Essex and Barking, Havering & Redbridge Supra-Network. In-patient and Community Neurological Rehabilitation Operational Policy
|
|
|
- Laurence Atkinson
- 5 years ago
- Views:
Transcription
1 Essex and Barking, Havering & Redbridge Supra-Network Brain & CNS NDSG In-patient and Community Neurological Rehabilitation Operational Policy Version 1.3 March 2012 Review Date March 2013 Author Kate Patience Macmillan AHP Lead Essex Cancer Network 1 V 1.3
2 Brain & CNS NSSG In-patient and Community Neurological Rehabilitation Operational Policy Agreement Cover Sheet This Constitution has been agreed by: Position: Name: Chair of the Brain & CNS NSSG, Trust Clinical Lead Dr K Madhavan Organisation: Date Agreed: 21 st March 2012 Southend University Hospital NHS Foundation Trust Position: Name: Chair of the Network Board Sheila Bremner Organisation: Date Agreed: 15 th May 2012 Position: Name: Neurorehabilitation Lead Kate Patience Organisation: Essex Cancer Network Date Agreed: 21 st March 2012 Position: Name: Trust Clinical Lead Dr Hafiz Algurafi Organisation: Basildon Date Agreed: 21 st March 2012 Essex Cancer Network 2 V 1.3
3 Position: Name: Trust Clinical Lead Dr Alan Lamont Organisation: Date Agreed: 21 st March 2012 Colchester Hospital University NHS Foundation Trust Position: Name: Trust Clinical Lead Dr Vivienne Loo Organisation: Mid Essex Hospital Trust Date Agreed: 21 st march 2012 Essex Cancer Network 3 V 1.3
4 Title: Neurological Rehabilitation Operational Policy incorporating guidelines for the referral and management of Brain & CNS cancer patients within regional and local in-patient and community rehabilitation facilities. Author: Kate Patience Macmillan AHP Lead Document Owner: Essex Cancer Network Swift House Hedgerows Business Park Chelmsford Essex CM2 5PF This document: March 2012 Essex Cancer Network 4 V 1.3
5 CONTENTS Contents Page 1. Introduction 6 2. Background 6 3. Description of the service Purpose and objectives Who the service is for (service users) Equality and diversity (Inclusion) 8 4. Rehabilitation Pathway 8 5. Operational details about how the 10 service will be delivered 5.1 Neurorehabilitation Team Members Neurorehabilitation Facilities within 11 ECN 5.3 Referral process Service provision Key working relationships Equipment provision Communication User Involvement Reference List Appendix 1 ECN Rehabilitation Pathway 19 for Brain & CNS Tumours (including MSCC) Essex Cancer Network 5 V 1.3
6 1.0 INTRODUCTION 1.1 In line with the Calman Hine report (1995), NHS cancer Plan (2000), NICE Improving Supportive and Palliative Care for Adults with Cancer (2004), NICE Improving Outcomes Guidance (IOG) for People with Brain and other CNS Tumours (2006), Cancer Reform Strategy (2007), Metastatic Spinal Cord Compression IOG (2008) and Improving Outcomes: A Guide for Cancer (2011) the purpose of this document is to provide clarity on the rehabilitation of patients with Brain & CNS tumours in Essex Cancer Network (ECN). The Essex Cancer Network Board is asked to formally approve this document on behalf of all its constituent organisations thereby ensuring uniformly high quality in primary, secondary and tertiary rehabilitation centres for all its patients, compliant with national guidance. 1.2 The Brain & CNS Peer Review Measures (11-1A-206k, 11-1D-111k) require a network wide operational policy for accessing neurorehabilitation facilities both in the acute and community setting, agreed by each locality. The Macmillan AHP Lead for the Essex Cancer Network (Kate Patience) worked with the Brain & CNS Network Site Specific Group and Rehabilitation Board to develop this document. 1.3 The AHP Lead is also a specialist oncology physiotherapist (Band 7) in North East Essex and is the area lead for neurorehabilitation (Peer Review Measure 11-1C-111k). The area lead for neuro-rehabilitation is a member of the CNMDT and NSSG and has the responsibility of overseeing and signposting access to acute, specialist in-patient neurological/spinal rehabilitation and community neuro-rehabilitation services for patients with brain and CNS tumours. 2.0 BACKGROUND 2.1 The ECRIC figures for the Essex Cancer Network ( ) show the annual average incidence of brain & CNS tumours was 163. Though primary brain tumours account for less than 2% of UK cancer diagnoses, more people under 40 die from a brain tumour than any other cancer. 2.2 The NICE IOGs for people with Brain & other CNS tumours (2006) and Metastatic Spinal Cord Compression (2008) state that patients with such tumours should have rapid access to Allied Health Professional (AHP) assessment & rehabilitation, including specialist neurorehabilitation where appropriate, as their condition changes. This includes the immediate access to, or provision of, specialist equipment as necessary. 2.3 The document will also cover neurological rehabilitation for patients requiring input as a result of paraneoplastic syndrome, a rare but potentially disabling condition from a variety of tumour sites which can cause a wide range of neurological deficits. 2.4 Cancer and its treatment can have a major impact on patients ability to carry on with their usual daily routines. Activities that most people take for granted, such as moving, speaking, eating, drinking and engaging in sexual activity, can all be severely impaired. 2.5 Tumours of the brain and CNS (including malignant spinal cord compression) can be highly complex due to poor prognosis, extent of disability, and experiences of long-term progressive, physical, cognitive and emotional problems. It is vital that consideration is given to the impact that such a diagnosis has and the wide ranging needs and support required throughout this period of care for both the patient and their support network. This requires an AHP workforce that is skilled in both physical and emotional issues to deal sensitively and competently with patients and their families/carers. Essex Cancer Network 6 V 1.3
7 2.6 Some tumours carry a good long-term prognosis, yet a patient s ability to live and function independently may be compromised and they may require ongoing rehabilitation services for a prolonged period of time. 2.7 Access to neurorehabilitation services should not be based on diagnosis or prognosis, but on the needs of the patient, rehabilitation potential and patient goals. Rehabilitation should be provided in the best location for the patient, whether that is an in-patient, out-patient or community setting. Specialist rehabilitation units should be considered if appropriate. The commissioning teams need to work closely with social service departments, primary, secondary and tertiary care providers to ensure that this aspect of the pathway is properly financed to meet patient needs in a timely manner. This should include rehabilitation for any signs and symptoms caused by the tumour and/or side effects from any treatments (including steroid induced myopathy). 2.8 Patients with spinal cord tumours should have the opportunity to undergo intensive rehabilitation in a specially adapted unit such as a spinal injuries unit, in order for them to achieve their maximum functional potential. Commissioners should ensure that patients with spinal tumours can be admitted to such units and that the treatment programme is appropriate to their needs. 2.9 The NICE Supportive and Palliative Care IOG describes a recommended model of rehabilitation assessment and support, with 4 levels of training and expertise for AHP groups. Level 1 indicates an assistant grade, Level 2 would describe generalist or rotational qualified staff, Level 3 is experienced AHPs with a basic level of cancer training, and Level 4 are advanced practitioners working solely or predominantly within cancer or palliative care with higher level training in the rehabilitation needs of people with cancer. The Brain & CNS IOG recommends that patients with brain and CNS tumours should be seen by Level 3 or 4 practitioners due to the complexity of the disease Cancer rehabilitation is gaining in profile, with developments such as the National Cancer Survivorship Initiative (NCSI) and NCAT Rehabilitation Pathways highlighting the need for intervention to improve quality of life and general health as much as possible. Studies have shown that functional improvements for people with brain and CNS tumours are comparable to rehabilitation effects for people after CVA and Traumatic Brain Injuries Rehabilitation in oncology should be offered from pre-diagnosis through to end of life and at all key stages in-between, as determined by the functional problems encountered by the patient and/or carer/family. Rehabilitation in oncology and palliative care aims to be: Preventative reducing the impact of expected disabilities and assistance in learning to cope with any disabilities Restorative returning the patient to pre-illness level without disability Supportive in the presence of persistent disease and the continual need for treatment, the goal is to limit functional loss and provide support Palliative further loss of function, put in place measures which eliminate or reduce complications and to provide support (symptom management) (Dietz, 1980) 2.12 Cancer rehabilitation attempts to maximise patients ability to function, to promote their independence and to help them adapt to their condition. It offers a major route to improving their quality of life, no matter how long or short the timescale. It aims to maximise dignity and reduce the extent to which cancer interferes with an individuals physical, psychosocial and economic functioning. (Macmillan AHP in Cancer Care Evidence Review, 2011) 2.13 The rehabilitation team also play a key role in the discharge planning of patients from acute and tertiary services, and this work should be commenced from admission and be co-ordinated by a named key worker. For many patients it may be appropriate for AHPs to be key workers, both in the acute and community setting, to ensure continuation of care. Essex Cancer Network 7 V 1.3
