Early instrumental predictors of long term neurodevelopmental impairment in newborns with perinatal asphyxia treated with therapeutic hypothermia
|
|
|
- Candice Hardy
- 5 years ago
- Views:
Transcription
1 SIGNA VITAE 218; 14(1): Early instrumental predictors of long term neurodevelopmental impairment in newborns with perinatal asphyxia treated with therapeutic hypothermia ALICE MONZANI 1, GIANLUCA COSI 2, GIULIA GENONI 1, MARIA LAVRANO 1, CIN- ZIA PERUZZI 3, ROBERTA POMELLA 3, FEDERICA FERRERO 2 1 Division of Pediatrics, Department of Health Sciences, Università del Piemonte Orientale, vara, Italy 2 Division of Neonatal Intensive Care Unit, Azienda Ospedaliero-Universitaria Maggiore della Carità, vara, Italy 3 Division of Child Neurology and Psychiatry, Azienda Ospedaliero-Universitaria Maggiore della Carità, vara, Italy Corresponding author Alice Monzani Division of Pediatrics Department of Health Sciences, Università del Piemonte Orientale V. Solaroli 17, 281 vara, Italy Phone: (39) Fax: (39) alice.monzani@med.uniupo.it ABSTRACT Background. Hypoxic-ischemic encephalopathy (HIE) is a leading cause of disability in full-term newborns. Long-term consequences of HIE, even when treated by hypothermia, are not easily predictable. Aims. To assess the potential role of electroencephalography and neuroimaging parameters as early predictors of neurodevelopmental outcome in HIE newborns treated with hypothermia. Methods. We retrospectively evaluated 13 HIE patients treated with hypothermia in January 212-September 214. We reviewed their amplitude-integrated electroencephalography (a-eeg) at 6, 12 and 24 hours (h), cranial ultrasonography (US) at 12, 72 h and >7 days of life (DOL) and brain magnetic resonance (MRI) performed at 7-28 DOL, according to validated scores. aeeg, US and MRI patterns were correlated to neurodevelopmental outcome at months, considered as negative if one of the following was present: Mental Development Index (MDI)<85, motor, visual or hearing impairment. Results. The severity of a-eeg, US and MRI alterations at each time point was not different according to the outcome. MDI was negatively correlated with aeeg score at 12h (R= -.571, p=.4) and with US score at 72h (R= -.63, p=.2). A positive correlation was found between aeeg score at 6h and US score at >7DOL (R=.69, p=.13). US alterations of the cortical matter at 72h were directly correlated with a-eeg score at 12h (R =.66, p=.28) and 24h (R=.65, p=.29). Conclusions. Early instrumental evaluations, in particular aeeg and US, seem to predict neurodevelopmental outcome at months in HIE newborns treated with hypothermia. Key words: asphyxia, hypoxic-ischemic encephalopathy, hypothermia, newborn INTRODUCTION Hypoxic-ischemic encephalopathy (HIE), following neonatal asphyxia, is a leading cause of neurological disability in newborns: (1) it can result in serious consequences such as death, cerebral palsy, epilepsy, cognitive, behavioural and developmental deficits. (2,3) Brain damage is an evolutionary process characterized by an acute stage of neuronal necrosis followed by a phase of reperfusion injury characterized by neural apoptosis. Hypothermic treatment limits brain damage, reducing mortality and disability at months of life. (4) However, long-term consequences of perinatal asphyxia are not easily predictable. (3) Therefore, the aim of this study was to assess the potential role of amplitude-integrated electroencephalography (a-eeg) background patterns, cranial ultrasonography (US) and cerebral magnetic resonance imaging (MRI) findings as early predictors of neurodevelopmental outcome at months in neonates undergoing therapeutic hypothermia for HIE. MATERIALS AND METHODS We retrospectively analysed data of all the patients who underwent hypothermic treatment from 1 January 212 to 3 September 214 in the Neonatal Intensive Care Unit of Maggiore della Carità University Hospital, vara, Italy. Hypothermic treatment was performed according to the current national guidelines for the management of HIE. (5,6) For each subject, a-eeg, cranial US and cerebral MRI, performed at scheduled time-points, were reviewed according to validated scores. (7-9) a-eeg A trained nurse or technician applied surface electrodes at C3-C4 locations according to the international 1 2 system. a-eeg was recorded for all the cooling period and for six hours after rewarming. a-eeg recordings were reviewed by a pediatric neurologist (C.P.) skilled in neonatal a-eeg and blinded to clinical factors. A severity score, based on the classification reported by Murray et al. (7) was assigned to tracings recorded at 6, 12 and 24 hours SIGNA VITAE 81
2 of life, as follows: Grade (normal a-eeg): continuous pattern with physiological characteristics Grade 1 (mildly abnormal): continuous pattern with slightly abnormal activity (slight asymmetry, mild depression voltage, poorly differentiated sleepwake cycle) Grade 2 (moderately abnormal): discontinuous activities with interburst <1 seconds, not differentiated sleepwake cycle, or clear asymmetry or asynchrony Grade 3 (severe abnormalities): discontinuous activities with interburst of 1-6 seconds, severe depression voltage, or lack of sleep-wake cycle Grade 4 (inactive/flat EEG): basic activities <1 microvolts or severe discontinuity with interburst range > 6 seconds. Cranial US Cranial US was performed for all patients at three time-points: t = (within 24 hours), t = 72 (at 72 hours) and t> 7 DOL (at 7-1 days of life). US images were blindly reviewed by a single neonatologist (G.C.) skilled in cerebral US. For each patient different anatomical sites were evaluated: basal ganglia, periventricular and subcortical white matter, cortical grey matter, and the severity of injuries was classified according to the severity score proposed by DeVries. (8) The basal ganglia were classified as: normal in the absence of ultrasound abnormalities, slightly altered in the presence of focal hemorrhage or hyperechogenicity of the lateral thalamus, moderately altered in the case of hyperechogenicity of the thalamus and putamen, seriously altered if the caudate and the entire thalamus were involved. The white and cortical substance were classified as: normal in the absence of ultrasound abnormalities, slightly altered in the case of focal hemorrhage of the periventricular white matter or widespread hyperechogenicity predominant in the paraventricular and parasagittal areas, moderately altered in the absence of cortical profile in one or both cerebral hemispheres, severely impaired in the case of diffuse hyperechogenicity of the white matter with greater involvement of the subcortical substance. Brain MRI Brain MRI was performed between 7 and 28 days of life and different anatomical sites were evaluated: posterior limb of the internal capsule (PLIC), basal ganglia, periventricular white matter and subcortical and cortical grey matter. The severity of injuries was classified according to the severity score proposed by Cheong JL et al. (9) The PLIC was classified as normal/ abnormal, where the abnormality was defined by the reduction or absence of the intensity signal on T1/T2 sequences and/ or by a reduced or increased diffusion in DWI sequences. The basal ganglia were classified as normal/moderately abnormal in the absence or minimum focal alterations of signal in T1/T2 sequences and/or normal diffusion characteristics, and moderately/severely altered in the case of multiple or diffuse signal alterations in T1/T2 sequences and/or qualitative abnormalities of DWI sequences. The white matter was classified as normal/mildly abnormal in the absence or minimal alterations on T1/ T2 sequences and/or in the case of normal diffusion characteristics in DWI sequences, and as moderately/severely abnormal in the case of signal alterations in T1/T2 or diffusion alterations in DWI sequences extending to the subcortical white matter or in more than three white matter areas. The cortical gray matter was classified as normal/mildly abnormal in the absence of signal alterations in T1/T2 or diffusion abnormalities in 2 or less areas (including the central sulcus, the inter-hemispheric fissure and the insular region), and moderately/severely abnormal in the case of more extensive involvement. Neurodevelopmental evaluation For all patients, a development evaluation was performed between 18 and 24 months of life by a pediatric neurologist (R.P.). Children were tested by Mental Development Index (MDI) of the Bayley Scales of Infant Development and classified according to their score as subjects with accelerated performance (MDI 115), within the normal range (MDI ), slightly delayed (MDI 7-84) and significantly delayed (MDI 69). (1) Neurological examination was performed according to Amiel Tison assessment, (11) and the presence of motor, hearing or