What to Expect in the Last Days of Life: A Guide for Caregivers
|
|
|
- Brett Rogers
- 6 years ago
- Views:
Transcription
1 Inside this guide: Physical changes and needs Eating and drinking 2 Pain 3 Restlessness, agitation and disorientation Mouth, nose and eye care Weakness and sleepiness Changes in breathing Looking after yourself Very near the time of death When your loved one dies What to Expect in the Last Days of Life: A Guide for Caregivers The end of a loved one's life is a challenging time, full of complicated emotions and concerns. As a caregiver, you may have many questions or feel uncertain about how best to meet your loved one's needs. These questions and concerns are a natural part of caring for someone approaching death. Knowing what to expect in the last days and hours of life can help you feel better prepared. We've put together this guide to help you care for yourself and your loved one during your last days and hours together at home. This information will also be useful if you are caring for someone in a hospital, hospice or another institution, like a long-term care home. We hope that this guide will help you to understand and attend to your loved one's changing needs, and to ease any fears and worries you may have. If you have any questions or concerns about this information, please talk with your doctor or nurse. It's a good idea to write down your questions so that you can remember them the next time you speak with your health-care providers. A University of Toronto affiliated patient care, teaching and research centre
2 Physical changes and needs At the end of life a person's body goes through many physical changes. These changes usually happen over a few days, but sometimes they happen very quickly and dramatically over the course of a few hours. A person can go from looking quite stable to looking as though he or she has only hours to live. Sometimes these changes may be stressful or disturbing, but they aren't usually medical emergencies. They are part of the normal process of dying. These physical changes are described in the following sections, along with some tips on how you can help manage them and keep your loved one as comfortable as possible. Eating and drinking At this time, your loved one will eat or drink very little, if at all. This is normal. At the end of life, people generally don't feel hungry or thirsty because the body s systems have slowed. The body loses its ability to use food and fluids and does not benefit from the nutrients in them. It's okay to offer fluids. First, raise their head off the pillow slightly to prevent gagging. Then, offer fluid in one or more of the following ways: For these reasons, if your loved one does not want to eat or drink, it's important to respect those wishes. It's natural to want to feed someone who is ill, but feeding a dying person will not ease their suffering, and will not extend life. In fact, food or drink can make a dying person feel nauseated and uncomfortable. Give a couple of sips of water from a syringe or baby cup with a spout. Place a couple of ice chips or a spoonful of crushed Popsicle in the mouth. Do not feed your loved one if they are very sleepy or cannot swallow properly. Food and water can get into their lungs, which can cause coughing and gagging, and can lead to congestion and pneumonia. Many family members ask about intravenous (or IV) feeding. In IV feeding, a doctor or nurse inserts a needle into a person's vein, and fluids are given directly through the vein. These fluids are usually water with salt or sugar added. We tend to not recommend the use of IV feeding, unless the person needs special medications that can be given only in this way. IV fluids do not provide much nutrition and in our experience sometimes make the dying process longer. Offer a sponge swab dipped in water for your loved one to suck. Your loved one may bite down on the sponge. This is a normal reaction. Continue to hold onto the stick; after a few moments, they will let go. Important notes Be careful not to force fluids or food on your loved one. If they cough or have trouble breathing during feeding, stop immediately. Don't be alarmed if their urine is dark in colour. As a person drinks less, urine becomes more concentrated and darker. 2
3 Pain Pain doesn't usually get worse at the end of life. In fact, a person may experience less pain as they become sleepier and move less. If your loved one can't tell you that they are in pain, you can look for body language that signals discomfort, such as a scrunched-up forehead, wincing, flinching, stiffening of the body or clenched teeth. If pain medication is being used, the dose or the way the medication is given may need to be adjusted as a person s condition changes. For example, if a person can no longer swallow, some pain medications can be provided in patch form, or through an IV or injection. If you think that your loved one's pain medication needs to be adjusted, contact the doctor or nurse. Sometimes, you may hear your loved one moan. Moaning happens most often as a dying person exhales, or when they are moved from side to side. This kind of moaning is not necessarily caused by pain it may be caused by a change in breathing. This is explained in more detail in the section on changes in breathing. Use pain medication as instructed by your doctor or nurse. Call your health-care provider if the medication doesn't seem to be working. Restlessness, agitation and disorientation At the end of life, people can often become very fidgety, restless, disoriented or distressed. They may feel frightened or threatened. It is also common for people near death to believe that they see things that are not there, such as animals or people who have died. They may appear confused and may not recognize familiar faces. Try not to feel insulted if your loved one doesn't seem to recognize you. This kind of confusion is normal and is not a sign that they feel differently about you. Talk to a member of the health-care team. The doctor or nurse can order medication to help ease distress. If your loved one is using a sedative, ensure that he or she is taking it as prescribed. Try to keep the room as quiet and peaceful as possible. Limit visual distractions, such as television and computer screens. Identify yourself by name, and speak clearly and audibly. Engage in calming activities like holding hands, playing quiet music or reading softly to your loved one. Your loved one may become more agitated if left alone. Ask whether they would like to have familiar faces around more often. Try not to argue or to correct or contradict what they say. This may be upsetting for both of you. Minimize confusion. Try to conduct only one conversation at a time and keep noise and chaos to a minimum. 3
4 Mouth, nose and eye care Near the end of life, the tongue, lips, nose and eyes can feel dry and uncomfortable. You may find that the person you are caring for often breathes through their mouth, which can make the dryness worse. Frequent mouth, nose and eye care will help ease the dryness and discomfort. Frequently clean and freshen the lining inside the mouth. You can use water or a solution made of salt, water and baking soda: Mix together 4 cups (1 litre) of water, ½ teaspoon of salt and 1 teaspoon of baking soda. Make a fresh batch of solution each day. Moisten a sponge-tipped swab with the solution and use the swab to clean and freshen the lining of the mouth, the gums and the tongue. Your nurse will show you how to do this. Your loved one may bite down on the sponge. This is a normal reaction. Continue to hold onto the stick; after a few moments, he or she will let go. Avoid using mouthwash that contains alcohol. It can increase dryness. Use lip balm to protect the lips. Important note: If your loved one is using oxygen, do not use petroleum jelly (like Vaseline) on the lips. The petroleum can degrade the washers for the oxygen valves. Moisten the nostrils with a water-based gel such as Secaris, which you can purchase at a pharmacy without a prescription. Water-based gels can be used safely with oxygen to moisten the nostrils. Moisten the eyes with artificial tears 3 or 4 times a day. Your nurse can show you how to do this. You can purchase artificial tears without a prescription at a pharmacy. 4
5 Weakness and sleepiness Your loved one may feel very weak and tired. People tend to sleep more as their illness progresses. At this time, it is common for people to: Spend all their time in bed Appear to be drowsy or in a light sleep most or all the time Be hard to wake up Talk very little or not at all. In some cases, your loved one may be in a coma. Someone is considered to be in a coma when they no longer respond to voice or touch. We don't know whether comatose patients are able to hear people talk to them or if they understand what's going on around them. They may be able to hear at times, so you can continue to talk to and touch your loved one to provide comfort. If your loved one is drowsy and sleeping a lot, you may be concerned that they are getting too much pain medication. In general, pain relief relaxes the body and allows the patient to sleep more restfully. Talk to your doctor or another member of the health-care team if you're concerned about possible effects of the pain medication. Help find the most comfortable position in bed. We have found that the two best positions are: Turned partly to the side. This position is helpful when a person is quite congested. To keep your loved one from rolling onto his or her back, use pillows to support the whole length of the back. Long body pillows are very useful and can be found at most department stores. Flat on the back with the head slightly elevated (about 30 ). Be careful not to raise their so high that they slide down in bed. The resulting friction can cause bed sores. Ask a nurse how best to position your loved one and adjust the bed. Change your loved one s position in the bed every 6 to 8 hours, switching between the positions they find most comfortable. Regularly changing position helps to reduce discomfort and prevents bed sores from developing. Your nurse or support worker will show you how to do this. Eliminate trips to the toilet by using disposable absorbent undergarments or by asking your doctor or nurse to insert a catheter. There may be some discomfort when the catheter is inserted, but there is usually no pain once it is in place. Talk to your loved one as if they can hear everything. Say everything you want to say. Continue to be affectionate and reassure the person that you are close by. 5
