Generalized Lymphadenopathy as Presenting Feature of Systemic Lupus Erythematosus: Case Report and Review of the Literature
|
|
|
- Buck Dorsey
- 6 years ago
- Views:
Transcription
1 Elmer ress Case Report J Clin Med Res. 2016;8(11): Generalized Lymphadenopathy as Presenting Feature of Systemic Lupus Erythematosus: Case Report and Review of the Literature Wais Afzal a, c, Talal Arab a, Tofura Ullah b, Katerina Teller a, Kaushik J. Doshi a Abstract Lymphadenopathy could represent a vast spectrum of etiologies including infectious and non-infectious diseases. Besides proper history taking, physical examination, and laboratory investigations, a tissue diagnosis is often necessary to unmask the cause of generalized lymphadenopathy. Here we present a 23-year-old woman who was admitted for diffuse generalized lymphadenopathy, fatigue, malaise, weight loss, nausea, and bilateral lower extremity edema. She reported a history of seizures as well as stroke 2 years prior with no other medical conditions present. Although malignant and infectious etiologies were initially the primary targets for workup, her history of seizures and stroke remained a dilemma. Extensive workup for malignant and infectious diseases was unrevealing; however, rheumatologic workup was eventually positive for systemic lupus erythematosus (SLE). This case illustrates that extensive generalized diffuse lymphadenopathy may be a presenting feature of SLE and should be considered in the differential diagnosis of patients presenting with diffuse lymphadenopathy and constitutional symptoms. Keywords: Lymphadenopathy; Systemic lupus erythematosus; Seizure; Stroke Introduction Lymphadenopathy could be the presenting feature of many ailments including infectious or non-infectious diseases. Infectious etiologies include viral, bacterial, fungal, parasitic, and rickettsial causes. Common causes of non-infectious lymphadenopathy include malignancy, sarcoidosis, connective tissue Manuscript accepted for publication September 02, 2016 a Department of Internal Medicine, Jamaica Hospital Medical Center, 8900 Van Wyck Expressway, Jamaica, NY 11418, USA b Department of Clinical Research, Jamaica Hospital Medical Center, 8900 Van Wyck Expressway, Jamaica, NY 11418, USA c Corresponding Author: Wais Afzal, Department of Internal Medicine, Jamaica Hospital Medical Center, 8900 Van Wyck Expressway, Jamaica, NY 11418, USA. wais.afzal@gmail.com doi: disease, and Kikuchi-Fujimoto disease. The initial approach to discern the cause of lymphadenopathy begins with proper history and physical examination followed by laboratory investigations. A tissue diagnosis is often necessary to unmask the cause of lymphadenopathy. Systemic lupus erythematosus (SLE) is a chronic multisystem autoimmune inflammatory disease with diverse clinical manifestations. It presents most often in young females. The diagnosis of SLE is established by the presence of four or more of the 11 American College of Rheumatology (ACR) criteria, none of which include lymphadenopathy. The precise prevalence of lymphadenopathy in SLE is unknown. There are several case reports suggesting that generalized lymphadenopathy could be the first manifestation of SLE [1-4]. Here we present a 23-year-old female who came to our hospital with diffuse generalized lymphadenopathy, fatigue, malaise, weight loss, nausea, and bilateral lower extremity edema. She underwent extensive workup for malignant, infectious, and immunologic diseases and was ultimately diagnosed with SLE. This case adds to the body of evidence suggesting that diffuse generalized lymphadenopathy may be the presenting feature of SLE. It should be considered in the differential diagnosis of patients presenting with diffuse lymphadenopathy and constitutional symptoms in select groups of patients, such as young women. Case Report A 23-year-old Afro-Jamaican woman presented with generalized lymphadenopathy of 7-8 months duration. She complained of gradual worsening fatigue, malaise, unintentional weight loss of 40 pounds, nausea, intermittent headaches, and progressively worsening bilateral lower extremity edema. She denied fever, chills, night sweats, loss of appetite, rash, sore throat, cough, and shortness of breath. At age 15, she had an episode of left facial palsy which lasted 7 months and resolved spontaneously. She experienced tonic-clonic seizures 2 years ago and had been on sodium valproate 200 mg daily since that time. Her last episode of seizures was 3 months ago. Two years prior, she suffered from ischemic stroke with residual left-sided weakness. She was never diagnosed with infectious diseases, sarcoidosis, or malignancies and had no family history of such. The patient lived most of her life in the Jamaican Republic and was visiting the United States. This is an open-access article distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited 819
2 Lupus Lymphadenopathy J Clin Med Res. 2016;8(11): Table 1. Initial Investigations Complete blood count Comprehensive metabolic panel Inflammatory and coagulation profile Endocrinology and nutrition Urine analysis WBC: 3,700/µL* Glucose: 81 mg/dl CRP :0.50 < mg/dl TSH: 4.67 µu/ml Color: yellow Neutrophils: 32.7%* BUN: 11 mg/dl ESR: 132 mm/h* Free T 4 : 2.23 ng/dl Appearance: clear Lymphocyte: 53.3%* Creatinine: 1.0 mg/dl D-dimer: 1,331 ng/ml* T 3 : 91.5 ng/dl Specific gravity: Monocytes: 11.7% Sodium: 135 meq/l PT: 9.1 s hcg: < 5.0 miu/ml ph: 6.0 Eosinophils: 0.0%* Potassium: 3.8 meq/l aptt: 30.4 s Folate: 4.8 ng/ml Protein: 500 mg/dl* Basophils: 2.3% Chloride: 110 meq/l* LDH: 964 U/L* Vitamin B12: 886 pg/ml Blood: negative Hemoglobin: 8.7 mg/dl* Bicarbonate: 25 meq/l Cholesterol: 364 mg/dl* Urobilinogen: < 2.0 EU Platelets: 96/µL* Calcium: 7.0 mg/dl Triglycerides: 580 mg/dl* WBC: 3/HPF Albumin: 1.5 g/dl* HDL: 44 mg/dl RBC: 3/HPF Bilirubin: 0.3 mg/dl Epithelial cells: 3/HPF AST: 33 U/L Hyaline casts: 4/LPF ALT: 23 U/L Mucous threads: rare ALP: 169 U/L* *Abnormal values. Physical examination revealed a well-developed, wellnourished young female in no acute distress with normal vital signs. Heart and lung examinations were unremarkable. Abdominal examination was consistent with hepatomegaly and mild splenomegaly. There was 2+ pitting edema of lower extremities up to shins left more than right. There were multiple painless, enlarged, soft, non-tender, freely movable lymph nodes in the cervical, axillary, and inguinal areas, the largest of which measured 5 4 cm. On neurological examination, she was found to have left facial droop, motor strength of 5/5 on right upper and lower extremities, and 3/5 on left upper and lower extremities. There was decreased sensation on the left side, and slow finger to nose on the left. She was limping and used a cane for ambulation. Her neurologic signs and symptoms were the sequelae of the ischemic stroke 2 years prior. She was admitted with possible diagnosis of malignancy versus infectious etiology. Nevertheless, the history of stroke in this young woman with no known cardiovascular risk factors remained a dilemma. Initial investigations are presented in Table 1. Considering diffuse lymphadenopathy on physical exami- Figure 1. (a) CT neck with IV contrast demonstrating multiple enlarged supraclavicular lymph nodes. (b) CT chest with IV contrast demonstrating enlarged axillary lymph nodes. (c) CT abdomen and pelvis with IV contrast demonstrating a hypodense lesion in the periphery of the spleen measuring cm. (d) CT abdomen and pelvis with IV contrast demonstrating multiple enlarged external iliac lymph nodes. 820
