table 2). Within the cheilectomy group, the outcomes of the procedures between active duty and non active duty patients were, respectively, as follows: RTD, 78.3% versus 100% (P ¼.512); RTA, 13.3 weeks versus 10.7 weeks (P ¼.182); mean MFS, 80.4 versus 98.0 (P ¼.163); and subjective patient satisfaction with the surgical procedure, 76.3% versus 100.0% (P ¼.482) (Table 3). In the decompressive osteotomy group, the outcomes of the procedures between active duty and non active duty patients were, respectively, as follows: RTD, 92.6% versus 100% (P ¼.557); RTA, 17.0 weeks versus 18.7 weeks (P ¼.830); mean MFS, 83.0 versus 90.6 (P ¼.231); and subjective patient satisfaction with the surgical procedure, 84.3% versus 88.9% (P ¼.798) (Table 4). Among patients in the arthrodesis group, the outcomes of the procedures between active duty and non active duty patients were, respectively, as follows: RTD, 70.0%, versus 92.3% (P ¼.136); RTA, 21.4 weeks versus 20.2 weeks (P ¼.720); mean MFS, 79.5 versus 83.5 (P ¼.5.34); and subjective patient satisfaction with the surgical procedure, 80.0% versus 76.9% (P ¼.615) (Table 5). Overall, five patients in the cheilectomy group were unable to return to duty, with all of these patients being active duty patients. Two of the five underwent fusion before leaving the military and successfully returned to full duty. Of these five patients, three were classified as having grade II disease before surgery and two patients had grade III disease. In the decompressive osteotomy group, the two active duty patients who did not return to duty were grade I before surgery. Within the arthrodesis group, of the six patients unable to return to duty, two were grade II and four were grade III before surgery (Table 6). Five of these patients were active duty and one was non active duty. Journal of the American Podiatric Medical Association Vol 108 No 4 July/August
5 Figure 2. Drago, Oloff, and Jacobs classification system. Discussion In our study, RTA time was the only statistically significant factor (P,.05), with cheilectomy having the quickest RTA at a mean of 12.9 weeks between all patients. This is not surprising, as this procedure does not rely on bone healing associated with an osteotomy or an arthrodesis. The decompressive osteotomy group had the highest RTD rate, satisfaction rate, and Maryland Foot Scores of all of the groups, although these differences were not statistically significant. Within this study, the decompressive osteotomy group was not inferior to the arthrodesis or cheilectomy procedure arms in outcomes measures, which stands in contrast to some of the results of other published studies. Decompressive osteotomies of the first metatarsal have had reported success rates in the literature ranging from 54% to 95%. 1,15-17 Our satisfaction rate of 85.2% falls within this range but is higher than the 73.3% reported by Roukis in a large systematic review. 15 Our satisfaction rate overall for the cheilectomy group was 80.0%, which is lower than rates reported in other published studies. A systematic review of cheilectomies by Roukis that included 23 studies showed a 91% success rate. 18 Coughlin and Shurnas found a 92% success rate among 93 patients with a 10-year follow-up. 14 Newer studies have also reported that there are good outcomes with a cheilectomy procedure in stage III hallux rigidus. 19 Lower satisfaction scores and outcomes are most likely attributable to the active duty patients who were included in this study; these patients have a much higher physical activity demand postoperatively than the general population included in the other studies. Active duty military patients have increased physical demands placed on them on a daily basis, that typically include wearing rucksacks (up to 100 pounds), running, wearing combat boots, deployments, and extensive high-impact activities. Even with these high demands, there was an overall RTD rate of 83.8% in the active duty patients across all three surgical groups. In an exhaustive review of the literature, we found no published outcome studies looking at hallux rigidus surgery in active duty military and scarce published studies looking at athletes. Mulier et al 20 published a study looking at athletes who had a cheilectomy procedure performed, and with a 5-year follow-up, they reported that 10% of the patients were unable to return to their sport because of the procedure and had an RTA of 11.5 weeks. Overall, in our study, with the exception of satisfaction rates in the arthrodesis group, non active duty patients had higher RTD rates, satisfaction rates, and Maryland Foot Scores compared with the active duty patients, although these 276 July/August 2018 Vol 108 No 4 Journal of the American Podiatric Medical Association
6 Table 1. Preoperative Grade of Hallux Rigidus by Group Surgical Group Grade I Grade II Grade III Grade IV Cheilectomy Decompressive osteotomy Arthrodesis Table 2. Comparison of Outcomes of Each Surgical Group Surgical Group No. of Feet RTD (%) Satisfied (%) Mean Postoperative MFS RTA (weeks) Cheilectomy Decompressive osteotomy Arthrodesis P value a Abbreviations: RTD, return to full duty/activity; MFS, Maryland Foot Score; RTA, return to full activity. a Statistically significant. Table 3. Comparison of Active Duty and Non Active Duty Patient Populations Within the Cheilectomy Group No. of Feet RTD (%) Satisfied (%) Mean Postoperative MFS RTA (weeks) AD Non-AD P value Abbreviations: RTD, return to full duty/activity; MFS, Maryland Foot Score; RTA, return to full activity; AD, active duty. Table 4. Comparison of Active Duty and Non Active Duty Patient Populations Within the Decompressive Osteotomy Group No. of Feet RTD (%) Satisfied (%) Mean Postoperative MFS RTA (weeks) AD Non-AD P value Abbreviations: RTD, return to full duty/activity; MFS, Maryland Foot Score; RTA, return to full activity; AD, active duty. Table 5. Comparison of Active Duty and Non Active Duty Patient Populations Within the Arthrodesis Group No. of Feet RTD (%) Satisfied (%) Mean Postoperative MFS RTA (weeks) AD Non-AD P value Abbreviations: RTD, return to full duty/activity; MFS, Maryland Foot Score; RTA, return to full activity; AD, active duty. Table 6. Number of Patients Unable to Return to Full Activity/Duty Surgical Group Grade I Grade II Grade III Grade IV Cheilectomy Decompressive osteotomy Arthrodesis Journal of the American Podiatric Medical Association Vol 108 No 4 July/August
7 differences were not statistically significant. We had one nonunion in the arthrodesis group (which occurred in a non active duty woman), for a fusion rate of 97%, which is comparable to the published literature showing fusion rates ranging from 92% to 96% in several large studies. 14,21,22 The average age of our patients at the time of surgery was 42.4 years, which is younger than in other studies reported in the literature. Peace and Hamilton 9 reported the mean age of onset as 43 years, with average surgical correction occurring at age 50. Most likely, this is caused by increased wear and tear on the first MTPJ resulting from increased amounts of high-impact activities that the active duty patient experiences on a daily basis. Trégouët, in a study of National Collegiate Athletic Association basketball players, agreed with the theory that a decrease in the range of motion at the first MTPJ was a result of long-term sporting activity. In addition, he supported the premise that repeated cyclic loads below the injury threshold produce a fatigue effect on the joint even without a known traumatic event. 