There is extensive evidence that a family history of alcoholism
|
|
|
- Rosalind Cole
- 5 years ago
- Views:
Transcription
1 Article Altered NMDA Glutamate Receptor Antagonist Response in Individuals With a Family Vulnerability to Alcoholism Ismene L. Petrakis, M.D. Diana Limoncelli, B.A. Ralitza Gueorguieva, Ph.D. Peter Jatlow, M.D. Nashaat N. Boutros, M.D. Louis Trevisan, M.D. Joel Gelernter, M.D. John H. Krystal, M.D. Objective: A family history of alcoholism is a risk factor for the development of ethanol dependence. Ethanol is an antagonist of the N-methyl-D-aspartate (NMDA) glutamate receptor, and alterations in NMDA receptor function are thought to be involved in ethanol abuse and dependence. The purpose of this study was to determine in healthy individuals with no ethanol dependence whether response to the NMDA receptor antagonist ketamine would differentiate those with a family history of ethanol dependence from those without such a family history. Method: Healthy subjects between the ages of 21 and 30 received 40-minute intravenous infusions of saline, low-dose ketamine (0.1 mg/kg), and high-dose ketamine (0.5 mg/kg) on three separate test days in a randomized order under doubleblind conditions. The healthy individuals with at least one first-degree relative and another first- or second-degree relative with ethanol dependence (N=16) were compared with those who had no family history of ethanol dependence in any firstor second-degree relative (N=29). Outcome measures included the Brief Psychiatric Rating Scale, Clinician-Administered Dissociative States Scale, verbal fluency, Hopkins Verbal Learning Test, a biphasic alcohol effects scale, visual analog scales of mood states, and ketamine levels. Results: During ketamine infusion, individuals with a family history of ethanol dependence showed an attenuated response in terms of perceptual alterations and dysphoric mood relative to those without such a family history. Conclusions: These data suggest that alterations in NMDA receptor function may contribute to subjective response to ethanol and therefore also to the risk of developing alcoholism. (Am J Psychiatry 2004; 161: ) There is extensive evidence that a family history of alcoholism is a risk factor for the development of ethanol problems (1). A substantial part of the tendency for ethanol dependence to run in families is attributable to genetic factors (2). Healthy individuals with a family history of ethanol dependence exhibit a relatively lower intensity of subjective intoxication, ataxia, body sway, or flushing to moderate doses of ethanol in a laboratory setting than do healthy individuals with no family history of alcoholism. These findings have clinical importance, since follow-up studies have shown that a reduced sensitivity to the dysphoric or adverse effects of ethanol is the single strongest predictor of the subsequent development of alcoholism (3). Antagonists of the N-methyl-D-aspartate (NMDA) receptor have provided an important mechanism for evaluating the pathophysiology of neuropsychiatric disorders, such as Alzheimer s disease, anxiety, depression, and schizophrenia. For example, administration of the NMDA antagonist ketamine to healthy subjects and the subsequent cognitive deficits (4, 5) and perceptual changes (6 9) have led to further understanding of the pathophysiology of schizophrenia (6 9). NMDA glutamate receptors are among the highest affinity ethanol targets in the brain (10). NMDA receptor antagonists substitute for ethanol in drug discrimination studies conducted in animals, particularly for higher ethanol doses (11 13). Postmortem studies of brain tissue suggest that certain subunits of NMDA receptors are increased in cortical structures of ethanol-dependent individuals (14), and in vivo ethanol withdrawal increases cerebrospinal fluid glutamate levels. The NMDA antagonist ketamine produced dose-related ethanol-like effects in recently detoxified ethanol-dependent patients, and the intensity and the degree of similarity of the ethanol-like effects of ketamine were greater at higher doses (7). Patients also showed reductions in their sensitivity to some of the negative effects (i.e., perceptual, mood, and cognitive effects) of ketamine (15). These group differences in ketamine response could reflect a response to prolonged ethanol exposure. However, ketamine response could also be a heritable trait marker for a family history of ethanol dependence. The purpose of the current study was to examine whether healthy individuals at increased familial risk to develop ethanol dependence exhibit alterations in NMDA receptor function. This objective was evaluated by comparing among healthy individuals the dose-related effects
2 PETRAKIS, LIMONCELLI, GUEORGUIEVA, ET AL. of the NMDA receptor antagonist ketamine in those with a strong family history of ethanol dependence versus those with no such family history. Method Subjects In this institutional review board-approved study, healthy individuals (N=45) were recruited by advertisements and compensated for their participation. The subjects included in the study 1) were between the ages of 21 30, 2) had no lifetime axis I psychiatric or substance use disorder, and 3) had biological mothers with no history of alcoholism, in order to ensure that any effects were not the result of direct toxicity of alcohol during pregnancy. Individuals with a history of consultation for an emotional difficulty, those with a psychiatric illness in a first- or second-degree relative, and those who were alcohol naive were excluded from participation. After signing informed consent, subjects underwent a screening that included the Structured Clinical Interview for DSM-III-R (SCID) (16) to rule out any axis I disorders and a physical screening to ensure they were medically healthy. Subjects were asked to report their alcohol consumption for the 30 days preceding the intake assessment. Family history was formally evaluated by interviewing the subject to obtain the psychiatric status (including substance abuse/dependence, mood disorder, etc.) of all firstand second-degree biological relatives (including parents) using a questionnaire based on the SCID (H.R. Kranzler, personal communication, 2002). Subjects with a family history of ethanol dependence (N=16) had a biological father and another first- or second-degree biological relative with history of alcoholism. The remaining subjects (N=29) had no family history of alcoholism in any first or second-degree relatives. Eighteen of these 29 subjects included in the data analysis were individuals who met entry criteria for this study but who participated in a previous near-identical ketamine study, described in another report (6). There were no significant differences between groups in age, weight, or years of education. Similarly, there was no significant difference in the amount of self-reported alcohol use between groups. Procedures Subjects completed 3 test days at least 3 days apart in a randomized order under double-blind conditions. Prior to the administration of any study medication, subjects were warned that ketamine had addictive potential and that its effects resembled the effects of ethanol. The individuals with a family history of ethanol dependence in particular were encouraged not to participate if they were concerned about their increased risk for the development of a substance use disorder. Prior to each test session, participants fasted overnight and remained in a fasting state during the test session. They were tested at approximately 8:30 a.m., and an intravenous line was placed at that time. On each test day, patients received a 40-minute intravenous infusion containing saline solution; ketamine hydrochloride, 0.1 mg/kg; or ketamine hydrochloride, 0.5 mg/kg (Ketalar, Parke-Davis, Kalamazoo, Mich.). This method of administration was similar to that reported previously in healthy subjects and ethanol-dependent patients (6, 7). Another intravenous catheter was placed and used for sampling plasma for hormonal analyses and to determine plasma ketamine levels. Blood was drawn to determine ketamine levels 10 and 80 minutes after the initiation of ketamine infusion. The order of multiple assessments was standardized. Psychosis, dysphoria, negative symptoms, and behavior changes were assessed by using the Brief Psychiatric Rating Scale (BPRS) (17) as in prior studies of ketamine effects (6, 7, 18). Four key BPRS items for the positive symptoms of psychosis were used: conceptual disorganization, hallucinatory behavior, suspiciousness, and unusual thought content. Dysphoria was derived from the BPRS anxious-depression factor, comprising the items anxiety, guilt feelings, depressive mood, somatic concern, tension, and motor retardation (19). Three BPRS items for negative symptoms were used: blunted affect, emotional withdrawal, and motor retardation. Behavior changes were derived from the BPRS activation subscale, which comprises the items of tension, mannerisms, and posturing and excitement (19). The BPRS was administered at baseline and 10, 40, 80, 110, and 230 minutes after the start of the infusion. The Clinician-Administered Dissociative States Scale (20), which has 19 self-reported items and eight observer-rated items scored from 0 (not at all) to 4 (extremely), was administered at baseline and after 10, 40, 80, 110, and 230 minutes. Mood ratings were assessed at 10, 20, 40, 80, 110, 170, and 230 minutes using visual analog scales. These scales are 100-mm visual analog scales marked proportionately to the perceived intensity of the subjective experience (0=not at all, 100=extremely) for the following mood states: depressed, high, anxious, drowsy, nauseous, and hungry. These mood rating scales have shown convergent validity with other measures of mood states during similar challenge studies (7, 21, 22). Subjective intoxication ratings were also assessed at 10, 20, 40, 80, 110, 170, and 230 minutes using visual analog scales. Ketamine-induced effects, which are similar to the effects of alcohol, were measured by a biphasic alcohol effects scale in which the ascending scale measured activating alcohollike symptoms such as euphoria while the descending scale measured sedation. Cognitive functions were assessed as follows. Verbal fluency was assessed by using a task that required subjects to generate as many words as possible during a 1-minute interval that began with a specified letter. Equivalent versions of this task were administered on the 3 test days at 20 minutes after the initiation of infusion by using letters equated for frequency in English (23). The Hopkins Verbal Learning Test is a word list learning test of verbal memory (24). This test is sensitive to the amnesic effects of NMDA antagonists and has the advantage of six different versions that permit multiple episodes of testing. The procedures associated with the test allow some degree of distinction between immediate recall, delayed recall (after 30 minutes), and recognition. This test was administered 20 minutes after infusion initiation. Samples for blood ketamine levels were drawn during the laboratory session by a research nurse 10 and 80 minutes after infusion initation. Samples were spun immediately and then frozen in airtight vials. Plasma ketamine concentrations were measured by reversed-phase high-performance liquid chromatography with ion pairing. Variation between days over a range (400 ng/ml to 20 ng/ml) varied from 2.1% to 7.8%. Data Analysis All analyses were performed by using SAS Version 8.2. Cumulative logit generalized estimating equation models for ordinal data were fitted in PROC GENMOD for the analysis of the BPRS, visual analog scale, and Clinician-Administered Dissociative States Scale data. Group (family history, no family history), dose (high, low, placebo), and time and all possible interactions of these variables were considered as predictors. Sex was included as a covariate. Independence working correlation matrix was assumed. The analysis was restricted only to dose levels and time points for which there was variability in the data. Alcohol consumption was considered as a covariate but was nonsignificant and dropped from the final model for parsimony. Model-based post hoc between-group comparisons of high-dose ketamine response were performed for the time points considered in the model. Betweengroup comparisons were also performed by using Fisher s exact test for all dose and time combinations, even the ones at which
