Autogenic Training as a behavioural approach to insomnia: a prospective cohort study
|
|
|
- Maude Blair
- 6 years ago
- Views:
Transcription
1 Primary Health Care Research & Development page 1 of 11 doi: /s Autogenic Training as a behavioural approach to insomnia: a prospective cohort study Ann Bowden 1, Ava Lorenc 2 and Nicola Robinson 2 1 Royal London Hospital for Integrated Medicine, University College London Hospitals, London, UK 2 Department of Allied Health Sciences, London South Bank University, London, UK RESEARCH Background: Insomnia is commonly associated with chronic health problems. Behavioural and cognitive factors often perpetuate a vicious cycle of anxiety and sleep disturbance, leading to long-term insomnia. National Institute for Health and Clinical Excellence currently recommends behavioural approaches before prescribing hypnotics. Behavioural approaches aim to treat underlying causes, but are not widely available. Research usually includes patients diagnosed with insomnia rather than secondary, co-morbid sleep- related problems. Aim: To examine the effectiveness of autogenic training (AT) as a non-drug approach to sleep-related problems associated with chronic ill health. Design: Prospective pre- and post-treatment cohort study. Setting: AT centre, Royal London Hospital for Integrated Medicine, University College London Hospitals NHS Foundation Trust. Methods: All patients referred for AT from April 2007 to April 2008 were invited to participate. Participants received standard 8-week training, with no specific focus on sleep. Sleep questionnaires were administered at four time points, Measure Your Medical Outcome Profile (MYMOP) and Hospital Anxiety and Depression Scale, before and after treatment. Results before and after treatment were compared. Camden and Islington Community Local Research and Ethics Committee approved the study. Results: The AT course was completed by 153 participants, of whom 73% were identified as having a sleep-related problem. Improvements in sleep patterns included: sleep onset latency (P ), falling asleep quicker after night waking (P, 0.001), feeling more refreshed (P, 0.001) and more energised on waking (P ). MYMOP symptom, well-being, anxiety and depression scores significantly improved (all P, 0.001). Conclusion: This study suggests that AT may improve sleep patterns for patients with various health conditions and reduce anxiety and depression, both of which may result from and cause insomnia. Improvements in sleep patterns occurred despite, or possibly due to, not focusing on sleep during training. AT may provide an approach to insomnia that could be incorporated into primary care. Key words: autogenic training; behavioural approach; insomnia; sleep Received 17 February 2010; accepted 11 April 2011 Introduction Correspondence to: Dr Ann Bowden, M.B., Ch.B, D.C.H., MFHom, Lead Clinician, Autogenic Therapy, Royal London Hospital for Integrated Medicine, University College London Hospitals, Great Ormond Street, London WC1N 3HR, UK. ann.bowden@uclh.nhs.uk r Cambridge University Press 2011 Insomnia is one of the most common problems presented to health-care professionals, with an estimated prevalence of 10 38% (National Institute for Health and Clinical Excellence (NICE), 2005).
2 2 Ann Bowden, Ava Lorenc and Nicola Robinson Sleep disturbances are considered insomnia once they become chronic. This may include difficulty in falling asleep, waking up frequently and waking up feeling un-refreshed (Morgan, 2008). Insomnia is associated with impaired social functioning, anxiety, delayed recovery from acute illness, depression and many non-specific physical symptoms (Luthe and Schultz, 1969; Morgan, 2008). Thus, it is costly both financially and in its impact on physical and psychological well-being (Chilcott and Shapiro, 1996; Szuba et al., 2003). A number of factors are associated with the increased risk of long-term sleep disturbance: high levels of psychological and physical arousal; a worrisome cognitive style (often familial); being female or of older age; individuals with long-term ill health; and those providing care at home for a dependent relative or spouse (Morgan, 2008). The most common causes of acute insomnia are loss through death, separation or divorce, physical illness, mental or emotional trauma (Szuba et al., 2003). The acute episode may need short-term medication, but for most people with appropriate support there will be resolution over time. For others, although the precipitating event has resolved, the sleep disturbance continues and it is at this point that cognitive and behavioural factors perpetuate the problem (Spielman et al., 1987). Maladaptive habits and unhelpful beliefs establish a vicious cycle in which anxiety about not sleeping becomes the focus of attention. Patients report that their lack of sleep makes them anxious and that their anxiety stops them from sleeping (Bowden, 2010). Prescribing a hypnotic has been a standard solution to insomnia (Murtagh and Greenwood, 1995) and can be effective and welcomed by patients desperate for a good night s sleep. However, despite the introduction of newer, better, safer and more expensive hypnotics over the past 50 years, they have not solved the problem of inability to sleep. A meta-analysis of hypnotics for older people with insomnia concluded that their use could not be justified in this group because of the risk of adverse effects (Glass et al., 2005). In addition, trials have shown that no drug is more effective than placebo for improving sleep, daytime functioning, cognition, falls and dependency (Glass et al., 2005). Ironically, the side effects of this group of drugs cognitive impairment, daytime sleepiness and depression are similar to the symptoms of insomnia (Holbrook, 2004). Patients with sleep-related problems tend to be well informed about the pros and cons of the longterm use of hypnotics and are likely to welcome alternatives. Behavioural (non-pharmacological) approaches attempt to address the underlying cause of insomnia and include relaxation-based interventions, such as stimulus control therapy, sleep hygiene education, cognitive behavioural therapy and mindfulness-based stress reduction, often in combination (Morin et al., 1994; Szuba et al., 2003). Relaxation methods focus primarily on reducing somatic arousal and the mental arousal of thoughts and worries. These methods include autogenic training (AT), progressive muscle relaxation and biofeedback. However, behavioural treatments for insomnia are not widely available at present. To enable implementation of current NICE guidelines for treating insomnia, there would need to be an increase in the number of appropriately trained staff within the NHS (Anonymous, 2004). AT is one of of the many complementary therapies provided at the NHS Royal London Hospital for Integrated Medicine (RLHIM). 1 It is a stress management technique particularly recommended for conditions in which stress plays a major role in producing or maintaining ill health (Stetter and Kupper, 2002). AT was developed by the German physician and psychiatrist J.H. Schultz in the early twentieth century and is based on his extensive work on hypnosis and sleep. AT is a psychophysiologically based form of autonomic self-regulation, a structured meditative practice. Here, the patient learns a set of six simple meditative exercises that focus the mind on the body s experience of relaxation, heaviness and warmth in the limbs, a calm heart beat, slower breathing, abdominal warmth and a cool forehead. This leads to a reduction in excessive sympathetic tone and a better balance between sympathetic and parasympathetic activity (Luthe and Schultz, 1969). Supporting this autogenic shift is a state of passive awareness, which is a non-striving, non-judgmental attitude with the ability to accept what is making possible the diminution of the effects of stressors both internal and external (Luthe and Schultz, 1969). Home 1 Formerly the Royal London Homeopathic Hospital.
3 Autogenic Training for insomnia 3 practice is a key component and emphasises the autogenic aspect (auto 5 self and genic 5 arising from ); the patient then comes to realise that it is their own process (Luthe and Schultz, 1969). Practice is an appointment with the self, and it is the patient who decides when and where to practise and how much time to devote to it (Luthe and Schultz, 1969). AT improves sleep latency, duration, efficiency, and reduces medication, daytime dysfunction, anxiety and depression (Nicassio and Bootzin, 1974; Coursey et al., 1980; Stam and Bultz, 1986; Wright et al., 2002; Hidderley and Holt, 2004). A randomised study found that AT significantly improved sleep latency compared with placebo (Nicassio and Bootzin, 1974). Two other studies compared AT with biofeedback and client-centred therapy (Engel-Sittenfeld et al., 1980) and with biofeedback and electrosleep (Coursey et al., 1980) and found significant improvements in insomnia, but no difference between treatments. All three studies used patients with a diagnosis of functional insomnia, in contrast to this study, which uses a sample of patients with a range of health conditions with incidentally high levels of insomnia. The pragmatic nature of this study s NHS setting is also novel. This study examines the effectiveness of AT as a self-management, non-drug approach to sleep disorders within NHS outpatient provision within the context of chronic ill health. Methods Study design This was a prospective, cohort study of AT for insomnia. Ethical approval was obtained from the Camden and Islington Community Local Research and Ethics Committee (reference no. 06/Q0511/106). The primary outcomes were related to sleep and were measured at four time points: at initial consultation, usually approximately 2.5 months before treatment (T1); at the start of treatment (T2); at the end of treatment (T3); and at followup (T4). Secondary outcomes were symptoms and well-being measured using Measure Your Medical Outcome Profile (MYMOP) and anxiety and depression measured using the Hospital Anxiety and Depression Scale (HADS) at T2 and T3. Participants acted as their own controls by comparing changes in scores during pre-treatment period (T1 T2) with changes during treatment (T2 T3). The pre-treatment period (T1 T2) was approximately 2.5 months, which was considered sufficient time to show significant changes in sleep parameters for this period. Setting and sample The