Upper Airway Collapsibility and Cephalometric Variables in Patients with Obstructive Sleep Apnea
|
|
|
- Oswald Freeman
- 6 years ago
- Views:
Transcription
1 Upper Airway Collapsibility and Cephalometric Variables in Patients with Obstructive Sleep Apnea EMILIA SFORZA, WILLIAM BACON, THOMAS WEISS, ANNE THIBAULT, CHRISTOPHE PETIAU, and JEAN KRIEGER Sleep Disorders Unit and Department of Clinical Dental Sciences, University Hospital, Strasbourg, France Increased pharyngeal collapsibility and abnormal anatomic structures have been postulated to contribute to the pathophysiology of obstructive sleep apnea (OSA) syndrome. It is unclear whether the abnormal craniofacial and soft tissue features may affect the pharyngeal collapsibility and contribute to the apnea density. In the present study we examine the relationship between pharyngeal collapsibility and cephalometric variables in a group of 57 male OSA patients. Pharyngeal collapsibility was measured during the night of nasal continuous positive airway pressure (ncpap) titration by analyzing the pressure flow relationship. Pharyngeal critical pressure (Pcrit) was calculated as the extrapolated pressure at zero flow. The patients, age yr, had an average apnea hypopnea index (AHI) of and a mean Pcrit of cm H 2 O. A significant correlation was found between Pcrit and the soft palate length (SPl) (r 0.27, p 0.04), the distance from the hyoid bone to the posterior pharyngeal wall (H-Ph) (r 0.29, p 0.03), and the distance from the hyoid bone to posterior nasal space (H-Pns) (r 0.32, p 0.02). While in obese patients Pcrit was related to SPl and neck circumference, the distance of the hyoid bone to the mandibular plane (H-MP) affected Pcrit in nonobese patients. Our results show that both pharyngeal soft tissue abnormalities and the lower position of the hyoid bone affect Pcrit in OSA patients, suggesting that an anatomic narrowing contributes to the upper airway collapsibility. Sforza E, Bacon W, Weiss T, Thibault A, Petiau C, Krieger J. Upper airway collapsibility and cephalometric variables in patients with obstructive sleep apnea. AM J RESPIR CRIT CARE MED 2000;161: The obstructive sleep apnea (OSA) syndrome results from repeated occlusion of the upper airway during sleep; however, it is still unclear why an individual s airway is obstructed during sleep. Previous studies have focused on anatomic factors as predictive factors in apnea density. Compared with control subjects and snorers, cephalographic evaluation in OSA patients has shown deviations in the position of the hyoid bone, in the dimensions of the posterior airway space, and in the diameter and length of the soft palate and the tongue (1 3). However, there is no consistent evidence that these differences in the upper airway anatomy have a substantial impact on the incidence of OSA. A considerable overlap in airway caliber is present between normals, snorers, and OSA patients (4) and facial bone and soft tissue abnormalities are unlikely to be major factors in obese groups (5, 6). Thus, the determinants of upper airway collapse are multiple, the airway anatomy being only one such determinant. Recently, the process of pharyngeal collapse has been explained by applying the Starling resistor concept to upper airway flow mechanisms. According to this model, the suction pressure applied to the downstream end of the collapsible tube can increase the flow only to a limited extent and the flow (Received in original form October 26, 1998 and in revised form June 30, 1999) Correspondence and requests for reprints should be addressed to Emilia Sforza, M.D., Ph.D., Laboratoire de Sommeil, Hôpital Belle-Idée, CH-1225 Genève, Switzerland. Am J Respir Crit Care Med Vol 161. pp , 2000 Internet address: mechanism depends essentially on the dynamic behavior of the collapsible segment, that is, the segment between soft palate and hypopharynx. Thus the air flows through the pharynx only when the upstream pressure exceeds a critical pressure. Many methods have been introduced to measure upper airway collapsibility, the most sensitive being the pharyngeal critical pressure (Pcrit). Positive values of Pcrit differentiate OSA patients from snorers (7) and Pcrit influences the density of the sleep-related breathing disorders (8). Although there are studies supporting the effect of neuromuscular control on pharyngeal collapsibility (9), we have no detailed data on the role of anatomic factors. Schwartz and colleagues have demonstrated in OSA patients treated by uvulopalatopharyngoplasty (UPPP) (10) a significant decrease in the apnea hypopnea index (AHI) only in patients in whom Pcrit becomes more negative. This suggests that anatomic alterations may be a contributing factor to upper airway collapsibility. To determine the relative influence on pharyngeal collapsibility of the anatomic factors, we measured Pcrit in a group of patients with OSA having cephalometry and we studied the possible relationship of Pcrit with some craniofacial and soft tissue variables. METHODS Among the consecutive patients referred to the sleep laboratory from March 1997 to March 1998 for assessment of possible sleep-disordered breathing, 130 were identified from the polysomnographic study register. The exclusion criteria were AHI 10 (17 subjects), fe-
2 348 AMERICAN JOURNAL OF RESPIRATORY AND CRITICAL CARE MEDICINE VOL male sex (20 subjects), previous treatment for sleep apnea with nasal continuous positive airway pressure (ncpap) (five patients), corrective upper airway surgery or cleft palate repair (five patients), and presence of craniofacial malformation (four patients). Patients with cephalograms with an intra- or interexaminer error of more than 1 mm or 1 (10 subjects) and patients showing mask and mouth leaks (12 patients) during the titration night were also excluded. Of the original sample, 57 male Caucasian patients met the selection criteria. The subjects were divided into two groups, obese (n 30) and nonobese (n 27), using a body mass index (BMI) 30 kg/m 2 as a cutoff score. Written informed consent was obtained before entry into the study. All patients had a full evaluation including polysomnography, blood gas analysis, respiratory function tests, and cephalometry. Neck circumference was measured in all subjects at the level of the superior border of the cricothyroid membrane in the upright position. Cephalometric radiographs, obtained according to a method described in our previous work (3, 11), were recorded in the sitting natural head posture (mirror technique) at the end-expiration phase and without swallowing. The radiographs were traced twice by two different investigators blinded to the subject s apnea frequency and Pcrit. The mean value of measurements for each patient was used for the calculation and the variables were assessed as angular (degree) or linear (millimeters) measures. The cephalometric variables were classified into four categories: soft tissue data, hyoid bone position data, airway size data (Figure 1A), and craniofacial data (Figure 1B). The following soft tissue variables were measured: the length of the soft palate (SPl) from the posterior nasal spine of the maxilla to the lower edge of the uvula; the soft palate width (Spw); the tongue length (Tl) measured from the lowest part of the epiglottis to the tip of the tongue; and the tongue width (Tw). Hyoid position variables included the distance of the hyoid bone to the mandibular plane (H-MP); the shortest distance of the hyoid bone to the posterior pharyngeal wall (H-Ph); and the distance of the hyoid bone from the posterior nasal spine (H-Pns) representing pharyngeal elongation. Upper airway size data were defined as the superior (SPAS) and inferior (IPAS) posterior airway space measured respectively as the shortest distance from the posterior pharyngeal wall to the posterior soft palate (SPAS) and to the dorsum of the tongue (IPAS). Bony measurements (Figure 1B) included: the length of the anterior cranial base from nasion to sella (SN); the angulation of the cranial base (BaSN); the sagittal dimension of the bony pharynx (BaPns); the maxillary position (SNA); the mandibular position (SNB); the difference in prognathism (ANB); the lower face height; the total face height; the angulation of the mandibular plane with the cranial base (SN-MP); the maxillary unit length (Ans-Pns) calculated as the distance between the medial condylar point of the maxilla to the tip of the posterior nasal spine; and the mandibular unit length (Cd-Gn) measured as the distance from the medial condylar of the mandible to gnathion, i.e., the most anterior inferior point of the mandibular symphysis. Polysomnographic Study Nocturnal recording was carried out for two nights, the first without ncpap and the second with ncpap, as part of the diagnostic workup. Polysomnography included an electroencephalogram, electro-oculogram, and electromyogram of chin muscles for conventional sleep staging. Breathing was analyzed with a pneumotachograph attached to a face mask. Oxygen saturation was measured continuously with an ear oximeter (Biox III; Ohmeda, Boulder, CO). Esophageal pressure was measured with a 10-cm latex balloon placed in the lower third of Figure 1. (A) Cephalometric landmarks and soft tissue, hyoid position, and airway size variables used in the study. Landmarks: Pns: posterior nasal spine; H: hyoid bone; MP: mandibular plane (tangent line from the symphysis to the inferior border of the mandibular angle). Variables: 1) SPl: the length of the soft palate; 2) Spw: the width of the soft palate; 3) Tl: the length of the base of the tongue; 4) Tw: the width of the tongue; 5) H-Ph: the distance from the hyoid bone to the posterior wall of the pharynx; 6) H-Pns: the distance from the hyoid bone to Pns; 7) H-MP: the distance from the hyoid bone to the mandibular plane; 8) SPAS: the upper posterior pharyngeal space; 9) IPAS: the lower posterior pharyngeal space. (B) Anatomic reference points and variables for craniofacial skeletal measurements. A: the most posterior midline point in the concavity between the anterior nasal spine and the lowest point on the alveolar bone overlying the maxillary incisors; B: the most posterior midline point on the anterior concavity of the mandibular symphysis; Ans: anterior nasal spine: the anterior tip of the sharp bony process of the maxilla at the lower margin of the anterior nasal opening; Ba: basion; Cd: condylion, i.e., the most posterior superior point on the curvature of the condylar head; Gn: gnation, i.e., the most anterior inferior point on the contour of the bony chin symphysis; Me: menton, i.e., the lowest point on the symphyseal shadow of the mandible; N: nasion; S: geometric center of the pituitary fossa. Skeletal variables: 10) SNA: maxillary protrusion; 11) SNB: mandibular prognathism; 12) ANB: maxillo-mandibular discrepancy; 13) BaSN: cranial base angle; 14) SN-MP: angle of facial divergence; 15) BaPns: upper pharynx bony opening; 16) total face height; 17) lower face height; 18) Ans-Pns: sagittal dimension of the maxilla; 19) Cd-Gn: overall length of the mandible.
