Lower Extremity Reconstruction
|
|
|
- Austen Gordon
- 5 years ago
- Views:
Transcription
1 1 Chapter 21 Overview: Lower Extremity Reconstruction Louis Carter This subject is also partially covered in the chapters Flaps for Wound Coverage and Perforator Flaps. This chapter will deal with reconstruction from the knee to the foot. Primary closure or delayed primary closure is ideal. If this is not possible then the most reliable method available should be used and not necessarily the simplest. If the wound is under tension after primary closure, then a more reliable method as a flap should be used. It is very important that every attempt should be made to close an acute clean wound immediately especially on the leg. Though wounds on the face and upper extremity may be closed within 24 hours if débrided and cleansed well, the 8 hour limit remains for lower extremity injures. If after an accident skin is missing but the wound is clean, then a skin graft or even a flap can be used to cover the wound immediately. A meshed graft works well. There is absolutely no need to delay closure in order for granulation tissue to develop. Contaminated wounds that cannot be closed acutely because of contamination should be closed within the first 7 days by delayed direct primary closure, skin grafts or flaps. After 7 days, the wound will then need radical débridement before closure unless a VAC is used. During the time the wound is left open it must be kept moist by methods described. (See chapter on Chronic Wounds). Care of the open fracture wound is dictated by the fracture type (See PAACS Orthopaedic Curriculum): Type I open fractures, small wounds, <1 cm. long, should be débrided and loosely closed if clean. Type II open fractures, > 1 cm. long, débrided and if possible the wound is closed very loosely over any exposed bone and a second look with repeat débridement should be done within hours. If the wound is clean after the second look, then it should be definitely closed by skin grafts, local fasciocutaneous or muscle flaps. Type III, >10 cm. long, débrided, with a second look hours for further débridement. Further débridements will likely be necessary but every
2 attempt should be made to close the wound as early as possible and definitely by 7 days. In Type III, if closure is delayed past 7 days, then a VAC may likely be necessary. As far as the timing of the closure is concerned, recent studies show that it is the quality of the wound that is important before the wound is closed, not necessarily the timing of the closure. As long as adequate debridement is done and the wound is clean, the wound can be closed and sooner you can do this the better. The many variables preclude definite statements regarding treatment of Type III open fractures. These variables include where the fracture occurred as in the farm or on the highway, contamination, length of time before débridement, adequacy and frequency of irrigations and débridements, tissue loss, stabilization, how well the tissues are kept moist, vascular damage, availability of VACs, etc. Method of débridement is found in the chapter on open fractures in the PAACS Orthopaedic Curriculum, pg. 6, 7. Many Type III injuries may need long term VAC use followed by flap coverage. Occasionally, Type III injuries maybe loosely and partially closed after débridement. A cephalosporin antibiotic should always be used and if microbiology is available, cultures should be obtained on admission with contaminated wounds. An aminoglycoside +/- penicillin is added if the wounds are severely contaminated, likely with gram-negative and anaerobic microorganisms. In any open fracture early stabilization is very important before wound closure. The fracture site should be covered as soon as there fixation of the fracture. If the wound is clean, SIGN nailing is an excellent method of fixation of long bones and this is available in many hospitals throughout Africa. If nailing is not possible then external fixation should be used. Both of these methods of stabilization allow for repeated débridements of the wound and allow for the use of a VAC and later flap coverage. When external fixation is used, care must be taken to apply it in such a way that VAC and flaps can be used. Bone should never be left exposed or it will desiccate. Wounds must be covered with moist dressings, dressings impregnated with silver sulfadiazine or a VAC, and definitively closed as soon as possible, preferably before 7 days post injury. Ideally a muscle flap is best but if not available then a fasciocutaneous flap. Muscle brings in a greater blood supply for débridement of wound and healing of fractures. 2
3 3 Flaps for Knee and Upper third of Tibia: Medial Gastrocnemius Flap is a Type I muscle flap supplied by the medial sural artery off the popliteal artery. It can be used to cover an exposed knee joint or the upper third of the tibia or it can be turned posteriorly into the popliteal fossa. Though it can be used as a myocutaneous flap it is a bulky flap when skin and subcutaneous tissue are added to the muscle and will leave a significant donor site deformity. It is an easy flap to elevate and it can be lengthened by dissecting up to its origin and even carefully dividing the origin at the medial femoral condyle. In order to cover the entire anterior knee and distally to the middle third of the tibia, the muscle may be passed beneath the gracilis, sartorius, and semitendinosus tendons (pes anserinus). If this is done, these tendons must be well freed up proximally and distally to ensure that there is no constricting pressure on the muscle and pedicle. The author will occasionally divide one or more of these tendons if necessary for complete coverage of a wound over the knee. These may be sacrificed without significant functional loss. The gastrocnemius muscle fascia may also be scored longitudinally with multiple parallel incisions through the fascia in order to gain additional width to cover the upper third of the tibia or the popliteal space. A small portion of the Achilles tendon is taken with the muscle so that the muscle flap can be securely inset into the surrounding tissue. In all reconstructions the muscle may be grafted immediately with a meshed skin. During muscle elevation care is taken not to injure the greater saphenous vein and saphenous nerve in the posterior midline. (Editor s Note: It is rarely necessary to pass the gastrocnemius beneath the muscles and tendons in the pes anserinus sartorius, gracilis and semitendinosus. No matter how much these tendons are freed up, there should still be concern about pressure on the gastrocnemius muscle.) It is also possible to use the lateral gastrocnemius muscle flap to cover lateral knee and tibial defects but because of the fibula, this muscle will not rotate to cover as much as desired. During elevation of the lateral gastrocnemius, great care is needed to protect the peroneal nerve. During elevation of both heads care is taken to preserve the sural nerve and lesser saphenous vein which lie in the midline between the heads of the gastrocnemius muscle. After the muscles have been inset skin grafting should be done immediately.
4 4 Fig 1 Fig 2 Open fracture of tibi al plateau. Woun d dé bri de d and medial gastrocnemius muscle flap with skin graft was used to cover the wound at the time of the original surgery and fixation Fig 3 Fig 4 Fig 5 Popliteal contracture with scarred skin over medial aspect of leg: medial gastrocnemius flap was used with longitudinal scoring of the muscle fascia and STSG. Scar was excised in this case Saphenous Flap and Cross Leg Flap are thin fasciocutaneous flaps supplied by the small saphenous artery which runs along with the saphenous vein on the medial side of the leg. This flap is an excellent flap for coverage of the popliteal fossa after a burn contracture release. Its anterior border is along the medial edge of the tibia and it can be taken posteriorly with an 8-10 cm. width. As in other fasciocutaneous flaps, the length can be taken approximately 3 X the width. The axis of rotation is at the level of the knee joint. Flaps less than 6 cm. wide can be closed but most of the time the donor site is closed with a meshed skin graft. This flap uses the superficial fascia not the fascia over the gastrocnemius muscle see center picture below with muscle fascia on muscle. This flap is also the one commonly used in the cross leg flap which still remains a valuable flap in Sub-Saharan Africa. (See Chapter on Burn Reconstruction) The donor site must be grafted and dressed before the inset of the flap. A stent dressing is applied using Vaseline or non-adherent gauze, wet cotton balls to hold the skin graft in the crevices, wet and dry gauze with stent sutures tied over this dressing to hold it in place. This is not a bulky dressing. The recipient area is usually the distal third of the leg, ankle or foot. With the knees flexed, it is important to immobilize the extremities with an external
5 fixator so that the flap is fixed into position and will not move. Any movement of the flap may disrupt the capillaries bridging the suture line. It is easy to elevate the legs with the external fixator. In addition, it is important to put the extremities and especially the knees through a full range of motion once the fixator is removed and the flap divided usually at three weeks. There is no absolute age limit for use of the cross leg flap though the older the patient is, the more difficulty there will be in regaining full range of motion. Final inset of the flap is best delayed for a week after division. (After flap division, the flap is loosely inset, but careful inset is performed a few days to a week later.) 5 Fig 6 Fig 7 Fig 8 Saphenous flap: the muscle fascia of the medial gastrocnemius muscle can be left on the muscle see arrow. The flap still contains the superficial fascia. The cross leg flap may also include the medial head of the gastrocnemius muscle when additional coverage is required. The muscle may be used to cover one area and the fasciocutaneous portion used for another area. Fig 9 Fig 10 Fig 11 Medial head of gastrocnemius muscle used to cover popliteal fossa when saphenous flap alone was not adequate.