study took place in the AT department at the RLHIM, University College London Hospitals NHS Foundation Trust. Patients were referred from primary care (35%), tertiary care (60%) and self-referral (5%). Referrals covered a wide range of health problems, in which stress is considered to play a major role. All patients who chose to start an AT course between April 2007 and April 2008 were invited to participate. Inclusion criteria for the course were based on a verbal agreement to attend the course, work in a group and engage in home practice. Patients who would not be able to understand or follow the instructions were excluded. For this study, no further inclusion or exclusion criteria were applied. Intervention All patients referred for AT, irrespective of their presenting complaint, had an initial assessment where health problems were discussed, the principles of AT and the necessity of home practice explained and possible benefits outlined. Training took place in a group setting with six to eight participants per group, eight weekly sessions of 2 h and follow-up at three months after training. AT courses were delivered as standard by three experienced AT practitioners. There was no particular emphasis, discussion or recommendation for dealing with sleep-related problems other than expectation and encouragement of standard AT practice. Consistency in the study was implicit as the three practitioners used exactly the same training model (British Autogenic Society, 2009). Outcome measures Three outcome measures were used: for primary outcomes, a sleep questionnaire based on the Pittsburgh sleep index was used (Buysse et al., 1989), which has been shown to be valid and reliable for healthy volunteers and those with depression and
4 4 Ann Bowden, Ava Lorenc and Nicola Robinson sleep disorders (Buysse et al., 1989); for secondary outcomes, MYMOP 2 a patient-generated measure was used, which was shown to be valid and responsive for patients in primary care and complementary therapy clinics (Paterson, 1996) and HADS 3 (Zigmond and Snaith, 1983), validated for physically ill patients (Herrmann, 1997). The sleep questionnaire included the following aspects: time taken to fall asleep (sleep latency), 4 number of night-time awakenings, 2 difficulties in getting back to sleep, 2 total sleep time, 2 feeling refreshed on waking, 2 dream recall 2 and previous day s energy. 2 Questionnaires also contained open-ended questions about patients perceived reasons for sleeprelated problems, as well as on the effects of AT on sleep. Participants completed the standard AT medical history form and feedback forms. Participants also received a study information pack and signed a consent form at the start of training. Data analysis Sleep data for the pre-treatment period (T1 T2) were compared with data for the treatment period (T2 T3). For MYMOP and HADS, scores at T2andT3werecompared.Pairedt-tests were used for normally distributed data (continuous variables and interval data). Non-parametric tests were used for non-normally distributed data: Wilcoxon signed-ranks test for interval data; and McNemar s test for interval variables with inconsistent intervals. In addition, an intention-to-treat analysis was performed, imputing missing values with the last available value carried forward. Analysis was performed using SPSS version 15 (SPSS Inc.). Results A total of 289 patients were referred to the AT service during the study period. Of these referrals, 84 did not start the course because of a variety of reasons including personal choice, and being unable to commit. Data are presented for the total of 153 participants who completed the AT course, that is, completed all eight sessions and one or more questionnaires at T3 (52 started but 2 Ordered categorical variable with consistent categories. 3 Continuous variable. 4 Ordinal variable categorised as deteriorated/stayed the same/ improved. Table 1 Demographic characteristics of participants Completed course (n 5 153) %(n) a Did not complete course (n 5 52) %(n) a Gender Female 75 (115) 83 (43) Male 18 (28) 15 (8) Missing (10) (1) Marital status Single 43 (61) 33 (17) Married 26 (37) 27 (14) Divorced (11) (4) Widowed (9) (2) Cohabiting (7) (2) Missing 12 (35) 25 (13) Education Primary school (1) 0 Secondary school 16 (25) 12 (6) Further education 66 (101) 79 (35) Missing (26) 21 (11) Age (years),18 (1) (9) 8 (4) (20) 25 (13) (38) 12 (6) (33) 25 (13) (17) (2) (7) (2) Missing (28) 23 (12) Medication b Homeopathic 29 (32) 30 (10) Antidepressants 22 (23) 21 (7) Cardiovascular 22 (23) 21 (7) Vitamins/minerals 13 (14) (2) Gastrointestinal 12 (12) 18 (6) Hypnotics 10 (11) 18 (6) Endocrine (thyroid, diabetes) 10 (11) 18 (6) NSAIDs (10) 0 Anxiolytics (8) (1) Respiratory (7) 0 Neurological (4) 0 Other 14 (15) 18 (6) NSAIDs 5 non-steroidal anti-inflammatory drugs. a Percentage was not calculated when n, 10. b Percentage of cases, many were on more than one type of medication. did not complete). Attrition at follow-up was high (only 32% of the 153 provided data at T4), and therefore no follow-up data are presented. There were 102 completed sets of sleep questionnaires, that is, 119 for MYMOP and 138 for HADS. Table 1 provides demographic characteristics of
5 Autogenic Training for insomnia 5 participants who completed the course and those who did not complete. The average length of pre-treatment period was 2.6 (SD 2.08) months, the average treatment period was 1.9 (SD 0.69) months and the average follow-up period was 3.69 (SD 2.19) months. Presenting health complaints The most common presenting complaints of those who completed the course (n 5 153) were anxiety/depression (64% of cases), cardiovascular disorders, mostly hypertension (15%), insomnia (13%), gynaecological problems, including premenstrual tension, polycystic ovaries, endometriosis and infertility (10%); musculoskeletal disorders including rheumatoid arthritis, osteoarthritis, fibromyalgia, pain tension syndrome (11%); and neurological disorders including multiple sclerosis and Parkinson s disease (6%). Associated problems included family and relationship dysfunction (40%), family illness or death (39%) and employment problems (12%). Frequency of and reasons for sleep-related problems A total of 112 (73% of those who completed the course) participants reported having a sleep-related problem: 17 as their presenting complaint; 95 on the pre-course questionnaire or sleep questionnaire. The reasons participants gave for their sleeprelated problems (open-ended question) were: worry/can t switch off (21%), stress (16%) or anxiety/depression (15%). Participants also reported pain, tension, family troubles, noise disturbances, snoring, menopausal flushes, work worries, medication, shift work, irritable bowel syndrome and bladder symptoms, reflux and nightmares as reasons for not sleeping. Sleep changes Comparing changes in the pre-treatment period (T1 T2) with changes in the treatment period (T2 T3), there were significant improvements for the primary outcomes of: time taken to fall asleep; difficulty getting back to sleep; energy levels; dream recall and feeling refreshed upon waking (Table 2). Analysis was repeated using intention-to-treat analysis, imputing missing values with the most recent data available, which increased the total number of cases to 121 time taken to fall asleep was no longer significant; difficulty getting back to sleep, feeling refreshed, dream recall and energy all remained significant; total hours asleep and number of night-time awakenings remained non-significant. Qualitative comments and feedback forms The comments in Box 1 show how participants appreciated AT as a self-management tool often to help them get to sleep or to get back to sleep when they wake up in the night. Qualitative data have been presented in more detail elsewhere (Robinson et al., 2010). The feedback forms indicate that one of the most important aspects of the training was group support, as well as relaxation and increased confidence. Improvements in anxiety and depression Anxiety/depression was reported by 64% (n 5 74) of participants as their most important current health problem. Figure 1 compares HADS scores from T2 to T3 (HADS was not administered at T1). Significant improvements were shown with a reduction of to 8.94 for anxiety (95% CI to 3.262, P, 0.001) and 7.35 to 5.28 (95% CI to 2.664, P, 0.001) for depression. Typical responses on the evaluation forms (in response to questions on change of symptoms or other changes following AT) illustrated the impact of the effects of AT on anxiety and depression (Box 2) MYMOP improvements All MYMOP scores (symptoms 1 and 2, activity and well-being) improved significantly (all P, 0.001) when comparing T2 with T3 (MYMOP was not administered at T1) (Table 3). Profile scores dropped by an average of 1.28 following treatment. Discussion Summary of the main findings and comparison with previous literature This study showed significant improvements in sleep following eight sessions of AT and personal
6 Table 2 Variable Changes in sleep variables comparing pre-treatment period (T1 T2) with treatment period (T2 T3) Pre-treatment control (T1 T2; completed both questionnaires, n 5 125) Deteriorated Stayed the same Improved Missing data Significance test and P-value Treatment (T2 T3; completed both questionnaires, n 5 111) Deteriorated Stayed the same Improved Missing data Significance test and P-value Significance test comparing changes during treatment with pre-treatment control and P-value (completed all questionnaires, n 5 102) Intention-to-treat analysis (n 5 121) Missing data Significance test and P-value x , x , Z , Time taken to fall x , x , P * 0 x , asleep a P P, 0.001* P ** Number of nighttime x , x , P x , awakenings a P P * P *** Time taken to get Z , Z , P, 0.001* 4 Z , back to sleep b P P, P, 0.001*, *** Total hours asleep c % CI to 0.22, P % CI to 20.01, P * 95% CI to 0.26, P % CI to 0.21, P *** Feeling refreshed on waking up d Z , P Z , P, 0.001* Z , P, 0.001* 7 Z , P,0.002*, *** Dream recal b Z , P * Z , P, 0.16 Z , P * 10 Z , P *, *** Energy (previous day) c % CI to 20.41, P % CI to 20.56, P, 0.001* 95% CI to 20.17, P * 2 95% CI to 20.03, P *, *** 6 Ann Bowden, Ava Lorenc and Nicola Robinson *Significant results; **lost significance; ***no change. T1 5 before treatment; T2 5 at the start of treatment; T3 5 at the end of treatment. a McNemars test. b Significance test. c Paired t-test. d Wilcoxon signed-rank test.
