2. Description of the activity
|
|
|
- Kellie Arnold
- 5 years ago
- Views:
Transcription
1 Curricular Components for GI EPA 1. EPA Title Care of infants, children and adolescents with acute and chronic liver diseases, biliary/cholestatic diseases, pancreatic disorders, and those requiring liver transplantation 2. Description of the activity 3. Judicious mapping to domains of competence 4. Competencies within each domain critical to entrustment decisions Practicing gastroenterologists/hepatologists must be trained to care for children and adolescents with acute and chronic hepatobiliary disease as well as liver transplantation and pancreatic disorders. Pediatric gastroenterologists/hepatologists need to be familiar with current knowledge of disease processes and presentations. Additionally, subspecialists should be able to manage acute issues as well as long-term chronic management including the transition of care. The specific functions which define this EPA include: Understanding and applying the epidemiology, pathophysiology, pathogenesis and natural history, of acute/chronic liver diseases, biliary diseases, liver transplantation and pancreatic disorders Interpreting and applying basic/translational and clinical research in hepatology, biliary and pancreatic disorders to the care of patients Recognizing and diagnosing children with suspected liver, biliary and pancreatic disorders in a variety of clinical presentations Managing children and adolescents with liver, biliary, pancreatic disorders, and liver transplantation including the acute presentations and emergencies as well as long-term management of complex chronic diseases Educating parents and children on liver, biliary and pancreatic diseases including cause, treatment, and clinical course. Leading, directing and coordinating care for children/adolescents with liver, biliary and pancreatic diseases within the medical system and the community X Patient Care X Medical Knowledge X Practice-based Learning and Improvement X Interpersonal and Communication Skills Professionalism System-based Practice X Personal and Professional Development PC 5: Performing complete physical exams PC 9: Counseling patients and families MK 1: Demonstrating knowledge MK 2: Practicing EBM PBLI 2: Setting goals PBLI 8: Developing teaching skills PBLI 10: Engaging in lifelong learning
2 ICS 2: Demonstrating insight into emotion PPD 8: Dealing with uncertainty 5. Curricular Components that support the functions of the EPA (knowledge, skills and attitudes needed to execute this EPA safely): Rationale/ Scope of Practice: Pediatric gastroenterologists care for patients with acute and chronic liver and biliary disorders, some of which may require liver transplantation, and pancreatic disorders. Acute and Chronic Hepatobiliary Diseases: Practicing subspecialists must be trained to care for children and adolescents with acute and chronic liver disease. Within the pediatric gastroenterology subspecialty, these relatively uncommon conditions account for a significant amount of morbidity and mortality. Pediatric gastroenterologists need to be familiar with current knowledge of liver disease processes. Additionally, subspecialists should be able to manage acute issues as well as long-term management of chronic illnesses including the transition of care. The diagnosis and treatment of acute and chronic liver disease requires the knowledge and understanding of anatomy, pathophysiology, epidemiology and diagnosis/management of these diseases that include acute liver failure, chronic liver failure, viral hepatitis, autoimmune hepatitis, fatty liver disease, congenital liver diseases, hepatic tumors, infectious/drug-induced hepatitis, other liver conditions. The diagnosis and treatment of diseases of the biliary tree, cholestatic liver disease and metabolic liver disease compose a significant proportion of practice for pediatric gastroenterologists. Due to the relative rarity of these conditions, pediatric gastroenterologists serve a key role as consultants to general pediatricians who encounter patients with signs/symptoms (e.g., jaundice, right upper quadrant (RUQ) pain) or findings (laboratory or radiographic abnormalities) suggestive of biliary/liver pathology. Pediatric gastroenterologists should be able to obtain key diagnostic information from patient history, physical examination and targeted studies (including labs, imaging, and procedures) to evaluate for biliary and liver pathology. Pediatric gastroenterologists planning clinical practice may choose to obtain proficiency with percutaneous liver biopsy to diagnose hepatobiliary pathology although not required, and some pediatric gastroenterologists may also work towards proficiency in endoscopic retrograde cholangiopancreatography (ERCP), though for most the key proficiency will be appropriate referral to a center that performs ERCP on children. Additionally, pediatric gastroenterologists must provide longitudinal care for patients with disorders of diseases of the bile ducts, cholestatic liver disease and metabolic liver disease. The pediatric gastroenterologist may serve as the point person in management in some of these rare diseases (e.g., biliary atresia, progressive familial intrahepatic cholestasis (PFIC), Alagille syndrome, biliary atresia, Crigler-Najjar syndrome, glycogen storage disease, and others), whereas they will be a part of a multidisciplinary team approach for others (e.g., cystic fibrosis, alpha-1 antitrypsin deficiency, mitochondrial disease). Liver Transplantation: Pediatric gastroenterologists participate in the care of children and adolescents who will have or have undergone a liver transplantation. Pediatric gastroenterologists should have a complete understanding of acute and chronic liver conditions requiring transplantation. Pediatric gastroenterologists should be familiar with the
3 indications for liver transplantation and participate in the pre-transplant work-up and preparation as well as post-transplant care. Pancreatic Diseases: Pediatric gastroenterologists must understand acute and chronic pancreatic diseases, including hereditary disorders that occur in the pediatric population. Pediatric gastroenterologists must be able to diagnose and treat pancreatic disorders and their complications, as well as demonstrate a thorough understanding of their pathophysiology. Pediatric gastroenterologists should have a thorough understanding of the spectrum of pancreatic disease including epidemiology, etiology, pathophysiology, natural history and disease management. These diseases include acute, acute recurrent, and chronic pancreatitis, including hereditary pancreatitis, autoimmune pancreatitis, pancreatitis due to toxic/metabolic causes, and pancreatitis due to anatomical variants. Genetic and metabolic pancreatic disorders that can affect both the endocrine and exocrine pancreatic function including cystic fibrosis, Schwachman-Diamond, and Johanson-Blizzard as well as other disorders of pancreatic dysfunction are also important considerations. In addition, pediatric gastroenterologists must be familiar with the normal anatomy and embryology of the pancreas including structural variants (e.g. pancreatic divisum, annular pancreas and pancreatic agenesis). Pediatric gastroenterologists must be able to care for pediatric patients of all ages with these conditions and unite a team of caregivers to provide exceptional patient care and must display skills of communication and life-long learning skills. Pediatric gastroenterologists must be sensitive to a wide variety of patient s backgrounds and beliefs in their caring for children with gastrointestinal disorders and must demonstrate a caring and empathetic attitude towards patients and families. Curricular components that support the functions of the EPA: Understanding and applying the epidemiology, pathogenesis and natural history, of acute/chronic liver diseases, biliary diseases, and pancreatic disorders Knows and understands the basic science of the acute and chronic liver disease etiologies including pathogenesis, genetics, and immunology. Understands the natural history of acute and chronic liver diseases. Understands the normal physiology of the liver, and understands liver enzyme and liver function tests and their abnormalities in disease. Demonstrates understanding of liver metabolic pathways, such as the urea cycle, glycogen synthesis and breakdown. Demonstrates knowledge of basic biliary anatomy and bile duct development. Differentiates between gallbladder/biliary infection and inflammation and directs management accordingly. Describes the normal physiology of bilirubin and bile acid metabolism, including synthesis, conjugation, excretion and recirculation, and factors that influence bile flow. Liver Transplantation
4 Knows and understands the clinical science of liver transplantation including indications, epidemiology, natural history, nutritional, gastrointestinal and surgical management and complications. Knows and understands the basic science of liver transplantation including immunology, genetics, post-transplant physiology and common disease processes after transplantation. Knows and understands the mechanism of action, side effects, and other complications of medications and treatments used before and after liver transplantation including steroids, immunomodulators, biologics, antivirals and other medications. Knows and understands the acute and chronic immunological consequences of liver transplantation including acute and chronic rejection, autoimmune post-transplant processes and other processes in relation to graft vs. host reactions. Pancreatic Disorders Knows and understands the normal anatomy of the pancreas and congenital variants. Knows and understands the physiology of pancreatic exocrine secretion of digestive enzymes, including the types of enzymes, their mechanisms of activation, regulation, and roles in digestion. Demonstrates knowledge of established and evolving biomedical, clinical and epidemiological sciences of pancreatic disorders, as well as the application of this knowledge to patient care. Knows and understands the epidemiology, etiology, pathophysiology, natural history, and management of acute and chronic pancreatitis. Demonstrates a basic understanding of the molecular genetics of pancreatic disease including but not limited to gallstone pancreatitis, hereditary pancreatitis and cystic fibrosis, their diagnosis and management. Interpreting and applying basic/translational and clinical research in hepatology, biliary and pancreatic disorders to the care of patients Applies evidence based medicine to the care of children with liver disease. Participates in lifelong learning as it relates to care of children with liver disease. Demonstrates use of available evidence to evaluate and optimize the care of patients with acute and chronic liver disease, biliary disorders, cholestatic liver disease and/or metabolic liver diseases. Knows and understands principles of evidence-based medicine, as applied to the management of hepatobiliary and metabolic disorders. Liver Transplantation Knows and understands research as it applies to liver transplantation, management pre and post transplantation, and transplant rejection. Applies evidence based medicine to the care of children with liver transplantation. Knows and understands medications used in transplantation.