23 This theory would presumably be supported in the active duty military population as well, because of the repetitive nature of their training and deployment environment. The active duty population usually has required daily physical training, marching, and carrying heavy weight (eg, rucksacks) contributing to the repeated cyclical loads to the first MTPJ. This combined with the less frequent contributing factors of macrotrauma and/or microtrauma related to jumping from a significant height out of large vehicles or on rough terrain, kicking in doors, and running with a combat load (.100 pounds) during combat operations can contribute to the early degeneration of the first MTPJ in a portion of our study group. The strengths of this study included a high rate of response to the telephone survey, with 80 of 104 patients (76.9%) contacted and willing to participate in the follow-up survey. As a result, a large sample size of 80 patients, with 95 feet having surgical procedures performed, was able to be obtained. This study also had a mean follow-up time of nearly 3 years (34.5 months) from the DOS to the date of the administration of the phone survey. Limitations of our study include its retrospective nature and the small sample size within the non active duty patient population, especially within the cheilectomy group. Larger prospective studies with preoperative outcome scores are needed to confirm our findings. Conclusions The findings of this study show that a decompressive osteotomy, cheilectomy, and first MTPJ arthrodesis are all reliable and effective procedures for treatment of hallux rigidus in both active duty and non active duty patients. No statistical difference was found between active duty and non active duty patients related to the outcome measures we used in this study. Active duty military personal, just like non active duty patients, can be effectively treated with these three surgical procedures for hallux rigidus and have a high rate of returning to their prior military activities. Financial Disclosure: None reported. Conflict of Interest: None reported. References 1. KILMARTIN TE: Phalangeal osteotomy versus first metatarsal decompression osteotomy for the surgical treatment of hallux rigidus: a prospective study of agematched and condition-matched patients. Foot Ankle Surg 44: 2, BONNEY G, MACNAB I: Hallux valgus and hallux rigidus: a critical survey of operative result. J Bone Joint Surg Br 34: 366, SHEREFF MD, BAUMHAUER JF: Hallux rigidus and osteoarthrosis of the first metatarsophalangeal joint. J Bone Joint Surg Am 80: 898, SCHNIRRING-JUDGE M, HEHEMANN D: The cheilectomy and its modifications. Clin Podiatr Med Surg 28: 305, LAMBRINUDI P: Metatarsus primus elevates. Proc R Soc Med 31: 1273, DRAGO JJ, OLOFF L, JACOBS AM: A comprehensive review of hallux limitus. J Foot Surg 23: 213, HATTRUP SJ, JOHNSON KA: Subjective results of hallux rigidus following treatment with cheilectomy. Clin Orthop Relat Res 226: 182, O MALLEY MJ, BASRAN HS, GU U, ET AL: Treatment of advanced stages of hallux rigidus with cheilectomy and phalangeal osteotomy. J Bone Joint Surg Am 95: 606, PEACE RA, HAMILTON GA: End stage hallux rigidus: cheilectomy, implant or arthrodesis? Clin Podiatr Med Surg 29: 341, COTTERIL JM: Stiffness of the great toe in adolescents. BMJ 1: 158, DURRANT M, SIEPERT K: Role of soft tissue structures as an etiology of hallux limitus. JAPMA 83: 173, SHARIFF R, MYERSON MS: The use of osteotomy in the management of hallux rigidus. Foot Ankle Clin 20: 493, KEISERMAN LS, SAMMARCO VJ, SAMMARCO GJ: Surgical treatment of the hallux rigidus. Foot Ankle Clin 10: 75, July/August 2018 Vol 108 No 4 Journal of the American Podiatric Medical Association
8 14. COUGHLIN MJ, SHURNAS PS: Hallux rigidus: grading and long-term results of operative treatment J Bone Joint Surg Am 85: 2072, ROUKIS TS: Clinical outcomes after isolate periarticular osteotomies of the first metatarsal for hallux rigidus: a systematic review. J Foot Ankle Surg 49: 553, MALERBA F, MILANI R, SARTORELLI E, ET AL: Distal oblique first metatarsal osteotomy in grade 3 hallux rigidus: a long-term followup. Foot Ankle Int 29: 677, RONCONI P, MONACHINO P, BALEANU PM, ET AL: Distal oblique osteotomy of the first metatarsal for the correction of hallux limitus and rigidus deformity. J Foot Ankle Surg 39: 154, ROUKIS TS: The need for surgical revision after isolated cheilectomy for hallux rigidus: a systematic review. J Foot Ankle Surg 49: 465, CETINKAYA E, YALCINKAYA M, SOKUCU S, ET AL: Cheilectomy as a first line surgical treatment option yields good functional results in grade III hallux rigidus. JAPMA 106: 22, MULIER T, STEENWERCKX A, THIENPONT E, ET AL: Results after cheilectomy in athletes with hallux rigidus. Foot Ankle Int 20: 232, GOUCHER NR, COUGHLIN MJ: Hallux metatarsophalangeal joint arthrodesis using dome-shaped reamers and dorsal plate fixation: a prospective study. Foot Ankle Int 27: 869, ROUKIS TS: Nonunion after arthrodesis of first metatarsal-phalangeal joint: a systematic review. J Foot Ankle Surg 50: 710, TRÉGOUËT P: An assessment of hallux limitus in university basketball players compared with noncompetitive individuals. JAPMA 104: 468, Journal of the American Podiatric Medical Association Vol 108 No 4 July/August
Disclosures. 55 year old Male 2/23/2018. Recurrent Hallux Rigidus: Options Other than Arthrodesis
 Recurrent Hallux Rigidus: Options Other than Arthrodesis Gregory C Berlet, MD FRCS(C), FAOA Orthopedic Foot and Ankle Columbus, Ohio Columbus, Ohio orthofootankle.com Disclosures Consultant/Speaker Bureau/Royalties/
Recurrent Hallux Rigidus: Options Other than Arthrodesis Gregory C Berlet, MD FRCS(C), FAOA Orthopedic Foot and Ankle Columbus, Ohio Columbus, Ohio orthofootankle.com Disclosures Consultant/Speaker Bureau/Royalties/
6/5/2018. Forefoot Disorders. Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) Hallux Rigidus
 Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Intermediate outcome of interpositional arthroplasty for the treatment of hallux rigidus. Anand Vora, MD
 Intermediate outcome of interpositional arthroplasty for the treatment of hallux rigidus Anand Vora, MD CONFLICT TO DISCLOSE Intermediate outcome of interpositional arthroplasty for the treatment of hallux
Intermediate outcome of interpositional arthroplasty for the treatment of hallux rigidus Anand Vora, MD CONFLICT TO DISCLOSE Intermediate outcome of interpositional arthroplasty for the treatment of hallux
We are IntechOpen, the first native scientific publisher of Open Access books. International authors and editors. Our authors are among the TOP 1%
 We are IntechOpen, the first native scientific publisher of Open Access books 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our authors are among the 151 Countries
We are IntechOpen, the first native scientific publisher of Open Access books 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our authors are among the 151 Countries
THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT. Miss Sue Kendall PhD FRCS (Orth&Trauma)
 THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT Miss Sue Kendall PhD FRCS (Orth&Trauma) Is Minimally Invasive Surgery of the foot a good idea? Minimally invasive surgery, keyhole surgery entering
THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT Miss Sue Kendall PhD FRCS (Orth&Trauma) Is Minimally Invasive Surgery of the foot a good idea? Minimally invasive surgery, keyhole surgery entering
innovative and comprehensive product line Metatarsophalangeal Joint Lower Hallux Limitus Hallux Rigidus Extremity
 Surgical Solutions innovative and comprehensive product line Metatarsophalangeal Joint Hallux Limitus Hallux Rigidus Lower Extremity Solutions Hallux Limitus and Hallux Rigidus Hallux limitus is a progressive
Surgical Solutions innovative and comprehensive product line Metatarsophalangeal Joint Hallux Limitus Hallux Rigidus Lower Extremity Solutions Hallux Limitus and Hallux Rigidus Hallux limitus is a progressive
NORTHERN OHIO FOUNDATION
 NORTHERN OHIO FOOT & ANKLE FOUNDATION! The!Northern!Ohio!Foot!and!Ankle!Journal!!!!!!!!!!!!!!!Official!Publication!of!the!NOFA!Foundation!! First MPJ Proximal Phalanx Hemi Implant Arthroplasty Literature
NORTHERN OHIO FOOT & ANKLE FOUNDATION! The!Northern!Ohio!Foot!and!Ankle!Journal!!!!!!!!!!!!!!!Official!Publication!of!the!NOFA!Foundation!! First MPJ Proximal Phalanx Hemi Implant Arthroplasty Literature
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity
 Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT
 C H A P T E R 1 5 HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT Joe T. Southerland, DPM Mickey D. Stapp, DPM INTRODUCTION Hemi-implant arthroplasty of the first metatarsophalangeal
C H A P T E R 1 5 HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT Joe T. Southerland, DPM Mickey D. Stapp, DPM INTRODUCTION Hemi-implant arthroplasty of the first metatarsophalangeal
Could this Research Change the Way You Treat Hallux Limitus?
