Review Article Current Controversies in Newer Therapies to Treat Birth Asphyxia
|
|
|
- Valentine Oliver
- 5 years ago
- Views:
Transcription
1 International Pediatrics Volume 2011, Article ID , 5 pages doi: /2011/ Review Article Current Controversies in Newer Therapies to Treat Birth Asphyxia Pia Wintermark Division of Newborn Medicine, Montreal Children s Hospital, McGill University, 2300 Rue Tupper, C-920, Montreal, QC, Canada H3H 1P3 Correspondence should be addressed to Pia Wintermark, pia.wintermark@blu .ch Received 24 August 2011; Accepted 28 September 2011 Academic Editor: Khalid N. Haque Copyright 2011 Pia Wintermark. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Despite major advances in monitoring technology and knowledge of fetal and neonatal pathophysiology, neonatal hypoxicischemic encephalopathy (HIE) remains one of the main causes of severe adverse neurological outcome in children. Until recently, there were no therapies other than supportive measures. Over the past several years, mild hypothermia has been proven to be safe to treat HIE. Unfortunately, this neuroprotective strategy seems efficient in preventing brain injury in some asphyxiated newborns, but not in all of them. Thus, there is increasing interest to rapidly understand how to refine hypothermia therapy and add neuroprotective or neurorestorative strategies. Several promising newer treatments to treat birth asphyxia and prevent its devastating neurological consequences are currently being tested. In this paper, the physiopathology behind HIE, the currently available treatment, the potential alternatives, and the next steps before implementation of these other treatments are reviewed. 1. Introduction Hypoxic-ischemic encephalopathy (HIE) is a serious brain injury due to birth asphyxia [1, 2]. HIE has a variety of perinatal causes of interrupted uterine and fetal blood flow and/or hypoxia, such as uterine rupture, placental abruption, and cord prolapse. However, most often, the exact timing and underlying cause remain unknown [3 5]. Its severity is also variable. Despite major advances in monitoring technology and knowledge of fetal and neonatal pathophysiology, birth asphyxia remains a serious condition that causes significant mortality and long-term morbidity. Causing 23% of all neonatal deaths worldwide [6, 7], it is one of the top 20 leading causes of burden of disease in all age groups (in terms of disability life adjusted years) by the World Health Organization [7]. Most deaths occur in the first week of life due to multiple organ failure or withdrawal of care due to the prospect of severe neurological impairments [8]. Moreover, children who survive birth asphyxia develop problems such as cerebral palsy, mental retardation, learning difficulties, and other disabilities [9]. Until recently, there were no therapies other than supportive measures for perinatal HIE. In the past several years, studies have been carried out to address the safety and efficacy of cooling in HIE [10 18]. Unfortunately, this neuroprotective strategy seems efficient in preventing brain injury in some asphyxiated newborns, but not in all of them. Thus, there is an increasing interest to rapidly understand the degree of brain injury and to possibly refine individual neuroprotective strategies or add neurorestorative strategies [19 23]. In this paper, the physiopathology behind HIE, the current available treatment, the potential alternatives, and the next steps before implementation of these other treatments are reviewed. 2. What Is Hypoxic-Ischemic Encephalopathy? Neonatal brain hypoxic-ischemic injury is an evolving process initiated by the hypoxic-ischemic insult leading to decreased blood flow to the brain (primary lesions), followed by the restoration of blood flow in an injured brain and the initiation of a cascade of pathways (secondary lesions, reperfusion injury ). This cascade includes accumulation of extracellular glutamate with excessive activation of glutamate receptors, calcium influx, and generation of reactive oxygen and nitrogen species, leading to cell death and definitive brain injuries [24]. This cascade is a primary target for neuroprotective interventions, but such interventions are currently limited by insufficient knowledge of the timing and
2 2 International Pediatrics Table 1: Potential therapies to treat birth asphyxia in newborns. Neuroprotective therapies: Hypothermia Drugs that might produce a synergistic neuroprotective effect with hypothermia: (i) anticonvulsant or antiexcitatory drugs: for example, phenobarbital, topiramate, bumetanide, magnesium sulphate, xenon (ii) anti-apoptotic drugs: for example, erythropoietin (iii) anti-calcium drugs: for example, xenon (iv) anti-inflammatory or antioxidative drugs: for example, melatonin, N-acetylcysteine Neurorestorative therapies: (i) erythropoietin (ii) cord blood and mesenchymal stem cells duration of the so-called therapeutic window in newborns [19, 21, 22]. 3. What Is the Current Available Treatment? As the only neuroprotective treatment to have been clinically tested in large randomized controlled trials to minimize brain injury in asphyxiated term newborns [10, 11, 13, 14, 17, 18], cooling is thought to be protective in newborns (Table 1) mainly by reducing brain perfusion and metabolism, as well as mitigating reperfusion injury, reducing excessive free radical production, depressing the immune response and various potentially harmful proinflammatory reactions, and suppress epileptic activity [25]. Some results also suggest that moderate hypothermia can prevent or delay apoptosis and might be able to extend the therapeutic window for other interventions [25]. Results of these clinical trials in newborns have shown that moderate hypothermia after birth asphyxia reduces the risk of death and disability at 18 months, with a number needed to treat of nine asphyxiated newborns to prevent brain injury in one of them [12, 15, 16]. There was no real difference in any of the outcomes between whole-body cooling versus selective head cooling [12, 15, 16]. Only little adverse affects have been observed with this therapy; the main ones were arrhythmia and thrombocytopenia [12, 15, 16]. However, it remains unclear why induced hypothermia seems effective in preventing brain injury and improving neurological outcome in some asphyxiated newborns (mainly those with moderate HIE), but not in others (mainly those with severe HIE) [11, 14]. A better understanding of why brain injury continues to develop despite hypothermia treatment in some asphyxiated newborns is required in order to create and test some more specifically adjunctive therapies. Furthermore, early identification of patients who will develop further brain injury despite this treatment would be of utmost importance in order to determine those who would benefit most from adjustments in their hypothermia therapy or from adjunctive neuroprotective or neurorestorative therapies [20, 23]. According to the trials described above, mild hypothermia to an esophageal temperature of 33.5 C must be started in an asphyxiated newborn within 6 hours of life and continued for 72 hours. This temperature and this timing are based on animal data; for example the 6-hour limit for cooling initiation comes from data suggesting that the effectiveness of cooling diminishes as time increases from the hypoxicischemic event to initiation of cooling, with the closing of the window at a time between 5.5 and 8 hours after the event [26]. However, as previously mentioned, the exact timing of the therapeutic window is not known in human newborns. Some authors are thus starting to suggest that there might be a benefit from later initiation of cooling and increased depth or duration of cooling, as well as prolonged rewarming strategies [19]. Determination of the exact timing of the therapeutic window in asphyxiated newborns needs to be further investigated [27]. Additional randomized controlled trials are required to test if adjustments of current guidelines of moderate hypothermia for asphyxiated newborns might be useful to prevent even more efficiently brain injury in these patients. Such trials are currently ongoing (e.g., late hypothermia for hypoxic-ischemic encephalopathy, ClinicalTrials.gov Identifier: NCT ), and results should be known in the near future. One of the main challenges of the current guidelines for cooling newborns with HIE is to initiate the hypothermia within the first 6 hours of birth. In many places around the world, newborns may be born at great distances from neonatal intensive care units offering cooling, preventing them from arriving there within the good timing. Specific protocols have to be developed in collaboration with the cooling centers of reference in order to start cooling safely and reliably prior to the transport at the birthing center and/or during transport, so that these patients can also benefit from this treatment [16, 19, 28]. In particular, continuous measurement of central temperature (esophageal or rectal) should be carefully monitored, in order to target the recommended temperature [16, 19, 28]. 4. What Are the Potential Alternatives? Studies of alternative treatments for neonatal HIE are becoming available, with the goal of further increasing the proven benefits of hypothermia, that is, to decrease eventual neonatal brain injury associated with neonatal asphyxia and thus improve future neurodevelopmental outcome. These alternatives include specific brain-oriented therapies, which are targeted to the critical events contributing to tissue damage in neonatal HIE (Table 1)[29]. They usually involve molecules that cross the blood-brain barrier and target mechanisms of injury, which are not (or are not completely) inhibited by hypothermia. These include anticonvulsant or antiexcitatory drugs (e.g., phenobarbital, topiramate, bumetanide, magnesium sulphate, and xenon), antiapoptotic drugs (e.g., erythropoietin), anticalcium drugs (e.g., xenon), or anti-inflammatory or antioxidative drugs (e.g., melatonin and N-acetylcysteine) [30 33]. The goal of these experimental therapies is to produce a synergistic neuroprotective effect with hypothermia [30 33].
