2004, Editrice Kurtis
|
|
|
- Daniela Baker
- 6 years ago
- Views:
Transcription
1 Aging Clinical and Experimental Research Acute geriatric intervention increases the number of patients able to live at home. A prospective randomized study Ingvild Saltvedt 1,2, Turi Saltnes 2, Ellen-Sofie Opdahl Mo 1, Peter Fayers 2,3, Stein Kaasa 2,4, and Olav Sletvold 1,5 1 Section of Geriatrics, Department of Internal Medicine, University Hospital of Trondheim, Trondheim, Norway, 2 Unit of Applied Clinical Research, Norwegian University of Science and Technology (NTNU), Trondheim, Norway, 3 Department of Public Health, University of Aberdeen, Scotland, 4 Palliative Medicine Unit, Department of Oncology and Radiotherapy, University Hospital of Trondheim, Trondheim, Norway, 5 Department of Clinical Neurosciences, Faculty of Medicine, NTNU, Trondheim, Norway ABSTRACT. Background and aims: In a previous publication, we showed that treatment of acutely sick, frail elderly patients in a Geriatric Evaluation and Management Unit (GEMU) reduced mortality considerably when compared with the general Medical Wards (MW). The aim of this presentation was to study the impact of treatment in a GEMU on health care utilization. Methods: Acutely sick, frail patients, 75 years or older, who had been admitted as emergencies to the Department of Internal Medicine were randomized either to treatment in the GEMU (n=127) or to continued treatment in the MW (n=127). While usual treatment was given in the MW, the GEMU emphasized interdisciplinary and comprehensive assessment of all relevant disorders, early mobilization/rehabilitation, and discharge planning. After discharge from hospital, no specific follow-up was offered to any of the groups. Results: Of all subjects, 101 (80%) GEMU and 79 (64%) MW patients were still living in their own homes at three months (p=0.005); at six months the number was 91 (72%) and 74 (60%) (p=0.04) respectively. Median length of index stay was 19 days in the GEMU and 13 days in the MW group (p<0.001). After the initial stay, there were no statistically significant differences in admissions to or time spent in institutions. Conclusions: The results indicate the overall positive treatment effect of acutely sick, frail elderly in a GEMU, i.e. patients treated in the GEMU had increased possibilities of living in their own homes, an effect that was mainly related to considerably reduced mortality in the GEMU group. (Aging Clin Exp Res 2004; 16: ) INTRODUCTION Demographic trends in all Western societies consistently show increasing numbers of elderly people in need of health care facilities. At the same time, progress in medical science is creating increased expectations and demands, leading to considerable pressure on health care systems. A central issue is of course that medical treatment should be appropriate. Although patients and society may be more concerned about the quality of survival than about death, it has been shown that old people may have at least as much as the young to gain from active diagnostic work-up and invasive treatments in terms of preventing immediate death (1). Previous research has shown that elderly patients in hospital experience underdiagnosis and misdiagnosis, increased risk of iatrogenic conditions, and functional decline (2-5). A meta-analysis published in 1993 showed that treatment in Geriatric Evaluation and Management Units (GEMUs) increased the chance of living in one s own home and improved survival (6). Later, three randomized studies on the effectiveness of GEMUs from acute care settings were published, but failed to replicate these findings (7-9), even though in the study of Landefeld et al. discharges to long-term care institutions were reduced (7) and in that of Asplund et al. the length of the initial hospital stay was shortened (8). Two former rehabilitation studies have shown reduced time spent in institutions and reduced mortality for GEMU patients as compared with usual care (10, 11). In a recent randomized rehabilitation study, patients were assigned to receive care either in a GEMU or usual inpatient care after their condition had been stabilized (12). The mean number of days in long-term care was slightly lower for the GEMU patients and, al- Key words: Frail elderly, geriatric evaluation and management unit (GEMU), health care utilization, hospitalization, randomized clinical trial. Correspondence: I. Saltvedt, MD, Section of Geriatrics, University Hospital of Trondheim, 7006 Trondheim, Norway. Ingvild.Saltvedt@medisin.ntnu.no Received July 8, 2003; accepted in revised form May 14, Aging Clin Exp Res, Vol. 16, No. 4
2 Acute geriatric intervention though there was a significant reduction in functional decline, there was no difference in survival. Many hospital wards are overcrowded by frail elderly patients otherwise ready for discharge, who have to stay in hospital awaiting transfer to extended care facilities (13). These so-called bed-blockers may have substantial consequences for the daily organization of medical units. However, discharge of frail elderly patients depends upon several factors such as patients function, family members ability to care for the patient, access to and quality of general practitioners, and extent and quality of home care nursing. Additionally, many of these patients will need acute specialized care in order to prevent repetitive re-hospitalization, and close collaboration between the hospital and primary health care system is necessary. A GEMU was established in 1994 at the Department of Internal Medicine (DIM) at the University Hospital of Trondheim, Norway. As the Department had already performed a randomized study showing the beneficial effects of establishing a stroke unit (14), it was decided to evaluate the GEMU through a randomized study comparing treatment in the GEMU with treatment in the general medical wards (MW). In a previous publication, it was shown that mortality in the GEMU group was reduced by 50% during six months of follow-up (15). The present analyses were undertaken to explore the use of health care resources in the given population. When planning the study, we had the following expectations for the intervention patients: 1) an increased number of patients would be able to live at home; 2) the number of readmissions to and time in hospital and nursing homes during a six-month period of follow-up would be reduced; 3) the length of the initial stay would be longer in the intervention group, due to more time-consuming assessment and intervention, when compared with standard practice at the DIM. After reduced mortality in the GEMU group was found, it was debated that, if life were prolonged in those patients who had the highest morbidity, it was likely that overall health care utilization would be higher in the GEMU group. Hence, it would be a positive finding if no differences in health care utilization could be found in the two groups. METHODS Hospital setting Patients were recruited from the DIM at the University Hospital of Trondheim, Norway. This hospital serves both as the regional hospital for Central Norway, and as the local hospital for about 200,000 inhabitants of the city of Trondheim and neighboring municipalities. The DIM consisted of nine different sections with a total of 190 beds, and more than 90% of all its admissions were emergencies. In April 1994, a nine-bed GEMU was established as a section within the DIM. Six months later the present study started. Patients were included between October 31, 1994 and November 13, Patient selection and randomization Frail patients 75 years or older admitted acutely to the DIM (local hospital patients) were screened for enrolment. Patients should not be too healthy or too sick to benefit from treatment in a GEMU. To target frail patients, at least one of the Winograd targeting criteria had to be met (acute impairment of single activity of daily living (ADL), imbalance/dizziness, impaired mobility, chronic disability, prolonged bedrest, falls, confusion, depression, mild/moderate dementia, weight loss, malnutrition, vision or hearing impairment, urinary incontinence, social/family problems, polypharmacy) (16). Patients were excluded if they had terminal illnesses, including known cancer with metastases, severe dementia, or lived in nursing homes, as were also those who had been fully independent and seemed to recover quickly from the acute illness precipitating the emergency admission. Further, patients were not included if discharge was planned within two days. Suitable patients were screened when there was a free bed in the GEMU. Randomization was executed after patients had given their informed consent. Permuted block randomization with unknown and varied block size was used. During the study period, 254 patients were recruited and randomly allocated, 127 to the GEMU and 127 to continued treatment in the general medical wards (MW) where they were already staying. Patients allocated to the GEMU were transferred on the day of inclusion. More details on study design and methods have been described in an earlier publication (15). Patient care The staff in the GEMU included one geriatrician, one resident, two occupational therapists, and one physiotherapist. The number of nurses was comparable with that in the MW. All professionals evaluated each patient, and short- and long-term goals were set through regular interdisciplinary meetings. Comprehensive assessment and treatment of all relevant illnesses, prevention of complications, and early mobilization were essential. Rehabilitation was initiated in the GEMU, but if long-lasting rehabilitation was indicated, patients were referred to a rehabilitation institution. Discharge planning started as early as possible, in collaboration with the patient, family caregivers, and community nurses. When necessary, nurses or occupational therapists arranged visits to patients homes to evaluate their ability to manage to live at home, and if technical arrangements, aids and assistance from the home services was required. The staff in the GEMU was also used for (time-consuming) study-re- Aging Clin Exp Res, Vol. 16, No
