NIH Public Access Author Manuscript Eur Urol. Author manuscript; available in PMC 2012 July 1.
|
|
|
- Bethanie Dorsey
- 5 years ago
- Views:
Transcription
1 NIH Public Access Author Manuscript Published in final edited form as: Eur Urol July ; 60(1): doi: /j.eururo Robot-Assisted Laparoscopic Partial Adrenalectomy for Pheochromocytoma: The National Cancer Institute Technique Kevin P. Asher, Gopal N. Gupta, Ronald Boris, Peter A. Pinto, W. Marston Linehan, and Gennady Bratslavsky * Urologic Oncology Branch, National Cancer Institute, National Institutes of Health, Bethesda, MD, USA Abstract Background Partial adrenalectomy has recently been advocated to preserve unaffected adrenal tissue during resection of pheochromocytoma. Objective To describe a robot-assisted laparoscopic partial adrenalectomy (RALPA) technique and to report on early functional and oncologic outcomes. Design, setting, and participants From 2007 to 2010, 15 RALPA were performed on 12 consecutive patients with pheochromocytoma. Follow-up data of >1 yr are available on 11 procedures. Median follow-up for the entire cohort was 17.3 mo (range: 6 45). Surgical procedure Positioning and port placement is designed for adequate reach and visualization of the upper retroperitoneum. The plane between the adrenal cortex and pheochromocytoma pseudocapsule is identified visually and with laparoscopic ultrasound. The tumor is dissected away from normal adrenal cortex, preserving normal adrenal tissue. Measurements Preoperative, perioperative, pathologic, and functional outcomes data were analyzed. * Corresponding author Urologic Oncology Branch, National Cancer Institute, Building 10 Room , Bethesda, MD USA , bratslag@mail.nih.gov. Publisher's Disclaimer: This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our customers we are providing this early version of the manuscript. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published in its final citable form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain. Author contributions: Gennady Bratslavsky had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. Study concept and design: Bratslavsky, Gupta, Asher. Acquisition of data: Asher, Boris, Gupta. Analysis and interpretation of data: Asher, Bratslavsky, Boris, Linehan, Pinto, Gupta. Drafting of the manuscript: Asher, Gupta, Bratslavsky. Critical revision of the manuscript for important intellectual content: Asher, Gupta, Bratslavsky. Statistical analysis: Asher, Bratslavsky. Obtaining funding: Bratslavsky, Linehan. Administrative, technical, or material support: Gupta. Supervision: Bratslavsky, Pinto, Linehan. Other (specify): None. Financial disclosures: I certify that all conflicts of interest, including specific financial interests and relationships and affiliations relevant to the subject matter or materials discussed in the manuscript (eg, employment/ affiliation, grants or funding, consultancies, honoraria, stock ownership or options, expert testimony, royalties, or patents filed, received, or pending), are the following: None. Funding/Support and role of the sponsor: None. The Surgery in Motion video accompanying this article can be found in the online version at <doi to be filled in by typesetter> and via Subscribers to the printed journal will find the Surgery in Motion DVD enclosed.
2 Asher et al. Page 2 Results and limitations Fourteen of 15 cases were completed robotically. Among 15 procedures, 4 were performed on a solitary adrenal gland. Four cases required resection of multiple tumors (up to six) with two performed in a solitary gland. The mean age of the patients was 30 yr, and the mean body mass index was 27. The mean operative time was 163 min, the median estimated blood loss was 161 ml, and the median tumor size was 2.7 cm (range: ). There was one conversion to an open procedure in a patient requiring reoperation on a solitary adrenal gland. One patient who underwent RALPA on a solitary adrenal gland required postoperative steroid supplementation at last follow-up. At a median follow-up of 17.3 mo (range: 6 45), there were no recurrences or metastatic events. Study limitations include small sample size and short follow-up. Conclusions RALPA for the treatment of pheochromocytoma is feasible and safe and provides encouraging functional and oncologic outcomes, even in patients with a solitary adrenal lesion or multiple ipsilateral lesions. Keywords Adrenalectomy; Laparoscopy; Partial adrenalectomy; Pheochromocytoma; Robotic surgery 1. Introduction Pheochromocytoma is an uncommon tumor with an incidence of approximately one or two per adults per year but is much more common in familial cancer syndromes, including von Hippel-Lindau (VHL), multiple endocrine neoplasia (MEN) type 2, and neurofibromatosis type I. Among VHL patients who develop pheochromocytomas, up to 47% will develop bilateral lesions [1]. Traditional surgical treatment for pheochromocytoma has been total adrenalectomy. Recent reports have described adrenal-sparing surgery as a surgical option for patients with hereditary cancer syndromes [2 7]. In addition, adrenalsparing surgery has also been described for sporadic adrenal masses, since, even in sporadic cases, other pathologic processes may affect the remaining solitary adrenal gland [8 11]. Laparoscopic approaches have become widely used for adrenal lesions [12 14], including several reports describing laparoscopic adrenal-sparing surgery utilizing both the transperitoneal and retroperitoneal approaches [15 17]. At our referral center, the majority of patients have hereditary conditions and may develop bilateral, multifocal adrenal lesions. Additionally, many patients have had prior adrenal surgery and some have multiple adrenal lesions. These patients afforded us a unique opportunity to evaluate robot-assisted, laparoscopic, partial adrenalectomy (RALPA) for pheochromocytoma. Here we describe our surgical technique and report early functional and oncologic outcomes. 2. Patients and methods We performed 15 RALPA procedures in 12 consecutive patients presenting with pheochromocytoma to the National Cancer Institute, US National Institutes of Health, from June 2007 through August All patients gave written consent regarding the surgical risks of the procedure and the risk for postoperative steroid replacement. The study protocol was approved by the institutional review board Inclusion and exclusion criteria All patients with an adrenal mass that had radiographic and biochemical features consistent with adrenal pheochromocytoma were included. Urine and serum catecholamine
3 Asher et al. Page 3 measurements, computed tomography scan, magnetic resonance imaging, and metaiodobenzylguanidine scan were obtained to confirm the diagnosis of pheochromocytoma. Tumors in a solitary adrenal gland or previous adrenal surgery (either ipsilateral or contralateral) did not exclude patients from the RALPA technique Data collection and follow-up 2.3. Surgical technique Patients demographics and perioperative variables, such as operative time, estimated blood loss (EBL), tumor size, and intraoperative blood pressure and pulse were reviewed. All patients had pheochromocytoma on final pathology. Complications were recorded and classified using the Clavien system. Follow-up consisted of clinic visits at 3 and 12 mo with cross-sectional imaging and biochemical measurements including urine and plasma catecholamine levels to assess for disease recurrence. In the immediate postoperative period, patients with solitary adrenal gland or with signs or symptoms suggestive of adrenal insufficiency were evaluated with an adrenocorticotropic hormone-based cortisol stimulation test. To assess the long-term functional outcome, we tabulated the clinical need for permanent steroid supplementation. Because of a large number of patients residing far away from our tertiary referral center, telephone follow-up was used in many cases Patient preparation Patients were prescribed a 2-wk, preoperative, oral adrenergic blockade consisting of phenoxybenzamine 10 mg twice daily and metyrosine 250 mg three times daily. Patients were encouraged to orally hydrate in the 2 wk prior to surgery. A magnesium-citrate bowel preparation was given the day before surgery. An arterial line was placed for blood pressure monitoring and two large-bore, peripheral intravenous catheters were placed. Blood pressure was carefully monitored intraoperatively to ensure hemodynamic stability during the procedure and specifically during tumor manipulation. We did not observe significant intraoperative blood pressure lability with this regimen, and therefore a central line was not routinely used Patient positioning Two technical modifications are used that distinguish the operative setup for RALPA from typically used robotic configurations for renal surgery. First, the patient is positioned in an extreme flank position, with the axis of the shoulders close to a 90 angle to the operating table. This positioning allows easier access to the adrenal gland, and is particularly important on the right side where pheochromocytoma is typically located retrocavally. Second, the robotic camera axis is placed above and lateral to the umbilicus facilitating better visualization of the upper retroperitoneum (Fig. 1) Port placement The port configuration is shown in the Figure 2. In most cases, a single 12-mm assistant port is used between the left robotic trocar and the camera port, but in obese patients, a second assistant port may be added. An additional 5-mm subxyphoid trocar is used for liver retraction in a right-sided case. The robotic cart is then brought in at a 45 angle in relationship to the table over the head of the patient with the working axis of the robot directed at the ipsilateral clavicle (Fig. 2) Instrumentation A 30 down lens is utilized throughout the operation. Monopolar scissors are placed in the right robotic arm and bipolar forceps in the left.