 Could this Research Change the Way You Treat Hallux Limitus? Lawrence Z. Huppin, D.P.M. Assistant Clinical Professor, Western University of Health Sciences, College of Podiatric Medicine Disclosure: Medical
Could this Research Change the Way You Treat Hallux Limitus? Lawrence Z. Huppin, D.P.M. Assistant Clinical Professor, Western University of Health Sciences, College of Podiatric Medicine Disclosure: Medical
First Metatarsal Head Osteochondral Defect Treatment with Particulated Juvenile Cartilage Allograft Transplantation
 First Metatarsal Head Osteochondral Defect Treatment with Particulated Juvenile Cartilage Allograft Transplantation Bryan Van Dyke, DO Gregory C. Berlet, MD Justin L. Daigre, MD Christopher F. Hyer, DPM,
First Metatarsal Head Osteochondral Defect Treatment with Particulated Juvenile Cartilage Allograft Transplantation Bryan Van Dyke, DO Gregory C. Berlet, MD Justin L. Daigre, MD Christopher F. Hyer, DPM,
Low Profile Medial Locking plate augmentation Lapidus Arthrodesis with an early weight bearing protocol: Clinical and Radiographic Analysis
 Low Profile Medial Locking plate augmentation Lapidus Arthrodesis with an early weight bearing protocol: Clinical and Radiographic Analysis James Cottom, DPM Anand Vora, MD Low Profile Medial Locking plate
Low Profile Medial Locking plate augmentation Lapidus Arthrodesis with an early weight bearing protocol: Clinical and Radiographic Analysis James Cottom, DPM Anand Vora, MD Low Profile Medial Locking plate
The Vilex Hemi-Implant: A Retrospective Analysis of 30 Patients in the Treatment of Hallux Rigidus
 Open Access Publication The Vilex Hemi-Implant: A Retrospective Analysis of 30 Patients in the Treatment of Hallux Rigidus by David M. Davidson, DPM 1, Kenneth T. Goldstein, DPM 2, James D. Yakel, DPM
Open Access Publication The Vilex Hemi-Implant: A Retrospective Analysis of 30 Patients in the Treatment of Hallux Rigidus by David M. Davidson, DPM 1, Kenneth T. Goldstein, DPM 2, James D. Yakel, DPM
Section 6: Preoperative Planning
 Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
A Patient s Guide to Hallux Rigidus
 A Patient s Guide to Hallux Rigidus Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER: The information in this booklet
A Patient s Guide to Hallux Rigidus Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER: The information in this booklet
Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity
 FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2012.0400 Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity Pascal F. Rippstein, MD; Young-Uk
FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2012.0400 Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity Pascal F. Rippstein, MD; Young-Uk
Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy
 CHAPTER 2 Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy Kevin Lam, DPM Rikhil Patel, DPM Thomas Merrill, DPM Hallux abducto valgus
CHAPTER 2 Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy Kevin Lam, DPM Rikhil Patel, DPM Thomas Merrill, DPM Hallux abducto valgus
Increased pressures at
 Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
Hallux Rigidus: Demographics, Etiology, and Radiographic Assessment
 FOOT &ANKLE INTERNATIONAL Copyright 2003 by the American Orthopaedic Foot & Ankle Society, Inc. Hallux Rigidus: Demographics, Etiology, and Radiographic Assessment Michael J. Coughlin, M.D.; Paul S. Shurnas,
FOOT &ANKLE INTERNATIONAL Copyright 2003 by the American Orthopaedic Foot & Ankle Society, Inc. Hallux Rigidus: Demographics, Etiology, and Radiographic Assessment Michael J. Coughlin, M.D.; Paul S. Shurnas,
A perspective on MPJ implant arthroplasty.
 A perspective on MPJ implant arthroplasty. The BioPro MPJ Hemi Implant System: +65 years of successful clinical use. Pre-op Post-op 20+ year implant survivorship 14 96% Survivorship 1 97% Patient Satisfaction
A perspective on MPJ implant arthroplasty. The BioPro MPJ Hemi Implant System: +65 years of successful clinical use. Pre-op Post-op 20+ year implant survivorship 14 96% Survivorship 1 97% Patient Satisfaction
PATIENT GUIDE FOR THE TREATMENT OF TOE ARTHRITIS
 arthrosurface.com PATIENT GUIDE FOR THE TREATMENT OF TOE ARTHRITIS A NATIONWIDE SURGEON SURVEY ON OVER 2,000 HEMICAP TOE PROCEDURES INCLUDES: Patient Function and Activity Milestones Patient Rehabilitation
arthrosurface.com PATIENT GUIDE FOR THE TREATMENT OF TOE ARTHRITIS A NATIONWIDE SURGEON SURVEY ON OVER 2,000 HEMICAP TOE PROCEDURES INCLUDES: Patient Function and Activity Milestones Patient Rehabilitation
Great Toe Joint Replacement Patient Guide
 Great Toe Joint Replacement Patient Guide The BioPro First MPJ Hemi Implant The proven long-term joint fusion alternative. Long-term use Clinically proven High implant survivorship Long-term implant survivorship
Great Toe Joint Replacement Patient Guide The BioPro First MPJ Hemi Implant The proven long-term joint fusion alternative. Long-term use Clinically proven High implant survivorship Long-term implant survivorship
Foot and ankle update
 Foot and ankle update Mr Ian Garnham Consultant Foot and Ankle Surgeon Whipps Cross University Hospital Hallux Rigidus Symptoms first ray and 1st MTP pain and swelling worse with push off or forced dorsiflexion
Foot and ankle update Mr Ian Garnham Consultant Foot and Ankle Surgeon Whipps Cross University Hospital Hallux Rigidus Symptoms first ray and 1st MTP pain and swelling worse with push off or forced dorsiflexion
19 Arthrodesis of the First Metatarsocuneiform Joint
 19 Arthrodesis of the First Metatarsocuneiform Joint CHARLES GUDAS Abduction of the first metatarsal to correct metatarsus primus varus and hallux valgus was first described by Albrecht in 1911. 1 Lapidus