5 Pancreatic Disorders Demonstrates use of available evidence to investigate, evaluate and improve the care of patients with pancreatic disorders. Knows and understands principles of evidence-based medicine, as applied to children with pancreatic disorders. Knows and understands that clinical practice guidelines are suggestions for clinical care and may be flexible and evolve with time. Explains clinical decisions in the context of evidence based medicine. Demonstrates knowledge of research that has been performed in patient care, diagnosis and pathophysiology in children with pancreatic disorders. Recognizing and diagnosing children with suspected liver, biliary and pancreatic disorders in a variety of clinical presentations Articulates the differential diagnosis of neonatal cholestasis, and formulates an appropriate evaluation and treatment plan. Demonstrates proficiency in the evaluation and treatment of infants, children and adolescents with cholestasis, including indications for genetic testing and available treatment options for pruritus. Knows the indications for surgical intervention, such as biliary diversion, or liver transplantation in this patient population. Knows and understands the initial diagnostic evaluation for metabolic liver disease, and coordinates care of these patients in consultation with the other medical professionals. Gathers essential and accurate information regarding risk factors such as intravenous injections, foreign travel, contact with jaundiced individuals, medications/toxin exposures, and sexual history in adolescents if sexually active. Gathers essential and accurate information from the patient/parent, focused on concerning signs and symptoms for potential hepatobiliary pathology (jaundice, acholic stool, failure to thrive, RUQ pain, pruritus, encephalopathy, etc.). Performs an initial appropriate physical examination, with evaluation for evidence of chronic liver disease including hepatomegaly, splenomegaly, ascites, and a complete neurological exam for evaluation of encephalopathy. Performs an appropriate initial diagnostic evaluation for a child with acute and chronic liver disease (including laboratory, imaging, and histological interpretation). Understands that the etiology for acute liver failure (ALF) is usually age dependent and thus the need for tailoring of initial work-up. Performs an appropriate initial diagnostic for a child with suspected biliary disease or cholestatic liver disease (laboratory testing and imaging) Explains the differences between acute and chronic liver disease. Demonstrates knowledge of the differential diagnosis for acute (e.g., acute infectious hepatitis, drug/toxin hepatitis, (ALF) and chronic liver disease (e.g., chronic viral hepatitis, autoimmune hepatitis, non-alcoholic steatohepatitis, congenital liver disease)
6 including clinical presentation and features, epidemiology, natural history and treatment (including liver transplantation). Recognizes the clinical and laboratory findings of a child in ALF and explains the management of ALF (including PICU support, prevention/treatment of complications, hepatic support and consideration for liver transplantation). Liver Transplantation Performs an appropriate initial workup for a child with liver or metabolic disease who may be a suitable candidate for liver transplantation, including laboratory tests, appropriate endoscopic evaluation, liver biopsy and pathology review, imaging, psychological and socio-economic evaluations. Appropriately contacts a hepatology transplant center for referral when indicated if located in a non-transplant center. Obtains a comprehensive history and physical exam focused on the appropriate systems for post-transplant children and adolescents. Pancreatic Disorders Obtains a detailed, complete and accurate history of pancreatic disorders and presentation of common pancreatic disorders such as acute and chronic pancreatitis as well as disorders of pancreatic exocrine dysfunction. Performs a physical exam that would appropriately identify signs of pancreatitis and/or pancreatic insufficiency and related systemic manifestations. Accurately assesses nature, acuity and severity of the clinical problem. Provides a comprehensive assessment of the medical issues that must be addressed for each patient. Orders necessary and appropriate laboratory and diagnostic tests in light of the clinical presentation and formulates a treatment plan based on the diagnosis. Managing children and adolescents with liver, biliary and pancreatic disorders including the acute presentations and emergencies as well as long-term management of complex chronic diseases Establishes the diagnosis, stages the disease and detects complications of liver disease. Develops an initial treatment plan with monitoring of medications and potential side effects. Recognizes remission and exacerbation in chronic liver disease and develops a treatment plan for disease exacerbations and maintenance therapy. Identifies patients in need of interventional diagnostics for hepatobiliary disease (including liver biopsy, endoscopic retrograde cholangiopancreatography (ERCP), percutaneous transhepatic cholangiogram) and describe the risks and benefits of each procedure. Recognizes clinical signs and symptoms in a patient presenting with acute or chronic liver disease that may be indicative of an underlying metabolic disorder.
7 Monitors for and recognizes complications of both acute and chronic liver disease. Performs endoscopy for esophageal varices if indicated (see Procedure EPA). Distinguishes among the various imaging modalities for liver disease including but not limited to abdominal radiography, ultrasonograpy with doppler, CT scans and MRI, including magnetic resonance cholangiopancreatography (MRCP) and/or ERCP and chooses the appropriate modality based on top diagnostic considerations. In consultation with pathology, correctly interprets liver biopsy findings, including identification of findings suggestive of biliary obstruction or metabolic liver disease. Knows and understands the use of treatment modalities for liver disease including: Steroids Immunomodulators Biologics Anti-virals Oral, enteral and parenteral nutrition Other medications (vitamins E, D, K, fish oil, etc) Pharmacotherapy in portal hypertension( e.g., Beta-blockers, octreotide) Endoscopic or surgical treatment for portal hypertension Aldosterone antagonist and diuretics for ascites Albumin infusion Pharmacotherapy for hepatic encephalopathy (e.g., lactulose, antibiotics) Non-conventional therapies, alternative medicine Liver transplantation Evolving therapies / new treatment modalities for hepatic support (eg. Molecular Absorbent Recirculating Systems, hepatocyte transplantation) Recognizes extra-intestinal manifestations of liver disease. Interprets pathology findings. Knows and understands health care maintenance and vaccinations in children with chronic liver disease and immunosuppression medical regimens. Recognizes and addresses psychosocial concerns. Explains the mechanism of action, side effects, and other complications of medications and treatments for chronic liver disease including immunosuppression medical regimens, nutritional and vitamin supplementation, and other medications. Knows and understands the extrahepatic manifestation of liver disease, including but not limited to neurological involvement, renal disease, and hematological disorders. Demonstrates knowledge of and recognizes complications of liver disease, including malnutrition and growth failure, pruritus, ascending cholangitis, portal hypertension, ascites, variceal bleeding, coagulopathy, hepatic encephalopathy, hepatorenal syndrome, hepatopulmonary syndrome, bacterial infections (spontaneous bacterial peritonitis) and hepatocellular carcinoma. Recognizes signs and symptoms of End Stage Liver Disease (ESLD) and appropriate timing to refer for liver transplantation. Identifies liver metabolic diseases that may lead to evaluation for liver transplantation Demonstrates knowledge regarding transmission and prevention strategies for the viral hepatitis.