8 3.0 DESCRIPTION OF THE SERVICE 3.1 AIMS AND OBJECTIVES This Operational Policy has been developed to ensure equality of rehabilitation services across the Essex cancer Network for people with primary and secondary brain tumours, central nervous system tumours, metastatic spinal cord compression and neurological disorders as a result of Paraneoplastic Syndrome The Brain & CNS NSSG and the Rehabilitation Board are to ensure that all patients diagnosed with Brain & CNS tumours and Metastatic Spinal Cord Compressions are managed within an appropriate multidisciplinary care pathway as described in this document. The NSSG and Rehabilitation Board will ensure that there is continuous improvement in service delivery including the rehabilitation pathway through their work plans All patients must be assessed for their rehabilitation needs and referred or signposted to appropriate services, regardless of location and stage on the cancer pathway. This document outlines the processes to be followed in ensuring correct rehabilitation for patients is accessed and delivered. 3.2 SERVICE USERS This policy covers all patients with tumours of the brain and central nervous system, and patients with metastatic spinal cord compression or neurological damage from paraneoplastic syndrome from any tumour site All grades of tumours are included within this operational policy, as people with low grade tumours may require neurorehabilitation for any neurological deficits caused by the tumour and/or treatments given and their rehabilitation needs must be taken into consideration All stages of the cancer pathway are covered by this policy, as patients may require intervention from diagnosis, through treatment and into the survivorship stage, which may be a curative or palliative pathway. This would include vocational rehabilitation where appropriate This document should be used by commissioners, cancer clinicians, CNSs, AHPs and the extended rehabilitation team to ensure prompt and appropriate referral to rehabilitation services which may require individually commissioned packages of care and equipment depending on the circumstances of each person. 3.3 EQUALITY AND DIVERSITY Neurorehabilitation facilities should be open to patients whose rehabilitation needs are caused by their tumour or its treatment and they should not be excluded from specialist services due to a cancer diagnosis or because of a palliative condition Due to the range of communication and mobility difficulties which may be caused as a result of brain and CNS tumours, services must ensure they offer a variety of methods for communication and accessibility to ensure that people are able to make appointments and access services. 4.0 REHABILITATION PATHWAY 4.1 The Essex and Barking, Havering & Redbrige (BHR) Supra-network Neuroscience MDT is hosted by BHR. The Essex Cancer Network MDT (CNMDT) is hosted by Southend University Hospital Foundation Trust. The Essex CNMDT is associated with the Neurosciences SMDT and Neurosurgical SMDT at Queens s hospital Romford and patients are pulled from this list to be discussed at the CNMDT to ensure continuation of care. All patients should be referred to the Essex Cancer Network 8 V 1.3
9 CNMDT for the supervision of the non-surgical aspects of their care including rehabilitation and specialist palliative care services (see diagram below). 4.2 The Neurosurgical MDT should have an AHP agreed as having responsibility for liaison with neurorehabilitation services in attendance as a core member (11-2K-201). This should be specified in the job plan of the person designated to cover this meeting, and they should have a named representative to cover when they are not able to attend. This person is responsible for ensuring that rehabilitation needs are discussed in the meeting and signposts to appropriate AHP services. 4.3 The cancer network MDT is the coordinating team for the non-surgical management of most adult patients with CNS tumours. The Brain & CNS Peer Review measures (11-2K-101) state that there should be an occupational therapist, speech and language therapist and a physiotherapist with time specified in their job plan for the care of patients with a CNS tumour as part of this CNMDT. 4.4 The CNMDT are responsible for nominating and recording a key worker to act as point of contact for patients, their relatives and carers. This should be agreed with the patient, their relatives and carers. The CNMDT will also and agree who is responsible for organising rehabilitation referrals. 4.5 The CNMDT member nominated responsible for referrals to rehabilitation services will enaure that referrals are completed and sent within 24 hours of the CNMDT meeting. A record of all referrals should be kept on the MDT proforma (outcomes sheet). 4.6 The CNMDT should refer to the Essex Cancer Network Rehabilitation Pathway for People with Brain and CNS Tumours for a list of triggers to referrals to the main rehabilitation AHP groups (Physiotherapy, Occupational Therapy, Speech and Language Therapy, Dietetics and Lymphoedema Therapists) to ensure that patients are referred to the appropriate services. This pathway can be found as appendix 1. A list of contact numbers for local teams can be found under section 5.6 of this document or within the AHPs in Cancer Service Directory. Essex Cancer Network 9 V 1.3
10 Supportive and Palliative care (Access throughout) Southend Hospital Initial presentation Broomfield Hospital Colchester Hospital Neurosciences SMDT at Queens Hospital, Romford Essex MDT Basildon Hospital Local diagnostic imaging Local Diagnostic Imaging Specialist Diagnostic Imaging Key: Patient referral for assessment / management Patient referral for diagnostic imaging 5.0 OPERATIONAL DETAILS OF SERVICE DELIVERY 5.1 NEUROREHABILITATION TEAM MEMBERS Neurorehabilitation services are provided by a range of allied health professionals (AHPs) including Physiotherapists Occupational therapists Speech and Language Therapists Dieticians The following health and social care professionals may also have a role in neurorehabilitation Nurses Primary health care team Neuropsychology, neuropsychiatry and psychological therapy Social services care manager/continuing care manager Orthotists/appliance officers Chaplaincy services Essex Cancer Network 10 V 1.3
11 The Cancer Network Macmillan AHP Lead will ensure that Level 4 specialist AHPs are available in each locality in the network and that patients are able to access them as and when appropriate. 5.2 NEUROREHABILITATION FACILITIES WITHIN ECN The NICE IOG for Brain & CNS Tumours (2006) states there should be provision of rehabilitation facilities inpatient, outpatient, domiciliary services, hydrotherapy, specialist neurorehabilitation services, and specialist palliative care services. Below is a table indicating the service provision across the Network. Area In-patient Community/ Out-patient Mid Essex North East South East Oncology ward team Stroke Unit (post-op) Oncology ward team Medical ward team Oncology ward team Neurorehab (Physio only) Neurorehab team (OT, Physio SLT) Physio (general community) Hydro No Yes Specialist Palliative Care AHPs OT and Physio at Farleigh Hospice OT and Physio at St Helena Hospice Specialist Neurorehabilitation Referred to Northwood Park for assessment Referred to Homerton for assessment No None available Referred to Northwick Park South West Pagglesham Ward team Palliative Care ward team Neurorehab team (physio only) Palliative OT Team (equipment only) Palliative Care OT (equipment only) Yes Very limited Physio input only Referred to Northwick Park Queens General ward teams Neurosurgical team Neuro PT, Community OT No OT and Physio at St Francis Hospice Referred to Homerton or Northwick Park For a more in depth listing and contact details see section 5.6 Communication The Brain and CNS IOG states that where there is no local provision of neurorehabilitation facilities, the network should provide a cancer network neuro-oncology rehabilitation team Almost all neuroscience centres in England and Wales (96%) reported having access to a specialist neurorehabilitation unit. Access to specialist neurorehabilitation units was much lower for oncology/radiotherapy units (60%). All patients with rehabilitation potential should be offered referral to appropriate rehabilitation services. If patients choose not to accept a referral to such a unit, this should be documented in their medical notes to ensure that this can be audited. Essex Cancer Network 11 V 1.3
12 5.2.4 Service providers should ensure that all patients admitted to hospital with MSCC, Brain and CNS tumours have access to a full range of healthcare professional support services for assessment, advice and rehabilitation Service providers should focus the rehabilitation of patients with MSCC, Brain & CNS tumours on their goals and desired outcomes, which could include promoting functional independence, participation in normal activities of daily life and aspects related to their quality of life Service providers should offer admission to a specialist rehabilitation unit to those patients with MSCC, Brain & CNS tumours who are most likely to benefit, for example, those with a good prognosis, a high activity tolerance and strong rehabilitation potential It must be noted that there is no provision for in-patient specialist neurorehabilitation within the Essex Cancer Network. Due to the long waiting lists and referral criteria for specialist units patients with brain and CNS tumours are rarely referred. The ECN Brain & CNS NSSG is in agreement that this is not justifiable as patients are being denied access to such facilities which may have a huge impact on quality of life. The Neuro-rehab Lead and NSSG Chair are therefore working with service providers to develop a business case to establish local specialist services to meet the needs of our population. 5.3 REFERRAL PROCESS FOR REHABILITATION SERVICES Service Users should be assessed for their rehabilitation needs at each key stage of the cancer pathway and at any point where there is a change in their condition. A holistic assessment using a recognised assessment tool should be performed by the key worker in order to determine and rehabilitation needs. Referrals to AHP services should be offered and a copy of any referrals should be kept in the patient s medical records and their own patient records where applicable There should be AHP input at NSMDT and CNMDT meetings to ensure that rehabilitation needs are discussed and ensure that appropriate services are signposted to. Decisions made at the meeting should be noted in the outcomes on the MDT proforma. Referrals should be made within 24 hours of the meeting by a person nominated at the meeting and a copy of the referral should be stored in the patient s medical notes. Teams should ensure they have relevant contact details for all local and regional services (as listed in section 5.6 of this document) For in-patients referrals should be made to the appropriate teams and responded to within an appropriate timescale as per local policy Patients meeting the on-call respiratory physiotherapy criteria (e.g. for aspiration or deteriorating post-operative respiratory complications) should be treated as per the local on-call physiotherapy service policy. Patients at risk of aspiration should be placed Nil By Mouth and should be assessed by a dietician and speech and language therapist within 24 hours of referral For patients with suspected MSCC, the ECN Care Pathway for Acute Management of Suspected Metastatic Spinal Cord Compression (MSCC) must be followed. Patients should be nursed flat in neutral spinal alignment (including log rolling) until spinal stability has been ensured. Following treatment, the protocol for mobilising patients safely should be followed (NICE MSCC IOG, 2008) Mobility and manual handling risk assessments should be performed within 72 hours of admission, and an appropriate management and treatment plan put into place which is communicated to all ward staff For service users transferred to the Neurosurgical Centre, the Occupational Therapy team at Queens will liaise with local OT teams to ensure that equipment required for discharge is organised and delivered in a timely manner to facilitate a timely and safe discharge. This will include carrying out any access visits required locally. Essex Cancer Network 12 V 1.3