6 Changes in breathing patterns As your loved one gets weaker, you may notice that their regular breathing patterns change. Breathing may speed up, sound shallow or become irregular. These changes are generally not due to a lack of oxygen. Just before death, your loved one s breathing will slow down. There may be gaps as long as 20 or 30 seconds between breaths. Inhaling may sound like gasping. This pattern of breathing can last for hours or days. Your loved one will not be aware of this change or be in any distress. If you have any concerns about changes in breathing patterns, please discuss them with the health-care team. You can help to reduce or stop the noise by positioning your loved one on their side in the fetal position on a flat bed. Long body pillows are very useful to support the back and prevent your loved one from rolling over. You can find them at most department stores. Noisy breathing When a person is in a coma or an extremely drowsy state, their breathing often sounds gurgly or congested, or like snoring. There may also be a soft, short moaning sound with each breath. These noises result from: A small amount of mucus or phlegm in the throat that builds up when a person is not conscious enough to cough The nearness of the mucus or phlegm to the vocal cords This change in breathing tends to occur anywhere from a few days to a few hours before a person dies. Although the sounds may be difficult to listen to, the person will not be in any distress and will not choke on the mucus or phlegm causing the sound. Oxygen will not help reduce or stop the noise. Sometimes people ask about using a suction machine to remove mucus. We generally do not recommend using these machines because the hose can cause gagging and vomiting. If there's concern that the dying person is uncomfortable, doctors can prescribe medicine to help. Please ask a member of your health-care team about this. 6
7 Looking after yourself The end of a loved one's life can be a time of worry and stress for you and your family. Throughout the course of your loved one's illness, it's likely that you have faced many challenges, both in terms of providing care and in dealing with your own grief and emotions. As their death approaches, you may experience a variety of feelings, including fear, worry, sorrow, comfort, peace and relief. You may also feel that your loved one is nearing the end of suffering. All of these feelings are normal. As a caregiver, you may be emotionally and physically exhausted. You may also be taking care of grieving children or other family members. As important as it is for you to look after your loved ones, you also need to care for yourself. Looking after yourself will help you to be a better caregiver for the people around you. You might also encourage your other family members to take good care of themselves. What you can do Remember to eat regularly and drink plenty of water to stay hydrated. Try to get some sleep. By allowing yourself enough time to rest, you will be better able to help your loved one and keep yourself healthy during this time. Give yourself permission to take a bit of time for yourself, away from the bedside of your loved one. Taking time for a hot shower or bath, a quiet walk, meditation or prayer can help ease your stress levels and renew your energy. If possible, surround yourself with supportive friends and relatives. Accept their offers for help and let yourself ask for help with things you need. People are often very eager to help during this difficult time. Say yes to offers of help with meals, housework, child care, grocery shopping, driving or sitting with the dying person while you take a short break. Discuss your fears and worries with your health care team. If you feel you need help coping with your grief, ask your family doctor or nurse for a referral to a support or counselling program. 7
8 Very near the time of death As death nears, a person's eyes may stay open, without blinking. There may be long pauses between breaths. You also may notice some of the following skin changes, which occur as blood circulation slows: The skin may become blue and blotchy The underside of the body may darken The skin around the mouth may appear bluish grey The face may be pale The nose, ears, hands, arms, feet and legs may feel cool to the touch The fingertips may darken. Do not worry if the nurse stops taking your loved one s blood pressure and pulse. These measures are less critical when a person is close to death. Occasionally, someone who is unresponsive may suddenly become more alert or have a surge in energy. For a short period of time, they may be talkative or more interested in food or visitors. If this temporary change occurs, they are not in any distress. Keep them comfortably warm if their skin feels cool to the touch. Avoid very loud noises. They may startle and disturb your loved one, and cause distress. Speaking at a normal level is fine. Say the things you want to say. Some people find it comforting to express thoughts and feelings at this time, such as: Reassuring your loved one that it's okay to die Letting him or her know how much they mean to you Saying "I love you" When your loved one dies How will I know death has occurred? You will know that your loved one has died because: Do not panic. You do not need to call police or 911. There will be no breathing, response, or pulse The eyelids may be slightly open and they will not blink Their pupils will be enlarged Their eyes will be fixed on a certain spot Their jaw will relax and their mouth will be slightly open There may be a release from the bowel or bladder. In the event that 911 is called, be sure to have your completed Do Not Resuscitate (DNR) form on hand, if you have one. This form will alert the authorities not to initiate cardiopulmonary resuscitation (CPR). 8
9 When should I call the palliative care physician? If your loved one dies between 7:00 a.m. and midnight, please page your palliative care doctor to arrange a time for them to come to your home. If your loved one dies between midnight and 7:00 a.m., we respectfully request that you wait until the morning to page us. Our palliative care team is available around the clock for urgent support during our care for your loved one, but we need to reserve a short amount of time for rest and emergency patient care. How long can I keep my deceased loved one at home? There is no need to hurry you can spend as much time with your loved one as you wish. You may prefer to keep your deceased loved one with you for a few hours or overnight, or you may prefer to have his or her body removed sooner. Either is fine. There are no legal reasons to remove your loved one immediately. Let the doctor know what you would prefer when you call. As time passes after a death, physical changes occur in the body that makes it difficult to change position. If you do decide to keep your loved one at home for a period of time, close their eyelids and move the person onto his or her back. A farewell gesture such as a hug or kiss or some words can help you honour the moment and say goodbye. When should I call the funeral home? After the doctor has arrived and filled out the necessary forms, you can call the funeral home. You may wish to select and make arrangements with the funeral home before your loved one dies. How can I support the work of the Temmy Latner Centre? Funeral homes often ask families if there is a charity they wish to support with memorial donations. You may wish to discuss this matter with your loved one and family members before the death. Often, people select a charity or cause that has had great meaning to them over the course of their lifetime or their illness. We would be honoured if you choose to direct donations in support of the Temmy Latner Centre for Palliative Care. Directing memorial donations to the Temmy Latner Centre will help us continue to provide the best possible palliative care in the home and in Mount Sinai Hospital, conduct leading-edge research and deliver valuable education to thousands of students and practicing health care professionals. If you would like to make an online donation, please visit our website at For cheque donations, please make cheques payable to Mount Sinai Hospital Foundation. For more information please call , or foundation@mtsinai.on.ca ****** We appreciate the important role that you and your family members have played in caring for and supporting your loved one through the many challenges that illness brings. We could not have managed to provide home care without your help, concern and sacrifice. If you have questions or concerns at any time, please speak to the doctor or nurse, or visit the Temmy Latner Centre website at ****** 9
Palliative Care Victoria The Process of Dying Page 1. The Process of Dying. What to expect and how to help
 Palliative Care Victoria The Process of Dying Page 1 The Process of Dying What to expect and how to help Palliative Care Victoria The Process of Dying Page 2 About dying Dying is a natural part of life.
