Journey s End: What to Expect and What to Do When Giving Care at the End of Life
|
|
|
- Jordan Park
- 5 years ago
- Views:
Transcription
1 Journey s End: What to Expect and What to Do When Giving Care at the End of Life
2 2009 Pathways Home Health & Hospice. All rights reserved.
3 Journey s End: What to Expect and What to Do Just as our lives take different paths, so do the ways we conclude those journeys. The end of life is as individual as the people around us. Many people aren t sure that they ll know what to do and whether they ll be able to manage in the final weeks of their loved one s life. Here we ll tell you about some of the things that often occur and that you may see, and we ll give you some suggestions for ways to comfort your loved one. Remember that Pathways Hospice is always just a phone call away. 1
4 Retreat from Activity and People Oftentimes, weeks or even months before a person s passing, he or she begins to communicate less and to withdraw from friends, family and surroundings. There may be less interest in visitors, TV, and other activities even from much loved family members. This decreased socialization may be an internal acceptance that the end of life is nearing. It may be part of your loved one s preparation to separate from this life. As the patient continues to retreat from the world, there will be more and more napping. Then more time is spent sleeping than awake, and eventually the person becomes difficult to wake. Near the end of life he or she may be unconscious; you are unable to wake them. When this turning inward begins there are some things you can do. Plan activities and visiting for times of day when your loved one seems most alert. Since hearing seems to remain until the very end, you can continue to reassure your loved one by talking to them in your usual tone of voice about what you re doing, how much you care, or things you want him or her to know. 2
5 It s a good idea to tell the patient what you are going to do before you do it. For example, Hi Alex, it s Maria and I m going to clean your mouth now. Remember not to say anything in front of the patient that you wouldn t say if the person were wide awake. Decreased Appetite There comes a time when nearly everyone who is very sick with a life-limiting illness loses their appetite, eats less, and eventually refuses food and water. Food symbolizes life and love and caring in all cultures. If we don t provide food, we may feel as though we are not doing all we can for our loved one. However, with advanced disease there is little desire or need for food. At this stage decline in appetite is normal. As body systems begin to wind down, so does the ability to digest foods. Flavors may start to taste different. Solid foods, especially meats, become unappetizing and too difficult to chew and digest. At some point, a person may prefer only liquids, and later, nothing at all. Sometimes people eat to make their caregivers feel better. For many, appetite comes and goes. 3
6 Allowing a loved one to refuse food is not starving him. Starvation occurs when an otherwise healthy person is hungry and food is not available. People nearing the end of life do not experience feelings of hunger that healthy people do. Let your loved one be the guide; he or she will let you know if he wants food or fluids. Offer food and fluids, but honor his or her refusal. If the person coughs and sputters when taking fluid or food, it may be time to stop trying to feed your loved one to prevent choking. The ability to swallow is lost near the end of life. You may want to talk to your Pathways Hospice nurse about this. People who can t speak will sometimes bite a straw or spoon, clamp their teeth closed, stash food in their cheeks, turn their heads to the side, or spit food out to let you know they don t want to eat. We can do no great things on this earth, only small things with great love. Mother Teresa 4
7 At about the same time a person begins to lose his appetite, you may see other changes more sleeping, periods of confusion, restlessness, and sometimes breathing changes. These are all part of the normal course at the end of life. Stopping eating does not cause these changes, but they often happen around the same time. Thirst By the time a person stops drinking, he or she is usually sleeping with an open mouth; this dries the mucous membranes. Your loved one may say he or she is thirsty, but doesn t really drink when water is offered. What we have learned is that people usually mean their mouths are dry. When we provide frequent mouth care (misting the mouth with water, wetting the tongue, and cleaning teeth and gums), they no longer complain of thirst. Feeding Tubes and IVs At a time when a person is naturally giving up fluids, using tube feedings and intravenous (IV) fluid may overload the body. This can cause uncomfortable symptoms such as swelling, shortness of breath (from fluid in the lungs), and increased saliva that can t be swallowed. Instead of making 5
8 the person feel better, these fluids may make your loved one feel worse. Feeding tubes do not necessarily prolong life, and they carry the added risk of aspiration pneumonia. This occurs when the liquid food is burped or bubbled up into the throat and is then breathed into the lungs. Disorientation As the body begins to shut down, changes happen that can make a dying person confused. Sometimes it becomes unimportant or difficult for the person to keep track of time and people. If the person simply forgets where he or she is, or forgets the date and is easily reoriented, gently remind him of where he is and the day, date, and time. If orienting the patient to the correct date or place agitates or upsets him, let it go. Some people seem disoriented to time in another way, sleeping during the day and awake at night. This may be caused by a fear of dying in one s sleep at night when no one will notice. It may seem safer to sleep when there are people around during the day. Or it may just be caused by too many daytime naps. 6
9 Pets may also help keep a person oriented. If there is a sudden disorientation, however, you should call your Pathways Hospice nurse. Confusion or Hallucinations Sometimes a person appears to be hallucinating seeing people and places that aren t visible to anyone else. Your loved one may have imaginary conversations, often with someone who has already died. At first glance you may think the patient is over-medicated or under-medicated, or that he is out of it. But if we listen carefully there may be meaningful messages in what sounds like rambling. The only way out of the desert is through it. African proverb 7
10 People nearing the end of life will sometimes talk about travel, as though they plan a journey. A person might ask about the bus schedule, whether the suitcase is packed, or if the road to the airport is open. This can actually be reassuring; it lets you know that your loved one is aware of the transition he or she will soon be making. Dying people occasionally seem to move seamlessly back and forth between this world and another. They may talk clearly to people that you know have already died, often close relatives or friends, and then turn and talk clearly to you. Another phenomenon is seeing a place that those in the room can t see. Or a patient may say he is ready to go home. At first you may want to answer, You ARE home. But the person is probably not talking about his or her physical, earthly home. Instead you may get a more meaningful response by asking, Are you ready to leave? or, Tell me about what is happening with you. There is no need to disagree or correct your loved one. These are normal experiences. There is no reason to speak louder than usual. If the patient is truly having hallucinations (like seeing bugs on the wall) the Hospice nurse can help. Adding or discontinuing medications can often relieve these symptoms. 8
11 Fever As the body becomes weaker, so does a person s internal thermostat. Often a person nearing death will have a slight fever. If it is less than 101 F., your loved one may not need any medication. A cool washcloth to the forehead and taking off a blanket may be all that s needed. If the fever is greater than 101 F., your nurse may suggest acetaminophen (Tylenol). As it lowers the temperature, the patient may perspire, and pajamas and sheets may need changing if they become damp. Your loved one may throw the covers off when the room seems comfortable to you. It s important to know that he or she may be warm even when you feel cool. Perhaps all that is needed now is a sheet and no blanket. Sometimes people become sweaty and clammy even without a fever. Hope is an orientation of the heart, of the spirit. It is not the belief that things will turn out well, but that things will make sense, however they turn out. Vaclav Havel 9
12 Incontinence Incontinence is the loss of control of the bowels or bladder that can sometimes occur as muscles in the lower body begin to relax. The overall caregiving goal is simply to keep the person clean, dry, and comfortable. Adult disposable briefs (these words may impart more dignity than saying diapers ) and under-pads on the bed may solve the problem. Your Pathways Hospice nurse or home health aide can show you how to change these for someone in bed. The nurse may suggest placing a catheter (a tube that drains into an enclosed plastic bag) into the bladder to keep the skin dry. A catheter is uncomfortable only for a few seconds while being placed. Then it generally isn t felt. People at the end of life make much less urine in the final few days, and the color is usually darker than normal. I am only one, but I am one. I cannot do everything, but still I can do something. Helen Keller 10
