GUIDELINES FOR MANAGING INSOMNIA IN PALLIATIVE CARE
|
|
|
- Griselda Cobb
- 6 years ago
- Views:
Transcription
1 GUIDELINES FOR MANAGING INSOMNIA IN PALLIATIVE CARE 1. GENERAL PRINCIPLES Insomnia may be a symptom or a syndrome. The diagnostic criteria are outlined in Table 1. Table 1 Diagnostic criteria for insomnia [Level 4] (adapted from Wilson et al 1 ) In all definitions, one criterion from each of columns A, B & C needs to be fulfilled. International Classification of Sleep Disorders (ICSD) 2 and Research Diagnostic Criteria for Insomnia (RDC) 3 Difficulty - Initiating - Maintaining - Waking up too early or - Sleep is chronically nonrestorative or poor in quality A B C Occurs despite adequate opportunity and circumstances for At least one form of daytime impairment 1. Fatigue or malaise 2. Poor attention, concentration or memory impairment 3. Social or vocational dysfunction or poor school performance 4. Mood disturbance or irritability 5. Daytime iness 6. Lack of motivation, energy or initiative reduction 7. Prone to errors or accidents at work or while driving 8. Tension headaches or gastrointestinal symptoms in response to loss 9. Concerns or worries about International Classification of Disease ICD-10 4 Difficulty in - Falling a - Maintaining or - Nonrefreshing 3 times a week and for longer than one month Marked personal distress or interference with personal functioning in daily living Diagnostic and Statistical Manual of Mental Disorders DSM- IV 5 Predominant complaint - Difficulty initiating - Difficulty maintaining or - Non-restorative For at least one month Clinically significant distress or impairment in social, occupational or other important areas of functioning.
2 Insomnia may be transient (less than 1 month), short term (1-6 months), or chronic ( more than 6 months). 1,2,4 Insomnia is one of the most frequent and distressing symptoms in cancer patients and the clinical impact on patients is often underestimated. 6-9 Insomnia in cancer patients may be linked to uncontrolled physical and / or psychological symptoms. 6-8, GUIDELINES It is important to take a history from all patients. The nature of any disturbance, its duration and effect on every day functioning should be documented in the case notes. 6,7,9 [Level 4] A cause of the disturbance should be identified where possible (see Table 2). 1,6-8,10-15 [Level 4] Table 2 Causes of Insomnia 1,6-8,10-15 [Level 4] Age related (i.e. extension of normal physiological changes) Bladder / bowel symptoms (e.g. nocturia, high output stoma, short bowel syndrome) Environmental (e.g. noise levels, light) Medication induced (e.g. diuretics, corticosteriods, psychostimulants, bronchodilators, stimulant anti-depressants) Medication withdrawal (e.g. benzodiazepines) Neurological (e.g. cognitive impairment, delirium, restless legs) Pain Psychiatric & Psychological (e.g. anxiety, hallucinations, nightmares, depression) Respiratory (e.g. breathlessness, obstructive apnoea) Substance withdrawal (e.g. alcohol, nicotine, recreational drugs) Metabolic (e.g. restless legs from low ferritin) Other uncontrolled symptoms (e.g. sweating, pruritus) Pain, depression and anxiety are common causes of insomnia and should be identified and treated as appropriate [Level 4] Drugs which may contribute to insomnia (e.g. corticosteroids, diuretics, stimulant antidepressants and other stimulants) should be reviewed and discontinued where possible. If corticosteroids are required they should be administered before 2pm. 6,7,16 [Level 4] The management of insomnia may include non-pharmacological and pharmacological measures. 1,6-8,14,15 [Level 4] Non-pharmacological measures are outlined in Table 3. 15,17
3 Table 3 Psychological and behavioural therapies for insomnia 15,17 [Level 4] Stimulus control therapy Behavioural recommendations designed to reinforce the association between the bed or bedroom and, and to strengthen a consistent -wake schedule: a) go to bed only when y; b) get out of bed when unable to ; c) use the bed for only (no reading, problem-solving in bed); d) arise at the same time every morning; e) avoid napping. Sleep restriction therapy A method that limits the time spent in bed as close as possible to the actual time, thereby producing a mild deprivation, which results in more consolidated. The window is gradually increased throughout a few days or weeks until optimum duration is achieved. Relaxation training Clinical procedures aimed at reduction of somatic tension (e.g, progressive muscle relaxation, autogenic training) or intrusive thoughts (e.g. imagery training, meditation) interfering with. Most relaxation techniques need professional guidance initially and daily practice for a few weeks. Sleep hygiene education General guidelines about health practices (e.g. diet, exercise, substance use) and environmental factors (e.g. light, noise, temperature) that might promote or interfere with : a) avoid stimulants (e.g. caffeine, nicotine) for several hours before bedtime b) avoid alcohol around bedtime as it fragments during the second half of the night; c) exercise regularly, it can deepen d) do not watch the clock; e) keep the bedroom environment dark, quiet, and comfortable. Cognitive therapy Psychotherapeutic method aimed at alleviating excessive worries and revising misconceptions about, insomnia, and daytime consequences. Specific targets include unrealistic expectations, fear of the consequences of insomnia, and misconceptions of the causes of insomnia. Cognitive behavioural therapy A combination of any of the above behavioural (e.g., restriction, stimulus control instructions, relaxation) and cognitive procedures. A ward environment conducive to will include: - A differentiation between light and dark during day time and night time hours. - Adapting timing of patient care interactions: e.g. clustering and quiet times. - Providing a structured bedtime routine. - Use of ear plugs and eye masks for unavoidable disruptions 18,19 [Level 4].
4 Pharmacological measures should be used with caution. Medication should be prescribed at the lowest possible dose and for the shortest period of time. Tables 4 and 5 list some of the commonly used drugs in the management of insomnia. 1,6,7,15,16,20-22 [Level 4] Table 4 Hypnotic drugs used in the management of insomnia 1,6,7,15,16,20-22 [Level 4] Medication Oral dose Class of drug Notes Lorazepam Temazepam 500microgram 1mg nocte (sublingual) 10mg 40mg nocte Short acting benzodiazepine Intermediate acting benzodiazepine Little hangover effect, promotes onset and maintenance Monitor for hangover effect. Promotes onset and maintenance Zopiclone 3.75mg 15mg nocte Short acting cyclopyrrolone Little hangover effect, promotes onset Table 5 Sedating drugs which may be used in the management of insomnia in the presence of other symptoms 1,6,7,15,16,20-22 [Level 4] Symptom Medication Oral dose Class of drug Notes Delirium Depression Pain Depression Pain Haloperidol Mirtazapine Amitriptyline Clonazepam See guidelines for management of delirium 7.5mg 15mg nocte 10mg 75mg nocte 500 microgram 8mg nocte Long acting dopamine antagonist Long acting NaSSA Tricyclic antidepressant Benzodiazepine Haloperidol may be used for the management of nightmares and hallucinations but it has little sedative effect. Useful if co-existing depression, lower doses more sedative e.g. 15mg Caution in cardiac disease, concurrent SSRI use, glaucoma and history of urinary retention Long acting benzodiazepine Caution must be exercised in older patients as many of the drugs used in the management of insomnia cause postural hypotension and urinary retention. These may in turn lead to poor mobility, falls and increasing agitation. 16,20 [Level 4] Zopiclone is a short acting cyclopyrrolone and aims to initiate. A dose of 7.5mg is recommended, with 3.75mg initially for older patients. Maximum