Palliative Care Victoria The Process of Dying Page 1 The Process of Dying What to expect and how to help Palliative Care Victoria The Process of Dying Page 2 About dying Dying is a natural part of life.
Preparing for Approaching Death
 Preparing for Approaching Death Old Colony Hospice created this guide for our hospice family and caregivers by revising and adapting the following journal article: Hospice Techniques: Preparing for the
Preparing for Approaching Death Old Colony Hospice created this guide for our hospice family and caregivers by revising and adapting the following journal article: Hospice Techniques: Preparing for the
Precious Moments. Giving comfort and support when someone you love is dying.
 Precious Moments Giving comfort and support when someone you love is dying www.stjoes.ca When someone you love is dying When someone you love is dying, you may want to know how you can provide comfort
Precious Moments Giving comfort and support when someone you love is dying www.stjoes.ca When someone you love is dying When someone you love is dying, you may want to know how you can provide comfort
Physical/Emotional Symptoms and Appropriate Comfort Measures
 Physical/Emotional Symptoms and Appropriate Comfort Measures A. Diminishing Appetite Page 2 B. Decreased Socialization Page 2 C. Sleeping Page 2 E. Changes in Pain Level Page 3 D. Incontinence Page 3 F.
Physical/Emotional Symptoms and Appropriate Comfort Measures A. Diminishing Appetite Page 2 B. Decreased Socialization Page 2 C. Sleeping Page 2 E. Changes in Pain Level Page 3 D. Incontinence Page 3 F.
What to expect in the last days and hours of life in the Intensive Care Unit (ICU)
 What to expect in the last days and hours of life in the Intensive Care Unit (ICU) Information for patients and caregivers Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca
What to expect in the last days and hours of life in the Intensive Care Unit (ICU) Information for patients and caregivers Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca
Preparing for the Death of a Loved One. Information for Patients & Visitors
 Preparing for the Death of a Loved One Information for Patients & Visitors This booklet is provided to help you know what to expect when your loved one is dying. It may help you to respond in ways that
Preparing for the Death of a Loved One Information for Patients & Visitors This booklet is provided to help you know what to expect when your loved one is dying. It may help you to respond in ways that
ALONG THE FINAL JOURNEY
 ALONG THE FINAL JOURNEY A Guide for families and caregivers TABLE OF CONTENTS STARTING THE JOURNEY...2 ALONG THE JOURNEY... 3 Physical/Emotional Symptoms and Appropriate Comfort Measures Diminishing Appetite...
ALONG THE FINAL JOURNEY A Guide for families and caregivers TABLE OF CONTENTS STARTING THE JOURNEY...2 ALONG THE JOURNEY... 3 Physical/Emotional Symptoms and Appropriate Comfort Measures Diminishing Appetite...
What to expect in the last few days of life
 What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 6 What can I do to help?... 7 Can friends and
What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 6 What can I do to help?... 7 Can friends and
What to expect in the last few days of life
 What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 7 What can I do to help?... 7 Can friends and
What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 7 What can I do to help?... 7 Can friends and
Coping with dying. Information for families and carers
 Coping with dying Information for families and carers This leaflet describes some of the physical changes that happen to people as they start to die. It also covers what will happen immediately following
Coping with dying Information for families and carers This leaflet describes some of the physical changes that happen to people as they start to die. It also covers what will happen immediately following
Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person
 Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person This brochure shares some simple ways you can help our care staff to prevent delirium, recognize
Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person This brochure shares some simple ways you can help our care staff to prevent delirium, recognize
When Someone Close To You Is Dying
 Remember that preparing for a death can be difficult. We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect. While
Remember that preparing for a death can be difficult. We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect. While
When Someone Close To You Is Dying
 Remember that preparing for a death can be difficult We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect While
Remember that preparing for a death can be difficult We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect While
Preparing for Approaching Death By North Central Florida Hospice, Inc.
 Preparing for Approaching Death By North Central Florida Hospice, Inc. When a person enters the final stage of the dying process, two different dynamics are at work which are closely interrelated and interdependent.
Preparing for Approaching Death By North Central Florida Hospice, Inc. When a person enters the final stage of the dying process, two different dynamics are at work which are closely interrelated and interdependent.
ALZHEIMER S DISEASE, DEMENTIA & DEPRESSION
 ALZHEIMER S DISEASE, DEMENTIA & DEPRESSION Daily Activities/Tasks As Alzheimer's disease and dementia progresses, activities like dressing, bathing, eating, and toileting may become harder to manage. Each
ALZHEIMER S DISEASE, DEMENTIA & DEPRESSION Daily Activities/Tasks As Alzheimer's disease and dementia progresses, activities like dressing, bathing, eating, and toileting may become harder to manage. Each
Delirium: Information for Patients and Families
 health information Delirium: Information for Patients and Families 605837 Alberta Health Services, (2016/11) Resources Delirium in the Older Person Family Guide: search delirium at viha.ca Go to myhealth.alberta.ca
health information Delirium: Information for Patients and Families 605837 Alberta Health Services, (2016/11) Resources Delirium in the Older Person Family Guide: search delirium at viha.ca Go to myhealth.alberta.ca
CHEMOTHERAPY. What should I expect?