6 6 Fig 12 Fig 13 Fig 14 Open ankle wound requiring cross leg or saphenous flap. Note: skin graft and stent dressing applie d be fore flap Middle Third Defects: Soleus Flap may be used to cover middle third tibial defects. This is a Type II muscle flap with blood supply from the posterior tibial artery for the medial half and the peroneal artery for the lateral half. Only the medial half of the soleus may be used, a hemi-soleus flap, or the entire muscle may be used. The author uses the entire soleus most of the time unless there is only a very small defect to cover over the tibia. The soleus muscle arises from the proximal tibia and the muscle often extends to the ankle. The muscle is deep to the gastrocnemius. In elevating the distal half of the muscle, care should be taken to carefully divide and ligate the minor pedicles from the posterior tibial artery and vein. One should ligate only the pedicles needed to allow transposition of the muscle to cover the defect. The distal half of the soleus muscle must be sharply dissected free from the gastrocnemius portion of the Achilles tendon. The lateral half of the soleus can be bluntly dissected free. As with the gastrocnemius, the soleus fascia can be scored longitudinally to increase its width. Fig 15 Fig 16 Fig 17 Open fracture junction of u ppe r and mi ddle third of tibi a: Soleus muscle was use d for reconstruction with meshed STSG. Note raw appearance of muscle in middle picture (arrow): this represents where muscle was sharply dissected from Achilles tendon (e nd of hemostat). Reconstruction performed 3 days after injury.
7 7 Fig 18 Fig 19 Fig 20 This is a similar case where soleus muscle was used for middle third tibial fracture. Note the scoring (arrow) of the muscle to increase the width. Fig 21 Fig 22 Fig 23 Reconstruction of large tibial defect with both medial gastrocnemius and soleus muscles. Patient will do well with lateral gastrocnemius. Note scoring of soleus muscle. The soleus has also been raised as a distally based flap on the distal perforators to cover small wounds on the distal third of the leg. This distally based flap is not reliable and the author does not recommend it. The plantaris tendon is located between the gastrocnemius and soleus. (See Chronic Wound
8 chapter where a soleus muscle was used acutely to cover the distal tibia in a severe lower leg injury.) Distal Third Tibial Defects: These are difficult to cover without microvascular capability. The following four techniques do not require microvascular techniques: The cross leg flap can be used to cover these defects but this requires 3-4 weeks of immobilization and multiple stages. The sural artery flap is a very reliable flap when it is taken with the parameters described below. Technique for the Sural Artery or Reversed Leg Flap: It is a reversed fasciocutaneous axial flap that may be used for coverage of the distal tibia, malleoli and heel. The classic flap is based on perforators from the Peroneal Artery to the Sural Artery with the axis of rotation at least 3 fingers breadth (5 cm.) above the lateral malleolus. So this flap may also be classified as a perforator flap. The pedicle must be at least 3 cm. wide and the maximum size of the flap is 9 cm. wide by 12 cm. long. The flap cannot extend proximally more than 20 cm. from the lateral malleolus unless it is delayed. The flap is very reliable if it is raised within these parameters. Some surgeons may prefer to stage the flap elevation and inset because of questionable reversed blood supply or the need to extend the flap proximally, beyond 20 cm, for distal coverage. The center of the flap is the short saphenous vein. Once this vein is found proximally between the two heads of the gastrocnemius, the flap can be outlined. 8 Fig 24 Fig 25 Postop view of reverse sural artery flap harvested as described above to cover posterior ankle wound. Superior edge of donor site is 22 cm. above lateral malleolus but flap was also de laye d once to allow radical débri dement of two week old wound
9 The sural nerve must be taken with the flap to ensure viability. The flap is taken deep to the muscle fascia of the Gastrocnemius but care is taken to preserve the paratenon over the Achilles tendon. In situations where the lateral side of the ankle is injured and when one is unsure about the zone of injury, one can take a wider flap based on perforators from both the peroneal and posterior tibial arteries and delay the flap (see below). 9 Fig 26 Fig 27 Fig 28 Chronic distal third wound 12 days ol d: woun d de bri de d three ti mes and the reverse posterior leg flap (modified reverse sural artery flap) was delayed and lengthened at each dé bri de me nt. The flap was based on mainly the posterior tibial artery because of the injury on the lateral side of the distal leg. Fig Sural Artery flap design, elevation, delay, inset and final result. Note VAC over heel and narrow pedicle. (Courtesy Dr. Blair Summitt)
10 10 Posterior Tibial Perforator Flaps These are excellent flaps for coverage of lower extremity wounds. It can be based on one or more perforators from the posterior tibial artery. A description of this flap is in the Perforator Flap chapter. Keystone Island Perforator Flaps These are island fasciocutaneous flaps taken in a keystone design adjacent to the defect. They are based on perforators adjacent in the tissue adjacent to the defect. (See under Perforator Flaps) Fasciocutaneous Flaps Many other fasciocutaneous flaps can be taken in the lower extremity. Unless based on a definite vessel or perforator but care must be taken not to take the flap longer than 2 X the width. Additional care should be taken to gently rotate the flap into position. If necessary the flap can be delayed once or twice to gain more length. A small backcut can also be made. Retrograde flaps can be taken based on known perforators. In all these flaps, delay may help maintain vascularity especially when used to cover large wounds or when there is the need to rotate the flap sharply for coverage. (Ideally the flap is never rotated acutely.) As long as the recipient wound is kept moist, closure can be delayed for several days. The use of the VAC (Vacuum Assisted Closure (Negative Pressure Therapy) is an excellent addition to the armamentarium of the plastic surgeon. The VAC can be used to clean wounds and create angiogenesis and granulation tissue over bone and tendons and prepare the wound for skin grafting. This technique is described in detail in the Chronic Wound and Wound Closure with VAC chapters. Using perforator flaps from the posterior tibial or peroneal arteries is a newer method and is described in the chapter on Perforator Flaps. In addition there is a newer variant of perforator flaps called the Keystone Island Perforator Flap. It is described at the end of the perforator flap chapter. Foot Defects: Dorsalis Pedis and M edial Plantar Flaps These are small fasciocutaneous flaps of the foot. The Dorsalis Pedis Flap is based on the Dorsalis Pedis Artery, the terminal branch of the Anterior
11 Tibial Artery. The flap can be taken from the anterior surface of the foot and it extends down to the MPJ level. This flap can be used to cover small foot defects and the medial and lateral malleolus. When harvesting the flap care must be taken to leave paratenon over the extensor tendons so that a skin graft will take. 11 Fig 35 Fig 36 Fig 37 Fig 38 Woun d over me di al malle olus: dé bri de d, dorsalis pe di s fla p rai sed and i nset. STSG The M edial Plantar Flap is taken from the instep of the sole of the foot and is supplied by the medial plantar artery, a branch of the posterior tibial artery. This vessel travels beneath the abductor hallucis tendon to supply the sole of the foot. The flap may be rotated to cover the heel with an axis of rotation at the medial malleolus. Terminal branches of the posterior tibial nerve may be taken with the flap to give a sensate heel reconstruction. This will require loupe magnification to dissect these branches from the digital nerves which are not sacrificed. Fig 39 Fig 40 Fig 41 Fig 42 Wound of the plantar we i ght be ari ng surface. Ra di ally dé bri de d and an innervated medial plantar flap raised and rotated to cover defect with a skin graft for donor site The main advantage of the medial plantar flap over other types of heel reconstruction and especially skin grafts is that it provides like tissue to cover the heel and it can also provide a sensate reconstruction. In elevating this
12 fascial flap the longitudinal fibrous septae must be divided. These run the length of the foot between the metatarsals and the plantar fascia. The neurovascular bundles lie on either side of the septae. The donor area, the instep of the foot, is a non-weight bearing portion of the foot and may be reconstructed with a skin graft. The foot needs to be immobilized and elevated in the postoperative period and weight bearing is not allowed for 3 weeks. 12 Fig 43 Fig 44 Medial plantar flap used to reconstruct the heel after excision of a malignant melanoma. An innervated flap was used. This patient refused amputation. Achilles tendon injuries (see Tendon Injuries) Acute open injuries can be repaired with several core weave sutures as in flexor tendon injuries or a Krachow whip stitch with a large braided nonabsorbable suture probably the largest available in the hospital (usually silk, Mersilene or Ethibond). It is best to expose the tendon through a medial incision. The ankle may then be casted in plantar flexion for 6-8 weeks. If the Achilles is avulsed off the calcaneus, it can be repaired using large anchors or with sutures passed through drill holes in the calcaneus. Acute closed ruptures can be treated open or closed with equally good results in recent literature studies. Krachow suture is shown below. Many now add a second suture to give four strands for both Achilles tendon and biceps tendon repairs.