4 Asher et al. Page Exposure of adrenal gland Right-sided exposure: Because of the extreme flank positioning, a direct approach to the right adrenal can be performed without bowel mobilization. The triangular liver ligament is divided as cranially as possible to release the liver, and the locking grasper (placed through the subxyphoid trocar) is used as a liver retractor. The posterior peritoneum overlying the upper pole of the adrenal is also divided to release the liver, which is then retracted more superiorly. Superior retraction on the liver is crucial for the right sided approach, as broad exposure of the supra-adrenal cava is essential to avoid hemorrhage and to optimize workspace. Occasionally, short hepatic veins may be divided to gain additional length of the vena cava. The lateral border of the inferior vena cava is identified, the adventitia over the cava is incised, and the dissection is carried until the right adrenal vein is encountered and then clipped and divided. Often, small accessory adrenal veins are identified and controlled with bipolar cautery or clips Left-sided exposure: The splenic flexure and a portion of the descending colon are mobilized. The lateral attachments of the spleen, as well as splenorenal ligaments, are divided. The spleen, bowel, and the pancreas are mobilized medially until the adrenal gland is clearly visualized. Depending on the location of the pheochromocytoma, the left adrenal veins may or may not be divided Identification of pheochromocytoma Once the adrenal gland has been identified, a laparoscopic ultrasound probe is used to identify the adrenal gland, the upper pole of the kidney, and the pheochromocytoma. On ultrasound, the pheochromocytoma appears as a homogenous, hypoechoic, well-demarcated lesion, distinct from the surrounding normal adrenal. The ultrasound is used to scan the entire adrenal gland to assess for occult multiple masses (Fig. 3). Once the mass is identified, the Gerota s fascia layer overlying the tumor is incised. Careful, gentle dissection is then used to identify the pheochromocytoma pseudocapsule within the normal adrenal gland. The robotic instruments are particularly helpful with minimizing the handling of normal adrenal tissue, which may help preserve the adrenal blood supply. Dissection of the superior and medial aspects of the adrenal gland is minimized, as these are the sites of arterial blood supply. If, due to the tumor location, superomedial dissection is needed, care must be taken to minimize dissection inferior to the adrenal within Gerota s fascia, as the blood supply from the vasculature in this region is necessary to maintain the viability of the residual unaffected adrenal gland. Once the mass is clearly visualized, the plane between normal adrenal tissue and pheochromocytoma pseudocapsule can be appreciated (Fig. 4) Resection of pheochromocytoma The mass is carefully enucleated, taking great care to keep the tumor pseudocapsule intact and to respect tissue planes. Gentle upward traction is provided with the bipolar forceps and blunt dissection in the proper plane is used to peel the tumor mass away with minimal tissue damage. Dissection into an incorrect plane may produce troublesome bleeding. Locking clips and pinpoint cautery are used for hemostasis. The entire specimen and tumor capsule are inspected to ensure complete resection. The adrenal bed is inspected for residual tumor visually and with laparoscopic ultrasound to ensure adequate hemostasis. A frozen section of the base is not routinely performed (Fig. 5 and 6).
5 Asher et al. Page 5 3. Results 4. Discussion A total of 15 RALPAs were performed in 12 patients. Patient characteristics are listed in Table 1. Ten of 12 patients had VHL disease, one patient had neurofibromatosis type 1, and the other had bilateral pheochromocytomas without a known genetic disorder. Median follow-up for the entire cohort was 17.3 mo (range: 6 45), and 11 procedures had >1 yr follow-up. Mean tumor size for the cohort was 2.7 cm. Four patients underwent RALPA with resection of multiple ipsilateral pheochromocytomas, ranging from two to six lesions. In addition, four patients had a solitary adrenal gland, and of these, two patients had multiple tumors resected (three and six tumors, respectively). Perioperative characteristics are listed in Table 2. Median blood loss was 161 ml. Mean total operative time from skin incision to closure was 163 min (range: ). Intraoperative hypertension or tachycardia was not observed with manipulation of the pheochromocytoma. There was one conversion to open partial adrenalectomy due to severe adhesions to the liver and repeated vena caval injuries requiring initially robotic, and then open repairs. They occurred during medial dissection of the adrenal in a patient with a solitary adrenal gland and prior adrenal surgery on the ipsilateral side. The same patient also had the only operative complication (Clavien grade 3) of the series: a bile leak that required a temporary drain for 5 d. At 16 mo postoperatively, this patient has no evidence of recurrence and does not require steroid supplementation. Of the total cohort of 15 patients, none had biochemical evidence of recurrent pheochromocytoma and 14 did not require long-term, postoperative, steroid supplementation. One patient, a 44-yr-old woman with a history of bilateral multifocal pheochromocytomas had resection of six masses in a solitary adrenal and has required steroid supplementation since the time of surgery, despite visual preservation of a small portion of unaffected adrenal. Pheochromocytoma has traditionally been surgically managed by total adrenalectomy. In this report we describe our technique of RALPA in detail. We have found this technique effective for the management of pheochromocytoma, even with multiple lesions or in the setting of a solitary adrenal gland, with promising functional and oncologic outcomes. Several technical considerations are important to successfully perform this procedure (Table 3). First, the patient must be positioned in an exaggerated flank position, with the axis of the shoulders almost perpendicular to the operating table. This exaggerated flank position is crucial to easily exposing the adrenal glands. This is in contrast to the robotic renal approach, where the patient is typically positioned in a 45 flank position. Second, the port arrangement should be rotated more laterally and more superiorly, with the camera axis pointed toward the ipsilateral clavicle. Again, this allows better access to the upper retroperitoneum. With these modifications, we typically do not have to mobilize the bowel on the right side and minimize bowel mobilization on the left. Third, on the right side, one must mobilize the liver as cephalad as possible, dividing not only the peritoneal attachments between the upper pole of the kidney and inferior liver surface, but dividing the triangular ligament as superiorly as possible. This allows access to the supra-adrenal vena cava on the right side. This area must be well exposed, as the short hepatic veins enter at this level and may cause hemorrhage if not appreciated. Fourth, the plane between the pheochromocytoma capsule and the surrounding adrenal parenchyma must be clearly visualized. The enhanced visualization of the three-dimensional laparoscopic view and the intraoperative ultrasound facilitate the identification of this plane. Once the correct dissection plane is identified and
6 Asher et al. Page 6 entered, the tumor enucleation is straightforward and minimal bleeding is typically encountered. Finally, the advantage of the robotic platform over traditional laparoscopy may best be appreciated during the tumor resection. As the remainder of the unaffected adrenal should be minimally dissected to preserve the blood supply, the articulation of the robotic instruments permits circumferential dissection around the tumor deep within the adrenal with minimal manipulation of the normal adrenal gland. Laparoscopic partial adrenalectomy has been increasingly utilized in recent years. Walz et al in 2004 reported the largest series in the published literature with 100 laparoscopic adrenalsparing procedures [17]. Their series used prone patient positioning and a retroperitoneal approach. The median operative time was 79 min and the EBL was 29 ml. At a mean follow-up of 51 mo there were no recurrences. In a subgroup of 15 patients with bilateral adrenal masses and hereditary syndromes (VHL, MEN, succinate dehydrogenase genes), one patient required postoperative steroid supplementation. These findings are similar to our results, in which one of 15 procedures resulted in steroid supplementation. However, 40% (6 of 15) of procedures in our cohort were performed in patients with a solitary gland or multifocal lesions. Patient selection as well as a learning curve can certainly explain our longer operative times. In our most recent RALPA cases, we completed the entire procedure in <60 min, which compares favorably with these reports and with those utilizing laparoscopic or robotic approaches [17,19]. A comprehensive literature review of partial adrenalectomy was performed by Kaye et al, reporting on 417 patients, including 319 laparoscopic partial adrenalectomies performed via a variety of approaches. Thirty-seven percent of these procedures were performed for pheochromocytoma. Mean operative time was 130 min and mean EBL was 72 ml. In the laparoscopic group, complications occurred in 7.3% of patients. Six of 133 (4.5%) patients required long-term steroid supplementation in this review [18]. These numbers are comparable to the findings of our series, despite our more challenging patient cohort, as described earlier. Recently, there have been several case reports of RALPA in the literature. Narmada et al reported on four patients undergoing partial adrenalectomy for pheochromocytoma using a transperitoneal, four- or five-port technique [19]. Their report, similar to our experience, emphasized the exaggerated flank positioning as a key operative step. They reported a mean blood loss of 97 ml and mean operative time of 77 min. All patients had a single lesion in this cohort and none had multifocal lesions. Kumar et al described a transperitoneal, robotic, partial adrenalectomy in a left-sided adrenal metastasis in a patient with renal-cell carcinoma and a previous right adrenalectomy [20]. The operative time was 90 min and blood loss was 50 ml. We also recently reported on a cohort of patients treated with transperitoneal RALPA for adrenal masses [21]. The present report focuses on our surgical technique for pheochromocytoma. In our cohort, EBL was slightly higher (161 ml) and operative times were longer (163 min) than in these other laparoscopic series. As mentioned above, these findings may be explained in part by patient selection as well as a learning curve, as the cases are frequently performed by the fellows in training. A strength of our study is the follow-up on functional outcomes. Only one of 15 patients in our cohort has required postoperative steroid supplementation. This is an encouraging result considering our challenging patient population and its propensity to developing bilateral, multifocal pheochromocytomas potentially requiring bilateral adrenalectomy. Three patients in this series had bilateral lesions at presentation and, after staged bilateral RALPA, each of these patients has no evidence of residual tumor and none require steroid supplementation. Finally, of four patients with a solitary adrenal gland, three patients did not require longterm treatment with steroid replacement after RALPA, indicating that the residual adrenal gland after RALPA was able to provide physiologic levels of endogenous steroids. These results are consistent with the findings of Sanford et al, evaluating outcomes of patients