13 Restlessness During the last day or two of life some people become restless and fidget. Your loved one may make repeated motions or pick at the sheets or air. You can reassure your loved one that you are there and won t leave him or her. Speak slowly and calmly in a soothing way. Reading to the patient, playing soft music, or massaging the hands or feet may be a comfort. You can gently brush their hair or just hold hands. It is not necessary to restrain a restless patient, but you may need to use bed rails or have someone sit with the person if he or she is very restless. Continuing to give pain medication is important. Although your loved one may no longer be able to tell you if he or she is having pain, we must do what we can to be sure the person remains as pain-free as possible. Sometimes a dying person is worried about who will take care of things when he or she is gone. Offering reassurance I ll make sure your plants are watered and Frank will take care of the cat. Or, I love you and I will miss you so much, but I will be okay. I don t want you to worry. Anna will help me with the checkbook. This reassurance can be very calming. 11
14 Surge of Energy An unexpected increase in the level of energy is a phenomenon that you may see in someone who has been weak, disoriented, and withdrawn. Your loved one may unexpectedly seem more awake, may feel like eating, may want to visit, or may want to get out of bed things he hasn t done for days or weeks. This surge of energy is sometimes subtle. It may be the patient gathering all his or her physical strength for one last full, bodily experience in this earthly life. It s easy to see how this can give the impression that the person is getting better. Enjoy this time with your loved one for what it is another opportunity to communicate in a meaningful way. The human spirit is stronger than anything that can happen to it. C.C. Scott 12
15 Breathing Changes As a person begins to slip from one world to another, breathing patterns often begin to change. Breathing may slow down or there may be rapid shallow breaths followed by periods of no breathing. These periods can last 5 to 30 seconds, or even up to a full minute. These changes usually mean that death will occur within hours or days. Breathing with pauses is not uncomfortable for the patient; it simply means the end is nearing. There isn t anything you need to do about this. The nurse will instruct you in the use of medication if the breathing is very rapid or seems labored. When the end is very near, you may see very slight movement of the jaw with each breath, and a gasping quality to the breaths. Sometimes when a person is so weak that he can t swallow his own saliva, it gathers in the back of the throat and makes a noisy, wet, rattling sound. Turning the patient side-to-side every five or ten minutes and raising and lowering the head of the bed sometimes help to move these secretions so that they drain out of the throat. This loud breathing isn t hard for your loved one, but it is sometimes hard to listen to. 13
16 Your nurse may suggest medication you can give to dry excessive secretions. At this point the patient is usually breathing with his or her mouth open. This may make the mouth very dry and frequent mouth care is a great comfort. If the breathing seems especially labored, your doctor may prescribe low dose morphine. This is safe and eases the workload for the heart and lungs and you will see more relaxed breathing. Grief is the price of love. M.A. Schreder Slowing Circulation Another change that you will see when death is just hours or a day or so away, is the slowing of circulation to the point that arms and legs begin to feel cooler than usual. The hands, feet and knees may have a blotchy, mottled look. Parts of the body that the patient is lying on may be darker than the rest, and the patient may appear pale and have a bluish cast around the lips, on the ear lobes, and under the fingernails. 14
17 This state doesn t cause any discomfort for your loved one, although it is another sign that he or she will soon pass on. You may use a warm blanket, gently continue to change the person s position, and very softly massage or stroke your loved one. This is a time to reassuringly tell the person that you are there, and that he or she won t be left alone, that you will stay at his side. How Will You Know When Death Has Occurred? When your loved one has passed away you will see no breathing and feel no heart beat. There will be no response to your voice or touch. The eyes will be partly open and the pupils will be large and staring. The jaw will relax and the mouth will open. There may be loss of bowel and bladder contents. What to Do When Death Has Occurred Although you may have felt well prepared, when your loved one dies it may still feel like a shock. This isn t an emergency; it s what you have been expecting. There is no need to call 911. The police do not need to be notified. 15
18 This is the time you may want to call a friend or relative that you ve arranged to be with you. Please call Pathways. We encourage you to accept Pathways help. Hospice staff is available 24 hours a day to help you through this time. A nurse can remove equipment (like tubes), bathe the patient, and prepare the body if you wish. Pathways can call the doctor, dispose of medications, and call the mortuary for you if you wish. Even if you don t want a nurse or social worker to visit, please call Pathways to let us know what has happened. We will call the coroner if it is necessary. You and your family can decide when you would like the mortuary to come. There is no hurry. It isn t necessary for the body to be removed immediately. When you come to the edge of all the light, and you know you are about to step off into the darkness of the unknown, faith is knowing one of two things will happen: either there will be something solid to stand on, or... you will be taught how to fly. Patrick Overton 16
19 It s okay to keep the body in the home for several hours. You may want time to sit and say goodbye, or need time for other relatives to come. Let the mortuary know when you are ready for them to come. Many people leave the room while the mortuary removes the body, but you may help if you wish, whichever feels right. The mortuary will let you know about making arrangements for services. This is all you have to do right now. Let others help you. Don t forget to eat. Don t be surprised if you have feelings of confusion, fear, numbness, anger, sadness, or relief. These are normal responses. Try to rest when you can. Now is the time to take care of your self. Support Pathways Hospice provides bereavement support for those who have lost a loved one. You may want to take advantage of Pathways support groups, remembrance and memorial services, counseling, newsletters and check-in calls. Your grief is just that your grief. Each of us grieves differently. There is no right or wrong way to grieve and no typical time frame for grieving. And if you feel you need support during this time, Pathways is here for you. 17
20 They are not dead who live in the hearts they leave behind. Tuscarora saying End-of-Life Timeline There is no set timeline for how life ends; for some it comes quickly, others may linger. There are many factors that affect when life will end. Among them are: the aggressiveness of the disease, whether the patient has expressed a readiness to die, and how long he or she has gone without food and fluids. However, the following timeline is somewhat typical. Six To Eight Weeks Retreat from people and activities Decreased appetite Increased fatigue and weakness More time spent sleeping One To Two Weeks Confusion or disorientation Sleeping most of the time Decreased blood pressure Great weakness Talking to people not present Eating and drinking very little 18
21 Last Few Days Less urine, darker color Pauses in breathing Surge of energy Restlessness, agitation Incontinence Difficulty waking Clammy skin No eating or drinking Little if any communication Hours Slight jaw movement with each breath Cold, blotchy hands and feet No pulse felt in the wrist Rattling noise with each breath Little or no communication Waxy, pale skin; bluish color around the lips Minutes Slowing, gasping breaths Very slow heart rate No response to voice or touch Glassy, unseeing eyes Darkening of parts of the body resting on bed When Death Has Occurred No breath or pulse Large, fixed pupils of the eyes Relaxed, open jaw Release of a small amount of urine or stool Muscle spasm or movement 19
22 Community based, not for profit
23 The printing of this guide was made possible through generous donations to Pathways Hospice Foundation, the philanthropic branch of the Pathways Family of Services. For more information about Pathways Hospice Foundation, please call or visit
24 When it s time for hospice care, remember you re not alone... we re always here to help Community based, not for profit
Physical/Emotional Symptoms and Appropriate Comfort Measures
 Physical/Emotional Symptoms and Appropriate Comfort Measures A. Diminishing Appetite Page 2 B. Decreased Socialization Page 2 C. Sleeping Page 2 E. Changes in Pain Level Page 3 D. Incontinence Page 3 F.