13 5.3.8 Patients requiring specialist neurological rehabilitation as an in-patient to improve function and quality of life should be referred to the regional rehabilitation centre as per the local policy. Patients must have rehabilitation potential but should not be excluded due to a cancer diagnosis or a palliative condition. A specialist neurorehabilitation centre should be available within the cancer network For out-patients, patients should be referred to the appropriate local rehabilitation services. For complex physical needs, this should be a neurorehabilitation team. For complex psychological needs this should be a specialist palliative care team at a hospice. For patients with general rehabilitation needs it may be more appropriate to use general rehabilitation teams, who would be able to access specialist advice from Level 4 practitioners in neurorehabilitation or specialist palliative care services if required Patients should be able to access neurorehabilitation and/or specialist palliative care services rapidly due to the nature of the disease which can cause rapid changes in condition. Teams should ensure that there are local policies in place to enable this rapid access to assessment, as this may prevent avoidable hospital or hospice admissions and enable patients to remain at home for as long as possible. Patients and/or their families and carers should have clear contact points for these services Referrals should be screened and prioritised by local teams as per local policy.. Any referrals not considered appropriate should be discussed with the referrer within 1 working week to enable alternative arrangements to be made Due to the complexity of neurological and cognitive deficits, patients should be offered domiciliary visits where required Service users should be provided with a range of methods communication to arrange appointments to ensure patients with sensory deficits or cognitive impairments have access to services Due to the overlap of complex physical and psychological needs for patients with brain & CNS tumours neurorehabilitation teams and specialist palliative care teams should meet regularly to discuss patients who may be under the shared care of both teams, as occurs with other conditions (e.g. Motor Neurone Disease) Service Users should also be referred to survivorship groups where appropriate, e.g. exercise groups or vocational rehabilitation projects to ensure general health and wellbeing is addressed. This may require onward referral to specialist services e.g. benefits service to access assistance with returning to work etc Patients coming to the end of treatment should continue to have access to rehabilitative therapies for an indefinite period, and should know how to initiate such access. 5.4 SERVICE PROVISION Physiotherapy Input Neurological assessment Mobility assessment Falls and balance assessment Prophylactic respiratory and thromboembolic input Respiratory physiotherapy Positioning and seating issues Vocational Rehabilitation Pain management Fatigue management Reduced exercise tolerance (including myopathy) Essex Cancer Network 13 V 1.3
14 Trachaeostomy care Breathlessness management Hydrotherapy Botox treatment Continence advice Occupational Therapy Input ADL assessments Neurological assessment Cognitive assessment Falls and balance assessment Positioning and seating issues Vocational Rehabilitation Fatigue and anxiety management Wheelchair assessment Splinting Dietetic input Nutritional assessment Dysphagia Nausea and vomiting Fatigue management Anorexia/cachexia Steroid induced diabetes Enteral feeding Diet modification (neurological bowel management) Speech and language therapy input Communication advice Vocal rehabilitation Dysphagia assessment and management 5.5 KEY WORKING RELATIONSHIPS Due to the complexity of tumours of the brain and CNS, there are many key working relationships. Patients should be given contact details for all relevant services. Local MDT teams should ensure that they have the contact details for all the local services held centrally and the neuroscience centre should have a copy of services from each locality The following should be on the key contact lists: CNSs Key workers Clinicians (Surgeons, Neurologists, Oncologists) MDT Co-ordinators Palliative Care Team Members Hospice services Support Groups Charities e.g. Headway, Brain Tumour UK For Teenagers and Young Adults, a contact at the Primary Treatment Centre (UCLH) Information centre Benefits service Physiotherapy teams Occupational Therapy Teams Orthotists Speech and Language Therapy Teams Essex Cancer Network 14 V 1.3
15 Dietetic and Nutrition services Network Rehabilitation Lead 5.6 EQUIPMENT PROVISION Patients should have holistic assessment at all key stages of the cancer pathway using a recognised holistic assessment tool which should highlight any functional problems which may require onward referral for further specialist assessment for equipment needs Providers should ensure suitable facilities and ready access to equipment to support effective and safe rehabilitation. They should ensure equipment is available to enable patients to continue their rehabilitation plan at home. Priority should be given to those patients who are dying Providers should ensure that patients requiring specialist seating have rapid access to assessment and provision of this equipment For larger items of equipment such as standing frames which may benefit patients, it may be necessary to access grants or charitable funding (e.g. Macmillan, Catalyst). This should be offered to patients in a timely manner to ensure full benefit Delays in accessing equipment and facilities may occur with failure to prioritise services required, particularly for patients at the end of life. The ECN Rehabilitation Board will work with the equipment services to develop a policy to ensure equipment is available to patients within 24 hours of the request at the end of life Providers should be able to demonstrate robust systems of forward planning for orders and delivery times, with capacity to anticipate individual patient needs for appliances such as appropriate wigs, splints and orthoses. A ready supply of appliances commonly needed by patients with particular conditions should be available. Patients should be made aware of the appropriate person to contact to obtain fresh supplies or to discuss problems or concerns. 5.7 COMMUNICATION Area Service Name Contact details Mid Essex North East Essex Physiotherapy (Acute) Occupational Therapy (Acute) Physiotherapy (Out patient Neurorehabilitation) Dietetic Department (Acute and Out-patient) Speech and Language Therapy (Acute and Oupatient) Specialist Palliative Care Physiotherapy (acute) Lisa Curtis Lead PT Planned Care Broomfield Hospital Senior OT (oncology) Broomfield Hospital Debbie Snell Lead PT Out-patients, Broomfield Hospital Broomfield Hospital Broomfield Hospital Helen Peter/Nikki Tuff, Senior OT/PT, Farleigh Hospice Amy Eade Senior Physiotherapist bleep 241 or Essex Cancer Network 15 V 1.3
16 Essex County Hospital Occupational Therapy (acute) Senior OT Essex County Hospital South East Essex Physiotherapy (outpatient Neurorehabilitation) Occupational Therapy (out-patient Neurorehabilitation) Dietetics (acute and community) Speech and Language Therapy (acute and community) Specialist Palliative Care Occupational Therapy (acute palliative) Jane Forster Specialist Physiotherapist Colchester General Hospital Cathy Chambers Specialist OT Colchester General Hospital Heather Copson Oncology Dietitian Essex County Hospital Ruth Myers Lead SLT Anglia Community Enterprise Kimberley Rice/Liz Ritson Senior PT/OT St Helena Hospice Beverley Kemp Senior OT Southend General Hospital or bleep (need to refer to full hospice services) Physiotherapy (Inpatient Neurorehabilitation) Joanne Lay Senior PT Southend General Hospital Dietetics (acute and community) Dietetic Team Southend Hospital Speech and Language Therapy (neuro community team) Speech and Language Therapy Team Southend Hospital South West Essex Occupational Therapy (Community) Physiotherapy (community) Occupational Therapy (Acute) Physiotherapy (Acute) Kerry Lockhart Clinical Lead, Duty OT Team South East Essex PCT Susanne Barton Specialist Physiotherapist Natasha York Specialist OT Basildon Hospital Sue Webb Specialist Physiotherapist Basildon Hospital ext ext bleep 6203 Occupational Therapy (Community) Matthew Goddard Specialist OT Basildon Speech and Language Therapy (acute & community) Dietetics (acute & community) Rebecca Kelso Speech and Language Therapist Basildon Hospital Dietetic Team Basildon Hospital ext ext Essex Cancer Network 16 V 1.3
17 Queens Hospital, Romford (Neurosurgical Centre) Physiotherapy (Outpatient Neurorehabilitation) Occupational Therapy (Team Lead) Physiotherapy (Neuro Team) Occupational Therapy (Neuro Team) Neurorehab Team Basildon Hospital Mark Mainwood Specialist OT Queens Hospital Charlotte Turnpenny Specialist Physio Claire Howley Specialist Neuro OT ext ext ext For emergency presentations transferring as in-patients between local hospitals and the neurosurgical centre there should be a telephone handover and a copy of patient notes and/or a treatment summary and patient goals Any telephone communication should be documented in the patient records or on relevant systems (e.g. System 1) Patients should be able to access appointments using a variety of communication styles, depending on the needs of the patient. Services should take this into account when making initial contact For service users with communication difficulties or cognitive impairment service providers should make use of carers, relatives or Power of Attorney in decision making process/communication with consent of the patient where appropriate A range of tools for communication taking into account patient needs, including information prescription, should be offered to all patients informing them of relevant services, contact details and important information (e.g. treatment information, exercise programmes etc) A discharge summary should be sent to the referrer, patient and GP advising of treatment given, goals (whether met or outstanding) and any onwards referrals required. 5.8 USER INVOLVEMENT The Brain & CNS NSSG and Rehabilitation Board should have 2 User Representatives (patients or carers) who are responsible for providing the patient perspective on any issues raised (11-1A-202K). If User Representatives are not available for the group, the User Facilitator for the Cancer Network will attend meetings to ensure that User views are taken into account. As the NSSG and Rehabilitation Board are responsible for producing and reviewing this document, service users will be involved in any service development There must also be a member of the CNMDT who should be nominated as having specific responsibility for users and carers issues and information (11-2K-101). Essex Cancer Network 17 V 1.3