 CHEMOTHERAPY What should I expect? WHAT IS CHEMOTHERAPY? Chemotherapy is treatment that uses drugs to stop the growth of cancer cells, either by killing the cells or by stopping them from dividing. Chemotherapy
CHEMOTHERAPY What should I expect? WHAT IS CHEMOTHERAPY? Chemotherapy is treatment that uses drugs to stop the growth of cancer cells, either by killing the cells or by stopping them from dividing. Chemotherapy
for the grieving process How to cope as your loved one nears the end stages of IPF
 Preparing yourself for the grieving process How to cope as your loved one nears the end stages of IPF 3 As your loved one nears the end stages of IPF, it s important that you be there for him or her as
Preparing yourself for the grieving process How to cope as your loved one nears the end stages of IPF 3 As your loved one nears the end stages of IPF, it s important that you be there for him or her as
Understanding and preventing delirium in older people
 Understanding and preventing delirium in older people Tips for family, whānau, and friends As people get older, especially if they are unwell or living with a dementia, they have greater risk of developing
Understanding and preventing delirium in older people Tips for family, whānau, and friends As people get older, especially if they are unwell or living with a dementia, they have greater risk of developing
Preventing delirium while in the hospital
 Preventing delirium while in the hospital What is delirium? When an older person becomes ill and goes into the hospital, there is an increased risk of developing delirium and other problems. Delirium is
Preventing delirium while in the hospital What is delirium? When an older person becomes ill and goes into the hospital, there is an increased risk of developing delirium and other problems. Delirium is
Managing Sleep Problems after Cancer
 Managing Sleep Problems after Cancer For cancer survivors Read this resource to learn about: What a sleep problem is What causes it What you can do to improve your sleep When to talk to your doctor Please
Managing Sleep Problems after Cancer For cancer survivors Read this resource to learn about: What a sleep problem is What causes it What you can do to improve your sleep When to talk to your doctor Please
Improving Your Sleep During Your Hospital Stay
 PATIENT & CAREGIVER EDUCATION Improving Your Sleep During Your Hospital Stay This information will help you improve your sleep during your hospital stay. Sleeping well at night can make you feel better
PATIENT & CAREGIVER EDUCATION Improving Your Sleep During Your Hospital Stay This information will help you improve your sleep during your hospital stay. Sleeping well at night can make you feel better
Coach on Call. Letting Go of Stress. A healthier life is on the line for you! How Does Stress Affect Me?
 Coach on Call How Does Stress Affect Me? Over time, stress can affect the way you feel, think, and act. You need some time when you are free of stress. You need ways to get relief from stress. Without
Coach on Call How Does Stress Affect Me? Over time, stress can affect the way you feel, think, and act. You need some time when you are free of stress. You need ways to get relief from stress. Without
S A M P L E. Is Near. When Death. Logo A CAREGIVER S GUIDE
 When Death Is Near A CAREGIVER S GUIDE Logo Updated 2019. 2008 by Hospice of Santa Cruz County. This booklet (published as When Death is Near and When the Time Comes) was created by Hospice of Santa Cruz
When Death Is Near A CAREGIVER S GUIDE Logo Updated 2019. 2008 by Hospice of Santa Cruz County. This booklet (published as When Death is Near and When the Time Comes) was created by Hospice of Santa Cruz
Approaching End of Life Some Thoughts... Information for Patients and Families
 Approaching End of Life Some Thoughts... Information for Patients and Families This pamphlet has been produced by the Cancer Care Program of North York General Hospital www.nygh.on.ca 4001 Leslie Street,
Approaching End of Life Some Thoughts... Information for Patients and Families This pamphlet has been produced by the Cancer Care Program of North York General Hospital www.nygh.on.ca 4001 Leslie Street,
INFORMATION FOR PATIENTS, CARERS AND FAMILIES. Coping with dying
 INFORMATION FOR PATIENTS, CARERS AND FAMILIES Coping with dying This leaflet describes some of the physical changes that happen to people as they start to die. It anticipates some of the questions you
INFORMATION FOR PATIENTS, CARERS AND FAMILIES Coping with dying This leaflet describes some of the physical changes that happen to people as they start to die. It anticipates some of the questions you
TAKING CARE OF YOUR FEELINGS
 TAKING CARE OF YOUR FEELINGS A burn injury causes changes in your life. Even though the event or accident that caused the burn may be over, you may still experience strong emotional or physical reactions.
TAKING CARE OF YOUR FEELINGS A burn injury causes changes in your life. Even though the event or accident that caused the burn may be over, you may still experience strong emotional or physical reactions.
First aid for seizures
 First aid for seizures What is epilepsy? Epilepsy is a tendency to have repeated seizures that begin in the brain. For most people with epilepsy their seizures will be controlled by medication. Around
First aid for seizures What is epilepsy? Epilepsy is a tendency to have repeated seizures that begin in the brain. For most people with epilepsy their seizures will be controlled by medication. Around
Pandemic FLU. What you need to know
 Pandemic FLU OR What you need to know Important note: Hygiene is the most important step in preventing the spread of flu. Pandemic Flu is it different to the normal flu? Yes it is a completely different
Pandemic FLU OR What you need to know Important note: Hygiene is the most important step in preventing the spread of flu. Pandemic Flu is it different to the normal flu? Yes it is a completely different
Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing
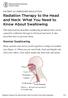 PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
Tobacco Cessation Toolkit
 You notice physical s, like moments of dizziness, sweating, hands trembling or a mild headache. When using tobacco, nicotine increases your heart rate (by about 10 20 beats per minute) and blood pressure.
You notice physical s, like moments of dizziness, sweating, hands trembling or a mild headache. When using tobacco, nicotine increases your heart rate (by about 10 20 beats per minute) and blood pressure.
Flu: What You Can Do. Caring for People at Home
 Flu: What You Can Do Caring for People at Home Flu: What You Can Do Caring for People at Home For more information, please visit: www.mass.gov/dph/flu CONTENTS: What is the flu? 2 table of contents Flu
Flu: What You Can Do Caring for People at Home Flu: What You Can Do Caring for People at Home For more information, please visit: www.mass.gov/dph/flu CONTENTS: What is the flu? 2 table of contents Flu
Ready to give up. Booklet 3
 Ready to give up Booklet 3 This booklet is written for people who have decided that they want to stop smoking. You can use this booklet on its own or go through it with the person who gave it to you. You
Ready to give up Booklet 3 This booklet is written for people who have decided that they want to stop smoking. You can use this booklet on its own or go through it with the person who gave it to you. You
Delirium Information for patients and relatives. Delirium is common Delirium is treatable Relatives can stay to help us
 Delirium Information for patients and relatives Delirium is common Delirium is treatable Relatives can stay to help us What is delirium? Delirium is caused by a disturbance of brain function. It is used
Delirium Information for patients and relatives Delirium is common Delirium is treatable Relatives can stay to help us What is delirium? Delirium is caused by a disturbance of brain function. It is used
Wellness along the Cancer Journey: Palliative Care Revised October 2015
 Wellness along the Cancer Journey: Palliative Care Revised October 2015 Chapter 3: Addressing Cancer Pain as a part of Palliative Care Palliative Care Rev. 10.8.15 Page 360 Addressing Cancer Pain as Part
Wellness along the Cancer Journey: Palliative Care Revised October 2015 Chapter 3: Addressing Cancer Pain as a part of Palliative Care Palliative Care Rev. 10.8.15 Page 360 Addressing Cancer Pain as Part
Journey towards new life...