7 Asher et al. Page 7 5. Conclusions requiring adrenal surgery on a solitary adrenal [22]. Given the risks associated with bilateral adrenalectomy and uncertain dosing with exogenous steroids, it appears that adrenal-sparing surgery offers these patients a significant benefit. Our described technique of robotic assistance may facilitate and allow for a wider acceptance of adrenal-sparing surgery, while conferring the benefits of a minimally invasive laparoscopic approach [23]. In general, our results are consistent with other published, laparoscopic, partial adrenalectomy series. In our experience, we have found that while the perioperative outcomes may not yet be significantly different than those of published laparoscopic series, the procedure may be technically easier to perform. Other studies have demonstrated that laparoscopic approaches for adrenal surgery are associated with decreased blood loss, shortened convalescent time, and decreased need for postoperative analgesia, as compared with open adrenalectomy, and we have observed the same benefits in the current series compared with our open experience [24]. The enhanced visualization and articulating dissecting instruments allow for a controlled, accurate enucleation, and use of a two-handed technique with assistance afforded by the robotic platform. The robotic approach is particularly well-suited for laparoscopic surgery that requires very precise dissection in a small space. Additionally, in our experience, the RALPA technique has been easily learned by urologic oncology fellows. There are several inherent limitations in the current study. It is retrospective and the sample size is small. The follow-up is limited and the long-term oncologic outcomes are not yet available. While this current report describing our technique does not yet demonstrate longterm oncologic efficacy, recent evidence suggests that partial adrenalectomy for pheochromocytoma may provide excellent, long-term, oncologic and functional outcomes [4]. Additionally, Kaye s review also demonstrates an evolving role for adrenal-sparing surgery [18]. The patients in this series have hereditary syndromes predisposing to the development of bilateral, multifocal adrenal pheochromocytomas, which may affect our perioperative outcome measures. Finally, our surgical team has significant experience in both open and laparoscopic partial adrenalectomy, which may have contributed to our perioperative outcomes in this series. RALPA for pheochromocytoma is a safe, technically feasible procedure that provides excellent short-term functional and oncologic outcomes. Our technique for RALPA may be used for patients with adrenal pheochromocytoma, including multifocal lesions, and is especially well suited to those with a solitary adrenal gland. The procedure may be applicable for other type of adrenal lesions. Longer follow-up is needed to assess long-term functional and oncologic outcomes. Supplementary Material References Refer to Web version on PubMed Central for supplementary material. 1. Vaughan, E.; Blumenfeld, J. Pathophysiology, evaluation, and medical management of adrenal disorders. In: Wein, A.; Kavoussi, L.; Novic, L., editors. Campbell-Walsh urology. ed. 9. Philadelphia, PA: Saunders Elsevier; p Al-Sobhi S, Peschel R, Zihak C, Bartsch G, Neumann H, Janetschek G. Laparoscopic partial adrenalectomy for recurrent pheochromocytoma after open partial adrenalectomy in von Hippel- Lindau disease. J Endourol. 2002; 16: [PubMed: ]
8 Asher et al. Page 8 3. Baghai M, Thompson GB, Young WF Jr, Grant CS, Michels VV, van Heerden JA. Pheochromocytomas and paragangliomas in von Hippel-Lindau disease: a role for laparoscopic and cortical-sparing surgery. Arch Surg. 2002; 137: [PubMed: ] 4. Benhammou JN, Boris RS, Pacak K, Pinto PA, Linehan WM, Bratslavsky G. Functional and oncologic outcomes of partial adrenalectomy for pheochromocytoma in patients with von Hippel- Lindau syndrome after at least 5 years of followup. J Urol. 2010; 184: [PubMed: ] 5. Neumann HP, Reincke M, Bender BU, Elsner R, Janetschek G. Preserved adrenocortical function after laparoscopic bilateral adrenal sparing surgery for hereditary pheochromocytoma. J Clin Endocrinol Metab. 1999; 84: [PubMed: ] 6. Roukounakis N, Dimas S, Kafetzis I, et al. Is preservation of the adrenal vein mandatory in laparoscopic adrenal-sparing surgery? JSLS. 2007; 11: [PubMed: ] 7. Walther MM, Keiser HR, Choyke PL, Rayford W, Lyne JC, Linehan WM. Management of hereditary pheochromocytoma in von Hippel-Lindau kindreds with partial adrenalectomy. J Urol. 1999; 161: [PubMed: ] 8. Bornstein SR. Predisposing factors for adrenal insufficiency. N Engl J Med. 2009; 360: [PubMed: ] 9. Jeschke K, Janetschek G, Peschel R, Schellander L, Bartsch G, Henning K. Laparoscopic partial adrenalectomy in patients with aldosterone-producing adenomas: indications, technique, and results. Urology. 2003; 61: [PubMed: ] 10. Kok KY, Yapp SK. Laparoscopic adrenal-sparing surgery for primary hyperaldosteronism due to aldosterone-producing adenoma. Surg Endosc. 2002; 16: [PubMed: ] 11. Sasagawa I, Suzuki Y, Itoh K, et al. Posterior retroperitoneoscopic partial adrenalectomy: clinical experience in 47 procedures. Eur Urol. 2003; 43: [PubMed: ] 12. Gumbs AA, Gagner M. Laparoscopic adrenalectomy. Best Pract Res Clin Endocrinol Metab. 2006; 20: [PubMed: ] 13. Jacobs JK, Goldstein RE, Geer RJ. Laparoscopic adrenalectomy. A new standard of care. Ann Surg. 1997; 225: [PubMed: ] 14. Lev-Chelouche D, Sagie B, Keidar A, Klausner JM, Szold A. Laparoscopic adrenalectomy: indications, technique, complications and follow-up. Isr Med Assoc J. 2003; 5: [PubMed: ] 15. Imai T, Tanaka Y, Kikumori T, et al. Laparoscopic partial adrenalectomy. Surg Endosc. 1999; 13: [PubMed: ] 16. Liao CH, Chueh SC, Wu KD, Hsieh MH, Chen J. Laparoscopic partial adrenalectomy for aldosterone-producing adenomas with needlescopic instruments. Urology. 2006; 68: [PubMed: ] 17. Walz MK, Peitgen K, Diesing D, et al. Partial versus total adrenalectomy by the posterior retroperitoneoscopic approach: early and long-term results of 325 consecutive procedures in primary adrenal neoplasias. World J Surg. 2004; 28: [PubMed: ] 18. Kaye DR, Storey BB, Pacak K, Pinto PA, Linehan WM, Bratslavsky G. Partial adrenalectomy: underused first line therapy for small adrenal tumors. J Urol. 2010; 184: [PubMed: ] 19. Narmada P, Rishi N, Prabhjo S, et al. Robot-assisted partial adrenalectomy for isolated adrenal metastasis. J Endourol. 2010; 24: [PubMed: ] 20. Kumar A, Hyams ES, Stifelman MD. Robot-assisted partial adrenalectomy for isolated adrenal metastasis. J Endourol. 2009; 23: [PubMed: ] 21. Boris RS, Gupta G, Linehan WM, Pinto PA, Bratslavsky G. Robot-assisted laparoscopic partial adrenalectomy: initial experience. Urology. In press. 22. Sanford TH, Storey BB, Linehan WM, Rogers CA, Pinto PA, Bratslavsky G. Outcomes and timing for intervention of partial adrenalectomy in patients with a solitary adrenal remnant and history of bilateral phaeochromocytomas. BJU Int. 2011; 107: [PubMed: ] 23. Asari R, Scheuba C, Kaczirek K, Niederle B. Estimated risk of pheochromocytoma recurrence after adrenal-sparing surgery in patients with multiple endocrine neoplasia type 2A. Arch Surg. 2006; 141: [PubMed: ]
9 Asher et al. Page Jacobsen NE, Campbell JB, Hobart MG. Laparoscopic versus open adrenalectomy for surgical adrenal disease. Can J Urol. 2003; 10: [PubMed: ]
10 Asher et al. Page 10 Fig. 1. Lateral and superior port placement. The camera port and the robotic axis are rotated superiorly and laterally to access the adrenal gland in the posterior retroperitoneum.
11 Asher et al. Page 11 Fig. 2. Port placement for robot-assisted laparoscopic partial adrenalectomy. This case was performed on an obese patient. In addition to the 5-mm trocar used between the camera port and right robotic port, another assistant port is placed between the camera and the left robotic port in patients with extreme obesity. A 5-mm subxyphoid port is used for liver retraction. Note the axis of the camera port directed at the ipsilateral clavicle.
12 Asher et al. Page 12 Fig. 3. Laparoscopic ultrasound aids in identifying pheochromocytoma. The pheochromocytoma appears as a well-demarcated, homogenous, dark mass that is distinct from the surrounding normal adrenal cortex.
13 Asher et al. Page 13 Fig. 4. Identification of the plane between normal adrenal cortex and pheochromocytoma. The enhanced visualization allows identification of the plane between tumor tissue and adjacent normal adrenal cortex. A plane of dissection can then be developed.
14 Asher et al. Page 14 Fig. 5. Dissection of tumor from uninvolved adrenal cortex. By following the pseudocapsule of the lesion, the pheochromocytoma is carefully enucleated. Locking laparoscopic clips are used to control small perforating vessels.
15 Asher et al. Page 15 Fig. 6. Minimal handling of normal adrenal tissue. The dissection is performed to maximize the separation of tumor tissue from the underlying uninvolved adrenal bed. The precise movements of the robotic instruments allow for minimal handling of normal adrenal tissue, which may help preserve blood supply and minimize long-term damage to normal healthy adrenal cortical tissue.
16 Asher et al. Page 16 Demographic and preoperative data Patients, No. 12 RAPLA, No. RAPLA with planned staged procedures, No RAPLA performed on right side, No. (%) 9 (60) Patient age, yr, mean (range) 30.0 ( ) Follow-up, mo, median (range) 17.3 (6 45) BMI, kg/m 2, mean (range) 27 (20 48) Procedures for multifocal lesions, No. (%) 4 (26) Procedures on solitary adrenal gland, No. (%) 4 (26) Table 1 RAPLA = robot-assisted laparoscopic partial adrenalectomy; BMI = body mass index.
