Original Article Local vs. general anesthesia for decompression for thoracic spinal stenosis
|
|
|
- Spencer Webster
- 5 years ago
- Views:
Transcription
1 Int J Clin Exp Med 2018;11(7): /ISSN: /IJCEM Original Article Local vs. general anesthesia for decompression for thoracic spinal stenosis Ye Zhao 1, Juan Xu 2 Departments of 1 Orthopedics, 2 Ultrasound, Cangzhou Central Hospital, Cangzhou, Hebei, China Received July 30, 2017; Accepted April 9, 2018; Epub July 15, 2018; Published July 30, 2018 Abstract: This research was aimed to assess the safety and efficacy of local and general anesthesia for decompression for thoracic spinal stenosis (TSS). From June 2005 to December 2015, 130 cases receiving decompression for TSS were chosen for a retrospective study. The efficacy and safety of the decompression operation under two anesthetic techniques were assessed by neurological function (JOA score), postoperative efficacy (Mann s standard) and incidence of complications. The incidence of complications (spinal cord injury), operation time, intraoperative blood loss, number of days in hospital and hospitalization costs were significantly lower in the local anesthesia group; the average JOA score at 2 weeks after operation was 7.92±1.09 in the local anesthesia group. The paired t-test showed that all indicators were significantly better in the local anesthesia group as compared with the general anesthesia group (P<0.05); For the local anesthesia group, there were 22 cases (33.8%) achieving excellent treatment effects, 32 cases (49.2%) good effects, 10 cases (15.4%) moderate effects, and 1 case (15.4%) poor effects. The excellent and good rate was much higher in the local anesthesia group than in the general anesthesia group (P<0.05); Multivariate conditional logistic regression indicated that general anesthesia was the independent risk factor of the operation effect (OR=1.611, P=0.015). Decompression for TSS under local anesthesia has a higher safety, lower incidence of complications and lower cost. Local anesthesia can greatly reduce neurological deterioration after surgery. This approach is ideal and noteworthy for elderly patients with poor tolerance of general anesthesia. Keywords: Decompression for thoracic spinal stenosis, local anesthesia, efficacy and safety, cohort study Introduction Thoracic spinal stenosis (TSS) is the condition of thoracic spinal canal narrowing due to congenital factors, degeneration, endocrine and systemic disorders. This is usually accompanied by spinal cord decompression and (or) poor blood supply to the spinal cord as a result of thoracic spinal degeneration [1-3]. As to the causes of TSS in China, over 80% of the TSS cases are related to ossification of ligamentum flavum (OLF); about 15% of the cases are related to thoracic disc herniation (TDH), and less than 5% of the cases are related to ossification of the posterior longitudinal ligament (OPLL) and other reasons [4-6]. Thoracic spinal cord compression is the presenting symptom. The patients may suffer from pain in the chest and back, unsteady walking, loss of skin sensation, thermohypesthesia, loss of muscle tone, muscular tension, positive pyramidal signs, weakening or loss of tendon reflex, or even paraplegia and incontinence at advanced stage of the disease [7, 8]. Surgery is the only radical cure for TSS so far. TSS, if not timely and properly treated, will cause irreversible damage to the spine and impair patients physical and psychological health. Most decompression for TSS is performed under general anesthesia [9], but this anesthesia approach is associated with the risk of neurological deterioration and postoperative cognitive dysfunction (POCD) [10]. Based on different anesthesia approach that was used, TSS cases matched for baseline information were equally divided into local anesthesia group and general anesthesia group, for a retrospective cohort study. The efficacy and safety of local anesthesia for decompression for TSS were assessed based on postoperative neurological recovery.
2 operations were undertaken by one surgeon. All cases had complete clinical data, physical examination data, baseline information and follow-up data. The study was approved by the Ethics Committee of Cangzhou Central Hospital and all patients were informed consent. 65 cases were included in the local anesthesia group. Equal number of cases who were matched for gender, age (±1 year), preoperative JOA score (±0.5) and etiology received general anesthesia. The retrospective cohort study was performed between these two groups. The research flow chart was seen in the Figure 1. Surgical method For the local anesthesia group, local infiltration anesthesia was performed using 0.5% lidocaine, and for the general anesthesia group, endotracheal intubation was performed first. For cases with simple OLF, en-bloc removal of the spinal canal via the posterior approach termed as thinned cap uncovering was carried out; for cases with simple OPLL and TDH, anterior decompression was performed; for cases of Figure 1. Consort chart showing flow of participants through the trial. OLF combined with OPLL or TDH, the decompression via the combined anterior-poste- Materials and methods rior approach and circumferential decompression were performed, respectively. General data From June 2005 to December 2015, a total of 130 TSS patients receiving decompression at our hospital were included. All of them were confirmed by clinical presentations and imaging findings (CT, MRI) and also by surgery, according to the diagnostic criteria. The conditions of thoracic spine fracture, tumors, cysts and spinal nerve root injury were excluded. All Both two groups were put under perioperative monitoring, and the drainage tube was kept unobstructed. The patients were inquired of sensation and mobility of the lower limbs every hour, and the neurological functions of the patients were closely observed. Wide-spectrum antibiotics were given to prevent infections, and microcirculation was improved by neurotrophin treatment. The patients took active flex Int J Clin Exp Med 2018;11(7):
3 Table 1. Comparison of baseline information between the two groups Factors Gender (n, %) LA group (n=65) GA group (n=65) Male 34 (54.0%) 34 (54.0%) - 1 Female 29 (46.0%) 29 (46.0%) Pathogenesis (n, %) Ossification of the yellow ligament 40 (64.62%) 40 (64.62%) - 1 Ossification of posterior longitudinal ligament 4 (6.15%) 4 (6.15%) Thoracic disc herniation 2 (3.07%) 2 (3.07%) Ossification of the posterior longitudinal ligament and ossification of the yellow ligament 10 (15.38%) 10 (15.38%) Ossification of the thoracic intervertebral disc with ossification of the yellow ligament 7 (10.77%) 7 (10.77%) Age (year) 59.1± ± Preoperative JOA score (score) 4.67± ± Course of disease (month) 26.3± ± Note: Comparison of observation indicators between the two groups using paired t-test and paired chi-square test. X 2 /t P Figure 2. The MRI of typical cases in the research. A: Ossification of the yellow ligament, B: Ossification of posterior longitudinal ligament, C: Protrusion of thoracic intervertebral disc, D: Ossification of the posterior longitudinal ligament and ossification of the yellow ligament, E: Ossification of the thoracic intervertebral disc with ossification of the yellow ligament. The arrow points to the position of the lesion. ion and extension exercises of the ankles and straight leg raising at early stage postoperatively to facilitate the recovery of muscular strength in the four limbs and to prevent adhesion. The patients were allowed movements out of bed at 2-3 weeks postoperatively, for functional exercises. Observation indicators (1) Demographic information; (2) Evaluation indicators: operation time, intraoperative blood loss, expenses and number of days in hospital; (3) course of disease, radiological classification, and preoperative assessment of neurological functions; (4) postoperative assessment of treatment effects, neurological functions and complications. Treatment effects were assessed based on clinical manifestations and symptoms in the last follow-up using Mann s standard [11]. Excellent efficacy was defined as full or near full recovery of sensation and mobility; good efficacy was defined as significant improvement in sensation and mobility with self-care ability; moderate efficacy was defined as alleviation of clinical symptoms, but without self-care ability; poor efficacy was defined as neither improvement nor deterioration of the symptoms Int J Clin Exp Med 2018;11(7):