3 I. Saltvedt, T. Saltnes, E-S. Opdahl Mo, et al. lated assessments in both groups during hospital stays and also during follow-up. Enrolled patients assigned to the MW were treated according to the routines of the DIM. Physiotherapy and occupational therapy were given when prescribed by the doctor, each therapist serving several wards. When considered appropriate by the hospital staff, arrangements for discharge were discussed with the community nurses. The health care system in Norway is public. In the municipality of Trondheim, at the time of this study, community nurses made the final decisions on the type and amount of service, including nursing home placement, offered to patients in both groups. Their decisions were based upon overall evaluation of patients medical and social situation, as well as the current availability of resources in the municipality, which had experienced a shortage of nursing home beds for years. After discharge from hospital, general practitioners were responsible for medical treatment in both groups. Baseline and outcome variables Sociodemographic characteristics were obtained through standard interviews with patients and caregivers. Information about diagnoses, hospital stays and number of readmissions to hospital was obtained from hospital records. Records of the Municipality of Trondheim gave information on nursing home admissions and duration of stays. Rehabilitation stays were registered partly from rehabilitation institutions records and partly from the National Registry. Official death certificates provided details on deaths. Sample size and statistical analysis Sample size estimations were based upon expected mortality reduction. It was estimated that one-year mortality would be 30% in the MW and 15% in the GEMU group, with α=0.05 and power 80%. This would require 113 patients in each group, and it was decided to include patients for one year or until this number of patients was reached (15). The chi-squared test was used for comparison of all categorical data. The Mann-Whitney U-test was used for comparison of age and time in institutions. Kaplan Meier plots and the log rank test were used for survival analyses and to compare time to readmission in hospital and time to nursing home placement. In order to estimate the magnitude of the treatment effect, Cox s proportional hazard model was used to estimate the hazard ratio (HR) of living at home. In this analysis individuals who were placed in permanent nursing homes or who died were regarded as experiencing a negative event in contrast to those still alive in their own homes. A p-value of less than 0.05 was considered statistically significant. All analyses were carried out by SPSS software version Ethics Participation in the trial was voluntary and according to the Helsinki Declaration. Written informed consent was obtained from all patients except those who were not able to write, when oral consent was accepted. If the patient was cognitively impaired, relatives also gave their written consent. The Regional Ethical Committee approved the protocol. RESULTS During the study period, 1426 patients aged 75 or more from the municipality of Trondheim were admitted to the Department of Internal Medicine. Of these, 254 (18%) were allocated to the study, with an identical number of patients in the two groups (Fig. 1). Five patients refused to participate, 1167 patients were not included either because they were not suitable for the study or because there was no free bed in the GEMU. One GEMU and two MW patients withdrew their consent after the index stay and were excluded from later analysis. Nursing home data were missing for ten GEMU and 16 MW patients; data on living location were missing for two MW patients (Fig. 1). Analysis Follow-up Allocation Admissions Patients 75 years from Trondheim admitted as emergencies, n=1426 Randomized, n=254 Allocated to GEMU, n=127 Lost to follow-up, n=1 (withdrew consent) Time in nursing homes, n=116 (missing n=10) Living location, n=126 All other analyses, n=126 Refused participation, n=5. Not suitable or no free bed in GEMU, n=1167 Allocated to MW, n=127 Lost to follow-up, n=2 (withdrew consent) Time in nursing homes, n=109 (missing n=16) Living location, n=123 (missing n=2) All other analyses, n=125 Figure 1 - Flow of study. GEMU: Geriatric Evaluation and Management Unit, MW: general Medical Wards. 302 Aging Clin Exp Res, Vol. 16, No. 4
4 Acute geriatric intervention Table 1 - Sociodemographic characteristics at baseline. GEMU (n=127) MW (n=127) Age, mean ±SD 82±5 82±5 Female 81 (64%) 84 (66%) Widowed/living alone 93 (73%) 85 (67%) Residence at time of inclusion Private home 115 (91%) 110 (87%) Sheltered housing 12 (9%) 17 (13%) Days in hospital before inclusion, 3.8 (±3.7) 4.6 (±4.3) mean (±SD) Previous diagnoses * Heart disease 46 (36%) 58 (46%) Infectious disease 30 (24%) 21 (17%) Gastrointestinal disorder 27 (21%) 22 (17%) Cerebrovascular disease 24 (19%) 17 (13%) Endocrine disease 20 (16%) 16 (13%) Airway disease 18 (14%) 9 (7%) Cancer 15 (12%) 12 (9%) Other 41 (32%) 44 (35%) No. of Winograd targeting criteria, 4 (3-5) 4 (3-5) median (iqr ) GEMU: Geriatric Evaluation and Management Unit. MW: general Medical Wards. *Diagnoses at earlier admissions to University Hospital of Trondheim. acute impairment of single activity of daily living (ADL), imbalance/dizziness, impaired mobility, chronic disability, prolonged bedrest, falls, confusion, depression, mild/moderate dementia, weight loss, malnutrition, vision or hearing impairment, urinary incontinence, social/family problems, polypharmacy (16). iqr= interquartile range. None of the differences were statistically significant. The GEMU and MW groups were comparable with respect to all demographic and clinical characteristics at baseline (Table 1). The mean number of days spent in hospital before entering the study was 3.8 (SD 3.7) in the GEMU and 4.6 (SD 4.3) in the MW, p=0.09. There were no differences in number of patients admitted to or time spent in hospital one year before inclusion in the study. At discharge, 38% of the GEMU patients and 7% of the MW patients had psychiatric diagnoses (mainly dementia, depression and delirium), p<0.001 (Table 2). There were no statistically significant differences in the distribution of the other diagnoses. Patients in the GEMU group had a median of three diagnoses at discharge, while in the MW group the median was two, p< As reported previously (15), the mortality in the GEMU and MW groups during the index stay was 8 (6%) and 17 (13%) (p=0.002), at three months 15 (12%) and 34 (27%) (p=0.004), and at six months 20 (16%) and 37 (29%) (p=0.02) respectively. After the index stay, a comparable number of patients in the GEMU and MW groups were discharged to their homes, 87 (73%) and 80 (73%); to rehabilitation institutions, 13 (11%) and 11 (10%); and to nursing homes, 15 (13%) and 15 (14%). Four (3%) patients in each group were transferred to another hospital department. Of those still alive, 10 (9%) GEMU and 11 (12%) MW patients were living in nursing homes at three months, and 15 (14%) and 12 (14%) at six months. The numbers living in their own homes were 101 (91%) in the GEMU group and 79 (88%) in the MW group at three months, and 91 (86%) and 74 (86%) at six months. Of all patients recruited in the study, 101 (80%) GEMU and 79 (64%) MW patients were living at home (p=0.005) at three months, and 91 (72%) and 74 (60%) (p=0.04) at six months. The hazard ratio (HR) of living at home versus living in nursing homes or having died, was 2.1 (95% CI ) after three months, and 1.6 (95% CI ) after six months, showing that the GEMU patients had significantly higher chances of living in their own homes. The partitioned survival curves (Fig. 2) show the proportion of observed time spent in nursing homes and hospital by the two groups. The proportion of observed time spent in hospital during the first weeks was higher in the GEMU group, because the index stay was longer (Fig. 3). The total length of the index stay had a median of 19 days (interquartile range 13 to 30) in the GEMU group and 13 days (interquartile range 7 to 18) in the MW group, p< Patients were not enrolled if discharge was planned within two days. Despite this criterion, 18 (14%) MW patients were discharged during this time period. After the index stay, the proportion of observed time spent in hospital and nursing homes had no statistically significant difference in the two groups (Fig. 2). Forty-one (35%) of the GEMU and 33 (31%) of the MW patients surviving the index stay were not readmitted to any kind of institution during follow-up (p=0.5). Each GEMU patient spent a mean of 35.4 (SD 48.5) days in institutions after the initial hospital stay, as compared with 30.9 (SD 47.3) days in the MW group (p=0.63). Table 2 - Diagnoses at discharge from index stay. GEMU MW (n=127) (n=127) n % n % Heart disease 72 (57) 69 (54) Infectious disease 20 (16) 25 (20) Gastrointestinal disease 22 (17) 15 (12) Cerebrovascular disease 38 (30) 28 (22) Endocrine disease 24 (19) 21 (17) Airway disease 17 (13) 12 (9) Cancer 12 (9) 10 (8) Psychiatric disorders* 48 (38) 9 (7) Other 51 (40) 68 (54) GEMU: Geriatric Evaluation and Management Unit., MW: general Medical Wards. *p< None of the other differences were statistically significant. Aging Clin Exp Res, Vol. 16, No