7 Autogenic Training for insomnia 7 Box 1 Quotes from the sleep questionnaire and evaluation form I worry less about sleeping It has definitely helped me to get better quality of sleep It has given me a coping mechanism for handling insomnia, knowledge that I possess this power is a great reassurance and calming in itself. It prevents a vicious cycle of insomnia and panic about having insomnia I have noticed I wake feeling more refreshed. Knowing I can use AT to get back to sleep if I need to Very good go off to sleep almost straight away after AT exercise very relaxing I am sleeping undisturbed!! AMAZING Outstanding! I was astounded but very pleased with the almost immediate effect AT had on my ability to fall asleep, its made a huge difference An excellent effect. It has been such a long time since I have had the pleasure and benefits of a good restful sleep. Long may it last I am more able to put the day s activities aside and relaxed. I feel calmer when I go to bed Likely presence of condition 10 Borderline presence of condition 5 0 Score for anxiety before course Score for depression before course Score for anxiety after course Score for depression after course Figure 1 Boxplot showing median scores and interquartile ranges for HADS scores daily home AT practice. These included: falling asleep quicker; getting back to sleep quicker after waking up in the night; feeling refreshed on waking up (most frequent improvement) and having more energy on waking up. When missing data were included in the intention-to-treat analysis, only results for time taken to fall asleep were affected. MYMOP scores also showed significant improvement in symptoms and well-being. Recruitment for the study was not restricted to patients presenting with insomnia; however, 73% of the patients did in fact have a sleep-related
8 8 Ann Bowden, Ava Lorenc and Nicola Robinson problem, and over half had co-morbid insomnia (a sleep-related problem secondary to their presenting complaint). Chronic symptoms can produce physiological and cognitive changes that are similar to those experienced as a result of prolonged stress (Sadigh, 2001). It is, therefore, not surprising that our findings confirm that people with chronic health problems often do not sleep, which then becomes an additional burden (Katon et al., 2007). Research generally focuses on individuals with primary insomnia, who are otherwise healthy and not on medication (Murtagh and Greenwood, 1995). In this study, participants were suffering from a wide range of chronic conditions, which included a high incidence of insomnia. Improvements in sleep occurred despite not specifically focusing on the Box 2 Quotes on changes following AT Feel a lot calmer and more centred/grounded Feel much happier I m not so anxiousy The repetitive thought are almost nil I attract more positive responses from others. Calmness and lack of panic are frequently remarked upon by family and close friends I can control my panic attacks I am coping better as I have a more positive outlook more control over my surroundings and a feeling of assertiveness with confidence able to handle stressful situations better, generally feel calmer problem. Any discussion about sleep was instigated by the participants; for example, reporting their first good night s sleep for a long time, or starting an AT exercise on going to bed and sleeping through until morning. In a group setting, these comments encourage and enhance the effects of AT practice and its possibilities. Our findings support observations by AT therapists that AT improves the sleep pattern. Some trainees who have not mentioned a sleep-related problem recognise the fact that they have a sleep deficit. Others find that AT exercise results in feeling refreshed with renewed energy. It has been observed in trainees with or without sleep disorders that after a few weeks of AT practice changes in sleeping patterns occur, primarily falling asleep more quickly, feeling more refreshed in the morning, improved mood and increased recall of dreams (Luthe and Schultz, 1969). Trainees report that they find their own way of practising at home, but the most significant changes are noticed when they practise regularly during the day (Luthe and Schultz, 1969). Each session acts as a power rest and breaks up the vicious cycle of increasing mental and physical tension, restlessness and anxiety, which can build up during the day and prevent sleep (Luthe and Schultz, 1969). The value placed on the group support element of AT by participants highlights that the essence of the AT group process is acceptance, respect and trust between the therapist and the individual and between the group members themselves (Bowden, 2010). Many participants who embarked on this AT course were experiencing great stresses in their lives and felt isolated with their symptoms. Feedback and Table 3 MYMOP scores a before versus after treatment MYMOP Before treatment After treatment P-value (before and after) c Mean (SD) Mean (SD) Symptom (1.310) 3.00 (1.408),0.001 Symptom (1.133) 2.73 (1.256),0.001 Activity 4.09 (1.301) 2.71 (1.376),0.001 Well-being 3.43 (1.187) 2.54 (1.231),0.001 Profile score b 3.90 (0.932) 2.62 (0.945),0.001 MYMOP 5 Measure Your Medical Outcome Profile. a Scale from 0 to 6, 0 is good as it can be, 6 is as bad as it can be. b Mean of all other scores. c Wilcoxon signed-rank test.
9 Autogenic Training for insomnia 9 modelling from other group members provide opportunities for social and cognitive reframing, and from this can ensue the development of greater self-esteem and self-confidence. Strengths and limitations of the study Unlike most studies on treatments for insomnia, participants for this study were not chosen for their sleep-related problems, yet there was a high prevalence of co-morbid insomnia. This recruitment strategy allowed us to show that AT can improve sleep despite sleep not being the focus of training. The study is subject to a number of limitations. Participants acted as their own controls, which cannot reliably confirm causal effects and may be subject to contamination by historical events. However, we felt that it would be unethical to randomise patients to treatment or no treatment groups as the study was pragmatic, taking place within a normal NHS clinic, in which the act of volunteering for the study was inherent in the expectation of doing the training. Another possible option would have been to use patients who declined the training as controls; however, this would have inevitably introduced confounding variables. We, therefore, chose to use the pre-treatment period as the control, which is an accepted methodology, and we believe that this is a legitimate and valid design for psychological and sociological research within service evaluation. It is possible that those who did not benefit from AT left the course or the study. However, intention-to-treat analysis (although this only added 19 cases) shows that the significance of results for six out of seven variables did not change. Dropout was usually due to patients ill health, problems involved in travelling to the hospital, unforeseen personal or work demands or patients failing to engage with the process. There were a number of missing and incomplete questionnaires that limited the findings. This was due to the pragmatic nature of the study, which took place in a time-limited NHS clinic. There were additional missing data for time taken to get back to sleep and dream recall, probably because of questionnaire layout and the inevitability of participants not answering all the questions on all questionnaires. A number of questions on the sleep questionnaire were categorical, and thus may not have been sensitive enough to identify smaller improvements, particularly dream recall. A further limitation was the variation in the length of the pre-treatment and follow-up periods (SD and 2.19 months, respectively). Future research may need to improve participant motivation regarding return of questionnaires and monitoring of individual s questionnaire completion, a common difficulty when using multiple questionnaires in a clinical setting. Attrition at follow-up (T4) was high, and therefore results could not be calculated, although intention-to-treat analysis suggests that the effect of dropout was minimal. The study took place at an NHS specialist hospital in Central London, and thus the study population was exclusive to those patients who could be referred and could travel (often long distances) to attend the sessions. Although previous research has shown that outcomes are not related to age or gender (Morin et al., 1994), it is likely that providing AT locally would result in its uptake by a wider patient population and in better follow-up. The group element of the training was valued by participants; however, there is a chance that interaction between participants within groups biased the results by increasing the chance of a type I error, although participants did complete questionnaires by themselves, mostly at home (Baldwin et al., 2005). Clinical implications The current NICE guidelines for treating insomnia in primary care recommend that behavioural approaches be considered before prescribing a hypnotic (NICE, 2005). The results of this study show improvements in sleep, anxiety and depression and general well-being in patients who completed an AT course in an NHS setting. Participants recognised improvements and described AT as a therapeutic tool, which is particularly helpful for inducing sleep and for getting back to sleep after waking up in the night. Fitting AT practice into busy lives can highlight behavioural and cognitive patterns that are maintaining ill health. With self-observed improvements in symptoms, patients are encouraged to see AT practice as a personal, internal, therapeutic resource that they can use as required. Continued practice is essential if health benefits are to be maintained.
10 10 Ann Bowden, Ava Lorenc and Nicola Robinson Dr Ann Bowden, previously a general practitioner, has considerable experience of the positive results of offering the training in General Practice and of introducing AT into primary care (Author, 2010). A two-year pilot project, commissioned by a Primary Care Group from the RLHIM, for anxiety, panic attacks and insomnia, showed similar results to the current study (Author, 2006). Future research This study shows very promising results for using AT to treat co-morbid insomnia. Studies using randomisation, separate control groups and comparison with other behavioural interventions and hypnotics are now needed. Studies focusing on specific disease populations could provide more insight into the treatment of insomnia as a secondary component. Conclusion This study suggests that AT can improve sleep patterns in participants with a wide range of health conditions and may reduce depression and anxiety, which can both result from and cause insomnia. The improvements in sleep were despite, and possibly due to, not focusing on sleep problems during training. This highlights how observation of nonspecific effects of an intervention can measure the holistic effect rather than simply the evaluation of effects on the presenting complaint. It also suggests that, as a drug-free treatment, AT may provide a more acceptable option for patients with chronic insomnia than taking hypnotics (Morin et al., 1994). As a structured eightsession group-based course, it also has the potential to be cost effective in the long term (Anonymous, 2004). Acknowledgements This study received 1000 from the RLHIM League of Friends. The authors have no conflict of interest to declare. The authors thank Tamara Callea and Chris Perrin, two of the AT therapists, who were generous with their time and provided invaluable help and support. They also thank Tom Kirby, Clinical Governance Manager, for support in setting up the project, and the RLHIM League of Friends for their donation to the study. The authors are very grateful to the patients who took part. References Anonymous. 2004: What s wrong with prescribing hypnotics? Drug and Therapeutics Bulletin 42, Bowden, A. 2006: AT as a non-drug approach to anxiety, panic attacks and insomnia. Journal of Holistic Care 1. Baldwin, S.A., Murray, D.M. and Shadish, W.R. 2005: Empirically supported treatments or type I errors? Problems with the analysis of data from group-administered treatments. Journal of Consulting and Clinical Psychology 73, British Autogenic Society. 2009: org.uk Bowden, A. 2010: Clinical roundup: how do you treat insomnia in your practice?: Autogenic Training. Alternative and Complementary Therapies 16, Buysse, D.J., Reynolds, C.F. III, Monk, T.H., Berman, S.R. and Kupfer, D.J. 1989: The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry Research 28, Chilcott, L.A. and Shapiro, C.M. 1996: The socioeconomic impact of insomnia: an overview. Pharmaeconomics 10, Coursey, R.D., Frankel, B.L., Gaarder, K.R. and Mott, D.E. 1980: A comparison of relaxation techniques with electrosleep therapy for chronic, sleep-onset insomnia a sleep-eeg study. Biofeedback and Self Regulation 5, Engel-Sittenfeld, P., Engel, R., Huber, H. and Zangl, K. 1980: Wirkmechanismen psychologischer Therapieverfahren bei der Behandlung chronischer Schlafstorungen [Effects of psychological therapy in the treatment of insomnia]. Zietschrift fur Klinische Psychologie 9, Glass, J., Lanctot, K.L., Herrmann, N., Sproule, B.A. and Busto, U.E. 2005: Sedative hypnotics in older people with insomnia: meta-analysis of risks and benefits. British Medical Journal 331, Herrmann, C. 1997: International experiences with the Hospital Anxiety and Depression Scale a review of validation data and clinical results. Journal of Psychosomatic Research 42, Hidderley, M. and Holt, M. 2004: A pilot randomized trial assessing the effects of autogenic training in early stage cancer patients in relation to psychological status and immune system responses. European Journal of Oncology Nursing 8, Holbrook, A.M. 2004: Editorial: treating insomnia. British Medical Journal 39. Katon, W., Lin, E.H. and Kroenke, K. 2007: The association of depression and anxiety with medical symptom burden in patients with chronic medical illness. General Hospital Psychiatry 29,
