T raumatic brain injury (TBI) is a
|
|
|
- Stephanie Dayna Johns
- 5 years ago
- Views:
Transcription
1 COMMENTARY 593 Head trauma... Intracranial injury in minor head trauma N Kuppermann... Commentary on the paper by Dunning et al (see page 653) T raumatic brain injury (TBI) is a leading cause of childhood death and disability worldwide. In the United States, childhood head trauma results in 3000 deaths, hospitalisations, and emergency department (ED) visits annually. 1 2 Children with seemingly minor head trauma, defined here by Glasgow Coma Scale (GCS) scores of 14 15, account for 40 59% of those with TBIs, 3 5 and present a perplexing problem to clinicians. Despite the frequency of childhood minor head trauma, there exists no highly accurate and reliable clinical scoring system for separating those children with minor head trauma at negligible risk of TBI from those at greater risk. Children with TBIs who present with signs of seemingly minor head trauma are at risk for delayed diagnosis and treatment, and such unrecognised TBIs are a source of preventable morbidity. 6 8 Nevertheless, although some TBIs in children with minor head trauma are initially unrecognised and therefore neuroimaging is delayed, a great many more children evaluated for minor head trauma receive unnecessary neuroimaging. More than 50% of children evaluated in EDs for head trauma in the United States undergo cranial computed tomography (CT) scanning, 1 and this percentage doubled between 1996 and Children with minor head trauma account for 70 85% of children who receive cranial CT scans during their ED evaluation for head trauma in the United States, 4 5 yet only 4 8% of these CT scans show TBI Furthermore, approximately 5% of those with positive CT scans undergo operative intervention. 4 9 Therefore CT scans are used inefficiently. Although CT scanning is the reference standard for diagnosing TBI and delayed recognition of TBI increases morbidity, overuse of CT scanning has important drawbacks. These include transporting the child away from the supervised setting of the ED, the occasional requirement for pharmacological sedation with its potential for complications, and additional health care costs and resource utilisation. The most important drawback of inappropriate CT utilisation, however, is radiation exposure that may lead to malignancy and other sequelae. CT scanning accounts for most (67%) of the collective effective radiation dosage from diagnostic imaging in the United States, although only 11% of all radiographic studies are CT scans. 13 The typical radiation dosage from a current paediatric cranial CT scan is times greater than that for a routine chest radiograph. 14 The estimates of lifetime attributable risk for fatal cancer from one current generation cranial CT scan ranges from 1 per 2000 scans for young infants to 1 per 5000 for those 10 years old Furthermore, for every case of fatal cancer caused by cranial CT scans, several cases of nonfatal cancer may be induced In addition, it has recently been reported that low doses of ionising radiation in infancy may adversely affect cognitive abilities in young adulthood. 18 Nevertheless, although the risks of radiation induced malignancy can be estimated, they are small for any given individual. It is apparent that both under-utilisation and over-utilisation of CT scanning have potential ill effects, and the use of CT scanning following blunt head trauma must be optimised. Unfortunately, there have been few published prospective studies on this topic in children, and none with the necessary size and patient diversity to ensure narrow confidence intervals around the estimates of model accuracy, and wide generalisability of the resulting model. As a consequence, there is substantial variation among ED physicians in the use of CT scans for the evaluation of these children, and the creation of a decision rule to assist with decision making for CT use is a priority among ED physicians. The lack of reliable data on risk factors for TBI in children with minor head trauma motivated Dunning et al to perform a meta-analysis of the literature, which is reported in this issue of Archives. 23 Using an appropriate, detailed search strategy, the authors identified 16 papers meeting criteria for inclusion in the meta-analysis. In the metaanalysis, the authors assessed the predictive effect of six clinical symptoms and signs, in addition to plain radiography, for identifying which children have intracranial haemorrhage after minor head trauma. The authors reported the pooled estimates for the relative risks of these seven individual criteria. They found that the variables with significant point estimates for risk of TBI were focal neurological findings, skull fracture, a reduced level of consciousness, and a history of loss of consciousness (with seizure trending towards significance). In the absence of rigorous prospectively acquired data, the meta-analysis by Dunning et al helps us focus on the areas of greatest uncertainty and controversy. There is little debate that a child with focal neurological signs or a depressed level of consciousness after head trauma needs emergent neuroimaging. In addition, several prospective paediatric studies have shown that signs of a skull fracture are significantly predictive of intracranial haemorrhage. 4 5 There is much more controversy, however, over the importance of headache, vomiting, and history of loss of consciousness. Readers must be cautious, however, of translating the findings of Dunning et al into clinical practice. As noted by the authors, the heterogeneous nature of the studies and the wide reported rates of intracranial haemorrhage limit the ability to pool the data and translate the results. Even the definition of minor head trauma itself varies between studies. Dunning et al defined minor head trauma as GCS scores of 13 15, whereas others have defined this as GCS scores of 14 15, 4 and GCS scores of In clinical practice, there is not substantial controversy over imaging children with GCS scores of 13, whereas there is great controversy over children with GCS scores of 15. In our experience, 26.5% (95% CI 14.9% to 41.1%) of children with GCS scores of 13 have intracranial haemorrhage versus 2.6% (95% CI 1.7% to 3.9%) of those with GCS scores of Another conundrum is the clinical assessment of pre-verbal children with minor head trauma. As noted by Dunning et al, certain variables cannot be used reliably in the assessment of these children, specifically headache, amnesia, and dizziness. It is unclear how headache was assessed in preverbal children in the studies compiled Abbreviations: CT, computed tomography; ED, emergency department; GCS, Glasgow Coma Scale; TBI, traumatic brain injury
2 594 COMMENTARY by Dunning et al. Furthermore, scalp haematoma is one of the most important clinical variables in the assessment of infants with minor head trauma, 3 24 and was not assessed in the metaanalysis by Dunning et al. The need for a separate neuroimaging decision rule for pre-verbal children is apparent. An additional important limitation to the clinical utility of the Dunning et al study is the univariate nature of the meta-analysis. Only by assessing the importance of particular variables in the presence or absence of other variables (through multivariable analysis) can one truly assess the independent predictive effect of any particular variable. Some variables which seem important in univariate analysis may no longer be important in the multivariable analysis. For example, it seems intuitive that a child with a history of loss of consciousness after head trauma has a greater risk of TBI than a child without this history. More controversial, however, is the child with an isolated loss of consciousness (that is, without any other symptoms or signs of TBI). Is this finding in isolation sufficiently predictive of intracranial haemorrhage to require neuroimaging? Several multivariable analyses that assessed this variable, including those in recent large prospective studies, suggest not. Similarly, other variables which appear not to be predictive in univariate analyses may in fact be predictive when in the presence of other variables. The variables headache and vomiting are not significant in the univariate metaanalysis of Dunning et al, but were important in recent large prospective multivariable studies on this topic. 4 9 This may be due to the insufficient characterisation of headache and vomiting in previous retrospective studies on the topic, as noted by Dunning et al. It may also be that these variables emerge as important only in the presence or absence of other variables. Finally, in a meta-analysis such as this, one cannot determine whether the absence of certain high risk factors decreases the overall risk of intracranial haemorrhage below the clinical threshold to obtain emergent neuroimaging. The Dunning et al study increases our knowledge base about prediction of TBI. It is nonetheless apparent, however, that accurate, sufficient and generalisable data on which to derive reliable evidence based guidelines for neuroimaging children with minor head trauma are still lacking. Fortunately, multicentre research networks in the United Kingdom, Canada, and in the United States have large ongoing studies to gather these data. The Pediatric Emergency Care Applied Research Network (PECARN), a research network of 25 hospital EDs in the United States, 26 will collect such data on approximately children with minor head trauma. Using these types of networks to conduct such studies will ensure adequate sample sizes, standardised data collection, appropriate multivariable analyses, and enrolment of a clinical cohort of suitable diversity to generalise the results. These studies will ultimately affect clinical decision making and improve the care of children with minor blunt head trauma. ACKNOWLEDGEMENTS The work and research reflected in this editorial were supported in part by a Distinguished Scholar grant from the United States United Kingdom Fulbright Commission. I gratefully thank and acknowledge their support. Arch Dis Child 2004;89: doi: /adc Correspondence to: Dr N Kuppermann, Division of Emergency Medicine, UC Davis Medical Center, 2315 Stockton Blvd, PSSB Bldg, Suite 2100, Sacramento, CA 98517, USA; nkuppermann@ucdavis.edu REFERENCES 1 National Center for Health Statistics Centers for Disease Control and Prevention. 2000; National Hospital Ambulatory Medical Care Survey, Emergency Department File. 2002; CD-ROM Series 13, No National Center for Injury Prevention and Control. Traumatic brain injury in the United States: Assessing outcomes in children. Centers for Disease Control and Prevention, Greenes DS, Schutzman SA. Clinical indicators of intracranial injury in head-injured infants. Pediatrics 1999;104: Palchak MJ, Holmes JF, Vance CW, et al. A decision rule for identifying children at low risk for brain injuries after blunt head trauma. Ann Emerg Med 2003;42: Quayle KS, Jaffe DM, Kuppermann N, et al. Diagnostic testing for acute head injury in children: when are head computed tomography and skull radiographs indicated? Pediatrics 1997;99:e Connors JM, Ruddy RM, McCall J, et al. Delayed diagnosis in pediatric blunt trauma. Pediatr Emerg Care 2001;17: Furnival RA, Woodward GA, Schunk JE. Delayed diagnosis of injury in pediatric trauma. Pediatrics 1996;98: Klauber MR, Marshall LF, Luerssen TG, et al. Determinants of head injury mortality: importance of the low risk patient. Neurosurgery 1989;24: Haydel MJ, Shembekar AD. Prediction of intracranial injury in children aged five years and older with loss of consciousness after minor head injury due to nontrivial mechanisms. Ann Emerg Med 2003;42: Davis RL, Mullen N, Makela M, et al. Cranial computed tomography scans in children after minimal head injury with loss of consciousness. Ann Emerg Med 1994;24: Homer CJ. American Academy of Pediatrics technical report: blunt head injury in children. Pediatrics 1999;104:e Schunk JE, Rodgerson JD, Woodward GA. The utility of head computed tomographic scanning in pediatric patients with normal neurologic examination in the emergency department. Pediatr Emerg Care 1996;12: Mettler FA Jr, Wiest PW, Locken JA, et al. CT scanning: patterns of use and dose. J Radiol Prot 2000;20: Accessed 12 February Brenner DJ. Estimating cancer risks from pediatric CT: going from the qualitative to the quantitative. Pediatr Radiol 2002;32: Brenner D, Elliston C, Hall E, et al. Estimated risks of radiation-induced fatal cancer from pediatric CT. AJR 2001;176: Faulkner K, Moores BM. Radiation dose and somatic risk from computed tomography. Acta Radiol 1987;28: Hall P, Adami HO, Trichopoulos D, et al. Effect of low doses of ionising radiation in infancy on cognitive function in adulthood: Swedish population based cohort study. BMJ 2004;328: Aitken ME, Herrerias CT, Davis R, et al. Minor head injury in children: current management practices of pediatricians, emergency physicians, and family physicians. Arch Pediatr Adolesc Med 1998;152: Klassen TP, Reed MH, Stiell IG, et al. Variation in utilization of computed tomography scanning for the investigation of minor head trauma in children: a Canadian experience. Acad Emerg Med 2000;7: Stiell IG, Wells GA, Vandemheen K, et al. Variation in ED use of computed tomography for patients with minor head injury. Ann Emerg Med 1997;30: Graham ID, Stiell IG, Laupacis A, et al. Emergency physicians attitudes toward and use of clinical decision rules for radiography. Acad Emerg Med 1998;5: Dunning J, Batchelor J, Stratford-Smith P, et al. A meta-analysis of variables that predict significant intracranial injury in minor head trauma. Arch Dis Child 2004;89: Greenes DS, Schutzman SA. Clinical significance of scalp abnormalities in asymptomatic headinjured infants. Pediatr Emerg Care 2001;17: Palchak MJ, Holmes JF, Vance CW, et al. Does an isolated history of loss of consciousness or amnesia predict brain injuries after blunt head trauma? Pediatrics, In press. 26 The Pediatric Emergency Care Applied Research Network. The Pediatric Emergency Care Applied Research Network (PECARN): rationale, development, and first steps. Acad Emerg Med 2003;10:661 8.