8 Applies quality measures to improve care of children with liver disease Liver Transplantation Accurately assesses nature, acuity and severity of the clinical post-transplant problems. Utilizes laboratory test, imaging studies and pathologic data to monitor patient posttransplant. Knows and understands the short- and long-term consequences of immunosuppressive therapy including steroids, immunomodulators, biologic/antibody therapy and other emerging therapies. Recognizes acute and chronic post-transplant complications: nutritional, metabolic, infectious, and surgical. Utilizes clinical practice guidelines in the care of post-transplant children. Pancreatic Disorders Performs continuing evaluation of patients to evaluate safety and efficacy of observations and treatment plan as instituted; orders additional studies and/or adjusts therapy as clinically indicated. Develops and carries out patient management plans and communicates with patient, family, primary as well as consulting physician, resident physicians, nursing staff, nutrition support team and other ancillary health service providers. Knows and understands the indications for and interprets laboratory results in the diagnosis and management of pancreatic diseases. Knows and understands the principles, utility, indications for and basic interpretation of all radiographic studies of the pancreas including their potential risks and benefits. Recognizes therapeutic options for the treatment of pancreatic disease including the role of nutritional therapy, pain management and endoscopic, radiographic and surgical intervention. Recognizes the indications for invasive testing of the pancreas including endoscopic ultrasound (EUS), ERCP and endoscopic management of pancreatic diseases. Educating parents and children on liver, biliary and pancreatic diseases including cause, treatment and clinical course. Educates parents and children on cause, treatment, and other aspects of liver disease including maintenance health check and cancer surveillance. Effectively communicates disease information, treatment plan, and outcome to parents and children. Assesses patient s and parents level of medical understanding and explains medical decision making in understandable terms. Creates a comfortable environment where parents can share sensitive history that may have influenced development of disease (toxic ingestions, consanguinity, etc.). Enables patients and parents to be comfortable asking questions and making suggestions.
9 Liver Transplantation Empathetically discusses the process of evaluation for liver transplantation and the ethics of the national organ donation system. Involves patient and their families in creating treatment plans. Ensures that the patient and their family understand the rationale for the plan of care. Encourages patient to freely discuss their care and concerns about medications and current management by exhibiting empathetic listening skills. Ensures that patients understand the correct way to administer their medications. Pancreatic Disorders Provides education to patients and families concerning the pathophysiology and manifestations of their gastrointestinal disease process. Discusses the proper use of prescribed medications and/or interventions (e.g., ERCP) including potential adverse effects. Effectively communicates disease information, treatment plan and outcome to patients and their families. Leading, directing and coordinating care for children/adolescents with liver, biliary and pancreatic diseases within the medical system and the community Chronic GI Disease (in general) Recognizes the importance of a biopsychosocial model of care for patients with chronic disease that addresses not only the physical but social, emotional, behavioral and mental health issues that often complicate chronic illness. Ensures that the patient and family are part of the interdisciplinary health care team and engages them in shared decision making. Acknowledges the anxiety that accompanies diagnosis and management of chronic disease and supports the patient/ family s emotional response to living with uncertainties through ongoing updates as knowledge becomes available and balancing difficult conversations with hope. Recognizes issues that may contribute to poor compliance or noncompliance and is able to recruit necessary resources to address these issues (i.e. health educator for health literacy issues, psychiatry/social work for depression, etc.). Coordinates care of children with acute and chronic hepatobiliary disease including PCPs, surgeons, psychologists/social workers, nutritionists, radiologists, and other medical professionals. Effectively communicates with other medical professionals involved in the care of patients with acute and chronic liver disease. Prepares for transition and appropriately transitions care in children with liver disease, biliary disease and metabolic disorders to adult gastroenterologists/hepatologists. Communicates effectively with all members of a multidisciplinary team, including nursing staff, medical assistants, pharmacy staff, social workers, primary care providers and other consultants (surgeons, radiologists, pathologists).
10 Practices high-quality, fiscally responsible and cost-effective health care by demonstrating consideration of costs to the patients families and the system in recommending diagnostic tests, treatments, and follow-up management. Advocates for patients within the health care system, particularly those in resource poor settings. Knows and understands the link between early and effective management of congenital hepatobiliary disease (e.g. biliary atresia, cystic fibrosis, primary hyperoxaluria, etc.) and prevention of secondary healthcare costs later in life. Educates health care professionals and the lay public on issues in management of hepatobiliary disease and acts as an advocate for recognition of disease (red flags) and management (best practices). Liver Transplantation Communicates management plans, in a timely fashion, to the patient, family, primary physician, resident physicians, nursing staff, nutrition team and other ancillary health service providers. Demonstrates an awareness of and responsiveness to the larger context and system of health care and the ability to effectively call on system resources to provide care that is of optimal value. Practices high-quality fiscally responsible and cost-effective health care by demonstrating consideration of costs to the patients families and the system in recommending diagnostic tests, treatments, and follow-up management. Advocates for patients within the health care system. Coordinates care of post-transplant children with primary care physicians, surgeons, psychologists, social workers, dietitians, radiologists, and other medical professionals. Transitions care of post-transplant children to adult gastroenterologists. Pancreatic Disorders Effectively communicates with other medical professionals involved in the care of the patient. Works effectively as a member or leader of a health care team coordinating care of the patient. Problems that generally require further consultation where the role of the subspecialist is to recognize and provide preliminary evaluation, and refer/co-manage. Liver Transplantation Endoscopic retrograde cholangiopancreatography (ERCP) Cholecystectomy Surgery for hepatic masses or other lesions Psychiatry/Psychology/Pain Medicine/Social work Anxiety/Depression Chronic pain
Entrustable Professional Activity
 Entrustable Professional Activity 1. EPA Title: Care of infants, children and adolescents with acute and chronic s 2. Description of Activity Practicing subspecialists must be trained to care for children
Entrustable Professional Activity 1. EPA Title: Care of infants, children and adolescents with acute and chronic s 2. Description of Activity Practicing subspecialists must be trained to care for children
Entrustable Professional Activity
 Entrustable Professional Activity 1. EPA Title: Care of infants, children and adolescents requiring liver 2. Description of Activity The pediatric gastroenterology trainee should participate in the care
Entrustable Professional Activity 1. EPA Title: Care of infants, children and adolescents requiring liver 2. Description of Activity The pediatric gastroenterology trainee should participate in the care
Entrustable Professional Activity
 Entrustable Professional Activity 1. Title: Care for infants, children, and adolescents with common outpatient GI, liver/biliary, pancreatic and nutritional issues 2. Description of Activity Pediatric
Entrustable Professional Activity 1. Title: Care for infants, children, and adolescents with common outpatient GI, liver/biliary, pancreatic and nutritional issues 2. Description of Activity Pediatric
Entrustable Professional Activity
 Entrustable Professional Activity 1. EPA Title: Care of infants, children and adolescents with inflammatory bowel disease 2. Description of Activity Practicing subspecialists must be trained to care for
Entrustable Professional Activity 1. EPA Title: Care of infants, children and adolescents with inflammatory bowel disease 2. Description of Activity Practicing subspecialists must be trained to care for
Overall Goals and Objectives for Transplant Hepatology EPAs:
 Overall Goals and Objectives for Transplant Hepatology EPAs: 1. DIAGNOSTIC LIST During the one-year Advanced Pediatric Transplant Hepatology Program, fellows are expected to develop comprehensive skills
Overall Goals and Objectives for Transplant Hepatology EPAs: 1. DIAGNOSTIC LIST During the one-year Advanced Pediatric Transplant Hepatology Program, fellows are expected to develop comprehensive skills
Transplant Hepatology
 Transplant Hepatology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified
Transplant Hepatology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified
Gastroenterology. Certification Examination Blueprint. Purpose of the exam
 Gastroenterology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified gastroenterologist
Gastroenterology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified gastroenterologist
EVALUATION & LISTING. Your Child s Liver Transplant Evaluation. What is the Liver?
