To protect patients exhibiting signs and symptoms of spinal injuries and those who have the potential for spinal injuries.
|
|
|
- Bernice Woods
- 5 years ago
- Views:
Transcription
1 POLICY T1 SPINAL MOTION RESTRICTION Effective Date: January 1, 2017 Last Review Date: January 1, 2017 New Policy Next Review Date: January 2019 Purpose: To protect patients exhibiting signs and symptoms of spinal injuries and those who have the potential for spinal injuries. Introduction: The term Spinal Motion Restriction best describes the procedure used to care for patients with possible spinal injuries. This includes A) Reduction of gross motor movement by the patient, B) Prevention of duplicating the damaging mechanism to the spine, and C) Regular reassessment of the motor, vascular, and sensory functions. This protocol has not been composed to clear patients who may or may not have spinal injuries in the field. This policy seeks to provide an evidence-based approach (whenever possible) that directs the careful practice of Spinal Motion Restriction through set criteria. This may include modified positioning for patients that have experienced traumatic injuries. Place these patients in Spinal Motion Restriction when the benefits outweigh the risks. When the benefits do not outweigh the risks, patients should not incur clinically unnecessary immobilization with hard collars and back boards based on tradition alone. The need for and degree of restriction or immobilization of the neck and spine should be assessed in every patient with any degree of traumatic injury. The utilization of back boards/long spine boards should be for patient movement to the stretcher and for those patients who exhibit signs and symptoms of spinal injury. Maintenance of in-line spinal alignment when moving the patient and appropriately securing them to the transport stretcher remains an important component of Spinal Motion Restriction. Spinal Injury Assessment: If a spinal injury is suspected (to the spinal cord or spinal column) use the following in assessing the patient. 1. Language Barrier: The inability to communicate through a language the provider and patient have in common. Using family members or bystanders (third party translators) to obtain assessment findings is not an ideal situation although acceptable. It is preferred when possible to use certified translators. 2. Age Extremes: Are defined as patients that are 7 years of age or younger and the elderly. Patients in these age demographics can be prone to unreliable medical history or communicating the events leading to the injury. If these patients have suffered a mechanism of injury compatible with possible spinal injury, they should be placed in Spinal Motion Restriction. Always use extra padding in the pediatric and geriatric populations. People are considered elderly if they have anatomic and/or physiologic degradations from normal baseline. 3. Altered Mentation: Any patient that is unable to appropriately answer questions used to determine the level of orientation. The use of Glasgow Coma Scale (GCS) and AVPU (Alert, Verbal, Purposeful, and Unresponsive) should not be the only method used. This is regardless of past medical Page: 1 of 6
2 history/condition(s) where altered mentation may be a baseline to the patient. In addition, any patient that cannot remember the events leading to the injury or a reported loss of consciousness should be placed in Spinal Motion Restriction. Remember that patients with head/brain injuries and acute stress reactions are considered unreliable in their examination. 4. Alcohol and/or Drug Ingestion: Any patient suspected to have used alcohol and/or drugs (e.g. narcotics, benzodiazepines, barbiturates, marijuana, and cocaine) should be considered at high risk for the potential of spinal injury with the appropriate mechanism. The provider s impression of clinical sobriety (use caution) can help guide whether the patient will be placed in Spinal Motion Restriction if they have suffered a mechanism of injury compatible with a possible spinal injury. Clinical sobriety is based upon the provider s judgement. There is no hard rule for what constitutes clinical sobriety. If there are questions or concerns the provider needs to contact the base hospital and/or their supervisor for guidance. Are there signs of impairment that limits the patient s capacity to make decisions and give a proper examination? 5. Neck, Spine, or Paraspinal Pain or Tenderness: Any patient that presents with pain or palpable tenderness in the spinal area from the base of the skull to the coccyx or paraspinal (adjacent to the spinal column) areas after suffering a mechanism of injury compatible with possible spinal injury, are to be placed in Spinal Motion Restriction. Don t force non-cooperative or combative patients into Spinal Motion Restriction or traditional spinal immobilization. 6. Spinal Deformities on Exam: When a deformity is found in the spinal area from the base of the skull to the coccyx that could have resulted from the sustained traumatic event, patients are to be placed in Spinal Motion Restriction. 7. Decreased Range of Motion/Sensation: Any patient that present with gross motor deficits, decreased or lost range of motion, numbness or tingling to any of the extremities after suffering a mechanism of injury compatible with a possible spinal injury, are to be placed in Spinal Motion Restriction. 8. Distracting Pain: Any injury not related to the potential spinal trauma that causes the patient not to focus on the provider s examination and/or questioning. The provider must use their best judgment when an injury exists that is taking away from the examination of the spinal area. 9. Trauma Criteria: If a patient meets trauma triage criteria apply traditional spinal immobilization that includes hard backboard. Please ensure that appropriate cushioning and padding are placed. An example is the kyphotic elderly patient that unless modified the spinal immobilization can cause greater harm than good. If there is concern that traditional spinal immobilization will cause undue harm, then contact base hospital for advice regarding modification. Remember that SMR (Spinal Motion Restriction) does not equal Traditional Spinal Immobilization with LSB (Long Spine Board). Spinal Examination Procedure: 1. This procedure details the spinal examination process and must be used in conjunction with the above Spinal Examination Assessment. 2. Spinal Motion Restriction does not take precedence over airway, respiratory, and cardiovascular stabilization of the critical trauma patient. 3. With the patient s spine supported to limit movement, begin palpation at the base of the skull (at the midline of the spine), and continue the palpation of the spinal column to include the sacrum (base of the spine). Palpate each individual vertebrae and the paraspinal musculature. Page: 2 of 6
3 4. Provide an extrication or rigid cervical collar and continue to maintain neutral in-line immobilization (not traction). 5. Explain to the patient what actions you are going to take. Ask the patient to immediately report any pain, numbness, or other neurologic findings and answer the questions with a yes or no rather than shaking their head. Have the patient repeat back their understanding to avoid patient moving themselves. 6. Moving the head into a neutral in-line position is contraindicated if: a. There is pain upon starting movement. b. There is muscle spasm or back pressure upon attempting movement. c. Patient holds head angulated (tilted) to the side and patient cannot move head. d. The head is rigidly held to one side. e. The maneuver cannot be safely achieved due to space or other consideration. f. In these cases, the patient shall have Spinal Motion Restriction in the position in which they are found. 7. On palpation of each vertebral body, look for evidence of pain and ask the patient if they are experiencing pain. If evidence of pain along the spinal column is encountered, the patient should have their spinal motion restricted. This does not necessarily mean placing them on a long hard spine board. The patient can be placed/secured to the gurney and have a cervical collar applied. Reminding the patient to limit their movement. 