Physical/Emotional Symptoms and Appropriate Comfort Measures A. Diminishing Appetite Page 2 B. Decreased Socialization Page 2 C. Sleeping Page 2 E. Changes in Pain Level Page 3 D. Incontinence Page 3 F.
Palliative Care Victoria The Process of Dying Page 1. The Process of Dying. What to expect and how to help
 Palliative Care Victoria The Process of Dying Page 1 The Process of Dying What to expect and how to help Palliative Care Victoria The Process of Dying Page 2 About dying Dying is a natural part of life.
Palliative Care Victoria The Process of Dying Page 1 The Process of Dying What to expect and how to help Palliative Care Victoria The Process of Dying Page 2 About dying Dying is a natural part of life.
ALONG THE FINAL JOURNEY
 ALONG THE FINAL JOURNEY A Guide for families and caregivers TABLE OF CONTENTS STARTING THE JOURNEY...2 ALONG THE JOURNEY... 3 Physical/Emotional Symptoms and Appropriate Comfort Measures Diminishing Appetite...
ALONG THE FINAL JOURNEY A Guide for families and caregivers TABLE OF CONTENTS STARTING THE JOURNEY...2 ALONG THE JOURNEY... 3 Physical/Emotional Symptoms and Appropriate Comfort Measures Diminishing Appetite...
What to expect in the last days and hours of life in the Intensive Care Unit (ICU)
 What to expect in the last days and hours of life in the Intensive Care Unit (ICU) Information for patients and caregivers Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca
What to expect in the last days and hours of life in the Intensive Care Unit (ICU) Information for patients and caregivers Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca
Preparing for Approaching Death
 Preparing for Approaching Death Old Colony Hospice created this guide for our hospice family and caregivers by revising and adapting the following journal article: Hospice Techniques: Preparing for the
Preparing for Approaching Death Old Colony Hospice created this guide for our hospice family and caregivers by revising and adapting the following journal article: Hospice Techniques: Preparing for the
Preparing for the Death of a Loved One. Information for Patients & Visitors
 Preparing for the Death of a Loved One Information for Patients & Visitors This booklet is provided to help you know what to expect when your loved one is dying. It may help you to respond in ways that
Preparing for the Death of a Loved One Information for Patients & Visitors This booklet is provided to help you know what to expect when your loved one is dying. It may help you to respond in ways that
What to expect in the last few days of life
 What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 7 What can I do to help?... 7 Can friends and
What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 7 What can I do to help?... 7 Can friends and
What to expect in the last few days of life
 What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 6 What can I do to help?... 7 Can friends and
What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 6 What can I do to help?... 7 Can friends and
Precious Moments. Giving comfort and support when someone you love is dying.
 Precious Moments Giving comfort and support when someone you love is dying www.stjoes.ca When someone you love is dying When someone you love is dying, you may want to know how you can provide comfort
Precious Moments Giving comfort and support when someone you love is dying www.stjoes.ca When someone you love is dying When someone you love is dying, you may want to know how you can provide comfort
Coping with dying. Information for families and carers
 Coping with dying Information for families and carers This leaflet describes some of the physical changes that happen to people as they start to die. It also covers what will happen immediately following
Coping with dying Information for families and carers This leaflet describes some of the physical changes that happen to people as they start to die. It also covers what will happen immediately following
S A M P L E. Is Near. When Death. Logo A CAREGIVER S GUIDE
 When Death Is Near A CAREGIVER S GUIDE Logo Updated 2019. 2008 by Hospice of Santa Cruz County. This booklet (published as When Death is Near and When the Time Comes) was created by Hospice of Santa Cruz
When Death Is Near A CAREGIVER S GUIDE Logo Updated 2019. 2008 by Hospice of Santa Cruz County. This booklet (published as When Death is Near and When the Time Comes) was created by Hospice of Santa Cruz
When Someone Close To You Is Dying
 Remember that preparing for a death can be difficult. We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect. While
Remember that preparing for a death can be difficult. We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect. While
When Someone Close To You Is Dying
 Remember that preparing for a death can be difficult We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect While
Remember that preparing for a death can be difficult We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect While
May the longtime sun shine upon you, All love surround you, And the pure light within you Guide you on your way.
 May the longtime sun shine upon you, All love surround you, And the pure light within you Guide you on your way. Introduction Dying is a natural part of life, but many people do not have experience caring
May the longtime sun shine upon you, All love surround you, And the pure light within you Guide you on your way. Introduction Dying is a natural part of life, but many people do not have experience caring
Preparing for Approaching Death By North Central Florida Hospice, Inc.
 Preparing for Approaching Death By North Central Florida Hospice, Inc. When a person enters the final stage of the dying process, two different dynamics are at work which are closely interrelated and interdependent.
Preparing for Approaching Death By North Central Florida Hospice, Inc. When a person enters the final stage of the dying process, two different dynamics are at work which are closely interrelated and interdependent.
Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person
 Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person This brochure shares some simple ways you can help our care staff to prevent delirium, recognize
Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person This brochure shares some simple ways you can help our care staff to prevent delirium, recognize
Coach on Call. Letting Go of Stress. A healthier life is on the line for you! How Does Stress Affect Me?
 Coach on Call How Does Stress Affect Me? Over time, stress can affect the way you feel, think, and act. You need some time when you are free of stress. You need ways to get relief from stress. Without
Coach on Call How Does Stress Affect Me? Over time, stress can affect the way you feel, think, and act. You need some time when you are free of stress. You need ways to get relief from stress. Without
for the grieving process How to cope as your loved one nears the end stages of IPF
 Preparing yourself for the grieving process How to cope as your loved one nears the end stages of IPF 3 As your loved one nears the end stages of IPF, it s important that you be there for him or her as
Preparing yourself for the grieving process How to cope as your loved one nears the end stages of IPF 3 As your loved one nears the end stages of IPF, it s important that you be there for him or her as
Delirium A guide for caregivers
 Delirium A guide for caregivers Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified health-care provider. Please consult your
Delirium A guide for caregivers Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified health-care provider. Please consult your
Ileal Conduit Diversion Surgery
 Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Delirium: Information for Patients and Families
 health information Delirium: Information for Patients and Families 605837 Alberta Health Services, (2016/11) Resources Delirium in the Older Person Family Guide: search delirium at viha.ca Go to myhealth.alberta.ca
health information Delirium: Information for Patients and Families 605837 Alberta Health Services, (2016/11) Resources Delirium in the Older Person Family Guide: search delirium at viha.ca Go to myhealth.alberta.ca
Anal Atresia FACTS: There is no known cause for anal atresia. Children with anal atresia can lead very happy lives post surgery!