3 Sforza, Bacon, Weiss, et al.: Cephalometry and Pharyngeal Critical Pressure 349 the esophagus, inflated with 1 ml of air and connected to a pressure transducer (Validyne MP 45; Validyne, Northridge, CA). During the titration night the nasal pressure (Pn) was measured through a side port in the nasal mask and a thermocouple was placed over the lips to ascertain that mouth breathing did not occur during the measurements. ncpap was increased from the initial value of 2 cm H 2 O with 1 cm H 2 O increments up to the efficacious level. Sleep was scored using the criteria of Rechtschaffen and Kales (12) for 10-s epochs and respiratory events were scored using standard criteria. Hypopneas were defined as a 50% or greater reduction in tidal volume from the baseline value lasting at least 10 s. The apnea index (AI) and the AHI were established as the ratio of the number of apneas and apneas hypopneas per hour of sleep. Apnea time was expressed as the sleep time spent in apnea. As indices of nocturnal hypoxemia we considered the mean Sa O2 (Sa O2 mean) during sleep and the minimal value recorded during sleep (Sa O2 min). During the ncpap titration night, we measured Pcrit according to described methods (8) by relating changes in maximal inspiratory airflow ( V I max ) to varying levels of ncpap (Pn) by least square regression analysis. The Pcrit was defined as the extrapolated pressure at zero flow. Measurements were made during light sleep (Stages 1 2 of non rapid eye movement [NREM] sleep) in the supine position. Recurrent obstructive apneas and hypopneas were always allowed to occur before initial changes in nasal pressure. Mask pressure was then raised in 1 cm H 2 O increments and at least 10 min of light sleep were observed before a subsequent rise in nasal pressure. During periods with hypopneas, the relationship between maximal airflow and nasal pressure was obtained by averaging the maximal flow for the last four breaths of an hypopnea. During periods free of apnea and hypopneas TABLE 1 ANTHROPOMETRIC, CLINICAL, AND CEPHALOMETRIC DATA OF ANALYZED PATIENTS Mean SD Range Age, yr BMI, kg/m Neck size, cm AHI, n/h AI, n/h Apnea time, min Mean Sa O2 % Pcrit, cm H 2 O SPI, mm Spw, mm TI, mm Tw, mm H-MP, mm H-Pns, mm H-Ph, mm SPAS, mm IPAS, mm SN, mm BaSN, BaPns, mm SNA, SNB, ANB, Lower face height, mm Total face height, mm Ans-Pns, mm Cd-Gn, mm SN-MP, Definition of abbreviations: AHI apnea hypopnea index; AI apnea index; ANB difference in prognathism; Ans-Pns maxillary unit length; BaSN angulation of the cranial base; BMI body mass index; Cd-Gn mandibular unit length; H-MP distance of the hyoid bone to the mandibular plane; H-Pns distance of hyoid bone to the posterior nasal spine; IPAS inferior posterior airway space; H-Ph shortest distance of the hyoid bone to the posterior pharyngeal wall; Pcrit pharyngeal critical pressure; SN length of the anterior cranial base from nasion to sella; SNA position of the maxilla; SNB position of the mandible; SN-MP angle of facial divergence; SPAS superior posterior airway space; SPl length of the soft palate; Spw soft palate width; Tl tongue length; Tw tongue width. but with flow limitation, defined as a reduced and plateaued inspiratory airflow while esophageal pressure was increasing, maximal inspiratory airflow was measured at each level of ncpap for several breaths. In all patients the r of the regression analysis was above Statistical Analysis Data were expressed as means SD. Bivariate correlation analysis using Pearson s correlation coefficient was used to find the variables correlated with Pcrit and multivariate regression analysis was done to define the contribution of anthropometric and cephalometric variables in explaining pharyngeal collapsibility. Obese and nonobese patients were compared using one-way analysis of variance. When a significant difference was found, individual means were compared using the Student-Newman-Keuls test. The statistical significance level selected for all analyses was p RESULTS Clinical, anthropometric, and cephalometric variables of the study group are shown in Table 1. The patients, age yr with a mean BMI of kg/m 2, had a mean AHI of ranging from 19 to 152 and a mean AI of The mean time of sleep spent in apnea was min ranging from 26 to 228. A wide range of nocturnal hypoxemia severity was present with a mean Sa O2 of % and a minimal Sa O2 of %. The mean neck circumference was cm. As a group, the patients had normal blood gases; eight patients were hypoxemic, defined as having a Pa O2 65 mm Hg (mean Pa O2 : mm Hg) and 15 were hypercapnic, with a Pa CO2 45 mm Hg (Pa CO2 : mm Hg). In each subject there was a significant linear relationship between the values of V I max and the corresponding Pn, with a TABLE 2 PEARSON S CORRELATION COEFFCIENTS OF RELATIONSHIPS BETWEEN Pcrit AND DIURNAL AND NOCTURNAL VARIABLES All Patients Obese Nonobese r p Value r p Value r p Value Age, yr NS NS NS AHI, n/h NS Apnea time, min BMI, kg/m NS NS Neck size, cm NS SPI, mm NS Spw, mm NS NS NS Tl, mm NS NS NS Tw, mm NS NS NS H-MP, mm NS H-Pns, mm NS H-Ph, mm NS SPAS, mm NS NS NS IPAS, mm NS NS NS SN, mm NS NS NS BaSN, NS NS NS BaPns, mm NS NS NS SNA, NS NS NS SNB, NS NS NS ANB, NS NS NS Lower face height, mm NS NS NS Total face height, mm NS NS NS Ans-Pns, mm NS NS NS Cd-Gn, mm NS NS NS SN-MP, NS NS NS Definition of abbreviation: NS not significant. For other definitions see Table 1.
4 350 AMERICAN JOURNAL OF RESPIRATORY AND CRITICAL CARE MEDICINE VOL correlation coefficient ranging from 0.90 to Calculated Pcrit values ranged from 0.3 to 4.7 with an average value of cm H 2 O. Table 2 reports the correlation coefficients of craniofacial variables, diurnal and nocturnal parameters, and Pcrit. As expected, Pcrit was highly correlated with AHI (r 0.52, p ) and apnea time (0.68, p 0.001). Regarding anthropomorphic variables, Pcrit was strongly correlated with the neck circumference (p 0.38, p 0.004) and with BMI (r 0.29, p 0.02), whereas no correlations were found with age (r 0.14, p ns). Correlation of Pcrit with the cephalometric variables indicated a higher linear relationship with the hyoid bone position (H-Ph: r 0.29, p 0.03; H-Pns: 0.32, p 0.02), and the SPl (r 0.27, p 0.04) and a near significant relationship with the H-MP (0.26, p 0.06). No relationships were found in our study sample between Pcrit, tongue length, or craniofacial data. With all variables in the regression analysis no cephalometric variable independently predicted Pcrit, neck circumference alone explaining the 14% of the variance in Pcrit. Because cephalometric cranial and soft tissue variables may differ in patients with and without obesity, the patients were classified as obese and nonobese according to a BMI 30. Table 3 shows the clinical, polygraphic, and cephalometric data of the patients according to BMI. Of the study group, 27 were nonobese and 30 had a BMI 30. Significant differences between groups were seen for AHI, apnea time, neck circumference, and Pcrit, with higher values in obese patients. Regarding craniofacial, hyoid bone position, and upper airway size data, there were no significant differences between groups except for ANB, which was greater in obese patients ( mm versus mm, p 0.009). No differences in pharyngeal soft tissue variables were seen between the two groups but obese patients had longer H-Ph ( mm versus mm). Correlation analysis (Table 2) in the nonobese patients showed that Pcrit was related to H-MP. In TABLE 3 ANTHROPOMETRIC, CLINICAL, AND CEPHALOMETRIC DATA OF OBESE AND NONOBESE PATIENTS Nonobese Obese p Value Age, yr NS Neck size, cm AHI, n/h Apnea time, min Pcrit, cm H 2 O SPI, mm NS Spw, mm NS Tl, mm NS Tw, mm NS H-MP, mm NS H-Pns, mm NS H-Ph, mm SPAS, mm NS IPAS, mm NS SN, mm NS BaSN, NS BaPns, mm NS SNA, NS SNB, NS ANB, Lower facial height, mm NS Total face height, mm NS Ans-Pns, mm NS Cd-Gn, mm NS SN-MP, NS For definitions of abbreviations, see Table 1. the obese group Pcrit was significantly related to neck circumference (r 0.38, p 0.04) and SPl (r 0.39, p 0.03). A near significant relationship was also present with H-Ph (r 0.34, p 0.07) and H-Pns (r 0.33, p 0.06) (Table 2). DISCUSSION In the present study we demonstrate significant correlation between Pcrit and anatomic variables assessed by cephalometry. Elongated soft palate and lower hyoid bone position increase the individual tendency to pharyngeal collapse, i.e., Pcrit, which in turn affects the frequency of sleep-related breathing disorders. Although the correlations between cephalometric variables and Pcrit are in the moderate range, they are consistent with the hypothesis of an influence of soft tissue configuration and anatomic narrowing on the pharyngeal collapsibility. Whereas airway compliance, pharyngeal muscular force, and anatomic variables may all influence upper airway configuration, the critical factors responsible for control of pharyngeal patency remain controversial. Two hypotheses have been proposed to explain the tendency of patients with OSA to collapse: a neural hypothesis implying reduced dilator muscle activity and an anatomic theory suggesting an anatomic narrowing of the upper airway. According to the neural hypothesis, the loss of wakefulness stimulus and changes in neuromuscular control (9) may account for the greater pharyngeal collapsibility in patients with OSA. It is generally assumed that upper airway muscle activity is modulated by chemical stimuli and by changes in upper airway pressure. Breathing through a narrow pharynx generates greater collapsing forces, and pharyngeal collapse would depend on the force of contraction of the upper airway muscles. The more forceful the pharyngeal muscle contraction, the less likely that collapse will occur. However, abnormalities in bony structure or fat deposition in the neck may contribute to low pharyngeal cross-sectional area. Increased upper airway compliance and collapsibility have been found in OSA patients (13), partially related to regional neck obesity (14). Moreover, anatomic abnormalities may influence the greater collapsibility in patients with OSA because closing pressure is elevated in micrognathic infants (15) and in patients with enlarged uvula (16). Furthermore, patients who responded to UPPP were those with enlarged and hypertrophic tonsils in whom Pcrit greatly decreased after surgery (10). Thus, it could be quite correctly argued that changes in soft tissue and body facial anatomy may interfere with upper airway collapsibility. In our patients with OSA, Pcrit was related to the length of the soft palate and the position of the hyoid arch, two structures that contribute to pharyngeal aperture and stability of the upper airway. Although this study does not provide definitive evidence concerning the mechanisms by which the anatomic variables interfere with upper airway collapsibility, our results provide interesting preliminary information that may be useful in future studies. The statistical comparison between the two groups showed that they did not differ for craniofacial architecture, and the pharyngeal soft tissue variables were also very similar. However, pharyngeal soft tissues, neck circumference, and hyoid bone compensation seemed to be involved in a different way in obese and nonobese patients. Because the site of the collapse in 80% of patients with OSA is at the upper pharyngeal level, we can postulate that the Pcrit would become more positive when the tongue impinges on an elongated soft palate. Obesity, through neck and soft tissue fat deposition, and increased pressure on the neck of submental adipose tissue, may predispose to upper airway obstruction (17). Thus the correlation between Pcrit and SPl in