visual impairment at months was recorded in order to set the grade of disability. Patients were divided into two groups according to their neurodevelopmental outcome at months, considered as negative if one of the following was present: Mental Development Index (MDI) score <85, motor, hearing or visual impairment. Statistical analysis Data are presented as numbers (percentages) or mean values (±SD). Differences between subjects with positive and negative neurodevelopmental outcome were evaluated by chi-square test (or Fischer test as appropriate) for categorical variables and by Mann-Whitney U test for continuous variables. Correlation analyses were performed by Spearman's rank test. A p value <.5 was considered significant. Statistical analysis was performed using SPSS version 17. (Chicago, IL, USA). RESULTS The study population consisted of 13 patients (M:F = 6:7). Out of 13 enrolled patients, 8 (61.5%) had a positive neurodevelopmental outcome (M:F = 6:2) and 5 (38.5%) had a negative outcome (M: F = 1: 4) at months. Characteristics of enrolled patients for the four items included in the definition of neurodevelopmental outcome (MDI score, motor, hearing and visual impairment) are shown in table 1. Mean MDI score at months was ± in the group with a positive outcome and 88.5 ± 2.4 in the negativeoutcome group. The a-eeg severity scores at 6, 12 and 24 hours were not different in subjects with positive and negative neurodevelopmental outcomes. Globally, there was an improving trend from 6 to 24 hours, with an increase in slight alterations at the expense of severe ones (table 2). In regard to the cranial US, the two groups of subjects with positive and negative neurodevelopmental outcomes did not differ in severity of alterations in any anatomical site and at any time (table 3). In regard to the brain MRI, the two groups did not differ in severity of alterations in any anatomical site. Severe anomalies were recorded at all sites in one patient belonging to the group with a negative outcome (table 4). CORRELATION ANALYSIS MDI score was negatively correlated with the severity of a-eeg alterations at 12 hours (R= -.571, p=.42, df=11 for twotailed test) and with the severity of cortical alterations evaluated by US at 72 hours (R= -.63, p=.21, df=11 for two-tailed test). The severity of US anomalies of the white matter at 7 DOL showed a direct correlation with the alterations of a-eeg recorded at 6 hours (R=.69, p=.13, df=11 for two-tailed test). The severity of US alterations of the corti- 82 SIGNA VITAE
3 cal matter at t=72h was directly correlated with the severity of a-eeg alterations at 12 hours (R=.66, p =.28, df=11 for two-tailed test) and at 24 hours (R=.65, p=.29, df=11 for two-tailed test). DISCUSSION Table 1. Global assessment at months of all subjects according to neurodevelopmental outcome. MDI score n pathological Slightly low Significantly low Motor impairment Hearing impairment Unknown Visual impairment MDI, Mental Development Index. This study aimed to analyse the presence of early anomalies detected by a-eeg, cranial US and brain MRI, in neonates undergoing therapeutic hypothermia for HIE, and to assess their potential prognostic value with respect to neurodevelopmental outcomes at months. Out of 13 newborns treated with therapeutic hypothermia for HIE, five had a negative outcome at months on the basis of a pathological MDI and/or the presence of motor, hearing and/or visual impairment. The first instrumental parameter taken into account was a-eeg recorded at 6, 12 and 24 hours of birth. difference was found in the a-eeg severity scores at each time point between subjects with positive and negative neurodevelopmental outcomes. However, it could be supposed that it may be due to the small sample size, as at all times the prevalence of subjects with severe/flat a-eeg tended to be higher in subjects with a negative outcome. An improving trend from 6 to 24 hours was also globally found, with an increase of the slight alterations at the expense of the severe ones, that, however, tended to persist into the negative outcome group. Moreover, the severity of a-eeg alterations at 12 hours was indirectly correlated to MDI at months, suggesting the potential prognostic value of a-eeg performed at 12 hours of life. Our findings are consistent with the results reported by Murray et al., (7) highlighting the improvement of EEG alterations from 6 to 48 hours and suggesting the importance of performing early EEG assessments as predictors of outcome after perinatal asphyxia, since normal or mildly abnormal EEG results within 6 hours of life were associated with normal neurodevelopmental outcomes at 24 months. Also, in the systematic review by van Laerhoven et al., (3) a-eeg was the most promising test with a sensitivity of 93% and a specificity of 9% in predicting long term neurodevelopmental outcomes. Regarding imaging methods, no significant difference was found in the severity score of US and MRI alterations at any time and in any site according to neurodevelopmental outcome. However, it should be pointed out that only one subject showed severe alterations at all anatomical sites both on US and MRI, and he developed severe neurological sequelae (cerebral palsy with spastic-dystonic quadriplegia, serious impaired motor functions, slurred speech and feeding difficulties). The severe alterations were not present on US imaging performed at 24 hours of life, and appeared starting from 72 hours, persisting at the following time-points. From a long-term perspective, correlation analysis 8 (1%) 8 (1%) 2 (4%) 1 (2%) 2 (4%) 2 (4%) 3 (6%) 1 (2%) 3 (6%) 1 (2%) 2 (4%) 3 (6%) Table 2. Distribution of a-eeg patterns at 6, 12 and 24 hours in all subjects divided according to positive or negative neurodevelopmental outcome. a-eeg at 6 hours (normal) (mildly impaired) 2 (moderately impaired) 7 (53.8%) 2 (4%) 3-4 (severe/flat) 5 (38.5%) 3 (6%) a-eeg at 12 hours (normal) (mildly impaired) 4 (3.8%) 4 (5%) 2 (moderately impaired) 5 (38.5%) 3 (6%) 3-4 (severe/flat) 4 (3.8%) 2 (4%) a-eeg at 24 hours (normal) (mildly impaired) 6 (46.2%) 3 (6%) 2 (moderately impaired) 3-4 (severe/flat) 2 (4%) showed that MDI at months was inversely correlated with the severity of US alterations of cortical matter at 72 hours, that was directly related with the severity of a-eeg alterations at 12 and 24 hours. Moreover, later alterations of the white matter, observed by cranial US at 7 DOL, showed a direct correlation with a-eeg alterations at 6 hours. Our data showed a tight interplay between a-eeg and cranial US in detecting anomalies following HIE. SIGNA VITAE 83
4 Previous data reported that cranial US has poor predictive accuracy, being highly examiner dependent, with a high false-positive rate. (7,12) However, due to its safety and availability at the bedside, it can be suggested that, in the presence of alterations on cranial US performed starting at 72 hours, neuroradiological imaging and clinical follow-up is highly recommended in newborns with HIE. Conversely, normal cranial US findings can be reassuring of a positive neurodevelopmental outcome. In our series, no correlation was found between MRI alterations and outcome indicators, probably due to the fact that only one subject displayed severe alterations on MRI. Our data are in contrast with those reported by van Laerhoven et al. (3) in their review, showing that brain MRI performed within two weeks of birth had the best sensitivity in predicting long term outcome. The main limitation of our study was the small sample size, but all newborns who underwent hypothermic treatment in the considered period were included in the analysis. In conclusion, our data confirm that a- EEG is the earliest method capable of identifying alterations with a prognostic neurodevelopmental value in newborns undergoing therapeutic hypothermia for HIE. Moreover, cranial US performed starting from 72 hours, even with the limitation of low accuracy, should be considered a useful imaging technique for identifying which subjects will be deserving of neurological follow-up. Table 3. Distribution of US patterns at, 72 hours and >7 days of life in all subjects, divided according to positive or negative neurodevelopmental outcomes. US at T= US at T=72h US at T>7 DOL 8 (1%) 8 (1%) 8 (1%) 5 (1%) 1 (2%) 3 (6%) 1 (2%) 4 (8%) 1 (2%) 4 (8%) 1 (2%) 3 (6%) 1 (2%) 1 (2%) 3 (6%) 1 (2%) 1 (2%) 4 (8%) 1 (2%) 3 (6%) 1 (2%) 1 (2%) 4 (8%) 1 (2%) DOL, days of life; US, ultrasound. 84 SIGNA VITAE