3 Afzal et al J Clin Med Res. 2016;8(11): Figure 2. (a) Right inguinal lymph node sample indicating numerous hyperplasic follicles (H&E, 10 magnification). (b) Right inguinal lymph node sample indicating hyperplastic follicles with prominent germinal centers and reactive lymphocytosis (H&E, 40 magnification). nation and pancytopenia on laboratory investigation, malignancy in particular lymphoma was considered the most likely diagnosis. Moreover, her hypoalbuminemia, proteinuria, and hyperlipidemia were concerning for possible nephrotic syndrome. A computed tomography (CT) scan of the head without contrast revealed an old infarct and encephalomalacia in the right posterior insula, right superior temporal gyrus and adjacent to parietal lobe, and old infarcts in the bilateral frontal lobes and left parietal lobe. Numerous enlarged cervical lymph nodes (Fig. 1a) with hypertrophy of nasopharyngeal soft tissues and palatine and lingual tonsils were seen. A CT of the chest with IV contrast showed bilateral axillary lymphadenopathy (Fig. 1b). Mediastinal and right hilar lymph nodes were also enlarged. CT scan of abdomen and pelvis with IV contrast indicated hepatomegaly (17.7 cm in length), mild splenomegaly (12.9 cm) anterior-posteriorly, a hypodense lesion in the periphery of the spleen ( cm), as well as posterior splenic contour nodularity (Fig. 1c). There was periportal, mesenteric, retroperitoneal, common iliac, pelvic sidewall, external iliac, and inguinal lymphadenopathy bilaterally as demonstrated by the CT scan of the abdomen and pelvis (Fig. 1d). Excisional lymph node biopsy was performed from the right inguinal area. The results of the biopsy were reported as reactive lymph node with follicular hyperplastic pattern and no evidence of lymphoma (Fig. 2a and b). Flow cytometry and marker results did not support malignancy. Acid-fast stain, bacterial, mycobacterial and fungal cultures were all reported as negative. Further investigations for human immunodeficiency virus (HIV 1 and 2), heterophile antibody, human T-cell lymphotropic virus (HTLV 1 and 2) antibodies, and purified protein derivative (PPD) were all negative. Anticardiolipin IgA and IgM antibodies were positive; however, anticardiolipin IgG was reported as negative. Antinuclear antibodies (ANA) were also positive with high titer of 1:1,280. Owing to proteinuria of 500 mg/dl on urine analysis, a 24-h urine protein was performed and found to be 4,338 mg/24 h. This was consistent with nephrotic syndrome. A complete panel of lupus serology was sent, and diagnosis of active lupus was confirmed (Table 2). Pulse dose of methylprednisolone 1 g IV was started for 3 days and switched to oral prednisone 60 mg daily. Despite encouragement, the patient refused to proceed with renal biopsy. Neurology evaluation was completed to assess possible causes of previous stroke with magnetic resonance angiography (MRA) of the brain, carotid Doppler, and transthoracic echocardiogram (TTE) with bubble study. MRA revealed multiple chronic small cerebral infarcts more on the right than left hemispheres and narrowing of right more than left middle cerebral arteries. Carotid arteries were less than 30% stenotic bilaterally suggesting lupus vasculitis as the possible cause of the ischemic stroke. The patient was discharged on prednisone 60 mg oral daily tapering dose, calcium and vitamin D supplement, aspirin 81 mg oral daily, lisinopril 2.5 mg oral daily, and atorvastatin 80 mg oral at night. She was also advised to continue sodium valproate and follow with rheumatology and nephrology clinics. The plan was to start mycophenolate mofetil and hydroxychloroquine and tapper off oral prednisone. Unfortunately, the patient did not follow with rheumatology clinic and was lost to follow-up. Discussion Lymphadenopathy could represent a vast spectrum of etiologies including infectious or non-infectious diseases. Some of the infectious causes include HIV, Castleman s disease, tuberculosis, brucellosis, and syphilis. Common causes of noninfectious etiologies of diffuse lymphadenopathy include lymphoma, sarcoidosis, connective tissue disease, and Kikuchi-Fujimoto disease. The initial approach to delineate the cause of lymphadenopathy begins with obtaining proper his- Table 2. Connective Tissue Disease Panel Test ANA ds-dna antibody SM antibody RNP antibody SS-A SS-B C3 C4 Rheumtoid factor Anti-CCP Results 1:1,280 homogenous 38 U/mL > 8 AI > 8 AI < 1.0 AI < 1.0 AI < 40 mg/dl 9.6 mg/dl Negative Negative 821
4 Lupus Lymphadenopathy J Clin Med Res. 2016;8(11): tory and physical examination. Laboratory investigations focusing on infections, malignancies, and immunological causes are of paramount importance and can lead to a proper diagnosis. Tissue diagnosis is often needed to unmask the cause of lymphadenopathy. Large-scale studies advocate for excisional biopsy as the gold standard method with minimal morbidity and mortality for rectifying benign and malignant causes of lymphadenopathy [5]. SLE is a chronic multisystem autoimmune inflammatory disease with diverse clinical manifestations. It most often affects young females. According to Systemic Lupus International Collaborating Clinics (SLICC) classification criteria, generalized lymphadenopathy is not considered a criterion for diagnosis [6]. The prevalence of generalized lymphadenopathy is by far less as seen in SLE patients previously [1]. The precise prevalence of lymphadenopathy in SLE patient is unknown. In one retrospective study of 90 SLE patients, 23 patients (26%) were found to have lymphadenopathy [7]. The same study indicated that SLE patients presenting with lymphadenopathy are more likely to manifest constitutional symptoms such as fever, fatigue, weight loss, cutaneous symptoms and signs, higher rates of hepatomegaly and splenomegaly, increased anti-dsdna antibodies, and decreased complement levels. This illustrates that lymphadenopathy is indicative of active disease. There are several case reports suggesting that generalized lymphadenopathy could be the first manifestation of SLE [1-4]. In the patient described in this report, all of these clinical features were seen with the exception of cutaneous manifestations. There was no history of rash, photosensitivity, oral ulcers, arthritis, or serositis. The diagnosis of SLE was established by ruling out other more common causes of lymphadenopathy, followed by her history of seizures, documented nephrotic range proteinuria, pancytopenia, positive high titers of ANA, anti-dsdna, anti-sm, low C3 and C4, and the presence of anticardiolipin IgM antibodies. At the histologic level, manifestations of SLE lymphadenopathy are non-specific and include follicular hyperplasia, scattered immunoblasts, and plasma cells with increased vascularity [8]. Biopsy result in our patient yielded similar findings. Lymph node biopsy, in addition to flow cytometry and markers, can exclude lymphoma as a cause of lymphadenopathy. Since our patient did not consent for renal biopsy, the degree of renal involvement could not be staged properly. Though lymphoma may not be an initial diagnosis, there is strong evidence demonstrating that patients with SLE are at increased risk of developing non-hodgkin lymphoma, Hodgkin lymphoma, leukemia, and some non-hematologic malignancies [9]. Thus, a lymph node biopsy is crucial even if the diagnosis of SLE is confirmed. Other diseases that need to be considered and ruled out in presence of generalized lymphadenopathy include sarcoidosis, Kikuchi-Fujimoto disease, and Castleman s disease. Sarcoidosis is a multisystem granulomatous disease with heterogeneous presentation characterized by cellular alteration in lung tissue and intrathoracic lymphadenopathy. Histopathologically, sarcoidosis causes widespread non-caseating granulomas, which is very specific to this disease. Elevated serum calcium is also seen. Sarcoidosis in this young woman with African roots was a possibility. However, absence of non-caseating granulomas on lymph node biopsy and normal serum calcium was not suggestive of this diagnosis. Kikuchi-Fujimoto disease, also known as histiocytic necrotizing lymphadenitis, is an extremely rare disease with worldwide distribution with high predilection for young Asian females and it is known to have favorable prognosis. Common clinical manifestations include fever, chills, upper respiratory symptoms, and lymphadenopathy with cervical lymphadenopathy the most common [10]. The characteristic lymph node histopathologic features of Kikuchi-Fujimoto disease include irregular paracortical areas of coagulative necrosis with abundant karyorrhectic debris, and abundance of histiocytes at the margin of the necrotic areas [11]. Our patient s lymph node biopsy did not have any of these features. There is evidence indicating Kikuchi-Fujimoto disease has a rare association with SLE, the diagnosis of which may precede, coincide or follow SLE [12]. Castleman s disease, a rare lymphoproliferative disorder, has an equal predilection for both sexes and may affect anyone from adolescence to seventh decade of life [13]. Clinical manifestations include fever, fatigue, night sweats, anemia, and lymphadenopathy. The extent of lymphadenopathy depends on if the