4 Table 2. Comparison of operation indicators between the two groups Group Operation time (min) Blood loss of the operation (ml) Hospitalization time (day) Hospitalization expenses (ten thousands RMB) LA ± ± ± ±0.67 GA ± ± ± ±0.82 T P <0.001 * <0.001 * * <0.001 * Note: * P<0.05, compared with the general anesthesia group using the paired t-test. Comparison of operation indicators between the two groups The operation time, intraoperative blood loss, number of days in hospital and medical expenses were significantly lower in the local anesthesia group, as compared with the general anesthesia group (P<0.05). See Table 2. The Japanese Orthopedic Association (JOA) scoring system of 11 points was used to assess the neurological status [12], which included a preoperative assessment of mobility and sensation of the lower limbs, sensation of the trunk and bladder function, as well as a postoperative assessment of neurological functions at 2 weeks postoperatively and in the last follow-up. All cases were followed up for at least 6 months after surgery, with an average of 29.6 months (6-35 months). The improvement rate of neurological functions was calculated as follows: (postoperative JOA score-preoperative JOA score)/(11-preoperative JOA score) 100%. The improvement rate 75% was considered excellent, 50%-74% good, 25%-49% moderate, and <25% poor. Statistical analysis Statistical analyses were performed using SPSS 20.0 software. Measurements were reported as mean ± standard deviation ( _ X ±s). Intergroup comparisons were conducted using paired t-test and analysis of variance. Counts were reported as number of cases (percentages, N (%)), and intergroup comparisons were conducted using paired chi-square test. Multivariate conditional logistic regression was carried out with significance level α set to Results Baseline information compared between the two groups The two groups of patients were comparable in gender, age, preoperative JOA score and course of disease (P>0.05). See Table 1. Typical cases detected by MRI were seen in Figure 2. Comparison of JOA score between the two groups Neurological functions and treatment effects were assessed by postoperative JOA score. The two groups showed significant difference in JOA score before operation, 2 weeks after operation and in the last follow-up (P<0.001). LSD test indicated that the JOA score at 2 weeks after operation and that in the last follow-up were all considerably higher as compared with the score before operation (P<0.001). This means that decompression for TSS is feasible whether under general anesthesia or local anesthesia; all cases achieved a remarkable improvement after the surgery. The average JOA score in the local anesthesia group at 2 weeks after operation was 7.92±1.09 and that in the last follow-up was 8.23±1.33; the recovery rate reached 56.24% in the last follow-up. The paired t-test showed that the observation indicators in the local anesthesia group were all higher than those in the general anesthesia group (P<0.001). It is apparent that the patients achieved better recovery of neurological function under local anesthesia (Table 3). Treatment effects and complications compared between the two groups The treatment effect was assessed based on clinical manifestations using Mann s standard. There were 22 cases (33.8%) achieved excellent effect, 32 cases (49.2%) achieved good effect, 10 cases (15.4%) achieved moderate effect and 1 case (15.4%) achieved poor effect in the local anesthesia group; the difference was of statistical significance (Table 4). There were 12 cases suffering from postoperative complications in the local anesthesia 7211 Int J Clin Exp Med 2018;11(7):
5 Table 3. Comparison of JOA score between the two groups Group Preoperative Two weeks after the operation Final follow-up (more than 6 months) The last follow-up recovery rate (%) LA 4.67± ±1.09 * 8.23±1.33 * 56.24± <0.001 GA 4.82± ±1.38 * 7.25±1.59 * 39.32± <0.001 T P <0.001 <0.001 < Note: JOA score within the same group at different time points was compared by variance analysis; LSD test was used for pairwise comparisons; * indicates comparison of JOA score within the same group at 2 weeks after operation and in the last follow-up; * P<0.05, between different groups at the same time point using paired t-test. Recovery rate: postoperative JOA score-preoperative JOA score)/(11-preoperative JOA score) 100%. F P Table 4. Comparison of postoperative treatment effects between the two groups Curative effect LA (n=65) GA (n=65) X 2 /t P Excellent 22 (33.8%) 14 (21.5%) * Good 32 (49.2%) 26 (40.0%) Moderate 10 (15.4%) 21 (32.3%) Poor 1 (1.5%) 4 (6.2%) Note: * P<0.05, compared with the general anesthesia group using the chi-square test. Treatment effects were assessed based on clinical manifestations and symptoms in the last follow-up using Mann s standard: Excellent efficacy was defined as full or near full recovery of sensation and mobility; good efficacy was defined as significant improvement in sensation and mobility with self-care ability; moderate efficacy was defined as alleviation of clinical symptoms, but without self-care ability; poor efficacy was defined as neither improvement nor deterioration of the symptoms. group; the incidence was 18.5% vs. 35.4% in the general anesthesia group (23 cases), indicating significant difference (P<0.05). Only 1 case in the local anesthesia group had deteriorating spinal cord injury after operation, as opposed to 7 cases who showed similar conditions in the general anesthesia group (P<0.05). Under local anesthesia, decompression of TSS can greatly reduce the spinal cord injury and achieve a better safety (Table 5). Multivariate conditional logistic regression for the influence factors of treatment effects To exclude the confounding factors, the baseline information and anesthesia approach were taken as independent variables; the treatment effect was taken as the dependent variable. Five potential influence factors (anesthesia method, age, course of disease, preoperative JOA score and other concurrent spinal cord diseases) were identified by regression analysis, as shown in Table 6. Among them, anesthesia method was the independent risk factor (OR= 1.611, P=0.015). The proportion of adverse effects after general anesthesia was times as much as that under local anesthesia. This means the decompression of TSS is safer and more effective under local anesthesia. Discussion Conservative treatment for TSS can only achieve a moderate effect because of poor supply to the thoracic spinal canal with stenosis. Thus surgical decompression offers the only hope for TSS patients [13, 14]. Much modified decompression has emerged recently to directly address the pathological factors causing spinal cord compression. We compared the treatment effect and efficacy of local anesthesia and general anesthesia for decompression of TSS and found that the JOA score at 2 weeks after surgery and that in the last follow-up were both higher than the preoperative JOA score for either the general anesthesia group and local anesthesia group (P<0.001); the improvement rate of the treatment effect reached 82.0% and 61.5% for the two groups, respectively. This result indicates that decompression is very effective for TSS. TSS is most common in the elderly people (the average age was 59.1±9.7 in the local anesthesia group), who are usually combined with organ dysfunction. Moreover, the surgery is very challenging because of the small buffer space in the thoracic spinal canal and spinal cord. Different surgical approaches are preferred for different causes of TSS, but no standard has been established yet. For this reason, surgical treatment for TSS may have a high incidence of complications including paraplegia, and the 7212 Int J Clin Exp Med 2018;11(7):
6 Table 5. Comparison of postoperative complications between the two groups Complications LA (n=65) GA (n=65) X 2 P Total of complications 12 (18.5%) 23 (35.4%) * Damage aggravated of spinal function 1 (1.5%) 7 (10.8%) * Pulmonary infection 4 (6.2%) 3 (4.6%) Leakage of cerebrospinal fluid 5 (7.7%) 7 (10.8%) Nerve root injury 2 (3.1%) 4 (6.2%) Incision fat liquefaction 0 (0.0%) 2 (3.1%) Note: * P<0.05, compared with the general anesthesia group using paired chi-square test. Table 6. Multivariate logistic regression analysis of postoperative curative effect in patients with thoracic spinal stenosis B S.E Wald X 2 P Exp (B) EXP (B) 95% C.I. Lower Limit Upper Limit Age (>65 years) < Course of disease (>25 months) < Preoperative JOA score (<5 score) < Combined with other spinal disorders Anesthesia (general anesthesia) prognosis is unpredictable [15, 16]. The choice of an appropriate anesthesia technique is very crucial for ensuring the treatment effect and safety of the decompression. General anesthesia has a higher risk for the elderly patients who are combined with organ degeneration, a decline in physical function and lower tolerance to anesthesia and surgery [17, 18]; besides, the incidence of POCD is also higher after general anesthesia for the elderly patients [19]. Spinal cord injury is another severe postoperative complication after decompression under general anesthesia [20, 21]. Constant efforts are being made to reduce the spinal cord injury caused by surgeries. It is reported that posterior float decompression inner fixation method under local anesthesia can achieve a better effect, with a less risk of spinal cord injury and higher safety as compared with the surgery under general anesthesia (P<0.05) [22]. To confirm this, we assessed the decompression of TSS under local anesthesia. A retrospective cohort study was performed with equal number of cases randomly assigned to local anesthesia group and general anesthesia group. Univariate regression showed that the average JOA score in the last follow-up was 8.23±1.33 and the recovery rate in the last follow-up was 56.24% for the local anesthesia group; the excellent and good rate was 82.0%. All these indicators were significantly improved as compared with the general anesthesia group. Logistic regression also indicated that general anesthesia was the risk independent factor of the treatment effect (OR=1.611, P=0.015). The incidence of complications, operation time, intraoperative blood loss, number of days in hospital, and hospital expenses were all considerably lower in the local anesthesia group as compared with the general anesthesia group (P<0.05). Only 1 case in the local anesthesia group had spinal cord injury after the operation, while 7 cases suffered similar conditions in the general anesthesia group; the difference in the incidence of complications was of statistical significance (P<0.05). We believe that decompression of TSS is safer and more effective under local anesthesia, with fewer postoperative complications and lower cost. Patients are more responsive to potential spinal cord injury under local anesthesia so that the surgeon can timely shift to safer procedures [23, 24]. This benefit is helpful for reducing postoperative neurological deterioration, especially for elderly patients who are intolerant to general anesthesia. Before decompression of TSS under local anesthesia, an effective communication with the 7213 Int J Clin Exp Med 2018;11(7):
