CT-Guided Transthoracic Needle Aspiration Biopsy of Small ( 20 mm) Solitary Pulmonary Nodules
|
|
|
- Susan Nichols
- 6 years ago
- Views:
Transcription
1 Yoshiharu Ohno 1 Hiroto Hatabu 2 Daisuke Takenaka 1 Takanori Higashino 1 Hirokazu Watanabe 1 Chiho Ohbayashi 3 Kazuro Sugimura 1 Received May 16, 2002; accepted after revision October 30, Department of Radiology, Kobe University Graduate School of Medicine, Kusunoki-cho, Chuo-ku, Kobe, Hyogo , Japan. Address correspondence to Y. Ohno. 2 Department of Radiology, Beth Israel Deaconess Medical Center, 330 Brookline Ave., Boston, MA Division of Pathology, Kobe University Hospital, Kusanoki-cho, Chuo-ku, Kobe, Hyogo , Japan. AJR 2003;180: X/03/ American Roentgen Ray Society CT-Guided Transthoracic Needle Aspiration Biopsy of Small ( 20 mm) Solitary Pulmonary Nodules OBJECTIVE. The purpose of our study was to determine the diagnostic accuracy and to analyze the factors influencing the diagnostic accuracy and incidences of pneumothorax and chest tube insertion rates for percutaneous CT-guided needle biopsy of small ( 20 mm) solitary pulmonary nodules. SUBJECTS AND METHODS. One hundred sixty-two patients with 162 small solitary pulmonary nodules underwent CT-guided transthoracic needle aspiration biopsy. The overall diagnostic accuracy, pneumothorax rate, and chest tube insertion rate were calculated. Factors influencing the diagnostic accuracy and pneumothorax rate were statistically evaluated. Influencing factors, diagnostic accuracies, pneumothorax rates, and chest tube insertion rates were statistically compared. RESULTS. Overall diagnostic accuracy, pneumothorax rate, and chest tube insertion rate were 77.2%, 28.4%, and 2.5%, respectively. Diagnostic accuracy was significantly affected by length of needle path and lesion size ( p < 0.05). The pneumothorax rate was significantly affected by the percentage of predicted forced expiratory volume in 1 sec, the number of punctures, and the needle path length ( p < 0.05). The chest tube insertion rate was significantly affected by the number of punctures ( p < 0.05). For diagnostic accuracy, needle path lengths of 40 mm or less and lesion sizes greater than 10 mm were significantly more accurate than other factors ( p < 0.05). For pneumothorax rates, a percentage of predicted forced expiratory volume in 1 sec of greater than 70%, a single puncture, and a needle path length of 40 mm or less were significantly lower than other factors ( p < 0.05). CONCLUSION. CT-guided transthoracic needle aspiration biopsy is a useful diagnostic tool for small solitary pulmonary nodules smaller than 20 mm in diameter. The diagnostic accuracy is significantly improved for large (> 10 mm) lesion size and short ( 40 mm) needle path length. R ecently, academic and public interest in lung cancer screening using low-dose CT has grown drastically. With the increased use of lung cancer screening with helical CT, an increased incidence of small lung cancer, especially small adenocarcinoma, has been reported in some countries [1 4]. According to current reports of CT screening for early lung cancer, the detection of small lung cancers may improve the prognosis of lung cancer patients [5 9]. However, the increased number of small solitary pulmonary nodules detected at CT screening has created a new problem in management. Repeated CT examination with evaluation of volume change of the small solitary pulmonary nodule is one of the solutions for management of solitary pulmonary nodules [10, 11]. However, when an increase in solitary pulmonary nodule size is recognized on follow-up CT examination, a pathologic diagnosis is mandated. Data about diagnostic accuracy and incidences of pneumothorax and chest tube insertion of percutaneous CT-guided needle biopsy in these cases of small solitary pulmonary nodules would provide critical information as to how to manage each case with a growing small solitary pulmonary nodule of 2 cm or less in diameter. Percutaneous CT-guided needle biopsy of the lung is a relatively safe and accurate method of diagnosing benign and malignant lesions of the chest [12 19]. Various reports have analyzed factors thought to influence the diagnostic accuracy and the complication rate of CT-guided transthoracic needle aspiration biopsy [15 20]. The diagnostic accuracy and the frequency of pneumothorax in CT-guided transthoracic needle aspiration biopsy are affected by many fac- AJR:180, June
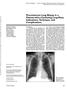
2 TABLE 1 Characteristics of 97 Male and 65 Female Patients Characteristic No. Lesion size (mm) > 80 7 Distance to pleura (mm) Needle approach Patient supine 86 Patient prone 76 Location Right upper lobe 36 Right middle lobe 18 Right lower lobe 37 Left upper lobe 38 Left lower lobe 33 Needle pleural angle ( ) No. of punctures % of predicted forced expiratory volume in 1 sec > Note. Patients were years old (mean ± SD, 66.6 ± 11.9 years). Ohno et al. tors, including size, depth, and number of needle paths. However, to our knowledge no major reports have evaluated factors influencing the diagnostic accuracy and the pneumothorax rate of small solitary nodules less than 20 mm in diameter. The purpose of our study was to provide basic data about diagnostic accuracy and incidence of pneumothorax and chest tube insertion with respect to percutaneous CT-guided needle biopsy of small solitary pulmonary nodules of 20 mm or less in diameter. Subjects and Methods Patients One hundred sixty-two patients with 162 small solitary pulmonary nodules with diameters of less than 20 mm 97 men and 65 women who were years old (mean ± SD, 67 ± 12 years) underwent CT-guided transthoracic needle aspiration biopsy in our hospital between April 1996 and July Patients characteristics are shown in Table 1. Diameters of all nodules, including adjacent ground-glass opacities, were measured on lung window settings. All patients underwent posteroanterior and lateral chest radiography in the erect position before the biopsy procedures. Follow-up erect posteroanterior and lateral chest radiographs were obtained immediately after biopsy, 2 4 hr later, and 24 hr later for evaluation of pneumothorax. The placement of a chest catheter or tube was considered in the event a patient became symptomatic or a large (> 30%) pneumothorax was found. Patients were generally observed, and the size of the pneumothorax was reevaluated every 7 days after the last follow-up examination if the patient was asymptomatic. However, if the pneumothorax increased (> 30%) on follow-up chest radiographs or if the patient became symptomatic or was found to have a large pneumothorax, a chest catheter or tube was placed. Pneumothorax size was determined on the basis of the criteria established by Rhea et al. [21]. Pulmonary function tests were performed according to American Thoracic Society standards [22, 23]. Pulmonary function tests and electrocardiography were performed before the CT-guided biopsy procedure (mean, 7 ± 2 days). The institutional review board approved the study, and informed consent was obtained from all patients before biopsy. CT-Guided Biopsy Techniques and Procedures For CT-guided biopsy, 62 examinations were conducted on a nonhelical CT scanner (TCT 300, Toshiba, Tokyo, Japan), and 100 examinations were conducted on a single-detector helical CT scanner (Somatom Plus 4 VB 40, Siemens, Forchheim, Germany) by two radiologists experienced in thoracic and interventional radiology. The scanning parameters of the TCT 300 scanner were 120 kvp, 200 ma, 3- to 5-mm collimation, and 3- to 5-mm section thickness. The scanning parameters of the Somatom Plus 4 VB 40 scanner were 120 kvp, ma, 3- to 5-mm collimation, 3- to 5-mm section thickness, and a table speed of 3 10 mm/sec (pitch, 1 2). Thirty-five biopsies were performed with IV-injected contrast media to avoid necrotic tissue, and cystic lesions were identified using prior diagnostic contrast-enhanced CT. A total of 40 ml of iodinated contrast agent (Omnipaque 300 [iohexol], Daiichi Seiyaku, Tokyo, Japan) was administrated IV at 2 ml/sec by a power injector (Auto Enhance-50, Nemoto, Tokyo, Japan) with a scanning delay of 20 sec on conventional CT. The remaining 60 ml of iodinated contrast agent was administrated at 1 ml/ sec during the initial puncture and check of the needle tip in the tumor. Unenhanced CT scans were reviewed with a lung window setting (window width, 1600 H; window level, 600 H) or with a mediastinal window setting (window width, 450 H; window level, 30 H). The contrast-enhanced CT scans were reviewed with a mediastinal window setting (window width, 450 H; window level, 40 H) for evaluation of the relationship between needle tip and intratumoral necrosis. All CT-guided aspiration cytologic examinations were performed with 9- to 15-cm, 22-gauge Westcott needles (MD TECH, Gainesville, FL). All biopsies were performed with the patient prone or supine, depending on the proximity of the lesion to the chest wall and considering the number of pleural surfaces to be crossed by the needle in choosing the biopsy route. With the patient in the prone position, the shoulders were abducted to move the scapulae laterally. A pillow was routinely placed under the patient s chest to open the intercostal spaces posteriorly, thereby permitting easier access to the lesions. The patient was instructed to stop breathing after normal inspiration at functional residual capacity. The importance of breath-holding was explained to each patient, and the technique was practiced before the procedure. The CT-guided biopsy procedure was as follows. CT images were obtained from the lung apices to the diaphragm for the detection of solitary pulmonary nodules at end-inspiration. The center of the lesion was positioned at the CT landmark using a radiopaque grid on the patient s skin. CT images were obtained again, and the puncture point was determined after we measured the distance from the skin surface to the pleura, the length of needle path, and the smallest angle between the pleura and the needle on the cathode-ray tube monitor of the imager (Fig. 1A). The needle path length was the length between the skin surface and the center of the solitary pulmonary nodule. The distance to the pleura was the distance from the skin surface of the initial puncture to the pleura. The needle pleural angle was formed between the skin surface of the initial puncture and the biopsy needle. The initial puncture was performed without penetrating the pleura. CT images were obtained to check the course of the biopsy needle (Fig. 1B). If the nodule was on the extended course of the needle track, the biopsy procedure was continued. If the nodule was not on the extended course of the needle track, the course or puncture site was changed. When the nodule was penetrated, the needle tip was checked and an aspiration specimen was obtained (Fig. 1C). The specimen was placed in 99% ethyl alcohol for cytologic examination. Then the on-site cytologist evalu AJR:180, June 2003