disease is unicentric or multicentric. The lymph node biopsy may reveal increased plasma cell proliferation within the follicles with increased vascularity [14]. Our patient s lymph node biopsy did not have any of these features. As discussed earlier, our patient was found to be negative for HIV-1 and 2, HTLV-1 and 2 antibodies, as well as infectious mononucleosis. Negative bacterial, fungal and mycobacterial cultures have effectively ruled out these as the cause. Testing for brucellosis and syphilis were never performed. Conclusion Lymphadenopathy could be seen in the course of SLE; however, it is not considered a diagnostic criterion for the disease. The prevalence of generalized lymphadenopathy in SLE is much less in comparison to cases encountered in the past. Evidence suggests that generalized lymphadenopathy could be indicative of active disease. In addition to proper history, physical examination, and laboratory investigations, a tissue diagnosis based on excisional lymph node biopsy is required to differentiate SLE lymphadenopathy from other diseases, particularly malignancy. Acknowledgments The authors are very thankful to Dr. Kam Newman at the National Institute of Arthritis and Musculoskeletal and Skin Diseases for the revision of the manuscript. Disclosure The manuscript, patient data, and imaging are reproduced in 822
5 Afzal et al J Clin Med Res. 2016;8(11): accordance with Jamaica Hospital Medical Center policies approved by internal IRB. Conflicts of Interest The authors declare that there are no conflicts of interest. References 1. Smith LW, Gelber AC, Petri M. Diffuse lymphadenopathy as the presenting manifestation of systemic lupus erythematosus. J Clin Rheumatol. 2013;19(7): Kitsanou M, Andreopoulou E, Bai MK, Elisaf M, Drosos AA. Extensive lymphadenopathy as the first clinical manifestation in systemic lupus erythematosus. Lupus. 2000;9(2): Shrestha D, Dhakal AK, Shiva RK, Shakya A, Shah SC, Shakya H. Systemic lupus erythematosus and granulomatous lymphadenopathy. BMC Pediatr. 2013;13: Gillmore R, Sin WY. Systemic lupus erythematosus mimicking lymphoma: the relevance of the clinical background in interpreting imaging studies. BMJ Case Rep. 2014; Ozkan EA, Goret CC, Ozdemir ZT, Yanik S, Goret NE, Dogan M, Cihan FG, et al. Evaluation of peripheral lymphadenopathy with excisional biopsy: six-year experience. Int J Clin Exp Pathol. 2015;8(11): Petri M, Orbai AM, Alarcon GS, Gordon C, Merrill JT, Fortin PR, Bruce IN, et al. Derivation and validation of the Systemic Lupus International Collaborating Clinics classification criteria for systemic lupus erythematosus. Arthritis Rheum. 2012;64(8): Shapira Y, Weinberger A, Wysenbeek AJ. Lymphadenopathy in systemic lupus erythematosus. Prevalence and relation to disease manifestations. Clin Rheumatol. 1996;15(4): Papadaki HA, Xylouri I, Katrinakis G, Foudoulakis A, Kritikos HD, Stathopoulos EN, Boumpas DT, et al. Non- Hodgkin's lymphoma in patients with systemic lupus erythematosus. Leuk Lymphoma. 2003;44(2): Cao L, Tong H, Xu G, Liu P, Meng H, Wang J, Zhao X, et al. Systemic lupus erythematous and malignancy risk: a meta-analysis. PLoS One. 2015;10(4):e Kucukardali Y, Solmazgul E, Kunter E, Oncul O, Yildirim S, Kaplan M. Kikuchi-Fujimoto Disease: analysis of 244 cases. Clin Rheumatol. 2007;26(1): Bosch X, Guilabert A, Miquel R, Campo E. Enigmatic Kikuchi-Fujimoto disease: a comprehensive review. Am J Clin Pathol. 2004;122(1): Santana A, Lessa B, Galrao L, Lima I, Santiago M. Kikuchi-Fujimoto's disease associated with systemic lupus erythematosus: case report and review of the literature. Clin Rheumatol. 2005;24(1): Barua A, Vachlas K, Milton R, Thorpe JA. Castleman's disease - a diagnostic dilemma. J Cardiothorac Surg. 2014;9: Casper C. The aetiology and management of Castleman disease at 50 years: translating pathophysiology to patient 823
9/13/2015. Nothing to disclose
 Jared Bozeman Kathleen Luskin MD Bipin Thapa MD Medical College of Wisconsin Milwaukee, Wisconsin Nothing to disclose 24 Year old previously healthy woman presenting from OSH Fatigue Weakness Neck swelling
Jared Bozeman Kathleen Luskin MD Bipin Thapa MD Medical College of Wisconsin Milwaukee, Wisconsin Nothing to disclose 24 Year old previously healthy woman presenting from OSH Fatigue Weakness Neck swelling
Case conference. Welcome Dr. Lawrence Tierney
 Case conference Welcome Dr. Lawrence Tierney Case: 18 year-old male CC) hamatomesis, Fever and cough HPI) 1 st admission One month ago, he admitted to our hospital because of hematemesis. He had weight
Case conference Welcome Dr. Lawrence Tierney Case: 18 year-old male CC) hamatomesis, Fever and cough HPI) 1 st admission One month ago, he admitted to our hospital because of hematemesis. He had weight
High Impact Rheumatology
 High Impact Rheumatology Systemic Lupus Erythematosus Bernard Rubin, DO MPH Case 1: History A 45-year-old woman presents with severe dyspnea and cough. She was in excellent health until 4 weeks ago when
High Impact Rheumatology Systemic Lupus Erythematosus Bernard Rubin, DO MPH Case 1: History A 45-year-old woman presents with severe dyspnea and cough. She was in excellent health until 4 weeks ago when
Fever in Lupus. 21 st April 2014
 Fever in Lupus 21 st April 2014 Fever in lupus Cause of fever N= 487 % SLE fever 206 42 Infection in SLE 265 54.5 Active SLE and infection 8 1.6 Tumor fever 4 0.8 Miscellaneous 4 0.8 Crucial Question Infection
Fever in Lupus 21 st April 2014 Fever in lupus Cause of fever N= 487 % SLE fever 206 42 Infection in SLE 265 54.5 Active SLE and infection 8 1.6 Tumor fever 4 0.8 Miscellaneous 4 0.8 Crucial Question Infection
Clinical outcome and predictive factors of recurrence among patients with Kikuchi s disease
 International Journal of Infectious Diseases (2009) 13, 322 326 http://intl.elsevierhealth.com/journals/ijid Clinical outcome and predictive factors of recurrence among patients with Kikuchi s disease
International Journal of Infectious Diseases (2009) 13, 322 326 http://intl.elsevierhealth.com/journals/ijid Clinical outcome and predictive factors of recurrence among patients with Kikuchi s disease
Pathology of Hematopoietic and Lymphoid tissue
 Pathology of Hematopoietic and Lymphoid tissue Peerayut Sitthichaiyakul, M.D. Department of Pathology and Forensic Medicine Faculty of Medicine, Naresuan University CONTENTS White blood cells and lymph
Pathology of Hematopoietic and Lymphoid tissue Peerayut Sitthichaiyakul, M.D. Department of Pathology and Forensic Medicine Faculty of Medicine, Naresuan University CONTENTS White blood cells and lymph
Abstracting Hematopoietic Neoplasms
 CASE 1: LYMPHOMA PHYSICAL EXAMINATION 43yo male with a history of lower gastrointestinal bleeding and melena undergoing colonoscopy and biopsy to rule out neoplasm versus inflammation. Patient had no other
CASE 1: LYMPHOMA PHYSICAL EXAMINATION 43yo male with a history of lower gastrointestinal bleeding and melena undergoing colonoscopy and biopsy to rule out neoplasm versus inflammation. Patient had no other
CPC. Chutika Srisuttiyakorn, M.D. Kobkul Aunhachoke, M.D. Phramongkutklao Hospital Bangkok, Thailand
 CPC Chutika Srisuttiyakorn, M.D. Kobkul Aunhachoke, M.D. Phramongkutklao Hospital Bangkok, Thailand A 53 year-old woman with fever, facial swelling and rashes on face, trunk and upper extremities for 3
CPC Chutika Srisuttiyakorn, M.D. Kobkul Aunhachoke, M.D. Phramongkutklao Hospital Bangkok, Thailand A 53 year-old woman with fever, facial swelling and rashes on face, trunk and upper extremities for 3
Case Report Traumatic Haemorrhagic Cervical Lymphadenopathy with Underlying Infectious Mononucleosis
 Hindawi Case Reports in Radiology Volume 2017, Article ID 3097414, 4 pages https://doi.org/10.1155/2017/3097414 Case Report Traumatic Haemorrhagic Cervical Lymphadenopathy with Underlying Infectious Mononucleosis
Hindawi Case Reports in Radiology Volume 2017, Article ID 3097414, 4 pages https://doi.org/10.1155/2017/3097414 Case Report Traumatic Haemorrhagic Cervical Lymphadenopathy with Underlying Infectious Mononucleosis
CASE-BASED SMALL GROUP DISCUSSION MHD II
 MHD II, Session 11, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD II Session 11 April 11, 2016 STUDENT COPY MHD II, Session 11, Student Copy Page 2 CASE HISTORY 1 Chief complaint: Our baby
MHD II, Session 11, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD II Session 11 April 11, 2016 STUDENT COPY MHD II, Session 11, Student Copy Page 2 CASE HISTORY 1 Chief complaint: Our baby