7 patients, pulmonary functional training, defecation training, and exercises in prone position are all measures to improve intraoperative cooperation and reduce fear, anxiety, muscular tension and fluctuation in blood pressure. If the patients are very sensitive to pain, a small dose of flurbiprofen with ketamine can be given at 30 min before surgery to enhance local anesthetic and analgesic effects. In addition to general anesthesia, age, course of disease, preoperative JOA score and other concurrent spinal cord diseases were also found to be the influence factors of the treatment effect. These factors also deserve attention in the decompression of TSS. Acknowledgements This work was supported by the Hebei Science and Technology Science and Technology Support Program ( ZD). Disclosure of conflict of interest None. Address correspondence to: Dr. Ye Zhao, Department of Orthopedics, Cangzhou Central Hospital, 16 Xinhua Road, Cangzhou , Hebei, China. Tel: ; Fax: ; zhaoyeczcp@163.com References [1] Barnett GH, Hardy RW Jr, Little JR, Bay JW, Sypert GW. Thoracic spinal canal stenosis. J Neurosurg 1987; 66: [2] Hou X, Sun C, Liu X, Liu Z, Qi Q, Guo Z, Li W, Zeng Y, Chen Z. Clinical features of thoracic spinal stenosis-associated myelopathy: a retrospective analysis of 427 cases. Clin Spine Surg 2016; 29: [3] Vleggeert-Lankamp C, Peul W. Surgical decompression of thoracic spinal stenosis in achondroplasia: indication and outcome. J Neurosurg Spine 2012; 17: [4] Jayakumar PN, Devi BI, Bhat DI, Das BS. Thoracic cord compression due to ossified hypertrophied ligamentum flavum. Neurol India 2002; 50: [5] Benvenutti-Regato M, De la Garza-Ramos R, Caro-Osorio E. Thoracic epidural spinal angiolipoma with coexisting lumbar spinal stenosis: Case report and review of the literature. Int J Spine Surg 2015; 9: [6] Shimokawa T, Miyamoto K, Hioki A, Masuda T, Akiyama H, Shimizu K. Trachea-thoracic vertebral body fistula causing spinal cord injury: a case report. Spine 1976; 39: E [7] Park BC, Min WK, Oh CW, Jeon IH, Kim SY, Kyung HS, Oh SH. Surgical outcome of thoracic myelopathy secondary to ossification of ligamentum flavum. Joint Bone Spine 2007; 74: [8] Liu X, Sun B, Xu Q, Che X, Hu J, Gu S, Shou J. Outcomes in treatment for primary spinal anaplastic ependymomas: a retrospective series of 20 patients. J Neurosurg Spine 2013; 19: [9] Somri M, Gaitini LA, Vaida SJ, Malatzkey S, Sabo E, Yudashkin M, Tome R. The effectiveness and safety of spinal anaesthesia in the pyloromyotomy procedure. Paediatr Anaesth 2003; 13: [10] Liu FJ, Chai Y, Shen Y, Xu JX, Du W, Zhang P. Posterior decompression with transforaminal interbody fusion for thoracic myelopathy due to ossification of the posterior longitudinal ligament and the ligamentum flavum at the same level. J Clin Neurosci 2013; 20: [11] Mann KS, Khosla VK, Gulati DR. Cervical spondylotic myelopathy treated by single-stage multilevel anterior decompression. A prospective study. J Neurosurg 1984; 60: [12] Kato S, Oshima Y, Oka H, Chikuda H, Takeshita Y, Miyoshi K, Kawamura N, Masuda K, Kunogi J, Okazaki R, Azuma S, Hara N, Tanaka S, Takeshita K. Comparison of the Japanese Orthopaedic Association (JOA) score and modified JOA (mjoa) score for the assessment of cervical myelopathy: a multicenter observational study. PLoS One 2015; 10: e [13] Matsuyama Y, Yoshihara H, Tsuji T, Sakai Y, Yukawa Y, Nakamura H, Ito K, Ishiguro N. Surgical outcome of ossification of the posterior longitudinal ligament (OPLL) of the thoracic spine: implication of the type of ossification and surgical options. J Spinal Disord Tech 2005; 18: [14] Yamazaki M, Okawa A, Fujiyoshi T, Furuya T, Koda M. Posterior decompression with instrumented fusion for thoracic myelopathy caused by ossification of the posterior longitudinal ligament. Eur Spine J 2010; 19: [15] He B, Yan L, Xu Z, Guo H, Liu T, Hao D. Treatment strategies for the surgical complications of thoracic spinal stenosis: a retrospective analysis of two hundred and eighty three cases. Int Orthop 2014; 38: [16] Sun J, Zhang C, Ning G, Li Y, Wang P, Feng S. Surgical strategies for ossified ligamentum flavum associated with dural ossification in thoracic spinal stenosis. J Clin Neurosci 2014; 21: [17] Ballard C, Jones E, Gauge N, Aarsland D, Nilsen OB, Saxby BK, Lowery D, Corbett A, Wesnes K, 7214 Int J Clin Exp Med 2018;11(7):
8 Katsaiti E, Arden J, Amoako D, Prophet N, Purushothaman B, Green D. Optimised anaesthesia to reduce post operative cognitive decline (POCD) in older patients undergoing elective surgery, a randomised controlled trial. PLoS One 2012; 7: e [18] Zywiel MG, Prabhu A, Perruccio AV, Gandhi R. The influence of anesthesia and pain management on cognitive dysfunction after joint arthroplasty: a systematic review. Clin Orthop Relat Res 2014; 472: [19] Rasmussen LS, Johnson T, Kuipers HM, Kristensen D, Siersma VD, Vila P, Jolles J, Papaioannou A, Abildstrom H, Silverstein JH, Bonal JA, Raeder J, Nielsen IK, Korttila K, Munoz L, Dodds C, Hanning CD, Moller JT. Does anaesthesia cause postoperative cognitive dysfunction? A randomised study of regional versus general anaesthesia in 438 elderly patients. Acta Anaesth Scand 2003; 47: [20] Palumbo MA, Hilibrand AS, Hart RA, Bohlman HH. Surgical treatment of thoracic spinal stenosis: a 2- to 9-year follow-up. Spine 1976; 26: [21] Chan AK, Winkler EA, Jacques L. Rate of perioperative neurological complications after surgery for cervical spinal cord stimulation. J Neurosurg Spine 2016; 25: [22] Beems T, van Dongen RT. Use of a tubular retractor system as a minimally invasive technique for epidural plate electrode placement under local anesthesia for spinal cord stimulation: technical note. Neurosurgery 2006; 58: ONS-E177. [23] Lee SE, Choi RM, Kee R, Lee KH, Jeon S, Jung JW, Kim WJ, Yoon JS. Epidural anesthesia for permanent spinal cord stimulation with a cylindrical type lead: a case series. Korean J Anesthesiol 2015; 68: [24] McLain RF, Kalfas I, Bell GR, Tetzlaff JE, Yoon HJ, Rana M. Comparison of spinal and general anesthesia in lumbar laminectomy surgery: a case-controlled analysis of 400 patients. J Neurosurg Spine 2005; 2: Int J Clin Exp Med 2018;11(7):
Junming Cao, Yongsheng Lin, Xiangbei Qi, Zhihong Wang, Yipeng Yang, Hehuan Xia, Bin Xu
 Int J Clin Exp Med 2018;11(2):741-746 www.ijcem.com /ISSN:1940-5901/IJCEM0067327 Original Article Effect of intramedullary signal intensity on T2-weighted magnetic resonance images on prognosis in patients
Int J Clin Exp Med 2018;11(2):741-746 www.ijcem.com /ISSN:1940-5901/IJCEM0067327 Original Article Effect of intramedullary signal intensity on T2-weighted magnetic resonance images on prognosis in patients
Comparative study on the effect of anterior and posterior decompression in the treatment of multi-segmental cervical spondylotic myelopathy
 92 Journal of Hainan Medical University 2016; 22(6): 92-96 Journal of Hainan Medical University http://www.jhmuweb.net/ Comparative study on the effect of anterior and posterior decompression in the treatment
92 Journal of Hainan Medical University 2016; 22(6): 92-96 Journal of Hainan Medical University http://www.jhmuweb.net/ Comparative study on the effect of anterior and posterior decompression in the treatment
Neurological manifestations of thoracic myelopathy in 203 patients
 Neurological manifestations of thoracic myelopathy in 203 patients Shota Takenaka* a, MD; Takashi Kaito b, MD; Noboru Hosono a, MD; Toshitada Miwa c, MD; Takenori Oda d, MD; Shinya Okuda d, MD; Tomoya
Neurological manifestations of thoracic myelopathy in 203 patients Shota Takenaka* a, MD; Takashi Kaito b, MD; Noboru Hosono a, MD; Toshitada Miwa c, MD; Takenori Oda d, MD; Shinya Okuda d, MD; Tomoya
S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA
 AN INSIGHT TO THE DILEMMA- CO-EXISTENCE OF OSSIFICAION OF POSTERIOR LONGITUDINAL LIGAMENT AND CERVICAL DISC PROLAPSE A SRI LANKAN EXPERIENCE S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA BACKGROUND
AN INSIGHT TO THE DILEMMA- CO-EXISTENCE OF OSSIFICAION OF POSTERIOR LONGITUDINAL LIGAMENT AND CERVICAL DISC PROLAPSE A SRI LANKAN EXPERIENCE S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA BACKGROUND
Is OPLL-induced canal stenosis a risk factor of cord injury in cervical trauma?