3 CT-Guided Biopsy of Solitary Pulmonary Nodules dicted forced expiratory volume in 1 sec ( 50%, 51 60%, 61 70%, 71 80%, and 81%). All quantitative data were evaluated on the cathode-ray tube monitor of the CT imager by two radiologists. The mean value was accepted for all quantitative data. Diagnostic accuracy and pneumothorax rate were statistically compared for each influencing factor using analysis of variance followed by Fisher s protected least significant difference test. A p value of less than 0.05 was determined to be significant. Statistical Analysis In our study, aspiration specimens were cytologically diagnosed into three groups by consensus among a cytologist and two pathologists as follows: negative for malignant cells, atypical cell with indeterminate or unknown malignant potential, and atypical cells suggestive of or positive for malignancy. Negative for malignant cells was considered the group for benign lesions, insufficient component was considered the group for atypical cells with indeterminate or unknown malignant potential, and malignant lesion was considered the group for atypical cells suggestive of or positive for malignancy. The overall diagnostic accuracy, pneumothorax rate, and chest tube insertion rate were determined. Positive findings at transthoracic needle aspiration biopsy of a solitary pulmonary nodule (including suspected malignancy) were considered to be true-positive in cases with surgical confirmation, when biopsy of another site revealed cancer with the same histologic characteristics, or when the lesion increased in size and other proven metastases were found. Negative findings at transthoracic needle aspiration biopsy were considered to be true-negative in cases with surgical confirmation, when the lesion subsequently disappeared or decreased in size with or without the administration of antibiotics, or when the lesion remained stable on follow-up CT for 24 months. Follow-up CT for cases with negative findings was scheduled 3, 6, 12, 18, and 24 months after the biopsy, during which changes in lesion size were assessed. Positive findings at transthoracic needle aspiration biopsy were considered to be false-positive if surgical resection yielded a benign diagnosis, if the lesion subsequently disappeared or decreased in size before surgical resection, or if the lesion remained stable on the follow-up CT for at least 24 months in cases in which the patient did not agree to surgical resection. Negative findings at transthoracic needle aspiration biopsy were considered to be false-negative if surgical resection yielded a malignant diagnosis; if the lesion increased in size; if other proven metastases were diagnosed on CT, MR imaging, or bone scintigraphy and proven by histologic examination of the biopsy specimen or resection; or if the specimen of transthoracic needle aspiration biopsy was insufficient. True-positive and true-negative cases were considered diagnosed cases. Falsepositive and false-negative cases were considered nondiagnosed cases. The overall diagnostic accuracy was calculated using the following formula: diagnostic accuracy (%) = number of solitary pulmonary nodules accurately diagnosed (true-positive + true-negative) / total number of solitary pulmonary nodules. Overall diagnostic accuracy, pneumothorax rate, and chest tube insertion rate of transthoracic biopsy were statistically evaluated with stepwise regression analysis with respect to the following factors: age, lesion size ( 10, 11 15, and mm), needle path length (the distance from the visceral pleura to the center of the lesion: 10, 11 20, 21 30, 31 40, 41 50, 51 60, 61 70, 71 80, and 81 mm), distance from the skin surface to the pleura (distance to pleura: 10, 11 20, 21 30, 31 40, and 41 mm), patient position (prone or supine) during needle approach, location of solitary pulmonary nodules (right upper, right middle, right lower, left upper, or left lower lobe), the smallest angle between the pleura and the needle (needle pleural angle: 10, 11 20, 21 30, 31 40, 41 50, 51 60, 61 70, 71 80, and ), number of puncture attempts, and percentage of pre- The overall diagnostic accuracy of CTguided transthoracic needle aspiration biopsy of small solitary pulmonary nodules was 77.2%. Of the 162 solitary pulmonary nodules, 103 diagnosed as malignant and 22 diagnosed as benign were true-positive and true-negative cases, respectively. The remaining 37 solitary pulmonary nodules (15 malignant, 22 benign) were false-positive and false-negative cases, respectively, and were correctly diagnosed at video-assisted thoracic surgery (n = 8), open lung biopsy (n = 9), sputum cytology (n = 7), and follow-up examination (n = 14). The false-positive cases included 17 organizing pneumonias and five active inflammations. The overall pneumothorax rate of CT-guided transthoracic needle aspiration biopsy of small solitary pulmonary nodules was 28.4%. The overall chest tube insertion rate was 2.5% In stepwise regression analysis, diagnostic accuracy was significantly affected by the needle path length and the lesion size (r = 0.54, r 2 = 0.29, p < 0.05). The pneumothorax rate was A B C ated whether the quantity of the specimen was sufficient for diagnosis. If the specimen quantity was sufficient, the procedure was finished. If the specimen was not sufficient, another puncture was performed until a sufficient specimen was obtained. Results Fig year-old woman with adenocarcinoma in right upper lobe diagnosed at conventional CT-guided biopsy (conventional method). CT images were obtained with radiopaque grid. A, Puncture point was determined after measuring distance from skin surface to pleura (distance between a and b), needle path length (distance between b and c), and smallest angle between pleura and needle (α) on cathode-ray tube monitor of imager. B, Initial puncture was performed without penetrating pleura. CT images were obtained to check course of biopsy needle. C, When solitary pulmonary nodule was penetrated, needle tip was checked and aspiration or histologic specimen was obtained. AJR:180, June
4 Ohno et al. Diagnostic Accuracy for TABLE 2 Each Range of Influencing Factors Factor Accuracy (%) a a a a a Lesion size (mm) b b a Significantly different from needle path lengths 40 mm (p < 0.05). b Significantly different from lesion sizes 10 mm (p < 0.05). significantly affected by the following three factors: percentage of predicted forced expiratory volume per 1 sec, the number of punctures, and needle path length (r = 0.59, r 2 = 0.35, p < 0.05). The chest tube insertion rate was significantly affected by the number of punctures (r = 0.43, r 2 = 0.23, p < 0.05). Diagnostic accuracies for each range of length of the needle path and lesion size are shown in Table 2. Diagnostic accuracy for needle path lengths of 40 mm or less was significantly greater than that for lengths greater than 40 mm (p < 0.05). Diagnostic accuracy for lesion size of 10 mm or less (52.0%) was significantly less than that of other sizes (11 15 mm, 74.4%; mm, 91.5%; p < 0.05). In the 10- mm-or-less group, 13 (nine malignant and four benign) of 25 solitary pulmonary nodules were true-positive and true-negative cases, respectively. The remaining 12 solitary pulmonary nodules (six malignant, six benign) were falsepositive and false-negative cases, respectively. In the more-than-10-mm and 15-mm-or-less groups, 58 (46 malignant and 12 benign) of 78 solitary pulmonary nodules were true-positive and true-negative cases, respectively. The remaining 20 solitary pulmonary nodules (seven malignant, 13 benign) were false-positive and false-negative cases, respectively. In the morethan-15-mm and 20-mm-or-less groups, 54 (48 malignant and six benign) of 59 solitary pulmonary nodules were true-positive and truenegative cases, respectively. The remaining five solitary pulmonary nodules (two malignant, three benign) were false-positive and false-negative cases, respectively. The pneumothorax rates for the percentage of predicted forced expiratory volume per 1 sec, number of punctures, and length of the needle path are shown in Table 3. The pneumothorax rate for patients whose percentage of predicted forced expiratory volume per 1 sec was greater than 70% was significantly lower than that for patients with a percentage of 70% or less ( p < 0.05). The pneumothorax rate for patients with single punctures was significantly lower than that for patients with more than one puncture ( p < ). Pneumothorax rates of patients who had needle path lengths of 40 mm or less were significantly lower than those of patients with lengths greater than 80 mm ( p < 0.05). The chest tube insertion rate for patients with three punctures (50%) was significantly greater than that of other groups (one puncture, 0.0%; two punctures, 0.3%; p < 0.05). Discussion Since Haaga and Alfidi [12] reported the first CT-guided biopsy in 1976, improved techniques have expanded the scope of thoracic lesions that are amenable to transthoracic biopsy [12 19, 24 32]. Percutaneous needle aspiration biopsy is a relatively safe and accurate means of diagnosing benign and malignant lesions of the chest [12 19, 24 32]. How to manage patients with growing solitary pulmonary nodules that are 20 mm or smaller is the ultimate question for radiologists and clinicians. The decisions depend on multiple factors including age, life style, coexisting medical problems, and experiences in each medical institution. When radiologists and clinicians consider using CT-guided transthoracic needle aspiration biopsy for small solitary pulmonary nodules, they should consider the impact that lesion size and the expected needle path length have on diagnostic accuracy. When transthoracic needle aspiration biopsy is performed, its accuracy must be explained carefully to the patients and referring physicians. Additionally, the association of pneumothorax rate with percentage of predicted forced expiratory volume in 1 sec, number of needle passes, and length of the needle path should be considered. The overall diagnostic accuracy (77.2%), pneumothorax rate (28.5%), and chest tube insertion rate (2.5%) of CT-guided transthoracic needle aspiration biopsy of small solitary pulmonary nodules were within the ranges of results of CT-guided biopsy reported in the literature, which include any size of solitary pulmonary nodule [12 19, 24 32]. Moreover, the diagnostic accuracy of small solitary pulmonary nodules smaller than 20 mm in diameter in our study was greater than that of fiberoptic bronchoscopy [33]. Our stepwise regression analysis suggested important factors that affect the diagnostic accuracy, pneumothorax rate, and chest tube insertion rate. Needle path length and lesion size significantly affect the diagnostic accuracy of CT-guided transthoracic needle aspiration biopsy of small solitary pulmonary nodules. Other factors