Scaglioni, Mario F; Rittirsch, Daniel; Giovanoli, Pietro
|
|
|
- Dorthy Carpenter
- 5 years ago
- Views:
Transcription
1 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich Year: 2018 Reconstruction of the heel, middle foot sole and plantar forefoot with the medial plantar artery perforator (MPAP) flap: clinical experience with 28 cases Scaglioni, Mario F; Rittirsch, Daniel; Giovanoli, Pietro Abstract: INTRODUCTION: Defects in the weight-bearing region of the foot sole can represent a substantial restriction in quality of life and pose a challenge for reconstructive plastic surgery.the purpose of this article is to report our experience with the use of medial plantar artery perforator (MPAP) flap for reconstruction of defects of the foot sole in 3 different regions: heel, middle foot sole and plantar forefoot. PATIENTS AND METHODS: From January 2003 to May 2016, 28 patients (13 males and 15 females) with an average age of 54 years (range 12 to 84 y.o.) received reconstruction with 28 MPAP flaps.26 flaps were harvested as pedicle perforator flaps and 2 as free perforator flaps. All flaps were raised from the ipsilateral instep area. The defect locations included the heel (20 cases), middle foot sole (4 cases) and forefoot (4 cases).the causes of reconstruction were tumors in 18 patients (64%), decubitus in 8 patients (29%) and trauma in 2 patients (7%). RESULTS: The flap sizes varied from cm to cm. All of the flaps survived completely after surgery, apart from one. The donor sites were all covered with a split-thickness skin graft. Follow-up observations were conducted for 4 to 12 months, and all patients had good functional recovery with satisfactory cosmetic results. CONCLUSION: The MPAP flap can be considered an optimal method of foot sole reconstruction not only for covering the weight-bearing area of the heel but also for the middle and forefoot plantar region. DOI: Posted at the Zurich Open Repository and Archive, University of Zurich ZORA URL: Journal Article Accepted Version Originally published at: Scaglioni, Mario F; Rittirsch, Daniel; Giovanoli, Pietro (2018). Reconstruction of the heel, middle foot sole and plantar forefoot with the medial plantar artery perforator (MPAP) flap: clinical experience with 28 cases. Plastic and Reconstructive Surgery, 141(1): DOI:
2 Plastic and Reconstructive Surgery Advance Online Article DOI: /PRS Reconstruction of the heel, middle foot sole and plantar forefoot with the medial plantar artery perforator (MPAP) flap: clinical experience with 28 cases. Mario F. Scaglioni MD 1, Daniel Rittirsch MD 1, Pietro Giovanoli MD 1 1 Department of Plastic and Hand Surgery, University Hospital Zurich, Zurich, Switzerland Running Head: Plantaris medialis artery perforator flap for total plantar foot reconstruction Corresponding Author: Mario F. Scaglioni, MD Department of Plastic and Hand Surgery, University Hospital Zurich, Zurich, Switzerland Address: Rämistraße 100, 8091, Zurich, Switzerland Telephone number: Mario.scaglioni@gmail.com Disclosure: The authors have no financial conflicts or commercial associations to disclose. 1
3 ABSTRACT Introduction: Defects in the weight-bearing region of the foot sole can represent a substantial restriction in quality of life and pose a challenge for reconstructive plastic surgery. The purpose of this article is to report our experience with the use of medial plantar artery perforator (MPAP) flap for reconstruction of defects of the foot sole in 3 different regions: heel, middle foot sole and plantar forefoot. Patients and Methods: From January 2003 to May 2016, 28 patients (13 males and 15 females) with an average age of 54 years (range 12 to 84 y.o.) received reconstruction with 28 MPAP flaps. 26 flaps were harvested as pedicle perforator flaps and 2 as free perforator flaps. All flaps were raised from the ipsilateral instep area. The defect locations included the heel (20 cases), middle foot sole (4 cases) and forefoot (4 cases). The causes of reconstruction were tumors in 18 patients (64%), decubitus in 8 patients (29%) and trauma in 2 patients (7%). Results: The flap sizes varied from cm to cm. All of the flaps survived completely after surgery, apart from one. The donor sites were all covered with a split-thickness skin graft. Follow-up observations were conducted for 4 to 12 months, and all patients had good functional recovery with satisfactory cosmetic results. Conclusion: The MPAP flap can be considered an optimal method of foot sole reconstruction not only for covering the weight-bearing area of the heel but also for the middle and forefoot plantar region. Keywords: Plantaris medialis artery perforator flap, plantar foot reconstruction, Instep flap, free flap 2
4 INTRODUCTION Soft tissue reconstruction of the foot sole has long been a reconstructive challenge not only to restore an aesthetic appearance but also to maintain function. In fact, defects of this region of the body can enormously hamper the patient s quality of life. Therefore, the choice of reconstruction of the weight-bearing plantar foot surface is very important. Due to the limited availability and mobility of the adjacent skin, defects involving the plantar foot area may require complex reconstruction procedures. One of the most important factors for skin resurfacing of the weight-bearing area of the foot sole is the provision of an adequate type of skin with similar properties, of thickness and sensitivity. 1 Many techniques, such as skin graft, local flaps, local pedicle flaps and free flaps, have been already described for the reconstruction of these regions; 2 13 however, the reconstructive options to improve outcomes are still under discussion and there is not a supreme procedure, which is considered as a gold standard; there are only few flaps which can withstand the stresses and loads posed each and every day by a person s body weight. Ideally, defects involving this area are optimally repaired using thin and pliable flaps. Based on basic plastic surgery principles to replace like with like, with minimal donor site morbidity and without sacrificing a major vessel, perforator flaps designed from the instep area of the foot represent a viable option. The term instep area refers to the hairless nonweight-bearing medial plantar region of the foot sole centered over the medial plantar artery. 14,15 The medial plantar artery perforator (MPAP) flap, which is harvested from this region, is therefore ideal for the reconstruction of soft tissue defects of the foot sole with minimal donor site morbidity. The MPAP can be defined as a perforator flap based on the superficial branch of the medial plantar artery (MPA). It can be used as a pedicle or free flap. 9 Moreover, it contains a sensitive branch of the medial plantar nerve which supplies the instep skin area and provides a new sensation in the defect region. 5,16 In this article we describe our 3
5 experience using the MPAP flap for the reconstruction of defects of the heel, the middle and the forefoot sole. PATIENTS AND METHODS Between January 2003 and May 2016, 28 patients underwent foot sole reconstructions with the MPAP flap. There were 13 male patients and 15 female patients. The average age of the patients was 54 years (range, years). The causes were various and included soft tissue defect after cancer resection in 18 cases, trauma in 2 cases and pressure sores in 8 cases. The defect locations were the heel in 20 patients and the middle plantar foot and forefoot in 4 patients, respectively. In all cases, the defect dimension and especially the weight-bearing surface precluded skin grafting and primary closure. The details of patients are presented in Table 1. Surgical technique All flaps were designed on the medial part of the sole, the so called instep area. To begin, a surface marking is done in the instep area and also a preoperatively Doppler probe detected the perforators from the superficial branch of the medial plantar artery system and proved the patency of the posterior tibial artery (PTA) and dorsalis pedis artery (DPA). Under tourniquet control without previous exsanguination, the first incision is made parallel to the abductor hallucis muscle, creating the medial border of the flap. When the flap is dissected laterally and suprafascially above the flexor hallucis muscle, several perforators of the medial plantar vessel can be readily identified through the intermuscular septum between the abductor hallucis muscle and the flexor digitorum muscle (brevis or longus) (Fig. 1). With the use of retractors, the medial plantar vessel is clearly exposed through the intermuscular space. The perforator is deeply dissected to the division of the medial plantar vessel. The lateral border of the MPAP flap is then incised and dissected, taking care to include the perforators. The perforator arteries are always small in the MPAP flap. The diameter of the perforated artery is approximately 0.4 to 0.8 mm and the pedicle length 4