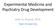
3 NDMA RECEPTOR FUNCTION AND ALCOHOLISM FIGURE 1. Psychotic Response Among Healthy Subjects During a 40-Minute, High-Dose (0.5 mg/kg) Ketamine Infusion, by Family History of Ethanol Dependence a 20 Subjects with a family history of ethanol dependence (N=16) Subjects with no family history of ethanol dependence (N=29) BPRS Positive Symptom Score b 80 Time From Initiation of Drug Infusion (minutes) a Horizontal lines represent group means. b Data collected from only 10 subjects with no family history of ethanol dependence at this time point. there was not enough variability to include the data in the general model. The verbal fluency data were analyzed by using a mixed model with fixed group, dose, and group-by-dose effects and a random subject effect in SAS PROC MIXED. The group-by-dose interaction was tested first and was followed by Bonferroni-adjusted individual comparisons. The ascending and descending scales of the biphasic alcohol effects scale were assessed log transformed, and each scale was analyzed with a mixed model with fixed effects of dose, group, and time and all possible interactions, a random subject effect, and heterogeneous autoregressive structure over time. Baseline was included as a covariate. The immediate recall data from the Hopkins Verbal Learning Test were analyzed by using a mixed model with fixed effects of group, dose, and time and a random subject effect. Perseverations and sex were used as covariates. Recognition and delay variables were tested with both 1) a mixed model with fixed effects of group and dose and a random subject effect, with immediate recall data as a covariate; and 2) a nonparametric model to test effects of treatment and family history. Ketamine levels were also assessed log transformed and analyzed with a mixed model with fixed effects of dose, group, and time and all possible interactions. Correlations between blood values and the main outcome variables were also analyzed by using a logistic model. Results Behavioral and Subjective Effects Psychotic response. Individuals with a family history of ethanol dependence had a blunted psychotic response to ketamine relative to those with no such family history (Figure 1). In the analysis of the four key positive symptom scores, scores were first clustered into low ( 4) or high ( 5) scores for analysis in a logistic regression generalized estimating equation model. However, for the placebo and low-dose ketamine (0.1 mg/kg) infusions, subjects in both groups exhibited low scores at almost all the time points. As a result, it was necessary to limit the analysis to the higher ketamine (0.5 mg/kg) dose. Within the ketamine 0.5 mg/kg test day, high responses were limited to the assessment made 10 minutes following the initiation of ketamine infusion. The effect of group was significant, with subjects who had no family history of alcoholism exhibiting greater response than those with a family history of ethanol dependence (Table 1). Dysphoria. Ketamine produced a more pronounced dysphoric mood response in individuals with no family history of ethanol dependence, as measured by the BPRS anxious-depression factor. In the analysis of this factor, scores were first clustered into low ( 6), medium (7, 8), or high ( 9) scores. The analysis was restricted to the 10- and 80- minute time points, which revealed a significant group-bydose-by-time interaction (Table 1). Negative symptoms. Subjects with no family history of ethanol dependence also exhibited more pronounced ketamine-induced negative symptoms (blunted affect, emotional withdrawal, and psychomotor retardation). In the analysis of these three key negative symptom scores, scores were first clustered into low ( 3) or high ( 4) scores. The model could only be fit to the high-dose ketamine comparisons. There was a significant group-by-time effect (Table 1). Two post hoc between-group comparisons at the 10- and 80-minute time points were performed; only the comparison at 80 minutes was significant (χ 2 =4.15, df=1, p<0.05), with the post hoc results confirmed by Fisher s exact test (p=0.055). Behavior changes. In the analysis of the BPRS activation subscale, scores were first clustered into low ( 3) or high ( 4) scores. The model could only fit to the high dose of ketamine and to the 10-minute time point. Although there were no significant group differences, there is some indication that the ketamine effect was sustained in the
4 PETRAKIS, LIMONCELLI, GUEORGUIEVA, ET AL. TABLE 1. Effects Over Time of a 40-Minute, High-Dose (0.5 mg/kg) Ketamine Infusion in Healthy Subjects, by Family History of Ethanol Dependence Score Subjects With No Family History of Ethanol Dependence (N=29) Subjects With a Family History of Ethanol Dependence (N=16) 10 Minutes 40 Minutes b 80 Minutes 10 Minutes 40 Minutes 80 Minutes Analysis a Effect Mean SD Mean SD Mean SD Mean SD Mean SD Mean SD Effect χ 2 df p Psychosis Group Dysphoria Group-bydose-by-time Negative symptoms Group-by-time Behavior changes 3.6 c Dissociation d Group-by-time a Cumulative logit generalized estimating equation models assessing the effects of group, dose, and time and all possible interactions. b N=10 for all effect measures except dissociation (N=11). c N=28. d For subjects with no history of ethanol dependence, N=27, 11, and 28 at 10, 40, and 80 minutes, respectively. For subjects with a family history of ethanol dependence, N=14 at 40 minutes. healthy subjects who had no family history of alcoholism relative to those with a family history of ethanol dependence. Post hoc analysis with Fisher s exact tests showed a significant between-group comparison at the high-dose 80-minute time point (p<0.02). Dissociation. The subjects with a family history of ethanol dependence had a blunted dissociative response to ketamine relative to those without such a family history, as measured by the Clinician-Administered Dissociative States Scale (Figure 2). In the analysis of the Clinician-Administered Dissociative States Scale scores, scores were first clustered into low (0 2), medium (3 10), high (11 25), or very high ( 26) scores. The analysis was restricted to the 10- and 80-minute time points. There was a significant group-by-time effect (Table 1) with significant betweengroup differences occurring at the 80-minute time point only (χ 2 =11.50, df=1, p=0.0007), which was confirmed by Fisher s exact test (p 0.01). Intensity of mood states. Subject ratings from the visual analog scale were categorized into five 20-mm increments (0 20, 21 40, etc.). On the basis of visual analog scale ratings for high and drowsy, ketamine produced significant euphoria (dose-by-time effect: (χ 2 =54.12, df=6, p<0.01). No group-related differences were significant in the analysis. There were no other significant effects for the other mood states assessed with the visual analog scale. Subjective intoxication. There were significant ketamine-induced effects, which are similar to the effects of alcohol, as measured by a biphasic alcohol effects scale. For both the ascending and descending scales, ketamine showed significant effects of dose (F=4.05, df=2, 56.9, p= 0.02 and F=19.1, df=2, 31.1, p<0.01, respectively), time (F= 3.33, df=6, 202, p<0.01; F=23.4, df=6, 159, p<0.01), and dose-by-time (F=3.02, df=12, 203, p<0.01; F=9.92, df=12, 130, p<0.01), but no group-related differences were significant in this analysis. Cognitive Effects On the Hopkins Verbal Learning Test, there was a significant ketamine effect on immediate recall (F=16.84, df=2, 234, p<0.001), with lower scores during the high dose relative to both the low dose and placebo (p<0.001, p<0.001). Although there was a significant group effect on immediate recall in which those individuals with a family history of ethanol dependence had lower scores than those without such a family history (F=8.78, df=1, 234, p<0.004), there was no significant dose-by-group effect. There was no significant group effect or dose effect for either delayed recall or recognition. On the verbal fluency test, there was not a significant group effect or a group-by-dose effect (F=1.67, df=2, 76.4, p=0.20). However, post hoc tests of the within-group dose effect showed a significant effect for individuals with no family history of ethanol dependence (F=5.72, df=2, 76.6, p=0.005) in which the higher the dose, the lower the verbal fluency scores; this was not seen in subjects with a family history of ethanol dependence (F=0.08, df=2, 76.2, p= 0.92). Blood Level Effects As expected, there were significant effects on ketamine plasma levels for dose (F=8.01, df=1, 90, p<0.001) and time (F=10.24, df=1, 90, p<0.001). However, there was no statistically significant difference in ketamine levels between individuals with a family history of ethanol dependence and those with no such family history. Ketamine blood levels were not significantly correlated with the intensity of the psychotic or dissociative responses. Discussion The principal finding from this study is that in healthy individuals with no ethanol dependence, response to the NMDA receptor antagonist ketamine was altered in those with a family history of ethanol dependence relative to those with no such family history. Specifically, these data show that individuals with a family history of ethanol de
5 NDMA RECEPTOR FUNCTION AND ALCOHOLISM FIGURE 2. Dissociative Response Among Healthy Subjects During a 40-Minute, High-Dose (0.5 mg/kg) Ketamine Infusion, by Family History of Ethanol Dependence a Total Score on Clinician-Administered Dissociative States Scale Subjects with a family history of ethanol dependence (N=15) Subjects with no family history of ethanol dependence (N=28) 10 b 40 c 80 Time From Initiation of Drug Infusion (minutes) a Horizontal lines represent group means. b Data were missing for one subject with no family history of ethanol dependence at this time point. c At this time point, data collected from only 11 subjects with no family history of ethanol dependence, and one subject with a family history of ethanol dependence had data missing. pendence exhibited blunted psychosis, dysphoric mood, negative symptom, and perceptual responses but sustained activation to ketamine relative to individuals with no such family history. The impact of possible confounding factors was considered. However, the groups were matched by age, and there were no significant differences in demographic characteristics except for sex, and this was added as a covariate to the models. Similarly, since there were no significant differences in ketamine plasma levels between the groups, nor was there a significant effect of plasma ketamine level on the intensity of the main outcome variables, our results are not likely to have arisen from group differences in drug metabolism. A second finding from this study is, as expected, that subjects as a group perceived ketamine to be similar to alcohol and experienced it as euphoric and sedating. However, there were no group differences in perceptions of similarity to alcohol or in experiences of sedation or being high. The data suggest that differences in ketamine response between the two groups are reflected in their distinct subjective responses to ethanol. The evidence supporting this interpretation is that both groups reported an equivalently high degree of similarity between the subjective effects of ketamine and their recollection of the subjective effects of ethanol. The similarity of the subjective effects of ketamine to