11 Autogenic Training for insomnia 11 Luthe, W. and Schultz, J.H. 1969: Autogenic therapy: applications in psychotherapy. New York: Gronne Statton. Morgan, K. 2008: Patients with insomnia should recieve sleep hygeine advice. Guidelines in Practice 11, Morin, C.M., Culbert, J.P. and Schwartz, S.M. 1994: Nonpharmacological interventions for insomnia: a metaanalysis of treatment efficacy. American Journal of Psychiatry 151, Murtagh, D.R. and Greenwood, K.M. 1995: Identifying effective psychological treatments for insomnia: a metaanalysis. Journal of Consulting and Clinical Psychology 63, Nicassio, P. and Bootzin, R. 1974: A comparison of progressive relaxation and autogenic training as treatments for insomnia. Journal of Abnormal Psychology 83, National Institute for Health and Clinical Excellence (NICE). 2005: Insomnia newer hypnotic drugs: Guidance TA77. London: NICE website Guidance TA77. Paterson, C. 1996: Measuring outcomes in primary care: a patient generated measure, MYMOP, compared with the SF-36 health survey. British Medical Journal 312, Robinson, N., Bowden, A. and Lorenc, A. 2010: Can improvements in sleep be used as an indicator of the wider benefits of Autogenic Training and CAM research in general? European Journal of Integrative Medicine 2, Sadigh, M.R. 2001: Autogenic Training: a mind body approach to the treatment of fibromyalgia and chronic pain syndromes. Philadelphia, PA: Haworth Medical Press. Spielman, A.J., Carruso, L.S. and Glovinsky, P.B. 1987: A behavioural perspective on insomnia treatment. The Psychiatric Clinics of North America 10, Stam, H.J. and Bultz, B.D. 1986: The treatment of severe insomnia in a cancer patient. Journal of Behaviour Therapy and Experimental Psychiatry 17, Stetter, F. and Kupper, S. 2002: Autogenic training: a metaanalysis of clinical outcome studies. Applied Psychophysiology and Biofeedback 27, Szuba, M.P., Kloos, J.D. and Dinges, D.F. 2003: Insomnia: principles and management. Cambridge: Cambridge University Press. Wright, S., Courtney, U. and Crowther, D. 2002: A quantitative and qualitative pilot study of the perceived benefits of autogenic training for a group of people with cancer 6. European Journal of Cancer Care (England) 11, Zigmond, A.S. and Snaith, R.P. 1983: The hospital anxiety and depression scale. Acta Psychiatrica Scandinavica 67,
Royal London Hospital for Integrated Medicine. Autogenic Training
 Royal London Hospital for Integrated Medicine Autogenic Training 1 If you would like this document in another language or format or require the services of an interpreter please contact Patient Services
Royal London Hospital for Integrated Medicine Autogenic Training 1 If you would like this document in another language or format or require the services of an interpreter please contact Patient Services
INSOMNIAS. Stephan Eisenschenk, MD Department of Neurology
 INSOMNIAS INSOMNIAS General criteria for insomnia A. Repeated difficulty with sleep initiation, duration, consolidation or quality. B. Adequate sleep opportunity, persistent sleep difficulty and associated
INSOMNIAS INSOMNIAS General criteria for insomnia A. Repeated difficulty with sleep initiation, duration, consolidation or quality. B. Adequate sleep opportunity, persistent sleep difficulty and associated
Copyright American Psychological Association
 Introduction Sleep is an essential part of life that most people take for granted. We assume that the mind and the body will naturally turn off when we decide to lie down in bed and rest. After about 8
Introduction Sleep is an essential part of life that most people take for granted. We assume that the mind and the body will naturally turn off when we decide to lie down in bed and rest. After about 8
Treating Insomnia in Primary Care. Judith R. Davidson Ph.D., C. Psych. Kingston Family Health Team
 Treating Insomnia in Primary Care Judith R. Davidson Ph.D., C. Psych. Kingston Family Health Team jdavidson@kfhn.net Disclosure statement Nothing to disclose A ruffled mind makes a restless pillow. ~ Charlotte
Treating Insomnia in Primary Care Judith R. Davidson Ph.D., C. Psych. Kingston Family Health Team jdavidson@kfhn.net Disclosure statement Nothing to disclose A ruffled mind makes a restless pillow. ~ Charlotte
Individual Planning: A Treatment Plan Overview for Individuals Sleep Disorder Problems.
 COURSES ARTICLE - THERAPYTOOLS.US Individual Planning: A Treatment Plan Overview for Individuals Sleep Disorder Problems. Individual Planning: A Treatment Plan Overview for Individuals Sleep Disorder Problems.
COURSES ARTICLE - THERAPYTOOLS.US Individual Planning: A Treatment Plan Overview for Individuals Sleep Disorder Problems. Individual Planning: A Treatment Plan Overview for Individuals Sleep Disorder Problems.
SLEEP DISORDERS CENTER QUESTIONNAIRE
 Carteret Health Care Patient's name DOB Gender: M F Date of Visit _ Referring physicians: Primary care providers: Please complete the following questionnaire by filling in the blanks and placing a check
Carteret Health Care Patient's name DOB Gender: M F Date of Visit _ Referring physicians: Primary care providers: Please complete the following questionnaire by filling in the blanks and placing a check
Insomnia. Learning Objectives. Disclosure 6/7/11. Research funding: NIH, Respironics, Embla Consulting: Elsevier
 Insomnia Teofilo Lee-Chiong MD Professor of Medicine National Jewish Health University of Colorado Denver School of Medicine Learning Objectives Learn about the causes of transient and chronic Learn how
Insomnia Teofilo Lee-Chiong MD Professor of Medicine National Jewish Health University of Colorado Denver School of Medicine Learning Objectives Learn about the causes of transient and chronic Learn how
 Sleep This factsheet is available in a downloadable PDF here. Table of Contents Introduction Insomnia How Long does Insomnia Last? How much Sleep should You get? Symptoms of Insomnia Causes of Insomnia
Sleep This factsheet is available in a downloadable PDF here. Table of Contents Introduction Insomnia How Long does Insomnia Last? How much Sleep should You get? Symptoms of Insomnia Causes of Insomnia
Sleep Insomnia Severity Index (SISI) Pittsburgh Sleep Quality Inventory. POMS Vigor subscale
 Physical GLOBAL HEALTH PROMIS completed already Sleep PROMIS-Sleep Sleep Insomnia Severity Index () Pittsburgh Sleep Quality Inventory 8 items 7 items 18 items Vigor Vigor subscale 6 items 1 Sleep- PROMIS
Physical GLOBAL HEALTH PROMIS completed already Sleep PROMIS-Sleep Sleep Insomnia Severity Index () Pittsburgh Sleep Quality Inventory 8 items 7 items 18 items Vigor Vigor subscale 6 items 1 Sleep- PROMIS
Cognitive-Behavioral Therapy for Insomnia
 Wisconsin Department of Health Services Wisconsin Public Psychiatry Network Teleconference (WPPNT) This teleconference is brought to you by the Wisconsin Department of Health Services (DHS) Bureau of Prevention,
Wisconsin Department of Health Services Wisconsin Public Psychiatry Network Teleconference (WPPNT) This teleconference is brought to you by the Wisconsin Department of Health Services (DHS) Bureau of Prevention,
WHOLE HEALTH: CHANGE THE CONVERSATION. Autogenic Training Clinical Tool
 Advancing Skills in the Delivery of Personalized, Proactive, Patient-Driven Care Autogenic Training Clinical Tool This document has been written for clinicians. The content was developed by the Integrative
Advancing Skills in the Delivery of Personalized, Proactive, Patient-Driven Care Autogenic Training Clinical Tool This document has been written for clinicians. The content was developed by the Integrative
Sleep & Relaxation. Session 1 Understanding Insomnia Sleep improvement techniques Try a new technique
 Sleep & Relaxation Sleep & Relaxation Session 1 Understanding Insomnia Sleep improvement techniques Try a new technique Session 2 Dealing with unhelpful thoughts Putting these techniques together for better
Sleep & Relaxation Sleep & Relaxation Session 1 Understanding Insomnia Sleep improvement techniques Try a new technique Session 2 Dealing with unhelpful thoughts Putting these techniques together for better
Sleep Center. Have you had a previous sleep study? Yes No If so, when and where? Name of facility Address
 Patient Label For office use only Appt date: Clinician: Sleep Center Main Campus Highlands Ranch Location 1400 Jackson Street 8671 S. Quebec St., Ste 120 Denver, CO 80206 Highlands Ranch, CO 80130 Leading
Patient Label For office use only Appt date: Clinician: Sleep Center Main Campus Highlands Ranch Location 1400 Jackson Street 8671 S. Quebec St., Ste 120 Denver, CO 80206 Highlands Ranch, CO 80130 Leading
Sleep Management in Parkinson s
 Sleep Management in Parkinson s Booklet 1 Introduction An introduction to Sleep Management in Parkinson s Sleep disturbances are commonly experienced by those with Parkinson s, and by the relatives and
Sleep Management in Parkinson s Booklet 1 Introduction An introduction to Sleep Management in Parkinson s Sleep disturbances are commonly experienced by those with Parkinson s, and by the relatives and
Insomnia. F r e q u e n t l y A s k e d Q u e s t i o n s
 Insomnia Q: What is insomnia? A: Insomnia is a common sleep disorder. If you have insomnia, you may: Lie awake for a long time and have trouble falling asleep Wake up a lot and have trouble returning to
Insomnia Q: What is insomnia? A: Insomnia is a common sleep disorder. If you have insomnia, you may: Lie awake for a long time and have trouble falling asleep Wake up a lot and have trouble returning to
ADHD clinic for adults Feedback on services for attention deficit hyperactivity disorder
 ADHD clinic for adults Feedback on services for attention deficit hyperactivity disorder Healthwatch Islington Healthwatch Islington is an independent organisation led by volunteers from the local community.
ADHD clinic for adults Feedback on services for attention deficit hyperactivity disorder Healthwatch Islington Healthwatch Islington is an independent organisation led by volunteers from the local community.
This is the published version of a paper published in Behavioural and Cognitive Psychotherapy.
 http://www.diva-portal.org This is the published version of a paper published in Behavioural and Cognitive Psychotherapy. Citation for the original published paper (version of record): Norell Clarke, A.,
http://www.diva-portal.org This is the published version of a paper published in Behavioural and Cognitive Psychotherapy. Citation for the original published paper (version of record): Norell Clarke, A.,
Cognitive behavioural therapy for insomnia
 Cognitive behavioural therapy for insomnia Item type Authors Citation Publisher Journal Article Ruth, Alan Ruth A. Cognitive behavioural therapy for insomnia. Nurs Gen Prac 2014 May 29-30, 32 Nursing in
Cognitive behavioural therapy for insomnia Item type Authors Citation Publisher Journal Article Ruth, Alan Ruth A. Cognitive behavioural therapy for insomnia. Nurs Gen Prac 2014 May 29-30, 32 Nursing in
Not sure if a talking therapy is for you?