8. Document motor, gross sensation, and circulation status on each of the extremities. This documentation includes the proximal and distal aspects of the extremities. This needs to be performed prior to, and a modified version after the patient is placed in spinal immobilization. Pre-immobilization Motor Examination a. Check finger adduction and abduction in both hands. b. Check bilateral grip strength c. Check wrist extension and flexion in both hands. d. Check flexion and extension at both elbows. e. Check the ability to shrug both shoulders. f. Check plantarflexion in both feet. g. Check dorsiflexion in both feet. h. Check flexion and extension at both knees. i. Check flexion and extension at both hips. Post-Immobilization Motor examination You can eliminate d, h, and I which are d) flexion and extension at the elbow, h) flexion and extension at the knees, and i) flexion and extension at the hips. 9. Check and document for abnormal sensations (e.g. paresthesia) in all extremities. Spinal Motion Restriction Procedure: A. Provide manual stabilization restricting gross motion while avoiding traction being placed on the spine in any direction. B. Correctly size the rigid cervical collar to additionally avoid traction being placed on the spine. Apply cervical collar. Page: 3 of 6
4 C. Always ensure that there is adequate padding and support for patients. This is especially true for the elderly and pediatric population. Abnormal flexion for the pediatric population can cause respiratory compromise. D. Extricate patient limiting flexion, extension, rotation and distraction of the spine. E. Obtain a baseline assessment of the patient s motor and sensory function prior to placement of Spinal Motion Restriction. The function of a long board/back board is for the transfer of patient from their vehicle or location to the EMS gurney/stretcher (except when they meet trauma triage criteria). The KED (Kendrick Extrication Device) can be used as appropriate if needed. F. Place patient on long board/back board. Whenever possible avoid rolling or log rolling the patient to the long board/back board. The patient should be fork-lifted to the extrication device and/or stretcher. Utilize multiple rescuers to maintain spinal column integrity of alignment. The patient should be placed on the board best suited to protect the airway. Pad any voids between the patient s body and long board/back board if needed (e.g. kyphotic patients and under pediatric patient s shoulder with large occiput). G. If needed the patient can be secured to the stretcher with the knees bent to decrease pressure and potential pain to the back/spine. There needs to be support behind the knees for this position. Complete a thorough physical evaluation and history prior to ensure there is no injury to the thoracic or lumbar spine. This needs to be documented in the Patient Care Record (PCR). H. Use straps, webbing, and another approved equipment to secure the patient. I. Obtain a second assessment of the patient s motor and sensory function after the patient has been secured to stretcher. Regularly reassess the patient s motor and sensory and respiratory quality throughout the duration of patient care if possible. J. If the capable patient is found to be pain free, ask the patient to turn their head first to one side (so that the chin is pointing toward the shoulder on the same side as the head is rotating) then, if pain free, to the other. If there is evidence of pain the patient should be placed in Spinal Motion Restriction. Special Considerations 1. Ambulatory patients at scene/self-extricated: Patients who are ambulatory at the scene of blunt trauma may not require either traditional spinal immobilization or Spinal Motion Restriction. They do need a full evaluation for spinal injury. The use of standing takedown is no longer recommended. If the examination indicates Spinal Motion Restriction, then act accordingly. 2. Axial Loading Accidents: An example of this mechanism is diving injury. These patients are at great risk for spinal injury. 3. Penetrating Trauma: Stabbings and gunshot wounds to the head, neck and/or torso SHOULD NOT receive traditional spinal immobilization unless there is one or more of the following: a. Obvious neurologic deficits to the extremities b. Significant secondary blunt mechanism of injury (e.g. fell down stairs after getting shot) c. Priapism d. Anatomic deformity to the spine. 4. Patients with acute or chronic dyspnea/ disease: Traditional spinal immobilization has been found to limit respiratory function with the greatest effect on the geriatric and pediatric patients. If not monitored these patients can respiratory arrest. Page: 4 of 6
5 5. Modified Traditional Spinal Immobilization: Any instance where placement or positioning of a patient on a spinal board becomes detrimental to the outcome of the patient s health or injury. Modified traditional spinal immobilization will consist of either a rigid cervical collar or object(s) (i.e. towels, blankets, blocks) to maintain the integrity of the cervical spine followed by placement in a position better suited for management of the concerns that did not allow traditional spinal immobilization standards. Always ensure adequate padding to prevent skin breakdown (this can occur rapidly). 6. Chronic versus New Onset Pain and/or Deficits: Always err on the side of precaution when dealing with new or chronic pain and/or neurologic deficits. Use Spinal Motion Restriction and precautions such as cervical collar and immobilization on the stretcher (provider judgement). 7. Isolated Cervical Pain: If after a complete physical evaluation and history the patient may be considered for being placed only in a cervical collar and alternative positions on the stretcher other than supine. The only complaint needs to be clearly documented as isolated neck pain with no associated issues including but not limited to numbness or weakness. There needs to be a normal physical examination that does not indicate neurologic findings. In addition, there needs to be no distracting injuries on physical examination. The patient still needs to be safely restrained/secured to prevent injury. 8. Pregnancy: These patients may need to be restrained on a hardboard allowing them to be placed in a left lateral position of at least 15 to 30 degrees. This will take the uterus off the inferior vena cava and improve the venous return. 9. Pediatric Patients and Car Seats: a. Always inspect the posterior aspect of children in care seats. Infants restrained in a rear-facing car seat may be immobilized and extricated in the car seat if the immobilization is secure and his/her condition allows (no signs of respiratory distress or shock). b. Children restrained in a car seat with a high back may be immobilized and extricated in the car seat; however once removed the child should be placed in spine motion restriction. c. Children restrained in a booster seat (without a back) need to be extricated and immobilized following the Spinal Motion Restriction procedure after clinical examination. d. Utilization of padded pediatric motion restricting boards, if available may be used for traditional pediatric spinal immobilization. 10. Combative Patients: Avoid methods that provoke increased spinal movement and/or combativeness. To prevent other potential damage let the patient position themselves. 11. Diseases that increase Risk: Patients that have osteoporosis, prior spinal fractures, arthritis, cancer, dialysis or underlying spinal or bone disease require the provider to be extra cautious. These patients are at higher risk for injury even in minor mechanisms secondary to their illness. Occasionally in patients who are extremely kyphotic the provider may need to be creative to immobilize these patients. In kyphotic patients if great care is not taken to carefully immobilize these patients great harm can occur to these patients. 12. Alternative Devices: The use of vacuum mattresses and/or other approved appropriate devices can be utilized. 13. Change of plane fall : This is defined as when a patient strikes his head while falling, causing sudden deceleration and hyperextension of the cervical spine. Take extra caution with these patients during the evaluation. 14. Spinal Immobilization While Transporting: If a patient that was deemed safe for transport without Spinal Motion Restriction per this policy develops spinal/paraspinal pain with neurological deficits during transport, the provider must use their best judgment factoring the severity, transport route and Page: 5 of 6