5 Sforza, Bacon, Weiss, et al.: Cephalometry and Pharyngeal Critical Pressure 351 obese patients is a reasonable finding. This supports the data of Schwartz and colleagues (18) who demonstrated changes in Pcrit in patients treated with weight loss. Assuming that hyoid bone position is crucial to pharyngeal patency, several hypotheses can be advanced to explain which factors influence the position of the hyoid bone and consequently Pcrit. An imbalance between suprahyoid and infrahyoid muscles may influence the hyoid bone position. Chronic snoring trauma and/or repetition of chemical and mechanical stimuli may produce morphological alterations in the pharyngeal dilator muscles (19, 20) or pharyngeal neuropathy (21, 22). The consequent changes in contractile properties (23) and the progressive loss in the compensatory muscular mechanisms maintaining upper airway patency (24) and influencing hyoid position may determine a greater pharyngeal collapsibility. Although no significant differences were found between obese and nonobese patients, nonobese patients had smaller H-Ph distance and smaller ANB. We know that mandibular protrusion increases upper airway caliber at the oropharynx and hypopharynx (25), mostly in nonobese patients, suggesting that the pharyngeal occlusion will more likely occur when the mandible is smaller or receded. From these data we can suggest that alteration in mandibular position may affect hyoid bone position and, thus, Pcrit. It remains also possible that other factors, besides anatomic and neuromuscular variables, may alter the position of the hyoid bone. In our group larger H-MP and larger H-Pns were found in obese patients having greater Pcrit. Thus obesity, by neck fat deposition, may shift the hyoid bone caudally altering the pharyngeal patency and leading to greater upper airway collapsibility. Although significant relationships do exist between the soft palate length, hyoid bone position, and Pcrit in our patients, the correlations are mostly in the moderate to lower range. It is likely that our failure to observe a clear relationship between Pcrit and cephalometric variables may be the result of other factors that we were unable to control. An important consideration in the present study is our ability to accurately assess upper airway collapsibility. Many methods have been used to measure pharyngeal collapsibility and the one most widely used is Pcrit. One problem in using Pcrit is the interference of anatomic and neuromuscular factors on this variable: mandibular advancement (26), sleep posture (27), tongue position, neck flexion and enlarged uvulas (16), may all affect the pharyngeal collapsibility. Thus, Pcrit may not adequately reflect the true individual pharyngeal collapsibility. The closing pressure (Pclose) has been introduced to improve the assessment of pharyngeal collapsibility. This is an entirely objective measure of pharyngeal properties obtained under general anesthesia (28) or during ncpap treatment (29) in which muscular influences are removed. By using Pclose these investigators demonstrated that the anatomic narrowing related to mandibular position (26) or to enlarged adenoids and tonsils (30) induces a higher collapsibility of the pharynx. Moreover, adenotonsillectomy (30) and mandibular advancement (26) may be therapeutic only when Pclose becomes more negative. These observations are in agreement with our results supporting the hypothesis that an anatomic narrowing predisposes to pharyngeal collapse. There are several other possible explanations why the airway of the awake patients did not strongly affect Pcrit in our sample. First, cephalometric data were obtained when the subject was awake and in the sitting position, and thus did not reflect the changes that could have occurred during sleep when the awake activation of pharyngeal muscles is removed and when the patient is supine. Even though tongue and soft palate thickness increases in supine position, a close relationship between upright and supine craniofacial and soft tissue measurements (31) is present. Second, cephalometry provides information for anteroposterior but not lateral pharyngeal structures that are implicated in the pharyngeal narrowing. Studies using magnetic resonance imaging techniques have demonstrated that differences between snorers and patients with OSA in airway caliber are more related to lateral pharyngeal wall size and thickness than to anteroposterior dimension (6). This finding is supported by previous studies showing that ncpap dilates the upper airway more laterally than in the anteroposterior direction (32) and that the fat deposition is greater in the lateral upper airways walls (33). Third, it is possible that the shape of the upper airway (34) and its elliptical orientation may predispose to pharyngeal collapse during sleep more than the airway size itself. Finally, we collected data in patients with severe OSA, and snorers or hypopneic patients were not analyzed. Because Pcrit is more frequently subatmospheric in individuals with snoring, it seems reasonable to expect a greater relationship when patients having negative values of Pcrit are considered. In summary, in analyzing the relationship between Pcrit and cephalometric variables we wondered whether patients with OSA had a more collapsible pharynx, dependent on anatomic variables. Overall, a relationship between Pcrit, hyoid bone position, and soft palate length was found in patients with severe OSA. Although these results should not be overstated, it could be quite correctly argued that changes in soft tissue and body facial anatomy may interfere with upper airway collapsibility. Further studies in sleeping condition would provide more information on the influence of the anatomic variables on the upper airway collapsibility. Acknowledgment : The writers thank Dr. A. Gold and F. Sériès for their helpful advice and the staff of the sleep laboratory for technical assistance. References 1. Partinen, M., C. Guilleminault, M. A. Quera-Salva, and A. Jamieson Obstructive sleep apnea and cephalometric roentgenograms: the role of anatomic upper airway abnormalities in the definition of abnormal breathing during sleep. Chest 93: Lyberg, T., O. Krogstadt, and G. Djupesland Cephalometric analysis in patients with obstructive sleep apnea syndrome: I. Skeletal morphology. J. Laryngol. Otol. 103: Bacon, W. H., J. C. Turlot, J. Krieger, and J. L. Stierle Cephalometric evaluation of pharyngeal obstructive factors in patients with sleep apnea syndrome. Angle Orthod. 60: Mathur, R., and N. J. Douglas Family studies in patients with the sleep apnea hypopnea syndrome. Ann. Intern. Med. 122: Nelson, S., and M. Hans Contribution of craniofacial risk factors in increasing apneic activity among obese and nonobese habitual snorers. Chest 111: Schwab, R. J., K. B. Guptka, W. B. Gefter, L. J. Metzger, E. A. Hoffman, and A. I. Pack Upper airway and soft tissue anatomy in normal subjects and patients with sleep-disordered breathing: significance of the lateral pharyngeal walls. Am. J. Respir. Crit. Care Med. 152: Gleadhill, I. C., A. R. Schwartz, N. Schubert, R. A. Wise, S. Permutt, and P. L. Smith Upper airway collapsibility in snorers and in patients with obstructive sleep apnea. Am. Rev. Respir. Dis. 143: Sforza, E., C. Petiau, T. Weiss, A. Thibault, and J. Krieger Pharyngeal critical pressure in patients with obstructive sleep apnea syndrome: clinical implications. Am. J. Respir. Crit. Care Med. 159: Horner, R. L., J. A. Innes, K. Murphy, and A. Guz Evidence for reflex upper airway dilator muscle activation by sudden negative pressure in man. J. Physiol. 436: Schwartz, A. R., N. Schubert, and W. Rothman Effect of uvulopalatopharyngoplasty on upper airway collapsibility in obstructive sleep apnea syndrome. Am. Rev. Respir. Dis. 145: Bacon, W. H., J. Krieger, J. C. Turlot, and J. L. Stierle Craniofacial characteristics in patients with obstructive sleep apneas syndrome. Cleft Palate J. 25:
6 352 AMERICAN JOURNAL OF RESPIRATORY AND CRITICAL CARE MEDICINE VOL Rechtschaffen, A., and A. Kales A manual of standardized terminology, technique and scoring system for sleep stages of human sleep. Los Angeles Brain Information Service. Brain Information Institute, UCLA. 13. Brown, I. G., T. D. Bradley, E. A. Phillipson, N. Zamel, and V. Hoffstein Pharyngeal compliance in snoring subjects with and without obstructive sleep apnea. Am. Rev. Respir. Dis. 132: Ryan, C. F., and L. L. Love Mechanical properties of the velopharynx in obese patients with obstructive sleep apnea. Am. J. Respir. Crit. Care Med. 154: Roberts, J. L., W. R. Reed, O. P. Mathew, A. A. Menon, and B. T. Thach Assessment of pharyngeal airway stability in normal and micrognathic infants. J. Appl. Physiol. 58: Morrison, D. L., S. H. Launois, S. Isono, T. R. Feroah, W. A. Whitelaw, and J. E. Remmers Pharyngeal narrowing and closing pressure in patients with obstructive sleep apnea. Am. Rev. Respir. Dis. 148: Ferguson, K. A., T. Ono, A. A. Lowe, C. F. Ryan, and J. A. Fleetham The relationship between obesity and craniofacial structure in obstructive sleep apnea. Chest 108: Schwartz, A. R., A. R. Gold, N. Schubert, A. Stryzak, R. A. Wise, S. Permutt, and P. L. Smith Effect of weight loss on upper airway collapsibility in obstructive sleep apnea. Am. Rev. Respir. Dis. 144: Smirne, S., S. Iannacone, L. Ferini-Strambi, M. Comola, E. Colombo, and R. Nemni Muscle fibre type and habitual snoring. Lancet 337: Friberg, D., T. Ansved, K. Borg, B. Carlsson-Nordlander, H. Larsson, and E. Svanborg Histological indications of a progressive snorers disease in an upper airway muscle. Am. J. Respir. Crit. Care Med. 157: Larsson, H., B. Carlsson-Nordlander, L. E. Linblad, O. Norbeck, and E. Svanborg Temperature threshold in the oropharynx of patients with obstructive sleep apnea syndrome. Am. Rev. Respir. Dis. 146: Woodson, B. T., J. C. Garancis, and R. J. Toohill Histopathological changes in snoring and obstructive sleep apnea syndrome. Laryngoscope 101: Series, F., C. Coté, J. A. Simoneau, S. St. Pierre, and I. Marc Upper airway collapsibility and contractile and metabolic characteristics of muscular uvula. FASEB J. 10: Mezzanotte, W. S., D. K. Tangel, and D. P. White Influence of sleep onset on upper-airway activity in apnea patients versus normal controls. Am. J. Respir. Crit. Care Med. 153: Ferguson, K. A., L. L. Love, and C. F. Ryan Effect of mandibular and tongue protrusion on upper airway size during wakefulness. Am. J. Respir. Crit. Care Med. 155: Isono, S., A. Tanaka, Y. Sho, A. Konno, and T. Nishino Advancement of the mandible improves velopharyngeal airway patency. J. Appl. Physiol. 