did not contribute to improved diagnostic accuracy. Moreover, needle path length influenced diagnostic accuracy more than lesion size did. In published reports, many investigators indicate that diagnostic accuracies of CTguided biopsies were influenced mainly by lesion size [15 19, 24 32]. To our knowledge, no major reports suggest that needle path length is a more important factor in diagnostic accuracy of CT-guided transthoracic needle aspiration biopsy. In addition, our results suggest that the solitary pulmonary nodules of 10 mm or less in diameter should be followed up by repeated CT because the diagnostic accuracy for these nodules is significantly lower than that for larger solitary pulmonary nodules. The percentage of predicted forced expiratory volume in 1 sec, the number of punctures, and the needle path length significantly affected pneumothorax rate; and the number of punctures significantly affected the chest tube insertion rate. The pneumothorax rate of CT-guided transthoracic needle aspiration biopsy of small solitary pulmonary nodules in our study was not influenced by other factors, although some investigators have suggested that lesion size, needle pleural angle, location of the nodule, and needle approach influence pneumothorax rates [15 20]. The percentage of predicted forced expiratory volume in 1 sec suggests the degree of chronic obstructive pulmonary disease in patients [23]. A lower percentage of predicted forced expiratory volume in 1 sec has been suggested as a factor influencing pneumothorax rates [16, 20, 34]. In our study, patients whose percentage of predicted forced expiratory volume in 1 sec was 70% or less had a greater risk of pneumothorax, which is compatible with previous reports [16, 20, 34]. However, in our study, the number of punctures and the needle path length also significantly affected the pneumothorax rate. In addition, the number of punctures significantly affected the chest tube insertion rate AJR:180, June 2003
5 CT-Guided Biopsy of Solitary Pulmonary Nodules Rate of Pneumothorax for TABLE 3 Each Range of Influencing Factors Pneumothorax Factor Rate (%) % of predicted forced expiratory volume in 1 sec a a a No. of punctures b b c a Significantly different from percentage of predicted forced expiratory volume in 1 sec of > 70% ( p < 0.05). b Significantly different from single puncture ( p < 0.05). c Significantly different from needle path length of 40 mm ( p < 0.05). These facts are not compatible with previous results [15 20]. Recently, some investigators applied a coaxial technique for CT-guided biopsy. In our study, we did not adapt a coaxial technique. Therefore, the number of punctures may have directly affected the pneumothorax rate and chest tube insertion rate in our study. In 122 of 164 cases, the on-site cytologist evaluated the specimen from a single puncture as being sufficient for diagnosis. However, in the remaining 40 cases, 12 specimens from single punctures were not sufficient for diagnosis, and the other 28 cases were evaluated as inaccurate targeting of the lesion on the cathode-ray tube monitor. In these cases, we had to repuncture to obtain another specimen. In these situations, the increased number of punctures increases the risk of pneumothorax and the necessity of chest tube insertion. The needle path length must be considered because a longer needle path tends to damage a larger part of the lung parenchyma between the pleura and the solitary pulmonary nodule. Therefore, needle path length may significantly increase the risk of pneumothorax. Hence, it is preferable to try an accurate single puncture of a small solitary pulmonary nodule and to plan the needle trajectory (path) to be 40 mm or less. In conclusion, CT-guided transthoracic needle aspiration biopsy is useful as a diagnostic tool for small solitary pulmonary nodules with diameters of less than 20 mm. The diagnostic accuracy is significantly improved for larger (>10 mm) lesion size and short ( 40 mm) needle path. Moreover, pneumothorax rates also significantly improved for a larger percentage of predicted forced expiratory volume in 1 sec (> 70%), single puncture, and short ( 40 mm) needle path. In addition, the chest tube insertion rate is significantly increased if the operator risks a third puncture. References 1. Barsky SH, Cameron R, Osann KE, Tomita D, Holmes EC. Rising incidence of bronchioloalveolar lung carcinoma and its unique clinicopathologic features. Cancer 1994;73: Valaitis J, Warren S, Gamble D. Increasing incidence of adenocarcinoma of the lung. Cancer 1981;47: Auerbach O, Garfinkel L. The changing pattern of lung carcinoma. Cancer 1991;68: Travis WD, Travis LB, Devesa SS. Lung cancer. Cancer 1995;75[suppl 1]: Sone S, Takashima S, Li F, et al. Mass screening for lung cancer with mobile spiral computed tomography scanner. Lancet 1998;351: Kaneko M, Eguchi K, Ohmatsu H, et al. Peripheral lung cancer: screening and detection with low-dose spiral CT versus radiography. Radiology 1996;201: Marshall D, Simpson KN, Earle CC, Chu C. Potential cost-effectiveness of one-time screening for lung cancer (LC) in a high risk cohort. Lung Cancer 2001;32: Henschke CI. Early Lung Cancer Action Project: overall design and findings from baseline screening. Cancer 2000;89[suppl]:S2474 S Henschke CI, Naidich DP, Yankelevitz DF, et al. Early Lung Cancer Action Project: initial findings on repeat screenings. Cancer 2001;92: Henschke CI, McCauley DI, Yankelevitz DF, et al. Early Lung Cancer Action Project: a summary of the findings on baseline screening. Oncologist 2001;6: Yankelevitz DF, Gupta R, Zhao B, Henschke CI. Small pulmonary nodules: evaluation with repeat CT preliminary experience. Radiology 1999;212: Haaga JR, Alfidi RJ. Precise biopsy localization by computer tomography. Radiology 1976;118: Cohan RH, Newman GE, Braun SD, Dunnick NR. CT assistance for fluoroscopically guided transthoracic needle aspiration biopsy. J Comput Assist Tomogr 1984;8: Moore EH. Technical aspects of needle aspiration lung biopsy: a personal perspective. Radiology 1998;208: Westcott JL. Direct percutaneous needle aspiration of localized pulmonary lesions: result in 422 patients. Radiology 1980;137: Kazerooni EA, Lim FT, Mikhail A, Martinez FJ. Risk of pneumothorax in CT-guided transthoracic needle aspiration biopsy of the lung. Radiology 1996;198: Garcia-Rio F, Pino JM, Casadevall J, et al. Use of spirometry to predict risk of pneumothorax in CTguided needle biopsy of the lung. J Comput Assist Tomogr 1996;20: Li H, Boiselle PM, Shepard J-AO, Trotman-Dickenson B, McLoud TC. Diagnostic accuracy and safety of CT-guided percutaneous needle aspiration biopsy of the lung: comparison of small and large pulmonary nodules. AJR 1996;167: Laurent F, Michel P, Latrabe V, Tunon de Lara M, Marthan R. Pneumothoraces and chest tube placement after CT-guided transthoracic lung biopsy using a coaxial technique: incidence and risk factors. AJR 1999;172: Ko JP, Shepard JO, Drucker EA, et al. Factors influencing pneumothorax rate at lung biopsy: are dwell time and angle of pleural puncture contributing factors? Radiology 2001;218: Rhea JT, DeLuca SA, Greene RE. Determining the size of pneumothorax in the upright patient. Radiology 1982;144: American Thoracic Society. Standardization of spirometry: 1987 update. Am Rev Respir Dis 1987;136: American Thoracic Society. Lung function testing: selection of reference values and interpretative strategies. Am Rev Respir Dis 1991;144: van Sonnenberg E, Casola G, Ho M, et al. Difficult thoracic lesions: CT-guided biopsy experience in 150 cases. Radiology 1988;167: Haaga JR, Reich NE, Havrilla TR, Alfidi RJ, Meaney TF. CT guided biopsy. Cleve Clin Q 1977;44: Khouri NF, Stitik FP, Erozan YS, et al. Transthoracic needle aspiration biopsy of benign and malignant lung lesions. AJR 1985;144: Fink I, Gamsu G, Harter LP. CT-guided aspiration biopsy of the thorax. J Comput Assist Tomogr 1982;6: Gatenby RA, Mulhern CB Jr, Broder GJ, Moldofsky PJ. Computed-tomographic-guided biopsy of small apical and peripheral upper-lobe lung masses. Radiology 1984;150: Sider L, Davis TM Jr. Hilar masses: evaluation with CT-guided biopsy after negative bronchoscopic examination. Radiology 1987;164: Stanley JH, Fish GD, Andriole JG, et al. Lung lesions: cytologic diagnosis by fine-needle biopsy. Radiology 1987;162: Perlmutt LM, Johnston WW, Dunnick NR. Percutaneous transthoracic needle aspiration: a review. AJR 1989;152: Laurent F, Latrabe V, Vergier B, Michel P. Percutaneous CT-guided biopsy of the lung: comparison between aspiration and automated cutting needles using a coaxial technique. Cardiovasc Intervent Radiol 2000;23: Baaklini WA, Reinoso MA, Gorin AB, Sharafkaneh A, Manian P. Diagnostic yield of fiberoptic bronchoscopy in evaluating solitary pulmonary nodules. Chest 2000;117: Anderson CL, Crespo JC, Lie TH. Risk of pneumothorax not increased by obstructive lung disease in percutaneous needle biopsy. Chest 1994;105: AJR:180, June
Percutaneous Needle Aspiration Biopsy (PCNA) of Pulmonary Lesions: Evaluation of a Reaspiration or a Rebiopsy (second PCNA) 1
 Percutaneous Needle Aspiration Biopsy (PCNA) of Pulmonary Lesions: Evaluation of a Reaspiration or a Rebiopsy (second PCNA) 1 In Jae Lee, M.D., Dong Gyu Kim, M.D. 2, Ki-Suck Jung, M.D. 2, Hyoung June Im,
Percutaneous Needle Aspiration Biopsy (PCNA) of Pulmonary Lesions: Evaluation of a Reaspiration or a Rebiopsy (second PCNA) 1 In Jae Lee, M.D., Dong Gyu Kim, M.D. 2, Ki-Suck Jung, M.D. 2, Hyoung June Im,
MATERIALS AND METHODS. We retrospectively reviewed a consecutive series
 Huanqi Li1 Phillip M. Boiselle1 2 Jo-Anne 0. Shepard1 Beatrice Trotman-Dickenson1 Theresa C. McLoud1 Received January 2, 1996; accepted after revision Febru ary 19, 1996. tchest Division, Department of
Huanqi Li1 Phillip M. Boiselle1 2 Jo-Anne 0. Shepard1 Beatrice Trotman-Dickenson1 Theresa C. McLoud1 Received January 2, 1996; accepted after revision Febru ary 19, 1996. tchest Division, Department of
Cardiopulmonary Imaging Original Research
 Cardiopulmonary Imaging Original Research Choi et al. Outcomes of Biopsies of Small Pulmonary Nodules Cardiopulmonary Imaging Original Research Sang Hyun Choi 1 Eun Jin Chae Ji-Eun Kim Eun Young Kim Sang
Cardiopulmonary Imaging Original Research Choi et al. Outcomes of Biopsies of Small Pulmonary Nodules Cardiopulmonary Imaging Original Research Sang Hyun Choi 1 Eun Jin Chae Ji-Eun Kim Eun Young Kim Sang
CT Fluoroscopy-Guided vs Multislice CT Biopsy ModeGuided Lung Biopies:a preliminary experience
 CT Fluoroscopy-Guided vs Multislice CT Biopsy ModeGuided Lung Biopies:a preliminary experience Poster No.: C-0097 Congress: ECR 2016 Type: Scientific Exhibit Authors: A. Casarin, G. Rech, C. Cicero, A.
CT Fluoroscopy-Guided vs Multislice CT Biopsy ModeGuided Lung Biopies:a preliminary experience Poster No.: C-0097 Congress: ECR 2016 Type: Scientific Exhibit Authors: A. Casarin, G. Rech, C. Cicero, A.