 Anal Atresia FACTS: Anal atresia affects 1 in 5,000 births and is slightly more common in boys. There is no known cause for this condition. With anal atresia, any of the following can occur: The anal passage
Anal Atresia FACTS: Anal atresia affects 1 in 5,000 births and is slightly more common in boys. There is no known cause for this condition. With anal atresia, any of the following can occur: The anal passage
wrha.mb.ca a conversation about tube feeding a guide for clients, families and friends healthcare professional guide Healthcare Professional Guide
 a conversation about tube feeding a guide for clients, families and friends healthcare professional guide Health Care Professional Guide Pamphlet Information Healthcare Professional Guide If you are reading
a conversation about tube feeding a guide for clients, families and friends healthcare professional guide Health Care Professional Guide Pamphlet Information Healthcare Professional Guide If you are reading
Understanding bone metastases and XGEVA
 Understanding bone metastases and XGEVA Contents About bone metastases 3 About XGEVA 5 Dealing with common side effects of XGEVA 8 FAs about living with bone metastases 9 Notes 10 About bone metastases
Understanding bone metastases and XGEVA Contents About bone metastases 3 About XGEVA 5 Dealing with common side effects of XGEVA 8 FAs about living with bone metastases 9 Notes 10 About bone metastases
Preventing delirium while in the hospital
 Preventing delirium while in the hospital What is delirium? When an older person becomes ill and goes into the hospital, there is an increased risk of developing delirium and other problems. Delirium is
Preventing delirium while in the hospital What is delirium? When an older person becomes ill and goes into the hospital, there is an increased risk of developing delirium and other problems. Delirium is
GASTRECTOMY. Date of Surgery. Please bring this booklet the day of your surgery. QHC#34
 GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
INFORMATION FOR PATIENTS, CARERS AND FAMILIES. Coping with dying
 INFORMATION FOR PATIENTS, CARERS AND FAMILIES Coping with dying This leaflet describes some of the physical changes that happen to people as they start to die. It anticipates some of the questions you
INFORMATION FOR PATIENTS, CARERS AND FAMILIES Coping with dying This leaflet describes some of the physical changes that happen to people as they start to die. It anticipates some of the questions you
Preparing for Death. A guide for families and caregivers as death approaches PALLIATIVE & END OF LIFE
 PALLIATIVE & END OF LIFE Preparing for Death A guide for families and caregivers as death approaches In this booklet you will learn about: Things to consider when a loved one is seriously ill Checklist
PALLIATIVE & END OF LIFE Preparing for Death A guide for families and caregivers as death approaches In this booklet you will learn about: Things to consider when a loved one is seriously ill Checklist
Keeping Home Safe WHAT CAN YOU DO?
 Keeping Home Safe or dementia may have trouble knowing what is dangerous or making safe decisions. By helping him or her feel more relaxed and less confused at home, you can help stop accidents. trip because
Keeping Home Safe or dementia may have trouble knowing what is dangerous or making safe decisions. By helping him or her feel more relaxed and less confused at home, you can help stop accidents. trip because
First Aid Preparedness Patsy Ramey, RN, BSN Clinical Resource Nurse Epilepsy Division
 First Aid Preparedness Patsy Ramey, RN, BSN Clinical Resource Nurse Epilepsy Division TRUST Time the seizure Remove glasses and anything tight around the neck Use something soft under their head STAY CALM
First Aid Preparedness Patsy Ramey, RN, BSN Clinical Resource Nurse Epilepsy Division TRUST Time the seizure Remove glasses and anything tight around the neck Use something soft under their head STAY CALM
Managing Other Medical Conditions
 Managing Other Medical Conditions When Dementia is Part of the Picture Terms You Will NEED to Know - Advanced directives - Living Will - DNR orders - Durable HC-POA - Palliative care - Hospice care - Comfort
Managing Other Medical Conditions When Dementia is Part of the Picture Terms You Will NEED to Know - Advanced directives - Living Will - DNR orders - Durable HC-POA - Palliative care - Hospice care - Comfort
*521634* Sleep History Questionnaire. Name of primary care doctor:
 *521634* Today s Date: Sleep History Questionnaire Appointment Date: Please answer the following questions before coming to your appointment. Please arrive 15 minutes early with this packet filled out.
*521634* Today s Date: Sleep History Questionnaire Appointment Date: Please answer the following questions before coming to your appointment. Please arrive 15 minutes early with this packet filled out.
Journey towards new life...