5 I. Saltvedt, T. Saltnes, E-S. Opdahl Mo, et al. Percentage Percentage GEMU MW In hospital In hospital At home At home Observation time (months) In nursing home In nursing home Figure 2 - Partitioned survival curves. Proportion of observed time that survivors spent in hospital, nursing homes and in own homes during six-month follow-up. GEMU: Geriatric Evaluation and Management Unit, MW: general Medical Wards. Forty-six (39%) of the GEMU and 42 (39%) of the MW patients surviving the index stay were readmitted to hospital during the six-month follow-up, and their mean number of days spent in hospital after the index stay was 18.9 (SD 17.9) and 15.2 (SD 16.8) respectively (p=0.26). There was no difference in time to the first readmission in the two groups. Within six months, 40 (35%) of the GEMU and 30 (28%) of the MW patients surviving the index stay had been in nursing homes (p=0.26). These GEMU and MW patients had spent a mean of 67.4 (SD 50.0) and 70.6 (SD 60.7) days respectively in nursing homes during the six-month follow-up (p=0.81). Twenty-two (19%) and 17 (16%) of these GEMU and MW patients respectively had been in nursing homes permanently. There was no difference in time from inclusion in the study to permanent nursing home placement, and there was no difference in time spent in rehabilitation institutions. The number of patients still living at home who received assistance from the community nurses was 58 (57%) in the GEMU and 43 (54%) in MW group at three months and 57 (63%) and 44 (59%) respectively at six months. DISCUSSION In contrast to other randomized trials from acute care settings (7-9, 17, 18), in this study an increased number of patients were still able to live in their own homes, an effect that was mainly related to the considerably reduced mortality in the GEMU group (Fig. 2). After the index stay, which was longer in the GEMU group, there were neither statistically significant differences in admissions to or days in hospital, nursing homes and rehabilitation institutions, nor in the percentage of patients who received assistance from the community nurses. The treatment of acutely sick frail elderly patients in the GEMU significantly reduced mortality, a result which has been discussed in a previous publication (15). The consequence of improved survival among frail elderly patients may theoretically be an increased number of patients in need of long-term care facilities and hospitalization, if life was prolonged in those who were the sickest and with the poorest function. However, our data demonstrate that the comprehensive one-time intervention performed in a GEMU by a multidisciplinary geriatric team increased survival with no extra need of home care services, rehabilitation, readmissions to hospital or nursing home stays, and this should be regarded as a positive finding. The index stay in the GEMU group was prolonged mainly due to a delay shortly after inclusion in the study (Fig. 3). There may be several explanations for this. Transfer of patients from another ward, the interdisciplinary approach, comprehensive medical examination, and the fact that the staff in the GEMU performed study-related assessments in both groups may all have prolonged the stay in the GEMU group. The short run-in period of six months after the GEMU was established, from scratch until the start of the trial, may also have contributed to an unnecessarily long index stay. However, Percentage of patients discharged Time from inclusion (days) GEMU MW Figure 3 - Length of index stay. GEMU: Geriatric Evaluation and Management Unit, MW: general Medical Wards. 304 Aging Clin Exp Res, Vol. 16, No. 4
6 Acute geriatric intervention continuous evaluation of the routines in the GEMU aimed at improving efficacy, and subsequently the length of stay has since been shortened considerably. The study design did not allow further analyses as to which elements in the intervention had impact on the outcomes. However, it is noteworthy that, although patients planned to be discharged within two days were excluded, 18 MW patients were discharged within this period (Fig. 3), showing that while discharge planning was emphasized in the GEMU group, this was not the case in the MW. Diagnoses given at discharge were usually confined to those relevant for that specific hospital stay, which means that the real number of diagnoses per patient are likely to be higher than reported. However, it was shown that patients in the GEMU group had more diagnoses at discharge, including an increased number of psychiatric diagnoses, than those in the MW group (Table 2). This is explained by the comprehensive assessment of all relevant disorders in the GEMU, not as a real difference between the two groups. In addition, internists are generally less engaged in geriatric conditions like cognitive decline and depression. Our intervention was based upon a conservative in-patient hospital approach, and the achievement of improved time spent at home is very encouraging. However, while designing the study, an important overall aim of the GEMU intervention was a general reduction of health care utilization by each patient, which was not achieved. Other randomized studies focusing on improved collaboration between hospital and community health care system have shown the following results: reduced length of hospital stay (18), reduced number of patients awaiting transfer to nursing homes (19), reduced number of unplanned readmissions (20-23), postponed permanent nursing home placement (18, 24), and increased number of days spent at home (18, 23). In hospitals coordinating geriatric and discharge planning services, a reduced percentage of beds occupied by patients awaiting long-term care placement has been shown (13). By combining GEMU treatment and post-discharge intervention, the meta-analysis of Stuck et al. showed increased ability to live at home (6). In the light of results from the present study and these findings, it seems that to reduce health care utilization, future treatment models should combine optimal in-hospital treatment with systematic follow-up of patients by the GEMU team, in collaboration with the primary health care system (25, 26). CONCLUSIONS This is the first study to demonstrate that treatment of acutely sick frail elderly patients in a GEMU can significantly improve survival (15) and increase the number of patients able to live in their own homes, yet without statistically significant extra demands on health care utilization after discharge from hospital. These results strongly support the introduction of GEMU facilities and a general change in the management of frail elderly patients in hospitals. ACKNOWLEDGEMENTS The authors thank the members of the staff in the Geriatric Evaluation and Management Unit for their enthusiasm and willingness during the study. The study was supported by the Norwegian Ministry of Health and Social Affairs and the Research Council of Norway. REFERENCES 1. Grimley EJ. 21st Century: Review: ageing and medicine. J Intern Med 2000; 247: Sager MA, Franke T, Inouye SK, et al. Functional outcomes of acute medical illness and hospitalization in older persons. Arch Intern Med 1996; 156: Steel K, Gertman PM, Crescenzi C, Anderson J. Iatrogenic illness on a general medical service at a university hospital. N Engl J Med 1981; 304: Gillick MR, Serrell NA, Gillick LS. Adverse consequences of hospitalization in the elderly. Soc Sci Med 1982; 16: Rubenstein LZ, Josephson K, Wieland GD, et al. Geriatric assessment on a subacute hospital ward. Clin Geriatr Med 1987; 3: Stuck AE, Siu AL, Wieland GD, Adams J, Rubenstein LZ. Comprehensive geriatric assessment: a meta-analysis of controlled trials. Lancet 1993; 342: Landefeld CS, Palmer RM, Kresevic DM, Fortinsky RH, Kowal J. A randomized trial of care in a hospital medical unit especially designed to improve the functional outcomes of acutely ill older patients. N Engl J Med 1995; 332: Asplund K, Gustafson Y, Jacobsson C, et al. Geriatric-based versus general wards for older acute medical patients: a randomized comparison of outcomes and use of resources. J Am Geriatr Soc 2000; 48: Counsell SR, Holder CM, Liebenauer LL, et al. Effects of a multicomponent intervention on functional outcomes and process of care in hospitalized older patients: a randomized controlled trial of Acute Care for Elders (ACE) in a community hospital. J Am Geriatr Soc 2000; 48: Rubenstein LZ, Josephson KR, Wieland GD, English PA, Sayre JA, Kane RL. Effectiveness of a geriatric evaluation unit. A randomized clinical trial. N Engl J Med 1984; 311: Applegate WB, Miller ST, Graney MJ, Elam JT, Burns R, Akins DE. A randomized, controlled trial of a geriatric assessment unit in a community rehabilitation hospital. N Engl J Med 1990; 322: Cohen HJ, Feussner JR, Weinberger M, et al. A controlled trial of inpatient and outpatient geriatric evaluation and management. N Engl J Med 2002; 346: Brymer CD, Kohm CA, Naglie G, et al. Do geriatric programs decrease long-term use of acute care beds? J Am Geriatr Soc 1995; 43: Indredavik B, Bakke F, Solberg R, Rokseth R, Haaheim LL, Holme I. Benefit of a stroke unit: a randomized controlled trial. Stroke 1991; 22: Saltvedt I, Mo ES, Fayers P, Kaasa S, Sletvold O. Reduced mortality in treating acutely sick, frail older patients in a geriatric evaluation and management unit. A prospective randomized trial. J Am Geriatr Soc 2002; 50: Aging Clin Exp Res, Vol. 16, No
7 I. Saltvedt, T. Saltnes, E-S. Opdahl Mo, et al. 16. Winograd CH, Gerety MB, Chung M, Goldstein MK, Dominguez F. Jr, Vallone R. Screening for frailty: criteria and predictors of outcomes. J Am Geriatr Soc 1991; 39: Harris RD, Henschke PJ, Popplewell PY, et al. A randomised study of outcomes in a defined group of acutely ill elderly patients managed in a geriatric assessment unit or a general medical unit. Aust NZ J Med 1991; 21: Nikolaus T, Specht-Leible N, Bach M, Oster P, Schlierf G. A randomized trial of comprehensive geriatric assessment and home intervention in the care of hospitalized patients. Age Ageing 1999; 28: Styrborn K. Early discharge planning for elderly patients in acute hospitals - an intervention study. Scand J Soc Med 1995; 23: Hansen FR, Poulsen H, Sorensen KH. A model of regular geriatric follow-up by home visits to selected patients discharged from a geriatric ward: a randomized controlled trial. Aging Clin Exp Res 1995; 7: Stewart S, Pearson S, Luke CG, Horowitz JD. Effects of homebased intervention on unplanned readmissions and out-of-hospital deaths. J Am Geriatr Soc 1998; 46: Naylor MD, Brooten D, Campbell R, et al. Comprehensive discharge planning and home follow-up of hospitalized elders: a randomized clinical trial. JAMA 1999; 281: Melin AL, Bygren LO. Efficacy of the rehabilitation of elderly primary health care patients after short-stay hospital treatment. Med Care 1992; 30: Hansen FR, Spedtsberg K, Schroll M. Geriatric follow-up by home visits after discharge from hospital: a randomized controlled trial. Age Ageing 1992; 21: Young J, Philp I. Future directions for geriatric medicine. Geriatricians must move with their patients into the community. BMJ 2000; 320: Boult C, Boult LB, Morishita L, Dowd B, Kane RL, Urdangarin CF. A randomized clinical trial of outpatient geriatric evaluation and management. J Am Geriatr Soc 2001; 49: Aging Clin Exp Res, Vol. 16, No. 4
Comprehensive Assessment of the Frail Older Patient
 Comprehensive Assessment of the Frail Older Patient Executive Summary Comprehensive geriatric assessment (CGA) is a multidimensional and usually interdisciplinary diagnostic process designed to determine
Comprehensive Assessment of the Frail Older Patient Executive Summary Comprehensive geriatric assessment (CGA) is a multidimensional and usually interdisciplinary diagnostic process designed to determine
Geriatric screening in acute care wards a novel method of providing care to elderly patients