 Journey towards new life... Dear Family, The staff of Maxville Manor accompanies you on this difficult journey. Our Residents are like family to us. In an effort to provide the support you need, we offer
Journey towards new life... Dear Family, The staff of Maxville Manor accompanies you on this difficult journey. Our Residents are like family to us. In an effort to provide the support you need, we offer
Management of Chronic Obstructive Lung Disease
 Management of Chronic Obstructive Lung Disease 慢性阻塞性肺病的治療與護理 Chapter Three Put Yourself in Control LEARNING HELPFUL WAYS TO BREATHE Learning helpful ways to breathe means learning to use your lungs smarter
Management of Chronic Obstructive Lung Disease 慢性阻塞性肺病的治療與護理 Chapter Three Put Yourself in Control LEARNING HELPFUL WAYS TO BREATHE Learning helpful ways to breathe means learning to use your lungs smarter
GASTRECTOMY. Date of Surgery. Please bring this booklet the day of your surgery. QHC#34
 GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
WHAT IS STRESS? increased muscle tension increased heart rate increased breathing rate increase in alertness to the slightest touch or sound
 EXAM STRESS WHAT IS STRESS? Stress is part of the body s natural response to a perceived threat. We all experience it from time to time. When we feel under threat, our bodies go into fight or flight response,
EXAM STRESS WHAT IS STRESS? Stress is part of the body s natural response to a perceived threat. We all experience it from time to time. When we feel under threat, our bodies go into fight or flight response,
Patient & Family Guide. Bowel Surgery.
 Patient & Family Guide 2016 Bowel Surgery www.nshealth.ca Bowel Surgery This pamphlet will answer some of your questions about your stay in hospital and care at home. We hope this information will help
Patient & Family Guide 2016 Bowel Surgery www.nshealth.ca Bowel Surgery This pamphlet will answer some of your questions about your stay in hospital and care at home. We hope this information will help
CARING FOR SICK PEOPLE AT HOME
 PANDEMIC INFLUENZA CARING FOR SICK PEOPLE AT HOME What is pandemic flu? Pandemic flu means that a new strain of influenza has spread all over the world and is affecting a large number of people. During
PANDEMIC INFLUENZA CARING FOR SICK PEOPLE AT HOME What is pandemic flu? Pandemic flu means that a new strain of influenza has spread all over the world and is affecting a large number of people. During
Journey s End: What to Expect and What to Do When Giving Care at the End of Life
 Journey s End: What to Expect and What to Do When Giving Care at the End of Life 2009 Pathways Home Health & Hospice. All rights reserved. Journey s End: What to Expect and What to Do Just as our lives
Journey s End: What to Expect and What to Do When Giving Care at the End of Life 2009 Pathways Home Health & Hospice. All rights reserved. Journey s End: What to Expect and What to Do Just as our lives
FACTSHEET F18 COPING WITH TIREDNESS
 COPING WITH TIREDNESS Many people with chest, heart and stroke conditions experience tiredness or fatigue. This factsheet explains some of the reasons why you might feel so tired. It also offers advice
COPING WITH TIREDNESS Many people with chest, heart and stroke conditions experience tiredness or fatigue. This factsheet explains some of the reasons why you might feel so tired. It also offers advice
ANESTHESIA. Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS
 ANESTHESIA & YOU Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS UNIQUE T he amount of pain a woman feels during labor may differ from that felt by another woman.
ANESTHESIA & YOU Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS UNIQUE T he amount of pain a woman feels during labor may differ from that felt by another woman.
How to look after your mouth. Cancer Services Information for patients
 How to look after your mouth Cancer Services Information for patients i Is my mouth at risk? There are many things that can affect your mouth. If you answer yes to any of the following, you may be at risk
How to look after your mouth Cancer Services Information for patients i Is my mouth at risk? There are many things that can affect your mouth. If you answer yes to any of the following, you may be at risk
Also there may be some increased saliva production by the autonomic nervous system.
 Introduction Possible problems What can be done? Too much saliva Too little saliva Thick saliva Further help Saliva Control Introduction This fact sheet is aimed at those affected by MSA and experiencing
Introduction Possible problems What can be done? Too much saliva Too little saliva Thick saliva Further help Saliva Control Introduction This fact sheet is aimed at those affected by MSA and experiencing
Methadone for Pain Control
 Palliative Care Guidelines Methadone for Pain Control Information for patients, relatives and carers - 1 - Methadone for Pain Management Other names Methadone Hydrochloride Oral Solution: Metharose, Physeptone
Palliative Care Guidelines Methadone for Pain Control Information for patients, relatives and carers - 1 - Methadone for Pain Management Other names Methadone Hydrochloride Oral Solution: Metharose, Physeptone
Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers
 Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers The Critical Care unit can be a frightening place for patients and visitors. Seeing a loved one attached
Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers The Critical Care unit can be a frightening place for patients and visitors. Seeing a loved one attached
Short-Term Side Effects from Head and Neck Radiation
 PATIENT EDUCATION patienteducation.osumc.edu Short-Term Side Effects from Head and Neck Radiation Side effects are problems caused by radiation therapy. These problems are different for each person and
PATIENT EDUCATION patienteducation.osumc.edu Short-Term Side Effects from Head and Neck Radiation Side effects are problems caused by radiation therapy. These problems are different for each person and
Preparing for Death. A guide for families and caregivers as death approaches PALLIATIVE & END OF LIFE
 PALLIATIVE & END OF LIFE Preparing for Death A guide for families and caregivers as death approaches In this booklet you will learn about: Things to consider when a loved one is seriously ill Checklist
PALLIATIVE & END OF LIFE Preparing for Death A guide for families and caregivers as death approaches In this booklet you will learn about: Things to consider when a loved one is seriously ill Checklist
Ileal Conduit Diversion Surgery
 Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Information for patients preparing for a tracheostomy at Toronto General Hospital
 Tracheostomy Information for patients preparing for a tracheostomy at Toronto General Hospital This booklet will answer the following questions: What is a tracheostomy or trach? Why do I need a tracheostomy?
Tracheostomy Information for patients preparing for a tracheostomy at Toronto General Hospital This booklet will answer the following questions: What is a tracheostomy or trach? Why do I need a tracheostomy?