6 approximately 4 to 6 cm. There is usually a separate branch arising from the medial plantar nerve or from the main trunk of the posterior tibial nerve. This branch again divides into 2. The medial of the 2 branches proceeds to supply the sensation of the medial side of the great toe and the lateral branch to supply the sensation of the instep area. The lateral branch supplying the instep area is easily separable from the main branch under loupe magnification. Smaller branches of the medial plantar nerve around the medial plantar aponeurosis are cut. Then, the flap is transposed or rotated in propeller fashion into the defect (Fig. 2). The donor site was covered by a split-thickness skin graft. Postoperatively, patients were maintained on strict bedrest with the foot elevated. At one week after surgery, patients were allowed to begin a dangling protocol, and at 2 weeks, patients began light weight-bearing on the operated foot with the assistance of physical therapy when indicated. RESULTS Twenty-eight MPAP flaps were performed. The dimensions of the flap skin paddle ranged from cm to cm. The average perforator number included in the flap was 1 (range, 1 2). The mean pedicle length was 5 cm with a range of 4 6 cm. Regarding the two free MPAP flaps, the recipient vessels were the branch of lateral plantar artery in 2 patients. The arterial anastomoses were performed in an end-to-end fashion. All the flaps survived completely, except for one, with a success rate of 96%. One MPAP distal based flap for forefoot reconstruction was lost due to poor vascular perfusion. No arterial nor venous thrombosis occurred in the free MPAP flaps. The follow-up time ranged from 4 to 12 months (mean: 9 months). The flaps healed well and the color matches were excellent. All donor sites were covered with a split-thickness skin graft, and no early nor late complications were encountered. None of the patients complained about the donor site scar. All patients returned to their original jobs and were satisfied with the functional results and cosmetic appearance. Eventually they could also wear regular footwear. Details are shown in Table 1. 5
7 Case 1: Coverage of heel defect A 55-year-old woman sustained a weight-bearing malignant melanoma on the left heel. After a wide excision, a tumor free defect measured 5 5 cm was noted (Fig. 3, above left). A 5 5 cm pedicle MPAP flap was harvested from the ipsilateral instep area based on one perforator. (Fig.3, above right). Then the flap was transferred to reconstruct the defect (Fig. 3, below left). The donor site was covered with split-thickness skin graft from the contralateral thigh. The flap survived completely and the donor site healed uneventfully. The follow-up time was 6 months. The patient had full functional recovery with acceptable cosmetic result (Fig. 3 below right). Case 2: Coverage of middle foot sole defect A 51-year-old man was diagnosed as malignant melanoma on the right middle foot sole. After wide excision, a tumor free defect measured 6 5 cm was noted (Fig. 4, above left). A cm pedicle MPAP flap was harvested from the ipsilateral instep area based on one perforator. (Fig. 4, above right). Then, the flap was propelled with 90 degree of rotation to reconstruct the defect (Fig. 4, below left). The donor site was covered with split-thickness skin graft from the contralateral thigh. At the 8-month follow-up, the flap counter, color and healing were excellent. The patient had full functional recovery with acceptable cosmetic result (Fig. 4, below right). Case 3: Coverage of a forefoot defect A 53-year-old woman was diagnosed as malignant melanoma on her right forefoot. After wide excision, a tumor free defect measured cm was noted (Fig. 5, above left). A 5 5 cm pedicled MPAP flap was harvested from the ipsilateral instep area based on the distal perforator of the MPA (Fig. 5, above right). Then the flap was rotated in propeller fashion of around 180 degrees to reconstruct the forefoot defect (Fig. 5, below). The donor site was covered with split-thickness skin graft from the contralateral thigh. Postoperatively, the patient had nothing negative to report regarding ambulation or at the donor site. The follow- 6
8 up time was 6 months. The patient had full functional recovery with acceptable cosmetic result. DISCUSSION Surgical reconstruction of soft tissue defect in the foot sole regions poses one of the greatest challenges for plastic surgery. The location of the defect enormously hampers the patient s quality of life and the peculiar anatomic structure of the plantar foot can make even a small defect a difficult task. In particular, due to the very robust and thick characteristic of the skin of this area, it can easily withstand the stresses and loads it is exposed to on a daily basis. Many soft tissue reconstructions of these areas have been described using traditional local and free flaps, and the common aim was to use a type of skin with similar properties to the original skin in order to guaranteeing appropriate coverage and function. 1,16 Since the description of the freestyle perforator concept and the perforasome theory pioneered by Wei and Mardini, the use of local perforator flaps has grown in popularity. 17 Hence, local perforator flaps based on the plantar medial artery have been successfully employed for plantar foot reconstruction, although the dimension of defect represents the main limitation. As described by Attinger et al. 18 in 2006, the foot sole is perfused by the medial plantar artery and the lateral plantar artery providing their own corresponding angiosome. The medial plantar artery perforator (MPAP) flap is based on the perforators arising from the superficial branch of the medial plantar artery. 19 As it has been already reported in the literature, the perforator nourishing the MPAP flap is constant and can be found between the adductor allucis muscle and the flexor digitorum brevis muscle in proximity of the navicular bone. 15,16,20 However, the number of suitable perforators and their caliber has not been described. Moreover, a cutaneous nerve, branch of the medial plantar nerve, can provide sensation if incorporated within the flap. 21 7
9 Due to the non-weight-bearing localization of the instep area, the MPAP flap, harvested from this region, represents an ideal method of reconstruction of soft tissue defects of the foot sole and has the great advantage that the donor site morbidity is very low The instep flap was first described in 1981 by Harrison and Morgan for soft tissue coverage of the heel. 22 Thereafter, in 1983 Morrison et al. 9 developed a free sensory instep flap with medial plantar artery for heel defects. Since then, it has gained more and more popularity for plantar foot reconstruction, and it has been employed as free flap for defect coverage of the hand and fingers as well It is important to clarify that the instep flap is based on the deep branch of the MPA and it is classified as a pedicle fasciocutaneous flap; contrarily, the MPAP flap is based on the perforators of the superficial branch of the MPA. 15,19 Only few reports described the use of the MPAP flap for plantar foot sole reconstruction. In this article, which covers a period of 13 years, we describe our experience with the use of the MPAP flap for soft tissue defect reconstruction of the heel, the middle part of the foot sole, and the forefoot plantar region. During the flap elevation we could always identify, in the septum between the abductor hallucis and the flexor digitorum brevis muscle, two perforators: one proximal, few centimeters after the exit of the MPA from the abductor hallucis muscle, and one more distal. However, the caliber of the perforators could be variable (around 0.4 to 0.8 mm); in 24 cases the proximal perforator was bigger than the distal perforator and the flap could be harvested based on only one perforator. In two cases (two heel reconstructions) 2 perforators were included in the flap because the distal perforator appeared dominant with a bigger caliber compared to the proximal one. About the forefoot defect, the distal perforator was the one to supply the vascularity of the pedicle MPAP flap. Usually a few cm distally to the distal perforator of the superficial branch of the MPA, perforators, that runs from the superficial branch of the MPA up to the dorsal foot, can be appreciated; these are the connecting branch 8