5 plasma concentration is achieved after 1½ - 2 hours and is not affected by food. The most common side effect is a metallic taste. Withdrawal and rebound insomnia have occasionally been observed on discontinuation of treatment, mainly in association with prolonged treatment. There may be an increased risk of falls. 16,20 [Level 4] All benzodiazepines have a significant side effect profile. These include dizziness, confusion, ataxia, dependence, paradoxical agitation and postural hypotension. 16,20 [Level 4] 3. STANDARDS 1. Assessment and documentation of a patient s quality of should be part of specialist palliative care assessment. 1,6-8 [Grade D] 2. For patients with insomnia, reversible causes should be identified, treated where appropriate and recorded in the case-notes. 1,6-8 [Grade D] 3. Phamacological and non-pharmacological measures taken to improve quality should be reviewed and effectiveness documented. 1,6,7,15,17,23 [Grade D] 4. Patients commenced on hypnotic medication should be reviewed within 7 days for inpatient settings and within 14 days for community setting. Ineffective medication should be discontinued following dose optimization 1,6-8 [Grade D] 4. REFERENCES 1. Wilson S, Nutt D, Alford C, Argyropoulos S, Baldwin D, Bateson A, et al. British Association for Psychopharmacology consensus statement on evidence-based treatment of insomnia, parasomnias and circadian rhythm disorders. Journal of Psychopharmacology 2010; 24(11): Diagnostic Classification Steering Committee, Thorp MJ, Chairman. ICSD- International Classification of Sleep Disorders: Diagnostic and Coding Manual. Rochester, Minnesota: American Sleep Disorders Association; Edinger J, Bonnet M, Bootzin R, Doghramji K, Dorsey C, Espie C, et al. Derivation of research diagnostic criteria for insomnia: Report of an American Academy of Sleep Medicine Work Group. Sleep 2004;27(8): ICD-10. The ICD-10 Classification of Mental and Behavioural Disorders - clinical descriptions and diagnostic guidelines.. First ed. Geneva: World Health Organization; American Psychiatric Association. Diagnostic and statistical manual of mental disorders: DSM-IV-TR. 4th ed., text revision ed. Washington, DC: American Psychiatric Association; Hugel H, Ellershaw J, Cook L, Skinner J, Irvine C. The prevalence, key causes and management of insomnia in palliative care patients. J Pain Symptom Manage 2004;27(4):
6 7. Kvale EA, Shuster JL. Sleep disturbance in supportive care of cancer: A review. J Palliat Med 2006;9(2): Sateia MJ, Lang BJ. Sleep and Cancer: Recent Developments. Curr Oncol Rep 2008;10(4): Stepanski E. Clinical evaluation and treatment of insomnia in patients with cancer. Comm Oncology 2007;4(4): Delgado-Guay M, Yennurajalingam S, Parsons H, Palmer JL, Bruera E. Association between self-reported disturbance and other symptoms in patients with advanced cancer. J Pain Symptom Manage 2011;41(5): Wells-Di Gregorio S, Gustin J, Marks D, Taylor R, Coller K, Magalang U. Worry as a Significant Predictor of Insomnia among Palliative Care Patients with Advanced Cancer. J Pain Symptom Manage 2010;39(2): Mystakidou K, Parpa E, Tsilika E, Gennatas C, Galanos A, Vlahos L. How is quality affected by the psychological and symptom distress of advanced cancer patients? Palliat Med 2009;23(1): Eyigor S, Eyigor C, Uslu R. Assessment of pain, fatigue, and quality of life (QoL) in elderly hospitalized cancer patients. Arch Gerontol Geriatr 2010;51(3):e57-e Morin CM, Savard J, Ouellet M, Daley M. Insomnia. Handbook of Psychology: John Wiley & Sons, Inc.; Morin CM, Benca R. Chronic insomnia. The Lancet 2012;379(9821): Twycross R, Wilcock A. Palliative Care Formulary. 4th ed. Nottingham: palliativedrugs.com; Morgenthaler, T., Kramer, M., Alessi, C., Friedman, L., Boehlecke, B., Brown, T., Coleman, J., Kapur, V., Lee-Chiong, T., Owens, J., Pancer, J., Swick,T. Practice parameters for the psychological and behavioral treatment of insomnia: An update. An American Academy of Sleep Medicine Report. Sleep 2006;29(11): Gibson J, Grealish L. Relating palliative care principles to the promotion of undisturbed in a hospice setting. Int J Palliat Nurs 2001;7(3): Richardson A, Thompson A, Coghill E, Chambers I, Turnock C. Development and implementation of a noise reduction intervention programme: a pre- and post-audit of three hospital wards. J Clin Nurs 2009;18(23): Joint Formulary Committee. British National Formulary 63. British Medical Association and Royal Pharmaceutical Society of Great Britain Hirst A, Sloan R. Benzodiazepines and related drugs for insomnia in palliative care. Cochrane database of systematic reviews 2002(4):CD
7 22. Henderson M, MacGregor E, Sykes N, Hotopt M. The use of benzodiazepines in palliative care. Palliat Med 2006;20(4): GUIDELINE DEVELOPMENT GROUP Lead Contributor Dr A Khodabukus, Academic Clinical Fellow and Specialty Registrar in Palliative Medicine, Marie Curie Hospice, Liverpool Contributors B Humphries, Clinical Nurse, Specialist in Palliative Care, Countess of Chester Hospital NHS, Foundation Trust, Chester. Dr C Irvine, Associate Specialist, Hospice of the Good Shepherd, Chester. Dr J Smith, Consultant in Palliative Medicine, Countess of Chester Hospital NHS Foundation Trust, Chester. Dr R Latten, Consultant in Palliative Medicine, Marie Curie Hospice, Liverpool. Dr P Swarbrick, Medical Director, St Mary's Hospice Ulverston Dr C Watt, Consultant in Palliative Medicine, St John s Hospice, Lancaster Invited Expert Dr J O Reilly, Consultant Respiratory Physician, Aintree University Hospitals NHS Trust, Liverpool Date of Guideline Production 2012 Date of Guideline Review July 2014 Date Posted on Network Website September 2014
MCCN Supra-Regional Audit of Insomnia Management in Palliative Care
 MCCN Supra-Regional Audit of Insomnia Management in Palliative Care Barbara Humphries Caroline Irvine Andrew Khodabukus Richard Latten Jenny Smith Phil Swarbrick Carolyn Watt - Countess of Chester Hospital
MCCN Supra-Regional Audit of Insomnia Management in Palliative Care Barbara Humphries Caroline Irvine Andrew Khodabukus Richard Latten Jenny Smith Phil Swarbrick Carolyn Watt - Countess of Chester Hospital
MCCN Supra-Regional Audit of Insomnia Management in Palliative Care
 MCCN Supra-Regional Audit of Insomnia Management in Palliative Care Barbara Humphries Caroline Irvine Andrew Khodabukus Richard Latten Jenny Smith Phil Swarbrick Carolyn Watt - Countess of Chester Hospital
MCCN Supra-Regional Audit of Insomnia Management in Palliative Care Barbara Humphries Caroline Irvine Andrew Khodabukus Richard Latten Jenny Smith Phil Swarbrick Carolyn Watt - Countess of Chester Hospital
Chronic Insomnia: DSM - V. Insomnia DSM - V. Patient Symptoms. Insomnia: Assessment and Overview of Management. Insomnia Management in the Digital Age
 Insomnia Management in the Digital Age Dr Anup Desai Sleep & Respiratory Medicine MBBS (syd), PhD (syd), FRACP Senior Staff Specialist, POW Hospital Medical Director, Sydney Sleep Centre Senior Lecturer,
Insomnia Management in the Digital Age Dr Anup Desai Sleep & Respiratory Medicine MBBS (syd), PhD (syd), FRACP Senior Staff Specialist, POW Hospital Medical Director, Sydney Sleep Centre Senior Lecturer,
Insomnia. Learning Objectives. Disclosure 6/7/11. Research funding: NIH, Respironics, Embla Consulting: Elsevier