13 13 Steps: Fig 45 Krachow suture for Achilles tendon repair (Figures courtesy of Kenneth A. Krackow MD) Summary: Flaps provide an excellent reconstruction of some difficult areas. There are many more flaps than listed here. These are the most commonly used extremity flaps. Knowledge of vascular anatomy is most important for successful elevation of a flap. Temporary immobilization and elevation of the extremity is important after any flap. In addition, the wounds should be dressed so that inspection of the flap may be carried out frequently during the first 24 hours. If there is a question of viability in the first 24 hours, the patient should be returned to the operating room. Frequently the flap can be salvaged if the problem is corrected early.
Versatility of Reverse Sural Artery Flap for Heel Reconstruction
 ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
Anatomy MCQs Week 13
 Anatomy MCQs Week 13 1. Posterior to the medial malleolus of the ankle: The neurovascular bundle lies between Tibialis Posterior and Flexor Digitorum Longus The tendon of Tibialis Posterior inserts into
Anatomy MCQs Week 13 1. Posterior to the medial malleolus of the ankle: The neurovascular bundle lies between Tibialis Posterior and Flexor Digitorum Longus The tendon of Tibialis Posterior inserts into
17 FibulA FlAP Tor Chiu fibula flap 153
 17 Fibula Flap Tor Chiu Fibula Flap 153 Fibula Flap FLAP TERRITORY This flap includes a segment of the fibular bone with or without the overlying skin island on the peroneal/ lateral aspect of the calf.
17 Fibula Flap Tor Chiu Fibula Flap 153 Fibula Flap FLAP TERRITORY This flap includes a segment of the fibular bone with or without the overlying skin island on the peroneal/ lateral aspect of the calf.
Knee Disarticulation Amputation
 Knee Disarticulation Amputation Pre-Op 64 year old man, previous spinal cord injury, diabetes, renal failure, and a history of spasticity with dynamic knee flexion contracture. He had an open left ankle
Knee Disarticulation Amputation Pre-Op 64 year old man, previous spinal cord injury, diabetes, renal failure, and a history of spasticity with dynamic knee flexion contracture. He had an open left ankle
Lower Limb Nerves. Clinical Anatomy
 Lower Limb Nerves Clinical Anatomy Lumbar Plexus Ventral rami L1 L4 Supplies: Abdominal wall External genitalia Anteromedial thigh Major nerves.. Lumbar Plexus Nerves relation to psoas m. : Obturator n.
Lower Limb Nerves Clinical Anatomy Lumbar Plexus Ventral rami L1 L4 Supplies: Abdominal wall External genitalia Anteromedial thigh Major nerves.. Lumbar Plexus Nerves relation to psoas m. : Obturator n.
The Transtibial Amputation
 The Transtibial Amputation Site of Previous Surgeries: Amputation indication: four unsuccessful previous surgeries. Patient experiences chronic pain and disfunction along with a limited range of motion.
The Transtibial Amputation Site of Previous Surgeries: Amputation indication: four unsuccessful previous surgeries. Patient experiences chronic pain and disfunction along with a limited range of motion.
Gastrocnemius Muscle Flap Coverage of Chronically= Infected Knee Joints
 Gastrocnemius Muscle Flap Coverage of Chronically= Infected Knee Joints ABSTRACT Chronically infected open knee joints present dif cult problem. Aggressive debridement of chronically infected soft tissue
Gastrocnemius Muscle Flap Coverage of Chronically= Infected Knee Joints ABSTRACT Chronically infected open knee joints present dif cult problem. Aggressive debridement of chronically infected soft tissue
Surgical Technique. Achilles Tendon Repair Using Conexa Reconstructive Tissue Matrix. conexatm. Surgical Technique Described by Tom Chang, DPM
 Surgical Technique Achilles Tendon Repair Using Conexa Reconstructive Tissue Matrix Surgical Technique Described by Tom Chang, DPM conexatm r e c o n s t r u c t i v e t i s s u e m a t r i x Achilles
Surgical Technique Achilles Tendon Repair Using Conexa Reconstructive Tissue Matrix Surgical Technique Described by Tom Chang, DPM conexatm r e c o n s t r u c t i v e t i s s u e m a t r i x Achilles
Leg. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Leg Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skin of the Leg Cutaneous Nerves Medially: The saphenous nerve, a branch of the femoral nerve supplies the skin on the medial surface
Leg Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skin of the Leg Cutaneous Nerves Medially: The saphenous nerve, a branch of the femoral nerve supplies the skin on the medial surface
Heel Defect Reconstruction using Local Vascularized Flaps: Results and Clinical Outcomes in 16 Patients
 JFS (P) Kuldeep Singh et al ORIGINL RTICLE 10.5005/jp-journals-10040-1083 Heel Defect Reconstruction using Local Vascularized Flaps: Results and Clinical Outcomes in 16 Patients 1 Kuldeep Singh, 2 Zile
JFS (P) Kuldeep Singh et al ORIGINL RTICLE 10.5005/jp-journals-10040-1083 Heel Defect Reconstruction using Local Vascularized Flaps: Results and Clinical Outcomes in 16 Patients 1 Kuldeep Singh, 2 Zile
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts
 Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Transfemoral Amputation
 Transfemoral Amputation Pre-Op: 42 year old male who sustained severe injuries in a motorcycle accident. Note: he is a previous renal transplant recipient and is on immunosuppressive treatments. His injuries
Transfemoral Amputation Pre-Op: 42 year old male who sustained severe injuries in a motorcycle accident. Note: he is a previous renal transplant recipient and is on immunosuppressive treatments. His injuries
Where should you palpate the pulse of different arteries in the lower limb?