18 REFERENCE LIST Dietz, J.H. (1980) Adaptive Rehabilitation in Cancer. Postgraduate Medicine, 68(1), National Council for Hospice and Specialist Palliative Care Services. Fulfilling Lives. Rehabilitation in palliative care. London: NCHSPCS. August Nice Guidance: MSCC, Supportive & Palliative Care, Brain & CNS Essex Cancer Network 18 V 1.3
19 AHP Diagnosis & Care Planning Treatment Post treatment Monitoring Palliative/end of life care Intervention Rehab Pathway p.2-3 Rehab Pathway p.3-5 Rehab Pathway p.6-7 Rehab Pathway p.7-9 Rehab Pathway p Team Local Hospital Teams Surgery Queens Hospital, Romford Radiotherapy Southend/Colchester Chemo- Broomfield, Colchester, Southend Physiotherapy Impaired mobility/function Respiratory problems Impaired upper limb function Falls Manual handling issues Seating/positioning problems Impaired balance Carer/family support Vocational rehab Reduced exercise tolerance Fatigue Trachaeostomy care Pain Local Hospital teams, neurorehabilitation teams or hospice Local Hospital teams, neurorehabilitation teams or hospice Breathlessness neurorehabilitation teams or hospice Occupational Therapy Concerns with ADL s and coping at home Anxiety Falls Manual handling issues Impaired upper limb function Seating/positioning problems Carer/family support Wheelchair assessment Fatigue Vocational rehabilitation Cognitive rehabilitation Essex Cancer Network 19 V 1.3
20 AHP Diagnosis & Care Planning Treatment Post treatment Monitoring Palliative/end of life care Intervention Rehab Pathway p.2-3 Rehab Pathway p.3-5 Rehab Pathway p.6-7 Rehab Pathway p.7-9 Rehab Pathway p Team Local Hospital Teams Surgery Queens Hospital, Romford Radiotherapy Southend/Colchester Chemo- Broomfield, Colchester, Southend Speech and Language Therapy Dietetics Communication problems with voice or speech Dysphagia Carer/family support Dysphagia Poor nutritional intake MUST score>2 Anorexia/cachexia Carer/family support Inter-operative language assessment Enteral feeding Fatigue Nausea & vomiting Taste changes Dry mouth Steroid induced diabetes Local Hospital teams, neurorehabilitation teams or hospice Local Hospital teams, neurorehabilitation teams or hospice If a diagnosis of lymphoedema is made at any point of the cancer journey the patient should be referred to the local Lymphoedema Service. Signs and symptoms include: neurorehabilitation teams or hospice Lymphoedema Swelling in the arms, hands, fingers, shoulders, chest, or legs. This may occur for the first time after a trauma (e.g. bruises, cuts, sunburn, and sports injuries), after an infection in the part of the body that was treated for cancer, or after an airplane trip lasting more than three hours. A "full" or heavy sensation in the arms or legs. Tightness of the skin. Decreased range of movement in the hand, wrist, or ankle. Difficulty fitting into clothing in one specific area, or new tightness of jewellery. Essex Cancer Network 20 V 1.3
ECN Rehabilitation Board Rehabilitation Needs Assessment
 1 ECN Rehabilitation Board Rehabilitation Needs Assessment (Peer Review Measure 11-1E-114v) Agreement Cover Sheet 2 The ECN Rehabilitation Needs Assessment has been agreed by: Position Name Organisation
1 ECN Rehabilitation Board Rehabilitation Needs Assessment (Peer Review Measure 11-1E-114v) Agreement Cover Sheet 2 The ECN Rehabilitation Needs Assessment has been agreed by: Position Name Organisation
National Cancer Action Team. Rehabilitation Care Pathway Brain CNS
 National Cancer Action Team Rehabilitation Care Pathway Brain CNS Rehabilitation Care Pathway Brain CNS Diagnosis & Care Planning Drop Down Pathways Dysphagia Mobility/ loss of function Intervention D1
National Cancer Action Team Rehabilitation Care Pathway Brain CNS Rehabilitation Care Pathway Brain CNS Diagnosis & Care Planning Drop Down Pathways Dysphagia Mobility/ loss of function Intervention D1
CANCER REHABILITATION PATHWAY - HAEMATOLOGY
 CANCER REHABILITATION PATHWAY - HAEMATOLOGY Statement: To be used in conjunction with Brain and CNS Rehabilitation Care Pathway as appropriate Diagnosis and Care Planning: The following symptom pathways
CANCER REHABILITATION PATHWAY - HAEMATOLOGY Statement: To be used in conjunction with Brain and CNS Rehabilitation Care Pathway as appropriate Diagnosis and Care Planning: The following symptom pathways
Lung Cancer and Rehabilitation
 Lung Cancer and Rehabilitation Report to Lung NSSG Sally Donaghey Macmillan AHP Lead, Ang CN sally.donaghey@suffolkpct.nhs.uk/tel: 01638 608218 Lung Cancer and Rehabilitation Evidence based Rehabilitation
Lung Cancer and Rehabilitation Report to Lung NSSG Sally Donaghey Macmillan AHP Lead, Ang CN sally.donaghey@suffolkpct.nhs.uk/tel: 01638 608218 Lung Cancer and Rehabilitation Evidence based Rehabilitation
INTERNAL VALIDATION REPORT (MULTI-DISCIPLINARY TEAM)
 INTERNAL VALIDATION REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MVCN EAST AND NORTH HERTFORDSHIRE Mount Vernon Cancer Centre Cancer Network MDT (11-2K-1) - 2011/12 Date Self Assessment Completed
INTERNAL VALIDATION REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MVCN EAST AND NORTH HERTFORDSHIRE Mount Vernon Cancer Centre Cancer Network MDT (11-2K-1) - 2011/12 Date Self Assessment Completed
Work Programme/Service Delivery Plan 2010/2013
 Essex and East Suffolk Gynaecological Cancer Network Site Specific Group Work Programme/Service Delivery Plan 2010/2013 Version Number 1.2 Author Members of the NSSG Date Written June 2010 Reviewed May
Essex and East Suffolk Gynaecological Cancer Network Site Specific Group Work Programme/Service Delivery Plan 2010/2013 Version Number 1.2 Author Members of the NSSG Date Written June 2010 Reviewed May
NATIONAL REHABILITATION HOSPITAL SPINAL CORD SYSTEM OF CARE (SCSC) OUTPATIENT SCOPE OF SERVICE
 NATIONAL REHABILITATION HOSPITAL SPINAL CORD SYSTEM OF CARE (SCSC) OUTPATIENT SCOPE OF SERVICE Introduction: The Spinal Cord System of Care (SCSC) at the National Rehabilitation Hospital (NRH) provides
NATIONAL REHABILITATION HOSPITAL SPINAL CORD SYSTEM OF CARE (SCSC) OUTPATIENT SCOPE OF SERVICE Introduction: The Spinal Cord System of Care (SCSC) at the National Rehabilitation Hospital (NRH) provides
Upper GI Cancer Network Site-Specific Group. Work Programme/Service Delivery Plan 2011/14
 Upper GI Cancer Network Site-Specific Group Work Programme/Service Delivery Plan 2011/14 1 UPPER GI NSSG Work Programme/Service Delivery Plan AGREEMENT COVER SHEET 2011/14 This Work Programme has been
Upper GI Cancer Network Site-Specific Group Work Programme/Service Delivery Plan 2011/14 1 UPPER GI NSSG Work Programme/Service Delivery Plan AGREEMENT COVER SHEET 2011/14 This Work Programme has been
Improving services for upper GI (OG) cancer Application template (Version 2)
 Trust Clinical lead Improving services for upper GI (OG) cancer Application template (Version 2) Managerial lead Date completed 14 June 2013 Barnet & Chase Farm Hospitals NHS Trust Dr Marta Carpani Upper
Trust Clinical lead Improving services for upper GI (OG) cancer Application template (Version 2) Managerial lead Date completed 14 June 2013 Barnet & Chase Farm Hospitals NHS Trust Dr Marta Carpani Upper
Brain Tumour Scoping project
 Brain Tumour Scoping project 2012-13 Kim Ainsworth, AHP Lead, North London Cancer Network Louise Platt, Therapy Team Lead Neurosurgery, NHNN Sharon Cavanagh, LWBC Lead, Living with and Beyond Cancer Quick
Brain Tumour Scoping project 2012-13 Kim Ainsworth, AHP Lead, North London Cancer Network Louise Platt, Therapy Team Lead Neurosurgery, NHNN Sharon Cavanagh, LWBC Lead, Living with and Beyond Cancer Quick
PATHWAY MANAGEMENT OF METASTATIC SPINAL CORD COMPRESSION (MSCC) THE CHRISTIE, GREATER MANCHESTER & CHESHIRE
 PATHWAY MANAGEMENT OF METASTATIC SPINAL CORD COMPRESSION (MSCC) THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: Dr V. Misra Version: Accountable Committee: V3 MSCC Network
PATHWAY MANAGEMENT OF METASTATIC SPINAL CORD COMPRESSION (MSCC) THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: Dr V. Misra Version: Accountable Committee: V3 MSCC Network
Freedom of Information Act Request Physiotherapy Services for Neurological Conditions
 Freedom of Information Act Request Physiotherapy Services for Neurological Conditions 1. In total how many physiotherapists does C&V UHB employ? s services 33 qualified paediatric physiotherapy staff in
Freedom of Information Act Request Physiotherapy Services for Neurological Conditions 1. In total how many physiotherapists does C&V UHB employ? s services 33 qualified paediatric physiotherapy staff in
Referral guide for acute oncology emergencies
 Referral guide for acute oncology emergencies 1 st Edition v 1.0 London Cancer March 2013 To be used in conjunction with London Cancer clinical guidelines for acute oncology emergencies; A Guide to Acute
Referral guide for acute oncology emergencies 1 st Edition v 1.0 London Cancer March 2013 To be used in conjunction with London Cancer clinical guidelines for acute oncology emergencies; A Guide to Acute
NATIONAL REHABILITATION HOSPITAL (NRH) THE SPINAL CORD SYSTEM OF CARE (SCSC) PROGRAMME INPATIENT SCOPE OF SERVICE
 NATIONAL REHABILITATION HOSPITAL (NRH) THE SPINAL CORD SYSTEM OF CARE (SCSC) PROGRAMME INPATIENT SCOPE OF SERVICE NATIONAL REHABILITATION HOSPITAL SCOPE OF SERVICE FOR THE SPINAL CORD SYSTEM OF CARE PROGRAMME
NATIONAL REHABILITATION HOSPITAL (NRH) THE SPINAL CORD SYSTEM OF CARE (SCSC) PROGRAMME INPATIENT SCOPE OF SERVICE NATIONAL REHABILITATION HOSPITAL SCOPE OF SERVICE FOR THE SPINAL CORD SYSTEM OF CARE PROGRAMME
National Cancer Action Team. Rehabilitation Care Pathway Poor Mobility and Loss of Function