3 COMMENTARY 595 Diagnosis... The need for caution in considering the diagnostic utility of antibasal ganglia antibodies in movement disorders H S Singer, J J Hong, C A Rippel, C A Pardo... Commentary on the paper by Church et al (see page 611) I Now this is not the end. It is not even the beginning of the end. But it is, perhaps, the end of the beginning. (Sir Winston Churchill, Speech in November 1942) n this issue, Church and colleagues discuss the possibility that immunological analyses of sera could serve as diagnostic markers for movement disorders associated with streptococcal infection. 1 These investigators have been at the forefront of studies evaluating antibasal ganglia antibodies (ABGA) in a variety of proposed poststreptococcal movement conditions. These studies have great potential, given that identification of a specific immune mechanism could lead to insights into pathophysiological mechanisms as well as the development of new therapies. Nevertheless, based on ongoing studies in our laboratory, we feel compelled to raise concerns about the reproducibility of ABGA results, about methodology, and about the inability to confirm serum microinfusion induced alterations of rodent behaviour. As described in the quotation from the wise leader and historian Winston Churchill, we believe that whereas important initial steps have been taken, the final solution has not been reached. The goal of this commentary is not to criticise existing reports, but to identify disparities in data and to emphasise the need for additional testing, before implementing ABGA screening for children with movement disorders. HYPOTHESIS AND REQUIREMENTS FOR CONFIRMATION In susceptible individuals, antibodies produced against the group A b haemolytic streptococcus (GABHS) cross-react with epitopes on neurones located in the basal ganglia, through a process of molecular mimicry, and cause movement abnormalities (chorea, tics, other). IAcceptance of the aforementioned poststreptococcal autoimmune hypothesis requires confirmation on two major levels: (1) epidemiological evidence showing a clear association between streptococcal infection and movement disorders; and (2) definitive evidence for an autoimmune mechanism. Since the focus of this commentary is on laboratory based approaches, the reader is referred to other sources for a discussion of clinical issues and requisites for documentation of a streptococcal infection. 2 4 Experimental affirmation of autoimmunity requires several factors, including the identification of autoantibodies, the presence of immunoglobulins at the pathological site, the induction of symptoms with autoantigens, passive transfer of the disorder to animal models, and a positive response to immunomodulatory therapy. 5 METHODS FOR EVALUATING ABGA ABGA have been measured in children with SC and TS by either enzyme linked immunosorbent assays (ELISA) or immunofluorescent methods. ELISA is generally selected because it is more specific than immunofluorescent techniques. 6 Western blot analyses, which permit detection of autoantibody activity against specific brain epitopes, have also been applied successfully. Lastly, the bilateral microinfusion of sera or IgG into rodent striatum has been suggested as a valuable method to assess the functional effect of ABGA obtained from individuals with movement disorders. Although each of the ABGA detection methods appears to be relatively straightforward, results are affected by the use of sera or IgG, brain region (caudate, putamen, or globus pallidus), condition of tissue (fresh or frozen), method of tissue preparation (with or without removal of lipids, that is, delipided), selection of tissue fractions (supernatant, pellet, or synaptosomes), method for Western blotting (electrochemiluminescence, ECL, or colorimetric detection), and several other factors (Singer et al, unpublished data). NOTEWORTHY LABORATORY DISCREPANCIES In their paper, Church and colleagues provide information on antibodies detected in 40 children in the UK presenting with movement disorders associated with streptococcal infections: 20 PANDAS, 16 SC, and four idiopathic movement disorders. 1 Pooled group results suggest that this cohort can be differentiated from a variety of disease controls by ELISA and Western immunoblotting methods. In contrast, results of similar immune assays performed on children with SC and PANDAS and compared to healthy controls, discussed below, have produced significantly different results. 7 8 ELISA In nine children with acute SC, age range years, assays performed on fresh brain tissues from caudate, putamen, and globus pallidus showed that optical density (OD) values were higher in SC patients than controls across all brain regions, but did not reach a level of significance. Although our results (33% above a negative cutoff) did not confirm the 95% positive rates reported by Church and colleagues, 6 the documented positive trend supports the possibility that inclusion of additional cases would identify a meaningful difference in SC. In contrast, however, two separate evaluations of ELISA in children with PANDAS have shown absolutely no difference from controls 8 (Singer et al, unpublished data). In the first evaluation, ELISA was measured on supernatant, pellet, and synaptosomal preparations from fresh postmortem caudate, putamen, and globus pallidus by using serum from 15 children with classic PANDAS (participants in the hallmark study by Swedo et al 9 ). This lack of correlation has been further confirmed in a second study of 40 additional cases of PANDAS. Thus, ELISA is unchanged in a population of children who have a proposed association with GABHS. Nevertheless, since ABGA are identified in normal individuals, it is possible that small changes could be missed or the serum might be obtained after symptoms have waned.... Abbreviations: ABGA, antibasal ganglia antibodies; GABHS, group A b haemolytic streptococcus; PANDAS, paediatric autoimmune neuropsychiatric disorders associated with streptococcal infections; SC, Sydenham s chorea; TS, Tourette syndrome
4 596 COMMENTARY Western immunoblotting In this technique, small amounts of brain protein are subjected to electrophoresis in acrylamide gels, the protein is transferred to nitrocellulose, exposed to serum, and then to an antihuman IgG secondary antibody that is conjugated to either horseradish peroxidase or a colorimetric agent. Resulting bands are then analysed by several techniques ranging from direct visual comparison (useful with minimal bands) to digital conversion of bands on each blot to peaks with assigned molecular weights and measurable peak heights and areas. Church and colleagues, using frozen tissue and a colorimetric assay, identified only a few bands in controls (limited reactivity against any basal ganglia antigens), but significantly more bands in poststreptococcal patients. 1 They suggest that specific MW bands (60, 45, 40 kda) are commonly detected in their movement disorder patients but not in controls. Their identification of similar bands in subjects with different clinical disorders raises questions of disease specificity. In addition, as shown in fig 1, the use of fresh postmortem tissue and an ECL detection system identifies many more bands than shown by the method used by Church and colleagues (frozen tissue and a colorometric detection system). This suggests that the methods selected can have an important influence on the detection of potential disease specific basal ganglia antigens. A further issue is that antigen binding, claimed to be associated with PANDAS and SC patients, is also found in controls. That is, in the evaluation of fresh postmortem tissue without lipids from 10 control subjects, binding was present at 60 kda in 100%, at 45 kda in 80%, and at 40 kda in 100%; binding in frozen delipided tissue was present in 100%, 30%, and 40%, respectively (Singer et al, unpublished data). Lastly, questions exist about the importance of Figure 1 Western blotting using sera and caudate supernatant. Numerous bands (antigen-antibody interactions) are observed in SC and PANDAS subjects and controls. a band at 60 kda, since epitopes at this same molecular weight are identified using only secondary antibody, without the addition of serum or IgG (fig 2). Western immunoblotting of serum from patients with SC, analysed by use of discriminant analysis of data vectors calculated from individual blots, has shown that patterns are significantly different from controls, most notably in caudate supernatant fractions. Numerous antigens contributed to this statistical difference, but the two most prominent molecular masses that distinguished the groups were at 126 and 113 kda. 7 In PANDAS, complex staining patterns were observed in all cases, but no differences from control were seen for either the number of bands or the total density of bands. Discriminant analyses did show small differences in mean data vectors between PANDAS and controls that were limited to the caudate supernatant preparation. These changes, however, were minimal compared to those detected between SC and controls. Whether differences in Western blotting offer specific insight into the pathophysiology of movement disorders or merely represent an epiphenomenon, remains undetermined. For example, children with the diagnosis of TS and no history of streptococcal associated exacerbations show prominent immunoblot differences. 10 To date, weaknesses in most ABGA studies include the analysis of antibody patterns at only a single point in time, rather than in longitudinal samples, and the failure to determine whether there is an association between ABGA and a streptococcal infection. Lastly, it should be recognised that measured autoantibody repertoires can be secondary immune responses to components of damaged tissue 11 rather than to the inciting pathological factor. Indirect immunofluorescence Studies in the Church and Singer laboratories have identified fluorescent binding in some patients with TS and PANDAS. Location of this positive binding remains unclear, ranging from axonal with sparing of the cell body to astroglial processes. Additional analyses with double labelled staining (antihuman IgG with GFAP or a neuronal indicator) are necessary to further identify the precise anatomical region. Similar positive binding has also been detected in controls. RODENT MICROINFUSION MODELS One of the major criteria for any neurological disorder to be recognised as autoimmune is the ability to transfer the disease passively to animals. Two studies, both frequently cited as supporting evidence for an autoimmune mechanism in paediatric movement disorders, have reported behavioural effects after the infusion of ABGA from subjects with TS into rodent striatum. That is, the microinfusion of sera containing increased antibodies into the ventral or ventrolateral striatum of rats significantly increases stereotypic behaviours (for example, licks and forepaw shakes) and in one study caused episodic utterances. 12 In contrast to the Figure 2 Two Western blotting methods using various caudate preparations and only secondary antibody. Despite the lack of serum (source of the primary antibody), bands are seen at 60 and 28 kda. Del., delipided.