 Journey towards new life... Dear Family, The staff of Maxville Manor accompanies you on this difficult journey. Our Residents are like family to us. In an effort to provide the support you need, we offer
Journey towards new life... Dear Family, The staff of Maxville Manor accompanies you on this difficult journey. Our Residents are like family to us. In an effort to provide the support you need, we offer
Surgical Instructions. Wisdom Tooth TREASURE VALLEY ORAL & FACIAL SURGERY
 TREASURE VALLEY ORAL & FACIAL SURGERY Surgical Instructions Wisdom Tooth 1000 North Curtis Road, Suite 103 Boise, ID 83706 Phone: 208-343-0909 Fax: 208-343-6282 TREASURE VALLEY ORAL & FACIAL SURGERY AFTER
TREASURE VALLEY ORAL & FACIAL SURGERY Surgical Instructions Wisdom Tooth 1000 North Curtis Road, Suite 103 Boise, ID 83706 Phone: 208-343-0909 Fax: 208-343-6282 TREASURE VALLEY ORAL & FACIAL SURGERY AFTER
Understanding and preventing delirium in older people
 Understanding and preventing delirium in older people Tips for family, whānau, and friends As people get older, especially if they are unwell or living with a dementia, they have greater risk of developing
Understanding and preventing delirium in older people Tips for family, whānau, and friends As people get older, especially if they are unwell or living with a dementia, they have greater risk of developing
CARING FOR YOUR CATHETER AT HOME
 CARING FOR YOUR CATHETER AT HOME After surgery (radical prostatectomy) for prostate cancer you will have a urinary catheter for a short period of time and will need to go home with the catheter still in
CARING FOR YOUR CATHETER AT HOME After surgery (radical prostatectomy) for prostate cancer you will have a urinary catheter for a short period of time and will need to go home with the catheter still in
CARING FOR PATIENTS WITH DEMENTIA:
 CARING FOR PATIENTS WITH DEMENTIA: LESSON PLAN Lesson overview Time: One hour This lesson teaches useful ways to work with patients who suffer from dementia. Learning goals At the end of this session,
CARING FOR PATIENTS WITH DEMENTIA: LESSON PLAN Lesson overview Time: One hour This lesson teaches useful ways to work with patients who suffer from dementia. Learning goals At the end of this session,
After Dental Extractions or Wisdom Teeth Removal
 Patient & Family Guide After Dental Extractions or Wisdom Teeth Removal 2017 Aussi disponible en français : Après l extraction des dents ou l enlèvement des dents de sagesse (FF85-1786) www.nshealth.ca
Patient & Family Guide After Dental Extractions or Wisdom Teeth Removal 2017 Aussi disponible en français : Après l extraction des dents ou l enlèvement des dents de sagesse (FF85-1786) www.nshealth.ca
Delirium Information for patients and relatives. Delirium is common Delirium is treatable Relatives can stay to help us
 Delirium Information for patients and relatives Delirium is common Delirium is treatable Relatives can stay to help us What is delirium? Delirium is caused by a disturbance of brain function. It is used
Delirium Information for patients and relatives Delirium is common Delirium is treatable Relatives can stay to help us What is delirium? Delirium is caused by a disturbance of brain function. It is used
University Counselling Service
 Bereavement The death of someone close can be devastating. There are no right or wrong reactions to death, the way you grieve will be unique to you. How you grieve will depend on many factors including
Bereavement The death of someone close can be devastating. There are no right or wrong reactions to death, the way you grieve will be unique to you. How you grieve will depend on many factors including
A Guide to Help You Reduce and Stop Using Tobacco
 Let s Talk Tobacco A Guide to Help You Reduce and Stop Using Tobacco Congratulations for taking this first step towards a healthier you! 1-866-710-QUIT (7848) albertaquits.ca It can be hard to stop using
Let s Talk Tobacco A Guide to Help You Reduce and Stop Using Tobacco Congratulations for taking this first step towards a healthier you! 1-866-710-QUIT (7848) albertaquits.ca It can be hard to stop using
Controlling Worries and Habits
 THINK GOOD FEEL GOOD Controlling Worries and Habits We often have obsessional thoughts that go round and round in our heads. Sometimes these thoughts keep happening and are about worrying things like germs,
THINK GOOD FEEL GOOD Controlling Worries and Habits We often have obsessional thoughts that go round and round in our heads. Sometimes these thoughts keep happening and are about worrying things like germs,
keep track of other information like warning discuss with your doctor, and numbers of signs for relapse, things you want to
 Helping you set your brain free from psychosis. www.heretohelp.bc.ca This book was written by Sophia Kelly and the BC Schizophrenia Society, for the BC Partners for Mental Health and Addictions Information.
Helping you set your brain free from psychosis. www.heretohelp.bc.ca This book was written by Sophia Kelly and the BC Schizophrenia Society, for the BC Partners for Mental Health and Addictions Information.
ALZHEIMER S DISEASE, DEMENTIA & DEPRESSION
 ALZHEIMER S DISEASE, DEMENTIA & DEPRESSION Daily Activities/Tasks As Alzheimer's disease and dementia progresses, activities like dressing, bathing, eating, and toileting may become harder to manage. Each
ALZHEIMER S DISEASE, DEMENTIA & DEPRESSION Daily Activities/Tasks As Alzheimer's disease and dementia progresses, activities like dressing, bathing, eating, and toileting may become harder to manage. Each
What is an Upper GI Endoscopy?
 What is an Upper GI Endoscopy? An upper GI endoscopy is a test your doctor does to see inside part of your digestive system. Your doctor will look at the inside of your esophagus (the tube that links your
What is an Upper GI Endoscopy? An upper GI endoscopy is a test your doctor does to see inside part of your digestive system. Your doctor will look at the inside of your esophagus (the tube that links your
Ready to give up. Booklet 3
 Ready to give up Booklet 3 This booklet is written for people who have decided that they want to stop smoking. You can use this booklet on its own or go through it with the person who gave it to you. You
Ready to give up Booklet 3 This booklet is written for people who have decided that they want to stop smoking. You can use this booklet on its own or go through it with the person who gave it to you. You
Understanding Your Own Grief Journey. Information for Teens
 Understanding Your Own Grief Journey Information for Teens Grief is a natural response to love and loss. People who are grieving experience a variety of feelings, sometimes in succession, sometimes at
Understanding Your Own Grief Journey Information for Teens Grief is a natural response to love and loss. People who are grieving experience a variety of feelings, sometimes in succession, sometimes at
CHEMOTHERAPY. What should I expect?
 CHEMOTHERAPY What should I expect? WHAT IS CHEMOTHERAPY? Chemotherapy is treatment that uses drugs to stop the growth of cancer cells, either by killing the cells or by stopping them from dividing. Chemotherapy
CHEMOTHERAPY What should I expect? WHAT IS CHEMOTHERAPY? Chemotherapy is treatment that uses drugs to stop the growth of cancer cells, either by killing the cells or by stopping them from dividing. Chemotherapy
Concussion & You. A Handbook for Parents and Kids DEVELOPED BY CONCUSSION EXPERTS AT HOLLAND BLOORVIEW KIDS REHABILITATION HOSPITAL
 Concussion & You A Handbook for Parents and Kids DEVELOPED BY CONCUSSION EXPERTS AT HOLLAND BLOORVIEW KIDS REHABILITATION HOSPITAL Trusted experts in youth concussion www.hollandbloorview.ca/concussion
Concussion & You A Handbook for Parents and Kids DEVELOPED BY CONCUSSION EXPERTS AT HOLLAND BLOORVIEW KIDS REHABILITATION HOSPITAL Trusted experts in youth concussion www.hollandbloorview.ca/concussion
severe croup university of alberta capital health stollery children s hospital
 severe croup university of alberta capital health stollery children s hospital A Message from Dr.William Craig Croup is an illness that affects young children. It can come on quite suddenly and can cause
severe croup university of alberta capital health stollery children s hospital A Message from Dr.William Craig Croup is an illness that affects young children. It can come on quite suddenly and can cause
SAFETYNET LEARNING TOOLS
 SAFETYNET LEARNING TOOLS Topic: Urinary Tract Infection Use the materials in this document to help others learn more about urinary tract infection. LEARNING TOOLS: 1. How to Say it Guide 2. Recognizing
SAFETYNET LEARNING TOOLS Topic: Urinary Tract Infection Use the materials in this document to help others learn more about urinary tract infection. LEARNING TOOLS: 1. How to Say it Guide 2. Recognizing
What is stress? Stress is an emotional/ bodily reaction to
 The Basics What is stress? What are some causes of stress? Stress is an emotional/ bodily reaction to a physical, psychological or emotional demand We all display stress in different ways Some stress is
The Basics What is stress? What are some causes of stress? Stress is an emotional/ bodily reaction to a physical, psychological or emotional demand We all display stress in different ways Some stress is
Seniors Helping Seniors September 7 & 12, 2016 Amy Abrams, MSW/MPH Education & Outreach Manager Alzheimer s San Diego
 Dementia Skills for In-Home Care Providers Seniors Helping Seniors September 7 & 12, 2016 Amy Abrams, MSW/MPH Education & Outreach Manager Alzheimer s San Diego Objectives Familiarity with the most common
Dementia Skills for In-Home Care Providers Seniors Helping Seniors September 7 & 12, 2016 Amy Abrams, MSW/MPH Education & Outreach Manager Alzheimer s San Diego Objectives Familiarity with the most common
TAKING CARE OF YOUR FEELINGS
 TAKING CARE OF YOUR FEELINGS A burn injury causes changes in your life. Even though the event or accident that caused the burn may be over, you may still experience strong emotional or physical reactions.