 South Tyneside NHS Foundation Trust Primary Care Mental Health Service Not sure if a talking therapy is for you? Take a look at the different types of therapy we have available to find out more about them.
South Tyneside NHS Foundation Trust Primary Care Mental Health Service Not sure if a talking therapy is for you? Take a look at the different types of therapy we have available to find out more about them.
CBT in the Treatment of Persistent Insomnia in Patients with Cancer
 CBT in the Treatment of Persistent Insomnia in Patients with Cancer Colin A Espie University of Glasgow Sleep Centre Sackler Institute of Psychobiological Research University of Glasgow Scotland UK Outline
CBT in the Treatment of Persistent Insomnia in Patients with Cancer Colin A Espie University of Glasgow Sleep Centre Sackler Institute of Psychobiological Research University of Glasgow Scotland UK Outline
SLEEP QUESTIONNAIRE. Please briefly describe your sleep or sleep problem:
 SLEEP QUESTIONNAIRE Your answers to the following questions will help us to obtain a better understanding of your sleep problems. Please answer every question to the best of your ability. It is helpful
SLEEP QUESTIONNAIRE Your answers to the following questions will help us to obtain a better understanding of your sleep problems. Please answer every question to the best of your ability. It is helpful
Art Lift, Gloucestershire. Evaluation Report: Executive Summary
 Art Lift, Gloucestershire Evaluation Report: Executive Summary University of Gloucestershire September 2011 Evaluation Team: Dr Diane Crone (Lead), Elaine O Connell (Research Student), Professor David
Art Lift, Gloucestershire Evaluation Report: Executive Summary University of Gloucestershire September 2011 Evaluation Team: Dr Diane Crone (Lead), Elaine O Connell (Research Student), Professor David
Guideline for Adult Insomnia
 Guideline for Adult Insomnia Exclusions This guideline does not apply to: Children under the age of 18 Pregnant and lactating women Geriatric patients: While the general principles of the diagnosis and
Guideline for Adult Insomnia Exclusions This guideline does not apply to: Children under the age of 18 Pregnant and lactating women Geriatric patients: While the general principles of the diagnosis and
Optimal Sleep Using NeurOptimal -Insomnia Studies
 Optimal Sleep Using NeurOptimal -Insomnia Studies Edward B. O'Malley, PhD, FAASM Diplomate, American Board of Sleep Medicine Managing Director, Sleep HealthCare of CT Fairfield, CT eomalley@sleephelathcarect.com
Optimal Sleep Using NeurOptimal -Insomnia Studies Edward B. O'Malley, PhD, FAASM Diplomate, American Board of Sleep Medicine Managing Director, Sleep HealthCare of CT Fairfield, CT eomalley@sleephelathcarect.com
Non-epileptic attacks
 Non-epileptic attacks A short guide for patients and families Information for patients Neurology Psychotherapy Service What are non-epileptic attacks? Non-epileptic attacks are episodes in which people
Non-epileptic attacks A short guide for patients and families Information for patients Neurology Psychotherapy Service What are non-epileptic attacks? Non-epileptic attacks are episodes in which people
PULMONARY & CRITICAL CARE CONSULTANTS OF AUSTIN 1305 West 34 th Street, Suite 400, Austin, TX Phone: Fax:
 Name: Sex: Age: Date: Date of Birth Height Weight Neck size Referring Physician: Primary Care MD: Main Sleep Complaint(s) trouble falling asleep trouble remaining asleep excessive sleepiness during the
Name: Sex: Age: Date: Date of Birth Height Weight Neck size Referring Physician: Primary Care MD: Main Sleep Complaint(s) trouble falling asleep trouble remaining asleep excessive sleepiness during the
Cognitive Behavioral Therapy for Insomnia. Melanie K. Leggett, PhD, CBSM Duke University Medical Center
 Cognitive Behavioral Therapy for Insomnia Melanie K. Leggett, PhD, CBSM Duke University Medical Center Disclosures I have no relevant financial relationship with the manufacturers of any commercial products
Cognitive Behavioral Therapy for Insomnia Melanie K. Leggett, PhD, CBSM Duke University Medical Center Disclosures I have no relevant financial relationship with the manufacturers of any commercial products
Autogenic Dynamics: Physiological, Psychological, and Research Matters Autogenic Training a review of the Meta-Analysis by Stetter and Kupper 2002
 Autogenic Dynamics: Physiological, Psychological, and Research Matters Autogenic Training a review of the Meta-Analysis by Stetter and Kupper 2002 l Preamble This paper reviews some of the more recent
Autogenic Dynamics: Physiological, Psychological, and Research Matters Autogenic Training a review of the Meta-Analysis by Stetter and Kupper 2002 l Preamble This paper reviews some of the more recent
Pittsburgh Insomnia Rating Scale University of Pittsburgh School of Medicine, Department of Psychiatry, All Rights Reserved.
 Pittsburgh Insomnia Rating Scale University of Pittsburgh School of Medicine, Department of Psychiatry, 2001. All Rights Reserved. Name ID# Date A. Overall sleep quality: Consider the quality of your sleep
Pittsburgh Insomnia Rating Scale University of Pittsburgh School of Medicine, Department of Psychiatry, 2001. All Rights Reserved. Name ID# Date A. Overall sleep quality: Consider the quality of your sleep
Associated Neurological Specialties and Sleep Disorder Center
 Sleep Center Questionnaire Name: Sex: Age: Date: Date of Birth: Height: Weight: Neck Size: Primary Care Physician: Referring Physician: Main Sleep Issues/Complaints Trouble falling asleep Trouble staying
Sleep Center Questionnaire Name: Sex: Age: Date: Date of Birth: Height: Weight: Neck Size: Primary Care Physician: Referring Physician: Main Sleep Issues/Complaints Trouble falling asleep Trouble staying
Sleep Medicine Questionnaire
 Please bring this completed questionnaire with you to your sleep medicine appointment. Our sleep medicine staff strives to understand your sleep symptoms, which may be complex in nature. Thank you for
Please bring this completed questionnaire with you to your sleep medicine appointment. Our sleep medicine staff strives to understand your sleep symptoms, which may be complex in nature. Thank you for
Improving Your Sleep Course. Session 4 Dealing With a Racing Mind
 Improving Your Sleep Course Session 4 Dealing With a Racing Mind Session 4 Dealing With a Racing Mind This session will: Help you to learn ways of overcoming the mental alertness, repetitive thoughts and
Improving Your Sleep Course Session 4 Dealing With a Racing Mind Session 4 Dealing With a Racing Mind This session will: Help you to learn ways of overcoming the mental alertness, repetitive thoughts and
SLEEP QUESTIONNAIRE. Name: Sex: Age: Date: DOB: / / SSN: - - Address: Referring Physician: Family Physician: Height: Weight: Neck Size: Phone:
 SLEEP QUESTIONNAIRE Name: Sex: Age: Date: DOB: / / SSN: - - Address: Referring Physician: Family Physician: Height: Weight: Neck Size: Phone: Please fill in the blanks, and check appropriate areas on the
SLEEP QUESTIONNAIRE Name: Sex: Age: Date: DOB: / / SSN: - - Address: Referring Physician: Family Physician: Height: Weight: Neck Size: Phone: Please fill in the blanks, and check appropriate areas on the
Improving Your Sleep Course. Session 1 Understanding Sleep and Assessing Your Difficulties
 Improving Your Sleep Course Session 1 Understanding Sleep and Assessing Your Difficulties Course Information Session Details Sessions Session 1 Session 2 Session 3 Session 4 Optional Review Session 5 Session
Improving Your Sleep Course Session 1 Understanding Sleep and Assessing Your Difficulties Course Information Session Details Sessions Session 1 Session 2 Session 3 Session 4 Optional Review Session 5 Session
11/15/2017. Disclosure. What is an EAP and History of Biofeedback at UCLA s Staff and Faculty Counseling Center
 From Good to Great: The Use of Biofeedback in Employee Assistance Programs as a Tool to Build Resilience in the Workplace by: Dr. J. Cherbosque. PhD, CEAP, Dr. S. Sideroff, PhD, and Beth Argus, MFT, CEAP
From Good to Great: The Use of Biofeedback in Employee Assistance Programs as a Tool to Build Resilience in the Workplace by: Dr. J. Cherbosque. PhD, CEAP, Dr. S. Sideroff, PhD, and Beth Argus, MFT, CEAP
YOU REALLY NEED TO SLEEP: Several methods to improve your sleep
 YOU REALLY NEED TO SLEEP: Several methods to improve your sleep Sleep is essential to our well-being. When humans fail to get good sleep over a period of time, numerous problems can occur. CAN T SLEEP!!
YOU REALLY NEED TO SLEEP: Several methods to improve your sleep Sleep is essential to our well-being. When humans fail to get good sleep over a period of time, numerous problems can occur. CAN T SLEEP!!