5 COMMENTARY 597 aforementioned, however, two additional studies have questioned the validity of the model. For example, microinfusion of sera from patients with TS and PANDAS into the same striatal sites as in prior reports, failed to induce any significant increase in either stereotypic behaviour or episodic utterances. 14 Lastly, a double blind, collaborative effort involving three institutions, showed no differences in behaviours between infusions of TS sera with high and low ABGA titres, but non-specific increases induced by continuous infusion (Singer et al, unpublished data). CONCLUSION In conclusion, although it is currently hypothesised that an autoimmune process is the underlying pathophysiological mechanism in several movement disorders, specific disease related brain autoantigens have not been identified. Furthermore, before accepting the pathogenic relevance of a monoclonal antibody, confirmation will require determination of regional and neuronal specificity, evidence of cross reactivity with streptococcal proteins, and documentation of passive transfer of the disorder. We believe that the proposal of an autoimmune ABGA mechanism for poststreptococcal neurological disorders deserves careful study, but emphasise that the use of ABGA as diagnostic markers is currently premature. For clinicians considering making the diagnosis of PANDAS, we suggest strict adherence to the formal published criteria, 10 recognition that the diagnosis requires longitudinal assessments, realisation that a single measurement of antistreptococcal antibodies has limited value, and that treatment with prophylactic antibiotics or immunomodulatory therapies is controversial and fraught with potential serious side effects. Until further clarification is available, we suggest that therapy should continue to focus on the use of standard approaches to control symptoms. Along with the scientific community, we anxiously await the result of longitudinal case-control studies now in progress. ACKNOWLEDGEMENTS Supported in part by funding from NIH RO1 NS37706, RO1 MH61940, and RO1 NS Arch Dis Child 2004;89: doi: /adc Authors affiliations H S Singer, J J Hong, C A Rippel, C A Pardo, Department of Neurology, Johns Hopkins University School of Medicine, Jefferson Street Building 124, 600 N Wolfe Street, Baltimore, MD, USA Correspondence to: Dr H S Singer, Division of Pediatric Neurology, Johns Hopkins Hospital, Jefferson Street Building 124, 600 N Wolfe Street, Baltimore, MD , USA; hsinger@jhmi.edu REFERENCES 1 Church AJ, Dale RC, Giovannoni G. Anti-basal ganglia antibodies: a possible diagnostic utility in idiopathic movement disorders? Arch Dis Child 2004;89: Singer HS, Loiselle C. PANDAS: a commentary. J Psychosom Res 2003;55: Kurlan R. Tourette s syndrome and PANDAS : will the relation bear out? Pediatric autoimmune neuropsychiatric disorders associated with streptococcal infection. Neurology 1998;50: Kaplan EL, Gerber MA. Group A, group C, and group G beta hemolytic streptococcal infections. In: Feigin RD, Cherry JD, eds. Textbook of pediatric infectious diseases, Vol. 1. Philadelphia: W. B. Saunders, 1998: Archelos JJ, Hartung HP. Pathogenetic role of autoantibodies in neurological diseases. Trends Neurosci 2000;23: Church AJ, Cardoso F, Dale RC, et al. Anti-basal ganglia antibodies in acute and persistent Sydenham s chorea. Neurology 2002;59: Singer HS, Loiselle CR, Lee O, et al. Antibasal ganglia antibody abnormalities in Sydenham chorea. J Neuroimmunol 2003;136: Singer HS, Loiselle CR, Lee O, et al. Anti-basal ganglia antibody abnormalities in PANDAS. Mov Disord 2004;19: Swedo SE, Leonard HL, Garvey M, et al. Pediatric autoimmune neuropsychiatric disorders associated with streptococcal infections: clinical description of the first 50 cases. Am J Psychiatry 1998;155: Singer HS, Giuliano JD, Hansen BH, et al. Antibodies against human putamen in children with Tourette syndrome. Neurology 1998;50: Bornstein NM, Aronovich B, Korczyn AD, et al. Antibodies to brain antigens following stroke. Neurology 2001;56: Hallett JJ, Harling-Berg CJ, Knopf PM, et al. Antistriatal antibodies in Tourette syndrome cause neuronal dysfunction. J Neuroimmunol 2000;111: Taylor JR, Morshed SA, Parveen S, et al. An animal model of Tourette s syndrome. Am J Psychiatry 2002;159: Loiselle CR, Lee O, Moran TH, et al. Striatal microinfusion of Tourette syndrome and PANDAS sera: failure to induce behavioral changes. Mov Disord 2004;19: IMAGES IN PAEDIATRICS... A novel cause of neck stiffness A 4 year old boy was referred to hospital with suspected meningitis. There was a four day history of neck stiffness and anorexia but also of drooling and dysphonia. Examination revealed him to be significantly dehydrated but alert and afebrile. There was no stridor. Serum urea and electrolytes were consistent with hypernatraemic dehydration: sodium 161 mm/l; urea 16.9 mm/l; creatinine 74 mm/l. A lateral radiograph of the neck showed a large foreign body in the proximal oesophagus at the level of cricopharyngeus (see fig). After appropriate fluid resuscitation, the foreign body was removed under general anaesthesia revealing a significant ulceration in the posterior superior pharynx and minor oedema of the arytenoids corresponding with P and A on the figure respectively. The child s parents identified the foreign body as a bolt recently noted to be absent from its hole in a bed-head. The postoperative recovery was swift and complete. The discharge weight was almost 15% greater than the weight on presentation. This case illustrates how cricopharyngeus ( the upper oesophageal sphincter ) is one of the three sites where oesophageal foreign bodies may lodge the other two sites being where the aortic arch descends anterior to the mid oesophagus and at the level of the cardiac sphincter. The case also serves as a reminder that young children can conceal a potential life threatening condition for several days. R Gupta, C Driver, S Turner Department of Child Health, University of Aberdeen, Foresterhill, Aberdeen AB25 2ZG, UK; s.w.turner@abdn.ac.uk
Pediatric head trauma: the evidence regarding indications for emergent neuroimaging
 DOI 10.1007/s00247-008-0996-5 ALARA: BUILDING BRIDGES BETWEEN RADIOLOGY AND EMERGENCY MEDICINE Pediatric head trauma: the evidence regarding indications for emergent neuroimaging Nathan Kuppermann Received:
DOI 10.1007/s00247-008-0996-5 ALARA: BUILDING BRIDGES BETWEEN RADIOLOGY AND EMERGENCY MEDICINE Pediatric head trauma: the evidence regarding indications for emergent neuroimaging Nathan Kuppermann Received:
Use of CT in minor traumatic brain injury. Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD
 Use of CT in minor traumatic brain injury Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD No financial or other conflicts of interest Epidemiology of traumatic brain injury (TBI) Risks associated
Use of CT in minor traumatic brain injury Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD No financial or other conflicts of interest Epidemiology of traumatic brain injury (TBI) Risks associated
G illes de la Tourette s syndrome is characterised by multiple. Tourette s syndrome: a cross sectional study to examine the PANDAS hypothesis PAPER