 Acta Orthop. Belg., 2014, 80, 567-574 ORIGINAL STUDY Is OPLL-induced canal stenosis a risk factor of cord injury in cervical trauma? Kyung-Jin Song, Chan-Il Park, Do-Yeon Kim, Young-Ran Jung, Kwang-Bok
Acta Orthop. Belg., 2014, 80, 567-574 ORIGINAL STUDY Is OPLL-induced canal stenosis a risk factor of cord injury in cervical trauma? Kyung-Jin Song, Chan-Il Park, Do-Yeon Kim, Young-Ran Jung, Kwang-Bok
Disclosures: T. Yoshii: None. T. Yamada: None. T. Taniyama: None. S. Sotome: None. T. Kato: None. S. Kawabata: None. A. Okawa: None.
 Dynamic Changes in Spinal Cord Compression by Cervical Ossification of the Posterior Longitudinal Ligament Evaluated by Kinematic Computed Tomography Myelogram Toshitaka Yoshii, Tsuyoshi Yamada, Takashi
Dynamic Changes in Spinal Cord Compression by Cervical Ossification of the Posterior Longitudinal Ligament Evaluated by Kinematic Computed Tomography Myelogram Toshitaka Yoshii, Tsuyoshi Yamada, Takashi
Clinical Results and Complications of Surgical Treatment for Thoracic Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament
 Clinical Results and Complications of Surgical Treatment for Thoracic Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament - A Multicenter Retrospective Study - Mitsumasa Hayashida,
Clinical Results and Complications of Surgical Treatment for Thoracic Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament - A Multicenter Retrospective Study - Mitsumasa Hayashida,
Int J Clin Exp Med 2016;9(5): /ISSN: /IJCEM Ye Zhao 1, Juan Xu 2, Shukui Li 1, Cai Cheng 1, Hongjiang Sun 1
 Int J Clin Exp Med 2016;9(5):8685-8691 www.ijcem.com /ISSN:1940-5901/IJCEM0020477 Original Article Comparative study on clinical efficacy of posterior laminectomy and a modified transfacet joints approach
Int J Clin Exp Med 2016;9(5):8685-8691 www.ijcem.com /ISSN:1940-5901/IJCEM0020477 Original Article Comparative study on clinical efficacy of posterior laminectomy and a modified transfacet joints approach
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE
 CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki 3), Masatsune Yamagata 1), Yoshikazu Ikeda 1), Fumitake Nakajima 1)
 Long-term results of anterior cervical corpectomy and arthrodesis for cervical degenerative diseases with more than ten years of follow-up Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki
Long-term results of anterior cervical corpectomy and arthrodesis for cervical degenerative diseases with more than ten years of follow-up Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki
흉추척수증을유발한황색인대골화증의골절 - 증례보고 -
 대한척추외과학회지제 14 권제 1 호 Journal of Korean Spine Surg. Vol. 14, No. 1, pp 52~56, 2007 흉추척수증을유발한황색인대골화증의골절 - 증례보고 - 하기용 김영훈 # 지원희 $ 가톨릭대학교의과대학강남성모병원정형외과, 성모자애병원정형외과 #, 강남성모병원영상의학과 $ Fracture of Ossification
대한척추외과학회지제 14 권제 1 호 Journal of Korean Spine Surg. Vol. 14, No. 1, pp 52~56, 2007 흉추척수증을유발한황색인대골화증의골절 - 증례보고 - 하기용 김영훈 # 지원희 $ 가톨릭대학교의과대학강남성모병원정형외과, 성모자애병원정형외과 #, 강남성모병원영상의학과 $ Fracture of Ossification
Life expectancy after cervical laminoplasty Causes of the fatal prognosis at the early stage (within 5 years)
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Life expectancy after cervical laminoplasty Causes of the fatal prognosis at the early stage (within 5 years) Yoshiharu Kawaguchi 1), Masato Nakano 1),
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Life expectancy after cervical laminoplasty Causes of the fatal prognosis at the early stage (within 5 years) Yoshiharu Kawaguchi 1), Masato Nakano 1),
Spinal canal stenosis Degenerative diseases F 06
 What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
decompression combined with interbody fusion and internal fixation for thoracic spinal stenosis
 Int J Clin Exp Med 2018;11(2):818-823 www.ijcem.com /ISSN:1940-5901/IJCEM0066999 Original Article Posterolateral decompression combined with interbody fusion and internal fixation for thoracic spinal stenosis
Int J Clin Exp Med 2018;11(2):818-823 www.ijcem.com /ISSN:1940-5901/IJCEM0066999 Original Article Posterolateral decompression combined with interbody fusion and internal fixation for thoracic spinal stenosis
Radiological pathogenesis of cervical myelopathy in 60 consecutive patients with cervical ossi cation of the posterior longitudinal ligament
 Spinal Cord (1999) 37, 853 ± 857 ã 1999 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/99 $15.00 http://www.stockton-press.co.uk/sc Radiological pathogenesis of cervical myelopathy
Spinal Cord (1999) 37, 853 ± 857 ã 1999 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/99 $15.00 http://www.stockton-press.co.uk/sc Radiological pathogenesis of cervical myelopathy
Bilateral Foot Drop Without Cauda Equinae Syndrome Due To L4-L5 Disc Prolapse: A Case Report
 ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 Bilateral Foot Drop Without Cauda Equinae Syndrome Due To L4-L5 Disc Prolapse: A Case Report R Ramnaryan, C Palinikumar Citation R Ramnaryan,
ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 Bilateral Foot Drop Without Cauda Equinae Syndrome Due To L4-L5 Disc Prolapse: A Case Report R Ramnaryan, C Palinikumar Citation R Ramnaryan,
Rick C. Sasso MD Professor Chief of Spine Surgery Clinical Orthopaedic Surgery Indiana University School of Medicine
 Cervical Myelopathy: Anterior Surgery is Best Rick C. Sasso MD Professor Chief of Surgery Clinical Orthopaedic Surgery University School of Medicine Disclosure: Research support-medtronic, Stryker, AO,
Cervical Myelopathy: Anterior Surgery is Best Rick C. Sasso MD Professor Chief of Surgery Clinical Orthopaedic Surgery University School of Medicine Disclosure: Research support-medtronic, Stryker, AO,
Case Report Two-year follow-up results of C2/3 Prestige-LP cervical disc replacement: first report
 Int J Clin Exp Med 2016;9(4):7349-7353 www.ijcem.com /ISSN:1940-5901/IJCEM0018962 Case Report Two-year follow-up results of C2/3 Prestige-LP cervical disc replacement: first report Yi Yang 1, Mengying
Int J Clin Exp Med 2016;9(4):7349-7353 www.ijcem.com /ISSN:1940-5901/IJCEM0018962 Case Report Two-year follow-up results of C2/3 Prestige-LP cervical disc replacement: first report Yi Yang 1, Mengying
Original Investigation. Byung-Wan CHOI. INTRODUCTION Ossification of the posterior longitudinal ligament ABSTRACT
 DOI: 10.5137/1019-5149.JTN.16196-15.1 Received: 25.09.2015 / Accepted: 07.12.2015 Published Online: 01.06.2016 Original Investigation Clinical and Radiological Characteristics of Ossification of the Posterior
DOI: 10.5137/1019-5149.JTN.16196-15.1 Received: 25.09.2015 / Accepted: 07.12.2015 Published Online: 01.06.2016 Original Investigation Clinical and Radiological Characteristics of Ossification of the Posterior
Neurological Surgery, P.C. Brings Progressive Spine Surgery to Long Island. Long Island
 Long Island A BUSINESS & PRACTICE MANAGEMENT MAGAZINE ABOUT PHYSICIANS FROM PHYSICIANS FOR PHYSICIANS Neurological Surgery, P.C. Brings Progressive Spine Surgery to Long Island Neurological Surgery, P.C.
Long Island A BUSINESS & PRACTICE MANAGEMENT MAGAZINE ABOUT PHYSICIANS FROM PHYSICIANS FOR PHYSICIANS Neurological Surgery, P.C. Brings Progressive Spine Surgery to Long Island Neurological Surgery, P.C.