6 time left in transport. If stopping transport to provide Spinal Motion Restriction or traditional spinal immobilization would be detrimental to the patient s outcome, the ambulance should proceed to the ED. If the provider determines that Spinal Motion Restriction or traditional spinal immobilization would benefit the patient s outcome and it can be safely completed, the ambulance may pull over and complete the procedure then continue with transport to ED. 15. Evaluation of Pre-Existing Spinal Immobilization: EMS providers in general should not remove patients who are in Spinal Motion Restriction that was placed by another EMS responder unless the immobilization compromises the patient s life or limb. A provider who is certified at a higher level of training/education may if deemed appropriate after completing a full spinal assessment per this protocol remove Spinal Motion Restriction. This needs to be reported to the Merced County EMS Agency. This needs to be conveyed to the receiving facility. 16. te: if the above occurs where a patient is removed from Spinal Motion Restriction, the provider MUST complete an online Incident Report and submit the form to Merced County EMS within 24 hours. The online Incident Report can be found on the EMS Agency web site at the following URL: Mechanisms that are considered high risk are as follows: high-speed MVC, falls greater than three times the patient s height, axial loading diving accidents, penetrating wounds in or near the spinal column, sports injuries to the head and/or neck, and the unconscious trauma patient. 18. Please remember that in the very young and very old, a normal examination may not be sufficient to rule-out spinal injury. 19. Consider also the change of plane mechanism in which a patient strikes their head while falling, causing a sudden deceleration and hyperextension of the cervical spine are at high risk. 20. Remember that ill-fitting equipment may be worse than no equipment at all. More harm may be caused by a cervical collar that hyperextends the cervical spine that has been injured than by omitting the collar altogether. Page: 6 of 6
7 Spinal Motion Restriction (SMR) Algorithm PEARLS A rigid cervical collar should not be placed or shall be removed if the 1. Collar creates airway compromise 2. Appropriate sized collar is unavailable 3. Collar increases pain 4. Patients anatomy precludes fitting a collar (i.e. severe curvature of the spine) 5. Patient is combative and fighting application of the collar * Patients already immobilized should remain immobilized * Patients with penetrating injuries do not require SMR unless they meet specific criteria in the algorithm * Long Spine Boards should be avoided in ambulatory patients * Elderly or kyphotic individuals requiring SMR may require vacuum immobilization devices * SMR does not take precedence over airway or cardiovascular stabilization * Leave helmets and shoulder pads in place unless they interfere with resuscitation Mechanism of Injury compatible with possible spinal injury Spinal deformity on exam Patient is 5 and under, or Elderly age extremes are prone to unreliable history (Consider SMR if any concerns) Penetrating injury With gross motor/sensory deficits Altered Level of Consciousness Intoxicated (Drugs and/or Alcohol) (Impairment/Lack of Capacity) Gross motor or sensory deficits Numbness, Tingling, Check CMS Cervical, Thoracic,Lumbar, Midline or Paraspinal Pain/Tenderness Spinal Immobilization Ambulatory patients and those that can selfextricate, are cooperative, can follow instructions and who have only midline cervical or thoracic pain may be placed in a rigid collar and secured to the ambulance gurney ( LSB Necessary) Distracting pain (Patient fixates on one location of pain) Language barrier preventing reliable exam (Consider SMR if any concerns) PATIENT DOES NOT REQUIRE SMR IF THE PATIENT DOES NOT MEET ANY OF THE CRITERIA ABOVE ONLY THEN MAY THE PATIENT BE TRANSPORTED WITHOUT SPINAL MOTION RESTRICTION OR TRADITIONAL SPINAL IMMOBILIZATION Mountain-Valley EMS Agency is acknowledged for its contribution to the development of this SMR Algorithm
XXX Spinal Motion Restriction
 Nor-Cal EMS Policy & Procedure Manual NAME OF MODULE XXX Purpose: The purpose of this protocol is to protect patients with signs and symptoms of spinal injuries and those who have the potential for spinal
Nor-Cal EMS Policy & Procedure Manual NAME OF MODULE XXX Purpose: The purpose of this protocol is to protect patients with signs and symptoms of spinal injuries and those who have the potential for spinal
10O SPLINTING OF INJURIES ADULT & PEDIATRIC. 10Oa: Axial/Spine with Selective Spinal Motion Restriction Adult & Pediatric:
 10O SPLINTING OF INJURIES ADULT & PEDIATRIC EMERGENCY MEDICAL RESPONDER EMT EMT-INTERMEDIATE 85 ADVANCED EMT PARAMEDIC 10Oa: Axial/Spine with Selective Spinal Motion Restriction Adult & Pediatric: Many
10O SPLINTING OF INJURIES ADULT & PEDIATRIC EMERGENCY MEDICAL RESPONDER EMT EMT-INTERMEDIATE 85 ADVANCED EMT PARAMEDIC 10Oa: Axial/Spine with Selective Spinal Motion Restriction Adult & Pediatric: Many
EMS Update Spinal Motion Restriction Training
 EMS Update Spinal Motion Restriction Training 700-M11 Spinal Motion Restriction Spinal Motion Restriction, also called SMR Formally known as Spinal Immobilization or C-Spine Effective February 9, 2016
EMS Update Spinal Motion Restriction Training 700-M11 Spinal Motion Restriction Spinal Motion Restriction, also called SMR Formally known as Spinal Immobilization or C-Spine Effective February 9, 2016
MEDICAL CONTROL POLICY STATEMENT/ADVISORY. Re: Spinal Injury Assessment & Spinal Precautions Procedure
 MEDICAL CONTROL POLICY STATEMENT/ADVISORY No. 2015-01 Date: January 20, 2015 Re: Spinal Injury Assessment & Spinal Precautions Procedure Office of the Medical Director Noel Wagner, MD, NREMT-P 1000 Houghton
MEDICAL CONTROL POLICY STATEMENT/ADVISORY No. 2015-01 Date: January 20, 2015 Re: Spinal Injury Assessment & Spinal Precautions Procedure Office of the Medical Director Noel Wagner, MD, NREMT-P 1000 Houghton
Overview. Overview. Chapter 30. Injuries to the Head and Spine 9/11/2012. Review of the Nervous and Skeletal Systems. Devices for Immobilization
 Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
SPINAL IMMOBILIZATION
 Spinal Immobilization Decision Assessment Recent studies have shown an increase in mortality for patients with isolated penetrating trauma who are spinally immobilized. Therefore spinal immobilization
Spinal Immobilization Decision Assessment Recent studies have shown an increase in mortality for patients with isolated penetrating trauma who are spinally immobilized. Therefore spinal immobilization
Selective Spine Assessment & Spinal Motion Restriction
 Selective Spine Assessment & Spinal Motion Restriction Supersedes: 02-09-15 Effective: 10-20-15 Spinal cord injury may be the result of direct blunt and/or penetrating trauma, compression forces (axial
Selective Spine Assessment & Spinal Motion Restriction Supersedes: 02-09-15 Effective: 10-20-15 Spinal cord injury may be the result of direct blunt and/or penetrating trauma, compression forces (axial
Shenandoah Co. Fire & Rescue. Injuries to. and Spine. December EMS Training Bill Streett Training Section Chief
 Shenandoah Co. Fire & Rescue Injuries to the Head and Spine December EMS Training Bill Streett Training Section Chief C.E. Card Information BLS Providers 2 Cards / Provider Category 1 Course # Blank Topic#
Shenandoah Co. Fire & Rescue Injuries to the Head and Spine December EMS Training Bill Streett Training Section Chief C.E. Card Information BLS Providers 2 Cards / Provider Category 1 Course # Blank Topic#
Chapter 32. Objectives. Objectives 01/09/2013. Spinal Column and Spinal Cord Trauma
 Chapter 32 Spinal Column and Spinal Cord Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1.
Chapter 32 Spinal Column and Spinal Cord Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1.