CT-Guided Fine-Needle Aspiration and Core Needle Biopsies of Pulmonary Lesions: A Single-Center Experience With 750 Biopsies in Japan
 Cardiopulmonary Imaging Original Research Takeshita et al. CT-Guided Biopsy of Pulmonary Lesions Cardiopulmonary Imaging Original Research Jumpei Takeshita 1 Katsuhiro Masago Ryoji Kato Akito Hata Reiko
Cardiopulmonary Imaging Original Research Takeshita et al. CT-Guided Biopsy of Pulmonary Lesions Cardiopulmonary Imaging Original Research Jumpei Takeshita 1 Katsuhiro Masago Ryoji Kato Akito Hata Reiko
Consensus of Percutaneous Lung Needle Biopsy Statement from Japanese Society of Lung Needle Biopsy
 IVR Jpn J Intervent Radiol 22:256-261, 2007. Consensus of Percutaneous Lung Needle Biopsy Statement from Japanese Society of Lung Needle Biopsy 2000CT CT 5 IVR CT 100 Europian radiology 5 CT EBM IC 1 2
IVR Jpn J Intervent Radiol 22:256-261, 2007. Consensus of Percutaneous Lung Needle Biopsy Statement from Japanese Society of Lung Needle Biopsy 2000CT CT 5 IVR CT 100 Europian radiology 5 CT EBM IC 1 2
CT-guided needle biopsy of lung lesions is a. Management of Pneumothorax After Percutaneous CT-Guided Lung Biopsy*
 Management of Pneumothorax After Percutaneous CT-Guided Lung Biopsy* Takuji Yamagami, MD, PhD; Toshiyuki Nakamura, MD; Shigeharu Iida, MD; Takeharu Kato, MD; and Tsunehiko Nishimura, MD, PhD Objectives:
Management of Pneumothorax After Percutaneous CT-Guided Lung Biopsy* Takuji Yamagami, MD, PhD; Toshiyuki Nakamura, MD; Shigeharu Iida, MD; Takeharu Kato, MD; and Tsunehiko Nishimura, MD, PhD Objectives:
Transthoracic needle biopsy of lung masses: a survey of techniques
 Clinical Radiology (2005) 60, 370 374 Transthoracic needle biopsy of lung masses: a survey of techniques G. Aviram a, *, D.S. Schwartz b, S. Meirsdorf a, G. Rosen a, J. Greif c, M. Graif a Departments
Clinical Radiology (2005) 60, 370 374 Transthoracic needle biopsy of lung masses: a survey of techniques G. Aviram a, *, D.S. Schwartz b, S. Meirsdorf a, G. Rosen a, J. Greif c, M. Graif a Departments
Risk of Pneumothorax in Post Lung Biopsy Patients: Is Short-Term Monitoring Necessary?
 Risk of Pneumothorax in Post Lung Biopsy Patients: Is Short-Term Monitoring Necessary? Poster No.: C-1852 Congress: ECR 2011 Type: Authors: Keywords: DOI: Scientific Exhibit R. Hayter, T. Berkmen; New
Risk of Pneumothorax in Post Lung Biopsy Patients: Is Short-Term Monitoring Necessary? Poster No.: C-1852 Congress: ECR 2011 Type: Authors: Keywords: DOI: Scientific Exhibit R. Hayter, T. Berkmen; New
Clinical Study Needle Gauge and Cytological Yield in CT-Guided Lung Biopsy
 International Scholarly Research Network ISRN Pulmonology Volume 2011, Article ID 970813, 4 pages doi:10.5402/2011/970813 Clinical Study Needle Gauge and Cytological Yield in CT-Guided Lung Biopsy William
International Scholarly Research Network ISRN Pulmonology Volume 2011, Article ID 970813, 4 pages doi:10.5402/2011/970813 Clinical Study Needle Gauge and Cytological Yield in CT-Guided Lung Biopsy William
PERCUTANEOUS CT GUIDED CUTTING NEEDLE BIOPSY OF LUNG LESIONS
 ORIGINAL ARTICLE PERCUTANEOUS CT GUIDED CUTTING NEEDLE BIOPSY OF LUNG LESIONS Abdur Rehman Khan, Arshad Javed, Mohammad Ejaz Department of Radiology and Department of Pulmonology, Postgraduate Medical
ORIGINAL ARTICLE PERCUTANEOUS CT GUIDED CUTTING NEEDLE BIOPSY OF LUNG LESIONS Abdur Rehman Khan, Arshad Javed, Mohammad Ejaz Department of Radiology and Department of Pulmonology, Postgraduate Medical
CT Screening for Lung Cancer for High Risk Patients
 CT Screening for Lung Cancer for High Risk Patients The recently published National Lung Cancer Screening Trial (NLST) showed that low-dose CT screening for lung cancer reduces mortality in high-risk patients
CT Screening for Lung Cancer for High Risk Patients The recently published National Lung Cancer Screening Trial (NLST) showed that low-dose CT screening for lung cancer reduces mortality in high-risk patients
Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit
 Page1 Original Article NJR 2011;1(1):1 7;Available online at www.nranepal.org Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit S
Page1 Original Article NJR 2011;1(1):1 7;Available online at www.nranepal.org Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit S
Accuracy and safety of CT guided transthoracic needle biopsy
 Original Article Accuracy and safety of CT guided transthoracic needle biopsy * Atheer A. Fadhil** FICMS-CABMS-FICMS (Pulm.), DMRD, FIBMS (Rad.), Fac Med Baghdad 2012; Vol. 54, No. 1 Received Dec.2011
Original Article Accuracy and safety of CT guided transthoracic needle biopsy * Atheer A. Fadhil** FICMS-CABMS-FICMS (Pulm.), DMRD, FIBMS (Rad.), Fac Med Baghdad 2012; Vol. 54, No. 1 Received Dec.2011
Computed tomography (CT) guided transthoracic
 Original Article 432 Three-step Needle Withdrawal Method: A Modified Technique for Reducing the Rate of Pneumothorax after CT-guided Lung Biopsy Hung-Jung Wang 1, MD; Ting-Kai Leung 1,2, MD; Chi-Ming Lee
Original Article 432 Three-step Needle Withdrawal Method: A Modified Technique for Reducing the Rate of Pneumothorax after CT-guided Lung Biopsy Hung-Jung Wang 1, MD; Ting-Kai Leung 1,2, MD; Chi-Ming Lee
CT-guided transthoracic needle biopsy induced complications - how to cut back?
 CT-guided transthoracic needle biopsy induced complications - how to cut back? Poster No.: C-0560 Congress: ECR 2014 Type: Educational Exhibit Authors: T. Boskovic, M. Stojanovic, S. Pena Karan, G. Vujasinovi#;
CT-guided transthoracic needle biopsy induced complications - how to cut back? Poster No.: C-0560 Congress: ECR 2014 Type: Educational Exhibit Authors: T. Boskovic, M. Stojanovic, S. Pena Karan, G. Vujasinovi#;
Combined Fluoroscopy- and CT-Guided Transthoracic Needle Biopsy Using a C-Arm Cone-Beam CT System: Comparison with Fluoroscopy-Guided Biopsy
 Original Article DOI: 10.3348/kjr.2011.12.1.89 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2011;12(1):89-96 Combined Fluoroscopy- and CT-Guided Transthoracic Needle Biopsy Using a C-Arm Cone-Beam CT
Original Article DOI: 10.3348/kjr.2011.12.1.89 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2011;12(1):89-96 Combined Fluoroscopy- and CT-Guided Transthoracic Needle Biopsy Using a C-Arm Cone-Beam CT
Small Pulmonary Nodules: Our Preliminary Experience in Volumetric Analysis of Doubling Times
 Small Pulmonary Nodules: Our Preliminary Experience in Volumetric Analysis of Doubling Times Andrea Borghesi, MD Davide Farina, MD Roberto Maroldi, MD Department of Radiology University of Brescia Brescia,
Small Pulmonary Nodules: Our Preliminary Experience in Volumetric Analysis of Doubling Times Andrea Borghesi, MD Davide Farina, MD Roberto Maroldi, MD Department of Radiology University of Brescia Brescia,
Transthoracic fine-needle aspiration biopsy of the lungs using a C-arm cone-beam CT system: diagnostic accuracy and postprocedural
 The British Journal of Radiology, 85 (2012), e217 e222 Transthoracic fine-needle aspiration biopsy of the lungs using a C-arm cone-beam CT system: diagnostic accuracy and postprocedural complications W
The British Journal of Radiology, 85 (2012), e217 e222 Transthoracic fine-needle aspiration biopsy of the lungs using a C-arm cone-beam CT system: diagnostic accuracy and postprocedural complications W
May-Lin Wilgus. A. Study Purpose and Rationale
 Utility of a Computer-Aided Diagnosis Program in the Evaluation of Solitary Pulmonary Nodules Detected on Computed Tomography Scans: A Prospective Observational Study May-Lin Wilgus A. Study Purpose and
Utility of a Computer-Aided Diagnosis Program in the Evaluation of Solitary Pulmonary Nodules Detected on Computed Tomography Scans: A Prospective Observational Study May-Lin Wilgus A. Study Purpose and
CT-Guided Thoracic Biopsy: Evaluating Diagnostic Yield and Complications
 Original Article 285 CT-Guided Thoracic Biopsy: Evaluating Diagnostic Yield and Complications Stanley EK Loh, 1 MBChB, MRCS, FRCR (UK), Donald DF Wu, 1 BSc, Sudhakar K Venkatesh, 1 MBBS, MD FRCR (UK),
Original Article 285 CT-Guided Thoracic Biopsy: Evaluating Diagnostic Yield and Complications Stanley EK Loh, 1 MBChB, MRCS, FRCR (UK), Donald DF Wu, 1 BSc, Sudhakar K Venkatesh, 1 MBBS, MD FRCR (UK),
Improved Diagnostic Efficacy by Rapid Cytology Test in Fluoroscopy-Guided Bronchoscopy
 ORIGINAL ARTICLE Improved Diagnostic Efficacy by Rapid Cytology Test in Fluoroscopy-Guided Bronchoscopy Junji Uchida, MD, Fumio Imamura, MD, Akemi Takenaka, CT, Mana Yoshimura, MD, Kiyonobu Ueno, MD, Kazuyuki