5 Table 4. Distribution of MRI patterns in all subjects, divided according to positive or negative neurodevelopmental outcomes. PLIC at MRI at MRI at MRI at MRI 8 (61.5%) 4 (3.8%) 3 (6%) 1 (2%) 1 (2%) 3 (6%) 1 (2%) 1 (2%) 3 (6%) 1 (2%) 1 (2%) 3 (6%) 1 (2%) 1 (2%) MRI, magnetic resonance imaging; PLIC, posterior limb of the internal capsule. REFERENCES 1. Douglas-Escobar M, Weiss MD. Hypoxic-ischemic encephalopathy: a review for the clinician. JAMA Pediatr 215;169: Kurinczuk JJ, White-Koning M, Badawi N. Epidemiology of neonatal encephalopathy and hypoxic-ischaemic encephalopathy. Early Hum Dev 21;86: van Laerhoven H, de Haan TR, Offringa M, Post B, van der Lee JH. Prognostic tests in term neonates with hypoxic-ischemic encephalopathy: a systematic review. Pediatrics 213;131: Edwards AD, Brocklehurst P, Gunn AJ, Halliday H, Juszczak E, Levene M, et al. Neurological outcomes at 18 months of age after moderate hypothermia for perinatal hypoxic ischaemic encephalopathy: synthesis and meta-analysis of trial data. BMJ 21;34:c Ancora G, Pomero G, Ferrari F. Raccomandazioni per l assistenza al neonato con encefalopatia ipossico-ischemica possibile candidato al trattamento ipotermico. Milano: Biomedia; Mosalli R. Whole body cooling for infants with hypoxic-ischemic encephalopathy. J Clin Neonatol 212;1: Murray DM, Boylan GB, Ryan CA, Connolly S. Early EEG findings in hypoxic-ischemic encephalopathy predict outcomes at 2 years. Pediatrics 29;124:e Govaert P, De Vries LS. An Atlas of Neonatal Brain Sonography. 2nd ed. London, Cambridge: Mac Keith Press; Cheong JL, Coleman L, Hunt RW, Lee KJ, Doyle LW, Inder TE, Jacobs SE. Infant Cooling Evaluation Collaboration. Prognostic utility of magnetic resonance imaging in neonatal hypoxic-ischemic encephalopathy: substudy of a randomized trial. Arch Pediatr Adolesc Med 212;166: Bayley NM. Bayley Scales of Infant Development. 2nd ed. San Antonio, TX: The Psychological Corporation; Amiel-Tison C, Gosselin J. Neurological Development from Birth to Six Years. Baltimore: John Hopkins UniversityPress; Reynolds PR, Dale RC, Cowan FM. Neonatal cranial ultrasound interpretation: a clinical audit. Arch Dis Child Fetal Neonatal Ed 21;84:F92-5. SIGNA VITAE 85
Correlation of Neurodevelopmental Outcome and brain MRI/EEG findings in term HIE infants
 Correlation of Neurodevelopmental Outcome and brain MRI/EEG findings in term HIE infants Ajou University School of Medicine Department of Pediatrics Moon Sung Park M.D. Hee Cheol Jo, M.D., Jang Hoon Lee,
Correlation of Neurodevelopmental Outcome and brain MRI/EEG findings in term HIE infants Ajou University School of Medicine Department of Pediatrics Moon Sung Park M.D. Hee Cheol Jo, M.D., Jang Hoon Lee,
Prognosis in. Encephalopathy. Hypoxic-Ischemic. Özge Aydemİr MD
 Prognosis in Hypoxic-Ischemic Encephalopathy Özge Aydemİr MD Major problems we have to face while caring infants with HIE are; Øto provide families with reliable information about outcome. Øto decide how
Prognosis in Hypoxic-Ischemic Encephalopathy Özge Aydemİr MD Major problems we have to face while caring infants with HIE are; Øto provide families with reliable information about outcome. Øto decide how
Predicting Outcomes in HIE. Naaz Merchant Consultant Neonatologist Beds & Herts Meeting 17/03/2016
 Predicting Outcomes in HIE Naaz Merchant Consultant Neonatologist Beds & Herts Meeting 17/03/2016 Interactive please! Case 1 Term, 3.5 kg Antenatal: Breech Labour/Delivery: Em CS failure to progress, mec
Predicting Outcomes in HIE Naaz Merchant Consultant Neonatologist Beds & Herts Meeting 17/03/2016 Interactive please! Case 1 Term, 3.5 kg Antenatal: Breech Labour/Delivery: Em CS failure to progress, mec
Queen Charlotte Hospital
 Queen Charlotte Hospital Neuroprotection for neonatal encephalopathy Neonatal encephalopathy accounts for 1 million deaths worldwide and even greater numbers of disabled survivors In countries with
Queen Charlotte Hospital Neuroprotection for neonatal encephalopathy Neonatal encephalopathy accounts for 1 million deaths worldwide and even greater numbers of disabled survivors In countries with
Study of correlation severity of hypoxic ischemic encephalopathy on MRI brain with clinical findings
 Radiology and Imaging Special Issue December 2017: Vol-7, Issue- 1, P 34-41 Original article: Study of correlation severity of hypoxic ischemic encephalopathy on MRI brain with clinical findings *Dr Ramaa
Radiology and Imaging Special Issue December 2017: Vol-7, Issue- 1, P 34-41 Original article: Study of correlation severity of hypoxic ischemic encephalopathy on MRI brain with clinical findings *Dr Ramaa
Perlman J, Clinics Perinatol 2006; 33: Underlying causal pathways. Antenatal Intrapartum Postpartum. Acute near total asphyxia
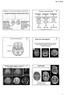 Perlman J, Clinics Perinatol 2006; 33:335-353 Underlying causal pathways Antenatal Intrapartum Postpartum Acute injury Subacute injury Associated problem Reduced fetal movements Placental insufficiency
Perlman J, Clinics Perinatol 2006; 33:335-353 Underlying causal pathways Antenatal Intrapartum Postpartum Acute injury Subacute injury Associated problem Reduced fetal movements Placental insufficiency
Imaging findings in neonates with hypoxic-ischaemic encephalopathy and terapeutic hypothermia.
 Imaging findings in neonates with hypoxic-ischaemic encephalopathy and terapeutic hypothermia. Poster No.: C-1577 Congress: ECR 2014 Type: Scientific Exhibit Authors: S. Manso Garcia, M. J. Velasco Marcos,
Imaging findings in neonates with hypoxic-ischaemic encephalopathy and terapeutic hypothermia. Poster No.: C-1577 Congress: ECR 2014 Type: Scientific Exhibit Authors: S. Manso Garcia, M. J. Velasco Marcos,
I t is increasingly recognised that arterial cerebral infarction
 F252 ORIGINAL ARTICLE Does cranial ultrasound imaging identify arterial cerebral infarction in term neonates? F Cowan, E Mercuri, F Groenendaal, L Bassi, D Ricci, M Rutherford, L de Vries... See end of
F252 ORIGINAL ARTICLE Does cranial ultrasound imaging identify arterial cerebral infarction in term neonates? F Cowan, E Mercuri, F Groenendaal, L Bassi, D Ricci, M Rutherford, L de Vries... See end of
Imaging findings in neonates with hypoxic-ischaemic encephalopathy and terapeutic hypothermia.
 Imaging findings in neonates with hypoxic-ischaemic encephalopathy and terapeutic hypothermia. Poster No.: C-1577 Congress: ECR 2014 Type: Scientific Exhibit Authors: S. Manso Garcia, M. J. Velasco Marcos,
Imaging findings in neonates with hypoxic-ischaemic encephalopathy and terapeutic hypothermia. Poster No.: C-1577 Congress: ECR 2014 Type: Scientific Exhibit Authors: S. Manso Garcia, M. J. Velasco Marcos,
Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy
 Original article: Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy *Dr Harshad Bhagat, ** Dr Ravindra Kawade, ***Dr Y.P.Sachdev *Junior Resident, Department Of Radiodiagnosis,
Original article: Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy *Dr Harshad Bhagat, ** Dr Ravindra Kawade, ***Dr Y.P.Sachdev *Junior Resident, Department Of Radiodiagnosis,
When? Incidence of neonatal seizures in a NICU population The incidence of seizures is higher in the neonatal period than in any other age group.
 Incidence of neonatal seizures in a NICU population The incidence of seizures is higher in the neonatal period than in any other age group. Standard EEG 2,3% 8.6% Standard EEG + aeeg Scher MS et al; Pediatrics
Incidence of neonatal seizures in a NICU population The incidence of seizures is higher in the neonatal period than in any other age group. Standard EEG 2,3% 8.6% Standard EEG + aeeg Scher MS et al; Pediatrics
Disclosures. Objectives. Definition: HIE. HIE: Incidence. Impact 9/10/2018. Hypoxic Ischemic Encephalopathy in the Neonate
 Disclosures Hypoxic Ischemic Encephalopathy in the Neonate No relevant financial relationships or conflicts of interest to disclose Franscesca Miquel-Verges MD 2018 Review therapies currently under research
Disclosures Hypoxic Ischemic Encephalopathy in the Neonate No relevant financial relationships or conflicts of interest to disclose Franscesca Miquel-Verges MD 2018 Review therapies currently under research
7 Simple Steps to Assess & Document any Neonatal aeeg
 7 Simple Steps to Assess & Document any Neonatal aeeg Created for you by: www.aeegcoach.com How to use the Seven Simple Steps Checklist Hi! It s Kathi Randall here Your aeeg coach. I m so excited to share
7 Simple Steps to Assess & Document any Neonatal aeeg Created for you by: www.aeegcoach.com How to use the Seven Simple Steps Checklist Hi! It s Kathi Randall here Your aeeg coach. I m so excited to share
Seizure burden and neurodevelopmental outcome in neonates with hypoxic ischemic encephalopathy
 DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE Seizure burden and neurodevelopmental outcome in neonates with hypoxic ischemic encephalopathy LIUDMILA KHAROSHANKAYA 1,2 NATHAN J STEVENSON 1
DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE Seizure burden and neurodevelopmental outcome in neonates with hypoxic ischemic encephalopathy LIUDMILA KHAROSHANKAYA 1,2 NATHAN J STEVENSON 1