Relaxation Techniques
 Relaxation is needed for good health. It gives your body and mind a chance to rest and recover from high-stress situations. Your heart rate slows down, blood pressure decreases and muscles relax. Relaxation
Relaxation is needed for good health. It gives your body and mind a chance to rest and recover from high-stress situations. Your heart rate slows down, blood pressure decreases and muscles relax. Relaxation
Pain Relief During Labor and Delivery
 Pain Relief During Labor and Delivery Each woman's labor is unique. The amount of pain a woman feels during labor may differ from that felt by another woman. Pain depends on many factors, such as the size
Pain Relief During Labor and Delivery Each woman's labor is unique. The amount of pain a woman feels during labor may differ from that felt by another woman. Pain depends on many factors, such as the size
For the Patient: Bendamustine Other names: TREANDA
 For the Patient: Bendamustine Other names: TREANDA Bendamustine (ben'' da mus' teen) is a drug that is used to treat some types of cancer (lymphoma). It is a clear liquid that is injected into a vein.
For the Patient: Bendamustine Other names: TREANDA Bendamustine (ben'' da mus' teen) is a drug that is used to treat some types of cancer (lymphoma). It is a clear liquid that is injected into a vein.
END-OF-LIFE DECISIONS HONORING THE WISHES OF A PERSON WITH ALZHEIMER S DISEASE
 END-OF-LIFE DECISIONS HONORING THE WISHES OF A PERSON WITH ALZHEIMER S DISEASE PREPARING FOR THE END OF LIFE When a person with late-stage Alzheimer s a degenerative brain disease nears the end of life
END-OF-LIFE DECISIONS HONORING THE WISHES OF A PERSON WITH ALZHEIMER S DISEASE PREPARING FOR THE END OF LIFE When a person with late-stage Alzheimer s a degenerative brain disease nears the end of life
Cirrhosis. How the Liver Works 3. What is Cirrhosis? 4. Symptoms of Cirrhosis 5. Managing your Cirrhosis Symptoms 6. How is Cirrhosis Treated?
 Cirrhosis Page How the Liver Works 3 What is Cirrhosis? 4 Symptoms of Cirrhosis 5 Managing your Cirrhosis Symptoms 6 How is Cirrhosis Treated? 12 Cirrhosis: Serious Illness- Serious Decisions 17 Other
Cirrhosis Page How the Liver Works 3 What is Cirrhosis? 4 Symptoms of Cirrhosis 5 Managing your Cirrhosis Symptoms 6 How is Cirrhosis Treated? 12 Cirrhosis: Serious Illness- Serious Decisions 17 Other
A Palliative Approach to Supporting Individuals and Families Living With Late and End-Stage Dementia. Dianna Drascic 2018 Alzheimer Symposium
 A Palliative Approach to Supporting Individuals and Families Living With Late and End-Stage Dementia Dianna Drascic 2018 Alzheimer Symposium Objectives Identify when a palliative approach becomes palliative
A Palliative Approach to Supporting Individuals and Families Living With Late and End-Stage Dementia Dianna Drascic 2018 Alzheimer Symposium Objectives Identify when a palliative approach becomes palliative
Understanding late stage dementia Understanding dementia
 Understanding late stage dementia About this factsheet This factsheet is for relatives of people diagnosed with dementia. It provides information about what to expect as dementia progresses to late stage.
Understanding late stage dementia About this factsheet This factsheet is for relatives of people diagnosed with dementia. It provides information about what to expect as dementia progresses to late stage.
PATIENT NAME: M.R. #: ACCT #: HOME TEL: WORK TEL: AGE: D.O.B.: OCCUPATION: HEIGHT: WEIGHT: NECK SIZE: GENDER EMERGENCY CONTACT: RELATIONSHIP: TEL:
 SLEEP DISORDERS INSTITUTE HOSPITAL: DePaul Building Street Address City, State Zip Tel: (202) 555-1212 Fax: (202) 555-1212 SLEEP QUESTIONNAIRE PATIENT NAME: M.R. #: ACCT #: STREET ADDRESS: CITY: STATE:
SLEEP DISORDERS INSTITUTE HOSPITAL: DePaul Building Street Address City, State Zip Tel: (202) 555-1212 Fax: (202) 555-1212 SLEEP QUESTIONNAIRE PATIENT NAME: M.R. #: ACCT #: STREET ADDRESS: CITY: STATE:
Total Thyroidectomy. Post-Surgery Instructions for: WHAT YOU SHOULD KNOW:
 Post-Surgery Instructions for: Orlando Health Surgical Group 14 West Gore Street Orlando, FL 32806 321-843-5001 Total Thyroidectomy Michael Kahky, MD, F.A.C.S Marc Demers, MD, F.A.C.S Jeffrey R. Smith,
Post-Surgery Instructions for: Orlando Health Surgical Group 14 West Gore Street Orlando, FL 32806 321-843-5001 Total Thyroidectomy Michael Kahky, MD, F.A.C.S Marc Demers, MD, F.A.C.S Jeffrey R. Smith,
Winter Health Tips for Vocalists
 Winter Health Tips for Vocalists The winter season is a busy time of the year for a lot of people. Along with changes in weather comes an increased potential for colds and upper respiratory ailments that
Winter Health Tips for Vocalists The winter season is a busy time of the year for a lot of people. Along with changes in weather comes an increased potential for colds and upper respiratory ailments that
There are many benefits to quitting for people with cancer even if the cancer diagnosis is not tobacco-related INCREASED
 Stopping tobacco use reduces your risk for disease and early death. There are health benefits at any age. YOU ARE NEVER TOO OLD TO QUIT. Health benefits begin immediately. INCREASED blood oxygen levels
Stopping tobacco use reduces your risk for disease and early death. There are health benefits at any age. YOU ARE NEVER TOO OLD TO QUIT. Health benefits begin immediately. INCREASED blood oxygen levels
A Guide to Help You Reduce and Stop Using Tobacco
 Let s Talk Tobacco A Guide to Help You Reduce and Stop Using Tobacco Congratulations for taking this first step towards a healthier you! 1-866-710-QUIT (7848) albertaquits.ca It can be hard to stop using
Let s Talk Tobacco A Guide to Help You Reduce and Stop Using Tobacco Congratulations for taking this first step towards a healthier you! 1-866-710-QUIT (7848) albertaquits.ca It can be hard to stop using
Enhanced Recovery Programme
 Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
Esophagectomy Surgery
 Esophagectomy Surgery What is esophagectomy surgery? Esophagectomy surgery is the removal part, or all, of the esophagus. The esophagus is the tube that your food goes down on the way to your stomach.
Esophagectomy Surgery What is esophagectomy surgery? Esophagectomy surgery is the removal part, or all, of the esophagus. The esophagus is the tube that your food goes down on the way to your stomach.
COMMUNICATION ISSUES IN PALLIATIVE CARE
 COMMUNICATION ISSUES IN PALLIATIVE CARE Palliative Care: Communication, Communication, Communication! Key Features of Communication in Appropriate setting Permission Palliative Care Be clear about topic
COMMUNICATION ISSUES IN PALLIATIVE CARE Palliative Care: Communication, Communication, Communication! Key Features of Communication in Appropriate setting Permission Palliative Care Be clear about topic
Tripler Army Medical Center Obstetric Anesthesia Service - FAQs
 Tripler Army Medical Center Obstetric Anesthesia Service - FAQs What is a labor epidural? A labor epidural is a thin tube (called an epidural catheter) placed in a woman s lower back by an anesthesia provider.