ORIGINAL ARTICLE Improved Diagnostic Efficacy by Rapid Cytology Test in Fluoroscopy-Guided Bronchoscopy Junji Uchida, MD, Fumio Imamura, MD, Akemi Takenaka, CT, Mana Yoshimura, MD, Kiyonobu Ueno, MD, Kazuyuki
Pneumothorax Post CT-guided Fine Needle Aspiration Biopsy for Lung Nodules: Our Experience in King Hussein Medical Center
 Pneumothorax Post CT-guided Fine Needle Aspiration Biopsy for Lung Nodules: Our Experience in King Hussein Medical Center Ala Qayet MD*, Laith Obaidat MD**, Mazin Al-Omari MD*, Ashraf Al-Tamimi MD^, Ahmad
Pneumothorax Post CT-guided Fine Needle Aspiration Biopsy for Lung Nodules: Our Experience in King Hussein Medical Center Ala Qayet MD*, Laith Obaidat MD**, Mazin Al-Omari MD*, Ashraf Al-Tamimi MD^, Ahmad
With recent advances in diagnostic imaging technologies,
 ORIGINAL ARTICLE Management of Ground-Glass Opacity Lesions Detected in Patients with Otherwise Operable Non-small Cell Lung Cancer Hong Kwan Kim, MD,* Yong Soo Choi, MD,* Kwhanmien Kim, MD,* Young Mog
ORIGINAL ARTICLE Management of Ground-Glass Opacity Lesions Detected in Patients with Otherwise Operable Non-small Cell Lung Cancer Hong Kwan Kim, MD,* Yong Soo Choi, MD,* Kwhanmien Kim, MD,* Young Mog
Diagnostic Correlation of Findings of Multidetector Computed Tomography and Fine Needle Aspiration Cytology in Lung Masses
 RESEARCH ARTICLE Diagnostic Correlation of Findings 10.5005/jp-journals-10057-0004 of MDCT and FNAC in Lung Masses Diagnostic Correlation of Findings of Multidetector Computed Tomography and Fine Needle
RESEARCH ARTICLE Diagnostic Correlation of Findings 10.5005/jp-journals-10057-0004 of MDCT and FNAC in Lung Masses Diagnostic Correlation of Findings of Multidetector Computed Tomography and Fine Needle
Blood path technique to reduce pneumothorax after CT guided lung biopsy
 Blood path technique to reduce pneumothorax after CT guided lung biopsy Poster No.: C-0753 Congress: ECR 2011 Type: Scientific Paper Authors: G. J. Mallarajapatna, N. Ramanna; Bangalore/IN Keywords: Interventional
Blood path technique to reduce pneumothorax after CT guided lung biopsy Poster No.: C-0753 Congress: ECR 2011 Type: Scientific Paper Authors: G. J. Mallarajapatna, N. Ramanna; Bangalore/IN Keywords: Interventional
Low-dose CT Lung Cancer Screening Guidelines for Pulmonary Nodules Management Version 2
 Low-dose CT Lung Cancer Screening Guidelines for Pulmonary Nodules Management Version 2 The Committee for Management of CT-screening-detected Pulmonary Nodules 2009-2011 The Japanese Society of CT Screening
Low-dose CT Lung Cancer Screening Guidelines for Pulmonary Nodules Management Version 2 The Committee for Management of CT-screening-detected Pulmonary Nodules 2009-2011 The Japanese Society of CT Screening
Small solid noncalcified pulmonary nodules detected by screening chest computed tomography
 Respiratory Medicine (2007) 101, 1880 1884 Small solid noncalcified pulmonary nodules detected by screening chest computed tomography Sang-Man Jin a,b, Seung-Ho Choi c, Chul-Gyu Yoo a,b, Young-Whan Kim
Respiratory Medicine (2007) 101, 1880 1884 Small solid noncalcified pulmonary nodules detected by screening chest computed tomography Sang-Man Jin a,b, Seung-Ho Choi c, Chul-Gyu Yoo a,b, Young-Whan Kim
CT-Guided Lung Biopsies: Pleural Blood Patching Reduces the Rate of Chest Tube Placement for Postbiopsy Pneumothorax
 Vascular and Interventional Radiology Original Research Wagner et al. Treatment of Postbiopsy Pneumothorax Vascular and Interventional Radiology Original Research FOCUS ON: Jason M. Wagner 1,2 J. Louis
Vascular and Interventional Radiology Original Research Wagner et al. Treatment of Postbiopsy Pneumothorax Vascular and Interventional Radiology Original Research FOCUS ON: Jason M. Wagner 1,2 J. Louis
Guidelines for the Management of Pulmonary Nodules Detected by Low-dose CT Lung Cancer Screening
 Guidelines for the Management of Pulmonary Nodules Detected by Low-dose CT Lung Cancer Screening 1. Introduction In January 2005, the Committee for Preparation of Clinical Practice Guidelines for the Management
Guidelines for the Management of Pulmonary Nodules Detected by Low-dose CT Lung Cancer Screening 1. Introduction In January 2005, the Committee for Preparation of Clinical Practice Guidelines for the Management
Computed tomography guided fine needle aspiration cytology of thoracic lesions: A retrospective analysis of 114 cases
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 47-52 Computed tomography guided fine needle aspiration cytology
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 47-52 Computed tomography guided fine needle aspiration cytology
Early Lung Cancer Action Project: A Summary of the Findings on Baseline Screening
 Early Lung Cancer Action Project: A Summary of the Findings on Baseline Screening CLAUDIA I. HENSCHKE, a DOROTHY I. MCCAULEY, b DAVID F. YANKELEVITZ, a DAVID P. NAIDICH, b GEORGEANN MCGUINNESS, b OLLI
Early Lung Cancer Action Project: A Summary of the Findings on Baseline Screening CLAUDIA I. HENSCHKE, a DOROTHY I. MCCAULEY, b DAVID F. YANKELEVITZ, a DAVID P. NAIDICH, b GEORGEANN MCGUINNESS, b OLLI
Role of CT imaging to evaluate solitary pulmonary nodule with extrapulmonary neoplasms
 Original Research Article Role of CT imaging to evaluate solitary pulmonary nodule with extrapulmonary neoplasms Anand Vachhani 1, Shashvat Modia 1*, Varun Garasia 1, Deepak Bhimani 1, C. Raychaudhuri
Original Research Article Role of CT imaging to evaluate solitary pulmonary nodule with extrapulmonary neoplasms Anand Vachhani 1, Shashvat Modia 1*, Varun Garasia 1, Deepak Bhimani 1, C. Raychaudhuri
geoffrey dick b.app.sci. (med.rad.) rmit deputy chief radiographer angliss hospital, melbourne ct supervisor angliss hospital, melbourne
 ct intervention tips geoffrey dick b.app.sci. (med.rad.) rmit deputy chief radiographer angliss hospital, melbourne ct supervisor angliss hospital, melbourne sessional lecturer monash university department
ct intervention tips geoffrey dick b.app.sci. (med.rad.) rmit deputy chief radiographer angliss hospital, melbourne ct supervisor angliss hospital, melbourne sessional lecturer monash university department
Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule
 Case Report on Aerodigestive Endoscopy Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule Jennifer L. Sullivan 1, Michael G. Martin 2, Benny Weksler 1 1 Division of
Case Report on Aerodigestive Endoscopy Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule Jennifer L. Sullivan 1, Michael G. Martin 2, Benny Weksler 1 1 Division of
Evaluation of the Efficacy and Safety of Percutaneous Biopsy of Lung
 82 The Open Respiratory Medicine Journal, 2012, 6, 82-88 Evaluation of the Efficacy and Safety of Percutaneous Biopsy of Lung Open Access Sean E. McSweeney, Kevin N. O Regan, Patrick D. Mc Laughlin, Lee
82 The Open Respiratory Medicine Journal, 2012, 6, 82-88 Evaluation of the Efficacy and Safety of Percutaneous Biopsy of Lung Open Access Sean E. McSweeney, Kevin N. O Regan, Patrick D. Mc Laughlin, Lee
Downloaded from by on 01/12/18 from IP address Copyright ARRS. For personal use only; all rights reserved
 Vascular and Interventional Radiology Original Research Hiraki et al. Complications After CT Fluoroscopy Guided Lung Biopsy Vascular and Interventional Radiology Original Research Takao Hiraki 1 Hidefumi
Vascular and Interventional Radiology Original Research Hiraki et al. Complications After CT Fluoroscopy Guided Lung Biopsy Vascular and Interventional Radiology Original Research Takao Hiraki 1 Hidefumi
CT Screening for Lung Cancer: Implication of Lung Biopsy Recommendations
 Cardiopulmonary Imaging Original Research Wagnetz et al. Lung Biopsy and CT Screening for Lung Cancer Cardiopulmonary Imaging Original Research Ute Wagnetz 1 Ravi J. Menezes 2 Scott Boerner 3 Narinder
Cardiopulmonary Imaging Original Research Wagnetz et al. Lung Biopsy and CT Screening for Lung Cancer Cardiopulmonary Imaging Original Research Ute Wagnetz 1 Ravi J. Menezes 2 Scott Boerner 3 Narinder
Xiaohuan Pan 1,2 *, Xinguan Yang 1,2 *, Jingxu Li 1,2, Xiao Dong 1,2, Jianxing He 2,3, Yubao Guan 1,2. Original Article
 Original Article Is a 5-mm diameter an appropriate cut-off value for the diagnosis of atypical adenomatous hyperplasia and adenocarcinoma in situ on chest computed tomography and pathological examination?
Original Article Is a 5-mm diameter an appropriate cut-off value for the diagnosis of atypical adenomatous hyperplasia and adenocarcinoma in situ on chest computed tomography and pathological examination?