Epilepsy in children with cerebral palsy
 Seizure 2003; 12: 110 114 doi:10.1016/s1059 1311(02)00255-8 Epilepsy in children with cerebral palsy A.K. GURURAJ, L. SZTRIHA, A. BENER,A.DAWODU & V. EAPEN Departments of Paediatrics, Community Medicine
Seizure 2003; 12: 110 114 doi:10.1016/s1059 1311(02)00255-8 Epilepsy in children with cerebral palsy A.K. GURURAJ, L. SZTRIHA, A. BENER,A.DAWODU & V. EAPEN Departments of Paediatrics, Community Medicine
Hypoxic ischemic brain injury in neonates - early MR imaging findings
 Hypoxic ischemic brain injury in neonates - early MR imaging findings Poster No.: C-1208 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit E.-M. Heursen, R. Reina Cubero, T. Guijo Hernandez,
Hypoxic ischemic brain injury in neonates - early MR imaging findings Poster No.: C-1208 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit E.-M. Heursen, R. Reina Cubero, T. Guijo Hernandez,
Analysis between clinical and MRI findings of childhood and teenages with epilepsy after hypoxic-ischemic encephalopathy in neonates periods
 Analysis between clinical and MRI findings of childhood and teenages with epilepsy after hypoxic-ischemic encephalopathy in neonates periods Poster No.: C-0401 Congress: ECR 2015 Type: Scientific Exhibit
Analysis between clinical and MRI findings of childhood and teenages with epilepsy after hypoxic-ischemic encephalopathy in neonates periods Poster No.: C-0401 Congress: ECR 2015 Type: Scientific Exhibit
Neuroimaging updates on neonatal hypoxic ischemic injury and hypothermia
 Neuroimaging updates on neonatal hypoxic ischemic injury and hypothermia Fabio Triulzi Neuroradiology Dept. Cà Granda Foundation Ospedale Maggiore Policlinico Università degli Studi, Milan ITALY Term Neonate
Neuroimaging updates on neonatal hypoxic ischemic injury and hypothermia Fabio Triulzi Neuroradiology Dept. Cà Granda Foundation Ospedale Maggiore Policlinico Università degli Studi, Milan ITALY Term Neonate
DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI Page 1 Page 2 perinatal events and brain damage in surviving
DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI Page 1 Page 2 perinatal events and brain damage in surviving
RESEARCH BRIEF. Prognostic Value of Resistive Index in Neonates with Hypoxic Ischemic
 RESEARCH BRIEF Prognostic Value of Resistive Index in Neonates with Hypoxic Ischemic A Senthil Kumar, Aparna Chandrasekaran, Rajamannar Asokan and *Kathirvelu Gopinathan From the Department of Neonatology,
RESEARCH BRIEF Prognostic Value of Resistive Index in Neonates with Hypoxic Ischemic A Senthil Kumar, Aparna Chandrasekaran, Rajamannar Asokan and *Kathirvelu Gopinathan From the Department of Neonatology,
Perinatal hypoxic-ischemic events cause hypoxic-ischemic encephalopathy (HIE) in at least 1 to 2/1000 term-born infants,
 General Movements in Full-Term Infants with Perinatal Asphyxia Are Related to Basal Ganglia and Thalamic Lesions Fabrizio Ferrari, MD, Alessandra Todeschini, MD, Isotta Guidotti, MD, Miriam Martinez-Biarge,
General Movements in Full-Term Infants with Perinatal Asphyxia Are Related to Basal Ganglia and Thalamic Lesions Fabrizio Ferrari, MD, Alessandra Todeschini, MD, Isotta Guidotti, MD, Miriam Martinez-Biarge,
Newborn Hypoxic Ischemic Brain Injury. Hisham Dahmoush, MBBCh FRCR Lucile Packard Children s Hospital at Stanford
 Newborn Hypoxic Ischemic Brain Injury Hisham Dahmoush, MBBCh FRCR Lucile Packard Children s Hospital at Stanford NO DISCLOSURES INTRODUCTION Neonatal hypoxic-ischemic encephalopathy (HIE) is a major cause
Newborn Hypoxic Ischemic Brain Injury Hisham Dahmoush, MBBCh FRCR Lucile Packard Children s Hospital at Stanford NO DISCLOSURES INTRODUCTION Neonatal hypoxic-ischemic encephalopathy (HIE) is a major cause
Objectives. Birth Depression Management. Birth Depression Terms
 Objectives Birth Depression Management Regional Perinatal Outreach Program 2016 Understand the terms and the clinical characteristics of birth depression. Be familiar with the evidence behind therapeutic
Objectives Birth Depression Management Regional Perinatal Outreach Program 2016 Understand the terms and the clinical characteristics of birth depression. Be familiar with the evidence behind therapeutic
Insults to the Developing Brain & Effect on Neurodevelopmental Outcomes
 Insults to the Developing Brain & Effect on Neurodevelopmental Outcomes Ira Adams-Chapman, MD Assistant Professor of Pediatrics Director, Developmental Progress Clinic Emory University School of Medicine
Insults to the Developing Brain & Effect on Neurodevelopmental Outcomes Ira Adams-Chapman, MD Assistant Professor of Pediatrics Director, Developmental Progress Clinic Emory University School of Medicine
The Clinical Spectrum and Prediction of Outcome in Hypoxic-Ischemic Encephalopathy
 Article neurology The Clinical Spectrum and Prediction of Outcome in Hypoxic-Ischemic Encephalopathy Walter C. Allan, MD* Objectives After completing this article, readers should be able to: 1. List the
Article neurology The Clinical Spectrum and Prediction of Outcome in Hypoxic-Ischemic Encephalopathy Walter C. Allan, MD* Objectives After completing this article, readers should be able to: 1. List the
SWISS SOCIETY OF NEONATOLOGY. Bart s syndrome with severe newborn encephalopathy: a delayed diagnosis
 SWISS SOCIETY OF NEONATOLOGY Bart s syndrome with severe newborn encephalopathy: a delayed diagnosis May 2003 2 Buettiker V, Hogan P, Badawi N, Department of Neonatology (BV, NB), Department of Dermatology
SWISS SOCIETY OF NEONATOLOGY Bart s syndrome with severe newborn encephalopathy: a delayed diagnosis May 2003 2 Buettiker V, Hogan P, Badawi N, Department of Neonatology (BV, NB), Department of Dermatology
Cerebral function monitoring in term or near term neonates at MDH: preliminary experience and proposal of a guideline
 Original Article Cerebral function monitoring in term or near term neonates at MDH: preliminary experience and proposal of a guideline Stephen Attard, Doriette Soler, Paul Soler Introduction: Cerebral
Original Article Cerebral function monitoring in term or near term neonates at MDH: preliminary experience and proposal of a guideline Stephen Attard, Doriette Soler, Paul Soler Introduction: Cerebral
TOO COOL OR NOT TOO COOL- THERAPEUTIC HYPOTHERMIA IN THE ICU SCCM TX 2017 TED WU MD PEDIATRIC CRITICAL CARE UNIVERSITY OF TEXAS HEALTH SAN ANTONIO
 TOO COOL OR NOT TOO COOL- THERAPEUTIC HYPOTHERMIA IN THE ICU SCCM TX 2017 TED WU MD PEDIATRIC CRITICAL CARE UNIVERSITY OF TEXAS HEALTH SAN ANTONIO DISCLOSURE I have no relationships with commercial companies
TOO COOL OR NOT TOO COOL- THERAPEUTIC HYPOTHERMIA IN THE ICU SCCM TX 2017 TED WU MD PEDIATRIC CRITICAL CARE UNIVERSITY OF TEXAS HEALTH SAN ANTONIO DISCLOSURE I have no relationships with commercial companies
Imaging the Premature Brain- New Knowledge
 Imaging the Premature Brain- New Knowledge Stein Magnus Aukland Haukeland University Hospital University of Bergen NORWAY No disclosure Imaging modalities O Skull X-ray O Computer Tomography O Cerebral
Imaging the Premature Brain- New Knowledge Stein Magnus Aukland Haukeland University Hospital University of Bergen NORWAY No disclosure Imaging modalities O Skull X-ray O Computer Tomography O Cerebral
Automated EEG discontinuity in cooled newborns predicts cerebral MRI and neurodevelopmental outcome
 Automated EEG discontinuity in cooled newborns predicts cerebral MRI and neurodevelopmental outcome Jonathan M Dunne 1, David Wertheim MA, PhD 2 ; Paul Clarke MD, FRCPCH 3 ; Olga Kapellou MRCPCH, MD, PhD
Automated EEG discontinuity in cooled newborns predicts cerebral MRI and neurodevelopmental outcome Jonathan M Dunne 1, David Wertheim MA, PhD 2 ; Paul Clarke MD, FRCPCH 3 ; Olga Kapellou MRCPCH, MD, PhD
Gerda van Wezel-Meijler Neonatal Cranial Ultrasonography
 Gerda van Wezel-Meijler Neonatal Cranial Ultrasonography Gerda van Wezel-Meijler Neonatal Cranial Ultrasonography Guidelines for the Procedure and Atlas of Normal Ultrasound Anatomy With 121 Figures and
Gerda van Wezel-Meijler Neonatal Cranial Ultrasonography Gerda van Wezel-Meijler Neonatal Cranial Ultrasonography Guidelines for the Procedure and Atlas of Normal Ultrasound Anatomy With 121 Figures and
Thais Agut 1*, Marisol León 1, Mónica Rebollo 2, Jordi Muchart 2, Gemma Arca 1 and Alfredo Garcia-Alix 1
 Agut et al. BMC Pediatrics 2014, 14:177 RESEARCH ARTICLE Open Access Early identification of brain injury in infants with hypoxic ischemic encephalopathy at high risk for severe impairments: accuracy of
Agut et al. BMC Pediatrics 2014, 14:177 RESEARCH ARTICLE Open Access Early identification of brain injury in infants with hypoxic ischemic encephalopathy at high risk for severe impairments: accuracy of
Is there a way to predict outcome in (near) term neonates with hypoxic-ischemic encephalopathy based on MR imaging?