79: Neill, A. M., S. M. Angus, D. Sajkov, and R. D. McEvoy Effects of sleep posture on upper airway stability in patients with obstructive sleep apnea. Am. J. Respir. Crit. Care Med. 155: Isono, S., J. E. Remmers, A. Tanaka, Y. Sho, J. Saro, and T. Nishino Anatomy of the pharynx in patients with obstructive sleep apnea and in normal subjects. J. Appl. Physiol. 82: Schwartz, A. R., C. R. O Donnell, J. Baron, N. Schubert, D. Alam, S. D. Samadi, and P. L. Smith The hypotonic upper airway in obstructive sleep apnea: role of structures and neuromuscular activity. Am. J. Respir. Crit. Care Med. 157: Isono, S., A. Shimada, M. Utsugi, A. Konno, and T. Nishino Comparison of static mechanical properties of the passive pharynx between normal children and children with sleep disordered breathing. Am. J. Respir. Crit. Care Med. 157: Pae, E. K., A. A. Lowe, K. Sasaki, C. Price, M. Tsuchiya, and J. A. Fleetham A cephalometric and electromyographic study of upper airway structures in the upright and supine positions. Am. J. Orthod. Dentofacial Orthop. 106: Schwab, R. J., A. I. Pack, K. B. Gupta, L. J. Metzger, E. Oh, J. E. Getsy, E. A. Hoffman, and W. B. Gefter Upper airway and soft tissue structural changes induced by CPAP in normal subjects. Am. J. Respir. Crit. Care Med. 154: Horner, R. L., R. H. Mohiaddin, D. G. Lowell, S. A. Shea, E. D. Burman, D. B. Longmore, and A. Guz Sites and sizes of fat deposits around the pharynx in obese patients with obstructive sleep apnea and weight matched controls. Eur. Respir. J. 2: Leiter, J. C Upper airway shape: is it important in the pathogenesis of obstructive sleep apnea? Am. J. Respir. Crit. Care Med. 153:
Pharyngeal Critical Pressure in Patients with Obstructive Sleep Apnea Syndrome Clinical Implications
 Pharyngeal Critical Pressure in Patients with Obstructive Sleep Apnea Syndrome Clinical Implications EMILIA SFORZA, CHRISTOPHE PETIAU, THOMAS WEISS, ANNE THIBAULT, and JEAN KRIEGER Sleep Disorders Unit,
Pharyngeal Critical Pressure in Patients with Obstructive Sleep Apnea Syndrome Clinical Implications EMILIA SFORZA, CHRISTOPHE PETIAU, THOMAS WEISS, ANNE THIBAULT, and JEAN KRIEGER Sleep Disorders Unit,
6. The Upper Airway. Anatomy of the Pharyngeal Airway in Sleep Apneics: Separating Anatomic Factors From Neuromuscular Factors
 Sleep, 16:S80-S84 1993 American Sleep Disorders Association and Sleep Research Society 6 The Upper Airway (a) Response to Anatomy Anatomy of the Pharyngeal Airway in Sleep Apneics: Separating Anatomic
Sleep, 16:S80-S84 1993 American Sleep Disorders Association and Sleep Research Society 6 The Upper Airway (a) Response to Anatomy Anatomy of the Pharyngeal Airway in Sleep Apneics: Separating Anatomic
Developmental Changes in Collapsibility of the Passive Pharynx during Infancy
 Developmental Changes in Collapsibility of the Passive Pharynx during Infancy SHIROH ISONO, ATSUKO TANAKA, TERUHIKO ISHIKAWA, and TAKASHI NISHINO Department of Anesthesiology, Chiba University School of
Developmental Changes in Collapsibility of the Passive Pharynx during Infancy SHIROH ISONO, ATSUKO TANAKA, TERUHIKO ISHIKAWA, and TAKASHI NISHINO Department of Anesthesiology, Chiba University School of
Comparative Effects of Two Oral Appliances on Upper Airway Structure in Obstructive Sleep Apnea
 COMPARISON OF EFFECTS OF ORAL APPLIANCES ON THE AIRWAY IN OSA Comparative Effects of Two Oral Appliances on Upper Airway Structure in Obstructive Sleep Apnea Kate Sutherland, PhD 1,2 ; Sheryn A. Deane,
COMPARISON OF EFFECTS OF ORAL APPLIANCES ON THE AIRWAY IN OSA Comparative Effects of Two Oral Appliances on Upper Airway Structure in Obstructive Sleep Apnea Kate Sutherland, PhD 1,2 ; Sheryn A. Deane,
P. Mayer*, J-L. Pépin*, G. Bettega**, D. Veale* +, G. Ferretti ++, C. Deschaux*, P. Lévy*
 Eur Respir J, 1996, 9, 181 189 DOI: 1.1183/931936.96.99181 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 93-1936 Relationship between body mass index,
Eur Respir J, 1996, 9, 181 189 DOI: 1.1183/931936.96.99181 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 93-1936 Relationship between body mass index,
Philip L. Smith, MD; Christopher P. O Donnell, PhD; Lawrence Allan, BS; and Alan R. Schwartz, MD
 A Physiologic Comparison of Nasal and Oral Positive Airway Pressure* Philip L. Smith, MD; Christopher P. O Donnell, PhD; Lawrence Allan, BS; and Alan R. Schwartz, MD Study objectives: The effectiveness
A Physiologic Comparison of Nasal and Oral Positive Airway Pressure* Philip L. Smith, MD; Christopher P. O Donnell, PhD; Lawrence Allan, BS; and Alan R. Schwartz, MD Study objectives: The effectiveness
New Perspectives on the Pathogenesis of OSA - Anatomic Perspective. New Perspectives on the Pathogenesis of OSA: Anatomic Perspective - Disclosures
 New Perspectives on the Pathogenesis of OSA - Anatomic Perspective Richard J. Schwab, M.D. Professor of Medicine Interim Chief, Division of Sleep Medicine Medical Director, Penn Sleep Centers University
New Perspectives on the Pathogenesis of OSA - Anatomic Perspective Richard J. Schwab, M.D. Professor of Medicine Interim Chief, Division of Sleep Medicine Medical Director, Penn Sleep Centers University
Sleep? 2: Pathophysiology of obstructive sleep apnoea/hypopnoea syndrome
 19 REVIEW SERIES Sleep? 2: Pathophysiology of obstructive sleep apnoea/hypopnoea syndrome R B Fogel, A Malhotra, D P White... The pathogenesis of airway obstruction in patients with obstructive sleep apnoea/hypopnoea
19 REVIEW SERIES Sleep? 2: Pathophysiology of obstructive sleep apnoea/hypopnoea syndrome R B Fogel, A Malhotra, D P White... The pathogenesis of airway obstruction in patients with obstructive sleep apnoea/hypopnoea
Jefferson Cephalometric Analysis--Face and Health Focused
 Jefferson Cephalometric Analysis--Face and Health Focused Google: Jefferson Ceph Analysis Video Instruction for video instruction. Note: video instruction teaches how to find Center O. Center O is now
Jefferson Cephalometric Analysis--Face and Health Focused Google: Jefferson Ceph Analysis Video Instruction for video instruction. Note: video instruction teaches how to find Center O. Center O is now
Sleep Diordered Breathing (Part 1)
 Sleep Diordered Breathing (Part 1) History (for more topics & presentations, visit ) Obstructive sleep apnea - first described by Charles Dickens in 1836 in Papers of the Pickwick Club, Dickens depicted
Sleep Diordered Breathing (Part 1) History (for more topics & presentations, visit ) Obstructive sleep apnea - first described by Charles Dickens in 1836 in Papers of the Pickwick Club, Dickens depicted
Brian Palmer, D.D.S, Kansas City, Missouri, USA. April, 2001
 Brian Palmer, D.D.S, Kansas City, Missouri, USA A1 April, 2001 Disclaimer The information in this presentation is for basic information only and is not to be construed as a diagnosis or treatment for any
Brian Palmer, D.D.S, Kansas City, Missouri, USA A1 April, 2001 Disclaimer The information in this presentation is for basic information only and is not to be construed as a diagnosis or treatment for any
Snorers and Non Snorers: A Comparative Study Using Cephalometric Analysis of Hard Tissues
 s and Non s: A Comparative Study Using Cephalometric Analysis of Hard Tissues 1 Nilotpol Kashyap Professor and Head, Department of Pedodontics and Preventive Dentistry, Rungta College of Dental Sciences
s and Non s: A Comparative Study Using Cephalometric Analysis of Hard Tissues 1 Nilotpol Kashyap Professor and Head, Department of Pedodontics and Preventive Dentistry, Rungta College of Dental Sciences
A correlation between a new angle (S-Gn-Go angle) with the facial height
 A correlation between a new angle (S-Gn-Go angle) with the facial height Esraa S. Jassim B.D.S., M.Sc. (1) Marwan S. Al-Daggistany B.D.S., M.Sc. (1) Jinan E. Saloom B.D.S., M.Sc. (1) ABSTRACT Background:
A correlation between a new angle (S-Gn-Go angle) with the facial height Esraa S. Jassim B.D.S., M.Sc. (1) Marwan S. Al-Daggistany B.D.S., M.Sc. (1) Jinan E. Saloom B.D.S., M.Sc. (1) ABSTRACT Background:
AJNR Am J Neuroradiol 26: , November/December 2005
 AJNR Am J Neuroradiol 26:2624 2629, November/December 2005 Evaluation of the Upper Airway Cross-sectional Area Changes in Different Degrees of Severity of Obstructive Sleep Apnea Syndrome: Cephalometric
AJNR Am J Neuroradiol 26:2624 2629, November/December 2005 Evaluation of the Upper Airway Cross-sectional Area Changes in Different Degrees of Severity of Obstructive Sleep Apnea Syndrome: Cephalometric
Dental and Skeletal Changes Associated with Long-term Mandibular Advancement
 SLEEP-RELATED BREATHING DISORDERS Dental and Skeletal Changes Associated with Long-term Mandibular Advancement C.J. Robertson BDS, MDS Department of Oral Sciences and Orthodontics, School of Dentistry,
SLEEP-RELATED BREATHING DISORDERS Dental and Skeletal Changes Associated with Long-term Mandibular Advancement C.J. Robertson BDS, MDS Department of Oral Sciences and Orthodontics, School of Dentistry,
More than 20 years ago, before obstructive sleep. Gender Differences in Sleep Apnea* The Role of Neck Circumference
 Gender Differences in Sleep Apnea* The Role of Neck Circumference David R. Dancey, MD; Patrick J. Hanly, MD; Christine Soong, BSc; Bert Lee, BSc; John Shepard, Jr., MD, FCCP; and Victor Hoffstein, PhD,
Gender Differences in Sleep Apnea* The Role of Neck Circumference David R. Dancey, MD; Patrick J. Hanly, MD; Christine Soong, BSc; Bert Lee, BSc; John Shepard, Jr., MD, FCCP; and Victor Hoffstein, PhD,
Effect of body position on tongue posture in awake patients with obstructive sleep apnoea
 Thorax 1997,52:255 259 255 Effect of body position on tongue posture in awake patients with obstructive sleep apnoea Keisuke Miyamoto, Murat M Özbek, Alan A Lowe, John A Fleetham Abstract Martin et al
Thorax 1997,52:255 259 255 Effect of body position on tongue posture in awake patients with obstructive sleep apnoea Keisuke Miyamoto, Murat M Özbek, Alan A Lowe, John A Fleetham Abstract Martin et al
ORIGINAL ARTICLE. for mild to moderate obstructive
 ORIGINAL ARTICLE An Investigation of Upper Airway Changes Associated With Mandibular Advancement Device Using Sleep Videofluoroscopy in Patients With Obstructive Sleep Apnea Chul Hee Lee, MD, PhD; Jeong-Whun
ORIGINAL ARTICLE An Investigation of Upper Airway Changes Associated With Mandibular Advancement Device Using Sleep Videofluoroscopy in Patients With Obstructive Sleep Apnea Chul Hee Lee, MD, PhD; Jeong-Whun
Increasing the Functional Residual Capacity May Reverse Obstructive Sleep Apnea
 Sleep 11(4):349-353, Raven Press, Ltd., New York 1988 Association of Professional Sleep Societies ncreasing the Functional Residual Capacity May Reverse Obstructive Sleep Apnea F. Series, Y. Cormier, N.