 602 PAPER Tourette s syndrome: a cross sectional study to examine the PANDAS hypothesis A J Church, R C Dale, A J Lees, G Giovannoni, M M Robertson... See end of article for authors affiliations... Correspondence
602 PAPER Tourette s syndrome: a cross sectional study to examine the PANDAS hypothesis A J Church, R C Dale, A J Lees, G Giovannoni, M M Robertson... See end of article for authors affiliations... Correspondence
Evidence-based Evaluation of Children with Blunt Head Trauma in the Emergency Department
 Evidence-based Evaluation of Children with Blunt Head Trauma in the Emergency Department Nathan Kuppermann, MD, MPH University of California, Davis School of Medicine Departments of Emergency Medicine
Evidence-based Evaluation of Children with Blunt Head Trauma in the Emergency Department Nathan Kuppermann, MD, MPH University of California, Davis School of Medicine Departments of Emergency Medicine
Title of Study: Childhood Head Trauma: A Neuroimaging Decision Rule
 1 Proposed Protocol: Title of Study: Childhood Head Trauma: A Neuroimaging Decision Rule Principal Investigator: Nathan Kuppermann, MD, MPH Purpose: The overall objective of this study is to develop a
1 Proposed Protocol: Title of Study: Childhood Head Trauma: A Neuroimaging Decision Rule Principal Investigator: Nathan Kuppermann, MD, MPH Purpose: The overall objective of this study is to develop a
Pediatric Autoimmune Neuropsychiatric Disorders Associated with Streptococcus (PANDAS) Brittany Andry, MD PGY III Pediatric Resident LSUHSC
 Pediatric Autoimmune Neuropsychiatric Disorders Associated with Streptococcus (PANDAS) Brittany Andry, MD PGY III Pediatric Resident LSUHSC Objectives Learn the diagnostic criteria of Pediatric Autoimmune
Pediatric Autoimmune Neuropsychiatric Disorders Associated with Streptococcus (PANDAS) Brittany Andry, MD PGY III Pediatric Resident LSUHSC Objectives Learn the diagnostic criteria of Pediatric Autoimmune
A bout million patients present to UK hospitals
 420 ORIGINAL ARTICLE Application of the Canadian CT head rules in managing minor head injuries in a UK emergency department: implications for the implementation of the NICE guidelines H Y Sultan, A Boyle,
420 ORIGINAL ARTICLE Application of the Canadian CT head rules in managing minor head injuries in a UK emergency department: implications for the implementation of the NICE guidelines H Y Sultan, A Boyle,
Author Manuscript. Received Date : 27-Oct Revised Date : 09-Jan-2017 Accepted Date : 31-Jan-2017
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 Received Date : 27-Oct-2016 Revised Date : 09-Jan-2017 Accepted Date : 31-Jan-2017 Article type ABSTRACT : Original Contribution
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 Received Date : 27-Oct-2016 Revised Date : 09-Jan-2017 Accepted Date : 31-Jan-2017 Article type ABSTRACT : Original Contribution
Derivation of the children s head injury algorithm for the prediction of important clinical events decision rule for head injury in children
 885 ORIGINAL ARTICLE Derivation of the children s head injury algorithm for the prediction of important clinical events decision rule for head injury in children J Dunning, J Patrick Daly, J-P Lomas, F
885 ORIGINAL ARTICLE Derivation of the children s head injury algorithm for the prediction of important clinical events decision rule for head injury in children J Dunning, J Patrick Daly, J-P Lomas, F
Can we abolish skull x-rays for head injury?
 ADC Online First, published on April 25, 2005 as 10.1136/adc.2004.053603 Can we abolish skull x-rays for head injury? Matthew J Reed, Jen G Browning, A. Graham Wilkinson & Tom Beattie Corresponding author:
ADC Online First, published on April 25, 2005 as 10.1136/adc.2004.053603 Can we abolish skull x-rays for head injury? Matthew J Reed, Jen G Browning, A. Graham Wilkinson & Tom Beattie Corresponding author:
정서적불안정을동반한 PANDAS 1 예
 KISEP Case Report J Korean Neuropsychiatr Assoc Vol 43, No 3 1 예 전남대학교병원정신과 양종철 A Case of PANDAS with Emotional Lability Jong-Chul Yang, MD, PhD Department of Psychiatry, Cheonnam National University Hospital,
KISEP Case Report J Korean Neuropsychiatr Assoc Vol 43, No 3 1 예 전남대학교병원정신과 양종철 A Case of PANDAS with Emotional Lability Jong-Chul Yang, MD, PhD Department of Psychiatry, Cheonnam National University Hospital,
Complicações neurológicas pós infecção por estreptococos (mitos e verdades) Silvia Tenembaum
 Complicações neurológicas pós infecção por estreptococos (mitos e verdades) Silvia Tenembaum Proposed pathophysiology of immune-mediated disorders Infection Tumor other Genetic predisposition 1. Molecular
Complicações neurológicas pós infecção por estreptococos (mitos e verdades) Silvia Tenembaum Proposed pathophysiology of immune-mediated disorders Infection Tumor other Genetic predisposition 1. Molecular
Management of Severe Traumatic Brain Injury
 Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
LOSS OF CONSCIOUSNESS & ASSESSMENT. Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT
 LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
O ne million patients are treated annually in United
 859 ORIGIAL ARTICLE Can we abolish skull x rays for head injury? M J Reed, J G Browning, A G Wilkinson, T Beattie... See end of article for authors affiliations... Correspondence to: Matthew J Reed, Accident
859 ORIGIAL ARTICLE Can we abolish skull x rays for head injury? M J Reed, J G Browning, A G Wilkinson, T Beattie... See end of article for authors affiliations... Correspondence to: Matthew J Reed, Accident
recommendations of the Royal College of
 Archives of Emergency Medicine, 1993, 10, 138-144 Skull X-ray after head injury: the recommendations of the Royal College of Surgeons Working Party Report in practice R. E. MACLAREN, H. I. GHOORAHOO &
Archives of Emergency Medicine, 1993, 10, 138-144 Skull X-ray after head injury: the recommendations of the Royal College of Surgeons Working Party Report in practice R. E. MACLAREN, H. I. GHOORAHOO &
Childhood Post-infectious Autoimmune Encephalitis. PANDA problems. Michael Daines, M.D. Pediatric Allergy-Immunology
 Childhood Post-infectious Autoimmune Encephalitis PANDA problems Michael Daines, M.D. Pediatric Allergy-Immunology Terms PANDAS Pediatric Autoimmune Neuropsychiatric Disorders Associated with Strep PANS
Childhood Post-infectious Autoimmune Encephalitis PANDA problems Michael Daines, M.D. Pediatric Allergy-Immunology Terms PANDAS Pediatric Autoimmune Neuropsychiatric Disorders Associated with Strep PANS
2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY
 Measure #416: Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 2 through 17 Years - National Quality Strategy Domain: Efficiency and Cost Reduction
Measure #416: Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 2 through 17 Years - National Quality Strategy Domain: Efficiency and Cost Reduction
P A N D A S. What is. Fact or Fiction PANDAS: Michael E. Pichichero, MD. Rochester General Hospital. Rochester, New York. Research Institute
 PANDAS: Fact or Fiction Michael E. Pichichero, MD Director Rochester General Hospital Research Institute and Legacy Pediatrics Rochester, New York What is P A N D A S Swedo SE. Am J Psychiatry. 1998;155:264-271.
PANDAS: Fact or Fiction Michael E. Pichichero, MD Director Rochester General Hospital Research Institute and Legacy Pediatrics Rochester, New York What is P A N D A S Swedo SE. Am J Psychiatry. 1998;155:264-271.