3 International Pediatrics 3 Most research efforts in neonatal neurology are currently targeted to neuroprotective strategies, but another concept is slowly emerging from the adult stroke literature. In adults, neurorestorative therapies (Table 1) are currently being developed to treat ischemic brain injury, including cerebral vasculature-based therapy combined with neuroprotection [34], as the more conventional strategies (antiapoptosis, anticalcium, anti-inflammation, and antioxidative injury) have been disappointingly ineffective in adult clinical trials. These neurorestorative therapies target the neurovascular unit, composed of functionally integrated cellular (including brain endothelial cells, astrocytes, pericytes and smooth muscle cells, neural stem cells, oligodendrocytes, and neurons) and acellular elements that form the basement membrane [35]. Thus, they lead to enhancement of restorative events, such as endogenous neurogenesis, angiogenesis, axonal sprouting, and synaptogenesis in the ischemic brain, explaining the potential for stimulation of brain plasticity and improvement in functional recovery [36, 37]. In adult models of stroke, these therapies have been shown to activate these processes and successfully reduce the size of the infarcted areas [38, 39] and are now being actively tested in human patients. The immature brain of a newborn is not simply a small adult brain, and the mechanisms underlying neonatal HIE is certainly very unique compared to the ones underlying adult stroke [40]. However, evidence is growing in the literature that such a systemic approach might also be useful to better treat neonatal brain injury. One such potential neurorestorative drug in newborns is erythropoietin, which has a recognized role in promoting neural regeneration and neurovascular remodeling [41]. A randomized controlled clinical trial is currently ongoing in human newborns to assess its efficiency (i.e., neonatal erythropoietin in asphyxiated term newborns, Clinical- Trials.gov Identifier: NCT ). Another promising alternative treatment of neonatal HIE utilizes cord blood and mesenchymal stem cells to replace neurons lost due to brain injury, as well as activate endogenous stem cells, and release growth factors, thus minimizing brain damage and promoting restoration [42, 43]. 5. What Are the Next Steps before Implementing These Treatments? These adjunctive therapies have until now mostly been tested only in animal models of HIE or in different populations of newborns (e.g., erythropoietin to reduce the need for blood transfusions in very low birthweight infants [44]). Only a few randomized-controlled studies using these treatments are currently available in human newborns with HIE, and they usually include only small numbers of patients [45]. Before implementation, these alternative therapies will need to prove their efficiency and safety in randomized-controlled clinical trials with appropriate sample size consideration and outcome variables. Determining the best timing and the best dosage range for these alternative treatments is also crucial to obtain their maximum efficiency. It has been hypothesized that hypothermia may buy additional time for neuroprotective drugs to act within an expanded therapeutic window [25]. However, for most of these alternative treatments, it remains to be determined when they will have the maximum synergistic effect with hypothermia treatment. For example, in the first randomized trial of erythropoietin in term newborns with HIE, the medication was given first within the first 24 hours of birth and thereafter every other day for 2 weeks; the results showed a significantly improved primary outcome (death or disability rate) at 18 months, suggesting that this medication may provide therapeutic effect over a longer period than the first 6 hours of life [45]. Further similar trials need to be performed for each of these other potential treatments. In addition, appropriate selection of the newborns most likely to respond to these adjunctive treatments is of utmost importance to demonstrate more quickly their efficacy. Planning for such trials should include early identification of newborns at risk of developing brain HI injury (whether or not hypothermia is administered). To this end, early biomarkers of future brain HI injury in newborns are required to adjust existing cooling guidelines or to add other therapeutic interventions. Ideally, regular evolution of such biomarkers should be known, so that the impact of these newer treatments may be assessed as soon as possible. Current biomarkers included clinical signs, neurological exam outcomes, and assessment of brain activity by amplitude-integrated electroencephalogram [14, 46, 47]. Recent studies suggest some other potential biomarkers, such as brain magnetic resonance imaging [27], near-infrared spectroscopy [47], or biochemical markers [48], which would help guide the adjustment of therapies. Adjustment of the hypothermia treatment or addition of new treatments should be performed according to the specific clinical and imaging findings of these patients. 6. Conclusions How to treat newborns with HIE following birth asphyxia has become one of today s hottest topics in neonatal medicine. Over the past decade, substantial progress has been made in neurointensive care for newborns. However, much remains to be done to improve these early positive results and reduce further the eventual neonatal brain injury and improve future neurodevelopmental outcome of newborns with a hypoxic-ischemic event at birth. Several promising new treatments for the prevention of the devastating neurological consequences of birth asphyxia are currently being tested, but further detailed animal and clinical studies are required before their safe application in human newborns with HIE. 7. Future Research Directions (i) Define early biomarkers of brain injury to target the newborns with HIE most vulnerable to brain injury despite hypothermia treatment. (ii) Determine if adjustments to current guidelines for mild hypothermia (i.e., cool later, lower, or longer) might be useful to further prevent brain injury.
4 4 International Pediatrics (iii) Determine the best timing and the best dosage range of administration of adjunctive treatments, in order to get their maximum efficiency. (iv) Study in more detail the synergistic effects of these various treatments to better target the different and specific needs of each asphyxiated newborn infant and decrease the eventual neonatal brain injury and thus improve future neurodevelopmental outcome. (v) Perform safety studies in human newborns with HIE for all these potential alternative treatments. Abbreviation HIE: hypoxic-ischemic encephalopathy. Conflict of Interests The authors declare that there is no conflict of interests affecting the content of this paper. Acknowledgment The author thanks Aaron Johnstone and Richard Gosselin for their thorough review of the paper. References [1] American Academy of Pediatrics, Relation between perinatal factors and neurological outcome, in Guidelines for Perinatal Care, pp , American Academy of Pediatrics, Elk Grove Village, Ill, USA, 3rd edition, [2] W.Oh,L.R.Blackmon,M.Escobedoetal., Useandabuseof the APGAR score, Pediatrics, vol. 98, no. 1, pp , [3] D. M. Ferriero, Medical progress: neonatal brain injury, The New England Medicine, vol. 351, no. 19, pp , [4] J. Grow and J. D. E. Barks, Pathogenesis of hypoxic-ischemic cerebral injury in the term infant: current concepts, Clinics in Perinatology, vol. 29, no. 4, pp , [5] M. Oskoui and M. I. Shevell, Cerebral palsy and the transition from pediatric to adult care, Continuum: Lifelong Learning in Neurology, vol. 15, no. 6, pp , [6] J. Bryce, C. Boschi-Pinto, K. Shibuya, and R. E. Black, WHO estimates of the causes of death in children, The Lancet, vol. 365, no. 9465, pp , [7] J. Lawn, K. Shibuya, and C. Stein, No cry at birth: global estimates of intrapartum stillbirths and intrapartum-related neonatal deaths, Bulletin of the World Health Organization, vol. 83, no. 6, pp , [8] D. Wilkinson, MRI and withdrawal of life support from newborn infants with hypoxic-ischemic encephalopathy, Pediatrics, vol. 126, no. 2, pp. e451 e458, [9] N. Al-Macki, S. P. Miller, N. Hall, and M. Shevell, The spectrum of abnormal neurologic outcomes subsequent to trerm intrapartum asphyxia, Pediatric Neurology, vol. 41, no. 6, pp , [10] D. Azzopardi, P. Brocklehurst, D. Edwards et al., The TOBY study: whole body hypothermia for the treatment of perinatal asphyxial encephalopathy: a randomised controlled trial, BMC Pediatrics, vol. 8, article 17, [11] D. V. Azzopardi, B. Strohm, A. D. Edwards et al., Moderate hypothermia to treat perinatal asphyxial encephalopathy, The New England Medicine, vol. 361, no. 14, pp , [12] A. D. Edwards, P. Brocklehurst, A. J. Gunn et al., Neurological outcomes at 18 months of age after moderate hypothermia for perinatal hypoxic ischaemic encephalopathy: synthesis and meta-analysis of trial data, British Medical Journal, vol. 340, p. c363, [13] D. J. Eicher, C. L. Wagner, L. P. Katikaneni et al., Moderate hypothermia in neonatal encephalopathy: efficacy outcomes, Pediatric Neurology, vol. 32, no. 1, pp , [14] P. D. Gluckman, J. S. Wyatt, D. Azzopardi et al., Selective head cooling with mild systemic hypothermia after neonatal encephalopathy: multicentre randomised trial, The Lancet, vol. 365, no. 9460, pp , [15] S. Jacobs, R. Hunt, W. Tarnow-Mordi, T. Inder, and P. Davis, Cooling for newborns with hypoxic ischaemic encephalopathy, Cochrane Database of Systematic Reviews, vol. 4, Article ID CD003311, [16] P. S. Shah, Hypothermia: a systematic review and metaanalysis of clinical trials, Seminars in Fetal and Neonatal Medicine, vol. 15, no. 5, pp , [17] S. Shankaran, A. R. Laptook, R. A. Ehrenkranz et al., Wholebody hypothermia for neonates with hypoxic-ischemic encephalopathy, The New England Medicine, vol. 353, no. 15, pp , [18] G. Simbruner, R. A. Mittal, F. Rohlmann et al., Systemic hypothermia after neonatal encephalopathy: outcomes of neo.neuro.network RCT, Pediatrics, vol. 126, no. 4, pp. e771 e778, [19] J. D. E. Barks, Current controversies in hypothermic neuroprotection, Seminars in Fetal and Neonatal Medicine, vol. 13, no. 1, pp , [20] F. F. Gonzalez and D. M. Ferriero, Neuroprotection in the newborn infant, Clinics in Perinatology, vol. 36, no. 4, pp , [21] R. D. Higgins, T. N. K. Raju, J. Perlman et al., Hypothermia and perinatal asphyxia: executive summary of the National Institute of Child Health and Human Development workshop, Pediatrics, vol. 148, no. 2, pp , [22] R. D. Higgins and S. Shankaran, Hypothermia for hypoxic ischemic encephalopathy in infants 36 weeks, Early Human Development, vol. 85, no. 10, pp. S49 S52, [23] M. I. Levene, Cool treatment for birth asphyxia, but what s next? Archives of Disease in Childhood: Fetal and Neonatal Edition, vol. 95, no. 3, pp. F154 F157, [24] J. M. Perlman, Brain injury in the term infant, Seminars in Perinatology, vol. 28, no. 6, pp , [25] K. H. Polderman, Induced hypothermia and fever control for prevention and treatment of neurological injuries, The Lancet, vol. 371, no. 9628, pp , [26] A. J. Gunn and T. R. Gunn, The pharmacology of neuronal rescue with cerebral hypothermia, Early Human Development, vol. 53, no. 1, pp , [27] P. Wintermark, A. Hansen, M. C. Gregas et al., Brain perfusion in asphyxiated newborns treated with therapeutic hypothermia, American Neuroradiology.In Press. [28]S.E.Jacobs,C.J.Morey,T.E.Inderetal., Whole-body hypothermia for term and near-term newborns with hypoxicischemic encephalopathy: a randomized controlled trial, Archives of Pediatrics & Adolescent Medicine, vol. 165, no. 8, pp , 2011.