Sleep 11(4):349-353, Raven Press, Ltd., New York 1988 Association of Professional Sleep Societies ncreasing the Functional Residual Capacity May Reverse Obstructive Sleep Apnea F. Series, Y. Cormier, N.
Differences of Upper Airway Morphology According to Obesity: Study with Cephalometry and Dynamic MD-CT
 Clinical and Experimental Otorhinolaryngology Vol. 3, No. 3: 147-152, September 2010 DOI 10.3342/ceo.2010.3.3.147 Original Article Differences of Upper Airway Morphology According to Obesity: Study with
Clinical and Experimental Otorhinolaryngology Vol. 3, No. 3: 147-152, September 2010 DOI 10.3342/ceo.2010.3.3.147 Original Article Differences of Upper Airway Morphology According to Obesity: Study with
Research Article EK Sign: A Wrinkling of Uvula and the Base of Uvula in Obstructive Sleep Apnea-Hypopnea Syndrome
 Sleep Disorders Volume 2015, Article ID 749068, 4 pages http://dx.doi.org/10.1155/2015/749068 Research Article EK Sign: A Wrinkling of Uvula and the Base of Uvula in Obstructive Sleep Apnea-Hypopnea Syndrome
Sleep Disorders Volume 2015, Article ID 749068, 4 pages http://dx.doi.org/10.1155/2015/749068 Research Article EK Sign: A Wrinkling of Uvula and the Base of Uvula in Obstructive Sleep Apnea-Hypopnea Syndrome
Cephalometric abnormalities in non-obese and obese patients with obstructive sleep apnoea
 Eur Respir J 1999; 13: 403±410 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 1999 European Respiratory Journal ISSN 0903-1936 Cephalometric abnormalities in non-obese and obese patients
Eur Respir J 1999; 13: 403±410 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 1999 European Respiratory Journal ISSN 0903-1936 Cephalometric abnormalities in non-obese and obese patients
Craniofacial morphology, head posture, and nasal respiratory resistance in obstructive sleep apnoea: an inter-ethnic comparison
 European Journal of Orthodontics 27 (2005) 91 97 European Journal of Orthodontics vol. 27 no. 1 doi: 10.1093/ejo/cjh077 European Orthodontic Society 2005; all rights reserved. Craniofacial morphology,
European Journal of Orthodontics 27 (2005) 91 97 European Journal of Orthodontics vol. 27 no. 1 doi: 10.1093/ejo/cjh077 European Orthodontic Society 2005; all rights reserved. Craniofacial morphology,
Patients with upper airway resistance syndrome
 Two-Point Palatal Discrimination in Patients With Upper Airway Resistance Syndrome, Obstructive Sleep Apnea Syndrome, and Normal Control Subjects* Christian Guilleminault, MD, BiolD; Kasey Li, MD, DDS;
Two-Point Palatal Discrimination in Patients With Upper Airway Resistance Syndrome, Obstructive Sleep Apnea Syndrome, and Normal Control Subjects* Christian Guilleminault, MD, BiolD; Kasey Li, MD, DDS;
Precision Sleep Medicine
 Precision Sleep Medicine Picking Winners Improves Outcomes and Avoids Side-Effects North American Dental Sleep Medicine Conference February 17-18, 2017 Clearwater Beach, FL John E. Remmers, MD Conflict
Precision Sleep Medicine Picking Winners Improves Outcomes and Avoids Side-Effects North American Dental Sleep Medicine Conference February 17-18, 2017 Clearwater Beach, FL John E. Remmers, MD Conflict
Pharyngeal shape and dimensions in healthy
 722 Pulmonary Division D Rodenstein Y Thomas G Liistro D C Stanescu Radiology Department G Dooms Electrophysiology Laboratory C Cuke G Aubert-Tulkens Cliniques Universitaires St Luc, Brussels, Belgium
722 Pulmonary Division D Rodenstein Y Thomas G Liistro D C Stanescu Radiology Department G Dooms Electrophysiology Laboratory C Cuke G Aubert-Tulkens Cliniques Universitaires St Luc, Brussels, Belgium
BTS sleep Course. Module 10 Therapies I: Mechanical Intervention Devices (Prepared by Debby Nicoll and Debbie Smith)
 BTS sleep Course Module 10 Therapies I: Mechanical Intervention Devices (Prepared by Debby Nicoll and Debbie Smith) S1: Overview of OSA Definition History Prevalence Pathophysiology Causes Consequences
BTS sleep Course Module 10 Therapies I: Mechanical Intervention Devices (Prepared by Debby Nicoll and Debbie Smith) S1: Overview of OSA Definition History Prevalence Pathophysiology Causes Consequences
Identification of Craniofacial Risk Factors for Obstructive Sleep Apnea Using Three-
 Identification of Craniofacial Risk Factors for Obstructive Sleep Apnea Using Three Dimensional MRI Luqi Chi, MD; FrancoisLouis Comyn, DMD; Nandita Mitra, PhD; Muredach P. Reilly, MD; Fei Wan, BS; Greg
Identification of Craniofacial Risk Factors for Obstructive Sleep Apnea Using Three Dimensional MRI Luqi Chi, MD; FrancoisLouis Comyn, DMD; Nandita Mitra, PhD; Muredach P. Reilly, MD; Fei Wan, BS; Greg
Morphological variations of soft palate and influence of age on it: A digital cephalometric study
 Original Research Article Morphological variations of soft palate and influence of age on it: A digital cephalometric study C. Vani 1*, T. Vinila Lakshmi 2, V. Dheeraj Roy 3 1 Professor, 2 Post graduate
Original Research Article Morphological variations of soft palate and influence of age on it: A digital cephalometric study C. Vani 1*, T. Vinila Lakshmi 2, V. Dheeraj Roy 3 1 Professor, 2 Post graduate
Three variables are important in the development
 Acoustic pharyngometry patterns of snoring and obstructive sleep apnea patients IBRAHIM KAMAL, BRIGADIER GEN, MD, MSC, Cairo, Egypt OBJECTIVE: Anatomic narrowing of the pharyngeal airway increases the
Acoustic pharyngometry patterns of snoring and obstructive sleep apnea patients IBRAHIM KAMAL, BRIGADIER GEN, MD, MSC, Cairo, Egypt OBJECTIVE: Anatomic narrowing of the pharyngeal airway increases the
Tongue Protrusion Strength in Arousal State Is Predictive of the Airway Patency in Obstructive Sleep Apnea
 Tohoku J. Exp. Med., 2015, 236, 241-245 Tongue Protrusion Strength in Obstructive Sleep Apnea 241 Tongue Protrusion Strength in Arousal State Is Predictive of the Airway Patency in Obstructive Sleep Apnea
Tohoku J. Exp. Med., 2015, 236, 241-245 Tongue Protrusion Strength in Obstructive Sleep Apnea 241 Tongue Protrusion Strength in Arousal State Is Predictive of the Airway Patency in Obstructive Sleep Apnea
Multiple Level Pharyngeal Surgery for Obstructive Sleep Apnoea
 O r i g i n a l A r t i c l e Singapore Med J 2001 Vol 42(4) : 160-164 Multiple Level Pharyngeal Surgery for Obstructive Sleep Apnoea P P Hsu, R H Brett Division of Otolaryngology Changi General Hospital
O r i g i n a l A r t i c l e Singapore Med J 2001 Vol 42(4) : 160-164 Multiple Level Pharyngeal Surgery for Obstructive Sleep Apnoea P P Hsu, R H Brett Division of Otolaryngology Changi General Hospital
Snoring, obstructive sleep apnea (OSA), and upper. impact of basic research on tomorrow. Snoring Imaging* Could Bernoulli Explain It All?
 impact of basic research on tomorrow Snoring Imaging* Could Bernoulli Explain It All? Igor Fajdiga, MD, PhD Study objectives: To identify upper airway changes in snoring using CT scanning, to clarify the
impact of basic research on tomorrow Snoring Imaging* Could Bernoulli Explain It All? Igor Fajdiga, MD, PhD Study objectives: To identify upper airway changes in snoring using CT scanning, to clarify the
OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update
 OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update David Claman, MD Professor of Medicine Director, UCSF Sleep Disorders Center 415-885-7886 Disclosures: None Chronic Sleep Deprivation (0 v 4 v 6 v 8 hrs)
OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update David Claman, MD Professor of Medicine Director, UCSF Sleep Disorders Center 415-885-7886 Disclosures: None Chronic Sleep Deprivation (0 v 4 v 6 v 8 hrs)
Airway and Airflow Characteristics In OSAS
 Airway and Airflow Characteristics In OSAS 16 th Annual Advances in Diagnostics and Treatment of Sleep Apnea and Snoring February 12-13, 2010 San Francisco, CA Nelson B. Powell M.D., D.D.S. Adjunct Clinical
Airway and Airflow Characteristics In OSAS 16 th Annual Advances in Diagnostics and Treatment of Sleep Apnea and Snoring February 12-13, 2010 San Francisco, CA Nelson B. Powell M.D., D.D.S. Adjunct Clinical
Obstructive sleep apnoea (OSA) has been. Heritability of upper airway dimensions derived using acoustic pharyngometry
 Eur Respir J 2008; 32: 1304 1308 DOI: 10.1183/09031936.00029808 CopyrightßERS Journals Ltd 2008 Heritability of upper airway dimensions derived using acoustic pharyngometry S.R. Patel*,#, J.M. Frame #,
Eur Respir J 2008; 32: 1304 1308 DOI: 10.1183/09031936.00029808 CopyrightßERS Journals Ltd 2008 Heritability of upper airway dimensions derived using acoustic pharyngometry S.R. Patel*,#, J.M. Frame #,
Sleep Disordered Breathing
 Sleep Disordered Breathing SDB SDB Is an Umbrella Term for Many Disorders characterized by a lack of drive to breathe Results n repetitive pauses in breathing with no effort Occurs for a minimum of 10
Sleep Disordered Breathing SDB SDB Is an Umbrella Term for Many Disorders characterized by a lack of drive to breathe Results n repetitive pauses in breathing with no effort Occurs for a minimum of 10
Clinical Papers. MRI s courtesy of Upper Airway Effects of Two Oral Appliances Sutherland et al
 Clinical Papers MRI s courtesy of Upper Airway Effects of Two Oral Appliances Sutherland et al Development Design MK 2 2005 First molded TSD 2.6mm silicone wall thickness PLEASE NOTE: This version of the
Clinical Papers MRI s courtesy of Upper Airway Effects of Two Oral Appliances Sutherland et al Development Design MK 2 2005 First molded TSD 2.6mm silicone wall thickness PLEASE NOTE: This version of the
SURGERY FOR SNORING AND MILD OBSTRUCTIVE SLEEP APNOEA
 SURGERY FOR SNORING AND MILD OBSTRUCTIVE SLEEP APNOEA INTRODUCTION Snoring with or without excessive daytime somnolence, restless sleep and periods of apnoea are all manifestations of sleep disordered
SURGERY FOR SNORING AND MILD OBSTRUCTIVE SLEEP APNOEA INTRODUCTION Snoring with or without excessive daytime somnolence, restless sleep and periods of apnoea are all manifestations of sleep disordered
Mandibular advancement oral appliance therapy for obstructive sleep apnoea: evect on awake calibre of the velopharynx
 972 Departments of Medicine and Clinical Dental Sciences, University of British Columbia, Vancouver, British Columbia, Canada CFRyan LLLove D Peat J A Fleetham AALowe Correspondence to: Dr CF Ryan, Division
972 Departments of Medicine and Clinical Dental Sciences, University of British Columbia, Vancouver, British Columbia, Canada CFRyan LLLove D Peat J A Fleetham AALowe Correspondence to: Dr CF Ryan, Division
University, India.) Corresponding author: Dr. Shubham Agarwal1
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 3 Ver.15 March. (2018), PP 59-63 www.iosrjournals.org Effect of Severity of OSA on Oxygen Saturation:
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 3 Ver.15 March. (2018), PP 59-63 www.iosrjournals.org Effect of Severity of OSA on Oxygen Saturation:
Long-term Dentofacial Changes in Chinese Obstructive Sleep Apnea Patients after Treatment with a Mandibular Advancement Device
 Original Article Long-term Dentofacial Changes in Chinese Obstructive Sleep Apnea Patients after Treatment with a Mandibular Advancement Device H. M. Hou a ; K. Sam b ;U.Hägg c ; A. B. M. Rabie d ; M.