TAKING CARE OF YOUR FEELINGS A burn injury causes changes in your life. Even though the event or accident that caused the burn may be over, you may still experience strong emotional or physical reactions.
Dealing with Depression Feature Article July 2008
 Dealing with Depression Feature Article July 2008 Marjorie and Ann were housemates for about three years. Everyone thought that they did not like each other very much. Direct support staff said that they
Dealing with Depression Feature Article July 2008 Marjorie and Ann were housemates for about three years. Everyone thought that they did not like each other very much. Direct support staff said that they
In most cases, behavioural and psychological symptoms can be successfully managed without medication.
 MEDICATION People with dementia often develop changes as their condition progresses. These include changes in their behaviour and feelings, the things they think and how they perceive the world. Collectively,
MEDICATION People with dementia often develop changes as their condition progresses. These include changes in their behaviour and feelings, the things they think and how they perceive the world. Collectively,
Patient Scheduled Letter Thunderbird Internal Medicine Sleep Center 5620 W. Thunderbird Rd., Suite C-1 Glendale, AZ (602)
 Patient Scheduled Letter Thunderbird Internal Medicine Sleep Center 5620 W. Thunderbird Rd., Suite C-1 Glendale, AZ 85306 (602) 938 6960 Dear Patient, Your Doctor has requested you be scheduled for a sleep
Patient Scheduled Letter Thunderbird Internal Medicine Sleep Center 5620 W. Thunderbird Rd., Suite C-1 Glendale, AZ 85306 (602) 938 6960 Dear Patient, Your Doctor has requested you be scheduled for a sleep
Post Operative Instructions: Wisdom Teeth
 The removal of impacted teeth is a serious surgical procedure. Post-operative care is very important. Unnecessary pain and the complications of infection and swelling can be minimized if the instructions
The removal of impacted teeth is a serious surgical procedure. Post-operative care is very important. Unnecessary pain and the complications of infection and swelling can be minimized if the instructions
RESOURCES FOR THE JOURNEY OF GRIEF. Is There Anything I Can Do? Supporting a Friend Who Is Grieving
 RESOURCES FOR THE JOURNEY OF GRIEF Is There Anything I Can Do? Supporting a Friend Who Is Grieving I can t even imagine what they re going through... Being a friend to someone whose loved one has died
RESOURCES FOR THE JOURNEY OF GRIEF Is There Anything I Can Do? Supporting a Friend Who Is Grieving I can t even imagine what they re going through... Being a friend to someone whose loved one has died
Dr. Nuelle Knee Replacement: Discharge Care Instructions
 Dr. Nuelle Knee Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your knee replacement surgery. We hope that you had a good stay with us. These discharge
Dr. Nuelle Knee Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your knee replacement surgery. We hope that you had a good stay with us. These discharge
THE INSPIRED LIVING MINDFULNESS MEDITATION PROGRAMME
 THE INSPIRED LIVING MINDFULNESS MEDITATION PROGRAMME 1 Foreword More and more research is proving that Mindfulness can help us to overcome addictions, stress, fear, anxiety and even depression. Mindfulness
THE INSPIRED LIVING MINDFULNESS MEDITATION PROGRAMME 1 Foreword More and more research is proving that Mindfulness can help us to overcome addictions, stress, fear, anxiety and even depression. Mindfulness
Total Thyroidectomy. Post-Surgery Instructions for: WHAT YOU SHOULD KNOW:
 Post-Surgery Instructions for: Orlando Health Surgical Group 14 West Gore Street Orlando, FL 32806 321-843-5001 Total Thyroidectomy Michael Kahky, MD, F.A.C.S Marc Demers, MD, F.A.C.S Jeffrey R. Smith,
Post-Surgery Instructions for: Orlando Health Surgical Group 14 West Gore Street Orlando, FL 32806 321-843-5001 Total Thyroidectomy Michael Kahky, MD, F.A.C.S Marc Demers, MD, F.A.C.S Jeffrey R. Smith,
AFSP SURVIVOR OUTREACH PROGRAM VOLUNTEER TRAINING HANDOUT
 AFSP SURVIVOR OUTREACH PROGRAM VOLUNTEER TRAINING HANDOUT Goals of the AFSP Survivor Outreach Program Suggested Answers To Frequently Asked Questions on Visits Roadblocks to Communication During Visits
AFSP SURVIVOR OUTREACH PROGRAM VOLUNTEER TRAINING HANDOUT Goals of the AFSP Survivor Outreach Program Suggested Answers To Frequently Asked Questions on Visits Roadblocks to Communication During Visits
Teaching Family and Friends in Your Community
 2 CHAPTER Teaching Family and Friends in Your Community 9 Old people can remember when there were fewer problems with teeth and gums. Children s teeth were stronger and adults kept their teeth longer.
2 CHAPTER Teaching Family and Friends in Your Community 9 Old people can remember when there were fewer problems with teeth and gums. Children s teeth were stronger and adults kept their teeth longer.
First Aid Preparedness. Patsy Ramey, RN, BSN Clinical Resource Nurse Epilepsy Division
 First Aid Preparedness Patsy Ramey, RN, BSN Clinical Resource Nurse Epilepsy Division Epilepsy Basics Seizures are a bit like an electrical brainstorm. The chaos that occurs in the brain during a seizure
First Aid Preparedness Patsy Ramey, RN, BSN Clinical Resource Nurse Epilepsy Division Epilepsy Basics Seizures are a bit like an electrical brainstorm. The chaos that occurs in the brain during a seizure
Beyond Cancer Moving On
 Beyond Cancer Moving On Today, people with cancer have a better chance at living a normal life than ever before in history. In fact, there are more than 10 million survivors people who have, or are living
Beyond Cancer Moving On Today, people with cancer have a better chance at living a normal life than ever before in history. In fact, there are more than 10 million survivors people who have, or are living
Tripler Army Medical Center Obstetric Anesthesia Service - FAQs
 Tripler Army Medical Center Obstetric Anesthesia Service - FAQs What is a labor epidural? A labor epidural is a thin tube (called an epidural catheter) placed in a woman s lower back by an anesthesia provider.
Tripler Army Medical Center Obstetric Anesthesia Service - FAQs What is a labor epidural? A labor epidural is a thin tube (called an epidural catheter) placed in a woman s lower back by an anesthesia provider.