 Chapter 5 Is there a way to predict outcome in (near) term neonates with hypoxic-ischemic encephalopathy based on MR imaging? Lishya Liauw Jeroen van der Grond Annette van den Berg-Huysmans Laura Laan
Chapter 5 Is there a way to predict outcome in (near) term neonates with hypoxic-ischemic encephalopathy based on MR imaging? Lishya Liauw Jeroen van der Grond Annette van den Berg-Huysmans Laura Laan
Running title: EEG, MRI and neurodevelopmental outcome in HIE. Word count manuscript body: Word count abstract: 226. Address correspondence to:
 Role of EEG background activity, seizure burden and MRI in predicting neurodevelopmental outcome in full-term infants with hypoxic-ischaemic encephalopathy in the era of therapeutic hypothermia. Lauren
Role of EEG background activity, seizure burden and MRI in predicting neurodevelopmental outcome in full-term infants with hypoxic-ischaemic encephalopathy in the era of therapeutic hypothermia. Lauren
Advanced magnetic resonance imaging for monitoring brain development and injury
 Advanced magnetic resonance imaging for monitoring brain development and injury Stéphane Sizonenko, MD-PhD Division of Development and Growth Department of Child and Adolescent Medicine Geneva University
Advanced magnetic resonance imaging for monitoring brain development and injury Stéphane Sizonenko, MD-PhD Division of Development and Growth Department of Child and Adolescent Medicine Geneva University
Utility of neuroradiographic imaging in predicting outcomes after neonatal extracorporeal membrane oxygenation
 Journal of Pediatric Surgery (2012) 47, 76 80 www.elsevier.com/locate/jpedsurg Utility of neuroradiographic imaging in predicting outcomes after neonatal extracorporeal membrane oxygenation Michael D.
Journal of Pediatric Surgery (2012) 47, 76 80 www.elsevier.com/locate/jpedsurg Utility of neuroradiographic imaging in predicting outcomes after neonatal extracorporeal membrane oxygenation Michael D.
The child with hemiplegic cerebral palsy thinking beyond the motor impairment. Dr Paul Eunson Edinburgh
 The child with hemiplegic cerebral palsy thinking beyond the motor impairment Dr Paul Eunson Edinburgh Content Coming to a diagnosis The importance of understanding the injury MRI scans Role of epilepsy
The child with hemiplegic cerebral palsy thinking beyond the motor impairment Dr Paul Eunson Edinburgh Content Coming to a diagnosis The importance of understanding the injury MRI scans Role of epilepsy
Neonatal Brain MRI and Motor Outcome at School Age in Children with Neonatal Encephalopathy: A Review of Personal Experience
 NEURAL PLASTICITY VOLUME 10, NO. 1-2, 2003 Neonatal Brain MRI and Motor Outcome at School Age in Children with Neonatal Encephalopathy: A Review of Personal Experience Eugenio Mercuri and Anna L. Barnett
NEURAL PLASTICITY VOLUME 10, NO. 1-2, 2003 Neonatal Brain MRI and Motor Outcome at School Age in Children with Neonatal Encephalopathy: A Review of Personal Experience Eugenio Mercuri and Anna L. Barnett
CEREBRAL FUNCTION MONITORING
 CEREBRAL FUNCTION MONITORING Introduction and Definitions The term amplitude integrated electroencephalography (aeeg) is used to denote a method for electro-cortical monitoring whereas cerebral function
CEREBRAL FUNCTION MONITORING Introduction and Definitions The term amplitude integrated electroencephalography (aeeg) is used to denote a method for electro-cortical monitoring whereas cerebral function
Chapter 7. Neuropediatrics 2007; 38 (5): Lara Leijser Alla Vein Lishya Liauw Tzipi Strauss Sylvia Veen Gerda van Wezel-Meijler
 Chapter 7 Prediction of short-term neurological outcome in full-term neonates with hypoxic-ischaemic encephalopathy based on combined use of electroencephalogram and neuro-imaging Lara Leijser Alla Vein
Chapter 7 Prediction of short-term neurological outcome in full-term neonates with hypoxic-ischaemic encephalopathy based on combined use of electroencephalogram and neuro-imaging Lara Leijser Alla Vein
Incidence and diagnosis of unilateral arterial cerebral infarction in newborn infants *
 J. Perinat. Med. 33 (2005) 170 175 Copyright by Walter de Gruyter Berlin New York. DOI 10.1515/JPM.2005.032 Short communication Incidence and diagnosis of unilateral arterial cerebral infarction in newborn
J. Perinat. Med. 33 (2005) 170 175 Copyright by Walter de Gruyter Berlin New York. DOI 10.1515/JPM.2005.032 Short communication Incidence and diagnosis of unilateral arterial cerebral infarction in newborn
Hypoxic-Ischemic Encephalopathy. TW de Witt University of Pretoria Department of Paediatrics Neonatology
 Hypoxic-Ischemic Encephalopathy TW de Witt University of Pretoria Department of Paediatrics Neonatology Background HIE remains a serious condition that causes significant mortality and longterm morbidity.
Hypoxic-Ischemic Encephalopathy TW de Witt University of Pretoria Department of Paediatrics Neonatology Background HIE remains a serious condition that causes significant mortality and longterm morbidity.
Swiss neonatal network and Follow up Group
 Swiss neonatal network and Follow up Group March 2011 Barbara Brotschi and Cornelia Hagmann Hypoxic ischaemic encephalopathy Neonatal encephalopathy due to perinatal hypoxiaischaemia: clinically defined
Swiss neonatal network and Follow up Group March 2011 Barbara Brotschi and Cornelia Hagmann Hypoxic ischaemic encephalopathy Neonatal encephalopathy due to perinatal hypoxiaischaemia: clinically defined
Articles. Funding UK Medical Research Council; UK Department of Health.
 Assessment of brain tissue injury after moderate hypothermia in neonates with hypoxic ischaemic encephalopathy: a nested substudy of a randomised controlled trial Mary Rutherford, Luca A Ramenghi, A David
Assessment of brain tissue injury after moderate hypothermia in neonates with hypoxic ischaemic encephalopathy: a nested substudy of a randomised controlled trial Mary Rutherford, Luca A Ramenghi, A David
Serum Lactate, Brain Magnetic Resonance Imaging and Outcome of Neonatal Hypoxic Ischemic Encephalopathy after Therapeutic Hypothermia
 Pediatrics and Neonatology (2016) 57, 35e40 Available online at www.sciencedirect.com ScienceDirect journal homepage: http://www.pediatr-neonatol.com ORIGINAL ARTICLE Serum Lactate, Brain Magnetic Resonance
Pediatrics and Neonatology (2016) 57, 35e40 Available online at www.sciencedirect.com ScienceDirect journal homepage: http://www.pediatr-neonatol.com ORIGINAL ARTICLE Serum Lactate, Brain Magnetic Resonance
INTRODUCING SOLITAIRE PLATINUM REVASCULARIZATION DEVICE ENHANCED VISIBILITY EXPANDED PORTFOLIO SEEING IS KNOWING. KNOWLEDGE IS CONFIDENCE.
 INTRODUCING SOLITAIRE PLATINUM REVASCULARIZATION DEVICE ENHANCED VISIBILITY EXPANDED PORTFOLIO 6X40MM SEEING IS KNOWING. KNOWLEDGE IS CONFIDENCE. www.medtronic.eu UC201708427 EE Medtronic 2017. All rights
INTRODUCING SOLITAIRE PLATINUM REVASCULARIZATION DEVICE ENHANCED VISIBILITY EXPANDED PORTFOLIO 6X40MM SEEING IS KNOWING. KNOWLEDGE IS CONFIDENCE. www.medtronic.eu UC201708427 EE Medtronic 2017. All rights
PEER REVIEW HISTORY ARTICLE DETAILS TITLE (PROVISIONAL)
 PEER REVIEW HISTORY BMJ Paediatrics Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form and are provided with free text boxes to elaborate
PEER REVIEW HISTORY BMJ Paediatrics Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form and are provided with free text boxes to elaborate
I have no relevant financial relationships with the manufacturers of any commercial products or provider of commercial CME services discussed in this
 Neonatal Seizures Dennis J. Dlugos, MD Pediatric Regional Epilepsy Program The Children s Hospital of Philadelphia Perelman School of Medicine at the University of Pennsylvania I have no relevant financial
Neonatal Seizures Dennis J. Dlugos, MD Pediatric Regional Epilepsy Program The Children s Hospital of Philadelphia Perelman School of Medicine at the University of Pennsylvania I have no relevant financial
Original Articles NEUROSONOGRAPHIC ABNORMALITIES IN NEONATES WITH HYPOXIC ISCHEMIC ENCEPHALOPATHY
 Original Articles NEUROSONOGRAPHIC ABNORMALITIES IN NEONATES WITH HYPOXIC ISCHEMIC ENCEPHALOPATHY N.K. Anand A.K. Gupta I.M.S. Lamba ABSTRACT Pattern of neurosonographic (NSG) abnormalities in 150 term
Original Articles NEUROSONOGRAPHIC ABNORMALITIES IN NEONATES WITH HYPOXIC ISCHEMIC ENCEPHALOPATHY N.K. Anand A.K. Gupta I.M.S. Lamba ABSTRACT Pattern of neurosonographic (NSG) abnormalities in 150 term
The Pharmacokinetics of Antiepileptics Drugs in Neonates with Hypoxic Ischemic Encephalopathy
 The Pharmacokinetics of Antiepileptics Drugs in Neonates with Hypoxic Ischemic Encephalopathy KELIANA O MARA, PHARMD FLORIDA NEONATAL NEUROLOGIC NETWORK STATE MEETING Objectives Describe seizures in hypoxic
The Pharmacokinetics of Antiepileptics Drugs in Neonates with Hypoxic Ischemic Encephalopathy KELIANA O MARA, PHARMD FLORIDA NEONATAL NEUROLOGIC NETWORK STATE MEETING Objectives Describe seizures in hypoxic
Pathophysiology Review. Hypoxic-Ischemic Encephalopathy & Therapeutic Hypothermia. Objectives. What is Hypoxic-Ischemic Encephalopathy?