 National Cancer Action Team Rehabilitation Care Pathway Poor Mobility and Loss of Function Diagnosis & Care Planning Assess respiratory status especially in people with preexisting respiratory disease
National Cancer Action Team Rehabilitation Care Pathway Poor Mobility and Loss of Function Diagnosis & Care Planning Assess respiratory status especially in people with preexisting respiratory disease
Ratified by: Care and Clinical Policies Date: 17 th February 2016
 Clinical Guideline Reference Number: 0803 Version 5 Title: Physiotherapy guidelines for the Management of People with Multiple Sclerosis Document Author: Henrieke Dimmendaal / Laura Shenton Date February
Clinical Guideline Reference Number: 0803 Version 5 Title: Physiotherapy guidelines for the Management of People with Multiple Sclerosis Document Author: Henrieke Dimmendaal / Laura Shenton Date February
2010 National Audit of Dementia (Care in General Hospitals)
 Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Barking, Havering and Redbridge Hospitals NHS Trust The 2010
Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Barking, Havering and Redbridge Hospitals NHS Trust The 2010
ACTION: FS to send a link to the directory of services
 London Cancer Rehabilitation ERG Date: Wednesday, 27 January 2016, 15:00 16:30 Venue: Boardroom, 3 rd Floor, 170 Tottenham Court Road, London, W1T 7HA Chair: Sharon Cavanagh 1. Welcome, Apologies and minutes
London Cancer Rehabilitation ERG Date: Wednesday, 27 January 2016, 15:00 16:30 Venue: Boardroom, 3 rd Floor, 170 Tottenham Court Road, London, W1T 7HA Chair: Sharon Cavanagh 1. Welcome, Apologies and minutes
Richard Watson, Chief Transformation Officer. Dr P Holloway, GP Clinical Lead for Cancer Lisa Parrish, Senior Transformation Lead
 GOVERNING BODY Agenda Item No. 08 Reference No. IESCCG 18-02 Date. 23 January 2018 Title Lead Chief Officer Author(s) Purpose Cancer Services Update Richard Watson, Chief Transformation Officer Dr P Holloway,
GOVERNING BODY Agenda Item No. 08 Reference No. IESCCG 18-02 Date. 23 January 2018 Title Lead Chief Officer Author(s) Purpose Cancer Services Update Richard Watson, Chief Transformation Officer Dr P Holloway,
NZ Organised Stroke Rehabilitation Service Specifications (in-patient and community)
 NZ Organised Stroke Rehabilitation Service Specifications (in-patient and community) Prepared by the National Stroke Network to outline minimum and strongly recommended standards for DHBs. Date: December
NZ Organised Stroke Rehabilitation Service Specifications (in-patient and community) Prepared by the National Stroke Network to outline minimum and strongly recommended standards for DHBs. Date: December
2010 National Audit of Dementia (Care in General Hospitals) Guy's and St Thomas' NHS Foundation Trust
 Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Guy's and St Thomas' NHS Foundation Trust The 2010 national
Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Guy's and St Thomas' NHS Foundation Trust The 2010 national
2010 National Audit of Dementia (Care in General Hospitals) North West London Hospitals NHS Trust
 Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: rth West London Hospitals NHS Trust The 2010 national audit
Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: rth West London Hospitals NHS Trust The 2010 national audit
HERTS VALLEYS CCG PALLIATIVE AND END OF LIFE CARE STRATEGY FOR ADULTS AND CHILDREN
 HERTS VALLEYS CCG PALLIATIVE AND END OF LIFE CARE STRATEGY FOR ADULTS AND CHILDREN 2016-2021 1 1. Introduction Herts Valleys Palliative and End of Life Care Strategy is guided by the End of Life Care Strategic
HERTS VALLEYS CCG PALLIATIVE AND END OF LIFE CARE STRATEGY FOR ADULTS AND CHILDREN 2016-2021 1 1. Introduction Herts Valleys Palliative and End of Life Care Strategy is guided by the End of Life Care Strategic
North Thames Teenager and Young Adults Cancer Network Coordinating Group (TYACNCG) Annual Report
 North Thames Teenager and Young Adults Cancer Network Coordinating Group (TYACNCG) Annual Report 2011-12 V0.9 Agreement Chair of the TYA Cancer Network (11-7A-201,202) Position: Divisional Director Name:
North Thames Teenager and Young Adults Cancer Network Coordinating Group (TYACNCG) Annual Report 2011-12 V0.9 Agreement Chair of the TYA Cancer Network (11-7A-201,202) Position: Divisional Director Name:
2010 National Audit of Dementia (Care in General Hospitals) Chelsea and Westminster Hospital NHS Foundation Trust
 Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: NHS Foundation Trust The 2010 national audit of dementia
Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: NHS Foundation Trust The 2010 national audit of dementia
Survivorship Guidelines. September 2013 (updated August 2015)
 Survivorship Guidelines September 2013 (updated August 2015) CONTENTS Contents 1 Introduction... 3 2 Background... 3 3 Recommendations and Rationale... 4 Appendix 1: Holistic Needs Assessment... 9 Appendix
Survivorship Guidelines September 2013 (updated August 2015) CONTENTS Contents 1 Introduction... 3 2 Background... 3 3 Recommendations and Rationale... 4 Appendix 1: Holistic Needs Assessment... 9 Appendix
Selective Dorsal Rhizotomy (SDR) Scotland Service Pathway
 Selective Dorsal Rhizotomy (SDR) Scotland Service Pathway This pathway should to be read in conjunction with the attached notes. The number in each text box refers to the note that relates to the specific
Selective Dorsal Rhizotomy (SDR) Scotland Service Pathway This pathway should to be read in conjunction with the attached notes. The number in each text box refers to the note that relates to the specific
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 Chronic fatigue syndrome myalgic encephalomyelitis elitis overview bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated
Chronic fatigue syndrome myalgic encephalomyelitis elitis overview bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated
Improving Outcomes for People with Sarcoma
 NHS National Institute for Health and Clinical Excellence Guidance on Cancer Services Improving Outcomes for People with Sarcoma List of All Recommendations March 2006 Developed for NICE by the National
NHS National Institute for Health and Clinical Excellence Guidance on Cancer Services Improving Outcomes for People with Sarcoma List of All Recommendations March 2006 Developed for NICE by the National
SPINAL CORD INJURY Rehab Definitions Framework Self-Assessment Tool inpatient rehab Survey for Spinal Cord Injury (SCI)
 SPINAL CORD INJURY Rehab s Framework Self-Assessment Tool inpatient rehab Survey for Spinal Cord Injury (SCI) INTRODUCTION: In response to a changing rehab landscape in which rehabilitation is offered
SPINAL CORD INJURY Rehab s Framework Self-Assessment Tool inpatient rehab Survey for Spinal Cord Injury (SCI) INTRODUCTION: In response to a changing rehab landscape in which rehabilitation is offered
South East Coast Operational Delivery Network. Critical Care Rehabilitation
 South East Coast Operational Delivery Networks Hosted by Medway Foundation Trust South East Coast Operational Delivery Network Background Critical Care Rehabilitation The optimisation of recovery from
South East Coast Operational Delivery Networks Hosted by Medway Foundation Trust South East Coast Operational Delivery Network Background Critical Care Rehabilitation The optimisation of recovery from
Realising the potential of AHPs to support those with cancer in the future
 Realising the potential of AHPs to support those with cancer in the future June Davis National cancer rehabilitation lead Macmillan Cancer Support 1 st June 2016 The shifting pattern of survival Total
Realising the potential of AHPs to support those with cancer in the future June Davis National cancer rehabilitation lead Macmillan Cancer Support 1 st June 2016 The shifting pattern of survival Total
Sentinel Stroke National Audit Programme (SSNAP)
 Sentinel Stroke National Audit Programme (SSNAP) Changes over Time: 4 years of data April 2013 March 2017 National results Based on stroke patients admitted to and/or discharged from hospital between April
Sentinel Stroke National Audit Programme (SSNAP) Changes over Time: 4 years of data April 2013 March 2017 National results Based on stroke patients admitted to and/or discharged from hospital between April
This specification should be read in conjunction with the Rotherham Hospice overall contract and schedules.
 Care Pathway/Service Commissioner Lead Provider Lead Period Applicability of Module E (Acute Services Requirements) Rotherham Palliative Medicine Service Gail Palmer Fiona Hendry 1 April 2011 31 March
Care Pathway/Service Commissioner Lead Provider Lead Period Applicability of Module E (Acute Services Requirements) Rotherham Palliative Medicine Service Gail Palmer Fiona Hendry 1 April 2011 31 March
MANAGEMENT OF PATIENTS WITH METASTATIC SPINAL CORD COMPRESSION
 CLINICAL POLICY MANAGEMENT OF PATIENTS WITH METASTATIC SPINAL CORD COMPRESSION DOCUMENT REF: PCLASCORD (Version No. 1.4) Name and designation of policy author(s) Approved by (committee, group, manager)
CLINICAL POLICY MANAGEMENT OF PATIENTS WITH METASTATIC SPINAL CORD COMPRESSION DOCUMENT REF: PCLASCORD (Version No. 1.4) Name and designation of policy author(s) Approved by (committee, group, manager)
Background and Context
 Background and Context People affected by cancer need information that is timely and relevant to enable them to make decisions. It can be difficult for patients and others affected by cancer to identify
Background and Context People affected by cancer need information that is timely and relevant to enable them to make decisions. It can be difficult for patients and others affected by cancer to identify
National information for commissioners on commissioning specialist level palliative care. Maureen McGinn, Senior Project Manager, RM Partners
 National information for commissioners on commissioning specialist level palliative care Maureen McGinn, Senior Project Manager, RM Partners National information for commissioners on commissioning specialist
National information for commissioners on commissioning specialist level palliative care Maureen McGinn, Senior Project Manager, RM Partners National information for commissioners on commissioning specialist
LCA Lung Clinical Forum. 21 st October 2014
 LCA Lung Clinical Forum 21 st October 2014 Welcome Dr Liz Sawicka Chair - LCA Lung Pathway Group Succession planning Dr Kate Haire Consultant in Public Health Medicine, LCA Commissioning Intentions for
LCA Lung Clinical Forum 21 st October 2014 Welcome Dr Liz Sawicka Chair - LCA Lung Pathway Group Succession planning Dr Kate Haire Consultant in Public Health Medicine, LCA Commissioning Intentions for
Commissioning Living with and Beyond Cancer in Yorkshire and Humber; an Overview.