Why Is Mommy Like She Is?
 Why Is Mommy Like She Is? A Book For Kids About PTSD Deployment Edition Patience H. C. Mason Patience Press High Springs, Florida PP Patience Press 2010 by Patience Mason All rights reserved. No part of
Why Is Mommy Like She Is? A Book For Kids About PTSD Deployment Edition Patience H. C. Mason Patience Press High Springs, Florida PP Patience Press 2010 by Patience Mason All rights reserved. No part of
The Fresco Institute for Parkinson's and Movement Disorders
 The Fresco Institute for Parkinson's and Movement Disorders Follow Up Patient Questionnaire Name: Date: Accompanied by: Do you smoke? CURRENT PAST NEVER Which neurological symptom bothers you most right
The Fresco Institute for Parkinson's and Movement Disorders Follow Up Patient Questionnaire Name: Date: Accompanied by: Do you smoke? CURRENT PAST NEVER Which neurological symptom bothers you most right
ANESTHESIA. Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS
 ANESTHESIA & YOU Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS UNIQUE T he amount of pain a woman feels during labor may differ from that felt by another woman.
ANESTHESIA & YOU Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS UNIQUE T he amount of pain a woman feels during labor may differ from that felt by another woman.
There For You. Your Compassionate Guide. World-Class Hospice Care Since 1979
 There For You Your Compassionate Guide World-Class Hospice Care Since 1979 What Is Hospice? Hospice is a type of care designed to provide support during an advanced illness. Hospice care focuses on comfort
There For You Your Compassionate Guide World-Class Hospice Care Since 1979 What Is Hospice? Hospice is a type of care designed to provide support during an advanced illness. Hospice care focuses on comfort
Lose Weight. without dieting.
 Lose Weight without dieting www.bronwendeklerk.com The Secret to Losing Weight Today I want to share a little secret with you. If you re reading this you have probably become despondent with dieting. Maybe
Lose Weight without dieting www.bronwendeklerk.com The Secret to Losing Weight Today I want to share a little secret with you. If you re reading this you have probably become despondent with dieting. Maybe
A Palliative Approach to Supporting Individuals and Families Living With Late and End-Stage Dementia. Dianna Drascic 2018 Alzheimer Symposium
 A Palliative Approach to Supporting Individuals and Families Living With Late and End-Stage Dementia Dianna Drascic 2018 Alzheimer Symposium Objectives Identify when a palliative approach becomes palliative
A Palliative Approach to Supporting Individuals and Families Living With Late and End-Stage Dementia Dianna Drascic 2018 Alzheimer Symposium Objectives Identify when a palliative approach becomes palliative
NEW PATIENT HOME CARE PACKET
 NEW PATIENT HOME CARE PACKET CORRECT POSTURE Correct posture is a very important component to your TMJ treatment and overall health. Poor posture can throw your head and spine off balance in relation to
NEW PATIENT HOME CARE PACKET CORRECT POSTURE Correct posture is a very important component to your TMJ treatment and overall health. Poor posture can throw your head and spine off balance in relation to
4.2 Later in Life Issues Coping, Treatment and Decision Making at the End of Life
 4.2 Later in Life Issues Coping, Treatment and Decision Making at the End of Life This Help Sheet offers information that can help when someone with Progressive Supranuclear Palsy (PSP) is at the end of
4.2 Later in Life Issues Coping, Treatment and Decision Making at the End of Life This Help Sheet offers information that can help when someone with Progressive Supranuclear Palsy (PSP) is at the end of
HOW WOULD I KNOW? WHAT CAN I DO?
 HOW WOULD I KNOW? WHAT CAN I DO? How to help someone with dementia who is in pain or distress Help! 1 Unusual behaviour may be a sign of pain or distress If you are giving care or support to somebody with
HOW WOULD I KNOW? WHAT CAN I DO? How to help someone with dementia who is in pain or distress Help! 1 Unusual behaviour may be a sign of pain or distress If you are giving care or support to somebody with
Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing
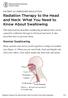 PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
Davy the Detective. Finding out about anaesthetics
 Davy the Detective Finding out about anaesthetics When Davy wants to know about something, he becomes a detective (with a little help from his friends). Information about anaesthesia for young people This
Davy the Detective Finding out about anaesthetics When Davy wants to know about something, he becomes a detective (with a little help from his friends). Information about anaesthesia for young people This
Sepsis 911 Leader Script
 Sepsis 911 Leader Script SLIDE 1 Sepsis 911 Welcome to Sepsis 9-1-1. My name is. I m speaking to you today about sepsis, something that you may not have heard of before you joined us today. You re not
Sepsis 911 Leader Script SLIDE 1 Sepsis 911 Welcome to Sepsis 9-1-1. My name is. I m speaking to you today about sepsis, something that you may not have heard of before you joined us today. You re not
9 INSTRUCTOR GUIDELINES
 STAGE: Ready to Quit You are a clinician in a family practice group and are seeing 16-yearold Nicole Green, one of your existing patients. She has asthma and has come to the office today for her yearly
STAGE: Ready to Quit You are a clinician in a family practice group and are seeing 16-yearold Nicole Green, one of your existing patients. She has asthma and has come to the office today for her yearly
Delirium. Script. So what are the signs and symptoms you are likely to see in this syndrome?
 Delirium Script Note: Script may vary slightly from the audio. Slide 2 Index Definition About delirium Signs and symptoms of delirium Why delirium occurs Risk Factors and causes of delirium Conditions
Delirium Script Note: Script may vary slightly from the audio. Slide 2 Index Definition About delirium Signs and symptoms of delirium Why delirium occurs Risk Factors and causes of delirium Conditions
Research has long suggested that 21 days is all it takes to start a new habit.
 Research has long suggested that 21 days is all it takes to start a new habit. 2 Introduction It s normal to feel a tad stressed from time to time. Life can be stressful. We all worry about things like
Research has long suggested that 21 days is all it takes to start a new habit. 2 Introduction It s normal to feel a tad stressed from time to time. Life can be stressful. We all worry about things like
University Staff Counselling Service
 University Staff Counselling Service Anxiety and Panic What is anxiety? Anxiety is a normal emotional and physiological response to feeling threatened, ranging from mild uneasiness and worry to severe
University Staff Counselling Service Anxiety and Panic What is anxiety? Anxiety is a normal emotional and physiological response to feeling threatened, ranging from mild uneasiness and worry to severe
When You re Having Surgery for a Fractured Hip
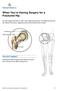 When You re Having Surgery for a Fractured Hip The hip includes the head or ball of the thigh bone (femur). The thigh bone fits into the socket of the pelvis. Ligaments and muscles hold the joint in place.
When You re Having Surgery for a Fractured Hip The hip includes the head or ball of the thigh bone (femur). The thigh bone fits into the socket of the pelvis. Ligaments and muscles hold the joint in place.