19 Arthrodesis of the First Metatarsocuneiform Joint CHARLES GUDAS Abduction of the first metatarsal to correct metatarsus primus varus and hallux valgus was first described by Albrecht in 1911. 1 Lapidus
Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint
 Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint Subject: Partial or Total Replacement of First Metatarsophalangeal (MTP) Joint Background: Underlying causes of disease or
Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint Subject: Partial or Total Replacement of First Metatarsophalangeal (MTP) Joint Background: Underlying causes of disease or
A Patient s Guide to Hallux Rigidus
 A Patient s Guide to Hallux Rigidus Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Hallux Rigidus Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled from a variety
Hallux Rigidus. Normal. Normal Arthritis Arthritis
 Richard M. Marks, MD Professor and Director Division of Foot and Ankle Department of Orthopaedic Surgery Medical College of Wisconsin Hallux Rigidus Explanation: Hallux Rigidus is characterized as degeneration
Richard M. Marks, MD Professor and Director Division of Foot and Ankle Department of Orthopaedic Surgery Medical College of Wisconsin Hallux Rigidus Explanation: Hallux Rigidus is characterized as degeneration
Preservation of the First Ray in Patients with Diabetes
 Preservation of the First Ray in Patients with Diabetes Surgical approaches are often necessary to off-load excessive pressure. By Derek Ley, DPM, and Barry Rosenblum, DPM Introduction In approaching diabetic
Preservation of the First Ray in Patients with Diabetes Surgical approaches are often necessary to off-load excessive pressure. By Derek Ley, DPM, and Barry Rosenblum, DPM Introduction In approaching diabetic
ABSTRACT. Key Words: Hallux Rigidus, toe, arthrodesis, fusion, arthroplasty, MTP, HemiCAP resurfacing. Level of Evidence: Review
 RESURFACING OF THE FIRST METATARSAL HEAD FOR THE TREATMENT OF HALLUX RIGIDUS: EVOLUTION OF IMPLANT DESIGN, REVIEW OF CLINICAL EXPERIENCE AND PRELIMINARY 5 YEAR RESULTS OF METATARSAL HEAD RESURFACING MTP
RESURFACING OF THE FIRST METATARSAL HEAD FOR THE TREATMENT OF HALLUX RIGIDUS: EVOLUTION OF IMPLANT DESIGN, REVIEW OF CLINICAL EXPERIENCE AND PRELIMINARY 5 YEAR RESULTS OF METATARSAL HEAD RESURFACING MTP
.org. Posterior Tibial Tendon Dysfunction. Anatomy. Cause. Symptoms
 Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
SURGEON SURVEY ON THE TREATMENT OF FIRST TOE ARTHRITIS
 arthrosurface.com SURGEON SURVEY ON THE TREATMENT OF FIRST TOE ARTHRITIS A Patient Guide to Surgeons Experiences INCLUDES: Patient Function and Activity Milestones Patient Rehabilitation & Physiotherapy
arthrosurface.com SURGEON SURVEY ON THE TREATMENT OF FIRST TOE ARTHRITIS A Patient Guide to Surgeons Experiences INCLUDES: Patient Function and Activity Milestones Patient Rehabilitation & Physiotherapy
Functional Hallux Limitus Orthotic Therapy for Hallux Valgus and Hallux Rigidus
 Pathology Specific Orthoses Evidence Based Orthotic Therapy: Functional Hallux Limitus Orthotic Therapy for Hallux Valgus and Hallux Rigidus Lawrence Z. Huppin, DPM California School of Podiatric Medicine
Pathology Specific Orthoses Evidence Based Orthotic Therapy: Functional Hallux Limitus Orthotic Therapy for Hallux Valgus and Hallux Rigidus Lawrence Z. Huppin, DPM California School of Podiatric Medicine
Geoffrey Watson, MD Matthew McKean, MD Siddhant K. Mehta, MD Thom A. Tarquinio, MD
 Geoffrey Watson, MD Matthew McKean, MD Siddhant K. Mehta, MD Thom A. Tarquinio, MD University of Mississippi Medical Center Jackson, Mississippi American Orthopaedic Foot & Ankle Society ANNUAL MEETING
Geoffrey Watson, MD Matthew McKean, MD Siddhant K. Mehta, MD Thom A. Tarquinio, MD University of Mississippi Medical Center Jackson, Mississippi American Orthopaedic Foot & Ankle Society ANNUAL MEETING
Hallux rigidus: Joint preserving alternatives to arthrodesis - a review of the literature
 Online Submissions: http://www.wjgnet.com/esps/ bpgoffice@wjgnet.com doi:10.5312/wjo.v5.i1.6 World J Orthop 2014 January 18; 5(1): 6-13 ISSN 2218-5836 (online) 2014 Baishideng Publishing Group Co., Limited.
Online Submissions: http://www.wjgnet.com/esps/ bpgoffice@wjgnet.com doi:10.5312/wjo.v5.i1.6 World J Orthop 2014 January 18; 5(1): 6-13 ISSN 2218-5836 (online) 2014 Baishideng Publishing Group Co., Limited.
1 st MTPJ Arthrodesis- The Influence of Joint Pathology Surface Preparation & Osteosynthesis Technique On Union Rates
 1 st MTPJ Arthrodesis- The Influence of Joint Pathology Surface Preparation & Osteosynthesis Technique On Union Rates Ghosh A, Mahadevan M, Korim MT, Allen PE, Bhatia M, Mangwani J Leicester General Hospital
1 st MTPJ Arthrodesis- The Influence of Joint Pathology Surface Preparation & Osteosynthesis Technique On Union Rates Ghosh A, Mahadevan M, Korim MT, Allen PE, Bhatia M, Mangwani J Leicester General Hospital
Weil osteotomy and flexor to extensor transfer for irreparable plantar plate tear: prospective study
 Weil osteotomy and flexor to extensor transfer for irreparable plantar plate tear: prospective study Daniel Baumfeld, MD Fernando Raduan, MD Fernanda Catena, MD Tania Mann, MD Caio Nery, MD Disclosure
Weil osteotomy and flexor to extensor transfer for irreparable plantar plate tear: prospective study Daniel Baumfeld, MD Fernando Raduan, MD Fernanda Catena, MD Tania Mann, MD Caio Nery, MD Disclosure
Hallux Valgus Deformity: Preoperative Radiologic Assessment
 119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
Mid-Term Results of Triple Osteotomy in Hallux Valgus with Highly Increased Distal Metatarsal Articular Angle
 AOFAS Annual Meeting 2012 The Korean Foot & Ankle Society Mid-Term Results of Triple Osteotomy in Hallux Valgus with Highly Increased Distal Metatarsal Articular Angle Kyung Tai Lee, M.D., Ki Won Young,