Tripler Army Medical Center Obstetric Anesthesia Service - FAQs What is a labor epidural? A labor epidural is a thin tube (called an epidural catheter) placed in a woman s lower back by an anesthesia provider.
Aging may affect memory by changing the way the brain stores information and by making it harder to recall stored information.
 Return to Web version Dementia Overview How does the brain store information? Information is stored in different parts of your memory. Information stored in recent memory may include what you ate for breakfast
Return to Web version Dementia Overview How does the brain store information? Information is stored in different parts of your memory. Information stored in recent memory may include what you ate for breakfast
Patient & Family Guide
 Patient & Family Guide 2017 After Your Wired Jaw Surgery (4.2 Plastic Surgery) www.nshealth.ca After Your Wired Jaw Surgery (4.2 Plastic Surgery) After your surgery, you will notice bars on your top and
Patient & Family Guide 2017 After Your Wired Jaw Surgery (4.2 Plastic Surgery) www.nshealth.ca After Your Wired Jaw Surgery (4.2 Plastic Surgery) After your surgery, you will notice bars on your top and
Methotrexate. About This Drug. Possible Side Effects. Warnings and Precautions
 Methotrexate About This Drug Methotrexate is used to treat cancer. This drug is given in the vein (IV). Possible Side Effects Soreness of the mouth and throat. You may have red areas, white patches, or
Methotrexate About This Drug Methotrexate is used to treat cancer. This drug is given in the vein (IV). Possible Side Effects Soreness of the mouth and throat. You may have red areas, white patches, or
21. Getting Tested for HIV
 21. Getting Tested for HIV Objectives By the end of this session, group members will be able to: Describe the process of HIV testing. List reasons for getting tested for HIV. Background notes It is not
21. Getting Tested for HIV Objectives By the end of this session, group members will be able to: Describe the process of HIV testing. List reasons for getting tested for HIV. Background notes It is not
Anxiety. A self help guide. East Cheshire Hospice Millbank Drive Macclesfield Cheshire SK10 3DR
 Anxiety A self help guide East Cheshire Hospice Millbank Drive Macclesfield Cheshire SK10 3DR Main reception: 01625 610364 Physiotherapy / OT 01625 665689 Fax: 01625 666995 www.eastcheshirehospice.org.uk
Anxiety A self help guide East Cheshire Hospice Millbank Drive Macclesfield Cheshire SK10 3DR Main reception: 01625 610364 Physiotherapy / OT 01625 665689 Fax: 01625 666995 www.eastcheshirehospice.org.uk
Your Kidney Health. Your Choices. Chronic Kidney Disease
 Your Kidney Health Your Choices Your doctor may have told you that you have chronic kidney disease (CKD or advanced kidney disease; or, you may be in kidney failure, and may have to make a decision about
Your Kidney Health Your Choices Your doctor may have told you that you have chronic kidney disease (CKD or advanced kidney disease; or, you may be in kidney failure, and may have to make a decision about
It is very common to get symptoms like cough, sore throat, runny nose and watery eyes. Usually when you
 A Publication of the National Center for Farmworker Health Let s Learn about Respiratory Infections It is very common to get symptoms like cough, sore throat, runny nose and watery eyes. Usually when you
A Publication of the National Center for Farmworker Health Let s Learn about Respiratory Infections It is very common to get symptoms like cough, sore throat, runny nose and watery eyes. Usually when you
Instructions for Patients Following Vitreoretinal Surgery Who Need to Posture
 Manchester Royal Eye Hospital Vitreoretinal Services Information for Patients Instructions for Patients Following Vitreoretinal Surgery Who Need to Posture Patient name: Hospital Number: Consultant: Surgery
Manchester Royal Eye Hospital Vitreoretinal Services Information for Patients Instructions for Patients Following Vitreoretinal Surgery Who Need to Posture Patient name: Hospital Number: Consultant: Surgery
Introduction. Today we hope to provide tips and resources to help balance the challenges of caregiving and ensure that everyone is being cared for.
 Caregiver Wellness Introduction Being a caregiver can be both rewarding and challenging. It s easy to forget to tend to your own needs while caring for your loved one, but it is incredibly important. Today
Caregiver Wellness Introduction Being a caregiver can be both rewarding and challenging. It s easy to forget to tend to your own needs while caring for your loved one, but it is incredibly important. Today
Anal Atresia FACTS: There is no known cause for anal atresia. Children with anal atresia can lead very happy lives post surgery!
 Anal Atresia FACTS: Anal atresia affects 1 in 5,000 births and is slightly more common in boys. There is no known cause for this condition. With anal atresia, any of the following can occur: The anal passage
Anal Atresia FACTS: Anal atresia affects 1 in 5,000 births and is slightly more common in boys. There is no known cause for this condition. With anal atresia, any of the following can occur: The anal passage
behaviors How to respond when dementia causes unpredictable behaviors
 behaviors How to respond when dementia causes unpredictable behaviors the compassion to care, the leadership to conquer how should i handle erratic behaviors? Alzheimer's disease and related dementias
behaviors How to respond when dementia causes unpredictable behaviors the compassion to care, the leadership to conquer how should i handle erratic behaviors? Alzheimer's disease and related dementias
About general anaesthesia Day Surgery Unit Patient Information Leaflet
 About general anaesthesia Day Surgery Unit Patient Information Leaflet Originator: Nahla Farid - Consultant Anaesthetist Date: November 2011 Version: 1 Date for Review: November 2014 DGOH Ref No: DGOH/PIL/00560
About general anaesthesia Day Surgery Unit Patient Information Leaflet Originator: Nahla Farid - Consultant Anaesthetist Date: November 2011 Version: 1 Date for Review: November 2014 DGOH Ref No: DGOH/PIL/00560
Enhanced Recovery Programme Liver surgery
 Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
HOW WOULD I KNOW? WHAT CAN I DO?
 HOW WOULD I KNOW? WHAT CAN I DO? How to help someone with dementia who is in pain or distress Help! 1 Unusual behaviour may be a sign of pain or distress If you are giving care or support to somebody with
HOW WOULD I KNOW? WHAT CAN I DO? How to help someone with dementia who is in pain or distress Help! 1 Unusual behaviour may be a sign of pain or distress If you are giving care or support to somebody with
Nasogastric Tube Patient Passport
 Nutrition and Dietetics Department Nasogastric Tube Patient Passport Please bring this booklet with you for all tube changes Patient Information If you need this information in another format or language
Nutrition and Dietetics Department Nasogastric Tube Patient Passport Please bring this booklet with you for all tube changes Patient Information If you need this information in another format or language
Hospice Journey. A guide of signs, symptoms and caregiving
 Hospice Journey A guide of signs, symptoms and caregiving 1 This book is a guide to help you through the dying journey a natural part of life. A variety of changes can be seen as a body prepares for death.