the subjective effects of ethanol was reported by both groups despite the fact that ketamine had a markedly different array of effects in these two groups. If alterations in NMDA receptor antagonist response did not extend to ethanol, one would have expected to find significant differences in the extent of ethanol similarity of ketamine effects in groups distinguished by their ketamine responses. Thus, the current data are also consistent with the extensive literature that suggests that subjects with versus those without a family history of ethanol dependence are distinguished by alterations in ethanol response that resemble their differences in ketamine response in the current study. However, an important limitation of the current study design was the absence of an ethanol test day that would have allowed for a direct comparison of ketamine and ethanol effects in these groups. A third finding is that ketamine produced some expected cognitive impairments, particularly in memory, but again there were no group differences in cognitive measures in the response to ketamine administration. Of note, however, was the group difference at baseline for one of the cognitive measures: individuals with a family history of ethanol dependence scored significantly lower on a test of verbal memory. Cognitive impairments and other soft neurologic signs in individuals with a family history of ethanol dependence relative to those with no such family history have long been of interest as potentially relevant factors that could contribute to the development of ethanol dependence (25). While many studies have found similarities between these groups in learning, memory, and verbal and total intelligence scores, differences in abstract reasoning and logic performance suggest the potential for underlying neurobiological abnormalities in neural circuitry (25). Further, an attenuation of ethanol-induced cognitive deficits has been found in individuals with a family history of ethanol dependence relative to those with no such family history (26). In this study, baseline differences in cognitive function did not influence ketamine response, suggesting that baseline learning and memory could not account for group differences in subjective ketamine responses. Additionally, individuals with a family history of ethanol dependence did not exhibit a reduced
6 PETRAKIS, LIMONCELLI, GUEORGUIEVA, ET AL. sensitivity to the ketamine-induced effects on cognitive function. Results from this study suggest that altered NMDA receptor function may contribute to the altered ethanol response in individuals with a family history of ethanol dependence relative to those with no such family history. These NMDA receptor functional changes include a shift in the reward valence of the actions of NMDA receptor antagonists, presumably including ethanol, toward the experience of a drug of predominately reduced dysphoric effects. The present results are also consistent with data from recently detoxified individuals (27) showing that when ethanol-dependent patients are subtyped, those with a family history of ethanol dependence show reduced ketamine induction of affect blunting, dysphoric mood, and impaired performance on the Wisconsin Card Sorting Test. However, other ketamine responses that discriminated healthy subjects with a family history of ethanol dependence from those without such a history did not differentiate ethanol-dependent patients with versus without a family history of ethanol dependence, including sustained or enhanced euphoria. These data suggest that family history of ethanol dependence and ethanol dependence convey convergent, but not overlapping, alterations in NMDA receptor function. Changes in the response to ketamine could reflect alterations in NMDA receptor function related to voltage-gated ion channels, NMDA receptor-related signal processing cascades, modulation of the phosphorylation state of NMDA receptor subunits, and shifts in the levels or posttranscriptional processing of NMDA receptor subunit mrnas or proteins (28). Alternatively, these responses could reflect network consequences of alterations in NMDA receptor function, such as the stimulation of the release of glutamate and dopamine (29). Clinical evidence has shown that drugs that attenuate glutamate release or glutamatergic excitability via blockade of voltage-gated cation channels reduce the dysphoric effects of ketamine and promote the euphoric effects of ketamine in both healthy subjects (30) and recovering ethanol-dependent patients (31). In fact, pretreatment with calcium channel blockers in individuals with no family history of ethanol dependence leads to a ketamine response that is more consistent with that of individuals who have a family history of ethanol dependence (30), suggesting that the alteration reflects dysfunction related to voltage-gated cation channels. Nevertheless, other mechanisms have not been definitively ruled out. A strength of this study is its use of a study design that mirrors previous work with ketamine, including similar doses and outcome measures, in ethanol-dependent individuals, so the results can be compared. However, there are several limitations to this study. First, individuals were recruited by advertisement, and family history of alcoholism was assessed by self-report. Interviewing affected relatives of subjects who claimed to have a positive family history in order to confirm the diagnosis of alcoholism was not done for practical reasons. Similarly, the recruitment of offspring of a treatment-seeking population would be more accurate but was ruled out because of practical reasons. Therefore, the diagnosis of alcohol dependence in the family member could not be confirmed. However, we surmise that bias in reporting familial affection is more likely to occur in the other direction, i.e., in failing to attribute deserved diagnoses to relatives, so the healthy sample may have included individuals with a family member with alcohol dependence that was unrecognized. In any event, if such errors occurred in either direction, they would tend to decrease the power of the study rather than lead to a positive finding. Second, although alcohol dependence is moderately heritable, not all individuals with a family history carry the risk of developing alcoholism, although for that reason we included only those with multiple family members with the diagnosis. Arguably, since we sampled only unaffected subjects past the major period of lifetime risk for developing alcohol dependence, the subjects we studied, who have successfully avoided developing alcohol dependence despite a family history, would be those among the at-risk population who have protective factors as well as risk factors. That is, our study design may have preferentially included individuals who were unlikely to become ethanol dependent despite their family history. Human subject considerations are thought to mandate the selection of such a sample. Third, the results could be explained by some confounding factor that was not tested, such as the presence of a personality disorder. In summary, this study reported alterations in response to the NMDA receptor antagonist ketamine between healthy subjects with a family history of ethanol dependence relative to those without such a family history. The subjects with a family history experienced dysphoric responses to ketamine that were markedly reduced and some mild enhancement in euphoria. An inherited underlying alteration in NMDA receptor antagonist response may have implications for the subsequent response of these individuals to ethanol ingestion. If NMDA antagonists are not perceived as unpleasant, it may shift the reward valence of ingestion of these substances. Clinically, these individuals may lack the warning signs to stop heavy drinking when consuming moderate amounts of alcohol. In the right environmental and social context, the loss of a potentially important brake on drinking may promote heavy drinking. The strength of the current findings suggest that future candidate gene investigations might concentrate on genes that influence glutamatergic function. In these studies, the response to ketamine or other NMDA receptor antagonists might prove to be a useful phenotype. Received Sept. 26, 2002; revisions received May 13 and Dec. 9, 2003; accepted Dec. 15, From the Department of Veterans Affairs Alcohol Research Center, VA Connecticut Healthcare System; the National Institute on Alcohol and Alcohol Abuse Center for the Trans
7 NDMA RECEPTOR FUNCTION AND ALCOHOLISM lational Neuroscience of Alcoholism, New Haven, Conn.; the Clinical Neuroscience Research Unit, Abraham Ribicoff Research Facilities, New Haven, Conn.; and the Departments of Psychiatry, Laboratory Medicine, and Epidemiology and Public Health (Division of Biostatistics), Yale University School of Medicine, New Haven, Conn. Address reprint requests to Dr. Petrakis, West Haven VA Medical Center (116- A), 950 Campbell Ave., West Haven, CT 06516; yale.edu ( ). Supported by grants from the National Institute on Alcohol Abuse and Alcoholism (1R01 AA , RO1 AA , KO2 AA , and P50 AA ) to Drs. Krystal and Petrakis; and Merit Review grants and funding from the Department of Veterans Affairs VA-Yale Alcohol Research Center to Drs. Krystal and Petrakis. The authors thank Rachel Alpert; William Ford; Angelina Genovese, R.N.C., M.B.A; Elizabeth O Donnell, R.N.; and Jane Zhang, Ph.D., for their contributions as well as the staffs of the Biostudies Unit and Substance Abuse Treatment Unit of VA Connecticut Healthcare System. References 1. Hesselbrock MN, Hesselbrock VM: Relationship of family history, antisocial personality disorder and personality traits in young men at risk for alcoholism. J Stud Alcohol 1992; 53: Kendler KS, Prescott CA, Neale MC, Pedersen NL: Temperance board registration for alcohol abuse in a national sample of Swedish male twins, born 1902 to Arch Gen Psychiatry 1997; 54: Schuckit MA, Smith TL: An 8-year follow-up of 450 sons of alcoholic and control subjects. Arch Gen Psychiatry 1996; 53: Ghoneim MM, Hinrichs JV, Mewaldt SP, Petersen RC: Ketamine: behavioral effects of subanesthetic doses. J Clin Psychopharmacol 1985; 5: Malhotra AK, Pinals DA, Weingartner H, Sirocco K, Missar CD, Pickar D, Breier A: NMDA receptor function and human cognition: the effects of ketamine in healthy volunteers. Neuropsychopharmacology 1996; 14: Krystal JH, Karper LP, Seibyl JP, Freeman GK, Delaney R, Bremner JD, Heninger GR, Bowers MB Jr, Charney DS: Subanesthetic effects of the noncompetitive NMDA antagonist, ketamine, in humans: psychotomimetic, perceptual, cognitive, and neuroendocrine responses. Arch Gen Psychiatry 1994; 51: Krystal JH, Petrakis IL, Webb E, Cooney NL, Karper LP, Namanworth S, Trevisan LA, Charney DS: Dose-related ethanol-like effects of the NMDA antagonist, ketamine, in recently detoxified alcoholics. Arch Gen Psychiatry 1998; 55: Adler CM, Goldberg TE, Malhotra AK, Pickar D, Breier A: Effects of ketamine on thought disorder, working memory, and semantic memory in healthy volunteers. Biol Psychiatry 1998; 43: Adler CM, Malhotra AK, Elman I, Goldberg T, Egan M, Pickar D, Breier A: Comparison of ketamine-induced thought disorder in healthy volunteers and thought disorder in schizophrenia. Am J Psychiatry 1999; 156: Grant KA, Lovinger DM: Cellular and behavioral neurobiology of alcohol: receptor-mediated neuronal processes. Clin Neurosci 1995; 3: Grant K: Strategies for understanding the pharmacological effects of ethanol with drug discrimination procedures. Pharmacol Biochem Behav 1999; 64: Butelman E, Baron S, Wods J: Ethanol effects in pigeons trained to discriminate MK-801, PCP or CGS Behav Pharmacol 1993; 4: Schechter M, Meehan S, Gordon T, McBurney D: The NMDA receptor antagonist MK-801 produces ethanol-like discrimination in the rat. Alcohol 1993; 10: Michaelis EK, Freed WJ, Galton N, Foye J, Michaelis ML, Phillips I, Kleinman JE: Glutamate receptor changes in brain synaptic membranes