Approach to diagnosis of metabolic diseases
|
|
|
- Kerrie Flowers
- 5 years ago
- Views:
Transcription
1 Translational Science of Rare Diseases 1 (2016) 3 22 DOI /TRD IOS Press 3 Approach to diagnosis of metabolic diseases Enid Gilbert-Barness a,b and Philip M. Farrell c,d, a Department of Pathology, Cell Biology, Pediatrics and Obstetrics and Gynecology, Tampa General Hospital, University of South Florida Morsani College of Medicine, Tampa, FL, USA b Pathology and Laboratory Medicine, Distinguished Medical Alumni Professor Emeritus, University of Wisconsin School of Medicine and Public Health, Madison, WI, USA c Department of Pediatrics and Population Health Sciences, University of Wisconsin School of Medicine and Public Health, Madison, WI, USA d Department of Pediatrics, University of South Florida Morsani College of Medicine, Tampa General Hospital, Tampa, FL, USA Abstract. Inborn errors of metabolism are generally categorized as rare diseases. Their presentations are often so subtle and insidious as to cause daunting diagnostic challenges for even the most astute clinicians. Thus, irreversible morbidity and preventable mortality have been unavoidable until recent decades because of delayed diagnoses. This unfortunate circumstance has led to newborn screening programs worldwide for 40 or more hereditary metabolic disorders beginning with the dramatic improvements for patients with phenylketonuria in the 1960 s. Increasingly sophisticated testing procedures such as tandem mass spectrometry and other multiplex technologies applied to dried blood spot specimens are now having greater impact without raising costs significantly. The advent of next generation sequencing methods is likely to stimulate further progress and lead to whole genome or exome sequencing as prenatal and neonatal screening expands further. With early diagnosis through screening and expedited therapies better outcomes are routinely possible, and even preventive therapies amounting to cures can be anticipated through research. Keywords: Gene, genetic mutations, inborn errors of metabolism, hyperglycemia 1. Conceptual overview The term inborn errors of metabolism was first used by Sir Archibald Garrod in his Croonian Lectures in 1908 [1] and in his monograph Inborn Errors of Metabolism in 1909 [2]. He defined these inborn errors as genetically determined diseases caused by blocks in the metabolic pathways due to deficient activity of an enzyme [3]. From Sir Garrod s observations of patients with alkaptonuria, albinism, cystinuria, and pentosuria, he developed the concept that certain diseases of lifelong duration arise because an enzyme governing a single metabolic step is reduced in activity or missing altogether [4]. Most of these disorders may be classified as rare diseases because newborn screening data show clearly that their incidence ranges from 1:4,000 for congenital hypothyroidism to >1:250,000 (many disorders such as Maple Syrup Urine Disease (branched chain ketoaciduria). Corresponding author: Philip M. Farrell, Departments of Pediatrics and Population Health Sciences, UW School of Medicine and Public Health, 600 Highland Ave, Madison, WI 53792, USA. Tel: ; Fax: ; pmfarrell@wisc.edu /16/$ IOS Press and the authors. All rights reserved This article is published online with Open Access and distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC 4.0).
2 4 E. Gilbert-Barness and P.M. Farrell / Approach to diagnosis of metabolic diseases The definition of an inborn error of metabolism is arbitrary. Scriver et al. [5] include several hundred diseases with definite biochemical genetic bases. McKusick s catalog [6] contains several thousand diseases and disease states whose genetic abnormalities are described or assumed. Scriver et al. [5] solved the problem of exclusivity by adding molecular before encompassing every disease of the textbook of the future. The 2nd Edition of Metabolic Diseases: Foundations of Clinical Management, Genetics, and Pathology [7] is limited to those diseases with either: 1) recognized biochemical abnormalities supplemented with pathologic and genetic information, and in which a mutation leads to an enzyme that causes a metabolic disease such as phenylketonuria (PKU); or 2) disorders associated with known genetic mutations that have altered cellular physiology such as the chloride channel defect in cystic fibrosis or caused severe structural, cellular, or subcellular abnormalities. Emphasis in the book has been given to the more common and/or well defined hereditary biochemical/metabolic disorders. Prototype conditions such as Lesch Nyhan Disease, an excellent example of a nucleotide (purine) metabolism disorder, are also emphasized. Investigation of the molecular functions of genes has determined that they control the cellular metabolic function in the pathogenesis of disease far beyond that commonly understood as a metabolic disease. The genetics of variant human phenotypes is discussed by Scriver et al. [5] and Champion [8]. The relationship between gene and enzyme was described as one gene, one enzyme by Beadle and Tatum [9 11]. Tatum expanded this concept as follows: 1) all biochemical processes in all organisms are under genetic control; 2) these biochemical processes are resolvable into series of individual stepwise reactions; 3) each biochemical reaction is under the ultimate control of a different single gene; and 4) mutation of a single gene results only in an alteration in the ability of the cell to carry out a single primary chemical reaction. Pauling et al. [12] discovered direct evidence that human mutations actually produce an alteration in the primary structure of proteins. Their seminal research revealed a valine substitution for glutamic acid in sickle cell hemoglobin. Ingram [13] showed that inborn errors of metabolism were caused by mutant genes that produced abnormal proteins whose functional activities were altered. It is estimated that some 30,000 genes constitute the human genome. A variety of genome maps are available, including some that are disease specific such as the cancer cell map [14]. The genome map is being constantly improved, with updated gene sequences and locations of intronic elements, revised lists of benign SNPs, additional reference genomes, databases of variant frequencies that are ethnicityspecific, and associations of specific genes with specific human diseases. In addition, combinations of genes can result in a metabolic error. Thus, although 7000 hereditary metabolic disorders are currently known, at least the same number of significant genetic errors as the number of genes seems theoretically possible, and an undetermined but large percentage of these may cause biochemical disorders with clinical impact. An estimation of genetic disease frequencies is shown in Table 1. Table 1 Estimation of genetic disease frequencies 1% of live-born infants have monogenic disease 5% of individuals under 25 can expect to have a disease due to a genetic component 6% 8% of hospitalized children have monogenic disease 29% 41% of hospitalized children have gene-influenced disease 60% of older individuals have genetically influenced diseases, if multifactorial diseases are included 100% of humans carry 6 8 lethal genes 20% 30% of all infant deaths are due to genetic disorders 30% 50% of post-neonatal deaths are due to congenital malformations 50% of mental retardation has a genetic basis
3 E. Gilbert-Barness and P.M. Farrell / Approach to diagnosis of metabolic diseases 5 2. Diagnostic strategies and tactics Clinical diagnosis of metabolic disease is made by specific tests, biochemical analyses, and histologic and genetic studies that are discussed by Leonard et al. [15] and Cleary et al. [16]. New methods such as next generation sequencing of genes [17, 18] and even whole genome sequencing [19, 20] are facilitating diagnoses and other goals such as genetic counseling. Clinicians seek diagnosis, effective treatment, an understanding of prognosis, and the capability to explain and counsel patients and their families. Parents and patients appreciate gaps in knowledge but may be left seriously disappointed or angry without a cure. Fortunately, our increased genetic knowledge and better understanding of molecular pathophysiology of the past two decades has led to dramatic improvements in therapies using novel methods such as small molecule modulators of defective proteins [e.g., CFTR modulators for cystic fibrosis [21], gene therapy [22], and stem cell infusions [23]]. Thus, investments in expedited diagnostic strategies such as newborn screening can pay great dividends when well targeted, highly effective therapies are available. Identification of inborn errors of metabolism provides the basis for diagnosis, prognosis, genetic counseling, and, in an increasing number of patients, targeted treatments aimed directly at the fundamental defect. Many infants and children present as medical emergencies and life-preserving treatment is begun before a definite diagnosis is available. Diagnosis should be made rapidly and the implications and complexities of treatment explained in detail. Metabolic disease is usually not suspected in patients until more common diseases are considered. Those children with a history of consanguinity or those in families with a history of unexplained death, multiple spontaneous abortions, or previously diagnosed metabolic diseases have an increased likelihood of a metabolic disease. Frequently, children (and some adults) with metabolic diseases are first seen as critically ill patients with non-specific findings. Dehydration, acidosis, vomiting, ammonemia, hypoglycemia, or seizures must be managed aggressively. Inborn metabolic errors may be suspected if response to emergency treatment is not as expected. Metabolic diseases can be divided into 3 main categories as listed in (Table 2). The majority of these disorders are inherited as autosomal recessive traits. Some such as Duchenne muscular dystrophy are X-linked. A few are inherited as dominant traits, and mitochondrial disorders form a genetically separate category. Mitochondrial enzymes are coded by both the maternal nuclear genome and by the mitochondrial DNA. Clinical findings associated with metabolic diseases are listed in Table 3. It has been well recognized that symptoms may be quite variable, even in a group of patients with the same mutation. Thus, it has become clear that genetic modifiers may alter the expression of signs/symptoms and that gene-environment and nutrition-metabolism relationships can also influence the disease liability of pathologic genetic mutations. The newborn with a severe metabolic abnormality may present with symptoms of apparent sepsis or asphyxia. These symptoms usually consist of irritability, failure to feed or suck, flaccidity, or coma. Previous miscarriages or sudden unexpected death in a sibling should trigger a screening investigation for metabolic disease. Sophisticated newborn screening using 4-5 blood spots on filter paper [ Guthrie cards named for Robert Guthrie, the originator of population-based newborn screening with dried blood spots [24]], combined with tandem mass spectrometry as discussed by Ziadeh et al. [25] and Millington et al. [26] or molecular analyses [21] can identify a number of life-threatening diseases with a single, multiplex assay. The hereditary metabolic diseases that can now be screened for from filter paper blood spots in the newborn are listed in Table 4. Recently, severe combined immuno (SCID) has been added in many regions as well as point of care screening methods such as oxygen saturation measurements for critical congenital heart diseases. Metabolic abnormalities may be suspected in infants with hydrops fetalis Table 3, or with placental abnormalities. Routine placental examination may disclose fetal metabolic storage disease by the
4 6 E. Gilbert-Barness and P.M. Farrell / Approach to diagnosis of metabolic diseases Table 2 Categories of metabolic disease (Examples) Large Complex Molecule Diseases Complex lipid degradation (Gaucher, Niemann-Pick, Tay-Sachs, metachromatic leukodystrophy) Glycoprotein degradation (fucosidase and mannosidase ) Mucopolysaccharidoses (Sanfilippo and Hurler syndrome) Lipofuscin storage disorders (Batten disease) Glycogen storage disease type I (von Gierke disease), type II (Pompe disease), type III (debrancher ) Peroxisomal disorders (Zellweger syndrome) Small Molecule Diseases Amino acid metabolism disorders (phenylketonuria, maple syrup urine disease, homocystinuria, tyrosinemia) Ammonia metabolism disorders (ornithine transcarbamylase ) Organic acid metabolism disorders (methylmalonic acidemia, propionic acidemia, isovaleric acidemia) Monosaccharides (galactosemia, hereditary fructose intolerance) Pyruvic and lactic acid metabolism disorders (primary lactic acidosis, mitochondrial disorders) Fatty acid metabolism disorders (medium-chain acyl-coa dehydrogenase ) Purines and pyrimidine metabolism disorders (Lesch-Nyhan syndrome) Vitamin and cofactor metabolism disorders (biotinidase ) Other Diseases Metal metabolism disorders (Wilson and Menkes disease, hemochromatosis) Lipoprotein metabolism disorders (Abetalipoproteinemia, familial hypercholesterolemia) Porphyrin metabolism disorders (porphyria) Membrane transport disorders (cystinuria, cystinosis) Intestinal disaccharidases Collagen and connective tissue disorders (Ehlers-Danlos disease, Marfan syndrome) Congenital adrenal hyperplasia Hyperinsulinism presence of vacuolations of syncytiotrophoblasts, intermediate trophoblasts, and stromal Hofbauer cells. Suspected metabolic errors in the newborn are emergencies and require prompt identification and treatment. After obtaining the appropriate specimens for testing, emergency treatment must be instituted. If the patient dies, regardless of age, preparation should be made for a metabolic disease autopsy as discussed by Ernst et al. [27]. Pregnancy may occur in patients with metabolic diseases. Some of these conditions can be teratogenic. Many such pregnancies can be successfully managed with treatment. Treatment of these disorders is discussed in each chapter. Examples of inborn errors of metabolism potentially occurring in high frequency among specific ethnic groups are listed in Table 5. However, it should be noted that some of these disorders are quite rare now in the era of prenatal diagnosis. For instance, the incidence of Tay Sachs disease in targeted Jewish populations is extremely low worldwide [28, 29]. The most common presentations of inborn errors are without gross physical anomalies and include disorders of amino acid, fatty acid, organic acid, and carbohydrate metabolism Table 6. Others present with dysmorphic features, neonatal deaths, self-mutilation, abnormal body or urine odor, hypotonia, deafness, or recurrent acidosis with or without ketosis. Failure to recognize and, when possible, treat these infants can result in irreversible neurologic damage. Diagnostic strategy consists of meticulous attention to history and physical examination followed by appropriate screening tests, including biochemistry, radiology, or other modalities, and specific enzyme, protein, or gene analysis. Special educational services for children with inborn errors of metabolism may be available and therefore accuracy of diagnosis is essential as discussed by Powell et al. [30].