 Insomnia Teofilo Lee-Chiong MD Professor of Medicine National Jewish Health University of Colorado Denver School of Medicine Learning Objectives Learn about the causes of transient and chronic Learn how
Insomnia Teofilo Lee-Chiong MD Professor of Medicine National Jewish Health University of Colorado Denver School of Medicine Learning Objectives Learn about the causes of transient and chronic Learn how
Treating Insomnia in Primary Care. Judith R. Davidson Ph.D., C. Psych. Kingston Family Health Team
 Treating Insomnia in Primary Care Judith R. Davidson Ph.D., C. Psych. Kingston Family Health Team jdavidson@kfhn.net Disclosure statement Nothing to disclose A ruffled mind makes a restless pillow. ~ Charlotte
Treating Insomnia in Primary Care Judith R. Davidson Ph.D., C. Psych. Kingston Family Health Team jdavidson@kfhn.net Disclosure statement Nothing to disclose A ruffled mind makes a restless pillow. ~ Charlotte
Dr Alex Bartle. Sleep Well Clinic
 Dr Alex Bartle Sleep Well Clinic Overview of Sleep Disorders Sleep: Why bother. Effect of Poor Quality or reduced Quantity of Sleep Common Sleep Disorders Management of Insomnia Medication vs CBTi Conclusion
Dr Alex Bartle Sleep Well Clinic Overview of Sleep Disorders Sleep: Why bother. Effect of Poor Quality or reduced Quantity of Sleep Common Sleep Disorders Management of Insomnia Medication vs CBTi Conclusion
Behavioral Sleep Medicine W 12:50p 3:50p, HPNP G103 CLP 7934 Section 03A4
 Behavioral Sleep Medicine W 12:50p 3:50p, HPNP G103 CLP 7934 Section 03A4 Fall 2013 Instructor: Office hours: Christina McCrae, PhD, CBSM Department of Clinical & Health Psychology HPNP, Room 3139 csmccrae@phhp.ufl.edu
Behavioral Sleep Medicine W 12:50p 3:50p, HPNP G103 CLP 7934 Section 03A4 Fall 2013 Instructor: Office hours: Christina McCrae, PhD, CBSM Department of Clinical & Health Psychology HPNP, Room 3139 csmccrae@phhp.ufl.edu
MMG003 GUIDELINES FOR THE USE OF HYPNOTICS FOR THE TREATMENT OF INSOMNIA
 MMG003 GUIDELINES FOR THE USE OF HYPNOTICS FOR THE TREATMENT OF INSOMNIA Page 1 of 11 Table of Contents Why we need this Guideline... 3 What the Policy is trying to do... 3 Which stakeholders have been
MMG003 GUIDELINES FOR THE USE OF HYPNOTICS FOR THE TREATMENT OF INSOMNIA Page 1 of 11 Table of Contents Why we need this Guideline... 3 What the Policy is trying to do... 3 Which stakeholders have been
Guideline for Adult Insomnia
 Guideline for Adult Insomnia Exclusions This guideline does not apply to: Children under the age of 18 Pregnant and lactating women Geriatric patients: While the general principles of the diagnosis and
Guideline for Adult Insomnia Exclusions This guideline does not apply to: Children under the age of 18 Pregnant and lactating women Geriatric patients: While the general principles of the diagnosis and
8/29/2013. Discuss Relation of Fatigue to Sleep Disturbance. Assessing and Treating Factors Contributing to Fatigue and Sleep Disturbance
 Timothy Pearman, Ph.D. Director, Supportive Oncology Robert H. Lurie Comprehensive Cancer Center Associate Professor of Medical Social Sciences and Psychiatry Northwestern University Feinberg School of
Timothy Pearman, Ph.D. Director, Supportive Oncology Robert H. Lurie Comprehensive Cancer Center Associate Professor of Medical Social Sciences and Psychiatry Northwestern University Feinberg School of
SLEEP-WAKE DISORDERS: INSOMNIA. Prof. Paz Gía-Portilla
 SLEEP-WAKE DISORDERS: INSOMNIA Prof. Paz Gía-Portilla SLEEP-WAKE DISORDERS AND ICD-10 Chapter V: Mental and Behavioural Disorders F51. Non-organic sleep disorders Chapter VI: Nervous System Illnesses G47.
SLEEP-WAKE DISORDERS: INSOMNIA Prof. Paz Gía-Portilla SLEEP-WAKE DISORDERS AND ICD-10 Chapter V: Mental and Behavioural Disorders F51. Non-organic sleep disorders Chapter VI: Nervous System Illnesses G47.
 Sleep This factsheet is available in a downloadable PDF here. Table of Contents Introduction Insomnia How Long does Insomnia Last? How much Sleep should You get? Symptoms of Insomnia Causes of Insomnia
Sleep This factsheet is available in a downloadable PDF here. Table of Contents Introduction Insomnia How Long does Insomnia Last? How much Sleep should You get? Symptoms of Insomnia Causes of Insomnia
Beyond Sleep Hygiene: Behavioral Approaches to Insomnia
 Beyond Sleep Hygiene: Behavioral Approaches to Insomnia Rocky Garrison, PhD, CBSM Damon Michael Williams, RN, PMHNP-BC In House Counseling Laughing Heart LLC 10201 SE Main St. 12 SE 14 th Ave. Suite 10
Beyond Sleep Hygiene: Behavioral Approaches to Insomnia Rocky Garrison, PhD, CBSM Damon Michael Williams, RN, PMHNP-BC In House Counseling Laughing Heart LLC 10201 SE Main St. 12 SE 14 th Ave. Suite 10
1. GUIDELINES FOR THE MANAGEMENT OF AGITATION IN ADVANCED CANCER
 1. GUIDELINES FOR THE MANAGEMENT OF AGITATION IN ADVANCED CANCER 1.1 GENERAL PRINCIPLES There are many causes of agitation in palliative care patients, which makes recommendations for treatment difficult.
1. GUIDELINES FOR THE MANAGEMENT OF AGITATION IN ADVANCED CANCER 1.1 GENERAL PRINCIPLES There are many causes of agitation in palliative care patients, which makes recommendations for treatment difficult.
Insomnia % of adults suffer from chronic and severe insomnia (Complaints of insomnia with daytime consequences)
 10-15% of adults suffer from chronic and severe insomnia (Complaints of insomnia with daytime consequences) 30 40% of adults complain of insomnia symptoms only 95% experience insomnia at some time in their
10-15% of adults suffer from chronic and severe insomnia (Complaints of insomnia with daytime consequences) 30 40% of adults complain of insomnia symptoms only 95% experience insomnia at some time in their
Sleep and Parkinson's Disease
 Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
INSOMNIAS. Stephan Eisenschenk, MD Department of Neurology
 INSOMNIAS INSOMNIAS General criteria for insomnia A. Repeated difficulty with sleep initiation, duration, consolidation or quality. B. Adequate sleep opportunity, persistent sleep difficulty and associated
INSOMNIAS INSOMNIAS General criteria for insomnia A. Repeated difficulty with sleep initiation, duration, consolidation or quality. B. Adequate sleep opportunity, persistent sleep difficulty and associated
Benzodiazepines and Hypnotics
 Benzodiazepines and Hypnotics Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date (when this version goes out of date):
Benzodiazepines and Hypnotics Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date (when this version goes out of date):
Zopiclone Orion. Date: , Version 1.2 PUBLIC SUMMARY OF THE RISK MANAGEMENT PLAN
 Zopiclone Orion Date: 16-11-2016, Version 1.2 PUBLIC SUMMARY OF THE RISK MANAGEMENT PLAN VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Insomnia (i.e. sleeplessness) is a common
Zopiclone Orion Date: 16-11-2016, Version 1.2 PUBLIC SUMMARY OF THE RISK MANAGEMENT PLAN VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Insomnia (i.e. sleeplessness) is a common
Insomnia. Dr Terri Henderson MBChB FCPsych
 Insomnia Dr Terri Henderson MBChB FCPsych Plan Basics of insomnia Pharmacology Medication CBT Details of insomnia Unsatisfactory sleep that impairs daytime well-being Starts with specific problem or change
Insomnia Dr Terri Henderson MBChB FCPsych Plan Basics of insomnia Pharmacology Medication CBT Details of insomnia Unsatisfactory sleep that impairs daytime well-being Starts with specific problem or change
Dr Alex Bartle. Director Sleep Well Clinic
 Dr Alex Bartle Director Sleep Well Clinic 1 Fatigue in the Workforce The structure of sleep Fatigue and sleep Consequences of fatigue Management of Shiftwork Conclusion Sleep Architecture REM NREM Rapid