Original Article Long-term Dentofacial Changes in Chinese Obstructive Sleep Apnea Patients after Treatment with a Mandibular Advancement Device H. M. Hou a ; K. Sam b ;U.Hägg c ; A. B. M. Rabie d ; M.
Upper Airway Collapsibility is Associated with Obesity and Hyoid Position
 pii: sp-00638-13 http://dx.doi.org/10.5665/sleep.4078 UPPER AIRWAY COLLAPSIBILITY IS ASSOCIATED WITH OBESITY AND HYOID POSITION Upper Airway Collapsibility is Associated with Obesity and Hyoid Position
pii: sp-00638-13 http://dx.doi.org/10.5665/sleep.4078 UPPER AIRWAY COLLAPSIBILITY IS ASSOCIATED WITH OBESITY AND HYOID POSITION Upper Airway Collapsibility is Associated with Obesity and Hyoid Position
Cephalometric Analysis
 Cephalometric Analysis of Maxillary and Mandibular Growth and Dento-Alveolar Change Part III In two previous articles in the PCSO Bulletin s Faculty Files, we discussed the benefits and limitations of
Cephalometric Analysis of Maxillary and Mandibular Growth and Dento-Alveolar Change Part III In two previous articles in the PCSO Bulletin s Faculty Files, we discussed the benefits and limitations of
U ntil recently the restoration of airflow which terminates
 861 SLEEP-DISORDERED BREATHING Mechanisms used to restore ventilation after partial upper airway collapse during sleep in humans Amy S Jordan, Andrew Wellman, Raphael C Heinzer, Yu-Lun Lo, Karen Schory,
861 SLEEP-DISORDERED BREATHING Mechanisms used to restore ventilation after partial upper airway collapse during sleep in humans Amy S Jordan, Andrew Wellman, Raphael C Heinzer, Yu-Lun Lo, Karen Schory,
The characteristics of profile facial types and its relation with mandibular rotation in a sample of Iraqi adults with different skeletal relations
 The characteristics of profile facial types and its relation with mandibular rotation in a sample of Iraqi adults with different skeletal relations Sara M. Al-Mashhadany, B.D.S., M.Sc. (1) Nagham M.J.
The characteristics of profile facial types and its relation with mandibular rotation in a sample of Iraqi adults with different skeletal relations Sara M. Al-Mashhadany, B.D.S., M.Sc. (1) Nagham M.J.
Reliability of A and B point for cephalometric analysis
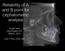 Reliability of A and B point for cephalometric analysis Angle East Washington DC March, 2015 Carl P Roy, DDS, MS 1 History Orthodontic profession has always attempted to classify malocclusions. A-P relationship
Reliability of A and B point for cephalometric analysis Angle East Washington DC March, 2015 Carl P Roy, DDS, MS 1 History Orthodontic profession has always attempted to classify malocclusions. A-P relationship
Head and Neck Physical Examination: Comparison Between Nonapneic and Obstructive Sleep Apnea Patients
 The Laryngoscope Lippincott Williams & Wilkins, Inc. 2005 The American Laryngological, Rhinological and Otological Society, Inc. Head and Neck Physical Examination: Comparison Between Nonapneic and Obstructive
The Laryngoscope Lippincott Williams & Wilkins, Inc. 2005 The American Laryngological, Rhinological and Otological Society, Inc. Head and Neck Physical Examination: Comparison Between Nonapneic and Obstructive
Effect of mandibular setback surgery on the posterior airway size
 Maija Liukkonen, DDS Assistant Professor Department of Oral Development and Orthodontics Institute of Dentistry University of Turku Kimmo Vähätalo, DDS Senior Oral and Maxillofacial Surgeon Timo Peltomäki,
Maija Liukkonen, DDS Assistant Professor Department of Oral Development and Orthodontics Institute of Dentistry University of Turku Kimmo Vähätalo, DDS Senior Oral and Maxillofacial Surgeon Timo Peltomäki,
Nasal obstruction as a risk factor for sleep apnoea syndrome
 Eur Respir J 2000; 16: 639±643 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 2000 European Respiratory Journal ISSN 0903-1936 Nasal obstruction as a risk factor for sleep apnoea syndrome
Eur Respir J 2000; 16: 639±643 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 2000 European Respiratory Journal ISSN 0903-1936 Nasal obstruction as a risk factor for sleep apnoea syndrome
Does the dimple point represent the margin of soft palate musculature?
 Asian Biomedicine Vol. 2 No. 5 October 2008;397-401 Brief Communication Does the dimple point represent the margin of soft palate musculature? Department of Otolaryngology, Faculty of Medicine, Chulalongkorn
Asian Biomedicine Vol. 2 No. 5 October 2008;397-401 Brief Communication Does the dimple point represent the margin of soft palate musculature? Department of Otolaryngology, Faculty of Medicine, Chulalongkorn
Obstructive sleep apnea (OSA)
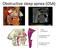 Obstructive sleep apnea (OSA) In a healthy sleeping child, the mouth is typically closed, the oral cavity is collapsed, and the nasopharynx and hypopharynx are patent with minimal wall motion Obstructive
Obstructive sleep apnea (OSA) In a healthy sleeping child, the mouth is typically closed, the oral cavity is collapsed, and the nasopharynx and hypopharynx are patent with minimal wall motion Obstructive
Management of OSA. saurabh maji
 Management of OSA saurabh maji INTRODUCTION Obstructive sleep apnea is a major public health problem Prevalence of OSAS in INDIA is 2.4% to 4.96% in men and 1% to 2 % in women In the rest of the world
Management of OSA saurabh maji INTRODUCTION Obstructive sleep apnea is a major public health problem Prevalence of OSAS in INDIA is 2.4% to 4.96% in men and 1% to 2 % in women In the rest of the world
Alexandria Workshop on
 Alexandria Workshop on 1 Snoring & OSA Surgery Course Director: Yassin Bahgat MD Claudio Vicini MD Course Board: Filippo Montevecchi MD Pietro Canzi MD Snoring & Obstructive ti Sleep Apnea The basic information
Alexandria Workshop on 1 Snoring & OSA Surgery Course Director: Yassin Bahgat MD Claudio Vicini MD Course Board: Filippo Montevecchi MD Pietro Canzi MD Snoring & Obstructive ti Sleep Apnea The basic information
Visceral fat accumulation as an important risk factor for obstructive sleep apnoea syndrome in obese subjects
 Journal of Internal Medicine 1997; 241: 11 18 Visceral fat accumulation as an important risk factor for obstructive sleep apnoea syndrome in obese subjects E. SHINOHARA, S. KIHARA, S. YAMASHITA, M. YAMANE,
Journal of Internal Medicine 1997; 241: 11 18 Visceral fat accumulation as an important risk factor for obstructive sleep apnoea syndrome in obese subjects E. SHINOHARA, S. KIHARA, S. YAMASHITA, M. YAMANE,
Neuromechanical control of upper airway patency during sleep
 J Appl Physiol 102: 547 556, 2007. First published September 28, 2006; doi:10.1152/japplphysiol.00282.2006. Neuromechanical control of upper airway patency during sleep Susheel P. Patil, Hartmut Schneider,
J Appl Physiol 102: 547 556, 2007. First published September 28, 2006; doi:10.1152/japplphysiol.00282.2006. Neuromechanical control of upper airway patency during sleep Susheel P. Patil, Hartmut Schneider,
Original Article. Chisato Iida-Kondo 1, Norio Yoshino 4, Tohru Kurabayashi 4, Shirou Mataki 2, Makoto Hasegawa 3 and Norimasa Kurosaki 1
 J Med Dent Sci 2006; 53: 119 126 Original Article Comparison of Tongue Volume/Oral Cavity Volume Ratio between Obstructive Sleep Apnea Syndrome Patients and Normal Adults Using Magnetic Resonance Imaging
J Med Dent Sci 2006; 53: 119 126 Original Article Comparison of Tongue Volume/Oral Cavity Volume Ratio between Obstructive Sleep Apnea Syndrome Patients and Normal Adults Using Magnetic Resonance Imaging
Surgical Options for the Successful Treatment of Obstructive Sleep Apnea
 Surgical Options for the Successful Treatment of Obstructive Sleep Apnea Benjamin J. Teitelbaum, MD, FACS Otolaryngology Head and Neck Surgery Saint Agnes Medical Center Fresno, California Terms Apnea
Surgical Options for the Successful Treatment of Obstructive Sleep Apnea Benjamin J. Teitelbaum, MD, FACS Otolaryngology Head and Neck Surgery Saint Agnes Medical Center Fresno, California Terms Apnea
Overnight fluid shifts in subjects with and without obstructive sleep apnea
 Original Article Overnight fluid shifts in subjects with and without obstructive sleep apnea Ning Ding 1 *, Wei Lin 2 *, Xi-Long Zhang 1, Wen-Xiao Ding 1, Bing Gu 3, Bu-Qing Ni 4, Wei Zhang 4, Shi-Jiang
Original Article Overnight fluid shifts in subjects with and without obstructive sleep apnea Ning Ding 1 *, Wei Lin 2 *, Xi-Long Zhang 1, Wen-Xiao Ding 1, Bing Gu 3, Bu-Qing Ni 4, Wei Zhang 4, Shi-Jiang
Contents. Section 1: Introduction and History. 1. Cephalometry in Orthodontics Section 2: Classification of Cephalometric Landmarks
 Contents Section 1: Introduction and History 1. Cephalometry in Orthodontics... 3 Technical Aspects 4 Cephalometric X-ray Tracing Techniques 4 Section 2: Classification of Cephalometric Landmarks 2. Classification
Contents Section 1: Introduction and History 1. Cephalometry in Orthodontics... 3 Technical Aspects 4 Cephalometric X-ray Tracing Techniques 4 Section 2: Classification of Cephalometric Landmarks 2. Classification
Mandibular Advancement Device : Long-term Effects on Apnea and Sleep
 Mandibular Advancement Device With Obstructive Sleep Apnea * in Patients : Long-term Effects on Apnea and Sleep Marie Marklund, Carin Sahlin, Hans Stenlund, Maurits Persson and Karl A. Franklin Chest 2001;120;162-169
Mandibular Advancement Device With Obstructive Sleep Apnea * in Patients : Long-term Effects on Apnea and Sleep Marie Marklund, Carin Sahlin, Hans Stenlund, Maurits Persson and Karl A. Franklin Chest 2001;120;162-169
Medicare C/D Medical Coverage Policy
 Medicare C/D Medical Coverage Policy Surgical Treatment of Obstructive Sleep Apnea Origination: June 26, 2000 Review Date: January 18, 2017 Next Review January, 2019 DESCRIPTION OF PROCEDURE OR SERVICE
Medicare C/D Medical Coverage Policy Surgical Treatment of Obstructive Sleep Apnea Origination: June 26, 2000 Review Date: January 18, 2017 Next Review January, 2019 DESCRIPTION OF PROCEDURE OR SERVICE
The Position of Anatomical Porion in Different Skeletal Relationships. Tarek. EL-Bialy* Ali. H. Hassan**