17 Asher et al. Page 17 Table 2 Perioperative, postoperative, and functional outcomes Perioperative Operative time, min, median (range) 163 ( ) EBL, ml, median (range) 161 (50 300) RAPLA requiring transfusion, No. 1 (7.5) Conversions to open procedure, No. (%) 1 (7.5) Intraoperative hypertensionortachycardia episodes, No. 0 Postoperative Largest tumor size, cm, median (range) 2.7 ( ) Local ordistant recurrence, No. 0 Functional RAPLA requiring steroid replacement postoperatively, No. (%) 1 (7.5) EBL = estimated blood loss; RAPLA = robot-assisted laparoscopic partial adrenalectomy.
18 Asher et al. Page 18 Table 3 Technical keys to success with robot-assisted laparoscopic partial adrenalectomy 1. Thorough preoperative blockade with phenoxybenzamine and metyrosine 2. Extreme flank positioning 3. Axis of robotic ports directed at ipsilateral clavicle 4. Identify adrenal vein and ligate if there is potential for injury 5. Identify adrenal pheochromocytoma visually and with laparoscopic ultrasound 6. Establish plane between pseudocapsule of lesion and normal adrenal 7. Minimize handling of tissue and use of cautery to preserve blood supply 8. Resect the mass along the pseudocapsule plane
Robot-Assisted Laparoscopic Partial Adrenalectomy for Pheochromocytoma: The National Cancer Institute Technique
 EUROPEAN UROLOGY 60 (2011) 118 124 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Robot-Assisted Laparoscopic Partial Adrenalectomy for Pheochromocytoma:
EUROPEAN UROLOGY 60 (2011) 118 124 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Robot-Assisted Laparoscopic Partial Adrenalectomy for Pheochromocytoma:
Chapter 2. Simple Nephrectomy. Please Give Three Tips for Laparoscopic Simple Nephrectomy. Dr. de la Rosette
 Chapter 2 Simple Nephrectomy Please Give Three Tips for Laparoscopic Simple Nephrectomy............. 39 How Does One Find the Renal Hilum during Transperitoneal Laparoscopic Nephrectomy?.................
Chapter 2 Simple Nephrectomy Please Give Three Tips for Laparoscopic Simple Nephrectomy............. 39 How Does One Find the Renal Hilum during Transperitoneal Laparoscopic Nephrectomy?.................
Partial Nephrectomy Techniques for Renal Preservation: Historical and Modern Approaches
 Partial Nephrectomy Techniques for Renal Preservation: Historical and Modern Approaches Cary N Robertson MD FACS Associate Professor Division of Urology Associate Director Urologic Oncology Duke Cancer
Partial Nephrectomy Techniques for Renal Preservation: Historical and Modern Approaches Cary N Robertson MD FACS Associate Professor Division of Urology Associate Director Urologic Oncology Duke Cancer
2 Adrenal Disease. Open Surgery. Andrew C. Novick SURGICAL ANATOMY
 Preface More than 125 years have passed since the basic contributions of John Hunter, Crawford Long, and Lord Lister transformed surgery into a sound science as well as a delicate art. Several great surgeons
Preface More than 125 years have passed since the basic contributions of John Hunter, Crawford Long, and Lord Lister transformed surgery into a sound science as well as a delicate art. Several great surgeons
Case Report Left Transperitoneal Adrenalectomy with a Laparoendoscopic Single-Site Surgery Combined Technique: Initial Case Reports
 Volume 2011, Article ID 651380, 4 pages doi:10.1155/2011/651380 Case Report Left Transperitoneal Adrenalectomy with a Laparoendoscopic Single-Site Surgery Combined Technique: Initial Case Reports Yasuhiro
Volume 2011, Article ID 651380, 4 pages doi:10.1155/2011/651380 Case Report Left Transperitoneal Adrenalectomy with a Laparoendoscopic Single-Site Surgery Combined Technique: Initial Case Reports Yasuhiro
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Guidelines for the Minimally Invasive Treatment of Adrenal Pathology
 SAGES Society of American Gastrointestinal and Endoscopic Surgeons http://www.sages.org Guidelines for the Minimally Invasive Treatment of Adrenal Pathology Author : SAGES Webmaster Dimitrios Stefanidis,
SAGES Society of American Gastrointestinal and Endoscopic Surgeons http://www.sages.org Guidelines for the Minimally Invasive Treatment of Adrenal Pathology Author : SAGES Webmaster Dimitrios Stefanidis,
Robotic Surgery for Upper Tract Urothelial Carcinoma. Li-Ming Su, MD
 Robotic Surgery for Upper Tract Urothelial Carcinoma Li-Ming Su, MD David A. Cofrin Professor of Urology, Associate Chairman of Clinical Affairs, Chief, Division of Robotic and Minimally Invasive Urologic
Robotic Surgery for Upper Tract Urothelial Carcinoma Li-Ming Su, MD David A. Cofrin Professor of Urology, Associate Chairman of Clinical Affairs, Chief, Division of Robotic and Minimally Invasive Urologic
RECURRENT ADRENAL DISEASE. Megan Applewhite Endorama 2/19/2015 SR , SC
 RECURRENT ADRENAL DISEASE Megan Applewhite Endorama 2/19/2015 SR 2412318, SC 3421561 Category: Adrenal Attendings: Angelos & Grogan PATIENT #1 36yo woman with a hx of Cushing s Syndrome and right adrenalectomy
RECURRENT ADRENAL DISEASE Megan Applewhite Endorama 2/19/2015 SR 2412318, SC 3421561 Category: Adrenal Attendings: Angelos & Grogan PATIENT #1 36yo woman with a hx of Cushing s Syndrome and right adrenalectomy
Initial Series of Robotic Radical Nephrectomy with Vena Caval Tumor Thrombectomy
 EUROPEAN UROLOGY 59 (2011) 652 656 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Series of the Month Initial Series of Robotic Radical Nephrectomy with Vena Caval Tumor
EUROPEAN UROLOGY 59 (2011) 652 656 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Series of the Month Initial Series of Robotic Radical Nephrectomy with Vena Caval Tumor
Bilateral laparoscopic partial adrenalectomy: A case presentation and review of the literature
 Himmelfarb Health Sciences Library, The George Washington University Health Sciences Research Commons Surgery Faculty Publications Surgery 4-2014 Bilateral laparoscopic partial adrenalectomy: A case presentation
Himmelfarb Health Sciences Library, The George Washington University Health Sciences Research Commons Surgery Faculty Publications Surgery 4-2014 Bilateral laparoscopic partial adrenalectomy: A case presentation
RADICAL CYSTECTOMY. Solutions for minimally invasive urologic surgery
 RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Intuitive motion RADICAL CYSTECTOMY Maintains the oncologic
RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Intuitive motion RADICAL CYSTECTOMY Maintains the oncologic
INGUINAL HERNIA REPAIR PROCEDURE GUIDE
 ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
Robotic-assisted ipsilateral adrenalectomy after robotic-assisted partial nephrectomy: a case report
 Case Report Page 1 of 5 Robotic-assisted ipsilateral adrenalectomy after robotic-assisted partial nephrectomy: a case report David P. Feng 1, Zuliang Feng 2, Amy N. Luckenbaugh 1, Svetlana Avulova 1, Daniel
Case Report Page 1 of 5 Robotic-assisted ipsilateral adrenalectomy after robotic-assisted partial nephrectomy: a case report David P. Feng 1, Zuliang Feng 2, Amy N. Luckenbaugh 1, Svetlana Avulova 1, Daniel
Health Sciences Centre, Team A, Dr. L. Bohacek (Endocrine Surgery) Medical Expert
 Health Sciences Centre, Team A, Dr. L. Bohacek (Endocrine Surgery) Introduction Medical Expert This is a three month PGY 1-5 rotation in which residents gain exposure in the care and management of patients
Health Sciences Centre, Team A, Dr. L. Bohacek (Endocrine Surgery) Introduction Medical Expert This is a three month PGY 1-5 rotation in which residents gain exposure in the care and management of patients
Surgical Technique. Laparoscopic Partial Adrenalectomy. Rezumat
 Surgical Technique Chirurgia (2017) 112: 77-81 No. 1, January - February Copyright Celsius http://dx.doi.org/10.21614/chirurgia.112.1.77 Adrian Miron 1,2, Cosmin Giulea 1,2, Mihai Nãdrãgea 1, Octavian
Surgical Technique Chirurgia (2017) 112: 77-81 No. 1, January - February Copyright Celsius http://dx.doi.org/10.21614/chirurgia.112.1.77 Adrian Miron 1,2, Cosmin Giulea 1,2, Mihai Nãdrãgea 1, Octavian
Initial Clinical Experience with Robot-Assisted Laparoscopic Partial Nephrectomy for Complex Renal Tumors
 Initial Clinical Experience with Robot-Assisted Laparoscopic Partial Nephrectomy for Complex Renal Tumors Kyung Hwa Choi, Cheol Kyu Oh, Wooju Jeong, Enrique Ian S. Lorenzo, Woong Kyu Han, Koon Ho Rha From
Initial Clinical Experience with Robot-Assisted Laparoscopic Partial Nephrectomy for Complex Renal Tumors Kyung Hwa Choi, Cheol Kyu Oh, Wooju Jeong, Enrique Ian S. Lorenzo, Woong Kyu Han, Koon Ho Rha From
Laparoscopic Radical Nephrectomy- the current gold standard
 Laparoscopic Radical Nephrectomy- the current gold standard Anoop M. Meraney, M.D Director, Urologic Oncology, Helen and Harry Gray Cancer Center, Hartford Hospital and Connecticut Surgical Group. Is it