5 International Pediatrics 5 [29] S. Shankaran and A. Laptook, Challenge of conducting trials of neuroprotection in the asphyxiated term infant, Seminars in Perinatology, vol. 27, no. 4, pp , [30] M. R. Cilio and D. M. Ferriero, Synergistic neuroprotective therapies with hypothermia, Seminars in Fetal and Neonatal Medicine, vol. 15, no. 5, pp , [31] M. V. Johnston, A. Fatemi, M. A. Wilson, and F. Northington, Treatment advances in neonatal neuroprotection and neurointensive care, The Lancet Neurology, vol. 10, no. 4, pp , [32] D. Kelen and N. J. Robertson, Experimental treatments for hypoxic ischaemic encephalopathy, Early Human Development, vol. 86, no. 6, pp , [33] F. van Bel and F. Groenendaal, Long-term pharmacologic neuroprotection after birth asphyxia: where do we stand? Neonatology, vol. 94, no. 3, pp , [34] J. Folkman, Angiogenesis: an organizing principle for drug discovery? Nature Reviews Drug Discovery, vol.6,no.4,pp , [35]G.J.delZoppo, Strokeandneurovascularprotection, The New England Medicine, vol. 354, no. 6, pp , [36] Y. Fan and G. Y. Yang, Therapeutic angiogenesis for brain ischemia: a brief review, Neuroimmune Pharmacology, vol. 2, no. 3, pp , [37] Z. G. Zhang and M. Chopp, Neurorestorative therapies for stroke: underlying mechanisms and translation to the clinic, The Lancet Neurology, vol. 8, no. 5, pp , [38] R. Zhang, L. Wang, L. Zhang et al., Nitric oxide enhances angiogenesis via the synthesis of vascular endothelial growth factor and cgmp after stroke in the rat, Circulation Research, vol. 92, no. 3, pp , [39] L. Zhang, R. L. Zhang, Y. Wang et al., Functional recovery in aged and young rats after embolic stroke: treatment with a phosphodiesterase type 5 inhibitor, Stroke, vol. 36, no. 4, pp , [40] F. E. Jensen, Developmental factors regulating susceptibility to perinatal brain injury and seizures, Current Opinion in Pediatrics, vol. 18, no. 6, pp , [41] T. Xiong, Y. Qu, D. Mu, and D. Ferriero, Erythropoietin for neonatal brain injury: opportunity and challenge, International Developmental Neuroscience,vol.29,no.6,pp , [42] I. S. Lee, K. Jung, M. Kim, and K. I. Park, Neural stem cells: properties and therapeutic potentials for hypoxic-ischemic brain injury in newborn infants, Pediatrics International, vol. 52, no. 6, pp , [43] P. M. Pimentel-Coelho and R. Mendez-Otero, Cell therapy for neonatal hypoxic-ischemic encephalopathy, Stem Cells and Development, vol. 19, no. 3, pp , [44] K. M. Shannon, J. F. Keith III, W. C. Mentzer et al., Recombinant human erythropoietin stimulates erythropoiesis and reduces erythrocyte transfusions in very low birth weight preterm infants, Pediatrics, vol. 95, no. 1, pp. 1 8, [45] C. Zhu, W. Kang, F. Xu et al., Erythropoietin improved neurologic outcomes in newborns with hypoxic-ischemic encephalopathy, Pediatrics, vol. 124, no. 2, pp. e218 e226, [46] N. Al Naqeeb, A. D. Edwards, F. M. Cowan, and D. Azzopardi, Assessment of neonatal encephalopathy by amplitudeintegrated electroencephalography, Pediatrics, vol. 103, no. 6, part 1, pp , [47] M. C. Toet and P. M. A. Lemmers, Brain monitoring in neonates, Early Human Development, vol. 85, no. 2, pp , [48] L. Bennet, L. Booth, and A. J. Gunn, Potential biomarkers for hypoxic-ischemic encephalopathy, Seminars in Fetal and Neonatal Medicine, vol. 15, no. 5, pp , 2010.
6 MEDIATORS of INFLAMMATION The Scientific World Journal Gastroenterology Research and Practice Diabetes Research International Endocrinology Immunology Research Disease Markers Submit your manuscripts at BioMed Research International PPAR Research Obesity Ophthalmology Evidence-Based Complementary and Alternative Medicine Stem Cells International Oncology Parkinson s Disease Computational and Mathematical Methods in Medicine AIDS Behavioural Neurology Research and Treatment Oxidative Medicine and Cellular Longevity
Neonatal Therapeutic Hypothermia. A Wasunna Professor of Neonatal Medicine and Pediatrics School of Medicine, University of Nairobi
 Neonatal Therapeutic Hypothermia A Wasunna Professor of Neonatal Medicine and Pediatrics School of Medicine, University of Nairobi Definition of Perinatal Asphyxia *No agreed universal definition ACOG/AAP
Neonatal Therapeutic Hypothermia A Wasunna Professor of Neonatal Medicine and Pediatrics School of Medicine, University of Nairobi Definition of Perinatal Asphyxia *No agreed universal definition ACOG/AAP
Too Cool? Hypoxic Ischemic Encephalopathy and Therapeutic Hypothermia. Lauren Sacco DNP, ARNP, NNP-BC
 Too Cool? Hypoxic Ischemic Encephalopathy and Therapeutic Hypothermia Lauren Sacco DNP, ARNP, NNP-BC Pathophysiology of HIE Occurs in two energy failure phases: First phase happens during the initial insult
Too Cool? Hypoxic Ischemic Encephalopathy and Therapeutic Hypothermia Lauren Sacco DNP, ARNP, NNP-BC Pathophysiology of HIE Occurs in two energy failure phases: First phase happens during the initial insult
Objectives. Birth Depression Management. Birth Depression Terms
 Objectives Birth Depression Management Regional Perinatal Outreach Program 2016 Understand the terms and the clinical characteristics of birth depression. Be familiar with the evidence behind therapeutic
Objectives Birth Depression Management Regional Perinatal Outreach Program 2016 Understand the terms and the clinical characteristics of birth depression. Be familiar with the evidence behind therapeutic
COOLING FOR HYPOXIC ISCHEMIC ENCEPHALOPATHY
 COOLING FOR HYPOXIC ISCHEMIC ENCEPHALOPATHY Roger F. Soll H. Wallace Professor of Neonatology University of Vermont 19 th International Symposium on Neonatology Sao Paulo, Brazil DISCLOSURE Roger F. Soll
COOLING FOR HYPOXIC ISCHEMIC ENCEPHALOPATHY Roger F. Soll H. Wallace Professor of Neonatology University of Vermont 19 th International Symposium on Neonatology Sao Paulo, Brazil DISCLOSURE Roger F. Soll
Temperature Correction of Blood Gas Measurements during Therapeutic Hypothermia: Is it Time to Chill Out?
 Temperature Correction of Blood Gas Measurements during Therapeutic Hypothermia: Is it Time to Chill Out? Dr. Elizabeth Zorn Dr. Gwenyth Fischer Dr. Martha Lyon Disclosures (ML) Speaking Honoraria Radiometer
Temperature Correction of Blood Gas Measurements during Therapeutic Hypothermia: Is it Time to Chill Out? Dr. Elizabeth Zorn Dr. Gwenyth Fischer Dr. Martha Lyon Disclosures (ML) Speaking Honoraria Radiometer
Effect of ALlopurinol in addition to hypothermia for hypoxic-ischemic Brain Injury on Neurocognitive Outcome. Axel Franz, Tübingen
 Effect of ALlopurinol in addition to hypothermia for hypoxic-ischemic Brain Injury on Neurocognitive Outcome Axel Franz, Tübingen Hypoxic-ischemic encephalopathy 1-2 / 1000 newborn suffer from moderate
Effect of ALlopurinol in addition to hypothermia for hypoxic-ischemic Brain Injury on Neurocognitive Outcome Axel Franz, Tübingen Hypoxic-ischemic encephalopathy 1-2 / 1000 newborn suffer from moderate
Running head: THERAPEUTIC HYPOTHERMIA AND TRANSPORT 1
 Running head: THERAPEUTIC HYPOTHERMIA AND TRANSPORT 1 Therapeutic Hypothermia for Neonatal Encephalopathy: Preparation for Transport to Cooling Center Teresa Z. Baker, DNP-S Annie L. Addison, FNP-S NURS
Running head: THERAPEUTIC HYPOTHERMIA AND TRANSPORT 1 Therapeutic Hypothermia for Neonatal Encephalopathy: Preparation for Transport to Cooling Center Teresa Z. Baker, DNP-S Annie L. Addison, FNP-S NURS
Pathophysiology Review. Hypoxic-Ischemic Encephalopathy & Therapeutic Hypothermia. Objectives. What is Hypoxic-Ischemic Encephalopathy?