EMS Spinal Assessment and Precautions
 EMS Spinal Assessment and Precautions Adapted from a presentation prepared by Chelsea C. White IV, MD, NREMT-P Medical Director, Bernalillo County Fire Department Robert M. Domeier, MD, EMS Medical Director,
EMS Spinal Assessment and Precautions Adapted from a presentation prepared by Chelsea C. White IV, MD, NREMT-P Medical Director, Bernalillo County Fire Department Robert M. Domeier, MD, EMS Medical Director,
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Injuries to the Head and Spine
 Injuries to the Head and Spine Anatomy Review Skull Protects the brain Made up of several bones with seam like sutures Regions of the scalp-frontal, occipital, parietal, temporal Bones of face Orbits Mandible
Injuries to the Head and Spine Anatomy Review Skull Protects the brain Made up of several bones with seam like sutures Regions of the scalp-frontal, occipital, parietal, temporal Bones of face Orbits Mandible
Cervical Spine Precautions A quick review. By Joseph Lewis, M.D. Medical Director, Honolulu EMS Board Certified in Emergency Medicine
 Cervical Spine Precautions A quick review By Joseph Lewis, M.D. Medical Director, Honolulu EMS Board Certified in Emergency Medicine 1 Goals of this Cervical Spine Immobilization In-service Learn Objectives:
Cervical Spine Precautions A quick review By Joseph Lewis, M.D. Medical Director, Honolulu EMS Board Certified in Emergency Medicine 1 Goals of this Cervical Spine Immobilization In-service Learn Objectives:
MEMORANDUM Date: To: From: Subject:
 COUNTY OF EL DORADO HEALTH & HUMAN SERVICES BOARD OF SUPERVISORS Director Chris Weston Program Manager II 931 Spring Street Placerville, CA 95667 530-621-6100 Phone / 530-295-2501 Fax 1360 Johnson Boulevard,
COUNTY OF EL DORADO HEALTH & HUMAN SERVICES BOARD OF SUPERVISORS Director Chris Weston Program Manager II 931 Spring Street Placerville, CA 95667 530-621-6100 Phone / 530-295-2501 Fax 1360 Johnson Boulevard,
Steve Blados M.Ed., NRP Linda Gibbens, M.S., ATC, LAT
 Steve Blados M.Ed., NRP Linda Gibbens, M.S., ATC, LAT The National Athletic Trainers Association has updated the recommendations pertaining to equipment removal of injured players when spinal immobilization
Steve Blados M.Ed., NRP Linda Gibbens, M.S., ATC, LAT The National Athletic Trainers Association has updated the recommendations pertaining to equipment removal of injured players when spinal immobilization
Heidi Lako-Adamson, MD, NRP, FAEMS FM Ambulance and Sanford EMS Education Medical Director
 Heidi Lako-Adamson, MD, NRP, FAEMS FM Ambulance and Sanford EMS Education Medical Director Spinal cord injury statistics. Definition of spinal motion restriction. Difference between spinal motion restriction
Heidi Lako-Adamson, MD, NRP, FAEMS FM Ambulance and Sanford EMS Education Medical Director Spinal cord injury statistics. Definition of spinal motion restriction. Difference between spinal motion restriction
Chapter 32. Injuries to the Spine by Pearson Education, Inc. Upper Saddle River, New Jersey
 Chapter Injuries to the Spine Topics Anatomy and physiology of the spine Spinal injuries Guidelines for immobilization Special considerations Enrichment Introduction Injuries to the spine are among the
Chapter Injuries to the Spine Topics Anatomy and physiology of the spine Spinal injuries Guidelines for immobilization Special considerations Enrichment Introduction Injuries to the spine are among the
Indications for cervical spine immobilisation: -
 Paediatric Trauma Cervical Spine Guidelines UHW Traumatic injuries of the cervical spine (C-spine) are uncommon in children. However, it is safer assume there is a cervical spine injury until examination
Paediatric Trauma Cervical Spine Guidelines UHW Traumatic injuries of the cervical spine (C-spine) are uncommon in children. However, it is safer assume there is a cervical spine injury until examination
3/10/17 Spinal a Injury 1
 Spinal Injury 1 'Paralysed' Watmough vows he'll have the backbone for Game Two after treatment for neck injury Watmough will have cortisone injected into his spine this morning to speed up the recovery
Spinal Injury 1 'Paralysed' Watmough vows he'll have the backbone for Game Two after treatment for neck injury Watmough will have cortisone injected into his spine this morning to speed up the recovery
Hatfield & McCoy Mine Safety Competition First-Aid Contest JULY 15, Page 1
 Hatfield & McCoy Mine Safety Competition First-Aid Contest JULY 15, 2014 Page 1 PROBLEM Billy is a maintenance person that has been conducting clean-up and service duties on the number one conveyor belt
Hatfield & McCoy Mine Safety Competition First-Aid Contest JULY 15, 2014 Page 1 PROBLEM Billy is a maintenance person that has been conducting clean-up and service duties on the number one conveyor belt
Pre-hospital Spinal Motion Restriction Standard update. Presented by: Dr. Tatiana Jevremovic CCFP (EM)(SEM), Dip.
 Pre-hospital Spinal Motion Restriction Standard update Presented by: Dr. Tatiana Jevremovic CCFP (EM)(SEM), Dip. Sport Med (CASEM) Dr. Thomas J. Pashby What is happening Pre-hospital Spinal Motion Restriction
Pre-hospital Spinal Motion Restriction Standard update Presented by: Dr. Tatiana Jevremovic CCFP (EM)(SEM), Dip. Sport Med (CASEM) Dr. Thomas J. Pashby What is happening Pre-hospital Spinal Motion Restriction
INTERNATIONAL TRAUMA LIFE SUPPORT
 INTERNATIONAL TRAUMA LIFE SUPPORT LONG BACKBOARD USE FOR SPINAL MOTION RESTRICTION OF THE TRAUMA PATIENT The guidelines and references contained in this document are current as of the date of publication
INTERNATIONAL TRAUMA LIFE SUPPORT LONG BACKBOARD USE FOR SPINAL MOTION RESTRICTION OF THE TRAUMA PATIENT The guidelines and references contained in this document are current as of the date of publication
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question.
 EPC Ch 24 Quiz w-key Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) Which of the following best explains the presentation and prognosis of
EPC Ch 24 Quiz w-key Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) Which of the following best explains the presentation and prognosis of
Injuries to the Head and Spine From Bradys Emergency Care 10 th Edition
 Injuries to the Head and Spine From Bradys Emergency Care 10 th Edition 1. When performing the four-rescuer log roll, which responder pulls the board into position? A.) Head B.) Waist C.) Knee D.) Shoulder
Injuries to the Head and Spine From Bradys Emergency Care 10 th Edition 1. When performing the four-rescuer log roll, which responder pulls the board into position? A.) Head B.) Waist C.) Knee D.) Shoulder
PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT
 PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT Board Approved June 2007 Revised December 2009 Revised July 2011 Revised June 2015 435 Hunter Street Fredericksburg, VA 22401
PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT Board Approved June 2007 Revised December 2009 Revised July 2011 Revised June 2015 435 Hunter Street Fredericksburg, VA 22401
MASSACHUSETTS DEPARTMENT OF PUBLIC HEALTH OFFICE OF EMERGENCY MEDICAL SERVICES Basic EMT Practical Examination Cardiac Arrest Management
 Basic EMT Practical Examination 6.0 - Cardiac Arrest Management Station 1 RESUSCITATION & DEFIBRILLATION No Point WHILE FUNCTIONING AS FIRST RESCUER: Point 1. Verbalizes or takes body substance isolation
Basic EMT Practical Examination 6.0 - Cardiac Arrest Management Station 1 RESUSCITATION & DEFIBRILLATION No Point WHILE FUNCTIONING AS FIRST RESCUER: Point 1. Verbalizes or takes body substance isolation
Controversies in Spinal Immobilization
 Controversies in Spinal Immobilization Ken Berumen, BSN, MD, FACEP Medical Director El Paso Fire Department Medical Director Emergency Services District #1 Network Director EM Sierra Providence Health
Controversies in Spinal Immobilization Ken Berumen, BSN, MD, FACEP Medical Director El Paso Fire Department Medical Director Emergency Services District #1 Network Director EM Sierra Providence Health
4/19/2017. Prehospital Spinal Care: Then. Prehospital Spinal Care: Then. Prehospital Spinal Care: Then. Prehospital Spinal Care: Then. Why Immobilize?