10 from dorsal to plantar foot and should be always spared and kept if a distal based MPAP is planned. Based on our experience, the selection of the perforators depends on the intraoperative findings: 1) for heel reconstruction the proximal perforator is the more suitable due its vicinity to the defect; however, if it has very small size, the second perforator can be included as well. 2) for middle plantar foot reconstruction actually the dissection of the MPA is less important than heel construction as the MPAP flap needs to be rotated in propeller fashion of around 90 degrees, and it is possible only by dissecting the proximal or distal perforator. The choice of the perforator depends on the its size. In our series in all four cases the proximal perforator was selected. 3) for forefoot plantar reconstruction between the first and third metatarsus, our first choice is the distal perforator of the MPA; however, if it is not to be trusted due to its very small size, the proximal perforator can be included. We usually tried to dissect only the perforator and to propeller the flap without divided the superficial branch of the MPA proximally, however sometimes it was not enough to reach the defect, and consequently we needed to dissect the superficial branch of the MPA and eventually to divide it proximally to gain more length. Before dividing it proximally, we always clamped temporarily the vessel proximally and checked the vascularity of the flap for few minutes. If no signs of congestion appeared, we proceeded with the division. In contrast, for forefoot plantar reconstruction between the third and fifth metatarsus, we proceeded for a free MPAP based on one dominant perforator. Comparing with the instep flap, the MPAP flap has no fascial component and can be based on 1 or 2 perforators allowing an extra propeller rotation with consequent increase of the pedicle length if necessary. About the flap donor site, it interesting to mention that our patient did not experienced early and late complications of the donor site area such as split-thickness skin graft loss, infection, 9
11 and contracture and pain; it might be due to the preservation of the fascia; however further investigations are warranted to address this point. Patient selection is an important aspect to achieve favorable results: the Doppler of the PTA, DPA and of the perforators of the superficial branch of the MPA were routinely performed in all our patients before the reconstruction, only if the indicators were positive the patient was selected for MPAP flap reconstruction. Certainly, patients that have no PTA nor DPA pulse, nor with diabetes nor a vascular disease should be considered to be at risk and not be a good candidate for this reconstruction procedure. The patients venous condition was investigated as well and none of our patients had venous incontinence. The limitation of the MPAP flap is that it is not suitable for the repair of a big defect involving more than two third of the plantar foot, our biggest flap was cm, which actually represents the whole instep area. However, it is usually big enough for middle and small defect coverage. In contrast the MPAP flap has several advantages: 1) optimal flap thickness and quality for plantar foot reconstruction, 2) good color and texture match, 3) minimal donor site morbidity, 4) lack of functional loss, 5) wide arc of rotation, 6) consistent and reliable vascular anatomy, 7) possibility of a sensible flap including the cutaneous nerve of the medial plantar nerve. Conclusions In summary, the MPAP flap can be elevated based on the perforators of the superficial branch of the MPA. The perforators location is constant and allows a proximal or distally based flap. The donor site morbidity is minimal. Furthermore, the MPAP flap can be used as a pedicle or free flap, and in both cases as a sensate flap as well. Our case series shows that the MPAP flap is an ideal and optimal method for covering small to medium size defects of the heel, middle foot sole and forefoot plantar region. 10
12 REFERENCES 1. Erdemir A, Sirimamilla PA, Halloran JP, van den Bogert AJ. An Elaborate Data Set Characterizing the Mechanical Response of the Foot. J Biomech Eng. 2009;131: Bach AD, Leffler M, Kneser U, Kopp J, Horch RE. The versatility of the distally based peroneus brevis muscle flap in reconstructive surgery of the foot and lower leg. Ann Plast Surg. 2007;58: Peek A, Giessler G a. Functional total and subtotal heel reconstruction with free composite osteofasciocutaneous groin flaps of the deep circumflex iliac vessels. Ann Plast Surg. 2006;56: Roblin P, Healy CMJ. Heel Reconstruction with a Medial Plantar V-Y Flap. Plast Reconstr Surg. 2007;119: Shanahan RE, Gingrass RP. Medial plantar sensory flap for coverage of heel defects. Plast Reconstr Surg. 1979;64: Ulusal BG, Lin Y Te, Yen JT, Ulusal AE, Lin CH. Reconstruction of foot defects with free lateral arm fasciocutaneous flaps: Analysis of fifty patients. Microsurgery. 2005;25: Yücel A, Senyuva C, Aydin Y, Cinar C, Güzel Z. Soft-tissue reconstruction of sole and heel defects with free tissue transfers. Ann Plast Surg. 2000;44: ; discussion Baker GL, Newton ED, Franklin JD. Fasciocutaneous island flap based on the medial plantar artery: clinical applications for leg, ankle, and forefoot. Plast Reconstr Surg. 1990;85: Morrison WA, Crabb DM, O Brien BM, Jenkins A. The instep of the foot as a fasciocutaneous island and as a free flap for heel defects. Plast Reconstr Surg. 1983;72:
13 10. Kim ES, Hwang JH, Kim KS, Lee SY. Plantar reconstruction using the medial sural artery perforator free flap. Ann Plast Surg. 2009;62: Kuran I, Turgut G, Bas L, Ozkan T, Bayri O, Gulgonen a. Comparison between sensitive and nonsensitive free flaps in reconstruction of the heel and plantar area. Plast Reconstr Surg. 2000;105: Ortak T, Ozdemir R, Ulusoy MG, et al. Reconstruction of heel defects with a proximally based abductor hallucis muscle flap. J Foot Ankle Surg. 2005;44: Taylor GA, Gilbert Hopson W. The Cross-Foot Flap. Plast Reconstr Surg. 1975;55: Siddiqi MA, Hafeez K, Cheema TA, Rashid H ur. The Medial Plantar Artery Flap: A Series of Cases over 14 Years. J Foot Ankle Surg. 2012;51: Yang D, Yang JF, Morris SF, Tang M, Nie C. Medial plantar artery perforator flap for soft-tissue reconstruction of the heel. Ann Plast Surg. 2011;67: Wan DC, Gabbay J, Levi B, Boyd JB, Granzow JW. Quality of innervation in sensate medial plantar flaps for heel reconstruction. Plast Reconstr Surg. 2011;127: Wei F-C, Mardini S. Free-style free flaps. Plast Reconstr Surg. 2004;114: Attinger CE, Evans KK, Bulan E, Blume P, Cooper P. Angiosomes of the foot and ankle and clinical implications for limb salvage: reconstruction, incisions, and revascularization. Plast Reconstr Surg. 2006;117:261S-293S. 19. Tsai F-C, Cheng M-H, Chen H-C, Wei F-C. Microsurgical medialis pedis flaps for reconstruction of soft-tissue defects in the hand. Ann Plast Surg. 2002;48: Koshima I, Narushima M, Mihara M, et al. Island medial plantar artery perforator flap for reconstruction of plantar defects. Ann Plast Surg. 2007;59: Mourougayan V. Medial plantar artery (instep flap) flap. Ann Plast Surg. 2006;56:
14 22. Harrison DH, Morgan BDG. The instep island flap to resurface plantar defects. Br J Plast Surg. 1981;34: Shanahan RE, Gingrass RP. Medial plantar sensory flap for coverage of heel defects. Plast Reconstr Surg Sep;64(3): Gu JH, Jeong S-H. Radical resection of a venous malformation in middle finger and immediate reconstruction using medial plantar artery perforator flap: a case report. Microsurgery. 2012;32: Huang SH, Wu SH, Lai CH, et al. Free medial plantar artery perforator flap for finger pulp reconstruction: Report of a series of 10 cases. Microsurgery. 2010;30: Lai C-H, Lai C-S, Huang S-H, Lin S-D, Chang K-P. Free medial plantar artery perforator flaps for the resurfacing of thumb defects. Ann Plast Surg. 2010;65: Chai Y-M, Wang C-Y, Wen G, Zeng B-F, Cai P-H, Han P. Combined medialis pedis and medial plantar fasciocutaneous flaps based on the medial plantar pedicle for reconstruction of complex soft tissue defects in the hand. Microsurgery. 2011;31:
15 Figure Legend Figure 1: the perforators of the superficial branch of the medial plantar artery (MPA) can be identified through the intermuscular septum between the abductor hallucis muscle and the flexor digitorum muscle. Arrows: proximal and distal perforators of the superficial branch of the MPA; star left: posterior tibial artery (PTA); dot middle: superficial branch of the MPA; triangle right: abductor halluces muscle. Figure 2: Range of applications of the MPAP flap with two constant perforators of the superficial branch of the medial plantar artery: Example A shows a defect in the forefoot area. The flap is rotated 180 and therefore, the blood supply comes retrograde from the dorsalis pedis artery. Example B shows a defect of the midfoot. The flap needs to be rotated 90 from the harvest site. Example C shows a defect of the heel. In order to cover the defect, the superficial branch of the medial plantar artery is tracked proximally until a sufficient length is needed for flap rotation. Triangle: superficial branch of the MPA, star: deep branch of the MPA. Figure 3: Defect measured 5 cm 5 cm after wide excision of the Melanoma in the left heel (above left). A 5 cm 5 cm pedicle MPAP flap was harvested from the ipsilateral instep area based on one perforator (above right). The MPAP flap was transferred to reconstruct the defect and the donor site was covered with split-thickness skin graft from the contralateral thigh (below left). Follow-up at 6 months post-operative (below right). Figure 4: Defect measured 6 cm 5 cm after wide excision of the Melanoma in the right middle foot sole (above left). A 6.5 cm 5. 5 cm pedicle MPAP flap was harvested from the ipsilateral instep area based on the proximal perforator (black arrow) (above right). The MPAP flap was propelled 90 degrees to covert the defect and the donor site was covered with split-thickness skin graft from the contralateral thigh (below left). Follow-up at 8 months post-operative (below right). 14
16 Figure 5: Defect measured 4 cm 4.5 cm after wide excision of the Melanoma in the right plantar forefoot (above left). Dissection of the distal MPAP perforator (above right). A 5 cm 5 cm pedicle MPAP flap was harvested from the ipsilateral instep area based on the distal perforator (below left). The MPAP flap was propelled 180 degrees to covert the defect and the donor site was covered with split-thickness skin graft from the contralateral thigh (below right). 15
17 Table. 1 Summary of the patients receiving MPAP flap for Heel, middle part and forefoot reconstruction No. Age/Sex Etiology Defect location Size Defect (cm) Type of MPAP-flap 1 55, W Ulcer Heel 5 x 5 proximal 2 65, M Tumor Heel 5 x 4.5 proximal 3 31, M Ulcer Heel 7 x 4 proximal 4 56, M Tumor Heel 2,8 x 3 proximal 5 83, W Tumor Heel 3.5 x 4 proximal 6 63, M Tumor Heel 3 x 3 proximal 7 63, W Tumor Heel 4 x 2 proximal 8 56, M Ulcer Heel 4 x 5 proximal 9 37, W Ulcer Heel 5 x 3 proximal 10 84, M Tumor Heel 5.5 x 9.5 proximal on 11 80, W Ulcer Heel 3 x 4 proximal 12 37, M Ulcer Heel 6 x 5 proximal 13 73, M Tumor Heel 4 x 4 proximal 14 52, W Ulcer Heel 3 x 4.5 proximal 15 22, W Trauma Heel 5,5 x 5,5 proximal 16 70, W Tumor Heel 4 x 3 proximal 17 48, M Tumor Heel 5 x 4 proximal 18 12, W Trauma Heel 6 x 7 proximal 19 63, M Ulcer Heel 7 x 5 proximal 20 44, W Tumor Heel 5 x 5 proximal 21 19, W Tumor Medial 5 x 5 proximal 22 68, W Tumor Medial 7 x 5 proximal 23 47, W Tumor Medial 4 x 4 proximal 24 51, M Tumor Medial 6 x 5 proximal 25 53, W Tumor Forefoot 2,5 x 2,5 distal pedicle based flap 26 73, W Tumor Forefoot 3 x 4,5 distal pedicle based flap 27 60, M Tumor Forefoot 5 x 4 free flap No. of Perforators MPAP harvest ing time (min.) Follow up Complication 1 P none 1 P 55 8 none 1 P none 1 P 45 6 none 1 P 50 6 none 1 P 40 9 none 1 P none 1 P none 1 P none 2 P + D 60 9 none 1 P 45 9 none 1 P 60 4 none 1 P none 1 P none 1 P 45 6 none 1 P none 1 P 55 8 none 2 P + D 60 8 none 1 P none 1 P 55 4 none 1 P 55 4 none 1 P none 1 P 55 6 none 1 P 55 9 none 1 D 75 9 none 1 D 1 P total lost none 28 58, M Tumor Forefoot 5 x 6 free flap 1 P 55 8 none
18 A C C EP TE D Figure 1 17
19 Figure 2 18
20 Figure 3 19
21 A C C EP TE D Figure 4 20
22 Figure 5 21
Versatility of Reverse Sural Artery Flap for Heel Reconstruction
 ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
Heel Defect Reconstruction using Local Vascularized Flaps: Results and Clinical Outcomes in 16 Patients
 JFS (P) Kuldeep Singh et al ORIGINL RTICLE 10.5005/jp-journals-10040-1083 Heel Defect Reconstruction using Local Vascularized Flaps: Results and Clinical Outcomes in 16 Patients 1 Kuldeep Singh, 2 Zile
JFS (P) Kuldeep Singh et al ORIGINL RTICLE 10.5005/jp-journals-10040-1083 Heel Defect Reconstruction using Local Vascularized Flaps: Results and Clinical Outcomes in 16 Patients 1 Kuldeep Singh, 2 Zile
The earlier clinic experience of the reverse-flow anterolateral thigh island flap
 British Journal of Plastic Surgery (2005) 58, 160 164 The earlier clinic experience of the reverse-flow anterolateral thigh island flap Gang Zhou, Qi-Xu Zhang*, Guang-Yu Chen Scar Multiple Treatment Centre,
British Journal of Plastic Surgery (2005) 58, 160 164 The earlier clinic experience of the reverse-flow anterolateral thigh island flap Gang Zhou, Qi-Xu Zhang*, Guang-Yu Chen Scar Multiple Treatment Centre,
Johannesburg, South Africa
 NEUROVASCULAR ISLAND FLAP IN THE TREATMENT OF TROPHIC ULCERATION OF THE HEEL By ISIDORE KAPLAN, F.R.C.S., F.R.C.S.(Ed.) Johannesburg, South Africa THE transfer of skin and subcutaneous tissue on a neurovascular
NEUROVASCULAR ISLAND FLAP IN THE TREATMENT OF TROPHIC ULCERATION OF THE HEEL By ISIDORE KAPLAN, F.R.C.S., F.R.C.S.(Ed.) Johannesburg, South Africa THE transfer of skin and subcutaneous tissue on a neurovascular
ORIGINAL ARTICLE DISTALLY BASED PERONEUS BREVIS MUSCLE FLAP FOR DISTAL LEG DEFECTS
 DISTALLY BASED PERONEUS BREVIS MUSCLE FLAP FOR DISTAL LEG DEFECTS Peddi Manjunath 1, Ramesha K.T 2, Smitha S Segu 3, Jainath 4, Shankarappa M 5 HOW TO CITE THIS ARTICLE: Peddi Manjunath, Ramesha KT, Smitha
DISTALLY BASED PERONEUS BREVIS MUSCLE FLAP FOR DISTAL LEG DEFECTS Peddi Manjunath 1, Ramesha K.T 2, Smitha S Segu 3, Jainath 4, Shankarappa M 5 HOW TO CITE THIS ARTICLE: Peddi Manjunath, Ramesha KT, Smitha
17 FibulA FlAP Tor Chiu fibula flap 153
 17 Fibula Flap Tor Chiu Fibula Flap 153 Fibula Flap FLAP TERRITORY This flap includes a segment of the fibular bone with or without the overlying skin island on the peroneal/ lateral aspect of the calf.
17 Fibula Flap Tor Chiu Fibula Flap 153 Fibula Flap FLAP TERRITORY This flap includes a segment of the fibular bone with or without the overlying skin island on the peroneal/ lateral aspect of the calf.
CHAPTER 16 LOWER EXTREMITY. Amanda K Silva, MD and Warren Ellsworth, MD, FACS
 CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
ABSTRACT. Key words: Flaps, Adipofascial, Lower limb reconstruction. Khaldoun J. Haddadin, MD*, Samer Y. Haddad, MD. Introduction.
 DISTALLY BASED ADIPOFASCIAL FLAPS: A VERSATILE FLAP FOR THE RECONSTRUCTION OF LOWER LEG AND PROXIMAL FOOT DEFECTS AT THE ROYAL JORDANIAN REHABILITATION CENTER Khaldoun J. Haddadin, MD*, Samer Y. Haddad,
DISTALLY BASED ADIPOFASCIAL FLAPS: A VERSATILE FLAP FOR THE RECONSTRUCTION OF LOWER LEG AND PROXIMAL FOOT DEFECTS AT THE ROYAL JORDANIAN REHABILITATION CENTER Khaldoun J. Haddadin, MD*, Samer Y. Haddad,
The distally-based island ulnar artery perforator flap for wrist defects
 Free full text on www.ijps.org Original Article The distally-based island ulnar artery perforator flap for wrist defects Durga Karki, A. K. Singh Post Graduate Department of Plastic and Reconstructive
Free full text on www.ijps.org Original Article The distally-based island ulnar artery perforator flap for wrist defects Durga Karki, A. K. Singh Post Graduate Department of Plastic and Reconstructive
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts
 Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Planning and outcome of soft tissue defects of the foot
 206; 2(4): 47-423 ISSN: 2395-958 IJOS 206; 2(4): 47-423 206 IJOS www.orthopaper.com Received: -08-206 Accepted: 2-09-206 Dr. Shuaib Ahmed Dr. Latheesh Leo Hand and Microvascular Surgery, Department of
206; 2(4): 47-423 ISSN: 2395-958 IJOS 206; 2(4): 47-423 206 IJOS www.orthopaper.com Received: -08-206 Accepted: 2-09-206 Dr. Shuaib Ahmed Dr. Latheesh Leo Hand and Microvascular Surgery, Department of
Soft Tissue Reconstruction of the Foot Using the Distally Based Island Pedicle Flap after Resection of Malignant Melanoma
 Original Article Clinics in Orthopedic Surgery 2010;2:244-249 doi:10.4055/cios.2010.2.4.244 Soft Tissue Reconstruction of the Foot Using the Distally Based Island Pedicle Flap after Resection of Malignant
Original Article Clinics in Orthopedic Surgery 2010;2:244-249 doi:10.4055/cios.2010.2.4.244 Soft Tissue Reconstruction of the Foot Using the Distally Based Island Pedicle Flap after Resection of Malignant
Sensate First Dorsal Metacarpal Artery Flap for Resurfacing Extensive Pulp Defects of the Thumb
 ORIGINAL ARTICLE Sensate First Dorsal Metacarpal Artery Flap for Resurfacing Extensive Pulp Defects of the Thumb Shun-Cheng Chang, MD, Shao-Liang Chen, MD, Tim-Mo Chen, MD, Chia-Jueng Chuang, MD, Tian-Yeu