 Geriatric screening in acute care wards a novel method of providing care to elderly patients JKH Luk, T Kwok, J Woo Objective. To assess a nurse-implemented geriatric screening system. Design. Descriptive
Geriatric screening in acute care wards a novel method of providing care to elderly patients JKH Luk, T Kwok, J Woo Objective. To assess a nurse-implemented geriatric screening system. Design. Descriptive
INPATIENT AND OUTPATIENT GERIATRIC EVALUATION AND MANAGEMENT. Special Article
 INPATIENT AND OUTPATIENT GERIATRIC EVALUATION AND MANAGEMENT Special Article A CONTROLLED TRIAL OF INPATIENT AND OUTPATIENT GERIATRIC EVALUATION AND MANAGEMENT HARVEY JAY COHEN, M.D., JOHN R. FEUSSNER,
INPATIENT AND OUTPATIENT GERIATRIC EVALUATION AND MANAGEMENT Special Article A CONTROLLED TRIAL OF INPATIENT AND OUTPATIENT GERIATRIC EVALUATION AND MANAGEMENT HARVEY JAY COHEN, M.D., JOHN R. FEUSSNER,
The Long-term Prognosis of Delirium
 The Long-term Prognosis of Jane McCusker, MD, DrPH, Professor, Epidemiology and Biostatistics, McGill University; Head, Clinical Epidemiology and Community Studies, St. Mary s Hospital, Montreal, QC. Nine
The Long-term Prognosis of Jane McCusker, MD, DrPH, Professor, Epidemiology and Biostatistics, McGill University; Head, Clinical Epidemiology and Community Studies, St. Mary s Hospital, Montreal, QC. Nine
Hospitalization- Associated Disability
 Hospitalization- Associated Disability Deborah Villarreal, MD Assistant Professor Geriatric and Palliative Medicine An Unfortunately Common Scenario Mrs.G 70 y/o BF DM type II, HTN, s/p CVA, OA, OP admitted
Hospitalization- Associated Disability Deborah Villarreal, MD Assistant Professor Geriatric and Palliative Medicine An Unfortunately Common Scenario Mrs.G 70 y/o BF DM type II, HTN, s/p CVA, OA, OP admitted
Health and independence Strategic Vision and Implementation Plan for the Shropshire Frail & Complex Service
 Enclosure 01 Health and independence Strategic Vision and Implementation Plan for the Shropshire Frail & Complex Service Frail &Complex Service The challenge to the local health & social care economy The
Enclosure 01 Health and independence Strategic Vision and Implementation Plan for the Shropshire Frail & Complex Service Frail &Complex Service The challenge to the local health & social care economy The
BED BLOCKERS: A STUDY ON THE ELDERLY PATIENTS IN A TEACHING HOSPITAL IN INDIA
 ISPUB.COM The Internet Journal of Health Volume 11 Number 1 BED BLOCKERS: A STUDY ON THE ELDERLY PATIENTS IN A TEACHING HOSPITAL IN INDIA P N., N Shinge, P S. Citation P N., N Shinge, P S.. BED BLOCKERS:
ISPUB.COM The Internet Journal of Health Volume 11 Number 1 BED BLOCKERS: A STUDY ON THE ELDERLY PATIENTS IN A TEACHING HOSPITAL IN INDIA P N., N Shinge, P S. Citation P N., N Shinge, P S.. BED BLOCKERS:
Healthcare, hospitals and the challenges of an ageing population
 Healthcare, hospitals and the challenges of an ageing population Prof David Oliver Vice President, RCP, London Past President, British Geriatrics Society Senior Visiting Fellow, King s Fund Consultant
Healthcare, hospitals and the challenges of an ageing population Prof David Oliver Vice President, RCP, London Past President, British Geriatrics Society Senior Visiting Fellow, King s Fund Consultant
International Journal of Gerontology
 International Journal of Gerontology 6 (2012) 112e116 Contents lists available at SciVerse ScienceDirect International Journal of Gerontology journal homepage: www.ijge-online.com Original Article Geriatric
International Journal of Gerontology 6 (2012) 112e116 Contents lists available at SciVerse ScienceDirect International Journal of Gerontology journal homepage: www.ijge-online.com Original Article Geriatric
Why New Thinking is Needed for Older Adults across the Rehabilitation Continuum
 Why New Thinking is Needed for Older Adults across the Rehabilitation Continuum Samir K. Sinha MD, DPhil, FRCPC Director of Geriatrics Mount Sinai and the University Health Network Hospitals Assistant
Why New Thinking is Needed for Older Adults across the Rehabilitation Continuum Samir K. Sinha MD, DPhil, FRCPC Director of Geriatrics Mount Sinai and the University Health Network Hospitals Assistant
Outcomes in GEM models of geriatric care: How do we measure success? Disclosure. Objectives. Geriatric Grand Rounds
 Geriatric Grand Rounds Tuesday, October 7, 2008 12:00 noon Dr. Bill Black Auditorium Glenrose Rehabilitation Hospital Outcomes in GEM models of geriatric care: How do we measure success? In keeping with
Geriatric Grand Rounds Tuesday, October 7, 2008 12:00 noon Dr. Bill Black Auditorium Glenrose Rehabilitation Hospital Outcomes in GEM models of geriatric care: How do we measure success? In keeping with
CHF Longitudinal Workgroup. Addressing readmissions from SNFs and other PAC settings 3/2/17
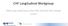 CHF Longitudinal Workgroup Addressing readmissions from SNFs and other PAC settings 3/2/17 Readmission Rate (%) Readmission Rate from SNF by Hospital (CHF) 16 14 13.6% 12 10 8 6 4 2 0 Mean = 6.3% 0% 0
CHF Longitudinal Workgroup Addressing readmissions from SNFs and other PAC settings 3/2/17 Readmission Rate (%) Readmission Rate from SNF by Hospital (CHF) 16 14 13.6% 12 10 8 6 4 2 0 Mean = 6.3% 0% 0
Evaluating Functional Status in Hospitalized Geriatric Patients. UCLA-Santa Monica Geriatric Medicine Didactic Lecture Series
 Evaluating Functional Status in Hospitalized Geriatric Patients UCLA-Santa Monica Geriatric Medicine Didactic Lecture Series Case 88 y.o. woman was admitted for a fall onto her hip. She is having trouble
Evaluating Functional Status in Hospitalized Geriatric Patients UCLA-Santa Monica Geriatric Medicine Didactic Lecture Series Case 88 y.o. woman was admitted for a fall onto her hip. She is having trouble
Quality of Acute Care for Older Persons with Dementia
 Quality of Acute Care for Older Persons with Dementia A Hospital-Based Pilot Study Chien-Liang Liu Center for Geriatrics and Gerontology, Taipei Veterans General Hospital, Taiwan 2013/04/20 Outline Background
Quality of Acute Care for Older Persons with Dementia A Hospital-Based Pilot Study Chien-Liang Liu Center for Geriatrics and Gerontology, Taipei Veterans General Hospital, Taiwan 2013/04/20 Outline Background
Improving Healthcare Utilization in Injured Older Adults
 Improving Healthcare Utilization in Injured Older Adults G ERIATRIC T R A U MA I N I T I AT I V E S AT S TA N F O R D H E A LT H C A R E J U LY 12, 2018 Objectives Background on Geriatric Trauma Population
Improving Healthcare Utilization in Injured Older Adults G ERIATRIC T R A U MA I N I T I AT I V E S AT S TA N F O R D H E A LT H C A R E J U LY 12, 2018 Objectives Background on Geriatric Trauma Population
Geriatrics and Cancer Care
 Geriatrics and Cancer Care Roger Wong, BMSc, MD, FRCPC, FACP Postgraduate Dean of Medical Education Clinical Professor, Division of Geriatric Medicine UBC Faculty of Medicine Disclosure No competing interests
Geriatrics and Cancer Care Roger Wong, BMSc, MD, FRCPC, FACP Postgraduate Dean of Medical Education Clinical Professor, Division of Geriatric Medicine UBC Faculty of Medicine Disclosure No competing interests
EMU A NEW MODEL OF EMERGENCY CARE FOR THE FRAIL & ELDERLY
 EMU A NEW MODEL OF EMERGENCY CARE FOR THE FRAIL & ELDERLY Geriatrics, General practice, Emergency medicine, Interface medicine SUMMARY An integrated, community emergency service specifically designed for
EMU A NEW MODEL OF EMERGENCY CARE FOR THE FRAIL & ELDERLY Geriatrics, General practice, Emergency medicine, Interface medicine SUMMARY An integrated, community emergency service specifically designed for
Management of the Frail Older Patients: What Are the Outcomes
 Management of the Frail Older Patients: What Are the Outcomes Professor Edwina Brown Imperial College Renal and Transplant Centre Hammersmith Hospital, London Increasing prevalence of old old on RRT RRT
Management of the Frail Older Patients: What Are the Outcomes Professor Edwina Brown Imperial College Renal and Transplant Centre Hammersmith Hospital, London Increasing prevalence of old old on RRT RRT
Delirium assessment and management. Dr Kim Jeffs Northern Health
 Delirium assessment and management Dr Kim Jeffs Northern Health What do you need to know? Epidemiology How big is the problem? Who is at risk? Assessment Tools for diagnosis Prevention Evidence base Management
Delirium assessment and management Dr Kim Jeffs Northern Health What do you need to know? Epidemiology How big is the problem? Who is at risk? Assessment Tools for diagnosis Prevention Evidence base Management
Breast cancer in the elderly - is there a role for the geriatrician?
 Breast cancer in the elderly - is there a role for the geriatrician? Workshop in Breast Cancer Surgery Aarhus 18 May 2016 Lone Winther Lietzen MD, PhD Department of Geriatrics, Geriatricians? Internal
Breast cancer in the elderly - is there a role for the geriatrician? Workshop in Breast Cancer Surgery Aarhus 18 May 2016 Lone Winther Lietzen MD, PhD Department of Geriatrics, Geriatricians? Internal
ACEing Age Old Issues in the Care of Older Canadians
 ACEing Age Old Issues in the Care of Older Canadians Dr. Samir K. Sinha MD, DPhil, FRCPC Peter and Shelagh Godsoe Chair in Geriatrics and Director of Geriatrics Sinai Health System and the University Health
ACEing Age Old Issues in the Care of Older Canadians Dr. Samir K. Sinha MD, DPhil, FRCPC Peter and Shelagh Godsoe Chair in Geriatrics and Director of Geriatrics Sinai Health System and the University Health
Edith Haage, PT, GCS NewCourtland Senior Services 10/26/2016. NEWCOURTLAND.org
 Edith Haage, PT, GCS NewCourtland Senior Services 10/26/2016 NEWCOURTLAND.org 1-888-530-4913 Edith Haage has disclosed she has no financial relationships. 1. Define frailty in geriatric clientele, including
Edith Haage, PT, GCS NewCourtland Senior Services 10/26/2016 NEWCOURTLAND.org 1-888-530-4913 Edith Haage has disclosed she has no financial relationships. 1. Define frailty in geriatric clientele, including
Understanding and Assessing for Frailty
 Understanding and Assessing for Frailty Dr Gloria Yu Clinical Head of Bexley Integrated Care Consultant Physician in Elderly, General and Stroke Medicine 8 July 2015 Learning objectives What is frailty?
Understanding and Assessing for Frailty Dr Gloria Yu Clinical Head of Bexley Integrated Care Consultant Physician in Elderly, General and Stroke Medicine 8 July 2015 Learning objectives What is frailty?
after acute care (inc. ED)?