 Hypoxic-Ischemic Encephalopathy & Therapeutic Hypothermia Nancy Couto Nurse Practitioner, NICU London Health Sciences Centre, Children s Hospital nancy.couto@lhsc.on.ca 2014 12 17 Objectives Review Pathophysiology
Hypoxic-Ischemic Encephalopathy & Therapeutic Hypothermia Nancy Couto Nurse Practitioner, NICU London Health Sciences Centre, Children s Hospital nancy.couto@lhsc.on.ca 2014 12 17 Objectives Review Pathophysiology
Predictive Value of Multimodality Evoked Potentials in Asphyxiated Term Newborns
 Ann Ali Abdel Kader et al. Predictive Value of Multimodality Evoked Potentials in Asphyxiated Term Newborns Ann Ali Abdel Kader 1, Saly El-Kholy 1, Dahlia El-Sebaie 2, Shahira Mostafa 1, Amira El-Gohary
Ann Ali Abdel Kader et al. Predictive Value of Multimodality Evoked Potentials in Asphyxiated Term Newborns Ann Ali Abdel Kader 1, Saly El-Kholy 1, Dahlia El-Sebaie 2, Shahira Mostafa 1, Amira El-Gohary
DWI assessment of ischemic changes in the fetal brain
 DWI assessment of ischemic changes in the fetal brain Dafi Bergman, 4 th year Medical student in the 4-year program, Sackler school of medicine B.Sc Life and Medical Sciences, Tel Aviv University Supervised
DWI assessment of ischemic changes in the fetal brain Dafi Bergman, 4 th year Medical student in the 4-year program, Sackler school of medicine B.Sc Life and Medical Sciences, Tel Aviv University Supervised
Neurodevelopmental Follow Up After Therapeutic Hypothermia for Perinatal Asphyxia
 ORIGINAL PAPER doi: 10.5455/medarh.2015.69.362-366 Med Arh. 2015 Dec; 69(6): 362-366 Received: August 25th 2015 Accepted: November 05th 2015 2015 Smail Zubcevic, Suada Heljic, Feriha Catibusic, Sajra Uzicanin,
ORIGINAL PAPER doi: 10.5455/medarh.2015.69.362-366 Med Arh. 2015 Dec; 69(6): 362-366 Received: August 25th 2015 Accepted: November 05th 2015 2015 Smail Zubcevic, Suada Heljic, Feriha Catibusic, Sajra Uzicanin,
Advancing Neurologic Care in the Intensive Care Nursery
 Article neurology Advancing Neurologic Care in the Intensive Care Nursery Hannah C. Glass, MDCM* AUTHOR DISCLOSURE Dr Glass has disclosed that she is supported by grant K23NS066137 from the National Institute
Article neurology Advancing Neurologic Care in the Intensive Care Nursery Hannah C. Glass, MDCM* AUTHOR DISCLOSURE Dr Glass has disclosed that she is supported by grant K23NS066137 from the National Institute
Ultrasonography and Magnetic Resonance Imaging of the Brain in Hypoxic Full-Term Newborns
 42 CONTINUING MEDICAL EDUCATION :42-9 Ultrasonography and Magnetic Resonance Imaging of the Brain in Hypoxic Full-Term Newborns Aušrelė Kudrevičienė 1, Saulius Lukoševičius 2, Jūratė Laurynaitienė 3, Vitalija
42 CONTINUING MEDICAL EDUCATION :42-9 Ultrasonography and Magnetic Resonance Imaging of the Brain in Hypoxic Full-Term Newborns Aušrelė Kudrevičienė 1, Saulius Lukoševičius 2, Jūratė Laurynaitienė 3, Vitalija
Articles. Heart rate variability in hypoxic ischemic encephalopathy during therapeutic hypothermia. Clinical Investigation
 nature publishing group Clinical Investigation Heart rate variability in hypoxic ischemic encephalopathy during therapeutic hypothermia Robert M. Goulding 1,2, Nathan J. Stevenson 1, Deirdre M. Murray
nature publishing group Clinical Investigation Heart rate variability in hypoxic ischemic encephalopathy during therapeutic hypothermia Robert M. Goulding 1,2, Nathan J. Stevenson 1, Deirdre M. Murray
ECMUS The Safety Committee of EFSUMB : Tutorial
 Neonatal cranial ultrasound Safety Aspects (2013) Prepared for ECMUS by B.J. van der Knoop, M.D. 1, J.I.P. de Vries, M.D., PhD 1, I.A. Zonnenberg, M.D. 2, J.I.M.L. Verbeke, M.D. 3 R.J. Vermeulen, M.D.,
Neonatal cranial ultrasound Safety Aspects (2013) Prepared for ECMUS by B.J. van der Knoop, M.D. 1, J.I.P. de Vries, M.D., PhD 1, I.A. Zonnenberg, M.D. 2, J.I.M.L. Verbeke, M.D. 3 R.J. Vermeulen, M.D.,
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of therapeutic hypothermia with intracorporeal temperature monitoring for hypoxic
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of therapeutic hypothermia with intracorporeal temperature monitoring for hypoxic
To evaluate the role of MRI in infants with suspected hypoxic ischemic encephalopathy and prognosticating neurological outcome at end of one year
 International Journal of Research in Medical Sciences Ramachandran S et al. Int J Res Med Sci. 2017 May;5(5):1893-1897 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research rticle DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20171813
International Journal of Research in Medical Sciences Ramachandran S et al. Int J Res Med Sci. 2017 May;5(5):1893-1897 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research rticle DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20171813
Neuroimaging in Cerebral Palsy Report from North India
 original ARTICLE Neuroimaging in Cerebral Palsy Report from North India How to Cite This Article: Aggarwal A, Mittal H, Debnath SKR, Rai A. Neuroimaging in Cerebral Palsy Report from North India. Iran
original ARTICLE Neuroimaging in Cerebral Palsy Report from North India How to Cite This Article: Aggarwal A, Mittal H, Debnath SKR, Rai A. Neuroimaging in Cerebral Palsy Report from North India. Iran
Insults to the Term Brain
 Insults to the Term Brain Monica Epelman, MD mepelman@nemours.org Literature comparing US and MR has deficiencies Retrospective studies Long time interval between US and MR exams in the same patient
Insults to the Term Brain Monica Epelman, MD mepelman@nemours.org Literature comparing US and MR has deficiencies Retrospective studies Long time interval between US and MR exams in the same patient
Department of Rehabilitation Medicine, CHA Bundang Medical Center, CHA University, Seongnam, Korea
 Original Article Ann Rehabil Med 2015;39(4):624-629 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2015.39.4.624 Annals of Rehabilitation Medicine Gross Motor Function Outcome After Intensive
Original Article Ann Rehabil Med 2015;39(4):624-629 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2015.39.4.624 Annals of Rehabilitation Medicine Gross Motor Function Outcome After Intensive
COOLING FOR HYPOXIC ISCHEMIC ENCEPHALOPATHY
 COOLING FOR HYPOXIC ISCHEMIC ENCEPHALOPATHY Roger F. Soll H. Wallace Professor of Neonatology University of Vermont 19 th International Symposium on Neonatology Sao Paulo, Brazil DISCLOSURE Roger F. Soll
COOLING FOR HYPOXIC ISCHEMIC ENCEPHALOPATHY Roger F. Soll H. Wallace Professor of Neonatology University of Vermont 19 th International Symposium on Neonatology Sao Paulo, Brazil DISCLOSURE Roger F. Soll
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC
 Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Cranial ultrasound abnormalities in full term infants in a postnatal ward: outcome at 12 and 18 months
 F128 Department of Paediatrics and Neonatal Medicine, Imperial College School of Medicine, Hammersmith Hospital, Du Cane Road, London W12 0HS, UK L Haataja E Mercuri FCowan L Dubowitz Correspondence to:
F128 Department of Paediatrics and Neonatal Medicine, Imperial College School of Medicine, Hammersmith Hospital, Du Cane Road, London W12 0HS, UK L Haataja E Mercuri FCowan L Dubowitz Correspondence to:
Neonatal Therapeutic Hypothermia. A Wasunna Professor of Neonatal Medicine and Pediatrics School of Medicine, University of Nairobi
 Neonatal Therapeutic Hypothermia A Wasunna Professor of Neonatal Medicine and Pediatrics School of Medicine, University of Nairobi Definition of Perinatal Asphyxia *No agreed universal definition ACOG/AAP
Neonatal Therapeutic Hypothermia A Wasunna Professor of Neonatal Medicine and Pediatrics School of Medicine, University of Nairobi Definition of Perinatal Asphyxia *No agreed universal definition ACOG/AAP
Serial 1- and 2-Dimensional Cerebral MRI Measurements in Full-Term Infants after Perinatal Asphyxia
 Original Paper Received: October 27, 2015 Accepted after revision: January 18, 2016 Published online: March 12, 2016 Serial 1- and 2-Dimensional Cerebral MRI Measurements in Full-Term Infants after Perinatal
Original Paper Received: October 27, 2015 Accepted after revision: January 18, 2016 Published online: March 12, 2016 Serial 1- and 2-Dimensional Cerebral MRI Measurements in Full-Term Infants after Perinatal
RESEARCH ARTICLE EVALUATION OF NEUROIMAGING IN CEREBRAL PALSY. S.H. Hasanpour avanji MD
 RESEARCH ARTICLE EVALUATION OF NEUROIMAGING IN CEREBRAL PALSY S.H. Hasanpour avanji MD Assistant Professor of Child Neurology, Iran University of Medical Sciences Corresponding Author: S.H. Hasanpour avanji
RESEARCH ARTICLE EVALUATION OF NEUROIMAGING IN CEREBRAL PALSY S.H. Hasanpour avanji MD Assistant Professor of Child Neurology, Iran University of Medical Sciences Corresponding Author: S.H. Hasanpour avanji
Fetal Heart Rate Monitoring Myths and Misperceptions s: Electronic Fetal Heart Rate Monitoring (EFM): Baseline Assumptions.