 EVALUATION & LISTING Your Child s Liver Transplant Evaluation The University of Michigan is a national leader in liver transplantation, as well as the surgical and medical management of patients with liver
EVALUATION & LISTING Your Child s Liver Transplant Evaluation The University of Michigan is a national leader in liver transplantation, as well as the surgical and medical management of patients with liver
GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint
 GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Gastroenterology MOC exam blueprint Based on feedback from physicians that MOC assessments
GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Gastroenterology MOC exam blueprint Based on feedback from physicians that MOC assessments
Jaundice. Agnieszka Dobrowolska- Zachwieja, MD, PhD
 Jaundice Agnieszka Dobrowolska- Zachwieja, MD, PhD Jaundice definition Jaundice, as in the French jaune, refers to the yellow discoloration of the skin. It arises from the abnormal accumulation of bilirubin
Jaundice Agnieszka Dobrowolska- Zachwieja, MD, PhD Jaundice definition Jaundice, as in the French jaune, refers to the yellow discoloration of the skin. It arises from the abnormal accumulation of bilirubin
Lahey Clinic Internal Medicine Residency Program: Curriculum for Gastroenterology
 Lahey Clinic Internal Medicine Residency Program: Curriculum for Gastroenterology Faculty representative: David L. Burns, MD, CNSP Resident representative: Tom Castiglione, MD Revision date: March 6, 2006
Lahey Clinic Internal Medicine Residency Program: Curriculum for Gastroenterology Faculty representative: David L. Burns, MD, CNSP Resident representative: Tom Castiglione, MD Revision date: March 6, 2006
During the course of the 12 month fellowship, candidates will attend at least one international liver meeting (generally AASLD).
 Hepatology and Liver Transplantation fellowship Length: 1 year Number of positions: 2 Type of fellowship: Clinical and Research Fellowship Director: Dr. Deschenes McGill University Health Centre Fellowship
Hepatology and Liver Transplantation fellowship Length: 1 year Number of positions: 2 Type of fellowship: Clinical and Research Fellowship Director: Dr. Deschenes McGill University Health Centre Fellowship
Primary Sclerosing Cholangitis and Cholestatic liver diseases. Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants
 Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
A Review of Liver Function Tests. James Gray Gastroenterology Vancouver
 A Review of Liver Function Tests James Gray Gastroenterology Vancouver Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted
A Review of Liver Function Tests James Gray Gastroenterology Vancouver Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted
LIVER CIRRHOSIS. The liver extracts nutrients from the blood and processes them for later use.
 LIVER CIRRHOSIS William Sanchez, M.D. & Jayant A. Talwalkar, M.D., M.P.H. Advanced Liver Disease Study Group Miles and Shirley Fiterman Center for Digestive Diseases Mayo College of Medicine Rochester,
LIVER CIRRHOSIS William Sanchez, M.D. & Jayant A. Talwalkar, M.D., M.P.H. Advanced Liver Disease Study Group Miles and Shirley Fiterman Center for Digestive Diseases Mayo College of Medicine Rochester,
Curricular Components for Infectious Diseases EPA
 Curricular Components for Infectious Diseases EPA 1. EPA Title Management of previously healthy patients with a pediatric infectious disease. 2. Description of the A key role for subspecialists is to provide
Curricular Components for Infectious Diseases EPA 1. EPA Title Management of previously healthy patients with a pediatric infectious disease. 2. Description of the A key role for subspecialists is to provide
Differentiate IgE-mediated food allergy from non-ige mediated food allergy. List the foods and formulas most commonly associated with food allergy.
 Gastroenterology Description: The resident will be exposed to various clinical symptoms and diseases of the gastrointestinal tract which are commonly seen by the gastroenterologist. The resident will be
Gastroenterology Description: The resident will be exposed to various clinical symptoms and diseases of the gastrointestinal tract which are commonly seen by the gastroenterologist. The resident will be
Gastroenterology Fellowship Program
 Gastroenterology Fellowship Program Outpatient Clinical Rotations I. Overview A. Three Year Continuity Clinic Experience All gastroenterology fellows will be required to have a ½ day continuity clinic
Gastroenterology Fellowship Program Outpatient Clinical Rotations I. Overview A. Three Year Continuity Clinic Experience All gastroenterology fellows will be required to have a ½ day continuity clinic
Curricular Components for Rheumatology EPA
 Curricular Components for Rheumatology EPA 1. EPA Title Manage patients with acute or chronic complex multi-system rheumatic disease in an ambulatory, emergency, or inpatient setting. 2. Description of
Curricular Components for Rheumatology EPA 1. EPA Title Manage patients with acute or chronic complex multi-system rheumatic disease in an ambulatory, emergency, or inpatient setting. 2. Description of
WEEK. MPharm Programme. Liver Biochemistry. Slide 1 of 49 MPHM14 Liver Biochemistry
 MPharm Programme Liver Biochemistry Slide 1 of 49 MPHM Liver Biochemistry Learning Outcomes Assess and evaluate the signs and symptoms of illness Assess and critically appraise a patients medication regimen,
MPharm Programme Liver Biochemistry Slide 1 of 49 MPHM Liver Biochemistry Learning Outcomes Assess and evaluate the signs and symptoms of illness Assess and critically appraise a patients medication regimen,
ACG Clinical Guideline: Primary Sclerosing Cholangitis
 ACG Clinical Guideline: Primary Sclerosing Cholangitis Keith D. Lindor, MD, FACG 1, Kris V. Kowdley, MD, FACG 2, and M. Edwyn Harrison, MD 3 1 College of Health Solutions, Arizona State University, Phoenix,
ACG Clinical Guideline: Primary Sclerosing Cholangitis Keith D. Lindor, MD, FACG 1, Kris V. Kowdley, MD, FACG 2, and M. Edwyn Harrison, MD 3 1 College of Health Solutions, Arizona State University, Phoenix,
PROGRESSIVE FAMILIAL INTRAHEPATIC CHOLESTASIS (PFIC)
 The Childhood Liver Disease Research Network strives to provide information and support to individuals and families affected by liver disease through its many research programs. PROGRESSIVE FAMILIAL INTRAHEPATIC
The Childhood Liver Disease Research Network strives to provide information and support to individuals and families affected by liver disease through its many research programs. PROGRESSIVE FAMILIAL INTRAHEPATIC
Gastrointestinal System: Accessory Organ Disorders
 Gastrointestinal System: Accessory Organ Disorders Mary DeLetter, PhD, RN Associate Professor Dept. of Baccalaureate and Graduate Nursing Eastern Kentucky University Disorders of Accessory Organs Portal
Gastrointestinal System: Accessory Organ Disorders Mary DeLetter, PhD, RN Associate Professor Dept. of Baccalaureate and Graduate Nursing Eastern Kentucky University Disorders of Accessory Organs Portal
Curricular Components for Hematology/Oncology EPA
 Curricular Components for Hematology/Oncology EPA 1. EPA Title Manage patients with hematology-oncology conditions, whether acute or chronic, simple or complex, in an ambulatory, emergency, or inpatient
Curricular Components for Hematology/Oncology EPA 1. EPA Title Manage patients with hematology-oncology conditions, whether acute or chronic, simple or complex, in an ambulatory, emergency, or inpatient
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Gastroenterology
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Gastroenterology 1. GOAL: Understand the role of the general pediatrician in the assessment and management of patients with
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Gastroenterology 1. GOAL: Understand the role of the general pediatrician in the assessment and management of patients with
List of NASPGHAN EPAs
 List of NASPGHAN EPAs 1. Care for infants, children, and adolescents with common outpatient GI, liver/biliary, pancreatic and nutritional issues 2. Perform medical procedures related to gastrointestinal
List of NASPGHAN EPAs 1. Care for infants, children, and adolescents with common outpatient GI, liver/biliary, pancreatic and nutritional issues 2. Perform medical procedures related to gastrointestinal
Noncalculous Biliary Disease Dean Abramson, M.D. Gastroenterologists, P.C. Cedar Rapids. Cholestasis
 Noncalculous Biliary Disease Dean Abramson, M.D. Gastroenterologists, P.C. Cedar Rapids Cholestasis Biochemical hallmark Impaired bile flow from liver to small intestine Alkaline phosphatase is primary
Noncalculous Biliary Disease Dean Abramson, M.D. Gastroenterologists, P.C. Cedar Rapids Cholestasis Biochemical hallmark Impaired bile flow from liver to small intestine Alkaline phosphatase is primary
Biliary tree dilation - and now what?
 Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Chronic Hepatic Disease
 Chronic Hepatic Disease 10 th Leading Cause of Death Liver Functions Energy Metabolism Protein Synthesis Solubilization, Transport, and Storage Protects and Clears drugs, damaged cells Causes of Liver
Chronic Hepatic Disease 10 th Leading Cause of Death Liver Functions Energy Metabolism Protein Synthesis Solubilization, Transport, and Storage Protects and Clears drugs, damaged cells Causes of Liver
Hepatocytes produce. Proteins Clotting factors Hormones. Bile Flow
 R.J.Bailey MD Hepatocytes produce Proteins Clotting factors Hormones Bile Flow Trouble.. for the liver! Trouble for the Liver Liver Gall Bladder Common Alcohol Hep C Fatty Liver Cancer Drugs Viruses Uncommon
R.J.Bailey MD Hepatocytes produce Proteins Clotting factors Hormones Bile Flow Trouble.. for the liver! Trouble for the Liver Liver Gall Bladder Common Alcohol Hep C Fatty Liver Cancer Drugs Viruses Uncommon
Histology. The pathology of the. bile ducts. pancreas. liver. The lecture in summary. Vt-2006
 Vt-2006 The pathology of the liver, bile ducts and pancreas Richard Palmqvist Docent, ST-läkare, Klin Pat Lab, Labcentrum The lecture in summary Introduction, histology & physiology in brief General phenomenon
Vt-2006 The pathology of the liver, bile ducts and pancreas Richard Palmqvist Docent, ST-läkare, Klin Pat Lab, Labcentrum The lecture in summary Introduction, histology & physiology in brief General phenomenon
Curricular Components for Cardiology EPA
 Curricular Components for Cardiology EPA 1. EPA Title 2. Description of the Activity Diagnosis and management of patients with acute congenital or acquired cardiac problems requiring intensive care. Upon
Curricular Components for Cardiology EPA 1. EPA Title 2. Description of the Activity Diagnosis and management of patients with acute congenital or acquired cardiac problems requiring intensive care. Upon
What Is Cirrhosis? CIRRHOSIS. Cirrhosis occurs when the liver is. by chronic conditions and diseases. permanently scarred or injured
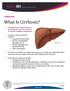 What Is Cirrhosis? Cirrhosis occurs when the liver is permanently scarred or injured by chronic conditions and diseases. Common causes of cirrhosis include: Long-term alcohol abuse. Chronic viral hepatitis
What Is Cirrhosis? Cirrhosis occurs when the liver is permanently scarred or injured by chronic conditions and diseases. Common causes of cirrhosis include: Long-term alcohol abuse. Chronic viral hepatitis
Overview of PSC Jayant A. Talwalkar, MD, MPH Associate Professor of Medicine Mayo Clinic Rochester, MN
 Overview of PSC Jayant A. Talwalkar, MD, MPH Associate Professor of Medicine Mayo Clinic Rochester, MN 2012 Annual Conference PSC Partners Seeking a Cure May 5, 2012 Primary Sclerosing Cholangitis Multifocal
Overview of PSC Jayant A. Talwalkar, MD, MPH Associate Professor of Medicine Mayo Clinic Rochester, MN 2012 Annual Conference PSC Partners Seeking a Cure May 5, 2012 Primary Sclerosing Cholangitis Multifocal
Jaundice Chris Wells Regional CMT teaching 6 th June 2017
 Jaundice Chris Wells Regional CMT teaching 6 th June 2017 By the end you will Have a systematic approach to the patient with jaundice Be able to diagnose the cause of jaundice Have a framework for managing
Jaundice Chris Wells Regional CMT teaching 6 th June 2017 By the end you will Have a systematic approach to the patient with jaundice Be able to diagnose the cause of jaundice Have a framework for managing
BILIARY ATRESIA. What is biliary atresia?
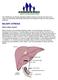 The Childhood Liver Disease Research Network strives to provide information and support to individuals and families affected by liver disease through its many research programs. BILIARY ATRESIA What is
The Childhood Liver Disease Research Network strives to provide information and support to individuals and families affected by liver disease through its many research programs. BILIARY ATRESIA What is
Approach to a case of Neonatal Cholestasis
 Approach to a case of Neonatal Cholestasis Ira Shah (Co-Incharge, Consultant Pediatrician, Pediatric Liver Clinic) Gunjan Narkhede (Resident in Pediatric Liver Clinic) Pediatric Hepatobiliary Clinic, B.J.Wadia
Approach to a case of Neonatal Cholestasis Ira Shah (Co-Incharge, Consultant Pediatrician, Pediatric Liver Clinic) Gunjan Narkhede (Resident in Pediatric Liver Clinic) Pediatric Hepatobiliary Clinic, B.J.Wadia
Liver failure &portal hypertension
 Liver failure &portal hypertension Objectives: by the end of this lecture each student should be able to : Diagnose liver failure (acute or chronic) List the causes of acute liver failure Diagnose and
Liver failure &portal hypertension Objectives: by the end of this lecture each student should be able to : Diagnose liver failure (acute or chronic) List the causes of acute liver failure Diagnose and
Cystic Biliary Atresia: Why Is It Important to Distinguish this from Congenital Choledochal Cyst?
 Bahrain Medical Bulletin, Vol. 36, No. 2, June 2014 Cystic Biliary Atresia: Why Is It Important to Distinguish this from Congenital Choledochal Cyst? Hussein Ahmed Mohammed Hamdy, MRCSEd, FEBPS* Hind Mustafa
Bahrain Medical Bulletin, Vol. 36, No. 2, June 2014 Cystic Biliary Atresia: Why Is It Important to Distinguish this from Congenital Choledochal Cyst? Hussein Ahmed Mohammed Hamdy, MRCSEd, FEBPS* Hind Mustafa
Original Policy Date 12:2013
 MP 6.01.30 Magnetic Resonance Cholangiopancreatography Medical Policy Section Radiology Is12:2013sue 3:2005 Original Policy Date 12:2013 Last Review Status/Date 12:2013 Return to Medical Policy Index Disclaimer
MP 6.01.30 Magnetic Resonance Cholangiopancreatography Medical Policy Section Radiology Is12:2013sue 3:2005 Original Policy Date 12:2013 Last Review Status/Date 12:2013 Return to Medical Policy Index Disclaimer
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Accelerated intravascular coagulation and fibrinolysis (AICF) in liver disease, 390 391 Acid suppression in liver disease, 403 404 ACLF.
Index Note: Page numbers of article titles are in boldface type. A Accelerated intravascular coagulation and fibrinolysis (AICF) in liver disease, 390 391 Acid suppression in liver disease, 403 404 ACLF.
Autoimmune Hepatobiliary Diseases PROF. DR. SABEHA ALBAYATI CABM,FRCP
 Autoimmune Hepatobiliary Diseases PROF. DR. SABEHA ALBAYATI CABM,FRCP Autoimmune hepatobiliary diseases The liver is an important target for immunemediated injury. Three disease phenotypes are recognized:
Autoimmune Hepatobiliary Diseases PROF. DR. SABEHA ALBAYATI CABM,FRCP Autoimmune hepatobiliary diseases The liver is an important target for immunemediated injury. Three disease phenotypes are recognized:
Imaging of liver and pancreas
 Imaging of liver and pancreas.. Disease of the liver Focal liver disease Diffusion liver disease Focal liver disease Benign Cyst Abscess Hemangioma FNH Hepatic adenoma HCC Malignant Fibrolamellar carcinoma
Imaging of liver and pancreas.. Disease of the liver Focal liver disease Diffusion liver disease Focal liver disease Benign Cyst Abscess Hemangioma FNH Hepatic adenoma HCC Malignant Fibrolamellar carcinoma
Liver Disease. By: Michael Martins
 Liver Disease By: Michael Martins Recently I have been getting a flurry of patients that have some serious liver complications. This week s literature review will be the dental management of the patients
Liver Disease By: Michael Martins Recently I have been getting a flurry of patients that have some serious liver complications. This week s literature review will be the dental management of the patients
DISEASE LEVEL MEDICAL EVIDENCE PROTOCOL
 DISEASE LEVEL MEDICAL EVIDENCE PROTOCOL 1. This Protocol sets out the medical evidence that must be delivered to the Administrator for proof of Disease Level. It is subject to such further and other Protocols
DISEASE LEVEL MEDICAL EVIDENCE PROTOCOL 1. This Protocol sets out the medical evidence that must be delivered to the Administrator for proof of Disease Level. It is subject to such further and other Protocols
CrackCast Episode 28 Jaundice
 CrackCast Episode 28 Jaundice Episode overview: 1) Describe heme metabolism 2) List common pre-hepatic/hepatic/post-hepatic causes of jaundice Wisecracks: 1) What are clinical signs of liver disease? 2)
CrackCast Episode 28 Jaundice Episode overview: 1) Describe heme metabolism 2) List common pre-hepatic/hepatic/post-hepatic causes of jaundice Wisecracks: 1) What are clinical signs of liver disease? 2)
Liver Disease in Cystic Fibrosis
 Liver Disease in Cystic Fibrosis Basic Overview Clinical Aspects Management What Is Cystic Fibrosis? Autosomal recessive disease W-1:3000, H-1:10,000, AA-1:15,000 Mutations of CFTR defective Cl - transport
Liver Disease in Cystic Fibrosis Basic Overview Clinical Aspects Management What Is Cystic Fibrosis? Autosomal recessive disease W-1:3000, H-1:10,000, AA-1:15,000 Mutations of CFTR defective Cl - transport
Approach to the Patient with Liver Disease
 Approach to the Patient with Liver Disease Diagnosis of liver disease Careful history taking Physical examination Laboratory tests Radiologic examination and imaging studies Liver biopsy Liver diseases
Approach to the Patient with Liver Disease Diagnosis of liver disease Careful history taking Physical examination Laboratory tests Radiologic examination and imaging studies Liver biopsy Liver diseases