 How to prevent early & unplanned hospital admission after acute care (inc. ED)? Luis Mieiro @luismieiro Consultant Geriatrician Forest Assessment Unit - Older People s Services Whipps Cross University
How to prevent early & unplanned hospital admission after acute care (inc. ED)? Luis Mieiro @luismieiro Consultant Geriatrician Forest Assessment Unit - Older People s Services Whipps Cross University
How to disseminate the Acute Care for Elders (ACE) model of care beyond one unit
 How to disseminate the Acute Care for Elders (ACE) model of care beyond one unit Roger Wong, BMSc, MD, FRCPC, FACP Clinical Professor, Division of Geriatric Medicine Associate Dean, Postgraduate Medical
How to disseminate the Acute Care for Elders (ACE) model of care beyond one unit Roger Wong, BMSc, MD, FRCPC, FACP Clinical Professor, Division of Geriatric Medicine Associate Dean, Postgraduate Medical
Quality Care for the Hospitalized Older Adult
 Quality Care for the Hospitalized Older Adult Quality Care for the Hospitalized Older Adult Shelley R McDonald, DO, PhD May 19 th, 2018 Objectives To define why the hospital is a dangerous place for older
Quality Care for the Hospitalized Older Adult Quality Care for the Hospitalized Older Adult Shelley R McDonald, DO, PhD May 19 th, 2018 Objectives To define why the hospital is a dangerous place for older
Ageing Well. The challenge of our ageing population. Martin Vernon NCD Older People. Find Recognise Assess Intervene Long-term.
 Ageing Well The challenge of our ageing population Martin Vernon NCD Older People 7 th June 2017 1 Projected UK age structure Foresight, 2016 2 Ageing impacts 15 million live with a long term condition
Ageing Well The challenge of our ageing population Martin Vernon NCD Older People 7 th June 2017 1 Projected UK age structure Foresight, 2016 2 Ageing impacts 15 million live with a long term condition
The Challenges of Managing the Older Persons
 IAG Presidential Oration The Challenges of Managing the Older Persons G.S. Shanthi Professor & Head, Department of Geriatric Medicine, Madras Medical College, Chennai Globally, due to shifting demographics,
IAG Presidential Oration The Challenges of Managing the Older Persons G.S. Shanthi Professor & Head, Department of Geriatric Medicine, Madras Medical College, Chennai Globally, due to shifting demographics,
Functional level at admission is a predictor of survival in older patients admitted to an acute geriatric unit
 Matzen et al. BMC Geriatrics 2012, 12:32 RESEARCH ARTICLE Open Access Functional level at admission is a predictor of survival in older patients admitted to an acute geriatric unit Lars E Matzen 1,2*,
Matzen et al. BMC Geriatrics 2012, 12:32 RESEARCH ARTICLE Open Access Functional level at admission is a predictor of survival in older patients admitted to an acute geriatric unit Lars E Matzen 1,2*,
PROVIDING BETTER CARE FOR OLDER CANADIANS OBJECTIVES
 PROVIDING BETTER CARE FOR OLDER CANADIANS CGS/ SQG SYMPOSIUM MARIE-JEANNE KERGOAT MD, FRCPC,TORONTO, APRIL 19TH 2013 OBJECTIVES Debate with other clinicians responsible for delivering care to vulnerable
PROVIDING BETTER CARE FOR OLDER CANADIANS CGS/ SQG SYMPOSIUM MARIE-JEANNE KERGOAT MD, FRCPC,TORONTO, APRIL 19TH 2013 OBJECTIVES Debate with other clinicians responsible for delivering care to vulnerable
How to prevent early & unplanned hospital readmission?
 How to prevent early & unplanned hospital readmission? - after subacute care K. Singler 21th September 2017 CONFLICT OF INTEREST DISCLOSURE I have no potential conflict of interest to report. K. Singler
How to prevent early & unplanned hospital readmission? - after subacute care K. Singler 21th September 2017 CONFLICT OF INTEREST DISCLOSURE I have no potential conflict of interest to report. K. Singler
4/26/2012. Laura Grooms, MD Assistant Professor Geriatric Medicine Department of Family and Geriatric Medicine University of Louisville April 20, 2012
 Laura Grooms, MD Assistant Professor Geriatric Medicine Department of Family and Geriatric Medicine University of Louisville April 20, 2012 Laura Grooms, MD Assistant Professor Geriatric Medicine Department
Laura Grooms, MD Assistant Professor Geriatric Medicine Department of Family and Geriatric Medicine University of Louisville April 20, 2012 Laura Grooms, MD Assistant Professor Geriatric Medicine Department
GRACE Team Care A New Model of Integrated Medical and Social Care for Older Persons
 GRACE Team Care A New Model of Integrated Medical and Social Care for Older Persons Steven R. Counsell, MD Mary Elizabeth Mitchell Professor and Director, Scientist, IU Center for Aging Research E-mail:
GRACE Team Care A New Model of Integrated Medical and Social Care for Older Persons Steven R. Counsell, MD Mary Elizabeth Mitchell Professor and Director, Scientist, IU Center for Aging Research E-mail:
Assessing the utility of simple measures of frailty in older hospital-based cardiology patients. by Yong Yong Tew (medical student)
 Assessing the utility of simple measures of frailty in older hospital-based cardiology patients by Yong Yong Tew (medical student) Declaration No conflict of interest. Ethical considerations Reviewed and
Assessing the utility of simple measures of frailty in older hospital-based cardiology patients by Yong Yong Tew (medical student) Declaration No conflict of interest. Ethical considerations Reviewed and
Delirium in the Elderly
 Delirium in the Elderly ELITE 2015 Mamata Yanamadala M.B.B.S, MS Division of Geriatrics Why should we care about delirium? It is: common associated with high mortality associated with increased morbidity
Delirium in the Elderly ELITE 2015 Mamata Yanamadala M.B.B.S, MS Division of Geriatrics Why should we care about delirium? It is: common associated with high mortality associated with increased morbidity
Integrating Medical and Social Support for Elderly System & Technology Enabled Service Innovations. Dr Christina MAW Hospital Authority, Hong Kong
 Integrating Medical and Social Support for Elderly System & Technology Enabled Service Innovations Dr Christina MAW Hospital Authority, Hong Kong Hospital Authority (HA) of Hong Kong A statutory body responsible
Integrating Medical and Social Support for Elderly System & Technology Enabled Service Innovations Dr Christina MAW Hospital Authority, Hong Kong Hospital Authority (HA) of Hong Kong A statutory body responsible
Innovative geriatric care: Integrating the Transitional Care Bridge Program in a new Co-Management Model for Frail Elderly
 Innovative geriatric care: Integrating the Transitional Care Bridge Program in a new Co-Management Model for Frail Elderly Herbert Habets, Walther Sipers, Bart Ament, Anneke van Dijk-de Vries, Erik van
Innovative geriatric care: Integrating the Transitional Care Bridge Program in a new Co-Management Model for Frail Elderly Herbert Habets, Walther Sipers, Bart Ament, Anneke van Dijk-de Vries, Erik van
Integration of palliative care into oncology
 1 Integration of palliative care into oncology Stein Kaasa European Palliative Care Research Centre, Faculty of Medicine, NTNU and Department of Oncology, St. Olavs Hospital, Trondheim University Hospital
1 Integration of palliative care into oncology Stein Kaasa European Palliative Care Research Centre, Faculty of Medicine, NTNU and Department of Oncology, St. Olavs Hospital, Trondheim University Hospital
Statistical analysis plan - The Oslo Study of Clonidine in Elderly Patients with Delirium; LUCID
 Statistical analysis plan - The Oslo Study of Clonidine in Elderly Patients with Delirium; LUCID Note: This statistical analysis plan was written prior to unblinding of randomisation / treatment allocation.
Statistical analysis plan - The Oslo Study of Clonidine in Elderly Patients with Delirium; LUCID Note: This statistical analysis plan was written prior to unblinding of randomisation / treatment allocation.
Delirium in the Elderly
 Delirium in the Elderly ELITE 2017 Liza Genao, MD Division of Geriatrics Why should we care about delirium? It is: common associated with high mortality associated with increased morbidity Very much under-recognized
Delirium in the Elderly ELITE 2017 Liza Genao, MD Division of Geriatrics Why should we care about delirium? It is: common associated with high mortality associated with increased morbidity Very much under-recognized
Comprehensive geriatric assessment (CGA)
 Comprehensive geriatric assessment (CGA) Mieke Deschodt, RN, PhD Lucky you, getting older in Europe - Multiplier event IC Dien Oostduinkerke, 5 June 2018 @mieke_deschodt 2 Outline Comprehensive geriatric
Comprehensive geriatric assessment (CGA) Mieke Deschodt, RN, PhD Lucky you, getting older in Europe - Multiplier event IC Dien Oostduinkerke, 5 June 2018 @mieke_deschodt 2 Outline Comprehensive geriatric
Do shared care wards work?
 Do shared care wards work? Prof Rowan H. Harwood Nottingham University Hospitals NHS Trust & University of Nottingham rowan.harwood@nuh.nhs.uk This presentation is on independent research funded by the
Do shared care wards work? Prof Rowan H. Harwood Nottingham University Hospitals NHS Trust & University of Nottingham rowan.harwood@nuh.nhs.uk This presentation is on independent research funded by the
The Risks of Hip Fracture in Older People from Private Homes and Institutions
 Age and Ageing 1996:25:381-385 The Risks of Hip Fracture in Older People from Private Homes and Institutions MEG BUTLER, ROBYN NORTON, TREVOR LEE-JOE, ADA CHENG, A. JOHN CAMPBELL Summary This study aimed
Age and Ageing 1996:25:381-385 The Risks of Hip Fracture in Older People from Private Homes and Institutions MEG BUTLER, ROBYN NORTON, TREVOR LEE-JOE, ADA CHENG, A. JOHN CAMPBELL Summary This study aimed
Inpatient Geriatric Evaluation and Management Units (GEMs) in the Veterans Health System: Diamonds in the Rough?