Hospice Journey A guide of signs, symptoms and caregiving 1 This book is a guide to help you through the dying journey a natural part of life. A variety of changes can be seen as a body prepares for death.
information The Enhanced Recovery Programme for Total Hip Replacement (1 of 6) What will happen before I come into hospital?
 information If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk. You are entitled
information If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk. You are entitled
A Guide to Help New Mothers Stay Smoke-Free
 A Guide to Help New Mothers Stay Smoke-Free 1 Welcome to motherhood! You have just been through a life-changing experience pregnancy and child birth. Having a plan to stay smoke-free is an important step.
A Guide to Help New Mothers Stay Smoke-Free 1 Welcome to motherhood! You have just been through a life-changing experience pregnancy and child birth. Having a plan to stay smoke-free is an important step.
Palliative Care Asking the questions that matter to me
 Palliative Care Asking the questions that matter to me THE PALLIATIVE HUB Adult This booklet has been developed by the Palliative Care Senior Nurses Network and adapted with permission from Palliative
Palliative Care Asking the questions that matter to me THE PALLIATIVE HUB Adult This booklet has been developed by the Palliative Care Senior Nurses Network and adapted with permission from Palliative
Oesophago-gastro duodenoscopy (OGD) Your appointment details, information about the examination and the consent form
 Gastroscopy Oesophago-gastro duodenoscopy (OGD) Your appointment details, information about the examination and the consent form Please bring this booklet with you to your appointment 1 2 Your appointment
Gastroscopy Oesophago-gastro duodenoscopy (OGD) Your appointment details, information about the examination and the consent form Please bring this booklet with you to your appointment 1 2 Your appointment
*521634* Sleep History Questionnaire. Name of primary care doctor:
 *521634* Today s Date: Sleep History Questionnaire Appointment Date: Please answer the following questions before coming to your appointment. Please arrive 15 minutes early with this packet filled out.
*521634* Today s Date: Sleep History Questionnaire Appointment Date: Please answer the following questions before coming to your appointment. Please arrive 15 minutes early with this packet filled out.
NEW PATIENT HOME CARE PACKET
 NEW PATIENT HOME CARE PACKET CORRECT POSTURE Correct posture is a very important component to your TMJ treatment and overall health. Poor posture can throw your head and spine off balance in relation to
NEW PATIENT HOME CARE PACKET CORRECT POSTURE Correct posture is a very important component to your TMJ treatment and overall health. Poor posture can throw your head and spine off balance in relation to
For the Patient: LUPUPE (Carboplatin Option)
 For the Patient: LUPUPE (Carboplatin Option) Other Names: Treatment of Cancer of Unknown Primary Involving the Thorax with Carboplatin and Etoposide LU = LUng PU = Primary Unknown PE = CarboPlatin, Etoposide
For the Patient: LUPUPE (Carboplatin Option) Other Names: Treatment of Cancer of Unknown Primary Involving the Thorax with Carboplatin and Etoposide LU = LUng PU = Primary Unknown PE = CarboPlatin, Etoposide
Be Fit for Life Series. Key Number Five Increase Metabolism
 Key #5 Increase Metabolism Page 1 of 9 Be Fit for Life Series Key Number Five Increase Metabolism Sit or lie in a safe and comfortable position I want you to close your eyes keep them closed until I ask
Key #5 Increase Metabolism Page 1 of 9 Be Fit for Life Series Key Number Five Increase Metabolism Sit or lie in a safe and comfortable position I want you to close your eyes keep them closed until I ask
Your Guide to a Smoke Free Future
 Your Guide to a Smoke Free Future If you smoke, or if you have quit within the past 2 months, then ask for our detailed handout which provides information on how to begin and maintain a smoke-free lifestyle.
Your Guide to a Smoke Free Future If you smoke, or if you have quit within the past 2 months, then ask for our detailed handout which provides information on how to begin and maintain a smoke-free lifestyle.
The Wellbeing Plus Course
 The Wellbeing Plus Course Resource: Good Sleep Guide The Wellbeing Plus Course was written by Professor Nick Titov and Dr Blake Dear The development of the Wellbeing Plus Course was funded by a research
The Wellbeing Plus Course Resource: Good Sleep Guide The Wellbeing Plus Course was written by Professor Nick Titov and Dr Blake Dear The development of the Wellbeing Plus Course was funded by a research
Delirium Information for relatives, carers and patients
 Delirium Information for relatives, carers and patients Contents Part A Introduction What is delirium? Quotes from relatives or carers showing what might happen to a patient suffering from delirium How
Delirium Information for relatives, carers and patients Contents Part A Introduction What is delirium? Quotes from relatives or carers showing what might happen to a patient suffering from delirium How
Bowel Resection Surgery (Open Method)
 Bowel Resection Surgery (Open Method) What is a bowel resection? A bowel resection is surgery to remove a part of the large or small intestine. These parts are shown on this diagram. small intestine large
Bowel Resection Surgery (Open Method) What is a bowel resection? A bowel resection is surgery to remove a part of the large or small intestine. These parts are shown on this diagram. small intestine large
SLEEP HISTORY QUESTIONNAIRE
 Date of birth: Today s date: Dear Patient: SLEEP HISTORY QUESTIONNAIRE Thank you for taking the time to fill out a sleep history questionnaire. This will help our healthcare team to provide the best possible
Date of birth: Today s date: Dear Patient: SLEEP HISTORY QUESTIONNAIRE Thank you for taking the time to fill out a sleep history questionnaire. This will help our healthcare team to provide the best possible
Insomnia. F r e q u e n t l y A s k e d Q u e s t i o n s
 Insomnia Q: What is insomnia? A: Insomnia is a common sleep disorder. If you have insomnia, you may: Lie awake for a long time and have trouble falling asleep Wake up a lot and have trouble returning to
Insomnia Q: What is insomnia? A: Insomnia is a common sleep disorder. If you have insomnia, you may: Lie awake for a long time and have trouble falling asleep Wake up a lot and have trouble returning to
Your anaesthetic for heart surgery
 Your anaesthetic for heart surgery Information for patients and carers First Edition 2018 www.rcoa.ac.uk/patientinfo This leaflet gives you information about your anaesthetic for adult heart (cardiac)
Your anaesthetic for heart surgery Information for patients and carers First Edition 2018 www.rcoa.ac.uk/patientinfo This leaflet gives you information about your anaesthetic for adult heart (cardiac)
wrha.mb.ca a conversation about tube feeding a guide for clients, families and friends healthcare professional guide Healthcare Professional Guide
 a conversation about tube feeding a guide for clients, families and friends healthcare professional guide Health Care Professional Guide Pamphlet Information Healthcare Professional Guide If you are reading
a conversation about tube feeding a guide for clients, families and friends healthcare professional guide Health Care Professional Guide Pamphlet Information Healthcare Professional Guide If you are reading