from human alcoholics. Neurochem Res 1990; 15: Krystal J, Karper L, D Souza DC, Webb E, Bennett A, Abi-Dargham A, Petrakis IL, Brenner L, Morrissey K, Abi-Saab D, Charney DS: Differentiating NMDA dysregulation in schizophrenia and alcoholism using ketamine. Schizophr Res 1995; 15: Spitzer RL, Williams JBW, Gibbon M, First MB: The Structured Clinical Interview for DSM-III-R (SCID), I: history, rationale, and description. Arch Gen Psychiatry 1992; 49: Overall JE, Gorham DR: The Brief Psychiatric Rating Scale. Psychol Rep 1962; 10: Krystal JH, D Souza DC, Karper LP, Bennett A, Abi-Dargham A, Abi-Saab D, Bowers MB Jr, Jatlow P, Heninger GR, Charney DS: Interactive effects of subanesthetic ketamine and haloperidol. Psychopharmacology (Berl) 1999; 145: Hedlund JL, Vieweg BW: The Brief Psychiatric Rating Scale (BPRS): a comprehensive review. J Operational Psychiatry 1980; 11: Bremner JD, Krystal JH, Putnam FW, Southwick SM, Marmar C, Charney DS, Mazure CM: Measurement of dissociative states with the Clinician-Administered Dissociative States Scale (CADSS). J Trauma Stress 1998; 11: Krystal JH, Webb E, Cooney NL, Kranzler HR, Southwick SW, Heninger GR, Charney DS: Serotonergic and noradrenergic dysregulation in alcoholism: m-chlorophenylpiperazine and yohimbine effects in recently detoxified alcoholics and healthy comparison subjects. Am J Psychiatry 1996; 153: Petrakis IL, Trevisan L, Boutros NN, Limoncelli D, Cooney NL, Krystal JH: Effect of tryptophan depletion on alcohol cue-induced craving in abstinent alcoholic patients. Alcohol Clin Exp Res 2001; 25: Borkowski JG, Benton AL, Spreen O: Word fluency and brain damage. Neuropsychologia 1967; 5: Brandt J: The Hopkins Verbal Learning Test: development of a new memory test with six equivalent forms. Clin Neuropsychol 1991; 5: Schuckit MA: A clinical model of genetic influences in alcohol dependence. J Stud Alcohol 1994; 55: Erblich J, Earleywine M: Children of alcoholics exhibit attenuated cognitive impairment during an ethanol challenge. Alcohol Clin Exp Res 1999; 23: Krystal JH, Petrakis IL, Limoncelli D, Webb E, Gueorgueva R, D Souza DC, Boutros N, Trevisan L, Charney DS: Altered NMDA glutamate receptor antagonist response in recovering ethanoldependent patients. Neuropsychopharmacology 2003; 28: Krystal JH, Petrakis IL, Mason G, Trevisan L, D Souza DC: N- methyl-d-aspartate glutamate receptors and alcoholism: reward, dependence, treatment, and vulnerability. Pharmacol Ther 2003; 99: Moghaddam B, Adams B, Verma A, Daly D: Activation of glutamatergic neurotransmission by ketamine: a novel step in the pathway from NMDA receptor blockade to dopaminergic and cognitive disruptions associated with the prefrontal cortex. J Neurosci 1997; 17: Anand A, Charney DS, Oren DA, Berman RM, Hu XS, Cappiello A, Krystal JH: Attenuation of the neuropsychiatric effects of ketamine with lamotrigine: support for hyperglutamatergic effects of N-methyl-D-aspartate receptor antagonists. Arch Gen Psychiatry 2000; 57: Krupitsky EM, Burakov AM, Romanova TN, Grinenko NI, Grinenko AY, Fletcher J, Petrakis IL, Krystal JH: Attenuation of ketamine effects by nimodipine pretreatment in recovering ethanol dependent men: psychopharmacologic implications of the interaction of NMDA and L-type calcium channel antagonists. Neuropsychopharmacology 2001; 25:
Effects of Ketamine on Healthy Participants and Individuals Suffering from Schizophrenia. John Smith. Physiological Foundations of Psychology 71733
 Effects of Ketamine on Healthy Participants and Individuals Suffering from Schizophrenia John Smith Physiological Foundations of Psychology 71733 Long Beach City College, Spring 2002 Abstract The purpose
Effects of Ketamine on Healthy Participants and Individuals Suffering from Schizophrenia John Smith Physiological Foundations of Psychology 71733 Long Beach City College, Spring 2002 Abstract The purpose
Effects of acute ketamine infusion on visual working memory encoding: a study using ERPs
 Effects of acute ketamine infusion on visual working memory encoding: a study using ERPs Corinna Haenschel Psychology, City University London, UK Partly Funded by: the Welsh Institute of Cognitive Neuroscience
Effects of acute ketamine infusion on visual working memory encoding: a study using ERPs Corinna Haenschel Psychology, City University London, UK Partly Funded by: the Welsh Institute of Cognitive Neuroscience
A preliminary naturalistic study of low-dose ketamine for depression and suicide ideation in the emergency department
 International Journal of Neuropsychopharmacology (2011), 14, 1127 1131. f CINP 2011 doi:10.1017/s1461145711000629 A preliminary naturalistic study of low-dose ketamine for depression and suicide ideation
International Journal of Neuropsychopharmacology (2011), 14, 1127 1131. f CINP 2011 doi:10.1017/s1461145711000629 A preliminary naturalistic study of low-dose ketamine for depression and suicide ideation
ΔTHC level. ΔTHC-COOH level
 Supplemental information 12 2 11 18 1 16 THC (ng/dl) A 9 8 7 6 5 4 3 2 1 5 1 15 2 Minutes 25 ΔTHC level B 14 12 1 8 6 4 2-2 -4 y = 11.92x + 42.11 R² =.1375 y =.196x + 29.63 R² =.2977 y =.1513x +.8471 R²
Supplemental information 12 2 11 18 1 16 THC (ng/dl) A 9 8 7 6 5 4 3 2 1 5 1 15 2 Minutes 25 ΔTHC level B 14 12 1 8 6 4 2-2 -4 y = 11.92x + 42.11 R² =.1375 y =.196x + 29.63 R² =.2977 y =.1513x +.8471 R²
Experimental Medicine and Psychiatry Drug Development. John H. Krystal, M.D. Yale University
 Experimental Medicine and Psychiatry Drug Development John H. Krystal, M.D. Yale University Four problems We don t know the disorders sufficiently The biology is complex and heterogeneous We have animal
Experimental Medicine and Psychiatry Drug Development John H. Krystal, M.D. Yale University Four problems We don t know the disorders sufficiently The biology is complex and heterogeneous We have animal
OUTCOMES OF DICHOTOMIZING A CONTINUOUS VARIABLE IN THE PSYCHIATRIC EARLY READMISSION PREDICTION MODEL. Ng CG
 ORIGINAL PAPER OUTCOMES OF DICHOTOMIZING A CONTINUOUS VARIABLE IN THE PSYCHIATRIC EARLY READMISSION PREDICTION MODEL Ng CG Department of Psychological Medicine, Faculty of Medicine, University Malaya,
ORIGINAL PAPER OUTCOMES OF DICHOTOMIZING A CONTINUOUS VARIABLE IN THE PSYCHIATRIC EARLY READMISSION PREDICTION MODEL Ng CG Department of Psychological Medicine, Faculty of Medicine, University Malaya,
The Neurobiology of Addiction
 The Neurobiology of Addiction Jodi Gilman, Ph.D. Center for Addiction Medicine Massachusetts General Hospital Associate Professor, Department of Psychiatry Harvard Medical School What is Addiction? commonly
The Neurobiology of Addiction Jodi Gilman, Ph.D. Center for Addiction Medicine Massachusetts General Hospital Associate Professor, Department of Psychiatry Harvard Medical School What is Addiction? commonly
Memantine Reverses Social Withdrawal Induced by Ketamine in Rats
 http://dx.doi.org/10.5607/en.2013.22.1.18 Exp Neurobiol. 2013 Mar;22(1):18-22. pissn 1226-2560 eissn 2093-8144 Original Article Memantine Reverses Social Withdrawal Induced by Ketamine in Rats Ezequiel
http://dx.doi.org/10.5607/en.2013.22.1.18 Exp Neurobiol. 2013 Mar;22(1):18-22. pissn 1226-2560 eissn 2093-8144 Original Article Memantine Reverses Social Withdrawal Induced by Ketamine in Rats Ezequiel
Neural model of emotional regulation structures - Circuits involving prefrontal cortex and subcortical limbic structures - MDE associated with
 Topics Brain and signalling changes in depression Ketamine activity in refractory depression Mechanism of Action New Data Dose finding Route of Administration Activity in Other Disorders Neural model of
Topics Brain and signalling changes in depression Ketamine activity in refractory depression Mechanism of Action New Data Dose finding Route of Administration Activity in Other Disorders Neural model of
MOLECULAR BIOLOGY OF DRUG ADDICTION. Sylvane Desrivières, SGDP Centre
 1 MOLECULAR BIOLOGY OF DRUG ADDICTION Sylvane Desrivières, SGDP Centre Reward 2 Humans, as well as other organisms engage in behaviours that are rewarding The pleasurable feelings provide positive reinforcement
1 MOLECULAR BIOLOGY OF DRUG ADDICTION Sylvane Desrivières, SGDP Centre Reward 2 Humans, as well as other organisms engage in behaviours that are rewarding The pleasurable feelings provide positive reinforcement
HHS Public Access Author manuscript Bipolar Disord. Author manuscript; available in PMC 2016 June 01.
 A single infusion of ketamine improves depression scores in patients with anxious bipolar depression Dawn F Ionescu a,b, David A Luckenbaugh c, Mark J Niciu c, Erica M Richards c, and Carlos A Zarate Jr
A single infusion of ketamine improves depression scores in patients with anxious bipolar depression Dawn F Ionescu a,b, David A Luckenbaugh c, Mark J Niciu c, Erica M Richards c, and Carlos A Zarate Jr
Carlos A. Zarate, Jr., M.D
 Performing valid analysis in sex differences and treatment response in depression vs. Multi-modal imaging and psychiatric stress testing: A strategy for translational psychopharmacology in mood disorders
Performing valid analysis in sex differences and treatment response in depression vs. Multi-modal imaging and psychiatric stress testing: A strategy for translational psychopharmacology in mood disorders
Relationship Between Stress and Substance Use Disorders: Neurobiologic Interface
 Relationship Between Stress and Substance Use Disorders: Neurobiologic Interface Kathleen Brady, M.D., Ph.D. Professor of Psychiatry Associate Dean of Clinical and Translational Research Medical University
Relationship Between Stress and Substance Use Disorders: Neurobiologic Interface Kathleen Brady, M.D., Ph.D. Professor of Psychiatry Associate Dean of Clinical and Translational Research Medical University
NIH Public Access Author Manuscript J Affect Disord. Author manuscript; available in PMC 2015 April 01.
 NIH Public Access Author Manuscript Published in final edited form as: J Affect Disord. 2014 April ; 159: 56 61. doi:10.1016/j.jad.2014.02.017. Do the dissociative side effects of ketamine mediate its
NIH Public Access Author Manuscript Published in final edited form as: J Affect Disord. 2014 April ; 159: 56 61. doi:10.1016/j.jad.2014.02.017. Do the dissociative side effects of ketamine mediate its
"The Drugs Don't Work" Eye Movements as Biomarkers in Psychopharmacology
 "The Drugs Don't Work" Eye Movements as Biomarkers in Psychopharmacology ESSEM, 11.9.2014 Ulrich Ettinger Department of Psychology University of Bonn Biomarkers and Model Systems What is a biomarker? What
"The Drugs Don't Work" Eye Movements as Biomarkers in Psychopharmacology ESSEM, 11.9.2014 Ulrich Ettinger Department of Psychology University of Bonn Biomarkers and Model Systems What is a biomarker? What
The role of family conflict as a moderator of alcoholism outcomes among offspring of alcoholics
 Washington University School of Medicine Digital Commons@Becker Posters 2004: Alcoholism and the Latest Genetics and Neuroscience Findings 2004 The role of family conflict as a moderator of alcoholism
Washington University School of Medicine Digital Commons@Becker Posters 2004: Alcoholism and the Latest Genetics and Neuroscience Findings 2004 The role of family conflict as a moderator of alcoholism
The Neurobiology of Psychiatric Disorders
 The Neurobiology of Psychiatric Disorders Vikaas S. Sohal, MD PhD Department of Psychiatry Center for Integrative Neuroscience Sloan Swartz Center for Theoretical Neurobiology Overview 1. Classification
The Neurobiology of Psychiatric Disorders Vikaas S. Sohal, MD PhD Department of Psychiatry Center for Integrative Neuroscience Sloan Swartz Center for Theoretical Neurobiology Overview 1. Classification
Addictive Properties of Caffeine. Roland R. Griffiths, Ph.D. Departments of Psychiatry and Neuroscience Johns Hopkins University School of Medicine
 Addictive Properties of Caffeine Roland R. Griffiths, Ph.D. Departments of Psychiatry and Neuroscience Johns Hopkins University School of Medicine Caffeine Subjective Effects Reinforcing Effects (i.e.