Avoidable Imaging Learning Collaborative: 2008 Mild Traumatic Brain Injury Clinical Policy Success Story BWH Head and PE CTs with Clinical Decision
 Avoidable Imaging Learning Collaborative: 2008 Mild Traumatic Brain Injury Clinical Policy Success Story BWH Head and PE CTs with Clinical Decision Support Using the Canadian CT Head Rule to Reduce Unnecessary
Avoidable Imaging Learning Collaborative: 2008 Mild Traumatic Brain Injury Clinical Policy Success Story BWH Head and PE CTs with Clinical Decision Support Using the Canadian CT Head Rule to Reduce Unnecessary
Head trauma is a common chief complaint among children visiting
 Discussions in Surgery Validation of the Sainte-Justine Head Trauma Pathway for children younger than two years of age Sarah Spénard Serge Gouin, MDCM Marianne Beaudin, MD Jocelyn Gravel, MD, MSc Partial
Discussions in Surgery Validation of the Sainte-Justine Head Trauma Pathway for children younger than two years of age Sarah Spénard Serge Gouin, MDCM Marianne Beaudin, MD Jocelyn Gravel, MD, MSc Partial
2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Efficiency
 Measure #416: Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 2 Through 17 Years - National Quality Strategy Domain: Efficiency and Cost Reduction
Measure #416: Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 2 Through 17 Years - National Quality Strategy Domain: Efficiency and Cost Reduction
Annually in the United States, 1 million patients will require
 ORIGINAL RESEARCH SPINE Screening Cervical Spine CT in the Emergency Department, Phase 2: A Prospective Assessment of Use B. Griffith, M. Kelly, P. Vallee, M. Slezak, J. Nagarwala, S. Krupp, C.P. Loeckner,
ORIGINAL RESEARCH SPINE Screening Cervical Spine CT in the Emergency Department, Phase 2: A Prospective Assessment of Use B. Griffith, M. Kelly, P. Vallee, M. Slezak, J. Nagarwala, S. Krupp, C.P. Loeckner,
Lumbar puncture. Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: ml Replenished: 4-6 h Routine LP (3-5 ml): <1h
 Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
Each year more than children are seen in hospital
 CMAJ Research CATCH: a clinical decision rule for the use of computed tomography in children with minor head injury Martin H. Osmond MD CM, Terry P. Klassen MD, George A. Wells PhD, Rhonda Correll RN,
CMAJ Research CATCH: a clinical decision rule for the use of computed tomography in children with minor head injury Martin H. Osmond MD CM, Terry P. Klassen MD, George A. Wells PhD, Rhonda Correll RN,
Critical care resources are often provided to the too well and as well as. to the too sick. The former include the patients admitted to an ICU
 Literature Review Critical care resources are often provided to the too well and as well as to the too sick. The former include the patients admitted to an ICU following major elective surgery for overnight
Literature Review Critical care resources are often provided to the too well and as well as to the too sick. The former include the patients admitted to an ICU following major elective surgery for overnight
Original Article. Emergency Department Evaluation of Ventricular Shunt Malfunction. Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH
 Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Measuring Overuse and Underuse of Brain CTs in Pediatric Patients with mtbi in Two Canadian Emergency Departments
 Measuring Overuse and Underuse of Brain CTs in Pediatric Patients with mtbi in Two Canadian Emergency Departments Martin Gariépy, PhD Dr Patrick Archambault Dr Jocelyn Gravel 2017 Quebec City, Quebec,
Measuring Overuse and Underuse of Brain CTs in Pediatric Patients with mtbi in Two Canadian Emergency Departments Martin Gariépy, PhD Dr Patrick Archambault Dr Jocelyn Gravel 2017 Quebec City, Quebec,
Reviewing the recent literature to answer clinical questions: Should I change my practice?
 Reviewing the recent literature to answer clinical questions: Should I change my practice? JILL MILLER, MD PEM ATTENDING CHKD ASSISTANT PROFESSOR PEDIATRICS, EVMS Objectives Review the literature to answer
Reviewing the recent literature to answer clinical questions: Should I change my practice? JILL MILLER, MD PEM ATTENDING CHKD ASSISTANT PROFESSOR PEDIATRICS, EVMS Objectives Review the literature to answer
Disclosure Statement. Dr. Kadish has no relevant financial relationships with any commercial interests mentioned in this talk.
 Disclosure Statement Dr. Kadish has no relevant financial relationships with any commercial interests mentioned in this talk. Head Trauma Evaluation Primary and secondary injury Disposition Sports related
Disclosure Statement Dr. Kadish has no relevant financial relationships with any commercial interests mentioned in this talk. Head Trauma Evaluation Primary and secondary injury Disposition Sports related
Pre-hospital Response to Trauma and Brain Injury. Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center
 Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Kristin s Head Trauma Board Questions 11/07/14
 Kristin s Head Trauma Board Questions { 11/07/14 A healthy 15 y/o boy was playing football at a park near his home with a group of friends when he tripped over a friend s leg while trying to catch a pass.
Kristin s Head Trauma Board Questions { 11/07/14 A healthy 15 y/o boy was playing football at a park near his home with a group of friends when he tripped over a friend s leg while trying to catch a pass.
DIAGNOSTIC PROCEDURES IN MILD TRAUMATIC BRAIN INJURY: RESULTS OF THE WHO COLLABORATING CENTRE TASK FORCE ON MILD TRAUMATIC BRAIN INJURY
 J Rehabil Med 2004; Suppl. 43: 61 75 DIAGNOSTIC PROCEDURES IN MILD TRAUMATIC BRAIN INJURY: RESULTS OF THE WHO COLLABORATING CENTRE TASK FORCE ON MILD TRAUMATIC BRAIN INJURY Jörgen Borg, 1 Lena Holm, 2
J Rehabil Med 2004; Suppl. 43: 61 75 DIAGNOSTIC PROCEDURES IN MILD TRAUMATIC BRAIN INJURY: RESULTS OF THE WHO COLLABORATING CENTRE TASK FORCE ON MILD TRAUMATIC BRAIN INJURY Jörgen Borg, 1 Lena Holm, 2
PANS-PANDAS An Update on Research and Clinical Management
 PANS-PANDAS An Update on Research and Clinical Management Kyle Williams, MD PhD Director, Pediatric Neuropsychiatry and Immunology Program Massachusetts General Hospital Clinical Case-PANDAS 10 y.o. male
PANS-PANDAS An Update on Research and Clinical Management Kyle Williams, MD PhD Director, Pediatric Neuropsychiatry and Immunology Program Massachusetts General Hospital Clinical Case-PANDAS 10 y.o. male
USE OF CT SCAN IN A CHILD WITH MTBI
 TO SCAN OR NOT TO SCAN USE OF CT SCAN IN A CHILD WITH MTBI LISA AYOUB-RODRIGUEZ MD PEDIATRIC HOSPITALIST MIKE LEE MD PEDIATRIC RESIDENT BERT JOHANSSON MD PEDIATRIC HOSPITALIST DISCLOSURES I M NOT A SURGEON
TO SCAN OR NOT TO SCAN USE OF CT SCAN IN A CHILD WITH MTBI LISA AYOUB-RODRIGUEZ MD PEDIATRIC HOSPITALIST MIKE LEE MD PEDIATRIC RESIDENT BERT JOHANSSON MD PEDIATRIC HOSPITALIST DISCLOSURES I M NOT A SURGEON
Pediatric Imaging Spine MRI and Spine CT Test Request Tip Sheet
 Pediatric Imaging Spine MRI and Spine CT MRI is almost always preferred over CT scan; if ordering CT, CLEARLY document why MRI is not appropriate. In cases of ongoing back pain, six weeks of conservative
Pediatric Imaging Spine MRI and Spine CT MRI is almost always preferred over CT scan; if ordering CT, CLEARLY document why MRI is not appropriate. In cases of ongoing back pain, six weeks of conservative
Imaging Biomarkers Significance S100B NSE. Admitted within 6 hours of injury and CT scan occurred after initial examination. N = 1,064 CT+ N = 50 4.
 Concussion Guidelines Step 1: Systematic Review of Prevalent Indicators Supplemental Content 7 Evidence Table. Included Studies For Key Question 4 Imaging and Biomarker Publications Medium Potential for
Concussion Guidelines Step 1: Systematic Review of Prevalent Indicators Supplemental Content 7 Evidence Table. Included Studies For Key Question 4 Imaging and Biomarker Publications Medium Potential for
Pediatric Imaging Spine MRI and Spine CT Test Request Tip Sheet
 Pediatric Imaging Spine MRI and Spine CT MRI is almost always preferred over CT scan; if ordering CT, CLEARLY document why MRI is not appropriate. In cases of back pain without red flags, six weeks of
Pediatric Imaging Spine MRI and Spine CT MRI is almost always preferred over CT scan; if ordering CT, CLEARLY document why MRI is not appropriate. In cases of back pain without red flags, six weeks of
A ccurate prediction of outcome in the acute and
 401 PAPER Predicting functional outcome in acute stroke: comparison of a simple six variable model with other predictive systems and informal clinical prediction C Counsell, M Dennis, M McDowall... See
401 PAPER Predicting functional outcome in acute stroke: comparison of a simple six variable model with other predictive systems and informal clinical prediction C Counsell, M Dennis, M McDowall... See
CLINICAL INVESTIGATIONS
 ACADEMIC EMERGENCY MEDICINE July 2000, Volume 7, Number 7 739 CLINICAL INVESTIGATIONS Variation in Utilization of Computed Tomography Scanning for the Investigation of Minor Head Trauma in Children: A
ACADEMIC EMERGENCY MEDICINE July 2000, Volume 7, Number 7 739 CLINICAL INVESTIGATIONS Variation in Utilization of Computed Tomography Scanning for the Investigation of Minor Head Trauma in Children: A
I would like to do today is to trace the evolution of PANDAS and all the iterations that have gone
 BASIL J. ZITELLI, MD 1 This is a difficult and controversial topic to present. Instead of true false, I ve fact, fiction or in between and we ll be talking about the alphabet soup as well. I don t have
BASIL J. ZITELLI, MD 1 This is a difficult and controversial topic to present. Instead of true false, I ve fact, fiction or in between and we ll be talking about the alphabet soup as well. I don t have
PANDAS: A Model for Autoimmune Neuropsychiatric Disorders.