5 E. Gilbert-Barness and P.M. Farrell / Approach to diagnosis of metabolic diseases 7 Table 3 Clinical findings associated with specific metabolic diseases Abdomen Hepatomegaly Galactosemia Glycogen storage disease, type 1 Hereditary fructose intolerance Fructose-1,6-diphosphatase Methylmalonic acidemia Propionic acidemia Glutaric acidemia, type II Very-long-chain acyl-coa Medium-chain acyl-coa Short-chain acyl-coa Long-chain 3-OH acyl-coa, dehydrogenase Carnitine transporter defect Carnitine palmityl transferase IoII Acylcarnitine translocase 3-hydroxy-3-methylglutaryl-CoA lyase Phosphoenolpyruvate carboxykinase Mitochondrial respiratory/electron transport chain defects Hereditary tyrosinemia, type I Argininosuccinicaciduria 1 -Antitrypsin Smith-Lemli-Opitz syndrome Zellweger syndrome Neonatal adrenoleukodystrophy Nieman-Pick disease, type C Hepatosplenomegaly GM 1 gangliosidosis I-cell disease Gaucher disease, type I Niemann-Pick disease, type A, C Galactosialidosis Sialidosis Mucopolysaccharidosis, type VII Wolman disease Pancreatitis Glycogen storage disease, type I Lipoprotein lipase Homocystinuria Hydroxymethylgiutaryl-CoA lyase Methylmalonic acidemia Propionic acidemia Pearson syndrome Chest Cardiomyopathy Glycogen storage disease, type I Glycogen storage disease, type II Glycogen storage disease, type III Electron transport chain abnormalities Disorders of fatty acid oxidation Mucopolysaccharidoses Myocardial infarction Familial Hypocholesterolemia Fabry disease Homocystinuria Menkes disease Diarrhea Lysinuric protein intolerance Shwachman syndrome Johansson Blizzard syndrome Pearson syndrome Congenital chloride diarrhea Glucose galactose malabsorption Lactase Sucrase Abetalipoproteinemia Wolman disease Diarrhea (Persistent) Sucrase isomaltase Acrodermatitis enteropathica Congenital folate malabsorption Dysmorphic Features Glutaric aciduria, type II Glomerulopathy Renal cystic dysplasia Cerebral dysgenesis Facial dysmorphism Congenital heart disease Genital anomalies Pyruvate dehydrogenase Microcephaly Fetal alcohol facies Agenesis of corpus callosum Peroxisomal Disorders Zellweger Syndrome Renal microcysts Epiphyseal calcification Facial dysmorphism Congenital heart disease Cerebral dysgenesis Hepatopathy Infantile Refsum disease Facial dysmorphism Hepatopathy Rhizomelic chondrodysplasia punctata
6 8 E. Gilbert-Barness and P.M. Farrell / Approach to diagnosis of metabolic diseases Table 3 (Continued) Facial dysmorphism Rhizomelic limb shortening GM 1 gangliosidosis Frontal bossing, low-set ears Congenital adrenal hyperplasia Ambiguous genitalia Sialidosis Coarse facial features, stippled epiphyses Mucolipidosis II Coarse facial features Mucopolysaccharidoses Coarse facial features Infantile sialic acid storage disease Coarse facial features -Hydroxyisobutyryl-CoA deacylase Congenital heart defects Agenesis of corpus callosum Dysmorphic facies Gaucher-like storage disease Arthrogryposis Muscle phosphorylase Arthrogryposis Smith-Lemli-Opitz syndrome Genital and digital abnormalities Ears Otic atrophy Pyruvate dehydrogenase com plex Leigh disease Zellweger syndrome Extremities Arthritis Alkaptonuria Gaucher disease, type I Lesch-Nyhan disease Farber disease I-cell disease Mucolipidosis III Homocystinuria Mucopolysaccharidosis IS, HS Bone or limb deformity Dyostosis Multiplex Hurler, Hurler-Scheie disease Hunter disease Sanfilippo disease GM1 gangliosidosis Mucolipidosis II, I-cell disease Mucolipidosis III Galactosialidosis Maroteaux-Lamy disease Sly disease Multiple sulfatase Osteoporosis and/or fractures Propionic acidemia Methylmalonic acidemia Glycogen storage disease, type I Homocystinuria Adenosine deaminase Lysinuric protein intolerance Menkes disease Infantile Refsum disease Gaucher disease I-cell disease Eyes Cataract Galactosemia Lowe syndrome Mitochondrial respiratory electron transport chain defects Zellweger syndrome Rhizomelic chondrodysplasia punctata Mevalonic aciduria Corneal Clouding I-cell disease Steroid sulfatase Dislocated lens Methionine synthetase Sulfite oxidase Macular cherry-red spot GM 1 gangliosidosis Galactosialidosis Niemann-Pick Disease, type A Tay-Sachs disease (GM 2 gangliosidosis) Retinitis pigmentosa Mitochondrial respiratory electron transport chain defects Methylmalonic acidemia/homocystinuria Sjögren-Larsson syndrome Zellweger syndrome Neonatal adrenoleukodystrophy Infantile Refsum disease Abetalipoproteinemia Long-chain 3-OH acyl-coa dehydrogenase Head Alopecia
7 E. Gilbert-Barness and P.M. Farrell / Approach to diagnosis of metabolic diseases 9 Table 3 (Continued) Multiple carboxylase Orotic aciduria Cerebral calcification Mevalonic aciduria Adrenoleukodystrophy Pearson syndrome Abnormalities of folate metabolism Abnormalities of folate metabolism L-2-Hydroxyglutaric aciduria Shwachman syndrome Biopterin abnormalities Johansson Blizzard syndrome Coarse facial features GM 1 gangliosidosis Hydrops fetalis I-cell disease Gaucher disease Mucopolysaccharidosis, type VII GM 1 gangliosidosis Sialidosis Salla disease Galactosialidosis Sialidosis Macrocephaly Wolman disease 4-Hydroxybutyric aciduria -Glucuronidase Glutaric aciduria, type I Congenital disorders of protein L-2-Hydroxyglutaric aciduria glycosylation Neonatal adrenoleukodystrophy Deficiencies of red cell Tay-Sachs disease glycolytic/pentose phosphate Hurler disease pathway enzymes (eg, Krabbe disease G6PDH, private Multiple sulfatase kinase ) Canavan disease Farber disease Mannosidosis Fumarase 3-Hydroxy-3-methylglutaric aciduria GSD IV Pyruvate carboxylase MPS VII (Sly disease) Multiple acyl-coa dehydrogenase MPS IVA (Morquio type A) Microcephaly Mucolipidosis I (Sialidosis) Short-chain Acyl-CoA dehydrogenase Mucolipidosis II (I-cell Mitochondrial respiratory electron transport chain defects disease) Leigh disease Neonatal hemochromatosis Steely hair Niemann-Pick C Menkes disease Primary carnitine Respiratory chain disorders Hematology Sialic acid storage disease Hematologic abnormalities Morquio syndrome Leukopenia with or without thrombopenia and anemia Neuraminidase Methylmalonic acidemia Myotonic dystrophy Propionic acidemia Perinatal iron storage syndrome Isovaleric acidemia Carnitine 3-Oxothiolase Niemann-Pick type C Abnormalities of folate metabolism I-cell disease Transcobalamin II Farber disease Shwachman syndrome Mucopolysaccharidosis type VII Pearson syndrome Carbohydrate-deficient glycoprotein storage Johansson Blizzard syndrome disease Megaloblastosis Cobalamin metabolic errors: Mouth and throat Methylmalonic acidemia Macroglossia Homocystinuria GM 1 gangliosidosis Transcobalamin II Macroglossia
8 10 E. Gilbert-Barness and P.M. Farrell / Approach to diagnosis of metabolic diseases Table 3 (Continued) Neurological MLD, Niemann-Pick A and B, and Gaucher, type III Gaucher disease, type II Glutaric acidemia, type I Krabbe disease Crigler-Najjar syndrome Phenylketonuria caused by a biopterin defect Stroke-like episodes Carbamoyl phosphate synthetase MELAS Carbohydrate deficient glycoprotein storage disease Ethylmalonic aciduria Fabry disease Glutaric aciduria, type I Homocystinuria Isovaleric acidemia Menkes disease 3-MTHF reductase Methylmalonic acidemia Ornithine transcarbamylase Propionic acidemia Purine nucleoside phosphorylase Odor Sweaty feet, strong Glutaric aciduria (type II) Isovaleric acidemia Mousy or musty Phenylketonuria Maple syrup Maple syrup urine disease Tomcat urine -Methylcrotonylglycinuria Cabbage Methionine malabsorption Rotting fish Trimethylaminuria Rancid fishy or cabbage Tyrosinemia Hoplike Oasthouse disease Swimming pool Hawkinsinuria Psychiatric Sanfilippo syndrome (MPS III) Hunter syndrome (MPS II) X-linked ALD Late-onset MLD Late-onset GM2 gangliosidosis Lesch-Nyhan syndrome Porphyria Wilson disease Cerebrotendinous xanthomatosis UCED Homocystinuria due to MTHF reductase Adult-onset NCL Skin Angiokeratoma Fabry disease GM 1 gangliosidosis Fucosidosis Galactosialidosis Sialidosis Desquamating, eczematous, or vesiculobullous lesions Acrodermatitis enteropathica Multiple carboxylase Methylmalonic acidemia Propionic acidemia Hepatoerythropoietic porphyria Congenital erythropoietic porphyria Ichthyosis Multiple sulfatase X-linked ichthyosis (steroid sulfatase ) Gaucher disease Krabbe disease Refsum disease Sjögren-Larsson syndrome Nodules Farber disease (Ceramidase ) Thick skin I-cell disease GM 2 gangliosidosis Mucopolysaccharidosis, type VII Sialidosis Galactosialidosis Xanthomas Familial hypercholesterolemia Lipoprotein lipase Niemann-pick disease ALD, adrenoleukodystrophy; MLD, metachromatic leukodystrophy; UCED, urea cycle enzyme defects; MTHF, methylenetetrahydrofolate; NCL, neuronal ceroid lipofuscinosis; MELAS, myoclonic epilepsy, lactic acidosis, and stroke.