Addictive Properties of Caffeine Roland R. Griffiths, Ph.D. Departments of Psychiatry and Neuroscience Johns Hopkins University School of Medicine Caffeine Subjective Effects Reinforcing Effects (i.e.
NIH Public Access Author Manuscript Psychiatry Clin Neurosci. Author manuscript; available in PMC 2010 November 1.
 NIH Public Access Author Manuscript Published in final edited form as: Psychiatry Clin Neurosci. 2003 October ; 57(5): 542 544. An Open Pilot Study of Gabapentin vs. Trazodone to Treat Insomnia in Alcoholic
NIH Public Access Author Manuscript Published in final edited form as: Psychiatry Clin Neurosci. 2003 October ; 57(5): 542 544. An Open Pilot Study of Gabapentin vs. Trazodone to Treat Insomnia in Alcoholic
8 Distinguishing Features of Primary Psychosis Versus Cannabis-Induced Psychosis
 8 Distinguishing Features of Primary Psychosis Versus Cannabis-Induced Psychosis Ruby S. Grewal, MD and Tony P. George, MD, FRCPC As cannabis consumption rises, there has been significant emerging evidence
8 Distinguishing Features of Primary Psychosis Versus Cannabis-Induced Psychosis Ruby S. Grewal, MD and Tony P. George, MD, FRCPC As cannabis consumption rises, there has been significant emerging evidence
Sensory Gating Measures. Auditory P50 Response Prepulse Inhibition of Startle (PPI) Bruce Turetsky, M.D. IOM Workshop June 22, 2010
 Sensory Gating Measures Auditory P50 Response Prepulse Inhibition of Startle (PPI) Bruce Turetsky, M.D. IOM Workshop June 22, 2010 Heuristically, sensory gating denotes the ability to filter out irrelevant
Sensory Gating Measures Auditory P50 Response Prepulse Inhibition of Startle (PPI) Bruce Turetsky, M.D. IOM Workshop June 22, 2010 Heuristically, sensory gating denotes the ability to filter out irrelevant
Individual Differences in Psychophysiological Reactivity in Adults with Childhood Abuse
 Clinical Psychology and Psychotherapy Clin. Psychol. Psychother. 9, 7 76 () Individual Differences in Psychophysiological Reactivity in Adults with Childhood Abuse Christian G. Schmahl, Bernet M. Elzinga
Clinical Psychology and Psychotherapy Clin. Psychol. Psychother. 9, 7 76 () Individual Differences in Psychophysiological Reactivity in Adults with Childhood Abuse Christian G. Schmahl, Bernet M. Elzinga
Supplementary Online Content
 Supplementary Online Content Subotnik KL, Casaus LR, Ventura J, et al. Long-acting injectable risperidone for relapse prevention and control of breakthrough symptoms after a recent first episode of schizophrenia:
Supplementary Online Content Subotnik KL, Casaus LR, Ventura J, et al. Long-acting injectable risperidone for relapse prevention and control of breakthrough symptoms after a recent first episode of schizophrenia:
Repeatable Battery for the Assessment of Neuropsychological Status as a Screening Test in Schizophrenia, I: Sensitivity, Reliability, and Validity
 Repeatable Battery for the Assessment of Neuropsychological Status as a Screening Test in Schizophrenia, I: Sensitivity, Reliability, and Validity James M. Gold, Ph.D., Caleb Queern, B.A., Virginia N.
Repeatable Battery for the Assessment of Neuropsychological Status as a Screening Test in Schizophrenia, I: Sensitivity, Reliability, and Validity James M. Gold, Ph.D., Caleb Queern, B.A., Virginia N.
Mood Disorders and Addictions: A shared biology?
 Mood Disorders and Addictions: A shared biology? Dr. Paul Stokes Clinical Senior Lecturer, Centre for Affective Disorders, Department of Psychological Medicine Disclosures No relevant disclosures: No paid
Mood Disorders and Addictions: A shared biology? Dr. Paul Stokes Clinical Senior Lecturer, Centre for Affective Disorders, Department of Psychological Medicine Disclosures No relevant disclosures: No paid
Mk-801 Administration in Adolescent Male Rats and Cocaine Conditioned Place
 Mk-801 Administration in Adolescent Male Rats and Cocaine Conditioned Place Preference Stephanie Willis, Jonnique Adjmul, Shabaaz Sandhu, Antoniette M. Maldonado-Devincci, Cheryl Kirsten ABSTRACT The present
Mk-801 Administration in Adolescent Male Rats and Cocaine Conditioned Place Preference Stephanie Willis, Jonnique Adjmul, Shabaaz Sandhu, Antoniette M. Maldonado-Devincci, Cheryl Kirsten ABSTRACT The present
Tracey G. Skale, MD Chief Medical Officer Greater Cincinnati Behavioral Health
 Schizophrenia: What Do We Know? Where Do We Go From Here? Tracey G. Skale, MD Chief Medical Officer Greater Cincinnati Behavioral Health Objectives Participants will be able to: Understand the clinical
Schizophrenia: What Do We Know? Where Do We Go From Here? Tracey G. Skale, MD Chief Medical Officer Greater Cincinnati Behavioral Health Objectives Participants will be able to: Understand the clinical
Persistent Insomnia, Abstinence, and Moderate Drinking in Alcohol-Dependent Individuals
 The American Journal on Addictions, 20: 435 440, 2011 Copyright C American Academy of Addiction Psychiatry ISSN: 1055-0496 print / 1521-0391 online DOI: 10.1111/j.1521-0391.2011.00152.x Persistent Insomnia,
The American Journal on Addictions, 20: 435 440, 2011 Copyright C American Academy of Addiction Psychiatry ISSN: 1055-0496 print / 1521-0391 online DOI: 10.1111/j.1521-0391.2011.00152.x Persistent Insomnia,
Word priming in schizophrenia: Associational and semantic influences
 Word priming in schizophrenia: Associational and semantic influences The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation
Word priming in schizophrenia: Associational and semantic influences The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation
Rating Mental Impairment with AMA Guides 6 th edition:
 Rating Mental Impairment with AMA Guides 6 th edition: Practical Considerations and Strategies CSME/CAPDA C-CAT Course, March 24, 2018 William H. Gnam, PhD, MD, FRCPC (william.gnam@gmail.com) Consultant
Rating Mental Impairment with AMA Guides 6 th edition: Practical Considerations and Strategies CSME/CAPDA C-CAT Course, March 24, 2018 William H. Gnam, PhD, MD, FRCPC (william.gnam@gmail.com) Consultant
substance use and mental disorders: one, the other, or both?
 substance use and mental disorders: one, the other, or both? Stephen Strobbe, PhD, RN, PMHCNS-BC, CARN-AP Dawn Farm Education Series St. Joe s Education Center, Ypsilanti, MI Tuesday, January 27, 2015
substance use and mental disorders: one, the other, or both? Stephen Strobbe, PhD, RN, PMHCNS-BC, CARN-AP Dawn Farm Education Series St. Joe s Education Center, Ypsilanti, MI Tuesday, January 27, 2015
RATING MENTAL WHOLE PERSON IMPAIRMENT UNDER THE NEW SABS: New Methods, New Challenges. CSME/CAPDA Conference, April 1, 2017
 RATING MENTAL WHOLE PERSON IMPAIRMENT UNDER THE NEW SABS: New Methods, New Challenges CSME/CAPDA Conference, April 1, 2017 William H. Gnam, PhD, MD, FRCPC (william.gnam@gmail.com) Consultant Psychiatrist
RATING MENTAL WHOLE PERSON IMPAIRMENT UNDER THE NEW SABS: New Methods, New Challenges CSME/CAPDA Conference, April 1, 2017 William H. Gnam, PhD, MD, FRCPC (william.gnam@gmail.com) Consultant Psychiatrist
Neurobiology of Addiction JeanAnne Johnson Talbert, DHA, APRN BC, FNP, CARN AP
 Neurobiology of Addiction JeanAnne Johnson Talbert, DHA, APRN BC, FNP, CARN AP Disclosures This speaker has no conflicts of interest to disclose Objectives Define drug abuse and addiction Identify the
Neurobiology of Addiction JeanAnne Johnson Talbert, DHA, APRN BC, FNP, CARN AP Disclosures This speaker has no conflicts of interest to disclose Objectives Define drug abuse and addiction Identify the
Schizophrenia FAHAD ALOSAIMI
 Schizophrenia FAHAD ALOSAIMI MBBS, SSC - PSYCH C ONSULTATION LIAISON PSYCHIATRIST K ING SAUD UNIVERSITY Schizophrenia - It is not a single disease but a group of disorders with heterogeneous etiologies.
Schizophrenia FAHAD ALOSAIMI MBBS, SSC - PSYCH C ONSULTATION LIAISON PSYCHIATRIST K ING SAUD UNIVERSITY Schizophrenia - It is not a single disease but a group of disorders with heterogeneous etiologies.