 Where should you palpate the pulse of different arteries in the lower limb? The femoral artery In the femoral triangle, its pulse is easily felt just inferior to the inguinal ligament midway between the
Where should you palpate the pulse of different arteries in the lower limb? The femoral artery In the femoral triangle, its pulse is easily felt just inferior to the inguinal ligament midway between the
Injuries to the Hands and Feet
 Injuries to the Hands and Feet Chapter 26 Injuries to the Hands and Feet Introduction Combat injuries to the hands and feet differ from those of the arms and legs in terms of mortality and morbidity. Death
Injuries to the Hands and Feet Chapter 26 Injuries to the Hands and Feet Introduction Combat injuries to the hands and feet differ from those of the arms and legs in terms of mortality and morbidity. Death
The Leg. Prof. Oluwadiya KS
 The Leg Prof. Oluwadiya KS www.oluwadiya.sitesled.com Compartments of the leg 4 Four Compartments: 1. Anterior compartment Deep fibular nerve Dorsiflexes the foot and toes 2. Lateral Compartment Superficial
The Leg Prof. Oluwadiya KS www.oluwadiya.sitesled.com Compartments of the leg 4 Four Compartments: 1. Anterior compartment Deep fibular nerve Dorsiflexes the foot and toes 2. Lateral Compartment Superficial
Fascial Turn-Down Flap Repair of Chronic Achilles Tendon Rupture
 19 Fascial Turn-Down Flap Repair of Chronic Achilles Tendon Rupture S. Ghosh, P. Laing, and Nicola Maffulli Introduction Fascial turn-down flaps can be used for an anatomic repair of chronic Achilles tendon
19 Fascial Turn-Down Flap Repair of Chronic Achilles Tendon Rupture S. Ghosh, P. Laing, and Nicola Maffulli Introduction Fascial turn-down flaps can be used for an anatomic repair of chronic Achilles tendon
Role Of Reverse Sural Artery Flap In Ankle, Foot And Leg Defects
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. VIII (May. 2016), PP 64-68 www.iosrjournals.org Role Of Reverse Sural Artery Flap In
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. VIII (May. 2016), PP 64-68 www.iosrjournals.org Role Of Reverse Sural Artery Flap In
HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS
 HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS October 22, 2010 D. LOWER LIMB MUSCLES 2. Lower limb compartments ANTERIOR THIGH COMPARTMENT General lfunction: Hip flexion, knee extension, other motions
HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS October 22, 2010 D. LOWER LIMB MUSCLES 2. Lower limb compartments ANTERIOR THIGH COMPARTMENT General lfunction: Hip flexion, knee extension, other motions
ORIGINAL ARTICLE DISTALLY BASED PERONEUS BREVIS MUSCLE FLAP FOR DISTAL LEG DEFECTS
 DISTALLY BASED PERONEUS BREVIS MUSCLE FLAP FOR DISTAL LEG DEFECTS Peddi Manjunath 1, Ramesha K.T 2, Smitha S Segu 3, Jainath 4, Shankarappa M 5 HOW TO CITE THIS ARTICLE: Peddi Manjunath, Ramesha KT, Smitha
DISTALLY BASED PERONEUS BREVIS MUSCLE FLAP FOR DISTAL LEG DEFECTS Peddi Manjunath 1, Ramesha K.T 2, Smitha S Segu 3, Jainath 4, Shankarappa M 5 HOW TO CITE THIS ARTICLE: Peddi Manjunath, Ramesha KT, Smitha
CHAPTER 16 LOWER EXTREMITY. Amanda K Silva, MD and Warren Ellsworth, MD, FACS
 CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
Transtibial Amputation with Extended Flap and Bone Bridging
 Transtibial Amputation with Extended Flap and Bone Bridging Pre-Op Plan: Amputation indication: four years status post a crush injury to his left foot. Patient experiences chronic pain and dysfunction
Transtibial Amputation with Extended Flap and Bone Bridging Pre-Op Plan: Amputation indication: four years status post a crush injury to his left foot. Patient experiences chronic pain and dysfunction
5.1 Identify, describe the attachments of and deduce the actions of the muscles of the thigh:
 5.1 Identify, describe the attachments of and deduce the actions of the muscles of the thigh: Anterior group Proximal attachment Distal attachment Sartorius ASIS» Upper part of shaft tibia (middle surface)»
5.1 Identify, describe the attachments of and deduce the actions of the muscles of the thigh: Anterior group Proximal attachment Distal attachment Sartorius ASIS» Upper part of shaft tibia (middle surface)»
Compartment Syndrome
 Compartment Syndrome Chapter 34 Compartment Syndrome Introduction Compartment syndrome may occur with an injury to any fascial compartment. The fascial defect caused by the injury may not be adequate to
Compartment Syndrome Chapter 34 Compartment Syndrome Introduction Compartment syndrome may occur with an injury to any fascial compartment. The fascial defect caused by the injury may not be adequate to
Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect of Upper and Middle Third Leg
 Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
TRANSTIBIAL AMPUTATION General Principles & Update on Surgical Techniques
 TRANSTIBIAL AMPUTATION General Principles & Update on Surgical Techniques Douglas G. Smith, MD Harborview Medical Center and University of Washington - Emeritus Prosthetic Research Study Amputee Coalition
TRANSTIBIAL AMPUTATION General Principles & Update on Surgical Techniques Douglas G. Smith, MD Harborview Medical Center and University of Washington - Emeritus Prosthetic Research Study Amputee Coalition
1-Muscles: 2-Blood supply: Branches of the profunda femoris artery. 3-Nerve supply: Sciatic nerve
 1-Muscles: B i c e p s f e m o r i s S e m i t e n d i n o s u s S e m i m e m b r a n o s u s a small part of the adductor magnus (h a m s t r i n g p a r t o r i s c h i a l p a r t ) 2-Blood supply:
1-Muscles: B i c e p s f e m o r i s S e m i t e n d i n o s u s S e m i m e m b r a n o s u s a small part of the adductor magnus (h a m s t r i n g p a r t o r i s c h i a l p a r t ) 2-Blood supply:
The Lower Limb VI: The Leg. Anatomy RHS 241 Lecture 6 Dr. Einas Al-Eisa
 The Lower Limb VI: The Leg Anatomy RHS 241 Lecture 6 Dr. Einas Al-Eisa Muscles of the leg Posterior compartment (superficial & deep): primary plantar flexors of the foot flexors of the toes Anterior compartment:
The Lower Limb VI: The Leg Anatomy RHS 241 Lecture 6 Dr. Einas Al-Eisa Muscles of the leg Posterior compartment (superficial & deep): primary plantar flexors of the foot flexors of the toes Anterior compartment:
موسى صالح عبد الرحمن الحنبلي أحمد سلمان
 8 موسى صالح عبد الرحمن الحنبلي أحمد سلمان 1 P a g e Today we will talk about a new region, which is the leg. And as always, we will start with studying the sensory innervation of the leg. What is the importance
8 موسى صالح عبد الرحمن الحنبلي أحمد سلمان 1 P a g e Today we will talk about a new region, which is the leg. And as always, we will start with studying the sensory innervation of the leg. What is the importance
Surgical Management of wounds, flaps, grafts, and scars
 Disclosures Surgical Management of wounds, flaps, grafts, and scars I have no financial disclosures Cherrie Heinrich, MD, FACS Department of Plastic Surgery Regions Hospital Assistant Professor University
Disclosures Surgical Management of wounds, flaps, grafts, and scars I have no financial disclosures Cherrie Heinrich, MD, FACS Department of Plastic Surgery Regions Hospital Assistant Professor University
Chronic Wounds and Ulcers
 1 Chapter 2 Chronic Wounds and Ulcers Louis Carter Chronic wounds are likely the greatest cause of morbidity and cost to both patients and hospitals in Africa. With more surgeons and the availability of
1 Chapter 2 Chronic Wounds and Ulcers Louis Carter Chronic wounds are likely the greatest cause of morbidity and cost to both patients and hospitals in Africa. With more surgeons and the availability of
Johannesburg, South Africa
 NEUROVASCULAR ISLAND FLAP IN THE TREATMENT OF TROPHIC ULCERATION OF THE HEEL By ISIDORE KAPLAN, F.R.C.S., F.R.C.S.(Ed.) Johannesburg, South Africa THE transfer of skin and subcutaneous tissue on a neurovascular
NEUROVASCULAR ISLAND FLAP IN THE TREATMENT OF TROPHIC ULCERATION OF THE HEEL By ISIDORE KAPLAN, F.R.C.S., F.R.C.S.(Ed.) Johannesburg, South Africa THE transfer of skin and subcutaneous tissue on a neurovascular
Distal Femoral Resection
 Distal Femoral Resection Annie Arteau, Bruno Fuchs Introduction This text is a general description of a distal femoral resection. Focus is on anatomical structures and muscle resection. Each femoral resection
Distal Femoral Resection Annie Arteau, Bruno Fuchs Introduction This text is a general description of a distal femoral resection. Focus is on anatomical structures and muscle resection. Each femoral resection
musculoskeletal system anatomy muscles of foot sheet done by: dina sawadha & mohammad abukabeer
 musculoskeletal system anatomy muscles of foot sheet done by: dina sawadha & mohammad abukabeer Extensor retinaculum : A- superior extensor retinaculum (SER) : originates from the distal ends of the tibia
musculoskeletal system anatomy muscles of foot sheet done by: dina sawadha & mohammad abukabeer Extensor retinaculum : A- superior extensor retinaculum (SER) : originates from the distal ends of the tibia
Muscles of the Hip 1. Tensor Fasciae Latae O: iliac crest I: lateral femoral condyle Action: abducts the thigh Nerve: gluteal nerve
 Muscles of the Hip 1. Tensor Fasciae Latae O: iliac crest I: lateral femoral condyle Action: abducts the thigh Nerve: gluteal nerve 2. Gluteus Maximus O: ilium I: femur Action: abduct the thigh Nerve:
Muscles of the Hip 1. Tensor Fasciae Latae O: iliac crest I: lateral femoral condyle Action: abducts the thigh Nerve: gluteal nerve 2. Gluteus Maximus O: ilium I: femur Action: abduct the thigh Nerve:
BOAST 4 Algorithm. 6th September 2013
 BOAST 4 Algorithm 6th September 2013 Background The British Orthopaedic Association and the British Association of Plastic, Reconstructive and Aesthetic Surgeons reviewed their 1997 guidance and published
BOAST 4 Algorithm 6th September 2013 Background The British Orthopaedic Association and the British Association of Plastic, Reconstructive and Aesthetic Surgeons reviewed their 1997 guidance and published
Understanding Leg Anatomy and Function THE UPPER LEG
 Understanding Leg Anatomy and Function THE UPPER LEG The long thigh bone is the femur. It connects to the pelvis to form the hip joint and then extends down to meet the tibia (shin bone) at the knee joint.