AOFAS Annual Meeting 2012 The Korean Foot & Ankle Society Mid-Term Results of Triple Osteotomy in Hallux Valgus with Highly Increased Distal Metatarsal Articular Angle Kyung Tai Lee, M.D., Ki Won Young,
Hallux Rigidus & Silastic Total Implants
 Hallux Rigidus & Silastic Total Implants JOSHUA L. MOORE, DPM FACFAS ASSISTANT DEAN OF EDUCATIONAL AFFAIRS TUSPM CLINICAL ASSISTANT PROFESSOR OF SURGERY Definitions Hallux Limitus 1 st MTPJ range of motion
Hallux Rigidus & Silastic Total Implants JOSHUA L. MOORE, DPM FACFAS ASSISTANT DEAN OF EDUCATIONAL AFFAIRS TUSPM CLINICAL ASSISTANT PROFESSOR OF SURGERY Definitions Hallux Limitus 1 st MTPJ range of motion
Osteotomy vs No Osteotomy Second Ray
 Osteotomy vs No Osteotomy Second Ray Michael D. Dujela DPM, FACFAS Fellowship Trained Foot and Ankle Surgeon Washington Orthopaedic Center, Centralia, WA Chairman, Education and Scientific Affairs Committee
Osteotomy vs No Osteotomy Second Ray Michael D. Dujela DPM, FACFAS Fellowship Trained Foot and Ankle Surgeon Washington Orthopaedic Center, Centralia, WA Chairman, Education and Scientific Affairs Committee
Hallux rigidus (Arthritis of the big toe joint) surgery
 Information for patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. This leaflet tells you about to treat
Information for patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. This leaflet tells you about to treat
High Rate of Recurrent Hallux Valgus Following Proximal Medial Opening Wedge Osteotomy for Correction of Moderate to Severe Deformity
 High Rate of Recurrent Hallux Valgus Following Proximal Medial Opening Wedge Osteotomy for Correction of Moderate to Severe Deformity Sravisht Iyer, MD 1 Constantine Demetracopoulos, MD Jeanne Yu, BS Sriniwasan
High Rate of Recurrent Hallux Valgus Following Proximal Medial Opening Wedge Osteotomy for Correction of Moderate to Severe Deformity Sravisht Iyer, MD 1 Constantine Demetracopoulos, MD Jeanne Yu, BS Sriniwasan
University of Groningen. Forefoot disorders Schrier, Joost
 University of Groningen Forefoot disorders Schrier, Joost IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document version
University of Groningen Forefoot disorders Schrier, Joost IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document version
RISK FACTORS FOR SUBOPTIMAL OUTCOMES IN HAMMERTOE SURGERY JACOB RANDICH BS
 RISK FACTORS FOR SUBOPTIMAL OUTCOMES IN HAMMERTOE SURGERY JACOB RANDICH BS RACHEL ALBRIGHT DPM, MOIZ HASSAN MS, ROBERT O KEEFE DPM, ERIN E. KLEIN DPM, MS, LOWELL WEIL JR. DPM, MBA, LOWELL WEIL SR. DPM,
RISK FACTORS FOR SUBOPTIMAL OUTCOMES IN HAMMERTOE SURGERY JACOB RANDICH BS RACHEL ALBRIGHT DPM, MOIZ HASSAN MS, ROBERT O KEEFE DPM, ERIN E. KLEIN DPM, MS, LOWELL WEIL JR. DPM, MBA, LOWELL WEIL SR. DPM,
Distraction Osteogenesis and Fusion for Failed First Metatarsophalangeal Joint Replacement: Case Series
 737481FAIXXX10.1177/1071100717737481Foot & Ankle InternationalDa Cunha et al research-article2017 Case Report Distraction Osteogenesis and Fusion for Failed First Metatarsophalangeal Joint Replacement:
737481FAIXXX10.1177/1071100717737481Foot & Ankle InternationalDa Cunha et al research-article2017 Case Report Distraction Osteogenesis and Fusion for Failed First Metatarsophalangeal Joint Replacement:
Matthew Beuchel MD 2 C. Luke Rust MD 3 Jessica Hooper MD 3
 A Prospective, Randomized,Controlled Trial Comparing Early- Weightbearing vs. Non-Weightbearing Following Modified Lapidus Arthrodesis Intermediate Results - Donald R. Bohay, MD, FACS Professor, Michigan
A Prospective, Randomized,Controlled Trial Comparing Early- Weightbearing vs. Non-Weightbearing Following Modified Lapidus Arthrodesis Intermediate Results - Donald R. Bohay, MD, FACS Professor, Michigan
MULTIPLE APPLICATIONS OF THE MINIRAIL
 C H A P T E R 2 1 MULTIPLE APPLICATIONS OF THE MINIRAIL Thomas J. Merrill, DPM James M. Losito, DPM Mario Cala, DPM Victor Herrera, DPM Alan E. Sotelo, DPM INTRODUCTION The unilateral MiniRail External
C H A P T E R 2 1 MULTIPLE APPLICATIONS OF THE MINIRAIL Thomas J. Merrill, DPM James M. Losito, DPM Mario Cala, DPM Victor Herrera, DPM Alan E. Sotelo, DPM INTRODUCTION The unilateral MiniRail External
Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months.
 Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months. Diagnosis: II MTP instability Demographics of MT instability Lesser MTP joint instability occurs
Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months. Diagnosis: II MTP instability Demographics of MT instability Lesser MTP joint instability occurs
1. Orthoapedic Associates of Michigan, PC, Grand Rapids, MI 2. Michigan State University College of Human Medicine, Grand Rapids, MI
 Second Metatarsal Osteotomy Shortening with Tarsometatarsal Arthrodesis: Comparison of Outcomes Between MSP TM Metatarsal Shortening System and Plates and Screws Donald R. Bohay, MD, FACS 1 ; John G. Anderson,
Second Metatarsal Osteotomy Shortening with Tarsometatarsal Arthrodesis: Comparison of Outcomes Between MSP TM Metatarsal Shortening System and Plates and Screws Donald R. Bohay, MD, FACS 1 ; John G. Anderson,
CLINICAL EXAM PREDICTORS OF PLANTAR PLATE TEARS
 CLINICAL EXAM PREDICTORS OF PLANTAR PLATE TEARS Erin E. Klein, DPM, MS Lowell Weil, Jr., DPM, MBA Lowell Scott Weil, Sr., DPM Jessica Knight, DPM Weil Foot & Ankle Institute Des Plaines, Illinois CLINICAL
CLINICAL EXAM PREDICTORS OF PLANTAR PLATE TEARS Erin E. Klein, DPM, MS Lowell Weil, Jr., DPM, MBA Lowell Scott Weil, Sr., DPM Jessica Knight, DPM Weil Foot & Ankle Institute Des Plaines, Illinois CLINICAL
Index. Clin Podiatr Med Surg 22 (2005) Note: Page numbers of article titles are in boldface type.