9 Acylcarnitines MS/MS Table 4 Newborn screening panel: Core panel and secondary targets Amino acids 9 Organic 5 Fatty Acid 6 Aminoacidopathies 3 Hemoglobinopathies 7 Other Genetic Acidemia Disorders Oxidation Defects Disorders Core panel Isovaleric academia Medium-chain acyl-coa Phenlketonuria Sickle cell anemia Congenital Hypothyroidism dehydrogenase (hemoglobin SS disease) Glutaric acidemia type I Very long-chain acyl-coa Maple syrup disease Biotinidase 3-hydroxy-3-methyl glutaric dehydrogenase Homocystinuria Hemoglobin Congenital adrenal aciduria (HMG) (due to cystathionine beta S/ -thalassemia hyperplasia Multiple carboxylase Long-chain L-3-hydroxy synthase ) Hemoglobin S/C disease (21-hydroxylase ) Methylmalonic acidemia acyl-coa dehydrogenase Citrullinemia Classical galactosemia (mutase ) 3-Methylcrotonyl-CoA Argininosuccinic academia Hearing loss carboxylase Trifunctional protein Tyrosinemia type I Cystic fibrosis Methylmalonic acidemia Carnitine uptake defect Severe combined (cobalamin disorders A&B) immuno Propionic acidemia B-Ketothiolase Secondary targets 6 More Organic 8 More Fatty Acid 8 More Other 2 Other Hereditary Acidemia Disorders Oxidation Defects Aminioacidopathies Hemoglobinopathies Metabolic Disorders Methylmalonic academia (cobalamin disorders C&D) Malonic academia Short-chain acyl-coa dehydrogenase Glutaric acidemia type II Medium/short-chain L-3-hydroxy acyl-coa dehydrogenase Benign hyperphenylalaninemia Tyrosinemia type II Defects of biopterin cofactor biosynthesis Variant hemoglobinopathies (including hemoglobin E) Galactokinase Galactose epimerase (Continued) E. Gilbert-Barness and P.M. Farrell / Approach to diagnosis of metabolic diseases 11
10 Table 4 (Continued) Secondary targets 6 More Organic 8 More Fatty Acid 8 More Other 2 Other Hereditary Acidemia Disorders Oxidation Defects Aminioacidopathies Hemoglobinopathies Metabolic Disorders Isobutyryl-CoA dehydrogenase 2-Methyl 3-hydroxy butyric aciduria 2-Methylbutyryl-CoA dehydrogenase 3-Methylglutaconic aciduria Medium-chain ketoacyl-coa thiolase Carnitine palmitoyltransferase II Carnitine: acylcarnitine translocase Carnitine palmitoyltransferase I (liver) Dienoyl-CoA reductase Argininemia Tyrosinemia type III Defects of biopterin cofactor regeneration Hypermethioninemia Citrullinemia type II From Newborn Screening: Toward a Uniform Screening Panel and System, Maternal and Child Health Bureau [Federal Register: March 8, 2005 (Volume 70, Number 44)]. [ 12 E. Gilbert-Barness and P.M. Farrell / Approach to diagnosis of metabolic diseases
11 E. Gilbert-Barness and P.M. Farrell / Approach to diagnosis of metabolic diseases 13 Table 5 Ethnic group incidence of inborn errors of metabolism Inborn Error Ethnic Group Estimated Incidence (per births) Hepatorenal tyrosinemia French-Canadians (Saguenay-Lac Saint-Jean region) 54 (before the introduction of preventive prenatal diagnosis) Tay-Sachs disease Canavan disease Ashkenazi Jews 33 (before the introduction of preventive prenatal diagnosis) Gaucher disease, type 1 Canavan disease Ashkenazi Jews 100 Phenylketonuria (PKU) Canavan disease Ashkenazi Jews 5 Yemenite Jews 19 Turkish 38.5 Porphyria variegata South African (white) 300 Congenital adrenal hyperplasia Yupik Eskimos 200 Glutaric aciduria, type 1 Ojibway Indians (Canada) >50 Maple syrup urine disease Mennonites (Pennsylvania) 568 From: Clarke JTR, (Ed.): A Clinical Guide to Inherited Metabolic Diseases 3rd ed., Cambridge University Press, Clinical investigation is augmented by a large number of common blood and urine tests (blood, sugar, urine ph, anion gap, cytopenia, liver function tests, sweat test, electroencephalogram, and radiography of bones). Radiologic examination may include X-rays, CT scans, and MR imaging. MRI scans should be substituted for CT scans whenever possible to avoid radiation exposure. Ophthalmologic and neurophysiologic investigations are often important. Laboratory findings in inborn errors of metabolism are listed in Table 7. Abnormal metabolites are shown in Table 8. Abnormalities in serum electrolytes can be caused by vomiting or diarrhea. Inclusion of bicarbonate and ph assessment may indicate a large anion gap due to the presence of organic acids. Electrolytes, however, may be normal with organic acidemias. Neutropenia or pancytopenia suggests the presence of one of the organic acidemias. A urinalysis may indicate the presence of reducing substances and the presence or absence of ketones. Ketonuria is not found in normal newborns. Urine ph above 5.0 in an acidotic infant may suggest renal tubular acidosis. Absence of ketones in association with hypoglycemia may indicate an error in fatty acid metabolism. It is helpful to save a small amount of frozen urine and plasma for later evaluation of keto acids, carnitine, and organic acids. Elevated serum ammonia levels are found in patients with liver disease and in those with errors of the urea cycle and several of the organic acidemias. Transient hyperammonemia occurs in some newborns, and this is reversible when treatment is prompt. Urea cycle errors are frequently associated with very low blood urea levels. Some metabolic disorders cause liver cirrhosis in infants and children and some liver disorders progress to stupor and coma. Liver function tests commonly indicate primary liver diseases. However, abnormal liver function test findings result from many of the metabolic diseases, including disorders of organic and amino acid metabolism, and many of the storage diseases. Elevated serum lactate is usually due to hypoxemia or poor perfusion and occurs with sepsis. It may be due, however, to improper technique in drawing blood without good blood flow. Lactic acid is produced in the anaerobic metabolism of glucose through pyruvate, which is then converted in the liver to glucose. Deficiency of pyruvate dehydrogenase complex is the most common error of metabolism that causes lactic acidosis.
12 14 E. Gilbert-Barness and P.M. Farrell / Approach to diagnosis of metabolic diseases Table 6 Laboratory findings in some inborn errors of metabolism Lactic acidosis ± Hyperammonemia Fructose-1,6-diphosphatase Increased anion gap Ornithine transcarbamylase Methylmalonic acidemia Hypoglycemia Propionic acidemia Carbamoyl phosphate Hyperinsulinism Isovaleric acidemia synthetase Glycogen storage disease, type I Multiple carboxylase Argininosuccini- Hereditary fructose intolerance Maple syrup urine disease caciduria Fructose-1,6-diphosphatase Glutaric acidemia, type I Citrullinemia Glutaric acidemia, type II Methylmalonic acidemia Glutaric acidemia, type I Short-chain acyl-coa Propionic acidemia Glutaric acidemia, type II dehydrogenase Isovaleric acidemia Very-long-chain acyl-coa Long-chain 3-OH acyl-coa Multiple carboxylase dehydrogenase dehydrogenase Glutaric acidemia, type II Medium-chain acyl-coa Ketothiolase Very-long-chain acyl-coa dehydrogenase Acetoacetate CoA ligase dehydrogenase Short-chain acyl-coa 3-hydroxy-3-methylglutaryl Medium-chain acyl-coa dehydrogenase CoA Iyase dehydrogenase Long-chain 3-OH acyl-coa Pyruvate dehydrogenase Short-chain acyl-coa dehydrogenase dehydrogenase complex Carnitine transporter defect Pyruvate carboxylase Acylcarnitine translocase Carnitine palmitoyl transferase I Phosphoenolpyruvate Ketosis Carnitine palmitoyl transferase II carboxykinase Methylmalonic acidemia Mitochondrial respiratory/electron Propionic acidemia Acylcarnitine translocase transport chain defects Isovaleric acidemia Ketothiolase Leigh disease Multiple carboxylase Acetoacetate-CoA ligase Hereditary galactosemia Maple syrup urine disease 3-hydroxy-3-methylglutaryl-CoA Glycogen storage disease, Glutaric acidemia, type II Iyase type I Short-chain acyl-coa dehydrogenase Hereditary galactosemia Hereditary fructose intolerance Neonatal hemochromatosis Fructose-1,6-diphosphatase Ketothiolase Mitochondrial respiratory/electron Acetoacetate-CoA ligase transport chain defects Hereditary tyrosinemia, Lipemia type I Pyruvate carboxylase Glycogen storage disease, type I Respiratory alkalosis Glycogen storage disease, type I Omithine transcarbamylase Carbamoyl phosphate synthetase Argininosuccinicaciduria Citrullinemia Myopathy can be caused by a few of the glycogen storage diseases or mitochondrial disorders. Muscle biopsy or fibroblast cultures may be diagnostic. Myoglobinuria may be present, and serum free carnitine may be decreased. Peroxisomal action is responsible for -oxidation of fatty acids, and results in developmental retardation. Peroxisomal disorders with such manifestations include Zellweger syndrome,
13 E. Gilbert-Barness and P.M. Farrell / Approach to diagnosis of metabolic diseases 15 Table 7 Laboratory evaluation for suspected inborn errors of metabolism Comments Initial Evaluation Blood tests CBC with differential Blood glucose Electrolytes, BUN, creatinine, uric acid Arterial blood gas Serum ammonia AST, ALT, bilirubin, PT LDH, aldolase, creatine, kinase Urine Tests Color, odor Urinalysis Reducing substances Myoglobin Specialized Tests Blood tests Quantitative plasma amino acids Lactate and pyruvate Acylcarnitine profile Urine Tests Qualitative urine organic acids Should be obtained from artery or vein without a tourniquet; the tube should be placed on ice for transport to the laboratory and analyzed immediately. If the plasma ammonia concentration is >100 micromol/l (1.7 mcg/ml), the measurement should be repeated immediately If the patient has signs or symptoms of myopathy If the patient has signs or symptoms of myopathy Plasma amino acid analysis must be performed quantitatively rather than qualitatively Lactate and pyruvate should be measured in arterial blood that is, transported on ice Analysis of acylcarnitine conjugates is performed by tandem mass spectrometry and can be measured in a plasma sample or a filter-paper bloodspot; serum is preferred because of inherent problems in quantitating compounds from a filter-paper blood spot Minimum of 2 to 5 ml in sterile container without preservative CBC: complete blood count; ALT: alanine aminotransferase; BUN: blood urea nitrogen; PT: prothrombin time; AST: aspartate aminotransferase; LDH: lactate dehydrogenase. If possible, blood and urine samples should be obtained for both the initial and specialized tests at the time of presentation. Samples for specialized tests should be processed and stored appropriately for further testing if indicated. adrenoleukodystrophy, and oxalosis [31]. Very-long-chain fatty acids are elevated in the serum with most forms of peroxisomal disorders. Many chemical screening programs such as determination of organic and amino acids, oligosaccharides, and glycosaminoglycans in blood and urine are available for diagnostic workup of suspected progressive degenerative metabolic diseases. Distinguishing biochemical findings of inborn errors of metabolism are shown in Table 9. Some inherited metabolic diseases significantly increase the risk of intercurrent illness. For example, recurrent treatment-resistant otitis media is a common problem in children with mucopolysaccharide storage diseases because distortion of the Eustachian tube and production of particularly tenacious