 Hypoxic-Ischemic Encephalopathy & Therapeutic Hypothermia Nancy Couto Nurse Practitioner, NICU London Health Sciences Centre, Children s Hospital nancy.couto@lhsc.on.ca 2014 12 17 Objectives Review Pathophysiology
Hypoxic-Ischemic Encephalopathy & Therapeutic Hypothermia Nancy Couto Nurse Practitioner, NICU London Health Sciences Centre, Children s Hospital nancy.couto@lhsc.on.ca 2014 12 17 Objectives Review Pathophysiology
Perinatal asphyxia: Pathophysiology and therapy
 Perinatal asphyxia: Pathophysiology and therapy Peter Davis Melbourne Australia With thanks to Dr Sue Jacobs Moderate or severe HIE Complicates ~1/1000 term live births: Mortality: >25% Major neurological
Perinatal asphyxia: Pathophysiology and therapy Peter Davis Melbourne Australia With thanks to Dr Sue Jacobs Moderate or severe HIE Complicates ~1/1000 term live births: Mortality: >25% Major neurological
Total Body Cooling & Hypoxic Ischemic Encephalopathy in the Neonate Kaleidoscope 2017
 Total Body Cooling & Hypoxic Ischemic Encephalopathy in the Neonate Kaleidoscope 2017 LEIGH ANN CATES PHD, APRN, NNP -BC, RRT-NPS, CHSE N E O N ATA L N U R S E P R A C T I T I O N E R - T E X A S C H I
Total Body Cooling & Hypoxic Ischemic Encephalopathy in the Neonate Kaleidoscope 2017 LEIGH ANN CATES PHD, APRN, NNP -BC, RRT-NPS, CHSE N E O N ATA L N U R S E P R A C T I T I O N E R - T E X A S C H I
TOO COOL OR NOT TOO COOL- THERAPEUTIC HYPOTHERMIA IN THE ICU SCCM TX 2017 TED WU MD PEDIATRIC CRITICAL CARE UNIVERSITY OF TEXAS HEALTH SAN ANTONIO
 TOO COOL OR NOT TOO COOL- THERAPEUTIC HYPOTHERMIA IN THE ICU SCCM TX 2017 TED WU MD PEDIATRIC CRITICAL CARE UNIVERSITY OF TEXAS HEALTH SAN ANTONIO DISCLOSURE I have no relationships with commercial companies
TOO COOL OR NOT TOO COOL- THERAPEUTIC HYPOTHERMIA IN THE ICU SCCM TX 2017 TED WU MD PEDIATRIC CRITICAL CARE UNIVERSITY OF TEXAS HEALTH SAN ANTONIO DISCLOSURE I have no relationships with commercial companies
ETIOLOGY AND PATHOGENESIS OF HYPOXIC-ISCHEMIC ENCEPHALOPATHY
 ETIOLOGY AND PATHOGENESIS OF HYPOXIC-ISCHEMIC ENCEPHALOPATHY HYPOXIC-ISCHEMIC ENCEPHALOPATHY Hypoxic-İschemic Encephalopathy Encephalopathy due to hypoxic-ischemic injury [Hypoxic-ischemic encephalopathy
ETIOLOGY AND PATHOGENESIS OF HYPOXIC-ISCHEMIC ENCEPHALOPATHY HYPOXIC-ISCHEMIC ENCEPHALOPATHY Hypoxic-İschemic Encephalopathy Encephalopathy due to hypoxic-ischemic injury [Hypoxic-ischemic encephalopathy
Disclosures. Objectives. Definition: HIE. HIE: Incidence. Impact 9/10/2018. Hypoxic Ischemic Encephalopathy in the Neonate
 Disclosures Hypoxic Ischemic Encephalopathy in the Neonate No relevant financial relationships or conflicts of interest to disclose Franscesca Miquel-Verges MD 2018 Review therapies currently under research
Disclosures Hypoxic Ischemic Encephalopathy in the Neonate No relevant financial relationships or conflicts of interest to disclose Franscesca Miquel-Verges MD 2018 Review therapies currently under research
Kimberly M. Thornton, 1,2 Hongying Dai, 3 Seth Septer, 2,4 and Joshua E. Petrikin 1,2. 1. Introduction
 International Pediatrics, Article ID 643689, 7 pages http://dx.doi.org/10.1155/2014/643689 Research Article Effects of Whole Body Therapeutic Hypothermia on Gastrointestinal Morbidity and Feeding Tolerance
International Pediatrics, Article ID 643689, 7 pages http://dx.doi.org/10.1155/2014/643689 Research Article Effects of Whole Body Therapeutic Hypothermia on Gastrointestinal Morbidity and Feeding Tolerance
Dysphagia in Encephalopathic Neonates Treated with Hypothermia
 Dysphagia in Encephalopathic Neonates Treated with Hypothermia A thesis submitted to the University of Arizona College of Medicine -- Phoenix in partial fulfillment of the requirements for the degree of
Dysphagia in Encephalopathic Neonates Treated with Hypothermia A thesis submitted to the University of Arizona College of Medicine -- Phoenix in partial fulfillment of the requirements for the degree of
REVIEW ARTICLE. Mohamed A. Tagin, MB BCh; Christy G. Woolcott, PhD; Michael J. Vincer, MD; Robin K. Whyte, MB; Dora A. Stinson, MD
 REVIEW ARTICLE ONLINE FIRST JOURNAL CLUB for Neonatal Hypoxic Ischemic Encephalopathy Scan for Author Audio Interview An Updated Systematic Review and Meta-analysis Mohamed A. Tagin, MB BCh; Christy G.
REVIEW ARTICLE ONLINE FIRST JOURNAL CLUB for Neonatal Hypoxic Ischemic Encephalopathy Scan for Author Audio Interview An Updated Systematic Review and Meta-analysis Mohamed A. Tagin, MB BCh; Christy G.
No social problems noted No past med hx Mother had spontaneous rupture of fetal membranes SB born on Needed to be resuscitated at birth
 No social problems noted No past med hx Mother had spontaneous rupture of fetal membranes SB born on 9-16-2011 Needed to be resuscitated at birth (included assisted vent) Had generalized edema and possible
No social problems noted No past med hx Mother had spontaneous rupture of fetal membranes SB born on 9-16-2011 Needed to be resuscitated at birth (included assisted vent) Had generalized edema and possible
REVIEW ARTICLE. Hypothermia to Treat Neonatal Hypoxic Ischemic Encephalopathy
 REVIEW ARTICLE Hypothermia to Treat Neonatal Hypoxic Ischemic Encephalopathy Systematic Review Prakesh S. Shah, MD, MSc, FRCPC; Arne Ohlsson, FRCPC, MSc; Max Perlman, FRCPC Objectives: To systematically
REVIEW ARTICLE Hypothermia to Treat Neonatal Hypoxic Ischemic Encephalopathy Systematic Review Prakesh S. Shah, MD, MSc, FRCPC; Arne Ohlsson, FRCPC, MSc; Max Perlman, FRCPC Objectives: To systematically
Serum Lactate, Brain Magnetic Resonance Imaging and Outcome of Neonatal Hypoxic Ischemic Encephalopathy after Therapeutic Hypothermia
 Pediatrics and Neonatology (2016) 57, 35e40 Available online at www.sciencedirect.com ScienceDirect journal homepage: http://www.pediatr-neonatol.com ORIGINAL ARTICLE Serum Lactate, Brain Magnetic Resonance
Pediatrics and Neonatology (2016) 57, 35e40 Available online at www.sciencedirect.com ScienceDirect journal homepage: http://www.pediatr-neonatol.com ORIGINAL ARTICLE Serum Lactate, Brain Magnetic Resonance
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of therapeutic hypothermia with intracorporeal temperature monitoring for hypoxic
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of therapeutic hypothermia with intracorporeal temperature monitoring for hypoxic
Neonatal HI brain injury is an evolving process initiated by
 ORIGINAL RESEARCH P. Wintermark A. Hansen M.C. Gregas J. Soul M. Labrecque R.L. Robertson S.K. Warfield Brain Perfusion in Asphyxiated Newborns Treated with Therapeutic Hypothermia BACKGROUND AND PURPOSE:
ORIGINAL RESEARCH P. Wintermark A. Hansen M.C. Gregas J. Soul M. Labrecque R.L. Robertson S.K. Warfield Brain Perfusion in Asphyxiated Newborns Treated with Therapeutic Hypothermia BACKGROUND AND PURPOSE:
Number: Policy *Please see amendment for Pennsylvania Medicaid at the end of this CPB.
 Number: 0812 Policy *Please see amendment for Pennsylvania Medicaid at the end of this CPB. Aetna considers total body cooling (TBC, also known as whole body cooling) and/or selective head cooling (SHC)
Number: 0812 Policy *Please see amendment for Pennsylvania Medicaid at the end of this CPB. Aetna considers total body cooling (TBC, also known as whole body cooling) and/or selective head cooling (SHC)
Does phenobarbital improve the effectiveness of therapeutic hypothermia in infants with hypoxic-ischemic encephalopathy?
 (2012) 32, 15 20 r 2012 Nature America, Inc. All rights reserved. 0743-8346/12 www.nature.com/jp ORIGINAL ARTICLE Does phenobarbital improve the effectiveness of therapeutic hypothermia in infants with
(2012) 32, 15 20 r 2012 Nature America, Inc. All rights reserved. 0743-8346/12 www.nature.com/jp ORIGINAL ARTICLE Does phenobarbital improve the effectiveness of therapeutic hypothermia in infants with
Neurodevelopmental Follow Up After Therapeutic Hypothermia for Perinatal Asphyxia
 ORIGINAL PAPER doi: 10.5455/medarh.2015.69.362-366 Med Arh. 2015 Dec; 69(6): 362-366 Received: August 25th 2015 Accepted: November 05th 2015 2015 Smail Zubcevic, Suada Heljic, Feriha Catibusic, Sajra Uzicanin,
ORIGINAL PAPER doi: 10.5455/medarh.2015.69.362-366 Med Arh. 2015 Dec; 69(6): 362-366 Received: August 25th 2015 Accepted: November 05th 2015 2015 Smail Zubcevic, Suada Heljic, Feriha Catibusic, Sajra Uzicanin,
Initiation of passive cooling at referring centre is most predictive of achieving early therapeutic hypothermia in asphyxiated newborns
 Paediatrics & Child Health, 2017, 264 268 doi: 10.1093/pch/pxx062 Original Article Advance Access publication 23 May 2017 Original Article Initiation of passive cooling at referring centre is most predictive
Paediatrics & Child Health, 2017, 264 268 doi: 10.1093/pch/pxx062 Original Article Advance Access publication 23 May 2017 Original Article Initiation of passive cooling at referring centre is most predictive
Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy
 Original article: Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy *Dr Harshad Bhagat, ** Dr Ravindra Kawade, ***Dr Y.P.Sachdev *Junior Resident, Department Of Radiodiagnosis,
Original article: Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy *Dr Harshad Bhagat, ** Dr Ravindra Kawade, ***Dr Y.P.Sachdev *Junior Resident, Department Of Radiodiagnosis,
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Hypoxic Ischemic Encephalopathy. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Hypoxic Ischemic Encephalopathy. These podcasts are designed to give medical students an overview of key topics in pediatrics.
DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI Page 1 Page 2 perinatal events and brain damage in surviving
DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI Page 1 Page 2 perinatal events and brain damage in surviving
Hypothermia: Neuroprotective Treatment of Hypoxic-Ischemic Encephalopathy. Serious perinatal asphyxia. Therapeutic hypothermia
 Therapeutic hypothermia Hypothermia: Neuroprotective Treatment of Hypoxic-Ischemic Encephalopathy Background of hypothermia Clinical application Floris Groenendaal Department of Neonatology Complications
Therapeutic hypothermia Hypothermia: Neuroprotective Treatment of Hypoxic-Ischemic Encephalopathy Background of hypothermia Clinical application Floris Groenendaal Department of Neonatology Complications
Too or Too Cold. Too Cold...Too Hot...Just Right. Temperature Control in Newborns. Temperature Balance in Newborns. Basics in the Delivery Room
 Too or Too Cold Neonatology Rediscovers Temperature Control Advances and Controversies in Clinical Pediatrics May 31, 2007 Terri A. Slagle Neonatology, CPMC Too Cold...Too Hot...Just Right Too Cold = Issues
Too or Too Cold Neonatology Rediscovers Temperature Control Advances and Controversies in Clinical Pediatrics May 31, 2007 Terri A. Slagle Neonatology, CPMC Too Cold...Too Hot...Just Right Too Cold = Issues
Natalia Gorelik 1, Ricardo Faingold 2, Alan Daneman 3, Monica Epelman 3,4. Original Article
 Original Article Intraventricular hemorrhage in term neonates with hypoxicischemic encephalopathy: a comparison study between neonates treated with and without hypothermia Natalia Gorelik 1, Ricardo Faingold
Original Article Intraventricular hemorrhage in term neonates with hypoxicischemic encephalopathy: a comparison study between neonates treated with and without hypothermia Natalia Gorelik 1, Ricardo Faingold
Hypoxic-Ischemic Encephalopathy. TW de Witt University of Pretoria Department of Paediatrics Neonatology
 Hypoxic-Ischemic Encephalopathy TW de Witt University of Pretoria Department of Paediatrics Neonatology Background HIE remains a serious condition that causes significant mortality and longterm morbidity.
Hypoxic-Ischemic Encephalopathy TW de Witt University of Pretoria Department of Paediatrics Neonatology Background HIE remains a serious condition that causes significant mortality and longterm morbidity.
Therapeutichypothermia headcooling and its Adverse Effects in Newborns with PerinatalAsphyxia
 International Research Journal of Applied and Basic Sciences 2013 Available online at www.irjabs.com ISSN 2251-838X / Vol, 5 (12): 1546-1551 Science Explorer Publications Therapeutichypothermia headcooling
International Research Journal of Applied and Basic Sciences 2013 Available online at www.irjabs.com ISSN 2251-838X / Vol, 5 (12): 1546-1551 Science Explorer Publications Therapeutichypothermia headcooling
Target group Term and near term infants with hypoxic ischaemic encephalopathy (HIE) and parents
 Topic Expert Group: Medical care and clinical practice Postnatal management of newborn infants with hypoxic ischaemic encephalopathy (HIE) Van Bel F, Hellström-Westas L, Zimmermann, L Buonocore G, Murray
Topic Expert Group: Medical care and clinical practice Postnatal management of newborn infants with hypoxic ischaemic encephalopathy (HIE) Van Bel F, Hellström-Westas L, Zimmermann, L Buonocore G, Murray
Birth Asphyxia. Perinatal Depression. Birth Asphyxia. Risk Factors maternal. Risk Factors fetal. Risk Factors Intrapartum 2/12/2011
 Birth Asphyxia Perinatal Depression Sara Brown, ARNP Children s Hospital and Regional Medical Center May occur in utero, during labor/delivery or during the neonatal period Condition of impaired blood
Birth Asphyxia Perinatal Depression Sara Brown, ARNP Children s Hospital and Regional Medical Center May occur in utero, during labor/delivery or during the neonatal period Condition of impaired blood
Queen Charlotte Hospital
 Queen Charlotte Hospital Neuroprotection for neonatal encephalopathy Neonatal encephalopathy accounts for 1 million deaths worldwide and even greater numbers of disabled survivors In countries with
Queen Charlotte Hospital Neuroprotection for neonatal encephalopathy Neonatal encephalopathy accounts for 1 million deaths worldwide and even greater numbers of disabled survivors In countries with
This lecture will provide an overview of the neurologic exam of a neonate in the context of clinical cases.
 A11a Neuro Nuggets from the Trenches Michael D. Weiss, MD Associate Professor Department of Pediatrics, Division of Neonatology University of Florida, Gainesville, FL The speaker has signed a disclosure
A11a Neuro Nuggets from the Trenches Michael D. Weiss, MD Associate Professor Department of Pediatrics, Division of Neonatology University of Florida, Gainesville, FL The speaker has signed a disclosure
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC
 Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Neuroprotective Strategies after Neonatal Hypoxic Ischemic Encephalopathy
 Int. J. Mol. Sci. 2015, 16, 22368-22401; doi:10.3390/ijms160922368 Review OPEN ACCESS International Journal of Molecular Sciences ISSN 1422-0067 www.mdpi.com/journal/ijms Neuroprotective Strategies after
Int. J. Mol. Sci. 2015, 16, 22368-22401; doi:10.3390/ijms160922368 Review OPEN ACCESS International Journal of Molecular Sciences ISSN 1422-0067 www.mdpi.com/journal/ijms Neuroprotective Strategies after
Serum creatine kinase and lactic dehydrogenase levels as useful markers of immediate and long-term outcome of perinatal asphyxia
 Serum creatine kinase and lactic dehydrogenase levels as useful markers of immediate and long-term outcome of perinatal asphyxia D H Karunatilaka 1, G W D S Amaratunga 2, K D N I Perera 3, V Caldera 4
Serum creatine kinase and lactic dehydrogenase levels as useful markers of immediate and long-term outcome of perinatal asphyxia D H Karunatilaka 1, G W D S Amaratunga 2, K D N I Perera 3, V Caldera 4
PEER REVIEW HISTORY ARTICLE DETAILS TITLE (PROVISIONAL)
 PEER REVIEW HISTORY BMJ Paediatrics Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form and are provided with free text boxes to elaborate
PEER REVIEW HISTORY BMJ Paediatrics Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form and are provided with free text boxes to elaborate
Clinical Study Incidence of Retinopathy of Prematurity in Extremely Premature Infants
 ISRN Pediatrics, Article ID 134347, 4 pages http://dx.doi.org/10.1155/2014/134347 Clinical Study Incidence of Retinopathy of Prematurity in Extremely Premature Infants Alparslan Fahin, Muhammed Fahin,
ISRN Pediatrics, Article ID 134347, 4 pages http://dx.doi.org/10.1155/2014/134347 Clinical Study Incidence of Retinopathy of Prematurity in Extremely Premature Infants Alparslan Fahin, Muhammed Fahin,
Perlman J, Clinics Perinatol 2006; 33: Underlying causal pathways. Antenatal Intrapartum Postpartum. Acute near total asphyxia
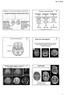 Perlman J, Clinics Perinatol 2006; 33:335-353 Underlying causal pathways Antenatal Intrapartum Postpartum Acute injury Subacute injury Associated problem Reduced fetal movements Placental insufficiency
Perlman J, Clinics Perinatol 2006; 33:335-353 Underlying causal pathways Antenatal Intrapartum Postpartum Acute injury Subacute injury Associated problem Reduced fetal movements Placental insufficiency
Therapeutic hypothermia for hypoxic ischemic encephalopathy using low-technology methods: A systematic review and meta-analysis
 Therapeutic hypothermia for hypoxic ischemic encephalopathy using low-technology methods: A systematic review and meta-analysis Rossouw G 1, Irlam J 2, Horn AR 1 1)Division of Neonatal Medicine, Department
Therapeutic hypothermia for hypoxic ischemic encephalopathy using low-technology methods: A systematic review and meta-analysis Rossouw G 1, Irlam J 2, Horn AR 1 1)Division of Neonatal Medicine, Department
Long-term neuroprotective effects of allopurinol after moderate perinatal asphyxia: follow-up of two randomised controlled trials
 1 Perinatal Center, Wilhelmina 2 Department of Neonatology, Leiden University Medical Center, Leiden, The Netherlands 3 Department of Neonatology, Beatrix Children s Hospital, University Medical Center
1 Perinatal Center, Wilhelmina 2 Department of Neonatology, Leiden University Medical Center, Leiden, The Netherlands 3 Department of Neonatology, Beatrix Children s Hospital, University Medical Center
Research Article Predictions of the Length of Lumbar Puncture Needles
 Computational and Mathematical Methods in Medicine, Article ID 732694, 5 pages http://dx.doi.org/10.1155/2014/732694 Research Article Predictions of the Length of Lumbar Puncture Needles Hon-Ping Ma, 1,2
Computational and Mathematical Methods in Medicine, Article ID 732694, 5 pages http://dx.doi.org/10.1155/2014/732694 Research Article Predictions of the Length of Lumbar Puncture Needles Hon-Ping Ma, 1,2
Therapeutic hypothermia in neonatal asphyxia
 FVV IN OBGYN, 2012, 4 (2): 133-139 New perspective Therapeutic hypothermia in neonatal asphyxia L. CORNETTE Head Department Neonatology, AZ Sint Jan Brugge-Oostende AV Ruddershove 10, 8000 Brugge, Belgium.
FVV IN OBGYN, 2012, 4 (2): 133-139 New perspective Therapeutic hypothermia in neonatal asphyxia L. CORNETTE Head Department Neonatology, AZ Sint Jan Brugge-Oostende AV Ruddershove 10, 8000 Brugge, Belgium.