Surgical Treatment for Ossification of the Posterior Longitudinal Ligament (OPLL) at the Thoracic Spine: Usefulness of the Posterior Approach
 REVIEW ARTICLE SPINE SURGERY AND RELATED RESEARCH Surgical Treatment for Ossification of the Posterior Longitudinal Ligament (OPLL) at the Thoracic Spine: Usefulness of the Posterior Approach Shigeru Hirabayashi,
REVIEW ARTICLE SPINE SURGERY AND RELATED RESEARCH Surgical Treatment for Ossification of the Posterior Longitudinal Ligament (OPLL) at the Thoracic Spine: Usefulness of the Posterior Approach Shigeru Hirabayashi,
Segmental stability following minimally invasive decompressive surgery with tubular retractor for lumbar spinal stenosis
 Segmental stability following minimally invasive decompressive surgery with tubular retractor for lumbar spinal stenosis Department of Spinal surgery, Research Institute for Brain and Blood Vessels-Akita
Segmental stability following minimally invasive decompressive surgery with tubular retractor for lumbar spinal stenosis Department of Spinal surgery, Research Institute for Brain and Blood Vessels-Akita
Cervical myelopathy is a common disease that is
 TECHNICAL NOTE J Neurosurg Spine 26:325 330, 2017 A novel technique to correct kyphosis in cervical myelopathy due to continuous-type ossification of the posterior longitudinal ligament Dong-Ho Lee, MD,
TECHNICAL NOTE J Neurosurg Spine 26:325 330, 2017 A novel technique to correct kyphosis in cervical myelopathy due to continuous-type ossification of the posterior longitudinal ligament Dong-Ho Lee, MD,
ASJ. Analysis of the Prevalence and Distribution of Cervical and Thoracic Compressive Lesions of the Spinal Cord in Lumbar Degenerative Disease
 Asian Spine Journal Asian Spine Clinical Journal Study Cervical and thoracic Asian compressive Spine J 2014;8(1):19-26 lesions in http://dx.doi.org/10.4184/asj.2014.8.1.19 lumbar degenerative disease 19
Asian Spine Journal Asian Spine Clinical Journal Study Cervical and thoracic Asian compressive Spine J 2014;8(1):19-26 lesions in http://dx.doi.org/10.4184/asj.2014.8.1.19 lumbar degenerative disease 19
A Structural Service Plan: Towards Better and Safer Spine Surgeries. Department of Orthopaedics & Traumatology Tuen Mun Hospital
 A Structural Service Plan: Towards Better and Safer Spine Surgeries Department of Orthopaedics & Traumatology Tuen Mun Hospital Cheung KK Wong CY Chan Andrew Tse Alfred Chow YY Department of Orthopaedics
A Structural Service Plan: Towards Better and Safer Spine Surgeries Department of Orthopaedics & Traumatology Tuen Mun Hospital Cheung KK Wong CY Chan Andrew Tse Alfred Chow YY Department of Orthopaedics
Int J Clin Exp Med 2018;11(2): /ISSN: /IJCEM Yi Yang, Hao Liu, Yueming Song, Tao Li
 Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Contributing factors affecting the prognosis surgical outcome for thoracic OLF
 Eur Spine J (2006) 15: 485 491 DOI 10.1007/s00586-005-0903-9 ORIGINAL ARTICLE Sung Uk Kuh Young Soo Kim Yong Eun Cho Byung Ho Jin Keun Su Kim Young Sul Yoon Dong Kyu Chin Contributing factors affecting
Eur Spine J (2006) 15: 485 491 DOI 10.1007/s00586-005-0903-9 ORIGINAL ARTICLE Sung Uk Kuh Young Soo Kim Yong Eun Cho Byung Ho Jin Keun Su Kim Young Sul Yoon Dong Kyu Chin Contributing factors affecting
Functional Outcome of Patients with Lumbar Intervertebral Disc Herniation after Minimally Invasive Microdiscectomy
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. II (July. 2017), PP 35-39 www.iosrjournals.org Functional Outcome of Patients with Lumbar
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. II (July. 2017), PP 35-39 www.iosrjournals.org Functional Outcome of Patients with Lumbar
Yoshifumi Kudo, 1 Tomoaki Toyone, 1 Toshiyuki Shirahata, 1 Tomoyuki Ozawa, 1 Akira Matsuoka, 1 Yoichi Jin, 2 and Katsunori Inagaki 1. 1.
 Case Reports in Orthopedics Volume 2016, Article ID 1250810, 5 pages http://dx.doi.org/10.1155/2016/1250810 Case Report A Case of Successful Foraminotomy for Severe Bilateral C5 Palsy following Posterior
Case Reports in Orthopedics Volume 2016, Article ID 1250810, 5 pages http://dx.doi.org/10.1155/2016/1250810 Case Report A Case of Successful Foraminotomy for Severe Bilateral C5 Palsy following Posterior
Retro-odontoid pseudotumors are mass lesions formed
 SURGICAL TECHNIQUE Microscopic Posterior Transdural Resection of Cervical Retro-Odontoid Pseudotumors Yasushi Fujiwara, MD, PhD,* Hideki Manabe,* Tadayoshi Sumida,w Nobuhiro Tanaka,z and Takahiko Hamasakiy
SURGICAL TECHNIQUE Microscopic Posterior Transdural Resection of Cervical Retro-Odontoid Pseudotumors Yasushi Fujiwara, MD, PhD,* Hideki Manabe,* Tadayoshi Sumida,w Nobuhiro Tanaka,z and Takahiko Hamasakiy
PREOPERATIVE RETROLISTHESIS IS A RISK FACTOR OF LUMBAR DISC HERNIATION AFTER FENESTRATION WITHOUT DISCECTOMY
 PREOPERATIVE RETROLISTHESIS IS A RISK FACTOR OF LUMBAR DISC HERNIATION AFTER FENESTRATION WITHOUT DISCECTOMY Shota Takenaka*, Noboru Hosono, Yoshihiro Mukai, Kosuke Tateishi, Takeshi Fuji Osaka Kosei-nenkin
PREOPERATIVE RETROLISTHESIS IS A RISK FACTOR OF LUMBAR DISC HERNIATION AFTER FENESTRATION WITHOUT DISCECTOMY Shota Takenaka*, Noboru Hosono, Yoshihiro Mukai, Kosuke Tateishi, Takeshi Fuji Osaka Kosei-nenkin
QF-78. S. Tanaka 1, T.Yokoyama 1, K.Takeuchi 1, K.Wada 2, T. Tanaka 2, S.Abrakawa 2, G.Kumagai 2, T.Asari 2, A.Ono 2, Y.
 QF-78 Patient-oriented outcomes after musclepreserving interlaminar decompression for patients with lumbar spinal canal stenosis: Multi-center study to identify risk factors for poor outcomes S. Tanaka
QF-78 Patient-oriented outcomes after musclepreserving interlaminar decompression for patients with lumbar spinal canal stenosis: Multi-center study to identify risk factors for poor outcomes S. Tanaka
Original Article Prognosis of Cervical Degenerative Myelopathy after Multilevel Anterior Cervical Discectomies and Fusion
 Egyptian Journal of Neurosurgery Volume 9 / No. / January - March 4 57-6 Original Article Prognosis of Cervical Degenerative Myelopathy after Multilevel Anterior Cervical Discectomies and Fusion Ahmed
Egyptian Journal of Neurosurgery Volume 9 / No. / January - March 4 57-6 Original Article Prognosis of Cervical Degenerative Myelopathy after Multilevel Anterior Cervical Discectomies and Fusion Ahmed
Lumbar spinal canal stenosis Degenerative diseases F 08
 What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
Effect of Swallowing Function After ROI-C Anterior Cervical Interbody Fusion
 Journal of Surgery 2016; 4(6): 141-145 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160406.14 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Effect of Swallowing Function After ROI-C
Journal of Surgery 2016; 4(6): 141-145 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160406.14 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Effect of Swallowing Function After ROI-C
Treatment for thoracic ossification of posterior longitudinal ligament with posterior circumferential decompression: complications and managements
 Yang et al. Journal of Orthopaedic Surgery and Research (2016) 11:153 DOI 10.1186/s13018-016-0489-4 RESEARCH ARTICLE Open Access Treatment for thoracic ossification of posterior longitudinal ligament with
Yang et al. Journal of Orthopaedic Surgery and Research (2016) 11:153 DOI 10.1186/s13018-016-0489-4 RESEARCH ARTICLE Open Access Treatment for thoracic ossification of posterior longitudinal ligament with
The Comparison of the Result of Epiduroscopic Laser Neural Decompression between FBSS or Not
 Original Article Korean J Pain 2014 January; Vol. 27, No. 1: 63-67 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2014.27.1.63 The Comparison of the Result of Epiduroscopic Laser Neural
Original Article Korean J Pain 2014 January; Vol. 27, No. 1: 63-67 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2014.27.1.63 The Comparison of the Result of Epiduroscopic Laser Neural
Risk factors for development of cervical spondylotic myelopathy: results of a systematic review
 Systematic review Risk factors for development of cervical spondylotic myelopathy 35 35 42 Risk factors for development of cervical spondylotic myelopathy: results of a systematic review Authors Anoushka
Systematic review Risk factors for development of cervical spondylotic myelopathy 35 35 42 Risk factors for development of cervical spondylotic myelopathy: results of a systematic review Authors Anoushka
Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia: A Case Series
 C a s e R e p o r t J. of Advanced Spine Surgery Volume 2, Number 2, pp 60~65 Journal of Advanced Spine Surgery JASS Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia:
C a s e R e p o r t J. of Advanced Spine Surgery Volume 2, Number 2, pp 60~65 Journal of Advanced Spine Surgery JASS Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia:
Minamide A*, Yoshida M*, Yamada H*, Hashizume H*, NakagawaY*, Iwasaki H*, Tsutsui S*, Hiroyuki Oka H**.