14 16 E. Gilbert-Barness and P.M. Farrell / Approach to diagnosis of metabolic diseases Table 8 Abnormal metabolites in metabolic disorders Disorder Organic Acidemias Methylmalonic academia Propionic academia Isovaleric academia Glutaric academia type I 3-Methylglutaconic aciduria 2-Hydroxy-3-methylbutyryl-CoA dehydrogenase 2-Hydroxyglutaric aciduria Disorders of Ketogenesis Medium chain acyl-coa dehydrogenase (MCAD) 3-ketothiolase 3-Hydroxy-3-methylglutaryl (HMG)-CoA lyase Other Disorders Canavan disease Glutaric academia type II (multiple acyl-coa dehydrogenase ) Mevalonate kinase Maple syrup urine disease Phenylketonuria Fumarase Glutathione synthetase deificneyc Biotinidase * Holocarboxylase synthetase Glycerol kinase Ethylmalonic encephalopathy Disorders of Uncertain Consequence 3-methylcrotonyl-CoA carboxlase Short chain acyl-coa dehydrogenase Abnormal Metabolite (s) Methylmalonic and methylcitric acids 3-Hydroxpropionic acid propionylglycine, methylcitric acid Isovalerylglycine Glutaric and 3-hydroxyglutaric acids 3-Methylglutaconic acid 2-Hydroxy-3-methylblutyric acid, tiglyglycine, 2-methyl-3-hydroxyacetoacetic acid 2-Hydroxyglutaric acid Hexanoylglycine and suberylglycine 2-hydroxy-3-methylbutyric acid, tiglyglycine, 2-methyl-3-hydroxyacetoacetic acid 3-Hydroxy-3-methylglutaric, 3-methylglutaric and 3-methylglutaconic acids N-acetylaspartic acid Glutaric and 2-hydroxyglutaric acids Mevalonic acid 2-Hydroxyisovaleric and 2-hydroxy-3-methylvaleric Phenylpyruvic and phenyllactic acids Fumaric acid 5-Oxoproline (pyroglutamic acid) 3-Hydroxyisovaleric acid, methylcitric acid, 3-methylcrotonlglycine, propionylglycine 3-Hydroxyisovaleric acid, methylcitric acid, 3-methylcrotonylglycine, propionylglycine Glycerol Ethylmalonic and methylsuccinic acids 3-methylcrotonylglycine Ethylmalonic acid, butyrylglycine Other abnormal metabolites may be seen in these disorders but those listed are the most characteristic for the diagnosis. mucus combine to create a favorable environment for bacterial colonization of the middle ear. The neutropenia that is a prominent feature of glycogen storage disease type Ib, and some of the organic acidopathies, predisposes to pyogenic infections. Classic galactosemia predisposes infants to neonatal Escherichia coli sepsis [32]. Major congenital malformations, such as meningomyelocele, complex congenital heart disease, and major congenital limb deformities, are not generally considered signs of an underlying inherited metabolic disease; however, some inherited metabolic conditions occur with dysmorphism so characteristic that a strong presumptive diagnosis can be made on physical examination alone [32]. A large
15 E. Gilbert-Barness and P.M. Farrell / Approach to diagnosis of metabolic diseases 17 Table 9 Distinguishing biochemical findings of inborn errors of metabolism Findings MSUD OA UCD DCM FAO MD PD LSD Metabolic acidosis ± ++ ± ± ± Respiratory alkalosis + Hyperammonemia ± + ++ ± Hypoglyclemia ± ± + + ± Ketones A/H H A A/H A/L A/H A A Lactic acidosis ± ± + ± ++ MSUD: maple syrup urine disease; OA: organic acidemias UCD: urea cycle disorders; DCM: disorders of carbohydrate metabolism; FAO: fatty acid oxidation disorders; MD: mitochondrial disorders; PD: peroxisomal disorders; LSD: lysosomal storage disorder. : usually absent; ±: sometimes present; +: usually present; ++: always present. A: appropriate; H: inappropriately high; L: inappropriately low. Adapted from: Weiner DL, Metabolic Emergencies. In: Textbook of Pediatric Emergency Medicine, 5th ed. Fleisher GR, Ludwig S, Henretig FM (Eds). Lippincott, Williams & Wilkins, Philadelphia, number of metabolic diseases present with gross abnormalities of appearance Table 10A and 10B. Many of these have lysosomal defects, and most will have hepatosplenomegaly. These include such diseases as mucopolysaccharidoses, sphingolipidoses, and other lysosomal storage diseases. These diseases are not acutely life-threatening. Children with these conditions commonly have developmental delay. Many appear normal at birth and progressively deteriorate Table 3. An important step between the clinical findings and the biochemical findings is the anatomic pathology, including histology, histochemistry, immunochemistry, and electron microscopy (EM). For example, screening peripheral blood for cytoplasmic vacuoles in the lymphocytes as shown in Fig. 1 may be the first indication of a storage disorder. Some metabolic disorders present as acute encephalopathy. The earliest signs of encephalopathy may be no more obvious than excessive drowsiness, unusual behavior, or some unsteadiness of gait. Acute or intermittent ataxia is a common sign of acute encephalopathy in older children with inborn errors of metabolism. A history of recurrent attacks of unsteadiness of gait or ataxia, especially when associated with vomiting or deterioration of consciousness, should stimulate investigation of a possible inherited metabolic disease Table 11 [25]. In addition to the biochemical tests of blood and urine, solid tissues and cell cultures may be needed for biochemical assays. A biopsy specimen should be divided for biochemical analysis and morphologic investigation. This is particularly important in liver, muscle, and intestinal biopsies and in skin biopsies made for the fibroblast cultures. Hypoglycemia occurs with starvation in young infants but also may indicate an error in gluconeogenesis, errors in fat metabolism and defects in hormone metabolism. A rapid response to glucose, especially in the presence of hepatomegaly, may suggest glycogen storage disease or fructose-1,6- diphosphatase. An approach to diagnosis when a patient presents with hypoglycemia is shown in Fig. 2. This algorithm will guide clinicians toward a proper sequence of diagnostic tests. Even after death, some of the techniques used in the living can be helpful in detecting inborn errors of metabolism. For example, even small amounts of urine may remain in the bladder and should be aspirated and saved. Tissues and body fluids should be obtained and maintained in a state suitable for the tests desired. New diseases and diagnostic tests are identified at a surprisingly rapid rate. Very few laboratories perform all the tests.
16 18 E. Gilbert-Barness and P.M. Farrell / Approach to diagnosis of metabolic diseases Table 10A Physical examination findings as clues to inborn errors of Metabolism Finding General Tall, long-limbed body habitus Head Coarse facial features (eg, hirsuitism prominent brow ridge, and gingival hypertrophy) Microcephaly Macrocephaly Hair Alopecia Sparse Kinky, brittle Eyes Cataracts Cherry red spot Corneal clouding Corneal opacity Dislocated lens Kayser-Fleischer rings Retitinitis pigmentosa Potential Inborn Error Homocysturia Oligosaccharidoses, mucopolysaccharidoses, mucolipidoses Untreated phenylketonuria (PKU), maternal PKU syndrome, congenital disorders of protein glycosylation, leukodystrophies (late, organic acidemias, urea cycle disorders, maple syrup urine disease Canavan disease, glutaric academia type I, oligosaccharidoses, mucopolysaccharidoses, mucolipidoses, Tay-Sachs (early) Biotinidase, vitamin D resistant rickets Biotinidase, Menkes disease Argininosuccinic aciduria and citrullinemia (due to arginine ), Menkes disease, mucopolysaccharidoses Oligosaccharidoses, Fabry diseiase, neuronal ceroid lipofuscinosis, galactosemia, Smith-Lemli-Opitz syndrome peroxisome bioigenesis defects, rhizomelic chondrodysplasia punctata, Wilson disease, errors of mitochondrial oxidative phosphorylation Tay-Sachs disease, Sandhoff disease, Sialidosis type I and type II, GM1-gangliosidosis, Niemann-Pick disease type A, Gaucher disease type 2, metachromatic leukodystrophy, galactosialidosis Oligosaccharidoses, mucopolysaccharidoses, mucolipidoses, Tangier, sialidosis Oligosaccharidoses, Fabry disease, steroid sulfatase (X-linked ichthyosis), Tangier, molybdenum cofactor, sulfite oxidase Homocystinuria, sulfite oxidase Wilson disease Abetalipoproteinemia, peroxisome biogenesis disorders of protein glycosylation, fatty acid oxidation defects, mitochondrial defects, mucopolysaccharidoses, Krabbe disease, Menkes disease, disorders of cobalamin (vitamin B12) transport and synthesis, ornithine aminotransferase Adapted from Wappner Rs, Hainline BE. Inborn errors of metabolism. In: Oski s Pediatrics, Principles and Practice, 3rd ed., McMillan JA, DeAngelis CD, Feigin RD, Warshaw JB (Eds), Lippincott, Williams and Wilkins, Philadelphia, Saudubray JM, Chappentier C. Clinical phenotypes: Diagnosis/algorithms. In: Metabolic and Molecular Bases of Inherited Disease, 8th ed, Scriver CR, Beaudet AL, Sly WS, Valle D (Eds), McGrall-Hill, New York, 2001.Lindor NM, Karnes PS. Initial assessment of infants and children with suspected inborn errors of metabolism. Mayo Clin Proc 70:987, Cleary MA, Green A. Developmental delay: when to suspect and how to investigate for an inborn error of metabolism, Arch Dis Child 90:1128, 2005.
17 E. Gilbert-Barness and P.M. Farrell / Approach to diagnosis of metabolic diseases 19 Table 10B Physical examination findings as clues to inborn errors of Metabolism Finding Hearing loss Mouth Gingival hyperplasia Chest Inverted nipples Abdomen Hepatosplenomegaly Hepatomegaly Musculoskeletal Arthritis Neurologic Dystonia Myopathy Paresthesia Peripheral neuropathy Psychoses Skin Hypopigmentation or absent pigment Angiokeratoma Dermatitis Edema Hirsutism Ichthyosis Photosentization Xanthomas Potential Inborn Error Peroxisomal disorders, mitochondrial disorders, lysosomal storage disorders, mucopolysaccharidoses Oligosaccharidoses, mucopolysaccharidoses, mucolipidoses Congenital disorders of protein glycosylation Lysosomal storage disease Glycogen storage diseases, carnitine palmitoyltransferase II (infantile form), peroxisomal disorders, mitochondrial DNA depletion disorders, tyrosinemia type I (hepatorenal), mucolipidoses, congenital disorders of protein glycosylation, longer chain fatty acid oxidation disorders Farber disease, purine metabolism disorders Glutaric acidemia I, organic acidemias, Wilson disease, mitochondrial disorders Fatty acid oxidation defects, mitochondrial disorders, Pompe disease and other glycogen storage diseases Fabry disease, sialidosis Congenital disorders of protein glycosylation, leukodystrophies, peroxisomal disorders, Tangier disease Adult MLD Tay-Sachs, homocystinuria, porphyrias, purine metabolism disorders Cystinosis, Menkes disease, phenylketonuria, sialidosis Fabry, fucosidosis, galactosialidosis, beta-mannosidosis, sialidosis Biotinidase, Hartup disease, phenylketonuria, prolidase GM1 gangliosidosis, prolidase Oligosaccharidoses, mucopolysaccharidoses, mucolipidoses Multiple sulfatase, isolated steroid sulfatase Porphyrias Hyperlipoproteinemias and other disorders of lipoproteins Adapted from Wappner Rs, Hainline BE. Inborn errors of metabolism. In: Oski s Pediatrics, Principles and Practice, 3rd ed., McMillan JA, DeAngelis CD, Feigin RD, Warshaw JB (Eds), Lippincott, Williams and Wilkins, Philadelphia, Saudubray JM, Chappentier C. Clinical phenotypes: Diagnosis/algorithms. In: Metabolic and Molecular Bases of Inherited Disease, 8th ed, Scriver CR, Beaudet AL, Sly WS, Valle D (Eds), McGrall-Hill, New York, 2001.Lindor NM, Karnes PS. Initial assessment of infants and children with suspected inborn errors of metabolism. Mayo Clin Proc 70:987, Cleary MA, Green A. Developmental delay: when to suspect and how to investigate for an inborn error of metabolism, Arch Dis Child 90:1128, 2005.
18 20 E. Gilbert-Barness and P.M. Farrell / Approach to diagnosis of metabolic diseases Fig. 1. Vacuolated lymphocyte in the peripheral blood of a patient with mannosidosis. Table 11 Differential diagnosis of acute encephalopathy in metabolic diseases UCED MSUD OAuria FAOD ETC Defects Metabolic acidosis 0 ± +++ ± ++ Plasma glucose N N or N Urinary ketones N 0 0 Plasma ammonia N N Plasma lactate N N ± Liver function ±N N N N Plasma carnitine N N N Plasma amino acids Abnormal BCAA glycine ± alanine Urinary organic acids N Abnormal Abnormal Abnormal N UCED, urea cycle enzyme defect; MSUD, maple syrup urine disease; OAuria, organic aciduria; FAOD, fatty acid oxidation defect; ETC, mitochondrial electron transport chain; BCAA, branched-chain amino acids;, elevated; decreased;+, present; ±, variably present; N, normal; O, not present. From: Clarke JTR, (Ed.): A Clinical Guide to Inherited Metabolic Diseases 3rd ed., Cambridge University Press, Further development of prenatal and neonatal screening As techniques such as next generation sequencing [17, 18] and whole genome sequencing are developed further for routine use, there will be many more commercial laboratories offering comprehensive testing as has already proved helpful for newborn intensive care units [19, 20]. However, reporting and ethical issues need to be resolved before whole genome sequencing can be used widely [33].