 Can FHR Monitoring Prevent Hypoxic-Ischemic Encephalopathy in the Newborn? Fetal Heart Rate Monitoring Myths and Misperceptions 1. Yes 2. No 72% Tekoa L. King CNM, MPH June 6, 2008 28% Yes No Objectives
Can FHR Monitoring Prevent Hypoxic-Ischemic Encephalopathy in the Newborn? Fetal Heart Rate Monitoring Myths and Misperceptions 1. Yes 2. No 72% Tekoa L. King CNM, MPH June 6, 2008 28% Yes No Objectives
Cerebellar Vermian Atrophy after Neonatal Hypoxic-Ischemic Encephalopathy
 AJNR Am J Neuroradiol 25:1008 1015, June/July 2004 Vermian Atrophy after Neonatal Hypoxic-Ischemic Encephalopathy Michael A. Sargent, Kenneth J. Poskitt, Elke H. Roland, Alan Hill, and Glenda Hendson BACKGROUND
AJNR Am J Neuroradiol 25:1008 1015, June/July 2004 Vermian Atrophy after Neonatal Hypoxic-Ischemic Encephalopathy Michael A. Sargent, Kenneth J. Poskitt, Elke H. Roland, Alan Hill, and Glenda Hendson BACKGROUND
Perinatal asphyxia: Pathophysiology and therapy
 Perinatal asphyxia: Pathophysiology and therapy Peter Davis Melbourne Australia With thanks to Dr Sue Jacobs Moderate or severe HIE Complicates ~1/1000 term live births: Mortality: >25% Major neurological
Perinatal asphyxia: Pathophysiology and therapy Peter Davis Melbourne Australia With thanks to Dr Sue Jacobs Moderate or severe HIE Complicates ~1/1000 term live births: Mortality: >25% Major neurological
Target group Term and near term infants with hypoxic ischaemic encephalopathy (HIE) and parents
 Topic Expert Group: Medical care and clinical practice Postnatal management of newborn infants with hypoxic ischaemic encephalopathy (HIE) Van Bel F, Hellström-Westas L, Zimmermann, L Buonocore G, Murray
Topic Expert Group: Medical care and clinical practice Postnatal management of newborn infants with hypoxic ischaemic encephalopathy (HIE) Van Bel F, Hellström-Westas L, Zimmermann, L Buonocore G, Murray
University of Bristol - Explore Bristol Research
 Elstad, M., Liu, X., & Thoresen, M. (2016). Heart rate response to therapeutic hypothermia in infants with hypoxic-ischaemic encephalopathy. Resuscitation, 106, 53-57. DOI: 10.1016/j.resuscitation.2016.06.023
Elstad, M., Liu, X., & Thoresen, M. (2016). Heart rate response to therapeutic hypothermia in infants with hypoxic-ischaemic encephalopathy. Resuscitation, 106, 53-57. DOI: 10.1016/j.resuscitation.2016.06.023
Reproducibility and Accuracy of MR Imaging of the Brain after Severe Birth Asphyxia
 AJNR Am J Neuroradiol : 8, August 999 Reproducibility and Accuracy of MR Imaging of the Brain after Severe Birth Asphyxia Phillipe Jouvet, Francis M. Cowan, Philip Cox, Edward Lazda, Mary A. Rutherford,
AJNR Am J Neuroradiol : 8, August 999 Reproducibility and Accuracy of MR Imaging of the Brain after Severe Birth Asphyxia Phillipe Jouvet, Francis M. Cowan, Philip Cox, Edward Lazda, Mary A. Rutherford,
Effects of Hypothermia for Perinatal Asphyxia on Childhood Outcomes
 The new england journal of medicine original article Effects of Hypothermia for Perinatal Asphyxia on Childhood Outcomes Denis Azzopardi, M.D., Brenda Strohm, R.N., Neil Marlow, D.M., Peter Brocklehurst,
The new england journal of medicine original article Effects of Hypothermia for Perinatal Asphyxia on Childhood Outcomes Denis Azzopardi, M.D., Brenda Strohm, R.N., Neil Marlow, D.M., Peter Brocklehurst,
Neonatal Hypoxic-Ischemic Injury: Ultrasound and Dynamic Color Doppler Sonography perfusion of the Brain and Abdomen with pathologic correlation.
 Neonatal Hypoxic-Ischemic Injury: Ultrasound and Dynamic Color Doppler Sonography perfusion of the Brain and Abdomen with pathologic correlation. Ricardo Faingold,MD Montreal Children s Hospital Medical
Neonatal Hypoxic-Ischemic Injury: Ultrasound and Dynamic Color Doppler Sonography perfusion of the Brain and Abdomen with pathologic correlation. Ricardo Faingold,MD Montreal Children s Hospital Medical
Does phenobarbital improve the effectiveness of therapeutic hypothermia in infants with hypoxic-ischemic encephalopathy?
 (2012) 32, 15 20 r 2012 Nature America, Inc. All rights reserved. 0743-8346/12 www.nature.com/jp ORIGINAL ARTICLE Does phenobarbital improve the effectiveness of therapeutic hypothermia in infants with
(2012) 32, 15 20 r 2012 Nature America, Inc. All rights reserved. 0743-8346/12 www.nature.com/jp ORIGINAL ARTICLE Does phenobarbital improve the effectiveness of therapeutic hypothermia in infants with
No social problems noted No past med hx Mother had spontaneous rupture of fetal membranes SB born on Needed to be resuscitated at birth
 No social problems noted No past med hx Mother had spontaneous rupture of fetal membranes SB born on 9-16-2011 Needed to be resuscitated at birth (included assisted vent) Had generalized edema and possible
No social problems noted No past med hx Mother had spontaneous rupture of fetal membranes SB born on 9-16-2011 Needed to be resuscitated at birth (included assisted vent) Had generalized edema and possible
Serum creatine kinase and lactic dehydrogenase levels as useful markers of immediate and long-term outcome of perinatal asphyxia
 Serum creatine kinase and lactic dehydrogenase levels as useful markers of immediate and long-term outcome of perinatal asphyxia D H Karunatilaka 1, G W D S Amaratunga 2, K D N I Perera 3, V Caldera 4
Serum creatine kinase and lactic dehydrogenase levels as useful markers of immediate and long-term outcome of perinatal asphyxia D H Karunatilaka 1, G W D S Amaratunga 2, K D N I Perera 3, V Caldera 4
Neurological outcome after perinatal asphyxia at term
 Section 1 Chapter 1 Scientific background Neurological outcome after perinatal asphyxia at term David Odd and Andrew Whitelaw Introduction It was nearly 150 years ago that an association between perinatal
Section 1 Chapter 1 Scientific background Neurological outcome after perinatal asphyxia at term David Odd and Andrew Whitelaw Introduction It was nearly 150 years ago that an association between perinatal
HYPOXIC ISCHEMIC ENCEPHALOPATHY AND THE OBSTETRICIAN
 HYPOXIC ISCHEMIC ENCEPHALOPATHY AND THE OBSTETRICIAN DISCLOSURE I have nothing to disclose and have no real or potential conflicts with this presentation and its content. Michael P. Nageotte, M.D. CASE:
HYPOXIC ISCHEMIC ENCEPHALOPATHY AND THE OBSTETRICIAN DISCLOSURE I have nothing to disclose and have no real or potential conflicts with this presentation and its content. Michael P. Nageotte, M.D. CASE:
These signs should lead to the administration of high concentrations of
 Hypoxic-ischemic encephalopathy (HIE); (cont.) Clinical manifestations; *Intrauterine; growth restriction and increased vascular resistances may be the st manifestation of fetal hypoxia. *During labor;
Hypoxic-ischemic encephalopathy (HIE); (cont.) Clinical manifestations; *Intrauterine; growth restriction and increased vascular resistances may be the st manifestation of fetal hypoxia. *During labor;
National follow-up program CPUP Pediatric Neurology paper form
 National follow-up program CPUP Pediatric Neurology paper form 110206 1 National Follow-Up program- CPUP Pediatric Neurology Personal nr (unique identifier): Last name: First name: Region child belongs
National follow-up program CPUP Pediatric Neurology paper form 110206 1 National Follow-Up program- CPUP Pediatric Neurology Personal nr (unique identifier): Last name: First name: Region child belongs
Hypoxic-ischemic encephalopathy has an incidence of
 Original Article Amplitude-Integrated EEG Is Useful in Predicting Neurodevelopmental Outcome in Full-Term Infants With Hypoxic-Ischemic Encephalopathy: A Meta-Analysis Journal of Child Neurology Volume
Original Article Amplitude-Integrated EEG Is Useful in Predicting Neurodevelopmental Outcome in Full-Term Infants With Hypoxic-Ischemic Encephalopathy: A Meta-Analysis Journal of Child Neurology Volume
Neurology. Access Center 24/7 access for referring physicians (866) 353-KIDS (5437)
 Neurology The Neurology practice at Valley Children s provides diagnostic services, medical treatment, and followup care to infants, children, and adolescents who have suspected or confirmed neurological
Neurology The Neurology practice at Valley Children s provides diagnostic services, medical treatment, and followup care to infants, children, and adolescents who have suspected or confirmed neurological
Cranial ultrasound findings in preterm infants predict the development of cerebral palsy
 Syddansk Universitet Cranial ultrasound findings in preterm infants predict the development of cerebral palsy Skovgaard, Ann Lawaetz; Zachariassen, Gitte Published in: Danish Medical Journal Publication
Syddansk Universitet Cranial ultrasound findings in preterm infants predict the development of cerebral palsy Skovgaard, Ann Lawaetz; Zachariassen, Gitte Published in: Danish Medical Journal Publication
MRI Lesions and Infants with Neonatal Encephalopathy. Is the Apgar Score Predictive?