Sleep Hygiene. William M. DeMayo, M.D. John P. Murtha Neuroscience and Pain Institute Conemaugh Health System Johnstown, PA
 Sleep Hygiene William M. DeMayo, M.D. John P. Murtha Neuroscience and Pain Institute Conemaugh Health System Johnstown, PA Why Is Sleep Important? Symptoms of Sleep Deprivation: Irritability / Poor Stress
Sleep Hygiene William M. DeMayo, M.D. John P. Murtha Neuroscience and Pain Institute Conemaugh Health System Johnstown, PA Why Is Sleep Important? Symptoms of Sleep Deprivation: Irritability / Poor Stress
New Patient Sleep Intake
 New Patient Sleep Intake Name: Date of Birth: Primary Care Physician: Date of Visit: Referring Physician and/or Other Physicians: Retail Pharmacy: Mail Order Pharmacy: Address: Mail Order Phone #: Phone
New Patient Sleep Intake Name: Date of Birth: Primary Care Physician: Date of Visit: Referring Physician and/or Other Physicians: Retail Pharmacy: Mail Order Pharmacy: Address: Mail Order Phone #: Phone
Study on sleep quality and associated psychosocial factors among elderly in a rural population of Kerala, India
 International Journal of Community Medicine and Public Health George S et al. Int J Community Med Public Health. 2018 Feb;5(2):526-531 http://www.ijcmph.com pissn 2394-6032 eissn 2394-6040 Original Research
International Journal of Community Medicine and Public Health George S et al. Int J Community Med Public Health. 2018 Feb;5(2):526-531 http://www.ijcmph.com pissn 2394-6032 eissn 2394-6040 Original Research
Oral Medicine Psychology Service
 Oral Medicine Psychology Service Information for patients Introduction The team in Oral Medicine includes oral medicine consultants, clinical fellows, clinical psychologists, specialist nurses and pain
Oral Medicine Psychology Service Information for patients Introduction The team in Oral Medicine includes oral medicine consultants, clinical fellows, clinical psychologists, specialist nurses and pain
INDEX. Group psychotherapy, described, 97 Group stimulus control, 29-47; see also Stimulus control (group setting)
 Index Abdominal breathing, 70; see also Breathing; Relaxation therapy Activation, sleep drive/responsivity, 6-9 Age level; see also Elderly circadian rhythms and, 68-69 delayed sleep phase syndrome and,
Index Abdominal breathing, 70; see also Breathing; Relaxation therapy Activation, sleep drive/responsivity, 6-9 Age level; see also Elderly circadian rhythms and, 68-69 delayed sleep phase syndrome and,
RESTore TM. Clinician Manual for Single User. Insomnia and Sleep Disorders. A step by step manual to help you guide your clients through the program
 RESTore TM Insomnia and Sleep Disorders Clinician Manual for Single User A step by step manual to help you guide your clients through the program Version 10 July, 2016 Table of Contents Introduction...
RESTore TM Insomnia and Sleep Disorders Clinician Manual for Single User A step by step manual to help you guide your clients through the program Version 10 July, 2016 Table of Contents Introduction...
Dr June Brown Senior Lecturer in Clinical Psychology Institute of Psychiatry
 Dr June Brown Senior Lecturer in Clinical Psychology Institute of Psychiatry Background to insomnia Design of study Methods Results Conclusions Where next? Insomnia is the most common mental health symptom
Dr June Brown Senior Lecturer in Clinical Psychology Institute of Psychiatry Background to insomnia Design of study Methods Results Conclusions Where next? Insomnia is the most common mental health symptom
President s Message. Patrick R. Steffen, Ph.D. Winter 2014 Contents: From the Editor
 ISMA-USA Newsletter President s Message Patrick R. Steffen, Ph.D. Winter 2014 Winter 2014 Contents: From the Editor 2 Getting to Know You: Dr. Tom McCutchen 2 Embracing Stress in Your Life: Dr. Tom McCutchen
ISMA-USA Newsletter President s Message Patrick R. Steffen, Ph.D. Winter 2014 Winter 2014 Contents: From the Editor 2 Getting to Know You: Dr. Tom McCutchen 2 Embracing Stress in Your Life: Dr. Tom McCutchen
Early Intervention Guidelines for Supporting School Anxiety. Information for Schools, Professionals and Parents/Carers
 Early Intervention Guidelines for Supporting School Anxiety Information for Schools, Professionals and Parents/Carers Aims To outline what anxiety is and when it becomes problematic for children and young
Early Intervention Guidelines for Supporting School Anxiety Information for Schools, Professionals and Parents/Carers Aims To outline what anxiety is and when it becomes problematic for children and young
This copyright in this form is owned by the University of Pittsburgh and may be reprinted without charge only for non-commercial research and
 This copyright in this form is owned by the University of Pittsburgh and may be reprinted without charge only for non-commercial research and educational purposes. You may not make changes or modifications
This copyright in this form is owned by the University of Pittsburgh and may be reprinted without charge only for non-commercial research and educational purposes. You may not make changes or modifications
Objectives. Disclosure. APNA 26th Annual Conference Session 2017: November 8, Kurtz 1. The speaker has no conflicts of interest to disclose
 Christine Kurtz, DNP, PMHCNS BC Valparaiso University Disclosure The speaker has no conflicts of interest to disclose Objectives The learner will Describe the rationale for and five therapies of CBT I
Christine Kurtz, DNP, PMHCNS BC Valparaiso University Disclosure The speaker has no conflicts of interest to disclose Objectives The learner will Describe the rationale for and five therapies of CBT I
Case Study 3. DSM Symptoms Present: [DSM criteria as evidenced by (with evidence from case study)]
![Case Study 3. DSM Symptoms Present: [DSM criteria as evidenced by (with evidence from case study)] Case Study 3. DSM Symptoms Present: [DSM criteria as evidenced by (with evidence from case study)]](/thumbs/87/96891346.jpg) Case Study 3 DSM Symptoms Present: [DSM criteria as evidenced by (with evidence from case study)] Insomnia Related to Generalized Anxiety Disorder A. The predominant complaint is difficulty initiating
Case Study 3 DSM Symptoms Present: [DSM criteria as evidenced by (with evidence from case study)] Insomnia Related to Generalized Anxiety Disorder A. The predominant complaint is difficulty initiating
Sleep and Ageing. Siobhan Banks PhD. Body and Brain at Work, Centre for Sleep Research University of South Australia
 Sleep and Ageing Siobhan Banks PhD Body and Brain at Work, Centre for Sleep Research University of South Australia Health and Active Ageing, 22 nd September 2015 Sleep and Aging How does sleep change as
Sleep and Ageing Siobhan Banks PhD Body and Brain at Work, Centre for Sleep Research University of South Australia Health and Active Ageing, 22 nd September 2015 Sleep and Aging How does sleep change as
VCU CENTER FOR SLEEP MEDICINE NEW PATIENT QUESTIONNAIRE
 VCU CENTER FOR SLEEP MEDICINE NEW PATIENT QUESTIONNAIRE Name:_ DOB: MR#: Date: Sex: Age: Height: Referring physician: Primary care physician: What is your primary sleep problem? Please explain any strange
VCU CENTER FOR SLEEP MEDICINE NEW PATIENT QUESTIONNAIRE Name:_ DOB: MR#: Date: Sex: Age: Height: Referring physician: Primary care physician: What is your primary sleep problem? Please explain any strange
Pain-related Distress: Recognition and Appropriate Interventions. Tamar Pincus Professor in psychology Royal Holloway University of London
 Pain-related Distress: Recognition and Appropriate Interventions Tamar Pincus Professor in psychology Royal Holloway University of London Remit (and limitations) of presentation Mostly, research in low
Pain-related Distress: Recognition and Appropriate Interventions Tamar Pincus Professor in psychology Royal Holloway University of London Remit (and limitations) of presentation Mostly, research in low
Sleeping your way to better mental health
 Sleeping your way to better mental health Liverpool PWP Master Class 28 th January 2015 Dr Sophie Bostock sophie@sleepio.com Sleep Matters What we ll cover today.. 1. Sleep and mental health are intimately
Sleeping your way to better mental health Liverpool PWP Master Class 28 th January 2015 Dr Sophie Bostock sophie@sleepio.com Sleep Matters What we ll cover today.. 1. Sleep and mental health are intimately
Managing Sleep Problems after Cancer
 Managing Sleep Problems after Cancer For cancer survivors Read this resource to learn about: What a sleep problem is What causes it What you can do to improve your sleep When to talk to your doctor Please
Managing Sleep Problems after Cancer For cancer survivors Read this resource to learn about: What a sleep problem is What causes it What you can do to improve your sleep When to talk to your doctor Please
Beyond Sleep Hygiene: Behavioral Approaches to Insomnia
 Beyond Sleep Hygiene: Behavioral Approaches to Insomnia Rocky Garrison, PhD, CBSM Damon Michael Williams, RN, PMHNP-BC In House Counseling Laughing Heart LLC 10201 SE Main St. 12 SE 14 th Ave. Suite 10
Beyond Sleep Hygiene: Behavioral Approaches to Insomnia Rocky Garrison, PhD, CBSM Damon Michael Williams, RN, PMHNP-BC In House Counseling Laughing Heart LLC 10201 SE Main St. 12 SE 14 th Ave. Suite 10
Managing Insomnia: an example sequence of CBT-based sessions for sleep treatment
 Managing Insomnia: an example sequence of CBT-based sessions for sleep treatment Session 1: Introduction and sleep assessment -Assess sleep problem (option: have client complete 20-item sleep questionnaire).
Managing Insomnia: an example sequence of CBT-based sessions for sleep treatment Session 1: Introduction and sleep assessment -Assess sleep problem (option: have client complete 20-item sleep questionnaire).
Depression Fact Sheet
 Depression Fact Sheet Please feel free to alter and use this fact sheet to spread awareness of depression, its causes and symptoms, and what can be done. What is Depression? Depression is an illness that
Depression Fact Sheet Please feel free to alter and use this fact sheet to spread awareness of depression, its causes and symptoms, and what can be done. What is Depression? Depression is an illness that
Sleep Center New Patient Questionnaire
 For office use only Appt date: Sleep Center Clinician: Main Campus Highlands Ranch Location 1400 Jackson Street 8671 S. Quebec St., Ste 120 Denver, CO 80206 Highlands Ranch, CO 80130 #1 respiratory hospital
For office use only Appt date: Sleep Center Clinician: Main Campus Highlands Ranch Location 1400 Jackson Street 8671 S. Quebec St., Ste 120 Denver, CO 80206 Highlands Ranch, CO 80130 #1 respiratory hospital
Sleep History Questionnaire B/P / Pulse: Neck Circum Wgt: Pulse Ox
 2700 Campus Drive, Ste 100 2412 E 117 th Street Plymouth, MN 55441 Burnsville, MN 55337 P 763.519.0634 F 763.519.0636 P 952.431.5011 F 952.431.5013 www.whitneysleepcenter.com Sleep History Questionnaire
2700 Campus Drive, Ste 100 2412 E 117 th Street Plymouth, MN 55441 Burnsville, MN 55337 P 763.519.0634 F 763.519.0636 P 952.431.5011 F 952.431.5013 www.whitneysleepcenter.com Sleep History Questionnaire
Introduction into Psychiatric Disorders. Dr Jon Spear- Psychiatrist
 Introduction into Psychiatric Disorders Dr Jon Spear- Psychiatrist Content Stress Major depressive disorder Adjustment disorder Generalised anxiety disorder Post traumatic stress disorder Borderline personality
Introduction into Psychiatric Disorders Dr Jon Spear- Psychiatrist Content Stress Major depressive disorder Adjustment disorder Generalised anxiety disorder Post traumatic stress disorder Borderline personality
Article printed from
 What Are Sleep Disorders? Sleep disorders are conditions that affect how much and how well you sleep. The causes range from poor habits that keep you awake to medical problems that disrupt your sleep cycle.