19 E. Gilbert-Barness and P.M. Farrell / Approach to diagnosis of metabolic diseases 21 Fig. 2. Approach to the differential diagnosis of hypoglycemia. Abbreviations: SGA, small for gestational age; IDM, infant of diabetic mother; HFI, hereditary fructose intolerance; AA, amino acids; OA, organic acids; FFA, free fatty acids; FAOD, fatty acid oxidation defect; hgh, human growth hormone; T4, thyroxine; GSD, glycogen storage disease; FDPase, fructose- 6-diphosphatase. Clarke JTR, (Ed.): A Clinical Guide to Inherited Metabolic Diseases 3rd ed., Cambridge University Press, References [1] A.E. Garrod, Inborn errors of metabolism (Croonian Lectures), Lancet 2 (1908), 1. [2] A.E. Garrod, Inborn Errors of Metabolism, London, 1909, Oxford University Press. [3] A.E. Garrod, Inborn Errors of Metabolism, London, 1923, Oxford University Press. [4] A.G. Bearn and E.D. Miller, Archibald Garrod and the development of the concept of inborn errors of metabolism. Bull Hist Med 53 (1979), [5] C.R. Scriver, A.L. Beaudet, W.S. Sly and D. Valle, editors: The Metabolic and Molecular Bases of Inherited Disease, 7th ed, New York, 1995, McGraw-Hill. [6] V.A. McKusick, Mendelian Inheritance in Man, 11th ed, Baltimore, 1994, The Johns Hopkins University Press. [7] E. Gilbert-Barness, L. Barness and P. Farrell (Eds.), Metabolic Diseases: Foundations of Clinical Management, Genetics, and Pathology. IOS Press, Amsterdam, In press. [8] M.O. Champion, An approach to the diagnosis of inherited metabolic disease. Arch Dis Child Educ Pract Ed 95 (2010), [9] G.W. Beadle, Biochemical genetics. Chem Rev 37 (1945), 15. [10] G.W. Beadle and E.L. Tatum, Genetic control of biochemical reactions in Neurospora. Proc Natl Acad Sci USA 27 (1941), [11] E.L. Tatum, A case history of biological research. Science 129 (1959),
INBORN ERRORS OF METABOLISM (IEM) IAP UG Teaching slides
 INBORN ERRORS OF METABOLISM (IEM) 1 OBJECTIVES What are IEMs? Categories When to suspect? History and clinical pointers Metabolic presentation Differential diagnosis Emergency and long term management
INBORN ERRORS OF METABOLISM (IEM) 1 OBJECTIVES What are IEMs? Categories When to suspect? History and clinical pointers Metabolic presentation Differential diagnosis Emergency and long term management
Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015
 Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015 Metabolic birth defects can cause physical problems, mental retardation and, in some cases, death. It is
Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015 Metabolic birth defects can cause physical problems, mental retardation and, in some cases, death. It is
BROADENING YOUR PATIENT S OPTIONS FOR GENETIC CARRIER SCREENING.
 BROADENING YOUR PATIENT S OPTIONS FOR GENETIC CARRIER SCREENING. The Inheritest SM Carrier Screen provides relevant genetic screening for many inherited diseases found throughout the pan-ethnic US population.
BROADENING YOUR PATIENT S OPTIONS FOR GENETIC CARRIER SCREENING. The Inheritest SM Carrier Screen provides relevant genetic screening for many inherited diseases found throughout the pan-ethnic US population.
7 Medical Genetics. Hemoglobinopathies. Hemoglobinopathies. Protein and Gene Structure. and Biochemical Genetics
 SESSION 7 Medical Genetics Hemoglobinopathies and Biochemical Genetics J a v a d F a s a J a m s h i d i U n i v e r s i t y o f M e d i c a l S c i e n c e s, N o v e m b e r 2 0 1 7 Hemoglobinopathies
SESSION 7 Medical Genetics Hemoglobinopathies and Biochemical Genetics J a v a d F a s a J a m s h i d i U n i v e r s i t y o f M e d i c a l S c i e n c e s, N o v e m b e r 2 0 1 7 Hemoglobinopathies
CHRONIC MYELOGENOUS LEUKEMIA
 CHRONIC MYELOGENOUS LEUKEMIA SHUFFLING THE GENETIC DECK IN CML 9 9 (q+) 22 Ph (22q-) bcr bcr-abl abl Fusion protein causes cancer GLEEVEC AND BCR-ABL FUSION PROTEIN GENETIC MEDICINE A. Genetic diseases
CHRONIC MYELOGENOUS LEUKEMIA SHUFFLING THE GENETIC DECK IN CML 9 9 (q+) 22 Ph (22q-) bcr bcr-abl abl Fusion protein causes cancer GLEEVEC AND BCR-ABL FUSION PROTEIN GENETIC MEDICINE A. Genetic diseases
Most common is the congenital adrenogenital syndrome (AGS) or congenital adrenal hyperplasia (CAH) due to 21-hydroxylase deficiency.
 Newborn Screening Examination parameters: TSH-neonatal (hypothyreosis), 17-OH progesterone (AGS), galactose (galactosemia), galactose-uridyl transferase (galacto semia), biotinidase (biotinidase ), phenylalanine
Newborn Screening Examination parameters: TSH-neonatal (hypothyreosis), 17-OH progesterone (AGS), galactose (galactosemia), galactose-uridyl transferase (galacto semia), biotinidase (biotinidase ), phenylalanine
For Your Baby s Health Department of Health
 Newborn Screening For Your Baby s Health Department of Health Why is my baby tested? To help make sure your baby will be as healthy as possible. The blood test provides important information about your
Newborn Screening For Your Baby s Health Department of Health Why is my baby tested? To help make sure your baby will be as healthy as possible. The blood test provides important information about your
All diseases on Foresight
 All diseases on Foresight Disease 11-Beta-Hydroxylase- Deficient Congenital Adrenal Hyperplasia 21-Hydroxylase-Deficient Congenital Adrenal Hyperplasia 3-Hydroxy-3-Methylglutaryl- CoA Lyase Deficiency
All diseases on Foresight Disease 11-Beta-Hydroxylase- Deficient Congenital Adrenal Hyperplasia 21-Hydroxylase-Deficient Congenital Adrenal Hyperplasia 3-Hydroxy-3-Methylglutaryl- CoA Lyase Deficiency
A. disorders of amino acid metabolism classical phenylketonuria and hyperphenylalaninemia
 OMIM # FULL NAME A. disorders of amino acid metabolism 1 261600 classical phenylketonuria and hyperphenylalaninemia 2 261640 phenylketonuria due to PTPS deficiency 3 261630 phenylketonuria due to DHPR
OMIM # FULL NAME A. disorders of amino acid metabolism 1 261600 classical phenylketonuria and hyperphenylalaninemia 2 261640 phenylketonuria due to PTPS deficiency 3 261630 phenylketonuria due to DHPR
Clinical Approach to Diagnosis of Lysosomal Storage Diseases
 Clinical Approach to Diagnosis of Lysosomal Storage Diseases M. Rohrbach, MD, PhD FMH Pädiatrie und FMH Medizinische Genetik Abteilung Stoffwechsel Universitätskinderklinik Zürich Lysosomal storage disorders
Clinical Approach to Diagnosis of Lysosomal Storage Diseases M. Rohrbach, MD, PhD FMH Pädiatrie und FMH Medizinische Genetik Abteilung Stoffwechsel Universitätskinderklinik Zürich Lysosomal storage disorders
The spectrum and outcome of the. neonates with inborn errors of. metabolism at a tertiary care hospital
 The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
Introduction to Organic Acidemias. Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.
 Introduction to Organic Acidemias Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.2014 A Brief Historical Overview Garrod, Archibald E. 1902. The Incidence of
Introduction to Organic Acidemias Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.2014 A Brief Historical Overview Garrod, Archibald E. 1902. The Incidence of
Newborn Screening: Blood Spot Disorders
 Newborn Screening: Blood Spot Disorders Arizona s Newborn Screening Program Program Overview Panel of Disorders Disorder Descriptions Program Components Hospitals ADHS Lab ADHS Follow-up ADHS Billing Medical
Newborn Screening: Blood Spot Disorders Arizona s Newborn Screening Program Program Overview Panel of Disorders Disorder Descriptions Program Components Hospitals ADHS Lab ADHS Follow-up ADHS Billing Medical
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis)
 Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Inborn Errors of Metabolism (IEM)
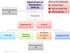 Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
Diagnose a broad range of metabolic disorders with a single test, Global MAPS
 PEDIATRIC Assessing or diagnosing a metabolic disorder commonly requires several tests. Global Metabolomic Assisted Pathway Screen, commonly known as Global MAPS, is a unifying test for analyzing hundreds
PEDIATRIC Assessing or diagnosing a metabolic disorder commonly requires several tests. Global Metabolomic Assisted Pathway Screen, commonly known as Global MAPS, is a unifying test for analyzing hundreds
Positive Newborn Screens: What do you do next?
 Positive Newborn Screens: What do you do next? James B. Gibson, MD, Ph.D. Biochemical Geneticist at Specially for Children Clinical Associate Professor of Pediatrics UTHSCSA Carla R. Scott, MD Pediatric
Positive Newborn Screens: What do you do next? James B. Gibson, MD, Ph.D. Biochemical Geneticist at Specially for Children Clinical Associate Professor of Pediatrics UTHSCSA Carla R. Scott, MD Pediatric
Newborn Screening in Manitoba. Information for Health Care Providers
 Newborn Screening in Manitoba Information for Health Care Providers Newborn screening: a healthy start leads to a healthier life Health care professionals have provided newborn screening for phenylketonuria
Newborn Screening in Manitoba Information for Health Care Providers Newborn screening: a healthy start leads to a healthier life Health care professionals have provided newborn screening for phenylketonuria
When users open the application interface, the starting page presents a disclaimer. Upon agreeing to the
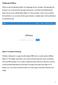 Walkthrough of IEMbase When users open the application interface, the starting page presents a disclaimer. Upon agreeing to the disclaimer, users are directed to the main page, which presents a search
Walkthrough of IEMbase When users open the application interface, the starting page presents a disclaimer. Upon agreeing to the disclaimer, users are directed to the main page, which presents a search
Metabolic Disorders. Chapter Thomson - Wadsworth
 Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism
 Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism Patricia Jones, PhD DABCC FACB UT Southwestern Medical Center Children s Medical Center Dallas, Texas Learning Objectives Justify
Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism Patricia Jones, PhD DABCC FACB UT Southwestern Medical Center Children s Medical Center Dallas, Texas Learning Objectives Justify
Overview of Newborn Screening, Potential Uses of Residual Dried Blood Spots, and Protection of Privacy
 Overview of Newborn Screening, Potential Uses of Residual Dried Blood Spots, and Protection of Privacy Alan R. Fleischman, M.D. Senior Vice President and Medical Director Chair, Federal Advisory Committee,
Overview of Newborn Screening, Potential Uses of Residual Dried Blood Spots, and Protection of Privacy Alan R. Fleischman, M.D. Senior Vice President and Medical Director Chair, Federal Advisory Committee,
Medical Foods for Inborn Errors of Metabolism
 Medical Foods for Inborn Errors of Metabolism Policy Number: Original Effective Date: MM.02.014 02/18/2000 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 08/23/2013 Section: Medicine Place(s)
Medical Foods for Inborn Errors of Metabolism Policy Number: Original Effective Date: MM.02.014 02/18/2000 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 08/23/2013 Section: Medicine Place(s)
MISSOURI DEPARTMENT OF HEALTH AND SENIOR SERVICES
 NEWBORN SCREENING Protecting your newborn MISSOURI DEPARTMENT OF HEALTH AND SENIOR SERVICES [ 1 ] NEWBORN SCREENING [ 2 ] FREQUENTLY ASKED QUESTIONS [ 4 ] DISORDERS INCLUDED IN NEWBORN SCREENING [ 12 ]
NEWBORN SCREENING Protecting your newborn MISSOURI DEPARTMENT OF HEALTH AND SENIOR SERVICES [ 1 ] NEWBORN SCREENING [ 2 ] FREQUENTLY ASKED QUESTIONS [ 4 ] DISORDERS INCLUDED IN NEWBORN SCREENING [ 12 ]
Inborn Error Of Metabolism :
 Inborn Error Of Metabolism : Inborn Error Of Metabolism inborn error of metabolism are a large group of hereditary biochemical diseases in which specific gene mutation cause abnormal or missing proteins
Inborn Error Of Metabolism : Inborn Error Of Metabolism inborn error of metabolism are a large group of hereditary biochemical diseases in which specific gene mutation cause abnormal or missing proteins
Training Syllabus CLINICAL SYLLABUS
 Training Syllabus CLINICAL SYLLABUS SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated July 2006 This syllabus is intended as a guide. Whilst the training should be comprehensive,
Training Syllabus CLINICAL SYLLABUS SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated July 2006 This syllabus is intended as a guide. Whilst the training should be comprehensive,
Testing Strategy for Inborn Errors of Metabolism in the Neonate Aditi I. Dagli, Roberto T. Zori and Bryce A. Heese. DOI: /neo.