Laparoscopic Radical Nephrectomy- the current gold standard Anoop M. Meraney, M.D Director, Urologic Oncology, Helen and Harry Gray Cancer Center, Hartford Hospital and Connecticut Surgical Group. Is it
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
Daniela Faivovich K., MS VII Universidad de Chile Gillian Lieberman, MD Harvard Medical School
 Daniela Faivovich K., MS VII Universidad de Chile Gillian Lieberman, MD Harvard Medical School May 21st, 2010 56 year old male patient History of hypertension, hyperlipidemia and insulin-resistance 2009:
Daniela Faivovich K., MS VII Universidad de Chile Gillian Lieberman, MD Harvard Medical School May 21st, 2010 56 year old male patient History of hypertension, hyperlipidemia and insulin-resistance 2009:
Sex: 女 Age: 51 Occupation: 無 Admission date:92/07/22
 Sex: 女 Age: 51 Occupation: 無 Admission date:92/07/22 Chief complaint Unknown fever for one month Hand tremor and left huge renal tumor was noted Present illness Suffered from fever for one month, hand
Sex: 女 Age: 51 Occupation: 無 Admission date:92/07/22 Chief complaint Unknown fever for one month Hand tremor and left huge renal tumor was noted Present illness Suffered from fever for one month, hand
Pheochromocytomas (PHEOs) are rare catecholamineproducing
 Usefulness of Standardized Uptake Values for Distinguishing Adrenal Glands with Pheochromocytoma from Normal Adrenal Glands by Use of 6- F-Fluorodopamine PET Henri J.L.M. Timmers 1,2, Jorge A. Carrasquillo
Usefulness of Standardized Uptake Values for Distinguishing Adrenal Glands with Pheochromocytoma from Normal Adrenal Glands by Use of 6- F-Fluorodopamine PET Henri J.L.M. Timmers 1,2, Jorge A. Carrasquillo
Laparoscopic Adrenalectomy in the Treatment of Pheochromocytoma 111
 Vol. Brazilian 1, Nº 3Journal of Videoendoscopic Surgery Original Article Laparoscopic Adrenalectomy in the Treatment of Pheochromocytoma 111 Laparoscopic Adrenalectomy in the Treatment of Pheochromocytoma:
Vol. Brazilian 1, Nº 3Journal of Videoendoscopic Surgery Original Article Laparoscopic Adrenalectomy in the Treatment of Pheochromocytoma 111 Laparoscopic Adrenalectomy in the Treatment of Pheochromocytoma:
Case Based Urology Learning Program
 Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 4 CBULP 2010 004 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 4 CBULP 2010 004 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Single-port endoscopic retroperitoneal adrenalectomy: initial experience
 Surgical Videosurgery Single-port endoscopic retroperitoneal adrenalectomy: initial experience Virgilijus Beiša, Gintaras Simutis, Karolis Lagunavičius, Kęstutis Strupas Clinic of Gastroenterology, Nephrourology
Surgical Videosurgery Single-port endoscopic retroperitoneal adrenalectomy: initial experience Virgilijus Beiša, Gintaras Simutis, Karolis Lagunavičius, Kęstutis Strupas Clinic of Gastroenterology, Nephrourology
RAPN. in T1b Renal Masses? A. Mottrie. G. Denaeyer, P. Schatteman, G. Novara
 RAPN in T1b Renal Masses? A. Mottrie G. Denaeyer, P. Schatteman, G. Novara Department of Urology O.L.V. Clinic Aalst OLV Vattikuti Robotic Surgery Institute Aalst Belgium Guidelines on Renal Cell Carcinoma
RAPN in T1b Renal Masses? A. Mottrie G. Denaeyer, P. Schatteman, G. Novara Department of Urology O.L.V. Clinic Aalst OLV Vattikuti Robotic Surgery Institute Aalst Belgium Guidelines on Renal Cell Carcinoma
The Leeds Teaching Hospitals NHS Trust Adrenalectomy
 n The Leeds Teaching Hospitals NHS Trust Adrenalectomy Information for patients This leaflet provides information on having an adrenalectomy, reasons for the procedure and alternatives to surgery, along
n The Leeds Teaching Hospitals NHS Trust Adrenalectomy Information for patients This leaflet provides information on having an adrenalectomy, reasons for the procedure and alternatives to surgery, along
Surgical management of the undescended testis is performed
 Undescended Testes/Orchiopexy James C.Y. Dunn, MD, PhD, 1 Akemi L. Kawaguchi, MD, 2 and Eric W. Fonkalsrud, MD 1 Surgical management of the undescended testis is performed to prevent the potential complications
Undescended Testes/Orchiopexy James C.Y. Dunn, MD, PhD, 1 Akemi L. Kawaguchi, MD, 2 and Eric W. Fonkalsrud, MD 1 Surgical management of the undescended testis is performed to prevent the potential complications
Laparoscopic Radical Nephrectomy for Renal Masses 7 Centimeters or Larger
 SCIENTIFIC PAPER Laparoscopic Radical Nephrectomy for Renal Masses 7 Centimeters or Larger James S. Rosoff, MD, Jay D. Raman, MD, R. Ernest Sosa, MD, Joseph J. Del Pizzo, MD ABSTRACT Objective: To report
SCIENTIFIC PAPER Laparoscopic Radical Nephrectomy for Renal Masses 7 Centimeters or Larger James S. Rosoff, MD, Jay D. Raman, MD, R. Ernest Sosa, MD, Joseph J. Del Pizzo, MD ABSTRACT Objective: To report
Patient Selection for Ablative Therapies. Adrian D Joyce Leeds UK
 Patient Selection for Ablative Adrian D Joyce Leeds UK Therapy Renal Cell Ca USA: 30,000 new cases annually >12,000 deaths RCC accounts for 3% of all adult malignancy 40% of patients will die from their
Patient Selection for Ablative Adrian D Joyce Leeds UK Therapy Renal Cell Ca USA: 30,000 new cases annually >12,000 deaths RCC accounts for 3% of all adult malignancy 40% of patients will die from their
Solitary Contralateral Adrenal Metastases after Nephrectomy for Renal Cell Carcinoma
 Original Report ISSN 1537-744X; DOI 10.1100/tsw.2004.39 Solitary Contralateral Adrenal after Nephrectomy for Renal Cell Carcinoma Nikolaos Antoniou, M.D. and Demetrios Karanastasis, M.D. General Hospital
Original Report ISSN 1537-744X; DOI 10.1100/tsw.2004.39 Solitary Contralateral Adrenal after Nephrectomy for Renal Cell Carcinoma Nikolaos Antoniou, M.D. and Demetrios Karanastasis, M.D. General Hospital
BJUI. Robotic nephrectomy for the treatment of benign and malignant disease
 . JOURNAL COMPILATION 2008 BJU INTERNATIONAL Laparoscopic and Robotic Urology ROGERS et al. BJUI BJU INTERNATIONAL Robotic nephrectomy for the treatment of benign and malignant disease Craig Rogers, Rajesh
. JOURNAL COMPILATION 2008 BJU INTERNATIONAL Laparoscopic and Robotic Urology ROGERS et al. BJUI BJU INTERNATIONAL Robotic nephrectomy for the treatment of benign and malignant disease Craig Rogers, Rajesh
Parenchyma-sparing lung resections are a potential therapeutic
 Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
ORIGINAL ARTICLE. Laparoscopic Posterior Adrenalectomy
 Laparoscopic Posterior Adrenalectomy Technical Considerations ORIGINAL ARTICLE Allan E. Siperstein, MD; Eren Berber, MD; Kristen L. Engle, MD; Quan-Yang Duh, MD; Orlo H. Clark, MD Hypothesis: Although
Laparoscopic Posterior Adrenalectomy Technical Considerations ORIGINAL ARTICLE Allan E. Siperstein, MD; Eren Berber, MD; Kristen L. Engle, MD; Quan-Yang Duh, MD; Orlo H. Clark, MD Hypothesis: Although
Robotics, Laparoscopy & Endosurgery
 Robotics, Laparoscopy and Endosurgery Robotics, Laparoscopy & Endosurgery How to preserve bladder neck during robotic radical prostatectomy? Abdullah Erdem Canda* Department of Urology, Yildirim Beyazit
Robotics, Laparoscopy and Endosurgery Robotics, Laparoscopy & Endosurgery How to preserve bladder neck during robotic radical prostatectomy? Abdullah Erdem Canda* Department of Urology, Yildirim Beyazit
Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation
 Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 61-70, Abr.-Jun., 2006 Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 61-70, Abr.-Jun., 2006 Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
LAPAROSCOPIC RADICAL NEPHRECTOMY FOR LARGE (GREATER THAN 7 CM, T2) RENAL TUMORS
 0022-5347/04/1726-2172/0 Vol. 172, 2172 2176, December 2004 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2004 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000140961.53335.04 LAPAROSCOPIC
0022-5347/04/1726-2172/0 Vol. 172, 2172 2176, December 2004 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2004 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000140961.53335.04 LAPAROSCOPIC
Challenges in RCC surgery. Treatment Goals. Surgical challenges. Management options in VHL associated RCCs
 Management options in VHL associated RCCs Challenges in RCC surgery JJ PATARD, MD, PhD Paris XI University Observation, Radical nephrectomy, Renal parenchymal sparing surgery, Open, laparoscopic, robotic
Management options in VHL associated RCCs Challenges in RCC surgery JJ PATARD, MD, PhD Paris XI University Observation, Radical nephrectomy, Renal parenchymal sparing surgery, Open, laparoscopic, robotic
Indications for Surgical Removal of Adrenal Glands
 The adrenal glands are orange-colored endocrine glands which are located on the top of both kidneys. The adrenal glands are triangular shaped and measure about one-half inch in height and 3 inches in length.