No Disclosures or Conflicts of Interest. Objectives. Overview. Therapeutic Hypothermia and other Potential Neuroprotective Strategies for HIE
 Therapeutic Hypothermia and other Potential Neuroprotective Strategies for HIE Alexis Davis, M.D. Medical Director, Neonatal Intensive Care Unit Lucile Packard Children s Hospital Clinical Associate Professor
Therapeutic Hypothermia and other Potential Neuroprotective Strategies for HIE Alexis Davis, M.D. Medical Director, Neonatal Intensive Care Unit Lucile Packard Children s Hospital Clinical Associate Professor
Advancing Neurologic Care in the Intensive Care Nursery
 Article neurology Advancing Neurologic Care in the Intensive Care Nursery Hannah C. Glass, MDCM* AUTHOR DISCLOSURE Dr Glass has disclosed that she is supported by grant K23NS066137 from the National Institute
Article neurology Advancing Neurologic Care in the Intensive Care Nursery Hannah C. Glass, MDCM* AUTHOR DISCLOSURE Dr Glass has disclosed that she is supported by grant K23NS066137 from the National Institute
When? Incidence of neonatal seizures in a NICU population The incidence of seizures is higher in the neonatal period than in any other age group.
 Incidence of neonatal seizures in a NICU population The incidence of seizures is higher in the neonatal period than in any other age group. Standard EEG 2,3% 8.6% Standard EEG + aeeg Scher MS et al; Pediatrics
Incidence of neonatal seizures in a NICU population The incidence of seizures is higher in the neonatal period than in any other age group. Standard EEG 2,3% 8.6% Standard EEG + aeeg Scher MS et al; Pediatrics
UK cooling TOBY. register. UK TOBY Cooling Register Protocol
 UK cooling TOBY register UK TOBY Cooling Register Protocol Version 3, 11th June 2007 1 Contents 1. Background 2 1.1 Perinatal asphyxial encephalopathy 2 1.2 Pathogenesis of perinatal asphyxial encephalopathy
UK cooling TOBY register UK TOBY Cooling Register Protocol Version 3, 11th June 2007 1 Contents 1. Background 2 1.1 Perinatal asphyxial encephalopathy 2 1.2 Pathogenesis of perinatal asphyxial encephalopathy
Intraventricular hemorrhage in asphyxiated newborns treated with hypothermia: a look into incidence, timing and risk factors
 Al Yazidi et al. BMC Pediatrics (2015) 15:106 DOI 10.1186/s12887-015-0415-7 RESEARCH ARTICLE Open Access Intraventricular hemorrhage in asphyxiated newborns treated with hypothermia: a look into incidence,
Al Yazidi et al. BMC Pediatrics (2015) 15:106 DOI 10.1186/s12887-015-0415-7 RESEARCH ARTICLE Open Access Intraventricular hemorrhage in asphyxiated newborns treated with hypothermia: a look into incidence,
Therapeutic Hypothermia for Hypoxic Ischaemic Encephalopathy in Singapore General Hospital: Two Patient Case Series and Review Of Literature
 case report Therapeutic Hypothermia for Hypoxic Ischaemic Encephalopathy in Singapore General Hospital: Two Patient Case Series and Review Of Literature Sridhar Arunachalam, MD, MRCPCH (UK); Woei Bing
case report Therapeutic Hypothermia for Hypoxic Ischaemic Encephalopathy in Singapore General Hospital: Two Patient Case Series and Review Of Literature Sridhar Arunachalam, MD, MRCPCH (UK); Woei Bing
Neonatal Encephalopathy: Treatment With Hypothermia Seetha Shankaran. DOI: /neo.11-2-e85
 Neonatal Encephalopathy: Treatment With Hypothermia Seetha Shankaran NeoReviews 2010;11;e85-e92 DOI: 10.1542/neo.11-2-e85 The online version of this article, along with updated information and services,
Neonatal Encephalopathy: Treatment With Hypothermia Seetha Shankaran NeoReviews 2010;11;e85-e92 DOI: 10.1542/neo.11-2-e85 The online version of this article, along with updated information and services,
University of Bristol - Explore Bristol Research
 Elstad, M., Liu, X., & Thoresen, M. (2016). Heart rate response to therapeutic hypothermia in infants with hypoxic-ischaemic encephalopathy. Resuscitation, 106, 53-57. DOI: 10.1016/j.resuscitation.2016.06.023
Elstad, M., Liu, X., & Thoresen, M. (2016). Heart rate response to therapeutic hypothermia in infants with hypoxic-ischaemic encephalopathy. Resuscitation, 106, 53-57. DOI: 10.1016/j.resuscitation.2016.06.023
How to combat brain injury in newborns hopes and challenges for regenerative therapies
 ISSN 2399-1534 RESEARCH FEATURES ISSUE 119 RESEARCHERS FEATURED: Dr C Webb; Dr T Tay; Prof Dr U Felderhoff- Müser; Dr C Hohmann & Dr A Winstead; Prof A Schwartzman; Dr J Foppen; Prof R Williams & Dr P
ISSN 2399-1534 RESEARCH FEATURES ISSUE 119 RESEARCHERS FEATURED: Dr C Webb; Dr T Tay; Prof Dr U Felderhoff- Müser; Dr C Hohmann & Dr A Winstead; Prof A Schwartzman; Dr J Foppen; Prof R Williams & Dr P
Relationship between acute kidney injury and brain MRI findings in asphyxiated newborns after therapeutic hypothermia
 nature publishing group Clinical Investigation Relationship between acute kidney injury and brain MRI findings in asphyxiated newborns after therapeutic hypothermia Subrata Sarkar 1, David J. Askenazi
nature publishing group Clinical Investigation Relationship between acute kidney injury and brain MRI findings in asphyxiated newborns after therapeutic hypothermia Subrata Sarkar 1, David J. Askenazi
Study of renal functions in neonatal asphyxia
 Original article: Study of renal functions in neonatal asphyxia *Dr. D.Y.Shrikhande, **Dr. Vivek Singh, **Dr. Amit Garg *Professor and Head, **Senior Resident Department of Pediatrics, Pravara Institute
Original article: Study of renal functions in neonatal asphyxia *Dr. D.Y.Shrikhande, **Dr. Vivek Singh, **Dr. Amit Garg *Professor and Head, **Senior Resident Department of Pediatrics, Pravara Institute
be able to identify newer adjunct therapies for management of infants with HIE.
 A7a Beyond Hypothermia: Emerging Therapies for Neuroprotection Rajan Wadhawan, MD, MMM, CPE, FAAP Chief of Neonatology Walt Disney Pavilion, Florida Hospital for Children Orlando, FL The speaker has signed
A7a Beyond Hypothermia: Emerging Therapies for Neuroprotection Rajan Wadhawan, MD, MMM, CPE, FAAP Chief of Neonatology Walt Disney Pavilion, Florida Hospital for Children Orlando, FL The speaker has signed
AMERICAN COLLEGE OF SURGEONS CRITICAL CARE REVIEW COURSE 2012 HOT TOPICS IN PEDIATRIC CRITICAL CARE
 AMERICAN COLLEGE OF SURGEONS CRITICAL CARE REVIEW COURSE 2012 HOT TOPICS IN PEDIATRIC CRITICAL CARE Karyn L. Butler, MD, FACS, FCCM Chief, Surgical Critical Care Hartford Hospital / University of Connecticut
AMERICAN COLLEGE OF SURGEONS CRITICAL CARE REVIEW COURSE 2012 HOT TOPICS IN PEDIATRIC CRITICAL CARE Karyn L. Butler, MD, FACS, FCCM Chief, Surgical Critical Care Hartford Hospital / University of Connecticut
NEONATOLOGY GIVES BACK WHAT OBSTETRICS TAKE AWAY. It is well-known that hypoxic and/or ischemic events during labor and
 NEONATOLOGY GIVES BACK WHAT OBSTETRICS TAKE AWAY I. Introduction It is well-known that hypoxic and/or ischemic events during labor and delivery can cause injury to the baby's brain. The mechanisms at first
NEONATOLOGY GIVES BACK WHAT OBSTETRICS TAKE AWAY I. Introduction It is well-known that hypoxic and/or ischemic events during labor and delivery can cause injury to the baby's brain. The mechanisms at first
University of Bristol - Explore Bristol Research
 Wang, H., Cheng, Z., Liao, Y., Li, J., Weber, J., Thomas, A., & Faul, C. FJ. (2017). Conjugated Microporous Polycarbazole Networks as Precursors for Nitrogen Enriched Microporous Carbons for CO2 Storage
Wang, H., Cheng, Z., Liao, Y., Li, J., Weber, J., Thomas, A., & Faul, C. FJ. (2017). Conjugated Microporous Polycarbazole Networks as Precursors for Nitrogen Enriched Microporous Carbons for CO2 Storage
Therapeu(c Hypothermia: The Status of its Use for Hypoxic-Ischemic Encephalopathy (HIE)
 Therapeu(c Hypothermia: The Status of its Use for Hypoxic-Ischemic Encephalopathy (HIE) Abbot R. Laptook, M.D. Medical Director, NICU Women and Infants Hospital of RI Professor of Pediatrics Alpert Medical
Therapeu(c Hypothermia: The Status of its Use for Hypoxic-Ischemic Encephalopathy (HIE) Abbot R. Laptook, M.D. Medical Director, NICU Women and Infants Hospital of RI Professor of Pediatrics Alpert Medical
Report CAEN Category 1A: Visit by the Applicant to Another Laboratory
 Report CAEN Category 1A: Visit by the Applicant to Another Laboratory Visitor: Gustavo Ferreira, Federal University of Rio de Janeiro, Brazil Host: Prof. Mary C. McKenna, University of Maryland, Baltimore,
Report CAEN Category 1A: Visit by the Applicant to Another Laboratory Visitor: Gustavo Ferreira, Federal University of Rio de Janeiro, Brazil Host: Prof. Mary C. McKenna, University of Maryland, Baltimore,
BMC Pediatrics. Open Access. Abstract
 BMC Pediatrics BioMed Central Research article A systematic review of cooling for neuroprotection in neonates with hypoxic ischemic encephalopathy are we there yet? Sven M Schulzke* 1,2, Shripada Rao 1
BMC Pediatrics BioMed Central Research article A systematic review of cooling for neuroprotection in neonates with hypoxic ischemic encephalopathy are we there yet? Sven M Schulzke* 1,2, Shripada Rao 1
7 Simple Steps to Assess & Document any Neonatal aeeg
 7 Simple Steps to Assess & Document any Neonatal aeeg Created for you by: www.aeegcoach.com How to use the Seven Simple Steps Checklist Hi! It s Kathi Randall here Your aeeg coach. I m so excited to share
7 Simple Steps to Assess & Document any Neonatal aeeg Created for you by: www.aeegcoach.com How to use the Seven Simple Steps Checklist Hi! It s Kathi Randall here Your aeeg coach. I m so excited to share
Thais Agut 1*, Marisol León 1, Mónica Rebollo 2, Jordi Muchart 2, Gemma Arca 1 and Alfredo Garcia-Alix 1
 Agut et al. BMC Pediatrics 2014, 14:177 RESEARCH ARTICLE Open Access Early identification of brain injury in infants with hypoxic ischemic encephalopathy at high risk for severe impairments: accuracy of
Agut et al. BMC Pediatrics 2014, 14:177 RESEARCH ARTICLE Open Access Early identification of brain injury in infants with hypoxic ischemic encephalopathy at high risk for severe impairments: accuracy of
Moving beyond therapeutic hypothermia
 Moving beyond therapeutic hypothermia #swaps2017 #foamneo @elisasmit_neo Elisa Smit, MD MRCPCH Consultant Neonatologist Cardiff and Vale University Health Board Honorary Researcher Neonatal Neuroscience
Moving beyond therapeutic hypothermia #swaps2017 #foamneo @elisasmit_neo Elisa Smit, MD MRCPCH Consultant Neonatologist Cardiff and Vale University Health Board Honorary Researcher Neonatal Neuroscience
Cerebral palsy? Cerebral palsies? Cerebral palsy spectrum disorder?