Supplemental Figures and Legends
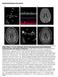 Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
CASE-BASED SMALL GROUP DISCUSSION
 MHD I, Session 13, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION SESSION 13 MHD I Autoimmunity November 10, 2016 STUDENT COPY MHD I, Session 13, STUDENT Copy Page 2 Case 1 CHIEF COMPLAINT: I am
MHD I, Session 13, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION SESSION 13 MHD I Autoimmunity November 10, 2016 STUDENT COPY MHD I, Session 13, STUDENT Copy Page 2 Case 1 CHIEF COMPLAINT: I am
Pathology of Hematopoietic and Lymphoid tissue
 CONTENTS Pathology of Hematopoietic and Lymphoid tissue White blood cells and lymph nodes Quantitative disorder of white blood cells Reactive lymphadenopathies Infectious lymphadenitis Tumor metastasis
CONTENTS Pathology of Hematopoietic and Lymphoid tissue White blood cells and lymph nodes Quantitative disorder of white blood cells Reactive lymphadenopathies Infectious lymphadenitis Tumor metastasis
MHD I SESSION X. Renal Disease
 MHD I, Session X, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION X Renal Disease Monday, November 11, 2013 MHD I, Session X, Student Copy Page 2 Case #1 Cc: I have had weeks of diarrhea
MHD I, Session X, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION X Renal Disease Monday, November 11, 2013 MHD I, Session X, Student Copy Page 2 Case #1 Cc: I have had weeks of diarrhea
Evaluation of Neck Mass. Disclosure. Learning Objectives 3/24/2014. Karen T. Pitman MD, FACS Banner MDACC, Gilbert AZ. Nothing to disclose
 Evaluation of Neck Mass Karen T. Pitman MD, FACS Banner MDACC, Gilbert AZ Nothing to disclose Disclosure Learning Objectives 1. Describe a systematic method to evaluate a patient with a neck mass 2. Select
Evaluation of Neck Mass Karen T. Pitman MD, FACS Banner MDACC, Gilbert AZ Nothing to disclose Disclosure Learning Objectives 1. Describe a systematic method to evaluate a patient with a neck mass 2. Select
CASE-BASED SMALL GROUP DISCUSSION
 MHD I, Session XII, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION Session XII MHD I Friday, November 15, 2013 STUDENT COPY MHD I, Session XII, Student Copy Page 2 Case 1 CHIEF COMPLAINT: I am very
MHD I, Session XII, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION Session XII MHD I Friday, November 15, 2013 STUDENT COPY MHD I, Session XII, Student Copy Page 2 Case 1 CHIEF COMPLAINT: I am very
Kikuchi-Fujimoto disease in inguinal lymph node - A rare site of occurrence
 Kandukuri Mahesh Kumar, V. Indira, V. Hari Shanker. Kikuchi-Fujimoto disease in inguinal lymph node - A rare site of Case Report Kikuchi-Fujimoto disease in inguinal lymph node - A rare site of occurrence
Kandukuri Mahesh Kumar, V. Indira, V. Hari Shanker. Kikuchi-Fujimoto disease in inguinal lymph node - A rare site of Case Report Kikuchi-Fujimoto disease in inguinal lymph node - A rare site of occurrence
Kikuchi s Disease. Safaa AlKhawaja* Khatoon Ali** Shameem Shareef ***
 Bahrain Medical Bulletin, Vol. 28, No. 3, September 2006 Kikuchi s Disease Safaa AlKhawaja* Khatoon Ali** Shameem Shareef *** Fifteen year old male presented with high grade intermittent fever and cervical
Bahrain Medical Bulletin, Vol. 28, No. 3, September 2006 Kikuchi s Disease Safaa AlKhawaja* Khatoon Ali** Shameem Shareef *** Fifteen year old male presented with high grade intermittent fever and cervical
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS LYMPHOMA. April 16, 2008
 MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS LYMPHOMA April 16, 2008 FACULTY COPY GOAL: Learn the appearance of normal peripheral blood elements and lymph nodes. Recognize abnormal peripheral blood
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS LYMPHOMA April 16, 2008 FACULTY COPY GOAL: Learn the appearance of normal peripheral blood elements and lymph nodes. Recognize abnormal peripheral blood
PROFILE OF PAEDIATRIC PATIENTS WITH CERVICAL LYMPHADENOPATHY: A STUDY FROM CENTRAL INDIA Jharna Mishra 1, M. Maheshwari 2, Roshan Chanchlani 3
 PROFILE OF PAEDIATRIC PATIENTS WITH CERVICAL LYMPHADENOPATHY: A STUDY FROM CENTRAL INDIA Jharna Mishra 1, M. Maheshwari 2, Roshan Chanchlani 3 HOW TO CITE THIS ARTICLE: Jharna Mishra, M. Maheshwari, Roshan
PROFILE OF PAEDIATRIC PATIENTS WITH CERVICAL LYMPHADENOPATHY: A STUDY FROM CENTRAL INDIA Jharna Mishra 1, M. Maheshwari 2, Roshan Chanchlani 3 HOW TO CITE THIS ARTICLE: Jharna Mishra, M. Maheshwari, Roshan
DISCUSSION BY: Dr M. R. Shakeebi, MD, Rheumatologist
 Case presentations Related to some Rheumatic Diseases Lab & Clinic i Programs, Tuesday, April 24, 2012 COORDINATOR: Dr M. Mahdi Mohammadi, LMD,PhD, Immunologist COORDINATOR: Dr M. Mahdi Mohammadi, LMD,PhD,
Case presentations Related to some Rheumatic Diseases Lab & Clinic i Programs, Tuesday, April 24, 2012 COORDINATOR: Dr M. Mahdi Mohammadi, LMD,PhD, Immunologist COORDINATOR: Dr M. Mahdi Mohammadi, LMD,PhD,
Test Result Reference Range Flag
 Date of Last Result Test Result Reference Range Flag Dec 07, 2016 25-Hydroxy Vitamin D Total 53 ng/ml 30-100 ng/ml Activated Partial Thromboplast Time Alanine Aminotransferase (ALT/SGPT) 25 sec 24-35 sec
Date of Last Result Test Result Reference Range Flag Dec 07, 2016 25-Hydroxy Vitamin D Total 53 ng/ml 30-100 ng/ml Activated Partial Thromboplast Time Alanine Aminotransferase (ALT/SGPT) 25 sec 24-35 sec
SLIDE SEMINAR NON NEOPLASTIC LYMPH NODE DISORDERS DR SHEILA NAIR CMC, VELLORE
 SLIDE SEMINAR NON NEOPLASTIC LYMPH NODE DISORDERS DR SHEILA NAIR CMC, VELLORE Case 1 34 year old male, mass right cervical region, for 4 years. No other significant findings. Grossly, the mass was well
SLIDE SEMINAR NON NEOPLASTIC LYMPH NODE DISORDERS DR SHEILA NAIR CMC, VELLORE Case 1 34 year old male, mass right cervical region, for 4 years. No other significant findings. Grossly, the mass was well
Dr. Venkateswari. R. Dr. Janani Sankar s unit Kanchi Kamakoti CHILDS Trust Hospital
 Dr. Venkateswari. R. Dr. Janani Sankar s unit Kanchi Kamakoti CHILDS Trust Hospital Acknowledgements: KKCTH Dr. Ramkumar Consultant Dermatologist Dr. Ramprakash Consultant Ophthalmologist Dr. Prasad Manne
Dr. Venkateswari. R. Dr. Janani Sankar s unit Kanchi Kamakoti CHILDS Trust Hospital Acknowledgements: KKCTH Dr. Ramkumar Consultant Dermatologist Dr. Ramprakash Consultant Ophthalmologist Dr. Prasad Manne
Lymphoma co existing with Tuberculosis granulomatous
 Available online at www.worldscientificnews.com WSN 90 (2017) 265-270 EISSN 2392-2192 SHORT COMMUNICATION Lymphoma co existing with Tuberculosis granulomatous Madeeha Subhan 1, *, Waleed Sadiq 2 1 Ayub
Available online at www.worldscientificnews.com WSN 90 (2017) 265-270 EISSN 2392-2192 SHORT COMMUNICATION Lymphoma co existing with Tuberculosis granulomatous Madeeha Subhan 1, *, Waleed Sadiq 2 1 Ayub
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 3/ Issue 37/Aug 21, 2014 Page 9580
 THE SPECTRUM OF CERVICAL LYMPHADENOPATHY IN CHILDREN: A STUDY IN RURAL NORTH INDIA Pawan Tiwari 1, Satya Kiran Kapoor 2, Madhu Tiwari 3, Yogesh Yadav 4 HOW TO CITE THIS ARTICLE: Pawan Tiwari, Satya Kiran
THE SPECTRUM OF CERVICAL LYMPHADENOPATHY IN CHILDREN: A STUDY IN RURAL NORTH INDIA Pawan Tiwari 1, Satya Kiran Kapoor 2, Madhu Tiwari 3, Yogesh Yadav 4 HOW TO CITE THIS ARTICLE: Pawan Tiwari, Satya Kiran
Case Report A Case of Relapsing Kikuchi-Fujimoto Disease
 Case Reports in Otolaryngology Volume 2013, Article ID 364795, 4 pages http://dx.doi.org/10.1155/2013/364795 Case Report A Case of Relapsing Kikuchi-Fujimoto Disease Talayeh Rezayat, Matthew B. Carroll,
Case Reports in Otolaryngology Volume 2013, Article ID 364795, 4 pages http://dx.doi.org/10.1155/2013/364795 Case Report A Case of Relapsing Kikuchi-Fujimoto Disease Talayeh Rezayat, Matthew B. Carroll,
Mr. I.K 58 years old
 Mr. I.K 58 years old Hospitalized because of marked pitting peripheral edema (bilateral crural and perimalleolar edema) and uncontrolled blood pressure (BP 150/100 mmhg under treatment). since age 54 years
Mr. I.K 58 years old Hospitalized because of marked pitting peripheral edema (bilateral crural and perimalleolar edema) and uncontrolled blood pressure (BP 150/100 mmhg under treatment). since age 54 years
Case presentation. Dr Rammohan Reddy 1 st year PG, Dept of DVL, Kamineni Institute of Medical Sciences, Narketpally.