 Efficacy of Posterior Segmental Decompression Surgery for Pincer Mechanism in Cervical Spondylotic Myelopathy -A retrospective case control study using propensity score matching Minamide A*, Yoshida M*,
Efficacy of Posterior Segmental Decompression Surgery for Pincer Mechanism in Cervical Spondylotic Myelopathy -A retrospective case control study using propensity score matching Minamide A*, Yoshida M*,
3D titanium interbody fusion cages sharx. White Paper
 3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
Transforaminal Endoscopic Decompression for a Giant Epidural Gas-Containing Pseudocyst: A Case Report and Literature Review
 Pain Physician 2017; 20:E445-E449 ISSN 2150-1149 Literature Review Transforaminal Endoscopic Decompression for a Giant Epidural Gas-Containing Pseudocyst: A Case Report and Literature Review Bin Zhu, MD,
Pain Physician 2017; 20:E445-E449 ISSN 2150-1149 Literature Review Transforaminal Endoscopic Decompression for a Giant Epidural Gas-Containing Pseudocyst: A Case Report and Literature Review Bin Zhu, MD,
Incidence of deep vein thrombosis after major spine surgeries with no mechanical or chemical prophylaxis
 29 29 33 Incidence of deep vein thrombosis after major spine surgeries with no mechanical or chemical prophylaxis Author Institution Sreedharan Namboothiri Kovai Medical Center and Hospitals, Coimbatore,
29 29 33 Incidence of deep vein thrombosis after major spine surgeries with no mechanical or chemical prophylaxis Author Institution Sreedharan Namboothiri Kovai Medical Center and Hospitals, Coimbatore,
Factors related to long-term outcome after decompressive surgery for ossification of the ligamentum flavum of the thoracic spine
 J Neurosurg (Spine 3) 99:251 256, 2003 Factors related to long-term outcome after decompressive surgery for ossification of the ligamentum flavum of the thoracic spine NAOHISA MIYAKOSHI, M.D., YOICHI SHIMADA,
J Neurosurg (Spine 3) 99:251 256, 2003 Factors related to long-term outcome after decompressive surgery for ossification of the ligamentum flavum of the thoracic spine NAOHISA MIYAKOSHI, M.D., YOICHI SHIMADA,
Range of motion of thoracic spine in sagittal plane
 DOI 10.1007/s00586-013-3088-7 ORIGINAL ARTICLE Range of motion of thoracic spine in sagittal plane Daigo Morita Yasutsugu Yukawa Hiroaki Nakashima Keigo Ito Go Yoshida Masaaki Machino Syunsuke Kanbara
DOI 10.1007/s00586-013-3088-7 ORIGINAL ARTICLE Range of motion of thoracic spine in sagittal plane Daigo Morita Yasutsugu Yukawa Hiroaki Nakashima Keigo Ito Go Yoshida Masaaki Machino Syunsuke Kanbara
Treatment of Two Level Artificial Disc Replacement for Cervical Spondylotic Myelopathy
 Journal of Minimally Invasive Spine JMISST Surgery and Technique 3(1):34-38, 2018 Case Report eissn 2508-2043 https://doi.org/10.21182/jmisst.2017.00269 www.jmisst.org for Cervical Spondylotic Myelopathy
Journal of Minimally Invasive Spine JMISST Surgery and Technique 3(1):34-38, 2018 Case Report eissn 2508-2043 https://doi.org/10.21182/jmisst.2017.00269 www.jmisst.org for Cervical Spondylotic Myelopathy
Ten Second Step Test" as a New Quantifiable Parameter of Cervical Myelopathy. Spine January 1, 2009; Volume 34; Issue 1; pp 82-86
 Ten Second Step Test" as a New Quantifiable Parameter of Cervical Myelopathy 1 Spine January 1, 2009; Volume 34; Issue 1; pp 82-86 Yukawa, Yasutsugu; Kato, Fumihiko; Ito, Keigo; Horie, Yumiko; Nakashima,
Ten Second Step Test" as a New Quantifiable Parameter of Cervical Myelopathy 1 Spine January 1, 2009; Volume 34; Issue 1; pp 82-86 Yukawa, Yasutsugu; Kato, Fumihiko; Ito, Keigo; Horie, Yumiko; Nakashima,
PARADIGM SPINE. Patient Information. Treatment of a Narrow Lumbar Spinal Canal
 PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012
 Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc disease: Is there a difference at 12 months?
 Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
VERTEBRAL COLUMN ANATOMY IN CNS COURSE
 VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
Anterior approach versus posterior approach for the treatment of multilevel cervical spondylotic myelopathy: a systemic review and meta-analysis
 Eur Spine J (201) 22:158 159 DOI 10.1007/s00586-01-2817-2 ORIGINAL ARTICLE Anterior approach versus posterior approach for the treatment of multilevel cervical spondylotic myelopathy: a systemic review
Eur Spine J (201) 22:158 159 DOI 10.1007/s00586-01-2817-2 ORIGINAL ARTICLE Anterior approach versus posterior approach for the treatment of multilevel cervical spondylotic myelopathy: a systemic review
Original Article Clinics in Orthopedic Surgery 2013;5:
 Original Article Clinics in Orthopedic Surgery 2013;5:129-133 http://dx.doi.org/10.4055/cios.2013.5.2.129 The Efficacy of Carotid Tubercle as an Anatomical Landmark for Identification of Cervical Spinal
Original Article Clinics in Orthopedic Surgery 2013;5:129-133 http://dx.doi.org/10.4055/cios.2013.5.2.129 The Efficacy of Carotid Tubercle as an Anatomical Landmark for Identification of Cervical Spinal
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy
 Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
ORIGINAL PAPER. Department of Orthopedic Surgery, Chubu Rosai Hospital, Nagoya, Japan ABSTRACT
 Nagoya J. Med. Sci. 77. 221 ~ 228, 2015 ORIGINAL PAPER RANGE OF MOTION DETERMINED BY MULTIDETECTOR-ROW COMPUTED TOMOGRAPHY IN PATIENTS WITH CERVICAL OSSIFICATION OF THE POSTERIOR LONGITUDINAL LIGAMENT
Nagoya J. Med. Sci. 77. 221 ~ 228, 2015 ORIGINAL PAPER RANGE OF MOTION DETERMINED BY MULTIDETECTOR-ROW COMPUTED TOMOGRAPHY IN PATIENTS WITH CERVICAL OSSIFICATION OF THE POSTERIOR LONGITUDINAL LIGAMENT
Appendix: Diagnostic Criteria for OPLL and Diagnosis and Treatment Algorithm
 Appendix: Diagstic Criteria for OPLL and Diagsis and Treatment Algorithm Diagstic Criteria for Ossification of the Posterior Longitudinal Ligament of the Cervical Spine (Proposed by the Committee for Development
Appendix: Diagstic Criteria for OPLL and Diagsis and Treatment Algorithm Diagstic Criteria for Ossification of the Posterior Longitudinal Ligament of the Cervical Spine (Proposed by the Committee for Development
Cervical spondylarthrotic myelopathy with early onset in Down's syndrome: five cases and a review of the literature
 283 Journal of Intellectual Disability Research VOLUME 43 PART 4 pp 283±288 AUGUST 1999 Cervical spondylarthrotic myelopathy with early onset in Down's syndrome: five cases and a review of the literature
283 Journal of Intellectual Disability Research VOLUME 43 PART 4 pp 283±288 AUGUST 1999 Cervical spondylarthrotic myelopathy with early onset in Down's syndrome: five cases and a review of the literature
Spinal Stenosis Surgical
 Spinal Stenosis Surgical Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
Spinal Stenosis Surgical Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
Orthopaedics and Rehabilitation Medicine Fuculty of Medical Sciences University of Fukui
 Quantitative analysis and prognostic value of changes in spinal cord signal intensity on magnetic resonance imaging in patients with cervical compressive myelopathy Orthopaedics and Rehabilitation Medicine
Quantitative analysis and prognostic value of changes in spinal cord signal intensity on magnetic resonance imaging in patients with cervical compressive myelopathy Orthopaedics and Rehabilitation Medicine
Dynamic Mri of the Cervical Spine An Important Tool in Planning Surgical Treatment of Cervical Compressive Myelopathy
 International Journal of Neurosurgery 2018; 2(1): 17-22 http://www.sciencepublishinggroup.com/j/ijn doi: 10.11648/j.ijn.20180201.14 Dynamic Mri of the Cervical Spine An Important Tool in Planning Surgical
International Journal of Neurosurgery 2018; 2(1): 17-22 http://www.sciencepublishinggroup.com/j/ijn doi: 10.11648/j.ijn.20180201.14 Dynamic Mri of the Cervical Spine An Important Tool in Planning Surgical
DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL
 SPINAL CHAPTER, NESON DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL INTRODUCTION DEGENERATIVE SPINAL DISEASE Gradual loss of normal structure and function of spine with time Also
SPINAL CHAPTER, NESON DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL INTRODUCTION DEGENERATIVE SPINAL DISEASE Gradual loss of normal structure and function of spine with time Also