Dr Alex Bartle Director Sleep Well Clinic 1 Fatigue in the Workforce The structure of sleep Fatigue and sleep Consequences of fatigue Management of Shiftwork Conclusion Sleep Architecture REM NREM Rapid
RECIPES FOR A GOOD NIGHT S SLEEP
 RECIPES FOR A GOOD NIGHT S SLEEP Maribeth Gallagher, PMHNP-BC, MS Hospice of the Valley Objectives: Describe the most common changes in sleep that occur in older adults. Discuss the possible negative effects
RECIPES FOR A GOOD NIGHT S SLEEP Maribeth Gallagher, PMHNP-BC, MS Hospice of the Valley Objectives: Describe the most common changes in sleep that occur in older adults. Discuss the possible negative effects
Cognitive-Behavioral Therapy for Insomnia
 Wisconsin Department of Health Services Wisconsin Public Psychiatry Network Teleconference (WPPNT) This teleconference is brought to you by the Wisconsin Department of Health Services (DHS) Bureau of Prevention,
Wisconsin Department of Health Services Wisconsin Public Psychiatry Network Teleconference (WPPNT) This teleconference is brought to you by the Wisconsin Department of Health Services (DHS) Bureau of Prevention,
Critical Care Pharmacological Management of Delirium
 Critical Care Pharmacological Management of Delirium Policy Title: in the Critical Care Unit Executive Summary: This policy provides guidance Pharmacological Management of delirium in the Critical Care
Critical Care Pharmacological Management of Delirium Policy Title: in the Critical Care Unit Executive Summary: This policy provides guidance Pharmacological Management of delirium in the Critical Care
SUMMARY OF PRODUCT CHARACTERISTICS FOR BENZODIAZEPINES AS ANXIOLYTICS OR HYPNOTICS
 SUMMARY OF PRODUCT CHARACTERISTICS FOR BENZODIAZEPINES AS ANXIOLYTICS OR HYPNOTICS Guideline Title Summary of Product Characteristics for Benzodiazepines as Anxiolytics or Hypnotics Legislative basis Directive
SUMMARY OF PRODUCT CHARACTERISTICS FOR BENZODIAZEPINES AS ANXIOLYTICS OR HYPNOTICS Guideline Title Summary of Product Characteristics for Benzodiazepines as Anxiolytics or Hypnotics Legislative basis Directive
Cognitive behavioural therapy for insomnia
 Cognitive behavioural therapy for insomnia Item type Authors Citation Publisher Journal Article Ruth, Alan Ruth A. Cognitive behavioural therapy for insomnia. Nurs Gen Prac 2014 May 29-30, 32 Nursing in
Cognitive behavioural therapy for insomnia Item type Authors Citation Publisher Journal Article Ruth, Alan Ruth A. Cognitive behavioural therapy for insomnia. Nurs Gen Prac 2014 May 29-30, 32 Nursing in
CPT David Shaha, MC US Army
 CPT David Shaha, MC US Army None Thoughts and comments are my own and do not represent the official policy of the Department of the Army, Department of Defense, or United States Government. Clinical Case
CPT David Shaha, MC US Army None Thoughts and comments are my own and do not represent the official policy of the Department of the Army, Department of Defense, or United States Government. Clinical Case
SLEEP DISORDERS. Kenneth C. Sassower, MD Division of Sleep Medicine; Department of Neurology Massachusetts General Hospital for Children
 SLEEP DISORDERS Kenneth C. Sassower, MD Division of Sleep Medicine; Department of Neurology Massachusetts General Hospital for Children Distinctive Features of Pediatric Sleep Daytime sleepiness uncommon
SLEEP DISORDERS Kenneth C. Sassower, MD Division of Sleep Medicine; Department of Neurology Massachusetts General Hospital for Children Distinctive Features of Pediatric Sleep Daytime sleepiness uncommon
John McLachlan. Clinical Lead Pulmonary Physiology & Sleep Medicine. President Elect, WA Branch Thoracic Society of Australia & NZ
 John McLachlan Respiratory & Sleep Physician @FSH Clinical Lead Pulmonary Physiology & Sleep Medicine Sleep Physician x 27 years Interest in Insomnia management President Elect, WA Branch Thoracic Society
John McLachlan Respiratory & Sleep Physician @FSH Clinical Lead Pulmonary Physiology & Sleep Medicine Sleep Physician x 27 years Interest in Insomnia management President Elect, WA Branch Thoracic Society
Sleep Hygiene. William M. DeMayo, M.D. John P. Murtha Neuroscience and Pain Institute Conemaugh Health System Johnstown, PA
 Sleep Hygiene William M. DeMayo, M.D. John P. Murtha Neuroscience and Pain Institute Conemaugh Health System Johnstown, PA Why Is Sleep Important? Symptoms of Sleep Deprivation: Irritability / Poor Stress
Sleep Hygiene William M. DeMayo, M.D. John P. Murtha Neuroscience and Pain Institute Conemaugh Health System Johnstown, PA Why Is Sleep Important? Symptoms of Sleep Deprivation: Irritability / Poor Stress
일차진료에서불면증치료 김종우. Primary Insomnia : DSM-IV criteria 경희대학교의과대학정신과학교실 MEMO. Diagnostic Criteria for Insomnia (ICSD-2) 개원의와함께하는임상강좌
 개원의와함께하는임상강좌 2011 일차진료에서불면증치료 경희대학교의과대학정신과학교실 김종우 Diagnostic Criteria for Insomnia (ICSD-2) International Classification of Sleep Disorders, 2nd Edition (ICSD-2) Primary Insomnia : DSM-IV criteria A. The
개원의와함께하는임상강좌 2011 일차진료에서불면증치료 경희대학교의과대학정신과학교실 김종우 Diagnostic Criteria for Insomnia (ICSD-2) International Classification of Sleep Disorders, 2nd Edition (ICSD-2) Primary Insomnia : DSM-IV criteria A. The
TOP 10 LIST OF SLEEP QUESTIONS. Kenneth C. Sassower, MD Sleep Disorders Unit Massachusetts General Hospital for Children
 TOP 10 LIST OF SLEEP QUESTIONS Kenneth C. Sassower, MD Sleep Disorders Unit Massachusetts General Hospital for Children QUESTION #1: ARE SLEEP ISSUES IN CHILDREN THE SAME AS IN ADULTS? Distinctive Features
TOP 10 LIST OF SLEEP QUESTIONS Kenneth C. Sassower, MD Sleep Disorders Unit Massachusetts General Hospital for Children QUESTION #1: ARE SLEEP ISSUES IN CHILDREN THE SAME AS IN ADULTS? Distinctive Features
HOW TO DEAL WITH SLEEP PROBLEMS
 The Handbook on Successful Ageing HOW TO DEAL WITH SLEEP PROBLEMS Up to 50% of the elderly complain of insomnia, but although such complaints are prevalent and are often accompanied by higher rates of
The Handbook on Successful Ageing HOW TO DEAL WITH SLEEP PROBLEMS Up to 50% of the elderly complain of insomnia, but although such complaints are prevalent and are often accompanied by higher rates of
Sleep Disorders. Guidance for Primary Care. National Advisory Group for Respiratory Managed Clinical Networks
 Sleep Disorders Guidance for Primary Care National Advisory Group for Respiratory Managed Clinical Networks Presentation Patient complaining of difficulty sleeping, ongoing fatigue, poor concentration
Sleep Disorders Guidance for Primary Care National Advisory Group for Respiratory Managed Clinical Networks Presentation Patient complaining of difficulty sleeping, ongoing fatigue, poor concentration
GUIDELINES FOR THE USE OF PSYCHOSTIMULANTS IN PALLIATIVE CARE
 GUIDELINES FOR THE USE OF PSYCHOSTIMULANTS IN PALLIATIVE CARE 36.1 GENERAL PRINCIPLES Current research evidence supports the use of psychostimulants in palliative care in four areas: depression; 1, 2 opioid
GUIDELINES FOR THE USE OF PSYCHOSTIMULANTS IN PALLIATIVE CARE 36.1 GENERAL PRINCIPLES Current research evidence supports the use of psychostimulants in palliative care in four areas: depression; 1, 2 opioid
Insomnia Disorder A Journey to the Land of No Nod
 Insomnia Disorder A Journey to the Land of No Nod JACQUELINE D. KLOSS, PH.D. P S Y C H O L O G I S T B R Y N M A W R P S Y C H O L O G I C A L A S S O C I A T E S B E H A V I O R A L S L E E P M E D I
Insomnia Disorder A Journey to the Land of No Nod JACQUELINE D. KLOSS, PH.D. P S Y C H O L O G I S T B R Y N M A W R P S Y C H O L O G I C A L A S S O C I A T E S B E H A V I O R A L S L E E P M E D I
HEALTH 3--DEPRESSION, SLEEP, AND HEALTH GOALS FOR LEADERS. To educate participants regarding the sleep wake cycle.