 Case presentation Dr Rammohan Reddy 1 st year PG, Dept of DVL, Kamineni Institute of Medical Sciences, Narketpally. Name : XXX Age : 33 years Sex : Female Occupation : Farmer IP no : 201608905 DOA : 15-02-2016
Case presentation Dr Rammohan Reddy 1 st year PG, Dept of DVL, Kamineni Institute of Medical Sciences, Narketpally. Name : XXX Age : 33 years Sex : Female Occupation : Farmer IP no : 201608905 DOA : 15-02-2016
A Rare case of Tubercular Gingivitis Case Report
 Case Report A Rare case of Tubercular Gingivitis Case Report *Dr. Ansh Chugh 1, Dr. Firoz A Hakkim 2, Dr. Rajesh. V 3, Dr. Raghava Sharma 4 1: JUNIOR RESIDENT IN GENERAL MEDICINE 2: SENIOR RESIDENT IN
Case Report A Rare case of Tubercular Gingivitis Case Report *Dr. Ansh Chugh 1, Dr. Firoz A Hakkim 2, Dr. Rajesh. V 3, Dr. Raghava Sharma 4 1: JUNIOR RESIDENT IN GENERAL MEDICINE 2: SENIOR RESIDENT IN
Kikuchi s disease (necrotizing lymphadenitis) presenting as acneiform eruption
 Journal of the Saudi Society of Dermatology & Dermatologic Surgery (2012) 16, 67 71 King Saud University Journal of the Saudi Society of Dermatology & Dermatologic Surgery www.ksu.edu.sa www.jssdds.org
Journal of the Saudi Society of Dermatology & Dermatologic Surgery (2012) 16, 67 71 King Saud University Journal of the Saudi Society of Dermatology & Dermatologic Surgery www.ksu.edu.sa www.jssdds.org
Tables of Normal Values (As of February 2005)
 Tables of Normal Values (As of February 2005) Note: Values and units of measurement listed in these Tables are derived from several resources. Substantial variation exists in the ranges quoted as normal
Tables of Normal Values (As of February 2005) Note: Values and units of measurement listed in these Tables are derived from several resources. Substantial variation exists in the ranges quoted as normal
EBV and Infectious Mononucleosis. Infectious Disease Definitions. Infectious Diseases
 Infectious Disease Definitions Infection when a microorganism invades a host and multiplies enough to disrupt normal function by causing signs and symptoms Pathogencity ability of an organism to cause
Infectious Disease Definitions Infection when a microorganism invades a host and multiplies enough to disrupt normal function by causing signs and symptoms Pathogencity ability of an organism to cause
Fever of unknown origin
 Fever of unknown origin Case B History of the present illness 75 years old women presented at our hospital with since months daily fevers between 38 to 39.5 Celsius (100.4-103.1 F) with night sweats. Her
Fever of unknown origin Case B History of the present illness 75 years old women presented at our hospital with since months daily fevers between 38 to 39.5 Celsius (100.4-103.1 F) with night sweats. Her
MULTI-SYSTEM SARCOIDOSIS CAUSING PANHYPOPITUITARISM: RAPID IMPROVEMENT WITH CORTICOSTEROID THERAPY Rashid Mahboob, MD; Ali A.
 ENDOCRINE PRACTICE Rapid Electronic Article in Press Rapid Electronic Articles in Press are preprinted manuscripts that have been reviewed and accepted for publication, but have yet to be edited, typeset
ENDOCRINE PRACTICE Rapid Electronic Article in Press Rapid Electronic Articles in Press are preprinted manuscripts that have been reviewed and accepted for publication, but have yet to be edited, typeset
AAM Case Discussion Guide Key Learning Objectives
 AAM Case Discussion Guide Key Learning Objectives List the differential diagnosis for a systemic disease presentation in a young person. Discuss the key elements of diagnosing systemic lupus erythematosus
AAM Case Discussion Guide Key Learning Objectives List the differential diagnosis for a systemic disease presentation in a young person. Discuss the key elements of diagnosing systemic lupus erythematosus
Case Report A Rare Case of Kikuchi Fujimoto s Disease with Subsequent Development of Systemic Lupus Erythematosus
 Case Reports in Rheumatology Volume 2012, Article ID 325062, 4 pages doi:10.1155/2012/325062 Case Report A Rare Case of Kikuchi Fujimoto s Disease with Subsequent Development of Systemic Lupus Erythematosus
Case Reports in Rheumatology Volume 2012, Article ID 325062, 4 pages doi:10.1155/2012/325062 Case Report A Rare Case of Kikuchi Fujimoto s Disease with Subsequent Development of Systemic Lupus Erythematosus
SB 6331 (scanned slide available) Keith Duncan; Mills-Peninsula Hospital 52-year-old male with painful right parotid mass.
 SB 6331 (scanned slide available) Keith Duncan; Mills-Peninsula Hospital 52-year-old male with painful right parotid mass. SB 6332 Shyam Raghavan/Don Born; Stanford 77-year-old male with right
SB 6331 (scanned slide available) Keith Duncan; Mills-Peninsula Hospital 52-year-old male with painful right parotid mass. SB 6332 Shyam Raghavan/Don Born; Stanford 77-year-old male with right
HISTOPATHOLOGIC FINDINGS OF LYMPH NODE BIOPSY CASES IN COMPARISON WITH CLINICAL FEATURES
 Original Article HISTOPATHOLOGIC FINDINGS OF LYMPH NODE BIOPSY CASES IN COMPARISON WITH CLINICAL FEATURES Shokouh Taghipour Zahir 1, Alireza Azimi 2 ABSTRACT Objective: To determine useful and important
Original Article HISTOPATHOLOGIC FINDINGS OF LYMPH NODE BIOPSY CASES IN COMPARISON WITH CLINICAL FEATURES Shokouh Taghipour Zahir 1, Alireza Azimi 2 ABSTRACT Objective: To determine useful and important
Lymphoma Case Scenario 1
 Lymphoma Case Scenario 1 HISTORY: A 23-year-old healthy female presented with a month-long history of persistent headache of increasing severity. She noted episodic nausea and vomiting in association with
Lymphoma Case Scenario 1 HISTORY: A 23-year-old healthy female presented with a month-long history of persistent headache of increasing severity. She noted episodic nausea and vomiting in association with
Lymphatic System Disorders
 Lymphatic System Disorders Lymphomas Malignant neoplasms involving lymphocyte proliferation in lymph nodes Specific causes not identified // Higher risk in adults who received radiation during childhood
Lymphatic System Disorders Lymphomas Malignant neoplasms involving lymphocyte proliferation in lymph nodes Specific causes not identified // Higher risk in adults who received radiation during childhood
Significance of Anti-C1q Antibodies in Patients with Systemic Lupus Erythematosus as A Marker of Disease Activity and Lupus Nephritis
 THE EGYPTIAN JOURNAL OF IMMUNOLOGY Vol. 23 (1), 2016 Page: 00-00 Significance of Anti-C1q Antibodies in Patients with Systemic Lupus Erythematosus as A Marker of Disease Activity and Lupus Nephritis 1
THE EGYPTIAN JOURNAL OF IMMUNOLOGY Vol. 23 (1), 2016 Page: 00-00 Significance of Anti-C1q Antibodies in Patients with Systemic Lupus Erythematosus as A Marker of Disease Activity and Lupus Nephritis 1
An Uncommon Presentation of Large B-cell Lymphoma of the kidney A Case Report and Literature Review
 An Uncommon Presentation of Large B-cell Lymphoma of the kidney A Case Report and Literature Review CHRISTOPHER ADILETTA M.D., AJAZ SHAWL M.D. ST. JOSEPH S HEALTH, SYRACUSE, NY Our Patient Case We present
An Uncommon Presentation of Large B-cell Lymphoma of the kidney A Case Report and Literature Review CHRISTOPHER ADILETTA M.D., AJAZ SHAWL M.D. ST. JOSEPH S HEALTH, SYRACUSE, NY Our Patient Case We present
SydPath Reference Intervals for Clinical Trials (Contract Pathology Unit) Unauthorised Copy
 HAEMATOLOGY APTT 1 150 M 25 35 sec APTT 1 150 F 25 35 sec Basophils Cord 2 weeks M 0.0 0.4 10^9/L Basophils Cord 2 weeks F 0.0 0.4 10^9/L Basophils 2 wks 3 mths M 0.0 0.2 10^9/L Basophils 2 wks 3 mths
HAEMATOLOGY APTT 1 150 M 25 35 sec APTT 1 150 F 25 35 sec Basophils Cord 2 weeks M 0.0 0.4 10^9/L Basophils Cord 2 weeks F 0.0 0.4 10^9/L Basophils 2 wks 3 mths M 0.0 0.2 10^9/L Basophils 2 wks 3 mths
Case Presentation VASCULITIS. Case Presentation. Case Presentation. Vasculitis
 Case Presentation VASCULITIS The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
Case Presentation VASCULITIS The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
YF Case Discussion Guide Key Learning Objectives
 YF Case Discussion Guide Key Learning Objectives List the differential diagnosis for a systemic disease presentation. Describe the key manifestations of disease on physical exam in a multisystem disease
YF Case Discussion Guide Key Learning Objectives List the differential diagnosis for a systemic disease presentation. Describe the key manifestations of disease on physical exam in a multisystem disease
Contents. vii. Preface... Acknowledgments... v xiii
 Contents Preface... Acknowledgments... v xiii SECTION I 1. Introduction... 3 Knowledge-Based Diagnosis... 4 Systematic Examination of the Lymph Node... 7 Cell Type Identification... 9 Cell Size and Cellularity...