 MRI Lesions and Infants with Neonatal Encephalopathy. Is the Apgar Score Predictive? E. Mercuri 1,2 M. Rutherford 1 A. Barnett 1 Chr. Foglia 1 L. Haataja 1,3 S. Counsell 4 F. Cowan 1 L. Dubowitz 1 150
MRI Lesions and Infants with Neonatal Encephalopathy. Is the Apgar Score Predictive? E. Mercuri 1,2 M. Rutherford 1 A. Barnett 1 Chr. Foglia 1 L. Haataja 1,3 S. Counsell 4 F. Cowan 1 L. Dubowitz 1 150
The tale of global hypoxic ischaemic injury
 The tale of global hypoxic ischaemic injury Poster No.: C-0400 Congress: ECR 2016 Type: Educational Exhibit Authors: L. M. Zammit, R. Grech ; Paola/MT, Dublin 9/IE Keywords: CNS, CT, MR, Education, Computer
The tale of global hypoxic ischaemic injury Poster No.: C-0400 Congress: ECR 2016 Type: Educational Exhibit Authors: L. M. Zammit, R. Grech ; Paola/MT, Dublin 9/IE Keywords: CNS, CT, MR, Education, Computer
1/29/2014. Kimberly Johnson Hatchett, MD PGY-4 11/15/13
 Kimberly Johnson Hatchett, MD PGY-4 11/15/13 History of Present Illness 14 month old previously healthy infant boy presented via EMS after being found by his mother to be breathing loudly and non-responsive.
Kimberly Johnson Hatchett, MD PGY-4 11/15/13 History of Present Illness 14 month old previously healthy infant boy presented via EMS after being found by his mother to be breathing loudly and non-responsive.
AMERICAN COLLEGE OF SURGEONS CRITICAL CARE REVIEW COURSE 2012 HOT TOPICS IN PEDIATRIC CRITICAL CARE
 AMERICAN COLLEGE OF SURGEONS CRITICAL CARE REVIEW COURSE 2012 HOT TOPICS IN PEDIATRIC CRITICAL CARE Karyn L. Butler, MD, FACS, FCCM Chief, Surgical Critical Care Hartford Hospital / University of Connecticut
AMERICAN COLLEGE OF SURGEONS CRITICAL CARE REVIEW COURSE 2012 HOT TOPICS IN PEDIATRIC CRITICAL CARE Karyn L. Butler, MD, FACS, FCCM Chief, Surgical Critical Care Hartford Hospital / University of Connecticut
Early Accurate Diagnosis & Early Intervention for Cerebral Palsy INTERNATIONAL RECOMMENDATIONS
 Early Accurate Diagnosis & Early Intervention for Cerebral Palsy INTERNATIONAL RECOMMENDATIONS Professor Iona Novak Cerebral Palsy Alliance Australia Neuroplasticity is fundamentally why we believe in
Early Accurate Diagnosis & Early Intervention for Cerebral Palsy INTERNATIONAL RECOMMENDATIONS Professor Iona Novak Cerebral Palsy Alliance Australia Neuroplasticity is fundamentally why we believe in
Hypoxic ischaemic encephalopathy
 Hypoxic ischaemic encephalopathy Frances Cowan Denis Azzopardi Abstract Encephalopathy occurring soon after birth continues to be a major complication in near- and full-term newborn infants. Early neonatal
Hypoxic ischaemic encephalopathy Frances Cowan Denis Azzopardi Abstract Encephalopathy occurring soon after birth continues to be a major complication in near- and full-term newborn infants. Early neonatal
Review Article Current Controversies in Newer Therapies to Treat Birth Asphyxia
 International Pediatrics Volume 2011, Article ID 848413, 5 pages doi:10.1155/2011/848413 Review Article Current Controversies in Newer Therapies to Treat Birth Asphyxia Pia Wintermark Division of Newborn
International Pediatrics Volume 2011, Article ID 848413, 5 pages doi:10.1155/2011/848413 Review Article Current Controversies in Newer Therapies to Treat Birth Asphyxia Pia Wintermark Division of Newborn
Predicting outcome using neonatal MRI in preterm infants. Manon Benders, neonatologist. Summer Conference on Neonatology in Provence
 Predicting outcome using neonatal MRI in preterm infants Manon Benders, neonatologist Summer Conference on Neonatology in Provence Avignon, France, 6 th - 9 th September 2017 the human brain the third
Predicting outcome using neonatal MRI in preterm infants Manon Benders, neonatologist Summer Conference on Neonatology in Provence Avignon, France, 6 th - 9 th September 2017 the human brain the third
The NeuroNICU From Concept to Clinical Service. MJ Harbert, MD Co-Director, NeuroNICU Service Rady Children s Hospital San Diego
 The NeuroNICU From Concept to Clinical Service MJ Harbert, MD Co-Director, NeuroNICU Service Rady Children s Hospital San Diego What is a NeuroNICU? Collaboration between Neonatology and Neurology Neonatal
The NeuroNICU From Concept to Clinical Service MJ Harbert, MD Co-Director, NeuroNICU Service Rady Children s Hospital San Diego What is a NeuroNICU? Collaboration between Neonatology and Neurology Neonatal
Long-term neurodevelopmental outcome with hypoxic-ischemic encephalopathy
 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2013 Long-term neurodevelopmental outcome with hypoxic-ischemic encephalopathy
Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2013 Long-term neurodevelopmental outcome with hypoxic-ischemic encephalopathy
Ultrasound examination of the neonatal brain
 Ultrasound examination of the neonatal brain Guideline for the performance and reporting of neonatal and preterm brain ultrasound examination, by the Finnish Perinatology Society and the Paediatric Radiology
Ultrasound examination of the neonatal brain Guideline for the performance and reporting of neonatal and preterm brain ultrasound examination, by the Finnish Perinatology Society and the Paediatric Radiology
UK cooling TOBY. register. UK TOBY Cooling Register Protocol
 UK cooling TOBY register UK TOBY Cooling Register Protocol Version 3, 11th June 2007 1 Contents 1. Background 2 1.1 Perinatal asphyxial encephalopathy 2 1.2 Pathogenesis of perinatal asphyxial encephalopathy
UK cooling TOBY register UK TOBY Cooling Register Protocol Version 3, 11th June 2007 1 Contents 1. Background 2 1.1 Perinatal asphyxial encephalopathy 2 1.2 Pathogenesis of perinatal asphyxial encephalopathy
University of Groningen
 University of Groningen Perinatal Anemia is Associated with Neonatal and Neurodevelopmental Outcomes in Infants with Moderate to Severe Perinatal Asphyxia Kalteren, Willemien S.; ter Horst, Hendrik J.;
University of Groningen Perinatal Anemia is Associated with Neonatal and Neurodevelopmental Outcomes in Infants with Moderate to Severe Perinatal Asphyxia Kalteren, Willemien S.; ter Horst, Hendrik J.;