 Management of Cervical Spine Injuries and Athletic Equipment Removal Gianluca Del Rossi, PhD, ATC Prehospital Spinal Care: Then While the exact origins of backboards in EMS are unclear, noted trauma surgeon
Management of Cervical Spine Injuries and Athletic Equipment Removal Gianluca Del Rossi, PhD, ATC Prehospital Spinal Care: Then While the exact origins of backboards in EMS are unclear, noted trauma surgeon
Lifting and Moving Patients
 1. Which of the following factors should be considered before lifting any patient? a. The weight of the patient b. Your physical limitations c. Communications 2. When lifting a patient, a basic principle
1. Which of the following factors should be considered before lifting any patient? a. The weight of the patient b. Your physical limitations c. Communications 2. When lifting a patient, a basic principle
Spinal or Suspected Spinal, Injury: Logrolling Technique with C- Spine Precautions
 Approved by: Spinal or Suspected Spinal, Injury: Logrolling Technique with C- Spine Precautions Vice President and Chief Medical Officer; and Vice President and Chief Operating Officer Corporate Policy
Approved by: Spinal or Suspected Spinal, Injury: Logrolling Technique with C- Spine Precautions Vice President and Chief Medical Officer; and Vice President and Chief Operating Officer Corporate Policy
Chapter 24 Spinal Trauma Introduction to Spinal Injuries (1 of 2) Annually 15,000 permanent spinal cord injuries Commonly men years old
 1 2 3 4 5 6 7 Chapter 24 Spinal Trauma Introduction to Spinal Injuries (1 of 2) Annually 15,000 permanent spinal cord injuries Commonly men 16-30 years old Mechanism of Injury: Vehicle crashes: 48% : 21%
1 2 3 4 5 6 7 Chapter 24 Spinal Trauma Introduction to Spinal Injuries (1 of 2) Annually 15,000 permanent spinal cord injuries Commonly men 16-30 years old Mechanism of Injury: Vehicle crashes: 48% : 21%
STOP THE MADDNESS! 4/19/2012. Mechanism of Injury A historical review of bad advice and dangerous dogma
 OBJECTIVES Discuss the inherent inaccuracy of using mechanism of injury as the primary indicator leading to spinal immobilization. STOP THE MADDNESS! Jim Morrissey, EMT-P Alameda County EMS PHCC FBI Tactical
OBJECTIVES Discuss the inherent inaccuracy of using mechanism of injury as the primary indicator leading to spinal immobilization. STOP THE MADDNESS! Jim Morrissey, EMT-P Alameda County EMS PHCC FBI Tactical
EMS SKILL NEUROLOGICAL EMERGENCY / SPINAL MOTION RESTRICTION (SMR) VEST TYPE EXTRICATION DEVICE FOR THE SEATED PATIENT
 EMS SKILL NEUROLOGICAL EMERGENCY / SPINAL MOTION RESTRICTION (SMR) VEST TYPE EXTRICATION DEVICE FOR THE SEATED PATIENT PERFORMANCE OBJECTIVES Demonstrate competency in performing and directing team members
EMS SKILL NEUROLOGICAL EMERGENCY / SPINAL MOTION RESTRICTION (SMR) VEST TYPE EXTRICATION DEVICE FOR THE SEATED PATIENT PERFORMANCE OBJECTIVES Demonstrate competency in performing and directing team members
Introduction. Objectives C-Spine: Where Are We Now? NAEMSP Medical Director Course 1/9/2013
 NAEMSP Medical Director Course 1/9/2013 Objectives C-Spine: Where Are We Now? Robert M. Domeier, MD EMS Medical Director Washtenaw/Livingston Medical Control Authority Department of Emergency Medicine
NAEMSP Medical Director Course 1/9/2013 Objectives C-Spine: Where Are We Now? Robert M. Domeier, MD EMS Medical Director Washtenaw/Livingston Medical Control Authority Department of Emergency Medicine
Pediatric Sports Emergencies. Asthma
 Pediatric Sports Emergencies Michele Kirk, MD JPS Sports Medicine Fellowship TCU Team Physician Two underlying factors: Inflammation Asthma Chronic Leads to structural changes Increase in airway smooth
Pediatric Sports Emergencies Michele Kirk, MD JPS Sports Medicine Fellowship TCU Team Physician Two underlying factors: Inflammation Asthma Chronic Leads to structural changes Increase in airway smooth
ESCAMBIA COUNTY TRAUMA TRANSPORT
 TRAUMA ALERT CRITERIA are established state mandated criteria. ADULT TRAUMA ALERT CRITERIA (Physical and anatomical characteristics of a person 16 years of age or older) Any 1 of the following: 1. Airway:
TRAUMA ALERT CRITERIA are established state mandated criteria. ADULT TRAUMA ALERT CRITERIA (Physical and anatomical characteristics of a person 16 years of age or older) Any 1 of the following: 1. Airway:
NEW SPINAL PRECAUTION STANDARDS
 NEW SPINAL PRECAUTION STANDARDS July 31, 2015 Dane Van Horn B.S., CCEMT-P Field Supervisor - Life EMS Ambulance Disclosure I have no relevant financial relationships or conflicts of interest to disclose
NEW SPINAL PRECAUTION STANDARDS July 31, 2015 Dane Van Horn B.S., CCEMT-P Field Supervisor - Life EMS Ambulance Disclosure I have no relevant financial relationships or conflicts of interest to disclose
Northwest Community EMS System Continuing Education Class Credit Questions for October 2014 Spine Motion Restriction (Didactic)
 Northwest Community EMS System Continuing Education Class Credit Questions for October 2014 Spine Motion Restriction (Didactic) Name (PRINT): Date submitted: Affiliation: Rating: [ ] Complete [ ] Incomplete
Northwest Community EMS System Continuing Education Class Credit Questions for October 2014 Spine Motion Restriction (Didactic) Name (PRINT): Date submitted: Affiliation: Rating: [ ] Complete [ ] Incomplete
Every day thousands of people become the accidental victims of trauma.
 Aurora Health Care South Region EMS 2010 2 nd Quarter CE Packet Spinal Cord Trauma Every day thousands of people become the accidental victims of trauma. Approximately 43,000 people die in motor vehicle
Aurora Health Care South Region EMS 2010 2 nd Quarter CE Packet Spinal Cord Trauma Every day thousands of people become the accidental victims of trauma. Approximately 43,000 people die in motor vehicle
Focused History and Physical Examination of the
 Henry: EMT Prehospital Care, Revised 3 rd Edition Lecture Notes Chapter 10: Focused History and Physical Examination of Trauma Patients Chapter 10 Focused History and Physical Examination of the Trauma
Henry: EMT Prehospital Care, Revised 3 rd Edition Lecture Notes Chapter 10: Focused History and Physical Examination of Trauma Patients Chapter 10 Focused History and Physical Examination of the Trauma
Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and
 1 2 3 4 5 Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and involuntary activities Voluntary activities
1 2 3 4 5 Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and involuntary activities Voluntary activities
Fractures of the Thoracic and Lumbar Spine
 A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
Spinal, or Suspected Spinal Injury
 Approved by: Spinal, or Suspected Spinal Injury Vice President and Chief Medical Officer; and Vice President and Chief Operating Officer Corporate Policy & Procedures Manual Number: VII-B-150 Date Approved
Approved by: Spinal, or Suspected Spinal Injury Vice President and Chief Medical Officer; and Vice President and Chief Operating Officer Corporate Policy & Procedures Manual Number: VII-B-150 Date Approved
Restore adequate respiratory and circulatory conditions. Reduce pain
 Pre-hospital management of the trauma patient is best performed by an integrated team focused on minimizing the time from injury to definitive care at an appropriate trauma center. Dispatchers, first responders,
Pre-hospital management of the trauma patient is best performed by an integrated team focused on minimizing the time from injury to definitive care at an appropriate trauma center. Dispatchers, first responders,
Position Statement for the Management of Patients with Potential Spinal Injuries
 Office of the Medical Director San Antonio Fire Department and UT Health San Antonio Dept. of Emergency Health Sciences Position Statement for the Management of Patients with Potential Spinal Injuries
Office of the Medical Director San Antonio Fire Department and UT Health San Antonio Dept. of Emergency Health Sciences Position Statement for the Management of Patients with Potential Spinal Injuries
3/14/2014 USED TO BE SIMPLE.. TO IMMOBILIZE OR NOT TO IMMOBILIZE.THAT IS THE QUESTION THE PROBLEM OLD THINKING
 USED TO BE SIMPLE.. TO IMMOBILIZE OR NOT TO IMMOBILIZE.THAT IS THE QUESTION Immobilization following injury used to be a simple decision--but no one was thinking. Up to 5 million people per year receive
USED TO BE SIMPLE.. TO IMMOBILIZE OR NOT TO IMMOBILIZE.THAT IS THE QUESTION Immobilization following injury used to be a simple decision--but no one was thinking. Up to 5 million people per year receive
Cervical Spine Injury Guidelines
 6/15/2018 Cervical Spine Injury Guidelines Benjamin Oshlag, MD, CAQSM Assistant Professor of Emergency Medicine Assistant Professor of Sports Medicine Columbia University Medical Center Nothing to Disclose
6/15/2018 Cervical Spine Injury Guidelines Benjamin Oshlag, MD, CAQSM Assistant Professor of Emergency Medicine Assistant Professor of Sports Medicine Columbia University Medical Center Nothing to Disclose
CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS
 CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS PRACTICAL STATIONS CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS 1. CARDIAC ARREST MANAGEMENT 2. AIRWAY & RESPIRATORY MANAGEMENT 3. SPINAL IMMOBILIZATION
CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS PRACTICAL STATIONS CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS 1. CARDIAC ARREST MANAGEMENT 2. AIRWAY & RESPIRATORY MANAGEMENT 3. SPINAL IMMOBILIZATION
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions
 Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What is caused by overexerting or tearing of a muscle? p. 375 A.) Dislocation B.) Sprain C.) Fracture *D.)