 HEALTH 3--DEPRESSION, SLEEP, AND HEALTH GOALS FOR LEADERS Talk about the relationship between depression, sleep, and health problems. To educate participants regarding the sleep wake cycle. To provide
HEALTH 3--DEPRESSION, SLEEP, AND HEALTH GOALS FOR LEADERS Talk about the relationship between depression, sleep, and health problems. To educate participants regarding the sleep wake cycle. To provide
Reduction in the Use of Night Sedation to Reduce the Risk of Falls
 Reduction in the Use of Night Sedation to Reduce the Risk of Falls Ms Margaret Hargraves Hospital Pharmacist Prince of Wales Hospital South Eastern Sydney Illawarra Area Health Service Objectives Falls
Reduction in the Use of Night Sedation to Reduce the Risk of Falls Ms Margaret Hargraves Hospital Pharmacist Prince of Wales Hospital South Eastern Sydney Illawarra Area Health Service Objectives Falls
Faculty/Presenter Disclosure
 A Little CBT I With My Tea Please: Cognitive Behavioural Therapy for insomnia (CBT I) and Its Use In the Treatment of Sleeplessness W. Jerome Alonso, MD Medical Director, Canadian Sleep Consultants Clinical
A Little CBT I With My Tea Please: Cognitive Behavioural Therapy for insomnia (CBT I) and Its Use In the Treatment of Sleeplessness W. Jerome Alonso, MD Medical Director, Canadian Sleep Consultants Clinical
Individual Planning: A Treatment Plan Overview for Individuals Sleep Disorder Problems.
 COURSES ARTICLE - THERAPYTOOLS.US Individual Planning: A Treatment Plan Overview for Individuals Sleep Disorder Problems. Individual Planning: A Treatment Plan Overview for Individuals Sleep Disorder Problems.
COURSES ARTICLE - THERAPYTOOLS.US Individual Planning: A Treatment Plan Overview for Individuals Sleep Disorder Problems. Individual Planning: A Treatment Plan Overview for Individuals Sleep Disorder Problems.
Sleep and Students. John Villa, DO Medical Director
 Sleep and Students John Villa, DO Medical Director Objectives: Importance and Benefits of Sleep States and Stages of the Sleep Cycle Sleep Needs, Patterns and Characteristics for All Ages Healthy Sleep
Sleep and Students John Villa, DO Medical Director Objectives: Importance and Benefits of Sleep States and Stages of the Sleep Cycle Sleep Needs, Patterns and Characteristics for All Ages Healthy Sleep
Therapeutic brief 18
 Therapeutic brief 18 Insomnia Management: Effective approaches for a common problem A large amount of research supports the benefits of nondrug therapies for insomnia. 1-4 Non-drug therapies based on behavioural
Therapeutic brief 18 Insomnia Management: Effective approaches for a common problem A large amount of research supports the benefits of nondrug therapies for insomnia. 1-4 Non-drug therapies based on behavioural
Insomnia. F r e q u e n t l y A s k e d Q u e s t i o n s
 Insomnia Q: What is insomnia? A: Insomnia is a common sleep disorder. If you have insomnia, you may: Lie awake for a long time and have trouble falling asleep Wake up a lot and have trouble returning to
Insomnia Q: What is insomnia? A: Insomnia is a common sleep disorder. If you have insomnia, you may: Lie awake for a long time and have trouble falling asleep Wake up a lot and have trouble returning to
INSOMNIA IN THE GERIATRIC POPULATION. Shannon Bush, MS4
 INSOMNIA IN THE GERIATRIC POPULATION Shannon Bush, MS4 CHANGES IN SLEEP ARCHITECTURE 2 Reduction in slow wave sleep (stage 3 and 4) Increase in lighter stages of sleep (stage 1 and 2) Decrease in REM sleep
INSOMNIA IN THE GERIATRIC POPULATION Shannon Bush, MS4 CHANGES IN SLEEP ARCHITECTURE 2 Reduction in slow wave sleep (stage 3 and 4) Increase in lighter stages of sleep (stage 1 and 2) Decrease in REM sleep
WHY CAN T I SLEEP? Deepti Chandran, MD
 WHY CAN T I SLEEP? Deepti Chandran, MD Sleep and Aging How does sleep change as we age? Do we need less sleep as we get older? Can a person expect to experience more sleep problems or have a sleep disorder
WHY CAN T I SLEEP? Deepti Chandran, MD Sleep and Aging How does sleep change as we age? Do we need less sleep as we get older? Can a person expect to experience more sleep problems or have a sleep disorder
Parkinson s Disease Associated Sleep Disturbance Ehsan M. Hadi, MD, MPH. Dignity Health Neurological Institute
 Parkinson s Disease Associated Sleep Disturbance Ehsan M. Hadi, MD, MPH. Dignity Health Neurological Institute Parkinson s Disease 2 nd most common neurodegenerative disorder Peak age at onset is 60 years
Parkinson s Disease Associated Sleep Disturbance Ehsan M. Hadi, MD, MPH. Dignity Health Neurological Institute Parkinson s Disease 2 nd most common neurodegenerative disorder Peak age at onset is 60 years
Cognitive Behavioral Therapy for Insomnia. Melanie K. Leggett, PhD, CBSM Duke University Medical Center
 Cognitive Behavioral Therapy for Insomnia Melanie K. Leggett, PhD, CBSM Duke University Medical Center Disclosures I have no relevant financial relationship with the manufacturers of any commercial products
Cognitive Behavioral Therapy for Insomnia Melanie K. Leggett, PhD, CBSM Duke University Medical Center Disclosures I have no relevant financial relationship with the manufacturers of any commercial products
Critical Care Pharmacological Management of Delirium
 Critical Care Pharmacological Management of Delirium Policy Title: in the Critical Care Unit Executive Summary: This policy provides guidance Pharmacological Management of delirium in the Critical Care
Critical Care Pharmacological Management of Delirium Policy Title: in the Critical Care Unit Executive Summary: This policy provides guidance Pharmacological Management of delirium in the Critical Care
How to Manage Insomnia with and without medications
 How to Manage Insomnia with and without medications Tatyana Gurvich, Pharm.D. USC School of Pharmacy UC Irvine SeniorHealth Center Insomnia: How common is it? 26-50% of adult population complain of insomnia
How to Manage Insomnia with and without medications Tatyana Gurvich, Pharm.D. USC School of Pharmacy UC Irvine SeniorHealth Center Insomnia: How common is it? 26-50% of adult population complain of insomnia
ADULT PRIMARY INSOMNIA
 Clinical Practice Guideline Adult Primary Insomnia: Diagnosis to Management 2007 Update This guideline was developed by a Clinical Practice Guidelines Working Group to assist physicians in the management
Clinical Practice Guideline Adult Primary Insomnia: Diagnosis to Management 2007 Update This guideline was developed by a Clinical Practice Guidelines Working Group to assist physicians in the management
Sleep Dysfunction in Multiple System Atrophy DR CALLUM DUPRE NEUROLOGY/SLEEP MEDICINE CAPITAL HEALTH SYSTEM
 Sleep Dysfunction in Multiple System Atrophy DR CALLUM DUPRE NEUROLOGY/SLEEP MEDICINE CAPITAL HEALTH SYSTEM Categories of Disturbance Sleep Breathing Disorders Parasomnias Sleepiness Insomnia Breathing?
Sleep Dysfunction in Multiple System Atrophy DR CALLUM DUPRE NEUROLOGY/SLEEP MEDICINE CAPITAL HEALTH SYSTEM Categories of Disturbance Sleep Breathing Disorders Parasomnias Sleepiness Insomnia Breathing?