Chapter 1 Introduction
 Chapter 1 Introduction Chapter 1-1 Chapter Highlights 1. This Manual is for You 2. What is Scleroderma? 3. Who gets Scleroderma? 4. What are the Early Symptoms of Scleroderma? 5. Is All Scleroderma the
Chapter 1 Introduction Chapter 1-1 Chapter Highlights 1. This Manual is for You 2. What is Scleroderma? 3. Who gets Scleroderma? 4. What are the Early Symptoms of Scleroderma? 5. Is All Scleroderma the
CARING FOR SICK PEOPLE AT HOME
 PANDEMIC INFLUENZA CARING FOR SICK PEOPLE AT HOME What is pandemic flu? Pandemic flu means that a new strain of influenza has spread all over the world and is affecting a large number of people. During
PANDEMIC INFLUENZA CARING FOR SICK PEOPLE AT HOME What is pandemic flu? Pandemic flu means that a new strain of influenza has spread all over the world and is affecting a large number of people. During
Lesson 9 Anxiety and Relaxation Techniques
 The following presentation was originally developed for individuals and families by Achieva (a Western PA service provider). Now offered as a webcast production, ODP is providing this valuable resource
The following presentation was originally developed for individuals and families by Achieva (a Western PA service provider). Now offered as a webcast production, ODP is providing this valuable resource
WICKING DEMENTIA RESEARCH & EDUCATION CENTRE. Prof. Fran McInerney RN, BAppSci, MA, PhD Professor of Dementia Studies and Education
 WICKING DEMENTIA RESEARCH & EDUCATION CENTRE Prof. Fran McInerney RN, BAppSci, MA, PhD Professor of Dementia Studies and Education Wicking Dementia Research & Education Centre Engaging families in a palliative
WICKING DEMENTIA RESEARCH & EDUCATION CENTRE Prof. Fran McInerney RN, BAppSci, MA, PhD Professor of Dementia Studies and Education Wicking Dementia Research & Education Centre Engaging families in a palliative
What to Expect in the Last Days of Life: A Guide for Caregivers
 Inside this guide: Physical changes and needs Eating and drinking 2 Pain 3 Restlessness, agitation and disorientation Mouth, nose and eye care Weakness and sleepiness Changes in breathing Looking after
Inside this guide: Physical changes and needs Eating and drinking 2 Pain 3 Restlessness, agitation and disorientation Mouth, nose and eye care Weakness and sleepiness Changes in breathing Looking after
Delirium Information for relatives, carers and patients
 Delirium Information for relatives, carers and patients Contents Part A Introduction What is delirium? Quotes from relatives or carers showing what might happen to a patient suffering from delirium How
Delirium Information for relatives, carers and patients Contents Part A Introduction What is delirium? Quotes from relatives or carers showing what might happen to a patient suffering from delirium How
CHILDHOOD C 3 HANGE CARE TOOL: PROVIDER REPORT
 Date: / / Patient s Project ID# For use as-needed in clinic visits A SURVEY TO LEARN ABOUT A PATIENT S NEEDS AND ABILITIES: Health care providers of children and adolescents aged 5 to 2 How is this patient
Date: / / Patient s Project ID# For use as-needed in clinic visits A SURVEY TO LEARN ABOUT A PATIENT S NEEDS AND ABILITIES: Health care providers of children and adolescents aged 5 to 2 How is this patient
Smoking and Quitting Assessment
 Smoking and Quitting Assessment A. Which of the following describes you? q I m not interested in trying to quit smoking. q I know I need to quit smoking, but I m not quite ready yet. q I m ready to quit
Smoking and Quitting Assessment A. Which of the following describes you? q I m not interested in trying to quit smoking. q I know I need to quit smoking, but I m not quite ready yet. q I m ready to quit
How to Work with the Patterns That Sustain Depression
 How to Work with the Patterns That Sustain Depression Module 5.2 - Transcript - pg. 1 How to Work with the Patterns That Sustain Depression How the Grieving Mind Fights Depression with Marsha Linehan,
How to Work with the Patterns That Sustain Depression Module 5.2 - Transcript - pg. 1 How to Work with the Patterns That Sustain Depression How the Grieving Mind Fights Depression with Marsha Linehan,
4/3/2014. Dame Cicely Sanders : Born in England Nursing Degree Social Work Degree Doctor Opened 1 st Stand Alone Hospice 1967
 Catherine Hausenfluke Independent Consultant 512-966-4955 Know More about Dying and Grief Come to Terms with Your Own Morality Understand Grief and What are the Rules Understand the Dying Process Relating
Catherine Hausenfluke Independent Consultant 512-966-4955 Know More about Dying and Grief Come to Terms with Your Own Morality Understand Grief and What are the Rules Understand the Dying Process Relating
Epidurals and spinals: information about their operation for anyone who may benefit from an epidural or spinal
 Information for patients pidurals and spinals: information about their operation for anyone who may benefit from an epidural or spinal This leaflet has been made using information from the Royal College
Information for patients pidurals and spinals: information about their operation for anyone who may benefit from an epidural or spinal This leaflet has been made using information from the Royal College
COMMUNICATION ISSUES IN PALLIATIVE CARE
 COMMUNICATION ISSUES IN PALLIATIVE CARE Palliative Care: Communication, Communication, Communication! Key Features of Communication in Appropriate setting Permission Palliative Care Be clear about topic
COMMUNICATION ISSUES IN PALLIATIVE CARE Palliative Care: Communication, Communication, Communication! Key Features of Communication in Appropriate setting Permission Palliative Care Be clear about topic
Psychological Sleep Services Sleep Assessment
 Psychological Sleep Services Sleep Assessment Name Date **************************************************** Insomnia Severity Index For each question, please CIRCLE the number that best describes your
Psychological Sleep Services Sleep Assessment Name Date **************************************************** Insomnia Severity Index For each question, please CIRCLE the number that best describes your
PNEUMONIA. Your Treatment and Recovery
 PNEUMONIA Your Treatment and Recovery Understanding Pneumonia Symptoms of Pneumonia Do you feel feverish and tired, with a cough that won t go away? If so, you may have pneumonia. This is a lung infection
PNEUMONIA Your Treatment and Recovery Understanding Pneumonia Symptoms of Pneumonia Do you feel feverish and tired, with a cough that won t go away? If so, you may have pneumonia. This is a lung infection
Principles and language suggestions for talking with patients
 SAFER MANAGEMENT OF OPIOIDS FOR CHRONIC PAIN: Principles and language suggestions for talking with patients Use these principles and language suggestions when discussing opioid risks and safety monitoring
SAFER MANAGEMENT OF OPIOIDS FOR CHRONIC PAIN: Principles and language suggestions for talking with patients Use these principles and language suggestions when discussing opioid risks and safety monitoring
The Recovery Journey after a PICU admission
 The Recovery Journey after a PICU admission A guide for families Introduction This booklet has been written for parents and young people who have experienced a Paediatric Intensive Care Unit (PICU) admission.
The Recovery Journey after a PICU admission A guide for families Introduction This booklet has been written for parents and young people who have experienced a Paediatric Intensive Care Unit (PICU) admission.