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What is caused by overexerting or tearing of a muscle? p. 375 A.) Dislocation B.) Sprain C.) Fracture *D.)
Patient Assessment. Chapter 8
 Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
Chapter 30 - Musculoskeletal_Trauma
 Introduction to Emergency Medical Care 1 OBJECTIVES 30.1 Define key terms introduced in this chapter. Slides 11 12, 19 20, 22 23, 37 30.2 Describe the anatomy of elements of the musculoskeletal system.
Introduction to Emergency Medical Care 1 OBJECTIVES 30.1 Define key terms introduced in this chapter. Slides 11 12, 19 20, 22 23, 37 30.2 Describe the anatomy of elements of the musculoskeletal system.
SIERRA-SACRAMENTO VALLEY EMS AGENCY PROGRAM POLICY
 SIERRA-SACRAMENTO VALLEY EMS AGENCY PROGRAM POLICY PURPOSE: To identify those patients who are at greatest risk for severe injury and determine the most appropriate facility to transport persons with different
SIERRA-SACRAMENTO VALLEY EMS AGENCY PROGRAM POLICY PURPOSE: To identify those patients who are at greatest risk for severe injury and determine the most appropriate facility to transport persons with different
Evaluation and Stabilization of the Athlete with Possible Spine Injury
 Evaluation and Stabilization of the Athlete with Possible Spine Injury Jeffrey H. Bohmer, MD, FACEP Emergency Physician Northwestern Medicine Central DuPage Hospital June 12, 2015 Introduction Goals: 1.
Evaluation and Stabilization of the Athlete with Possible Spine Injury Jeffrey H. Bohmer, MD, FACEP Emergency Physician Northwestern Medicine Central DuPage Hospital June 12, 2015 Introduction Goals: 1.
SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services OBJECTIVES DEFINITION 11/8/2017. Identify SCIWORA.
 SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services Identify SCIWORA. OBJECTIVES Identify the population at risk. To identify anatomic and physiologic reasons for SCIWORA. To
SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services Identify SCIWORA. OBJECTIVES Identify the population at risk. To identify anatomic and physiologic reasons for SCIWORA. To
11. Spinal cord injury
 11. Spinal cord injury Introduction Always think spinal (vertebral) and/or spinal cord injury (SCI) in children with trauma. Remember SCIWORA cord injury may be present without abnormalities on routine
11. Spinal cord injury Introduction Always think spinal (vertebral) and/or spinal cord injury (SCI) in children with trauma. Remember SCIWORA cord injury may be present without abnormalities on routine
BUKU PANDUAN INSTRUKTUR SKILLS LEARNING SISTEM EMERGENSI DAN TRAUMATOLOGI STABILISASI DAN TRANSPORTASI
 BUKU PANDUAN INSTRUKTUR SKILLS LEARNING SISTEM EMERGENSI DAN TRAUMATOLOGI STABILISASI DAN TRANSPORTASI KOORDINATOR SKILLS LAB SISTEM EMERGENSI DAN TRAUMATAOLOGI FAKULTAS KEDOKTERAN UNIVERSITAS HASANUDDIN
BUKU PANDUAN INSTRUKTUR SKILLS LEARNING SISTEM EMERGENSI DAN TRAUMATOLOGI STABILISASI DAN TRANSPORTASI KOORDINATOR SKILLS LAB SISTEM EMERGENSI DAN TRAUMATAOLOGI FAKULTAS KEDOKTERAN UNIVERSITAS HASANUDDIN
Competency Log Professional Responder Courses
 Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
4 inch laceration traversing down the front of forearm. Fracture of lower leg midway between knee and ankle
 2 inch wound on forehead 3 inch wound on top of shoulder islocated elbow in flexed position 4 inch laceration traversing down the front of forearm 3 inch wound on inner thigh Fracture of lower leg midway
2 inch wound on forehead 3 inch wound on top of shoulder islocated elbow in flexed position 4 inch laceration traversing down the front of forearm 3 inch wound on inner thigh Fracture of lower leg midway
CLINICAL MANUAL. Trauma System Activation Trauma Code Criteria
 CLINICAL MANUAL Policy Number: CM T-28 Approved by: Nursing Congress, Management Forum Issue Date: 09/1999 Applies to: Downtown Value(s): Respect, Integrity, Innovation Page(s): 1 of 4 Trauma System Activation
CLINICAL MANUAL Policy Number: CM T-28 Approved by: Nursing Congress, Management Forum Issue Date: 09/1999 Applies to: Downtown Value(s): Respect, Integrity, Innovation Page(s): 1 of 4 Trauma System Activation
Pre-hospital Trauma Life Support. Rattiya Banjungam Emergency Physician, Khon Kaen Hospital
 Pre-hospital Trauma Life Support Rattiya Banjungam Emergency Physician, Khon Kaen Hospital Golden principles of Prehospital Trauma Care Golden Hour There is a golden hour if you are critically injured,
Pre-hospital Trauma Life Support Rattiya Banjungam Emergency Physician, Khon Kaen Hospital Golden principles of Prehospital Trauma Care Golden Hour There is a golden hour if you are critically injured,
County of Santa Clara Emergency Medical Services System
 County of Santa Clara Emergency Medical Services System EMS System Policy Change Coversheet EMS SYSTEM POLICY CHANGE COVERSHEET Policy Number and Name: 605: Prehospital Trauma Triage Date: May 27, 2014
County of Santa Clara Emergency Medical Services System EMS System Policy Change Coversheet EMS SYSTEM POLICY CHANGE COVERSHEET Policy Number and Name: 605: Prehospital Trauma Triage Date: May 27, 2014
SEMINOLE COUNTY EMS PROVISIONAL EMT SKILLS VERIFICATION
 The following individual has completed the Seminole County EMS Provisional EMT Skills Verification check in the following areas: Oxygen, Airway and Ventilation Skills ALS Assistance Trauma Management Medical
The following individual has completed the Seminole County EMS Provisional EMT Skills Verification check in the following areas: Oxygen, Airway and Ventilation Skills ALS Assistance Trauma Management Medical
SAN LUIS OBISPO COUNTY EMERGENCY MEDICAL SERVICES AGENCY PREHOSPITAL POLICY
 SAN LUIS OBISPO COUNTY EMERGENCY MEDICAL SERVICES AGENCY PREHOSPITAL POLICY Policy Reference No: 153 [01/08/2013] Formerly Policy No: 201.3 Effective Date: 11/01/2012 Review Date: 03/01/2014 TRAUMA PATIENT
SAN LUIS OBISPO COUNTY EMERGENCY MEDICAL SERVICES AGENCY PREHOSPITAL POLICY Policy Reference No: 153 [01/08/2013] Formerly Policy No: 201.3 Effective Date: 11/01/2012 Review Date: 03/01/2014 TRAUMA PATIENT
GOALS: To be able to assure proper patient selection in spinal motion restriction
 CLINICAL STANDARD OF PRACTICE APPROVED BY: MAB MEDICAL DIRECTOR: Dr. James Cameron REVIEW DATE: April 16, 2014 REVIEWED: REVISED: February 18, 2015 TITLE: Pre-hospital spinal motion restriction (Revised
CLINICAL STANDARD OF PRACTICE APPROVED BY: MAB MEDICAL DIRECTOR: Dr. James Cameron REVIEW DATE: April 16, 2014 REVIEWED: REVISED: February 18, 2015 TITLE: Pre-hospital spinal motion restriction (Revised
Commonwealth Health Corporation NEXT
 Commonwealth Health Corporation This computer-based learning (CBL) module details important aspects of musculoskeletal disorders, body mechanics and ergonomics in the workplace. It examines: what causes
Commonwealth Health Corporation This computer-based learning (CBL) module details important aspects of musculoskeletal disorders, body mechanics and ergonomics in the workplace. It examines: what causes
The Spine.