Lumbar Disc Prolapse. Dr. Ahmed Salah Eldin Hassan. Professor of Neurosurgery & Consultant spinal surgeon
 Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018
 EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018 Marc J. Levine, MD Rothman Institute Director Spine Surgery Program
EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018 Marc J. Levine, MD Rothman Institute Director Spine Surgery Program
Cervical spondylotic myelopathy (CSM) is a
 WScJ 4: 1-5, 2013 Functional Evaluation Using the Modified Japanese Orthopedic Association Score (mjoa) for Cervical Spondylotic Myelopathy by Age, Gender, and Type of Disease Parisa Azimi 1*, Sohrab Shahzadi
WScJ 4: 1-5, 2013 Functional Evaluation Using the Modified Japanese Orthopedic Association Score (mjoa) for Cervical Spondylotic Myelopathy by Age, Gender, and Type of Disease Parisa Azimi 1*, Sohrab Shahzadi
Case Report Delayed myelopathy secondary to stab wound with a retained blade tip within the laminae: case report
 Int J Clin Exp Med 2015;8(9):16787-16792 www.ijcem.com /ISSN:1940-5901/IJCEM0012160 Case Report Delayed myelopathy secondary to stab wound with a retained blade tip within the laminae: case report Hui
Int J Clin Exp Med 2015;8(9):16787-16792 www.ijcem.com /ISSN:1940-5901/IJCEM0012160 Case Report Delayed myelopathy secondary to stab wound with a retained blade tip within the laminae: case report Hui
Cervical intervertebral disc disease Degenerative diseases F 04
 Cervical intervertebral disc disease Degenerative diseases F 04 How is a herniated cervical intervertebral disc treated? Conservative treatment is generally sufficient for mild symptoms not complicated
Cervical intervertebral disc disease Degenerative diseases F 04 How is a herniated cervical intervertebral disc treated? Conservative treatment is generally sufficient for mild symptoms not complicated
Surgical outcomes for lumbar spinal canal stenosis with coexisting cervical stenosis (tandem spinal stenosis): a retrospective analysis of 565 cases
 Yamada et al. Journal of Orthopaedic Surgery and Research (2018) 13:60 https://doi.org/10.1186/s13018-018-0765-6 RESEARCH ARTICLE Open Access Surgical outcomes for lumbar spinal canal stenosis with coexisting
Yamada et al. Journal of Orthopaedic Surgery and Research (2018) 13:60 https://doi.org/10.1186/s13018-018-0765-6 RESEARCH ARTICLE Open Access Surgical outcomes for lumbar spinal canal stenosis with coexisting
Risk Factors for Hinge Fracture Associated with Surgery Following Cervical Open-Door Laminoplasty
 CLINICAL ARTICLE Korean J Neurotrauma 18;14(2):118-122 pissn 2234-8999 / eissn 2288-2243 https://doi.org/1.134/kjnt.18.14.2.118 Risk Factors for Hinge Fracture Associated with Surgery Following Cervical
CLINICAL ARTICLE Korean J Neurotrauma 18;14(2):118-122 pissn 2234-8999 / eissn 2288-2243 https://doi.org/1.134/kjnt.18.14.2.118 Risk Factors for Hinge Fracture Associated with Surgery Following Cervical
Department of Neurological Surgery, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea
 online ML Comm CLINICAL ARTICLE Korean J Neurotrauma 2014;10(2):60-65 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2014.10.2.60 Midline Splitting Cervical Laminoplasty Using Allogeneic
online ML Comm CLINICAL ARTICLE Korean J Neurotrauma 2014;10(2):60-65 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2014.10.2.60 Midline Splitting Cervical Laminoplasty Using Allogeneic
CMEARTICLE * * * Wen Qi Tan 1, BEng, Bak Siew Steven Wong 2, MBChB, MMed
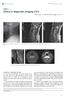 Singapore Med J 2015; 56(7): 373-378 doi: 10.11622/smedj.2015107 CMEARTICLE Clinics in diagnostic imaging (161) Wen Qi Tan 1, BEng, Bak Siew Steven Wong 2, MBChB, MMed 2a 2b Fig. 1 Lateral radiograph of
Singapore Med J 2015; 56(7): 373-378 doi: 10.11622/smedj.2015107 CMEARTICLE Clinics in diagnostic imaging (161) Wen Qi Tan 1, BEng, Bak Siew Steven Wong 2, MBChB, MMed 2a 2b Fig. 1 Lateral radiograph of
Degenerative Disease of the Spine
 Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
Abstract Study Design Systematic review. Weerasak Singhatanadgige 1 Worawat Limthongkul 1 Frank Valone III 2 Wicharn Yingsakmongkol 1 K.
 702 Review Article GLOBAL SPINE JOURNAL THIEME Outcomes following or Fusion in Patients with Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament: A Systematic Review Weerasak Singhatanadgige
702 Review Article GLOBAL SPINE JOURNAL THIEME Outcomes following or Fusion in Patients with Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament: A Systematic Review Weerasak Singhatanadgige
4/28/2015 DR. TRACY W. PRICE, D.C. PPI due to injury or illness AMA GUIDES TO THE EVALUATION OF PERMANENT IMPAIRMENT 5 TH EDITION
 DR. TRACY W. PRICE, D.C CHAPEL HILL CHIROPRACTIC CENTER, INC. 1520 HOME AVE. AKRON, OH 44310 PH.330.630.1500: FAX.330.630.9303 EMAIL: DOCKTRACY@AOL.COM WEB: AKRONCHHIRO.COM AMA GUIDES TO THE EVALUATION
DR. TRACY W. PRICE, D.C CHAPEL HILL CHIROPRACTIC CENTER, INC. 1520 HOME AVE. AKRON, OH 44310 PH.330.630.1500: FAX.330.630.9303 EMAIL: DOCKTRACY@AOL.COM WEB: AKRONCHHIRO.COM AMA GUIDES TO THE EVALUATION
Corporate Medical Policy
 Corporate Medical Policy Image-Guided Minimally Invasive Decompression (IG-MLD) for File Name: Origination: Last CAP Review: Next CAP Review: Last Review: image-guided_minimally_invasive_decompression_for_spinal_stenosis
Corporate Medical Policy Image-Guided Minimally Invasive Decompression (IG-MLD) for File Name: Origination: Last CAP Review: Next CAP Review: Last Review: image-guided_minimally_invasive_decompression_for_spinal_stenosis
/ 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66
 1425 / 66 / 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66 2011 1 10 20 n-ha/pa66 8 12 22 80 51 1 24 4 L 4 5 8 L 5 S 1 9 L 4 S 1 3 3 5 9 3 X CT Oswestry ODI SF-36 20 6 9 7 3 d 3 6 P < 0.01P > 0.05 3 9 4
1425 / 66 / 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66 2011 1 10 20 n-ha/pa66 8 12 22 80 51 1 24 4 L 4 5 8 L 5 S 1 9 L 4 S 1 3 3 5 9 3 X CT Oswestry ODI SF-36 20 6 9 7 3 d 3 6 P < 0.01P > 0.05 3 9 4
Usefulness of Intraoperative Computed Tomography in Complication Management after Spine Surgery
 THIEME Techniques in Neurosurgery 193 Usefulness of Intraoperative Computed Tomography in Complication Management after Spine Surgery Johannes Kerschbaumer 1 Christian Franz Freyschlag 1 Marcel Seiz-Rosenhagen
THIEME Techniques in Neurosurgery 193 Usefulness of Intraoperative Computed Tomography in Complication Management after Spine Surgery Johannes Kerschbaumer 1 Christian Franz Freyschlag 1 Marcel Seiz-Rosenhagen
A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES
 A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES Takahiro Tsutsumimoto, Mutsuki Yui, Masashi Uehara, Hiroki Ohba, Hiroshi Ohta, Hidemi
A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES Takahiro Tsutsumimoto, Mutsuki Yui, Masashi Uehara, Hiroki Ohba, Hiroshi Ohta, Hidemi
Posterior Thoracic Corpectomies with Cage Reconstruction for Metastatic Spinal Tumors: Comparing the MiniOpen Approach to the Open Approach
 Posterior Thoracic Corpectomies with Cage Reconstruction for Metastatic Spinal Tumors: Comparing the MiniOpen Approach to the Open Approach Darryl Lau, MD and Dean Chou, MD Department of Neurological Surgery
Posterior Thoracic Corpectomies with Cage Reconstruction for Metastatic Spinal Tumors: Comparing the MiniOpen Approach to the Open Approach Darryl Lau, MD and Dean Chou, MD Department of Neurological Surgery
Asymmetrical degenerative marrow (Modic) changes in cervical spine: prevalence, correlative factors, and surgical outcomes
 Gao et al. Journal of Orthopaedic Surgery and Research (2018) 13:85 https://doi.org/10.1186/s13018-018-0807-0 RESEARCH ARTICLE Open Access Asymmetrical degenerative marrow (Modic) changes in cervical spine:
Gao et al. Journal of Orthopaedic Surgery and Research (2018) 13:85 https://doi.org/10.1186/s13018-018-0807-0 RESEARCH ARTICLE Open Access Asymmetrical degenerative marrow (Modic) changes in cervical spine:
Yoshii et al. Journal of Orthopaedic Surgery and Research (2017) 12:12 DOI /s