INDEX. Group psychotherapy, described, 97 Group stimulus control, 29-47; see also Stimulus control (group setting)
 Index Abdominal breathing, 70; see also Breathing; Relaxation therapy Activation, sleep drive/responsivity, 6-9 Age level; see also Elderly circadian rhythms and, 68-69 delayed sleep phase syndrome and,
Index Abdominal breathing, 70; see also Breathing; Relaxation therapy Activation, sleep drive/responsivity, 6-9 Age level; see also Elderly circadian rhythms and, 68-69 delayed sleep phase syndrome and,
PRACTICAL MANAGEMENT OF INSOMNIA IN THE OFFICE
 PRACTICAL MANAGEMENT OF INSOMNIA IN THE OFFICE NORAH VINCENT, PHD., C. PSYCH. PSYCHOLOGIST, WINNIPEG REGIONAL HEALTH AUTHORITY PROFESSOR, DEPARTMENT OF CLINICAL HEALTH PSYCHOLOGY, UNIVERSITY OF MANITOBA
PRACTICAL MANAGEMENT OF INSOMNIA IN THE OFFICE NORAH VINCENT, PHD., C. PSYCH. PSYCHOLOGIST, WINNIPEG REGIONAL HEALTH AUTHORITY PROFESSOR, DEPARTMENT OF CLINICAL HEALTH PSYCHOLOGY, UNIVERSITY OF MANITOBA
Insomnia Management Guideline
 Insomnia Management Guideline Guideline Development This document is an update of existing guidance and has been developed by Barnsley CCG Medicines Management Team in consultation with colleagues from
Insomnia Management Guideline Guideline Development This document is an update of existing guidance and has been developed by Barnsley CCG Medicines Management Team in consultation with colleagues from
CONQUERING INSOMNIA & ACHIEVING SLEEP WELLNESS
 CONQUERING INSOMNIA & ACHIEVING SLEEP WELLNESS "Sleep is the golden chain that ties health and our bodies together." ~ Thomas Dekker ~ Under recognized & Under treated Insomnia Facts Negatively Affects
CONQUERING INSOMNIA & ACHIEVING SLEEP WELLNESS "Sleep is the golden chain that ties health and our bodies together." ~ Thomas Dekker ~ Under recognized & Under treated Insomnia Facts Negatively Affects
Reference document. Sleep disorders
 Reference document Sleep disorders Table of contents Introduction 2 Definition 2 Myths 2 Major determinants 2 Major sleep disorders 3 The consequences of sleep deprivation 3 Tips for better sleep 4 Conclusion
Reference document Sleep disorders Table of contents Introduction 2 Definition 2 Myths 2 Major determinants 2 Major sleep disorders 3 The consequences of sleep deprivation 3 Tips for better sleep 4 Conclusion
The Wellbeing Plus Course
 The Wellbeing Plus Course Resource: Good Sleep Guide The Wellbeing Plus Course was written by Professor Nick Titov and Dr Blake Dear The development of the Wellbeing Plus Course was funded by a research
The Wellbeing Plus Course Resource: Good Sleep Guide The Wellbeing Plus Course was written by Professor Nick Titov and Dr Blake Dear The development of the Wellbeing Plus Course was funded by a research
Learning Objectives. Management of Insomnia. Impact of Chronic Insomnia. Insomnia: Definitions. Measurement of Goals. Goals of Therapy 9/29/2017
 Learning Objectives Characterize insomnia and its negative effects Management of Insomnia Discuss the goals of treatment Summarize guidelines of management of insomnia including non-pharmacologic and pharmacologic
Learning Objectives Characterize insomnia and its negative effects Management of Insomnia Discuss the goals of treatment Summarize guidelines of management of insomnia including non-pharmacologic and pharmacologic
Psychiatric Treatment of the Concussed Athlete
 Psychiatric Treatment of the Concussed Athlete Eastern Athletic Trainers Association January 11 th, 2015 Alexander S. Strauss, MD Centra, P.C. E-MAIL: DRSTRAUSS@ALEXSTRAUSSMD.COM Evidence Mounts Linking
Psychiatric Treatment of the Concussed Athlete Eastern Athletic Trainers Association January 11 th, 2015 Alexander S. Strauss, MD Centra, P.C. E-MAIL: DRSTRAUSS@ALEXSTRAUSSMD.COM Evidence Mounts Linking
Treating sleep disorders
 Treating sleep disorders Sue Wilson Centre for Neuropsychopharmacology Imperial College London sue.wilson@imperial.ac.uk Suggested algorithm for treatment of insomnia Diagnosis of insomnia Associated with
Treating sleep disorders Sue Wilson Centre for Neuropsychopharmacology Imperial College London sue.wilson@imperial.ac.uk Suggested algorithm for treatment of insomnia Diagnosis of insomnia Associated with
A good night s sleep
 A good night s sleep Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm A good night
A good night s sleep Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm A good night
Get on the Road to Better Health Recognizing the Dangers of Sleep Apnea
 Get on the Road to Better Health You Will Learn About The importance and benefits of sleep Sleep deprivation and its consequences The prevalence, symptoms, and treatments for major sleep problems/ disorders
Get on the Road to Better Health You Will Learn About The importance and benefits of sleep Sleep deprivation and its consequences The prevalence, symptoms, and treatments for major sleep problems/ disorders
Dr Alex Bartle. Medical Director Sleep Well Clinic Christchurch
 Dr Alex Bartle Medical Director Sleep Well Clinic Christchurch 8:30-9:25 WS #191: Sleep Disorders in The Elderly 9:35-10:30 WS #203: Sleep Disorders in The Elderly (Repeated) REM - Rapid Eye Movement
Dr Alex Bartle Medical Director Sleep Well Clinic Christchurch 8:30-9:25 WS #191: Sleep Disorders in The Elderly 9:35-10:30 WS #203: Sleep Disorders in The Elderly (Repeated) REM - Rapid Eye Movement
INTRINSIC SLEEP DISORDERS. Excessive daytime sleepiness (EDS) is a common complaint. Causes of EDS are numerous and include:
 INTRINSIC SLEEP DISORDERS Introduction Excessive daytime sleepiness (EDS) is a common complaint. Causes of EDS are numerous and include: Intrinsic sleep disorders (e.g. narcolepsy, obstructive sleep apnoea/hypopnea
INTRINSIC SLEEP DISORDERS Introduction Excessive daytime sleepiness (EDS) is a common complaint. Causes of EDS are numerous and include: Intrinsic sleep disorders (e.g. narcolepsy, obstructive sleep apnoea/hypopnea
May 27, Gosia Eve Phillips, MD
 May 27, 2015 Gosia Eve Phillips, MD Diplomate, American Board of Psychiatry and Neurology Assistant Professor of Medicine, Dalhousie University Medical Director, MedSleep Atlantic >50% of MS patients suffer
May 27, 2015 Gosia Eve Phillips, MD Diplomate, American Board of Psychiatry and Neurology Assistant Professor of Medicine, Dalhousie University Medical Director, MedSleep Atlantic >50% of MS patients suffer
OBJECTIVES. The psychiatric, medical, and neurologic causes of sleep problems. Office-based and objective methods of evaluating sleep
 SLEEP ISSUES 1 OBJECTIVES 2 Know and understand: Age-related changes in sleep The psychiatric, medical, and neurologic causes of sleep problems Office-based and objective methods of evaluating sleep Appropriate
SLEEP ISSUES 1 OBJECTIVES 2 Know and understand: Age-related changes in sleep The psychiatric, medical, and neurologic causes of sleep problems Office-based and objective methods of evaluating sleep Appropriate
Insomnia treatment. Sleep hygiene education sleep hygiene teaches good sleeping habits. This includes:
 Insomnia treatment INSOMNIA OVERVIEW insomnia is defined as difficulty falling asleep, difficulty staying asleep, or waking up early in the morning and not being able to return to sleep. In general, people
Insomnia treatment INSOMNIA OVERVIEW insomnia is defined as difficulty falling asleep, difficulty staying asleep, or waking up early in the morning and not being able to return to sleep. In general, people
What is the economic burden associated with poor sleep?