Understanding Leg Anatomy and Function THE UPPER LEG The long thigh bone is the femur. It connects to the pelvis to form the hip joint and then extends down to meet the tibia (shin bone) at the knee joint.
Contents of the Posterior Fascial Compartment of the Thigh
 Contents of the Posterior Fascial Compartment of the Thigh 1-Muscles: B i c e p s f e m o r i s S e m i t e n d i n o s u s S e m i m e m b r a n o s u s a small part of the adductor magnus (h a m s t
Contents of the Posterior Fascial Compartment of the Thigh 1-Muscles: B i c e p s f e m o r i s S e m i t e n d i n o s u s S e m i m e m b r a n o s u s a small part of the adductor magnus (h a m s t
musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer
 musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer #Sacral plexus : emerges from the ventral rami of the spinal segments L4 - S4 and provides motor and
musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer #Sacral plexus : emerges from the ventral rami of the spinal segments L4 - S4 and provides motor and
Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function
 Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function Vinay Gundlapalli, MD, a John W. Gillespie III, MD, b and Chris D. Tzarnas, MD, FACS c a
Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function Vinay Gundlapalli, MD, a John W. Gillespie III, MD, b and Chris D. Tzarnas, MD, FACS c a
ANKLE PLANTAR FLEXION
 ANKLE PLANTAR FLEXION Evaluation and Measurements By Isabelle Devreux 1 Ankle Plantar Flexion: Gastrocnemius and Soleus ROM: 0 to 40-45 A. Soleus: Origin: Posterior of head of fibula and proximal1/3 of
ANKLE PLANTAR FLEXION Evaluation and Measurements By Isabelle Devreux 1 Ankle Plantar Flexion: Gastrocnemius and Soleus ROM: 0 to 40-45 A. Soleus: Origin: Posterior of head of fibula and proximal1/3 of
BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK Musculoskeletal Anatomy & Kinesiology KNEE & ANKLE MUSCLES
 BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK Musculoskeletal Anatomy & Kinesiology KNEE & ANKLE MUSCLES MSAK201-I Session 3 1) REVIEW a) THIGH, LEG, ANKLE & FOOT i) Tibia Medial Malleolus
BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK Musculoskeletal Anatomy & Kinesiology KNEE & ANKLE MUSCLES MSAK201-I Session 3 1) REVIEW a) THIGH, LEG, ANKLE & FOOT i) Tibia Medial Malleolus
New 2010 CPT Codes (italic font represents a new or revised code/description)
 New 2010 CPT Codes (italic font represents a new or revised code/description) 14301 Adjacent tissue transfer or rearrangement, any area; defect 30.1 sq cm to 60.0 sq cm 14302 each additional 30.0 sq cm,
New 2010 CPT Codes (italic font represents a new or revised code/description) 14301 Adjacent tissue transfer or rearrangement, any area; defect 30.1 sq cm to 60.0 sq cm 14302 each additional 30.0 sq cm,
ABSTRACT. Key words: Flaps, Adipofascial, Lower limb reconstruction. Khaldoun J. Haddadin, MD*, Samer Y. Haddad, MD. Introduction.
 DISTALLY BASED ADIPOFASCIAL FLAPS: A VERSATILE FLAP FOR THE RECONSTRUCTION OF LOWER LEG AND PROXIMAL FOOT DEFECTS AT THE ROYAL JORDANIAN REHABILITATION CENTER Khaldoun J. Haddadin, MD*, Samer Y. Haddad,
DISTALLY BASED ADIPOFASCIAL FLAPS: A VERSATILE FLAP FOR THE RECONSTRUCTION OF LOWER LEG AND PROXIMAL FOOT DEFECTS AT THE ROYAL JORDANIAN REHABILITATION CENTER Khaldoun J. Haddadin, MD*, Samer Y. Haddad,
Therapeutic Foot Care Certificate Program Part I: Online Home Study Program
 Therapeutic Foot Care Certificate Program Part I: Online Home Study Program 1 Anatomy And Terminology Of The Lower Extremity Joan E. Edelstein, MA, PT, FISPO Associate Professor of Clinical Physical Therapy
Therapeutic Foot Care Certificate Program Part I: Online Home Study Program 1 Anatomy And Terminology Of The Lower Extremity Joan E. Edelstein, MA, PT, FISPO Associate Professor of Clinical Physical Therapy
Injuries to the Hands and Feet
 Injuries to the Hands and Feet Chapter 24 Injuries to the Hands and Feet Introduction Combat injuries to the hands and feet differ from those of the arms and legs in terms of mortality and morbidity. The
Injuries to the Hands and Feet Chapter 24 Injuries to the Hands and Feet Introduction Combat injuries to the hands and feet differ from those of the arms and legs in terms of mortality and morbidity. The
Transfemoral Amputation
 Transfemoral Amputation Preop This 26 year old male sustained a gunshot wound to the left thigh. He was treated emergently with revascularization and fasciotomies. He was transferred to our regional trauma
Transfemoral Amputation Preop This 26 year old male sustained a gunshot wound to the left thigh. He was treated emergently with revascularization and fasciotomies. He was transferred to our regional trauma
Amputations. Chapter 23
 Amputations Chapter 23 Amputations Introduction Battle casualties who sustain amputations have the most severe extremity injuries. Historically, 1 in 3 patients with a major amputation (proximal to the
Amputations Chapter 23 Amputations Introduction Battle casualties who sustain amputations have the most severe extremity injuries. Historically, 1 in 3 patients with a major amputation (proximal to the
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 Introduction Compartment Syndromes of the Leg Related to Athletic Activity Mark M. Casillas, M.D. Consequences of a misdiagnosis persistence of a performance limitation loss of function/compartment loss
Introduction Compartment Syndromes of the Leg Related to Athletic Activity Mark M. Casillas, M.D. Consequences of a misdiagnosis persistence of a performance limitation loss of function/compartment loss
The earlier clinic experience of the reverse-flow anterolateral thigh island flap
 British Journal of Plastic Surgery (2005) 58, 160 164 The earlier clinic experience of the reverse-flow anterolateral thigh island flap Gang Zhou, Qi-Xu Zhang*, Guang-Yu Chen Scar Multiple Treatment Centre,
British Journal of Plastic Surgery (2005) 58, 160 164 The earlier clinic experience of the reverse-flow anterolateral thigh island flap Gang Zhou, Qi-Xu Zhang*, Guang-Yu Chen Scar Multiple Treatment Centre,
Femoral Artery. Its entrance to the thigh Position Midway between ASIS and pubic symphysis
 Lower Limb Vessels Lecture Objectives Describe the major arteries of the lower limb. Describe the deep and superficial veins of the lower limb. Describe the topographical relationships of the arteries
Lower Limb Vessels Lecture Objectives Describe the major arteries of the lower limb. Describe the deep and superficial veins of the lower limb. Describe the topographical relationships of the arteries
DISSECTION SCHEDULE. Session I - Hip (Front) & Thigh (Superficial)
 DISSECTION SCHEDULE Session I - Hip (Front) & Thigh (Superficial) Surface anatomy Inguinal region Gluteal region Thigh Leg Foot bones Hip bone Femur Superficial fascia Great saphenous vein Superficial
DISSECTION SCHEDULE Session I - Hip (Front) & Thigh (Superficial) Surface anatomy Inguinal region Gluteal region Thigh Leg Foot bones Hip bone Femur Superficial fascia Great saphenous vein Superficial
EndoBlade Soft Tissue Release System
 Surgical Technique Endoscopic Gastroc Recession Endoscopic Plantar Fascia Release EndoBlade Soft Tissue Release System Endoscopic Gastroc Recession Arthrex has developed a comprehensive, completely disposable
Surgical Technique Endoscopic Gastroc Recession Endoscopic Plantar Fascia Release EndoBlade Soft Tissue Release System Endoscopic Gastroc Recession Arthrex has developed a comprehensive, completely disposable
Clarification of Terms
 Clarification of Terms The plantar aspect of the foot refers to the role or its bottom The dorsal aspect refers to the top or its superior portion The ankle and foot perform three main functions: 1. shock