 Journal ofgerontologv: MEDICAL SCIENCES 1994, Vol. 49, No. 5,'M195-M200 In the Public Domain Inpatient Geriatric Evaluation and Management Units (GEMs) in the Veterans Health System: Diamonds in the Rough?
Journal ofgerontologv: MEDICAL SCIENCES 1994, Vol. 49, No. 5,'M195-M200 In the Public Domain Inpatient Geriatric Evaluation and Management Units (GEMs) in the Veterans Health System: Diamonds in the Rough?
Geriatric Medicine I) OBJECTIVES
 Geriatric Medicine I) OBJECTIVES 1 To provide a broad training and in-depth experience at a level sufficient for trainees to acquire competence and professionalism required of a specialist in Geriatric
Geriatric Medicine I) OBJECTIVES 1 To provide a broad training and in-depth experience at a level sufficient for trainees to acquire competence and professionalism required of a specialist in Geriatric
1338 THE NEW ENGLAND JOURNAL OF MEDICINE May 18, 1995 SPECIAL ARTICLES
 1338 THE NEW ENGLAND JOURNAL OF MEDICINE May 18, 1995 SPECIAL ARTICLES A RANDOMIZED TRIAL OF CARE IN A HOSPITAL MEDICAL UNIT ESPECIALLY DESIGNED TO IMPROVE THE FUNCTIONAL OUTCOMES OF ACUTELY ILL OLDER
1338 THE NEW ENGLAND JOURNAL OF MEDICINE May 18, 1995 SPECIAL ARTICLES A RANDOMIZED TRIAL OF CARE IN A HOSPITAL MEDICAL UNIT ESPECIALLY DESIGNED TO IMPROVE THE FUNCTIONAL OUTCOMES OF ACUTELY ILL OLDER
It is a challenge to organize a healthcare service that can
 Stroke Unit Care Combined With Early Supported Discharge Long-Term Follow-Up of a Randomized Controlled Trial Hild Fjærtoft, RPT; Bent Indredavik, MD, PhD; Stian Lydersen, PhD Background and Purpose Early
Stroke Unit Care Combined With Early Supported Discharge Long-Term Follow-Up of a Randomized Controlled Trial Hild Fjærtoft, RPT; Bent Indredavik, MD, PhD; Stian Lydersen, PhD Background and Purpose Early
Creating a Hospital Nurse-Driven Mobility Program - Why and How Physical Therapist Should Lead the Way
 Creating a Hospital Nurse-Driven Mobility Program - Why and How Physical Therapist Should Lead the Way, GCS University of North Georgia Grady Health System The Problem The Solution The How To F u n c t
Creating a Hospital Nurse-Driven Mobility Program - Why and How Physical Therapist Should Lead the Way, GCS University of North Georgia Grady Health System The Problem The Solution The How To F u n c t
Differences between ''geriatric" and "medical" patients aged 75 and over
 The Ulster Medical Journal, Volume 62, No. 1, pp. 4-10, April 1993. Differences between ''geriatric" and "medical" patients aged 75 and over Maree Todd, Vivienne Crawford, R W Stout Accepted 20 December
The Ulster Medical Journal, Volume 62, No. 1, pp. 4-10, April 1993. Differences between ''geriatric" and "medical" patients aged 75 and over Maree Todd, Vivienne Crawford, R W Stout Accepted 20 December
Rehabilitation - Reducing costs and hospital stay. Dr Elizabeth Aitken Consultant Physician
 Rehabilitation - Reducing costs and hospital stay Dr Elizabeth Aitken Consultant Physician What factors affect outcome? Comorbidities Cardiac Respiratory Neurological Nutritional issues Diabetes Anaemia
Rehabilitation - Reducing costs and hospital stay Dr Elizabeth Aitken Consultant Physician What factors affect outcome? Comorbidities Cardiac Respiratory Neurological Nutritional issues Diabetes Anaemia
Integration of Palliative and Oncology Care in patients with lung and other
 1 Integration of Palliative and Oncology Care in patients with lung and other thoracic cancer: referral criteria and clinical care pathways. A. Caraceni, C. Brunelli, S. Lo Dico, E. Zecca, P. Bracchi,
1 Integration of Palliative and Oncology Care in patients with lung and other thoracic cancer: referral criteria and clinical care pathways. A. Caraceni, C. Brunelli, S. Lo Dico, E. Zecca, P. Bracchi,
Positive impact of stroke unit establishment on patient recovery in Firoozgar hospital
 Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Positive impact of stroke unit establishment on patient recovery in Firoozgar hospital Masoud
Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Positive impact of stroke unit establishment on patient recovery in Firoozgar hospital Masoud
*GERIATRIC FELLOWSHIP COMPETENCY CHECKLIST EDUCATIONAL GOALS:
 *GERIATRIC FELLOWSHIP COMPETENCY CHECKLIST EDUCATIONAL GOALS: The goal of geriatric fellowship training is to prepare fellows for competency in the following core areas: Check and record date completed
*GERIATRIC FELLOWSHIP COMPETENCY CHECKLIST EDUCATIONAL GOALS: The goal of geriatric fellowship training is to prepare fellows for competency in the following core areas: Check and record date completed
One-year health and care costs after hip fracture for home-dwelling elderly in Norway. Results from the Trondheim Hip Fracture Trial
 One-year health and care costs after hip fracture for home-dwelling elderly in Norway. Results from the Trondheim Hip Fracture Trial Liv Faksvåg Hektoen 1, Ingvild Saltvedt 2,3, Olav Sletvold 2, 3, Jorunn
One-year health and care costs after hip fracture for home-dwelling elderly in Norway. Results from the Trondheim Hip Fracture Trial Liv Faksvåg Hektoen 1, Ingvild Saltvedt 2,3, Olav Sletvold 2, 3, Jorunn
Functional status and social support network as risk factors for hospital readmission in Heart Failure
 Functional status and social support network as risk factors for hospital readmission in Heart Failure Sílvia Alexandra Duarte Centro Hospitalar de Trás os Montes e Alto Douro, Vila Real, Portugal CONFLICT
Functional status and social support network as risk factors for hospital readmission in Heart Failure Sílvia Alexandra Duarte Centro Hospitalar de Trás os Montes e Alto Douro, Vila Real, Portugal CONFLICT
Frailty and Rehabilitation: How We Utilized FIM Data to Develop Risk Models
 Frailty and Rehabilitation: How We Utilized FIM Data to Develop Risk Models User Groups 2015 Orlando, Florida March 19, 2015 Las Vegas, Nevada May 7, 2015 Pam Roberts, PhD, OTR/L, SCFES, FAOTA, CPHQ, FNAP
Frailty and Rehabilitation: How We Utilized FIM Data to Develop Risk Models User Groups 2015 Orlando, Florida March 19, 2015 Las Vegas, Nevada May 7, 2015 Pam Roberts, PhD, OTR/L, SCFES, FAOTA, CPHQ, FNAP
public health crisis! Understanding frailty at population level!
 Frailty as an emerging public health crisis! Understanding frailty at population level! Dr Rónán O Caoimh, MB, MRCPI, MSc, PhD Senior Lecturer in Geriatric Medicine 08/03/2017 A brief history of frailty...
Frailty as an emerging public health crisis! Understanding frailty at population level! Dr Rónán O Caoimh, MB, MRCPI, MSc, PhD Senior Lecturer in Geriatric Medicine 08/03/2017 A brief history of frailty...