 Testing Strategy for Inborn Errors of Metabolism in the Neonate Aditi I. Dagli, Roberto T. Zori and Bryce A. Heese Neoreviews 2008;9;e291 DOI: 10.1542/neo.9-7-e291 The online version of this article, along
Testing Strategy for Inborn Errors of Metabolism in the Neonate Aditi I. Dagli, Roberto T. Zori and Bryce A. Heese Neoreviews 2008;9;e291 DOI: 10.1542/neo.9-7-e291 The online version of this article, along
HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up
 HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up Dr. Josephine Chong Clinical Professional Consultant Centre of Inborn Errors
HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up Dr. Josephine Chong Clinical Professional Consultant Centre of Inborn Errors
[R23-13-MET/HRG] STATE OF RHODE ISLAND AND PROVIDENCE PLANTATIONS DEPARTMENT OF HEALTH. February October October 1992 (E) September 1995
![[R23-13-MET/HRG] STATE OF RHODE ISLAND AND PROVIDENCE PLANTATIONS DEPARTMENT OF HEALTH. February October October 1992 (E) September 1995 [R23-13-MET/HRG] STATE OF RHODE ISLAND AND PROVIDENCE PLANTATIONS DEPARTMENT OF HEALTH. February October October 1992 (E) September 1995](/thumbs/95/122505027.jpg) RULES AND REGULATIONS PERTAINING TO THE NEWBORN METABOLIC, ENDOCRINE, AND HEMOGLOBINOPATHY SCREENING PROGRAM AND THE NEWBORN HEARING LOSS SCREENING PROGRAM [R23-13-MET/HRG] STATE OF RHODE ISLAND AND PROVIDENCE
RULES AND REGULATIONS PERTAINING TO THE NEWBORN METABOLIC, ENDOCRINE, AND HEMOGLOBINOPATHY SCREENING PROGRAM AND THE NEWBORN HEARING LOSS SCREENING PROGRAM [R23-13-MET/HRG] STATE OF RHODE ISLAND AND PROVIDENCE
Newborn Screening: Focus on Treatment
 Newborn Screening: Focus on Treatment Alan R. Fleischman, M.D. Senior Vice President and Medical Director March of Dimes National Conference of State Legislatures July 21, 2008 Newborn Screening: A Public
Newborn Screening: Focus on Treatment Alan R. Fleischman, M.D. Senior Vice President and Medical Director March of Dimes National Conference of State Legislatures July 21, 2008 Newborn Screening: A Public
Metabolic Disorders Screened Overseas but not Screened in Australia Condition Features Inherited Diagnosis Treatment Newborn Screen
 Metabolic Disorders ed Overseas but not ed in Australia Biotinidase Deficiency Severe form causes seizures & delay Biotin can prevent complications NZ, USA Tyrosinaemia Type I Coma & death before age 10
Metabolic Disorders ed Overseas but not ed in Australia Biotinidase Deficiency Severe form causes seizures & delay Biotin can prevent complications NZ, USA Tyrosinaemia Type I Coma & death before age 10
Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition
 Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition Introduction Review clinical findings that may be suspicious of a metabolic
Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition Introduction Review clinical findings that may be suspicious of a metabolic
NEWBORN SCREENING. health.mo.gov/newbornscreening MISSOURI DEPARTMENT OF HEALTH AND SENIOR SERVICES
 NEWBORN SCREENING health.mo.gov/newbornscreening MISSOURI DEPARTMENT OF HEALTH AND SENIOR SERVICES Table of Contents NEWBORN SCREENING...1 FREQUENTLY ASKED QUESTIONS...2 DISORDERS INCLUDED IN NEWBORN SCREENING...4
NEWBORN SCREENING health.mo.gov/newbornscreening MISSOURI DEPARTMENT OF HEALTH AND SENIOR SERVICES Table of Contents NEWBORN SCREENING...1 FREQUENTLY ASKED QUESTIONS...2 DISORDERS INCLUDED IN NEWBORN SCREENING...4
A Lawyer s Perspective on Genetic Screening Performed by Cryobanks
 A Lawyer s Perspective on Genetic Screening Performed by Cryobanks As a lawyer practicing in the area of sperm bank litigation, I have, unfortunately, represented too many couples that conceived a child
A Lawyer s Perspective on Genetic Screening Performed by Cryobanks As a lawyer practicing in the area of sperm bank litigation, I have, unfortunately, represented too many couples that conceived a child
Beyond the case for NBS in South Africa. Chris Vorster 28/05/2016
 Beyond the case for NBS in South Africa Chris Vorster 28/05/2016 The case for NBS in SA Economic justification Cost Utility analysis = Cost/QALY GDP/Capita Immediate implementation (WHO) Political justification
Beyond the case for NBS in South Africa Chris Vorster 28/05/2016 The case for NBS in SA Economic justification Cost Utility analysis = Cost/QALY GDP/Capita Immediate implementation (WHO) Political justification
Newborn screening for congenital metabolic diseases Optional out-of-pocket tests Information Sheet
 Newborn screening for congenital metabolic diseases Optional out-of-pocket tests Information Sheet Website:www.tipn.org.tw Telephone:(02)85962050 Ext. 401-403 Service line:(02)85962065 Fax:(02)85962067
Newborn screening for congenital metabolic diseases Optional out-of-pocket tests Information Sheet Website:www.tipn.org.tw Telephone:(02)85962050 Ext. 401-403 Service line:(02)85962065 Fax:(02)85962067
HEREDITARY METABOLIC DISEASES
 HEREDITARY METABOLIC DISEASES Particular risk factors are: Advanced maternal age (e.g. Down's syndrome) Family history of inherited diseases (e.g. fragile X syndrome, Huntington's chorea) Previous child
HEREDITARY METABOLIC DISEASES Particular risk factors are: Advanced maternal age (e.g. Down's syndrome) Family history of inherited diseases (e.g. fragile X syndrome, Huntington's chorea) Previous child
The role of the laboratory in diagnosing lysosomal disorders
 The role of the laboratory in diagnosing lysosomal disorders Dr Guy Besley, formerly Willink Biochemical Genetics Unit, Manchester Children s Hospital, Manchester M27 4HA, UK. Lysosomal disorders What
The role of the laboratory in diagnosing lysosomal disorders Dr Guy Besley, formerly Willink Biochemical Genetics Unit, Manchester Children s Hospital, Manchester M27 4HA, UK. Lysosomal disorders What
Inborn Errors of Metabolism Clinical Approach to Diagnosis and Treatment
 Case Scenario: 15 year old girl presented in ED with aggressive behaviour and hallucinations. No associated fever, vomiting, seizures or developmental concerns Previously well Inborn Errors of Metabolism
Case Scenario: 15 year old girl presented in ED with aggressive behaviour and hallucinations. No associated fever, vomiting, seizures or developmental concerns Previously well Inborn Errors of Metabolism
Metabolic Changes in ASD. Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius
 Metabolic Changes in ASD Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius 12 patients 3 Autism: Ages 3/3/3.7 3 PDD: Ages 3/3/6 3 Asperger: Ages 6/7/15.1 3 Speech delay and Sensory Problems (SHL):
Metabolic Changes in ASD Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius 12 patients 3 Autism: Ages 3/3/3.7 3 PDD: Ages 3/3/6 3 Asperger: Ages 6/7/15.1 3 Speech delay and Sensory Problems (SHL):
NEWBORN SCREENING. in Massachusetts: Answers for You and Your Baby. University of Massachusetts Medical School
 University of Massachusetts Medical School NEWBORN SCREENING in Massachusetts: Answers for You and Your Baby New England Newborn Screening Program Biotech 4, 2nd Floor UMass Medical School 377 Plantation
University of Massachusetts Medical School NEWBORN SCREENING in Massachusetts: Answers for You and Your Baby New England Newborn Screening Program Biotech 4, 2nd Floor UMass Medical School 377 Plantation
Date of commencement: February Principal Investigator Dr. Jayesh J. Sheth CASE RECORD FORM
 ICMR-FRIGE-MULTICENTRIC LSDs Project Foundation for Research in Genetics & Endocrinology [FRIGE], FRIGE House, Jodhpur Gam road, Satellite, Ahmedabad-380015 Tel no: 079-26921414, Fax no: 079-26921415 E-mail:
ICMR-FRIGE-MULTICENTRIC LSDs Project Foundation for Research in Genetics & Endocrinology [FRIGE], FRIGE House, Jodhpur Gam road, Satellite, Ahmedabad-380015 Tel no: 079-26921414, Fax no: 079-26921415 E-mail:
Summary. Syndromic versus Etiologic. Definitions. Why does it matter? ASD=autism
 Summary It is becoming clear that multiple genes with complex interactions underlie autism spectrum (ASD). A small subset of people with ASD, however, actually suffer from rare single-gene Important to
Summary It is becoming clear that multiple genes with complex interactions underlie autism spectrum (ASD). A small subset of people with ASD, however, actually suffer from rare single-gene Important to
Inborn Errors of Metabolism in the Emergency Department. Will Davies June 2014
 Inborn Errors of Metabolism in the Emergency Department Will Davies June 2014 Inborn Errors of Metabolism in the Emergency Department Overview Although individually rare, altogether they are 1:1000-2500
Inborn Errors of Metabolism in the Emergency Department Will Davies June 2014 Inborn Errors of Metabolism in the Emergency Department Overview Although individually rare, altogether they are 1:1000-2500
What s New in Newborn Screening?
 What s New in Newborn Screening? Funded by: Illinois Department of Public Health Information on Newborn Screening Newborn screening in Illinois is mandated and administered by the Illinois Department of
What s New in Newborn Screening? Funded by: Illinois Department of Public Health Information on Newborn Screening Newborn screening in Illinois is mandated and administered by the Illinois Department of
Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD
 Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD April 24, 2017 SAP 2017 Buenos Aires Genetic disorders are rare why
Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD April 24, 2017 SAP 2017 Buenos Aires Genetic disorders are rare why
NEWBORN SCREENING. in Massachusetts: Information for You and Your Baby. University of Massachusetts Medical School
 University of Massachusetts Medical School NEWBORN SCREENING in Massachusetts: Information for You and Your Baby New England Newborn Screening Program Biotech 4, 2nd Floor UMass Medical School 377 Plantation
University of Massachusetts Medical School NEWBORN SCREENING in Massachusetts: Information for You and Your Baby New England Newborn Screening Program Biotech 4, 2nd Floor UMass Medical School 377 Plantation
Best Practice Guidelines for the Biochemical Investigation of Patients with Foetal and Neonatal Hydrops
 National Metabolic Biochemistry Network Best Practice Guidelines for the Biochemical Investigation of Patients with Foetal and Neonatal Hydrops INTRODUCTION Hydrops is defined as the presence of skin oedema
National Metabolic Biochemistry Network Best Practice Guidelines for the Biochemical Investigation of Patients with Foetal and Neonatal Hydrops INTRODUCTION Hydrops is defined as the presence of skin oedema
NEWBORN METABOLIC SCREEN, MINNESOTA
 Lab Dept: Test Name: Chemistry NEWBORN METABOLIC SCREEN, MINNESOTA General Information Lab Order Codes: Synonyms: CPT Codes: Test Includes: PKUN Newborn Screen for Hyopothyroidism, Phenylketonuria (PKU),
Lab Dept: Test Name: Chemistry NEWBORN METABOLIC SCREEN, MINNESOTA General Information Lab Order Codes: Synonyms: CPT Codes: Test Includes: PKUN Newborn Screen for Hyopothyroidism, Phenylketonuria (PKU),
What s New in Newborn Screening?