Clarification of Terms The plantar aspect of the foot refers to the role or its bottom The dorsal aspect refers to the top or its superior portion The ankle and foot perform three main functions: 1. shock
MUSCLES OF THE LOWER LIMBS
 MUSCLES OF THE LOWER LIMBS Naming, location and general function Dr. Nabil khouri ROLES THAT SHOULD NOT BE FORGOTTEN Most anterior compartment muscles of the hip and thigh Flexor of the femur at the hip
MUSCLES OF THE LOWER LIMBS Naming, location and general function Dr. Nabil khouri ROLES THAT SHOULD NOT BE FORGOTTEN Most anterior compartment muscles of the hip and thigh Flexor of the femur at the hip
Gross Anatomy Coloring Book Series. Lower Extremity Arteries
 Gross Anatomy Coloring Book Series Lower Extremity Arteries 1 Femoral Artery and Associated Branches For the life of the flesh is in the blood. Leviticus 17:11 Femoral Artery and Associated Branches After
Gross Anatomy Coloring Book Series Lower Extremity Arteries 1 Femoral Artery and Associated Branches For the life of the flesh is in the blood. Leviticus 17:11 Femoral Artery and Associated Branches After
Mohammad Ashraf. Abdulrahman Al-Hanbali. Ahmad Salman. 1 P a g e
 - 7 Mohammad Ashraf Abdulrahman Al-Hanbali Ahmad Salman 1 P a g e Structures under the cover of Gluteus Maximus: 1-Bones: Ileum, Femur (Head, greater trochanter and gluteal tuberosity), Ischium (ischial
- 7 Mohammad Ashraf Abdulrahman Al-Hanbali Ahmad Salman 1 P a g e Structures under the cover of Gluteus Maximus: 1-Bones: Ileum, Femur (Head, greater trochanter and gluteal tuberosity), Ischium (ischial
The gastrocnemius with soleus bi-muscle flap
 The British Association of Plastic Surgeons (2004) 57, 77 82 The gastrocnemius with soleus bi-muscle flap Ikuo Hyodo a, *, Bin Nakayama b, Mitsuru Takahashi c, Kazuhiro Toriyama d, Yuzuru Kamei d, Shuhei
The British Association of Plastic Surgeons (2004) 57, 77 82 The gastrocnemius with soleus bi-muscle flap Ikuo Hyodo a, *, Bin Nakayama b, Mitsuru Takahashi c, Kazuhiro Toriyama d, Yuzuru Kamei d, Shuhei
Introduction to Anatomy. Dr. Maher Hadidi. Laith Al-Hawajreh. Mar/25 th /2013
 Introduction to Anatomy Dr. Maher Hadidi Laith Al-Hawajreh 22 Mar/25 th /2013 Lower limb - The leg The skeleton of the leg is formed by two bones: 1) Medial: Tibia 2) Lateral: Fibula The two bones are
Introduction to Anatomy Dr. Maher Hadidi Laith Al-Hawajreh 22 Mar/25 th /2013 Lower limb - The leg The skeleton of the leg is formed by two bones: 1) Medial: Tibia 2) Lateral: Fibula The two bones are
Hip and Knee Approaches
 Hip and Knee Approaches Professor VLADIMIR STAVREV, MD, PhD, DMSc GEORGI MINEV MD DEPARTMENT OF ORTHOPEDICS AND TRAUMATOLOGY, MEDICAL UNIVERSITY -PLOVDIV Anterior View Hip Joint Posterior View - Hip Joint
Hip and Knee Approaches Professor VLADIMIR STAVREV, MD, PhD, DMSc GEORGI MINEV MD DEPARTMENT OF ORTHOPEDICS AND TRAUMATOLOGY, MEDICAL UNIVERSITY -PLOVDIV Anterior View Hip Joint Posterior View - Hip Joint
Human Anatomy Biology 351
 Human Anatomy Biology 351 Lower Limb Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average, between
Human Anatomy Biology 351 Lower Limb Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average, between
ACHILLES TENDON REPAIRS. Priya Parthasarathy, DPM
 ACHILLES TENDON REPAIRS Priya Parthasarathy, DPM DISCLOSURES NO CONFLICTS OF INTEREST ANATOMY 10-12 cm long 0.5-1.0 cm diameter Avascular zone 2-6 cm proximal to insertion Fibers rotate 90 degrees at insertion
ACHILLES TENDON REPAIRS Priya Parthasarathy, DPM DISCLOSURES NO CONFLICTS OF INTEREST ANATOMY 10-12 cm long 0.5-1.0 cm diameter Avascular zone 2-6 cm proximal to insertion Fibers rotate 90 degrees at insertion
Lecture 09. Popliteal Fossa. BY Dr Farooq Khan Aurakzai
 Lecture 09 Popliteal Fossa BY Dr Farooq Khan Aurakzai Dated: 14.02.2018 What is popliteus? Introduction Anything relating to, or near the part of the leg behind the knee. From New Latin popliteus the muscle
Lecture 09 Popliteal Fossa BY Dr Farooq Khan Aurakzai Dated: 14.02.2018 What is popliteus? Introduction Anything relating to, or near the part of the leg behind the knee. From New Latin popliteus the muscle
Copyright 2012 by The McGraw-Hill Companies, Inc. All rights reserved. McGraw-Hill/Irwin
 CHAPTER 8: THE LOWER EXTREMITY: KNEE, ANKLE, AND FOOT KINESIOLOGY Scientific Basis of Human Motion, 12 th edition Hamilton, Weimar & Luttgens Presentation Created by TK Koesterer, Ph.D., ATC Humboldt State
CHAPTER 8: THE LOWER EXTREMITY: KNEE, ANKLE, AND FOOT KINESIOLOGY Scientific Basis of Human Motion, 12 th edition Hamilton, Weimar & Luttgens Presentation Created by TK Koesterer, Ph.D., ATC Humboldt State
FACTS 1. Most need only Gastro aponeurotic release [in positive Silverskiold test]
![FACTS 1. Most need only Gastro aponeurotic release [in positive Silverskiold test] FACTS 1. Most need only Gastro aponeurotic release [in positive Silverskiold test]](/thumbs/83/88335212.jpg) FOOT IN CEREBRAL PALSY GAIT IN CEREBRAL PALSY I True Equinus II Jump gait III Apparent Equinus IV Crouch gait Group I True Equinus Extended hip and knee Equinus at ankle II Jump Gait [commonest] Equinus
FOOT IN CEREBRAL PALSY GAIT IN CEREBRAL PALSY I True Equinus II Jump gait III Apparent Equinus IV Crouch gait Group I True Equinus Extended hip and knee Equinus at ankle II Jump Gait [commonest] Equinus
fig fig For the following diagrams
 fig. 1271 For the following diagrams Please draw small circles at the following points (pts in bold are main syllabus pts): Liver-1 Liver-2 Liver-3 Liver-4 Spleen-4 Spleen-5 Stomach-41 Stomach-42 Stomach-43
fig. 1271 For the following diagrams Please draw small circles at the following points (pts in bold are main syllabus pts): Liver-1 Liver-2 Liver-3 Liver-4 Spleen-4 Spleen-5 Stomach-41 Stomach-42 Stomach-43
The thigh. Prof. Oluwadiya KS
 The thigh Prof. Oluwadiya KS www.oluwadiya.com The Thigh: Boundaries The thigh is the region of the lower limb that is approximately between the hip and knee joints Anteriorly, it is separated from the
The thigh Prof. Oluwadiya KS www.oluwadiya.com The Thigh: Boundaries The thigh is the region of the lower limb that is approximately between the hip and knee joints Anteriorly, it is separated from the
1. A worker falls from a height and lands on his feet. Radiographs reveal a fracture of the sustentaculum tali. The muscle passing immediately
 1. A worker falls from a height and lands on his feet. Radiographs reveal a fracture of the sustentaculum tali. The muscle passing immediately beneath it that would be adversely affected is the: fibularis
1. A worker falls from a height and lands on his feet. Radiographs reveal a fracture of the sustentaculum tali. The muscle passing immediately beneath it that would be adversely affected is the: fibularis
Lumbar Plexus. Ventral rami L1 L4 Supplies: Major nerves.. Abdominal wall External genitalia Anteromedial thigh
 Lower Limb Nerves Lectures Objectives Describe the structure and relationships of the plexuses of the lower limb. Describe the course, relationships and structures supplied for the major nerves of the
Lower Limb Nerves Lectures Objectives Describe the structure and relationships of the plexuses of the lower limb. Describe the course, relationships and structures supplied for the major nerves of the
Muscles of the lower extremities. Dr. Nabil khouri MD, MSc, Ph.D
 Muscles of the lower extremities Dr. Nabil khouri MD, MSc, Ph.D Posterior leg Popliteal fossa Boundaries Biceps femoris (superior-lateral) Semitendinosis and semimembranosis (superior-medial) Gastrocnemius
Muscles of the lower extremities Dr. Nabil khouri MD, MSc, Ph.D Posterior leg Popliteal fossa Boundaries Biceps femoris (superior-lateral) Semitendinosis and semimembranosis (superior-medial) Gastrocnemius
Alberta Health Care Insurance Plan. Schedule Of Anaesthetic Rates Applicable To Podiatric Surgery. Procedure List. As Of.