The adrenal glands are orange-colored endocrine glands which are located on the top of both kidneys. The adrenal glands are triangular shaped and measure about one-half inch in height and 3 inches in length.
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
Alexander C Vlantis. Selective Neck Dissection 33
 05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
Organ-Preserving Endoscopic Kidney Cancer Resection
 european urology 50 (2006) 732 737 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Organ-Preserving Endoscopic Kidney Cancer Resection Elmar Heinrich, Tobias
european urology 50 (2006) 732 737 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Organ-Preserving Endoscopic Kidney Cancer Resection Elmar Heinrich, Tobias
RPLND: Tips and Tricks
 RPLND: Tips and Tricks Andrew J. Stephenson, MD FACS FRCS(C) Director, Center for Urologic Oncology Glickman Urological & Kidney Institute Cleveland Clinic, Cleveland, OH RPLND: Keys to success Knowledge
RPLND: Tips and Tricks Andrew J. Stephenson, MD FACS FRCS(C) Director, Center for Urologic Oncology Glickman Urological & Kidney Institute Cleveland Clinic, Cleveland, OH RPLND: Keys to success Knowledge
Guidelines for Laparoscopic Resection of Curable Colon and Rectal Cancer
 SAGES Society of American Gastrointestinal and Endoscopic Surgeons http://www.sages.org Guidelines for Laparoscopic Resection of Curable Colon and Rectal Cancer Author : SAGES Webmaster PREAMBLE The following
SAGES Society of American Gastrointestinal and Endoscopic Surgeons http://www.sages.org Guidelines for Laparoscopic Resection of Curable Colon and Rectal Cancer Author : SAGES Webmaster PREAMBLE The following
THE FACTS YOU NEED TO KNOW
 PHEOCHROMOCYTOMA THE FACTS YOU NEED TO KNOW Pheochromocytoma is a part of the pheochromocytoma and paraganglioma group of syndromes. A pheochromocytoma is a tumor arising in the adrenal gland medulla.
PHEOCHROMOCYTOMA THE FACTS YOU NEED TO KNOW Pheochromocytoma is a part of the pheochromocytoma and paraganglioma group of syndromes. A pheochromocytoma is a tumor arising in the adrenal gland medulla.
Retroperitoneoscopic Radical Nephrectomy: Initial Experience
 Retroperitoneoscopic Radical Nephrectomy: Initial Experience A. Hasegan 1, D. Bratu 2, V. Pirvut 1, I. Mihai 1, N. Grigore 1 1 Lucian Blaga University of Sibiu, Department of Urology 2 Lucian Blaga University
Retroperitoneoscopic Radical Nephrectomy: Initial Experience A. Hasegan 1, D. Bratu 2, V. Pirvut 1, I. Mihai 1, N. Grigore 1 1 Lucian Blaga University of Sibiu, Department of Urology 2 Lucian Blaga University
Differences in Left and Right Laparoscopic Adrenalectomy
 SCIENTIFIC PAPER Differences in Left and Right Laparoscopic Adrenalectomy Jocelyn M. Rieder, MD, Alan A. Nisbet, MD, Melanie C. Wuerstle, MD, Viet Q. Tran, MD, Eric O. Kwon, MD, Gary W. Chien, MD ABSTRACT
SCIENTIFIC PAPER Differences in Left and Right Laparoscopic Adrenalectomy Jocelyn M. Rieder, MD, Alan A. Nisbet, MD, Melanie C. Wuerstle, MD, Viet Q. Tran, MD, Eric O. Kwon, MD, Gary W. Chien, MD ABSTRACT
Department of Urology, Columbia University School of Medicine, New York, NY
 Laparoscopic Partial Nephrectomy Jaime Landman, MD Associate Professor of Urology Director of Minimally Invasive Urology Columbia University Department of Urology Department of Urology, Columbia University
Laparoscopic Partial Nephrectomy Jaime Landman, MD Associate Professor of Urology Director of Minimally Invasive Urology Columbia University Department of Urology Department of Urology, Columbia University
Laparoscopic total mesorectal excision (TME) with electric hook for rectal cancer
 Technical Note Page 1 of 8 Laparoscopic total mesorectal excision (TME) with electric hook for rectal cancer Gong Chen, Rong-Xin Zhang, Zhi-Tao Xiao Department of Colorectal Surgery, Sun Yat-sen University
Technical Note Page 1 of 8 Laparoscopic total mesorectal excision (TME) with electric hook for rectal cancer Gong Chen, Rong-Xin Zhang, Zhi-Tao Xiao Department of Colorectal Surgery, Sun Yat-sen University
NIH Public Access Author Manuscript Eur Urol. Author manuscript; available in PMC 2009 March 1.
 NIH Public Access Author Manuscript Published in final edited form as: Eur Urol. 2008 March ; 53(3): 514 521. doi:10.1016/j.eururo.2007.09.047. ROBOTIC PARTIAL NEPHRECTOMY FOR COMPLEX RENAL TUMORS: SURGICAL
NIH Public Access Author Manuscript Published in final edited form as: Eur Urol. 2008 March ; 53(3): 514 521. doi:10.1016/j.eururo.2007.09.047. ROBOTIC PARTIAL NEPHRECTOMY FOR COMPLEX RENAL TUMORS: SURGICAL
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
IVC THROMBECTOMY: OPEN
 IVC THROMBECTOMY: OPEN Gennady Bratslavsky, M.D. Professor and Chairman Department of Urology SUNY Upstate Medical University Syracuse, NY Disclosures None I am not an ideal candidate to argue for open
IVC THROMBECTOMY: OPEN Gennady Bratslavsky, M.D. Professor and Chairman Department of Urology SUNY Upstate Medical University Syracuse, NY Disclosures None I am not an ideal candidate to argue for open
Kidney Case # 1 DISCHARGE SUMMARY. Date: 08/25/2010. Admitted: 08/19/2010 Discharged: 08/25/2010
 DISCHARGE SUMMARY Kidney Case # 1 Date: 08/25/2010 Admitted: 08/19/2010 Discharged: 08/25/2010 Admission Diagnosis: Left renal mass, suspicious, with renal cell carcinoma Discharge Diagnosis: Left renal
DISCHARGE SUMMARY Kidney Case # 1 Date: 08/25/2010 Admitted: 08/19/2010 Discharged: 08/25/2010 Admission Diagnosis: Left renal mass, suspicious, with renal cell carcinoma Discharge Diagnosis: Left renal
RADICAL CYSTECTOMY. Solutions for minimally invasive urologic surgery
 RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation 3D HD Vision 3D HD visualization facilitates accurate
RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation 3D HD Vision 3D HD visualization facilitates accurate
Procedure related complications and how to prevent them
 Procedure related complications and how to prevent them Rama Jayanthi, M.D. Section of Urology Nationwide Children s Hospital The Ohio State University Retroperitoneoscopic surgery Inadvertent peritoneal
Procedure related complications and how to prevent them Rama Jayanthi, M.D. Section of Urology Nationwide Children s Hospital The Ohio State University Retroperitoneoscopic surgery Inadvertent peritoneal
Robotic distal ureterectomy with psoas hitch and ureteroneocystostomy: Surgical technique and outcomes
 Asian Journal of Urology (2015) 2, 123e127 HOSTED BY Available online at www.sciencedirect.com ScienceDirect journal homepage: www.elsevier.com/locate/ajur CASE REPORT Robotic distal with psoas hitch and
Asian Journal of Urology (2015) 2, 123e127 HOSTED BY Available online at www.sciencedirect.com ScienceDirect journal homepage: www.elsevier.com/locate/ajur CASE REPORT Robotic distal with psoas hitch and
Management of pediatric pheochromocytoma
 Jemis, 4 (1) 2016 Management of pediatric pheochromocytoma A review of the literature C. Muriello C. Gambardella G. Siciliano G. Izzo E. Tartaglia D. Esposito S. Reina R. Patrone L. Santini G. Conzo Table
Jemis, 4 (1) 2016 Management of pediatric pheochromocytoma A review of the literature C. Muriello C. Gambardella G. Siciliano G. Izzo E. Tartaglia D. Esposito S. Reina R. Patrone L. Santini G. Conzo Table
Subtotal Adrenalectomy for Phaeochromocytoma 69. Subtotal Adrenalectomy for Phaeochromocytoma in Multiple Endocrine Neoplasia Type 2A
 Subtotal Adrenalectomy for Phaeochromocytoma 69 6 Subtotal Adrenalectomy for Phaeochromocytoma in Multiple Endocrine Neoplasia Type 2A 70 Chapter 6 Abstract Objective: To describe our surgical technique
Subtotal Adrenalectomy for Phaeochromocytoma 69 6 Subtotal Adrenalectomy for Phaeochromocytoma in Multiple Endocrine Neoplasia Type 2A 70 Chapter 6 Abstract Objective: To describe our surgical technique
Lower pole approach in retroperitoneal laparoscopic radical nephrectomy: a new approach for the management of renal vascular pedicle
 Yuan et al. World Journal of Surgical Oncology (2018) 16:31 https://doi.org/10.1186/s12957-018-1324-7 RESEARCH Open Access Lower pole approach in retroperitoneal laparoscopic radical nephrectomy: a new
Yuan et al. World Journal of Surgical Oncology (2018) 16:31 https://doi.org/10.1186/s12957-018-1324-7 RESEARCH Open Access Lower pole approach in retroperitoneal laparoscopic radical nephrectomy: a new
New technologies in Endocrine Surgery
 New technologies in Endocrine Surgery 1. Nerve monitoring 2. New technologies in Endocrine Surgery Jessica E. Gosnell MD Post graduate course in General Surgery March 28, 2012 1 2 Recurrent laryngeal nerve