 The Position of Anatomical Porion in Different Skeletal Relationships Tarek. EL-Bialy* Ali. H. Hassan** Abstract Previous research has shown that the position of glenoid fossa differs in different skeletal
The Position of Anatomical Porion in Different Skeletal Relationships Tarek. EL-Bialy* Ali. H. Hassan** Abstract Previous research has shown that the position of glenoid fossa differs in different skeletal
Using the Pathophysiology of Obstructive Sleep Apnea (OSA) to Teach Cardiopulmonary Integration
 Using the Pathophysiology of Obstructive Sleep Apnea (OSA) to Teach Cardiopulmonary Integration Michael G. Levitzky, Ph.D. Department of Physiology Louisiana State University Health Sciences Center 1901
Using the Pathophysiology of Obstructive Sleep Apnea (OSA) to Teach Cardiopulmonary Integration Michael G. Levitzky, Ph.D. Department of Physiology Louisiana State University Health Sciences Center 1901
High Flow Nasal Cannula in Children During Sleep. Brian McGinley M.D. Associate Professor of Pediatrics University of Utah
 High Flow Nasal Cannula in Children During Sleep Brian McGinley M.D. Associate Professor of Pediatrics University of Utah Disclosures Conflicts of Interest: None Will discuss a product that is commercially
High Flow Nasal Cannula in Children During Sleep Brian McGinley M.D. Associate Professor of Pediatrics University of Utah Disclosures Conflicts of Interest: None Will discuss a product that is commercially
Obstructive Sleep Apnea- Hypopnea Syndrome and Snoring: Surgical Options
 Obstructive Sleep Apnea- Hypopnea Syndrome and Snoring: Surgical Options Joshua L. Kessler, MD, FACS Boston ENT Associates Clinical Instructor, Otology and Laryngology Harvard Medical School Why Consider
Obstructive Sleep Apnea- Hypopnea Syndrome and Snoring: Surgical Options Joshua L. Kessler, MD, FACS Boston ENT Associates Clinical Instructor, Otology and Laryngology Harvard Medical School Why Consider
Obstructive sleep apnea hypopnea syndrome (OSAS) is SCIENTIFIC INVESTIGATIONS
 http://dx.doi.org/10.5664/jcsm.3164 Palatal Sensory Threshold Reflects Nocturnal Hypoxemia and Airway Occlusion in Snorers and Obstructive Sleep Apnea Patients Sang-Wook Kim, M.D., Ph.D. 1,2 ; Hyun Woo
http://dx.doi.org/10.5664/jcsm.3164 Palatal Sensory Threshold Reflects Nocturnal Hypoxemia and Airway Occlusion in Snorers and Obstructive Sleep Apnea Patients Sang-Wook Kim, M.D., Ph.D. 1,2 ; Hyun Woo
SANDHYA CA SHYAM LOHAKARE Professor, Orthodontics Department, Chattisgarh Dental College & Research Centre, Rajnandgaon, C.G
 International Journal of Applied and Natural Sciences (IJANS) ISSN(P): 2319-4014; ISSN(E): 2319-4022 Vol. 5, Issue 6, Oct Nov 2016; 49-58 IASET CEPHALOMETRIC STUDY OF UPPER AND LOWER PHARYNGEAL AIRWAYS
International Journal of Applied and Natural Sciences (IJANS) ISSN(P): 2319-4014; ISSN(E): 2319-4022 Vol. 5, Issue 6, Oct Nov 2016; 49-58 IASET CEPHALOMETRIC STUDY OF UPPER AND LOWER PHARYNGEAL AIRWAYS
An update on childhood sleep-disordered breathing
 An update on childhood sleep-disordered breathing แพทย หญ งวนพร อน นตเสร ภาคว ชาก มารเวชศาสตร คณะแพทยศาสตร มหาว ทยาล ยสงขลานคร นทร Sleep-disordered breathing Primary snoring Upper airway resistance syndrome
An update on childhood sleep-disordered breathing แพทย หญ งวนพร อน นตเสร ภาคว ชาก มารเวชศาสตร คณะแพทยศาสตร มหาว ทยาล ยสงขลานคร นทร Sleep-disordered breathing Primary snoring Upper airway resistance syndrome
College & Hospital, DPU Vidyapeeth Pimpri, Pune, India. *Corresponding Author:
 Original Research Article DOI: 10.18231/2278-3784.2017.0001 Evaluation of changes in maxillary arch dimensions, Posterior Transverse Inter Arch Discrepancy (PTID), upper and lower incisor inclination in
Original Research Article DOI: 10.18231/2278-3784.2017.0001 Evaluation of changes in maxillary arch dimensions, Posterior Transverse Inter Arch Discrepancy (PTID), upper and lower incisor inclination in
Performance Characteristics of Upper Airway Critical Collapsing Pressure Measurements during Sleep
 UPPER AIRWAY CRITICAL COLLAPSING PRESSURE DURING SLEEP Performance Characteristics of Upper Airway Critical Collapsing Pressure Measurements during Sleep Jason P. Kirkness, PhD 1 ; Leigh A. Peterson, MHS
UPPER AIRWAY CRITICAL COLLAPSING PRESSURE DURING SLEEP Performance Characteristics of Upper Airway Critical Collapsing Pressure Measurements during Sleep Jason P. Kirkness, PhD 1 ; Leigh A. Peterson, MHS
Ioannis Kollias and Olaf Krogstad Department of Orthodontics, University of Oslo, Norway
 European Journal of Orthodontics 21 (1999) 345 355 1999 European Orthodontic Society Adult craniocervical and pharyngeal changes a longitudinal cephalometric study between 22 and 42 years of age. Part
European Journal of Orthodontics 21 (1999) 345 355 1999 European Orthodontic Society Adult craniocervical and pharyngeal changes a longitudinal cephalometric study between 22 and 42 years of age. Part
Clinical Study Changes in the Upper and Lower Pharyngeal Airway Spaces Associated with Rapid Maxillary Expansion
 International Scholarly Research Network ISRN Dentistry Volume 2012, Article ID 290964, 5 pages doi:10.5402/2012/290964 Clinical Study Changes in the Upper and Lower Pharyngeal Airway Spaces Associated
International Scholarly Research Network ISRN Dentistry Volume 2012, Article ID 290964, 5 pages doi:10.5402/2012/290964 Clinical Study Changes in the Upper and Lower Pharyngeal Airway Spaces Associated
EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS
 EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS Dr. Masatoshi Sana Year: ESLO 01 RÉSUMÉ OF CASE 8 CASE CATEGORY: TRANS / VERTICAL DISCREPANCY NAME: Akiko T. BORN : 15/03/1973 SEX: F PRE-TREATMENT RECORDS: AGE:
EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS Dr. Masatoshi Sana Year: ESLO 01 RÉSUMÉ OF CASE 8 CASE CATEGORY: TRANS / VERTICAL DISCREPANCY NAME: Akiko T. BORN : 15/03/1973 SEX: F PRE-TREATMENT RECORDS: AGE:
Obstructive sleep apnea (OSA) is characterized by. Quality of Life in Patients with Obstructive Sleep Apnea*
 Quality of Life in Patients with Obstructive Sleep Apnea* Effect of Nasal Continuous Positive Airway Pressure A Prospective Study Carolyn D Ambrosio, MD; Teri Bowman, MD; and Vahid Mohsenin, MD Background:
Quality of Life in Patients with Obstructive Sleep Apnea* Effect of Nasal Continuous Positive Airway Pressure A Prospective Study Carolyn D Ambrosio, MD; Teri Bowman, MD; and Vahid Mohsenin, MD Background:
Diverse Morphologies of Soft Palate in Normal Individuals: A Cephalometric Perspective
 10.5005/jp-journals-10011-1252 RESEARCH ARTICLE Diverse Morphologies of Soft Palate in Normal Individuals: A Cephalometric Perspective Kruthika S Guttal, Rohit Breh, Ramaprakasha Bhat, Krishna N Burde,
10.5005/jp-journals-10011-1252 RESEARCH ARTICLE Diverse Morphologies of Soft Palate in Normal Individuals: A Cephalometric Perspective Kruthika S Guttal, Rohit Breh, Ramaprakasha Bhat, Krishna N Burde,
Nasal pressure recording in the diagnosis of sleep apnoea hypopnoea syndrome
 56 Unité de Recherche, Centre de Pneumologie de l Hôpital Laval, Université Laval, Québec, Canada F Sériès I Marc Correspondence to: Dr F Sériès, Centre de Pneumologie, 2725 Chemin Sainte Foy, Sainte Foy
56 Unité de Recherche, Centre de Pneumologie de l Hôpital Laval, Université Laval, Québec, Canada F Sériès I Marc Correspondence to: Dr F Sériès, Centre de Pneumologie, 2725 Chemin Sainte Foy, Sainte Foy
The effect of tooth agenesis on dentofacial structures
 European Journal of Orthodontics 19 (1997) 71 78 9 1997 European Orthodontic Society The effect of on dentofacial structures Sema Yª and Tuba Department of Orthodontics, Faculty of Dentistry, Gazi University,
European Journal of Orthodontics 19 (1997) 71 78 9 1997 European Orthodontic Society The effect of on dentofacial structures Sema Yª and Tuba Department of Orthodontics, Faculty of Dentistry, Gazi University,
Upper airway sagittal dimensions in obstructive sleep apnea (OSA) patients and severity of the disease
 Stomatologija, Baltic Dental and Maxillofacial Journal, 13:123-7, 2011 Upper airway sagittal dimensions in obstructive sleep apnea (OSA) patients and severity of the disease Juris Svaza, Andrejs Skagers,
Stomatologija, Baltic Dental and Maxillofacial Journal, 13:123-7, 2011 Upper airway sagittal dimensions in obstructive sleep apnea (OSA) patients and severity of the disease Juris Svaza, Andrejs Skagers,
Does a correlation exist between nasal airway volume and craniofacial morphology: A cone beam computed tomography study
 Original Research Does a correlation exist between nasal airway volume and craniofacial morphology: A cone beam computed tomography study Jeenal V Gupta, Makhija PG, Gupta KC 1 Departments of Orthodontics
Original Research Does a correlation exist between nasal airway volume and craniofacial morphology: A cone beam computed tomography study Jeenal V Gupta, Makhija PG, Gupta KC 1 Departments of Orthodontics
Postnatal Growth. The study of growth in growing children is for two reasons : -For health and nutrition assessment
 Growth of The Soft Tissues Postnatal Growth Postnatal growth is defined as the first 20 years of growth after birth krogman 1972 The study of growth in growing children is for two reasons : -For health
Growth of The Soft Tissues Postnatal Growth Postnatal growth is defined as the first 20 years of growth after birth krogman 1972 The study of growth in growing children is for two reasons : -For health
LATERAL CEPHALOMETRIC EVALUATION IN CLEFT PALATE PATIENTS
 POLSKI PRZEGLĄD CHIRURGICZNY 2009, 81, 1, 23 27 10.2478/v10035-009-0004-2 LATERAL CEPHALOMETRIC EVALUATION IN CLEFT PALATE PATIENTS PRADEEP JAIN, ANAND AGARWAL, ARVIND SRIVASTAVA Department of Plastic
POLSKI PRZEGLĄD CHIRURGICZNY 2009, 81, 1, 23 27 10.2478/v10035-009-0004-2 LATERAL CEPHALOMETRIC EVALUATION IN CLEFT PALATE PATIENTS PRADEEP JAIN, ANAND AGARWAL, ARVIND SRIVASTAVA Department of Plastic
Overview. Goal of Evaluation. DISE: Identifying the Sites of Obstruction in OSA. Characterize disorder to guide effective treatment.