ORIGINAL ARTICLE Sensate First Dorsal Metacarpal Artery Flap for Resurfacing Extensive Pulp Defects of the Thumb Shun-Cheng Chang, MD, Shao-Liang Chen, MD, Tim-Mo Chen, MD, Chia-Jueng Chuang, MD, Tian-Yeu
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty
 CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function
 Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function Vinay Gundlapalli, MD, a John W. Gillespie III, MD, b and Chris D. Tzarnas, MD, FACS c a
Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function Vinay Gundlapalli, MD, a John W. Gillespie III, MD, b and Chris D. Tzarnas, MD, FACS c a
Kuwabara, Kaoru; Nonaka, Takashi; H. Citation Journal of Clinical Urology, 7(5),
 NAOSITE: Nagasaki University's Ac Title Author(s) Gluteal-fold adipofascial perforato fistula reconstruction Fujioka, Masaki; Hayashida, Kenji; Kuwabara, Kaoru; Nonaka, Takashi; H Citation Journal of Clinical
NAOSITE: Nagasaki University's Ac Title Author(s) Gluteal-fold adipofascial perforato fistula reconstruction Fujioka, Masaki; Hayashida, Kenji; Kuwabara, Kaoru; Nonaka, Takashi; H Citation Journal of Clinical
Hyperbaric oxygen therapy and surgical delay improve flap survival of reverse pedicle flaps for lower third leg and foot reconstruction
 Original Article Plastic and Aesthetic Research Hyperbaric oxygen therapy and surgical delay improve flap survival of reverse pedicle flaps for lower third leg and foot reconstruction Pradeoth Mukundan
Original Article Plastic and Aesthetic Research Hyperbaric oxygen therapy and surgical delay improve flap survival of reverse pedicle flaps for lower third leg and foot reconstruction Pradeoth Mukundan
Jonathan A. Dunne, MBChB, MRCS, a Daniel J. Wilks, MBChB, MRCS, b and Jeremy M. Rawlins, MBChB, MPhil, FRCS (Plast) c INTRODUCTION
 CASE REPORT A Previously Discounted Flap Now Reconsidered: MatriDerm and Split-Thickness Skin Grafting for Tendon Cover Following Dorsalis Pedis Fasciocutaneous Flap in Lower Limb Trauma Jonathan A. Dunne,
CASE REPORT A Previously Discounted Flap Now Reconsidered: MatriDerm and Split-Thickness Skin Grafting for Tendon Cover Following Dorsalis Pedis Fasciocutaneous Flap in Lower Limb Trauma Jonathan A. Dunne,
Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect of Upper and Middle Third Leg
 Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
Closure of Chronic Heel Ulcer by Simple V-Y Flap
 Egypt, J. Plast. Reconstr. Surg., Vol. 40, No. 1, January: 97-101, 2016 Closure of Chronic Heel Ulcer by Simple V-Y lap ESA TAAN,.D.; AYAN ARHAT,.D.; OUSTAA EKY,.D. and AHOUD NASI,.D. The Department of
Egypt, J. Plast. Reconstr. Surg., Vol. 40, No. 1, January: 97-101, 2016 Closure of Chronic Heel Ulcer by Simple V-Y lap ESA TAAN,.D.; AYAN ARHAT,.D.; OUSTAA EKY,.D. and AHOUD NASI,.D. The Department of
The plantar aponeurosis
 Anatomy of the foot The plantar aponeurosis Is a triangular thickening of the deep fascia Its apex is attached to the medial and lateral tubercles of the calcaneum. The base of the aponeurosis divides
Anatomy of the foot The plantar aponeurosis Is a triangular thickening of the deep fascia Its apex is attached to the medial and lateral tubercles of the calcaneum. The base of the aponeurosis divides
Interesting Case Series. Reconstruction of Dorsal Wrist Defects
 Interesting Case Series Reconstruction of Dorsal Wrist Defects Maelee Yang, BS, and Joseph Meyerson, MD The Ohio State University Wexner Medical Center, Columbus Correspondence: maelee.yang@osumc.edu Keywords:
Interesting Case Series Reconstruction of Dorsal Wrist Defects Maelee Yang, BS, and Joseph Meyerson, MD The Ohio State University Wexner Medical Center, Columbus Correspondence: maelee.yang@osumc.edu Keywords:
Distally Based Sural Artery Adipofascial Flap based on a Single Sural Nerve Branch: Anatomy and Clinical Applications
 Distally Based Sural Artery Adipofascial Flap based on a Single Sural Nerve Branch: Anatomy and Clinical Applications Wan Loong James Mok 1, Yong Chen Por 1, Bien Keem Tan 2 1 Department of Plastic, Reconstructive
Distally Based Sural Artery Adipofascial Flap based on a Single Sural Nerve Branch: Anatomy and Clinical Applications Wan Loong James Mok 1, Yong Chen Por 1, Bien Keem Tan 2 1 Department of Plastic, Reconstructive
Role Of Reverse Sural Artery Flap In Ankle, Foot And Leg Defects
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. VIII (May. 2016), PP 64-68 www.iosrjournals.org Role Of Reverse Sural Artery Flap In
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. VIII (May. 2016), PP 64-68 www.iosrjournals.org Role Of Reverse Sural Artery Flap In
The free thoracodorsal artery perforator flap in head and neck reconstruction
 European Annals of Otorhinolaryngology, Head and Neck diseases (2012) 129, 167 171 Available online at www.sciencedirect.com TECHNICAL NOTE The free thoracodorsal artery perforator flap in head and neck
European Annals of Otorhinolaryngology, Head and Neck diseases (2012) 129, 167 171 Available online at www.sciencedirect.com TECHNICAL NOTE The free thoracodorsal artery perforator flap in head and neck
MEDIAL SURAL ARTERY PERFORATOR FLAP FOR TONGUE AND FLOOR OF MOUTH RECONSTRUCTION. Adequate speech and swallowing are dependent
 ORIGINAL ARTICLE MEDIAL SURAL ARTERY PERFORATOR FLAP FOR TONGUE AND FLOOR OF MOUTH RECONSTRUCTION Shao-Liang Chen, MD, 1 Tim-Mo Chen, MD, 1 Niann-Tzyy Dai, MD, 1 Yi-Jan Hsia, DDS, MDSC, 2 Yaoh-Shiang Lin,
ORIGINAL ARTICLE MEDIAL SURAL ARTERY PERFORATOR FLAP FOR TONGUE AND FLOOR OF MOUTH RECONSTRUCTION Shao-Liang Chen, MD, 1 Tim-Mo Chen, MD, 1 Niann-Tzyy Dai, MD, 1 Yi-Jan Hsia, DDS, MDSC, 2 Yaoh-Shiang Lin,
Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study
 Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study Raphael Sinna, MD, a Hassene Hajji, MD, b Quentin Qassemyar,
Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study Raphael Sinna, MD, a Hassene Hajji, MD, b Quentin Qassemyar,
JPRAS Open 3 (2015) 1e5. Contents lists available at ScienceDirect. JPRAS Open. journal homepage:
 JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
Mentosternal Contracture Treated With an Occipito-Scapular Flap in a 5-year-old Boy: A Case Report
 Mentosternal Contracture Treated With an Occipito-Scapular Flap in a 5-year-old Boy: A Case Report Armin Kraus, MD, Hans-Eberhard Schaller, MD, and Hans-Oliver Rennekampff, MD Department for Hand, Plastic,
Mentosternal Contracture Treated With an Occipito-Scapular Flap in a 5-year-old Boy: A Case Report Armin Kraus, MD, Hans-Eberhard Schaller, MD, and Hans-Oliver Rennekampff, MD Department for Hand, Plastic,
THE pedicled flap, commonly used by the plastic surgeon in the reconstruction
 THE PEDICLE!) SKIN FLAP ROBIN ANDERSON, M.D. Department of Plastic Surgery THE pedicled flap, commonly used by the plastic surgeon in the reconstruction of skin and soft tissue defects, differs from the
THE PEDICLE!) SKIN FLAP ROBIN ANDERSON, M.D. Department of Plastic Surgery THE pedicled flap, commonly used by the plastic surgeon in the reconstruction of skin and soft tissue defects, differs from the
Lower Extremity Reconstruction
 1 Chapter 21 Overview: Lower Extremity Reconstruction Louis Carter This subject is also partially covered in the chapters Flaps for Wound Coverage and Perforator Flaps. This chapter will deal with reconstruction
1 Chapter 21 Overview: Lower Extremity Reconstruction Louis Carter This subject is also partially covered in the chapters Flaps for Wound Coverage and Perforator Flaps. This chapter will deal with reconstruction
Pedicled medial sural perforator flap for the reconstruction of knee defects
 International Wound Journal ISSN 1742-4801 ORIGINAL ARTICLE Pedicled medial sural perforator flap for the reconstruction of knee defects I-Han Chiang 1, Chia-Chun Wu 2, Shyi-Gen Chen 1 & Chih-Hsin Wang
International Wound Journal ISSN 1742-4801 ORIGINAL ARTICLE Pedicled medial sural perforator flap for the reconstruction of knee defects I-Han Chiang 1, Chia-Chun Wu 2, Shyi-Gen Chen 1 & Chih-Hsin Wang
Limb salvage surgery following resection of a melanoma: Foot and ankle reconstruction using cutaneous flaps
 1966 Limb salvage surgery following resection of a melanoma: Foot and ankle reconstruction using cutaneous flaps JIAN FENG LIU 1*, LI RONG ZHAO 2*, LAI JIN LU 1, LEI CHEN 1, ZHI GANG LIU 1, XU GONG 1 and
1966 Limb salvage surgery following resection of a melanoma: Foot and ankle reconstruction using cutaneous flaps JIAN FENG LIU 1*, LI RONG ZHAO 2*, LAI JIN LU 1, LEI CHEN 1, ZHI GANG LIU 1, XU GONG 1 and
Anatomical study. Clinical study. R. Ogawa, H. Hyakusoku, M. Murakami, R. Aoki, K. Tanuma* and D. G. Pennington?