New technologies in Endocrine Surgery 1. Nerve monitoring 2. New technologies in Endocrine Surgery Jessica E. Gosnell MD Post graduate course in General Surgery March 28, 2012 1 2 Recurrent laryngeal nerve
ADRENAL INCIDENTALOMA. Jamii St. Julien
 ADRENAL INCIDENTALOMA Jamii St. Julien Outline Definition Differential Evaluation Treatment Follow up Questions Case Definition The phenomenon of detecting an otherwise unsuspected adrenal mass on radiologic
ADRENAL INCIDENTALOMA Jamii St. Julien Outline Definition Differential Evaluation Treatment Follow up Questions Case Definition The phenomenon of detecting an otherwise unsuspected adrenal mass on radiologic
Pheochromocytoma AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGY ILLINOIS CHAPTER OCTOBER 13, 2018
 Pheochromocytoma AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGY ILLINOIS CHAPTER OCTOBER 13, 2018 Steven A. De Jong, M.D., FACS, FACE Professor and Vice Chair of Surgery Chief, Division of General Surgery
Pheochromocytoma AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGY ILLINOIS CHAPTER OCTOBER 13, 2018 Steven A. De Jong, M.D., FACS, FACE Professor and Vice Chair of Surgery Chief, Division of General Surgery
Vincenzo Ficarra 1,2,3. Associate Editor BJU International
 Partial Nephrectomy for RCC Vincenzo Ficarra 1,2,3 1 Director Department of Urology University of Udine, Italy 2 Associate Editor BJU International 3 Scientific Director OLV Robotic Surgery Institute,
Partial Nephrectomy for RCC Vincenzo Ficarra 1,2,3 1 Director Department of Urology University of Udine, Italy 2 Associate Editor BJU International 3 Scientific Director OLV Robotic Surgery Institute,
Retroperitoneal Laparoscopic Radical Nephroureterectomy for High Urothelial Tumours
 Retroperitoneal Laparoscopic Radical Nephroureterectomy for High Urothelial Tumours A. Hașegan 1, V. Pîrvuț 1, I. Mihai 1, N. Grigore 1 1 Lucian Blaga University of Sibiu, Faculty of Medicine Clinical
Retroperitoneal Laparoscopic Radical Nephroureterectomy for High Urothelial Tumours A. Hașegan 1, V. Pîrvuț 1, I. Mihai 1, N. Grigore 1 1 Lucian Blaga University of Sibiu, Faculty of Medicine Clinical
THE HIGHS AND LOWS OF ADRENAL GLAND PATHOLOGY
 THE HIGHS AND LOWS OF ADRENAL GLAND PATHOLOGY Symptoms of Adrenal Gland Disorders 2 Depends on whether it is making too much or too little hormone And on what you Google! Symptoms include obesity, skin
THE HIGHS AND LOWS OF ADRENAL GLAND PATHOLOGY Symptoms of Adrenal Gland Disorders 2 Depends on whether it is making too much or too little hormone And on what you Google! Symptoms include obesity, skin
da Vinci Prostatectomy
 da Vinci Prostatectomy Justin T. Lee MD Director of Robotic Surgery Urology Associates of North Texas (UANT) USMD Prostate Cancer Center (www.usmdpcc.com) Prostate Cancer Facts Prostate cancer Leading
da Vinci Prostatectomy Justin T. Lee MD Director of Robotic Surgery Urology Associates of North Texas (UANT) USMD Prostate Cancer Center (www.usmdpcc.com) Prostate Cancer Facts Prostate cancer Leading
Superior mediastinal paraganglioma associated with von Hippel-Lindau syndrome: report of a case
 Takahashi et al. World Journal of Surgical Oncology 2014, 12:74 WORLD JOURNAL OF SURGICAL ONCOLOGY CASE REPORT Open Access Superior mediastinal paraganglioma associated with von Hippel-Lindau syndrome:
Takahashi et al. World Journal of Surgical Oncology 2014, 12:74 WORLD JOURNAL OF SURGICAL ONCOLOGY CASE REPORT Open Access Superior mediastinal paraganglioma associated with von Hippel-Lindau syndrome:
Surgical Management of VHL-related Renal Cancers. Disclosures. Glossary. Overview. none
 Surgical Management of VHL-related Renal Cancers Disclosures Presentation to the VHL Family Alliance Annual Meeting, Denver, CO October 20, 2018 none Adam R. Metwalli, M.D. Professor & Chief, Division
Surgical Management of VHL-related Renal Cancers Disclosures Presentation to the VHL Family Alliance Annual Meeting, Denver, CO October 20, 2018 none Adam R. Metwalli, M.D. Professor & Chief, Division
Laparoscopic Right Colectomy
 Laparoscopic Right Colectomy Shawnee Mission Medical Center February 22, 2011 Hi, and welcome to the program. My name is Dr. Sanjay Thekkeurumbil, and I m a colorectal surgeon at Shawnee Mission Medical
Laparoscopic Right Colectomy Shawnee Mission Medical Center February 22, 2011 Hi, and welcome to the program. My name is Dr. Sanjay Thekkeurumbil, and I m a colorectal surgeon at Shawnee Mission Medical
Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery
 SCIENTIFIC PAPER Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery Steven J. Binenbaum, MD, Michael A. Goldfarb, MD ABSTRACT Background: Inadvertent enterotomy (IE) in laparoscopic abdominal
SCIENTIFIC PAPER Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery Steven J. Binenbaum, MD, Michael A. Goldfarb, MD ABSTRACT Background: Inadvertent enterotomy (IE) in laparoscopic abdominal
The abdominal Esophagus, Stomach and the Duodenum. Prof. Oluwadiya KS
 The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
Kidney Case 1 SURGICAL PATHOLOGY REPORT
 Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Financial and Other Disclosures
 Financial and Other Disclosures Off-label use of drugs, devices, or other agents: None Data from IRB-approved human research is not presented I have the following financial interests or relationships to
Financial and Other Disclosures Off-label use of drugs, devices, or other agents: None Data from IRB-approved human research is not presented I have the following financial interests or relationships to
Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit Urinary Diversion
 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Study of the Month Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit
available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Study of the Month Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit
Ruijin robotic thoracic surgery: S segmentectomy of the left upper lobe
 Case Report Page 1 of 5 Ruijin robotic thoracic surgery: S 1+2+3 segmentectomy of the left upper lobe Han Wu, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Hailei Du, Dingpei Han, Kai Chen,
Case Report Page 1 of 5 Ruijin robotic thoracic surgery: S 1+2+3 segmentectomy of the left upper lobe Han Wu, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Hailei Du, Dingpei Han, Kai Chen,
Transperitoneal Laparoscopic Nephrectomy for Autosomal Dominant Polycystic Kidney Disease
 SCIENTIFIC PAPER Transperitoneal Laparoscopic Nephrectomy for Autosomal Dominant Polycystic Kidney Disease Grégory Verhoest, MD, Arnaud Delreux, MD, Romain Mathieu, MD, Jean-Jacques Patard, MD, Cécile
SCIENTIFIC PAPER Transperitoneal Laparoscopic Nephrectomy for Autosomal Dominant Polycystic Kidney Disease Grégory Verhoest, MD, Arnaud Delreux, MD, Romain Mathieu, MD, Jean-Jacques Patard, MD, Cécile
Who are Candidates for Laparoscopic or Open Radical Nephrectomy. Arieh Shalhav
 Who are Candidates for Laparoscopic or Open Radical Nephrectomy Arieh Shalhav Fritz Duda Chair of Urologic Surgery Professor of Surgery and the Comprehensive Cancer Research Center Who are Candidates for
Who are Candidates for Laparoscopic or Open Radical Nephrectomy Arieh Shalhav Fritz Duda Chair of Urologic Surgery Professor of Surgery and the Comprehensive Cancer Research Center Who are Candidates for
Florida Cancer Specialist & Research Institute, Sebastian and Vero Beach, Fl, USA 3
 Evaluation of Perioperative Outcomes and Renal Function after Robotic Assisted Laparoscopic Partial Nephrectomy Off/On Clamp: Comparison of ct1a versus ct1b Renal Masses Hugo H Davila 1-4*, Raul E Storey
Evaluation of Perioperative Outcomes and Renal Function after Robotic Assisted Laparoscopic Partial Nephrectomy Off/On Clamp: Comparison of ct1a versus ct1b Renal Masses Hugo H Davila 1-4*, Raul E Storey
Laparoendoscopic Single-Site Nephrectomy Using Standard Laparoscopic Instruments
 Laparoendoscopic Single-Site Nephrectomy Using Standard Laparoscopic Instruments Our Initial Experience LAPAROSCOPIC UROLOGY Alireza Aminsharifi, Bahman Goshtasbi, Firoozeh Afsar Department of Urology,
Laparoendoscopic Single-Site Nephrectomy Using Standard Laparoscopic Instruments Our Initial Experience LAPAROSCOPIC UROLOGY Alireza Aminsharifi, Bahman Goshtasbi, Firoozeh Afsar Department of Urology,
Cover Page. The following handle holds various files of this Leiden University dissertation:
 Cover Page The following handle holds various files of this Leiden University dissertation: http://hdl.handle.net/1887/6119 Author: Spruit, E.N. Title: Increasing the efficiency of laparoscopic surgical