 Commissioning Living with and Beyond Cancer in Yorkshire and Humber; an Overview. Document Title An Overview of Commissioning Living with and Beyond Cancer in Yorkshire and Humber Version number: 1 First
Commissioning Living with and Beyond Cancer in Yorkshire and Humber; an Overview. Document Title An Overview of Commissioning Living with and Beyond Cancer in Yorkshire and Humber Version number: 1 First
Integrated Cancer Services Action Plan. Colchester Hospital University NHS Foundation Trust 31 March 2014
 Integrated Cancer Services Action Plan Colchester Hospital University NHS Foundation Trust 31 March KEY Implemented, clearly evidenced and externally approved On Track to deliver Some issues narrative
Integrated Cancer Services Action Plan Colchester Hospital University NHS Foundation Trust 31 March KEY Implemented, clearly evidenced and externally approved On Track to deliver Some issues narrative
LCA Mental Health & Psychological Support Mapping
 LCA Mental Health & Psychological Support Mapping November 2013 Contents 1 Introduction... 3 2 Method... 3 3 Results... 3 3.1 Information Centres... 3 3.2 Training and Education... 5 3.3 Level Two Supervision...
LCA Mental Health & Psychological Support Mapping November 2013 Contents 1 Introduction... 3 2 Method... 3 3 Results... 3 3.1 Information Centres... 3 3.2 Training and Education... 5 3.3 Level Two Supervision...
North Somerset Autism Strategy
 North Somerset Autism Strategy Approved by: Ratification date: Review date: September 2017 1 Contents 1 Introduction and background... 3 2 Defining Autism...Error! Bookmark not defined. 3 National and
North Somerset Autism Strategy Approved by: Ratification date: Review date: September 2017 1 Contents 1 Introduction and background... 3 2 Defining Autism...Error! Bookmark not defined. 3 National and
ESSEX AND EAST SUFFOLK GYNAECOLOGICAL CANCER NETWORK SITE SPECIFIC GROUP. Friday, 14 th December 2012 at 2.00pm -4.00pm TA Centre Chelmsford
 ESSEX AND EAST SUFFOLK GYNAECOLOGICAL CANCER NETWORK SITE SPECIFIC GROUP Friday, 14 th December 2012 at 2.00pm -4.00pm TA Centre Chelmsford MINUTES Present: Mr Barnaby Rufford (Chair) BR Consultant Gynae
ESSEX AND EAST SUFFOLK GYNAECOLOGICAL CANCER NETWORK SITE SPECIFIC GROUP Friday, 14 th December 2012 at 2.00pm -4.00pm TA Centre Chelmsford MINUTES Present: Mr Barnaby Rufford (Chair) BR Consultant Gynae
ESSEX AND EAST SUFFOLK GYNAECOLOGICAL CANCER NETWORK SITE SPECIFIC GROUP
 ESSEX AND EAST SUFFOLK GYNAECOLOGICAL CANCER NETWORK SITE SPECIFIC GROUP Friday, 4 th November 2011 at 1.30pm-4.30pm Swift House, Board & Middle, CM2 5PF Present: MINUTES Mr Khalil Razvi (Chair) KR Consultant
ESSEX AND EAST SUFFOLK GYNAECOLOGICAL CANCER NETWORK SITE SPECIFIC GROUP Friday, 4 th November 2011 at 1.30pm-4.30pm Swift House, Board & Middle, CM2 5PF Present: MINUTES Mr Khalil Razvi (Chair) KR Consultant
Aiming for Excellence in Stroke Care
 Training Centre in Sub-acute Care (TRACS WA) Aiming for Excellence in Stroke Care A tool for quality improvement in stroke care Developed by TRAining Centre in Subacute Care (TRACS WA) February 2016 For
Training Centre in Sub-acute Care (TRACS WA) Aiming for Excellence in Stroke Care A tool for quality improvement in stroke care Developed by TRAining Centre in Subacute Care (TRACS WA) February 2016 For
WAHT-T&O-006 It is the responsibility of every individual to check that this is the latest version/copy of this document.
 OPERATIONAL GUIDELINES FOR OCCUPATIONAL THERAPY ASSESSMENT AND TREATMENT OF ADULTS WITH TRAUMATIC HEAD INJURY ADMITTED/TRANSFERRED OR ATTENDING A&E AT WORCESTERSHIRE ROYAL HOSPITAL This guidance does t
OPERATIONAL GUIDELINES FOR OCCUPATIONAL THERAPY ASSESSMENT AND TREATMENT OF ADULTS WITH TRAUMATIC HEAD INJURY ADMITTED/TRANSFERRED OR ATTENDING A&E AT WORCESTERSHIRE ROYAL HOSPITAL This guidance does t
Essex Cancer Network
 Thyroid NSSG Constitution Version 2 July 2012 Date NSSG Sign Off Date Essex Cancer Network Board Sign Off Signed (Chair H&N NSSG) 17 th July 2012 Signed (Chair ECN Board) Date for Review July 2013 Draft
Thyroid NSSG Constitution Version 2 July 2012 Date NSSG Sign Off Date Essex Cancer Network Board Sign Off Signed (Chair H&N NSSG) 17 th July 2012 Signed (Chair ECN Board) Date for Review July 2013 Draft
A. Service Specification
 A. Service Specification Service Specification No: 1767 Service Adult Highly Specialist Pain Management Services Commissioner Lead For local completion Lead For local completion 1. Scope 1.1 Prescribed
A. Service Specification Service Specification No: 1767 Service Adult Highly Specialist Pain Management Services Commissioner Lead For local completion Lead For local completion 1. Scope 1.1 Prescribed
Palliative Care Emergencies
 Palliative Care Emergencies LAURA BARNFIELD What might constitute an emergency in Palliative Care? 1 Palliative Care Emergencies Major haemorrhage Metastatic Spinal Cord Compression (MSCC) Superior Vena
Palliative Care Emergencies LAURA BARNFIELD What might constitute an emergency in Palliative Care? 1 Palliative Care Emergencies Major haemorrhage Metastatic Spinal Cord Compression (MSCC) Superior Vena
What to expect following spinal cord injury. Information for patients Therapy Services
 What to expect following spinal cord injury Information for patients Therapy Services Introduction This leaflet aims to explain what spinal cord injury is and what to expect over the next few months. What
What to expect following spinal cord injury Information for patients Therapy Services Introduction This leaflet aims to explain what spinal cord injury is and what to expect over the next few months. What
REPORT TO CLINICAL COMMISSIONING GROUP
 REPORT TO CLINICAL COMMISSIONING GROUP 12th December 2012 Agenda No. 6.2 Title of Document: Report Author/s: Lead Director/ Clinical Lead: Contact details: Commissioning Model for Dementia Care Dr Aryan
REPORT TO CLINICAL COMMISSIONING GROUP 12th December 2012 Agenda No. 6.2 Title of Document: Report Author/s: Lead Director/ Clinical Lead: Contact details: Commissioning Model for Dementia Care Dr Aryan
2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL)
 B3d 2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification B3d No.
B3d 2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification B3d No.
02/GMS/0030 ADULT EPILEPSY SERVICE CCP for General Medical and Surgical POOLE HOSPITAL NHS FOUNDATION TRUST
 Service Specification No. Service Commissioner Leads 02/GMS/0030 ADULT EPILEPSY SERVICE CCP for General Medical and Surgical Provider Lead POOLE HOSPITAL NHS FOUNDATION TRUST Period 1 April 2013 to 31
Service Specification No. Service Commissioner Leads 02/GMS/0030 ADULT EPILEPSY SERVICE CCP for General Medical and Surgical Provider Lead POOLE HOSPITAL NHS FOUNDATION TRUST Period 1 April 2013 to 31
National Cancer Peer Review Programme
 National Cancer Peer Review Programme Julia Hill Acting Deputy National Co-ordinator What is Cancer Peer Review? A quality assurance process for cancer services. An integral part of Improving Outcomes
National Cancer Peer Review Programme Julia Hill Acting Deputy National Co-ordinator What is Cancer Peer Review? A quality assurance process for cancer services. An integral part of Improving Outcomes
Update on Management of Malignant Spinal Cord Compression. Heino Hugel Consultant in Palliative Medicine University Hospital Aintree
 Update on Management of Malignant Spinal Cord Compression Heino Hugel Consultant in Palliative Medicine University Hospital Aintree Current Guidelines The symptoms of MSCC may be subtle and therefore careful
Update on Management of Malignant Spinal Cord Compression Heino Hugel Consultant in Palliative Medicine University Hospital Aintree Current Guidelines The symptoms of MSCC may be subtle and therefore careful
CP80 Version: V01. Acute Oncology Management Service Date approved: 8 th May 2015 Date ratified: 1 st June 2015 Review date: 1 st June 2017
 STANDARD OPERATING PROCEDURE (SOP) AND PATHWAY FOR THE MANAGEMENT OF PATIENTS WITH METASTATIC SPINAL CORD COMPRESSION (MSCC) WITHIN THE CHRISTIE (Refer to the Manchester Cancer Network MSCC Pathway flowchart)
STANDARD OPERATING PROCEDURE (SOP) AND PATHWAY FOR THE MANAGEMENT OF PATIENTS WITH METASTATIC SPINAL CORD COMPRESSION (MSCC) WITHIN THE CHRISTIE (Refer to the Manchester Cancer Network MSCC Pathway flowchart)
Proposed Neurosciences National Structure. Accountability Framework Neurological Alliance (Feedback Loop) National Advisory Group (Neurosciences)
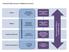 Accountability Framework Neurological Alliance (Feedback Loop) Proposed s National Structure National NHS England National Medical Director National Advisory Group (s) Regional NHS England Sub-Regional
Accountability Framework Neurological Alliance (Feedback Loop) Proposed s National Structure National NHS England National Medical Director National Advisory Group (s) Regional NHS England Sub-Regional
A Best Practice Clinical Care Pathway for Major Amputation Surgery
 A Best Practice Clinical Care Pathway for Major Amputation Surgery April 2016 Introduction The perioperative mortality rate after major lower limb amputation in the UK is unacceptably high in modern medical
A Best Practice Clinical Care Pathway for Major Amputation Surgery April 2016 Introduction The perioperative mortality rate after major lower limb amputation in the UK is unacceptably high in modern medical
PREVIOUS EMPLOYMENT. Associate OT : CJ Occupational Therapy * Assessment and treatment for adults with neurological conditions
 CURRICULUM VITAE Katie Hanagarth Green Owl Therapy Office 3, 36 Greenhill Street Stratford-upon-Avon CV37 6LE Tel: 01789 413960 / 07966 573317 Email: katie@greenowltherapy.co.uk - Web: www.greenowltherapy.co.uk