Clinical Implications for Four Drugs of the DSM-IV Distinction Between Substance Dependence With and Without a Physiological Component
 Clinical Implications for Four Drugs of the DSM-IV Distinction Between Substance Dependence With and Without a Physiological Component Marc A. Schuckit, M.D., Jean-Bernard Daeppen, M.D., George P. Danko,
Clinical Implications for Four Drugs of the DSM-IV Distinction Between Substance Dependence With and Without a Physiological Component Marc A. Schuckit, M.D., Jean-Bernard Daeppen, M.D., George P. Danko,
Cannabis for Medical Use: Body and Mind
 Cannabis for Medical Use: Body and Mind Shaul Schreiber, MD Division of Psychiatry, Tel Aviv Sourasky Medical Center; Tel Aviv University Sackler Faculty of Medicine; Sagol School of Neuroscience, Israel
Cannabis for Medical Use: Body and Mind Shaul Schreiber, MD Division of Psychiatry, Tel Aviv Sourasky Medical Center; Tel Aviv University Sackler Faculty of Medicine; Sagol School of Neuroscience, Israel
Do we still believe in the dopamine hypothesis? New data bring new evidence
 International Journal of Neuropsychopharmacology (24), 7 (Supplement 1), S1 S5. Copyright f 24 CINP DOI : 1.117/S146114574411 Do we still believe in the dopamine hypothesis? New data bring new evidence
International Journal of Neuropsychopharmacology (24), 7 (Supplement 1), S1 S5. Copyright f 24 CINP DOI : 1.117/S146114574411 Do we still believe in the dopamine hypothesis? New data bring new evidence
ESSENTIAL PSYCHOPHARMACOLOGY, Neurobiology of Schizophrenia Carl Salzman MD Montreal
 ESSENTIAL PSYCHOPHARMACOLOGY, 2011 Neurobiology of Schizophrenia Carl Salzman MD Montreal EVOLVING CONCEPTS OF SCHIZOPHRENIA Psychotic illness with delusions, hallucinations, thought disorder and deterioration;
ESSENTIAL PSYCHOPHARMACOLOGY, 2011 Neurobiology of Schizophrenia Carl Salzman MD Montreal EVOLVING CONCEPTS OF SCHIZOPHRENIA Psychotic illness with delusions, hallucinations, thought disorder and deterioration;
Interactive effects of subanesthetic ketamine and subhypnotic lorazepam in humans
 Psychopharmacology (1998) 135 : 213 229 Springer-Verlag 1998 ORIGINAL INVESTIGATION John H. Krystal Laurence P. Karper Alexandre Bennett D. Cyril D Souza Anissa Abi-Dargham Kristen Morrissey Danielle Abi-Saab
Psychopharmacology (1998) 135 : 213 229 Springer-Verlag 1998 ORIGINAL INVESTIGATION John H. Krystal Laurence P. Karper Alexandre Bennett D. Cyril D Souza Anissa Abi-Dargham Kristen Morrissey Danielle Abi-Saab
Prospective assessment of treatment use by patients with personality disorders
 Wesleyan University From the SelectedWorks of Charles A. Sanislow, Ph.D. February, 2006 Prospective assessment of treatment use by Donna S. Bender Andrew E. Skodol Maria E. Pagano Ingrid R. Dyck Carlos
Wesleyan University From the SelectedWorks of Charles A. Sanislow, Ph.D. February, 2006 Prospective assessment of treatment use by Donna S. Bender Andrew E. Skodol Maria E. Pagano Ingrid R. Dyck Carlos
Hallucinogens as Treatment? Preliminary Data with Ketamine. Elias Dakwar, MD Columbia University College of Physicians and Surgeons 19 October, 2017
 Hallucinogens as Treatment? Preliminary Data with Ketamine Elias Dakwar, MD Columbia University College of Physicians and Surgeons 19 October, 2017 Disclosures Elias Dakwar has received funding from NIDA
Hallucinogens as Treatment? Preliminary Data with Ketamine Elias Dakwar, MD Columbia University College of Physicians and Surgeons 19 October, 2017 Disclosures Elias Dakwar has received funding from NIDA
Acute Effects of Ketamine on Memory Systems and Psychotic Symptoms in Healthy Volunteers
 (2004) 29, 208 218 & 2004 Nature Publishing Group All rights reserved 0893-133X/04 $25.00 www.neuropsychopharmacology.org Acute Effects of Ketamine on Memory Systems and Psychotic Symptoms in Healthy Volunteers
(2004) 29, 208 218 & 2004 Nature Publishing Group All rights reserved 0893-133X/04 $25.00 www.neuropsychopharmacology.org Acute Effects of Ketamine on Memory Systems and Psychotic Symptoms in Healthy Volunteers
Dichotic listening in schizotypal personality disorder: Evidence for gender and laterality effects
 Dichotic listening in schizotypal personality disorder: Evidence for gender and laterality effects The Harvard community has made this article openly available. Please share how this access benefits you.
Dichotic listening in schizotypal personality disorder: Evidence for gender and laterality effects The Harvard community has made this article openly available. Please share how this access benefits you.
Effects of sodium nitroprusside in the prevention of schizophrenia-like symptoms induced by ketamine A translational double-blind study
 Original article Effects of sodium nitroprusside in the prevention of schizophrenia-like symptoms induced by ketamine A translational double-blind study Tatiana M. N. Rezende 1, João Paulo Maia-de-Oliveira,3,
Original article Effects of sodium nitroprusside in the prevention of schizophrenia-like symptoms induced by ketamine A translational double-blind study Tatiana M. N. Rezende 1, João Paulo Maia-de-Oliveira,3,
Amino Acid Neurotransmitters. Paul Glue
 Amino Acid Neurotransmitters Paul Glue Objectives Review: Relative abundance of AAs vs monoamines Pharmacology of glutamate, GABA Postulated role of glutamate, GABA dysfunction in neuropsych disorders
Amino Acid Neurotransmitters Paul Glue Objectives Review: Relative abundance of AAs vs monoamines Pharmacology of glutamate, GABA Postulated role of glutamate, GABA dysfunction in neuropsych disorders
Schizophrenia. Nikita Verma 2017 Page 1
 Schizophrenia It is a severe psychiatric disorder with symptoms of emotional instability, detachment from reality and withdrawal into self. It is an umbrella term used to outline a range of different psychiatric
Schizophrenia It is a severe psychiatric disorder with symptoms of emotional instability, detachment from reality and withdrawal into self. It is an umbrella term used to outline a range of different psychiatric
Personality disorders as predictors of treatment outcome in a sample of alcohol dependent veterans with comorbid axis I disorders
 Washington University School of Medicine Digital Commons@Becker Posters 2005: Alcoholism and Comorbidity 2005 Personality disorders as predictors of treatment outcome in a sample of alcohol dependent veterans
Washington University School of Medicine Digital Commons@Becker Posters 2005: Alcoholism and Comorbidity 2005 Personality disorders as predictors of treatment outcome in a sample of alcohol dependent veterans
Beacon Health Strategies Comorbid Mental Health and Substance Use Disorder Screening Program Description
 Purpose The purpose of Beacon s Comorbid Mental Health Substance Use Disorder Screening Program is to establish a formal process of assessing and ensuring early detection and treatment cooccurring mental
Purpose The purpose of Beacon s Comorbid Mental Health Substance Use Disorder Screening Program is to establish a formal process of assessing and ensuring early detection and treatment cooccurring mental
EVALUATION OF WORRY IN PATIENTS WITH SCHIZOPHRENIA AND PERSECUTORY DELUSION COMPARED WITH GENERAL POPULATION
 Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 7 (56) No. 1-2014 EVALUATION OF WORRY IN PATIENTS WITH SCHIZOPHRENIA AND PERSECUTORY DELUSION COMPARED WITH GENERAL POPULATION
Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 7 (56) No. 1-2014 EVALUATION OF WORRY IN PATIENTS WITH SCHIZOPHRENIA AND PERSECUTORY DELUSION COMPARED WITH GENERAL POPULATION
NEUROBIOLOGY ALCOHOLISM
 NEUROBIOLOGY ALCOHOLISM THERE HAS BEEN A MAJOR THEORETICAL SHIFT IN MEDICATION DEVELOPMENT IN ALCOHOLISM Driven by animal models of intermittent ethanol administration followed by termination, then access
NEUROBIOLOGY ALCOHOLISM THERE HAS BEEN A MAJOR THEORETICAL SHIFT IN MEDICATION DEVELOPMENT IN ALCOHOLISM Driven by animal models of intermittent ethanol administration followed by termination, then access
CHAPTER 5 NEUROPSYCHOLOGICAL PROFILE OF ALZHEIMER S DISEASE
 CHAPTER 5 NEUROPSYCHOLOGICAL PROFILE OF ALZHEIMER S DISEASE 5.1 GENERAL BACKGROUND Neuropsychological assessment plays a crucial role in the assessment of cognitive decline in older age. In India, there
CHAPTER 5 NEUROPSYCHOLOGICAL PROFILE OF ALZHEIMER S DISEASE 5.1 GENERAL BACKGROUND Neuropsychological assessment plays a crucial role in the assessment of cognitive decline in older age. In India, there
Concurrent Disorders
 Concurrent Disorders Dr. Christy Sutherland MD CCFP dipabam Medical Director, PHS Community Services Methadone/Buprenorphine 101 Workshop April 1, 2017 Overview Introduction Epidemiology Treatment Principles
Concurrent Disorders Dr. Christy Sutherland MD CCFP dipabam Medical Director, PHS Community Services Methadone/Buprenorphine 101 Workshop April 1, 2017 Overview Introduction Epidemiology Treatment Principles
Biomarkers in Schizophrenia
 Biomarkers in Schizophrenia David A. Lewis, MD Translational Neuroscience Program Department of Psychiatry NIMH Conte Center for the Neuroscience of Mental Disorders University of Pittsburgh Disease Process
Biomarkers in Schizophrenia David A. Lewis, MD Translational Neuroscience Program Department of Psychiatry NIMH Conte Center for the Neuroscience of Mental Disorders University of Pittsburgh Disease Process
One important measure of the clinical relevance of a
 Article Five-Year Clinical Course Associated With DSM-IV Alcohol Abuse or Dependence in a Large Group of Men and Women Marc A. Schuckit, M.D. Tom L. Smith, Ph.D. George P. Danko, Ph.D. Kathleen K. Bucholz,
Article Five-Year Clinical Course Associated With DSM-IV Alcohol Abuse or Dependence in a Large Group of Men and Women Marc A. Schuckit, M.D. Tom L. Smith, Ph.D. George P. Danko, Ph.D. Kathleen K. Bucholz,
C81ADD Psychology of Addiction. Alcohol. Ethyl alcohol (ethanol) School of Psychology. Tobias Bast.
 C81ADD Psychology of Addiction Alcohol Ethyl alcohol (ethanol) Tobias Bast School of Psychology tobias.bast@nottingham.ac.uk 1 Selected aspects of the psychopharmacology of alcohol (ethanol) Primary neuropharmacological
C81ADD Psychology of Addiction Alcohol Ethyl alcohol (ethanol) Tobias Bast School of Psychology tobias.bast@nottingham.ac.uk 1 Selected aspects of the psychopharmacology of alcohol (ethanol) Primary neuropharmacological
#CHAIR2016. September 15 17, 2016 The Biltmore Hotel Miami, FL. Sponsored by
 #CHAIR2016 September 15 17, 2016 The Biltmore Hotel Miami, FL Sponsored by Bending the Illness Curve: A New Treatment Model for Early Stage Psychoses Jeffrey A. Lieberman, M.D. Columbia University College
#CHAIR2016 September 15 17, 2016 The Biltmore Hotel Miami, FL Sponsored by Bending the Illness Curve: A New Treatment Model for Early Stage Psychoses Jeffrey A. Lieberman, M.D. Columbia University College
BroadcastMed Bipolar, Borderline, Both? Diagnostic/Formulation Issues in Mood and Personality Disorders
 BroadcastMed Bipolar, Borderline, Both? Diagnostic/Formulation Issues in Mood and Personality Disorders BRIAN PALMER: Hi. My name is Brian Palmer. I'm a psychiatrist here at Mayo Clinic. Today, we'd like
BroadcastMed Bipolar, Borderline, Both? Diagnostic/Formulation Issues in Mood and Personality Disorders BRIAN PALMER: Hi. My name is Brian Palmer. I'm a psychiatrist here at Mayo Clinic. Today, we'd like
Schizophrenia: New Concepts for Therapeutic Discovery
 Schizophrenia: New Concepts for Therapeutic Discovery William T. Carpenter, M.D. Professor of Psychiatry and Pharmacology University of Maryland School of Medicine Department of Psychiatry Maryland Psychiatric
Schizophrenia: New Concepts for Therapeutic Discovery William T. Carpenter, M.D. Professor of Psychiatry and Pharmacology University of Maryland School of Medicine Department of Psychiatry Maryland Psychiatric
Clinical Policy Title: Ketamine for treatment-resistant depression
 Clinical Policy Title: Ketamine for treatment-resistant depression Clinical Policy Number: 00.02.13 Effective Date: January 1, 2016 Initial Review Date: August 19, 2015 Most Recent Review Date: January
Clinical Policy Title: Ketamine for treatment-resistant depression Clinical Policy Number: 00.02.13 Effective Date: January 1, 2016 Initial Review Date: August 19, 2015 Most Recent Review Date: January
Nature, prevalence and clinical significance. Barcelona, Spain
 Nature, prevalence and clinical significance Jaime Kulisevsky Barcelona, Spain 1 Non motor (neuropsychiatric) symptoms are an integral part of Parkinson s s disease (PD) Affective disorders And are associated
Nature, prevalence and clinical significance Jaime Kulisevsky Barcelona, Spain 1 Non motor (neuropsychiatric) symptoms are an integral part of Parkinson s s disease (PD) Affective disorders And are associated
Diagnostic orphans for alcohol use disorders in a treatment-seeking psychiatric sample
 Available online at www.sciencedirect.com Drug and Alcohol Dependence 96 (2008) 187 191 Short communication Diagnostic orphans for alcohol use disorders in a treatment-seeking psychiatric sample Lara A.