 AS@W...SLEEP AND DEPRESSION How does depression affect sleep? Depressed mood can significantly impact sleep. Some people find it difficult to fall asleep or stay asleep. Others find that they wake up much
AS@W...SLEEP AND DEPRESSION How does depression affect sleep? Depressed mood can significantly impact sleep. Some people find it difficult to fall asleep or stay asleep. Others find that they wake up much
Guidelines MANAGEMENT OF MAJOR DEPRESSIVE DISORDER (MDD)
 MANAGEMENT OF MAJOR DEPRESSIVE DISORDER (MDD) Guidelines CH Lim, B Baizury, on behalf of Development Group Clinical Practice Guidelines Management of Major Depressive Disorder A. Introduction Major depressive
MANAGEMENT OF MAJOR DEPRESSIVE DISORDER (MDD) Guidelines CH Lim, B Baizury, on behalf of Development Group Clinical Practice Guidelines Management of Major Depressive Disorder A. Introduction Major depressive
HEALTHY LIFESTYLE, HEALTHY SLEEP. There are many different sleep disorders, and almost all of them can be improved with lifestyle changes.
 HEALTHY LIFESTYLE, HEALTHY SLEEP There are many different sleep disorders, and almost all of them can be improved with lifestyle changes. HEALTHY LIFESTYLE, HEALTHY SLEEP There are many different sleep
HEALTHY LIFESTYLE, HEALTHY SLEEP There are many different sleep disorders, and almost all of them can be improved with lifestyle changes. HEALTHY LIFESTYLE, HEALTHY SLEEP There are many different sleep
AGING CHANGES IN SLEEP
 OBJECTIVES: Understand the common age-related changes in sleep Discuss the evaluation of the older person with sleep complaints Identify sleep apnea, PLMS, RLS, and REM sleep disorders and their treatments
OBJECTIVES: Understand the common age-related changes in sleep Discuss the evaluation of the older person with sleep complaints Identify sleep apnea, PLMS, RLS, and REM sleep disorders and their treatments
KEY MESSAGES. It is often under-recognised and 30-50% of MDD cases in primary care and medical settings are not detected.
 KEY MESSAGES Major depressive disorder (MDD) is a significant mental health problem that disrupts a person s mood and affects his psychosocial and occupational functioning. It is often under-recognised
KEY MESSAGES Major depressive disorder (MDD) is a significant mental health problem that disrupts a person s mood and affects his psychosocial and occupational functioning. It is often under-recognised
NEUROPATHIC CANCER PAIN STANDARDS AND GUIDELINES
 NEUROPATHIC CANCER PAIN STANDARDS AND GUIDELINES GENERAL PRINCIPLES Neuropathic pain may be relieved in the majority of patients by multimodal management A careful history and examination are essential.
NEUROPATHIC CANCER PAIN STANDARDS AND GUIDELINES GENERAL PRINCIPLES Neuropathic pain may be relieved in the majority of patients by multimodal management A careful history and examination are essential.
INSOMNIA IN GERIATRICS. Presented By: Sara Kamalfar MD, Geriatrics Medicine Fellow
 INSOMNIA IN GERIATRICS Presented By: Sara Kamalfar MD, Geriatrics Medicine Fellow Insomnia Insomnia is the inability to fall asleep, the inability to stay asleep, or waking up earlier than desired. To
INSOMNIA IN GERIATRICS Presented By: Sara Kamalfar MD, Geriatrics Medicine Fellow Insomnia Insomnia is the inability to fall asleep, the inability to stay asleep, or waking up earlier than desired. To
Introduction. v Insomnia is very prevalent in acute (30-50%) and chronic forms (10-15%). v Insomnia is often ignored as a symptom of other disorders.
 Introduction v Insomnia is very prevalent in acute (30-50%) and chronic forms (10-15%). v Insomnia is often ignored as a symptom of other disorders. v Insomnia is a risk factor for psychiatric and medical
Introduction v Insomnia is very prevalent in acute (30-50%) and chronic forms (10-15%). v Insomnia is often ignored as a symptom of other disorders. v Insomnia is a risk factor for psychiatric and medical
European PSUR Work Sharing Project CORE SAFETY PROFILE. Lendormin, 0.25mg, tablets Brotizolam
 European PSUR Work Sharing Project CORE SAFETY PROFILE Lendormin, 0.25mg, tablets Brotizolam 4.2 Posology and method of administration Unless otherwise prescribed by the physician, the following dosages
European PSUR Work Sharing Project CORE SAFETY PROFILE Lendormin, 0.25mg, tablets Brotizolam 4.2 Posology and method of administration Unless otherwise prescribed by the physician, the following dosages
M0BCore Safety Profile. Active substance: Bromazepam Pharmaceutical form(s)/strength: Tablets 6 mg FR/H/PSUR/0066/001 Date of FAR:
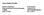 M0BCore Safety Profile Active substance: Bromazepam Pharmaceutical form(s)/strength: Tablets 6 mg P-RMS: FR/H/PSUR/0066/001 Date of FAR: 26.11.2013 4.3 Contraindications Bromazepam must not be administered
M0BCore Safety Profile Active substance: Bromazepam Pharmaceutical form(s)/strength: Tablets 6 mg P-RMS: FR/H/PSUR/0066/001 Date of FAR: 26.11.2013 4.3 Contraindications Bromazepam must not be administered
Sleep and Traumatic Brain Injury (TBI)
 Sleep and Traumatic Brain Injury (TBI) A resource for individuals with traumatic brain injury and their supporters This presentation is based on TBI Model Systems research and was developed with support
Sleep and Traumatic Brain Injury (TBI) A resource for individuals with traumatic brain injury and their supporters This presentation is based on TBI Model Systems research and was developed with support
Sleep and Ageing. Siobhan Banks PhD. Body and Brain at Work, Centre for Sleep Research University of South Australia
 Sleep and Ageing Siobhan Banks PhD Body and Brain at Work, Centre for Sleep Research University of South Australia Health and Active Ageing, 22 nd September 2015 Sleep and Aging How does sleep change as
Sleep and Ageing Siobhan Banks PhD Body and Brain at Work, Centre for Sleep Research University of South Australia Health and Active Ageing, 22 nd September 2015 Sleep and Aging How does sleep change as
Sleep and Insomnia 2/8/2018. Presented by. Marie Rataj, MSN, APRN, ANP. Objectives. Everything you wanted to know
 Sleep and Insomnia Everything you wanted to know Presented by Marie Rataj, MSN, APRN, ANP Objectives Develop a basic knowledge of normal sleep and differentiate from abnormal sleep Develop basic understanding
Sleep and Insomnia Everything you wanted to know Presented by Marie Rataj, MSN, APRN, ANP Objectives Develop a basic knowledge of normal sleep and differentiate from abnormal sleep Develop basic understanding
Improving Your Sleep Course. Session 1 Understanding Sleep and Assessing Your Difficulties
 Improving Your Sleep Course Session 1 Understanding Sleep and Assessing Your Difficulties Course Information Session Details Sessions Session 1 Session 2 Session 3 Session 4 Optional Review Session 5 Session
Improving Your Sleep Course Session 1 Understanding Sleep and Assessing Your Difficulties Course Information Session Details Sessions Session 1 Session 2 Session 3 Session 4 Optional Review Session 5 Session
6/3/2015. Insomnia An Integrative Approach. Objectives. Why An Integrative Approach? Integrative Model. Definition. Short-term Insomnia
 Insomnia An Integrative Approach Jeffrey S. Jump, M.D. Medical Director CHI Memorial Integrative Medicine Associates Objectives Understand the importance of sleep to health Identify patients with insomnia
Insomnia An Integrative Approach Jeffrey S. Jump, M.D. Medical Director CHI Memorial Integrative Medicine Associates Objectives Understand the importance of sleep to health Identify patients with insomnia
Many people with physical
 FACTSHEET How to Sleep Better Many people with physical disabilities suffer from sleep disturbances, and sleep tends to become more disrupted as we get older. Not sleeping well can negatively impact your
FACTSHEET How to Sleep Better Many people with physical disabilities suffer from sleep disturbances, and sleep tends to become more disrupted as we get older. Not sleeping well can negatively impact your
Objectives. Types of Sleep Problems in Developmental Disorders