CURRICULUM VITAE Katie Hanagarth Green Owl Therapy Office 3, 36 Greenhill Street Stratford-upon-Avon CV37 6LE Tel: 01789 413960 / 07966 573317 Email: katie@greenowltherapy.co.uk - Web: www.greenowltherapy.co.uk
SPINAL CORD INJURY Rehab Definitions Framework Self-Assessment Tool Outpatient/ambulatory rehab Survey for Spinal Cord Injury (SCI)
 SPINAL CORD INJURY Rehab s Framework Self-Assessment Tool Outpatient/ambulatory rehab Survey for Spinal Cord Injury (SCI) INTRODUCTION: In response to a changing rehab landscape in which rehabilitation
SPINAL CORD INJURY Rehab s Framework Self-Assessment Tool Outpatient/ambulatory rehab Survey for Spinal Cord Injury (SCI) INTRODUCTION: In response to a changing rehab landscape in which rehabilitation
All about the adult cystic fibrosis service
 All about the adult cystic fibrosis service All about the adult cystic fibrosis service Lay Introduction to Cystic Fibrosis Service Specification Since April 2013, NHS England has taken on direct responsibility
All about the adult cystic fibrosis service All about the adult cystic fibrosis service Lay Introduction to Cystic Fibrosis Service Specification Since April 2013, NHS England has taken on direct responsibility
NELFT NHS Foundation Trust About us
 NELFT NHS Foundation Trust About us Best care by the best people Here at NELFT, our top priority is your health and wellbeing. So whether you are experiencing a physical or mental health condition, NELFT
NELFT NHS Foundation Trust About us Best care by the best people Here at NELFT, our top priority is your health and wellbeing. So whether you are experiencing a physical or mental health condition, NELFT
MCIP Recruitment Pack
 MCIP Recruitment Pack Page 1 of 13 Welcome Thank you for the interest you have shown in the MCIP Programme. An exciting partnership has been established to redesign cancer care in Manchester. Funded by
MCIP Recruitment Pack Page 1 of 13 Welcome Thank you for the interest you have shown in the MCIP Programme. An exciting partnership has been established to redesign cancer care in Manchester. Funded by
Occupational Therapy and Physiotherapy in Stroke and Neurology Inpatient Services
 Occupational Therapy and Physiotherapy in Stroke and Neurology Inpatient Services Information for patients Welcome to the Stroke and Neurology inpatient therapy team. As part of your stay you may be assessed
Occupational Therapy and Physiotherapy in Stroke and Neurology Inpatient Services Information for patients Welcome to the Stroke and Neurology inpatient therapy team. As part of your stay you may be assessed
Collation of responses to GW. 1. Please state the definitions that you use for different forms of palliative and end of life services
 Collation of responses to GW 1. Please state the definitions that you use for different forms of palliative and end of life services Palliative care is the active holistic care of patients with advanced
Collation of responses to GW 1. Please state the definitions that you use for different forms of palliative and end of life services Palliative care is the active holistic care of patients with advanced
South Tees Hospitals NHS Foundation Trust. Excellence in dementia care across general hospital and community settings. Competency framework
 South Tees Hospitals NHS Foundation Trust Excellence in dementia care across general hospital and community settings. Competency framework 2013-2018 Written and compiled by Helen Robinson-Clinical Educator
South Tees Hospitals NHS Foundation Trust Excellence in dementia care across general hospital and community settings. Competency framework 2013-2018 Written and compiled by Helen Robinson-Clinical Educator
National Peer Review Report: Brain and CNS Cancer Services Report 2012/2013
 National Peer Review Programme National Peer Review Report: Brain and CNS Cancer Services Report 2012/2013 www.nationalpeerreview.nhs.uk Brain and CNS Cancer Network (Non-Surgical) MDTs) Overall Performance
National Peer Review Programme National Peer Review Report: Brain and CNS Cancer Services Report 2012/2013 www.nationalpeerreview.nhs.uk Brain and CNS Cancer Network (Non-Surgical) MDTs) Overall Performance
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM)
 SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician ASWCN TAUNTON AND SOMERSET Taunton Lung MDT (11-2C-1) - 2011/12 Dr Sarah Foster Compliance Self Assessment LUNG MDT
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician ASWCN TAUNTON AND SOMERSET Taunton Lung MDT (11-2C-1) - 2011/12 Dr Sarah Foster Compliance Self Assessment LUNG MDT
PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM)
 PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM) Network Organisation (Trust) Team DCN POOLE Poole THYROID ONLY MDT (11-2I-2) - 2011/12 Peer Review Visit Date 18th August 2011 Compliance THYROID ONLY
PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM) Network Organisation (Trust) Team DCN POOLE Poole THYROID ONLY MDT (11-2I-2) - 2011/12 Peer Review Visit Date 18th August 2011 Compliance THYROID ONLY
National Standards for Acute Oncology Services
 Cancer National Specialist Advisory Group National Standards for Acute Oncology Services June 2016 TABLE OF CONTENTS 1. PURPOSE... 2 2. INTRODUCTION... 2 3. STRATEGIC CONTEXT... 4 4. SCOPE OF ACUTE ONCOLOGY
Cancer National Specialist Advisory Group National Standards for Acute Oncology Services June 2016 TABLE OF CONTENTS 1. PURPOSE... 2 2. INTRODUCTION... 2 3. STRATEGIC CONTEXT... 4 4. SCOPE OF ACUTE ONCOLOGY
Test and Learn Community Frailty Service for frail housebound patients and those living in care homes in South Gloucestershire
 Test and Learn Community Frailty Service for frail housebound patients and those living in care homes in South Gloucestershire Introduction This document introduces South Gloucestershire Clinical Commissioning
Test and Learn Community Frailty Service for frail housebound patients and those living in care homes in South Gloucestershire Introduction This document introduces South Gloucestershire Clinical Commissioning
FRAILTY PATIENT FOCUS GROUP
 FRAILTY PATIENT FOCUS GROUP Community House, Bromley 28 November 2016-10am to 12noon In attendance: 7 Patient and Healthwatch representatives: 4 CCG representatives: Dr Ruchira Paranjape went through the
FRAILTY PATIENT FOCUS GROUP Community House, Bromley 28 November 2016-10am to 12noon In attendance: 7 Patient and Healthwatch representatives: 4 CCG representatives: Dr Ruchira Paranjape went through the
The Ayrshire Hospice
 Strategy 2010-2015 Welcome... The Ayrshire Hospice : Strategy 2010-2015 Index 05 06 08 09 10 12 15 17 19 Foreword Our vision and purpose Our guiding principles Our achievements 1989-2010 Our priorities
Strategy 2010-2015 Welcome... The Ayrshire Hospice : Strategy 2010-2015 Index 05 06 08 09 10 12 15 17 19 Foreword Our vision and purpose Our guiding principles Our achievements 1989-2010 Our priorities
ESSEX AND EAST SUFFOLK GYNAECOLOGICAL CANCER NETWORK SITE SPECIFIC GROUP
 ESSEX AND EAST SUFFOLK GYNAECOLOGICAL CANCER NETWORK SITE SPECIFIC GROUP Friday, 7 th September 2012 at 1.30pm-4.30pm Swift House, Board & Middle, CM2 5PF Present: MINUTES Mr Khalil Razvi (Chair) KR Consultant
ESSEX AND EAST SUFFOLK GYNAECOLOGICAL CANCER NETWORK SITE SPECIFIC GROUP Friday, 7 th September 2012 at 1.30pm-4.30pm Swift House, Board & Middle, CM2 5PF Present: MINUTES Mr Khalil Razvi (Chair) KR Consultant
The NHS Cancer Plan: A Progress Report
 DEPARTMENT OF HEALTH The NHS Cancer Plan: A Progress Report LONDON: The Stationery Office 9.25 Ordered by the House of Commons to be printed on 7 March 2005 REPORT BY THE COMPTROLLER AND AUDITOR GENERAL
DEPARTMENT OF HEALTH The NHS Cancer Plan: A Progress Report LONDON: The Stationery Office 9.25 Ordered by the House of Commons to be printed on 7 March 2005 REPORT BY THE COMPTROLLER AND AUDITOR GENERAL
SECTION B THE SERVICES
 SECTION B THE SERVICES 2012/13 NHS STANDARD CONTRACT- SECTION B THE SERVICES (Amended 14 February 2012) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. 1.2 Service Commissioner Lead
SECTION B THE SERVICES 2012/13 NHS STANDARD CONTRACT- SECTION B THE SERVICES (Amended 14 February 2012) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. 1.2 Service Commissioner Lead
Stroke Rehab Definitions Framework Self-Assessment Tool Acute Integrated Stroke Unit
 rth & East GTA Stroke Network Stroke Rehab Definitions Framework Self-Assessment Tool Acute Integrated Stroke Unit Purpose of the Self-Assessment Tool: The GTA Rehab Network and the GTA regions of the
rth & East GTA Stroke Network Stroke Rehab Definitions Framework Self-Assessment Tool Acute Integrated Stroke Unit Purpose of the Self-Assessment Tool: The GTA Rehab Network and the GTA regions of the
Contents Introduction Context nationally and locally What is a health and wellbeing event?... 4
 Living With and Beyond Cancer Merseyside and Cheshire Health and Wellbeing Clinic Event Guidance January 2017 Contents 1 1. Introduction... 2 2. Context nationally and locally... 3 3. What is a health
Living With and Beyond Cancer Merseyside and Cheshire Health and Wellbeing Clinic Event Guidance January 2017 Contents 1 1. Introduction... 2 2. Context nationally and locally... 3 3. What is a health
Exclude referred pain from the neck, diaphragm, heart, lungs, & polymyalgia rheumatica YES. NSAIDs/analgesics as required
 Shoulder Pain Clinical Presentation info for GPs who refer into PAH more info History and Examination Exclude referred pain from the neck, diaphragm, heart, lungs, & polymyalgia rheumatica more info for
Shoulder Pain Clinical Presentation info for GPs who refer into PAH more info History and Examination Exclude referred pain from the neck, diaphragm, heart, lungs, & polymyalgia rheumatica more info for