What Are Sleep Disorders? Sleep disorders are conditions that affect how much and how well you sleep. The causes range from poor habits that keep you awake to medical problems that disrupt your sleep cycle.
WELCOME TO THE NORTHSHORE UNIVERSITY HEALTHSYSTEM SLEEP CENTERS
 WELCOME TO THE NORTHSHORE UNIVERSITY HEALTHSYSTEM SLEEP CENTERS Prior to your office visit, we request that you complete this questionnaire. It asks questions not only about your sleeping habits and behavior
WELCOME TO THE NORTHSHORE UNIVERSITY HEALTHSYSTEM SLEEP CENTERS Prior to your office visit, we request that you complete this questionnaire. It asks questions not only about your sleeping habits and behavior
Overcoming Extreme Challenges. How NeurOptimal can be an answer for our veterans
 Overcoming Extreme Challenges How NeurOptimal can be an answer for our veterans Operation giving back! Astonishing improvement of our clients suffering from trauma.! High need of help for veterans and
Overcoming Extreme Challenges How NeurOptimal can be an answer for our veterans Operation giving back! Astonishing improvement of our clients suffering from trauma.! High need of help for veterans and
Revised Standards. S 1a: The service routinely collects data on age, gender and ethnicity for each person referred for psychological therapy.
 Revised Standards S 1a: The service routinely collects data on age, gender and ethnicity for each person referred for psychological therapy. S1b: People starting treatment with psychological therapy are
Revised Standards S 1a: The service routinely collects data on age, gender and ethnicity for each person referred for psychological therapy. S1b: People starting treatment with psychological therapy are
Psychological Sleep Services Sleep Assessment
 Psychological Sleep Services Sleep Assessment Name Date **************************************************** Insomnia Severity Index For each question, please CIRCLE the number that best describes your
Psychological Sleep Services Sleep Assessment Name Date **************************************************** Insomnia Severity Index For each question, please CIRCLE the number that best describes your
Sleep Questionnaire Name: Sex: Age: Da te: Da te of birth: Height: Weight: Neck siz e: Ref erring Physician: Primary Car e MD:
 www.myvcmf.com 1133 E. Stanley Blvd., Suite 101 Livermore, CA 94550 925 454-4280 5725 W. Las Positas Blvd., Suite 110 Pleasanton, CA 94588 925-416-6767 Sleep Questionnaire Name: Sex: Age: Da te: Da te
www.myvcmf.com 1133 E. Stanley Blvd., Suite 101 Livermore, CA 94550 925 454-4280 5725 W. Las Positas Blvd., Suite 110 Pleasanton, CA 94588 925-416-6767 Sleep Questionnaire Name: Sex: Age: Da te: Da te
THIBODAUX REGIONAL SLEEP DISORDERS CENTER 604 N ACADIA ROAD, Suite 210 THIBODAUX, LA 70301
 Name:_ Date: Address: Phone (home): Work: Marital Status: Date of Birth: Height: Weight: In case of emergency contact: ************************************************************************ Social Security#:
Name:_ Date: Address: Phone (home): Work: Marital Status: Date of Birth: Height: Weight: In case of emergency contact: ************************************************************************ Social Security#:
Coping with Advanced Stage Heart Failure and LVAD/Transplant. Kristin Kuntz, Ph.D. Department of Psychiatry and Behavioral Health
 Coping with Advanced Stage Heart Failure and LVAD/Transplant Kristin Kuntz, Ph.D. Department of Psychiatry and Behavioral Health What is Health Psychology? Health psychology focuses on how biology, psychology,
Coping with Advanced Stage Heart Failure and LVAD/Transplant Kristin Kuntz, Ph.D. Department of Psychiatry and Behavioral Health What is Health Psychology? Health psychology focuses on how biology, psychology,
Chronic Insomnia: DSM - V. Insomnia DSM - V. Patient Symptoms. Insomnia: Assessment and Overview of Management. Insomnia Management in the Digital Age
 Insomnia Management in the Digital Age Dr Anup Desai Sleep & Respiratory Medicine MBBS (syd), PhD (syd), FRACP Senior Staff Specialist, POW Hospital Medical Director, Sydney Sleep Centre Senior Lecturer,
Insomnia Management in the Digital Age Dr Anup Desai Sleep & Respiratory Medicine MBBS (syd), PhD (syd), FRACP Senior Staff Specialist, POW Hospital Medical Director, Sydney Sleep Centre Senior Lecturer,
Hearing Voices Group. Introduction. And. Background information. David DddddFreemanvvvvvvvvv
 Hearing Voices Group Introduction And Background information David DddddFreemanvvvvvvvvv Contents Hearing Voices Group Rationale Inclusion criteria for hearing voices group Structure of Group Process The
Hearing Voices Group Introduction And Background information David DddddFreemanvvvvvvvvv Contents Hearing Voices Group Rationale Inclusion criteria for hearing voices group Structure of Group Process The
604 NORTH ACADIA ROAD, Suite 210 THIBODAUX, LA SLEEP HISTORY QUESTIONNAIRE
 604 NORTH ACADIA ROAD, Suite 210 THIBODAUX, LA 70301 985-493-4759 SLEEP HISTORY QUESTIONNAIRE DATE: / / NAME: AGE (First) (Middle) (Last) ADDRESS: (Street) (City) (State) (Zip) PHONE: Home( ) Work:( )
604 NORTH ACADIA ROAD, Suite 210 THIBODAUX, LA 70301 985-493-4759 SLEEP HISTORY QUESTIONNAIRE DATE: / / NAME: AGE (First) (Middle) (Last) ADDRESS: (Street) (City) (State) (Zip) PHONE: Home( ) Work:( )
Nebraska Bariatric Medicine 8207 Northwoods Dr., Suite 101 Lincoln, NE MEDICAL HISTORY
 Nebraska Bariatric Medicine 8207 rthwoods Dr., Suite 101 Lincoln, NE 68505 MEDICAL HISTORY Name Today s Date The following page allows you to complete what we call a weight timeline. This is a very valuable
Nebraska Bariatric Medicine 8207 rthwoods Dr., Suite 101 Lincoln, NE 68505 MEDICAL HISTORY Name Today s Date The following page allows you to complete what we call a weight timeline. This is a very valuable
Awake. Rapid Eye Movement (REM) or dreaming sleep. Normally, we go through Stages 2 to 5 a few times every night, before waking up in the morning.
 Narcolepsy Need-to-Know Guide Childhood Narcolepsy This guide provides information for parents or carers of children and young people with narcolepsy. It aims to promote a clear understanding of the condition
Narcolepsy Need-to-Know Guide Childhood Narcolepsy This guide provides information for parents or carers of children and young people with narcolepsy. It aims to promote a clear understanding of the condition
Problem Solving
 www.working-minds.org.uk Problem Solving Problem Solving The psychological importance of effective problem solving is very underestimated and is often taken for granted. As human beings, we assume that
www.working-minds.org.uk Problem Solving Problem Solving The psychological importance of effective problem solving is very underestimated and is often taken for granted. As human beings, we assume that
Bi-directional Relationship Between Poor Sleep and Work-related Stress: Management through transformational leadership and work organization
 Bi-directional Relationship Between Poor Sleep and Work-related Stress: Management through transformational leadership and work organization Sleep & its Importance Most vital episode of human life! Psychological
Bi-directional Relationship Between Poor Sleep and Work-related Stress: Management through transformational leadership and work organization Sleep & its Importance Most vital episode of human life! Psychological
Baptist Health Floyd 1850 State Street New Albany, IN Sleep Disorders Center Lung & Sleep Specialists. Date of Birth: Age:
 Page 1 of 7 GENERAL INFORMATION Name: Date of Birth: Age: Social Security #: Sex: Height: Weight: Address: City: State: Zip: Home Phone: Cell Phone: Work Phone: Employer s Name: Marital Status: Married
Page 1 of 7 GENERAL INFORMATION Name: Date of Birth: Age: Social Security #: Sex: Height: Weight: Address: City: State: Zip: Home Phone: Cell Phone: Work Phone: Employer s Name: Marital Status: Married
Goals. Brief Behavioural Interventions for Insomnia. What is insomnia? RCPsych International Congress, London 2014
 Brief Behavioural Interventions for Insomnia RCPsych International Congress, London 2014 Dr David O Regan PhD MRCPsych, ST5 Higher Trainee Insomnia Clinic, Royal London Hospital for Integrated Medicine
Brief Behavioural Interventions for Insomnia RCPsych International Congress, London 2014 Dr David O Regan PhD MRCPsych, ST5 Higher Trainee Insomnia Clinic, Royal London Hospital for Integrated Medicine
The Reasons for Insomnia and the Ways to Fight It
 The Reasons for Insomnia and the Ways to Fight It Insomnia is a relatively common sleep disorder, which is indicated by insufficient duration or unsatisfactory quality of sleep over an extended period.
The Reasons for Insomnia and the Ways to Fight It Insomnia is a relatively common sleep disorder, which is indicated by insufficient duration or unsatisfactory quality of sleep over an extended period.