 Objectives Sleep Problems in the Child with Neurodevelopmental Disorders AACPDM September 11, 2014 BRK-3 Golda Milo-Manson MD, MHSc, FRCP(C) Holland Bloorview Kids Rehabilitation Hospital Toronto, Canada
Objectives Sleep Problems in the Child with Neurodevelopmental Disorders AACPDM September 11, 2014 BRK-3 Golda Milo-Manson MD, MHSc, FRCP(C) Holland Bloorview Kids Rehabilitation Hospital Toronto, Canada
Benzodiazepines: risks, benefits or dependence
 Benzodiazepines: risks, benefits or dependence A re-evaluation Council Report CR 59 January 1997 Royal College of Psychiatrists, London Due for review: January 2002 1 Contents A College Statement 3 Benefits
Benzodiazepines: risks, benefits or dependence A re-evaluation Council Report CR 59 January 1997 Royal College of Psychiatrists, London Due for review: January 2002 1 Contents A College Statement 3 Benefits
Managing Insomnia Disorder A Review of the Research for Adults
 Managing Insomnia Disorder A Review of the Research for Adults e Is This Information Right for Me? This information is right for you if: Your health care professional said you have insomnia disorder (said
Managing Insomnia Disorder A Review of the Research for Adults e Is This Information Right for Me? This information is right for you if: Your health care professional said you have insomnia disorder (said
MMG035 Symptom Management Guidelines for a Person thought to be in the Last Few Days and Hours of Life
 MMG035 Symptom Management Guidelines for a Person thought to be in the Last Few Days and Hours of Life The following pages are guidelines for the management of common symptoms for a person thought to be
MMG035 Symptom Management Guidelines for a Person thought to be in the Last Few Days and Hours of Life The following pages are guidelines for the management of common symptoms for a person thought to be
Programme. Why bother? The effects of sleep loss. Common Sleep Disorders, Identification and investigation Treatments
 Programme. Why bother? The effects of sleep loss. Common Sleep Disorders, Identification and investigation Treatments Brief (but important ) questions. Why bother? The three Pillars of health: - Nutrition
Programme. Why bother? The effects of sleep loss. Common Sleep Disorders, Identification and investigation Treatments Brief (but important ) questions. Why bother? The three Pillars of health: - Nutrition
Appendix 4B - Guidance for the use of Pharmacological Agents for the Treatment of Depression in Adults (18 years and over)
 Appendix 4B - Guidance for the use of Pharmacological Agents for the Treatment of Depression in Adults (18 years and over) Introduction / Background Treatment comes after diagnosis Diagnosis is based on
Appendix 4B - Guidance for the use of Pharmacological Agents for the Treatment of Depression in Adults (18 years and over) Introduction / Background Treatment comes after diagnosis Diagnosis is based on
Managing Sleep Problems after Cancer
 Managing Sleep Problems after Cancer For cancer survivors Read this resource to learn about: What a sleep problem is What causes it What you can do to improve your sleep When to talk to your doctor Please
Managing Sleep Problems after Cancer For cancer survivors Read this resource to learn about: What a sleep problem is What causes it What you can do to improve your sleep When to talk to your doctor Please
KU LEUVEN. Liesbet Van Houdenhove Clinical Psychologist Student Health Center KU Leuven
 SLEEPLESS @ KU LEUVEN Liesbet Van Houdenhove Clinical Psychologist Student Health Center KU Leuven Background Impaired sleep is a frequent and important health problem in college students Prevalence rates
SLEEPLESS @ KU LEUVEN Liesbet Van Houdenhove Clinical Psychologist Student Health Center KU Leuven Background Impaired sleep is a frequent and important health problem in college students Prevalence rates
Summary of Delirium Clinical Practice Guideline Recommendations Post Operative
 Summary of Delirium Clinical Practice Guideline Recommendations Post Operative Intensive Care Unit Clinical Practice Guideline for Postoperative Clinical Practice Guidelines for the Delirium in Older Adults;
Summary of Delirium Clinical Practice Guideline Recommendations Post Operative Intensive Care Unit Clinical Practice Guideline for Postoperative Clinical Practice Guidelines for the Delirium in Older Adults;
Learning Objectives. Delirium. Delirium. Delirium. Terminal Restlessness 3/28/2016
 Terminal Restlessness Dr. Christopher Churchill St. Cloud VA Health Care System EC&R Service Line Director & Medical Director Hospice & Palliative Care March 31, 2016 Learning Objectives Different Terminology
Terminal Restlessness Dr. Christopher Churchill St. Cloud VA Health Care System EC&R Service Line Director & Medical Director Hospice & Palliative Care March 31, 2016 Learning Objectives Different Terminology
Disclosures. Speaker: Teva, UCB, Purdue Advisory Board: Welltrinsic Sleep Network Consultant: Vapotherm, Inc. National Interpretor: Novasom
 So PAP Doesn t Work Rochelle Goldberg, MD, FAASM, FCCP Diplomat, American Board of Sleep Medicine Director Sleep Medicine Services Main Line Health Systems Lankenau Medical Center and Paoli Hospital Disclosures
So PAP Doesn t Work Rochelle Goldberg, MD, FAASM, FCCP Diplomat, American Board of Sleep Medicine Director Sleep Medicine Services Main Line Health Systems Lankenau Medical Center and Paoli Hospital Disclosures
Sleep, tiredness, lack of energy: heart sink symptoms
 Sleep, tiredness, lack of energy: heart sink symptoms Abstract Problematic sleep is a widespread issue and insomnia is the commonest complaint. The diagnosis of insomnia requires thorough history-taking
Sleep, tiredness, lack of energy: heart sink symptoms Abstract Problematic sleep is a widespread issue and insomnia is the commonest complaint. The diagnosis of insomnia requires thorough history-taking
Achieving better sleep
 Achieving better sleep A patient s guide 1 Sleep problems are common and affect a large proportion of people at some time in their lives. One question often asked is How much sleep do I need? for which
Achieving better sleep A patient s guide 1 Sleep problems are common and affect a large proportion of people at some time in their lives. One question often asked is How much sleep do I need? for which
Caring for the Mind: Managing Depression and Anxiety. Highlights from 2017 ONS Congress
 Caring for the Mind: Managing Depression and Anxiety Highlights from 2017 ONS Congress Mood and Anxiety Disorders: Symptoms of mood disorders Non-reactive mood, worthlessness, guilt, loss of interest,
Caring for the Mind: Managing Depression and Anxiety Highlights from 2017 ONS Congress Mood and Anxiety Disorders: Symptoms of mood disorders Non-reactive mood, worthlessness, guilt, loss of interest,
FATIGUE MANAGEMENT & MITIGATION
 FATIGUE MANAGEMENT & MITIGATION PAM JAGER DIRECTOR OF EDUCATION & DEVELOPMENT GRMEP OBJECTIVES By the end of this presentation participants will: Understand ACGME requirements for fatigue management &
FATIGUE MANAGEMENT & MITIGATION PAM JAGER DIRECTOR OF EDUCATION & DEVELOPMENT GRMEP OBJECTIVES By the end of this presentation participants will: Understand ACGME requirements for fatigue management &
Insomnia. St. Joseph s Annual Family Practice Refresher March 1, Robert J. Ostrander, M.D
 St. Joseph s Annual Family Practice Refresher March 1, 2018 Robert J. Ostrander, M.D If in bed I say, When shall I arise? then the night drags on; I am filled with restlessness until the dawn. Job 7:4
St. Joseph s Annual Family Practice Refresher March 1, 2018 Robert J. Ostrander, M.D If in bed I say, When shall I arise? then the night drags on; I am filled with restlessness until the dawn. Job 7:4
Let s Sleep On It: Developing a Healthy Sleep Pattern. The Presenter. Session Overview
 Let s Sleep On It: Developing a Healthy Sleep Pattern The Presenter Gina Crome Gina has extensive personnel management experience, acting as Director of Implementation at CME Incorporated and Director
Let s Sleep On It: Developing a Healthy Sleep Pattern The Presenter Gina Crome Gina has extensive personnel management experience, acting as Director of Implementation at CME Incorporated and Director