 Page 1 of 11 PANDAS: A Model for Autoimmune Neuropsychiatric Disorders. Susan E. Swedo, MD, and Paul J. Grant, MD Primary Psychiatry. 2004;11(4):28-33 Faculty Affiliations and Disclosures Dr. Swedo is
Page 1 of 11 PANDAS: A Model for Autoimmune Neuropsychiatric Disorders. Susan E. Swedo, MD, and Paul J. Grant, MD Primary Psychiatry. 2004;11(4):28-33 Faculty Affiliations and Disclosures Dr. Swedo is
The AHEAD Study: Managing anticoagulatedpatients who suffer head injury
 AHEAD Study The AHEAD Study: Managing anticoagulatedpatients who suffer head injury Suzanne Mason 1,2, Maxine Kuczawski 1, Matthew Stevenson 1, Dawn Teare 1, Michael Holmes 1, ShammiRamlakhan 1, Steve
AHEAD Study The AHEAD Study: Managing anticoagulatedpatients who suffer head injury Suzanne Mason 1,2, Maxine Kuczawski 1, Matthew Stevenson 1, Dawn Teare 1, Michael Holmes 1, ShammiRamlakhan 1, Steve
8/29/2011. Brain Injury Incidence: 200/100,000. Prehospital Brain Injury Mortality Incidence: 20/100,000
 Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
The Yield of Head CT in Syncope: A Pilot Study
 The Yield of Head CT in Syncope: A Pilot Study The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Published Version Accessed
The Yield of Head CT in Syncope: A Pilot Study The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Published Version Accessed
Neuroimaging for Pediatric Head Trauma: Do Patient and Hospital Characteristics Influence Who Gets Imaged?
 Neuroimaging for Pediatric Head Trauma: Do Patient and Hospital Characteristics Influence Who Gets Imaged? The Harvard community has made this article openly available. Please share how this access benefits
Neuroimaging for Pediatric Head Trauma: Do Patient and Hospital Characteristics Influence Who Gets Imaged? The Harvard community has made this article openly available. Please share how this access benefits
Canadian C-spine Rule and the National Emergency X-Radiography Utilization Low-Risk Criteria for C-spine radiography in young trauma patients
 Journal of Pediatric Surgery (2009) 44, 987 991 www.elsevier.com/locate/jpedsurg Canadian C-spine Rule and the National Emergency X-Radiography Utilization Low-Risk Criteria for C-spine radiography in
Journal of Pediatric Surgery (2009) 44, 987 991 www.elsevier.com/locate/jpedsurg Canadian C-spine Rule and the National Emergency X-Radiography Utilization Low-Risk Criteria for C-spine radiography in
emeasure Title Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 18 Years and Older
 emeasure Title Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 18 Years and Older emeasure Identifier (Measure Authoring Tool) NQF Number Measurement
emeasure Title Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 18 Years and Older emeasure Identifier (Measure Authoring Tool) NQF Number Measurement
INFLAMMATION AND AUTOIMMUNITY IN PEDIATRIC ANXIETY AND MOVEMENT DISORDERS
 INFLAMMATION AND AUTOIMMUNITY IN PEDIATRIC ANXIETY AND MOVEMENT DISORDERS Kyle Williams, MD, PhD Director, Pediatric Neuropsychiatry and Immunology Program Massachusetts General Hospital For Children DISCLOSURES
INFLAMMATION AND AUTOIMMUNITY IN PEDIATRIC ANXIETY AND MOVEMENT DISORDERS Kyle Williams, MD, PhD Director, Pediatric Neuropsychiatry and Immunology Program Massachusetts General Hospital For Children DISCLOSURES
Neurosurgery (Orthopaedic PGY-1) Goals. Objectives
 Neurosurgery (Orthopaedic PGY-1) Length: 1 month of PGY-1 (Orthopaedic Designated Residents) or 1 month of PGY-2, -3, or -4 year Location: The Queen's Medical Center Primary Supervisor: William Obana,
Neurosurgery (Orthopaedic PGY-1) Length: 1 month of PGY-1 (Orthopaedic Designated Residents) or 1 month of PGY-2, -3, or -4 year Location: The Queen's Medical Center Primary Supervisor: William Obana,
The Use of Bedside Ultrasound in the Detection of Skull Fractures in Pediatric Patients
 Pacific University CommonKnowledge School of Physician Assistant Studies Theses, Dissertations and Capstone Projects Summer 8-8-2015 The Use of Bedside Ultrasound in the Detection of Skull Fractures in
Pacific University CommonKnowledge School of Physician Assistant Studies Theses, Dissertations and Capstone Projects Summer 8-8-2015 The Use of Bedside Ultrasound in the Detection of Skull Fractures in
Infection-Associated Neurological Syndromes
 Infection-Associated Neurological Syndromes Anand P, MD PhD Medical Director, BloodCenter of Wisconsin Assistant Professor, Medical College of Wisconsin ASFA Annual Meeting San Antonio, TX, May 8th, 2015
Infection-Associated Neurological Syndromes Anand P, MD PhD Medical Director, BloodCenter of Wisconsin Assistant Professor, Medical College of Wisconsin ASFA Annual Meeting San Antonio, TX, May 8th, 2015
HEPARIN-INDUCED THROMBOCYTOPENIA (HIT)
 HEPARIN-INDUCED THROMBOCYTOPENIA (HIT) OBJECTIVE: To assist clinicians with the investigation and management of suspected and documented heparin-induced thrombocytopenia (HIT). BACKGROUND: HIT is a transient,
HEPARIN-INDUCED THROMBOCYTOPENIA (HIT) OBJECTIVE: To assist clinicians with the investigation and management of suspected and documented heparin-induced thrombocytopenia (HIT). BACKGROUND: HIT is a transient,
Centers for Disease Control and Prevention Guideline on the Diagnosis and Management of Mild Traumatic Brain Injury Among Children September 2018
 Centers for Disease Control and Prevention Guideline on the Diagnosis and Management of Mild Traumatic Brain Injury Among Children September 2018 Nothing to Disclose CDC Guidelines- Objective Question-
Centers for Disease Control and Prevention Guideline on the Diagnosis and Management of Mild Traumatic Brain Injury Among Children September 2018 Nothing to Disclose CDC Guidelines- Objective Question-
Kyle Williams, MD, PhD Director, Pediatric Neuropsychiatry and Immunology Program Massachusetts General Hospital For Children
 Pediatric Autoimmune Neuropsychiatric Disorder Associated with Streptococcal infections (PANDAS): An Inflammatory Hypothesis for Pediatric Obsessive Compulsive Disorder Kyle Williams, MD, PhD Director,
Pediatric Autoimmune Neuropsychiatric Disorder Associated with Streptococcal infections (PANDAS): An Inflammatory Hypothesis for Pediatric Obsessive Compulsive Disorder Kyle Williams, MD, PhD Director,
The risk of a bleed after delayed head injury presentation to the ED: systematic review protocol. Correspondence to:
 The risk of a bleed after delayed head injury presentation to the ED: systematic review protocol. Carl Marincowitz, Christopher M. Smith, William Townend Emergency Department, Hull Royal, Hull, UK Correspondence
The risk of a bleed after delayed head injury presentation to the ED: systematic review protocol. Carl Marincowitz, Christopher M. Smith, William Townend Emergency Department, Hull Royal, Hull, UK Correspondence
Adherence to Head Computed Tomography Guidelines for Mild Traumatic Brain Injury
 Original Research Adherence to Head Computed Tomography Guidelines for Mild Traumatic Brain Injury Landon A. Jones, MD* Eric J. Morley, MD, MS William D. Grant, EdD* Susan M. Wojcik, PhD* William F. Paolo,
Original Research Adherence to Head Computed Tomography Guidelines for Mild Traumatic Brain Injury Landon A. Jones, MD* Eric J. Morley, MD, MS William D. Grant, EdD* Susan M. Wojcik, PhD* William F. Paolo,
WP01 Longitudinal Onset and Course Cohort Studies (Leader: UCL / A. Schrag): Objectives
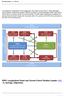 To facilitate the organisation and management, the project is structured in Work packages which together comprise the project. EMTICS consists of 12 work packages (WPs). Each WP is carried out by a varying
To facilitate the organisation and management, the project is structured in Work packages which together comprise the project. EMTICS consists of 12 work packages (WPs). Each WP is carried out by a varying
UTILIZATION MANAGEMENT POLICY AND PROCEDURE MANUAL
 University of Florida, Pediatric Integrated Care System UTILIZATION MANAGEMENT POLICY AND PROCEDURE MANUAL Policy: Program(s): Approval Criteria for Neuroimaging of Headaches Title XIX and Title XXI Effective
University of Florida, Pediatric Integrated Care System UTILIZATION MANAGEMENT POLICY AND PROCEDURE MANUAL Policy: Program(s): Approval Criteria for Neuroimaging of Headaches Title XIX and Title XXI Effective
Episode 66 Backboard and Collar Nightmares from EMU Conference. The Risks Associated with Backboard & Collar
 However, backboards and collars are not without risk: Episode 66 Backboard and Collar Nightmares from EMU Conference With Dr. Kylie Bosman Prepared by Dr., edited by Dr. Kylie Bosman & Anton Helman, May
However, backboards and collars are not without risk: Episode 66 Backboard and Collar Nightmares from EMU Conference With Dr. Kylie Bosman Prepared by Dr., edited by Dr. Kylie Bosman & Anton Helman, May
How can the clinical manifestations of autism shed light on environmental etiologies?