Loren Ketai, MD; Mathurn Malby, BS; Kirk Jordan, MD; Andrew Meholic, MD; and Julie Locken, MD
 Small Nodules Detected on Chest Radiography* Does Size Predict Calcification? Loren Ketai, MD; Mathurn Malby, BS; Kirk Jordan, MD; Andrew Meholic, MD; and Julie Locken, MD Study objectives: To determine
Small Nodules Detected on Chest Radiography* Does Size Predict Calcification? Loren Ketai, MD; Mathurn Malby, BS; Kirk Jordan, MD; Andrew Meholic, MD; and Julie Locken, MD Study objectives: To determine
Single Plane Fluoroscopic Guided Biopsy of Thoracic Lesions
 Single Plane Fluoroscopic Guided Biopsy of Thoracic Lesions Abstract Pages with reference to book, From 73 To 77 Sarwat Hussain ( The Aga Khan University Medical Center, Karachi. ) Single plane fluoroscoyic
Single Plane Fluoroscopic Guided Biopsy of Thoracic Lesions Abstract Pages with reference to book, From 73 To 77 Sarwat Hussain ( The Aga Khan University Medical Center, Karachi. ) Single plane fluoroscoyic
Screening for lung cancer with low-dose computed tomography
 Original Article Radiographic and Clinical Characterization of False Negative Results from CT-Guided Needle Biopsies of Lung Nodules Brian D. Gelbman, MD,* Mathew D. Cham, MD, Won Kim, MD,* Daniel M. Libby,
Original Article Radiographic and Clinical Characterization of False Negative Results from CT-Guided Needle Biopsies of Lung Nodules Brian D. Gelbman, MD,* Mathew D. Cham, MD, Won Kim, MD,* Daniel M. Libby,
Results of three-year mass screening programme for lung cancer using mobile low-dose spiral computed tomography scanner
 doi: 10.1054/ bjoc.2000.1531 available online at http://www.idealibrary.com on http://www.bjcancer.com Results of three-year mass screening programme for lung cancer using mobile low-dose spiral computed
doi: 10.1054/ bjoc.2000.1531 available online at http://www.idealibrary.com on http://www.bjcancer.com Results of three-year mass screening programme for lung cancer using mobile low-dose spiral computed
Electromagnetic navigational bronchoscopy in patients with solitary pulmonary nodules
 Original article Electromagnetic navigational bronchoscopy in patients with solitary pulmonary nodules Samuel Copeland MD, Shrinivas Kambali MD, Gilbert Berdine MD, Raed Alalawi MD Abstract Background:
Original article Electromagnetic navigational bronchoscopy in patients with solitary pulmonary nodules Samuel Copeland MD, Shrinivas Kambali MD, Gilbert Berdine MD, Raed Alalawi MD Abstract Background:
Management of Multiple Pure Ground-Glass Opacity Lesions in Patients with Bronchioloalveolar Carcinoma
 ORIGINAL ARTICLE Management of Multiple Pure Ground-Glass Opacity Lesions in Patients with Bronchioloalveolar Carcinoma Hong Kwan Kim, MD,* Yong Soo Choi, MD,* Jhingook Kim, MD, PhD,* Young Mog Shim, MD,
ORIGINAL ARTICLE Management of Multiple Pure Ground-Glass Opacity Lesions in Patients with Bronchioloalveolar Carcinoma Hong Kwan Kim, MD,* Yong Soo Choi, MD,* Jhingook Kim, MD, PhD,* Young Mog Shim, MD,
Risk of Pleural Recurrence After Computed Tomographic-Guided Percutaneous Needle Biopsy in Stage I Lung Cancer Patients
 GENERAL THORACIC Risk of Pleural Recurrence After Computed Tomographic-Guided Percutaneous Needle Biopsy in Stage I Lung Cancer Patients Masayoshi Inoue, MD, PhD, Osamu Honda, MD, PhD, Noriyuki Tomiyama,
GENERAL THORACIC Risk of Pleural Recurrence After Computed Tomographic-Guided Percutaneous Needle Biopsy in Stage I Lung Cancer Patients Masayoshi Inoue, MD, PhD, Osamu Honda, MD, PhD, Noriyuki Tomiyama,
CT Screening for Lung Cancer: Frequency and Significance of Part-Solid and Nonsolid Nodules
 Claudia I. Henschke 1 David F. Yankelevitz 1 Rosna Mirtcheva 1 Georgeann McGuinness 2 Dorothy McCauley 1 0lli S. Miettinen 3 for the ELCAP Group Received June 19, 2001; accepted after revision November
Claudia I. Henschke 1 David F. Yankelevitz 1 Rosna Mirtcheva 1 Georgeann McGuinness 2 Dorothy McCauley 1 0lli S. Miettinen 3 for the ELCAP Group Received June 19, 2001; accepted after revision November
American College Of Radiology ACR Appropriateness Criteria WORK-UP OF THE SOLITARY PULMONARY NODULE
 This document is provided to you by the American College of Radiology. We strive to deliver this information in a convenient and effective manner. After you finish reviewing the criteria, please provide
This document is provided to you by the American College of Radiology. We strive to deliver this information in a convenient and effective manner. After you finish reviewing the criteria, please provide
Percutaneous Lung Biopsy in the Molecular Profiling Era: A Survey of Current Practices
 Percutaneous Lung Biopsy in the Molecular Profiling Era: A Survey of Current Practices PHILLIP GUICHET, B.A. 1, FEREIDOUN ABTIN, M.D. 2, CHRISTOPHER LEE, M.D. 1 1 KECK SCHOOL OF MEDICINE OF USC, DEPT OF
Percutaneous Lung Biopsy in the Molecular Profiling Era: A Survey of Current Practices PHILLIP GUICHET, B.A. 1, FEREIDOUN ABTIN, M.D. 2, CHRISTOPHER LEE, M.D. 1 1 KECK SCHOOL OF MEDICINE OF USC, DEPT OF
Imaging Decisions Start Here SM
 Owing to its high resolution and wide anatomic coverage, dynamic first-pass perfusion 320-detector-row CT outperforms PET/CT for distinguishing benign from malignant lung nodules, researchers from Japan
Owing to its high resolution and wide anatomic coverage, dynamic first-pass perfusion 320-detector-row CT outperforms PET/CT for distinguishing benign from malignant lung nodules, researchers from Japan
Percutaneous CT-guided biopsy of hilar lesions: Diagnostic accuracy and complication rate
 Percutaneous CT-guided biopsy of hilar lesions: Diagnostic accuracy and complication rate Poster No.: C-1878 Congress: ECR 2010 Type: Scientific Exhibit Topic: Interventional Radiology Authors: M. C. Freund
Percutaneous CT-guided biopsy of hilar lesions: Diagnostic accuracy and complication rate Poster No.: C-1878 Congress: ECR 2010 Type: Scientific Exhibit Topic: Interventional Radiology Authors: M. C. Freund
The Computed Tomography-Guided Adrenal Biopsy
 The Computed Tomography-Guided Adrenal Biopsy An Alternative to Surgery in Adrenal Mass Diagnosis WILLIAM A. BERKMAN, MD,'$ MICHAEL E. BERNARDINO, MD,' CHARLES W. SEWELL, MD,t R. BARTON PRICE, MD,' AND
The Computed Tomography-Guided Adrenal Biopsy An Alternative to Surgery in Adrenal Mass Diagnosis WILLIAM A. BERKMAN, MD,'$ MICHAEL E. BERNARDINO, MD,' CHARLES W. SEWELL, MD,t R. BARTON PRICE, MD,' AND
Relative Survival Rate
 5X Su r vi val Th r ou gh Ear l y Det ect i on Cancer Stage I II III IV Relative Survival Rate 55,2% 28% 8% 2% 90% TIME AND COST IS W AITING IN LINE OBJ ECTIVES Reduce Screening Time By Reduce Screening
5X Su r vi val Th r ou gh Ear l y Det ect i on Cancer Stage I II III IV Relative Survival Rate 55,2% 28% 8% 2% 90% TIME AND COST IS W AITING IN LINE OBJ ECTIVES Reduce Screening Time By Reduce Screening
Computer-Aided Detection in Screening CT for
 Yuan et al. Screening CT for Pulmonary Chest Imaging Original Research C M E D E N T U R I C L I M G I N G JR 2006; 186:1280 1287 0361 803X/06/1865 1280 merican Roentgen Ray Society Y O Ren Yuan 1 Patrick
Yuan et al. Screening CT for Pulmonary Chest Imaging Original Research C M E D E N T U R I C L I M G I N G JR 2006; 186:1280 1287 0361 803X/06/1865 1280 merican Roentgen Ray Society Y O Ren Yuan 1 Patrick
Computerized tomography guided percutaneous transthoracic fine needle aspiration of lung lesions
 Original Research Article Computerized tomography guided percutaneous transthoracic fine needle aspiration of lung lesions Sunita Bajaj 1*, Sandeep R Saboo 2 1 Associate Professor, Department of Radiology,
Original Research Article Computerized tomography guided percutaneous transthoracic fine needle aspiration of lung lesions Sunita Bajaj 1*, Sandeep R Saboo 2 1 Associate Professor, Department of Radiology,
Percutaneous Lung Biopsy in a Patient with a Cavitating Lung Mass: Indications, Technique, and Complications
 Interventional Radiology Case Conference Chest Imaging Interventional Radiology Case Conference Massachusetts General Hospital Michael M. Maher 1,2 Mannudeep K. Kalra 2 Ross L. Titton 2 Giles W. Boland
Interventional Radiology Case Conference Chest Imaging Interventional Radiology Case Conference Massachusetts General Hospital Michael M. Maher 1,2 Mannudeep K. Kalra 2 Ross L. Titton 2 Giles W. Boland
Adam J. Hansen, MD UHC Thoracic Surgery
 Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Risk Factors for Severity of Pneumothorax after CT-Guided Percutaneous Lung Biopsy using the Single-Needle Method
 Hiroshima J. Med. Sci. Vol. 59, No. 3, 43-50, September, 2010 HIJM 59-9 43 Risk Factors for Severity of Pneumothorax after CT-Guided Percutaneous Lung Biopsy using the Single-Needle Method Hideaki KAKIZAWA1,*),
Hiroshima J. Med. Sci. Vol. 59, No. 3, 43-50, September, 2010 HIJM 59-9 43 Risk Factors for Severity of Pneumothorax after CT-Guided Percutaneous Lung Biopsy using the Single-Needle Method Hideaki KAKIZAWA1,*),
OBJECTIVES. Solitary Solid Spiculated Nodule. What would you do next? Case Based Discussion: State of the Art Management of Lung Nodules.