What is Acute Oncology? Kay McCallum Acute Oncology Advanced Nurse Practitioner John Radcliffe Hospital Oxford September 2015
 What is Acute Oncology? Kay McCallum Acute Oncology Advanced Nurse Practitioner John Radcliffe Hospital Oxford September 2015 What is Acute Oncology? Outline of Talk Concept of Acute Oncology Service (AOS)
What is Acute Oncology? Kay McCallum Acute Oncology Advanced Nurse Practitioner John Radcliffe Hospital Oxford September 2015 What is Acute Oncology? Outline of Talk Concept of Acute Oncology Service (AOS)
National Standards for Sarcoma Services
 National Standards for Sarcoma Services 2009 TABLE OF CONTENTS 1. INTRODUCTION TO THE NATIONAL CANCER STANDARDS...2 2. METHODOLOGY...4 3. FORMAT...4 4. INTRODUCTION TO SARCOMA...5 STANDARDS TOPIC: ORGANISATION...10
National Standards for Sarcoma Services 2009 TABLE OF CONTENTS 1. INTRODUCTION TO THE NATIONAL CANCER STANDARDS...2 2. METHODOLOGY...4 3. FORMAT...4 4. INTRODUCTION TO SARCOMA...5 STANDARDS TOPIC: ORGANISATION...10
National Standards for Sarcoma Services 2009
 National Standards for Sarcoma Services 2009 Crown copyright July 2010 F1101011 Contents 1. Introduction to the National Cancer Standards 2. Methodology 3. Format 4. Introduction to Sarcoma Standards Topic:
National Standards for Sarcoma Services 2009 Crown copyright July 2010 F1101011 Contents 1. Introduction to the National Cancer Standards 2. Methodology 3. Format 4. Introduction to Sarcoma Standards Topic:
Essex Cancer Network Partnership. Tuesday, 31 st January am-1.00pm at Swift House, Middle & Annexe M I N U T E S
 Essex Cancer Network Partnership Tuesday, 31 st January 2012 10.00am-1.00pm at Swift House, Middle & Annexe Present M I N U T E S Ken Aldred (Chair) KA St Helena Hospice Partnership Michael Scanes MS Partnership
Essex Cancer Network Partnership Tuesday, 31 st January 2012 10.00am-1.00pm at Swift House, Middle & Annexe Present M I N U T E S Ken Aldred (Chair) KA St Helena Hospice Partnership Michael Scanes MS Partnership
North Thames Children and Young People s Cancer Network
 North Thames Children and Young People s Cancer Network CCN Initial Referral Protocol Relevant Children s Cancer Measure: 14-7A-115 Created: May 2010 Version: 2.1 Last Updated: May 2015 Referral Form only
North Thames Children and Young People s Cancer Network CCN Initial Referral Protocol Relevant Children s Cancer Measure: 14-7A-115 Created: May 2010 Version: 2.1 Last Updated: May 2015 Referral Form only
Commissioning for Better Outcomes in COPD
 Commissioning for Better Outcomes in COPD Dr Matt Kearney Primary Care & Public Health Advisor Respiratory Programme, Department of Health General Practitioner, Runcorn November 2011 What are the Commissioning
Commissioning for Better Outcomes in COPD Dr Matt Kearney Primary Care & Public Health Advisor Respiratory Programme, Department of Health General Practitioner, Runcorn November 2011 What are the Commissioning
Who we are and what we do
 Who we are and what we do Introduction Art therapists Dietitians Drama therapists Music therapists Occupational therapists Orthoptists Introduction Art therapists Dietitians Drama therapists Music therapists
Who we are and what we do Introduction Art therapists Dietitians Drama therapists Music therapists Occupational therapists Orthoptists Introduction Art therapists Dietitians Drama therapists Music therapists
Manual for Cancer Services 2008: Northern Ireland - Colorectal Measures
 National Cancer Action Team National Cancer Peer Review Programme Manual for Cancer Services 2008: Northern Ireland - Colorectal Measures NORTHERN IRELAND - COLORECTAL MEASURES GATEWAY No. XXXX - JUN 2009
National Cancer Action Team National Cancer Peer Review Programme Manual for Cancer Services 2008: Northern Ireland - Colorectal Measures NORTHERN IRELAND - COLORECTAL MEASURES GATEWAY No. XXXX - JUN 2009
Promoting Excellence: A framework for all health and social services staff working with people with Dementia, their families and carers
 Promoting Excellence: A framework for all health and social services staff working with people with Dementia, their families and carers Mapped to the NHS Knowledge and Skills Framework () Background and
Promoting Excellence: A framework for all health and social services staff working with people with Dementia, their families and carers Mapped to the NHS Knowledge and Skills Framework () Background and
Cancer Transformation Programme
 Cancer Transformation Programme Introduction to and supporting documentation for VALUE BASED TRANSFORMATION FUNDING SITE SELECTION November 2016 1 Introduction and Contents The Planning Guidance for 2017-2019
Cancer Transformation Programme Introduction to and supporting documentation for VALUE BASED TRANSFORMATION FUNDING SITE SELECTION November 2016 1 Introduction and Contents The Planning Guidance for 2017-2019
Progress Review of Five Cancer Services at Colchester Hospital University NHS Foundation Trust
 Progress Review of Five Cancer Services at Colchester Hospital University NHS Foundation Trust 1 2 Progress Review of Five Cancer Services at Colchester Hospital University NHS Foundation Trust NHS England
Progress Review of Five Cancer Services at Colchester Hospital University NHS Foundation Trust 1 2 Progress Review of Five Cancer Services at Colchester Hospital University NHS Foundation Trust NHS England
We need to talk about Palliative Care. Pancreatic Cancer UK
 We need to talk about Palliative Care Pancreatic Cancer UK 1. Pancreatic Cancer UK welcomes the opportunity to respond to the Health and Sport Committee s inquiry on palliative care. About Pancreatic Cancer
We need to talk about Palliative Care Pancreatic Cancer UK 1. Pancreatic Cancer UK welcomes the opportunity to respond to the Health and Sport Committee s inquiry on palliative care. About Pancreatic Cancer
Criteria and Guidance for Referral to Specialist Palliative Care Services
 Criteria and Guidance for Referral to Specialist Palliative Care Services March 2014 Introduction This guidance is for health professionals caring for patients who may need referral to specialist palliative
Criteria and Guidance for Referral to Specialist Palliative Care Services March 2014 Introduction This guidance is for health professionals caring for patients who may need referral to specialist palliative
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM)
 SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician NECN NORTH TEES AND HARTLEPOOL North Tees And Hartlepool Lung MDT (11-2C-1) - 2011/12 Dr D N Leitch Compliance Self
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician NECN NORTH TEES AND HARTLEPOOL North Tees And Hartlepool Lung MDT (11-2C-1) - 2011/12 Dr D N Leitch Compliance Self
Enter & View WDP Havering Drug and alcohol dependency services 11 October 2016
 Enter & View WDP Havering Drug and alcohol dependency services 11 October 2016 Healthwatch Havering is the operating name of Havering Healthwatch Limited A company limited by guarantee Registered in England
Enter & View WDP Havering Drug and alcohol dependency services 11 October 2016 Healthwatch Havering is the operating name of Havering Healthwatch Limited A company limited by guarantee Registered in England
All Wales Standards for Accessible Communication and Information for People with Sensory Loss
 All Wales Standards for Accessible Communication and Information for People with Sensory Loss Published July 2013 by NHS Wales All Wales Standards for Accessible Communication and Information for People
All Wales Standards for Accessible Communication and Information for People with Sensory Loss Published July 2013 by NHS Wales All Wales Standards for Accessible Communication and Information for People
Artificial nutrition and rehabilitation for head and neck cancer patients in the community setting
 Artificial nutrition and rehabilitation for head and neck cancer patients in the community setting Mary Mc Clenaghan Advanced Specialist Head and Neck Dietitian, South London Community Head and Neck Team,
Artificial nutrition and rehabilitation for head and neck cancer patients in the community setting Mary Mc Clenaghan Advanced Specialist Head and Neck Dietitian, South London Community Head and Neck Team,
I write in response to your request for information in relation to physiotherapy services within NHS Lothian.
 Lothian NHS Board = Waverley Gate 2-4 Waterloo Place Edinburgh EH1 3EG = Telephone: 0131 536 9000 www.nhslothian.scot.nhs.uk www.nhslothian.scot.nhs.uk Dear FREEDOM OF INFORMATION PHYSIOTHERAPY Date: 15/08/2016
Lothian NHS Board = Waverley Gate 2-4 Waterloo Place Edinburgh EH1 3EG = Telephone: 0131 536 9000 www.nhslothian.scot.nhs.uk www.nhslothian.scot.nhs.uk Dear FREEDOM OF INFORMATION PHYSIOTHERAPY Date: 15/08/2016
Dementia Strategy. Contents
 Section Dementia Strategy Contents Page 1. Introduction 2 2. Context of Northern and Eastern Devon 2 3. Our Values and Principles 3 4. Key Result Areas 5 5. Needs Analysis 6 6. Model of Service Delivery
Section Dementia Strategy Contents Page 1. Introduction 2 2. Context of Northern and Eastern Devon 2 3. Our Values and Principles 3 4. Key Result Areas 5 5. Needs Analysis 6 6. Model of Service Delivery
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM)
 SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician GMCN ROYAL WOLVERHAMPTON HOSPITALS The Royal Wolverhampton Hospitals Trust Lung MDT (11-2C-1) - 2011/12 Dr Angela Morgan
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician GMCN ROYAL WOLVERHAMPTON HOSPITALS The Royal Wolverhampton Hospitals Trust Lung MDT (11-2C-1) - 2011/12 Dr Angela Morgan