 Teamwork makes the dream work Nationaal symposium van Belgische CP-centra 18/02/2019 Cerebral palsy? Cerebral palsies? Cerebral palsy spectrum disorder? Faes Franny Dienst Kinderneurologie UZ Gent Centrum
Teamwork makes the dream work Nationaal symposium van Belgische CP-centra 18/02/2019 Cerebral palsy? Cerebral palsies? Cerebral palsy spectrum disorder? Faes Franny Dienst Kinderneurologie UZ Gent Centrum
BIRTH TRAUMA LITIGATION: PROVING THE CAUSE OF NEWBORN NEUROLOGIC INJURY 1 By Richard C. Halpern
 BIRTH TRAUMA LITIGATION: PROVING THE CAUSE OF NEWBORN NEUROLOGIC INJURY 1 By Richard C. Halpern Proving the cause of newborn neurologic injury in birth trauma litigation, an essential step to a successful
BIRTH TRAUMA LITIGATION: PROVING THE CAUSE OF NEWBORN NEUROLOGIC INJURY 1 By Richard C. Halpern Proving the cause of newborn neurologic injury in birth trauma litigation, an essential step to a successful
jamapediatrics.com (Reprinted) JAMA Pediatrics Published online February 16, 2015 E1
 Clinical Review & Education Review A Review for the Clinician Martha Douglas-Escobar, MD; Michael D. Weiss, MD IMPORTANCE Hypoxic-ischemic encephalopathy (HIE) occurs in 1 to 8 per 1000 live births in
Clinical Review & Education Review A Review for the Clinician Martha Douglas-Escobar, MD; Michael D. Weiss, MD IMPORTANCE Hypoxic-ischemic encephalopathy (HIE) occurs in 1 to 8 per 1000 live births in
Case Report Complete Obstruction of Endotracheal Tube in an Infant with a Retropharyngeal and Anterior Mediastinal Abscess
 Hindawi Case Reports in Pediatrics Volume 2017, Article ID 1848945, 4 pages https://doi.org/10.1155/2017/1848945 Case Report Complete Obstruction of Endotracheal Tube in an Infant with a Retropharyngeal
Hindawi Case Reports in Pediatrics Volume 2017, Article ID 1848945, 4 pages https://doi.org/10.1155/2017/1848945 Case Report Complete Obstruction of Endotracheal Tube in an Infant with a Retropharyngeal
Imaging findings in neonates with hypoxic-ischaemic encephalopathy and terapeutic hypothermia.
 Imaging findings in neonates with hypoxic-ischaemic encephalopathy and terapeutic hypothermia. Poster No.: C-1577 Congress: ECR 2014 Type: Scientific Exhibit Authors: S. Manso Garcia, M. J. Velasco Marcos,
Imaging findings in neonates with hypoxic-ischaemic encephalopathy and terapeutic hypothermia. Poster No.: C-1577 Congress: ECR 2014 Type: Scientific Exhibit Authors: S. Manso Garcia, M. J. Velasco Marcos,
Perinatal Depression. Lauren Sacco DNP, ARNP Seattle Children s
 Perinatal Depression Lauren Sacco DNP, ARNP Seattle Children s Birth Asphyxia May occur in utero, during labor/delivery or during the neonatal period Condition of impaired blood gas exchange that leads
Perinatal Depression Lauren Sacco DNP, ARNP Seattle Children s Birth Asphyxia May occur in utero, during labor/delivery or during the neonatal period Condition of impaired blood gas exchange that leads
Newborn Hypoxic Ischemic Brain Injury. Hisham Dahmoush, MBBCh FRCR Lucile Packard Children s Hospital at Stanford
 Newborn Hypoxic Ischemic Brain Injury Hisham Dahmoush, MBBCh FRCR Lucile Packard Children s Hospital at Stanford NO DISCLOSURES INTRODUCTION Neonatal hypoxic-ischemic encephalopathy (HIE) is a major cause
Newborn Hypoxic Ischemic Brain Injury Hisham Dahmoush, MBBCh FRCR Lucile Packard Children s Hospital at Stanford NO DISCLOSURES INTRODUCTION Neonatal hypoxic-ischemic encephalopathy (HIE) is a major cause
TLC March 27, Shawn Hollinger-Neonatal Fellow CHEO
 TLC March 27, 2013 Presented/Prepared by: Shawn Hollinger, PGY5 Neonatal-Perinatal Medicine Resident - University of Ottawa With slides/images from Dr. Brigitte Lemyre Associate Professor of Pediatrics
TLC March 27, 2013 Presented/Prepared by: Shawn Hollinger, PGY5 Neonatal-Perinatal Medicine Resident - University of Ottawa With slides/images from Dr. Brigitte Lemyre Associate Professor of Pediatrics
Seizure burden and neurodevelopmental outcome in neonates with hypoxic ischemic encephalopathy
 DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE Seizure burden and neurodevelopmental outcome in neonates with hypoxic ischemic encephalopathy LIUDMILA KHAROSHANKAYA 1,2 NATHAN J STEVENSON 1
DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE Seizure burden and neurodevelopmental outcome in neonates with hypoxic ischemic encephalopathy LIUDMILA KHAROSHANKAYA 1,2 NATHAN J STEVENSON 1
Hypothermia Plus: New NeuroProtective Strategies with Stem Cells
 Hypothermia Plus: New NeuroProtective Strategies with Stem Cells The BEST of IPOKRaTES: an Update in Neonatology Leuven, Belgium, September 17-20, 2014 Clinical Background Perinatal Hypoxia-Ischemia (Birth
Hypothermia Plus: New NeuroProtective Strategies with Stem Cells The BEST of IPOKRaTES: an Update in Neonatology Leuven, Belgium, September 17-20, 2014 Clinical Background Perinatal Hypoxia-Ischemia (Birth
Hypoxic ischaemic encephalopathy
 Hypoxic ischaemic encephalopathy Frances Cowan Denis Azzopardi Abstract Encephalopathy occurring soon after birth continues to be a major complication in near- and full-term newborn infants. Early neonatal
Hypoxic ischaemic encephalopathy Frances Cowan Denis Azzopardi Abstract Encephalopathy occurring soon after birth continues to be a major complication in near- and full-term newborn infants. Early neonatal
Neonatal Hypoxic-Ischemic Injury: Ultrasound and Dynamic Color Doppler Sonography perfusion of the Brain and Abdomen with pathologic correlation.
 Neonatal Hypoxic-Ischemic Injury: Ultrasound and Dynamic Color Doppler Sonography perfusion of the Brain and Abdomen with pathologic correlation. Ricardo Faingold,MD Montreal Children s Hospital Medical
Neonatal Hypoxic-Ischemic Injury: Ultrasound and Dynamic Color Doppler Sonography perfusion of the Brain and Abdomen with pathologic correlation. Ricardo Faingold,MD Montreal Children s Hospital Medical
TREATMENT OF HYPOXIC ISCHEMIC ENCEPALOPATHY AND CEREBRAL HYPOTHERMIA
 TREATMENT OF HYPOXIC ISCHEMIC ENCEPALOPATHY AND CEREBRAL HYPOTHERMIA F. Emre CANPOLAT MD NICU, Ministry of Health, Zekai Tahir Burak Maternity and Teaching Hospital, Ankara, TURKEY Disclosure statement
TREATMENT OF HYPOXIC ISCHEMIC ENCEPALOPATHY AND CEREBRAL HYPOTHERMIA F. Emre CANPOLAT MD NICU, Ministry of Health, Zekai Tahir Burak Maternity and Teaching Hospital, Ankara, TURKEY Disclosure statement
Research Article Clinical Outcome of a Novel Anti-CD6 Biologic Itolizumab in Patients of Psoriasis with Comorbid Conditions
 Dermatology Research and Practice Volume 2, Article ID 13326, 4 pages http://dx.doi.org/.1155/2/13326 Research Article Clinical Outcome of a Novel Anti-CD6 Biologic Itolizumab in Patients of Psoriasis
Dermatology Research and Practice Volume 2, Article ID 13326, 4 pages http://dx.doi.org/.1155/2/13326 Research Article Clinical Outcome of a Novel Anti-CD6 Biologic Itolizumab in Patients of Psoriasis
FINDINGS IDENTIFY. cause. this nerve cell death in infant mice. that: The brain. and even to recover. more
 Embargoed until November 17, 11:30 a.m. ET Press Room, November 15 19: (202) 249-4125 Contacts: Sara Harris, (202) 962-4087 Todd Bentsen, (202) 962-4086 BRAIN RESEARCH FINDINGS IDENTIFY NEW TREATMENTS
Embargoed until November 17, 11:30 a.m. ET Press Room, November 15 19: (202) 249-4125 Contacts: Sara Harris, (202) 962-4087 Todd Bentsen, (202) 962-4086 BRAIN RESEARCH FINDINGS IDENTIFY NEW TREATMENTS
Original Article THERAPEUTIC EFFICACY OF MAGNESIUM SULPHATE ON NEUROLOGICAL OUTCOME OF NEONATES WITH SEVERE BIRTH ASPHYXIA
 Original Article ON NEUROLOGICAL OUTCOME OF NEONATES WITH SEVERE BIRTH ASPHYXIA 1 2 3 Nisar Khan Sajid, Muhammad Junaid, Saeed Ahmed 1 Associate Professor of Paediatrics Aziz Fatima Medical & Dental College
Original Article ON NEUROLOGICAL OUTCOME OF NEONATES WITH SEVERE BIRTH ASPHYXIA 1 2 3 Nisar Khan Sajid, Muhammad Junaid, Saeed Ahmed 1 Associate Professor of Paediatrics Aziz Fatima Medical & Dental College
1. Arai Y et al., Combinatorial effects of neuroinflammation and genetic background in the pathophysiology of developmental disorders.