Contents Preface... Acknowledgments... v xiii SECTION I 1. Introduction... 3 Knowledge-Based Diagnosis... 4 Systematic Examination of the Lymph Node... 7 Cell Type Identification... 9 Cell Size and Cellularity...
MANAGING THE PATIENT WITH POSITIVE ANA
 MANAGING THE PATIENT WITH POSITIVE ANA Rafael F. Rivas-Chacon, M.D. Disclosures Grant/Research support for: Pfizer Study JIA A3921104 Tofacitinib not related to this presentation 1 Positive Antinuclear
MANAGING THE PATIENT WITH POSITIVE ANA Rafael F. Rivas-Chacon, M.D. Disclosures Grant/Research support for: Pfizer Study JIA A3921104 Tofacitinib not related to this presentation 1 Positive Antinuclear
Case Presentation. Rafid Asfar, MD
 Case Presentation Rafid Asfar, MD Introduction ANCA associated vasculitis may be localized or systemic, and can involve the eyes Ocular manifestations can occur in the absence of systemic disease in persons
Case Presentation Rafid Asfar, MD Introduction ANCA associated vasculitis may be localized or systemic, and can involve the eyes Ocular manifestations can occur in the absence of systemic disease in persons
LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center
 LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center Lymphoma is cancer of the lymphatic system. The lymphatic system is made up of organs all over the body that make up and store cells
LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center Lymphoma is cancer of the lymphatic system. The lymphatic system is made up of organs all over the body that make up and store cells
1.) 3 yr old FS Siamese cat: 3 day history of lethargy, anorexia. Dyspneic, thin, febrile.
 1.) 3 yr old FS Siamese cat: 3 day history of lethargy, anorexia. Dyspneic, thin, febrile. NUCLEATED CELLS 19.5 High 4.0-14.0 x 10^3/ul METAMYELOCYTES 9 % 1.8 High 0.0-0.0 x 10^3/ul BAND NEUTROPHILS 61
1.) 3 yr old FS Siamese cat: 3 day history of lethargy, anorexia. Dyspneic, thin, febrile. NUCLEATED CELLS 19.5 High 4.0-14.0 x 10^3/ul METAMYELOCYTES 9 % 1.8 High 0.0-0.0 x 10^3/ul BAND NEUTROPHILS 61
9/25/2013 SYSTEMIC LUPUS ERYTHEMATOSUS (SLE)
 SYSTEMIC LUPUS ERYTHEMATOSUS (SLE) 1 Other Types of Lupus Discoid Lupus Erythematosus Lupus Pernio --- Sarcoidosis Lupus Vulgaris --- Tuberculosis of the face Manifestations of SLE Fever Rashes Arthritis
SYSTEMIC LUPUS ERYTHEMATOSUS (SLE) 1 Other Types of Lupus Discoid Lupus Erythematosus Lupus Pernio --- Sarcoidosis Lupus Vulgaris --- Tuberculosis of the face Manifestations of SLE Fever Rashes Arthritis
VASCULITIS. Case Presentation. Case Presentation
 VASCULITIS Case Presentation The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
VASCULITIS Case Presentation The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
ACHIEVING EXCELLENCE IN ABSTRACTING: LYMPHOMA
 ACHIEVING EXCELLENCE IN ABSTRACTING: LYMPHOMA ACHIEVING EXCELLENCE IN ABSTRACTING LYMPHOMA Recoding Audit Performed in 2009 260 cases audited 17 data items audited per case 4420 possible discrepancies
ACHIEVING EXCELLENCE IN ABSTRACTING: LYMPHOMA ACHIEVING EXCELLENCE IN ABSTRACTING LYMPHOMA Recoding Audit Performed in 2009 260 cases audited 17 data items audited per case 4420 possible discrepancies
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING
 AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
NEW RCPCH REFERENCE RANGES-
 s vary between populations and age groups and it is important to always check the reference Haematology: Haemoglobin Male 130 175 g/l 0 6 days 145-220 g/l Female 115 165 g/l 7 days 140-186 g/l 8 days 3
s vary between populations and age groups and it is important to always check the reference Haematology: Haemoglobin Male 130 175 g/l 0 6 days 145-220 g/l Female 115 165 g/l 7 days 140-186 g/l 8 days 3
Difficult Diagnosis: Case History. 7 months prior, she happened to have undergone a C-spine MRI after a car accident
 Relevant Disclosures: None Difficult Diagnosis: Recent Advances in Neurology 2013 Jeffrey M. Gelfand, MD Assistant Professor UCSF Neuroinflammation and MS Center UCSF Department of Neurology Case History
Relevant Disclosures: None Difficult Diagnosis: Recent Advances in Neurology 2013 Jeffrey M. Gelfand, MD Assistant Professor UCSF Neuroinflammation and MS Center UCSF Department of Neurology Case History
Management of acute alcoholic hepatitis
 Management of acute alcoholic hepatitis Yesim ALAHDAB Marmara University Hospital, Istanbul/TURKEY 5 th European Young Hepatologists Workshop August, 27-29, 2015 Moulin de Vernègues, France 1.4L ALCOHOL
Management of acute alcoholic hepatitis Yesim ALAHDAB Marmara University Hospital, Istanbul/TURKEY 5 th European Young Hepatologists Workshop August, 27-29, 2015 Moulin de Vernègues, France 1.4L ALCOHOL
Easy Trick to Spot Leukemia for Pediatricians
 Easy Trick to Spot Leukemia for Pediatricians Piya Rujkijyanont, MD Division of Hematology-Oncology Department of Pediatrics Phramongkutklao Hospital Most Common Pediatric Cancers Age 0-14 Leukemia 32%
Easy Trick to Spot Leukemia for Pediatricians Piya Rujkijyanont, MD Division of Hematology-Oncology Department of Pediatrics Phramongkutklao Hospital Most Common Pediatric Cancers Age 0-14 Leukemia 32%
Scleritis LEN V KOH OD
 Scleritis LEN V KOH OD 2014 PUCO 1 Introduction A painful, destructive, and potentially blinding disorder Highly symptomatic High association with systemic disease Immunosuppresssive agents 2014 PUCO 2
Scleritis LEN V KOH OD 2014 PUCO 1 Introduction A painful, destructive, and potentially blinding disorder Highly symptomatic High association with systemic disease Immunosuppresssive agents 2014 PUCO 2
Documentation Dissection
 History of Present Illness: Documentation Dissection The patient is a 50-year-old male c/o symptoms for past 4 months 1, severe 2 bloating and stomach cramps, some nausea, vomiting, diarrhea. In last 3
History of Present Illness: Documentation Dissection The patient is a 50-year-old male c/o symptoms for past 4 months 1, severe 2 bloating and stomach cramps, some nausea, vomiting, diarrhea. In last 3
Infectious Mononucleosis The Virus Pathophysiology: Age: History: Fever. Lymphadenopathy
 Infectious Mononucleosis The Virus A member of the Herpesvirus family Infects human B lymphocytes Herpes viruses contain double-stranded DNA, and they have an icosahedral capsid and a glycoprotein-containing
Infectious Mononucleosis The Virus A member of the Herpesvirus family Infects human B lymphocytes Herpes viruses contain double-stranded DNA, and they have an icosahedral capsid and a glycoprotein-containing
Systemic examination
 PROLONGED FEVER IN AN ADOLESCENT BOY Dr.Praveena Lionel, DNB PG, Dr.Kannan (HOD) Railway Hospital, Perambur History 11 yrs old adolescent boy was admitted with c/o Fever -1 wk Myalgia -1 wk Arthralgia
PROLONGED FEVER IN AN ADOLESCENT BOY Dr.Praveena Lionel, DNB PG, Dr.Kannan (HOD) Railway Hospital, Perambur History 11 yrs old adolescent boy was admitted with c/o Fever -1 wk Myalgia -1 wk Arthralgia
CLINICAL VIGNETTE Sarcoidosis: A Case Study Gloria Kim, M.D.