 Alberta Health Care Insurance Plan Procedure List As Of 01 April 2016 Alberta Health Care Insurance Plan Page i Generated 2016/03/22 TABLE OF CONTENTS As of 2016/04/01 07 PHYSICAL MEDICINE, REHABILITATION,
Alberta Health Care Insurance Plan Procedure List As Of 01 April 2016 Alberta Health Care Insurance Plan Page i Generated 2016/03/22 TABLE OF CONTENTS As of 2016/04/01 07 PHYSICAL MEDICINE, REHABILITATION,
~, /' ~::'~ EXTENSOR HALLUCIS LONGUS. Leg-anterolateral :.:~ / ~\,
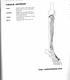 TIBIALIS ANTERIOR Lateral condyle of tibia, upper half of lateral surface of tibia, interosseous membrane Medial side and plantar surface of medial cuneiform bone, and base of first metatarsal bone Dorsiflexes
TIBIALIS ANTERIOR Lateral condyle of tibia, upper half of lateral surface of tibia, interosseous membrane Medial side and plantar surface of medial cuneiform bone, and base of first metatarsal bone Dorsiflexes
Technique Guide. VersiTomic. ReelX STT Double-Row Achilles G-Lok. J. Martin Leland III, M.D. J. Martin Leland III, M.D. Proximal Biceps Tenodesis
 Technique Guide VersiTomic ReelX STT Double-Row Achilles G-Lok Tendon Sub-Pectoral Repair Proximal Biceps Tenodesis J. Martin Leland III, M.D. J. Martin Leland III, M.D. The opinions expressed are those
Technique Guide VersiTomic ReelX STT Double-Row Achilles G-Lok Tendon Sub-Pectoral Repair Proximal Biceps Tenodesis J. Martin Leland III, M.D. J. Martin Leland III, M.D. The opinions expressed are those
Alberta Health Care Insurance Plan. Schedule Of Anaesthetic Rates Applicable To Podiatry. Procedure List. As Of. 01 April Government of Alberta
 Alberta Health Care Insurance Plan Procedure List As Of 01 April 2017 Alberta Health Care Insurance Plan Page i Generated 2017/03/14 TABLE OF CONTENTS As of 2017/04/01 II. OPERATIONS ON THE NERVOUS SYSTEM.......................
Alberta Health Care Insurance Plan Procedure List As Of 01 April 2017 Alberta Health Care Insurance Plan Page i Generated 2017/03/14 TABLE OF CONTENTS As of 2017/04/01 II. OPERATIONS ON THE NERVOUS SYSTEM.......................
حسام أبو عوض. - Ahmad. 1 P a g e
 - 9 حسام أبو عوض - - Ahmad 1 P a g e In the last lecture, we finished discussing the superficial part of the posterior compartment and the popliteus muscle of the deep layer[reminder: The entire posterior
- 9 حسام أبو عوض - - Ahmad 1 P a g e In the last lecture, we finished discussing the superficial part of the posterior compartment and the popliteus muscle of the deep layer[reminder: The entire posterior
Wound coverage of plantar metatarsal ulcers in leprosy using a toe web flap
 Free full text on www.ijps.org Original Article Wound coverage of plantar metatarsal ulcers in leprosy using a toe web flap J. Joshua, V. Chakraborthy Premananda Memorial Leprosy Hospital, The Leprosy
Free full text on www.ijps.org Original Article Wound coverage of plantar metatarsal ulcers in leprosy using a toe web flap J. Joshua, V. Chakraborthy Premananda Memorial Leprosy Hospital, The Leprosy
PUT YOUR BEST FOOT FORWARD
 PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
To describe he knee joint, ligaments, structure & To list the main features of other lower limb joints
 To describe he knee joint, ligaments, structure & neurovascular supply To demonstrate the ankle joint anatomy To list the main features of other lower limb joints To list main groups of lymph nodes in
To describe he knee joint, ligaments, structure & neurovascular supply To demonstrate the ankle joint anatomy To list the main features of other lower limb joints To list main groups of lymph nodes in
lesser trochanter of femur lesser trochanter of femur iliotibial tract (connective tissue) medial surface of proximal tibia
 LOWER LIMB MUSCLES OF THE APPENDICULAR SKELETON The muscles that act on the lower limb fall into three groups: those that move the thigh, those that move the lower leg, and those that move the ankle, foot,
LOWER LIMB MUSCLES OF THE APPENDICULAR SKELETON The muscles that act on the lower limb fall into three groups: those that move the thigh, those that move the lower leg, and those that move the ankle, foot,
Thomas Zgonis a, *, Douglas T. Cromack b, Thomas S. Roukis c, Joann Orphanos d, Vasilios D. Polyzois e CASE REPORT. Introduction.
 Injury Extra (2007) 38, 187 192 www.elsevier.com/locate/inext CASE REPORT Severe degloving injury of the sole and heel treated by a reverse flow sural artery neurofasciocutaneous flap and a modified off-loading
Injury Extra (2007) 38, 187 192 www.elsevier.com/locate/inext CASE REPORT Severe degloving injury of the sole and heel treated by a reverse flow sural artery neurofasciocutaneous flap and a modified off-loading
Quillen College of Medicine
 Ea s t T e n n e s s e e St a t e Un i v e r s i t y Quillen College of Medicine Failing to prepare is preparing to fail. John Wooden, UCL A Dr. Tom Kwasigroch Associate Dean Director, Medical Human Gross
Ea s t T e n n e s s e e St a t e Un i v e r s i t y Quillen College of Medicine Failing to prepare is preparing to fail. John Wooden, UCL A Dr. Tom Kwasigroch Associate Dean Director, Medical Human Gross
VENOUS DRAINAGE OF THE LOWER LIMB
 Anatomy of the lower limb Superficial veins & nerve injuries Dr. Hayder VENOUS DRAINAGE OF THE LOWER LIMB The venous drainage of the lower limb is of huge clinical & surgical importance. Since the venous
Anatomy of the lower limb Superficial veins & nerve injuries Dr. Hayder VENOUS DRAINAGE OF THE LOWER LIMB The venous drainage of the lower limb is of huge clinical & surgical importance. Since the venous
Principle Management of Wound and Fracture in Emergency Department
 Principle Management of Wound and Fracture in Emergency Department Presented in Clinical Update Seminar January 15 th 2011 dr. Tedjo Rukmoyo, SpOT (K) Spine Initial Management ATLS Procedure A : airway
Principle Management of Wound and Fracture in Emergency Department Presented in Clinical Update Seminar January 15 th 2011 dr. Tedjo Rukmoyo, SpOT (K) Spine Initial Management ATLS Procedure A : airway
Distally Based Sural Artery Adipofascial Flap based on a Single Sural Nerve Branch: Anatomy and Clinical Applications
 Distally Based Sural Artery Adipofascial Flap based on a Single Sural Nerve Branch: Anatomy and Clinical Applications Wan Loong James Mok 1, Yong Chen Por 1, Bien Keem Tan 2 1 Department of Plastic, Reconstructive
Distally Based Sural Artery Adipofascial Flap based on a Single Sural Nerve Branch: Anatomy and Clinical Applications Wan Loong James Mok 1, Yong Chen Por 1, Bien Keem Tan 2 1 Department of Plastic, Reconstructive
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
The Muscular System. Chapter 10 Part D. PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College
 Chapter 10 Part D The Muscular System Annie Leibovitz/Contact Press Images PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College Table 10.14: Muscles Crossing the Hip and
Chapter 10 Part D The Muscular System Annie Leibovitz/Contact Press Images PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College Table 10.14: Muscles Crossing the Hip and
Copyright 2004, Yoshiyuki Shiratori. All right reserved.