 Poster Presentations 10 th Hershey Conference 1. Arai Y et al., Combinatorial effects of neuroinflammation and genetic background in the pathophysiology of developmental disorders. 2. Azhan A et al., Do
Poster Presentations 10 th Hershey Conference 1. Arai Y et al., Combinatorial effects of neuroinflammation and genetic background in the pathophysiology of developmental disorders. 2. Azhan A et al., Do
Hypoxic-ischemic encephalopathy has an incidence of
 Original Article Amplitude-Integrated EEG Is Useful in Predicting Neurodevelopmental Outcome in Full-Term Infants With Hypoxic-Ischemic Encephalopathy: A Meta-Analysis Journal of Child Neurology Volume
Original Article Amplitude-Integrated EEG Is Useful in Predicting Neurodevelopmental Outcome in Full-Term Infants With Hypoxic-Ischemic Encephalopathy: A Meta-Analysis Journal of Child Neurology Volume
State of Florida Systemic Supportive Care Guidelines. Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology
 State of Florida Systemic Supportive Care Guidelines Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology I. FEN 1. What intravenous fluids should be initiated upon admission
State of Florida Systemic Supportive Care Guidelines Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology I. FEN 1. What intravenous fluids should be initiated upon admission
Ipotermia terapeutica nel bambino: manca l evidenza?
 Ipotermia terapeutica nel bambino: manca l evidenza? Andrea Moscatelli UOSD Terapia Intensiva Neonatale e Pediatrica Dipartimento Integrato di Alta Intensita` di Cura e Chirurgia Istituto Giannina Gaslini
Ipotermia terapeutica nel bambino: manca l evidenza? Andrea Moscatelli UOSD Terapia Intensiva Neonatale e Pediatrica Dipartimento Integrato di Alta Intensita` di Cura e Chirurgia Istituto Giannina Gaslini
Therapeutic Hypothermia: Treatment for Hypoxic-Ischemic Encephalopathy in the NICU
 Therapeutic Hypothermia: Treatment for Hypoxic-Ischemic Encephalopathy in the NICU Denise M. Casey, RN, MS, CCRN, CPNP Nancy Tella, RN, BSN, CCRN Rachel Turesky, RN, BSN Michelle Labrecque, RN, MSN, CCRN
Therapeutic Hypothermia: Treatment for Hypoxic-Ischemic Encephalopathy in the NICU Denise M. Casey, RN, MS, CCRN, CPNP Nancy Tella, RN, BSN, CCRN Rachel Turesky, RN, BSN Michelle Labrecque, RN, MSN, CCRN
Research Article Predictive Factors for Medical Consultation for Sore Throat in Adults with Recurrent Pharyngotonsillitis
 International Otolaryngology Volume 2016, Article ID 6095689, 5 pages http://dx.doi.org/10.1155/2016/6095689 Research Article Predictive Factors for Medical Consultation for Sore Throat in Adults with
International Otolaryngology Volume 2016, Article ID 6095689, 5 pages http://dx.doi.org/10.1155/2016/6095689 Research Article Predictive Factors for Medical Consultation for Sore Throat in Adults with
Conference Paper Antithrombotic Therapy in Patients with Acute Coronary Syndromes: Biological Markers and Personalized Medicine
 Conference Papers in Medicine, Article ID 719, pages http://dx.doi.org/1.1155/13/719 Conference Paper Antithrombotic Therapy in Patients with Acute Coronary Syndromes: Biological Markers and Personalized
Conference Papers in Medicine, Article ID 719, pages http://dx.doi.org/1.1155/13/719 Conference Paper Antithrombotic Therapy in Patients with Acute Coronary Syndromes: Biological Markers and Personalized
Childhood Outcomes after Hypothermia for Neonatal Encephalopathy
 T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article Childhood Outcomes after Hypothermia for Neonatal Encephalopathy Seetha Shankaran, M.D., Athina Pappas, M.D., Scott A. McDonald, B.S.,
T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article Childhood Outcomes after Hypothermia for Neonatal Encephalopathy Seetha Shankaran, M.D., Athina Pappas, M.D., Scott A. McDonald, B.S.,
REVIEWS. A new neurological focus in neonatal intensive care. Sonia L. Bonifacio, Hannah C. Glass, Susan Peloquin and Donna M.
 A new neurological focus in neonatal intensive care Sonia L. Bonifacio, Hannah C. Glass, Susan Peloquin and Donna M. Ferriero Abstract Advances in the care of high-risk newborn babies have contributed
A new neurological focus in neonatal intensive care Sonia L. Bonifacio, Hannah C. Glass, Susan Peloquin and Donna M. Ferriero Abstract Advances in the care of high-risk newborn babies have contributed
Automated System for Detecting Neonatal Brain Injuries
 Snapshots of Postgraduate Research at University College Cork 2016 Automated System for Detecting Neonatal Brain Injuries Rehan Ahmed Dept. of Electrical and Electronics Engineering,, UCC The most dangerous
Snapshots of Postgraduate Research at University College Cork 2016 Automated System for Detecting Neonatal Brain Injuries Rehan Ahmed Dept. of Electrical and Electronics Engineering,, UCC The most dangerous
INTRODUCING SOLITAIRE PLATINUM REVASCULARIZATION DEVICE ENHANCED VISIBILITY EXPANDED PORTFOLIO SEEING IS KNOWING. KNOWLEDGE IS CONFIDENCE.
 INTRODUCING SOLITAIRE PLATINUM REVASCULARIZATION DEVICE ENHANCED VISIBILITY EXPANDED PORTFOLIO 6X40MM SEEING IS KNOWING. KNOWLEDGE IS CONFIDENCE. www.medtronic.eu UC201708427 EE Medtronic 2017. All rights
INTRODUCING SOLITAIRE PLATINUM REVASCULARIZATION DEVICE ENHANCED VISIBILITY EXPANDED PORTFOLIO 6X40MM SEEING IS KNOWING. KNOWLEDGE IS CONFIDENCE. www.medtronic.eu UC201708427 EE Medtronic 2017. All rights
Running title: EEG, MRI and neurodevelopmental outcome in HIE. Word count manuscript body: Word count abstract: 226. Address correspondence to:
 Role of EEG background activity, seizure burden and MRI in predicting neurodevelopmental outcome in full-term infants with hypoxic-ischaemic encephalopathy in the era of therapeutic hypothermia. Lauren
Role of EEG background activity, seizure burden and MRI in predicting neurodevelopmental outcome in full-term infants with hypoxic-ischaemic encephalopathy in the era of therapeutic hypothermia. Lauren
Retrospectıve analysıs for newborn ınfants wıth hypoxıc-ıschemıc encephalopathy
 Basic Research Journal of Medicine and Clinical Sciences ISSN 2315-6864 Vol. 1(2) pp. 19-24 September 2012 Available online http//www.basicresearchjournals.org Copyright 2012 Basic Research Journal Full
Basic Research Journal of Medicine and Clinical Sciences ISSN 2315-6864 Vol. 1(2) pp. 19-24 September 2012 Available online http//www.basicresearchjournals.org Copyright 2012 Basic Research Journal Full
The wufless-ness of glutamate!
 The wufless-ness of glutamate! EXCITOTOXINS are substances, usually acidic amino acids, that react with specialized receptors in the brain in such a way as to lead to destruction of certain types of neurons.
The wufless-ness of glutamate! EXCITOTOXINS are substances, usually acidic amino acids, that react with specialized receptors in the brain in such a way as to lead to destruction of certain types of neurons.
1/29/2014. Kimberly Johnson Hatchett, MD PGY-4 11/15/13
 Kimberly Johnson Hatchett, MD PGY-4 11/15/13 History of Present Illness 14 month old previously healthy infant boy presented via EMS after being found by his mother to be breathing loudly and non-responsive.
Kimberly Johnson Hatchett, MD PGY-4 11/15/13 History of Present Illness 14 month old previously healthy infant boy presented via EMS after being found by his mother to be breathing loudly and non-responsive.
The Clinical Spectrum and Prediction of Outcome in Hypoxic-Ischemic Encephalopathy
 Article neurology The Clinical Spectrum and Prediction of Outcome in Hypoxic-Ischemic Encephalopathy Walter C. Allan, MD* Objectives After completing this article, readers should be able to: 1. List the
Article neurology The Clinical Spectrum and Prediction of Outcome in Hypoxic-Ischemic Encephalopathy Walter C. Allan, MD* Objectives After completing this article, readers should be able to: 1. List the