Available online at www.sciencedirect.com Drug and Alcohol Dependence 96 (2008) 187 191 Short communication Diagnostic orphans for alcohol use disorders in a treatment-seeking psychiatric sample Lara A.
S P O U S A L R ES E M B L A N C E I N PSYCHOPATHOLOGY: A C O M PA R I SO N O F PA R E N T S O F C H I LD R E N W I T H A N D WITHOUT PSYCHOPATHOLOGY
 Aggregation of psychopathology in a clinical sample of children and their parents S P O U S A L R ES E M B L A N C E I N PSYCHOPATHOLOGY: A C O M PA R I SO N O F PA R E N T S O F C H I LD R E N W I T H
Aggregation of psychopathology in a clinical sample of children and their parents S P O U S A L R ES E M B L A N C E I N PSYCHOPATHOLOGY: A C O M PA R I SO N O F PA R E N T S O F C H I LD R E N W I T H
9/16/2016. I would feel comfortable dispensing/prescribing varenicline to a patient with a mental health disorder. Learning Objectives
 The Smoking Gun: for Smoking Cessation in Patients with Mental Health Disorders BRENDON HOGAN, PHARMD PGY2 PSYCHIATRIC PHARMACY RESIDENT CTVHCS, TEMPLE, TX 09/23/2016 I would feel comfortable dispensing/prescribing
The Smoking Gun: for Smoking Cessation in Patients with Mental Health Disorders BRENDON HOGAN, PHARMD PGY2 PSYCHIATRIC PHARMACY RESIDENT CTVHCS, TEMPLE, TX 09/23/2016 I would feel comfortable dispensing/prescribing
Tobacco Dependence Treatment From Neurobiology through Public Policy
 Tobacco Dependence Treatment From Neurobiology through Public Policy Mary Ellen Wewers, PhD, MPH, RN Professor Emerita The Ohio State University College of Public Health Disclosures Funding from the National
Tobacco Dependence Treatment From Neurobiology through Public Policy Mary Ellen Wewers, PhD, MPH, RN Professor Emerita The Ohio State University College of Public Health Disclosures Funding from the National
Relationship of ketamine s antidepressant and psychotomimetic effects in unipolar depression
 Activitas Nervosa Superior Rediviva Volume 55 No. 1 2 2013 ORIGINAL ARTICLE Relationship of ketamine s antidepressant and psychotomimetic effects in unipolar depression Peter Sos, Monika Klirova, Tomas
Activitas Nervosa Superior Rediviva Volume 55 No. 1 2 2013 ORIGINAL ARTICLE Relationship of ketamine s antidepressant and psychotomimetic effects in unipolar depression Peter Sos, Monika Klirova, Tomas
Comorbidity With Substance Abuse P a g e 1
 Comorbidity With Substance Abuse P a g e 1 Comorbidity With Substance Abuse Introduction This interesting session provided an overview of recent findings in the diagnosis and treatment of several psychiatric
Comorbidity With Substance Abuse P a g e 1 Comorbidity With Substance Abuse Introduction This interesting session provided an overview of recent findings in the diagnosis and treatment of several psychiatric
Comorbidity of Depression and Other Diseases
 Comorbidity of Depression and Other Diseases JMAJ 44(5): 225 229, 2001 Masaru MIMURA Associate Professor, Department of Psychiatry, Showa University, School of Medicine Abstract: This paper outlines the
Comorbidity of Depression and Other Diseases JMAJ 44(5): 225 229, 2001 Masaru MIMURA Associate Professor, Department of Psychiatry, Showa University, School of Medicine Abstract: This paper outlines the
ADHD & Addictions -What We Know
 ADHD & Addictions -What We Know Dr. David Teplin, Psy.D., C.Psych. 4th CADDAC Annual Conference, Toronto October 14, 2012 1 Introduction Adult ADHD commonly co-exists with several other disorders, including
ADHD & Addictions -What We Know Dr. David Teplin, Psy.D., C.Psych. 4th CADDAC Annual Conference, Toronto October 14, 2012 1 Introduction Adult ADHD commonly co-exists with several other disorders, including
Study Guide Unit 3 Psych 2022, Fall 2003
 Psychological Disorders: General Study Guide Unit 3 Psych 2022, Fall 2003 1. What are psychological disorders? 2. What was the main treatment for some psychological disorders prior to the 1950 s? 3. What
Psychological Disorders: General Study Guide Unit 3 Psych 2022, Fall 2003 1. What are psychological disorders? 2. What was the main treatment for some psychological disorders prior to the 1950 s? 3. What
Understanding and Treating Behavioral Addictions
 Understanding and Treating Behavioral Addictions Jon Grant, MD, JD, MPH Professor of Psychiatry and Behavioral Neuroscience University of Chicago Chicago, Illinois Disclosure The faculty have been informed
Understanding and Treating Behavioral Addictions Jon Grant, MD, JD, MPH Professor of Psychiatry and Behavioral Neuroscience University of Chicago Chicago, Illinois Disclosure The faculty have been informed
Effects of "Mere Exposure" on Learning and Affect
 Journal ot Personality and Social Psychology 1975, Vol. 31, No. 1, 7-12 Effects of "Mere Exposure" on Learning and Affect David J. Stang Queens College of the City University of New York The mediating
Journal ot Personality and Social Psychology 1975, Vol. 31, No. 1, 7-12 Effects of "Mere Exposure" on Learning and Affect David J. Stang Queens College of the City University of New York The mediating
Shift 1, 8 July 2018, 09:30-13:00
 Shift 1, 8 July 2018, 09:30-13:00 CNS patterning A001-A014 Stem cells: basic biology and postnatal neurogenesis - part I Development of neural systems: Molecular and genetic characterisationa Epigenetic
Shift 1, 8 July 2018, 09:30-13:00 CNS patterning A001-A014 Stem cells: basic biology and postnatal neurogenesis - part I Development of neural systems: Molecular and genetic characterisationa Epigenetic
Serotonin System May Have Potential as a Target for Cocaine Medications
 NIDA - Publications - NIDA Notes - Vol. 21, No. 3 - Research Findings of 4 http://www.drugabuse.gov/nida_notes/nnvol21n3/serotonin.html 9/26/2011 3:45 PM NIDA NEWS NIDA Home > Publications > NIDA Notes
NIDA - Publications - NIDA Notes - Vol. 21, No. 3 - Research Findings of 4 http://www.drugabuse.gov/nida_notes/nnvol21n3/serotonin.html 9/26/2011 3:45 PM NIDA NEWS NIDA Home > Publications > NIDA Notes
Brief Psychiatric Rating Scale-Anchored (BPRS-A)
 Brief Psychiatric Rating Scale-Anchored (BPRS-A) Questionnaire Supplement to the Study Data Tabulation Model Implementation Guide for Human Clinical Trials Prepared by CDISC Questionnaire Sub-team Notes
Brief Psychiatric Rating Scale-Anchored (BPRS-A) Questionnaire Supplement to the Study Data Tabulation Model Implementation Guide for Human Clinical Trials Prepared by CDISC Questionnaire Sub-team Notes
Neurobiology of Addiction and Recovery. R. Dewayne Book, M.D. Medical Director Fellowship Hall Greensboro, North Carolina
 Neurobiology of Addiction and Recovery R. Dewayne Book, M.D. Medical Director Fellowship Hall Greensboro, North Carolina 1 Addiction Drug Addiction results from adaptations in specific brain neurons caused
Neurobiology of Addiction and Recovery R. Dewayne Book, M.D. Medical Director Fellowship Hall Greensboro, North Carolina 1 Addiction Drug Addiction results from adaptations in specific brain neurons caused
Treatment of AD with Stabilized Oral NADH: Preliminary Findings
 MS # 200 000 128 Treatment of AD with Stabilized Oral NADH: Preliminary Findings G.G. Kay, PhD, V. N. Starbuck, PhD and S. L. Cohan, MD, PhD Department of Neurology, Georgetown University School of Medicine
MS # 200 000 128 Treatment of AD with Stabilized Oral NADH: Preliminary Findings G.G. Kay, PhD, V. N. Starbuck, PhD and S. L. Cohan, MD, PhD Department of Neurology, Georgetown University School of Medicine
Trends, Tactics and Toxicity: Marijuana Movement on Missouri College Campuses. Janice Putnam PhD, RN Amy Kiger MS, ABD Kelly Skinner DNP, FNP-C
 Trends, Tactics and Toxicity: Marijuana Movement on Missouri College Campuses Janice Putnam PhD, RN Amy Kiger MS, ABD Kelly Skinner DNP, FNP-C 1 Marijuana/Cannabis Marijuana use is growing in popularity
Trends, Tactics and Toxicity: Marijuana Movement on Missouri College Campuses Janice Putnam PhD, RN Amy Kiger MS, ABD Kelly Skinner DNP, FNP-C 1 Marijuana/Cannabis Marijuana use is growing in popularity
PSY/NEU338: Animal learning and decision making: Psychological, computational and neural perspectives
 Too much dopamine can be bad for you: 1I. Latent inhibition and schizophrenia PSY/NEU338: Animal learning and decision making: Psychological, computational and neural perspectives thanks to Ina Weiner
Too much dopamine can be bad for you: 1I. Latent inhibition and schizophrenia PSY/NEU338: Animal learning and decision making: Psychological, computational and neural perspectives thanks to Ina Weiner
Main Questions. Why study addiction? Substance Use Disorders, Part 1 Alecia Schweinsburg, MA Abnromal Psychology, Fall Substance Use Disorders
 Substance Use Disorders Main Questions Why study addiction? What is addiction? Why do people become addicted? What do alcohol and drugs do? How do we treat substance use disorders? Why study addiction?