 Clin Podiatr Med Surg 22 (2005) 309 314 Index Note: Page numbers of article titles are in boldface type. A Abductor digiti minimi muscle, myectomy of, for tailor s bunionette, 243 Achilles tendon, lengthening
Clin Podiatr Med Surg 22 (2005) 309 314 Index Note: Page numbers of article titles are in boldface type. A Abductor digiti minimi muscle, myectomy of, for tailor s bunionette, 243 Achilles tendon, lengthening
Long Oblique Distal Osteotomy of the Fifth Metatarsal for Correction of Tailor s Bunion: A Retrospective Review
 Long Oblique Distal Osteotomy of the Fifth Metatarsal for Correction of Tailor s Bunion: A Retrospective Review Barry P. London, DPM, 1 Stephen F. Stern, DPM, 2 Mark A. Quist, DPM, 3 Robert K. Lee, DPM,
Long Oblique Distal Osteotomy of the Fifth Metatarsal for Correction of Tailor s Bunion: A Retrospective Review Barry P. London, DPM, 1 Stephen F. Stern, DPM, 2 Mark A. Quist, DPM, 3 Robert K. Lee, DPM,
First metatarsophalangeal hemiarthroplasty for hallux rigidus
 DOI 10.1007/s00264-010-1012-x ORIGINAL PAPER First metatarsophalangeal hemiarthroplasty for hallux rigidus Eric Giza & Martin Sullivan & Dan Ocel & Gregory Lundeen & Matt Mitchell & Lauren Frizzell Received:
DOI 10.1007/s00264-010-1012-x ORIGINAL PAPER First metatarsophalangeal hemiarthroplasty for hallux rigidus Eric Giza & Martin Sullivan & Dan Ocel & Gregory Lundeen & Matt Mitchell & Lauren Frizzell Received:
SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT
 C H A P T E R 1 7 SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT William D. Fishco, DPM, MS INTRODUCTION Arthroereisis is a surgical procedure designed to limit the motion of a joint. Subtalar joint arthroereisis
C H A P T E R 1 7 SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT William D. Fishco, DPM, MS INTRODUCTION Arthroereisis is a surgical procedure designed to limit the motion of a joint. Subtalar joint arthroereisis
Synthetic Cartilage Implant for 1st MTP Osteoarthritis: The Difference is DATA
 Synthetic Cartilage Implant for 1st MTP Osteoarthritis: The Difference is DATA This educational activity is supported by an educational grant from Cartiva, Inc. Faculty Peter A. Blume, DPM, FACFAS Attending
Synthetic Cartilage Implant for 1st MTP Osteoarthritis: The Difference is DATA This educational activity is supported by an educational grant from Cartiva, Inc. Faculty Peter A. Blume, DPM, FACFAS Attending
Joint Preserving Surgery in Severe Forefoot Disorders
 Joint Preserving Surgery in Severe Forefoot Disorders J ORTHOP TRAUMA SURG REL RES 4 (12) 2008 Review article LOUIS S. BAROUK*, PIERRE BAROUK** * 39, Chemin de la Roche, 33370, Yvrac, France ** Clinique
Joint Preserving Surgery in Severe Forefoot Disorders J ORTHOP TRAUMA SURG REL RES 4 (12) 2008 Review article LOUIS S. BAROUK*, PIERRE BAROUK** * 39, Chemin de la Roche, 33370, Yvrac, France ** Clinique
Common Foot and Ankle Conditions: How Can You Find Relief?
 Common Foot and Ankle Conditions: How Can You Find Relief? Your Feet and Ankles are Workhorses They bear a lot of weight They perform various movements Common Conditions That Cause Foot/Ankle Pain Plantar
Common Foot and Ankle Conditions: How Can You Find Relief? Your Feet and Ankles are Workhorses They bear a lot of weight They perform various movements Common Conditions That Cause Foot/Ankle Pain Plantar
CURRICULUM VITAE. East Lansing, Michigan B.S. Biochemistry. Michigan State University
 NAME: EDUCATION: Michigan State University East Lansing, Michigan 1979-1983 B.S. Biochemistry Michigan State University College of Osteopathic Medicine East Lansing, Michigan Top 20% Class Standing 1983-1987
NAME: EDUCATION: Michigan State University East Lansing, Michigan 1979-1983 B.S. Biochemistry Michigan State University College of Osteopathic Medicine East Lansing, Michigan Top 20% Class Standing 1983-1987
ORTHOLOC 3Di. Foot Reconstruction System SURGIC AL TECHNIQUE
 ORTHOLOC 3Di Foot Reconstruction System S C R E W TA R G E T I N G G U I D E SURGIC AL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: ORTHOLOC
ORTHOLOC 3Di Foot Reconstruction System S C R E W TA R G E T I N G G U I D E SURGIC AL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: ORTHOLOC
1 st MP Arthrodesis. - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA
 1 st MP Arthrodesis - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA Hallux Limitus Dorsal Bunion Spasm of Short Flexor Immobility of Sesamoids DJD of 1 st MPJ Hallus Limitus Plantar
1 st MP Arthrodesis - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA Hallux Limitus Dorsal Bunion Spasm of Short Flexor Immobility of Sesamoids DJD of 1 st MPJ Hallus Limitus Plantar
HALLUX LIMITUS VS. TURF TOE
 VS. TURF TOE EATA Conference 2015 { Dr Jim Sullivan DPM ATC North Smithfield Podiatry Foot and Ankle Consultant: University of Rhode Island Athletics Providence College Athletics Providence Bruins USA
VS. TURF TOE EATA Conference 2015 { Dr Jim Sullivan DPM ATC North Smithfield Podiatry Foot and Ankle Consultant: University of Rhode Island Athletics Providence College Athletics Providence Bruins USA
A finite-element analysis study of the metatarsophalangeal joint of the hallux rigidus
 A finite-element analysis study of the metatarsophalangeal joint of the hallux rigidus R. Flavin, T. Halpin, R. O Sullivan, D. FitzPatrick, A. Ivankovic, M. M. Stephens From Cappagh National Orthopaedic
A finite-element analysis study of the metatarsophalangeal joint of the hallux rigidus R. Flavin, T. Halpin, R. O Sullivan, D. FitzPatrick, A. Ivankovic, M. M. Stephens From Cappagh National Orthopaedic
Minimally Invasive Bunion Surgery: Methods and Outcomes
 Minimally Invasive Bunion Surgery: Methods and Outcomes Hummira H. Abawi, DPM Diplomate ABPM, AACFAS Instructor of Orthopedics, University of Maryland Medical Center Director of Education, Maryland VA
Minimally Invasive Bunion Surgery: Methods and Outcomes Hummira H. Abawi, DPM Diplomate ABPM, AACFAS Instructor of Orthopedics, University of Maryland Medical Center Director of Education, Maryland VA
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus
 Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
)221( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE
 )221( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE First Metatarsophalangeal Joint Arthrodesis: A Retrospective Comparison of Crossed-screws, Locking and Non-Locking Plate
)221( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE First Metatarsophalangeal Joint Arthrodesis: A Retrospective Comparison of Crossed-screws, Locking and Non-Locking Plate
Modified Proximal Scarf Osteotomy for Hallux Valgus
 Original Article Clinics in Orthopedic Surgery 2018;10:479-483 https://doi.org/10.4055/cios.2018.10.4.479 Modified Proximal Scarf Osteotomy for Hallux Valgus Ki Won Young, MD, Hong Seop Lee, MD, Seong
Original Article Clinics in Orthopedic Surgery 2018;10:479-483 https://doi.org/10.4055/cios.2018.10.4.479 Modified Proximal Scarf Osteotomy for Hallux Valgus Ki Won Young, MD, Hong Seop Lee, MD, Seong
Investigation performed at Orthopaedic Hospital Gersthof, Vienna, Austria
 1131 COPYRIGHT 2004 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Salvage of a Failed Keller Resection Arthroplasty BY FELIX MACHACEK JR., MD, MARK E. EASLEY, MD, FLORIAN GRUBER, MD, PETER RITSCHL,
1131 COPYRIGHT 2004 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Salvage of a Failed Keller Resection Arthroplasty BY FELIX MACHACEK JR., MD, MARK E. EASLEY, MD, FLORIAN GRUBER, MD, PETER RITSCHL,
Locked Versus Nonlocked Plate Fixation For Hallux MTP Arthrodesis
 FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2011.0704 Locked Versus Nonlocked Plate Fixation For Hallux MTP Arthrodesis Kenneth J. Hunt, MD; J. Kent Ellington, MD, MS; Robert B. Anderson, MD; Bruce E. Cohen,
FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2011.0704 Locked Versus Nonlocked Plate Fixation For Hallux MTP Arthrodesis Kenneth J. Hunt, MD; J. Kent Ellington, MD, MS; Robert B. Anderson, MD; Bruce E. Cohen,
Length of the Sesamoids and Their Distance From the Metatarsophalangeal Joint Space in Feet With Incipient Hallux Limitus
 ORIGINAL ARTICLES Length of the Sesamoids and Their Distance From the Metatarsophalangeal Joint Space in Feet With Incipient Hallux Limitus Pedro V. Munuera, LicPod, PhD* Gabriel Domínguez, LicPod, PhD*
ORIGINAL ARTICLES Length of the Sesamoids and Their Distance From the Metatarsophalangeal Joint Space in Feet With Incipient Hallux Limitus Pedro V. Munuera, LicPod, PhD* Gabriel Domínguez, LicPod, PhD*
Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot.
 Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot. Compression technology Variable angle locking technology Anatomic and
Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot. Compression technology Variable angle locking technology Anatomic and
Surgical Off-loading. Reiber et al Goals of Diabetic Foot Surgery 4/28/2012. The most common causal pathway to a diabetic foot ulceration
 Reiber et al. 1999 Surgical Off-loading The most common causal pathway to a diabetic foot ulceration Alex Reyzelman DPM Associate Professor California School of Podiatric Medicine at Samuel Merritt University
Reiber et al. 1999 Surgical Off-loading The most common causal pathway to a diabetic foot ulceration Alex Reyzelman DPM Associate Professor California School of Podiatric Medicine at Samuel Merritt University
The Effect of Hallux Abducto Valgus Surgery on the Sesamoid Apparatus Position
 1999 WILLIAM J. STICKEL GOLD AWARD The Effect of Hallux Abducto Valgus Surgery on the Sesamoid Apparatus Position MOLLY S. JUDGE, DPM* STEPHAN LAPOINTE, DPM, PhD GERARD V. YU, DPM JEFFREY E. SHOOK, DPM
1999 WILLIAM J. STICKEL GOLD AWARD The Effect of Hallux Abducto Valgus Surgery on the Sesamoid Apparatus Position MOLLY S. JUDGE, DPM* STEPHAN LAPOINTE, DPM, PhD GERARD V. YU, DPM JEFFREY E. SHOOK, DPM
The bunionette the epidemiological and results from technical Ludloff study. Mário Kuhn Adames Gustavo Batista Birro Rafael da Silveira Basso
 The bunionette the epidemiological and results from technical Ludloff study Mário Kuhn Adames Gustavo Batista Birro Rafael da Silveira Basso NO CONFLICT DISCLOSE The bunionette the epidemiological and
The bunionette the epidemiological and results from technical Ludloff study Mário Kuhn Adames Gustavo Batista Birro Rafael da Silveira Basso NO CONFLICT DISCLOSE The bunionette the epidemiological and
5 COMMON CONDITIONS IN THE FOOT & ANKLE
 5 COMMON CONDITIONS IN THE FOOT & ANKLE MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA IN A NUTSHELL ~ ALL ANATOMY & BIOMECHANICS >90% OF CONDITIONS IN FOOT & ANKLE DIAGNISED FROM GOOD
5 COMMON CONDITIONS IN THE FOOT & ANKLE MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA IN A NUTSHELL ~ ALL ANATOMY & BIOMECHANICS >90% OF CONDITIONS IN FOOT & ANKLE DIAGNISED FROM GOOD
Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot
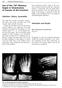 168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
Foot & Ankle Disorders
 Foot & Ankle Disorders Hillingdon PGMC 6-7-2013 Htwe Zaw FRCS (Tr&Orth) Consultant Foot & Ankle and Trauma Surgeon Hillingdon Hospitals NHS Foundation Trust Overview Anatomy: hindfoot-midfoot coupling
Foot & Ankle Disorders Hillingdon PGMC 6-7-2013 Htwe Zaw FRCS (Tr&Orth) Consultant Foot & Ankle and Trauma Surgeon Hillingdon Hospitals NHS Foundation Trust Overview Anatomy: hindfoot-midfoot coupling
Are you living with toe pain?
 Are you living with toe pain? Unlike a toe fusion, the Arthrosurface Joint Restoration Systems can allow you to resume full activity and preserves the natural anatomy of your joint. Find out if the Arthrosurface
Are you living with toe pain? Unlike a toe fusion, the Arthrosurface Joint Restoration Systems can allow you to resume full activity and preserves the natural anatomy of your joint. Find out if the Arthrosurface
Bunion Surgery. This article provides information on surgery for bunions. For more general information: Bunions (topic.cfm? topic=a00155).
 Bunion Surgery This article provides information on surgery for bunions. For more general information: Bunions (topic.cfm? topic=a00155). Most people with bunions find pain relief with simple treatments
Bunion Surgery This article provides information on surgery for bunions. For more general information: Bunions (topic.cfm? topic=a00155). Most people with bunions find pain relief with simple treatments
Diseases of the Musculoskeletal System and Connective Tissue M00 M50 (Part 2)
 Diseases of the Musculoskeletal System and Connective Tissue M00 M50 (Part 2) Presented by Lawrence Santi, DPM, FASPS Webinar 4b: Thursday, March 6, 2014 1 APMA Educational Information: ICD-10 Webinars
Diseases of the Musculoskeletal System and Connective Tissue M00 M50 (Part 2) Presented by Lawrence Santi, DPM, FASPS Webinar 4b: Thursday, March 6, 2014 1 APMA Educational Information: ICD-10 Webinars
Can modification of the Weil osteotomy reduce the risk of dorsiflexion contracture? -A biomechanical cadaveric analysis
 Can modification of the Weil osteotomy reduce the risk of dorsiflexion contracture? -A biomechanical cadaveric analysis Anthony Perera University Hospital of Wales, UK Oscar Helguera-Mendoza Hospital Puerto
Can modification of the Weil osteotomy reduce the risk of dorsiflexion contracture? -A biomechanical cadaveric analysis Anthony Perera University Hospital of Wales, UK Oscar Helguera-Mendoza Hospital Puerto
Merete BLP. Surgical Technique. - Bunion Locking Plate - Low Profile Locking Bone Plate System
 Merete BLP - Bunion Locking Plate - Low Profile Locking Bone Plate System Surgical Technique Merete Medical, Inc. 49 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 www.merete-medical.com - Surgical
Merete BLP - Bunion Locking Plate - Low Profile Locking Bone Plate System Surgical Technique Merete Medical, Inc. 49 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 www.merete-medical.com - Surgical
FREIBERG S INFRACTION TREATMENT WITH METATARSAL NECK DORSAL CLOSING WEDGE OSTEOTOMY: REPORT OF TWO CASES
 FREIBERG S INFRACTION TREATMENT WITH METATARSAL NECK DORSAL CLOSING WEDGE OSTEOTOMY: REPORT OF TWO CASES Sung-Yen Lin, 1 Yuh-Min Cheng, 1,2 and Peng-Ju Huang 1,2 1 Department of Orthopedics, Kaohsiung
FREIBERG S INFRACTION TREATMENT WITH METATARSAL NECK DORSAL CLOSING WEDGE OSTEOTOMY: REPORT OF TWO CASES Sung-Yen Lin, 1 Yuh-Min Cheng, 1,2 and Peng-Ju Huang 1,2 1 Department of Orthopedics, Kaohsiung
Immediate full weight bearing after tarsometata arthrodesis in correcting severe hallux valgus deformity - is it achievable?