 Organ Imaging : September 25 2015 OBJECTIVES Case Based Discussion: State of the Art Management of Lung Nodules Dr. Elsie T. Nguyen Dr. Kazuhiro Yasufuku 1. To review guidelines for follow up and management
Organ Imaging : September 25 2015 OBJECTIVES Case Based Discussion: State of the Art Management of Lung Nodules Dr. Elsie T. Nguyen Dr. Kazuhiro Yasufuku 1. To review guidelines for follow up and management
Proportion and characteristics of transient nodules in a retrospective analysis of pulmonary nodules
 Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Proportion and characteristics of transient nodules in a retrospective analysis of pulmonary nodules Jin-Yeong Yu 1, Boram Lee 1, Sunmi Ju 1, Eun-Young Kim
Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Proportion and characteristics of transient nodules in a retrospective analysis of pulmonary nodules Jin-Yeong Yu 1, Boram Lee 1, Sunmi Ju 1, Eun-Young Kim
Comparison of three mathematical prediction models in patients with a solitary pulmonary nodule
 Original Article Comparison of three mathematical prediction models in patients with a solitary pulmonary nodule Xuan Zhang*, Hong-Hong Yan, Jun-Tao Lin, Ze-Hua Wu, Jia Liu, Xu-Wei Cao, Xue-Ning Yang From
Original Article Comparison of three mathematical prediction models in patients with a solitary pulmonary nodule Xuan Zhang*, Hong-Hong Yan, Jun-Tao Lin, Ze-Hua Wu, Jia Liu, Xu-Wei Cao, Xue-Ning Yang From
CT Findings of Surgically Resected Pleomorphic Carcinoma of the Lung in 30 Patients
 Kim et al. CT of Pleomorphic Carcinoma of the Lung Chest Imaging Clinical Observations Tae Sung Kim 1 Joungho Han 2 Kyung Soo Lee 1 Yeon Joo Jeong 1 Seo Hyun Kwak 1 Hong Sik Byun 1 Myung Jin Chung 1 Hojoong
Kim et al. CT of Pleomorphic Carcinoma of the Lung Chest Imaging Clinical Observations Tae Sung Kim 1 Joungho Han 2 Kyung Soo Lee 1 Yeon Joo Jeong 1 Seo Hyun Kwak 1 Hong Sik Byun 1 Myung Jin Chung 1 Hojoong
Electromagnetic Navigation Bronchoscopy Performed by Thoracic Surgeons: One Center s Early Success
 Electromagnetic Navigation Bronchoscopy Performed by Thoracic Surgeons: One Center s Early Success Daryl Phillip Pearlstein, MD, Curtis C. Quinn, MD, Charles C. Burtis, BS, Kwang Woo Ahn, PhD, and Aaron
Electromagnetic Navigation Bronchoscopy Performed by Thoracic Surgeons: One Center s Early Success Daryl Phillip Pearlstein, MD, Curtis C. Quinn, MD, Charles C. Burtis, BS, Kwang Woo Ahn, PhD, and Aaron
Characteristics of Subsolid Pulmonary Nodules Showing Growth During Follow-up With CT Scanning
 CHEST Original Research Characteristics of Subsolid Pulmonary Nodules Showing Growth During Follow-up With CT Scanning Haruhisa Matsuguma, MD ; Kiyoshi Mori, MD ; Rie Nakahara, MD ; Haruko Suzuki, MD ;
CHEST Original Research Characteristics of Subsolid Pulmonary Nodules Showing Growth During Follow-up With CT Scanning Haruhisa Matsuguma, MD ; Kiyoshi Mori, MD ; Rie Nakahara, MD ; Haruko Suzuki, MD ;
Radiofrequency ablation combined with conventional radiotherapy: a treatment option for patients with medically inoperable lung cancer
 Radiofrequency ablation combined with conventional radiotherapy: a treatment option for patients with medically inoperable lung cancer Poster No.: C-0654 Congress: ECR 2011 Type: Scientific Paper Authors:
Radiofrequency ablation combined with conventional radiotherapy: a treatment option for patients with medically inoperable lung cancer Poster No.: C-0654 Congress: ECR 2011 Type: Scientific Paper Authors:
Malignant solitary pulmonary nodules: assessment of mass growth rate and doubling time at follow-up CT
 Original Article Malignant solitary pulmonary nodules: assessment of mass growth rate and doubling time at follow-up CT Jingxu Li*, Tingting Xia*, Xinguan Yang, Xiao Dong, Jiamin Liang, Nanshan Zhong,
Original Article Malignant solitary pulmonary nodules: assessment of mass growth rate and doubling time at follow-up CT Jingxu Li*, Tingting Xia*, Xinguan Yang, Xiao Dong, Jiamin Liang, Nanshan Zhong,
Radial endobronchial ultrasound (EBUS), performed during
 Original Article Can Computed Tomography Characteristics Predict Outcomes in Patients Undergoing Radial Endobronchial Ultrasound-Guided Biopsy of Peripheral Lung Lesions? Matthew Evison,* Philip A.J. Crosbie,*
Original Article Can Computed Tomography Characteristics Predict Outcomes in Patients Undergoing Radial Endobronchial Ultrasound-Guided Biopsy of Peripheral Lung Lesions? Matthew Evison,* Philip A.J. Crosbie,*
The Spectrum of Management of Pulmonary Ground Glass Nodules
 The Spectrum of Management of Pulmonary Ground Glass Nodules Stanley S Siegelman CT Society 10/26/2011 No financial disclosures. Noguchi M et al. Cancer 75: 2844-2852, 1995. 236 surgically resected peripheral
The Spectrum of Management of Pulmonary Ground Glass Nodules Stanley S Siegelman CT Society 10/26/2011 No financial disclosures. Noguchi M et al. Cancer 75: 2844-2852, 1995. 236 surgically resected peripheral
Mayo Clinic College of Medicine, Rochester, Minnesota, USA
 The Oncologist Lung Cancer Commentary: CT Screening for Lung Cancer Caveat Emptor JAMES R. JETT,DAVID E. MIDTHUN Mayo Clinic College of Medicine, Rochester, Minnesota, USA Key Words. CT screening Early
The Oncologist Lung Cancer Commentary: CT Screening for Lung Cancer Caveat Emptor JAMES R. JETT,DAVID E. MIDTHUN Mayo Clinic College of Medicine, Rochester, Minnesota, USA Key Words. CT screening Early
September 2014 Imaging Case of the Month. Michael B. Gotway, MD. Department of Radiology Mayo Clinic Arizona Scottsdale, AZ
 September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
Small Pulmonary Nodules: Volume Measurement at Chest CT Phantom Study 1
 Jane P. Ko, MD Henry Rusinek, PhD Erika L. Jacobs, MD James S. Babb, PhD Margrit Betke, PhD Georgeann McGuinness, MD David P. Naidich, MD Index terms: Computed tomography (CT), image processing, 60.12117
Jane P. Ko, MD Henry Rusinek, PhD Erika L. Jacobs, MD James S. Babb, PhD Margrit Betke, PhD Georgeann McGuinness, MD David P. Naidich, MD Index terms: Computed tomography (CT), image processing, 60.12117
Thoracic CT pattern in lung cancer: correlation of CT and pathologic diagnosis
 19 th Congress of APSR PG of Lung Cancer (ESAP): Update of Lung Cancer Thoracic CT pattern in lung cancer: correlation of CT and pathologic diagnosis Kazuma Kishi, M.D. Department of Respiratory Medicine,
19 th Congress of APSR PG of Lung Cancer (ESAP): Update of Lung Cancer Thoracic CT pattern in lung cancer: correlation of CT and pathologic diagnosis Kazuma Kishi, M.D. Department of Respiratory Medicine,
ORIGINAL PAPER APPLICATION OF SUBSECOND ROTATION SCAN TO HELICAL CT FOR LUNG CANCER SCREENING
 Nagoya J. Med. Sci. 68. 139 ~ 145, 2006 ORIGINAL PAPER APPLICATION OF SUBSECOND ROTATION SCAN TO HELICAL CT FOR LUNG CANCER SCREENING YOSHINE MORI, 1 SHIGEKI ITOH, 2 MITSURU IKEDA, 2 AKIKO SAWAKI, 1 KOUJIRO
Nagoya J. Med. Sci. 68. 139 ~ 145, 2006 ORIGINAL PAPER APPLICATION OF SUBSECOND ROTATION SCAN TO HELICAL CT FOR LUNG CANCER SCREENING YOSHINE MORI, 1 SHIGEKI ITOH, 2 MITSURU IKEDA, 2 AKIKO SAWAKI, 1 KOUJIRO
Diagnostic performance of percutaneous lung biopsy using automated biopsy. ground-glass opacity lesions
 ARTICLE INFORMATION 2013 The Authors Received: 26 August 2012 Revised: 31 October 2012 Accepted: 21 November 2012 doi: 10.1259/bjr.20120447 Cite this article as: Yamagami T, Yoshimatsu R, Miura H, Yamada
ARTICLE INFORMATION 2013 The Authors Received: 26 August 2012 Revised: 31 October 2012 Accepted: 21 November 2012 doi: 10.1259/bjr.20120447 Cite this article as: Yamagami T, Yoshimatsu R, Miura H, Yamada
Projected Outcomes Using Different Nodule Sizes to Define a Positive CT Lung Cancer Screening Examination
 DOI:10.1093/jnci/dju284 First published online October 20, 2014 The Author 2014. Published by Oxford University Press. All rights reserved. For Permissions, please e-mail: journals.permissions@oup.com.
DOI:10.1093/jnci/dju284 First published online October 20, 2014 The Author 2014. Published by Oxford University Press. All rights reserved. For Permissions, please e-mail: journals.permissions@oup.com.
Impalpable Pulmonary Nodules With Ground-Glass Opacity* Success for Making Pathologic Sections With Preoperative Marking by Lipiodol
 CHEST Impalpable Pulmonary Nodules With Ground-Glass Opacity* Success for Making Pathologic Sections With Preoperative Marking by Lipiodol Original Research Koei Ikeda, MD, PhD; Hiroaki Nomori, MD, PhD;
CHEST Impalpable Pulmonary Nodules With Ground-Glass Opacity* Success for Making Pathologic Sections With Preoperative Marking by Lipiodol Original Research Koei Ikeda, MD, PhD; Hiroaki Nomori, MD, PhD;
Radiological staging of lung cancer. Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh
 Radiological staging of lung cancer Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh Bronchogenic Carcinoma Accounts for 14% of new cancer diagnoses in 2012. Estimated to kill ~150,000
Radiological staging of lung cancer Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh Bronchogenic Carcinoma Accounts for 14% of new cancer diagnoses in 2012. Estimated to kill ~150,000
Differentiation of Pleural Effusions From Parenchymal Opacities: Accuracy of Bedside Chest Radiography
 Cardiopulmonary Imaging Original Research Kitazono et al. Chest Radiography of Pleural Effusions Cardiopulmonary Imaging Original Research Mary T. Kitazono 1 Charles T. Lau Andrea N. Parada Pooja Renjen
Cardiopulmonary Imaging Original Research Kitazono et al. Chest Radiography of Pleural Effusions Cardiopulmonary Imaging Original Research Mary T. Kitazono 1 Charles T. Lau Andrea N. Parada Pooja Renjen
Gold Anchor enables safe reach to inner organs
 Gold Anchor enables safe reach to inner organs Fine needles for cytology have been used >50 years in all parts of the human body with no to very little harm Gold Anchor comes pre-loaded in needles of the
Gold Anchor enables safe reach to inner organs Fine needles for cytology have been used >50 years in all parts of the human body with no to very little harm Gold Anchor comes pre-loaded in needles of the
Imprint cytology improves accuracy of CT-guided percutaneous transthoracic