 What s New in Newborn Screening? Funded by: Illinois Department of Public Health Information on Newborn Screening Newborn screening in Illinois is administered by the Illinois Department of Public Health.
What s New in Newborn Screening? Funded by: Illinois Department of Public Health Information on Newborn Screening Newborn screening in Illinois is administered by the Illinois Department of Public Health.
Pathophysiology. Tutorial 1 Genetic Diseases
 Pathophysiology Tutorial 1 Genetic Diseases ILOs Analyze genetic pedigrees and recognize the mode of inheritance of diseases. Differentiate between patterns of inheritance based on the type of the protein
Pathophysiology Tutorial 1 Genetic Diseases ILOs Analyze genetic pedigrees and recognize the mode of inheritance of diseases. Differentiate between patterns of inheritance based on the type of the protein
PREDICAGEN LLC REPORT
 The report below is a scientific interpretation of the DNA variants (referred as RS numbers) to the customer by a third party (for example 23andMe). The report should not be considered exclusive, because
The report below is a scientific interpretation of the DNA variants (referred as RS numbers) to the customer by a third party (for example 23andMe). The report should not be considered exclusive, because
Further expansion of the neonatal screening panel in the Netherlands
 Further expansion of the neonatal screening panel in the Netherlands J.Gerard Loeber APHL-NBSGT, St.Louis (MO), USA 290216 Population Area Newborns 6.01 million 0.35:1 16.8 million 180,693 sq km 4.3:1
Further expansion of the neonatal screening panel in the Netherlands J.Gerard Loeber APHL-NBSGT, St.Louis (MO), USA 290216 Population Area Newborns 6.01 million 0.35:1 16.8 million 180,693 sq km 4.3:1
Inborn Errors of Metabolism. Metabolic Pathway. Digestion and Fasting. How is Expanded Newborn Screening Different? MS/MS. The body is a factory.
 Inborn Errors of Metabolism The body is a factory. Inborn errors of metabolism are rare genetic disorders in which the body cannot properly turn food into energy. The disorders are usually caused by defects
Inborn Errors of Metabolism The body is a factory. Inborn errors of metabolism are rare genetic disorders in which the body cannot properly turn food into energy. The disorders are usually caused by defects
COMMON INHERITED METABOLIC CONDITIONS IN SOUTH AFRICA DIAGNOSING RARE DISEASE IN GENETICALLY UNIQUE AND UNDERSTUDIED POPULATION GROUPS
 COMMON INHERITED METABOLIC CONDITIONS IN SOUTH AFRICA DIAGNOSING RARE DISEASE IN GENETICALLY UNIQUE AND UNDERSTUDIED POPULATION GROUPS S MELDAU, G VAN DER WATT INHERITED METABOLIC DISEASES GROUP UCT /
COMMON INHERITED METABOLIC CONDITIONS IN SOUTH AFRICA DIAGNOSING RARE DISEASE IN GENETICALLY UNIQUE AND UNDERSTUDIED POPULATION GROUPS S MELDAU, G VAN DER WATT INHERITED METABOLIC DISEASES GROUP UCT /
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children
 National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
(f) "Birthing center" means any facility that is licensed by the Georgia Department of Community Health as a birthing center;
 Ga. Comp. R. & Regs. r. 511-5-5-.02 Definitions Rule 511-5-5-.02. Definitions (a) "Abnormal test result" is a test result from blood testing or physiologic monitoring that is outside the screening limits
Ga. Comp. R. & Regs. r. 511-5-5-.02 Definitions Rule 511-5-5-.02. Definitions (a) "Abnormal test result" is a test result from blood testing or physiologic monitoring that is outside the screening limits
Urea Cycle Defects. Dr Mick Henderson. Biochemical Genetics Leeds Teaching Hospitals Trust. MetBioNet IEM Introductory Training
 Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
Presentation and investigation of mitochondrial disease in children
 Presentation and investigation of mitochondrial disease in children Andrew Morris Willink Unit, Manchester Mitochondrial function Carbohydrate Fat Respiratory chain Energy Mitochondria are the product
Presentation and investigation of mitochondrial disease in children Andrew Morris Willink Unit, Manchester Mitochondrial function Carbohydrate Fat Respiratory chain Energy Mitochondria are the product
Considerations in Choosing Screening Conditions: One (US) Approach
 22 Plenary Considerations in Choosing Screening Conditions: One (US) Approach Bradford L Therrell Jr, 1,2 MS, PhD Abstract The lack of a national policy on newborn screening (NBS) in the United States
22 Plenary Considerations in Choosing Screening Conditions: One (US) Approach Bradford L Therrell Jr, 1,2 MS, PhD Abstract The lack of a national policy on newborn screening (NBS) in the United States
Title: Assessing Recommendations Related To Timeliness of Newborn Screening
 Title: Assessing Recommendations Related To Timeliness of Newborn Screening Purpose: In January 2014, the Secretary s Discretionary Advisory Committee on Heritable Diseases on Newborns and Children (Committee)
Title: Assessing Recommendations Related To Timeliness of Newborn Screening Purpose: In January 2014, the Secretary s Discretionary Advisory Committee on Heritable Diseases on Newborns and Children (Committee)
Doenças Hereditárias do Metabolismo: de Garrod às Ciências Ómicas
 Doenças Hereditárias do Metabolismo: de Garrod às Ciências Ómicas Isabel Tavares de Almeida Lab. Met & Gen. FFULisboa XIII Curso Básico de Doenças Hereditárias do Metabolismo Coimbra, 5 a 7 Dezembro 2016
Doenças Hereditárias do Metabolismo: de Garrod às Ciências Ómicas Isabel Tavares de Almeida Lab. Met & Gen. FFULisboa XIII Curso Básico de Doenças Hereditárias do Metabolismo Coimbra, 5 a 7 Dezembro 2016
A Guide for Prenatal Educators
 A Guide for Prenatal Educators Why Teach Newborn Screening This booklet is designed to make it easy for you, a prenatal educator, to effectively inform expectant parents about newborn screening. All of
A Guide for Prenatal Educators Why Teach Newborn Screening This booklet is designed to make it easy for you, a prenatal educator, to effectively inform expectant parents about newborn screening. All of
Dysmorphology Guy Besley
 Dysmorphology Guy Besley Willink Biochemical Genetics Unit, Manchester Children s s Hospital Dysmorphic presentation Congenital malformation Disorder of embryogenesis Intrauterine insult infection; chromosomal/genetic
Dysmorphology Guy Besley Willink Biochemical Genetics Unit, Manchester Children s s Hospital Dysmorphic presentation Congenital malformation Disorder of embryogenesis Intrauterine insult infection; chromosomal/genetic
Genetic Diseases. SCPA202: Basic Pathology
 Genetic Diseases SCPA202: Basic Pathology Amornrat N. Jensen, Ph.D. Department of Pathobiology School of Science, Mahidol University amornrat.nar@mahidol.ac.th Genetic disease An illness caused by abnormalities
Genetic Diseases SCPA202: Basic Pathology Amornrat N. Jensen, Ph.D. Department of Pathobiology School of Science, Mahidol University amornrat.nar@mahidol.ac.th Genetic disease An illness caused by abnormalities
SELECTIVE VULNERABILITY (HYPOXIA AND HYPOGLYCEMIA)
 DEFICIENCY OF METABOLITE -HYPOXIA AND HYPOGLYCEMIA -HYPOVITAMINOSIS SELECTIVE VULNERABILITY (HYPOXIA AND HYPOGLYCEMIA) -SPECIFIC CELL TYPE NEURONS>OLIGODENDROCYTES>ASTROCYTES -SPECIFIC BRAIN REGION PYRAMIDAL
DEFICIENCY OF METABOLITE -HYPOXIA AND HYPOGLYCEMIA -HYPOVITAMINOSIS SELECTIVE VULNERABILITY (HYPOXIA AND HYPOGLYCEMIA) -SPECIFIC CELL TYPE NEURONS>OLIGODENDROCYTES>ASTROCYTES -SPECIFIC BRAIN REGION PYRAMIDAL
CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE. Bwee Tien Poll-The Amsterdam UMC The Netherlands
 CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE Bwee Tien Poll-The Amsterdam UMC The Netherlands FRAMEWORK OF PRINCIPALS 1. Problem-oriented clinical approach 2. Biomarkers in plasma, urine, CSF
CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE Bwee Tien Poll-The Amsterdam UMC The Netherlands FRAMEWORK OF PRINCIPALS 1. Problem-oriented clinical approach 2. Biomarkers in plasma, urine, CSF
FABRY DISEASE 12/30/2012. Ataxia-Telangiectasia. Ophthalmologic Signs of Genetic Neurological Disease
 Ophthalmologic Signs of Genetic Neurological Disease ES ROACH,MD. Ophthalmologic Signs of Genetic Neurological Disease Conjunctival lesions Corneal lesions Lesions of iris & lens Retinal vascular lesions
Ophthalmologic Signs of Genetic Neurological Disease ES ROACH,MD. Ophthalmologic Signs of Genetic Neurological Disease Conjunctival lesions Corneal lesions Lesions of iris & lens Retinal vascular lesions
The Compelling Benefits of Routine 2 nd NBS: A Fifteen-Year Review in Washington State. Saving lives with a simple blood spot
 The Compelling Benefits of Routine 2 nd NBS: A Fifteen-Year Review in Washington State Caroline T. Nucup-Villaruz, MD Primary Author NBS Consultant - Disorder FU Santosh Shaunak Co-Author & Presenter Laboratory
The Compelling Benefits of Routine 2 nd NBS: A Fifteen-Year Review in Washington State Caroline T. Nucup-Villaruz, MD Primary Author NBS Consultant - Disorder FU Santosh Shaunak Co-Author & Presenter Laboratory
23andMe Reports GENETIC HEALTH RISK REPORTS. Increased risk for breast and ovarian cancer. function
 1 23andMe Reports GENETIC HEALTH RISK REPORTS BRCA1/BRCA2 Late-Onset Alzheimer's Disease Parkinson's Disease Age-Related Macular Degeneration Alpha-1 Antitrypsin Deficiency Celiac Disease G6PD Deficiency
1 23andMe Reports GENETIC HEALTH RISK REPORTS BRCA1/BRCA2 Late-Onset Alzheimer's Disease Parkinson's Disease Age-Related Macular Degeneration Alpha-1 Antitrypsin Deficiency Celiac Disease G6PD Deficiency
Oxidation of Long Chain Fatty Acids
 Oxidation of Long Chain Fatty Acids Dr NC Bird Oxidation of long chain fatty acids is the primary source of energy supply in man and animals. Hibernating animals utilise fat stores to maintain body heat,
Oxidation of Long Chain Fatty Acids Dr NC Bird Oxidation of long chain fatty acids is the primary source of energy supply in man and animals. Hibernating animals utilise fat stores to maintain body heat,
SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE
 SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated December 2014: Vassili Valayannopoulos and Andrew Morris Paediatrics is an independent medical specialty based on the knowledge and
SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated December 2014: Vassili Valayannopoulos and Andrew Morris Paediatrics is an independent medical specialty based on the knowledge and
GUIDE TO NEWBORN SCREENING PROGRAMME
 \ GUIDE TO NEWBORN SCREENING PROGRAMME 1 MEDILAB PROFILE MEDILAB, the leading independent provider of Clinical Laboratory Diagnostic Services in Cyprus, was established in 1980 by Mr. C. Pavlides and has
\ GUIDE TO NEWBORN SCREENING PROGRAMME 1 MEDILAB PROFILE MEDILAB, the leading independent provider of Clinical Laboratory Diagnostic Services in Cyprus, was established in 1980 by Mr. C. Pavlides and has
Genetic Testing FOR DISEASES OF INCREASED FREQUENCY IN THE ASHKENAZI JEWISH POPULATION
 Carrier Screening and Diagnostic Testing for the Ashkenazi Jewish Population Genetic Testing FOR DISEASES OF INCREASED FREQUENCY IN THE ASHKENAZI JEWISH POPULATION Our Science. Your Care. An extensive
Carrier Screening and Diagnostic Testing for the Ashkenazi Jewish Population Genetic Testing FOR DISEASES OF INCREASED FREQUENCY IN THE ASHKENAZI JEWISH POPULATION Our Science. Your Care. An extensive