 Ankle and Leg Evaluation 1. History Chief Complaint: A. What happened? B. Is it a sharp or dull pain? C. How long have you had the pain? D. Can you pinpoint the pain? E. Do you have any numbness or tingling?
Ankle and Leg Evaluation 1. History Chief Complaint: A. What happened? B. Is it a sharp or dull pain? C. How long have you had the pain? D. Can you pinpoint the pain? E. Do you have any numbness or tingling?
DISTANT FLAPS KEY FIGURES:
 Chapter 14 DISTANT FLAPS KEY FIGURES: Chest flap Cross arm flap Cross leg flap Design of groin flap Examples of groin flap Examples of free flaps A distant flap involves moving tissue (skin, fascia, muscle,
Chapter 14 DISTANT FLAPS KEY FIGURES: Chest flap Cross arm flap Cross leg flap Design of groin flap Examples of groin flap Examples of free flaps A distant flap involves moving tissue (skin, fascia, muscle,
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Osteosynthesis involving a joint Thomas P Rüedi
 Osteosynthesis involving a joint Thomas P Rüedi How to use this handout? The left column contains the information given during the lecture. The column at the right gives you space to make personal notes.
Osteosynthesis involving a joint Thomas P Rüedi How to use this handout? The left column contains the information given during the lecture. The column at the right gives you space to make personal notes.
CHAPTER 8: THE BIOMECHANICS OF THE HUMAN LOWER EXTREMITY
 CHAPTER 8: THE BIOMECHANICS OF THE HUMAN LOWER EXTREMITY _ 1. The hip joint is the articulation between the and the. A. femur, acetabulum B. femur, spine C. femur, tibia _ 2. Which of the following is
CHAPTER 8: THE BIOMECHANICS OF THE HUMAN LOWER EXTREMITY _ 1. The hip joint is the articulation between the and the. A. femur, acetabulum B. femur, spine C. femur, tibia _ 2. Which of the following is
EGR Endoscopic Gastrocnemius Recession. Operative technique
 Endoscopic Gastrocnemius Recession Operative technique Endoscopic Gastrocnemius Recession Table of contents Introduction 3 Operative technique 4 This publication sets forth detailed recommended procedures
Endoscopic Gastrocnemius Recession Operative technique Endoscopic Gastrocnemius Recession Table of contents Introduction 3 Operative technique 4 This publication sets forth detailed recommended procedures
Human Anatomy Biology 351
 Human Anatomy Biology 351 Lower Limb Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average, between
Human Anatomy Biology 351 Lower Limb Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average, between
Partial Heel Pad Avulsion with Open Calcaneal Tuberosity Fracture with Tendo-achilles Rupture: A Case Report
 Case Report Journal of Orthopaedic Case Reports 2016 Sep-Oct: 6(4):44-48 Partial Heel Pad Avulsion with Open Calcaneal Tuberosity Fracture with Tendo-achilles Rupture: A Case Report Shameem Ahmed 1, Syed
Case Report Journal of Orthopaedic Case Reports 2016 Sep-Oct: 6(4):44-48 Partial Heel Pad Avulsion with Open Calcaneal Tuberosity Fracture with Tendo-achilles Rupture: A Case Report Shameem Ahmed 1, Syed
Lower limb summary. Anterior compartment of the thigh. Done By: Laith Qashou. Doctor_2016
 Lower limb summary Done By: Laith Qashou Doctor_2016 Anterior compartment of the thigh Sartorius Anterior superior iliac spine Upper medial surface of shaft of tibia 1. Flexes, abducts, laterally rotates
Lower limb summary Done By: Laith Qashou Doctor_2016 Anterior compartment of the thigh Sartorius Anterior superior iliac spine Upper medial surface of shaft of tibia 1. Flexes, abducts, laterally rotates
Muscles of Lesson Five. Muscular Nomenclature and Kinesiology - Two. Muscles of Lesson Five, cont. Chapter 16
 Chapter 16 Muscular Nomenclature and Kinesiology - Two Lessons 5-6 Muscles of Lesson Five Iliopsoas (psoas major, iliacus) Hip outward rotators (piriformis, gemellus superior, gemellus inferior, obturator
Chapter 16 Muscular Nomenclature and Kinesiology - Two Lessons 5-6 Muscles of Lesson Five Iliopsoas (psoas major, iliacus) Hip outward rotators (piriformis, gemellus superior, gemellus inferior, obturator
Pedicled medial sural perforator flap for the reconstruction of knee defects
 International Wound Journal ISSN 1742-4801 ORIGINAL ARTICLE Pedicled medial sural perforator flap for the reconstruction of knee defects I-Han Chiang 1, Chia-Chun Wu 2, Shyi-Gen Chen 1 & Chih-Hsin Wang
International Wound Journal ISSN 1742-4801 ORIGINAL ARTICLE Pedicled medial sural perforator flap for the reconstruction of knee defects I-Han Chiang 1, Chia-Chun Wu 2, Shyi-Gen Chen 1 & Chih-Hsin Wang
Toe walking gives rise to parental concern. Therefore, toe-walkers are often referred at the 3 years of age.
 IDIOPATHIC TOE WALKING Toe walking is a common feature in immature gait and is considered normal up to 3 years of age. As walking ability improves, initial contact is made with the heel. Toe walking gives
IDIOPATHIC TOE WALKING Toe walking is a common feature in immature gait and is considered normal up to 3 years of age. As walking ability improves, initial contact is made with the heel. Toe walking gives
Located Deep to Flexor Retinaculum on medial aspect of ankle. Posterior to Posterior Tibial Artery. Tom, Dick, and Very Nervous Harry
 ANKLE BLOCK ANESTHESIA GREGORY CLARK D.P.M. HEAD, SECTION OF PODIATRY SCRIPPS CLINIC LA JOLLA, CALIFORNIA A METHOD BY WHICH ONE MAY PROVIDE AN ANESTHETIC BLOCK TO THE FOOT OR ANKLE WITH A MINIMUM OF PATIENT
ANKLE BLOCK ANESTHESIA GREGORY CLARK D.P.M. HEAD, SECTION OF PODIATRY SCRIPPS CLINIC LA JOLLA, CALIFORNIA A METHOD BY WHICH ONE MAY PROVIDE AN ANESTHETIC BLOCK TO THE FOOT OR ANKLE WITH A MINIMUM OF PATIENT
TransFx External Fixation System Large and Intermediate Surgical Technique
 TransFx External Fixation System Large and Intermediate Surgical Technique TransFx External Fixation System Large and Intermediate Surgical Technique 1 Surgical Technique For TransFx External Fixation
TransFx External Fixation System Large and Intermediate Surgical Technique TransFx External Fixation System Large and Intermediate Surgical Technique 1 Surgical Technique For TransFx External Fixation