1. Discuss the basic pathophysiology of end-stage liver and kidney failure.
 TRANSPLANT SURGERY ROTATION (PGY1, 2) A. Medical Knowledge Goal: The resident will achieve a detailed knowledge of the evaluation and treatment of a variety of disease processes. The resident will be exposed
TRANSPLANT SURGERY ROTATION (PGY1, 2) A. Medical Knowledge Goal: The resident will achieve a detailed knowledge of the evaluation and treatment of a variety of disease processes. The resident will be exposed
Gall bladder cancer. Information for patients Hepatobiliary
 Gall bladder cancer Information for patients Hepatobiliary page 2 of 12 Who will provide my care? You will be cared for by a number of professionals who work together. These professionals will be specialist
Gall bladder cancer Information for patients Hepatobiliary page 2 of 12 Who will provide my care? You will be cared for by a number of professionals who work together. These professionals will be specialist
Biliary Atresia. Karen F. Murray, MD Professor of Pediatrics Director, Hepatobiliary Program Seattle Children s
 Biliary Atresia Karen F. Murray, MD Professor of Pediatrics Director, Hepatobiliary Program Seattle Children s Biliary Atresia Incidence: 1/8,000-15,000 live births Girls > boys 1.5:1 The most common cause
Biliary Atresia Karen F. Murray, MD Professor of Pediatrics Director, Hepatobiliary Program Seattle Children s Biliary Atresia Incidence: 1/8,000-15,000 live births Girls > boys 1.5:1 The most common cause
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ACLF. See Acute-on-chronic liver failure (ACLF) Acute kidney injury (AKI) in ACLF patients, 967 Acute liver failure (ALF), 957 964 causes
Index Note: Page numbers of article titles are in boldface type. A ACLF. See Acute-on-chronic liver failure (ACLF) Acute kidney injury (AKI) in ACLF patients, 967 Acute liver failure (ALF), 957 964 causes
Pictorial review of Benign Biliary tract abnormality on MRCP/MRI Liver with Endoscopic (including splyglass) and Endoscopic Ultrasound correlation
 Pictorial review of Benign Biliary tract abnormality on MRCP/MRI Liver with Endoscopic (including splyglass) and Endoscopic Ultrasound correlation Poster No.: C-2617 Congress: ECR 2015 Type: Educational
Pictorial review of Benign Biliary tract abnormality on MRCP/MRI Liver with Endoscopic (including splyglass) and Endoscopic Ultrasound correlation Poster No.: C-2617 Congress: ECR 2015 Type: Educational
Esophageal Disorders. Gastrointestinal Diseases. Peptic Ulcer Disease. Wireless capsule endoscopy. Diseases of the Small Intestine 7/24/2010
 Esophageal Disorders Gastrointestinal Diseases Fernando Vega, MD HIHIM 409 Dysphagia Difficulty Swallowing and passing food from mouth via the esophagus Diagnostic aids: Endoscopy, Barium x ray, Cineradiology,
Esophageal Disorders Gastrointestinal Diseases Fernando Vega, MD HIHIM 409 Dysphagia Difficulty Swallowing and passing food from mouth via the esophagus Diagnostic aids: Endoscopy, Barium x ray, Cineradiology,
Pediatric PSC A children s tale
 Pediatric PSC A children s tale September 8 th PSC Partners seeking a cure Tamir Miloh Assistant Professor Pediatric Hepatology Mount Sinai Hospital, NY Incidence Primary Sclerosing Cholangitis (PSC) ;
Pediatric PSC A children s tale September 8 th PSC Partners seeking a cure Tamir Miloh Assistant Professor Pediatric Hepatology Mount Sinai Hospital, NY Incidence Primary Sclerosing Cholangitis (PSC) ;
What Are Gallstones? GALLSTONES. Gallstones are pieces of hard, solid matter that form over time in. the gallbladder of some people.
 What Are Gallstones? Gallstones are pieces of hard, solid matter that form over time in the gallbladder of some people. The gallbladder sits under the liver and stores bile (a key digestive juice ). Gallstones
What Are Gallstones? Gallstones are pieces of hard, solid matter that form over time in the gallbladder of some people. The gallbladder sits under the liver and stores bile (a key digestive juice ). Gallstones
Pancreatic Cancer (1 of 5)
 i If you need your information in another language or medium (audio, large print, etc) please contact Customer Care on 0800 374 208 or send an email to: customercare@ salisbury.nhs.uk You are entitled
i If you need your information in another language or medium (audio, large print, etc) please contact Customer Care on 0800 374 208 or send an email to: customercare@ salisbury.nhs.uk You are entitled
Cirrhosis of the Liver
 235 60th Street, West New York, NJ 07093 T: (201) 854-4646 F: (201) 854-4647 810 Main Street, Hackensack, NJ 07601 T: (201) 488-0095 Cirrhosis of the Liver The liver, the largest organ in the body, is
235 60th Street, West New York, NJ 07093 T: (201) 854-4646 F: (201) 854-4647 810 Main Street, Hackensack, NJ 07601 T: (201) 488-0095 Cirrhosis of the Liver The liver, the largest organ in the body, is
Cholangiocarcinoma (Bile Duct Cancer)
 Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Gastrointestinal, Hepatic, and Nutritional Challenges in FA
 Gastrointestinal, Hepatic, and Nutritional Challenges in FA Sarah Jane Schwarzenberg, MD Pediatric Gastroenterology, Hepatology and Nutrition June 29, 2014 GI problems in FA 5% have gastrointestinal tract
Gastrointestinal, Hepatic, and Nutritional Challenges in FA Sarah Jane Schwarzenberg, MD Pediatric Gastroenterology, Hepatology and Nutrition June 29, 2014 GI problems in FA 5% have gastrointestinal tract
Pediatric Primary Sclerosing Cholangitis and Potential Therapies
 Pediatric Primary Sclerosing Cholangitis and Potential Therapies Philip Rosenthal, M.D. Professor of Pediatrics & Surgery University of California, San Francisco DISCLOSURE I have the following financial
Pediatric Primary Sclerosing Cholangitis and Potential Therapies Philip Rosenthal, M.D. Professor of Pediatrics & Surgery University of California, San Francisco DISCLOSURE I have the following financial
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute variceal bleeding management of, 251 262 balloon tamponade of esophagus in, 257 258 endoscopic therapies in, 255 257. See also Endoscopy,
Index Note: Page numbers of article titles are in boldface type. A Acute variceal bleeding management of, 251 262 balloon tamponade of esophagus in, 257 258 endoscopic therapies in, 255 257. See also Endoscopy,
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons
 General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: UPPER GI & HPB - HEPATIC, PANCREATIC & BILIARY
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: UPPER GI & HPB - HEPATIC, PANCREATIC & BILIARY
Figure 2: Post-cholecystectomy biliary-like pain
 Figure 2: Post-cholecystectomy biliary-like pain 1 patient with recurrent episodes of pain (not daily), in the epigastrium/right upper quadrant, lasting >30 mins, building to a steady level, interrupting
Figure 2: Post-cholecystectomy biliary-like pain 1 patient with recurrent episodes of pain (not daily), in the epigastrium/right upper quadrant, lasting >30 mins, building to a steady level, interrupting
Liver Cancer (Hepatocellular Carcinoma or HCC) Overview
 Liver Cancer (Hepatocellular Carcinoma or HCC) Overview Recent advances in liver cancer care seek to address the rising incidence of liver cancer, which has steadily increased over the past three decades.