 Immediate full weight bearing after tarsometata arthrodesis in correcting severe hallux valgus deformity - is it achievable? Burg Giebichenstein. KunstHochschule Halle Leopoldina Presentation title: Immediate
Immediate full weight bearing after tarsometata arthrodesis in correcting severe hallux valgus deformity - is it achievable? Burg Giebichenstein. KunstHochschule Halle Leopoldina Presentation title: Immediate
Clinical Policy Title: Hammer toe surgery
 Clinical Policy Title: Hammer toe surgery Clinical Policy Number: 18.03.04 Effective Date: July 1, 2016 Initial Review Date: July 15, 2016 Most Recent Review Date: May 1, 2018 Next Review Date: May 2019
Clinical Policy Title: Hammer toe surgery Clinical Policy Number: 18.03.04 Effective Date: July 1, 2016 Initial Review Date: July 15, 2016 Most Recent Review Date: May 1, 2018 Next Review Date: May 2019
Moderate to severe hallux valgus deformity: correction with proximal crescentic osteotomy and distal soft-tissue release
 Arch Orthop Trauma Surg (2000) 120 : 397 402 Springer-Verlag 2000 ORIGINAL ARTICLE R. Zettl H.-J. Trnka M. Easley M. Salzer P. Ritschl Moderate to severe hallux valgus deformity: correction with proximal
Arch Orthop Trauma Surg (2000) 120 : 397 402 Springer-Verlag 2000 ORIGINAL ARTICLE R. Zettl H.-J. Trnka M. Easley M. Salzer P. Ritschl Moderate to severe hallux valgus deformity: correction with proximal
LAPIDUS What is Old is New
 LAPIDUS What is Old is New Alan Jay Block, DPM, MS, FASPS, FACFAS Fellowship trained in Advanced Ankle Techniques Adjunct Professor Dept Of Orthopeadics The Ohio State University Board Member The Ohio
LAPIDUS What is Old is New Alan Jay Block, DPM, MS, FASPS, FACFAS Fellowship trained in Advanced Ankle Techniques Adjunct Professor Dept Of Orthopeadics The Ohio State University Board Member The Ohio
Metatarsophalangeal joint replacement for hallux rigidus: a developing field
 OPN issue 168 Metatarsophalangeal joint replacement for hallux rigidus: a developing field Maire-Clare Killen, Liam McEntee, Mohan Emmanuel, Prasad Karpe and Rajiv Limaye describe the use of arthroplasty
OPN issue 168 Metatarsophalangeal joint replacement for hallux rigidus: a developing field Maire-Clare Killen, Liam McEntee, Mohan Emmanuel, Prasad Karpe and Rajiv Limaye describe the use of arthroplasty
pedcat Clinical Case Studies
 pedcat Clinical Case Studies C u r v e B e a m 1 7 5 T i t u s A v e, S u i t e 3 0 0 W a r r i n g t o n, P A 1 8 9 7 6 267-4 8 3-8081 w w w. c u r v e b e a m. c o m PedCAT: Clinical Evidence of diagnostic
pedcat Clinical Case Studies C u r v e B e a m 1 7 5 T i t u s A v e, S u i t e 3 0 0 W a r r i n g t o n, P A 1 8 9 7 6 267-4 8 3-8081 w w w. c u r v e b e a m. c o m PedCAT: Clinical Evidence of diagnostic
Surgical correction of Hallux Valgus
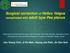 Surgical correction of Hallux Valgus complicated with adult type Pes planus Department of Orthopedic Surgery, Inje University, Ilsan Paik Hospital, Goyang-si, Korea * W Institute for Foot and Ankle Diseases
Surgical correction of Hallux Valgus complicated with adult type Pes planus Department of Orthopedic Surgery, Inje University, Ilsan Paik Hospital, Goyang-si, Korea * W Institute for Foot and Ankle Diseases
TURF TOE IN A TAEKWANDOO PLAYER: CASE REPORT
 Journal of Sports Science and Medicine (2004) 3, 96-100 http://www.jssm.org Case report TURF TOE IN A TAEKWANDOO PLAYER: CASE REPORT Namık Sahin 1, Teoman Atici 1, Sadik M. Bilgen 2 and Omer F. Bilgen
Journal of Sports Science and Medicine (2004) 3, 96-100 http://www.jssm.org Case report TURF TOE IN A TAEKWANDOO PLAYER: CASE REPORT Namık Sahin 1, Teoman Atici 1, Sadik M. Bilgen 2 and Omer F. Bilgen
Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair
 Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair Carlos Villas, MD, PhD, 1 Javier Del Río, MD, 3 Andres
Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair Carlos Villas, MD, PhD, 1 Javier Del Río, MD, 3 Andres
The American Academy of Foot & Ankle Osteosynthesis. presents
 The American Academy of Foot & Ankle Osteosynthesis presents Comprehensive Course of Internal Fixation for Reconstructive Surgery and Trauma of the Foot & Ankle September 4-6, 2014 Goodlett Farms Innovation
The American Academy of Foot & Ankle Osteosynthesis presents Comprehensive Course of Internal Fixation for Reconstructive Surgery and Trauma of the Foot & Ankle September 4-6, 2014 Goodlett Farms Innovation
Synthetic Cartilage Implants for Joint Pain
 Synthetic Cartilage Implants for Joint Pain Policy Number: 7.01.160 Last Review: 3/2018 Origination: 2/2018 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Synthetic Cartilage Implants for Joint Pain Policy Number: 7.01.160 Last Review: 3/2018 Origination: 2/2018 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
A Patient s Guide to Bunions. Foot and Ankle Center of Massachusetts, P.C.
 A Patient s Guide to Bunions Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written and professionally
A Patient s Guide to Bunions Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written and professionally
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow.
 Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Bunions. Compliments of: Institute of Sports Medicine & Orthopaedics
 A Patient s Guide to Bunions 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Bunions 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet is compiled
RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS
 C H A P T E R 1 7 RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS Michelle L. Butterworth, DPM Michael S. Downey, DPM Digital deformities are one of the most common entities we face as foot and
C H A P T E R 1 7 RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS Michelle L. Butterworth, DPM Michael S. Downey, DPM Digital deformities are one of the most common entities we face as foot and
Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities
 Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities NO DISCLOSURES Objectives The main objectives of any procedure in hallux abducto valgus surgery are to correct the deformity,
Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities NO DISCLOSURES Objectives The main objectives of any procedure in hallux abducto valgus surgery are to correct the deformity,
Salvage of first metatarsophalangeal joint arthroplasty complications
 Foot Ankle Clin N Am 8 (2003) 37 48 Salvage of first metatarsophalangeal joint arthroplasty complications Judith F. Baumhauer, MD*, Benedict F. DiGiovanni, MD Orthopedic Department, University of Rochester
Foot Ankle Clin N Am 8 (2003) 37 48 Salvage of first metatarsophalangeal joint arthroplasty complications Judith F. Baumhauer, MD*, Benedict F. DiGiovanni, MD Orthopedic Department, University of Rochester