 CLINICAL VIGNETTE Sarcoidosis: A Case Study Gloria Kim, M.D. Case Report A 56-year-old female presented to her primary care physician with complaints of dyspnea on exertion and increasing cough. She reported
CLINICAL VIGNETTE Sarcoidosis: A Case Study Gloria Kim, M.D. Case Report A 56-year-old female presented to her primary care physician with complaints of dyspnea on exertion and increasing cough. She reported
UNUSUAL PRESENTATIONS OF SYSTEMIC LUPUS ERYTHEMATOSUS
 UNUSUAL PRESENTATIONS OF SYSTEMIC LUPUS ERYTHEMATOSUS Presenter- Dr. Meghana B S Prof Dr. NAGARAJA B S Prof Dr. NIRMALA A C Dr. SIVARANJANI H Dr. B C PRAKASH Dr. MUMTAZ ALI KHAN A 60 year old lady, k/c/o
UNUSUAL PRESENTATIONS OF SYSTEMIC LUPUS ERYTHEMATOSUS Presenter- Dr. Meghana B S Prof Dr. NAGARAJA B S Prof Dr. NIRMALA A C Dr. SIVARANJANI H Dr. B C PRAKASH Dr. MUMTAZ ALI KHAN A 60 year old lady, k/c/o
Dr Vidya Devarajan DNB(Gen Med),FNB(ID), Fellowship ID,SCE (UK) Consultant ID Apollo Cancer Hospital
 Dr Vidya Devarajan DNB(Gen Med),FNB(ID), Fellowship ID,SCE (UK) Consultant ID Apollo Cancer Hospital Knowledge of nodal distribution and anatomic drainage Provide an approach to the patient with peripheral
Dr Vidya Devarajan DNB(Gen Med),FNB(ID), Fellowship ID,SCE (UK) Consultant ID Apollo Cancer Hospital Knowledge of nodal distribution and anatomic drainage Provide an approach to the patient with peripheral
Warm Autoantibodies in a Patient with Hemophagocytic Lymphohistiocytosis: A Case Report
 Warm Autoantibodies in a Patient with Hemophagocytic Lymphohistiocytosis: A Case Report Emily Coberly, MD Department of Pathology and Anatomical Sciences University of Missouri Columbia April 30, 2013
Warm Autoantibodies in a Patient with Hemophagocytic Lymphohistiocytosis: A Case Report Emily Coberly, MD Department of Pathology and Anatomical Sciences University of Missouri Columbia April 30, 2013
Subject ID: I N D # # U A * Consent Date: Day Month Year
 IND Study # Eligibility Checklist Pg 1 of 15 Instructions: Check the appropriate box for each Inclusion and Exclusion Criterion below. Each criterion must be marked and all protocol criteria have to be
IND Study # Eligibility Checklist Pg 1 of 15 Instructions: Check the appropriate box for each Inclusion and Exclusion Criterion below. Each criterion must be marked and all protocol criteria have to be
88-year-old Female with Lymphadenopathy. Faizi Ali, MD
 88-year-old Female with Lymphadenopathy Faizi Ali, MD Clinical History A 88-year-old caucasian female presented to our hospital with the complaints of nausea, vomiting,diarrhea, shortness of breath and
88-year-old Female with Lymphadenopathy Faizi Ali, MD Clinical History A 88-year-old caucasian female presented to our hospital with the complaints of nausea, vomiting,diarrhea, shortness of breath and
Committee Approval Date: May 9, 2014 Next Review Date: May 2015
 Medication Policy Manual Policy No: dru248 Topic: Benlysta, belimumab Date of Origin: May 13, 2011 Committee Approval Date: May 9, 2014 Next Review Date: May 2015 Effective Date: June 1, 2014 IMPORTANT
Medication Policy Manual Policy No: dru248 Topic: Benlysta, belimumab Date of Origin: May 13, 2011 Committee Approval Date: May 9, 2014 Next Review Date: May 2015 Effective Date: June 1, 2014 IMPORTANT
Case 5 15-year-old male
 Case 5 15-year-old male Present illness: Six months ago, abnormality of ECG was incidentally detected by annual health check. His blood level of γ-gtp, HbA1c and norepinephrine were elevated; however,
Case 5 15-year-old male Present illness: Six months ago, abnormality of ECG was incidentally detected by annual health check. His blood level of γ-gtp, HbA1c and norepinephrine were elevated; however,
Case Report Internal Jugular Vein Thrombosis in Isolated Tuberculous Cervical Lymphadenopathy
 Volume 2016, Article ID 5184196, 4 pages http://dx.doi.org/10.1155/2016/5184196 Case Report Internal Jugular Vein Thrombosis in Isolated Tuberculous Cervical Lymphadenopathy Sanjay Khaladkar, Avadhesh
Volume 2016, Article ID 5184196, 4 pages http://dx.doi.org/10.1155/2016/5184196 Case Report Internal Jugular Vein Thrombosis in Isolated Tuberculous Cervical Lymphadenopathy Sanjay Khaladkar, Avadhesh
Severe falciparum malaria with hypophosphataemia and presumed hypophosphatemia induced rhabdomyolysis: a case report
 142 Case Report Severe falciparum malaria with hypophosphataemia and presumed hypophosphatemia induced rhabdomyolysis: a case report M Perera, V Samarawickrama, K Lokuketagoda, K Thirumavalavan Sri Lankan
142 Case Report Severe falciparum malaria with hypophosphataemia and presumed hypophosphatemia induced rhabdomyolysis: a case report M Perera, V Samarawickrama, K Lokuketagoda, K Thirumavalavan Sri Lankan
POSTGRADUATE INSTITUTE OF MEDICINE UNIVERSITY OF COLOMBO
 POSTGRADUATE INSTITUTE OF MEDICINE UNIVERSITY OF COLOMBO Selection Examination for Enrolment to the in-service Training Programme in Postgraduate Certificate in Basic Laboratory Sciences leading to the
POSTGRADUATE INSTITUTE OF MEDICINE UNIVERSITY OF COLOMBO Selection Examination for Enrolment to the in-service Training Programme in Postgraduate Certificate in Basic Laboratory Sciences leading to the
Infections and nonmicrobial inflammatory stimuli can cause leukocytosis (as seen in Lab 1) as well as lymph node enlargement (lymphadenopathy).
 LAB 5: LYMPHOID TISSUE AND SKIN The focus of this week s lab will be pathology of the lymphoid tissue and skin. The lymphoid organs include the thymus, spleen, and lymph nodes. Abnormalities in the lymph
LAB 5: LYMPHOID TISSUE AND SKIN The focus of this week s lab will be pathology of the lymphoid tissue and skin. The lymphoid organs include the thymus, spleen, and lymph nodes. Abnormalities in the lymph
ACP Rheumatology Pearls. Adam Q Carlson MD Assistant Professor UVA Rheumatology
 ACP Rheumatology Pearls Adam Q Carlson MD Assistant Professor UVA Rheumatology Disclosures I have no personal or professional disclosures Case #1 27 yo woman with a history of systemic lupus complicated
ACP Rheumatology Pearls Adam Q Carlson MD Assistant Professor UVA Rheumatology Disclosures I have no personal or professional disclosures Case #1 27 yo woman with a history of systemic lupus complicated
Budsakorn Darawankul, MD. Maharat Nakhon Ratchasima Hospital
 Budsakorn Darawankul, MD. Maharat Nakhon Ratchasima Hospital Outline What is ANA? How to detect ANA? Clinical application Common autoantibody in ANA diseases Outline What is ANA? How to detect ANA? Clinical
Budsakorn Darawankul, MD. Maharat Nakhon Ratchasima Hospital Outline What is ANA? How to detect ANA? Clinical application Common autoantibody in ANA diseases Outline What is ANA? How to detect ANA? Clinical
COMPANY OR UNIVERSITY
 CONTRIBUTOR NAME Daniel Heinrich, DVM CONTRIBUTOR EMAIL dheinric@umn.edu COAUTHORS Jed Overmann, DVM, DACVP; Davis Seelig DVM, PhD, DACVP & Matthew Sturos, DVM COMPANY OR UNIVERSITY University of Minnesota
CONTRIBUTOR NAME Daniel Heinrich, DVM CONTRIBUTOR EMAIL dheinric@umn.edu COAUTHORS Jed Overmann, DVM, DACVP; Davis Seelig DVM, PhD, DACVP & Matthew Sturos, DVM COMPANY OR UNIVERSITY University of Minnesota
The focus of this week s lab will be pathology of the cardiovascular system.