 British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
TRANSPOSITIONAL ADIPOFASCIAL FLAPS FOR COMPLICATED ACUTE FINGER INJURIES
 K.B. Poon, S.H. Chien, G.T. Lin, et al TRANSPSITINAL ADIPFASCIAL FLAPS FR CMPLICATED ACUTE FINGER INJURIES Kein Boon Poon, Song-Hsiung Chien, 1 Gau-Tyan Lin, 1 and Yin-Chih Fu 1 Department of rthopaedic
K.B. Poon, S.H. Chien, G.T. Lin, et al TRANSPSITINAL ADIPFASCIAL FLAPS FR CMPLICATED ACUTE FINGER INJURIES Kein Boon Poon, Song-Hsiung Chien, 1 Gau-Tyan Lin, 1 and Yin-Chih Fu 1 Department of rthopaedic
The gastrocnemius with soleus bi-muscle flap
 The British Association of Plastic Surgeons (2004) 57, 77 82 The gastrocnemius with soleus bi-muscle flap Ikuo Hyodo a, *, Bin Nakayama b, Mitsuru Takahashi c, Kazuhiro Toriyama d, Yuzuru Kamei d, Shuhei
The British Association of Plastic Surgeons (2004) 57, 77 82 The gastrocnemius with soleus bi-muscle flap Ikuo Hyodo a, *, Bin Nakayama b, Mitsuru Takahashi c, Kazuhiro Toriyama d, Yuzuru Kamei d, Shuhei
Injuries to the Hands and Feet
 Injuries to the Hands and Feet Chapter 26 Injuries to the Hands and Feet Introduction Combat injuries to the hands and feet differ from those of the arms and legs in terms of mortality and morbidity. Death
Injuries to the Hands and Feet Chapter 26 Injuries to the Hands and Feet Introduction Combat injuries to the hands and feet differ from those of the arms and legs in terms of mortality and morbidity. Death
Anatomy MCQs Week 13
 Anatomy MCQs Week 13 1. Posterior to the medial malleolus of the ankle: The neurovascular bundle lies between Tibialis Posterior and Flexor Digitorum Longus The tendon of Tibialis Posterior inserts into
Anatomy MCQs Week 13 1. Posterior to the medial malleolus of the ankle: The neurovascular bundle lies between Tibialis Posterior and Flexor Digitorum Longus The tendon of Tibialis Posterior inserts into
Femoral Artery. Its entrance to the thigh Position Midway between ASIS and pubic symphysis
 Lower Limb Vessels Lecture Objectives Describe the major arteries of the lower limb. Describe the deep and superficial veins of the lower limb. Describe the topographical relationships of the arteries
Lower Limb Vessels Lecture Objectives Describe the major arteries of the lower limb. Describe the deep and superficial veins of the lower limb. Describe the topographical relationships of the arteries
Reverse Adipofascial Radial Forearm Flap Surgery for Soft-Tissue Reconstruction of Hand Defects
 Reverse Adipofascial Radial Forearm Flap Surgery for Soft-Tissue Reconstruction of Hand Defects Osman Akdag, MD, a Mehtap Karamese, MD, a Muhammed NebilSelimoglu, MD, a Ahmet Akatekin, MD, a Malik Abacı,
Reverse Adipofascial Radial Forearm Flap Surgery for Soft-Tissue Reconstruction of Hand Defects Osman Akdag, MD, a Mehtap Karamese, MD, a Muhammed NebilSelimoglu, MD, a Ahmet Akatekin, MD, a Malik Abacı,
The Foot. Dr. Wegdan Moh.Mustafa Medicine Faculty Assistant Professor Mob:
 The Foot Dr. Wegdan Moh.Mustafa Medicine Faculty Assistant Professor Mob: 0127155717 The skeleton of the foot Cutaneous innervations Sole of foot layers of muscles First layer -Abductor hallucis -Flexor
The Foot Dr. Wegdan Moh.Mustafa Medicine Faculty Assistant Professor Mob: 0127155717 The skeleton of the foot Cutaneous innervations Sole of foot layers of muscles First layer -Abductor hallucis -Flexor
Clinical teaching/experi ence. Lectures/semina rs/conferences Self-directed. learning. Clinical teaching/experi ence
 Regional Medical Center (The MED) Plastic Surgery PGY-3 By the end of the Plastic Surgery at the MED, the PGY-3 residents are expected to expand and cultivate knowledge and skills developed during previous
Regional Medical Center (The MED) Plastic Surgery PGY-3 By the end of the Plastic Surgery at the MED, the PGY-3 residents are expected to expand and cultivate knowledge and skills developed during previous
Role of free tissue transfer in management of chronic venous ulcer
 Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
musculoskeletal system anatomy muscles of foot sheet done by: dina sawadha & mohammad abukabeer
 musculoskeletal system anatomy muscles of foot sheet done by: dina sawadha & mohammad abukabeer Extensor retinaculum : A- superior extensor retinaculum (SER) : originates from the distal ends of the tibia
musculoskeletal system anatomy muscles of foot sheet done by: dina sawadha & mohammad abukabeer Extensor retinaculum : A- superior extensor retinaculum (SER) : originates from the distal ends of the tibia
Tor Chiu. Deep Inferior Epigastric Artery Perforator Flap 161
 18 Deep Inferior Epigastric Artery Perforator Flap Tor Chiu Deep Inferior Epigastric Artery Perforator Flap 161 Deep Inferior Epigastric Artery Perforator Flap FLAP TERRITORY The deep inferior epigastric
18 Deep Inferior Epigastric Artery Perforator Flap Tor Chiu Deep Inferior Epigastric Artery Perforator Flap 161 Deep Inferior Epigastric Artery Perforator Flap FLAP TERRITORY The deep inferior epigastric
Propeller perforator flaps for finger reconstruction
 Technical Note Page 1 of 7 Propeller perforator flaps for finger reconstruction Alexandru Valentin Georgescu, Ileana Rodica Matei Department of Plastic Surgery, University of Medicine Iuliu Hatieganu Cluj
Technical Note Page 1 of 7 Propeller perforator flaps for finger reconstruction Alexandru Valentin Georgescu, Ileana Rodica Matei Department of Plastic Surgery, University of Medicine Iuliu Hatieganu Cluj
Increased SuccessRate in Delayed Reverse Sural Artery Flap
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 9 Ver. IV (Sep. 2017), PP 24-28 www.iosrjournals.org Increased SuccessRate in Delayed Reverse
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 9 Ver. IV (Sep. 2017), PP 24-28 www.iosrjournals.org Increased SuccessRate in Delayed Reverse
Perforator flaps for reconstruction of lower limb defects
 International Surgery Journal Yasir M et al. Int Surg J. 2016 Nov;3(4):2109-2114 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20163583
International Surgery Journal Yasir M et al. Int Surg J. 2016 Nov;3(4):2109-2114 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20163583
Surgical Anatomy of the Medial Sural Artery Perforator Flap
 555 Surgical Anatomy of the Medial Sural Artery Perforator Flap Man-Zhi Wong, M.B.B.S., M.R.C.S., M.Med. 1 Chin-Ho Wong, M.B.B.S., M.R.C.S., M.Med., F.A.M.S. 2 Bien-Keem Tan, M.B.B.S., F.R.C.S., F.A.M.S.
555 Surgical Anatomy of the Medial Sural Artery Perforator Flap Man-Zhi Wong, M.B.B.S., M.R.C.S., M.Med. 1 Chin-Ho Wong, M.B.B.S., M.R.C.S., M.Med., F.A.M.S. 2 Bien-Keem Tan, M.B.B.S., F.R.C.S., F.A.M.S.
What s New in Fingertip Injuries. Gordon A. Brody, MD SOAR Redwood City
 What s New in Fingertip Injuries Gordon A. Brody, MD SOAR Redwood City Goals of Treatment Durable Sensate Aesthetic Preserve Length Preserve Mobility Goals of Treatment Pain and Worker s Compensation are
What s New in Fingertip Injuries Gordon A. Brody, MD SOAR Redwood City Goals of Treatment Durable Sensate Aesthetic Preserve Length Preserve Mobility Goals of Treatment Pain and Worker s Compensation are
New 2010 CPT Codes (italic font represents a new or revised code/description)
 New 2010 CPT Codes (italic font represents a new or revised code/description) 14301 Adjacent tissue transfer or rearrangement, any area; defect 30.1 sq cm to 60.0 sq cm 14302 each additional 30.0 sq cm,
New 2010 CPT Codes (italic font represents a new or revised code/description) 14301 Adjacent tissue transfer or rearrangement, any area; defect 30.1 sq cm to 60.0 sq cm 14302 each additional 30.0 sq cm,
Endoscopic assisted harvest of the pedicled pectoralis major muscle flap
 British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
Evaluation of the Posterior Interosseous Artery Flap in Reconstructing Hand Defects
 POSTERIOR THE IRAQI POSTGRADUATE INTEROSSEOUS MEDICAL ARTERY JOURNAL FLAP Evaluation of the Posterior Interosseous Artery Flap in Reconstructing Hand Defects Osam Ahmed Ibraheem, Mahdi Hameed Abood, Heider
POSTERIOR THE IRAQI POSTGRADUATE INTEROSSEOUS MEDICAL ARTERY JOURNAL FLAP Evaluation of the Posterior Interosseous Artery Flap in Reconstructing Hand Defects Osam Ahmed Ibraheem, Mahdi Hameed Abood, Heider
Where should you palpate the pulse of different arteries in the lower limb?