 How can the clinical manifestations of autism shed light on environmental etiologies? Susan E. Swedo, M.D. Pediatric & Developmental Neuropsychiatry Branch National Institute of Mental Health Department
How can the clinical manifestations of autism shed light on environmental etiologies? Susan E. Swedo, M.D. Pediatric & Developmental Neuropsychiatry Branch National Institute of Mental Health Department
Child Neurology Elective PL1 Rotation
 PL1 Rotation The neurology elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
PL1 Rotation The neurology elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
Instructional Course #34. Review of Neuropharmacology in Pediatric Brain Injury. John Pelegano MD Jilda Vargus-Adams MD, MSc Micah Baird MD
 Instructional Course #34 Review of Neuropharmacology in Pediatric Brain Injury John Pelegano MD Jilda Vargus-Adams MD, MSc Micah Baird MD Outline of Course 1. Introduction John Pelegano MD 2. Neuropharmocologic
Instructional Course #34 Review of Neuropharmacology in Pediatric Brain Injury John Pelegano MD Jilda Vargus-Adams MD, MSc Micah Baird MD Outline of Course 1. Introduction John Pelegano MD 2. Neuropharmocologic
The Abdominal plain film: A justified 21st century imaging investigation?
 The Abdominal plain film: A justified 21st century imaging investigation? Poster No.: C-0877 Congress: ECR 2012 Type: Authors: Keywords: DOI: Scientific Exhibit Z. J. Hussain 1, H. F. D'Costa 2 ; 1 Oxford/UK,
The Abdominal plain film: A justified 21st century imaging investigation? Poster No.: C-0877 Congress: ECR 2012 Type: Authors: Keywords: DOI: Scientific Exhibit Z. J. Hussain 1, H. F. D'Costa 2 ; 1 Oxford/UK,
Head injury in children
 Head injury in children Michael Kim, MD Department of Emergency Medicine University of Wisconsin- Madison #1 cause of death and disability Bimodal distribution 62,000 hospitalization 564,000 ED visits
Head injury in children Michael Kim, MD Department of Emergency Medicine University of Wisconsin- Madison #1 cause of death and disability Bimodal distribution 62,000 hospitalization 564,000 ED visits
Canadian CT head rule and New Orleans Criteria in mild traumatic brain injury: comparison at a tertiary referral hospital in Japan
 DOI 10.1186/s40064-016-1781-9 RESEARCH Open Access Canadian CT head rule and New Orleans Criteria in mild traumatic brain injury: comparison at a tertiary referral hospital in Japan Daddy Mata Mbemba 1,2,
DOI 10.1186/s40064-016-1781-9 RESEARCH Open Access Canadian CT head rule and New Orleans Criteria in mild traumatic brain injury: comparison at a tertiary referral hospital in Japan Daddy Mata Mbemba 1,2,
RESEARCH ARTICLE IS LUMBAR PUNCTURE ALWAYS NECESSARY IN THE FEBRILE CHILD WITH CONVULSION?
 RESEARCH ARTICLE IS LUMBAR PUNCTURE ALWAYS NECESSARY IN THE FEBRILE CHILD WITH CONVULSION? MR. Salehi Omrani MD¹, MR. Edraki MD 2, M. Alizadeh MD 3 Abstract: Objective Febrile convulsion is the most common
RESEARCH ARTICLE IS LUMBAR PUNCTURE ALWAYS NECESSARY IN THE FEBRILE CHILD WITH CONVULSION? MR. Salehi Omrani MD¹, MR. Edraki MD 2, M. Alizadeh MD 3 Abstract: Objective Febrile convulsion is the most common
Research Article Analysis of Repeated CT Scan Need in Blunt Head Trauma
 Hindawi Publishing Corporation Emergency Medicine International Volume 2013, Article ID 916253, 5 pages http://dx.doi.org/10.1155/2013/916253 Research Article Analysis of Repeated CT Scan Need in Blunt
Hindawi Publishing Corporation Emergency Medicine International Volume 2013, Article ID 916253, 5 pages http://dx.doi.org/10.1155/2013/916253 Research Article Analysis of Repeated CT Scan Need in Blunt
CERVICAL SPINE CLEARANCE
 DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
CEWT (Children s Epilepsy Workstream in Trent) Guidelines process.
 ttingham Children s Hospital ttingham University Hospitals Seizure with Fever Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author)
ttingham Children s Hospital ttingham University Hospitals Seizure with Fever Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author)
Clarifying Murky Waters: Head Injuries in Children
 Clarifying Murky Waters: Head Injuries in Children Judith R. Klein, MD, FACEP Assistant Professor of Emergency Medicine UCSF-SFGH Emergency Services 1 Case #1: Newborn Leo 2 month old dropped 4 feet onto
Clarifying Murky Waters: Head Injuries in Children Judith R. Klein, MD, FACEP Assistant Professor of Emergency Medicine UCSF-SFGH Emergency Services 1 Case #1: Newborn Leo 2 month old dropped 4 feet onto
Head injuries. Severity of head injuries
 Head injuries ED Teaching day 23 rd October Severity of head injuries Minor GCS 14-15 Must not have any of the following: Amnesia 10min Neurological sign or symptom Skull fracture (clinically or radiologically)
Head injuries ED Teaching day 23 rd October Severity of head injuries Minor GCS 14-15 Must not have any of the following: Amnesia 10min Neurological sign or symptom Skull fracture (clinically or radiologically)
Analysis of pediatric head injury from falls
 Neurosurg Focus 8 (1):Article 3, 2000 Analysis of pediatric head injury from falls K. ANTHONY KIM, MICHAEL Y. WANG, M.D., PAMELA M. GRIFFITH, R.N.C., SUSAN SUMMERS, R.N., AND MICHAEL L. LEVY, M.D. Division
Neurosurg Focus 8 (1):Article 3, 2000 Analysis of pediatric head injury from falls K. ANTHONY KIM, MICHAEL Y. WANG, M.D., PAMELA M. GRIFFITH, R.N.C., SUSAN SUMMERS, R.N., AND MICHAEL L. LEVY, M.D. Division
:: Closed Head Injury in Adults
 ADULT TRAUMA CLINICAL PRACTICE GUIDELINES Initial Management of :: Closed Head Injury in Adults Suggested citation: Dr Duncan Reed 2007, Adult Trauma Clinical Practice Guidelines, Initial Management of
ADULT TRAUMA CLINICAL PRACTICE GUIDELINES Initial Management of :: Closed Head Injury in Adults Suggested citation: Dr Duncan Reed 2007, Adult Trauma Clinical Practice Guidelines, Initial Management of
Spine MRI and Spine CT Test Request Tip Sheet
 Spine MRI and Spine CT With/Without Contrast CT, MRI The study considered best for a specific clinical scenario should be ordered. The second study should be done ONLY if the first study does not provide
Spine MRI and Spine CT With/Without Contrast CT, MRI The study considered best for a specific clinical scenario should be ordered. The second study should be done ONLY if the first study does not provide
Update sulle lesioni emorragiche posttraumatiche
 Update sulle lesioni emorragiche posttraumatiche Corrado Iaccarino Neurochirurgia-Neurotraumatologia AOU Parma Neurochirurgia d'urgenza IRCCS ASMN Reggio Emilia LAW UPDATING This document provides recommendations
Update sulle lesioni emorragiche posttraumatiche Corrado Iaccarino Neurochirurgia-Neurotraumatologia AOU Parma Neurochirurgia d'urgenza IRCCS ASMN Reggio Emilia LAW UPDATING This document provides recommendations
Debra Pennington, MD Director of Imaging Dell Children s Medical Center
 Debra Pennington, MD Director of Imaging Dell Children s Medical Center 1 Gray (Gy) is 1 J of radiation energy/ 1 kg matter (physical quantity absorbed dose) Diagnostic imaging doses in mgy (.001 Gy)
Debra Pennington, MD Director of Imaging Dell Children s Medical Center 1 Gray (Gy) is 1 J of radiation energy/ 1 kg matter (physical quantity absorbed dose) Diagnostic imaging doses in mgy (.001 Gy)
Learning Objectives 1. TBI Severity & Evaluation Tools. Clinical Diagnosis of TBI. Learning Objectives 2 3/3/2015. Define TBI severity using GCS
 Learning Objectives 1 TBI Severity & Evaluation Tools Define TBI severity using GCS and PTA Describe functional prognosis after moderate to severe TBI using trends and threshold values Jennifer M Zumsteg,
Learning Objectives 1 TBI Severity & Evaluation Tools Define TBI severity using GCS and PTA Describe functional prognosis after moderate to severe TBI using trends and threshold values Jennifer M Zumsteg,
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Efficiency
 Quality ID #419: Overuse Of Neuroimaging For Patients With Primary Headache And A Normal Neurological Examination National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL
Quality ID #419: Overuse Of Neuroimaging For Patients With Primary Headache And A Normal Neurological Examination National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL
SUDANESE JOURNAL OF PAEDIATRICS 2014; Vol 14, Issue No. 1
 Education and Practice Case Report and Literature Review Managing traumatic brain injury in children: When do we need a computed tomography of the head? Mohammed A Kambal (1), Manal E Abou (2), Iman Al
Education and Practice Case Report and Literature Review Managing traumatic brain injury in children: When do we need a computed tomography of the head? Mohammed A Kambal (1), Manal E Abou (2), Iman Al
KEVIN J. BIANCHINI, PH.D., ABPN
 KEVIN J. BIANCHINI, PH.D., ABPN Slick et al., 1999 Bianchini et al., 2005 4 4 Criterion A: Evidence of significant external incentive Criterion B: Evidence from physical evaluation 1. Probable effort
KEVIN J. BIANCHINI, PH.D., ABPN Slick et al., 1999 Bianchini et al., 2005 4 4 Criterion A: Evidence of significant external incentive Criterion B: Evidence from physical evaluation 1. Probable effort
Epilepsy after two different neurosurgical approaches
 Journal ofneurology, Neurosurgery, and Psychiatry, 1976, 39, 1052-1056 Epilepsy after two different neurosurgical approaches to the treatment of ruptured intracranial aneurysm R. J. CABRAL, T. T. KING,
Journal ofneurology, Neurosurgery, and Psychiatry, 1976, 39, 1052-1056 Epilepsy after two different neurosurgical approaches to the treatment of ruptured intracranial aneurysm R. J. CABRAL, T. T. KING,
Andrzej Żyluk 1, Agnieszka Mazur 1, Bernard Piotuch 1, Krzysztof Safranow 2
 POLSKI PRZEGLĄD CHIRURGICZNY 2013, 85, 12, 699 705 10.2478/pjs-2013-0107 Analysis of the reliability of clinical examination in predicting traumatic cerebral lesions and skull fractures in patients with
POLSKI PRZEGLĄD CHIRURGICZNY 2013, 85, 12, 699 705 10.2478/pjs-2013-0107 Analysis of the reliability of clinical examination in predicting traumatic cerebral lesions and skull fractures in patients with
Concussions. Recognition, Management, and Care
 Concussions Recognition, Management, and Care Sports Concussion: Complex, pathophysiological process affecting the brain, induced by traumatic bio-mechanical forces. 1 1.6-3.8 million concussions occur
Concussions Recognition, Management, and Care Sports Concussion: Complex, pathophysiological process affecting the brain, induced by traumatic bio-mechanical forces. 1 1.6-3.8 million concussions occur
The research questions are presented in priority order, and are further elaborated with lay summaries and three-part questions where applicable.