 The Spine www.fisiokinesiterapia.biz Characteristics of Vertebrae Cervical Spine 1 and 2 Sacrum and Coccyx Curves Lordotic in the Spine Kyphotic Lordotic Ligamentous Support Muscles of the Spine Spinal
The Spine www.fisiokinesiterapia.biz Characteristics of Vertebrae Cervical Spine 1 and 2 Sacrum and Coccyx Curves Lordotic in the Spine Kyphotic Lordotic Ligamentous Support Muscles of the Spine Spinal
By: Kurt Bloomstrand, MD. EMS Medical Director
 By: Kurt Bloomstrand, MD EMS Medical Director Review anatomy and physiology List the mechanisms of injury that cause a high index of suspicion for the possibility of spine injury Discuss historical perspectives
By: Kurt Bloomstrand, MD EMS Medical Director Review anatomy and physiology List the mechanisms of injury that cause a high index of suspicion for the possibility of spine injury Discuss historical perspectives
The Assessment & Management of Spine & Spinal Cord Injuries in the Field:
 The Assessment & Management of Spine & Spinal Cord Injuries in the Field: Where We Started, Where We are Now, & Why WMTC Wilderness Medicine Training Center International Paul Nicolazzo Director Wilderness
The Assessment & Management of Spine & Spinal Cord Injuries in the Field: Where We Started, Where We are Now, & Why WMTC Wilderness Medicine Training Center International Paul Nicolazzo Director Wilderness
Chapter 5. Learning Objectives. Learning Objectives 9/18/2012. Lifting and Moving Patients. Define body mechanics
 Chapter 5 Lifting and Moving Patients Learning Objectives Define body mechanics Discuss guidelines/safety precautions to follow when lifting patient Explain rationale for properly lifting/moving patients
Chapter 5 Lifting and Moving Patients Learning Objectives Define body mechanics Discuss guidelines/safety precautions to follow when lifting patient Explain rationale for properly lifting/moving patients
IRECA BLS Challenge 2015 Scenario 1
 Scenario 1 Team Name Team Number Captain Name Judge 1 # Judge 2 # JUDGE S SHEET Overview: This scenario challenges the competitors to use basic triage techniques and then to do the most good for the most
Scenario 1 Team Name Team Number Captain Name Judge 1 # Judge 2 # JUDGE S SHEET Overview: This scenario challenges the competitors to use basic triage techniques and then to do the most good for the most
Musculoskeletal System
 CHAPTER 28 Musculoskeletal Injuries Musculoskeletal System Anatomy & Physiology Bones provide framework. Joints allow for bending. Muscles allow for movement. Cartilage provides flexibility. Tendons connect
CHAPTER 28 Musculoskeletal Injuries Musculoskeletal System Anatomy & Physiology Bones provide framework. Joints allow for bending. Muscles allow for movement. Cartilage provides flexibility. Tendons connect
CHAPTER 28 Musculoskeletal Injuries
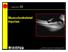 CHAPTER 28 Musculoskeletal Injuries Musculoskeletal System Anatomy & Physiology Bones provide framework. Joints allow for bending. Muscles allow for movement. Cartilage provides flexibility. Tendons connect
CHAPTER 28 Musculoskeletal Injuries Musculoskeletal System Anatomy & Physiology Bones provide framework. Joints allow for bending. Muscles allow for movement. Cartilage provides flexibility. Tendons connect
Chapter 8 - Lifting and Moving Patients
 1 Chapter 8 Lifting and Moving Patients 2 3 4 5 6 7 8 9 National EMS Education Standard Competencies EMS Operations Knowledge of operational roles and responsibilities to ensure patient, public, and personnel
1 Chapter 8 Lifting and Moving Patients 2 3 4 5 6 7 8 9 National EMS Education Standard Competencies EMS Operations Knowledge of operational roles and responsibilities to ensure patient, public, and personnel
Musculoskeletal Trauma. Lesson Goal. Lesson Objectives 9/10/2012. Recognize and manage patients with musculoskeletal trauma
 Musculoskeletal Trauma Lesson Goal Recognize and manage patients with musculoskeletal trauma Lesson Objectives Describe function of muscular system Describe composition of muscular system Describe, compare,
Musculoskeletal Trauma Lesson Goal Recognize and manage patients with musculoskeletal trauma Lesson Objectives Describe function of muscular system Describe composition of muscular system Describe, compare,
Chapter 12. Learning Objectives. Learning Objectives 9/11/2012. Musculoskeletal Injuries
 Chapter 12 Musculoskeletal Injuries Learning Objectives Describe the anatomy and function of the musculoskeletal system Demonstrate the assessment and management of a patient with a suspected musculoskeletal
Chapter 12 Musculoskeletal Injuries Learning Objectives Describe the anatomy and function of the musculoskeletal system Demonstrate the assessment and management of a patient with a suspected musculoskeletal
ITLS Pediatric Provider Course Advanced Pre-Test
 ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
North West London Trauma Network Spinal Pathway and Protocols
 North West London Trauma Network Spinal Pathway and Protocols 1. Spinal Clearance in the Trauma Patient Inclusions: All trauma patients who are not alert and orientated, unable to cooperate (including
North West London Trauma Network Spinal Pathway and Protocols 1. Spinal Clearance in the Trauma Patient Inclusions: All trauma patients who are not alert and orientated, unable to cooperate (including
Selective Spinal Immobilization
 Selective Spinal Immobilization Objectives Understand the background of spinal immobilization. Understand the rationale for developing a current selective spinal immobilization protocol. Review the data
Selective Spinal Immobilization Objectives Understand the background of spinal immobilization. Understand the rationale for developing a current selective spinal immobilization protocol. Review the data
Airway Adjuncts and Suction
 Airway Adjuncts and Suction Oropharyngeal Airway Selects appropriately sized airway. Measures airway. Inserts airway without pushing the tongue posteriorly. Examiner States: patient is gagging and becoming
Airway Adjuncts and Suction Oropharyngeal Airway Selects appropriately sized airway. Measures airway. Inserts airway without pushing the tongue posteriorly. Examiner States: patient is gagging and becoming
Maximal isokinetic and isometric muscle strength of major muscle groups related to age, body weight, height, and sex in 178 healthy subjects
 Maximal isokinetic and isometric muscle strength of major muscle groups related to age, body weight, height, and sex in 178 healthy subjects Test protocol Muscle test procedures. Prior to each test participants
Maximal isokinetic and isometric muscle strength of major muscle groups related to age, body weight, height, and sex in 178 healthy subjects Test protocol Muscle test procedures. Prior to each test participants
1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles. Striated Skeletal. Smooth
 1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles Striated Skeletal Smooth 3 Anatomy and Physiology of the Musculoskeletal System 4 Skeletal System 5 Skeletal System Functions
1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles Striated Skeletal Smooth 3 Anatomy and Physiology of the Musculoskeletal System 4 Skeletal System 5 Skeletal System Functions
9/15/2015. Introduction (1 of 3) Chapter 8. Introduction (2 of 3) What is the difference? Scene Size-up (1 of 2) Patient Assessment
 Introduction (1 of 3) Chapter 8 Patient Assessment Patient assessment is very important. EMTs must master the patient assessment process. Patient assessment is used, to some degree, in every patient encounter.