 Where should you palpate the pulse of different arteries in the lower limb? The femoral artery In the femoral triangle, its pulse is easily felt just inferior to the inguinal ligament midway between the
Where should you palpate the pulse of different arteries in the lower limb? The femoral artery In the femoral triangle, its pulse is easily felt just inferior to the inguinal ligament midway between the
CASE REPORT Omentum Free Flap Anastomosed to Arterial Bypass in Open Knee Dislocation: Case Report and Discussion
 CASE REPORT Omentum Free Flap Anastomosed to Arterial Bypass in Open Knee Dislocation: Case Report and Discussion Julien Pauchot, MD, PhD, a Emilie Ducroux, MD, b Grégoire Leclerc, MD, a Laurent Obert,
CASE REPORT Omentum Free Flap Anastomosed to Arterial Bypass in Open Knee Dislocation: Case Report and Discussion Julien Pauchot, MD, PhD, a Emilie Ducroux, MD, b Grégoire Leclerc, MD, a Laurent Obert,
Gross Anatomy Coloring Book Series. Lower Extremity Arteries
 Gross Anatomy Coloring Book Series Lower Extremity Arteries 1 Femoral Artery and Associated Branches For the life of the flesh is in the blood. Leviticus 17:11 Femoral Artery and Associated Branches After
Gross Anatomy Coloring Book Series Lower Extremity Arteries 1 Femoral Artery and Associated Branches For the life of the flesh is in the blood. Leviticus 17:11 Femoral Artery and Associated Branches After
Will it heal? How to assess the probability of wound healing
 Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
Original Article Lateral tarsal flap with a reverse dorsalis pedis artery pedicle: an approach in repair and reconstructive surgery
 Int J Clin Exp Med 2016;9(6):11334-11340 www.ijcem.com /ISSN:1940-5901/IJCEM0021713 Original Article Lateral tarsal flap with a reverse dorsalis pedis artery pedicle: an approach in repair and reconstructive
Int J Clin Exp Med 2016;9(6):11334-11340 www.ijcem.com /ISSN:1940-5901/IJCEM0021713 Original Article Lateral tarsal flap with a reverse dorsalis pedis artery pedicle: an approach in repair and reconstructive
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 Introduction Compartment Syndromes of the Leg Related to Athletic Activity Mark M. Casillas, M.D. Consequences of a misdiagnosis persistence of a performance limitation loss of function/compartment loss
Introduction Compartment Syndromes of the Leg Related to Athletic Activity Mark M. Casillas, M.D. Consequences of a misdiagnosis persistence of a performance limitation loss of function/compartment loss
The Leg. Prof. Oluwadiya KS
 The Leg Prof. Oluwadiya KS www.oluwadiya.sitesled.com Compartments of the leg 4 Four Compartments: 1. Anterior compartment Deep fibular nerve Dorsiflexes the foot and toes 2. Lateral Compartment Superficial
The Leg Prof. Oluwadiya KS www.oluwadiya.sitesled.com Compartments of the leg 4 Four Compartments: 1. Anterior compartment Deep fibular nerve Dorsiflexes the foot and toes 2. Lateral Compartment Superficial
Interesting Case Series. Scalp Reconstruction With Free Latissimus Dorsi Muscle
 Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
Distally based anterolateral thigh flap pedicled on the oblique branch of the lateral circumflex femoral artery
 Original Article Page 1 of 8 Distally based anterolateral thigh flap pedicled on the oblique branch of the lateral circumflex femoral artery Yuanbo Liu, Mengqing Zang, Shan Zhu, Bo Chen, Shanshan Li, Bingjian
Original Article Page 1 of 8 Distally based anterolateral thigh flap pedicled on the oblique branch of the lateral circumflex femoral artery Yuanbo Liu, Mengqing Zang, Shan Zhu, Bo Chen, Shanshan Li, Bingjian
Wound coverage of plantar metatarsal ulcers in leprosy using a toe web flap
 Free full text on www.ijps.org Original Article Wound coverage of plantar metatarsal ulcers in leprosy using a toe web flap J. Joshua, V. Chakraborthy Premananda Memorial Leprosy Hospital, The Leprosy
Free full text on www.ijps.org Original Article Wound coverage of plantar metatarsal ulcers in leprosy using a toe web flap J. Joshua, V. Chakraborthy Premananda Memorial Leprosy Hospital, The Leprosy
~, /' ~::'~ EXTENSOR HALLUCIS LONGUS. Leg-anterolateral :.:~ / ~\,
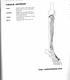 TIBIALIS ANTERIOR Lateral condyle of tibia, upper half of lateral surface of tibia, interosseous membrane Medial side and plantar surface of medial cuneiform bone, and base of first metatarsal bone Dorsiflexes
TIBIALIS ANTERIOR Lateral condyle of tibia, upper half of lateral surface of tibia, interosseous membrane Medial side and plantar surface of medial cuneiform bone, and base of first metatarsal bone Dorsiflexes
Leg. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Leg Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skin of the Leg Cutaneous Nerves Medially: The saphenous nerve, a branch of the femoral nerve supplies the skin on the medial surface
Leg Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skin of the Leg Cutaneous Nerves Medially: The saphenous nerve, a branch of the femoral nerve supplies the skin on the medial surface
Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage
 Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage Shareef Jandali, MD, and David W. Low, MD Division of Plastic Surgery, University of Pennsylvania Health System, Philadelphia Correspondence:
Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage Shareef Jandali, MD, and David W. Low, MD Division of Plastic Surgery, University of Pennsylvania Health System, Philadelphia Correspondence:
The myofascial compartments of the foot
 The myofascial compartments of the foot A CADAVER STUDY Z. X. Ling, V. P. Kumar From the National University of Singapore, Republic of Singapore Compartment syndrome of the foot requires urgent surgical
The myofascial compartments of the foot A CADAVER STUDY Z. X. Ling, V. P. Kumar From the National University of Singapore, Republic of Singapore Compartment syndrome of the foot requires urgent surgical
The gluteal perforator-based flap in repair of pressure sores
 The British Association of Plastic Surgeons (2004) 57, 342 347 CASE REPORTS The gluteal perforator-based flap in repair of pressure sores Çilingir Meltem*, Çelik Esra, Fındık Hasan, Duman Ali Department
The British Association of Plastic Surgeons (2004) 57, 342 347 CASE REPORTS The gluteal perforator-based flap in repair of pressure sores Çilingir Meltem*, Çelik Esra, Fındık Hasan, Duman Ali Department
Organization of the Lower Limb
 Organization of the Lower Limb Limb Development Lower limb develops in an aterolateral position at the level of the L2 to S3 trunk segments Great toe positioned cephalic direction with the soles of the
Organization of the Lower Limb Limb Development Lower limb develops in an aterolateral position at the level of the L2 to S3 trunk segments Great toe positioned cephalic direction with the soles of the
Lower Limb Nerves. Clinical Anatomy
 Lower Limb Nerves Clinical Anatomy Lumbar Plexus Ventral rami L1 L4 Supplies: Abdominal wall External genitalia Anteromedial thigh Major nerves.. Lumbar Plexus Nerves relation to psoas m. : Obturator n.
Lower Limb Nerves Clinical Anatomy Lumbar Plexus Ventral rami L1 L4 Supplies: Abdominal wall External genitalia Anteromedial thigh Major nerves.. Lumbar Plexus Nerves relation to psoas m. : Obturator n.
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
JMSCR Vol 07 Issue 01 Page January 2019
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v7i1.36 Original Article A Study on the
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v7i1.36 Original Article A Study on the
A new operative technique for dissecting perforator vessel in perforator flap: a better way to minimize donor-site morbidity
 Original Article Page 1 of 7 A new operative technique for dissecting perforator vessel in perforator flap: a better way to minimize donor-site morbidity Limin Qing, Panfeng Wu, Zhouzheng Bing, Fang Yu,
Original Article Page 1 of 7 A new operative technique for dissecting perforator vessel in perforator flap: a better way to minimize donor-site morbidity Limin Qing, Panfeng Wu, Zhouzheng Bing, Fang Yu,
HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS
 HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS October 22, 2010 D. LOWER LIMB MUSCLES 2. Lower limb compartments ANTERIOR THIGH COMPARTMENT General lfunction: Hip flexion, knee extension, other motions
HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS October 22, 2010 D. LOWER LIMB MUSCLES 2. Lower limb compartments ANTERIOR THIGH COMPARTMENT General lfunction: Hip flexion, knee extension, other motions
The homodigital neurovascular antegrade island flap. for fingertip reconstruction in children and
 Acta Orthop. Belg., 2011, 77, 598-602 ORIGINAL STUDY The homodigital neurovascular antegrade island flap for fingertip reconstruction in children Bingqi WAng, Lei CHEn, Laijin LU, Zhigang LiU, Zhixin ZHAng,
Acta Orthop. Belg., 2011, 77, 598-602 ORIGINAL STUDY The homodigital neurovascular antegrade island flap for fingertip reconstruction in children Bingqi WAng, Lei CHEn, Laijin LU, Zhigang LiU, Zhixin ZHAng,
Primary closure of the deltopectoral flap-donor site without skin grafting
 Primary closure of the deltopectoral flap-donor site without skin grafting Received: 4/3/2013 Accepted: 14/5/2013 Introduction Reliable and simultaneous reconstruction of head-and-neck defects has been
Primary closure of the deltopectoral flap-donor site without skin grafting Received: 4/3/2013 Accepted: 14/5/2013 Introduction Reliable and simultaneous reconstruction of head-and-neck defects has been
موسى صالح عبد الرحمن الحنبلي أحمد سلمان
 8 موسى صالح عبد الرحمن الحنبلي أحمد سلمان 1 P a g e Today we will talk about a new region, which is the leg. And as always, we will start with studying the sensory innervation of the leg. What is the importance
8 موسى صالح عبد الرحمن الحنبلي أحمد سلمان 1 P a g e Today we will talk about a new region, which is the leg. And as always, we will start with studying the sensory innervation of the leg. What is the importance
Perforator-based propeller flaps treating loss of substance in the lower limb
 J Orthopaed Traumatol (2011) 12:93 99 DOI 10.1007/s10195-011-0136-0 ORIGINAL ARTICLE Perforator-based propeller flaps treating loss of substance in the lower limb Pierluigi Tos Marco Innocenti Stefano
J Orthopaed Traumatol (2011) 12:93 99 DOI 10.1007/s10195-011-0136-0 ORIGINAL ARTICLE Perforator-based propeller flaps treating loss of substance in the lower limb Pierluigi Tos Marco Innocenti Stefano
Thomas Zgonis a, *, Douglas T. Cromack b, Thomas S. Roukis c, Joann Orphanos d, Vasilios D. Polyzois e CASE REPORT. Introduction.