Cover Page The following handle holds various files of this Leiden University dissertation: http://hdl.handle.net/1887/6119 Author: Spruit, E.N. Title: Increasing the efficiency of laparoscopic surgical
Accessory Glands of Digestive System
 Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
Laparoscopic adrenalectomy for pheochromocytoma is more difficult compared to other adrenal tumors
 Original paper Videosurgery Laparoscopic adrenalectomy for pheochromocytoma is more difficult compared to other adrenal tumors Michał Natkaniec 1, Michał Pędziwiatr 1, Mateusz Wierdak 1,2, Magdalena Białas
Original paper Videosurgery Laparoscopic adrenalectomy for pheochromocytoma is more difficult compared to other adrenal tumors Michał Natkaniec 1, Michał Pędziwiatr 1, Mateusz Wierdak 1,2, Magdalena Białas
Minimally Invasive Esophagectomy
 Minimally Invasive Esophagectomy M A R K B E R R Y, M D A S S O C I AT E P R O F E S S O R D E PA R T M E N T OF C A R D I O T H O R A C I C S U R G E R Y S TA N F O R D U N I V E R S I T Y S E P T E M
Minimally Invasive Esophagectomy M A R K B E R R Y, M D A S S O C I AT E P R O F E S S O R D E PA R T M E N T OF C A R D I O T H O R A C I C S U R G E R Y S TA N F O R D U N I V E R S I T Y S E P T E M
MDCT signs differentiating retroperitoneal and intraperitoneal lesions- diagnostic pearls
 MDCT signs differentiating retroperitoneal and intraperitoneal lesions- diagnostic pearls Poster No.: C-0987 Congress: ECR 2015 Type: Educational Exhibit Authors: D. V. Bhargavi, R. Avantsa, P. Kala; Bangalore/IN
MDCT signs differentiating retroperitoneal and intraperitoneal lesions- diagnostic pearls Poster No.: C-0987 Congress: ECR 2015 Type: Educational Exhibit Authors: D. V. Bhargavi, R. Avantsa, P. Kala; Bangalore/IN
Oncourology COMPLICATIONS OF PARTIAL NEPHRECTOMY AT OPERATIVE TREATMENT OF RENAL CELL CARCINOMA
 1 Oncourology COMPLICATIONS OF PARTIAL NEPHRECTOMY AT OPERATIVE TREATMENT OF RENAL CELL CARCINOMA Address: Eduard Oleksandrovych Stakhovsky, 03022, Kyiv, Lomonosova Str., 33/43, National Cancer Institute
1 Oncourology COMPLICATIONS OF PARTIAL NEPHRECTOMY AT OPERATIVE TREATMENT OF RENAL CELL CARCINOMA Address: Eduard Oleksandrovych Stakhovsky, 03022, Kyiv, Lomonosova Str., 33/43, National Cancer Institute
Thyroidectomy. Siu Kwan Ng. Modified Radical Neck Dissection Type II 47
 06 Thyroidectomy Siu Kwan Ng Modified Radical Neck Dissection Type II 47 Thyroidectomy STEP 1. EXPOSING THE THYROID GLAND The collar incision Figure 1 (curvilinear skin crease incision) is made at 1.5-2
06 Thyroidectomy Siu Kwan Ng Modified Radical Neck Dissection Type II 47 Thyroidectomy STEP 1. EXPOSING THE THYROID GLAND The collar incision Figure 1 (curvilinear skin crease incision) is made at 1.5-2
Laparoscopic Adrenalectomy: Surgical Technique
 WJOLS Laparoscopic drenalectomy: Surgical Technique REVIEW RTICLE Laparoscopic drenalectomy: Surgical Technique Thawatchai Tullavardhana Department of Surgery, Faculty of Medicine, Srinakarinwirot University,
WJOLS Laparoscopic drenalectomy: Surgical Technique REVIEW RTICLE Laparoscopic drenalectomy: Surgical Technique Thawatchai Tullavardhana Department of Surgery, Faculty of Medicine, Srinakarinwirot University,
What is the role of partial nephrectomy in the context of active surveillance and renal ablation?
 What is the role of partial nephrectomy in the context of active surveillance and renal ablation? Dogu Teber Department of Urology University Hospital Heidelberg Coming from Heidelberg obligates to speak
What is the role of partial nephrectomy in the context of active surveillance and renal ablation? Dogu Teber Department of Urology University Hospital Heidelberg Coming from Heidelberg obligates to speak
EndoRelease ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM
 EndoRelease ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM SURGICAL TECHNIQUE Up p e r Ex t r e m i t y So l u t i o n s ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM Description: The EndoRelease Endoscopic Cubital
EndoRelease ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM SURGICAL TECHNIQUE Up p e r Ex t r e m i t y So l u t i o n s ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM Description: The EndoRelease Endoscopic Cubital
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of laparoscopic partial nephrectomy 308 Introduction This overview has been
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of laparoscopic partial nephrectomy 308 Introduction This overview has been
Technique of Laparoscopic-Endoscopic Single-Site Surgery Radical Nephrectomy
 EUROPEAN UROLOGY 56 (2009) 644 650 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Technique of Laparoscopic-Endoscopic Single-Site Surgery Radical Nephrectomy
EUROPEAN UROLOGY 56 (2009) 644 650 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Technique of Laparoscopic-Endoscopic Single-Site Surgery Radical Nephrectomy
Robot Assisted Rectopexy
 1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
Single-stage laparoscopic surgery for bilateral organ tumors using a transumbilical approach with a zigzag incision: a report of two cases
 Kato et al. BMC Urology (2018) 18:28 https://doi.org/10.1186/s12894-018-0343-6 CASE REPORT Single-stage laparoscopic surgery for bilateral organ tumors using a transumbilical approach with a zigzag incision:
Kato et al. BMC Urology (2018) 18:28 https://doi.org/10.1186/s12894-018-0343-6 CASE REPORT Single-stage laparoscopic surgery for bilateral organ tumors using a transumbilical approach with a zigzag incision:
Guidelines, Policies and Statements D5 Statement on Abdominal Scanning
 Guidelines, Policies and Statements D5 Statement on Abdominal Scanning Disclaimer and Copyright The ASUM Standards of Practice Board have made every effort to ensure that this Guideline/Policy/Statement
Guidelines, Policies and Statements D5 Statement on Abdominal Scanning Disclaimer and Copyright The ASUM Standards of Practice Board have made every effort to ensure that this Guideline/Policy/Statement
Alexander C Vlantis. Total Laryngectomy 57
 07 Total Laryngectomy Alexander C Vlantis Total Laryngectomy 57 Total Laryngectomy STEP 1 INCISION AND POSITION OF STOMA A superiorly based apron flap incision is marked with the horizontal limb placed
07 Total Laryngectomy Alexander C Vlantis Total Laryngectomy 57 Total Laryngectomy STEP 1 INCISION AND POSITION OF STOMA A superiorly based apron flap incision is marked with the horizontal limb placed
Off-clamp robot-assisted partial nephrectomy for complex renal tumors
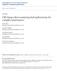 Washington University School of Medicine Digital Commons@Becker Open Access Publications 8-30-2012 Off-clamp robot-assisted partial nephrectomy for complex renal tumors Eric H. Kim Youssef S. Tanagho Gurdarshan
Washington University School of Medicine Digital Commons@Becker Open Access Publications 8-30-2012 Off-clamp robot-assisted partial nephrectomy for complex renal tumors Eric H. Kim Youssef S. Tanagho Gurdarshan
Anesthetic Management of a Child with Malignant Hypertension Secondary to a Renal Paraganglioma and Concomitant Renal Artery Stenosis
 Anesthetic Management of a Child with Malignant Hypertension Secondary to a Renal Paraganglioma and Concomitant Renal Artery Stenosis Moderators: Joel Stockman, MD, Ellen Choi, MD Objectives: 1. Identify
Anesthetic Management of a Child with Malignant Hypertension Secondary to a Renal Paraganglioma and Concomitant Renal Artery Stenosis Moderators: Joel Stockman, MD, Ellen Choi, MD Objectives: 1. Identify
Robot-assisted laparoscopic rectal resection
 Journal of Visceral Surgery (2014) 151, 377 387 Available online at ScienceDirect www.sciencedirect.com SURGICAL TECHNIQUE Robot-assisted laparoscopic rectal resection A. Valverde, N. Goasguen, O. Oberlin
Journal of Visceral Surgery (2014) 151, 377 387 Available online at ScienceDirect www.sciencedirect.com SURGICAL TECHNIQUE Robot-assisted laparoscopic rectal resection A. Valverde, N. Goasguen, O. Oberlin
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
Bilateral Renal Angiomyolipomas with Invasion of the Renal Vein: A Case Report
 Case Study TheScientificWorldJOURNAL (2008) 8, 145 148 TSW Urology ISSN 1537-744X; DOI 10.1100/tsw.2008.29 Bilateral Renal Angiomyolipomas with Invasion of the Renal Vein: A Case Report C. Blick, N. Ravindranath,
Case Study TheScientificWorldJOURNAL (2008) 8, 145 148 TSW Urology ISSN 1537-744X; DOI 10.1100/tsw.2008.29 Bilateral Renal Angiomyolipomas with Invasion of the Renal Vein: A Case Report C. Blick, N. Ravindranath,