Newborn Screening in Washington State Saving lives with a simple blood spot
 Newborn Screening in Washington State Saving lives with a simple blood spot Ashleigh Ragsdale, MPH Gauri Gupta, MScPH Objectives Newborn Screening Overview Process and Law Completing Collection Cards Video
Newborn Screening in Washington State Saving lives with a simple blood spot Ashleigh Ragsdale, MPH Gauri Gupta, MScPH Objectives Newborn Screening Overview Process and Law Completing Collection Cards Video
D evelopmental disabilities occur in approximately
 1128 REVIEW Developmental delay: when to suspect and how to investigate for an inborn error of metabolism M A Cleary, A Green... The purpose of this review is to provide a practical guideline on the suspicion
1128 REVIEW Developmental delay: when to suspect and how to investigate for an inborn error of metabolism M A Cleary, A Green... The purpose of this review is to provide a practical guideline on the suspicion
Fatty Acid Oxidation Disorders- an update. Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London
 Fatty Acid Oxidation Disorders- an update Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London An update. Overview of metabolism Clinical presentation and outcome Diagnostic
Fatty Acid Oxidation Disorders- an update Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London An update. Overview of metabolism Clinical presentation and outcome Diagnostic
Amino Acid Oxidation and the Urea Cycle
 Amino Acid Oxidation and the Urea Cycle Amino Acids: Final class of biomolecules whose oxidation contributes significantly to the generation of energy Undergo oxidation in three metabolic circumstances
Amino Acid Oxidation and the Urea Cycle Amino Acids: Final class of biomolecules whose oxidation contributes significantly to the generation of energy Undergo oxidation in three metabolic circumstances
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Genetics
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Genetics 1. GOAL: Understand the role of the pediatrician in preventing genetic disease, and in counseling and screening
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Genetics 1. GOAL: Understand the role of the pediatrician in preventing genetic disease, and in counseling and screening
Inborn Errors of Metabolism (IEM) An Indian Perspective
 Symposium on Fest - Schrift for Late Dr. P.M. Udani Inborn Errors of Metabolism (IEM) An Indian Perspective N.B. Kumta Department of Pediatrics, KEM Hospital, Mumbai, Maharashtra, India. Abstract. The
Symposium on Fest - Schrift for Late Dr. P.M. Udani Inborn Errors of Metabolism (IEM) An Indian Perspective N.B. Kumta Department of Pediatrics, KEM Hospital, Mumbai, Maharashtra, India. Abstract. The
Metabolic Emergencies and the Pediatrician
 Metabolic Emergencies and the Pediatrician Stephen G. Kahler, MD Professor of Pediatrics Section of Genetics and Metabolism, UAMS and ACH Hot Springs, AR March 8, 2012 INHERITED METABOLIC DISORDERS HOW
Metabolic Emergencies and the Pediatrician Stephen G. Kahler, MD Professor of Pediatrics Section of Genetics and Metabolism, UAMS and ACH Hot Springs, AR March 8, 2012 INHERITED METABOLIC DISORDERS HOW
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE
 THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
Table S5. Disease pairs that have a significant comorbidity and are connected in either KEGG or BiGG database
 Table S5. Disease pairs that have a significant comorbidity and are connected in either KEGG or BiGG database Coincide nce Expected coincidence Maximum possible comorbidity Disease1 Disease2 Link(KEGG)
Table S5. Disease pairs that have a significant comorbidity and are connected in either KEGG or BiGG database Coincide nce Expected coincidence Maximum possible comorbidity Disease1 Disease2 Link(KEGG)
Most common metabolic disorders in childhood. Neonatal screening and diagnostic approach to the. Inborn errors of metabolism (IEM)
 Department of Pediatrics and Developmental Disorders Medical University of Bialystok Most common metabolic disorders in childhood. Neonatal screening and diagnostic approach to the inborn errors of metabolism
Department of Pediatrics and Developmental Disorders Medical University of Bialystok Most common metabolic disorders in childhood. Neonatal screening and diagnostic approach to the inborn errors of metabolism
Newborn Screening: What s New?
 Newborn Screening: What s New? Patricia M. Jones, PhD (Department of Pathology, University of Texas Southwestern Medical Center and Children s Medical Center of Dallas, Dallas, TX) DOI: 10.1309/LMOOXWVPSM5FC3B6
Newborn Screening: What s New? Patricia M. Jones, PhD (Department of Pathology, University of Texas Southwestern Medical Center and Children s Medical Center of Dallas, Dallas, TX) DOI: 10.1309/LMOOXWVPSM5FC3B6
CLINICAL AND HUMAN TESTING
 CLINICAL AND HUMAN TESTING CARRIER SCREENING FOR FAMILY PLANNING Let knowledge be your guide. Identify genetic conditions before or during a pregnancy to help predict the chances of having a child with
CLINICAL AND HUMAN TESTING CARRIER SCREENING FOR FAMILY PLANNING Let knowledge be your guide. Identify genetic conditions before or during a pregnancy to help predict the chances of having a child with
The laboratory investigation of lactic acidaemia. J Bonham/T Laing
 The laboratory investigation of lactic acidaemia J Bonham/T Laing Reference range Typical ranges for blood lactate are: Newborn 0.3-2.2 mmol/l Nielsen J et al1 1994 1-12mo 0.9-1.8 mmol/l Bonnefont et al
The laboratory investigation of lactic acidaemia J Bonham/T Laing Reference range Typical ranges for blood lactate are: Newborn 0.3-2.2 mmol/l Nielsen J et al1 1994 1-12mo 0.9-1.8 mmol/l Bonnefont et al
Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff
 Training Syllabus LABORATORY SYLLABUS Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff This syllabus is intended as a guide. Whilst the training
Training Syllabus LABORATORY SYLLABUS Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff This syllabus is intended as a guide. Whilst the training
PROTEIN METABOLISM: SPECIFIC WAYS OF AMINO ACIDS CATABOLISM AND SYNTHESIS
 PROTEIN METABOLISM: SPECIFIC WAYS OF AMINO ACIDS CATABOLISM AND SYNTHESIS SPECIFIC WAYS OF AMINO ACID CATABOLISM After removing of amino group the carbon skeletons of amino acids are transformed into metabolic
PROTEIN METABOLISM: SPECIFIC WAYS OF AMINO ACIDS CATABOLISM AND SYNTHESIS SPECIFIC WAYS OF AMINO ACID CATABOLISM After removing of amino group the carbon skeletons of amino acids are transformed into metabolic
Inborn error of metabolism
 Inborn error of metabolism The lecture is given by Dr Kefah Al qa qa, Consultant metabolic pediatrician, in Queen Rania Al Abdulla children hospital, on Thursday 11/12/2014. Let s tart Metabolism: refers
Inborn error of metabolism The lecture is given by Dr Kefah Al qa qa, Consultant metabolic pediatrician, in Queen Rania Al Abdulla children hospital, on Thursday 11/12/2014. Let s tart Metabolism: refers
N.I.R.M.A.N. Dr. ANIL B. JALAN (MD DCH MCPS) Test list Oct 2017
 Tests and Profiles Tests Method Sample Needed TAT Genetic Consultation / - All samples to be sent at 2 8 C. Counseling 1 Urine MRST - 15 ml Urine 24 hrs 2 Sr. Ammonia, Lactate, Sugar Fuji Dry Chem 2 ml
Tests and Profiles Tests Method Sample Needed TAT Genetic Consultation / - All samples to be sent at 2 8 C. Counseling 1 Urine MRST - 15 ml Urine 24 hrs 2 Sr. Ammonia, Lactate, Sugar Fuji Dry Chem 2 ml
Metabolism of pentoses, glycogen, fructose and galactose. Jana Novotna
 Metabolism of pentoses, glycogen, fructose and galactose Jana Novotna 1. The Pentose Phosphate Pathway The pentose phosphate pathway (PPP): (hexose monophosphate or 6-phosphogluconate patway) Process that
Metabolism of pentoses, glycogen, fructose and galactose Jana Novotna 1. The Pentose Phosphate Pathway The pentose phosphate pathway (PPP): (hexose monophosphate or 6-phosphogluconate patway) Process that
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review -
 Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital
 e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital Fatty Acids Fatty acids are a major source of energy and body fat is an energy dense material. They
e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital Fatty Acids Fatty acids are a major source of energy and body fat is an energy dense material. They
Neonatal manifestations of lysosomal storage diseases
 Neonatal manifestations of lysosomal storage diseases Nadia ALhashmi MD Metabolic &genetic disorder Royal hospital 2 nd Oman international pediatric and neonatal conference 13 th -15 th April 2017 Muscat
Neonatal manifestations of lysosomal storage diseases Nadia ALhashmi MD Metabolic &genetic disorder Royal hospital 2 nd Oman international pediatric and neonatal conference 13 th -15 th April 2017 Muscat
Acute Management of Sick Infants with Suspected Inborn Errors of Metabolism
 Indian J Pediatr (July 2011) 78(7):854 859 DOI 10.1007/s12098-011-0422-0 SYMPOSIUM ON PICU PROTOCOLS OF AIIMS Acute Management of Sick Infants with Suspected Inborn Errors of Metabolism Neerja Gupta Madhulika
Indian J Pediatr (July 2011) 78(7):854 859 DOI 10.1007/s12098-011-0422-0 SYMPOSIUM ON PICU PROTOCOLS OF AIIMS Acute Management of Sick Infants with Suspected Inborn Errors of Metabolism Neerja Gupta Madhulika
Inborn errors of metabolism
 ESPEN Congress Nice 2010 From child to adult nutrition Inborn errors of metabolism Pascal Crenn Inborn errors of metabolism: from child to adult Pascal Crenn Hôpital Raymond Poincaré 92380 Garches. France
ESPEN Congress Nice 2010 From child to adult nutrition Inborn errors of metabolism Pascal Crenn Inborn errors of metabolism: from child to adult Pascal Crenn Hôpital Raymond Poincaré 92380 Garches. France
BIOTIN (BIOTINIDASE) DEFICIENCY Marc E. Tischler, PhD; University of Arizona
 BIOTIN (BIOTINIDASE) DEFICIENCY Marc E. Tischler, PhD; University of Arizona BIOTIN (BIOTINIDASE) DEFICIENCY biotin in the body is recycled by its removal from carboxylase enzymes to which it is attached
BIOTIN (BIOTINIDASE) DEFICIENCY Marc E. Tischler, PhD; University of Arizona BIOTIN (BIOTINIDASE) DEFICIENCY biotin in the body is recycled by its removal from carboxylase enzymes to which it is attached
Assessing the follow-up of BART hemoglobin reported by the Wisconsin Newborn Screening Laboratory
 Assessing the follow-up of BART hemoglobin reported by the Wisconsin Newborn Screening Laboratory Bao Yang MPH Candidate Background The Wisconsin Newborn Screening (NBS) Laboratory screens 70,000 babies
Assessing the follow-up of BART hemoglobin reported by the Wisconsin Newborn Screening Laboratory Bao Yang MPH Candidate Background The Wisconsin Newborn Screening (NBS) Laboratory screens 70,000 babies
The Israeli population carrier screening program. Joël Zlotogora MD, PhD Hadassah medical school Hebrew University Jerusalem
 The Israeli population carrier screening program Joël Zlotogora MD, PhD Hadassah medical school Hebrew University Jerusalem The Israeli population 2015 8,134,500 inhabitants Jews (75.1%) Ashkenazi, non
The Israeli population carrier screening program Joël Zlotogora MD, PhD Hadassah medical school Hebrew University Jerusalem The Israeli population 2015 8,134,500 inhabitants Jews (75.1%) Ashkenazi, non