 LAB 3: THE MUSCLE AND CARDIOVASCULAR SYSTEM The focus of this week s lab will be pathology of the cardiovascular system. The cases we will cover are: A. Atherosclerosis Refer to virtual slide p_8, should
LAB 3: THE MUSCLE AND CARDIOVASCULAR SYSTEM The focus of this week s lab will be pathology of the cardiovascular system. The cases we will cover are: A. Atherosclerosis Refer to virtual slide p_8, should
Australian and New Zealand College of Veterinary Scientists. Membership Examination. Small Animal Medicine Paper 1
 Australian and New Zealand College of Veterinary Scientists Membership Examination June 2017 Small Animal Medicine Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours after perusal Answer
Australian and New Zealand College of Veterinary Scientists Membership Examination June 2017 Small Animal Medicine Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours after perusal Answer
Case Report A case of EBV positive diffuse large B-cell lymphoma of the adolescent
 Int J Clin Exp Med 2014;7(1):307-311 www.ijcem.com /ISSN:1940-5901/IJCEM1311029 Case Report A case of EBV positive diffuse large B-cell lymphoma of the adolescent Qilin Ao 2, Ying Wang 1, Sanpeng Xu 2,
Int J Clin Exp Med 2014;7(1):307-311 www.ijcem.com /ISSN:1940-5901/IJCEM1311029 Case Report A case of EBV positive diffuse large B-cell lymphoma of the adolescent Qilin Ao 2, Ying Wang 1, Sanpeng Xu 2,
Summary Article: Lupus (Systemic Lupus Erythematosus) from Harvard Medical School Health Topics A-Z
 Topic Page: Systemic Lupus Erythematosus Summary Article: Lupus (Systemic Lupus Erythematosus) from Harvard Medical School Health Topics A-Z What Is It? Lupus is thought to develop when the immune system
Topic Page: Systemic Lupus Erythematosus Summary Article: Lupus (Systemic Lupus Erythematosus) from Harvard Medical School Health Topics A-Z What Is It? Lupus is thought to develop when the immune system
Pulmonary Sarcoidosis - Radiological Evaluation
 Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
( Rosai Dorfman disease)
 Sinus histiocytosis with massive lymphadenopathy ( Rosai Dorfman disease) BIBI SHAIN SHAMSIAN Rosai Dorfman disease Rosai-Dorfman Disease (RDD) or Sinus Histiocytosis with massive lymhadenopathy (SHML):
Sinus histiocytosis with massive lymphadenopathy ( Rosai Dorfman disease) BIBI SHAIN SHAMSIAN Rosai Dorfman disease Rosai-Dorfman Disease (RDD) or Sinus Histiocytosis with massive lymhadenopathy (SHML):
AAF Case Discussion Guide Key Learning Objectives
 AAF Case Discussion Guide Key Learning Objectives List the differential diagnosis for a systemic disease presentation with multisystem involvement. Identify the key questions from the history to look for
AAF Case Discussion Guide Key Learning Objectives List the differential diagnosis for a systemic disease presentation with multisystem involvement. Identify the key questions from the history to look for
Vasculitis. Edward Dwyer, M.D. Division of Rheumatology. Vasculitis
 Edward Dwyer, M.D. Division of Rheumatology VASCULITIS is a primary inflammatory disease process of the vasculature Determinants of the Clinical Manifestations of : Target organ involved Size of vessel
Edward Dwyer, M.D. Division of Rheumatology VASCULITIS is a primary inflammatory disease process of the vasculature Determinants of the Clinical Manifestations of : Target organ involved Size of vessel
A RARE NEUROLOGICAL PRESENTATION OF SLE. Dr Yoganand M N Dr Prithvi P Nayak
 A RARE NEUROLOGICAL PRESENTATION OF SLE Dr Jayachandra Dr Yoganand M N Dr Prithvi P Nayak Presenter: Dr Shambhavi K R CHIEF COMPLAINTS A 30 year old lady hailing from Nepal presented to OPD with complaints
A RARE NEUROLOGICAL PRESENTATION OF SLE Dr Jayachandra Dr Yoganand M N Dr Prithvi P Nayak Presenter: Dr Shambhavi K R CHIEF COMPLAINTS A 30 year old lady hailing from Nepal presented to OPD with complaints
LEUKAEMIA and LYMPHOMA. Dr Mubarak Abdelrahman Assistant Professor Jazan University
 LEUKAEMIA and LYMPHOMA Dr Mubarak Abdelrahman Assistant Professor Jazan University OBJECTIVES Identify etiology and epidemiology for leukemia and lymphoma. Discuss common types of leukemia. Distinguish
LEUKAEMIA and LYMPHOMA Dr Mubarak Abdelrahman Assistant Professor Jazan University OBJECTIVES Identify etiology and epidemiology for leukemia and lymphoma. Discuss common types of leukemia. Distinguish
THE URINARY SYSTEM. The cases we will cover are:
 THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
THE URINARY SYSTEM. The cases we will cover are:
 THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD. Part 1
 HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD Part 1 NONNEOPLASTIC DISEASES OF THE WHITE BLOOD CELLS There are five major types of WBCs in the blood: neutrophils,
HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD Part 1 NONNEOPLASTIC DISEASES OF THE WHITE BLOOD CELLS There are five major types of WBCs in the blood: neutrophils,
HASPI Medical Biology Lab 03
 Patient 1001 is a 42-year-old female that is experiencing severe heartburn, abdominal pain, bloating, nausea, and vomiting. Ulcers Bleeding sores in the stomach or intestine Gallbladder Disease Gallstones
Patient 1001 is a 42-year-old female that is experiencing severe heartburn, abdominal pain, bloating, nausea, and vomiting. Ulcers Bleeding sores in the stomach or intestine Gallbladder Disease Gallstones
FINE NEEDLE ASPIRATION (FNAC) AS A DIAGNOSTIC TOOL IN PAEDIATRIC LYMPHADENOPATHY.
 IJCRR Vol 06 issue 01 Section: Healthcare Category: Research Received on: 16/10/13 Revised on: 18/11/13 Accepted on: 20/12/13 FINE NEEDLE ASPIRATION (FNAC) AS A DIAGNOSTIC TOOL IN PAEDIATRIC Heming Agrawal,
IJCRR Vol 06 issue 01 Section: Healthcare Category: Research Received on: 16/10/13 Revised on: 18/11/13 Accepted on: 20/12/13 FINE NEEDLE ASPIRATION (FNAC) AS A DIAGNOSTIC TOOL IN PAEDIATRIC Heming Agrawal,
CASE-BASED SMALL GROUP DISCUSSION
 MHD II, Session XII, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION Session XII MHD II April 21, 2014 STUDENT COPY Helpful Resource: ACP Medicine online available through LUHS Library Infectious
MHD II, Session XII, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION Session XII MHD II April 21, 2014 STUDENT COPY Helpful Resource: ACP Medicine online available through LUHS Library Infectious
PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert.
 PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. GENERIC DRUG NAME / COMPOUND NUMBER: Tofacitinib / CP-690,550
PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. GENERIC DRUG NAME / COMPOUND NUMBER: Tofacitinib / CP-690,550
Systemic Lupus Erythematosus
 Systemic Lupus Erythematosus Marc C. Hochberg, MD, MPH Professor of Medicine and Head, Division of Rheumatology University of Maryland School of Medicine CASE: HISTORY A 26-year-old woman is seen for migratory
Systemic Lupus Erythematosus Marc C. Hochberg, MD, MPH Professor of Medicine and Head, Division of Rheumatology University of Maryland School of Medicine CASE: HISTORY A 26-year-old woman is seen for migratory
Clinical Radiological Pathological Conference
 Clinical Radiological Pathological Conference CASE 1: A 59-year-old female Housekeeper Live in Phuket, Thailand Progressive dyspnea for 1 year Present illness 1 year PTA : She developed dyspnea on exertion
Clinical Radiological Pathological Conference CASE 1: A 59-year-old female Housekeeper Live in Phuket, Thailand Progressive dyspnea for 1 year Present illness 1 year PTA : She developed dyspnea on exertion
Systemic lupus erythematosus (SLE) is a chronic, autoimmune
 115 Focal Neurological Deficits due to a Contrast Enhancing Lesion in a Patient with Systemic Lupus Erythematosus Case report and Review of Literature Sundeep Srikakulam, M.D., and Anca Askanase, M.D.,
115 Focal Neurological Deficits due to a Contrast Enhancing Lesion in a Patient with Systemic Lupus Erythematosus Case report and Review of Literature Sundeep Srikakulam, M.D., and Anca Askanase, M.D.,
Hamilton Regional Laboratory Medicine Program
 Created: April 2002 of Review: February 2004 of Review: June 2006 of Review: July 2007, St. Joseph s Healthcare went live with Meditech as of June18, 2007. of Review: August 2009 of Review: December 2011;
Created: April 2002 of Review: February 2004 of Review: June 2006 of Review: July 2007, St. Joseph s Healthcare went live with Meditech as of June18, 2007. of Review: August 2009 of Review: December 2011;