Substance Use Disorders Main Questions Why study addiction? What is addiction? Why do people become addicted? What do alcohol and drugs do? How do we treat substance use disorders? Why study addiction?
Tobacco Addiction: Neurobiology and Its Clinical Implications
 Tobacco Addiction: Neurobiology and Its Clinical Implications Robert M. Anthenelli, M.D. Professor and Executive Vice Chair Director, Pacific Treatment and Research Center Department of Psychiatry University
Tobacco Addiction: Neurobiology and Its Clinical Implications Robert M. Anthenelli, M.D. Professor and Executive Vice Chair Director, Pacific Treatment and Research Center Department of Psychiatry University
Restless Legs Syndrome (RLS) is a common yet
 Restless Legs Syndrome is Associated with DSM-IV Major Depressive Disorder and Panic Disorder in the Community Hochang B. Lee, M.D. Wayne A. Hening, M.D, Ph.D. Richard P. Allen, Ph.D. Amanda E. Kalaydjian,
Restless Legs Syndrome is Associated with DSM-IV Major Depressive Disorder and Panic Disorder in the Community Hochang B. Lee, M.D. Wayne A. Hening, M.D, Ph.D. Richard P. Allen, Ph.D. Amanda E. Kalaydjian,
Understanding Addiction: Why Can t Those Affected Just Say No?
 Understanding Addiction: Why Can t Those Affected Just Say No? 1 The Stigma of Addiction There continues to be a stigma surrounding addiction even among health care workers. Consider the negative opinions
Understanding Addiction: Why Can t Those Affected Just Say No? 1 The Stigma of Addiction There continues to be a stigma surrounding addiction even among health care workers. Consider the negative opinions
Defense mechanisms and symptom severity in panic disorder
 ACTA BIOMED 2010; 81: 30-34 Mattioli 1885 O R I G I N A L A R T I C L E Defense mechanisms and symptom severity in panic disorder Marco Fario, Sonja Aprile, Chiara Cabrino, Carlo Maggini, Carlo Marchesi
ACTA BIOMED 2010; 81: 30-34 Mattioli 1885 O R I G I N A L A R T I C L E Defense mechanisms and symptom severity in panic disorder Marco Fario, Sonja Aprile, Chiara Cabrino, Carlo Maggini, Carlo Marchesi
Schizophrenia and Related Psychotic Disorders
 and Related Psychotic Disorders Anand K. Pandurangi, MD Professor & Chair, Div. of Inpatient Psychiatry Director, Program VCU Medical Center 1 Kraeplin 1896 Dementia Praecox. Single, Homogenous Disorder
and Related Psychotic Disorders Anand K. Pandurangi, MD Professor & Chair, Div. of Inpatient Psychiatry Director, Program VCU Medical Center 1 Kraeplin 1896 Dementia Praecox. Single, Homogenous Disorder
Management of Tobacco Dependence. Dr. Lokesh Kumar Singh Associate Professor Department of Psychiatry AIIMS, Raipur
 Management of Tobacco Dependence Dr. Lokesh Kumar Singh Associate Professor Department of Psychiatry AIIMS, Raipur Difficult to identify any other condition that presents such a mix of lethality, prevalence,
Management of Tobacco Dependence Dr. Lokesh Kumar Singh Associate Professor Department of Psychiatry AIIMS, Raipur Difficult to identify any other condition that presents such a mix of lethality, prevalence,
Genetic and Environmental Contributions to Obesity and Binge Eating
 Genetic and Environmental Contributions to Obesity and Binge Eating Cynthia M. Bulik,* Patrick F. Sullivan, and Kenneth S. Kendler Virginia Institute for Psychiatric and Behavioral Genetics of Virginia
Genetic and Environmental Contributions to Obesity and Binge Eating Cynthia M. Bulik,* Patrick F. Sullivan, and Kenneth S. Kendler Virginia Institute for Psychiatric and Behavioral Genetics of Virginia
Does the Use of Oral Amphetamines Reduce Cocaine Use in Cocaine-Dependent Individuals?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2016 Does the Use of Oral Amphetamines Reduce
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2016 Does the Use of Oral Amphetamines Reduce
Psychosis and Agitation in Dementia
 Psychosis and Agitation in Dementia Dilip V. Jeste, MD Estelle & Edgar Levi Chair in Aging, Director, Stein Institute for Research on Aging, Distinguished Professor of Psychiatry & Neurosciences, University
Psychosis and Agitation in Dementia Dilip V. Jeste, MD Estelle & Edgar Levi Chair in Aging, Director, Stein Institute for Research on Aging, Distinguished Professor of Psychiatry & Neurosciences, University
Brief Psychiatric Rating Scale-Anchored (BPRS-A)
 Brief Psychiatric Rating Scale-Anchored (BPRS-A) Questionnaire Supplement to the Study Data Tabulation Model Implementation Guide for Human Clinical Trials Prepared by CDISC Questionnaire Sub-team Notes
Brief Psychiatric Rating Scale-Anchored (BPRS-A) Questionnaire Supplement to the Study Data Tabulation Model Implementation Guide for Human Clinical Trials Prepared by CDISC Questionnaire Sub-team Notes
The Neurobiology of Schizophrenia
 The Neurobiology of Schizophrenia Dost Ongur, MD PhD Neither I nor my spouse/partner has a relevant financial relationship with a commercial interest to disclose. What is Psychosis? Response Language Affect
The Neurobiology of Schizophrenia Dost Ongur, MD PhD Neither I nor my spouse/partner has a relevant financial relationship with a commercial interest to disclose. What is Psychosis? Response Language Affect
ALCOHOL SENSITIVITY AND ALCOHOL CRAVING
 RAY, MESKEW-STACER, AND HUTCHISON 379 The Relationship Between Prospective Self-Rating of Alcohol Sensitivity and Craving and Experimental Results From Two Alcohol Challenge Studies* LARA A. RAY, M.A.,
RAY, MESKEW-STACER, AND HUTCHISON 379 The Relationship Between Prospective Self-Rating of Alcohol Sensitivity and Craving and Experimental Results From Two Alcohol Challenge Studies* LARA A. RAY, M.A.,
Panic disorder and anxiety symptoms are hypothesized
 Article Anxiety in Major Depression: Relationship to Suicide Attempts Giovanni P.A. Placidi, M.D. Maria A. Oquendo, M.D. Kevin M. Malone, M.D. Beth Brodsky, Ph.D. Steven P. Ellis, Ph.D. J. John Mann, M.D.
Article Anxiety in Major Depression: Relationship to Suicide Attempts Giovanni P.A. Placidi, M.D. Maria A. Oquendo, M.D. Kevin M. Malone, M.D. Beth Brodsky, Ph.D. Steven P. Ellis, Ph.D. J. John Mann, M.D.
Dr. Meldon Kahan. Women s College Hospital. with PIA LAW
 with PIA LAW and Toronto ABI Network Dr. Meldon Kahan Women s College Hospital Dr. Meldon Kahan is an Associate Professor in the Department of Family Medicine at University of Toronto, and Medical Director
with PIA LAW and Toronto ABI Network Dr. Meldon Kahan Women s College Hospital Dr. Meldon Kahan is an Associate Professor in the Department of Family Medicine at University of Toronto, and Medical Director
The N-methyl-d-aspartate (NMDA) of glutamate
 Small-Dose Ketamine Improves the Postoperative State of Depressed Patients Akira Kudoh, MD*, Yoko Takahira, Hiroshi Katagai, MD, and Tomoko Takazawa, MD *Department of Anesthesiology, Hakodate Watanabe
Small-Dose Ketamine Improves the Postoperative State of Depressed Patients Akira Kudoh, MD*, Yoko Takahira, Hiroshi Katagai, MD, and Tomoko Takazawa, MD *Department of Anesthesiology, Hakodate Watanabe
In the general population, men are more physically aggressive
 Article Gender Differences in Violent Behaviors: Relationship to Clinical Symptoms and Psychosocial Factors Menahem Krakowski, M.D., Ph.D. Pal Czobor, Ph.D. Objective: Men are more violent than women in
Article Gender Differences in Violent Behaviors: Relationship to Clinical Symptoms and Psychosocial Factors Menahem Krakowski, M.D., Ph.D. Pal Czobor, Ph.D. Objective: Men are more violent than women in
Psychopathology in patients with schizophrenia attending a psychiatry outpatient clinic at a tertiary care hospital
 Original paper Psychopathology in patients with schizophrenia attending a psychiatry outpatient clinic at a tertiary care hospital Hiranya Wijesundara, Madhubhashinee Dayabandara, Arjuna Ellepola and Raveen
Original paper Psychopathology in patients with schizophrenia attending a psychiatry outpatient clinic at a tertiary care hospital Hiranya Wijesundara, Madhubhashinee Dayabandara, Arjuna Ellepola and Raveen
Psychotropic Drugs in the Pipeline. Norman Sussman, M.D. Professor of Psychiatry New York University School of Medicine
 Psychotropic Drugs in the Pipeline Norman Sussman, M.D. Professor of Psychiatry New York University School of Medicine Norman Sussman, MD No Conflict of Interest to Declare Antidepressant Pipeline We need
Psychotropic Drugs in the Pipeline Norman Sussman, M.D. Professor of Psychiatry New York University School of Medicine Norman Sussman, MD No Conflict of Interest to Declare Antidepressant Pipeline We need
(Seng, et al., 2013). Studies have reported prevalence rates ranging from 1 to 30 percent of
 POSTPARTUM POSTTRAUMATIC STRESS DISORDER Introduction Recent research suggests that childbirth may be a significant cause of PTSD in women (Seng, et al., 2013). Studies have reported prevalence rates ranging
POSTPARTUM POSTTRAUMATIC STRESS DISORDER Introduction Recent research suggests that childbirth may be a significant cause of PTSD in women (Seng, et al., 2013). Studies have reported prevalence rates ranging
Ø We used a standard dose of 5 instead of 3 mci in order to ensure optimal signal to noise in the data
 Differentiation of the effects of an AMPA potentiator on regional brain metabolism between working memory and control tasks: A functional PET (fpet) study. *G. V. WILLIAMS 1,3, B. M. ROBERTS 1,3, D. E.
Differentiation of the effects of an AMPA potentiator on regional brain metabolism between working memory and control tasks: A functional PET (fpet) study. *G. V. WILLIAMS 1,3, B. M. ROBERTS 1,3, D. E.
ADHD and Substance Use Disorders: An Intoxicating Combination
 ADHD and Substance Use Disorders: An Intoxicating Combination Timothy E. Wilens, MD Chief, Division of Child & Adolescent Psychiatry Director, Center for Addiction Medicine Massachusetts General Hospital
ADHD and Substance Use Disorders: An Intoxicating Combination Timothy E. Wilens, MD Chief, Division of Child & Adolescent Psychiatry Director, Center for Addiction Medicine Massachusetts General Hospital