FALLS PREVENTION. S H I R L E Y H U A N G, M S c, M D, F R C P C
 FALLS PREVENTION S H I R L E Y H U A N G, M S c, M D, F R C P C S T A F F G E R I A T R I C I A N T H E O T T A W A H O S P I T A L B R U Y E R E C O N T I N U I N G C A R E W I N C H E S T E R D I S T
FALLS PREVENTION S H I R L E Y H U A N G, M S c, M D, F R C P C S T A F F G E R I A T R I C I A N T H E O T T A W A H O S P I T A L B R U Y E R E C O N T I N U I N G C A R E W I N C H E S T E R D I S T
Managing and streaming of all admissions The Heartlands experience
 Managing and streaming of all admissions The Heartlands experience Dr Marwa Mattar, ST6 Acute Medicine Dr Ariyur Balaji, Clinical Lead Acute Medicine BHH Why is this important? Unprecedented demand for
Managing and streaming of all admissions The Heartlands experience Dr Marwa Mattar, ST6 Acute Medicine Dr Ariyur Balaji, Clinical Lead Acute Medicine BHH Why is this important? Unprecedented demand for
RHSC 501 Section W Section Instructor: Heidi Schwellnus Critically Appraised Topic Barbara Holuboff. November 11, 2010
 1 RHSC 501 Section 002-2010W Section Instructor: Heidi Schwellnus Critically Appraised Topic Barbara Holuboff 10275097 November 11, 2010 Masters of Rehabilitation Sciences University of British Columbia
1 RHSC 501 Section 002-2010W Section Instructor: Heidi Schwellnus Critically Appraised Topic Barbara Holuboff 10275097 November 11, 2010 Masters of Rehabilitation Sciences University of British Columbia
Drug use in long term care. Graziano Onder Centro Medicina Invecchiamento Università Cattolica Sacro Cuore, Rome
 Drug use in long term care Graziano Onder Centro Medicina Invecchiamento Università Cattolica Sacro Cuore, Rome Polypharmacy in nursing home (USA) Concurrent use of 9 medications was reported for 39.7%
Drug use in long term care Graziano Onder Centro Medicina Invecchiamento Università Cattolica Sacro Cuore, Rome Polypharmacy in nursing home (USA) Concurrent use of 9 medications was reported for 39.7%
Feasibility of Implementing Advance Directive in Hong Kong Chinese Elderly People
 Asia Pacific Regional Conference in End-of-Life and Palliative Care in Long Term Care Settings Feasibility of Implementing Advance Directive in Hong Kong Chinese Elderly People Dr. Patrick CHIU MBBS (HK),
Asia Pacific Regional Conference in End-of-Life and Palliative Care in Long Term Care Settings Feasibility of Implementing Advance Directive in Hong Kong Chinese Elderly People Dr. Patrick CHIU MBBS (HK),
Young onset dementia service Doncaster
 Young onset dementia service Doncaster RDaSH Older People s Mental Health Services Introduction The following procedures and protocols will govern the operational working and function of the Doncaster
Young onset dementia service Doncaster RDaSH Older People s Mental Health Services Introduction The following procedures and protocols will govern the operational working and function of the Doncaster
Appendix 1: Service self-assessment
 Appendix 1: Service self-assessment Frailty Screening Are we delivering high-quality care for frail older people? We are assessing for frailty in people aged 65+ at every entry into the service using a
Appendix 1: Service self-assessment Frailty Screening Are we delivering high-quality care for frail older people? We are assessing for frailty in people aged 65+ at every entry into the service using a
ASSESS & RESTORE SHARED PROVINCIAL INDICATORS AND TECHNICAL SPECIFICATIONS
 Shared Provincial s & ASSESS & RESTORE SHARED PROVINCIAL INDICATORS AND TECHNICAL SPECIFICATIONS January 2018 0 P a g e J a n u a r y 2 0 1 8 Shared Provincial s & BACKGROUND To evaluate the impact of
Shared Provincial s & ASSESS & RESTORE SHARED PROVINCIAL INDICATORS AND TECHNICAL SPECIFICATIONS January 2018 0 P a g e J a n u a r y 2 0 1 8 Shared Provincial s & BACKGROUND To evaluate the impact of
Evaluation of the functional independence for stroke survivors in the community
 Asian J Gerontol Geriatr 2009; 4: 24 9 Evaluation of the functional independence for stroke survivors in the community ORIGINAL ARTICLE CKC Chan Bsc, DWC Chan Msc, SKM Wong MBA, MAIS, BA, PDOT ABSTRACT
Asian J Gerontol Geriatr 2009; 4: 24 9 Evaluation of the functional independence for stroke survivors in the community ORIGINAL ARTICLE CKC Chan Bsc, DWC Chan Msc, SKM Wong MBA, MAIS, BA, PDOT ABSTRACT
Professor Brian Draper
 Understanding what s different for patients with dementia in acute care hospitals coalface implications Psychiatry Professor Brian Draper UNSW & Prince of Wales Hospital, Randwick Background Previous analyses
Understanding what s different for patients with dementia in acute care hospitals coalface implications Psychiatry Professor Brian Draper UNSW & Prince of Wales Hospital, Randwick Background Previous analyses
Acute care for older people with frailty
 Acute care for older people with frailty Professor Simon Conroy Clinical lead, Acute Frailty Network, England Geriatrician, University Hospitals of Leicester Worldview that will colour this talk Demography
Acute care for older people with frailty Professor Simon Conroy Clinical lead, Acute Frailty Network, England Geriatrician, University Hospitals of Leicester Worldview that will colour this talk Demography
Basic Standards for Residency/Fellowship Training in Geriatric Psychiatry
 Basic Standards for Residency/Fellowship Training in Geriatric Psychiatry American Osteopathic Association and American College of Osteopathic Neurologists and Psychiatrists Approved 2/2005 Revised 2/2008,
Basic Standards for Residency/Fellowship Training in Geriatric Psychiatry American Osteopathic Association and American College of Osteopathic Neurologists and Psychiatrists Approved 2/2005 Revised 2/2008,
Cumulated Ambulation Score to evaluate mobility is feasible in geriatric patients and in patients with hip fracture
 Cumulated Ambulation Score to evaluate mobility is feasible in geriatric patients and in patients with hip fracture Morten Tange Kristensen 1, 2,Thomas Linding Jakobsen 3, 4, Jesper Westphal Nielsen 1,
Cumulated Ambulation Score to evaluate mobility is feasible in geriatric patients and in patients with hip fracture Morten Tange Kristensen 1, 2,Thomas Linding Jakobsen 3, 4, Jesper Westphal Nielsen 1,
SHRUGs national report Information & Statistics Division The National Health Service in Scotland Edinburgh June 2000
 Scottish Health Resource Utilisation Groups SHRUGs national report 1999 Information & Statistics Division The National Health Service in Scotland Edinburgh June 2000 Contents -- click on the section of
Scottish Health Resource Utilisation Groups SHRUGs national report 1999 Information & Statistics Division The National Health Service in Scotland Edinburgh June 2000 Contents -- click on the section of
Holy Cross Health Meeting the Needs of the Senior Population. Judith Rogers, RNC, MSN, PhD President, Holy Cross Hospital February, 2016
 Holy Cross Health Meeting the Needs of the Senior Population Judith Rogers, RNC, MSN, PhD President, Holy Cross Hospital February, 2016 Service Area Holy Cross Hospital s service area includes about 1.7
Holy Cross Health Meeting the Needs of the Senior Population Judith Rogers, RNC, MSN, PhD President, Holy Cross Hospital February, 2016 Service Area Holy Cross Hospital s service area includes about 1.7
What can we learn from the AVERT trial (so far)?
 South West Stroke Network Event, 29 th April, 2015 What can we learn from the AVERT trial (so far)? Peter Langhorne, Professor of stroke care, Glasgow University Disclosure PL was AVERT investigator and
South West Stroke Network Event, 29 th April, 2015 What can we learn from the AVERT trial (so far)? Peter Langhorne, Professor of stroke care, Glasgow University Disclosure PL was AVERT investigator and
Appendix E : Evidence table 9 Rehabilitation: Other Key Documents
 Appendix E : Evidence table 9 Rehabilitation: Other Key Documents 1. Cameron et al. Geriatric rehabilitation following following fractures in older people: a systematic review. Health Technology Assessment
Appendix E : Evidence table 9 Rehabilitation: Other Key Documents 1. Cameron et al. Geriatric rehabilitation following following fractures in older people: a systematic review. Health Technology Assessment
NZ Organised Stroke Rehabilitation Service Specifications (in-patient and community)
 NZ Organised Stroke Rehabilitation Service Specifications (in-patient and community) Prepared by the National Stroke Network to outline minimum and strongly recommended standards for DHBs. Date: December
NZ Organised Stroke Rehabilitation Service Specifications (in-patient and community) Prepared by the National Stroke Network to outline minimum and strongly recommended standards for DHBs. Date: December
The OPRAA Cohort. Emma Reynish
 The OPRAA Cohort Emma Reynish Chair of Dementia Research, Faculty of Social Science, University of Stirling. Consultant Geriatrician, Royal Infirmary Edinburgh, NHS Lothian Standardised Assessment of older
The OPRAA Cohort Emma Reynish Chair of Dementia Research, Faculty of Social Science, University of Stirling. Consultant Geriatrician, Royal Infirmary Edinburgh, NHS Lothian Standardised Assessment of older
Aged Care and Health Services Research. A/Prof Kwang Lim Sep 2016
 Aged Care and Health Services Research A/Prof Kwang Lim Sep 2016 Accumulating evidence 20% of health care interventions is based on hard evidence. Feasibility of doing randomised controlled trials on all
Aged Care and Health Services Research A/Prof Kwang Lim Sep 2016 Accumulating evidence 20% of health care interventions is based on hard evidence. Feasibility of doing randomised controlled trials on all
ONLINE DATA SUPPLEMENT - ASTHMA INTERVENTION PROGRAM PREVENTS READMISSIONS IN HIGH HEALTHCARE UTILIZERS
 R2 (REVISED MANUSCRIPT BLUE 200208-877OC) ONLINE DATA SUPPLEMENT - ASTHMA INTERVENTION PROGRAM PREVENTS READMISSIONS IN HIGH HEALTHCARE UTILIZERS Mario Castro, M.D., M.P.H. Nina A. Zimmermann R.N. Sue
R2 (REVISED MANUSCRIPT BLUE 200208-877OC) ONLINE DATA SUPPLEMENT - ASTHMA INTERVENTION PROGRAM PREVENTS READMISSIONS IN HIGH HEALTHCARE UTILIZERS Mario Castro, M.D., M.P.H. Nina A. Zimmermann R.N. Sue
Geriatric screening tools in older patients with cancer
 Geriatric screening tools in older patients with cancer Pr. Elena Paillaud Henri Mondor hospital, Créteil, France University Paris-Est Créteil CONFLICT OF INTEREST DISCLOSURE I have the following potential
Geriatric screening tools in older patients with cancer Pr. Elena Paillaud Henri Mondor hospital, Créteil, France University Paris-Est Créteil CONFLICT OF INTEREST DISCLOSURE I have the following potential
JAMA, January 11, 2012 Vol 307, No. 2
 JAMA, January 11, 2012 Vol 307, No. 2 Dementia is associated with increased rates and often poorer outcomes of hospitalization Worsening cognitive status Adequate chronic disease management is more difficult
JAMA, January 11, 2012 Vol 307, No. 2 Dementia is associated with increased rates and often poorer outcomes of hospitalization Worsening cognitive status Adequate chronic disease management is more difficult
Strategies for Enhancing Sepsis Survivorship
 Strategies for Enhancing Sepsis Survivorship Hallie Prescott, MD, MSc Ohio Hospital Association August 16, 2016 Disclosures I have no relevant financial conflicts of interest Key Funding NIH/NIGMS American
Strategies for Enhancing Sepsis Survivorship Hallie Prescott, MD, MSc Ohio Hospital Association August 16, 2016 Disclosures I have no relevant financial conflicts of interest Key Funding NIH/NIGMS American
Acute care for older people with frailty
 Acute care for older people with frailty Professor Simon Conroy Clinical lead, Acute Frailty Network, England Geriatrician, University Hospitals of Leicester Why acute frailty? Demography Absence of immortality
Acute care for older people with frailty Professor Simon Conroy Clinical lead, Acute Frailty Network, England Geriatrician, University Hospitals of Leicester Why acute frailty? Demography Absence of immortality
Continence, falls and the frailty syndrome. Anne Foley - BGS Bladders and Bowel Health 2012
 Continence, falls and the frailty syndrome Outline Frailty Geriatric syndromes and giants Aetiology What can be done? The future Frailty Frailty Frailty (noun): The state of being weak in health or body
Continence, falls and the frailty syndrome Outline Frailty Geriatric syndromes and giants Aetiology What can be done? The future Frailty Frailty Frailty (noun): The state of being weak in health or body
La complessità di un reparto di geriatria
 4 marzo 2011 La complessità di un reparto di geriatria Renzo Rozzini The Future of Geriatrics Looks Bright The world is aging! Robert L. Kane, MD University of Minnesota School of Public Health What
4 marzo 2011 La complessità di un reparto di geriatria Renzo Rozzini The Future of Geriatrics Looks Bright The world is aging! Robert L. Kane, MD University of Minnesota School of Public Health What
Division of Medicine. Department of Geriatric Medicine. Staff. Jerry Ciocon, M.D., F.A.C.P., F.A.C.A., A.G.S.F. Diana J. Galindo, M.D.