 Yoshii et al. Journal of Orthopaedic Surgery and Research (2017) 12:12 DOI 10.1186/s13018-017-0515-1 TECHNICAL NOTE Open Access Intraoperative evaluation using mobile computed tomography in anterior cervical
Yoshii et al. Journal of Orthopaedic Surgery and Research (2017) 12:12 DOI 10.1186/s13018-017-0515-1 TECHNICAL NOTE Open Access Intraoperative evaluation using mobile computed tomography in anterior cervical
Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine
 Neurol Med Chir (Tokyo) 51, 484 489, 2011 Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine Manabu SASAKI, 1 Masanori AOKI, 2 Kazuya NISHIOKA, 3 and Toshiki YOSHIMINE 4 1 Department
Neurol Med Chir (Tokyo) 51, 484 489, 2011 Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine Manabu SASAKI, 1 Masanori AOKI, 2 Kazuya NISHIOKA, 3 and Toshiki YOSHIMINE 4 1 Department
Unanswered Questions. Laminoplasty is best
 Laminoplasty is best Wellington K. Hsu, MD Clifford C. Raisbeck Distinguished Professor of Orthopaedic Surgery Director of Research Department of Orthopaedic Surgery Northwestern University Feinberg School
Laminoplasty is best Wellington K. Hsu, MD Clifford C. Raisbeck Distinguished Professor of Orthopaedic Surgery Director of Research Department of Orthopaedic Surgery Northwestern University Feinberg School
Endogenous-Lesioned Cervical Disc Herniation: A Retrospective Review of 9 Cases
 Int Surg 2011;96:363 370 Endogenous-Lesioned Cervical Disc Herniation: A Retrospective Review of 9 Cases Zifeng Zhang 1, Yushu Bai 2, Tiesheng Hou 2 1 School of Naval Architecture, Ocean & Civil Engineering,
Int Surg 2011;96:363 370 Endogenous-Lesioned Cervical Disc Herniation: A Retrospective Review of 9 Cases Zifeng Zhang 1, Yushu Bai 2, Tiesheng Hou 2 1 School of Naval Architecture, Ocean & Civil Engineering,
CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY
 CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY A NEUROSURGEON S VIEW A Preventable Journey to a wheelchair bound-life Dr H. BOODHOO F.C.S (Neurosurgery) Cervical Spondylosis Spinal Osteoarthritis
CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY A NEUROSURGEON S VIEW A Preventable Journey to a wheelchair bound-life Dr H. BOODHOO F.C.S (Neurosurgery) Cervical Spondylosis Spinal Osteoarthritis
Cervical corpectomy for sub-axial retro-vertebral body lesions
 Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion
 Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Surgical Neurology International
 Surgical Neurology International SNI: Spine, a supplement to Surgical Neurology International OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: Nancy E. Epstein,
Surgical Neurology International SNI: Spine, a supplement to Surgical Neurology International OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: Nancy E. Epstein,
Case Report Two-year follow-up results of artificial disc replacement C7-T1
 Int J Clin Exp Med 2016;9(2):4748-4753 www.ijcem.com /ISSN:1940-5901/IJCEM0018942 Case Report Two-year follow-up results of artificial disc replacement C7-T1 Yi Yang 1, Litai Ma 1, Shan Wu 1, Ying Hong
Int J Clin Exp Med 2016;9(2):4748-4753 www.ijcem.com /ISSN:1940-5901/IJCEM0018942 Case Report Two-year follow-up results of artificial disc replacement C7-T1 Yi Yang 1, Litai Ma 1, Shan Wu 1, Ying Hong
Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS NASS COVERAGE POLICY RECOMMENDATIONS TASKFORCE
 NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
Lumbar disc prolapse. Done by : Areej Al-Hadidi
 Lumbar disc prolapse Done by : Areej Al-Hadidi Anatomy of IVD IVD is composed of two components: 1. anulus fibrosus : it is the outer fibrous layer (fibrocartilage ) **It is comressible &tough 2. nucleus
Lumbar disc prolapse Done by : Areej Al-Hadidi Anatomy of IVD IVD is composed of two components: 1. anulus fibrosus : it is the outer fibrous layer (fibrocartilage ) **It is comressible &tough 2. nucleus
Is unilateral pedicle screw fixation superior than bilateral pedicle screw fixation for lumbar degenerative diseases: a meta-analysis
 Lu et al. Journal of Orthopaedic Surgery and Research (2018) 13:296 https://doi.org/10.1186/s13018-018-1004-x SYSTEMATIC REVIEW Open Access Is unilateral pedicle screw fixation superior than bilateral
Lu et al. Journal of Orthopaedic Surgery and Research (2018) 13:296 https://doi.org/10.1186/s13018-018-1004-x SYSTEMATIC REVIEW Open Access Is unilateral pedicle screw fixation superior than bilateral
Estimation of Stellate Ganglion Block Injection Point Using the Cricoid Cartilage as Landmark Through X-ray Review
 Original Article Korean J Pain 2011 September; Vol. 24, No. 3: 141-145 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2011.24.3.141 Estimation of Stellate Ganglion Block Injection Point
Original Article Korean J Pain 2011 September; Vol. 24, No. 3: 141-145 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2011.24.3.141 Estimation of Stellate Ganglion Block Injection Point
Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics
 Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics Yoshiro Nanjo, Hideki Nagashima, Shinji Tanishima,Tokumitsu Mihara,
Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics Yoshiro Nanjo, Hideki Nagashima, Shinji Tanishima,Tokumitsu Mihara,
2016 OPAM Mid-Year Educational Conference, sponsored by AOCOPM Thursday, March 10, 2016 C-1
 Long-term Outcomes of Lumbar Fusion Among Workers Compensation Subjects : An Historical Cohort Study Trang Nguyen M.D., Ph.D. David C. Randolph M.D, M.P.H. James Talmage MD Paul Succop PhD Russell Travis
Long-term Outcomes of Lumbar Fusion Among Workers Compensation Subjects : An Historical Cohort Study Trang Nguyen M.D., Ph.D. David C. Randolph M.D, M.P.H. James Talmage MD Paul Succop PhD Russell Travis
Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with and without Instrumentation
 Document heading doi: 10.21276/apjhs.2017.4.1.18 Research Article Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with without Instrumentation ABSTRACT Sanjay
Document heading doi: 10.21276/apjhs.2017.4.1.18 Research Article Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with without Instrumentation ABSTRACT Sanjay
) ACDF. (Japanese Orthopaedic Association,JOA) ACCF (175.4±12.1ml VS 201.3±80.4ml) ACDF JOA VAS (P=0.000),ACCF :A : X(2015)
 2015 25 5 Chinese Journal of Spine and Spinal Cord,2015,Vol.25,No.5 433 1, 2, 2, 3, 3 (1 ;2 466000 ;3 466000 ) : (anterior cervical discectomy and fusion,acdf) (anterior cervical corpectomy and fusion,accf)
2015 25 5 Chinese Journal of Spine and Spinal Cord,2015,Vol.25,No.5 433 1, 2, 2, 3, 3 (1 ;2 466000 ;3 466000 ) : (anterior cervical discectomy and fusion,acdf) (anterior cervical corpectomy and fusion,accf)
Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with Thoracolumbar Fractures
 Journal of Clinical and Nursing Research 2018, 2(1): 23-27 Journal of Clinical and Nursing Research Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with
Journal of Clinical and Nursing Research 2018, 2(1): 23-27 Journal of Clinical and Nursing Research Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with
Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic resonance imaging study evidence
 See the Editorial and the Response in this issue, p 1. J Neurosurg (Spine 1) 100:2 6, 2004 Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic
See the Editorial and the Response in this issue, p 1. J Neurosurg (Spine 1) 100:2 6, 2004 Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic
Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion. Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD
 ORIGINAL ARTICLE Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD Study Design: A prospective study assessing
ORIGINAL ARTICLE Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD Study Design: A prospective study assessing
Intraoperative spinal cord monitoring with Tce-MEP for cervical laminoplasty
 Intraoperative spinal cord monitoring with Tce-MEP for cervical laminoplasty Nobuhiro Tanaka 1, 2), Kazuyoshi Nakanishi 2), Naosuke Kamei 2), Toshio Nakamae 2), Shinji Kotaka 2), Yoshinori Fujimoto 1),
Intraoperative spinal cord monitoring with Tce-MEP for cervical laminoplasty Nobuhiro Tanaka 1, 2), Kazuyoshi Nakanishi 2), Naosuke Kamei 2), Toshio Nakamae 2), Shinji Kotaka 2), Yoshinori Fujimoto 1),