Liver Cancer (Hepatocellular Carcinoma or HCC) Overview Recent advances in liver cancer care seek to address the rising incidence of liver cancer, which has steadily increased over the past three decades.
Observational Medical Outcomes Partnership
 Implications of Health Outcomes of Interest Definitions: Acute Liver Injury Case Study Judy Racoosin, Patrick Ryan on behalf of OMOP Research Team Observational Medical Outcomes Partnership Established
Implications of Health Outcomes of Interest Definitions: Acute Liver Injury Case Study Judy Racoosin, Patrick Ryan on behalf of OMOP Research Team Observational Medical Outcomes Partnership Established
Dhanpat Jain Yale University School of Medicine, New Haven, CT
 Dhanpat Jain Yale University School of Medicine, New Haven, CT Case history 15 years old female presented with fatigue. Found to have features suggestive of cirrhosis with esophageal varices, splenomegaly
Dhanpat Jain Yale University School of Medicine, New Haven, CT Case history 15 years old female presented with fatigue. Found to have features suggestive of cirrhosis with esophageal varices, splenomegaly
What to do with abnormal LFTs? Andrew M Smith Hepatobiliary Surgeon
 What to do with abnormal LFTs? Andrew M Smith Hepatobiliary Surgeon "it looks like there's something wrong.with your television set. Matt Groenig, creator of The Simpsons Probability of an abnormal screening
What to do with abnormal LFTs? Andrew M Smith Hepatobiliary Surgeon "it looks like there's something wrong.with your television set. Matt Groenig, creator of The Simpsons Probability of an abnormal screening
Hepatitis C Virus (HCV): Current Screening Guidelines and Treatment Approaches
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/hepatitis-c-virus-hcvcurrent-screening-guidelines-treatment-approaches/9514/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/hepatitis-c-virus-hcvcurrent-screening-guidelines-treatment-approaches/9514/
End Stage Liver Disease & Disease Specific Indications for Liver Transplant. Susan Kang, RN, MSN, ANP-BC
 End Stage Liver Disease & Disease Specific Indications for Liver Transplant Susan Kang, RN, MSN, ANP-BC Introduction (https://www.srtr.org) What does the liver do? STORAGE METABOLIC DETOXIFICATION SYNTHETIC
End Stage Liver Disease & Disease Specific Indications for Liver Transplant Susan Kang, RN, MSN, ANP-BC Introduction (https://www.srtr.org) What does the liver do? STORAGE METABOLIC DETOXIFICATION SYNTHETIC
End Stage Liver Disease & Disease Specific Indications for Liver Transplant Susan Kang, RN, MSN, ANP BC
 End Stage Liver Disease & Disease Specific Indications for Liver Transplant Susan Kang, RN, MSN, ANP BC Introduction (https://www.srtr.org) 1 What does the liver do? STORAGE METABOLIC DETOXIFICATION SYNTHETIC
End Stage Liver Disease & Disease Specific Indications for Liver Transplant Susan Kang, RN, MSN, ANP BC Introduction (https://www.srtr.org) 1 What does the liver do? STORAGE METABOLIC DETOXIFICATION SYNTHETIC
Appendix 5. EFSUMB Newsletter. Gastroenterological Ultrasound
 EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
The Continuum of Care for Advanced Liver Disease: Partnering with the Liver Specialist. K V Speeg, MD, PhD UT Health San Antonio
 The Continuum of Care for Advanced Liver Disease: Partnering with the Liver Specialist K V Speeg, MD, PhD UT Health San Antonio Objectives Review staging of liver disease Review consequences of end-stage
The Continuum of Care for Advanced Liver Disease: Partnering with the Liver Specialist K V Speeg, MD, PhD UT Health San Antonio Objectives Review staging of liver disease Review consequences of end-stage
Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association
 CIRRHOSIS AND PORTAL HYPERTENSION Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association WHAT IS CIRRHOSIS? What is Cirrhosis? DEFINITION OF CIRRHOSIS
CIRRHOSIS AND PORTAL HYPERTENSION Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association WHAT IS CIRRHOSIS? What is Cirrhosis? DEFINITION OF CIRRHOSIS
Jaundice , The Patient Education Institute, Inc. syf80102 Last reviewed: 05/05/2017 1
 Jaundice Introduction Jaundice causes your skin and the whites of your eyes to turn yellow. Too much bilirubin causes jaundice. Bilirubin is a yellow chemical in hemoglobin, the substance that carries
Jaundice Introduction Jaundice causes your skin and the whites of your eyes to turn yellow. Too much bilirubin causes jaundice. Bilirubin is a yellow chemical in hemoglobin, the substance that carries
Curriculum: Goals and Objectives Department of Medicine Harbor-UCLA Medical Center
 MEDICAL ONCOLOGY AND HEMATOLOGY (R2, R3) A. The PURPOSE of this rotation is to afford medical residents a broad clinical and training experience in the clinical diagnosis and management of common adult
MEDICAL ONCOLOGY AND HEMATOLOGY (R2, R3) A. The PURPOSE of this rotation is to afford medical residents a broad clinical and training experience in the clinical diagnosis and management of common adult
Hepatobiliary investigations
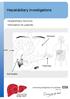 Hepatobiliary investigations Hepatobiliary Services Information for patients Liver i Stomach Pancreas Gall bladder Introduction You have been referred to the Hepatobiliary Unit. We specialise in procedures
Hepatobiliary investigations Hepatobiliary Services Information for patients Liver i Stomach Pancreas Gall bladder Introduction You have been referred to the Hepatobiliary Unit. We specialise in procedures
Alpha-1 Liver Disease
 Alpha-1 Liver Disease Jeffrey Teckman, M.D. Professor of Pediatrics and Biochemistry Associate Chair of Pediatrics for Research Director, Pediatric Gastroenterology and Hepatology St. Louis University
Alpha-1 Liver Disease Jeffrey Teckman, M.D. Professor of Pediatrics and Biochemistry Associate Chair of Pediatrics for Research Director, Pediatric Gastroenterology and Hepatology St. Louis University
What Is Pancreatitis?