 DISE: Identifying the Sites of Obstruction in OSA Eric J. Kezirian, MD, MPH Director, Division of Sleep Surgery Otolaryngology Head and Neck Surgery University of California, San Francisco ekezirian@ohns.ucsf.edu
DISE: Identifying the Sites of Obstruction in OSA Eric J. Kezirian, MD, MPH Director, Division of Sleep Surgery Otolaryngology Head and Neck Surgery University of California, San Francisco ekezirian@ohns.ucsf.edu
Soft and Hard Tissue Changes after Bimaxillary Surgery in Chinese Class III Patients
 Original Article Soft and Hard Tissue Changes after Bimaxillary Surgery in Chinese Class III Patients Ming Tak Chew a Abstract: Cephalometric studies have shown that the Chinese race tends to have a greater
Original Article Soft and Hard Tissue Changes after Bimaxillary Surgery in Chinese Class III Patients Ming Tak Chew a Abstract: Cephalometric studies have shown that the Chinese race tends to have a greater
Acoustic Reflection: Review and Clinical Applications for Sleep- Disordered Breathing
 REVIEW ARTICLE Acoustic Reflection: Review and Clinical Applications for Sleep- Disordered Breathing John S. Viviano, D.D.S. 1 ABSTRACT Sleep-disordered breathing (SDB) affects more than 4% of the adult
REVIEW ARTICLE Acoustic Reflection: Review and Clinical Applications for Sleep- Disordered Breathing John S. Viviano, D.D.S. 1 ABSTRACT Sleep-disordered breathing (SDB) affects more than 4% of the adult
Effects of Airway Problems on Maxillary Growth: A Review
 Effects of Airway Problems on Maxillary Growth: A Review Ahmet Yalcin Gungor a Hakan Turkkahraman b Abstract The volume of air passing through the nose and nasopharinx is limited by its shape and diameter.
Effects of Airway Problems on Maxillary Growth: A Review Ahmet Yalcin Gungor a Hakan Turkkahraman b Abstract The volume of air passing through the nose and nasopharinx is limited by its shape and diameter.
Maxillomandibular Volume Influences the Relationship between Weight Loss and Improvement in Obstructive Sleep Apnea
 pii: sp-00167-15 http://dx.doi.org/10.5665/sleep.5314 SLEEP DISORDERED BREATHING Maxillomandibular Volume Influences the Relationship between Weight Loss and Improvement in Obstructive Sleep Apnea Kate
pii: sp-00167-15 http://dx.doi.org/10.5665/sleep.5314 SLEEP DISORDERED BREATHING Maxillomandibular Volume Influences the Relationship between Weight Loss and Improvement in Obstructive Sleep Apnea Kate
An orthodontic oral appliance
 Original Article An orthodontic oral appliance A randomized, controlled pilot study Marie Marklund a ; Per Erik Legrell b ABSTRACT Objective: This pilot study was performed to test the hypothesis that
Original Article An orthodontic oral appliance A randomized, controlled pilot study Marie Marklund a ; Per Erik Legrell b ABSTRACT Objective: This pilot study was performed to test the hypothesis that
Research Article. Jigar R. Doshi, Kalyani Trivedi, Tarulatha Shyagali,
 Research Article Predictability of Yen Angle & Appraisal of Various Cephalometric Parameters in the Assessment of Sagittal Relationship between Maxilla and Mandible in Angle s Class II Malocclusion Jigar
Research Article Predictability of Yen Angle & Appraisal of Various Cephalometric Parameters in the Assessment of Sagittal Relationship between Maxilla and Mandible in Angle s Class II Malocclusion Jigar
Materials and Methods
 Anesthesiology 2002; 97:786 93 2002 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Collapsibility of the Upper Airway during Anesthesia with Isoflurane Peter R. Eastwood,
Anesthesiology 2002; 97:786 93 2002 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Collapsibility of the Upper Airway during Anesthesia with Isoflurane Peter R. Eastwood,
The Mandibular Advancement Device and Patient Selection in the Treatment of Obstructive Sleep Apnea
 ORIGINAL ARTICLE The Mandibular Advancement Device and Patient Selection in the Treatment of Obstructive Sleep Apnea Chul Hee Lee, MD; Ji-Hun Mo, MD; Ik-Joon Choi, MD; Hyun Jong Lee, MD; Beom Seok Seo,
ORIGINAL ARTICLE The Mandibular Advancement Device and Patient Selection in the Treatment of Obstructive Sleep Apnea Chul Hee Lee, MD; Ji-Hun Mo, MD; Ik-Joon Choi, MD; Hyun Jong Lee, MD; Beom Seok Seo,
Pathophysiology and Clinical Presentation of Sleep Apnea
 Pathophysiology and Clinical Presentation of Sleep Apnea Allan I. Pack, M.B., Ch.B., Ph.D. Division of Sleep Medicine/Department of Medicine Center for Sleep and Respiratory Neurobiology University of
Pathophysiology and Clinical Presentation of Sleep Apnea Allan I. Pack, M.B., Ch.B., Ph.D. Division of Sleep Medicine/Department of Medicine Center for Sleep and Respiratory Neurobiology University of
Polysomnography (PSG) (Sleep Studies), Sleep Center
 Policy Number: 1036 Policy History Approve Date: 07/09/2015 Effective Date: 07/09/2015 Preauthorization All Plans Benefit plans vary in coverage and some plans may not provide coverage for certain service(s)
Policy Number: 1036 Policy History Approve Date: 07/09/2015 Effective Date: 07/09/2015 Preauthorization All Plans Benefit plans vary in coverage and some plans may not provide coverage for certain service(s)
Soft tissue hypopharyngeal surgery for obstructive sleep apnea syndrome
 Oral Maxillofacial Surg Clin N Am 14 (2002) 371 376 Soft tissue hypopharyngeal surgery for obstructive sleep apnea syndrome B. Tucker Woodson, MD, FACS, ABSM Department of Otolaryngology and Human Communication,
Oral Maxillofacial Surg Clin N Am 14 (2002) 371 376 Soft tissue hypopharyngeal surgery for obstructive sleep apnea syndrome B. Tucker Woodson, MD, FACS, ABSM Department of Otolaryngology and Human Communication,
ORTHOGNATHIC SURGERY
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-16 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-16 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Effects of different surgical procedures on the pharyngeal space with mandibular prognathism
 J Osaka Dent Univ 2015 (October) ; 49 (2) : 143 148. Effects of different surgical procedures on the pharyngeal space with mandibular prognathism Yutaka Yamada and Naoyuki Matsumoto Department of Orthodontics,
J Osaka Dent Univ 2015 (October) ; 49 (2) : 143 148. Effects of different surgical procedures on the pharyngeal space with mandibular prognathism Yutaka Yamada and Naoyuki Matsumoto Department of Orthodontics,
Three dimensional evaluation of upper airway volume in children with different dental and skeletal malocclusions
 ORIGINAL ARTICLE Three dimensional evaluation of upper airway volume in children with different dental and skeletal malocclusions Kula, Katherine 1, Ahn, Eun Jeong 1, Halum, Stacey 2, Dillehay, Kendall
ORIGINAL ARTICLE Three dimensional evaluation of upper airway volume in children with different dental and skeletal malocclusions Kula, Katherine 1, Ahn, Eun Jeong 1, Halum, Stacey 2, Dillehay, Kendall
Ped e iat a r t i r c c S lee e p e A p A nea e a Surg r er e y
 Airway Imaging in Pediatric OSA Kasey Li, MD, DDS, FACS Stanford University Sleep Medicine Program The airway is smaller in children with OSA compared to controls The adenoid and tonsils are larger and
Airway Imaging in Pediatric OSA Kasey Li, MD, DDS, FACS Stanford University Sleep Medicine Program The airway is smaller in children with OSA compared to controls The adenoid and tonsils are larger and
Sleep Apnea and Body Position during Sleep
 Sleep 11(1):9-99, Raven Press, Ltd" New York 1988 Association of Professional Sleep Societies Sleep Apnea and Body Position during Sleep C. F. George, T. W. Millar, and M. H. Kryger Department / Respiratory
Sleep 11(1):9-99, Raven Press, Ltd" New York 1988 Association of Professional Sleep Societies Sleep Apnea and Body Position during Sleep C. F. George, T. W. Millar, and M. H. Kryger Department / Respiratory