 ERJ Express. Published on October 10, 2007 as doi: 10.1183/09031936.00038907 Imprint cytology improves accuracy of CT-guided percutaneous transthoracic needle biopsy Yeun-Chung Chang, M.D., Ph.D. 1, ycc5566@ntu.edu.tw
ERJ Express. Published on October 10, 2007 as doi: 10.1183/09031936.00038907 Imprint cytology improves accuracy of CT-guided percutaneous transthoracic needle biopsy Yeun-Chung Chang, M.D., Ph.D. 1, ycc5566@ntu.edu.tw
Chapter 11. Summary and general discussion
 Chapter 11 Summary and general discussion Low Dose Computed Tomography of the Chest: Applications and Limitations INTRODUCTION The introduction of spiral, multidetector-row computed tomography (CT) has
Chapter 11 Summary and general discussion Low Dose Computed Tomography of the Chest: Applications and Limitations INTRODUCTION The introduction of spiral, multidetector-row computed tomography (CT) has
MANAGEMENT RECOMMENDATIONS
 1 MANAGEMENT RECOMMENDATIONS 1. Adrenal masses!!!!!!! page 2 2. Liver Masses!!!!!!! page 3 3. Obstetric US Soft Markers for Aneuploidy!! pages 4-6 4. Ovarian and Adnexal Cysts!!!!! pages 7-10 5. Pancreatic
1 MANAGEMENT RECOMMENDATIONS 1. Adrenal masses!!!!!!! page 2 2. Liver Masses!!!!!!! page 3 3. Obstetric US Soft Markers for Aneuploidy!! pages 4-6 4. Ovarian and Adnexal Cysts!!!!! pages 7-10 5. Pancreatic
What to Do with Small Lung Nodules Hanh Vu Nghiem, MD William Beaumont Hospital Royal Oak, Michigan
 What to Do with Small Lung Nodules Hanh Vu Nghiem, MD William Beaumont Hospital Royal Oak, Michigan Small Lung Nodules What to do with small lung nodules? We biopsy them when requested What are our accuracy
What to Do with Small Lung Nodules Hanh Vu Nghiem, MD William Beaumont Hospital Royal Oak, Michigan Small Lung Nodules What to do with small lung nodules? We biopsy them when requested What are our accuracy
Natural History of Pure Ground-Glass Opacity After Long-Term Follow-up of More Than 2 Years
 Natural History of Pure Ground-Glass Opacity After Long-Term Follow-up of More Than 2 Years Ken Kodama, MD, Masahiko Higashiyama, MD, Hideoki Yokouchi, MD, Koji Takami, MD, Keiko Kuriyama, MD, Yoko Kusunoki,
Natural History of Pure Ground-Glass Opacity After Long-Term Follow-up of More Than 2 Years Ken Kodama, MD, Masahiko Higashiyama, MD, Hideoki Yokouchi, MD, Koji Takami, MD, Keiko Kuriyama, MD, Yoko Kusunoki,
Variable Presentations of Thoracic Biopsy Related Hemothorax
 Universal Journal of Clinical Medicine 1(2): 22-27, 2013 DOI: 10.13189/ujcm.2013.010202 http://www.hrpub.org Variable Presentations of Thoracic Biopsy Related Hemothorax Brent Weinberg, Lori Watumull,
Universal Journal of Clinical Medicine 1(2): 22-27, 2013 DOI: 10.13189/ujcm.2013.010202 http://www.hrpub.org Variable Presentations of Thoracic Biopsy Related Hemothorax Brent Weinberg, Lori Watumull,
Shodayu Takashima 1 Shusuke Sone 2 Feng Li 1 Yuichiro Maruyama 1 Minoru Hasegawa 1 Tsuyoshi Matsushita 1 Fumiyoshi Takayama 2 Masumi Kadoya 1
 Small Solitary Pulmonary Nodules ( 1 cm) Detected at Population- Based CT Screening for Lung Cancer: Reliable High-Resolution CT Features of Benign Lesions Shodayu Takashima 1 Shusuke Sone 2 Feng Li 1
Small Solitary Pulmonary Nodules ( 1 cm) Detected at Population- Based CT Screening for Lung Cancer: Reliable High-Resolution CT Features of Benign Lesions Shodayu Takashima 1 Shusuke Sone 2 Feng Li 1
ORIGINAL ARTICLE. Abstract. Introduction
 ORIGINAL ARTICLE Virtual Bronchoscopic Navigation Improves the Diagnostic Yield of Radial-Endobronchial Ultrasound for Peripheral Pulmonary Lesions with Involved Bronchi on CT Fumihiro Asano 1, Naofumi
ORIGINAL ARTICLE Virtual Bronchoscopic Navigation Improves the Diagnostic Yield of Radial-Endobronchial Ultrasound for Peripheral Pulmonary Lesions with Involved Bronchi on CT Fumihiro Asano 1, Naofumi
Necrotizing Granuloma of the Lung: Imaging Characteristics and Imaging-Guided Diagnosis
 Necrotizing Granuloma of the Lung Chest Imaging Clinical Observations Rennae Thiessen 1 Jean M. Seely 1 Frederick R. K. Matzinger 1 Prachi garwal 1,2 Karen L. urns 3 Carole J. Dennie 1 Rebecca Peterson
Necrotizing Granuloma of the Lung Chest Imaging Clinical Observations Rennae Thiessen 1 Jean M. Seely 1 Frederick R. K. Matzinger 1 Prachi garwal 1,2 Karen L. urns 3 Carole J. Dennie 1 Rebecca Peterson
Percutaneous needle biopsies (PNB) are widely used
 GENERAL THORACIC Risk of Pleural Recurrence After Needle Biopsy in Patients With Resected Early Stage Lung Cancer Haruhisa Matsuguma, MD, Rie Nakahara, MD, Tetsuro Kondo, MD, Yukari Kamiyama, MD, Kiyoshi
GENERAL THORACIC Risk of Pleural Recurrence After Needle Biopsy in Patients With Resected Early Stage Lung Cancer Haruhisa Matsuguma, MD, Rie Nakahara, MD, Tetsuro Kondo, MD, Yukari Kamiyama, MD, Kiyoshi
CT-Guided Percutaneous Lung Biopsies in Patients With Suspicion for Infection May Yield Clinically Useful Information
 Vascular and Interventional Radiology Original Research Haas et al. CT-Guided Percutaneous Lung Biopsies Vascular and Interventional Radiology Original Research Brian M. Haas 1 Joshua D. Clayton Brett
Vascular and Interventional Radiology Original Research Haas et al. CT-Guided Percutaneous Lung Biopsies Vascular and Interventional Radiology Original Research Brian M. Haas 1 Joshua D. Clayton Brett
Use of percutaneous needle biopsy in the investigation
 Thorax 1987;42:967-971 Use of percutaneous needle biopsy in the investigation of solitary pulmonary nodules A R L PENKETH, A A ROBINSON, V BARKER, C D R FLOWER From the East Anglian Regional Cardiothoracic
Thorax 1987;42:967-971 Use of percutaneous needle biopsy in the investigation of solitary pulmonary nodules A R L PENKETH, A A ROBINSON, V BARKER, C D R FLOWER From the East Anglian Regional Cardiothoracic
Diagnostic challenge: Sclerosing Hemangioma of the Lung. Department of Medicine, Division of Pulmonary and Critical Care, Lincoln Medical and
 Diagnostic challenge: Sclerosing Hemangioma of the Lung. S. Arias M.D, R. Loganathan M.D, FCCP Department of Medicine, Division of Pulmonary and Critical Care, Lincoln Medical and Mental Health Center/Weill
Diagnostic challenge: Sclerosing Hemangioma of the Lung. S. Arias M.D, R. Loganathan M.D, FCCP Department of Medicine, Division of Pulmonary and Critical Care, Lincoln Medical and Mental Health Center/Weill
Copyright 2007 IEEE. Reprinted from 4th IEEE International Symposium on Biomedical Imaging: From Nano to Macro, April 2007.
 Copyright 27 IEEE. Reprinted from 4th IEEE International Symposium on Biomedical Imaging: From Nano to Macro, April 27. This material is posted here with permission of the IEEE. Such permission of the
Copyright 27 IEEE. Reprinted from 4th IEEE International Symposium on Biomedical Imaging: From Nano to Macro, April 27. This material is posted here with permission of the IEEE. Such permission of the
T hese guidelines have been developed at the
 920 BTS GUIDELINES Guidelines for radiologically guided lung biopsy A Manhire, Chairman, M Charig, C Clelland, F Gleeson, R Miller, H Moss, K Pointon, C Richardson, E Sawicka... See end of article for
920 BTS GUIDELINES Guidelines for radiologically guided lung biopsy A Manhire, Chairman, M Charig, C Clelland, F Gleeson, R Miller, H Moss, K Pointon, C Richardson, E Sawicka... See end of article for
LYMPH NODE METASTASIS IN SMALL PERIPHERAL ADENOCARCINOMA OF THE LUNG
 LYMPH NODE METASTASIS IN SMALL PERIPHERAL ADENOCARCINOMA OF THE LUNG Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Takehiro Watanabe, MD a Yuzo Kurita, MD b Akira Yokoyama, MD b Keiichi
LYMPH NODE METASTASIS IN SMALL PERIPHERAL ADENOCARCINOMA OF THE LUNG Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Takehiro Watanabe, MD a Yuzo Kurita, MD b Akira Yokoyama, MD b Keiichi
Peripheral Lung Adenocarcinoma: Correlation of Thin-Section CT Findings with Histologic Prognostic Factors and Survival 1
 Thoracic Imaging Takatoshi Aoki, MD Yoshinori Tomoda, MD Hideyuki Watanabe, MD Hajime Nakata, MD Takahiko Kasai, MD Hiroshi Hashimoto, MD Mantaro Kodate, MD Toshihiro Osaki, MD Kosei Yasumoto, MD Peripheral
Thoracic Imaging Takatoshi Aoki, MD Yoshinori Tomoda, MD Hideyuki Watanabe, MD Hajime Nakata, MD Takahiko Kasai, MD Hiroshi Hashimoto, MD Mantaro Kodate, MD Toshihiro Osaki, MD Kosei Yasumoto, MD Peripheral
Since the introduction of low-dose helical computed tomography
 Original Article Prognostic Impact of Tumor Size Eliminating the Ground Glass Opacity Component Modified Clinical T Descriptors of the Tumor, Node, Metastasis Classification of Lung Cancer Shota Nakamura,
Original Article Prognostic Impact of Tumor Size Eliminating the Ground Glass Opacity Component Modified Clinical T Descriptors of the Tumor, Node, Metastasis Classification of Lung Cancer Shota Nakamura,
American College of Radiology ACR Appropriateness Criteria
 American College of Radiology ACR Criteria Radiologic Management of Thoracic Nodules and Masses Variant 1: Middle-aged patient (35 60 years old) with an incidental 1.5-cm lung nodule. The lesion was smooth.
American College of Radiology ACR Criteria Radiologic Management of Thoracic Nodules and Masses Variant 1: Middle-aged patient (35 60 years old) with an incidental 1.5-cm lung nodule. The lesion was smooth.
Computer tomography guided lung biopsy using interactive breath-hold control: a randomized study
 Original Article Page 1 of 6 Computer tomography guided lung biopsy using interactive breath-hold control: a randomized study Haseem Ashraf 1,2,3, Shella Krag-Andersen 1, Matiullah Naqibullah 1, Valentina
Original Article Page 1 of 6 Computer tomography guided lung biopsy using interactive breath-hold control: a randomized study Haseem Ashraf 1,2,3, Shella Krag-Andersen 1, Matiullah Naqibullah 1, Valentina
May 2017 Imaging Case of the Month. Prasad M. Panse, MD and Michael B. Gotway, MD. Department of Radiology Mayo Clinic Arizona Scottsdale, Arizona USA
 May 2017 Imaging Case of the Month Prasad M. Panse, MD and Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, Arizona USA Clinical History: A 32-year-old man presented for routine
May 2017 Imaging Case of the Month Prasad M. Panse, MD and Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, Arizona USA Clinical History: A 32-year-old man presented for routine