 Injury Extra (2007) 38, 187 192 www.elsevier.com/locate/inext CASE REPORT Severe degloving injury of the sole and heel treated by a reverse flow sural artery neurofasciocutaneous flap and a modified off-loading
Injury Extra (2007) 38, 187 192 www.elsevier.com/locate/inext CASE REPORT Severe degloving injury of the sole and heel treated by a reverse flow sural artery neurofasciocutaneous flap and a modified off-loading
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study
 Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps
 Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Gastrocnemius Muscle Flap Coverage of Chronically= Infected Knee Joints
 Gastrocnemius Muscle Flap Coverage of Chronically= Infected Knee Joints ABSTRACT Chronically infected open knee joints present dif cult problem. Aggressive debridement of chronically infected soft tissue
Gastrocnemius Muscle Flap Coverage of Chronically= Infected Knee Joints ABSTRACT Chronically infected open knee joints present dif cult problem. Aggressive debridement of chronically infected soft tissue
The Lower Limb VI: The Leg. Anatomy RHS 241 Lecture 6 Dr. Einas Al-Eisa
 The Lower Limb VI: The Leg Anatomy RHS 241 Lecture 6 Dr. Einas Al-Eisa Muscles of the leg Posterior compartment (superficial & deep): primary plantar flexors of the foot flexors of the toes Anterior compartment:
The Lower Limb VI: The Leg Anatomy RHS 241 Lecture 6 Dr. Einas Al-Eisa Muscles of the leg Posterior compartment (superficial & deep): primary plantar flexors of the foot flexors of the toes Anterior compartment:
Medical Journal of the Volume 20 Islamic Republic of Iran Number 3 Fall 1385 November Original Articles
 Medical Journal of the Volume 0 Islamic Republic of Iran Number 3 Fall 38 November 00 Original Articles ANATOMY OF THE SUPERFICIAL INFERIOR EPIGASTRIC ARTERY FLAP MAHDI FATHI, M.D., EBRAHIM HATAMIPOUR,
Medical Journal of the Volume 0 Islamic Republic of Iran Number 3 Fall 38 November 00 Original Articles ANATOMY OF THE SUPERFICIAL INFERIOR EPIGASTRIC ARTERY FLAP MAHDI FATHI, M.D., EBRAHIM HATAMIPOUR,
Combined tongue flap and V Y advancement flap for lower lip defects
 British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
Muscles of the Gluteal Region
 Muscles of the Gluteal Region 1 Some of the most powerful in the body Extend the thigh during forceful extension Stabilize the iliotibial band and thoracolumbar fascia Related to shoulders and arms because
Muscles of the Gluteal Region 1 Some of the most powerful in the body Extend the thigh during forceful extension Stabilize the iliotibial band and thoracolumbar fascia Related to shoulders and arms because
The University Of Jordan Faculty Of Medicine FOOT. Dr.Ahmed Salman Assistant Prof. of Anatomy. The University Of Jordan
 The University Of Jordan Faculty Of Medicine FOOT Dr.Ahmed Salman Assistant Prof. of Anatomy. The University Of Jordan Tarsal Tunnel Syndrome Due to compression of Tibial nerve as it travels through the
The University Of Jordan Faculty Of Medicine FOOT Dr.Ahmed Salman Assistant Prof. of Anatomy. The University Of Jordan Tarsal Tunnel Syndrome Due to compression of Tibial nerve as it travels through the
A systematic approach to the failed plastic surgical reconstruction of the diabetic foot
 æiefs PROCEEDINGS A systematic approach to the failed plastic surgical reconstruction of the diabetic foot Ioannis I. Ignatiadis, MD, PhD 1 *, Vassiliki A. Tsiampa, MD 2 and Apostolos E. Papalois, PhD
æiefs PROCEEDINGS A systematic approach to the failed plastic surgical reconstruction of the diabetic foot Ioannis I. Ignatiadis, MD, PhD 1 *, Vassiliki A. Tsiampa, MD 2 and Apostolos E. Papalois, PhD
The lumbar artery perforator based island flap: anatomical study and case reports
 British Journal of Plastic Surgery (1999), 52, 541 546 1999 The British Association of Plastic Surgeons The lumbar artery perforator based island flap: anatomical study and case reports H. Kato*, M. Hasegawa,
British Journal of Plastic Surgery (1999), 52, 541 546 1999 The British Association of Plastic Surgeons The lumbar artery perforator based island flap: anatomical study and case reports H. Kato*, M. Hasegawa,
Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes
 DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
DISSECTION SCHEDULE. Session I - Hip (Front) & Thigh (Superficial)
 DISSECTION SCHEDULE Session I - Hip (Front) & Thigh (Superficial) Surface anatomy Inguinal region Gluteal region Thigh Leg Foot bones Hip bone Femur Superficial fascia Great saphenous vein Superficial
DISSECTION SCHEDULE Session I - Hip (Front) & Thigh (Superficial) Surface anatomy Inguinal region Gluteal region Thigh Leg Foot bones Hip bone Femur Superficial fascia Great saphenous vein Superficial
THERE IS NO PROOF FOR THE ANGIOSOME CONCEPT
 THERE IS NO PROOF FOR THE ANGIOSOME CONCEPT Peter Huppert Professor of Radiology and Neuroradiology Department of Radiology, Neuroradiology and Nuclear Medicine Klinikum Darmstadt Academic Teaching Hospital
THERE IS NO PROOF FOR THE ANGIOSOME CONCEPT Peter Huppert Professor of Radiology and Neuroradiology Department of Radiology, Neuroradiology and Nuclear Medicine Klinikum Darmstadt Academic Teaching Hospital
Organization of the Lower Limb
 Organization of the Lower Limb Most illustrations from: Thieme Atlas of Anatomy: Musculoskeletal System. M Schuenke, et al, 2006. Anatomy: A Regional Atlas of the Human Body. Carmine Clemente, 4th edition.
Organization of the Lower Limb Most illustrations from: Thieme Atlas of Anatomy: Musculoskeletal System. M Schuenke, et al, 2006. Anatomy: A Regional Atlas of the Human Body. Carmine Clemente, 4th edition.
Malignant soft tissue tumor, wide excision, and sural flap
 CASE REPORT Magetsari et al. 1 PEER REVIEWED OPEN ACCESS Malignant soft tissue tumor, wide excision, and sural flap Rahadyan Magetsari, Yudha Mathan Sakti, Arie Nugroho ABSTRACT Introduction: Soft tissue
CASE REPORT Magetsari et al. 1 PEER REVIEWED OPEN ACCESS Malignant soft tissue tumor, wide excision, and sural flap Rahadyan Magetsari, Yudha Mathan Sakti, Arie Nugroho ABSTRACT Introduction: Soft tissue
Reconstruction of axillary scar contractures retrospective study of 124 cases over 25 years
 British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
PUT YOUR BEST FOOT FORWARD
 PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
Foot. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Foot Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Dorsum of the Foot Sole of the Foot Plantar aponeurosis It is a triangular thickening of deep fascia in the sole of the foot Attachments:
Foot Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Dorsum of the Foot Sole of the Foot Plantar aponeurosis It is a triangular thickening of deep fascia in the sole of the foot Attachments:
Anatomy of the lower limb
 Anatomy of the lower limb Arches & sole of the foot Dr. Hayder ARCHES OF THE FOOT The foot as a mechanical unit performs two major functions: - It acts as a pliable platform to support the body weigh during
Anatomy of the lower limb Arches & sole of the foot Dr. Hayder ARCHES OF THE FOOT The foot as a mechanical unit performs two major functions: - It acts as a pliable platform to support the body weigh during
Surgical Management of wounds, flaps, grafts, and scars
 Disclosures Surgical Management of wounds, flaps, grafts, and scars I have no financial disclosures Cherrie Heinrich, MD, FACS Department of Plastic Surgery Regions Hospital Assistant Professor University
Disclosures Surgical Management of wounds, flaps, grafts, and scars I have no financial disclosures Cherrie Heinrich, MD, FACS Department of Plastic Surgery Regions Hospital Assistant Professor University
Critical Limb Ischemia A Collaborative Approach to Patient Care. Christopher LeSar, MD Vascular Institute of Chattanooga July 28, 2017
 Critical Limb Ischemia A Collaborative Approach to Patient Care Christopher LeSar, MD Vascular Institute of Chattanooga July 28, 2017 Surgeons idea Surgeons idea represents the final stage of peripheral
Critical Limb Ischemia A Collaborative Approach to Patient Care Christopher LeSar, MD Vascular Institute of Chattanooga July 28, 2017 Surgeons idea Surgeons idea represents the final stage of peripheral