Introduction (1 of 3) Chapter 8 Patient Assessment Patient assessment is very important. EMTs must master the patient assessment process. Patient assessment is used, to some degree, in every patient encounter.
Kinetic Energy Energy in Motion KE = Mass (weight) X Velocity (speed)² 2 Double Weight = Energy Double Speed = Energy IS THE GREATEST DETERMINANT
 1 Chapter 17 Blunt Trauma 2 Introduction to Blunt Trauma Most common cause of trauma death and disability exchange between an object and the human body, without intrusion through the skin 3 Blunt trauma
1 Chapter 17 Blunt Trauma 2 Introduction to Blunt Trauma Most common cause of trauma death and disability exchange between an object and the human body, without intrusion through the skin 3 Blunt trauma
the back book Your Guide to a Healthy Back
 the back book Your Guide to a Healthy Back anatomy Your spine s job is to: Support your upper body and neck Increase flexibility of your spine Protect your spinal cord There are 6 primary components of
the back book Your Guide to a Healthy Back anatomy Your spine s job is to: Support your upper body and neck Increase flexibility of your spine Protect your spinal cord There are 6 primary components of
Chapter 24. Learning Objectives. Learning Objectives 9/18/2012. Injuries to the Head and Spine
 Chapter 24 Injuries to the Head and Spine Learning Objectives State components of the nervous system List functions of the central nervous system Define structure of the skeletal system as it relates to
Chapter 24 Injuries to the Head and Spine Learning Objectives State components of the nervous system List functions of the central nervous system Define structure of the skeletal system as it relates to
Emergency Care Progress Log
 Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
Assessment of the Trauma Patient
 CHAPTER 10 Assessment of the Trauma Patient Overall Assessment Scheme Scene Size-Up Initial Assessment Trauma Physical Exam Vital Signs & SAMPLE History Medical SAMPLE History Physical Exam & Vital Signs
CHAPTER 10 Assessment of the Trauma Patient Overall Assessment Scheme Scene Size-Up Initial Assessment Trauma Physical Exam Vital Signs & SAMPLE History Medical SAMPLE History Physical Exam & Vital Signs
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions
 Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What do injuries to the shoulder often produce? p. 393 *A.) Anterior dislocation B.) Superior dislocation
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What do injuries to the shoulder often produce? p. 393 *A.) Anterior dislocation B.) Superior dislocation
Acute spinal cord injury
 Acute spinal cord injury Thakul Oearsakul Songklanagarind hospital Hat Yai Songkhla Introduction New SCI 10000-12000 cases Approximately 4.0-5.3 per 100000 population Common causes of traumatic SCI :Motor
Acute spinal cord injury Thakul Oearsakul Songklanagarind hospital Hat Yai Songkhla Introduction New SCI 10000-12000 cases Approximately 4.0-5.3 per 100000 population Common causes of traumatic SCI :Motor
Position Statement from the National Ski Patrol Medical Advisory Committee on the Selective Use of Backboards for Possible Spinal Injuries
 Position Statement from the National Ski Patrol Medical Advisory Committee on the Selective Use of Backboards for Possible Spinal Injuries Approved by the NSP Medical Committee 3/8/ 2017 Approved by the
Position Statement from the National Ski Patrol Medical Advisory Committee on the Selective Use of Backboards for Possible Spinal Injuries Approved by the NSP Medical Committee 3/8/ 2017 Approved by the
Contraindicated and High-Risk Exercises
 Contraindicated and High-Risk Exercises Young sub Kwon, Ph.D. ACSM RCEP, NSCA CSCS,*D Exercise Physiology Laboratory The University of New Mexico Albuquerque, NM, USA Introduction Any activity selected
Contraindicated and High-Risk Exercises Young sub Kwon, Ph.D. ACSM RCEP, NSCA CSCS,*D Exercise Physiology Laboratory The University of New Mexico Albuquerque, NM, USA Introduction Any activity selected
SPINE EVALUATION AND CLEARANCE Basic Principles
 SPINE EVALUATION AND CLEARANCE Basic Principles General 1. Entire spine is immobilized during primary survey. 2. Radiographic clearance of the spine is not required before emergent surgical procedures.
SPINE EVALUATION AND CLEARANCE Basic Principles General 1. Entire spine is immobilized during primary survey. 2. Radiographic clearance of the spine is not required before emergent surgical procedures.
Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles
 1 2 3 4 5 6 7 Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles Striated Skeletal Smooth Anatomy and Physiology of the Musculoskeletal System Skeletal System Skeletal System Functions
1 2 3 4 5 6 7 Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles Striated Skeletal Smooth Anatomy and Physiology of the Musculoskeletal System Skeletal System Skeletal System Functions
Chapter 7 EMERGENCY PLAN AND INITIAL INJURY EVALUATION
 Chapter 7 EMERGENCY PLAN AND INITIAL INJURY EVALUATION Major Concepts. Proper planning of an emergency response is essential for appropriate first aid management of an injury. Anything that can be done
Chapter 7 EMERGENCY PLAN AND INITIAL INJURY EVALUATION Major Concepts. Proper planning of an emergency response is essential for appropriate first aid management of an injury. Anything that can be done
PTA 210 PTA Techniques. Patient Positioning and Draping
 PTA 210 PTA Techniques Patient Positioning and Draping Review Last Lecture 5 vital signs you are responsible for? What is patency? How do you test it? Pressing too hard with HR can cause Contraindications
PTA 210 PTA Techniques Patient Positioning and Draping Review Last Lecture 5 vital signs you are responsible for? What is patency? How do you test it? Pressing too hard with HR can cause Contraindications
D. Pre-Hospital Trauma Triage and Bypass Algorithm
 D. Pre-Hospital Trauma Triage and Bypass Algorithm Hospital bypass is defined as transporting the patient to the nearest hospital that has the appropriate level of care for the patient s suspected severity
D. Pre-Hospital Trauma Triage and Bypass Algorithm Hospital bypass is defined as transporting the patient to the nearest hospital that has the appropriate level of care for the patient s suspected severity
Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing
 1 2 3 4 5 6 Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing D-Disability Chief complaint and/or Mechanism
1 2 3 4 5 6 Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing D-Disability Chief complaint and/or Mechanism
Cases from the Streets. Kelly Buchanan MD, ATC/L EMS Fellow December, 2011
 Cases from the Streets Kelly Buchanan MD, ATC/L EMS Fellow December, 2011 The Scene Car vs Light Pole, 35 mph, front right side damage 10 with no PCI + airbag deployment, starring on windshield Given the
Cases from the Streets Kelly Buchanan MD, ATC/L EMS Fellow December, 2011 The Scene Car vs Light Pole, 35 mph, front right side damage 10 with no PCI + airbag deployment, starring on windshield Given the
Follow your protocols!
 By Will Dunn, BA, NRP, CCEMTP & Myles Sibley, BA, NREMT P Eagle County Paramedic Services, Eagle County, CO. FIELD ASSESSMENT AND TREATMENT OF CLOSED HEAD AND SPINAL INJURY Follow your protocols! Objectives
By Will Dunn, BA, NRP, CCEMTP & Myles Sibley, BA, NREMT P Eagle County Paramedic Services, Eagle County, CO. FIELD ASSESSMENT AND TREATMENT OF CLOSED HEAD AND SPINAL INJURY Follow your protocols! Objectives