 Top 30 Emergency Medicine Research Priorities 23 January 2017 The rankings were established by consensus at the final prioritisation workshop run by the James Lind Alliance Emergency Medicine Priority
Top 30 Emergency Medicine Research Priorities 23 January 2017 The rankings were established by consensus at the final prioritisation workshop run by the James Lind Alliance Emergency Medicine Priority
Redgrave JN, Coutts SB, Schulz UG et al. Systematic review of associations between the presence of acute ischemic lesions on
 6. Imaging in TIA 6.1 What type of brain imaging should be used in suspected TIA? 6.2 Which patients with suspected TIA should be referred for urgent brain imaging? Evidence Tables IMAG1: After TIA/minor
6. Imaging in TIA 6.1 What type of brain imaging should be used in suspected TIA? 6.2 Which patients with suspected TIA should be referred for urgent brain imaging? Evidence Tables IMAG1: After TIA/minor
Just Clear Them The Approach to Medical Clearance
 Just Clear Them The Approach to Medical Clearance Dr. Nalin Ahluwalia MD CCFP(EM) Associate Chief of Staff Emergency Physician Oakville Trafalgar Memorial Hospital My Disclosures None! Exemplary patient
Just Clear Them The Approach to Medical Clearance Dr. Nalin Ahluwalia MD CCFP(EM) Associate Chief of Staff Emergency Physician Oakville Trafalgar Memorial Hospital My Disclosures None! Exemplary patient
Spine MRI and Spine CT Test Request Tip Sheet
 Spine MRI and Spine CT With/Without Contrast CT, MRI The study considered best for a specific clinical scenario should be ordered. The second study should be done ONLY if the first study does not provide
Spine MRI and Spine CT With/Without Contrast CT, MRI The study considered best for a specific clinical scenario should be ordered. The second study should be done ONLY if the first study does not provide
Clinical Decision Rules to Rule Out Subarachnoid Hemorrhage for Acute Headache FREE
 Clinical Decision Rules to Rule Out Subarachnoid Hemorrhage for Acute Headache FREE Jeffrey J. Perry, MD, MSc1; Ian G. Stiell, MD, MSc1; Marco L. A. Sivilotti, MD, MSc5,6; Michael J. Bullard, MD11; Corinne
Clinical Decision Rules to Rule Out Subarachnoid Hemorrhage for Acute Headache FREE Jeffrey J. Perry, MD, MSc1; Ian G. Stiell, MD, MSc1; Marco L. A. Sivilotti, MD, MSc5,6; Michael J. Bullard, MD11; Corinne
Algorithms for managing the common trauma patient
 ALGORITHMS Algorithms for managing the common trauma patient J John, MB ChB Department of Urology, Frere Hospital, East London Hospital Complex, East London, South Africa Corresponding author: J John (jeffveenajohn@gmail.com)
ALGORITHMS Algorithms for managing the common trauma patient J John, MB ChB Department of Urology, Frere Hospital, East London Hospital Complex, East London, South Africa Corresponding author: J John (jeffveenajohn@gmail.com)
Spine MRI and Spine CT Test Request Tip Sheet
 Spine MRI and Spine CT With/Without Contrast CT, MRI Studies should NOT be ordered simultaneously as dual studies (i.e., with and without contrast). Radiation exposure is doubled and both views are rarely
Spine MRI and Spine CT With/Without Contrast CT, MRI Studies should NOT be ordered simultaneously as dual studies (i.e., with and without contrast). Radiation exposure is doubled and both views are rarely
Specific Issues in Pediatric OCD: Treatment and Adulthood Outcome
 Specific Issues in Pediatric OCD: Treatment and Adulthood Outcome Michael H. Bloch M.D., M.S. Assistant Director, Yale OCD Clinic Assistant Professor, Yale Child Study Center Michael.bloch@yale.edu Objectives
Specific Issues in Pediatric OCD: Treatment and Adulthood Outcome Michael H. Bloch M.D., M.S. Assistant Director, Yale OCD Clinic Assistant Professor, Yale Child Study Center Michael.bloch@yale.edu Objectives
Hit head, on blood thinner-wife wants CT. Will Davies June 2014
 Hit head, on blood thinner-wife wants CT Will Davies June 2014 Selection of Adults with Head Injury for CT Scan Early management of head injury: summary of updated NICE guidance. Hodgkinson S, Pollit V,
Hit head, on blood thinner-wife wants CT Will Davies June 2014 Selection of Adults with Head Injury for CT Scan Early management of head injury: summary of updated NICE guidance. Hodgkinson S, Pollit V,
USASOC Neurocognitive Testing and Post Injury Evaluation and Treatment Clinical Practice Guideline (CPG)
 USASOC Neurocognitive Testing and Post Injury Evaluation and Treatment Clinical Practice Guideline (CPG) Note: The intent of this CPG is to serve as general guidance for medics and medical officers. It
USASOC Neurocognitive Testing and Post Injury Evaluation and Treatment Clinical Practice Guideline (CPG) Note: The intent of this CPG is to serve as general guidance for medics and medical officers. It
Traumatic brain injuries are caused by external mechanical forces such as: - Falls - Transport-related accidents - Assault
 PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
NEWS. In this Issue: November Clinical Conversation: Understanding PANS and PANDAS. Leadership: John Straus, MD Founding Director
 February 2019 NEWS November Clinical Conversation: Understanding PANS and PANDAS Clinical Conversation: November 20, 2018 Presented by Michele Casoli Reardon, MD, MCPAP Medical Director and Pediatric Liaison,
February 2019 NEWS November Clinical Conversation: Understanding PANS and PANDAS Clinical Conversation: November 20, 2018 Presented by Michele Casoli Reardon, MD, MCPAP Medical Director and Pediatric Liaison,
Spine MRI and Spine CT Test Request Tip Sheet
 Spine MRI and Spine CT MRI is almost always preferred over CT scan; if ordering CT, CLEARLY document why MRI is not appropriate. In cases of back pain without red flags, six weeks of multimodality supervised
Spine MRI and Spine CT MRI is almost always preferred over CT scan; if ordering CT, CLEARLY document why MRI is not appropriate. In cases of back pain without red flags, six weeks of multimodality supervised
Correlation of Computed Tomography findings with Glassgow Coma Scale in patients with acute traumatic brain injury
 Journal of College of Medical Sciences-Nepal, 2014, Vol-10, No-2 ABSTRACT OBJECTIVE To correlate Computed Tomography (CT) findings with Glasgow Coma Scale (GCS) in patients with acute traumatic brain injury
Journal of College of Medical Sciences-Nepal, 2014, Vol-10, No-2 ABSTRACT OBJECTIVE To correlate Computed Tomography (CT) findings with Glasgow Coma Scale (GCS) in patients with acute traumatic brain injury
EDUCATIONAL COMMENTARY THROAT CULTURES LEARNING OUTCOMES. Upon completion of this exercise, the participant should be able to:
 EDUCATIONAL COMMENTARY THROAT CULTURES LEARNING OUTCOMES Upon completion of this exercise, the participant should be able to: distinguish three types of hemolysis produced by bacterial colonies. discuss
EDUCATIONAL COMMENTARY THROAT CULTURES LEARNING OUTCOMES Upon completion of this exercise, the participant should be able to: distinguish three types of hemolysis produced by bacterial colonies. discuss
Acute cerebral MCA ischemia with secondary severe head injury and acute intracerebral and subdural haematoma. Case report
 214 Balasa et al - Acute cerebral MCA ischemia Acute cerebral MCA ischemia with secondary severe head injury and acute intracerebral and subdural haematoma. Case report D. Balasa 1, A. Tunas 1, I. Rusu
214 Balasa et al - Acute cerebral MCA ischemia Acute cerebral MCA ischemia with secondary severe head injury and acute intracerebral and subdural haematoma. Case report D. Balasa 1, A. Tunas 1, I. Rusu