Biopsychosocial Characteristics of Somatoform Disorders
 Contemporary Psychiatric-Mental Health Nursing Chapter 19 Somatoform and Sleep Disorders Biopsychosocial Characteristics of Somatoform Disorders Unconscious transformation of emotions into physical symptoms
Contemporary Psychiatric-Mental Health Nursing Chapter 19 Somatoform and Sleep Disorders Biopsychosocial Characteristics of Somatoform Disorders Unconscious transformation of emotions into physical symptoms
Case Study. Salus. May 2010
 Case Study Salus May 2010 Background Based within Coatbridge, Salus consists of one of the largest NHS based multidisciplinary teams in Scotland. Through its various services Salus Case Management Services
Case Study Salus May 2010 Background Based within Coatbridge, Salus consists of one of the largest NHS based multidisciplinary teams in Scotland. Through its various services Salus Case Management Services
SLEEP & MEDICAL HISTORY QUESTIONNAIRE
 SLEEP & MEDICAL HISTORY QUESTIONNAIRE Patient Name Sex Age Date Please complete the following questionnaire by placing a check in the appropriate areas and filling in the blanks. My Main Sleep Complaint(s)
SLEEP & MEDICAL HISTORY QUESTIONNAIRE Patient Name Sex Age Date Please complete the following questionnaire by placing a check in the appropriate areas and filling in the blanks. My Main Sleep Complaint(s)
Chronic Fatigue Syndrome (CFS) / Myalgic Encephalomyelitis/Encephalopathy (ME)
 Chronic Fatigue Syndrome (CFS) / Myalgic Encephalomyelitis/Encephalopathy (ME) This intervention (and hence this listing of competences) assumes that practitioners are familiar with, and able to deploy,
Chronic Fatigue Syndrome (CFS) / Myalgic Encephalomyelitis/Encephalopathy (ME) This intervention (and hence this listing of competences) assumes that practitioners are familiar with, and able to deploy,
Cognitive Behavioral Therapy for Chronic Insomnia: State of the Science Versus Current Clinical
 Running Title: Cognitive Behavioral Therapy for Chronic Insomnia Cognitive Behavioral Therapy for Chronic Insomnia: State of the Science Versus Current Clinical Practices This article was published online
Running Title: Cognitive Behavioral Therapy for Chronic Insomnia Cognitive Behavioral Therapy for Chronic Insomnia: State of the Science Versus Current Clinical Practices This article was published online
Developing a new treatment approach to binge eating and weight management. Clinical Psychology Forum, Number 244, April 2013.
 Developing a new treatment approach to binge eating and weight management Clinical Psychology Forum, Number 244, April 2013 Dr Marie Prince 1 Contents Service information Binge Eating Disorder Binge Eating
Developing a new treatment approach to binge eating and weight management Clinical Psychology Forum, Number 244, April 2013 Dr Marie Prince 1 Contents Service information Binge Eating Disorder Binge Eating
Exposure Therapy. in Low Intensity CBT. Marie Chellingsworth, Dr Paul Farrand & Gemma Wilson. Marie Chellingsworth, Dr Paul Farrand & Gemma Wilson
 Exposure Therapy in Low Intensity CBT Marie Chellingsworth, Dr Paul Farrand & Gemma Wilson CONTENTS Part 1 What is Exposure Therapy? Exposure Therapy Stages Part 2 Doing Exposure Therapy The Four Rules
Exposure Therapy in Low Intensity CBT Marie Chellingsworth, Dr Paul Farrand & Gemma Wilson CONTENTS Part 1 What is Exposure Therapy? Exposure Therapy Stages Part 2 Doing Exposure Therapy The Four Rules
Individual Planning: A Treatment Plan Overview for Individuals with Somatization Disorder
 COURSES ARTICLE - THERAPYTOOLS.US Individual Planning: A Treatment Plan Overview for Individuals with Somatization Disorder Individual Planning: A Treatment Plan Overview for Individuals with Somatization
COURSES ARTICLE - THERAPYTOOLS.US Individual Planning: A Treatment Plan Overview for Individuals with Somatization Disorder Individual Planning: A Treatment Plan Overview for Individuals with Somatization
How To Cure Insomnia: Discover How To Cure Insomnia Without Drug Or Alcohol, How To Get A Good Night's Sleep And Be Well Rested For Life By Sally M.
 How To Cure Insomnia: Discover How To Cure Insomnia Without Drug Or Alcohol, How To Get A Good Night's Sleep And Be Well Rested For Life By Sally M. Dennis Lack of Sleep and the Immune System - WebMD -
How To Cure Insomnia: Discover How To Cure Insomnia Without Drug Or Alcohol, How To Get A Good Night's Sleep And Be Well Rested For Life By Sally M. Dennis Lack of Sleep and the Immune System - WebMD -
Coach on Call. Please give me a call if you have more questions about this or other topics.
 Coach on Call It was great to talk with you. Thank you for your interest in. I hope you find this tip sheet helpful. Please give me a call if you have more questions about this or other topics. As your
Coach on Call It was great to talk with you. Thank you for your interest in. I hope you find this tip sheet helpful. Please give me a call if you have more questions about this or other topics. As your
Sleep Disorders. Guidance for Primary Care. National Advisory Group for Respiratory Managed Clinical Networks
 Sleep Disorders Guidance for Primary Care National Advisory Group for Respiratory Managed Clinical Networks Presentation Patient complaining of difficulty sleeping, ongoing fatigue, poor concentration
Sleep Disorders Guidance for Primary Care National Advisory Group for Respiratory Managed Clinical Networks Presentation Patient complaining of difficulty sleeping, ongoing fatigue, poor concentration
Homeopathy FAQ (November 2015)
 Homeopathy FAQ (November 2015) What's Homeopathy and who uses the service? Homeopathy is the system of medicine which is based on the principle that you can treat like with like, that is, a substance which
Homeopathy FAQ (November 2015) What's Homeopathy and who uses the service? Homeopathy is the system of medicine which is based on the principle that you can treat like with like, that is, a substance which
Sleep Health Center. You have been scheduled for an Insomnia Treatment Program consultation to further discuss your
 Sleep Health Center You have been scheduled for an Insomnia Treatment Program consultation to further discuss your sleep. In the week preceding your appointment, please take the time to complete the enclosed
Sleep Health Center You have been scheduled for an Insomnia Treatment Program consultation to further discuss your sleep. In the week preceding your appointment, please take the time to complete the enclosed
Sleep Self-Assessment
 We are pleased you are taking the time to become more aware of your sleep patterns and discover strategies for improving your sleep. You deserve to get a good night s sleep we re here to help! The following
We are pleased you are taking the time to become more aware of your sleep patterns and discover strategies for improving your sleep. You deserve to get a good night s sleep we re here to help! The following
Living well with and beyond cancer Information, support and practical advice to help you through treatment and beyond
 Living well with and beyond cancer Information, support and practical advice to help you through treatment and beyond Exceptional healthcare, personally delivered Introduction to this booklet Receiving
Living well with and beyond cancer Information, support and practical advice to help you through treatment and beyond Exceptional healthcare, personally delivered Introduction to this booklet Receiving
Assessment and management of selfharm
 Assessment and management of selfharm procedure Version: 1.1 Consultation Approved by: Medical Director, CAMHS Director, Director of Quality, Patient Experience and Adult services Medical Director Date
Assessment and management of selfharm procedure Version: 1.1 Consultation Approved by: Medical Director, CAMHS Director, Director of Quality, Patient Experience and Adult services Medical Director Date
Fatigue management guidelines
 Contents Introduction...2 1. What is the purpose of this guide?...2 2. What is fatigue?...3 3. Why does fatigue matter to taxi drivers?...3 4. Fatigue management responsibilities for drivers... 3 5. Effects
Contents Introduction...2 1. What is the purpose of this guide?...2 2. What is fatigue?...3 3. Why does fatigue matter to taxi drivers?...3 4. Fatigue management responsibilities for drivers... 3 5. Effects
Using Hypnotherapy & Hypnosis To Reduce Insomnia & Sleep Disorders
 Using Hypnotherapy & Hypnosis To Reduce Insomnia & Sleep Disorders As A General Rule, Think Of All Symptoms Such as Sleep Disorders & Insomnia From Two Perspectives How Can I Treat That Problem? How Can
Using Hypnotherapy & Hypnosis To Reduce Insomnia & Sleep Disorders As A General Rule, Think Of All Symptoms Such as Sleep Disorders & Insomnia From Two Perspectives How Can I Treat That Problem? How Can
Sleep History Questionnaire. Sleep Disorders Center Duke University Medical Center. General Information. Age: Sex: F M (select one)
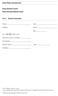 Sleep History Questionnaire Sleep Disorders Center Duke University Medical Center Part I: General Information Name: Address: Date: Phone: Age: Sex: F M (select one) Education (years of school): Occupation:
Sleep History Questionnaire Sleep Disorders Center Duke University Medical Center Part I: General Information Name: Address: Date: Phone: Age: Sex: F M (select one) Education (years of school): Occupation:
Are Somatisation Disorders any use to clinicians or patients? February 13th 2013 Charlotte Feinmann
 Are Somatisation Disorders any use to clinicians or patients? February 13th 2013 Charlotte Feinmann Outline Context and Definitions Changing Classification Changing Medical Attitudes Understanding Psychological
Are Somatisation Disorders any use to clinicians or patients? February 13th 2013 Charlotte Feinmann Outline Context and Definitions Changing Classification Changing Medical Attitudes Understanding Psychological
Depression, Anxiety, and the Adolescent Athlete: Introduction to Identification and Treatment
 Depression, Anxiety, and the Adolescent Athlete: Introduction to Identification and Treatment Jamie E. Pardini, PhD Sports Medicine and Concussion Specialists Banner University Medical Center-Phoenix University
Depression, Anxiety, and the Adolescent Athlete: Introduction to Identification and Treatment Jamie E. Pardini, PhD Sports Medicine and Concussion Specialists Banner University Medical Center-Phoenix University
SEPTEMBER 2010 Recovery discussion Topic Boundaries
 SEPTEMBER 2010 Recovery discussion Topic Boundaries One of the differences between Peers and other clinical staff is the language that we use. Peer based learning and literature talks about people and
SEPTEMBER 2010 Recovery discussion Topic Boundaries One of the differences between Peers and other clinical staff is the language that we use. Peer based learning and literature talks about people and
Dr Alex Bartle. Sleep Well Clinic
 Dr Alex Bartle Sleep Well Clinic Overview of Sleep Disorders Sleep: Why bother. Effect of Poor Quality or reduced Quantity of Sleep Common Sleep Disorders Management of Insomnia Medication vs CBTi Conclusion
Dr Alex Bartle Sleep Well Clinic Overview of Sleep Disorders Sleep: Why bother. Effect of Poor Quality or reduced Quantity of Sleep Common Sleep Disorders Management of Insomnia Medication vs CBTi Conclusion