 What Is Pancreatitis? Pancreatitis is inflammation (swelling) of the pancreas that is most often caused by gallstones or alcohol abuse. There are other causes that your gastroenterologist will look for,
What Is Pancreatitis? Pancreatitis is inflammation (swelling) of the pancreas that is most often caused by gallstones or alcohol abuse. There are other causes that your gastroenterologist will look for,
Int. J. Pharm. Sci. Rev. Res., 46(1), September - October 2017; Article No. 07, Pages: 37-41
 Research Article Assessment of Clinical Profile and Prescription Pattern of Drugs in Alcoholic Liver Disease and Hepatitis in a Tertiary Care Hospital Christeena James*, Dr.ShirishInamdar, Dr.Bharathi
Research Article Assessment of Clinical Profile and Prescription Pattern of Drugs in Alcoholic Liver Disease and Hepatitis in a Tertiary Care Hospital Christeena James*, Dr.ShirishInamdar, Dr.Bharathi
ACG Clinical Guideline: Evaluation of Abnormal Liver Chemistries
 ACG Clinical Guideline: Evaluation of Abnormal Liver Chemistries Ashwani K. Singal, MD, MS, FACG 1, Ramon Bataller, MD, PhD, FACG 2, Joseph Ahn, MD, MS, FACG (GRADE Methodologist) 3, Patrick S. Kamath,
ACG Clinical Guideline: Evaluation of Abnormal Liver Chemistries Ashwani K. Singal, MD, MS, FACG 1, Ramon Bataller, MD, PhD, FACG 2, Joseph Ahn, MD, MS, FACG (GRADE Methodologist) 3, Patrick S. Kamath,
The Pancreas. Basic Anatomy. Endocrine pancreas. Exocrine pancreas. Pancreas vasculature. Islets of Langerhans. Acinar cells Ductal System
 SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
General Surgery PURPLE SERVICE MUHC-RVH Site
 Preamble HPB is a clinical teaching unit with several different vocations: It regroups all solid organ Transplantation as well as most advanced Hepatobiliary and Pancreatic clinical activities performed
Preamble HPB is a clinical teaching unit with several different vocations: It regroups all solid organ Transplantation as well as most advanced Hepatobiliary and Pancreatic clinical activities performed
Curricular Components for General Pediatrics EPA EPA Title Assess and manage patients with common behavior/mental health problems
 Curricular Components for General Pediatrics EPA 9 1. EPA Title Assess and manage patients with common behavior/mental health problems 2. Description of the activity Mental health and behavioral issues
Curricular Components for General Pediatrics EPA 9 1. EPA Title Assess and manage patients with common behavior/mental health problems 2. Description of the activity Mental health and behavioral issues
Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
 Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Neonatal Cholestasis. What is Cholestasis? Congenital and Pediatric liver diseases 4/26/18
 Congenital and Pediatric liver diseases Nitika Gupta, M.D. Personal/Professional Financial Relationships with Industry in the past year External Industry Relationships * Equity, stock, or options in biomedical
Congenital and Pediatric liver diseases Nitika Gupta, M.D. Personal/Professional Financial Relationships with Industry in the past year External Industry Relationships * Equity, stock, or options in biomedical
Diagnosis of chronic Pancreatitis. Christoph Beglinger, University Hospital Basel, Switzerland
 Diagnosis of chronic Pancreatitis Christoph Beglinger, University Hospital Basel, Switzerland Pancreatitis Pancreas Pancreas - an organ that makes bicarbonate to neutralize gastric acid, enzymes to digest
Diagnosis of chronic Pancreatitis Christoph Beglinger, University Hospital Basel, Switzerland Pancreatitis Pancreas Pancreas - an organ that makes bicarbonate to neutralize gastric acid, enzymes to digest
This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated.
 A-Z of medical words This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated. Absorption: once your food has been broken down,
A-Z of medical words This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated. Absorption: once your food has been broken down,
Alpha-1 Antitrypsin Deficiency: Liver Disease
 Alpha-1 Antitrypsin Deficiency: Liver Disease Who is at risk to develop Alpha-1 liver disease? Alpha-1 liver disease may affect children and adults who have abnormal Alpha-1 antitrypsin genes. Keys to
Alpha-1 Antitrypsin Deficiency: Liver Disease Who is at risk to develop Alpha-1 liver disease? Alpha-1 liver disease may affect children and adults who have abnormal Alpha-1 antitrypsin genes. Keys to
Certified Clinical Transplant Nurse (CCTN) * Detailed Content Outline
 I. PRETRANSPLANTATION CARE 9 11 3 23 A. Evaluate End-Stage Organ Failure 1 1 1 3 1. History and physical assessment 2. Vital signs and / or hemodynamic parameters 3. Lab values 4. Diagnostic tests B. Monitor
I. PRETRANSPLANTATION CARE 9 11 3 23 A. Evaluate End-Stage Organ Failure 1 1 1 3 1. History and physical assessment 2. Vital signs and / or hemodynamic parameters 3. Lab values 4. Diagnostic tests B. Monitor
Together, putting patients first
 The Role of a Gastroenterologist in the Diagnosis and Management of Pancreatic Cancer Sarah Jowett, Consultant Gastroenterologist Bradford Teaching Hospitals Trust Leeds Regional Study Day, 12 September
The Role of a Gastroenterologist in the Diagnosis and Management of Pancreatic Cancer Sarah Jowett, Consultant Gastroenterologist Bradford Teaching Hospitals Trust Leeds Regional Study Day, 12 September
Patient Information Leaflet Liver Transplantation Assessment
 Patient Information Leaflet Liver Transplantation Assessment South West Liver Unit Derriford Hospital Plymouth PL6 8DH Tel: 01752 431320 Information about Liver Transplantation: Your specialist may recommend
Patient Information Leaflet Liver Transplantation Assessment South West Liver Unit Derriford Hospital Plymouth PL6 8DH Tel: 01752 431320 Information about Liver Transplantation: Your specialist may recommend
JAUNDICE. Zdeněk Fryšák 3rd Clinic of Internal Medicine Nephrology-Rheumatology-Endocrinology Faculty Hospital Olomouc
 JAUNDICE Zdeněk Fryšák 3rd Clinic of Internal Medicine Nephrology-Rheumatology-Endocrinology Faculty Hospital Olomouc Definition of Jaundice Icterus A yellowish staining of the skin, sclerae and deeper
JAUNDICE Zdeněk Fryšák 3rd Clinic of Internal Medicine Nephrology-Rheumatology-Endocrinology Faculty Hospital Olomouc Definition of Jaundice Icterus A yellowish staining of the skin, sclerae and deeper
Natural history of α-1-atd in children
 Natural history of α-1-atd in children Agnieszka Bakuła Dpt of Gastroenterology, Hepatology, Nutrition Disorders and Paediatrics The Children s Memorial Health Institute Warsaw, Poland Topics to be discussed
Natural history of α-1-atd in children Agnieszka Bakuła Dpt of Gastroenterology, Hepatology, Nutrition Disorders and Paediatrics The Children s Memorial Health Institute Warsaw, Poland Topics to be discussed
Biliary Atresia. Who is at risk for biliary atresia?
 Biliary Atresia Biliary atresia is a life-threatening condition in infants in which the bile ducts inside or outside the liver do not have normal openings. Bile ducts in the liver, also called hepatic
Biliary Atresia Biliary atresia is a life-threatening condition in infants in which the bile ducts inside or outside the liver do not have normal openings. Bile ducts in the liver, also called hepatic
Evaluation Process for Liver Transplant Candidates
 Evaluation Process for Liver Transplant Candidates 2 Objectives Identify components of the liver transplant referral to evaluation Describe the role of the liver transplant coordinator Describe selection
Evaluation Process for Liver Transplant Candidates 2 Objectives Identify components of the liver transplant referral to evaluation Describe the role of the liver transplant coordinator Describe selection
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons
 General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: TRANSPLANTATION 7-Nov-2016 DEVELOPED BY: Daryl
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: TRANSPLANTATION 7-Nov-2016 DEVELOPED BY: Daryl
Rokitansky-Aschoff sinuses are epithelial invaginations in the gallbladder wall that from as a result of increased gallbladder pressures.
 Anatomy The complexity of the biliary tree can be broken down into much simpler segments. The intrahepatic ducts converge to form the right and left hepatic ducts which exit the liver and join to become
Anatomy The complexity of the biliary tree can be broken down into much simpler segments. The intrahepatic ducts converge to form the right and left hepatic ducts which exit the liver and join to become
Key Points: Autoimmune Liver Disease: Update for Pathologists from the Hepatologist s Perspective. Jenny Heathcote, MD. University of Toronto
 Autoimmune Liver Disease: Update for Pathologists from the Hepatologist s Perspective Jenny Heathcote, MD University of Toronto Key Points: AILD comprise autoimmune hepatitis, primary biliary cirrhosis
Autoimmune Liver Disease: Update for Pathologists from the Hepatologist s Perspective Jenny Heathcote, MD University of Toronto Key Points: AILD comprise autoimmune hepatitis, primary biliary cirrhosis
following the last documented transfusion; thereafter, evaluate the residual impairment(s).
 Adult Listings 5.01 Category of Impairments, Digestive System 5.02 Gastrointestinal hemorrhaging from any cause, requiring blood transfusion (with or without hospitalization) of at least 2 units of blood
Adult Listings 5.01 Category of Impairments, Digestive System 5.02 Gastrointestinal hemorrhaging from any cause, requiring blood transfusion (with or without hospitalization) of at least 2 units of blood