 Division of Medicine Department of Geriatric Medicine Staff Jerry Ciocon, M.D., F.A.C.P., F.A.C.A., A.G.S.F. Diana J. Galindo, M.D. 1 Chairman s Letter We are all getting older, and providing the care
Division of Medicine Department of Geriatric Medicine Staff Jerry Ciocon, M.D., F.A.C.P., F.A.C.A., A.G.S.F. Diana J. Galindo, M.D. 1 Chairman s Letter We are all getting older, and providing the care
This is the author s final accepted version.
 Smart, R., Carter, B., McGovern, J., Luckman, S., Connelly, A., Hewitt, J., Quasim, T. and Moug, S. (2017) Frailty exists in younger adults admitted as surgical emergency leading to adverse outcomes. Journal
Smart, R., Carter, B., McGovern, J., Luckman, S., Connelly, A., Hewitt, J., Quasim, T. and Moug, S. (2017) Frailty exists in younger adults admitted as surgical emergency leading to adverse outcomes. Journal
People at the centre of health and care
 People at the centre of health and care Improving Care for Older People in Acute Care F is for Frailty F is for Frailty Identification and co-ordination of care for frail older people Starting point -
People at the centre of health and care Improving Care for Older People in Acute Care F is for Frailty F is for Frailty Identification and co-ordination of care for frail older people Starting point -
Restoring function in community dwelling older adults: Balancing risk, frailty and medical complexity
 Restoring function in community dwelling older adults: Balancing risk, frailty and medical complexity Dr. Jo-Anne Clarke Geriatrician, North East Specialized Geriatric Services Disclosure Faculty: Jo-
Restoring function in community dwelling older adults: Balancing risk, frailty and medical complexity Dr. Jo-Anne Clarke Geriatrician, North East Specialized Geriatric Services Disclosure Faculty: Jo-
2003, Editrice Kurtis
 Aging Clinical and Experimental Research (Aging 15: 142-147, 2003), Prediction of falls among older people in residential care facilities by the Downton index Erik Rosendahl, Lillemor Lundin-Olsson, Kristina
Aging Clinical and Experimental Research (Aging 15: 142-147, 2003), Prediction of falls among older people in residential care facilities by the Downton index Erik Rosendahl, Lillemor Lundin-Olsson, Kristina
The number of elderly patients and their associated
 The Impact of Social Vulnerability and Level of Psychiatric Dysfunction PETER DE JONGE, PH.D., FRITS J. HUYSE, M.D., PH.D. G. MAARTEN-FRISO RUINEMANS, M.SC., FRIEDERICH C. STIEFEL, M.D. JOHN S. LYONS,
The Impact of Social Vulnerability and Level of Psychiatric Dysfunction PETER DE JONGE, PH.D., FRITS J. HUYSE, M.D., PH.D. G. MAARTEN-FRISO RUINEMANS, M.SC., FRIEDERICH C. STIEFEL, M.D. JOHN S. LYONS,
RESEARCH. Inpatient rehabilitation specifically designed for geriatric patients: systematic review and meta-analysis of randomised controlled trials
 1 Department of Geriatrics, Inselspital, of Bern Hospital, Freiburgstrasse 10, CH-3010 Bern, Switzerland 2 Rehabilitation Centre Klinik Valens, CH-7317 Valens, Switzerland 3 Institute of Social and Preventive
1 Department of Geriatrics, Inselspital, of Bern Hospital, Freiburgstrasse 10, CH-3010 Bern, Switzerland 2 Rehabilitation Centre Klinik Valens, CH-7317 Valens, Switzerland 3 Institute of Social and Preventive
Care That Works: Geriatric Resources for Assessment and Care of Elders (GRACE)
 Care That Works: Geriatric Resources for Assessment and Care of Elders (GRACE) April 2018 Care That Works: Geriatric Resources for Assessment and Care of Elders (GRACE) This is the second in an occasional
Care That Works: Geriatric Resources for Assessment and Care of Elders (GRACE) April 2018 Care That Works: Geriatric Resources for Assessment and Care of Elders (GRACE) This is the second in an occasional
Virtual Mentor American Medical Association Journal of Ethics May 2014, Volume 16, Number 5:
 Virtual Mentor American Medical Association Journal of Ethics May 2014, Volume 16, Number 5: 385-389. HISTORY OF MEDICINE Geriatric Medicine: History of a Young Specialty Mary Ann Forciea, MD The fascination
Virtual Mentor American Medical Association Journal of Ethics May 2014, Volume 16, Number 5: 385-389. HISTORY OF MEDICINE Geriatric Medicine: History of a Young Specialty Mary Ann Forciea, MD The fascination
Prognostic Factors for Return to Work, Sickness Benefits, and Transitions Between These States: A 4-year Follow-up After Work-Related Rehabilitation
 J Occup Rehabil (2014) 24:199 212 DOI 10.1007/s10926-013-9466-5 Prognostic Factors for Return to Work, Sickness Benefits, and Transitions Between These States: A 4-year Follow-up After Work-Related Rehabilitation
J Occup Rehabil (2014) 24:199 212 DOI 10.1007/s10926-013-9466-5 Prognostic Factors for Return to Work, Sickness Benefits, and Transitions Between These States: A 4-year Follow-up After Work-Related Rehabilitation
20 Years of Community Geriatric Assessment Service
 20 Years of Community Geriatric Assessment Service Dr CP Wong JP MBBS FRCP FRCPE FRCPG FHKAM FHKCP Specialist in Geriatric Medicine Private Practice Outline Geriatric Assessment Breaking the Walls 20 Years
20 Years of Community Geriatric Assessment Service Dr CP Wong JP MBBS FRCP FRCPE FRCPG FHKAM FHKCP Specialist in Geriatric Medicine Private Practice Outline Geriatric Assessment Breaking the Walls 20 Years
Natural Language Question Activity
 Teacher s Manual Natural Language Question Activity Write Your Own Medical Adventure provided by: 2012 Reynolds Grantee 10 th Annual Meeting TEXAS Training Excellence in Aging Studies Division of Geriatric
Teacher s Manual Natural Language Question Activity Write Your Own Medical Adventure provided by: 2012 Reynolds Grantee 10 th Annual Meeting TEXAS Training Excellence in Aging Studies Division of Geriatric
STROKE REHABILITATION: PREDICTING INPATIENT LENGTH OF STAY AND DISCHARGE PLACEMENT
 STROKE HKJOT REHABILITATION 2004;14:3 11 STROKE REHABILITATION: PREDICTING INPATIENT LENGTH OF STAY AND DISCHARGE PLACEMENT Fung Mei Ling Background: Stroke is the third leading cause of death in Hong
STROKE HKJOT REHABILITATION 2004;14:3 11 STROKE REHABILITATION: PREDICTING INPATIENT LENGTH OF STAY AND DISCHARGE PLACEMENT Fung Mei Ling Background: Stroke is the third leading cause of death in Hong
Integrating Geriatrics Innovations into Health Care
 Integrating Geriatrics Innovations into Health Care Mark A. Supiano, M.D. Professor and Chief, Division of Geriatric Medicine Director, Salt Lake City Geriatric Research Education and Clinical Center Executive
Integrating Geriatrics Innovations into Health Care Mark A. Supiano, M.D. Professor and Chief, Division of Geriatric Medicine Director, Salt Lake City Geriatric Research Education and Clinical Center Executive
The Geriatrician in the Trauma Service. Trauma Quality Improvement Program (TQIP) Annual Scientific Meeting and Training 2013
 The Geriatrician in the Trauma Service Trauma Quality Improvement Program (TQIP) Annual Scientific Meeting and Training 2013 Challenges of the Geriatric Trauma Patient Challenges of the Geriatric Patient
The Geriatrician in the Trauma Service Trauma Quality Improvement Program (TQIP) Annual Scientific Meeting and Training 2013 Challenges of the Geriatric Trauma Patient Challenges of the Geriatric Patient
Delirium. A Geriatric Syndrome. Jonathan McCaleb, MD, CMD, HMDC UNSOM, Assistant Professor of Medicine Geriatrics / Hospice & Palliative Medicine
 Delirium A Geriatric Syndrome Jonathan McCaleb, MD, CMD, HMDC UNSOM, Assistant Professor of Medicine Geriatrics / Hospice & Palliative Medicine Introduction Common Serious Unrecognized: a medical emergency
Delirium A Geriatric Syndrome Jonathan McCaleb, MD, CMD, HMDC UNSOM, Assistant Professor of Medicine Geriatrics / Hospice & Palliative Medicine Introduction Common Serious Unrecognized: a medical emergency
